User login
Severe Asthma Guidelines
Hemorrhagic Lacrimation and Epistaxis: Rare Findings in Acute Hemorrhagic Edema of Infancy
To the Editor:
Hemorrhagic lacrimation and epistaxis are dramatic presentations with a narrow differential diagnosis. It rarely has been reported to present alongside the more typical features of acute hemorrhagic edema of infancy (AHEI), which is a benign self-limited leukocytoclastic vasculitis most often seen in children aged 4 months to 2 years. Extracutaneous involvement rarely is seen in AHEI, though joint, gastrointestinal tract, and renal involvement have been reported.1 Most patients present with edematous, annular, or cockade purpuric vasculitic lesions classically involving the face and distal extremities with relative sparing of the trunk. We present a case of a well-appearing, 10-month-old infant boy with hemorrhagic vasculitic lesions, acral edema, and an associated episode of hemorrhagic lacrimation and epistaxis.
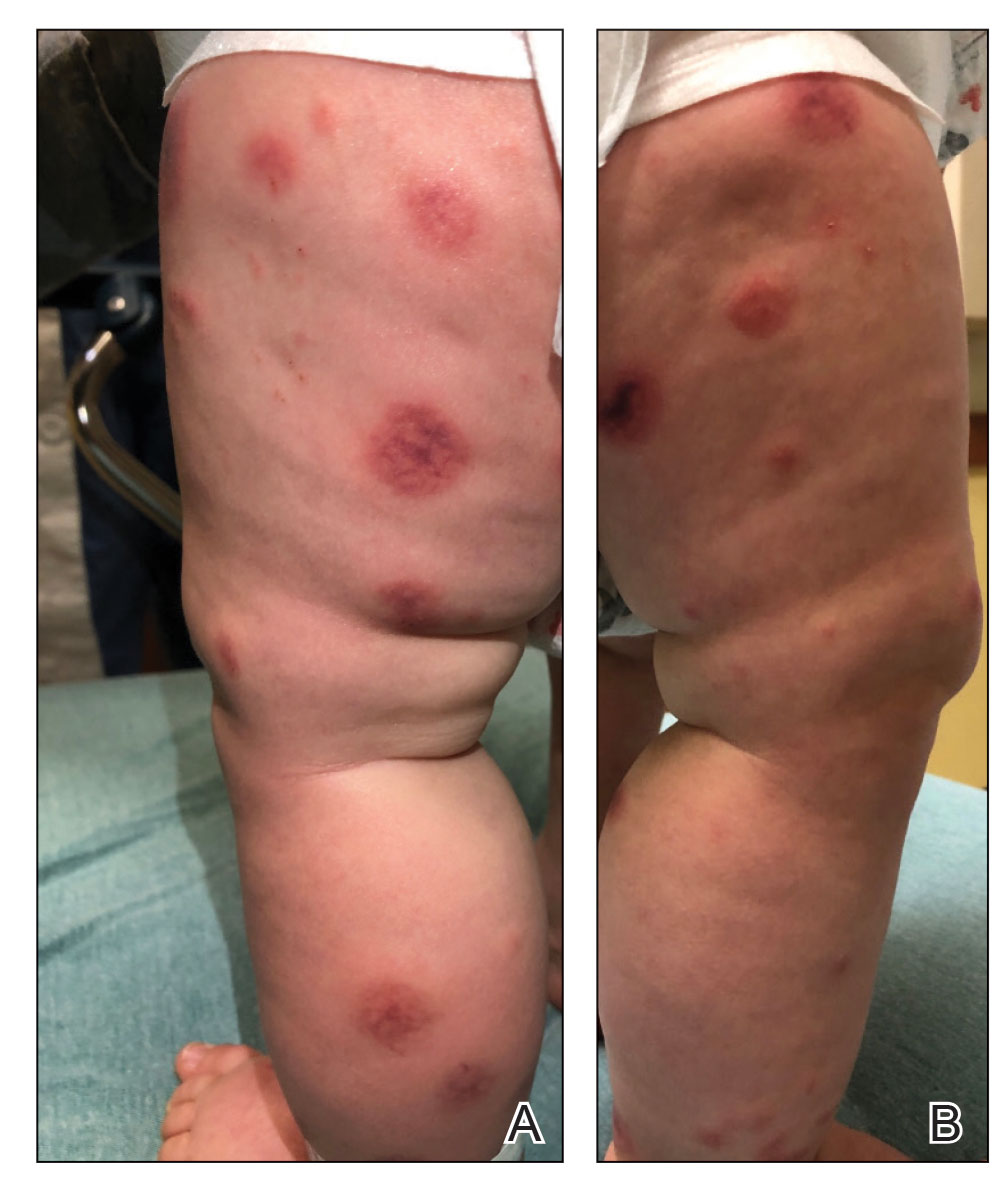
A 10-month-old infant boy who was otherwise healthy presented to the emergency department (ED) with an acute-onset, progressively worsening cutaneous eruption of 2 days’ duration. A thorough history revealed that the eruption initially had presented as several small, bright-red papules on the thighs. The eruption subsequently spread to involve the buttocks, legs, and arms (Figures 1 and 2). The parents also noted that the patient had experienced an episode of bloody tears and epistaxis that lasted a few minutes at the pediatrician’s office earlier that morning, a finding that prompted the urgent referral to the ED.
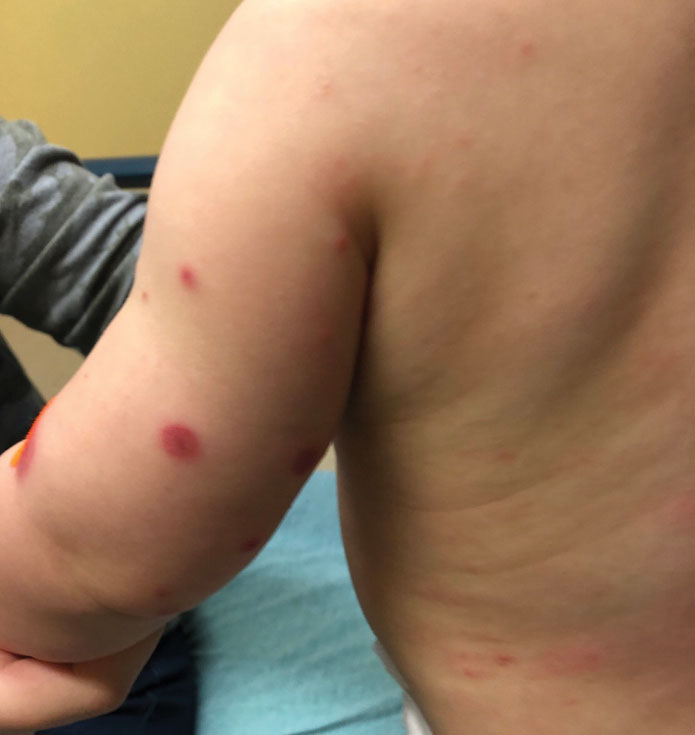
Dermatology was then consulted. A review of systems was notable for rhinorrhea and diarrhea during the week leading to the eruption. The patient’s parents denied fevers, decreased oral intake, or a recent course of antibiotics. The patient’s medical history was notable only for atopic dermatitis treated with emollients and occasional topical steroids. The parents denied recent travel or vaccinations. Physical examination showed an afebrile, well-appearing infant with multiple nontender, slightly edematous, circular, purpuric papules and plaques scattered on the buttocks and extremities with edema on the dorsal feet. The remainder of the patient’s workup in the ED was notable for mild elevations in C-reactive protein levels (1.4 mg/dL [reference range, 0–1.2 mg/dL]) and an elevated erythrocyte sedimentation rate (22 mm/h [reference range, 2–12 mm/h]). A complete blood cell count; liver function tests; urinalysis; and coagulation studies, including prothrombin, partial thromboplastin time, and international normalized ratio, were unremarkable. Acute hemorrhagic edema of infancy was diagnosed based on the clinical manifestations.
Acute hemorrhagic edema of infancy (also known as Finkelstein disease, medallionlike purpura, Seidemayer syndrome, infantile postinfectious irislike purpura and edema, and purpura en cocarde avec oedeme) is believed to result from an immune complex–related reaction, often in the setting of an upper respiratory tract infection; medications, especially antibiotics; or vaccinations. The condition previously was considered a benign form of Henoch-Schönlein purpura; however, it is now recognized as its own clinical entity. Acute hemorrhagic edema of infancy commonly affects children between the ages of 4 months and 2 years. The incidence peaks in the winter months, and males tend to be more affected than females.1
Acute hemorrhagic edema of infancy is clinically characterized by a triad of large purpuric lesions, low-grade fever, and peripheral acral edema. Edema can develop on the hands, feet, and genitalia. Importantly, facial edema has been noted to precede skin lesions.2 Coin-shaped or targetoid hemorrhagic and purpuric lesions in a cockade or rosette pattern with scalloped margins typically begin on the distal extremities and tend to spread proximally. The lesions are variable in size but have been reported to be as large as 5 cm in diameter. Although joint pain, bloody diarrhea, hematuria, and proteinuria can accompany AHEI, most cases are devoid of systemic symptoms.3 Hemorrhagic lacrimation and epistaxis—both present in our patient—are rare findings with AHEI. It is likely that most providers, including dermatologists, may be unfamiliar with these striking clinical findings. Although the pathophysiology of hemorrhagic lacrimation and epistaxis has not been formally investigated, we postulate that it likely is related to the formation of immune complexes that lead to small vessel vasculitis, underpinning the characteristic findings in AHEI.4,5 This reasoning is supported by the complete resolution of symptoms corresponding with clinical clearance of the cutaneous vasculitis in 2 prior cases4,5 as well as in our patient who did not have a relapse of symptoms following cessation of the cutaneous eruption at a pediatric follow-up appointment 2 weeks later.
