User login
Disruptive physicians: Is this an HR or MEC issue?
it can greatly lower staff morale and compromise patient care. Addressing this behavior head-on is imperative, experts said, but knowing which route to take is not always clear.
Physician leaders may wonder: When is this a human resources (HR) issue and when should the medical executive committee (MEC) step in?
The answer depends on the circumstances and the employment status of the physician in question, said Mark Peters, a labor and employment attorney based in Nashville, Tenn.
“There are a couple of different considerations when deciding how, or more accurately who, should address disruptive physician behavior in the workplace,” Mr. Peters said in an interview. “The first consideration is whether the physician is employed by the health care entity or is a contractor. Typically, absent an employment relationship with the physician, human resources is not involved directly with the physician and the issue is handled through the MEC.”
However, in some cases both HR and the MEC may become involved. For instance, if the complaint is made by an employee, HR would likely get involved – regardless of whether the disruptive physician is a contractor – because employers have a legal duty to ensure a “hostile-free environment,” Mr. Peters said.
The hospital may also ask that the MEC intervene to ensure the medical staff understands all of the facts and can weigh in on whether the doctor is being treated fairly by the hospital, he said.
There are a range of advantages and disadvantages to each resolution path, said Jeffrey Moseley, a health law attorney based in Franklin, Tenn. The HR route usually means dealing with a single point person and typically the issue is resolved more swiftly. Going through the MEC, on the other hand, often takes months. The MEC path also means more people will be involved, and it’s possible the case may become more political, depending on the culture of the MEC.
“If you have to end up taking an action, the employment setting may be a quicker way to address the issue than going through the medical staff side,” Mr. Moseley said in an interview. “Most medical staffs, if they were to try to restrict or revoke privileges, they are going to have to go through a fair hearing and appeals, [which] can take 6 months easily. The downside to the employment side is you don’t get all the immunities that you get on the medical staff side.”
A disruptive physician issue handled by the MEC as a peer review matter or professional review action is protected under the Healthcare Quality Improvement Act, which shields the medical staff and/or hospital from civil damages in the event that they are sued. Additionally, information disclosed during the MEC process that is part of the peer review privilege is confidential and not necessarily discoverable by plaintiff’s attorneys in a subsequent court case.
The way the MEC handles the issue often hinges on the makeup of the committee, Mr. Moseley noted. In his experience, older medical staffs tend to be more sensitive to the accused physician and question whether the behavior is egregious. Older physicians are generally used to a more “captain of the ship” leadership style, with the doctor as the authority figure. Younger staffs are generally more sensitive to concerns about a hostile work environment and lean toward a team approach to health care.
“If your leadership on the medical staff is a [group of older doctors] versus a mix or younger docs, they might be more or less receptive to discipline [for] a behavioral issue, based on their worldview,” he said.
Disruptive behavior is best avoided by implementing sensitivity training and employing a zero tolerance policy for unprofessional behavior that applies to all staff members from the highest revenue generators to the lowest, no exceptions, Mr. Peters advised. “A top down culture that expects and requires professionalism amongst all medical staff [is key].”
it can greatly lower staff morale and compromise patient care. Addressing this behavior head-on is imperative, experts said, but knowing which route to take is not always clear.
Physician leaders may wonder: When is this a human resources (HR) issue and when should the medical executive committee (MEC) step in?
The answer depends on the circumstances and the employment status of the physician in question, said Mark Peters, a labor and employment attorney based in Nashville, Tenn.
“There are a couple of different considerations when deciding how, or more accurately who, should address disruptive physician behavior in the workplace,” Mr. Peters said in an interview. “The first consideration is whether the physician is employed by the health care entity or is a contractor. Typically, absent an employment relationship with the physician, human resources is not involved directly with the physician and the issue is handled through the MEC.”
However, in some cases both HR and the MEC may become involved. For instance, if the complaint is made by an employee, HR would likely get involved – regardless of whether the disruptive physician is a contractor – because employers have a legal duty to ensure a “hostile-free environment,” Mr. Peters said.
The hospital may also ask that the MEC intervene to ensure the medical staff understands all of the facts and can weigh in on whether the doctor is being treated fairly by the hospital, he said.
There are a range of advantages and disadvantages to each resolution path, said Jeffrey Moseley, a health law attorney based in Franklin, Tenn. The HR route usually means dealing with a single point person and typically the issue is resolved more swiftly. Going through the MEC, on the other hand, often takes months. The MEC path also means more people will be involved, and it’s possible the case may become more political, depending on the culture of the MEC.
“If you have to end up taking an action, the employment setting may be a quicker way to address the issue than going through the medical staff side,” Mr. Moseley said in an interview. “Most medical staffs, if they were to try to restrict or revoke privileges, they are going to have to go through a fair hearing and appeals, [which] can take 6 months easily. The downside to the employment side is you don’t get all the immunities that you get on the medical staff side.”
A disruptive physician issue handled by the MEC as a peer review matter or professional review action is protected under the Healthcare Quality Improvement Act, which shields the medical staff and/or hospital from civil damages in the event that they are sued. Additionally, information disclosed during the MEC process that is part of the peer review privilege is confidential and not necessarily discoverable by plaintiff’s attorneys in a subsequent court case.
The way the MEC handles the issue often hinges on the makeup of the committee, Mr. Moseley noted. In his experience, older medical staffs tend to be more sensitive to the accused physician and question whether the behavior is egregious. Older physicians are generally used to a more “captain of the ship” leadership style, with the doctor as the authority figure. Younger staffs are generally more sensitive to concerns about a hostile work environment and lean toward a team approach to health care.
“If your leadership on the medical staff is a [group of older doctors] versus a mix or younger docs, they might be more or less receptive to discipline [for] a behavioral issue, based on their worldview,” he said.
Disruptive behavior is best avoided by implementing sensitivity training and employing a zero tolerance policy for unprofessional behavior that applies to all staff members from the highest revenue generators to the lowest, no exceptions, Mr. Peters advised. “A top down culture that expects and requires professionalism amongst all medical staff [is key].”
it can greatly lower staff morale and compromise patient care. Addressing this behavior head-on is imperative, experts said, but knowing which route to take is not always clear.
Physician leaders may wonder: When is this a human resources (HR) issue and when should the medical executive committee (MEC) step in?
The answer depends on the circumstances and the employment status of the physician in question, said Mark Peters, a labor and employment attorney based in Nashville, Tenn.
“There are a couple of different considerations when deciding how, or more accurately who, should address disruptive physician behavior in the workplace,” Mr. Peters said in an interview. “The first consideration is whether the physician is employed by the health care entity or is a contractor. Typically, absent an employment relationship with the physician, human resources is not involved directly with the physician and the issue is handled through the MEC.”
However, in some cases both HR and the MEC may become involved. For instance, if the complaint is made by an employee, HR would likely get involved – regardless of whether the disruptive physician is a contractor – because employers have a legal duty to ensure a “hostile-free environment,” Mr. Peters said.
The hospital may also ask that the MEC intervene to ensure the medical staff understands all of the facts and can weigh in on whether the doctor is being treated fairly by the hospital, he said.
There are a range of advantages and disadvantages to each resolution path, said Jeffrey Moseley, a health law attorney based in Franklin, Tenn. The HR route usually means dealing with a single point person and typically the issue is resolved more swiftly. Going through the MEC, on the other hand, often takes months. The MEC path also means more people will be involved, and it’s possible the case may become more political, depending on the culture of the MEC.
“If you have to end up taking an action, the employment setting may be a quicker way to address the issue than going through the medical staff side,” Mr. Moseley said in an interview. “Most medical staffs, if they were to try to restrict or revoke privileges, they are going to have to go through a fair hearing and appeals, [which] can take 6 months easily. The downside to the employment side is you don’t get all the immunities that you get on the medical staff side.”
A disruptive physician issue handled by the MEC as a peer review matter or professional review action is protected under the Healthcare Quality Improvement Act, which shields the medical staff and/or hospital from civil damages in the event that they are sued. Additionally, information disclosed during the MEC process that is part of the peer review privilege is confidential and not necessarily discoverable by plaintiff’s attorneys in a subsequent court case.
The way the MEC handles the issue often hinges on the makeup of the committee, Mr. Moseley noted. In his experience, older medical staffs tend to be more sensitive to the accused physician and question whether the behavior is egregious. Older physicians are generally used to a more “captain of the ship” leadership style, with the doctor as the authority figure. Younger staffs are generally more sensitive to concerns about a hostile work environment and lean toward a team approach to health care.
“If your leadership on the medical staff is a [group of older doctors] versus a mix or younger docs, they might be more or less receptive to discipline [for] a behavioral issue, based on their worldview,” he said.
Disruptive behavior is best avoided by implementing sensitivity training and employing a zero tolerance policy for unprofessional behavior that applies to all staff members from the highest revenue generators to the lowest, no exceptions, Mr. Peters advised. “A top down culture that expects and requires professionalism amongst all medical staff [is key].”
Pruritus linked to wide variety of cancers
A wide variety of hematologic, dermatologic, and solid organ malignancies are associated with pruritus, a large, single-center, retrospective study suggests.
Blacks with pruritus had a higher odds ratio of hematologic malignancies, among others, while whites had higher likelihood of liver, gastrointestinal, respiratory and gynecologic cancers, results of the study show.
The results by race help address a gap in the literature, according to Shawn G. Kwatra, MD, of Johns Hopkins University, Baltimore, and his coinvestigators.
“Little is known about the association between pruritus and malignancy among different ethnic groups,” Dr. Kwatra and his coauthors wrote in the Journal of the American Academy of Dermatology.
The study shows a stronger association with more types of malignancies than has been reported previously, according to the investigators.
“The main difference is that prior studies focused on diagnosis of malignancy after the onset of pruritus, while our study includes malignancies diagnosed on or after pruritus onset,” they wrote.
Retrospective data for the study, which came from the Johns Hopkins Health System, included 16,925 patients aged 18 years or older who presented with itching or pruritus between April 4, 2013 and Dec. 31, 2017.
Of those 16,925 patients, 2,903 were also diagnosed with a concomitant malignancy during that time period. Compared with patients with no itching diagnosis during that time period, the pruritus patients more likely to have a concomitant malignancy, with an OR of 5.76 (95% confidence interval, 5.53-6.00), Dr. Kwatra and his colleagues found.
Malignancies most strongly associated with pruritus included those of the skin, liver, gallbladder and biliary tract, and hematopoietic system.
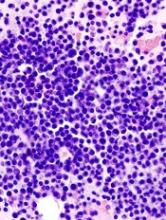
Among hematologic malignancies, pruritus was most strongly linked to myeloid leukemia and primary cutaneous lymphoma, while among skin cancers, squamous cell carcinoma was most strongly linked.
Whites had higher odds of any malignancy versus blacks, according to investigators, with ORs of 6.12 (95% CI, 5.81-6.46) and 5.61 (95% CI, 5.21-6.04), respectively.
Blacks with pruritus had higher ORs for hematologic and soft tissue malignancies including those of the muscle, fat, and peripheral nerve, investigators said, while whites had higher ORs for skin and liver malignancies.
The investigators also looked at the prevalence of skin eruptions in patients with pruritus and malignancy. “Eruption is variable by malignancy type and points to differing underlying mechanisms of pruritus,” they reported.
The highest rates of skin eruption were in patients with myeloid leukemia at 66%, followed by bone cancers at 58%, lymphocytic leukemia at 57%, multiple myeloma at 53%, and bronchus at 53%. The lowest rates of skin eruption were in patients with gallbladder and biliary tract, colon, pancreas, and liver malignancies.
Dr. Kwatra reported that he is an advisory board member for Menlo Therapeutics and Trevi Therapeutics.
SOURCE: Kwatra SG et al. J Am Acad Dermatol. 2018 Sep 11. doi: 10.1016/j.jaad.2018.08.044.
A wide variety of hematologic, dermatologic, and solid organ malignancies are associated with pruritus, a large, single-center, retrospective study suggests.
Blacks with pruritus had a higher odds ratio of hematologic malignancies, among others, while whites had higher likelihood of liver, gastrointestinal, respiratory and gynecologic cancers, results of the study show.
The results by race help address a gap in the literature, according to Shawn G. Kwatra, MD, of Johns Hopkins University, Baltimore, and his coinvestigators.
“Little is known about the association between pruritus and malignancy among different ethnic groups,” Dr. Kwatra and his coauthors wrote in the Journal of the American Academy of Dermatology.
The study shows a stronger association with more types of malignancies than has been reported previously, according to the investigators.
“The main difference is that prior studies focused on diagnosis of malignancy after the onset of pruritus, while our study includes malignancies diagnosed on or after pruritus onset,” they wrote.
Retrospective data for the study, which came from the Johns Hopkins Health System, included 16,925 patients aged 18 years or older who presented with itching or pruritus between April 4, 2013 and Dec. 31, 2017.
Of those 16,925 patients, 2,903 were also diagnosed with a concomitant malignancy during that time period. Compared with patients with no itching diagnosis during that time period, the pruritus patients more likely to have a concomitant malignancy, with an OR of 5.76 (95% confidence interval, 5.53-6.00), Dr. Kwatra and his colleagues found.
Malignancies most strongly associated with pruritus included those of the skin, liver, gallbladder and biliary tract, and hematopoietic system.
