User login
Monofilament suture works best for cesarean closure
LAS VEGAS – A monofilament suture led to substantially fewer wound complications than a braided suture for closing nonemergency cesarean incisions in a head-to-head trial with 520 evaluable women.
Cesarean incision closure with a braided, polyglactin 910 suture (Vicryl) led to 65% more wound complications than the monofilament poliglecaprone 25 suture (Monocryl), Arin M. Buresch, MD, said at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
This is the first randomized, controlled trial to compare these two suture types, according to Dr. Buresch, and she highlighted the need for caution about changing practice based on results from a single study. But based in large part on these results, which were gathered at Montefiore Medical Center in New York, the obstetrical staff at Montefiore is now primarily using the monofilament, poliglecaprone 25 suture, she said.
The study enrolled 550 pregnant women at 37 weeks’ gestation or greater during May 2015 to July 2016. Participants were either scheduled for an elective cesarean delivery or underwent a nonemergency, indicated cesarean after labor began but without significant maternal or fetal distress. The study excluded emergency cesareans as well as women with a recent urogenital infection, chronic or injected steroid use, or a vertical skin incision. The enrolled women averaged 31 years old, and their average body mass index was 34 kg/m2. The demographic and clinical profile of the two randomized groups closely matched.
The study’s primary endpoint was the incidence of a wound complication during 30 days following delivery. A complication could be a surgical site infection, hematoma, seroma, or wound separation. Of the 550 women randomized, 520 were available for complete 30-day follow-up.
The results showed that wound complications occurred in 9% of the 263 women treated with the poliglecaprone 25 monofilament suture and in 14% of the 257 treated with the polyglactin 910 braided suture, a statistically significant difference, Dr. Buresch reported. The relative risk for a complication increased by 65% with the braided suture, compared with patients treated with monofilament sutures. Treating 18 patients with the monofilament suture prevented one wound complication, on average.
A subgroup analysis showed that the poliglecaprone 25 suture was effective at reducing wound complications in women who underwent elective cesarean deliveries, but among the 17% of participants who had begun labor at the time of their cesarean delivery the monofilament suture conferred no significant advantage, compared with the braided suture. Benefit from the poliglecaprone 25 monofilament occurred about equally across the entire range of body mass index among the women in the study, Dr. Buresch said.
Dr. Buresch had no disclosures.
[email protected]
On Twitter @mitchelzoler
LAS VEGAS – A monofilament suture led to substantially fewer wound complications than a braided suture for closing nonemergency cesarean incisions in a head-to-head trial with 520 evaluable women.
Cesarean incision closure with a braided, polyglactin 910 suture (Vicryl) led to 65% more wound complications than the monofilament poliglecaprone 25 suture (Monocryl), Arin M. Buresch, MD, said at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
This is the first randomized, controlled trial to compare these two suture types, according to Dr. Buresch, and she highlighted the need for caution about changing practice based on results from a single study. But based in large part on these results, which were gathered at Montefiore Medical Center in New York, the obstetrical staff at Montefiore is now primarily using the monofilament, poliglecaprone 25 suture, she said.
The study enrolled 550 pregnant women at 37 weeks’ gestation or greater during May 2015 to July 2016. Participants were either scheduled for an elective cesarean delivery or underwent a nonemergency, indicated cesarean after labor began but without significant maternal or fetal distress. The study excluded emergency cesareans as well as women with a recent urogenital infection, chronic or injected steroid use, or a vertical skin incision. The enrolled women averaged 31 years old, and their average body mass index was 34 kg/m2. The demographic and clinical profile of the two randomized groups closely matched.
The study’s primary endpoint was the incidence of a wound complication during 30 days following delivery. A complication could be a surgical site infection, hematoma, seroma, or wound separation. Of the 550 women randomized, 520 were available for complete 30-day follow-up.
The results showed that wound complications occurred in 9% of the 263 women treated with the poliglecaprone 25 monofilament suture and in 14% of the 257 treated with the polyglactin 910 braided suture, a statistically significant difference, Dr. Buresch reported. The relative risk for a complication increased by 65% with the braided suture, compared with patients treated with monofilament sutures. Treating 18 patients with the monofilament suture prevented one wound complication, on average.
A subgroup analysis showed that the poliglecaprone 25 suture was effective at reducing wound complications in women who underwent elective cesarean deliveries, but among the 17% of participants who had begun labor at the time of their cesarean delivery the monofilament suture conferred no significant advantage, compared with the braided suture. Benefit from the poliglecaprone 25 monofilament occurred about equally across the entire range of body mass index among the women in the study, Dr. Buresch said.
Dr. Buresch had no disclosures.
[email protected]
On Twitter @mitchelzoler
LAS VEGAS – A monofilament suture led to substantially fewer wound complications than a braided suture for closing nonemergency cesarean incisions in a head-to-head trial with 520 evaluable women.
Cesarean incision closure with a braided, polyglactin 910 suture (Vicryl) led to 65% more wound complications than the monofilament poliglecaprone 25 suture (Monocryl), Arin M. Buresch, MD, said at the annual Pregnancy Meeting sponsored by the Society for Maternal-Fetal Medicine.
This is the first randomized, controlled trial to compare these two suture types, according to Dr. Buresch, and she highlighted the need for caution about changing practice based on results from a single study. But based in large part on these results, which were gathered at Montefiore Medical Center in New York, the obstetrical staff at Montefiore is now primarily using the monofilament, poliglecaprone 25 suture, she said.
The study enrolled 550 pregnant women at 37 weeks’ gestation or greater during May 2015 to July 2016. Participants were either scheduled for an elective cesarean delivery or underwent a nonemergency, indicated cesarean after labor began but without significant maternal or fetal distress. The study excluded emergency cesareans as well as women with a recent urogenital infection, chronic or injected steroid use, or a vertical skin incision. The enrolled women averaged 31 years old, and their average body mass index was 34 kg/m2. The demographic and clinical profile of the two randomized groups closely matched.
The study’s primary endpoint was the incidence of a wound complication during 30 days following delivery. A complication could be a surgical site infection, hematoma, seroma, or wound separation. Of the 550 women randomized, 520 were available for complete 30-day follow-up.
The results showed that wound complications occurred in 9% of the 263 women treated with the poliglecaprone 25 monofilament suture and in 14% of the 257 treated with the polyglactin 910 braided suture, a statistically significant difference, Dr. Buresch reported. The relative risk for a complication increased by 65% with the braided suture, compared with patients treated with monofilament sutures. Treating 18 patients with the monofilament suture prevented one wound complication, on average.
A subgroup analysis showed that the poliglecaprone 25 suture was effective at reducing wound complications in women who underwent elective cesarean deliveries, but among the 17% of participants who had begun labor at the time of their cesarean delivery the monofilament suture conferred no significant advantage, compared with the braided suture. Benefit from the poliglecaprone 25 monofilament occurred about equally across the entire range of body mass index among the women in the study, Dr. Buresch said.
Dr. Buresch had no disclosures.
[email protected]
On Twitter @mitchelzoler
Megamerger rulings may chill future consolidations
Expect a chilling effect on future health care consolidations after two health insurance megamergers were blocked by federal courts, analysts say.
A federal judge barred a merger between Aetna and Humana on Jan. 23, followed by a Feb. 8 decision that blocked Anthem and Cigna from consolidating. Both rulings called the deals anticompetitive.
“Both of these decisions are likely to chill future mergers,” Mr. Dahlquist said in an interview. “We have the FTC [Federal Trade Commission] winning on the provider side. Now we have the DOJ [Department of Justice] winning on the insurer side. While they are different players in the marketplace, the law that is being applied is very similar, if not the same. The one-sided victories by the government are creating a situation of imbalance.”
Ruling positive and negative for providers
Anthem’s proposed $54 billion merger with Cigna would have been the largest insurer consolidation in history. The merger, along with Aetna’s $37 billion plan to purchase Humana, would have reduced the number of major U.S. health insurers from five to three, reshaping the industry. The Department of Justice and a number of states immediately opposed the mergers, arguing the consolidations would significantly reduce competition to the detriment of patients. Judges ultimately agreed.
“The [insurers] already have a huge market position so they can already hammer [providers] with low rates,” Mr. Greer said in an interview. “The reason why [the rulings are] such a big win for providers, is there won’t be this huge concentration of power. Anthem may not be able to hammer them quite as much as if they would’ve merged with Cigna.”
However, the rulings may discourage future health care consolidations between insurers and among health providers, Mr. Dahlquist noted. In recent years, the government has scored a series of legal wins that have blocked provider mergers. In 2013 for example, the Federal Trade Commission successfully stopped the acquisition of Palmyra Medical Center by Phoebe Putney Memorial Hospital (Albany, Ga.), followed by a 2014 win that barred St. Luke’s Health System’s acquisition of Saltzer Medical Group (Nampa, Idaho), an independent physician practice. In 2016, the FTC successfully blocked the merger of Penn State Hershey (Pa.) Medical Center’s merger with PinnacleHealth System (Harrisburg, Penn.).
“Every merger needs to be looked at [based on] the facts of that merger, and the facts of that case, the markets they compete in, [and] the markets they want to expand into,” Mr. Dahlquist said. “That’s why you shouldn’t look at all mergers of health care providers or health insurers as inherently bad, and I think that’s what these [decisions] are unfortunately driving toward.”
A broader takeaway is that the insurance industry needs to develop a better business model, said Barak D. Richman, PhD, an antitrust expert and law professor at Duke University in Durham, N.C. Mr. Richman consulted with several state departments of insurance as they were reviewing the Anthem-Cigna mergers.
“The general story here is that the insurance industry, over a number of years, has been consolidating and has reached a point where it now has passed a threshold where antitrust scrutiny will be very real,” Mr. Richman said in an interview. “One thing that the court cases revealed is that there is a certain prevailing business model in insurance which is: Get as big as you can, balance risk through volume, and use buying leverage to negotiate favorable prices from providers. It looks like that business model has reached its limits and really is not going to be sustainable any longer.”
The current market demands business models that center on value, not volume, Mr. Richman continued. Insurance companies will need to be more deliberate and analytical about how to provide value to patients and generate cost effective care.
“That really is the takeaway, that we need a real shift in the business of health insurance,” he said.
Anthem banking on new administration
Since the rulings, Aetna and Humana have chosen not to appeal and have mutually ended their merger agreement. Cigna is seeking to terminate its agreement with Anthem, but Anthem is fighting the dissolution. The insurance giant is looking toward the Trump administration to potentially turn the case around.
To enforce the termination, Cigna is suing Anthem in the Delaware Court of Chancery seeking a declaratory judgment that Cigna has lawfully terminated the contract, according to an announcement by Cigna. Anthem, meanwhile, is seeking a temporary restraining order to enjoin Cigna from terminating its contract.
“Anthem believes there is still sufficient time and a viable path forward potentially to complete the transaction that will save millions of Americans more than $2 billion in annual medical costs and deliver significant value to shareholders,” according to a company statement. “In addition to filing this lawsuit, Anthem is pursuing an expedited appeal of the District Court’s decision and is committed to completing this value-creating merger either through a successful appeal or through settlement with the new leadership at the Department of Justice.”
Part of that new leadership could include Makan Delrahim, a former Anthem lobbyist now serving as deputy White House counsel. He is rumored to be a top contender to lead the DOJ’s antitrust division.
Records also show that Indiana insurance regulators were supportive of the Anthem-Cigna deal while Vice President Pence was governor of Indiana and that Anthem contributed $100,000 to President Trump’s inaugural committee, according to Senate lobbying reports.
“A lot of folks are talking about the possibility that Trump will appoint people at both the FTC and DOJ antitrust devision [who] are Republicans and tend to be more business friendly, which would mean that maybe some of these mergers would be more likely to make it and less likely to be challenged,” he said.
On the other hand, a couple of leadership changes will not likely reverse the country’s historic antitrust enforcement, Mr. Dahlquist said.
“I don’t believe you’re going to see a systemic shift in the antitrust enforcement policy of this country,” he said. “Even one change at the top is not going to [create] upheaval within the ranks at the FTC and DOJ. The government is on a winning streak; I think that’s going to continue in the short term.”
“I don’t expect to see any change in the government’s approach in continuing to challenge anticompetitive health care transactions,” Ms. Feinstein said during at interview at the meeting.
[email protected]
On Twitter @legal_med
Expect a chilling effect on future health care consolidations after two health insurance megamergers were blocked by federal courts, analysts say.
A federal judge barred a merger between Aetna and Humana on Jan. 23, followed by a Feb. 8 decision that blocked Anthem and Cigna from consolidating. Both rulings called the deals anticompetitive.
“Both of these decisions are likely to chill future mergers,” Mr. Dahlquist said in an interview. “We have the FTC [Federal Trade Commission] winning on the provider side. Now we have the DOJ [Department of Justice] winning on the insurer side. While they are different players in the marketplace, the law that is being applied is very similar, if not the same. The one-sided victories by the government are creating a situation of imbalance.”
Ruling positive and negative for providers
Anthem’s proposed $54 billion merger with Cigna would have been the largest insurer consolidation in history. The merger, along with Aetna’s $37 billion plan to purchase Humana, would have reduced the number of major U.S. health insurers from five to three, reshaping the industry. The Department of Justice and a number of states immediately opposed the mergers, arguing the consolidations would significantly reduce competition to the detriment of patients. Judges ultimately agreed.
“The [insurers] already have a huge market position so they can already hammer [providers] with low rates,” Mr. Greer said in an interview. “The reason why [the rulings are] such a big win for providers, is there won’t be this huge concentration of power. Anthem may not be able to hammer them quite as much as if they would’ve merged with Cigna.”
However, the rulings may discourage future health care consolidations between insurers and among health providers, Mr. Dahlquist noted. In recent years, the government has scored a series of legal wins that have blocked provider mergers. In 2013 for example, the Federal Trade Commission successfully stopped the acquisition of Palmyra Medical Center by Phoebe Putney Memorial Hospital (Albany, Ga.), followed by a 2014 win that barred St. Luke’s Health System’s acquisition of Saltzer Medical Group (Nampa, Idaho), an independent physician practice. In 2016, the FTC successfully blocked the merger of Penn State Hershey (Pa.) Medical Center’s merger with PinnacleHealth System (Harrisburg, Penn.).
“Every merger needs to be looked at [based on] the facts of that merger, and the facts of that case, the markets they compete in, [and] the markets they want to expand into,” Mr. Dahlquist said. “That’s why you shouldn’t look at all mergers of health care providers or health insurers as inherently bad, and I think that’s what these [decisions] are unfortunately driving toward.”
A broader takeaway is that the insurance industry needs to develop a better business model, said Barak D. Richman, PhD, an antitrust expert and law professor at Duke University in Durham, N.C. Mr. Richman consulted with several state departments of insurance as they were reviewing the Anthem-Cigna mergers.
“The general story here is that the insurance industry, over a number of years, has been consolidating and has reached a point where it now has passed a threshold where antitrust scrutiny will be very real,” Mr. Richman said in an interview. “One thing that the court cases revealed is that there is a certain prevailing business model in insurance which is: Get as big as you can, balance risk through volume, and use buying leverage to negotiate favorable prices from providers. It looks like that business model has reached its limits and really is not going to be sustainable any longer.”
The current market demands business models that center on value, not volume, Mr. Richman continued. Insurance companies will need to be more deliberate and analytical about how to provide value to patients and generate cost effective care.
“That really is the takeaway, that we need a real shift in the business of health insurance,” he said.
Anthem banking on new administration
Since the rulings, Aetna and Humana have chosen not to appeal and have mutually ended their merger agreement. Cigna is seeking to terminate its agreement with Anthem, but Anthem is fighting the dissolution. The insurance giant is looking toward the Trump administration to potentially turn the case around.
To enforce the termination, Cigna is suing Anthem in the Delaware Court of Chancery seeking a declaratory judgment that Cigna has lawfully terminated the contract, according to an announcement by Cigna. Anthem, meanwhile, is seeking a temporary restraining order to enjoin Cigna from terminating its contract.
“Anthem believes there is still sufficient time and a viable path forward potentially to complete the transaction that will save millions of Americans more than $2 billion in annual medical costs and deliver significant value to shareholders,” according to a company statement. “In addition to filing this lawsuit, Anthem is pursuing an expedited appeal of the District Court’s decision and is committed to completing this value-creating merger either through a successful appeal or through settlement with the new leadership at the Department of Justice.”
Part of that new leadership could include Makan Delrahim, a former Anthem lobbyist now serving as deputy White House counsel. He is rumored to be a top contender to lead the DOJ’s antitrust division.
Records also show that Indiana insurance regulators were supportive of the Anthem-Cigna deal while Vice President Pence was governor of Indiana and that Anthem contributed $100,000 to President Trump’s inaugural committee, according to Senate lobbying reports.
“A lot of folks are talking about the possibility that Trump will appoint people at both the FTC and DOJ antitrust devision [who] are Republicans and tend to be more business friendly, which would mean that maybe some of these mergers would be more likely to make it and less likely to be challenged,” he said.
On the other hand, a couple of leadership changes will not likely reverse the country’s historic antitrust enforcement, Mr. Dahlquist said.
