User login
AGA to FDA: We support new labeling recommendations for probiotics
In a new comment letter to FDA, AGA commends FDA’s recent draft guidance – “Policy Regarding Quantitative Labeling of Dietary Supplements Containing Live Microbials” – clarifying the expectations of probiotics manufacturers who choose to specify the amount of a live microbial component in their product in colony forming units (CFUs).
Though manufacturers are not currently required to report CFUs, AGA feels strongly that all manufacturers of probiotic supplements should voluntarily report the composition of live microbials in their products as CFUs.
However, reporting CFUs alone provides insufficient information to consumers and health care professionals who may recommend probiotic supplements to their patients. In our comment letter, AGA encourages FDA to expand what information manufacturers are required to include. In addition to the conditions already outlined in FDA’s draft guidance, AGA recommends including the conditions of storage as well as an expiration or “use by” date.
We acknowledge that researchers are evaluating other methods and units of measure besides CFUs for not only live microbials but also microbial bioactivity. However, in the absence of a widely accepted alternative, which may take several years to develop and adopt, AGA strongly encourages FDA and manufacturers to take the small step forward of using CFUs now rather than waiting for another solution to emerge.
Probiotics have been an important focus for the AGA Center for Gut Microbiome Research and Education due to the need for evidence-based guidance for health care providers and their patients. The center will continue to work to educate physicians, patients and industry on best practices to ensure safe use of probiotics.
In a new comment letter to FDA, AGA commends FDA’s recent draft guidance – “Policy Regarding Quantitative Labeling of Dietary Supplements Containing Live Microbials” – clarifying the expectations of probiotics manufacturers who choose to specify the amount of a live microbial component in their product in colony forming units (CFUs).
Though manufacturers are not currently required to report CFUs, AGA feels strongly that all manufacturers of probiotic supplements should voluntarily report the composition of live microbials in their products as CFUs.
However, reporting CFUs alone provides insufficient information to consumers and health care professionals who may recommend probiotic supplements to their patients. In our comment letter, AGA encourages FDA to expand what information manufacturers are required to include. In addition to the conditions already outlined in FDA’s draft guidance, AGA recommends including the conditions of storage as well as an expiration or “use by” date.
We acknowledge that researchers are evaluating other methods and units of measure besides CFUs for not only live microbials but also microbial bioactivity. However, in the absence of a widely accepted alternative, which may take several years to develop and adopt, AGA strongly encourages FDA and manufacturers to take the small step forward of using CFUs now rather than waiting for another solution to emerge.
Probiotics have been an important focus for the AGA Center for Gut Microbiome Research and Education due to the need for evidence-based guidance for health care providers and their patients. The center will continue to work to educate physicians, patients and industry on best practices to ensure safe use of probiotics.
In a new comment letter to FDA, AGA commends FDA’s recent draft guidance – “Policy Regarding Quantitative Labeling of Dietary Supplements Containing Live Microbials” – clarifying the expectations of probiotics manufacturers who choose to specify the amount of a live microbial component in their product in colony forming units (CFUs).
Though manufacturers are not currently required to report CFUs, AGA feels strongly that all manufacturers of probiotic supplements should voluntarily report the composition of live microbials in their products as CFUs.
However, reporting CFUs alone provides insufficient information to consumers and health care professionals who may recommend probiotic supplements to their patients. In our comment letter, AGA encourages FDA to expand what information manufacturers are required to include. In addition to the conditions already outlined in FDA’s draft guidance, AGA recommends including the conditions of storage as well as an expiration or “use by” date.
We acknowledge that researchers are evaluating other methods and units of measure besides CFUs for not only live microbials but also microbial bioactivity. However, in the absence of a widely accepted alternative, which may take several years to develop and adopt, AGA strongly encourages FDA and manufacturers to take the small step forward of using CFUs now rather than waiting for another solution to emerge.
Probiotics have been an important focus for the AGA Center for Gut Microbiome Research and Education due to the need for evidence-based guidance for health care providers and their patients. The center will continue to work to educate physicians, patients and industry on best practices to ensure safe use of probiotics.
No change in postoperative pain with restrictive opioid protocol
Opioid prescriptions after gynecologic surgery can be significantly reduced without impacting postoperative pain scores or complication rates, according to a paper published in JAMA Network Open.
A tertiary care comprehensive care center implemented an ultrarestrictive opioid prescription protocol (UROPP) then evaluated the outcomes in a case-control study involving 605 women undergoing gynecologic surgery, compared with 626 controls treated before implementation of the new protocol.
The ultrarestrictive protocol was prompted by frequent inquiries from patients who had used very little of their prescribed opioids after surgery and wanted to know what to do with the unused pills.
The new protocol involved a short preoperative counseling session about postoperative pain management. Following that, ambulatory surgery, minimally invasive surgery, or laparotomy patients were prescribed a 7-day supply of nonopioid pain relief. Laparotomy patients were also prescribed a 3-day supply of an oral opioid.
Any patients who required more than five opioid doses in the 24 hours before discharge were also prescribed a 3-day supply of opioid pain medication as needed, and all patients had the option of requesting an additional 3-day opioid refill.
Researchers saw no significant differences between the two groups in mean postoperative pain scores 2 weeks after surgery, and a similar number of patients in each group requested an opioid refill. There was also no significant difference in the number of postoperative complications between groups.
Implementation of the ultrarestrictive protocol was associated with significant declines in the mean number of opioid pills prescribed dropped from 31.7 to 3.5 in all surgical cases, from 43.6 to 12.1 in the laparotomy group, from 38.4 to 1.3 in the minimally invasive surgery group, and from 13.9 to 0.2 in patients who underwent ambulatory surgery.
“These data suggest that the implementation of a UROPP in a large surgical service is feasible and safe and was associated with a significantly decreased number of opioids dispensed during the perioperative period, particularly among opioid-naive patients,” wrote Jaron Mark, MD, of the department of gynecologic oncology at Roswell Park Comprehensive Cancer Center, Buffalo, N.Y., and his coauthors. “The opioid-sparing effect was also marked and statistically significant in the laparotomy group, where most patients remained physically active and recovered well with no negative sequelae or elevated pain score after surgery.”
The researchers also noted that patients who were discharged home with an opioid prescription were more likely to call and request a refill within 30 days, compared with patients who did not receive opioids at discharge.
The study was supported by the Roswell Park Comprehensive Cancer Center, the National Cancer Institute and the Roswell Park Alliance Foundation. Two authors reported receiving fees and nonfinancial support from the private sector unrelated to the study.
SOURCE: Mark J et al. JAMA Netw Open. 2018 Dec 7. doi: 10.1001/jamanetworkopen.2018.5452.
The ultrarestrictive postoperative opioid prescribing protocol described in this study is a promising strategy for reducing opioid prescribing without increasing pain and limiting the potential for diversion and misuse of opioids. An important element of this protocol is the preoperative counseling, because setting patient expectations is likely to be an important factor in improving postoperative outcomes.
It is also worth noting that this study focused on patients undergoing major and minor gynecologic surgery, so more research is needed to explore these outcomes particularly among patients undergoing procedures that may be associated with a higher risk of persistent postoperative pain and/or opioid use. It is also a management strategy explored in patients at low risk of chronic postoperative opioid use, but a similar pathway should be developed and explored in more high-risk patients.
Dr. Jennifer M. Hah is from the department of anesthesiology, perioperative, and pain management at Stanford University (Calif.). These comments are taken from an accompanying editorial (JAMA Network Open. 2018 Dec 7. doi: 10.1001/jamanetworkopen.2018.5432). No conflicts of interest were reported.
The ultrarestrictive postoperative opioid prescribing protocol described in this study is a promising strategy for reducing opioid prescribing without increasing pain and limiting the potential for diversion and misuse of opioids. An important element of this protocol is the preoperative counseling, because setting patient expectations is likely to be an important factor in improving postoperative outcomes.
It is also worth noting that this study focused on patients undergoing major and minor gynecologic surgery, so more research is needed to explore these outcomes particularly among patients undergoing procedures that may be associated with a higher risk of persistent postoperative pain and/or opioid use. It is also a management strategy explored in patients at low risk of chronic postoperative opioid use, but a similar pathway should be developed and explored in more high-risk patients.
Dr. Jennifer M. Hah is from the department of anesthesiology, perioperative, and pain management at Stanford University (Calif.). These comments are taken from an accompanying editorial (JAMA Network Open. 2018 Dec 7. doi: 10.1001/jamanetworkopen.2018.5432). No conflicts of interest were reported.
The ultrarestrictive postoperative opioid prescribing protocol described in this study is a promising strategy for reducing opioid prescribing without increasing pain and limiting the potential for diversion and misuse of opioids. An important element of this protocol is the preoperative counseling, because setting patient expectations is likely to be an important factor in improving postoperative outcomes.
It is also worth noting that this study focused on patients undergoing major and minor gynecologic surgery, so more research is needed to explore these outcomes particularly among patients undergoing procedures that may be associated with a higher risk of persistent postoperative pain and/or opioid use. It is also a management strategy explored in patients at low risk of chronic postoperative opioid use, but a similar pathway should be developed and explored in more high-risk patients.
Dr. Jennifer M. Hah is from the department of anesthesiology, perioperative, and pain management at Stanford University (Calif.). These comments are taken from an accompanying editorial (JAMA Network Open. 2018 Dec 7. doi: 10.1001/jamanetworkopen.2018.5432). No conflicts of interest were reported.
Opioid prescriptions after gynecologic surgery can be significantly reduced without impacting postoperative pain scores or complication rates, according to a paper published in JAMA Network Open.
A tertiary care comprehensive care center implemented an ultrarestrictive opioid prescription protocol (UROPP) then evaluated the outcomes in a case-control study involving 605 women undergoing gynecologic surgery, compared with 626 controls treated before implementation of the new protocol.
The ultrarestrictive protocol was prompted by frequent inquiries from patients who had used very little of their prescribed opioids after surgery and wanted to know what to do with the unused pills.
The new protocol involved a short preoperative counseling session about postoperative pain management. Following that, ambulatory surgery, minimally invasive surgery, or laparotomy patients were prescribed a 7-day supply of nonopioid pain relief. Laparotomy patients were also prescribed a 3-day supply of an oral opioid.
Any patients who required more than five opioid doses in the 24 hours before discharge were also prescribed a 3-day supply of opioid pain medication as needed, and all patients had the option of requesting an additional 3-day opioid refill.
Researchers saw no significant differences between the two groups in mean postoperative pain scores 2 weeks after surgery, and a similar number of patients in each group requested an opioid refill. There was also no significant difference in the number of postoperative complications between groups.
Implementation of the ultrarestrictive protocol was associated with significant declines in the mean number of opioid pills prescribed dropped from 31.7 to 3.5 in all surgical cases, from 43.6 to 12.1 in the laparotomy group, from 38.4 to 1.3 in the minimally invasive surgery group, and from 13.9 to 0.2 in patients who underwent ambulatory surgery.
“These data suggest that the implementation of a UROPP in a large surgical service is feasible and safe and was associated with a significantly decreased number of opioids dispensed during the perioperative period, particularly among opioid-naive patients,” wrote Jaron Mark, MD, of the department of gynecologic oncology at Roswell Park Comprehensive Cancer Center, Buffalo, N.Y., and his coauthors. “The opioid-sparing effect was also marked and statistically significant in the laparotomy group, where most patients remained physically active and recovered well with no negative sequelae or elevated pain score after surgery.”
The researchers also noted that patients who were discharged home with an opioid prescription were more likely to call and request a refill within 30 days, compared with patients who did not receive opioids at discharge.
The study was supported by the Roswell Park Comprehensive Cancer Center, the National Cancer Institute and the Roswell Park Alliance Foundation. Two authors reported receiving fees and nonfinancial support from the private sector unrelated to the study.
SOURCE: Mark J et al. JAMA Netw Open. 2018 Dec 7. doi: 10.1001/jamanetworkopen.2018.5452.
Opioid prescriptions after gynecologic surgery can be significantly reduced without impacting postoperative pain scores or complication rates, according to a paper published in JAMA Network Open.
A tertiary care comprehensive care center implemented an ultrarestrictive opioid prescription protocol (UROPP) then evaluated the outcomes in a case-control study involving 605 women undergoing gynecologic surgery, compared with 626 controls treated before implementation of the new protocol.
The ultrarestrictive protocol was prompted by frequent inquiries from patients who had used very little of their prescribed opioids after surgery and wanted to know what to do with the unused pills.
The new protocol involved a short preoperative counseling session about postoperative pain management. Following that, ambulatory surgery, minimally invasive surgery, or laparotomy patients were prescribed a 7-day supply of nonopioid pain relief. Laparotomy patients were also prescribed a 3-day supply of an oral opioid.
Any patients who required more than five opioid doses in the 24 hours before discharge were also prescribed a 3-day supply of opioid pain medication as needed, and all patients had the option of requesting an additional 3-day opioid refill.
Researchers saw no significant differences between the two groups in mean postoperative pain scores 2 weeks after surgery, and a similar number of patients in each group requested an opioid refill. There was also no significant difference in the number of postoperative complications between groups.
Implementation of the ultrarestrictive protocol was associated with significant declines in the mean number of opioid pills prescribed dropped from 31.7 to 3.5 in all surgical cases, from 43.6 to 12.1 in the laparotomy group, from 38.4 to 1.3 in the minimally invasive surgery group, and from 13.9 to 0.2 in patients who underwent ambulatory surgery.
“These data suggest that the implementation of a UROPP in a large surgical service is feasible and safe and was associated with a significantly decreased number of opioids dispensed during the perioperative period, particularly among opioid-naive patients,” wrote Jaron Mark, MD, of the department of gynecologic oncology at Roswell Park Comprehensive Cancer Center, Buffalo, N.Y., and his coauthors. “The opioid-sparing effect was also marked and statistically significant in the laparotomy group, where most patients remained physically active and recovered well with no negative sequelae or elevated pain score after surgery.”
The researchers also noted that patients who were discharged home with an opioid prescription were more likely to call and request a refill within 30 days, compared with patients who did not receive opioids at discharge.
