User login
Primary Effusion Lymphoma: An Infiltrative Plaque in a Patient With HIV
To the Editor:
A 47-year-old man presented to the dermatology service with an asymptomatic plaque on the right thigh of 2 months’ duration. He had a medical history of HIV and Kaposi sarcoma as well as a recently relapsed primary effusion lymphoma (PEL) subsequent to an allogeneic bone marrow transplant. He initially was diagnosed with PEL 3 years prior to the current presentation during a workup for fever and weight loss. Imaging at the time demonstrated a bladder mass, which was biopsied and demonstrated PEL. Further imaging demonstrated both sinus and bone marrow involvement. Prior to dermatologic consultation, he had been treated with 6 cycles of etoposide, prednisolone, vincristine, cyclophosphamide, and doxorubicin (EPOCH); 6 cycles of brentuximab; 4 cycles of rituximab with gemcitabine and oxaliplatin; and 2 cycles of ifosfamide, carboplatin, and etoposide. Despite these therapies, he had 3 relapses, and oncology determined the need for a matched unrelated donor allogeneic stem cell transplant for his PEL.
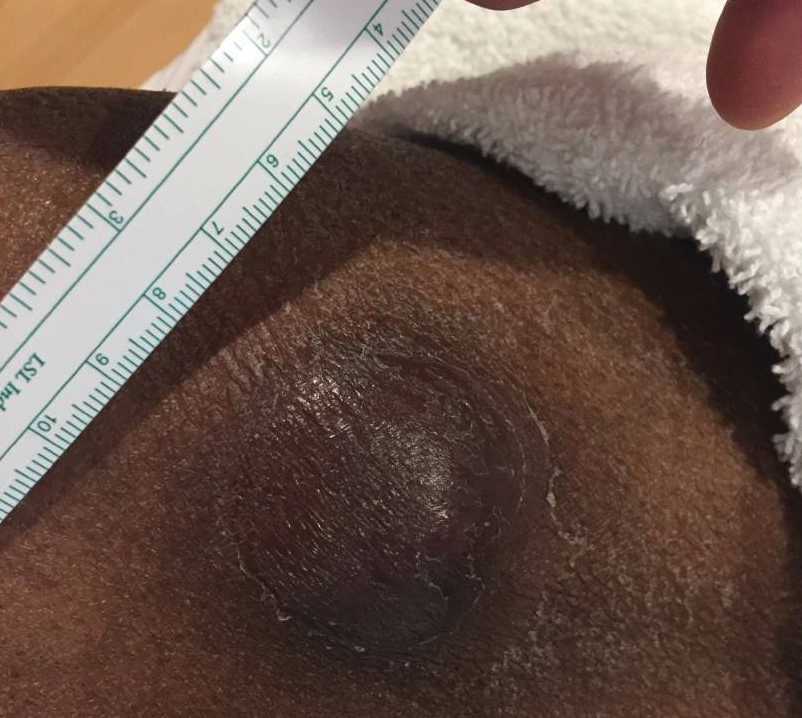
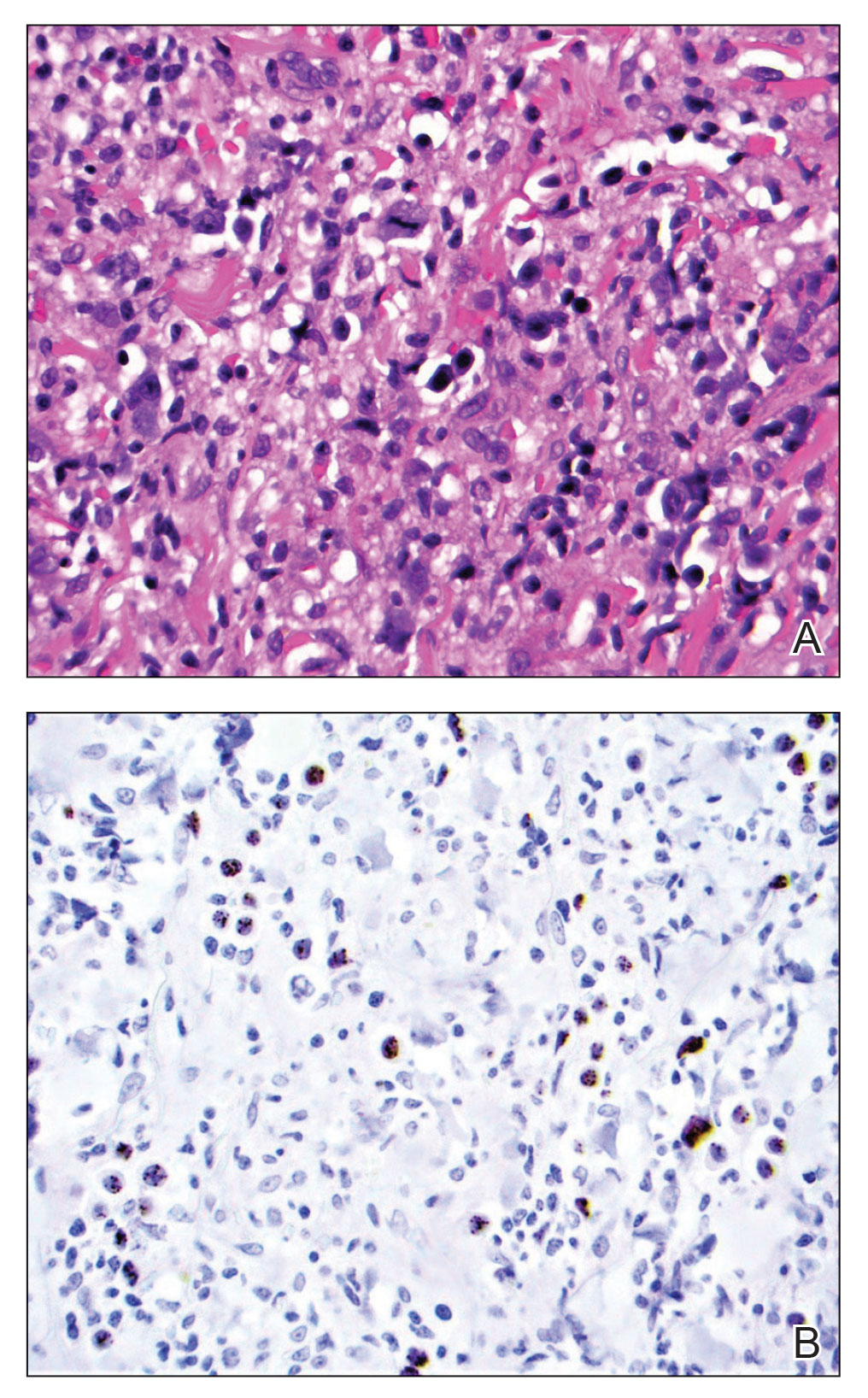
At the time of dermatology consultation, the patient was being managed on daratumumab and bortezomib. Physical examination revealed an infiltrative plaque on the right inferomedial thigh measuring approximately 6.0 cm (largest dimension) with a small amount of peripheral scale (Figure 1). An ultrasound revealed notable subcutaneous tissue edema and increased vascularity without a discrete mass or fluid collection. A 4-mm punch biopsy demonstrated a dense infiltrate comprised of collections of histiocytes admixed with scattered plasma cells and mature lymphoid aggregates. Additionally, rare enlarged plasmablastic cells with scant basophilic cytoplasm and slightly irregular nuclear contours were visualized (Figure 2A). Immunohistochemistry was positive for CD3 with a normal CD4:CD8 ratio, CD68-highlighted histiocytes within the lymphoid aggregates, and human herpesvirus 8 (HHV-8)(or Kaposi sarcoma–associated herpesvirus) demonstrated stippled nuclear staining within the scattered large cells (Figure 2B). Epstein-Barr virus–encoded RNA staining was negative, though the area of interest was lost on deeper sectioning of the tissue block. The histopathologic findings were consistent with cutaneous extracavitary PEL. Shortly after this diagnosis, he died from disease complications.
Primary effusion lymphoma is an aggressive non-Hodgkin B-cell lymphoma that was first described by Knowles et al1 in 1989. Primary effusion lymphoma occurs exclusively in the setting of HHV-8 infection and typically is associated with chronic immunosuppression related to HIV/AIDS. Cases that are negative for HIV-1 are rare but have been reported in organ transplant recipients and elderly men from areas with a high prevalence of HHV-8 infections. Most HIV-associated cases show concurrent Epstein-Barr virus infection, though the pathogenic meaning of this co-infection remains unclear.2,3
Primary effusion lymphoma classically presents as an isolated effusion of malignant lymphoid cells within body cavities in the absence of solid tumor masses. The pleural, peritoneal, and pericardial spaces most commonly are involved. Extracavitary PEL, a rare variant, may present as a solid mass without effusion. In general, extracavitary tumors may occur in the setting of de novo malignancy or recurrent PEL.4 Cutaneous manifestations associated with extracavitary PEL are rare; 4 cases have been described in which skin lesions were the heralding sign of the disease.3 Interestingly, despite obligatory underlying HHV-8 infection, a review by Pielasinski et al3 noted only 2 patients with cutaneous PEL who had prior or concurrent Kaposi sarcoma. This heterogeneity in HHV-8–related phenotypes may be related to differences in microRNA expression, but further study is needed.5
The diagnosis of PEL relies on histologic, immunophenotypic, and molecular analysis of the affected tissue. The malignant cells typically are large with round to irregular nuclei. These cells may demonstrate a variety of appearances, including anaplastic, plasmablastic, and immunoblastic morphologies.6,7 The immunophenotype displays CD45 positivity and markers of lymphocyte activation (CD30, CD38, CD71), while typical B-cell (CD19, CD20, CD79a) and T-cell (CD3, CD4, CD8) markers often are absent.6-8 Human herpesvirus 8 detection by polymerase chain reaction testing of the peripheral blood or by immunohistochemistry staining of the affected tissue is required for diagnosis.6,7 Epstein-Barr virus infection may be detected via in situ hybridization, though it is not required for diagnosis.
The overall prognosis for PEL is poor; Brimo et al6 reported a median survival of less than 6 months, and Guillet et al9 reported 5-year overall survival (OS) for PEL vs extracavitary PEL to be 43% vs 39%. Another review noted variation in survival contingent on the number of body cavities involved; patients with a single body cavity involved experienced a median OS of 18 months, whereas patients with multiple involved cavities experienced a median OS of 4 months,7 possibly due to the limited study of treatment regimens or disease aggressiveness. Even in cases of successful initial treatment, relapse within 6 to 8 months is common. Extracavitary PEL may have improved disease-free survival relative to classic PEL, though the data were less clear for OS.9 Limitations of the Guillet et al9 study included a small sample size, the impossibility to randomize to disease type, and loss of power on the log-rank test for OS in the setting of possible nonproportional hazards (crossing survival curves). Overall, prognostic differences between the groups may be challenging to ascertain until further data are obtained.
As with many HIV-associated neoplasms, antiretroviral treatment (ART) for HIV-positive patients affords a better prognosis when used in addition to therapy directed at malignancy.7 The general approach is for concurrent ART with systemic therapies such as rituximab, cyclophosphamide, doxorubicin, vincristine, and prednisone for the rare CD20+ cases, and cyclophosphamide, doxorubicin, vincristine, and prednisone (CHOP) or dose-adjusted EPOCH therapy in the more common CD20− PEL cases. Narkhede et al7 suggested avoidance of methotrexate in patients with effusions because of increased toxicity, but it is unclear if this recommendation is applicable in extracavitary PEL patients without an effusion. Additionally, second-line treatment modalities include radiation for solid PEL masses, HHV-8–targeted antivirals, and stem cell transplantation, though evidence is limited. Of note, there is a phase I-II trial (ClinicalTrials.gov identifier NCT02911142) ongoing for treatment-naïve PEL patients involving the experimental treatment DA-EPOCH-R plus lenalidomide, but the trial is ongoing.10
We report a case of cutaneous PEL in a patient with a history of Kaposi sarcoma. The patient’s deterioration and ultimate death despite initial treatment with EPOCH and bone marrow transplantation followed by final management with daratumumab and bortezomib confirm other reports that PEL has a poor prognosis and that optimal treatments are not well delineated for these patients. In general, the current approach is to utilize ART for HIV-positive patients and to then implement chemotherapy such as CHOP. Without continued research and careful planning of treatments, data will remain limited on how best to serve patients with PEL.
- Knowles DM, Inghirami G, Ubriaco A, et al. Molecular genetic analysis of three AIDS-associated neoplasms of uncertain lineage demonstrates their B-cell derivation and the possible pathogenetic role of the Epstein-Barr virus. Blood. 1989;73:792-799.
- Kugasia IAR, Kumar A, Khatri A, et al. Primary effusion lymphoma of the pleural space: report of a rare complication of cardiac transplant with review of the literature. Transpl Infect Dis. 2019;21:E13005.
- Pielasinski U, Santonja C, Rodriguez-Pinilla SM, et al. Extracavitary primary effusion lymphoma presenting as a cutaneous tumor: a case report and literature review. J Cutan Pathol. 2014;41:745-753.
- Boulanger E, Meignin V, Afonso PV, et al. Extracavitary tumor after primary effusion lymphoma: relapse or second distinct lymphoma? Haematologica. 2007;92:1275-1276.
- Goncalves PH, Uldrick TS, Yarchoan R. HIV-associated Kaposi sarcoma and related diseases. AIDS. 2017;31:1903-1916.
- Brimo F, Michel RP, Khetani K, et al. Primary effusion lymphoma: a series of 4 cases and review of the literature with emphasis on cytomorphologic and immunocytochemical differential diagnosis. Cancer. 2007;111:224-233.
- Narkhede M, Arora S, Ujjani C. Primary effusion lymphoma: current perspectives. Onco Targets Ther. 2018;11:3747-3754.
- Chen YB, Rahemtullah A, Hochberg E. Primary effusion lymphoma. Oncologist. 2007;12:569-576.
- Guillet S, Gerard L, Meignin V, et al. Classic and extracavitary primary effusion lymphoma in 51 HIV-infected patients from a single institution. Am J Hematol. 2016;91:233-237.
To the Editor:
A 47-year-old man presented to the dermatology service with an asymptomatic plaque on the right thigh of 2 months’ duration. He had a medical history of HIV and Kaposi sarcoma as well as a recently relapsed primary effusion lymphoma (PEL) subsequent to an allogeneic bone marrow transplant. He initially was diagnosed with PEL 3 years prior to the current presentation during a workup for fever and weight loss. Imaging at the time demonstrated a bladder mass, which was biopsied and demonstrated PEL. Further imaging demonstrated both sinus and bone marrow involvement. Prior to dermatologic consultation, he had been treated with 6 cycles of etoposide, prednisolone, vincristine, cyclophosphamide, and doxorubicin (EPOCH); 6 cycles of brentuximab; 4 cycles of rituximab with gemcitabine and oxaliplatin; and 2 cycles of ifosfamide, carboplatin, and etoposide. Despite these therapies, he had 3 relapses, and oncology determined the need for a matched unrelated donor allogeneic stem cell transplant for his PEL.

At the time of dermatology consultation, the patient was being managed on daratumumab and bortezomib. Physical examination revealed an infiltrative plaque on the right inferomedial thigh measuring approximately 6.0 cm (largest dimension) with a small amount of peripheral scale (Figure 1). An ultrasound revealed notable subcutaneous tissue edema and increased vascularity without a discrete mass or fluid collection. A 4-mm punch biopsy demonstrated a dense infiltrate comprised of collections of histiocytes admixed with scattered plasma cells and mature lymphoid aggregates. Additionally, rare enlarged plasmablastic cells with scant basophilic cytoplasm and slightly irregular nuclear contours were visualized (Figure 2A). Immunohistochemistry was positive for CD3 with a normal CD4:CD8 ratio, CD68-highlighted histiocytes within the lymphoid aggregates, and human herpesvirus 8 (HHV-8)(or Kaposi sarcoma–associated herpesvirus) demonstrated stippled nuclear staining within the scattered large cells (Figure 2B). Epstein-Barr virus–encoded RNA staining was negative, though the area of interest was lost on deeper sectioning of the tissue block. The histopathologic findings were consistent with cutaneous extracavitary PEL. Shortly after this diagnosis, he died from disease complications.

