User login
Novel vascular sheath detects periprocedural bleeds
LAS VEGAS – A set of electrodes arrayed in a standard, vascular-access catheter sheath accurately alerted operators to access-site bleeding in a first-in-human study with 60 patients treated at any of five U.S. centers.
“The Early Bird bleed-monitoring system was safe, easily incorporated in standard flow of work, and demonstrated the capacity to detect bleeding before progression to a more severe or symptomatic phase,” Philippe Généreux, MD, said at the Society for Cardiovascular Angiography & Interventions annual scientific sessions. The study in 60 patients undergoing standard intravascular procedures via femoral-artery access – most often transcatheter aortic valve replacement – showed that an alert for access-site bleeding occurred with a Cohen’s kappa of 0.84, compared with CT imaging for bleeding, a score that shows “almost perfect” concordance between the two methods, noted Dr. Généreux, an interventional cardiologist and director of the structural heart program at Morristown (N.J.) Medical Center.
The study protocol called for keeping the sheath in place for up to 12 hours post procedure, and in practice the sheath remained in place for an average of about 160 minutes post procedure; 31% of the bleeds occurred during the procedure, with the remaining 69% occurring later. Another notable finding from the CT imaging at the time of sheath removal was that only 4 of the 60 patients had absolutely no bleeding, while 34 patients (57%) had blood infiltration at the access site and 22 patients (37%) had an access-site hematoma. No patients had retroperitoneal bleeding, but the system is designed to also detect bleeding within that space.
The Early Bird system received de novo classification as a new device from the Food and Drug Administration in March 2019; based on this, Saranas – the company developing the device – will likely start U.S. marketing before the end of 2019, Dr. Généreux said during a press briefing. The company is planning a registry of cases that use the device to collect data on patient outcomes to try to eventually document the clinical impact and cost-effectiveness of the system. Until now, standard of care has been to identify vascular-access associated bleeds once they become overt or symptomatic. If bleeds are identified at an earlier stage they could potentially be resolved before symptoms develop or become severe and hence provide a potential opportunity for cost savings.
Although the current study did not target specific types of patients, it makes sense in routine practice to target the device to patients at high risk for either developing a bleed or complications secondary to a bleed, such as patients undergoing transcatheter aortic valve replacement, patients receiving a mechanical circulatory assist device, or patients scheduled for complex procedures that will use multiple sheaths, he said.
The Early Bird sheath is 30 cm long, and is placed through the left or right femoral vein to the bifurcation of the iliac artery. (In the current study, more than 80% of the 60 treated patients had the sheath placed in their right femoral vein.) The access sheath for the catheters involved in the procedures themselves were most often placed in the left or right femoral artery. Electrodes within the Early Bird sheath detect leaked blood by its impact on bioimpedance of the tissue surrounding the sheath, with the system able to roughly gauge the volume of released blood based on the local level of bioimpedance change.
A couple of years ago, Dr. Généreux and his associates documented an 18% incidence of bleeding complications among 17,672 U.S. patients who underwent a transcatheter procedure with a large-bore catheter during 2013-2014 using data collected by the National Inpatient Sample (JAMA Cardiol. 2017 Jul;2[7]:798-802). Their analysis also documented that the patients with bleeding-related complications had in-hospital costs that averaged more than 50% higher than the costs for patients without bleeding complications, findings that raised the possibility that earlier identification of a bleed, before severe complications ensured, could be both cost effective and beneficial to patients, Dr. Généreux said.
Dr. Généreux has been a consultant to Saranas and to several other companies. He is also chief medical officer for Saranas and has an equity interest in the company.
SOURCE: Généreux P. SCAI 2019, Abstract 5713.
LAS VEGAS – A set of electrodes arrayed in a standard, vascular-access catheter sheath accurately alerted operators to access-site bleeding in a first-in-human study with 60 patients treated at any of five U.S. centers.
“The Early Bird bleed-monitoring system was safe, easily incorporated in standard flow of work, and demonstrated the capacity to detect bleeding before progression to a more severe or symptomatic phase,” Philippe Généreux, MD, said at the Society for Cardiovascular Angiography & Interventions annual scientific sessions. The study in 60 patients undergoing standard intravascular procedures via femoral-artery access – most often transcatheter aortic valve replacement – showed that an alert for access-site bleeding occurred with a Cohen’s kappa of 0.84, compared with CT imaging for bleeding, a score that shows “almost perfect” concordance between the two methods, noted Dr. Généreux, an interventional cardiologist and director of the structural heart program at Morristown (N.J.) Medical Center.
The study protocol called for keeping the sheath in place for up to 12 hours post procedure, and in practice the sheath remained in place for an average of about 160 minutes post procedure; 31% of the bleeds occurred during the procedure, with the remaining 69% occurring later. Another notable finding from the CT imaging at the time of sheath removal was that only 4 of the 60 patients had absolutely no bleeding, while 34 patients (57%) had blood infiltration at the access site and 22 patients (37%) had an access-site hematoma. No patients had retroperitoneal bleeding, but the system is designed to also detect bleeding within that space.
The Early Bird system received de novo classification as a new device from the Food and Drug Administration in March 2019; based on this, Saranas – the company developing the device – will likely start U.S. marketing before the end of 2019, Dr. Généreux said during a press briefing. The company is planning a registry of cases that use the device to collect data on patient outcomes to try to eventually document the clinical impact and cost-effectiveness of the system. Until now, standard of care has been to identify vascular-access associated bleeds once they become overt or symptomatic. If bleeds are identified at an earlier stage they could potentially be resolved before symptoms develop or become severe and hence provide a potential opportunity for cost savings.
Although the current study did not target specific types of patients, it makes sense in routine practice to target the device to patients at high risk for either developing a bleed or complications secondary to a bleed, such as patients undergoing transcatheter aortic valve replacement, patients receiving a mechanical circulatory assist device, or patients scheduled for complex procedures that will use multiple sheaths, he said.
The Early Bird sheath is 30 cm long, and is placed through the left or right femoral vein to the bifurcation of the iliac artery. (In the current study, more than 80% of the 60 treated patients had the sheath placed in their right femoral vein.) The access sheath for the catheters involved in the procedures themselves were most often placed in the left or right femoral artery. Electrodes within the Early Bird sheath detect leaked blood by its impact on bioimpedance of the tissue surrounding the sheath, with the system able to roughly gauge the volume of released blood based on the local level of bioimpedance change.
A couple of years ago, Dr. Généreux and his associates documented an 18% incidence of bleeding complications among 17,672 U.S. patients who underwent a transcatheter procedure with a large-bore catheter during 2013-2014 using data collected by the National Inpatient Sample (JAMA Cardiol. 2017 Jul;2[7]:798-802). Their analysis also documented that the patients with bleeding-related complications had in-hospital costs that averaged more than 50% higher than the costs for patients without bleeding complications, findings that raised the possibility that earlier identification of a bleed, before severe complications ensured, could be both cost effective and beneficial to patients, Dr. Généreux said.
Dr. Généreux has been a consultant to Saranas and to several other companies. He is also chief medical officer for Saranas and has an equity interest in the company.
SOURCE: Généreux P. SCAI 2019, Abstract 5713.
LAS VEGAS – A set of electrodes arrayed in a standard, vascular-access catheter sheath accurately alerted operators to access-site bleeding in a first-in-human study with 60 patients treated at any of five U.S. centers.
“The Early Bird bleed-monitoring system was safe, easily incorporated in standard flow of work, and demonstrated the capacity to detect bleeding before progression to a more severe or symptomatic phase,” Philippe Généreux, MD, said at the Society for Cardiovascular Angiography & Interventions annual scientific sessions. The study in 60 patients undergoing standard intravascular procedures via femoral-artery access – most often transcatheter aortic valve replacement – showed that an alert for access-site bleeding occurred with a Cohen’s kappa of 0.84, compared with CT imaging for bleeding, a score that shows “almost perfect” concordance between the two methods, noted Dr. Généreux, an interventional cardiologist and director of the structural heart program at Morristown (N.J.) Medical Center.
The study protocol called for keeping the sheath in place for up to 12 hours post procedure, and in practice the sheath remained in place for an average of about 160 minutes post procedure; 31% of the bleeds occurred during the procedure, with the remaining 69% occurring later. Another notable finding from the CT imaging at the time of sheath removal was that only 4 of the 60 patients had absolutely no bleeding, while 34 patients (57%) had blood infiltration at the access site and 22 patients (37%) had an access-site hematoma. No patients had retroperitoneal bleeding, but the system is designed to also detect bleeding within that space.
The Early Bird system received de novo classification as a new device from the Food and Drug Administration in March 2019; based on this, Saranas – the company developing the device – will likely start U.S. marketing before the end of 2019, Dr. Généreux said during a press briefing. The company is planning a registry of cases that use the device to collect data on patient outcomes to try to eventually document the clinical impact and cost-effectiveness of the system. Until now, standard of care has been to identify vascular-access associated bleeds once they become overt or symptomatic. If bleeds are identified at an earlier stage they could potentially be resolved before symptoms develop or become severe and hence provide a potential opportunity for cost savings.
Although the current study did not target specific types of patients, it makes sense in routine practice to target the device to patients at high risk for either developing a bleed or complications secondary to a bleed, such as patients undergoing transcatheter aortic valve replacement, patients receiving a mechanical circulatory assist device, or patients scheduled for complex procedures that will use multiple sheaths, he said.
The Early Bird sheath is 30 cm long, and is placed through the left or right femoral vein to the bifurcation of the iliac artery. (In the current study, more than 80% of the 60 treated patients had the sheath placed in their right femoral vein.) The access sheath for the catheters involved in the procedures themselves were most often placed in the left or right femoral artery. Electrodes within the Early Bird sheath detect leaked blood by its impact on bioimpedance of the tissue surrounding the sheath, with the system able to roughly gauge the volume of released blood based on the local level of bioimpedance change.
A couple of years ago, Dr. Généreux and his associates documented an 18% incidence of bleeding complications among 17,672 U.S. patients who underwent a transcatheter procedure with a large-bore catheter during 2013-2014 using data collected by the National Inpatient Sample (JAMA Cardiol. 2017 Jul;2[7]:798-802). Their analysis also documented that the patients with bleeding-related complications had in-hospital costs that averaged more than 50% higher than the costs for patients without bleeding complications, findings that raised the possibility that earlier identification of a bleed, before severe complications ensured, could be both cost effective and beneficial to patients, Dr. Généreux said.
Dr. Généreux has been a consultant to Saranas and to several other companies. He is also chief medical officer for Saranas and has an equity interest in the company.
SOURCE: Généreux P. SCAI 2019, Abstract 5713.
REPORTING FROM SCAI 2019
Severe respiratory failure strikes healthy teens on trimethoprim-sulfamethoxazole
TMP-SMX, a frequently prescribed antibiotic, has been associated with “idiosyncratic adverse drug reactions, including cutaneous reactions and hypersensitivity syndromes,” but pulmonary complications are rare, especially in children, wrote Jenna O. Miller, MD, of the University of Missouri–Kansas City and colleagues.
In a case series published in Pediatrics, the researchers described the patients, who were aged 13-18 years; the 18-year-old was male, the others were female. Four of the patients (three females, one male) were taking TMP-SMX for acne vulgaris. One of these patients, a 13-year-old girl, underwent a bilateral lung and heart transplant after developing interstitial lung disease and died as a result of solid organ transplant complications. The other death occurred in a 15-year-old girl who was taking TMP-SMX to treat a urinary tract infection. This patient developed interstitial lung disease and died of complications from the disease while awaiting a lung transplant.
“In all cases, patients were transferred to academic medical facilities, and pediatric pulmonologists and infectious diseases specialists performed extensive evaluations,” the researchers wrote. The patients did not improve when the drug was discontinued, and four of the five were considered or listed for organ transplants. The spectrum of disease was varied among the patients, and the pathophysiology remains poorly understood.
Although no clinical test could confirm causality between TMP-SMX and ARDS in the five teens, “the extensive negative workup, paired with recent TMP-SMX exposure and similarity among these cases, raises the possibility that the observed ARDS was TMP-SMX triggered,” they wrote.
The researchers had no financial conflicts to disclose.
SOURCE: Miller JO et al. Pediatrics. 2019 May 29. doi: 10.1542/peds.2018.3242.
TMP-SMX, a frequently prescribed antibiotic, has been associated with “idiosyncratic adverse drug reactions, including cutaneous reactions and hypersensitivity syndromes,” but pulmonary complications are rare, especially in children, wrote Jenna O. Miller, MD, of the University of Missouri–Kansas City and colleagues.
