User login
Medication compliance
Introduction
Stimulant medications are an important part of attention-deficit/hyperactivity disorder (ADHD) treatment for most affected children and teens. But studies suggest that children and teens may not take their prescribed medication anywhere from 13% to as much as 64% of the time. As teenagers develop an appropriate increased desire for autonomy, they wish to have greater participation in their medication decisions, sometimes to the dismay of their parents.
Case
Will is an engaging young man who has been on stimulants for many years. However, he is frequently in conflict with his parents over an array of issues, including being annoyed at being reminded to take his medications. Although he is willing to take medication some of the time, he often forgets. He commonly fails to complete his homework, a further source of conflict.
Discussion
Parents can get frustrated with their teens and drawn into a control struggle over medication and other issues. Teenagers want to have more control of their lives, and sometimes this takes the form of not wanting to take medication. The No. 1 goal is to help the family move away from digging themselves further into conflict, and instead to have a genuine discussion about the pros and cons of medication.
This starts with listening seriously to the teenager. It helps to reassure teens that you are not going to get mad at them for not taking medication, but that instead you really value the information about how often they are taking it and, if they are skipping some doses or not taking it at all, the reason for that.
It is crucial to find out the real reason why someone is not taking his medication. Sometimes teens are genuinely forgetting. Here it can be helpful to be sure that the medication has to be taken as few times a day as possible, and then to set some kind of alarm reminder. This is one area where the omnipresence of cell phones is very useful. Help parents and teens negotiate about whether the parent will remind the teen, as repeated reminders can be irritating. Divided pill containers help both the parent and teen know whether the medication has been taken or not. If you formulate a plan with the family, write it down so that you can ask next time how it worked out, because if you are asking someone to make a behavior change, it is important to pay attention to whether they did it or not.
Other times it is clear that the teen doesn’t want to take the medication. In this situation, it is important to get the specifics. It is key to convey that the teen’s point of view is very important.
Reasons for not wanting to take a medication include some type of side effect, embarrassment about having to take the medication in school, inconvenience, or a general feeling that the teen doesn’t want to be on medication.
A genuinely collaborative attitude is the best approach. Restate what you have heard from the teen about his or her viewpoint. Help the parents state their concerns (for instance, about school success, driving safety, or the potential for impulsive behavior) in a noncritical manner. Then outline options and discuss the possible pros and cons of the different choices, including going off the medication as one option. By considering this as an option, you will have an opportunity to discuss what the drawbacks, as well as the advantages, might be.
When it comes to ADHD, there are many choices. These can include trying a different stimulant or using a nonstimulant such as atomoxetine or an alpha-adrenergic agonist. Because these medications have very different side effect profiles, they may be more acceptable to the teenager, although they also may have different efficacy. There are also psychotherapeutic options such as organizational skills training. By discussing a variety of choices and listening to the teen’s concerns and hopes, the teenager is engaged in taking responsibility for his own choices.
Once a choice is decided upon, it is important to follow up and review how well the plan is working and revise if necessary.
When to consult
If parents and teens are unable to participate in discussion and come up with a plan, family therapy to improve communication and address parenting issues can be recommended.
Dr. Hall is assistant professor of psychiatry and pediatrics at the University of Vermont, Burlington. Dr. Hall said that she had no relevant financial disclosures. To comment, e-mail her at [email protected].
Introduction
Stimulant medications are an important part of attention-deficit/hyperactivity disorder (ADHD) treatment for most affected children and teens. But studies suggest that children and teens may not take their prescribed medication anywhere from 13% to as much as 64% of the time. As teenagers develop an appropriate increased desire for autonomy, they wish to have greater participation in their medication decisions, sometimes to the dismay of their parents.
Case
Will is an engaging young man who has been on stimulants for many years. However, he is frequently in conflict with his parents over an array of issues, including being annoyed at being reminded to take his medications. Although he is willing to take medication some of the time, he often forgets. He commonly fails to complete his homework, a further source of conflict.
Discussion
Parents can get frustrated with their teens and drawn into a control struggle over medication and other issues. Teenagers want to have more control of their lives, and sometimes this takes the form of not wanting to take medication. The No. 1 goal is to help the family move away from digging themselves further into conflict, and instead to have a genuine discussion about the pros and cons of medication.
This starts with listening seriously to the teenager. It helps to reassure teens that you are not going to get mad at them for not taking medication, but that instead you really value the information about how often they are taking it and, if they are skipping some doses or not taking it at all, the reason for that.
It is crucial to find out the real reason why someone is not taking his medication. Sometimes teens are genuinely forgetting. Here it can be helpful to be sure that the medication has to be taken as few times a day as possible, and then to set some kind of alarm reminder. This is one area where the omnipresence of cell phones is very useful. Help parents and teens negotiate about whether the parent will remind the teen, as repeated reminders can be irritating. Divided pill containers help both the parent and teen know whether the medication has been taken or not. If you formulate a plan with the family, write it down so that you can ask next time how it worked out, because if you are asking someone to make a behavior change, it is important to pay attention to whether they did it or not.
Other times it is clear that the teen doesn’t want to take the medication. In this situation, it is important to get the specifics. It is key to convey that the teen’s point of view is very important.
Reasons for not wanting to take a medication include some type of side effect, embarrassment about having to take the medication in school, inconvenience, or a general feeling that the teen doesn’t want to be on medication.
A genuinely collaborative attitude is the best approach. Restate what you have heard from the teen about his or her viewpoint. Help the parents state their concerns (for instance, about school success, driving safety, or the potential for impulsive behavior) in a noncritical manner. Then outline options and discuss the possible pros and cons of the different choices, including going off the medication as one option. By considering this as an option, you will have an opportunity to discuss what the drawbacks, as well as the advantages, might be.
When it comes to ADHD, there are many choices. These can include trying a different stimulant or using a nonstimulant such as atomoxetine or an alpha-adrenergic agonist. Because these medications have very different side effect profiles, they may be more acceptable to the teenager, although they also may have different efficacy. There are also psychotherapeutic options such as organizational skills training. By discussing a variety of choices and listening to the teen’s concerns and hopes, the teenager is engaged in taking responsibility for his own choices.
Once a choice is decided upon, it is important to follow up and review how well the plan is working and revise if necessary.
When to consult
If parents and teens are unable to participate in discussion and come up with a plan, family therapy to improve communication and address parenting issues can be recommended.
Dr. Hall is assistant professor of psychiatry and pediatrics at the University of Vermont, Burlington. Dr. Hall said that she had no relevant financial disclosures. To comment, e-mail her at [email protected].
Introduction
Stimulant medications are an important part of attention-deficit/hyperactivity disorder (ADHD) treatment for most affected children and teens. But studies suggest that children and teens may not take their prescribed medication anywhere from 13% to as much as 64% of the time. As teenagers develop an appropriate increased desire for autonomy, they wish to have greater participation in their medication decisions, sometimes to the dismay of their parents.
Case
Will is an engaging young man who has been on stimulants for many years. However, he is frequently in conflict with his parents over an array of issues, including being annoyed at being reminded to take his medications. Although he is willing to take medication some of the time, he often forgets. He commonly fails to complete his homework, a further source of conflict.
Discussion
Parents can get frustrated with their teens and drawn into a control struggle over medication and other issues. Teenagers want to have more control of their lives, and sometimes this takes the form of not wanting to take medication. The No. 1 goal is to help the family move away from digging themselves further into conflict, and instead to have a genuine discussion about the pros and cons of medication.
This starts with listening seriously to the teenager. It helps to reassure teens that you are not going to get mad at them for not taking medication, but that instead you really value the information about how often they are taking it and, if they are skipping some doses or not taking it at all, the reason for that.
It is crucial to find out the real reason why someone is not taking his medication. Sometimes teens are genuinely forgetting. Here it can be helpful to be sure that the medication has to be taken as few times a day as possible, and then to set some kind of alarm reminder. This is one area where the omnipresence of cell phones is very useful. Help parents and teens negotiate about whether the parent will remind the teen, as repeated reminders can be irritating. Divided pill containers help both the parent and teen know whether the medication has been taken or not. If you formulate a plan with the family, write it down so that you can ask next time how it worked out, because if you are asking someone to make a behavior change, it is important to pay attention to whether they did it or not.
Other times it is clear that the teen doesn’t want to take the medication. In this situation, it is important to get the specifics. It is key to convey that the teen’s point of view is very important.
Reasons for not wanting to take a medication include some type of side effect, embarrassment about having to take the medication in school, inconvenience, or a general feeling that the teen doesn’t want to be on medication.
A genuinely collaborative attitude is the best approach. Restate what you have heard from the teen about his or her viewpoint. Help the parents state their concerns (for instance, about school success, driving safety, or the potential for impulsive behavior) in a noncritical manner. Then outline options and discuss the possible pros and cons of the different choices, including going off the medication as one option. By considering this as an option, you will have an opportunity to discuss what the drawbacks, as well as the advantages, might be.
When it comes to ADHD, there are many choices. These can include trying a different stimulant or using a nonstimulant such as atomoxetine or an alpha-adrenergic agonist. Because these medications have very different side effect profiles, they may be more acceptable to the teenager, although they also may have different efficacy. There are also psychotherapeutic options such as organizational skills training. By discussing a variety of choices and listening to the teen’s concerns and hopes, the teenager is engaged in taking responsibility for his own choices.
Once a choice is decided upon, it is important to follow up and review how well the plan is working and revise if necessary.
When to consult
If parents and teens are unable to participate in discussion and come up with a plan, family therapy to improve communication and address parenting issues can be recommended.
Dr. Hall is assistant professor of psychiatry and pediatrics at the University of Vermont, Burlington. Dr. Hall said that she had no relevant financial disclosures. To comment, e-mail her at [email protected].
Mortality, outcomes good in AAA repair in octogenarians
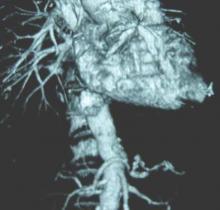
SCOTTSDALE, ARIZ.– Abdominal aortic aneurysm repair in patients 80 years and older can be performed safely and with good medium-term survival rates, a prospective single-site study has shown.
Perioperative mortality in elective and emergent AAA repair for octogenarians was 2% and 35%, respectively, with a median survival rate of 19 months in both groups.
According to these data, “Patients shouldn’t be turned down for aneurysm repair on the basis of their age alone,” Dr. Christopher M. Lamb, a vascular surgery fellow at the University of California Davis Medical Center in Sacramento, said during a presentation at this year’s Southern Association for Vascular Surgery annual meeting.
“However, whether we should be doing these procedures is a different question, and I don’t think these data allow us to answer that question properly.”Dr. Lamb and his colleagues reviewed the records of 847 consecutive patients aged 80 years or older, seen between April 2005 and February 2014 for any type of AAA repair. Cases were sorted according to whether they were elective, ruptured, or urgent but unruptured. A total of 226 patients met the study’s age criteria; there were nearly seven men for every woman, all with a median age of 83 years. Of the elective AAA repair arm of the study, 131 patients (116 men) with a median age of 82 years had an endovascular repair, while the rest underwent open surgical repair. The combined 30-day mortality rate for these patients was 2.3%, with no significant difference between either the endovascular aneurysm repair (EVAR) or the open surgical repair (OSR) patients (1.9% vs. 4.2%; P = .458). The median survival of all elective repair patients was 19 months (interquartile range, 10-35), with no difference seen between the two groups (P = .113)Of the 65 patients (53 men) with ruptured AAA, the median age was 83 years. A third had open repair (32.3%), while the rest had EVAR. The combined 30-day mortality rate was 35.4% but was significantly higher after OSR (52.4% vs. 27.3%; P = .048). The median survival rate was 6 months (IQR, 6-42) when 30-day mortality rates were excluded. The median survival rates in patients who lived longer than 30 days was significantly higher in OSR patients (42.5 months vs. 11 months; P = .019).
Of the 23 men and 7 women with symptomatic but unruptured AAA, all but 1 had EVAR. At 30 days, there was one diverticular perforation–related postoperative death in the EVAR group, which had a median survival rate of 29 months. There being only a single patient in the OSR group obviated a comparative median survival rate analysis.
A subanalysis of the final 20 months of the study showed that 41% of octogenarians seeking any type of AAA repair at the site were rejected (48 rejections vs. 69 repairs). Those who were rejected for repair tended to be older, with a median age of 86 years vs. 83 years for patients who underwent repair (P = .0004).
