User login
PA defends against license suspension for COVID treatment
The suspension stemmed from allegations against Scott C. Miller, PA-C, by at least six COVID patients, including some who weren’t his patients or whom he never examined and a few who later died from the virus, according to the Washington Medical Commission.
“Miller’s treatment of COVID-19 patients fell below the standard of care,” the suspension report states. “Miller began a public campaign promoting ivermectin as a curative for COVID-19, and prescribing it without adequate examination to at least one person, with no reliable clinical studies that establish its efficacy in preventing or treating COVID-19.”
Mr. Miller has until early November to respond to the allegations. On his clinic’s website, Mr. Miller stated, “In response to the charges, I want to reassure all of you that the initial attacks against me have been brought on by a small handful of people that have no ties to our medical practice, and by pharmacies and hospitals that have a zero tolerance policy on family members asking that I help them advocate for loved ones that have been admitted and written off in our current system of dismissiveness and neglect.”
Mr. Miller also expressed gratitude for the support he has received recently. A GoFundMe campaign to raise money for Mr. Miller’s legal fund had raised more than $59,000 at press time. His GoFundMe page had been shared 2,400 times. He has more than 550 followers and more than 400 donors.
“I don’t know that I have the words to adequately describe the deep sense of love and connection I have received from you, the families I serve, and those that have reached out to me in this deeply challenging time,” he wrote on the clinic website.
Mr. Miller has spoken publicly about his anti-mask views and his support for ivermectin, according to the commission report. As part of the suspension, he was charged with making “misleading representations regarding the efficacy of non-FDA approved treatment and mask use.”
In one case that was cited in the report, a 39-year-old patient contacted the pediatric clinic, and Mr. Miller spoke with the patient by phone. The patient reported that he had tested positive for COVID. Mr. Miller advised the patient to take supplements, including vitamin D and C, zinc, and melatonin, and he prescribed ivermectin, dexamethasone, and azithromycin. He did not perform an exam, verify the information that the patient had provided, advise the patient regarding interactions, or order follow-up testing, the report states.
Other charges against Mr. Miller include harassing hospital staff by making threatening statements about hospitals and doctors who treat COVID-19 patients and misrepresenting his original 2013 license application. He denied on the application that he was being investigated by another licensing board. At the time, the California Physician Assistant Board was investigating him for providing medical care and prescribing without a supervising doctor’s authorization and without conducting physical exams, among other charges.
A version of this article first appeared on Medscape.com.
The suspension stemmed from allegations against Scott C. Miller, PA-C, by at least six COVID patients, including some who weren’t his patients or whom he never examined and a few who later died from the virus, according to the Washington Medical Commission.
“Miller’s treatment of COVID-19 patients fell below the standard of care,” the suspension report states. “Miller began a public campaign promoting ivermectin as a curative for COVID-19, and prescribing it without adequate examination to at least one person, with no reliable clinical studies that establish its efficacy in preventing or treating COVID-19.”
Mr. Miller has until early November to respond to the allegations. On his clinic’s website, Mr. Miller stated, “In response to the charges, I want to reassure all of you that the initial attacks against me have been brought on by a small handful of people that have no ties to our medical practice, and by pharmacies and hospitals that have a zero tolerance policy on family members asking that I help them advocate for loved ones that have been admitted and written off in our current system of dismissiveness and neglect.”
Mr. Miller also expressed gratitude for the support he has received recently. A GoFundMe campaign to raise money for Mr. Miller’s legal fund had raised more than $59,000 at press time. His GoFundMe page had been shared 2,400 times. He has more than 550 followers and more than 400 donors.
“I don’t know that I have the words to adequately describe the deep sense of love and connection I have received from you, the families I serve, and those that have reached out to me in this deeply challenging time,” he wrote on the clinic website.
Mr. Miller has spoken publicly about his anti-mask views and his support for ivermectin, according to the commission report. As part of the suspension, he was charged with making “misleading representations regarding the efficacy of non-FDA approved treatment and mask use.”
In one case that was cited in the report, a 39-year-old patient contacted the pediatric clinic, and Mr. Miller spoke with the patient by phone. The patient reported that he had tested positive for COVID. Mr. Miller advised the patient to take supplements, including vitamin D and C, zinc, and melatonin, and he prescribed ivermectin, dexamethasone, and azithromycin. He did not perform an exam, verify the information that the patient had provided, advise the patient regarding interactions, or order follow-up testing, the report states.
Other charges against Mr. Miller include harassing hospital staff by making threatening statements about hospitals and doctors who treat COVID-19 patients and misrepresenting his original 2013 license application. He denied on the application that he was being investigated by another licensing board. At the time, the California Physician Assistant Board was investigating him for providing medical care and prescribing without a supervising doctor’s authorization and without conducting physical exams, among other charges.
A version of this article first appeared on Medscape.com.
The suspension stemmed from allegations against Scott C. Miller, PA-C, by at least six COVID patients, including some who weren’t his patients or whom he never examined and a few who later died from the virus, according to the Washington Medical Commission.
“Miller’s treatment of COVID-19 patients fell below the standard of care,” the suspension report states. “Miller began a public campaign promoting ivermectin as a curative for COVID-19, and prescribing it without adequate examination to at least one person, with no reliable clinical studies that establish its efficacy in preventing or treating COVID-19.”
Mr. Miller has until early November to respond to the allegations. On his clinic’s website, Mr. Miller stated, “In response to the charges, I want to reassure all of you that the initial attacks against me have been brought on by a small handful of people that have no ties to our medical practice, and by pharmacies and hospitals that have a zero tolerance policy on family members asking that I help them advocate for loved ones that have been admitted and written off in our current system of dismissiveness and neglect.”
Mr. Miller also expressed gratitude for the support he has received recently. A GoFundMe campaign to raise money for Mr. Miller’s legal fund had raised more than $59,000 at press time. His GoFundMe page had been shared 2,400 times. He has more than 550 followers and more than 400 donors.
“I don’t know that I have the words to adequately describe the deep sense of love and connection I have received from you, the families I serve, and those that have reached out to me in this deeply challenging time,” he wrote on the clinic website.
Mr. Miller has spoken publicly about his anti-mask views and his support for ivermectin, according to the commission report. As part of the suspension, he was charged with making “misleading representations regarding the efficacy of non-FDA approved treatment and mask use.”
In one case that was cited in the report, a 39-year-old patient contacted the pediatric clinic, and Mr. Miller spoke with the patient by phone. The patient reported that he had tested positive for COVID. Mr. Miller advised the patient to take supplements, including vitamin D and C, zinc, and melatonin, and he prescribed ivermectin, dexamethasone, and azithromycin. He did not perform an exam, verify the information that the patient had provided, advise the patient regarding interactions, or order follow-up testing, the report states.
Other charges against Mr. Miller include harassing hospital staff by making threatening statements about hospitals and doctors who treat COVID-19 patients and misrepresenting his original 2013 license application. He denied on the application that he was being investigated by another licensing board. At the time, the California Physician Assistant Board was investigating him for providing medical care and prescribing without a supervising doctor’s authorization and without conducting physical exams, among other charges.
A version of this article first appeared on Medscape.com.
Open ICUs giveth and taketh away
Background: Some academic medical centers and many community centers use “open” ICU models in which primary services longitudinally follow patients into the ICU with intensivist comanagement.
Design: Semistructured interviews with 12 hospitalists and 8 intensivists.
Setting: Open 16-bed ICUs at the University of California, San Francisco. Teams round separately at the bedside and are informally encouraged to check in daily.
Synopsis: The authors iteratively developed the interview questions. Participants were selected using purposive sampling. The main themes were communication, education, and structure. Communication was challenging among teams as well as with patients and families. The open ICU was felt to affect handoffs and care continuity positively. Hospitalists focused more on longitudinal relationships, smoother transitions, and opportunities to observe disease evolution. Intensivists focused more on fragmentation during the ICU stay and noted cognitive disengagement among some team members with certain aspects of patient care. Intensivists did not identify any educational or structural benefits of the open ICU model.
This is the first qualitative study of hospitalist and intensivist perceptions of the open ICU model. The most significant limitation is the risk of bias from the single-center design and purposive sampling. These findings have implications for other models of medical comanagement.
Bottom line: Open ICU models offer a mix of communication, educational, and structural barriers as well as opportunities. Role clarity may help optimize the open ICU model.
Citation: Santhosh L and Sewell J. Hospital and intensivist experiences of the “open” intensive care unit environment: A qualitative exploration. J Gen Intern Med. 2020;35(8):2338-46.
Dr. Sweigart is a hospitalist at the Lexington (Ky.) VA Health Care System.
Background: Some academic medical centers and many community centers use “open” ICU models in which primary services longitudinally follow patients into the ICU with intensivist comanagement.
Design: Semistructured interviews with 12 hospitalists and 8 intensivists.
Setting: Open 16-bed ICUs at the University of California, San Francisco. Teams round separately at the bedside and are informally encouraged to check in daily.
Synopsis: The authors iteratively developed the interview questions. Participants were selected using purposive sampling. The main themes were communication, education, and structure. Communication was challenging among teams as well as with patients and families. The open ICU was felt to affect handoffs and care continuity positively. Hospitalists focused more on longitudinal relationships, smoother transitions, and opportunities to observe disease evolution. Intensivists focused more on fragmentation during the ICU stay and noted cognitive disengagement among some team members with certain aspects of patient care. Intensivists did not identify any educational or structural benefits of the open ICU model.
This is the first qualitative study of hospitalist and intensivist perceptions of the open ICU model. The most significant limitation is the risk of bias from the single-center design and purposive sampling. These findings have implications for other models of medical comanagement.
Bottom line: Open ICU models offer a mix of communication, educational, and structural barriers as well as opportunities. Role clarity may help optimize the open ICU model.
Citation: Santhosh L and Sewell J. Hospital and intensivist experiences of the “open” intensive care unit environment: A qualitative exploration. J Gen Intern Med. 2020;35(8):2338-46.
Dr. Sweigart is a hospitalist at the Lexington (Ky.) VA Health Care System.
Background: Some academic medical centers and many community centers use “open” ICU models in which primary services longitudinally follow patients into the ICU with intensivist comanagement.
Design: Semistructured interviews with 12 hospitalists and 8 intensivists.
Setting: Open 16-bed ICUs at the University of California, San Francisco. Teams round separately at the bedside and are informally encouraged to check in daily.
Synopsis: The authors iteratively developed the interview questions. Participants were selected using purposive sampling. The main themes were communication, education, and structure. Communication was challenging among teams as well as with patients and families. The open ICU was felt to affect handoffs and care continuity positively. Hospitalists focused more on longitudinal relationships, smoother transitions, and opportunities to observe disease evolution. Intensivists focused more on fragmentation during the ICU stay and noted cognitive disengagement among some team members with certain aspects of patient care. Intensivists did not identify any educational or structural benefits of the open ICU model.