“I don’t believe you’re going to see a systemic shift in the antitrust enforcement policy of this country,” he said. “Even one change at the top is not going to [create] upheaval within the ranks at the FTC and DOJ. The government is on a winning streak; I think that’s going to continue in the short term.”
“I don’t expect to see any change in the government’s approach in continuing to challenge anticompetitive health care transactions,” Ms. Feinstein said during at interview at the meeting.
[email protected]
On Twitter @legal_med
Expect a chilling effect on future health care consolidations after two health insurance megamergers were blocked by federal courts, analysts say.
A federal judge barred a merger between Aetna and Humana on Jan. 23, followed by a Feb. 8 decision that blocked Anthem and Cigna from consolidating. Both rulings called the deals anticompetitive.
“Both of these decisions are likely to chill future mergers,” Mr. Dahlquist said in an interview. “We have the FTC [Federal Trade Commission] winning on the provider side. Now we have the DOJ [Department of Justice] winning on the insurer side. While they are different players in the marketplace, the law that is being applied is very similar, if not the same. The one-sided victories by the government are creating a situation of imbalance.”
Ruling positive and negative for providers
Anthem’s proposed $54 billion merger with Cigna would have been the largest insurer consolidation in history. The merger, along with Aetna’s $37 billion plan to purchase Humana, would have reduced the number of major U.S. health insurers from five to three, reshaping the industry. The Department of Justice and a number of states immediately opposed the mergers, arguing the consolidations would significantly reduce competition to the detriment of patients. Judges ultimately agreed.
“The [insurers] already have a huge market position so they can already hammer [providers] with low rates,” Mr. Greer said in an interview. “The reason why [the rulings are] such a big win for providers, is there won’t be this huge concentration of power. Anthem may not be able to hammer them quite as much as if they would’ve merged with Cigna.”
However, the rulings may discourage future health care consolidations between insurers and among health providers, Mr. Dahlquist noted. In recent years, the government has scored a series of legal wins that have blocked provider mergers. In 2013 for example, the Federal Trade Commission successfully stopped the acquisition of Palmyra Medical Center by Phoebe Putney Memorial Hospital (Albany, Ga.), followed by a 2014 win that barred St. Luke’s Health System’s acquisition of Saltzer Medical Group (Nampa, Idaho), an independent physician practice. In 2016, the FTC successfully blocked the merger of Penn State Hershey (Pa.) Medical Center’s merger with PinnacleHealth System (Harrisburg, Penn.).
“Every merger needs to be looked at [based on] the facts of that merger, and the facts of that case, the markets they compete in, [and] the markets they want to expand into,” Mr. Dahlquist said. “That’s why you shouldn’t look at all mergers of health care providers or health insurers as inherently bad, and I think that’s what these [decisions] are unfortunately driving toward.”
A broader takeaway is that the insurance industry needs to develop a better business model, said Barak D. Richman, PhD, an antitrust expert and law professor at Duke University in Durham, N.C. Mr. Richman consulted with several state departments of insurance as they were reviewing the Anthem-Cigna mergers.
“The general story here is that the insurance industry, over a number of years, has been consolidating and has reached a point where it now has passed a threshold where antitrust scrutiny will be very real,” Mr. Richman said in an interview. “One thing that the court cases revealed is that there is a certain prevailing business model in insurance which is: Get as big as you can, balance risk through volume, and use buying leverage to negotiate favorable prices from providers. It looks like that business model has reached its limits and really is not going to be sustainable any longer.”
The current market demands business models that center on value, not volume, Mr. Richman continued. Insurance companies will need to be more deliberate and analytical about how to provide value to patients and generate cost effective care.
“That really is the takeaway, that we need a real shift in the business of health insurance,” he said.
Anthem banking on new administration
Since the rulings, Aetna and Humana have chosen not to appeal and have mutually ended their merger agreement. Cigna is seeking to terminate its agreement with Anthem, but Anthem is fighting the dissolution. The insurance giant is looking toward the Trump administration to potentially turn the case around.
To enforce the termination, Cigna is suing Anthem in the Delaware Court of Chancery seeking a declaratory judgment that Cigna has lawfully terminated the contract, according to an announcement by Cigna. Anthem, meanwhile, is seeking a temporary restraining order to enjoin Cigna from terminating its contract.
“Anthem believes there is still sufficient time and a viable path forward potentially to complete the transaction that will save millions of Americans more than $2 billion in annual medical costs and deliver significant value to shareholders,” according to a company statement. “In addition to filing this lawsuit, Anthem is pursuing an expedited appeal of the District Court’s decision and is committed to completing this value-creating merger either through a successful appeal or through settlement with the new leadership at the Department of Justice.”
Part of that new leadership could include Makan Delrahim, a former Anthem lobbyist now serving as deputy White House counsel. He is rumored to be a top contender to lead the DOJ’s antitrust division.
Records also show that Indiana insurance regulators were supportive of the Anthem-Cigna deal while Vice President Pence was governor of Indiana and that Anthem contributed $100,000 to President Trump’s inaugural committee, according to Senate lobbying reports.
“A lot of folks are talking about the possibility that Trump will appoint people at both the FTC and DOJ antitrust devision [who] are Republicans and tend to be more business friendly, which would mean that maybe some of these mergers would be more likely to make it and less likely to be challenged,” he said.
On the other hand, a couple of leadership changes will not likely reverse the country’s historic antitrust enforcement, Mr. Dahlquist said.
“I don’t believe you’re going to see a systemic shift in the antitrust enforcement policy of this country,” he said. “Even one change at the top is not going to [create] upheaval within the ranks at the FTC and DOJ. The government is on a winning streak; I think that’s going to continue in the short term.”
“I don’t expect to see any change in the government’s approach in continuing to challenge anticompetitive health care transactions,” Ms. Feinstein said during at interview at the meeting.
[email protected]
On Twitter @legal_med
rFVII didn’t improve hemorrhagic stroke outcomes in twin trials
HOUSTON – Acute hemostatic treatment with a clotting protein didn’t improve either short- or long-term outcomes in patients with intracerebral hemorrhage (ICH), according to findings from twin studies.
When given to patients who displayed a high-risk imaging marker suggestive of active bleeding, recombinant activated blood coagulation factor VII (rFVII) didn’t significantly reduce 24-hour hemorrhage volume or improve 90-day stroke outcomes, relative to placebo, David Gladstone, MD, said at the International Stroke Conference sponsored by the American Heart Association.
This isn’t the first time rFVII has been investigated as an acute treatment for ICH, said Dr. Gladstone, director of the Sunnybrook Regional Stroke Prevention Clinic and the Rapid Transient Ischemic Attack Clinic, Toronto. In the large phase III FAST trial, rFVII reduced growth of the hematoma but did not improve survival or functional outcome in an unselected population.
Their determination was the genesis of the two studies, SPOTLIGHT (Canada) and STOP-IT (United States), that Dr. Gladstone reported at the meeting.
Both studies stratified patients using the “spot sign,” a relatively new imaging biomarker thought to reflect active bleeding in the ICH hematoma. The hyperintense signal can be easily seen on cerebral angiography.
“It shows up like a flashlight as a bright spot in the margin of the hematoma,” Dr. Gladstone said. “When we see this, we know this patient has a possible active bleed that is likely to expand and get worse. They are at highest risk for ICH expansion and should be the best candidates for hemostatic therapy.”
Spot-negative patients, on the other hand, are at low risk for ICH expansion and would not benefit from hemostatic therapy, he said.
Both SPOTLIGHT and STOP-IT stratified their subjects by the presence of this sign. Spot-positive patients were randomized to placebo or to a single intravenous bolus of 80 mcg/kg rFVII given in the emergency department and within 6.5 hours of stroke onset. Spot-negative patients were enrolled in a prospective observational cohort, which provided data to support the sign’s use as a predictor of outcome.
In order to obtain the most focused patient population, the investigators imposed a number of exclusion criteria – a choice that may have contributed to the lackluster results, Dr. Gladstone noted. Exclusion criteria were brain stem ICH; ICH with secondary cause, such as a tumor or trauma; additional treatments such as plasma or prothrombin; acute coronary ischemia; history of other strokes, angioplasty, or stenting; past thrombotic events; a Glasgow Coma Scale of less than 8; or a modified Rankin Scale (mRS) score more than 2.
These stringent criteria, plus the uncommon nature of ICH events, compared with other cerebrovascular events, made recruitment a struggle, Dr. Gladstone said. After 6 years, the trials together managed to enroll only 69 spot-positive and 72 spot-negative patients. At that point, both studies were stopped because of the low numbers and because they had run out of money.
The studies’ primary efficacy endpoint was 24-hour ICH volume. Secondary outcomes were 24-hour total ICH plus intraventricular hemorrhage volumes, 90-day mRS of 5-6, and comparisons between the spot-negative and spot-positive groups. The primary safety outcome was acute myocardial infarction, ischemic stroke, or pulmonary embolism within 4 days of treatment.
Patients were a mean of about 70 years, although spot-positive patients were older than were spot-negative patients (71 years vs. 61 years). Spot-positive patients were also less likely to have a Glasgow coma score of 15-16 (56% vs. 66%). The National Institutes of Health Stroke Scale score was a mean of 16 in the spot-positive group and 10 in the spot-negative group. Intraventricular hemorrhage was also more common in the spot-positive group (44% vs. 18%).
After researchers adjusted for baseline ICH volume and onset-to-needle time, rFVII exerted no significant effect on either 24-hour ICH volume or 24-hour total volume.
In the treated group, median ICH volume increased from 16 mL at baseline to 22 mL by 24 hours. In the placebo group, it increased from 20 mL at baseline to 29 mL at 24 hours (between-group difference, P = 0.9).
In the treated group, the median total volume (ICH plus intraventricular hemorrhage) increased from 24 mL at baseline to 26 mL at 24 hours. In the placebo group, it increased from 25 mL at baseline to 31 mL at 24 hours later (between-group difference, P = .9).
There was no significant difference in the number of patients who had a volume increase of more than 6 mL or more than 33% (41% vs. 43%, respectively).
In contrast, spot-negative patients had lower baseline and 24-hour total hematoma volumes. In the spot-negative group, total volumes increased from a median of 13 mL at baseline to 14 mL at 24 hours. Significantly fewer spot-negative patients than spot-positive patients experienced hematoma growth of more than 6 mL or 33% (11% vs. 43%, respectively.)
However, the spot sign was a very good predictor of continued bleeding. In all spot-positive patients, median ICH volume expanded 9 mL over 24 hours (from 20 mL at baseline to 29 mL at 24 hours), compared with a median ICH expansion of only 1 mL over 24 hours (from 12 mL to 13 mL) for spot-negative patients.
There were no significant differences in 90-day mRS scores between the treated and placebo groups. One-fifth of each group (20%) had a score of 1-2, and one-fifth died. mRS scores of 3-5 were also similar between the groups.
Despite similar scores, other factors showed that the spot-negative patients did significantly better. Only 6% of this group died. More than a third (38%) had an mRS of 0-1 at 90 days.
Dr. Gladstone was not pleased about the treatment time intervals, which were prolonged, compared with those that have been achieved with antithrombotic therapy in ischemic stroke.
Time from stroke onset to the emergency department was similar in both spot-positive groups taking rFVIIa and spot-positive placebo patients (64 and 66 minutes, respectively). Onset-to-CT time was significantly longer in the rFVIIa patients than in placebo patients (89 vs. 83 minutes, respectively). Door-to-needle time also was longer in the rFVIIa patients than in the placebo patients (104 vs. 87 minutes, respectively), as was onset-to-needle time (195 vs. 161 minutes, respectively).
Only 37% of spot-positive patients receiving rFVIIa were treated in less than 3 hours – significantly less than the 65% that were treated that quickly in the spot-positive placebo group.
rFVII had a positive safety profile, with no significant events related to the study medication. No patient had a heart attack or pulmonary embolism within 4 days. An ischemic stroke developed in one patient in the placebo group. One patient had a possible thrombosis in the middle cerebral artery, but this was asymptomatic.
“What we are left with is that the spot sign predicted final ICH volume, but the magnitude of ICH expansion was small, less than we expected,” Dr. Gladstone said. “The median absolute ICH volume increase overall was only 2.5 mm, which is surprisingly small for this group of patients. And I do believe that treatment was administered too late, after most of the ICH expansion had already happened.”
Nonetheless, “there is much to learn here,” he said. “The biggest issue I think is that treatment was just too little, too late. We need to be catching these patients at a much earlier phase to make a difference, and that is probably the largest reason we didn’t see a difference.”
On the upside, the spot sign “was a statistically significant predictor of final ICH volumes,” Dr. Gladstone said. It’s an easy sign to catch, and it’s obvious on an imaging study that’s routinely acquired for stroke patients.
“We are also beginning to understand that there are many different types of spot signs associated with different kinds of bleeding at different times,” he noted. “We need to understand this variation further, and this should allow us to characterize the patients who are likely to be big bleeders.”
SPOTLIGHT was funded by the Canadian Institutes of Health Research, the Ontario Stroke Network, and the Ontario Ministry of Research, Innovation, and Science. STOP-IT was funded by the National Institute of Neurological Disorders and Stroke.
Dr. Gladstone had no financial disclosures.
[email protected]
On Twitter @alz_gal
HOUSTON – Acute hemostatic treatment with a clotting protein didn’t improve either short- or long-term outcomes in patients with intracerebral hemorrhage (ICH), according to findings from twin studies.
When given to patients who displayed a high-risk imaging marker suggestive of active bleeding, recombinant activated blood coagulation factor VII (rFVII) didn’t significantly reduce 24-hour hemorrhage volume or improve 90-day stroke outcomes, relative to placebo, David Gladstone, MD, said at the International Stroke Conference sponsored by the American Heart Association.
This isn’t the first time rFVII has been investigated as an acute treatment for ICH, said Dr. Gladstone, director of the Sunnybrook Regional Stroke Prevention Clinic and the Rapid Transient Ischemic Attack Clinic, Toronto. In the large phase III FAST trial, rFVII reduced growth of the hematoma but did not improve survival or functional outcome in an unselected population.
Their determination was the genesis of the two studies, SPOTLIGHT (Canada) and STOP-IT (United States), that Dr. Gladstone reported at the meeting.
Both studies stratified patients using the “spot sign,” a relatively new imaging biomarker thought to reflect active bleeding in the ICH hematoma. The hyperintense signal can be easily seen on cerebral angiography.
“It shows up like a flashlight as a bright spot in the margin of the hematoma,” Dr. Gladstone said. “When we see this, we know this patient has a possible active bleed that is likely to expand and get worse. They are at highest risk for ICH expansion and should be the best candidates for hemostatic therapy.”
Spot-negative patients, on the other hand, are at low risk for ICH expansion and would not benefit from hemostatic therapy, he said.
Both SPOTLIGHT and STOP-IT stratified their subjects by the presence of this sign. Spot-positive patients were randomized to placebo or to a single intravenous bolus of 80 mcg/kg rFVII given in the emergency department and within 6.5 hours of stroke onset. Spot-negative patients were enrolled in a prospective observational cohort, which provided data to support the sign’s use as a predictor of outcome.
In order to obtain the most focused patient population, the investigators imposed a number of exclusion criteria – a choice that may have contributed to the lackluster results, Dr. Gladstone noted. Exclusion criteria were brain stem ICH; ICH with secondary cause, such as a tumor or trauma; additional treatments such as plasma or prothrombin; acute coronary ischemia; history of other strokes, angioplasty, or stenting; past thrombotic events; a Glasgow Coma Scale of less than 8; or a modified Rankin Scale (mRS) score more than 2.
These stringent criteria, plus the uncommon nature of ICH events, compared with other cerebrovascular events, made recruitment a struggle, Dr. Gladstone said. After 6 years, the trials together managed to enroll only 69 spot-positive and 72 spot-negative patients. At that point, both studies were stopped because of the low numbers and because they had run out of money.
The studies’ primary efficacy endpoint was 24-hour ICH volume. Secondary outcomes were 24-hour total ICH plus intraventricular hemorrhage volumes, 90-day mRS of 5-6, and comparisons between the spot-negative and spot-positive groups. The primary safety outcome was acute myocardial infarction, ischemic stroke, or pulmonary embolism within 4 days of treatment.
Patients were a mean of about 70 years, although spot-positive patients were older than were spot-negative patients (71 years vs. 61 years). Spot-positive patients were also less likely to have a Glasgow coma score of 15-16 (56% vs. 66%). The National Institutes of Health Stroke Scale score was a mean of 16 in the spot-positive group and 10 in the spot-negative group. Intraventricular hemorrhage was also more common in the spot-positive group (44% vs. 18%).
After researchers adjusted for baseline ICH volume and onset-to-needle time, rFVII exerted no significant effect on either 24-hour ICH volume or 24-hour total volume.
In the treated group, median ICH volume increased from 16 mL at baseline to 22 mL by 24 hours. In the placebo group, it increased from 20 mL at baseline to 29 mL at 24 hours (between-group difference, P = 0.9).
In the treated group, the median total volume (ICH plus intraventricular hemorrhage) increased from 24 mL at baseline to 26 mL at 24 hours. In the placebo group, it increased from 25 mL at baseline to 31 mL at 24 hours later (between-group difference, P = .9).