Primary effusion lymphoma is an aggressive non-Hodgkin B-cell lymphoma that was first described by Knowles et al1 in 1989. Primary effusion lymphoma occurs exclusively in the setting of HHV-8 infection and typically is associated with chronic immunosuppression related to HIV/AIDS. Cases that are negative for HIV-1 are rare but have been reported in organ transplant recipients and elderly men from areas with a high prevalence of HHV-8 infections. Most HIV-associated cases show concurrent Epstein-Barr virus infection, though the pathogenic meaning of this co-infection remains unclear.2,3
Primary effusion lymphoma classically presents as an isolated effusion of malignant lymphoid cells within body cavities in the absence of solid tumor masses. The pleural, peritoneal, and pericardial spaces most commonly are involved. Extracavitary PEL, a rare variant, may present as a solid mass without effusion. In general, extracavitary tumors may occur in the setting of de novo malignancy or recurrent PEL.4 Cutaneous manifestations associated with extracavitary PEL are rare; 4 cases have been described in which skin lesions were the heralding sign of the disease.3 Interestingly, despite obligatory underlying HHV-8 infection, a review by Pielasinski et al3 noted only 2 patients with cutaneous PEL who had prior or concurrent Kaposi sarcoma. This heterogeneity in HHV-8–related phenotypes may be related to differences in microRNA expression, but further study is needed.5
The diagnosis of PEL relies on histologic, immunophenotypic, and molecular analysis of the affected tissue. The malignant cells typically are large with round to irregular nuclei. These cells may demonstrate a variety of appearances, including anaplastic, plasmablastic, and immunoblastic morphologies.6,7 The immunophenotype displays CD45 positivity and markers of lymphocyte activation (CD30, CD38, CD71), while typical B-cell (CD19, CD20, CD79a) and T-cell (CD3, CD4, CD8) markers often are absent.6-8 Human herpesvirus 8 detection by polymerase chain reaction testing of the peripheral blood or by immunohistochemistry staining of the affected tissue is required for diagnosis.6,7 Epstein-Barr virus infection may be detected via in situ hybridization, though it is not required for diagnosis.
The overall prognosis for PEL is poor; Brimo et al6 reported a median survival of less than 6 months, and Guillet et al9 reported 5-year overall survival (OS) for PEL vs extracavitary PEL to be 43% vs 39%. Another review noted variation in survival contingent on the number of body cavities involved; patients with a single body cavity involved experienced a median OS of 18 months, whereas patients with multiple involved cavities experienced a median OS of 4 months,7 possibly due to the limited study of treatment regimens or disease aggressiveness. Even in cases of successful initial treatment, relapse within 6 to 8 months is common. Extracavitary PEL may have improved disease-free survival relative to classic PEL, though the data were less clear for OS.9 Limitations of the Guillet et al9 study included a small sample size, the impossibility to randomize to disease type, and loss of power on the log-rank test for OS in the setting of possible nonproportional hazards (crossing survival curves). Overall, prognostic differences between the groups may be challenging to ascertain until further data are obtained.
As with many HIV-associated neoplasms, antiretroviral treatment (ART) for HIV-positive patients affords a better prognosis when used in addition to therapy directed at malignancy.7 The general approach is for concurrent ART with systemic therapies such as rituximab, cyclophosphamide, doxorubicin, vincristine, and prednisone for the rare CD20+ cases, and cyclophosphamide, doxorubicin, vincristine, and prednisone (CHOP) or dose-adjusted EPOCH therapy in the more common CD20− PEL cases. Narkhede et al7 suggested avoidance of methotrexate in patients with effusions because of increased toxicity, but it is unclear if this recommendation is applicable in extracavitary PEL patients without an effusion. Additionally, second-line treatment modalities include radiation for solid PEL masses, HHV-8–targeted antivirals, and stem cell transplantation, though evidence is limited. Of note, there is a phase I-II trial (ClinicalTrials.gov identifier NCT02911142) ongoing for treatment-naïve PEL patients involving the experimental treatment DA-EPOCH-R plus lenalidomide, but the trial is ongoing.10
We report a case of cutaneous PEL in a patient with a history of Kaposi sarcoma. The patient’s deterioration and ultimate death despite initial treatment with EPOCH and bone marrow transplantation followed by final management with daratumumab and bortezomib confirm other reports that PEL has a poor prognosis and that optimal treatments are not well delineated for these patients. In general, the current approach is to utilize ART for HIV-positive patients and to then implement chemotherapy such as CHOP. Without continued research and careful planning of treatments, data will remain limited on how best to serve patients with PEL.
To the Editor:
A 47-year-old man presented to the dermatology service with an asymptomatic plaque on the right thigh of 2 months’ duration. He had a medical history of HIV and Kaposi sarcoma as well as a recently relapsed primary effusion lymphoma (PEL) subsequent to an allogeneic bone marrow transplant. He initially was diagnosed with PEL 3 years prior to the current presentation during a workup for fever and weight loss. Imaging at the time demonstrated a bladder mass, which was biopsied and demonstrated PEL. Further imaging demonstrated both sinus and bone marrow involvement. Prior to dermatologic consultation, he had been treated with 6 cycles of etoposide, prednisolone, vincristine, cyclophosphamide, and doxorubicin (EPOCH); 6 cycles of brentuximab; 4 cycles of rituximab with gemcitabine and oxaliplatin; and 2 cycles of ifosfamide, carboplatin, and etoposide. Despite these therapies, he had 3 relapses, and oncology determined the need for a matched unrelated donor allogeneic stem cell transplant for his PEL.

At the time of dermatology consultation, the patient was being managed on daratumumab and bortezomib. Physical examination revealed an infiltrative plaque on the right inferomedial thigh measuring approximately 6.0 cm (largest dimension) with a small amount of peripheral scale (Figure 1). An ultrasound revealed notable subcutaneous tissue edema and increased vascularity without a discrete mass or fluid collection. A 4-mm punch biopsy demonstrated a dense infiltrate comprised of collections of histiocytes admixed with scattered plasma cells and mature lymphoid aggregates. Additionally, rare enlarged plasmablastic cells with scant basophilic cytoplasm and slightly irregular nuclear contours were visualized (Figure 2A). Immunohistochemistry was positive for CD3 with a normal CD4:CD8 ratio, CD68-highlighted histiocytes within the lymphoid aggregates, and human herpesvirus 8 (HHV-8)(or Kaposi sarcoma–associated herpesvirus) demonstrated stippled nuclear staining within the scattered large cells (Figure 2B). Epstein-Barr virus–encoded RNA staining was negative, though the area of interest was lost on deeper sectioning of the tissue block. The histopathologic findings were consistent with cutaneous extracavitary PEL. Shortly after this diagnosis, he died from disease complications.

Primary effusion lymphoma is an aggressive non-Hodgkin B-cell lymphoma that was first described by Knowles et al1 in 1989. Primary effusion lymphoma occurs exclusively in the setting of HHV-8 infection and typically is associated with chronic immunosuppression related to HIV/AIDS. Cases that are negative for HIV-1 are rare but have been reported in organ transplant recipients and elderly men from areas with a high prevalence of HHV-8 infections. Most HIV-associated cases show concurrent Epstein-Barr virus infection, though the pathogenic meaning of this co-infection remains unclear.2,3
Primary effusion lymphoma classically presents as an isolated effusion of malignant lymphoid cells within body cavities in the absence of solid tumor masses. The pleural, peritoneal, and pericardial spaces most commonly are involved. Extracavitary PEL, a rare variant, may present as a solid mass without effusion. In general, extracavitary tumors may occur in the setting of de novo malignancy or recurrent PEL.4 Cutaneous manifestations associated with extracavitary PEL are rare; 4 cases have been described in which skin lesions were the heralding sign of the disease.3 Interestingly, despite obligatory underlying HHV-8 infection, a review by Pielasinski et al3 noted only 2 patients with cutaneous PEL who had prior or concurrent Kaposi sarcoma. This heterogeneity in HHV-8–related phenotypes may be related to differences in microRNA expression, but further study is needed.5
The diagnosis of PEL relies on histologic, immunophenotypic, and molecular analysis of the affected tissue. The malignant cells typically are large with round to irregular nuclei. These cells may demonstrate a variety of appearances, including anaplastic, plasmablastic, and immunoblastic morphologies.6,7 The immunophenotype displays CD45 positivity and markers of lymphocyte activation (CD30, CD38, CD71), while typical B-cell (CD19, CD20, CD79a) and T-cell (CD3, CD4, CD8) markers often are absent.6-8 Human herpesvirus 8 detection by polymerase chain reaction testing of the peripheral blood or by immunohistochemistry staining of the affected tissue is required for diagnosis.6,7 Epstein-Barr virus infection may be detected via in situ hybridization, though it is not required for diagnosis.
The overall prognosis for PEL is poor; Brimo et al6 reported a median survival of less than 6 months, and Guillet et al9 reported 5-year overall survival (OS) for PEL vs extracavitary PEL to be 43% vs 39%. Another review noted variation in survival contingent on the number of body cavities involved; patients with a single body cavity involved experienced a median OS of 18 months, whereas patients with multiple involved cavities experienced a median OS of 4 months,7 possibly due to the limited study of treatment regimens or disease aggressiveness. Even in cases of successful initial treatment, relapse within 6 to 8 months is common. Extracavitary PEL may have improved disease-free survival relative to classic PEL, though the data were less clear for OS.9 Limitations of the Guillet et al9 study included a small sample size, the impossibility to randomize to disease type, and loss of power on the log-rank test for OS in the setting of possible nonproportional hazards (crossing survival curves). Overall, prognostic differences between the groups may be challenging to ascertain until further data are obtained.
As with many HIV-associated neoplasms, antiretroviral treatment (ART) for HIV-positive patients affords a better prognosis when used in addition to therapy directed at malignancy.7 The general approach is for concurrent ART with systemic therapies such as rituximab, cyclophosphamide, doxorubicin, vincristine, and prednisone for the rare CD20+ cases, and cyclophosphamide, doxorubicin, vincristine, and prednisone (CHOP) or dose-adjusted EPOCH therapy in the more common CD20− PEL cases. Narkhede et al7 suggested avoidance of methotrexate in patients with effusions because of increased toxicity, but it is unclear if this recommendation is applicable in extracavitary PEL patients without an effusion. Additionally, second-line treatment modalities include radiation for solid PEL masses, HHV-8–targeted antivirals, and stem cell transplantation, though evidence is limited. Of note, there is a phase I-II trial (ClinicalTrials.gov identifier NCT02911142) ongoing for treatment-naïve PEL patients involving the experimental treatment DA-EPOCH-R plus lenalidomide, but the trial is ongoing.10
We report a case of cutaneous PEL in a patient with a history of Kaposi sarcoma. The patient’s deterioration and ultimate death despite initial treatment with EPOCH and bone marrow transplantation followed by final management with daratumumab and bortezomib confirm other reports that PEL has a poor prognosis and that optimal treatments are not well delineated for these patients. In general, the current approach is to utilize ART for HIV-positive patients and to then implement chemotherapy such as CHOP. Without continued research and careful planning of treatments, data will remain limited on how best to serve patients with PEL.
- Knowles DM, Inghirami G, Ubriaco A, et al. Molecular genetic analysis of three AIDS-associated neoplasms of uncertain lineage demonstrates their B-cell derivation and the possible pathogenetic role of the Epstein-Barr virus. Blood. 1989;73:792-799.
- Kugasia IAR, Kumar A, Khatri A, et al. Primary effusion lymphoma of the pleural space: report of a rare complication of cardiac transplant with review of the literature. Transpl Infect Dis. 2019;21:E13005.
- Pielasinski U, Santonja C, Rodriguez-Pinilla SM, et al. Extracavitary primary effusion lymphoma presenting as a cutaneous tumor: a case report and literature review. J Cutan Pathol. 2014;41:745-753.
- Boulanger E, Meignin V, Afonso PV, et al. Extracavitary tumor after primary effusion lymphoma: relapse or second distinct lymphoma? Haematologica. 2007;92:1275-1276.
- Goncalves PH, Uldrick TS, Yarchoan R. HIV-associated Kaposi sarcoma and related diseases. AIDS. 2017;31:1903-1916.
- Brimo F, Michel RP, Khetani K, et al. Primary effusion lymphoma: a series of 4 cases and review of the literature with emphasis on cytomorphologic and immunocytochemical differential diagnosis. Cancer. 2007;111:224-233.
- Narkhede M, Arora S, Ujjani C. Primary effusion lymphoma: current perspectives. Onco Targets Ther. 2018;11:3747-3754.
- Chen YB, Rahemtullah A, Hochberg E. Primary effusion lymphoma. Oncologist. 2007;12:569-576.
- Guillet S, Gerard L, Meignin V, et al. Classic and extracavitary primary effusion lymphoma in 51 HIV-infected patients from a single institution. Am J Hematol. 2016;91:233-237.
- Knowles DM, Inghirami G, Ubriaco A, et al. Molecular genetic analysis of three AIDS-associated neoplasms of uncertain lineage demonstrates their B-cell derivation and the possible pathogenetic role of the Epstein-Barr virus. Blood. 1989;73:792-799.
- Kugasia IAR, Kumar A, Khatri A, et al. Primary effusion lymphoma of the pleural space: report of a rare complication of cardiac transplant with review of the literature. Transpl Infect Dis. 2019;21:E13005.
- Pielasinski U, Santonja C, Rodriguez-Pinilla SM, et al. Extracavitary primary effusion lymphoma presenting as a cutaneous tumor: a case report and literature review. J Cutan Pathol. 2014;41:745-753.
- Boulanger E, Meignin V, Afonso PV, et al. Extracavitary tumor after primary effusion lymphoma: relapse or second distinct lymphoma? Haematologica. 2007;92:1275-1276.
- Goncalves PH, Uldrick TS, Yarchoan R. HIV-associated Kaposi sarcoma and related diseases. AIDS. 2017;31:1903-1916.
- Brimo F, Michel RP, Khetani K, et al. Primary effusion lymphoma: a series of 4 cases and review of the literature with emphasis on cytomorphologic and immunocytochemical differential diagnosis. Cancer. 2007;111:224-233.
- Narkhede M, Arora S, Ujjani C. Primary effusion lymphoma: current perspectives. Onco Targets Ther. 2018;11:3747-3754.
- Chen YB, Rahemtullah A, Hochberg E. Primary effusion lymphoma. Oncologist. 2007;12:569-576.
- Guillet S, Gerard L, Meignin V, et al. Classic and extracavitary primary effusion lymphoma in 51 HIV-infected patients from a single institution. Am J Hematol. 2016;91:233-237.
Practice Points
- Extracavitary primary effusion lymphoma is an aggressive non-Hodgkin B-cell lymphoma that occurs solely in the presence of human herpesvirus 8 infection and typically is associated with HIV/AIDS.
- Diagnosis necessitates a thorough workup and correlation of histologic, molecular, and immunophenotypic analysis.
- Antiretroviral therapy in HIV-positive patients and intensive chemotherapy regimens are the current recommended treatments. Despite newer targeted agents, the prognosis remains poor.
ILD risk elevated in RA, PsA after starting biologic or targeted synthetic DMARDs
MILAN – Patients with psoriatic arthritis (PsA) who are using biologic and targeted synthetic disease-modifying antirheumatic drugs (b/tsDMARDs) have fivefold higher risk for interstitial lung disease (ILD) than does the general population, according to the first study to explore risk of ILD in this particular patient group.
The study also found 10-fold higher risk of ILD in patients with RA who were starting a b/tsDMARD, compared with the general population, while the addition of methotrexate did not appear to be associated with increased risk for ILD in either RA nor PsA.
Sella Aarrestad Provan, MD, of the Center for Treatment of Rheumatic and Musculoskeletal Diseases at Diakonhjemmet Hospital, Oslo, presented the results at the annual European Congress of Rheumatology.
Explaining the motivation for the study, Dr. Aarrestad Provan said that, in RA, methotrexate’s role in ILD development remained unclear, while some small studies linked b/tsDMARDs with risk for ILD. “In PsA, very few studies have explored the risk of ILD, and no systematic studies have looked at ILD risk factors in this disease.”
The researchers analyzed patient data from hospital and death registries across five Nordic countries (Denmark, Norway, Finland, Iceland, and Sweden) and compared them with general population controls. They calculated risk ratios for people who developed ILD within 5 years of starting a b/tsDMARD (with or without methotrexate).
A total of 37,010 patients with RA, 12,341 with PsA, and 569,451 members of the general population were included in the analysis, with respective disease durations of 10 and 8.9 years. Methotrexate was used along with b/tsDMARDs in 49% of patients with RA and 41% with PsA, and most patients were already on methotrexate when b/tsDMARDs were started. The tumor necrosis factor inhibitor etanercept (Enbrel) was the most commonly used b/tsDMARD in both RA and PsA, followed by infliximab (Remicade and biosimilars) and adalimumab (Humira and biosimilars).
The incidence of ILD within 5 years of starting a b/tsDMARD was 0.8% in patients with RA, 0.2% with PsA, and 0.1% in the general population, and these findings generated hazard ratios of 10.1 (95% confidence interval, 8.6-11.9) for RA and 5.0 (95% CI, 3.4-7.4) for PsA, compared with the general population as reference.
