User login
Listen Now: Dr. Peter Jamieson Discusses Evolution of Hospital Medicine in Canada
Peter Jamieson, MD, medical director of Foothills Medical Center in Calgary, Alberta, talks about hospital medicine's evolution Canada away from the term “hospitalist” and toward the
establishment and development of a core curriculum and credential of added competency in hospital medicine.
Peter Jamieson, MD, medical director of Foothills Medical Center in Calgary, Alberta, talks about hospital medicine's evolution Canada away from the term “hospitalist” and toward the
establishment and development of a core curriculum and credential of added competency in hospital medicine.
Peter Jamieson, MD, medical director of Foothills Medical Center in Calgary, Alberta, talks about hospital medicine's evolution Canada away from the term “hospitalist” and toward the
establishment and development of a core curriculum and credential of added competency in hospital medicine.
Listen Now: Dr. Henry Feldman Discusses Advancing Hospital Medicine Globally
Henry Feldman, MD, a hospitalist at Beth Israel Deaconess Medical Center in Boston, talks about his work with hospitalists overseas to help advance their medical informatics, diabetes care, stroke care, and dissemination of “Open Notes” policies.
Henry Feldman, MD, a hospitalist at Beth Israel Deaconess Medical Center in Boston, talks about his work with hospitalists overseas to help advance their medical informatics, diabetes care, stroke care, and dissemination of “Open Notes” policies.
Henry Feldman, MD, a hospitalist at Beth Israel Deaconess Medical Center in Boston, talks about his work with hospitalists overseas to help advance their medical informatics, diabetes care, stroke care, and dissemination of “Open Notes” policies.
New Studies Find RIPC Ineffective
NEW YORK - The theory that heart surgery can be made safer by periodically cutting off blood flow to an arm has been called into serious question.
Two large randomized studies, published online by the New England Journal of Medicine and presented on Oct. 5 at the European Society of Intensive Care Medicine Congress in Berlin, show that the technique, known as remote ischemic preconditioning (RIPC), made no difference in terms of the risk of death, heart attack, or kidney failure after surgery.
"The conclusions from both trials are definitive: remote ischemic preconditioning is ineffective in adults undergoing on-pump cardiac surgery," wrote Dr. Michael Zaugg and Dr. Eliana Lucchinetti of the University of Alberta in Edmonton, Canada, in a Journal editorial.
But the chief author of one of the studies, Dr. Patrick Meybohm of University Hospital Frankfurt in Germany, said research on the technique will likely continue because propofol was used as an anesthetic, which may have muted the effect, and patients who were excluded because of recent heart attack or severe liver or kidney disease might benefit.
"Other RIPC protocols (e.g., involving lower-limb RIPC, a longer duration of ischemia, or more cycles) may still be protective. Thus future studies should focus on these confounders," he said by email.
Evidence supporting the technique has been mixed, although tests that have looked at serum cardiac and renal biomarkers have suggested that cutting off flow to an extremity during on-pump surgery might offer better outcomes.
"The underlying hypothesis is that RIPC may attenuate organ injury by releasing various molecules such as damage-associated molecular patterns, adenosin, etc. etc., and that the body's own mediators may then induce natural defenses such as bioenergetic down-regulation and temporary cell-cycle arrest," Meybohm said. "These defenses, once engaged, can then protect the organs during subsequent inflammatory or ischemic stress."
The two studies, known as ERICCA and the RIPHeart, both included a sham group so the surgeons would not know which of the unconscious patients were getting their arm circulation cut off by a blood pressure cuff during the operation. Virtually all the patients were sedated with intravenous propofol.
ERICCA, the larger of the two, was conducted in the UK at 30 cardiac surgery centers on people undergoing coronary artery bypass graft surgery with or without valve replacement.
In the active treatment group, the blood was cut off from the arm for five minutes and restored for five minutes. The cycle was repeated three more times. In the control group, the inflation valve was left open.
Ultimately, 26.5% of the 801 patients in the test group died from cardiovascular causes, experienced a myocardial infarction, required coronary revascularization or experienced a stroke 12 months after randomization. The rate was 27.7% for the 811 in the control group (p=0.58).
There were no significant differences for those individual measures, nor on secondary measures such as the rate of acute kidney injury, troponin levels, length of stay in the ICU, or amount of time spent in the hospital.
The research team, led by Dr. Derek Hausenloy of University College in London, did not find any evidence that preconditioning produced serious side effects.
The RIPHeart study, conducted at 14 German hospitals by Dr. Meybohm and colleagues, randomized 1,403 patients and used a composite endpoint of death, heart attack, stroke, or acute renal failure up to the time of hospital discharge or a maximum of 14 days. A secondary analysis followed the volunteers for three months.
To disguise which patients were receiving preconditioning and which were not, cuffs were placed on each patient's arm and on a dummy arm, both covered by surgical drapes. Only one cuff was inflated.
Again, the endpoint rates in the two groups were the same - 14.3% with preconditioning and 14.6% with sham preconditioning. Analyzing the individual elements of the composite endpoint also show no advantage either way.
No significant differences were seen "in the level of troponin release, the duration of mechanical ventilation, the length of stay in the intensive care unit or the hospital, new onset of atrial fibrillation, and the incidence of postoperative delirium," the team concluded.
"In addition, no significant differences between treatment groups were found at the 30-day and 90-day follow-up," they wrote.
They also saw no adverse events. In their editorial, Drs. Zaugg and Lucchinetti speculated that the technique might be risky in patients with highly unstable coronary plaques because there was a small, albeit nonsignificant, increase in deaths from cardiovascular causes in one of the two studies.
Dr. Meybohm said he didn't think that speculation was warranted.
"Current data do not strongly support the hypothesis that RIPC may do more harm than good," he said. "There are preliminary results from about two-three studies, but there are also nearly a hundred studies demonstrating reduced biomarkers of organ ischemia/reperfusion injury, and positive/neutral effects."
The ERICCA study was funded by the Efficacy and Evaluation Program and the British Heart Foundation; the RIPHeart study was funded by the German Research Foundation.
NEW YORK - The theory that heart surgery can be made safer by periodically cutting off blood flow to an arm has been called into serious question.
Two large randomized studies, published online by the New England Journal of Medicine and presented on Oct. 5 at the European Society of Intensive Care Medicine Congress in Berlin, show that the technique, known as remote ischemic preconditioning (RIPC), made no difference in terms of the risk of death, heart attack, or kidney failure after surgery.
"The conclusions from both trials are definitive: remote ischemic preconditioning is ineffective in adults undergoing on-pump cardiac surgery," wrote Dr. Michael Zaugg and Dr. Eliana Lucchinetti of the University of Alberta in Edmonton, Canada, in a Journal editorial.
But the chief author of one of the studies, Dr. Patrick Meybohm of University Hospital Frankfurt in Germany, said research on the technique will likely continue because propofol was used as an anesthetic, which may have muted the effect, and patients who were excluded because of recent heart attack or severe liver or kidney disease might benefit.
"Other RIPC protocols (e.g., involving lower-limb RIPC, a longer duration of ischemia, or more cycles) may still be protective. Thus future studies should focus on these confounders," he said by email.
Evidence supporting the technique has been mixed, although tests that have looked at serum cardiac and renal biomarkers have suggested that cutting off flow to an extremity during on-pump surgery might offer better outcomes.
"The underlying hypothesis is that RIPC may attenuate organ injury by releasing various molecules such as damage-associated molecular patterns, adenosin, etc. etc., and that the body's own mediators may then induce natural defenses such as bioenergetic down-regulation and temporary cell-cycle arrest," Meybohm said. "These defenses, once engaged, can then protect the organs during subsequent inflammatory or ischemic stress."
The two studies, known as ERICCA and the RIPHeart, both included a sham group so the surgeons would not know which of the unconscious patients were getting their arm circulation cut off by a blood pressure cuff during the operation. Virtually all the patients were sedated with intravenous propofol.
ERICCA, the larger of the two, was conducted in the UK at 30 cardiac surgery centers on people undergoing coronary artery bypass graft surgery with or without valve replacement.
In the active treatment group, the blood was cut off from the arm for five minutes and restored for five minutes. The cycle was repeated three more times. In the control group, the inflation valve was left open.
Ultimately, 26.5% of the 801 patients in the test group died from cardiovascular causes, experienced a myocardial infarction, required coronary revascularization or experienced a stroke 12 months after randomization. The rate was 27.7% for the 811 in the control group (p=0.58).
There were no significant differences for those individual measures, nor on secondary measures such as the rate of acute kidney injury, troponin levels, length of stay in the ICU, or amount of time spent in the hospital.