Acute hemorrhagic edema of infancy is a clinical diagnosis; however, a skin biopsy can be performed to confirm the clinical suspicion and rule out more serious conditions. Histopathologic examination reveals a leukocytoclastic vasculitis involving the capillaries and postcapillary venules of the upper and mid dermis. Laboratory test results usually are nonspecific but can help distinguish AHEI from more serious diseases. The erythrocyte sedimentation rate and C-reactive protein level may be slightly elevated in infants with AHEI. Urinalysis and stool guaiac tests also can be performed to evaluate for any renal or gastrointestinal involvement.6
The differential diagnosis includes IgA vasculitis, erythema multiforme, acute meningococcemia, urticarial vasculitis, Kawasaki disease, and child abuse. IgA vasculitis often presents with more systemic involvement, with abdominal pain, vomiting, hematemesis, diarrhea, and hematochezia occurring in up to 50% of patients. The cutaneous findings of erythema multiforme classically are confined to the limbs and face, and edema of the extremities typically is not seen. Patients with acute meningococcemia appear toxic with high fevers, malaise, and possible septic shock.5
Acute hemorrhagic edema of infancy is a self-limited condition typically lasting 1 to 3 weeks and requires only supportive care.7 Antibiotics should be given to treat concurrent bacterial infections, and antihistamines and steroids may be useful for symptomatic relief. Importantly, however, systemic corticosteroids do not appear to conclusively alter the disease course.8
Acute hemorrhagic edema of infancy is a rare benign leukocytoclastic vasculitis with a striking presentation often seen following an upper respiratory tract infection or course of antibiotics. Our case demonstrates that on rare occasions, AHEI may be accompanied by hemorrhagic lacrimation and epistaxis—findings that can be quite alarming to both parents and medical providers. Nonetheless, patients and their caretakers should be assured that the condition is self-limited and resolves without permanent sequalae.
- Emerich PS, Prebianchi PA, Motta LL, et al. Acute hemorrhagic edema of infancy: report of three cases. An Bras Dermatol. 2011;86:1181-1184.
- Avhad G, Ghuge P, Jerajani H. Acute hemorrhagic edema of infancy. Indian Dermatol Online J. 2014;5:356-357.
- Krause I, Lazarov A, Rachmel A, et al. Acute haemorrhagic oedema of infancy, a benign variant of leucocytoclastic vasculitis. Acta Paediatr. 1996;85:114-117.
- Sneller H, Vega C, Zemel L, et al. Acute hemorrhagic edema of infancy with associated hemorrhagic lacrimation. Pediatr Emerg Care. 2021;37:E70-E72. doi:10.1097/PEC.0000000000001542
- Mreish S, Al-Tatari H. Hemorrhagic lacrimation and epistaxis in acute hemorrhagic edema of infancy. Case Rep Pediatr. 2016;2016:9762185. doi:10.1155/2016/9762185
- Savino F, Lupica MM, Tarasco V, et al. Acute hemorrhagic edema of infancy: a troubling cutaneous presentation with a self-limiting course. Pediatr Dermatol. 2013;30:E149-E152.
- Fiore E, Rizzi M, Ragazzi M, et al. Acute hemorrhagic edema of young children (cockade purpura and edema): a case series and systematic review. J Am Acad Dermatol. 2008;59:684-695.
- Acute hemorrhagic edema of young children: a concise narrative review. Eur J Pediatr. 2011;170:1507-1511.
To the Editor:
Hemorrhagic lacrimation and epistaxis are dramatic presentations with a narrow differential diagnosis. It rarely has been reported to present alongside the more typical features of acute hemorrhagic edema of infancy (AHEI), which is a benign self-limited leukocytoclastic vasculitis most often seen in children aged 4 months to 2 years. Extracutaneous involvement rarely is seen in AHEI, though joint, gastrointestinal tract, and renal involvement have been reported.1 Most patients present with edematous, annular, or cockade purpuric vasculitic lesions classically involving the face and distal extremities with relative sparing of the trunk. We present a case of a well-appearing, 10-month-old infant boy with hemorrhagic vasculitic lesions, acral edema, and an associated episode of hemorrhagic lacrimation and epistaxis.

A 10-month-old infant boy who was otherwise healthy presented to the emergency department (ED) with an acute-onset, progressively worsening cutaneous eruption of 2 days’ duration. A thorough history revealed that the eruption initially had presented as several small, bright-red papules on the thighs. The eruption subsequently spread to involve the buttocks, legs, and arms (Figures 1 and 2). The parents also noted that the patient had experienced an episode of bloody tears and epistaxis that lasted a few minutes at the pediatrician’s office earlier that morning, a finding that prompted the urgent referral to the ED.

Dermatology was then consulted. A review of systems was notable for rhinorrhea and diarrhea during the week leading to the eruption. The patient’s parents denied fevers, decreased oral intake, or a recent course of antibiotics. The patient’s medical history was notable only for atopic dermatitis treated with emollients and occasional topical steroids. The parents denied recent travel or vaccinations. Physical examination showed an afebrile, well-appearing infant with multiple nontender, slightly edematous, circular, purpuric papules and plaques scattered on the buttocks and extremities with edema on the dorsal feet. The remainder of the patient’s workup in the ED was notable for mild elevations in C-reactive protein levels (1.4 mg/dL [reference range, 0–1.2 mg/dL]) and an elevated erythrocyte sedimentation rate (22 mm/h [reference range, 2–12 mm/h]). A complete blood cell count; liver function tests; urinalysis; and coagulation studies, including prothrombin, partial thromboplastin time, and international normalized ratio, were unremarkable. Acute hemorrhagic edema of infancy was diagnosed based on the clinical manifestations.
Acute hemorrhagic edema of infancy (also known as Finkelstein disease, medallionlike purpura, Seidemayer syndrome, infantile postinfectious irislike purpura and edema, and purpura en cocarde avec oedeme) is believed to result from an immune complex–related reaction, often in the setting of an upper respiratory tract infection; medications, especially antibiotics; or vaccinations. The condition previously was considered a benign form of Henoch-Schönlein purpura; however, it is now recognized as its own clinical entity. Acute hemorrhagic edema of infancy commonly affects children between the ages of 4 months and 2 years. The incidence peaks in the winter months, and males tend to be more affected than females.1
Acute hemorrhagic edema of infancy is clinically characterized by a triad of large purpuric lesions, low-grade fever, and peripheral acral edema. Edema can develop on the hands, feet, and genitalia. Importantly, facial edema has been noted to precede skin lesions.2 Coin-shaped or targetoid hemorrhagic and purpuric lesions in a cockade or rosette pattern with scalloped margins typically begin on the distal extremities and tend to spread proximally. The lesions are variable in size but have been reported to be as large as 5 cm in diameter. Although joint pain, bloody diarrhea, hematuria, and proteinuria can accompany AHEI, most cases are devoid of systemic symptoms.3 Hemorrhagic lacrimation and epistaxis—both present in our patient—are rare findings with AHEI. It is likely that most providers, including dermatologists, may be unfamiliar with these striking clinical findings. Although the pathophysiology of hemorrhagic lacrimation and epistaxis has not been formally investigated, we postulate that it likely is related to the formation of immune complexes that lead to small vessel vasculitis, underpinning the characteristic findings in AHEI.4,5 This reasoning is supported by the complete resolution of symptoms corresponding with clinical clearance of the cutaneous vasculitis in 2 prior cases4,5 as well as in our patient who did not have a relapse of symptoms following cessation of the cutaneous eruption at a pediatric follow-up appointment 2 weeks later.
Acute hemorrhagic edema of infancy is a clinical diagnosis; however, a skin biopsy can be performed to confirm the clinical suspicion and rule out more serious conditions. Histopathologic examination reveals a leukocytoclastic vasculitis involving the capillaries and postcapillary venules of the upper and mid dermis. Laboratory test results usually are nonspecific but can help distinguish AHEI from more serious diseases. The erythrocyte sedimentation rate and C-reactive protein level may be slightly elevated in infants with AHEI. Urinalysis and stool guaiac tests also can be performed to evaluate for any renal or gastrointestinal involvement.6
The differential diagnosis includes IgA vasculitis, erythema multiforme, acute meningococcemia, urticarial vasculitis, Kawasaki disease, and child abuse. IgA vasculitis often presents with more systemic involvement, with abdominal pain, vomiting, hematemesis, diarrhea, and hematochezia occurring in up to 50% of patients. The cutaneous findings of erythema multiforme classically are confined to the limbs and face, and edema of the extremities typically is not seen. Patients with acute meningococcemia appear toxic with high fevers, malaise, and possible septic shock.5
Acute hemorrhagic edema of infancy is a self-limited condition typically lasting 1 to 3 weeks and requires only supportive care.7 Antibiotics should be given to treat concurrent bacterial infections, and antihistamines and steroids may be useful for symptomatic relief. Importantly, however, systemic corticosteroids do not appear to conclusively alter the disease course.8
Acute hemorrhagic edema of infancy is a rare benign leukocytoclastic vasculitis with a striking presentation often seen following an upper respiratory tract infection or course of antibiotics. Our case demonstrates that on rare occasions, AHEI may be accompanied by hemorrhagic lacrimation and epistaxis—findings that can be quite alarming to both parents and medical providers. Nonetheless, patients and their caretakers should be assured that the condition is self-limited and resolves without permanent sequalae.