When the risk for ILD was explored according to methotrexate use in RA patients, “there was no signal of increased risk across patients using methotrexate,” Dr. Aarrestad Provan reported. When risk of ILD was explored according to b/tsDMARD use in RA patients, a signal of increased risk was observed with rituximab, she noted, “but upon adjusting for age, sex, and comorbidities, this association was no longer significant, but was still numerically increased.”
Iain McInnes, MD, PhD, vice principal, professor of rheumatology, and head of the College of Medical, Veterinary and Life Sciences at the University of Glasgow, remarked that he “loves results that are unexpected” and thanked the researcher for such an “important study.”
“For years, we’ve been interested in the potential for DMARDs to impact interstitial lung disease, with potential that drugs could make it worse, or better,” he said. “This study is wonderful and novel because first of all, there hasn’t, until now, been a direct comparison between RA and PsA in quite this way, and secondly, we haven’t really assessed whether there is a drug-related risk in PsA. Note that drug related does not necessarily imply causality.”
Regarding mechanisms, Dr. McInnes added that “epidemiologic studies suggest that PsA often coexists with the presence of cardiometabolic syndrome and obesity, which has a higher prevalence in PsA than in RA. Obesity is also related to ILD. As such, it begs the question of whether cardiometabolic, diabetes, or obesity-related features may give us a clue as to what is going on in these PsA patients.”
The research was supported by NordForsk and FOREUM. Dr. Aarrestad Provan reported serving as a consultant to Boehringer Ingelheim and Novartis and receiving grant/research support from Boehringer Ingelheim. Dr. McInnes declared no disclosures relevant to this study.
MILAN – Patients with psoriatic arthritis (PsA) who are using biologic and targeted synthetic disease-modifying antirheumatic drugs (b/tsDMARDs) have fivefold higher risk for interstitial lung disease (ILD) than does the general population, according to the first study to explore risk of ILD in this particular patient group.
The study also found 10-fold higher risk of ILD in patients with RA who were starting a b/tsDMARD, compared with the general population, while the addition of methotrexate did not appear to be associated with increased risk for ILD in either RA nor PsA.
Sella Aarrestad Provan, MD, of the Center for Treatment of Rheumatic and Musculoskeletal Diseases at Diakonhjemmet Hospital, Oslo, presented the results at the annual European Congress of Rheumatology.
Explaining the motivation for the study, Dr. Aarrestad Provan said that, in RA, methotrexate’s role in ILD development remained unclear, while some small studies linked b/tsDMARDs with risk for ILD. “In PsA, very few studies have explored the risk of ILD, and no systematic studies have looked at ILD risk factors in this disease.”
The researchers analyzed patient data from hospital and death registries across five Nordic countries (Denmark, Norway, Finland, Iceland, and Sweden) and compared them with general population controls. They calculated risk ratios for people who developed ILD within 5 years of starting a b/tsDMARD (with or without methotrexate).
A total of 37,010 patients with RA, 12,341 with PsA, and 569,451 members of the general population were included in the analysis, with respective disease durations of 10 and 8.9 years. Methotrexate was used along with b/tsDMARDs in 49% of patients with RA and 41% with PsA, and most patients were already on methotrexate when b/tsDMARDs were started. The tumor necrosis factor inhibitor etanercept (Enbrel) was the most commonly used b/tsDMARD in both RA and PsA, followed by infliximab (Remicade and biosimilars) and adalimumab (Humira and biosimilars).
The incidence of ILD within 5 years of starting a b/tsDMARD was 0.8% in patients with RA, 0.2% with PsA, and 0.1% in the general population, and these findings generated hazard ratios of 10.1 (95% confidence interval, 8.6-11.9) for RA and 5.0 (95% CI, 3.4-7.4) for PsA, compared with the general population as reference.
When the risk for ILD was explored according to methotrexate use in RA patients, “there was no signal of increased risk across patients using methotrexate,” Dr. Aarrestad Provan reported. When risk of ILD was explored according to b/tsDMARD use in RA patients, a signal of increased risk was observed with rituximab, she noted, “but upon adjusting for age, sex, and comorbidities, this association was no longer significant, but was still numerically increased.”
Iain McInnes, MD, PhD, vice principal, professor of rheumatology, and head of the College of Medical, Veterinary and Life Sciences at the University of Glasgow, remarked that he “loves results that are unexpected” and thanked the researcher for such an “important study.”
“For years, we’ve been interested in the potential for DMARDs to impact interstitial lung disease, with potential that drugs could make it worse, or better,” he said. “This study is wonderful and novel because first of all, there hasn’t, until now, been a direct comparison between RA and PsA in quite this way, and secondly, we haven’t really assessed whether there is a drug-related risk in PsA. Note that drug related does not necessarily imply causality.”
Regarding mechanisms, Dr. McInnes added that “epidemiologic studies suggest that PsA often coexists with the presence of cardiometabolic syndrome and obesity, which has a higher prevalence in PsA than in RA. Obesity is also related to ILD. As such, it begs the question of whether cardiometabolic, diabetes, or obesity-related features may give us a clue as to what is going on in these PsA patients.”
The research was supported by NordForsk and FOREUM. Dr. Aarrestad Provan reported serving as a consultant to Boehringer Ingelheim and Novartis and receiving grant/research support from Boehringer Ingelheim. Dr. McInnes declared no disclosures relevant to this study.
MILAN – Patients with psoriatic arthritis (PsA) who are using biologic and targeted synthetic disease-modifying antirheumatic drugs (b/tsDMARDs) have fivefold higher risk for interstitial lung disease (ILD) than does the general population, according to the first study to explore risk of ILD in this particular patient group.
The study also found 10-fold higher risk of ILD in patients with RA who were starting a b/tsDMARD, compared with the general population, while the addition of methotrexate did not appear to be associated with increased risk for ILD in either RA nor PsA.
Sella Aarrestad Provan, MD, of the Center for Treatment of Rheumatic and Musculoskeletal Diseases at Diakonhjemmet Hospital, Oslo, presented the results at the annual European Congress of Rheumatology.
Explaining the motivation for the study, Dr. Aarrestad Provan said that, in RA, methotrexate’s role in ILD development remained unclear, while some small studies linked b/tsDMARDs with risk for ILD. “In PsA, very few studies have explored the risk of ILD, and no systematic studies have looked at ILD risk factors in this disease.”
The researchers analyzed patient data from hospital and death registries across five Nordic countries (Denmark, Norway, Finland, Iceland, and Sweden) and compared them with general population controls. They calculated risk ratios for people who developed ILD within 5 years of starting a b/tsDMARD (with or without methotrexate).
A total of 37,010 patients with RA, 12,341 with PsA, and 569,451 members of the general population were included in the analysis, with respective disease durations of 10 and 8.9 years. Methotrexate was used along with b/tsDMARDs in 49% of patients with RA and 41% with PsA, and most patients were already on methotrexate when b/tsDMARDs were started. The tumor necrosis factor inhibitor etanercept (Enbrel) was the most commonly used b/tsDMARD in both RA and PsA, followed by infliximab (Remicade and biosimilars) and adalimumab (Humira and biosimilars).
The incidence of ILD within 5 years of starting a b/tsDMARD was 0.8% in patients with RA, 0.2% with PsA, and 0.1% in the general population, and these findings generated hazard ratios of 10.1 (95% confidence interval, 8.6-11.9) for RA and 5.0 (95% CI, 3.4-7.4) for PsA, compared with the general population as reference.
When the risk for ILD was explored according to methotrexate use in RA patients, “there was no signal of increased risk across patients using methotrexate,” Dr. Aarrestad Provan reported. When risk of ILD was explored according to b/tsDMARD use in RA patients, a signal of increased risk was observed with rituximab, she noted, “but upon adjusting for age, sex, and comorbidities, this association was no longer significant, but was still numerically increased.”
Iain McInnes, MD, PhD, vice principal, professor of rheumatology, and head of the College of Medical, Veterinary and Life Sciences at the University of Glasgow, remarked that he “loves results that are unexpected” and thanked the researcher for such an “important study.”
“For years, we’ve been interested in the potential for DMARDs to impact interstitial lung disease, with potential that drugs could make it worse, or better,” he said. “This study is wonderful and novel because first of all, there hasn’t, until now, been a direct comparison between RA and PsA in quite this way, and secondly, we haven’t really assessed whether there is a drug-related risk in PsA. Note that drug related does not necessarily imply causality.”
Regarding mechanisms, Dr. McInnes added that “epidemiologic studies suggest that PsA often coexists with the presence of cardiometabolic syndrome and obesity, which has a higher prevalence in PsA than in RA. Obesity is also related to ILD. As such, it begs the question of whether cardiometabolic, diabetes, or obesity-related features may give us a clue as to what is going on in these PsA patients.”
The research was supported by NordForsk and FOREUM. Dr. Aarrestad Provan reported serving as a consultant to Boehringer Ingelheim and Novartis and receiving grant/research support from Boehringer Ingelheim. Dr. McInnes declared no disclosures relevant to this study.
AT EULAR 2023
Minimally invasive vs. open surgery in pancreatic cancer
, suggest results from the international DIPLOMA study.
In the trial, around 260 patients were randomly assigned to undergo either open surgery or minimally invasive laparoscopic or robot-assisted surgery. Rates of complete tumor removal were comparable between the groups.
In addition, the disease-free and overall survival rates at 3 years were nearly identical.
“For pancreatic cancer, we have proven for the first time that minimally invasive distal pancreatectomy is as good as open surgery,” commented principal investigator Mohammad Abu Hilal, MD, PhD, surgical director at the Instituto Ospedaliero Fondazione Poliambulanza in Brescia, Italy.
“Our research provides reassurance for surgeons and can help patients by giving them the information they need to have a conversation with their doctor about how they want to be treated,” he added.
Dr. Hilal was speaking at a press briefing ahead of the annual meeting of the American Society of Clinical Oncology, where the study will be presented (abstract 4163) on June 5.
The study was not able to show that there was a benefit in terms of shorter hospital stays or greater functional recovery with the minimally invasive approach, Dr. Hilal noted, but he suggested that this could be because of differences in postoperative procedures between the participating centers.
He said in an interview that minimally invasive surgery is becoming “very common all over the world,” particularly in the United States, and that randomized controlled trials are “always the last step” in convincing people to use the technique.
He also emphasized that the “best results are obtained in high-volume centers where surgeons do more than at least 50 pancreatic resections a year,” because the minimally invasive approach is “quite complex and difficult,” more so than open surgery.
“This confirmatory study proves that minimally invasive surgical techniques are a safe and effective option for resectable pancreatic cancer,” commented ASCO expert Jennifer F. Tseng, MD, chair of surgery at Boston University and surgeon-in-chief at the Boston Medical Center. It may also “provide benefits like faster recovery time and less infection risk, without increasing cancer risk.”
The results from this trial “will help both surgeons and patients feel comfortable that minimally invasive surgery, in expert hands, is not inferior to open surgery,” she commented in a statement.
Minimally invasive surgery
Only around 12% of patients with pancreatic cancer are diagnosed when the disease is at an early enough stage for surgical resection to be a possibility, Dr. Hilal noted. Minimally invasive pancreatectomy, particularly the distal procedure, was introduced around 25 years ago, but it was initially used only for benign tumors or borderline malignancies.
It took another 10 years before it was considered in cases of confirmed malignancies, “and the main reason for this delay was concerns about the oncological efficiency” of MIDP in terms of its ability to achieve radical resection and an adequate lymph node yield. At the same time, some concerns about minimally invasive surgery for cancer were raised because of results from randomized trials in other cancer types, such as hysterectomy for cervical cancer. Some studies showed worse survival after minimally invasive surgery than after open surgery.
In recent years, use of minimally invasive techniques for pancreatic cancer has become an increasingly “hot topic in many surgical forums,” Dr. Hilal said.
So his team set out to investigate the approach in a phase 3 noninferiority trial. The investigators focused on patients who had an indication for elective distal pancreatectomy plus splenectomy because of proven or highly suspected pancreatic ductal adenocarcinoma in the pancreatic body or tail.
Patients from 35 centers in 12 countries were recruited between May 2018 and May 2021 and were randomly assigned to undergo either MIDP or open distal pancreatectomy.
Patients, nurses, and pathologists were blinded to the surgical procedure by covering of the abdominal wall.
None of the patients underwent adjuvant or neoadjuvant chemotherapy.
Following the procedure, the patients were followed up at 2 weeks and at 1, 3, 6, and 12 months, and a CT scan was performed at 12 months. A range of assessments was performed at each visit, including quality of life measures.
From 1,146 patients initially screened, 261 patients were included.
A few patients withdrew; 131 patients underwent MIDP, and 127 underwent open surgery and were included in the intention-to-treat analysis. Of those, 129 and 125, respectively, were included in the follow-up analysis.
The results confirmed the noninferiority of MIDP, compared with open surgery, with a rate of R0 radical resection (defined as ≥ 1 mm distance between the tumor and the surgical margin) of 73% vs. 69% (P = .039).
In addition, the lymph node yield was comparable between the two approaches, at an average of 22 nodes for MIDP vs. 23 for open surgery (P = .89), and the time to functional recovery was identical, at 5 days for both (P = .22).
The rate of intraperitoneal recurrence was found to be 41% with MIDP, compared with 38% for patients who underwent open surgery.
Dr. Hilal also showed that the rate of serious adverse events, such as bleeding or organ damage, was similar between the two procedures, at 18% with minimally invasive surgery vs. 22% for the open procedure.
Turning to the survival curves, he noted that it is “very clear” that the two procedures achieved near-identical results, at a hazard ratio of 0.99 (P = .94) for overall survival and 0.97 (P = .88) for disease-free survival when comparing MIDP with open surgery.
The researchers will continue to follow up the patients for 3-5 years and will analyze the lymph nodes retrieved to determine whether removal of the spleen is necessary.
The study was funded by Medtronic and Ethicon. Dr. Hilal has relationships with Ethicon and Medtronic. Dr. Tseng has relationships with Aegerion, Amgen, AstraZeneca, Bristol-Myers Squibb, Cubist, Curadel Surgical Innovations, Daiichi Sankyo/Lilly, GlaxoSmithKline, Intarcia Therapeutics, Merck, MyoKardia, PanTher Therapeutics, Pfizer, Quest Diagnostics, Sanofi, Vertex, and Zeus.
A version of this article first appeared on Medscape.com.
, suggest results from the international DIPLOMA study.
In the trial, around 260 patients were randomly assigned to undergo either open surgery or minimally invasive laparoscopic or robot-assisted surgery. Rates of complete tumor removal were comparable between the groups.
In addition, the disease-free and overall survival rates at 3 years were nearly identical.
“For pancreatic cancer, we have proven for the first time that minimally invasive distal pancreatectomy is as good as open surgery,” commented principal investigator Mohammad Abu Hilal, MD, PhD, surgical director at the Instituto Ospedaliero Fondazione Poliambulanza in Brescia, Italy.
“Our research provides reassurance for surgeons and can help patients by giving them the information they need to have a conversation with their doctor about how they want to be treated,” he added.
Dr. Hilal was speaking at a press briefing ahead of the annual meeting of the American Society of Clinical Oncology, where the study will be presented (abstract 4163) on June 5.
The study was not able to show that there was a benefit in terms of shorter hospital stays or greater functional recovery with the minimally invasive approach, Dr. Hilal noted, but he suggested that this could be because of differences in postoperative procedures between the participating centers.
He said in an interview that minimally invasive surgery is becoming “very common all over the world,” particularly in the United States, and that randomized controlled trials are “always the last step” in convincing people to use the technique.
He also emphasized that the “best results are obtained in high-volume centers where surgeons do more than at least 50 pancreatic resections a year,” because the minimally invasive approach is “quite complex and difficult,” more so than open surgery.
“This confirmatory study proves that minimally invasive surgical techniques are a safe and effective option for resectable pancreatic cancer,” commented ASCO expert Jennifer F. Tseng, MD, chair of surgery at Boston University and surgeon-in-chief at the Boston Medical Center. It may also “provide benefits like faster recovery time and less infection risk, without increasing cancer risk.”
The results from this trial “will help both surgeons and patients feel comfortable that minimally invasive surgery, in expert hands, is not inferior to open surgery,” she commented in a statement.
Minimally invasive surgery
Only around 12% of patients with pancreatic cancer are diagnosed when the disease is at an early enough stage for surgical resection to be a possibility, Dr. Hilal noted. Minimally invasive pancreatectomy, particularly the distal procedure, was introduced around 25 years ago, but it was initially used only for benign tumors or borderline malignancies.