There was no significant difference in the number of patients who had a volume increase of more than 6 mL or more than 33% (41% vs. 43%, respectively).
In contrast, spot-negative patients had lower baseline and 24-hour total hematoma volumes. In the spot-negative group, total volumes increased from a median of 13 mL at baseline to 14 mL at 24 hours. Significantly fewer spot-negative patients than spot-positive patients experienced hematoma growth of more than 6 mL or 33% (11% vs. 43%, respectively.)
However, the spot sign was a very good predictor of continued bleeding. In all spot-positive patients, median ICH volume expanded 9 mL over 24 hours (from 20 mL at baseline to 29 mL at 24 hours), compared with a median ICH expansion of only 1 mL over 24 hours (from 12 mL to 13 mL) for spot-negative patients.
There were no significant differences in 90-day mRS scores between the treated and placebo groups. One-fifth of each group (20%) had a score of 1-2, and one-fifth died. mRS scores of 3-5 were also similar between the groups.
Despite similar scores, other factors showed that the spot-negative patients did significantly better. Only 6% of this group died. More than a third (38%) had an mRS of 0-1 at 90 days.
Dr. Gladstone was not pleased about the treatment time intervals, which were prolonged, compared with those that have been achieved with antithrombotic therapy in ischemic stroke.
Time from stroke onset to the emergency department was similar in both spot-positive groups taking rFVIIa and spot-positive placebo patients (64 and 66 minutes, respectively). Onset-to-CT time was significantly longer in the rFVIIa patients than in placebo patients (89 vs. 83 minutes, respectively). Door-to-needle time also was longer in the rFVIIa patients than in the placebo patients (104 vs. 87 minutes, respectively), as was onset-to-needle time (195 vs. 161 minutes, respectively).
Only 37% of spot-positive patients receiving rFVIIa were treated in less than 3 hours – significantly less than the 65% that were treated that quickly in the spot-positive placebo group.
rFVII had a positive safety profile, with no significant events related to the study medication. No patient had a heart attack or pulmonary embolism within 4 days. An ischemic stroke developed in one patient in the placebo group. One patient had a possible thrombosis in the middle cerebral artery, but this was asymptomatic.
“What we are left with is that the spot sign predicted final ICH volume, but the magnitude of ICH expansion was small, less than we expected,” Dr. Gladstone said. “The median absolute ICH volume increase overall was only 2.5 mm, which is surprisingly small for this group of patients. And I do believe that treatment was administered too late, after most of the ICH expansion had already happened.”
Nonetheless, “there is much to learn here,” he said. “The biggest issue I think is that treatment was just too little, too late. We need to be catching these patients at a much earlier phase to make a difference, and that is probably the largest reason we didn’t see a difference.”
On the upside, the spot sign “was a statistically significant predictor of final ICH volumes,” Dr. Gladstone said. It’s an easy sign to catch, and it’s obvious on an imaging study that’s routinely acquired for stroke patients.
“We are also beginning to understand that there are many different types of spot signs associated with different kinds of bleeding at different times,” he noted. “We need to understand this variation further, and this should allow us to characterize the patients who are likely to be big bleeders.”
SPOTLIGHT was funded by the Canadian Institutes of Health Research, the Ontario Stroke Network, and the Ontario Ministry of Research, Innovation, and Science. STOP-IT was funded by the National Institute of Neurological Disorders and Stroke.
Dr. Gladstone had no financial disclosures.
[email protected]
On Twitter @alz_gal
HOUSTON – Acute hemostatic treatment with a clotting protein didn’t improve either short- or long-term outcomes in patients with intracerebral hemorrhage (ICH), according to findings from twin studies.
When given to patients who displayed a high-risk imaging marker suggestive of active bleeding, recombinant activated blood coagulation factor VII (rFVII) didn’t significantly reduce 24-hour hemorrhage volume or improve 90-day stroke outcomes, relative to placebo, David Gladstone, MD, said at the International Stroke Conference sponsored by the American Heart Association.
This isn’t the first time rFVII has been investigated as an acute treatment for ICH, said Dr. Gladstone, director of the Sunnybrook Regional Stroke Prevention Clinic and the Rapid Transient Ischemic Attack Clinic, Toronto. In the large phase III FAST trial, rFVII reduced growth of the hematoma but did not improve survival or functional outcome in an unselected population.
Their determination was the genesis of the two studies, SPOTLIGHT (Canada) and STOP-IT (United States), that Dr. Gladstone reported at the meeting.
Both studies stratified patients using the “spot sign,” a relatively new imaging biomarker thought to reflect active bleeding in the ICH hematoma. The hyperintense signal can be easily seen on cerebral angiography.
“It shows up like a flashlight as a bright spot in the margin of the hematoma,” Dr. Gladstone said. “When we see this, we know this patient has a possible active bleed that is likely to expand and get worse. They are at highest risk for ICH expansion and should be the best candidates for hemostatic therapy.”
Spot-negative patients, on the other hand, are at low risk for ICH expansion and would not benefit from hemostatic therapy, he said.
Both SPOTLIGHT and STOP-IT stratified their subjects by the presence of this sign. Spot-positive patients were randomized to placebo or to a single intravenous bolus of 80 mcg/kg rFVII given in the emergency department and within 6.5 hours of stroke onset. Spot-negative patients were enrolled in a prospective observational cohort, which provided data to support the sign’s use as a predictor of outcome.
In order to obtain the most focused patient population, the investigators imposed a number of exclusion criteria – a choice that may have contributed to the lackluster results, Dr. Gladstone noted. Exclusion criteria were brain stem ICH; ICH with secondary cause, such as a tumor or trauma; additional treatments such as plasma or prothrombin; acute coronary ischemia; history of other strokes, angioplasty, or stenting; past thrombotic events; a Glasgow Coma Scale of less than 8; or a modified Rankin Scale (mRS) score more than 2.
These stringent criteria, plus the uncommon nature of ICH events, compared with other cerebrovascular events, made recruitment a struggle, Dr. Gladstone said. After 6 years, the trials together managed to enroll only 69 spot-positive and 72 spot-negative patients. At that point, both studies were stopped because of the low numbers and because they had run out of money.
The studies’ primary efficacy endpoint was 24-hour ICH volume. Secondary outcomes were 24-hour total ICH plus intraventricular hemorrhage volumes, 90-day mRS of 5-6, and comparisons between the spot-negative and spot-positive groups. The primary safety outcome was acute myocardial infarction, ischemic stroke, or pulmonary embolism within 4 days of treatment.
Patients were a mean of about 70 years, although spot-positive patients were older than were spot-negative patients (71 years vs. 61 years). Spot-positive patients were also less likely to have a Glasgow coma score of 15-16 (56% vs. 66%). The National Institutes of Health Stroke Scale score was a mean of 16 in the spot-positive group and 10 in the spot-negative group. Intraventricular hemorrhage was also more common in the spot-positive group (44% vs. 18%).
After researchers adjusted for baseline ICH volume and onset-to-needle time, rFVII exerted no significant effect on either 24-hour ICH volume or 24-hour total volume.
In the treated group, median ICH volume increased from 16 mL at baseline to 22 mL by 24 hours. In the placebo group, it increased from 20 mL at baseline to 29 mL at 24 hours (between-group difference, P = 0.9).
In the treated group, the median total volume (ICH plus intraventricular hemorrhage) increased from 24 mL at baseline to 26 mL at 24 hours. In the placebo group, it increased from 25 mL at baseline to 31 mL at 24 hours later (between-group difference, P = .9).
There was no significant difference in the number of patients who had a volume increase of more than 6 mL or more than 33% (41% vs. 43%, respectively).
In contrast, spot-negative patients had lower baseline and 24-hour total hematoma volumes. In the spot-negative group, total volumes increased from a median of 13 mL at baseline to 14 mL at 24 hours. Significantly fewer spot-negative patients than spot-positive patients experienced hematoma growth of more than 6 mL or 33% (11% vs. 43%, respectively.)
However, the spot sign was a very good predictor of continued bleeding. In all spot-positive patients, median ICH volume expanded 9 mL over 24 hours (from 20 mL at baseline to 29 mL at 24 hours), compared with a median ICH expansion of only 1 mL over 24 hours (from 12 mL to 13 mL) for spot-negative patients.
There were no significant differences in 90-day mRS scores between the treated and placebo groups. One-fifth of each group (20%) had a score of 1-2, and one-fifth died. mRS scores of 3-5 were also similar between the groups.
Despite similar scores, other factors showed that the spot-negative patients did significantly better. Only 6% of this group died. More than a third (38%) had an mRS of 0-1 at 90 days.
Dr. Gladstone was not pleased about the treatment time intervals, which were prolonged, compared with those that have been achieved with antithrombotic therapy in ischemic stroke.
Time from stroke onset to the emergency department was similar in both spot-positive groups taking rFVIIa and spot-positive placebo patients (64 and 66 minutes, respectively). Onset-to-CT time was significantly longer in the rFVIIa patients than in placebo patients (89 vs. 83 minutes, respectively). Door-to-needle time also was longer in the rFVIIa patients than in the placebo patients (104 vs. 87 minutes, respectively), as was onset-to-needle time (195 vs. 161 minutes, respectively).
Only 37% of spot-positive patients receiving rFVIIa were treated in less than 3 hours – significantly less than the 65% that were treated that quickly in the spot-positive placebo group.
rFVII had a positive safety profile, with no significant events related to the study medication. No patient had a heart attack or pulmonary embolism within 4 days. An ischemic stroke developed in one patient in the placebo group. One patient had a possible thrombosis in the middle cerebral artery, but this was asymptomatic.
“What we are left with is that the spot sign predicted final ICH volume, but the magnitude of ICH expansion was small, less than we expected,” Dr. Gladstone said. “The median absolute ICH volume increase overall was only 2.5 mm, which is surprisingly small for this group of patients. And I do believe that treatment was administered too late, after most of the ICH expansion had already happened.”
Nonetheless, “there is much to learn here,” he said. “The biggest issue I think is that treatment was just too little, too late. We need to be catching these patients at a much earlier phase to make a difference, and that is probably the largest reason we didn’t see a difference.”
On the upside, the spot sign “was a statistically significant predictor of final ICH volumes,” Dr. Gladstone said. It’s an easy sign to catch, and it’s obvious on an imaging study that’s routinely acquired for stroke patients.
“We are also beginning to understand that there are many different types of spot signs associated with different kinds of bleeding at different times,” he noted. “We need to understand this variation further, and this should allow us to characterize the patients who are likely to be big bleeders.”
SPOTLIGHT was funded by the Canadian Institutes of Health Research, the Ontario Stroke Network, and the Ontario Ministry of Research, Innovation, and Science. STOP-IT was funded by the National Institute of Neurological Disorders and Stroke.
Dr. Gladstone had no financial disclosures.
[email protected]
On Twitter @alz_gal
Key clinical point:
Major finding: In the treated group, median ICH volume increased from 16 mL at baseline to 22 mL at 24 hours. In the placebo group, it increased from 20 mL to 29 mL (between-group difference, P = .9).
Data source: SPOTLIGHT and STOP-IT enrolled 141 patients.
Disclosures: SPOTLIGHT was funded by the Canadian Institutes of Health Research, the Ontario Stroke Network, and the Ontario Ministry of Research, Innovation, and Science. STOP-IT was funded by the National Institute of Neurological Disorders and Stroke.
Follow-up data support using mesh for umbilical hernia repair
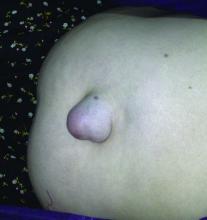
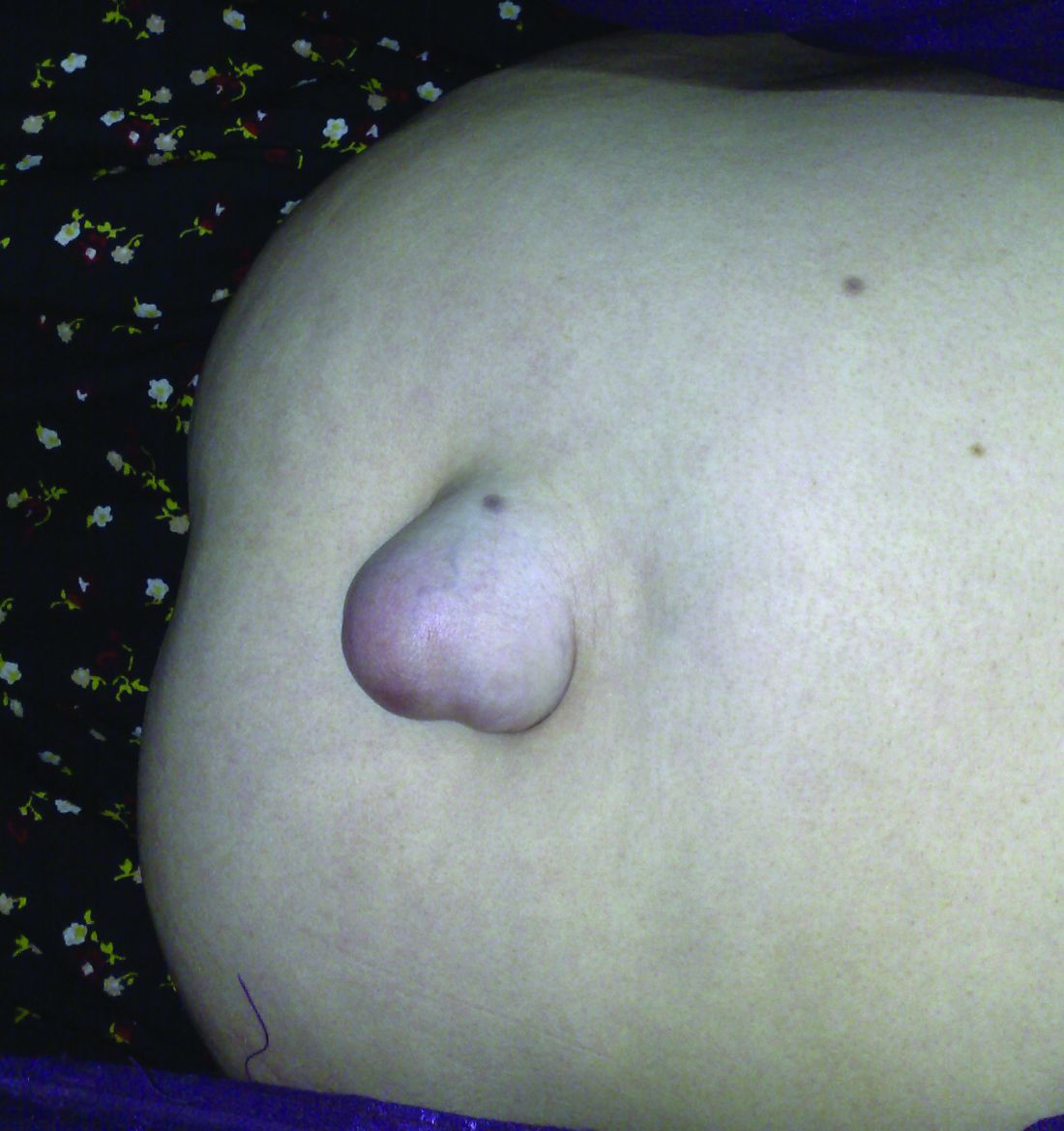
Patients with umbilical hernias and multiple comorbidities should be considered for mesh repair to reduce the risk of recurrence, say the authors of a study of the factors associated with umbilical hernia recurrence after repair.
The retrospective cohort study, published in JAMA Surgery, examined recurrence and mortality outcomes in 332 military veteran patients who underwent primary umbilical hernia repair between 1998 and 2008 and followed until June 2014.
The overall recurrence rate was 6% and a mean recurrence time after index repair of 3.1 years. The recurrence rate was significantly higher among patients who underwent primary suture repair, compared with those who underwent mesh repair (9.8% vs. 2.4%, P = .04). Mesh repair decreased the risk of recurrence more than threefold, compared with primary suture repair (odds ratio, 0.28; 95% confidence interval, 0.08-0.95).
Patients with ascites had a significantly greater risk of recurrence, compared with those without ascites (20% vs. 5.1%, P = .02), as did those with liver disease (35% vs. 13.8%, P = .02), and diabetes (55% vs. 32.7%).
“This information suggests that umbilical hernias should be repaired using mesh, especially if a patient has multiple comorbidities that are significantly associated with recurrence, such as obesity, diabetes, liver disease, and ascites,” wrote Divya A. Shankar, a medical student at Boston University School of Medicine, and her coauthors (JAMA Surg. 2017 Jan 25. doi: 10.1001/jamasurg.2016.5052).
Among these patients, only 1 died within 30 days, but the study captured mortality in this group over 6-16 years after their hernia surgery. Mortality rate in the group was 27% through the follow-up period. However, older individuals, smokers, patients with liver disease and ascites, and those who had to undergo emergency or semi-urgent repair or who required intraoperative bowel resection had significantly increased long-term mortality rates.
“Although there is a trend toward higher mortality rates in patients who underwent emergency repair, it is difficult to interpret whether the deaths were related to the emergency or to underlying medical conditions given that the etiology of the majority of these deaths is unknown,” the authors wrote.