Dr. Lamb noted that although the findings demonstrate acceptable overall safety rates for the entire cohort, without a control group of patients that did not have AAA repair, it would be hard to draw a definite conclusion about the utility of the findings, and that more data were warranted; however, the potential for limited long-term survival with what previous reports have suggested may include “a reduced quality of life for a good part of it, possibly raises the question that these patients should be treated conservatively, more often.”
The rejection rate data prompted the presentation’s discussant, Dr. William D. Jordan Jr., section chief of vascular surgery at the University of Alabama at Birmingham and the presentation’s discussant, to challenge the findings and asked whether a single surgeon selected the patients.
“You said there is not a selection bias in your study, but I beg to differ. Perhaps all these kinds of studies have a selection bias, and I believe they should. We should select the appropriate patients for the appropriate procedure at the appropriate time, with the appropriate expectation of outcome. Bias in this setting may be seen as good,” Dr. Jordan said.Dr. Lamb responded that the treatment algorithm at the site for all patients with a confirmed AAA of 5.5 cm or greater included CT imaging that is reviewed by a multidisciplinary team comprising vascular surgeons and interventional radiologists, who then evaluated the patients according to their physiology and anatomy, as well as their comorbidities, with the intention that whenever possible, EVAR rather than open repair would be performed.
As to whether there was a bias toward not repairing AAA in older patients, Dr. Lamb said it was incumbent on any health system to evaluate a procedure’s cost-effectiveness, but that, “the life expectancy of a vascular patient is often more limited than I think we’d like to believe ... we don’t know what the natural history of these patients’ life expectancy is. We don’t know from these data what the cause of death was, but anecdotally, we didn’t see hundreds of patients return with ruptured aneurysms after an EVAR.”
“I would truly like to see how many [of these patients] who make it out of the hospital return to normal living within 6 months,” Dr. Samuel R. Money, chair of surgery at the Mayo Clinic in Scottsdale, Ariz., said in an interview following the presentation. “At some point, the question becomes ‘Can we afford to spend $100,000 dollars to keep a 90-year-old patient alive for 6 more months?’ Can this society sustain the cost of that?”
On Twitter @whitneymcknight
This discussion is provocative and raises some interesting points. Obviously cost-effectiveness considerations are important, and our country does not have unlimited funds to spend on medical care. And perhaps there are some elderly and frail individuals who should not have their AAAs repaired electively because the risk of rupture during the patients’ remaining months or years of life is small.
This is particularly true if the patient’s AAA is less than 7 cm and his or her anatomy and condition are unsuitable for an easy repair. However, if the AAA is large and threatening, and the patient has the possibility of living several years, elective repair is justified and reasonable – especially if it can be accomplished endovascularly. As someone who is near 80 [years old], I could not feel more strongly about this, and I would maintain this view if I were near 90 and healthy.

|
Dr. Frank J. Veith |
I hold the same view even more strongly regarding a ruptured AAA. In this setting, the alternative management is nontreatment, which is uniformly fatal. The common term “palliative treatment” for such nontreatment is a misleading misnomer. No sane, reasonably healthy elderly patient would knowingly choose such nontreatment when a good alternative with well over an even chance of living a lot longer is offered. That good alternative – again especially if it can be performed endovascularly – should be offered, and our health system should pay for it and compensate by saving money on unnecessary SFA [superficial femoral artery] stents and carotid procedures.
Dr. Frank J. Veith is professor of surgery at New York University Medical Center and the Cleveland Clinic and is an associate medical editor for Vascular Specialist.
This discussion is provocative and raises some interesting points. Obviously cost-effectiveness considerations are important, and our country does not have unlimited funds to spend on medical care. And perhaps there are some elderly and frail individuals who should not have their AAAs repaired electively because the risk of rupture during the patients’ remaining months or years of life is small.
This is particularly true if the patient’s AAA is less than 7 cm and his or her anatomy and condition are unsuitable for an easy repair. However, if the AAA is large and threatening, and the patient has the possibility of living several years, elective repair is justified and reasonable – especially if it can be accomplished endovascularly. As someone who is near 80 [years old], I could not feel more strongly about this, and I would maintain this view if I were near 90 and healthy.

|
Dr. Frank J. Veith |
I hold the same view even more strongly regarding a ruptured AAA. In this setting, the alternative management is nontreatment, which is uniformly fatal. The common term “palliative treatment” for such nontreatment is a misleading misnomer. No sane, reasonably healthy elderly patient would knowingly choose such nontreatment when a good alternative with well over an even chance of living a lot longer is offered. That good alternative – again especially if it can be performed endovascularly – should be offered, and our health system should pay for it and compensate by saving money on unnecessary SFA [superficial femoral artery] stents and carotid procedures.
Dr. Frank J. Veith is professor of surgery at New York University Medical Center and the Cleveland Clinic and is an associate medical editor for Vascular Specialist.
This discussion is provocative and raises some interesting points. Obviously cost-effectiveness considerations are important, and our country does not have unlimited funds to spend on medical care. And perhaps there are some elderly and frail individuals who should not have their AAAs repaired electively because the risk of rupture during the patients’ remaining months or years of life is small.
This is particularly true if the patient’s AAA is less than 7 cm and his or her anatomy and condition are unsuitable for an easy repair. However, if the AAA is large and threatening, and the patient has the possibility of living several years, elective repair is justified and reasonable – especially if it can be accomplished endovascularly. As someone who is near 80 [years old], I could not feel more strongly about this, and I would maintain this view if I were near 90 and healthy.

|
Dr. Frank J. Veith |
I hold the same view even more strongly regarding a ruptured AAA. In this setting, the alternative management is nontreatment, which is uniformly fatal. The common term “palliative treatment” for such nontreatment is a misleading misnomer. No sane, reasonably healthy elderly patient would knowingly choose such nontreatment when a good alternative with well over an even chance of living a lot longer is offered. That good alternative – again especially if it can be performed endovascularly – should be offered, and our health system should pay for it and compensate by saving money on unnecessary SFA [superficial femoral artery] stents and carotid procedures.
Dr. Frank J. Veith is professor of surgery at New York University Medical Center and the Cleveland Clinic and is an associate medical editor for Vascular Specialist.
SCOTTSDALE, ARIZ.– Abdominal aortic aneurysm repair in patients 80 years and older can be performed safely and with good medium-term survival rates, a prospective single-site study has shown.
Perioperative mortality in elective and emergent AAA repair for octogenarians was 2% and 35%, respectively, with a median survival rate of 19 months in both groups.
According to these data, “Patients shouldn’t be turned down for aneurysm repair on the basis of their age alone,” Dr. Christopher M. Lamb, a vascular surgery fellow at the University of California Davis Medical Center in Sacramento, said during a presentation at this year’s Southern Association for Vascular Surgery annual meeting.
“However, whether we should be doing these procedures is a different question, and I don’t think these data allow us to answer that question properly.”Dr. Lamb and his colleagues reviewed the records of 847 consecutive patients aged 80 years or older, seen between April 2005 and February 2014 for any type of AAA repair. Cases were sorted according to whether they were elective, ruptured, or urgent but unruptured. A total of 226 patients met the study’s age criteria; there were nearly seven men for every woman, all with a median age of 83 years. Of the elective AAA repair arm of the study, 131 patients (116 men) with a median age of 82 years had an endovascular repair, while the rest underwent open surgical repair. The combined 30-day mortality rate for these patients was 2.3%, with no significant difference between either the endovascular aneurysm repair (EVAR) or the open surgical repair (OSR) patients (1.9% vs. 4.2%; P = .458). The median survival of all elective repair patients was 19 months (interquartile range, 10-35), with no difference seen between the two groups (P = .113)Of the 65 patients (53 men) with ruptured AAA, the median age was 83 years. A third had open repair (32.3%), while the rest had EVAR. The combined 30-day mortality rate was 35.4% but was significantly higher after OSR (52.4% vs. 27.3%; P = .048). The median survival rate was 6 months (IQR, 6-42) when 30-day mortality rates were excluded. The median survival rates in patients who lived longer than 30 days was significantly higher in OSR patients (42.5 months vs. 11 months; P = .019).
Of the 23 men and 7 women with symptomatic but unruptured AAA, all but 1 had EVAR. At 30 days, there was one diverticular perforation–related postoperative death in the EVAR group, which had a median survival rate of 29 months. There being only a single patient in the OSR group obviated a comparative median survival rate analysis.
A subanalysis of the final 20 months of the study showed that 41% of octogenarians seeking any type of AAA repair at the site were rejected (48 rejections vs. 69 repairs). Those who were rejected for repair tended to be older, with a median age of 86 years vs. 83 years for patients who underwent repair (P = .0004).
Dr. Lamb noted that although the findings demonstrate acceptable overall safety rates for the entire cohort, without a control group of patients that did not have AAA repair, it would be hard to draw a definite conclusion about the utility of the findings, and that more data were warranted; however, the potential for limited long-term survival with what previous reports have suggested may include “a reduced quality of life for a good part of it, possibly raises the question that these patients should be treated conservatively, more often.”
The rejection rate data prompted the presentation’s discussant, Dr. William D. Jordan Jr., section chief of vascular surgery at the University of Alabama at Birmingham and the presentation’s discussant, to challenge the findings and asked whether a single surgeon selected the patients.
“You said there is not a selection bias in your study, but I beg to differ. Perhaps all these kinds of studies have a selection bias, and I believe they should. We should select the appropriate patients for the appropriate procedure at the appropriate time, with the appropriate expectation of outcome. Bias in this setting may be seen as good,” Dr. Jordan said.Dr. Lamb responded that the treatment algorithm at the site for all patients with a confirmed AAA of 5.5 cm or greater included CT imaging that is reviewed by a multidisciplinary team comprising vascular surgeons and interventional radiologists, who then evaluated the patients according to their physiology and anatomy, as well as their comorbidities, with the intention that whenever possible, EVAR rather than open repair would be performed.
As to whether there was a bias toward not repairing AAA in older patients, Dr. Lamb said it was incumbent on any health system to evaluate a procedure’s cost-effectiveness, but that, “the life expectancy of a vascular patient is often more limited than I think we’d like to believe ... we don’t know what the natural history of these patients’ life expectancy is. We don’t know from these data what the cause of death was, but anecdotally, we didn’t see hundreds of patients return with ruptured aneurysms after an EVAR.”
“I would truly like to see how many [of these patients] who make it out of the hospital return to normal living within 6 months,” Dr. Samuel R. Money, chair of surgery at the Mayo Clinic in Scottsdale, Ariz., said in an interview following the presentation. “At some point, the question becomes ‘Can we afford to spend $100,000 dollars to keep a 90-year-old patient alive for 6 more months?’ Can this society sustain the cost of that?”
On Twitter @whitneymcknight
SCOTTSDALE, ARIZ.– Abdominal aortic aneurysm repair in patients 80 years and older can be performed safely and with good medium-term survival rates, a prospective single-site study has shown.
Perioperative mortality in elective and emergent AAA repair for octogenarians was 2% and 35%, respectively, with a median survival rate of 19 months in both groups.
According to these data, “Patients shouldn’t be turned down for aneurysm repair on the basis of their age alone,” Dr. Christopher M. Lamb, a vascular surgery fellow at the University of California Davis Medical Center in Sacramento, said during a presentation at this year’s Southern Association for Vascular Surgery annual meeting.
“However, whether we should be doing these procedures is a different question, and I don’t think these data allow us to answer that question properly.”Dr. Lamb and his colleagues reviewed the records of 847 consecutive patients aged 80 years or older, seen between April 2005 and February 2014 for any type of AAA repair. Cases were sorted according to whether they were elective, ruptured, or urgent but unruptured. A total of 226 patients met the study’s age criteria; there were nearly seven men for every woman, all with a median age of 83 years. Of the elective AAA repair arm of the study, 131 patients (116 men) with a median age of 82 years had an endovascular repair, while the rest underwent open surgical repair. The combined 30-day mortality rate for these patients was 2.3%, with no significant difference between either the endovascular aneurysm repair (EVAR) or the open surgical repair (OSR) patients (1.9% vs. 4.2%; P = .458). The median survival of all elective repair patients was 19 months (interquartile range, 10-35), with no difference seen between the two groups (P = .113)Of the 65 patients (53 men) with ruptured AAA, the median age was 83 years. A third had open repair (32.3%), while the rest had EVAR. The combined 30-day mortality rate was 35.4% but was significantly higher after OSR (52.4% vs. 27.3%; P = .048). The median survival rate was 6 months (IQR, 6-42) when 30-day mortality rates were excluded. The median survival rates in patients who lived longer than 30 days was significantly higher in OSR patients (42.5 months vs. 11 months; P = .019).