To the Editor:
Hemorrhagic lacrimation and epistaxis are dramatic presentations with a narrow differential diagnosis. It rarely has been reported to present alongside the more typical features of acute hemorrhagic edema of infancy (AHEI), which is a benign self-limited leukocytoclastic vasculitis most often seen in children aged 4 months to 2 years. Extracutaneous involvement rarely is seen in AHEI, though joint, gastrointestinal tract, and renal involvement have been reported.1 Most patients present with edematous, annular, or cockade purpuric vasculitic lesions classically involving the face and distal extremities with relative sparing of the trunk. We present a case of a well-appearing, 10-month-old infant boy with hemorrhagic vasculitic lesions, acral edema, and an associated episode of hemorrhagic lacrimation and epistaxis.

A 10-month-old infant boy who was otherwise healthy presented to the emergency department (ED) with an acute-onset, progressively worsening cutaneous eruption of 2 days’ duration. A thorough history revealed that the eruption initially had presented as several small, bright-red papules on the thighs. The eruption subsequently spread to involve the buttocks, legs, and arms (Figures 1 and 2). The parents also noted that the patient had experienced an episode of bloody tears and epistaxis that lasted a few minutes at the pediatrician’s office earlier that morning, a finding that prompted the urgent referral to the ED.

Dermatology was then consulted. A review of systems was notable for rhinorrhea and diarrhea during the week leading to the eruption. The patient’s parents denied fevers, decreased oral intake, or a recent course of antibiotics. The patient’s medical history was notable only for atopic dermatitis treated with emollients and occasional topical steroids. The parents denied recent travel or vaccinations. Physical examination showed an afebrile, well-appearing infant with multiple nontender, slightly edematous, circular, purpuric papules and plaques scattered on the buttocks and extremities with edema on the dorsal feet. The remainder of the patient’s workup in the ED was notable for mild elevations in C-reactive protein levels (1.4 mg/dL [reference range, 0–1.2 mg/dL]) and an elevated erythrocyte sedimentation rate (22 mm/h [reference range, 2–12 mm/h]). A complete blood cell count; liver function tests; urinalysis; and coagulation studies, including prothrombin, partial thromboplastin time, and international normalized ratio, were unremarkable. Acute hemorrhagic edema of infancy was diagnosed based on the clinical manifestations.
Acute hemorrhagic edema of infancy (also known as Finkelstein disease, medallionlike purpura, Seidemayer syndrome, infantile postinfectious irislike purpura and edema, and purpura en cocarde avec oedeme) is believed to result from an immune complex–related reaction, often in the setting of an upper respiratory tract infection; medications, especially antibiotics; or vaccinations. The condition previously was considered a benign form of Henoch-Schönlein purpura; however, it is now recognized as its own clinical entity. Acute hemorrhagic edema of infancy commonly affects children between the ages of 4 months and 2 years. The incidence peaks in the winter months, and males tend to be more affected than females.1
Acute hemorrhagic edema of infancy is clinically characterized by a triad of large purpuric lesions, low-grade fever, and peripheral acral edema. Edema can develop on the hands, feet, and genitalia. Importantly, facial edema has been noted to precede skin lesions.2 Coin-shaped or targetoid hemorrhagic and purpuric lesions in a cockade or rosette pattern with scalloped margins typically begin on the distal extremities and tend to spread proximally. The lesions are variable in size but have been reported to be as large as 5 cm in diameter. Although joint pain, bloody diarrhea, hematuria, and proteinuria can accompany AHEI, most cases are devoid of systemic symptoms.3 Hemorrhagic lacrimation and epistaxis—both present in our patient—are rare findings with AHEI. It is likely that most providers, including dermatologists, may be unfamiliar with these striking clinical findings. Although the pathophysiology of hemorrhagic lacrimation and epistaxis has not been formally investigated, we postulate that it likely is related to the formation of immune complexes that lead to small vessel vasculitis, underpinning the characteristic findings in AHEI.4,5 This reasoning is supported by the complete resolution of symptoms corresponding with clinical clearance of the cutaneous vasculitis in 2 prior cases4,5 as well as in our patient who did not have a relapse of symptoms following cessation of the cutaneous eruption at a pediatric follow-up appointment 2 weeks later.
Acute hemorrhagic edema of infancy is a clinical diagnosis; however, a skin biopsy can be performed to confirm the clinical suspicion and rule out more serious conditions. Histopathologic examination reveals a leukocytoclastic vasculitis involving the capillaries and postcapillary venules of the upper and mid dermis. Laboratory test results usually are nonspecific but can help distinguish AHEI from more serious diseases. The erythrocyte sedimentation rate and C-reactive protein level may be slightly elevated in infants with AHEI. Urinalysis and stool guaiac tests also can be performed to evaluate for any renal or gastrointestinal involvement.6
The differential diagnosis includes IgA vasculitis, erythema multiforme, acute meningococcemia, urticarial vasculitis, Kawasaki disease, and child abuse. IgA vasculitis often presents with more systemic involvement, with abdominal pain, vomiting, hematemesis, diarrhea, and hematochezia occurring in up to 50% of patients. The cutaneous findings of erythema multiforme classically are confined to the limbs and face, and edema of the extremities typically is not seen. Patients with acute meningococcemia appear toxic with high fevers, malaise, and possible septic shock.5
Acute hemorrhagic edema of infancy is a self-limited condition typically lasting 1 to 3 weeks and requires only supportive care.7 Antibiotics should be given to treat concurrent bacterial infections, and antihistamines and steroids may be useful for symptomatic relief. Importantly, however, systemic corticosteroids do not appear to conclusively alter the disease course.8
Acute hemorrhagic edema of infancy is a rare benign leukocytoclastic vasculitis with a striking presentation often seen following an upper respiratory tract infection or course of antibiotics. Our case demonstrates that on rare occasions, AHEI may be accompanied by hemorrhagic lacrimation and epistaxis—findings that can be quite alarming to both parents and medical providers. Nonetheless, patients and their caretakers should be assured that the condition is self-limited and resolves without permanent sequalae.
- Emerich PS, Prebianchi PA, Motta LL, et al. Acute hemorrhagic edema of infancy: report of three cases. An Bras Dermatol. 2011;86:1181-1184.
- Avhad G, Ghuge P, Jerajani H. Acute hemorrhagic edema of infancy. Indian Dermatol Online J. 2014;5:356-357.
- Krause I, Lazarov A, Rachmel A, et al. Acute haemorrhagic oedema of infancy, a benign variant of leucocytoclastic vasculitis. Acta Paediatr. 1996;85:114-117.
- Sneller H, Vega C, Zemel L, et al. Acute hemorrhagic edema of infancy with associated hemorrhagic lacrimation. Pediatr Emerg Care. 2021;37:E70-E72. doi:10.1097/PEC.0000000000001542
- Mreish S, Al-Tatari H. Hemorrhagic lacrimation and epistaxis in acute hemorrhagic edema of infancy. Case Rep Pediatr. 2016;2016:9762185. doi:10.1155/2016/9762185
- Savino F, Lupica MM, Tarasco V, et al. Acute hemorrhagic edema of infancy: a troubling cutaneous presentation with a self-limiting course. Pediatr Dermatol. 2013;30:E149-E152.
- Fiore E, Rizzi M, Ragazzi M, et al. Acute hemorrhagic edema of young children (cockade purpura and edema): a case series and systematic review. J Am Acad Dermatol. 2008;59:684-695.
- Acute hemorrhagic edema of young children: a concise narrative review. Eur J Pediatr. 2011;170:1507-1511.
- Emerich PS, Prebianchi PA, Motta LL, et al. Acute hemorrhagic edema of infancy: report of three cases. An Bras Dermatol. 2011;86:1181-1184.
- Avhad G, Ghuge P, Jerajani H. Acute hemorrhagic edema of infancy. Indian Dermatol Online J. 2014;5:356-357.
- Krause I, Lazarov A, Rachmel A, et al. Acute haemorrhagic oedema of infancy, a benign variant of leucocytoclastic vasculitis. Acta Paediatr. 1996;85:114-117.
- Sneller H, Vega C, Zemel L, et al. Acute hemorrhagic edema of infancy with associated hemorrhagic lacrimation. Pediatr Emerg Care. 2021;37:E70-E72. doi:10.1097/PEC.0000000000001542
- Mreish S, Al-Tatari H. Hemorrhagic lacrimation and epistaxis in acute hemorrhagic edema of infancy. Case Rep Pediatr. 2016;2016:9762185. doi:10.1155/2016/9762185
- Savino F, Lupica MM, Tarasco V, et al. Acute hemorrhagic edema of infancy: a troubling cutaneous presentation with a self-limiting course. Pediatr Dermatol. 2013;30:E149-E152.
- Fiore E, Rizzi M, Ragazzi M, et al. Acute hemorrhagic edema of young children (cockade purpura and edema): a case series and systematic review. J Am Acad Dermatol. 2008;59:684-695.
- Acute hemorrhagic edema of young children: a concise narrative review. Eur J Pediatr. 2011;170:1507-1511.
PRACTICE POINTS
- Acute hemorrhagic edema of infancy (AHEI) is clinically characterized by a triad of large purpuric lesions, low-grade fever, and peripheral acral edema. Although joint pain, bloody diarrhea, hematuria, and proteinuria can accompany AHEI, most cases are devoid of systemic symptoms.
