User login
Hernia repair: Studies don’t support use of higher-cost biological mesh
The jury is still out on the costs and efficacy of biological mesh implants for abdominal wall hernia repair, according to a systematic review of the literature.
Of 20 articles that met search criteria, only 3 were comparative studies and none was a randomized clinical trial. In fact, most were case series involving convenience samples of patients at single institutions, Dr. Sergio Huerta of the University of Texas Southwestern Medical Center, Dallas, and his colleagues reported online Jan. 27 in JAMA Surgery.
The authors used multiple electronic databases to identify articles published between 1948 and June 30, 2015, on the use of biological mesh materials for reinforcement of the abdominal wall for hernia repair. Included were 14 articles that described outcomes with human acellular dermal matrix, 2 that reported results for porcine collagen intestinal submucosa derivatives, 3 that reported on porcine acelluar collagen skin derivatives, and 1 that described results for bovine pericardium.
Several problems were noted with respect to the studies, including widely varying follow-up time, operative technique, types of mesh used, and patient selection criteria. Also, outcome measures were not reported consistently across studies.
In addition, 16 of the 20 studies that met search criteria did not report investigator conflicts of interest, the authors reported (JAMA Surg. 2016 Jan 27. doi: 10.10001/jamasurg.2015.5234).
Notably, all the meshes used in the studies were approved by the Food and Drug Administration and were considered to be comparable to a group of nonbiological predicate devices, which cost up to 25% less than the biological equivalents, they noted.
“We were unable to find any evidence that supported the use of expensive biological material relative to low-cost synthetic mesh. In fact, with one exception, the biological materials became commercially available by showing that these materials were equivalent to low-cost established synthetic mesh material in an FDA 510(k) approval process. This process does not require phase 0 through IV clinical trials as required for drugs or biological agents,” they wrote, noting that the one material that bypassed the 510(k) process (Alloderm) was not required to demonstrate equivalence because it was classified as human transplanted tissue.
Biological mesh materials were introduced in the 1990s to minimize the risk of complications commonly seen with the use of synthetic mesh for abdominal wall hernia repair – one of the most common procedures performed by general surgeons, the authors explained.
“Because the outcomes for biological mesh material are perceived to be better than those for polymer-based prosthetic mesh replacement materials, the use of biological grafts increased exponentially without clear clinical evidence of efficacy,” they wrote.
The current review suggests that the evidence remains insufficient to determine whether cost and clinical benefits exist.
“It is generally assumed that FDA-approved drug or biological agents have been rigorously evaluated and that there is demonstrable safety and efficacy. This is not the case for 510(k) medical devices. Before using a new medical device, physicians should know the approval basis for the device and recognize that if it is a 510(k) device neither safety nor efficacy is ensured,” they said, adding that physicians should assume such devices are no better than predicate devices to which they are equivalent, and that “there can be no justification for purchasing a more expensive device when a lower-cost predicate device, which is equivalent, is available.”
Though limited by certain factors such as lack of access to detailed FDA information such as the specific criteria used to determine equivalence, and a lack of published literature on the full market penetration of biological mesh materials vs. nonbiological counterparts, the authors maintained that until evidence demonstrates superiority of biological materials, the expense associated with their use cannot be justified.
This study was supported by the Hudson-Penn Endowment fund at the University of Texas Southwestern Medical Center. The authors reported having no relevant financial disclosures.
Balancing the need for innovation against the practicalities of demonstrating clinical benefit for novel ideas is a fundamental problem in surgery – a problem highlighted by Heurta et al., Dr. Benjamin K. Poulose and his colleagues said in an editorial.
“This issue is particularly timely given an unsustainable trajectory of health care spending in the United States,” they wrote (JAMA Surg 2016 Jan 27. doi: 10.1001/jamasurg2015.5236).
Like the authors of the literature review, the editorial authors stressed the importance of understanding the limitations of the 510(k) process, and noted that surgeons should consider that the FDA sees them as “the group responsible for understanding and evaluating the data before using expensive medical devices.
“Understanding who is in charge of making sure that the devices that we use during surgery are safe and effective is critical. Likely, it will require a collaborative effort of the FDA, medical device companies, and physicians,” they wrote. Establishing a more formal system of postmarketing surveillance for higher-risk medical devices will benefit patients, they added. Current efforts suffer from reliance on self-reporting and lack of standardized data collection.
Postmarketing surveillance can be greatly improved by directly linking medical device approval with the support of high-quality registries, and the end result should provide transparent data for monitoring effectiveness and safety to drive value-based care and maintain innovation, they said.
Dr. Poulose is with Vanderbilt University Medical Center, Nashville, Tenn. Dr. Poulose reported receiving personal fees from Ariste Medical for consulting work, and research grants from Bard-Davol outside the submitted work.
Balancing the need for innovation against the practicalities of demonstrating clinical benefit for novel ideas is a fundamental problem in surgery – a problem highlighted by Heurta et al., Dr. Benjamin K. Poulose and his colleagues said in an editorial.
“This issue is particularly timely given an unsustainable trajectory of health care spending in the United States,” they wrote (JAMA Surg 2016 Jan 27. doi: 10.1001/jamasurg2015.5236).
Like the authors of the literature review, the editorial authors stressed the importance of understanding the limitations of the 510(k) process, and noted that surgeons should consider that the FDA sees them as “the group responsible for understanding and evaluating the data before using expensive medical devices.
“Understanding who is in charge of making sure that the devices that we use during surgery are safe and effective is critical. Likely, it will require a collaborative effort of the FDA, medical device companies, and physicians,” they wrote. Establishing a more formal system of postmarketing surveillance for higher-risk medical devices will benefit patients, they added. Current efforts suffer from reliance on self-reporting and lack of standardized data collection.
Postmarketing surveillance can be greatly improved by directly linking medical device approval with the support of high-quality registries, and the end result should provide transparent data for monitoring effectiveness and safety to drive value-based care and maintain innovation, they said.
Dr. Poulose is with Vanderbilt University Medical Center, Nashville, Tenn. Dr. Poulose reported receiving personal fees from Ariste Medical for consulting work, and research grants from Bard-Davol outside the submitted work.
Balancing the need for innovation against the practicalities of demonstrating clinical benefit for novel ideas is a fundamental problem in surgery – a problem highlighted by Heurta et al., Dr. Benjamin K. Poulose and his colleagues said in an editorial.
“This issue is particularly timely given an unsustainable trajectory of health care spending in the United States,” they wrote (JAMA Surg 2016 Jan 27. doi: 10.1001/jamasurg2015.5236).
Like the authors of the literature review, the editorial authors stressed the importance of understanding the limitations of the 510(k) process, and noted that surgeons should consider that the FDA sees them as “the group responsible for understanding and evaluating the data before using expensive medical devices.
“Understanding who is in charge of making sure that the devices that we use during surgery are safe and effective is critical. Likely, it will require a collaborative effort of the FDA, medical device companies, and physicians,” they wrote. Establishing a more formal system of postmarketing surveillance for higher-risk medical devices will benefit patients, they added. Current efforts suffer from reliance on self-reporting and lack of standardized data collection.
Postmarketing surveillance can be greatly improved by directly linking medical device approval with the support of high-quality registries, and the end result should provide transparent data for monitoring effectiveness and safety to drive value-based care and maintain innovation, they said.
Dr. Poulose is with Vanderbilt University Medical Center, Nashville, Tenn. Dr. Poulose reported receiving personal fees from Ariste Medical for consulting work, and research grants from Bard-Davol outside the submitted work.
The jury is still out on the costs and efficacy of biological mesh implants for abdominal wall hernia repair, according to a systematic review of the literature.
Of 20 articles that met search criteria, only 3 were comparative studies and none was a randomized clinical trial. In fact, most were case series involving convenience samples of patients at single institutions, Dr. Sergio Huerta of the University of Texas Southwestern Medical Center, Dallas, and his colleagues reported online Jan. 27 in JAMA Surgery.
The authors used multiple electronic databases to identify articles published between 1948 and June 30, 2015, on the use of biological mesh materials for reinforcement of the abdominal wall for hernia repair. Included were 14 articles that described outcomes with human acellular dermal matrix, 2 that reported results for porcine collagen intestinal submucosa derivatives, 3 that reported on porcine acelluar collagen skin derivatives, and 1 that described results for bovine pericardium.
Several problems were noted with respect to the studies, including widely varying follow-up time, operative technique, types of mesh used, and patient selection criteria. Also, outcome measures were not reported consistently across studies.
In addition, 16 of the 20 studies that met search criteria did not report investigator conflicts of interest, the authors reported (JAMA Surg. 2016 Jan 27. doi: 10.10001/jamasurg.2015.5234).
Notably, all the meshes used in the studies were approved by the Food and Drug Administration and were considered to be comparable to a group of nonbiological predicate devices, which cost up to 25% less than the biological equivalents, they noted.
“We were unable to find any evidence that supported the use of expensive biological material relative to low-cost synthetic mesh. In fact, with one exception, the biological materials became commercially available by showing that these materials were equivalent to low-cost established synthetic mesh material in an FDA 510(k) approval process. This process does not require phase 0 through IV clinical trials as required for drugs or biological agents,” they wrote, noting that the one material that bypassed the 510(k) process (Alloderm) was not required to demonstrate equivalence because it was classified as human transplanted tissue.
Biological mesh materials were introduced in the 1990s to minimize the risk of complications commonly seen with the use of synthetic mesh for abdominal wall hernia repair – one of the most common procedures performed by general surgeons, the authors explained.
“Because the outcomes for biological mesh material are perceived to be better than those for polymer-based prosthetic mesh replacement materials, the use of biological grafts increased exponentially without clear clinical evidence of efficacy,” they wrote.
The current review suggests that the evidence remains insufficient to determine whether cost and clinical benefits exist.
“It is generally assumed that FDA-approved drug or biological agents have been rigorously evaluated and that there is demonstrable safety and efficacy. This is not the case for 510(k) medical devices. Before using a new medical device, physicians should know the approval basis for the device and recognize that if it is a 510(k) device neither safety nor efficacy is ensured,” they said, adding that physicians should assume such devices are no better than predicate devices to which they are equivalent, and that “there can be no justification for purchasing a more expensive device when a lower-cost predicate device, which is equivalent, is available.”
Though limited by certain factors such as lack of access to detailed FDA information such as the specific criteria used to determine equivalence, and a lack of published literature on the full market penetration of biological mesh materials vs. nonbiological counterparts, the authors maintained that until evidence demonstrates superiority of biological materials, the expense associated with their use cannot be justified.
This study was supported by the Hudson-Penn Endowment fund at the University of Texas Southwestern Medical Center. The authors reported having no relevant financial disclosures.
The jury is still out on the costs and efficacy of biological mesh implants for abdominal wall hernia repair, according to a systematic review of the literature.
Of 20 articles that met search criteria, only 3 were comparative studies and none was a randomized clinical trial. In fact, most were case series involving convenience samples of patients at single institutions, Dr. Sergio Huerta of the University of Texas Southwestern Medical Center, Dallas, and his colleagues reported online Jan. 27 in JAMA Surgery.
The authors used multiple electronic databases to identify articles published between 1948 and June 30, 2015, on the use of biological mesh materials for reinforcement of the abdominal wall for hernia repair. Included were 14 articles that described outcomes with human acellular dermal matrix, 2 that reported results for porcine collagen intestinal submucosa derivatives, 3 that reported on porcine acelluar collagen skin derivatives, and 1 that described results for bovine pericardium.
Several problems were noted with respect to the studies, including widely varying follow-up time, operative technique, types of mesh used, and patient selection criteria. Also, outcome measures were not reported consistently across studies.
In addition, 16 of the 20 studies that met search criteria did not report investigator conflicts of interest, the authors reported (JAMA Surg. 2016 Jan 27. doi: 10.10001/jamasurg.2015.5234).
Notably, all the meshes used in the studies were approved by the Food and Drug Administration and were considered to be comparable to a group of nonbiological predicate devices, which cost up to 25% less than the biological equivalents, they noted.
“We were unable to find any evidence that supported the use of expensive biological material relative to low-cost synthetic mesh. In fact, with one exception, the biological materials became commercially available by showing that these materials were equivalent to low-cost established synthetic mesh material in an FDA 510(k) approval process. This process does not require phase 0 through IV clinical trials as required for drugs or biological agents,” they wrote, noting that the one material that bypassed the 510(k) process (Alloderm) was not required to demonstrate equivalence because it was classified as human transplanted tissue.
Biological mesh materials were introduced in the 1990s to minimize the risk of complications commonly seen with the use of synthetic mesh for abdominal wall hernia repair – one of the most common procedures performed by general surgeons, the authors explained.
“Because the outcomes for biological mesh material are perceived to be better than those for polymer-based prosthetic mesh replacement materials, the use of biological grafts increased exponentially without clear clinical evidence of efficacy,” they wrote.
The current review suggests that the evidence remains insufficient to determine whether cost and clinical benefits exist.
“It is generally assumed that FDA-approved drug or biological agents have been rigorously evaluated and that there is demonstrable safety and efficacy. This is not the case for 510(k) medical devices. Before using a new medical device, physicians should know the approval basis for the device and recognize that if it is a 510(k) device neither safety nor efficacy is ensured,” they said, adding that physicians should assume such devices are no better than predicate devices to which they are equivalent, and that “there can be no justification for purchasing a more expensive device when a lower-cost predicate device, which is equivalent, is available.”
Though limited by certain factors such as lack of access to detailed FDA information such as the specific criteria used to determine equivalence, and a lack of published literature on the full market penetration of biological mesh materials vs. nonbiological counterparts, the authors maintained that until evidence demonstrates superiority of biological materials, the expense associated with their use cannot be justified.
This study was supported by the Hudson-Penn Endowment fund at the University of Texas Southwestern Medical Center. The authors reported having no relevant financial disclosures.
FROM JAMA SURGERY
Key clinical point: The jury is still out on the costs and efficacy of biological mesh implants for abdominal wall hernia repair, and the expense associated with their use cannot be justified at this time, a systematic review of the literature suggested.
Major finding: Available evidence remains insufficient to determine whether cost and clinical benefits exist with the use of biological mesh for abdominal wall hernia repair.
Data source: A systematic review of the literature, yielding 20 eligible studies.
Disclosures: This study was supported by the Hudson-Penn Endowment fund at University of Texas Southwestern Medical Center. The authors reported having no relevant financial disclosures.
Level 1 activation reduces LOS, mortality in geriatric trauma
SAN ANTONIO – Automatically bumping elderly Level 2 trauma patients to Level 1 status reduced mortality and emergency department lengths of stay at Indiana University Health Methodist Hospital, Indianapolis.
Like trauma services elsewhere, the Methodist team is trying to figure out how best to handle the coming increase in elderly patients as the Baby Boom generation ages. It’s known that older trauma patients tend to be undertriaged. To improve the situation, “we need to respond quickly with a lot of resources up front so we don’t delay diagnosis” and treatment, said investigator Dr. Peter Hammer, assistant professor of surgery at Indiana University, Indianapolis.
The solution Methodist has tried since October 2013 is a Level 1 response to any patient aged 70 years or older who meets Level 2 criteria, regardless of vital sign stability or injury mechanism. With Level 1, trauma attendings, residents, respiratory therapists, clinical pharmacists, and others are at the bedside within 15 minutes and CT services and operating rooms are on standby, among other measures. Compared with the 1,271 patients aged 70 years or older treated in the almost 2 years before the change, the 998 treated in the year and a half afterwards were, after controlling for age, comorbidities, and injury severity scores (ISS), more likely to leave the ED in less than 2 hours (odds ratio, 1.614; 95% confidence interval, 1.088-2.394) and less likely to die (OR, 0.689, 95% CI, 0.484-0.979).
The before and after groups were similar, with a mean age of 81 years, a mean ISS of 12.2, a high comorbidity burden, and, for most, a blunt injury: 8.3% died in the before group, versus 7.6% in the after group. The shorter ED stays occurred despite a nursing staff reduction in 2014. Patients who went into cardiac arrest before arrival or died in the ED were excluded from the analysis.
“A simple, focused intervention of a higher level of trauma activation can decrease ED length of stay and in-hospital mortality in elderly trauma patients,” Dr. Hammer said at the annual scientific assembly of the Eastern Association for the Surgery of Trauma.
Among many initiatives as many trauma centers gear up for aging baby boomers, others are trying age as a criteria for higher activation, too, and recent guidelines from EAST recommend a lower threshold for trauma activation for patients 65 years or older, among other steps.
