User login
Revolutionizing Quality Improvement in Hospital Medicine
As the senior physician advisor to SHM’s Center for Hospital Innovation and Improvement, Eric Howell, MD, SFHM, bridges the gap between clinical expertise and project support and development. The Hospitalist recently had a conversation with Dr. Howell, a past president of SHM, to learn more about his role and how the Center for Hospital Innovation and Improvement is revolutionizing quality improvement (QI) in hospital medicine.
Question: What is your role as the senior physician advisor to The Center for Hospital Innovation and Improvement?
Answer: I see my role as the intersection of a Venn diagram; one circle involves my clinical know-how, and the other includes the proposals brought to the Center for Hospital Innovation and Improvement by hospitalists and healthcare professionals. Where those two circles intersect is where I am able to use my experience from the front line of patient care to validate potential projects.
In addition to project assessment, I monitor the pulse of healthcare professionals and hospital leadership to ensure we are meeting their needs, including our efforts of convening a recent summit, where hospitalist clinicians … weighed in on how our team could help them improve. I plan to share this feedback in an upcoming feature, centered on emerging topics in hospital medicine, including care transitions, high-risk medications, advance care planning, and others.
Q: Given your clinical experience and involvement with SHM, how would you say hospitalists are positioned to improve quality, safety, and patient outcomes?

appropriate prescribing practices, which will aid in slowing the emergence of antibiotic-resistant bacteria and prevent the spread of resistant infections.
—Dr. Howell
A: We possess the necessary ingredients to develop a recipe for success in QI from both a clinical and an operational perspective. Hospital medicine is still a young, innovative field that is extremely open to change. Anyone who knows QI knows that it is all about effectively managing and responding to change. Hospitalists also are aware of how to operate in a highly matrixed environment and to collaborate as part of an interdisciplinary team, which are invaluable assets to implementing QI initiatives successfully and proactively monitoring their impact.
Q: What are the biggest assets the Center for Hospital Innovation and Improvement can offer hospitalists in their mission to improve patient care?
A: Our team has resources to help hospitalists improve their skills at whatever stage they are in their careers. If you are just beginning or trying to learn new things independently, you can explore the web-based materials and resource rooms. They are publicly accessible resources that can assist in informing quality improvement efforts in the hospital. For those looking to expand their skills in a more hands-on way, we offer a mentored implementation program, where hospitalists can receive guidance from expert mentors in a number of different clinical areas.
Q: How can the Center for Hospital Innovation and Improvement help hospitalists address emerging challenges in hospital medicine?
A: You cannot talk about the Center for Hospital Innovation and Improvement without mentioning signature mentored implementation programs like Project BOOST, focused on effective care transitions, and glycemic control—they are juggernauts for SHM’s portfolio because of their proven track records and sustainable frameworks for driving positive change. These two alone have already been implemented at over 400 facilities, with more inquiries each day.
With support from The Milbank Foundation, The Hastings Center and SHM have joined forces and will create new skills-based training resources and a QI framework to improve end-of-life care in the hospital. Our goal is to equip hospital clinicians with the requisite tools to provide adequate palliative care, especially given the policy landscape related to advance care planning discussions.
As antibiotic resistance emerges as a global issue, antibiotic stewardship has continued to be a high priority for hospitalists. After attending the related White House forum earlier this year, SHM committed to cultivating initiatives that emphasize appropriate prescribing practices, which will aid in slowing the emergence of antibiotic-resistant bacteria and prevent the spread of resistant infections. SHM looks forward to making noteworthy contributions to this initiative, promoting awareness and behavior change through the “Fight the Resistance” campaign.
Q: What is one major takeaway about The Center for Hospital Innovation and Improvement hospitalists should know?
A: The Center for Hospital Innovation and Improvement is not an exclusive club—rather, it is like an open farmers’ market. Anyone with any amount of expertise can get resources through collaboration and partnership. Whether it is residents trying to improve the house staff or professors at major academic centers looking for research partners, The Center for Hospital Innovation and Improvement will welcome you to collaborate and link you to valuable resources.
Brett Radler is SHM’s communications coordinator.
As the senior physician advisor to SHM’s Center for Hospital Innovation and Improvement, Eric Howell, MD, SFHM, bridges the gap between clinical expertise and project support and development. The Hospitalist recently had a conversation with Dr. Howell, a past president of SHM, to learn more about his role and how the Center for Hospital Innovation and Improvement is revolutionizing quality improvement (QI) in hospital medicine.
Question: What is your role as the senior physician advisor to The Center for Hospital Innovation and Improvement?
Answer: I see my role as the intersection of a Venn diagram; one circle involves my clinical know-how, and the other includes the proposals brought to the Center for Hospital Innovation and Improvement by hospitalists and healthcare professionals. Where those two circles intersect is where I am able to use my experience from the front line of patient care to validate potential projects.
In addition to project assessment, I monitor the pulse of healthcare professionals and hospital leadership to ensure we are meeting their needs, including our efforts of convening a recent summit, where hospitalist clinicians … weighed in on how our team could help them improve. I plan to share this feedback in an upcoming feature, centered on emerging topics in hospital medicine, including care transitions, high-risk medications, advance care planning, and others.
Q: Given your clinical experience and involvement with SHM, how would you say hospitalists are positioned to improve quality, safety, and patient outcomes?

appropriate prescribing practices, which will aid in slowing the emergence of antibiotic-resistant bacteria and prevent the spread of resistant infections.
—Dr. Howell
A: We possess the necessary ingredients to develop a recipe for success in QI from both a clinical and an operational perspective. Hospital medicine is still a young, innovative field that is extremely open to change. Anyone who knows QI knows that it is all about effectively managing and responding to change. Hospitalists also are aware of how to operate in a highly matrixed environment and to collaborate as part of an interdisciplinary team, which are invaluable assets to implementing QI initiatives successfully and proactively monitoring their impact.
Q: What are the biggest assets the Center for Hospital Innovation and Improvement can offer hospitalists in their mission to improve patient care?
A: Our team has resources to help hospitalists improve their skills at whatever stage they are in their careers. If you are just beginning or trying to learn new things independently, you can explore the web-based materials and resource rooms. They are publicly accessible resources that can assist in informing quality improvement efforts in the hospital. For those looking to expand their skills in a more hands-on way, we offer a mentored implementation program, where hospitalists can receive guidance from expert mentors in a number of different clinical areas.
Q: How can the Center for Hospital Innovation and Improvement help hospitalists address emerging challenges in hospital medicine?
A: You cannot talk about the Center for Hospital Innovation and Improvement without mentioning signature mentored implementation programs like Project BOOST, focused on effective care transitions, and glycemic control—they are juggernauts for SHM’s portfolio because of their proven track records and sustainable frameworks for driving positive change. These two alone have already been implemented at over 400 facilities, with more inquiries each day.
With support from The Milbank Foundation, The Hastings Center and SHM have joined forces and will create new skills-based training resources and a QI framework to improve end-of-life care in the hospital. Our goal is to equip hospital clinicians with the requisite tools to provide adequate palliative care, especially given the policy landscape related to advance care planning discussions.
As antibiotic resistance emerges as a global issue, antibiotic stewardship has continued to be a high priority for hospitalists. After attending the related White House forum earlier this year, SHM committed to cultivating initiatives that emphasize appropriate prescribing practices, which will aid in slowing the emergence of antibiotic-resistant bacteria and prevent the spread of resistant infections. SHM looks forward to making noteworthy contributions to this initiative, promoting awareness and behavior change through the “Fight the Resistance” campaign.
Q: What is one major takeaway about The Center for Hospital Innovation and Improvement hospitalists should know?
A: The Center for Hospital Innovation and Improvement is not an exclusive club—rather, it is like an open farmers’ market. Anyone with any amount of expertise can get resources through collaboration and partnership. Whether it is residents trying to improve the house staff or professors at major academic centers looking for research partners, The Center for Hospital Innovation and Improvement will welcome you to collaborate and link you to valuable resources.
Brett Radler is SHM’s communications coordinator.
As the senior physician advisor to SHM’s Center for Hospital Innovation and Improvement, Eric Howell, MD, SFHM, bridges the gap between clinical expertise and project support and development. The Hospitalist recently had a conversation with Dr. Howell, a past president of SHM, to learn more about his role and how the Center for Hospital Innovation and Improvement is revolutionizing quality improvement (QI) in hospital medicine.
Question: What is your role as the senior physician advisor to The Center for Hospital Innovation and Improvement?
Answer: I see my role as the intersection of a Venn diagram; one circle involves my clinical know-how, and the other includes the proposals brought to the Center for Hospital Innovation and Improvement by hospitalists and healthcare professionals. Where those two circles intersect is where I am able to use my experience from the front line of patient care to validate potential projects.
In addition to project assessment, I monitor the pulse of healthcare professionals and hospital leadership to ensure we are meeting their needs, including our efforts of convening a recent summit, where hospitalist clinicians … weighed in on how our team could help them improve. I plan to share this feedback in an upcoming feature, centered on emerging topics in hospital medicine, including care transitions, high-risk medications, advance care planning, and others.
Q: Given your clinical experience and involvement with SHM, how would you say hospitalists are positioned to improve quality, safety, and patient outcomes?