- It is a self-limited condition typically lasting 1 to 3 weeks and requires only supportive care.
- On rare occasions, AHEI may be accompanied by hemorrhagic lacrimation and epistaxis. Patients should be assured that the condition is self-limited and resolves without permanent sequalae.
Can a ‘smart’ skin patch detect early neurodegenerative diseases?
A new “smart patch” composed of microneedles that can detect proinflammatory markers via simulated skin interstitial fluid (ISF) may help diagnose neurodegenerative disorders such as Alzheimer’s disease and Parkinson’s disease very early on.
Originally developed to deliver medications and vaccines via the skin in a minimally invasive manner, the microneedle arrays were fitted with molecular sensors that, when placed on the skin, detect neuroinflammatory biomarkers such as interleukin-6 in as little as 6 minutes.
The literature suggests that these biomarkers of neurodegenerative disease are present years before patients become symptomatic, said study investigator Sanjiv Sharma, PhD.
“Neurodegenerative disorders such as Parkinson’s disease and Alzheimer’s disease are [characterized by] progressive loss in nerve cell and brain cells, which leads to memory problems and a loss of mental ability. That is why early diagnosis is key to preventing the loss of brain tissue in dementia, which can go undetected for years,” added Dr. Sharma, who is a lecturer in medical engineering at Swansea (Wales) University.
Dr. Sharma developed the patch with scientists at the Polytechnic of Porto (Portugal) School of Engineering in Portugal. In 2022, they designed, and are currently testing, a microneedle patch that will deliver the COVID vaccine.
The investigators describe their research on the patch’s ability to detect IL-6 in an article published in ACS Omega.
At-home diagnosis?
“The skin is the largest organ in the body – it contains more skin interstitial fluid than the total blood volume,” Dr. Sharma noted. “This fluid is an ultrafiltrate of blood and holds biomarkers that complement other biofluids, such as sweat, saliva, and urine. It can be sampled in a minimally invasive manner and used either for point-of-care testing or real-time using microneedle devices.”
Dr. Sharma and associates tested the microneedle patch in artificial ISF that contained the inflammatory cytokine IL-6. They found that the patch accurately detected IL-6 concentrations as low as 1 pg/mL in the fabricated ISF solution.
“In general, the transdermal sensor presented here showed simplicity in designing, short measuring time, high accuracy, and low detection limit. This approach seems a successful tool for the screening of inflammatory biomarkers in point of care testing wherein the skin acts as a window to the body,” the investigators reported.
Dr. Sharma noted that early detection of neurodegenerative diseases is crucial, as once symptoms appear, the disease may have already progressed significantly, and meaningful intervention is challenging.
The device has yet to be tested in humans, which is the next step, said Dr. Sharma.
“We will have to test the hypothesis through extensive preclinical and clinical studies to determine if bloodless, transdermal (skin) diagnostics can offer a cost-effective device that could allow testing in simpler settings such as a clinician’s practice or even home settings,” he noted.
Early days
Commenting on the research, David K. Simon, MD, PhD, professor of neurology at Harvard Medical School, Boston, said it is “a promising step regarding validation of a potentially beneficial method for rapidly and accurately measuring IL-6.”
However, he added, “many additional steps are needed to validate the method in actual human skin and to determine whether or not measuring these biomarkers in skin will be useful in studies of neurodegenerative diseases.”
He noted that one study limitation is that inflammatory cytokines such as IL-6 are highly nonspecific, and levels are elevated in various diseases associated with inflammation.
“It is highly unlikely that measuring IL-6 will be useful as a diagnostic tool. However, it does have potential as a biomarker for measuring the impact of treatments aimed at reducing inflammation. As the authors point out, it’s more likely that clinicians will require a panel of biomarkers rather than only measuring IL-6,” he said.
The study was funded by Fundação para a Ciência e Tecnologia. The investigators disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
A new “smart patch” composed of microneedles that can detect proinflammatory markers via simulated skin interstitial fluid (ISF) may help diagnose neurodegenerative disorders such as Alzheimer’s disease and Parkinson’s disease very early on.
Originally developed to deliver medications and vaccines via the skin in a minimally invasive manner, the microneedle arrays were fitted with molecular sensors that, when placed on the skin, detect neuroinflammatory biomarkers such as interleukin-6 in as little as 6 minutes.
The literature suggests that these biomarkers of neurodegenerative disease are present years before patients become symptomatic, said study investigator Sanjiv Sharma, PhD.
“Neurodegenerative disorders such as Parkinson’s disease and Alzheimer’s disease are [characterized by] progressive loss in nerve cell and brain cells, which leads to memory problems and a loss of mental ability. That is why early diagnosis is key to preventing the loss of brain tissue in dementia, which can go undetected for years,” added Dr. Sharma, who is a lecturer in medical engineering at Swansea (Wales) University.
Dr. Sharma developed the patch with scientists at the Polytechnic of Porto (Portugal) School of Engineering in Portugal. In 2022, they designed, and are currently testing, a microneedle patch that will deliver the COVID vaccine.
The investigators describe their research on the patch’s ability to detect IL-6 in an article published in ACS Omega.
At-home diagnosis?
“The skin is the largest organ in the body – it contains more skin interstitial fluid than the total blood volume,” Dr. Sharma noted. “This fluid is an ultrafiltrate of blood and holds biomarkers that complement other biofluids, such as sweat, saliva, and urine. It can be sampled in a minimally invasive manner and used either for point-of-care testing or real-time using microneedle devices.”
Dr. Sharma and associates tested the microneedle patch in artificial ISF that contained the inflammatory cytokine IL-6. They found that the patch accurately detected IL-6 concentrations as low as 1 pg/mL in the fabricated ISF solution.
“In general, the transdermal sensor presented here showed simplicity in designing, short measuring time, high accuracy, and low detection limit. This approach seems a successful tool for the screening of inflammatory biomarkers in point of care testing wherein the skin acts as a window to the body,” the investigators reported.
Dr. Sharma noted that early detection of neurodegenerative diseases is crucial, as once symptoms appear, the disease may have already progressed significantly, and meaningful intervention is challenging.
The device has yet to be tested in humans, which is the next step, said Dr. Sharma.
“We will have to test the hypothesis through extensive preclinical and clinical studies to determine if bloodless, transdermal (skin) diagnostics can offer a cost-effective device that could allow testing in simpler settings such as a clinician’s practice or even home settings,” he noted.
Early days
Commenting on the research, David K. Simon, MD, PhD, professor of neurology at Harvard Medical School, Boston, said it is “a promising step regarding validation of a potentially beneficial method for rapidly and accurately measuring IL-6.”
However, he added, “many additional steps are needed to validate the method in actual human skin and to determine whether or not measuring these biomarkers in skin will be useful in studies of neurodegenerative diseases.”
He noted that one study limitation is that inflammatory cytokines such as IL-6 are highly nonspecific, and levels are elevated in various diseases associated with inflammation.
“It is highly unlikely that measuring IL-6 will be useful as a diagnostic tool. However, it does have potential as a biomarker for measuring the impact of treatments aimed at reducing inflammation. As the authors point out, it’s more likely that clinicians will require a panel of biomarkers rather than only measuring IL-6,” he said.
The study was funded by Fundação para a Ciência e Tecnologia. The investigators disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
A new “smart patch” composed of microneedles that can detect proinflammatory markers via simulated skin interstitial fluid (ISF) may help diagnose neurodegenerative disorders such as Alzheimer’s disease and Parkinson’s disease very early on.
Originally developed to deliver medications and vaccines via the skin in a minimally invasive manner, the microneedle arrays were fitted with molecular sensors that, when placed on the skin, detect neuroinflammatory biomarkers such as interleukin-6 in as little as 6 minutes.
The literature suggests that these biomarkers of neurodegenerative disease are present years before patients become symptomatic, said study investigator Sanjiv Sharma, PhD.
“Neurodegenerative disorders such as Parkinson’s disease and Alzheimer’s disease are [characterized by] progressive loss in nerve cell and brain cells, which leads to memory problems and a loss of mental ability. That is why early diagnosis is key to preventing the loss of brain tissue in dementia, which can go undetected for years,” added Dr. Sharma, who is a lecturer in medical engineering at Swansea (Wales) University.
Dr. Sharma developed the patch with scientists at the Polytechnic of Porto (Portugal) School of Engineering in Portugal. In 2022, they designed, and are currently testing, a microneedle patch that will deliver the COVID vaccine.
The investigators describe their research on the patch’s ability to detect IL-6 in an article published in ACS Omega.
At-home diagnosis?
“The skin is the largest organ in the body – it contains more skin interstitial fluid than the total blood volume,” Dr. Sharma noted. “This fluid is an ultrafiltrate of blood and holds biomarkers that complement other biofluids, such as sweat, saliva, and urine. It can be sampled in a minimally invasive manner and used either for point-of-care testing or real-time using microneedle devices.”
Dr. Sharma and associates tested the microneedle patch in artificial ISF that contained the inflammatory cytokine IL-6. They found that the patch accurately detected IL-6 concentrations as low as 1 pg/mL in the fabricated ISF solution.
“In general, the transdermal sensor presented here showed simplicity in designing, short measuring time, high accuracy, and low detection limit. This approach seems a successful tool for the screening of inflammatory biomarkers in point of care testing wherein the skin acts as a window to the body,” the investigators reported.
Dr. Sharma noted that early detection of neurodegenerative diseases is crucial, as once symptoms appear, the disease may have already progressed significantly, and meaningful intervention is challenging.