In a case series published in Pediatrics, the researchers described the patients, who were aged 13-18 years; the 18-year-old was male, the others were female. Four of the patients (three females, one male) were taking TMP-SMX for acne vulgaris. One of these patients, a 13-year-old girl, underwent a bilateral lung and heart transplant after developing interstitial lung disease and died as a result of solid organ transplant complications. The other death occurred in a 15-year-old girl who was taking TMP-SMX to treat a urinary tract infection. This patient developed interstitial lung disease and died of complications from the disease while awaiting a lung transplant.
“In all cases, patients were transferred to academic medical facilities, and pediatric pulmonologists and infectious diseases specialists performed extensive evaluations,” the researchers wrote. The patients did not improve when the drug was discontinued, and four of the five were considered or listed for organ transplants. The spectrum of disease was varied among the patients, and the pathophysiology remains poorly understood.
Although no clinical test could confirm causality between TMP-SMX and ARDS in the five teens, “the extensive negative workup, paired with recent TMP-SMX exposure and similarity among these cases, raises the possibility that the observed ARDS was TMP-SMX triggered,” they wrote.
The researchers had no financial conflicts to disclose.
SOURCE: Miller JO et al. Pediatrics. 2019 May 29. doi: 10.1542/peds.2018.3242.
TMP-SMX, a frequently prescribed antibiotic, has been associated with “idiosyncratic adverse drug reactions, including cutaneous reactions and hypersensitivity syndromes,” but pulmonary complications are rare, especially in children, wrote Jenna O. Miller, MD, of the University of Missouri–Kansas City and colleagues.
In a case series published in Pediatrics, the researchers described the patients, who were aged 13-18 years; the 18-year-old was male, the others were female. Four of the patients (three females, one male) were taking TMP-SMX for acne vulgaris. One of these patients, a 13-year-old girl, underwent a bilateral lung and heart transplant after developing interstitial lung disease and died as a result of solid organ transplant complications. The other death occurred in a 15-year-old girl who was taking TMP-SMX to treat a urinary tract infection. This patient developed interstitial lung disease and died of complications from the disease while awaiting a lung transplant.
“In all cases, patients were transferred to academic medical facilities, and pediatric pulmonologists and infectious diseases specialists performed extensive evaluations,” the researchers wrote. The patients did not improve when the drug was discontinued, and four of the five were considered or listed for organ transplants. The spectrum of disease was varied among the patients, and the pathophysiology remains poorly understood.
Although no clinical test could confirm causality between TMP-SMX and ARDS in the five teens, “the extensive negative workup, paired with recent TMP-SMX exposure and similarity among these cases, raises the possibility that the observed ARDS was TMP-SMX triggered,” they wrote.
The researchers had no financial conflicts to disclose.
SOURCE: Miller JO et al. Pediatrics. 2019 May 29. doi: 10.1542/peds.2018.3242.
FROM PEDIATRICS
Incidence of adult diabetes drops, prevalence remains stable
according to a review of Centers for Disease Control and Prevention data.
It’s the longest plateau in prevalence since the 1980s, and the longest period of declining incidence ever recorded. The findings suggest that efforts “to stem the tide of type 2 diabetes may be working ... [but] we still have a very long way to go,” investigator Ann Albright, PhD, director of the CDC Division of Diabetes Translation, said in a press statement.
However, the authors noted that “obesity and severe obesity trends have generally increased over the past 10 years, and prediabetes remains unchanged and high, affecting 84 million U.S. adults, or 34% of the US adult population,” and they emphasized the need for continued focus on prevention for type 2 diabetes and diabetes complications, as well as better screening and detection of the disease.
Dr Albright and her colleagues reviewed the CDC’s annual National Health Interview Survey data from 1980-2017. Diabetes diagnoses were by self-report, and the data did not distinguish between type 1 and type 2 disease, although it is known that about 95% of diabetes cases are type 2 (BMJ Open Diab Res Care. 2019 May 28;7:e000657. doi:10.1136/bmjdrc-2019-000657).
New cases declined from a high of 1.73 million in 2008 to 1.34 million in 2017, a drop of 3.1% a year, from 7.8 to 6 new cases/1,000 adults. The findings were driven largely by decreasing incidence in non-Hispanic whites.
Prevalence peaked at 8.2/100 adults in 2009, and has remained there since, possibly because people with diabetes are living longer with the disease, the investigators said.
Similar prevalence trends were seen across age, racial, education, and ethnic groups, and in both men and women. The findings were all statistically significant.
The drop in incidence corresponds with flat or downward trends in several type 2 risk factors, including sugar, soda, and total calorie intake, and physical inactivity. In 2010, the American Diabetes Association recommended hemoglobin A1c for diabetes diagnosis, which might have also decreased the incidence because it is less sensitive than traditional fasting blood glucose. Increased screening in recent years might have depleted the pool of new cases as well, the authors said.
The CDC has been emphasizing type 2 education and prevention through its National Diabetes Prevention Program, which might also have helped.
There was no external funding for the survey, and the investigators reported no disclosures or conflicts of interest.
SOURCE: Benoit SR et al. BMJ Open Diab Res Care. 2019 May 28. doi:10.1136/bmjdrc-2019-000657
according to a review of Centers for Disease Control and Prevention data.
It’s the longest plateau in prevalence since the 1980s, and the longest period of declining incidence ever recorded. The findings suggest that efforts “to stem the tide of type 2 diabetes may be working ... [but] we still have a very long way to go,” investigator Ann Albright, PhD, director of the CDC Division of Diabetes Translation, said in a press statement.
However, the authors noted that “obesity and severe obesity trends have generally increased over the past 10 years, and prediabetes remains unchanged and high, affecting 84 million U.S. adults, or 34% of the US adult population,” and they emphasized the need for continued focus on prevention for type 2 diabetes and diabetes complications, as well as better screening and detection of the disease.
Dr Albright and her colleagues reviewed the CDC’s annual National Health Interview Survey data from 1980-2017. Diabetes diagnoses were by self-report, and the data did not distinguish between type 1 and type 2 disease, although it is known that about 95% of diabetes cases are type 2 (BMJ Open Diab Res Care. 2019 May 28;7:e000657. doi:10.1136/bmjdrc-2019-000657).
New cases declined from a high of 1.73 million in 2008 to 1.34 million in 2017, a drop of 3.1% a year, from 7.8 to 6 new cases/1,000 adults. The findings were driven largely by decreasing incidence in non-Hispanic whites.
Prevalence peaked at 8.2/100 adults in 2009, and has remained there since, possibly because people with diabetes are living longer with the disease, the investigators said.
Similar prevalence trends were seen across age, racial, education, and ethnic groups, and in both men and women. The findings were all statistically significant.
The drop in incidence corresponds with flat or downward trends in several type 2 risk factors, including sugar, soda, and total calorie intake, and physical inactivity. In 2010, the American Diabetes Association recommended hemoglobin A1c for diabetes diagnosis, which might have also decreased the incidence because it is less sensitive than traditional fasting blood glucose. Increased screening in recent years might have depleted the pool of new cases as well, the authors said.
The CDC has been emphasizing type 2 education and prevention through its National Diabetes Prevention Program, which might also have helped.
There was no external funding for the survey, and the investigators reported no disclosures or conflicts of interest.
SOURCE: Benoit SR et al. BMJ Open Diab Res Care. 2019 May 28. doi:10.1136/bmjdrc-2019-000657
according to a review of Centers for Disease Control and Prevention data.
It’s the longest plateau in prevalence since the 1980s, and the longest period of declining incidence ever recorded. The findings suggest that efforts “to stem the tide of type 2 diabetes may be working ... [but] we still have a very long way to go,” investigator Ann Albright, PhD, director of the CDC Division of Diabetes Translation, said in a press statement.
However, the authors noted that “obesity and severe obesity trends have generally increased over the past 10 years, and prediabetes remains unchanged and high, affecting 84 million U.S. adults, or 34% of the US adult population,” and they emphasized the need for continued focus on prevention for type 2 diabetes and diabetes complications, as well as better screening and detection of the disease.
Dr Albright and her colleagues reviewed the CDC’s annual National Health Interview Survey data from 1980-2017. Diabetes diagnoses were by self-report, and the data did not distinguish between type 1 and type 2 disease, although it is known that about 95% of diabetes cases are type 2 (BMJ Open Diab Res Care. 2019 May 28;7:e000657. doi:10.1136/bmjdrc-2019-000657).
New cases declined from a high of 1.73 million in 2008 to 1.34 million in 2017, a drop of 3.1% a year, from 7.8 to 6 new cases/1,000 adults. The findings were driven largely by decreasing incidence in non-Hispanic whites.
Prevalence peaked at 8.2/100 adults in 2009, and has remained there since, possibly because people with diabetes are living longer with the disease, the investigators said.
Similar prevalence trends were seen across age, racial, education, and ethnic groups, and in both men and women. The findings were all statistically significant.
The drop in incidence corresponds with flat or downward trends in several type 2 risk factors, including sugar, soda, and total calorie intake, and physical inactivity. In 2010, the American Diabetes Association recommended hemoglobin A1c for diabetes diagnosis, which might have also decreased the incidence because it is less sensitive than traditional fasting blood glucose. Increased screening in recent years might have depleted the pool of new cases as well, the authors said.
The CDC has been emphasizing type 2 education and prevention through its National Diabetes Prevention Program, which might also have helped.
There was no external funding for the survey, and the investigators reported no disclosures or conflicts of interest.
SOURCE: Benoit SR et al. BMJ Open Diab Res Care. 2019 May 28. doi:10.1136/bmjdrc-2019-000657
FROM BMJ OPEN DIABETES RESEARCH & CARE
Part 4: Talking to Older Patients About Sex and STIs
Having established that there is a documented increase in sexually transmitted infections (STIs) among older Americans, and furthermore recognizing that a contributing factor to this trend may be communication gaps between patients and their health care providers, I now want to address the “What do we do about it?” aspect of our discussion. As clinicians, we know that the core focus around infectious diseases of any kind is prevention.
There are 3 types of prevention, as noted by Fos and Fine in Introduction to Public Health, all of which fit into our current topic: primary (eliminating risk factors), secondary (early detection), and tertiary (eliminating or moderating disability associated with advanced disease).1 The following recommendations fall into at least one of these categories.
1. All clinicians need to be involved in educating older Americans about the risks for STIs. Providers should routinely ask seniors if they are sexually active and should be prepared to recommend appropriate screening and education resources. Essentially, older adults should be getting the same basic “safe sex” education that younger people receive: learning about STIs, from recognizing the signs to understanding how STIs complicate other chronic medical conditions.2,3
2. Seniors also need education on the importance—and proper use—of condoms. Furthermore, we should go a step further and ensure that free condoms are distributed in places where seniors live and congregate. People older than 60 report the lowest condom use of any population.2,3
3. Information on STI detection and treatment options needs to be well publicized. For example, Medicare provides free STI screenings and low-cost treatments. We need to make sure our older patients are aware of this benefit and encourage them to make use of it.
4. Older Americans should be screened for STIs, regardless of age, per CDC guidelines. Seniors should get annual testing if they have new sexual partners—which means they must be asked the difficult questions.
And that’s the crux of the issue: Family members and clinicians may find it uncomfortable to have this conversation with Grandpa or Grandma. But there should be a dialogue to ensure they are aware of their risk for STIs, as well as how to prevent them.3 A well-known NP colleague reminded me of the importance of emphasizing to our older patients that anything discussed within the encounter is confidential and will not be disclosed without their permission. She starts off her conversations with patients by saying, “A lot of people your age experience …” or “Please don’t be insulted if I ask you about …” or “Is it OK if I ask you a few very personal questions?”
Continue to: It is critical...
It is critical to keep an open mind and accepting attitude when discussing sexuality or intimate issues with older patients. Paying attention to patients’ verbal and nonverbal cues is also essential. Clinicians should never assume older adults are sexually inactive, no longer care about sex, or are necessarily heterosexual. There was an excellent article in the Journal of Family Practice a few years ago on “How to discuss sex with elderly patients” that is worth rereading. In it, the authors suggest using the PLISSIT model to facilitate a conversation with your elderly patient. As explained in the article, the acronym “is a reminder to seek Permission to discuss sexuality, share Limited information about sexual issues that affect the older adult, provide Specific Suggestions to improve sexual health, and offer to provide a referral for Intensive Therapy if needed.”4 The Table offers some examples of how to address each step of PLISSIT.

So, as we wrap up our examination of this issue, I encourage you to open this dialogue with your older patients. In light of the increasing number of older patients with STIs, it is essential for clinicians to obtain an accurate and complete sexual history for patients of any age. That starts with asking the appropriate questions, preferably in a manner that puts the patient at ease to share important details. If you have additional ideas about what we can do to reverse this STI trend, please share them with me at [email protected].
1. Goldstein RL, Goldstein K, Dwelle TL. Introduction to Public Health. 2nd ed. New York, NY: Springer Publishing Co; 2015.