Among hematologic malignancies, pruritus was most strongly linked to myeloid leukemia and primary cutaneous lymphoma, while among skin cancers, squamous cell carcinoma was most strongly linked.
Whites had higher odds of any malignancy versus blacks, according to investigators, with ORs of 6.12 (95% CI, 5.81-6.46) and 5.61 (95% CI, 5.21-6.04), respectively.
Blacks with pruritus had higher ORs for hematologic and soft tissue malignancies including those of the muscle, fat, and peripheral nerve, investigators said, while whites had higher ORs for skin and liver malignancies.
The investigators also looked at the prevalence of skin eruptions in patients with pruritus and malignancy. “Eruption is variable by malignancy type and points to differing underlying mechanisms of pruritus,” they reported.
The highest rates of skin eruption were in patients with myeloid leukemia at 66%, followed by bone cancers at 58%, lymphocytic leukemia at 57%, multiple myeloma at 53%, and bronchus at 53%. The lowest rates of skin eruption were in patients with gallbladder and biliary tract, colon, pancreas, and liver malignancies.
Dr. Kwatra reported that he is an advisory board member for Menlo Therapeutics and Trevi Therapeutics.
SOURCE: Kwatra SG et al. J Am Acad Dermatol. 2018 Sep 11. doi: 10.1016/j.jaad.2018.08.044.
A wide variety of hematologic, dermatologic, and solid organ malignancies are associated with pruritus, a large, single-center, retrospective study suggests.
Blacks with pruritus had a higher odds ratio of hematologic malignancies, among others, while whites had higher likelihood of liver, gastrointestinal, respiratory and gynecologic cancers, results of the study show.
The results by race help address a gap in the literature, according to Shawn G. Kwatra, MD, of Johns Hopkins University, Baltimore, and his coinvestigators.
“Little is known about the association between pruritus and malignancy among different ethnic groups,” Dr. Kwatra and his coauthors wrote in the Journal of the American Academy of Dermatology.
The study shows a stronger association with more types of malignancies than has been reported previously, according to the investigators.
“The main difference is that prior studies focused on diagnosis of malignancy after the onset of pruritus, while our study includes malignancies diagnosed on or after pruritus onset,” they wrote.
Retrospective data for the study, which came from the Johns Hopkins Health System, included 16,925 patients aged 18 years or older who presented with itching or pruritus between April 4, 2013 and Dec. 31, 2017.
Of those 16,925 patients, 2,903 were also diagnosed with a concomitant malignancy during that time period. Compared with patients with no itching diagnosis during that time period, the pruritus patients more likely to have a concomitant malignancy, with an OR of 5.76 (95% confidence interval, 5.53-6.00), Dr. Kwatra and his colleagues found.
Malignancies most strongly associated with pruritus included those of the skin, liver, gallbladder and biliary tract, and hematopoietic system.
Among hematologic malignancies, pruritus was most strongly linked to myeloid leukemia and primary cutaneous lymphoma, while among skin cancers, squamous cell carcinoma was most strongly linked.
Whites had higher odds of any malignancy versus blacks, according to investigators, with ORs of 6.12 (95% CI, 5.81-6.46) and 5.61 (95% CI, 5.21-6.04), respectively.
Blacks with pruritus had higher ORs for hematologic and soft tissue malignancies including those of the muscle, fat, and peripheral nerve, investigators said, while whites had higher ORs for skin and liver malignancies.
The investigators also looked at the prevalence of skin eruptions in patients with pruritus and malignancy. “Eruption is variable by malignancy type and points to differing underlying mechanisms of pruritus,” they reported.
The highest rates of skin eruption were in patients with myeloid leukemia at 66%, followed by bone cancers at 58%, lymphocytic leukemia at 57%, multiple myeloma at 53%, and bronchus at 53%. The lowest rates of skin eruption were in patients with gallbladder and biliary tract, colon, pancreas, and liver malignancies.
Dr. Kwatra reported that he is an advisory board member for Menlo Therapeutics and Trevi Therapeutics.
SOURCE: Kwatra SG et al. J Am Acad Dermatol. 2018 Sep 11. doi: 10.1016/j.jaad.2018.08.044.
FROM THE JOURNAL OF THE AMERICAN ACADEMY OF DERMATOLOGY
Key clinical point:
Major finding: Blacks with pruritus had higher odds ratios for hematologic and soft tissue malignancies, while whites had higher ORs for skin and liver malignancies.
Study details: A retrospective study of 16,925 adults with itching or pruritus seen at a tertiary care center.
Disclosures: Dr. Kwatra reported serving as an advisory board member for Menlo Therapeutics and Trevi Therapeutics.
Source: Kwatra SG et al. J Am Acad Dermatol. 2018 Sep 11. doi: 10.1016/j.jaad.2018.08.044.
Repeat MRI not useful in suspected axial spondyloarthritis
Patients with chronic back pain suspected of having axial spondyloarthritis (axSpA) should not undergo follow-up MRI of the sacroiliac joint (MRI-SI) within a year if they had a negative baseline MRI-SI, according to investigators.
It is very unlikely that a follow-up MRI-SI will yield new results, reported Pauline A. Bakker, MD, of the department of rheumatology at Leiden University Medical Centre, the Netherlands, and her colleagues.
Since gender and HLA-B27 status were closely associated with MRI-SI positivity, these factors should be considered when deciding to repeat an MRI-SI.
“Over the last decade, MRI rapidly gained ground and proved to be an important imaging technique in the diagnostic process of [nonradiographic] axial spondyloarthritis,” the investigators wrote in Arthritis and Rheumatology. “It has been shown that MRI can detect the early inflammatory stages of sacroiliitis months to years before structural damage can be detected on a conventional radiograph.”
Although MRI represents a diagnostic leap forward, questions of clinical application remain. “For example… if an MRI is completely normal and there is still a clinical suspicion of axSpA, should the MRI be repeated? And if so, after what period of follow-up? Or does this not contribute to the diagnostic process?”
To answer these questions, the investigators observed the “evolution of MRI lesions over a 3-month and 1-year time frame” in patients with early chronic back pain and suspected axSpA.
The prospective study involved 188 patients from the Spondyloarthritis Caught Early (SPACE) cohort. The authors commented that this is “an ideal cohort… since it includes a population of patients with back pain of short duration referred to rheumatologists with a suspicion of SpA [but without the mandatory presence of a single or multiple SpA features].”
Enrolled patients had chronic back pain lasting between 3 months and 2 years, with onset beginning between 16 and 45 years of age. Each underwent physical examination (including evaluation of other SpA features), MRI and radiographs of the sacroiliac joints, and HLA-B27 testing. If patients fulfilled axSpA criteria or had possible axSpA (at least one SpA feature), then they proceeded into the follow-up phase of the study, which included repeat MRI-SI at 3 months and 1 year.
Among enrolled patients, slightly more than one-third were male, almost half were HLA-B27 positive, and about three-quarters had Assessment of Spondyloarthritis International Society–defined inflammatory back pain. Mean age was 31 years; 31 (16.5%) patients were MRI-SI positive.
Of patients that were MRI-SI positive at baseline, 11.1% and 37.9% had a negative MRI-SI at 3 months and 1 year, respectively. The authors noted that this change “was partly induced by the start of anti-TNF [tumor necrosis factor] therapy.” In patients who were MRI-SI negative at baseline, 4.3% and 7.2% were positive at 3 months and 1 year, respectively.
“A very small percentage of patients become positive… which indicates that the usefulness of repeating an MRI-SI in the diagnostic process after 3 months or 1 year is very limited,” the authors wrote.
Gender and HLA-B27 status were independently associated with a positive MRI-SI at any point in time. About 43% of HLA-B27-positive men had a positive MRI-SI, compared with just 7% of HLA-B27-negative women. The investigators advised that these associations be considered when deciding upon repeat MRI-SI.
“If a clinical suspicion [of axSpA] remains [for example, a patient develops other SpA features] it might be worthwhile to consider redoing an MRI in HLA-B27 positive patients,” the investigators wrote. “Likewise, there is a statistically significant difference between male and female patients with a negative baseline MRI, namely that in male patients more often a positive MRI at follow-up is seen [difference: 12% in men, 3% in women].”
The researchers reported having no conflicts of interest.
SOURCE: Bakker PA et al. Arthritis Rheumatol. 2018 Sep 11. doi: 10.1002/art.40718.
Patients with chronic back pain suspected of having axial spondyloarthritis (axSpA) should not undergo follow-up MRI of the sacroiliac joint (MRI-SI) within a year if they had a negative baseline MRI-SI, according to investigators.
It is very unlikely that a follow-up MRI-SI will yield new results, reported Pauline A. Bakker, MD, of the department of rheumatology at Leiden University Medical Centre, the Netherlands, and her colleagues.
Since gender and HLA-B27 status were closely associated with MRI-SI positivity, these factors should be considered when deciding to repeat an MRI-SI.
“Over the last decade, MRI rapidly gained ground and proved to be an important imaging technique in the diagnostic process of [nonradiographic] axial spondyloarthritis,” the investigators wrote in Arthritis and Rheumatology. “It has been shown that MRI can detect the early inflammatory stages of sacroiliitis months to years before structural damage can be detected on a conventional radiograph.”
Although MRI represents a diagnostic leap forward, questions of clinical application remain. “For example… if an MRI is completely normal and there is still a clinical suspicion of axSpA, should the MRI be repeated? And if so, after what period of follow-up? Or does this not contribute to the diagnostic process?”
To answer these questions, the investigators observed the “evolution of MRI lesions over a 3-month and 1-year time frame” in patients with early chronic back pain and suspected axSpA.
The prospective study involved 188 patients from the Spondyloarthritis Caught Early (SPACE) cohort. The authors commented that this is “an ideal cohort… since it includes a population of patients with back pain of short duration referred to rheumatologists with a suspicion of SpA [but without the mandatory presence of a single or multiple SpA features].”
Enrolled patients had chronic back pain lasting between 3 months and 2 years, with onset beginning between 16 and 45 years of age. Each underwent physical examination (including evaluation of other SpA features), MRI and radiographs of the sacroiliac joints, and HLA-B27 testing. If patients fulfilled axSpA criteria or had possible axSpA (at least one SpA feature), then they proceeded into the follow-up phase of the study, which included repeat MRI-SI at 3 months and 1 year.
Among enrolled patients, slightly more than one-third were male, almost half were HLA-B27 positive, and about three-quarters had Assessment of Spondyloarthritis International Society–defined inflammatory back pain. Mean age was 31 years; 31 (16.5%) patients were MRI-SI positive.
Of patients that were MRI-SI positive at baseline, 11.1% and 37.9% had a negative MRI-SI at 3 months and 1 year, respectively. The authors noted that this change “was partly induced by the start of anti-TNF [tumor necrosis factor] therapy.” In patients who were MRI-SI negative at baseline, 4.3% and 7.2% were positive at 3 months and 1 year, respectively.
“A very small percentage of patients become positive… which indicates that the usefulness of repeating an MRI-SI in the diagnostic process after 3 months or 1 year is very limited,” the authors wrote.
Gender and HLA-B27 status were independently associated with a positive MRI-SI at any point in time. About 43% of HLA-B27-positive men had a positive MRI-SI, compared with just 7% of HLA-B27-negative women. The investigators advised that these associations be considered when deciding upon repeat MRI-SI.
“If a clinical suspicion [of axSpA] remains [for example, a patient develops other SpA features] it might be worthwhile to consider redoing an MRI in HLA-B27 positive patients,” the investigators wrote. “Likewise, there is a statistically significant difference between male and female patients with a negative baseline MRI, namely that in male patients more often a positive MRI at follow-up is seen [difference: 12% in men, 3% in women].”
The researchers reported having no conflicts of interest.
SOURCE: Bakker PA et al. Arthritis Rheumatol. 2018 Sep 11. doi: 10.1002/art.40718.
Patients with chronic back pain suspected of having axial spondyloarthritis (axSpA) should not undergo follow-up MRI of the sacroiliac joint (MRI-SI) within a year if they had a negative baseline MRI-SI, according to investigators.
It is very unlikely that a follow-up MRI-SI will yield new results, reported Pauline A. Bakker, MD, of the department of rheumatology at Leiden University Medical Centre, the Netherlands, and her colleagues.
Since gender and HLA-B27 status were closely associated with MRI-SI positivity, these factors should be considered when deciding to repeat an MRI-SI.
“Over the last decade, MRI rapidly gained ground and proved to be an important imaging technique in the diagnostic process of [nonradiographic] axial spondyloarthritis,” the investigators wrote in Arthritis and Rheumatology. “It has been shown that MRI can detect the early inflammatory stages of sacroiliitis months to years before structural damage can be detected on a conventional radiograph.”
Although MRI represents a diagnostic leap forward, questions of clinical application remain. “For example… if an MRI is completely normal and there is still a clinical suspicion of axSpA, should the MRI be repeated? And if so, after what period of follow-up? Or does this not contribute to the diagnostic process?”
To answer these questions, the investigators observed the “evolution of MRI lesions over a 3-month and 1-year time frame” in patients with early chronic back pain and suspected axSpA.
The prospective study involved 188 patients from the Spondyloarthritis Caught Early (SPACE) cohort. The authors commented that this is “an ideal cohort… since it includes a population of patients with back pain of short duration referred to rheumatologists with a suspicion of SpA [but without the mandatory presence of a single or multiple SpA features].”
