User login
Decreasing RBC transfusions saves center $1 million
Researchers have reported that interventions designed to decrease the need for red blood cell (RBC) transfusions proved effective when implemented at an academic medical center, and they resulted in an annual cost savings of more than $1 million.
The interventions included educational tools, a “best practice advisory,” and changes to the computerized provider order entry system.
They enabled the medical center to reduce multi-unit transfusions by 67.1% and transfusions for patients with hemoglobin (Hb) values of at least 7 g/dL by 47.4%.
Ian Jenkins, MD, of University of California San Diego (UCSD) Health, and his colleagues reported these results in The Joint Commission Journal on Quality and Patient Safety.
This work began with a multidisciplinary team at UCSD Health reviewing the transfusion literature on clinical trials, meta-analyses, guidelines, and improvement efforts.
The team used the information gleaned from this review and implemented the following interventions in an attempt to reduce unnecessary RBC transfusions:
- Educational tools (handouts, a video, PowerPoint presentations, etc)
- Enhancements to the health system’s computerized provider order entry system (eg, changing default RBC dose from 2 units to 1 unit)
- A “best practice advisory” intended to reduce unnecessary blood product use and costs by using real-time clinical decision support, a process for providing information at the point of care to help inform decisions about a patient’s care.
To assess the impact of their interventions, the researchers evaluated data on most non-infant, inpatient RBC transfusions given at UCSD Health between January 1, 2014, and September 30, 2016.
They excluded units given to patients with gastrointestinal bleeding and units given within 12 hours of a surgical procedure. The team said they excluded these transfusions because of the higher probability of unstable blood volume or special circumstances that might justify off-protocol transfusion.
The researchers then calculated the rate of inpatient RBC units transfused per 1000 patient-days (without exclusions), the percentage of inpatient RBC units transfused for patients with Hb ≥ 7 g/dL, and the percentage of multi-unit RBC transfusions, divided into 3 periods:
- Pre-intervention or baseline (January 1, 2014–September 30, 2014)
- During the intervention (October 1, 2014–April 30, 2015)
- Post-intervention (May 1, 2015–September 30, 2016).
There were 36,386 RBC units administered during the study period, which was 464,424 patient days.
Multi-unit transfusions decreased from 59.9% at baseline to 41.7% during the intervention period and 19.7% during the post-intervention period (P<0.0001).
Transfusions in patients with Hb values ≥ 7 g/dL decreased from 72.3% at baseline to 57.8% during the intervention period and 38.0% during the post-intervention period (P<0.0001).
The total RBC transfusion rate (units per 1000 patient-days) decreased from 89.8 at baseline to 78.1 during the intervention period and 72.7 during the post-intervention period (P<0.0001).
The estimated savings, based on a cost of $250 per RBC unit, was about $1,050,750 per year. ![]()
Researchers have reported that interventions designed to decrease the need for red blood cell (RBC) transfusions proved effective when implemented at an academic medical center, and they resulted in an annual cost savings of more than $1 million.
The interventions included educational tools, a “best practice advisory,” and changes to the computerized provider order entry system.
They enabled the medical center to reduce multi-unit transfusions by 67.1% and transfusions for patients with hemoglobin (Hb) values of at least 7 g/dL by 47.4%.
Ian Jenkins, MD, of University of California San Diego (UCSD) Health, and his colleagues reported these results in The Joint Commission Journal on Quality and Patient Safety.
This work began with a multidisciplinary team at UCSD Health reviewing the transfusion literature on clinical trials, meta-analyses, guidelines, and improvement efforts.
The team used the information gleaned from this review and implemented the following interventions in an attempt to reduce unnecessary RBC transfusions:
- Educational tools (handouts, a video, PowerPoint presentations, etc)
- Enhancements to the health system’s computerized provider order entry system (eg, changing default RBC dose from 2 units to 1 unit)
- A “best practice advisory” intended to reduce unnecessary blood product use and costs by using real-time clinical decision support, a process for providing information at the point of care to help inform decisions about a patient’s care.
To assess the impact of their interventions, the researchers evaluated data on most non-infant, inpatient RBC transfusions given at UCSD Health between January 1, 2014, and September 30, 2016.
They excluded units given to patients with gastrointestinal bleeding and units given within 12 hours of a surgical procedure. The team said they excluded these transfusions because of the higher probability of unstable blood volume or special circumstances that might justify off-protocol transfusion.
The researchers then calculated the rate of inpatient RBC units transfused per 1000 patient-days (without exclusions), the percentage of inpatient RBC units transfused for patients with Hb ≥ 7 g/dL, and the percentage of multi-unit RBC transfusions, divided into 3 periods:
- Pre-intervention or baseline (January 1, 2014–September 30, 2014)
- During the intervention (October 1, 2014–April 30, 2015)
- Post-intervention (May 1, 2015–September 30, 2016).
There were 36,386 RBC units administered during the study period, which was 464,424 patient days.
Multi-unit transfusions decreased from 59.9% at baseline to 41.7% during the intervention period and 19.7% during the post-intervention period (P<0.0001).
Transfusions in patients with Hb values ≥ 7 g/dL decreased from 72.3% at baseline to 57.8% during the intervention period and 38.0% during the post-intervention period (P<0.0001).
The total RBC transfusion rate (units per 1000 patient-days) decreased from 89.8 at baseline to 78.1 during the intervention period and 72.7 during the post-intervention period (P<0.0001).
The estimated savings, based on a cost of $250 per RBC unit, was about $1,050,750 per year. ![]()
Researchers have reported that interventions designed to decrease the need for red blood cell (RBC) transfusions proved effective when implemented at an academic medical center, and they resulted in an annual cost savings of more than $1 million.
The interventions included educational tools, a “best practice advisory,” and changes to the computerized provider order entry system.
They enabled the medical center to reduce multi-unit transfusions by 67.1% and transfusions for patients with hemoglobin (Hb) values of at least 7 g/dL by 47.4%.
Ian Jenkins, MD, of University of California San Diego (UCSD) Health, and his colleagues reported these results in The Joint Commission Journal on Quality and Patient Safety.
This work began with a multidisciplinary team at UCSD Health reviewing the transfusion literature on clinical trials, meta-analyses, guidelines, and improvement efforts.
The team used the information gleaned from this review and implemented the following interventions in an attempt to reduce unnecessary RBC transfusions:
- Educational tools (handouts, a video, PowerPoint presentations, etc)
- Enhancements to the health system’s computerized provider order entry system (eg, changing default RBC dose from 2 units to 1 unit)
- A “best practice advisory” intended to reduce unnecessary blood product use and costs by using real-time clinical decision support, a process for providing information at the point of care to help inform decisions about a patient’s care.
To assess the impact of their interventions, the researchers evaluated data on most non-infant, inpatient RBC transfusions given at UCSD Health between January 1, 2014, and September 30, 2016.
They excluded units given to patients with gastrointestinal bleeding and units given within 12 hours of a surgical procedure. The team said they excluded these transfusions because of the higher probability of unstable blood volume or special circumstances that might justify off-protocol transfusion.
The researchers then calculated the rate of inpatient RBC units transfused per 1000 patient-days (without exclusions), the percentage of inpatient RBC units transfused for patients with Hb ≥ 7 g/dL, and the percentage of multi-unit RBC transfusions, divided into 3 periods:
- Pre-intervention or baseline (January 1, 2014–September 30, 2014)
- During the intervention (October 1, 2014–April 30, 2015)
- Post-intervention (May 1, 2015–September 30, 2016).
There were 36,386 RBC units administered during the study period, which was 464,424 patient days.
Multi-unit transfusions decreased from 59.9% at baseline to 41.7% during the intervention period and 19.7% during the post-intervention period (P<0.0001).
Transfusions in patients with Hb values ≥ 7 g/dL decreased from 72.3% at baseline to 57.8% during the intervention period and 38.0% during the post-intervention period (P<0.0001).
The total RBC transfusion rate (units per 1000 patient-days) decreased from 89.8 at baseline to 78.1 during the intervention period and 72.7 during the post-intervention period (P<0.0001).
The estimated savings, based on a cost of $250 per RBC unit, was about $1,050,750 per year. ![]()
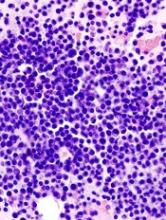
GEP classifier predicts risk in MM
A gene expression profiling (GEP) classifier can accurately identify high- and low-risk patients with multiple myeloma (MM), according to research published in Clinical Lymphoma, Myeloma and Leukemia.
The GEP classifier is known as SKY92, and researchers found they could accurately identify high-risk MM patients using SKY92 alone.
By combining SKY92 with the International Staging System (ISS), the team was able to identify low-risk MM patients as well.
“We have demonstrated the prognostic value of SKY92 not only as a marker of high risk, but also as a marker of low risk when combined with ISS,” said study author Erik H. van Beers, PhD, vice president of genomics at SkylineDx, the company that developed SKY92.
“Both validated markers may serve as the basis for the discovery of improved individualized therapies for patients with multiple myeloma.”
Dr van Beers and his colleagues compared 8 risk-assessment platforms to analyze gene expression data from 91 newly diagnosed MM patients. The patients were included in an independent dataset amassed by the Multiple Myeloma Research Foundation and the Multiple Myeloma Genomics Initiative (MMRF/MMGI).
The researchers used the GEP classifiers SKY92, UAMS70, UAMS80, IFM15, HM19, Cancer Testis Antigen, Centrosome Index, and Proliferation Index to identify high-risk patients.
Of the 8 classifiers, SKY92 identified the largest proportion (21%) of high-risk cases and also attained the highest Cox proportional hazard ratio (8.2) for overall survival (OS).
Additionally, SKY92 predicted 9 of the 13 (60%) deaths that occurred at 2 years and 16 of the 31 (52%) deaths at 5 years, a predictive rate that was higher than any of the other classifiers.
Dr van Beers and his colleagues also combined the SKY92 standard-risk classifier with the ISS to identify low-risk patients in the MMRF/MMGI cohort. This combination was recently identified as a marker for detecting low-risk MM.*
The SKY92/ISS marker identified 42% of patients as low risk, with their median OS not reached at 96 months. The low-risk classification was strongly supported by the achieved hazard ratio of 10.
“The MMRF/MMGI dataset was not part of our previous discovery*, which demonstrated that the combination of SKY92 and ISS identifies the lowest-risk patients with high accuracy and leaves the smallest proportion of patients identified as intermediate risk,” Dr van Beers said. “Thus, the dataset remained available for independent validation—an important factor in the adoption of gene expression profiling tools.”
“We are pleased to have validated the SKY92/ISS low-risk marker by applying it to the well-characterized MMRF/MMGI cohort,” added study author Rafael Fonseca, MD, of the Mayo Clinic in Scottsdale, Arizona. “Our findings further strengthen the prognostic utility of the combination marker.” ![]()
*Kuiper R, van Duin M, van Vliet, MH, et al. Prediction of high- and low-risk multiple myeloma based on gene expression and the International Staging System. Blood. 2015;126(17):1996-2004.
A gene expression profiling (GEP) classifier can accurately identify high- and low-risk patients with multiple myeloma (MM), according to research published in Clinical Lymphoma, Myeloma and Leukemia.
The GEP classifier is known as SKY92, and researchers found they could accurately identify high-risk MM patients using SKY92 alone.
By combining SKY92 with the International Staging System (ISS), the team was able to identify low-risk MM patients as well.
“We have demonstrated the prognostic value of SKY92 not only as a marker of high risk, but also as a marker of low risk when combined with ISS,” said study author Erik H. van Beers, PhD, vice president of genomics at SkylineDx, the company that developed SKY92.
“Both validated markers may serve as the basis for the discovery of improved individualized therapies for patients with multiple myeloma.”
Dr van Beers and his colleagues compared 8 risk-assessment platforms to analyze gene expression data from 91 newly diagnosed MM patients. The patients were included in an independent dataset amassed by the Multiple Myeloma Research Foundation and the Multiple Myeloma Genomics Initiative (MMRF/MMGI).
The researchers used the GEP classifiers SKY92, UAMS70, UAMS80, IFM15, HM19, Cancer Testis Antigen, Centrosome Index, and Proliferation Index to identify high-risk patients.
Of the 8 classifiers, SKY92 identified the largest proportion (21%) of high-risk cases and also attained the highest Cox proportional hazard ratio (8.2) for overall survival (OS).
Additionally, SKY92 predicted 9 of the 13 (60%) deaths that occurred at 2 years and 16 of the 31 (52%) deaths at 5 years, a predictive rate that was higher than any of the other classifiers.
Dr van Beers and his colleagues also combined the SKY92 standard-risk classifier with the ISS to identify low-risk patients in the MMRF/MMGI cohort. This combination was recently identified as a marker for detecting low-risk MM.*
The SKY92/ISS marker identified 42% of patients as low risk, with their median OS not reached at 96 months. The low-risk classification was strongly supported by the achieved hazard ratio of 10.
“The MMRF/MMGI dataset was not part of our previous discovery*, which demonstrated that the combination of SKY92 and ISS identifies the lowest-risk patients with high accuracy and leaves the smallest proportion of patients identified as intermediate risk,” Dr van Beers said. “Thus, the dataset remained available for independent validation—an important factor in the adoption of gene expression profiling tools.”
“We are pleased to have validated the SKY92/ISS low-risk marker by applying it to the well-characterized MMRF/MMGI cohort,” added study author Rafael Fonseca, MD, of the Mayo Clinic in Scottsdale, Arizona. “Our findings further strengthen the prognostic utility of the combination marker.” ![]()
*Kuiper R, van Duin M, van Vliet, MH, et al. Prediction of high- and low-risk multiple myeloma based on gene expression and the International Staging System. Blood. 2015;126(17):1996-2004.