Of the 23 men and 7 women with symptomatic but unruptured AAA, all but 1 had EVAR. At 30 days, there was one diverticular perforation–related postoperative death in the EVAR group, which had a median survival rate of 29 months. There being only a single patient in the OSR group obviated a comparative median survival rate analysis.
A subanalysis of the final 20 months of the study showed that 41% of octogenarians seeking any type of AAA repair at the site were rejected (48 rejections vs. 69 repairs). Those who were rejected for repair tended to be older, with a median age of 86 years vs. 83 years for patients who underwent repair (P = .0004).
Dr. Lamb noted that although the findings demonstrate acceptable overall safety rates for the entire cohort, without a control group of patients that did not have AAA repair, it would be hard to draw a definite conclusion about the utility of the findings, and that more data were warranted; however, the potential for limited long-term survival with what previous reports have suggested may include “a reduced quality of life for a good part of it, possibly raises the question that these patients should be treated conservatively, more often.”
The rejection rate data prompted the presentation’s discussant, Dr. William D. Jordan Jr., section chief of vascular surgery at the University of Alabama at Birmingham and the presentation’s discussant, to challenge the findings and asked whether a single surgeon selected the patients.
“You said there is not a selection bias in your study, but I beg to differ. Perhaps all these kinds of studies have a selection bias, and I believe they should. We should select the appropriate patients for the appropriate procedure at the appropriate time, with the appropriate expectation of outcome. Bias in this setting may be seen as good,” Dr. Jordan said.Dr. Lamb responded that the treatment algorithm at the site for all patients with a confirmed AAA of 5.5 cm or greater included CT imaging that is reviewed by a multidisciplinary team comprising vascular surgeons and interventional radiologists, who then evaluated the patients according to their physiology and anatomy, as well as their comorbidities, with the intention that whenever possible, EVAR rather than open repair would be performed.
As to whether there was a bias toward not repairing AAA in older patients, Dr. Lamb said it was incumbent on any health system to evaluate a procedure’s cost-effectiveness, but that, “the life expectancy of a vascular patient is often more limited than I think we’d like to believe ... we don’t know what the natural history of these patients’ life expectancy is. We don’t know from these data what the cause of death was, but anecdotally, we didn’t see hundreds of patients return with ruptured aneurysms after an EVAR.”
“I would truly like to see how many [of these patients] who make it out of the hospital return to normal living within 6 months,” Dr. Samuel R. Money, chair of surgery at the Mayo Clinic in Scottsdale, Ariz., said in an interview following the presentation. “At some point, the question becomes ‘Can we afford to spend $100,000 dollars to keep a 90-year-old patient alive for 6 more months?’ Can this society sustain the cost of that?”
On Twitter @whitneymcknight
Helping parents manage rules across two homes
A major challenge faced by parents is the task of setting basic ground rules and expectations for their children, and then enforcing these with limits, rewards, and consequences. This task is made far more difficult when parents are separated or divorced. Agreeing upon and enforcing rules in separate homes often becomes burdened by the angry baggage that led to the divorce. When a family in your practice is going through a divorce, you have an opportunity to provide the parents with valuable strategies to manage rules effectively so that conflict is minimized.
Many happily married parents who communicate very well on most matters struggle to get on the same page when negotiating rules and limits. One parent’s sense of what is an appropriate bedtime, how children should help with chores, or even how often they can have sweets can become a deeply held belief and might be very different than their spouse’s opinions. Sometimes, a parent has old anger about how they were raised and finds it hard to distinguish what might have been better for them, compared with what is best for their own child. Cultural and family differences on how much choice children should have at different ages, criteria and severity of any consequences for misbehavior, and opportunities for redemption or amnesty all add complexity to the discussion. Once they have found common ground on what makes sense for their joint rules, values, and needs of their child, they have to manage enforcing rules and limits, agreeing upon appropriate rewards and punishments, and bearing the inevitable distress of their children when facing a limit or consequence. And, of course, once parents think they have it all figured out, their children react and grow, and they must reset the rules, expectations, and consequences.
When parents get separated or divorced, this process becomes considerably more difficult. Negotiating new rules or limits is very difficult when communication is hampered by conflict. Parental guilt about the divorce itself, anger at old hurts or disputes about money and custody, missing the child between visits, and remarriages all add baggage to the discussion of a reasonable bedtime or consequences for a poor grade at school. If the divorce required aggressive negotiation between lawyers, appointment of a guardian ad Litem to manage ongoing disputes involving the children, or a court case to reach resolution, the tensions between parents can be intense, enduring, and with no issue too small to add fuel to the arguments. Enforcing limits is much harder for a single parent than when there are two parents doing the enforcement. And divorced parents, already feeling guilty and insecure, are more likely to suspend rules or limits so that they don’t have to be the “bad parent.” For the child or children, the stress and disruptions that come with divorce can cause an increase in regressed or disrespectful behavior. While it can be a time when limits are increasingly tested, being reasonable and consistent in enforcing limits becomes more important, as it provides reassuring steadiness in the midst of turbulent change.
Let’s take the example of a 12-year-old coming home from school with poor grades. One parent may see the need for a tutor, but might be using that approach as part of a financial attack if the other parent has to pay for it. The other parent may want to limit the use of computer games or access to television until the grades go up. And one may expect movement from a D to a C average while the other may expect A’s, period. Is the poor grade based on lack of ability, effort, an attempt to get attention, a reaction to the divorce, or preoccupation with ongoing parental discord? What is the impact on the child if in one home there is a tutor and a C expectation, and in the other there is no tutor, no computer use, no TV... and these change every time the child moves from one home to the other? A child striving to overcome a poor grade needs calm, consistent, patient, and optimistic support, rather than managing the increased tension across two homes or feeling like the cause of increased conflict. Virtually any reasonable approach is better for the child than each parent doing something different as a reflection of ongoing tension. Pediatricians can be extraordinarily helpful to their patient if they can get divorced parents to agree on a single approach that is based on their child’s needs rather than past and ongoing angers. The emotional damage of ongoing discord is far worse than any C average.
As the pediatrician to a family managing divorce, you may be one of the few authority figures whom both parents and the children all still respect and trust. You are in a strong position to ask a parent during an appointment how rules and limits are being managed across two homes. Find out if they have a clear plan for handling routine communication about the children, whether about summer camps or a new curfew, so that they don’t default to communicating only once there is a crisis. See if rules are a vehicle for ongoing parental fighting so that a minor difference (an 8 o’clock bedtime in one house versus 9 o’clock in the other) carries a high emotional charge. Find out if there are certain rules that have become very hard to enforce, or if their child has been testing limits more. Ask if there has been a consequence enforced in one home, but not in another. Often simply providing a calm affirmation that increased limit testing is normal in children after a divorce is very reassuring for parents. Remind them that providing reasonably consistent rules and limits will be very helpful to their children during this period, the opposite of making them a “bad parent.”
Some divorced parents will become more rigid about rules, managing any infraction or extenuating circumstance more like a contract negotiation. These parents might benefit from a suggestion that consistency and simplicity are the keys to effective rules across two households. Rules also provide an opportunity to listen to their children’s thoughts and feelings and share the family’s values that are the basis for the rules. Parents should be curious about their children’s opinions and be ready to show thoughtful flexibility when rules become outdated or special circumstances exist.
You can suggest a rule the parents should follow. While they can talk honestly about what each parent may struggle with or acknowledge clear differences in style or personality, they should strive to never vilify the other parent. Even in circumstances in which it is very difficult for two parents to collaborate, sharing grievances with the children will only be painful and confusing for them.
Lastly, pediatricians can discuss the long-term goals that all parents, even those alienated from each other, share. Children will do best when they have a positive, honest, warm relationship with each parent, and do not carry responsibility for negotiating conflict between their parents. Ultimately, more autonomy and fewer rules will be an important part of the child’s adolescence. Discord between parents, sabotaging of rules and consequences, and explicit contempt for their children’s other parent all will lead to children feeling burdened, having lower self-esteem, and being at greater risk for serious problems in school, emotionally or with substances as they grow into adolescents and young adults. If you are frustrated in your effort to protect children from ongoing discord, suggest a referral to a mental health clinician with expertise helping parents after a divorce.
Dr. Swick is an attending psychiatrist in the division of child psychiatry at Massachusetts General Hospital, Boston, and director of the Parenting at a Challenging Time (PACT) Program at the Vernon Cancer Center at Newton Wellesley Hospital, also in Boston. Dr. Jellinek is professor of psychiatry and of pediatrics at Harvard Medical School, Boston. E-mail them at [email protected].
A major challenge faced by parents is the task of setting basic ground rules and expectations for their children, and then enforcing these with limits, rewards, and consequences. This task is made far more difficult when parents are separated or divorced. Agreeing upon and enforcing rules in separate homes often becomes burdened by the angry baggage that led to the divorce. When a family in your practice is going through a divorce, you have an opportunity to provide the parents with valuable strategies to manage rules effectively so that conflict is minimized.
Many happily married parents who communicate very well on most matters struggle to get on the same page when negotiating rules and limits. One parent’s sense of what is an appropriate bedtime, how children should help with chores, or even how often they can have sweets can become a deeply held belief and might be very different than their spouse’s opinions. Sometimes, a parent has old anger about how they were raised and finds it hard to distinguish what might have been better for them, compared with what is best for their own child. Cultural and family differences on how much choice children should have at different ages, criteria and severity of any consequences for misbehavior, and opportunities for redemption or amnesty all add complexity to the discussion. Once they have found common ground on what makes sense for their joint rules, values, and needs of their child, they have to manage enforcing rules and limits, agreeing upon appropriate rewards and punishments, and bearing the inevitable distress of their children when facing a limit or consequence. And, of course, once parents think they have it all figured out, their children react and grow, and they must reset the rules, expectations, and consequences.
When parents get separated or divorced, this process becomes considerably more difficult. Negotiating new rules or limits is very difficult when communication is hampered by conflict. Parental guilt about the divorce itself, anger at old hurts or disputes about money and custody, missing the child between visits, and remarriages all add baggage to the discussion of a reasonable bedtime or consequences for a poor grade at school. If the divorce required aggressive negotiation between lawyers, appointment of a guardian ad Litem to manage ongoing disputes involving the children, or a court case to reach resolution, the tensions between parents can be intense, enduring, and with no issue too small to add fuel to the arguments. Enforcing limits is much harder for a single parent than when there are two parents doing the enforcement. And divorced parents, already feeling guilty and insecure, are more likely to suspend rules or limits so that they don’t have to be the “bad parent.” For the child or children, the stress and disruptions that come with divorce can cause an increase in regressed or disrespectful behavior. While it can be a time when limits are increasingly tested, being reasonable and consistent in enforcing limits becomes more important, as it provides reassuring steadiness in the midst of turbulent change.
Let’s take the example of a 12-year-old coming home from school with poor grades. One parent may see the need for a tutor, but might be using that approach as part of a financial attack if the other parent has to pay for it. The other parent may want to limit the use of computer games or access to television until the grades go up. And one may expect movement from a D to a C average while the other may expect A’s, period. Is the poor grade based on lack of ability, effort, an attempt to get attention, a reaction to the divorce, or preoccupation with ongoing parental discord? What is the impact on the child if in one home there is a tutor and a C expectation, and in the other there is no tutor, no computer use, no TV... and these change every time the child moves from one home to the other? A child striving to overcome a poor grade needs calm, consistent, patient, and optimistic support, rather than managing the increased tension across two homes or feeling like the cause of increased conflict. Virtually any reasonable approach is better for the child than each parent doing something different as a reflection of ongoing tension. Pediatricians can be extraordinarily helpful to their patient if they can get divorced parents to agree on a single approach that is based on their child’s needs rather than past and ongoing angers. The emotional damage of ongoing discord is far worse than any C average.
As the pediatrician to a family managing divorce, you may be one of the few authority figures whom both parents and the children all still respect and trust. You are in a strong position to ask a parent during an appointment how rules and limits are being managed across two homes. Find out if they have a clear plan for handling routine communication about the children, whether about summer camps or a new curfew, so that they don’t default to communicating only once there is a crisis. See if rules are a vehicle for ongoing parental fighting so that a minor difference (an 8 o’clock bedtime in one house versus 9 o’clock in the other) carries a high emotional charge. Find out if there are certain rules that have become very hard to enforce, or if their child has been testing limits more. Ask if there has been a consequence enforced in one home, but not in another. Often simply providing a calm affirmation that increased limit testing is normal in children after a divorce is very reassuring for parents. Remind them that providing reasonably consistent rules and limits will be very helpful to their children during this period, the opposite of making them a “bad parent.”