appropriate prescribing practices, which will aid in slowing the emergence of antibiotic-resistant bacteria and prevent the spread of resistant infections.
—Dr. Howell
A: We possess the necessary ingredients to develop a recipe for success in QI from both a clinical and an operational perspective. Hospital medicine is still a young, innovative field that is extremely open to change. Anyone who knows QI knows that it is all about effectively managing and responding to change. Hospitalists also are aware of how to operate in a highly matrixed environment and to collaborate as part of an interdisciplinary team, which are invaluable assets to implementing QI initiatives successfully and proactively monitoring their impact.
Q: What are the biggest assets the Center for Hospital Innovation and Improvement can offer hospitalists in their mission to improve patient care?
A: Our team has resources to help hospitalists improve their skills at whatever stage they are in their careers. If you are just beginning or trying to learn new things independently, you can explore the web-based materials and resource rooms. They are publicly accessible resources that can assist in informing quality improvement efforts in the hospital. For those looking to expand their skills in a more hands-on way, we offer a mentored implementation program, where hospitalists can receive guidance from expert mentors in a number of different clinical areas.
Q: How can the Center for Hospital Innovation and Improvement help hospitalists address emerging challenges in hospital medicine?
A: You cannot talk about the Center for Hospital Innovation and Improvement without mentioning signature mentored implementation programs like Project BOOST, focused on effective care transitions, and glycemic control—they are juggernauts for SHM’s portfolio because of their proven track records and sustainable frameworks for driving positive change. These two alone have already been implemented at over 400 facilities, with more inquiries each day.
With support from The Milbank Foundation, The Hastings Center and SHM have joined forces and will create new skills-based training resources and a QI framework to improve end-of-life care in the hospital. Our goal is to equip hospital clinicians with the requisite tools to provide adequate palliative care, especially given the policy landscape related to advance care planning discussions.
As antibiotic resistance emerges as a global issue, antibiotic stewardship has continued to be a high priority for hospitalists. After attending the related White House forum earlier this year, SHM committed to cultivating initiatives that emphasize appropriate prescribing practices, which will aid in slowing the emergence of antibiotic-resistant bacteria and prevent the spread of resistant infections. SHM looks forward to making noteworthy contributions to this initiative, promoting awareness and behavior change through the “Fight the Resistance” campaign.
Q: What is one major takeaway about The Center for Hospital Innovation and Improvement hospitalists should know?
A: The Center for Hospital Innovation and Improvement is not an exclusive club—rather, it is like an open farmers’ market. Anyone with any amount of expertise can get resources through collaboration and partnership. Whether it is residents trying to improve the house staff or professors at major academic centers looking for research partners, The Center for Hospital Innovation and Improvement will welcome you to collaborate and link you to valuable resources.
Brett Radler is SHM’s communications coordinator.
Risk Adjusting Readmissions: Coming Soon?
Nearly three-quarters of hospitals will be receiving penalties from the Centers for Medicare and Medicaid Services (CMS) in 2016 for excess readmissions, having failed to prevent enough patients from returning to the hospital 30 days post-discharge. With so many hospitals impacted by penalties, it is understandable that the underlying methodology of the Hospital Readmissions Reduction Program (HRRP) is coming under intense scrutiny.
Research published in JAMA Internal Medicine in September hit upon many of the myriad factors—often outside of the hospital or providers’ control—that influence whether a patient is readmitted to the hospital. This information adds weight to criticism of the measures included in the HRRP and asserts the need to refine or reform the measures to better account for readmissions preventable through the interventions of the healthcare system. The behavior these measures are meant to curb, including poor quality care, inadequate access to follow-up or medications, and gaps in transitions of care, are not identifiable within broad-based, all-cause readmission measures. Instead, hospitals are being penalized for all readmissions, a majority of which may be attributable to community or patient-related factors, such as sociodemographic or housing status, among other variables.
A growing consensus on two fronts asserts that these measures, as currently structured, might not be appropriate for use in pay-for-performance programs. Measure developers, bolstered by a recent decision by the National Quality Forum to institute a trial run of risk adjusting measures for sociodemographic status, are exploring the impact of using different available variables to enhance risk adjusting their measures. Measures for readmissions are at the front of the line of these efforts. Although it is only in the beginning stages, this work could change the foundation of all quality measures used in pay-for-performance programs.
In Congress, legislation has been introduced in both the House of Representatives and the Senate aiming to refine the HRRP through additional risk adjustments. The Establishing Beneficiary Equity in the Hospital Readmission Program Act of 2015 (H.R. 1343 and S. 688), introduced by Rep. Jim Renacci (R-Ohio) and Sen. Joe Manchin (D-W.V.), would create immediate relief for hospitals by implementing risk adjustment for dual-eligible patients and the socioeconomic status of the hospital’s patients. At the same time, when reports that are currently in progress about risk adjustment in readmission measures and the use of a 30-day window for categorizing readmissions are completed, CMS would be required to incorporate their findings into the risk adjustment in the HRRP in the future.
SHM is supporting both of these pathways toward improving risk adjustment in readmissions measures. By engaging in the measure process and advocating for the passage of legislation to refine risk adjustment, SHM has taken a stand. The goal of reducing preventable readmissions is too important to use imprecise metrics that seem to penalize the hospitals serving the nation’s neediest patients.
As hospitalists on the front line, you can join SHM in advocating for these common sense, and necessary, changes to the HRRP.
Visit SHM’s Legislative Action Center to send a message to Congress in support of the Establishing Beneficiary Equity in the Hospital Readmission Program Act of 2015.
Joshua Lapps is SHM’s government relations manager.
Nearly three-quarters of hospitals will be receiving penalties from the Centers for Medicare and Medicaid Services (CMS) in 2016 for excess readmissions, having failed to prevent enough patients from returning to the hospital 30 days post-discharge. With so many hospitals impacted by penalties, it is understandable that the underlying methodology of the Hospital Readmissions Reduction Program (HRRP) is coming under intense scrutiny.
Research published in JAMA Internal Medicine in September hit upon many of the myriad factors—often outside of the hospital or providers’ control—that influence whether a patient is readmitted to the hospital. This information adds weight to criticism of the measures included in the HRRP and asserts the need to refine or reform the measures to better account for readmissions preventable through the interventions of the healthcare system. The behavior these measures are meant to curb, including poor quality care, inadequate access to follow-up or medications, and gaps in transitions of care, are not identifiable within broad-based, all-cause readmission measures. Instead, hospitals are being penalized for all readmissions, a majority of which may be attributable to community or patient-related factors, such as sociodemographic or housing status, among other variables.
A growing consensus on two fronts asserts that these measures, as currently structured, might not be appropriate for use in pay-for-performance programs. Measure developers, bolstered by a recent decision by the National Quality Forum to institute a trial run of risk adjusting measures for sociodemographic status, are exploring the impact of using different available variables to enhance risk adjusting their measures. Measures for readmissions are at the front of the line of these efforts. Although it is only in the beginning stages, this work could change the foundation of all quality measures used in pay-for-performance programs.
In Congress, legislation has been introduced in both the House of Representatives and the Senate aiming to refine the HRRP through additional risk adjustments. The Establishing Beneficiary Equity in the Hospital Readmission Program Act of 2015 (H.R. 1343 and S. 688), introduced by Rep. Jim Renacci (R-Ohio) and Sen. Joe Manchin (D-W.V.), would create immediate relief for hospitals by implementing risk adjustment for dual-eligible patients and the socioeconomic status of the hospital’s patients. At the same time, when reports that are currently in progress about risk adjustment in readmission measures and the use of a 30-day window for categorizing readmissions are completed, CMS would be required to incorporate their findings into the risk adjustment in the HRRP in the future.
SHM is supporting both of these pathways toward improving risk adjustment in readmissions measures. By engaging in the measure process and advocating for the passage of legislation to refine risk adjustment, SHM has taken a stand. The goal of reducing preventable readmissions is too important to use imprecise metrics that seem to penalize the hospitals serving the nation’s neediest patients.
As hospitalists on the front line, you can join SHM in advocating for these common sense, and necessary, changes to the HRRP.
Visit SHM’s Legislative Action Center to send a message to Congress in support of the Establishing Beneficiary Equity in the Hospital Readmission Program Act of 2015.
Joshua Lapps is SHM’s government relations manager.
Nearly three-quarters of hospitals will be receiving penalties from the Centers for Medicare and Medicaid Services (CMS) in 2016 for excess readmissions, having failed to prevent enough patients from returning to the hospital 30 days post-discharge. With so many hospitals impacted by penalties, it is understandable that the underlying methodology of the Hospital Readmissions Reduction Program (HRRP) is coming under intense scrutiny.
Research published in JAMA Internal Medicine in September hit upon many of the myriad factors—often outside of the hospital or providers’ control—that influence whether a patient is readmitted to the hospital. This information adds weight to criticism of the measures included in the HRRP and asserts the need to refine or reform the measures to better account for readmissions preventable through the interventions of the healthcare system. The behavior these measures are meant to curb, including poor quality care, inadequate access to follow-up or medications, and gaps in transitions of care, are not identifiable within broad-based, all-cause readmission measures. Instead, hospitals are being penalized for all readmissions, a majority of which may be attributable to community or patient-related factors, such as sociodemographic or housing status, among other variables.
A growing consensus on two fronts asserts that these measures, as currently structured, might not be appropriate for use in pay-for-performance programs. Measure developers, bolstered by a recent decision by the National Quality Forum to institute a trial run of risk adjusting measures for sociodemographic status, are exploring the impact of using different available variables to enhance risk adjusting their measures. Measures for readmissions are at the front of the line of these efforts. Although it is only in the beginning stages, this work could change the foundation of all quality measures used in pay-for-performance programs.
In Congress, legislation has been introduced in both the House of Representatives and the Senate aiming to refine the HRRP through additional risk adjustments. The Establishing Beneficiary Equity in the Hospital Readmission Program Act of 2015 (H.R. 1343 and S. 688), introduced by Rep. Jim Renacci (R-Ohio) and Sen. Joe Manchin (D-W.V.), would create immediate relief for hospitals by implementing risk adjustment for dual-eligible patients and the socioeconomic status of the hospital’s patients. At the same time, when reports that are currently in progress about risk adjustment in readmission measures and the use of a 30-day window for categorizing readmissions are completed, CMS would be required to incorporate their findings into the risk adjustment in the HRRP in the future.
SHM is supporting both of these pathways toward improving risk adjustment in readmissions measures. By engaging in the measure process and advocating for the passage of legislation to refine risk adjustment, SHM has taken a stand. The goal of reducing preventable readmissions is too important to use imprecise metrics that seem to penalize the hospitals serving the nation’s neediest patients.
As hospitalists on the front line, you can join SHM in advocating for these common sense, and necessary, changes to the HRRP.
Visit SHM’s Legislative Action Center to send a message to Congress in support of the Establishing Beneficiary Equity in the Hospital Readmission Program Act of 2015.
Joshua Lapps is SHM’s government relations manager.
Which Hospitalist Should Bill for Inpatient Stays with Multiple Providers?
During a facility stay, a patient could be attended to by more than one hospitalist. For example, perhaps one hospitalist is the admitting physician, but the patient has a three-day stay and may be seen by three different hospitalists. Are there any guidelines as to which physician should be billed on the facility claim? Thank you for any remarks, suggestions, or references.
—Anonymous
Dr. Hospitalist responds:
Most of us can definitely relate to the concerns you have about properly billing during the patient’s hospital stay. By facility claim, I’m assuming you mean the physician’s bill for services rendered to a hospitalized patient. After querying the Centers for Medicare and Medicaid (CMS) website and discussing the question with several of our coding and billing gurus, as far as I can tell, there are no specific guidelines pertaining to which physician in a multiphysician group should bill. CMS guidelines are clear that you should only bill for the services you provide. CMS is very specific about allowing only one physician of the same specialty billing per day (reference the CMS Manual, Chapter 12, 30.6.9-Payment for Inpatient Hospital Visits).
In our very large group, we bill daily for the individual inpatient services we provide. That way, when the bill goes out, the clinician author is responsible for its validity and can support the level of care as documented.
Billing and coding is such an arduous process, I can’t imagine attempting it without an electronic interface. Most hospitalist groups have some form of electronic billing software that has integrated checks and balances to catch the common mistakes. Improper billing done by anyone in the group can expose the entire group to an audit. With ICD-10 now upon us, this becomes ever more important.
Good luck!
Do you have a problem or concern that you’d like Dr. Hospitalist to address? Email your questions to [email protected].
During a facility stay, a patient could be attended to by more than one hospitalist. For example, perhaps one hospitalist is the admitting physician, but the patient has a three-day stay and may be seen by three different hospitalists. Are there any guidelines as to which physician should be billed on the facility claim? Thank you for any remarks, suggestions, or references.
—Anonymous
Dr. Hospitalist responds:
Most of us can definitely relate to the concerns you have about properly billing during the patient’s hospital stay. By facility claim, I’m assuming you mean the physician’s bill for services rendered to a hospitalized patient. After querying the Centers for Medicare and Medicaid (CMS) website and discussing the question with several of our coding and billing gurus, as far as I can tell, there are no specific guidelines pertaining to which physician in a multiphysician group should bill. CMS guidelines are clear that you should only bill for the services you provide. CMS is very specific about allowing only one physician of the same specialty billing per day (reference the CMS Manual, Chapter 12, 30.6.9-Payment for Inpatient Hospital Visits).
In our very large group, we bill daily for the individual inpatient services we provide. That way, when the bill goes out, the clinician author is responsible for its validity and can support the level of care as documented.
Billing and coding is such an arduous process, I can’t imagine attempting it without an electronic interface. Most hospitalist groups have some form of electronic billing software that has integrated checks and balances to catch the common mistakes. Improper billing done by anyone in the group can expose the entire group to an audit. With ICD-10 now upon us, this becomes ever more important.
Good luck!
Do you have a problem or concern that you’d like Dr. Hospitalist to address? Email your questions to [email protected].
During a facility stay, a patient could be attended to by more than one hospitalist. For example, perhaps one hospitalist is the admitting physician, but the patient has a three-day stay and may be seen by three different hospitalists. Are there any guidelines as to which physician should be billed on the facility claim? Thank you for any remarks, suggestions, or references.
—Anonymous
Dr. Hospitalist responds:
Most of us can definitely relate to the concerns you have about properly billing during the patient’s hospital stay. By facility claim, I’m assuming you mean the physician’s bill for services rendered to a hospitalized patient. After querying the Centers for Medicare and Medicaid (CMS) website and discussing the question with several of our coding and billing gurus, as far as I can tell, there are no specific guidelines pertaining to which physician in a multiphysician group should bill. CMS guidelines are clear that you should only bill for the services you provide. CMS is very specific about allowing only one physician of the same specialty billing per day (reference the CMS Manual, Chapter 12, 30.6.9-Payment for Inpatient Hospital Visits).
In our very large group, we bill daily for the individual inpatient services we provide. That way, when the bill goes out, the clinician author is responsible for its validity and can support the level of care as documented.
Billing and coding is such an arduous process, I can’t imagine attempting it without an electronic interface. Most hospitalist groups have some form of electronic billing software that has integrated checks and balances to catch the common mistakes. Improper billing done by anyone in the group can expose the entire group to an audit. With ICD-10 now upon us, this becomes ever more important.
Good luck!
Do you have a problem or concern that you’d like Dr. Hospitalist to address? Email your questions to [email protected].
Eliminations Hospitalist Groups Should Consider
Editor’s note: Second in a continuing series of articles exploring ways hospitalist groups can cut back.
In last month’s column, I made the case that most hospitalist groups should think about doing away with a morning meeting to distribute overnight admissions and changing a daytime admitter shift into another rounder and having all of the day rounders share admissions. Here I’ll describe additional things in place at some hospitalist groups that should probably be eliminated.
Obscuring Attending Hospitalist Name
Some hospitalist groups admit patients to the “blue team” or “gold team” or use a similar system. I encountered one place that had a fuchsia team. Such designations typically take the place of the attending physician’s name and can be convenient when one hospitalist goes off service and is replaced by another; the team name stays the same. Even if the attending hospitalist makes up the entire team (i.e., no residents or students), some groups use the “team” name rather than the attending hospitalist name.
But when the patient’s chart, sign on the door, and other identifying materials all refer only to the team that is caring for the patient, the patients, their families, and most hospital staff don’t have an easy way to identify the responsible physician. Say a worried daughter steps into the hall to ask the nurse, “Which doctor is taking care of my dad?” The nurse might readily see that the blue team is responsible but may not know which hospitalist is working on the blue team today and might have to walk back to the nursing station to look over a sheet of paper (a “decoder ring”) to figure out the hospitalist’s name.
This scenario has all kinds of drawbacks. To the daughter, the name of the doctor in charge is a big deal. It doesn’t inspire confidence if the nurse can’t readily say who that is. And the busy nurse might forget to investigate and provide the name to the daughter in a timely way.
I think groups using a system like this should seriously consider replacing team names with the attending hospitalist name and updating that name in the medical record, whether that is an EHR, a paper chart, or some other form, every time that doctor rotates off service and is replaced by another. Hospital staff, patients, and families should always see the name of the attending physician and not an uninformative color or nondescript team name.
It will require work for someone, the hospitalist in many cases, to go into the EHR and write an order or send a message to ensure that the hospitalist name is kept current every time one doctor replaces another. But it’s worth the effort.
Day Hospitalists Should Round on Patients Admitted after Midnight
Although not exactly common, I’ve come across this scenario often enough that it’s worth mentioning.
Hospitalists, sometimes with a hint of indignity or even chest thumping, have told me they don’t visit or round on patients admitted after midnight by their night doctor. “You can’t bill for a second visit on the same calendar day,” they explain, firmly. “So if I can’t get paid to see the patient, then I won’t.”
This is just crazy.
For one thing, these same doctors are typically employed by the hospital and are being paid to provide whatever care patients need. I think they’ve just latched onto the “can’t bill another visit” as an excuse to get out of some work.
Don’t forget that many of these patients may wait over 30 hours from their admitting visit to the first follow-up visit; this delay is at the beginning of their hospital stay, when they might be most unstable. And it delays initiation of discharge planning and other important steps in patient care.
I don’t see any room for meaningful debate on this. The rounder who picks up a patient admitted the night before should always make a full rounding visit, even if the admission was after midnight.
But if the visit isn’t billable, you are freed from the typical billing-related documentation requirements. No need to document detail in the note that doesn’t meaningfully contribute to the care of the patient. For example, you might omit a chief complaint for this encounter.
Daytime Triage Doctor
Practices larger than about 20 full-time equivalents often have one daytime doctor hold a “triage” or “hot” pager, which others call to make a new referral. This triage doctor will hear about all referrals and keep track of and contact the hospitalist responsible for the next new patient. This can be a very busy job and often comes on top of a full clinical load for that doctor.
As I mentioned in my July 2015 and December 2010 articles, in many or most groups, a clerical person could take over this function, at least during business hours.
Vacation Time
In many or most cases, hospitalists that have specified vacation time are not getting a better deal than those that have no vacation time. What really matters is how many shifts you’re responsible for in a year. For the days you aren’t on shift, in most hospitalist groups it really doesn’t matter whether you label some of them as vacation days or CME days.
I discussed this issue in greater detail in my March 2007 article.
But if you’re in the 30% of hospitalist groups that have a vacation (or PTO) provision currently and it works well, then there certainly isn’t a compelling reason to change or do away with it.

Editor’s note: Second in a continuing series of articles exploring ways hospitalist groups can cut back.
In last month’s column, I made the case that most hospitalist groups should think about doing away with a morning meeting to distribute overnight admissions and changing a daytime admitter shift into another rounder and having all of the day rounders share admissions. Here I’ll describe additional things in place at some hospitalist groups that should probably be eliminated.
Obscuring Attending Hospitalist Name
Some hospitalist groups admit patients to the “blue team” or “gold team” or use a similar system. I encountered one place that had a fuchsia team. Such designations typically take the place of the attending physician’s name and can be convenient when one hospitalist goes off service and is replaced by another; the team name stays the same. Even if the attending hospitalist makes up the entire team (i.e., no residents or students), some groups use the “team” name rather than the attending hospitalist name.
But when the patient’s chart, sign on the door, and other identifying materials all refer only to the team that is caring for the patient, the patients, their families, and most hospital staff don’t have an easy way to identify the responsible physician. Say a worried daughter steps into the hall to ask the nurse, “Which doctor is taking care of my dad?” The nurse might readily see that the blue team is responsible but may not know which hospitalist is working on the blue team today and might have to walk back to the nursing station to look over a sheet of paper (a “decoder ring”) to figure out the hospitalist’s name.
This scenario has all kinds of drawbacks. To the daughter, the name of the doctor in charge is a big deal. It doesn’t inspire confidence if the nurse can’t readily say who that is. And the busy nurse might forget to investigate and provide the name to the daughter in a timely way.
I think groups using a system like this should seriously consider replacing team names with the attending hospitalist name and updating that name in the medical record, whether that is an EHR, a paper chart, or some other form, every time that doctor rotates off service and is replaced by another. Hospital staff, patients, and families should always see the name of the attending physician and not an uninformative color or nondescript team name.
It will require work for someone, the hospitalist in many cases, to go into the EHR and write an order or send a message to ensure that the hospitalist name is kept current every time one doctor replaces another. But it’s worth the effort.
Day Hospitalists Should Round on Patients Admitted after Midnight
Although not exactly common, I’ve come across this scenario often enough that it’s worth mentioning.
Hospitalists, sometimes with a hint of indignity or even chest thumping, have told me they don’t visit or round on patients admitted after midnight by their night doctor. “You can’t bill for a second visit on the same calendar day,” they explain, firmly. “So if I can’t get paid to see the patient, then I won’t.”
This is just crazy.
For one thing, these same doctors are typically employed by the hospital and are being paid to provide whatever care patients need. I think they’ve just latched onto the “can’t bill another visit” as an excuse to get out of some work.
Don’t forget that many of these patients may wait over 30 hours from their admitting visit to the first follow-up visit; this delay is at the beginning of their hospital stay, when they might be most unstable. And it delays initiation of discharge planning and other important steps in patient care.
I don’t see any room for meaningful debate on this. The rounder who picks up a patient admitted the night before should always make a full rounding visit, even if the admission was after midnight.
But if the visit isn’t billable, you are freed from the typical billing-related documentation requirements. No need to document detail in the note that doesn’t meaningfully contribute to the care of the patient. For example, you might omit a chief complaint for this encounter.
Daytime Triage Doctor
Practices larger than about 20 full-time equivalents often have one daytime doctor hold a “triage” or “hot” pager, which others call to make a new referral. This triage doctor will hear about all referrals and keep track of and contact the hospitalist responsible for the next new patient. This can be a very busy job and often comes on top of a full clinical load for that doctor.
As I mentioned in my July 2015 and December 2010 articles, in many or most groups, a clerical person could take over this function, at least during business hours.
Vacation Time
In many or most cases, hospitalists that have specified vacation time are not getting a better deal than those that have no vacation time. What really matters is how many shifts you’re responsible for in a year. For the days you aren’t on shift, in most hospitalist groups it really doesn’t matter whether you label some of them as vacation days or CME days.
I discussed this issue in greater detail in my March 2007 article.
But if you’re in the 30% of hospitalist groups that have a vacation (or PTO) provision currently and it works well, then there certainly isn’t a compelling reason to change or do away with it.