The study was supported by the Roswell Park Comprehensive Cancer Center, the National Cancer Institute and the Roswell Park Alliance Foundation. Two authors reported receiving fees and nonfinancial support from the private sector unrelated to the study.
SOURCE: Mark J et al. JAMA Netw Open. 2018 Dec 7. doi: 10.1001/jamanetworkopen.2018.5452.
Key clinical point: A ultrarestrictive postoperative opioid protocol is not associated with higher postoperative pain scores.
Major finding: The protocol achieves significant reductions in opioid use.
Study details: A case-control study in 1,231 women undergoing gynecologic surgery.
Disclosures: The study was supported by the Roswell Park Comprehensive Cancer Center, the National Cancer Institute, and the Roswell Park Alliance Foundation. Two authors reported receiving fees and nonfinancial support from the private sector unrelated to the study.
Source: Mark J et al. JAMA Netw Open. 2018 Dec 7. doi: 10.1001/jamanetworkopen.2018.5452.
Firibastat looking good for difficult-to-treat hypertension
CHICAGO – Firibastat, a first-in-class oral antihypertensive drug, proved safe, effective, and well-tolerated in NEW-HOPE, a phase 2b clinical trial focused on an understudied and underserved patient population composed largely of overweight or obese, high-risk, hypertensive racial minorities,
Firibastat is the first brain aminopeptidase A inhibitor. It selectively and specifically inhibits conversion of angiotensin II to angiotensin III, which exerts tonic stimulation over blood pressure. Decreased angiotensin III means less release of vasopressin, reduced sympathetic nervous system activity, and increased baroreflex activity, all of which add up to lower blood pressure, Keith C. Ferdinand, MD, explained at the American Heart Association scientific sessions.
NEW-HOPE (Novel Evaluation With QGC001 in Hypertensive Overweight Patients of Multiple Ethnic origins) was an open-label multicenter study including 254 middle-aged or older hypertensive patients. Two-thirds were obese, the rest overweight. Participants had a mean body mass index of 33 kg/m2 and a baseline automated office blood pressure (AOBP) of 153.9/91.5 mm Hg. A total of 46% were women, and 38% were black. Indeed, blacks and other minorities made up 54% of the NEW-HOPE population.
“Minority populations in many of the clinical trials in hypertension have been underrepresented,” observed Dr. Ferdinand, professor of medicine at Tulane University in New Orleans.
After a 2-week washout period, all patients were placed on firibastat at 250 mg b.i.d. for 2 weeks. If at that point their AOBP was more than 140/90 mm Hg they were bumped up to 500 mg b.i.d. Hydrochlorothiazide at 25 mg/day could be added 1 month into the trial if a patient’s systolic blood pressure was 160 mm Hg or more or their diastolic blood pressure was at least 100 mm Hg. Of note, 85% of patients were able to remain on firibastat monotherapy throughout the study.
The primary endpoint was change from baseline in systolic AOBP at 8 weeks. By week 8, the mean systolic blood pressure (SBP) had fallen by 9.7 mm Hg from a baseline of 153.9, which in hypertension circles is deemed a clinically meaningful improvement. Mean diastolic AOBP fell from 91.5 to 87.2 mm Hg, for a 4.3–mm Hg reduction.
“The diastolic number was smaller, but remember, this was a middle-aged and older population, and SBP is the most important endpoint in patients of that age, not just in clinical trials but in terms of its effects on morbidity and mortality,” Dr. Ferdinand said.
A word about the rigorous AOBP protocol used in NEW-HOPE: It was similar to that used in the landmark SPRINT trial. Patients were required to rest seated with back support in a quiet room with no talking for 5 minutes. Then six measurements were taken at 1-minute intervals, with patients’ legs uncrossed and feet on the floor the whole time. The first measurement was discarded, and the next five were averaged.
“This correlates very well with daytime ambulatory blood pressure, which is the gold standard,” the cardiologist noted.
In a prespecified subgroup analysis, systolic AOBP was reduced significantly more in obese than in overweight patients. Black patients averaged a 10.5–mm Hg decrease, nonblacks a 4.1–mm Hg reduction. But black patients also averaged a 2.0 kg/m2 higher body mass index.
“ACE inhibitors and angiotensin receptor blockers have been shown to be less efficacious in black patients. Firibastat, however, had similar effects in both black and nonblack patients. And this is probably one of the main take-away points of the study: This is a drug based on the phenotype of obesity and increased blood pressure, and the drug had efficacy regardless of self-identified race,” the cardiologist continued.
The most common treatment-emergent adverse events were headache in 4% of patients and skin reactions in 3%. There were no cases of angioedema. The only serious adverse event was one case of erythema multiforme. There were no clinically meaningful changes in any laboratory parameters.
Based upon these encouraging results, a pivotal phase 3 clinical trial is being planned in patients with difficult-to-treat or resistant hypertension. Dr. Ferdinand sees firibastat as being particularly useful as part of a two-drug treatment strategy, probably with the addition of a calcium channel blocker or potent diuretic, since “two drugs is the way to go in resistant hypertension.”
Audience members called the study “very hopeful,” but wondered about the absence of a placebo control arm. Reservations were also voiced about the need for twice-daily dosing of firibastat because it’s well established that adherence drops off when an antihypertensive agent has to be taken more than once daily.
Dr. Ferdinand said the lack of a placebo arm in NEW-HOPE was endorsed by the Food and Drug Administration because of ethical concerns surrounding use of a placebo in a high-risk population such as this. Obesity is known to increase the risk of resistant hypertension fivefold. Obesity is more common in blacks and Hispanics, with a prevalence of 47%, than in whites, where the prevalence is 38%.
As for the b.i.d. dosing, Quantum Genomics, the company that sponsored NEW-HOPE, is developing a sustained-release, once-daily formulation of firibastat that’s better suited for clinical practice, he added.
NEW-HOPE was carried out in collaboration with the Association of Black Cardiologists. Dr. Ferdinand reported serving as a consultant to Quantum Genomics and a handful of other pharmaceutical companies.
CHICAGO – Firibastat, a first-in-class oral antihypertensive drug, proved safe, effective, and well-tolerated in NEW-HOPE, a phase 2b clinical trial focused on an understudied and underserved patient population composed largely of overweight or obese, high-risk, hypertensive racial minorities,
Firibastat is the first brain aminopeptidase A inhibitor. It selectively and specifically inhibits conversion of angiotensin II to angiotensin III, which exerts tonic stimulation over blood pressure. Decreased angiotensin III means less release of vasopressin, reduced sympathetic nervous system activity, and increased baroreflex activity, all of which add up to lower blood pressure, Keith C. Ferdinand, MD, explained at the American Heart Association scientific sessions.
NEW-HOPE (Novel Evaluation With QGC001 in Hypertensive Overweight Patients of Multiple Ethnic origins) was an open-label multicenter study including 254 middle-aged or older hypertensive patients. Two-thirds were obese, the rest overweight. Participants had a mean body mass index of 33 kg/m2 and a baseline automated office blood pressure (AOBP) of 153.9/91.5 mm Hg. A total of 46% were women, and 38% were black. Indeed, blacks and other minorities made up 54% of the NEW-HOPE population.
“Minority populations in many of the clinical trials in hypertension have been underrepresented,” observed Dr. Ferdinand, professor of medicine at Tulane University in New Orleans.
After a 2-week washout period, all patients were placed on firibastat at 250 mg b.i.d. for 2 weeks. If at that point their AOBP was more than 140/90 mm Hg they were bumped up to 500 mg b.i.d. Hydrochlorothiazide at 25 mg/day could be added 1 month into the trial if a patient’s systolic blood pressure was 160 mm Hg or more or their diastolic blood pressure was at least 100 mm Hg. Of note, 85% of patients were able to remain on firibastat monotherapy throughout the study.
The primary endpoint was change from baseline in systolic AOBP at 8 weeks. By week 8, the mean systolic blood pressure (SBP) had fallen by 9.7 mm Hg from a baseline of 153.9, which in hypertension circles is deemed a clinically meaningful improvement. Mean diastolic AOBP fell from 91.5 to 87.2 mm Hg, for a 4.3–mm Hg reduction.
“The diastolic number was smaller, but remember, this was a middle-aged and older population, and SBP is the most important endpoint in patients of that age, not just in clinical trials but in terms of its effects on morbidity and mortality,” Dr. Ferdinand said.
A word about the rigorous AOBP protocol used in NEW-HOPE: It was similar to that used in the landmark SPRINT trial. Patients were required to rest seated with back support in a quiet room with no talking for 5 minutes. Then six measurements were taken at 1-minute intervals, with patients’ legs uncrossed and feet on the floor the whole time. The first measurement was discarded, and the next five were averaged.
“This correlates very well with daytime ambulatory blood pressure, which is the gold standard,” the cardiologist noted.
In a prespecified subgroup analysis, systolic AOBP was reduced significantly more in obese than in overweight patients. Black patients averaged a 10.5–mm Hg decrease, nonblacks a 4.1–mm Hg reduction. But black patients also averaged a 2.0 kg/m2 higher body mass index.
“ACE inhibitors and angiotensin receptor blockers have been shown to be less efficacious in black patients. Firibastat, however, had similar effects in both black and nonblack patients. And this is probably one of the main take-away points of the study: This is a drug based on the phenotype of obesity and increased blood pressure, and the drug had efficacy regardless of self-identified race,” the cardiologist continued.
The most common treatment-emergent adverse events were headache in 4% of patients and skin reactions in 3%. There were no cases of angioedema. The only serious adverse event was one case of erythema multiforme. There were no clinically meaningful changes in any laboratory parameters.
Based upon these encouraging results, a pivotal phase 3 clinical trial is being planned in patients with difficult-to-treat or resistant hypertension. Dr. Ferdinand sees firibastat as being particularly useful as part of a two-drug treatment strategy, probably with the addition of a calcium channel blocker or potent diuretic, since “two drugs is the way to go in resistant hypertension.”
Audience members called the study “very hopeful,” but wondered about the absence of a placebo control arm. Reservations were also voiced about the need for twice-daily dosing of firibastat because it’s well established that adherence drops off when an antihypertensive agent has to be taken more than once daily.
Dr. Ferdinand said the lack of a placebo arm in NEW-HOPE was endorsed by the Food and Drug Administration because of ethical concerns surrounding use of a placebo in a high-risk population such as this. Obesity is known to increase the risk of resistant hypertension fivefold. Obesity is more common in blacks and Hispanics, with a prevalence of 47%, than in whites, where the prevalence is 38%.
As for the b.i.d. dosing, Quantum Genomics, the company that sponsored NEW-HOPE, is developing a sustained-release, once-daily formulation of firibastat that’s better suited for clinical practice, he added.
NEW-HOPE was carried out in collaboration with the Association of Black Cardiologists. Dr. Ferdinand reported serving as a consultant to Quantum Genomics and a handful of other pharmaceutical companies.
CHICAGO – Firibastat, a first-in-class oral antihypertensive drug, proved safe, effective, and well-tolerated in NEW-HOPE, a phase 2b clinical trial focused on an understudied and underserved patient population composed largely of overweight or obese, high-risk, hypertensive racial minorities,
Firibastat is the first brain aminopeptidase A inhibitor. It selectively and specifically inhibits conversion of angiotensin II to angiotensin III, which exerts tonic stimulation over blood pressure. Decreased angiotensin III means less release of vasopressin, reduced sympathetic nervous system activity, and increased baroreflex activity, all of which add up to lower blood pressure, Keith C. Ferdinand, MD, explained at the American Heart Association scientific sessions.
NEW-HOPE (Novel Evaluation With QGC001 in Hypertensive Overweight Patients of Multiple Ethnic origins) was an open-label multicenter study including 254 middle-aged or older hypertensive patients. Two-thirds were obese, the rest overweight. Participants had a mean body mass index of 33 kg/m2 and a baseline automated office blood pressure (AOBP) of 153.9/91.5 mm Hg. A total of 46% were women, and 38% were black. Indeed, blacks and other minorities made up 54% of the NEW-HOPE population.
“Minority populations in many of the clinical trials in hypertension have been underrepresented,” observed Dr. Ferdinand, professor of medicine at Tulane University in New Orleans.
After a 2-week washout period, all patients were placed on firibastat at 250 mg b.i.d. for 2 weeks. If at that point their AOBP was more than 140/90 mm Hg they were bumped up to 500 mg b.i.d. Hydrochlorothiazide at 25 mg/day could be added 1 month into the trial if a patient’s systolic blood pressure was 160 mm Hg or more or their diastolic blood pressure was at least 100 mm Hg. Of note, 85% of patients were able to remain on firibastat monotherapy throughout the study.
The primary endpoint was change from baseline in systolic AOBP at 8 weeks. By week 8, the mean systolic blood pressure (SBP) had fallen by 9.7 mm Hg from a baseline of 153.9, which in hypertension circles is deemed a clinically meaningful improvement. Mean diastolic AOBP fell from 91.5 to 87.2 mm Hg, for a 4.3–mm Hg reduction.
“The diastolic number was smaller, but remember, this was a middle-aged and older population, and SBP is the most important endpoint in patients of that age, not just in clinical trials but in terms of its effects on morbidity and mortality,” Dr. Ferdinand said.
A word about the rigorous AOBP protocol used in NEW-HOPE: It was similar to that used in the landmark SPRINT trial. Patients were required to rest seated with back support in a quiet room with no talking for 5 minutes. Then six measurements were taken at 1-minute intervals, with patients’ legs uncrossed and feet on the floor the whole time. The first measurement was discarded, and the next five were averaged.
“This correlates very well with daytime ambulatory blood pressure, which is the gold standard,” the cardiologist noted.
In a prespecified subgroup analysis, systolic AOBP was reduced significantly more in obese than in overweight patients. Black patients averaged a 10.5–mm Hg decrease, nonblacks a 4.1–mm Hg reduction. But black patients also averaged a 2.0 kg/m2 higher body mass index.
“ACE inhibitors and angiotensin receptor blockers have been shown to be less efficacious in black patients. Firibastat, however, had similar effects in both black and nonblack patients. And this is probably one of the main take-away points of the study: This is a drug based on the phenotype of obesity and increased blood pressure, and the drug had efficacy regardless of self-identified race,” the cardiologist continued.