Among the deaths, 43 (48%) were from unknown causes, 18 (20%) were cancer related, 12 (13%) were related to renal disease, and 3 (3.3%) were related to sepsis.
Researchers found that patients with a history of hernias were significantly less likely to have an umbilical hernia recurrence, although a greater percentage of these patients – 61% – received mesh in contrast to the 44% of patients without a history of hernia.
Defect size did not appear to affect the rate of recurrence but the authors noted that defect size was only recorded in about half of the patients in the study.
“Because there was no significant difference between these groups, we are unable to conclude whether the size of defects should play a role in a surgeon’s decision to use mesh,” they wrote.
Sixty-one patients (18%) had at least one complication within 30 days of the repair, with the most common being seroma (9.6%), surgical site infection (6.9%) and hematoma (2.4%). Two patients experienced a mesh infection and three experienced ascites leaks. The rate of complications was slightly, but not significantly, higher in the patients who received mesh repair, compared with the primary suture repair.
“A surprise finding was that patient who underwent emergent or semi-emergent repair had a 2.2 times increased odds of death. Twenty deaths occurred more than 30 days after emergent or semi-urgent repair and 12 (60%) were secondary to unknown causes and 5 (25%) were secondary to liver disease,” the investigators noted.
“Interestingly, 193 (58%) patients who underwent umbilical hernia repair had other hernias that were either repaired before the index repair or developed postoperatively. Therefore, we propose that umbilical hernias may be a type of ‘field defect’ and we support the idea of that abnormal collegan metabolism could play a role in hernia development. ...We speculate that surgeons might be more inclined to use mesh in a patients with a history of other hernias.”
Despite the potential for complications, “elective hernia repair with mesh should be considered in patients with multiple comorbidities given that the use of mesh offers protection from recurrence without major morbidity.”
The study was supported by the VA Healthcare System. No conflicts of interest were declared.
Patients with umbilical hernias and multiple comorbidities should be considered for mesh repair to reduce the risk of recurrence, say the authors of a study of the factors associated with umbilical hernia recurrence after repair.
The retrospective cohort study, published in JAMA Surgery, examined recurrence and mortality outcomes in 332 military veteran patients who underwent primary umbilical hernia repair between 1998 and 2008 and followed until June 2014.
The overall recurrence rate was 6% and a mean recurrence time after index repair of 3.1 years. The recurrence rate was significantly higher among patients who underwent primary suture repair, compared with those who underwent mesh repair (9.8% vs. 2.4%, P = .04). Mesh repair decreased the risk of recurrence more than threefold, compared with primary suture repair (odds ratio, 0.28; 95% confidence interval, 0.08-0.95).
Patients with ascites had a significantly greater risk of recurrence, compared with those without ascites (20% vs. 5.1%, P = .02), as did those with liver disease (35% vs. 13.8%, P = .02), and diabetes (55% vs. 32.7%).
“This information suggests that umbilical hernias should be repaired using mesh, especially if a patient has multiple comorbidities that are significantly associated with recurrence, such as obesity, diabetes, liver disease, and ascites,” wrote Divya A. Shankar, a medical student at Boston University School of Medicine, and her coauthors (JAMA Surg. 2017 Jan 25. doi: 10.1001/jamasurg.2016.5052).
Among these patients, only 1 died within 30 days, but the study captured mortality in this group over 6-16 years after their hernia surgery. Mortality rate in the group was 27% through the follow-up period. However, older individuals, smokers, patients with liver disease and ascites, and those who had to undergo emergency or semi-urgent repair or who required intraoperative bowel resection had significantly increased long-term mortality rates.
“Although there is a trend toward higher mortality rates in patients who underwent emergency repair, it is difficult to interpret whether the deaths were related to the emergency or to underlying medical conditions given that the etiology of the majority of these deaths is unknown,” the authors wrote.
Among the deaths, 43 (48%) were from unknown causes, 18 (20%) were cancer related, 12 (13%) were related to renal disease, and 3 (3.3%) were related to sepsis.
Researchers found that patients with a history of hernias were significantly less likely to have an umbilical hernia recurrence, although a greater percentage of these patients – 61% – received mesh in contrast to the 44% of patients without a history of hernia.
Defect size did not appear to affect the rate of recurrence but the authors noted that defect size was only recorded in about half of the patients in the study.
“Because there was no significant difference between these groups, we are unable to conclude whether the size of defects should play a role in a surgeon’s decision to use mesh,” they wrote.
Sixty-one patients (18%) had at least one complication within 30 days of the repair, with the most common being seroma (9.6%), surgical site infection (6.9%) and hematoma (2.4%). Two patients experienced a mesh infection and three experienced ascites leaks. The rate of complications was slightly, but not significantly, higher in the patients who received mesh repair, compared with the primary suture repair.
“A surprise finding was that patient who underwent emergent or semi-emergent repair had a 2.2 times increased odds of death. Twenty deaths occurred more than 30 days after emergent or semi-urgent repair and 12 (60%) were secondary to unknown causes and 5 (25%) were secondary to liver disease,” the investigators noted.
“Interestingly, 193 (58%) patients who underwent umbilical hernia repair had other hernias that were either repaired before the index repair or developed postoperatively. Therefore, we propose that umbilical hernias may be a type of ‘field defect’ and we support the idea of that abnormal collegan metabolism could play a role in hernia development. ...We speculate that surgeons might be more inclined to use mesh in a patients with a history of other hernias.”
Despite the potential for complications, “elective hernia repair with mesh should be considered in patients with multiple comorbidities given that the use of mesh offers protection from recurrence without major morbidity.”
The study was supported by the VA Healthcare System. No conflicts of interest were declared.
Patients with umbilical hernias and multiple comorbidities should be considered for mesh repair to reduce the risk of recurrence, say the authors of a study of the factors associated with umbilical hernia recurrence after repair.
The retrospective cohort study, published in JAMA Surgery, examined recurrence and mortality outcomes in 332 military veteran patients who underwent primary umbilical hernia repair between 1998 and 2008 and followed until June 2014.
The overall recurrence rate was 6% and a mean recurrence time after index repair of 3.1 years. The recurrence rate was significantly higher among patients who underwent primary suture repair, compared with those who underwent mesh repair (9.8% vs. 2.4%, P = .04). Mesh repair decreased the risk of recurrence more than threefold, compared with primary suture repair (odds ratio, 0.28; 95% confidence interval, 0.08-0.95).
Patients with ascites had a significantly greater risk of recurrence, compared with those without ascites (20% vs. 5.1%, P = .02), as did those with liver disease (35% vs. 13.8%, P = .02), and diabetes (55% vs. 32.7%).
“This information suggests that umbilical hernias should be repaired using mesh, especially if a patient has multiple comorbidities that are significantly associated with recurrence, such as obesity, diabetes, liver disease, and ascites,” wrote Divya A. Shankar, a medical student at Boston University School of Medicine, and her coauthors (JAMA Surg. 2017 Jan 25. doi: 10.1001/jamasurg.2016.5052).
Among these patients, only 1 died within 30 days, but the study captured mortality in this group over 6-16 years after their hernia surgery. Mortality rate in the group was 27% through the follow-up period. However, older individuals, smokers, patients with liver disease and ascites, and those who had to undergo emergency or semi-urgent repair or who required intraoperative bowel resection had significantly increased long-term mortality rates.
“Although there is a trend toward higher mortality rates in patients who underwent emergency repair, it is difficult to interpret whether the deaths were related to the emergency or to underlying medical conditions given that the etiology of the majority of these deaths is unknown,” the authors wrote.
Among the deaths, 43 (48%) were from unknown causes, 18 (20%) were cancer related, 12 (13%) were related to renal disease, and 3 (3.3%) were related to sepsis.
Researchers found that patients with a history of hernias were significantly less likely to have an umbilical hernia recurrence, although a greater percentage of these patients – 61% – received mesh in contrast to the 44% of patients without a history of hernia.
Defect size did not appear to affect the rate of recurrence but the authors noted that defect size was only recorded in about half of the patients in the study.
“Because there was no significant difference between these groups, we are unable to conclude whether the size of defects should play a role in a surgeon’s decision to use mesh,” they wrote.
Sixty-one patients (18%) had at least one complication within 30 days of the repair, with the most common being seroma (9.6%), surgical site infection (6.9%) and hematoma (2.4%). Two patients experienced a mesh infection and three experienced ascites leaks. The rate of complications was slightly, but not significantly, higher in the patients who received mesh repair, compared with the primary suture repair.
“A surprise finding was that patient who underwent emergent or semi-emergent repair had a 2.2 times increased odds of death. Twenty deaths occurred more than 30 days after emergent or semi-urgent repair and 12 (60%) were secondary to unknown causes and 5 (25%) were secondary to liver disease,” the investigators noted.
“Interestingly, 193 (58%) patients who underwent umbilical hernia repair had other hernias that were either repaired before the index repair or developed postoperatively. Therefore, we propose that umbilical hernias may be a type of ‘field defect’ and we support the idea of that abnormal collegan metabolism could play a role in hernia development. ...We speculate that surgeons might be more inclined to use mesh in a patients with a history of other hernias.”
Despite the potential for complications, “elective hernia repair with mesh should be considered in patients with multiple comorbidities given that the use of mesh offers protection from recurrence without major morbidity.”
The study was supported by the VA Healthcare System. No conflicts of interest were declared.
FROM JAMA SURGERY
Older recreational endurance athletes face sky-high AF risk
SNOWMASS, COLO. – , N. A. Mark Estes III, MD, said at the Annual Cardiovascular Conference at Snowmass.
“I see a very large number of former collegiate or professional athletes who come to me in their 40s, 50s, and 60s having recently developed A-fib. These are mainly men who’ve been doing high-intensity endurance exercise,” said Dr. Estes, professor of medicine and director of the New England Cardiac Arrhythmia Center at Tufts University in Boston.
This is an aspect of the athletic heart syndrome that has gone understudied and underappreciated, according to Dr. Estes, who asserted, “The best available evidence suggests that exercise, if excessive, is probably harmful. I know that’s heresy.”
He is coauthor of a forthcoming review on this topic to be published in the Journal of the American College of Cardiology – Electrophysiology. In it, he and his coauthors analyzed more than a half dozen published observational epidemiologic studies and concluded that the collective data show a classic J-shaped curve describes the relationship between physical activity level and risk of developing AF, but only in men. The risk is roughly 25% lower in men who regularly engage in moderate physical activity as defined in American Heart Association/American College of Cardiology guidelines, compared with that of sedentary men. But the AF risk shoots up dramatically in men who focus on intense exercise.
“As you get into the high-intensity/high-endurance end of the spectrum – typically more than 5 hours per week at greater than 80% of peak heart rate – the risk of A-fib increases up to 10-fold,” according to Dr. Estes.
“These are new data. They are important data. I think these data should impact the way we counsel people about exercise, particularly men who like to get into that high-intensity/high-endurance range,” the cardiologist continued.
This J-curve doesn’t apply to women, for reasons unclear. The analysis by Dr. Estes and his colleagues documented that women who engage in moderate physical activity have a lower risk of developing AF than do sedentary women, but unlike in men, the AF risk is lower still in women who favor high-intensity exercise.
“Maybe the explanation is in part endocrinologic differences, maybe in part due to women having smaller left atria and therefore less left atrial wall stress, less fibrosis. We really don’t know, but I think the observation, based on epidemiologic data, is valid,” he said.
Proposed multifactorial mechanisms for the increased incidence of AF in aging endurance athletes hinge in part upon basic science studies. These mechanisms include atrial inflammation and fibrosis, atrial enlargement, increased vagal tone, sympathetic nervous system stimulation, pulmonary vein triggers, genetic predisposition, and use of performance-enhancing substances.
Dr. Estes’ presentation struck a responsive chord with the audience. Numerous cardiologists rose to chime in that they, too, have encountered new-onset AF in middle-aged patients, friends, and medical colleagues who are serious cyclists, marathoners, and devotees of other forms of high-intensity endurance exercise to the tune of 10-20 hours per weekly.
“I know an electrophysiologist in his 60s who probably does 20 hours per week of spin and Cross-Fit classes and who is just now going into A-fib. How should I counsel him about this?” one audience member asked.
“You can’t tell these people to stop exercising,” Dr. Estes replied. “It’s so much a part of their identity. Their endorphin levels go down, and they feel depressed.”
For these patients he stresses what he called “the virtue of moderation.”
“If they have clinically important symptoms, many times we’ll decondition them. Often their symptoms will improve, and, in some instances, the A-fib will actually clear up and we don’t even need to go to any medical therapy,” Dr. Estes said.
His exercise prescription for deconditioning such patients is “basically nothing more than a moderate jog, a 10-minute mile. They should be able to carry on a conversation, with a peak heart rate no more than 60% of their maximum.”
If drug therapy is required, he favors rate control with beta blockers, as these patients generally don’t tolerate antiarrhythmic agents very well.
“Our threshold for AF ablation in these people is quite low because the response rate is high in paroxysmal AF in the absence of underlying structural heart disease,” he added.
Dr. Robert A. Vogel, who has been a consultant to the National Football League for a decade, commented, “I agree that you can exercise too much. These are the super-elite triathletes and so forth. A few of these folks not only get A-fib, but we’ve shown they can get accelerated atherosclerosis due to pervasive endothelial dysfunction caused by excessive athletics.”
“However, nothing here should be construed as saying exercise is bad for you. Athletes, even drug-taking cyclists and football players, actually live longer than similar nonathletes,” said Dr. Vogel, a cardiologist at the University of Colorado, Denver.
Dr. Estes was quick to agree.
“The cardiovascular benefits of exercise resoundingly overwhelm the adverse effects in that small group that experiences adverse effects,” he said.
Dr. Estes reported serving as a consultant to Boston Scientific, Medtronic, and St. Jude Medical.
SNOWMASS, COLO. – , N. A. Mark Estes III, MD, said at the Annual Cardiovascular Conference at Snowmass.
“I see a very large number of former collegiate or professional athletes who come to me in their 40s, 50s, and 60s having recently developed A-fib. These are mainly men who’ve been doing high-intensity endurance exercise,” said Dr. Estes, professor of medicine and director of the New England Cardiac Arrhythmia Center at Tufts University in Boston.
This is an aspect of the athletic heart syndrome that has gone understudied and underappreciated, according to Dr. Estes, who asserted, “The best available evidence suggests that exercise, if excessive, is probably harmful. I know that’s heresy.”
He is coauthor of a forthcoming review on this topic to be published in the Journal of the American College of Cardiology – Electrophysiology. In it, he and his coauthors analyzed more than a half dozen published observational epidemiologic studies and concluded that the collective data show a classic J-shaped curve describes the relationship between physical activity level and risk of developing AF, but only in men. The risk is roughly 25% lower in men who regularly engage in moderate physical activity as defined in American Heart Association/American College of Cardiology guidelines, compared with that of sedentary men. But the AF risk shoots up dramatically in men who focus on intense exercise.
“As you get into the high-intensity/high-endurance end of the spectrum – typically more than 5 hours per week at greater than 80% of peak heart rate – the risk of A-fib increases up to 10-fold,” according to Dr. Estes.
“These are new data. They are important data. I think these data should impact the way we counsel people about exercise, particularly men who like to get into that high-intensity/high-endurance range,” the cardiologist continued.
This J-curve doesn’t apply to women, for reasons unclear. The analysis by Dr. Estes and his colleagues documented that women who engage in moderate physical activity have a lower risk of developing AF than do sedentary women, but unlike in men, the AF risk is lower still in women who favor high-intensity exercise.
“Maybe the explanation is in part endocrinologic differences, maybe in part due to women having smaller left atria and therefore less left atrial wall stress, less fibrosis. We really don’t know, but I think the observation, based on epidemiologic data, is valid,” he said.
Proposed multifactorial mechanisms for the increased incidence of AF in aging endurance athletes hinge in part upon basic science studies. These mechanisms include atrial inflammation and fibrosis, atrial enlargement, increased vagal tone, sympathetic nervous system stimulation, pulmonary vein triggers, genetic predisposition, and use of performance-enhancing substances.
Dr. Estes’ presentation struck a responsive chord with the audience. Numerous cardiologists rose to chime in that they, too, have encountered new-onset AF in middle-aged patients, friends, and medical colleagues who are serious cyclists, marathoners, and devotees of other forms of high-intensity endurance exercise to the tune of 10-20 hours per weekly.
“I know an electrophysiologist in his 60s who probably does 20 hours per week of spin and Cross-Fit classes and who is just now going into A-fib. How should I counsel him about this?” one audience member asked.
“You can’t tell these people to stop exercising,” Dr. Estes replied. “It’s so much a part of their identity. Their endorphin levels go down, and they feel depressed.”
For these patients he stresses what he called “the virtue of moderation.”
“If they have clinically important symptoms, many times we’ll decondition them. Often their symptoms will improve, and, in some instances, the A-fib will actually clear up and we don’t even need to go to any medical therapy,” Dr. Estes said.
His exercise prescription for deconditioning such patients is “basically nothing more than a moderate jog, a 10-minute mile. They should be able to carry on a conversation, with a peak heart rate no more than 60% of their maximum.”