The device has yet to be tested in humans, which is the next step, said Dr. Sharma.
“We will have to test the hypothesis through extensive preclinical and clinical studies to determine if bloodless, transdermal (skin) diagnostics can offer a cost-effective device that could allow testing in simpler settings such as a clinician’s practice or even home settings,” he noted.
Early days
Commenting on the research, David K. Simon, MD, PhD, professor of neurology at Harvard Medical School, Boston, said it is “a promising step regarding validation of a potentially beneficial method for rapidly and accurately measuring IL-6.”
However, he added, “many additional steps are needed to validate the method in actual human skin and to determine whether or not measuring these biomarkers in skin will be useful in studies of neurodegenerative diseases.”
He noted that one study limitation is that inflammatory cytokines such as IL-6 are highly nonspecific, and levels are elevated in various diseases associated with inflammation.
“It is highly unlikely that measuring IL-6 will be useful as a diagnostic tool. However, it does have potential as a biomarker for measuring the impact of treatments aimed at reducing inflammation. As the authors point out, it’s more likely that clinicians will require a panel of biomarkers rather than only measuring IL-6,” he said.
The study was funded by Fundação para a Ciência e Tecnologia. The investigators disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM ACS OMEGA
Biosimilar equal to natalizumab for relapsing remitting MS
An agent biologically similar to the humanized monoclonal antibody natalizumab is as effective and safe as the original reference drug for relapsing remitting multiple sclerosis (RRMS) – and has a similar level of immunogenicity, new research shows.
The investigators noted that these phase 3 trial findings are the final stage in the regulatory approval process.
“There will be a biosimilar that with respect to all parameters – efficacy, side effects, immunogenicity – doesn’t differ from the original drug and will probably be an option to consider to reduce treatment costs in MS,” said lead investigator Bernhard Hemmer, MD, a professor in the department of neurology, Technical University of Munich (Germany).
The findings were published online in JAMA Neurology.
Potential cost savings
Disease-modifying therapies (DMTs), particularly targeted biologics, have revolutionized the treatment of MS, including RRMS. Natalizumab, which was the first targeted biologic therapy approved for RRMS, is very effective and widely used, Dr. Hemmer said.
However, this and other DMTs are costly. Biosimilars, which are medicines clinically similar to an already marketed reference biologic medicine, can address this issue. In the areas of rheumatology and oncology, biosimilars have already demonstrated significant cost savings and improved treatment access.
The biosimilar natalizumab (biosim-NTZ), developed by Polpharma Biologics, is the first biosimilar monoclonal antibody therapy to be developed for MS.
Health authorities such as the Food and Drug Administration require comparative phase 3 studies to confirm there are no clinically relevant differences between a proposed biosimilar and its reference medicine.
The new multicenter, phase 3, double-blind, randomized trial – known as Antelope – included 264 adult patients with RRMS at 48 centers in seven Eastern European countries. Most study participants were women (61.4%), and their mean age was 36.7 years.
All study participants were randomly assigned to receive intravenous infusions every 4 weeks of 300 mg of biosim-NTZ or reference natalizumab (ref-NTZ) for a total of 12 infusions.
At week 24, 30 patients were switched from ref-NTZ to biosim-NTZ for the remainder of their infusions. Including such a population is required by regulatory agencies to ensure switching patients from a drug they’ve been taking to a new biosimilar does not introduce any concerns, said Dr. Hemmer.
Comparable efficacy, safety profile
The primary efficacy endpoint was the cumulative number of new active brain lesions on MRI.
At baseline, 48.1% of the biosimilar group and 45.9% of the reference drug group had at least one gadolinium-enhancing lesion. In addition, 96.9% of the biosimilar group had more than 15 T2 lesions, compared with 96.2% of the reference group.
At week 24, the mean difference between biosim-NTZ and ref-NTZ in the cumulative number of new active lesions was 0.17 (least square means, 0.34 vs. 0.45), with a 95% confidence interval of –0.61 to 0.94 and a point estimate within the prespecified margins of ± 2.1.
The annualized relapse rate for biosim-NTZ and ref-NTZ was similar at 24 weeks (0.21 vs. 0.15), as well as at 48 weeks (0.17 vs. 0.13). For Expanded Disability Status Scale scores, which were similar between treatment groups at baseline (mean, 3.4 vs. 3.2), change at 24 and 48 weeks was minimal and similar in both groups.
The safety profile was as expected for patients with RRMS receiving natalizumab. There were few adverse events of special interest, with similar proportions across all treatment groups.
The overall adverse-event profile for patients who switched from ref-NTZ to biosim-NTZ was similar to patients continuing ref-NTZ treatment and did not indicate any new or increased risks associated with switching.
Rates of treatment-emergent adverse events (TEAEs) were similar, at 64.9% for biosim-NTZ, 68.9% for ref-NTZ, and 73.3% for the switch group. The most-reported TEAEs among all treatment groups were nervous system disorders and infections and infestations.
Progressive multifocal leukoencephalopathy (PML), a rare and potentially fatal demyelinating disease of the central nervous system, is associated with some DMTs – notably ref-NTZ. It is caused by infection with the John Cunningham virus (JCV) (also referred to as human polyomavirus), the researchers noted.
As per the study protocol, no participant had a JCV-positive index of more than 1.5 at baseline. Proportions of patients positive for anti-JCV antibodies were similarly distributed between treatment groups throughout the study.
Similar immunogenicity
There was strong concordance regarding positivity for treatment-emergent antidrug antibodies between the biosim-NTZ and ref-NTZ groups (79.4% and 74.0%). This was also the case for antinatalizumab-neutralizing antibodies (69.0% and 66.2%).
“There was nothing that indicated immunogenicity is different” between the two agents, said Dr. Hemmer.
While this might change “when you look at longer time periods,” antibodies to natalizumab usually develop “very early on,” he added.
Dr. Hemmer noted that this comparison of the proposed biosimilar with the reference drug had no real surprises.
“If the immunogenicity is the same, the mode of action is the same, and the dose is the same, you would expect to have a similar clinical effect and also a similar side-effect profile, which is indeed the case,” he said.
Dr. Hemmer added that he has no insight as to when the drug might be approved but believes developers expect that to occur sometime this year.
Welcome results
Commenting on the study results, Torge Rempe, MD, assistant professor in the department of neurology, University of Florida, Gainesville, and the William T. And Janice M. Neely professor for research in MS, said he welcomes these new results showing the biosimilar matched the reference medication.
“The authors report no significant difference in their primary endpoint of cumulative number of active lesions as well as their secondary clinical endpoints of annualized relapse rate and changes from baseline Expanded Disability Status Scale scores,” said Dr. Rempe, who was not involved with the research.
The study also showed the reported adverse events were similar between the biosimilar and reference natalizumab, he noted.
However, although no cases of PML were uncovered during the study period, further research is needed to determine long-term safety in this area, Dr. Rempe said.
Finally, he agreed that the development of biosimilars such as this one addresses the issue of high annual costs for DMTs, an area of concern in the field of MS.
The study was funded by Polpharma Biologics. Dr. Hemmer has reported receiving personal fees from Polpharma and Sandoz during the conduct of the study and personal fees from Novartis, Biocom, and TG Therapeutics outside the submitted work. He has also received a patent for genetic determinants of antibodies against interferon-beta and a patent for KIR4.1 antibodies in MS; served on scientific advisory boards for Novartis; served as a data monitoring and safety committee member for AllergyCare, Polpharma Biologics, Sandoz, and TG Therapeutics; and received speaker honoraria from Desitin, grants from Regeneron for MS research, and funding from the Multiple MS EU consortium, the CLINSPECT-M consortium, and the German Research Foundation. Dr. Rempe has reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
An agent biologically similar to the humanized monoclonal antibody natalizumab is as effective and safe as the original reference drug for relapsing remitting multiple sclerosis (RRMS) – and has a similar level of immunogenicity, new research shows.
The investigators noted that these phase 3 trial findings are the final stage in the regulatory approval process.
“There will be a biosimilar that with respect to all parameters – efficacy, side effects, immunogenicity – doesn’t differ from the original drug and will probably be an option to consider to reduce treatment costs in MS,” said lead investigator Bernhard Hemmer, MD, a professor in the department of neurology, Technical University of Munich (Germany).
The findings were published online in JAMA Neurology.
Potential cost savings
Disease-modifying therapies (DMTs), particularly targeted biologics, have revolutionized the treatment of MS, including RRMS. Natalizumab, which was the first targeted biologic therapy approved for RRMS, is very effective and widely used, Dr. Hemmer said.
However, this and other DMTs are costly. Biosimilars, which are medicines clinically similar to an already marketed reference biologic medicine, can address this issue. In the areas of rheumatology and oncology, biosimilars have already demonstrated significant cost savings and improved treatment access.
The biosimilar natalizumab (biosim-NTZ), developed by Polpharma Biologics, is the first biosimilar monoclonal antibody therapy to be developed for MS.
Health authorities such as the Food and Drug Administration require comparative phase 3 studies to confirm there are no clinically relevant differences between a proposed biosimilar and its reference medicine.
The new multicenter, phase 3, double-blind, randomized trial – known as Antelope – included 264 adult patients with RRMS at 48 centers in seven Eastern European countries. Most study participants were women (61.4%), and their mean age was 36.7 years.
All study participants were randomly assigned to receive intravenous infusions every 4 weeks of 300 mg of biosim-NTZ or reference natalizumab (ref-NTZ) for a total of 12 infusions.