2. Cohen JK. STDs on the rise among senior. Becker's Hospital Review. May 18, 2018. www.beckershospitalreview.com/population-health/stds-on-the-rise-among-seniors.html. Accessed May 22, 2019.
3. Humphrey D. Seniors at high risk for sexually transmitted diseases [STDs]. HomeHelpers. March 31, 2018. https://www.homehelpershomecare.com/clearwater/blog/2018/13/seniors-at-high-risk-for-sexually-transmitted-diseases-stds. Accessed Mary 22, 2019.
4. Omole F, Fresh EM, Sow C, et al. How to discuss sex with elderly patients. J Fam Pract. 2014;63(4):E1-E4.
Having established that there is a documented increase in sexually transmitted infections (STIs) among older Americans, and furthermore recognizing that a contributing factor to this trend may be communication gaps between patients and their health care providers, I now want to address the “What do we do about it?” aspect of our discussion. As clinicians, we know that the core focus around infectious diseases of any kind is prevention.
There are 3 types of prevention, as noted by Fos and Fine in Introduction to Public Health, all of which fit into our current topic: primary (eliminating risk factors), secondary (early detection), and tertiary (eliminating or moderating disability associated with advanced disease).1 The following recommendations fall into at least one of these categories.
1. All clinicians need to be involved in educating older Americans about the risks for STIs. Providers should routinely ask seniors if they are sexually active and should be prepared to recommend appropriate screening and education resources. Essentially, older adults should be getting the same basic “safe sex” education that younger people receive: learning about STIs, from recognizing the signs to understanding how STIs complicate other chronic medical conditions.2,3
2. Seniors also need education on the importance—and proper use—of condoms. Furthermore, we should go a step further and ensure that free condoms are distributed in places where seniors live and congregate. People older than 60 report the lowest condom use of any population.2,3
3. Information on STI detection and treatment options needs to be well publicized. For example, Medicare provides free STI screenings and low-cost treatments. We need to make sure our older patients are aware of this benefit and encourage them to make use of it.
4. Older Americans should be screened for STIs, regardless of age, per CDC guidelines. Seniors should get annual testing if they have new sexual partners—which means they must be asked the difficult questions.
And that’s the crux of the issue: Family members and clinicians may find it uncomfortable to have this conversation with Grandpa or Grandma. But there should be a dialogue to ensure they are aware of their risk for STIs, as well as how to prevent them.3 A well-known NP colleague reminded me of the importance of emphasizing to our older patients that anything discussed within the encounter is confidential and will not be disclosed without their permission. She starts off her conversations with patients by saying, “A lot of people your age experience …” or “Please don’t be insulted if I ask you about …” or “Is it OK if I ask you a few very personal questions?”
Continue to: It is critical...
It is critical to keep an open mind and accepting attitude when discussing sexuality or intimate issues with older patients. Paying attention to patients’ verbal and nonverbal cues is also essential. Clinicians should never assume older adults are sexually inactive, no longer care about sex, or are necessarily heterosexual. There was an excellent article in the Journal of Family Practice a few years ago on “How to discuss sex with elderly patients” that is worth rereading. In it, the authors suggest using the PLISSIT model to facilitate a conversation with your elderly patient. As explained in the article, the acronym “is a reminder to seek Permission to discuss sexuality, share Limited information about sexual issues that affect the older adult, provide Specific Suggestions to improve sexual health, and offer to provide a referral for Intensive Therapy if needed.”4 The Table offers some examples of how to address each step of PLISSIT.

So, as we wrap up our examination of this issue, I encourage you to open this dialogue with your older patients. In light of the increasing number of older patients with STIs, it is essential for clinicians to obtain an accurate and complete sexual history for patients of any age. That starts with asking the appropriate questions, preferably in a manner that puts the patient at ease to share important details. If you have additional ideas about what we can do to reverse this STI trend, please share them with me at [email protected].
Having established that there is a documented increase in sexually transmitted infections (STIs) among older Americans, and furthermore recognizing that a contributing factor to this trend may be communication gaps between patients and their health care providers, I now want to address the “What do we do about it?” aspect of our discussion. As clinicians, we know that the core focus around infectious diseases of any kind is prevention.
There are 3 types of prevention, as noted by Fos and Fine in Introduction to Public Health, all of which fit into our current topic: primary (eliminating risk factors), secondary (early detection), and tertiary (eliminating or moderating disability associated with advanced disease).1 The following recommendations fall into at least one of these categories.
1. All clinicians need to be involved in educating older Americans about the risks for STIs. Providers should routinely ask seniors if they are sexually active and should be prepared to recommend appropriate screening and education resources. Essentially, older adults should be getting the same basic “safe sex” education that younger people receive: learning about STIs, from recognizing the signs to understanding how STIs complicate other chronic medical conditions.2,3
2. Seniors also need education on the importance—and proper use—of condoms. Furthermore, we should go a step further and ensure that free condoms are distributed in places where seniors live and congregate. People older than 60 report the lowest condom use of any population.2,3
3. Information on STI detection and treatment options needs to be well publicized. For example, Medicare provides free STI screenings and low-cost treatments. We need to make sure our older patients are aware of this benefit and encourage them to make use of it.
4. Older Americans should be screened for STIs, regardless of age, per CDC guidelines. Seniors should get annual testing if they have new sexual partners—which means they must be asked the difficult questions.
And that’s the crux of the issue: Family members and clinicians may find it uncomfortable to have this conversation with Grandpa or Grandma. But there should be a dialogue to ensure they are aware of their risk for STIs, as well as how to prevent them.3 A well-known NP colleague reminded me of the importance of emphasizing to our older patients that anything discussed within the encounter is confidential and will not be disclosed without their permission. She starts off her conversations with patients by saying, “A lot of people your age experience …” or “Please don’t be insulted if I ask you about …” or “Is it OK if I ask you a few very personal questions?”
Continue to: It is critical...
It is critical to keep an open mind and accepting attitude when discussing sexuality or intimate issues with older patients. Paying attention to patients’ verbal and nonverbal cues is also essential. Clinicians should never assume older adults are sexually inactive, no longer care about sex, or are necessarily heterosexual. There was an excellent article in the Journal of Family Practice a few years ago on “How to discuss sex with elderly patients” that is worth rereading. In it, the authors suggest using the PLISSIT model to facilitate a conversation with your elderly patient. As explained in the article, the acronym “is a reminder to seek Permission to discuss sexuality, share Limited information about sexual issues that affect the older adult, provide Specific Suggestions to improve sexual health, and offer to provide a referral for Intensive Therapy if needed.”4 The Table offers some examples of how to address each step of PLISSIT.

So, as we wrap up our examination of this issue, I encourage you to open this dialogue with your older patients. In light of the increasing number of older patients with STIs, it is essential for clinicians to obtain an accurate and complete sexual history for patients of any age. That starts with asking the appropriate questions, preferably in a manner that puts the patient at ease to share important details. If you have additional ideas about what we can do to reverse this STI trend, please share them with me at [email protected].
1. Goldstein RL, Goldstein K, Dwelle TL. Introduction to Public Health. 2nd ed. New York, NY: Springer Publishing Co; 2015.
2. Cohen JK. STDs on the rise among senior. Becker's Hospital Review. May 18, 2018. www.beckershospitalreview.com/population-health/stds-on-the-rise-among-seniors.html. Accessed May 22, 2019.
3. Humphrey D. Seniors at high risk for sexually transmitted diseases [STDs]. HomeHelpers. March 31, 2018. https://www.homehelpershomecare.com/clearwater/blog/2018/13/seniors-at-high-risk-for-sexually-transmitted-diseases-stds. Accessed Mary 22, 2019.
4. Omole F, Fresh EM, Sow C, et al. How to discuss sex with elderly patients. J Fam Pract. 2014;63(4):E1-E4.
1. Goldstein RL, Goldstein K, Dwelle TL. Introduction to Public Health. 2nd ed. New York, NY: Springer Publishing Co; 2015.
2. Cohen JK. STDs on the rise among senior. Becker's Hospital Review. May 18, 2018. www.beckershospitalreview.com/population-health/stds-on-the-rise-among-seniors.html. Accessed May 22, 2019.
3. Humphrey D. Seniors at high risk for sexually transmitted diseases [STDs]. HomeHelpers. March 31, 2018. https://www.homehelpershomecare.com/clearwater/blog/2018/13/seniors-at-high-risk-for-sexually-transmitted-diseases-stds. Accessed Mary 22, 2019.
4. Omole F, Fresh EM, Sow C, et al. How to discuss sex with elderly patients. J Fam Pract. 2014;63(4):E1-E4.
Energy drinks increase BP and disrupt the heart’s electrical activity
Consuming caffeinated energy drinks leads to a prolonged QT interval and an increase in blood pressure, according to a study of young volunteers who had their hearts tested after drinking either energy drinks or placebo.
“Further investigation is warranted on whether an individual ingredient or a unique combination leads to the observed electrophysiological and hemodynamic changes,” wrote Sachin A. Shah of the University of the Pacific, Stockton, Calif., and coinvestigators. The study was published in the Journal of the American Heart Association.
To analyze electrocardiographic changes in the heart after consumption of 300 mg of caffeine plus other energy drink ingredients, the researchers assigned 34 healthy volunteers with an average age of 22 years to consume two 16-ounce bottles of either Drink A, a commercially available energy drink, Drink B, a different brand of energy drink, or a placebo drink for 3 days, followed by a 6-day washout period. Before and for 4 hours after consuming the beverages, volunteers had their hearts measured via ECG to test for differences in QT interval. Their blood pressures also were recorded.
Compared with placebo, the Drink A group had a 6.1 ms increase in QT interval and the Drink B group had a 7.7 ms rise. The maximum changes from baseline in corrected QT interval for Drink A, Drink B, and placebo were 17.9 ms, 19.6 ms, and 11.9 ms, respectively; both differences were statistically significant. Volunteers in Drink A and Drink B groups also had statistically significant increases of 5 mm Hg in systolic and 4 mm Hg in diastolic blood pressure after energy drink consumption, compared with placebo.
Both energy drinks used in the study contained caffeine (about 300 mg), taurine, glucuronolactone, and B vitamins. The investigators said that caffeine at doses under 400 mg is not expected to induce any electrocardiographic changes.
The coauthors noted their study’s limitations, including not investigating the effects of different doses and the possibility that consuming two 16-ounce bottles is an unrealistic real-world volume. That said, they noted that 16% of respondents to a 2,040-person survey admitted to consuming more than two energy drinks a day. In addition, though not every brand was tested, the researchers stated that, “the class of energy drinks, rather than one particular product, warrants use with caution.”
Dr. Shah reported serving as an expert witness in legal cases related to caffeinated energy drinks. The other authors reported no conflicts of interest.
SOURCE: Shah SA et al. J Am Heart Assoc. 2019 May 29.
Consuming caffeinated energy drinks leads to a prolonged QT interval and an increase in blood pressure, according to a study of young volunteers who had their hearts tested after drinking either energy drinks or placebo.
“Further investigation is warranted on whether an individual ingredient or a unique combination leads to the observed electrophysiological and hemodynamic changes,” wrote Sachin A. Shah of the University of the Pacific, Stockton, Calif., and coinvestigators. The study was published in the Journal of the American Heart Association.
To analyze electrocardiographic changes in the heart after consumption of 300 mg of caffeine plus other energy drink ingredients, the researchers assigned 34 healthy volunteers with an average age of 22 years to consume two 16-ounce bottles of either Drink A, a commercially available energy drink, Drink B, a different brand of energy drink, or a placebo drink for 3 days, followed by a 6-day washout period. Before and for 4 hours after consuming the beverages, volunteers had their hearts measured via ECG to test for differences in QT interval. Their blood pressures also were recorded.
Compared with placebo, the Drink A group had a 6.1 ms increase in QT interval and the Drink B group had a 7.7 ms rise. The maximum changes from baseline in corrected QT interval for Drink A, Drink B, and placebo were 17.9 ms, 19.6 ms, and 11.9 ms, respectively; both differences were statistically significant. Volunteers in Drink A and Drink B groups also had statistically significant increases of 5 mm Hg in systolic and 4 mm Hg in diastolic blood pressure after energy drink consumption, compared with placebo.
Both energy drinks used in the study contained caffeine (about 300 mg), taurine, glucuronolactone, and B vitamins. The investigators said that caffeine at doses under 400 mg is not expected to induce any electrocardiographic changes.
The coauthors noted their study’s limitations, including not investigating the effects of different doses and the possibility that consuming two 16-ounce bottles is an unrealistic real-world volume. That said, they noted that 16% of respondents to a 2,040-person survey admitted to consuming more than two energy drinks a day. In addition, though not every brand was tested, the researchers stated that, “the class of energy drinks, rather than one particular product, warrants use with caution.”
Dr. Shah reported serving as an expert witness in legal cases related to caffeinated energy drinks. The other authors reported no conflicts of interest.