Some divorced parents will become more rigid about rules, managing any infraction or extenuating circumstance more like a contract negotiation. These parents might benefit from a suggestion that consistency and simplicity are the keys to effective rules across two households. Rules also provide an opportunity to listen to their children’s thoughts and feelings and share the family’s values that are the basis for the rules. Parents should be curious about their children’s opinions and be ready to show thoughtful flexibility when rules become outdated or special circumstances exist.
You can suggest a rule the parents should follow. While they can talk honestly about what each parent may struggle with or acknowledge clear differences in style or personality, they should strive to never vilify the other parent. Even in circumstances in which it is very difficult for two parents to collaborate, sharing grievances with the children will only be painful and confusing for them.
Lastly, pediatricians can discuss the long-term goals that all parents, even those alienated from each other, share. Children will do best when they have a positive, honest, warm relationship with each parent, and do not carry responsibility for negotiating conflict between their parents. Ultimately, more autonomy and fewer rules will be an important part of the child’s adolescence. Discord between parents, sabotaging of rules and consequences, and explicit contempt for their children’s other parent all will lead to children feeling burdened, having lower self-esteem, and being at greater risk for serious problems in school, emotionally or with substances as they grow into adolescents and young adults. If you are frustrated in your effort to protect children from ongoing discord, suggest a referral to a mental health clinician with expertise helping parents after a divorce.
Dr. Swick is an attending psychiatrist in the division of child psychiatry at Massachusetts General Hospital, Boston, and director of the Parenting at a Challenging Time (PACT) Program at the Vernon Cancer Center at Newton Wellesley Hospital, also in Boston. Dr. Jellinek is professor of psychiatry and of pediatrics at Harvard Medical School, Boston. E-mail them at [email protected].
A major challenge faced by parents is the task of setting basic ground rules and expectations for their children, and then enforcing these with limits, rewards, and consequences. This task is made far more difficult when parents are separated or divorced. Agreeing upon and enforcing rules in separate homes often becomes burdened by the angry baggage that led to the divorce. When a family in your practice is going through a divorce, you have an opportunity to provide the parents with valuable strategies to manage rules effectively so that conflict is minimized.
Many happily married parents who communicate very well on most matters struggle to get on the same page when negotiating rules and limits. One parent’s sense of what is an appropriate bedtime, how children should help with chores, or even how often they can have sweets can become a deeply held belief and might be very different than their spouse’s opinions. Sometimes, a parent has old anger about how they were raised and finds it hard to distinguish what might have been better for them, compared with what is best for their own child. Cultural and family differences on how much choice children should have at different ages, criteria and severity of any consequences for misbehavior, and opportunities for redemption or amnesty all add complexity to the discussion. Once they have found common ground on what makes sense for their joint rules, values, and needs of their child, they have to manage enforcing rules and limits, agreeing upon appropriate rewards and punishments, and bearing the inevitable distress of their children when facing a limit or consequence. And, of course, once parents think they have it all figured out, their children react and grow, and they must reset the rules, expectations, and consequences.
When parents get separated or divorced, this process becomes considerably more difficult. Negotiating new rules or limits is very difficult when communication is hampered by conflict. Parental guilt about the divorce itself, anger at old hurts or disputes about money and custody, missing the child between visits, and remarriages all add baggage to the discussion of a reasonable bedtime or consequences for a poor grade at school. If the divorce required aggressive negotiation between lawyers, appointment of a guardian ad Litem to manage ongoing disputes involving the children, or a court case to reach resolution, the tensions between parents can be intense, enduring, and with no issue too small to add fuel to the arguments. Enforcing limits is much harder for a single parent than when there are two parents doing the enforcement. And divorced parents, already feeling guilty and insecure, are more likely to suspend rules or limits so that they don’t have to be the “bad parent.” For the child or children, the stress and disruptions that come with divorce can cause an increase in regressed or disrespectful behavior. While it can be a time when limits are increasingly tested, being reasonable and consistent in enforcing limits becomes more important, as it provides reassuring steadiness in the midst of turbulent change.
Let’s take the example of a 12-year-old coming home from school with poor grades. One parent may see the need for a tutor, but might be using that approach as part of a financial attack if the other parent has to pay for it. The other parent may want to limit the use of computer games or access to television until the grades go up. And one may expect movement from a D to a C average while the other may expect A’s, period. Is the poor grade based on lack of ability, effort, an attempt to get attention, a reaction to the divorce, or preoccupation with ongoing parental discord? What is the impact on the child if in one home there is a tutor and a C expectation, and in the other there is no tutor, no computer use, no TV... and these change every time the child moves from one home to the other? A child striving to overcome a poor grade needs calm, consistent, patient, and optimistic support, rather than managing the increased tension across two homes or feeling like the cause of increased conflict. Virtually any reasonable approach is better for the child than each parent doing something different as a reflection of ongoing tension. Pediatricians can be extraordinarily helpful to their patient if they can get divorced parents to agree on a single approach that is based on their child’s needs rather than past and ongoing angers. The emotional damage of ongoing discord is far worse than any C average.
As the pediatrician to a family managing divorce, you may be one of the few authority figures whom both parents and the children all still respect and trust. You are in a strong position to ask a parent during an appointment how rules and limits are being managed across two homes. Find out if they have a clear plan for handling routine communication about the children, whether about summer camps or a new curfew, so that they don’t default to communicating only once there is a crisis. See if rules are a vehicle for ongoing parental fighting so that a minor difference (an 8 o’clock bedtime in one house versus 9 o’clock in the other) carries a high emotional charge. Find out if there are certain rules that have become very hard to enforce, or if their child has been testing limits more. Ask if there has been a consequence enforced in one home, but not in another. Often simply providing a calm affirmation that increased limit testing is normal in children after a divorce is very reassuring for parents. Remind them that providing reasonably consistent rules and limits will be very helpful to their children during this period, the opposite of making them a “bad parent.”
Some divorced parents will become more rigid about rules, managing any infraction or extenuating circumstance more like a contract negotiation. These parents might benefit from a suggestion that consistency and simplicity are the keys to effective rules across two households. Rules also provide an opportunity to listen to their children’s thoughts and feelings and share the family’s values that are the basis for the rules. Parents should be curious about their children’s opinions and be ready to show thoughtful flexibility when rules become outdated or special circumstances exist.
You can suggest a rule the parents should follow. While they can talk honestly about what each parent may struggle with or acknowledge clear differences in style or personality, they should strive to never vilify the other parent. Even in circumstances in which it is very difficult for two parents to collaborate, sharing grievances with the children will only be painful and confusing for them.
Lastly, pediatricians can discuss the long-term goals that all parents, even those alienated from each other, share. Children will do best when they have a positive, honest, warm relationship with each parent, and do not carry responsibility for negotiating conflict between their parents. Ultimately, more autonomy and fewer rules will be an important part of the child’s adolescence. Discord between parents, sabotaging of rules and consequences, and explicit contempt for their children’s other parent all will lead to children feeling burdened, having lower self-esteem, and being at greater risk for serious problems in school, emotionally or with substances as they grow into adolescents and young adults. If you are frustrated in your effort to protect children from ongoing discord, suggest a referral to a mental health clinician with expertise helping parents after a divorce.
Dr. Swick is an attending psychiatrist in the division of child psychiatry at Massachusetts General Hospital, Boston, and director of the Parenting at a Challenging Time (PACT) Program at the Vernon Cancer Center at Newton Wellesley Hospital, also in Boston. Dr. Jellinek is professor of psychiatry and of pediatrics at Harvard Medical School, Boston. E-mail them at [email protected].
Is the wedding still on?
“So tell me, Kathy,” I asked as I walked in. “Is the wedding still on?”
“Yes!” she said.
I was kidding, of course. I wanted to defuse the tension every bride feels as her big day approaches. With her nuptials 2 months off, Kathy was here for an acne tune-up.
Good news: no new pimples. Though Kathy had stopped squeezing her old ones, their marks were fading slowly. Brides don’t want to depend on makeup or Photoshop.
Her current regimen was a topical antibiotic in the morning and a retinoid at night. The question was whether to add or change anything.
“Maybe we should consider adding an oral medicine to help speed healing?” I asked. Then I watched her eyes. Her frown gave me my answer.
“I’d prefer to avoid oral medications unless I absolutely need them,” Kathy said.
“No problem,” I said. “You’re doing well, and we still have 2 months for the marks you have to fade.” I arranged to see her again shortly before the wedding, for any last-minute adjustments.
Outside the exam room, I took my student aside. “That’s how you negotiate,” I told her.
“Some young women approach their weddings in a kind of panic. They want to do whatever it takes to speed healing. If Kathy had felt that way, and I told her things were fine as they were, she would have been upset. ‘Isn’t there something else we can do, maybe something to take by mouth?’ she’d have asked.
“Instead, Kathy felt the opposite,” I told my student. “When patients have a specific problem, you can make a shrewd guess about how aggressive they want to be in addressing it. But you can’t be sure. That means watching their eyes and body language when making suggestions.
“Of course, not every medical condition is negotiable. Sometimes, the matter is so urgent or dire that there really is only one thing to do. Then you have to be more direct. But many situations are not so clear cut. You and the patient will have choices. Which is best may depend less on the medical condition than on the patient’s mindset and circumstances.
“Your job is to know the options, watch their eyes, and negotiate,” I said.
My student nodded, probably noticing that this is not standard clinical advice. In school, they teach you to make the right diagnosis and prescribe the treatment of choice. Anything else would be substandard care, a dereliction of professional duty.
Nowadays, teachers – and insurers – go in for algorithms, cookbook medicine. If the patient has this, do this. If that, do that. “How do you treat acne?” students often ask at the start of their rotation. “Can you give me a decision tree?”
These days more and more doctors spend their visit time clicking tablets or laptops. If the patient has acne, they are checking off vital data points like:
• Are there pimples, pustules, whiteheads, blackheads, cysts?
• How many of each?
• Where they are – face, chest, back?
This information is supposed to objectively describe and grade the patient’s acne. You click what is important: what you can count and measure.
Here is what electronic medical records do not have you click off:
• Is the patient getting married soon?
• Is she afraid of oral antibiotics because she’s heard they wreck your immune system and make you sick?
• Have her friends recommended an acne cream they are sure is the best thing since sliced tretinoin?
They don’t make boxes for what goes on inside people’s brains. You can’t count or measure that, and if you can’t count it, it doesn’t count.
So doctors click what they tell us to. As we click the keyboard, we are not looking at the patient’s face. So we don’t know whether the patient is buying what we have to offer.
More medical treatment than we care to admit is – or should be – a process of negotiation. Negotiating means looking people in the eye and hearing what they say and the way they say it. That way you know not only what they have, but what they want. In Kathy’s case, that would be a wedding to remember.
As she proceeds in her career, my student may do more than counting pimples and grading acne. At any rate, I hope so.
Dr. Rockoff practices dermatology in Brookline, Mass., and is a longtime contributor to Dermatology News. He serves on the clinical faculty at Tufts University, Boston, and has taught senior medical students and other trainees for 30 years.
“So tell me, Kathy,” I asked as I walked in. “Is the wedding still on?”
“Yes!” she said.
I was kidding, of course. I wanted to defuse the tension every bride feels as her big day approaches. With her nuptials 2 months off, Kathy was here for an acne tune-up.
Good news: no new pimples. Though Kathy had stopped squeezing her old ones, their marks were fading slowly. Brides don’t want to depend on makeup or Photoshop.
Her current regimen was a topical antibiotic in the morning and a retinoid at night. The question was whether to add or change anything.
“Maybe we should consider adding an oral medicine to help speed healing?” I asked. Then I watched her eyes. Her frown gave me my answer.
“I’d prefer to avoid oral medications unless I absolutely need them,” Kathy said.
“No problem,” I said. “You’re doing well, and we still have 2 months for the marks you have to fade.” I arranged to see her again shortly before the wedding, for any last-minute adjustments.
Outside the exam room, I took my student aside. “That’s how you negotiate,” I told her.
“Some young women approach their weddings in a kind of panic. They want to do whatever it takes to speed healing. If Kathy had felt that way, and I told her things were fine as they were, she would have been upset. ‘Isn’t there something else we can do, maybe something to take by mouth?’ she’d have asked.
“Instead, Kathy felt the opposite,” I told my student. “When patients have a specific problem, you can make a shrewd guess about how aggressive they want to be in addressing it. But you can’t be sure. That means watching their eyes and body language when making suggestions.
