User login
Worsening cognitive impairments
The history and findings in this case are suggestive of Alzheimer's disease (AD).
AD is the most common type of dementia. It is characterized by cognitive and behavioral impairment that significantly impairs a patient's social and occupational functioning. The predominant AD pathogenesis hypothesis suggests that AD is largely caused by the accumulation of insoluble amyloid beta deposits and neurofibrillary tangles induced by highly phosphorylated tau proteins in the neocortex, hippocampus, and amygdala, as well as significant loss of neurons and synapses, which leads to brain atrophy. Estimates suggest that approximately 6.2 million people ≥ 65 years of age have AD and that by 2060, the number of Americans with AD may increase to 13.8 million, the result of an aging population and the lack of effective prevention and treatment strategies. AD is a chronic disease that confers tremendous emotional and economic burdens to individuals, families, and society.
Insidiously progressive memory loss is commonly seen in patients presenting with AD. As the disease progresses over the course of several years, other areas of cognition are impaired. Patients may develop language disorders (eg, anomic aphasia or anomia) and impairment in visuospatial skills and executive functions. Slowly progressive behavioral changes are also observed in many individuals with AD.
Criteria for the clinical diagnosis of AD (eg, insidious onset of cognitive impairment, clear history of worsening symptoms) have been developed and are frequently employed. Among individuals who meet the core clinical criteria for probable AD dementia, biomarker evidence may help to increase the certainty that AD is the basis of the clinical dementia syndrome. Several cerebrospinal fluid and blood biomarkers have shown excellent diagnostic ability by identifying tau pathology and cerebral amyloid beta for AD. Neuroimaging is becoming increasingly important for identifying the underlying causes of cognitive impairment. Currently, MRI is considered the preferred neuroimaging modality for AD as it enables accurate measurement of the three-dimensional volume of brain structures, particularly the size of the hippocampus and related regions. CT may be used when MRI is not possible, such as in a patient with a pacemaker.
PET is increasingly being used as a noninvasive method for depicting tau pathology deposition and distribution in patients with cognitive impairment. In 2020, the US Food and Drug Administration approved the first tau PET tracer, 18F-flortaucipir, a significant achievement in improving AD diagnosis.
Currently, the only therapies available for AD are symptomatic therapies. Cholinesterase inhibitors and a partial N-methyl-d-aspartate antagonist are the standard medical treatment for AD. Recently approved antiamyloid therapies are also available for patients with mild cognitive impairment or mild dementia. These include aducanumab, a first-in-class amyloid beta–directed antibody that was approved in 2021; and lecanemab, another amyloid beta–directed antibody that was approved in 2023. Both aducanumab and lecanemab are recommended for the treatment of patients with mild cognitive impairment or mild dementia stage of disease, the population in which the safety and efficacy of these newer agents were demonstrated in clinical trials.
Psychotropic agents are often used to treat the secondary symptoms of AD, such as depression, agitation, aggression, hallucinations, delusions, and/or sleep disorders, which can be problematic. Behavioral interventions, including patient-centered approaches and caregiver training, may also be beneficial for managing the cognitive and behavioral manifestations of AD. These modalities are often used in combination with pharmacologic interventions, such as anxiolytics for anxiety and agitation, neuroleptics for delusions or hallucinations, and antidepressants or mood stabilizers for mood disorders and specific manifestations (eg, episodes of anger or rage). Regular physical activity and exercise is also emerging as a potential strategy for delaying AD progression and possibly conferring a protective effect on brain health.
Behavioral interventions, including patient-centered approaches and caregiver training, may also be beneficial for managing the cognitive and behavioral manifestations of AD. These modalities are often used in combination with pharmacologic interventions, such as anxiolytics for anxiety and agitation, neuroleptics for delusions or hallucinations, and antidepressants or mood stabilizers for mood disorders and specific manifestations (eg, episodes of anger or rage). Regular physical activity and exercise is also emerging as a potential strategy for delaying AD progression and possibly conferring a protective effect on brain health.
Jasvinder Chawla, MD, Professor of Neurology, Loyola University Medical Center, Maywood; Director, Clinical Neurophysiology Lab, Department of Neurology, Hines VA Hospital, Hines, IL.
Jasvinder Chawla, MD, has disclosed no relevant financial relationships.
Image Quizzes are fictional or fictionalized clinical scenarios intended to provide evidence-based educational takeaways.
The history and findings in this case are suggestive of Alzheimer's disease (AD).
AD is the most common type of dementia. It is characterized by cognitive and behavioral impairment that significantly impairs a patient's social and occupational functioning. The predominant AD pathogenesis hypothesis suggests that AD is largely caused by the accumulation of insoluble amyloid beta deposits and neurofibrillary tangles induced by highly phosphorylated tau proteins in the neocortex, hippocampus, and amygdala, as well as significant loss of neurons and synapses, which leads to brain atrophy. Estimates suggest that approximately 6.2 million people ≥ 65 years of age have AD and that by 2060, the number of Americans with AD may increase to 13.8 million, the result of an aging population and the lack of effective prevention and treatment strategies. AD is a chronic disease that confers tremendous emotional and economic burdens to individuals, families, and society.
Insidiously progressive memory loss is commonly seen in patients presenting with AD. As the disease progresses over the course of several years, other areas of cognition are impaired. Patients may develop language disorders (eg, anomic aphasia or anomia) and impairment in visuospatial skills and executive functions. Slowly progressive behavioral changes are also observed in many individuals with AD.
Criteria for the clinical diagnosis of AD (eg, insidious onset of cognitive impairment, clear history of worsening symptoms) have been developed and are frequently employed. Among individuals who meet the core clinical criteria for probable AD dementia, biomarker evidence may help to increase the certainty that AD is the basis of the clinical dementia syndrome. Several cerebrospinal fluid and blood biomarkers have shown excellent diagnostic ability by identifying tau pathology and cerebral amyloid beta for AD. Neuroimaging is becoming increasingly important for identifying the underlying causes of cognitive impairment. Currently, MRI is considered the preferred neuroimaging modality for AD as it enables accurate measurement of the three-dimensional volume of brain structures, particularly the size of the hippocampus and related regions. CT may be used when MRI is not possible, such as in a patient with a pacemaker.
PET is increasingly being used as a noninvasive method for depicting tau pathology deposition and distribution in patients with cognitive impairment. In 2020, the US Food and Drug Administration approved the first tau PET tracer, 18F-flortaucipir, a significant achievement in improving AD diagnosis.
Currently, the only therapies available for AD are symptomatic therapies. Cholinesterase inhibitors and a partial N-methyl-d-aspartate antagonist are the standard medical treatment for AD. Recently approved antiamyloid therapies are also available for patients with mild cognitive impairment or mild dementia. These include aducanumab, a first-in-class amyloid beta–directed antibody that was approved in 2021; and lecanemab, another amyloid beta–directed antibody that was approved in 2023. Both aducanumab and lecanemab are recommended for the treatment of patients with mild cognitive impairment or mild dementia stage of disease, the population in which the safety and efficacy of these newer agents were demonstrated in clinical trials.
Psychotropic agents are often used to treat the secondary symptoms of AD, such as depression, agitation, aggression, hallucinations, delusions, and/or sleep disorders, which can be problematic. Behavioral interventions, including patient-centered approaches and caregiver training, may also be beneficial for managing the cognitive and behavioral manifestations of AD. These modalities are often used in combination with pharmacologic interventions, such as anxiolytics for anxiety and agitation, neuroleptics for delusions or hallucinations, and antidepressants or mood stabilizers for mood disorders and specific manifestations (eg, episodes of anger or rage). Regular physical activity and exercise is also emerging as a potential strategy for delaying AD progression and possibly conferring a protective effect on brain health.
Behavioral interventions, including patient-centered approaches and caregiver training, may also be beneficial for managing the cognitive and behavioral manifestations of AD. These modalities are often used in combination with pharmacologic interventions, such as anxiolytics for anxiety and agitation, neuroleptics for delusions or hallucinations, and antidepressants or mood stabilizers for mood disorders and specific manifestations (eg, episodes of anger or rage). Regular physical activity and exercise is also emerging as a potential strategy for delaying AD progression and possibly conferring a protective effect on brain health.
Jasvinder Chawla, MD, Professor of Neurology, Loyola University Medical Center, Maywood; Director, Clinical Neurophysiology Lab, Department of Neurology, Hines VA Hospital, Hines, IL.
Jasvinder Chawla, MD, has disclosed no relevant financial relationships.
Image Quizzes are fictional or fictionalized clinical scenarios intended to provide evidence-based educational takeaways.
The history and findings in this case are suggestive of Alzheimer's disease (AD).
AD is the most common type of dementia. It is characterized by cognitive and behavioral impairment that significantly impairs a patient's social and occupational functioning. The predominant AD pathogenesis hypothesis suggests that AD is largely caused by the accumulation of insoluble amyloid beta deposits and neurofibrillary tangles induced by highly phosphorylated tau proteins in the neocortex, hippocampus, and amygdala, as well as significant loss of neurons and synapses, which leads to brain atrophy. Estimates suggest that approximately 6.2 million people ≥ 65 years of age have AD and that by 2060, the number of Americans with AD may increase to 13.8 million, the result of an aging population and the lack of effective prevention and treatment strategies. AD is a chronic disease that confers tremendous emotional and economic burdens to individuals, families, and society.
Insidiously progressive memory loss is commonly seen in patients presenting with AD. As the disease progresses over the course of several years, other areas of cognition are impaired. Patients may develop language disorders (eg, anomic aphasia or anomia) and impairment in visuospatial skills and executive functions. Slowly progressive behavioral changes are also observed in many individuals with AD.
Criteria for the clinical diagnosis of AD (eg, insidious onset of cognitive impairment, clear history of worsening symptoms) have been developed and are frequently employed. Among individuals who meet the core clinical criteria for probable AD dementia, biomarker evidence may help to increase the certainty that AD is the basis of the clinical dementia syndrome. Several cerebrospinal fluid and blood biomarkers have shown excellent diagnostic ability by identifying tau pathology and cerebral amyloid beta for AD. Neuroimaging is becoming increasingly important for identifying the underlying causes of cognitive impairment. Currently, MRI is considered the preferred neuroimaging modality for AD as it enables accurate measurement of the three-dimensional volume of brain structures, particularly the size of the hippocampus and related regions. CT may be used when MRI is not possible, such as in a patient with a pacemaker.
PET is increasingly being used as a noninvasive method for depicting tau pathology deposition and distribution in patients with cognitive impairment. In 2020, the US Food and Drug Administration approved the first tau PET tracer, 18F-flortaucipir, a significant achievement in improving AD diagnosis.
Currently, the only therapies available for AD are symptomatic therapies. Cholinesterase inhibitors and a partial N-methyl-d-aspartate antagonist are the standard medical treatment for AD. Recently approved antiamyloid therapies are also available for patients with mild cognitive impairment or mild dementia. These include aducanumab, a first-in-class amyloid beta–directed antibody that was approved in 2021; and lecanemab, another amyloid beta–directed antibody that was approved in 2023. Both aducanumab and lecanemab are recommended for the treatment of patients with mild cognitive impairment or mild dementia stage of disease, the population in which the safety and efficacy of these newer agents were demonstrated in clinical trials.
Psychotropic agents are often used to treat the secondary symptoms of AD, such as depression, agitation, aggression, hallucinations, delusions, and/or sleep disorders, which can be problematic. Behavioral interventions, including patient-centered approaches and caregiver training, may also be beneficial for managing the cognitive and behavioral manifestations of AD. These modalities are often used in combination with pharmacologic interventions, such as anxiolytics for anxiety and agitation, neuroleptics for delusions or hallucinations, and antidepressants or mood stabilizers for mood disorders and specific manifestations (eg, episodes of anger or rage). Regular physical activity and exercise is also emerging as a potential strategy for delaying AD progression and possibly conferring a protective effect on brain health.
Behavioral interventions, including patient-centered approaches and caregiver training, may also be beneficial for managing the cognitive and behavioral manifestations of AD. These modalities are often used in combination with pharmacologic interventions, such as anxiolytics for anxiety and agitation, neuroleptics for delusions or hallucinations, and antidepressants or mood stabilizers for mood disorders and specific manifestations (eg, episodes of anger or rage). Regular physical activity and exercise is also emerging as a potential strategy for delaying AD progression and possibly conferring a protective effect on brain health.
Jasvinder Chawla, MD, Professor of Neurology, Loyola University Medical Center, Maywood; Director, Clinical Neurophysiology Lab, Department of Neurology, Hines VA Hospital, Hines, IL.
Jasvinder Chawla, MD, has disclosed no relevant financial relationships.
Image Quizzes are fictional or fictionalized clinical scenarios intended to provide evidence-based educational takeaways.
A 73-year-old male restaurant manager presents with concerns of progressively worsening cognitive impairment. The patient's symptoms began approximately 2 years ago. At that time, he attributed them to normal aging. Recently, however, he has begun to have increasing difficulties at work. On several occasions, he has forgotten to place important supply orders and has made errors with staff scheduling. His wife reports that he frequently misplaces items at home, such as his cell phone and car keys, and has been experiencing noticeable deficits with his short-term memory. In addition, he has been "unlike himself" for quite some time, with uncharacteristic episodes of depression, anxiety, and emotional lability. The patient's past medical history is significant for mild obesity, hypertension, and dyslipidemia. There is no history of neurotoxic exposure, head injuries, strokes, or seizures. His family history is negative for dementia. Current medications include rosuvastatin 40 mg/d and metoprolol 100 mg/d. His current height and weight are 5 ft 11 in and 223 lb (BMI 31.1).
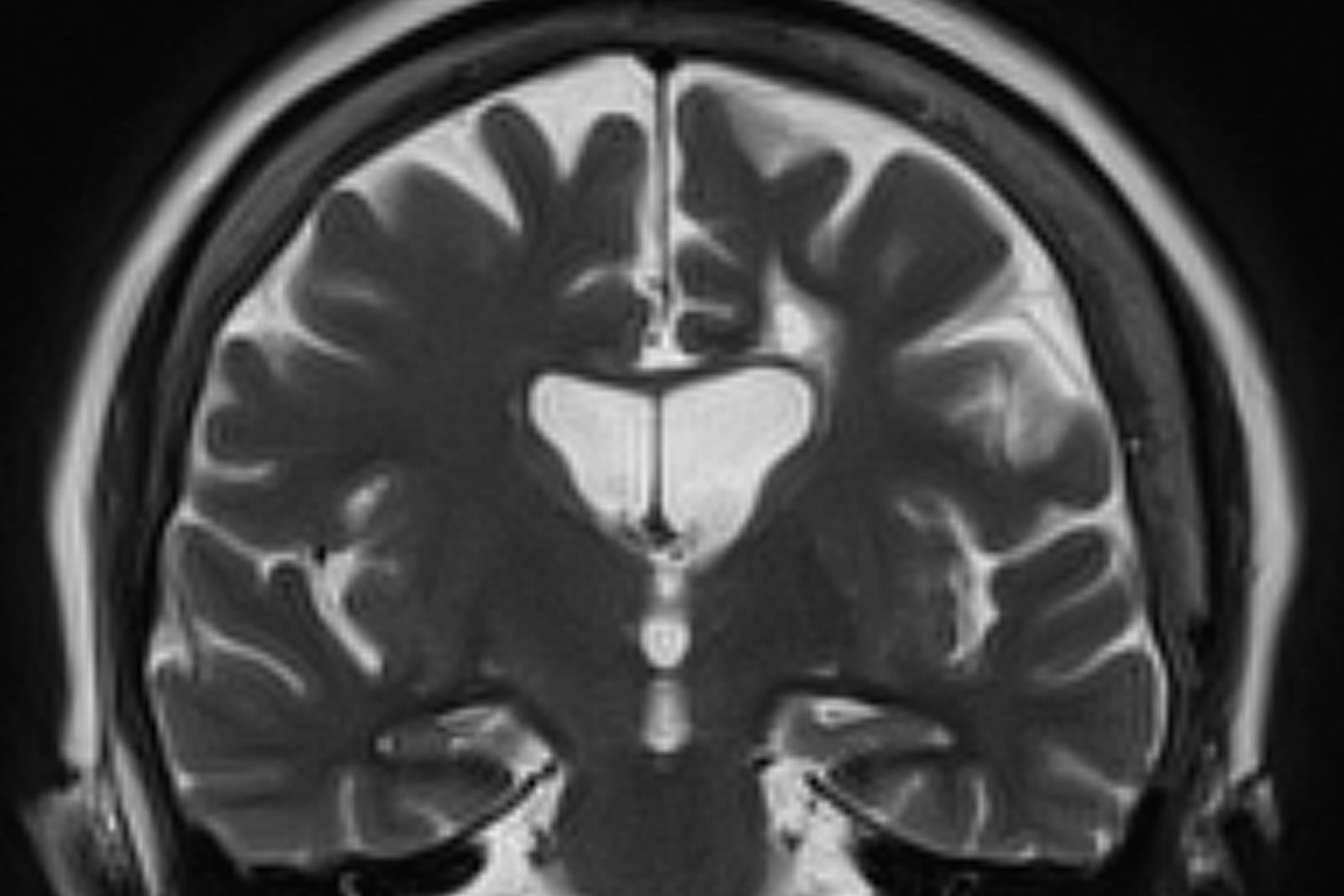
No abnormalities are noted on physical exam; the patient's blood pressure, pulse oximetry, and heart rate are within normal ranges. Laboratory tests are within normal ranges, except for elevated levels of fasting blood glucose level (119 mg/dL) and A1c (6.3%). The patient scores 19 on the Montreal Cognitive Assessment test. His clinician orders MRI scanning, which reveals generalized atrophy of brain tissue and an accentuated loss of tissue involving the temporal lobes.
Nonpharmacologic therapies for T2D: Five things to know
According to the Centers for Disease Control and Prevention National Diabetes Statistic Report, there are more than 37 million adults aged 18 years or older with diabetes in the United States, representing 14.7% of the adult population. Approximately 90%-95% of people diagnosed with diabetes have type 2 diabetes (T2D). An increasing aging population with T2D and a disparate incidence and burden of disease in African American and Hispanic populations raise important care considerations in effective disease assessment and management, especially in primary care, where the majority of diabetes management occurs.
This extends to the need for quality patient education in an effort to give persons with diabetes a better understanding of what it’s like to live with the disease.
Here are five things to know about nonpharmacologic therapies for effective T2D management.
1. Understand and treat the person before the disease.
Diabetes is a complex and unrelenting disease of self-management, requiring an individualized care approach to achieve optimal health outcomes and quality of life for persons living with this condition. Over 90% of care is provided by the person with diabetes, therefore understanding the lived world of the person with diabetes and its connected impact on self-care is critical to establishing effective treatment recommendations, especially for people from racial and ethnic minority groups and lower socioeconomic status where diabetes disparities are highest. Disease prevalence, cost of care, and disease burden are driven by social determinants of health (SDOH) factors that need to be assessed, and strategies addressing causative factors need to be implemented. SDOH factors, including the built environment, safety, financial status, education, food access, health care access, and social support, directly affect the ability of a person with diabetes to effectively implement treatment recommendations, including access to new medications. The adoption of a shared decision-making approach is key to person-centered care. Shared decision-making promotes a positive communication feedback loop, therapeutic patient-care team relationship, and collaborative plan of care between the person with diabetes and the care team. It also supports the establishment of mutual respect between the person with diabetes and the care team members. This cultivates the strong, open, and authentic partnership needed for effective chronic disease management.
2. Quality diabetes education is the foundation for effective self-care.
Diabetes self-management education and support (DSMES) is a fundamental component of diabetes care and ensures patients have the knowledge, skills, motivation, and resources necessary for effectively managing this condition. Despite treatment advances and the evidence base for DSMES, less than 5% of Medicare beneficiaries and 6.8% of privately insured beneficiaries have utilized its services, and this is a likely contributor to the lack of improvement for achieving national diabetes clinical targets. The Association of Diabetes Care and Education Specialists (ADCES7) Self-Care Behaviors provides an evidence-based framework for an optimal DSMES curriculum, incorporating the self-care behaviors of healthy coping (e.g., having a positive attitude toward diabetes self-management), nutritious eating, being active, taking medication, monitoring, reducing risk, and problem-solving.