The research team, led by Dr. Derek Hausenloy of University College in London, did not find any evidence that preconditioning produced serious side effects.
The RIPHeart study, conducted at 14 German hospitals by Dr. Meybohm and colleagues, randomized 1,403 patients and used a composite endpoint of death, heart attack, stroke, or acute renal failure up to the time of hospital discharge or a maximum of 14 days. A secondary analysis followed the volunteers for three months.
To disguise which patients were receiving preconditioning and which were not, cuffs were placed on each patient's arm and on a dummy arm, both covered by surgical drapes. Only one cuff was inflated.
Again, the endpoint rates in the two groups were the same - 14.3% with preconditioning and 14.6% with sham preconditioning. Analyzing the individual elements of the composite endpoint also show no advantage either way.
No significant differences were seen "in the level of troponin release, the duration of mechanical ventilation, the length of stay in the intensive care unit or the hospital, new onset of atrial fibrillation, and the incidence of postoperative delirium," the team concluded.
"In addition, no significant differences between treatment groups were found at the 30-day and 90-day follow-up," they wrote.
They also saw no adverse events. In their editorial, Drs. Zaugg and Lucchinetti speculated that the technique might be risky in patients with highly unstable coronary plaques because there was a small, albeit nonsignificant, increase in deaths from cardiovascular causes in one of the two studies.
Dr. Meybohm said he didn't think that speculation was warranted.
"Current data do not strongly support the hypothesis that RIPC may do more harm than good," he said. "There are preliminary results from about two-three studies, but there are also nearly a hundred studies demonstrating reduced biomarkers of organ ischemia/reperfusion injury, and positive/neutral effects."
The ERICCA study was funded by the Efficacy and Evaluation Program and the British Heart Foundation; the RIPHeart study was funded by the German Research Foundation.
NEW YORK - The theory that heart surgery can be made safer by periodically cutting off blood flow to an arm has been called into serious question.
Two large randomized studies, published online by the New England Journal of Medicine and presented on Oct. 5 at the European Society of Intensive Care Medicine Congress in Berlin, show that the technique, known as remote ischemic preconditioning (RIPC), made no difference in terms of the risk of death, heart attack, or kidney failure after surgery.
"The conclusions from both trials are definitive: remote ischemic preconditioning is ineffective in adults undergoing on-pump cardiac surgery," wrote Dr. Michael Zaugg and Dr. Eliana Lucchinetti of the University of Alberta in Edmonton, Canada, in a Journal editorial.
But the chief author of one of the studies, Dr. Patrick Meybohm of University Hospital Frankfurt in Germany, said research on the technique will likely continue because propofol was used as an anesthetic, which may have muted the effect, and patients who were excluded because of recent heart attack or severe liver or kidney disease might benefit.
"Other RIPC protocols (e.g., involving lower-limb RIPC, a longer duration of ischemia, or more cycles) may still be protective. Thus future studies should focus on these confounders," he said by email.
Evidence supporting the technique has been mixed, although tests that have looked at serum cardiac and renal biomarkers have suggested that cutting off flow to an extremity during on-pump surgery might offer better outcomes.
"The underlying hypothesis is that RIPC may attenuate organ injury by releasing various molecules such as damage-associated molecular patterns, adenosin, etc. etc., and that the body's own mediators may then induce natural defenses such as bioenergetic down-regulation and temporary cell-cycle arrest," Meybohm said. "These defenses, once engaged, can then protect the organs during subsequent inflammatory or ischemic stress."
The two studies, known as ERICCA and the RIPHeart, both included a sham group so the surgeons would not know which of the unconscious patients were getting their arm circulation cut off by a blood pressure cuff during the operation. Virtually all the patients were sedated with intravenous propofol.
ERICCA, the larger of the two, was conducted in the UK at 30 cardiac surgery centers on people undergoing coronary artery bypass graft surgery with or without valve replacement.
In the active treatment group, the blood was cut off from the arm for five minutes and restored for five minutes. The cycle was repeated three more times. In the control group, the inflation valve was left open.
Ultimately, 26.5% of the 801 patients in the test group died from cardiovascular causes, experienced a myocardial infarction, required coronary revascularization or experienced a stroke 12 months after randomization. The rate was 27.7% for the 811 in the control group (p=0.58).
There were no significant differences for those individual measures, nor on secondary measures such as the rate of acute kidney injury, troponin levels, length of stay in the ICU, or amount of time spent in the hospital.
The research team, led by Dr. Derek Hausenloy of University College in London, did not find any evidence that preconditioning produced serious side effects.
The RIPHeart study, conducted at 14 German hospitals by Dr. Meybohm and colleagues, randomized 1,403 patients and used a composite endpoint of death, heart attack, stroke, or acute renal failure up to the time of hospital discharge or a maximum of 14 days. A secondary analysis followed the volunteers for three months.
To disguise which patients were receiving preconditioning and which were not, cuffs were placed on each patient's arm and on a dummy arm, both covered by surgical drapes. Only one cuff was inflated.
Again, the endpoint rates in the two groups were the same - 14.3% with preconditioning and 14.6% with sham preconditioning. Analyzing the individual elements of the composite endpoint also show no advantage either way.
No significant differences were seen "in the level of troponin release, the duration of mechanical ventilation, the length of stay in the intensive care unit or the hospital, new onset of atrial fibrillation, and the incidence of postoperative delirium," the team concluded.
"In addition, no significant differences between treatment groups were found at the 30-day and 90-day follow-up," they wrote.
They also saw no adverse events. In their editorial, Drs. Zaugg and Lucchinetti speculated that the technique might be risky in patients with highly unstable coronary plaques because there was a small, albeit nonsignificant, increase in deaths from cardiovascular causes in one of the two studies.
Dr. Meybohm said he didn't think that speculation was warranted.
"Current data do not strongly support the hypothesis that RIPC may do more harm than good," he said. "There are preliminary results from about two-three studies, but there are also nearly a hundred studies demonstrating reduced biomarkers of organ ischemia/reperfusion injury, and positive/neutral effects."
The ERICCA study was funded by the Efficacy and Evaluation Program and the British Heart Foundation; the RIPHeart study was funded by the German Research Foundation.
Listen Now: Antimicrobial Stewardship Programs and Hospital Medicine
Dr. Jonathan Zenilman, chief of infectious diseases at Johns Hopkins Bayview Medical Center in Baltimore, discusses details of Bayview’s antibiotic stewardship program and the challenge of getting such programs funded.
Dr. Jonathan Zenilman, chief of infectious diseases at Johns Hopkins Bayview Medical Center in Baltimore, discusses details of Bayview’s antibiotic stewardship program and the challenge of getting such programs funded.
Dr. Jonathan Zenilman, chief of infectious diseases at Johns Hopkins Bayview Medical Center in Baltimore, discusses details of Bayview’s antibiotic stewardship program and the challenge of getting such programs funded.
Canada Develops Core Competencies for Hospitalists
The Canadian Society of Hospital Medicine is spearheading an initiative called the Core Competencies in Hospitalist Medicine Document Project, which could be used to clarify what the field is, update certification processes, and define its future growth.
Neither the Royal College of Physicians and Surgeons of Canada nor the College of Family Physicians of Canada is likely to pursue board certification for a subspecialty in hospital medicine, says Peter Jamieson, MD, CCFP, FCFP, a hospitalist at Foothills Medical Center in Calgary, Alberta.
“If you think about hospital medicine as a construct—and take the focus off the person and put it instead onto the patient and onto the work, then you can describe the necessary competencies,” Dr. Jamieson says. “What are the preparation, the evaluation, and all of the associated functions? We want to be clear about what this job really is. We don’t have to be defined by training in a particular specialty.”
Writing and reviewing the competencies has been assigned to large physician working groups, with a well-defined process for validation, Dr. Jamieson says.
“Next steps will include elaborating the evaluation criteria, the learning objectives, and those sorts of things. That’s all going on right now,” he explains. “Our objective is to have all of them in a publishable format within the next year or so. Then we’ll need to get the regulatory folks to agree that this represents a subset of practice and a discrete and obtainable set of skills.
“As time goes by, it will become more and more obvious that hospital medicine is a discrete set of skills—not that any doctor couldn’t obtain those skills, but in order to obtain and maintain them you will need some training through a professional development pathway that creates and maintains the professional competencies.” TH
The Canadian Society of Hospital Medicine is spearheading an initiative called the Core Competencies in Hospitalist Medicine Document Project, which could be used to clarify what the field is, update certification processes, and define its future growth.