The most common treatment-emergent adverse events were headache in 4% of patients and skin reactions in 3%. There were no cases of angioedema. The only serious adverse event was one case of erythema multiforme. There were no clinically meaningful changes in any laboratory parameters.
Based upon these encouraging results, a pivotal phase 3 clinical trial is being planned in patients with difficult-to-treat or resistant hypertension. Dr. Ferdinand sees firibastat as being particularly useful as part of a two-drug treatment strategy, probably with the addition of a calcium channel blocker or potent diuretic, since “two drugs is the way to go in resistant hypertension.”
Audience members called the study “very hopeful,” but wondered about the absence of a placebo control arm. Reservations were also voiced about the need for twice-daily dosing of firibastat because it’s well established that adherence drops off when an antihypertensive agent has to be taken more than once daily.
Dr. Ferdinand said the lack of a placebo arm in NEW-HOPE was endorsed by the Food and Drug Administration because of ethical concerns surrounding use of a placebo in a high-risk population such as this. Obesity is known to increase the risk of resistant hypertension fivefold. Obesity is more common in blacks and Hispanics, with a prevalence of 47%, than in whites, where the prevalence is 38%.
As for the b.i.d. dosing, Quantum Genomics, the company that sponsored NEW-HOPE, is developing a sustained-release, once-daily formulation of firibastat that’s better suited for clinical practice, he added.
NEW-HOPE was carried out in collaboration with the Association of Black Cardiologists. Dr. Ferdinand reported serving as a consultant to Quantum Genomics and a handful of other pharmaceutical companies.
REPORTING FROM THE AHA SCIENTIFIC SESSIONS
Key clinical point: A first-in-class oral brain angiotensin III inhibitor shows considerable promise in difficult-to-treat hypertension.
Major finding: Mean systolic blood pressure fell by 9.7 mm Hg at 8 weeks from a baseline of 153.9 mm Hg in response to firibastat.
Study details: This 8-week, open-label, multicenter trial included 254 obese or overweight patients with difficult-to-treat hypertension.
Disclosures: The presenter reported serving as a consultant to Quantum Genomics, the study sponsor.
Older breast cancer patients given adjuvant chemo live longer
SAN ANTONIO – captured in the National Cancer Database.
“Data for elderly patients in clinical trials is limited. The NCCN [National Comprehensive Cancer Network] guidelines note that there is limited data to make chemotherapy recommendations for those older than 70 years of age,” commented first author Shreya Sinha, MD, an oncology fellow at the State University of New York, Syracuse. Furthermore, the few studies assessing adjuvant chemotherapy benefit among geriatric breast cancer patients have had conflicting results.
In the new study, reported at the San Antonio Breast Cancer Symposium, older women with stage I-III breast cancer who received adjuvant chemotherapy had a nearly 40% reduction in the adjusted risk of death relative to counterparts who did not receive adjuvant chemotherapy. Benefit was seen across disease stages and across hormone receptor statuses.
Patients’ fitness to receive chemotherapy and their causes of death could not be determined, Dr. Sinha acknowledged. Therefore, chemotherapy’s role in the observed survival difference is not definitive.
“In general, when we are treating our elderly population, we have to take physiologic age into consideration when coming up with a treatment plan,” she said. However, “we also have to use chemotherapy toxicity prediction calculators,” such as the Cancer and Aging Research Group tool and the Chemotherapy Risk Assessment Scale for High-Age Patients.
In addition, gene-based assays, such as Oncotype DX and MammaPrint, which were not taken into account for the study, can be applied to estimate the likely benefit of chemotherapy and further inform the treatment decision.
“It can’t be that chemotherapy is making these patients live longer. It has to be that the doctors know not to give chemotherapy to those who are going to die soon,” speculated symposium attendee Steven E. Vogl, MD, an oncologist at Montefiore Medical Center, New York.
He therefore wondered if the amount of chemotherapy received was related to survival. “If it was a chemotherapy effect, then more is probably better, and if it’s a selection effect at the time of initiation, then more probably wouldn’t be better.”
“These are the issues we run into when we use the National Cancer Database or such large databases,” Dr. Sinha replied. “We don’t necessarily have the information on how much chemotherapy the patients received. It really is based on if they received chemotherapy or not.”
Study details
The 160,676 patients studied were treated for stage I-III breast cancer during 2004-2015 and were included regardless of hormone receptor status and HER2 status.
Overall, 60.45% received adjuvant chemotherapy, Dr. Sinha reported. Mean age was 70.7 years among chemotherapy recipients and 75.5 years among nonrecipients.
Women were more likely to receive adjuvant chemotherapy if they had a tumor grade of 2 or 3 (adjusted odds ratios, 1.88 and 3.51), had a tumor negative for both estrogen and progesterone receptors or just progesterone receptors (aOR, 2.72 and 1.70), had private insurance versus Medicaid or Medicare (aOR, 1.40 and 1.20), or received radiation therapy (aOR, 2.55).
Women were less likely to receive adjuvant chemotherapy if they had stage 1 or 2 disease (aOR, 0.23 and 0.56; P less than .0001 for each), were older than 80 years (aOR, 0.105; P less than .0001), had undergone lumpectomy versus mastectomy (aOR, 0.82; P = .0011), were treated in an academic versus community program (aOR, 0.93; P = .0007), or had a Charlson/Deyo comorbidity score of 3 or higher (aOR, 0.38; P less than .0001).
Median overall survival was 144.9 months with and 112.6 months without adjuvant chemotherapy. The difference translated to a significantly reduced risk of death for the women given adjuvant chemotherapy (adjusted hazard ratio, 0.617; P less than .0001). The corresponding 10-year overall survival rates were 59.5% and 46.7%.
The reduced risk of death with adjuvant chemotherapy was evident in women with stage 1 disease (aHR, 0.801), stage 2 disease (aHR, 0.608), and stage 3 disease (aHR, 0.666) (P less than .0001 for all). It was also evident in those with tumors positive for both estrogen and progesterone receptors (aHR, 0.649), negative for progesterone receptors only (aHR, 0.609), and negative for both (aHR, 0.547) (P less than .0001 for all).
“The HER2/neu patient unfortunately was not well defined since there was no data [on that marker] before 2010,” Dr. Sinha noted
Dr. Sinha reported no relevant conflicts of interest. The study received funding from the Research Foundation of SUNY.
SOURCE: Sinha S et al. SABCS 2018, Abstract GS2-02.
SAN ANTONIO – captured in the National Cancer Database.
“Data for elderly patients in clinical trials is limited. The NCCN [National Comprehensive Cancer Network] guidelines note that there is limited data to make chemotherapy recommendations for those older than 70 years of age,” commented first author Shreya Sinha, MD, an oncology fellow at the State University of New York, Syracuse. Furthermore, the few studies assessing adjuvant chemotherapy benefit among geriatric breast cancer patients have had conflicting results.
In the new study, reported at the San Antonio Breast Cancer Symposium, older women with stage I-III breast cancer who received adjuvant chemotherapy had a nearly 40% reduction in the adjusted risk of death relative to counterparts who did not receive adjuvant chemotherapy. Benefit was seen across disease stages and across hormone receptor statuses.
Patients’ fitness to receive chemotherapy and their causes of death could not be determined, Dr. Sinha acknowledged. Therefore, chemotherapy’s role in the observed survival difference is not definitive.
“In general, when we are treating our elderly population, we have to take physiologic age into consideration when coming up with a treatment plan,” she said. However, “we also have to use chemotherapy toxicity prediction calculators,” such as the Cancer and Aging Research Group tool and the Chemotherapy Risk Assessment Scale for High-Age Patients.
In addition, gene-based assays, such as Oncotype DX and MammaPrint, which were not taken into account for the study, can be applied to estimate the likely benefit of chemotherapy and further inform the treatment decision.
“It can’t be that chemotherapy is making these patients live longer. It has to be that the doctors know not to give chemotherapy to those who are going to die soon,” speculated symposium attendee Steven E. Vogl, MD, an oncologist at Montefiore Medical Center, New York.
He therefore wondered if the amount of chemotherapy received was related to survival. “If it was a chemotherapy effect, then more is probably better, and if it’s a selection effect at the time of initiation, then more probably wouldn’t be better.”
“These are the issues we run into when we use the National Cancer Database or such large databases,” Dr. Sinha replied. “We don’t necessarily have the information on how much chemotherapy the patients received. It really is based on if they received chemotherapy or not.”
Study details
The 160,676 patients studied were treated for stage I-III breast cancer during 2004-2015 and were included regardless of hormone receptor status and HER2 status.
Overall, 60.45% received adjuvant chemotherapy, Dr. Sinha reported. Mean age was 70.7 years among chemotherapy recipients and 75.5 years among nonrecipients.
Women were more likely to receive adjuvant chemotherapy if they had a tumor grade of 2 or 3 (adjusted odds ratios, 1.88 and 3.51), had a tumor negative for both estrogen and progesterone receptors or just progesterone receptors (aOR, 2.72 and 1.70), had private insurance versus Medicaid or Medicare (aOR, 1.40 and 1.20), or received radiation therapy (aOR, 2.55).
Women were less likely to receive adjuvant chemotherapy if they had stage 1 or 2 disease (aOR, 0.23 and 0.56; P less than .0001 for each), were older than 80 years (aOR, 0.105; P less than .0001), had undergone lumpectomy versus mastectomy (aOR, 0.82; P = .0011), were treated in an academic versus community program (aOR, 0.93; P = .0007), or had a Charlson/Deyo comorbidity score of 3 or higher (aOR, 0.38; P less than .0001).
Median overall survival was 144.9 months with and 112.6 months without adjuvant chemotherapy. The difference translated to a significantly reduced risk of death for the women given adjuvant chemotherapy (adjusted hazard ratio, 0.617; P less than .0001). The corresponding 10-year overall survival rates were 59.5% and 46.7%.
The reduced risk of death with adjuvant chemotherapy was evident in women with stage 1 disease (aHR, 0.801), stage 2 disease (aHR, 0.608), and stage 3 disease (aHR, 0.666) (P less than .0001 for all). It was also evident in those with tumors positive for both estrogen and progesterone receptors (aHR, 0.649), negative for progesterone receptors only (aHR, 0.609), and negative for both (aHR, 0.547) (P less than .0001 for all).
“The HER2/neu patient unfortunately was not well defined since there was no data [on that marker] before 2010,” Dr. Sinha noted
Dr. Sinha reported no relevant conflicts of interest. The study received funding from the Research Foundation of SUNY.
SOURCE: Sinha S et al. SABCS 2018, Abstract GS2-02.
SAN ANTONIO – captured in the National Cancer Database.
“Data for elderly patients in clinical trials is limited. The NCCN [National Comprehensive Cancer Network] guidelines note that there is limited data to make chemotherapy recommendations for those older than 70 years of age,” commented first author Shreya Sinha, MD, an oncology fellow at the State University of New York, Syracuse. Furthermore, the few studies assessing adjuvant chemotherapy benefit among geriatric breast cancer patients have had conflicting results.
In the new study, reported at the San Antonio Breast Cancer Symposium, older women with stage I-III breast cancer who received adjuvant chemotherapy had a nearly 40% reduction in the adjusted risk of death relative to counterparts who did not receive adjuvant chemotherapy. Benefit was seen across disease stages and across hormone receptor statuses.
Patients’ fitness to receive chemotherapy and their causes of death could not be determined, Dr. Sinha acknowledged. Therefore, chemotherapy’s role in the observed survival difference is not definitive.
“In general, when we are treating our elderly population, we have to take physiologic age into consideration when coming up with a treatment plan,” she said. However, “we also have to use chemotherapy toxicity prediction calculators,” such as the Cancer and Aging Research Group tool and the Chemotherapy Risk Assessment Scale for High-Age Patients.
In addition, gene-based assays, such as Oncotype DX and MammaPrint, which were not taken into account for the study, can be applied to estimate the likely benefit of chemotherapy and further inform the treatment decision.
“It can’t be that chemotherapy is making these patients live longer. It has to be that the doctors know not to give chemotherapy to those who are going to die soon,” speculated symposium attendee Steven E. Vogl, MD, an oncologist at Montefiore Medical Center, New York.
He therefore wondered if the amount of chemotherapy received was related to survival. “If it was a chemotherapy effect, then more is probably better, and if it’s a selection effect at the time of initiation, then more probably wouldn’t be better.”
“These are the issues we run into when we use the National Cancer Database or such large databases,” Dr. Sinha replied. “We don’t necessarily have the information on how much chemotherapy the patients received. It really is based on if they received chemotherapy or not.”
Study details
The 160,676 patients studied were treated for stage I-III breast cancer during 2004-2015 and were included regardless of hormone receptor status and HER2 status.
Overall, 60.45% received adjuvant chemotherapy, Dr. Sinha reported. Mean age was 70.7 years among chemotherapy recipients and 75.5 years among nonrecipients.
Women were more likely to receive adjuvant chemotherapy if they had a tumor grade of 2 or 3 (adjusted odds ratios, 1.88 and 3.51), had a tumor negative for both estrogen and progesterone receptors or just progesterone receptors (aOR, 2.72 and 1.70), had private insurance versus Medicaid or Medicare (aOR, 1.40 and 1.20), or received radiation therapy (aOR, 2.55).
Women were less likely to receive adjuvant chemotherapy if they had stage 1 or 2 disease (aOR, 0.23 and 0.56; P less than .0001 for each), were older than 80 years (aOR, 0.105; P less than .0001), had undergone lumpectomy versus mastectomy (aOR, 0.82; P = .0011), were treated in an academic versus community program (aOR, 0.93; P = .0007), or had a Charlson/Deyo comorbidity score of 3 or higher (aOR, 0.38; P less than .0001).
Median overall survival was 144.9 months with and 112.6 months without adjuvant chemotherapy. The difference translated to a significantly reduced risk of death for the women given adjuvant chemotherapy (adjusted hazard ratio, 0.617; P less than .0001). The corresponding 10-year overall survival rates were 59.5% and 46.7%.