A gene expression profiling (GEP) classifier can accurately identify high- and low-risk patients with multiple myeloma (MM), according to research published in Clinical Lymphoma, Myeloma and Leukemia.
The GEP classifier is known as SKY92, and researchers found they could accurately identify high-risk MM patients using SKY92 alone.
By combining SKY92 with the International Staging System (ISS), the team was able to identify low-risk MM patients as well.
“We have demonstrated the prognostic value of SKY92 not only as a marker of high risk, but also as a marker of low risk when combined with ISS,” said study author Erik H. van Beers, PhD, vice president of genomics at SkylineDx, the company that developed SKY92.
“Both validated markers may serve as the basis for the discovery of improved individualized therapies for patients with multiple myeloma.”
Dr van Beers and his colleagues compared 8 risk-assessment platforms to analyze gene expression data from 91 newly diagnosed MM patients. The patients were included in an independent dataset amassed by the Multiple Myeloma Research Foundation and the Multiple Myeloma Genomics Initiative (MMRF/MMGI).
The researchers used the GEP classifiers SKY92, UAMS70, UAMS80, IFM15, HM19, Cancer Testis Antigen, Centrosome Index, and Proliferation Index to identify high-risk patients.
Of the 8 classifiers, SKY92 identified the largest proportion (21%) of high-risk cases and also attained the highest Cox proportional hazard ratio (8.2) for overall survival (OS).
Additionally, SKY92 predicted 9 of the 13 (60%) deaths that occurred at 2 years and 16 of the 31 (52%) deaths at 5 years, a predictive rate that was higher than any of the other classifiers.
Dr van Beers and his colleagues also combined the SKY92 standard-risk classifier with the ISS to identify low-risk patients in the MMRF/MMGI cohort. This combination was recently identified as a marker for detecting low-risk MM.*
The SKY92/ISS marker identified 42% of patients as low risk, with their median OS not reached at 96 months. The low-risk classification was strongly supported by the achieved hazard ratio of 10.
“The MMRF/MMGI dataset was not part of our previous discovery*, which demonstrated that the combination of SKY92 and ISS identifies the lowest-risk patients with high accuracy and leaves the smallest proportion of patients identified as intermediate risk,” Dr van Beers said. “Thus, the dataset remained available for independent validation—an important factor in the adoption of gene expression profiling tools.”
“We are pleased to have validated the SKY92/ISS low-risk marker by applying it to the well-characterized MMRF/MMGI cohort,” added study author Rafael Fonseca, MD, of the Mayo Clinic in Scottsdale, Arizona. “Our findings further strengthen the prognostic utility of the combination marker.” ![]()
*Kuiper R, van Duin M, van Vliet, MH, et al. Prediction of high- and low-risk multiple myeloma based on gene expression and the International Staging System. Blood. 2015;126(17):1996-2004.
Product granted fast track designation for aTTP
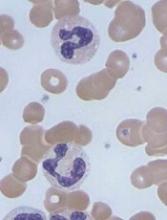
The US Food and Drug Administration (FDA) has granted fast track designation to caplacizumab, an anti-von Willebrand factor (vWF) nanobody being developed for the treatment of acquired thrombotic thrombocytopenic purpura (aTTP).
The FDA’s fast track program is designed to facilitate the development and expedite the review of products intended to treat or prevent serious or life-threatening conditions and address unmet medical need.
Through the fast track program, a product may be eligible for priority review. In addition, the company developing the product may be allowed to submit sections of the new drug application or biologics license application on a rolling basis as data become available.
Fast track designation also provides the company with opportunities for more frequent meetings and written communications with the FDA.
About caplacizumab
Caplacizumab is a bivalent anti-vWF nanobody being developed by Ablynx. Caplacizumab works by blocking the interaction of ultra-large vWF multimers with platelets, having an immediate effect on platelet aggregation and the ensuing formation and accumulation of the micro-clots that cause the severe thrombocytopenia, tissue ischemia, and organ dysfunction that occurs in patients with aTTP.
Researchers evaluated the efficacy and safety of caplacizumab, given with standard care for aTTP, in the phase 2 TITAN trial.
The trial enrolled 75 patients with aTTP. They all received the standard of care—daily plasma exchange and immunosuppressive therapy. Thirty-six patients were randomized to receive caplacizumab as well, and 39 were randomized to placebo.
The study’s primary endpoint was time to response (platelet count normalization). Patients in the caplacizumab arm had a 39% reduction in the median time to response compared to patients in the placebo arm (P=0.005).
The rate of confirmed response was 86.1% (n=31) in the caplacizumab arm and 71.8% (n=28) in the placebo arm.
There were more relapses in the caplacizumab arm than the placebo arm—8 (22.2%) and 0, respectively. Relapse was defined as a TTP event occurring more than 30 days after the end of daily plasma exchange.
There were fewer exacerbations in the caplacizumab arm than the placebo arm—3 (8.3%) and 11 (28.2%), respectively. Exacerbation was defined as recurrent thrombocytopenia within 30 days of the end of daily plasma exchange that required re-initiation of daily exchange.
The rate of adverse events thought to be related to the study drug was 17% in the caplacizumab arm and 11% in the placebo arm. The rate of events that were possibly related was 54% and 8%, respectively.
A lower proportion of subjects in the caplacizumab arm experienced one or more major thromboembolic events or died, compared to the placebo arm—11.4% and 43.2%, respectively.
In addition, fewer caplacizumab-treated patients were refractory to treatment—5.7% vs 21.6%.
There were 2 deaths in the placebo arm, and both of those patients were refractory to treatment. There were no deaths reported in the caplacizumab arm.
Now, researchers are evaluating caplacizumab in the phase 3 HERCULES trial (NCT02553317). Results from this study are anticipated in the second half of 2017 are expected to support a planned biologics license application filing in the US in 2018. ![]()
The US Food and Drug Administration (FDA) has granted fast track designation to caplacizumab, an anti-von Willebrand factor (vWF) nanobody being developed for the treatment of acquired thrombotic thrombocytopenic purpura (aTTP).
The FDA’s fast track program is designed to facilitate the development and expedite the review of products intended to treat or prevent serious or life-threatening conditions and address unmet medical need.
Through the fast track program, a product may be eligible for priority review. In addition, the company developing the product may be allowed to submit sections of the new drug application or biologics license application on a rolling basis as data become available.
Fast track designation also provides the company with opportunities for more frequent meetings and written communications with the FDA.
About caplacizumab
Caplacizumab is a bivalent anti-vWF nanobody being developed by Ablynx. Caplacizumab works by blocking the interaction of ultra-large vWF multimers with platelets, having an immediate effect on platelet aggregation and the ensuing formation and accumulation of the micro-clots that cause the severe thrombocytopenia, tissue ischemia, and organ dysfunction that occurs in patients with aTTP.
Researchers evaluated the efficacy and safety of caplacizumab, given with standard care for aTTP, in the phase 2 TITAN trial.
The trial enrolled 75 patients with aTTP. They all received the standard of care—daily plasma exchange and immunosuppressive therapy. Thirty-six patients were randomized to receive caplacizumab as well, and 39 were randomized to placebo.
The study’s primary endpoint was time to response (platelet count normalization). Patients in the caplacizumab arm had a 39% reduction in the median time to response compared to patients in the placebo arm (P=0.005).
The rate of confirmed response was 86.1% (n=31) in the caplacizumab arm and 71.8% (n=28) in the placebo arm.
There were more relapses in the caplacizumab arm than the placebo arm—8 (22.2%) and 0, respectively. Relapse was defined as a TTP event occurring more than 30 days after the end of daily plasma exchange.
There were fewer exacerbations in the caplacizumab arm than the placebo arm—3 (8.3%) and 11 (28.2%), respectively. Exacerbation was defined as recurrent thrombocytopenia within 30 days of the end of daily plasma exchange that required re-initiation of daily exchange.
The rate of adverse events thought to be related to the study drug was 17% in the caplacizumab arm and 11% in the placebo arm. The rate of events that were possibly related was 54% and 8%, respectively.
A lower proportion of subjects in the caplacizumab arm experienced one or more major thromboembolic events or died, compared to the placebo arm—11.4% and 43.2%, respectively.
In addition, fewer caplacizumab-treated patients were refractory to treatment—5.7% vs 21.6%.
There were 2 deaths in the placebo arm, and both of those patients were refractory to treatment. There were no deaths reported in the caplacizumab arm.
Now, researchers are evaluating caplacizumab in the phase 3 HERCULES trial (NCT02553317). Results from this study are anticipated in the second half of 2017 are expected to support a planned biologics license application filing in the US in 2018. ![]()
The US Food and Drug Administration (FDA) has granted fast track designation to caplacizumab, an anti-von Willebrand factor (vWF) nanobody being developed for the treatment of acquired thrombotic thrombocytopenic purpura (aTTP).
The FDA’s fast track program is designed to facilitate the development and expedite the review of products intended to treat or prevent serious or life-threatening conditions and address unmet medical need.
Through the fast track program, a product may be eligible for priority review. In addition, the company developing the product may be allowed to submit sections of the new drug application or biologics license application on a rolling basis as data become available.
Fast track designation also provides the company with opportunities for more frequent meetings and written communications with the FDA.
About caplacizumab
Caplacizumab is a bivalent anti-vWF nanobody being developed by Ablynx. Caplacizumab works by blocking the interaction of ultra-large vWF multimers with platelets, having an immediate effect on platelet aggregation and the ensuing formation and accumulation of the micro-clots that cause the severe thrombocytopenia, tissue ischemia, and organ dysfunction that occurs in patients with aTTP.
Researchers evaluated the efficacy and safety of caplacizumab, given with standard care for aTTP, in the phase 2 TITAN trial.
The trial enrolled 75 patients with aTTP. They all received the standard of care—daily plasma exchange and immunosuppressive therapy. Thirty-six patients were randomized to receive caplacizumab as well, and 39 were randomized to placebo.
The study’s primary endpoint was time to response (platelet count normalization). Patients in the caplacizumab arm had a 39% reduction in the median time to response compared to patients in the placebo arm (P=0.005).
The rate of confirmed response was 86.1% (n=31) in the caplacizumab arm and 71.8% (n=28) in the placebo arm.
There were more relapses in the caplacizumab arm than the placebo arm—8 (22.2%) and 0, respectively. Relapse was defined as a TTP event occurring more than 30 days after the end of daily plasma exchange.
There were fewer exacerbations in the caplacizumab arm than the placebo arm—3 (8.3%) and 11 (28.2%), respectively. Exacerbation was defined as recurrent thrombocytopenia within 30 days of the end of daily plasma exchange that required re-initiation of daily exchange.
The rate of adverse events thought to be related to the study drug was 17% in the caplacizumab arm and 11% in the placebo arm. The rate of events that were possibly related was 54% and 8%, respectively.
A lower proportion of subjects in the caplacizumab arm experienced one or more major thromboembolic events or died, compared to the placebo arm—11.4% and 43.2%, respectively.
In addition, fewer caplacizumab-treated patients were refractory to treatment—5.7% vs 21.6%.
There were 2 deaths in the placebo arm, and both of those patients were refractory to treatment. There were no deaths reported in the caplacizumab arm.
Now, researchers are evaluating caplacizumab in the phase 3 HERCULES trial (NCT02553317). Results from this study are anticipated in the second half of 2017 are expected to support a planned biologics license application filing in the US in 2018. ![]()
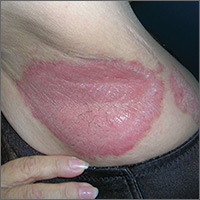
Bilateral axillary rash
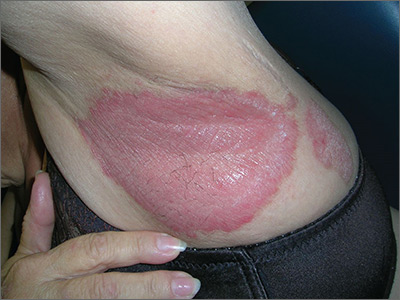
The FP diagnosed inverse psoriasis. Important clues that pointed to the diagnosis included the history of the rash not resolving with antifungal medications or after stopping use of deodorant (evidence that this was unlikely to be contact dermatitis), along with the fingernail pits.
Inverse psoriasis is found in the intertriginous areas of the axillae, groin, inframammary folds, and intergluteal fold. “Inverse” refers to the fact that the distribution is not on extensor surfaces, but in areas of body folds. Morphologically, the lesions have little to no visible scale and, therefore, are not easily recognized as psoriasis. The color is generally pink to red, but can be hyperpigmented in dark-skinned individuals.
Inverse psoriasis often mimics Candida and tinea infections; when antifungal medicines are not working, always consider inverse psoriasis. Not all erythematous plaques in the axillae are fungal. It helps to look for clues such as nail changes (such as the pits noted with this patient) or subtle plaques on the elbows, knees, or umbilicus to make the diagnosis of psoriasis.
Treatment consists of a mid- to high-potency topical steroid. The choice of vehicle can be based on patient preference; creams and ointments both work to treat inverse psoriasis.
In this case, the FP prescribed a mid-potency topical corticosteroid (0.1% triamcinolone ointment) to be applied twice daily. Both the FP and the patient agreed that an ointment, rather than a cream, would be the better option. While the ointment can be greasy, creams often have an alcohol base and are thus more likely than a petrolatum ointment to sting.
The FP also checked for psoriasis risk factors and discovered that the patient was neither smoking nor drinking alcohol. However, the patient was overweight and agreed to improve her diet and exercise for reasonable weight loss.