Neither the Royal College of Physicians and Surgeons of Canada nor the College of Family Physicians of Canada is likely to pursue board certification for a subspecialty in hospital medicine, says Peter Jamieson, MD, CCFP, FCFP, a hospitalist at Foothills Medical Center in Calgary, Alberta.
“If you think about hospital medicine as a construct—and take the focus off the person and put it instead onto the patient and onto the work, then you can describe the necessary competencies,” Dr. Jamieson says. “What are the preparation, the evaluation, and all of the associated functions? We want to be clear about what this job really is. We don’t have to be defined by training in a particular specialty.”
Writing and reviewing the competencies has been assigned to large physician working groups, with a well-defined process for validation, Dr. Jamieson says.
“Next steps will include elaborating the evaluation criteria, the learning objectives, and those sorts of things. That’s all going on right now,” he explains. “Our objective is to have all of them in a publishable format within the next year or so. Then we’ll need to get the regulatory folks to agree that this represents a subset of practice and a discrete and obtainable set of skills.
“As time goes by, it will become more and more obvious that hospital medicine is a discrete set of skills—not that any doctor couldn’t obtain those skills, but in order to obtain and maintain them you will need some training through a professional development pathway that creates and maintains the professional competencies.” TH
The Canadian Society of Hospital Medicine is spearheading an initiative called the Core Competencies in Hospitalist Medicine Document Project, which could be used to clarify what the field is, update certification processes, and define its future growth.
Neither the Royal College of Physicians and Surgeons of Canada nor the College of Family Physicians of Canada is likely to pursue board certification for a subspecialty in hospital medicine, says Peter Jamieson, MD, CCFP, FCFP, a hospitalist at Foothills Medical Center in Calgary, Alberta.
“If you think about hospital medicine as a construct—and take the focus off the person and put it instead onto the patient and onto the work, then you can describe the necessary competencies,” Dr. Jamieson says. “What are the preparation, the evaluation, and all of the associated functions? We want to be clear about what this job really is. We don’t have to be defined by training in a particular specialty.”
Writing and reviewing the competencies has been assigned to large physician working groups, with a well-defined process for validation, Dr. Jamieson says.
“Next steps will include elaborating the evaluation criteria, the learning objectives, and those sorts of things. That’s all going on right now,” he explains. “Our objective is to have all of them in a publishable format within the next year or so. Then we’ll need to get the regulatory folks to agree that this represents a subset of practice and a discrete and obtainable set of skills.
“As time goes by, it will become more and more obvious that hospital medicine is a discrete set of skills—not that any doctor couldn’t obtain those skills, but in order to obtain and maintain them you will need some training through a professional development pathway that creates and maintains the professional competencies.” TH
CDC to celebrate best blood clot prevention strategies
The Centers for Disease Control and Prevention has launched a program to honor hospitals, health systems, and managed care organizations that have implemented effective strategies to prevent health care–associated blood clots.
The HA-VTE Prevention Challenge invites provider organizations around the world to submit evidence of demonstrated successful use of venous thromboembolism (VTE) prevention strategies and interventions. VTE leads to approximately 100,000 premature deaths in the United States every year, according to the CDC, yet as many as 70% of HA-VTEs are preventable, although fewer than half of hospital patients receive appropriate prevention. Indeed, about half of all blood clots happen after a recent hospital stay or surgery.
“Doctors and nurses in hospitals and other health care settings can save lives by implementing the best practices discovered through this challenge,” Dr. Tom Frieden, CDC director, said in a statement. “Tell us about what you are doing and what’s helping prevent blood clots, so we can advance science and save lives together.”
The purpose of the challenge is to highlight the systems, processes, and staffing that contribute to exceptional VTE prevention, according to the CDC. Processes may include the implementation of protocols, risk assessments, and the use of health information technology and clinical decision support tools. Seven of the highest scoring U.S. non-federal hospitals, multihospital systems, hospital networks, and managed care organizations will be recognized as HA-VTE Prevention Champions and will receive a cash award of $10,000 each. Winning submissions from U.S. federal and international entities will be eligible for nonmonetary recognition.
The CDC will accept submissions from Nov. 2, 2015, until Jan. 10, 2016. Winners will be announced in March 2016.
For more information, visit the HA-VTE Prevention Challenge website.
On Twitter: @richpizzi
The Centers for Disease Control and Prevention has launched a program to honor hospitals, health systems, and managed care organizations that have implemented effective strategies to prevent health care–associated blood clots.
The HA-VTE Prevention Challenge invites provider organizations around the world to submit evidence of demonstrated successful use of venous thromboembolism (VTE) prevention strategies and interventions. VTE leads to approximately 100,000 premature deaths in the United States every year, according to the CDC, yet as many as 70% of HA-VTEs are preventable, although fewer than half of hospital patients receive appropriate prevention. Indeed, about half of all blood clots happen after a recent hospital stay or surgery.
“Doctors and nurses in hospitals and other health care settings can save lives by implementing the best practices discovered through this challenge,” Dr. Tom Frieden, CDC director, said in a statement. “Tell us about what you are doing and what’s helping prevent blood clots, so we can advance science and save lives together.”
The purpose of the challenge is to highlight the systems, processes, and staffing that contribute to exceptional VTE prevention, according to the CDC. Processes may include the implementation of protocols, risk assessments, and the use of health information technology and clinical decision support tools. Seven of the highest scoring U.S. non-federal hospitals, multihospital systems, hospital networks, and managed care organizations will be recognized as HA-VTE Prevention Champions and will receive a cash award of $10,000 each. Winning submissions from U.S. federal and international entities will be eligible for nonmonetary recognition.
The CDC will accept submissions from Nov. 2, 2015, until Jan. 10, 2016. Winners will be announced in March 2016.
For more information, visit the HA-VTE Prevention Challenge website.
On Twitter: @richpizzi
The Centers for Disease Control and Prevention has launched a program to honor hospitals, health systems, and managed care organizations that have implemented effective strategies to prevent health care–associated blood clots.
The HA-VTE Prevention Challenge invites provider organizations around the world to submit evidence of demonstrated successful use of venous thromboembolism (VTE) prevention strategies and interventions. VTE leads to approximately 100,000 premature deaths in the United States every year, according to the CDC, yet as many as 70% of HA-VTEs are preventable, although fewer than half of hospital patients receive appropriate prevention. Indeed, about half of all blood clots happen after a recent hospital stay or surgery.
“Doctors and nurses in hospitals and other health care settings can save lives by implementing the best practices discovered through this challenge,” Dr. Tom Frieden, CDC director, said in a statement. “Tell us about what you are doing and what’s helping prevent blood clots, so we can advance science and save lives together.”
The purpose of the challenge is to highlight the systems, processes, and staffing that contribute to exceptional VTE prevention, according to the CDC. Processes may include the implementation of protocols, risk assessments, and the use of health information technology and clinical decision support tools. Seven of the highest scoring U.S. non-federal hospitals, multihospital systems, hospital networks, and managed care organizations will be recognized as HA-VTE Prevention Champions and will receive a cash award of $10,000 each. Winning submissions from U.S. federal and international entities will be eligible for nonmonetary recognition.
The CDC will accept submissions from Nov. 2, 2015, until Jan. 10, 2016. Winners will be announced in March 2016.
For more information, visit the HA-VTE Prevention Challenge website.
On Twitter: @richpizzi
FROM THE SVS: Society responds to recent PAD study
A written statement from the SVS:
The Society for Vascular Surgery, with more than 5,000 vascular surgeon and allied health members, reviewed with interest the study of Thomas T. Tsai, et al entitled “The Contemporary Safety and Effectiveness of Lower Extremity Bypass Surgery and Peripheral Endovascular Interventions in the Treatment of Symptomatic Peripheral Arterial Disease.”
Over the last decade there has been a dramatic evolution in the treatment of peripheral arterial disease with less invasive endovascular therapy far surpassing conventional open surgery as the first line therapy in the majority of cases. According to Dr. Bruce A. Perler, President of the Society for Vascular Surgery, “Vascular surgeons are truly comprehensive vascular specialists who perform both endovascular and open vascular surgical procedures, as well as medical management, and therefore have a unique perspective on the relative risks and benefits of treatment options for peripheral arterial disease.” Utilizing a community-based registry including more than 1,800 patients, Tsai, et al. found that while endovascular therapy was associated with fewer complications in the 30 day peri-procedural period, the rate of target lesion revascularization was significantly higher at one and three years following the procedure.