Enrolled patients had chronic back pain lasting between 3 months and 2 years, with onset beginning between 16 and 45 years of age. Each underwent physical examination (including evaluation of other SpA features), MRI and radiographs of the sacroiliac joints, and HLA-B27 testing. If patients fulfilled axSpA criteria or had possible axSpA (at least one SpA feature), then they proceeded into the follow-up phase of the study, which included repeat MRI-SI at 3 months and 1 year.
Among enrolled patients, slightly more than one-third were male, almost half were HLA-B27 positive, and about three-quarters had Assessment of Spondyloarthritis International Society–defined inflammatory back pain. Mean age was 31 years; 31 (16.5%) patients were MRI-SI positive.
Of patients that were MRI-SI positive at baseline, 11.1% and 37.9% had a negative MRI-SI at 3 months and 1 year, respectively. The authors noted that this change “was partly induced by the start of anti-TNF [tumor necrosis factor] therapy.” In patients who were MRI-SI negative at baseline, 4.3% and 7.2% were positive at 3 months and 1 year, respectively.
“A very small percentage of patients become positive… which indicates that the usefulness of repeating an MRI-SI in the diagnostic process after 3 months or 1 year is very limited,” the authors wrote.
Gender and HLA-B27 status were independently associated with a positive MRI-SI at any point in time. About 43% of HLA-B27-positive men had a positive MRI-SI, compared with just 7% of HLA-B27-negative women. The investigators advised that these associations be considered when deciding upon repeat MRI-SI.
“If a clinical suspicion [of axSpA] remains [for example, a patient develops other SpA features] it might be worthwhile to consider redoing an MRI in HLA-B27 positive patients,” the investigators wrote. “Likewise, there is a statistically significant difference between male and female patients with a negative baseline MRI, namely that in male patients more often a positive MRI at follow-up is seen [difference: 12% in men, 3% in women].”
The researchers reported having no conflicts of interest.
SOURCE: Bakker PA et al. Arthritis Rheumatol. 2018 Sep 11. doi: 10.1002/art.40718.
FROM ARTHRITIS & RHEUMATOLOGY
Key clinical point:
Major finding: In patients who had a negative baseline MRI of the sacroiliac joints, the maximum likelihood of a follow-up MRI being positive was 7%.
Study details: A prospective study involving 188 patients (from the Spondyloarthritis Caught Early cohort) with early chronic back pain suspected of axial spondyloarthritis.
Disclosures: The researchers reported having no financial disclosures.
Source: Bakker PA et al. Arthritis Rheumatol. 2018 Sep 11. doi: 10.1002/art.40718.
Natural history is comparable for astrovirus, sapovirus, norovirus
ATLANTA – Astrovirus and sapovirus in children visiting the ED with acute gastroenteritis have a similar natural history, which is also similar to that of norovirus, according to findings from a prospective cohort study.
Thanks to the increased use of molecular diagnostic testing, astrovirus and sapovirus (AsV and SaV) recently gained new appreciation as a cause of gastroenteritis, but little is known about their natural history.
The current findings from the Alberta Provincial Pediatric Enteric Infection Team (APPETITE) study provide some longitudinal insight regarding that history, Gillian A. M. Tarr, PhD, of the University of Calgary (Alta.), and her colleagues noted in a poster presentation at the International Conference on Emerging Infectious Diseases.
The investigators tested rectal swabs and stool samples from 2,590 children under age 18 years who had experienced at least three episodes of diarrhea and/or vomiting in 24 hours. AsV was detected in 84 children (3.2%), SaV was detected in 229 (8.8%), and norovirus (NoV) was detected in 655 (25%). After excluding those with coinfection, a total of 54, 144, and 478 children with AsV, SaV, and NoV, respectively, were included.
Vomiting occurred in 83%, 92%, and 98%; diarrhea occurred in 94%, 79% and 75%; and blood was present in the stool in 4.0%, 7.0%, and 3.5%, of those with AsV, SaV, and NoV, respectively, they reported.
The median maximal vomiting episodes per day was slightly lower for AsV versus SaV and NoV (about 3 vs. 5 and 7, respectively); the median maximal diarrhea episodes was slightly higher for AsV (about 5 vs. 4 for both SaV and NoV).
Vomiting duration was similar for AsV and SaV (about 3 days) and slightly longer than for NoV (about 2 days); median diarrhea duration was about 5 days for all three viruses.
“Most AsV cases present with both vomiting and diarrhea; most SaV cases present with vomiting and only approximately half with diarrhea,” the investigators wrote.
APPETITE study participants were enrolled from the EDs of two large children’s hospitals from December 2014 to May 2018. All were tested for 18 enteric pathogens and information on patient symptoms, medications, and potential exposures at enrollment and at 14 days was provided by patients and parents/guardians.
“We compared the natural histories of AsV and SaV to that of NoV, and found that all are comparable. These data provide a clearer picture than previously available of the duration and intensity of cardinal gastroenteritis symptoms associated with AsV and SaV infections,” they concluded.
Dr. Tarr reported having no financial disclosures.
ATLANTA – Astrovirus and sapovirus in children visiting the ED with acute gastroenteritis have a similar natural history, which is also similar to that of norovirus, according to findings from a prospective cohort study.
Thanks to the increased use of molecular diagnostic testing, astrovirus and sapovirus (AsV and SaV) recently gained new appreciation as a cause of gastroenteritis, but little is known about their natural history.
The current findings from the Alberta Provincial Pediatric Enteric Infection Team (APPETITE) study provide some longitudinal insight regarding that history, Gillian A. M. Tarr, PhD, of the University of Calgary (Alta.), and her colleagues noted in a poster presentation at the International Conference on Emerging Infectious Diseases.
The investigators tested rectal swabs and stool samples from 2,590 children under age 18 years who had experienced at least three episodes of diarrhea and/or vomiting in 24 hours. AsV was detected in 84 children (3.2%), SaV was detected in 229 (8.8%), and norovirus (NoV) was detected in 655 (25%). After excluding those with coinfection, a total of 54, 144, and 478 children with AsV, SaV, and NoV, respectively, were included.
Vomiting occurred in 83%, 92%, and 98%; diarrhea occurred in 94%, 79% and 75%; and blood was present in the stool in 4.0%, 7.0%, and 3.5%, of those with AsV, SaV, and NoV, respectively, they reported.
The median maximal vomiting episodes per day was slightly lower for AsV versus SaV and NoV (about 3 vs. 5 and 7, respectively); the median maximal diarrhea episodes was slightly higher for AsV (about 5 vs. 4 for both SaV and NoV).
Vomiting duration was similar for AsV and SaV (about 3 days) and slightly longer than for NoV (about 2 days); median diarrhea duration was about 5 days for all three viruses.
“Most AsV cases present with both vomiting and diarrhea; most SaV cases present with vomiting and only approximately half with diarrhea,” the investigators wrote.
APPETITE study participants were enrolled from the EDs of two large children’s hospitals from December 2014 to May 2018. All were tested for 18 enteric pathogens and information on patient symptoms, medications, and potential exposures at enrollment and at 14 days was provided by patients and parents/guardians.
“We compared the natural histories of AsV and SaV to that of NoV, and found that all are comparable. These data provide a clearer picture than previously available of the duration and intensity of cardinal gastroenteritis symptoms associated with AsV and SaV infections,” they concluded.
Dr. Tarr reported having no financial disclosures.
ATLANTA – Astrovirus and sapovirus in children visiting the ED with acute gastroenteritis have a similar natural history, which is also similar to that of norovirus, according to findings from a prospective cohort study.
Thanks to the increased use of molecular diagnostic testing, astrovirus and sapovirus (AsV and SaV) recently gained new appreciation as a cause of gastroenteritis, but little is known about their natural history.
The current findings from the Alberta Provincial Pediatric Enteric Infection Team (APPETITE) study provide some longitudinal insight regarding that history, Gillian A. M. Tarr, PhD, of the University of Calgary (Alta.), and her colleagues noted in a poster presentation at the International Conference on Emerging Infectious Diseases.
The investigators tested rectal swabs and stool samples from 2,590 children under age 18 years who had experienced at least three episodes of diarrhea and/or vomiting in 24 hours. AsV was detected in 84 children (3.2%), SaV was detected in 229 (8.8%), and norovirus (NoV) was detected in 655 (25%). After excluding those with coinfection, a total of 54, 144, and 478 children with AsV, SaV, and NoV, respectively, were included.
Vomiting occurred in 83%, 92%, and 98%; diarrhea occurred in 94%, 79% and 75%; and blood was present in the stool in 4.0%, 7.0%, and 3.5%, of those with AsV, SaV, and NoV, respectively, they reported.
The median maximal vomiting episodes per day was slightly lower for AsV versus SaV and NoV (about 3 vs. 5 and 7, respectively); the median maximal diarrhea episodes was slightly higher for AsV (about 5 vs. 4 for both SaV and NoV).
Vomiting duration was similar for AsV and SaV (about 3 days) and slightly longer than for NoV (about 2 days); median diarrhea duration was about 5 days for all three viruses.
“Most AsV cases present with both vomiting and diarrhea; most SaV cases present with vomiting and only approximately half with diarrhea,” the investigators wrote.
APPETITE study participants were enrolled from the EDs of two large children’s hospitals from December 2014 to May 2018. All were tested for 18 enteric pathogens and information on patient symptoms, medications, and potential exposures at enrollment and at 14 days was provided by patients and parents/guardians.
“We compared the natural histories of AsV and SaV to that of NoV, and found that all are comparable. These data provide a clearer picture than previously available of the duration and intensity of cardinal gastroenteritis symptoms associated with AsV and SaV infections,” they concluded.
Dr. Tarr reported having no financial disclosures.
REPORTING FROM ICEID 2018
Key clinical point:
Major finding: Vomiting lasted about 3 days for astrovirus and sapovirus and 2 days for norovirus; diarrhea lasted about 5 days for all three viruses.
Study details: A prospective cohort study of 2,590 children.
Disclosures: Dr. Tarr reported having no financial disclosures.
Noninvasive fat removal devices continue to gain popularity
SAN DIEGO – Noninvasive fat removal, such as laser treatment and cryolipolysis, is here to stay.
That’s what Mathew M. Avram, MD, JD, told attendees at the annual Masters of Aesthetics Symposium.
“It does not compare to liposuction, but many patients prefer these devices because there’s less downtime,” he said. “They don’t want pain. They don’t want time away from work.”
In the decade or so since the inception of the noninvasive body contouring field, noninvasive and minimally invasive devices have become far more popular than traditional liposuction, said Dr. Avram, director of laser, cosmetics, and dermatologic surgery at Massachusetts General Hospital in Boston. “It’s not even close. Among American Society for Dermatologic Surgery [ASDS] members, for every 1 liposuction, there are over 10 noninvasive body sculpting treatments.”
There were 408,000 body-sculpting procedures performed in 2017. More than half of those (208,000) were cryolipolysis, followed by use of radiofrequency (89,000), deoxycholic acid (46,000), laser lipolysis (25,000), “other” procedures (25,000), and tumescent liposuction (15,000), according to data from the ASDS.
“Each treatment has improved in efficacy with time,” Dr. Avram said.
Devices currently cleared by the Food and Drug Administration for the noninvasive removal of fat include ultrasound, lasers, low-level laser therapy, cryolipolysis, and radiofrequency. One of the most common is low-level laser therapy.
“There are several different devices on the market, but there’s no good histology to confirm mechanism of action, so you question what the efficacy is,” said Dr. Avram, who is also the immediate past president of the American Society for Laser Medicine and Surgery.
SculpSure
In the traditional laser domain, the one most commonly used for fat removal is SculpSure, an FDA-cleared hyperthermic 1,060-nm diode laser. It features four flat, nonsuction applicators, a contact cooling system, and it enables the user to treat more than one area in a 25-minute session. There is minimal absorption by melanin.
“You shouldn’t treat over tattoos, however, because if there’s black ink, the tattoo will absorb the wavelength,” Dr. Avram said. “It’s safe in all skin types and there are a variety of different configurations you can use to treat the desired area.”
Initially there is a 4-minute warm-up cycle to achieve the target temperature. Over the next 21 minutes, 1,060-nm energy is delivered via proprietary modulation, alternating between heat and cooling.
“There is definitely some pain with this device,” he said. “Whether or not it’s a relevant endpoint is not known at this point. But typically, if you’re destroying fat with heat there should be some pain. It’s relieved by a period of cooling. A submental fat treatment is now available. I have not personally used it, but it’s the same technology.”
CoolSculpting
Another popular technology is cryolipolysis (CoolSculpting), which was developed at Massachusetts General Hospital by R. Rox Anderson, MD, and Dieter Manstein, MD, PhD.
It’s FDA cleared for noninvasive fat removal and there have been more than 6 million cryolipolysis treatments performed around the world. The purported mechanism of action is selective crystallization of lipids and fat cells at temperatures below freezing. An inflammatory process results in fat reduction over 2-4 months.
“When it first started, cryolipolysis was designed to treat local areas like love handles in males,” Dr. Avram said. “Over time, applicators have been designed to treat different areas, most recently, one for the posterior upper arms and above the knees. There is now a larger, faster CoolSculpting applicator which results in a 35-minute treatment. It’s a little larger, there’s a little less pain, a lower temperature, and it’s a little bit more effective. This has been helpful in our practice in terms of getting more treatment cycles in a visit.”