At her follow-up 2 months later, the patient’s psoriasis was 90% better. She had also lost 5 pounds. While discussing treatment options, a joint decision was made to try a higher-potency topical steroid ointment with the goal of 100% clearance. The patient understood the risk of skin atrophy and was given instructions to return to the mid-potency steroid once the higher-potency steroid achieved satisfactory results.
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Usatine R. Psoriasis. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013: 878-895.
To learn more about the Color Atlas of Family Medicine, see: www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/
You can now get the second edition of the Color Atlas of Family Medicine as an app by clicking on this link: usatinemedia.com

The FP diagnosed inverse psoriasis. Important clues that pointed to the diagnosis included the history of the rash not resolving with antifungal medications or after stopping use of deodorant (evidence that this was unlikely to be contact dermatitis), along with the fingernail pits.
Inverse psoriasis is found in the intertriginous areas of the axillae, groin, inframammary folds, and intergluteal fold. “Inverse” refers to the fact that the distribution is not on extensor surfaces, but in areas of body folds. Morphologically, the lesions have little to no visible scale and, therefore, are not easily recognized as psoriasis. The color is generally pink to red, but can be hyperpigmented in dark-skinned individuals.
Inverse psoriasis often mimics Candida and tinea infections; when antifungal medicines are not working, always consider inverse psoriasis. Not all erythematous plaques in the axillae are fungal. It helps to look for clues such as nail changes (such as the pits noted with this patient) or subtle plaques on the elbows, knees, or umbilicus to make the diagnosis of psoriasis.
Treatment consists of a mid- to high-potency topical steroid. The choice of vehicle can be based on patient preference; creams and ointments both work to treat inverse psoriasis.
In this case, the FP prescribed a mid-potency topical corticosteroid (0.1% triamcinolone ointment) to be applied twice daily. Both the FP and the patient agreed that an ointment, rather than a cream, would be the better option. While the ointment can be greasy, creams often have an alcohol base and are thus more likely than a petrolatum ointment to sting.
The FP also checked for psoriasis risk factors and discovered that the patient was neither smoking nor drinking alcohol. However, the patient was overweight and agreed to improve her diet and exercise for reasonable weight loss.
At her follow-up 2 months later, the patient’s psoriasis was 90% better. She had also lost 5 pounds. While discussing treatment options, a joint decision was made to try a higher-potency topical steroid ointment with the goal of 100% clearance. The patient understood the risk of skin atrophy and was given instructions to return to the mid-potency steroid once the higher-potency steroid achieved satisfactory results.
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Usatine R. Psoriasis. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013: 878-895.
To learn more about the Color Atlas of Family Medicine, see: www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/
You can now get the second edition of the Color Atlas of Family Medicine as an app by clicking on this link: usatinemedia.com

The FP diagnosed inverse psoriasis. Important clues that pointed to the diagnosis included the history of the rash not resolving with antifungal medications or after stopping use of deodorant (evidence that this was unlikely to be contact dermatitis), along with the fingernail pits.
Inverse psoriasis is found in the intertriginous areas of the axillae, groin, inframammary folds, and intergluteal fold. “Inverse” refers to the fact that the distribution is not on extensor surfaces, but in areas of body folds. Morphologically, the lesions have little to no visible scale and, therefore, are not easily recognized as psoriasis. The color is generally pink to red, but can be hyperpigmented in dark-skinned individuals.
Inverse psoriasis often mimics Candida and tinea infections; when antifungal medicines are not working, always consider inverse psoriasis. Not all erythematous plaques in the axillae are fungal. It helps to look for clues such as nail changes (such as the pits noted with this patient) or subtle plaques on the elbows, knees, or umbilicus to make the diagnosis of psoriasis.
Treatment consists of a mid- to high-potency topical steroid. The choice of vehicle can be based on patient preference; creams and ointments both work to treat inverse psoriasis.
In this case, the FP prescribed a mid-potency topical corticosteroid (0.1% triamcinolone ointment) to be applied twice daily. Both the FP and the patient agreed that an ointment, rather than a cream, would be the better option. While the ointment can be greasy, creams often have an alcohol base and are thus more likely than a petrolatum ointment to sting.
The FP also checked for psoriasis risk factors and discovered that the patient was neither smoking nor drinking alcohol. However, the patient was overweight and agreed to improve her diet and exercise for reasonable weight loss.
At her follow-up 2 months later, the patient’s psoriasis was 90% better. She had also lost 5 pounds. While discussing treatment options, a joint decision was made to try a higher-potency topical steroid ointment with the goal of 100% clearance. The patient understood the risk of skin atrophy and was given instructions to return to the mid-potency steroid once the higher-potency steroid achieved satisfactory results.
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Usatine R. Psoriasis. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013: 878-895.
To learn more about the Color Atlas of Family Medicine, see: www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/
You can now get the second edition of the Color Atlas of Family Medicine as an app by clicking on this link: usatinemedia.com
C diff infection among U.S. ED patients
Title: C. diff infection common in emergency department patients, even without risk factors.
Clinical Question: Should all emergency department (ED) patients with diarrhea, without vomiting, get tested for Clostridium difficile?
Background: C. difficile infection has been described in low-risk patients in retrospective studies, but the prevalence in a prospective cohort has not been evaluated.
Setting: Ten urban, university-affiliated EDs in the United States between 2010 and 2013.
Synopsis: 422 patients met the inclusion of criteria of age older than 2, at least three diarrhea episodes in 24 hours, and absence of vomiting. The prevalence of C. difficile by stool culture and toxin assay was 10.2% (43/422; 95% CI, 7.7%-13.4%). The prevalence was 6.9% among patients without traditional risk factors defined as prior history of C. difficile, overnight health care stay, or antibiotic exposure in the last 3 months. The biggest limitation for this study is that the prevalence of C. difficile in the “low-risk” group may be overestimated given that factors such as use of antacids, history of inflammatory bowel disease, and immune suppression were not considered traditional risk factors. Also, 15 of the C. difficile samples were obtained via rectal swab, which is not standard of diagnosis.
Bottom Line: The absence of traditional risk factors does not exclude the presence of C. difficile infection, which should be considered in ED patients with diarrhea and no vomiting.
Citation: Abrahamian FM, Talan DA, Krishnadasan A, Citron DM, Paulick AL, Anderson LJ, et al. Clostridium difficile infection among U.S. emergency department patients with diarrhea and no vomiting. Ann Emerg Med. 2017; doi: 10.1016/j.annemergmed.2016.12.013.
Dr. Ayoubieh is assistant professor in the division of hospital medicine at the University of New Mexico.
Title: C. diff infection common in emergency department patients, even without risk factors.
Clinical Question: Should all emergency department (ED) patients with diarrhea, without vomiting, get tested for Clostridium difficile?
Background: C. difficile infection has been described in low-risk patients in retrospective studies, but the prevalence in a prospective cohort has not been evaluated.
Setting: Ten urban, university-affiliated EDs in the United States between 2010 and 2013.
Synopsis: 422 patients met the inclusion of criteria of age older than 2, at least three diarrhea episodes in 24 hours, and absence of vomiting. The prevalence of C. difficile by stool culture and toxin assay was 10.2% (43/422; 95% CI, 7.7%-13.4%). The prevalence was 6.9% among patients without traditional risk factors defined as prior history of C. difficile, overnight health care stay, or antibiotic exposure in the last 3 months. The biggest limitation for this study is that the prevalence of C. difficile in the “low-risk” group may be overestimated given that factors such as use of antacids, history of inflammatory bowel disease, and immune suppression were not considered traditional risk factors. Also, 15 of the C. difficile samples were obtained via rectal swab, which is not standard of diagnosis.
Bottom Line: The absence of traditional risk factors does not exclude the presence of C. difficile infection, which should be considered in ED patients with diarrhea and no vomiting.
Citation: Abrahamian FM, Talan DA, Krishnadasan A, Citron DM, Paulick AL, Anderson LJ, et al. Clostridium difficile infection among U.S. emergency department patients with diarrhea and no vomiting. Ann Emerg Med. 2017; doi: 10.1016/j.annemergmed.2016.12.013.
Dr. Ayoubieh is assistant professor in the division of hospital medicine at the University of New Mexico.
Title: C. diff infection common in emergency department patients, even without risk factors.
Clinical Question: Should all emergency department (ED) patients with diarrhea, without vomiting, get tested for Clostridium difficile?
Background: C. difficile infection has been described in low-risk patients in retrospective studies, but the prevalence in a prospective cohort has not been evaluated.
Setting: Ten urban, university-affiliated EDs in the United States between 2010 and 2013.
Synopsis: 422 patients met the inclusion of criteria of age older than 2, at least three diarrhea episodes in 24 hours, and absence of vomiting. The prevalence of C. difficile by stool culture and toxin assay was 10.2% (43/422; 95% CI, 7.7%-13.4%). The prevalence was 6.9% among patients without traditional risk factors defined as prior history of C. difficile, overnight health care stay, or antibiotic exposure in the last 3 months. The biggest limitation for this study is that the prevalence of C. difficile in the “low-risk” group may be overestimated given that factors such as use of antacids, history of inflammatory bowel disease, and immune suppression were not considered traditional risk factors. Also, 15 of the C. difficile samples were obtained via rectal swab, which is not standard of diagnosis.
Bottom Line: The absence of traditional risk factors does not exclude the presence of C. difficile infection, which should be considered in ED patients with diarrhea and no vomiting.
Citation: Abrahamian FM, Talan DA, Krishnadasan A, Citron DM, Paulick AL, Anderson LJ, et al. Clostridium difficile infection among U.S. emergency department patients with diarrhea and no vomiting. Ann Emerg Med. 2017; doi: 10.1016/j.annemergmed.2016.12.013.
Dr. Ayoubieh is assistant professor in the division of hospital medicine at the University of New Mexico.
Youth perfectionism: Too much of a good thing
SAN FRANCISCO – Maladaptive perfectionism contributes to and is a risk factor for many common psychiatric disorders in children and adolescents, panelists said at the annual conference of the Anxiety and Depression Association of America.
“Perfectionism isn’t a disorder, it’s a personality style. Some of the kids who come in don’t meet criteria for any psychiatric disorder, they just have this personality style that really warrants treatment, because it is getting in the way of their living happy and productive lives. But I would say most of the time we see overlap with DSM Axis I disorders,” said Deborah Ledley, PhD, a clinical psychologist at the Children’s and Adult Center for OCD and Anxiety in Plymouth Meeting, Pa.
“Basically, when people present with multiple disorders and underlying perfectionism, it might actually be more effective to target the perfectionism, rather than treating each disorder sequentially,” according to Dr. Ledley. “Do we really need to treat social anxiety and panic disorder, and a subclinical eating disorder, or can we say, ‘This person is a perfectionist – let us treat that and see if we can remit all those disorders.’”
That strategy often has proved successful for Dr. Ledley and her fellow panelist Lynne Siqueland, PhD, who also practices at the center. Both specialize in cognitive-behavioral therapy (CBT). They were quick to note that there are essentially no published studies on CBT for pediatric perfectionism. Nonetheless, they have found CBT to be quite effective in clinical practice, with the caveat that the standard, full-speed-ahead, 12-sessions-and-we’re done manualized approach to CBT as often applied to anxiety disorders, depression, and other CBT-amenable disorders will not work for perfectionistic youths.
Dr. Ledley agreed. “We are not rushing with these patients,” she said. “This is so different from the way we are with an OCD patient, for example. When I have an OCD patient, I have the initial session with the parents, then an assessment session with the kid, then in the next session, I do some psychoeducation, and in the session after that, I’m doing exposures, because I work fast. Working with perfectionist kids is different: I have to earn their trust. I tell them a lot of stories about patients I’ve worked with who are just like them.”
How to spot maladaptive perfectionism
When the therapists meet with the parents for the first time – generally without the kids present – what they hear over and over again is, “My child is wound like a spring.” These are generally children who excel at everything: school, sports, music lessons, and other activities. And they are stressed out.
“These are the kids who are working on their Beethoven at age 8, trying to master the Moonlight Sonata. But the parents say the child is too hard on himself, freaking out over a grade less than 100% on a small quiz,” Dr. Ledley observed.
Sometimes, though, perfectionism backfires even in grade school, and the parents’ concern is not that their child is super accomplished yet not enjoying it, but rather that their kid has great potential and never gets anything done because of procrastination or an inability to hand in work that is less than perfect.
Dr. Ledley said when she first meets a perfectionist child, she typically sees a kid who looks perfect, has impeccable manners, and is mature beyond their years.
“They’re invested in coming across as successful in every way. They definitely do not let their guard down when you first meet them. But with these kids who look so perfect, we feel that there’s this fragility and fear, and delicacy lurking just below the surface. It’s almost like they’re afraid they’re going to break because they’re so held together,” according to the psychologist.
Once trust has been established and the youth has drawn up a requested list of the pros and cons of their perfectionism, Dr. Siqueland said, she hears a familiar refrain: “No freedom, no fun, no choice, no time for friends, tired all the time, and no sleep. That’s the usual list of the kids.”
The notion that hard-driving parents typically are at fault for pushing their child into perfectionism is a misconception.
“In our practice, I would say it’s self-induced perfectionism in 75% of cases,” according to Dr. Siqueland.
Treatment tips
After spending considerable time establishing rapport with a perfectionist youth, Dr. Ledley and Dr. Siqueland emphasize three key messages:
1. While on the surface your perfectionist strategy makes sense, enabling you to bask in positive feedback from teachers, coaches, friends, and in some cases your parents, it simply can’t be kept up long term.