There are four core times to implement and adapt referral for DSMES: (1) at diagnosis, (2) annually or when not meeting targets, (3) when complications arise, and (4) with transitions in life and care. DSMES referrals should be made for programs accredited by the ADCES or American Diabetes Association (ADA) and led by expert Certified Diabetes Care and Education Specialists (CDCES). The multidisciplinary composition and clinical skill level of CDCES make them a highly valued member of the diabetes care team. CDCES have demonstrated not only diabetes education expertise but are involved in broader health care roles to include population health management, technology integration, mitigation of therapeutic inertia, quality improvement activity, and delivery of cost-effective care.
3. Establish a strong foundation in lifestyle medicine.
Lifestyle medicine encompasses healthy eating, physical activity, restorative sleep, stress management, avoidance of risky behaviors, and positive social connections. It has also been strongly connected as a primary modality to prevent and treat chronic conditions like T2D. Lifestyle modifications have been noted in reducing the incidence of developing diabetes, reversing disease, improving clinical markers such as A1c and lipids, weight reduction, reducing use of medications, and improving quality of life. The multidisciplinary care team and CDCES can support the empowerment of individuals with T2D to develop the life skills and knowledge needed to establish positive self-care behaviors and successfully achieve health goals. Lifestyle medicine is not a replacement for pharmacologic interventions but rather serves as an adjunct when medication management is required.
4. Harness technology in diabetes treatment and care delivery.
Diabetes technology is advancing swiftly and includes glucose monitors, medication delivery devices, data-sharing platforms, and disease self-management applications. Combined with education and support, diabetes technology has been shown to have a positive clinical and personal impact on disease outcomes and quality of life. Regardless of its benefits, at times technology can seem overwhelming for the person with diabetes and the care team. Diabetes Care and Education Specialists (DCES) can support the care team and people living with diabetes to effectively identify, implement, and evaluate patient-centered diabetes technologies, as well as implement processes to drive clinical efficiencies and sustainability. Patient-generated health data reports can provide the care team with effective and proficient evaluation of diabetes care and needed treatment changes.
The expansion of telehealth during the COVID-19 pandemic, including real-time and asynchronous approaches, coupled with in-person care team visits, has resulted in improved access to diabetes care and education. Moreover, there continues to be an expanding health system focus on improving access to care beyond traditional brick and mortar solutions. Telehealth poses one possible access solution for people living with diabetes for whom factors such as transportation, remote geographies, and physical limitations affect their ability to attend in-person care visits.
5. Assess and address diabetes-related distress.
The persistent nature of diabetes self-care expectations and the impact on lifestyle behaviors, medication adherence, and glycemic control demands the need for assessment and treatment of diabetes-related distress (DRD). DRD can be expressed as shame, guilt, anger, fear, and frustration in combination with the everyday context of life priorities and stressors. An assessment of diabetes distress, utilizing a simple scale, should be included as part of an annual therapeutic diabetes care plan. The ADA Standards of Care in Diabetes recommends assessing patients’ psychological and social situations as an ongoing part of medical management, including an annual screening for depression and other psychological problems. The prevalence of depression is nearly twice as high in people with T2D than in the general population and can significantly influence patients’ ability to self-manage their diabetes and achieve healthy outcomes. Assessment and treatment of psychosocial components of care can result in significant improvements in A1c and other positive outcomes, including quality of life.
Kellie M. Rodriguez, director of the global diabetes program at Parkland Health, Dallas, Tex., disclosed ties with the Association of Diabetes Care and Education Specialists.
A version of this article originally appeared on Medscape.com.
According to the Centers for Disease Control and Prevention National Diabetes Statistic Report, there are more than 37 million adults aged 18 years or older with diabetes in the United States, representing 14.7% of the adult population. Approximately 90%-95% of people diagnosed with diabetes have type 2 diabetes (T2D). An increasing aging population with T2D and a disparate incidence and burden of disease in African American and Hispanic populations raise important care considerations in effective disease assessment and management, especially in primary care, where the majority of diabetes management occurs.
This extends to the need for quality patient education in an effort to give persons with diabetes a better understanding of what it’s like to live with the disease.
Here are five things to know about nonpharmacologic therapies for effective T2D management.
1. Understand and treat the person before the disease.
Diabetes is a complex and unrelenting disease of self-management, requiring an individualized care approach to achieve optimal health outcomes and quality of life for persons living with this condition. Over 90% of care is provided by the person with diabetes, therefore understanding the lived world of the person with diabetes and its connected impact on self-care is critical to establishing effective treatment recommendations, especially for people from racial and ethnic minority groups and lower socioeconomic status where diabetes disparities are highest. Disease prevalence, cost of care, and disease burden are driven by social determinants of health (SDOH) factors that need to be assessed, and strategies addressing causative factors need to be implemented. SDOH factors, including the built environment, safety, financial status, education, food access, health care access, and social support, directly affect the ability of a person with diabetes to effectively implement treatment recommendations, including access to new medications. The adoption of a shared decision-making approach is key to person-centered care. Shared decision-making promotes a positive communication feedback loop, therapeutic patient-care team relationship, and collaborative plan of care between the person with diabetes and the care team. It also supports the establishment of mutual respect between the person with diabetes and the care team members. This cultivates the strong, open, and authentic partnership needed for effective chronic disease management.
2. Quality diabetes education is the foundation for effective self-care.
Diabetes self-management education and support (DSMES) is a fundamental component of diabetes care and ensures patients have the knowledge, skills, motivation, and resources necessary for effectively managing this condition. Despite treatment advances and the evidence base for DSMES, less than 5% of Medicare beneficiaries and 6.8% of privately insured beneficiaries have utilized its services, and this is a likely contributor to the lack of improvement for achieving national diabetes clinical targets. The Association of Diabetes Care and Education Specialists (ADCES7) Self-Care Behaviors provides an evidence-based framework for an optimal DSMES curriculum, incorporating the self-care behaviors of healthy coping (e.g., having a positive attitude toward diabetes self-management), nutritious eating, being active, taking medication, monitoring, reducing risk, and problem-solving.
There are four core times to implement and adapt referral for DSMES: (1) at diagnosis, (2) annually or when not meeting targets, (3) when complications arise, and (4) with transitions in life and care. DSMES referrals should be made for programs accredited by the ADCES or American Diabetes Association (ADA) and led by expert Certified Diabetes Care and Education Specialists (CDCES). The multidisciplinary composition and clinical skill level of CDCES make them a highly valued member of the diabetes care team. CDCES have demonstrated not only diabetes education expertise but are involved in broader health care roles to include population health management, technology integration, mitigation of therapeutic inertia, quality improvement activity, and delivery of cost-effective care.
3. Establish a strong foundation in lifestyle medicine.
Lifestyle medicine encompasses healthy eating, physical activity, restorative sleep, stress management, avoidance of risky behaviors, and positive social connections. It has also been strongly connected as a primary modality to prevent and treat chronic conditions like T2D. Lifestyle modifications have been noted in reducing the incidence of developing diabetes, reversing disease, improving clinical markers such as A1c and lipids, weight reduction, reducing use of medications, and improving quality of life. The multidisciplinary care team and CDCES can support the empowerment of individuals with T2D to develop the life skills and knowledge needed to establish positive self-care behaviors and successfully achieve health goals. Lifestyle medicine is not a replacement for pharmacologic interventions but rather serves as an adjunct when medication management is required.
4. Harness technology in diabetes treatment and care delivery.
Diabetes technology is advancing swiftly and includes glucose monitors, medication delivery devices, data-sharing platforms, and disease self-management applications. Combined with education and support, diabetes technology has been shown to have a positive clinical and personal impact on disease outcomes and quality of life. Regardless of its benefits, at times technology can seem overwhelming for the person with diabetes and the care team. Diabetes Care and Education Specialists (DCES) can support the care team and people living with diabetes to effectively identify, implement, and evaluate patient-centered diabetes technologies, as well as implement processes to drive clinical efficiencies and sustainability. Patient-generated health data reports can provide the care team with effective and proficient evaluation of diabetes care and needed treatment changes.
The expansion of telehealth during the COVID-19 pandemic, including real-time and asynchronous approaches, coupled with in-person care team visits, has resulted in improved access to diabetes care and education. Moreover, there continues to be an expanding health system focus on improving access to care beyond traditional brick and mortar solutions. Telehealth poses one possible access solution for people living with diabetes for whom factors such as transportation, remote geographies, and physical limitations affect their ability to attend in-person care visits.
5. Assess and address diabetes-related distress.
The persistent nature of diabetes self-care expectations and the impact on lifestyle behaviors, medication adherence, and glycemic control demands the need for assessment and treatment of diabetes-related distress (DRD). DRD can be expressed as shame, guilt, anger, fear, and frustration in combination with the everyday context of life priorities and stressors. An assessment of diabetes distress, utilizing a simple scale, should be included as part of an annual therapeutic diabetes care plan. The ADA Standards of Care in Diabetes recommends assessing patients’ psychological and social situations as an ongoing part of medical management, including an annual screening for depression and other psychological problems. The prevalence of depression is nearly twice as high in people with T2D than in the general population and can significantly influence patients’ ability to self-manage their diabetes and achieve healthy outcomes. Assessment and treatment of psychosocial components of care can result in significant improvements in A1c and other positive outcomes, including quality of life.
Kellie M. Rodriguez, director of the global diabetes program at Parkland Health, Dallas, Tex., disclosed ties with the Association of Diabetes Care and Education Specialists.
A version of this article originally appeared on Medscape.com.
According to the Centers for Disease Control and Prevention National Diabetes Statistic Report, there are more than 37 million adults aged 18 years or older with diabetes in the United States, representing 14.7% of the adult population. Approximately 90%-95% of people diagnosed with diabetes have type 2 diabetes (T2D). An increasing aging population with T2D and a disparate incidence and burden of disease in African American and Hispanic populations raise important care considerations in effective disease assessment and management, especially in primary care, where the majority of diabetes management occurs.
This extends to the need for quality patient education in an effort to give persons with diabetes a better understanding of what it’s like to live with the disease.
Here are five things to know about nonpharmacologic therapies for effective T2D management.
1. Understand and treat the person before the disease.
Diabetes is a complex and unrelenting disease of self-management, requiring an individualized care approach to achieve optimal health outcomes and quality of life for persons living with this condition. Over 90% of care is provided by the person with diabetes, therefore understanding the lived world of the person with diabetes and its connected impact on self-care is critical to establishing effective treatment recommendations, especially for people from racial and ethnic minority groups and lower socioeconomic status where diabetes disparities are highest. Disease prevalence, cost of care, and disease burden are driven by social determinants of health (SDOH) factors that need to be assessed, and strategies addressing causative factors need to be implemented. SDOH factors, including the built environment, safety, financial status, education, food access, health care access, and social support, directly affect the ability of a person with diabetes to effectively implement treatment recommendations, including access to new medications. The adoption of a shared decision-making approach is key to person-centered care. Shared decision-making promotes a positive communication feedback loop, therapeutic patient-care team relationship, and collaborative plan of care between the person with diabetes and the care team. It also supports the establishment of mutual respect between the person with diabetes and the care team members. This cultivates the strong, open, and authentic partnership needed for effective chronic disease management.
2. Quality diabetes education is the foundation for effective self-care.
Diabetes self-management education and support (DSMES) is a fundamental component of diabetes care and ensures patients have the knowledge, skills, motivation, and resources necessary for effectively managing this condition. Despite treatment advances and the evidence base for DSMES, less than 5% of Medicare beneficiaries and 6.8% of privately insured beneficiaries have utilized its services, and this is a likely contributor to the lack of improvement for achieving national diabetes clinical targets. The Association of Diabetes Care and Education Specialists (ADCES7) Self-Care Behaviors provides an evidence-based framework for an optimal DSMES curriculum, incorporating the self-care behaviors of healthy coping (e.g., having a positive attitude toward diabetes self-management), nutritious eating, being active, taking medication, monitoring, reducing risk, and problem-solving.
There are four core times to implement and adapt referral for DSMES: (1) at diagnosis, (2) annually or when not meeting targets, (3) when complications arise, and (4) with transitions in life and care. DSMES referrals should be made for programs accredited by the ADCES or American Diabetes Association (ADA) and led by expert Certified Diabetes Care and Education Specialists (CDCES). The multidisciplinary composition and clinical skill level of CDCES make them a highly valued member of the diabetes care team. CDCES have demonstrated not only diabetes education expertise but are involved in broader health care roles to include population health management, technology integration, mitigation of therapeutic inertia, quality improvement activity, and delivery of cost-effective care.
3. Establish a strong foundation in lifestyle medicine.
Lifestyle medicine encompasses healthy eating, physical activity, restorative sleep, stress management, avoidance of risky behaviors, and positive social connections. It has also been strongly connected as a primary modality to prevent and treat chronic conditions like T2D. Lifestyle modifications have been noted in reducing the incidence of developing diabetes, reversing disease, improving clinical markers such as A1c and lipids, weight reduction, reducing use of medications, and improving quality of life. The multidisciplinary care team and CDCES can support the empowerment of individuals with T2D to develop the life skills and knowledge needed to establish positive self-care behaviors and successfully achieve health goals. Lifestyle medicine is not a replacement for pharmacologic interventions but rather serves as an adjunct when medication management is required.
4. Harness technology in diabetes treatment and care delivery.
Diabetes technology is advancing swiftly and includes glucose monitors, medication delivery devices, data-sharing platforms, and disease self-management applications. Combined with education and support, diabetes technology has been shown to have a positive clinical and personal impact on disease outcomes and quality of life. Regardless of its benefits, at times technology can seem overwhelming for the person with diabetes and the care team. Diabetes Care and Education Specialists (DCES) can support the care team and people living with diabetes to effectively identify, implement, and evaluate patient-centered diabetes technologies, as well as implement processes to drive clinical efficiencies and sustainability. Patient-generated health data reports can provide the care team with effective and proficient evaluation of diabetes care and needed treatment changes.
The expansion of telehealth during the COVID-19 pandemic, including real-time and asynchronous approaches, coupled with in-person care team visits, has resulted in improved access to diabetes care and education. Moreover, there continues to be an expanding health system focus on improving access to care beyond traditional brick and mortar solutions. Telehealth poses one possible access solution for people living with diabetes for whom factors such as transportation, remote geographies, and physical limitations affect their ability to attend in-person care visits.
5. Assess and address diabetes-related distress.
The persistent nature of diabetes self-care expectations and the impact on lifestyle behaviors, medication adherence, and glycemic control demands the need for assessment and treatment of diabetes-related distress (DRD). DRD can be expressed as shame, guilt, anger, fear, and frustration in combination with the everyday context of life priorities and stressors. An assessment of diabetes distress, utilizing a simple scale, should be included as part of an annual therapeutic diabetes care plan. The ADA Standards of Care in Diabetes recommends assessing patients’ psychological and social situations as an ongoing part of medical management, including an annual screening for depression and other psychological problems. The prevalence of depression is nearly twice as high in people with T2D than in the general population and can significantly influence patients’ ability to self-manage their diabetes and achieve healthy outcomes. Assessment and treatment of psychosocial components of care can result in significant improvements in A1c and other positive outcomes, including quality of life.
Kellie M. Rodriguez, director of the global diabetes program at Parkland Health, Dallas, Tex., disclosed ties with the Association of Diabetes Care and Education Specialists.
A version of this article originally appeared on Medscape.com.
Mixed results on two treatments for erectile dysfunction
presented at the annual meeting of the American Urological Association.
In a single-blind prospective study that evaluated low-intensity shock-wave therapy, researchers randomly assigned 36 men with ED to receive mechanical therapy (n = 22) or sham treatment (n = 14) on their flaccid penises.
The patients in arm 1 of the study received three treatments of 5,000 shocks (4 Hz, 0.12 mJ/mm2) with the UroGold 1000 device (SoftWave) at weeks 0, 3, and 6. Those in arm 2 received a regimen of 5,000 shocks at week 0 and 3,000 at weeks 2 and 3, which was repeated 3 weeks later. Patients who completed sham treatment were unblinded and crossed over to the opposite arm for active treatment.
At weeks 20 and 32, the researchers assessed changes in gray-scale ultrasound erectile tissue homogeneity of the corpora cavernosa using visual grading scores as well as changes in color Duplex Doppler ultrasound assessments of artery blood flow parameters between baseline and follow-up.
Better blood flow – But is that enough?
After shock-wave therapy, more men experienced either improvements in or no worsening of blood flow parameters relative to baseline than after sham treatment. The decrease in end-diastolic volume was statistically significant for men in the active treatment arm 2 at week 32 (P = .003), according to the researchers.
The number of men whose visual grading scores for ultrasound gray-scale images improved in the proximal region was consistently higher with active treatment than with placebo (arm 1: 88.9% vs. 11.1%; arm 2: 40% vs. 20%), with statistical significance in arm 1 at weeks 20 (P = .005) and 32 (P = .001). Patients who received sham treatment and who subsequently received active shock-wave therapy also had improved scores on gray-scale ultrasound (arm 1: 33.3% vs. 11.1%; arm 2: 40% vs. 20%).
Scores on the International Index of Erectile Function (IIEF) were nominally higher for men in active treatment whose visual grading scores had improved compared with those who did not show improvement.
The most common adverse event was transient discomfort after the shock-wave treatment, according to the researchers.
The study provides “a glimpse into the concept” that the mechanotransduction from a shock wave results in biochemical changes, including “activation of stem cells within the corpus cavernosum,” said Irwin Goldstein, MD, director of San Diego Sexual Medicine and clinical professor of surgery at the University of California, San Diego, who led the trial. “If I can activate stem cells,” he added, “theoretically, I can improve the health of tissue.”
Dr. Goldstein noted that the study is the first to use before-and-after objective gray-scale ultrasound imaging along with color Doppler ultrasound. “We could see gray scale changes and peak systolic velocity changes even with a small group,” he said.
Dr. Goldstein added that the trial is the first in which zero energy was used in the sham phase instead of less energy than active treatment. With the sham treatment, there was no benefit on the gray scale, which he said is “very important.”
He said his team is in the process of submitting a proposal for a larger prospective trial to confirm the findings.
Although the results are promising, the study did not evaluate what matters most to men, said Louis Kuritzky, MD, a family medicine physician and assistant professor emeritus at HCA UCF Family Medicine Residency, in Gainesville, Fla.
“Men don’t care what the flow velocity is – they care [whether] they get an erection sufficient for penetration and completion of intercourse. That trial did not look at those endpoints. It looked at surrogates. Those are encouraging, but that’s not what I think a clinician would base their decision upon about whether or not a patient should possibly participate in shock therapy.”
Plasma injections a bust
The trial that assessed platelet-rich plasma was not encouraging. The results of the prospective, double-blind, randomized, placebo-controlled trial suggest that PRP is safe but not effective.
A proprietary version of the PRP injection is marketed as the “Priapus shot,” or the “P-shot,” despite a lack of solid evidence the therapy helps.
Brian Ledesma, MD, an andrology research fellow at the University of Miami, led the study, which received a “best abstract” award at the meeting. “We wanted to actually check and see – does this work or not?” Dr. Ledesma said of PRP injections generally.
Dr. Ledesma and his colleagues randomly assigned 61 men with mild to moderate ED to receive two intracavernosal injections of PRP 1 month apart (n = 28) or placebo treatment (n = 33). The primary outcome was change in IIEF score and the percentage of men meeting minimum clinically important difference (MCID) at 1 month. Complete data were available for 24 men who received PRP and for 28 who received placebo injections.