Postprocedurally, massage may improve clinical results by mobilizing lipid crystals created from treatment.
Extracorporeal shock wave therapy
Another modality to consider is extracorporeal shock wave therapy, which is the application of mechanically generated external sound waves. “It’s not the same as ultrasound or focused ultrasound, and it’s FDA cleared for the treatment of cellulite,” Dr. Avram said.
EmSculpt
A newer innovation, known as High Intensity Focused Electromagnetic (HIFEM) technology (EmSculpt), induces 20,000 forced muscle contractions per session, which leads to supramaximal contractions that can’t be achieved through normal voluntary muscle action.
“The idea is that you’re getting hypertrophy of the muscle to get volumetric growth,” he said. “There’s believed to be a cascaded apoptotic effect, inducing apoptosis and fat disruption.”
Dr. Avram added that HIFEM is nonionizing, nonradiating, nonthermal, and it does not affect sensory nerves. “It’s designed to only stimulate motor neurons. Time will tell in terms of what the ultimate results are with that device.”
truSculpt
Some clinicians are using monopolar radiofrequency with truSculpt, the proprietary delivery of deep radiofrequency energy. This device increases fat temperature between 6 and 10 degrees Celsius with dual frequency at 1 and 2 MHz.
Published data show that 45 degrees Celsius sustained for 3 minutes resulted in a 60% loss of adipose tissue viability (Lasers Surg Med. 2009;41:745-50; Lasers Surg Med. 2010;42:361-70).
“The heat delivery induces cell apoptosis, leading to the removal of those cells by natural healing processes,” said Dr. Avram, who added that he has not used the device. “We need more clinical data to assess this as well.”
Selective photothermolysis
Another technology being evaluated for fat removal is selective photothermolysis, a concept developed at Massachusetts General Hospital in 1983. It extends the theory of selective photothermolysis to target the lipids that make up subcutaneous fat.
“The theory is that you must select a wavelength well absorbed by the target chromophore with a pulse duration shorter than the target’s thermal relaxation time,” Dr. Avram explained. “This produces selective, localized heating with focal destruction of the target with minimal damage to the surrounding tissue. It requires a deeply penetrating wavelength.”
Lipids are a tempting target “because they heat quickly and easily and they do not lose their heat easily to surrounding structures. You want to target fat selectively and confine thermal damage effectively,” he said.
Nearly 10 years ago, Dr. Avram and his associates evaluated the effects of noninvasive 1,210-nm laser exposure on the adipose tissue of 24 patients with skin types 1-5 (Laser Surg Med. 2009;41:401-7).
“The laser pulses were painful, which limited the efficacy,” he said.
The contact cooling device failed in some subjects, and two patients had bulla, but no scarring. Histologic evidence of laser-induced fat damage was observed in 89% of test sites at 4-7 weeks, but dermal damage was also seen.
“This was the first study to show histologic evidence of laser-induced damage to subcutaneous fat,” Dr. Avram said.
Development of selective photothermolysis technology fell off the wayside after the Great Recession of 2008, but it is still being evaluated at Massachusetts General Hospital and other centers.
To optimize the technology, Dr. Avram said that longer pulse durations may target larger volumes of fat. “Cooling is essential to protect the epidermis, as well as to control pain.”
Injectables
Injectables provide a new, minimally invasive means to achieve noninvasive fat removal, Dr. Avram noted.
“Many injectables of questionable efficacy and safety had been available internationally for years,” he said, but none had FDA clearance until 2015, when the agency gave ATX-101 (Kybella) the nod.
ATX-101 is a nonanimal-derived formulation of deoxycholic acid that causes preferential adipocytolysis. Data from a phase 3 trial presented at the 2014 American Society of Plastic Surgery and the American Society of Aesthetic Plastic Surgery meetings showed a statistically significant reduction in submental fat among subjects who received ATX-101, compared with placebo. It requires an average of 2-4 treatments.
“In my experience, it tends not to require that many, but based on MRI, as well as clinician and patient-reported outcomes, there are significant improvements in the visual impact of chin fat,” Dr. Avram said.
Most adverse events are mild to moderate in severity, primarily bruising, pain, and a sensation of numbness to the anesthesia. “They decrease in incidence and severity over successive treatments, and they infrequently lead to discontinuation of treatment,” he said.
For submental fat, clinicians can combine cryolipolysis and deoxycholic acid. “Here, the idea is to assess the amount of fat targeted for treatment,” Dr. Avram said. “If the fat fills the cryolipolysis cup, use cryolipolysis alone. If the fat does not fill the cup, inject deoxycholic acid for a more targeted treatment. If there is residual fat after cryolipolysis, consider treating more focally with deoxycholic acid.”
Both treatments can produce temporary marginal mandibular nerve injury. “It’s not common, but that’s something to include in your consent forms,” he said.
Dr. Avram reported that he has received consulting fees from Allergan, Merz Pharma, Sciton, Soliton, and Zalea. He also reported having ownership and/or shareholder interest in Cytrellis Biosystems, Invasix, and Zalea.
[email protected]
SAN DIEGO – Noninvasive fat removal, such as laser treatment and cryolipolysis, is here to stay.
That’s what Mathew M. Avram, MD, JD, told attendees at the annual Masters of Aesthetics Symposium.
“It does not compare to liposuction, but many patients prefer these devices because there’s less downtime,” he said. “They don’t want pain. They don’t want time away from work.”
In the decade or so since the inception of the noninvasive body contouring field, noninvasive and minimally invasive devices have become far more popular than traditional liposuction, said Dr. Avram, director of laser, cosmetics, and dermatologic surgery at Massachusetts General Hospital in Boston. “It’s not even close. Among American Society for Dermatologic Surgery [ASDS] members, for every 1 liposuction, there are over 10 noninvasive body sculpting treatments.”
There were 408,000 body-sculpting procedures performed in 2017. More than half of those (208,000) were cryolipolysis, followed by use of radiofrequency (89,000), deoxycholic acid (46,000), laser lipolysis (25,000), “other” procedures (25,000), and tumescent liposuction (15,000), according to data from the ASDS.
“Each treatment has improved in efficacy with time,” Dr. Avram said.
Devices currently cleared by the Food and Drug Administration for the noninvasive removal of fat include ultrasound, lasers, low-level laser therapy, cryolipolysis, and radiofrequency. One of the most common is low-level laser therapy.
“There are several different devices on the market, but there’s no good histology to confirm mechanism of action, so you question what the efficacy is,” said Dr. Avram, who is also the immediate past president of the American Society for Laser Medicine and Surgery.
SculpSure
In the traditional laser domain, the one most commonly used for fat removal is SculpSure, an FDA-cleared hyperthermic 1,060-nm diode laser. It features four flat, nonsuction applicators, a contact cooling system, and it enables the user to treat more than one area in a 25-minute session. There is minimal absorption by melanin.
“You shouldn’t treat over tattoos, however, because if there’s black ink, the tattoo will absorb the wavelength,” Dr. Avram said. “It’s safe in all skin types and there are a variety of different configurations you can use to treat the desired area.”
Initially there is a 4-minute warm-up cycle to achieve the target temperature. Over the next 21 minutes, 1,060-nm energy is delivered via proprietary modulation, alternating between heat and cooling.
“There is definitely some pain with this device,” he said. “Whether or not it’s a relevant endpoint is not known at this point. But typically, if you’re destroying fat with heat there should be some pain. It’s relieved by a period of cooling. A submental fat treatment is now available. I have not personally used it, but it’s the same technology.”
CoolSculpting
Another popular technology is cryolipolysis (CoolSculpting), which was developed at Massachusetts General Hospital by R. Rox Anderson, MD, and Dieter Manstein, MD, PhD.
It’s FDA cleared for noninvasive fat removal and there have been more than 6 million cryolipolysis treatments performed around the world. The purported mechanism of action is selective crystallization of lipids and fat cells at temperatures below freezing. An inflammatory process results in fat reduction over 2-4 months.
“When it first started, cryolipolysis was designed to treat local areas like love handles in males,” Dr. Avram said. “Over time, applicators have been designed to treat different areas, most recently, one for the posterior upper arms and above the knees. There is now a larger, faster CoolSculpting applicator which results in a 35-minute treatment. It’s a little larger, there’s a little less pain, a lower temperature, and it’s a little bit more effective. This has been helpful in our practice in terms of getting more treatment cycles in a visit.”
Postprocedurally, massage may improve clinical results by mobilizing lipid crystals created from treatment.
Extracorporeal shock wave therapy
Another modality to consider is extracorporeal shock wave therapy, which is the application of mechanically generated external sound waves. “It’s not the same as ultrasound or focused ultrasound, and it’s FDA cleared for the treatment of cellulite,” Dr. Avram said.
EmSculpt
A newer innovation, known as High Intensity Focused Electromagnetic (HIFEM) technology (EmSculpt), induces 20,000 forced muscle contractions per session, which leads to supramaximal contractions that can’t be achieved through normal voluntary muscle action.
“The idea is that you’re getting hypertrophy of the muscle to get volumetric growth,” he said. “There’s believed to be a cascaded apoptotic effect, inducing apoptosis and fat disruption.”
Dr. Avram added that HIFEM is nonionizing, nonradiating, nonthermal, and it does not affect sensory nerves. “It’s designed to only stimulate motor neurons. Time will tell in terms of what the ultimate results are with that device.”
truSculpt
Some clinicians are using monopolar radiofrequency with truSculpt, the proprietary delivery of deep radiofrequency energy. This device increases fat temperature between 6 and 10 degrees Celsius with dual frequency at 1 and 2 MHz.
Published data show that 45 degrees Celsius sustained for 3 minutes resulted in a 60% loss of adipose tissue viability (Lasers Surg Med. 2009;41:745-50; Lasers Surg Med. 2010;42:361-70).
“The heat delivery induces cell apoptosis, leading to the removal of those cells by natural healing processes,” said Dr. Avram, who added that he has not used the device. “We need more clinical data to assess this as well.”
Selective photothermolysis
Another technology being evaluated for fat removal is selective photothermolysis, a concept developed at Massachusetts General Hospital in 1983. It extends the theory of selective photothermolysis to target the lipids that make up subcutaneous fat.
“The theory is that you must select a wavelength well absorbed by the target chromophore with a pulse duration shorter than the target’s thermal relaxation time,” Dr. Avram explained. “This produces selective, localized heating with focal destruction of the target with minimal damage to the surrounding tissue. It requires a deeply penetrating wavelength.”
Lipids are a tempting target “because they heat quickly and easily and they do not lose their heat easily to surrounding structures. You want to target fat selectively and confine thermal damage effectively,” he said.
Nearly 10 years ago, Dr. Avram and his associates evaluated the effects of noninvasive 1,210-nm laser exposure on the adipose tissue of 24 patients with skin types 1-5 (Laser Surg Med. 2009;41:401-7).
“The laser pulses were painful, which limited the efficacy,” he said.
The contact cooling device failed in some subjects, and two patients had bulla, but no scarring. Histologic evidence of laser-induced fat damage was observed in 89% of test sites at 4-7 weeks, but dermal damage was also seen.
“This was the first study to show histologic evidence of laser-induced damage to subcutaneous fat,” Dr. Avram said.
Development of selective photothermolysis technology fell off the wayside after the Great Recession of 2008, but it is still being evaluated at Massachusetts General Hospital and other centers.
To optimize the technology, Dr. Avram said that longer pulse durations may target larger volumes of fat. “Cooling is essential to protect the epidermis, as well as to control pain.”
Injectables
Injectables provide a new, minimally invasive means to achieve noninvasive fat removal, Dr. Avram noted.
“Many injectables of questionable efficacy and safety had been available internationally for years,” he said, but none had FDA clearance until 2015, when the agency gave ATX-101 (Kybella) the nod.
ATX-101 is a nonanimal-derived formulation of deoxycholic acid that causes preferential adipocytolysis. Data from a phase 3 trial presented at the 2014 American Society of Plastic Surgery and the American Society of Aesthetic Plastic Surgery meetings showed a statistically significant reduction in submental fat among subjects who received ATX-101, compared with placebo. It requires an average of 2-4 treatments.
“In my experience, it tends not to require that many, but based on MRI, as well as clinician and patient-reported outcomes, there are significant improvements in the visual impact of chin fat,” Dr. Avram said.
Most adverse events are mild to moderate in severity, primarily bruising, pain, and a sensation of numbness to the anesthesia. “They decrease in incidence and severity over successive treatments, and they infrequently lead to discontinuation of treatment,” he said.
For submental fat, clinicians can combine cryolipolysis and deoxycholic acid. “Here, the idea is to assess the amount of fat targeted for treatment,” Dr. Avram said. “If the fat fills the cryolipolysis cup, use cryolipolysis alone. If the fat does not fill the cup, inject deoxycholic acid for a more targeted treatment. If there is residual fat after cryolipolysis, consider treating more focally with deoxycholic acid.”
Both treatments can produce temporary marginal mandibular nerve injury. “It’s not common, but that’s something to include in your consent forms,” he said.
Dr. Avram reported that he has received consulting fees from Allergan, Merz Pharma, Sciton, Soliton, and Zalea. He also reported having ownership and/or shareholder interest in Cytrellis Biosystems, Invasix, and Zalea.
[email protected]
SAN DIEGO – Noninvasive fat removal, such as laser treatment and cryolipolysis, is here to stay.