“To the ones who really want to go to college and med school, I just say, ‘It’s not going to work there. You’ll not survive college. Or maybe college, but certainly not med school. So are you going to fix it now or fix it later? If you want med school as a goal, let’s help you get there,’ ” Dr. Siqueland said.
2. Therapy is not about changing your values.
“They fear that, if they don’t push and sacrifice, they’re going to be average, or even a slacker – and slacker might be worse than average,” Dr. Siqueland continued.
“We tell them it’s OK to have a drive for excellence, to go after your dream, and to take pride in good work well done. These are your values, and that’s great. We are not in the business of turning you into a slacker,” Dr. Ledley added.
3. Perfectionism takes away choices.
Therapy is all about helping you to live your life rather than having anxiety order you around. You can learn to have freedom, fun, choice, and sleep while in most cases doing as well as or better than before on your grades.
For clinicians who are inexperienced in addressing perfectionism in youth, Dr. Ledley and Dr. Siqueland recommended as a useful primer “The Perfectionism Workbook for Teens” (Oakland, Calif.: New Harbinger Publications, 2016).
They reported having no financial conflicts of interest.
SAN FRANCISCO – Maladaptive perfectionism contributes to and is a risk factor for many common psychiatric disorders in children and adolescents, panelists said at the annual conference of the Anxiety and Depression Association of America.
“Perfectionism isn’t a disorder, it’s a personality style. Some of the kids who come in don’t meet criteria for any psychiatric disorder, they just have this personality style that really warrants treatment, because it is getting in the way of their living happy and productive lives. But I would say most of the time we see overlap with DSM Axis I disorders,” said Deborah Ledley, PhD, a clinical psychologist at the Children’s and Adult Center for OCD and Anxiety in Plymouth Meeting, Pa.
“Basically, when people present with multiple disorders and underlying perfectionism, it might actually be more effective to target the perfectionism, rather than treating each disorder sequentially,” according to Dr. Ledley. “Do we really need to treat social anxiety and panic disorder, and a subclinical eating disorder, or can we say, ‘This person is a perfectionist – let us treat that and see if we can remit all those disorders.’”
That strategy often has proved successful for Dr. Ledley and her fellow panelist Lynne Siqueland, PhD, who also practices at the center. Both specialize in cognitive-behavioral therapy (CBT). They were quick to note that there are essentially no published studies on CBT for pediatric perfectionism. Nonetheless, they have found CBT to be quite effective in clinical practice, with the caveat that the standard, full-speed-ahead, 12-sessions-and-we’re done manualized approach to CBT as often applied to anxiety disorders, depression, and other CBT-amenable disorders will not work for perfectionistic youths.
Dr. Ledley agreed. “We are not rushing with these patients,” she said. “This is so different from the way we are with an OCD patient, for example. When I have an OCD patient, I have the initial session with the parents, then an assessment session with the kid, then in the next session, I do some psychoeducation, and in the session after that, I’m doing exposures, because I work fast. Working with perfectionist kids is different: I have to earn their trust. I tell them a lot of stories about patients I’ve worked with who are just like them.”
How to spot maladaptive perfectionism
When the therapists meet with the parents for the first time – generally without the kids present – what they hear over and over again is, “My child is wound like a spring.” These are generally children who excel at everything: school, sports, music lessons, and other activities. And they are stressed out.
“These are the kids who are working on their Beethoven at age 8, trying to master the Moonlight Sonata. But the parents say the child is too hard on himself, freaking out over a grade less than 100% on a small quiz,” Dr. Ledley observed.
Sometimes, though, perfectionism backfires even in grade school, and the parents’ concern is not that their child is super accomplished yet not enjoying it, but rather that their kid has great potential and never gets anything done because of procrastination or an inability to hand in work that is less than perfect.
Dr. Ledley said when she first meets a perfectionist child, she typically sees a kid who looks perfect, has impeccable manners, and is mature beyond their years.
“They’re invested in coming across as successful in every way. They definitely do not let their guard down when you first meet them. But with these kids who look so perfect, we feel that there’s this fragility and fear, and delicacy lurking just below the surface. It’s almost like they’re afraid they’re going to break because they’re so held together,” according to the psychologist.
Once trust has been established and the youth has drawn up a requested list of the pros and cons of their perfectionism, Dr. Siqueland said, she hears a familiar refrain: “No freedom, no fun, no choice, no time for friends, tired all the time, and no sleep. That’s the usual list of the kids.”
The notion that hard-driving parents typically are at fault for pushing their child into perfectionism is a misconception.
“In our practice, I would say it’s self-induced perfectionism in 75% of cases,” according to Dr. Siqueland.
Treatment tips
After spending considerable time establishing rapport with a perfectionist youth, Dr. Ledley and Dr. Siqueland emphasize three key messages:
1. While on the surface your perfectionist strategy makes sense, enabling you to bask in positive feedback from teachers, coaches, friends, and in some cases your parents, it simply can’t be kept up long term.
“To the ones who really want to go to college and med school, I just say, ‘It’s not going to work there. You’ll not survive college. Or maybe college, but certainly not med school. So are you going to fix it now or fix it later? If you want med school as a goal, let’s help you get there,’ ” Dr. Siqueland said.
2. Therapy is not about changing your values.
“They fear that, if they don’t push and sacrifice, they’re going to be average, or even a slacker – and slacker might be worse than average,” Dr. Siqueland continued.
“We tell them it’s OK to have a drive for excellence, to go after your dream, and to take pride in good work well done. These are your values, and that’s great. We are not in the business of turning you into a slacker,” Dr. Ledley added.
3. Perfectionism takes away choices.
Therapy is all about helping you to live your life rather than having anxiety order you around. You can learn to have freedom, fun, choice, and sleep while in most cases doing as well as or better than before on your grades.
For clinicians who are inexperienced in addressing perfectionism in youth, Dr. Ledley and Dr. Siqueland recommended as a useful primer “The Perfectionism Workbook for Teens” (Oakland, Calif.: New Harbinger Publications, 2016).
They reported having no financial conflicts of interest.
SAN FRANCISCO – Maladaptive perfectionism contributes to and is a risk factor for many common psychiatric disorders in children and adolescents, panelists said at the annual conference of the Anxiety and Depression Association of America.
“Perfectionism isn’t a disorder, it’s a personality style. Some of the kids who come in don’t meet criteria for any psychiatric disorder, they just have this personality style that really warrants treatment, because it is getting in the way of their living happy and productive lives. But I would say most of the time we see overlap with DSM Axis I disorders,” said Deborah Ledley, PhD, a clinical psychologist at the Children’s and Adult Center for OCD and Anxiety in Plymouth Meeting, Pa.
“Basically, when people present with multiple disorders and underlying perfectionism, it might actually be more effective to target the perfectionism, rather than treating each disorder sequentially,” according to Dr. Ledley. “Do we really need to treat social anxiety and panic disorder, and a subclinical eating disorder, or can we say, ‘This person is a perfectionist – let us treat that and see if we can remit all those disorders.’”
That strategy often has proved successful for Dr. Ledley and her fellow panelist Lynne Siqueland, PhD, who also practices at the center. Both specialize in cognitive-behavioral therapy (CBT). They were quick to note that there are essentially no published studies on CBT for pediatric perfectionism. Nonetheless, they have found CBT to be quite effective in clinical practice, with the caveat that the standard, full-speed-ahead, 12-sessions-and-we’re done manualized approach to CBT as often applied to anxiety disorders, depression, and other CBT-amenable disorders will not work for perfectionistic youths.
Dr. Ledley agreed. “We are not rushing with these patients,” she said. “This is so different from the way we are with an OCD patient, for example. When I have an OCD patient, I have the initial session with the parents, then an assessment session with the kid, then in the next session, I do some psychoeducation, and in the session after that, I’m doing exposures, because I work fast. Working with perfectionist kids is different: I have to earn their trust. I tell them a lot of stories about patients I’ve worked with who are just like them.”
How to spot maladaptive perfectionism
When the therapists meet with the parents for the first time – generally without the kids present – what they hear over and over again is, “My child is wound like a spring.” These are generally children who excel at everything: school, sports, music lessons, and other activities. And they are stressed out.
“These are the kids who are working on their Beethoven at age 8, trying to master the Moonlight Sonata. But the parents say the child is too hard on himself, freaking out over a grade less than 100% on a small quiz,” Dr. Ledley observed.
Sometimes, though, perfectionism backfires even in grade school, and the parents’ concern is not that their child is super accomplished yet not enjoying it, but rather that their kid has great potential and never gets anything done because of procrastination or an inability to hand in work that is less than perfect.
Dr. Ledley said when she first meets a perfectionist child, she typically sees a kid who looks perfect, has impeccable manners, and is mature beyond their years.
“They’re invested in coming across as successful in every way. They definitely do not let their guard down when you first meet them. But with these kids who look so perfect, we feel that there’s this fragility and fear, and delicacy lurking just below the surface. It’s almost like they’re afraid they’re going to break because they’re so held together,” according to the psychologist.
Once trust has been established and the youth has drawn up a requested list of the pros and cons of their perfectionism, Dr. Siqueland said, she hears a familiar refrain: “No freedom, no fun, no choice, no time for friends, tired all the time, and no sleep. That’s the usual list of the kids.”
The notion that hard-driving parents typically are at fault for pushing their child into perfectionism is a misconception.
“In our practice, I would say it’s self-induced perfectionism in 75% of cases,” according to Dr. Siqueland.
Treatment tips
After spending considerable time establishing rapport with a perfectionist youth, Dr. Ledley and Dr. Siqueland emphasize three key messages:
1. While on the surface your perfectionist strategy makes sense, enabling you to bask in positive feedback from teachers, coaches, friends, and in some cases your parents, it simply can’t be kept up long term.
“To the ones who really want to go to college and med school, I just say, ‘It’s not going to work there. You’ll not survive college. Or maybe college, but certainly not med school. So are you going to fix it now or fix it later? If you want med school as a goal, let’s help you get there,’ ” Dr. Siqueland said.
2. Therapy is not about changing your values.
“They fear that, if they don’t push and sacrifice, they’re going to be average, or even a slacker – and slacker might be worse than average,” Dr. Siqueland continued.
“We tell them it’s OK to have a drive for excellence, to go after your dream, and to take pride in good work well done. These are your values, and that’s great. We are not in the business of turning you into a slacker,” Dr. Ledley added.
3. Perfectionism takes away choices.
Therapy is all about helping you to live your life rather than having anxiety order you around. You can learn to have freedom, fun, choice, and sleep while in most cases doing as well as or better than before on your grades.
For clinicians who are inexperienced in addressing perfectionism in youth, Dr. Ledley and Dr. Siqueland recommended as a useful primer “The Perfectionism Workbook for Teens” (Oakland, Calif.: New Harbinger Publications, 2016).
They reported having no financial conflicts of interest.
EXPERT ANALYSIS FROM THE ANXIETY AND DEPRESSION CONFERENCE 2017
FLT3-L level may point to relapsed/refractory multiple myeloma
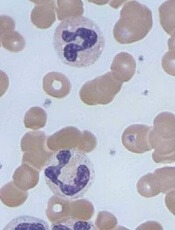
FLT3-ligand (FLT3-L) levels exceeding 92 pg/mL in bone marrow and 121 pg/mL in peripheral blood are associated with relapsed and refractory disease in patients with multiple myeloma, Normann Steiner, MD, and his colleagues report in a study published in PLoS ONE.
In the study of 14 patients with monoclonal gamm opathy of undetermined significance (MGUS), 42 patients with newly diagnosed myeloma, and 27 patients with relapsed/refractory myeloma, there was a 61% probability that patients with FLT3-L levels above 92 pg/mL in bone marrow had relapsed or refractory multiple myeloma and a 79% probability that those with FLT3-L levels of 92 pg/mL or less had not relapsed and were not refractory. Based on FLT3-L levels in peripheral blood, values of 121 pg/mL or more were associated with a 71% probability of relapsed or refractory disease. The likelihood of not having relapses or refractory disease was 87% for patients with values less than 121 pg/mL.
“FLT3-L could be useful as a marker to identify (relapsed or refractory multiple myeloma) patients and should be evaluated as a potential target for future therapy strategies,” Dr. Steiner of Innsbruck (Austria) Medical University, and his fellow researchers wrote in PLoS ONE.
The researchers obtained bone marrow aspirates from all patients. Peripheral blood was examined from 4 MGUS patients, 31 patients with newly diagnosed myeloma, and 16 patients with relapsed or refractory myeloma. Peripheral blood was also obtained from 16 control subjects.
The levels of four potential risk factors were measured – soluble TIE2, FLT3-L, endostatin, and osteoactivin. The most significant association with risk was seen with FLT3-L levels.
Expression of soluble TIE2 in bone marrow differed significantly among the three patient cohorts and may be driven by the same factors that influence FLT3-L levels. However, soluble TIE2 levels were not as effective at differentiating patients at risk for disease progression, the researchers wrote.
Soluble TIE2 expression in bone marrow was highest in MGUS patients (median 4003.97 pg/mL) in comparison to relapsed or refractory disease (median 2223.26 pg/mL; P = .03) and to newly diagnosed patients with myeloma (median 861.98 pg/mL; P less than .001). A statistically significant difference among bone marrow levels of soluble TIE2 was observed for newly diagnosed patients and those with relapsed or refractory disease (P = .03).
However, soluble TIE2 in peripheral blood plasma did not differ significantly in the three cohorts nor did it differ between patients and controls.