SOURCE: Shah SA et al. J Am Heart Assoc. 2019 May 29.
Consuming caffeinated energy drinks leads to a prolonged QT interval and an increase in blood pressure, according to a study of young volunteers who had their hearts tested after drinking either energy drinks or placebo.
“Further investigation is warranted on whether an individual ingredient or a unique combination leads to the observed electrophysiological and hemodynamic changes,” wrote Sachin A. Shah of the University of the Pacific, Stockton, Calif., and coinvestigators. The study was published in the Journal of the American Heart Association.
To analyze electrocardiographic changes in the heart after consumption of 300 mg of caffeine plus other energy drink ingredients, the researchers assigned 34 healthy volunteers with an average age of 22 years to consume two 16-ounce bottles of either Drink A, a commercially available energy drink, Drink B, a different brand of energy drink, or a placebo drink for 3 days, followed by a 6-day washout period. Before and for 4 hours after consuming the beverages, volunteers had their hearts measured via ECG to test for differences in QT interval. Their blood pressures also were recorded.
Compared with placebo, the Drink A group had a 6.1 ms increase in QT interval and the Drink B group had a 7.7 ms rise. The maximum changes from baseline in corrected QT interval for Drink A, Drink B, and placebo were 17.9 ms, 19.6 ms, and 11.9 ms, respectively; both differences were statistically significant. Volunteers in Drink A and Drink B groups also had statistically significant increases of 5 mm Hg in systolic and 4 mm Hg in diastolic blood pressure after energy drink consumption, compared with placebo.
Both energy drinks used in the study contained caffeine (about 300 mg), taurine, glucuronolactone, and B vitamins. The investigators said that caffeine at doses under 400 mg is not expected to induce any electrocardiographic changes.
The coauthors noted their study’s limitations, including not investigating the effects of different doses and the possibility that consuming two 16-ounce bottles is an unrealistic real-world volume. That said, they noted that 16% of respondents to a 2,040-person survey admitted to consuming more than two energy drinks a day. In addition, though not every brand was tested, the researchers stated that, “the class of energy drinks, rather than one particular product, warrants use with caution.”
Dr. Shah reported serving as an expert witness in legal cases related to caffeinated energy drinks. The other authors reported no conflicts of interest.
SOURCE: Shah SA et al. J Am Heart Assoc. 2019 May 29.
FROM THE JOURNAL OF THE AMERICAN HEART ASSOCIATION
Key clinical point:
Major finding: Compared with placebo, consuming two different energy drinks led to significant QT interval increases of 6.1 ms and 7.7 ms.
Study details: A randomized, double-blind crossover study of 34 healthy volunteers who had their hearts measured via electrocardiogram after consuming energy drink or placebo.
Disclosures: Dr. Shah reported serving as an expert witness in legal cases related to caffeinated energy drinks. The other authors reported no conflicts of interest.
Source: Shah SA et al. J Am Heart Assoc. 2019 May 29.
Supreme Court upholds part of Indiana abortion law
In a three-page, unsigned opinion issued May 28, justices wrote that Indiana has a legitimate interest in proper disposition of fetal remains and that the state’s burial/cremation mandate is rational. However, justices said they would not take up the second part of the law regarding abortions based on race, sex, or disability because not enough appeals courts have decided the issue. The court emphasized it was not expressing any view on the merits of the second question.
The opinion stems from an antiabortion measure signed into law by then–Indiana Governor Mike Pence (R) in 2016. According to the law, the health facility where an abortion occurred is required to dispose of fetal remains either by cremation or internment unless the woman or an associated party take possession of the remains. The measure allows the woman or associated party to choose a location of final disposition provided that the parties pay the costs for such arrangements. The second part of the law prohibits an abortion from being performed solely because of the fetus’s expected race, sex, diagnosis, or disability.
Planned Parenthood of Indiana and Kentucky sued over the law, arguing that the measure was unconstitutional. Indiana officials countered the disposal requirements provided fetuses dignity in death and that the law’s abortion restrictions prevented discrimination of particular fetuses in light of technological advances in genetic screening. In 2018, a three-judge panel of the Court of Appeals for the 7th Circuit struck down the entire law. The panel wrote that well-established Supreme Court precedent allows a woman to terminate her pregnancy for any reason and that the Indiana law invaded a woman’s privacy by examining the underlying basis of her decision for an abortion.
In the Supreme Court’s May 28 filing, Justice Ruth Bader Ginsburg and Justice Sonia Sotomayor wrote separately, each stating they would have upheld the lower court’s ban of the entire law. Justice Clarence Thomas, meanwhile, wrote a lengthy separate opinion, agreeing with the court’s decision, but expressing concern over the use of abortion as a “tool of modern-day eugenics.”
“The court will soon need to confront the constitutionality of laws like Indiana’s,” Justice Thomas wrote. “Enshrining a constitutional right to an abortion based solely on the race, sex or disability of an unborn child, as Planned Parenthood advocates, would constitutionalize the views of the 20th-century eugenics movement.”
The Supreme Court’s decision on the Indiana law comes just weeks after two other stringent state abortion measures were signed into law. On May 7, 2019, Georgia Gov. Brian Kemp (R) signed into law a statute that bars physicians from performing an abortion after a heartbeat is detected – usually at about 6 weeks of pregnancy. On May 15, Alabama Gov. Kay Ivey (R) signed a law that would ban abortion at every pregnancy stage and penalize physicians with a Class A felony for performing an abortion and charge them with a Class C felony for attempting to perform an abortion.
Analysts say the Alabama law, in particular, could land in front of the Supreme Court as a direct challenge to Roe v. Wade. Abortion critics have been encouraged by the Supreme Court appointment of right-leaning Justice Brett M. Kavanaugh and hope the Alabama measure will drive the Supreme Court to reconsider its central holding in Roe, court watchers said.
In a three-page, unsigned opinion issued May 28, justices wrote that Indiana has a legitimate interest in proper disposition of fetal remains and that the state’s burial/cremation mandate is rational. However, justices said they would not take up the second part of the law regarding abortions based on race, sex, or disability because not enough appeals courts have decided the issue. The court emphasized it was not expressing any view on the merits of the second question.
The opinion stems from an antiabortion measure signed into law by then–Indiana Governor Mike Pence (R) in 2016. According to the law, the health facility where an abortion occurred is required to dispose of fetal remains either by cremation or internment unless the woman or an associated party take possession of the remains. The measure allows the woman or associated party to choose a location of final disposition provided that the parties pay the costs for such arrangements. The second part of the law prohibits an abortion from being performed solely because of the fetus’s expected race, sex, diagnosis, or disability.
Planned Parenthood of Indiana and Kentucky sued over the law, arguing that the measure was unconstitutional. Indiana officials countered the disposal requirements provided fetuses dignity in death and that the law’s abortion restrictions prevented discrimination of particular fetuses in light of technological advances in genetic screening. In 2018, a three-judge panel of the Court of Appeals for the 7th Circuit struck down the entire law. The panel wrote that well-established Supreme Court precedent allows a woman to terminate her pregnancy for any reason and that the Indiana law invaded a woman’s privacy by examining the underlying basis of her decision for an abortion.
In the Supreme Court’s May 28 filing, Justice Ruth Bader Ginsburg and Justice Sonia Sotomayor wrote separately, each stating they would have upheld the lower court’s ban of the entire law. Justice Clarence Thomas, meanwhile, wrote a lengthy separate opinion, agreeing with the court’s decision, but expressing concern over the use of abortion as a “tool of modern-day eugenics.”
“The court will soon need to confront the constitutionality of laws like Indiana’s,” Justice Thomas wrote. “Enshrining a constitutional right to an abortion based solely on the race, sex or disability of an unborn child, as Planned Parenthood advocates, would constitutionalize the views of the 20th-century eugenics movement.”
The Supreme Court’s decision on the Indiana law comes just weeks after two other stringent state abortion measures were signed into law. On May 7, 2019, Georgia Gov. Brian Kemp (R) signed into law a statute that bars physicians from performing an abortion after a heartbeat is detected – usually at about 6 weeks of pregnancy. On May 15, Alabama Gov. Kay Ivey (R) signed a law that would ban abortion at every pregnancy stage and penalize physicians with a Class A felony for performing an abortion and charge them with a Class C felony for attempting to perform an abortion.
Analysts say the Alabama law, in particular, could land in front of the Supreme Court as a direct challenge to Roe v. Wade. Abortion critics have been encouraged by the Supreme Court appointment of right-leaning Justice Brett M. Kavanaugh and hope the Alabama measure will drive the Supreme Court to reconsider its central holding in Roe, court watchers said.
In a three-page, unsigned opinion issued May 28, justices wrote that Indiana has a legitimate interest in proper disposition of fetal remains and that the state’s burial/cremation mandate is rational. However, justices said they would not take up the second part of the law regarding abortions based on race, sex, or disability because not enough appeals courts have decided the issue. The court emphasized it was not expressing any view on the merits of the second question.
The opinion stems from an antiabortion measure signed into law by then–Indiana Governor Mike Pence (R) in 2016. According to the law, the health facility where an abortion occurred is required to dispose of fetal remains either by cremation or internment unless the woman or an associated party take possession of the remains. The measure allows the woman or associated party to choose a location of final disposition provided that the parties pay the costs for such arrangements. The second part of the law prohibits an abortion from being performed solely because of the fetus’s expected race, sex, diagnosis, or disability.
Planned Parenthood of Indiana and Kentucky sued over the law, arguing that the measure was unconstitutional. Indiana officials countered the disposal requirements provided fetuses dignity in death and that the law’s abortion restrictions prevented discrimination of particular fetuses in light of technological advances in genetic screening. In 2018, a three-judge panel of the Court of Appeals for the 7th Circuit struck down the entire law. The panel wrote that well-established Supreme Court precedent allows a woman to terminate her pregnancy for any reason and that the Indiana law invaded a woman’s privacy by examining the underlying basis of her decision for an abortion.
In the Supreme Court’s May 28 filing, Justice Ruth Bader Ginsburg and Justice Sonia Sotomayor wrote separately, each stating they would have upheld the lower court’s ban of the entire law. Justice Clarence Thomas, meanwhile, wrote a lengthy separate opinion, agreeing with the court’s decision, but expressing concern over the use of abortion as a “tool of modern-day eugenics.”
“The court will soon need to confront the constitutionality of laws like Indiana’s,” Justice Thomas wrote. “Enshrining a constitutional right to an abortion based solely on the race, sex or disability of an unborn child, as Planned Parenthood advocates, would constitutionalize the views of the 20th-century eugenics movement.”
The Supreme Court’s decision on the Indiana law comes just weeks after two other stringent state abortion measures were signed into law. On May 7, 2019, Georgia Gov. Brian Kemp (R) signed into law a statute that bars physicians from performing an abortion after a heartbeat is detected – usually at about 6 weeks of pregnancy. On May 15, Alabama Gov. Kay Ivey (R) signed a law that would ban abortion at every pregnancy stage and penalize physicians with a Class A felony for performing an abortion and charge them with a Class C felony for attempting to perform an abortion.
Analysts say the Alabama law, in particular, could land in front of the Supreme Court as a direct challenge to Roe v. Wade. Abortion critics have been encouraged by the Supreme Court appointment of right-leaning Justice Brett M. Kavanaugh and hope the Alabama measure will drive the Supreme Court to reconsider its central holding in Roe, court watchers said.
Psoriatic Arthritis Journal Scan: May 2019
The contribution of joint and skin improvements to the health-related quality of life of patients with psoriatic arthritis: a post hoc analysis of two randomised controlled studies.
Kavanaugh A, Gottlieb A, Morita A, et al. Ann Rheum Dis. 2019 May 21.
An integrated analysis to determine the contribution of joint and skin improvements to health-related quality of life (HRQoL) in patients with psoriatic arthritis (PsA). Optimal improvements in patients' HRQoL were dependent on successful treatment of both joint and skin symptoms.
Content validity and psychometric evaluation of Functional Assessment of Chronic Illness Therapy-Fatigue in patients with psoriatic arthritis.
Cella D, Wilson H, Shalhoub H, et al. J Patient Rep Outcomes. 2019 May 20;3(1):30.
One-on-one semi-structured qualitative interviews with adult patients evaluated the measurement properties (e.g., content validity, reliability, and ability to detect change) of the Functional Assessment of Chronic Illness Therapy (FACIT)-Fatigue scale in patients with active psoriatic arthritis (PsA). Fatigue was confirmed to be an important symptom to patients with PsA, and FACIT-Fatigue was found to be a reliable and valid measure in this population.
Birth Outcomes and Disease Activity during Pregnancy in a Prospective Cohort of Women with Psoriatic Arthritis and Ankylosing Spondylitis.
