User login
Targeting disease stem cells in AML, MDS
Image by Robert Paulson
The cell surface molecule CD99 occurs more frequently than normal on stem cells responsible for acute myeloid leukemia (AML) and myelodysplastic syndromes (MDS), according to research published in Science Translational Medicine.
Building on this discovery, researchers designed anti-CD99 monoclonal antibodies (mAbs).
In vitro and in vivo experiments
showed that these mAbs can recognize
and destroy AML and MDS stem/progenitor cells.
“Our findings not only identify a new molecule expressed on stem cells that drive these human malignancies, but we show that antibodies against this target can directly kill human AML stem cells,” said study author Christopher Y. Park, MD, PhD, of NYU Langone Medical Center in New York, New York.
“While we still have important details to work out, CD99 is likely to be an exploitable therapeutic target for most AML and MDS patients, and we are working urgently to finalize a therapy for human testing.”
Dr Park and his colleagues first examined stem cell populations from 79 patients with AML and 24 with MDS. More than 80% of stem cells in both groups expressed high levels of CD99.
The levels were so high that leukemia stem cells could be cleanly separated from normal hematopoietic stem cells in AML samples.
Upon confirming that CD99 was abundant on AML and MDS stem cells, the researchers made several anti-CD99 mAbs and tested them in vitro and in mouse models.
The mAbs destroyed AML and MDS stem cells by causing a sudden spike in the activity of SRC family kinases—a group of proteins that are implicated in invasion, tumor progression, and metastasis in a variety of cancers.
However, the mAbs had minimal effects on normal hematopoietic stem cells.
“With the appropriate support, we believe we can rapidly determine the best antibodies for use in patients, produce them at the quality needed to verify our results, and apply for permission to begin clinical trials,” Dr Park said. ![]()

Image by Robert Paulson
The cell surface molecule CD99 occurs more frequently than normal on stem cells responsible for acute myeloid leukemia (AML) and myelodysplastic syndromes (MDS), according to research published in Science Translational Medicine.
Building on this discovery, researchers designed anti-CD99 monoclonal antibodies (mAbs).
In vitro and in vivo experiments
showed that these mAbs can recognize
and destroy AML and MDS stem/progenitor cells.
“Our findings not only identify a new molecule expressed on stem cells that drive these human malignancies, but we show that antibodies against this target can directly kill human AML stem cells,” said study author Christopher Y. Park, MD, PhD, of NYU Langone Medical Center in New York, New York.
“While we still have important details to work out, CD99 is likely to be an exploitable therapeutic target for most AML and MDS patients, and we are working urgently to finalize a therapy for human testing.”
Dr Park and his colleagues first examined stem cell populations from 79 patients with AML and 24 with MDS. More than 80% of stem cells in both groups expressed high levels of CD99.
The levels were so high that leukemia stem cells could be cleanly separated from normal hematopoietic stem cells in AML samples.
Upon confirming that CD99 was abundant on AML and MDS stem cells, the researchers made several anti-CD99 mAbs and tested them in vitro and in mouse models.
The mAbs destroyed AML and MDS stem cells by causing a sudden spike in the activity of SRC family kinases—a group of proteins that are implicated in invasion, tumor progression, and metastasis in a variety of cancers.
However, the mAbs had minimal effects on normal hematopoietic stem cells.
“With the appropriate support, we believe we can rapidly determine the best antibodies for use in patients, produce them at the quality needed to verify our results, and apply for permission to begin clinical trials,” Dr Park said. ![]()

Image by Robert Paulson
The cell surface molecule CD99 occurs more frequently than normal on stem cells responsible for acute myeloid leukemia (AML) and myelodysplastic syndromes (MDS), according to research published in Science Translational Medicine.
Building on this discovery, researchers designed anti-CD99 monoclonal antibodies (mAbs).
In vitro and in vivo experiments
showed that these mAbs can recognize
and destroy AML and MDS stem/progenitor cells.
“Our findings not only identify a new molecule expressed on stem cells that drive these human malignancies, but we show that antibodies against this target can directly kill human AML stem cells,” said study author Christopher Y. Park, MD, PhD, of NYU Langone Medical Center in New York, New York.
“While we still have important details to work out, CD99 is likely to be an exploitable therapeutic target for most AML and MDS patients, and we are working urgently to finalize a therapy for human testing.”
Dr Park and his colleagues first examined stem cell populations from 79 patients with AML and 24 with MDS. More than 80% of stem cells in both groups expressed high levels of CD99.
The levels were so high that leukemia stem cells could be cleanly separated from normal hematopoietic stem cells in AML samples.
Upon confirming that CD99 was abundant on AML and MDS stem cells, the researchers made several anti-CD99 mAbs and tested them in vitro and in mouse models.
The mAbs destroyed AML and MDS stem cells by causing a sudden spike in the activity of SRC family kinases—a group of proteins that are implicated in invasion, tumor progression, and metastasis in a variety of cancers.
However, the mAbs had minimal effects on normal hematopoietic stem cells.
“With the appropriate support, we believe we can rapidly determine the best antibodies for use in patients, produce them at the quality needed to verify our results, and apply for permission to begin clinical trials,” Dr Park said. ![]()
Gene therapy granted breakthrough designation to treat hemophilia B

Image by Spencer Phillips
The US Food and Drug Administration (FDA) has granted breakthrough therapy designation for the investigational gene therapy AMT-060 as a treatment for patients with severe hemophilia B.
AMT-060 consists of a codon-optimized wild-type factor IX (FIX) gene cassette, the LP1 liver promoter, and an AAV5 viral vector manufactured by uniQure using its proprietary insect cell-based technology platform. uniQure is the company developing AMT-060.
The FDA’s breakthrough therapy designation is intended to expedite the development and review of new treatments for serious or life-threatening conditions.
Breakthrough designation entitles the company developing a therapy to more intensive FDA guidance on an efficient and accelerated development program, as well as eligibility for other actions to expedite FDA review, such as a rolling submission and priority review.
To earn breakthrough designation, a treatment must show encouraging early clinical results demonstrating substantial improvement over available therapies with regard to a clinically significant endpoint, or it must fulfill an unmet need.
Phase 1/2 trial
The breakthrough designation for AMT-060 is based on results from an ongoing phase 1/2 study. Updated data from this study were recently presented at the 2016 ASH Annual Meeting (abstract 2314).
In this trial, researchers are testing AMT-060 in 10 patients. All patients had severe or moderately severe hemophilia at baseline, including documented FIX levels less than 1% to 2% of normal, and required chronic infusions of prophylactic or on-demand FIX therapy at the time of enrollment.
Each patient received a 1-time, 30-minute, intravenous dose of AMT-060, without the use of corticosteroids. Five patients received AMT-060 at 5 x 1012 gc/kg, and 5 received AMT-060 at 2 x 1013 gc/kg.
The data presented at ASH included up to 52 weeks of follow-up from the low-dose cohort and up to 31 weeks of follow-up from the higher-dose cohort.
Data from the higher-dose cohort show a dose response with improvement in disease state in all 5 patients. Four patients who previously required prophylactic FIX replacement therapy were able to stop this therapy.
As of the data cutoff date for the ASH presentation, 1 unconfirmed spontaneous bleed had been reported during an aggregate of 94 weeks of follow-up after the discontinuation of prophylaxis.
Researchers previously reported that 4 patients in the low-dose cohort were able to discontinue prophylactic therapy. The 1 patient who
remained on prophylaxis sustained an improved disease
phenotype and also required materially less FIX concentrate after
treatment with AMT-060.
According to uniQure, all 5 patients in the low-dose cohort continue to maintain “constant and clinically meaningful” levels of FIX activity for up to 52 weeks post-treatment. In fact, there were no spontaneous bleeds in these patients in the last 14 weeks of observation.
uniQure also said AMT-060 continues to be well-tolerated, and there have been no severe adverse events.
Three patients (2 in the higher-dose cohort and 1 previously reported from the low-dose cohort) experienced mild, asymptomatic elevations of alanine aminotransferase and received a tapering course of corticosteroids per protocol.
These temporary alanine aminotransferase elevations were not associated with any loss of endogenous FIX activity or T-cell response to the AAV5 capsid.
None of the patients in either cohort have developed inhibitory antibodies against FIX, and none of the patients screened tested positive for anti-AAV5 antibodies. ![]()

Image by Spencer Phillips
The US Food and Drug Administration (FDA) has granted breakthrough therapy designation for the investigational gene therapy AMT-060 as a treatment for patients with severe hemophilia B.
AMT-060 consists of a codon-optimized wild-type factor IX (FIX) gene cassette, the LP1 liver promoter, and an AAV5 viral vector manufactured by uniQure using its proprietary insect cell-based technology platform. uniQure is the company developing AMT-060.
The FDA’s breakthrough therapy designation is intended to expedite the development and review of new treatments for serious or life-threatening conditions.
Breakthrough designation entitles the company developing a therapy to more intensive FDA guidance on an efficient and accelerated development program, as well as eligibility for other actions to expedite FDA review, such as a rolling submission and priority review.
To earn breakthrough designation, a treatment must show encouraging early clinical results demonstrating substantial improvement over available therapies with regard to a clinically significant endpoint, or it must fulfill an unmet need.
Phase 1/2 trial
The breakthrough designation for AMT-060 is based on results from an ongoing phase 1/2 study. Updated data from this study were recently presented at the 2016 ASH Annual Meeting (abstract 2314).
In this trial, researchers are testing AMT-060 in 10 patients. All patients had severe or moderately severe hemophilia at baseline, including documented FIX levels less than 1% to 2% of normal, and required chronic infusions of prophylactic or on-demand FIX therapy at the time of enrollment.
Each patient received a 1-time, 30-minute, intravenous dose of AMT-060, without the use of corticosteroids. Five patients received AMT-060 at 5 x 1012 gc/kg, and 5 received AMT-060 at 2 x 1013 gc/kg.
The data presented at ASH included up to 52 weeks of follow-up from the low-dose cohort and up to 31 weeks of follow-up from the higher-dose cohort.
Data from the higher-dose cohort show a dose response with improvement in disease state in all 5 patients. Four patients who previously required prophylactic FIX replacement therapy were able to stop this therapy.
As of the data cutoff date for the ASH presentation, 1 unconfirmed spontaneous bleed had been reported during an aggregate of 94 weeks of follow-up after the discontinuation of prophylaxis.
Researchers previously reported that 4 patients in the low-dose cohort were able to discontinue prophylactic therapy. The 1 patient who
remained on prophylaxis sustained an improved disease
phenotype and also required materially less FIX concentrate after
treatment with AMT-060.
According to uniQure, all 5 patients in the low-dose cohort continue to maintain “constant and clinically meaningful” levels of FIX activity for up to 52 weeks post-treatment. In fact, there were no spontaneous bleeds in these patients in the last 14 weeks of observation.
uniQure also said AMT-060 continues to be well-tolerated, and there have been no severe adverse events.
Three patients (2 in the higher-dose cohort and 1 previously reported from the low-dose cohort) experienced mild, asymptomatic elevations of alanine aminotransferase and received a tapering course of corticosteroids per protocol.
These temporary alanine aminotransferase elevations were not associated with any loss of endogenous FIX activity or T-cell response to the AAV5 capsid.
None of the patients in either cohort have developed inhibitory antibodies against FIX, and none of the patients screened tested positive for anti-AAV5 antibodies. ![]()

Image by Spencer Phillips
The US Food and Drug Administration (FDA) has granted breakthrough therapy designation for the investigational gene therapy AMT-060 as a treatment for patients with severe hemophilia B.
AMT-060 consists of a codon-optimized wild-type factor IX (FIX) gene cassette, the LP1 liver promoter, and an AAV5 viral vector manufactured by uniQure using its proprietary insect cell-based technology platform. uniQure is the company developing AMT-060.
The FDA’s breakthrough therapy designation is intended to expedite the development and review of new treatments for serious or life-threatening conditions.
Breakthrough designation entitles the company developing a therapy to more intensive FDA guidance on an efficient and accelerated development program, as well as eligibility for other actions to expedite FDA review, such as a rolling submission and priority review.
To earn breakthrough designation, a treatment must show encouraging early clinical results demonstrating substantial improvement over available therapies with regard to a clinically significant endpoint, or it must fulfill an unmet need.
Phase 1/2 trial
The breakthrough designation for AMT-060 is based on results from an ongoing phase 1/2 study. Updated data from this study were recently presented at the 2016 ASH Annual Meeting (abstract 2314).
In this trial, researchers are testing AMT-060 in 10 patients. All patients had severe or moderately severe hemophilia at baseline, including documented FIX levels less than 1% to 2% of normal, and required chronic infusions of prophylactic or on-demand FIX therapy at the time of enrollment.
Each patient received a 1-time, 30-minute, intravenous dose of AMT-060, without the use of corticosteroids. Five patients received AMT-060 at 5 x 1012 gc/kg, and 5 received AMT-060 at 2 x 1013 gc/kg.
The data presented at ASH included up to 52 weeks of follow-up from the low-dose cohort and up to 31 weeks of follow-up from the higher-dose cohort.
Data from the higher-dose cohort show a dose response with improvement in disease state in all 5 patients. Four patients who previously required prophylactic FIX replacement therapy were able to stop this therapy.
As of the data cutoff date for the ASH presentation, 1 unconfirmed spontaneous bleed had been reported during an aggregate of 94 weeks of follow-up after the discontinuation of prophylaxis.