With more expertise and resources to brought to bear, it’s not surprising that Level 1 patients left the ED sooner, but it’s unclear what role that played in reducing mortality. “I wouldn’t hazard [to say] that shorter lengths of stay necessarily” saved lives, Dr. Hammer said.
Before the intervention, just 4.8% of geriatric patients left the ED within 2 hours, versus 6.5% afterwards. The numbers are low because, “as in most hospitals, there are more trauma patients than beds. [Reducing ED] length or stay [remains] an ongoing project” at Methodist, and not just for the elderly. “The ED is always overcrowded come afternoon and into the evening,” Dr. Hammer said.
That’s one of the reasons management supported the project. “They like the concept of getting patients moved through quickly. We have a lot of resources in the ED, so there doesn’t seem to be much of a slowdown” with increased Level 1 activation. It probably costs more up front, “but the hope is we’ll save money on the back end with lower mortality and shorter ED stays,” he said.
The investigators had no disclosures.
SAN ANTONIO – Automatically bumping elderly Level 2 trauma patients to Level 1 status reduced mortality and emergency department lengths of stay at Indiana University Health Methodist Hospital, Indianapolis.
Like trauma services elsewhere, the Methodist team is trying to figure out how best to handle the coming increase in elderly patients as the Baby Boom generation ages. It’s known that older trauma patients tend to be undertriaged. To improve the situation, “we need to respond quickly with a lot of resources up front so we don’t delay diagnosis” and treatment, said investigator Dr. Peter Hammer, assistant professor of surgery at Indiana University, Indianapolis.
The solution Methodist has tried since October 2013 is a Level 1 response to any patient aged 70 years or older who meets Level 2 criteria, regardless of vital sign stability or injury mechanism. With Level 1, trauma attendings, residents, respiratory therapists, clinical pharmacists, and others are at the bedside within 15 minutes and CT services and operating rooms are on standby, among other measures. Compared with the 1,271 patients aged 70 years or older treated in the almost 2 years before the change, the 998 treated in the year and a half afterwards were, after controlling for age, comorbidities, and injury severity scores (ISS), more likely to leave the ED in less than 2 hours (odds ratio, 1.614; 95% confidence interval, 1.088-2.394) and less likely to die (OR, 0.689, 95% CI, 0.484-0.979).
The before and after groups were similar, with a mean age of 81 years, a mean ISS of 12.2, a high comorbidity burden, and, for most, a blunt injury: 8.3% died in the before group, versus 7.6% in the after group. The shorter ED stays occurred despite a nursing staff reduction in 2014. Patients who went into cardiac arrest before arrival or died in the ED were excluded from the analysis.
“A simple, focused intervention of a higher level of trauma activation can decrease ED length of stay and in-hospital mortality in elderly trauma patients,” Dr. Hammer said at the annual scientific assembly of the Eastern Association for the Surgery of Trauma.
Among many initiatives as many trauma centers gear up for aging baby boomers, others are trying age as a criteria for higher activation, too, and recent guidelines from EAST recommend a lower threshold for trauma activation for patients 65 years or older, among other steps.
With more expertise and resources to brought to bear, it’s not surprising that Level 1 patients left the ED sooner, but it’s unclear what role that played in reducing mortality. “I wouldn’t hazard [to say] that shorter lengths of stay necessarily” saved lives, Dr. Hammer said.
Before the intervention, just 4.8% of geriatric patients left the ED within 2 hours, versus 6.5% afterwards. The numbers are low because, “as in most hospitals, there are more trauma patients than beds. [Reducing ED] length or stay [remains] an ongoing project” at Methodist, and not just for the elderly. “The ED is always overcrowded come afternoon and into the evening,” Dr. Hammer said.
That’s one of the reasons management supported the project. “They like the concept of getting patients moved through quickly. We have a lot of resources in the ED, so there doesn’t seem to be much of a slowdown” with increased Level 1 activation. It probably costs more up front, “but the hope is we’ll save money on the back end with lower mortality and shorter ED stays,” he said.
The investigators had no disclosures.
SAN ANTONIO – Automatically bumping elderly Level 2 trauma patients to Level 1 status reduced mortality and emergency department lengths of stay at Indiana University Health Methodist Hospital, Indianapolis.
Like trauma services elsewhere, the Methodist team is trying to figure out how best to handle the coming increase in elderly patients as the Baby Boom generation ages. It’s known that older trauma patients tend to be undertriaged. To improve the situation, “we need to respond quickly with a lot of resources up front so we don’t delay diagnosis” and treatment, said investigator Dr. Peter Hammer, assistant professor of surgery at Indiana University, Indianapolis.
The solution Methodist has tried since October 2013 is a Level 1 response to any patient aged 70 years or older who meets Level 2 criteria, regardless of vital sign stability or injury mechanism. With Level 1, trauma attendings, residents, respiratory therapists, clinical pharmacists, and others are at the bedside within 15 minutes and CT services and operating rooms are on standby, among other measures. Compared with the 1,271 patients aged 70 years or older treated in the almost 2 years before the change, the 998 treated in the year and a half afterwards were, after controlling for age, comorbidities, and injury severity scores (ISS), more likely to leave the ED in less than 2 hours (odds ratio, 1.614; 95% confidence interval, 1.088-2.394) and less likely to die (OR, 0.689, 95% CI, 0.484-0.979).
The before and after groups were similar, with a mean age of 81 years, a mean ISS of 12.2, a high comorbidity burden, and, for most, a blunt injury: 8.3% died in the before group, versus 7.6% in the after group. The shorter ED stays occurred despite a nursing staff reduction in 2014. Patients who went into cardiac arrest before arrival or died in the ED were excluded from the analysis.
“A simple, focused intervention of a higher level of trauma activation can decrease ED length of stay and in-hospital mortality in elderly trauma patients,” Dr. Hammer said at the annual scientific assembly of the Eastern Association for the Surgery of Trauma.
Among many initiatives as many trauma centers gear up for aging baby boomers, others are trying age as a criteria for higher activation, too, and recent guidelines from EAST recommend a lower threshold for trauma activation for patients 65 years or older, among other steps.
With more expertise and resources to brought to bear, it’s not surprising that Level 1 patients left the ED sooner, but it’s unclear what role that played in reducing mortality. “I wouldn’t hazard [to say] that shorter lengths of stay necessarily” saved lives, Dr. Hammer said.
Before the intervention, just 4.8% of geriatric patients left the ED within 2 hours, versus 6.5% afterwards. The numbers are low because, “as in most hospitals, there are more trauma patients than beds. [Reducing ED] length or stay [remains] an ongoing project” at Methodist, and not just for the elderly. “The ED is always overcrowded come afternoon and into the evening,” Dr. Hammer said.
That’s one of the reasons management supported the project. “They like the concept of getting patients moved through quickly. We have a lot of resources in the ED, so there doesn’t seem to be much of a slowdown” with increased Level 1 activation. It probably costs more up front, “but the hope is we’ll save money on the back end with lower mortality and shorter ED stays,” he said.
The investigators had no disclosures.
AT THE EAST SCIENTIFIC ASSEMBLY
Key clinical point: Consider treating Level 2 elderly trauma patients at Level 1 status.
Major finding: The 998 Level 2 elderly trauma patients treated as Level 1, after controlling for age, comorbidities, and injury severity scores, were more likely to leave the ED in less than 2 hours and were less likely to die, compared with patients treated in the previous 2 years.
Data source: More than 2,000 trauma patients aged 70 years or older.
Disclosures: The investigators had no disclosures.
Behavior problems in youth: Are things worse today than in the past?
Every generation of adults seems to worry that the next generation of youth is in trouble. The perception of kids today is no different, with theories abounding as to why the mental health of the newest generation is slipping, compared with previous standards. From mobile phones to helicopter parents, it might seem like a foregone conclusion that our current crop of young people is destined to be insecure, inattentive, and unable to cope with challenges and stress. Many news headlines on the latest mass shooting or standardized test results often seem to confirm these widespread concerns.
Pediatricians often hear parents lamenting the “good old days” when such things as corporal punishment were more easily accepted to help keep kids in line. But taking a step back, it may be worth a more objective look to examine the assumption that child behavioral problems are worse than ever. Measuring overall mental health is not an easy task, but looking at several important metrics indicate that things may not be nearly as bad as many people think.
Substance use
From the latest data from the Monitoring the Future Study, one of the nation’s most reliable sources on teen substance use, the use of both alcohol and tobacco among youth is at the lowest level since the study began in 1975. Use of drugs like heroin and ecstasy also are declining. The only major exception to this trend seems to be cannabis use, which has generally shown stable rates during this climate of marijuana decriminalization and, for some states, legalization.
Teen pregnancy rates
One area where there continues to be sustained progress is in teen pregnancy. According to the government’s Centers for Disease Control and Prevention, the overall pregnancy rate among adolescent females has been cut in half from 1991 to 2011, across many different ethnic groups. The rate fell from 61.8/1,000 teenagers aged 15-19 years to 31.3/1,000 teenagers.
Delinquency
Far fewer adolescents are being held against their will in juvenile detention centers. The number of youth who are incarcerated have dropped from a high of 381/100,000 in 1995 to 225/100,000 in 2010, according to a report by the Annie E. Casey Foundation.
Bullying
Bullying has been increasingly recognized as the public health problem that it is. The use of online technology also has created many new settings in which bullying can take place. Nevertheless, there is reason to be optimistic. From the National Center for Education Statistics and the National Crime Victimization Survey, the number of students who report being bullied at school has dropped from 32% in 2007 to an all-time low of 22% in 2013. Another recent study reached similar conclusions for bullying and many other forms of child victimization between 2003 and 2011 (JAMA Pediatr. 2014 Jun;168[6]:540-6).
Suicide
According to the CDC, the rate of completed suicide in youth peaked in the early1990s and then dropped and stabilized before starting to creep up again over the past 5 or so years. The trends are somewhat different, based on gender and the specific age group that is examined. The majority of completed youth suicides occur in males, with current rates still well below those historical highs.
Psychiatric disorders
This one is particularly tricky. While the rates of many specific psychiatric disorders such as ADHD and bipolar disorder have been rising in youth, as well as the use of psychiatric medications, it is much less clear whether this represents a true rise in these disorders versus other factors such as improved detection and a lower diagnostic threshold. One study by Achenbach et al. that measured quantitative levels of child behavior problems from the same rating scale over a 23-year time span found some increases in overall levels from the 1970s to the early 1990s, but then levels began to fall by the end of the millennium (J Abnorm Child Psychol. 2003 Feb;31[1]:1-11).
Of course, these hopeful trends in many significant areas do not mean that these problems have been overcome. While much work remains to be done on many fronts, it is still worth keeping in mind that the overall condition of youth mental health may not be as dire as we might be led to believe and that there is evidence that our efforts, perhaps, are leading to some progress.
Dr. Rettew is associate professor of psychiatry and pediatrics at the University of Vermont, Burlington. He said he has no relevant financial disclosures. Follow him on Twitter @pedipsych. E-mail him at [email protected].
Every generation of adults seems to worry that the next generation of youth is in trouble. The perception of kids today is no different, with theories abounding as to why the mental health of the newest generation is slipping, compared with previous standards. From mobile phones to helicopter parents, it might seem like a foregone conclusion that our current crop of young people is destined to be insecure, inattentive, and unable to cope with challenges and stress. Many news headlines on the latest mass shooting or standardized test results often seem to confirm these widespread concerns.
Pediatricians often hear parents lamenting the “good old days” when such things as corporal punishment were more easily accepted to help keep kids in line. But taking a step back, it may be worth a more objective look to examine the assumption that child behavioral problems are worse than ever. Measuring overall mental health is not an easy task, but looking at several important metrics indicate that things may not be nearly as bad as many people think.
Substance use
From the latest data from the Monitoring the Future Study, one of the nation’s most reliable sources on teen substance use, the use of both alcohol and tobacco among youth is at the lowest level since the study began in 1975. Use of drugs like heroin and ecstasy also are declining. The only major exception to this trend seems to be cannabis use, which has generally shown stable rates during this climate of marijuana decriminalization and, for some states, legalization.
Teen pregnancy rates
One area where there continues to be sustained progress is in teen pregnancy. According to the government’s Centers for Disease Control and Prevention, the overall pregnancy rate among adolescent females has been cut in half from 1991 to 2011, across many different ethnic groups. The rate fell from 61.8/1,000 teenagers aged 15-19 years to 31.3/1,000 teenagers.
Delinquency
Far fewer adolescents are being held against their will in juvenile detention centers. The number of youth who are incarcerated have dropped from a high of 381/100,000 in 1995 to 225/100,000 in 2010, according to a report by the Annie E. Casey Foundation.
Bullying
Bullying has been increasingly recognized as the public health problem that it is. The use of online technology also has created many new settings in which bullying can take place. Nevertheless, there is reason to be optimistic. From the National Center for Education Statistics and the National Crime Victimization Survey, the number of students who report being bullied at school has dropped from 32% in 2007 to an all-time low of 22% in 2013. Another recent study reached similar conclusions for bullying and many other forms of child victimization between 2003 and 2011 (JAMA Pediatr. 2014 Jun;168[6]:540-6).
Suicide
According to the CDC, the rate of completed suicide in youth peaked in the early1990s and then dropped and stabilized before starting to creep up again over the past 5 or so years. The trends are somewhat different, based on gender and the specific age group that is examined. The majority of completed youth suicides occur in males, with current rates still well below those historical highs.
Psychiatric disorders
This one is particularly tricky. While the rates of many specific psychiatric disorders such as ADHD and bipolar disorder have been rising in youth, as well as the use of psychiatric medications, it is much less clear whether this represents a true rise in these disorders versus other factors such as improved detection and a lower diagnostic threshold. One study by Achenbach et al. that measured quantitative levels of child behavior problems from the same rating scale over a 23-year time span found some increases in overall levels from the 1970s to the early 1990s, but then levels began to fall by the end of the millennium (J Abnorm Child Psychol. 2003 Feb;31[1]:1-11).
Of course, these hopeful trends in many significant areas do not mean that these problems have been overcome. While much work remains to be done on many fronts, it is still worth keeping in mind that the overall condition of youth mental health may not be as dire as we might be led to believe and that there is evidence that our efforts, perhaps, are leading to some progress.
Dr. Rettew is associate professor of psychiatry and pediatrics at the University of Vermont, Burlington. He said he has no relevant financial disclosures. Follow him on Twitter @pedipsych. E-mail him at [email protected].
Every generation of adults seems to worry that the next generation of youth is in trouble. The perception of kids today is no different, with theories abounding as to why the mental health of the newest generation is slipping, compared with previous standards. From mobile phones to helicopter parents, it might seem like a foregone conclusion that our current crop of young people is destined to be insecure, inattentive, and unable to cope with challenges and stress. Many news headlines on the latest mass shooting or standardized test results often seem to confirm these widespread concerns.
Pediatricians often hear parents lamenting the “good old days” when such things as corporal punishment were more easily accepted to help keep kids in line. But taking a step back, it may be worth a more objective look to examine the assumption that child behavioral problems are worse than ever. Measuring overall mental health is not an easy task, but looking at several important metrics indicate that things may not be nearly as bad as many people think.
Substance use
From the latest data from the Monitoring the Future Study, one of the nation’s most reliable sources on teen substance use, the use of both alcohol and tobacco among youth is at the lowest level since the study began in 1975. Use of drugs like heroin and ecstasy also are declining. The only major exception to this trend seems to be cannabis use, which has generally shown stable rates during this climate of marijuana decriminalization and, for some states, legalization.
Teen pregnancy rates
One area where there continues to be sustained progress is in teen pregnancy. According to the government’s Centers for Disease Control and Prevention, the overall pregnancy rate among adolescent females has been cut in half from 1991 to 2011, across many different ethnic groups. The rate fell from 61.8/1,000 teenagers aged 15-19 years to 31.3/1,000 teenagers.
Delinquency
Far fewer adolescents are being held against their will in juvenile detention centers. The number of youth who are incarcerated have dropped from a high of 381/100,000 in 1995 to 225/100,000 in 2010, according to a report by the Annie E. Casey Foundation.
Bullying
Bullying has been increasingly recognized as the public health problem that it is. The use of online technology also has created many new settings in which bullying can take place. Nevertheless, there is reason to be optimistic. From the National Center for Education Statistics and the National Crime Victimization Survey, the number of students who report being bullied at school has dropped from 32% in 2007 to an all-time low of 22% in 2013. Another recent study reached similar conclusions for bullying and many other forms of child victimization between 2003 and 2011 (JAMA Pediatr. 2014 Jun;168[6]:540-6).