This is the first qualitative study of hospitalist and intensivist perceptions of the open ICU model. The most significant limitation is the risk of bias from the single-center design and purposive sampling. These findings have implications for other models of medical comanagement.
Bottom line: Open ICU models offer a mix of communication, educational, and structural barriers as well as opportunities. Role clarity may help optimize the open ICU model.
Citation: Santhosh L and Sewell J. Hospital and intensivist experiences of the “open” intensive care unit environment: A qualitative exploration. J Gen Intern Med. 2020;35(8):2338-46.
Dr. Sweigart is a hospitalist at the Lexington (Ky.) VA Health Care System.
Priming tremelimumab dose regimen shows promising benefit-risk profile in HCC
The novel regimen featuring a single, priming dose of tremelimumab “displayed the most encouraging benefit-risk profile,” wrote Robin Kate Kelley, MD, of the University of California, San Francisco, and colleagues in the Journal of Clinical Oncology. “These findings suggest that a single dose of tremelimumab may be sufficient to activate the tumor-fighting potential of the immune system.”
The incidence of HCC has been increasing worldwide over the last 20 years. HCC most commonly occurs in people with liver disease, particularly in those with chronic hepatitis B and C and although rare, HCC is the ninth-leading cause of cancer deaths in the United States. The 1-year survival rates in patients with HCC are less than 50%.
Atezolizumab plus bevacizumab gained regulatory approval in 2020 for the treatment of unresectable HCC. Several other immunotherapy-containing regimens are being evaluated, including immune checkpoint inhibitors combined with antiangiogenic agents. Immune checkpoint inhibitors – programmed death–ligand 1 and cytotoxic T-lymphocyte–associated antigen-4 – have shown promise in unresectable HCC, but they are insufficient as single agents and anti–CTLA-4 can be accompanied by challenging toxicities.
In this phase 1/2 study, researchers evaluated tremelimumab (anti–CTLA-4) and durvalumab (anti–PD-L1) as monotherapies and in combination, including a regimen featuring a single, priming dose of tremelimumab and durvalumab followed by durvalumab every 4 weeks. A total of 332 patients with HCC who had progressed on, were intolerant to, or refused sorafenib were randomly assigned to receive one of the four regimens. The primary endpoint was safety.
While the priming doses regimen showed the best benefit-risk profile, all regimens were found to be tolerable and clinically active.
Specifically, in patients on the priming dose, durvalumab, tremelimumab and combination regimes, grade 3 or higher treatment-related adverse events occurred in 37.8%, 20.8%, 43.5%, and 24.4%, respectively. For secondary endpoints, objective response rates were 24.0%, 10.6%, 7.2%, and 9.5%, respectively. The median overall survival was 18.7, 13.6, 15.1, and 11.3 months, respectively.
The priming dose regimen stimulated CD8+ T-cell production, which the authors suggested enhanced response and efficacy.
This novel regimen “may offer distinct differentiating features beyond demonstration of durable objective responses and promising overall survival, including a favorable safety profile with a relatively low steroid requirement, rare [antidrug antibody] formation, and a single, priming dose of tremelimumab followed by monthly durvalumab administration schedule,” the authors wrote. “Moreover, the absence of an antiangiogenic partner allows for treatment of patients who are contraindicated for antiangiogenics because of bleeding risks or comorbidities like cardiovascular disease.”
Another study, recently published in the Journal of Clinical Oncology, showed that donafenib was superior to sorafenib in improving overall survival, along with improved safety and tolerability, rendering it a potential first-line monotherapy for patients with advanced HCC.
The tremelimumab/durvalumab study was funded by AstraZeneca.
The novel regimen featuring a single, priming dose of tremelimumab “displayed the most encouraging benefit-risk profile,” wrote Robin Kate Kelley, MD, of the University of California, San Francisco, and colleagues in the Journal of Clinical Oncology. “These findings suggest that a single dose of tremelimumab may be sufficient to activate the tumor-fighting potential of the immune system.”
The incidence of HCC has been increasing worldwide over the last 20 years. HCC most commonly occurs in people with liver disease, particularly in those with chronic hepatitis B and C and although rare, HCC is the ninth-leading cause of cancer deaths in the United States. The 1-year survival rates in patients with HCC are less than 50%.
Atezolizumab plus bevacizumab gained regulatory approval in 2020 for the treatment of unresectable HCC. Several other immunotherapy-containing regimens are being evaluated, including immune checkpoint inhibitors combined with antiangiogenic agents. Immune checkpoint inhibitors – programmed death–ligand 1 and cytotoxic T-lymphocyte–associated antigen-4 – have shown promise in unresectable HCC, but they are insufficient as single agents and anti–CTLA-4 can be accompanied by challenging toxicities.
In this phase 1/2 study, researchers evaluated tremelimumab (anti–CTLA-4) and durvalumab (anti–PD-L1) as monotherapies and in combination, including a regimen featuring a single, priming dose of tremelimumab and durvalumab followed by durvalumab every 4 weeks. A total of 332 patients with HCC who had progressed on, were intolerant to, or refused sorafenib were randomly assigned to receive one of the four regimens. The primary endpoint was safety.
While the priming doses regimen showed the best benefit-risk profile, all regimens were found to be tolerable and clinically active.
Specifically, in patients on the priming dose, durvalumab, tremelimumab and combination regimes, grade 3 or higher treatment-related adverse events occurred in 37.8%, 20.8%, 43.5%, and 24.4%, respectively. For secondary endpoints, objective response rates were 24.0%, 10.6%, 7.2%, and 9.5%, respectively. The median overall survival was 18.7, 13.6, 15.1, and 11.3 months, respectively.
The priming dose regimen stimulated CD8+ T-cell production, which the authors suggested enhanced response and efficacy.
This novel regimen “may offer distinct differentiating features beyond demonstration of durable objective responses and promising overall survival, including a favorable safety profile with a relatively low steroid requirement, rare [antidrug antibody] formation, and a single, priming dose of tremelimumab followed by monthly durvalumab administration schedule,” the authors wrote. “Moreover, the absence of an antiangiogenic partner allows for treatment of patients who are contraindicated for antiangiogenics because of bleeding risks or comorbidities like cardiovascular disease.”
Another study, recently published in the Journal of Clinical Oncology, showed that donafenib was superior to sorafenib in improving overall survival, along with improved safety and tolerability, rendering it a potential first-line monotherapy for patients with advanced HCC.
The tremelimumab/durvalumab study was funded by AstraZeneca.
The novel regimen featuring a single, priming dose of tremelimumab “displayed the most encouraging benefit-risk profile,” wrote Robin Kate Kelley, MD, of the University of California, San Francisco, and colleagues in the Journal of Clinical Oncology. “These findings suggest that a single dose of tremelimumab may be sufficient to activate the tumor-fighting potential of the immune system.”
The incidence of HCC has been increasing worldwide over the last 20 years. HCC most commonly occurs in people with liver disease, particularly in those with chronic hepatitis B and C and although rare, HCC is the ninth-leading cause of cancer deaths in the United States. The 1-year survival rates in patients with HCC are less than 50%.
Atezolizumab plus bevacizumab gained regulatory approval in 2020 for the treatment of unresectable HCC. Several other immunotherapy-containing regimens are being evaluated, including immune checkpoint inhibitors combined with antiangiogenic agents. Immune checkpoint inhibitors – programmed death–ligand 1 and cytotoxic T-lymphocyte–associated antigen-4 – have shown promise in unresectable HCC, but they are insufficient as single agents and anti–CTLA-4 can be accompanied by challenging toxicities.
In this phase 1/2 study, researchers evaluated tremelimumab (anti–CTLA-4) and durvalumab (anti–PD-L1) as monotherapies and in combination, including a regimen featuring a single, priming dose of tremelimumab and durvalumab followed by durvalumab every 4 weeks. A total of 332 patients with HCC who had progressed on, were intolerant to, or refused sorafenib were randomly assigned to receive one of the four regimens. The primary endpoint was safety.
While the priming doses regimen showed the best benefit-risk profile, all regimens were found to be tolerable and clinically active.
Specifically, in patients on the priming dose, durvalumab, tremelimumab and combination regimes, grade 3 or higher treatment-related adverse events occurred in 37.8%, 20.8%, 43.5%, and 24.4%, respectively. For secondary endpoints, objective response rates were 24.0%, 10.6%, 7.2%, and 9.5%, respectively. The median overall survival was 18.7, 13.6, 15.1, and 11.3 months, respectively.
The priming dose regimen stimulated CD8+ T-cell production, which the authors suggested enhanced response and efficacy.
This novel regimen “may offer distinct differentiating features beyond demonstration of durable objective responses and promising overall survival, including a favorable safety profile with a relatively low steroid requirement, rare [antidrug antibody] formation, and a single, priming dose of tremelimumab followed by monthly durvalumab administration schedule,” the authors wrote. “Moreover, the absence of an antiangiogenic partner allows for treatment of patients who are contraindicated for antiangiogenics because of bleeding risks or comorbidities like cardiovascular disease.”
Another study, recently published in the Journal of Clinical Oncology, showed that donafenib was superior to sorafenib in improving overall survival, along with improved safety and tolerability, rendering it a potential first-line monotherapy for patients with advanced HCC.
The tremelimumab/durvalumab study was funded by AstraZeneca.
FROM THE JOURNAL OF CLINICAL ONCOLOGY
Life-threatening paradoxical bronchospasm may escape recognition in patients with COPD or asthma
according to a researcher who reviewed spirometry test results from U.S. military veterans.
Nearly 1.5% of the tests met the criteria for paradoxical bronchospasm, which refers to airway constriction that may rapidly occur after inhalation of a short-acting beta2 agonist (SABA) such as albuterol.
However, none of those reports alluded to paradoxical bronchospasm, said investigator Malvika Kaul, MD, fellow in the department of pulmonary and critical care at the University of Illinois at Chicago and the Jesse Brown Veterans Affairs Medical Center, also in Chicago.
“Paradoxical bronchospasm was neither recognized nor reported in any spirometry test results,” Dr. Kaul said in an online poster presentation at the annual meeting of the American College of Chest Physicians, held virtually this year.
By recognizing paradoxical bronchospasm, health care providers could address its clinical implications and identify potential alternative management options, according to Dr. Kaul.
“We hope in the future, education of clinicians about this phenomena is emphasized,” Dr. Kaul said in her presentation.
Recognizing paradoxical bronchospasm
In an interview, Dr. Kaul said she began researching paradoxical bronchospasm after encountering a patient who had an acute reaction to albuterol during a pulmonary function test.
“I was not taught about it, and I wasn’t recognizing that pattern very frequently in my patients,” she said.
Prescribing information for Food and Drug Administration–approved SABAs include a warning that life-threatening paradoxical bronchospasm may occur, said Dr. Kaul.
If paradoxical bronchospasm occurs, the patient should discontinue the medication immediately and start on alternative therapy, according to the available prescribing information for albuterol sulfate.