Editor’s note: Second in a continuing series of articles exploring ways hospitalist groups can cut back.
In last month’s column, I made the case that most hospitalist groups should think about doing away with a morning meeting to distribute overnight admissions and changing a daytime admitter shift into another rounder and having all of the day rounders share admissions. Here I’ll describe additional things in place at some hospitalist groups that should probably be eliminated.
Obscuring Attending Hospitalist Name
Some hospitalist groups admit patients to the “blue team” or “gold team” or use a similar system. I encountered one place that had a fuchsia team. Such designations typically take the place of the attending physician’s name and can be convenient when one hospitalist goes off service and is replaced by another; the team name stays the same. Even if the attending hospitalist makes up the entire team (i.e., no residents or students), some groups use the “team” name rather than the attending hospitalist name.
But when the patient’s chart, sign on the door, and other identifying materials all refer only to the team that is caring for the patient, the patients, their families, and most hospital staff don’t have an easy way to identify the responsible physician. Say a worried daughter steps into the hall to ask the nurse, “Which doctor is taking care of my dad?” The nurse might readily see that the blue team is responsible but may not know which hospitalist is working on the blue team today and might have to walk back to the nursing station to look over a sheet of paper (a “decoder ring”) to figure out the hospitalist’s name.
This scenario has all kinds of drawbacks. To the daughter, the name of the doctor in charge is a big deal. It doesn’t inspire confidence if the nurse can’t readily say who that is. And the busy nurse might forget to investigate and provide the name to the daughter in a timely way.
I think groups using a system like this should seriously consider replacing team names with the attending hospitalist name and updating that name in the medical record, whether that is an EHR, a paper chart, or some other form, every time that doctor rotates off service and is replaced by another. Hospital staff, patients, and families should always see the name of the attending physician and not an uninformative color or nondescript team name.
It will require work for someone, the hospitalist in many cases, to go into the EHR and write an order or send a message to ensure that the hospitalist name is kept current every time one doctor replaces another. But it’s worth the effort.
Day Hospitalists Should Round on Patients Admitted after Midnight
Although not exactly common, I’ve come across this scenario often enough that it’s worth mentioning.
Hospitalists, sometimes with a hint of indignity or even chest thumping, have told me they don’t visit or round on patients admitted after midnight by their night doctor. “You can’t bill for a second visit on the same calendar day,” they explain, firmly. “So if I can’t get paid to see the patient, then I won’t.”
This is just crazy.
For one thing, these same doctors are typically employed by the hospital and are being paid to provide whatever care patients need. I think they’ve just latched onto the “can’t bill another visit” as an excuse to get out of some work.
Don’t forget that many of these patients may wait over 30 hours from their admitting visit to the first follow-up visit; this delay is at the beginning of their hospital stay, when they might be most unstable. And it delays initiation of discharge planning and other important steps in patient care.
I don’t see any room for meaningful debate on this. The rounder who picks up a patient admitted the night before should always make a full rounding visit, even if the admission was after midnight.
But if the visit isn’t billable, you are freed from the typical billing-related documentation requirements. No need to document detail in the note that doesn’t meaningfully contribute to the care of the patient. For example, you might omit a chief complaint for this encounter.
Daytime Triage Doctor
Practices larger than about 20 full-time equivalents often have one daytime doctor hold a “triage” or “hot” pager, which others call to make a new referral. This triage doctor will hear about all referrals and keep track of and contact the hospitalist responsible for the next new patient. This can be a very busy job and often comes on top of a full clinical load for that doctor.
As I mentioned in my July 2015 and December 2010 articles, in many or most groups, a clerical person could take over this function, at least during business hours.
Vacation Time
In many or most cases, hospitalists that have specified vacation time are not getting a better deal than those that have no vacation time. What really matters is how many shifts you’re responsible for in a year. For the days you aren’t on shift, in most hospitalist groups it really doesn’t matter whether you label some of them as vacation days or CME days.
I discussed this issue in greater detail in my March 2007 article.
But if you’re in the 30% of hospitalist groups that have a vacation (or PTO) provision currently and it works well, then there certainly isn’t a compelling reason to change or do away with it.

Medicare’s Readmission Reduction Program Cuts $420M to U.S. Hospitals This Year
It’s that time of year again … the time when hospitals around the country are being notified of their 30-day readmission penalties from the Centers for Medicare and Medicaid Services (CMS). Now in the fourth year of the program, many hospitals have come to dread the announcement of how much they are being penalized each year.1
This year, the readmission reduction program will decrease Medicare payments within a total of 2,592 U.S. hospitals, for a combined total of $420 million. This year’s program included readmissions from July 2011 to June 2014; the program uses a three-year rolling average for its calculations.2
The readmission program, which initially was implemented through the Affordable Care Act in 2012, aimed to penalize hospitals with higher than expected 30-day readmission rates on select conditions (currently heart attack, heart failure, pneumonia, COPD, and hip/knee replacements). Medicare estimates that it spends $17 billion a year in avoidable readmissions, which prompted the initial support for the program. For each condition, CMS calculates expected readmission rates (based on risk adjustment models that include age, severity of illness, and comorbid conditions) and observed rates, and then calculates an “excess readmission ratio” for each hospital. Based on the overall ratio, the hospital is penalized up to 3% of its Medicare payments for all inpatient stays for that fiscal year. Each year, CMS reassesses the readmission rates for hospitals and readjusts the magnitude of the penalty. The purpose of the program is to incent hospitals to invest in discharge planning and care coordination efforts and do everything possible to avoid readmissions.1
Who Gets Penalized?
This year, most eligible hospitals were penalized to some extent, and all but 209 of the hospitals that were penalized last year were penalized again.
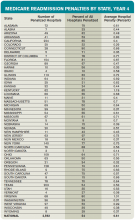
The average Medicare payment reduction will be 0.61% per patient stay.
A total of 506 hospitals will lose at least 1% of their Medicare payments, and 38 hospitals will receive the maximum 3% penalty.
Unfortunately, safety net hospitals were about 60% more likely than other hospitals to have been penalized in all three years of the program. In addition, hospitals with the lowest profit margins were 36% more likely to be penalized than those with higher margins.
Some states were disproportionately affected, with at least three-quarters of hospitals affected in Alabama, Connecticut, Florida, Massachusetts, New Jersey, New York, Rhode Island, South Carolina, Virginia, and the District of Columbia. States that fared the best were Idaho, Iowa, Kansas, Montana, Nebraska, North Dakota, and South Dakota.
Most of the 2,232 hospitals that avoided a penalty were spared because they were exempted from the program (Veterans Affairs hospitals, children’s hospitals, critical access hospitals, or those with too few Medicare patients), not because of exceptional performance.
Does the Program Work?
Despite criticism, there is no doubt that this program has forced hospitals to pay keen attention to transitions of care and avoidable readmissions. And it does appear to be an effective strategy for CMS to achieve its goals; there has been an overall decrease in 30-day readmission rates among Medicare recipients since the program began, in all types of hospitals.
Compared to 2012, there were 100,000 fewer readmissions among Medicare beneficiaries in the U.S. in 2013. As such, there is no evidence that the program will be discontinued, although it will hopefully be altered in some key aspects.3
What the Future Holds
The program has been criticized on many fronts. For one, it recalculates a three-year rolling average each year, which makes it incredibly difficult to “wash out” older (poor) performance and get off the penalty list.
In addition, critics have pointed out that the program fails to take into account the socioeconomic background of patients when assessing readmission penalties. Many argue that social determinants of readmissions that are beyond the immediate control of a hospital system can have a huge impact on readmission rates.
The National Quality Forum is examining the impact of these factors on readmissions, but this evaluation likely will take years.
In the meantime, the Hospital Readmissions Program Accuracy and Accountability Act of 2014 has been introduced as a bill that would require CMS to factor socioeconomic status into the equation when determining readmission penalties.
What All This Means for Hospitalists
All of us working within the confines of the current program can do a few things to improve our understanding and our hospitals’ performance:
- If your hospital is one that incurred a penalty, know that most “eligible” hospitals also incurred a penalty.
- Look at how your hospital fared within your state and find out if you are above or below average in the amount.3
- Continue to focus on exemplary care transition protocols, policies, and programs within your hospital system, because the penalties are unlikely to go away and are very likely to expand over time.
- Support any advocacy efforts toward improving risk adjustment methodologies for readmissions; all hospitals are likely to benefit from more accurate risk adjustments.

References
- Centers for Medicare and Medicaid Services. Readmissions reduction program. Accessed October 3, 2015.
- Rau J. Half of nation’s hospitals fail again to escape Medicare’s readmissions penalties. August 3, 2015. Accessed October 3, 2015.
- Medpac. The hospital readmission penalty: how well is it working?. Accessed October 3, 2015.
It’s that time of year again … the time when hospitals around the country are being notified of their 30-day readmission penalties from the Centers for Medicare and Medicaid Services (CMS). Now in the fourth year of the program, many hospitals have come to dread the announcement of how much they are being penalized each year.1
This year, the readmission reduction program will decrease Medicare payments within a total of 2,592 U.S. hospitals, for a combined total of $420 million. This year’s program included readmissions from July 2011 to June 2014; the program uses a three-year rolling average for its calculations.2
The readmission program, which initially was implemented through the Affordable Care Act in 2012, aimed to penalize hospitals with higher than expected 30-day readmission rates on select conditions (currently heart attack, heart failure, pneumonia, COPD, and hip/knee replacements). Medicare estimates that it spends $17 billion a year in avoidable readmissions, which prompted the initial support for the program. For each condition, CMS calculates expected readmission rates (based on risk adjustment models that include age, severity of illness, and comorbid conditions) and observed rates, and then calculates an “excess readmission ratio” for each hospital. Based on the overall ratio, the hospital is penalized up to 3% of its Medicare payments for all inpatient stays for that fiscal year. Each year, CMS reassesses the readmission rates for hospitals and readjusts the magnitude of the penalty. The purpose of the program is to incent hospitals to invest in discharge planning and care coordination efforts and do everything possible to avoid readmissions.1
Who Gets Penalized?
This year, most eligible hospitals were penalized to some extent, and all but 209 of the hospitals that were penalized last year were penalized again.
The average Medicare payment reduction will be 0.61% per patient stay.
A total of 506 hospitals will lose at least 1% of their Medicare payments, and 38 hospitals will receive the maximum 3% penalty.
Unfortunately, safety net hospitals were about 60% more likely than other hospitals to have been penalized in all three years of the program. In addition, hospitals with the lowest profit margins were 36% more likely to be penalized than those with higher margins.
Some states were disproportionately affected, with at least three-quarters of hospitals affected in Alabama, Connecticut, Florida, Massachusetts, New Jersey, New York, Rhode Island, South Carolina, Virginia, and the District of Columbia. States that fared the best were Idaho, Iowa, Kansas, Montana, Nebraska, North Dakota, and South Dakota.
Most of the 2,232 hospitals that avoided a penalty were spared because they were exempted from the program (Veterans Affairs hospitals, children’s hospitals, critical access hospitals, or those with too few Medicare patients), not because of exceptional performance.
Does the Program Work?
Despite criticism, there is no doubt that this program has forced hospitals to pay keen attention to transitions of care and avoidable readmissions. And it does appear to be an effective strategy for CMS to achieve its goals; there has been an overall decrease in 30-day readmission rates among Medicare recipients since the program began, in all types of hospitals.
Compared to 2012, there were 100,000 fewer readmissions among Medicare beneficiaries in the U.S. in 2013. As such, there is no evidence that the program will be discontinued, although it will hopefully be altered in some key aspects.3
What the Future Holds
The program has been criticized on many fronts. For one, it recalculates a three-year rolling average each year, which makes it incredibly difficult to “wash out” older (poor) performance and get off the penalty list.
In addition, critics have pointed out that the program fails to take into account the socioeconomic background of patients when assessing readmission penalties. Many argue that social determinants of readmissions that are beyond the immediate control of a hospital system can have a huge impact on readmission rates.
The National Quality Forum is examining the impact of these factors on readmissions, but this evaluation likely will take years.
In the meantime, the Hospital Readmissions Program Accuracy and Accountability Act of 2014 has been introduced as a bill that would require CMS to factor socioeconomic status into the equation when determining readmission penalties.
What All This Means for Hospitalists
All of us working within the confines of the current program can do a few things to improve our understanding and our hospitals’ performance:
- If your hospital is one that incurred a penalty, know that most “eligible” hospitals also incurred a penalty.
- Look at how your hospital fared within your state and find out if you are above or below average in the amount.3
- Continue to focus on exemplary care transition protocols, policies, and programs within your hospital system, because the penalties are unlikely to go away and are very likely to expand over time.
- Support any advocacy efforts toward improving risk adjustment methodologies for readmissions; all hospitals are likely to benefit from more accurate risk adjustments.

References
- Centers for Medicare and Medicaid Services. Readmissions reduction program. Accessed October 3, 2015.
- Rau J. Half of nation’s hospitals fail again to escape Medicare’s readmissions penalties. August 3, 2015. Accessed October 3, 2015.
- Medpac. The hospital readmission penalty: how well is it working?. Accessed October 3, 2015.
It’s that time of year again … the time when hospitals around the country are being notified of their 30-day readmission penalties from the Centers for Medicare and Medicaid Services (CMS). Now in the fourth year of the program, many hospitals have come to dread the announcement of how much they are being penalized each year.1
This year, the readmission reduction program will decrease Medicare payments within a total of 2,592 U.S. hospitals, for a combined total of $420 million. This year’s program included readmissions from July 2011 to June 2014; the program uses a three-year rolling average for its calculations.2
The readmission program, which initially was implemented through the Affordable Care Act in 2012, aimed to penalize hospitals with higher than expected 30-day readmission rates on select conditions (currently heart attack, heart failure, pneumonia, COPD, and hip/knee replacements). Medicare estimates that it spends $17 billion a year in avoidable readmissions, which prompted the initial support for the program. For each condition, CMS calculates expected readmission rates (based on risk adjustment models that include age, severity of illness, and comorbid conditions) and observed rates, and then calculates an “excess readmission ratio” for each hospital. Based on the overall ratio, the hospital is penalized up to 3% of its Medicare payments for all inpatient stays for that fiscal year. Each year, CMS reassesses the readmission rates for hospitals and readjusts the magnitude of the penalty. The purpose of the program is to incent hospitals to invest in discharge planning and care coordination efforts and do everything possible to avoid readmissions.1
Who Gets Penalized?
This year, most eligible hospitals were penalized to some extent, and all but 209 of the hospitals that were penalized last year were penalized again.
The average Medicare payment reduction will be 0.61% per patient stay.
A total of 506 hospitals will lose at least 1% of their Medicare payments, and 38 hospitals will receive the maximum 3% penalty.
Unfortunately, safety net hospitals were about 60% more likely than other hospitals to have been penalized in all three years of the program. In addition, hospitals with the lowest profit margins were 36% more likely to be penalized than those with higher margins.
Some states were disproportionately affected, with at least three-quarters of hospitals affected in Alabama, Connecticut, Florida, Massachusetts, New Jersey, New York, Rhode Island, South Carolina, Virginia, and the District of Columbia. States that fared the best were Idaho, Iowa, Kansas, Montana, Nebraska, North Dakota, and South Dakota.
Most of the 2,232 hospitals that avoided a penalty were spared because they were exempted from the program (Veterans Affairs hospitals, children’s hospitals, critical access hospitals, or those with too few Medicare patients), not because of exceptional performance.
Does the Program Work?
Despite criticism, there is no doubt that this program has forced hospitals to pay keen attention to transitions of care and avoidable readmissions. And it does appear to be an effective strategy for CMS to achieve its goals; there has been an overall decrease in 30-day readmission rates among Medicare recipients since the program began, in all types of hospitals.
Compared to 2012, there were 100,000 fewer readmissions among Medicare beneficiaries in the U.S. in 2013. As such, there is no evidence that the program will be discontinued, although it will hopefully be altered in some key aspects.3
What the Future Holds
The program has been criticized on many fronts. For one, it recalculates a three-year rolling average each year, which makes it incredibly difficult to “wash out” older (poor) performance and get off the penalty list.
In addition, critics have pointed out that the program fails to take into account the socioeconomic background of patients when assessing readmission penalties. Many argue that social determinants of readmissions that are beyond the immediate control of a hospital system can have a huge impact on readmission rates.
The National Quality Forum is examining the impact of these factors on readmissions, but this evaluation likely will take years.
In the meantime, the Hospital Readmissions Program Accuracy and Accountability Act of 2014 has been introduced as a bill that would require CMS to factor socioeconomic status into the equation when determining readmission penalties.
What All This Means for Hospitalists
All of us working within the confines of the current program can do a few things to improve our understanding and our hospitals’ performance:
- If your hospital is one that incurred a penalty, know that most “eligible” hospitals also incurred a penalty.
- Look at how your hospital fared within your state and find out if you are above or below average in the amount.3
- Continue to focus on exemplary care transition protocols, policies, and programs within your hospital system, because the penalties are unlikely to go away and are very likely to expand over time.
- Support any advocacy efforts toward improving risk adjustment methodologies for readmissions; all hospitals are likely to benefit from more accurate risk adjustments.

References
- Centers for Medicare and Medicaid Services. Readmissions reduction program. Accessed October 3, 2015.
- Rau J. Half of nation’s hospitals fail again to escape Medicare’s readmissions penalties. August 3, 2015. Accessed October 3, 2015.
- Medpac. The hospital readmission penalty: how well is it working?. Accessed October 3, 2015.
SHM Holding Roundtable for Hospitalist Practice Administrators
Are you a hospitalist practice administrator in a new role? SHM can help—and the upcoming roundtable discussion presented by Glenn Appelbaum, CHE, CPA, and Heather Fordyce, BS, on December 9 can help you find the resources to enable you to manage your practice effectively and efficiently. For details and to pre-register, visit the “Practice Administrators”.
Are you a hospitalist practice administrator in a new role? SHM can help—and the upcoming roundtable discussion presented by Glenn Appelbaum, CHE, CPA, and Heather Fordyce, BS, on December 9 can help you find the resources to enable you to manage your practice effectively and efficiently. For details and to pre-register, visit the “Practice Administrators”.
Are you a hospitalist practice administrator in a new role? SHM can help—and the upcoming roundtable discussion presented by Glenn Appelbaum, CHE, CPA, and Heather Fordyce, BS, on December 9 can help you find the resources to enable you to manage your practice effectively and efficiently. For details and to pre-register, visit the “Practice Administrators”.
Antimicrobial Stewardship Resources Often Lacking in Hospitalists' Routines
The best antibiotic stewardship programs weave improvements into the routines of hospitalists. But at the end of the day, developing and overseeing these important programs does require some level of time and money. And setting aside that time and money has been the exception rather than the rule.
According to early results from an SHM survey, nine of 123 hospitalists said that they are compensated for work on antimicrobial stewardship programs at their hospitals. That’s a mere 7%. Only 10 out of 122 respondents said they have “protected time” for work on an antimicrobial stewardship program. That’s about 8%. And it’s possible that the survey results are actually skewed somewhat, receiving responses from more proactive centers. One hundred fifteen out of 178 respondents, or 65%, said that they have an antimicrobial stewardship program at their centers.
Arjun Srinivasan, the CDC’s associate director for healthcare-associated infection prevention programs, says he has found that typically about half of U.S. hospitals have such programs. Eric Howell, MD, SFHM, director of the collaborative inpatient medicine service at Johns Hopkins Bayview Medical Center in Baltimore, says change can be a slow process, but he expects initiatives like SHM’s new antibiotic stewardship campaign to help tip the scales toward more resources and more change. It’s a matter of “making the case that, No. 1, this is a problem and, No. 2, there are solutions out there and, No. 3, these solutions are cost effective, as well as improving quality.” Demonstrating the effects on cost and outcomes, he says, is “likely the tipping point [where] we will see real change.”