Suicide
According to the CDC, the rate of completed suicide in youth peaked in the early1990s and then dropped and stabilized before starting to creep up again over the past 5 or so years. The trends are somewhat different, based on gender and the specific age group that is examined. The majority of completed youth suicides occur in males, with current rates still well below those historical highs.
Psychiatric disorders
This one is particularly tricky. While the rates of many specific psychiatric disorders such as ADHD and bipolar disorder have been rising in youth, as well as the use of psychiatric medications, it is much less clear whether this represents a true rise in these disorders versus other factors such as improved detection and a lower diagnostic threshold. One study by Achenbach et al. that measured quantitative levels of child behavior problems from the same rating scale over a 23-year time span found some increases in overall levels from the 1970s to the early 1990s, but then levels began to fall by the end of the millennium (J Abnorm Child Psychol. 2003 Feb;31[1]:1-11).
Of course, these hopeful trends in many significant areas do not mean that these problems have been overcome. While much work remains to be done on many fronts, it is still worth keeping in mind that the overall condition of youth mental health may not be as dire as we might be led to believe and that there is evidence that our efforts, perhaps, are leading to some progress.
Dr. Rettew is associate professor of psychiatry and pediatrics at the University of Vermont, Burlington. He said he has no relevant financial disclosures. Follow him on Twitter @pedipsych. E-mail him at [email protected].
Study reveals how Tregs protect themselves
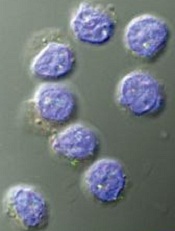
Image by Kathryn Iacono
Researchers say they have discovered how regulatory T cells (Tregs) remain intact and functional during activation.
The team found that once Tregs are activated, they are protected by autophagy, which maintains metabolic balance.
Hongbo Chi, PhD, of St. Jude Children’s Hospital in Memphis, Tennessee, and his colleagues described this discovery in Nature Immunology.
Until this study, no one knew how Tregs maintained themselves when activated.
“Regulatory T cells are very specialized cells that require activation to perform their function in curtailing undesirable immune responses,” Dr Chi explained. “But this activation is a double-edged sword, in that this very activation can destabilize them. They need to modulate this activation, or they will lose their stability and many of them will die. That could damage immune function.”
Dr Chi and his colleagues performed imaging studies in activated Tregs and found that autophagy was functional in the cells.
In experiments with mice, the researchers deleted Atg7 or Atg5, genes whose functions are necessary for autophagy in Tregs.
The mice showed key characteristics of Treg malfunction, including inflammatory and autoimmune disorders. The mice also more readily cleared tumors from their bodies, due to activated immune systems.
Dr Chi said that eliminating autophagy also affected the fate of Tregs.
“Once those T cells lack autophagy activity, they tend to undergo excessive cell death,” he said. “But even for the remaining surviving cells, they tend to be overly activated and lose their identity because they start to behave like non-regulatory T cells. That is why loss of autophagy in regulatory T cells produces a 2-fold effect on both survival and stability.”
Detailed analysis also revealed how the elimination of autophagy affected the basic energy-producing metabolic pathways of Tregs, compromising their function.
Dr Chi said this new understanding of autophagy’s role in Tregs could enable a 2-fold approach to immune therapy for cancers. Namely, by strengthening tumor-associated immune responses, targeting Treg autophagy could act in synergy with strategies that block autophagy in tumor cells.
In this study, the researchers used a transplanted colon cancer cell line. In further studies, they plan to explore the role of autophagy in immune reactions toward other tumor cell types to determine whether such therapies might be effective in a broad range of cancers.
The team also hopes to gain a better understanding of the detailed biochemical mechanisms regulating how autophagy connects to the cell’s metabolic pathways. ![]()

Image by Kathryn Iacono
Researchers say they have discovered how regulatory T cells (Tregs) remain intact and functional during activation.
The team found that once Tregs are activated, they are protected by autophagy, which maintains metabolic balance.
Hongbo Chi, PhD, of St. Jude Children’s Hospital in Memphis, Tennessee, and his colleagues described this discovery in Nature Immunology.
Until this study, no one knew how Tregs maintained themselves when activated.
“Regulatory T cells are very specialized cells that require activation to perform their function in curtailing undesirable immune responses,” Dr Chi explained. “But this activation is a double-edged sword, in that this very activation can destabilize them. They need to modulate this activation, or they will lose their stability and many of them will die. That could damage immune function.”
Dr Chi and his colleagues performed imaging studies in activated Tregs and found that autophagy was functional in the cells.
In experiments with mice, the researchers deleted Atg7 or Atg5, genes whose functions are necessary for autophagy in Tregs.
The mice showed key characteristics of Treg malfunction, including inflammatory and autoimmune disorders. The mice also more readily cleared tumors from their bodies, due to activated immune systems.
Dr Chi said that eliminating autophagy also affected the fate of Tregs.
“Once those T cells lack autophagy activity, they tend to undergo excessive cell death,” he said. “But even for the remaining surviving cells, they tend to be overly activated and lose their identity because they start to behave like non-regulatory T cells. That is why loss of autophagy in regulatory T cells produces a 2-fold effect on both survival and stability.”
Detailed analysis also revealed how the elimination of autophagy affected the basic energy-producing metabolic pathways of Tregs, compromising their function.
Dr Chi said this new understanding of autophagy’s role in Tregs could enable a 2-fold approach to immune therapy for cancers. Namely, by strengthening tumor-associated immune responses, targeting Treg autophagy could act in synergy with strategies that block autophagy in tumor cells.
In this study, the researchers used a transplanted colon cancer cell line. In further studies, they plan to explore the role of autophagy in immune reactions toward other tumor cell types to determine whether such therapies might be effective in a broad range of cancers.
The team also hopes to gain a better understanding of the detailed biochemical mechanisms regulating how autophagy connects to the cell’s metabolic pathways. ![]()

Image by Kathryn Iacono
Researchers say they have discovered how regulatory T cells (Tregs) remain intact and functional during activation.
The team found that once Tregs are activated, they are protected by autophagy, which maintains metabolic balance.
Hongbo Chi, PhD, of St. Jude Children’s Hospital in Memphis, Tennessee, and his colleagues described this discovery in Nature Immunology.
Until this study, no one knew how Tregs maintained themselves when activated.
“Regulatory T cells are very specialized cells that require activation to perform their function in curtailing undesirable immune responses,” Dr Chi explained. “But this activation is a double-edged sword, in that this very activation can destabilize them. They need to modulate this activation, or they will lose their stability and many of them will die. That could damage immune function.”
Dr Chi and his colleagues performed imaging studies in activated Tregs and found that autophagy was functional in the cells.
In experiments with mice, the researchers deleted Atg7 or Atg5, genes whose functions are necessary for autophagy in Tregs.
The mice showed key characteristics of Treg malfunction, including inflammatory and autoimmune disorders. The mice also more readily cleared tumors from their bodies, due to activated immune systems.
Dr Chi said that eliminating autophagy also affected the fate of Tregs.
“Once those T cells lack autophagy activity, they tend to undergo excessive cell death,” he said. “But even for the remaining surviving cells, they tend to be overly activated and lose their identity because they start to behave like non-regulatory T cells. That is why loss of autophagy in regulatory T cells produces a 2-fold effect on both survival and stability.”
Detailed analysis also revealed how the elimination of autophagy affected the basic energy-producing metabolic pathways of Tregs, compromising their function.
Dr Chi said this new understanding of autophagy’s role in Tregs could enable a 2-fold approach to immune therapy for cancers. Namely, by strengthening tumor-associated immune responses, targeting Treg autophagy could act in synergy with strategies that block autophagy in tumor cells.
In this study, the researchers used a transplanted colon cancer cell line. In further studies, they plan to explore the role of autophagy in immune reactions toward other tumor cell types to determine whether such therapies might be effective in a broad range of cancers.
The team also hopes to gain a better understanding of the detailed biochemical mechanisms regulating how autophagy connects to the cell’s metabolic pathways. ![]()
What Are Best Practices for Patients Discharged against Medical Advice?
Case No. 1
A 41-year-old woman with a history of asthma presents to the emergency department (ED) with shortness of breath and wheezing. She is diagnosed with a mild asthma exacerbation. After three albuterol nebulizer treatments, she still has wheezing on physical examination but appears comfortable and has no oxygen requirement. She has a primary medical doctor at the hospital and follows up with her regularly.
The hospitalist recommends that she stay in the hospital for further treatment, but the patient says she has a nebulizer machine at home and asks to be discharged. In addition, she is worried about her frail elderly mother, for whom she is the primary caretaker. The hospitalist acknowledges her concerns but continues to recommend that she remain in the hospital for additional care and monitoring. She becomes visibly upset and insists that she must return home. She asks for prescriptions for albuterol and prednisone and is discharged against medical advice (AMA).
Case No. 2
A 52-year-old man with a history of hypertension and diabetes presents to the ED with left foot pain. He frequently presents with this complaint but often leaves AMA before treatment is completed. He has no known physical address or telephone number and has no known outpatient healthcare providers. Physical examination reveals several ulcers on the dorsum of the foot, one with purulent drainage, and generalized lower extremity pallor. His left leg is cool to the touch, and vascular surgery is consulted for suspected limb-threatening ischemia; IV antibiotics are started for suspected osteomyelitis.
During the interview, he states that he wishes to leave the hospital because he has “things to take care of.” The hospitalist recommends that he remain in the hospital for limb-preserving surgery and antibiotics. He then explains that he is homeless and needs to return to his shelter to keep his bed. He is able to articulate the risks of premature discharge and the medical concerns, and it is determined that he has the capacity to participate in discharge planning. The hospitalist therefore discharges him AMA.
Background
AMA discharges represent 1%–2% of all inpatient discharges.¹,² Despite being a small percentage of total discharges, these patients have disproportionately high healthcare costs. One study reported that healthcare costs among these patients were 56% higher than expected.² Furthermore, AMA patients suffer higher than expected rates of morbidity, mortality, and hospital readmission.
For example, in one case-control study in an urban teaching hospital, patients discharged AMA from the general medicine service had a 21% 15-day readmission rate compared to a 3% readmission rate among age, gender, and diagnosis-matched controls.3,4,5
Additionally, history of AMA discharge appears to confer risk of increased future utilization of healthcare resources. In a cohort study of hospital admissions among HIV-infected patients with high rates of intravenous drug abuse, patients discharged AMA (13% of the cohort) were not only more likely to be readmitted within 30 days for a related diagnosis (odds ratio = 5.0) but also were more likely to have increased length of stay during the year following the index admission.6
These studies highlight the barriers to safe and effective transitions of care for this vulnerable population and demonstrate the increased burden that this population places on the health system.
Several retrospective studies have identified psychosocial and demographic risk factors associated with AMA discharge. These include younger age, male sex, substance abuse, lack of a primary care physician or health insurance, and history of previous AMA discharge.1,3,7,8 Insurance status is also associated with AMA discharge, with increased odds of AMA discharge among Medicare and Medicaid patients and patients without health insurance.9,10
Of note, one study found that race did not act as an independent predictor of AMA discharge when adjusted for age, gender, and socioeconomic factors.11
The AMA population is clinically heterogeneous. Among patients with pneumonia, for example, Saitz et al showed that a patient’s documented clinical severity did not independently predict AMA discharge, suggesting that there is great clinical heterogeneity even among AMA patients with similar admission diagnoses.12
These studies highlight the clinical and demographic heterogeneity within this population, suggesting that patients discharged AMA require individualized attention from hospitalists and other healthcare providers.
Patients describe numerous motivations for leaving the hospital prematurely, including needing to pick up public-assistance checks, personal financial issues, and familial obligations.13 Interestingly, in the cohort of HIV patients referenced above, discharge on the day welfare checks were distributed was an independent predictor of AMA discharge.6 In focus groups composed of patients discharged AMA and their treating nurses and physicians, several themes were identified as potential contributors to AMA discharge, including drug addiction, pain management issues, external obligations, wait time, the physician’s bedside manner, being in a teaching hospital, and communication issues.14
Clearly, patients have a diversity of reasons for requesting to be discharged AMA, and further research is necessary to define clear and potentially modifiable risk factors.
Discussion
The clinical scenarios outlined above present two patients with very different clinical presentations and outpatient support systems as well as demonstrate the great variability in clinical risk at the time of discharge AMA. These examples emphasize the importance of an individualized approach to care for each patient.
In Case No. 1, the patient is admitted with a mild asthma exacerbation with persistent bronchospasm, though she clinically appears well and has reliable follow-up. In contrast, in Case No. 2, the patient has life-threatening disease and no established primary care physician or mechanism for outpatient care. These examples demonstrate extremes on the clinical and psychosocial spectrum of patients requesting an “early” discharge and suggest that no two patients at risk of AMA discharge are the same. Patient 1 could likely be safely managed at home with close outpatient follow-up, while Patient 2 presents a high-risk scenario with very few safe outpatient treatment options.
We suggest that an individualized approach be taken for each patient, with attention to both clinical and psychosocial risk. In clinically low-risk cases (e.g., Case No. 1), an approach that prioritizes shared decision making and coordination with the outpatient care team may be preferable to an AMA discharge, particularly given the often adversarial nature of the later.2 In such cases, a collaborative approach may provide greater opportunity for harm reduction, provision of appropriate prescriptions, and follow-up appointments. In clinically high-risk patients such as Case No. 2, however, premature discharge is clearly inappropriate. Even in such clinically high-risk cases, however, we argue that a collaborative strategy aimed at identifying and addressing the patient’s psychosocial concerns is appropriate, as such an approach promotes shared decision making, builds trust between the patient and the care team, and therefore may facilitate improved follow-up at the time of discharge. Research is needed to formally assess the optimal approach for this patient population, including impact on rates of AMA discharge and the quality of post-discharge follow-up.
At present, the decision to classify a discharge as AMA falls solely on the treating provider, and we suspect that there is great variability in practice patterns, particularly as there are few established professional society practice guidelines regarding this difficult issue. As with all discharges from the hospital, the burden falls on the provider to engage the patient in shared decision making and ensure that the patient has the capacity to understand the risks and benefits of the proposed treatment plan. It is in this spirit that simply “filling out an AMA form” does not provide legal protection to a physician who does not adequately explain the full risks and benefits of refusal of inpatient treatment.2,15
We propose that a high-quality AMA discharge be defined as a discharge in which the patient is informed of the clinical team’s determination that further hospitalization is required but elects to leave the hospital, and it includes a clear discussion of the risks of outpatient treatment, a determination of capacity, and an exploration of safe alternative care plans that could satisfy both the patient’s medical and social needs. This definition places the burden on hospitalists and other providers to fully explore the motivations behind a patient’s request to leave the hospital and treats psychosocial motivators for premature discharge as variables in the complex risk-benefit analysis that underlies the informed consent discussion prior to AMA discharge.
Furthermore, AMA discharge does not obviate a physician’s responsibility to advocate for a patient’s well-being, and therefore an AMA discharge should be accompanied by reasonable efforts to coordinate a patient’s ongoing outpatient care. Of note, this approach is consistent with previous reviews and attempts to balance the physician’s duty to honor a patient’s autonomy with the responsibility to protect the patient from harm.2,16
Conclusion
Patients discharged AMA are a diverse population at markedly increased risk of morbidity, readmissions, and subsequent healthcare cost. We argue that in all cases of a potential premature discharge, a collaborative and patient-centered approach is crucial. Such an approach allows the provider to identify and address the patient’s concerns regarding further inpatient care, to explore possible safe outpatient treatment options, to document patient capacity, and to provide appropriate harm-reduction measures such as prescriptions.
Further research into the current practice patterns of hospitalists and other providers is necessary to allow for the formulation and adoption of best practices and implementation of appropriate harm-reduction strategies. TH
Dr. Tummalapalli is an internal medicine resident in the department of medicine at Icahn School of Medicine at Mount Sinai in New York City. Dr. Goodman is a hospitalist in the division of hospital medicine, department of medicine, at the Icahn School of Medicine at Mount Sinai.
References
- Aliyu ZY. Discharge against medical advice: sociodemographic, clinical and financial perspectives. Int J Clin Pract. 2002;56(5):325-327.
- Kahle CH, Rubio ML, Santos RA. Discharges against medical advice: considerations for the hospitalist and the patient. Hospital Medicine Clinics. 2015;4(3):421-429.