In contrast to TIE2 and FLT3-L, levels of endostatin were lowest (median 146.50 ng/mL) in bone marrow plasma samples of patients with relapsed or refractory disease. Levels were higher in MGUS patients (median 190.37 mg/dL) than in newly diagnosed myeloma patients (median 170.15 mg/mL; P = .5).
Similar to soluble TIE2, plasma levels of endostatin in peripheral blood did not differ significantly in the three patient cohorts. Measurements of endostatin in bone marrow and peripheral blood correlated significantly (P less than .001), and peripheral blood levels differed significantly (P less than .001) for patients and control persons.
Osteoactivin expression was highest in the MGUS cohort, with median bone marrow plasma levels of 36 ng/mL as compared with median levels of 24.92 ng/mL in newly diagnosed myeloma patients and 22.30 ng/mL in patients with relapsed or refractory myeloma. Osteoactivin levels in peripheral blood did not differ significantly in the three cohorts, but differed between patients and control subjects. Osteoactivin measures in bone marrow and peripheral blood correlated significantly.
Citation: Steiner N, et al. High levels of FLT3-ligand in bone marrow and peripheral blood of patients with advanced multiple myeloma. PLoS ONE 2017 Jul 20;12:e0181487. doi. org/10.1371/journal.pone.0181487.
[email protected]
On Twitter @maryjodales
FLT3-ligand (FLT3-L) levels exceeding 92 pg/mL in bone marrow and 121 pg/mL in peripheral blood are associated with relapsed and refractory disease in patients with multiple myeloma, Normann Steiner, MD, and his colleagues report in a study published in PLoS ONE.
In the study of 14 patients with monoclonal gamm opathy of undetermined significance (MGUS), 42 patients with newly diagnosed myeloma, and 27 patients with relapsed/refractory myeloma, there was a 61% probability that patients with FLT3-L levels above 92 pg/mL in bone marrow had relapsed or refractory multiple myeloma and a 79% probability that those with FLT3-L levels of 92 pg/mL or less had not relapsed and were not refractory. Based on FLT3-L levels in peripheral blood, values of 121 pg/mL or more were associated with a 71% probability of relapsed or refractory disease. The likelihood of not having relapses or refractory disease was 87% for patients with values less than 121 pg/mL.
“FLT3-L could be useful as a marker to identify (relapsed or refractory multiple myeloma) patients and should be evaluated as a potential target for future therapy strategies,” Dr. Steiner of Innsbruck (Austria) Medical University, and his fellow researchers wrote in PLoS ONE.
The researchers obtained bone marrow aspirates from all patients. Peripheral blood was examined from 4 MGUS patients, 31 patients with newly diagnosed myeloma, and 16 patients with relapsed or refractory myeloma. Peripheral blood was also obtained from 16 control subjects.
The levels of four potential risk factors were measured – soluble TIE2, FLT3-L, endostatin, and osteoactivin. The most significant association with risk was seen with FLT3-L levels.
Expression of soluble TIE2 in bone marrow differed significantly among the three patient cohorts and may be driven by the same factors that influence FLT3-L levels. However, soluble TIE2 levels were not as effective at differentiating patients at risk for disease progression, the researchers wrote.
Soluble TIE2 expression in bone marrow was highest in MGUS patients (median 4003.97 pg/mL) in comparison to relapsed or refractory disease (median 2223.26 pg/mL; P = .03) and to newly diagnosed patients with myeloma (median 861.98 pg/mL; P less than .001). A statistically significant difference among bone marrow levels of soluble TIE2 was observed for newly diagnosed patients and those with relapsed or refractory disease (P = .03).
However, soluble TIE2 in peripheral blood plasma did not differ significantly in the three cohorts nor did it differ between patients and controls.
In contrast to TIE2 and FLT3-L, levels of endostatin were lowest (median 146.50 ng/mL) in bone marrow plasma samples of patients with relapsed or refractory disease. Levels were higher in MGUS patients (median 190.37 mg/dL) than in newly diagnosed myeloma patients (median 170.15 mg/mL; P = .5).
Similar to soluble TIE2, plasma levels of endostatin in peripheral blood did not differ significantly in the three patient cohorts. Measurements of endostatin in bone marrow and peripheral blood correlated significantly (P less than .001), and peripheral blood levels differed significantly (P less than .001) for patients and control persons.
Osteoactivin expression was highest in the MGUS cohort, with median bone marrow plasma levels of 36 ng/mL as compared with median levels of 24.92 ng/mL in newly diagnosed myeloma patients and 22.30 ng/mL in patients with relapsed or refractory myeloma. Osteoactivin levels in peripheral blood did not differ significantly in the three cohorts, but differed between patients and control subjects. Osteoactivin measures in bone marrow and peripheral blood correlated significantly.
Citation: Steiner N, et al. High levels of FLT3-ligand in bone marrow and peripheral blood of patients with advanced multiple myeloma. PLoS ONE 2017 Jul 20;12:e0181487. doi. org/10.1371/journal.pone.0181487.
[email protected]
On Twitter @maryjodales
FLT3-ligand (FLT3-L) levels exceeding 92 pg/mL in bone marrow and 121 pg/mL in peripheral blood are associated with relapsed and refractory disease in patients with multiple myeloma, Normann Steiner, MD, and his colleagues report in a study published in PLoS ONE.
In the study of 14 patients with monoclonal gamm opathy of undetermined significance (MGUS), 42 patients with newly diagnosed myeloma, and 27 patients with relapsed/refractory myeloma, there was a 61% probability that patients with FLT3-L levels above 92 pg/mL in bone marrow had relapsed or refractory multiple myeloma and a 79% probability that those with FLT3-L levels of 92 pg/mL or less had not relapsed and were not refractory. Based on FLT3-L levels in peripheral blood, values of 121 pg/mL or more were associated with a 71% probability of relapsed or refractory disease. The likelihood of not having relapses or refractory disease was 87% for patients with values less than 121 pg/mL.
“FLT3-L could be useful as a marker to identify (relapsed or refractory multiple myeloma) patients and should be evaluated as a potential target for future therapy strategies,” Dr. Steiner of Innsbruck (Austria) Medical University, and his fellow researchers wrote in PLoS ONE.
The researchers obtained bone marrow aspirates from all patients. Peripheral blood was examined from 4 MGUS patients, 31 patients with newly diagnosed myeloma, and 16 patients with relapsed or refractory myeloma. Peripheral blood was also obtained from 16 control subjects.
The levels of four potential risk factors were measured – soluble TIE2, FLT3-L, endostatin, and osteoactivin. The most significant association with risk was seen with FLT3-L levels.
Expression of soluble TIE2 in bone marrow differed significantly among the three patient cohorts and may be driven by the same factors that influence FLT3-L levels. However, soluble TIE2 levels were not as effective at differentiating patients at risk for disease progression, the researchers wrote.
Soluble TIE2 expression in bone marrow was highest in MGUS patients (median 4003.97 pg/mL) in comparison to relapsed or refractory disease (median 2223.26 pg/mL; P = .03) and to newly diagnosed patients with myeloma (median 861.98 pg/mL; P less than .001). A statistically significant difference among bone marrow levels of soluble TIE2 was observed for newly diagnosed patients and those with relapsed or refractory disease (P = .03).
However, soluble TIE2 in peripheral blood plasma did not differ significantly in the three cohorts nor did it differ between patients and controls.
In contrast to TIE2 and FLT3-L, levels of endostatin were lowest (median 146.50 ng/mL) in bone marrow plasma samples of patients with relapsed or refractory disease. Levels were higher in MGUS patients (median 190.37 mg/dL) than in newly diagnosed myeloma patients (median 170.15 mg/mL; P = .5).
Similar to soluble TIE2, plasma levels of endostatin in peripheral blood did not differ significantly in the three patient cohorts. Measurements of endostatin in bone marrow and peripheral blood correlated significantly (P less than .001), and peripheral blood levels differed significantly (P less than .001) for patients and control persons.
Osteoactivin expression was highest in the MGUS cohort, with median bone marrow plasma levels of 36 ng/mL as compared with median levels of 24.92 ng/mL in newly diagnosed myeloma patients and 22.30 ng/mL in patients with relapsed or refractory myeloma. Osteoactivin levels in peripheral blood did not differ significantly in the three cohorts, but differed between patients and control subjects. Osteoactivin measures in bone marrow and peripheral blood correlated significantly.
Citation: Steiner N, et al. High levels of FLT3-ligand in bone marrow and peripheral blood of patients with advanced multiple myeloma. PLoS ONE 2017 Jul 20;12:e0181487. doi. org/10.1371/journal.pone.0181487.
[email protected]
On Twitter @maryjodales
FROM PLOS ONE
Key clinical point: .
Major finding: There was a 61% probability that patients with FLT3-L levels above 92 pg/mL in bone marrow had relapsed or refractory multiple myeloma and a 79% probability that those with FLT3-L levels of 92 pg/mL or less had not relapsed and were not refractory.
Data source: A study of 14 patients with monoclonal gammopathy of undetermined significance, 42 patients with newly diagnosed myeloma, and 27 patients with relapsed/refractory myeloma, plus 16 control subjects.
Disclosures: The study was not sponsored, and the authors had no relevant disclosures.
Citation: Steiner N, et al. High levels of FLT3-ligand in bone marrow and peripheral blood of patients with advanced multiple myeloma. PLoS ONE 2017 Jul 20;12:e0181487. doi. org/10.1371/journal.pone.0181487
Modifiable risk factors account for most of the dementia risk imposed by low socioeconomic status
LONDON – Twelve modifiable risk factors appear to account for more than half of the variation in dementia risk associated with socioeconomic status.
When integrated into an 18-point risk score, dubbed the “Lifestyle for Brain Health” (LIBRA) index, they accurately predicted dementia risk in more than 6,300 subjects who were followed for 7 years: Dementia risk increased by 30% for every 1-point increase on the LIBRA score, Sebastian Koehler, PhD, said at the Alzheimer’s Association International Conference.
According to Public Health England, 52% of citizens choose dementia prevention as a top health priority, but almost the same number believe that “there is nothing anyone can do to reduce their risk of getting dementia.” The LIBRA score could be employed as a public health measure to counteract that misunderstanding, he said.
“We can reduce the gap in risk that’s related to low socioeconomic status by improving health in that group. But we know that public health measures and messages are taken up much better by those with higher socioeconomic status. We think the first step is to raise awareness among this group that there is something we can do about dementia risk. And then we can reach out to this vulnerable group and design measures and messages that speak to both their needs and their resources.”
The 12 risk and protective factors were originally identified by epidemiologist Kay Deckers of Maastricht University, who drew them from a large meta-analysis published in 2015 (Int J Geriatr Psychiatry. 2015 Mar;30[3]:234-46).
They are the following:
• Diabetes.
• Hypertension.
• High cholesterol.
• Smoking.
• Obesity.
• Physical inactivity.
• Depression.
• Coronary heart disease.
• Kidney disease.
• Diet.
• Alcohol.
• Mental activity.
Dr. Koehler and his colleagues used them to create the weighted LIBRA score, which computes an 18-point risk level ranging from –5.9 (lower risk) to 12.7 (higher risk). Among the factors that reduce dementia risk are high cognitive activity, healthy diet or Mediterranean diet, and low-moderate alcohol intake. The others all increased risk. Each of the factors was assigned a point value based on its percentage of risk reduction or increase. For example, high cognitive activity reduced risk by more than 3 points, but depression increased it by 2 points. The investigators then validated this score on 6,346 participants in the English Longitudinal Study of Ageing, who were followed for up to 7 years.
Dr. Koehler’s study, however, was not just a LIBRA validation study. He wanted to correlate these protective and endangering factors with each subject’s socioeconomic status, and determine how much of the risk difference generally accredited to wealth was related to the LIBRA factors.
After 7 years, about 9% of the study sample developed incident dementia. These subjects were significantly older than those who didn’t (77 vs. 64 years). They were more likely to have lower education attainment (58% vs. 37%), and more likely to be poor (44% vs. 29%).
On the LIBRA risk factors, the participants who developed dementia were significantly more likely to have heart disease, diabetes, hypercholesterolemia, hypertension, and depression, although not significantly more likely to be obese or to smoke.
On the LIBRA protective factors, they were significantly less likely to be low-moderate alcohol users (37% vs. 57%), to have high cognitive activity (17% vs. 45%), and significantly more likely to be physically inactive (59% vs. 24%).
Two survival curves compared the incidence of dementia related to wealth and LIBRA score. Subjects of low socioeconomic status experienced an increase in dementia risk very similar to those with high LIBRA scores. Dr. Koehler also conducted three analyses that examined the effects of wealth on dementia risk: the total effect of wealth, the direct effect of wealth, and what he called the “indirect wealth effect.” This examined the impact of wealth on LIBRA scores, followed by the effect of these scores on dementia risk.
This final model concluded that 56% of the risk imposed by low socioeconomic status was actually attributable to LIBRA scores. In other words, low socioeconomic status was directly tied to both increases in physical and mental risk factors, and decreases in physical and mental protective factors.
“Health inequalities influencing dementia risk exist because of socioeconomic differences between people,” Dr. Koehler said. “People with less wealth have a higher frequency of being exposed to risk factors for dementia that are potentially treatable.”
The LIBRA study is part of a larger dementia prevention study called Innovative, Midlife Intervention for Dementia Deterrence (In-MINDD). Dr. Koehler had no financial disclosures.
[email protected]
On Twitter @alz_gal
LONDON – Twelve modifiable risk factors appear to account for more than half of the variation in dementia risk associated with socioeconomic status.