If drug therapy is required, he favors rate control with beta blockers, as these patients generally don’t tolerate antiarrhythmic agents very well.
“Our threshold for AF ablation in these people is quite low because the response rate is high in paroxysmal AF in the absence of underlying structural heart disease,” he added.
Dr. Robert A. Vogel, who has been a consultant to the National Football League for a decade, commented, “I agree that you can exercise too much. These are the super-elite triathletes and so forth. A few of these folks not only get A-fib, but we’ve shown they can get accelerated atherosclerosis due to pervasive endothelial dysfunction caused by excessive athletics.”
“However, nothing here should be construed as saying exercise is bad for you. Athletes, even drug-taking cyclists and football players, actually live longer than similar nonathletes,” said Dr. Vogel, a cardiologist at the University of Colorado, Denver.
Dr. Estes was quick to agree.
“The cardiovascular benefits of exercise resoundingly overwhelm the adverse effects in that small group that experiences adverse effects,” he said.
Dr. Estes reported serving as a consultant to Boston Scientific, Medtronic, and St. Jude Medical.
SNOWMASS, COLO. – , N. A. Mark Estes III, MD, said at the Annual Cardiovascular Conference at Snowmass.
“I see a very large number of former collegiate or professional athletes who come to me in their 40s, 50s, and 60s having recently developed A-fib. These are mainly men who’ve been doing high-intensity endurance exercise,” said Dr. Estes, professor of medicine and director of the New England Cardiac Arrhythmia Center at Tufts University in Boston.
This is an aspect of the athletic heart syndrome that has gone understudied and underappreciated, according to Dr. Estes, who asserted, “The best available evidence suggests that exercise, if excessive, is probably harmful. I know that’s heresy.”
He is coauthor of a forthcoming review on this topic to be published in the Journal of the American College of Cardiology – Electrophysiology. In it, he and his coauthors analyzed more than a half dozen published observational epidemiologic studies and concluded that the collective data show a classic J-shaped curve describes the relationship between physical activity level and risk of developing AF, but only in men. The risk is roughly 25% lower in men who regularly engage in moderate physical activity as defined in American Heart Association/American College of Cardiology guidelines, compared with that of sedentary men. But the AF risk shoots up dramatically in men who focus on intense exercise.
“As you get into the high-intensity/high-endurance end of the spectrum – typically more than 5 hours per week at greater than 80% of peak heart rate – the risk of A-fib increases up to 10-fold,” according to Dr. Estes.
“These are new data. They are important data. I think these data should impact the way we counsel people about exercise, particularly men who like to get into that high-intensity/high-endurance range,” the cardiologist continued.
This J-curve doesn’t apply to women, for reasons unclear. The analysis by Dr. Estes and his colleagues documented that women who engage in moderate physical activity have a lower risk of developing AF than do sedentary women, but unlike in men, the AF risk is lower still in women who favor high-intensity exercise.
“Maybe the explanation is in part endocrinologic differences, maybe in part due to women having smaller left atria and therefore less left atrial wall stress, less fibrosis. We really don’t know, but I think the observation, based on epidemiologic data, is valid,” he said.
Proposed multifactorial mechanisms for the increased incidence of AF in aging endurance athletes hinge in part upon basic science studies. These mechanisms include atrial inflammation and fibrosis, atrial enlargement, increased vagal tone, sympathetic nervous system stimulation, pulmonary vein triggers, genetic predisposition, and use of performance-enhancing substances.
Dr. Estes’ presentation struck a responsive chord with the audience. Numerous cardiologists rose to chime in that they, too, have encountered new-onset AF in middle-aged patients, friends, and medical colleagues who are serious cyclists, marathoners, and devotees of other forms of high-intensity endurance exercise to the tune of 10-20 hours per weekly.
“I know an electrophysiologist in his 60s who probably does 20 hours per week of spin and Cross-Fit classes and who is just now going into A-fib. How should I counsel him about this?” one audience member asked.
“You can’t tell these people to stop exercising,” Dr. Estes replied. “It’s so much a part of their identity. Their endorphin levels go down, and they feel depressed.”
For these patients he stresses what he called “the virtue of moderation.”
“If they have clinically important symptoms, many times we’ll decondition them. Often their symptoms will improve, and, in some instances, the A-fib will actually clear up and we don’t even need to go to any medical therapy,” Dr. Estes said.
His exercise prescription for deconditioning such patients is “basically nothing more than a moderate jog, a 10-minute mile. They should be able to carry on a conversation, with a peak heart rate no more than 60% of their maximum.”
If drug therapy is required, he favors rate control with beta blockers, as these patients generally don’t tolerate antiarrhythmic agents very well.
“Our threshold for AF ablation in these people is quite low because the response rate is high in paroxysmal AF in the absence of underlying structural heart disease,” he added.
Dr. Robert A. Vogel, who has been a consultant to the National Football League for a decade, commented, “I agree that you can exercise too much. These are the super-elite triathletes and so forth. A few of these folks not only get A-fib, but we’ve shown they can get accelerated atherosclerosis due to pervasive endothelial dysfunction caused by excessive athletics.”
“However, nothing here should be construed as saying exercise is bad for you. Athletes, even drug-taking cyclists and football players, actually live longer than similar nonathletes,” said Dr. Vogel, a cardiologist at the University of Colorado, Denver.
Dr. Estes was quick to agree.
“The cardiovascular benefits of exercise resoundingly overwhelm the adverse effects in that small group that experiences adverse effects,” he said.
Dr. Estes reported serving as a consultant to Boston Scientific, Medtronic, and St. Jude Medical.
EXPERT ANALYSIS FROM THE CARDIOVASCULAR CONFERENCE AT SNOWMASS
Updated SSI prevention guidance highlights glucose control, MRSA
The guidelines for controlling surgical site infections have been updated to reflect evidence-based findings of a collaboration between surgeons and infection control experts from the American College of Surgeons, the ACS National Surgical Quality Improvement Program, and the Surgical Infection Society.
Updated strategies to reduce the risk of surgical site infections (SSIs) include perioperative glucose control in all patients and the use of oral antibiotics as an element of colon procedures, according to guidelines published in Journal of the American College of Surgeons (J Am Coll Surg. 2017;224:59-74).
Surgical site infections now account for 20% of all hospital-acquired infections, wrote lead author Kristen A. Ban, MD, a surgical resident at Loyola University Medical Center, Maywood, Ill., and her colleagues.
The most recent guidelines for preventing surgical site infections came from the Centers for Disease Control and Prevention in 1999; “the CDC has been working on an update since 2011, but this has been incredibly slow,” E. Patchen Dellinger, MD, of the University of Washington, Seattle, one of the guidelines’ authors, said in an interview. “A publication should be coming out sometime this year, but in the meantime, it was useful to have something for clinicians to refer to,” he said.
The researchers used PubMed to review specific topics in the SSI literature and address knowledge gaps.
Based on their findings, the new guidelines add recommendations to previous versions that address SSI prevention in the prehospital setting, at the hospital, and after discharge. The level of evidence to support each guideline varies; the researchers strongly recommend certain points, such as perioperative glucose control for all patients, not only those with diabetes; other recommendations such as postoperative showering 12 hours after surgery vs. delayed showering are left to the surgeon’s discretion.
“The changes/new recommendations since the 1999 guideline include the recommendation for the use of oral antibiotics with mechanical bowel prep for colon operations (in combination with intravenous prophylactic antibiotics), the control of perioperative glucose levels in ALL patients (not just diabetics), the maintenance of normothermia in the OR, the use of wound protectors for clean-contaminated cases, the use of antimicrobial sutures, and the use of increased FiO2 levels for intubated patients,” Dr. Dellinger said. These new elements also will be recommended when the updated CDC guidelines are released, and already have been recommended in recent guidelines from the World Health Organization, he added.
Guidelines for prehospital interventions include smoking cessation 4-6 weeks before surgery, preoperative bathing with chlorhexidine, glucose control for diabetes patients, MRSA screening, and bowel preparation (combining mechanical and antibiotic) for all elective colectomies.
Recommended hospital interventions include the following:
• Intraoperative normothermia.
• Use of wound protectors in open abdominal surgery.
• Use of triclosan antibiotic sutures.
• Supplemental oxygen.
• Antibiotic prophylaxis when indicated.
• Glucose control for all patients perioperatively.
• Hair removal only when necessary, avoiding a razor if possible.
• Alcohol-based skin preparation when possible.
• Surgical hand scrub.
• Facility scrub laundering and use of a skull cap if minimal hair is exposed.
• Use of double gloves and changing gloves before incision closure in colorectal cases.
• Use of new instruments for closure in colorectal cases.
• Purse string closure of stoma sites.
• Use of topical antibiotics as part of wound care.
• Using wound vacuum therapy over stapled skin.
Data on interventions after hospital discharge that may reduce SSI incidence are limited, the researchers said. No specific wound care protocols or surveillance methods have been identified. However, “promising new methods of surveillance are being explored, many of which use smartphone technology to help patients send their surgeon daily photos or updates,” they noted.
“Strategies to decrease SSI are multimodal and occur across a range of settings under the supervision of numerous providers,” the researchers wrote. “Ensuring high compliance with these risk-reduction strategies is crucial to the success of SSI reduction efforts,” they added.
However, changes to surgical practice don’t happen overnight, Dr. Dellinger said. “If all of these are actually adapted it should decrease SSI rates in all areas,” he noted. “Oral antibiotics for colorectal cases and glucose control for all patients will probably make the biggest benefit if actually adopted,” he said.
“We could use some better studies on the precise timing of parenteral prophylactic antibiotics,” said Dr. Dellinger. “One such study has been submitted from Switzerland and should be published sometime this year. Hard evidence on the best timing is missing although observational data allows some of us to come to conclusions on that,” he said. “Additional studies on perioperative oxygenation where fluid management and temperature management are better controlled would be helpful, and more and better studies are need for antimicrobial sutures,” he added.
The authors had nothing to disclose relevant to the scope of the guidelines. Outside the scope of this work, Dr. Dellinger disclosed serving on the advisory boards for 3M, Melinta, and Theravance, as well as receiving a grant from Motif for a clinical trial of iclaprim vs. vancomycin for the treatment of skin and soft tissue infections.
The guidelines for controlling surgical site infections have been updated to reflect evidence-based findings of a collaboration between surgeons and infection control experts from the American College of Surgeons, the ACS National Surgical Quality Improvement Program, and the Surgical Infection Society.
Updated strategies to reduce the risk of surgical site infections (SSIs) include perioperative glucose control in all patients and the use of oral antibiotics as an element of colon procedures, according to guidelines published in Journal of the American College of Surgeons (J Am Coll Surg. 2017;224:59-74).
Surgical site infections now account for 20% of all hospital-acquired infections, wrote lead author Kristen A. Ban, MD, a surgical resident at Loyola University Medical Center, Maywood, Ill., and her colleagues.
The most recent guidelines for preventing surgical site infections came from the Centers for Disease Control and Prevention in 1999; “the CDC has been working on an update since 2011, but this has been incredibly slow,” E. Patchen Dellinger, MD, of the University of Washington, Seattle, one of the guidelines’ authors, said in an interview. “A publication should be coming out sometime this year, but in the meantime, it was useful to have something for clinicians to refer to,” he said.
The researchers used PubMed to review specific topics in the SSI literature and address knowledge gaps.
Based on their findings, the new guidelines add recommendations to previous versions that address SSI prevention in the prehospital setting, at the hospital, and after discharge. The level of evidence to support each guideline varies; the researchers strongly recommend certain points, such as perioperative glucose control for all patients, not only those with diabetes; other recommendations such as postoperative showering 12 hours after surgery vs. delayed showering are left to the surgeon’s discretion.
“The changes/new recommendations since the 1999 guideline include the recommendation for the use of oral antibiotics with mechanical bowel prep for colon operations (in combination with intravenous prophylactic antibiotics), the control of perioperative glucose levels in ALL patients (not just diabetics), the maintenance of normothermia in the OR, the use of wound protectors for clean-contaminated cases, the use of antimicrobial sutures, and the use of increased FiO2 levels for intubated patients,” Dr. Dellinger said. These new elements also will be recommended when the updated CDC guidelines are released, and already have been recommended in recent guidelines from the World Health Organization, he added.
Guidelines for prehospital interventions include smoking cessation 4-6 weeks before surgery, preoperative bathing with chlorhexidine, glucose control for diabetes patients, MRSA screening, and bowel preparation (combining mechanical and antibiotic) for all elective colectomies.
Recommended hospital interventions include the following:
• Intraoperative normothermia.
• Use of wound protectors in open abdominal surgery.
• Use of triclosan antibiotic sutures.
• Supplemental oxygen.
• Antibiotic prophylaxis when indicated.
• Glucose control for all patients perioperatively.
• Hair removal only when necessary, avoiding a razor if possible.
• Alcohol-based skin preparation when possible.
• Surgical hand scrub.
• Facility scrub laundering and use of a skull cap if minimal hair is exposed.
• Use of double gloves and changing gloves before incision closure in colorectal cases.
• Use of new instruments for closure in colorectal cases.
• Purse string closure of stoma sites.
• Use of topical antibiotics as part of wound care.
• Using wound vacuum therapy over stapled skin.
Data on interventions after hospital discharge that may reduce SSI incidence are limited, the researchers said. No specific wound care protocols or surveillance methods have been identified. However, “promising new methods of surveillance are being explored, many of which use smartphone technology to help patients send their surgeon daily photos or updates,” they noted.
“Strategies to decrease SSI are multimodal and occur across a range of settings under the supervision of numerous providers,” the researchers wrote. “Ensuring high compliance with these risk-reduction strategies is crucial to the success of SSI reduction efforts,” they added.
However, changes to surgical practice don’t happen overnight, Dr. Dellinger said. “If all of these are actually adapted it should decrease SSI rates in all areas,” he noted. “Oral antibiotics for colorectal cases and glucose control for all patients will probably make the biggest benefit if actually adopted,” he said.
“We could use some better studies on the precise timing of parenteral prophylactic antibiotics,” said Dr. Dellinger. “One such study has been submitted from Switzerland and should be published sometime this year. Hard evidence on the best timing is missing although observational data allows some of us to come to conclusions on that,” he said. “Additional studies on perioperative oxygenation where fluid management and temperature management are better controlled would be helpful, and more and better studies are need for antimicrobial sutures,” he added.
The authors had nothing to disclose relevant to the scope of the guidelines. Outside the scope of this work, Dr. Dellinger disclosed serving on the advisory boards for 3M, Melinta, and Theravance, as well as receiving a grant from Motif for a clinical trial of iclaprim vs. vancomycin for the treatment of skin and soft tissue infections.
The guidelines for controlling surgical site infections have been updated to reflect evidence-based findings of a collaboration between surgeons and infection control experts from the American College of Surgeons, the ACS National Surgical Quality Improvement Program, and the Surgical Infection Society.
Updated strategies to reduce the risk of surgical site infections (SSIs) include perioperative glucose control in all patients and the use of oral antibiotics as an element of colon procedures, according to guidelines published in Journal of the American College of Surgeons (J Am Coll Surg. 2017;224:59-74).
Surgical site infections now account for 20% of all hospital-acquired infections, wrote lead author Kristen A. Ban, MD, a surgical resident at Loyola University Medical Center, Maywood, Ill., and her colleagues.
The most recent guidelines for preventing surgical site infections came from the Centers for Disease Control and Prevention in 1999; “the CDC has been working on an update since 2011, but this has been incredibly slow,” E. Patchen Dellinger, MD, of the University of Washington, Seattle, one of the guidelines’ authors, said in an interview. “A publication should be coming out sometime this year, but in the meantime, it was useful to have something for clinicians to refer to,” he said.
The researchers used PubMed to review specific topics in the SSI literature and address knowledge gaps.
Based on their findings, the new guidelines add recommendations to previous versions that address SSI prevention in the prehospital setting, at the hospital, and after discharge. The level of evidence to support each guideline varies; the researchers strongly recommend certain points, such as perioperative glucose control for all patients, not only those with diabetes; other recommendations such as postoperative showering 12 hours after surgery vs. delayed showering are left to the surgeon’s discretion.
“The changes/new recommendations since the 1999 guideline include the recommendation for the use of oral antibiotics with mechanical bowel prep for colon operations (in combination with intravenous prophylactic antibiotics), the control of perioperative glucose levels in ALL patients (not just diabetics), the maintenance of normothermia in the OR, the use of wound protectors for clean-contaminated cases, the use of antimicrobial sutures, and the use of increased FiO2 levels for intubated patients,” Dr. Dellinger said. These new elements also will be recommended when the updated CDC guidelines are released, and already have been recommended in recent guidelines from the World Health Organization, he added.
Guidelines for prehospital interventions include smoking cessation 4-6 weeks before surgery, preoperative bathing with chlorhexidine, glucose control for diabetes patients, MRSA screening, and bowel preparation (combining mechanical and antibiotic) for all elective colectomies.
Recommended hospital interventions include the following:
• Intraoperative normothermia.
• Use of wound protectors in open abdominal surgery.
• Use of triclosan antibiotic sutures.
• Supplemental oxygen.
• Antibiotic prophylaxis when indicated.
• Glucose control for all patients perioperatively.
• Hair removal only when necessary, avoiding a razor if possible.