“Of course, not every medical condition is negotiable. Sometimes, the matter is so urgent or dire that there really is only one thing to do. Then you have to be more direct. But many situations are not so clear cut. You and the patient will have choices. Which is best may depend less on the medical condition than on the patient’s mindset and circumstances.
“Your job is to know the options, watch their eyes, and negotiate,” I said.
My student nodded, probably noticing that this is not standard clinical advice. In school, they teach you to make the right diagnosis and prescribe the treatment of choice. Anything else would be substandard care, a dereliction of professional duty.
Nowadays, teachers – and insurers – go in for algorithms, cookbook medicine. If the patient has this, do this. If that, do that. “How do you treat acne?” students often ask at the start of their rotation. “Can you give me a decision tree?”
These days more and more doctors spend their visit time clicking tablets or laptops. If the patient has acne, they are checking off vital data points like:
• Are there pimples, pustules, whiteheads, blackheads, cysts?
• How many of each?
• Where they are – face, chest, back?
This information is supposed to objectively describe and grade the patient’s acne. You click what is important: what you can count and measure.
Here is what electronic medical records do not have you click off:
• Is the patient getting married soon?
• Is she afraid of oral antibiotics because she’s heard they wreck your immune system and make you sick?
• Have her friends recommended an acne cream they are sure is the best thing since sliced tretinoin?
They don’t make boxes for what goes on inside people’s brains. You can’t count or measure that, and if you can’t count it, it doesn’t count.
So doctors click what they tell us to. As we click the keyboard, we are not looking at the patient’s face. So we don’t know whether the patient is buying what we have to offer.
More medical treatment than we care to admit is – or should be – a process of negotiation. Negotiating means looking people in the eye and hearing what they say and the way they say it. That way you know not only what they have, but what they want. In Kathy’s case, that would be a wedding to remember.
As she proceeds in her career, my student may do more than counting pimples and grading acne. At any rate, I hope so.
Dr. Rockoff practices dermatology in Brookline, Mass., and is a longtime contributor to Dermatology News. He serves on the clinical faculty at Tufts University, Boston, and has taught senior medical students and other trainees for 30 years.
“So tell me, Kathy,” I asked as I walked in. “Is the wedding still on?”
“Yes!” she said.
I was kidding, of course. I wanted to defuse the tension every bride feels as her big day approaches. With her nuptials 2 months off, Kathy was here for an acne tune-up.
Good news: no new pimples. Though Kathy had stopped squeezing her old ones, their marks were fading slowly. Brides don’t want to depend on makeup or Photoshop.
Her current regimen was a topical antibiotic in the morning and a retinoid at night. The question was whether to add or change anything.
“Maybe we should consider adding an oral medicine to help speed healing?” I asked. Then I watched her eyes. Her frown gave me my answer.
“I’d prefer to avoid oral medications unless I absolutely need them,” Kathy said.
“No problem,” I said. “You’re doing well, and we still have 2 months for the marks you have to fade.” I arranged to see her again shortly before the wedding, for any last-minute adjustments.
Outside the exam room, I took my student aside. “That’s how you negotiate,” I told her.
“Some young women approach their weddings in a kind of panic. They want to do whatever it takes to speed healing. If Kathy had felt that way, and I told her things were fine as they were, she would have been upset. ‘Isn’t there something else we can do, maybe something to take by mouth?’ she’d have asked.
“Instead, Kathy felt the opposite,” I told my student. “When patients have a specific problem, you can make a shrewd guess about how aggressive they want to be in addressing it. But you can’t be sure. That means watching their eyes and body language when making suggestions.
“Of course, not every medical condition is negotiable. Sometimes, the matter is so urgent or dire that there really is only one thing to do. Then you have to be more direct. But many situations are not so clear cut. You and the patient will have choices. Which is best may depend less on the medical condition than on the patient’s mindset and circumstances.
“Your job is to know the options, watch their eyes, and negotiate,” I said.
My student nodded, probably noticing that this is not standard clinical advice. In school, they teach you to make the right diagnosis and prescribe the treatment of choice. Anything else would be substandard care, a dereliction of professional duty.
Nowadays, teachers – and insurers – go in for algorithms, cookbook medicine. If the patient has this, do this. If that, do that. “How do you treat acne?” students often ask at the start of their rotation. “Can you give me a decision tree?”
These days more and more doctors spend their visit time clicking tablets or laptops. If the patient has acne, they are checking off vital data points like:
• Are there pimples, pustules, whiteheads, blackheads, cysts?
• How many of each?
• Where they are – face, chest, back?
This information is supposed to objectively describe and grade the patient’s acne. You click what is important: what you can count and measure.
Here is what electronic medical records do not have you click off:
• Is the patient getting married soon?
• Is she afraid of oral antibiotics because she’s heard they wreck your immune system and make you sick?
• Have her friends recommended an acne cream they are sure is the best thing since sliced tretinoin?
They don’t make boxes for what goes on inside people’s brains. You can’t count or measure that, and if you can’t count it, it doesn’t count.
So doctors click what they tell us to. As we click the keyboard, we are not looking at the patient’s face. So we don’t know whether the patient is buying what we have to offer.
More medical treatment than we care to admit is – or should be – a process of negotiation. Negotiating means looking people in the eye and hearing what they say and the way they say it. That way you know not only what they have, but what they want. In Kathy’s case, that would be a wedding to remember.
As she proceeds in her career, my student may do more than counting pimples and grading acne. At any rate, I hope so.
Dr. Rockoff practices dermatology in Brookline, Mass., and is a longtime contributor to Dermatology News. He serves on the clinical faculty at Tufts University, Boston, and has taught senior medical students and other trainees for 30 years.
Plantago major
For centuries, the leaves of Plantago major have been used in most regions of the world in traditional medical treatment of wounds and various diseases, including cutaneous conditions (J. Ethnopharmacol. 2000;71:1-21). P. major, also known as broadleaf plantain or greater plantain, is a member of the Plantaginaceae family, which is now widely dispersed throughout the world, though native to much of Europe as well as northern and central Asia. The Norwegian and Swedish name for the plant, groblad, means “healing leaves” (J. Ethnopharmacol. 2000;71:1-21). It was brought to the Americas by Europeans during the colonial period. Native Americans referred to it as the “white man’s footprint,” which inspired the genus name Plantago from the Latin planta (foot) (J. Ethnopharmacol. 2000;71:1-21).
Among the biologically active constituents of P. major are polysaccharides, lipids, caffeic acid derivatives, flavonoids (apigenin, luteolin, scutellarin, baicalein, nepetin, hispidulin, plantagoside), iridoid glycosides (aucubin, catalpol), terpenoids, and alkaloids (J. Ethnopharmacol. 2000;71:1-21; Medical Herbalism: The Science and Practice of Herbal Medicine, 2003, Healing Arts Press). In an ethnopharmacologic and folk medicine survey study of 1,225 residents of the Atlantic coast of Colombia completed in 2011, Gómez-Estrada et al. found that P. major was one of the plants traditionally used to treat inflammation; it also was used to treat kidney pain and eye injuries (J. Ethnobiol. Ethnomed. 2011;7:27). P. major also is traditionally used as a mucilage and bulk laxative (Principles and Practice of Phytotherapy: Modern Herbal Medicine, 2013, Churchill Livingstone).
Extracts of the plant have been associated with myriad biologic activities, including wound healing, anti-inflammatory, antimicrobial, analgesic, antioxidant, immunomodulating, and antiulcerogenic action, which Samuelsen suggested may account for the use of the botanical in traditional medicine (J. Ethnopharmacol. 2000;71:1-21; Medical Herbalism: The Science and Practice of Herbal Medicine, 2003, Healing Arts Press). In fact, the range of biologic properties attributed to P. major also includes astringent, anesthetic, antihelminthic, analeptic, antihistaminic, antirheumatic, antiviral, antitumor, antiulcer, diuretic, hypotensive, and expectorant activity (Exp. Biol. Med. [Maywood] 2012;237:1379-86). Though not the most popular botanical for this indication, P. major is among the plants used in the treatment of cutaneous leishmanial ulcers in Bahia, Brazil, where Leishmania brazilenesis is endemic (Rev. Soc. Bras. Med. Trop. 1996;29:229-32). Other dermatologic uses in traditional medicine include eczema, cuts, hemorrhoids, ulcerations, and wounds (Medical Herbalism: The Science and Practice of Herbal Medicine, 2003, Healing Arts Press).
Wound healing
The use of P. major for wound healing dates back to the first century, as described by the Greek physician Dioscorides in “De Materia Medica” (J. Ethnopharmacol. 2000;71:1-21).
In 2011, Krasnov et al. developed an experimental model for characterizing proteins and showed that a newly discovered group of tissue-specific biogregulating proteins found previously in animal tissues was also present in P. major and responsible for the wound-healing activity associated with the plant (Prikl Biokhim. Mikrobiol. 2011;47:146-53).
The next year, Thomé et al. investigated and compared the wound-healing effects of P. major and Siparuna guianensis with a commercial product used in Brazil. Mice with cervical dorsal area wounds were treated with the botanical ingredients and the commercial product. Decreases in the wound area occurred earliest in mice treated with P. major, with complete closure (by day 15) seen only in this group. The investigators concluded that their findings support the traditional application of P. major, which shows potential as a viable wound-healing agent (Exp. Biol. Med. [Maywood] 2012;237:1379-86).
Conclusion
The numerous biologic properties of P. major are well established. In addition, use of the plant in traditional medicine for some cutaneous indications warrants consideration for modern therapeutic usage. Much more research is necessary, however, to elucidate the potential incorporation of this botanical into standard topical preparations for any of various skin conditions.
Dr. Baumann is chief executive officer of the Baumann Cosmetic & Research Institute in the Design District in Miami. She founded the Cosmetic Dermatology Center at the University of Miami in 1997. Dr. Baumann wrote the textbook “Cosmetic Dermatology: Principles and Practice” (New York: McGraw-Hill, 2002), and a book for consumers, “The Skin Type Solution” (New York: Bantam Dell, 2006). She has contributed to the Cosmeceutical Critique column in Dermatology News since January 2001. Her latest book, “Cosmeceuticals and Cosmetic Ingredients,” was published in November 2014. Dr. Baumann has received funding for clinical grants from Allergan, Aveeno, Avon Products, Evolus, Galderma, GlaxoSmithKline, Kythera Biopharmaceuticals, Mary Kay, Medicis Pharmaceuticals, Neutrogena, Philosophy, Topix Pharmaceuticals, and Unilever.
For centuries, the leaves of Plantago major have been used in most regions of the world in traditional medical treatment of wounds and various diseases, including cutaneous conditions (J. Ethnopharmacol. 2000;71:1-21). P. major, also known as broadleaf plantain or greater plantain, is a member of the Plantaginaceae family, which is now widely dispersed throughout the world, though native to much of Europe as well as northern and central Asia. The Norwegian and Swedish name for the plant, groblad, means “healing leaves” (J. Ethnopharmacol. 2000;71:1-21). It was brought to the Americas by Europeans during the colonial period. Native Americans referred to it as the “white man’s footprint,” which inspired the genus name Plantago from the Latin planta (foot) (J. Ethnopharmacol. 2000;71:1-21).
Among the biologically active constituents of P. major are polysaccharides, lipids, caffeic acid derivatives, flavonoids (apigenin, luteolin, scutellarin, baicalein, nepetin, hispidulin, plantagoside), iridoid glycosides (aucubin, catalpol), terpenoids, and alkaloids (J. Ethnopharmacol. 2000;71:1-21; Medical Herbalism: The Science and Practice of Herbal Medicine, 2003, Healing Arts Press). In an ethnopharmacologic and folk medicine survey study of 1,225 residents of the Atlantic coast of Colombia completed in 2011, Gómez-Estrada et al. found that P. major was one of the plants traditionally used to treat inflammation; it also was used to treat kidney pain and eye injuries (J. Ethnobiol. Ethnomed. 2011;7:27). P. major also is traditionally used as a mucilage and bulk laxative (Principles and Practice of Phytotherapy: Modern Herbal Medicine, 2013, Churchill Livingstone).