Researchers previously reported that 4 patients in the low-dose cohort were able to discontinue prophylactic therapy. The 1 patient who
remained on prophylaxis sustained an improved disease
phenotype and also required materially less FIX concentrate after
treatment with AMT-060.
According to uniQure, all 5 patients in the low-dose cohort continue to maintain “constant and clinically meaningful” levels of FIX activity for up to 52 weeks post-treatment. In fact, there were no spontaneous bleeds in these patients in the last 14 weeks of observation.
uniQure also said AMT-060 continues to be well-tolerated, and there have been no severe adverse events.
Three patients (2 in the higher-dose cohort and 1 previously reported from the low-dose cohort) experienced mild, asymptomatic elevations of alanine aminotransferase and received a tapering course of corticosteroids per protocol.
These temporary alanine aminotransferase elevations were not associated with any loss of endogenous FIX activity or T-cell response to the AAV5 capsid.
None of the patients in either cohort have developed inhibitory antibodies against FIX, and none of the patients screened tested positive for anti-AAV5 antibodies. ![]()
Long-term oxygen for COPD with moderate desaturation
Clinical question: Does using supplemental oxygen in patients with stable chronic obstructive pulmonary disease (COPD) result in a longer time to death or first hospitalization?
Background: Previous trials have shown that use of long-term, supplemental oxygen in COPD and severe resting hypoxia reduced mortality, however, data is inconclusive if its use in mild-moderate COPD has the same effect.
Study design: Parallel-group, randomized, unblinded clinical trial.
Synopsis: Researchers randomized 738 patients from 42 outpatient centers with stable COPD and moderate resting desaturation (SpO2, 89%-93%) or moderate exercise induced desaturation (6-minute walk test, SpO2 greater than 80% for five minutes, and greater than 90% for 10 seconds) to long-term supplemental oxygen or no supplemental oxygen. Time-to-event analysis found no differences in the composite primary outcome of death or first hospitalization (HR, 0.94; 95% confidence interval, 0.79-1.12), or in any other secondary outcomes of COPD exacerbations, or COPD-related or all-cause hospitalizations.
Limitations included lack of blinding, possible exclusion of patients with higher COPD severity, and lack of assessment of immediate effects of oxygen on symptoms or exercise performance.
Bottom line: Long-term, supplemental oxygen provided no benefit in mortality or time to first hospitalization among other outcomes in patients with stable COPD and resting or exercise-induced moderate desaturations.
Citation: The Long-Term Oxygen Treatment Trial Research Group. A randomized trial of long-term oxygen for COPD with moderate desaturation. N Engl J Med. 2016;375:1617-27.
Dr. Ciarkowski is a clinical instructor at the University of Utah School of Medicine and an academic hospitalist at the University of Utah Hospital.
Clinical question: Does using supplemental oxygen in patients with stable chronic obstructive pulmonary disease (COPD) result in a longer time to death or first hospitalization?
Background: Previous trials have shown that use of long-term, supplemental oxygen in COPD and severe resting hypoxia reduced mortality, however, data is inconclusive if its use in mild-moderate COPD has the same effect.
Study design: Parallel-group, randomized, unblinded clinical trial.
Synopsis: Researchers randomized 738 patients from 42 outpatient centers with stable COPD and moderate resting desaturation (SpO2, 89%-93%) or moderate exercise induced desaturation (6-minute walk test, SpO2 greater than 80% for five minutes, and greater than 90% for 10 seconds) to long-term supplemental oxygen or no supplemental oxygen. Time-to-event analysis found no differences in the composite primary outcome of death or first hospitalization (HR, 0.94; 95% confidence interval, 0.79-1.12), or in any other secondary outcomes of COPD exacerbations, or COPD-related or all-cause hospitalizations.
Limitations included lack of blinding, possible exclusion of patients with higher COPD severity, and lack of assessment of immediate effects of oxygen on symptoms or exercise performance.
Bottom line: Long-term, supplemental oxygen provided no benefit in mortality or time to first hospitalization among other outcomes in patients with stable COPD and resting or exercise-induced moderate desaturations.
Citation: The Long-Term Oxygen Treatment Trial Research Group. A randomized trial of long-term oxygen for COPD with moderate desaturation. N Engl J Med. 2016;375:1617-27.
Dr. Ciarkowski is a clinical instructor at the University of Utah School of Medicine and an academic hospitalist at the University of Utah Hospital.
Clinical question: Does using supplemental oxygen in patients with stable chronic obstructive pulmonary disease (COPD) result in a longer time to death or first hospitalization?
Background: Previous trials have shown that use of long-term, supplemental oxygen in COPD and severe resting hypoxia reduced mortality, however, data is inconclusive if its use in mild-moderate COPD has the same effect.
Study design: Parallel-group, randomized, unblinded clinical trial.
Synopsis: Researchers randomized 738 patients from 42 outpatient centers with stable COPD and moderate resting desaturation (SpO2, 89%-93%) or moderate exercise induced desaturation (6-minute walk test, SpO2 greater than 80% for five minutes, and greater than 90% for 10 seconds) to long-term supplemental oxygen or no supplemental oxygen. Time-to-event analysis found no differences in the composite primary outcome of death or first hospitalization (HR, 0.94; 95% confidence interval, 0.79-1.12), or in any other secondary outcomes of COPD exacerbations, or COPD-related or all-cause hospitalizations.
Limitations included lack of blinding, possible exclusion of patients with higher COPD severity, and lack of assessment of immediate effects of oxygen on symptoms or exercise performance.
Bottom line: Long-term, supplemental oxygen provided no benefit in mortality or time to first hospitalization among other outcomes in patients with stable COPD and resting or exercise-induced moderate desaturations.
Citation: The Long-Term Oxygen Treatment Trial Research Group. A randomized trial of long-term oxygen for COPD with moderate desaturation. N Engl J Med. 2016;375:1617-27.
Dr. Ciarkowski is a clinical instructor at the University of Utah School of Medicine and an academic hospitalist at the University of Utah Hospital.
Breath test aims to sniff out GEJ cancers
AMSTERDAM – A test that samples exhaled breath and looks for the presence of just five volatile organic compounds shows promise as an inexpensive method for screening patients with suspected cancers of the gastroesophageal junction (GEJ), investigators from the United Kingdom reported.
In a multicenter clinical trial testing breath samples from patients with adenocarcinoma of the GEJ and matched controls, the test had an overall sensitivity of 80% and specificity of 81% for adenocarcinoma of the GEJ, said Sheraz R. Markar, MD, PhD, from Imperial College London.
If the test can be validated in larger studies, it could increase the number of patients screened and has the potential to save medical costs by reducing the number of unnecessary endoscopies and by catching GEJ cancers at earlier, potentially curable stages, he said.
The test uses selected ion flow tube mass spectrometry, or SIFT-MS to identify the olfactory signatures of specific chemical components among the millions of possible odors in a sample of air.
The investigators previously identified 13 volatile organic compounds (VOCs) associated with GEJ cancers and through additional analysis pared the number down to five: butyric acid, pentanoic acid, hexanoic acid, butanal, and decanal.
In tests of the five-VOC breath model, they found it had an area under the curve (AUC) of the receiver operating characteristic of 0.90, sensitivity of 84%, and a specificity of 88%.
They then sought to validate the model in a multicenter blinded study. They enrolled 163 treatment-naive patients diagnosed with nonmetastatic GEJ cancer (stages I-III), and 172 controls matched on a 1:1 basis.
Breath samples from all participants were collected in steel breath bags and sent to a central lab for SIFT-MS analysis. A statistician blinded to patient diagnosis then determined cancer risk based on previously determined odds ratios for each VOC.
The investigators used quality assurance measures to minimize the risk of errors, including sampling of the ambient air where the samples were collected, training of all researchers in uniform breath collection technique, and calibration to water.
They found that in this validation study, four of the five VOCs were significantly dysregulated in cases, compared with controls; pentanoic acid was the exception. The AUC was 0.85, with a sensitivity of 80% and specificity of 81%.
Looking at the association between VOCs and demographics of the patients as possible confounders, they saw that hexanoic acid levels could be affected by smoking history, and that butanal could be affected by smoking, white race, or history of using an ACE inhibitor.
Dr. Markar said that among the strengths of the study are that is was adequately powered, performed in multiple centers, and had quality assurance measures in place. In addition, the results compared well with results from the use of a cytosponge.
He acknowledged, however, that there were more late- than early-stage cancers among patients in the study, and that the 80% sensitivity level meant that one in five cancers would be missed.
Nonetheless, if the test is refined and can be further validated in an unenriched population, it could serve as an endoscopy triage test, he said.
He noted that we are just beginning to understand the importance of smell, the “most primitive” of the five senses, in relation to human health and joked that, just as many airports have drug-sniffing dogs, clinical practices could have patient-sniffing dogs that could be used to direct patients to the right specialist.
He was not involved in the study, but commented on it as part of a media briefing.
The study was supported by the UK National Institute for Health Research. The authors reported no competing interests.
AMSTERDAM – A test that samples exhaled breath and looks for the presence of just five volatile organic compounds shows promise as an inexpensive method for screening patients with suspected cancers of the gastroesophageal junction (GEJ), investigators from the United Kingdom reported.
In a multicenter clinical trial testing breath samples from patients with adenocarcinoma of the GEJ and matched controls, the test had an overall sensitivity of 80% and specificity of 81% for adenocarcinoma of the GEJ, said Sheraz R. Markar, MD, PhD, from Imperial College London.
If the test can be validated in larger studies, it could increase the number of patients screened and has the potential to save medical costs by reducing the number of unnecessary endoscopies and by catching GEJ cancers at earlier, potentially curable stages, he said.
The test uses selected ion flow tube mass spectrometry, or SIFT-MS to identify the olfactory signatures of specific chemical components among the millions of possible odors in a sample of air.
The investigators previously identified 13 volatile organic compounds (VOCs) associated with GEJ cancers and through additional analysis pared the number down to five: butyric acid, pentanoic acid, hexanoic acid, butanal, and decanal.
In tests of the five-VOC breath model, they found it had an area under the curve (AUC) of the receiver operating characteristic of 0.90, sensitivity of 84%, and a specificity of 88%.
They then sought to validate the model in a multicenter blinded study. They enrolled 163 treatment-naive patients diagnosed with nonmetastatic GEJ cancer (stages I-III), and 172 controls matched on a 1:1 basis.
Breath samples from all participants were collected in steel breath bags and sent to a central lab for SIFT-MS analysis. A statistician blinded to patient diagnosis then determined cancer risk based on previously determined odds ratios for each VOC.
The investigators used quality assurance measures to minimize the risk of errors, including sampling of the ambient air where the samples were collected, training of all researchers in uniform breath collection technique, and calibration to water.
They found that in this validation study, four of the five VOCs were significantly dysregulated in cases, compared with controls; pentanoic acid was the exception. The AUC was 0.85, with a sensitivity of 80% and specificity of 81%.
Looking at the association between VOCs and demographics of the patients as possible confounders, they saw that hexanoic acid levels could be affected by smoking history, and that butanal could be affected by smoking, white race, or history of using an ACE inhibitor.
Dr. Markar said that among the strengths of the study are that is was adequately powered, performed in multiple centers, and had quality assurance measures in place. In addition, the results compared well with results from the use of a cytosponge.
He acknowledged, however, that there were more late- than early-stage cancers among patients in the study, and that the 80% sensitivity level meant that one in five cancers would be missed.
Nonetheless, if the test is refined and can be further validated in an unenriched population, it could serve as an endoscopy triage test, he said.
He noted that we are just beginning to understand the importance of smell, the “most primitive” of the five senses, in relation to human health and joked that, just as many airports have drug-sniffing dogs, clinical practices could have patient-sniffing dogs that could be used to direct patients to the right specialist.
He was not involved in the study, but commented on it as part of a media briefing.
The study was supported by the UK National Institute for Health Research. The authors reported no competing interests.
AMSTERDAM – A test that samples exhaled breath and looks for the presence of just five volatile organic compounds shows promise as an inexpensive method for screening patients with suspected cancers of the gastroesophageal junction (GEJ), investigators from the United Kingdom reported.
In a multicenter clinical trial testing breath samples from patients with adenocarcinoma of the GEJ and matched controls, the test had an overall sensitivity of 80% and specificity of 81% for adenocarcinoma of the GEJ, said Sheraz R. Markar, MD, PhD, from Imperial College London.
If the test can be validated in larger studies, it could increase the number of patients screened and has the potential to save medical costs by reducing the number of unnecessary endoscopies and by catching GEJ cancers at earlier, potentially curable stages, he said.
The test uses selected ion flow tube mass spectrometry, or SIFT-MS to identify the olfactory signatures of specific chemical components among the millions of possible odors in a sample of air.
The investigators previously identified 13 volatile organic compounds (VOCs) associated with GEJ cancers and through additional analysis pared the number down to five: butyric acid, pentanoic acid, hexanoic acid, butanal, and decanal.
In tests of the five-VOC breath model, they found it had an area under the curve (AUC) of the receiver operating characteristic of 0.90, sensitivity of 84%, and a specificity of 88%.
They then sought to validate the model in a multicenter blinded study. They enrolled 163 treatment-naive patients diagnosed with nonmetastatic GEJ cancer (stages I-III), and 172 controls matched on a 1:1 basis.
Breath samples from all participants were collected in steel breath bags and sent to a central lab for SIFT-MS analysis. A statistician blinded to patient diagnosis then determined cancer risk based on previously determined odds ratios for each VOC.
The investigators used quality assurance measures to minimize the risk of errors, including sampling of the ambient air where the samples were collected, training of all researchers in uniform breath collection technique, and calibration to water.