According to Dr. Perler, “These results are not unexpected, and are certainly consistent with the information we’ve been developing from our Vascular Quality Initiative which now includes more than 300,000 cases. While the less invasive approach to treating arterial occlusive disease would be expected to be associated with a lower rate of complications, and this is obviously appealing to patients and practitioners, the implications of the higher rate of subsequent reinterventions should not be ignored and will become an increasingly important consideration as we enter this era of value- based reimbursement with an emphasis on longitudinal care and bundled payments in the American health care system. In other words, will the lower rate of early complications be more than counterbalanced by a need for repeat interventions and greater costs mid- and long-term.”
The Society for Vascular Surgery has had a long-standing interest in cost efficacy analyses of treatment options. “As we continue to develop and publish clinical practice guidelines, in the future we will be including the relative costs of alternate treatment options in assessing and determining the most appropriate treatment option for our patients. In that regard, this study raises important questions that our research will address,” Dr. Perler said.
A written statement from the SVS:
The Society for Vascular Surgery, with more than 5,000 vascular surgeon and allied health members, reviewed with interest the study of Thomas T. Tsai, et al entitled “The Contemporary Safety and Effectiveness of Lower Extremity Bypass Surgery and Peripheral Endovascular Interventions in the Treatment of Symptomatic Peripheral Arterial Disease.”
Over the last decade there has been a dramatic evolution in the treatment of peripheral arterial disease with less invasive endovascular therapy far surpassing conventional open surgery as the first line therapy in the majority of cases. According to Dr. Bruce A. Perler, President of the Society for Vascular Surgery, “Vascular surgeons are truly comprehensive vascular specialists who perform both endovascular and open vascular surgical procedures, as well as medical management, and therefore have a unique perspective on the relative risks and benefits of treatment options for peripheral arterial disease.” Utilizing a community-based registry including more than 1,800 patients, Tsai, et al. found that while endovascular therapy was associated with fewer complications in the 30 day peri-procedural period, the rate of target lesion revascularization was significantly higher at one and three years following the procedure.
According to Dr. Perler, “These results are not unexpected, and are certainly consistent with the information we’ve been developing from our Vascular Quality Initiative which now includes more than 300,000 cases. While the less invasive approach to treating arterial occlusive disease would be expected to be associated with a lower rate of complications, and this is obviously appealing to patients and practitioners, the implications of the higher rate of subsequent reinterventions should not be ignored and will become an increasingly important consideration as we enter this era of value- based reimbursement with an emphasis on longitudinal care and bundled payments in the American health care system. In other words, will the lower rate of early complications be more than counterbalanced by a need for repeat interventions and greater costs mid- and long-term.”
The Society for Vascular Surgery has had a long-standing interest in cost efficacy analyses of treatment options. “As we continue to develop and publish clinical practice guidelines, in the future we will be including the relative costs of alternate treatment options in assessing and determining the most appropriate treatment option for our patients. In that regard, this study raises important questions that our research will address,” Dr. Perler said.
A written statement from the SVS:
The Society for Vascular Surgery, with more than 5,000 vascular surgeon and allied health members, reviewed with interest the study of Thomas T. Tsai, et al entitled “The Contemporary Safety and Effectiveness of Lower Extremity Bypass Surgery and Peripheral Endovascular Interventions in the Treatment of Symptomatic Peripheral Arterial Disease.”
Over the last decade there has been a dramatic evolution in the treatment of peripheral arterial disease with less invasive endovascular therapy far surpassing conventional open surgery as the first line therapy in the majority of cases. According to Dr. Bruce A. Perler, President of the Society for Vascular Surgery, “Vascular surgeons are truly comprehensive vascular specialists who perform both endovascular and open vascular surgical procedures, as well as medical management, and therefore have a unique perspective on the relative risks and benefits of treatment options for peripheral arterial disease.” Utilizing a community-based registry including more than 1,800 patients, Tsai, et al. found that while endovascular therapy was associated with fewer complications in the 30 day peri-procedural period, the rate of target lesion revascularization was significantly higher at one and three years following the procedure.
According to Dr. Perler, “These results are not unexpected, and are certainly consistent with the information we’ve been developing from our Vascular Quality Initiative which now includes more than 300,000 cases. While the less invasive approach to treating arterial occlusive disease would be expected to be associated with a lower rate of complications, and this is obviously appealing to patients and practitioners, the implications of the higher rate of subsequent reinterventions should not be ignored and will become an increasingly important consideration as we enter this era of value- based reimbursement with an emphasis on longitudinal care and bundled payments in the American health care system. In other words, will the lower rate of early complications be more than counterbalanced by a need for repeat interventions and greater costs mid- and long-term.”
The Society for Vascular Surgery has had a long-standing interest in cost efficacy analyses of treatment options. “As we continue to develop and publish clinical practice guidelines, in the future we will be including the relative costs of alternate treatment options in assessing and determining the most appropriate treatment option for our patients. In that regard, this study raises important questions that our research will address,” Dr. Perler said.
Survey: 3 in 10 MSMs don’t comply with UK blood donor policy
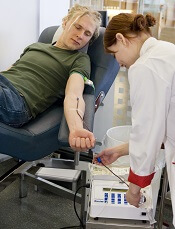
Photo by Marja Helander
ANAHEIM—A survey of UK blood donors suggests that as many as 30% of donors who are men who have sex with men (MSM) may not be compliant with the MSM blood donor policy.
The UK’s policy requires that MSMs do not donate blood if they have engaged in sexual activity with another male in the last 12 months.
But the survey indicates that as many as 3 in 10 MSMs are disregarding this policy.
The research also suggests that MSMs who do not comply with the policy engage in riskier sexual behavior than non-MSM male blood donors.
However, the researchers found no increase in the number of sexually transmitted infections present in the blood supply since the donation policy for MSMs changed from a lifetime ban to a 12-month deferral period.
The infections evaluated include human immunodeficiency virus (HIV), hepatitis C virus (HCV), hepatitis B virus (HBV), and syphilis.
The researchers also emphasized that the prevalence of HIV-positive blood donations in the UK remains low.
Katie Davidson, of Public Health England in London, presented these findings at the 2015 AABB Annual Meeting (abstract S36-030E*).
She noted that, in 2011, the blood services of England, Wales, and Scotland changed the blood donor policy for MSMs from a lifetime ban to a 12-month deferral since last male-to-male sex.
Before this policy change took effect, the blood services estimated that the change would mean 2679 MSMs would be newly eligible to donate blood (0.7% of male donors), and 8 of these donors would have HIV. So there would be a 0.5% increase in HIV risk.
“But what was clear was that these predictions in terms of HIV risk would be very dependent upon compliance,” Davidson said. “And what we mean by compliance is that a donor understands the rule, applies it correctly, and discloses any relevant information when they’re asked.”
To investigate donor behavior and compliance, Davidson and her colleagues conducted a large-scale, anonymous, web-based survey of blood donors.
Each month for 1 year (2013), all eligible new blood donors and at least an equal number of repeat blood donors in the UK were invited, via email, to complete an online questionnaire asking about their sexual history and compliance with the 12-month deferral policy for MSM (if applicable).
The researchers also looked at UK surveillance data on infections (HIV, HBV, HCV, and syphilis) in new and repeat blood donors over 6 years, comparing the incidence of infections before and after the policy change took effect (3 years pre- and post-change).
Donation and compliance
Among 65,439 survey respondents, 22,776 (35%) were male, and 242 (1%) were MSMs. Among the MSMs, 73 reported male-to-male sex within the last 12 months (non-compliance), and 181 said it had been more than 12 months since their last male-to-male sexual encounter.
The researchers adjusted these proportions for differences among the respondents and the donor population and extrapolated the data to the whole UK donor population.
The team estimated that, among 488,523 UK donors, there would be 5471 MSMs. Of the MSM donors, 3713 would be eligible under the new policy, and 1759 would be non-compliant.
So MSM compliance with the 12-month deferral policy would be 99.7% among all male donors but 70.4% of the MSM population.
“So 3 in every 10 MSMs donating blood in the UK shouldn’t be, [according to the estimates],” Davidson said.
The survey asked non-compliant MSM donors to provide their reasons for non-compliance, and many gave more than 1 reason.
“The reasons seemed to be associated, mostly, with self-assessment of their own risk [of transmitting infection] to be low,” Davidson said. “So that was based on the fact that they were in a monogamous relationship, they used condoms, practiced safe sex, or had regular [sexual health] screenings.”
However, there were some donors who regarded the policy as unimportant or said they didn’t agree with it. And there were some donors who didn’t declare their sexual behavior because they knew they wouldn’t be allowed to donate if they did.
Sexual behavior
Among all male respondents who reported having sex within the last 12 months, MSMs were more likely than men who had only female sexual partners to report having sex with more than 1 partner. Fifty percent of MSMs had more than 1 sexual partner in the last 12 months, as did 9.1% of male donors with only female sexual partners.