There was no significant difference in outcomes between the groups. IIEF scores changed from 17.4 (95% confidence interval [CI], –15.8 to 19.0) to 21 (95% CI, 17.9-24.0) for men who received PRP and from 18.6 (95% CI, 17.3-19.8) to 21.6 (95% CI, 19.1-24.1) for men in the placebo group (P = .756). Fourteen men (58.3%) in the PRP group, compared with 15 (53.6%) in the placebo group, met MCID. No differences were seen in mean penile Doppler parameters between PRP and placebo. The two adverse events reported in the trial were minor – a hematoma and “a new plaque that did not cause any curvature of the penis,” Dr. Ledesma said.
Platelet-rich plasma may be “really popular, but, objectively speaking, so far, we don’t have any evidence showing that it actually works.”
The study showed that “PRP was not more efficacious than placebo.” This treatment is “really popular, but, objectively speaking, so far, we don’t have any evidence showing that it actually works.”
Based on these findings, he said, “We would recommend sticking to the data primary care providers should tell their patients, ‘Don’t waste your money,’ because it’s pretty expensive.”
Dr. Kuritzky said more studies are needed for a definitive answer. “I think the results of PRP have been largely disappointing across most of the spheres of influence in which it’s been tried. So, it’s not so surprising to me that this trial would, again, not prove efficacious, but I’d have to hold judgment, dependent upon other trials,” he said.
Dr. Ledesma and his colleagues are conducting a prospective, randomized, double-blind trial “investigating whether PRP combined with shock-wave therapy could make a difference.” He said the trial, which is funded by the National Institutes of Health, is in the enrollment phase; results are expected in mid-2024.
Charles Runels, MD, who pioneered the P-Shot and other popular cosmetic procedures, defended the effectiveness of the injections.
“One of the legitimate criticisms of all of the review articles regarding PRP therapies in every field is that there is a significant variability in what people call PRP. The P-Shot represents a very specific protocol in the methods of preparing PRP, activating PRP, and injecting the PRP – all of which differ significantly from what was done in Ledesma’s study and which could account for their lack of results,” Dr. Runels said in an interview.
Dr. Runels added that “multiple studies” do show benefit of the injection of PRP for both erectile dysfunction and Peyronie’s disease and support the success of his protocol. “Also, all of our providers – there are over 3,000 people in our Cellular Medicine Association – offer money back to our patients if there are not satisfactory results,” he said.
Dr. Kuritzky said that when patients ask him about investigational treatments for ED, he tells them to stick to the more traditional approaches, such as phosphodiesterase type 5 inhibitors, intracorporeal injections, and vacuum devices.
But, he added, if other therapies are shown to be safe and effective “in a large population of men with diverse etiologies associated with their erectile dysfunction, including advanced age, diabetes, dyslipidemia, hypertension, cigarette smoking, then I think [they] could be recommended on a more consistent basis.”
Both studies were independently supported. Dr. Goldstein, Dr. Kuritzky, and Dr. Ledesma reported no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
presented at the annual meeting of the American Urological Association.
In a single-blind prospective study that evaluated low-intensity shock-wave therapy, researchers randomly assigned 36 men with ED to receive mechanical therapy (n = 22) or sham treatment (n = 14) on their flaccid penises.
The patients in arm 1 of the study received three treatments of 5,000 shocks (4 Hz, 0.12 mJ/mm2) with the UroGold 1000 device (SoftWave) at weeks 0, 3, and 6. Those in arm 2 received a regimen of 5,000 shocks at week 0 and 3,000 at weeks 2 and 3, which was repeated 3 weeks later. Patients who completed sham treatment were unblinded and crossed over to the opposite arm for active treatment.
At weeks 20 and 32, the researchers assessed changes in gray-scale ultrasound erectile tissue homogeneity of the corpora cavernosa using visual grading scores as well as changes in color Duplex Doppler ultrasound assessments of artery blood flow parameters between baseline and follow-up.
Better blood flow – But is that enough?
After shock-wave therapy, more men experienced either improvements in or no worsening of blood flow parameters relative to baseline than after sham treatment. The decrease in end-diastolic volume was statistically significant for men in the active treatment arm 2 at week 32 (P = .003), according to the researchers.
The number of men whose visual grading scores for ultrasound gray-scale images improved in the proximal region was consistently higher with active treatment than with placebo (arm 1: 88.9% vs. 11.1%; arm 2: 40% vs. 20%), with statistical significance in arm 1 at weeks 20 (P = .005) and 32 (P = .001). Patients who received sham treatment and who subsequently received active shock-wave therapy also had improved scores on gray-scale ultrasound (arm 1: 33.3% vs. 11.1%; arm 2: 40% vs. 20%).
Scores on the International Index of Erectile Function (IIEF) were nominally higher for men in active treatment whose visual grading scores had improved compared with those who did not show improvement.
The most common adverse event was transient discomfort after the shock-wave treatment, according to the researchers.
The study provides “a glimpse into the concept” that the mechanotransduction from a shock wave results in biochemical changes, including “activation of stem cells within the corpus cavernosum,” said Irwin Goldstein, MD, director of San Diego Sexual Medicine and clinical professor of surgery at the University of California, San Diego, who led the trial. “If I can activate stem cells,” he added, “theoretically, I can improve the health of tissue.”
Dr. Goldstein noted that the study is the first to use before-and-after objective gray-scale ultrasound imaging along with color Doppler ultrasound. “We could see gray scale changes and peak systolic velocity changes even with a small group,” he said.
Dr. Goldstein added that the trial is the first in which zero energy was used in the sham phase instead of less energy than active treatment. With the sham treatment, there was no benefit on the gray scale, which he said is “very important.”
He said his team is in the process of submitting a proposal for a larger prospective trial to confirm the findings.
Although the results are promising, the study did not evaluate what matters most to men, said Louis Kuritzky, MD, a family medicine physician and assistant professor emeritus at HCA UCF Family Medicine Residency, in Gainesville, Fla.
“Men don’t care what the flow velocity is – they care [whether] they get an erection sufficient for penetration and completion of intercourse. That trial did not look at those endpoints. It looked at surrogates. Those are encouraging, but that’s not what I think a clinician would base their decision upon about whether or not a patient should possibly participate in shock therapy.”
Plasma injections a bust
The trial that assessed platelet-rich plasma was not encouraging. The results of the prospective, double-blind, randomized, placebo-controlled trial suggest that PRP is safe but not effective.
A proprietary version of the PRP injection is marketed as the “Priapus shot,” or the “P-shot,” despite a lack of solid evidence the therapy helps.
Brian Ledesma, MD, an andrology research fellow at the University of Miami, led the study, which received a “best abstract” award at the meeting. “We wanted to actually check and see – does this work or not?” Dr. Ledesma said of PRP injections generally.
Dr. Ledesma and his colleagues randomly assigned 61 men with mild to moderate ED to receive two intracavernosal injections of PRP 1 month apart (n = 28) or placebo treatment (n = 33). The primary outcome was change in IIEF score and the percentage of men meeting minimum clinically important difference (MCID) at 1 month. Complete data were available for 24 men who received PRP and for 28 who received placebo injections.
There was no significant difference in outcomes between the groups. IIEF scores changed from 17.4 (95% confidence interval [CI], –15.8 to 19.0) to 21 (95% CI, 17.9-24.0) for men who received PRP and from 18.6 (95% CI, 17.3-19.8) to 21.6 (95% CI, 19.1-24.1) for men in the placebo group (P = .756). Fourteen men (58.3%) in the PRP group, compared with 15 (53.6%) in the placebo group, met MCID. No differences were seen in mean penile Doppler parameters between PRP and placebo. The two adverse events reported in the trial were minor – a hematoma and “a new plaque that did not cause any curvature of the penis,” Dr. Ledesma said.
Platelet-rich plasma may be “really popular, but, objectively speaking, so far, we don’t have any evidence showing that it actually works.”
The study showed that “PRP was not more efficacious than placebo.” This treatment is “really popular, but, objectively speaking, so far, we don’t have any evidence showing that it actually works.”
Based on these findings, he said, “We would recommend sticking to the data primary care providers should tell their patients, ‘Don’t waste your money,’ because it’s pretty expensive.”
Dr. Kuritzky said more studies are needed for a definitive answer. “I think the results of PRP have been largely disappointing across most of the spheres of influence in which it’s been tried. So, it’s not so surprising to me that this trial would, again, not prove efficacious, but I’d have to hold judgment, dependent upon other trials,” he said.
Dr. Ledesma and his colleagues are conducting a prospective, randomized, double-blind trial “investigating whether PRP combined with shock-wave therapy could make a difference.” He said the trial, which is funded by the National Institutes of Health, is in the enrollment phase; results are expected in mid-2024.
Charles Runels, MD, who pioneered the P-Shot and other popular cosmetic procedures, defended the effectiveness of the injections.
“One of the legitimate criticisms of all of the review articles regarding PRP therapies in every field is that there is a significant variability in what people call PRP. The P-Shot represents a very specific protocol in the methods of preparing PRP, activating PRP, and injecting the PRP – all of which differ significantly from what was done in Ledesma’s study and which could account for their lack of results,” Dr. Runels said in an interview.
Dr. Runels added that “multiple studies” do show benefit of the injection of PRP for both erectile dysfunction and Peyronie’s disease and support the success of his protocol. “Also, all of our providers – there are over 3,000 people in our Cellular Medicine Association – offer money back to our patients if there are not satisfactory results,” he said.
Dr. Kuritzky said that when patients ask him about investigational treatments for ED, he tells them to stick to the more traditional approaches, such as phosphodiesterase type 5 inhibitors, intracorporeal injections, and vacuum devices.
But, he added, if other therapies are shown to be safe and effective “in a large population of men with diverse etiologies associated with their erectile dysfunction, including advanced age, diabetes, dyslipidemia, hypertension, cigarette smoking, then I think [they] could be recommended on a more consistent basis.”
Both studies were independently supported. Dr. Goldstein, Dr. Kuritzky, and Dr. Ledesma reported no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
presented at the annual meeting of the American Urological Association.
In a single-blind prospective study that evaluated low-intensity shock-wave therapy, researchers randomly assigned 36 men with ED to receive mechanical therapy (n = 22) or sham treatment (n = 14) on their flaccid penises.
The patients in arm 1 of the study received three treatments of 5,000 shocks (4 Hz, 0.12 mJ/mm2) with the UroGold 1000 device (SoftWave) at weeks 0, 3, and 6. Those in arm 2 received a regimen of 5,000 shocks at week 0 and 3,000 at weeks 2 and 3, which was repeated 3 weeks later. Patients who completed sham treatment were unblinded and crossed over to the opposite arm for active treatment.
At weeks 20 and 32, the researchers assessed changes in gray-scale ultrasound erectile tissue homogeneity of the corpora cavernosa using visual grading scores as well as changes in color Duplex Doppler ultrasound assessments of artery blood flow parameters between baseline and follow-up.
Better blood flow – But is that enough?
After shock-wave therapy, more men experienced either improvements in or no worsening of blood flow parameters relative to baseline than after sham treatment. The decrease in end-diastolic volume was statistically significant for men in the active treatment arm 2 at week 32 (P = .003), according to the researchers.
The number of men whose visual grading scores for ultrasound gray-scale images improved in the proximal region was consistently higher with active treatment than with placebo (arm 1: 88.9% vs. 11.1%; arm 2: 40% vs. 20%), with statistical significance in arm 1 at weeks 20 (P = .005) and 32 (P = .001). Patients who received sham treatment and who subsequently received active shock-wave therapy also had improved scores on gray-scale ultrasound (arm 1: 33.3% vs. 11.1%; arm 2: 40% vs. 20%).
Scores on the International Index of Erectile Function (IIEF) were nominally higher for men in active treatment whose visual grading scores had improved compared with those who did not show improvement.
The most common adverse event was transient discomfort after the shock-wave treatment, according to the researchers.
The study provides “a glimpse into the concept” that the mechanotransduction from a shock wave results in biochemical changes, including “activation of stem cells within the corpus cavernosum,” said Irwin Goldstein, MD, director of San Diego Sexual Medicine and clinical professor of surgery at the University of California, San Diego, who led the trial. “If I can activate stem cells,” he added, “theoretically, I can improve the health of tissue.”
Dr. Goldstein noted that the study is the first to use before-and-after objective gray-scale ultrasound imaging along with color Doppler ultrasound. “We could see gray scale changes and peak systolic velocity changes even with a small group,” he said.
Dr. Goldstein added that the trial is the first in which zero energy was used in the sham phase instead of less energy than active treatment. With the sham treatment, there was no benefit on the gray scale, which he said is “very important.”
He said his team is in the process of submitting a proposal for a larger prospective trial to confirm the findings.
Although the results are promising, the study did not evaluate what matters most to men, said Louis Kuritzky, MD, a family medicine physician and assistant professor emeritus at HCA UCF Family Medicine Residency, in Gainesville, Fla.
“Men don’t care what the flow velocity is – they care [whether] they get an erection sufficient for penetration and completion of intercourse. That trial did not look at those endpoints. It looked at surrogates. Those are encouraging, but that’s not what I think a clinician would base their decision upon about whether or not a patient should possibly participate in shock therapy.”
Plasma injections a bust
The trial that assessed platelet-rich plasma was not encouraging. The results of the prospective, double-blind, randomized, placebo-controlled trial suggest that PRP is safe but not effective.
A proprietary version of the PRP injection is marketed as the “Priapus shot,” or the “P-shot,” despite a lack of solid evidence the therapy helps.
Brian Ledesma, MD, an andrology research fellow at the University of Miami, led the study, which received a “best abstract” award at the meeting. “We wanted to actually check and see – does this work or not?” Dr. Ledesma said of PRP injections generally.
Dr. Ledesma and his colleagues randomly assigned 61 men with mild to moderate ED to receive two intracavernosal injections of PRP 1 month apart (n = 28) or placebo treatment (n = 33). The primary outcome was change in IIEF score and the percentage of men meeting minimum clinically important difference (MCID) at 1 month. Complete data were available for 24 men who received PRP and for 28 who received placebo injections.
There was no significant difference in outcomes between the groups. IIEF scores changed from 17.4 (95% confidence interval [CI], –15.8 to 19.0) to 21 (95% CI, 17.9-24.0) for men who received PRP and from 18.6 (95% CI, 17.3-19.8) to 21.6 (95% CI, 19.1-24.1) for men in the placebo group (P = .756). Fourteen men (58.3%) in the PRP group, compared with 15 (53.6%) in the placebo group, met MCID. No differences were seen in mean penile Doppler parameters between PRP and placebo. The two adverse events reported in the trial were minor – a hematoma and “a new plaque that did not cause any curvature of the penis,” Dr. Ledesma said.
Platelet-rich plasma may be “really popular, but, objectively speaking, so far, we don’t have any evidence showing that it actually works.”
The study showed that “PRP was not more efficacious than placebo.” This treatment is “really popular, but, objectively speaking, so far, we don’t have any evidence showing that it actually works.”
Based on these findings, he said, “We would recommend sticking to the data primary care providers should tell their patients, ‘Don’t waste your money,’ because it’s pretty expensive.”
Dr. Kuritzky said more studies are needed for a definitive answer. “I think the results of PRP have been largely disappointing across most of the spheres of influence in which it’s been tried. So, it’s not so surprising to me that this trial would, again, not prove efficacious, but I’d have to hold judgment, dependent upon other trials,” he said.
Dr. Ledesma and his colleagues are conducting a prospective, randomized, double-blind trial “investigating whether PRP combined with shock-wave therapy could make a difference.” He said the trial, which is funded by the National Institutes of Health, is in the enrollment phase; results are expected in mid-2024.
Charles Runels, MD, who pioneered the P-Shot and other popular cosmetic procedures, defended the effectiveness of the injections.
“One of the legitimate criticisms of all of the review articles regarding PRP therapies in every field is that there is a significant variability in what people call PRP. The P-Shot represents a very specific protocol in the methods of preparing PRP, activating PRP, and injecting the PRP – all of which differ significantly from what was done in Ledesma’s study and which could account for their lack of results,” Dr. Runels said in an interview.
Dr. Runels added that “multiple studies” do show benefit of the injection of PRP for both erectile dysfunction and Peyronie’s disease and support the success of his protocol. “Also, all of our providers – there are over 3,000 people in our Cellular Medicine Association – offer money back to our patients if there are not satisfactory results,” he said.
Dr. Kuritzky said that when patients ask him about investigational treatments for ED, he tells them to stick to the more traditional approaches, such as phosphodiesterase type 5 inhibitors, intracorporeal injections, and vacuum devices.
But, he added, if other therapies are shown to be safe and effective “in a large population of men with diverse etiologies associated with their erectile dysfunction, including advanced age, diabetes, dyslipidemia, hypertension, cigarette smoking, then I think [they] could be recommended on a more consistent basis.”
Both studies were independently supported. Dr. Goldstein, Dr. Kuritzky, and Dr. Ledesma reported no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
FROM AUA 2023
Deep sleep may mitigate the impact of Alzheimer’s pathology
Investigators found that deep sleep, also known as non-REM (NREM) slow-wave sleep, can protect memory function in cognitively normal adults with a high beta-amyloid burden.
“Think of deep sleep almost like a life raft that keeps memory afloat, rather than memory getting dragged down by the weight of Alzheimer’s disease pathology,” senior investigator Matthew Walker, PhD, professor of neuroscience and psychology, University of California, Berkeley, said in a news release.
The study was published online in BMC Medicine.
Resilience factor
Studying resilience to existing brain pathology is “an exciting new research direction,” lead author Zsófia Zavecz, PhD, with the Center for Human Sleep Science at the University of California, Berkeley, said in an interview.
“That is, what factors explain the individual differences in cognitive function despite the same level of brain pathology, and how do some people with significant pathology have largely preserved memory?” she added.
The study included 62 cognitively normal older adults from the Berkeley Aging Cohort Study.
Sleep EEG recordings were obtained over 2 nights in a sleep lab and PET scans were used to quantify beta-amyloid. Half of the participants had high beta-amyloid burden and half were beta-amyloid negative.
After the sleep studies, all participants completed a memory task involving matching names to faces.
The results suggest that deep NREM slow-wave sleep significantly moderates the effect of beta-amyloid status on memory function.
Specifically, NREM slow-wave activity selectively supported superior memory function in adults with high beta-amyloid burden, who are most in need of cognitive reserve (B = 2.694, P = .019), the researchers report.
In contrast, adults without significant beta-amyloid pathological burden – and thus without the same need for cognitive reserve – did not similarly benefit from NREM slow-wave activity (B = –0.115, P = .876).
The findings remained significant after adjusting for age, sex, body mass index, gray matter atrophy, and previously identified cognitive reserve factors, such as education and physical activity.
Dr. Zavecz said there are several potential reasons why deep sleep may support cognitive reserve.
One is that during deep sleep specifically, memories are replayed in the brain, and this results in a “neural reorganization” that helps stabilize the memory and make it more permanent.
“Other explanations include deep sleep’s role in maintaining homeostasis in the brain’s capacity to form new neural connections and providing an optimal brain state for the clearance of toxins interfering with healthy brain functioning,” she noted.
“The extent to which sleep could offer a protective buffer against severe cognitive impairment remains to be tested. However, this study is the first step in hopefully a series of new research that will investigate sleep as a cognitive reserve factor,” said Dr. Zavecz.
Encouraging data
Reached for comment, Percy Griffin, PhD, Alzheimer’s Association director of scientific engagement, said although the study sample is small, the results are “encouraging because sleep is a modifiable factor and can therefore be targeted.”
“More work is needed in a larger population before we can fully leverage this stage of sleep to reduce the risk of developing cognitive decline,” Dr. Griffin said.
Also weighing in on this research, Shaheen Lakhan, MD, PhD, a neurologist and researcher in Boston, said the study is “exciting on two fronts – we may have an additional marker for the development of Alzheimer’s disease to predict risk and track disease, but also targets for early intervention with sleep architecture–enhancing therapies, be they drug, device, or digital.”
“For the sake of our brain health, we all must get very familiar with the concept of cognitive or brain reserve,” said Dr. Lakhan, who was not involved in the study.