They found that in this validation study, four of the five VOCs were significantly dysregulated in cases, compared with controls; pentanoic acid was the exception. The AUC was 0.85, with a sensitivity of 80% and specificity of 81%.
Looking at the association between VOCs and demographics of the patients as possible confounders, they saw that hexanoic acid levels could be affected by smoking history, and that butanal could be affected by smoking, white race, or history of using an ACE inhibitor.
Dr. Markar said that among the strengths of the study are that is was adequately powered, performed in multiple centers, and had quality assurance measures in place. In addition, the results compared well with results from the use of a cytosponge.
He acknowledged, however, that there were more late- than early-stage cancers among patients in the study, and that the 80% sensitivity level meant that one in five cancers would be missed.
Nonetheless, if the test is refined and can be further validated in an unenriched population, it could serve as an endoscopy triage test, he said.
He noted that we are just beginning to understand the importance of smell, the “most primitive” of the five senses, in relation to human health and joked that, just as many airports have drug-sniffing dogs, clinical practices could have patient-sniffing dogs that could be used to direct patients to the right specialist.
He was not involved in the study, but commented on it as part of a media briefing.
The study was supported by the UK National Institute for Health Research. The authors reported no competing interests.
Key clinical point: Breath analysis may be able detect early cancers of the gastroesophagel junction.
Major finding: A breath test had 80% sensitivity and 81% specificity for GEJ cancer.
Data source: Multicenter case-control study with 335 participants.
Disclosures: The study was supported by the UK National Institute for Health Research. The authors reported no competing interests.
Even small weight loss can improve long-term atrial fib ablation success
ORLANDO – Excess body weight exerts a major negative impact on the likelihood of remaining free of atrial fibrillation long term after an ablation procedure, according to a new set of data and a review of published studies.
“Just losing 3 pounds can dramatically improve the long-term success of an ablation when compared to a weight gain,” reported John D. Day, MD, medical director, Intermountain Heart Rhythm Specialists, Salt Lake City, at the annual International AF Symposium.
“As BMI goes up, long-term success in controlling AF goes down. The difference at 1 year may not be a big deal, but if you follow patients for a long time, weight control is a very big deal,” Dr. Day advised. He emphasized repeatedly, “We are just talking about a few pounds” for a favorable effect.
New data presented at the meeting supported the message. In the study, ablation outcomes in relationship to body mass index (BMI) were evaluated in 2,715 AF patients undergoing 3,742 ablations. Patients were stratified into five groups by BMI: less than 25 kg/m2, 25 to less than 30; 30 to less than 35; 35 to less than 40, and at least 40.
As BMI increased from less than 25 to at least 40, there were significant increases in left atrial size (P less than .005), CHADS2 scores (P = .002), persistent AF (P less than .0001), and longstanding AF (P less than .0001). Unlike persistent and long-term AF, rates of paroxysmal AF fell (48% to 16.3%; P less than .0001).
Not surprisingly and consistent with other published reports, increasing BMI was associated with increases in many of the key risk factors for AF in the study.
Specifically, as BMI increased from less than 25 to at least 40, the proportion of patients with cardiomyopathy climbed from 7.6% to 12.4% (P less than .001), hypertension climbed from 41% to 72.9% (P less than .0001), diabetes climbed from 4.3% to 23.3% (P less than .0001), and sleep apnea climbed from 7.0% to 46.9% (P less than .0001).
Dr. Day cited the LEGACY trial as one of the most influential studies associating weight loss with a reduction in AF burden (J Am Coll Cardiol. 2015 May 26;65[20]:2159-69). In that study, weight loss of at least 10% resulted in a sixfold increased likelihood of AF-free survival. Independent of AF, Dr. Day also pointed out that the sense of well-being among patients who achieved weight loss improved 200%.
Recognizing that major weight loss is difficult to achieve, Dr. Day repeatedly returned to the theme of weight control.
He cited one study in which AF patients were randomized to a weight loss program or usual care. In the usual care group, which included physician advice to lose weight, there was a small but significant weight loss. Even though the effect of that weight loss on AF burden was a fraction of that achieved in the group that achieved greater reductions in weight on active management, it, too, was significant, according to Dr. Day.
“Even brief physician advice can have a meaningful influence on waist circumference,” said Dr. Day, who urged physicians to inform their AF patients about the benefits of weight loss. Failing to do so might deprive patients of achieving the very modest reductions in weight loss required to improve their likelihood of freedom from AF, he added.
Dr. Winkle had no relevant financial relationships. Dr. Day reported a financial relationship with St. Jude Medical.
ORLANDO – Excess body weight exerts a major negative impact on the likelihood of remaining free of atrial fibrillation long term after an ablation procedure, according to a new set of data and a review of published studies.
“Just losing 3 pounds can dramatically improve the long-term success of an ablation when compared to a weight gain,” reported John D. Day, MD, medical director, Intermountain Heart Rhythm Specialists, Salt Lake City, at the annual International AF Symposium.
“As BMI goes up, long-term success in controlling AF goes down. The difference at 1 year may not be a big deal, but if you follow patients for a long time, weight control is a very big deal,” Dr. Day advised. He emphasized repeatedly, “We are just talking about a few pounds” for a favorable effect.
New data presented at the meeting supported the message. In the study, ablation outcomes in relationship to body mass index (BMI) were evaluated in 2,715 AF patients undergoing 3,742 ablations. Patients were stratified into five groups by BMI: less than 25 kg/m2, 25 to less than 30; 30 to less than 35; 35 to less than 40, and at least 40.
As BMI increased from less than 25 to at least 40, there were significant increases in left atrial size (P less than .005), CHADS2 scores (P = .002), persistent AF (P less than .0001), and longstanding AF (P less than .0001). Unlike persistent and long-term AF, rates of paroxysmal AF fell (48% to 16.3%; P less than .0001).
Not surprisingly and consistent with other published reports, increasing BMI was associated with increases in many of the key risk factors for AF in the study.
Specifically, as BMI increased from less than 25 to at least 40, the proportion of patients with cardiomyopathy climbed from 7.6% to 12.4% (P less than .001), hypertension climbed from 41% to 72.9% (P less than .0001), diabetes climbed from 4.3% to 23.3% (P less than .0001), and sleep apnea climbed from 7.0% to 46.9% (P less than .0001).
Dr. Day cited the LEGACY trial as one of the most influential studies associating weight loss with a reduction in AF burden (J Am Coll Cardiol. 2015 May 26;65[20]:2159-69). In that study, weight loss of at least 10% resulted in a sixfold increased likelihood of AF-free survival. Independent of AF, Dr. Day also pointed out that the sense of well-being among patients who achieved weight loss improved 200%.
Recognizing that major weight loss is difficult to achieve, Dr. Day repeatedly returned to the theme of weight control.
He cited one study in which AF patients were randomized to a weight loss program or usual care. In the usual care group, which included physician advice to lose weight, there was a small but significant weight loss. Even though the effect of that weight loss on AF burden was a fraction of that achieved in the group that achieved greater reductions in weight on active management, it, too, was significant, according to Dr. Day.
“Even brief physician advice can have a meaningful influence on waist circumference,” said Dr. Day, who urged physicians to inform their AF patients about the benefits of weight loss. Failing to do so might deprive patients of achieving the very modest reductions in weight loss required to improve their likelihood of freedom from AF, he added.
Dr. Winkle had no relevant financial relationships. Dr. Day reported a financial relationship with St. Jude Medical.
ORLANDO – Excess body weight exerts a major negative impact on the likelihood of remaining free of atrial fibrillation long term after an ablation procedure, according to a new set of data and a review of published studies.
“Just losing 3 pounds can dramatically improve the long-term success of an ablation when compared to a weight gain,” reported John D. Day, MD, medical director, Intermountain Heart Rhythm Specialists, Salt Lake City, at the annual International AF Symposium.
“As BMI goes up, long-term success in controlling AF goes down. The difference at 1 year may not be a big deal, but if you follow patients for a long time, weight control is a very big deal,” Dr. Day advised. He emphasized repeatedly, “We are just talking about a few pounds” for a favorable effect.
New data presented at the meeting supported the message. In the study, ablation outcomes in relationship to body mass index (BMI) were evaluated in 2,715 AF patients undergoing 3,742 ablations. Patients were stratified into five groups by BMI: less than 25 kg/m2, 25 to less than 30; 30 to less than 35; 35 to less than 40, and at least 40.
As BMI increased from less than 25 to at least 40, there were significant increases in left atrial size (P less than .005), CHADS2 scores (P = .002), persistent AF (P less than .0001), and longstanding AF (P less than .0001). Unlike persistent and long-term AF, rates of paroxysmal AF fell (48% to 16.3%; P less than .0001).
Not surprisingly and consistent with other published reports, increasing BMI was associated with increases in many of the key risk factors for AF in the study.
Specifically, as BMI increased from less than 25 to at least 40, the proportion of patients with cardiomyopathy climbed from 7.6% to 12.4% (P less than .001), hypertension climbed from 41% to 72.9% (P less than .0001), diabetes climbed from 4.3% to 23.3% (P less than .0001), and sleep apnea climbed from 7.0% to 46.9% (P less than .0001).
Dr. Day cited the LEGACY trial as one of the most influential studies associating weight loss with a reduction in AF burden (J Am Coll Cardiol. 2015 May 26;65[20]:2159-69). In that study, weight loss of at least 10% resulted in a sixfold increased likelihood of AF-free survival. Independent of AF, Dr. Day also pointed out that the sense of well-being among patients who achieved weight loss improved 200%.
Recognizing that major weight loss is difficult to achieve, Dr. Day repeatedly returned to the theme of weight control.
He cited one study in which AF patients were randomized to a weight loss program or usual care. In the usual care group, which included physician advice to lose weight, there was a small but significant weight loss. Even though the effect of that weight loss on AF burden was a fraction of that achieved in the group that achieved greater reductions in weight on active management, it, too, was significant, according to Dr. Day.
“Even brief physician advice can have a meaningful influence on waist circumference,” said Dr. Day, who urged physicians to inform their AF patients about the benefits of weight loss. Failing to do so might deprive patients of achieving the very modest reductions in weight loss required to improve their likelihood of freedom from AF, he added.
Dr. Winkle had no relevant financial relationships. Dr. Day reported a financial relationship with St. Jude Medical.
Key clinical point: New data expand evidence that obesity reduces long-term success of ablation for atrial fibrillation.
Major finding: Freedom from AF 5 years after ablation fell from 70% in patients with a BMI of less than 35 kg/m2 to 57% in those with BMIs of at least 35.
Data source: A retrospective observational study.
Disclosures: Dr. Winkle had no relevant financial relationships; Dr. Day reported a financial relationship with St. Jude Medical.
Residual disease burden is prognostic across breast cancer phenotypes
The Residual Cancer Burden (RCB), a standardized measure of residual disease in pathologic resection specimens following neoadjuvant chemotherapy, was found to be prognostic of long-term survival across all three phenotypic subtypes when it was applied to five breast cancer cohorts totaling 1,158 patients from a single institution, investigators report in the Journal of Clinical Oncology.
If the findings of this retrospective cohort analysis are validated in other cohorts, it would indicate that assessing patients’ RCB index could add “meaningful information to pretreatement clinical and pathologic information and posttreatment yp stage [American Joint Commission on Cancer stage],” said W. Fraser Symmans, MD, of the University of Texas M.D. Anderson Cancer Center, Houston, and his associates.
Residual disease is categorized into four groups: an index of zero (RCB-0) reflects a complete pathologic response to neoadjuvant treatment, RCB-I indicates minimal residual disease, RCB-II indicates moderate residual disease, and RCB-III indicates extensive residual disease. The investigators reviewed pathology specimens to determine the RCB index in a cohort of 219 patients followed for 13 years, a cohort of 262 patients followed for 9 years, a cohort of 342 patients followed for 7 years, a cohort of 132 patients followed for more than 16 years, and a cohort of 203 patients followed for 7 years.
They found that the RCB index predicted the risk of relapse or death across all five cohorts, regardless of other clinical and pathologic variables such as tumor stage or grade, patient age, and type of surgery (J Clin Oncol. 2017 Jan 30. doi: 10.1200/JCO.2015.63.1010).
RCB also was predictive regardless of whether patients had triple-negative disease, HR-positive/HER2-negative disease, HER2-positive disease treated with paclitaxel plus combined fluorouracil, doxorubicin, and cyclophosphamide alone, or HER2-positive disease treated with paclitaxel plus combined fluorouracil, doxorubicin, and cyclophosphamide plus trastuzumab.
In two especially high-risk groups of patients – those with triple-negative breast cancer and those with HER2-positive breast cancer – RCB was the only or the most important predictor of survival. Approximately half of the patients with triple-negative disease had an index of RCB-0 or RCB-I and a good prognosis, while those with an RCB-II or RCB-III index had poor survival, Dr. Symmans and his associates said.
The authors use their main finding – that RCB index provides additional and independent prognostic information to yp stage and other clinical factors – to support their opinion that clinicians should be provided this information.
Sibylle Loibl, MD, is with the German Breast Group in Neu-Isenburg, Germany. Carsten Denkert, MD, is with the German Breast Group and with Charite University Hospital, Berlin. They reported having no relevant financial disclosures. Dr. Loibl and Dr. Denkert made these remarks in an editorial accompanying Dr. Symmans’ report (J Clin Oncol. 2017 Jan 30. doi: 10.1200/JCO.2016.71.3503).
The authors use their main finding – that RCB index provides additional and independent prognostic information to yp stage and other clinical factors – to support their opinion that clinicians should be provided this information.