- Baptist AP, Warrier I, Arora R, Ager J, Massanari RM. Hospitalized patients with asthma who leave against medical advice: characteristics, reasons, and outcomes. J Allergy Clin Immunol. 2007;119(4):924-929.
- Hwang SW, Li J, Gupta R, Chien V, Martin RE. What happens to patients who leave hospital against medical advice? CMAJ. 2003;168(4):417-420.
- Glasgow JM, Vaughn-Sarrazin MV, Kaboli PJ. Leaving against medical advice (AMA): risk of 30-day mortality and hospital readmission. J Gen Int Med. 2010;25(9):926-929.
- Anis AH, Sun H, Guh DP, Palepu A, Schechter MT, O’Shaughnessy MV. Leaving hospital against medical advice among HIV-positive patients. CMAJ. 2002;167(6):633-637.
- Jeremiah J, O’Sullivan P, Stein MD. Who leaves against medical advice? J Gen Int Med. 1995; 10(7);403-405.
- O’Hara D, Hart W, McDonald I. Leaving hospital against medical advice. J Qual Clin Pract.1996;16(3):157-164.
- Ibrahim SA, Kwoh CK, Krishnan E. Factors associated with patients who leave acute-care hospitals against medical advice. Am J Public Health. 2007;97(12): 2204-2208.
- Weingart SN, Davis RB, Phillips RS. Patients discharged against medical advice from a general medicine service. J Gen Intern Med. 1998;13(8):568-571.
- Franks P, Meldrum S, Fiscella K. Discharges against medical advice: are race/ethnicity predictors? J Gen Intern Med. 2006;21(9):955-960.
- Saitz R, Ghali WA, Moskowitz MA. Characteristics of patients with pneumonia who are discharged from hospitals against medical advice. Am J Med. 1999;107(5):507-509.
- Alfandre, DJ. “I’m going home”: discharges against medical advice. Mayo Clin Proc. 2009;84(3):255-260.
- Onukwugha E, Saunders E, Mullins CD, Pradel FG, Zuckerman M, Weir MR. Reasons for discharges against medical advice: a qualitative study. Qual Saf Health Care. 2010;19(5):420-424. doi: 10.1136/qshc.2009.036269.
- Battenfeld v. Gregory, 589 A.2d 1059, 1061 (N.J. Super. Ct. App. Div. 1991).
- Berger J. Discharge against medical advice: ethical considerations and professional obligations. J Hosp Med. 2008;3(5):403-408.
Case No. 1
A 41-year-old woman with a history of asthma presents to the emergency department (ED) with shortness of breath and wheezing. She is diagnosed with a mild asthma exacerbation. After three albuterol nebulizer treatments, she still has wheezing on physical examination but appears comfortable and has no oxygen requirement. She has a primary medical doctor at the hospital and follows up with her regularly.
The hospitalist recommends that she stay in the hospital for further treatment, but the patient says she has a nebulizer machine at home and asks to be discharged. In addition, she is worried about her frail elderly mother, for whom she is the primary caretaker. The hospitalist acknowledges her concerns but continues to recommend that she remain in the hospital for additional care and monitoring. She becomes visibly upset and insists that she must return home. She asks for prescriptions for albuterol and prednisone and is discharged against medical advice (AMA).
Case No. 2
A 52-year-old man with a history of hypertension and diabetes presents to the ED with left foot pain. He frequently presents with this complaint but often leaves AMA before treatment is completed. He has no known physical address or telephone number and has no known outpatient healthcare providers. Physical examination reveals several ulcers on the dorsum of the foot, one with purulent drainage, and generalized lower extremity pallor. His left leg is cool to the touch, and vascular surgery is consulted for suspected limb-threatening ischemia; IV antibiotics are started for suspected osteomyelitis.
During the interview, he states that he wishes to leave the hospital because he has “things to take care of.” The hospitalist recommends that he remain in the hospital for limb-preserving surgery and antibiotics. He then explains that he is homeless and needs to return to his shelter to keep his bed. He is able to articulate the risks of premature discharge and the medical concerns, and it is determined that he has the capacity to participate in discharge planning. The hospitalist therefore discharges him AMA.
Background
AMA discharges represent 1%–2% of all inpatient discharges.¹,² Despite being a small percentage of total discharges, these patients have disproportionately high healthcare costs. One study reported that healthcare costs among these patients were 56% higher than expected.² Furthermore, AMA patients suffer higher than expected rates of morbidity, mortality, and hospital readmission.
For example, in one case-control study in an urban teaching hospital, patients discharged AMA from the general medicine service had a 21% 15-day readmission rate compared to a 3% readmission rate among age, gender, and diagnosis-matched controls.3,4,5
Additionally, history of AMA discharge appears to confer risk of increased future utilization of healthcare resources. In a cohort study of hospital admissions among HIV-infected patients with high rates of intravenous drug abuse, patients discharged AMA (13% of the cohort) were not only more likely to be readmitted within 30 days for a related diagnosis (odds ratio = 5.0) but also were more likely to have increased length of stay during the year following the index admission.6
These studies highlight the barriers to safe and effective transitions of care for this vulnerable population and demonstrate the increased burden that this population places on the health system.
Several retrospective studies have identified psychosocial and demographic risk factors associated with AMA discharge. These include younger age, male sex, substance abuse, lack of a primary care physician or health insurance, and history of previous AMA discharge.1,3,7,8 Insurance status is also associated with AMA discharge, with increased odds of AMA discharge among Medicare and Medicaid patients and patients without health insurance.9,10
Of note, one study found that race did not act as an independent predictor of AMA discharge when adjusted for age, gender, and socioeconomic factors.11
The AMA population is clinically heterogeneous. Among patients with pneumonia, for example, Saitz et al showed that a patient’s documented clinical severity did not independently predict AMA discharge, suggesting that there is great clinical heterogeneity even among AMA patients with similar admission diagnoses.12
These studies highlight the clinical and demographic heterogeneity within this population, suggesting that patients discharged AMA require individualized attention from hospitalists and other healthcare providers.
Patients describe numerous motivations for leaving the hospital prematurely, including needing to pick up public-assistance checks, personal financial issues, and familial obligations.13 Interestingly, in the cohort of HIV patients referenced above, discharge on the day welfare checks were distributed was an independent predictor of AMA discharge.6 In focus groups composed of patients discharged AMA and their treating nurses and physicians, several themes were identified as potential contributors to AMA discharge, including drug addiction, pain management issues, external obligations, wait time, the physician’s bedside manner, being in a teaching hospital, and communication issues.14
Clearly, patients have a diversity of reasons for requesting to be discharged AMA, and further research is necessary to define clear and potentially modifiable risk factors.
Discussion
The clinical scenarios outlined above present two patients with very different clinical presentations and outpatient support systems as well as demonstrate the great variability in clinical risk at the time of discharge AMA. These examples emphasize the importance of an individualized approach to care for each patient.
In Case No. 1, the patient is admitted with a mild asthma exacerbation with persistent bronchospasm, though she clinically appears well and has reliable follow-up. In contrast, in Case No. 2, the patient has life-threatening disease and no established primary care physician or mechanism for outpatient care. These examples demonstrate extremes on the clinical and psychosocial spectrum of patients requesting an “early” discharge and suggest that no two patients at risk of AMA discharge are the same. Patient 1 could likely be safely managed at home with close outpatient follow-up, while Patient 2 presents a high-risk scenario with very few safe outpatient treatment options.
We suggest that an individualized approach be taken for each patient, with attention to both clinical and psychosocial risk. In clinically low-risk cases (e.g., Case No. 1), an approach that prioritizes shared decision making and coordination with the outpatient care team may be preferable to an AMA discharge, particularly given the often adversarial nature of the later.2 In such cases, a collaborative approach may provide greater opportunity for harm reduction, provision of appropriate prescriptions, and follow-up appointments. In clinically high-risk patients such as Case No. 2, however, premature discharge is clearly inappropriate. Even in such clinically high-risk cases, however, we argue that a collaborative strategy aimed at identifying and addressing the patient’s psychosocial concerns is appropriate, as such an approach promotes shared decision making, builds trust between the patient and the care team, and therefore may facilitate improved follow-up at the time of discharge. Research is needed to formally assess the optimal approach for this patient population, including impact on rates of AMA discharge and the quality of post-discharge follow-up.
At present, the decision to classify a discharge as AMA falls solely on the treating provider, and we suspect that there is great variability in practice patterns, particularly as there are few established professional society practice guidelines regarding this difficult issue. As with all discharges from the hospital, the burden falls on the provider to engage the patient in shared decision making and ensure that the patient has the capacity to understand the risks and benefits of the proposed treatment plan. It is in this spirit that simply “filling out an AMA form” does not provide legal protection to a physician who does not adequately explain the full risks and benefits of refusal of inpatient treatment.2,15
We propose that a high-quality AMA discharge be defined as a discharge in which the patient is informed of the clinical team’s determination that further hospitalization is required but elects to leave the hospital, and it includes a clear discussion of the risks of outpatient treatment, a determination of capacity, and an exploration of safe alternative care plans that could satisfy both the patient’s medical and social needs. This definition places the burden on hospitalists and other providers to fully explore the motivations behind a patient’s request to leave the hospital and treats psychosocial motivators for premature discharge as variables in the complex risk-benefit analysis that underlies the informed consent discussion prior to AMA discharge.
Furthermore, AMA discharge does not obviate a physician’s responsibility to advocate for a patient’s well-being, and therefore an AMA discharge should be accompanied by reasonable efforts to coordinate a patient’s ongoing outpatient care. Of note, this approach is consistent with previous reviews and attempts to balance the physician’s duty to honor a patient’s autonomy with the responsibility to protect the patient from harm.2,16
Conclusion
Patients discharged AMA are a diverse population at markedly increased risk of morbidity, readmissions, and subsequent healthcare cost. We argue that in all cases of a potential premature discharge, a collaborative and patient-centered approach is crucial. Such an approach allows the provider to identify and address the patient’s concerns regarding further inpatient care, to explore possible safe outpatient treatment options, to document patient capacity, and to provide appropriate harm-reduction measures such as prescriptions.
Further research into the current practice patterns of hospitalists and other providers is necessary to allow for the formulation and adoption of best practices and implementation of appropriate harm-reduction strategies. TH
Dr. Tummalapalli is an internal medicine resident in the department of medicine at Icahn School of Medicine at Mount Sinai in New York City. Dr. Goodman is a hospitalist in the division of hospital medicine, department of medicine, at the Icahn School of Medicine at Mount Sinai.
References
- Aliyu ZY. Discharge against medical advice: sociodemographic, clinical and financial perspectives. Int J Clin Pract. 2002;56(5):325-327.
- Kahle CH, Rubio ML, Santos RA. Discharges against medical advice: considerations for the hospitalist and the patient. Hospital Medicine Clinics. 2015;4(3):421-429.
- Baptist AP, Warrier I, Arora R, Ager J, Massanari RM. Hospitalized patients with asthma who leave against medical advice: characteristics, reasons, and outcomes. J Allergy Clin Immunol. 2007;119(4):924-929.
- Hwang SW, Li J, Gupta R, Chien V, Martin RE. What happens to patients who leave hospital against medical advice? CMAJ. 2003;168(4):417-420.
- Glasgow JM, Vaughn-Sarrazin MV, Kaboli PJ. Leaving against medical advice (AMA): risk of 30-day mortality and hospital readmission. J Gen Int Med. 2010;25(9):926-929.
- Anis AH, Sun H, Guh DP, Palepu A, Schechter MT, O’Shaughnessy MV. Leaving hospital against medical advice among HIV-positive patients. CMAJ. 2002;167(6):633-637.
- Jeremiah J, O’Sullivan P, Stein MD. Who leaves against medical advice? J Gen Int Med. 1995; 10(7);403-405.
- O’Hara D, Hart W, McDonald I. Leaving hospital against medical advice. J Qual Clin Pract.1996;16(3):157-164.
- Ibrahim SA, Kwoh CK, Krishnan E. Factors associated with patients who leave acute-care hospitals against medical advice. Am J Public Health. 2007;97(12): 2204-2208.
- Weingart SN, Davis RB, Phillips RS. Patients discharged against medical advice from a general medicine service. J Gen Intern Med. 1998;13(8):568-571.
- Franks P, Meldrum S, Fiscella K. Discharges against medical advice: are race/ethnicity predictors? J Gen Intern Med. 2006;21(9):955-960.
- Saitz R, Ghali WA, Moskowitz MA. Characteristics of patients with pneumonia who are discharged from hospitals against medical advice. Am J Med. 1999;107(5):507-509.
- Alfandre, DJ. “I’m going home”: discharges against medical advice. Mayo Clin Proc. 2009;84(3):255-260.
- Onukwugha E, Saunders E, Mullins CD, Pradel FG, Zuckerman M, Weir MR. Reasons for discharges against medical advice: a qualitative study. Qual Saf Health Care. 2010;19(5):420-424. doi: 10.1136/qshc.2009.036269.
- Battenfeld v. Gregory, 589 A.2d 1059, 1061 (N.J. Super. Ct. App. Div. 1991).
- Berger J. Discharge against medical advice: ethical considerations and professional obligations. J Hosp Med. 2008;3(5):403-408.
Case No. 1
A 41-year-old woman with a history of asthma presents to the emergency department (ED) with shortness of breath and wheezing. She is diagnosed with a mild asthma exacerbation. After three albuterol nebulizer treatments, she still has wheezing on physical examination but appears comfortable and has no oxygen requirement. She has a primary medical doctor at the hospital and follows up with her regularly.
The hospitalist recommends that she stay in the hospital for further treatment, but the patient says she has a nebulizer machine at home and asks to be discharged. In addition, she is worried about her frail elderly mother, for whom she is the primary caretaker. The hospitalist acknowledges her concerns but continues to recommend that she remain in the hospital for additional care and monitoring. She becomes visibly upset and insists that she must return home. She asks for prescriptions for albuterol and prednisone and is discharged against medical advice (AMA).
Case No. 2
A 52-year-old man with a history of hypertension and diabetes presents to the ED with left foot pain. He frequently presents with this complaint but often leaves AMA before treatment is completed. He has no known physical address or telephone number and has no known outpatient healthcare providers. Physical examination reveals several ulcers on the dorsum of the foot, one with purulent drainage, and generalized lower extremity pallor. His left leg is cool to the touch, and vascular surgery is consulted for suspected limb-threatening ischemia; IV antibiotics are started for suspected osteomyelitis.
During the interview, he states that he wishes to leave the hospital because he has “things to take care of.” The hospitalist recommends that he remain in the hospital for limb-preserving surgery and antibiotics. He then explains that he is homeless and needs to return to his shelter to keep his bed. He is able to articulate the risks of premature discharge and the medical concerns, and it is determined that he has the capacity to participate in discharge planning. The hospitalist therefore discharges him AMA.
Background
AMA discharges represent 1%–2% of all inpatient discharges.¹,² Despite being a small percentage of total discharges, these patients have disproportionately high healthcare costs. One study reported that healthcare costs among these patients were 56% higher than expected.² Furthermore, AMA patients suffer higher than expected rates of morbidity, mortality, and hospital readmission.
For example, in one case-control study in an urban teaching hospital, patients discharged AMA from the general medicine service had a 21% 15-day readmission rate compared to a 3% readmission rate among age, gender, and diagnosis-matched controls.3,4,5
Additionally, history of AMA discharge appears to confer risk of increased future utilization of healthcare resources. In a cohort study of hospital admissions among HIV-infected patients with high rates of intravenous drug abuse, patients discharged AMA (13% of the cohort) were not only more likely to be readmitted within 30 days for a related diagnosis (odds ratio = 5.0) but also were more likely to have increased length of stay during the year following the index admission.6
These studies highlight the barriers to safe and effective transitions of care for this vulnerable population and demonstrate the increased burden that this population places on the health system.
Several retrospective studies have identified psychosocial and demographic risk factors associated with AMA discharge. These include younger age, male sex, substance abuse, lack of a primary care physician or health insurance, and history of previous AMA discharge.1,3,7,8 Insurance status is also associated with AMA discharge, with increased odds of AMA discharge among Medicare and Medicaid patients and patients without health insurance.9,10
Of note, one study found that race did not act as an independent predictor of AMA discharge when adjusted for age, gender, and socioeconomic factors.11
The AMA population is clinically heterogeneous. Among patients with pneumonia, for example, Saitz et al showed that a patient’s documented clinical severity did not independently predict AMA discharge, suggesting that there is great clinical heterogeneity even among AMA patients with similar admission diagnoses.12
These studies highlight the clinical and demographic heterogeneity within this population, suggesting that patients discharged AMA require individualized attention from hospitalists and other healthcare providers.