Smith CJF, Bandoli G, Kavanaugh A, Chambers CD. Arthritis Care Res (Hoboken). 2019 May 10.
Women with PsA and AS have increased risk for selected adverse pregnancy outcomes. Compared to healthy controls (n=717), PsA (n = 117) was associated with increased risk for moderate preterm delivery (32-36 weeks' gestation), oligohydramnios, and Caesarean delivery. Active disease and corticosteroid use may increase the risk for some adverse pregnancy outcomes in women with these conditions.
Differential synovial tissue biomarkers among psoriatic arthritis and rheumatoid factor/anti-citrulline antibody-negative rheumatoid arthritis.
Alivernini S, Bruno D, Tolusso B, et al. Arthritis Res Ther. 2019 May 9;21(1):116.
The aim of the study was to identify synovial tissue (ST) biomarkers differentially expressed in PsA and seronegative rheumatoid arthritis and test their predictive value of therapeutic response. Histological analysis of ST may help to solve the clinical overlap between the two diseases and provides prognostic data about the therapy success.
Psoriatic arthritis - new perspectives.
Krakowski P, Gerkowicz A, Piertrzak A, et al. Arch Med Sci. 2019 May;15(3):580-589.
The management of PsA requires the care of a multidisciplinary team, which should include dermatologists, rheumatologists, physiotherapists, and orthopedic surgeons. PsA should be diagnosed as early as possible to slow down joint damage and progression of disability.
The contribution of joint and skin improvements to the health-related quality of life of patients with psoriatic arthritis: a post hoc analysis of two randomised controlled studies.
Kavanaugh A, Gottlieb A, Morita A, et al. Ann Rheum Dis. 2019 May 21.
An integrated analysis to determine the contribution of joint and skin improvements to health-related quality of life (HRQoL) in patients with psoriatic arthritis (PsA). Optimal improvements in patients' HRQoL were dependent on successful treatment of both joint and skin symptoms.
Content validity and psychometric evaluation of Functional Assessment of Chronic Illness Therapy-Fatigue in patients with psoriatic arthritis.
Cella D, Wilson H, Shalhoub H, et al. J Patient Rep Outcomes. 2019 May 20;3(1):30.
One-on-one semi-structured qualitative interviews with adult patients evaluated the measurement properties (e.g., content validity, reliability, and ability to detect change) of the Functional Assessment of Chronic Illness Therapy (FACIT)-Fatigue scale in patients with active psoriatic arthritis (PsA). Fatigue was confirmed to be an important symptom to patients with PsA, and FACIT-Fatigue was found to be a reliable and valid measure in this population.
Birth Outcomes and Disease Activity during Pregnancy in a Prospective Cohort of Women with Psoriatic Arthritis and Ankylosing Spondylitis.
Smith CJF, Bandoli G, Kavanaugh A, Chambers CD. Arthritis Care Res (Hoboken). 2019 May 10.
Women with PsA and AS have increased risk for selected adverse pregnancy outcomes. Compared to healthy controls (n=717), PsA (n = 117) was associated with increased risk for moderate preterm delivery (32-36 weeks' gestation), oligohydramnios, and Caesarean delivery. Active disease and corticosteroid use may increase the risk for some adverse pregnancy outcomes in women with these conditions.
Differential synovial tissue biomarkers among psoriatic arthritis and rheumatoid factor/anti-citrulline antibody-negative rheumatoid arthritis.
Alivernini S, Bruno D, Tolusso B, et al. Arthritis Res Ther. 2019 May 9;21(1):116.
The aim of the study was to identify synovial tissue (ST) biomarkers differentially expressed in PsA and seronegative rheumatoid arthritis and test their predictive value of therapeutic response. Histological analysis of ST may help to solve the clinical overlap between the two diseases and provides prognostic data about the therapy success.
Psoriatic arthritis - new perspectives.
Krakowski P, Gerkowicz A, Piertrzak A, et al. Arch Med Sci. 2019 May;15(3):580-589.
The management of PsA requires the care of a multidisciplinary team, which should include dermatologists, rheumatologists, physiotherapists, and orthopedic surgeons. PsA should be diagnosed as early as possible to slow down joint damage and progression of disability.
The contribution of joint and skin improvements to the health-related quality of life of patients with psoriatic arthritis: a post hoc analysis of two randomised controlled studies.
Kavanaugh A, Gottlieb A, Morita A, et al. Ann Rheum Dis. 2019 May 21.
An integrated analysis to determine the contribution of joint and skin improvements to health-related quality of life (HRQoL) in patients with psoriatic arthritis (PsA). Optimal improvements in patients' HRQoL were dependent on successful treatment of both joint and skin symptoms.
Content validity and psychometric evaluation of Functional Assessment of Chronic Illness Therapy-Fatigue in patients with psoriatic arthritis.
Cella D, Wilson H, Shalhoub H, et al. J Patient Rep Outcomes. 2019 May 20;3(1):30.
One-on-one semi-structured qualitative interviews with adult patients evaluated the measurement properties (e.g., content validity, reliability, and ability to detect change) of the Functional Assessment of Chronic Illness Therapy (FACIT)-Fatigue scale in patients with active psoriatic arthritis (PsA). Fatigue was confirmed to be an important symptom to patients with PsA, and FACIT-Fatigue was found to be a reliable and valid measure in this population.
Birth Outcomes and Disease Activity during Pregnancy in a Prospective Cohort of Women with Psoriatic Arthritis and Ankylosing Spondylitis.
Smith CJF, Bandoli G, Kavanaugh A, Chambers CD. Arthritis Care Res (Hoboken). 2019 May 10.
Women with PsA and AS have increased risk for selected adverse pregnancy outcomes. Compared to healthy controls (n=717), PsA (n = 117) was associated with increased risk for moderate preterm delivery (32-36 weeks' gestation), oligohydramnios, and Caesarean delivery. Active disease and corticosteroid use may increase the risk for some adverse pregnancy outcomes in women with these conditions.
Differential synovial tissue biomarkers among psoriatic arthritis and rheumatoid factor/anti-citrulline antibody-negative rheumatoid arthritis.
Alivernini S, Bruno D, Tolusso B, et al. Arthritis Res Ther. 2019 May 9;21(1):116.
The aim of the study was to identify synovial tissue (ST) biomarkers differentially expressed in PsA and seronegative rheumatoid arthritis and test their predictive value of therapeutic response. Histological analysis of ST may help to solve the clinical overlap between the two diseases and provides prognostic data about the therapy success.
Psoriatic arthritis - new perspectives.
Krakowski P, Gerkowicz A, Piertrzak A, et al. Arch Med Sci. 2019 May;15(3):580-589.
The management of PsA requires the care of a multidisciplinary team, which should include dermatologists, rheumatologists, physiotherapists, and orthopedic surgeons. PsA should be diagnosed as early as possible to slow down joint damage and progression of disability.
Asymptomatic, Slowly Enlarging Papule on the Nipple
The Diagnosis: Erosive Adenomatosis of the Nipple
Biopsy of the lesion revealed proliferative sections of glandular epithelium demonstrating apocrine differentiation, connecting to the epidermis and traversing throughout the entire dermis of the specimen (Figure). There were papillary projections of dilated ducts with a retained layer of myoepithelial cells surrounding the epithelial layers. Cytologic atypia was not appreciated. The patient was diagnosed with erosive adenomatosis of the nipple (EAN), also known as nipple adenoma. The lesion subsequently was treated and cleared with Mohs micrographic surgery (MMS). At 8-month follow-up there was no clinical recurrence of the lesion, and the patient was satisfied with the overall cosmetic appearance and conservation of the areola. The patient was followed clinically with annual breast examinations and mammography to monitor future recurrence.

Erosive adenomatosis of the nipple is an uncommon benign proliferative process of the lactiferous ducts of the nipple. Recognizing EAN is important because it resembles malignant breast diseases such as Paget disease of the nipple and invasive breast carcinoma. Due to these similarities, early cases of EAN have resulted in unnecessary mastectomies before the benignity of the condition was established.1 Accurate diagnosis is important to both the patient and the clinician for treatment planning as well as psychosocial consequences associated with the potential removal of this anatomically and cosmetically sensitive area.
Reviewing the literature on EAN is complicated by the variety of terms used to describe this condition, including but not limited to nipple adenoma, nipple duct adenoma, papillary adenoma of the nipple, and florid papillomatosis of the nipple. In 1955, Jones2 described EAN using the term florid papillomatosis of the nipple ducts. In 1962, Handley and Thackray1 argued that adenoma of the nipple was a more descriptive term because it more closely described the appearance of a sweat gland adenoma. They reasoned that adenoma of the nipple is a separate process from ductal papilloma due to the adenomatous proliferation into the nipple stroma rather than the lumen of the nipple ducts.1 The term adenoma of the nipple was further supported in 1965 by Taylor and Robertson.3 In 1959, Le Gal et al4 used the term erosive adenomatosis of the nipple to describe the erosive nature of nipple adenoma. The term nipple adenoma was published in the 2012 WHO Classification of Tumors of the Breast with 4 common histologic subtypes.5,6
Erosive adenomatosis of the nipple is clinically indistinguishable from Paget disease of the nipple, thus biopsy is essential for accurate diagnosis. In contrast to Paget disease, EAN tends to present in younger patients and progresses more slowly, and symptoms may be exacerbated around menstruation.1 Case reports demonstrate that patients may wait years before seeking medical attention for EAN.1,3,7,8 Presenting symptoms may include inflammation, crusting, nipple skin erosion, itching, and pain. Serous or sanguineous discharge from the lesions also is commonly reported. Palpation may reveal a small, hard, or elastic nodule within or underlying the nipple. In addition to Paget disease, EAN may resemble squamous cell carcinoma of the nipple, eczema, psoriasis, or a skin infection.6 Axillary lymphadenopathy is not present in the absence of a concomitant breast malignancy.8 On biopsy, nipple adenoma represents ductal proliferation of glandular structures within the stroma of the nipple that is well circumscribed but without borders. The erosive appearance of the lesion is produced by extensions of the glandular epithelium on the surface of the nipple.1,6 Specific to EAN is the presence of 2 cell types: an inner columnar epithelium and an outer cuboidal myoepithelium. These 2 cell types are present in normal lactiferous ducts; however, normal ducts are highly organized compared to EAN.9
After confirmation of EAN by nipple biopsy, complete surgical excision has been the gold standard for treatment, followed by reconstructive surgery.6 Handley and Thackray1 advocated for total excision of the nipple and areola with an underlying wedge of breast tissue to facilitate wound closure. More recently, successful alternative forms of treatment have been utilized to minimize disfiguring surgery. Alternative treatments include MMS,8 cryotherapy,10 and nipple splitting enucleation.6 Treatment with MMS has resulted in nipple sparing with the least amount of surface area sacrificed (1.1 cm2).9 Our case and prior case reports demonstrate that the tissue sparing potential of MMS is appropriate for the treatment of EAN, though traditionally it has been reserved for more malignant tumors. Preserving this sensitive area is both cosmetically and psychologically advantageous for the patient and thus should be considered when reviewing treatment options for EAN.
- Handley RS, Thackray AC. Adenoma of nipple. Br J Cancer. 1962;16:187-194.
- Jones DB. Florid papillomatosis of the nipple ducts. Cancer. 1955;8:315-319.
- Taylor HB, Robertson AG. Adenomas of the nipple. Cancer. 1965:18:995-1002.
- Le Gal Y, Gros CM, Bader P. Erosive adenomatosis of the nipple [in French]. Ann Anat Pathol (Paris). 1959;4:292-304.
- Eusebi V, Lester S. Tumours of the nipple. In: Lakhani SR, Ellis IO, Schnitt SJ, et al, eds. WHO Classification of Tumours of the Breast. Lyon, France: IARC; 2012.
- Spohn GP, Trotter SC, Tozbician G, et al. Nipple adenoma in a female patient presenting with persistent erythema of the right nipple skin: case report, review of the literature, clinical implications, and relevancy to health care providers who evaluate and treat patients with dermatologic conditions of the breast skin. BMC Dermatol. 2016;16:4.
- Kowal R, Miller CJ, Elenitsas R. Eroded patch on the nipple of a 57-year-old woman. Arch Dermatol. 2008;144:933-938.
- Van Mierlo PL, Geelen GM, Neumann HA. Mohs micrographic surgery for an erosive adenomatosis of the nipple. Dermatol Surg. 1998;24:681-683.
- Brankov N, Nino T, Hsiang D, et al. Utilizing Mohs surgery for tissue preservation in erosive adenomatosis of the nipple. Dermatol Surg. 2016;42:684-686.
- Kuflik EG. Erosive adenomatosis of the nipple treated with cryosurgery. J Am Acad Dermatol. 1998;38:270-271.