That’s what Mathew M. Avram, MD, JD, told attendees at the annual Masters of Aesthetics Symposium.
“It does not compare to liposuction, but many patients prefer these devices because there’s less downtime,” he said. “They don’t want pain. They don’t want time away from work.”
In the decade or so since the inception of the noninvasive body contouring field, noninvasive and minimally invasive devices have become far more popular than traditional liposuction, said Dr. Avram, director of laser, cosmetics, and dermatologic surgery at Massachusetts General Hospital in Boston. “It’s not even close. Among American Society for Dermatologic Surgery [ASDS] members, for every 1 liposuction, there are over 10 noninvasive body sculpting treatments.”
There were 408,000 body-sculpting procedures performed in 2017. More than half of those (208,000) were cryolipolysis, followed by use of radiofrequency (89,000), deoxycholic acid (46,000), laser lipolysis (25,000), “other” procedures (25,000), and tumescent liposuction (15,000), according to data from the ASDS.
“Each treatment has improved in efficacy with time,” Dr. Avram said.
Devices currently cleared by the Food and Drug Administration for the noninvasive removal of fat include ultrasound, lasers, low-level laser therapy, cryolipolysis, and radiofrequency. One of the most common is low-level laser therapy.
“There are several different devices on the market, but there’s no good histology to confirm mechanism of action, so you question what the efficacy is,” said Dr. Avram, who is also the immediate past president of the American Society for Laser Medicine and Surgery.
SculpSure
In the traditional laser domain, the one most commonly used for fat removal is SculpSure, an FDA-cleared hyperthermic 1,060-nm diode laser. It features four flat, nonsuction applicators, a contact cooling system, and it enables the user to treat more than one area in a 25-minute session. There is minimal absorption by melanin.
“You shouldn’t treat over tattoos, however, because if there’s black ink, the tattoo will absorb the wavelength,” Dr. Avram said. “It’s safe in all skin types and there are a variety of different configurations you can use to treat the desired area.”
Initially there is a 4-minute warm-up cycle to achieve the target temperature. Over the next 21 minutes, 1,060-nm energy is delivered via proprietary modulation, alternating between heat and cooling.
“There is definitely some pain with this device,” he said. “Whether or not it’s a relevant endpoint is not known at this point. But typically, if you’re destroying fat with heat there should be some pain. It’s relieved by a period of cooling. A submental fat treatment is now available. I have not personally used it, but it’s the same technology.”
CoolSculpting
Another popular technology is cryolipolysis (CoolSculpting), which was developed at Massachusetts General Hospital by R. Rox Anderson, MD, and Dieter Manstein, MD, PhD.
It’s FDA cleared for noninvasive fat removal and there have been more than 6 million cryolipolysis treatments performed around the world. The purported mechanism of action is selective crystallization of lipids and fat cells at temperatures below freezing. An inflammatory process results in fat reduction over 2-4 months.
“When it first started, cryolipolysis was designed to treat local areas like love handles in males,” Dr. Avram said. “Over time, applicators have been designed to treat different areas, most recently, one for the posterior upper arms and above the knees. There is now a larger, faster CoolSculpting applicator which results in a 35-minute treatment. It’s a little larger, there’s a little less pain, a lower temperature, and it’s a little bit more effective. This has been helpful in our practice in terms of getting more treatment cycles in a visit.”
Postprocedurally, massage may improve clinical results by mobilizing lipid crystals created from treatment.
Extracorporeal shock wave therapy
Another modality to consider is extracorporeal shock wave therapy, which is the application of mechanically generated external sound waves. “It’s not the same as ultrasound or focused ultrasound, and it’s FDA cleared for the treatment of cellulite,” Dr. Avram said.
EmSculpt
A newer innovation, known as High Intensity Focused Electromagnetic (HIFEM) technology (EmSculpt), induces 20,000 forced muscle contractions per session, which leads to supramaximal contractions that can’t be achieved through normal voluntary muscle action.
“The idea is that you’re getting hypertrophy of the muscle to get volumetric growth,” he said. “There’s believed to be a cascaded apoptotic effect, inducing apoptosis and fat disruption.”
Dr. Avram added that HIFEM is nonionizing, nonradiating, nonthermal, and it does not affect sensory nerves. “It’s designed to only stimulate motor neurons. Time will tell in terms of what the ultimate results are with that device.”
truSculpt
Some clinicians are using monopolar radiofrequency with truSculpt, the proprietary delivery of deep radiofrequency energy. This device increases fat temperature between 6 and 10 degrees Celsius with dual frequency at 1 and 2 MHz.
Published data show that 45 degrees Celsius sustained for 3 minutes resulted in a 60% loss of adipose tissue viability (Lasers Surg Med. 2009;41:745-50; Lasers Surg Med. 2010;42:361-70).
“The heat delivery induces cell apoptosis, leading to the removal of those cells by natural healing processes,” said Dr. Avram, who added that he has not used the device. “We need more clinical data to assess this as well.”
Selective photothermolysis
Another technology being evaluated for fat removal is selective photothermolysis, a concept developed at Massachusetts General Hospital in 1983. It extends the theory of selective photothermolysis to target the lipids that make up subcutaneous fat.
“The theory is that you must select a wavelength well absorbed by the target chromophore with a pulse duration shorter than the target’s thermal relaxation time,” Dr. Avram explained. “This produces selective, localized heating with focal destruction of the target with minimal damage to the surrounding tissue. It requires a deeply penetrating wavelength.”
Lipids are a tempting target “because they heat quickly and easily and they do not lose their heat easily to surrounding structures. You want to target fat selectively and confine thermal damage effectively,” he said.
Nearly 10 years ago, Dr. Avram and his associates evaluated the effects of noninvasive 1,210-nm laser exposure on the adipose tissue of 24 patients with skin types 1-5 (Laser Surg Med. 2009;41:401-7).
“The laser pulses were painful, which limited the efficacy,” he said.
The contact cooling device failed in some subjects, and two patients had bulla, but no scarring. Histologic evidence of laser-induced fat damage was observed in 89% of test sites at 4-7 weeks, but dermal damage was also seen.
“This was the first study to show histologic evidence of laser-induced damage to subcutaneous fat,” Dr. Avram said.
Development of selective photothermolysis technology fell off the wayside after the Great Recession of 2008, but it is still being evaluated at Massachusetts General Hospital and other centers.
To optimize the technology, Dr. Avram said that longer pulse durations may target larger volumes of fat. “Cooling is essential to protect the epidermis, as well as to control pain.”
Injectables
Injectables provide a new, minimally invasive means to achieve noninvasive fat removal, Dr. Avram noted.
“Many injectables of questionable efficacy and safety had been available internationally for years,” he said, but none had FDA clearance until 2015, when the agency gave ATX-101 (Kybella) the nod.
ATX-101 is a nonanimal-derived formulation of deoxycholic acid that causes preferential adipocytolysis. Data from a phase 3 trial presented at the 2014 American Society of Plastic Surgery and the American Society of Aesthetic Plastic Surgery meetings showed a statistically significant reduction in submental fat among subjects who received ATX-101, compared with placebo. It requires an average of 2-4 treatments.
“In my experience, it tends not to require that many, but based on MRI, as well as clinician and patient-reported outcomes, there are significant improvements in the visual impact of chin fat,” Dr. Avram said.
Most adverse events are mild to moderate in severity, primarily bruising, pain, and a sensation of numbness to the anesthesia. “They decrease in incidence and severity over successive treatments, and they infrequently lead to discontinuation of treatment,” he said.
For submental fat, clinicians can combine cryolipolysis and deoxycholic acid. “Here, the idea is to assess the amount of fat targeted for treatment,” Dr. Avram said. “If the fat fills the cryolipolysis cup, use cryolipolysis alone. If the fat does not fill the cup, inject deoxycholic acid for a more targeted treatment. If there is residual fat after cryolipolysis, consider treating more focally with deoxycholic acid.”
Both treatments can produce temporary marginal mandibular nerve injury. “It’s not common, but that’s something to include in your consent forms,” he said.
Dr. Avram reported that he has received consulting fees from Allergan, Merz Pharma, Sciton, Soliton, and Zalea. He also reported having ownership and/or shareholder interest in Cytrellis Biosystems, Invasix, and Zalea.
[email protected]
EXPERT ANALYSIS FROM MOAS 2018
Years after ALLHAT, alpha-blocker use still common, risky
CHICAGO – The risk of cardiovascular and hypotension-related events is higher with alpha-blockers than with other hypertension drugs, but almost 20 years after the pivotal ALLHAT trial first raised safety concerns, they are still widely used, according to investigators from the University of Ottawa.
ALLHAT (Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial) linked the alpha-blocker doxazosin (Cardura) to an increased risk of heart failure and stroke, which led to the early cessation of the doxazosin arm. Guidelines no longer include alpha-blockers among the primary options for hypertension (JAMA. 2000;283[15]:1967-75).
However, there’s been some doubt about ALLHAT; doxazosin patients had diuretics withdrawn as part of the study, which might have contributed to the increased risks. “A lot of arguments have been made that perhaps alpha-blockers aren’t that bad and maybe should still be used, so we took a second look,” said lead investigator and nephrologist Swapnil Hiremath, MD, an assistant professor of medicine at the University of Ottawa.
What he and his team found “confirmed and expanded on the findings of ALLHAT.” Apart from a few specific situations, “don’t prescribe alpha-blockers. If a patient is on an alpha-blocker, consider prescribing an alternative,” Dr. Hiremath said at the joint scientific sessions of the American Heart Association Council on Hypertension, AHA Council on Kidney in Cardiovascular Disease, and American Society of Hypertension.
The drugs are still widely used, according to the team’s review of Ontario health data. From 1995 to 2015, nearly 81,000 patients were prescribed alpha-blockers for hypertension, sometimes as monotherapy, with no real downward trend in prescriptions over time.
There are some selected indications for alpha-blockers, including intolerance of other antihypertensives, pheochromocytoma management, and resistant hypertension. “So I thought maybe there would be 5,000 or 10,000. The fact that we found almost 81,000 was an eye-opener. I’m pretty sure 81,000 patients in Ontario don’t have resistant hypertension,” Dr. Hiremath said.
Patients with benign prostatic hypertrophy, another indication, were excluded from the study.
Before ALLHAT, alpha-blockers were considered first-line drugs, so maybe prescribers are just “sticking with something they know and are familiar with,” he said.
To assess the risks of continued use, the investigators used propensity scoring to match 69,092 patients prescribed alpha-blockers to 69,092 who were prescribed other antihypertensives, based on age, comorbidities, date of treatment, and a slew of other potential confounders. Patients were considered to be on an alpha-blocker only when they were filling prescriptions for the drugs. If they were not filling prescriptions they flipped into the unexposed arm.
The incident rates of ED visits and hospitalizations for hypotension and related complications – syncope, falls, and fractures – were markedly higher among alpha-blocker users. After adjusting for the total number of antihypertensives patients were on, those on alpha-blockers were 34% more likely to go to the ED or be hospitalized for hypotension, 49% more likely for syncope, 27% more likely for falls, and 41% more likely for fractures. First-dose effects don’t explain the findings; patients were often on alpha-blockers for years beforehand.
Alpha-blocker patients were also 26% more likely to have a major cardiovascular event, including heart failure and MI. The risks were greatest in those older than age 85 years. The results were all statistically significant.
About 9,000 alpha-blocker patients had a fracture versus 3,351 matched patients on other antihypertensives; “9,000 patients out of 70,000 is a huge number. These drugs are useful in some situations, but be careful,” Dr. Hiremath said.
“This is observational data, but it’s consistent with ALLHAT, and the outcomes are even worse. We didn’t in [subsequent] guidelines say that you should [never] use an alpha-blocker in hypertension. Maybe we should have,” said ALLHAT investigator William Cushman, MD, a professor of medicine and physiology at the University of Tennessee, Memphis.
There was no industry funding for the work, and the investigators reported having no financial disclosures. Dr. Cushman wasn’t involved in the work.
SOURCE: Hiremath S et al. Joint Hypertension 2018, Abstract P375.
CHICAGO – The risk of cardiovascular and hypotension-related events is higher with alpha-blockers than with other hypertension drugs, but almost 20 years after the pivotal ALLHAT trial first raised safety concerns, they are still widely used, according to investigators from the University of Ottawa.
ALLHAT (Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial) linked the alpha-blocker doxazosin (Cardura) to an increased risk of heart failure and stroke, which led to the early cessation of the doxazosin arm. Guidelines no longer include alpha-blockers among the primary options for hypertension (JAMA. 2000;283[15]:1967-75).
However, there’s been some doubt about ALLHAT; doxazosin patients had diuretics withdrawn as part of the study, which might have contributed to the increased risks. “A lot of arguments have been made that perhaps alpha-blockers aren’t that bad and maybe should still be used, so we took a second look,” said lead investigator and nephrologist Swapnil Hiremath, MD, an assistant professor of medicine at the University of Ottawa.
What he and his team found “confirmed and expanded on the findings of ALLHAT.” Apart from a few specific situations, “don’t prescribe alpha-blockers. If a patient is on an alpha-blocker, consider prescribing an alternative,” Dr. Hiremath said at the joint scientific sessions of the American Heart Association Council on Hypertension, AHA Council on Kidney in Cardiovascular Disease, and American Society of Hypertension.