Ten percent of MSMs reported paying for sex, as did 0.3% of non-MSMs. None of the MSMs reported having a partner who was HIV-positive, and less than 0.1% of non-MSMs said they had an HIV-positive partner.
Eleven percent of MSMs said they had a history of sexually transmitted infection, as did less than 0.1% of non-MSMs.
“So among the responders, there was very low numbers who reported a high-risk partner in the last 12 months,” Davidson noted. “But there was some suggestion, among these low numbers, that this was more common in the MSMs than the non-MSMs.”
She also acknowledged that some donors were unsure about whether they had a high-risk partner in the last 12 months.
Infections
The UK surveillance data on infections encompassed HIV, HBV, HCV, and syphilis.
In all, 3,667,408 blood donations from males were tested for infection in the 3 years prior to the MSM donor policy change, and 3,066,076 donations were tested in the 3 years after the change was implemented.
There were 428 donors who reported having an infection risk before the change and 268 who did so after. There were 577 donors who actually had an infection before the change and 434 who did after. And there were 32 infected MSM donors before the change and 34 after.
“So the number of male donors fell post-change by approximately 20%, [and] the total number of infected donors . . . fell by almost 30%,” Davidson noted.
“However, the number of MSM infected donors marginally increased, [and] the proportion of male infected donors who were MSMs, among all of those who reported a risk, increased from 7% [32/428] to 13% [34/268]. So there seems to be some impact [on infection] from MSMs, but the numbers are very small, and these differences are not significant.”
Predictions and HIV infection
Finally, the researchers compared their predictions from before the MSM blood donor policy change to the actual data after the change. This comparison assumed that the absolute number of compliant MSMs did not change after the policy changed.
In 2007, the group predicted there would be about 2 million blood donations, including 2679 from MSMs. In reality, in 2014, there were 1.9 million blood donations, including 3126 from MSMs.
The researchers predicted the number of HIV-positive donations would be 30, including 8 from MSMs. In reality, in 2014, there were 13 HIV-positive donations, including 1 from an MSM.
So the predicted HIV prevalence per 100,000 donations was 1.4, and the actual HIV prevalence was 0.7. The predicted HIV incidence per 100,000 person-years was 0.9, and the actual HIV incidence was 0.7.
The predicted HIV risk was 0.022 per 100,000, and the actual HIV risk was 0.016 per 100,000.
“So the estimated risk of HIV post-change remains very low,” Davidson noted, adding that she and her colleagues will continue to monitor the impact of the policy change. ![]()
*Data in the abstract differ from data presented at the meeting.

Photo by Marja Helander
ANAHEIM—A survey of UK blood donors suggests that as many as 30% of donors who are men who have sex with men (MSM) may not be compliant with the MSM blood donor policy.
The UK’s policy requires that MSMs do not donate blood if they have engaged in sexual activity with another male in the last 12 months.
But the survey indicates that as many as 3 in 10 MSMs are disregarding this policy.
The research also suggests that MSMs who do not comply with the policy engage in riskier sexual behavior than non-MSM male blood donors.
However, the researchers found no increase in the number of sexually transmitted infections present in the blood supply since the donation policy for MSMs changed from a lifetime ban to a 12-month deferral period.
The infections evaluated include human immunodeficiency virus (HIV), hepatitis C virus (HCV), hepatitis B virus (HBV), and syphilis.
The researchers also emphasized that the prevalence of HIV-positive blood donations in the UK remains low.
Katie Davidson, of Public Health England in London, presented these findings at the 2015 AABB Annual Meeting (abstract S36-030E*).
She noted that, in 2011, the blood services of England, Wales, and Scotland changed the blood donor policy for MSMs from a lifetime ban to a 12-month deferral since last male-to-male sex.
Before this policy change took effect, the blood services estimated that the change would mean 2679 MSMs would be newly eligible to donate blood (0.7% of male donors), and 8 of these donors would have HIV. So there would be a 0.5% increase in HIV risk.
“But what was clear was that these predictions in terms of HIV risk would be very dependent upon compliance,” Davidson said. “And what we mean by compliance is that a donor understands the rule, applies it correctly, and discloses any relevant information when they’re asked.”
To investigate donor behavior and compliance, Davidson and her colleagues conducted a large-scale, anonymous, web-based survey of blood donors.
Each month for 1 year (2013), all eligible new blood donors and at least an equal number of repeat blood donors in the UK were invited, via email, to complete an online questionnaire asking about their sexual history and compliance with the 12-month deferral policy for MSM (if applicable).
The researchers also looked at UK surveillance data on infections (HIV, HBV, HCV, and syphilis) in new and repeat blood donors over 6 years, comparing the incidence of infections before and after the policy change took effect (3 years pre- and post-change).
Donation and compliance
Among 65,439 survey respondents, 22,776 (35%) were male, and 242 (1%) were MSMs. Among the MSMs, 73 reported male-to-male sex within the last 12 months (non-compliance), and 181 said it had been more than 12 months since their last male-to-male sexual encounter.
The researchers adjusted these proportions for differences among the respondents and the donor population and extrapolated the data to the whole UK donor population.
The team estimated that, among 488,523 UK donors, there would be 5471 MSMs. Of the MSM donors, 3713 would be eligible under the new policy, and 1759 would be non-compliant.
So MSM compliance with the 12-month deferral policy would be 99.7% among all male donors but 70.4% of the MSM population.
“So 3 in every 10 MSMs donating blood in the UK shouldn’t be, [according to the estimates],” Davidson said.
The survey asked non-compliant MSM donors to provide their reasons for non-compliance, and many gave more than 1 reason.
“The reasons seemed to be associated, mostly, with self-assessment of their own risk [of transmitting infection] to be low,” Davidson said. “So that was based on the fact that they were in a monogamous relationship, they used condoms, practiced safe sex, or had regular [sexual health] screenings.”
However, there were some donors who regarded the policy as unimportant or said they didn’t agree with it. And there were some donors who didn’t declare their sexual behavior because they knew they wouldn’t be allowed to donate if they did.
Sexual behavior
Among all male respondents who reported having sex within the last 12 months, MSMs were more likely than men who had only female sexual partners to report having sex with more than 1 partner. Fifty percent of MSMs had more than 1 sexual partner in the last 12 months, as did 9.1% of male donors with only female sexual partners.
Ten percent of MSMs reported paying for sex, as did 0.3% of non-MSMs. None of the MSMs reported having a partner who was HIV-positive, and less than 0.1% of non-MSMs said they had an HIV-positive partner.
Eleven percent of MSMs said they had a history of sexually transmitted infection, as did less than 0.1% of non-MSMs.
“So among the responders, there was very low numbers who reported a high-risk partner in the last 12 months,” Davidson noted. “But there was some suggestion, among these low numbers, that this was more common in the MSMs than the non-MSMs.”
She also acknowledged that some donors were unsure about whether they had a high-risk partner in the last 12 months.
Infections
The UK surveillance data on infections encompassed HIV, HBV, HCV, and syphilis.
In all, 3,667,408 blood donations from males were tested for infection in the 3 years prior to the MSM donor policy change, and 3,066,076 donations were tested in the 3 years after the change was implemented.
There were 428 donors who reported having an infection risk before the change and 268 who did so after. There were 577 donors who actually had an infection before the change and 434 who did after. And there were 32 infected MSM donors before the change and 34 after.
“So the number of male donors fell post-change by approximately 20%, [and] the total number of infected donors . . . fell by almost 30%,” Davidson noted.
“However, the number of MSM infected donors marginally increased, [and] the proportion of male infected donors who were MSMs, among all of those who reported a risk, increased from 7% [32/428] to 13% [34/268]. So there seems to be some impact [on infection] from MSMs, but the numbers are very small, and these differences are not significant.”
Predictions and HIV infection
Finally, the researchers compared their predictions from before the MSM blood donor policy change to the actual data after the change. This comparison assumed that the absolute number of compliant MSMs did not change after the policy changed.
In 2007, the group predicted there would be about 2 million blood donations, including 2679 from MSMs. In reality, in 2014, there were 1.9 million blood donations, including 3126 from MSMs.
The researchers predicted the number of HIV-positive donations would be 30, including 8 from MSMs. In reality, in 2014, there were 13 HIV-positive donations, including 1 from an MSM.
So the predicted HIV prevalence per 100,000 donations was 1.4, and the actual HIV prevalence was 0.7. The predicted HIV incidence per 100,000 person-years was 0.9, and the actual HIV incidence was 0.7.
The predicted HIV risk was 0.022 per 100,000, and the actual HIV risk was 0.016 per 100,000.