• Alcohol-based skin preparation when possible.
• Surgical hand scrub.
• Facility scrub laundering and use of a skull cap if minimal hair is exposed.
• Use of double gloves and changing gloves before incision closure in colorectal cases.
• Use of new instruments for closure in colorectal cases.
• Purse string closure of stoma sites.
• Use of topical antibiotics as part of wound care.
• Using wound vacuum therapy over stapled skin.
Data on interventions after hospital discharge that may reduce SSI incidence are limited, the researchers said. No specific wound care protocols or surveillance methods have been identified. However, “promising new methods of surveillance are being explored, many of which use smartphone technology to help patients send their surgeon daily photos or updates,” they noted.
“Strategies to decrease SSI are multimodal and occur across a range of settings under the supervision of numerous providers,” the researchers wrote. “Ensuring high compliance with these risk-reduction strategies is crucial to the success of SSI reduction efforts,” they added.
However, changes to surgical practice don’t happen overnight, Dr. Dellinger said. “If all of these are actually adapted it should decrease SSI rates in all areas,” he noted. “Oral antibiotics for colorectal cases and glucose control for all patients will probably make the biggest benefit if actually adopted,” he said.
“We could use some better studies on the precise timing of parenteral prophylactic antibiotics,” said Dr. Dellinger. “One such study has been submitted from Switzerland and should be published sometime this year. Hard evidence on the best timing is missing although observational data allows some of us to come to conclusions on that,” he said. “Additional studies on perioperative oxygenation where fluid management and temperature management are better controlled would be helpful, and more and better studies are need for antimicrobial sutures,” he added.
The authors had nothing to disclose relevant to the scope of the guidelines. Outside the scope of this work, Dr. Dellinger disclosed serving on the advisory boards for 3M, Melinta, and Theravance, as well as receiving a grant from Motif for a clinical trial of iclaprim vs. vancomycin for the treatment of skin and soft tissue infections.
FROM THE JOURNAL OF THE AMERICAN COLLEGE OF SURGEONS
Prediction: LVADs will rule end-stage heart failure
SNOWMASS, COLO. – Multifaceted progress in mechanical circulatory support as long-term therapy in end-stage heart failure is happening at a brisk pace, Y. Joseph C. Woo, MD, reported at the Annual Cardiovascular Conference at Snowmass.
declared Dr. Woo, professor and chair of the department of cardiothoracic surgery at Stanford (Calif.) University.
That’s quite a prediction, especially considering the source: Stanford is where the late Dr. Norman Shumway – widely considered “the father of heart transplantation” – performed the first adult heart transplant in the United States in 1968.
Dr. Woo was coauthor of an American Heart Association policy statement on the future of cardiovascular disease in the United States, which forecast a 25% increase in heart failure between 2010 and 2030 (Circulation. 2011 Mar 1;123[8]:933-44). There is simply no way that heart transplantation can begin to meet the projected growing need for effective therapy in patients with end-stage disease.
Here’s what Dr. Woo sees as the future of MCS:
Minimally invasive implantation
At Stanford, LVAD implantations are now routinely done off-pump on a beating heart.
“We clamp only when there is a sound reason, like the presence of left ventricular thrombus, where you run the risk of embolization without the cross clamp,” the surgeon said.
Concomitant valvular surgery
At Stanford and other centers of excellence, surgeons perform additional procedures as warranted while they implant an LVAD, including atrial fibrillation ablation, revascularization of the right heart coronaries, patent foramen ovale closure, and repair of the tricuspid, pulmonic, or aortic valves.
Enhanced right ventricular management
Survival is greatly impaired if a patient with an LVAD later requires the addition of a right ventricular assist device. This realization has led to the development of multiple preoperative risk scoring systems by the Stanford group (Ann Thorac Surg. 2013 Sep;96[3]:857-63) and others, including investigators at the Deutsche Herzzentrum Berlin, the world’s busiest heart transplant center. The purpose is to identify upfront those patients who are likely to later develop right heart failure so they can receive biventricular MCS from the start.
Adjunctive biologic therapies
Intramyocardial injection of 25 million allogeneic mesenchymal precursor cells during LVAD implantation appeared to be safe and showed a promising efficacy signal in a 30-patient, multicenter, double-blind, placebo-controlled, National Institutes of Health–sponsored proof of concept study in which Dr. Woo was a coinvestigator (Circulation. 2014 Jun 3;129[22]:2287-96).
The goal of this research effort is to provide a cell therapy assist to the LVAD as a bridge to recovery of left ventricular function such that the device might eventually no longer be needed, he explained.
These cells are immune privileged. They can be transplanted into recipients without need for immunosuppressive therapy or HLA matching, basically as an off the shelf product. Rather than transforming into cardiomyocytes, it appears that the mechanism by which the donor cells enhance cardiac performance in heart failure is via secretion of a shower of growth and angiogenic factors.
Based upon the encouraging results of the initial study, a 90-patient, phase II, double-blind clinical trial is underway. In order to better evaluate efficacy, this time the patients will receive 150 million mesenchymal precursor cells rather than 25 million.
New technologies
The developmental pipeline is chock full of MCS devices. The trend is to go smaller and simpler. HeartWare is developing a miniaturized version of its approved continuous flow centrifugal force LVAD. The ReliantHeart aVAD, an intraventricular device less than 2.5 cm in diameter, is approved in Europe and under study in the U.S. The Thoratec HeartMate III is a smaller version of the HeartMate II, which is FDA-approved as destination therapy. And the Circulite Synergy micropump, designed to provide partial circulatory support to patients who don’t require a full-force LVAD, is the size of a AA battery.
Dr. Woo reported having no financial conflicts.
[email protected]
SNOWMASS, COLO. – Multifaceted progress in mechanical circulatory support as long-term therapy in end-stage heart failure is happening at a brisk pace, Y. Joseph C. Woo, MD, reported at the Annual Cardiovascular Conference at Snowmass.
declared Dr. Woo, professor and chair of the department of cardiothoracic surgery at Stanford (Calif.) University.
That’s quite a prediction, especially considering the source: Stanford is where the late Dr. Norman Shumway – widely considered “the father of heart transplantation” – performed the first adult heart transplant in the United States in 1968.
Dr. Woo was coauthor of an American Heart Association policy statement on the future of cardiovascular disease in the United States, which forecast a 25% increase in heart failure between 2010 and 2030 (Circulation. 2011 Mar 1;123[8]:933-44). There is simply no way that heart transplantation can begin to meet the projected growing need for effective therapy in patients with end-stage disease.
Here’s what Dr. Woo sees as the future of MCS:
Minimally invasive implantation
At Stanford, LVAD implantations are now routinely done off-pump on a beating heart.
“We clamp only when there is a sound reason, like the presence of left ventricular thrombus, where you run the risk of embolization without the cross clamp,” the surgeon said.
Concomitant valvular surgery
At Stanford and other centers of excellence, surgeons perform additional procedures as warranted while they implant an LVAD, including atrial fibrillation ablation, revascularization of the right heart coronaries, patent foramen ovale closure, and repair of the tricuspid, pulmonic, or aortic valves.
Enhanced right ventricular management
Survival is greatly impaired if a patient with an LVAD later requires the addition of a right ventricular assist device. This realization has led to the development of multiple preoperative risk scoring systems by the Stanford group (Ann Thorac Surg. 2013 Sep;96[3]:857-63) and others, including investigators at the Deutsche Herzzentrum Berlin, the world’s busiest heart transplant center. The purpose is to identify upfront those patients who are likely to later develop right heart failure so they can receive biventricular MCS from the start.
Adjunctive biologic therapies
Intramyocardial injection of 25 million allogeneic mesenchymal precursor cells during LVAD implantation appeared to be safe and showed a promising efficacy signal in a 30-patient, multicenter, double-blind, placebo-controlled, National Institutes of Health–sponsored proof of concept study in which Dr. Woo was a coinvestigator (Circulation. 2014 Jun 3;129[22]:2287-96).
The goal of this research effort is to provide a cell therapy assist to the LVAD as a bridge to recovery of left ventricular function such that the device might eventually no longer be needed, he explained.
These cells are immune privileged. They can be transplanted into recipients without need for immunosuppressive therapy or HLA matching, basically as an off the shelf product. Rather than transforming into cardiomyocytes, it appears that the mechanism by which the donor cells enhance cardiac performance in heart failure is via secretion of a shower of growth and angiogenic factors.
Based upon the encouraging results of the initial study, a 90-patient, phase II, double-blind clinical trial is underway. In order to better evaluate efficacy, this time the patients will receive 150 million mesenchymal precursor cells rather than 25 million.
New technologies
The developmental pipeline is chock full of MCS devices. The trend is to go smaller and simpler. HeartWare is developing a miniaturized version of its approved continuous flow centrifugal force LVAD. The ReliantHeart aVAD, an intraventricular device less than 2.5 cm in diameter, is approved in Europe and under study in the U.S. The Thoratec HeartMate III is a smaller version of the HeartMate II, which is FDA-approved as destination therapy. And the Circulite Synergy micropump, designed to provide partial circulatory support to patients who don’t require a full-force LVAD, is the size of a AA battery.
Dr. Woo reported having no financial conflicts.
[email protected]
SNOWMASS, COLO. – Multifaceted progress in mechanical circulatory support as long-term therapy in end-stage heart failure is happening at a brisk pace, Y. Joseph C. Woo, MD, reported at the Annual Cardiovascular Conference at Snowmass.
declared Dr. Woo, professor and chair of the department of cardiothoracic surgery at Stanford (Calif.) University.
That’s quite a prediction, especially considering the source: Stanford is where the late Dr. Norman Shumway – widely considered “the father of heart transplantation” – performed the first adult heart transplant in the United States in 1968.
Dr. Woo was coauthor of an American Heart Association policy statement on the future of cardiovascular disease in the United States, which forecast a 25% increase in heart failure between 2010 and 2030 (Circulation. 2011 Mar 1;123[8]:933-44). There is simply no way that heart transplantation can begin to meet the projected growing need for effective therapy in patients with end-stage disease.
Here’s what Dr. Woo sees as the future of MCS:
Minimally invasive implantation
At Stanford, LVAD implantations are now routinely done off-pump on a beating heart.
“We clamp only when there is a sound reason, like the presence of left ventricular thrombus, where you run the risk of embolization without the cross clamp,” the surgeon said.
Concomitant valvular surgery
At Stanford and other centers of excellence, surgeons perform additional procedures as warranted while they implant an LVAD, including atrial fibrillation ablation, revascularization of the right heart coronaries, patent foramen ovale closure, and repair of the tricuspid, pulmonic, or aortic valves.
Enhanced right ventricular management
Survival is greatly impaired if a patient with an LVAD later requires the addition of a right ventricular assist device. This realization has led to the development of multiple preoperative risk scoring systems by the Stanford group (Ann Thorac Surg. 2013 Sep;96[3]:857-63) and others, including investigators at the Deutsche Herzzentrum Berlin, the world’s busiest heart transplant center. The purpose is to identify upfront those patients who are likely to later develop right heart failure so they can receive biventricular MCS from the start.
Adjunctive biologic therapies
Intramyocardial injection of 25 million allogeneic mesenchymal precursor cells during LVAD implantation appeared to be safe and showed a promising efficacy signal in a 30-patient, multicenter, double-blind, placebo-controlled, National Institutes of Health–sponsored proof of concept study in which Dr. Woo was a coinvestigator (Circulation. 2014 Jun 3;129[22]:2287-96).
The goal of this research effort is to provide a cell therapy assist to the LVAD as a bridge to recovery of left ventricular function such that the device might eventually no longer be needed, he explained.
These cells are immune privileged. They can be transplanted into recipients without need for immunosuppressive therapy or HLA matching, basically as an off the shelf product. Rather than transforming into cardiomyocytes, it appears that the mechanism by which the donor cells enhance cardiac performance in heart failure is via secretion of a shower of growth and angiogenic factors.
Based upon the encouraging results of the initial study, a 90-patient, phase II, double-blind clinical trial is underway. In order to better evaluate efficacy, this time the patients will receive 150 million mesenchymal precursor cells rather than 25 million.
New technologies
The developmental pipeline is chock full of MCS devices. The trend is to go smaller and simpler. HeartWare is developing a miniaturized version of its approved continuous flow centrifugal force LVAD. The ReliantHeart aVAD, an intraventricular device less than 2.5 cm in diameter, is approved in Europe and under study in the U.S. The Thoratec HeartMate III is a smaller version of the HeartMate II, which is FDA-approved as destination therapy. And the Circulite Synergy micropump, designed to provide partial circulatory support to patients who don’t require a full-force LVAD, is the size of a AA battery.
Dr. Woo reported having no financial conflicts.
[email protected]
EXPERT ANALYSIS FROM THE CARDIOVASCULAR CONFERENCE AT SNOWMASS
Risk considerations for suicidal physicians
EXPERT ANALYSIS AT THE NPA PSYCHOPHARMACOLOGY UPDATE
LAS VEGAS – Michael F. Myers, MD, found a common thread in interviews with loved ones, friends, and colleagues of physicians who have taken their own lives: About 10%-15% of the decedents never sought help beforehand.
“They’ve gone from illness to death without any care,” Dr. Myers, a psychiatrist, said at the annual psychopharmacology update held by the Nevada Psychiatric Association.
In a new book based on the interviews, “Why Physicians Die by Suicide: Lessons Learned From Their Families and Others Who Cared” (Amazon, 2017), Dr. Myers combined stories from his own clinical practice and qualitative interviews with about 75 men and women to explore reasons why physicians might choose to take their own lives. “Our nonpsychiatric medical colleagues are really anxious to have information from us, because we’re living in an age of burnout; roughly 50% of U.S. physicians suffer from burnout,” he said. In addition to perspectives from bereaved loved ones and former medical colleagues, the book includes insights from others who are affected when doctors die by suicide: their medical training directors, employers, medical students, treating psychiatrists, and patients.
According to the American Foundation for Suicide Prevention, 300-400 physicians take their own lives every year, the equivalent of two to three medical school classes. “That’s a doctor a day we lose to suicide,” said Dr. Myers, a professor of clinical psychiatry at State University of New York, Brooklyn, who specializes in physician health. Compared with the general population, the suicide rate ratio is 2.27 among female physicians and 1.41 among male physicians (Am J Psychiatry. 2004;161[12]:2295-2302), and an estimated 85%-90% of those who carry out a suicide have a psychiatric illness such as major depressive disorder, bipolar disorder, alcohol use and substance use disorder, and borderline personality disorder. Other triggers common to physicians, Dr. Myers said, include other kinds of personality disorders, burnout, untreated anxiety disorders, substance/medication-induced depressive disorder (especially in clinicians who have been self-medicating), and posttraumatic stress disorder.
Additional risk considerations to keep in mind for physician patients include a family history of mood disorders, a sense of professional isolation, coping with lawsuits and/or medical license investigations, previous history of a depressive episode, and a previous suicide attempt. “Sometimes, it’s hard to get this information from a new physician who’s sitting opposite you,” Dr. Myers noted. “We mustn’t forget that there’s a lot of shame, embarrassment, and guilt that’s attached to previous suicide attempts.”
Suicide risk also is elevated for physicians with treatment-refractory psychiatric illness. “It troubles me when a physician is being treated by a generalist, the patient is not doing well, and he or she is not being referred for a second opinion or has never been referred to a psychopharmacologist,” he said. “It’s important that be done, because you know how difficult many of your patients can be. It’s important to have the expertise of a psychopharmacologist. I believe that physician patients will welcome that [second opinion], even if they have to travel 200 miles for it.”
The list of risk considerations for suicidal physicians also includes undiagnosed and untreated bipolar I or II disorder, rapid cycling bipolar disorder, and mixed affective states. “These are important things that can make our patients ill very quickly,” he said. Impulsivity is another consideration, as are severe sleep deprivation, circadian rhythm disturbances, and acute suicidal affective disturbance, which has emerged as a condition to consider in future revisions of DSM-5. “What you see in this condition is an individual becoming suicidal within minutes or hours,” Dr. Myers explained. “It’s usually an agitated state with insomnia and overvalued ideas or delusions that they are completely untreatable and hopeless. Physicians are no different than anyone else in that kind of state.” He emphasized that the stigma attached to mental illness in physicians is pernicious, because untreated mental illness is a key driver of suicide. After one of Dr. Myers’s patients took his own life, his son told Dr. Myers, “My father just hated being a patient. He felt so ashamed. I tried hard, too, but my support wasn’t enough.”
Inadequate treatment can occur for physician patients because of transference and countertransference dynamics “that muddle the treatment dyad,” Dr. Myers added. “We must be mindful of the many issues that are going on when we treat our own.”
In his 2005 book “Why People Die By Suicide,” psychologist Thomas Joiner, PhD, described three key reasons why people choose to take their own lives. The first is “perceived burdensomeness,” or a sense that one is a burden on others. “When I see it in my physician patients, it’s when they have a sense of being a burden on their family and feel they are no longer serving a purpose,” Dr. Myers said. The second reason is “failed belongingness,” or a sense that one does not belong to a valued social group. “This resonates with me,” Dr. Myers said. “Sometimes in therapy sessions, my physician patients will say ‘Don’t call me Dr. Smith anymore; I’m Mr. Smith.’ They’ve removed themselves from the field because they don’t feel like they belong anymore. That’s the unworthiness that physicians can feel.”