The Diagnosis: Erosive Adenomatosis of the Nipple
Biopsy of the lesion revealed proliferative sections of glandular epithelium demonstrating apocrine differentiation, connecting to the epidermis and traversing throughout the entire dermis of the specimen (Figure). There were papillary projections of dilated ducts with a retained layer of myoepithelial cells surrounding the epithelial layers. Cytologic atypia was not appreciated. The patient was diagnosed with erosive adenomatosis of the nipple (EAN), also known as nipple adenoma. The lesion subsequently was treated and cleared with Mohs micrographic surgery (MMS). At 8-month follow-up there was no clinical recurrence of the lesion, and the patient was satisfied with the overall cosmetic appearance and conservation of the areola. The patient was followed clinically with annual breast examinations and mammography to monitor future recurrence.

Erosive adenomatosis of the nipple is an uncommon benign proliferative process of the lactiferous ducts of the nipple. Recognizing EAN is important because it resembles malignant breast diseases such as Paget disease of the nipple and invasive breast carcinoma. Due to these similarities, early cases of EAN have resulted in unnecessary mastectomies before the benignity of the condition was established.1 Accurate diagnosis is important to both the patient and the clinician for treatment planning as well as psychosocial consequences associated with the potential removal of this anatomically and cosmetically sensitive area.
Reviewing the literature on EAN is complicated by the variety of terms used to describe this condition, including but not limited to nipple adenoma, nipple duct adenoma, papillary adenoma of the nipple, and florid papillomatosis of the nipple. In 1955, Jones2 described EAN using the term florid papillomatosis of the nipple ducts. In 1962, Handley and Thackray1 argued that adenoma of the nipple was a more descriptive term because it more closely described the appearance of a sweat gland adenoma. They reasoned that adenoma of the nipple is a separate process from ductal papilloma due to the adenomatous proliferation into the nipple stroma rather than the lumen of the nipple ducts.1 The term adenoma of the nipple was further supported in 1965 by Taylor and Robertson.3 In 1959, Le Gal et al4 used the term erosive adenomatosis of the nipple to describe the erosive nature of nipple adenoma. The term nipple adenoma was published in the 2012 WHO Classification of Tumors of the Breast with 4 common histologic subtypes.5,6
Erosive adenomatosis of the nipple is clinically indistinguishable from Paget disease of the nipple, thus biopsy is essential for accurate diagnosis. In contrast to Paget disease, EAN tends to present in younger patients and progresses more slowly, and symptoms may be exacerbated around menstruation.1 Case reports demonstrate that patients may wait years before seeking medical attention for EAN.1,3,7,8 Presenting symptoms may include inflammation, crusting, nipple skin erosion, itching, and pain. Serous or sanguineous discharge from the lesions also is commonly reported. Palpation may reveal a small, hard, or elastic nodule within or underlying the nipple. In addition to Paget disease, EAN may resemble squamous cell carcinoma of the nipple, eczema, psoriasis, or a skin infection.6 Axillary lymphadenopathy is not present in the absence of a concomitant breast malignancy.8 On biopsy, nipple adenoma represents ductal proliferation of glandular structures within the stroma of the nipple that is well circumscribed but without borders. The erosive appearance of the lesion is produced by extensions of the glandular epithelium on the surface of the nipple.1,6 Specific to EAN is the presence of 2 cell types: an inner columnar epithelium and an outer cuboidal myoepithelium. These 2 cell types are present in normal lactiferous ducts; however, normal ducts are highly organized compared to EAN.9
After confirmation of EAN by nipple biopsy, complete surgical excision has been the gold standard for treatment, followed by reconstructive surgery.6 Handley and Thackray1 advocated for total excision of the nipple and areola with an underlying wedge of breast tissue to facilitate wound closure. More recently, successful alternative forms of treatment have been utilized to minimize disfiguring surgery. Alternative treatments include MMS,8 cryotherapy,10 and nipple splitting enucleation.6 Treatment with MMS has resulted in nipple sparing with the least amount of surface area sacrificed (1.1 cm2).9 Our case and prior case reports demonstrate that the tissue sparing potential of MMS is appropriate for the treatment of EAN, though traditionally it has been reserved for more malignant tumors. Preserving this sensitive area is both cosmetically and psychologically advantageous for the patient and thus should be considered when reviewing treatment options for EAN.
The Diagnosis: Erosive Adenomatosis of the Nipple
Biopsy of the lesion revealed proliferative sections of glandular epithelium demonstrating apocrine differentiation, connecting to the epidermis and traversing throughout the entire dermis of the specimen (Figure). There were papillary projections of dilated ducts with a retained layer of myoepithelial cells surrounding the epithelial layers. Cytologic atypia was not appreciated. The patient was diagnosed with erosive adenomatosis of the nipple (EAN), also known as nipple adenoma. The lesion subsequently was treated and cleared with Mohs micrographic surgery (MMS). At 8-month follow-up there was no clinical recurrence of the lesion, and the patient was satisfied with the overall cosmetic appearance and conservation of the areola. The patient was followed clinically with annual breast examinations and mammography to monitor future recurrence.

Erosive adenomatosis of the nipple is an uncommon benign proliferative process of the lactiferous ducts of the nipple. Recognizing EAN is important because it resembles malignant breast diseases such as Paget disease of the nipple and invasive breast carcinoma. Due to these similarities, early cases of EAN have resulted in unnecessary mastectomies before the benignity of the condition was established.1 Accurate diagnosis is important to both the patient and the clinician for treatment planning as well as psychosocial consequences associated with the potential removal of this anatomically and cosmetically sensitive area.
Reviewing the literature on EAN is complicated by the variety of terms used to describe this condition, including but not limited to nipple adenoma, nipple duct adenoma, papillary adenoma of the nipple, and florid papillomatosis of the nipple. In 1955, Jones2 described EAN using the term florid papillomatosis of the nipple ducts. In 1962, Handley and Thackray1 argued that adenoma of the nipple was a more descriptive term because it more closely described the appearance of a sweat gland adenoma. They reasoned that adenoma of the nipple is a separate process from ductal papilloma due to the adenomatous proliferation into the nipple stroma rather than the lumen of the nipple ducts.1 The term adenoma of the nipple was further supported in 1965 by Taylor and Robertson.3 In 1959, Le Gal et al4 used the term erosive adenomatosis of the nipple to describe the erosive nature of nipple adenoma. The term nipple adenoma was published in the 2012 WHO Classification of Tumors of the Breast with 4 common histologic subtypes.5,6
Erosive adenomatosis of the nipple is clinically indistinguishable from Paget disease of the nipple, thus biopsy is essential for accurate diagnosis. In contrast to Paget disease, EAN tends to present in younger patients and progresses more slowly, and symptoms may be exacerbated around menstruation.1 Case reports demonstrate that patients may wait years before seeking medical attention for EAN.1,3,7,8 Presenting symptoms may include inflammation, crusting, nipple skin erosion, itching, and pain. Serous or sanguineous discharge from the lesions also is commonly reported. Palpation may reveal a small, hard, or elastic nodule within or underlying the nipple. In addition to Paget disease, EAN may resemble squamous cell carcinoma of the nipple, eczema, psoriasis, or a skin infection.6 Axillary lymphadenopathy is not present in the absence of a concomitant breast malignancy.8 On biopsy, nipple adenoma represents ductal proliferation of glandular structures within the stroma of the nipple that is well circumscribed but without borders. The erosive appearance of the lesion is produced by extensions of the glandular epithelium on the surface of the nipple.1,6 Specific to EAN is the presence of 2 cell types: an inner columnar epithelium and an outer cuboidal myoepithelium. These 2 cell types are present in normal lactiferous ducts; however, normal ducts are highly organized compared to EAN.9
After confirmation of EAN by nipple biopsy, complete surgical excision has been the gold standard for treatment, followed by reconstructive surgery.6 Handley and Thackray1 advocated for total excision of the nipple and areola with an underlying wedge of breast tissue to facilitate wound closure. More recently, successful alternative forms of treatment have been utilized to minimize disfiguring surgery. Alternative treatments include MMS,8 cryotherapy,10 and nipple splitting enucleation.6 Treatment with MMS has resulted in nipple sparing with the least amount of surface area sacrificed (1.1 cm2).9 Our case and prior case reports demonstrate that the tissue sparing potential of MMS is appropriate for the treatment of EAN, though traditionally it has been reserved for more malignant tumors. Preserving this sensitive area is both cosmetically and psychologically advantageous for the patient and thus should be considered when reviewing treatment options for EAN.
- Handley RS, Thackray AC. Adenoma of nipple. Br J Cancer. 1962;16:187-194.
- Jones DB. Florid papillomatosis of the nipple ducts. Cancer. 1955;8:315-319.
- Taylor HB, Robertson AG. Adenomas of the nipple. Cancer. 1965:18:995-1002.
- Le Gal Y, Gros CM, Bader P. Erosive adenomatosis of the nipple [in French]. Ann Anat Pathol (Paris). 1959;4:292-304.
- Eusebi V, Lester S. Tumours of the nipple. In: Lakhani SR, Ellis IO, Schnitt SJ, et al, eds. WHO Classification of Tumours of the Breast. Lyon, France: IARC; 2012.
- Spohn GP, Trotter SC, Tozbician G, et al. Nipple adenoma in a female patient presenting with persistent erythema of the right nipple skin: case report, review of the literature, clinical implications, and relevancy to health care providers who evaluate and treat patients with dermatologic conditions of the breast skin. BMC Dermatol. 2016;16:4.
- Kowal R, Miller CJ, Elenitsas R. Eroded patch on the nipple of a 57-year-old woman. Arch Dermatol. 2008;144:933-938.
- Van Mierlo PL, Geelen GM, Neumann HA. Mohs micrographic surgery for an erosive adenomatosis of the nipple. Dermatol Surg. 1998;24:681-683.
- Brankov N, Nino T, Hsiang D, et al. Utilizing Mohs surgery for tissue preservation in erosive adenomatosis of the nipple. Dermatol Surg. 2016;42:684-686.
- Kuflik EG. Erosive adenomatosis of the nipple treated with cryosurgery. J Am Acad Dermatol. 1998;38:270-271.
- Handley RS, Thackray AC. Adenoma of nipple. Br J Cancer. 1962;16:187-194.
- Jones DB. Florid papillomatosis of the nipple ducts. Cancer. 1955;8:315-319.
- Taylor HB, Robertson AG. Adenomas of the nipple. Cancer. 1965:18:995-1002.
- Le Gal Y, Gros CM, Bader P. Erosive adenomatosis of the nipple [in French]. Ann Anat Pathol (Paris). 1959;4:292-304.
- Eusebi V, Lester S. Tumours of the nipple. In: Lakhani SR, Ellis IO, Schnitt SJ, et al, eds. WHO Classification of Tumours of the Breast. Lyon, France: IARC; 2012.
- Spohn GP, Trotter SC, Tozbician G, et al. Nipple adenoma in a female patient presenting with persistent erythema of the right nipple skin: case report, review of the literature, clinical implications, and relevancy to health care providers who evaluate and treat patients with dermatologic conditions of the breast skin. BMC Dermatol. 2016;16:4.
- Kowal R, Miller CJ, Elenitsas R. Eroded patch on the nipple of a 57-year-old woman. Arch Dermatol. 2008;144:933-938.
- Van Mierlo PL, Geelen GM, Neumann HA. Mohs micrographic surgery for an erosive adenomatosis of the nipple. Dermatol Surg. 1998;24:681-683.
- Brankov N, Nino T, Hsiang D, et al. Utilizing Mohs surgery for tissue preservation in erosive adenomatosis of the nipple. Dermatol Surg. 2016;42:684-686.
- Kuflik EG. Erosive adenomatosis of the nipple treated with cryosurgery. J Am Acad Dermatol. 1998;38:270-271.