Paradoxical bronchospasm has been linked to worsened respiratory outcomes, including more frequent exacerbations, in patients with obstructive lung diseases, according to Dr. Kaul.
Two previous large studies pegged the prevalence of paradoxical bronchospasm at around 4.5% in patients with COPD or asthma, but “it has not been reported or addressed in high-risk population, such as veterans who have high prevalence of obstructive lung diseases like COPD,” Dr. Kaul said.
Latest study results
Dr. Kaul described a retrospective analysis of 1,150 pre- and postbronchodilator spirometry tests conducted in patients with COPD or asthma at the Jesse Brown VA Medical Center between 2017 and 2020.
A positive paradoxical bronchodilator response was defined as a decrease of least 12% and 200 mL in forced expiratory volume in 1 second and forced vital capacity from baseline after four puffs of albuterol were inhaled, Dr. Kaul said.
Out of 18 reviewed spirometry results that met the criteria, none of the test results reported or recognized paradoxical bronchospasm, according to Dr. Kaul.
Those meeting the criteria were predominantly COPD patients, according to Dr. Kaul, who said 12 had an underlying diagnosis COPD, 4 had asthma, and 2 had COPD and asthma.
Of the 18 patients, 13 were African American, and all but 1 of the 18 patients had a current or past smoking history, according to reported data.
A history of obstructive sleep apnea was reported in nine patients, and history of gastroesophageal reflux disease was also reported in nine patients. Eleven patients had emphysema.
Greater awareness needed
Results of this study emphasize the need to recognize potential cases paradoxical bronchospasm in clinical practice, as well as a need for more research, according to Allen J. Blaivas, DO, FCCP, chair of the CHEST Airway Disorders NetWork.
“It’s something to be on the alert for, and certainly be aware that, if your patient is telling you that they feel worse, we shouldn’t just pooh-pooh it,” said Dr. Blaivas, who is medical director of the intensive care unit at the East Orange campus of the VA New Jersey Health Care System.
Further research could focus on breaking down whether patients with suspected paradoxical bronchospasm are using metered-dose inhalers or nebulizers, whether or not they are also taking inhaled corticosteroids, and whether prospective testing can confirm paradoxical bronchospasm in patients who report tightness after using a SABA, he said in an interview.
Dr. Kaul and coauthor Israel Rubinstein, MD had no relevant relationships to disclose. Dr. Blaivas had no relevant relationships to disclose.
according to a researcher who reviewed spirometry test results from U.S. military veterans.
Nearly 1.5% of the tests met the criteria for paradoxical bronchospasm, which refers to airway constriction that may rapidly occur after inhalation of a short-acting beta2 agonist (SABA) such as albuterol.
However, none of those reports alluded to paradoxical bronchospasm, said investigator Malvika Kaul, MD, fellow in the department of pulmonary and critical care at the University of Illinois at Chicago and the Jesse Brown Veterans Affairs Medical Center, also in Chicago.
“Paradoxical bronchospasm was neither recognized nor reported in any spirometry test results,” Dr. Kaul said in an online poster presentation at the annual meeting of the American College of Chest Physicians, held virtually this year.
By recognizing paradoxical bronchospasm, health care providers could address its clinical implications and identify potential alternative management options, according to Dr. Kaul.
“We hope in the future, education of clinicians about this phenomena is emphasized,” Dr. Kaul said in her presentation.
Recognizing paradoxical bronchospasm
In an interview, Dr. Kaul said she began researching paradoxical bronchospasm after encountering a patient who had an acute reaction to albuterol during a pulmonary function test.
“I was not taught about it, and I wasn’t recognizing that pattern very frequently in my patients,” she said.
Prescribing information for Food and Drug Administration–approved SABAs include a warning that life-threatening paradoxical bronchospasm may occur, said Dr. Kaul.
If paradoxical bronchospasm occurs, the patient should discontinue the medication immediately and start on alternative therapy, according to the available prescribing information for albuterol sulfate.
Paradoxical bronchospasm has been linked to worsened respiratory outcomes, including more frequent exacerbations, in patients with obstructive lung diseases, according to Dr. Kaul.
Two previous large studies pegged the prevalence of paradoxical bronchospasm at around 4.5% in patients with COPD or asthma, but “it has not been reported or addressed in high-risk population, such as veterans who have high prevalence of obstructive lung diseases like COPD,” Dr. Kaul said.
Latest study results
Dr. Kaul described a retrospective analysis of 1,150 pre- and postbronchodilator spirometry tests conducted in patients with COPD or asthma at the Jesse Brown VA Medical Center between 2017 and 2020.
A positive paradoxical bronchodilator response was defined as a decrease of least 12% and 200 mL in forced expiratory volume in 1 second and forced vital capacity from baseline after four puffs of albuterol were inhaled, Dr. Kaul said.
Out of 18 reviewed spirometry results that met the criteria, none of the test results reported or recognized paradoxical bronchospasm, according to Dr. Kaul.
Those meeting the criteria were predominantly COPD patients, according to Dr. Kaul, who said 12 had an underlying diagnosis COPD, 4 had asthma, and 2 had COPD and asthma.
Of the 18 patients, 13 were African American, and all but 1 of the 18 patients had a current or past smoking history, according to reported data.
A history of obstructive sleep apnea was reported in nine patients, and history of gastroesophageal reflux disease was also reported in nine patients. Eleven patients had emphysema.
Greater awareness needed
Results of this study emphasize the need to recognize potential cases paradoxical bronchospasm in clinical practice, as well as a need for more research, according to Allen J. Blaivas, DO, FCCP, chair of the CHEST Airway Disorders NetWork.
“It’s something to be on the alert for, and certainly be aware that, if your patient is telling you that they feel worse, we shouldn’t just pooh-pooh it,” said Dr. Blaivas, who is medical director of the intensive care unit at the East Orange campus of the VA New Jersey Health Care System.
Further research could focus on breaking down whether patients with suspected paradoxical bronchospasm are using metered-dose inhalers or nebulizers, whether or not they are also taking inhaled corticosteroids, and whether prospective testing can confirm paradoxical bronchospasm in patients who report tightness after using a SABA, he said in an interview.
Dr. Kaul and coauthor Israel Rubinstein, MD had no relevant relationships to disclose. Dr. Blaivas had no relevant relationships to disclose.
according to a researcher who reviewed spirometry test results from U.S. military veterans.
Nearly 1.5% of the tests met the criteria for paradoxical bronchospasm, which refers to airway constriction that may rapidly occur after inhalation of a short-acting beta2 agonist (SABA) such as albuterol.
However, none of those reports alluded to paradoxical bronchospasm, said investigator Malvika Kaul, MD, fellow in the department of pulmonary and critical care at the University of Illinois at Chicago and the Jesse Brown Veterans Affairs Medical Center, also in Chicago.
“Paradoxical bronchospasm was neither recognized nor reported in any spirometry test results,” Dr. Kaul said in an online poster presentation at the annual meeting of the American College of Chest Physicians, held virtually this year.
By recognizing paradoxical bronchospasm, health care providers could address its clinical implications and identify potential alternative management options, according to Dr. Kaul.
“We hope in the future, education of clinicians about this phenomena is emphasized,” Dr. Kaul said in her presentation.
Recognizing paradoxical bronchospasm
In an interview, Dr. Kaul said she began researching paradoxical bronchospasm after encountering a patient who had an acute reaction to albuterol during a pulmonary function test.
“I was not taught about it, and I wasn’t recognizing that pattern very frequently in my patients,” she said.
Prescribing information for Food and Drug Administration–approved SABAs include a warning that life-threatening paradoxical bronchospasm may occur, said Dr. Kaul.
If paradoxical bronchospasm occurs, the patient should discontinue the medication immediately and start on alternative therapy, according to the available prescribing information for albuterol sulfate.
Paradoxical bronchospasm has been linked to worsened respiratory outcomes, including more frequent exacerbations, in patients with obstructive lung diseases, according to Dr. Kaul.
Two previous large studies pegged the prevalence of paradoxical bronchospasm at around 4.5% in patients with COPD or asthma, but “it has not been reported or addressed in high-risk population, such as veterans who have high prevalence of obstructive lung diseases like COPD,” Dr. Kaul said.
Latest study results
Dr. Kaul described a retrospective analysis of 1,150 pre- and postbronchodilator spirometry tests conducted in patients with COPD or asthma at the Jesse Brown VA Medical Center between 2017 and 2020.
A positive paradoxical bronchodilator response was defined as a decrease of least 12% and 200 mL in forced expiratory volume in 1 second and forced vital capacity from baseline after four puffs of albuterol were inhaled, Dr. Kaul said.
Out of 18 reviewed spirometry results that met the criteria, none of the test results reported or recognized paradoxical bronchospasm, according to Dr. Kaul.
Those meeting the criteria were predominantly COPD patients, according to Dr. Kaul, who said 12 had an underlying diagnosis COPD, 4 had asthma, and 2 had COPD and asthma.
Of the 18 patients, 13 were African American, and all but 1 of the 18 patients had a current or past smoking history, according to reported data.
A history of obstructive sleep apnea was reported in nine patients, and history of gastroesophageal reflux disease was also reported in nine patients. Eleven patients had emphysema.
Greater awareness needed
Results of this study emphasize the need to recognize potential cases paradoxical bronchospasm in clinical practice, as well as a need for more research, according to Allen J. Blaivas, DO, FCCP, chair of the CHEST Airway Disorders NetWork.
“It’s something to be on the alert for, and certainly be aware that, if your patient is telling you that they feel worse, we shouldn’t just pooh-pooh it,” said Dr. Blaivas, who is medical director of the intensive care unit at the East Orange campus of the VA New Jersey Health Care System.
Further research could focus on breaking down whether patients with suspected paradoxical bronchospasm are using metered-dose inhalers or nebulizers, whether or not they are also taking inhaled corticosteroids, and whether prospective testing can confirm paradoxical bronchospasm in patients who report tightness after using a SABA, he said in an interview.
Dr. Kaul and coauthor Israel Rubinstein, MD had no relevant relationships to disclose. Dr. Blaivas had no relevant relationships to disclose.
FROM CHEST 2021
Generalized Pustular Psoriasis: An Uncommon Diagnosis Carrying an Outsize Burden of Disease
In this supplement to Dermatology News, Alan Menter, MD discusses best practices for the rare, severe, and chronic autoinflammatory disease known as Generalized Pustular Psoriasis (GPP).
Read More
In this supplement to Dermatology News, Alan Menter, MD discusses best practices for the rare, severe, and chronic autoinflammatory disease known as Generalized Pustular Psoriasis (GPP).
Read More
In this supplement to Dermatology News, Alan Menter, MD discusses best practices for the rare, severe, and chronic autoinflammatory disease known as Generalized Pustular Psoriasis (GPP).