It took another 10 years before it was considered in cases of confirmed malignancies, “and the main reason for this delay was concerns about the oncological efficiency” of MIDP in terms of its ability to achieve radical resection and an adequate lymph node yield. At the same time, some concerns about minimally invasive surgery for cancer were raised because of results from randomized trials in other cancer types, such as hysterectomy for cervical cancer. Some studies showed worse survival after minimally invasive surgery than after open surgery.
In recent years, use of minimally invasive techniques for pancreatic cancer has become an increasingly “hot topic in many surgical forums,” Dr. Hilal said.
So his team set out to investigate the approach in a phase 3 noninferiority trial. The investigators focused on patients who had an indication for elective distal pancreatectomy plus splenectomy because of proven or highly suspected pancreatic ductal adenocarcinoma in the pancreatic body or tail.
Patients from 35 centers in 12 countries were recruited between May 2018 and May 2021 and were randomly assigned to undergo either MIDP or open distal pancreatectomy.
Patients, nurses, and pathologists were blinded to the surgical procedure by covering of the abdominal wall.
None of the patients underwent adjuvant or neoadjuvant chemotherapy.
Following the procedure, the patients were followed up at 2 weeks and at 1, 3, 6, and 12 months, and a CT scan was performed at 12 months. A range of assessments was performed at each visit, including quality of life measures.
From 1,146 patients initially screened, 261 patients were included.
A few patients withdrew; 131 patients underwent MIDP, and 127 underwent open surgery and were included in the intention-to-treat analysis. Of those, 129 and 125, respectively, were included in the follow-up analysis.
The results confirmed the noninferiority of MIDP, compared with open surgery, with a rate of R0 radical resection (defined as ≥ 1 mm distance between the tumor and the surgical margin) of 73% vs. 69% (P = .039).
In addition, the lymph node yield was comparable between the two approaches, at an average of 22 nodes for MIDP vs. 23 for open surgery (P = .89), and the time to functional recovery was identical, at 5 days for both (P = .22).
The rate of intraperitoneal recurrence was found to be 41% with MIDP, compared with 38% for patients who underwent open surgery.
Dr. Hilal also showed that the rate of serious adverse events, such as bleeding or organ damage, was similar between the two procedures, at 18% with minimally invasive surgery vs. 22% for the open procedure.
Turning to the survival curves, he noted that it is “very clear” that the two procedures achieved near-identical results, at a hazard ratio of 0.99 (P = .94) for overall survival and 0.97 (P = .88) for disease-free survival when comparing MIDP with open surgery.
The researchers will continue to follow up the patients for 3-5 years and will analyze the lymph nodes retrieved to determine whether removal of the spleen is necessary.
The study was funded by Medtronic and Ethicon. Dr. Hilal has relationships with Ethicon and Medtronic. Dr. Tseng has relationships with Aegerion, Amgen, AstraZeneca, Bristol-Myers Squibb, Cubist, Curadel Surgical Innovations, Daiichi Sankyo/Lilly, GlaxoSmithKline, Intarcia Therapeutics, Merck, MyoKardia, PanTher Therapeutics, Pfizer, Quest Diagnostics, Sanofi, Vertex, and Zeus.
A version of this article first appeared on Medscape.com.
, suggest results from the international DIPLOMA study.
In the trial, around 260 patients were randomly assigned to undergo either open surgery or minimally invasive laparoscopic or robot-assisted surgery. Rates of complete tumor removal were comparable between the groups.
In addition, the disease-free and overall survival rates at 3 years were nearly identical.
“For pancreatic cancer, we have proven for the first time that minimally invasive distal pancreatectomy is as good as open surgery,” commented principal investigator Mohammad Abu Hilal, MD, PhD, surgical director at the Instituto Ospedaliero Fondazione Poliambulanza in Brescia, Italy.
“Our research provides reassurance for surgeons and can help patients by giving them the information they need to have a conversation with their doctor about how they want to be treated,” he added.
Dr. Hilal was speaking at a press briefing ahead of the annual meeting of the American Society of Clinical Oncology, where the study will be presented (abstract 4163) on June 5.
The study was not able to show that there was a benefit in terms of shorter hospital stays or greater functional recovery with the minimally invasive approach, Dr. Hilal noted, but he suggested that this could be because of differences in postoperative procedures between the participating centers.
He said in an interview that minimally invasive surgery is becoming “very common all over the world,” particularly in the United States, and that randomized controlled trials are “always the last step” in convincing people to use the technique.
He also emphasized that the “best results are obtained in high-volume centers where surgeons do more than at least 50 pancreatic resections a year,” because the minimally invasive approach is “quite complex and difficult,” more so than open surgery.
“This confirmatory study proves that minimally invasive surgical techniques are a safe and effective option for resectable pancreatic cancer,” commented ASCO expert Jennifer F. Tseng, MD, chair of surgery at Boston University and surgeon-in-chief at the Boston Medical Center. It may also “provide benefits like faster recovery time and less infection risk, without increasing cancer risk.”
The results from this trial “will help both surgeons and patients feel comfortable that minimally invasive surgery, in expert hands, is not inferior to open surgery,” she commented in a statement.
Minimally invasive surgery
Only around 12% of patients with pancreatic cancer are diagnosed when the disease is at an early enough stage for surgical resection to be a possibility, Dr. Hilal noted. Minimally invasive pancreatectomy, particularly the distal procedure, was introduced around 25 years ago, but it was initially used only for benign tumors or borderline malignancies.
It took another 10 years before it was considered in cases of confirmed malignancies, “and the main reason for this delay was concerns about the oncological efficiency” of MIDP in terms of its ability to achieve radical resection and an adequate lymph node yield. At the same time, some concerns about minimally invasive surgery for cancer were raised because of results from randomized trials in other cancer types, such as hysterectomy for cervical cancer. Some studies showed worse survival after minimally invasive surgery than after open surgery.
In recent years, use of minimally invasive techniques for pancreatic cancer has become an increasingly “hot topic in many surgical forums,” Dr. Hilal said.
So his team set out to investigate the approach in a phase 3 noninferiority trial. The investigators focused on patients who had an indication for elective distal pancreatectomy plus splenectomy because of proven or highly suspected pancreatic ductal adenocarcinoma in the pancreatic body or tail.
Patients from 35 centers in 12 countries were recruited between May 2018 and May 2021 and were randomly assigned to undergo either MIDP or open distal pancreatectomy.
Patients, nurses, and pathologists were blinded to the surgical procedure by covering of the abdominal wall.
None of the patients underwent adjuvant or neoadjuvant chemotherapy.
Following the procedure, the patients were followed up at 2 weeks and at 1, 3, 6, and 12 months, and a CT scan was performed at 12 months. A range of assessments was performed at each visit, including quality of life measures.
From 1,146 patients initially screened, 261 patients were included.
A few patients withdrew; 131 patients underwent MIDP, and 127 underwent open surgery and were included in the intention-to-treat analysis. Of those, 129 and 125, respectively, were included in the follow-up analysis.
The results confirmed the noninferiority of MIDP, compared with open surgery, with a rate of R0 radical resection (defined as ≥ 1 mm distance between the tumor and the surgical margin) of 73% vs. 69% (P = .039).
In addition, the lymph node yield was comparable between the two approaches, at an average of 22 nodes for MIDP vs. 23 for open surgery (P = .89), and the time to functional recovery was identical, at 5 days for both (P = .22).
The rate of intraperitoneal recurrence was found to be 41% with MIDP, compared with 38% for patients who underwent open surgery.
Dr. Hilal also showed that the rate of serious adverse events, such as bleeding or organ damage, was similar between the two procedures, at 18% with minimally invasive surgery vs. 22% for the open procedure.
Turning to the survival curves, he noted that it is “very clear” that the two procedures achieved near-identical results, at a hazard ratio of 0.99 (P = .94) for overall survival and 0.97 (P = .88) for disease-free survival when comparing MIDP with open surgery.
The researchers will continue to follow up the patients for 3-5 years and will analyze the lymph nodes retrieved to determine whether removal of the spleen is necessary.
The study was funded by Medtronic and Ethicon. Dr. Hilal has relationships with Ethicon and Medtronic. Dr. Tseng has relationships with Aegerion, Amgen, AstraZeneca, Bristol-Myers Squibb, Cubist, Curadel Surgical Innovations, Daiichi Sankyo/Lilly, GlaxoSmithKline, Intarcia Therapeutics, Merck, MyoKardia, PanTher Therapeutics, Pfizer, Quest Diagnostics, Sanofi, Vertex, and Zeus.
A version of this article first appeared on Medscape.com.
FROM ASCO 2023
Warning on use of sotorasib after ICI in lung cancer
because of the risk of increased toxicity.
Sotorasib is indicated for adults with locally advanced or metastatic NSCLC who carry a KRASG12C mutation, which occurs in about 13% of cases.
Since its approval in 2021, sotorasib has emerged as “a new standard of care” for such patients after chemotherapy and anti–PD-L1 failure, the investigators say.
The new warning comes after the team compared 48 patients who received an anti–PD-L1 – most often pembrolizumab alone or in combination with platinum-based chemotherapy – before sotorasib with a control group of 54 patients who either didn’t receive an anti–PD-L1 before sotorasib or had at least one other treatment in between.
The team found that sequential anti–PD-L1 and sotorasib therapy significantly increased the risk of severe sotorasib-related hepatotoxicity and also the risk of non-liver adverse events, typically in patients who received sotorasib within 30 days of an anti–PD-L1.
“We suggest avoiding starting sotorasib within 30 days from the last anti–PD-(L)1 infusion,” say senior author Michaël Duruisseaux, MD, PhD, Louis Pradel Hospital, Bron, France, and collegues.
The findings should also “prompt a close monitoring for the development of hepatotoxicity and non-liver AEs [in] patients who receive sotorasib after anti–PD-(L)1,” they add.
The study was published in the Journal of Thoracic Oncology.
Actionable findings
“I consider the results to be highly credible and informative to my own practice,” said Jack West, MD, a thoracic medical oncologist at the City of Hope outside of Los Angeles, said in an interview.
The findings “may lead me to favor a trial of docetaxel as an intervening therapy for patients who have very recently discontinued immunotherapy, deferring sotorasib at least a few weeks and ideally several months,” Dr. West commented. “I think this is a particularly reasonable approach when we remember that sotorasib conferred no improvement in overall survival at all over docetaxel in the CodeBreaK 200 trial in KRASG12C-mutated NSCLC.”
Overall, the study “corroborates what we’ve seen in the limited first-line experience of sotorasib combined with immunotherapy and also echoes our experience of other targeted therapies, such as osimertinib administered in the weeks just after patients received immunotherapy, which is known to be associated with life-threatening pneumonitis,” he said.
Jared Weiss, MD, a thoracic medical oncologist at the University of North Carolina, Chapel Hill, said that given the long half-life of immune checkpoint inhibitors, “it is quite understandable that the toxicity challenges we previously saw with concurrent administration of immunotherapy and certain targeted therapies would be recapitulated in patients who had a relatively short interval between prior checkpoint inhibitor therapy and sotorasib.”
Even so, because of the aggressiveness of NSCLC, long treatment delays between immunotherapy and sotorasib therapy are “not a favored option.”
Like Dr. West, Dr. Weiss said docetaxel (with or without ramucirumab) is a sound intervening alternative.
Another option is to use adagrasib in the second line instead of sotorasib, Dr. Weiss suggested. It’s also a KRASG12C inhibitor but hasn’t so far been associated with severe hepatotoxicity, he said.
Hossein Borghaei, DO, a thoracic medical oncologist at Fox Chase Cancer Center, Philadelphia, agrees with his colleagues and thinks that what the French team found “is real.”
As the investigators suggest, “it might be that sotorasib leads to an inflammatory microenvironment that causes hepatotoxicity in the presence of a checkpoint inhibitor. In that case,” a lower dose of sotorasib might help reduce toxicity while remaining effective, Dr. Broghaei suggested.
Study details
The French team was prompted to investigate the issue by a report of life-threatening hepatitis in a patient with NSCLC for whom sotorasib therapy was initiated 14 weeks after treatment with pembrolizumab, as well as by “the long story of adverse events ... observed with sequential use of [immune checkpoint inhibitors] and targeted therapy.”
Like Dr. Weiss, they note that severe hepatotoxicity after anti–PD-L1 therapy has not, to date, been reported for other KRASG12C inhibitors.
Patients in the study were treated outside of clinical trials at 16 medical centers in France.
Half of the patients (24/48) who were treated immediately with an anti–PD-L1 after sotorasib therapy developed grade 3 or higher sotorasib-related adverse events, including 16 (33%) with severe sotorasib-related hepatotoxicity. Severe diarrhea and fatigue were also more frequent with sequential therapy.
Severe events typically occurred within 30 days of the last anti–PD-L1 infusion and to a lesser extent within 31-60 days.
In the control arm, the rate of severe sotorasib-related adverse events was 13% (7/54). Six patients (11%) experienced severe hepatotoxicity. There was one sotorasib-related death in the sequential therapy arm, which was due to toxic epidermal necrosis. No deaths occurred in the control group.
The two groups were balanced with respect to history of daily alcohol consumption and the presence of liver metastasis. More patients in the control arm had a history of hepatobiliary disease.
The study received no outside funding. Many of the authors report ties with pharmaceutical companies, including to Amgen, the maker of sotorasib, and Mirati Therapeutics, the maker of adagrasib. Dr. Weiss was an adagrasib investigator for Mirati. Dr. West is a regular contribiutor to Medscape and is an adviser for Amgen and Mirati as well as a speaker for Amgen. Dr. Borghaei reported extensive company ties. He has received research support, travel funding, and consulting fees from Amgen as well as consulting fees from Mirati.
A version of this article first appeared on Medscape.com.
because of the risk of increased toxicity.
Sotorasib is indicated for adults with locally advanced or metastatic NSCLC who carry a KRASG12C mutation, which occurs in about 13% of cases.
Since its approval in 2021, sotorasib has emerged as “a new standard of care” for such patients after chemotherapy and anti–PD-L1 failure, the investigators say.
The new warning comes after the team compared 48 patients who received an anti–PD-L1 – most often pembrolizumab alone or in combination with platinum-based chemotherapy – before sotorasib with a control group of 54 patients who either didn’t receive an anti–PD-L1 before sotorasib or had at least one other treatment in between.
The team found that sequential anti–PD-L1 and sotorasib therapy significantly increased the risk of severe sotorasib-related hepatotoxicity and also the risk of non-liver adverse events, typically in patients who received sotorasib within 30 days of an anti–PD-L1.
“We suggest avoiding starting sotorasib within 30 days from the last anti–PD-(L)1 infusion,” say senior author Michaël Duruisseaux, MD, PhD, Louis Pradel Hospital, Bron, France, and collegues.
The findings should also “prompt a close monitoring for the development of hepatotoxicity and non-liver AEs [in] patients who receive sotorasib after anti–PD-(L)1,” they add.
The study was published in the Journal of Thoracic Oncology.
Actionable findings
“I consider the results to be highly credible and informative to my own practice,” said Jack West, MD, a thoracic medical oncologist at the City of Hope outside of Los Angeles, said in an interview.
The findings “may lead me to favor a trial of docetaxel as an intervening therapy for patients who have very recently discontinued immunotherapy, deferring sotorasib at least a few weeks and ideally several months,” Dr. West commented. “I think this is a particularly reasonable approach when we remember that sotorasib conferred no improvement in overall survival at all over docetaxel in the CodeBreaK 200 trial in KRASG12C-mutated NSCLC.”
Overall, the study “corroborates what we’ve seen in the limited first-line experience of sotorasib combined with immunotherapy and also echoes our experience of other targeted therapies, such as osimertinib administered in the weeks just after patients received immunotherapy, which is known to be associated with life-threatening pneumonitis,” he said.
Jared Weiss, MD, a thoracic medical oncologist at the University of North Carolina, Chapel Hill, said that given the long half-life of immune checkpoint inhibitors, “it is quite understandable that the toxicity challenges we previously saw with concurrent administration of immunotherapy and certain targeted therapies would be recapitulated in patients who had a relatively short interval between prior checkpoint inhibitor therapy and sotorasib.”
Even so, because of the aggressiveness of NSCLC, long treatment delays between immunotherapy and sotorasib therapy are “not a favored option.”
Like Dr. West, Dr. Weiss said docetaxel (with or without ramucirumab) is a sound intervening alternative.
Another option is to use adagrasib in the second line instead of sotorasib, Dr. Weiss suggested. It’s also a KRASG12C inhibitor but hasn’t so far been associated with severe hepatotoxicity, he said.
Hossein Borghaei, DO, a thoracic medical oncologist at Fox Chase Cancer Center, Philadelphia, agrees with his colleagues and thinks that what the French team found “is real.”