Sibylle Loibl, MD, is with the German Breast Group in Neu-Isenburg, Germany. Carsten Denkert, MD, is with the German Breast Group and with Charite University Hospital, Berlin. They reported having no relevant financial disclosures. Dr. Loibl and Dr. Denkert made these remarks in an editorial accompanying Dr. Symmans’ report (J Clin Oncol. 2017 Jan 30. doi: 10.1200/JCO.2016.71.3503).
The authors use their main finding – that RCB index provides additional and independent prognostic information to yp stage and other clinical factors – to support their opinion that clinicians should be provided this information.
Sibylle Loibl, MD, is with the German Breast Group in Neu-Isenburg, Germany. Carsten Denkert, MD, is with the German Breast Group and with Charite University Hospital, Berlin. They reported having no relevant financial disclosures. Dr. Loibl and Dr. Denkert made these remarks in an editorial accompanying Dr. Symmans’ report (J Clin Oncol. 2017 Jan 30. doi: 10.1200/JCO.2016.71.3503).
The Residual Cancer Burden (RCB), a standardized measure of residual disease in pathologic resection specimens following neoadjuvant chemotherapy, was found to be prognostic of long-term survival across all three phenotypic subtypes when it was applied to five breast cancer cohorts totaling 1,158 patients from a single institution, investigators report in the Journal of Clinical Oncology.
If the findings of this retrospective cohort analysis are validated in other cohorts, it would indicate that assessing patients’ RCB index could add “meaningful information to pretreatement clinical and pathologic information and posttreatment yp stage [American Joint Commission on Cancer stage],” said W. Fraser Symmans, MD, of the University of Texas M.D. Anderson Cancer Center, Houston, and his associates.
Residual disease is categorized into four groups: an index of zero (RCB-0) reflects a complete pathologic response to neoadjuvant treatment, RCB-I indicates minimal residual disease, RCB-II indicates moderate residual disease, and RCB-III indicates extensive residual disease. The investigators reviewed pathology specimens to determine the RCB index in a cohort of 219 patients followed for 13 years, a cohort of 262 patients followed for 9 years, a cohort of 342 patients followed for 7 years, a cohort of 132 patients followed for more than 16 years, and a cohort of 203 patients followed for 7 years.
They found that the RCB index predicted the risk of relapse or death across all five cohorts, regardless of other clinical and pathologic variables such as tumor stage or grade, patient age, and type of surgery (J Clin Oncol. 2017 Jan 30. doi: 10.1200/JCO.2015.63.1010).
RCB also was predictive regardless of whether patients had triple-negative disease, HR-positive/HER2-negative disease, HER2-positive disease treated with paclitaxel plus combined fluorouracil, doxorubicin, and cyclophosphamide alone, or HER2-positive disease treated with paclitaxel plus combined fluorouracil, doxorubicin, and cyclophosphamide plus trastuzumab.
In two especially high-risk groups of patients – those with triple-negative breast cancer and those with HER2-positive breast cancer – RCB was the only or the most important predictor of survival. Approximately half of the patients with triple-negative disease had an index of RCB-0 or RCB-I and a good prognosis, while those with an RCB-II or RCB-III index had poor survival, Dr. Symmans and his associates said.
The Residual Cancer Burden (RCB), a standardized measure of residual disease in pathologic resection specimens following neoadjuvant chemotherapy, was found to be prognostic of long-term survival across all three phenotypic subtypes when it was applied to five breast cancer cohorts totaling 1,158 patients from a single institution, investigators report in the Journal of Clinical Oncology.
If the findings of this retrospective cohort analysis are validated in other cohorts, it would indicate that assessing patients’ RCB index could add “meaningful information to pretreatement clinical and pathologic information and posttreatment yp stage [American Joint Commission on Cancer stage],” said W. Fraser Symmans, MD, of the University of Texas M.D. Anderson Cancer Center, Houston, and his associates.
Residual disease is categorized into four groups: an index of zero (RCB-0) reflects a complete pathologic response to neoadjuvant treatment, RCB-I indicates minimal residual disease, RCB-II indicates moderate residual disease, and RCB-III indicates extensive residual disease. The investigators reviewed pathology specimens to determine the RCB index in a cohort of 219 patients followed for 13 years, a cohort of 262 patients followed for 9 years, a cohort of 342 patients followed for 7 years, a cohort of 132 patients followed for more than 16 years, and a cohort of 203 patients followed for 7 years.
They found that the RCB index predicted the risk of relapse or death across all five cohorts, regardless of other clinical and pathologic variables such as tumor stage or grade, patient age, and type of surgery (J Clin Oncol. 2017 Jan 30. doi: 10.1200/JCO.2015.63.1010).
RCB also was predictive regardless of whether patients had triple-negative disease, HR-positive/HER2-negative disease, HER2-positive disease treated with paclitaxel plus combined fluorouracil, doxorubicin, and cyclophosphamide alone, or HER2-positive disease treated with paclitaxel plus combined fluorouracil, doxorubicin, and cyclophosphamide plus trastuzumab.
In two especially high-risk groups of patients – those with triple-negative breast cancer and those with HER2-positive breast cancer – RCB was the only or the most important predictor of survival. Approximately half of the patients with triple-negative disease had an index of RCB-0 or RCB-I and a good prognosis, while those with an RCB-II or RCB-III index had poor survival, Dr. Symmans and his associates said.
FROM THE JOURNAL OF CLINICAL ONCOLOGY
Key clinical point: The RCB measure is prognostic of long-term survival across all three phenotypic subtypes of breast cancer.
Major finding: The RCB index predicted the risk of relapse or death across five cohorts at a single institution, regardless of other clinical and pathologic variables such as tumor stage or grade, patient age, and type of surgery.
Data source: A retrospective cohort study assessing the RCB’s ability to predict long-term survival using data from five breast cancer cohorts (1,158 patients) with 6-17 years of follow-up.
Disclosures: This study was supported by the Department of Defense Congressionally Directed Funds for Breast Cancer Research, the Breast Cancer Research Foundation, Susan G. Komen for the Cure, and the Nellie B. Connally Breast Center at M.D. Anderson Cancer Center. Dr. Symmans reported ties to ISIS Pharmaceuticals, Nuvera Biosciences, Affymetrix, Celgene, Genentech, and AbbVie, and his associates reported ties to numerous industry sources.
Adding bevacizumab improves PFS in extensive SCLC
Adding the antiangiogenic agent bevacizumab to standard first-line chemotherapy improves progression-free survival in extensive small-cell lung cancer, according to a report published online Jan. 30.
In what they described as the first prospective randomized, controlled phase III trial comparing these two approaches, researchers studied 204 adults who had extensive SCLC, including brain and bone metastases, at 29 medical centers in Italy. These participants (mean age, 64 years) were randomly assigned to receive a combination of standard cisplatin, etoposide, and bevacizumab every 3 weeks or cisplatin and etoposide chemotherapy every 3 weeks. Patients who developed cisplatin contraindications or toxicity related to the drug could substitute carboplatin. In the experimental arm of the study, patients could opt to continue bevacizumab alone as maintenance therapy for a maximum of 18 cycles. Forty-one patients (42%) did so, said Marcello Tiseo, MD, PhD, of Azienda Ospedaliero Universitaria, Parma, Italy, and his associates.
After a median follow-up of 35 months, the median progression-free survival was 5.7 months with standard therapy and 6.7 months with add-on bevacizumab (hazard ratio, 0.72; 95% confidence interval, 0.54 to 0.97; P = .030). However, adding bevacizumab did not significantly improve overall survival, which was the primary endpoint of the trial. A subgroup analysis showed that bevacizumab significantly extended overall survival among men (HR, 0.55) but not among women (HR, 1.55), an association that has been reported in previous studies, Dr. Tiseo and his associates said (J Clin Oncol. 2017 Jan 30. doi:10.1200/JCO.2016.69.4844).
These findings, together with those of other investigators assessing the same class of agents, justify “further studies with novel and better antiangiogenic agents in extensive SCLC, particularly in the maintenance setting,” they added.
This trial was supported by the Agenzia Italiana del Farmaco. Dr. Tiseo reported serving as a consultant for AstraZeneca, Eli Lilly, Boehringer Ingelheim, Novartis, Bristol-Myers Squibb, Pierre Fabre, and Otsuka; his associates reported ties to numerous industry sources.
Adding the antiangiogenic agent bevacizumab to standard first-line chemotherapy improves progression-free survival in extensive small-cell lung cancer, according to a report published online Jan. 30.
In what they described as the first prospective randomized, controlled phase III trial comparing these two approaches, researchers studied 204 adults who had extensive SCLC, including brain and bone metastases, at 29 medical centers in Italy. These participants (mean age, 64 years) were randomly assigned to receive a combination of standard cisplatin, etoposide, and bevacizumab every 3 weeks or cisplatin and etoposide chemotherapy every 3 weeks. Patients who developed cisplatin contraindications or toxicity related to the drug could substitute carboplatin. In the experimental arm of the study, patients could opt to continue bevacizumab alone as maintenance therapy for a maximum of 18 cycles. Forty-one patients (42%) did so, said Marcello Tiseo, MD, PhD, of Azienda Ospedaliero Universitaria, Parma, Italy, and his associates.
After a median follow-up of 35 months, the median progression-free survival was 5.7 months with standard therapy and 6.7 months with add-on bevacizumab (hazard ratio, 0.72; 95% confidence interval, 0.54 to 0.97; P = .030). However, adding bevacizumab did not significantly improve overall survival, which was the primary endpoint of the trial. A subgroup analysis showed that bevacizumab significantly extended overall survival among men (HR, 0.55) but not among women (HR, 1.55), an association that has been reported in previous studies, Dr. Tiseo and his associates said (J Clin Oncol. 2017 Jan 30. doi:10.1200/JCO.2016.69.4844).
These findings, together with those of other investigators assessing the same class of agents, justify “further studies with novel and better antiangiogenic agents in extensive SCLC, particularly in the maintenance setting,” they added.
This trial was supported by the Agenzia Italiana del Farmaco. Dr. Tiseo reported serving as a consultant for AstraZeneca, Eli Lilly, Boehringer Ingelheim, Novartis, Bristol-Myers Squibb, Pierre Fabre, and Otsuka; his associates reported ties to numerous industry sources.
Adding the antiangiogenic agent bevacizumab to standard first-line chemotherapy improves progression-free survival in extensive small-cell lung cancer, according to a report published online Jan. 30.
In what they described as the first prospective randomized, controlled phase III trial comparing these two approaches, researchers studied 204 adults who had extensive SCLC, including brain and bone metastases, at 29 medical centers in Italy. These participants (mean age, 64 years) were randomly assigned to receive a combination of standard cisplatin, etoposide, and bevacizumab every 3 weeks or cisplatin and etoposide chemotherapy every 3 weeks. Patients who developed cisplatin contraindications or toxicity related to the drug could substitute carboplatin. In the experimental arm of the study, patients could opt to continue bevacizumab alone as maintenance therapy for a maximum of 18 cycles. Forty-one patients (42%) did so, said Marcello Tiseo, MD, PhD, of Azienda Ospedaliero Universitaria, Parma, Italy, and his associates.
After a median follow-up of 35 months, the median progression-free survival was 5.7 months with standard therapy and 6.7 months with add-on bevacizumab (hazard ratio, 0.72; 95% confidence interval, 0.54 to 0.97; P = .030). However, adding bevacizumab did not significantly improve overall survival, which was the primary endpoint of the trial. A subgroup analysis showed that bevacizumab significantly extended overall survival among men (HR, 0.55) but not among women (HR, 1.55), an association that has been reported in previous studies, Dr. Tiseo and his associates said (J Clin Oncol. 2017 Jan 30. doi:10.1200/JCO.2016.69.4844).
These findings, together with those of other investigators assessing the same class of agents, justify “further studies with novel and better antiangiogenic agents in extensive SCLC, particularly in the maintenance setting,” they added.
This trial was supported by the Agenzia Italiana del Farmaco. Dr. Tiseo reported serving as a consultant for AstraZeneca, Eli Lilly, Boehringer Ingelheim, Novartis, Bristol-Myers Squibb, Pierre Fabre, and Otsuka; his associates reported ties to numerous industry sources.
FROM THE JOURNAL OF CLINICAL ONCOLOGY
Key clinical point: Adding bevacizumab to standard first-line chemotherapy improves progression-free survival in extensive small-cell lung cancer.
Major finding: After a median follow-up of 35 months, the median progression-free survival was 5.7 months with standard therapy and 6.7 months with add-on bevacizumab (hazard ratio, 0.72; 95% confidence interval, 0.54 to 0.97; P = .030).
Data source: A multicenter open-label randomized, controlled phase III trial involving 204 adults in Italy.
Disclosures: This trial was supported by the Agenzia Italiana del Farmaco. Dr. Tiseo reported serving as a consultant for AstraZeneca, Eli Lilly, Boehringer Ingelheim, Novartis, Bristol-Myers Squibb, Pierre Fabre, and Otsuka; his associates reported ties to numerous industry sources.