Read More
MS and (non-COVID) vaccinations: consensus recommendations
by the European Committee for Treatment and Research in Multiple Sclerosis (ECTRIMS) and the European Academy of Neurology (EAN).
The document, announced at the annual ECTRIMS meeting, proposes a standard for vaccination in patients with MS, including a global vaccination strategy for the general MS patient population and selected subpopulations.
The document does not include any recommendations regarding vaccination against COVID-19, which is the subject of a separate report, announced at the annual meeting.
The main conclusions in the new report are as follows:
- Vaccinations in general are considered safe for patients with MS and do not modify disease activity/progression.
- Live attenuated vaccines, however, are contraindicated with immunosuppressants.
- Inactivated vaccines can be used safely, but their efficacy may be decreased with immunosuppressants.
- Vaccinations should be considered early in MS management before using immunosuppressants whenever possible.
Presenting the vaccination consensus document, Susana Otero-Romero, MD, from the Multiple Sclerosis Center of Catalonia, Spain, explained that vaccination has become an important part of the risk management strategy in patients with MS treated with highly active drugs but that questions remain as to when and whether to introduce a particular vaccine and which disease-modifying treatments affect vaccine response.
“The current reference tool has been developed to help professionals to decide on the best vaccination strategy for their patients,” she said.
The consensus document recommends that, in general, vaccination should be performed at the time of diagnosis of MS or in the early stages of the disease to prevent future delays in starting therapies.
“Ideally, vaccination should take place before the onset of disease-modifying treatment,” Dr. Otero-Romero said. The consensus document recommends inactivated vaccines to be given 2-3 weeks before immunosuppressive therapy is started, and live attenuated vaccines at least 4 weeks beforehand.
In the case of relapse, vaccination should be delayed until clinical resolution or stabilization if possible, the consensus statement recommends.
Serological testing for vaccine-induced antibody titers can be performed 1-2 months after the last dose of the vaccine (suggested for hepatitis B, measles, mumps, and varicella). For attenuated live vaccines, serological tests should be done before starting immunosuppressive therapy. In the case of insufficient response, consideration should be given to administering a booster dose of the vaccine, except for hepatitis B, in which a complete revaccination is recommended, according to the document.
As for vaccination during immunosuppressive therapy, this is considered safe for patients on interferon or glatiramer acetate when indicated, the report says.
Vaccination should ideally be avoided in patients on dimethyl fumarate, teriflunomide (Aubagio) or natalizumab (Tysabri), although it can be considered in exceptional cases when the potential risk of acquiring the infection is greater than the risk of developing vaccine-related infections (unless the absolute lymphocyte count is below 800/mm3), it adds.
Vaccination should be avoided in patients on S1P modulators (for example, fingolimod [Gilenya]), anti-CD20 therapies, and before immune restoration for cladribine (Leustatin) and alemtuzumab (Lemtrada).
In the case of patients stopping immunosuppressive therapy, inactivated vaccines can be given any time after the discontinuation of therapy but preferably after immune restoration. Live attenuated vaccines should only be administered after a safety interval ensures immune restoration has been met.
Which vaccines?
On which vaccines are needed in patients with MS, the consensus document recommends the same routine vaccination schedule as for the general population. In addition, it advises influenza and pneumococcal vaccination if patients are immunosuppressed or have significant disability.
It also recommends human papillomavirus vaccine in women and men independent of their age if they are to be treated with alemtuzumab, fingolimod, cladribine, or anti-CD20 drugs. Hepatitis B vaccination is also advised in patients treated with anti-CD20 drugs.
Special populations: pregnancy/elderly
In patients with MS who are pregnant, inactivated flu vaccine can be given in any trimester at the start of the flu season, and vaccination against diphtheria, tetanus, and pertussis can be given during the third trimester, the report says. Live attenuated vaccines should be completed at least 1 month before pregnancy or after delivery and 4-6 weeks prior to the initiation of immunosuppressive therapy.
Elderly patients with MS should receive flu and pneumococcal vaccines annually and would also benefit from the inactivated herpes zoster vaccine.
Travel vaccines
On vaccinations needed for travel, the report recommends that patients with MS consult a specialized travel clinic or vaccination expert and start immunizations 2-3 months before departure. Patients with MS with or without immunosuppressive therapy can receive hepatitis A, rabies, Japanese encephalitis, tic-borne encephalitis, polio, and inactivated typhoid vaccine. But yellow fever and oral typhoid are contraindicated in patients on immunosuppressive therapies.
A version of this article first appeared on Medscape.com.
by the European Committee for Treatment and Research in Multiple Sclerosis (ECTRIMS) and the European Academy of Neurology (EAN).
The document, announced at the annual ECTRIMS meeting, proposes a standard for vaccination in patients with MS, including a global vaccination strategy for the general MS patient population and selected subpopulations.
The document does not include any recommendations regarding vaccination against COVID-19, which is the subject of a separate report, announced at the annual meeting.
The main conclusions in the new report are as follows:
- Vaccinations in general are considered safe for patients with MS and do not modify disease activity/progression.
- Live attenuated vaccines, however, are contraindicated with immunosuppressants.
- Inactivated vaccines can be used safely, but their efficacy may be decreased with immunosuppressants.
- Vaccinations should be considered early in MS management before using immunosuppressants whenever possible.
Presenting the vaccination consensus document, Susana Otero-Romero, MD, from the Multiple Sclerosis Center of Catalonia, Spain, explained that vaccination has become an important part of the risk management strategy in patients with MS treated with highly active drugs but that questions remain as to when and whether to introduce a particular vaccine and which disease-modifying treatments affect vaccine response.
“The current reference tool has been developed to help professionals to decide on the best vaccination strategy for their patients,” she said.
The consensus document recommends that, in general, vaccination should be performed at the time of diagnosis of MS or in the early stages of the disease to prevent future delays in starting therapies.
“Ideally, vaccination should take place before the onset of disease-modifying treatment,” Dr. Otero-Romero said. The consensus document recommends inactivated vaccines to be given 2-3 weeks before immunosuppressive therapy is started, and live attenuated vaccines at least 4 weeks beforehand.
In the case of relapse, vaccination should be delayed until clinical resolution or stabilization if possible, the consensus statement recommends.
Serological testing for vaccine-induced antibody titers can be performed 1-2 months after the last dose of the vaccine (suggested for hepatitis B, measles, mumps, and varicella). For attenuated live vaccines, serological tests should be done before starting immunosuppressive therapy. In the case of insufficient response, consideration should be given to administering a booster dose of the vaccine, except for hepatitis B, in which a complete revaccination is recommended, according to the document.
As for vaccination during immunosuppressive therapy, this is considered safe for patients on interferon or glatiramer acetate when indicated, the report says.
Vaccination should ideally be avoided in patients on dimethyl fumarate, teriflunomide (Aubagio) or natalizumab (Tysabri), although it can be considered in exceptional cases when the potential risk of acquiring the infection is greater than the risk of developing vaccine-related infections (unless the absolute lymphocyte count is below 800/mm3), it adds.
Vaccination should be avoided in patients on S1P modulators (for example, fingolimod [Gilenya]), anti-CD20 therapies, and before immune restoration for cladribine (Leustatin) and alemtuzumab (Lemtrada).
In the case of patients stopping immunosuppressive therapy, inactivated vaccines can be given any time after the discontinuation of therapy but preferably after immune restoration. Live attenuated vaccines should only be administered after a safety interval ensures immune restoration has been met.
Which vaccines?
On which vaccines are needed in patients with MS, the consensus document recommends the same routine vaccination schedule as for the general population. In addition, it advises influenza and pneumococcal vaccination if patients are immunosuppressed or have significant disability.
It also recommends human papillomavirus vaccine in women and men independent of their age if they are to be treated with alemtuzumab, fingolimod, cladribine, or anti-CD20 drugs. Hepatitis B vaccination is also advised in patients treated with anti-CD20 drugs.
Special populations: pregnancy/elderly
In patients with MS who are pregnant, inactivated flu vaccine can be given in any trimester at the start of the flu season, and vaccination against diphtheria, tetanus, and pertussis can be given during the third trimester, the report says. Live attenuated vaccines should be completed at least 1 month before pregnancy or after delivery and 4-6 weeks prior to the initiation of immunosuppressive therapy.
Elderly patients with MS should receive flu and pneumococcal vaccines annually and would also benefit from the inactivated herpes zoster vaccine.
Travel vaccines
On vaccinations needed for travel, the report recommends that patients with MS consult a specialized travel clinic or vaccination expert and start immunizations 2-3 months before departure. Patients with MS with or without immunosuppressive therapy can receive hepatitis A, rabies, Japanese encephalitis, tic-borne encephalitis, polio, and inactivated typhoid vaccine. But yellow fever and oral typhoid are contraindicated in patients on immunosuppressive therapies.
A version of this article first appeared on Medscape.com.
by the European Committee for Treatment and Research in Multiple Sclerosis (ECTRIMS) and the European Academy of Neurology (EAN).
The document, announced at the annual ECTRIMS meeting, proposes a standard for vaccination in patients with MS, including a global vaccination strategy for the general MS patient population and selected subpopulations.
The document does not include any recommendations regarding vaccination against COVID-19, which is the subject of a separate report, announced at the annual meeting.
The main conclusions in the new report are as follows:
- Vaccinations in general are considered safe for patients with MS and do not modify disease activity/progression.
- Live attenuated vaccines, however, are contraindicated with immunosuppressants.
- Inactivated vaccines can be used safely, but their efficacy may be decreased with immunosuppressants.
- Vaccinations should be considered early in MS management before using immunosuppressants whenever possible.
Presenting the vaccination consensus document, Susana Otero-Romero, MD, from the Multiple Sclerosis Center of Catalonia, Spain, explained that vaccination has become an important part of the risk management strategy in patients with MS treated with highly active drugs but that questions remain as to when and whether to introduce a particular vaccine and which disease-modifying treatments affect vaccine response.
“The current reference tool has been developed to help professionals to decide on the best vaccination strategy for their patients,” she said.
The consensus document recommends that, in general, vaccination should be performed at the time of diagnosis of MS or in the early stages of the disease to prevent future delays in starting therapies.
“Ideally, vaccination should take place before the onset of disease-modifying treatment,” Dr. Otero-Romero said. The consensus document recommends inactivated vaccines to be given 2-3 weeks before immunosuppressive therapy is started, and live attenuated vaccines at least 4 weeks beforehand.
In the case of relapse, vaccination should be delayed until clinical resolution or stabilization if possible, the consensus statement recommends.
Serological testing for vaccine-induced antibody titers can be performed 1-2 months after the last dose of the vaccine (suggested for hepatitis B, measles, mumps, and varicella). For attenuated live vaccines, serological tests should be done before starting immunosuppressive therapy. In the case of insufficient response, consideration should be given to administering a booster dose of the vaccine, except for hepatitis B, in which a complete revaccination is recommended, according to the document.