As the investigators suggest, “it might be that sotorasib leads to an inflammatory microenvironment that causes hepatotoxicity in the presence of a checkpoint inhibitor. In that case,” a lower dose of sotorasib might help reduce toxicity while remaining effective, Dr. Broghaei suggested.
Study details
The French team was prompted to investigate the issue by a report of life-threatening hepatitis in a patient with NSCLC for whom sotorasib therapy was initiated 14 weeks after treatment with pembrolizumab, as well as by “the long story of adverse events ... observed with sequential use of [immune checkpoint inhibitors] and targeted therapy.”
Like Dr. Weiss, they note that severe hepatotoxicity after anti–PD-L1 therapy has not, to date, been reported for other KRASG12C inhibitors.
Patients in the study were treated outside of clinical trials at 16 medical centers in France.
Half of the patients (24/48) who were treated immediately with an anti–PD-L1 after sotorasib therapy developed grade 3 or higher sotorasib-related adverse events, including 16 (33%) with severe sotorasib-related hepatotoxicity. Severe diarrhea and fatigue were also more frequent with sequential therapy.
Severe events typically occurred within 30 days of the last anti–PD-L1 infusion and to a lesser extent within 31-60 days.
In the control arm, the rate of severe sotorasib-related adverse events was 13% (7/54). Six patients (11%) experienced severe hepatotoxicity. There was one sotorasib-related death in the sequential therapy arm, which was due to toxic epidermal necrosis. No deaths occurred in the control group.
The two groups were balanced with respect to history of daily alcohol consumption and the presence of liver metastasis. More patients in the control arm had a history of hepatobiliary disease.
The study received no outside funding. Many of the authors report ties with pharmaceutical companies, including to Amgen, the maker of sotorasib, and Mirati Therapeutics, the maker of adagrasib. Dr. Weiss was an adagrasib investigator for Mirati. Dr. West is a regular contribiutor to Medscape and is an adviser for Amgen and Mirati as well as a speaker for Amgen. Dr. Borghaei reported extensive company ties. He has received research support, travel funding, and consulting fees from Amgen as well as consulting fees from Mirati.
A version of this article first appeared on Medscape.com.
because of the risk of increased toxicity.
Sotorasib is indicated for adults with locally advanced or metastatic NSCLC who carry a KRASG12C mutation, which occurs in about 13% of cases.
Since its approval in 2021, sotorasib has emerged as “a new standard of care” for such patients after chemotherapy and anti–PD-L1 failure, the investigators say.
The new warning comes after the team compared 48 patients who received an anti–PD-L1 – most often pembrolizumab alone or in combination with platinum-based chemotherapy – before sotorasib with a control group of 54 patients who either didn’t receive an anti–PD-L1 before sotorasib or had at least one other treatment in between.
The team found that sequential anti–PD-L1 and sotorasib therapy significantly increased the risk of severe sotorasib-related hepatotoxicity and also the risk of non-liver adverse events, typically in patients who received sotorasib within 30 days of an anti–PD-L1.
“We suggest avoiding starting sotorasib within 30 days from the last anti–PD-(L)1 infusion,” say senior author Michaël Duruisseaux, MD, PhD, Louis Pradel Hospital, Bron, France, and collegues.
The findings should also “prompt a close monitoring for the development of hepatotoxicity and non-liver AEs [in] patients who receive sotorasib after anti–PD-(L)1,” they add.
The study was published in the Journal of Thoracic Oncology.
Actionable findings
“I consider the results to be highly credible and informative to my own practice,” said Jack West, MD, a thoracic medical oncologist at the City of Hope outside of Los Angeles, said in an interview.
The findings “may lead me to favor a trial of docetaxel as an intervening therapy for patients who have very recently discontinued immunotherapy, deferring sotorasib at least a few weeks and ideally several months,” Dr. West commented. “I think this is a particularly reasonable approach when we remember that sotorasib conferred no improvement in overall survival at all over docetaxel in the CodeBreaK 200 trial in KRASG12C-mutated NSCLC.”
Overall, the study “corroborates what we’ve seen in the limited first-line experience of sotorasib combined with immunotherapy and also echoes our experience of other targeted therapies, such as osimertinib administered in the weeks just after patients received immunotherapy, which is known to be associated with life-threatening pneumonitis,” he said.
Jared Weiss, MD, a thoracic medical oncologist at the University of North Carolina, Chapel Hill, said that given the long half-life of immune checkpoint inhibitors, “it is quite understandable that the toxicity challenges we previously saw with concurrent administration of immunotherapy and certain targeted therapies would be recapitulated in patients who had a relatively short interval between prior checkpoint inhibitor therapy and sotorasib.”
Even so, because of the aggressiveness of NSCLC, long treatment delays between immunotherapy and sotorasib therapy are “not a favored option.”
Like Dr. West, Dr. Weiss said docetaxel (with or without ramucirumab) is a sound intervening alternative.
Another option is to use adagrasib in the second line instead of sotorasib, Dr. Weiss suggested. It’s also a KRASG12C inhibitor but hasn’t so far been associated with severe hepatotoxicity, he said.
Hossein Borghaei, DO, a thoracic medical oncologist at Fox Chase Cancer Center, Philadelphia, agrees with his colleagues and thinks that what the French team found “is real.”
As the investigators suggest, “it might be that sotorasib leads to an inflammatory microenvironment that causes hepatotoxicity in the presence of a checkpoint inhibitor. In that case,” a lower dose of sotorasib might help reduce toxicity while remaining effective, Dr. Broghaei suggested.
Study details
The French team was prompted to investigate the issue by a report of life-threatening hepatitis in a patient with NSCLC for whom sotorasib therapy was initiated 14 weeks after treatment with pembrolizumab, as well as by “the long story of adverse events ... observed with sequential use of [immune checkpoint inhibitors] and targeted therapy.”
Like Dr. Weiss, they note that severe hepatotoxicity after anti–PD-L1 therapy has not, to date, been reported for other KRASG12C inhibitors.
Patients in the study were treated outside of clinical trials at 16 medical centers in France.
Half of the patients (24/48) who were treated immediately with an anti–PD-L1 after sotorasib therapy developed grade 3 or higher sotorasib-related adverse events, including 16 (33%) with severe sotorasib-related hepatotoxicity. Severe diarrhea and fatigue were also more frequent with sequential therapy.
Severe events typically occurred within 30 days of the last anti–PD-L1 infusion and to a lesser extent within 31-60 days.
In the control arm, the rate of severe sotorasib-related adverse events was 13% (7/54). Six patients (11%) experienced severe hepatotoxicity. There was one sotorasib-related death in the sequential therapy arm, which was due to toxic epidermal necrosis. No deaths occurred in the control group.
The two groups were balanced with respect to history of daily alcohol consumption and the presence of liver metastasis. More patients in the control arm had a history of hepatobiliary disease.
The study received no outside funding. Many of the authors report ties with pharmaceutical companies, including to Amgen, the maker of sotorasib, and Mirati Therapeutics, the maker of adagrasib. Dr. Weiss was an adagrasib investigator for Mirati. Dr. West is a regular contribiutor to Medscape and is an adviser for Amgen and Mirati as well as a speaker for Amgen. Dr. Borghaei reported extensive company ties. He has received research support, travel funding, and consulting fees from Amgen as well as consulting fees from Mirati.
A version of this article first appeared on Medscape.com.
FROM THE JOURNAL OF THORACIC ONCOLOGY
Posluma approved for PET imaging in prostate cancer
The product is approved for use in men with suspected metastasis who are candidates for definitive therapy and for men with suspected recurrence, as evidenced by elevations in serum prostate-specific antigen (PSA) level, according to a press release from marketer Blue Earth Diagnostics.
Posluma binds prostate-specific membrane antigen (PSMA), which is usually overexpressed on prostate cancer cells, and tags the cells with fluorine-18 (F18), a positron emitter. Because of the radiolabeling, PET imaging can be used to gauge the extent of disease.
Posluma will be available in the United States in June 2023 from Blue Earth’s U.S. manufacturer and distributor, PETNET Solutions.
Blue Earth says that its new agent, which was known as 18F-rhPSMA-7.3 PET during trials, “is the first and only FDA-approved, PSMA-targeted imaging agent developed with proprietary radiohybrid technology.”
However, a similar product is currently on the U.S. market – the PSMA PET imaging radiopharmaceutical gallium-68 gozetotide (Illuccix, Locometz), which has the same two indications. Gozetotide is also indicated for metastatic prostate cancer amenable to lutetium Lu 177 vipivotide tetraxetan PSMA-directed therapy.
Approval based on two single-arm trials
Posluma’s approval was based on two single-arm trials from Blue Earth.
In the LIGHTHOUSE trial, 296 men underwent Posluma PET imaging before radical prostatectomy with pelvic lymph node dissection. About a quarter turned out to have positive nodes on pathology.
Posluma’s sensitivity for predicting positive nodes was low, ranging from 23% to 30% among three readers who were blinded to clinical information, but its specificity was high, ranging from 93% to 97%, according to the product labeling.
“The study showed that Posluma PET provided clinically valuable information prior to surgery that would likely result in management changes for these patients,” said investigator Brian Chapin, MD, a urologist at the University of Texas MD Anderson Cancer Center, Houston, in the company press release.
The second trial, SPOTLIGHT, included 389 men suspected of experiencing recurrence on the basis of elevations in PSA.
Posluma PET’s ability to detect true recurrence was compared with use of histology or other imaging techniques, including CT, MRI, technetium-99m bone scan, and fluciclovine F18 PET. In regions deemed positive for recurrence on Posluma PET by three readers, 46%-60% were positive by the other techniques, the labeling says.
Overall, the “results demonstrated high detection rates ... even at low PSA levels,” Blue Earth said.
Adverse events were minimal in the trials. The most frequent were diarrhea (0.7%), increases in blood pressure (0.5%), and injection-site pain (0.4%).
The product labeling warns that Posluma PET contributes to patients’ overall long-term cumulative radiation exposure and that interpretation with respect to recurrence may differ among readers.
The labeling also cautions that “a negative image does not rule out the presence of prostate cancer and a positive image does not confirm the presence of prostate cancer. ... Uptake is not specific for prostate cancer and may occur in other types of cancer, in nonmalignant processes, and in normal tissues.”
In addition, it notes that androgen deprivation therapy “and other therapies targeting the androgen pathway, such as androgen receptor antagonists, may result in changes in uptake of flotufolastat F18 in prostate cancer.”
The labeling for gozetotide carries the same warnings and precautions.
A version of this article first appeared on Medscape.com.
The product is approved for use in men with suspected metastasis who are candidates for definitive therapy and for men with suspected recurrence, as evidenced by elevations in serum prostate-specific antigen (PSA) level, according to a press release from marketer Blue Earth Diagnostics.
Posluma binds prostate-specific membrane antigen (PSMA), which is usually overexpressed on prostate cancer cells, and tags the cells with fluorine-18 (F18), a positron emitter. Because of the radiolabeling, PET imaging can be used to gauge the extent of disease.
Posluma will be available in the United States in June 2023 from Blue Earth’s U.S. manufacturer and distributor, PETNET Solutions.
Blue Earth says that its new agent, which was known as 18F-rhPSMA-7.3 PET during trials, “is the first and only FDA-approved, PSMA-targeted imaging agent developed with proprietary radiohybrid technology.”
However, a similar product is currently on the U.S. market – the PSMA PET imaging radiopharmaceutical gallium-68 gozetotide (Illuccix, Locometz), which has the same two indications. Gozetotide is also indicated for metastatic prostate cancer amenable to lutetium Lu 177 vipivotide tetraxetan PSMA-directed therapy.
Approval based on two single-arm trials
Posluma’s approval was based on two single-arm trials from Blue Earth.
In the LIGHTHOUSE trial, 296 men underwent Posluma PET imaging before radical prostatectomy with pelvic lymph node dissection. About a quarter turned out to have positive nodes on pathology.
Posluma’s sensitivity for predicting positive nodes was low, ranging from 23% to 30% among three readers who were blinded to clinical information, but its specificity was high, ranging from 93% to 97%, according to the product labeling.
“The study showed that Posluma PET provided clinically valuable information prior to surgery that would likely result in management changes for these patients,” said investigator Brian Chapin, MD, a urologist at the University of Texas MD Anderson Cancer Center, Houston, in the company press release.
The second trial, SPOTLIGHT, included 389 men suspected of experiencing recurrence on the basis of elevations in PSA.
Posluma PET’s ability to detect true recurrence was compared with use of histology or other imaging techniques, including CT, MRI, technetium-99m bone scan, and fluciclovine F18 PET. In regions deemed positive for recurrence on Posluma PET by three readers, 46%-60% were positive by the other techniques, the labeling says.
Overall, the “results demonstrated high detection rates ... even at low PSA levels,” Blue Earth said.
Adverse events were minimal in the trials. The most frequent were diarrhea (0.7%), increases in blood pressure (0.5%), and injection-site pain (0.4%).
The product labeling warns that Posluma PET contributes to patients’ overall long-term cumulative radiation exposure and that interpretation with respect to recurrence may differ among readers.
The labeling also cautions that “a negative image does not rule out the presence of prostate cancer and a positive image does not confirm the presence of prostate cancer. ... Uptake is not specific for prostate cancer and may occur in other types of cancer, in nonmalignant processes, and in normal tissues.”
In addition, it notes that androgen deprivation therapy “and other therapies targeting the androgen pathway, such as androgen receptor antagonists, may result in changes in uptake of flotufolastat F18 in prostate cancer.”
The labeling for gozetotide carries the same warnings and precautions.
A version of this article first appeared on Medscape.com.
The product is approved for use in men with suspected metastasis who are candidates for definitive therapy and for men with suspected recurrence, as evidenced by elevations in serum prostate-specific antigen (PSA) level, according to a press release from marketer Blue Earth Diagnostics.
Posluma binds prostate-specific membrane antigen (PSMA), which is usually overexpressed on prostate cancer cells, and tags the cells with fluorine-18 (F18), a positron emitter. Because of the radiolabeling, PET imaging can be used to gauge the extent of disease.
Posluma will be available in the United States in June 2023 from Blue Earth’s U.S. manufacturer and distributor, PETNET Solutions.
Blue Earth says that its new agent, which was known as 18F-rhPSMA-7.3 PET during trials, “is the first and only FDA-approved, PSMA-targeted imaging agent developed with proprietary radiohybrid technology.”
However, a similar product is currently on the U.S. market – the PSMA PET imaging radiopharmaceutical gallium-68 gozetotide (Illuccix, Locometz), which has the same two indications. Gozetotide is also indicated for metastatic prostate cancer amenable to lutetium Lu 177 vipivotide tetraxetan PSMA-directed therapy.
Approval based on two single-arm trials
Posluma’s approval was based on two single-arm trials from Blue Earth.
In the LIGHTHOUSE trial, 296 men underwent Posluma PET imaging before radical prostatectomy with pelvic lymph node dissection. About a quarter turned out to have positive nodes on pathology.
Posluma’s sensitivity for predicting positive nodes was low, ranging from 23% to 30% among three readers who were blinded to clinical information, but its specificity was high, ranging from 93% to 97%, according to the product labeling.
“The study showed that Posluma PET provided clinically valuable information prior to surgery that would likely result in management changes for these patients,” said investigator Brian Chapin, MD, a urologist at the University of Texas MD Anderson Cancer Center, Houston, in the company press release.
The second trial, SPOTLIGHT, included 389 men suspected of experiencing recurrence on the basis of elevations in PSA.
Posluma PET’s ability to detect true recurrence was compared with use of histology or other imaging techniques, including CT, MRI, technetium-99m bone scan, and fluciclovine F18 PET. In regions deemed positive for recurrence on Posluma PET by three readers, 46%-60% were positive by the other techniques, the labeling says.
Overall, the “results demonstrated high detection rates ... even at low PSA levels,” Blue Earth said.
Adverse events were minimal in the trials. The most frequent were diarrhea (0.7%), increases in blood pressure (0.5%), and injection-site pain (0.4%).
The product labeling warns that Posluma PET contributes to patients’ overall long-term cumulative radiation exposure and that interpretation with respect to recurrence may differ among readers.
The labeling also cautions that “a negative image does not rule out the presence of prostate cancer and a positive image does not confirm the presence of prostate cancer. ... Uptake is not specific for prostate cancer and may occur in other types of cancer, in nonmalignant processes, and in normal tissues.”
In addition, it notes that androgen deprivation therapy “and other therapies targeting the androgen pathway, such as androgen receptor antagonists, may result in changes in uptake of flotufolastat F18 in prostate cancer.”
The labeling for gozetotide carries the same warnings and precautions.
A version of this article first appeared on Medscape.com.
Regular exercise may boost pain tolerance
new research suggests.