“If we don’t change, we’re going to run out of antibiotics,” says Dr. Howell, who is also senior physician advisor to SHM’s Center for Hospital Innovation and Improvement. “People are sort of really panic-stricken. And that fear is helping to motivate them to drive change, too.”
Jonathan Zenilman, MD, chief of the division of infectious diseases at Bayview, says that his team worked with a non-Hopkins hospital in Delaware and found they saved about $80,000 a year just by eliminating the use of ertapenem for pre-operative prophylaxis for abdominal surgery. Numbers like that, he says, show that the case for savings can be made to hospital administration. Then again, it’s often easier to make the case before a program is started—and harder to keep it going after that first year.
“Between the second and the third year, you’re not going to generate much savings, if anything,” he says. If a new administrator is in place, it can be a challenge to get them to realize that costs will go back up once a program is dismantled.
“They look at this as an additional business model,” Dr. Zenilman explains. “They’ll say, ‘Where does my revenue offset the costs?’ And sometimes they just don’t get the value proposition…It needs to be pitched as a value proposition and not as a revenue proposition.”
The culture change toward value in the U.S. is helping, though, he says. “Now the business case is easier,” he says, “because there’s clearly this regulatory push towards doing it.” TH
The best antibiotic stewardship programs weave improvements into the routines of hospitalists. But at the end of the day, developing and overseeing these important programs does require some level of time and money. And setting aside that time and money has been the exception rather than the rule.
According to early results from an SHM survey, nine of 123 hospitalists said that they are compensated for work on antimicrobial stewardship programs at their hospitals. That’s a mere 7%. Only 10 out of 122 respondents said they have “protected time” for work on an antimicrobial stewardship program. That’s about 8%. And it’s possible that the survey results are actually skewed somewhat, receiving responses from more proactive centers. One hundred fifteen out of 178 respondents, or 65%, said that they have an antimicrobial stewardship program at their centers.
Arjun Srinivasan, the CDC’s associate director for healthcare-associated infection prevention programs, says he has found that typically about half of U.S. hospitals have such programs. Eric Howell, MD, SFHM, director of the collaborative inpatient medicine service at Johns Hopkins Bayview Medical Center in Baltimore, says change can be a slow process, but he expects initiatives like SHM’s new antibiotic stewardship campaign to help tip the scales toward more resources and more change. It’s a matter of “making the case that, No. 1, this is a problem and, No. 2, there are solutions out there and, No. 3, these solutions are cost effective, as well as improving quality.” Demonstrating the effects on cost and outcomes, he says, is “likely the tipping point [where] we will see real change.”

“If we don’t change, we’re going to run out of antibiotics,” says Dr. Howell, who is also senior physician advisor to SHM’s Center for Hospital Innovation and Improvement. “People are sort of really panic-stricken. And that fear is helping to motivate them to drive change, too.”
Jonathan Zenilman, MD, chief of the division of infectious diseases at Bayview, says that his team worked with a non-Hopkins hospital in Delaware and found they saved about $80,000 a year just by eliminating the use of ertapenem for pre-operative prophylaxis for abdominal surgery. Numbers like that, he says, show that the case for savings can be made to hospital administration. Then again, it’s often easier to make the case before a program is started—and harder to keep it going after that first year.
“Between the second and the third year, you’re not going to generate much savings, if anything,” he says. If a new administrator is in place, it can be a challenge to get them to realize that costs will go back up once a program is dismantled.
“They look at this as an additional business model,” Dr. Zenilman explains. “They’ll say, ‘Where does my revenue offset the costs?’ And sometimes they just don’t get the value proposition…It needs to be pitched as a value proposition and not as a revenue proposition.”
The culture change toward value in the U.S. is helping, though, he says. “Now the business case is easier,” he says, “because there’s clearly this regulatory push towards doing it.” TH
The best antibiotic stewardship programs weave improvements into the routines of hospitalists. But at the end of the day, developing and overseeing these important programs does require some level of time and money. And setting aside that time and money has been the exception rather than the rule.
According to early results from an SHM survey, nine of 123 hospitalists said that they are compensated for work on antimicrobial stewardship programs at their hospitals. That’s a mere 7%. Only 10 out of 122 respondents said they have “protected time” for work on an antimicrobial stewardship program. That’s about 8%. And it’s possible that the survey results are actually skewed somewhat, receiving responses from more proactive centers. One hundred fifteen out of 178 respondents, or 65%, said that they have an antimicrobial stewardship program at their centers.
Arjun Srinivasan, the CDC’s associate director for healthcare-associated infection prevention programs, says he has found that typically about half of U.S. hospitals have such programs. Eric Howell, MD, SFHM, director of the collaborative inpatient medicine service at Johns Hopkins Bayview Medical Center in Baltimore, says change can be a slow process, but he expects initiatives like SHM’s new antibiotic stewardship campaign to help tip the scales toward more resources and more change. It’s a matter of “making the case that, No. 1, this is a problem and, No. 2, there are solutions out there and, No. 3, these solutions are cost effective, as well as improving quality.” Demonstrating the effects on cost and outcomes, he says, is “likely the tipping point [where] we will see real change.”

“If we don’t change, we’re going to run out of antibiotics,” says Dr. Howell, who is also senior physician advisor to SHM’s Center for Hospital Innovation and Improvement. “People are sort of really panic-stricken. And that fear is helping to motivate them to drive change, too.”
Jonathan Zenilman, MD, chief of the division of infectious diseases at Bayview, says that his team worked with a non-Hopkins hospital in Delaware and found they saved about $80,000 a year just by eliminating the use of ertapenem for pre-operative prophylaxis for abdominal surgery. Numbers like that, he says, show that the case for savings can be made to hospital administration. Then again, it’s often easier to make the case before a program is started—and harder to keep it going after that first year.
“Between the second and the third year, you’re not going to generate much savings, if anything,” he says. If a new administrator is in place, it can be a challenge to get them to realize that costs will go back up once a program is dismantled.
“They look at this as an additional business model,” Dr. Zenilman explains. “They’ll say, ‘Where does my revenue offset the costs?’ And sometimes they just don’t get the value proposition…It needs to be pitched as a value proposition and not as a revenue proposition.”
The culture change toward value in the U.S. is helping, though, he says. “Now the business case is easier,” he says, “because there’s clearly this regulatory push towards doing it.” TH
Society of Hospital Medicine Launches Antimicrobial Stewardship Campaign
In 2006, infectious disease specialists and pharmacists at Johns Hopkins Bayview Medical Center in Baltimore took a look at the pharmacy budget and were jarred by the numbers.
“The proportion of the pharmacy budget that was antimicrobials was much larger than we would expect,” says Jonathan Zenilman, MD, chief of infectious diseases at Bayview.
The pharmacy and ID teams implemented antibiotic stewardship tools, including medication reassessments after two or three days and quicker conversion to oral drugs when appropriate. They also did something that was fairly new at the time: A hospitalist was incorporated into the team. The tactic was employed out of need—the ID department was stretched too thin—but it made perfect sense, Dr. Zenilman says. Most of the patients seen by hospitalists have bread-and-butter conditions that comprise a lot of the center’s antibiotic use.
“Patients on a typical hospital medicine series are not on advanced antifungals and complicated antibiotic regimens,” he says.
The arrangement worked: The center achieved a more than 50% reduction in the main target drug, Zosyn, and a hospitalist is still typically part of the antibiotic stewardship team.
That might have been a new concept then, but fast forward a decade: ID and public health experts are increasingly seeing hospitalists as central to the effort to limit antibiotic overuse and stall the development of drug resistance in antimicrobial organisms.
Now, SHM is about to launch a campaign to get more hospitalists to see themselves as central to that effort. SHM will formally kick off the “Fight the Resistance” campaign on November 9. It’s an awareness and behavior change campaign that builds on SHM’s participation in a White House forum on antibiotic resistance that was held in June.

“We wanted to not only enhance awareness among hospitalists about what appropriate antimicrobial prescribing is, but also to change behaviors and ultimately change culture to facilitate appropriate antibiotic use,” says Jenna Goldstein, director of SHM’s Center for Hospital Innovation and Improvement (CHII), who is leading the initiative along with Mobola Owolabi, SHM project manager.
Behavior Change
The society will provide educational inserts hospitalists can use at their hospitals, as well as downloadable posters that will help raise awareness on appropriate antibiotic use. The campaign will be highlighted in SHM’s online and social media presence.
Hospitalists will be asked to make behavior changes in their antibiotic-related practices that will promote better stewardship, such as taking an antibiotic “timeout” during which usage is revisited and changed or discontinued if antibiotic use is not appropriate.
“We’re specifically asking hospitalists to engage in behavior changes and we plan to assess outcomes and results after implementation,” Goldstein says. “Our ultimate goal, although we realize this is a much longer-term goal and certainly more arduous to measure, is to change the culture in the hospital related to prescribing, so that hospitalists are prescribing only when appropriate, only when there’s an indicated infection, and according to the evidence base for prescribing antimicrobials for their patients.”

Future plans will include developing a mentored implementation program in which SHM will provide guidance for hospitalists who want to develop or improve a stewardship program at their hospital. The guidance will be based in part on the CDC’s “Core Elements of Hospital Antibiotic Stewardship Programs,” a kind of guidebook on antibiotic stewardship.1
Read more about antibiotic stewardship resources.
Eric Howell, MD, SFHM, director of the collaborative inpatient medicine service at Bayview, associate professor of medicine at Johns Hopkins University School of Medicine, and CHII’s senior physician advisor, says it’s time for hospitalists to take on a bigger role.
“Doing ‘just in case’ antibiotics is really not appropriate and should be strongly discouraged, unless the risks are very high for a specific patient,” he says. A past president of SHM, Dr. Howell has long advocated that hospitalists take the time to explain the risk of excessive antibiotic use to their patients, even on a busy day.
“It’s our duty as physicians to make sure our patients get the best care possible, and often that means the physicians themselves have to do the educating,” he says. “I would say that, in general, it doesn’t take that much time. Having a conversation with your patient to educate them about anything—heart failure, diabetes, appropriate antibiotics—must be built into the care that we provide our patients somehow.”
That communication doesn’t necessarily have to be performed by the hospitalist, he notes. The pharmacist, nurse, or written material can relay this information. But somewhere along the line, he says, the antibiotic education must happen.
SHM’s initiative should help, simply because “knowledge is good,” says Dr. Zenilman, the ID expert at Hopkins Bayview. Key to success, he says, will be what happens when hospitalists are taking care of a patient—will they actually be willing to cut their regimens?
“People overuse antibiotics, sometimes not out of education issues, but because they’re anxious,” Dr. Zenilman says. “The more challenging part is getting people to deal with the uncertainty and recognizing intuitively that overuse has enormous complications.”
The literature is now replete with studies showing how antibiotic stewardship measures help curb resistance, eliminate incorrect antibiotic prescribing, lower antibiotic use, and lower costs.
A web-based program was projected to save almost $400,000 a year linked to restricted antibiotic use at Johns Hopkins, according to a 2008 study.2
In Canada, according to a 2007 study, a program including recommendations for alternative drugs and shorter, guideline-based treatment durations helped reduce Clostridium difficile infections by 60% over a two-year period.3
An analysis published in August, using data from the CDC’s National Healthcare Safety Network and Emerging Infections Program, concluded that a nationwide infection control and antibiotic stewardship intervention could, over five years, avoid an estimated 619,000 hospital-acquired infections from carbapenem-resistant Enterobacteriaceae, multidrug-resistant Pseudomonas aeruginosa, invasive methicillin-resistant Staphylococcus aureus (MRSA), or C. diff.4
In spite of the evidence, preliminary results of a recent SHM survey on antibiotic stewardship found very little support, in terms of money and protected time, for hospitalists to be involved in antibiotic stewardship programs.
UM’s Success Story
A kind of microcosm of what is possible can be seen at the University of Michigan. There, Scott Flanders, MD, MHM, clinical professor of internal medicine and past president of SHM, has led an effort, along with the CDC and the Institute for Healthcare Improvement, to look at hospitalist-led interventions for smarter antimicrobial use.

Hospitalists in several programs around the country were asked to focus on a few key improvement strategies that are believed to improve use. For instance, when guidelines give a range of duration of dosing, physicians often lean toward the higher end (when the range is seven to 21 days, the default was typically closer to 21), even when that might not be necessary in a given situation. So, more specific guidelines for common situations were applied.
Hospitalists also worked to improve documentation to make antibiotic use more visible at the point of care: which drug it is, when it was started, what day of therapy it is that day, how many more days are left.
An antibiotic “timeout” at 48 to 72 hours was implemented to determine whether the treatment course should be maintained, changed, or eliminated.
The idea was for hospitalists to track this as part of the usual care process.
“We didn’t want people to create whole new systems to do these things,” says Dr. Flanders, who has consulted with SHM for its stewardship initiative. “We wanted people, for example, to use their multidisciplinary rounds that they were already having to just add one thing to the checklist.”
The process was shown to be workable. All steps of the stewardship protocol were performed 70% of the time after the initiative began, compared with just 20% of the time before it began, Dr. Flanders says. Additionally, about 25% of patients had a “significant and important” change made to their antibiotic treatment following the “timeout.”

“During this timeout, a lot of action happened,” Dr. Flanders says. More study is needed to show exactly how much of a change occurred and whether it led to cost savings, he says, but “I suspect it will.”
Much-Anticipated Partnership
Arjun Srinivasan, MD, associate director for healthcare-associated infection prevention programs at the CDC, says he is eager to continue to work with SHM on its antibiotic stewardship efforts, but he cautions that hospitalists should not try to do too much too quickly in implementing change.
“Success generally comes from starting small, from starting with a focused approach to something that you know is a problem in your facility,” Dr. Srinivasan says. “When you try to delve into everything all at once, you can very quickly get overwhelmed.”
Although smaller centers might have less manpower and face a bigger challenge in leading a stewardship program, it can be done, he says.
“We see some very small hospitals that have fantastic stewardship programs and some very small hospitals that are struggling,” he says. “We know it’s doable across the spectrum of the sizes of hospital.”
Hospitalists, he adds, “are the tip of the spear. They are probably prescribing most of the antibiotics [for inpatients] … and diagnosing most of the infections. So arming them with the information they need, working with them to develop a process that makes prescribing optimal and most efficient is obviously hugely beneficial.
“You’re going to have a tremendous impact by reaching that particular group.”
Tom Collins is a freelance writer in South Florida.
References
- Centers for Disease Control and Prevention. Core elements of hospital antibiotic stewardship programs. May 7, 2015. Accessed October 6, 2015.
- Agwu AL, Lee CK, Jain SK. A World Wide Web-based antimicrobial stewardship program improves efficiency, communication, and user satisfaction and reduces cost in a tertiary care pediatric medical center. Clin Infect Dis. 2008 Sep 15;47(6):747-753.
- Valiquette L, Cossette B, Garant MP, Diab H, Pépin J. Impact of a reduction in the use of high-risk antibiotics on the course of an epidemic of Clostridium difficile-associated disease caused by the hypervirulent NAP1/027 strain. Clin Infect Dis. 2007;45 Suppl 2:S112-S121.
- Slayton RB, Toth D, Lee BY, et al. Vital signs: estimated effects of a coordinated approach for action to reduce antibiotic-resistant infections in health care facilities - United States. MMWR Morb Mortal Wkly Rep. 2015;64(30):826-831.
In 2006, infectious disease specialists and pharmacists at Johns Hopkins Bayview Medical Center in Baltimore took a look at the pharmacy budget and were jarred by the numbers.
“The proportion of the pharmacy budget that was antimicrobials was much larger than we would expect,” says Jonathan Zenilman, MD, chief of infectious diseases at Bayview.
The pharmacy and ID teams implemented antibiotic stewardship tools, including medication reassessments after two or three days and quicker conversion to oral drugs when appropriate. They also did something that was fairly new at the time: A hospitalist was incorporated into the team. The tactic was employed out of need—the ID department was stretched too thin—but it made perfect sense, Dr. Zenilman says. Most of the patients seen by hospitalists have bread-and-butter conditions that comprise a lot of the center’s antibiotic use.
“Patients on a typical hospital medicine series are not on advanced antifungals and complicated antibiotic regimens,” he says.
The arrangement worked: The center achieved a more than 50% reduction in the main target drug, Zosyn, and a hospitalist is still typically part of the antibiotic stewardship team.
That might have been a new concept then, but fast forward a decade: ID and public health experts are increasingly seeing hospitalists as central to the effort to limit antibiotic overuse and stall the development of drug resistance in antimicrobial organisms.
Now, SHM is about to launch a campaign to get more hospitalists to see themselves as central to that effort. SHM will formally kick off the “Fight the Resistance” campaign on November 9. It’s an awareness and behavior change campaign that builds on SHM’s participation in a White House forum on antibiotic resistance that was held in June.