February Hot Threads in ACS Communities
Your colleagues already have a lot to say in 2017. Here are the top discussion threads in ACS Communities just prior to press time (communities in which the threads appear are listed in parentheses):
1. Care for the Vulnerable vs Cash for the Powerful... (General Surgery)
2. Car lease or buy (General Surgery)
3. Interval cholecystectomy (General Surgery)
4. Enemy of good is better (General Surgery)
5. Crushed meds and elixirs (Bariatric Surgery)
6. Unsuspected cancer on reduction mammoplasty (Breast Surgery)
7. UC with sigmoid tumor (Colon and Rectal Surgery)
8. Transverse colostomy problems (Colon and Rectal Surgery)
9. Complex anal fistula (Colon and Rectal Surgery)
10. Ethical dilemma (Trauma Surgery)
To join communities, log in to ACS Communities at http://acscommunities.facs.org/home, go to “Browse All Communities” near the top of any page, and click the blue “Join” button next to the community you’d like to join. If you have any questions, please send them to [email protected].
Your colleagues already have a lot to say in 2017. Here are the top discussion threads in ACS Communities just prior to press time (communities in which the threads appear are listed in parentheses):
1. Care for the Vulnerable vs Cash for the Powerful... (General Surgery)
2. Car lease or buy (General Surgery)
3. Interval cholecystectomy (General Surgery)
4. Enemy of good is better (General Surgery)
5. Crushed meds and elixirs (Bariatric Surgery)
6. Unsuspected cancer on reduction mammoplasty (Breast Surgery)
7. UC with sigmoid tumor (Colon and Rectal Surgery)
8. Transverse colostomy problems (Colon and Rectal Surgery)
9. Complex anal fistula (Colon and Rectal Surgery)
10. Ethical dilemma (Trauma Surgery)
To join communities, log in to ACS Communities at http://acscommunities.facs.org/home, go to “Browse All Communities” near the top of any page, and click the blue “Join” button next to the community you’d like to join. If you have any questions, please send them to [email protected].
Your colleagues already have a lot to say in 2017. Here are the top discussion threads in ACS Communities just prior to press time (communities in which the threads appear are listed in parentheses):
1. Care for the Vulnerable vs Cash for the Powerful... (General Surgery)
2. Car lease or buy (General Surgery)
3. Interval cholecystectomy (General Surgery)
4. Enemy of good is better (General Surgery)
5. Crushed meds and elixirs (Bariatric Surgery)
6. Unsuspected cancer on reduction mammoplasty (Breast Surgery)
7. UC with sigmoid tumor (Colon and Rectal Surgery)
8. Transverse colostomy problems (Colon and Rectal Surgery)
9. Complex anal fistula (Colon and Rectal Surgery)
10. Ethical dilemma (Trauma Surgery)
To join communities, log in to ACS Communities at http://acscommunities.facs.org/home, go to “Browse All Communities” near the top of any page, and click the blue “Join” button next to the community you’d like to join. If you have any questions, please send them to [email protected].
Increase brings flu activity back to seasonal high
for the week ending Jan. 21, compared with three states the week before, according to the Centers for Disease Control and Prevention.
Alabama, Kansas, New Jersey, Oklahoma, and South Carolina were at level 10 on the CDC’s 1-10 scale of ILI activity, with Oklahoma reaching that level for the third consecutive week. Georgia (level 9) and Louisiana, Minnesota, Missouri, and Tennessee (level 8) were also in the “high” range, the CDC reported.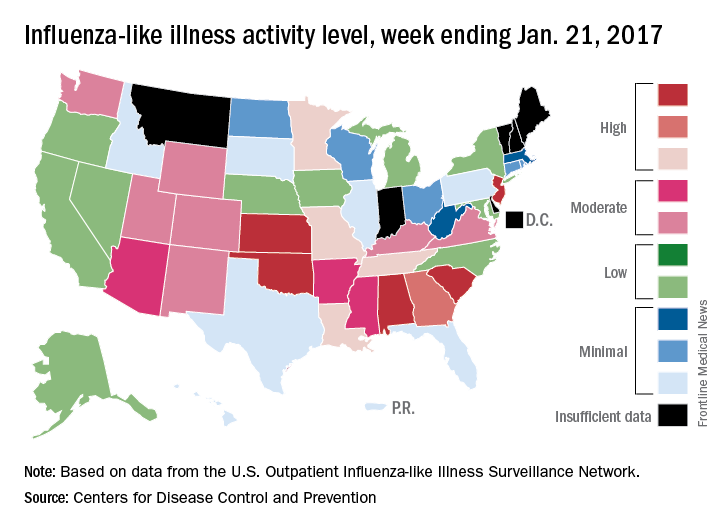
Three flu-related pediatric deaths were reported for the week, although two occurred during the week ending Jan. 14. The two earlier deaths were associated with an influenza A (H3) virus, and the more recent death was associated with an influenza B virus. For the 2016-2017 season so far, there have been a total of eight pediatric deaths, the CDC said.
for the week ending Jan. 21, compared with three states the week before, according to the Centers for Disease Control and Prevention.
Alabama, Kansas, New Jersey, Oklahoma, and South Carolina were at level 10 on the CDC’s 1-10 scale of ILI activity, with Oklahoma reaching that level for the third consecutive week. Georgia (level 9) and Louisiana, Minnesota, Missouri, and Tennessee (level 8) were also in the “high” range, the CDC reported.
Three flu-related pediatric deaths were reported for the week, although two occurred during the week ending Jan. 14. The two earlier deaths were associated with an influenza A (H3) virus, and the more recent death was associated with an influenza B virus. For the 2016-2017 season so far, there have been a total of eight pediatric deaths, the CDC said.
for the week ending Jan. 21, compared with three states the week before, according to the Centers for Disease Control and Prevention.
Alabama, Kansas, New Jersey, Oklahoma, and South Carolina were at level 10 on the CDC’s 1-10 scale of ILI activity, with Oklahoma reaching that level for the third consecutive week. Georgia (level 9) and Louisiana, Minnesota, Missouri, and Tennessee (level 8) were also in the “high” range, the CDC reported.
Three flu-related pediatric deaths were reported for the week, although two occurred during the week ending Jan. 14. The two earlier deaths were associated with an influenza A (H3) virus, and the more recent death was associated with an influenza B virus. For the 2016-2017 season so far, there have been a total of eight pediatric deaths, the CDC said.
Musculoskeletal Hand Pain Group Visits: An Adaptive Health Care Model
From Cooper Medical School of Rowan University (Dr. Patel, Dr. Fuller) and Cooper University Hospital (Dr. Kaufman), Camden, NJ.
Abstract
- Objective: To describe an adaptive musculoskeletal hand clinic that offers accessible and economically viable musculoskeletal care for an underserved, urban population.
- Methods: Descriptive report.
- Results: An enhanced access group visit model was developed offering both nonsurgical and surgical care pathways for patients with musculoskeletal disorders of the hand. Both patient education and care were provided in the group environment. Staffing included an orthopedic surgeon, nurse practitioner, medical student, orthopedic technician, and medical assistant. Over a 12-month period, group visit efficiency improved to accommodate an equivalent number of patients as compared to the traditional model. Access (time to appointment) was improved in the group visit. The model allows for the addition of non-physician clinical staff to improve access and limit costs in a manner not feasible with traditional office visits.
- Conclusion: A group visit model may offer a sustainable process to increase patient access to musculoskeletal subspecialty care and accommodate care of greater numbers of patients while maintaining quality. The group model offers flexible staffing, enhanced access, and educational benefit.
Key words: Group medical visit, team-based care, hand pain, access, underserved populations.
Group visits are a relatively new health care delivery model [1–3]. The term is applied to a wide variety of visits designed for groups of patients, rather than individual patient-provider appointments. The group visit format has been used for various disease- or condition-specific populations. Group visits can increase access to care and have been associated with improved clinical outcomes [4].
The Urban Health Institute, a dedicated business unit at Cooper University Health System in Camden, NJ, was established to focus on care of the underserved. The business unit is working to reduce cost of care delivery, increase access, and improve quality through the use of workflow redesign, task shifting, dashboards, and other methods. With a large startup grant from the Nicholson Foundation, the Urban Health Institute launched the Cooper Advanced Care Center to provide the local under-served population with access to a collaborative practice of 23 medical and surgical specialties under one roof. The center incorporates traditional one-on-one provider visits with innovative models of care, including group visits. Multiple partners were required in the group visit design and implementation starting with buy-in from Cooper Health System’s leadership for existing space to be redesigned for the group visit activities.
The Cooper Advanced Care Center, which had high no-show rates of 30% to 40%, and low reimbursement for a primarily Medicaid and self-pay population, initially operated at a financial loss. Meanwhile, most physicians had extended lag time until their next available appointment. In a traditional patient–physician office visit, additional physician time is required to increase access to care. This costly solution is often not financially viable. Group visits were considered as a means of using an interdisciplinary team to increase access while controlling or decreasing the per-visit cost.
Musculoskeletal medicine was identified as an area of need in part due to limited access to care. Patients were waiting more than 2 months to see a musculoskeletal specialist and were being scheduled beyond capacity in our existing traditional weekly hand and knee/sports medicine clinics. Within musculoskeletal medicine, 4 areas of musculoskeletal medicine were considered for group visits: back pain, knee pain, hand pain, and foot and ankle disorders. The decision was made to focus the subspecialty musculoskeletal clinic on disorders of the hand and wrist to provide nonsurgical and surgical care options for atraumatic and traumatic disorders of the hand in a teaching environment at an urban hospital. The purpose of this article is to discuss the design and implementation of a hand pain group visit model to increase access to care without increasing cost.
Setting and Patients
Camden City, New Jersey, is a medically underserved, resource-poor community. The population is 48% African American and 47% Hispanic and nearly 40% of individuals live below the poverty level [5]. The group visit was intentionally set up as a means to provide access to the un- or underinsured. Patients attending the group visits were 33% African American, 33% Hispanic, and 30% Caucasian. Most patients had Medicaid insurance (67%) with the remaining patients covered by commercial insurance (15%), dual Medicare/Medicaid (11%), Medicare (5%), or self pay (2%).
Group Visit Staffing and Structure
In a traditional office visit, used nearly ubiquitously in outpatient medical offices, patients arrive at individual appointment times for a prescribed time encounter with the physician, are registered and roomed by support staff, and are then seen by a clinician for diagnosis and treatment. While assistants and trainees participate in the patient’s care with attending physician supervision, the majority of direct care falls to the physician. Access is coupled to physician availability; increasing access to care requires crowding the schedule with additional patients. We used this model as the benchmark for volume and scheduling against which to compare the group visit.
The group visit staffing was the same as for the traditional visit: hand surgeon, nurse practitioner, orthopedic technician, medical student, and medical assistant. However, each clinical session consists of four 1-hour, consecutive group visits scheduled once a month on a Monday morning. Up to 10 people could be scheduled for each 1-hour group visit. We continued to offer our traditional office visit clinic on the other 3 Mondays in the month.
The hand surgeon begins the group visit with a 10-minute educational session and group discussion held in a meeting room. He reviews common disorders of the hand, including carpal tunnel syndrome, trigger fingers, hand arthritis, cysts, sprains and fractures, how they are treated, and risks and benefits of treatments. Patients sign a confidentiality agreement at check-in. Time is allowed for questions and experiential sharing is encouraged. Expectations are set at the start of the visit to honor each patient’s input to provide a safe environment for asking questions and expressing concerns about their shared health condition to enhance the learning experience [6]. A medical assistant enters the chief complaint using an electronic standardized questionnaire into the EMR along with basic vital signs for each patient either prior to, during, or after the group presentation.
After the group educational session with the surgeon, patients transition to a large, open clinical room with 6 separate workstations, each consisting of a small table with 4 chairs and a laptop computer. Small procedures can be performed on the table (suture removal, dressing changes, injections) and the table is appropriately sized to accommodate a care provider, the patient, and their support person(s). Tables are spaced comfortably such that conversations do not carry much from one to the other. The clinical space has white noise speakers for sound dampening while patients receive individual history, vital signs, physical examination, and review of relevant studies. Patients may see the clinicians in a private exam room if they wish or require.
In a traditional office setting, workflow through the major tasks (check-in, data gathering, diagnosis, treatment) is often linear, as dictated by the configuration of individual patient rooms and the patient’s expectations of a traditional doctor’s visit. In the group visit, major tasks are performed simultaneously by the advance practice providers (nurse practitioners, physician assistants) in conjunction with supervision of the attending physician. The workstations (tables, chairs, laptops) in the open clinical room allows for greater efficiency; providers can easily transition to other tasks from one workstation to another during time that may have been spent waiting for other team members in the more linear, traditional clinic. For example, while waiting for the attending physician’s approval of a diagnosis and treatment plan for one patient, a nurse practitioner may be able to begin assessing and gathering data with a second patient until the physician becomes available.
Scheduling and Access
A primary aim of the group visit pilot was to develop a model of care delivery that allowed scheduling beyond capacity for the traditional office hand clinic. At the inception of the group visit, all patients were offered a visit in either the traditional office or group visit model by our scheduling secretaries based upon availability, with emphasis on scheduling a defined underserved population into the group visit.
In traditional 1:1 appointments, the number of people who can access care is dependent on physician availability. The team-based model uncouples the number of scheduled patients from the physician availability, allowing increased efficiency in the model and/or additional staff to increase the number of patients the group visit can accommodate. Thus, patients were essentially guaranteed an appointment in the next clinic because there was no cap on the number of patients that could be scheduled into the group visit. If the number of patients exceeded the limit of 10 per hour, a non-physician clinician was added to accommodate the patient demand. As our group visit matures, the ability to increase the staffing model enables patients to get care without adding more physician time.
Task Shifting
A central pillar of making the group visit a sustainable model for more accessible care is shifting tasks to non-physician health care workers. Adding specialist time enhances access but drives up the cost of care. Non-physician clinical staff members in subspecialty orthopedic offices with experience diagnosing and treating common conditions are capable of providing the standard of care for those conditions with variable physician oversight [7].