Extracts of the plant have been associated with myriad biologic activities, including wound healing, anti-inflammatory, antimicrobial, analgesic, antioxidant, immunomodulating, and antiulcerogenic action, which Samuelsen suggested may account for the use of the botanical in traditional medicine (J. Ethnopharmacol. 2000;71:1-21; Medical Herbalism: The Science and Practice of Herbal Medicine, 2003, Healing Arts Press). In fact, the range of biologic properties attributed to P. major also includes astringent, anesthetic, antihelminthic, analeptic, antihistaminic, antirheumatic, antiviral, antitumor, antiulcer, diuretic, hypotensive, and expectorant activity (Exp. Biol. Med. [Maywood] 2012;237:1379-86). Though not the most popular botanical for this indication, P. major is among the plants used in the treatment of cutaneous leishmanial ulcers in Bahia, Brazil, where Leishmania brazilenesis is endemic (Rev. Soc. Bras. Med. Trop. 1996;29:229-32). Other dermatologic uses in traditional medicine include eczema, cuts, hemorrhoids, ulcerations, and wounds (Medical Herbalism: The Science and Practice of Herbal Medicine, 2003, Healing Arts Press).
Wound healing
The use of P. major for wound healing dates back to the first century, as described by the Greek physician Dioscorides in “De Materia Medica” (J. Ethnopharmacol. 2000;71:1-21).
In 2011, Krasnov et al. developed an experimental model for characterizing proteins and showed that a newly discovered group of tissue-specific biogregulating proteins found previously in animal tissues was also present in P. major and responsible for the wound-healing activity associated with the plant (Prikl Biokhim. Mikrobiol. 2011;47:146-53).
The next year, Thomé et al. investigated and compared the wound-healing effects of P. major and Siparuna guianensis with a commercial product used in Brazil. Mice with cervical dorsal area wounds were treated with the botanical ingredients and the commercial product. Decreases in the wound area occurred earliest in mice treated with P. major, with complete closure (by day 15) seen only in this group. The investigators concluded that their findings support the traditional application of P. major, which shows potential as a viable wound-healing agent (Exp. Biol. Med. [Maywood] 2012;237:1379-86).
Conclusion
The numerous biologic properties of P. major are well established. In addition, use of the plant in traditional medicine for some cutaneous indications warrants consideration for modern therapeutic usage. Much more research is necessary, however, to elucidate the potential incorporation of this botanical into standard topical preparations for any of various skin conditions.
Dr. Baumann is chief executive officer of the Baumann Cosmetic & Research Institute in the Design District in Miami. She founded the Cosmetic Dermatology Center at the University of Miami in 1997. Dr. Baumann wrote the textbook “Cosmetic Dermatology: Principles and Practice” (New York: McGraw-Hill, 2002), and a book for consumers, “The Skin Type Solution” (New York: Bantam Dell, 2006). She has contributed to the Cosmeceutical Critique column in Dermatology News since January 2001. Her latest book, “Cosmeceuticals and Cosmetic Ingredients,” was published in November 2014. Dr. Baumann has received funding for clinical grants from Allergan, Aveeno, Avon Products, Evolus, Galderma, GlaxoSmithKline, Kythera Biopharmaceuticals, Mary Kay, Medicis Pharmaceuticals, Neutrogena, Philosophy, Topix Pharmaceuticals, and Unilever.
For centuries, the leaves of Plantago major have been used in most regions of the world in traditional medical treatment of wounds and various diseases, including cutaneous conditions (J. Ethnopharmacol. 2000;71:1-21). P. major, also known as broadleaf plantain or greater plantain, is a member of the Plantaginaceae family, which is now widely dispersed throughout the world, though native to much of Europe as well as northern and central Asia. The Norwegian and Swedish name for the plant, groblad, means “healing leaves” (J. Ethnopharmacol. 2000;71:1-21). It was brought to the Americas by Europeans during the colonial period. Native Americans referred to it as the “white man’s footprint,” which inspired the genus name Plantago from the Latin planta (foot) (J. Ethnopharmacol. 2000;71:1-21).
Among the biologically active constituents of P. major are polysaccharides, lipids, caffeic acid derivatives, flavonoids (apigenin, luteolin, scutellarin, baicalein, nepetin, hispidulin, plantagoside), iridoid glycosides (aucubin, catalpol), terpenoids, and alkaloids (J. Ethnopharmacol. 2000;71:1-21; Medical Herbalism: The Science and Practice of Herbal Medicine, 2003, Healing Arts Press). In an ethnopharmacologic and folk medicine survey study of 1,225 residents of the Atlantic coast of Colombia completed in 2011, Gómez-Estrada et al. found that P. major was one of the plants traditionally used to treat inflammation; it also was used to treat kidney pain and eye injuries (J. Ethnobiol. Ethnomed. 2011;7:27). P. major also is traditionally used as a mucilage and bulk laxative (Principles and Practice of Phytotherapy: Modern Herbal Medicine, 2013, Churchill Livingstone).
Extracts of the plant have been associated with myriad biologic activities, including wound healing, anti-inflammatory, antimicrobial, analgesic, antioxidant, immunomodulating, and antiulcerogenic action, which Samuelsen suggested may account for the use of the botanical in traditional medicine (J. Ethnopharmacol. 2000;71:1-21; Medical Herbalism: The Science and Practice of Herbal Medicine, 2003, Healing Arts Press). In fact, the range of biologic properties attributed to P. major also includes astringent, anesthetic, antihelminthic, analeptic, antihistaminic, antirheumatic, antiviral, antitumor, antiulcer, diuretic, hypotensive, and expectorant activity (Exp. Biol. Med. [Maywood] 2012;237:1379-86). Though not the most popular botanical for this indication, P. major is among the plants used in the treatment of cutaneous leishmanial ulcers in Bahia, Brazil, where Leishmania brazilenesis is endemic (Rev. Soc. Bras. Med. Trop. 1996;29:229-32). Other dermatologic uses in traditional medicine include eczema, cuts, hemorrhoids, ulcerations, and wounds (Medical Herbalism: The Science and Practice of Herbal Medicine, 2003, Healing Arts Press).
Wound healing
The use of P. major for wound healing dates back to the first century, as described by the Greek physician Dioscorides in “De Materia Medica” (J. Ethnopharmacol. 2000;71:1-21).
In 2011, Krasnov et al. developed an experimental model for characterizing proteins and showed that a newly discovered group of tissue-specific biogregulating proteins found previously in animal tissues was also present in P. major and responsible for the wound-healing activity associated with the plant (Prikl Biokhim. Mikrobiol. 2011;47:146-53).
The next year, Thomé et al. investigated and compared the wound-healing effects of P. major and Siparuna guianensis with a commercial product used in Brazil. Mice with cervical dorsal area wounds were treated with the botanical ingredients and the commercial product. Decreases in the wound area occurred earliest in mice treated with P. major, with complete closure (by day 15) seen only in this group. The investigators concluded that their findings support the traditional application of P. major, which shows potential as a viable wound-healing agent (Exp. Biol. Med. [Maywood] 2012;237:1379-86).
Conclusion
The numerous biologic properties of P. major are well established. In addition, use of the plant in traditional medicine for some cutaneous indications warrants consideration for modern therapeutic usage. Much more research is necessary, however, to elucidate the potential incorporation of this botanical into standard topical preparations for any of various skin conditions.
Dr. Baumann is chief executive officer of the Baumann Cosmetic & Research Institute in the Design District in Miami. She founded the Cosmetic Dermatology Center at the University of Miami in 1997. Dr. Baumann wrote the textbook “Cosmetic Dermatology: Principles and Practice” (New York: McGraw-Hill, 2002), and a book for consumers, “The Skin Type Solution” (New York: Bantam Dell, 2006). She has contributed to the Cosmeceutical Critique column in Dermatology News since January 2001. Her latest book, “Cosmeceuticals and Cosmetic Ingredients,” was published in November 2014. Dr. Baumann has received funding for clinical grants from Allergan, Aveeno, Avon Products, Evolus, Galderma, GlaxoSmithKline, Kythera Biopharmaceuticals, Mary Kay, Medicis Pharmaceuticals, Neutrogena, Philosophy, Topix Pharmaceuticals, and Unilever.
DIAGNOSING CTD IN CLINICAL PRACTICE
This educational video is sponsored by Exagen Diagnostics, Inc.
For more information, please read the supplement below.
This educational supplement to Rheumatology News is supported by Exagen Diagnostics, Inc.
Nimesh Dayal, MD
Arthritis Center of Orlando
Ocoee, FL
John Goldman, MD, MACR, FACP, CCD
Chief of Rheumatology
Emory St. Joseph’s Hospital
Atlanta, GA
Richard Haddad, MD, FACR
Clinical Assistant Professor of Medicine
Rutgers/Robert Wood Johnson
Red Bank, NJ
Patricia Hopkins, MD
Private Practice
Quincy, MA
James Mossell, DO
Tift Regional Medical Center
Tifton, GA
This educational video is sponsored by Exagen Diagnostics, Inc.
For more information, please read the supplement below.
This educational supplement to Rheumatology News is supported by Exagen Diagnostics, Inc.
Nimesh Dayal, MD
Arthritis Center of Orlando
Ocoee, FL
John Goldman, MD, MACR, FACP, CCD
Chief of Rheumatology
Emory St. Joseph’s Hospital
Atlanta, GA
Richard Haddad, MD, FACR
Clinical Assistant Professor of Medicine
Rutgers/Robert Wood Johnson
Red Bank, NJ
Patricia Hopkins, MD
Private Practice
Quincy, MA
James Mossell, DO
Tift Regional Medical Center
Tifton, GA
This educational video is sponsored by Exagen Diagnostics, Inc.
For more information, please read the supplement below.
This educational supplement to Rheumatology News is supported by Exagen Diagnostics, Inc.
Nimesh Dayal, MD
Arthritis Center of Orlando
Ocoee, FL
John Goldman, MD, MACR, FACP, CCD
Chief of Rheumatology
Emory St. Joseph’s Hospital
Atlanta, GA
Richard Haddad, MD, FACR
Clinical Assistant Professor of Medicine
Rutgers/Robert Wood Johnson
Red Bank, NJ
Patricia Hopkins, MD
Private Practice
Quincy, MA
James Mossell, DO
Tift Regional Medical Center
Tifton, GA
A new treatment approach for ALK- ALCL?
Investigators say they have uncovered a new approach for treating ALK-negative anaplastic large cell lymphoma (ALCL).
Results of genomic analyses indicated that many cases of ALK-negative ALCL may be driven by alterations in the JAK/STAT3 pathway, and in vivo
experiments showed the disease can be inhibited by compounds that target this pathway.
The investigators believe these compounds could be more effective than current therapies.
“Current therapies for this form of lymphoma fail to work in the majority of cases,” said Raul Rabadan, PhD, of Columbia University in New York, New York.
“However, now that we know the mutations that drive a significant percentage of cases, we can envision a new, personalized genomic approach to the treatment of ALK-negative ALCL.”
Dr Rabadan and his colleagues recounted their discovery of the mutations in Cancer Cell.
The team had sequenced the exomes and RNA of cancer cells from 155 patients with ALCL and 74 control subjects with other types of lymphoma.
Results revealed mutations in either JAK1 or STAT3 in about 20% of the 88 patients with ALK-negative ALCL. Of that 20%, 38% had mutations in both genes.
The investigators also detected the presence of several novel gene fusions (NFκB2-ROS1, NFκB2-TYK2, NCOC2-ROS1, and PABPC4-TYK2), some of which appear to activate the JAK/STAT3 pathway (NFκB2-ROS1 and NFκB2-TYK2).
Patients with these fusions did not have JAK1 or STAT3 mutations, which suggests the fusions are an independent cause of ALK-negative ALCL.
To confirm whether JAK1 and STAT3 mutations can cause ALK-negative ALCL, the investigators induced these mutations in normal human cells. The mutations did, in fact, lead to diseased cells.
Finally, the team tested JAK/STAT3 pathway inhibitors—ruxolitinib and PUH71—in mouse models of ALK-negative ALCL. And they found that both drugs significantly inhibited tumor growth.
“Our findings demonstrate that drugs targeting the JAK/STAT3 pathway offer a viable therapeutic strategy in a subset of patients with ALCL,” Dr Rabadan said.
“A couple of JAK/STAT3 inhibitors have been approved by the FDA for the treatment of psoriasis and rheumatoid arthritis, and several more are currently in clinical trials. These could be tested in patients whose genetic profile matches those we identified in our study.” ![]()

Investigators say they have uncovered a new approach for treating ALK-negative anaplastic large cell lymphoma (ALCL).
Results of genomic analyses indicated that many cases of ALK-negative ALCL may be driven by alterations in the JAK/STAT3 pathway, and in vivo
experiments showed the disease can be inhibited by compounds that target this pathway.
The investigators believe these compounds could be more effective than current therapies.
“Current therapies for this form of lymphoma fail to work in the majority of cases,” said Raul Rabadan, PhD, of Columbia University in New York, New York.