The third reason is “learned fearlessness,” or the acquired capability to enact self-injury. Dr. Myers likened it to “the kind of exposure to pain and fear that people also might learn through such experiences as mountain climbing, performing surgery, fighting in wars, or being afflicted with anorexia.”
If you suspect that a physician patient is engaged in suicidal thinking and planning, Dr. Myers advises framing your mental health assessment in the context of trust and mutual respect. “Please don’t be seduced by somebody who’s squeaky clean in the area of suicidality,” he said. “That individual may just not be sharing with you yet. You’re going to have to be firm and parental at times. There’s a lot of terror and shame that can lurk behind those symptomatic behaviors. That’s where you’ll use your expertise. I have found that there are many physicians out there who welcome you to go in that ‘dark place’ with them. For them to be able to share those scary thoughts with someone can enhance the therapeutic alliance.” The inquiry should include questions about potential means and methods, including access to firearms, stockpiled and/or self-prescribed medications, and medications ordered online or stolen/diverted from the workplace. Timely and careful documentation are essential, he said.
The plan for treating suicidal physicians should include obtaining old records and speaking with former treating professionals. “If you get pushback from the patient, say, ‘This is about me wanting to be thorough in my assessment and treatment plan with you,’ ” Dr. Myers said. “There is no substitute for a detailed mental status evaluation, collateral information, clinical intuition, experience, and consultation.” Hospitalizing the physician patient should be judicious and in consultation with others. “If you’re not sure, get a second opinion, because it can be life-saving,” he said, “but if done inappropriately, you can turn them off psychiatry for the rest of their lives. Make sure you’re not just panicking and worrying about some sort of medical-legal risk.”
In cases of split treatment, ensure regular contact with the psychotherapist and document all communication and any changes in status, medication, or psychotherapy modality change.
Dr. Myers cited many ways that psychiatrists can educate their colleagues about burnout, depression, and the risk of suicide. These include offering to give grand rounds or a lecture on the topic, serving on your local CME planning committee, joining your institute’s physician wellness team, serving on your state’s physician health program, and offering to facilitate a group for physicians after a physician colleague has died by suicide. “Postvention is prevention for the next generation,” Dr. Myers said, quoting Edwin S. Shneidman, PhD, founder of the American Association of Suicidology. “By taking care of ourselves and accepting the painful reality of physician suicide, we reach out to those left behind and make a difference. You become a change agent – someone who is part of the movement to stop doctors from killing themselves.”
Dr. Myers disclosed that he has received funding from the Medical Education Speakers Network.
EXPERT ANALYSIS AT THE NPA PSYCHOPHARMACOLOGY UPDATE
LAS VEGAS – Michael F. Myers, MD, found a common thread in interviews with loved ones, friends, and colleagues of physicians who have taken their own lives: About 10%-15% of the decedents never sought help beforehand.
“They’ve gone from illness to death without any care,” Dr. Myers, a psychiatrist, said at the annual psychopharmacology update held by the Nevada Psychiatric Association.
In a new book based on the interviews, “Why Physicians Die by Suicide: Lessons Learned From Their Families and Others Who Cared” (Amazon, 2017), Dr. Myers combined stories from his own clinical practice and qualitative interviews with about 75 men and women to explore reasons why physicians might choose to take their own lives. “Our nonpsychiatric medical colleagues are really anxious to have information from us, because we’re living in an age of burnout; roughly 50% of U.S. physicians suffer from burnout,” he said. In addition to perspectives from bereaved loved ones and former medical colleagues, the book includes insights from others who are affected when doctors die by suicide: their medical training directors, employers, medical students, treating psychiatrists, and patients.
According to the American Foundation for Suicide Prevention, 300-400 physicians take their own lives every year, the equivalent of two to three medical school classes. “That’s a doctor a day we lose to suicide,” said Dr. Myers, a professor of clinical psychiatry at State University of New York, Brooklyn, who specializes in physician health. Compared with the general population, the suicide rate ratio is 2.27 among female physicians and 1.41 among male physicians (Am J Psychiatry. 2004;161[12]:2295-2302), and an estimated 85%-90% of those who carry out a suicide have a psychiatric illness such as major depressive disorder, bipolar disorder, alcohol use and substance use disorder, and borderline personality disorder. Other triggers common to physicians, Dr. Myers said, include other kinds of personality disorders, burnout, untreated anxiety disorders, substance/medication-induced depressive disorder (especially in clinicians who have been self-medicating), and posttraumatic stress disorder.
Additional risk considerations to keep in mind for physician patients include a family history of mood disorders, a sense of professional isolation, coping with lawsuits and/or medical license investigations, previous history of a depressive episode, and a previous suicide attempt. “Sometimes, it’s hard to get this information from a new physician who’s sitting opposite you,” Dr. Myers noted. “We mustn’t forget that there’s a lot of shame, embarrassment, and guilt that’s attached to previous suicide attempts.”
Suicide risk also is elevated for physicians with treatment-refractory psychiatric illness. “It troubles me when a physician is being treated by a generalist, the patient is not doing well, and he or she is not being referred for a second opinion or has never been referred to a psychopharmacologist,” he said. “It’s important that be done, because you know how difficult many of your patients can be. It’s important to have the expertise of a psychopharmacologist. I believe that physician patients will welcome that [second opinion], even if they have to travel 200 miles for it.”
The list of risk considerations for suicidal physicians also includes undiagnosed and untreated bipolar I or II disorder, rapid cycling bipolar disorder, and mixed affective states. “These are important things that can make our patients ill very quickly,” he said. Impulsivity is another consideration, as are severe sleep deprivation, circadian rhythm disturbances, and acute suicidal affective disturbance, which has emerged as a condition to consider in future revisions of DSM-5. “What you see in this condition is an individual becoming suicidal within minutes or hours,” Dr. Myers explained. “It’s usually an agitated state with insomnia and overvalued ideas or delusions that they are completely untreatable and hopeless. Physicians are no different than anyone else in that kind of state.” He emphasized that the stigma attached to mental illness in physicians is pernicious, because untreated mental illness is a key driver of suicide. After one of Dr. Myers’s patients took his own life, his son told Dr. Myers, “My father just hated being a patient. He felt so ashamed. I tried hard, too, but my support wasn’t enough.”
Inadequate treatment can occur for physician patients because of transference and countertransference dynamics “that muddle the treatment dyad,” Dr. Myers added. “We must be mindful of the many issues that are going on when we treat our own.”
In his 2005 book “Why People Die By Suicide,” psychologist Thomas Joiner, PhD, described three key reasons why people choose to take their own lives. The first is “perceived burdensomeness,” or a sense that one is a burden on others. “When I see it in my physician patients, it’s when they have a sense of being a burden on their family and feel they are no longer serving a purpose,” Dr. Myers said. The second reason is “failed belongingness,” or a sense that one does not belong to a valued social group. “This resonates with me,” Dr. Myers said. “Sometimes in therapy sessions, my physician patients will say ‘Don’t call me Dr. Smith anymore; I’m Mr. Smith.’ They’ve removed themselves from the field because they don’t feel like they belong anymore. That’s the unworthiness that physicians can feel.”
The third reason is “learned fearlessness,” or the acquired capability to enact self-injury. Dr. Myers likened it to “the kind of exposure to pain and fear that people also might learn through such experiences as mountain climbing, performing surgery, fighting in wars, or being afflicted with anorexia.”
If you suspect that a physician patient is engaged in suicidal thinking and planning, Dr. Myers advises framing your mental health assessment in the context of trust and mutual respect. “Please don’t be seduced by somebody who’s squeaky clean in the area of suicidality,” he said. “That individual may just not be sharing with you yet. You’re going to have to be firm and parental at times. There’s a lot of terror and shame that can lurk behind those symptomatic behaviors. That’s where you’ll use your expertise. I have found that there are many physicians out there who welcome you to go in that ‘dark place’ with them. For them to be able to share those scary thoughts with someone can enhance the therapeutic alliance.” The inquiry should include questions about potential means and methods, including access to firearms, stockpiled and/or self-prescribed medications, and medications ordered online or stolen/diverted from the workplace. Timely and careful documentation are essential, he said.
The plan for treating suicidal physicians should include obtaining old records and speaking with former treating professionals. “If you get pushback from the patient, say, ‘This is about me wanting to be thorough in my assessment and treatment plan with you,’ ” Dr. Myers said. “There is no substitute for a detailed mental status evaluation, collateral information, clinical intuition, experience, and consultation.” Hospitalizing the physician patient should be judicious and in consultation with others. “If you’re not sure, get a second opinion, because it can be life-saving,” he said, “but if done inappropriately, you can turn them off psychiatry for the rest of their lives. Make sure you’re not just panicking and worrying about some sort of medical-legal risk.”
In cases of split treatment, ensure regular contact with the psychotherapist and document all communication and any changes in status, medication, or psychotherapy modality change.
Dr. Myers cited many ways that psychiatrists can educate their colleagues about burnout, depression, and the risk of suicide. These include offering to give grand rounds or a lecture on the topic, serving on your local CME planning committee, joining your institute’s physician wellness team, serving on your state’s physician health program, and offering to facilitate a group for physicians after a physician colleague has died by suicide. “Postvention is prevention for the next generation,” Dr. Myers said, quoting Edwin S. Shneidman, PhD, founder of the American Association of Suicidology. “By taking care of ourselves and accepting the painful reality of physician suicide, we reach out to those left behind and make a difference. You become a change agent – someone who is part of the movement to stop doctors from killing themselves.”
Dr. Myers disclosed that he has received funding from the Medical Education Speakers Network.
EXPERT ANALYSIS AT THE NPA PSYCHOPHARMACOLOGY UPDATE
LAS VEGAS – Michael F. Myers, MD, found a common thread in interviews with loved ones, friends, and colleagues of physicians who have taken their own lives: About 10%-15% of the decedents never sought help beforehand.
“They’ve gone from illness to death without any care,” Dr. Myers, a psychiatrist, said at the annual psychopharmacology update held by the Nevada Psychiatric Association.
In a new book based on the interviews, “Why Physicians Die by Suicide: Lessons Learned From Their Families and Others Who Cared” (Amazon, 2017), Dr. Myers combined stories from his own clinical practice and qualitative interviews with about 75 men and women to explore reasons why physicians might choose to take their own lives. “Our nonpsychiatric medical colleagues are really anxious to have information from us, because we’re living in an age of burnout; roughly 50% of U.S. physicians suffer from burnout,” he said. In addition to perspectives from bereaved loved ones and former medical colleagues, the book includes insights from others who are affected when doctors die by suicide: their medical training directors, employers, medical students, treating psychiatrists, and patients.
According to the American Foundation for Suicide Prevention, 300-400 physicians take their own lives every year, the equivalent of two to three medical school classes. “That’s a doctor a day we lose to suicide,” said Dr. Myers, a professor of clinical psychiatry at State University of New York, Brooklyn, who specializes in physician health. Compared with the general population, the suicide rate ratio is 2.27 among female physicians and 1.41 among male physicians (Am J Psychiatry. 2004;161[12]:2295-2302), and an estimated 85%-90% of those who carry out a suicide have a psychiatric illness such as major depressive disorder, bipolar disorder, alcohol use and substance use disorder, and borderline personality disorder. Other triggers common to physicians, Dr. Myers said, include other kinds of personality disorders, burnout, untreated anxiety disorders, substance/medication-induced depressive disorder (especially in clinicians who have been self-medicating), and posttraumatic stress disorder.
Additional risk considerations to keep in mind for physician patients include a family history of mood disorders, a sense of professional isolation, coping with lawsuits and/or medical license investigations, previous history of a depressive episode, and a previous suicide attempt. “Sometimes, it’s hard to get this information from a new physician who’s sitting opposite you,” Dr. Myers noted. “We mustn’t forget that there’s a lot of shame, embarrassment, and guilt that’s attached to previous suicide attempts.”
Suicide risk also is elevated for physicians with treatment-refractory psychiatric illness. “It troubles me when a physician is being treated by a generalist, the patient is not doing well, and he or she is not being referred for a second opinion or has never been referred to a psychopharmacologist,” he said. “It’s important that be done, because you know how difficult many of your patients can be. It’s important to have the expertise of a psychopharmacologist. I believe that physician patients will welcome that [second opinion], even if they have to travel 200 miles for it.”
The list of risk considerations for suicidal physicians also includes undiagnosed and untreated bipolar I or II disorder, rapid cycling bipolar disorder, and mixed affective states. “These are important things that can make our patients ill very quickly,” he said. Impulsivity is another consideration, as are severe sleep deprivation, circadian rhythm disturbances, and acute suicidal affective disturbance, which has emerged as a condition to consider in future revisions of DSM-5. “What you see in this condition is an individual becoming suicidal within minutes or hours,” Dr. Myers explained. “It’s usually an agitated state with insomnia and overvalued ideas or delusions that they are completely untreatable and hopeless. Physicians are no different than anyone else in that kind of state.” He emphasized that the stigma attached to mental illness in physicians is pernicious, because untreated mental illness is a key driver of suicide. After one of Dr. Myers’s patients took his own life, his son told Dr. Myers, “My father just hated being a patient. He felt so ashamed. I tried hard, too, but my support wasn’t enough.”
Inadequate treatment can occur for physician patients because of transference and countertransference dynamics “that muddle the treatment dyad,” Dr. Myers added. “We must be mindful of the many issues that are going on when we treat our own.”
In his 2005 book “Why People Die By Suicide,” psychologist Thomas Joiner, PhD, described three key reasons why people choose to take their own lives. The first is “perceived burdensomeness,” or a sense that one is a burden on others. “When I see it in my physician patients, it’s when they have a sense of being a burden on their family and feel they are no longer serving a purpose,” Dr. Myers said. The second reason is “failed belongingness,” or a sense that one does not belong to a valued social group. “This resonates with me,” Dr. Myers said. “Sometimes in therapy sessions, my physician patients will say ‘Don’t call me Dr. Smith anymore; I’m Mr. Smith.’ They’ve removed themselves from the field because they don’t feel like they belong anymore. That’s the unworthiness that physicians can feel.”
The third reason is “learned fearlessness,” or the acquired capability to enact self-injury. Dr. Myers likened it to “the kind of exposure to pain and fear that people also might learn through such experiences as mountain climbing, performing surgery, fighting in wars, or being afflicted with anorexia.”
If you suspect that a physician patient is engaged in suicidal thinking and planning, Dr. Myers advises framing your mental health assessment in the context of trust and mutual respect. “Please don’t be seduced by somebody who’s squeaky clean in the area of suicidality,” he said. “That individual may just not be sharing with you yet. You’re going to have to be firm and parental at times. There’s a lot of terror and shame that can lurk behind those symptomatic behaviors. That’s where you’ll use your expertise. I have found that there are many physicians out there who welcome you to go in that ‘dark place’ with them. For them to be able to share those scary thoughts with someone can enhance the therapeutic alliance.” The inquiry should include questions about potential means and methods, including access to firearms, stockpiled and/or self-prescribed medications, and medications ordered online or stolen/diverted from the workplace. Timely and careful documentation are essential, he said.
The plan for treating suicidal physicians should include obtaining old records and speaking with former treating professionals. “If you get pushback from the patient, say, ‘This is about me wanting to be thorough in my assessment and treatment plan with you,’ ” Dr. Myers said. “There is no substitute for a detailed mental status evaluation, collateral information, clinical intuition, experience, and consultation.” Hospitalizing the physician patient should be judicious and in consultation with others. “If you’re not sure, get a second opinion, because it can be life-saving,” he said, “but if done inappropriately, you can turn them off psychiatry for the rest of their lives. Make sure you’re not just panicking and worrying about some sort of medical-legal risk.”
In cases of split treatment, ensure regular contact with the psychotherapist and document all communication and any changes in status, medication, or psychotherapy modality change.
Dr. Myers cited many ways that psychiatrists can educate their colleagues about burnout, depression, and the risk of suicide. These include offering to give grand rounds or a lecture on the topic, serving on your local CME planning committee, joining your institute’s physician wellness team, serving on your state’s physician health program, and offering to facilitate a group for physicians after a physician colleague has died by suicide. “Postvention is prevention for the next generation,” Dr. Myers said, quoting Edwin S. Shneidman, PhD, founder of the American Association of Suicidology. “By taking care of ourselves and accepting the painful reality of physician suicide, we reach out to those left behind and make a difference. You become a change agent – someone who is part of the movement to stop doctors from killing themselves.”
Dr. Myers disclosed that he has received funding from the Medical Education Speakers Network.
Follistatin, endoglin predict postallogeneic HCT NRM
ORLANDO – A composite score based on day 28 plasma levels of the angiogenic factors follistatin and endoglin predicts 1-year nonrelapse mortality in patients who have undergone myeloablative allogeneic hematopoietic cell transplantation, based on findings from the randomized Blood and Marrow Transplant Clinical Trials Network acute graft-versus-host prophylaxis study 0402 (BMT CTN 0402).