The reduced risk of death with adjuvant chemotherapy was evident in women with stage 1 disease (aHR, 0.801), stage 2 disease (aHR, 0.608), and stage 3 disease (aHR, 0.666) (P less than .0001 for all). It was also evident in those with tumors positive for both estrogen and progesterone receptors (aHR, 0.649), negative for progesterone receptors only (aHR, 0.609), and negative for both (aHR, 0.547) (P less than .0001 for all).
“The HER2/neu patient unfortunately was not well defined since there was no data [on that marker] before 2010,” Dr. Sinha noted
Dr. Sinha reported no relevant conflicts of interest. The study received funding from the Research Foundation of SUNY.
SOURCE: Sinha S et al. SABCS 2018, Abstract GS2-02.
REPORTING FROM SABCS 2018
Key clinical point: Older patients with early breast cancer who are given adjuvant chemotherapy live longer.
Major finding: Receipt of adjuvant chemotherapy was associated with a reduced risk of death after taking into account factors such as age and comorbidity burden (adjusted hazard ratio, 0.617; P less than .0001).
Study details: A retrospective cohort study of 160,676 breast cancer patients aged 65 years and older with stage I-III disease.
Disclosures: Dr. Sinha reported no relevant conflicts of interest. The study received funding from the Research Foundation of SUNY.
Source: Sinha S et al. SABCS 2018, Abstract GS2-02.
Early maladaptive schemas increase suicide risk, ideation in bipolar
The entitlement, social isolation, and defectiveness early maladaptive schemas (EMSs) were associated with increased suicide risk and ideation in patients with bipolar disorder, according to Vahid Khosravani of Shahid Beheshti University of Medical Sciences, Tehran, Iran, and his associates.
“These findings were in line with previous studies (J Nerv Ment Dis. 2016 Mar. 204[3]:236-9) showing higher scores of social isolation and entitlement in [bipolar disorder] patients with suicide attempts than those without such attempts,” Mr. Khosravani and his associates wrote in Psychiatry Research.
For the study, 100 inpatients with bipolar disorder completed the Young Schema Questionnaire–Short Form (YSQ-SF), the Bipolar Depression Rating Scale (BDRS), the Young Mania Rating Scale (YMRS), and the Beck Scale for Suicidal Ideation (BSSI). Of that group, 59% had attempted suicide and 59% had a BSSI score of 6 or higher, indicating high suicidal risk, reported Mr. Khosravani and his associates.
; they also had higher levels of depressive and hypomanic/manic symptoms. Current suicide ideation was associated with higher entitlement and defectiveness EMS scores, as well as with increased hypomanic/manic symptoms.
“The findings suggest that manic symptoms as well as specific EMSs including social isolation, entitlement, and defectiveness emerge as potentially implicated in suicidality in BD patients,” the investigators noted. “Therefore, providing social support in the economic, social, political, cultural, and educational spheres may be a factor in preventing suicide.”
Mr. Khosravani and his associates said their study received no funding from public, commercial, or nonprofit agencies. The investigators declared no conflicts of interest.
SOURCE: Khosravani V et al. Psychiatry Res. 2019 Jan. (271):351-9.
The entitlement, social isolation, and defectiveness early maladaptive schemas (EMSs) were associated with increased suicide risk and ideation in patients with bipolar disorder, according to Vahid Khosravani of Shahid Beheshti University of Medical Sciences, Tehran, Iran, and his associates.
“These findings were in line with previous studies (J Nerv Ment Dis. 2016 Mar. 204[3]:236-9) showing higher scores of social isolation and entitlement in [bipolar disorder] patients with suicide attempts than those without such attempts,” Mr. Khosravani and his associates wrote in Psychiatry Research.
For the study, 100 inpatients with bipolar disorder completed the Young Schema Questionnaire–Short Form (YSQ-SF), the Bipolar Depression Rating Scale (BDRS), the Young Mania Rating Scale (YMRS), and the Beck Scale for Suicidal Ideation (BSSI). Of that group, 59% had attempted suicide and 59% had a BSSI score of 6 or higher, indicating high suicidal risk, reported Mr. Khosravani and his associates.
; they also had higher levels of depressive and hypomanic/manic symptoms. Current suicide ideation was associated with higher entitlement and defectiveness EMS scores, as well as with increased hypomanic/manic symptoms.
“The findings suggest that manic symptoms as well as specific EMSs including social isolation, entitlement, and defectiveness emerge as potentially implicated in suicidality in BD patients,” the investigators noted. “Therefore, providing social support in the economic, social, political, cultural, and educational spheres may be a factor in preventing suicide.”
Mr. Khosravani and his associates said their study received no funding from public, commercial, or nonprofit agencies. The investigators declared no conflicts of interest.
SOURCE: Khosravani V et al. Psychiatry Res. 2019 Jan. (271):351-9.
The entitlement, social isolation, and defectiveness early maladaptive schemas (EMSs) were associated with increased suicide risk and ideation in patients with bipolar disorder, according to Vahid Khosravani of Shahid Beheshti University of Medical Sciences, Tehran, Iran, and his associates.
“These findings were in line with previous studies (J Nerv Ment Dis. 2016 Mar. 204[3]:236-9) showing higher scores of social isolation and entitlement in [bipolar disorder] patients with suicide attempts than those without such attempts,” Mr. Khosravani and his associates wrote in Psychiatry Research.
For the study, 100 inpatients with bipolar disorder completed the Young Schema Questionnaire–Short Form (YSQ-SF), the Bipolar Depression Rating Scale (BDRS), the Young Mania Rating Scale (YMRS), and the Beck Scale for Suicidal Ideation (BSSI). Of that group, 59% had attempted suicide and 59% had a BSSI score of 6 or higher, indicating high suicidal risk, reported Mr. Khosravani and his associates.
; they also had higher levels of depressive and hypomanic/manic symptoms. Current suicide ideation was associated with higher entitlement and defectiveness EMS scores, as well as with increased hypomanic/manic symptoms.
“The findings suggest that manic symptoms as well as specific EMSs including social isolation, entitlement, and defectiveness emerge as potentially implicated in suicidality in BD patients,” the investigators noted. “Therefore, providing social support in the economic, social, political, cultural, and educational spheres may be a factor in preventing suicide.”
Mr. Khosravani and his associates said their study received no funding from public, commercial, or nonprofit agencies. The investigators declared no conflicts of interest.
SOURCE: Khosravani V et al. Psychiatry Res. 2019 Jan. (271):351-9.
FROM PSYCHIATRY RESEARCH
Jakinib explosion for RA: Where do they fit in clinical practice?
CHICAGO – A measure of clarity regarding how the emerging class of oral Janus kinase inhibitors might fit into clinical practice for treatment of rheumatoid arthritis was supplied by a fusillade of five consecutive strongly positive phase 3 trials presented during a single session at the annual meeting of the American College of Rheumatology.
The session featured three randomized, double-blind, phase 3 trials of the Janus kinase inhibitor (JAKi) upadacitinib in more than 3,200 participants in three different clinical scenarios, known as the SELECT-COMPARE, SELECT-EARLY, and SELECT-MONOTHERAPY trials, along with two Japanese phase 3 trials of peficitinib, a JAK1 and -3 inhibitor, in a total of more than 1,000 rheumatoid arthritis patients.
Upadacitinib
SELECT-COMPARE: Roy M. Fleischmann, MD, presented the findings of this trial in which 1,629 patients with active RA inadequately responsive to methotrexate were randomized 2:2:1 to 26 weeks of once-daily oral upadacitinib at 15 mg, placebo, or 40 mg of adalimumab (Humira) by subcutaneous injection every 2 weeks, all on top of background stable doses of methotrexate.
Upadacitinib, a JAK1 selective agent, was the clear winner, trouncing placebo, unsurprisingly, but more importantly also proving statistically superior to adalimumab – the current go-to drug in patients with an insufficient response to methotrexate – in terms of across-the-board improvement in RA signs and symptoms, quality-of-life measures, and physical function. This result, coupled with the similarly positive findings of a trial of oral baricitinib (Olumiant) versus adalimumab in inadequate responders to methotrexate alone, and a third positive trial of oral tofacitinib (Xeljanz), have altered Dr. Fleischmann’s treatment philosophy.
“I think that these studies have changed the treatment paradigm. And I think if access – that is, costs – were the same, given a choice, if it were me, I would actually use a JAK inhibitor before I would use adalimumab, based on the results of these multiple studies in different populations,” said Dr. Fleischmann, a rheumatologist at the University of Texas Southwestern Medical Center, Dallas.
The two coprimary endpoints in SELECT-COMPARE were the week 12 American College of Rheumatology–defined 20% level of response (ACR 20) and a 28-joint Disease Activity Score based on C-reactive protein (DAS28-CRP). The ACR 20 response rate was 70.5% with upadacitinib 15 mg, significantly better than the 63% rate with adalimumab and the 36.4% rate with placebo. Similarly, the ACR 50 rate at 12 weeks was 45.2% with upadacitinib versus 29.1% with adalimumab, and ACR 70 rates were 24.9% and 13.5%, respectively.
“These are not small differences,” the rheumatologist observed. “That ACR 70 rate is almost doubled with upadacitinib.”
The rate for DAS28-CRP less than 2.6 at week 12 was 28.7% with upadacitinib, compared with 18% with adalimumab.
Improvements in pain scores and the Health Assessment Questionnaire Disability Index were also significantly greater with the JAKi, both at weeks 12 and 26.
As in the other two SELECT phase 3 trials presented at the meeting, the response to upadacitinib was quick: The JAKi was superior to placebo on the efficacy endpoints by week 2, and superior to adalimumab by week 4.
The week-12 Boolean remission rate, a stringent measure, was 9.8% in the upadacitinib group, more than twice the 4% rate with adalimumab. At week 26, the rates were 18.1% and 9.8%, respectively, a finding Dr. Fleischmann deemed “very impressive.”
Radiographic disease progression as measured by change in modified total Sharp score (mTSS) at week 26 was 0.92 with placebo, 0.24 with upadacitinib, and slightly better at 0.1 with adalimumab. Adalimumab was also slightly better than baricitinib by this metric in a separate randomized trial. But that’s not a deal breaker for Dr. Fleischmann.
“It’s a 0.1–Sharp unit difference over 6 months. So by the time a patient would be able to tell the difference clinically, if my calculation is correct they’ll be 712 years old,” he quipped.
Serious infection rates through 26 weeks were similar in the upadacitinib and adalimumab study arms, with both being higher than placebo. Venous thromboembolism occurred in one patient on placebo, two on upadacitinib, and three on adalimumab.
SELECT-EARLY: This trial involved 947 methotrexate-naive patients with moderately to severely active RA deemed at baseline to be at high risk for disease progression. They were randomized to upadacitinib at 15 or 30 mg once daily or to methotrexate monotherapy. The markers utilized for high-risk disease were positive serology, an elevated CRP, and/or erosions at baseline, explained Ronald van Vollenhoven, MD, PhD, professor of rheumatology at the University of Amsterdam.
The coprimary endpoints were the week 12 ACR 50 and DAS28-CRP-less-than-2.6 response rates. ACR 50 was achieved in 28.3% of patients on methotrexate, 52.1% on the lower dose of upadacitinib, and 56.4% on upadacitinib 30 mg. The corresponding week 24 rates were 33.4%, 60.3%, and 65.6%.
The week 12 DAS28-CRP-less-than-2.6 rates were 13.7%, 35.6%, and 40.8%. By week 24, the rates had improved to 18.5%, 48.3%, and 50%.
Other functional, clinical, and quality-of-life endpoints followed suit. There was no radiographic progression over the course of 24 weeks in 77.7% of patients on methotrexate, 87.5% on upadacitinib 15 mg, and 89.3% on the JAKi at 30 mg.
The safety profile of upadacitinib was generally similar to that of methotrexate. Decreases in hemoglobin and neutrophils were more common in the high-dose upadacitinib group, while increased transaminase levels and reduced lymphocytes occurred more often with methotrexate.
Asked if the SELECT-EARLY results will lead to a change in the major guidelines for treatment of early RA, Dr. van Vollenhoven replied: “The advent of JAKis is changing the treatment of RA. Right now the positioning of JAKis is a big point of discussion: Should they be second or third or even fourth line? But it’s clear that methotrexate stands undisputed as the first-line treatment for RA in clinical practice. That has to do in part with lots and lots of experience, the fact that some patients do well with methotrexate, the convenience, but also the pricing.”
The goal in SELECT-EARLY was to test an individualized approach in which JAKis, which are clearly more effective than methotrexate, might be reserved as first-line therapy for the subgroup of patients with compelling markers for worse prognosis, and who are therefore less likely to turn out to be methotrexate responders.
“The markers we used aren’t good enough yet to engage in individualized treatment with a very specific drug, but we’re all trying very hard to find out who needs which treatment at which point in time,” the rheumatologist said.
SELECT-MONOTHERAPY: This trial randomized 648 patients with active RA and insufficient response to methotrexate to double-blind monotherapy with once-daily upadacitinib at 15 or 30 mg or to continued methotrexate.
Once again, upadacitinib achieved all of its primary and secondary endpoints. The week 14 ACR 20 rates for methotrexate and low- and high-dose upadacitinib were 41.2%, 67.7%, and 71.2%, respectively, with DAS28-CRP-less-than-or-equal-to-3.2 rates of 19.4%, 44.7%, and 53%. Remission as defined by a Clinical Disease Activity Index (CDAI) score of 2.8 or less was achieved in 1% of patients on methotrexate, 15% on upadacitinib 15 mg, and nearly 20% with upadacitinib 30 mg, reported Josef S. Smolen, MD, professor of medicine and chairman of rheumatology at the Medical University of Vienna.
Peficitinib
Yoshiya Tanaka, MD, PhD, professor and chairman of the department of internal medicine at the University of Occupational and Environmental Health in Kitakyushu, Japan, presented the findings of two pivotal phase 3, placebo-controlled, double-blind clinical trials of peficitinib at 100 or 150 mg once daily in 1,025 Asian patients with active RA insufficiently responsive to methotrexate or other disease-modifying antirheumatic drugs. Both studies were positive for all the key endpoints. Based upon these results, the drug’s developer, Astellas Pharma, has filed for Japanese regulatory approval of peficitinib.