As for vaccination during immunosuppressive therapy, this is considered safe for patients on interferon or glatiramer acetate when indicated, the report says.
Vaccination should ideally be avoided in patients on dimethyl fumarate, teriflunomide (Aubagio) or natalizumab (Tysabri), although it can be considered in exceptional cases when the potential risk of acquiring the infection is greater than the risk of developing vaccine-related infections (unless the absolute lymphocyte count is below 800/mm3), it adds.
Vaccination should be avoided in patients on S1P modulators (for example, fingolimod [Gilenya]), anti-CD20 therapies, and before immune restoration for cladribine (Leustatin) and alemtuzumab (Lemtrada).
In the case of patients stopping immunosuppressive therapy, inactivated vaccines can be given any time after the discontinuation of therapy but preferably after immune restoration. Live attenuated vaccines should only be administered after a safety interval ensures immune restoration has been met.
Which vaccines?
On which vaccines are needed in patients with MS, the consensus document recommends the same routine vaccination schedule as for the general population. In addition, it advises influenza and pneumococcal vaccination if patients are immunosuppressed or have significant disability.
It also recommends human papillomavirus vaccine in women and men independent of their age if they are to be treated with alemtuzumab, fingolimod, cladribine, or anti-CD20 drugs. Hepatitis B vaccination is also advised in patients treated with anti-CD20 drugs.
Special populations: pregnancy/elderly
In patients with MS who are pregnant, inactivated flu vaccine can be given in any trimester at the start of the flu season, and vaccination against diphtheria, tetanus, and pertussis can be given during the third trimester, the report says. Live attenuated vaccines should be completed at least 1 month before pregnancy or after delivery and 4-6 weeks prior to the initiation of immunosuppressive therapy.
Elderly patients with MS should receive flu and pneumococcal vaccines annually and would also benefit from the inactivated herpes zoster vaccine.
Travel vaccines
On vaccinations needed for travel, the report recommends that patients with MS consult a specialized travel clinic or vaccination expert and start immunizations 2-3 months before departure. Patients with MS with or without immunosuppressive therapy can receive hepatitis A, rabies, Japanese encephalitis, tic-borne encephalitis, polio, and inactivated typhoid vaccine. But yellow fever and oral typhoid are contraindicated in patients on immunosuppressive therapies.
A version of this article first appeared on Medscape.com.
From ECTRIMS 2021
Facing Up to the Diagnosis
ANSWER
All of these items were rightly considered to be in the differential for this lesion, so the answer is choice “f.”
DISCUSSION
Individuals with type IV skin are less likely than those with types II and III to develop skin cancer. So, although cancer was definitely in the differential, the other items were considered just as, if not more, likely in this case.
The only way to sort through these diagnostic possibilities was to perform a biopsy. In this case, the entire lesion was removed by saucerization technique, under local anesthesia. The specimen provided would be adequate to detect any cancer, which a smaller specimen could easily miss.
The pathology results showed pigmented basal cell carcinoma. Given the patient’s extensive history of sun exposure, and the steady growth of the lesion, this was hardly a surprise. But prior to the biopsy, one could just as easily imagine the lesion to be, for example, a wart.
The take-home message is obvious: Nothing can take the place of biopsy in establishing a precise diagnosis. With that information in hand, the patient was referred for consultation with a Mohs surgeon. Surgical removal and closure would likely set him back several thousand dollars and leave a considerable scar.
ANSWER
All of these items were rightly considered to be in the differential for this lesion, so the answer is choice “f.”
DISCUSSION
Individuals with type IV skin are less likely than those with types II and III to develop skin cancer. So, although cancer was definitely in the differential, the other items were considered just as, if not more, likely in this case.
The only way to sort through these diagnostic possibilities was to perform a biopsy. In this case, the entire lesion was removed by saucerization technique, under local anesthesia. The specimen provided would be adequate to detect any cancer, which a smaller specimen could easily miss.
The pathology results showed pigmented basal cell carcinoma. Given the patient’s extensive history of sun exposure, and the steady growth of the lesion, this was hardly a surprise. But prior to the biopsy, one could just as easily imagine the lesion to be, for example, a wart.
The take-home message is obvious: Nothing can take the place of biopsy in establishing a precise diagnosis. With that information in hand, the patient was referred for consultation with a Mohs surgeon. Surgical removal and closure would likely set him back several thousand dollars and leave a considerable scar.
ANSWER
All of these items were rightly considered to be in the differential for this lesion, so the answer is choice “f.”
DISCUSSION
Individuals with type IV skin are less likely than those with types II and III to develop skin cancer. So, although cancer was definitely in the differential, the other items were considered just as, if not more, likely in this case.
The only way to sort through these diagnostic possibilities was to perform a biopsy. In this case, the entire lesion was removed by saucerization technique, under local anesthesia. The specimen provided would be adequate to detect any cancer, which a smaller specimen could easily miss.
The pathology results showed pigmented basal cell carcinoma. Given the patient’s extensive history of sun exposure, and the steady growth of the lesion, this was hardly a surprise. But prior to the biopsy, one could just as easily imagine the lesion to be, for example, a wart.
The take-home message is obvious: Nothing can take the place of biopsy in establishing a precise diagnosis. With that information in hand, the patient was referred for consultation with a Mohs surgeon. Surgical removal and closure would likely set him back several thousand dollars and leave a considerable scar.
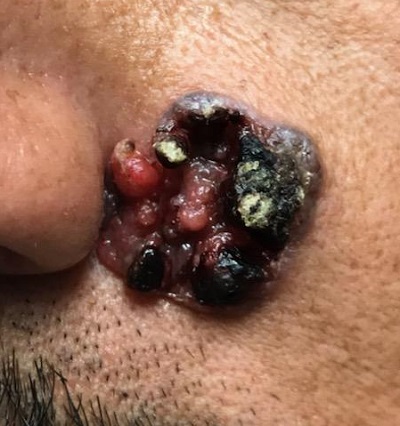
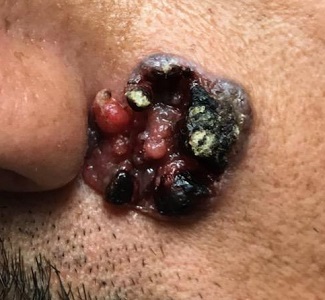
“Like a berry,” was how a 38-year-old Hispanic man described the lesion that had been slowly growing on his face for 4 years. His family was alarmed by it, but he reasoned that since it didn’t hurt and the surrounding area wasn’t especially red, it likely wasn’t much of a problem.
The patient worked as roofer up to 7 days per week when the weather was good and had been doing so since he was old enough to work. He had no insurance and was not inclined to spend money on a health care visit. When his wife finally convinced him to go to the urgent care clinic, he paid $100 just to be told he needed to see a dermatologist. He was so disgusted he almost refused to wait the 6 weeks it took to get into the dermatology office.
The patient, who had type IV skin with little evidence of sun damage, had an obvious, large, coarsely mamillated nodule on the left upper nasolabial area. The lesion measured 1.8 cm and was reddish blue. It was moderately firm, but no increased warmth could be detected. No nodes could be felt in the area. His skin elsewhere was free of any notable changes.
Mortality in 2nd wave higher with ECMO for COVID-ARDS
For patients with refractory acute respiratory distress syndrome (ARDS) caused by COVID-19 infections, extracorporeal membrane oxygenation (ECMO) may be the treatment of last resort.
But for reasons that aren’t clear, in the second wave of the COVID-19 pandemic at a major teaching hospital, the mortality rate of patients on ECMO for COVID-induced ARDS was significantly higher than it was during the first wave, despite changes in drug therapy and clinical management, reported Rohit Reddy, BS, a second-year medical student, and colleagues at Thomas Jefferson University Hospital in Philadelphia.
During the first wave, from April to September 2020, the survival rate of patients while on ECMO in their ICUs was 67%. In contrast, for patients treated during the second wave, from November 2020 to March 2021, the ECMO survival rate was 31% (P = .003).
The 30-day survival rates were also higher in the first wave compared with the second, at 54% versus 31%, but this difference was not statistically significant.
“More research is required to develop stricter inclusion/exclusion criteria and to improve pre-ECMO management in order to improve outcomes,” Mr. Reddy said in a narrated poster presented at the annual meeting of the American College of Chest Physicians, held virtually this year.
ARDS severity higher
ARDS is a major complication of COVID-19 infections, and there is evidence to suggest that COVID-associated ARDS is more severe than ARDS caused by other causes, the investigators noted.
“ECMO, which has been used as a rescue therapy in prior viral outbreaks, has been used to support certain patients with refractory ARDS due to COVID-19, but evidence for its efficacy is limited. Respiratory failure remained a highly concerning complication in the second wave of the COVID-19 pandemic, but it is unclear how the evolution of the disease and pharmacologic utility has affected the clinical utility of ECMO,” Mr. Reddy said.
To see whether changes in disease course or in treatment could explain changes in outcomes for patients with COVID-related ARDS, the investigators compared characteristics and outcomes for patients treated in the first versus second waves of the pandemic. Their study did not include data from patients infected with the Delta variant of the SARS-CoV-2 virus, which became the predominant viral strain later in 2021.
The study included data on 28 patients treated during the first wave, and 13 during the second. The sample included 28 men and 13 women with a mean age of 51 years.
All patients had venovenous ECMO, with cannulation in the femoral or internal jugular veins; some patients received ECMO via a single double-lumen cannula.
There were no significant differences between the two time periods in patient comorbidities prior to initiation of ECMO.
Patients in the second wave were significantly more likely to receive steroids (54% vs. 100%; P = .003) and remdesivir (39% vs. 85%; P = .007). Prone positioning before ECMO was also significantly more frequent in the second wave (11% vs. 85%; P < .001).
Patients in the second wave stayed on ECMO longer – median 20 days versus 14 days for first-wave patients – but as noted before, ECMO mortality rates were significantly higher during the second wave. During the first wave, 33% of patients died while on ECMO, compared with 69% in the second wave (P = .03). Respective 30-day mortality rates were 46% versus 69% (ns).
Rates of complications during ECMO were generally comparable between the groups, including acute renal failure (39% in the first wave vs 38% in the second), sepsis (32% vs. 23%), bacterial pneumonia (11% vs. 8%), and gastrointestinal bleeding (21% vs. 15%). However, significantly more patients in the second wave had cerebral vascular accidents (4% vs. 23%; P = .050).
Senior author Hitoshi Hirose, MD, PhD, professor of surgery at Thomas Jefferson University, said in an interview that the difference in outcomes was likely caused by changes in pre-ECMO therapy between the first and second waves.
“Our study showed the incidence of sepsis had a large impact on the patient outcomes,” he wrote. “We speculate that sepsis was attributed to use of immune modulation therapy. The prevention of the sepsis would be key to improve survival of ECMO for COVID 19.”