“We wanted to not only enhance awareness among hospitalists about what appropriate antimicrobial prescribing is, but also to change behaviors and ultimately change culture to facilitate appropriate antibiotic use,” says Jenna Goldstein, director of SHM’s Center for Hospital Innovation and Improvement (CHII), who is leading the initiative along with Mobola Owolabi, SHM project manager.
Behavior Change
The society will provide educational inserts hospitalists can use at their hospitals, as well as downloadable posters that will help raise awareness on appropriate antibiotic use. The campaign will be highlighted in SHM’s online and social media presence.
Hospitalists will be asked to make behavior changes in their antibiotic-related practices that will promote better stewardship, such as taking an antibiotic “timeout” during which usage is revisited and changed or discontinued if antibiotic use is not appropriate.
“We’re specifically asking hospitalists to engage in behavior changes and we plan to assess outcomes and results after implementation,” Goldstein says. “Our ultimate goal, although we realize this is a much longer-term goal and certainly more arduous to measure, is to change the culture in the hospital related to prescribing, so that hospitalists are prescribing only when appropriate, only when there’s an indicated infection, and according to the evidence base for prescribing antimicrobials for their patients.”

Future plans will include developing a mentored implementation program in which SHM will provide guidance for hospitalists who want to develop or improve a stewardship program at their hospital. The guidance will be based in part on the CDC’s “Core Elements of Hospital Antibiotic Stewardship Programs,” a kind of guidebook on antibiotic stewardship.1
Read more about antibiotic stewardship resources.
Eric Howell, MD, SFHM, director of the collaborative inpatient medicine service at Bayview, associate professor of medicine at Johns Hopkins University School of Medicine, and CHII’s senior physician advisor, says it’s time for hospitalists to take on a bigger role.
“Doing ‘just in case’ antibiotics is really not appropriate and should be strongly discouraged, unless the risks are very high for a specific patient,” he says. A past president of SHM, Dr. Howell has long advocated that hospitalists take the time to explain the risk of excessive antibiotic use to their patients, even on a busy day.
“It’s our duty as physicians to make sure our patients get the best care possible, and often that means the physicians themselves have to do the educating,” he says. “I would say that, in general, it doesn’t take that much time. Having a conversation with your patient to educate them about anything—heart failure, diabetes, appropriate antibiotics—must be built into the care that we provide our patients somehow.”
That communication doesn’t necessarily have to be performed by the hospitalist, he notes. The pharmacist, nurse, or written material can relay this information. But somewhere along the line, he says, the antibiotic education must happen.
SHM’s initiative should help, simply because “knowledge is good,” says Dr. Zenilman, the ID expert at Hopkins Bayview. Key to success, he says, will be what happens when hospitalists are taking care of a patient—will they actually be willing to cut their regimens?
“People overuse antibiotics, sometimes not out of education issues, but because they’re anxious,” Dr. Zenilman says. “The more challenging part is getting people to deal with the uncertainty and recognizing intuitively that overuse has enormous complications.”
The literature is now replete with studies showing how antibiotic stewardship measures help curb resistance, eliminate incorrect antibiotic prescribing, lower antibiotic use, and lower costs.
A web-based program was projected to save almost $400,000 a year linked to restricted antibiotic use at Johns Hopkins, according to a 2008 study.2
In Canada, according to a 2007 study, a program including recommendations for alternative drugs and shorter, guideline-based treatment durations helped reduce Clostridium difficile infections by 60% over a two-year period.3
An analysis published in August, using data from the CDC’s National Healthcare Safety Network and Emerging Infections Program, concluded that a nationwide infection control and antibiotic stewardship intervention could, over five years, avoid an estimated 619,000 hospital-acquired infections from carbapenem-resistant Enterobacteriaceae, multidrug-resistant Pseudomonas aeruginosa, invasive methicillin-resistant Staphylococcus aureus (MRSA), or C. diff.4
In spite of the evidence, preliminary results of a recent SHM survey on antibiotic stewardship found very little support, in terms of money and protected time, for hospitalists to be involved in antibiotic stewardship programs.
UM’s Success Story
A kind of microcosm of what is possible can be seen at the University of Michigan. There, Scott Flanders, MD, MHM, clinical professor of internal medicine and past president of SHM, has led an effort, along with the CDC and the Institute for Healthcare Improvement, to look at hospitalist-led interventions for smarter antimicrobial use.

Hospitalists in several programs around the country were asked to focus on a few key improvement strategies that are believed to improve use. For instance, when guidelines give a range of duration of dosing, physicians often lean toward the higher end (when the range is seven to 21 days, the default was typically closer to 21), even when that might not be necessary in a given situation. So, more specific guidelines for common situations were applied.
Hospitalists also worked to improve documentation to make antibiotic use more visible at the point of care: which drug it is, when it was started, what day of therapy it is that day, how many more days are left.
An antibiotic “timeout” at 48 to 72 hours was implemented to determine whether the treatment course should be maintained, changed, or eliminated.
The idea was for hospitalists to track this as part of the usual care process.
“We didn’t want people to create whole new systems to do these things,” says Dr. Flanders, who has consulted with SHM for its stewardship initiative. “We wanted people, for example, to use their multidisciplinary rounds that they were already having to just add one thing to the checklist.”
The process was shown to be workable. All steps of the stewardship protocol were performed 70% of the time after the initiative began, compared with just 20% of the time before it began, Dr. Flanders says. Additionally, about 25% of patients had a “significant and important” change made to their antibiotic treatment following the “timeout.”

“During this timeout, a lot of action happened,” Dr. Flanders says. More study is needed to show exactly how much of a change occurred and whether it led to cost savings, he says, but “I suspect it will.”
Much-Anticipated Partnership
Arjun Srinivasan, MD, associate director for healthcare-associated infection prevention programs at the CDC, says he is eager to continue to work with SHM on its antibiotic stewardship efforts, but he cautions that hospitalists should not try to do too much too quickly in implementing change.
“Success generally comes from starting small, from starting with a focused approach to something that you know is a problem in your facility,” Dr. Srinivasan says. “When you try to delve into everything all at once, you can very quickly get overwhelmed.”
Although smaller centers might have less manpower and face a bigger challenge in leading a stewardship program, it can be done, he says.
“We see some very small hospitals that have fantastic stewardship programs and some very small hospitals that are struggling,” he says. “We know it’s doable across the spectrum of the sizes of hospital.”
Hospitalists, he adds, “are the tip of the spear. They are probably prescribing most of the antibiotics [for inpatients] … and diagnosing most of the infections. So arming them with the information they need, working with them to develop a process that makes prescribing optimal and most efficient is obviously hugely beneficial.
“You’re going to have a tremendous impact by reaching that particular group.”
Tom Collins is a freelance writer in South Florida.
References
- Centers for Disease Control and Prevention. Core elements of hospital antibiotic stewardship programs. May 7, 2015. Accessed October 6, 2015.
- Agwu AL, Lee CK, Jain SK. A World Wide Web-based antimicrobial stewardship program improves efficiency, communication, and user satisfaction and reduces cost in a tertiary care pediatric medical center. Clin Infect Dis. 2008 Sep 15;47(6):747-753.
- Valiquette L, Cossette B, Garant MP, Diab H, Pépin J. Impact of a reduction in the use of high-risk antibiotics on the course of an epidemic of Clostridium difficile-associated disease caused by the hypervirulent NAP1/027 strain. Clin Infect Dis. 2007;45 Suppl 2:S112-S121.
- Slayton RB, Toth D, Lee BY, et al. Vital signs: estimated effects of a coordinated approach for action to reduce antibiotic-resistant infections in health care facilities - United States. MMWR Morb Mortal Wkly Rep. 2015;64(30):826-831.
In 2006, infectious disease specialists and pharmacists at Johns Hopkins Bayview Medical Center in Baltimore took a look at the pharmacy budget and were jarred by the numbers.
“The proportion of the pharmacy budget that was antimicrobials was much larger than we would expect,” says Jonathan Zenilman, MD, chief of infectious diseases at Bayview.
The pharmacy and ID teams implemented antibiotic stewardship tools, including medication reassessments after two or three days and quicker conversion to oral drugs when appropriate. They also did something that was fairly new at the time: A hospitalist was incorporated into the team. The tactic was employed out of need—the ID department was stretched too thin—but it made perfect sense, Dr. Zenilman says. Most of the patients seen by hospitalists have bread-and-butter conditions that comprise a lot of the center’s antibiotic use.
“Patients on a typical hospital medicine series are not on advanced antifungals and complicated antibiotic regimens,” he says.
The arrangement worked: The center achieved a more than 50% reduction in the main target drug, Zosyn, and a hospitalist is still typically part of the antibiotic stewardship team.
That might have been a new concept then, but fast forward a decade: ID and public health experts are increasingly seeing hospitalists as central to the effort to limit antibiotic overuse and stall the development of drug resistance in antimicrobial organisms.
Now, SHM is about to launch a campaign to get more hospitalists to see themselves as central to that effort. SHM will formally kick off the “Fight the Resistance” campaign on November 9. It’s an awareness and behavior change campaign that builds on SHM’s participation in a White House forum on antibiotic resistance that was held in June.

“We wanted to not only enhance awareness among hospitalists about what appropriate antimicrobial prescribing is, but also to change behaviors and ultimately change culture to facilitate appropriate antibiotic use,” says Jenna Goldstein, director of SHM’s Center for Hospital Innovation and Improvement (CHII), who is leading the initiative along with Mobola Owolabi, SHM project manager.
Behavior Change
The society will provide educational inserts hospitalists can use at their hospitals, as well as downloadable posters that will help raise awareness on appropriate antibiotic use. The campaign will be highlighted in SHM’s online and social media presence.
Hospitalists will be asked to make behavior changes in their antibiotic-related practices that will promote better stewardship, such as taking an antibiotic “timeout” during which usage is revisited and changed or discontinued if antibiotic use is not appropriate.
“We’re specifically asking hospitalists to engage in behavior changes and we plan to assess outcomes and results after implementation,” Goldstein says. “Our ultimate goal, although we realize this is a much longer-term goal and certainly more arduous to measure, is to change the culture in the hospital related to prescribing, so that hospitalists are prescribing only when appropriate, only when there’s an indicated infection, and according to the evidence base for prescribing antimicrobials for their patients.”

Future plans will include developing a mentored implementation program in which SHM will provide guidance for hospitalists who want to develop or improve a stewardship program at their hospital. The guidance will be based in part on the CDC’s “Core Elements of Hospital Antibiotic Stewardship Programs,” a kind of guidebook on antibiotic stewardship.1
Read more about antibiotic stewardship resources.
Eric Howell, MD, SFHM, director of the collaborative inpatient medicine service at Bayview, associate professor of medicine at Johns Hopkins University School of Medicine, and CHII’s senior physician advisor, says it’s time for hospitalists to take on a bigger role.
“Doing ‘just in case’ antibiotics is really not appropriate and should be strongly discouraged, unless the risks are very high for a specific patient,” he says. A past president of SHM, Dr. Howell has long advocated that hospitalists take the time to explain the risk of excessive antibiotic use to their patients, even on a busy day.
“It’s our duty as physicians to make sure our patients get the best care possible, and often that means the physicians themselves have to do the educating,” he says. “I would say that, in general, it doesn’t take that much time. Having a conversation with your patient to educate them about anything—heart failure, diabetes, appropriate antibiotics—must be built into the care that we provide our patients somehow.”
That communication doesn’t necessarily have to be performed by the hospitalist, he notes. The pharmacist, nurse, or written material can relay this information. But somewhere along the line, he says, the antibiotic education must happen.
SHM’s initiative should help, simply because “knowledge is good,” says Dr. Zenilman, the ID expert at Hopkins Bayview. Key to success, he says, will be what happens when hospitalists are taking care of a patient—will they actually be willing to cut their regimens?
“People overuse antibiotics, sometimes not out of education issues, but because they’re anxious,” Dr. Zenilman says. “The more challenging part is getting people to deal with the uncertainty and recognizing intuitively that overuse has enormous complications.”
The literature is now replete with studies showing how antibiotic stewardship measures help curb resistance, eliminate incorrect antibiotic prescribing, lower antibiotic use, and lower costs.
A web-based program was projected to save almost $400,000 a year linked to restricted antibiotic use at Johns Hopkins, according to a 2008 study.2
In Canada, according to a 2007 study, a program including recommendations for alternative drugs and shorter, guideline-based treatment durations helped reduce Clostridium difficile infections by 60% over a two-year period.3
An analysis published in August, using data from the CDC’s National Healthcare Safety Network and Emerging Infections Program, concluded that a nationwide infection control and antibiotic stewardship intervention could, over five years, avoid an estimated 619,000 hospital-acquired infections from carbapenem-resistant Enterobacteriaceae, multidrug-resistant Pseudomonas aeruginosa, invasive methicillin-resistant Staphylococcus aureus (MRSA), or C. diff.4
In spite of the evidence, preliminary results of a recent SHM survey on antibiotic stewardship found very little support, in terms of money and protected time, for hospitalists to be involved in antibiotic stewardship programs.
UM’s Success Story
A kind of microcosm of what is possible can be seen at the University of Michigan. There, Scott Flanders, MD, MHM, clinical professor of internal medicine and past president of SHM, has led an effort, along with the CDC and the Institute for Healthcare Improvement, to look at hospitalist-led interventions for smarter antimicrobial use.

Hospitalists in several programs around the country were asked to focus on a few key improvement strategies that are believed to improve use. For instance, when guidelines give a range of duration of dosing, physicians often lean toward the higher end (when the range is seven to 21 days, the default was typically closer to 21), even when that might not be necessary in a given situation. So, more specific guidelines for common situations were applied.
Hospitalists also worked to improve documentation to make antibiotic use more visible at the point of care: which drug it is, when it was started, what day of therapy it is that day, how many more days are left.
An antibiotic “timeout” at 48 to 72 hours was implemented to determine whether the treatment course should be maintained, changed, or eliminated.
The idea was for hospitalists to track this as part of the usual care process.
“We didn’t want people to create whole new systems to do these things,” says Dr. Flanders, who has consulted with SHM for its stewardship initiative. “We wanted people, for example, to use their multidisciplinary rounds that they were already having to just add one thing to the checklist.”
The process was shown to be workable. All steps of the stewardship protocol were performed 70% of the time after the initiative began, compared with just 20% of the time before it began, Dr. Flanders says. Additionally, about 25% of patients had a “significant and important” change made to their antibiotic treatment following the “timeout.”

“During this timeout, a lot of action happened,” Dr. Flanders says. More study is needed to show exactly how much of a change occurred and whether it led to cost savings, he says, but “I suspect it will.”
Much-Anticipated Partnership
Arjun Srinivasan, MD, associate director for healthcare-associated infection prevention programs at the CDC, says he is eager to continue to work with SHM on its antibiotic stewardship efforts, but he cautions that hospitalists should not try to do too much too quickly in implementing change.
“Success generally comes from starting small, from starting with a focused approach to something that you know is a problem in your facility,” Dr. Srinivasan says. “When you try to delve into everything all at once, you can very quickly get overwhelmed.”
Although smaller centers might have less manpower and face a bigger challenge in leading a stewardship program, it can be done, he says.
“We see some very small hospitals that have fantastic stewardship programs and some very small hospitals that are struggling,” he says. “We know it’s doable across the spectrum of the sizes of hospital.”
Hospitalists, he adds, “are the tip of the spear. They are probably prescribing most of the antibiotics [for inpatients] … and diagnosing most of the infections. So arming them with the information they need, working with them to develop a process that makes prescribing optimal and most efficient is obviously hugely beneficial.
“You’re going to have a tremendous impact by reaching that particular group.”
Tom Collins is a freelance writer in South Florida.
References
- Centers for Disease Control and Prevention. Core elements of hospital antibiotic stewardship programs. May 7, 2015. Accessed October 6, 2015.
- Agwu AL, Lee CK, Jain SK. A World Wide Web-based antimicrobial stewardship program improves efficiency, communication, and user satisfaction and reduces cost in a tertiary care pediatric medical center. Clin Infect Dis. 2008 Sep 15;47(6):747-753.
- Valiquette L, Cossette B, Garant MP, Diab H, Pépin J. Impact of a reduction in the use of high-risk antibiotics on the course of an epidemic of Clostridium difficile-associated disease caused by the hypervirulent NAP1/027 strain. Clin Infect Dis. 2007;45 Suppl 2:S112-S121.
- Slayton RB, Toth D, Lee BY, et al. Vital signs: estimated effects of a coordinated approach for action to reduce antibiotic-resistant infections in health care facilities - United States. MMWR Morb Mortal Wkly Rep. 2015;64(30):826-831.
Hospital Medicine Flourishing Around the World
Since last September, Anand Kartha, MD, MS, has headed the hospital medicine (HM) program at 600-bed Hamad General Hospital, the flagship facility for eight-hospital Hamad Medical Corporation in Doha, Qatar, a small nation of 1.8 million people located on the northeast corner of the Arabian Peninsula.
“Qatar has a world-class healthcare system,” he says. “But to me, it sometimes feels like 1999, with the beginnings of the hospitalist movement as a new model of care.”
Dr. Kartha, a native of India who trained at the University of Pittsburgh Medical Center Mercy and Boston University School of Medicine, was recruited by Hamad Medical Corporation to develop hospital medicine in response to the growing complexity of inpatient care—and of patients served.
“Hospital medicine, delivered 24/7 by attending physicians, is an important element of the Health Ministry’s strategy and vision,” he says. “They looked at Australian, British, and American health systems, trying to put together the best from each—adapted to local sensitivities.
“One reason I came here was to expand the hospitalist model and be part of its extraordinary growth and development.”
Dr. Kartha also participates in medical research and residency training. His group now employs 30 attending physicians, half of them recent hires from the U.S. and the U.K.
As in the U.S., international drivers for the hospitalist model of care include pressures to improve efficiency, throughput, and quality of care. Those drivers are especially in focus at Hamad General, which Dr. Kartha says has one of the busiest EDs in the world.
Hospital medicine programs are springing up in other parts of the world, too, often inspired by the success of the HM model in the U.S. Hospitalist pioneers from other countries pore over the published research and visit the U.S. to attend conferences like SHM’s annual meeting, with its programming for international members, or to complete fellowships or other trainings. U.S. hospitalists are invited to speak to groups in other countries. Some, like Dr. Kartha, are being tapped to build hospitalist programs around the globe.