“However, now that we know the mutations that drive a significant percentage of cases, we can envision a new, personalized genomic approach to the treatment of ALK-negative ALCL.”
Dr Rabadan and his colleagues recounted their discovery of the mutations in Cancer Cell.
The team had sequenced the exomes and RNA of cancer cells from 155 patients with ALCL and 74 control subjects with other types of lymphoma.
Results revealed mutations in either JAK1 or STAT3 in about 20% of the 88 patients with ALK-negative ALCL. Of that 20%, 38% had mutations in both genes.
The investigators also detected the presence of several novel gene fusions (NFκB2-ROS1, NFκB2-TYK2, NCOC2-ROS1, and PABPC4-TYK2), some of which appear to activate the JAK/STAT3 pathway (NFκB2-ROS1 and NFκB2-TYK2).
Patients with these fusions did not have JAK1 or STAT3 mutations, which suggests the fusions are an independent cause of ALK-negative ALCL.
To confirm whether JAK1 and STAT3 mutations can cause ALK-negative ALCL, the investigators induced these mutations in normal human cells. The mutations did, in fact, lead to diseased cells.
Finally, the team tested JAK/STAT3 pathway inhibitors—ruxolitinib and PUH71—in mouse models of ALK-negative ALCL. And they found that both drugs significantly inhibited tumor growth.
“Our findings demonstrate that drugs targeting the JAK/STAT3 pathway offer a viable therapeutic strategy in a subset of patients with ALCL,” Dr Rabadan said.
“A couple of JAK/STAT3 inhibitors have been approved by the FDA for the treatment of psoriasis and rheumatoid arthritis, and several more are currently in clinical trials. These could be tested in patients whose genetic profile matches those we identified in our study.” ![]()

Investigators say they have uncovered a new approach for treating ALK-negative anaplastic large cell lymphoma (ALCL).
Results of genomic analyses indicated that many cases of ALK-negative ALCL may be driven by alterations in the JAK/STAT3 pathway, and in vivo
experiments showed the disease can be inhibited by compounds that target this pathway.
The investigators believe these compounds could be more effective than current therapies.
“Current therapies for this form of lymphoma fail to work in the majority of cases,” said Raul Rabadan, PhD, of Columbia University in New York, New York.
“However, now that we know the mutations that drive a significant percentage of cases, we can envision a new, personalized genomic approach to the treatment of ALK-negative ALCL.”
Dr Rabadan and his colleagues recounted their discovery of the mutations in Cancer Cell.
The team had sequenced the exomes and RNA of cancer cells from 155 patients with ALCL and 74 control subjects with other types of lymphoma.
Results revealed mutations in either JAK1 or STAT3 in about 20% of the 88 patients with ALK-negative ALCL. Of that 20%, 38% had mutations in both genes.
The investigators also detected the presence of several novel gene fusions (NFκB2-ROS1, NFκB2-TYK2, NCOC2-ROS1, and PABPC4-TYK2), some of which appear to activate the JAK/STAT3 pathway (NFκB2-ROS1 and NFκB2-TYK2).
Patients with these fusions did not have JAK1 or STAT3 mutations, which suggests the fusions are an independent cause of ALK-negative ALCL.
To confirm whether JAK1 and STAT3 mutations can cause ALK-negative ALCL, the investigators induced these mutations in normal human cells. The mutations did, in fact, lead to diseased cells.
Finally, the team tested JAK/STAT3 pathway inhibitors—ruxolitinib and PUH71—in mouse models of ALK-negative ALCL. And they found that both drugs significantly inhibited tumor growth.
“Our findings demonstrate that drugs targeting the JAK/STAT3 pathway offer a viable therapeutic strategy in a subset of patients with ALCL,” Dr Rabadan said.
“A couple of JAK/STAT3 inhibitors have been approved by the FDA for the treatment of psoriasis and rheumatoid arthritis, and several more are currently in clinical trials. These could be tested in patients whose genetic profile matches those we identified in our study.” ![]()
Combo improves PFS in untreated CLL

Results of a phase 3 study suggest that adding ofatumumab to chlorambucil can improve progression-free survival (PFS) in treatment-naïve patients with chronic lymphocytic leukemia (CLL).
Ofatumumab plus chlorambucil improved the median PFS by 71% compared to chlorambucil alone.
The combination also improved the overall response rate, duration of response, and time to next treatment.
However, patients in the combination arm had a higher rate of grade 3 or greater adverse events (AEs).
Researchers reported these results in The Lancet. The study, known as COMPLEMENT 1, was funded by GlaxoSmithKline and Genmab A/S.
The study included 447 patients with previously untreated CLL for whom fludarabine-based therapy was considered inappropriate. Patients were randomized to treatment with up to 12 cycles of ofatumumab in combination with chlorambucil (n=221) or up to 12 cycles of chlorambucil alone (n=226).
The study’s primary endpoint was the median PFS, which was 22.4 months in the combination arm and 13.1 months in the chlorambucil arm (hazard ratio [HR]=0.57, P<0.0001). This improvement in PFS was observed in most subgroups, irrespective of age, gender, disease stage, and prognostic factors.
As for secondary endpoints, patients in the combination arm had a higher overall response rate than patients in the chlorambucil arm—82% and 69%, respectively (odds ratio=2.16, P=0.001).
And combination treatment increased the duration of response compared to chlorambucil alone—22.1 months and 13.2 months, respectively (HR=0.56, P<0.001).
Patients in the combination arm also experienced a significantly longer time to next therapy compared to the chlorambucil arm—39.8 months and 24.7 months, respectively (HR=0.49, P<0.0001).
Safety data
The most common AEs (occurring in at least 2% of patients) were neutropenia, thrombocytopenia, anemia, infections, and infusion-related reactions.
Neutropenia occurred more frequently in the combination arm (27% vs 18%), as did infusion-related reactions (67% vs 0%) and infections (46% vs 42%). But thrombocytopenia and anemia were more frequent in the chlorambucil arm (26% vs 14% and 13% vs 9%, respectively).
The incidence of grade 3 or greater AEs was higher in the combination arm than the chlorambucil arm—50% and 43%, respectively.
Grade 3/4 infusion-related reactions occurred in 10% of patients in the combination arm, leading to drug withdrawal in 3% of patients and hospitalization in 2% of patients. No fatal infusion-related reactions were reported.
The most common infections were respiratory tract infections, with an incidence of 27% in the combination arm and 31% in the chlorambucil arm. There were similar frequencies of sepsis (3% and 2%, respectively) and opportunistic infections between the arms (4% and 5%, respectively).
The incidence of AEs leading to treatment withdrawal was 13% in both arms. And the incidence of death during treatment or within 60 days after the last dose was 3% in both arms.
These data formed the basis for regulatory approvals of ofatumumab (Arzerra) in the US and European Union, as well as the recent inclusion of ofatumumab plus chlorambucil in the National Comprehensive Cancer Network treatment guidelines. ![]()

Results of a phase 3 study suggest that adding ofatumumab to chlorambucil can improve progression-free survival (PFS) in treatment-naïve patients with chronic lymphocytic leukemia (CLL).
Ofatumumab plus chlorambucil improved the median PFS by 71% compared to chlorambucil alone.
The combination also improved the overall response rate, duration of response, and time to next treatment.
However, patients in the combination arm had a higher rate of grade 3 or greater adverse events (AEs).
Researchers reported these results in The Lancet. The study, known as COMPLEMENT 1, was funded by GlaxoSmithKline and Genmab A/S.
The study included 447 patients with previously untreated CLL for whom fludarabine-based therapy was considered inappropriate. Patients were randomized to treatment with up to 12 cycles of ofatumumab in combination with chlorambucil (n=221) or up to 12 cycles of chlorambucil alone (n=226).
The study’s primary endpoint was the median PFS, which was 22.4 months in the combination arm and 13.1 months in the chlorambucil arm (hazard ratio [HR]=0.57, P<0.0001). This improvement in PFS was observed in most subgroups, irrespective of age, gender, disease stage, and prognostic factors.
As for secondary endpoints, patients in the combination arm had a higher overall response rate than patients in the chlorambucil arm—82% and 69%, respectively (odds ratio=2.16, P=0.001).
And combination treatment increased the duration of response compared to chlorambucil alone—22.1 months and 13.2 months, respectively (HR=0.56, P<0.001).
Patients in the combination arm also experienced a significantly longer time to next therapy compared to the chlorambucil arm—39.8 months and 24.7 months, respectively (HR=0.49, P<0.0001).
Safety data
The most common AEs (occurring in at least 2% of patients) were neutropenia, thrombocytopenia, anemia, infections, and infusion-related reactions.
Neutropenia occurred more frequently in the combination arm (27% vs 18%), as did infusion-related reactions (67% vs 0%) and infections (46% vs 42%). But thrombocytopenia and anemia were more frequent in the chlorambucil arm (26% vs 14% and 13% vs 9%, respectively).
The incidence of grade 3 or greater AEs was higher in the combination arm than the chlorambucil arm—50% and 43%, respectively.
Grade 3/4 infusion-related reactions occurred in 10% of patients in the combination arm, leading to drug withdrawal in 3% of patients and hospitalization in 2% of patients. No fatal infusion-related reactions were reported.
The most common infections were respiratory tract infections, with an incidence of 27% in the combination arm and 31% in the chlorambucil arm. There were similar frequencies of sepsis (3% and 2%, respectively) and opportunistic infections between the arms (4% and 5%, respectively).
The incidence of AEs leading to treatment withdrawal was 13% in both arms. And the incidence of death during treatment or within 60 days after the last dose was 3% in both arms.
These data formed the basis for regulatory approvals of ofatumumab (Arzerra) in the US and European Union, as well as the recent inclusion of ofatumumab plus chlorambucil in the National Comprehensive Cancer Network treatment guidelines. ![]()

Results of a phase 3 study suggest that adding ofatumumab to chlorambucil can improve progression-free survival (PFS) in treatment-naïve patients with chronic lymphocytic leukemia (CLL).
Ofatumumab plus chlorambucil improved the median PFS by 71% compared to chlorambucil alone.
The combination also improved the overall response rate, duration of response, and time to next treatment.
However, patients in the combination arm had a higher rate of grade 3 or greater adverse events (AEs).
Researchers reported these results in The Lancet. The study, known as COMPLEMENT 1, was funded by GlaxoSmithKline and Genmab A/S.
The study included 447 patients with previously untreated CLL for whom fludarabine-based therapy was considered inappropriate. Patients were randomized to treatment with up to 12 cycles of ofatumumab in combination with chlorambucil (n=221) or up to 12 cycles of chlorambucil alone (n=226).
The study’s primary endpoint was the median PFS, which was 22.4 months in the combination arm and 13.1 months in the chlorambucil arm (hazard ratio [HR]=0.57, P<0.0001). This improvement in PFS was observed in most subgroups, irrespective of age, gender, disease stage, and prognostic factors.
As for secondary endpoints, patients in the combination arm had a higher overall response rate than patients in the chlorambucil arm—82% and 69%, respectively (odds ratio=2.16, P=0.001).
And combination treatment increased the duration of response compared to chlorambucil alone—22.1 months and 13.2 months, respectively (HR=0.56, P<0.001).
Patients in the combination arm also experienced a significantly longer time to next therapy compared to the chlorambucil arm—39.8 months and 24.7 months, respectively (HR=0.49, P<0.0001).
Safety data
The most common AEs (occurring in at least 2% of patients) were neutropenia, thrombocytopenia, anemia, infections, and infusion-related reactions.
Neutropenia occurred more frequently in the combination arm (27% vs 18%), as did infusion-related reactions (67% vs 0%) and infections (46% vs 42%). But thrombocytopenia and anemia were more frequent in the chlorambucil arm (26% vs 14% and 13% vs 9%, respectively).
The incidence of grade 3 or greater AEs was higher in the combination arm than the chlorambucil arm—50% and 43%, respectively.
Grade 3/4 infusion-related reactions occurred in 10% of patients in the combination arm, leading to drug withdrawal in 3% of patients and hospitalization in 2% of patients. No fatal infusion-related reactions were reported.
The most common infections were respiratory tract infections, with an incidence of 27% in the combination arm and 31% in the chlorambucil arm. There were similar frequencies of sepsis (3% and 2%, respectively) and opportunistic infections between the arms (4% and 5%, respectively).
The incidence of AEs leading to treatment withdrawal was 13% in both arms. And the incidence of death during treatment or within 60 days after the last dose was 3% in both arms.