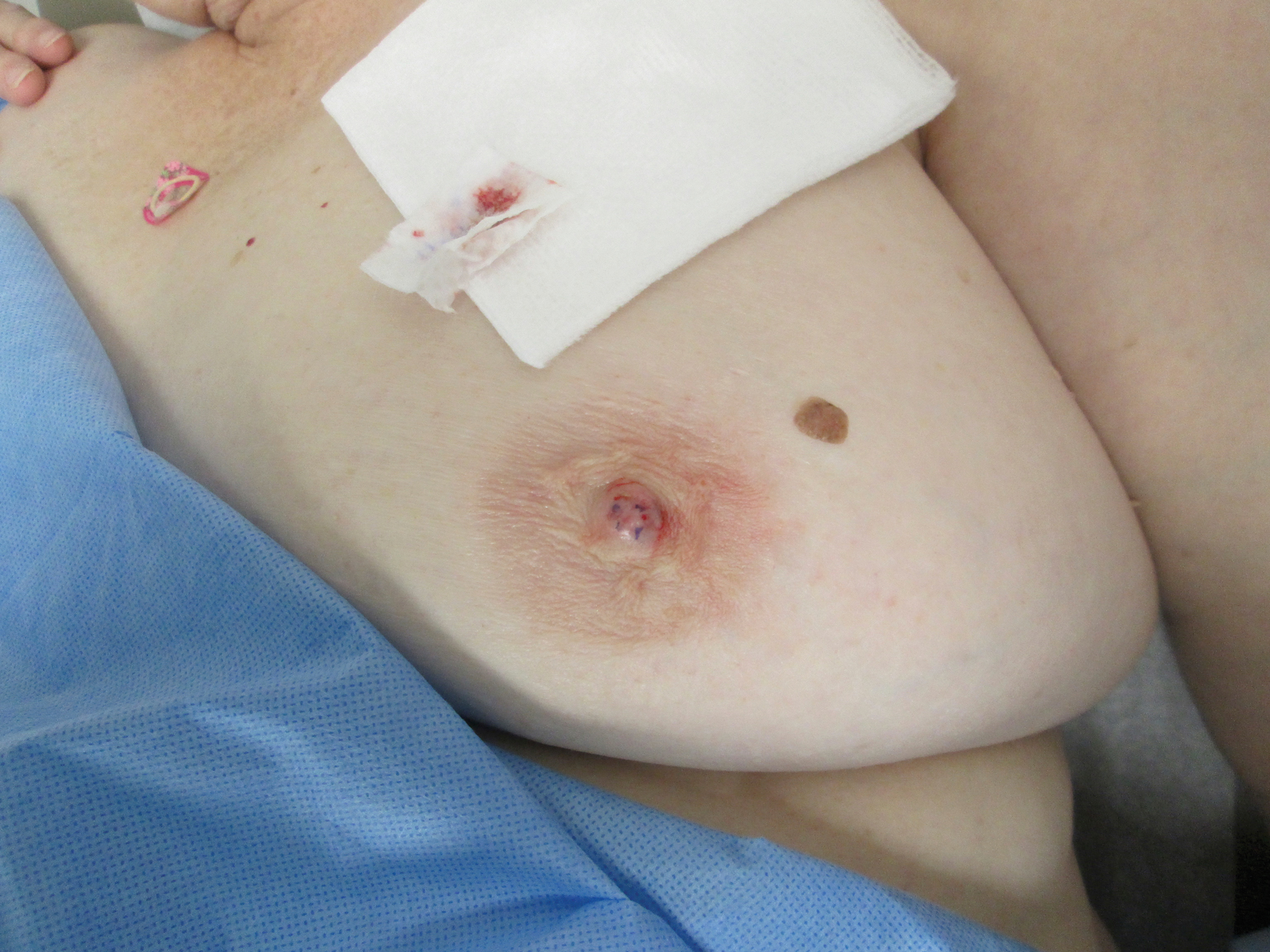
A 61-year-old woman presented with an asymptomatic, slowly enlarging, 9-mm, firm, red papule on the left nipple of 2 years' duration. She had no notable medical history, including a BI-RADS (Breast Imaging Reporting and Data System) mammogram score of 2 that was suggestive of benign findings 2 years prior. A repeat mammogram ordered by radiology and completed before presenting to dermatology had a BI-RADS score of 4, noting a concerning feature in the area of the lesion and prompting a biopsy.
FDA expands use of Vraylar to treatment of bipolar-associated depressive episodes
The Food and Drug Administration on May 28 approved a supplemental New Drug Application for cariprazine (Vraylar) for the treatment of depressive episodes associated with bipolar I disorder.
Approval for the expanded label was based on results of the RGH-MD-53, RGH-MD-54, and RGH-MD-56 clinical trials, in which cariprazine was compared with placebo over a 6-week period in patients with bipolar I disorder. In all three trials, patients receiving 1.5 mg cariprazine had significantly greater improvement in their Montgomery-Åsberg Depression Rating scale after 6 weeks, compared with patients receiving placebo.
Cariprazine previously was indicated for the treatment of manic or mixed episodes associated with bipolar I disorder in adults. The most common adverse reactions reported in the clinical trials were nausea, akathisia, restlessness, and extrapyramidal symptoms; these symptoms are similar to those on the Vraylar label.
“Treating bipolar disorder can be very difficult, because people living with the illness experience a range of depressive and manic symptoms, sometimes both at the same time, and , specifically manic, mixed, and depressive episodes, with just one medication,” Stephen M. Stahl, MD, PhD, professor of psychiatry at the University of California, San Diego, said in the press release.
Find the full press release on the Allergan website.
The Food and Drug Administration on May 28 approved a supplemental New Drug Application for cariprazine (Vraylar) for the treatment of depressive episodes associated with bipolar I disorder.
Approval for the expanded label was based on results of the RGH-MD-53, RGH-MD-54, and RGH-MD-56 clinical trials, in which cariprazine was compared with placebo over a 6-week period in patients with bipolar I disorder. In all three trials, patients receiving 1.5 mg cariprazine had significantly greater improvement in their Montgomery-Åsberg Depression Rating scale after 6 weeks, compared with patients receiving placebo.
Cariprazine previously was indicated for the treatment of manic or mixed episodes associated with bipolar I disorder in adults. The most common adverse reactions reported in the clinical trials were nausea, akathisia, restlessness, and extrapyramidal symptoms; these symptoms are similar to those on the Vraylar label.
“Treating bipolar disorder can be very difficult, because people living with the illness experience a range of depressive and manic symptoms, sometimes both at the same time, and , specifically manic, mixed, and depressive episodes, with just one medication,” Stephen M. Stahl, MD, PhD, professor of psychiatry at the University of California, San Diego, said in the press release.
Find the full press release on the Allergan website.
The Food and Drug Administration on May 28 approved a supplemental New Drug Application for cariprazine (Vraylar) for the treatment of depressive episodes associated with bipolar I disorder.
Approval for the expanded label was based on results of the RGH-MD-53, RGH-MD-54, and RGH-MD-56 clinical trials, in which cariprazine was compared with placebo over a 6-week period in patients with bipolar I disorder. In all three trials, patients receiving 1.5 mg cariprazine had significantly greater improvement in their Montgomery-Åsberg Depression Rating scale after 6 weeks, compared with patients receiving placebo.
Cariprazine previously was indicated for the treatment of manic or mixed episodes associated with bipolar I disorder in adults. The most common adverse reactions reported in the clinical trials were nausea, akathisia, restlessness, and extrapyramidal symptoms; these symptoms are similar to those on the Vraylar label.
“Treating bipolar disorder can be very difficult, because people living with the illness experience a range of depressive and manic symptoms, sometimes both at the same time, and , specifically manic, mixed, and depressive episodes, with just one medication,” Stephen M. Stahl, MD, PhD, professor of psychiatry at the University of California, San Diego, said in the press release.
Find the full press release on the Allergan website.
Building better flu vaccines is daunting
LJUBLJANA, SLOVENIA – Don’t hold your breath waiting for a substantially better, more reliably effective influenza vaccine.
That was a key cautionary message provided by vaccine expert Edward A. Belongia, MD, at the annual meeting of the European Society for Paediatric Infectious Diseases.
The effectiveness of seasonal influenza vaccine varies from 10% to 60% year by year, leaving enormous room for improvement. But many obstacles exist to developing a more consistent and reliably effective version of the seasonal influenza vaccine. And the lofty goal of creating a universal vaccine is even more ambitious, although the National Institute of Allergy and Infectious Diseases has declared it to be a top priority and mapped out a strategic plan for getting there (J Infect Dis. 2018 Jul 2;218[3]:347-54).
“Ultimately the Holy Grail is a universal flu vaccine that would provide pan-A and pan-B protection that would last for more than 1 year, with protection against avian and pandemic viruses, and would work for both children and adults. We are nowhere near that. Every 5 years someone says we’re 5 years away, and then 5 years go by and we’re still 5 years away. So I’m not making any predictions on that,” said Dr. Belongia, director of the Center for Clinical Epidemiology and Population Health at the Marshfield (Wisc.) Clinic Research Institute, which is part of the U.S. Influenza Vaccine Effectiveness Network.
One of the big problems in creating a more effective flu vaccine, particularly for children, is the H3N2 virus subtype. Dr. Belongia was first author of a systematic review and meta-analysis of studies of more than a dozen recent flu seasons showing that although vaccine effectiveness against H3N2 varied widely from year to year, it was consistently lower than against influenza type B and H1N1 (Lancet Infect Dis. 2016 Aug;16[8]:942-51).
And that’s especially true in children and adolescents. Notably, in the 2014-2015 U.S. flu season, vaccine effectiveness against H3N2 in children aged 6 months to 8 years was low at 23%, but shockingly lower at a mere 7% in the 9- to 17-year-olds. Whereas in the 2017-2018 season, vaccine effectiveness against H3N2 in the 9- to 17-year-olds jumped to 46% while remaining low but consistent at 22% in the younger children.
“We see a very different age pattern here for the older children compared to the younger children, and quite frankly we don’t really understand what’s doing this,” said Dr. Belongia.
What is well understood, however, is that the problematic performance of influenza vaccines when it comes to protecting against H3N2 is a complicated matter stemming from three sources: the virus itself; the current egg-based vaccine manufacturing methodology, which is now 7 decades old; and host factors.
That troublesome H3N2 virus
Antigenic evolution of the H3N2 virus occurs at a 5- to 6-fold higher rate than for influenza B virus and roughly 17-fold faster than for H1N1. That high mutation rate makes for a moving target that’s a real problem when trying to keep a vaccine current. Also, the globular head of the virus is prone to glycosylation, which enables the virus to evade immune detection.
Vaccine-related factors
It’s likely that the availability of the flu vaccine for the upcoming 2019-2020 season is going to be delayed because of late selection of the strains for inclusion. The World Health Organization ordinarily selects strains for vaccines for the Northern Hemisphere in February, giving vaccine manufacturers 6-8 months to produce their vaccines and ship them in time for administration from September through November. This year, however, the WHO delayed selection of the H3N2 component until March because of the high level of antigenic and genetic diversity of circulating strains.
“This hasn’t happened since 2003 – it’s a very rare occurrence – but it does increase the potential that there’s going to be a delay in the availability of the vaccine in the fall,” he explained.
Eventually, the WHO selected a new clade 3C.3a virus called A/Kansas/14/2017 for the 2019-2020 vaccine. It should cover the circulating strains of H3N2 “reasonably well,” according to the physician.
Another issue: H3N2 has become adapted to the mammalian environment, so growing the virus in eggs introduces strong selection pressure for mutations leading to reduced vaccine effectiveness. Yet only two flu vaccines licensed in the United States are manufactured without eggs: Flucelvax, marketed by Seqirus for patients aged 4 years and up, and Sanofi’s Flublok, which is licensed for individuals who are 18 years of age or older. Studies are underway looking at the relative effectiveness of egg-based versus cell culture-manufactured flu vaccines in real-world settings.
Host factors
Hemagglutinin imprinting, sometimes referred to as “original antigenic sin,” is a decades-old concept whereby early childhood exposure to influenza viruses shapes future vaccine response.
“It suggests there could be some birth cohort effects in vaccine responsiveness, depending on what was circulating in the first 2-3 years after birth. It would complicate vaccine strategy quite a bit if you had to have different strategies for different birth cohorts,” Dr. Belongia observed.
Another host factor issue is the controversial topic of negative interference stemming from repeated vaccinations. It’s unclear how important this is in the real world, because studies have been inconsistent. Reassuringly, Dr. Belongia and coworkers found no association between prior-season influenza vaccination and diminished vaccine effectiveness in 3,369 U.S. children aged 2-17 years studied during the 2013-14 through 2015-16 flu seasons (JAMA Netw Open. 2018 Oct 5;1[6]:e183742. doi: 10.1001/jamanetworkopen.2018.3742).
“We found no suggestion at all of a problem with being vaccinated two seasons in a row,” according to Dr. Belongia.
How to build a better influenza vaccine for children
“I would say that even before we get to a universal vaccine, the next generation of flu vaccines that are more effective are not going to be manufactured using eggs, although we’re not real close to that. But I think that’s eventually where we’re going,” he said.
“I think it’s going to take a systems biology approach in order to really understand the adaptive immune response to infection and vaccination in early life. That means a much more detailed understanding of what is underlying the imprinting mechanisms and what is the adaptive response to repeated vaccination and infection. I think this is going to take prospective infant cohort studies; the National Institutes of Health is funding some that will begin within the next year,” Dr. Belongia added.
Many investigational approaches to improving influenza virus subtype-level protection are being explored. These include novel adjuvants, nanoparticle vaccines, computationally optimized broadly reactive antigens, and standardization of neuraminidase content.
And as for the much-desired universal flu vaccine?