At week 24, 30 patients were switched from ref-NTZ to biosim-NTZ for the remainder of their infusions. Including such a population is required by regulatory agencies to ensure switching patients from a drug they’ve been taking to a new biosimilar does not introduce any concerns, said Dr. Hemmer.
Comparable efficacy, safety profile
The primary efficacy endpoint was the cumulative number of new active brain lesions on MRI.
At baseline, 48.1% of the biosimilar group and 45.9% of the reference drug group had at least one gadolinium-enhancing lesion. In addition, 96.9% of the biosimilar group had more than 15 T2 lesions, compared with 96.2% of the reference group.
At week 24, the mean difference between biosim-NTZ and ref-NTZ in the cumulative number of new active lesions was 0.17 (least square means, 0.34 vs. 0.45), with a 95% confidence interval of –0.61 to 0.94 and a point estimate within the prespecified margins of ± 2.1.
The annualized relapse rate for biosim-NTZ and ref-NTZ was similar at 24 weeks (0.21 vs. 0.15), as well as at 48 weeks (0.17 vs. 0.13). For Expanded Disability Status Scale scores, which were similar between treatment groups at baseline (mean, 3.4 vs. 3.2), change at 24 and 48 weeks was minimal and similar in both groups.
The safety profile was as expected for patients with RRMS receiving natalizumab. There were few adverse events of special interest, with similar proportions across all treatment groups.
The overall adverse-event profile for patients who switched from ref-NTZ to biosim-NTZ was similar to patients continuing ref-NTZ treatment and did not indicate any new or increased risks associated with switching.
Rates of treatment-emergent adverse events (TEAEs) were similar, at 64.9% for biosim-NTZ, 68.9% for ref-NTZ, and 73.3% for the switch group. The most-reported TEAEs among all treatment groups were nervous system disorders and infections and infestations.
Progressive multifocal leukoencephalopathy (PML), a rare and potentially fatal demyelinating disease of the central nervous system, is associated with some DMTs – notably ref-NTZ. It is caused by infection with the John Cunningham virus (JCV) (also referred to as human polyomavirus), the researchers noted.
As per the study protocol, no participant had a JCV-positive index of more than 1.5 at baseline. Proportions of patients positive for anti-JCV antibodies were similarly distributed between treatment groups throughout the study.
Similar immunogenicity
There was strong concordance regarding positivity for treatment-emergent antidrug antibodies between the biosim-NTZ and ref-NTZ groups (79.4% and 74.0%). This was also the case for antinatalizumab-neutralizing antibodies (69.0% and 66.2%).
“There was nothing that indicated immunogenicity is different” between the two agents, said Dr. Hemmer.
While this might change “when you look at longer time periods,” antibodies to natalizumab usually develop “very early on,” he added.
Dr. Hemmer noted that this comparison of the proposed biosimilar with the reference drug had no real surprises.
“If the immunogenicity is the same, the mode of action is the same, and the dose is the same, you would expect to have a similar clinical effect and also a similar side-effect profile, which is indeed the case,” he said.
Dr. Hemmer added that he has no insight as to when the drug might be approved but believes developers expect that to occur sometime this year.
Welcome results
Commenting on the study results, Torge Rempe, MD, assistant professor in the department of neurology, University of Florida, Gainesville, and the William T. And Janice M. Neely professor for research in MS, said he welcomes these new results showing the biosimilar matched the reference medication.
“The authors report no significant difference in their primary endpoint of cumulative number of active lesions as well as their secondary clinical endpoints of annualized relapse rate and changes from baseline Expanded Disability Status Scale scores,” said Dr. Rempe, who was not involved with the research.
The study also showed the reported adverse events were similar between the biosimilar and reference natalizumab, he noted.
However, although no cases of PML were uncovered during the study period, further research is needed to determine long-term safety in this area, Dr. Rempe said.
Finally, he agreed that the development of biosimilars such as this one addresses the issue of high annual costs for DMTs, an area of concern in the field of MS.
The study was funded by Polpharma Biologics. Dr. Hemmer has reported receiving personal fees from Polpharma and Sandoz during the conduct of the study and personal fees from Novartis, Biocom, and TG Therapeutics outside the submitted work. He has also received a patent for genetic determinants of antibodies against interferon-beta and a patent for KIR4.1 antibodies in MS; served on scientific advisory boards for Novartis; served as a data monitoring and safety committee member for AllergyCare, Polpharma Biologics, Sandoz, and TG Therapeutics; and received speaker honoraria from Desitin, grants from Regeneron for MS research, and funding from the Multiple MS EU consortium, the CLINSPECT-M consortium, and the German Research Foundation. Dr. Rempe has reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
An agent biologically similar to the humanized monoclonal antibody natalizumab is as effective and safe as the original reference drug for relapsing remitting multiple sclerosis (RRMS) – and has a similar level of immunogenicity, new research shows.
The investigators noted that these phase 3 trial findings are the final stage in the regulatory approval process.
“There will be a biosimilar that with respect to all parameters – efficacy, side effects, immunogenicity – doesn’t differ from the original drug and will probably be an option to consider to reduce treatment costs in MS,” said lead investigator Bernhard Hemmer, MD, a professor in the department of neurology, Technical University of Munich (Germany).
The findings were published online in JAMA Neurology.
Potential cost savings
Disease-modifying therapies (DMTs), particularly targeted biologics, have revolutionized the treatment of MS, including RRMS. Natalizumab, which was the first targeted biologic therapy approved for RRMS, is very effective and widely used, Dr. Hemmer said.
However, this and other DMTs are costly. Biosimilars, which are medicines clinically similar to an already marketed reference biologic medicine, can address this issue. In the areas of rheumatology and oncology, biosimilars have already demonstrated significant cost savings and improved treatment access.
The biosimilar natalizumab (biosim-NTZ), developed by Polpharma Biologics, is the first biosimilar monoclonal antibody therapy to be developed for MS.
Health authorities such as the Food and Drug Administration require comparative phase 3 studies to confirm there are no clinically relevant differences between a proposed biosimilar and its reference medicine.
The new multicenter, phase 3, double-blind, randomized trial – known as Antelope – included 264 adult patients with RRMS at 48 centers in seven Eastern European countries. Most study participants were women (61.4%), and their mean age was 36.7 years.
All study participants were randomly assigned to receive intravenous infusions every 4 weeks of 300 mg of biosim-NTZ or reference natalizumab (ref-NTZ) for a total of 12 infusions.
At week 24, 30 patients were switched from ref-NTZ to biosim-NTZ for the remainder of their infusions. Including such a population is required by regulatory agencies to ensure switching patients from a drug they’ve been taking to a new biosimilar does not introduce any concerns, said Dr. Hemmer.
Comparable efficacy, safety profile
The primary efficacy endpoint was the cumulative number of new active brain lesions on MRI.
At baseline, 48.1% of the biosimilar group and 45.9% of the reference drug group had at least one gadolinium-enhancing lesion. In addition, 96.9% of the biosimilar group had more than 15 T2 lesions, compared with 96.2% of the reference group.
At week 24, the mean difference between biosim-NTZ and ref-NTZ in the cumulative number of new active lesions was 0.17 (least square means, 0.34 vs. 0.45), with a 95% confidence interval of –0.61 to 0.94 and a point estimate within the prespecified margins of ± 2.1.
The annualized relapse rate for biosim-NTZ and ref-NTZ was similar at 24 weeks (0.21 vs. 0.15), as well as at 48 weeks (0.17 vs. 0.13). For Expanded Disability Status Scale scores, which were similar between treatment groups at baseline (mean, 3.4 vs. 3.2), change at 24 and 48 weeks was minimal and similar in both groups.
The safety profile was as expected for patients with RRMS receiving natalizumab. There were few adverse events of special interest, with similar proportions across all treatment groups.
The overall adverse-event profile for patients who switched from ref-NTZ to biosim-NTZ was similar to patients continuing ref-NTZ treatment and did not indicate any new or increased risks associated with switching.
Rates of treatment-emergent adverse events (TEAEs) were similar, at 64.9% for biosim-NTZ, 68.9% for ref-NTZ, and 73.3% for the switch group. The most-reported TEAEs among all treatment groups were nervous system disorders and infections and infestations.
Progressive multifocal leukoencephalopathy (PML), a rare and potentially fatal demyelinating disease of the central nervous system, is associated with some DMTs – notably ref-NTZ. It is caused by infection with the John Cunningham virus (JCV) (also referred to as human polyomavirus), the researchers noted.
As per the study protocol, no participant had a JCV-positive index of more than 1.5 at baseline. Proportions of patients positive for anti-JCV antibodies were similarly distributed between treatment groups throughout the study.
Similar immunogenicity
There was strong concordance regarding positivity for treatment-emergent antidrug antibodies between the biosim-NTZ and ref-NTZ groups (79.4% and 74.0%). This was also the case for antinatalizumab-neutralizing antibodies (69.0% and 66.2%).
“There was nothing that indicated immunogenicity is different” between the two agents, said Dr. Hemmer.
While this might change “when you look at longer time periods,” antibodies to natalizumab usually develop “very early on,” he added.
Dr. Hemmer noted that this comparison of the proposed biosimilar with the reference drug had no real surprises.
“If the immunogenicity is the same, the mode of action is the same, and the dose is the same, you would expect to have a similar clinical effect and also a similar side-effect profile, which is indeed the case,” he said.
Dr. Hemmer added that he has no insight as to when the drug might be approved but believes developers expect that to occur sometime this year.
Welcome results
Commenting on the study results, Torge Rempe, MD, assistant professor in the department of neurology, University of Florida, Gainesville, and the William T. And Janice M. Neely professor for research in MS, said he welcomes these new results showing the biosimilar matched the reference medication.