The drugs are still widely used, according to the team’s review of Ontario health data. From 1995 to 2015, nearly 81,000 patients were prescribed alpha-blockers for hypertension, sometimes as monotherapy, with no real downward trend in prescriptions over time.
There are some selected indications for alpha-blockers, including intolerance of other antihypertensives, pheochromocytoma management, and resistant hypertension. “So I thought maybe there would be 5,000 or 10,000. The fact that we found almost 81,000 was an eye-opener. I’m pretty sure 81,000 patients in Ontario don’t have resistant hypertension,” Dr. Hiremath said.
Patients with benign prostatic hypertrophy, another indication, were excluded from the study.
Before ALLHAT, alpha-blockers were considered first-line drugs, so maybe prescribers are just “sticking with something they know and are familiar with,” he said.
To assess the risks of continued use, the investigators used propensity scoring to match 69,092 patients prescribed alpha-blockers to 69,092 who were prescribed other antihypertensives, based on age, comorbidities, date of treatment, and a slew of other potential confounders. Patients were considered to be on an alpha-blocker only when they were filling prescriptions for the drugs. If they were not filling prescriptions they flipped into the unexposed arm.
The incident rates of ED visits and hospitalizations for hypotension and related complications – syncope, falls, and fractures – were markedly higher among alpha-blocker users. After adjusting for the total number of antihypertensives patients were on, those on alpha-blockers were 34% more likely to go to the ED or be hospitalized for hypotension, 49% more likely for syncope, 27% more likely for falls, and 41% more likely for fractures. First-dose effects don’t explain the findings; patients were often on alpha-blockers for years beforehand.
Alpha-blocker patients were also 26% more likely to have a major cardiovascular event, including heart failure and MI. The risks were greatest in those older than age 85 years. The results were all statistically significant.
About 9,000 alpha-blocker patients had a fracture versus 3,351 matched patients on other antihypertensives; “9,000 patients out of 70,000 is a huge number. These drugs are useful in some situations, but be careful,” Dr. Hiremath said.
“This is observational data, but it’s consistent with ALLHAT, and the outcomes are even worse. We didn’t in [subsequent] guidelines say that you should [never] use an alpha-blocker in hypertension. Maybe we should have,” said ALLHAT investigator William Cushman, MD, a professor of medicine and physiology at the University of Tennessee, Memphis.
There was no industry funding for the work, and the investigators reported having no financial disclosures. Dr. Cushman wasn’t involved in the work.
SOURCE: Hiremath S et al. Joint Hypertension 2018, Abstract P375.
CHICAGO – The risk of cardiovascular and hypotension-related events is higher with alpha-blockers than with other hypertension drugs, but almost 20 years after the pivotal ALLHAT trial first raised safety concerns, they are still widely used, according to investigators from the University of Ottawa.
ALLHAT (Antihypertensive and Lipid-Lowering Treatment to Prevent Heart Attack Trial) linked the alpha-blocker doxazosin (Cardura) to an increased risk of heart failure and stroke, which led to the early cessation of the doxazosin arm. Guidelines no longer include alpha-blockers among the primary options for hypertension (JAMA. 2000;283[15]:1967-75).
However, there’s been some doubt about ALLHAT; doxazosin patients had diuretics withdrawn as part of the study, which might have contributed to the increased risks. “A lot of arguments have been made that perhaps alpha-blockers aren’t that bad and maybe should still be used, so we took a second look,” said lead investigator and nephrologist Swapnil Hiremath, MD, an assistant professor of medicine at the University of Ottawa.
What he and his team found “confirmed and expanded on the findings of ALLHAT.” Apart from a few specific situations, “don’t prescribe alpha-blockers. If a patient is on an alpha-blocker, consider prescribing an alternative,” Dr. Hiremath said at the joint scientific sessions of the American Heart Association Council on Hypertension, AHA Council on Kidney in Cardiovascular Disease, and American Society of Hypertension.
The drugs are still widely used, according to the team’s review of Ontario health data. From 1995 to 2015, nearly 81,000 patients were prescribed alpha-blockers for hypertension, sometimes as monotherapy, with no real downward trend in prescriptions over time.
There are some selected indications for alpha-blockers, including intolerance of other antihypertensives, pheochromocytoma management, and resistant hypertension. “So I thought maybe there would be 5,000 or 10,000. The fact that we found almost 81,000 was an eye-opener. I’m pretty sure 81,000 patients in Ontario don’t have resistant hypertension,” Dr. Hiremath said.
Patients with benign prostatic hypertrophy, another indication, were excluded from the study.
Before ALLHAT, alpha-blockers were considered first-line drugs, so maybe prescribers are just “sticking with something they know and are familiar with,” he said.
To assess the risks of continued use, the investigators used propensity scoring to match 69,092 patients prescribed alpha-blockers to 69,092 who were prescribed other antihypertensives, based on age, comorbidities, date of treatment, and a slew of other potential confounders. Patients were considered to be on an alpha-blocker only when they were filling prescriptions for the drugs. If they were not filling prescriptions they flipped into the unexposed arm.
The incident rates of ED visits and hospitalizations for hypotension and related complications – syncope, falls, and fractures – were markedly higher among alpha-blocker users. After adjusting for the total number of antihypertensives patients were on, those on alpha-blockers were 34% more likely to go to the ED or be hospitalized for hypotension, 49% more likely for syncope, 27% more likely for falls, and 41% more likely for fractures. First-dose effects don’t explain the findings; patients were often on alpha-blockers for years beforehand.
Alpha-blocker patients were also 26% more likely to have a major cardiovascular event, including heart failure and MI. The risks were greatest in those older than age 85 years. The results were all statistically significant.
About 9,000 alpha-blocker patients had a fracture versus 3,351 matched patients on other antihypertensives; “9,000 patients out of 70,000 is a huge number. These drugs are useful in some situations, but be careful,” Dr. Hiremath said.
“This is observational data, but it’s consistent with ALLHAT, and the outcomes are even worse. We didn’t in [subsequent] guidelines say that you should [never] use an alpha-blocker in hypertension. Maybe we should have,” said ALLHAT investigator William Cushman, MD, a professor of medicine and physiology at the University of Tennessee, Memphis.
There was no industry funding for the work, and the investigators reported having no financial disclosures. Dr. Cushman wasn’t involved in the work.
SOURCE: Hiremath S et al. Joint Hypertension 2018, Abstract P375.
REPORTING FROM JOINT HYPERTENSION 2018
Key clinical point:
Major finding: Patients on alpha-blockers, versus other antihypertensives, were 26% more likely to have a major cardiovascular event, including heart failure and MI.
Study details: A propensity score matching study involving about 140,000 patients.
Disclosures: There was no industry funding for the work, and the investigators reported having no financial disclosures.
Source: Hiremath S et al. Joint Hypertension 2018, Abstract P375.
FDA approves Ajovy for migraine prevention
The .
Fremanezumab-vfrm is an injectable anti–calcitonin gene-related peptide monoclonal antibody, the first ever approved by the FDA. It can be administered at a 225-mg dose every month or at a 675-mg dose every 3 months, according to a press release from Teva, the drug’s manufacturer.
FDA approval was based on results from two, phase 3 trials in patients with disabling migraines, one of which involved fremanezumab-vfrm alone, with the other involving the injection in tandem with an oral treatment.
In both trials, patients experienced a reduction of monthly migraine days over a 12-week period. The most common adverse event in both trials was injection site reactions.
“Migraine is a disabling neurological disease that affects more than 36 million people in the United States. About 40 percent of people living with migraine may be appropriate candidates for preventive treatment, yet the majority of them are untreated. I am pleased to have another treatment option that may allow my patients to experience fewer monthly migraine days,” Stephen Silberstein, MD, director of the Jefferson Headache Center at Thomas Jefferson University Hospital in Philadelphia, said in the Teva press release.
The .
Fremanezumab-vfrm is an injectable anti–calcitonin gene-related peptide monoclonal antibody, the first ever approved by the FDA. It can be administered at a 225-mg dose every month or at a 675-mg dose every 3 months, according to a press release from Teva, the drug’s manufacturer.
FDA approval was based on results from two, phase 3 trials in patients with disabling migraines, one of which involved fremanezumab-vfrm alone, with the other involving the injection in tandem with an oral treatment.
In both trials, patients experienced a reduction of monthly migraine days over a 12-week period. The most common adverse event in both trials was injection site reactions.
“Migraine is a disabling neurological disease that affects more than 36 million people in the United States. About 40 percent of people living with migraine may be appropriate candidates for preventive treatment, yet the majority of them are untreated. I am pleased to have another treatment option that may allow my patients to experience fewer monthly migraine days,” Stephen Silberstein, MD, director of the Jefferson Headache Center at Thomas Jefferson University Hospital in Philadelphia, said in the Teva press release.
The .
Fremanezumab-vfrm is an injectable anti–calcitonin gene-related peptide monoclonal antibody, the first ever approved by the FDA. It can be administered at a 225-mg dose every month or at a 675-mg dose every 3 months, according to a press release from Teva, the drug’s manufacturer.
FDA approval was based on results from two, phase 3 trials in patients with disabling migraines, one of which involved fremanezumab-vfrm alone, with the other involving the injection in tandem with an oral treatment.
In both trials, patients experienced a reduction of monthly migraine days over a 12-week period. The most common adverse event in both trials was injection site reactions.
“Migraine is a disabling neurological disease that affects more than 36 million people in the United States. About 40 percent of people living with migraine may be appropriate candidates for preventive treatment, yet the majority of them are untreated. I am pleased to have another treatment option that may allow my patients to experience fewer monthly migraine days,” Stephen Silberstein, MD, director of the Jefferson Headache Center at Thomas Jefferson University Hospital in Philadelphia, said in the Teva press release.
Von Willebrand disease product approved in Europe
The European Commission has granted Shire marketing authorization for vonicog alfa (Veyvondi), a recombinant von Willebrand factor (rVWF) product.
The European Commission (EC) approved vonicog alfa for the treatment of bleeding events and treatment/prevention of surgical bleeding in adults with von Willebrand disease (VWD) when desmopressin treatment alone is ineffective or not indicated.
The product was approved in the United States in 2015 for on-demand treatment and control of bleeding episodes in adults.
The approval means Shire is authorized to market vonicog alfa in the European Union as well as in Iceland, Lichtenstein, and Norway.
The EC’s approval of vonicog alfa was based on outcomes from three clinical trials. This includes a phase 1 study and a pair of phase 3 trials – one in a surgical setting and one in a nonsurgical setting.
Data from these studies are available in the Summary of Product Characteristics for vonicog alfa.The phase 1 trial (NCT00816660) enrolled patients with type 3 or severe type 1 VWD.
The goal was to assess the safety and pharmacokinetics of vonicog alfa combined at a fixed ratio with recombinant factor VIII – referred to as “rVWF-rFVIII.” The researchers compared rVWF-rFVIII with plasma-derived (pd) VWF combined with pdFVIII (pdVWF-pdFVIII).
The safety analysis included 32 patients who received rVWF-rFVIII. There were no thrombotic events, serious adverse events, or new cases of inhibitors to VWF or FVIII in these patients.
The pharmacokinetic analysis included 19 patients. The researchers said the pharmacokinetics of rVWF ristocetin cofactor activity, VWF antigen, and collagen-binding activity were similar with rVWF-rFVIII and pdVWF-pdFVIII.
FVIII levels were higher after infusion with rVWF-rFVIII than with pdVWF-pdFVIII, even after 72 hours. These results were published in Blood (2013 Aug 1;122[5]:648-57).The phase 3 nonsurgical study (NCT01410227) included 49 patients with VWD who received vonicog alfa with or without rFVIII.
All participants had successful treatment of bleeding episodes. Nearly all (96.9%) treated bleeds were given an “excellent” efficacy rating and most (81.8%) were resolved with a single infusion of vonicog alfa; the treatment had a mean half-life of 21.9 hours.
There were eight adverse events considered related to vonicog alfa, two of which were serious. There were no thrombotic events, no treatment-related binding or neutralizing antibodies against VWF, and no neutralizing antibodies against FVIII. These results were published in Blood (2015 Oct 22;126[17]:2038-46).
The phase 3 surgical trial (NCT02283268) enrolled 15 adults with severe VWD who were undergoing elective surgical procedures.
Patients received vonicog alfa at 40-60 IU per kg of body weight 12-24 hours before surgery. Within 3 hours of surgery, each patient’s FVIII level (FVIII:C) was assessed, with a target of 30 IU/dL for minor surgeries and 60 IU/dL for major surgeries.
Within an hour of surgery, patients received a dose of vonicog alfa, with or without rFVIII, depending on the target FVIII:C levels at the 3-hour assessment.
A total of 10 patients received rVWF alone, 12 did not receive any preoperative rFVIII, and 2 did not receive rVWF postoperatively.
The study’s primary endpoint was met. Vonicog alfa demonstrated overall hemostatic efficacy, as assessed 24 hours after the last perioperative infusion or the completion of the study visit, whichever occurred earlier.
One patient developed deep vein thrombosis 3 days after undergoing hip replacement surgery; another tested positive for binding antibodies to VWF. None of the patients developed binding antibodies against potential impurities such as rFurin, CHO protein, or mouse IgG. These results were presented at the at the World Federation of Hemophilia World Congress in May 2018.
The European Commission has granted Shire marketing authorization for vonicog alfa (Veyvondi), a recombinant von Willebrand factor (rVWF) product.