Hospital medicine can be introduced from the top down as a strategy by the public health system or from the bottom up by pioneers and advocates at the grassroots level.
Ron Greeno, MD, MHM, FCCP, has been active in hospital medicine since before the term “hospitalist” was coined. Currently chief strategy officer with IPC Healthcare, Inc., he was a founder in 1993 of Cogent Healthcare, which recently merged with Sound Physicians in Tacoma, Wash. Dr. Greeno says he is fascinated by the growth in international hospital medicine.
“I have been impressed at the number of countries that are represented at SHM [meetings] and the enthusiasm they show as they talk about their experiences,” he says. “What I see in these young, enthusiastic physicians from around the world is they are not naïve, but they are very idealistic. Their descriptions of their struggles remind me of our early days in Southern California.
“The international representatives at SHM all recognize the need for data. Every one of them feels their hospitalist model has advantages for their health system. But everybody’s struggling with the need for more resources. That’s the same in the U.S.”
Similarities and Differences
Many aspects of the experience in Qatar have been surprisingly familiar for Dr. Kartha.
“We are a Joint Commission-accredited hospital,” he says. “Our residency program is accredited by the American College of Graduate Medical Education. We are the flagship hospital for Weill Cornell Medical College in Qatar.”
The workday of a hospitalist at Hamad General is strikingly similar to the one he knew as an academic hospitalist in Boston.
“Models we are introducing include extended hours coverage, evenings and weekends, proactive discharge planning, and co-management with specialists,” he says. The health system is also rolling out an electronic health record.
Still, his adaptation to a new medical system has generated many curiosities in the sports-mad, fully wired-for-Internet nation, which has the world’s highest per capita standard of living.
“Every now and then, I look around and think: ‘This isn’t Kansas anymore, Toto,’” Dr. Kartha says, adding that he has learned about important cultural and religious beliefs and traditions that affect patients’ attitudes toward health and healing.
Arpana Vidyarthi, MD, associate professor in the Duke-NUS Graduate Medical School in Singapore, previously worked as a hospitalist at the University of California-San Francisco (UCSF) before moving to Singapore in 2011. She thinks “pockets” of hospital medicine are being practiced all over the world “in response to local needs.”
“The model is manifest in a diverse fashion throughout the United States, yet it is agile enough to be adapted around the world and be truly relevant,” Dr. Vidyarthi says. “But local tradition and the way hospitals are structured will determine how the model is established.”
Traditionally, medical specialists, often without a central physician to coordinate care, manage inpatients in Singapore, according to Dr. Vidyarthi. At discharge, they are referred to numerous subspecialists and to a public health clinic. Half of hospital wards are staffed by “super-specialists,” the other half by general internists who see patients both in the clinic and in the hospital, she says.
“This is not hospital medicine as we know it in the United States,” she says, “but different models are evolving.”
Ten years ago, physicians from Singapore visited UCSF to observe how hospital medicine was practiced there. A family medicine hospitalist program was piloted in 2006 at Singapore General Hospital. The program helped reduce lengths of stay and costs of care without adversely affecting mortality or readmissions.1
Kheng-Hock Lee, MD, one of the researchers and president of the Singapore College of Family Physicians, says that defining a generalist role for hospital medicine in Singapore has been difficult.
“When I call myself a hospitalist here, there is a strong reaction from some who perceive it as profit driven,” Dr. Vidyarthi says. “Clearly, there is a need for a generalist physician at the center of the patient experience, to manage the complexity of the patient as a whole person, as well as the hospital system. That is where it’s emerging within internal medicine, whether it’s called hospital medicine or not.”
For the past year, Dr. Vidyarthi has been working at Singapore General.
“The concept of the academic hospitalist is new here. People are able to see when I’m on service that I do things differently. This is because of the hospitalist mindset I brought from the United States,” she says. “Because I have a systems lens, I organize my day differently than the other doctors. I teach concurrently with clinical care, delegate responsibilities and accountabilities, and focus on discharge from the first day of admission.
“In general, my team is happier and my patients have lower lengths of stay.”
Defining a Specialized Expertise
Whatever you call it, there is a need around the world for physicians to practice in hospitals—to help standardize care, improve quality and patient safety, and prevent waste. Peter Jamieson, MD, a family physician in Calgary, Alberta, Canada, and medical director of the Foothills Medical Centre, has worked as a hospitalist since 1997. He didn’t call himself a hospitalist at first, “but the concept is becoming better socialized and more widely recognized in Canada.”
The Canadian Society of Hospital Medicine, founded in 2001 and affiliated with SHM, has about 1,300 members.
“I’d say we’re more the same than different compared with the United States, with a similar focus on quality of care,” Dr. Jamieson says.
Interestingly, he says the moniker “hospitalist” is not helping the development—and recognition—of Canadians who practice hospital-based medicine. It’s a refrain echoed for years by many in the U.S.
“As leaders in hospital medicine in Canada, we’d prefer to move away from the term ‘hospitalist’ and toward ‘specialist’ or ‘expert in hospital medicine,’” he says. “That takes us more in the direction we want to go in defining the mission of hospital medicine.

“First of all, in Canada and other places, there’s a bit of baggage attached to the term ‘hospitalist.’ These other terms help us get away from some of the historical assumptions of what people thought a hospitalist was—based on educational background.”
In Canada, that has largely been family medicine. Hospital medicine advocates are now exploring the best preparation for practicing the specialty.
“We want to define the mission around competency, rather than board certification,” Dr. Jamieson explains.
Listen to Dr. Jamieson discuss the evolution of hospital medicine in Canada.
The days when the majority of Canadian primary care providers would join the staff of a hospital and continue to manage their patients’ care during the hospital stay are long gone, he adds. In smaller and rural hospitals, the family doctor may still be the physician of record, although the number of such hospitals is dwindling.
HM clinicians generally are not employed by the hospital but often are sole practitioners with independent corporations or organized into groups that associate for the sake of the practice, signing a common contract with the hospital. Depending on provincial law, most hospitalist groups have leaders appointed and compensated by the hospital for scheduling and coordination.
On top of billing fee-for-service to the provincial health authority, hospitalists may also receive a stipend from the hospital, collectively or individually.
“There is a recognition that the physician fee schedule has not kept pace with the demands of hospital medicine, and that stipend also covers other services performed in the hospital,” Dr. Jamieson says.
Vandad Yousefi, MD, CCFP, FHM, hospitalist at Vancouver General Hospital in British Columbia, Canada, and co-founder and CEO of Hospitalist Consulting Solutions, has researched the development of hospital medicine in Canada and says that, even more than in the U.S., it was driven by the withdrawal of PCPs from hospitals, which created a vacuum.2,3
“For a lot of programs I’ve consulted with, the crisis point happened when physicians resigned en masse from hospital staffs,” he says.
Another driver is an increase in “unattached” hospitalized patients, which in Canada means they don’t have a specific medical provider willing to supply their inpatient attending-level care. In his surveys of typologies of roles played by hospitalists, Dr. Yousefi has observed a lot of variation in program models—not just between academic centers, teaching hospitals, and rural hospitals, but also within each category.
“These differences in programs make it hard to benchmark,” he says.
Hospitalist—or House Officer?
The Netherlands also has “hospitalists,” although they also refer to themselves as “house officers,” says Marijke Timmermans, a doctoral student in epidemiology at the Scientific Institute for Quality of Healthcare at Radboud University Medical Center in Nijmegen. As part of a long-standing system of post-graduate, on-the-job training for doctors, Dutch hospitalists typically are medical residents who perform the medical care of hospitalized patients, but not as the physician of record.
Timmermans is studying the growing role of physician assistants (PAs) in managing hospitalized patients in response to demands for better continuity of care. Although the PA concept is little more than a decade old in the Netherlands, there are 1,000 PAs, with about half filling a hospitalist role under the supervision of a medical specialist. Timmermans’ research looks at the effectiveness and quality of care with PAs under a mixed model of PA and physician, compared with physician alone.4

In the Netherlands, the patient’s PCP does not assume medical management responsibility while the patient is hospitalized, although PCP visits might be made to reassure the patient and advise the hospital-based team. As in the U.S., the hospitalist will try to communicate with the primary care doctor at discharge and, if possible, schedule follow-up visits for the discharged patient at a clinic on the hospital campus.
A new experiment is underway in four Dutch hospitals. It’s a three-year medical education curriculum to train “hospital doctors” (ziekenhuisarts). The new medical specialty, with general medical training, will assume more responsibility for ward care in the hospital. Timmermans says it is not yet known how these professionals will relate to other professionals in the hospital.
Joseph Li, MD, SFHM, head of hospital medicine at Beth Israel Deaconess Medical Center in Boston and past president of SHM, notes a key distinction between hospitalists as they are commonly understood in the U.S. and house officers: House officers don’t assume medical responsibility for the patient’s care.
“A house officer is not a hospitalist as we understand it—but even in this country, terminology varies and means different things in different hospitals,” Dr. Li says.
The Acute Medical Unit
In the U.K., a different model has emerged over the past two decades. It is called the acute medical unit [PDF] (AMU) and is staffed by dedicated consultants.5 The AMU fits functionally between the hospital’s ED, or front door admissions, and specialty care units within the hospital.
Patients generally are admitted to the AMU for a maximum of 72 hours for medical work-ups, with consultations as needed by specialists. They should be seen twice a day by the acute medical consultant, who is responsible for the delivery and direction of their care. Then they either go home or get transferred to a specialty unit within the hospital, with specialty care organized in a manner broadly similar to the U.S.
This frontloading of medical attention at admission allows patients to be worked up and turned around quickly, says Derek Bell, MD, head of acute medicine at Imperial College London and a founder in 2000 of the U.K.’s Society for Acute Medicine. Dr. Bell suggests that this system developed to ensure a safe haven for medical patients who are unstable or require ongoing investigation and treatment. A national “four-hour rule,” designed to reduce overcrowding in EDs, means that patients need to either go home or be admitted within four hours of presentation to the hospital.
U.K. hospitals also employ a registrar, a senior trainee who supervises junior and resident doctors. Hospital physicians are salaried and employed by “provider organizations,” which can be a single hospital or a collection of hospitals.
“My hospital admits about 30 to 35 medical patients per day, and we have two consultants working during the day just doing acute medicine, along with two registrars, one for emergency patients, two intermediate grade doctors, and two junior residents,” Dr. Bell says.
Acute medicine consultants generally do weekday shifts, with one consultant on call per night.
A few hospitals have embedded PCPs, who know the local system and can facilitate communication with the patient’s family doctor. “This model is well recognized but is not common,” Dr. Bell says.
What’s Happening Elsewhere?
In Australia, public hospitals in New South Wales generated positive results for a hospitalist pilot program in 2007, but also encountered some resistance from the Australian Medical Association and others concerned about its potential impact on such existing roles as career medical officer, PCP, and general physician, and on the provision of medical training in hospitals.6
Hospital medicine has grown since then, but slowly, with individual institutions successfully employing hospitalists at various levels. The fledgling specialty has yet to take off nationally, says Mary G.T. Webber, MBBS, a past president of the Australasian Society of Career Medical Officers. Dr. Webber practices hospital medicine at Ryde Hospital in suburban Sydney, where she has found the mix of clinical care, system development, and mentoring roles offered by the service personally rewarding. She has been frustrated with a lack of progress for the hospitalist movement overall in Australia.
“The concept of a rural generalist is already well accepted in Australia, and hospital medicine is the next logical iteration of the medical generalist,” Dr. Webber says. This need has been supported by the NSW Ministry of Health through a Hospital Skills Program, and, more recently, the successful implementation of a master’s degree for experienced nonspecialist doctors through the Senior Hospitalist Initiative at the University of Newcastle.

“Once you adopt a system view of patient care in hospitals, there is no going back,” says Dr. Webber, who was lead author of the hospital skills program curriculum in hospital medicine. “This is an idea whose time has come.”
A pioneering hospitalist program at National Taiwan University Hospital in Taipei (NTUH) was established by internists with diverse specializations in pulmonology, nephrology, infectious diseases, and family medicine and is led by Hung-Bin Tsai, MD, and Nin-Chieh Hsu, MD.7,8 Because of relatively low salaries for generalist physicians and a national health insurance program that incentivizes patient access to specialists, 95% of internal medicine doctors in Taiwan have chosen to subspecialize, Dr. Hsu says.
Other barriers to the dissemination of hospital medicine in Taiwan include a shortage of internal medicine residents and resident work-hour restrictions mandated by the country’s Ministry of Health, with resulting heavy work schedules for internal medicine attending physicians, who average 64 hours per week. Advocates believe the hospitalist model could help promote better work-life-salary balance for inpatient physicians.
“We are trying to persuade the Ministry of Health to pay a fair reimbursement for inpatient care,” Dr. Hsu says.
The pioneer hospitalist program at NTUH, developed in 2009 in a 36-bed, hospitalist-run ward, now 70 beds, has this year been joined by more than 20 other hospital medicine programs under an initiative of the Ministry of Health. Auspiciously, the chief of the pioneer hospitalist program at NTUH, Wen-je Ko, MD, PhD, was elected mayor of Taipei earlier this year. A Taiwanese Society of Hospital Medicine should be up and running by late 2015, says Dr. Tsai, who is its chief facilitator. When that happens, organizers expect hospital medicine to finally take off in Taiwan.
The Future Is Now
When Dr. Greeno talks to international hospitalists, he says, “If you’re doing a good job, that creates value for somebody. Find out who that is—that’s where you need to go to get your resources, financial or otherwise. Is it your individual hospital or your national health system? Everybody wants to deliver better care at lower cost. When you do that, that’s your driver for growth.”
Something about the hospitalist model, he adds, “just makes sense.”
“There are people virtually everywhere who are very enthusiastic about it. We in the United States can learn a lot from their enthusiasm,” he says. “It will evolve in different ways. The future is already here; it’s just unevenly distributed.”
Larry Beresford is a freelance writer in Alameda, Calif.
References
- Hock Lee K, Yang Y, Soong Yang K, Chi Ong B, Seong Ng H. Bringing generalists into the hospital: outcomes of a family medicine hospitalist model in Singapore. J Hosp Med. 2011;6(3):115-121.
- Yousefi V, Chong CAKY. Does implementation of a hospitalist program in a Canadian community hospital improve measures of quality of care and utilization? An observational comparative analysis of hospitalists vs. traditional care providers. BMC Health Serv Res. 2013;13:204.
- Timmermans MJC, van Vught AJAH, Wensing M, Laurant MGH. The effectiveness of substitution of hospital ward care from medical doctors to physician assistants: a study protocol. BMC Health Serv Res.; 2014;14:43.
- Black C. Acute medicine: making it work for patients. Hosp Med. 2004;65(8):493-496.
- Australian Medical Association. AMA Position Statement: Hospitalists – 2008. October 21, 2008. Accessed October 5, 2015.
- Shu CC, Lin JW, Lin YF, Hsu NC, Ko WJ. Evaluating the performance of a hospitalist system in Taiwan: A pioneer study for nationwide health insurance in Asia. J Hosp Med. 2011;6(7):378-382.
- Shu CC, Hsu NC, Lin YF, Wang JY, Lin JW, Ko WJ. Integrated postdischarge transitional care in a hospitalist system to improve discharge outcome: an experimental study. BMC Med. 2011;9:96.
- Carmona-Torre F, Martinez-Urbistondo D, Landecho MF, Lucena JF. Surviving sepsis in an intermediate care unit. Lancet Infect Dis. 2013;13(4):294-295.
- Lucena JF, Alegre F, Rodil R, et al. Results of a retrospective observational study of intermediate care staffed by hospitalists: impact on mortality, co-management, and teaching. J Hosp Med. 2012;7(5):411-415.
Since last September, Anand Kartha, MD, MS, has headed the hospital medicine (HM) program at 600-bed Hamad General Hospital, the flagship facility for eight-hospital Hamad Medical Corporation in Doha, Qatar, a small nation of 1.8 million people located on the northeast corner of the Arabian Peninsula.
“Qatar has a world-class healthcare system,” he says. “But to me, it sometimes feels like 1999, with the beginnings of the hospitalist movement as a new model of care.”
Dr. Kartha, a native of India who trained at the University of Pittsburgh Medical Center Mercy and Boston University School of Medicine, was recruited by Hamad Medical Corporation to develop hospital medicine in response to the growing complexity of inpatient care—and of patients served.
“Hospital medicine, delivered 24/7 by attending physicians, is an important element of the Health Ministry’s strategy and vision,” he says. “They looked at Australian, British, and American health systems, trying to put together the best from each—adapted to local sensitivities.
“One reason I came here was to expand the hospitalist model and be part of its extraordinary growth and development.”
Dr. Kartha also participates in medical research and residency training. His group now employs 30 attending physicians, half of them recent hires from the U.S. and the U.K.
As in the U.S., international drivers for the hospitalist model of care include pressures to improve efficiency, throughput, and quality of care. Those drivers are especially in focus at Hamad General, which Dr. Kartha says has one of the busiest EDs in the world.
Hospital medicine programs are springing up in other parts of the world, too, often inspired by the success of the HM model in the U.S. Hospitalist pioneers from other countries pore over the published research and visit the U.S. to attend conferences like SHM’s annual meeting, with its programming for international members, or to complete fellowships or other trainings. U.S. hospitalists are invited to speak to groups in other countries. Some, like Dr. Kartha, are being tapped to build hospitalist programs around the globe.