Patients describe numerous motivations for leaving the hospital prematurely, including needing to pick up public-assistance checks, personal financial issues, and familial obligations.13 Interestingly, in the cohort of HIV patients referenced above, discharge on the day welfare checks were distributed was an independent predictor of AMA discharge.6 In focus groups composed of patients discharged AMA and their treating nurses and physicians, several themes were identified as potential contributors to AMA discharge, including drug addiction, pain management issues, external obligations, wait time, the physician’s bedside manner, being in a teaching hospital, and communication issues.14
Clearly, patients have a diversity of reasons for requesting to be discharged AMA, and further research is necessary to define clear and potentially modifiable risk factors.
Discussion
The clinical scenarios outlined above present two patients with very different clinical presentations and outpatient support systems as well as demonstrate the great variability in clinical risk at the time of discharge AMA. These examples emphasize the importance of an individualized approach to care for each patient.
In Case No. 1, the patient is admitted with a mild asthma exacerbation with persistent bronchospasm, though she clinically appears well and has reliable follow-up. In contrast, in Case No. 2, the patient has life-threatening disease and no established primary care physician or mechanism for outpatient care. These examples demonstrate extremes on the clinical and psychosocial spectrum of patients requesting an “early” discharge and suggest that no two patients at risk of AMA discharge are the same. Patient 1 could likely be safely managed at home with close outpatient follow-up, while Patient 2 presents a high-risk scenario with very few safe outpatient treatment options.
We suggest that an individualized approach be taken for each patient, with attention to both clinical and psychosocial risk. In clinically low-risk cases (e.g., Case No. 1), an approach that prioritizes shared decision making and coordination with the outpatient care team may be preferable to an AMA discharge, particularly given the often adversarial nature of the later.2 In such cases, a collaborative approach may provide greater opportunity for harm reduction, provision of appropriate prescriptions, and follow-up appointments. In clinically high-risk patients such as Case No. 2, however, premature discharge is clearly inappropriate. Even in such clinically high-risk cases, however, we argue that a collaborative strategy aimed at identifying and addressing the patient’s psychosocial concerns is appropriate, as such an approach promotes shared decision making, builds trust between the patient and the care team, and therefore may facilitate improved follow-up at the time of discharge. Research is needed to formally assess the optimal approach for this patient population, including impact on rates of AMA discharge and the quality of post-discharge follow-up.
At present, the decision to classify a discharge as AMA falls solely on the treating provider, and we suspect that there is great variability in practice patterns, particularly as there are few established professional society practice guidelines regarding this difficult issue. As with all discharges from the hospital, the burden falls on the provider to engage the patient in shared decision making and ensure that the patient has the capacity to understand the risks and benefits of the proposed treatment plan. It is in this spirit that simply “filling out an AMA form” does not provide legal protection to a physician who does not adequately explain the full risks and benefits of refusal of inpatient treatment.2,15
We propose that a high-quality AMA discharge be defined as a discharge in which the patient is informed of the clinical team’s determination that further hospitalization is required but elects to leave the hospital, and it includes a clear discussion of the risks of outpatient treatment, a determination of capacity, and an exploration of safe alternative care plans that could satisfy both the patient’s medical and social needs. This definition places the burden on hospitalists and other providers to fully explore the motivations behind a patient’s request to leave the hospital and treats psychosocial motivators for premature discharge as variables in the complex risk-benefit analysis that underlies the informed consent discussion prior to AMA discharge.
Furthermore, AMA discharge does not obviate a physician’s responsibility to advocate for a patient’s well-being, and therefore an AMA discharge should be accompanied by reasonable efforts to coordinate a patient’s ongoing outpatient care. Of note, this approach is consistent with previous reviews and attempts to balance the physician’s duty to honor a patient’s autonomy with the responsibility to protect the patient from harm.2,16
Conclusion
Patients discharged AMA are a diverse population at markedly increased risk of morbidity, readmissions, and subsequent healthcare cost. We argue that in all cases of a potential premature discharge, a collaborative and patient-centered approach is crucial. Such an approach allows the provider to identify and address the patient’s concerns regarding further inpatient care, to explore possible safe outpatient treatment options, to document patient capacity, and to provide appropriate harm-reduction measures such as prescriptions.
Further research into the current practice patterns of hospitalists and other providers is necessary to allow for the formulation and adoption of best practices and implementation of appropriate harm-reduction strategies. TH
Dr. Tummalapalli is an internal medicine resident in the department of medicine at Icahn School of Medicine at Mount Sinai in New York City. Dr. Goodman is a hospitalist in the division of hospital medicine, department of medicine, at the Icahn School of Medicine at Mount Sinai.
References
- Aliyu ZY. Discharge against medical advice: sociodemographic, clinical and financial perspectives. Int J Clin Pract. 2002;56(5):325-327.
- Kahle CH, Rubio ML, Santos RA. Discharges against medical advice: considerations for the hospitalist and the patient. Hospital Medicine Clinics. 2015;4(3):421-429.
- Baptist AP, Warrier I, Arora R, Ager J, Massanari RM. Hospitalized patients with asthma who leave against medical advice: characteristics, reasons, and outcomes. J Allergy Clin Immunol. 2007;119(4):924-929.
- Hwang SW, Li J, Gupta R, Chien V, Martin RE. What happens to patients who leave hospital against medical advice? CMAJ. 2003;168(4):417-420.
- Glasgow JM, Vaughn-Sarrazin MV, Kaboli PJ. Leaving against medical advice (AMA): risk of 30-day mortality and hospital readmission. J Gen Int Med. 2010;25(9):926-929.
- Anis AH, Sun H, Guh DP, Palepu A, Schechter MT, O’Shaughnessy MV. Leaving hospital against medical advice among HIV-positive patients. CMAJ. 2002;167(6):633-637.
- Jeremiah J, O’Sullivan P, Stein MD. Who leaves against medical advice? J Gen Int Med. 1995; 10(7);403-405.
- O’Hara D, Hart W, McDonald I. Leaving hospital against medical advice. J Qual Clin Pract.1996;16(3):157-164.
- Ibrahim SA, Kwoh CK, Krishnan E. Factors associated with patients who leave acute-care hospitals against medical advice. Am J Public Health. 2007;97(12): 2204-2208.
- Weingart SN, Davis RB, Phillips RS. Patients discharged against medical advice from a general medicine service. J Gen Intern Med. 1998;13(8):568-571.
- Franks P, Meldrum S, Fiscella K. Discharges against medical advice: are race/ethnicity predictors? J Gen Intern Med. 2006;21(9):955-960.
- Saitz R, Ghali WA, Moskowitz MA. Characteristics of patients with pneumonia who are discharged from hospitals against medical advice. Am J Med. 1999;107(5):507-509.
- Alfandre, DJ. “I’m going home”: discharges against medical advice. Mayo Clin Proc. 2009;84(3):255-260.
- Onukwugha E, Saunders E, Mullins CD, Pradel FG, Zuckerman M, Weir MR. Reasons for discharges against medical advice: a qualitative study. Qual Saf Health Care. 2010;19(5):420-424. doi: 10.1136/qshc.2009.036269.
- Battenfeld v. Gregory, 589 A.2d 1059, 1061 (N.J. Super. Ct. App. Div. 1991).
- Berger J. Discharge against medical advice: ethical considerations and professional obligations. J Hosp Med. 2008;3(5):403-408.
Malaria test granted CE mark

Image by Peter H. Seeberger
A malaria test called illumigene® Malaria has received the CE mark, which suggests it meets European health and safety standards.
illumigene Malaria is a molecular test that involves the use of loop-mediated isothermal amplification (LAMP) technology.
According to the test’s developers, it provides results in under an hour, doesn’t require a high level technical expertise, and is up to 80,000 times more sensitive than conventional malaria tests.
illumigene Malaria was developed by Meridian Bioscience, Inc., with technical assistance from the US Centers for Disease Control and Prevention (CDC) and Cheikh Anta Diop University in Dakar, Senegal.
“illumigene Malaria has the potential to change current practices,” said Daouda NDIAYE, PharmD, PhD, of Cheikh Anta Diop University.
“Faster and more accurate diagnosis is vital in the fight against malaria. Earlier diagnosis enables the correct treatment to be prescribed, which leads to better clinical outcomes for the person with malaria and keeps malaria treatments for the right people.”
“Because of submicroscopic parasitemia carriage among the populations, a robust, sensitive, and field-community-deployable screening tool is needed to track the malaria reservoir in pre-elimination regions. illumigene Malaria shows this capacity.”
illumigene Malaria uses LAMP technology to amplify DNA and detect the presence of the malaria parasite.
LAMP technology is isothermal and can be used at room temperature without the need to heat reagents or the material being tested, unlike the rapid diagnostic tests currently used in malaria, which use polymerase chain reaction technology. illumigene Malaria does not require refrigeration.
Meridian Bioscience has worked with experts at the CDC and the Cheikh Anta Diop University of Dakar during the development of illumigene Malaria and collaborated with these organizations to design clinical trials.
According to Meridian, data from more than 200 patients in Senegal validated the performance of illumigene Malaria. The test demonstrated 100% sensitivity and detected infected patients that were missed by conventional testing methods.
Meridian said illumigene Malaria will be distributed in the European, Middle Eastern, and African regions by Meridian Bioscience Europe and in additional international markets by the company’s global distribution network. ![]()

Image by Peter H. Seeberger
A malaria test called illumigene® Malaria has received the CE mark, which suggests it meets European health and safety standards.
illumigene Malaria is a molecular test that involves the use of loop-mediated isothermal amplification (LAMP) technology.
According to the test’s developers, it provides results in under an hour, doesn’t require a high level technical expertise, and is up to 80,000 times more sensitive than conventional malaria tests.
illumigene Malaria was developed by Meridian Bioscience, Inc., with technical assistance from the US Centers for Disease Control and Prevention (CDC) and Cheikh Anta Diop University in Dakar, Senegal.
“illumigene Malaria has the potential to change current practices,” said Daouda NDIAYE, PharmD, PhD, of Cheikh Anta Diop University.
“Faster and more accurate diagnosis is vital in the fight against malaria. Earlier diagnosis enables the correct treatment to be prescribed, which leads to better clinical outcomes for the person with malaria and keeps malaria treatments for the right people.”
“Because of submicroscopic parasitemia carriage among the populations, a robust, sensitive, and field-community-deployable screening tool is needed to track the malaria reservoir in pre-elimination regions. illumigene Malaria shows this capacity.”
illumigene Malaria uses LAMP technology to amplify DNA and detect the presence of the malaria parasite.
LAMP technology is isothermal and can be used at room temperature without the need to heat reagents or the material being tested, unlike the rapid diagnostic tests currently used in malaria, which use polymerase chain reaction technology. illumigene Malaria does not require refrigeration.
Meridian Bioscience has worked with experts at the CDC and the Cheikh Anta Diop University of Dakar during the development of illumigene Malaria and collaborated with these organizations to design clinical trials.
According to Meridian, data from more than 200 patients in Senegal validated the performance of illumigene Malaria. The test demonstrated 100% sensitivity and detected infected patients that were missed by conventional testing methods.
Meridian said illumigene Malaria will be distributed in the European, Middle Eastern, and African regions by Meridian Bioscience Europe and in additional international markets by the company’s global distribution network. ![]()

Image by Peter H. Seeberger
A malaria test called illumigene® Malaria has received the CE mark, which suggests it meets European health and safety standards.
illumigene Malaria is a molecular test that involves the use of loop-mediated isothermal amplification (LAMP) technology.
According to the test’s developers, it provides results in under an hour, doesn’t require a high level technical expertise, and is up to 80,000 times more sensitive than conventional malaria tests.
illumigene Malaria was developed by Meridian Bioscience, Inc., with technical assistance from the US Centers for Disease Control and Prevention (CDC) and Cheikh Anta Diop University in Dakar, Senegal.
“illumigene Malaria has the potential to change current practices,” said Daouda NDIAYE, PharmD, PhD, of Cheikh Anta Diop University.
“Faster and more accurate diagnosis is vital in the fight against malaria. Earlier diagnosis enables the correct treatment to be prescribed, which leads to better clinical outcomes for the person with malaria and keeps malaria treatments for the right people.”
“Because of submicroscopic parasitemia carriage among the populations, a robust, sensitive, and field-community-deployable screening tool is needed to track the malaria reservoir in pre-elimination regions. illumigene Malaria shows this capacity.”
illumigene Malaria uses LAMP technology to amplify DNA and detect the presence of the malaria parasite.
LAMP technology is isothermal and can be used at room temperature without the need to heat reagents or the material being tested, unlike the rapid diagnostic tests currently used in malaria, which use polymerase chain reaction technology. illumigene Malaria does not require refrigeration.
Meridian Bioscience has worked with experts at the CDC and the Cheikh Anta Diop University of Dakar during the development of illumigene Malaria and collaborated with these organizations to design clinical trials.
According to Meridian, data from more than 200 patients in Senegal validated the performance of illumigene Malaria. The test demonstrated 100% sensitivity and detected infected patients that were missed by conventional testing methods.
Meridian said illumigene Malaria will be distributed in the European, Middle Eastern, and African regions by Meridian Bioscience Europe and in additional international markets by the company’s global distribution network. ![]()
Compounds could treat leukemia, lymphoma

apoptosis in cancer cells
Preclinical research suggests a new class of small-molecule inhibitors could potentially treat leukemias and lymphomas.
Researchers identified compounds targeting the Mdm2–MdmX RING–RING interaction as a new class of E3 ligase inhibitors.
Experiments showed that these compounds, dubbed MMRis, can induce apoptosis in leukemia and lymphoma cells.
The researchers detailed these experiments in Cell Death and Disease.
“We are excited about the unique activities of these compounds and will continue to focus our research efforts on development of their clinical potential,” said study author Xinjiang Wang, PhD, of Roswell Park Cancer Institute in Buffalo, New York.
“These compounds kill cancer cells. [They don’t] just stop cancer cell growth temporarily. These types of agents offer the promise of therapeutic benefit.”
Dr Wang and his colleagues found that MMRis specifically inhibit Mdm2–MdmX E3 ligase activity toward Mdm2 and p53 substrates.
The team said MMRis have an advantage over p53-activating agents that are currently in use as cancer therapies.
That is because MMRis activate the pro-apoptotic function of the p53 pathway, whereas current p53-activating agents temporarily prevent cancer growth but don’t damage existing cancer cells or prevent cancer growth long-term.
The researchers found that 2 MMRi compounds—MMRi6 and its analog, MMRi64—can disrupt Mdm2–MdmX interactions and activate p53 in vitro.
And MMRi64 selectively induces the apoptotic arm of the p53 pathway in leukemia and lymphoma cells.
The team noted that, unlike Nutlin3a, MMRi64 only induces expression of the pro-apoptotic gene PUMA, with minimal induction of the growth-arresting gene p21. However, combining MMRi64 and Nutlin3a produces a synergistic apoptotic effect.
“This study opens a new area for anticancer drug development,” Dr Wang said. “MMRi compounds also can be used as a tool for better understanding the anti-death mechanisms developed by cancer cells.”
“We are moving the research of MMRi compounds forward using both preclinical models and human cancer cell lines. Our hope is that further development of clinically useful MMRi will eventually provide a new treatment option for cancer patients.” ![]()

apoptosis in cancer cells
Preclinical research suggests a new class of small-molecule inhibitors could potentially treat leukemias and lymphomas.
Researchers identified compounds targeting the Mdm2–MdmX RING–RING interaction as a new class of E3 ligase inhibitors.
Experiments showed that these compounds, dubbed MMRis, can induce apoptosis in leukemia and lymphoma cells.
The researchers detailed these experiments in Cell Death and Disease.
“We are excited about the unique activities of these compounds and will continue to focus our research efforts on development of their clinical potential,” said study author Xinjiang Wang, PhD, of Roswell Park Cancer Institute in Buffalo, New York.
“These compounds kill cancer cells. [They don’t] just stop cancer cell growth temporarily. These types of agents offer the promise of therapeutic benefit.”
Dr Wang and his colleagues found that MMRis specifically inhibit Mdm2–MdmX E3 ligase activity toward Mdm2 and p53 substrates.
The team said MMRis have an advantage over p53-activating agents that are currently in use as cancer therapies.
That is because MMRis activate the pro-apoptotic function of the p53 pathway, whereas current p53-activating agents temporarily prevent cancer growth but don’t damage existing cancer cells or prevent cancer growth long-term.