“So the estimated risk of HIV post-change remains very low,” Davidson noted, adding that she and her colleagues will continue to monitor the impact of the policy change. ![]()
*Data in the abstract differ from data presented at the meeting.

Photo by Marja Helander
ANAHEIM—A survey of UK blood donors suggests that as many as 30% of donors who are men who have sex with men (MSM) may not be compliant with the MSM blood donor policy.
The UK’s policy requires that MSMs do not donate blood if they have engaged in sexual activity with another male in the last 12 months.
But the survey indicates that as many as 3 in 10 MSMs are disregarding this policy.
The research also suggests that MSMs who do not comply with the policy engage in riskier sexual behavior than non-MSM male blood donors.
However, the researchers found no increase in the number of sexually transmitted infections present in the blood supply since the donation policy for MSMs changed from a lifetime ban to a 12-month deferral period.
The infections evaluated include human immunodeficiency virus (HIV), hepatitis C virus (HCV), hepatitis B virus (HBV), and syphilis.
The researchers also emphasized that the prevalence of HIV-positive blood donations in the UK remains low.
Katie Davidson, of Public Health England in London, presented these findings at the 2015 AABB Annual Meeting (abstract S36-030E*).
She noted that, in 2011, the blood services of England, Wales, and Scotland changed the blood donor policy for MSMs from a lifetime ban to a 12-month deferral since last male-to-male sex.
Before this policy change took effect, the blood services estimated that the change would mean 2679 MSMs would be newly eligible to donate blood (0.7% of male donors), and 8 of these donors would have HIV. So there would be a 0.5% increase in HIV risk.
“But what was clear was that these predictions in terms of HIV risk would be very dependent upon compliance,” Davidson said. “And what we mean by compliance is that a donor understands the rule, applies it correctly, and discloses any relevant information when they’re asked.”
To investigate donor behavior and compliance, Davidson and her colleagues conducted a large-scale, anonymous, web-based survey of blood donors.
Each month for 1 year (2013), all eligible new blood donors and at least an equal number of repeat blood donors in the UK were invited, via email, to complete an online questionnaire asking about their sexual history and compliance with the 12-month deferral policy for MSM (if applicable).
The researchers also looked at UK surveillance data on infections (HIV, HBV, HCV, and syphilis) in new and repeat blood donors over 6 years, comparing the incidence of infections before and after the policy change took effect (3 years pre- and post-change).
Donation and compliance
Among 65,439 survey respondents, 22,776 (35%) were male, and 242 (1%) were MSMs. Among the MSMs, 73 reported male-to-male sex within the last 12 months (non-compliance), and 181 said it had been more than 12 months since their last male-to-male sexual encounter.
The researchers adjusted these proportions for differences among the respondents and the donor population and extrapolated the data to the whole UK donor population.
The team estimated that, among 488,523 UK donors, there would be 5471 MSMs. Of the MSM donors, 3713 would be eligible under the new policy, and 1759 would be non-compliant.
So MSM compliance with the 12-month deferral policy would be 99.7% among all male donors but 70.4% of the MSM population.
“So 3 in every 10 MSMs donating blood in the UK shouldn’t be, [according to the estimates],” Davidson said.
The survey asked non-compliant MSM donors to provide their reasons for non-compliance, and many gave more than 1 reason.
“The reasons seemed to be associated, mostly, with self-assessment of their own risk [of transmitting infection] to be low,” Davidson said. “So that was based on the fact that they were in a monogamous relationship, they used condoms, practiced safe sex, or had regular [sexual health] screenings.”
However, there were some donors who regarded the policy as unimportant or said they didn’t agree with it. And there were some donors who didn’t declare their sexual behavior because they knew they wouldn’t be allowed to donate if they did.
Sexual behavior
Among all male respondents who reported having sex within the last 12 months, MSMs were more likely than men who had only female sexual partners to report having sex with more than 1 partner. Fifty percent of MSMs had more than 1 sexual partner in the last 12 months, as did 9.1% of male donors with only female sexual partners.
Ten percent of MSMs reported paying for sex, as did 0.3% of non-MSMs. None of the MSMs reported having a partner who was HIV-positive, and less than 0.1% of non-MSMs said they had an HIV-positive partner.
Eleven percent of MSMs said they had a history of sexually transmitted infection, as did less than 0.1% of non-MSMs.
“So among the responders, there was very low numbers who reported a high-risk partner in the last 12 months,” Davidson noted. “But there was some suggestion, among these low numbers, that this was more common in the MSMs than the non-MSMs.”
She also acknowledged that some donors were unsure about whether they had a high-risk partner in the last 12 months.
Infections
The UK surveillance data on infections encompassed HIV, HBV, HCV, and syphilis.
In all, 3,667,408 blood donations from males were tested for infection in the 3 years prior to the MSM donor policy change, and 3,066,076 donations were tested in the 3 years after the change was implemented.
There were 428 donors who reported having an infection risk before the change and 268 who did so after. There were 577 donors who actually had an infection before the change and 434 who did after. And there were 32 infected MSM donors before the change and 34 after.
“So the number of male donors fell post-change by approximately 20%, [and] the total number of infected donors . . . fell by almost 30%,” Davidson noted.
“However, the number of MSM infected donors marginally increased, [and] the proportion of male infected donors who were MSMs, among all of those who reported a risk, increased from 7% [32/428] to 13% [34/268]. So there seems to be some impact [on infection] from MSMs, but the numbers are very small, and these differences are not significant.”
Predictions and HIV infection
Finally, the researchers compared their predictions from before the MSM blood donor policy change to the actual data after the change. This comparison assumed that the absolute number of compliant MSMs did not change after the policy changed.
In 2007, the group predicted there would be about 2 million blood donations, including 2679 from MSMs. In reality, in 2014, there were 1.9 million blood donations, including 3126 from MSMs.
The researchers predicted the number of HIV-positive donations would be 30, including 8 from MSMs. In reality, in 2014, there were 13 HIV-positive donations, including 1 from an MSM.
So the predicted HIV prevalence per 100,000 donations was 1.4, and the actual HIV prevalence was 0.7. The predicted HIV incidence per 100,000 person-years was 0.9, and the actual HIV incidence was 0.7.
The predicted HIV risk was 0.022 per 100,000, and the actual HIV risk was 0.016 per 100,000.
“So the estimated risk of HIV post-change remains very low,” Davidson noted, adding that she and her colleagues will continue to monitor the impact of the policy change. ![]()
*Data in the abstract differ from data presented at the meeting.
Duo solves mystery regarding FVIII

Turner and Joel Moake
Photo from Rice University
A pair of researchers solved a long-standing mystery about where factor VIII (FVIII) is made, stored, and deployed in the body, according to an article published in PLOS ONE.
The duo found that FVIII is synthesized in glomerular microvascular endothelial cells (GMVECs) and human umbilical vein endothelial cells (HUVECs).
FVIII and von Willebrand factor (VWF) are stored in Weibel-Palade bodies (WPBs) in both of these cell types. And stimulated GMVECs and HUVECs secrete cell-anchored, ultra-large VWF strings with FVIII bound to them.
The researchers said these findings may lead to improved therapy for hemophilia A.
“Great clinical advances have been made over the past 50 years, in spite of our lack of understanding of where FVIII was made and stored,” said study author Joel Moake, MD, of Rice University in Houston, Texas.
“Understanding how the body makes, stores, and deploys the protein will be increasingly important in the future as physicians look to develop gene therapies that could free patients from a reliance on regular injections of FVIII.”
The FVIII research in Dr Moake’s lab began in early 2014 and was based on a hunch by lead author Nancy Turner, who specializes in the study of endothelial cells.
“Endothelial cells are the gate-controllers for the blood system, and, to me, they make all the exciting proteins,” she said. “They’re right on the surface next to the blood, and they constantly interact with the plasma. Similar to circulating cells, they produce their own defensive proteins to fight infections.”
Though Turner had not previously studied FVIII, she had done extensive experiments on VWF, which is made in endothelial cells and stored in WPBs. And VWF and FVIII are often bound together.
Based on her prior work, Turner was intrigued by a pair of 2014 studies that examined FVIII in mouse endothelial cells and showed that FVIII was produced in the endothelial cells within the liver, and not in the liver cells.
“They stopped short of saying that FVIII was stored in endothelial cells, but they suggested the possibility,” she said. “One of the papers was very elegant, and I liked it a lot, but it made a statement that really bothered me.”
The paper explained that FVIII had been found in a half-dozen types of endothelial cell types, but never HUVECs, the type of endothelial cell found in large veins.