Hospital medicine can be introduced from the top down as a strategy by the public health system or from the bottom up by pioneers and advocates at the grassroots level.
Ron Greeno, MD, MHM, FCCP, has been active in hospital medicine since before the term “hospitalist” was coined. Currently chief strategy officer with IPC Healthcare, Inc., he was a founder in 1993 of Cogent Healthcare, which recently merged with Sound Physicians in Tacoma, Wash. Dr. Greeno says he is fascinated by the growth in international hospital medicine.
“I have been impressed at the number of countries that are represented at SHM [meetings] and the enthusiasm they show as they talk about their experiences,” he says. “What I see in these young, enthusiastic physicians from around the world is they are not naïve, but they are very idealistic. Their descriptions of their struggles remind me of our early days in Southern California.
“The international representatives at SHM all recognize the need for data. Every one of them feels their hospitalist model has advantages for their health system. But everybody’s struggling with the need for more resources. That’s the same in the U.S.”
Similarities and Differences
Many aspects of the experience in Qatar have been surprisingly familiar for Dr. Kartha.
“We are a Joint Commission-accredited hospital,” he says. “Our residency program is accredited by the American College of Graduate Medical Education. We are the flagship hospital for Weill Cornell Medical College in Qatar.”
The workday of a hospitalist at Hamad General is strikingly similar to the one he knew as an academic hospitalist in Boston.
“Models we are introducing include extended hours coverage, evenings and weekends, proactive discharge planning, and co-management with specialists,” he says. The health system is also rolling out an electronic health record.
Still, his adaptation to a new medical system has generated many curiosities in the sports-mad, fully wired-for-Internet nation, which has the world’s highest per capita standard of living.
“Every now and then, I look around and think: ‘This isn’t Kansas anymore, Toto,’” Dr. Kartha says, adding that he has learned about important cultural and religious beliefs and traditions that affect patients’ attitudes toward health and healing.
Arpana Vidyarthi, MD, associate professor in the Duke-NUS Graduate Medical School in Singapore, previously worked as a hospitalist at the University of California-San Francisco (UCSF) before moving to Singapore in 2011. She thinks “pockets” of hospital medicine are being practiced all over the world “in response to local needs.”
“The model is manifest in a diverse fashion throughout the United States, yet it is agile enough to be adapted around the world and be truly relevant,” Dr. Vidyarthi says. “But local tradition and the way hospitals are structured will determine how the model is established.”
Traditionally, medical specialists, often without a central physician to coordinate care, manage inpatients in Singapore, according to Dr. Vidyarthi. At discharge, they are referred to numerous subspecialists and to a public health clinic. Half of hospital wards are staffed by “super-specialists,” the other half by general internists who see patients both in the clinic and in the hospital, she says.
“This is not hospital medicine as we know it in the United States,” she says, “but different models are evolving.”
Ten years ago, physicians from Singapore visited UCSF to observe how hospital medicine was practiced there. A family medicine hospitalist program was piloted in 2006 at Singapore General Hospital. The program helped reduce lengths of stay and costs of care without adversely affecting mortality or readmissions.1
Kheng-Hock Lee, MD, one of the researchers and president of the Singapore College of Family Physicians, says that defining a generalist role for hospital medicine in Singapore has been difficult.
“When I call myself a hospitalist here, there is a strong reaction from some who perceive it as profit driven,” Dr. Vidyarthi says. “Clearly, there is a need for a generalist physician at the center of the patient experience, to manage the complexity of the patient as a whole person, as well as the hospital system. That is where it’s emerging within internal medicine, whether it’s called hospital medicine or not.”
For the past year, Dr. Vidyarthi has been working at Singapore General.
“The concept of the academic hospitalist is new here. People are able to see when I’m on service that I do things differently. This is because of the hospitalist mindset I brought from the United States,” she says. “Because I have a systems lens, I organize my day differently than the other doctors. I teach concurrently with clinical care, delegate responsibilities and accountabilities, and focus on discharge from the first day of admission.
“In general, my team is happier and my patients have lower lengths of stay.”
Defining a Specialized Expertise
Whatever you call it, there is a need around the world for physicians to practice in hospitals—to help standardize care, improve quality and patient safety, and prevent waste. Peter Jamieson, MD, a family physician in Calgary, Alberta, Canada, and medical director of the Foothills Medical Centre, has worked as a hospitalist since 1997. He didn’t call himself a hospitalist at first, “but the concept is becoming better socialized and more widely recognized in Canada.”
The Canadian Society of Hospital Medicine, founded in 2001 and affiliated with SHM, has about 1,300 members.
“I’d say we’re more the same than different compared with the United States, with a similar focus on quality of care,” Dr. Jamieson says.
Interestingly, he says the moniker “hospitalist” is not helping the development—and recognition—of Canadians who practice hospital-based medicine. It’s a refrain echoed for years by many in the U.S.
“As leaders in hospital medicine in Canada, we’d prefer to move away from the term ‘hospitalist’ and toward ‘specialist’ or ‘expert in hospital medicine,’” he says. “That takes us more in the direction we want to go in defining the mission of hospital medicine.

“First of all, in Canada and other places, there’s a bit of baggage attached to the term ‘hospitalist.’ These other terms help us get away from some of the historical assumptions of what people thought a hospitalist was—based on educational background.”
In Canada, that has largely been family medicine. Hospital medicine advocates are now exploring the best preparation for practicing the specialty.
“We want to define the mission around competency, rather than board certification,” Dr. Jamieson explains.
Listen to Dr. Jamieson discuss the evolution of hospital medicine in Canada.
The days when the majority of Canadian primary care providers would join the staff of a hospital and continue to manage their patients’ care during the hospital stay are long gone, he adds. In smaller and rural hospitals, the family doctor may still be the physician of record, although the number of such hospitals is dwindling.
HM clinicians generally are not employed by the hospital but often are sole practitioners with independent corporations or organized into groups that associate for the sake of the practice, signing a common contract with the hospital. Depending on provincial law, most hospitalist groups have leaders appointed and compensated by the hospital for scheduling and coordination.
On top of billing fee-for-service to the provincial health authority, hospitalists may also receive a stipend from the hospital, collectively or individually.
“There is a recognition that the physician fee schedule has not kept pace with the demands of hospital medicine, and that stipend also covers other services performed in the hospital,” Dr. Jamieson says.
Vandad Yousefi, MD, CCFP, FHM, hospitalist at Vancouver General Hospital in British Columbia, Canada, and co-founder and CEO of Hospitalist Consulting Solutions, has researched the development of hospital medicine in Canada and says that, even more than in the U.S., it was driven by the withdrawal of PCPs from hospitals, which created a vacuum.2,3
“For a lot of programs I’ve consulted with, the crisis point happened when physicians resigned en masse from hospital staffs,” he says.
Another driver is an increase in “unattached” hospitalized patients, which in Canada means they don’t have a specific medical provider willing to supply their inpatient attending-level care. In his surveys of typologies of roles played by hospitalists, Dr. Yousefi has observed a lot of variation in program models—not just between academic centers, teaching hospitals, and rural hospitals, but also within each category.
“These differences in programs make it hard to benchmark,” he says.
Hospitalist—or House Officer?
The Netherlands also has “hospitalists,” although they also refer to themselves as “house officers,” says Marijke Timmermans, a doctoral student in epidemiology at the Scientific Institute for Quality of Healthcare at Radboud University Medical Center in Nijmegen. As part of a long-standing system of post-graduate, on-the-job training for doctors, Dutch hospitalists typically are medical residents who perform the medical care of hospitalized patients, but not as the physician of record.
Timmermans is studying the growing role of physician assistants (PAs) in managing hospitalized patients in response to demands for better continuity of care. Although the PA concept is little more than a decade old in the Netherlands, there are 1,000 PAs, with about half filling a hospitalist role under the supervision of a medical specialist. Timmermans’ research looks at the effectiveness and quality of care with PAs under a mixed model of PA and physician, compared with physician alone.4

In the Netherlands, the patient’s PCP does not assume medical management responsibility while the patient is hospitalized, although PCP visits might be made to reassure the patient and advise the hospital-based team. As in the U.S., the hospitalist will try to communicate with the primary care doctor at discharge and, if possible, schedule follow-up visits for the discharged patient at a clinic on the hospital campus.
A new experiment is underway in four Dutch hospitals. It’s a three-year medical education curriculum to train “hospital doctors” (ziekenhuisarts). The new medical specialty, with general medical training, will assume more responsibility for ward care in the hospital. Timmermans says it is not yet known how these professionals will relate to other professionals in the hospital.
Joseph Li, MD, SFHM, head of hospital medicine at Beth Israel Deaconess Medical Center in Boston and past president of SHM, notes a key distinction between hospitalists as they are commonly understood in the U.S. and house officers: House officers don’t assume medical responsibility for the patient’s care.
“A house officer is not a hospitalist as we understand it—but even in this country, terminology varies and means different things in different hospitals,” Dr. Li says.
The Acute Medical Unit
In the U.K., a different model has emerged over the past two decades. It is called the acute medical unit [PDF] (AMU) and is staffed by dedicated consultants.5 The AMU fits functionally between the hospital’s ED, or front door admissions, and specialty care units within the hospital.
Patients generally are admitted to the AMU for a maximum of 72 hours for medical work-ups, with consultations as needed by specialists. They should be seen twice a day by the acute medical consultant, who is responsible for the delivery and direction of their care. Then they either go home or get transferred to a specialty unit within the hospital, with specialty care organized in a manner broadly similar to the U.S.
This frontloading of medical attention at admission allows patients to be worked up and turned around quickly, says Derek Bell, MD, head of acute medicine at Imperial College London and a founder in 2000 of the U.K.’s Society for Acute Medicine. Dr. Bell suggests that this system developed to ensure a safe haven for medical patients who are unstable or require ongoing investigation and treatment. A national “four-hour rule,” designed to reduce overcrowding in EDs, means that patients need to either go home or be admitted within four hours of presentation to the hospital.
U.K. hospitals also employ a registrar, a senior trainee who supervises junior and resident doctors. Hospital physicians are salaried and employed by “provider organizations,” which can be a single hospital or a collection of hospitals.
“My hospital admits about 30 to 35 medical patients per day, and we have two consultants working during the day just doing acute medicine, along with two registrars, one for emergency patients, two intermediate grade doctors, and two junior residents,” Dr. Bell says.
Acute medicine consultants generally do weekday shifts, with one consultant on call per night.
A few hospitals have embedded PCPs, who know the local system and can facilitate communication with the patient’s family doctor. “This model is well recognized but is not common,” Dr. Bell says.
What’s Happening Elsewhere?
In Australia, public hospitals in New South Wales generated positive results for a hospitalist pilot program in 2007, but also encountered some resistance from the Australian Medical Association and others concerned about its potential impact on such existing roles as career medical officer, PCP, and general physician, and on the provision of medical training in hospitals.6
Hospital medicine has grown since then, but slowly, with individual institutions successfully employing hospitalists at various levels. The fledgling specialty has yet to take off nationally, says Mary G.T. Webber, MBBS, a past president of the Australasian Society of Career Medical Officers. Dr. Webber practices hospital medicine at Ryde Hospital in suburban Sydney, where she has found the mix of clinical care, system development, and mentoring roles offered by the service personally rewarding. She has been frustrated with a lack of progress for the hospitalist movement overall in Australia.
“The concept of a rural generalist is already well accepted in Australia, and hospital medicine is the next logical iteration of the medical generalist,” Dr. Webber says. This need has been supported by the NSW Ministry of Health through a Hospital Skills Program, and, more recently, the successful implementation of a master’s degree for experienced nonspecialist doctors through the Senior Hospitalist Initiative at the University of Newcastle.

“Once you adopt a system view of patient care in hospitals, there is no going back,” says Dr. Webber, who was lead author of the hospital skills program curriculum in hospital medicine. “This is an idea whose time has come.”
A pioneering hospitalist program at National Taiwan University Hospital in Taipei (NTUH) was established by internists with diverse specializations in pulmonology, nephrology, infectious diseases, and family medicine and is led by Hung-Bin Tsai, MD, and Nin-Chieh Hsu, MD.7,8 Because of relatively low salaries for generalist physicians and a national health insurance program that incentivizes patient access to specialists, 95% of internal medicine doctors in Taiwan have chosen to subspecialize, Dr. Hsu says.
Other barriers to the dissemination of hospital medicine in Taiwan include a shortage of internal medicine residents and resident work-hour restrictions mandated by the country’s Ministry of Health, with resulting heavy work schedules for internal medicine attending physicians, who average 64 hours per week. Advocates believe the hospitalist model could help promote better work-life-salary balance for inpatient physicians.
“We are trying to persuade the Ministry of Health to pay a fair reimbursement for inpatient care,” Dr. Hsu says.
The pioneer hospitalist program at NTUH, developed in 2009 in a 36-bed, hospitalist-run ward, now 70 beds, has this year been joined by more than 20 other hospital medicine programs under an initiative of the Ministry of Health. Auspiciously, the chief of the pioneer hospitalist program at NTUH, Wen-je Ko, MD, PhD, was elected mayor of Taipei earlier this year. A Taiwanese Society of Hospital Medicine should be up and running by late 2015, says Dr. Tsai, who is its chief facilitator. When that happens, organizers expect hospital medicine to finally take off in Taiwan.
The Future Is Now
When Dr. Greeno talks to international hospitalists, he says, “If you’re doing a good job, that creates value for somebody. Find out who that is—that’s where you need to go to get your resources, financial or otherwise. Is it your individual hospital or your national health system? Everybody wants to deliver better care at lower cost. When you do that, that’s your driver for growth.”
Something about the hospitalist model, he adds, “just makes sense.”
“There are people virtually everywhere who are very enthusiastic about it. We in the United States can learn a lot from their enthusiasm,” he says. “It will evolve in different ways. The future is already here; it’s just unevenly distributed.”
Larry Beresford is a freelance writer in Alameda, Calif.
References
- Hock Lee K, Yang Y, Soong Yang K, Chi Ong B, Seong Ng H. Bringing generalists into the hospital: outcomes of a family medicine hospitalist model in Singapore. J Hosp Med. 2011;6(3):115-121.
- Yousefi V, Chong CAKY. Does implementation of a hospitalist program in a Canadian community hospital improve measures of quality of care and utilization? An observational comparative analysis of hospitalists vs. traditional care providers. BMC Health Serv Res. 2013;13:204.
- Timmermans MJC, van Vught AJAH, Wensing M, Laurant MGH. The effectiveness of substitution of hospital ward care from medical doctors to physician assistants: a study protocol. BMC Health Serv Res.; 2014;14:43.
- Black C. Acute medicine: making it work for patients. Hosp Med. 2004;65(8):493-496.
- Australian Medical Association. AMA Position Statement: Hospitalists – 2008. October 21, 2008. Accessed October 5, 2015.
- Shu CC, Lin JW, Lin YF, Hsu NC, Ko WJ. Evaluating the performance of a hospitalist system in Taiwan: A pioneer study for nationwide health insurance in Asia. J Hosp Med. 2011;6(7):378-382.
- Shu CC, Hsu NC, Lin YF, Wang JY, Lin JW, Ko WJ. Integrated postdischarge transitional care in a hospitalist system to improve discharge outcome: an experimental study. BMC Med. 2011;9:96.
- Carmona-Torre F, Martinez-Urbistondo D, Landecho MF, Lucena JF. Surviving sepsis in an intermediate care unit. Lancet Infect Dis. 2013;13(4):294-295.
- Lucena JF, Alegre F, Rodil R, et al. Results of a retrospective observational study of intermediate care staffed by hospitalists: impact on mortality, co-management, and teaching. J Hosp Med. 2012;7(5):411-415.
Since last September, Anand Kartha, MD, MS, has headed the hospital medicine (HM) program at 600-bed Hamad General Hospital, the flagship facility for eight-hospital Hamad Medical Corporation in Doha, Qatar, a small nation of 1.8 million people located on the northeast corner of the Arabian Peninsula.
“Qatar has a world-class healthcare system,” he says. “But to me, it sometimes feels like 1999, with the beginnings of the hospitalist movement as a new model of care.”
Dr. Kartha, a native of India who trained at the University of Pittsburgh Medical Center Mercy and Boston University School of Medicine, was recruited by Hamad Medical Corporation to develop hospital medicine in response to the growing complexity of inpatient care—and of patients served.
“Hospital medicine, delivered 24/7 by attending physicians, is an important element of the Health Ministry’s strategy and vision,” he says. “They looked at Australian, British, and American health systems, trying to put together the best from each—adapted to local sensitivities.
“One reason I came here was to expand the hospitalist model and be part of its extraordinary growth and development.”
Dr. Kartha also participates in medical research and residency training. His group now employs 30 attending physicians, half of them recent hires from the U.S. and the U.K.
As in the U.S., international drivers for the hospitalist model of care include pressures to improve efficiency, throughput, and quality of care. Those drivers are especially in focus at Hamad General, which Dr. Kartha says has one of the busiest EDs in the world.
Hospital medicine programs are springing up in other parts of the world, too, often inspired by the success of the HM model in the U.S. Hospitalist pioneers from other countries pore over the published research and visit the U.S. to attend conferences like SHM’s annual meeting, with its programming for international members, or to complete fellowships or other trainings. U.S. hospitalists are invited to speak to groups in other countries. Some, like Dr. Kartha, are being tapped to build hospitalist programs around the globe.