In a large observational study of more than 10,000 adults, researchers found those who consistently engage in moderate to vigorous physical activity over the 7- to 8-year study period reported the highest pain tolerance. However, the results also showed that even light exercise was associated with greater pain tolerance.
“There were indications that both total amount of physical activity over time, as well as the direction of change in activity level over time matters to how high your pain tolerance is,” lead investigator Anders Pedersen Årnes, PT, MPH, research fellow and adviser at the University Hospital of North Norway, affiliated with the University of Tromsø, said in an interview. “As an observational study, this points toward the possibility that increased physical activity might increase pain tolerance.”
The findings were published online in PLOS One.
Anything is better than nothing
The researchers drew from the prospective, population-based Tromsø health study, a health survey that draws on surveys conducted periodically since 1974 among residents in northern Norway.
The study included 10,732 participants who completed surveys in 2007-2008 and again in 2015-2016.
Data on physical activity, experimental pain tolerance, sex, sociodemographic covariates, and chronic pain was collected through questionnaires, biological samples and clinical examination.
Pain tolerance was measured using the cold-pressor test (CPT), in which participants submerge their hand in icy water for as long as possible.
CPT tolerance was 7%, 14%, and 16% higher respectively for light, moderate, and vigorous consistent exercise across the two surveys versus the sedentary group.
“Engaging in habitual physical activity in leisure time is associated with higher pain tolerance,” Mr. Årnes said. “Any kind of activity over time is better than being sedentary.”
The researchers also found that people who were sedentary at baseline who reported greater physical activity at follow-up also had higher pain tolerance than those who remained sedentary, although this finding was not statistically significant.
This highest pain tolerance was noted in people who engaged in moderate to vigorous exercise over time, with a 20.4-second longer performance in the CPT than those who were consistently sedentary (P < .001; 95% confidence interval, 13.7-27.1).
There was no significant difference in pain tolerance between men and women and all participants experienced a decline in tolerance over time.
“Results indicate that a positive change in physical activity level over time was associated with higher pain tolerance,” Mr. Årnes said. “Your total activity level might decide how much, as more seems to be better.”
More work needed
The long follow-up and large number of patients are two strengths of the study, Steven Cohen, MD, chief of pain medicine and professor of anesthesiology, neurology, physical medicine & rehabilitation and psychiatry at Johns Hopkins University, Baltimore, said in an interview.
“This study explored the relationship between general physical activity levels and one form of acute pain, but data from other studies show a benefit for other forms of pain,” said Dr. Cohen, who was not part of the research. “Taken together, this suggests that exercise is beneficial for individuals living with pain.”
The findings demonstrate an association between exercise and pain tolerance and other research has shown evidence of a cause-and-effect relationship, Dr. Cohen said. However, “more work is needed to determine what mediates these effects.”
Questions also remain about how exercise might impact tolerance or risk for chronic pain, he added.
Investigators are now working on a follow-up study of how the effect of exercise on pain tolerance might influence chronic pain risk, Mr. Årnes said.
The study received no specific funding. Mr. Årnes and Dr. Cohen reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
new research suggests.
In a large observational study of more than 10,000 adults, researchers found those who consistently engage in moderate to vigorous physical activity over the 7- to 8-year study period reported the highest pain tolerance. However, the results also showed that even light exercise was associated with greater pain tolerance.
“There were indications that both total amount of physical activity over time, as well as the direction of change in activity level over time matters to how high your pain tolerance is,” lead investigator Anders Pedersen Årnes, PT, MPH, research fellow and adviser at the University Hospital of North Norway, affiliated with the University of Tromsø, said in an interview. “As an observational study, this points toward the possibility that increased physical activity might increase pain tolerance.”
The findings were published online in PLOS One.
Anything is better than nothing
The researchers drew from the prospective, population-based Tromsø health study, a health survey that draws on surveys conducted periodically since 1974 among residents in northern Norway.
The study included 10,732 participants who completed surveys in 2007-2008 and again in 2015-2016.
Data on physical activity, experimental pain tolerance, sex, sociodemographic covariates, and chronic pain was collected through questionnaires, biological samples and clinical examination.
Pain tolerance was measured using the cold-pressor test (CPT), in which participants submerge their hand in icy water for as long as possible.
CPT tolerance was 7%, 14%, and 16% higher respectively for light, moderate, and vigorous consistent exercise across the two surveys versus the sedentary group.
“Engaging in habitual physical activity in leisure time is associated with higher pain tolerance,” Mr. Årnes said. “Any kind of activity over time is better than being sedentary.”
The researchers also found that people who were sedentary at baseline who reported greater physical activity at follow-up also had higher pain tolerance than those who remained sedentary, although this finding was not statistically significant.
This highest pain tolerance was noted in people who engaged in moderate to vigorous exercise over time, with a 20.4-second longer performance in the CPT than those who were consistently sedentary (P < .001; 95% confidence interval, 13.7-27.1).
There was no significant difference in pain tolerance between men and women and all participants experienced a decline in tolerance over time.
“Results indicate that a positive change in physical activity level over time was associated with higher pain tolerance,” Mr. Årnes said. “Your total activity level might decide how much, as more seems to be better.”
More work needed
The long follow-up and large number of patients are two strengths of the study, Steven Cohen, MD, chief of pain medicine and professor of anesthesiology, neurology, physical medicine & rehabilitation and psychiatry at Johns Hopkins University, Baltimore, said in an interview.
“This study explored the relationship between general physical activity levels and one form of acute pain, but data from other studies show a benefit for other forms of pain,” said Dr. Cohen, who was not part of the research. “Taken together, this suggests that exercise is beneficial for individuals living with pain.”
The findings demonstrate an association between exercise and pain tolerance and other research has shown evidence of a cause-and-effect relationship, Dr. Cohen said. However, “more work is needed to determine what mediates these effects.”
Questions also remain about how exercise might impact tolerance or risk for chronic pain, he added.
Investigators are now working on a follow-up study of how the effect of exercise on pain tolerance might influence chronic pain risk, Mr. Årnes said.
The study received no specific funding. Mr. Årnes and Dr. Cohen reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
new research suggests.
In a large observational study of more than 10,000 adults, researchers found those who consistently engage in moderate to vigorous physical activity over the 7- to 8-year study period reported the highest pain tolerance. However, the results also showed that even light exercise was associated with greater pain tolerance.
“There were indications that both total amount of physical activity over time, as well as the direction of change in activity level over time matters to how high your pain tolerance is,” lead investigator Anders Pedersen Årnes, PT, MPH, research fellow and adviser at the University Hospital of North Norway, affiliated with the University of Tromsø, said in an interview. “As an observational study, this points toward the possibility that increased physical activity might increase pain tolerance.”
The findings were published online in PLOS One.
Anything is better than nothing
The researchers drew from the prospective, population-based Tromsø health study, a health survey that draws on surveys conducted periodically since 1974 among residents in northern Norway.
The study included 10,732 participants who completed surveys in 2007-2008 and again in 2015-2016.
Data on physical activity, experimental pain tolerance, sex, sociodemographic covariates, and chronic pain was collected through questionnaires, biological samples and clinical examination.
Pain tolerance was measured using the cold-pressor test (CPT), in which participants submerge their hand in icy water for as long as possible.
CPT tolerance was 7%, 14%, and 16% higher respectively for light, moderate, and vigorous consistent exercise across the two surveys versus the sedentary group.
“Engaging in habitual physical activity in leisure time is associated with higher pain tolerance,” Mr. Årnes said. “Any kind of activity over time is better than being sedentary.”
The researchers also found that people who were sedentary at baseline who reported greater physical activity at follow-up also had higher pain tolerance than those who remained sedentary, although this finding was not statistically significant.
This highest pain tolerance was noted in people who engaged in moderate to vigorous exercise over time, with a 20.4-second longer performance in the CPT than those who were consistently sedentary (P < .001; 95% confidence interval, 13.7-27.1).
There was no significant difference in pain tolerance between men and women and all participants experienced a decline in tolerance over time.
“Results indicate that a positive change in physical activity level over time was associated with higher pain tolerance,” Mr. Årnes said. “Your total activity level might decide how much, as more seems to be better.”
More work needed
The long follow-up and large number of patients are two strengths of the study, Steven Cohen, MD, chief of pain medicine and professor of anesthesiology, neurology, physical medicine & rehabilitation and psychiatry at Johns Hopkins University, Baltimore, said in an interview.
“This study explored the relationship between general physical activity levels and one form of acute pain, but data from other studies show a benefit for other forms of pain,” said Dr. Cohen, who was not part of the research. “Taken together, this suggests that exercise is beneficial for individuals living with pain.”
The findings demonstrate an association between exercise and pain tolerance and other research has shown evidence of a cause-and-effect relationship, Dr. Cohen said. However, “more work is needed to determine what mediates these effects.”
Questions also remain about how exercise might impact tolerance or risk for chronic pain, he added.
Investigators are now working on a follow-up study of how the effect of exercise on pain tolerance might influence chronic pain risk, Mr. Årnes said.
The study received no specific funding. Mr. Årnes and Dr. Cohen reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM PLOS ONE
Weight-control surgery surging among children and teens, report says
.
Metabolic and bariatric surgeries have been on the rise among youths aged 10 to 19 since 2016, the report says. From 2020 to 2021, the number shot up by 19%.
The procedures change parts of the digestive system, helping the person feel more full and less hungry – thereby contributing to weight loss.
Among American children, obesity affects 20%, or 15 million people between 2 and 19. In addition, more are becoming afflicted with severe obesity, with a body mass index 20% higher than the marker for obesity.
“Behavioral lifestyle interventions alone do not result in long-term, clinically important weight loss among youth with severe obesity,” the study’s authors wrote. “Metabolic and bariatric surgery (MBS) is a safe and effective treatment.”
The American Academy of Pediatrics updated its guidelines for the treatment of obesity this year for the first time in 15 years, CNN reported. “The new guidelines urge prompt use of behavior therapy and lifestyle changes and, for the first time, recommend surgery and medications for some young people,” CNN wrote.
Black and Hispanic children have higher rates of childhood obesity, the CDC says. Use of surgeries rose 42% among Black youths and 53% among Hispanic youths between 2020 and 2021.
A version of this article first appeared on WebMD.com.
.
Metabolic and bariatric surgeries have been on the rise among youths aged 10 to 19 since 2016, the report says. From 2020 to 2021, the number shot up by 19%.
The procedures change parts of the digestive system, helping the person feel more full and less hungry – thereby contributing to weight loss.
Among American children, obesity affects 20%, or 15 million people between 2 and 19. In addition, more are becoming afflicted with severe obesity, with a body mass index 20% higher than the marker for obesity.
“Behavioral lifestyle interventions alone do not result in long-term, clinically important weight loss among youth with severe obesity,” the study’s authors wrote. “Metabolic and bariatric surgery (MBS) is a safe and effective treatment.”
The American Academy of Pediatrics updated its guidelines for the treatment of obesity this year for the first time in 15 years, CNN reported. “The new guidelines urge prompt use of behavior therapy and lifestyle changes and, for the first time, recommend surgery and medications for some young people,” CNN wrote.
Black and Hispanic children have higher rates of childhood obesity, the CDC says. Use of surgeries rose 42% among Black youths and 53% among Hispanic youths between 2020 and 2021.
A version of this article first appeared on WebMD.com.
.
Metabolic and bariatric surgeries have been on the rise among youths aged 10 to 19 since 2016, the report says. From 2020 to 2021, the number shot up by 19%.
The procedures change parts of the digestive system, helping the person feel more full and less hungry – thereby contributing to weight loss.
Among American children, obesity affects 20%, or 15 million people between 2 and 19. In addition, more are becoming afflicted with severe obesity, with a body mass index 20% higher than the marker for obesity.
“Behavioral lifestyle interventions alone do not result in long-term, clinically important weight loss among youth with severe obesity,” the study’s authors wrote. “Metabolic and bariatric surgery (MBS) is a safe and effective treatment.”
The American Academy of Pediatrics updated its guidelines for the treatment of obesity this year for the first time in 15 years, CNN reported. “The new guidelines urge prompt use of behavior therapy and lifestyle changes and, for the first time, recommend surgery and medications for some young people,” CNN wrote.
Black and Hispanic children have higher rates of childhood obesity, the CDC says. Use of surgeries rose 42% among Black youths and 53% among Hispanic youths between 2020 and 2021.
A version of this article first appeared on WebMD.com.
FROM JAMA PEDIATRICS
What's your diagnosis?
Answer to ‘What’s your diagnosis?’: Gastric adenocarcinoma and proximal polyposis of the stomach syndrome.
Fundic gland polyps (FGPs) are the most common gastric polyps and when occurring in the sporadic setting are typically benign; however, FGPs that occur in gastrointestinal polyposis syndromes such as familial adenomatosis polyposis can progress to adenocarcinoma and require surveillance. Therefore, it is important to distinguish sporadic versus syndromic fundic gland polyposis. Gastric adenocarcinoma and proximal polyposis of the stomach is a recently described condition that significantly increases the risk of developing invasive gastric adenocarcinoma from FGPs. Diagnostic criteria include (1) gastric polyposis restricted to the body and fundus with no small bowel or colonic involvement, (2) >100 gastric polyps or >30 polyps in a first-degree relative, (3) histology consistent with FGP with areas of dysplasia, (4) a family history consistent with an autosomal-dominant pattern of inheritance, and (5) exclusion of other syndromes and proton pump inhibitor use.1 Unlike familial adenomatosis polyposis, the polyposis is restricted to the oxyntic mucosa of the gastric body and fundus with sparing of the gastric antrum, small bowel, and colon. The genetic basis of the disease has been attributed to a point mutation in the APC gene promotor IB region leading to a loss of tumor suppressor function.2 Typical histology shows large FGPs with areas of low-grade and high-grade dysplasia, as seen in our patient.
There are few data on the natural history of gastric adenocarcinoma and proximal polyposis of the stomach, but effective surveillance is limited by the degree of polyposis. There are multiple reports of hidden adenocarcinoma on surgically resected specimens, as well as rapid progression to metastatic adenocarcinoma despite adequate diagnosis and surveillance.1,3 Therefore, total gastrectomy should be offered to patients who are surgical candidates. Our patient underwent genetic testing that revealed a point mutation in the APC promotor IB. He declined surgical intervention and opted for surveillance endoscopy every 6 months.
References
1. Worthley D.L. et al. Gut. 2012;61:774-9
2. Li J et al. Am J Hum Genet. 2016;98:830-42
3. Rudloff U. Clin Exp Gastroenterol. 2018;11:447-59
Answer to ‘What’s your diagnosis?’: Gastric adenocarcinoma and proximal polyposis of the stomach syndrome.
Fundic gland polyps (FGPs) are the most common gastric polyps and when occurring in the sporadic setting are typically benign; however, FGPs that occur in gastrointestinal polyposis syndromes such as familial adenomatosis polyposis can progress to adenocarcinoma and require surveillance. Therefore, it is important to distinguish sporadic versus syndromic fundic gland polyposis. Gastric adenocarcinoma and proximal polyposis of the stomach is a recently described condition that significantly increases the risk of developing invasive gastric adenocarcinoma from FGPs. Diagnostic criteria include (1) gastric polyposis restricted to the body and fundus with no small bowel or colonic involvement, (2) >100 gastric polyps or >30 polyps in a first-degree relative, (3) histology consistent with FGP with areas of dysplasia, (4) a family history consistent with an autosomal-dominant pattern of inheritance, and (5) exclusion of other syndromes and proton pump inhibitor use.1 Unlike familial adenomatosis polyposis, the polyposis is restricted to the oxyntic mucosa of the gastric body and fundus with sparing of the gastric antrum, small bowel, and colon. The genetic basis of the disease has been attributed to a point mutation in the APC gene promotor IB region leading to a loss of tumor suppressor function.2 Typical histology shows large FGPs with areas of low-grade and high-grade dysplasia, as seen in our patient.
There are few data on the natural history of gastric adenocarcinoma and proximal polyposis of the stomach, but effective surveillance is limited by the degree of polyposis. There are multiple reports of hidden adenocarcinoma on surgically resected specimens, as well as rapid progression to metastatic adenocarcinoma despite adequate diagnosis and surveillance.1,3 Therefore, total gastrectomy should be offered to patients who are surgical candidates. Our patient underwent genetic testing that revealed a point mutation in the APC promotor IB. He declined surgical intervention and opted for surveillance endoscopy every 6 months.
References
1. Worthley D.L. et al. Gut. 2012;61:774-9
2. Li J et al. Am J Hum Genet. 2016;98:830-42
3. Rudloff U. Clin Exp Gastroenterol. 2018;11:447-59
Answer to ‘What’s your diagnosis?’: Gastric adenocarcinoma and proximal polyposis of the stomach syndrome.