The European Commission (EC) approved vonicog alfa for the treatment of bleeding events and treatment/prevention of surgical bleeding in adults with von Willebrand disease (VWD) when desmopressin treatment alone is ineffective or not indicated.
The product was approved in the United States in 2015 for on-demand treatment and control of bleeding episodes in adults.
The approval means Shire is authorized to market vonicog alfa in the European Union as well as in Iceland, Lichtenstein, and Norway.
The EC’s approval of vonicog alfa was based on outcomes from three clinical trials. This includes a phase 1 study and a pair of phase 3 trials – one in a surgical setting and one in a nonsurgical setting.
Data from these studies are available in the Summary of Product Characteristics for vonicog alfa.The phase 1 trial (NCT00816660) enrolled patients with type 3 or severe type 1 VWD.
The goal was to assess the safety and pharmacokinetics of vonicog alfa combined at a fixed ratio with recombinant factor VIII – referred to as “rVWF-rFVIII.” The researchers compared rVWF-rFVIII with plasma-derived (pd) VWF combined with pdFVIII (pdVWF-pdFVIII).
The safety analysis included 32 patients who received rVWF-rFVIII. There were no thrombotic events, serious adverse events, or new cases of inhibitors to VWF or FVIII in these patients.
The pharmacokinetic analysis included 19 patients. The researchers said the pharmacokinetics of rVWF ristocetin cofactor activity, VWF antigen, and collagen-binding activity were similar with rVWF-rFVIII and pdVWF-pdFVIII.
FVIII levels were higher after infusion with rVWF-rFVIII than with pdVWF-pdFVIII, even after 72 hours. These results were published in Blood (2013 Aug 1;122[5]:648-57).The phase 3 nonsurgical study (NCT01410227) included 49 patients with VWD who received vonicog alfa with or without rFVIII.
All participants had successful treatment of bleeding episodes. Nearly all (96.9%) treated bleeds were given an “excellent” efficacy rating and most (81.8%) were resolved with a single infusion of vonicog alfa; the treatment had a mean half-life of 21.9 hours.
There were eight adverse events considered related to vonicog alfa, two of which were serious. There were no thrombotic events, no treatment-related binding or neutralizing antibodies against VWF, and no neutralizing antibodies against FVIII. These results were published in Blood (2015 Oct 22;126[17]:2038-46).
The phase 3 surgical trial (NCT02283268) enrolled 15 adults with severe VWD who were undergoing elective surgical procedures.
Patients received vonicog alfa at 40-60 IU per kg of body weight 12-24 hours before surgery. Within 3 hours of surgery, each patient’s FVIII level (FVIII:C) was assessed, with a target of 30 IU/dL for minor surgeries and 60 IU/dL for major surgeries.
Within an hour of surgery, patients received a dose of vonicog alfa, with or without rFVIII, depending on the target FVIII:C levels at the 3-hour assessment.
A total of 10 patients received rVWF alone, 12 did not receive any preoperative rFVIII, and 2 did not receive rVWF postoperatively.
The study’s primary endpoint was met. Vonicog alfa demonstrated overall hemostatic efficacy, as assessed 24 hours after the last perioperative infusion or the completion of the study visit, whichever occurred earlier.
One patient developed deep vein thrombosis 3 days after undergoing hip replacement surgery; another tested positive for binding antibodies to VWF. None of the patients developed binding antibodies against potential impurities such as rFurin, CHO protein, or mouse IgG. These results were presented at the at the World Federation of Hemophilia World Congress in May 2018.
The European Commission has granted Shire marketing authorization for vonicog alfa (Veyvondi), a recombinant von Willebrand factor (rVWF) product.
The European Commission (EC) approved vonicog alfa for the treatment of bleeding events and treatment/prevention of surgical bleeding in adults with von Willebrand disease (VWD) when desmopressin treatment alone is ineffective or not indicated.
The product was approved in the United States in 2015 for on-demand treatment and control of bleeding episodes in adults.
The approval means Shire is authorized to market vonicog alfa in the European Union as well as in Iceland, Lichtenstein, and Norway.
The EC’s approval of vonicog alfa was based on outcomes from three clinical trials. This includes a phase 1 study and a pair of phase 3 trials – one in a surgical setting and one in a nonsurgical setting.
Data from these studies are available in the Summary of Product Characteristics for vonicog alfa.The phase 1 trial (NCT00816660) enrolled patients with type 3 or severe type 1 VWD.
The goal was to assess the safety and pharmacokinetics of vonicog alfa combined at a fixed ratio with recombinant factor VIII – referred to as “rVWF-rFVIII.” The researchers compared rVWF-rFVIII with plasma-derived (pd) VWF combined with pdFVIII (pdVWF-pdFVIII).
The safety analysis included 32 patients who received rVWF-rFVIII. There were no thrombotic events, serious adverse events, or new cases of inhibitors to VWF or FVIII in these patients.
The pharmacokinetic analysis included 19 patients. The researchers said the pharmacokinetics of rVWF ristocetin cofactor activity, VWF antigen, and collagen-binding activity were similar with rVWF-rFVIII and pdVWF-pdFVIII.
FVIII levels were higher after infusion with rVWF-rFVIII than with pdVWF-pdFVIII, even after 72 hours. These results were published in Blood (2013 Aug 1;122[5]:648-57).The phase 3 nonsurgical study (NCT01410227) included 49 patients with VWD who received vonicog alfa with or without rFVIII.
All participants had successful treatment of bleeding episodes. Nearly all (96.9%) treated bleeds were given an “excellent” efficacy rating and most (81.8%) were resolved with a single infusion of vonicog alfa; the treatment had a mean half-life of 21.9 hours.
There were eight adverse events considered related to vonicog alfa, two of which were serious. There were no thrombotic events, no treatment-related binding or neutralizing antibodies against VWF, and no neutralizing antibodies against FVIII. These results were published in Blood (2015 Oct 22;126[17]:2038-46).
The phase 3 surgical trial (NCT02283268) enrolled 15 adults with severe VWD who were undergoing elective surgical procedures.
Patients received vonicog alfa at 40-60 IU per kg of body weight 12-24 hours before surgery. Within 3 hours of surgery, each patient’s FVIII level (FVIII:C) was assessed, with a target of 30 IU/dL for minor surgeries and 60 IU/dL for major surgeries.
Within an hour of surgery, patients received a dose of vonicog alfa, with or without rFVIII, depending on the target FVIII:C levels at the 3-hour assessment.
A total of 10 patients received rVWF alone, 12 did not receive any preoperative rFVIII, and 2 did not receive rVWF postoperatively.
The study’s primary endpoint was met. Vonicog alfa demonstrated overall hemostatic efficacy, as assessed 24 hours after the last perioperative infusion or the completion of the study visit, whichever occurred earlier.
One patient developed deep vein thrombosis 3 days after undergoing hip replacement surgery; another tested positive for binding antibodies to VWF. None of the patients developed binding antibodies against potential impurities such as rFurin, CHO protein, or mouse IgG. These results were presented at the at the World Federation of Hemophilia World Congress in May 2018.
Study suggests “alarming” diabetes med discontinuation
ORLANDO – Most patients with type 2 diabetes mellitus stop taking their medication within a year, and nearly one-third stop within the first 3 months, a retrospective analysis of claims data for more than 324,000 patients suggests.
The findings in this population of commercially insured adults are startling and highlight a need for interventions to improve treatment persistence, according to Lisa Latts, MD, deputy chief health officer for IBM Watson Health in Cambridge, Mass.
Dr. Latts and her colleagues reviewed medication claims data for 324,136 patients with at least one diagnosis for type 2 diabetes mellitus and one outpatient pharmacy claim for a type 2 diabetes medication after at least 12 prior months without such a claim.
Of those patients, 58% discontinued treatment within 12 months, 31% discontinued within the first 3 months, and 44% discontinued within 6 months, Dr. Latts reported at the annual scientific sessions of the American Diabetes Association.
“Less than half of those patients who discontinued had a restart within the following year. So what we’re seeing here is a huge percentage of individuals who had a diagnosis of type 2 diabetes, were prescribed a medication, and then did not continue the medication,” she said.
Of those who discontinued within the 12-month follow-up, 27% restarted therapy within 60 days and 39% restarted therapy anytime during the 12-month follow-up (mean treatment gap, 107 days). Of those who discontinued by 3 months, 45% restarted within a year (mean treatment gap, 112 days), and of those who discontinued by 6 months, 44% restarted within a year (mean treatment gap, 119 days).
Patients included in the review, which was a collaborative effort of IBM Watson Health and the ADA, had at least 12 months of continuous enrollment in the Truven Health MarketScan Commercial and Medicare Supplemental Databases between 2013 and 2017, before and after the therapy initiation date.
They had a mean age of 55 years, with 28% aged 45-54 years and 35% aged 55-64 years. About 46% were women, and all had at least one diagnosis for type 2 diabetes mellitus during the study period and at least one outpatient pharmacy claim for a type 2 diabetes medication that was prescribed to be taken for at least 30 days.
“As you would expect, far and away the majority [68%] were given metformin,” Dr. Latts said.
Other prescribed treatments after the initial diagnosis included sulfonylureas (7%), insulin (6%), dipeptidyl peptidase–4 inhibitors (6%), sodium-glucose cotransporter 2 inhibitors (1.5%), and a variety of combination treatments – typically metformin plus sulfonylureas (5%).
This study provides real-world evidence that a majority of patients with type 2 diabetes discontinue their treatment within 1 year – an important finding given that medication persistence is imperative for successful treatment, Dr. Latts said. She noted that prior research has shown treatment discontinuation of prescribed medication within the first year is common for a number of chronic disease treatments and is associated with poor clinical outcomes.
“If you treat diabetes, this is alarming,” she said. “These are people who should be on a diabetes med, their doctor probably thinks they’re on a diabetes med, and they’re not taking it.”
The findings are limited by factors associated with the use of administrative claims data, such as possible coding inaccuracies and missed cases in which patients paid out of pocket for medications through low-cost pharmacy offers, as well as by the 12-month window used for the study. She added that the findings may not be generalizable to uninsured or Medicare patients.
Nevertheless, the findings are concerning and may reflect misunderstandings among patients about the need to refill prescriptions after the initial supply runs out, or may relate to side effects that patients don’t report to their physicians, Sherita Golden, MD, of Johns Hopkins University, Baltimore, said during a question-and-answer period following Dr. Latts’ presentation.
“I do treat patients with diabetes so I am very alarmed,” she said, adding that there is a need to improve communication between patients and physicians about treatment and side effects.
Dr. Latts reported relationships with Medtronic, Novo Nordisk, and Sanofi. Her coauthors from IBM Watson and the ADA all reported having no financial disclosures.
SOURCE: Latts L et al. ADA 2018, Abstract 135-OR.
ORLANDO – Most patients with type 2 diabetes mellitus stop taking their medication within a year, and nearly one-third stop within the first 3 months, a retrospective analysis of claims data for more than 324,000 patients suggests.
The findings in this population of commercially insured adults are startling and highlight a need for interventions to improve treatment persistence, according to Lisa Latts, MD, deputy chief health officer for IBM Watson Health in Cambridge, Mass.
Dr. Latts and her colleagues reviewed medication claims data for 324,136 patients with at least one diagnosis for type 2 diabetes mellitus and one outpatient pharmacy claim for a type 2 diabetes medication after at least 12 prior months without such a claim.
Of those patients, 58% discontinued treatment within 12 months, 31% discontinued within the first 3 months, and 44% discontinued within 6 months, Dr. Latts reported at the annual scientific sessions of the American Diabetes Association.
“Less than half of those patients who discontinued had a restart within the following year. So what we’re seeing here is a huge percentage of individuals who had a diagnosis of type 2 diabetes, were prescribed a medication, and then did not continue the medication,” she said.
Of those who discontinued within the 12-month follow-up, 27% restarted therapy within 60 days and 39% restarted therapy anytime during the 12-month follow-up (mean treatment gap, 107 days). Of those who discontinued by 3 months, 45% restarted within a year (mean treatment gap, 112 days), and of those who discontinued by 6 months, 44% restarted within a year (mean treatment gap, 119 days).
Patients included in the review, which was a collaborative effort of IBM Watson Health and the ADA, had at least 12 months of continuous enrollment in the Truven Health MarketScan Commercial and Medicare Supplemental Databases between 2013 and 2017, before and after the therapy initiation date.
They had a mean age of 55 years, with 28% aged 45-54 years and 35% aged 55-64 years. About 46% were women, and all had at least one diagnosis for type 2 diabetes mellitus during the study period and at least one outpatient pharmacy claim for a type 2 diabetes medication that was prescribed to be taken for at least 30 days.
“As you would expect, far and away the majority [68%] were given metformin,” Dr. Latts said.
Other prescribed treatments after the initial diagnosis included sulfonylureas (7%), insulin (6%), dipeptidyl peptidase–4 inhibitors (6%), sodium-glucose cotransporter 2 inhibitors (1.5%), and a variety of combination treatments – typically metformin plus sulfonylureas (5%).
This study provides real-world evidence that a majority of patients with type 2 diabetes discontinue their treatment within 1 year – an important finding given that medication persistence is imperative for successful treatment, Dr. Latts said. She noted that prior research has shown treatment discontinuation of prescribed medication within the first year is common for a number of chronic disease treatments and is associated with poor clinical outcomes.