In the group visit, there is a deliberate assignment of patients to clinical staff by the physician based on anticipated level of care required. Given the attending physician’s experience with the most common disorders related to hand pain, it is possible to anticipate the approximate complexity of care required for each patient based on the nature and duration of the presenting complaint. With some degree of clinical supervision by the physician, members of the team operate maximally independently to assist patients. The nurse practitioner can operate largely autonomously in the group visit. The overall goal is to encourage all team members to function at the top of their licenses and abilities. Task shifting in this manner increases the productivity of all members of the team and minimizes redundancy. Despite more autonomy of mid-level providers and support staff in the group visit, there is still direct supervision of care by the attending physician.
The current body of literature in task shifting to non-physician health care workers has mostly concerned low-income countries with marked physician and provider shortages [8]. However, given the increased patient volume already seen with the Affordable Care Act and further expected increases, the health care system is likely to see provider shortages, especially in primary care [9–11]. This will necessitate the adoption of strategies to increase access, maintain quality care, and decrease systemic cost. Task shifting provides one such strategy.
Patient Satisfaction
One concern with shifting clinical duties to non-physician clinical staff is patient satisfaction. An abbreviated interaction with physicians can make patients dissatisfied with medical care independent of eventual clinical outcome [12]. However, it has also been demonstrated in an outpatient hand surgery clinic that quality of time spent with the physician may have a greater impact on satisfaction than quantity of time [13].
Our group visit is structured to allow high physician-patient visibility and interaction. The introductory remarks by the physician engage patients with the physician early in the visit and establish a group and individual rapport. The physician introduces the clinical team and the idea of patients being seen by other clinical staff up front, which establishes comfort for later patient–staff interaction. This is also an important time for patient education, which has been shown as a significant determinant of patient satisfaction in the outpatient setting [14]. The patient education at the beginning of the visit answers questions by one person that another person may not have considered, and generates patient questions to be addressed individually with a clinician. One common example is when a person considering carpal tunnel surgery hears from a person who has recently completed the procedure and can talk about their operative experience.
In the group room, the physician and staff can move between patients quickly and efficiently without waiting for turnover of rooms and resources. The structure of the visit allows staff to dedicate more time to patient care by bypassing the extra time required when patients are roomed individually. The group/communal structure also allows patients to see the staff at work, as compared to time spent waiting alone in an exam room in the traditional office. This enables patients to appreciate the efforts of the clinical staff and avoids giving the impression that the physician is inattentive or cursory in patient interaction.
Medical Education
An important consideration at any academic medical center is education. However, education often introduces redundancies and inefficiency into the medical care visit. The work a trainee does is either extensively overseen or the clinical questions are repeated by a supervising provider. However, it is possible to increase efficiency and utility of trainees in the group visit setting while maintaining educational value.
Given the relatively narrow scope and the nature of conditions encountered in the hand clinic, medical decision making for many patients is limited to a “straightforward” or “low complexity” level. These designations assume a limited number of diagnoses, management options, and amount and complexity of diagnostic workup. Most importantly, risk of complications or morbidity/mortality at these levels is minimal to low. For these conditions, a supervising physician can allow a trainee more independence to practice employing simple treatment and management guidelines and progress to working independently when addressing simpler conditions as the trainee’s experience grows. As independence grows, trainees can build confidence in medical management as well as focus on other core educational competencies once they are comfortable with the evaluation and management of a limited scope of conditions. Conditions such as trigger fingers, hand arthritis, ganglion cysts, and carpal tunnel are those the trainee is likely to encounter in a primary care practice. While there may be a decrease in direct physician teaching, the trainee gains clinical autonomy and experience in educational core competencies such as patient communication, patient education, systems-based practice, procedural skill, cultural competency, and interdisciplinary teamwork [15,16].
Lessons Learned
The success of the group visit required buy-in from hospital and physician leadership, the clinical team, and multiple partners in the hospital system. The hospital administration supported group visits as an integral component of the Urban Health Institute. Buy-in from key hospital leadership ensured resources and dedicated space for the group visit program. Grant support allowed additional programmatic support to acquire the necessary assistance from information services, EMR support, legal, and marketing. Physician buy-in was the most significant piece to the success of an individual group visit. Accepting the movement away from physician autonomy to team-based care is challenging for many providers. Physician willingness to start a high-demand group visit, recognition of the start-up inefficiencies, and working with the administrative and clinical team on program improvement strategies has succeeded in launching a sustaining group visit model.
Conclusion
There is a need for an adaptive and economically viable model of patient care to meet increasing demand, as well as provide care for indigent populations in a way that is more economically sustainable than providing care through the emergency department. The development and implementation of an urban hand group visit at our institution has demonstrated that such a model, based on group visit models more commonly seen in primary care, can be effectively implemented in a subspecialty care setting. This model is capable of increasing patient access to care and effectively handling increased patient volume with room for cost-effective growth in the future, all while maintaining quality of care. We anticipate further subspecialty clinics within hand pain to emerge, such as a group visit dedicated specifically to carpal tunnel syndrome or hand arthritis. This will allow each group to be more focused and will streamline education and mutual support among the patients.
Corresponding author: Steven Kaufman, MD, 3 Cooper Plaza, Suite 211, Camden, NJ 08103, [email protected].
Funding/support: The Nicholson Foundation.
Financial disclosures: None reported.
1. Gardiner P, Dresner D, Barnett KG, et al. Medical group visits: a feasibility study to manage patients with chronic pain in an underserved urban clinic. Glob Adv Health Med 2014;3:20–6.
2. Remick RA, Remick AK. Do patients really prefer individual outpatient follow-up visits, compared with group medical visits?. Can J Psychiatry 2014;59:50–3.
3. Thompson C, Meeuwisse I, Dahlke R, Drummond N. Group medical visits in primary care for patients with diabetes and low socioeconomic status: users’ perspectives and lessons for practitioners. Can J Diabetes 2014;38:198–204.
4. Eisenstat S, Lipps SA, Carlson K, Ulman K. Putting group visits into practice: a practical overview to preparation, implementation, and maintenance of group visits at Massachusetts General Hospital. Women’s Health Associates, The John D. Stoeckle Center for Primary Care Innovation, Massachusetts General Hospital; January 2012.
5. U.S. Census Bureau. State and city Quickfacts: Camden (city), New Jersey. Accessed 29 Sep 2015 at http://quickfacts.census.gov/qfd/states/34/3410000.html.
6. Slocum YS. A survey of expectations about group therapy among clinical and nonclinical populations. Int J Group Psychother 1987;37:39–54.
7. Newhouse RP, Stanik-hutt J, White KM, et al. Advanced practice nurse outcomes 1990-2008: a systematic review. Nurs Econ 2011;29:230–50.
8. Joshi R, Alim M, Kengne AP, et al. Task shifting for non-communicable disease management in low and middle income countries--a systematic review. PLoS ONE 2014;9:e103754.
9. Hofer AN, Abraham JM, Moscovice I. Expansion of coverage under the Patient Protection and Affordable Care Act and primary care utilization. Milbank Q 2011;89:69–89.
10. Kushnir T, Greenberg D, Madjar N, et al. Is burnout associated with referral rates among primary care physicians in community clinics?. Fam Pract 2014;31:44–50.
11. Calfee RP, Shah CM, Canham CD, et al. The influence of insurance status on access to and utilization of a tertiary hand surgery referral center. J Bone Joint Surg Am 2012;94:2177–84.
12. Lin CT, Albertson GA, Schilling LM, et al. Is patients’ perception of time spent with the physician a determinant of ambulatory patient satisfaction?. Arch Intern Med 2001;161:1437–42.
13. Teunis T, Thornton ER, Jayakumar P, Ring D. Time seeing a hand surgeon is not associated with patient satisfaction. Clin Orthop Relat Res 2014.
14. Murdock A, Griffin B. How is patient education linked to patient satisfaction?. Nursing 2013;43:43–5.
15. Accreditation Council for Graduate Medical Education. Common program requirements. Approved 2014. Available at www.acgme.org/Portals/0/PFAssets/ProgramRequirements/CPRs_07012016.pdf.
16. Liaison Committee on Medical Education. Functions and structure of a medical school: standards for accreditation of medical education programs leading to the M.D. degree. [updated June 2013]. Available at www.lcme.org/publications/functions.pdf.
17. Perla RJ, Provost LP, Murray SK. The run chart: a simple analytical tool for learning from variation in healthcare processes. BMJ Qual Saf 2011;20:46–51.
From Cooper Medical School of Rowan University (Dr. Patel, Dr. Fuller) and Cooper University Hospital (Dr. Kaufman), Camden, NJ.
Abstract
- Objective: To describe an adaptive musculoskeletal hand clinic that offers accessible and economically viable musculoskeletal care for an underserved, urban population.
- Methods: Descriptive report.
- Results: An enhanced access group visit model was developed offering both nonsurgical and surgical care pathways for patients with musculoskeletal disorders of the hand. Both patient education and care were provided in the group environment. Staffing included an orthopedic surgeon, nurse practitioner, medical student, orthopedic technician, and medical assistant. Over a 12-month period, group visit efficiency improved to accommodate an equivalent number of patients as compared to the traditional model. Access (time to appointment) was improved in the group visit. The model allows for the addition of non-physician clinical staff to improve access and limit costs in a manner not feasible with traditional office visits.
- Conclusion: A group visit model may offer a sustainable process to increase patient access to musculoskeletal subspecialty care and accommodate care of greater numbers of patients while maintaining quality. The group model offers flexible staffing, enhanced access, and educational benefit.
Key words: Group medical visit, team-based care, hand pain, access, underserved populations.
Group visits are a relatively new health care delivery model [1–3]. The term is applied to a wide variety of visits designed for groups of patients, rather than individual patient-provider appointments. The group visit format has been used for various disease- or condition-specific populations. Group visits can increase access to care and have been associated with improved clinical outcomes [4].
The Urban Health Institute, a dedicated business unit at Cooper University Health System in Camden, NJ, was established to focus on care of the underserved. The business unit is working to reduce cost of care delivery, increase access, and improve quality through the use of workflow redesign, task shifting, dashboards, and other methods. With a large startup grant from the Nicholson Foundation, the Urban Health Institute launched the Cooper Advanced Care Center to provide the local under-served population with access to a collaborative practice of 23 medical and surgical specialties under one roof. The center incorporates traditional one-on-one provider visits with innovative models of care, including group visits. Multiple partners were required in the group visit design and implementation starting with buy-in from Cooper Health System’s leadership for existing space to be redesigned for the group visit activities.
The Cooper Advanced Care Center, which had high no-show rates of 30% to 40%, and low reimbursement for a primarily Medicaid and self-pay population, initially operated at a financial loss. Meanwhile, most physicians had extended lag time until their next available appointment. In a traditional patient–physician office visit, additional physician time is required to increase access to care. This costly solution is often not financially viable. Group visits were considered as a means of using an interdisciplinary team to increase access while controlling or decreasing the per-visit cost.
Musculoskeletal medicine was identified as an area of need in part due to limited access to care. Patients were waiting more than 2 months to see a musculoskeletal specialist and were being scheduled beyond capacity in our existing traditional weekly hand and knee/sports medicine clinics. Within musculoskeletal medicine, 4 areas of musculoskeletal medicine were considered for group visits: back pain, knee pain, hand pain, and foot and ankle disorders. The decision was made to focus the subspecialty musculoskeletal clinic on disorders of the hand and wrist to provide nonsurgical and surgical care options for atraumatic and traumatic disorders of the hand in a teaching environment at an urban hospital. The purpose of this article is to discuss the design and implementation of a hand pain group visit model to increase access to care without increasing cost.
Setting and Patients
Camden City, New Jersey, is a medically underserved, resource-poor community. The population is 48% African American and 47% Hispanic and nearly 40% of individuals live below the poverty level [5]. The group visit was intentionally set up as a means to provide access to the un- or underinsured. Patients attending the group visits were 33% African American, 33% Hispanic, and 30% Caucasian. Most patients had Medicaid insurance (67%) with the remaining patients covered by commercial insurance (15%), dual Medicare/Medicaid (11%), Medicare (5%), or self pay (2%).
Group Visit Staffing and Structure
In a traditional office visit, used nearly ubiquitously in outpatient medical offices, patients arrive at individual appointment times for a prescribed time encounter with the physician, are registered and roomed by support staff, and are then seen by a clinician for diagnosis and treatment. While assistants and trainees participate in the patient’s care with attending physician supervision, the majority of direct care falls to the physician. Access is coupled to physician availability; increasing access to care requires crowding the schedule with additional patients. We used this model as the benchmark for volume and scheduling against which to compare the group visit.
The group visit staffing was the same as for the traditional visit: hand surgeon, nurse practitioner, orthopedic technician, medical student, and medical assistant. However, each clinical session consists of four 1-hour, consecutive group visits scheduled once a month on a Monday morning. Up to 10 people could be scheduled for each 1-hour group visit. We continued to offer our traditional office visit clinic on the other 3 Mondays in the month.
The hand surgeon begins the group visit with a 10-minute educational session and group discussion held in a meeting room. He reviews common disorders of the hand, including carpal tunnel syndrome, trigger fingers, hand arthritis, cysts, sprains and fractures, how they are treated, and risks and benefits of treatments. Patients sign a confidentiality agreement at check-in. Time is allowed for questions and experiential sharing is encouraged. Expectations are set at the start of the visit to honor each patient’s input to provide a safe environment for asking questions and expressing concerns about their shared health condition to enhance the learning experience [6]. A medical assistant enters the chief complaint using an electronic standardized questionnaire into the EMR along with basic vital signs for each patient either prior to, during, or after the group presentation.