“It’s possible that the explanation for this is that patients in the second wave were sicker in a way that wasn’t adequately measured in the first wave,” CHEST 2021 program cochair Christopher Carroll, MD, FCCP, from Connecticut Children’s Medical Center in Hartford, said in an interview.
The differences may also have been attributable to changes in virulence, or to clinical decisions to put sicker patients on ECMO, he said.
Casey Cable, MD, MSc, a pulmonary disease and critical care specialist at Virginia Commonwealth Medical Center in Richmond, also speculated in an interview that second-wave patients may have been sicker.
“One interesting piece of this story is that we now know a lot more – we know about the use of steroids plus or minus remdesivir and proning, and patients received a large majority of those treatments but still got put on ECMO,” she said. “I wonder if there is a subset of really sick patients, and no matter what we treat with – steroids, proning – whatever we do they’re just not going to do well.”
Both Dr. Carroll and Dr. Cable emphasized the importance of ECMO as a rescue therapy for patients with severe, refractory ARDS associated with COVID-19 or other diseases.
Neither Dr. Carroll nor Dr. Cable were involved in the study.
No study funding was reported. Mr. Reddy, Dr. Hirose, Dr. Carroll, and Dr. Cable disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
For patients with refractory acute respiratory distress syndrome (ARDS) caused by COVID-19 infections, extracorporeal membrane oxygenation (ECMO) may be the treatment of last resort.
But for reasons that aren’t clear, in the second wave of the COVID-19 pandemic at a major teaching hospital, the mortality rate of patients on ECMO for COVID-induced ARDS was significantly higher than it was during the first wave, despite changes in drug therapy and clinical management, reported Rohit Reddy, BS, a second-year medical student, and colleagues at Thomas Jefferson University Hospital in Philadelphia.
During the first wave, from April to September 2020, the survival rate of patients while on ECMO in their ICUs was 67%. In contrast, for patients treated during the second wave, from November 2020 to March 2021, the ECMO survival rate was 31% (P = .003).
The 30-day survival rates were also higher in the first wave compared with the second, at 54% versus 31%, but this difference was not statistically significant.
“More research is required to develop stricter inclusion/exclusion criteria and to improve pre-ECMO management in order to improve outcomes,” Mr. Reddy said in a narrated poster presented at the annual meeting of the American College of Chest Physicians, held virtually this year.
ARDS severity higher
ARDS is a major complication of COVID-19 infections, and there is evidence to suggest that COVID-associated ARDS is more severe than ARDS caused by other causes, the investigators noted.
“ECMO, which has been used as a rescue therapy in prior viral outbreaks, has been used to support certain patients with refractory ARDS due to COVID-19, but evidence for its efficacy is limited. Respiratory failure remained a highly concerning complication in the second wave of the COVID-19 pandemic, but it is unclear how the evolution of the disease and pharmacologic utility has affected the clinical utility of ECMO,” Mr. Reddy said.
To see whether changes in disease course or in treatment could explain changes in outcomes for patients with COVID-related ARDS, the investigators compared characteristics and outcomes for patients treated in the first versus second waves of the pandemic. Their study did not include data from patients infected with the Delta variant of the SARS-CoV-2 virus, which became the predominant viral strain later in 2021.
The study included data on 28 patients treated during the first wave, and 13 during the second. The sample included 28 men and 13 women with a mean age of 51 years.
All patients had venovenous ECMO, with cannulation in the femoral or internal jugular veins; some patients received ECMO via a single double-lumen cannula.
There were no significant differences between the two time periods in patient comorbidities prior to initiation of ECMO.
Patients in the second wave were significantly more likely to receive steroids (54% vs. 100%; P = .003) and remdesivir (39% vs. 85%; P = .007). Prone positioning before ECMO was also significantly more frequent in the second wave (11% vs. 85%; P < .001).
Patients in the second wave stayed on ECMO longer – median 20 days versus 14 days for first-wave patients – but as noted before, ECMO mortality rates were significantly higher during the second wave. During the first wave, 33% of patients died while on ECMO, compared with 69% in the second wave (P = .03). Respective 30-day mortality rates were 46% versus 69% (ns).
Rates of complications during ECMO were generally comparable between the groups, including acute renal failure (39% in the first wave vs 38% in the second), sepsis (32% vs. 23%), bacterial pneumonia (11% vs. 8%), and gastrointestinal bleeding (21% vs. 15%). However, significantly more patients in the second wave had cerebral vascular accidents (4% vs. 23%; P = .050).
Senior author Hitoshi Hirose, MD, PhD, professor of surgery at Thomas Jefferson University, said in an interview that the difference in outcomes was likely caused by changes in pre-ECMO therapy between the first and second waves.
“Our study showed the incidence of sepsis had a large impact on the patient outcomes,” he wrote. “We speculate that sepsis was attributed to use of immune modulation therapy. The prevention of the sepsis would be key to improve survival of ECMO for COVID 19.”
“It’s possible that the explanation for this is that patients in the second wave were sicker in a way that wasn’t adequately measured in the first wave,” CHEST 2021 program cochair Christopher Carroll, MD, FCCP, from Connecticut Children’s Medical Center in Hartford, said in an interview.
The differences may also have been attributable to changes in virulence, or to clinical decisions to put sicker patients on ECMO, he said.
Casey Cable, MD, MSc, a pulmonary disease and critical care specialist at Virginia Commonwealth Medical Center in Richmond, also speculated in an interview that second-wave patients may have been sicker.
“One interesting piece of this story is that we now know a lot more – we know about the use of steroids plus or minus remdesivir and proning, and patients received a large majority of those treatments but still got put on ECMO,” she said. “I wonder if there is a subset of really sick patients, and no matter what we treat with – steroids, proning – whatever we do they’re just not going to do well.”
Both Dr. Carroll and Dr. Cable emphasized the importance of ECMO as a rescue therapy for patients with severe, refractory ARDS associated with COVID-19 or other diseases.
Neither Dr. Carroll nor Dr. Cable were involved in the study.
No study funding was reported. Mr. Reddy, Dr. Hirose, Dr. Carroll, and Dr. Cable disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
For patients with refractory acute respiratory distress syndrome (ARDS) caused by COVID-19 infections, extracorporeal membrane oxygenation (ECMO) may be the treatment of last resort.
But for reasons that aren’t clear, in the second wave of the COVID-19 pandemic at a major teaching hospital, the mortality rate of patients on ECMO for COVID-induced ARDS was significantly higher than it was during the first wave, despite changes in drug therapy and clinical management, reported Rohit Reddy, BS, a second-year medical student, and colleagues at Thomas Jefferson University Hospital in Philadelphia.
During the first wave, from April to September 2020, the survival rate of patients while on ECMO in their ICUs was 67%. In contrast, for patients treated during the second wave, from November 2020 to March 2021, the ECMO survival rate was 31% (P = .003).
The 30-day survival rates were also higher in the first wave compared with the second, at 54% versus 31%, but this difference was not statistically significant.
“More research is required to develop stricter inclusion/exclusion criteria and to improve pre-ECMO management in order to improve outcomes,” Mr. Reddy said in a narrated poster presented at the annual meeting of the American College of Chest Physicians, held virtually this year.
ARDS severity higher
ARDS is a major complication of COVID-19 infections, and there is evidence to suggest that COVID-associated ARDS is more severe than ARDS caused by other causes, the investigators noted.
“ECMO, which has been used as a rescue therapy in prior viral outbreaks, has been used to support certain patients with refractory ARDS due to COVID-19, but evidence for its efficacy is limited. Respiratory failure remained a highly concerning complication in the second wave of the COVID-19 pandemic, but it is unclear how the evolution of the disease and pharmacologic utility has affected the clinical utility of ECMO,” Mr. Reddy said.
To see whether changes in disease course or in treatment could explain changes in outcomes for patients with COVID-related ARDS, the investigators compared characteristics and outcomes for patients treated in the first versus second waves of the pandemic. Their study did not include data from patients infected with the Delta variant of the SARS-CoV-2 virus, which became the predominant viral strain later in 2021.
The study included data on 28 patients treated during the first wave, and 13 during the second. The sample included 28 men and 13 women with a mean age of 51 years.
All patients had venovenous ECMO, with cannulation in the femoral or internal jugular veins; some patients received ECMO via a single double-lumen cannula.
There were no significant differences between the two time periods in patient comorbidities prior to initiation of ECMO.
Patients in the second wave were significantly more likely to receive steroids (54% vs. 100%; P = .003) and remdesivir (39% vs. 85%; P = .007). Prone positioning before ECMO was also significantly more frequent in the second wave (11% vs. 85%; P < .001).
Patients in the second wave stayed on ECMO longer – median 20 days versus 14 days for first-wave patients – but as noted before, ECMO mortality rates were significantly higher during the second wave. During the first wave, 33% of patients died while on ECMO, compared with 69% in the second wave (P = .03). Respective 30-day mortality rates were 46% versus 69% (ns).
Rates of complications during ECMO were generally comparable between the groups, including acute renal failure (39% in the first wave vs 38% in the second), sepsis (32% vs. 23%), bacterial pneumonia (11% vs. 8%), and gastrointestinal bleeding (21% vs. 15%). However, significantly more patients in the second wave had cerebral vascular accidents (4% vs. 23%; P = .050).
Senior author Hitoshi Hirose, MD, PhD, professor of surgery at Thomas Jefferson University, said in an interview that the difference in outcomes was likely caused by changes in pre-ECMO therapy between the first and second waves.
“Our study showed the incidence of sepsis had a large impact on the patient outcomes,” he wrote. “We speculate that sepsis was attributed to use of immune modulation therapy. The prevention of the sepsis would be key to improve survival of ECMO for COVID 19.”
“It’s possible that the explanation for this is that patients in the second wave were sicker in a way that wasn’t adequately measured in the first wave,” CHEST 2021 program cochair Christopher Carroll, MD, FCCP, from Connecticut Children’s Medical Center in Hartford, said in an interview.
The differences may also have been attributable to changes in virulence, or to clinical decisions to put sicker patients on ECMO, he said.
Casey Cable, MD, MSc, a pulmonary disease and critical care specialist at Virginia Commonwealth Medical Center in Richmond, also speculated in an interview that second-wave patients may have been sicker.
“One interesting piece of this story is that we now know a lot more – we know about the use of steroids plus or minus remdesivir and proning, and patients received a large majority of those treatments but still got put on ECMO,” she said. “I wonder if there is a subset of really sick patients, and no matter what we treat with – steroids, proning – whatever we do they’re just not going to do well.”
Both Dr. Carroll and Dr. Cable emphasized the importance of ECMO as a rescue therapy for patients with severe, refractory ARDS associated with COVID-19 or other diseases.
Neither Dr. Carroll nor Dr. Cable were involved in the study.
No study funding was reported. Mr. Reddy, Dr. Hirose, Dr. Carroll, and Dr. Cable disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Rituximab more effective than other MS treatments?
, according to new research.