Elevations in these factors at day 28 may reflect susceptibility to regimen-related and other toxicities that adversely affect tissue repair and survival, Shernan Holtan, MD, said at the combined annual meetings of the Center for International Blood & Marrow Transplant Research and the American Society for Blood and Marrow Transplantation.
“Without important trophic angiogenic factors, the body may not be able to heal well after injury such as graft-versus-host disease [GVHD]. We previously reported that such angiogenic factors are indeed altered at the onset of acute graft-versus-host disease based upon samples from BMT CTN 0302 and 0802,” said Dr. Holtan of the University of Minnesota, Minneapolis. “Specifically, we found that repair factors of epidermal growth factor and VEGF-A are low at the onset of acute GVHD, and that damage-associated angiogenic factors are high at the onset of acute graft-versus-host disease.”
These damage-associated factors include follistatin, endoglin, placental growth factor, and angiopoietin-2, she added.
Based on the previous results, Dr. Holtan and her colleagues hypothesized that a pattern of tissue damage as illustrated by these markers at 28 days after treatment would be associated with 1-year nonrelapse mortality.
Of 221 patients from BMT CTN 0402 with pretreatment and day 28 plasma samples available for analysis, 25 had died at 1 year of causes unrelated to relapse. In a univariate analysis, nonrelapse mortality was associated with levels of follistatin, endoglin, and angiopoietin-2. When combined to assess for an overall pattern of damage, only follistatin and endoglin were significantly associated with nonrelapse mortality.
The relative risk of death unrelated to relapse was 4.5-fold higher in patients with the highest score (score of 3) on multivariate regression analysis of follistatin and endoglin levels. Grade II-IV acute GVHD was not significantly associated with 1-year nonrelapse mortality in multivariate analyses, but age over 50 years was.
“Notably, the composite score was a better predictor than any factor alone,” Dr. Holtan said.
The composite score was also predictive of the development of acute GVHD.
“We found that a moderate score of 2 was associated with a 2.3-fold increased risk of acute GVHD prior to day 100. Interestingly, the higher score [3] was not associated with acute GVHD. There was no association of the composite score with chronic GVHD,” she said.
The risk of nonrelapse mortality was less than 10% in patients with a composite score of 1.
Among patients in the study with a score of 3, more than half of the deaths were related to organ toxicity, including liver failure and respiratory failure, which were predominantly infection-related. Those with a low composite score had very few deaths associated with organ toxicity, she noted.
While there are many unanswered questions, these findings highlight possible opportunities to improve survival after allogeneic hematopoietic cell transplantation that warrant further study, she said.
“We need to learn how to constrain this angiogenic inflammatory response with the ultimate goal of hopefully identifying novel treatment strategies to mitigate nonrelapse mortality in our patients,” she concluded.
Dr. Holtan is an investigator for Alexion and is site principal investigator on the GI GVHD clinical trial.
ORLANDO – A composite score based on day 28 plasma levels of the angiogenic factors follistatin and endoglin predicts 1-year nonrelapse mortality in patients who have undergone myeloablative allogeneic hematopoietic cell transplantation, based on findings from the randomized Blood and Marrow Transplant Clinical Trials Network acute graft-versus-host prophylaxis study 0402 (BMT CTN 0402).
Elevations in these factors at day 28 may reflect susceptibility to regimen-related and other toxicities that adversely affect tissue repair and survival, Shernan Holtan, MD, said at the combined annual meetings of the Center for International Blood & Marrow Transplant Research and the American Society for Blood and Marrow Transplantation.
“Without important trophic angiogenic factors, the body may not be able to heal well after injury such as graft-versus-host disease [GVHD]. We previously reported that such angiogenic factors are indeed altered at the onset of acute graft-versus-host disease based upon samples from BMT CTN 0302 and 0802,” said Dr. Holtan of the University of Minnesota, Minneapolis. “Specifically, we found that repair factors of epidermal growth factor and VEGF-A are low at the onset of acute GVHD, and that damage-associated angiogenic factors are high at the onset of acute graft-versus-host disease.”
These damage-associated factors include follistatin, endoglin, placental growth factor, and angiopoietin-2, she added.
Based on the previous results, Dr. Holtan and her colleagues hypothesized that a pattern of tissue damage as illustrated by these markers at 28 days after treatment would be associated with 1-year nonrelapse mortality.
Of 221 patients from BMT CTN 0402 with pretreatment and day 28 plasma samples available for analysis, 25 had died at 1 year of causes unrelated to relapse. In a univariate analysis, nonrelapse mortality was associated with levels of follistatin, endoglin, and angiopoietin-2. When combined to assess for an overall pattern of damage, only follistatin and endoglin were significantly associated with nonrelapse mortality.
The relative risk of death unrelated to relapse was 4.5-fold higher in patients with the highest score (score of 3) on multivariate regression analysis of follistatin and endoglin levels. Grade II-IV acute GVHD was not significantly associated with 1-year nonrelapse mortality in multivariate analyses, but age over 50 years was.
“Notably, the composite score was a better predictor than any factor alone,” Dr. Holtan said.
The composite score was also predictive of the development of acute GVHD.
“We found that a moderate score of 2 was associated with a 2.3-fold increased risk of acute GVHD prior to day 100. Interestingly, the higher score [3] was not associated with acute GVHD. There was no association of the composite score with chronic GVHD,” she said.
The risk of nonrelapse mortality was less than 10% in patients with a composite score of 1.
Among patients in the study with a score of 3, more than half of the deaths were related to organ toxicity, including liver failure and respiratory failure, which were predominantly infection-related. Those with a low composite score had very few deaths associated with organ toxicity, she noted.
While there are many unanswered questions, these findings highlight possible opportunities to improve survival after allogeneic hematopoietic cell transplantation that warrant further study, she said.
“We need to learn how to constrain this angiogenic inflammatory response with the ultimate goal of hopefully identifying novel treatment strategies to mitigate nonrelapse mortality in our patients,” she concluded.
Dr. Holtan is an investigator for Alexion and is site principal investigator on the GI GVHD clinical trial.
ORLANDO – A composite score based on day 28 plasma levels of the angiogenic factors follistatin and endoglin predicts 1-year nonrelapse mortality in patients who have undergone myeloablative allogeneic hematopoietic cell transplantation, based on findings from the randomized Blood and Marrow Transplant Clinical Trials Network acute graft-versus-host prophylaxis study 0402 (BMT CTN 0402).
Elevations in these factors at day 28 may reflect susceptibility to regimen-related and other toxicities that adversely affect tissue repair and survival, Shernan Holtan, MD, said at the combined annual meetings of the Center for International Blood & Marrow Transplant Research and the American Society for Blood and Marrow Transplantation.
“Without important trophic angiogenic factors, the body may not be able to heal well after injury such as graft-versus-host disease [GVHD]. We previously reported that such angiogenic factors are indeed altered at the onset of acute graft-versus-host disease based upon samples from BMT CTN 0302 and 0802,” said Dr. Holtan of the University of Minnesota, Minneapolis. “Specifically, we found that repair factors of epidermal growth factor and VEGF-A are low at the onset of acute GVHD, and that damage-associated angiogenic factors are high at the onset of acute graft-versus-host disease.”
These damage-associated factors include follistatin, endoglin, placental growth factor, and angiopoietin-2, she added.
Based on the previous results, Dr. Holtan and her colleagues hypothesized that a pattern of tissue damage as illustrated by these markers at 28 days after treatment would be associated with 1-year nonrelapse mortality.
Of 221 patients from BMT CTN 0402 with pretreatment and day 28 plasma samples available for analysis, 25 had died at 1 year of causes unrelated to relapse. In a univariate analysis, nonrelapse mortality was associated with levels of follistatin, endoglin, and angiopoietin-2. When combined to assess for an overall pattern of damage, only follistatin and endoglin were significantly associated with nonrelapse mortality.
The relative risk of death unrelated to relapse was 4.5-fold higher in patients with the highest score (score of 3) on multivariate regression analysis of follistatin and endoglin levels. Grade II-IV acute GVHD was not significantly associated with 1-year nonrelapse mortality in multivariate analyses, but age over 50 years was.
“Notably, the composite score was a better predictor than any factor alone,” Dr. Holtan said.
The composite score was also predictive of the development of acute GVHD.
“We found that a moderate score of 2 was associated with a 2.3-fold increased risk of acute GVHD prior to day 100. Interestingly, the higher score [3] was not associated with acute GVHD. There was no association of the composite score with chronic GVHD,” she said.
The risk of nonrelapse mortality was less than 10% in patients with a composite score of 1.
Among patients in the study with a score of 3, more than half of the deaths were related to organ toxicity, including liver failure and respiratory failure, which were predominantly infection-related. Those with a low composite score had very few deaths associated with organ toxicity, she noted.
While there are many unanswered questions, these findings highlight possible opportunities to improve survival after allogeneic hematopoietic cell transplantation that warrant further study, she said.
“We need to learn how to constrain this angiogenic inflammatory response with the ultimate goal of hopefully identifying novel treatment strategies to mitigate nonrelapse mortality in our patients,” she concluded.
Dr. Holtan is an investigator for Alexion and is site principal investigator on the GI GVHD clinical trial.
AT THE 2017 BMT TANDEM MEETINGS
Key clinical point:
Major finding: Patients with a composite score of 3 had a 4.5-fold higher relative risk of nonrelapse mortality.
Data source: The randomized BMT CTN 0402 study of 221 patients.
Disclosures: Dr. Holtan is an investigator for Alexion and is site principal investigator on the GI GVHD clinical trial.
Expert to psychiatrists: Collaborative care is here to stay
SCOTTSDALE, ARIZ. – Whether or not the Affordable Care Act (ACA) is repealed, replaced, reviled, or revered should not deter psychiatrists and primary care physicians from seeking to work together, according to a leading expert on integrating mental health care in medical practice.
“Community-based psychiatrists should be focused on finding ways to help create integrated models of care, both in health systems and in other settings, to provide mental health specialty support for primary care providers, regardless of whatever else is going on [in Washington],” Paul Summergrad, MD, said in an interview at the annual meeting of the American College of Psychiatrists.
“If Medicaid expansion is replaced with block grants, that would lead to less care in general for Medicaid recipients,” Dr. Summergrad said in the interview. “It depends on how the states would view their costs of care, and how they would view the medical psychiatric issues.”
Since Medicaid is the largest payer of mental and behavioral health services in the country with reimbursable models of collaborative care, cutting funding for those services would sting. “There’s evidence that addressing mental and behavioral health issues keeps medical costs low,” said Dr. Summergrad, a past president of the American Psychiatric Association.
In his talk, Dr. Summergrad pointed to the now decade-old IMPACT study (Improving Mood: Promoting Access to Collaborative Treatment) which showed that patients screened for depression when presenting with chronic medical issues had lower overall medical costs over time.
He also referred to a more recent study in a large Utah health system that showed overall cost savings, far-fewer emergency department admissions, and better patient outcomes across a wide range of medical issues, which were achieved when mental health services were integrated into routine care: in all, a $12 million investment resulted in $52 million in savings after 4 years (JAMA. 2016;316[8]:826-34). “Utah is not exactly a blue state, but it worked for them,” Dr. Summergrad said. The key was that physicians “embraced normalizing mental health care,” he said.
As for how any changes to the Medicare Access and CHIP Reauthorization Act, which is predicated largely on team-based care for higher reimbursements, Dr. Summergrad said cash-only psychiatrists should be thinking about how to collaborate with primary care providers. “I think the important message at this point is that, however this works, we’ll have to think about integrated care.”
In an interview, Lee H. Beecher, MD, agreed. In fact, Dr. Beecher said that, in his state of Minnesota, engaging with patients on a cash-only basis is the only way a psychiatrist can have a private practice and provide valuable, essential communication with primary care physicians. “Direct-pay physicians are uniquely able to actively facilitate communication,” said Dr. Beecher, president of the nonprofit Minnesota Physician-Patient Alliance. “Most of this is done by phone, directly, with the primary care clinician – rather than inputting and sending an electronic health record.”
Dr. Summergrad had no relevant disclosures.
[email protected]
On Twitter @whitneymcknight
SCOTTSDALE, ARIZ. – Whether or not the Affordable Care Act (ACA) is repealed, replaced, reviled, or revered should not deter psychiatrists and primary care physicians from seeking to work together, according to a leading expert on integrating mental health care in medical practice.
“Community-based psychiatrists should be focused on finding ways to help create integrated models of care, both in health systems and in other settings, to provide mental health specialty support for primary care providers, regardless of whatever else is going on [in Washington],” Paul Summergrad, MD, said in an interview at the annual meeting of the American College of Psychiatrists.
“If Medicaid expansion is replaced with block grants, that would lead to less care in general for Medicaid recipients,” Dr. Summergrad said in the interview. “It depends on how the states would view their costs of care, and how they would view the medical psychiatric issues.”
Since Medicaid is the largest payer of mental and behavioral health services in the country with reimbursable models of collaborative care, cutting funding for those services would sting. “There’s evidence that addressing mental and behavioral health issues keeps medical costs low,” said Dr. Summergrad, a past president of the American Psychiatric Association.
In his talk, Dr. Summergrad pointed to the now decade-old IMPACT study (Improving Mood: Promoting Access to Collaborative Treatment) which showed that patients screened for depression when presenting with chronic medical issues had lower overall medical costs over time.
He also referred to a more recent study in a large Utah health system that showed overall cost savings, far-fewer emergency department admissions, and better patient outcomes across a wide range of medical issues, which were achieved when mental health services were integrated into routine care: in all, a $12 million investment resulted in $52 million in savings after 4 years (JAMA. 2016;316[8]:826-34). “Utah is not exactly a blue state, but it worked for them,” Dr. Summergrad said. The key was that physicians “embraced normalizing mental health care,” he said.
As for how any changes to the Medicare Access and CHIP Reauthorization Act, which is predicated largely on team-based care for higher reimbursements, Dr. Summergrad said cash-only psychiatrists should be thinking about how to collaborate with primary care providers. “I think the important message at this point is that, however this works, we’ll have to think about integrated care.”
In an interview, Lee H. Beecher, MD, agreed. In fact, Dr. Beecher said that, in his state of Minnesota, engaging with patients on a cash-only basis is the only way a psychiatrist can have a private practice and provide valuable, essential communication with primary care physicians. “Direct-pay physicians are uniquely able to actively facilitate communication,” said Dr. Beecher, president of the nonprofit Minnesota Physician-Patient Alliance. “Most of this is done by phone, directly, with the primary care clinician – rather than inputting and sending an electronic health record.”
Dr. Summergrad had no relevant disclosures.
[email protected]
On Twitter @whitneymcknight
SCOTTSDALE, ARIZ. – Whether or not the Affordable Care Act (ACA) is repealed, replaced, reviled, or revered should not deter psychiatrists and primary care physicians from seeking to work together, according to a leading expert on integrating mental health care in medical practice.
“Community-based psychiatrists should be focused on finding ways to help create integrated models of care, both in health systems and in other settings, to provide mental health specialty support for primary care providers, regardless of whatever else is going on [in Washington],” Paul Summergrad, MD, said in an interview at the annual meeting of the American College of Psychiatrists.
“If Medicaid expansion is replaced with block grants, that would lead to less care in general for Medicaid recipients,” Dr. Summergrad said in the interview. “It depends on how the states would view their costs of care, and how they would view the medical psychiatric issues.”
Since Medicaid is the largest payer of mental and behavioral health services in the country with reimbursable models of collaborative care, cutting funding for those services would sting. “There’s evidence that addressing mental and behavioral health issues keeps medical costs low,” said Dr. Summergrad, a past president of the American Psychiatric Association.
In his talk, Dr. Summergrad pointed to the now decade-old IMPACT study (Improving Mood: Promoting Access to Collaborative Treatment) which showed that patients screened for depression when presenting with chronic medical issues had lower overall medical costs over time.
He also referred to a more recent study in a large Utah health system that showed overall cost savings, far-fewer emergency department admissions, and better patient outcomes across a wide range of medical issues, which were achieved when mental health services were integrated into routine care: in all, a $12 million investment resulted in $52 million in savings after 4 years (JAMA. 2016;316[8]:826-34). “Utah is not exactly a blue state, but it worked for them,” Dr. Summergrad said. The key was that physicians “embraced normalizing mental health care,” he said.
As for how any changes to the Medicare Access and CHIP Reauthorization Act, which is predicated largely on team-based care for higher reimbursements, Dr. Summergrad said cash-only psychiatrists should be thinking about how to collaborate with primary care providers. “I think the important message at this point is that, however this works, we’ll have to think about integrated care.”
In an interview, Lee H. Beecher, MD, agreed. In fact, Dr. Beecher said that, in his state of Minnesota, engaging with patients on a cash-only basis is the only way a psychiatrist can have a private practice and provide valuable, essential communication with primary care physicians. “Direct-pay physicians are uniquely able to actively facilitate communication,” said Dr. Beecher, president of the nonprofit Minnesota Physician-Patient Alliance. “Most of this is done by phone, directly, with the primary care clinician – rather than inputting and sending an electronic health record.”
Dr. Summergrad had no relevant disclosures.
[email protected]
On Twitter @whitneymcknight
EXPERT ANALYSIS AT THE AMERICAN COLLEGE OF PSYCHIATRISTS ANNUAL MEETING