When integrated into an 18-point risk score, dubbed the “Lifestyle for Brain Health” (LIBRA) index, they accurately predicted dementia risk in more than 6,300 subjects who were followed for 7 years: Dementia risk increased by 30% for every 1-point increase on the LIBRA score, Sebastian Koehler, PhD, said at the Alzheimer’s Association International Conference.
According to Public Health England, 52% of citizens choose dementia prevention as a top health priority, but almost the same number believe that “there is nothing anyone can do to reduce their risk of getting dementia.” The LIBRA score could be employed as a public health measure to counteract that misunderstanding, he said.
“We can reduce the gap in risk that’s related to low socioeconomic status by improving health in that group. But we know that public health measures and messages are taken up much better by those with higher socioeconomic status. We think the first step is to raise awareness among this group that there is something we can do about dementia risk. And then we can reach out to this vulnerable group and design measures and messages that speak to both their needs and their resources.”
The 12 risk and protective factors were originally identified by epidemiologist Kay Deckers of Maastricht University, who drew them from a large meta-analysis published in 2015 (Int J Geriatr Psychiatry. 2015 Mar;30[3]:234-46).
They are the following:
• Diabetes.
• Hypertension.
• High cholesterol.
• Smoking.
• Obesity.
• Physical inactivity.
• Depression.
• Coronary heart disease.
• Kidney disease.
• Diet.
• Alcohol.
• Mental activity.
Dr. Koehler and his colleagues used them to create the weighted LIBRA score, which computes an 18-point risk level ranging from –5.9 (lower risk) to 12.7 (higher risk). Among the factors that reduce dementia risk are high cognitive activity, healthy diet or Mediterranean diet, and low-moderate alcohol intake. The others all increased risk. Each of the factors was assigned a point value based on its percentage of risk reduction or increase. For example, high cognitive activity reduced risk by more than 3 points, but depression increased it by 2 points. The investigators then validated this score on 6,346 participants in the English Longitudinal Study of Ageing, who were followed for up to 7 years.
Dr. Koehler’s study, however, was not just a LIBRA validation study. He wanted to correlate these protective and endangering factors with each subject’s socioeconomic status, and determine how much of the risk difference generally accredited to wealth was related to the LIBRA factors.
After 7 years, about 9% of the study sample developed incident dementia. These subjects were significantly older than those who didn’t (77 vs. 64 years). They were more likely to have lower education attainment (58% vs. 37%), and more likely to be poor (44% vs. 29%).
On the LIBRA risk factors, the participants who developed dementia were significantly more likely to have heart disease, diabetes, hypercholesterolemia, hypertension, and depression, although not significantly more likely to be obese or to smoke.
On the LIBRA protective factors, they were significantly less likely to be low-moderate alcohol users (37% vs. 57%), to have high cognitive activity (17% vs. 45%), and significantly more likely to be physically inactive (59% vs. 24%).
Two survival curves compared the incidence of dementia related to wealth and LIBRA score. Subjects of low socioeconomic status experienced an increase in dementia risk very similar to those with high LIBRA scores. Dr. Koehler also conducted three analyses that examined the effects of wealth on dementia risk: the total effect of wealth, the direct effect of wealth, and what he called the “indirect wealth effect.” This examined the impact of wealth on LIBRA scores, followed by the effect of these scores on dementia risk.
This final model concluded that 56% of the risk imposed by low socioeconomic status was actually attributable to LIBRA scores. In other words, low socioeconomic status was directly tied to both increases in physical and mental risk factors, and decreases in physical and mental protective factors.
“Health inequalities influencing dementia risk exist because of socioeconomic differences between people,” Dr. Koehler said. “People with less wealth have a higher frequency of being exposed to risk factors for dementia that are potentially treatable.”
The LIBRA study is part of a larger dementia prevention study called Innovative, Midlife Intervention for Dementia Deterrence (In-MINDD). Dr. Koehler had no financial disclosures.
[email protected]
On Twitter @alz_gal
LONDON – Twelve modifiable risk factors appear to account for more than half of the variation in dementia risk associated with socioeconomic status.
When integrated into an 18-point risk score, dubbed the “Lifestyle for Brain Health” (LIBRA) index, they accurately predicted dementia risk in more than 6,300 subjects who were followed for 7 years: Dementia risk increased by 30% for every 1-point increase on the LIBRA score, Sebastian Koehler, PhD, said at the Alzheimer’s Association International Conference.
According to Public Health England, 52% of citizens choose dementia prevention as a top health priority, but almost the same number believe that “there is nothing anyone can do to reduce their risk of getting dementia.” The LIBRA score could be employed as a public health measure to counteract that misunderstanding, he said.
“We can reduce the gap in risk that’s related to low socioeconomic status by improving health in that group. But we know that public health measures and messages are taken up much better by those with higher socioeconomic status. We think the first step is to raise awareness among this group that there is something we can do about dementia risk. And then we can reach out to this vulnerable group and design measures and messages that speak to both their needs and their resources.”
The 12 risk and protective factors were originally identified by epidemiologist Kay Deckers of Maastricht University, who drew them from a large meta-analysis published in 2015 (Int J Geriatr Psychiatry. 2015 Mar;30[3]:234-46).
They are the following:
• Diabetes.
• Hypertension.
• High cholesterol.
• Smoking.
• Obesity.
• Physical inactivity.
• Depression.
• Coronary heart disease.
• Kidney disease.
• Diet.
• Alcohol.
• Mental activity.
Dr. Koehler and his colleagues used them to create the weighted LIBRA score, which computes an 18-point risk level ranging from –5.9 (lower risk) to 12.7 (higher risk). Among the factors that reduce dementia risk are high cognitive activity, healthy diet or Mediterranean diet, and low-moderate alcohol intake. The others all increased risk. Each of the factors was assigned a point value based on its percentage of risk reduction or increase. For example, high cognitive activity reduced risk by more than 3 points, but depression increased it by 2 points. The investigators then validated this score on 6,346 participants in the English Longitudinal Study of Ageing, who were followed for up to 7 years.
Dr. Koehler’s study, however, was not just a LIBRA validation study. He wanted to correlate these protective and endangering factors with each subject’s socioeconomic status, and determine how much of the risk difference generally accredited to wealth was related to the LIBRA factors.
After 7 years, about 9% of the study sample developed incident dementia. These subjects were significantly older than those who didn’t (77 vs. 64 years). They were more likely to have lower education attainment (58% vs. 37%), and more likely to be poor (44% vs. 29%).
On the LIBRA risk factors, the participants who developed dementia were significantly more likely to have heart disease, diabetes, hypercholesterolemia, hypertension, and depression, although not significantly more likely to be obese or to smoke.
On the LIBRA protective factors, they were significantly less likely to be low-moderate alcohol users (37% vs. 57%), to have high cognitive activity (17% vs. 45%), and significantly more likely to be physically inactive (59% vs. 24%).
Two survival curves compared the incidence of dementia related to wealth and LIBRA score. Subjects of low socioeconomic status experienced an increase in dementia risk very similar to those with high LIBRA scores. Dr. Koehler also conducted three analyses that examined the effects of wealth on dementia risk: the total effect of wealth, the direct effect of wealth, and what he called the “indirect wealth effect.” This examined the impact of wealth on LIBRA scores, followed by the effect of these scores on dementia risk.
This final model concluded that 56% of the risk imposed by low socioeconomic status was actually attributable to LIBRA scores. In other words, low socioeconomic status was directly tied to both increases in physical and mental risk factors, and decreases in physical and mental protective factors.
“Health inequalities influencing dementia risk exist because of socioeconomic differences between people,” Dr. Koehler said. “People with less wealth have a higher frequency of being exposed to risk factors for dementia that are potentially treatable.”
The LIBRA study is part of a larger dementia prevention study called Innovative, Midlife Intervention for Dementia Deterrence (In-MINDD). Dr. Koehler had no financial disclosures.
[email protected]
On Twitter @alz_gal
AT AAIC 2017
Key clinical point:
Major finding: The factors accounted for 56% of the risk imposed by low SES.
Data source: The LIBRA validation study comprised more than 6,300 subjects.
Disclosures: The LIBRA study is part of a larger dementia prevention study called In-MINDD. Dr. Koehler had no financial disclosures.
Abiraterone plus ADT boosts prostate cancer survival
In findings that are being hailed as practice changing, men with metastatic prostate cancer had a near 40% lower risk of death when they were treated with a combination of abiraterone acetate (Zytiga), androgen deprivation therapy, and prednisone or prednisolone, compared with ADT alone.
After a median follow-up of 30.4 months, median overall survival for men with newly diagnosed metastatic, castration-sensitive prostate cancer treated with ADT plus dual placebos was 34.7 months, vs. not reached for men treated with ADT, abiraterone, and prednisone in the LATITUDE trial. Similarly, in the STAMPEDE trial, men with newly diagnosed locally advanced or metastatic disease who were randomized to ADT with abiraterone and prednisolone had a 37% reduction in their risk for death and a 79% reduction in their risk for treatment failure, compared with men randomized to ADT alone.
The majority of men with metastatic castration-sensitive prostate cancer who are started on androgen deprivation therapy with a luteinizing hormone–releasing hormone (LHRH) analog with or without a first-generation androgen receptor inhibitor will have responses to therapy, but within a median of 1-year most will progress to castration-resistant disease, noted Karim Fizazi, MD, from the Gustave Roussy Cancer Institute at the University of Paris Sud, Villejuif, France, and coinvestigators of the LATITUDE trial.
“Resistance to androgen-deprivation therapy is largely driven by the reactivation of androgen receptor signaling through persistent adrenal androgen production, upregulation of intratumoral testosterone production, modification of the biologic characteristics of androgen receptors, and steroidogenic parallel pathways,” they wrote.
Although ADT and docetaxel is the standard of care for men with metastatic castration-sensitive disease who are eligible for chemotherapy, data from real-world practice suggest that patients with this presentation are older than those enrolled in clinical trials, and may not be able to tolerate the toxicities that occur when docetaxel is added to ADT, they noted.
Abiraterone, in combination with prednisone, has been shown to increase overall survival (OS) in men with metastatic castration-resistant prostate cancer who have not undergone chemotherapy, and among patients who had previously been treated with docetaxel.
The drug is thought to exert its antitumor effects through a combination of androgen receptor antagonism and blockade of steroidogenic enzymes, the investigators wrote.
The LATITUDE trial
LATITUDE investigators from 235 sites in 34 countries in Europe, Asia/Pacific, Latin America and Canada enrolled 1,199 patients with newly diagnosed metastatic castration-sensitive prostate cancer and randomly assigned them to receive either abiraterone and prednisone plus ADT (597 patients), or ADT plus dual placebos (602).
At a planned interim analysis at a median follow-up of 30.4 months, after 406 patients had died, median OS, a co-primary end point, had not been reached among patients in the abiraterone group, compared with 34.7 months for patients assigned to ADT/placebo. This difference translates into a hazard ratio for death of 0.62 (P less than .001).
The median duration of radiographic progression-free survival (PFS), the other primary end point, was 33.0 months among patients treated with abiraterone vs. 14.8 months for those treated with placebo (HR for disease progression or death, 0.47; P less than .001)
Abiraterone was also associated with significantly better outcomes in all secondary endpoints, including time until pain progression, subsequent therapy, initiation of chemotherapy, and prostate-specific antigen (PSA) progression (P less than .001 for each comparison).
The frequency of adverse events leading to treatment discontinuation was 12% for patients in the abiraterone group vs. 10% for those in the placebo group. Rates of grade 3 or 4 hypertension and hypokalemia were higher among patients who received abiraterone.
Based on the trial results, the independent data and safety monitoring committee unanimously recommended unblinding of the trial and allowing patients in the placebo group to receive abiraterone.
The STAMPEDE trial
The STAMPEDE (Systemic Therapy in Advancing or Metastatic Prostate Cancer: Evaluation of Drug Efficacy) trial was designed to test whether adding other therapies to ADT can improve OS in the first-line setting for men with locally advanced or metastatic prostate cancer.
The investigators enrolled 1,917 patients with either newly diagnosed node-positive or metastatic prostate cancer, high-risk locally advanced disease, or relapsed, high-risk disease following radical surgery or radiotherapy.
In all, 95% of patients had newly diagnosed disease; 52% had metastatic disease, 20% had node-positive or node-indeterminate nonmetastatic disease, and 28% had node-negative nonmetastatic disease.
After a median follow-up of 40 months, there had been 184 deaths among the 960 patients assigned to received ADT plus abiraterone and prednisolone, compared with 262 deaths among 957 patients assigned to ADT alone. The respective 3-year survival rates were 83% vs. 76%, translating into a HR of 0.63 (P less than .001) favoring abiraterone. The respective hazard ratios for abiraterone in patients with metastatic and nonmetastatic disease were 0.75 and 0.61, respectively.
Failure-free survival (no radiologic, clinical, or prostate-specific antigen progression or prostate cancer death) also favored abiraterone, with a HR of 0.29, compared with ADT alone (P less than .001). The respective hazard ratios for patients with nonmetastatic disease and metastatic disease were 0.21 and 0.31, respectively.
Grade 3 or greater adverse events occurred in 47% of patients on abiraterone, and in 33% of patients treated with ADT alone. There nine deaths on treatment in the abiraterone group, including two cases of pneumonia (one with sepsis), two strokes, and one case each of dyspnea, lower respiratory tract infection, liver failure, pulmonary hemorrhage, and chest infections.
There were three deaths in the ADT alone group, two from myocardial infarctions and one from bronchopneumonia.