“The authors report no significant difference in their primary endpoint of cumulative number of active lesions as well as their secondary clinical endpoints of annualized relapse rate and changes from baseline Expanded Disability Status Scale scores,” said Dr. Rempe, who was not involved with the research.
The study also showed the reported adverse events were similar between the biosimilar and reference natalizumab, he noted.
However, although no cases of PML were uncovered during the study period, further research is needed to determine long-term safety in this area, Dr. Rempe said.
Finally, he agreed that the development of biosimilars such as this one addresses the issue of high annual costs for DMTs, an area of concern in the field of MS.
The study was funded by Polpharma Biologics. Dr. Hemmer has reported receiving personal fees from Polpharma and Sandoz during the conduct of the study and personal fees from Novartis, Biocom, and TG Therapeutics outside the submitted work. He has also received a patent for genetic determinants of antibodies against interferon-beta and a patent for KIR4.1 antibodies in MS; served on scientific advisory boards for Novartis; served as a data monitoring and safety committee member for AllergyCare, Polpharma Biologics, Sandoz, and TG Therapeutics; and received speaker honoraria from Desitin, grants from Regeneron for MS research, and funding from the Multiple MS EU consortium, the CLINSPECT-M consortium, and the German Research Foundation. Dr. Rempe has reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM JAMA NEUROLOGY
Atopic Dermatitis Medication
Metastatic Breast Cancer Workup
The future of GI
Dear friends,
Since the last issue of The New Gastroenterologist, the GI Fellowship Match has occurred and CONGRATULATIONS to the Class of 2026! You’ve all been on an arduous journey to get here, and it’s really time to slow down and soak up as much as you can. For those who did not match, do not give up, because you are still the future of GI!
This issue of TNG is particularly special to me, because it marks my first official selection of articles as I embark on my own TNG journey, and the theme is the future of GI. In the “In Focus” article this quarter, Dr. Eugenia N. Uche-Anya and Dr. Tyler M. Berzin review the vast and emerging advances of artificial intelligence (AI) in colonoscopy, its role in augmenting patient care, obstacles in incorporating AI into current practice, and the future of AI in gastroenterology and hepatology. One important aspect of developing our future in these technologies includes getting involved with industry. Dr. Raman Muthusamy gives practical tips on developing and navigating relationships with industry, with highlights on understanding intellectual property and conflicts of interest.
Continuing our trek into the future of GI, telemedicine came into the fold with the COVID-19 pandemic, and it is clearly here to stay. Dr. Russ R. Arjal repositions telemedicine as a way to increase access to care and optimize practice revenue, with the aim of improving patient outcomes in the future.
Last, to ground this issue clinically, Dr. Jason Kwon and Dr. Paul T. Kroner review the gastrointestinal, hepatic, and pancreaticobiliary adverse manifestations and management of immune checkpoint inhibitors, especially now that immunotherapies have revolutionized the treatment of cancer. As gastroenterologists, we are and will be seeing more and more of these adverse events.
If you are interested in contributing or have ideas for future TNG topics, please contact me ([email protected]). You may also contact Jillian Schweitzer ([email protected]), managing editor of TNG.
Until next time, I leave you with a historical fun fact: Philipp Bozzini is credited with having developed the first endoscope in 1805, called the Lichtleiter (German for “light conductor”), using a candle as its light source. Adolf Kussmaul, however, developed the first rigid gastroscope in 1868, recruiting a sword-swallower in his first demonstration.
Yours truly,
Judy A. Trieu, MD, MPH
Editor-in-Chief
Advanced Endoscopy Fellow
Division of Gastroenterology & Hepatology
University of North Carolina at Chapel Hill
Dear friends,
Since the last issue of The New Gastroenterologist, the GI Fellowship Match has occurred and CONGRATULATIONS to the Class of 2026! You’ve all been on an arduous journey to get here, and it’s really time to slow down and soak up as much as you can. For those who did not match, do not give up, because you are still the future of GI!
This issue of TNG is particularly special to me, because it marks my first official selection of articles as I embark on my own TNG journey, and the theme is the future of GI. In the “In Focus” article this quarter, Dr. Eugenia N. Uche-Anya and Dr. Tyler M. Berzin review the vast and emerging advances of artificial intelligence (AI) in colonoscopy, its role in augmenting patient care, obstacles in incorporating AI into current practice, and the future of AI in gastroenterology and hepatology. One important aspect of developing our future in these technologies includes getting involved with industry. Dr. Raman Muthusamy gives practical tips on developing and navigating relationships with industry, with highlights on understanding intellectual property and conflicts of interest.
Continuing our trek into the future of GI, telemedicine came into the fold with the COVID-19 pandemic, and it is clearly here to stay. Dr. Russ R. Arjal repositions telemedicine as a way to increase access to care and optimize practice revenue, with the aim of improving patient outcomes in the future.
Last, to ground this issue clinically, Dr. Jason Kwon and Dr. Paul T. Kroner review the gastrointestinal, hepatic, and pancreaticobiliary adverse manifestations and management of immune checkpoint inhibitors, especially now that immunotherapies have revolutionized the treatment of cancer. As gastroenterologists, we are and will be seeing more and more of these adverse events.
If you are interested in contributing or have ideas for future TNG topics, please contact me ([email protected]). You may also contact Jillian Schweitzer ([email protected]), managing editor of TNG.
Until next time, I leave you with a historical fun fact: Philipp Bozzini is credited with having developed the first endoscope in 1805, called the Lichtleiter (German for “light conductor”), using a candle as its light source. Adolf Kussmaul, however, developed the first rigid gastroscope in 1868, recruiting a sword-swallower in his first demonstration.
Yours truly,
Judy A. Trieu, MD, MPH
Editor-in-Chief
Advanced Endoscopy Fellow
Division of Gastroenterology & Hepatology
University of North Carolina at Chapel Hill
Dear friends,
Since the last issue of The New Gastroenterologist, the GI Fellowship Match has occurred and CONGRATULATIONS to the Class of 2026! You’ve all been on an arduous journey to get here, and it’s really time to slow down and soak up as much as you can. For those who did not match, do not give up, because you are still the future of GI!
This issue of TNG is particularly special to me, because it marks my first official selection of articles as I embark on my own TNG journey, and the theme is the future of GI. In the “In Focus” article this quarter, Dr. Eugenia N. Uche-Anya and Dr. Tyler M. Berzin review the vast and emerging advances of artificial intelligence (AI) in colonoscopy, its role in augmenting patient care, obstacles in incorporating AI into current practice, and the future of AI in gastroenterology and hepatology. One important aspect of developing our future in these technologies includes getting involved with industry. Dr. Raman Muthusamy gives practical tips on developing and navigating relationships with industry, with highlights on understanding intellectual property and conflicts of interest.
Continuing our trek into the future of GI, telemedicine came into the fold with the COVID-19 pandemic, and it is clearly here to stay. Dr. Russ R. Arjal repositions telemedicine as a way to increase access to care and optimize practice revenue, with the aim of improving patient outcomes in the future.
Last, to ground this issue clinically, Dr. Jason Kwon and Dr. Paul T. Kroner review the gastrointestinal, hepatic, and pancreaticobiliary adverse manifestations and management of immune checkpoint inhibitors, especially now that immunotherapies have revolutionized the treatment of cancer. As gastroenterologists, we are and will be seeing more and more of these adverse events.
If you are interested in contributing or have ideas for future TNG topics, please contact me ([email protected]). You may also contact Jillian Schweitzer ([email protected]), managing editor of TNG.
Until next time, I leave you with a historical fun fact: Philipp Bozzini is credited with having developed the first endoscope in 1805, called the Lichtleiter (German for “light conductor”), using a candle as its light source. Adolf Kussmaul, however, developed the first rigid gastroscope in 1868, recruiting a sword-swallower in his first demonstration.
Yours truly,
Judy A. Trieu, MD, MPH
Editor-in-Chief
Advanced Endoscopy Fellow
Division of Gastroenterology & Hepatology
University of North Carolina at Chapel Hill
Investing in GI innovation
Innovations in biomedical technology – from modern endoscopic devices and techniques to harnessing the microbiome to prevent and treat disease – have fundamentally changed the way in which we practice medicine and significantly improved the lives of our patients. In our February issue, we are pleased to highlight the launch of AGA’s GI Opportunity Fund, a new investment vehicle that provides AGA members and others a direct pathway to support development of promising, early-stage innovations by funding carefully vetted, cutting-edge start-up companies. We hope you will enjoy learning more about this exciting new initiative, which recently made its first major investment.
I want to thank GIHN Associate Editor Dr. Janice Jou for agreeing to spearhead this new column as its section editor – again, we invite you to nominate your colleagues, mentees, and others to be featured in future Member Spotlight columns.
We also highlight several recent papers published in AGA’s flagship journals, including a study assessing clinical outcomes and adverse events in patients receiving oral vs. colonic fecal microbiota transplant (FMT) for recurrent C. difficile infection, and another evaluating the cost-effectiveness of earlier colorectal cancer screening in patients with obesity. On the policy front, we summarize GI-relevant portions of the $1.7 trillion FY 2023 Omnibus Appropriations bill, signed into law on Dec. 30, 2022, by President Biden, and assess its impact on Medicare payments, continuation of support for telehealth/virtual care, and NIH-funding. We hope you enjoy reading these and other articles presented in our February issue.
Don’t forget to register for DDW 2023, May 6-9, 2023, in Chicago – general registration is now open!