The researchers found that 2 MMRi compounds—MMRi6 and its analog, MMRi64—can disrupt Mdm2–MdmX interactions and activate p53 in vitro.
And MMRi64 selectively induces the apoptotic arm of the p53 pathway in leukemia and lymphoma cells.
The team noted that, unlike Nutlin3a, MMRi64 only induces expression of the pro-apoptotic gene PUMA, with minimal induction of the growth-arresting gene p21. However, combining MMRi64 and Nutlin3a produces a synergistic apoptotic effect.
“This study opens a new area for anticancer drug development,” Dr Wang said. “MMRi compounds also can be used as a tool for better understanding the anti-death mechanisms developed by cancer cells.”
“We are moving the research of MMRi compounds forward using both preclinical models and human cancer cell lines. Our hope is that further development of clinically useful MMRi will eventually provide a new treatment option for cancer patients.” ![]()

apoptosis in cancer cells
Preclinical research suggests a new class of small-molecule inhibitors could potentially treat leukemias and lymphomas.
Researchers identified compounds targeting the Mdm2–MdmX RING–RING interaction as a new class of E3 ligase inhibitors.
Experiments showed that these compounds, dubbed MMRis, can induce apoptosis in leukemia and lymphoma cells.
The researchers detailed these experiments in Cell Death and Disease.
“We are excited about the unique activities of these compounds and will continue to focus our research efforts on development of their clinical potential,” said study author Xinjiang Wang, PhD, of Roswell Park Cancer Institute in Buffalo, New York.
“These compounds kill cancer cells. [They don’t] just stop cancer cell growth temporarily. These types of agents offer the promise of therapeutic benefit.”
Dr Wang and his colleagues found that MMRis specifically inhibit Mdm2–MdmX E3 ligase activity toward Mdm2 and p53 substrates.
The team said MMRis have an advantage over p53-activating agents that are currently in use as cancer therapies.
That is because MMRis activate the pro-apoptotic function of the p53 pathway, whereas current p53-activating agents temporarily prevent cancer growth but don’t damage existing cancer cells or prevent cancer growth long-term.
The researchers found that 2 MMRi compounds—MMRi6 and its analog, MMRi64—can disrupt Mdm2–MdmX interactions and activate p53 in vitro.
And MMRi64 selectively induces the apoptotic arm of the p53 pathway in leukemia and lymphoma cells.
The team noted that, unlike Nutlin3a, MMRi64 only induces expression of the pro-apoptotic gene PUMA, with minimal induction of the growth-arresting gene p21. However, combining MMRi64 and Nutlin3a produces a synergistic apoptotic effect.
“This study opens a new area for anticancer drug development,” Dr Wang said. “MMRi compounds also can be used as a tool for better understanding the anti-death mechanisms developed by cancer cells.”
“We are moving the research of MMRi compounds forward using both preclinical models and human cancer cell lines. Our hope is that further development of clinically useful MMRi will eventually provide a new treatment option for cancer patients.” ![]()
Leukemia death rates expected to fall in EU

receiving chemotherapy
Photo by Rhoda Baer
Projections for 2016 suggest that leukemia deaths are on the decline in the European Union (EU), particularly for children and young adults.
Leukemia death rates are expected to fall 19% in men and 16% in women in 2016, when compared to 2007 data.
Rates are projected to fall 38% in boys and 20% in girls ages 0 to 14, 26% in men and 22% in women ages 15 to 44, and 19% in men and women ages 45 to 69.
Researchers said improvements in management, multidrug chemotherapy, immunotherapies, stem cell transplants, radiotherapy, and targeted therapies have all contributed to improvements in survival for leukemia patients.
However, some leukemias remain hard to treat, particularly those that are more common in adults and the elderly.
“Predictions of death rates from leukemia are complicated by the fact that leukemias are a varied collection of blood cancers, with some being more treatable than others,” said study author Carlo La Vecchia, MD, of the University of Milan in Italy.
“However, the important falls in overall death rates from this group of diseases are very encouraging and are a testament to the hard work of researchers and clinicians in developing and implementing better diagnosis and treatments.”
Dr Vecchia and his colleagues reported the results of this research in Annals of Oncology.
The researchers looked at cancer deaths in the EU as a whole and in the 6 largest countries—France, Germany, Italy, Poland, Spain, and the UK.
The team assessed mortality for all cancers and looked at individual data for cancers of the stomach, intestines, pancreas, lung, prostate, breast, and uterus (including cervix), as well as leukemias.
All cancers
The researchers’ projections suggest that total cancer mortality rates will decrease for both sexes in 2016, despite a rise in the absolute number of deaths due to the aging population. The team said the median age of the total EU population was 41 in 2011 and will be 42 in 2016.
So a total of 1,359,500 EU citizens are expected to die of cancer in 2016—753,600 men and 605,900 women. This is compared to 1,314,787 cancer deaths in 2011—734,259 men and 580,528 women.
The age-standardized mortality rates for 2016 are 133.5 per 100,000 men and 85.2 per 100,000 women, compared to 144.6 per 100,000 men and 88.1 per 100,000 women in 2011.
So that’s a 7.7% fall in cancer death rates for men and a 3.3% fall for women from 2011 through 2016, despite a 3.3% increase in the absolute number of cancer deaths.
Leukemias
The researchers predict that, in 2016, age-standardized leukemia mortality rates will be 3.95 per 100,000 men and 2.46 per 100,000 women.
In comparison, the age-standardized mortality rates for 2000-2004 were 5.23 for men and 3.20 for women. The rates for 2005-2009 were 4.85 for men and 2.92 for women.
For males ages 0 to 14, the age-standardized mortality rates are 1.10 for 2000-2004, 0.87 for 2005-2009, and 0.54 for 2016. For females in this age group, the rates are 0.85 for 2000-2004, 0.69 for 2005-2009, and 0.55 for 2016.
For males ages 15 to 44, the age-standardized mortality rates are 1.50 for 2000-2004, 1.28 for 2005-2009, and 0.95 for 2016. For females, the rates are 1.07 for 2000-2004, 0.92 for 2005-2009, and 0.72 for 2016.
For males ages 45 to 69, the age-standardized mortality rates are 9.19 for 2000-2004, 8.39 for 2005-2009, and 6.79 for 2016. For females, the rates are 5.74 for 2000-2004, 5.12 for 2005-2009, and 4.16 for 2016. ![]()

receiving chemotherapy
Photo by Rhoda Baer
Projections for 2016 suggest that leukemia deaths are on the decline in the European Union (EU), particularly for children and young adults.
Leukemia death rates are expected to fall 19% in men and 16% in women in 2016, when compared to 2007 data.
Rates are projected to fall 38% in boys and 20% in girls ages 0 to 14, 26% in men and 22% in women ages 15 to 44, and 19% in men and women ages 45 to 69.
Researchers said improvements in management, multidrug chemotherapy, immunotherapies, stem cell transplants, radiotherapy, and targeted therapies have all contributed to improvements in survival for leukemia patients.
However, some leukemias remain hard to treat, particularly those that are more common in adults and the elderly.
“Predictions of death rates from leukemia are complicated by the fact that leukemias are a varied collection of blood cancers, with some being more treatable than others,” said study author Carlo La Vecchia, MD, of the University of Milan in Italy.
“However, the important falls in overall death rates from this group of diseases are very encouraging and are a testament to the hard work of researchers and clinicians in developing and implementing better diagnosis and treatments.”
Dr Vecchia and his colleagues reported the results of this research in Annals of Oncology.
The researchers looked at cancer deaths in the EU as a whole and in the 6 largest countries—France, Germany, Italy, Poland, Spain, and the UK.
The team assessed mortality for all cancers and looked at individual data for cancers of the stomach, intestines, pancreas, lung, prostate, breast, and uterus (including cervix), as well as leukemias.
All cancers
The researchers’ projections suggest that total cancer mortality rates will decrease for both sexes in 2016, despite a rise in the absolute number of deaths due to the aging population. The team said the median age of the total EU population was 41 in 2011 and will be 42 in 2016.
So a total of 1,359,500 EU citizens are expected to die of cancer in 2016—753,600 men and 605,900 women. This is compared to 1,314,787 cancer deaths in 2011—734,259 men and 580,528 women.
The age-standardized mortality rates for 2016 are 133.5 per 100,000 men and 85.2 per 100,000 women, compared to 144.6 per 100,000 men and 88.1 per 100,000 women in 2011.
So that’s a 7.7% fall in cancer death rates for men and a 3.3% fall for women from 2011 through 2016, despite a 3.3% increase in the absolute number of cancer deaths.
Leukemias
The researchers predict that, in 2016, age-standardized leukemia mortality rates will be 3.95 per 100,000 men and 2.46 per 100,000 women.
In comparison, the age-standardized mortality rates for 2000-2004 were 5.23 for men and 3.20 for women. The rates for 2005-2009 were 4.85 for men and 2.92 for women.
For males ages 0 to 14, the age-standardized mortality rates are 1.10 for 2000-2004, 0.87 for 2005-2009, and 0.54 for 2016. For females in this age group, the rates are 0.85 for 2000-2004, 0.69 for 2005-2009, and 0.55 for 2016.
For males ages 15 to 44, the age-standardized mortality rates are 1.50 for 2000-2004, 1.28 for 2005-2009, and 0.95 for 2016. For females, the rates are 1.07 for 2000-2004, 0.92 for 2005-2009, and 0.72 for 2016.
For males ages 45 to 69, the age-standardized mortality rates are 9.19 for 2000-2004, 8.39 for 2005-2009, and 6.79 for 2016. For females, the rates are 5.74 for 2000-2004, 5.12 for 2005-2009, and 4.16 for 2016. ![]()

receiving chemotherapy
Photo by Rhoda Baer
Projections for 2016 suggest that leukemia deaths are on the decline in the European Union (EU), particularly for children and young adults.
Leukemia death rates are expected to fall 19% in men and 16% in women in 2016, when compared to 2007 data.
Rates are projected to fall 38% in boys and 20% in girls ages 0 to 14, 26% in men and 22% in women ages 15 to 44, and 19% in men and women ages 45 to 69.
Researchers said improvements in management, multidrug chemotherapy, immunotherapies, stem cell transplants, radiotherapy, and targeted therapies have all contributed to improvements in survival for leukemia patients.
However, some leukemias remain hard to treat, particularly those that are more common in adults and the elderly.
“Predictions of death rates from leukemia are complicated by the fact that leukemias are a varied collection of blood cancers, with some being more treatable than others,” said study author Carlo La Vecchia, MD, of the University of Milan in Italy.
“However, the important falls in overall death rates from this group of diseases are very encouraging and are a testament to the hard work of researchers and clinicians in developing and implementing better diagnosis and treatments.”
Dr Vecchia and his colleagues reported the results of this research in Annals of Oncology.
The researchers looked at cancer deaths in the EU as a whole and in the 6 largest countries—France, Germany, Italy, Poland, Spain, and the UK.
The team assessed mortality for all cancers and looked at individual data for cancers of the stomach, intestines, pancreas, lung, prostate, breast, and uterus (including cervix), as well as leukemias.
All cancers
The researchers’ projections suggest that total cancer mortality rates will decrease for both sexes in 2016, despite a rise in the absolute number of deaths due to the aging population. The team said the median age of the total EU population was 41 in 2011 and will be 42 in 2016.
So a total of 1,359,500 EU citizens are expected to die of cancer in 2016—753,600 men and 605,900 women. This is compared to 1,314,787 cancer deaths in 2011—734,259 men and 580,528 women.
The age-standardized mortality rates for 2016 are 133.5 per 100,000 men and 85.2 per 100,000 women, compared to 144.6 per 100,000 men and 88.1 per 100,000 women in 2011.
So that’s a 7.7% fall in cancer death rates for men and a 3.3% fall for women from 2011 through 2016, despite a 3.3% increase in the absolute number of cancer deaths.
Leukemias
The researchers predict that, in 2016, age-standardized leukemia mortality rates will be 3.95 per 100,000 men and 2.46 per 100,000 women.
In comparison, the age-standardized mortality rates for 2000-2004 were 5.23 for men and 3.20 for women. The rates for 2005-2009 were 4.85 for men and 2.92 for women.
For males ages 0 to 14, the age-standardized mortality rates are 1.10 for 2000-2004, 0.87 for 2005-2009, and 0.54 for 2016. For females in this age group, the rates are 0.85 for 2000-2004, 0.69 for 2005-2009, and 0.55 for 2016.
For males ages 15 to 44, the age-standardized mortality rates are 1.50 for 2000-2004, 1.28 for 2005-2009, and 0.95 for 2016. For females, the rates are 1.07 for 2000-2004, 0.92 for 2005-2009, and 0.72 for 2016.
For males ages 45 to 69, the age-standardized mortality rates are 9.19 for 2000-2004, 8.39 for 2005-2009, and 6.79 for 2016. For females, the rates are 5.74 for 2000-2004, 5.12 for 2005-2009, and 4.16 for 2016. ![]()
Carotid Artery Ultrasound for Syncope
The Things We Do for No Reason (TWDFNR) series reviews practices which have become common parts of hospital care but which may provide little value to our patients. Practices reviewed in the TWDFNR series do not represent black and white conclusions or clinical practice standards, but are meant as a starting place for research and active discussions among hospitalists and patients. We invite you to be part of that discussion. https://www.choosingwisely.org/

CASE PRESENTATION
A 66‐year‐old man with a history of hypertension is hospitalized for a transient loss of consciousness while shopping at a farmers market with his wife on a hot summer day. He recalls feeling lightheaded seconds before he lost consciousness. He had no chest pain, diaphoresis, dyspnea, shaking movements, slurred speech, or head trauma. He felt mildly fatigued following the episode, but has since returned to his baseline. Physical examination, including a thorough cardiac and neurological examination, is normal. The hospitalist ponders whether to order a carotid artery ultrasound as part of a syncope evaluation.
BRIEF OVERVIEW
Syncope is defined as a rapid onset loss of consciousness of short duration as a result of global cerebral hypoperfusion with loss of postural tone, which is followed by spontaneous and complete recovery.[1] This definition describes syncope as a symptom rather than a disease. The challenge for providers is to determine the etiology of the syncope along with its attendant risk of morbidity and mortality. Given the wide variety of etiologies and concern over potentially missing an important etiology, diagnostic testing can become elaborate, expensive, and frequently low yield.
In the adult population, it is believed that approximately 35% of individuals will experience a syncopal episode in their lifetime.[2] As a result, syncope accounts for 1% to 3% of all emergency department visits and 1% to 6% of hospital admissions from emergency departments in the United States.[3, 4] The incidence and rate of hospitalization increase with age, as does the risk of mortality.[5, 6] There are 3 main types of syncope: cardiac, neurocardiogenic (vasovagal), and orthostatic. The presence of associated signs or symptoms with the syncope helps to differentiate the type and complexity of the syncope, while helping guide the diagnostic evaluation. Simple syncope is defined as the absence of focal neurological deficits or other signs or symptoms suggestive of transient ischemic attack (TIA) or cerebrovascular accident (CVA).[7] A differential diagnosis for a transient loss of consciousness that includes TIA and CVA will prompt a very different evaluation.
WHY YOU MIGHT THINK ORDERING CAROTID ARTERY ULTRASOUNDS FOR SYNCOPE EVALUATION ARE HELPFUL
Carotid artery ultrasounds are used to assess the extracranial carotid arteries for the presence of stenosis and to determine the direction of blood flow. The use of carotid artery ultrasound as a diagnostic tool in the evaluation of syncope can be traced to multiple articles from the 1980s. These articles noted the utility of screening patients with dizziness, lightheadedness, or syncope using carotid artery ultrasound due to possible decreased flow in the carotid artery circulation affecting cerebral perfusion.[8, 9] An association was noted between these symptoms and the presence of carotid artery stenosis. Further, a 1997 position paper from the American College of Physicians recommended that carotid artery or transcranial ultrasonography be reserved for syncope patients with carotid artery bruits or a history of neurovascular signs or symptoms.[10] More recent studies reveal carotid artery ultrasounds are still being performed regularly in syncope patients. In 2 studies evaluating syncope in the elderly, approximately 13% to 16% of syncope patients had a carotid artery ultrasound performed in an effort to identify an etiology.[7, 11]
Additionally, practitioners sometimes choose to perform carotid artery ultrasound in the evaluation of carotid sinus hypersensitivity. The carotid artery ultrasound can assess for the presence of stenosis or atheroma prior to performing carotid sinus massage, although the rate of persistent neurological complications from carotid sinus massage is estimated to occur in 1:1000 patients.[12]
WHY THERE IS NO REASON TO ORDER CAROTID ARTERY ULTRASOUNDS FOR THE EVALUATION OF SIMPLE SYNCOPE
Carotid artery ultrasounds are unlikely to determine the etiology of the syncope. We should expect a high‐value test to reveal an etiology for the syncope episodes at a significant rate. In the 2009 study by Mendu et al. at YaleNew Haven Hospital, 267 ultrasounds were performed on 2106 syncope admissions of high‐risk elderly patients (1920 total patients).[11] Of the 267 ultrasounds, only 2 of the tests (0.8%) helped to determine an etiology. Although 46% of the ultrasounds had abnormal findings, the measuring stick for these studies should be whether they uncover the etiology for syncope, not whether they find other unrelated vascular disease. In contrast, performing postural blood pressures helped to determine an etiology 15% to 21% of the time, depending on the criteria used to define an abnormal drop in postural blood pressures.