LATITUDE was supported by Janssen Research and Development. Dr. Fizazi reported having no relevant conflicts of interest. Multiple coauthors reported personal fees or other support from Janssen and other companies. STAMPEDE was supported by Cancer Research UK, Medical Research Council, Astellas Pharma, Clovis Oncology, Janssen, Novartis, Pfizer, and Sanofi-Aventis. Lead author Nicholas D. James, PhD, reports receiving support, fees, grants and/or other considerations from Astellas Pharma, Novartis, Pfizer, Clovis Oncology, and Sanofi-Aventis. Multiple coauthors reported similar relationships with various entities.
The LATITUDE and STAMPEDE research teams report encouraging improvements in the initial treatment of men with advanced prostate cancer. Metastatic, castration-sensitive prostate cancer is diagnosed in a small proportion of men with prostate cancer at initial presentation and is disproportionately represented in lethal prostate cancer. The findings of these two trials suggest that therapeutically relevant biologic features of this form of cancer are shared with castration-resistant prostate cancer and raise the broader question of whether earlier application of approved life-prolonging therapies will further improve outcomes.
The reports support the hypothesis that more complete suppression of androgen signaling with abiraterone acetate plus prednisone added to a luteinizing hormone–releasing hormone (LHRH) agonist lengthens survival of men with metastatic, castration-sensitive prostate cancer. The findings are in line with the efficacy of abiraterone plus LHRH agonist therapy as a preoperative treatment. Confidence in the conclusion stems from the observation that treatment with abiraterone plus an LHRH agonist was superior to an LHRH agonist alone in these two large studies among patients with distant metastases, including those with nonosseous visceral metastases. The reported toxic effects of the combination therapy relative to those observed with the LHRH agonist alone did not adversely affect outcomes. The findings may extend to second-generation androgen-receptor inhibitors or combinations with abiraterone currently under study. This practice-changing evidence supports the conclusion that men with metastatic, castration-sensitive prostate cancer, particularly those with more than three bone metastases on conventional imaging, should be treated with abiraterone plus an LHRH agonist.
Christopher J. Logothetis, MD, University of Texas MD Anderson Cancer Center, Houston. This comment is excerpted from an editorial accompanying the studies (N Engl J Med. 2017 Jul 27. doi: 10.1056/NEJMe1704992).
The LATITUDE and STAMPEDE research teams report encouraging improvements in the initial treatment of men with advanced prostate cancer. Metastatic, castration-sensitive prostate cancer is diagnosed in a small proportion of men with prostate cancer at initial presentation and is disproportionately represented in lethal prostate cancer. The findings of these two trials suggest that therapeutically relevant biologic features of this form of cancer are shared with castration-resistant prostate cancer and raise the broader question of whether earlier application of approved life-prolonging therapies will further improve outcomes.
The reports support the hypothesis that more complete suppression of androgen signaling with abiraterone acetate plus prednisone added to a luteinizing hormone–releasing hormone (LHRH) agonist lengthens survival of men with metastatic, castration-sensitive prostate cancer. The findings are in line with the efficacy of abiraterone plus LHRH agonist therapy as a preoperative treatment. Confidence in the conclusion stems from the observation that treatment with abiraterone plus an LHRH agonist was superior to an LHRH agonist alone in these two large studies among patients with distant metastases, including those with nonosseous visceral metastases. The reported toxic effects of the combination therapy relative to those observed with the LHRH agonist alone did not adversely affect outcomes. The findings may extend to second-generation androgen-receptor inhibitors or combinations with abiraterone currently under study. This practice-changing evidence supports the conclusion that men with metastatic, castration-sensitive prostate cancer, particularly those with more than three bone metastases on conventional imaging, should be treated with abiraterone plus an LHRH agonist.
Christopher J. Logothetis, MD, University of Texas MD Anderson Cancer Center, Houston. This comment is excerpted from an editorial accompanying the studies (N Engl J Med. 2017 Jul 27. doi: 10.1056/NEJMe1704992).
The LATITUDE and STAMPEDE research teams report encouraging improvements in the initial treatment of men with advanced prostate cancer. Metastatic, castration-sensitive prostate cancer is diagnosed in a small proportion of men with prostate cancer at initial presentation and is disproportionately represented in lethal prostate cancer. The findings of these two trials suggest that therapeutically relevant biologic features of this form of cancer are shared with castration-resistant prostate cancer and raise the broader question of whether earlier application of approved life-prolonging therapies will further improve outcomes.
The reports support the hypothesis that more complete suppression of androgen signaling with abiraterone acetate plus prednisone added to a luteinizing hormone–releasing hormone (LHRH) agonist lengthens survival of men with metastatic, castration-sensitive prostate cancer. The findings are in line with the efficacy of abiraterone plus LHRH agonist therapy as a preoperative treatment. Confidence in the conclusion stems from the observation that treatment with abiraterone plus an LHRH agonist was superior to an LHRH agonist alone in these two large studies among patients with distant metastases, including those with nonosseous visceral metastases. The reported toxic effects of the combination therapy relative to those observed with the LHRH agonist alone did not adversely affect outcomes. The findings may extend to second-generation androgen-receptor inhibitors or combinations with abiraterone currently under study. This practice-changing evidence supports the conclusion that men with metastatic, castration-sensitive prostate cancer, particularly those with more than three bone metastases on conventional imaging, should be treated with abiraterone plus an LHRH agonist.
Christopher J. Logothetis, MD, University of Texas MD Anderson Cancer Center, Houston. This comment is excerpted from an editorial accompanying the studies (N Engl J Med. 2017 Jul 27. doi: 10.1056/NEJMe1704992).
In findings that are being hailed as practice changing, men with metastatic prostate cancer had a near 40% lower risk of death when they were treated with a combination of abiraterone acetate (Zytiga), androgen deprivation therapy, and prednisone or prednisolone, compared with ADT alone.
After a median follow-up of 30.4 months, median overall survival for men with newly diagnosed metastatic, castration-sensitive prostate cancer treated with ADT plus dual placebos was 34.7 months, vs. not reached for men treated with ADT, abiraterone, and prednisone in the LATITUDE trial. Similarly, in the STAMPEDE trial, men with newly diagnosed locally advanced or metastatic disease who were randomized to ADT with abiraterone and prednisolone had a 37% reduction in their risk for death and a 79% reduction in their risk for treatment failure, compared with men randomized to ADT alone.
The majority of men with metastatic castration-sensitive prostate cancer who are started on androgen deprivation therapy with a luteinizing hormone–releasing hormone (LHRH) analog with or without a first-generation androgen receptor inhibitor will have responses to therapy, but within a median of 1-year most will progress to castration-resistant disease, noted Karim Fizazi, MD, from the Gustave Roussy Cancer Institute at the University of Paris Sud, Villejuif, France, and coinvestigators of the LATITUDE trial.
“Resistance to androgen-deprivation therapy is largely driven by the reactivation of androgen receptor signaling through persistent adrenal androgen production, upregulation of intratumoral testosterone production, modification of the biologic characteristics of androgen receptors, and steroidogenic parallel pathways,” they wrote.
Although ADT and docetaxel is the standard of care for men with metastatic castration-sensitive disease who are eligible for chemotherapy, data from real-world practice suggest that patients with this presentation are older than those enrolled in clinical trials, and may not be able to tolerate the toxicities that occur when docetaxel is added to ADT, they noted.
Abiraterone, in combination with prednisone, has been shown to increase overall survival (OS) in men with metastatic castration-resistant prostate cancer who have not undergone chemotherapy, and among patients who had previously been treated with docetaxel.
The drug is thought to exert its antitumor effects through a combination of androgen receptor antagonism and blockade of steroidogenic enzymes, the investigators wrote.
The LATITUDE trial
LATITUDE investigators from 235 sites in 34 countries in Europe, Asia/Pacific, Latin America and Canada enrolled 1,199 patients with newly diagnosed metastatic castration-sensitive prostate cancer and randomly assigned them to receive either abiraterone and prednisone plus ADT (597 patients), or ADT plus dual placebos (602).
At a planned interim analysis at a median follow-up of 30.4 months, after 406 patients had died, median OS, a co-primary end point, had not been reached among patients in the abiraterone group, compared with 34.7 months for patients assigned to ADT/placebo. This difference translates into a hazard ratio for death of 0.62 (P less than .001).
The median duration of radiographic progression-free survival (PFS), the other primary end point, was 33.0 months among patients treated with abiraterone vs. 14.8 months for those treated with placebo (HR for disease progression or death, 0.47; P less than .001)
Abiraterone was also associated with significantly better outcomes in all secondary endpoints, including time until pain progression, subsequent therapy, initiation of chemotherapy, and prostate-specific antigen (PSA) progression (P less than .001 for each comparison).
The frequency of adverse events leading to treatment discontinuation was 12% for patients in the abiraterone group vs. 10% for those in the placebo group. Rates of grade 3 or 4 hypertension and hypokalemia were higher among patients who received abiraterone.
Based on the trial results, the independent data and safety monitoring committee unanimously recommended unblinding of the trial and allowing patients in the placebo group to receive abiraterone.
The STAMPEDE trial
The STAMPEDE (Systemic Therapy in Advancing or Metastatic Prostate Cancer: Evaluation of Drug Efficacy) trial was designed to test whether adding other therapies to ADT can improve OS in the first-line setting for men with locally advanced or metastatic prostate cancer.
The investigators enrolled 1,917 patients with either newly diagnosed node-positive or metastatic prostate cancer, high-risk locally advanced disease, or relapsed, high-risk disease following radical surgery or radiotherapy.
In all, 95% of patients had newly diagnosed disease; 52% had metastatic disease, 20% had node-positive or node-indeterminate nonmetastatic disease, and 28% had node-negative nonmetastatic disease.
After a median follow-up of 40 months, there had been 184 deaths among the 960 patients assigned to received ADT plus abiraterone and prednisolone, compared with 262 deaths among 957 patients assigned to ADT alone. The respective 3-year survival rates were 83% vs. 76%, translating into a HR of 0.63 (P less than .001) favoring abiraterone. The respective hazard ratios for abiraterone in patients with metastatic and nonmetastatic disease were 0.75 and 0.61, respectively.
Failure-free survival (no radiologic, clinical, or prostate-specific antigen progression or prostate cancer death) also favored abiraterone, with a HR of 0.29, compared with ADT alone (P less than .001). The respective hazard ratios for patients with nonmetastatic disease and metastatic disease were 0.21 and 0.31, respectively.
Grade 3 or greater adverse events occurred in 47% of patients on abiraterone, and in 33% of patients treated with ADT alone. There nine deaths on treatment in the abiraterone group, including two cases of pneumonia (one with sepsis), two strokes, and one case each of dyspnea, lower respiratory tract infection, liver failure, pulmonary hemorrhage, and chest infections.
There were three deaths in the ADT alone group, two from myocardial infarctions and one from bronchopneumonia.
LATITUDE was supported by Janssen Research and Development. Dr. Fizazi reported having no relevant conflicts of interest. Multiple coauthors reported personal fees or other support from Janssen and other companies. STAMPEDE was supported by Cancer Research UK, Medical Research Council, Astellas Pharma, Clovis Oncology, Janssen, Novartis, Pfizer, and Sanofi-Aventis. Lead author Nicholas D. James, PhD, reports receiving support, fees, grants and/or other considerations from Astellas Pharma, Novartis, Pfizer, Clovis Oncology, and Sanofi-Aventis. Multiple coauthors reported similar relationships with various entities.
In findings that are being hailed as practice changing, men with metastatic prostate cancer had a near 40% lower risk of death when they were treated with a combination of abiraterone acetate (Zytiga), androgen deprivation therapy, and prednisone or prednisolone, compared with ADT alone.
After a median follow-up of 30.4 months, median overall survival for men with newly diagnosed metastatic, castration-sensitive prostate cancer treated with ADT plus dual placebos was 34.7 months, vs. not reached for men treated with ADT, abiraterone, and prednisone in the LATITUDE trial. Similarly, in the STAMPEDE trial, men with newly diagnosed locally advanced or metastatic disease who were randomized to ADT with abiraterone and prednisolone had a 37% reduction in their risk for death and a 79% reduction in their risk for treatment failure, compared with men randomized to ADT alone.
The majority of men with metastatic castration-sensitive prostate cancer who are started on androgen deprivation therapy with a luteinizing hormone–releasing hormone (LHRH) analog with or without a first-generation androgen receptor inhibitor will have responses to therapy, but within a median of 1-year most will progress to castration-resistant disease, noted Karim Fizazi, MD, from the Gustave Roussy Cancer Institute at the University of Paris Sud, Villejuif, France, and coinvestigators of the LATITUDE trial.
“Resistance to androgen-deprivation therapy is largely driven by the reactivation of androgen receptor signaling through persistent adrenal androgen production, upregulation of intratumoral testosterone production, modification of the biologic characteristics of androgen receptors, and steroidogenic parallel pathways,” they wrote.
Although ADT and docetaxel is the standard of care for men with metastatic castration-sensitive disease who are eligible for chemotherapy, data from real-world practice suggest that patients with this presentation are older than those enrolled in clinical trials, and may not be able to tolerate the toxicities that occur when docetaxel is added to ADT, they noted.
Abiraterone, in combination with prednisone, has been shown to increase overall survival (OS) in men with metastatic castration-resistant prostate cancer who have not undergone chemotherapy, and among patients who had previously been treated with docetaxel.
The drug is thought to exert its antitumor effects through a combination of androgen receptor antagonism and blockade of steroidogenic enzymes, the investigators wrote.
The LATITUDE trial
LATITUDE investigators from 235 sites in 34 countries in Europe, Asia/Pacific, Latin America and Canada enrolled 1,199 patients with newly diagnosed metastatic castration-sensitive prostate cancer and randomly assigned them to receive either abiraterone and prednisone plus ADT (597 patients), or ADT plus dual placebos (602).