Which oral JAKi to use?
Some audience members, numbed by the parade of positive results, asked the investigators for guidance as to which JAKi to choose, and when.
“The upadacitinib dataset mirrors the two approved oral JAKis. The data all look very similar,” said Stanley B. Cohen, MD, codirector of the division of rheumatology at Presbyterian Hospital in Dallas and a former ACR president. “All the JAKis are effective; the safety profiles are similar. Can you help clinicians know what differentiates them? Why should I choose one or the other?”
Dr. Tanaka replied that, although much gets made of the between-agent differences in selectivity for JAK1, 2, and/or 3 inhibition, “In the human body we cannot see much difference in safety and efficacy.”
If indeed such differences exist, head-to-head randomized trials will be required to ferret them out, noted Dr. Fleischmann.
Dr. Smolen indicated rheumatologists ought to rejoice in the looming prospect of a fistful of JAKis to choose from.
“I always wondered which beta-blocker to use, and I always wondered which cholesterol-lowering drug to use, and which NSAID to use – and interestingly enough, one NSAID will work in you but not in me, and another will work in me but not in you. So I think we should be pleased that we will have several oral JAKis to choose from,” he said.
Dr. Fleischmann got in the final word: “The answer to your question is the way we always answer it in the office. It’s access. Whichever one has the best access for the patient is the one you would select.”
The SELECT trials were sponsored by AbbVie, and all the upadacitinib investigators reported receiving research funds from and serving as paid consultants to that company and numerous others. Dr. Tanaka reported receiving research grants from and serving as a paid consultant to Astellas Pharma and close to a dozen other pharmaceutical companies.
CHICAGO – A measure of clarity regarding how the emerging class of oral Janus kinase inhibitors might fit into clinical practice for treatment of rheumatoid arthritis was supplied by a fusillade of five consecutive strongly positive phase 3 trials presented during a single session at the annual meeting of the American College of Rheumatology.
The session featured three randomized, double-blind, phase 3 trials of the Janus kinase inhibitor (JAKi) upadacitinib in more than 3,200 participants in three different clinical scenarios, known as the SELECT-COMPARE, SELECT-EARLY, and SELECT-MONOTHERAPY trials, along with two Japanese phase 3 trials of peficitinib, a JAK1 and -3 inhibitor, in a total of more than 1,000 rheumatoid arthritis patients.
Upadacitinib
SELECT-COMPARE: Roy M. Fleischmann, MD, presented the findings of this trial in which 1,629 patients with active RA inadequately responsive to methotrexate were randomized 2:2:1 to 26 weeks of once-daily oral upadacitinib at 15 mg, placebo, or 40 mg of adalimumab (Humira) by subcutaneous injection every 2 weeks, all on top of background stable doses of methotrexate.
Upadacitinib, a JAK1 selective agent, was the clear winner, trouncing placebo, unsurprisingly, but more importantly also proving statistically superior to adalimumab – the current go-to drug in patients with an insufficient response to methotrexate – in terms of across-the-board improvement in RA signs and symptoms, quality-of-life measures, and physical function. This result, coupled with the similarly positive findings of a trial of oral baricitinib (Olumiant) versus adalimumab in inadequate responders to methotrexate alone, and a third positive trial of oral tofacitinib (Xeljanz), have altered Dr. Fleischmann’s treatment philosophy.
“I think that these studies have changed the treatment paradigm. And I think if access – that is, costs – were the same, given a choice, if it were me, I would actually use a JAK inhibitor before I would use adalimumab, based on the results of these multiple studies in different populations,” said Dr. Fleischmann, a rheumatologist at the University of Texas Southwestern Medical Center, Dallas.
The two coprimary endpoints in SELECT-COMPARE were the week 12 American College of Rheumatology–defined 20% level of response (ACR 20) and a 28-joint Disease Activity Score based on C-reactive protein (DAS28-CRP). The ACR 20 response rate was 70.5% with upadacitinib 15 mg, significantly better than the 63% rate with adalimumab and the 36.4% rate with placebo. Similarly, the ACR 50 rate at 12 weeks was 45.2% with upadacitinib versus 29.1% with adalimumab, and ACR 70 rates were 24.9% and 13.5%, respectively.
“These are not small differences,” the rheumatologist observed. “That ACR 70 rate is almost doubled with upadacitinib.”
The rate for DAS28-CRP less than 2.6 at week 12 was 28.7% with upadacitinib, compared with 18% with adalimumab.
Improvements in pain scores and the Health Assessment Questionnaire Disability Index were also significantly greater with the JAKi, both at weeks 12 and 26.
As in the other two SELECT phase 3 trials presented at the meeting, the response to upadacitinib was quick: The JAKi was superior to placebo on the efficacy endpoints by week 2, and superior to adalimumab by week 4.
The week-12 Boolean remission rate, a stringent measure, was 9.8% in the upadacitinib group, more than twice the 4% rate with adalimumab. At week 26, the rates were 18.1% and 9.8%, respectively, a finding Dr. Fleischmann deemed “very impressive.”
Radiographic disease progression as measured by change in modified total Sharp score (mTSS) at week 26 was 0.92 with placebo, 0.24 with upadacitinib, and slightly better at 0.1 with adalimumab. Adalimumab was also slightly better than baricitinib by this metric in a separate randomized trial. But that’s not a deal breaker for Dr. Fleischmann.
“It’s a 0.1–Sharp unit difference over 6 months. So by the time a patient would be able to tell the difference clinically, if my calculation is correct they’ll be 712 years old,” he quipped.
Serious infection rates through 26 weeks were similar in the upadacitinib and adalimumab study arms, with both being higher than placebo. Venous thromboembolism occurred in one patient on placebo, two on upadacitinib, and three on adalimumab.
SELECT-EARLY: This trial involved 947 methotrexate-naive patients with moderately to severely active RA deemed at baseline to be at high risk for disease progression. They were randomized to upadacitinib at 15 or 30 mg once daily or to methotrexate monotherapy. The markers utilized for high-risk disease were positive serology, an elevated CRP, and/or erosions at baseline, explained Ronald van Vollenhoven, MD, PhD, professor of rheumatology at the University of Amsterdam.
The coprimary endpoints were the week 12 ACR 50 and DAS28-CRP-less-than-2.6 response rates. ACR 50 was achieved in 28.3% of patients on methotrexate, 52.1% on the lower dose of upadacitinib, and 56.4% on upadacitinib 30 mg. The corresponding week 24 rates were 33.4%, 60.3%, and 65.6%.
The week 12 DAS28-CRP-less-than-2.6 rates were 13.7%, 35.6%, and 40.8%. By week 24, the rates had improved to 18.5%, 48.3%, and 50%.
Other functional, clinical, and quality-of-life endpoints followed suit. There was no radiographic progression over the course of 24 weeks in 77.7% of patients on methotrexate, 87.5% on upadacitinib 15 mg, and 89.3% on the JAKi at 30 mg.
The safety profile of upadacitinib was generally similar to that of methotrexate. Decreases in hemoglobin and neutrophils were more common in the high-dose upadacitinib group, while increased transaminase levels and reduced lymphocytes occurred more often with methotrexate.
Asked if the SELECT-EARLY results will lead to a change in the major guidelines for treatment of early RA, Dr. van Vollenhoven replied: “The advent of JAKis is changing the treatment of RA. Right now the positioning of JAKis is a big point of discussion: Should they be second or third or even fourth line? But it’s clear that methotrexate stands undisputed as the first-line treatment for RA in clinical practice. That has to do in part with lots and lots of experience, the fact that some patients do well with methotrexate, the convenience, but also the pricing.”
The goal in SELECT-EARLY was to test an individualized approach in which JAKis, which are clearly more effective than methotrexate, might be reserved as first-line therapy for the subgroup of patients with compelling markers for worse prognosis, and who are therefore less likely to turn out to be methotrexate responders.
“The markers we used aren’t good enough yet to engage in individualized treatment with a very specific drug, but we’re all trying very hard to find out who needs which treatment at which point in time,” the rheumatologist said.
SELECT-MONOTHERAPY: This trial randomized 648 patients with active RA and insufficient response to methotrexate to double-blind monotherapy with once-daily upadacitinib at 15 or 30 mg or to continued methotrexate.
Once again, upadacitinib achieved all of its primary and secondary endpoints. The week 14 ACR 20 rates for methotrexate and low- and high-dose upadacitinib were 41.2%, 67.7%, and 71.2%, respectively, with DAS28-CRP-less-than-or-equal-to-3.2 rates of 19.4%, 44.7%, and 53%. Remission as defined by a Clinical Disease Activity Index (CDAI) score of 2.8 or less was achieved in 1% of patients on methotrexate, 15% on upadacitinib 15 mg, and nearly 20% with upadacitinib 30 mg, reported Josef S. Smolen, MD, professor of medicine and chairman of rheumatology at the Medical University of Vienna.
Peficitinib
Yoshiya Tanaka, MD, PhD, professor and chairman of the department of internal medicine at the University of Occupational and Environmental Health in Kitakyushu, Japan, presented the findings of two pivotal phase 3, placebo-controlled, double-blind clinical trials of peficitinib at 100 or 150 mg once daily in 1,025 Asian patients with active RA insufficiently responsive to methotrexate or other disease-modifying antirheumatic drugs. Both studies were positive for all the key endpoints. Based upon these results, the drug’s developer, Astellas Pharma, has filed for Japanese regulatory approval of peficitinib.
Which oral JAKi to use?
Some audience members, numbed by the parade of positive results, asked the investigators for guidance as to which JAKi to choose, and when.
“The upadacitinib dataset mirrors the two approved oral JAKis. The data all look very similar,” said Stanley B. Cohen, MD, codirector of the division of rheumatology at Presbyterian Hospital in Dallas and a former ACR president. “All the JAKis are effective; the safety profiles are similar. Can you help clinicians know what differentiates them? Why should I choose one or the other?”
Dr. Tanaka replied that, although much gets made of the between-agent differences in selectivity for JAK1, 2, and/or 3 inhibition, “In the human body we cannot see much difference in safety and efficacy.”
If indeed such differences exist, head-to-head randomized trials will be required to ferret them out, noted Dr. Fleischmann.
Dr. Smolen indicated rheumatologists ought to rejoice in the looming prospect of a fistful of JAKis to choose from.
“I always wondered which beta-blocker to use, and I always wondered which cholesterol-lowering drug to use, and which NSAID to use – and interestingly enough, one NSAID will work in you but not in me, and another will work in me but not in you. So I think we should be pleased that we will have several oral JAKis to choose from,” he said.
Dr. Fleischmann got in the final word: “The answer to your question is the way we always answer it in the office. It’s access. Whichever one has the best access for the patient is the one you would select.”
The SELECT trials were sponsored by AbbVie, and all the upadacitinib investigators reported receiving research funds from and serving as paid consultants to that company and numerous others. Dr. Tanaka reported receiving research grants from and serving as a paid consultant to Astellas Pharma and close to a dozen other pharmaceutical companies.
CHICAGO – A measure of clarity regarding how the emerging class of oral Janus kinase inhibitors might fit into clinical practice for treatment of rheumatoid arthritis was supplied by a fusillade of five consecutive strongly positive phase 3 trials presented during a single session at the annual meeting of the American College of Rheumatology.
The session featured three randomized, double-blind, phase 3 trials of the Janus kinase inhibitor (JAKi) upadacitinib in more than 3,200 participants in three different clinical scenarios, known as the SELECT-COMPARE, SELECT-EARLY, and SELECT-MONOTHERAPY trials, along with two Japanese phase 3 trials of peficitinib, a JAK1 and -3 inhibitor, in a total of more than 1,000 rheumatoid arthritis patients.
Upadacitinib
SELECT-COMPARE: Roy M. Fleischmann, MD, presented the findings of this trial in which 1,629 patients with active RA inadequately responsive to methotrexate were randomized 2:2:1 to 26 weeks of once-daily oral upadacitinib at 15 mg, placebo, or 40 mg of adalimumab (Humira) by subcutaneous injection every 2 weeks, all on top of background stable doses of methotrexate.
Upadacitinib, a JAK1 selective agent, was the clear winner, trouncing placebo, unsurprisingly, but more importantly also proving statistically superior to adalimumab – the current go-to drug in patients with an insufficient response to methotrexate – in terms of across-the-board improvement in RA signs and symptoms, quality-of-life measures, and physical function. This result, coupled with the similarly positive findings of a trial of oral baricitinib (Olumiant) versus adalimumab in inadequate responders to methotrexate alone, and a third positive trial of oral tofacitinib (Xeljanz), have altered Dr. Fleischmann’s treatment philosophy.
“I think that these studies have changed the treatment paradigm. And I think if access – that is, costs – were the same, given a choice, if it were me, I would actually use a JAK inhibitor before I would use adalimumab, based on the results of these multiple studies in different populations,” said Dr. Fleischmann, a rheumatologist at the University of Texas Southwestern Medical Center, Dallas.
The two coprimary endpoints in SELECT-COMPARE were the week 12 American College of Rheumatology–defined 20% level of response (ACR 20) and a 28-joint Disease Activity Score based on C-reactive protein (DAS28-CRP). The ACR 20 response rate was 70.5% with upadacitinib 15 mg, significantly better than the 63% rate with adalimumab and the 36.4% rate with placebo. Similarly, the ACR 50 rate at 12 weeks was 45.2% with upadacitinib versus 29.1% with adalimumab, and ACR 70 rates were 24.9% and 13.5%, respectively.
“These are not small differences,” the rheumatologist observed. “That ACR 70 rate is almost doubled with upadacitinib.”
The rate for DAS28-CRP less than 2.6 at week 12 was 28.7% with upadacitinib, compared with 18% with adalimumab.
Improvements in pain scores and the Health Assessment Questionnaire Disability Index were also significantly greater with the JAKi, both at weeks 12 and 26.
As in the other two SELECT phase 3 trials presented at the meeting, the response to upadacitinib was quick: The JAKi was superior to placebo on the efficacy endpoints by week 2, and superior to adalimumab by week 4.