Hospital medicine can be introduced from the top down as a strategy by the public health system or from the bottom up by pioneers and advocates at the grassroots level.
Ron Greeno, MD, MHM, FCCP, has been active in hospital medicine since before the term “hospitalist” was coined. Currently chief strategy officer with IPC Healthcare, Inc., he was a founder in 1993 of Cogent Healthcare, which recently merged with Sound Physicians in Tacoma, Wash. Dr. Greeno says he is fascinated by the growth in international hospital medicine.
“I have been impressed at the number of countries that are represented at SHM [meetings] and the enthusiasm they show as they talk about their experiences,” he says. “What I see in these young, enthusiastic physicians from around the world is they are not naïve, but they are very idealistic. Their descriptions of their struggles remind me of our early days in Southern California.
“The international representatives at SHM all recognize the need for data. Every one of them feels their hospitalist model has advantages for their health system. But everybody’s struggling with the need for more resources. That’s the same in the U.S.”
Similarities and Differences
Many aspects of the experience in Qatar have been surprisingly familiar for Dr. Kartha.
“We are a Joint Commission-accredited hospital,” he says. “Our residency program is accredited by the American College of Graduate Medical Education. We are the flagship hospital for Weill Cornell Medical College in Qatar.”
The workday of a hospitalist at Hamad General is strikingly similar to the one he knew as an academic hospitalist in Boston.
“Models we are introducing include extended hours coverage, evenings and weekends, proactive discharge planning, and co-management with specialists,” he says. The health system is also rolling out an electronic health record.
Still, his adaptation to a new medical system has generated many curiosities in the sports-mad, fully wired-for-Internet nation, which has the world’s highest per capita standard of living.
“Every now and then, I look around and think: ‘This isn’t Kansas anymore, Toto,’” Dr. Kartha says, adding that he has learned about important cultural and religious beliefs and traditions that affect patients’ attitudes toward health and healing.
Arpana Vidyarthi, MD, associate professor in the Duke-NUS Graduate Medical School in Singapore, previously worked as a hospitalist at the University of California-San Francisco (UCSF) before moving to Singapore in 2011. She thinks “pockets” of hospital medicine are being practiced all over the world “in response to local needs.”
“The model is manifest in a diverse fashion throughout the United States, yet it is agile enough to be adapted around the world and be truly relevant,” Dr. Vidyarthi says. “But local tradition and the way hospitals are structured will determine how the model is established.”
Traditionally, medical specialists, often without a central physician to coordinate care, manage inpatients in Singapore, according to Dr. Vidyarthi. At discharge, they are referred to numerous subspecialists and to a public health clinic. Half of hospital wards are staffed by “super-specialists,” the other half by general internists who see patients both in the clinic and in the hospital, she says.
“This is not hospital medicine as we know it in the United States,” she says, “but different models are evolving.”
Ten years ago, physicians from Singapore visited UCSF to observe how hospital medicine was practiced there. A family medicine hospitalist program was piloted in 2006 at Singapore General Hospital. The program helped reduce lengths of stay and costs of care without adversely affecting mortality or readmissions.1
Kheng-Hock Lee, MD, one of the researchers and president of the Singapore College of Family Physicians, says that defining a generalist role for hospital medicine in Singapore has been difficult.
“When I call myself a hospitalist here, there is a strong reaction from some who perceive it as profit driven,” Dr. Vidyarthi says. “Clearly, there is a need for a generalist physician at the center of the patient experience, to manage the complexity of the patient as a whole person, as well as the hospital system. That is where it’s emerging within internal medicine, whether it’s called hospital medicine or not.”
For the past year, Dr. Vidyarthi has been working at Singapore General.
“The concept of the academic hospitalist is new here. People are able to see when I’m on service that I do things differently. This is because of the hospitalist mindset I brought from the United States,” she says. “Because I have a systems lens, I organize my day differently than the other doctors. I teach concurrently with clinical care, delegate responsibilities and accountabilities, and focus on discharge from the first day of admission.
“In general, my team is happier and my patients have lower lengths of stay.”
Defining a Specialized Expertise
Whatever you call it, there is a need around the world for physicians to practice in hospitals—to help standardize care, improve quality and patient safety, and prevent waste. Peter Jamieson, MD, a family physician in Calgary, Alberta, Canada, and medical director of the Foothills Medical Centre, has worked as a hospitalist since 1997. He didn’t call himself a hospitalist at first, “but the concept is becoming better socialized and more widely recognized in Canada.”
The Canadian Society of Hospital Medicine, founded in 2001 and affiliated with SHM, has about 1,300 members.
“I’d say we’re more the same than different compared with the United States, with a similar focus on quality of care,” Dr. Jamieson says.
Interestingly, he says the moniker “hospitalist” is not helping the development—and recognition—of Canadians who practice hospital-based medicine. It’s a refrain echoed for years by many in the U.S.
“As leaders in hospital medicine in Canada, we’d prefer to move away from the term ‘hospitalist’ and toward ‘specialist’ or ‘expert in hospital medicine,’” he says. “That takes us more in the direction we want to go in defining the mission of hospital medicine.

“First of all, in Canada and other places, there’s a bit of baggage attached to the term ‘hospitalist.’ These other terms help us get away from some of the historical assumptions of what people thought a hospitalist was—based on educational background.”
In Canada, that has largely been family medicine. Hospital medicine advocates are now exploring the best preparation for practicing the specialty.
“We want to define the mission around competency, rather than board certification,” Dr. Jamieson explains.
Listen to Dr. Jamieson discuss the evolution of hospital medicine in Canada.
The days when the majority of Canadian primary care providers would join the staff of a hospital and continue to manage their patients’ care during the hospital stay are long gone, he adds. In smaller and rural hospitals, the family doctor may still be the physician of record, although the number of such hospitals is dwindling.
HM clinicians generally are not employed by the hospital but often are sole practitioners with independent corporations or organized into groups that associate for the sake of the practice, signing a common contract with the hospital. Depending on provincial law, most hospitalist groups have leaders appointed and compensated by the hospital for scheduling and coordination.
On top of billing fee-for-service to the provincial health authority, hospitalists may also receive a stipend from the hospital, collectively or individually.
“There is a recognition that the physician fee schedule has not kept pace with the demands of hospital medicine, and that stipend also covers other services performed in the hospital,” Dr. Jamieson says.
Vandad Yousefi, MD, CCFP, FHM, hospitalist at Vancouver General Hospital in British Columbia, Canada, and co-founder and CEO of Hospitalist Consulting Solutions, has researched the development of hospital medicine in Canada and says that, even more than in the U.S., it was driven by the withdrawal of PCPs from hospitals, which created a vacuum.2,3
“For a lot of programs I’ve consulted with, the crisis point happened when physicians resigned en masse from hospital staffs,” he says.
Another driver is an increase in “unattached” hospitalized patients, which in Canada means they don’t have a specific medical provider willing to supply their inpatient attending-level care. In his surveys of typologies of roles played by hospitalists, Dr. Yousefi has observed a lot of variation in program models—not just between academic centers, teaching hospitals, and rural hospitals, but also within each category.
“These differences in programs make it hard to benchmark,” he says.
Hospitalist—or House Officer?
The Netherlands also has “hospitalists,” although they also refer to themselves as “house officers,” says Marijke Timmermans, a doctoral student in epidemiology at the Scientific Institute for Quality of Healthcare at Radboud University Medical Center in Nijmegen. As part of a long-standing system of post-graduate, on-the-job training for doctors, Dutch hospitalists typically are medical residents who perform the medical care of hospitalized patients, but not as the physician of record.
Timmermans is studying the growing role of physician assistants (PAs) in managing hospitalized patients in response to demands for better continuity of care. Although the PA concept is little more than a decade old in the Netherlands, there are 1,000 PAs, with about half filling a hospitalist role under the supervision of a medical specialist. Timmermans’ research looks at the effectiveness and quality of care with PAs under a mixed model of PA and physician, compared with physician alone.4

In the Netherlands, the patient’s PCP does not assume medical management responsibility while the patient is hospitalized, although PCP visits might be made to reassure the patient and advise the hospital-based team. As in the U.S., the hospitalist will try to communicate with the primary care doctor at discharge and, if possible, schedule follow-up visits for the discharged patient at a clinic on the hospital campus.
A new experiment is underway in four Dutch hospitals. It’s a three-year medical education curriculum to train “hospital doctors” (ziekenhuisarts). The new medical specialty, with general medical training, will assume more responsibility for ward care in the hospital. Timmermans says it is not yet known how these professionals will relate to other professionals in the hospital.
Joseph Li, MD, SFHM, head of hospital medicine at Beth Israel Deaconess Medical Center in Boston and past president of SHM, notes a key distinction between hospitalists as they are commonly understood in the U.S. and house officers: House officers don’t assume medical responsibility for the patient’s care.
“A house officer is not a hospitalist as we understand it—but even in this country, terminology varies and means different things in different hospitals,” Dr. Li says.
The Acute Medical Unit
In the U.K., a different model has emerged over the past two decades. It is called the acute medical unit [PDF] (AMU) and is staffed by dedicated consultants.5 The AMU fits functionally between the hospital’s ED, or front door admissions, and specialty care units within the hospital.
Patients generally are admitted to the AMU for a maximum of 72 hours for medical work-ups, with consultations as needed by specialists. They should be seen twice a day by the acute medical consultant, who is responsible for the delivery and direction of their care. Then they either go home or get transferred to a specialty unit within the hospital, with specialty care organized in a manner broadly similar to the U.S.
This frontloading of medical attention at admission allows patients to be worked up and turned around quickly, says Derek Bell, MD, head of acute medicine at Imperial College London and a founder in 2000 of the U.K.’s Society for Acute Medicine. Dr. Bell suggests that this system developed to ensure a safe haven for medical patients who are unstable or require ongoing investigation and treatment. A national “four-hour rule,” designed to reduce overcrowding in EDs, means that patients need to either go home or be admitted within four hours of presentation to the hospital.
U.K. hospitals also employ a registrar, a senior trainee who supervises junior and resident doctors. Hospital physicians are salaried and employed by “provider organizations,” which can be a single hospital or a collection of hospitals.
“My hospital admits about 30 to 35 medical patients per day, and we have two consultants working during the day just doing acute medicine, along with two registrars, one for emergency patients, two intermediate grade doctors, and two junior residents,” Dr. Bell says.
Acute medicine consultants generally do weekday shifts, with one consultant on call per night.
A few hospitals have embedded PCPs, who know the local system and can facilitate communication with the patient’s family doctor. “This model is well recognized but is not common,” Dr. Bell says.
What’s Happening Elsewhere?
In Australia, public hospitals in New South Wales generated positive results for a hospitalist pilot program in 2007, but also encountered some resistance from the Australian Medical Association and others concerned about its potential impact on such existing roles as career medical officer, PCP, and general physician, and on the provision of medical training in hospitals.6
Hospital medicine has grown since then, but slowly, with individual institutions successfully employing hospitalists at various levels. The fledgling specialty has yet to take off nationally, says Mary G.T. Webber, MBBS, a past president of the Australasian Society of Career Medical Officers. Dr. Webber practices hospital medicine at Ryde Hospital in suburban Sydney, where she has found the mix of clinical care, system development, and mentoring roles offered by the service personally rewarding. She has been frustrated with a lack of progress for the hospitalist movement overall in Australia.
“The concept of a rural generalist is already well accepted in Australia, and hospital medicine is the next logical iteration of the medical generalist,” Dr. Webber says. This need has been supported by the NSW Ministry of Health through a Hospital Skills Program, and, more recently, the successful implementation of a master’s degree for experienced nonspecialist doctors through the Senior Hospitalist Initiative at the University of Newcastle.

“Once you adopt a system view of patient care in hospitals, there is no going back,” says Dr. Webber, who was lead author of the hospital skills program curriculum in hospital medicine. “This is an idea whose time has come.”
A pioneering hospitalist program at National Taiwan University Hospital in Taipei (NTUH) was established by internists with diverse specializations in pulmonology, nephrology, infectious diseases, and family medicine and is led by Hung-Bin Tsai, MD, and Nin-Chieh Hsu, MD.7,8 Because of relatively low salaries for generalist physicians and a national health insurance program that incentivizes patient access to specialists, 95% of internal medicine doctors in Taiwan have chosen to subspecialize, Dr. Hsu says.
Other barriers to the dissemination of hospital medicine in Taiwan include a shortage of internal medicine residents and resident work-hour restrictions mandated by the country’s Ministry of Health, with resulting heavy work schedules for internal medicine attending physicians, who average 64 hours per week. Advocates believe the hospitalist model could help promote better work-life-salary balance for inpatient physicians.
“We are trying to persuade the Ministry of Health to pay a fair reimbursement for inpatient care,” Dr. Hsu says.
The pioneer hospitalist program at NTUH, developed in 2009 in a 36-bed, hospitalist-run ward, now 70 beds, has this year been joined by more than 20 other hospital medicine programs under an initiative of the Ministry of Health. Auspiciously, the chief of the pioneer hospitalist program at NTUH, Wen-je Ko, MD, PhD, was elected mayor of Taipei earlier this year. A Taiwanese Society of Hospital Medicine should be up and running by late 2015, says Dr. Tsai, who is its chief facilitator. When that happens, organizers expect hospital medicine to finally take off in Taiwan.
The Future Is Now
When Dr. Greeno talks to international hospitalists, he says, “If you’re doing a good job, that creates value for somebody. Find out who that is—that’s where you need to go to get your resources, financial or otherwise. Is it your individual hospital or your national health system? Everybody wants to deliver better care at lower cost. When you do that, that’s your driver for growth.”
Something about the hospitalist model, he adds, “just makes sense.”
“There are people virtually everywhere who are very enthusiastic about it. We in the United States can learn a lot from their enthusiasm,” he says. “It will evolve in different ways. The future is already here; it’s just unevenly distributed.”
Larry Beresford is a freelance writer in Alameda, Calif.
References
- Hock Lee K, Yang Y, Soong Yang K, Chi Ong B, Seong Ng H. Bringing generalists into the hospital: outcomes of a family medicine hospitalist model in Singapore. J Hosp Med. 2011;6(3):115-121.
- Yousefi V, Chong CAKY. Does implementation of a hospitalist program in a Canadian community hospital improve measures of quality of care and utilization? An observational comparative analysis of hospitalists vs. traditional care providers. BMC Health Serv Res. 2013;13:204.
- Timmermans MJC, van Vught AJAH, Wensing M, Laurant MGH. The effectiveness of substitution of hospital ward care from medical doctors to physician assistants: a study protocol. BMC Health Serv Res.; 2014;14:43.
- Black C. Acute medicine: making it work for patients. Hosp Med. 2004;65(8):493-496.
- Australian Medical Association. AMA Position Statement: Hospitalists – 2008. October 21, 2008. Accessed October 5, 2015.
- Shu CC, Lin JW, Lin YF, Hsu NC, Ko WJ. Evaluating the performance of a hospitalist system in Taiwan: A pioneer study for nationwide health insurance in Asia. J Hosp Med. 2011;6(7):378-382.
- Shu CC, Hsu NC, Lin YF, Wang JY, Lin JW, Ko WJ. Integrated postdischarge transitional care in a hospitalist system to improve discharge outcome: an experimental study. BMC Med. 2011;9:96.
- Carmona-Torre F, Martinez-Urbistondo D, Landecho MF, Lucena JF. Surviving sepsis in an intermediate care unit. Lancet Infect Dis. 2013;13(4):294-295.
- Lucena JF, Alegre F, Rodil R, et al. Results of a retrospective observational study of intermediate care staffed by hospitalists: impact on mortality, co-management, and teaching. J Hosp Med. 2012;7(5):411-415.