At a planned interim analysis at a median follow-up of 30.4 months, after 406 patients had died, median OS, a co-primary end point, had not been reached among patients in the abiraterone group, compared with 34.7 months for patients assigned to ADT/placebo. This difference translates into a hazard ratio for death of 0.62 (P less than .001).
The median duration of radiographic progression-free survival (PFS), the other primary end point, was 33.0 months among patients treated with abiraterone vs. 14.8 months for those treated with placebo (HR for disease progression or death, 0.47; P less than .001)
Abiraterone was also associated with significantly better outcomes in all secondary endpoints, including time until pain progression, subsequent therapy, initiation of chemotherapy, and prostate-specific antigen (PSA) progression (P less than .001 for each comparison).
The frequency of adverse events leading to treatment discontinuation was 12% for patients in the abiraterone group vs. 10% for those in the placebo group. Rates of grade 3 or 4 hypertension and hypokalemia were higher among patients who received abiraterone.
Based on the trial results, the independent data and safety monitoring committee unanimously recommended unblinding of the trial and allowing patients in the placebo group to receive abiraterone.
The STAMPEDE trial
The STAMPEDE (Systemic Therapy in Advancing or Metastatic Prostate Cancer: Evaluation of Drug Efficacy) trial was designed to test whether adding other therapies to ADT can improve OS in the first-line setting for men with locally advanced or metastatic prostate cancer.
The investigators enrolled 1,917 patients with either newly diagnosed node-positive or metastatic prostate cancer, high-risk locally advanced disease, or relapsed, high-risk disease following radical surgery or radiotherapy.
In all, 95% of patients had newly diagnosed disease; 52% had metastatic disease, 20% had node-positive or node-indeterminate nonmetastatic disease, and 28% had node-negative nonmetastatic disease.
After a median follow-up of 40 months, there had been 184 deaths among the 960 patients assigned to received ADT plus abiraterone and prednisolone, compared with 262 deaths among 957 patients assigned to ADT alone. The respective 3-year survival rates were 83% vs. 76%, translating into a HR of 0.63 (P less than .001) favoring abiraterone. The respective hazard ratios for abiraterone in patients with metastatic and nonmetastatic disease were 0.75 and 0.61, respectively.
Failure-free survival (no radiologic, clinical, or prostate-specific antigen progression or prostate cancer death) also favored abiraterone, with a HR of 0.29, compared with ADT alone (P less than .001). The respective hazard ratios for patients with nonmetastatic disease and metastatic disease were 0.21 and 0.31, respectively.
Grade 3 or greater adverse events occurred in 47% of patients on abiraterone, and in 33% of patients treated with ADT alone. There nine deaths on treatment in the abiraterone group, including two cases of pneumonia (one with sepsis), two strokes, and one case each of dyspnea, lower respiratory tract infection, liver failure, pulmonary hemorrhage, and chest infections.
There were three deaths in the ADT alone group, two from myocardial infarctions and one from bronchopneumonia.
LATITUDE was supported by Janssen Research and Development. Dr. Fizazi reported having no relevant conflicts of interest. Multiple coauthors reported personal fees or other support from Janssen and other companies. STAMPEDE was supported by Cancer Research UK, Medical Research Council, Astellas Pharma, Clovis Oncology, Janssen, Novartis, Pfizer, and Sanofi-Aventis. Lead author Nicholas D. James, PhD, reports receiving support, fees, grants and/or other considerations from Astellas Pharma, Novartis, Pfizer, Clovis Oncology, and Sanofi-Aventis. Multiple coauthors reported similar relationships with various entities.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Key clinical point: Adding abiraterone acetate to androgen deprivation therapy (ADT) significantly improved overall survival in men with metastatic prostate cancer.
Major finding: The hazard ratio for death with abiraterone/ADT vs. ADT alone in LATITUDE was 0.62, and in STAMPEDE was 0.63.
Data source: Randomized LATITUDE study in 1,199 men with metastatic castration-sensitive prostate cancer. Randomized STAMPEDE trial in 1,917 patients with newly diagnosed node-positive or metastatic prostate cancer, high-risk locally advanced disease, or relapsed, high-risk disease.
Disclosures: LATITUDE was supported by Janssen Research and Development. Dr. Fizazi reported having no relevant conflicts of interest. Multiple coauthors reported personal fees or other support from Janssen and other companies. STAMPEDE was supported by Cancer Research UK, Medical Research Council, Astellas Pharma, Clovis Oncology, Janssen, Novartis, Pfizer, and Sanofi-Aventis. Lead author Nicholas D. James, PhD, reports receiving support, fees, grants and/or other considerations from Astellas Pharma, Novartis, Pfizer, Clovis Oncology, and Sanofi-Aventis. Multiple coauthors reported similar relationships with various entities.
Developments in celiac disease and wheat-sensitivity disorders
Celiac disease remained a rare disease until this century. “When I went to medical school, people from Ireland, the Netherlands, and other Northern Europeans had celiac disease. The prevalence of celiac disease has increased in the United States and worldwide.
Advances have been made in the understanding of celiac disease pathogenesis over the past few decades regarding the host genotype, currently restricted to the HLA genes, the delivery mode of gluten, type of feeding, time of feeding, and possibly antibiotics modulating the microbiome. The DQ2 genes are necessary but are insufficient to explain the development of celiac disease. About 40% of the burden of celiac disease is related to the HLA-DQ2.2, 2.5, and 8 genes. In spite of many genomewide association studies, no key molecules have been identified that play a significant role in causing the disease to date.
The association of enteric infections and celiac disease may explain why genetically susceptible individuals that are exposed to gluten from childhood do not all develop the disease in early childhood. The average age of diagnosis of celiac disease in modern times is the mid-40s, and the individuals have been eating gluten all their lives, so it’s not clear why and when people develop celiac disease. It has been postulated that enteric infection could modulate the immune system, cause breaches in the mucosal barrier, and alters of the microbiome, thus triggering the disease. A study recently published in Science supports the role of reovirus as a trigger for celiac disease and results from the TEDDY study group published in Clinical Gastroenterology and Hepatology suggest that rotavirus vaccination could reduce celiac disease autoimmunity in susceptible children.
While the mechanisms underlying nonceliac gluten sensitivity or wheat sensitivity are still unclear, the terms “encompass individuals who report symptoms or alterations in health that are related to perceived gluten or wheat ingestion.” These symptoms could stem from fructose or fructans in wheat starch (FODMAPs), which could lead to symptoms similar to irritable bowel syndrome or other functional GI disorders. North American data show that more and more people without a diagnosis of celiac disease are consuming gluten-free products. Researchers have postulated that the pathophysiology of these conditions could include activation of the innate immune system, increased permeability, mucosal inflammation, basophil and eosinophil activation, antigliadin antibody elevation, and wheat amyloid trypsin inhibitors, but data have been inconsistent. The recommendation for diagnosing nonceliac gluten or wheat sensitivity is a double-blind placebo-controlled gluten trial to assess gluten-induced symptoms after excluding celiac disease or wheat allergy, but this testing is rarely available in North America. A recent study published in Clinical Gastroenterology and Hepatology demonstrated the limitations of this testing. The gluten-free diet is now very popular, but some drawbacks have emerged. These include an increased risk for cardiovascular disorders linked to the diet according to a recent study published in BMJ, and increased levels of heavy metals in urine and blood found in insecticide used on rice, according to a recent study published in Epidemiology. Further studies are needed to corroborate these recall diet studies.
Dr. Crowe is a clinical professor of medicine in the department of gastroenterology, University of California, San Diego. She reports financial relationships with UpToDate, Ferring, and Otsuka. She made her comments during the AGA Institute Presidential Plenary at the Annual Digestive Disease Week.
Celiac disease remained a rare disease until this century. “When I went to medical school, people from Ireland, the Netherlands, and other Northern Europeans had celiac disease. The prevalence of celiac disease has increased in the United States and worldwide.
Advances have been made in the understanding of celiac disease pathogenesis over the past few decades regarding the host genotype, currently restricted to the HLA genes, the delivery mode of gluten, type of feeding, time of feeding, and possibly antibiotics modulating the microbiome. The DQ2 genes are necessary but are insufficient to explain the development of celiac disease. About 40% of the burden of celiac disease is related to the HLA-DQ2.2, 2.5, and 8 genes. In spite of many genomewide association studies, no key molecules have been identified that play a significant role in causing the disease to date.
The association of enteric infections and celiac disease may explain why genetically susceptible individuals that are exposed to gluten from childhood do not all develop the disease in early childhood. The average age of diagnosis of celiac disease in modern times is the mid-40s, and the individuals have been eating gluten all their lives, so it’s not clear why and when people develop celiac disease. It has been postulated that enteric infection could modulate the immune system, cause breaches in the mucosal barrier, and alters of the microbiome, thus triggering the disease. A study recently published in Science supports the role of reovirus as a trigger for celiac disease and results from the TEDDY study group published in Clinical Gastroenterology and Hepatology suggest that rotavirus vaccination could reduce celiac disease autoimmunity in susceptible children.
While the mechanisms underlying nonceliac gluten sensitivity or wheat sensitivity are still unclear, the terms “encompass individuals who report symptoms or alterations in health that are related to perceived gluten or wheat ingestion.” These symptoms could stem from fructose or fructans in wheat starch (FODMAPs), which could lead to symptoms similar to irritable bowel syndrome or other functional GI disorders. North American data show that more and more people without a diagnosis of celiac disease are consuming gluten-free products. Researchers have postulated that the pathophysiology of these conditions could include activation of the innate immune system, increased permeability, mucosal inflammation, basophil and eosinophil activation, antigliadin antibody elevation, and wheat amyloid trypsin inhibitors, but data have been inconsistent. The recommendation for diagnosing nonceliac gluten or wheat sensitivity is a double-blind placebo-controlled gluten trial to assess gluten-induced symptoms after excluding celiac disease or wheat allergy, but this testing is rarely available in North America. A recent study published in Clinical Gastroenterology and Hepatology demonstrated the limitations of this testing. The gluten-free diet is now very popular, but some drawbacks have emerged. These include an increased risk for cardiovascular disorders linked to the diet according to a recent study published in BMJ, and increased levels of heavy metals in urine and blood found in insecticide used on rice, according to a recent study published in Epidemiology. Further studies are needed to corroborate these recall diet studies.
Dr. Crowe is a clinical professor of medicine in the department of gastroenterology, University of California, San Diego. She reports financial relationships with UpToDate, Ferring, and Otsuka. She made her comments during the AGA Institute Presidential Plenary at the Annual Digestive Disease Week.
Celiac disease remained a rare disease until this century. “When I went to medical school, people from Ireland, the Netherlands, and other Northern Europeans had celiac disease. The prevalence of celiac disease has increased in the United States and worldwide.
Advances have been made in the understanding of celiac disease pathogenesis over the past few decades regarding the host genotype, currently restricted to the HLA genes, the delivery mode of gluten, type of feeding, time of feeding, and possibly antibiotics modulating the microbiome. The DQ2 genes are necessary but are insufficient to explain the development of celiac disease. About 40% of the burden of celiac disease is related to the HLA-DQ2.2, 2.5, and 8 genes. In spite of many genomewide association studies, no key molecules have been identified that play a significant role in causing the disease to date.
The association of enteric infections and celiac disease may explain why genetically susceptible individuals that are exposed to gluten from childhood do not all develop the disease in early childhood. The average age of diagnosis of celiac disease in modern times is the mid-40s, and the individuals have been eating gluten all their lives, so it’s not clear why and when people develop celiac disease. It has been postulated that enteric infection could modulate the immune system, cause breaches in the mucosal barrier, and alters of the microbiome, thus triggering the disease. A study recently published in Science supports the role of reovirus as a trigger for celiac disease and results from the TEDDY study group published in Clinical Gastroenterology and Hepatology suggest that rotavirus vaccination could reduce celiac disease autoimmunity in susceptible children.
While the mechanisms underlying nonceliac gluten sensitivity or wheat sensitivity are still unclear, the terms “encompass individuals who report symptoms or alterations in health that are related to perceived gluten or wheat ingestion.” These symptoms could stem from fructose or fructans in wheat starch (FODMAPs), which could lead to symptoms similar to irritable bowel syndrome or other functional GI disorders. North American data show that more and more people without a diagnosis of celiac disease are consuming gluten-free products. Researchers have postulated that the pathophysiology of these conditions could include activation of the innate immune system, increased permeability, mucosal inflammation, basophil and eosinophil activation, antigliadin antibody elevation, and wheat amyloid trypsin inhibitors, but data have been inconsistent. The recommendation for diagnosing nonceliac gluten or wheat sensitivity is a double-blind placebo-controlled gluten trial to assess gluten-induced symptoms after excluding celiac disease or wheat allergy, but this testing is rarely available in North America. A recent study published in Clinical Gastroenterology and Hepatology demonstrated the limitations of this testing. The gluten-free diet is now very popular, but some drawbacks have emerged. These include an increased risk for cardiovascular disorders linked to the diet according to a recent study published in BMJ, and increased levels of heavy metals in urine and blood found in insecticide used on rice, according to a recent study published in Epidemiology. Further studies are needed to corroborate these recall diet studies.
Dr. Crowe is a clinical professor of medicine in the department of gastroenterology, University of California, San Diego. She reports financial relationships with UpToDate, Ferring, and Otsuka. She made her comments during the AGA Institute Presidential Plenary at the Annual Digestive Disease Week.