The week-12 Boolean remission rate, a stringent measure, was 9.8% in the upadacitinib group, more than twice the 4% rate with adalimumab. At week 26, the rates were 18.1% and 9.8%, respectively, a finding Dr. Fleischmann deemed “very impressive.”
Radiographic disease progression as measured by change in modified total Sharp score (mTSS) at week 26 was 0.92 with placebo, 0.24 with upadacitinib, and slightly better at 0.1 with adalimumab. Adalimumab was also slightly better than baricitinib by this metric in a separate randomized trial. But that’s not a deal breaker for Dr. Fleischmann.
“It’s a 0.1–Sharp unit difference over 6 months. So by the time a patient would be able to tell the difference clinically, if my calculation is correct they’ll be 712 years old,” he quipped.
Serious infection rates through 26 weeks were similar in the upadacitinib and adalimumab study arms, with both being higher than placebo. Venous thromboembolism occurred in one patient on placebo, two on upadacitinib, and three on adalimumab.
SELECT-EARLY: This trial involved 947 methotrexate-naive patients with moderately to severely active RA deemed at baseline to be at high risk for disease progression. They were randomized to upadacitinib at 15 or 30 mg once daily or to methotrexate monotherapy. The markers utilized for high-risk disease were positive serology, an elevated CRP, and/or erosions at baseline, explained Ronald van Vollenhoven, MD, PhD, professor of rheumatology at the University of Amsterdam.
The coprimary endpoints were the week 12 ACR 50 and DAS28-CRP-less-than-2.6 response rates. ACR 50 was achieved in 28.3% of patients on methotrexate, 52.1% on the lower dose of upadacitinib, and 56.4% on upadacitinib 30 mg. The corresponding week 24 rates were 33.4%, 60.3%, and 65.6%.
The week 12 DAS28-CRP-less-than-2.6 rates were 13.7%, 35.6%, and 40.8%. By week 24, the rates had improved to 18.5%, 48.3%, and 50%.
Other functional, clinical, and quality-of-life endpoints followed suit. There was no radiographic progression over the course of 24 weeks in 77.7% of patients on methotrexate, 87.5% on upadacitinib 15 mg, and 89.3% on the JAKi at 30 mg.
The safety profile of upadacitinib was generally similar to that of methotrexate. Decreases in hemoglobin and neutrophils were more common in the high-dose upadacitinib group, while increased transaminase levels and reduced lymphocytes occurred more often with methotrexate.
Asked if the SELECT-EARLY results will lead to a change in the major guidelines for treatment of early RA, Dr. van Vollenhoven replied: “The advent of JAKis is changing the treatment of RA. Right now the positioning of JAKis is a big point of discussion: Should they be second or third or even fourth line? But it’s clear that methotrexate stands undisputed as the first-line treatment for RA in clinical practice. That has to do in part with lots and lots of experience, the fact that some patients do well with methotrexate, the convenience, but also the pricing.”
The goal in SELECT-EARLY was to test an individualized approach in which JAKis, which are clearly more effective than methotrexate, might be reserved as first-line therapy for the subgroup of patients with compelling markers for worse prognosis, and who are therefore less likely to turn out to be methotrexate responders.
“The markers we used aren’t good enough yet to engage in individualized treatment with a very specific drug, but we’re all trying very hard to find out who needs which treatment at which point in time,” the rheumatologist said.
SELECT-MONOTHERAPY: This trial randomized 648 patients with active RA and insufficient response to methotrexate to double-blind monotherapy with once-daily upadacitinib at 15 or 30 mg or to continued methotrexate.
Once again, upadacitinib achieved all of its primary and secondary endpoints. The week 14 ACR 20 rates for methotrexate and low- and high-dose upadacitinib were 41.2%, 67.7%, and 71.2%, respectively, with DAS28-CRP-less-than-or-equal-to-3.2 rates of 19.4%, 44.7%, and 53%. Remission as defined by a Clinical Disease Activity Index (CDAI) score of 2.8 or less was achieved in 1% of patients on methotrexate, 15% on upadacitinib 15 mg, and nearly 20% with upadacitinib 30 mg, reported Josef S. Smolen, MD, professor of medicine and chairman of rheumatology at the Medical University of Vienna.
Peficitinib
Yoshiya Tanaka, MD, PhD, professor and chairman of the department of internal medicine at the University of Occupational and Environmental Health in Kitakyushu, Japan, presented the findings of two pivotal phase 3, placebo-controlled, double-blind clinical trials of peficitinib at 100 or 150 mg once daily in 1,025 Asian patients with active RA insufficiently responsive to methotrexate or other disease-modifying antirheumatic drugs. Both studies were positive for all the key endpoints. Based upon these results, the drug’s developer, Astellas Pharma, has filed for Japanese regulatory approval of peficitinib.
Which oral JAKi to use?
Some audience members, numbed by the parade of positive results, asked the investigators for guidance as to which JAKi to choose, and when.
“The upadacitinib dataset mirrors the two approved oral JAKis. The data all look very similar,” said Stanley B. Cohen, MD, codirector of the division of rheumatology at Presbyterian Hospital in Dallas and a former ACR president. “All the JAKis are effective; the safety profiles are similar. Can you help clinicians know what differentiates them? Why should I choose one or the other?”
Dr. Tanaka replied that, although much gets made of the between-agent differences in selectivity for JAK1, 2, and/or 3 inhibition, “In the human body we cannot see much difference in safety and efficacy.”
If indeed such differences exist, head-to-head randomized trials will be required to ferret them out, noted Dr. Fleischmann.
Dr. Smolen indicated rheumatologists ought to rejoice in the looming prospect of a fistful of JAKis to choose from.
“I always wondered which beta-blocker to use, and I always wondered which cholesterol-lowering drug to use, and which NSAID to use – and interestingly enough, one NSAID will work in you but not in me, and another will work in me but not in you. So I think we should be pleased that we will have several oral JAKis to choose from,” he said.
Dr. Fleischmann got in the final word: “The answer to your question is the way we always answer it in the office. It’s access. Whichever one has the best access for the patient is the one you would select.”
The SELECT trials were sponsored by AbbVie, and all the upadacitinib investigators reported receiving research funds from and serving as paid consultants to that company and numerous others. Dr. Tanaka reported receiving research grants from and serving as a paid consultant to Astellas Pharma and close to a dozen other pharmaceutical companies.
REPORTING FROM THE ACR ANNUAL MEETING
Risk of second cancers in Hodgkin lymphoma survivors
Survivors of childhood Hodgkin lymphoma (HL) have a 14-fold higher risk of second cancers compared to the general population, according to new research.
The subsequent malignant neoplasms (SMNs) observed in HL survivors tended to follow specific patterns depending on the patient’s age at treatment, sex, treatment modality, and region of the body treated.
And although the risk of SMNs appears to be somewhat lower for HL patients treated in more recent decades, it is still significantly higher than the risk in the general population, according to investigators.
Anna S. Holmqvist, MD, PhD, of the University of Lund in Sweden, and her colleagues conducted this research and reported the results in Cancer.
The investigators looked at data from the Late Effects Study Group, a multinational cohort of patients age 16 or younger who were treated for HL and other cancers from 1955 through 1986.
The current report is the third update from an expanded cohort including data on 1,136 patients with a median follow-up of 26.6 years. The median patient age at diagnosis was 11 years (range, birth to 16 years), and the patients were followed for 23,212 person-years after HL diagnosis.
In all, 162 patients developed 196 SMNs, including breast cancer (n=54), basal cell carcinoma (n=34), thyroid cancer (n=30), colorectal cancer (n=15), lung cancer (n=11), and other malignancies (n=40). The disease site was not available in 12 cases.
The cumulative incidence of any SMN 40 years after HL diagnosis was 26.4%. By age 50, the cumulative incidence of any SMN was 27.2%.
The standardized incidence ratio for the entire cohort was 14.0, compared with the general population as derived from the Surveillance, Epidemiology and End Results database.
Risk factors by cancer type
Females treated with chest radiotherapy between the ages of 10 and 16 who did not receive alkylating agents or received low doses of alkylating agents had the highest risk of developing breast cancer. The cumulative incidence of breast cancer by age 50 was 45.3% in these patients.
The patients with the highest risk for subsequent lung cancer were males treated with chest radiotherapy before age 10. The cumulative incidence of lung cancer by age 50 was 4.2% in these patients.
Patients with the highest risk for colorectal cancer had received abdominal/pelvic radiotherapy and high-dose alkylating agents. The cumulative incidence of colorectal cancer by age 50 was 9.5% in these patients.
Patients with the highest risk for thyroid cancers were females who had been treated with radiotherapy to the neck before the age of 10. The cumulative incidence of thyroid cancer by age 50 was 17.3% in these patients.
The investigators noted that HL patients treated more recently are likely to have received lower doses and volumes of radiotherapy compared to patients treated in the 1950s, ’60s and ’70s.
“However, for the cohort of patients treated between 1955 and 1986, it is clear that continued surveillance for SMNs is essential because their risk continues to increase as these survivors enter their fourth and subsequent decades of life,” the investigators wrote.
They did not report a funding source for this research or make any conflict-of-interest disclosures.
Survivors of childhood Hodgkin lymphoma (HL) have a 14-fold higher risk of second cancers compared to the general population, according to new research.
The subsequent malignant neoplasms (SMNs) observed in HL survivors tended to follow specific patterns depending on the patient’s age at treatment, sex, treatment modality, and region of the body treated.
And although the risk of SMNs appears to be somewhat lower for HL patients treated in more recent decades, it is still significantly higher than the risk in the general population, according to investigators.
Anna S. Holmqvist, MD, PhD, of the University of Lund in Sweden, and her colleagues conducted this research and reported the results in Cancer.
The investigators looked at data from the Late Effects Study Group, a multinational cohort of patients age 16 or younger who were treated for HL and other cancers from 1955 through 1986.
The current report is the third update from an expanded cohort including data on 1,136 patients with a median follow-up of 26.6 years. The median patient age at diagnosis was 11 years (range, birth to 16 years), and the patients were followed for 23,212 person-years after HL diagnosis.
In all, 162 patients developed 196 SMNs, including breast cancer (n=54), basal cell carcinoma (n=34), thyroid cancer (n=30), colorectal cancer (n=15), lung cancer (n=11), and other malignancies (n=40). The disease site was not available in 12 cases.
The cumulative incidence of any SMN 40 years after HL diagnosis was 26.4%. By age 50, the cumulative incidence of any SMN was 27.2%.
The standardized incidence ratio for the entire cohort was 14.0, compared with the general population as derived from the Surveillance, Epidemiology and End Results database.
Risk factors by cancer type
Females treated with chest radiotherapy between the ages of 10 and 16 who did not receive alkylating agents or received low doses of alkylating agents had the highest risk of developing breast cancer. The cumulative incidence of breast cancer by age 50 was 45.3% in these patients.
The patients with the highest risk for subsequent lung cancer were males treated with chest radiotherapy before age 10. The cumulative incidence of lung cancer by age 50 was 4.2% in these patients.
Patients with the highest risk for colorectal cancer had received abdominal/pelvic radiotherapy and high-dose alkylating agents. The cumulative incidence of colorectal cancer by age 50 was 9.5% in these patients.
Patients with the highest risk for thyroid cancers were females who had been treated with radiotherapy to the neck before the age of 10. The cumulative incidence of thyroid cancer by age 50 was 17.3% in these patients.
The investigators noted that HL patients treated more recently are likely to have received lower doses and volumes of radiotherapy compared to patients treated in the 1950s, ’60s and ’70s.
“However, for the cohort of patients treated between 1955 and 1986, it is clear that continued surveillance for SMNs is essential because their risk continues to increase as these survivors enter their fourth and subsequent decades of life,” the investigators wrote.
They did not report a funding source for this research or make any conflict-of-interest disclosures.
Survivors of childhood Hodgkin lymphoma (HL) have a 14-fold higher risk of second cancers compared to the general population, according to new research.
The subsequent malignant neoplasms (SMNs) observed in HL survivors tended to follow specific patterns depending on the patient’s age at treatment, sex, treatment modality, and region of the body treated.
And although the risk of SMNs appears to be somewhat lower for HL patients treated in more recent decades, it is still significantly higher than the risk in the general population, according to investigators.
Anna S. Holmqvist, MD, PhD, of the University of Lund in Sweden, and her colleagues conducted this research and reported the results in Cancer.
The investigators looked at data from the Late Effects Study Group, a multinational cohort of patients age 16 or younger who were treated for HL and other cancers from 1955 through 1986.
The current report is the third update from an expanded cohort including data on 1,136 patients with a median follow-up of 26.6 years. The median patient age at diagnosis was 11 years (range, birth to 16 years), and the patients were followed for 23,212 person-years after HL diagnosis.
In all, 162 patients developed 196 SMNs, including breast cancer (n=54), basal cell carcinoma (n=34), thyroid cancer (n=30), colorectal cancer (n=15), lung cancer (n=11), and other malignancies (n=40). The disease site was not available in 12 cases.
The cumulative incidence of any SMN 40 years after HL diagnosis was 26.4%. By age 50, the cumulative incidence of any SMN was 27.2%.
The standardized incidence ratio for the entire cohort was 14.0, compared with the general population as derived from the Surveillance, Epidemiology and End Results database.
Risk factors by cancer type
Females treated with chest radiotherapy between the ages of 10 and 16 who did not receive alkylating agents or received low doses of alkylating agents had the highest risk of developing breast cancer. The cumulative incidence of breast cancer by age 50 was 45.3% in these patients.
The patients with the highest risk for subsequent lung cancer were males treated with chest radiotherapy before age 10. The cumulative incidence of lung cancer by age 50 was 4.2% in these patients.
Patients with the highest risk for colorectal cancer had received abdominal/pelvic radiotherapy and high-dose alkylating agents. The cumulative incidence of colorectal cancer by age 50 was 9.5% in these patients.
Patients with the highest risk for thyroid cancers were females who had been treated with radiotherapy to the neck before the age of 10. The cumulative incidence of thyroid cancer by age 50 was 17.3% in these patients.