“If you treat diabetes, this is alarming,” she said. “These are people who should be on a diabetes med, their doctor probably thinks they’re on a diabetes med, and they’re not taking it.”
The findings are limited by factors associated with the use of administrative claims data, such as possible coding inaccuracies and missed cases in which patients paid out of pocket for medications through low-cost pharmacy offers, as well as by the 12-month window used for the study. She added that the findings may not be generalizable to uninsured or Medicare patients.
Nevertheless, the findings are concerning and may reflect misunderstandings among patients about the need to refill prescriptions after the initial supply runs out, or may relate to side effects that patients don’t report to their physicians, Sherita Golden, MD, of Johns Hopkins University, Baltimore, said during a question-and-answer period following Dr. Latts’ presentation.
“I do treat patients with diabetes so I am very alarmed,” she said, adding that there is a need to improve communication between patients and physicians about treatment and side effects.
Dr. Latts reported relationships with Medtronic, Novo Nordisk, and Sanofi. Her coauthors from IBM Watson and the ADA all reported having no financial disclosures.
SOURCE: Latts L et al. ADA 2018, Abstract 135-OR.
ORLANDO – Most patients with type 2 diabetes mellitus stop taking their medication within a year, and nearly one-third stop within the first 3 months, a retrospective analysis of claims data for more than 324,000 patients suggests.
The findings in this population of commercially insured adults are startling and highlight a need for interventions to improve treatment persistence, according to Lisa Latts, MD, deputy chief health officer for IBM Watson Health in Cambridge, Mass.
Dr. Latts and her colleagues reviewed medication claims data for 324,136 patients with at least one diagnosis for type 2 diabetes mellitus and one outpatient pharmacy claim for a type 2 diabetes medication after at least 12 prior months without such a claim.
Of those patients, 58% discontinued treatment within 12 months, 31% discontinued within the first 3 months, and 44% discontinued within 6 months, Dr. Latts reported at the annual scientific sessions of the American Diabetes Association.
“Less than half of those patients who discontinued had a restart within the following year. So what we’re seeing here is a huge percentage of individuals who had a diagnosis of type 2 diabetes, were prescribed a medication, and then did not continue the medication,” she said.
Of those who discontinued within the 12-month follow-up, 27% restarted therapy within 60 days and 39% restarted therapy anytime during the 12-month follow-up (mean treatment gap, 107 days). Of those who discontinued by 3 months, 45% restarted within a year (mean treatment gap, 112 days), and of those who discontinued by 6 months, 44% restarted within a year (mean treatment gap, 119 days).
Patients included in the review, which was a collaborative effort of IBM Watson Health and the ADA, had at least 12 months of continuous enrollment in the Truven Health MarketScan Commercial and Medicare Supplemental Databases between 2013 and 2017, before and after the therapy initiation date.
They had a mean age of 55 years, with 28% aged 45-54 years and 35% aged 55-64 years. About 46% were women, and all had at least one diagnosis for type 2 diabetes mellitus during the study period and at least one outpatient pharmacy claim for a type 2 diabetes medication that was prescribed to be taken for at least 30 days.
“As you would expect, far and away the majority [68%] were given metformin,” Dr. Latts said.
Other prescribed treatments after the initial diagnosis included sulfonylureas (7%), insulin (6%), dipeptidyl peptidase–4 inhibitors (6%), sodium-glucose cotransporter 2 inhibitors (1.5%), and a variety of combination treatments – typically metformin plus sulfonylureas (5%).
This study provides real-world evidence that a majority of patients with type 2 diabetes discontinue their treatment within 1 year – an important finding given that medication persistence is imperative for successful treatment, Dr. Latts said. She noted that prior research has shown treatment discontinuation of prescribed medication within the first year is common for a number of chronic disease treatments and is associated with poor clinical outcomes.
“If you treat diabetes, this is alarming,” she said. “These are people who should be on a diabetes med, their doctor probably thinks they’re on a diabetes med, and they’re not taking it.”
The findings are limited by factors associated with the use of administrative claims data, such as possible coding inaccuracies and missed cases in which patients paid out of pocket for medications through low-cost pharmacy offers, as well as by the 12-month window used for the study. She added that the findings may not be generalizable to uninsured or Medicare patients.
Nevertheless, the findings are concerning and may reflect misunderstandings among patients about the need to refill prescriptions after the initial supply runs out, or may relate to side effects that patients don’t report to their physicians, Sherita Golden, MD, of Johns Hopkins University, Baltimore, said during a question-and-answer period following Dr. Latts’ presentation.
“I do treat patients with diabetes so I am very alarmed,” she said, adding that there is a need to improve communication between patients and physicians about treatment and side effects.
Dr. Latts reported relationships with Medtronic, Novo Nordisk, and Sanofi. Her coauthors from IBM Watson and the ADA all reported having no financial disclosures.
SOURCE: Latts L et al. ADA 2018, Abstract 135-OR.
REPORTING FROM ADA 2018
Key clinical point:
Major finding: In total, 58% of patients discontinued treatment within 12 months, and just 39% of those patients restarted within 1 year.
Study details: An analysis of claims data for more than 324,000 patients.
Disclosures: Dr. Latts reported relationships with Medtronic, Novo Nordisk, and Sanofi. Her coauthors from IBM Watson and the American Diabetes Association all reported having no financial disclosures.
Source: Latts L et al. ADA 2018, Abstract 135-OR.
CAR T-cell therapy elicits responses in MM
BOSTON—Early results from a phase 1 trial suggest the chimeric antigen receptor (CAR) T-cell therapy P-BCMA-101 can produce responses in patients with relapsed/refractory multiple myeloma (MM).
All 11 patients treated have experienced some clinical response, with 8 patients achieving a partial response (PR) or better.
The most common adverse events were neutropenia and thrombocytopenia. One patient was suspected to have cytokine release syndrome, but the condition resolved without use of tociluzimab or steroids.
These results were presented at the 2018 CAR-TCR Summit by Eric Ostertag, MD, PhD, chief executive officer of Poseida Therapeutics Inc., the company developing P-BCMA-101.
Dr. Ostertag presented data on 11 patients with heavily pretreated MM. They had a median of six prior therapies. Their median age was 60, and 73% were considered high risk.
Prior to receiving P-BCMA-101, patients received conditioning with fludarabine (30 mg/m2) and cyclophosphamide (300 mg/m2) for 3 days.
Patients were then treated across three dose groups with average CAR T-cell doses of 51×106 (n=3), 152×106 (n=7), and 430×106 (n=1).
As of August 10, 2018, all 11 patients were still on study.
There were no dose-limiting toxicities. Eight patients developed neutropenia, and 5 had thrombocytopenia.
Researchers suspected cytokine release syndrome in one patient, but the condition resolved without tociluzimab or steroid treatment. There was no neurotoxicity reported, and none of the patients required admission to an intensive care unit.
All patients showed improvement in biomarkers following treatment.
Ten patients were evaluable for response by International Myeloma Working Group criteria. Seven of these patients achieved at least a PR, including very good partial responses (VGPRs) and stringent complete response (CR).
The eleventh patient also responded to treatment, but this patient has oligosecretory disease and was only evaluable by PET. The patient had a near-CR by PET.
Poseida Therapeutics would not disclose additional details regarding how many patients achieved a PR, VGPR, or CR, but the company plans to release more information on response at an upcoming meeting.
“The latest data results show that P-BCMA-101 induces deep responses in a heavily pretreated population with relapsed/refractory multiple myeloma, with some patients reaching VGPR and even stringent CR at early efficacy assessments,” Dr. Ostertag said.
“We believe our advantages of a purified product, where all cells express the CAR molecule, and a product with high levels of stem cell memory T cells, producing a more gradual and prolonged immune response against tumor cells, provide a significantly better therapeutic index when compared with other CAR-T therapeutics. We are also encouraged that P-BCMA-101 is demonstrating significant efficacy even at doses that have been ineffective for other anti-BCMA CAR-T therapies and that our response rates continue to improve as the dose increases.”
This study (NCT03288493) is funded by the California Institute for Regenerative Medicine and Poseida Therapeutics.
BOSTON—Early results from a phase 1 trial suggest the chimeric antigen receptor (CAR) T-cell therapy P-BCMA-101 can produce responses in patients with relapsed/refractory multiple myeloma (MM).
All 11 patients treated have experienced some clinical response, with 8 patients achieving a partial response (PR) or better.
The most common adverse events were neutropenia and thrombocytopenia. One patient was suspected to have cytokine release syndrome, but the condition resolved without use of tociluzimab or steroids.
These results were presented at the 2018 CAR-TCR Summit by Eric Ostertag, MD, PhD, chief executive officer of Poseida Therapeutics Inc., the company developing P-BCMA-101.
Dr. Ostertag presented data on 11 patients with heavily pretreated MM. They had a median of six prior therapies. Their median age was 60, and 73% were considered high risk.
Prior to receiving P-BCMA-101, patients received conditioning with fludarabine (30 mg/m2) and cyclophosphamide (300 mg/m2) for 3 days.
Patients were then treated across three dose groups with average CAR T-cell doses of 51×106 (n=3), 152×106 (n=7), and 430×106 (n=1).
As of August 10, 2018, all 11 patients were still on study.
There were no dose-limiting toxicities. Eight patients developed neutropenia, and 5 had thrombocytopenia.
Researchers suspected cytokine release syndrome in one patient, but the condition resolved without tociluzimab or steroid treatment. There was no neurotoxicity reported, and none of the patients required admission to an intensive care unit.
All patients showed improvement in biomarkers following treatment.
Ten patients were evaluable for response by International Myeloma Working Group criteria. Seven of these patients achieved at least a PR, including very good partial responses (VGPRs) and stringent complete response (CR).
The eleventh patient also responded to treatment, but this patient has oligosecretory disease and was only evaluable by PET. The patient had a near-CR by PET.
Poseida Therapeutics would not disclose additional details regarding how many patients achieved a PR, VGPR, or CR, but the company plans to release more information on response at an upcoming meeting.
“The latest data results show that P-BCMA-101 induces deep responses in a heavily pretreated population with relapsed/refractory multiple myeloma, with some patients reaching VGPR and even stringent CR at early efficacy assessments,” Dr. Ostertag said.
“We believe our advantages of a purified product, where all cells express the CAR molecule, and a product with high levels of stem cell memory T cells, producing a more gradual and prolonged immune response against tumor cells, provide a significantly better therapeutic index when compared with other CAR-T therapeutics. We are also encouraged that P-BCMA-101 is demonstrating significant efficacy even at doses that have been ineffective for other anti-BCMA CAR-T therapies and that our response rates continue to improve as the dose increases.”
This study (NCT03288493) is funded by the California Institute for Regenerative Medicine and Poseida Therapeutics.
BOSTON—Early results from a phase 1 trial suggest the chimeric antigen receptor (CAR) T-cell therapy P-BCMA-101 can produce responses in patients with relapsed/refractory multiple myeloma (MM).
All 11 patients treated have experienced some clinical response, with 8 patients achieving a partial response (PR) or better.
The most common adverse events were neutropenia and thrombocytopenia. One patient was suspected to have cytokine release syndrome, but the condition resolved without use of tociluzimab or steroids.
These results were presented at the 2018 CAR-TCR Summit by Eric Ostertag, MD, PhD, chief executive officer of Poseida Therapeutics Inc., the company developing P-BCMA-101.
Dr. Ostertag presented data on 11 patients with heavily pretreated MM. They had a median of six prior therapies. Their median age was 60, and 73% were considered high risk.
Prior to receiving P-BCMA-101, patients received conditioning with fludarabine (30 mg/m2) and cyclophosphamide (300 mg/m2) for 3 days.
Patients were then treated across three dose groups with average CAR T-cell doses of 51×106 (n=3), 152×106 (n=7), and 430×106 (n=1).
As of August 10, 2018, all 11 patients were still on study.
There were no dose-limiting toxicities. Eight patients developed neutropenia, and 5 had thrombocytopenia.
Researchers suspected cytokine release syndrome in one patient, but the condition resolved without tociluzimab or steroid treatment. There was no neurotoxicity reported, and none of the patients required admission to an intensive care unit.
All patients showed improvement in biomarkers following treatment.
Ten patients were evaluable for response by International Myeloma Working Group criteria. Seven of these patients achieved at least a PR, including very good partial responses (VGPRs) and stringent complete response (CR).
The eleventh patient also responded to treatment, but this patient has oligosecretory disease and was only evaluable by PET. The patient had a near-CR by PET.
Poseida Therapeutics would not disclose additional details regarding how many patients achieved a PR, VGPR, or CR, but the company plans to release more information on response at an upcoming meeting.
“The latest data results show that P-BCMA-101 induces deep responses in a heavily pretreated population with relapsed/refractory multiple myeloma, with some patients reaching VGPR and even stringent CR at early efficacy assessments,” Dr. Ostertag said.
“We believe our advantages of a purified product, where all cells express the CAR molecule, and a product with high levels of stem cell memory T cells, producing a more gradual and prolonged immune response against tumor cells, provide a significantly better therapeutic index when compared with other CAR-T therapeutics. We are also encouraged that P-BCMA-101 is demonstrating significant efficacy even at doses that have been ineffective for other anti-BCMA CAR-T therapies and that our response rates continue to improve as the dose increases.”
This study (NCT03288493) is funded by the California Institute for Regenerative Medicine and Poseida Therapeutics.