“Brain reserve refers to our ability to buttress against the threat of dementia and classically it’s been associated with ongoing brain stimulation (i.e., higher education, cognitively demanding job),” he noted.
“This line of research now opens the door that optimal sleep health – especially deep NREM slow wave sleep – correlates with greater brain reserve against Alzheimer’s disease,” Dr. Lakhan said.
The study was supported by the National Institutes of Health and the University of California, Berkeley. Dr. Walker serves as an advisor to and has equity interest in Bryte, Shuni, Oura, and StimScience. Dr. Zavecz and Dr. Lakhan report no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
Investigators found that deep sleep, also known as non-REM (NREM) slow-wave sleep, can protect memory function in cognitively normal adults with a high beta-amyloid burden.
“Think of deep sleep almost like a life raft that keeps memory afloat, rather than memory getting dragged down by the weight of Alzheimer’s disease pathology,” senior investigator Matthew Walker, PhD, professor of neuroscience and psychology, University of California, Berkeley, said in a news release.
The study was published online in BMC Medicine.
Resilience factor
Studying resilience to existing brain pathology is “an exciting new research direction,” lead author Zsófia Zavecz, PhD, with the Center for Human Sleep Science at the University of California, Berkeley, said in an interview.
“That is, what factors explain the individual differences in cognitive function despite the same level of brain pathology, and how do some people with significant pathology have largely preserved memory?” she added.
The study included 62 cognitively normal older adults from the Berkeley Aging Cohort Study.
Sleep EEG recordings were obtained over 2 nights in a sleep lab and PET scans were used to quantify beta-amyloid. Half of the participants had high beta-amyloid burden and half were beta-amyloid negative.
After the sleep studies, all participants completed a memory task involving matching names to faces.
The results suggest that deep NREM slow-wave sleep significantly moderates the effect of beta-amyloid status on memory function.
Specifically, NREM slow-wave activity selectively supported superior memory function in adults with high beta-amyloid burden, who are most in need of cognitive reserve (B = 2.694, P = .019), the researchers report.
In contrast, adults without significant beta-amyloid pathological burden – and thus without the same need for cognitive reserve – did not similarly benefit from NREM slow-wave activity (B = –0.115, P = .876).
The findings remained significant after adjusting for age, sex, body mass index, gray matter atrophy, and previously identified cognitive reserve factors, such as education and physical activity.
Dr. Zavecz said there are several potential reasons why deep sleep may support cognitive reserve.
One is that during deep sleep specifically, memories are replayed in the brain, and this results in a “neural reorganization” that helps stabilize the memory and make it more permanent.
“Other explanations include deep sleep’s role in maintaining homeostasis in the brain’s capacity to form new neural connections and providing an optimal brain state for the clearance of toxins interfering with healthy brain functioning,” she noted.
“The extent to which sleep could offer a protective buffer against severe cognitive impairment remains to be tested. However, this study is the first step in hopefully a series of new research that will investigate sleep as a cognitive reserve factor,” said Dr. Zavecz.
Encouraging data
Reached for comment, Percy Griffin, PhD, Alzheimer’s Association director of scientific engagement, said although the study sample is small, the results are “encouraging because sleep is a modifiable factor and can therefore be targeted.”
“More work is needed in a larger population before we can fully leverage this stage of sleep to reduce the risk of developing cognitive decline,” Dr. Griffin said.
Also weighing in on this research, Shaheen Lakhan, MD, PhD, a neurologist and researcher in Boston, said the study is “exciting on two fronts – we may have an additional marker for the development of Alzheimer’s disease to predict risk and track disease, but also targets for early intervention with sleep architecture–enhancing therapies, be they drug, device, or digital.”
“For the sake of our brain health, we all must get very familiar with the concept of cognitive or brain reserve,” said Dr. Lakhan, who was not involved in the study.
“Brain reserve refers to our ability to buttress against the threat of dementia and classically it’s been associated with ongoing brain stimulation (i.e., higher education, cognitively demanding job),” he noted.
“This line of research now opens the door that optimal sleep health – especially deep NREM slow wave sleep – correlates with greater brain reserve against Alzheimer’s disease,” Dr. Lakhan said.
The study was supported by the National Institutes of Health and the University of California, Berkeley. Dr. Walker serves as an advisor to and has equity interest in Bryte, Shuni, Oura, and StimScience. Dr. Zavecz and Dr. Lakhan report no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
Investigators found that deep sleep, also known as non-REM (NREM) slow-wave sleep, can protect memory function in cognitively normal adults with a high beta-amyloid burden.
“Think of deep sleep almost like a life raft that keeps memory afloat, rather than memory getting dragged down by the weight of Alzheimer’s disease pathology,” senior investigator Matthew Walker, PhD, professor of neuroscience and psychology, University of California, Berkeley, said in a news release.
The study was published online in BMC Medicine.
Resilience factor
Studying resilience to existing brain pathology is “an exciting new research direction,” lead author Zsófia Zavecz, PhD, with the Center for Human Sleep Science at the University of California, Berkeley, said in an interview.
“That is, what factors explain the individual differences in cognitive function despite the same level of brain pathology, and how do some people with significant pathology have largely preserved memory?” she added.
The study included 62 cognitively normal older adults from the Berkeley Aging Cohort Study.
Sleep EEG recordings were obtained over 2 nights in a sleep lab and PET scans were used to quantify beta-amyloid. Half of the participants had high beta-amyloid burden and half were beta-amyloid negative.
After the sleep studies, all participants completed a memory task involving matching names to faces.
The results suggest that deep NREM slow-wave sleep significantly moderates the effect of beta-amyloid status on memory function.
Specifically, NREM slow-wave activity selectively supported superior memory function in adults with high beta-amyloid burden, who are most in need of cognitive reserve (B = 2.694, P = .019), the researchers report.
In contrast, adults without significant beta-amyloid pathological burden – and thus without the same need for cognitive reserve – did not similarly benefit from NREM slow-wave activity (B = –0.115, P = .876).
The findings remained significant after adjusting for age, sex, body mass index, gray matter atrophy, and previously identified cognitive reserve factors, such as education and physical activity.
Dr. Zavecz said there are several potential reasons why deep sleep may support cognitive reserve.
One is that during deep sleep specifically, memories are replayed in the brain, and this results in a “neural reorganization” that helps stabilize the memory and make it more permanent.
“Other explanations include deep sleep’s role in maintaining homeostasis in the brain’s capacity to form new neural connections and providing an optimal brain state for the clearance of toxins interfering with healthy brain functioning,” she noted.
“The extent to which sleep could offer a protective buffer against severe cognitive impairment remains to be tested. However, this study is the first step in hopefully a series of new research that will investigate sleep as a cognitive reserve factor,” said Dr. Zavecz.
Encouraging data
Reached for comment, Percy Griffin, PhD, Alzheimer’s Association director of scientific engagement, said although the study sample is small, the results are “encouraging because sleep is a modifiable factor and can therefore be targeted.”
“More work is needed in a larger population before we can fully leverage this stage of sleep to reduce the risk of developing cognitive decline,” Dr. Griffin said.
Also weighing in on this research, Shaheen Lakhan, MD, PhD, a neurologist and researcher in Boston, said the study is “exciting on two fronts – we may have an additional marker for the development of Alzheimer’s disease to predict risk and track disease, but also targets for early intervention with sleep architecture–enhancing therapies, be they drug, device, or digital.”
“For the sake of our brain health, we all must get very familiar with the concept of cognitive or brain reserve,” said Dr. Lakhan, who was not involved in the study.
“Brain reserve refers to our ability to buttress against the threat of dementia and classically it’s been associated with ongoing brain stimulation (i.e., higher education, cognitively demanding job),” he noted.
“This line of research now opens the door that optimal sleep health – especially deep NREM slow wave sleep – correlates with greater brain reserve against Alzheimer’s disease,” Dr. Lakhan said.
The study was supported by the National Institutes of Health and the University of California, Berkeley. Dr. Walker serves as an advisor to and has equity interest in Bryte, Shuni, Oura, and StimScience. Dr. Zavecz and Dr. Lakhan report no relevant financial relationships.
A version of this article originally appeared on Medscape.com.
FROM BMC MEDICINE
Parkinson’s in Marines linked to toxic drinking water at Camp Lejeune
in Jacksonville, N.C.
In one of the best-documented, large-scale contaminations in U.S. history, the drinking water at the Marine Corps base was contaminated with TCE and other volatile organic compounds from about 1953 to 1987.
The new study of more than 340,000 service members found the risk of PD was 70% higher in Marines stationed at Camp Lejeune in North Carolina during the years 1975-1985, compared with Marines stationed at Camp Pendleton in Oceanside, Calif.
“This is by far the largest study to look at the association of TCE and PD and the evidence is pretty strong,” lead investigator Samuel M. Goldman, MD, MPH, with University of California, San Francisco, said in an interview.
The link is supported by animal models that show that TCE can induce a neurodegenerative syndrome that is “very similar pathologically to what we see in PD,” Dr. Goldman said.
The study was published online in JAMA Neurology.
‘Hundreds of thousands’ at risk
At Camp Lejeune during the years 1975-1985, the period of maximal contamination, the estimated monthly median TCE level was more than 70-fold the Environmental Protection Agency maximum contaminant level. Maximum contaminant levels were also exceeded for perchloroethylene (PCE) and vinyl chloride.
Dr. Goldman and colleagues had health data on 158,122 veterans – 84,824 from Camp Lejeune and 73,298 from Camp Pendleton – who served for at least 3 months between 1975 and 1985, with follow up from Jan. 1, 1997, to Feb. 17, 2021.
Demographic characteristics were similar between the two groups; most were White men with an average age of 59 years.
A total of 430 veterans had PD: 279 from Camp Lejeune (prevalence, 0.33%) and 151 from Camp Pendleton (prevalence, 0.21%).
In multivariable models, Camp Lejeune veterans had a 70% higher risk for PD (odds ratio, 1.70; 95% confidence interval, 1.39-2.07; P < .001).
“Remarkably,” the researchers noted, among veterans without PD, residence at Camp Lejeune was also associated with a significantly higher risk of having several well-established prodromal features of PD, including tremor, suggesting they may be in a prediagnostic phase of evolving PD pathology.
Importantly, they added, in addition to the exposed service members, “hundreds of thousands of family members and civilian workers exposed to contaminated water at Camp Lejeune may also be at increased risk of PD, cancers, and other health consequences. Continued prospective follow-up of this population is essential.”
‘An unreasonable risk’
The new study supports a prior, and much smaller, study by Dr. Goldman and colleagues showing TCE exposure was associated with a sixfold increased risk for PD.
TCE is a ubiquitous environmental contaminant. The EPA Toxics Release Inventory estimates 2.05 million pounds of TCE was released into the environment from industrial sites in 2017.
In an accompanying editorial, E. Ray Dorsey, MD, with the University of Rochester (N.Y.) and coauthors noted the work of Dr. Goldman and colleagues “increases the certainty” that environmental exposure to TCE and the similar compound PCE “contribute importantly to the cause of the world’s fastest-growing brain disease.”
In December, the EPA found that PCE posed “an unreasonable risk” to human health, and 1 month later, it reached the same conclusion for TCE.
“These actions could lay the foundation for increased regulation and possibly a ban of these two chemicals that have contributed to immeasurable death and disability for generations,” Dr. Dorsey and colleagues noted.
“A U.S. ban would be a step forward but would not address the tens of thousands of TCE/PCE-contaminated sites in the U.S. and around the world or the rising global use of the toxic solvents,” they added.
This research was supported by Department of Veterans Affairs. Dr. Goldman reported no relevant financial relationships. Dr. Dorsey has received personal fees from organizations including the American Neurological Association, Elsevier, International Parkinson and Movement Disorder Society, Massachusetts Medical Society, Michael J. Fox Foundation, National Institutes of Health, and WebMD, as well as numerous pharmaceutical companies.
A version of this article originally appeared on Medscape.com.
in Jacksonville, N.C.
In one of the best-documented, large-scale contaminations in U.S. history, the drinking water at the Marine Corps base was contaminated with TCE and other volatile organic compounds from about 1953 to 1987.
The new study of more than 340,000 service members found the risk of PD was 70% higher in Marines stationed at Camp Lejeune in North Carolina during the years 1975-1985, compared with Marines stationed at Camp Pendleton in Oceanside, Calif.
“This is by far the largest study to look at the association of TCE and PD and the evidence is pretty strong,” lead investigator Samuel M. Goldman, MD, MPH, with University of California, San Francisco, said in an interview.
The link is supported by animal models that show that TCE can induce a neurodegenerative syndrome that is “very similar pathologically to what we see in PD,” Dr. Goldman said.
The study was published online in JAMA Neurology.
‘Hundreds of thousands’ at risk
At Camp Lejeune during the years 1975-1985, the period of maximal contamination, the estimated monthly median TCE level was more than 70-fold the Environmental Protection Agency maximum contaminant level. Maximum contaminant levels were also exceeded for perchloroethylene (PCE) and vinyl chloride.
Dr. Goldman and colleagues had health data on 158,122 veterans – 84,824 from Camp Lejeune and 73,298 from Camp Pendleton – who served for at least 3 months between 1975 and 1985, with follow up from Jan. 1, 1997, to Feb. 17, 2021.
Demographic characteristics were similar between the two groups; most were White men with an average age of 59 years.
A total of 430 veterans had PD: 279 from Camp Lejeune (prevalence, 0.33%) and 151 from Camp Pendleton (prevalence, 0.21%).
In multivariable models, Camp Lejeune veterans had a 70% higher risk for PD (odds ratio, 1.70; 95% confidence interval, 1.39-2.07; P < .001).
“Remarkably,” the researchers noted, among veterans without PD, residence at Camp Lejeune was also associated with a significantly higher risk of having several well-established prodromal features of PD, including tremor, suggesting they may be in a prediagnostic phase of evolving PD pathology.
Importantly, they added, in addition to the exposed service members, “hundreds of thousands of family members and civilian workers exposed to contaminated water at Camp Lejeune may also be at increased risk of PD, cancers, and other health consequences. Continued prospective follow-up of this population is essential.”
‘An unreasonable risk’
The new study supports a prior, and much smaller, study by Dr. Goldman and colleagues showing TCE exposure was associated with a sixfold increased risk for PD.
TCE is a ubiquitous environmental contaminant. The EPA Toxics Release Inventory estimates 2.05 million pounds of TCE was released into the environment from industrial sites in 2017.
In an accompanying editorial, E. Ray Dorsey, MD, with the University of Rochester (N.Y.) and coauthors noted the work of Dr. Goldman and colleagues “increases the certainty” that environmental exposure to TCE and the similar compound PCE “contribute importantly to the cause of the world’s fastest-growing brain disease.”
In December, the EPA found that PCE posed “an unreasonable risk” to human health, and 1 month later, it reached the same conclusion for TCE.
“These actions could lay the foundation for increased regulation and possibly a ban of these two chemicals that have contributed to immeasurable death and disability for generations,” Dr. Dorsey and colleagues noted.
“A U.S. ban would be a step forward but would not address the tens of thousands of TCE/PCE-contaminated sites in the U.S. and around the world or the rising global use of the toxic solvents,” they added.
This research was supported by Department of Veterans Affairs. Dr. Goldman reported no relevant financial relationships. Dr. Dorsey has received personal fees from organizations including the American Neurological Association, Elsevier, International Parkinson and Movement Disorder Society, Massachusetts Medical Society, Michael J. Fox Foundation, National Institutes of Health, and WebMD, as well as numerous pharmaceutical companies.
A version of this article originally appeared on Medscape.com.
in Jacksonville, N.C.
In one of the best-documented, large-scale contaminations in U.S. history, the drinking water at the Marine Corps base was contaminated with TCE and other volatile organic compounds from about 1953 to 1987.
The new study of more than 340,000 service members found the risk of PD was 70% higher in Marines stationed at Camp Lejeune in North Carolina during the years 1975-1985, compared with Marines stationed at Camp Pendleton in Oceanside, Calif.
“This is by far the largest study to look at the association of TCE and PD and the evidence is pretty strong,” lead investigator Samuel M. Goldman, MD, MPH, with University of California, San Francisco, said in an interview.
The link is supported by animal models that show that TCE can induce a neurodegenerative syndrome that is “very similar pathologically to what we see in PD,” Dr. Goldman said.
The study was published online in JAMA Neurology.
‘Hundreds of thousands’ at risk
At Camp Lejeune during the years 1975-1985, the period of maximal contamination, the estimated monthly median TCE level was more than 70-fold the Environmental Protection Agency maximum contaminant level. Maximum contaminant levels were also exceeded for perchloroethylene (PCE) and vinyl chloride.
Dr. Goldman and colleagues had health data on 158,122 veterans – 84,824 from Camp Lejeune and 73,298 from Camp Pendleton – who served for at least 3 months between 1975 and 1985, with follow up from Jan. 1, 1997, to Feb. 17, 2021.
Demographic characteristics were similar between the two groups; most were White men with an average age of 59 years.
A total of 430 veterans had PD: 279 from Camp Lejeune (prevalence, 0.33%) and 151 from Camp Pendleton (prevalence, 0.21%).
In multivariable models, Camp Lejeune veterans had a 70% higher risk for PD (odds ratio, 1.70; 95% confidence interval, 1.39-2.07; P < .001).
“Remarkably,” the researchers noted, among veterans without PD, residence at Camp Lejeune was also associated with a significantly higher risk of having several well-established prodromal features of PD, including tremor, suggesting they may be in a prediagnostic phase of evolving PD pathology.
Importantly, they added, in addition to the exposed service members, “hundreds of thousands of family members and civilian workers exposed to contaminated water at Camp Lejeune may also be at increased risk of PD, cancers, and other health consequences. Continued prospective follow-up of this population is essential.”
‘An unreasonable risk’
The new study supports a prior, and much smaller, study by Dr. Goldman and colleagues showing TCE exposure was associated with a sixfold increased risk for PD.
TCE is a ubiquitous environmental contaminant. The EPA Toxics Release Inventory estimates 2.05 million pounds of TCE was released into the environment from industrial sites in 2017.
In an accompanying editorial, E. Ray Dorsey, MD, with the University of Rochester (N.Y.) and coauthors noted the work of Dr. Goldman and colleagues “increases the certainty” that environmental exposure to TCE and the similar compound PCE “contribute importantly to the cause of the world’s fastest-growing brain disease.”
In December, the EPA found that PCE posed “an unreasonable risk” to human health, and 1 month later, it reached the same conclusion for TCE.
“These actions could lay the foundation for increased regulation and possibly a ban of these two chemicals that have contributed to immeasurable death and disability for generations,” Dr. Dorsey and colleagues noted.
“A U.S. ban would be a step forward but would not address the tens of thousands of TCE/PCE-contaminated sites in the U.S. and around the world or the rising global use of the toxic solvents,” they added.
This research was supported by Department of Veterans Affairs. Dr. Goldman reported no relevant financial relationships. Dr. Dorsey has received personal fees from organizations including the American Neurological Association, Elsevier, International Parkinson and Movement Disorder Society, Massachusetts Medical Society, Michael J. Fox Foundation, National Institutes of Health, and WebMD, as well as numerous pharmaceutical companies.
A version of this article originally appeared on Medscape.com.
FROM JAMA NEUROLOGY
Video-based AI tool estimates LVEF from angiograms
a new study suggests.
In the test dataset, the video-based algorithm, called a deep neural network (DNN), discriminated reduced LVEF (< 40%) with an area under the receiver operating characteristic curve of 0.911.
In the external validation dataset, the DNN discriminated reduced LVEF with an AUROC of 0.906. However, the DNN tended to overestimate low LVEFs and to underestimate high LVEFs.
“We know the findings will be unexpected for cardiologists who don’t typically expect to get an estimate of systolic function or pump function just from an angiogram,” principal investigator Geoffrey H. Tison, MD, of the University of California, San Francisco, said in an interview.