Similarly, in the 2005 study by Schnipper et al. at Massachusetts General Hospital, only 140 of 4199 adult patients (3.3%) who presented as either inpatients or outpatients for syncope or presyncope were referred for neurovascular testing.[13] Carotid artery ultrasound was performed in 109 of these patients, and the study neurologist could invoke cerebrovascular lesions as potential factors for syncope in only 2 patients, both of whom had syncope and focal neurologic symptoms. Moreover, both of the patients had severe cardiovascular disease (severe ischemic cardiomyopathy with complete heart block following coronary bypass surgery in 1 and aortic stenosis with decreased left ventricular ejection fraction in the other). It is quite possible that the ultrasounds did not find the etiology for any of the 140 high‐risk patients with syncope in the study.
In addition, the 2014 study by Scott et al. at Brigham and Women's Hospital analyzed carotid artery duplex ultrasounds performed on 313 inpatients and outpatients with syncope over a 5‐year period, excluding those with focal neurological deficits or carotid bruits.[7] Although 48 of the 313 patients (15.4%) were diagnosed with carotid stenosis of greater than 50%, the carotid artery ultrasound did not reveal a causal diagnosis in any patients. On the other hand, 7 patients had a change in medical management, and 1 patient underwent carotid endarterectomy following the carotid artery ultrasound, which was incidental to what prompted the evaluation.
Mendu et al. calculated the cost per test affecting the diagnosis or management of syncope (although diagnosis is the only important parameter). The cost per test was calculated as the charge per test multiplied by the cost‐to‐charge ratio of 0.34, based on the 2007 YaleNew Haven Hospital cost‐to‐charge ratio.[11] For carotid artery ultrasound, the cost per test was $19,580 to affect diagnosis or management as compared to $23 to $33 for postural blood pressures. Combining these findings with the results from the Schnipper et al. and Scott et al. articles, where carotid artery ultrasounds may not have found the cause of syncope in any of the patients, it seems clear that obtaining a carotid artery ultrasound in the evaluation of simple syncope is a low‐value proposition.
Many low‐value tests, like carotid artery ultrasounds, suffer from both upfront costs, as calculated in the Mendu et al. study, and downstream costs triggered by the testing itself. Performing carotid artery ultrasounds in elderly high‐risk syncope populations is likely to reveal asymptomatic carotid artery vascular disease, which may lead to more unwarranted testing or treatments in light of the initial indication for the test. In the Mendu et al. article, 122 (46%) of the 267 carotid artery ultrasounds performed on elderly patients admitted with syncope were abnormal. Abnormal findings were defined as any abnormality that was not seen on prior testing as written in the test reports. Similarly, Schnipper et al. found that 40% of the 140 highly selected patients had mild‐to‐severe carotid vascular disease.
National guideline recommendations are aligned with these findings. The National Institute for Health and Clinical Excellence Guideline for the Management of Transient Loss of Consciousness does not include carotid artery ultrasound in the summary of clinical recommendations.[14] Furthermore, the American Academy of Neurology Choosing Wisely campaign's recommendation 2 is: Do not perform imaging of the carotid arteries for simple syncope without other neurologic symptoms.[15]
WHAT YOU SHOULD DO INSTEAD: CHECK POSTURAL BLOOD PRESSURES
As is true for most of medicine, greater focus should be paid to the history and physical examination during the initial evaluation of the patient with syncope. Take great care to determine which patients have a history or symptoms concerning for neurologic or cardiac etiologies. Use this information to guide further diagnostic testing. Additionally, orthostatic testing is too often overlooked as an important diagnostic study. As described in the Mendu et al. study, orthostatic testing is inexpensive and effective, helping to determine an etiology 15% to 21% of the time. Carotid artery ultrasounds should be reserved for those patients with transient or permanent focal neurological symptoms.
RECOMMENDATIONS
- In patients suspected of syncope in the absence of other neurologic symptoms, carotid artery ultrasound should not be included in the diagnostic evaluation.
- Utilize postural blood pressures in the initial evaluation of syncope as an inexpensive and high‐value component of the physical examination.
- For patients with acute neurological findings in the setting of possible syncope, evaluate the patient for stroke.
- Use the history and physical examination to guide further evaluation.
CONCLUSION
Carotid artery ultrasounds should not be used to evaluate the cause of syncope in an effort to find incident symptomatic carotid vascular disease. Carotid artery ultrasounds rarely help determine the etiology of the syncopal episode and are more likely to find asymptomatic carotid vascular disease in the elderly population. The identification of carotid vascular disease can lead to further inappropriate testing and treatments unrelated to the indication for testing.
Acknowledgment
Disclosure: Nothing to report.
Do you think this is a low‐value practice? Is this truly a Thing We Do for No Reason? Share what you do in your practice and join in the conversation online by retweeting it on Twitter (#TWDFNR) and liking it on Facebook. We invite you to propose ideas for other Things We Do for No Reason topics by emailing [email protected].
- . Syncope. N Engl J Med. 2000;313(25):1856–1862.
- , , , , , . Lifetime cumulative incidence of syncope in the general population: a study of 549 Dutch subjects aged 35–60 years. J Cardiovasc Electrophysiol. 2006;17(11):1172–1176.
- . Evaluation and management of patients with syncope. JAMA. 1992;268(18):2553–2560.
- , , . Characteristics and admission patterns of patients presenting with syncope to U.S. emergency departments, 1992 to 2000. Acad Emerg Med. 2004;11:1029–1034.
- , . An approach to the evaluation and management of syncope in adults. BMJ. 2010;340:c880.
- , , , et al. Incidence and prognosis of syncope. N Engl J Med. 2002;347(12):878–885.
- , , , , . Choosing wisely for syncope: low‐value carotid ultrasound use. J Am Heart Assoc. 2014;3(4):e001063.
- , , . Hemodynamics of the carotid‐artery circulation in the elderly “dizzy” patient. J Am Geriatr Soc. 1981;29(9):402–406.
- . Clinical applications of noninvasive carotid artery testing. J Am Coll Cardiol. 1985;5(1):137–148.
- , , , , , . Diagnosing syncope. Part 2: unexplained syncope. Clinical efficacy assessment project of the American College of Physicians. Ann Intern Med. 1997;127(1):76–86.
- , , , , . Yield of diagnostic tests in evaluating syncopal episodes in older patients. Arch Intern Med. 2009;169(14):1299–1305.
- , , , , , . Complications of carotid sinus massage—a prospective series of older patients. Age Ageing. 2000;29(5):413–417.
- , , , . Diagnostic yield and utility of neurovascular ultrasonography in the evaluation of patients with syncope. Mayo Clin Proc. 2005;80(4):480–488.
- , , , et al. Transient Loss of Consciousness (‘Blackouts’) Management in Adults and Young People. NICE Clinical Guidelines, No. 109. London, UK: National Clinical Guideline Centre for Acute and Chronic Conditions, Royal College of Physicians; 2010.
- , , , et al. The American Academy of Neurology's top five choosing wisely recommendations. Neurology. 2013;81(11):1004–1011.
The Things We Do for No Reason (TWDFNR) series reviews practices which have become common parts of hospital care but which may provide little value to our patients. Practices reviewed in the TWDFNR series do not represent black and white conclusions or clinical practice standards, but are meant as a starting place for research and active discussions among hospitalists and patients. We invite you to be part of that discussion. https://www.choosingwisely.org/

CASE PRESENTATION
A 66‐year‐old man with a history of hypertension is hospitalized for a transient loss of consciousness while shopping at a farmers market with his wife on a hot summer day. He recalls feeling lightheaded seconds before he lost consciousness. He had no chest pain, diaphoresis, dyspnea, shaking movements, slurred speech, or head trauma. He felt mildly fatigued following the episode, but has since returned to his baseline. Physical examination, including a thorough cardiac and neurological examination, is normal. The hospitalist ponders whether to order a carotid artery ultrasound as part of a syncope evaluation.
BRIEF OVERVIEW
Syncope is defined as a rapid onset loss of consciousness of short duration as a result of global cerebral hypoperfusion with loss of postural tone, which is followed by spontaneous and complete recovery.[1] This definition describes syncope as a symptom rather than a disease. The challenge for providers is to determine the etiology of the syncope along with its attendant risk of morbidity and mortality. Given the wide variety of etiologies and concern over potentially missing an important etiology, diagnostic testing can become elaborate, expensive, and frequently low yield.
In the adult population, it is believed that approximately 35% of individuals will experience a syncopal episode in their lifetime.[2] As a result, syncope accounts for 1% to 3% of all emergency department visits and 1% to 6% of hospital admissions from emergency departments in the United States.[3, 4] The incidence and rate of hospitalization increase with age, as does the risk of mortality.[5, 6] There are 3 main types of syncope: cardiac, neurocardiogenic (vasovagal), and orthostatic. The presence of associated signs or symptoms with the syncope helps to differentiate the type and complexity of the syncope, while helping guide the diagnostic evaluation. Simple syncope is defined as the absence of focal neurological deficits or other signs or symptoms suggestive of transient ischemic attack (TIA) or cerebrovascular accident (CVA).[7] A differential diagnosis for a transient loss of consciousness that includes TIA and CVA will prompt a very different evaluation.
WHY YOU MIGHT THINK ORDERING CAROTID ARTERY ULTRASOUNDS FOR SYNCOPE EVALUATION ARE HELPFUL
Carotid artery ultrasounds are used to assess the extracranial carotid arteries for the presence of stenosis and to determine the direction of blood flow. The use of carotid artery ultrasound as a diagnostic tool in the evaluation of syncope can be traced to multiple articles from the 1980s. These articles noted the utility of screening patients with dizziness, lightheadedness, or syncope using carotid artery ultrasound due to possible decreased flow in the carotid artery circulation affecting cerebral perfusion.[8, 9] An association was noted between these symptoms and the presence of carotid artery stenosis. Further, a 1997 position paper from the American College of Physicians recommended that carotid artery or transcranial ultrasonography be reserved for syncope patients with carotid artery bruits or a history of neurovascular signs or symptoms.[10] More recent studies reveal carotid artery ultrasounds are still being performed regularly in syncope patients. In 2 studies evaluating syncope in the elderly, approximately 13% to 16% of syncope patients had a carotid artery ultrasound performed in an effort to identify an etiology.[7, 11]
Additionally, practitioners sometimes choose to perform carotid artery ultrasound in the evaluation of carotid sinus hypersensitivity. The carotid artery ultrasound can assess for the presence of stenosis or atheroma prior to performing carotid sinus massage, although the rate of persistent neurological complications from carotid sinus massage is estimated to occur in 1:1000 patients.[12]
WHY THERE IS NO REASON TO ORDER CAROTID ARTERY ULTRASOUNDS FOR THE EVALUATION OF SIMPLE SYNCOPE
Carotid artery ultrasounds are unlikely to determine the etiology of the syncope. We should expect a high‐value test to reveal an etiology for the syncope episodes at a significant rate. In the 2009 study by Mendu et al. at YaleNew Haven Hospital, 267 ultrasounds were performed on 2106 syncope admissions of high‐risk elderly patients (1920 total patients).[11] Of the 267 ultrasounds, only 2 of the tests (0.8%) helped to determine an etiology. Although 46% of the ultrasounds had abnormal findings, the measuring stick for these studies should be whether they uncover the etiology for syncope, not whether they find other unrelated vascular disease. In contrast, performing postural blood pressures helped to determine an etiology 15% to 21% of the time, depending on the criteria used to define an abnormal drop in postural blood pressures.
Similarly, in the 2005 study by Schnipper et al. at Massachusetts General Hospital, only 140 of 4199 adult patients (3.3%) who presented as either inpatients or outpatients for syncope or presyncope were referred for neurovascular testing.[13] Carotid artery ultrasound was performed in 109 of these patients, and the study neurologist could invoke cerebrovascular lesions as potential factors for syncope in only 2 patients, both of whom had syncope and focal neurologic symptoms. Moreover, both of the patients had severe cardiovascular disease (severe ischemic cardiomyopathy with complete heart block following coronary bypass surgery in 1 and aortic stenosis with decreased left ventricular ejection fraction in the other). It is quite possible that the ultrasounds did not find the etiology for any of the 140 high‐risk patients with syncope in the study.
In addition, the 2014 study by Scott et al. at Brigham and Women's Hospital analyzed carotid artery duplex ultrasounds performed on 313 inpatients and outpatients with syncope over a 5‐year period, excluding those with focal neurological deficits or carotid bruits.[7] Although 48 of the 313 patients (15.4%) were diagnosed with carotid stenosis of greater than 50%, the carotid artery ultrasound did not reveal a causal diagnosis in any patients. On the other hand, 7 patients had a change in medical management, and 1 patient underwent carotid endarterectomy following the carotid artery ultrasound, which was incidental to what prompted the evaluation.
Mendu et al. calculated the cost per test affecting the diagnosis or management of syncope (although diagnosis is the only important parameter). The cost per test was calculated as the charge per test multiplied by the cost‐to‐charge ratio of 0.34, based on the 2007 YaleNew Haven Hospital cost‐to‐charge ratio.[11] For carotid artery ultrasound, the cost per test was $19,580 to affect diagnosis or management as compared to $23 to $33 for postural blood pressures. Combining these findings with the results from the Schnipper et al. and Scott et al. articles, where carotid artery ultrasounds may not have found the cause of syncope in any of the patients, it seems clear that obtaining a carotid artery ultrasound in the evaluation of simple syncope is a low‐value proposition.
Many low‐value tests, like carotid artery ultrasounds, suffer from both upfront costs, as calculated in the Mendu et al. study, and downstream costs triggered by the testing itself. Performing carotid artery ultrasounds in elderly high‐risk syncope populations is likely to reveal asymptomatic carotid artery vascular disease, which may lead to more unwarranted testing or treatments in light of the initial indication for the test. In the Mendu et al. article, 122 (46%) of the 267 carotid artery ultrasounds performed on elderly patients admitted with syncope were abnormal. Abnormal findings were defined as any abnormality that was not seen on prior testing as written in the test reports. Similarly, Schnipper et al. found that 40% of the 140 highly selected patients had mild‐to‐severe carotid vascular disease.
National guideline recommendations are aligned with these findings. The National Institute for Health and Clinical Excellence Guideline for the Management of Transient Loss of Consciousness does not include carotid artery ultrasound in the summary of clinical recommendations.[14] Furthermore, the American Academy of Neurology Choosing Wisely campaign's recommendation 2 is: Do not perform imaging of the carotid arteries for simple syncope without other neurologic symptoms.[15]
WHAT YOU SHOULD DO INSTEAD: CHECK POSTURAL BLOOD PRESSURES
As is true for most of medicine, greater focus should be paid to the history and physical examination during the initial evaluation of the patient with syncope. Take great care to determine which patients have a history or symptoms concerning for neurologic or cardiac etiologies. Use this information to guide further diagnostic testing. Additionally, orthostatic testing is too often overlooked as an important diagnostic study. As described in the Mendu et al. study, orthostatic testing is inexpensive and effective, helping to determine an etiology 15% to 21% of the time. Carotid artery ultrasounds should be reserved for those patients with transient or permanent focal neurological symptoms.
RECOMMENDATIONS
- In patients suspected of syncope in the absence of other neurologic symptoms, carotid artery ultrasound should not be included in the diagnostic evaluation.
- Utilize postural blood pressures in the initial evaluation of syncope as an inexpensive and high‐value component of the physical examination.
- For patients with acute neurological findings in the setting of possible syncope, evaluate the patient for stroke.