“HUVECs are the generic human endothelial cells that [researchers] use the first time they do anything,” Turner said. “They’re cheap. They’re easy to work with, and they’ve been the model for endothelial cells for, I don’t know, at least 50 years.”
“So far, everything I’ve ever looked at in endothelial cells has been consistent. The different types might have different amounts of something, but they’re very similar. There hasn’t been anything that was wholly different from one type to another. Not yet. So I thought, ‘OK, fine. I’m already doing gene-expression experiments. I might as well just throw FVIII in there and see.”
The experiments she was conducting involved both HUVECs and GMVECs, which are found in the smallest capillaries of the kidney. Turner was conducting an extensive analysis to see how protein production differed in the 2 varieties.
She examined the cells for FVIII messenger RNA and found that it was present, which meant it was possible the cells were making the protein. She then ordered a fluorescent antibody designed to detect FVIII.
“I did the experiment and looked, and not only was it there, but it was bright, easy to see, and it worked perfectly the first time,” Turner said. “I thought, ‘What have people been doing for 20 or 30 years? Why couldn’t they see this?’ And then I thought, ‘This was too easy. No one is going to believe me.’”
So Turner set about running controls to rule out mistakes. Were the antibodies interfering with one another? Was there any contamination? Was the microscope working correctly? Could the reading be a false-positive, an inadvertent result of another reaction she hadn’t expected?
“No. 1, I had to convince myself,” she said. “I am always skeptical if something is too easy. I have reviewed many, many papers, and I can always find what people do wrong.”
Once she had convinced herself, she and Dr Moake had to convince the paper’s referees. As she’d expected, they were skeptical. She said the bulk of the work over the past year involved doing a number of controls to remove any doubts about the findings.
In the end, the research confirmed that FVIII was made in both HUVECs and GMVECs. Moreover, Turner found that FVIII, like VWF, is both stored and secreted from WPBs.
Dr Moake said the discovery has clear implications for any future treatments that aim to repair genetic defects in patients with hemophilia A.
“Now that we recognize that FVIII is normally synthesized in endothelial cells and stored in Weibel-Palade bodies,” Dr Moake said, “those become the precise, most effective physiological targets for gene delivery.” ![]()

Turner and Joel Moake
Photo from Rice University
A pair of researchers solved a long-standing mystery about where factor VIII (FVIII) is made, stored, and deployed in the body, according to an article published in PLOS ONE.
The duo found that FVIII is synthesized in glomerular microvascular endothelial cells (GMVECs) and human umbilical vein endothelial cells (HUVECs).
FVIII and von Willebrand factor (VWF) are stored in Weibel-Palade bodies (WPBs) in both of these cell types. And stimulated GMVECs and HUVECs secrete cell-anchored, ultra-large VWF strings with FVIII bound to them.
The researchers said these findings may lead to improved therapy for hemophilia A.
“Great clinical advances have been made over the past 50 years, in spite of our lack of understanding of where FVIII was made and stored,” said study author Joel Moake, MD, of Rice University in Houston, Texas.
“Understanding how the body makes, stores, and deploys the protein will be increasingly important in the future as physicians look to develop gene therapies that could free patients from a reliance on regular injections of FVIII.”
The FVIII research in Dr Moake’s lab began in early 2014 and was based on a hunch by lead author Nancy Turner, who specializes in the study of endothelial cells.
“Endothelial cells are the gate-controllers for the blood system, and, to me, they make all the exciting proteins,” she said. “They’re right on the surface next to the blood, and they constantly interact with the plasma. Similar to circulating cells, they produce their own defensive proteins to fight infections.”
Though Turner had not previously studied FVIII, she had done extensive experiments on VWF, which is made in endothelial cells and stored in WPBs. And VWF and FVIII are often bound together.
Based on her prior work, Turner was intrigued by a pair of 2014 studies that examined FVIII in mouse endothelial cells and showed that FVIII was produced in the endothelial cells within the liver, and not in the liver cells.
“They stopped short of saying that FVIII was stored in endothelial cells, but they suggested the possibility,” she said. “One of the papers was very elegant, and I liked it a lot, but it made a statement that really bothered me.”
The paper explained that FVIII had been found in a half-dozen types of endothelial cell types, but never HUVECs, the type of endothelial cell found in large veins.
“HUVECs are the generic human endothelial cells that [researchers] use the first time they do anything,” Turner said. “They’re cheap. They’re easy to work with, and they’ve been the model for endothelial cells for, I don’t know, at least 50 years.”
“So far, everything I’ve ever looked at in endothelial cells has been consistent. The different types might have different amounts of something, but they’re very similar. There hasn’t been anything that was wholly different from one type to another. Not yet. So I thought, ‘OK, fine. I’m already doing gene-expression experiments. I might as well just throw FVIII in there and see.”
The experiments she was conducting involved both HUVECs and GMVECs, which are found in the smallest capillaries of the kidney. Turner was conducting an extensive analysis to see how protein production differed in the 2 varieties.
She examined the cells for FVIII messenger RNA and found that it was present, which meant it was possible the cells were making the protein. She then ordered a fluorescent antibody designed to detect FVIII.
“I did the experiment and looked, and not only was it there, but it was bright, easy to see, and it worked perfectly the first time,” Turner said. “I thought, ‘What have people been doing for 20 or 30 years? Why couldn’t they see this?’ And then I thought, ‘This was too easy. No one is going to believe me.’”
So Turner set about running controls to rule out mistakes. Were the antibodies interfering with one another? Was there any contamination? Was the microscope working correctly? Could the reading be a false-positive, an inadvertent result of another reaction she hadn’t expected?
“No. 1, I had to convince myself,” she said. “I am always skeptical if something is too easy. I have reviewed many, many papers, and I can always find what people do wrong.”
Once she had convinced herself, she and Dr Moake had to convince the paper’s referees. As she’d expected, they were skeptical. She said the bulk of the work over the past year involved doing a number of controls to remove any doubts about the findings.
In the end, the research confirmed that FVIII was made in both HUVECs and GMVECs. Moreover, Turner found that FVIII, like VWF, is both stored and secreted from WPBs.
Dr Moake said the discovery has clear implications for any future treatments that aim to repair genetic defects in patients with hemophilia A.
“Now that we recognize that FVIII is normally synthesized in endothelial cells and stored in Weibel-Palade bodies,” Dr Moake said, “those become the precise, most effective physiological targets for gene delivery.” ![]()

Turner and Joel Moake
Photo from Rice University
A pair of researchers solved a long-standing mystery about where factor VIII (FVIII) is made, stored, and deployed in the body, according to an article published in PLOS ONE.
The duo found that FVIII is synthesized in glomerular microvascular endothelial cells (GMVECs) and human umbilical vein endothelial cells (HUVECs).
FVIII and von Willebrand factor (VWF) are stored in Weibel-Palade bodies (WPBs) in both of these cell types. And stimulated GMVECs and HUVECs secrete cell-anchored, ultra-large VWF strings with FVIII bound to them.
The researchers said these findings may lead to improved therapy for hemophilia A.
“Great clinical advances have been made over the past 50 years, in spite of our lack of understanding of where FVIII was made and stored,” said study author Joel Moake, MD, of Rice University in Houston, Texas.
“Understanding how the body makes, stores, and deploys the protein will be increasingly important in the future as physicians look to develop gene therapies that could free patients from a reliance on regular injections of FVIII.”
The FVIII research in Dr Moake’s lab began in early 2014 and was based on a hunch by lead author Nancy Turner, who specializes in the study of endothelial cells.
“Endothelial cells are the gate-controllers for the blood system, and, to me, they make all the exciting proteins,” she said. “They’re right on the surface next to the blood, and they constantly interact with the plasma. Similar to circulating cells, they produce their own defensive proteins to fight infections.”
Though Turner had not previously studied FVIII, she had done extensive experiments on VWF, which is made in endothelial cells and stored in WPBs. And VWF and FVIII are often bound together.
Based on her prior work, Turner was intrigued by a pair of 2014 studies that examined FVIII in mouse endothelial cells and showed that FVIII was produced in the endothelial cells within the liver, and not in the liver cells.
“They stopped short of saying that FVIII was stored in endothelial cells, but they suggested the possibility,” she said. “One of the papers was very elegant, and I liked it a lot, but it made a statement that really bothered me.”
The paper explained that FVIII had been found in a half-dozen types of endothelial cell types, but never HUVECs, the type of endothelial cell found in large veins.
“HUVECs are the generic human endothelial cells that [researchers] use the first time they do anything,” Turner said. “They’re cheap. They’re easy to work with, and they’ve been the model for endothelial cells for, I don’t know, at least 50 years.”