The investigators noted that HL patients treated more recently are likely to have received lower doses and volumes of radiotherapy compared to patients treated in the 1950s, ’60s and ’70s.
“However, for the cohort of patients treated between 1955 and 1986, it is clear that continued surveillance for SMNs is essential because their risk continues to increase as these survivors enter their fourth and subsequent decades of life,” the investigators wrote.
They did not report a funding source for this research or make any conflict-of-interest disclosures.
Growth on right hand
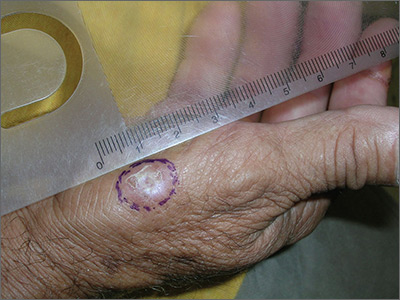
The FP recognized that this could be a wart but was concerned that it might be a squamous cell carcinoma (SCC) related to HPV and sun exposure.
He performed a shave biopsy and the pathology report indicated it was an SCC in situ. (See the Watch & Learn video on “Shave biopsy.”) At the follow-up visit, the FP reviewed the patient’s treatment options, which included topical 5% fluorouracil, topical imiquimod, and surgical excision. He also explained that the topical treatments were off label, so these options might have a lower success rate than the surgery.
The patient chose to have the surgery, even though he’d be out of work while the excision site was healing. The FP provided counseling about sun avoidance, the consistent use of a hat outdoors, and the use of sunscreens when exposed to the sun. He also referred the patient to a dermatologist who had extensive experience doing skin cancer surgery.
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Karnes J, Usatine R. Squamous cell carcinoma. In: Usatine R, Smith M, Mayeaux EJ, et al. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013:999-1007.
To learn more about the Color Atlas of Family Medicine, see: www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/.
The new third edition will be available in January 2019: https://www.amazon.com/Color-Atlas-Synopsis-Family-Medicine/dp/1259862046/.
You can also get the second edition of the Color Atlas of Family Medicine as an app by clicking on this link: usatinemedia.com.

The FP recognized that this could be a wart but was concerned that it might be a squamous cell carcinoma (SCC) related to HPV and sun exposure.
He performed a shave biopsy and the pathology report indicated it was an SCC in situ. (See the Watch & Learn video on “Shave biopsy.”) At the follow-up visit, the FP reviewed the patient’s treatment options, which included topical 5% fluorouracil, topical imiquimod, and surgical excision. He also explained that the topical treatments were off label, so these options might have a lower success rate than the surgery.
The patient chose to have the surgery, even though he’d be out of work while the excision site was healing. The FP provided counseling about sun avoidance, the consistent use of a hat outdoors, and the use of sunscreens when exposed to the sun. He also referred the patient to a dermatologist who had extensive experience doing skin cancer surgery.
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Karnes J, Usatine R. Squamous cell carcinoma. In: Usatine R, Smith M, Mayeaux EJ, et al. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013:999-1007.
To learn more about the Color Atlas of Family Medicine, see: www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/.
The new third edition will be available in January 2019: https://www.amazon.com/Color-Atlas-Synopsis-Family-Medicine/dp/1259862046/.
You can also get the second edition of the Color Atlas of Family Medicine as an app by clicking on this link: usatinemedia.com.

The FP recognized that this could be a wart but was concerned that it might be a squamous cell carcinoma (SCC) related to HPV and sun exposure.
He performed a shave biopsy and the pathology report indicated it was an SCC in situ. (See the Watch & Learn video on “Shave biopsy.”) At the follow-up visit, the FP reviewed the patient’s treatment options, which included topical 5% fluorouracil, topical imiquimod, and surgical excision. He also explained that the topical treatments were off label, so these options might have a lower success rate than the surgery.
The patient chose to have the surgery, even though he’d be out of work while the excision site was healing. The FP provided counseling about sun avoidance, the consistent use of a hat outdoors, and the use of sunscreens when exposed to the sun. He also referred the patient to a dermatologist who had extensive experience doing skin cancer surgery.
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Karnes J, Usatine R. Squamous cell carcinoma. In: Usatine R, Smith M, Mayeaux EJ, et al. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013:999-1007.
To learn more about the Color Atlas of Family Medicine, see: www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/.
The new third edition will be available in January 2019: https://www.amazon.com/Color-Atlas-Synopsis-Family-Medicine/dp/1259862046/.
You can also get the second edition of the Color Atlas of Family Medicine as an app by clicking on this link: usatinemedia.com.
Report criticizes VA’s suicide prevention efforts; author shares depression-fighting strategies
The suicide rate among veterans is almost double that of the general American population. It has been rising among those who served in the wars in Iraq and Afghanistan.
Rep. Tim Walz, the Minnesota Democrat who requested the investigation, reportedly said in a statement. “Unfortunately, VA failed to do that.”
Mr. Walz was referring to a failure in prevention efforts that was detailed in a Government Accountability Office report released recently and was the subject of an article in the New York Times. The report blames bureaucratic confusion and an absence of leadership – epitomized by several department vacancies.
“This is such an important issue; we need to be throwing everything we can at it,” said Caitin Thompson, PhD. She was director of the VA’s suicide prevention efforts but resigned in frustration in mid-2017. “It’s so ludicrous that money would be sitting on the table. Outreach is one of the first ways to engage with veterans and families about ways to get help. If we don’t have that, what do we have?”
Surviving the holidays with depression
The postcard image of the Christmas season is that of joyous celebration with family and friends. For many people, however, this image is false. Many complain about feelings of stress imposed by familial obligations, pressure to conform to those postcard myths, and the financial toll that all of that holiday largesse can exact.
Now add depression to this mix. How can those burdened by depression find some joy at this time of year? In a recent article in the Huffington Post, author Andrea Loewen advises staying away from social media and focusing on the positive.
“[Social media] is a double-edged sword: Either I see all the amazing things everyone else is doing and feel jealous/insignificant/left out, or I see that no one else is really posting and assume they must be too busy having incredible quality time with their families while I’m the unengaged loser scrolling Instagram,” Ms. Loewen wrote. “Either way, it’s bad news.”
One concrete practice that she engages in is taking a few minutes to think about and write down the positive things that happened each day.
“The list includes everything, big and small: from the thoughtful gift I wasn’t expecting to the simple observation that a friend seemed happy to see me,” Ms. Loewen wrote. “Depending on where I’m at in my depression, those seemingly tiny details can be vital reminders I hold a valuable place in the world.”
Artist perpetuates persistent myth
In some ways, Kanye West embraces his diagnosis of bipolar disorder. He calls the illness his “superpower,” and the art on his new album, “Ye,” includes the phrase: “I hate being Bi-Polar/it’s awesome.” But his decision to abandon his medications promotes a myth, Amanda Mull wrote in an opinion piece in the Atlantic.
“In apparently quitting his psychiatric medication for the sake of his creativity, Mr. West is promoting one of mental health’s most persistent and dangerous myths: that suffering is necessary for great art,” Ms. Mull wrote.
Philip R. Muskin, MD, who is affiliated with the department of psychiatry at Columbia University in New York, agreed that linking mental turmoil with creative genius is indeed problematic. “Creative people are not creative when they’re depressed, or so manic that no one can tolerate being with them and they start to merge into psychosis, or when they’re filled with numbing anxiety,” he said in the Atlantic article.
Esmé Weijun Wang concurred and offered a counterview to that of Mr. West. A novelist who has written about living with schizoaffective disorder, she said: “It may be true that mental illness has given me insights with which to work, creatively speaking, but it’s also made me too sick to use that creativity. The voice in my head that says, ‘Die, die, die’ is not a voice that encourages putting together a short story.”
For his part, Mr. West’s decision to stop taking his medicine threatens to undermine his own mental health. And his public musings could drive others away from treatment.
“Antiopioid backlash” causes pain
An article by Fox News has highlighted the daily toll that opioid addiction is exacting on Americans. Government efforts aimed at quelling the use of opioids by targeting availability have had the unintended consequence of the cut-off of prescriptions by many physicians. With that route turned off, many people are turning to other sources for pain relief – or are being left with no relief.
One person in the article related how his wife is unable to obtain pain relief for her neurologic and spinal diseases. “A welcome death has become a discussion,” he said.
Meanwhile, a 69-year-old veteran said the Department of Veterans Affairs ended his pain medication. “I now buy heroin on the street.”
Another person in the article, Herb Erne III, wrote: “As a nurse, I have seen addicts and the other end of opioid abuse. But there is another side to this crisis that people are not talking about, those that actually need pain medications but cannot get them because of the ‘fear factor’ of running afoul of the antiopioid – including legal ones taken safely under medical supervision – backlash.
“The chronically ill who do not abuse, who do not divert, have become the unintended victims of misguided and overzealous efforts by policy- and regulation-making bodies in the government,” he said.
Grandparents filling void
An article in the Detroit News reported on more carnage of the opioid crisis. In Michigan and elsewhere nationwide, increasing numbers of parents with opioid addiction are unable to safely care for their children or have died because of an overdose. Grandparents are stepping in to assume care.
Results of a national survey involving more than 1,000 grandparents found that 20% are the daily caregivers to their grandchildren. They can be on their own, without any financial aid from state or national programs. Other children without grandparents can be diverted to foster care.
It’s a role few grandparents anticipated. “Our system as a whole is messed up. It tears at my heart,” 47-year-old Christina Wasilewski said in the article. “Everyone keeps saying children are resilient, but only to a point.”
Ms. Wasilewski and her husband assumed care for their granddaughter when they discovered her in physical distress from lack of care.
In Michigan, the increase in the rate of opioid-related deaths slowed in 2017 but deaths still rose 9% from 2016 , according to the Michigan Department of Health & Human Services. The prior year the death rate was 35%. In Michigan, grandparents raising their grandchildren do not have legal parental rights for this care, including the right to seek medical care and to pursue educational options.
Ms. Wasilewski’s concern about these trends led her to launch the Caregiver Cafe, a support group for grandparents raising their grandchildren.
The suicide rate among veterans is almost double that of the general American population. It has been rising among those who served in the wars in Iraq and Afghanistan.
Rep. Tim Walz, the Minnesota Democrat who requested the investigation, reportedly said in a statement. “Unfortunately, VA failed to do that.”
Mr. Walz was referring to a failure in prevention efforts that was detailed in a Government Accountability Office report released recently and was the subject of an article in the New York Times. The report blames bureaucratic confusion and an absence of leadership – epitomized by several department vacancies.
“This is such an important issue; we need to be throwing everything we can at it,” said Caitin Thompson, PhD. She was director of the VA’s suicide prevention efforts but resigned in frustration in mid-2017. “It’s so ludicrous that money would be sitting on the table. Outreach is one of the first ways to engage with veterans and families about ways to get help. If we don’t have that, what do we have?”
Surviving the holidays with depression
The postcard image of the Christmas season is that of joyous celebration with family and friends. For many people, however, this image is false. Many complain about feelings of stress imposed by familial obligations, pressure to conform to those postcard myths, and the financial toll that all of that holiday largesse can exact.
Now add depression to this mix. How can those burdened by depression find some joy at this time of year? In a recent article in the Huffington Post, author Andrea Loewen advises staying away from social media and focusing on the positive.
“[Social media] is a double-edged sword: Either I see all the amazing things everyone else is doing and feel jealous/insignificant/left out, or I see that no one else is really posting and assume they must be too busy having incredible quality time with their families while I’m the unengaged loser scrolling Instagram,” Ms. Loewen wrote. “Either way, it’s bad news.”
One concrete practice that she engages in is taking a few minutes to think about and write down the positive things that happened each day.
“The list includes everything, big and small: from the thoughtful gift I wasn’t expecting to the simple observation that a friend seemed happy to see me,” Ms. Loewen wrote. “Depending on where I’m at in my depression, those seemingly tiny details can be vital reminders I hold a valuable place in the world.”
Artist perpetuates persistent myth
In some ways, Kanye West embraces his diagnosis of bipolar disorder. He calls the illness his “superpower,” and the art on his new album, “Ye,” includes the phrase: “I hate being Bi-Polar/it’s awesome.” But his decision to abandon his medications promotes a myth, Amanda Mull wrote in an opinion piece in the Atlantic.
“In apparently quitting his psychiatric medication for the sake of his creativity, Mr. West is promoting one of mental health’s most persistent and dangerous myths: that suffering is necessary for great art,” Ms. Mull wrote.
Philip R. Muskin, MD, who is affiliated with the department of psychiatry at Columbia University in New York, agreed that linking mental turmoil with creative genius is indeed problematic. “Creative people are not creative when they’re depressed, or so manic that no one can tolerate being with them and they start to merge into psychosis, or when they’re filled with numbing anxiety,” he said in the Atlantic article.
Esmé Weijun Wang concurred and offered a counterview to that of Mr. West. A novelist who has written about living with schizoaffective disorder, she said: “It may be true that mental illness has given me insights with which to work, creatively speaking, but it’s also made me too sick to use that creativity. The voice in my head that says, ‘Die, die, die’ is not a voice that encourages putting together a short story.”
For his part, Mr. West’s decision to stop taking his medicine threatens to undermine his own mental health. And his public musings could drive others away from treatment.
“Antiopioid backlash” causes pain
An article by Fox News has highlighted the daily toll that opioid addiction is exacting on Americans. Government efforts aimed at quelling the use of opioids by targeting availability have had the unintended consequence of the cut-off of prescriptions by many physicians. With that route turned off, many people are turning to other sources for pain relief – or are being left with no relief.
One person in the article related how his wife is unable to obtain pain relief for her neurologic and spinal diseases. “A welcome death has become a discussion,” he said.
Meanwhile, a 69-year-old veteran said the Department of Veterans Affairs ended his pain medication. “I now buy heroin on the street.”
Another person in the article, Herb Erne III, wrote: “As a nurse, I have seen addicts and the other end of opioid abuse. But there is another side to this crisis that people are not talking about, those that actually need pain medications but cannot get them because of the ‘fear factor’ of running afoul of the antiopioid – including legal ones taken safely under medical supervision – backlash.