These data formed the basis for regulatory approvals of ofatumumab (Arzerra) in the US and European Union, as well as the recent inclusion of ofatumumab plus chlorambucil in the National Comprehensive Cancer Network treatment guidelines. ![]()
Study illustrates challenges of parsing genetic data

Photo courtesy of NIGMS
A study of genes associated with bleeding disorders suggests it can be challenging to gauge the clinical significance of novel gene variants.
Researchers analyzed genomic data from more than 16,000 subjects, looking for missense variants in the integrin aIIbß3 receptor subunit genes ITGA2B and ITGB3.
Although the team identified close to 200 novel variants in these genes, they found it difficult to determine the functional impact of the variants.
Barry S. Coller, MD, of The Rockefeller University in New York, New York, and his colleagues described this research in PNAS.
The team analyzed genomic data from 16,108 people and found that about 1.3% of the individuals had missense variants in ITGA2B, ITGB3, or both genes.
To determine which of these missense variants were newly discovered, the researchers looked for 111 variants that were previously reported as being associated with Glanzmann thrombasthenia, 20 variants that were associated with alloimmune thrombocytopenia, and 5 variants that were associated with aniso/macrothrombocytopenia.
The results suggested the team had discovered 114 novel missense variants in ITGA2B and 68 novel variants in ITGB3. And they did not find any of the previously reported variants in the 2 genes.
“This means the disease-causing mutations previously reported are very rare and, thus, probably first appeared relatively recently—that is, in the past several hundred years,” Dr Coller said.
The researchers then used 3 different algorithms to try to predict the proportion of the missense variants that would likely have a negative impact on a person’s health by causing excess bleeding.
They got a wide range of results. Depending on the algorithm and other variables, between 27% and 71% of variants were predicted to be harmful.
To test the validity of the predictions, the team took a closer look at 3 of the variants that affect amino acids previously associated with Glanzmann thrombasthenia.
They found that 2 of the variants—aIIb P176H and ß3 C547G—severely reduced aIIbß3 expression. The third variant—aIIb P943A—partially reduced aIIbß3 expression but had no effect on fibrinogen binding.
These results show how challenging it can be to interpret genetic data, Dr Coller said.
“Some variants of these 2 genes will likely be obviously deleterious, but it may be impossible to predict whether others are deleterious,” he noted. “In those cases, we will need to use additional information to judge the likelihood of a mutation being deleterious, and, in many cases, there will be residual uncertainty.” ![]()

Photo courtesy of NIGMS
A study of genes associated with bleeding disorders suggests it can be challenging to gauge the clinical significance of novel gene variants.
Researchers analyzed genomic data from more than 16,000 subjects, looking for missense variants in the integrin aIIbß3 receptor subunit genes ITGA2B and ITGB3.
Although the team identified close to 200 novel variants in these genes, they found it difficult to determine the functional impact of the variants.
Barry S. Coller, MD, of The Rockefeller University in New York, New York, and his colleagues described this research in PNAS.
The team analyzed genomic data from 16,108 people and found that about 1.3% of the individuals had missense variants in ITGA2B, ITGB3, or both genes.
To determine which of these missense variants were newly discovered, the researchers looked for 111 variants that were previously reported as being associated with Glanzmann thrombasthenia, 20 variants that were associated with alloimmune thrombocytopenia, and 5 variants that were associated with aniso/macrothrombocytopenia.
The results suggested the team had discovered 114 novel missense variants in ITGA2B and 68 novel variants in ITGB3. And they did not find any of the previously reported variants in the 2 genes.
“This means the disease-causing mutations previously reported are very rare and, thus, probably first appeared relatively recently—that is, in the past several hundred years,” Dr Coller said.
The researchers then used 3 different algorithms to try to predict the proportion of the missense variants that would likely have a negative impact on a person’s health by causing excess bleeding.
They got a wide range of results. Depending on the algorithm and other variables, between 27% and 71% of variants were predicted to be harmful.
To test the validity of the predictions, the team took a closer look at 3 of the variants that affect amino acids previously associated with Glanzmann thrombasthenia.
They found that 2 of the variants—aIIb P176H and ß3 C547G—severely reduced aIIbß3 expression. The third variant—aIIb P943A—partially reduced aIIbß3 expression but had no effect on fibrinogen binding.
These results show how challenging it can be to interpret genetic data, Dr Coller said.
“Some variants of these 2 genes will likely be obviously deleterious, but it may be impossible to predict whether others are deleterious,” he noted. “In those cases, we will need to use additional information to judge the likelihood of a mutation being deleterious, and, in many cases, there will be residual uncertainty.” ![]()

Photo courtesy of NIGMS
A study of genes associated with bleeding disorders suggests it can be challenging to gauge the clinical significance of novel gene variants.
Researchers analyzed genomic data from more than 16,000 subjects, looking for missense variants in the integrin aIIbß3 receptor subunit genes ITGA2B and ITGB3.
Although the team identified close to 200 novel variants in these genes, they found it difficult to determine the functional impact of the variants.
Barry S. Coller, MD, of The Rockefeller University in New York, New York, and his colleagues described this research in PNAS.
The team analyzed genomic data from 16,108 people and found that about 1.3% of the individuals had missense variants in ITGA2B, ITGB3, or both genes.
To determine which of these missense variants were newly discovered, the researchers looked for 111 variants that were previously reported as being associated with Glanzmann thrombasthenia, 20 variants that were associated with alloimmune thrombocytopenia, and 5 variants that were associated with aniso/macrothrombocytopenia.
The results suggested the team had discovered 114 novel missense variants in ITGA2B and 68 novel variants in ITGB3. And they did not find any of the previously reported variants in the 2 genes.
“This means the disease-causing mutations previously reported are very rare and, thus, probably first appeared relatively recently—that is, in the past several hundred years,” Dr Coller said.
The researchers then used 3 different algorithms to try to predict the proportion of the missense variants that would likely have a negative impact on a person’s health by causing excess bleeding.
They got a wide range of results. Depending on the algorithm and other variables, between 27% and 71% of variants were predicted to be harmful.
To test the validity of the predictions, the team took a closer look at 3 of the variants that affect amino acids previously associated with Glanzmann thrombasthenia.
They found that 2 of the variants—aIIb P176H and ß3 C547G—severely reduced aIIbß3 expression. The third variant—aIIb P943A—partially reduced aIIbß3 expression but had no effect on fibrinogen binding.
These results show how challenging it can be to interpret genetic data, Dr Coller said.
“Some variants of these 2 genes will likely be obviously deleterious, but it may be impossible to predict whether others are deleterious,” he noted. “In those cases, we will need to use additional information to judge the likelihood of a mutation being deleterious, and, in many cases, there will be residual uncertainty.” ![]()
SGR repeal dubbed ‘victory’ for cancer patients

chemotherapy
Photo by Rhoda Baer
A bill that repeals the sustainable growth rate (SGR) formula for physician reimbursement under Medicare is a victory for cancer patients, according to oncologist groups.
The bill—known as H.R.2—passed both the US House of Representatives and the Senate with an overwhelming majority. It must still be signed into law by President Obama, but he has indicated he will sign it.
By repealing the SGR payment methodology, the bill will prevent a 21.2% reduction in physician reimbursement rates.
“Today’s courageous vote by the US Senate to finally end the sustainable growth rate formula is a vote for the millions of patients with cancer who depend on Medicare to help them fight their disease,” said Peter Paul Yu, MD, president of the American Society of Clinical Oncology.
“With Congress passing this historic legislation to finally end the 13-year SGR roller coaster ride, Medicare beneficiaries and their physicians can breathe easier knowing that they will no longer face the perennial threat of payment cuts that risk disruption of care and cause anxiety among patients.”
Under H.R. 2, Medicare’s physician reimbursements will increase by 0.5% in the second half of 2015, then an additional 0.5% annually from 2016 through the end of 2019. The 2019 rates will be maintained through 2025 with no additional increases.
The bill also includes comprehensive structural changes to Medicare’s reimbursement model that aim to promote physician participation in clinical quality improvement activities and value-based care that will take full effect in 2019.
Current Medicare programs that reward electronic health records, quality reporting, the value-based modifier, and meaningful use will be merged by 2019 to encourage participation and to reduce the administrative burden.
The bill also ensures the Children’s Health Insurance Program will receive funding for 2 more years and allocates $7.2 billion for community health centers.
“[P]assage of this legislation represents a long-awaited, historic victory for our patients,” said Bruce G. Haffty, MD, chair of the American Society for Radiation Oncology’s board of directors.
“Permanently repealing the SGR and replacing it with a stabilized reimbursement plan focused on quality will strengthen Medicare and allow us to enhance cancer care for the more than 1 million patients treated with radiation therapy each year.” ![]()

chemotherapy
Photo by Rhoda Baer
A bill that repeals the sustainable growth rate (SGR) formula for physician reimbursement under Medicare is a victory for cancer patients, according to oncologist groups.
The bill—known as H.R.2—passed both the US House of Representatives and the Senate with an overwhelming majority. It must still be signed into law by President Obama, but he has indicated he will sign it.
By repealing the SGR payment methodology, the bill will prevent a 21.2% reduction in physician reimbursement rates.
“Today’s courageous vote by the US Senate to finally end the sustainable growth rate formula is a vote for the millions of patients with cancer who depend on Medicare to help them fight their disease,” said Peter Paul Yu, MD, president of the American Society of Clinical Oncology.
“With Congress passing this historic legislation to finally end the 13-year SGR roller coaster ride, Medicare beneficiaries and their physicians can breathe easier knowing that they will no longer face the perennial threat of payment cuts that risk disruption of care and cause anxiety among patients.”
Under H.R. 2, Medicare’s physician reimbursements will increase by 0.5% in the second half of 2015, then an additional 0.5% annually from 2016 through the end of 2019. The 2019 rates will be maintained through 2025 with no additional increases.
The bill also includes comprehensive structural changes to Medicare’s reimbursement model that aim to promote physician participation in clinical quality improvement activities and value-based care that will take full effect in 2019.
Current Medicare programs that reward electronic health records, quality reporting, the value-based modifier, and meaningful use will be merged by 2019 to encourage participation and to reduce the administrative burden.
The bill also ensures the Children’s Health Insurance Program will receive funding for 2 more years and allocates $7.2 billion for community health centers.
“[P]assage of this legislation represents a long-awaited, historic victory for our patients,” said Bruce G. Haffty, MD, chair of the American Society for Radiation Oncology’s board of directors.
“Permanently repealing the SGR and replacing it with a stabilized reimbursement plan focused on quality will strengthen Medicare and allow us to enhance cancer care for the more than 1 million patients treated with radiation therapy each year.” ![]()

chemotherapy
Photo by Rhoda Baer
A bill that repeals the sustainable growth rate (SGR) formula for physician reimbursement under Medicare is a victory for cancer patients, according to oncologist groups.
The bill—known as H.R.2—passed both the US House of Representatives and the Senate with an overwhelming majority. It must still be signed into law by President Obama, but he has indicated he will sign it.
By repealing the SGR payment methodology, the bill will prevent a 21.2% reduction in physician reimbursement rates.
“Today’s courageous vote by the US Senate to finally end the sustainable growth rate formula is a vote for the millions of patients with cancer who depend on Medicare to help them fight their disease,” said Peter Paul Yu, MD, president of the American Society of Clinical Oncology.
“With Congress passing this historic legislation to finally end the 13-year SGR roller coaster ride, Medicare beneficiaries and their physicians can breathe easier knowing that they will no longer face the perennial threat of payment cuts that risk disruption of care and cause anxiety among patients.”
Under H.R. 2, Medicare’s physician reimbursements will increase by 0.5% in the second half of 2015, then an additional 0.5% annually from 2016 through the end of 2019. The 2019 rates will be maintained through 2025 with no additional increases.
The bill also includes comprehensive structural changes to Medicare’s reimbursement model that aim to promote physician participation in clinical quality improvement activities and value-based care that will take full effect in 2019.
Current Medicare programs that reward electronic health records, quality reporting, the value-based modifier, and meaningful use will be merged by 2019 to encourage participation and to reduce the administrative burden.
The bill also ensures the Children’s Health Insurance Program will receive funding for 2 more years and allocates $7.2 billion for community health centers.
“[P]assage of this legislation represents a long-awaited, historic victory for our patients,” said Bruce G. Haffty, MD, chair of the American Society for Radiation Oncology’s board of directors.
“Permanently repealing the SGR and replacing it with a stabilized reimbursement plan focused on quality will strengthen Medicare and allow us to enhance cancer care for the more than 1 million patients treated with radiation therapy each year.” ![]()