In fact, he noted, “one of the challenges we face is a lack of trust by the health care community. They may not understand what drives the predictions behind our models. We have to translate that information in such a way that physicians trust that the algorithm is using the right features from the data they feed in to make the predictions.”
To help bolster that trust, “we display the ‘Model Facts,’ a nutrition-style label that describes how we train the algorithm, how it was validated, and the inclusion and exclusion criteria,” added lead author Robert Avram, MD, of the University of Montreal.
Model Facts is a safeguard against inappropriate use of the algorithm, Dr. Avram said. For example, if the algorithm was trained on patients between the ages of 40 and 90 and a clinician fed in data for a 35-year-old, a pop-up would appear warning the physician that the data being inputted are different from the data the algorithm was trained and validated on, and so any prediction “should be taken with a grain of salt.”
The study was published online in JAMA Cardiology.
Additional procedure
LVEF can be determined before coronary angiography with transthoracic echocardiography, but that is not always available, particularly for patients being seen emergently for acute coronary syndromes, the researchers wrote. LVEF can also be assessed using left ventriculography, an additional procedure that requires insertion of a pigtail catheter into the left ventricle and injection of more contrast and longer radiation exposure.
“Novel methods to assess LVEF at the point of care during coronary angiography would expand the available options to perform this important physiologic determination,” they wrote. “Video-based deep neural networks can learn subtle patterns from medical data to accomplish certain tasks beyond what physicians can achieve with that data, providing an opportunity to assess cardiac systolic function in real time from standard angiographic images without additional cost or procedures.”
The investigators conducted a cross-sectional study using UCSF patient data from 2012 to 2019. Data were randomly categorized into training, development, and test datasets.
External validation data were obtained from the University of Ottawa Heart Institute.
All adult patients who received a coronary angiogram and a transthoracic echocardiogram (TTE) within 3 months before or 1 month after receiving the angiogram were included.
A total of 4,042 angiograms with corresponding TTE LVEF from 3,679 UCSF patients were included in the analysis. The mean age of the patients was 64.3 years, and 65% were men.
The researchers’ video-based DNN, called CathEF, was used to discriminate reduced LVEF and to predict a continuous LVEF percentage from standard angiogram videos of the left coronary artery.
In the UCSF test dataset, CathEF discriminated reduced LVEF with an AUROC of 0.911; the diagnostic odds ratio for reduced LVEF was 22.7.
Furthermore, the CathEF-predicted that LVEF had a mean absolute error (MAE) of 8.5%, compared with TTE LVEF.
The CathEF-predicted LVEF differed 5% or less in comparison with the TTE LVEF in 38% of the test dataset studies; however, differences greater than 15% were seen in 15.2% of cases.
In the external validation, CathEF discriminated reduced LVEF with an AUROC of 0.906 and an MAE of 7%.
CathEF performance was consistent irrespective of patient characteristics, including sex, body mass index, low estimated glomerular filtration rate (< 45), acute coronary syndromes, obstructive coronary artery disease, and left ventricular hypertrophy.
However, as noted, it tended to overestimate low LVEFs and to underestimate high LVEFs.
“Further research can improve accuracy and reduce the variability of DNNs to maximize their clinical utility,” the authors concluded.
A validation study is underway at the Montreal Heart Institute, and similar studies are planned at UCSF and McGill University, Dr. Tison said. “We expect to present preliminary findings at medical conferences either before the end of the year or maybe for the American College of Cardiology meeting in March 2024.”
Potentially improved outcomes
In a comment, Alfonso H. Waller, MD, a member of the American College of Cardiology’s Imaging Council and director of cardiac imaging at New Jersey Medical School, Newark, said that, “at some centers, in patients presenting with an acute ST-segment elevation myocardial infarction, some argue that assessment of myocardial and valvular function with [left ventriculography] grams may provide important prognostic information and in part may help guide the management of the patient.
“Therefore, this novel approach may provide information that is not usually available without performing a classic LV gram ... [and] may lead to improved delivery of care, earlier therapies, and potentially improved outcomes and quality of life.”
If the technology is available in real time, “it could enable real-time, dynamic assessment of cardiac function during coronary angiography, which may be particularly helpful in acute STEMI cases where baseline cardiac function and renal function may be unknown and additional contrast may be detrimental,” he said.
However, patients who might benefit most from the technology are those with severely reduced LVEF, “and unfortunately, the LVEF may be overestimated in this group,” he said.
Dr. Waller also noted that the model was developed using echocardiograms obtained 3 months before or up to 1 month after the angiogram, during which time “LVEF may change significantly. Typically, if someone presents with an acute coronary syndrome, there can be myocardial stunning, which can lead to regional wall motion abnormalities and lowering of LVEF.”
The validation study is evaluating patients with acute coronary syndrome for whom an echocardiogram was performed within 48 hours of the angiogram, he added.
The study was supported by grants from the Fonds de la Recherche en Santé du Québec, the Montreal Heart Institute Research Centre, the Montreal Heart Institute Foundation, the Des Groseillers-Bérard Research Chair, the National Institutes of Health, and the Heart and Stroke Foundation of Ontario. Dr. Tison, Dr. Avram, and Dr. Waller disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
a new study suggests.
In the test dataset, the video-based algorithm, called a deep neural network (DNN), discriminated reduced LVEF (< 40%) with an area under the receiver operating characteristic curve of 0.911.
In the external validation dataset, the DNN discriminated reduced LVEF with an AUROC of 0.906. However, the DNN tended to overestimate low LVEFs and to underestimate high LVEFs.
“We know the findings will be unexpected for cardiologists who don’t typically expect to get an estimate of systolic function or pump function just from an angiogram,” principal investigator Geoffrey H. Tison, MD, of the University of California, San Francisco, said in an interview.
In fact, he noted, “one of the challenges we face is a lack of trust by the health care community. They may not understand what drives the predictions behind our models. We have to translate that information in such a way that physicians trust that the algorithm is using the right features from the data they feed in to make the predictions.”
To help bolster that trust, “we display the ‘Model Facts,’ a nutrition-style label that describes how we train the algorithm, how it was validated, and the inclusion and exclusion criteria,” added lead author Robert Avram, MD, of the University of Montreal.
Model Facts is a safeguard against inappropriate use of the algorithm, Dr. Avram said. For example, if the algorithm was trained on patients between the ages of 40 and 90 and a clinician fed in data for a 35-year-old, a pop-up would appear warning the physician that the data being inputted are different from the data the algorithm was trained and validated on, and so any prediction “should be taken with a grain of salt.”
The study was published online in JAMA Cardiology.
Additional procedure
LVEF can be determined before coronary angiography with transthoracic echocardiography, but that is not always available, particularly for patients being seen emergently for acute coronary syndromes, the researchers wrote. LVEF can also be assessed using left ventriculography, an additional procedure that requires insertion of a pigtail catheter into the left ventricle and injection of more contrast and longer radiation exposure.
“Novel methods to assess LVEF at the point of care during coronary angiography would expand the available options to perform this important physiologic determination,” they wrote. “Video-based deep neural networks can learn subtle patterns from medical data to accomplish certain tasks beyond what physicians can achieve with that data, providing an opportunity to assess cardiac systolic function in real time from standard angiographic images without additional cost or procedures.”
The investigators conducted a cross-sectional study using UCSF patient data from 2012 to 2019. Data were randomly categorized into training, development, and test datasets.
External validation data were obtained from the University of Ottawa Heart Institute.
All adult patients who received a coronary angiogram and a transthoracic echocardiogram (TTE) within 3 months before or 1 month after receiving the angiogram were included.
A total of 4,042 angiograms with corresponding TTE LVEF from 3,679 UCSF patients were included in the analysis. The mean age of the patients was 64.3 years, and 65% were men.
The researchers’ video-based DNN, called CathEF, was used to discriminate reduced LVEF and to predict a continuous LVEF percentage from standard angiogram videos of the left coronary artery.
In the UCSF test dataset, CathEF discriminated reduced LVEF with an AUROC of 0.911; the diagnostic odds ratio for reduced LVEF was 22.7.
Furthermore, the CathEF-predicted that LVEF had a mean absolute error (MAE) of 8.5%, compared with TTE LVEF.
The CathEF-predicted LVEF differed 5% or less in comparison with the TTE LVEF in 38% of the test dataset studies; however, differences greater than 15% were seen in 15.2% of cases.
In the external validation, CathEF discriminated reduced LVEF with an AUROC of 0.906 and an MAE of 7%.
CathEF performance was consistent irrespective of patient characteristics, including sex, body mass index, low estimated glomerular filtration rate (< 45), acute coronary syndromes, obstructive coronary artery disease, and left ventricular hypertrophy.
However, as noted, it tended to overestimate low LVEFs and to underestimate high LVEFs.
“Further research can improve accuracy and reduce the variability of DNNs to maximize their clinical utility,” the authors concluded.
A validation study is underway at the Montreal Heart Institute, and similar studies are planned at UCSF and McGill University, Dr. Tison said. “We expect to present preliminary findings at medical conferences either before the end of the year or maybe for the American College of Cardiology meeting in March 2024.”
Potentially improved outcomes
In a comment, Alfonso H. Waller, MD, a member of the American College of Cardiology’s Imaging Council and director of cardiac imaging at New Jersey Medical School, Newark, said that, “at some centers, in patients presenting with an acute ST-segment elevation myocardial infarction, some argue that assessment of myocardial and valvular function with [left ventriculography] grams may provide important prognostic information and in part may help guide the management of the patient.
“Therefore, this novel approach may provide information that is not usually available without performing a classic LV gram ... [and] may lead to improved delivery of care, earlier therapies, and potentially improved outcomes and quality of life.”
If the technology is available in real time, “it could enable real-time, dynamic assessment of cardiac function during coronary angiography, which may be particularly helpful in acute STEMI cases where baseline cardiac function and renal function may be unknown and additional contrast may be detrimental,” he said.
However, patients who might benefit most from the technology are those with severely reduced LVEF, “and unfortunately, the LVEF may be overestimated in this group,” he said.
Dr. Waller also noted that the model was developed using echocardiograms obtained 3 months before or up to 1 month after the angiogram, during which time “LVEF may change significantly. Typically, if someone presents with an acute coronary syndrome, there can be myocardial stunning, which can lead to regional wall motion abnormalities and lowering of LVEF.”
The validation study is evaluating patients with acute coronary syndrome for whom an echocardiogram was performed within 48 hours of the angiogram, he added.
The study was supported by grants from the Fonds de la Recherche en Santé du Québec, the Montreal Heart Institute Research Centre, the Montreal Heart Institute Foundation, the Des Groseillers-Bérard Research Chair, the National Institutes of Health, and the Heart and Stroke Foundation of Ontario. Dr. Tison, Dr. Avram, and Dr. Waller disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
a new study suggests.
In the test dataset, the video-based algorithm, called a deep neural network (DNN), discriminated reduced LVEF (< 40%) with an area under the receiver operating characteristic curve of 0.911.
In the external validation dataset, the DNN discriminated reduced LVEF with an AUROC of 0.906. However, the DNN tended to overestimate low LVEFs and to underestimate high LVEFs.
“We know the findings will be unexpected for cardiologists who don’t typically expect to get an estimate of systolic function or pump function just from an angiogram,” principal investigator Geoffrey H. Tison, MD, of the University of California, San Francisco, said in an interview.
In fact, he noted, “one of the challenges we face is a lack of trust by the health care community. They may not understand what drives the predictions behind our models. We have to translate that information in such a way that physicians trust that the algorithm is using the right features from the data they feed in to make the predictions.”
To help bolster that trust, “we display the ‘Model Facts,’ a nutrition-style label that describes how we train the algorithm, how it was validated, and the inclusion and exclusion criteria,” added lead author Robert Avram, MD, of the University of Montreal.
Model Facts is a safeguard against inappropriate use of the algorithm, Dr. Avram said. For example, if the algorithm was trained on patients between the ages of 40 and 90 and a clinician fed in data for a 35-year-old, a pop-up would appear warning the physician that the data being inputted are different from the data the algorithm was trained and validated on, and so any prediction “should be taken with a grain of salt.”
The study was published online in JAMA Cardiology.
Additional procedure
LVEF can be determined before coronary angiography with transthoracic echocardiography, but that is not always available, particularly for patients being seen emergently for acute coronary syndromes, the researchers wrote. LVEF can also be assessed using left ventriculography, an additional procedure that requires insertion of a pigtail catheter into the left ventricle and injection of more contrast and longer radiation exposure.
“Novel methods to assess LVEF at the point of care during coronary angiography would expand the available options to perform this important physiologic determination,” they wrote. “Video-based deep neural networks can learn subtle patterns from medical data to accomplish certain tasks beyond what physicians can achieve with that data, providing an opportunity to assess cardiac systolic function in real time from standard angiographic images without additional cost or procedures.”
The investigators conducted a cross-sectional study using UCSF patient data from 2012 to 2019. Data were randomly categorized into training, development, and test datasets.
External validation data were obtained from the University of Ottawa Heart Institute.
All adult patients who received a coronary angiogram and a transthoracic echocardiogram (TTE) within 3 months before or 1 month after receiving the angiogram were included.
A total of 4,042 angiograms with corresponding TTE LVEF from 3,679 UCSF patients were included in the analysis. The mean age of the patients was 64.3 years, and 65% were men.
The researchers’ video-based DNN, called CathEF, was used to discriminate reduced LVEF and to predict a continuous LVEF percentage from standard angiogram videos of the left coronary artery.
In the UCSF test dataset, CathEF discriminated reduced LVEF with an AUROC of 0.911; the diagnostic odds ratio for reduced LVEF was 22.7.
Furthermore, the CathEF-predicted that LVEF had a mean absolute error (MAE) of 8.5%, compared with TTE LVEF.
The CathEF-predicted LVEF differed 5% or less in comparison with the TTE LVEF in 38% of the test dataset studies; however, differences greater than 15% were seen in 15.2% of cases.
In the external validation, CathEF discriminated reduced LVEF with an AUROC of 0.906 and an MAE of 7%.
CathEF performance was consistent irrespective of patient characteristics, including sex, body mass index, low estimated glomerular filtration rate (< 45), acute coronary syndromes, obstructive coronary artery disease, and left ventricular hypertrophy.
However, as noted, it tended to overestimate low LVEFs and to underestimate high LVEFs.
“Further research can improve accuracy and reduce the variability of DNNs to maximize their clinical utility,” the authors concluded.
A validation study is underway at the Montreal Heart Institute, and similar studies are planned at UCSF and McGill University, Dr. Tison said. “We expect to present preliminary findings at medical conferences either before the end of the year or maybe for the American College of Cardiology meeting in March 2024.”
Potentially improved outcomes
In a comment, Alfonso H. Waller, MD, a member of the American College of Cardiology’s Imaging Council and director of cardiac imaging at New Jersey Medical School, Newark, said that, “at some centers, in patients presenting with an acute ST-segment elevation myocardial infarction, some argue that assessment of myocardial and valvular function with [left ventriculography] grams may provide important prognostic information and in part may help guide the management of the patient.
“Therefore, this novel approach may provide information that is not usually available without performing a classic LV gram ... [and] may lead to improved delivery of care, earlier therapies, and potentially improved outcomes and quality of life.”
If the technology is available in real time, “it could enable real-time, dynamic assessment of cardiac function during coronary angiography, which may be particularly helpful in acute STEMI cases where baseline cardiac function and renal function may be unknown and additional contrast may be detrimental,” he said.
However, patients who might benefit most from the technology are those with severely reduced LVEF, “and unfortunately, the LVEF may be overestimated in this group,” he said.
Dr. Waller also noted that the model was developed using echocardiograms obtained 3 months before or up to 1 month after the angiogram, during which time “LVEF may change significantly. Typically, if someone presents with an acute coronary syndrome, there can be myocardial stunning, which can lead to regional wall motion abnormalities and lowering of LVEF.”
The validation study is evaluating patients with acute coronary syndrome for whom an echocardiogram was performed within 48 hours of the angiogram, he added.
The study was supported by grants from the Fonds de la Recherche en Santé du Québec, the Montreal Heart Institute Research Centre, the Montreal Heart Institute Foundation, the Des Groseillers-Bérard Research Chair, the National Institutes of Health, and the Heart and Stroke Foundation of Ontario. Dr. Tison, Dr. Avram, and Dr. Waller disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM JAMA CARDIOLOGY
Foot ulcers red flag for eye disease in diabetes
Sores on the feet can signal problems with the eyes in patients with diabetes.
Prior research and anecdotal experience show that diabetic foot ulcers and diabetic retinopathy frequently co-occur.
David J. Ramsey, MD, PhD, MPH, director of ophthalmic research at Lahey Hospital & Medical Center, Burlington, Mass., said when clinicians detect either condition, they should involve a team that can intervene to help protect a patient’s vision and mobility.
For example, they should ensure patients receive comprehensive eye and foot evaluations and help them optimize diabetes management.
The new study, presented at the annual meeting of the Association for Research in Vision and Ophthalmology, “adds an important dimension” to understanding the association between the conditions, said Dr. Ramsey, who recently reviewed correlations between diabetic foot ulcers and diabetic retinopathy and their underlying causes.
“Patients with diabetic foot ulcers appear to receive less attention to their diabetic retinopathy and may receive fewer treatments with eye injections targeting vascular endothelial growth factor (VEGF), an important driver of progression of diabetic retinopathy,” said Dr. Ramsey, who is also an associate professor of ophthalmology at Tufts University School of Medicine, Boston. He was not involved in the study presented at ARVO 2023.
In the new study, Christopher T. Zhu, a medical student at UT Health San Antonio, and colleagues analyzed data from 426 eyes of 213 patients with type 2 diabetes who had had at least two eye exams between 2012 and 2022; 72 of the patients had diabetic foot ulcers. Patients were followed for about 4 years on average.
Patients with diabetic foot ulcers had a higher percentage of eyes with macular edema on their initial exam (32.6% vs. 28%). By the final exam, the percentage of eyes with macular edema was significantly greater in the group with diabetic foot ulcers (64.6% vs. 37.6%; P < .0001), Mr. Zhu’s group reported.
Eyes with nonproliferative diabetic retinopathy progressed to proliferative diabetic retinopathy, the worst grade, at a higher rate in the group with foot ulcers (50.6% vs. 35.6%; P = .03). In addition, patients with foot ulcers were more likely to experience vitreous hemorrhage (55.6% vs. 38.7%), the researchers found.
Despite patients with foot ulcers tending to have worse disease, they received fewer treatments for retinopathy. Those without ulcers received an average of 6.9 anti-VEGF injections per eye, while those with ulcers averaged 4.3.
Foot ulcers may hinder the ability of patients to get to appointments to receive the injections, Mr. Zhu and colleagues wrote. “For many patients in our part of the country [South Texas], a lack of transportation is a particular barrier to health care access,” Mr. Zhu told this news organization.
Mr. Zhu’s team conducted their study after noticing that patients with diabetes and foot ulcers who presented to their eye clinics “appeared to progress faster to worse grades of retinopathy” than patients with diabetes who did not have ulcers.
“Similar to how foot ulcers develop due to a severe disruption in blood flow [vascular] and a loss of sensation [neurologic], diabetic retinopathy may have a relation to microvascular disease, neurologic degeneration, and inflammation,” he said.
The findings confirm “that poor perfusion of the eye and foot are linked and can cause ischemic retinopathy leading to the development of proliferative diabetic retinopathy and vitreous hemorrhages, both serious, vision-threatening conditions,” Dr. Ramsey said.
To some extent, fewer treatments with anti-VEGF agents may account for why patients with foot ulcers have more eye complications, Dr. Ramsey added. “Additional research needs to be done to further dissect the cause and the effect, but it’s a very important finding that we need to increase awareness about,” he said.
Dr. Ramsey and Mr. Zhu reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Sores on the feet can signal problems with the eyes in patients with diabetes.
Prior research and anecdotal experience show that diabetic foot ulcers and diabetic retinopathy frequently co-occur.