After the group educational session with the surgeon, patients transition to a large, open clinical room with 6 separate workstations, each consisting of a small table with 4 chairs and a laptop computer. Small procedures can be performed on the table (suture removal, dressing changes, injections) and the table is appropriately sized to accommodate a care provider, the patient, and their support person(s). Tables are spaced comfortably such that conversations do not carry much from one to the other. The clinical space has white noise speakers for sound dampening while patients receive individual history, vital signs, physical examination, and review of relevant studies. Patients may see the clinicians in a private exam room if they wish or require.
In a traditional office setting, workflow through the major tasks (check-in, data gathering, diagnosis, treatment) is often linear, as dictated by the configuration of individual patient rooms and the patient’s expectations of a traditional doctor’s visit. In the group visit, major tasks are performed simultaneously by the advance practice providers (nurse practitioners, physician assistants) in conjunction with supervision of the attending physician. The workstations (tables, chairs, laptops) in the open clinical room allows for greater efficiency; providers can easily transition to other tasks from one workstation to another during time that may have been spent waiting for other team members in the more linear, traditional clinic. For example, while waiting for the attending physician’s approval of a diagnosis and treatment plan for one patient, a nurse practitioner may be able to begin assessing and gathering data with a second patient until the physician becomes available.
Scheduling and Access
A primary aim of the group visit pilot was to develop a model of care delivery that allowed scheduling beyond capacity for the traditional office hand clinic. At the inception of the group visit, all patients were offered a visit in either the traditional office or group visit model by our scheduling secretaries based upon availability, with emphasis on scheduling a defined underserved population into the group visit.
In traditional 1:1 appointments, the number of people who can access care is dependent on physician availability. The team-based model uncouples the number of scheduled patients from the physician availability, allowing increased efficiency in the model and/or additional staff to increase the number of patients the group visit can accommodate. Thus, patients were essentially guaranteed an appointment in the next clinic because there was no cap on the number of patients that could be scheduled into the group visit. If the number of patients exceeded the limit of 10 per hour, a non-physician clinician was added to accommodate the patient demand. As our group visit matures, the ability to increase the staffing model enables patients to get care without adding more physician time.
Task Shifting
A central pillar of making the group visit a sustainable model for more accessible care is shifting tasks to non-physician health care workers. Adding specialist time enhances access but drives up the cost of care. Non-physician clinical staff members in subspecialty orthopedic offices with experience diagnosing and treating common conditions are capable of providing the standard of care for those conditions with variable physician oversight [7].
In the group visit, there is a deliberate assignment of patients to clinical staff by the physician based on anticipated level of care required. Given the attending physician’s experience with the most common disorders related to hand pain, it is possible to anticipate the approximate complexity of care required for each patient based on the nature and duration of the presenting complaint. With some degree of clinical supervision by the physician, members of the team operate maximally independently to assist patients. The nurse practitioner can operate largely autonomously in the group visit. The overall goal is to encourage all team members to function at the top of their licenses and abilities. Task shifting in this manner increases the productivity of all members of the team and minimizes redundancy. Despite more autonomy of mid-level providers and support staff in the group visit, there is still direct supervision of care by the attending physician.
The current body of literature in task shifting to non-physician health care workers has mostly concerned low-income countries with marked physician and provider shortages [8]. However, given the increased patient volume already seen with the Affordable Care Act and further expected increases, the health care system is likely to see provider shortages, especially in primary care [9–11]. This will necessitate the adoption of strategies to increase access, maintain quality care, and decrease systemic cost. Task shifting provides one such strategy.
Patient Satisfaction
One concern with shifting clinical duties to non-physician clinical staff is patient satisfaction. An abbreviated interaction with physicians can make patients dissatisfied with medical care independent of eventual clinical outcome [12]. However, it has also been demonstrated in an outpatient hand surgery clinic that quality of time spent with the physician may have a greater impact on satisfaction than quantity of time [13].
Our group visit is structured to allow high physician-patient visibility and interaction. The introductory remarks by the physician engage patients with the physician early in the visit and establish a group and individual rapport. The physician introduces the clinical team and the idea of patients being seen by other clinical staff up front, which establishes comfort for later patient–staff interaction. This is also an important time for patient education, which has been shown as a significant determinant of patient satisfaction in the outpatient setting [14]. The patient education at the beginning of the visit answers questions by one person that another person may not have considered, and generates patient questions to be addressed individually with a clinician. One common example is when a person considering carpal tunnel surgery hears from a person who has recently completed the procedure and can talk about their operative experience.
In the group room, the physician and staff can move between patients quickly and efficiently without waiting for turnover of rooms and resources. The structure of the visit allows staff to dedicate more time to patient care by bypassing the extra time required when patients are roomed individually. The group/communal structure also allows patients to see the staff at work, as compared to time spent waiting alone in an exam room in the traditional office. This enables patients to appreciate the efforts of the clinical staff and avoids giving the impression that the physician is inattentive or cursory in patient interaction.
Medical Education
An important consideration at any academic medical center is education. However, education often introduces redundancies and inefficiency into the medical care visit. The work a trainee does is either extensively overseen or the clinical questions are repeated by a supervising provider. However, it is possible to increase efficiency and utility of trainees in the group visit setting while maintaining educational value.
Given the relatively narrow scope and the nature of conditions encountered in the hand clinic, medical decision making for many patients is limited to a “straightforward” or “low complexity” level. These designations assume a limited number of diagnoses, management options, and amount and complexity of diagnostic workup. Most importantly, risk of complications or morbidity/mortality at these levels is minimal to low. For these conditions, a supervising physician can allow a trainee more independence to practice employing simple treatment and management guidelines and progress to working independently when addressing simpler conditions as the trainee’s experience grows. As independence grows, trainees can build confidence in medical management as well as focus on other core educational competencies once they are comfortable with the evaluation and management of a limited scope of conditions. Conditions such as trigger fingers, hand arthritis, ganglion cysts, and carpal tunnel are those the trainee is likely to encounter in a primary care practice. While there may be a decrease in direct physician teaching, the trainee gains clinical autonomy and experience in educational core competencies such as patient communication, patient education, systems-based practice, procedural skill, cultural competency, and interdisciplinary teamwork [15,16].
Lessons Learned
The success of the group visit required buy-in from hospital and physician leadership, the clinical team, and multiple partners in the hospital system. The hospital administration supported group visits as an integral component of the Urban Health Institute. Buy-in from key hospital leadership ensured resources and dedicated space for the group visit program. Grant support allowed additional programmatic support to acquire the necessary assistance from information services, EMR support, legal, and marketing. Physician buy-in was the most significant piece to the success of an individual group visit. Accepting the movement away from physician autonomy to team-based care is challenging for many providers. Physician willingness to start a high-demand group visit, recognition of the start-up inefficiencies, and working with the administrative and clinical team on program improvement strategies has succeeded in launching a sustaining group visit model.
Conclusion
There is a need for an adaptive and economically viable model of patient care to meet increasing demand, as well as provide care for indigent populations in a way that is more economically sustainable than providing care through the emergency department. The development and implementation of an urban hand group visit at our institution has demonstrated that such a model, based on group visit models more commonly seen in primary care, can be effectively implemented in a subspecialty care setting. This model is capable of increasing patient access to care and effectively handling increased patient volume with room for cost-effective growth in the future, all while maintaining quality of care. We anticipate further subspecialty clinics within hand pain to emerge, such as a group visit dedicated specifically to carpal tunnel syndrome or hand arthritis. This will allow each group to be more focused and will streamline education and mutual support among the patients.
Corresponding author: Steven Kaufman, MD, 3 Cooper Plaza, Suite 211, Camden, NJ 08103, [email protected].
Funding/support: The Nicholson Foundation.
Financial disclosures: None reported.
From Cooper Medical School of Rowan University (Dr. Patel, Dr. Fuller) and Cooper University Hospital (Dr. Kaufman), Camden, NJ.
Abstract
- Objective: To describe an adaptive musculoskeletal hand clinic that offers accessible and economically viable musculoskeletal care for an underserved, urban population.
- Methods: Descriptive report.
- Results: An enhanced access group visit model was developed offering both nonsurgical and surgical care pathways for patients with musculoskeletal disorders of the hand. Both patient education and care were provided in the group environment. Staffing included an orthopedic surgeon, nurse practitioner, medical student, orthopedic technician, and medical assistant. Over a 12-month period, group visit efficiency improved to accommodate an equivalent number of patients as compared to the traditional model. Access (time to appointment) was improved in the group visit. The model allows for the addition of non-physician clinical staff to improve access and limit costs in a manner not feasible with traditional office visits.
- Conclusion: A group visit model may offer a sustainable process to increase patient access to musculoskeletal subspecialty care and accommodate care of greater numbers of patients while maintaining quality. The group model offers flexible staffing, enhanced access, and educational benefit.
Key words: Group medical visit, team-based care, hand pain, access, underserved populations.
Group visits are a relatively new health care delivery model [1–3]. The term is applied to a wide variety of visits designed for groups of patients, rather than individual patient-provider appointments. The group visit format has been used for various disease- or condition-specific populations. Group visits can increase access to care and have been associated with improved clinical outcomes [4].
The Urban Health Institute, a dedicated business unit at Cooper University Health System in Camden, NJ, was established to focus on care of the underserved. The business unit is working to reduce cost of care delivery, increase access, and improve quality through the use of workflow redesign, task shifting, dashboards, and other methods. With a large startup grant from the Nicholson Foundation, the Urban Health Institute launched the Cooper Advanced Care Center to provide the local under-served population with access to a collaborative practice of 23 medical and surgical specialties under one roof. The center incorporates traditional one-on-one provider visits with innovative models of care, including group visits. Multiple partners were required in the group visit design and implementation starting with buy-in from Cooper Health System’s leadership for existing space to be redesigned for the group visit activities.
The Cooper Advanced Care Center, which had high no-show rates of 30% to 40%, and low reimbursement for a primarily Medicaid and self-pay population, initially operated at a financial loss. Meanwhile, most physicians had extended lag time until their next available appointment. In a traditional patient–physician office visit, additional physician time is required to increase access to care. This costly solution is often not financially viable. Group visits were considered as a means of using an interdisciplinary team to increase access while controlling or decreasing the per-visit cost.
Musculoskeletal medicine was identified as an area of need in part due to limited access to care. Patients were waiting more than 2 months to see a musculoskeletal specialist and were being scheduled beyond capacity in our existing traditional weekly hand and knee/sports medicine clinics. Within musculoskeletal medicine, 4 areas of musculoskeletal medicine were considered for group visits: back pain, knee pain, hand pain, and foot and ankle disorders. The decision was made to focus the subspecialty musculoskeletal clinic on disorders of the hand and wrist to provide nonsurgical and surgical care options for atraumatic and traumatic disorders of the hand in a teaching environment at an urban hospital. The purpose of this article is to discuss the design and implementation of a hand pain group visit model to increase access to care without increasing cost.
Setting and Patients
Camden City, New Jersey, is a medically underserved, resource-poor community. The population is 48% African American and 47% Hispanic and nearly 40% of individuals live below the poverty level [5]. The group visit was intentionally set up as a means to provide access to the un- or underinsured. Patients attending the group visits were 33% African American, 33% Hispanic, and 30% Caucasian. Most patients had Medicaid insurance (67%) with the remaining patients covered by commercial insurance (15%), dual Medicare/Medicaid (11%), Medicare (5%), or self pay (2%).
Group Visit Staffing and Structure
In a traditional office visit, used nearly ubiquitously in outpatient medical offices, patients arrive at individual appointment times for a prescribed time encounter with the physician, are registered and roomed by support staff, and are then seen by a clinician for diagnosis and treatment. While assistants and trainees participate in the patient’s care with attending physician supervision, the majority of direct care falls to the physician. Access is coupled to physician availability; increasing access to care requires crowding the schedule with additional patients. We used this model as the benchmark for volume and scheduling against which to compare the group visit.
The group visit staffing was the same as for the traditional visit: hand surgeon, nurse practitioner, orthopedic technician, medical student, and medical assistant. However, each clinical session consists of four 1-hour, consecutive group visits scheduled once a month on a Monday morning. Up to 10 people could be scheduled for each 1-hour group visit. We continued to offer our traditional office visit clinic on the other 3 Mondays in the month.
The hand surgeon begins the group visit with a 10-minute educational session and group discussion held in a meeting room. He reviews common disorders of the hand, including carpal tunnel syndrome, trigger fingers, hand arthritis, cysts, sprains and fractures, how they are treated, and risks and benefits of treatments. Patients sign a confidentiality agreement at check-in. Time is allowed for questions and experiential sharing is encouraged. Expectations are set at the start of the visit to honor each patient’s input to provide a safe environment for asking questions and expressing concerns about their shared health condition to enhance the learning experience [6]. A medical assistant enters the chief complaint using an electronic standardized questionnaire into the EMR along with basic vital signs for each patient either prior to, during, or after the group presentation.
After the group educational session with the surgeon, patients transition to a large, open clinical room with 6 separate workstations, each consisting of a small table with 4 chairs and a laptop computer. Small procedures can be performed on the table (suture removal, dressing changes, injections) and the table is appropriately sized to accommodate a care provider, the patient, and their support person(s). Tables are spaced comfortably such that conversations do not carry much from one to the other. The clinical space has white noise speakers for sound dampening while patients receive individual history, vital signs, physical examination, and review of relevant studies. Patients may see the clinicians in a private exam room if they wish or require.