Fundic gland polyps (FGPs) are the most common gastric polyps and when occurring in the sporadic setting are typically benign; however, FGPs that occur in gastrointestinal polyposis syndromes such as familial adenomatosis polyposis can progress to adenocarcinoma and require surveillance. Therefore, it is important to distinguish sporadic versus syndromic fundic gland polyposis. Gastric adenocarcinoma and proximal polyposis of the stomach is a recently described condition that significantly increases the risk of developing invasive gastric adenocarcinoma from FGPs. Diagnostic criteria include (1) gastric polyposis restricted to the body and fundus with no small bowel or colonic involvement, (2) >100 gastric polyps or >30 polyps in a first-degree relative, (3) histology consistent with FGP with areas of dysplasia, (4) a family history consistent with an autosomal-dominant pattern of inheritance, and (5) exclusion of other syndromes and proton pump inhibitor use.1 Unlike familial adenomatosis polyposis, the polyposis is restricted to the oxyntic mucosa of the gastric body and fundus with sparing of the gastric antrum, small bowel, and colon. The genetic basis of the disease has been attributed to a point mutation in the APC gene promotor IB region leading to a loss of tumor suppressor function.2 Typical histology shows large FGPs with areas of low-grade and high-grade dysplasia, as seen in our patient.
There are few data on the natural history of gastric adenocarcinoma and proximal polyposis of the stomach, but effective surveillance is limited by the degree of polyposis. There are multiple reports of hidden adenocarcinoma on surgically resected specimens, as well as rapid progression to metastatic adenocarcinoma despite adequate diagnosis and surveillance.1,3 Therefore, total gastrectomy should be offered to patients who are surgical candidates. Our patient underwent genetic testing that revealed a point mutation in the APC promotor IB. He declined surgical intervention and opted for surveillance endoscopy every 6 months.
References
1. Worthley D.L. et al. Gut. 2012;61:774-9
2. Li J et al. Am J Hum Genet. 2016;98:830-42
3. Rudloff U. Clin Exp Gastroenterol. 2018;11:447-59
A 72-year-old man with compensated cirrhosis owing to autoimmune hepatitis presented for evaluation of an indeterminate gastric lesion found during an otherwise normal endoscopic retrograde cholangiopancreatography performed for incidental ductal dilation seen on cross-sectional imaging. He did not endorse any abdominal pain, dyspepsia, or weight loss and was not on a proton pump inhibitor. Family history was notable for a daughter diagnosed with metastatic gastric adenocarcinoma at the age of 44 years.
Upper endoscopy showed innumerable sessile polyps of variable size carpeting the gastric body and fundus (Figure A) with a large, mound-like mass lesion in the fundus (Figure A, arrow and inset). Echoendoscopy revealed a hypoechoic, noncircumferential mass restricted to the mucosal surface with well-defined borders (Figure B, arrow). A technically challenging, piecemeal endoscopic mucosal resection was performed. The patient also underwent a colonoscopy that was unremarkable. Pathology of the gastric lesion was consistent with a fundic gland polyp (Figure C, arrowheads) containing low-grade and high-grade dysplasia (Figure C, arrows).
What is the most likely diagnosis?
Positive top-line results for cannabinoid-based med for nerve pain
, new top-line results released by Zelira Therapeutics suggest.
“The implications of these results for patients are incredibly promising,” principal investigator Bryan Doner, DO, medical director of HealthyWays Integrated Wellness Solutions, Gibsonia, Pa., said in a news release.
“Through this rigorously designed study, we have demonstrated that ZLT-L-007 is a safe, effective, and well-tolerated alternative for patients who would typically seek a Lyrica-level of pain relief,” he added.
The observational, nonblinded trial tested the efficacy, safety, and tolerability of ZLT-L-007 against pregabalin in 60 adults with diabetic nerve pain.
The study had three groups with 20 patients each (pregabalin alone, pregabalin plus ZLT-L-007, and ZLT-L-007 alone).
Top-line results show the study met its primary endpoint for change in daily pain severity as measured by the percent change from baseline at 30, 60, and 90 days on the Numerical Rating Scale.
For the pregabalin-only group, there was a reduction in symptom severity at all follow-up points, ranging from 20% to 35% (median percent change from baseline), the company said.
For the ZLT-L-007 only group, there was about a 33% reduction in symptom severity at 30 days, and 71% and 78% reduction, respectively, at 60 and 90 days, suggesting a larger improvement in symptom severity than with pregabalin alone, the company said.
For the pregabalin plus ZLT-L-007 group, there was a moderate 20% reduction in symptom severity at 30 days, but a larger reduction at 60 and 90 days (50% and 72%, respectively), which indicates substantially greater improvement in symptom severity than with pregabalin alone, the company said.
The study also met secondary endpoints, including significant decreases in daily pain severity as measured by the Visual Analog Scale and measurable changes in the short-form McGill Pain Questionnaire and Neuropathic Pain Symptom Inventory.
Dr. Doner noted that the top-line data showed “no serious adverse events, and participants’ blood pressure and other safety vitals remained unaffected throughout. This confirms that ZLT-L-007 is a well-tolerated product that delivers statistically significant pain relief, surpassing the levels achieved by Lyrica.”
The company plans to report additional insights from the full study, as they become available, during fiscal year 2023-2024.
A version of this article first appeared on Medscape.com.
, new top-line results released by Zelira Therapeutics suggest.
“The implications of these results for patients are incredibly promising,” principal investigator Bryan Doner, DO, medical director of HealthyWays Integrated Wellness Solutions, Gibsonia, Pa., said in a news release.
“Through this rigorously designed study, we have demonstrated that ZLT-L-007 is a safe, effective, and well-tolerated alternative for patients who would typically seek a Lyrica-level of pain relief,” he added.
The observational, nonblinded trial tested the efficacy, safety, and tolerability of ZLT-L-007 against pregabalin in 60 adults with diabetic nerve pain.
The study had three groups with 20 patients each (pregabalin alone, pregabalin plus ZLT-L-007, and ZLT-L-007 alone).
Top-line results show the study met its primary endpoint for change in daily pain severity as measured by the percent change from baseline at 30, 60, and 90 days on the Numerical Rating Scale.
For the pregabalin-only group, there was a reduction in symptom severity at all follow-up points, ranging from 20% to 35% (median percent change from baseline), the company said.
For the ZLT-L-007 only group, there was about a 33% reduction in symptom severity at 30 days, and 71% and 78% reduction, respectively, at 60 and 90 days, suggesting a larger improvement in symptom severity than with pregabalin alone, the company said.
For the pregabalin plus ZLT-L-007 group, there was a moderate 20% reduction in symptom severity at 30 days, but a larger reduction at 60 and 90 days (50% and 72%, respectively), which indicates substantially greater improvement in symptom severity than with pregabalin alone, the company said.
The study also met secondary endpoints, including significant decreases in daily pain severity as measured by the Visual Analog Scale and measurable changes in the short-form McGill Pain Questionnaire and Neuropathic Pain Symptom Inventory.
Dr. Doner noted that the top-line data showed “no serious adverse events, and participants’ blood pressure and other safety vitals remained unaffected throughout. This confirms that ZLT-L-007 is a well-tolerated product that delivers statistically significant pain relief, surpassing the levels achieved by Lyrica.”
The company plans to report additional insights from the full study, as they become available, during fiscal year 2023-2024.
A version of this article first appeared on Medscape.com.
, new top-line results released by Zelira Therapeutics suggest.
“The implications of these results for patients are incredibly promising,” principal investigator Bryan Doner, DO, medical director of HealthyWays Integrated Wellness Solutions, Gibsonia, Pa., said in a news release.
“Through this rigorously designed study, we have demonstrated that ZLT-L-007 is a safe, effective, and well-tolerated alternative for patients who would typically seek a Lyrica-level of pain relief,” he added.
The observational, nonblinded trial tested the efficacy, safety, and tolerability of ZLT-L-007 against pregabalin in 60 adults with diabetic nerve pain.
The study had three groups with 20 patients each (pregabalin alone, pregabalin plus ZLT-L-007, and ZLT-L-007 alone).
Top-line results show the study met its primary endpoint for change in daily pain severity as measured by the percent change from baseline at 30, 60, and 90 days on the Numerical Rating Scale.
For the pregabalin-only group, there was a reduction in symptom severity at all follow-up points, ranging from 20% to 35% (median percent change from baseline), the company said.
For the ZLT-L-007 only group, there was about a 33% reduction in symptom severity at 30 days, and 71% and 78% reduction, respectively, at 60 and 90 days, suggesting a larger improvement in symptom severity than with pregabalin alone, the company said.
For the pregabalin plus ZLT-L-007 group, there was a moderate 20% reduction in symptom severity at 30 days, but a larger reduction at 60 and 90 days (50% and 72%, respectively), which indicates substantially greater improvement in symptom severity than with pregabalin alone, the company said.
The study also met secondary endpoints, including significant decreases in daily pain severity as measured by the Visual Analog Scale and measurable changes in the short-form McGill Pain Questionnaire and Neuropathic Pain Symptom Inventory.
Dr. Doner noted that the top-line data showed “no serious adverse events, and participants’ blood pressure and other safety vitals remained unaffected throughout. This confirms that ZLT-L-007 is a well-tolerated product that delivers statistically significant pain relief, surpassing the levels achieved by Lyrica.”
The company plans to report additional insights from the full study, as they become available, during fiscal year 2023-2024.
A version of this article first appeared on Medscape.com.
How a medical recoding may limit cancer patients’ options for breast reconstruction
On June 1, the Centers for Medicare & Medicaid Services plans to reexamine how doctors are paid for a type of breast reconstruction known as DIEP flap, in which skin, fat, and blood vessels are harvested from a woman’s abdomen to create a new breast.
The procedure offers potential advantages over implants and operations that take muscle from the abdomen. But it’s also more expensive. If patients go outside an insurance network for the operation, it can cost more than $50,000. And, if insurers pay significantly less for the surgery as a result of the government’s decision, some in-network surgeons would stop offering it, a plastic surgeons group has argued.
The DIEP flap controversy, spotlighted by CBS News in January, illustrates arcane and indirect ways the federal government can influence which medical options are available – even to people with private insurance. Often, the answers come down to billing codes – which identify specific medical services on forms doctors submit for reimbursement – and the competing pleas of groups whose interests are riding on them.
Medical coding is the backbone for “how business gets done in medicine,” said Karen Joynt Maddox, MD, MPH, a physician at Washington University in St. Louis who researches health economics and policy.
CMS, the agency overseeing Medicare and Medicaid, maintains a list of codes representing thousands of medical services and products. It regularly evaluates whether to add codes or revise or remove existing ones. In 2022, it decided to eliminate a code that has enabled doctors to collect much more money for DIEP flap operations than for simpler types of breast reconstruction.
In 2006, CMS established an “S” code – S2068 – for what was then a relatively new procedure: breast reconstructions with deep inferior epigastric perforator flap (DIEP flap). S codes temporarily fill gaps in a parallel system of billing codes known as CPT codes, which are maintained by the American Medical Association.
Codes don’t dictate the amounts private insurers pay for medical services; those reimbursements are generally worked out between insurance companies and medical providers. However, using the narrowly targeted S code, doctors and hospitals have been able to distinguish DIEP flap surgeries, which require complex microsurgical skills, from other forms of breast reconstruction that take less time to perform and generally yield lower insurance reimbursements.
CMS announced in 2022 that it planned to eliminate the S code at the end of 2024 – a move some doctors say would slash the amount surgeons are paid. (To be precise, CMS announced it would eliminate a series of three S codes for similar procedures, but some of the more outspoken critics have focused on one of them, S2068.) The agency’s decision is already changing the landscape of reconstructive surgery and creating anxiety for breast cancer patients.
Kate Getz, a single mother in Morton, Ill., learned she had cancer in January at age 30. As she grappled with her diagnosis, it was overwhelming to think about what her body would look like over the long term. She pictured herself getting married one day and wondered “how on earth I would be able to wear a wedding dress with only having one breast left,” she said.
She thought a DIEP flap was her best option and worried about having to undergo repeated surgeries if she got implants instead. Implants generally need to be replaced every 10 years or so. But after she spent more than a month trying to get answers about how her DIEP flap surgery would be covered, Ms. Getz’s insurer, Cigna, informed her it would use a lower-paying CPT code to reimburse her physician, Ms. Getz said. As far as she could see, that would have made it impossible for Ms. Getz to obtain the surgery.
Paying out of pocket was “not even an option.”
“I’m a single mom. We get by, right? But I’m not, not wealthy by any means,” she said.
Cost is not necessarily the only hurdle patients seeking DIEP flaps must overcome. Citing the complexity of the procedure, Ms. Getz said, a local plastic surgeon told her it would be difficult for him to perform. She ended up traveling from Illinois to Texas for the surgery.
The government’s plan to eliminate the three S codes was driven by the Blue Cross Blue Shield Association, a major lobbying organization for health insurance companies. In 2021, the group asked CMS to discontinue the codes, arguing that they were no longer needed because the AMA had updated a CPT code to explicitly include DIEP flap surgery and the related operations, according to a CMS document.
For years, the AMA advised doctors that the CPT code was appropriate for DIEP flap procedures. But after the government’s decision, at least two major insurance companies told doctors they would no longer reimburse them under the higher-paying codes, prompting a backlash.
Physicians and advocacy groups for breast cancer patients, such as the nonprofit organization Susan G. Komen, have argued that many plastic surgeons would stop providing DIEP flap procedures for women with private insurance because they wouldn’t get paid enough.
Lawmakers from both parties have asked the agency to keep the S code, including Rep. Debbie Wasserman Schultz (D-Fla.) and Sen. Amy Klobuchar (D-Minn.), who have had breast cancer, and Sen. Marsha Blackburn (R-Tenn.).
CMS at its June 1 meeting will consider whether to keep the three S codes or delay their expiration.
In a May 30 statement, Blue Cross Blue Shield Association spokesperson Kelly Parsons reiterated the organization’s view that “there is no longer a need to keep the S codes.”
In a profit-driven health care system, there’s a tug of war over reimbursements between providers and insurance companies, often at the expense of patients, said Dr. Joynt Maddox.
“We’re in this sort of constant battle” between hospital chains and insurance companies “about who’s going to wield more power at the bargaining table,” Dr. Joynt Maddox said. “And the clinical piece of that often gets lost, because it’s not often the clinical benefit and the clinical priority and the patient centeredness that’s at the middle of these conversations.”
Elisabeth Potter, MD, a plastic surgeon who specializes in DIEP flap surgeries, decided to perform Ms. Getz’s surgery at whatever price Cigna would pay.
According to Fair Health, a nonprofit that provides information on health care costs, in Austin, Tex. – where Dr. Potter is based – an insurer might pay an in-network doctor $9,323 for the surgery when it’s billed using the CPT code and $18,037 under the S code. Those amounts are not averages; rather, Fair Health estimated that 80% of payment rates are lower than or equal to those amounts.
Dr. Potter said her Cigna reimbursement “is significantly lower.”
Weeks before her May surgery, Ms. Getz received big news – Cigna had reversed itself and would cover her surgery under the S code. It “felt like a real victory,” she said.
But she still fears for other patients.
“I’m still asking these companies to do right by women,” Ms. Getz said. “I’m still asking them to provide the procedures we need to reimburse them at rates where women have access to them regardless of their wealth.”
In a statement, Cigna spokesperson Justine Sessions said the insurer remains “committed to ensuring that our customers have affordable coverage and access to the full range of breast reconstruction procedures and to quality surgeons who perform these complex surgeries.”
Medical costs that health insurers cover generally are passed along to consumers in the form of premiums, deductibles, and other out-of-pocket expenses.
For any type of breast reconstruction, there are benefits, risks, and trade-offs. A 2018 paper published in JAMA Surgery found that women who underwent DIEP flap surgery had higher odds of developing “reoperative complications” within 2 years than those who received artificial implants. However, DIEP flaps had lower odds of infection than implants.
Implants carry risks of additional surgery, pain, rupture, and even an uncommon type of immune system cancer.
Other flap procedures that take muscle from the abdomen can leave women with weakened abdominal walls and increase their risk of developing a hernia.
Academic research shows that insurance reimbursement affects which women can access DIEP flap breast reconstruction, creating a two-tiered system for private health insurance versus government programs like Medicare and Medicaid. Private insurance generally pays physicians more than government coverage, and Medicare doesn’t use S codes.
Lynn Damitz, a physician and board vice president of health policy and advocacy for the American Society of Plastic Surgeons, said the group supports continuing the S code temporarily or indefinitely. If reimbursements drop, some doctors won’t perform DIEP flaps anymore.
A study published in February found that, of patients who used their own tissue for breast reconstruction, privately insured patients were more likely than publicly insured patients to receive DIEP flap reconstruction.