The risk for a first relapse was 6 times higher in patients receiving interferon beta or glatiramer acetate, compared with those receiving rituximab. But the level of disability at 3 years was only marginally different between the drugs studied.
The small differences in Expanded Disability Status Scale (EDSS) score are surprising, said investigator Peter Alping, a clinical assistant and doctoral student in the Department of Clinical Neuroscience at the Karolinska Institutet, Stockholm, as he presented the data. “It could be that we have too-short follow-up, so that EDSS doesn’t have time to diverge between therapies.”
He presented the findings at the annual meeting of the European Committee for Treatment and Research in Multiple Sclerosis (ECTRIMS).
COMBAT-MS study
Direct comparisons of disease-modifying therapies (DMTs) for MS can help neurologists choose the most appropriate treatment for a given patient. To compare the effectiveness of the most common initial DMTs administered in Sweden, the researchers examined data from the COMBAT-MS study.
They identified all patients who initiated an injectable therapy (interferon beta or glatiramer acetate), dimethyl fumarate, natalizumab, or rituximab as a first treatment between Jan. 1, 2011, and Dec. 14, 2020. Eligible participants had prospectively recorded outcome data in the Swedish MS Register. Follow-up for a participant continued even if the participant stopped receiving therapy.
The investigators replaced missing data using multiple imputation. They adjusted for potential confounders using stabilized inverse probability of treatment weighting with baseline variables. These variables included age, sex, disease duration, geographical region, EDSS score, and relapses.
Rituximab reduced relapses
The researchers included 1,938 first-ever treatment episodes in their analysis. Of this group, 858 were associated with injectables, 339 with dimethyl fumarate, 269 with natalizumab, and 472 with rituximab.
Participants’ baseline characteristics differed by the DMT that they used. Patients who initiated natalizumab were the youngest, had the shortest disease duration, and had the most previous relapses.
For each outcome, the investigators compared all other therapies with rituximab. After they adjusted the data, they found that the hazard ratio for first relapse was 6.0 for injectables, 2.9 for dimethyl fumarate, and 1.8 for natalizumab.
In the adjusted model, the MRI lesion rate ratio for injectables, compared with rituximab, was 4.5. The rate ratio was 4.8 for dimethyl fumarate and 1.9 for natalizumab.
But differences in EDSS score at 3 years from treatment initiation were small. EDSS score in patients who received injectables was 0.24 points higher, compared with those receiving rituximab. EDSS score was 0.05 points higher in patients receiving dimethyl fumarate and 0.01 points lower in patients receiving natalizumab.
The risk for treatment discontinuation, however, differed significantly between therapies. The HR for treatment discontinuation was 32.7 for injectables, 20.3 for dimethyl fumarate, and 16.3 for natalizumab, compared with rituximab.
Among patients receiving dimethyl fumarate and injectables, the main reasons for discontinuing therapy were inadequate effect and adverse events. The main reason for discontinuation among patients receiving natalizumab was categorized as “other reason,” which mostly reflected John Cunningham virus positivity and concern for developing progressive multifocal leukoencephalopathy.
‘The uncertainty continues’
“These differences that we see in the effectiveness can be somewhat surprising, especially when it comes to natalizumab,” which is considered very effective, said Mr. Alping. The vulnerable period that occurs after switching from natalizumab may partly explain the difference. “This is something to keep in mind when starting patients on natalizumab treatment in the clinic,” Mr. Alping added.
Although rituximab is not indicated for MS, many clinics are using it in this population, said Robert Fox, MD, staff neurologist at the Mellen Center for MS and vice chair for research at the Neurological Institute of Cleveland Clinic, both in Cleveland, Ohio. Dr. Fox was not involved in the study.
“Assessing the generalizability of the study outside Sweden will be important,” he added, “but I would be surprised if their findings did not hold up to external validation.”
The way that the researchers addressed missing data could affect the interpretation of the findings. “Depending upon how much data was missing, their imputation methods may have a high level of uncertainty,” said Dr. Fox.
The researchers’ adjustments for baseline differences also raise questions. “Even though MRI was an outcome, it doesn’t appear they adjusted for baseline differences in MRI between the groups,” Dr. Fox observed.
Moreover, the study was conducted over a long period of time. “We know there are time effects in MS, with a very different disease activity expected from patients over time,” said Dr. Fox. For example, relapse rates in placebo groups of MS trials tend to decline over time. “This time effect likely impacted their results.”
But the disability findings may be the most important part of the study, according to Dr. Fox. The lack of significant difference in disability progression between therapies “highlights that a couple relapses or lesions on MRI may be too small to translate into long-term differences in disability progression,” he said.
“The long-term implications of small differences in relapse and MRI outcomes may be very small,” Dr. Fox went on. “Thus, the uncertainty continues around escalation treatment versus initial highly effective treatment paradigms.”
The Patient-Centered Outcomes Research Institute, the Swedish Research Council, and NEURO Sweden funded this study. Mr. Alping disclosed no relevant financial relationships. Dr. Fox receives consulting fees from the companies that manufacture all the therapies analyzed in the study.
A version of this article first appeared on Medscape.com.
, according to new research.
The risk for a first relapse was 6 times higher in patients receiving interferon beta or glatiramer acetate, compared with those receiving rituximab. But the level of disability at 3 years was only marginally different between the drugs studied.
The small differences in Expanded Disability Status Scale (EDSS) score are surprising, said investigator Peter Alping, a clinical assistant and doctoral student in the Department of Clinical Neuroscience at the Karolinska Institutet, Stockholm, as he presented the data. “It could be that we have too-short follow-up, so that EDSS doesn’t have time to diverge between therapies.”
He presented the findings at the annual meeting of the European Committee for Treatment and Research in Multiple Sclerosis (ECTRIMS).
COMBAT-MS study
Direct comparisons of disease-modifying therapies (DMTs) for MS can help neurologists choose the most appropriate treatment for a given patient. To compare the effectiveness of the most common initial DMTs administered in Sweden, the researchers examined data from the COMBAT-MS study.
They identified all patients who initiated an injectable therapy (interferon beta or glatiramer acetate), dimethyl fumarate, natalizumab, or rituximab as a first treatment between Jan. 1, 2011, and Dec. 14, 2020. Eligible participants had prospectively recorded outcome data in the Swedish MS Register. Follow-up for a participant continued even if the participant stopped receiving therapy.
The investigators replaced missing data using multiple imputation. They adjusted for potential confounders using stabilized inverse probability of treatment weighting with baseline variables. These variables included age, sex, disease duration, geographical region, EDSS score, and relapses.
Rituximab reduced relapses
The researchers included 1,938 first-ever treatment episodes in their analysis. Of this group, 858 were associated with injectables, 339 with dimethyl fumarate, 269 with natalizumab, and 472 with rituximab.
Participants’ baseline characteristics differed by the DMT that they used. Patients who initiated natalizumab were the youngest, had the shortest disease duration, and had the most previous relapses.
For each outcome, the investigators compared all other therapies with rituximab. After they adjusted the data, they found that the hazard ratio for first relapse was 6.0 for injectables, 2.9 for dimethyl fumarate, and 1.8 for natalizumab.
In the adjusted model, the MRI lesion rate ratio for injectables, compared with rituximab, was 4.5. The rate ratio was 4.8 for dimethyl fumarate and 1.9 for natalizumab.
But differences in EDSS score at 3 years from treatment initiation were small. EDSS score in patients who received injectables was 0.24 points higher, compared with those receiving rituximab. EDSS score was 0.05 points higher in patients receiving dimethyl fumarate and 0.01 points lower in patients receiving natalizumab.
The risk for treatment discontinuation, however, differed significantly between therapies. The HR for treatment discontinuation was 32.7 for injectables, 20.3 for dimethyl fumarate, and 16.3 for natalizumab, compared with rituximab.
Among patients receiving dimethyl fumarate and injectables, the main reasons for discontinuing therapy were inadequate effect and adverse events. The main reason for discontinuation among patients receiving natalizumab was categorized as “other reason,” which mostly reflected John Cunningham virus positivity and concern for developing progressive multifocal leukoencephalopathy.
‘The uncertainty continues’
“These differences that we see in the effectiveness can be somewhat surprising, especially when it comes to natalizumab,” which is considered very effective, said Mr. Alping. The vulnerable period that occurs after switching from natalizumab may partly explain the difference. “This is something to keep in mind when starting patients on natalizumab treatment in the clinic,” Mr. Alping added.
Although rituximab is not indicated for MS, many clinics are using it in this population, said Robert Fox, MD, staff neurologist at the Mellen Center for MS and vice chair for research at the Neurological Institute of Cleveland Clinic, both in Cleveland, Ohio. Dr. Fox was not involved in the study.
“Assessing the generalizability of the study outside Sweden will be important,” he added, “but I would be surprised if their findings did not hold up to external validation.”
The way that the researchers addressed missing data could affect the interpretation of the findings. “Depending upon how much data was missing, their imputation methods may have a high level of uncertainty,” said Dr. Fox.
The researchers’ adjustments for baseline differences also raise questions. “Even though MRI was an outcome, it doesn’t appear they adjusted for baseline differences in MRI between the groups,” Dr. Fox observed.
Moreover, the study was conducted over a long period of time. “We know there are time effects in MS, with a very different disease activity expected from patients over time,” said Dr. Fox. For example, relapse rates in placebo groups of MS trials tend to decline over time. “This time effect likely impacted their results.”
But the disability findings may be the most important part of the study, according to Dr. Fox. The lack of significant difference in disability progression between therapies “highlights that a couple relapses or lesions on MRI may be too small to translate into long-term differences in disability progression,” he said.
“The long-term implications of small differences in relapse and MRI outcomes may be very small,” Dr. Fox went on. “Thus, the uncertainty continues around escalation treatment versus initial highly effective treatment paradigms.”
The Patient-Centered Outcomes Research Institute, the Swedish Research Council, and NEURO Sweden funded this study. Mr. Alping disclosed no relevant financial relationships. Dr. Fox receives consulting fees from the companies that manufacture all the therapies analyzed in the study.
A version of this article first appeared on Medscape.com.
, according to new research.
The risk for a first relapse was 6 times higher in patients receiving interferon beta or glatiramer acetate, compared with those receiving rituximab. But the level of disability at 3 years was only marginally different between the drugs studied.
The small differences in Expanded Disability Status Scale (EDSS) score are surprising, said investigator Peter Alping, a clinical assistant and doctoral student in the Department of Clinical Neuroscience at the Karolinska Institutet, Stockholm, as he presented the data. “It could be that we have too-short follow-up, so that EDSS doesn’t have time to diverge between therapies.”
He presented the findings at the annual meeting of the European Committee for Treatment and Research in Multiple Sclerosis (ECTRIMS).
COMBAT-MS study
Direct comparisons of disease-modifying therapies (DMTs) for MS can help neurologists choose the most appropriate treatment for a given patient. To compare the effectiveness of the most common initial DMTs administered in Sweden, the researchers examined data from the COMBAT-MS study.