In a traditional office setting, workflow through the major tasks (check-in, data gathering, diagnosis, treatment) is often linear, as dictated by the configuration of individual patient rooms and the patient’s expectations of a traditional doctor’s visit. In the group visit, major tasks are performed simultaneously by the advance practice providers (nurse practitioners, physician assistants) in conjunction with supervision of the attending physician. The workstations (tables, chairs, laptops) in the open clinical room allows for greater efficiency; providers can easily transition to other tasks from one workstation to another during time that may have been spent waiting for other team members in the more linear, traditional clinic. For example, while waiting for the attending physician’s approval of a diagnosis and treatment plan for one patient, a nurse practitioner may be able to begin assessing and gathering data with a second patient until the physician becomes available.
Scheduling and Access
A primary aim of the group visit pilot was to develop a model of care delivery that allowed scheduling beyond capacity for the traditional office hand clinic. At the inception of the group visit, all patients were offered a visit in either the traditional office or group visit model by our scheduling secretaries based upon availability, with emphasis on scheduling a defined underserved population into the group visit.
In traditional 1:1 appointments, the number of people who can access care is dependent on physician availability. The team-based model uncouples the number of scheduled patients from the physician availability, allowing increased efficiency in the model and/or additional staff to increase the number of patients the group visit can accommodate. Thus, patients were essentially guaranteed an appointment in the next clinic because there was no cap on the number of patients that could be scheduled into the group visit. If the number of patients exceeded the limit of 10 per hour, a non-physician clinician was added to accommodate the patient demand. As our group visit matures, the ability to increase the staffing model enables patients to get care without adding more physician time.
Task Shifting
A central pillar of making the group visit a sustainable model for more accessible care is shifting tasks to non-physician health care workers. Adding specialist time enhances access but drives up the cost of care. Non-physician clinical staff members in subspecialty orthopedic offices with experience diagnosing and treating common conditions are capable of providing the standard of care for those conditions with variable physician oversight [7].
In the group visit, there is a deliberate assignment of patients to clinical staff by the physician based on anticipated level of care required. Given the attending physician’s experience with the most common disorders related to hand pain, it is possible to anticipate the approximate complexity of care required for each patient based on the nature and duration of the presenting complaint. With some degree of clinical supervision by the physician, members of the team operate maximally independently to assist patients. The nurse practitioner can operate largely autonomously in the group visit. The overall goal is to encourage all team members to function at the top of their licenses and abilities. Task shifting in this manner increases the productivity of all members of the team and minimizes redundancy. Despite more autonomy of mid-level providers and support staff in the group visit, there is still direct supervision of care by the attending physician.
The current body of literature in task shifting to non-physician health care workers has mostly concerned low-income countries with marked physician and provider shortages [8]. However, given the increased patient volume already seen with the Affordable Care Act and further expected increases, the health care system is likely to see provider shortages, especially in primary care [9–11]. This will necessitate the adoption of strategies to increase access, maintain quality care, and decrease systemic cost. Task shifting provides one such strategy.
Patient Satisfaction
One concern with shifting clinical duties to non-physician clinical staff is patient satisfaction. An abbreviated interaction with physicians can make patients dissatisfied with medical care independent of eventual clinical outcome [12]. However, it has also been demonstrated in an outpatient hand surgery clinic that quality of time spent with the physician may have a greater impact on satisfaction than quantity of time [13].
Our group visit is structured to allow high physician-patient visibility and interaction. The introductory remarks by the physician engage patients with the physician early in the visit and establish a group and individual rapport. The physician introduces the clinical team and the idea of patients being seen by other clinical staff up front, which establishes comfort for later patient–staff interaction. This is also an important time for patient education, which has been shown as a significant determinant of patient satisfaction in the outpatient setting [14]. The patient education at the beginning of the visit answers questions by one person that another person may not have considered, and generates patient questions to be addressed individually with a clinician. One common example is when a person considering carpal tunnel surgery hears from a person who has recently completed the procedure and can talk about their operative experience.
In the group room, the physician and staff can move between patients quickly and efficiently without waiting for turnover of rooms and resources. The structure of the visit allows staff to dedicate more time to patient care by bypassing the extra time required when patients are roomed individually. The group/communal structure also allows patients to see the staff at work, as compared to time spent waiting alone in an exam room in the traditional office. This enables patients to appreciate the efforts of the clinical staff and avoids giving the impression that the physician is inattentive or cursory in patient interaction.
Medical Education
An important consideration at any academic medical center is education. However, education often introduces redundancies and inefficiency into the medical care visit. The work a trainee does is either extensively overseen or the clinical questions are repeated by a supervising provider. However, it is possible to increase efficiency and utility of trainees in the group visit setting while maintaining educational value.
Given the relatively narrow scope and the nature of conditions encountered in the hand clinic, medical decision making for many patients is limited to a “straightforward” or “low complexity” level. These designations assume a limited number of diagnoses, management options, and amount and complexity of diagnostic workup. Most importantly, risk of complications or morbidity/mortality at these levels is minimal to low. For these conditions, a supervising physician can allow a trainee more independence to practice employing simple treatment and management guidelines and progress to working independently when addressing simpler conditions as the trainee’s experience grows. As independence grows, trainees can build confidence in medical management as well as focus on other core educational competencies once they are comfortable with the evaluation and management of a limited scope of conditions. Conditions such as trigger fingers, hand arthritis, ganglion cysts, and carpal tunnel are those the trainee is likely to encounter in a primary care practice. While there may be a decrease in direct physician teaching, the trainee gains clinical autonomy and experience in educational core competencies such as patient communication, patient education, systems-based practice, procedural skill, cultural competency, and interdisciplinary teamwork [15,16].
Lessons Learned
The success of the group visit required buy-in from hospital and physician leadership, the clinical team, and multiple partners in the hospital system. The hospital administration supported group visits as an integral component of the Urban Health Institute. Buy-in from key hospital leadership ensured resources and dedicated space for the group visit program. Grant support allowed additional programmatic support to acquire the necessary assistance from information services, EMR support, legal, and marketing. Physician buy-in was the most significant piece to the success of an individual group visit. Accepting the movement away from physician autonomy to team-based care is challenging for many providers. Physician willingness to start a high-demand group visit, recognition of the start-up inefficiencies, and working with the administrative and clinical team on program improvement strategies has succeeded in launching a sustaining group visit model.
Conclusion
There is a need for an adaptive and economically viable model of patient care to meet increasing demand, as well as provide care for indigent populations in a way that is more economically sustainable than providing care through the emergency department. The development and implementation of an urban hand group visit at our institution has demonstrated that such a model, based on group visit models more commonly seen in primary care, can be effectively implemented in a subspecialty care setting. This model is capable of increasing patient access to care and effectively handling increased patient volume with room for cost-effective growth in the future, all while maintaining quality of care. We anticipate further subspecialty clinics within hand pain to emerge, such as a group visit dedicated specifically to carpal tunnel syndrome or hand arthritis. This will allow each group to be more focused and will streamline education and mutual support among the patients.
Corresponding author: Steven Kaufman, MD, 3 Cooper Plaza, Suite 211, Camden, NJ 08103, [email protected].
Funding/support: The Nicholson Foundation.
Financial disclosures: None reported.
1. Gardiner P, Dresner D, Barnett KG, et al. Medical group visits: a feasibility study to manage patients with chronic pain in an underserved urban clinic. Glob Adv Health Med 2014;3:20–6.
2. Remick RA, Remick AK. Do patients really prefer individual outpatient follow-up visits, compared with group medical visits?. Can J Psychiatry 2014;59:50–3.
3. Thompson C, Meeuwisse I, Dahlke R, Drummond N. Group medical visits in primary care for patients with diabetes and low socioeconomic status: users’ perspectives and lessons for practitioners. Can J Diabetes 2014;38:198–204.
4. Eisenstat S, Lipps SA, Carlson K, Ulman K. Putting group visits into practice: a practical overview to preparation, implementation, and maintenance of group visits at Massachusetts General Hospital. Women’s Health Associates, The John D. Stoeckle Center for Primary Care Innovation, Massachusetts General Hospital; January 2012.
5. U.S. Census Bureau. State and city Quickfacts: Camden (city), New Jersey. Accessed 29 Sep 2015 at http://quickfacts.census.gov/qfd/states/34/3410000.html.
6. Slocum YS. A survey of expectations about group therapy among clinical and nonclinical populations. Int J Group Psychother 1987;37:39–54.
7. Newhouse RP, Stanik-hutt J, White KM, et al. Advanced practice nurse outcomes 1990-2008: a systematic review. Nurs Econ 2011;29:230–50.
8. Joshi R, Alim M, Kengne AP, et al. Task shifting for non-communicable disease management in low and middle income countries--a systematic review. PLoS ONE 2014;9:e103754.
9. Hofer AN, Abraham JM, Moscovice I. Expansion of coverage under the Patient Protection and Affordable Care Act and primary care utilization. Milbank Q 2011;89:69–89.
10. Kushnir T, Greenberg D, Madjar N, et al. Is burnout associated with referral rates among primary care physicians in community clinics?. Fam Pract 2014;31:44–50.
11. Calfee RP, Shah CM, Canham CD, et al. The influence of insurance status on access to and utilization of a tertiary hand surgery referral center. J Bone Joint Surg Am 2012;94:2177–84.
12. Lin CT, Albertson GA, Schilling LM, et al. Is patients’ perception of time spent with the physician a determinant of ambulatory patient satisfaction?. Arch Intern Med 2001;161:1437–42.
13. Teunis T, Thornton ER, Jayakumar P, Ring D. Time seeing a hand surgeon is not associated with patient satisfaction. Clin Orthop Relat Res 2014.
14. Murdock A, Griffin B. How is patient education linked to patient satisfaction?. Nursing 2013;43:43–5.
15. Accreditation Council for Graduate Medical Education. Common program requirements. Approved 2014. Available at www.acgme.org/Portals/0/PFAssets/ProgramRequirements/CPRs_07012016.pdf.
16. Liaison Committee on Medical Education. Functions and structure of a medical school: standards for accreditation of medical education programs leading to the M.D. degree. [updated June 2013]. Available at www.lcme.org/publications/functions.pdf.
17. Perla RJ, Provost LP, Murray SK. The run chart: a simple analytical tool for learning from variation in healthcare processes. BMJ Qual Saf 2011;20:46–51.
1. Gardiner P, Dresner D, Barnett KG, et al. Medical group visits: a feasibility study to manage patients with chronic pain in an underserved urban clinic. Glob Adv Health Med 2014;3:20–6.
2. Remick RA, Remick AK. Do patients really prefer individual outpatient follow-up visits, compared with group medical visits?. Can J Psychiatry 2014;59:50–3.
3. Thompson C, Meeuwisse I, Dahlke R, Drummond N. Group medical visits in primary care for patients with diabetes and low socioeconomic status: users’ perspectives and lessons for practitioners. Can J Diabetes 2014;38:198–204.
4. Eisenstat S, Lipps SA, Carlson K, Ulman K. Putting group visits into practice: a practical overview to preparation, implementation, and maintenance of group visits at Massachusetts General Hospital. Women’s Health Associates, The John D. Stoeckle Center for Primary Care Innovation, Massachusetts General Hospital; January 2012.
5. U.S. Census Bureau. State and city Quickfacts: Camden (city), New Jersey. Accessed 29 Sep 2015 at http://quickfacts.census.gov/qfd/states/34/3410000.html.
6. Slocum YS. A survey of expectations about group therapy among clinical and nonclinical populations. Int J Group Psychother 1987;37:39–54.
7. Newhouse RP, Stanik-hutt J, White KM, et al. Advanced practice nurse outcomes 1990-2008: a systematic review. Nurs Econ 2011;29:230–50.
8. Joshi R, Alim M, Kengne AP, et al. Task shifting for non-communicable disease management in low and middle income countries--a systematic review. PLoS ONE 2014;9:e103754.
9. Hofer AN, Abraham JM, Moscovice I. Expansion of coverage under the Patient Protection and Affordable Care Act and primary care utilization. Milbank Q 2011;89:69–89.
10. Kushnir T, Greenberg D, Madjar N, et al. Is burnout associated with referral rates among primary care physicians in community clinics?. Fam Pract 2014;31:44–50.
11. Calfee RP, Shah CM, Canham CD, et al. The influence of insurance status on access to and utilization of a tertiary hand surgery referral center. J Bone Joint Surg Am 2012;94:2177–84.
12. Lin CT, Albertson GA, Schilling LM, et al. Is patients’ perception of time spent with the physician a determinant of ambulatory patient satisfaction?. Arch Intern Med 2001;161:1437–42.
13. Teunis T, Thornton ER, Jayakumar P, Ring D. Time seeing a hand surgeon is not associated with patient satisfaction. Clin Orthop Relat Res 2014.
14. Murdock A, Griffin B. How is patient education linked to patient satisfaction?. Nursing 2013;43:43–5.
15. Accreditation Council for Graduate Medical Education. Common program requirements. Approved 2014. Available at www.acgme.org/Portals/0/PFAssets/ProgramRequirements/CPRs_07012016.pdf.
16. Liaison Committee on Medical Education. Functions and structure of a medical school: standards for accreditation of medical education programs leading to the M.D. degree. [updated June 2013]. Available at www.lcme.org/publications/functions.pdf.
17. Perla RJ, Provost LP, Murray SK. The run chart: a simple analytical tool for learning from variation in healthcare processes. BMJ Qual Saf 2011;20:46–51.