- Use the history and physical examination to guide further evaluation.
CONCLUSION
Carotid artery ultrasounds should not be used to evaluate the cause of syncope in an effort to find incident symptomatic carotid vascular disease. Carotid artery ultrasounds rarely help determine the etiology of the syncopal episode and are more likely to find asymptomatic carotid vascular disease in the elderly population. The identification of carotid vascular disease can lead to further inappropriate testing and treatments unrelated to the indication for testing.
Acknowledgment
Disclosure: Nothing to report.
Do you think this is a low‐value practice? Is this truly a Thing We Do for No Reason? Share what you do in your practice and join in the conversation online by retweeting it on Twitter (#TWDFNR) and liking it on Facebook. We invite you to propose ideas for other Things We Do for No Reason topics by emailing [email protected].
The Things We Do for No Reason (TWDFNR) series reviews practices which have become common parts of hospital care but which may provide little value to our patients. Practices reviewed in the TWDFNR series do not represent black and white conclusions or clinical practice standards, but are meant as a starting place for research and active discussions among hospitalists and patients. We invite you to be part of that discussion. https://www.choosingwisely.org/

CASE PRESENTATION
A 66‐year‐old man with a history of hypertension is hospitalized for a transient loss of consciousness while shopping at a farmers market with his wife on a hot summer day. He recalls feeling lightheaded seconds before he lost consciousness. He had no chest pain, diaphoresis, dyspnea, shaking movements, slurred speech, or head trauma. He felt mildly fatigued following the episode, but has since returned to his baseline. Physical examination, including a thorough cardiac and neurological examination, is normal. The hospitalist ponders whether to order a carotid artery ultrasound as part of a syncope evaluation.
BRIEF OVERVIEW
Syncope is defined as a rapid onset loss of consciousness of short duration as a result of global cerebral hypoperfusion with loss of postural tone, which is followed by spontaneous and complete recovery.[1] This definition describes syncope as a symptom rather than a disease. The challenge for providers is to determine the etiology of the syncope along with its attendant risk of morbidity and mortality. Given the wide variety of etiologies and concern over potentially missing an important etiology, diagnostic testing can become elaborate, expensive, and frequently low yield.
In the adult population, it is believed that approximately 35% of individuals will experience a syncopal episode in their lifetime.[2] As a result, syncope accounts for 1% to 3% of all emergency department visits and 1% to 6% of hospital admissions from emergency departments in the United States.[3, 4] The incidence and rate of hospitalization increase with age, as does the risk of mortality.[5, 6] There are 3 main types of syncope: cardiac, neurocardiogenic (vasovagal), and orthostatic. The presence of associated signs or symptoms with the syncope helps to differentiate the type and complexity of the syncope, while helping guide the diagnostic evaluation. Simple syncope is defined as the absence of focal neurological deficits or other signs or symptoms suggestive of transient ischemic attack (TIA) or cerebrovascular accident (CVA).[7] A differential diagnosis for a transient loss of consciousness that includes TIA and CVA will prompt a very different evaluation.
WHY YOU MIGHT THINK ORDERING CAROTID ARTERY ULTRASOUNDS FOR SYNCOPE EVALUATION ARE HELPFUL
Carotid artery ultrasounds are used to assess the extracranial carotid arteries for the presence of stenosis and to determine the direction of blood flow. The use of carotid artery ultrasound as a diagnostic tool in the evaluation of syncope can be traced to multiple articles from the 1980s. These articles noted the utility of screening patients with dizziness, lightheadedness, or syncope using carotid artery ultrasound due to possible decreased flow in the carotid artery circulation affecting cerebral perfusion.[8, 9] An association was noted between these symptoms and the presence of carotid artery stenosis. Further, a 1997 position paper from the American College of Physicians recommended that carotid artery or transcranial ultrasonography be reserved for syncope patients with carotid artery bruits or a history of neurovascular signs or symptoms.[10] More recent studies reveal carotid artery ultrasounds are still being performed regularly in syncope patients. In 2 studies evaluating syncope in the elderly, approximately 13% to 16% of syncope patients had a carotid artery ultrasound performed in an effort to identify an etiology.[7, 11]
Additionally, practitioners sometimes choose to perform carotid artery ultrasound in the evaluation of carotid sinus hypersensitivity. The carotid artery ultrasound can assess for the presence of stenosis or atheroma prior to performing carotid sinus massage, although the rate of persistent neurological complications from carotid sinus massage is estimated to occur in 1:1000 patients.[12]
WHY THERE IS NO REASON TO ORDER CAROTID ARTERY ULTRASOUNDS FOR THE EVALUATION OF SIMPLE SYNCOPE
Carotid artery ultrasounds are unlikely to determine the etiology of the syncope. We should expect a high‐value test to reveal an etiology for the syncope episodes at a significant rate. In the 2009 study by Mendu et al. at YaleNew Haven Hospital, 267 ultrasounds were performed on 2106 syncope admissions of high‐risk elderly patients (1920 total patients).[11] Of the 267 ultrasounds, only 2 of the tests (0.8%) helped to determine an etiology. Although 46% of the ultrasounds had abnormal findings, the measuring stick for these studies should be whether they uncover the etiology for syncope, not whether they find other unrelated vascular disease. In contrast, performing postural blood pressures helped to determine an etiology 15% to 21% of the time, depending on the criteria used to define an abnormal drop in postural blood pressures.
Similarly, in the 2005 study by Schnipper et al. at Massachusetts General Hospital, only 140 of 4199 adult patients (3.3%) who presented as either inpatients or outpatients for syncope or presyncope were referred for neurovascular testing.[13] Carotid artery ultrasound was performed in 109 of these patients, and the study neurologist could invoke cerebrovascular lesions as potential factors for syncope in only 2 patients, both of whom had syncope and focal neurologic symptoms. Moreover, both of the patients had severe cardiovascular disease (severe ischemic cardiomyopathy with complete heart block following coronary bypass surgery in 1 and aortic stenosis with decreased left ventricular ejection fraction in the other). It is quite possible that the ultrasounds did not find the etiology for any of the 140 high‐risk patients with syncope in the study.
In addition, the 2014 study by Scott et al. at Brigham and Women's Hospital analyzed carotid artery duplex ultrasounds performed on 313 inpatients and outpatients with syncope over a 5‐year period, excluding those with focal neurological deficits or carotid bruits.[7] Although 48 of the 313 patients (15.4%) were diagnosed with carotid stenosis of greater than 50%, the carotid artery ultrasound did not reveal a causal diagnosis in any patients. On the other hand, 7 patients had a change in medical management, and 1 patient underwent carotid endarterectomy following the carotid artery ultrasound, which was incidental to what prompted the evaluation.
Mendu et al. calculated the cost per test affecting the diagnosis or management of syncope (although diagnosis is the only important parameter). The cost per test was calculated as the charge per test multiplied by the cost‐to‐charge ratio of 0.34, based on the 2007 YaleNew Haven Hospital cost‐to‐charge ratio.[11] For carotid artery ultrasound, the cost per test was $19,580 to affect diagnosis or management as compared to $23 to $33 for postural blood pressures. Combining these findings with the results from the Schnipper et al. and Scott et al. articles, where carotid artery ultrasounds may not have found the cause of syncope in any of the patients, it seems clear that obtaining a carotid artery ultrasound in the evaluation of simple syncope is a low‐value proposition.
Many low‐value tests, like carotid artery ultrasounds, suffer from both upfront costs, as calculated in the Mendu et al. study, and downstream costs triggered by the testing itself. Performing carotid artery ultrasounds in elderly high‐risk syncope populations is likely to reveal asymptomatic carotid artery vascular disease, which may lead to more unwarranted testing or treatments in light of the initial indication for the test. In the Mendu et al. article, 122 (46%) of the 267 carotid artery ultrasounds performed on elderly patients admitted with syncope were abnormal. Abnormal findings were defined as any abnormality that was not seen on prior testing as written in the test reports. Similarly, Schnipper et al. found that 40% of the 140 highly selected patients had mild‐to‐severe carotid vascular disease.
National guideline recommendations are aligned with these findings. The National Institute for Health and Clinical Excellence Guideline for the Management of Transient Loss of Consciousness does not include carotid artery ultrasound in the summary of clinical recommendations.[14] Furthermore, the American Academy of Neurology Choosing Wisely campaign's recommendation 2 is: Do not perform imaging of the carotid arteries for simple syncope without other neurologic symptoms.[15]
WHAT YOU SHOULD DO INSTEAD: CHECK POSTURAL BLOOD PRESSURES
As is true for most of medicine, greater focus should be paid to the history and physical examination during the initial evaluation of the patient with syncope. Take great care to determine which patients have a history or symptoms concerning for neurologic or cardiac etiologies. Use this information to guide further diagnostic testing. Additionally, orthostatic testing is too often overlooked as an important diagnostic study. As described in the Mendu et al. study, orthostatic testing is inexpensive and effective, helping to determine an etiology 15% to 21% of the time. Carotid artery ultrasounds should be reserved for those patients with transient or permanent focal neurological symptoms.
RECOMMENDATIONS
- In patients suspected of syncope in the absence of other neurologic symptoms, carotid artery ultrasound should not be included in the diagnostic evaluation.
- Utilize postural blood pressures in the initial evaluation of syncope as an inexpensive and high‐value component of the physical examination.
- For patients with acute neurological findings in the setting of possible syncope, evaluate the patient for stroke.
- Use the history and physical examination to guide further evaluation.
CONCLUSION
Carotid artery ultrasounds should not be used to evaluate the cause of syncope in an effort to find incident symptomatic carotid vascular disease. Carotid artery ultrasounds rarely help determine the etiology of the syncopal episode and are more likely to find asymptomatic carotid vascular disease in the elderly population. The identification of carotid vascular disease can lead to further inappropriate testing and treatments unrelated to the indication for testing.
Acknowledgment
Disclosure: Nothing to report.
Do you think this is a low‐value practice? Is this truly a Thing We Do for No Reason? Share what you do in your practice and join in the conversation online by retweeting it on Twitter (#TWDFNR) and liking it on Facebook. We invite you to propose ideas for other Things We Do for No Reason topics by emailing [email protected].
- . Syncope. N Engl J Med. 2000;313(25):1856–1862.
- , , , , , . Lifetime cumulative incidence of syncope in the general population: a study of 549 Dutch subjects aged 35–60 years. J Cardiovasc Electrophysiol. 2006;17(11):1172–1176.
- . Evaluation and management of patients with syncope. JAMA. 1992;268(18):2553–2560.
- , , . Characteristics and admission patterns of patients presenting with syncope to U.S. emergency departments, 1992 to 2000. Acad Emerg Med. 2004;11:1029–1034.
- , . An approach to the evaluation and management of syncope in adults. BMJ. 2010;340:c880.
- , , , et al. Incidence and prognosis of syncope. N Engl J Med. 2002;347(12):878–885.
- , , , , . Choosing wisely for syncope: low‐value carotid ultrasound use. J Am Heart Assoc. 2014;3(4):e001063.
- , , . Hemodynamics of the carotid‐artery circulation in the elderly “dizzy” patient. J Am Geriatr Soc. 1981;29(9):402–406.
- . Clinical applications of noninvasive carotid artery testing. J Am Coll Cardiol. 1985;5(1):137–148.
- , , , , , . Diagnosing syncope. Part 2: unexplained syncope. Clinical efficacy assessment project of the American College of Physicians. Ann Intern Med. 1997;127(1):76–86.
- , , , , . Yield of diagnostic tests in evaluating syncopal episodes in older patients. Arch Intern Med. 2009;169(14):1299–1305.
- , , , , , . Complications of carotid sinus massage—a prospective series of older patients. Age Ageing. 2000;29(5):413–417.
- , , , . Diagnostic yield and utility of neurovascular ultrasonography in the evaluation of patients with syncope. Mayo Clin Proc. 2005;80(4):480–488.
- , , , et al. Transient Loss of Consciousness (‘Blackouts’) Management in Adults and Young People. NICE Clinical Guidelines, No. 109. London, UK: National Clinical Guideline Centre for Acute and Chronic Conditions, Royal College of Physicians; 2010.
- , , , et al. The American Academy of Neurology's top five choosing wisely recommendations. Neurology. 2013;81(11):1004–1011.
- . Syncope. N Engl J Med. 2000;313(25):1856–1862.
- , , , , , . Lifetime cumulative incidence of syncope in the general population: a study of 549 Dutch subjects aged 35–60 years. J Cardiovasc Electrophysiol. 2006;17(11):1172–1176.
- . Evaluation and management of patients with syncope. JAMA. 1992;268(18):2553–2560.
- , , . Characteristics and admission patterns of patients presenting with syncope to U.S. emergency departments, 1992 to 2000. Acad Emerg Med. 2004;11:1029–1034.
- , . An approach to the evaluation and management of syncope in adults. BMJ. 2010;340:c880.
- , , , et al. Incidence and prognosis of syncope. N Engl J Med. 2002;347(12):878–885.
- , , , , . Choosing wisely for syncope: low‐value carotid ultrasound use. J Am Heart Assoc. 2014;3(4):e001063.
- , , . Hemodynamics of the carotid‐artery circulation in the elderly “dizzy” patient. J Am Geriatr Soc. 1981;29(9):402–406.
- . Clinical applications of noninvasive carotid artery testing. J Am Coll Cardiol. 1985;5(1):137–148.
- , , , , , . Diagnosing syncope. Part 2: unexplained syncope. Clinical efficacy assessment project of the American College of Physicians. Ann Intern Med. 1997;127(1):76–86.
- , , , , . Yield of diagnostic tests in evaluating syncopal episodes in older patients. Arch Intern Med. 2009;169(14):1299–1305.
- , , , , , . Complications of carotid sinus massage—a prospective series of older patients. Age Ageing. 2000;29(5):413–417.
- , , , . Diagnostic yield and utility of neurovascular ultrasonography in the evaluation of patients with syncope. Mayo Clin Proc. 2005;80(4):480–488.
- , , , et al. Transient Loss of Consciousness (‘Blackouts’) Management in Adults and Young People. NICE Clinical Guidelines, No. 109. London, UK: National Clinical Guideline Centre for Acute and Chronic Conditions, Royal College of Physicians; 2010.
- , , , et al. The American Academy of Neurology's top five choosing wisely recommendations. Neurology. 2013;81(11):1004–1011.
© 2015 Society of Hospital Medicine
David Henry's JCSO podcast, January 2016
In his January podcast for The Journal of Community and Supportive Oncology, Editor-in-Chief Dr David Henry discusses a Commentary by Dr Thomas Strouse on the use on cannabinoids in the cancer treatment setting and a Community Translations article on the recent approval of idarucizumab as the first specific oral anticoagulant reversal agent. Also included in the line-up are two Review articles, one on new therapies for antiemetic prophylaxis for chemotherapy-induced nausea and vomiting and another on the management of epidermal growth factor receptor inhibitor-associated rash; and Original Reports on cyclical hypofractionated radiotherapy for palliative treatment in locally advanced head and neck cancer and on the impact of surgery for early-stage non-small-cell lung cancer on patient quality of life.
Listen to the podcast below.
In his January podcast for The Journal of Community and Supportive Oncology, Editor-in-Chief Dr David Henry discusses a Commentary by Dr Thomas Strouse on the use on cannabinoids in the cancer treatment setting and a Community Translations article on the recent approval of idarucizumab as the first specific oral anticoagulant reversal agent. Also included in the line-up are two Review articles, one on new therapies for antiemetic prophylaxis for chemotherapy-induced nausea and vomiting and another on the management of epidermal growth factor receptor inhibitor-associated rash; and Original Reports on cyclical hypofractionated radiotherapy for palliative treatment in locally advanced head and neck cancer and on the impact of surgery for early-stage non-small-cell lung cancer on patient quality of life.
Listen to the podcast below.
In his January podcast for The Journal of Community and Supportive Oncology, Editor-in-Chief Dr David Henry discusses a Commentary by Dr Thomas Strouse on the use on cannabinoids in the cancer treatment setting and a Community Translations article on the recent approval of idarucizumab as the first specific oral anticoagulant reversal agent. Also included in the line-up are two Review articles, one on new therapies for antiemetic prophylaxis for chemotherapy-induced nausea and vomiting and another on the management of epidermal growth factor receptor inhibitor-associated rash; and Original Reports on cyclical hypofractionated radiotherapy for palliative treatment in locally advanced head and neck cancer and on the impact of surgery for early-stage non-small-cell lung cancer on patient quality of life.
Listen to the podcast below.