David J. Ramsey, MD, PhD, MPH, director of ophthalmic research at Lahey Hospital & Medical Center, Burlington, Mass., said when clinicians detect either condition, they should involve a team that can intervene to help protect a patient’s vision and mobility.
For example, they should ensure patients receive comprehensive eye and foot evaluations and help them optimize diabetes management.
The new study, presented at the annual meeting of the Association for Research in Vision and Ophthalmology, “adds an important dimension” to understanding the association between the conditions, said Dr. Ramsey, who recently reviewed correlations between diabetic foot ulcers and diabetic retinopathy and their underlying causes.
“Patients with diabetic foot ulcers appear to receive less attention to their diabetic retinopathy and may receive fewer treatments with eye injections targeting vascular endothelial growth factor (VEGF), an important driver of progression of diabetic retinopathy,” said Dr. Ramsey, who is also an associate professor of ophthalmology at Tufts University School of Medicine, Boston. He was not involved in the study presented at ARVO 2023.
In the new study, Christopher T. Zhu, a medical student at UT Health San Antonio, and colleagues analyzed data from 426 eyes of 213 patients with type 2 diabetes who had had at least two eye exams between 2012 and 2022; 72 of the patients had diabetic foot ulcers. Patients were followed for about 4 years on average.
Patients with diabetic foot ulcers had a higher percentage of eyes with macular edema on their initial exam (32.6% vs. 28%). By the final exam, the percentage of eyes with macular edema was significantly greater in the group with diabetic foot ulcers (64.6% vs. 37.6%; P < .0001), Mr. Zhu’s group reported.
Eyes with nonproliferative diabetic retinopathy progressed to proliferative diabetic retinopathy, the worst grade, at a higher rate in the group with foot ulcers (50.6% vs. 35.6%; P = .03). In addition, patients with foot ulcers were more likely to experience vitreous hemorrhage (55.6% vs. 38.7%), the researchers found.
Despite patients with foot ulcers tending to have worse disease, they received fewer treatments for retinopathy. Those without ulcers received an average of 6.9 anti-VEGF injections per eye, while those with ulcers averaged 4.3.
Foot ulcers may hinder the ability of patients to get to appointments to receive the injections, Mr. Zhu and colleagues wrote. “For many patients in our part of the country [South Texas], a lack of transportation is a particular barrier to health care access,” Mr. Zhu told this news organization.
Mr. Zhu’s team conducted their study after noticing that patients with diabetes and foot ulcers who presented to their eye clinics “appeared to progress faster to worse grades of retinopathy” than patients with diabetes who did not have ulcers.
“Similar to how foot ulcers develop due to a severe disruption in blood flow [vascular] and a loss of sensation [neurologic], diabetic retinopathy may have a relation to microvascular disease, neurologic degeneration, and inflammation,” he said.
The findings confirm “that poor perfusion of the eye and foot are linked and can cause ischemic retinopathy leading to the development of proliferative diabetic retinopathy and vitreous hemorrhages, both serious, vision-threatening conditions,” Dr. Ramsey said.
To some extent, fewer treatments with anti-VEGF agents may account for why patients with foot ulcers have more eye complications, Dr. Ramsey added. “Additional research needs to be done to further dissect the cause and the effect, but it’s a very important finding that we need to increase awareness about,” he said.
Dr. Ramsey and Mr. Zhu reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Sores on the feet can signal problems with the eyes in patients with diabetes.
Prior research and anecdotal experience show that diabetic foot ulcers and diabetic retinopathy frequently co-occur.
David J. Ramsey, MD, PhD, MPH, director of ophthalmic research at Lahey Hospital & Medical Center, Burlington, Mass., said when clinicians detect either condition, they should involve a team that can intervene to help protect a patient’s vision and mobility.
For example, they should ensure patients receive comprehensive eye and foot evaluations and help them optimize diabetes management.
The new study, presented at the annual meeting of the Association for Research in Vision and Ophthalmology, “adds an important dimension” to understanding the association between the conditions, said Dr. Ramsey, who recently reviewed correlations between diabetic foot ulcers and diabetic retinopathy and their underlying causes.
“Patients with diabetic foot ulcers appear to receive less attention to their diabetic retinopathy and may receive fewer treatments with eye injections targeting vascular endothelial growth factor (VEGF), an important driver of progression of diabetic retinopathy,” said Dr. Ramsey, who is also an associate professor of ophthalmology at Tufts University School of Medicine, Boston. He was not involved in the study presented at ARVO 2023.
In the new study, Christopher T. Zhu, a medical student at UT Health San Antonio, and colleagues analyzed data from 426 eyes of 213 patients with type 2 diabetes who had had at least two eye exams between 2012 and 2022; 72 of the patients had diabetic foot ulcers. Patients were followed for about 4 years on average.
Patients with diabetic foot ulcers had a higher percentage of eyes with macular edema on their initial exam (32.6% vs. 28%). By the final exam, the percentage of eyes with macular edema was significantly greater in the group with diabetic foot ulcers (64.6% vs. 37.6%; P < .0001), Mr. Zhu’s group reported.
Eyes with nonproliferative diabetic retinopathy progressed to proliferative diabetic retinopathy, the worst grade, at a higher rate in the group with foot ulcers (50.6% vs. 35.6%; P = .03). In addition, patients with foot ulcers were more likely to experience vitreous hemorrhage (55.6% vs. 38.7%), the researchers found.
Despite patients with foot ulcers tending to have worse disease, they received fewer treatments for retinopathy. Those without ulcers received an average of 6.9 anti-VEGF injections per eye, while those with ulcers averaged 4.3.
Foot ulcers may hinder the ability of patients to get to appointments to receive the injections, Mr. Zhu and colleagues wrote. “For many patients in our part of the country [South Texas], a lack of transportation is a particular barrier to health care access,” Mr. Zhu told this news organization.
Mr. Zhu’s team conducted their study after noticing that patients with diabetes and foot ulcers who presented to their eye clinics “appeared to progress faster to worse grades of retinopathy” than patients with diabetes who did not have ulcers.
“Similar to how foot ulcers develop due to a severe disruption in blood flow [vascular] and a loss of sensation [neurologic], diabetic retinopathy may have a relation to microvascular disease, neurologic degeneration, and inflammation,” he said.
The findings confirm “that poor perfusion of the eye and foot are linked and can cause ischemic retinopathy leading to the development of proliferative diabetic retinopathy and vitreous hemorrhages, both serious, vision-threatening conditions,” Dr. Ramsey said.
To some extent, fewer treatments with anti-VEGF agents may account for why patients with foot ulcers have more eye complications, Dr. Ramsey added. “Additional research needs to be done to further dissect the cause and the effect, but it’s a very important finding that we need to increase awareness about,” he said.
Dr. Ramsey and Mr. Zhu reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM ARVO 2023
Hyperbaric oxygen may improve heart function in long COVID
.
Patients with reduced left ventricular global longitudinal strain (GLS) at baseline who received HBOT had a significant increase in GLS, compared with those who received sham treatment.
GLS is a measure of systolic function that is thought to be a predictor of heart failure–related outcomes.
The study also showed that global work efficiency (GWE) and the global work index (GWI) increased in HBOT-treated patients, though not significantly.
“HBOT is an effective treatment for diabetic foot ulcers, decompression sickness in divers, and other conditions, such as cognitive impairment after stroke,” Marina Leitman, MD, of the Sackler School of Medicine, Tel Aviv, said in an interview. Her team also studied HBOT in asymptomatic older patients and found that the treatment seemed to improve left ventricular end systolic function.
“We should open our minds to thinking about this treatment for another indication,” she said. “That is the basis of precision medicine. We have this treatment and know it can be effective for cardiac pathology.
“Now we can say that post-COVID syndrome patients probably should be evaluated with echocardiography and GLS, which is the main parameter that showed improvement in our study,” she added. “If GLS is below normal values, these patients can benefit from HBOT, although additional research is needed to determine the optimal number of sessions.”
Dr. Leitman presented the study at the European Association of Cardiovascular Imaging 2023, a scientific congress of the European Society of Cardiology.
Biomarker changes
The study enrolled 60 hospitalized and nonhospitalized post-COVID syndrome patients with ongoing symptoms for at least 3 months after having mild to moderate symptomatic COVID-19.
Participants were randomized to receive HBOT or a sham procedure five times per week for 8 weeks, for a total of 40 sessions. They underwent echocardiography at baseline and 1-3 weeks after the final session to assess GLS.
The HBOT group received 100% oxygen through a mask at a pressure of two atmospheres for 90 minutes, with 5-minute air breaks every 20 minutes.
The sham group received 21% oxygen by mask at one atmosphere for 90 minutes.
At baseline, 29 participants (48%) had reduced GLS, despite having a normal ejection fraction, Dr. Leitman said. Of those, 16 (53%) were in the HBOT group and 13 (43%) were in the sham group.
The average GLS at baseline across all participants was –17.8%; a normal value is about –20%.
In the HBOT group, GLS increased significantly from –17.8% at baseline to –20.2% after HBOT. In the sham group, GLS was –17.8% at baseline and –19.1% at the end of the study, with no statistically significant difference between the two measurements.
In addition, GWE increased overall after HBOT from 96.3 to 97.1.
Dr. Leitman’s poster showed GLS and myocardial work indices before and after HBOT in a 45-year-old patient. Prior to treatment, GLS was –19%; GWE was 96%; and GWI was 1,833 mm Hg.
After HBOT treatment, GLS was –22%; GWE, 98%; and GWI, 1,911 mm Hg.
Clinical relevance unclear
Scott Gorenstein, MD, associate professor in the department of surgery and medical director of wound care and hyperbaric medicine at NYU Langone–Long Island, New York, commented on the study for this news organization.
“The approach certainly warrants studying, but the benefit is difficult to assess,” he said. “We still don’t understand the mechanism of long COVID, so it’s difficult to go from there to say that HBOT will be an effective therapy.”
That said, he added, “This is probably the best study I’ve seen in that it’s a randomized controlled trial, rather than a case series.”
Nevertheless, he noted, “We have no idea from this study whether the change in GLS is clinically relevant. As a clinician, I can’t now say that HBOT is going to improve heart failure secondary to long COVID. We don’t know whether the participants were New York heart failure class 3 or 4, for example, and all of a sudden went from really sick to really good.”
“There are many interventions that may change markers of cardiac function or inflammation,” he said. “But if they don’t make a difference in quantity or quality of life, is the treatment really valuable?”
Dr. Gorenstein said he would have no problem treating a patient with mild to moderate COVID-related heart failure with HBOT, since his own team’s study conducted near the outset of the pandemic showed it was safe. “But HBOT is an expensive treatment in the U.S. and there still are some risks and side effects, albeit very, very low.”
The study received no funding. Dr. Leitman and Dr. Gorenstein have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
.
Patients with reduced left ventricular global longitudinal strain (GLS) at baseline who received HBOT had a significant increase in GLS, compared with those who received sham treatment.
GLS is a measure of systolic function that is thought to be a predictor of heart failure–related outcomes.
The study also showed that global work efficiency (GWE) and the global work index (GWI) increased in HBOT-treated patients, though not significantly.
“HBOT is an effective treatment for diabetic foot ulcers, decompression sickness in divers, and other conditions, such as cognitive impairment after stroke,” Marina Leitman, MD, of the Sackler School of Medicine, Tel Aviv, said in an interview. Her team also studied HBOT in asymptomatic older patients and found that the treatment seemed to improve left ventricular end systolic function.
“We should open our minds to thinking about this treatment for another indication,” she said. “That is the basis of precision medicine. We have this treatment and know it can be effective for cardiac pathology.
“Now we can say that post-COVID syndrome patients probably should be evaluated with echocardiography and GLS, which is the main parameter that showed improvement in our study,” she added. “If GLS is below normal values, these patients can benefit from HBOT, although additional research is needed to determine the optimal number of sessions.”
Dr. Leitman presented the study at the European Association of Cardiovascular Imaging 2023, a scientific congress of the European Society of Cardiology.
Biomarker changes
The study enrolled 60 hospitalized and nonhospitalized post-COVID syndrome patients with ongoing symptoms for at least 3 months after having mild to moderate symptomatic COVID-19.
Participants were randomized to receive HBOT or a sham procedure five times per week for 8 weeks, for a total of 40 sessions. They underwent echocardiography at baseline and 1-3 weeks after the final session to assess GLS.
The HBOT group received 100% oxygen through a mask at a pressure of two atmospheres for 90 minutes, with 5-minute air breaks every 20 minutes.
The sham group received 21% oxygen by mask at one atmosphere for 90 minutes.
At baseline, 29 participants (48%) had reduced GLS, despite having a normal ejection fraction, Dr. Leitman said. Of those, 16 (53%) were in the HBOT group and 13 (43%) were in the sham group.
The average GLS at baseline across all participants was –17.8%; a normal value is about –20%.
In the HBOT group, GLS increased significantly from –17.8% at baseline to –20.2% after HBOT. In the sham group, GLS was –17.8% at baseline and –19.1% at the end of the study, with no statistically significant difference between the two measurements.
In addition, GWE increased overall after HBOT from 96.3 to 97.1.
Dr. Leitman’s poster showed GLS and myocardial work indices before and after HBOT in a 45-year-old patient. Prior to treatment, GLS was –19%; GWE was 96%; and GWI was 1,833 mm Hg.
After HBOT treatment, GLS was –22%; GWE, 98%; and GWI, 1,911 mm Hg.
Clinical relevance unclear
Scott Gorenstein, MD, associate professor in the department of surgery and medical director of wound care and hyperbaric medicine at NYU Langone–Long Island, New York, commented on the study for this news organization.
“The approach certainly warrants studying, but the benefit is difficult to assess,” he said. “We still don’t understand the mechanism of long COVID, so it’s difficult to go from there to say that HBOT will be an effective therapy.”
That said, he added, “This is probably the best study I’ve seen in that it’s a randomized controlled trial, rather than a case series.”
Nevertheless, he noted, “We have no idea from this study whether the change in GLS is clinically relevant. As a clinician, I can’t now say that HBOT is going to improve heart failure secondary to long COVID. We don’t know whether the participants were New York heart failure class 3 or 4, for example, and all of a sudden went from really sick to really good.”
“There are many interventions that may change markers of cardiac function or inflammation,” he said. “But if they don’t make a difference in quantity or quality of life, is the treatment really valuable?”
Dr. Gorenstein said he would have no problem treating a patient with mild to moderate COVID-related heart failure with HBOT, since his own team’s study conducted near the outset of the pandemic showed it was safe. “But HBOT is an expensive treatment in the U.S. and there still are some risks and side effects, albeit very, very low.”
The study received no funding. Dr. Leitman and Dr. Gorenstein have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
.
Patients with reduced left ventricular global longitudinal strain (GLS) at baseline who received HBOT had a significant increase in GLS, compared with those who received sham treatment.
GLS is a measure of systolic function that is thought to be a predictor of heart failure–related outcomes.
The study also showed that global work efficiency (GWE) and the global work index (GWI) increased in HBOT-treated patients, though not significantly.
“HBOT is an effective treatment for diabetic foot ulcers, decompression sickness in divers, and other conditions, such as cognitive impairment after stroke,” Marina Leitman, MD, of the Sackler School of Medicine, Tel Aviv, said in an interview. Her team also studied HBOT in asymptomatic older patients and found that the treatment seemed to improve left ventricular end systolic function.
“We should open our minds to thinking about this treatment for another indication,” she said. “That is the basis of precision medicine. We have this treatment and know it can be effective for cardiac pathology.
“Now we can say that post-COVID syndrome patients probably should be evaluated with echocardiography and GLS, which is the main parameter that showed improvement in our study,” she added. “If GLS is below normal values, these patients can benefit from HBOT, although additional research is needed to determine the optimal number of sessions.”
Dr. Leitman presented the study at the European Association of Cardiovascular Imaging 2023, a scientific congress of the European Society of Cardiology.
Biomarker changes
The study enrolled 60 hospitalized and nonhospitalized post-COVID syndrome patients with ongoing symptoms for at least 3 months after having mild to moderate symptomatic COVID-19.
Participants were randomized to receive HBOT or a sham procedure five times per week for 8 weeks, for a total of 40 sessions. They underwent echocardiography at baseline and 1-3 weeks after the final session to assess GLS.
The HBOT group received 100% oxygen through a mask at a pressure of two atmospheres for 90 minutes, with 5-minute air breaks every 20 minutes.
The sham group received 21% oxygen by mask at one atmosphere for 90 minutes.
At baseline, 29 participants (48%) had reduced GLS, despite having a normal ejection fraction, Dr. Leitman said. Of those, 16 (53%) were in the HBOT group and 13 (43%) were in the sham group.
The average GLS at baseline across all participants was –17.8%; a normal value is about –20%.
In the HBOT group, GLS increased significantly from –17.8% at baseline to –20.2% after HBOT. In the sham group, GLS was –17.8% at baseline and –19.1% at the end of the study, with no statistically significant difference between the two measurements.
In addition, GWE increased overall after HBOT from 96.3 to 97.1.
Dr. Leitman’s poster showed GLS and myocardial work indices before and after HBOT in a 45-year-old patient. Prior to treatment, GLS was –19%; GWE was 96%; and GWI was 1,833 mm Hg.
After HBOT treatment, GLS was –22%; GWE, 98%; and GWI, 1,911 mm Hg.
Clinical relevance unclear
Scott Gorenstein, MD, associate professor in the department of surgery and medical director of wound care and hyperbaric medicine at NYU Langone–Long Island, New York, commented on the study for this news organization.
“The approach certainly warrants studying, but the benefit is difficult to assess,” he said. “We still don’t understand the mechanism of long COVID, so it’s difficult to go from there to say that HBOT will be an effective therapy.”
That said, he added, “This is probably the best study I’ve seen in that it’s a randomized controlled trial, rather than a case series.”
Nevertheless, he noted, “We have no idea from this study whether the change in GLS is clinically relevant. As a clinician, I can’t now say that HBOT is going to improve heart failure secondary to long COVID. We don’t know whether the participants were New York heart failure class 3 or 4, for example, and all of a sudden went from really sick to really good.”
“There are many interventions that may change markers of cardiac function or inflammation,” he said. “But if they don’t make a difference in quantity or quality of life, is the treatment really valuable?”
Dr. Gorenstein said he would have no problem treating a patient with mild to moderate COVID-related heart failure with HBOT, since his own team’s study conducted near the outset of the pandemic showed it was safe. “But HBOT is an expensive treatment in the U.S. and there still are some risks and side effects, albeit very, very low.”
The study received no funding. Dr. Leitman and Dr. Gorenstein have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM EACVI 2023
Overcoming death anxiety: Understanding our lives and legacies
Disappointment – “I failed this exam, my life is ruined” or regret – “I am getting a divorce, I wasted so much of my life.” Patients present with a wide variety of complaints that can be understood as a form of death anxiety.
Fundamentally, patients come to see us to understand and explain their lives. One can reinterpret this as a patient asking, “If I died today, would my life have been good enough?” or “When I die, how will I look back at this moment in time and judge the choices I made?”
Other patients come to us attempting to use the same maladaptive defenses that did not serve them well in the past in the hopes of achieving a new outcome that will validate their lives. While it may be understandable that a child dissociates when facing abuse, hoping that this defense mechanism – as an adult – will work, it is unlikely to be fruitful and will certainly not validate or repair the past. This hope to repair one’s past can be interpreted as a fear of death – “I cannot die without correcting this.” This psychic conflict can intensify if one does not adopt a more adaptive understanding of his or her life.
Death anxiety is the feeling associated with the finality of life. Not only is life final, but a constant reminder of that fact is the idea that any one moment is final. Other than in science fiction, one cannot return to a prior moment and repair the past in the hope of a better future. Time goes only in one direction and death is the natural outcome of all life.
Death may have some evolutionary purpose that encourages the promotion of newer and more fitter genes, but one doesn’t have to consider its origin and reason to admit death’s constancy throughout humanity. People die and that is an anxiety-provoking fact of life. Death anxiety can feel especially tangible in our connected world. In a world of constant news, it can feel – for many people – that if your house wasn’t displaced because of global warming or that you are not a war refugee, you don’t deserve to be seen and heard.