“So far, everything I’ve ever looked at in endothelial cells has been consistent. The different types might have different amounts of something, but they’re very similar. There hasn’t been anything that was wholly different from one type to another. Not yet. So I thought, ‘OK, fine. I’m already doing gene-expression experiments. I might as well just throw FVIII in there and see.”
The experiments she was conducting involved both HUVECs and GMVECs, which are found in the smallest capillaries of the kidney. Turner was conducting an extensive analysis to see how protein production differed in the 2 varieties.
She examined the cells for FVIII messenger RNA and found that it was present, which meant it was possible the cells were making the protein. She then ordered a fluorescent antibody designed to detect FVIII.
“I did the experiment and looked, and not only was it there, but it was bright, easy to see, and it worked perfectly the first time,” Turner said. “I thought, ‘What have people been doing for 20 or 30 years? Why couldn’t they see this?’ And then I thought, ‘This was too easy. No one is going to believe me.’”
So Turner set about running controls to rule out mistakes. Were the antibodies interfering with one another? Was there any contamination? Was the microscope working correctly? Could the reading be a false-positive, an inadvertent result of another reaction she hadn’t expected?
“No. 1, I had to convince myself,” she said. “I am always skeptical if something is too easy. I have reviewed many, many papers, and I can always find what people do wrong.”
Once she had convinced herself, she and Dr Moake had to convince the paper’s referees. As she’d expected, they were skeptical. She said the bulk of the work over the past year involved doing a number of controls to remove any doubts about the findings.
In the end, the research confirmed that FVIII was made in both HUVECs and GMVECs. Moreover, Turner found that FVIII, like VWF, is both stored and secreted from WPBs.
Dr Moake said the discovery has clear implications for any future treatments that aim to repair genetic defects in patients with hemophilia A.
“Now that we recognize that FVIII is normally synthesized in endothelial cells and stored in Weibel-Palade bodies,” Dr Moake said, “those become the precise, most effective physiological targets for gene delivery.” ![]()
A new category of cytopenias

New research suggests that clonality may underlie the cytopenias observed in patients with idiopathic cytopenias of undetermined significance (ICUS).
So researchers say these patients should be classified as having clonal cytopenias of undetermined significance (CCUS).
The team believes that recognition of CCUS as a clinical entity would help identify it as a formally defined diagnostic group and could aid future studies.
“We don’t know to what extent patients who have low blood counts and mutations are at increased risk of developing an overt malignancy,” said Rafael Bejar, MD, PhD, of the UCSD Moores Cancer Center in La Jolla, California.
“We hope that by defining CCUS, future studies will follow these patients to learn what these mutations mean for their future, as their genetically abnormal cells may represent early stages of subsequent blood cancers.”
Dr Bejar and his colleagues defined CCUS in Blood. Their research was funded, in part, by Genoptix Medical Laboratory, and several study authors are employees of Genoptix.
The researchers prospectively examined bone marrow samples from 144 patients with unexplained cytopenias. Seventeen percent of these patients were diagnosed with myelodysplastic syndromes (MDS), 15% with ICUS and some evidence of dysplasia, and 69% with ICUS and no dysplasia.
The team then sequenced patient samples looking for mutations in 22 frequently mutated myeloid malignancy genes. They identified somatic mutations in 71% of MDS patients, 62% of patients with ICUS and some dysplasia, and 20% of ICUS patients with no dysplasia.
Overall, 35% of ICUS patients carried a somatic mutation or chromosomal abnormality indicative of clonal hematopoiesis.
To build upon these findings, the researchers performed a retrospective analysis of data from 91 patients with lower-risk MDS and 249 patients with ICUS.
The team identified mutations in 79% of patients with MDS, 45% of patients with ICUS and dysplasia, and 17% of patients with ICUS and no dysplasia.
The researchers said the spectrum of mutated genes was similar among the 3 groups. The exception was SF3B1, which was rarely mutated in patients without dysplasia.
The team added that variant allele fractions were comparable between clonal ICUS (CCUS) and MDS, and the same was true for the patients’ mean age and blood counts. But CCUS was a more frequent diagnosis than MDS.
Dr Bejar and his colleagues said larger, carefully controlled studies will be needed to confirm the findings of this research. ![]()

New research suggests that clonality may underlie the cytopenias observed in patients with idiopathic cytopenias of undetermined significance (ICUS).
So researchers say these patients should be classified as having clonal cytopenias of undetermined significance (CCUS).
The team believes that recognition of CCUS as a clinical entity would help identify it as a formally defined diagnostic group and could aid future studies.
“We don’t know to what extent patients who have low blood counts and mutations are at increased risk of developing an overt malignancy,” said Rafael Bejar, MD, PhD, of the UCSD Moores Cancer Center in La Jolla, California.
“We hope that by defining CCUS, future studies will follow these patients to learn what these mutations mean for their future, as their genetically abnormal cells may represent early stages of subsequent blood cancers.”
Dr Bejar and his colleagues defined CCUS in Blood. Their research was funded, in part, by Genoptix Medical Laboratory, and several study authors are employees of Genoptix.
The researchers prospectively examined bone marrow samples from 144 patients with unexplained cytopenias. Seventeen percent of these patients were diagnosed with myelodysplastic syndromes (MDS), 15% with ICUS and some evidence of dysplasia, and 69% with ICUS and no dysplasia.
The team then sequenced patient samples looking for mutations in 22 frequently mutated myeloid malignancy genes. They identified somatic mutations in 71% of MDS patients, 62% of patients with ICUS and some dysplasia, and 20% of ICUS patients with no dysplasia.
Overall, 35% of ICUS patients carried a somatic mutation or chromosomal abnormality indicative of clonal hematopoiesis.
To build upon these findings, the researchers performed a retrospective analysis of data from 91 patients with lower-risk MDS and 249 patients with ICUS.
The team identified mutations in 79% of patients with MDS, 45% of patients with ICUS and dysplasia, and 17% of patients with ICUS and no dysplasia.
The researchers said the spectrum of mutated genes was similar among the 3 groups. The exception was SF3B1, which was rarely mutated in patients without dysplasia.
The team added that variant allele fractions were comparable between clonal ICUS (CCUS) and MDS, and the same was true for the patients’ mean age and blood counts. But CCUS was a more frequent diagnosis than MDS.
Dr Bejar and his colleagues said larger, carefully controlled studies will be needed to confirm the findings of this research. ![]()

New research suggests that clonality may underlie the cytopenias observed in patients with idiopathic cytopenias of undetermined significance (ICUS).
So researchers say these patients should be classified as having clonal cytopenias of undetermined significance (CCUS).
The team believes that recognition of CCUS as a clinical entity would help identify it as a formally defined diagnostic group and could aid future studies.
“We don’t know to what extent patients who have low blood counts and mutations are at increased risk of developing an overt malignancy,” said Rafael Bejar, MD, PhD, of the UCSD Moores Cancer Center in La Jolla, California.
“We hope that by defining CCUS, future studies will follow these patients to learn what these mutations mean for their future, as their genetically abnormal cells may represent early stages of subsequent blood cancers.”
Dr Bejar and his colleagues defined CCUS in Blood. Their research was funded, in part, by Genoptix Medical Laboratory, and several study authors are employees of Genoptix.
The researchers prospectively examined bone marrow samples from 144 patients with unexplained cytopenias. Seventeen percent of these patients were diagnosed with myelodysplastic syndromes (MDS), 15% with ICUS and some evidence of dysplasia, and 69% with ICUS and no dysplasia.
The team then sequenced patient samples looking for mutations in 22 frequently mutated myeloid malignancy genes. They identified somatic mutations in 71% of MDS patients, 62% of patients with ICUS and some dysplasia, and 20% of ICUS patients with no dysplasia.
Overall, 35% of ICUS patients carried a somatic mutation or chromosomal abnormality indicative of clonal hematopoiesis.
To build upon these findings, the researchers performed a retrospective analysis of data from 91 patients with lower-risk MDS and 249 patients with ICUS.
The team identified mutations in 79% of patients with MDS, 45% of patients with ICUS and dysplasia, and 17% of patients with ICUS and no dysplasia.
The researchers said the spectrum of mutated genes was similar among the 3 groups. The exception was SF3B1, which was rarely mutated in patients without dysplasia.
The team added that variant allele fractions were comparable between clonal ICUS (CCUS) and MDS, and the same was true for the patients’ mean age and blood counts. But CCUS was a more frequent diagnosis than MDS.
Dr Bejar and his colleagues said larger, carefully controlled studies will be needed to confirm the findings of this research. ![]()