To Dr. Potter, that shows what will happen if private insurance payments plummet. “If you’re a Medicare provider and you’re not paid to do DIEP flaps, you never tell a patient that it’s an option. You won’t perform it,” Dr. Potter said. “If you take private insurance and all of a sudden your reimbursement rate is cut from $15,000 down to $3,500, you’re not going to do that surgery. And I’m not saying that that’s the right thing to do, but that’s what happens.”
KHN (Kaiser Health News) is a national newsroom that produces in-depth journalism about health issues. Together with Policy Analysis and Polling, KHN is one of the three major operating programs at KFF (Kaiser Family Foundation). KFF is an endowed nonprofit organization providing information on health issues to the nation.
On June 1, the Centers for Medicare & Medicaid Services plans to reexamine how doctors are paid for a type of breast reconstruction known as DIEP flap, in which skin, fat, and blood vessels are harvested from a woman’s abdomen to create a new breast.
The procedure offers potential advantages over implants and operations that take muscle from the abdomen. But it’s also more expensive. If patients go outside an insurance network for the operation, it can cost more than $50,000. And, if insurers pay significantly less for the surgery as a result of the government’s decision, some in-network surgeons would stop offering it, a plastic surgeons group has argued.
The DIEP flap controversy, spotlighted by CBS News in January, illustrates arcane and indirect ways the federal government can influence which medical options are available – even to people with private insurance. Often, the answers come down to billing codes – which identify specific medical services on forms doctors submit for reimbursement – and the competing pleas of groups whose interests are riding on them.
Medical coding is the backbone for “how business gets done in medicine,” said Karen Joynt Maddox, MD, MPH, a physician at Washington University in St. Louis who researches health economics and policy.
CMS, the agency overseeing Medicare and Medicaid, maintains a list of codes representing thousands of medical services and products. It regularly evaluates whether to add codes or revise or remove existing ones. In 2022, it decided to eliminate a code that has enabled doctors to collect much more money for DIEP flap operations than for simpler types of breast reconstruction.
In 2006, CMS established an “S” code – S2068 – for what was then a relatively new procedure: breast reconstructions with deep inferior epigastric perforator flap (DIEP flap). S codes temporarily fill gaps in a parallel system of billing codes known as CPT codes, which are maintained by the American Medical Association.
Codes don’t dictate the amounts private insurers pay for medical services; those reimbursements are generally worked out between insurance companies and medical providers. However, using the narrowly targeted S code, doctors and hospitals have been able to distinguish DIEP flap surgeries, which require complex microsurgical skills, from other forms of breast reconstruction that take less time to perform and generally yield lower insurance reimbursements.
CMS announced in 2022 that it planned to eliminate the S code at the end of 2024 – a move some doctors say would slash the amount surgeons are paid. (To be precise, CMS announced it would eliminate a series of three S codes for similar procedures, but some of the more outspoken critics have focused on one of them, S2068.) The agency’s decision is already changing the landscape of reconstructive surgery and creating anxiety for breast cancer patients.
Kate Getz, a single mother in Morton, Ill., learned she had cancer in January at age 30. As she grappled with her diagnosis, it was overwhelming to think about what her body would look like over the long term. She pictured herself getting married one day and wondered “how on earth I would be able to wear a wedding dress with only having one breast left,” she said.
She thought a DIEP flap was her best option and worried about having to undergo repeated surgeries if she got implants instead. Implants generally need to be replaced every 10 years or so. But after she spent more than a month trying to get answers about how her DIEP flap surgery would be covered, Ms. Getz’s insurer, Cigna, informed her it would use a lower-paying CPT code to reimburse her physician, Ms. Getz said. As far as she could see, that would have made it impossible for Ms. Getz to obtain the surgery.
Paying out of pocket was “not even an option.”
“I’m a single mom. We get by, right? But I’m not, not wealthy by any means,” she said.
Cost is not necessarily the only hurdle patients seeking DIEP flaps must overcome. Citing the complexity of the procedure, Ms. Getz said, a local plastic surgeon told her it would be difficult for him to perform. She ended up traveling from Illinois to Texas for the surgery.
The government’s plan to eliminate the three S codes was driven by the Blue Cross Blue Shield Association, a major lobbying organization for health insurance companies. In 2021, the group asked CMS to discontinue the codes, arguing that they were no longer needed because the AMA had updated a CPT code to explicitly include DIEP flap surgery and the related operations, according to a CMS document.
For years, the AMA advised doctors that the CPT code was appropriate for DIEP flap procedures. But after the government’s decision, at least two major insurance companies told doctors they would no longer reimburse them under the higher-paying codes, prompting a backlash.
Physicians and advocacy groups for breast cancer patients, such as the nonprofit organization Susan G. Komen, have argued that many plastic surgeons would stop providing DIEP flap procedures for women with private insurance because they wouldn’t get paid enough.
Lawmakers from both parties have asked the agency to keep the S code, including Rep. Debbie Wasserman Schultz (D-Fla.) and Sen. Amy Klobuchar (D-Minn.), who have had breast cancer, and Sen. Marsha Blackburn (R-Tenn.).
CMS at its June 1 meeting will consider whether to keep the three S codes or delay their expiration.
In a May 30 statement, Blue Cross Blue Shield Association spokesperson Kelly Parsons reiterated the organization’s view that “there is no longer a need to keep the S codes.”
In a profit-driven health care system, there’s a tug of war over reimbursements between providers and insurance companies, often at the expense of patients, said Dr. Joynt Maddox.
“We’re in this sort of constant battle” between hospital chains and insurance companies “about who’s going to wield more power at the bargaining table,” Dr. Joynt Maddox said. “And the clinical piece of that often gets lost, because it’s not often the clinical benefit and the clinical priority and the patient centeredness that’s at the middle of these conversations.”
Elisabeth Potter, MD, a plastic surgeon who specializes in DIEP flap surgeries, decided to perform Ms. Getz’s surgery at whatever price Cigna would pay.
According to Fair Health, a nonprofit that provides information on health care costs, in Austin, Tex. – where Dr. Potter is based – an insurer might pay an in-network doctor $9,323 for the surgery when it’s billed using the CPT code and $18,037 under the S code. Those amounts are not averages; rather, Fair Health estimated that 80% of payment rates are lower than or equal to those amounts.
Dr. Potter said her Cigna reimbursement “is significantly lower.”
Weeks before her May surgery, Ms. Getz received big news – Cigna had reversed itself and would cover her surgery under the S code. It “felt like a real victory,” she said.
But she still fears for other patients.
“I’m still asking these companies to do right by women,” Ms. Getz said. “I’m still asking them to provide the procedures we need to reimburse them at rates where women have access to them regardless of their wealth.”
In a statement, Cigna spokesperson Justine Sessions said the insurer remains “committed to ensuring that our customers have affordable coverage and access to the full range of breast reconstruction procedures and to quality surgeons who perform these complex surgeries.”
Medical costs that health insurers cover generally are passed along to consumers in the form of premiums, deductibles, and other out-of-pocket expenses.
For any type of breast reconstruction, there are benefits, risks, and trade-offs. A 2018 paper published in JAMA Surgery found that women who underwent DIEP flap surgery had higher odds of developing “reoperative complications” within 2 years than those who received artificial implants. However, DIEP flaps had lower odds of infection than implants.
Implants carry risks of additional surgery, pain, rupture, and even an uncommon type of immune system cancer.
Other flap procedures that take muscle from the abdomen can leave women with weakened abdominal walls and increase their risk of developing a hernia.
Academic research shows that insurance reimbursement affects which women can access DIEP flap breast reconstruction, creating a two-tiered system for private health insurance versus government programs like Medicare and Medicaid. Private insurance generally pays physicians more than government coverage, and Medicare doesn’t use S codes.
Lynn Damitz, a physician and board vice president of health policy and advocacy for the American Society of Plastic Surgeons, said the group supports continuing the S code temporarily or indefinitely. If reimbursements drop, some doctors won’t perform DIEP flaps anymore.
A study published in February found that, of patients who used their own tissue for breast reconstruction, privately insured patients were more likely than publicly insured patients to receive DIEP flap reconstruction.
To Dr. Potter, that shows what will happen if private insurance payments plummet. “If you’re a Medicare provider and you’re not paid to do DIEP flaps, you never tell a patient that it’s an option. You won’t perform it,” Dr. Potter said. “If you take private insurance and all of a sudden your reimbursement rate is cut from $15,000 down to $3,500, you’re not going to do that surgery. And I’m not saying that that’s the right thing to do, but that’s what happens.”
KHN (Kaiser Health News) is a national newsroom that produces in-depth journalism about health issues. Together with Policy Analysis and Polling, KHN is one of the three major operating programs at KFF (Kaiser Family Foundation). KFF is an endowed nonprofit organization providing information on health issues to the nation.
On June 1, the Centers for Medicare & Medicaid Services plans to reexamine how doctors are paid for a type of breast reconstruction known as DIEP flap, in which skin, fat, and blood vessels are harvested from a woman’s abdomen to create a new breast.
The procedure offers potential advantages over implants and operations that take muscle from the abdomen. But it’s also more expensive. If patients go outside an insurance network for the operation, it can cost more than $50,000. And, if insurers pay significantly less for the surgery as a result of the government’s decision, some in-network surgeons would stop offering it, a plastic surgeons group has argued.
The DIEP flap controversy, spotlighted by CBS News in January, illustrates arcane and indirect ways the federal government can influence which medical options are available – even to people with private insurance. Often, the answers come down to billing codes – which identify specific medical services on forms doctors submit for reimbursement – and the competing pleas of groups whose interests are riding on them.
Medical coding is the backbone for “how business gets done in medicine,” said Karen Joynt Maddox, MD, MPH, a physician at Washington University in St. Louis who researches health economics and policy.
CMS, the agency overseeing Medicare and Medicaid, maintains a list of codes representing thousands of medical services and products. It regularly evaluates whether to add codes or revise or remove existing ones. In 2022, it decided to eliminate a code that has enabled doctors to collect much more money for DIEP flap operations than for simpler types of breast reconstruction.
In 2006, CMS established an “S” code – S2068 – for what was then a relatively new procedure: breast reconstructions with deep inferior epigastric perforator flap (DIEP flap). S codes temporarily fill gaps in a parallel system of billing codes known as CPT codes, which are maintained by the American Medical Association.
Codes don’t dictate the amounts private insurers pay for medical services; those reimbursements are generally worked out between insurance companies and medical providers. However, using the narrowly targeted S code, doctors and hospitals have been able to distinguish DIEP flap surgeries, which require complex microsurgical skills, from other forms of breast reconstruction that take less time to perform and generally yield lower insurance reimbursements.
CMS announced in 2022 that it planned to eliminate the S code at the end of 2024 – a move some doctors say would slash the amount surgeons are paid. (To be precise, CMS announced it would eliminate a series of three S codes for similar procedures, but some of the more outspoken critics have focused on one of them, S2068.) The agency’s decision is already changing the landscape of reconstructive surgery and creating anxiety for breast cancer patients.
Kate Getz, a single mother in Morton, Ill., learned she had cancer in January at age 30. As she grappled with her diagnosis, it was overwhelming to think about what her body would look like over the long term. She pictured herself getting married one day and wondered “how on earth I would be able to wear a wedding dress with only having one breast left,” she said.
She thought a DIEP flap was her best option and worried about having to undergo repeated surgeries if she got implants instead. Implants generally need to be replaced every 10 years or so. But after she spent more than a month trying to get answers about how her DIEP flap surgery would be covered, Ms. Getz’s insurer, Cigna, informed her it would use a lower-paying CPT code to reimburse her physician, Ms. Getz said. As far as she could see, that would have made it impossible for Ms. Getz to obtain the surgery.
Paying out of pocket was “not even an option.”
“I’m a single mom. We get by, right? But I’m not, not wealthy by any means,” she said.
Cost is not necessarily the only hurdle patients seeking DIEP flaps must overcome. Citing the complexity of the procedure, Ms. Getz said, a local plastic surgeon told her it would be difficult for him to perform. She ended up traveling from Illinois to Texas for the surgery.
The government’s plan to eliminate the three S codes was driven by the Blue Cross Blue Shield Association, a major lobbying organization for health insurance companies. In 2021, the group asked CMS to discontinue the codes, arguing that they were no longer needed because the AMA had updated a CPT code to explicitly include DIEP flap surgery and the related operations, according to a CMS document.
For years, the AMA advised doctors that the CPT code was appropriate for DIEP flap procedures. But after the government’s decision, at least two major insurance companies told doctors they would no longer reimburse them under the higher-paying codes, prompting a backlash.
Physicians and advocacy groups for breast cancer patients, such as the nonprofit organization Susan G. Komen, have argued that many plastic surgeons would stop providing DIEP flap procedures for women with private insurance because they wouldn’t get paid enough.
Lawmakers from both parties have asked the agency to keep the S code, including Rep. Debbie Wasserman Schultz (D-Fla.) and Sen. Amy Klobuchar (D-Minn.), who have had breast cancer, and Sen. Marsha Blackburn (R-Tenn.).
CMS at its June 1 meeting will consider whether to keep the three S codes or delay their expiration.
In a May 30 statement, Blue Cross Blue Shield Association spokesperson Kelly Parsons reiterated the organization’s view that “there is no longer a need to keep the S codes.”
In a profit-driven health care system, there’s a tug of war over reimbursements between providers and insurance companies, often at the expense of patients, said Dr. Joynt Maddox.
“We’re in this sort of constant battle” between hospital chains and insurance companies “about who’s going to wield more power at the bargaining table,” Dr. Joynt Maddox said. “And the clinical piece of that often gets lost, because it’s not often the clinical benefit and the clinical priority and the patient centeredness that’s at the middle of these conversations.”
Elisabeth Potter, MD, a plastic surgeon who specializes in DIEP flap surgeries, decided to perform Ms. Getz’s surgery at whatever price Cigna would pay.
According to Fair Health, a nonprofit that provides information on health care costs, in Austin, Tex. – where Dr. Potter is based – an insurer might pay an in-network doctor $9,323 for the surgery when it’s billed using the CPT code and $18,037 under the S code. Those amounts are not averages; rather, Fair Health estimated that 80% of payment rates are lower than or equal to those amounts.
Dr. Potter said her Cigna reimbursement “is significantly lower.”
Weeks before her May surgery, Ms. Getz received big news – Cigna had reversed itself and would cover her surgery under the S code. It “felt like a real victory,” she said.
But she still fears for other patients.
“I’m still asking these companies to do right by women,” Ms. Getz said. “I’m still asking them to provide the procedures we need to reimburse them at rates where women have access to them regardless of their wealth.”
In a statement, Cigna spokesperson Justine Sessions said the insurer remains “committed to ensuring that our customers have affordable coverage and access to the full range of breast reconstruction procedures and to quality surgeons who perform these complex surgeries.”
Medical costs that health insurers cover generally are passed along to consumers in the form of premiums, deductibles, and other out-of-pocket expenses.
For any type of breast reconstruction, there are benefits, risks, and trade-offs. A 2018 paper published in JAMA Surgery found that women who underwent DIEP flap surgery had higher odds of developing “reoperative complications” within 2 years than those who received artificial implants. However, DIEP flaps had lower odds of infection than implants.
Implants carry risks of additional surgery, pain, rupture, and even an uncommon type of immune system cancer.
Other flap procedures that take muscle from the abdomen can leave women with weakened abdominal walls and increase their risk of developing a hernia.
Academic research shows that insurance reimbursement affects which women can access DIEP flap breast reconstruction, creating a two-tiered system for private health insurance versus government programs like Medicare and Medicaid. Private insurance generally pays physicians more than government coverage, and Medicare doesn’t use S codes.
Lynn Damitz, a physician and board vice president of health policy and advocacy for the American Society of Plastic Surgeons, said the group supports continuing the S code temporarily or indefinitely. If reimbursements drop, some doctors won’t perform DIEP flaps anymore.
A study published in February found that, of patients who used their own tissue for breast reconstruction, privately insured patients were more likely than publicly insured patients to receive DIEP flap reconstruction.
To Dr. Potter, that shows what will happen if private insurance payments plummet. “If you’re a Medicare provider and you’re not paid to do DIEP flaps, you never tell a patient that it’s an option. You won’t perform it,” Dr. Potter said. “If you take private insurance and all of a sudden your reimbursement rate is cut from $15,000 down to $3,500, you’re not going to do that surgery. And I’m not saying that that’s the right thing to do, but that’s what happens.”
KHN (Kaiser Health News) is a national newsroom that produces in-depth journalism about health issues. Together with Policy Analysis and Polling, KHN is one of the three major operating programs at KFF (Kaiser Family Foundation). KFF is an endowed nonprofit organization providing information on health issues to the nation.