This can be a particularly strong feeling for and among physicians, who don’t think that the mental health challenges generated by their own tough circumstances deserve to be labeled a mental disorder, so they designate themselves as having “burnout”1 – as they don’t deserve the sympathy of having the clinically significant impairments of “depression.” Our traumas don’t seem important enough to deserve notice, and thus we may feel like we could die without ever having truly mattered.
This can also be applied in the reverse fashion. Certain individuals, like celebrities, live such extravagant lives that our simpler achievements can feel futile in comparison. While the neighbor’s grass has always felt greener, we are now constantly exposed to perfectly manicured lawns on social media. When compounded, the idea that our successes and our pains are both simultaneously irrelevant can lead one to have very palpable death anxiety – my life will never matter if none of the things I do matter, or my life will never matter because I will never achieve the requisite number of “likes” or “views” on social media required to believe that one’s life was worth living.
A way of alleviating death anxiety can be through the concept of legacy, or what we leave behind. How will people remember me? Will people remember me, or will I disappear like a shadow into the distant memory of my near and dear ones? The idea of being forgotten or lost to memory is intolerable to some and can be a strong driving force to “make a name” for oneself. For those who crave fame, whether a celebrity or a generous alumnus, part of this is likely related to remaining well known after death. After all, one can argue that you are not truly dead as long as you continue to live in the memory and/or genes of others.
Legacy thus serves as a form of posthumous transitional object; a way of calming our fears about how we will be remembered. For many, reconciling their feelings towards their legacy is an avenue to tame death anxiety.
A case study
The case of Mr. B illustrates this. As a 72-year-old male with a long history of generalized anxiety, he once had a nightmare as a child, similar to the plot of Sleeping Beauty. In his dream, he walks up a spiral staircase in a castle and touches the spindle on a spinning wheel, thus ending his life. The dream was vivid and marked him.
His fear of death has subsequently reared its head throughout his life. In more recent years, he has suffered from cardiovascular disease. Although he is now quite stable on his current cardiac medications, he is constantly fearful that he will experience a cardiac event while asleep and suddenly die. He is so anxious about not waking up in the morning that falling asleep is nearly impossible.
Mr. B is single, with no close family besides a sister who lives in another state. He has a dog and few friends. He worries about what will happen to his dog if he doesn’t wake up in the morning, but perhaps most distressing to him is “there’s so much left for me to do, I have so much to write!” As an accomplished author, he continues to write, and hopes to publish many more novels in his lifetime. It is unsurprising that someone without a strong social network may fear death and feel pressured to somehow make a mark on the world before the curtain falls. It is scary to think that even without us, life goes on.
By bringing to Mr. B’s attention that his ever-present anxiety is rooted in fear of death, he was able to gain more insight into his own defensive behaviors. By confronting his death anxiety and processing his definition of a life well lived together in therapy, he’s acknowledged his lack of social connection as demoralizing, and has made significant strides to remedy this. He’s been able to focus on a more fulfilling life day to day, with less emphasis on his to-do list and aspirations. Instead, he’s connected more with his faith and members of his church. He’s gotten close to several neighbors and enjoys long dinners with them on his back patio.
At a recent meeting, he confessed that he feels “lighter” and not as fearful about sudden cardiac death, and thus has noticed that his overall anxiety has diminished greatly. He concluded that experiencing meaningful relationships in the present moment would give him greater joy than spending his remaining time engaged in preserving a future identity for himself. It seems elementary, but if we look within, we may find that we all suffer similarly: How much of our daily actions, thoughts, and fears are tied to the looming threat of death?
Conclusion
While modern psychiatry continues to advance with better understandings of our neurobiology, improved knowledge of pathophysiological processes of mental illness, and expanding discovery of novel pharmacotherapeutics, the modern psychiatrist should not forget fundamental truths of behavior and humanity that were once the staple of psychiatry.
Death anxiety is one of those truths; it is the ultimate stressor that we will all face and should be regular study and practice for psychiatrists. In this article, we explored some of those facets most meaningful to us but recommend you expand your study to the many more available.
Patients often come to physicians seeking validation of their lives or trying to use the same maladaptive defense mechanisms that did not serve them well in the past to achieve a better outcome.
In today’s world, death anxiety can feel palpable due to the constant exposure to global news and social media that can make us feel irrelevant. However, legacy, or what we leave behind, can serve as a way to alleviate death anxiety. For many, reconciling their feelings toward their legacy is an avenue to tame death anxiety. Therapy can help individuals gain insight into their defensive behaviors and process their definition of a life well lived. By focusing on a life worth living, individuals can alleviate their death anxiety and gain a sense of fulfillment.
Dr. Akkoor is a psychiatry resident at the University of California, San Diego. She is interested in immigrant mental health, ethics, consultation-liaison psychiatry, and medical education. Dr. Badre is a clinical and forensic psychiatrist in San Diego. He holds teaching positions at the University of California, San Diego, and the University of San Diego. He teaches medical education, psychopharmacology, ethics in psychiatry, and correctional care. Dr. Badre can be reached at his website, BadreMD.com. Dr. Badre and Dr. Akkoor have no conflicts of interest.
Reference
1. Badre N. Burnout: A concept that rebrands mental illness for professionals. Clinical Psychiatry News. 2020 Mar 5.
Disappointment – “I failed this exam, my life is ruined” or regret – “I am getting a divorce, I wasted so much of my life.” Patients present with a wide variety of complaints that can be understood as a form of death anxiety.
Fundamentally, patients come to see us to understand and explain their lives. One can reinterpret this as a patient asking, “If I died today, would my life have been good enough?” or “When I die, how will I look back at this moment in time and judge the choices I made?”
Other patients come to us attempting to use the same maladaptive defenses that did not serve them well in the past in the hopes of achieving a new outcome that will validate their lives. While it may be understandable that a child dissociates when facing abuse, hoping that this defense mechanism – as an adult – will work, it is unlikely to be fruitful and will certainly not validate or repair the past. This hope to repair one’s past can be interpreted as a fear of death – “I cannot die without correcting this.” This psychic conflict can intensify if one does not adopt a more adaptive understanding of his or her life.
Death anxiety is the feeling associated with the finality of life. Not only is life final, but a constant reminder of that fact is the idea that any one moment is final. Other than in science fiction, one cannot return to a prior moment and repair the past in the hope of a better future. Time goes only in one direction and death is the natural outcome of all life.
Death may have some evolutionary purpose that encourages the promotion of newer and more fitter genes, but one doesn’t have to consider its origin and reason to admit death’s constancy throughout humanity. People die and that is an anxiety-provoking fact of life. Death anxiety can feel especially tangible in our connected world. In a world of constant news, it can feel – for many people – that if your house wasn’t displaced because of global warming or that you are not a war refugee, you don’t deserve to be seen and heard.
This can be a particularly strong feeling for and among physicians, who don’t think that the mental health challenges generated by their own tough circumstances deserve to be labeled a mental disorder, so they designate themselves as having “burnout”1 – as they don’t deserve the sympathy of having the clinically significant impairments of “depression.” Our traumas don’t seem important enough to deserve notice, and thus we may feel like we could die without ever having truly mattered.
This can also be applied in the reverse fashion. Certain individuals, like celebrities, live such extravagant lives that our simpler achievements can feel futile in comparison. While the neighbor’s grass has always felt greener, we are now constantly exposed to perfectly manicured lawns on social media. When compounded, the idea that our successes and our pains are both simultaneously irrelevant can lead one to have very palpable death anxiety – my life will never matter if none of the things I do matter, or my life will never matter because I will never achieve the requisite number of “likes” or “views” on social media required to believe that one’s life was worth living.
A way of alleviating death anxiety can be through the concept of legacy, or what we leave behind. How will people remember me? Will people remember me, or will I disappear like a shadow into the distant memory of my near and dear ones? The idea of being forgotten or lost to memory is intolerable to some and can be a strong driving force to “make a name” for oneself. For those who crave fame, whether a celebrity or a generous alumnus, part of this is likely related to remaining well known after death. After all, one can argue that you are not truly dead as long as you continue to live in the memory and/or genes of others.
Legacy thus serves as a form of posthumous transitional object; a way of calming our fears about how we will be remembered. For many, reconciling their feelings towards their legacy is an avenue to tame death anxiety.
A case study
The case of Mr. B illustrates this. As a 72-year-old male with a long history of generalized anxiety, he once had a nightmare as a child, similar to the plot of Sleeping Beauty. In his dream, he walks up a spiral staircase in a castle and touches the spindle on a spinning wheel, thus ending his life. The dream was vivid and marked him.
His fear of death has subsequently reared its head throughout his life. In more recent years, he has suffered from cardiovascular disease. Although he is now quite stable on his current cardiac medications, he is constantly fearful that he will experience a cardiac event while asleep and suddenly die. He is so anxious about not waking up in the morning that falling asleep is nearly impossible.
Mr. B is single, with no close family besides a sister who lives in another state. He has a dog and few friends. He worries about what will happen to his dog if he doesn’t wake up in the morning, but perhaps most distressing to him is “there’s so much left for me to do, I have so much to write!” As an accomplished author, he continues to write, and hopes to publish many more novels in his lifetime. It is unsurprising that someone without a strong social network may fear death and feel pressured to somehow make a mark on the world before the curtain falls. It is scary to think that even without us, life goes on.
By bringing to Mr. B’s attention that his ever-present anxiety is rooted in fear of death, he was able to gain more insight into his own defensive behaviors. By confronting his death anxiety and processing his definition of a life well lived together in therapy, he’s acknowledged his lack of social connection as demoralizing, and has made significant strides to remedy this. He’s been able to focus on a more fulfilling life day to day, with less emphasis on his to-do list and aspirations. Instead, he’s connected more with his faith and members of his church. He’s gotten close to several neighbors and enjoys long dinners with them on his back patio.
At a recent meeting, he confessed that he feels “lighter” and not as fearful about sudden cardiac death, and thus has noticed that his overall anxiety has diminished greatly. He concluded that experiencing meaningful relationships in the present moment would give him greater joy than spending his remaining time engaged in preserving a future identity for himself. It seems elementary, but if we look within, we may find that we all suffer similarly: How much of our daily actions, thoughts, and fears are tied to the looming threat of death?
Conclusion
While modern psychiatry continues to advance with better understandings of our neurobiology, improved knowledge of pathophysiological processes of mental illness, and expanding discovery of novel pharmacotherapeutics, the modern psychiatrist should not forget fundamental truths of behavior and humanity that were once the staple of psychiatry.
Death anxiety is one of those truths; it is the ultimate stressor that we will all face and should be regular study and practice for psychiatrists. In this article, we explored some of those facets most meaningful to us but recommend you expand your study to the many more available.
Patients often come to physicians seeking validation of their lives or trying to use the same maladaptive defense mechanisms that did not serve them well in the past to achieve a better outcome.
In today’s world, death anxiety can feel palpable due to the constant exposure to global news and social media that can make us feel irrelevant. However, legacy, or what we leave behind, can serve as a way to alleviate death anxiety. For many, reconciling their feelings toward their legacy is an avenue to tame death anxiety. Therapy can help individuals gain insight into their defensive behaviors and process their definition of a life well lived. By focusing on a life worth living, individuals can alleviate their death anxiety and gain a sense of fulfillment.
Dr. Akkoor is a psychiatry resident at the University of California, San Diego. She is interested in immigrant mental health, ethics, consultation-liaison psychiatry, and medical education. Dr. Badre is a clinical and forensic psychiatrist in San Diego. He holds teaching positions at the University of California, San Diego, and the University of San Diego. He teaches medical education, psychopharmacology, ethics in psychiatry, and correctional care. Dr. Badre can be reached at his website, BadreMD.com. Dr. Badre and Dr. Akkoor have no conflicts of interest.
Reference
1. Badre N. Burnout: A concept that rebrands mental illness for professionals. Clinical Psychiatry News. 2020 Mar 5.
Disappointment – “I failed this exam, my life is ruined” or regret – “I am getting a divorce, I wasted so much of my life.” Patients present with a wide variety of complaints that can be understood as a form of death anxiety.
Fundamentally, patients come to see us to understand and explain their lives. One can reinterpret this as a patient asking, “If I died today, would my life have been good enough?” or “When I die, how will I look back at this moment in time and judge the choices I made?”
Other patients come to us attempting to use the same maladaptive defenses that did not serve them well in the past in the hopes of achieving a new outcome that will validate their lives. While it may be understandable that a child dissociates when facing abuse, hoping that this defense mechanism – as an adult – will work, it is unlikely to be fruitful and will certainly not validate or repair the past. This hope to repair one’s past can be interpreted as a fear of death – “I cannot die without correcting this.” This psychic conflict can intensify if one does not adopt a more adaptive understanding of his or her life.
Death anxiety is the feeling associated with the finality of life. Not only is life final, but a constant reminder of that fact is the idea that any one moment is final. Other than in science fiction, one cannot return to a prior moment and repair the past in the hope of a better future. Time goes only in one direction and death is the natural outcome of all life.
Death may have some evolutionary purpose that encourages the promotion of newer and more fitter genes, but one doesn’t have to consider its origin and reason to admit death’s constancy throughout humanity. People die and that is an anxiety-provoking fact of life. Death anxiety can feel especially tangible in our connected world. In a world of constant news, it can feel – for many people – that if your house wasn’t displaced because of global warming or that you are not a war refugee, you don’t deserve to be seen and heard.
This can be a particularly strong feeling for and among physicians, who don’t think that the mental health challenges generated by their own tough circumstances deserve to be labeled a mental disorder, so they designate themselves as having “burnout”1 – as they don’t deserve the sympathy of having the clinically significant impairments of “depression.” Our traumas don’t seem important enough to deserve notice, and thus we may feel like we could die without ever having truly mattered.
This can also be applied in the reverse fashion. Certain individuals, like celebrities, live such extravagant lives that our simpler achievements can feel futile in comparison. While the neighbor’s grass has always felt greener, we are now constantly exposed to perfectly manicured lawns on social media. When compounded, the idea that our successes and our pains are both simultaneously irrelevant can lead one to have very palpable death anxiety – my life will never matter if none of the things I do matter, or my life will never matter because I will never achieve the requisite number of “likes” or “views” on social media required to believe that one’s life was worth living.
A way of alleviating death anxiety can be through the concept of legacy, or what we leave behind. How will people remember me? Will people remember me, or will I disappear like a shadow into the distant memory of my near and dear ones? The idea of being forgotten or lost to memory is intolerable to some and can be a strong driving force to “make a name” for oneself. For those who crave fame, whether a celebrity or a generous alumnus, part of this is likely related to remaining well known after death. After all, one can argue that you are not truly dead as long as you continue to live in the memory and/or genes of others.
Legacy thus serves as a form of posthumous transitional object; a way of calming our fears about how we will be remembered. For many, reconciling their feelings towards their legacy is an avenue to tame death anxiety.
A case study
The case of Mr. B illustrates this. As a 72-year-old male with a long history of generalized anxiety, he once had a nightmare as a child, similar to the plot of Sleeping Beauty. In his dream, he walks up a spiral staircase in a castle and touches the spindle on a spinning wheel, thus ending his life. The dream was vivid and marked him.
His fear of death has subsequently reared its head throughout his life. In more recent years, he has suffered from cardiovascular disease. Although he is now quite stable on his current cardiac medications, he is constantly fearful that he will experience a cardiac event while asleep and suddenly die. He is so anxious about not waking up in the morning that falling asleep is nearly impossible.
Mr. B is single, with no close family besides a sister who lives in another state. He has a dog and few friends. He worries about what will happen to his dog if he doesn’t wake up in the morning, but perhaps most distressing to him is “there’s so much left for me to do, I have so much to write!” As an accomplished author, he continues to write, and hopes to publish many more novels in his lifetime. It is unsurprising that someone without a strong social network may fear death and feel pressured to somehow make a mark on the world before the curtain falls. It is scary to think that even without us, life goes on.
By bringing to Mr. B’s attention that his ever-present anxiety is rooted in fear of death, he was able to gain more insight into his own defensive behaviors. By confronting his death anxiety and processing his definition of a life well lived together in therapy, he’s acknowledged his lack of social connection as demoralizing, and has made significant strides to remedy this. He’s been able to focus on a more fulfilling life day to day, with less emphasis on his to-do list and aspirations. Instead, he’s connected more with his faith and members of his church. He’s gotten close to several neighbors and enjoys long dinners with them on his back patio.
At a recent meeting, he confessed that he feels “lighter” and not as fearful about sudden cardiac death, and thus has noticed that his overall anxiety has diminished greatly. He concluded that experiencing meaningful relationships in the present moment would give him greater joy than spending his remaining time engaged in preserving a future identity for himself. It seems elementary, but if we look within, we may find that we all suffer similarly: How much of our daily actions, thoughts, and fears are tied to the looming threat of death?
Conclusion
While modern psychiatry continues to advance with better understandings of our neurobiology, improved knowledge of pathophysiological processes of mental illness, and expanding discovery of novel pharmacotherapeutics, the modern psychiatrist should not forget fundamental truths of behavior and humanity that were once the staple of psychiatry.
Death anxiety is one of those truths; it is the ultimate stressor that we will all face and should be regular study and practice for psychiatrists. In this article, we explored some of those facets most meaningful to us but recommend you expand your study to the many more available.
Patients often come to physicians seeking validation of their lives or trying to use the same maladaptive defense mechanisms that did not serve them well in the past to achieve a better outcome.
In today’s world, death anxiety can feel palpable due to the constant exposure to global news and social media that can make us feel irrelevant. However, legacy, or what we leave behind, can serve as a way to alleviate death anxiety. For many, reconciling their feelings toward their legacy is an avenue to tame death anxiety. Therapy can help individuals gain insight into their defensive behaviors and process their definition of a life well lived. By focusing on a life worth living, individuals can alleviate their death anxiety and gain a sense of fulfillment.
Dr. Akkoor is a psychiatry resident at the University of California, San Diego. She is interested in immigrant mental health, ethics, consultation-liaison psychiatry, and medical education. Dr. Badre is a clinical and forensic psychiatrist in San Diego. He holds teaching positions at the University of California, San Diego, and the University of San Diego. He teaches medical education, psychopharmacology, ethics in psychiatry, and correctional care. Dr. Badre can be reached at his website, BadreMD.com. Dr. Badre and Dr. Akkoor have no conflicts of interest.
Reference
1. Badre N. Burnout: A concept that rebrands mental illness for professionals. Clinical Psychiatry News. 2020 Mar 5.
Preventing breaks and falls in older adults
LONG BEACH, CALIF. – Ms. S had recently arrived home after a stay at a skilled nursing facility to recover from a hip fracture resulting from osteoporosis. For many patients, follow-up care would have included a DEXA scan or a prescription for a bisphosphonate from a primary care clinician not trained in geriatrics.
But the 85-year-old received care that went further and that is considered best practice for the management of geriatric fractures: A physical therapist visited her after discharge and provided education on the importance of maintaining mobility. Ms. S also underwent assessment for fall risk and gait balance, and a team of multidisciplinary clinicians managed other factors, from postural hypotension to footwear and foot problems.
Sonja Rosen, MD, professor of medicine and chief of geriatric medicine at Cedars-Sinai Medical Center, Los Angeles, talked about Ms. S as part of a panel discussion on applying the “Geriatric 5Ms” for patients with osteoporosis at the annual meeting of the American Geriatrics Society.
“You have to figure out why they are falling and help them not fall again,” Dr. Rosen said.
Approximately 10 million Americans have osteoporosis, and another 44 million have low bone density. One in two women and up to one in four men will experience a bone fracture as a result of osteoporosis, according to the Bone Health and Osteoporosis Foundation.
, which involves considering the care preferences and goals for health care outcomes of individuals.