“The chronically ill who do not abuse, who do not divert, have become the unintended victims of misguided and overzealous efforts by policy- and regulation-making bodies in the government,” he said.
Grandparents filling void
An article in the Detroit News reported on more carnage of the opioid crisis. In Michigan and elsewhere nationwide, increasing numbers of parents with opioid addiction are unable to safely care for their children or have died because of an overdose. Grandparents are stepping in to assume care.
Results of a national survey involving more than 1,000 grandparents found that 20% are the daily caregivers to their grandchildren. They can be on their own, without any financial aid from state or national programs. Other children without grandparents can be diverted to foster care.
It’s a role few grandparents anticipated. “Our system as a whole is messed up. It tears at my heart,” 47-year-old Christina Wasilewski said in the article. “Everyone keeps saying children are resilient, but only to a point.”
Ms. Wasilewski and her husband assumed care for their granddaughter when they discovered her in physical distress from lack of care.
In Michigan, the increase in the rate of opioid-related deaths slowed in 2017 but deaths still rose 9% from 2016 , according to the Michigan Department of Health & Human Services. The prior year the death rate was 35%. In Michigan, grandparents raising their grandchildren do not have legal parental rights for this care, including the right to seek medical care and to pursue educational options.
Ms. Wasilewski’s concern about these trends led her to launch the Caregiver Cafe, a support group for grandparents raising their grandchildren.
The suicide rate among veterans is almost double that of the general American population. It has been rising among those who served in the wars in Iraq and Afghanistan.
Rep. Tim Walz, the Minnesota Democrat who requested the investigation, reportedly said in a statement. “Unfortunately, VA failed to do that.”
Mr. Walz was referring to a failure in prevention efforts that was detailed in a Government Accountability Office report released recently and was the subject of an article in the New York Times. The report blames bureaucratic confusion and an absence of leadership – epitomized by several department vacancies.
“This is such an important issue; we need to be throwing everything we can at it,” said Caitin Thompson, PhD. She was director of the VA’s suicide prevention efforts but resigned in frustration in mid-2017. “It’s so ludicrous that money would be sitting on the table. Outreach is one of the first ways to engage with veterans and families about ways to get help. If we don’t have that, what do we have?”
Surviving the holidays with depression
The postcard image of the Christmas season is that of joyous celebration with family and friends. For many people, however, this image is false. Many complain about feelings of stress imposed by familial obligations, pressure to conform to those postcard myths, and the financial toll that all of that holiday largesse can exact.
Now add depression to this mix. How can those burdened by depression find some joy at this time of year? In a recent article in the Huffington Post, author Andrea Loewen advises staying away from social media and focusing on the positive.
“[Social media] is a double-edged sword: Either I see all the amazing things everyone else is doing and feel jealous/insignificant/left out, or I see that no one else is really posting and assume they must be too busy having incredible quality time with their families while I’m the unengaged loser scrolling Instagram,” Ms. Loewen wrote. “Either way, it’s bad news.”
One concrete practice that she engages in is taking a few minutes to think about and write down the positive things that happened each day.
“The list includes everything, big and small: from the thoughtful gift I wasn’t expecting to the simple observation that a friend seemed happy to see me,” Ms. Loewen wrote. “Depending on where I’m at in my depression, those seemingly tiny details can be vital reminders I hold a valuable place in the world.”
Artist perpetuates persistent myth
In some ways, Kanye West embraces his diagnosis of bipolar disorder. He calls the illness his “superpower,” and the art on his new album, “Ye,” includes the phrase: “I hate being Bi-Polar/it’s awesome.” But his decision to abandon his medications promotes a myth, Amanda Mull wrote in an opinion piece in the Atlantic.
“In apparently quitting his psychiatric medication for the sake of his creativity, Mr. West is promoting one of mental health’s most persistent and dangerous myths: that suffering is necessary for great art,” Ms. Mull wrote.
Philip R. Muskin, MD, who is affiliated with the department of psychiatry at Columbia University in New York, agreed that linking mental turmoil with creative genius is indeed problematic. “Creative people are not creative when they’re depressed, or so manic that no one can tolerate being with them and they start to merge into psychosis, or when they’re filled with numbing anxiety,” he said in the Atlantic article.
Esmé Weijun Wang concurred and offered a counterview to that of Mr. West. A novelist who has written about living with schizoaffective disorder, she said: “It may be true that mental illness has given me insights with which to work, creatively speaking, but it’s also made me too sick to use that creativity. The voice in my head that says, ‘Die, die, die’ is not a voice that encourages putting together a short story.”
For his part, Mr. West’s decision to stop taking his medicine threatens to undermine his own mental health. And his public musings could drive others away from treatment.
“Antiopioid backlash” causes pain
An article by Fox News has highlighted the daily toll that opioid addiction is exacting on Americans. Government efforts aimed at quelling the use of opioids by targeting availability have had the unintended consequence of the cut-off of prescriptions by many physicians. With that route turned off, many people are turning to other sources for pain relief – or are being left with no relief.
One person in the article related how his wife is unable to obtain pain relief for her neurologic and spinal diseases. “A welcome death has become a discussion,” he said.
Meanwhile, a 69-year-old veteran said the Department of Veterans Affairs ended his pain medication. “I now buy heroin on the street.”
Another person in the article, Herb Erne III, wrote: “As a nurse, I have seen addicts and the other end of opioid abuse. But there is another side to this crisis that people are not talking about, those that actually need pain medications but cannot get them because of the ‘fear factor’ of running afoul of the antiopioid – including legal ones taken safely under medical supervision – backlash.
“The chronically ill who do not abuse, who do not divert, have become the unintended victims of misguided and overzealous efforts by policy- and regulation-making bodies in the government,” he said.
Grandparents filling void
An article in the Detroit News reported on more carnage of the opioid crisis. In Michigan and elsewhere nationwide, increasing numbers of parents with opioid addiction are unable to safely care for their children or have died because of an overdose. Grandparents are stepping in to assume care.
Results of a national survey involving more than 1,000 grandparents found that 20% are the daily caregivers to their grandchildren. They can be on their own, without any financial aid from state or national programs. Other children without grandparents can be diverted to foster care.
It’s a role few grandparents anticipated. “Our system as a whole is messed up. It tears at my heart,” 47-year-old Christina Wasilewski said in the article. “Everyone keeps saying children are resilient, but only to a point.”
Ms. Wasilewski and her husband assumed care for their granddaughter when they discovered her in physical distress from lack of care.
In Michigan, the increase in the rate of opioid-related deaths slowed in 2017 but deaths still rose 9% from 2016 , according to the Michigan Department of Health & Human Services. The prior year the death rate was 35%. In Michigan, grandparents raising their grandchildren do not have legal parental rights for this care, including the right to seek medical care and to pursue educational options.
Ms. Wasilewski’s concern about these trends led her to launch the Caregiver Cafe, a support group for grandparents raising their grandchildren.
Tofacitinib tackles cutaneous sarcoidosis
Tofacitinib significantly improved skin lesions associated with cutaneous sarcoidosis, according to a case report published in the New England Journal of Medicine.
Treatment options for cutaneous sarcoidosis are limited, as are data on the effectiveness of alternatives to prednisone, which is often the first choice despite adverse effects, wrote William Damsky, MD, of Yale University in New Haven, Conn., and his colleagues.
Previous studies have suggested involvement of the JAK-STAT pathway in sarcoidosis; therefore, the researchers treated a patient who had refractory cutaneous sarcoidosis with oral tofacitinib. The treatment significantly improved the patient’s skin lesions both clinically and histologically.
The patient was a 48-year-old woman with a history of cutaneous and pulmonary sarcoidosis and treatment-resistant skin lesions. At the time of the case report, she had no pulmonary symptoms and no ophthalmologic issues, but presented with pink-brown indurated papules and plaques, and some alopecia on her scalp (N Engl J Med. 2018;379:2540-6).
The patient had not responded to other medications including glucocorticoids, minocycline, hydroxychloroquine, methotrexate, adalimumab, tacrolimus, and apremilast. With her consent, the patient received off-label tofacitinib at 5 mg twice daily. The lesions began to improve, but treatment was discontinued because of insurance issues. When treatment resumed, the patient’s Cutaneous Sarcoidosis Activity and Morphology Instrument (CSAMI) score, used to assess disease activity, was 85 on a scale of 0 to 165; this score dropped to 53 after 4 months of treatment.
In addition, two samples collected after 10 months of treatment showed histologic resolution of granulomas.
Although the findings must be replicated in other patients, the results suggest that “the dysregulation of JAK-STAT–dependent cytokines (e.g., interferon-gamma) is pathogenically involved in cutaneous sarcoidosis and, probably, in sarcoidosis in general,” the researchers said.
Dr. Damsky disclosed a financial relationship with Eli Lilly, and research funding from the Dermatology Foundation and the National Institutes of Health. The study was supported by the Ranjini and Ajay Poddar Resource Fund for Dermatologic Diseases Research, the National Institutes of Health, and the Dermatology Foundation.
SOURCE: Damsky W et al. N Engl J Med. 2018;379:2540-6.
Tofacitinib significantly improved skin lesions associated with cutaneous sarcoidosis, according to a case report published in the New England Journal of Medicine.
Treatment options for cutaneous sarcoidosis are limited, as are data on the effectiveness of alternatives to prednisone, which is often the first choice despite adverse effects, wrote William Damsky, MD, of Yale University in New Haven, Conn., and his colleagues.
Previous studies have suggested involvement of the JAK-STAT pathway in sarcoidosis; therefore, the researchers treated a patient who had refractory cutaneous sarcoidosis with oral tofacitinib. The treatment significantly improved the patient’s skin lesions both clinically and histologically.
The patient was a 48-year-old woman with a history of cutaneous and pulmonary sarcoidosis and treatment-resistant skin lesions. At the time of the case report, she had no pulmonary symptoms and no ophthalmologic issues, but presented with pink-brown indurated papules and plaques, and some alopecia on her scalp (N Engl J Med. 2018;379:2540-6).
The patient had not responded to other medications including glucocorticoids, minocycline, hydroxychloroquine, methotrexate, adalimumab, tacrolimus, and apremilast. With her consent, the patient received off-label tofacitinib at 5 mg twice daily. The lesions began to improve, but treatment was discontinued because of insurance issues. When treatment resumed, the patient’s Cutaneous Sarcoidosis Activity and Morphology Instrument (CSAMI) score, used to assess disease activity, was 85 on a scale of 0 to 165; this score dropped to 53 after 4 months of treatment.
In addition, two samples collected after 10 months of treatment showed histologic resolution of granulomas.
Although the findings must be replicated in other patients, the results suggest that “the dysregulation of JAK-STAT–dependent cytokines (e.g., interferon-gamma) is pathogenically involved in cutaneous sarcoidosis and, probably, in sarcoidosis in general,” the researchers said.
Dr. Damsky disclosed a financial relationship with Eli Lilly, and research funding from the Dermatology Foundation and the National Institutes of Health. The study was supported by the Ranjini and Ajay Poddar Resource Fund for Dermatologic Diseases Research, the National Institutes of Health, and the Dermatology Foundation.
SOURCE: Damsky W et al. N Engl J Med. 2018;379:2540-6.
Tofacitinib significantly improved skin lesions associated with cutaneous sarcoidosis, according to a case report published in the New England Journal of Medicine.
Treatment options for cutaneous sarcoidosis are limited, as are data on the effectiveness of alternatives to prednisone, which is often the first choice despite adverse effects, wrote William Damsky, MD, of Yale University in New Haven, Conn., and his colleagues.
Previous studies have suggested involvement of the JAK-STAT pathway in sarcoidosis; therefore, the researchers treated a patient who had refractory cutaneous sarcoidosis with oral tofacitinib. The treatment significantly improved the patient’s skin lesions both clinically and histologically.
The patient was a 48-year-old woman with a history of cutaneous and pulmonary sarcoidosis and treatment-resistant skin lesions. At the time of the case report, she had no pulmonary symptoms and no ophthalmologic issues, but presented with pink-brown indurated papules and plaques, and some alopecia on her scalp (N Engl J Med. 2018;379:2540-6).
The patient had not responded to other medications including glucocorticoids, minocycline, hydroxychloroquine, methotrexate, adalimumab, tacrolimus, and apremilast. With her consent, the patient received off-label tofacitinib at 5 mg twice daily. The lesions began to improve, but treatment was discontinued because of insurance issues. When treatment resumed, the patient’s Cutaneous Sarcoidosis Activity and Morphology Instrument (CSAMI) score, used to assess disease activity, was 85 on a scale of 0 to 165; this score dropped to 53 after 4 months of treatment.
In addition, two samples collected after 10 months of treatment showed histologic resolution of granulomas.
Although the findings must be replicated in other patients, the results suggest that “the dysregulation of JAK-STAT–dependent cytokines (e.g., interferon-gamma) is pathogenically involved in cutaneous sarcoidosis and, probably, in sarcoidosis in general,” the researchers said.
Dr. Damsky disclosed a financial relationship with Eli Lilly, and research funding from the Dermatology Foundation and the National Institutes of Health. The study was supported by the Ranjini and Ajay Poddar Resource Fund for Dermatologic Diseases Research, the National Institutes of Health, and the Dermatology Foundation.
SOURCE: Damsky W et al. N Engl J Med. 2018;379:2540-6.
FROM NEW ENGLAND JOURNAL OF MEDICINE
Key clinical point: A 48-year-old woman with sarcoidosis showed significant improvement in her skin on treatment with tofacitinib.
Major finding: The patient’s disease activity score on the CSAMI went from 85 to 53 after 4 months of therapy.
Study details: Case report of a 48-year-old woman with cutaneous and pulmonary sarcoidosis and treatment-resistant skin lesions.
Disclosures: Dr. Damsky disclosed a financial relationship with Eli Lilly, and research funding from the Dermatology Foundation and the National Institutes of Health. The study was supported by the Ranjini and Ajay Poddar Resource Fund for Dermatologic Diseases Research, the National Institutes of Health, and the Dermatology Foundation.
Source: Damsky W et al. N Engl J Med. 2018;379:2540-6.