“I will say that if a universal vaccine is going to work it’s probably going to work first in children. They have a much shorter immune history and their antibody landscape is a lot smaller, so you have a much better opportunity, I think, to generate a broad response to a universal vaccine compared to adults, who have much more complex immune landscapes,” he said.
Dr. Belongia reported having no financial conflicts regarding his presentation.
LJUBLJANA, SLOVENIA – Don’t hold your breath waiting for a substantially better, more reliably effective influenza vaccine.
That was a key cautionary message provided by vaccine expert Edward A. Belongia, MD, at the annual meeting of the European Society for Paediatric Infectious Diseases.
The effectiveness of seasonal influenza vaccine varies from 10% to 60% year by year, leaving enormous room for improvement. But many obstacles exist to developing a more consistent and reliably effective version of the seasonal influenza vaccine. And the lofty goal of creating a universal vaccine is even more ambitious, although the National Institute of Allergy and Infectious Diseases has declared it to be a top priority and mapped out a strategic plan for getting there (J Infect Dis. 2018 Jul 2;218[3]:347-54).
“Ultimately the Holy Grail is a universal flu vaccine that would provide pan-A and pan-B protection that would last for more than 1 year, with protection against avian and pandemic viruses, and would work for both children and adults. We are nowhere near that. Every 5 years someone says we’re 5 years away, and then 5 years go by and we’re still 5 years away. So I’m not making any predictions on that,” said Dr. Belongia, director of the Center for Clinical Epidemiology and Population Health at the Marshfield (Wisc.) Clinic Research Institute, which is part of the U.S. Influenza Vaccine Effectiveness Network.
One of the big problems in creating a more effective flu vaccine, particularly for children, is the H3N2 virus subtype. Dr. Belongia was first author of a systematic review and meta-analysis of studies of more than a dozen recent flu seasons showing that although vaccine effectiveness against H3N2 varied widely from year to year, it was consistently lower than against influenza type B and H1N1 (Lancet Infect Dis. 2016 Aug;16[8]:942-51).
And that’s especially true in children and adolescents. Notably, in the 2014-2015 U.S. flu season, vaccine effectiveness against H3N2 in children aged 6 months to 8 years was low at 23%, but shockingly lower at a mere 7% in the 9- to 17-year-olds. Whereas in the 2017-2018 season, vaccine effectiveness against H3N2 in the 9- to 17-year-olds jumped to 46% while remaining low but consistent at 22% in the younger children.
“We see a very different age pattern here for the older children compared to the younger children, and quite frankly we don’t really understand what’s doing this,” said Dr. Belongia.
What is well understood, however, is that the problematic performance of influenza vaccines when it comes to protecting against H3N2 is a complicated matter stemming from three sources: the virus itself; the current egg-based vaccine manufacturing methodology, which is now 7 decades old; and host factors.
That troublesome H3N2 virus
Antigenic evolution of the H3N2 virus occurs at a 5- to 6-fold higher rate than for influenza B virus and roughly 17-fold faster than for H1N1. That high mutation rate makes for a moving target that’s a real problem when trying to keep a vaccine current. Also, the globular head of the virus is prone to glycosylation, which enables the virus to evade immune detection.
Vaccine-related factors
It’s likely that the availability of the flu vaccine for the upcoming 2019-2020 season is going to be delayed because of late selection of the strains for inclusion. The World Health Organization ordinarily selects strains for vaccines for the Northern Hemisphere in February, giving vaccine manufacturers 6-8 months to produce their vaccines and ship them in time for administration from September through November. This year, however, the WHO delayed selection of the H3N2 component until March because of the high level of antigenic and genetic diversity of circulating strains.
“This hasn’t happened since 2003 – it’s a very rare occurrence – but it does increase the potential that there’s going to be a delay in the availability of the vaccine in the fall,” he explained.
Eventually, the WHO selected a new clade 3C.3a virus called A/Kansas/14/2017 for the 2019-2020 vaccine. It should cover the circulating strains of H3N2 “reasonably well,” according to the physician.
Another issue: H3N2 has become adapted to the mammalian environment, so growing the virus in eggs introduces strong selection pressure for mutations leading to reduced vaccine effectiveness. Yet only two flu vaccines licensed in the United States are manufactured without eggs: Flucelvax, marketed by Seqirus for patients aged 4 years and up, and Sanofi’s Flublok, which is licensed for individuals who are 18 years of age or older. Studies are underway looking at the relative effectiveness of egg-based versus cell culture-manufactured flu vaccines in real-world settings.
Host factors
Hemagglutinin imprinting, sometimes referred to as “original antigenic sin,” is a decades-old concept whereby early childhood exposure to influenza viruses shapes future vaccine response.
“It suggests there could be some birth cohort effects in vaccine responsiveness, depending on what was circulating in the first 2-3 years after birth. It would complicate vaccine strategy quite a bit if you had to have different strategies for different birth cohorts,” Dr. Belongia observed.
Another host factor issue is the controversial topic of negative interference stemming from repeated vaccinations. It’s unclear how important this is in the real world, because studies have been inconsistent. Reassuringly, Dr. Belongia and coworkers found no association between prior-season influenza vaccination and diminished vaccine effectiveness in 3,369 U.S. children aged 2-17 years studied during the 2013-14 through 2015-16 flu seasons (JAMA Netw Open. 2018 Oct 5;1[6]:e183742. doi: 10.1001/jamanetworkopen.2018.3742).
“We found no suggestion at all of a problem with being vaccinated two seasons in a row,” according to Dr. Belongia.
How to build a better influenza vaccine for children
“I would say that even before we get to a universal vaccine, the next generation of flu vaccines that are more effective are not going to be manufactured using eggs, although we’re not real close to that. But I think that’s eventually where we’re going,” he said.
“I think it’s going to take a systems biology approach in order to really understand the adaptive immune response to infection and vaccination in early life. That means a much more detailed understanding of what is underlying the imprinting mechanisms and what is the adaptive response to repeated vaccination and infection. I think this is going to take prospective infant cohort studies; the National Institutes of Health is funding some that will begin within the next year,” Dr. Belongia added.
Many investigational approaches to improving influenza virus subtype-level protection are being explored. These include novel adjuvants, nanoparticle vaccines, computationally optimized broadly reactive antigens, and standardization of neuraminidase content.
And as for the much-desired universal flu vaccine?
“I will say that if a universal vaccine is going to work it’s probably going to work first in children. They have a much shorter immune history and their antibody landscape is a lot smaller, so you have a much better opportunity, I think, to generate a broad response to a universal vaccine compared to adults, who have much more complex immune landscapes,” he said.
Dr. Belongia reported having no financial conflicts regarding his presentation.
LJUBLJANA, SLOVENIA – Don’t hold your breath waiting for a substantially better, more reliably effective influenza vaccine.
That was a key cautionary message provided by vaccine expert Edward A. Belongia, MD, at the annual meeting of the European Society for Paediatric Infectious Diseases.
The effectiveness of seasonal influenza vaccine varies from 10% to 60% year by year, leaving enormous room for improvement. But many obstacles exist to developing a more consistent and reliably effective version of the seasonal influenza vaccine. And the lofty goal of creating a universal vaccine is even more ambitious, although the National Institute of Allergy and Infectious Diseases has declared it to be a top priority and mapped out a strategic plan for getting there (J Infect Dis. 2018 Jul 2;218[3]:347-54).
“Ultimately the Holy Grail is a universal flu vaccine that would provide pan-A and pan-B protection that would last for more than 1 year, with protection against avian and pandemic viruses, and would work for both children and adults. We are nowhere near that. Every 5 years someone says we’re 5 years away, and then 5 years go by and we’re still 5 years away. So I’m not making any predictions on that,” said Dr. Belongia, director of the Center for Clinical Epidemiology and Population Health at the Marshfield (Wisc.) Clinic Research Institute, which is part of the U.S. Influenza Vaccine Effectiveness Network.
One of the big problems in creating a more effective flu vaccine, particularly for children, is the H3N2 virus subtype. Dr. Belongia was first author of a systematic review and meta-analysis of studies of more than a dozen recent flu seasons showing that although vaccine effectiveness against H3N2 varied widely from year to year, it was consistently lower than against influenza type B and H1N1 (Lancet Infect Dis. 2016 Aug;16[8]:942-51).
And that’s especially true in children and adolescents. Notably, in the 2014-2015 U.S. flu season, vaccine effectiveness against H3N2 in children aged 6 months to 8 years was low at 23%, but shockingly lower at a mere 7% in the 9- to 17-year-olds. Whereas in the 2017-2018 season, vaccine effectiveness against H3N2 in the 9- to 17-year-olds jumped to 46% while remaining low but consistent at 22% in the younger children.
“We see a very different age pattern here for the older children compared to the younger children, and quite frankly we don’t really understand what’s doing this,” said Dr. Belongia.
What is well understood, however, is that the problematic performance of influenza vaccines when it comes to protecting against H3N2 is a complicated matter stemming from three sources: the virus itself; the current egg-based vaccine manufacturing methodology, which is now 7 decades old; and host factors.
That troublesome H3N2 virus
Antigenic evolution of the H3N2 virus occurs at a 5- to 6-fold higher rate than for influenza B virus and roughly 17-fold faster than for H1N1. That high mutation rate makes for a moving target that’s a real problem when trying to keep a vaccine current. Also, the globular head of the virus is prone to glycosylation, which enables the virus to evade immune detection.
Vaccine-related factors
It’s likely that the availability of the flu vaccine for the upcoming 2019-2020 season is going to be delayed because of late selection of the strains for inclusion. The World Health Organization ordinarily selects strains for vaccines for the Northern Hemisphere in February, giving vaccine manufacturers 6-8 months to produce their vaccines and ship them in time for administration from September through November. This year, however, the WHO delayed selection of the H3N2 component until March because of the high level of antigenic and genetic diversity of circulating strains.
“This hasn’t happened since 2003 – it’s a very rare occurrence – but it does increase the potential that there’s going to be a delay in the availability of the vaccine in the fall,” he explained.
Eventually, the WHO selected a new clade 3C.3a virus called A/Kansas/14/2017 for the 2019-2020 vaccine. It should cover the circulating strains of H3N2 “reasonably well,” according to the physician.
Another issue: H3N2 has become adapted to the mammalian environment, so growing the virus in eggs introduces strong selection pressure for mutations leading to reduced vaccine effectiveness. Yet only two flu vaccines licensed in the United States are manufactured without eggs: Flucelvax, marketed by Seqirus for patients aged 4 years and up, and Sanofi’s Flublok, which is licensed for individuals who are 18 years of age or older. Studies are underway looking at the relative effectiveness of egg-based versus cell culture-manufactured flu vaccines in real-world settings.
Host factors
Hemagglutinin imprinting, sometimes referred to as “original antigenic sin,” is a decades-old concept whereby early childhood exposure to influenza viruses shapes future vaccine response.
“It suggests there could be some birth cohort effects in vaccine responsiveness, depending on what was circulating in the first 2-3 years after birth. It would complicate vaccine strategy quite a bit if you had to have different strategies for different birth cohorts,” Dr. Belongia observed.
Another host factor issue is the controversial topic of negative interference stemming from repeated vaccinations. It’s unclear how important this is in the real world, because studies have been inconsistent. Reassuringly, Dr. Belongia and coworkers found no association between prior-season influenza vaccination and diminished vaccine effectiveness in 3,369 U.S. children aged 2-17 years studied during the 2013-14 through 2015-16 flu seasons (JAMA Netw Open. 2018 Oct 5;1[6]:e183742. doi: 10.1001/jamanetworkopen.2018.3742).
“We found no suggestion at all of a problem with being vaccinated two seasons in a row,” according to Dr. Belongia.
How to build a better influenza vaccine for children
“I would say that even before we get to a universal vaccine, the next generation of flu vaccines that are more effective are not going to be manufactured using eggs, although we’re not real close to that. But I think that’s eventually where we’re going,” he said.
“I think it’s going to take a systems biology approach in order to really understand the adaptive immune response to infection and vaccination in early life. That means a much more detailed understanding of what is underlying the imprinting mechanisms and what is the adaptive response to repeated vaccination and infection. I think this is going to take prospective infant cohort studies; the National Institutes of Health is funding some that will begin within the next year,” Dr. Belongia added.
Many investigational approaches to improving influenza virus subtype-level protection are being explored. These include novel adjuvants, nanoparticle vaccines, computationally optimized broadly reactive antigens, and standardization of neuraminidase content.
And as for the much-desired universal flu vaccine?
“I will say that if a universal vaccine is going to work it’s probably going to work first in children. They have a much shorter immune history and their antibody landscape is a lot smaller, so you have a much better opportunity, I think, to generate a broad response to a universal vaccine compared to adults, who have much more complex immune landscapes,” he said.
Dr. Belongia reported having no financial conflicts regarding his presentation.
REPORTING FROM ESPID 2019