Ms. S eventually visited a geriatrician through the Cedars-Sinai Geriatric Fracture Program, which has been shown to lower costs and shorten hospital stays. In the program, she was advised to use a walker. Initially, she saw the aid as a hindrance – she felt she should be able to walk without it, like before. But with education, she learned that it is impossible to predict falls and that the walking aid could reduce her risk of a stumble.
Dr. Rosen said clinicians should address any vision problems, prescriptions for psychotropic drugs,which can affect balance, and heart rate and rhythm abnormalities, and they should suggest modifications to the home environment, such as installing grab bars in showers and removing rugs that can easily be tripped over.
The program at Cedars-Sinai, like similar initiatives, offers a team with resources that some clinicians may not have access to, such as a care coordinator and bone-health coach. But health care providers can utilize aspects, such as making referrals to community exercise classes.
Dr. Rosen and her colleagues studied the effects of such exercise programs and found that the programs lessen loneliness and social isolation. Fear of falling decreased in 75% of participants, “which is so key to these postfracture patients in getting back out into the world and engaging in their prior level of functional status,” Dr. Rosen said.
The second ‘M’: Medication management
The second “M,” medications, can help clinicians sequence osteoporosis drugs, depending on patient characteristics and scenarios.
Cathleen Colon-Emeric, MD, MHS, chief of geriatrics at Duke University, in Durham, N.C., dived into the case history of Ms. S, who had hypertension and insomnia in addition to osteoporosis.
First-line treatment for Ms. S – and for most patients – was an oral bisphosphonate, Dr. Colon-Emeric said. Compared with placebo, the drugs decrease the risk of overall osteoporotic fractures by nearly 40% (odds ratio, 0.62). But the medications are linked to injury of the esophageal mucosa. This risk is decreased when a patient stays upright for 30 minutes after taking oral bisphosphonates. Dr. Colon-Emeric displayed a slide of a woman receiving a pedicure at a nail salon.
“The picture of the pedicure is to share the wonderful idea I got from one skilled nursing facility I was working with, who makes sure they do safe administration to prevent esophagitis in their patients by having them all go to a spa day, where they all sit up and get their nails done while they wait their 30 minutes [after taking the pill] sitting up safely,” Dr. Colon-Emeric said.
This strategy drew applause from the audience.
Dr. Colon-Emeric advised that clinicians use judgment in the interpretation of results from the Fracture Risk Assessment Tool (FRAX). Incorporating race into estimates of fracture risk has pros and cons. While there are racial and ethnic differences in average bone density, the data for race calibrations to estimate risk are dated, she said. Clinicians should compare FRAX estimates with and without race input to help patients understand a range of risks.
Some patients may be reluctant to begin taking osteoporosis drugs because of misinformation originating from inaccurate news reports or anecdotes from friends. Dr. Colon-Emeric advised clinicians to remind patients that one in five who experience a fracture will have another injury in the following 2 years.
“A major osteoporotic fracture is akin to a heart attack; it has a very similar 1-year mortality rate and a very similar rate of a subsequent secondary event,” Dr. Colon-Emeric said. “We have a class of medications that decrease both those risks by nearly a third.”
Shared decision-making can help patients understand the risks and benefits of treatment, she said.
“People are really scared about the side effects,” Michelle Keller, PhD, MPH, a research scientist at Cedars-Sinai who attended the session, said. “The idea that a “bone attack” is like a heart attack gets the message across.”
Mind and multicomplexity
Medical complexity of a patient must be considered when making decisions on treatment, according to Joshua Niznik, PharmD, PhD, assistant professor of medicine in the Center for Aging and Health at the University of North Carolina at Chapel Hill.
“Medical complexity is an acknowledgment of the entire person, the burden of their multiple chronic conditions, advanced illnesses, and also their biopsychosocial needs and how those together might augment treatment selection and decision-making,” Dr. Niznik said.
Studies by Dr. Niznik and others have shown that swallowing difficulties, severe dementia, and being older than 90 are linked with a lower likelihood of receiving treatment for osteoporosis.
But therapies for fracture prevention, especially bisphosphonates, appear to be at least as effective for adults with medical complexity as they are for people without such conditions, Dr. Niznik said. Physicians must consider the potential treatment burden and the likelihood of benefit, he said.
Dr. Niznik’s research has shown a lack of strong evidence on how clinicians can manage patients in nursing homes. In some cases, deprescribing is reasonable, such as for patients who have undergone treatment for several years and whose life expectancy is less than 2 years.
“In the absence of any of those, if they are not already treated for osteoporosis, it makes sense to initiate treatment at that time,” Dr. Niznik said.
Matters most: Patient input
Clinicians need to educate patients on how long they must undergo a treatment before they experience benefits, according to Sarah D. Berry, MD, MPH, associate professor of medicine at Harvard Medical School, in Boston.
A meta-analysis of studies that included more than 20,000 women who were randomly assigned to receive bisphosphonate or placebo found that one nonvertebral fracture was avoided during a 12-month period for every 100 persons treated. One hip fracture was avoided during a 20-month period for every 200 patients treated.
“In general, in persons with a 2-year life expectancy, time to benefit favors bisphosphonate use,” Dr. Berry said. “Anabolics may have an even quicker time to benefit.”
Dr. Berry said a shared a decision-making model can help clinicians facilitate discussions that help patients prioritize goals and compare options while considering results, benefits, and harms. And she offered a final tip: Use tools with absolute risk reduction to convey risks and benefits, as the relative risk calculations overestimate how effective treatment will be.
Dr. Rosen has disclosed no relevant financial relationships. Dr. Colon-Emeric has received grants from the National Institutes of Health and VA Health Services Research and Development Funding; has served as endpoint adjudication chair for UCB Pharma; and has received royalties from Wolters Kluwer. Dr. Niznik has received funding from the National Institute of Aging and the Centers for Disease Control and Prevention. Dr. Berry has received funding from the NIH and royalties from Wolters Kluwer.
A version of this article originally appeared on Medscape.com.
LONG BEACH, CALIF. – Ms. S had recently arrived home after a stay at a skilled nursing facility to recover from a hip fracture resulting from osteoporosis. For many patients, follow-up care would have included a DEXA scan or a prescription for a bisphosphonate from a primary care clinician not trained in geriatrics.
But the 85-year-old received care that went further and that is considered best practice for the management of geriatric fractures: A physical therapist visited her after discharge and provided education on the importance of maintaining mobility. Ms. S also underwent assessment for fall risk and gait balance, and a team of multidisciplinary clinicians managed other factors, from postural hypotension to footwear and foot problems.
Sonja Rosen, MD, professor of medicine and chief of geriatric medicine at Cedars-Sinai Medical Center, Los Angeles, talked about Ms. S as part of a panel discussion on applying the “Geriatric 5Ms” for patients with osteoporosis at the annual meeting of the American Geriatrics Society.
“You have to figure out why they are falling and help them not fall again,” Dr. Rosen said.
Approximately 10 million Americans have osteoporosis, and another 44 million have low bone density. One in two women and up to one in four men will experience a bone fracture as a result of osteoporosis, according to the Bone Health and Osteoporosis Foundation.
, which involves considering the care preferences and goals for health care outcomes of individuals.
Ms. S eventually visited a geriatrician through the Cedars-Sinai Geriatric Fracture Program, which has been shown to lower costs and shorten hospital stays. In the program, she was advised to use a walker. Initially, she saw the aid as a hindrance – she felt she should be able to walk without it, like before. But with education, she learned that it is impossible to predict falls and that the walking aid could reduce her risk of a stumble.
Dr. Rosen said clinicians should address any vision problems, prescriptions for psychotropic drugs,which can affect balance, and heart rate and rhythm abnormalities, and they should suggest modifications to the home environment, such as installing grab bars in showers and removing rugs that can easily be tripped over.
The program at Cedars-Sinai, like similar initiatives, offers a team with resources that some clinicians may not have access to, such as a care coordinator and bone-health coach. But health care providers can utilize aspects, such as making referrals to community exercise classes.
Dr. Rosen and her colleagues studied the effects of such exercise programs and found that the programs lessen loneliness and social isolation. Fear of falling decreased in 75% of participants, “which is so key to these postfracture patients in getting back out into the world and engaging in their prior level of functional status,” Dr. Rosen said.
The second ‘M’: Medication management
The second “M,” medications, can help clinicians sequence osteoporosis drugs, depending on patient characteristics and scenarios.
Cathleen Colon-Emeric, MD, MHS, chief of geriatrics at Duke University, in Durham, N.C., dived into the case history of Ms. S, who had hypertension and insomnia in addition to osteoporosis.
First-line treatment for Ms. S – and for most patients – was an oral bisphosphonate, Dr. Colon-Emeric said. Compared with placebo, the drugs decrease the risk of overall osteoporotic fractures by nearly 40% (odds ratio, 0.62). But the medications are linked to injury of the esophageal mucosa. This risk is decreased when a patient stays upright for 30 minutes after taking oral bisphosphonates. Dr. Colon-Emeric displayed a slide of a woman receiving a pedicure at a nail salon.
“The picture of the pedicure is to share the wonderful idea I got from one skilled nursing facility I was working with, who makes sure they do safe administration to prevent esophagitis in their patients by having them all go to a spa day, where they all sit up and get their nails done while they wait their 30 minutes [after taking the pill] sitting up safely,” Dr. Colon-Emeric said.
This strategy drew applause from the audience.
Dr. Colon-Emeric advised that clinicians use judgment in the interpretation of results from the Fracture Risk Assessment Tool (FRAX). Incorporating race into estimates of fracture risk has pros and cons. While there are racial and ethnic differences in average bone density, the data for race calibrations to estimate risk are dated, she said. Clinicians should compare FRAX estimates with and without race input to help patients understand a range of risks.
Some patients may be reluctant to begin taking osteoporosis drugs because of misinformation originating from inaccurate news reports or anecdotes from friends. Dr. Colon-Emeric advised clinicians to remind patients that one in five who experience a fracture will have another injury in the following 2 years.
“A major osteoporotic fracture is akin to a heart attack; it has a very similar 1-year mortality rate and a very similar rate of a subsequent secondary event,” Dr. Colon-Emeric said. “We have a class of medications that decrease both those risks by nearly a third.”
Shared decision-making can help patients understand the risks and benefits of treatment, she said.
“People are really scared about the side effects,” Michelle Keller, PhD, MPH, a research scientist at Cedars-Sinai who attended the session, said. “The idea that a “bone attack” is like a heart attack gets the message across.”
Mind and multicomplexity
Medical complexity of a patient must be considered when making decisions on treatment, according to Joshua Niznik, PharmD, PhD, assistant professor of medicine in the Center for Aging and Health at the University of North Carolina at Chapel Hill.
“Medical complexity is an acknowledgment of the entire person, the burden of their multiple chronic conditions, advanced illnesses, and also their biopsychosocial needs and how those together might augment treatment selection and decision-making,” Dr. Niznik said.
Studies by Dr. Niznik and others have shown that swallowing difficulties, severe dementia, and being older than 90 are linked with a lower likelihood of receiving treatment for osteoporosis.
But therapies for fracture prevention, especially bisphosphonates, appear to be at least as effective for adults with medical complexity as they are for people without such conditions, Dr. Niznik said. Physicians must consider the potential treatment burden and the likelihood of benefit, he said.
Dr. Niznik’s research has shown a lack of strong evidence on how clinicians can manage patients in nursing homes. In some cases, deprescribing is reasonable, such as for patients who have undergone treatment for several years and whose life expectancy is less than 2 years.
“In the absence of any of those, if they are not already treated for osteoporosis, it makes sense to initiate treatment at that time,” Dr. Niznik said.
Matters most: Patient input
Clinicians need to educate patients on how long they must undergo a treatment before they experience benefits, according to Sarah D. Berry, MD, MPH, associate professor of medicine at Harvard Medical School, in Boston.
A meta-analysis of studies that included more than 20,000 women who were randomly assigned to receive bisphosphonate or placebo found that one nonvertebral fracture was avoided during a 12-month period for every 100 persons treated. One hip fracture was avoided during a 20-month period for every 200 patients treated.
“In general, in persons with a 2-year life expectancy, time to benefit favors bisphosphonate use,” Dr. Berry said. “Anabolics may have an even quicker time to benefit.”
Dr. Berry said a shared a decision-making model can help clinicians facilitate discussions that help patients prioritize goals and compare options while considering results, benefits, and harms. And she offered a final tip: Use tools with absolute risk reduction to convey risks and benefits, as the relative risk calculations overestimate how effective treatment will be.
Dr. Rosen has disclosed no relevant financial relationships. Dr. Colon-Emeric has received grants from the National Institutes of Health and VA Health Services Research and Development Funding; has served as endpoint adjudication chair for UCB Pharma; and has received royalties from Wolters Kluwer. Dr. Niznik has received funding from the National Institute of Aging and the Centers for Disease Control and Prevention. Dr. Berry has received funding from the NIH and royalties from Wolters Kluwer.
A version of this article originally appeared on Medscape.com.
LONG BEACH, CALIF. – Ms. S had recently arrived home after a stay at a skilled nursing facility to recover from a hip fracture resulting from osteoporosis. For many patients, follow-up care would have included a DEXA scan or a prescription for a bisphosphonate from a primary care clinician not trained in geriatrics.
But the 85-year-old received care that went further and that is considered best practice for the management of geriatric fractures: A physical therapist visited her after discharge and provided education on the importance of maintaining mobility. Ms. S also underwent assessment for fall risk and gait balance, and a team of multidisciplinary clinicians managed other factors, from postural hypotension to footwear and foot problems.
Sonja Rosen, MD, professor of medicine and chief of geriatric medicine at Cedars-Sinai Medical Center, Los Angeles, talked about Ms. S as part of a panel discussion on applying the “Geriatric 5Ms” for patients with osteoporosis at the annual meeting of the American Geriatrics Society.
“You have to figure out why they are falling and help them not fall again,” Dr. Rosen said.
Approximately 10 million Americans have osteoporosis, and another 44 million have low bone density. One in two women and up to one in four men will experience a bone fracture as a result of osteoporosis, according to the Bone Health and Osteoporosis Foundation.
, which involves considering the care preferences and goals for health care outcomes of individuals.
Ms. S eventually visited a geriatrician through the Cedars-Sinai Geriatric Fracture Program, which has been shown to lower costs and shorten hospital stays. In the program, she was advised to use a walker. Initially, she saw the aid as a hindrance – she felt she should be able to walk without it, like before. But with education, she learned that it is impossible to predict falls and that the walking aid could reduce her risk of a stumble.
Dr. Rosen said clinicians should address any vision problems, prescriptions for psychotropic drugs,which can affect balance, and heart rate and rhythm abnormalities, and they should suggest modifications to the home environment, such as installing grab bars in showers and removing rugs that can easily be tripped over.
The program at Cedars-Sinai, like similar initiatives, offers a team with resources that some clinicians may not have access to, such as a care coordinator and bone-health coach. But health care providers can utilize aspects, such as making referrals to community exercise classes.
Dr. Rosen and her colleagues studied the effects of such exercise programs and found that the programs lessen loneliness and social isolation. Fear of falling decreased in 75% of participants, “which is so key to these postfracture patients in getting back out into the world and engaging in their prior level of functional status,” Dr. Rosen said.
The second ‘M’: Medication management
The second “M,” medications, can help clinicians sequence osteoporosis drugs, depending on patient characteristics and scenarios.
Cathleen Colon-Emeric, MD, MHS, chief of geriatrics at Duke University, in Durham, N.C., dived into the case history of Ms. S, who had hypertension and insomnia in addition to osteoporosis.
First-line treatment for Ms. S – and for most patients – was an oral bisphosphonate, Dr. Colon-Emeric said. Compared with placebo, the drugs decrease the risk of overall osteoporotic fractures by nearly 40% (odds ratio, 0.62). But the medications are linked to injury of the esophageal mucosa. This risk is decreased when a patient stays upright for 30 minutes after taking oral bisphosphonates. Dr. Colon-Emeric displayed a slide of a woman receiving a pedicure at a nail salon.
“The picture of the pedicure is to share the wonderful idea I got from one skilled nursing facility I was working with, who makes sure they do safe administration to prevent esophagitis in their patients by having them all go to a spa day, where they all sit up and get their nails done while they wait their 30 minutes [after taking the pill] sitting up safely,” Dr. Colon-Emeric said.
This strategy drew applause from the audience.
Dr. Colon-Emeric advised that clinicians use judgment in the interpretation of results from the Fracture Risk Assessment Tool (FRAX). Incorporating race into estimates of fracture risk has pros and cons. While there are racial and ethnic differences in average bone density, the data for race calibrations to estimate risk are dated, she said. Clinicians should compare FRAX estimates with and without race input to help patients understand a range of risks.
Some patients may be reluctant to begin taking osteoporosis drugs because of misinformation originating from inaccurate news reports or anecdotes from friends. Dr. Colon-Emeric advised clinicians to remind patients that one in five who experience a fracture will have another injury in the following 2 years.
“A major osteoporotic fracture is akin to a heart attack; it has a very similar 1-year mortality rate and a very similar rate of a subsequent secondary event,” Dr. Colon-Emeric said. “We have a class of medications that decrease both those risks by nearly a third.”
Shared decision-making can help patients understand the risks and benefits of treatment, she said.
“People are really scared about the side effects,” Michelle Keller, PhD, MPH, a research scientist at Cedars-Sinai who attended the session, said. “The idea that a “bone attack” is like a heart attack gets the message across.”
Mind and multicomplexity
Medical complexity of a patient must be considered when making decisions on treatment, according to Joshua Niznik, PharmD, PhD, assistant professor of medicine in the Center for Aging and Health at the University of North Carolina at Chapel Hill.
“Medical complexity is an acknowledgment of the entire person, the burden of their multiple chronic conditions, advanced illnesses, and also their biopsychosocial needs and how those together might augment treatment selection and decision-making,” Dr. Niznik said.
Studies by Dr. Niznik and others have shown that swallowing difficulties, severe dementia, and being older than 90 are linked with a lower likelihood of receiving treatment for osteoporosis.
But therapies for fracture prevention, especially bisphosphonates, appear to be at least as effective for adults with medical complexity as they are for people without such conditions, Dr. Niznik said. Physicians must consider the potential treatment burden and the likelihood of benefit, he said.
Dr. Niznik’s research has shown a lack of strong evidence on how clinicians can manage patients in nursing homes. In some cases, deprescribing is reasonable, such as for patients who have undergone treatment for several years and whose life expectancy is less than 2 years.
“In the absence of any of those, if they are not already treated for osteoporosis, it makes sense to initiate treatment at that time,” Dr. Niznik said.
Matters most: Patient input
Clinicians need to educate patients on how long they must undergo a treatment before they experience benefits, according to Sarah D. Berry, MD, MPH, associate professor of medicine at Harvard Medical School, in Boston.
A meta-analysis of studies that included more than 20,000 women who were randomly assigned to receive bisphosphonate or placebo found that one nonvertebral fracture was avoided during a 12-month period for every 100 persons treated. One hip fracture was avoided during a 20-month period for every 200 patients treated.
“In general, in persons with a 2-year life expectancy, time to benefit favors bisphosphonate use,” Dr. Berry said. “Anabolics may have an even quicker time to benefit.”
Dr. Berry said a shared a decision-making model can help clinicians facilitate discussions that help patients prioritize goals and compare options while considering results, benefits, and harms. And she offered a final tip: Use tools with absolute risk reduction to convey risks and benefits, as the relative risk calculations overestimate how effective treatment will be.
Dr. Rosen has disclosed no relevant financial relationships. Dr. Colon-Emeric has received grants from the National Institutes of Health and VA Health Services Research and Development Funding; has served as endpoint adjudication chair for UCB Pharma; and has received royalties from Wolters Kluwer. Dr. Niznik has received funding from the National Institute of Aging and the Centers for Disease Control and Prevention. Dr. Berry has received funding from the NIH and royalties from Wolters Kluwer.
A version of this article originally appeared on Medscape.com.
AT AGS 2023