They identified all patients who initiated an injectable therapy (interferon beta or glatiramer acetate), dimethyl fumarate, natalizumab, or rituximab as a first treatment between Jan. 1, 2011, and Dec. 14, 2020. Eligible participants had prospectively recorded outcome data in the Swedish MS Register. Follow-up for a participant continued even if the participant stopped receiving therapy.
The investigators replaced missing data using multiple imputation. They adjusted for potential confounders using stabilized inverse probability of treatment weighting with baseline variables. These variables included age, sex, disease duration, geographical region, EDSS score, and relapses.
Rituximab reduced relapses
The researchers included 1,938 first-ever treatment episodes in their analysis. Of this group, 858 were associated with injectables, 339 with dimethyl fumarate, 269 with natalizumab, and 472 with rituximab.
Participants’ baseline characteristics differed by the DMT that they used. Patients who initiated natalizumab were the youngest, had the shortest disease duration, and had the most previous relapses.
For each outcome, the investigators compared all other therapies with rituximab. After they adjusted the data, they found that the hazard ratio for first relapse was 6.0 for injectables, 2.9 for dimethyl fumarate, and 1.8 for natalizumab.
In the adjusted model, the MRI lesion rate ratio for injectables, compared with rituximab, was 4.5. The rate ratio was 4.8 for dimethyl fumarate and 1.9 for natalizumab.
But differences in EDSS score at 3 years from treatment initiation were small. EDSS score in patients who received injectables was 0.24 points higher, compared with those receiving rituximab. EDSS score was 0.05 points higher in patients receiving dimethyl fumarate and 0.01 points lower in patients receiving natalizumab.
The risk for treatment discontinuation, however, differed significantly between therapies. The HR for treatment discontinuation was 32.7 for injectables, 20.3 for dimethyl fumarate, and 16.3 for natalizumab, compared with rituximab.
Among patients receiving dimethyl fumarate and injectables, the main reasons for discontinuing therapy were inadequate effect and adverse events. The main reason for discontinuation among patients receiving natalizumab was categorized as “other reason,” which mostly reflected John Cunningham virus positivity and concern for developing progressive multifocal leukoencephalopathy.
‘The uncertainty continues’
“These differences that we see in the effectiveness can be somewhat surprising, especially when it comes to natalizumab,” which is considered very effective, said Mr. Alping. The vulnerable period that occurs after switching from natalizumab may partly explain the difference. “This is something to keep in mind when starting patients on natalizumab treatment in the clinic,” Mr. Alping added.
Although rituximab is not indicated for MS, many clinics are using it in this population, said Robert Fox, MD, staff neurologist at the Mellen Center for MS and vice chair for research at the Neurological Institute of Cleveland Clinic, both in Cleveland, Ohio. Dr. Fox was not involved in the study.
“Assessing the generalizability of the study outside Sweden will be important,” he added, “but I would be surprised if their findings did not hold up to external validation.”
The way that the researchers addressed missing data could affect the interpretation of the findings. “Depending upon how much data was missing, their imputation methods may have a high level of uncertainty,” said Dr. Fox.
The researchers’ adjustments for baseline differences also raise questions. “Even though MRI was an outcome, it doesn’t appear they adjusted for baseline differences in MRI between the groups,” Dr. Fox observed.
Moreover, the study was conducted over a long period of time. “We know there are time effects in MS, with a very different disease activity expected from patients over time,” said Dr. Fox. For example, relapse rates in placebo groups of MS trials tend to decline over time. “This time effect likely impacted their results.”
But the disability findings may be the most important part of the study, according to Dr. Fox. The lack of significant difference in disability progression between therapies “highlights that a couple relapses or lesions on MRI may be too small to translate into long-term differences in disability progression,” he said.
“The long-term implications of small differences in relapse and MRI outcomes may be very small,” Dr. Fox went on. “Thus, the uncertainty continues around escalation treatment versus initial highly effective treatment paradigms.”
The Patient-Centered Outcomes Research Institute, the Swedish Research Council, and NEURO Sweden funded this study. Mr. Alping disclosed no relevant financial relationships. Dr. Fox receives consulting fees from the companies that manufacture all the therapies analyzed in the study.
A version of this article first appeared on Medscape.com.
From ECTRIMS 2021
States can reserve COVID shots for kids 5-11 this week
States can preorder COVID-19 vaccine doses for younger children this week as they begin to set up vaccination campaigns for ages 5-11.
Vaccine advisory groups for the FDA and CDC are scheduled to discuss and approve the Pfizer shot for kids in the next three weeks. To help states and cities prepare for the rollout, the CDC issued guidance on how to set up expanded vaccination programs.
Immunization program managers can begin ordering doses on Wednesday, according to the guidance. The vials won’t be delivered until the FDA and CDC authorize the shot, but registering now will help federal officials ship doses quickly once they’re available.
Pharmacies in every state will be able to give COVID-19 shots to children, but they can only use doses that are prepared specifically for children. Ages 5-11 will need a 10-microgram dose, which is one-third of the dose administered to ages 12 and older. The guidance warns that doctors should not try to split up or fraction the adult doses.
The CDC guidance also recommends that pediatricians and family practice doctors should serve as primary places to give shots to kids. The document mentions other options, such as vaccination clinics at schools, but doesn’t endorse them as the first choice for vaccinating kids.
The CDC hasn’t yet addressed questions around whether kids should be required to get vaccinated to attend school. The decision will likely be left to state and city officials.
Federal health officials aren’t yet sure how many parents and guardians will seek shots for their younger kids right away, the AP reported. Demand may be high at first for some families, but it may not be as high as when shots first became available for adults, Marcus Plescia, MD, chief medical officer of the Association of State and Territorial Health Officials, told The Associated Press.
“We’re going to have potentially a very busy, and perhaps modestly chaotic time,” he said.
When vaccines were first authorized for adults, hospitals and pharmacies received priority for ordering shots. Some doctors felt left out. This time, however, the CDC has said that pediatricians will receive higher priority and be able to receive shipments quickly.
As the vaccine rollout begins, health officials should consider logistical concerns to address racial and economic disparities for younger kids, Richard Besser, MD, president and CEO of the Robert Wood Johnson Foundation and a former acting director of the CDC, told the AP.
If parents or guardians can’t leave work to take their kids to a pharmacy or doctor’s office, for instance, their kids may not receive a shot quickly – or at all.
“It’s really important that we recognize the barriers to vaccinations,” he said.
A version of this article first appeared on WebMD.com.
States can preorder COVID-19 vaccine doses for younger children this week as they begin to set up vaccination campaigns for ages 5-11.
Vaccine advisory groups for the FDA and CDC are scheduled to discuss and approve the Pfizer shot for kids in the next three weeks. To help states and cities prepare for the rollout, the CDC issued guidance on how to set up expanded vaccination programs.
Immunization program managers can begin ordering doses on Wednesday, according to the guidance. The vials won’t be delivered until the FDA and CDC authorize the shot, but registering now will help federal officials ship doses quickly once they’re available.
Pharmacies in every state will be able to give COVID-19 shots to children, but they can only use doses that are prepared specifically for children. Ages 5-11 will need a 10-microgram dose, which is one-third of the dose administered to ages 12 and older. The guidance warns that doctors should not try to split up or fraction the adult doses.
The CDC guidance also recommends that pediatricians and family practice doctors should serve as primary places to give shots to kids. The document mentions other options, such as vaccination clinics at schools, but doesn’t endorse them as the first choice for vaccinating kids.
The CDC hasn’t yet addressed questions around whether kids should be required to get vaccinated to attend school. The decision will likely be left to state and city officials.
Federal health officials aren’t yet sure how many parents and guardians will seek shots for their younger kids right away, the AP reported. Demand may be high at first for some families, but it may not be as high as when shots first became available for adults, Marcus Plescia, MD, chief medical officer of the Association of State and Territorial Health Officials, told The Associated Press.
“We’re going to have potentially a very busy, and perhaps modestly chaotic time,” he said.
When vaccines were first authorized for adults, hospitals and pharmacies received priority for ordering shots. Some doctors felt left out. This time, however, the CDC has said that pediatricians will receive higher priority and be able to receive shipments quickly.
As the vaccine rollout begins, health officials should consider logistical concerns to address racial and economic disparities for younger kids, Richard Besser, MD, president and CEO of the Robert Wood Johnson Foundation and a former acting director of the CDC, told the AP.
If parents or guardians can’t leave work to take their kids to a pharmacy or doctor’s office, for instance, their kids may not receive a shot quickly – or at all.
“It’s really important that we recognize the barriers to vaccinations,” he said.
A version of this article first appeared on WebMD.com.
States can preorder COVID-19 vaccine doses for younger children this week as they begin to set up vaccination campaigns for ages 5-11.
Vaccine advisory groups for the FDA and CDC are scheduled to discuss and approve the Pfizer shot for kids in the next three weeks. To help states and cities prepare for the rollout, the CDC issued guidance on how to set up expanded vaccination programs.
Immunization program managers can begin ordering doses on Wednesday, according to the guidance. The vials won’t be delivered until the FDA and CDC authorize the shot, but registering now will help federal officials ship doses quickly once they’re available.
Pharmacies in every state will be able to give COVID-19 shots to children, but they can only use doses that are prepared specifically for children. Ages 5-11 will need a 10-microgram dose, which is one-third of the dose administered to ages 12 and older. The guidance warns that doctors should not try to split up or fraction the adult doses.
The CDC guidance also recommends that pediatricians and family practice doctors should serve as primary places to give shots to kids. The document mentions other options, such as vaccination clinics at schools, but doesn’t endorse them as the first choice for vaccinating kids.
The CDC hasn’t yet addressed questions around whether kids should be required to get vaccinated to attend school. The decision will likely be left to state and city officials.
Federal health officials aren’t yet sure how many parents and guardians will seek shots for their younger kids right away, the AP reported. Demand may be high at first for some families, but it may not be as high as when shots first became available for adults, Marcus Plescia, MD, chief medical officer of the Association of State and Territorial Health Officials, told The Associated Press.
“We’re going to have potentially a very busy, and perhaps modestly chaotic time,” he said.
When vaccines were first authorized for adults, hospitals and pharmacies received priority for ordering shots. Some doctors felt left out. This time, however, the CDC has said that pediatricians will receive higher priority and be able to receive shipments quickly.
As the vaccine rollout begins, health officials should consider logistical concerns to address racial and economic disparities for younger kids, Richard Besser, MD, president and CEO of the Robert Wood Johnson Foundation and a former acting director of the CDC, told the AP.
If parents or guardians can’t leave work to take their kids to a pharmacy or doctor’s office, for instance, their kids may not receive a shot quickly – or at all.
“It’s really important that we recognize the barriers to vaccinations,” he said.
A version of this article first appeared on WebMD.com.