Megan A. Adams, MD, JD, MSc
Editor-in-Chief
Innovations in biomedical technology – from modern endoscopic devices and techniques to harnessing the microbiome to prevent and treat disease – have fundamentally changed the way in which we practice medicine and significantly improved the lives of our patients. In our February issue, we are pleased to highlight the launch of AGA’s GI Opportunity Fund, a new investment vehicle that provides AGA members and others a direct pathway to support development of promising, early-stage innovations by funding carefully vetted, cutting-edge start-up companies. We hope you will enjoy learning more about this exciting new initiative, which recently made its first major investment.
I want to thank GIHN Associate Editor Dr. Janice Jou for agreeing to spearhead this new column as its section editor – again, we invite you to nominate your colleagues, mentees, and others to be featured in future Member Spotlight columns.
We also highlight several recent papers published in AGA’s flagship journals, including a study assessing clinical outcomes and adverse events in patients receiving oral vs. colonic fecal microbiota transplant (FMT) for recurrent C. difficile infection, and another evaluating the cost-effectiveness of earlier colorectal cancer screening in patients with obesity. On the policy front, we summarize GI-relevant portions of the $1.7 trillion FY 2023 Omnibus Appropriations bill, signed into law on Dec. 30, 2022, by President Biden, and assess its impact on Medicare payments, continuation of support for telehealth/virtual care, and NIH-funding. We hope you enjoy reading these and other articles presented in our February issue.
Don’t forget to register for DDW 2023, May 6-9, 2023, in Chicago – general registration is now open!
Megan A. Adams, MD, JD, MSc
Editor-in-Chief
Innovations in biomedical technology – from modern endoscopic devices and techniques to harnessing the microbiome to prevent and treat disease – have fundamentally changed the way in which we practice medicine and significantly improved the lives of our patients. In our February issue, we are pleased to highlight the launch of AGA’s GI Opportunity Fund, a new investment vehicle that provides AGA members and others a direct pathway to support development of promising, early-stage innovations by funding carefully vetted, cutting-edge start-up companies. We hope you will enjoy learning more about this exciting new initiative, which recently made its first major investment.
I want to thank GIHN Associate Editor Dr. Janice Jou for agreeing to spearhead this new column as its section editor – again, we invite you to nominate your colleagues, mentees, and others to be featured in future Member Spotlight columns.
We also highlight several recent papers published in AGA’s flagship journals, including a study assessing clinical outcomes and adverse events in patients receiving oral vs. colonic fecal microbiota transplant (FMT) for recurrent C. difficile infection, and another evaluating the cost-effectiveness of earlier colorectal cancer screening in patients with obesity. On the policy front, we summarize GI-relevant portions of the $1.7 trillion FY 2023 Omnibus Appropriations bill, signed into law on Dec. 30, 2022, by President Biden, and assess its impact on Medicare payments, continuation of support for telehealth/virtual care, and NIH-funding. We hope you enjoy reading these and other articles presented in our February issue.
Don’t forget to register for DDW 2023, May 6-9, 2023, in Chicago – general registration is now open!
Megan A. Adams, MD, JD, MSc
Editor-in-Chief
Setting higher standards for digital health technologies
“It’s influenced the way I see medicine and the work that I do around identifying quality, not in the conventional context in a hospital or a clinic, but applying that lens to the world of technology,” said Dr. Mathews, assistant professor of medicine at Johns Hopkins Medicine in Baltimore.
Bringing greater visibility to digital health technologies is part of his life’s work.
“There is now an expectation that high quality must be part of the development process of these new technologies,” said Dr. Mathews.
In particular, he’d like to see noninvasive diagnostic technologies in the gastroenterology world become more patient-centric.
Bringing somebody into the hospital is often inconvenient and disruptive. The field is heading toward technologies that can be used in the home or in an outpatient setting. “I have some research in that area, and I’d love to see it ultimately reach the patient at the bedside, if possible.”
Dr. Mathews is a member of the AGA Center for GI Innovation and Technology and a previous mentee in the Future Leaders Program.
In an interview, Dr. Mathews discussed his push to validate health technologies in the GI field and to make them more transparent to physicians and patients.
Question: Why did you choose GI?
Answer: I think the world of gastroenterology offers a tremendous amount of diversity in the way we manage and treat patients. There’s a huge spectrum of disease. There’s also the procedural aspect, which is very different from a lot of other medical specialties. For me particularly, there’s the opportunity to work on technology as it relates to GI, as well as research in that space.
Q: It seems like gastroenterology involves a lot of detective work. Would you say that’s true?
A: When you think of something like abdominal pain or GI symptoms, any place in the body can cause those symptoms to be present. You have to think broadly about all of the contributing factors, the whole patient as it relates to travel, pets, exposures, food, diet. You really can’t be myopic when you think about all the potential causes.
The name of the game is to provide answers whenever possible, but I will settle for getting someone feeling better, even if we don’t have the answer etched in stone.
Q: What gives you the most joy in your day-to-day practice?
A: I work in an academic institution at Johns Hopkins. I really enjoy the direct connection with patients. I’ve switched mostly to a hospital-based practice, which means I’m getting patients at their sickest. It’s really a privilege to provide an opportunity for improvement or support in that context. I also enjoy the teaching and training of the next generation of folks that are going into this field. There’s so much to learn, and I think trying to set that example and teach by doing is a great opportunity, and I really enjoy that as well.
Q: Describe your biggest practice-related challenge and what you’re doing to address it.A: One of my focus areas on the research front is about providing greater transparency and validation around health technologies. How do patients know which health technologies to use? How do doctors know which ones to recommend or advocate for?
Q: Can you give an example of a technology of concern?
A: Looking at oncology and mobile apps, one study I coauthored in 2021 found that well over half did not meet physician or patient expectations. These were the most popular and highest rated apps available at the time. It shows that there’s a real disconnect between what the end users – the doctors and the patients – want from these solutions and what’s actually being provided.
There’s a flood of different solutions that are out there, and there really isn’t a streamlined way to know, as a clinician or as a patient, which ones really make a difference clinically and which ones are going to be helpful for you. And that’s been the focus of my research – understanding ways to evaluate technologies that are not so burdensome as to be purely in the realm of academics, but to be pragmatic.
Q: Who has had the strongest influence on your life?
A: I would say my spouse. She’s an academic physician at Hopkins. One of the things she has shown me is the importance of finding alignment in what you do professionally with the sort of goals that you have or the values that you hold as an individual. That’s why I’ve done some nontraditional things in my academic career. It’s really been in search of finding that alignment that matches my interests and goals, as opposed to just doing something because it’s a popular thing to do.
Lightning Round
Favorite sport: Soccer
What song do you have to sing along with when you hear it? 80s pop music
Introvert or extrovert? Introvert
Favorite holiday: Christmas
Optimist or pessimist? Realist
Dr. Mathews is on LinkedIn . His health tech blog is Digital Differential.
“It’s influenced the way I see medicine and the work that I do around identifying quality, not in the conventional context in a hospital or a clinic, but applying that lens to the world of technology,” said Dr. Mathews, assistant professor of medicine at Johns Hopkins Medicine in Baltimore.
Bringing greater visibility to digital health technologies is part of his life’s work.
“There is now an expectation that high quality must be part of the development process of these new technologies,” said Dr. Mathews.
In particular, he’d like to see noninvasive diagnostic technologies in the gastroenterology world become more patient-centric.
Bringing somebody into the hospital is often inconvenient and disruptive. The field is heading toward technologies that can be used in the home or in an outpatient setting. “I have some research in that area, and I’d love to see it ultimately reach the patient at the bedside, if possible.”
Dr. Mathews is a member of the AGA Center for GI Innovation and Technology and a previous mentee in the Future Leaders Program.
In an interview, Dr. Mathews discussed his push to validate health technologies in the GI field and to make them more transparent to physicians and patients.
Question: Why did you choose GI?
Answer: I think the world of gastroenterology offers a tremendous amount of diversity in the way we manage and treat patients. There’s a huge spectrum of disease. There’s also the procedural aspect, which is very different from a lot of other medical specialties. For me particularly, there’s the opportunity to work on technology as it relates to GI, as well as research in that space.
Q: It seems like gastroenterology involves a lot of detective work. Would you say that’s true?
A: When you think of something like abdominal pain or GI symptoms, any place in the body can cause those symptoms to be present. You have to think broadly about all of the contributing factors, the whole patient as it relates to travel, pets, exposures, food, diet. You really can’t be myopic when you think about all the potential causes.
The name of the game is to provide answers whenever possible, but I will settle for getting someone feeling better, even if we don’t have the answer etched in stone.
Q: What gives you the most joy in your day-to-day practice?
A: I work in an academic institution at Johns Hopkins. I really enjoy the direct connection with patients. I’ve switched mostly to a hospital-based practice, which means I’m getting patients at their sickest. It’s really a privilege to provide an opportunity for improvement or support in that context. I also enjoy the teaching and training of the next generation of folks that are going into this field. There’s so much to learn, and I think trying to set that example and teach by doing is a great opportunity, and I really enjoy that as well.
Q: Describe your biggest practice-related challenge and what you’re doing to address it.A: One of my focus areas on the research front is about providing greater transparency and validation around health technologies. How do patients know which health technologies to use? How do doctors know which ones to recommend or advocate for?
Q: Can you give an example of a technology of concern?
A: Looking at oncology and mobile apps, one study I coauthored in 2021 found that well over half did not meet physician or patient expectations. These were the most popular and highest rated apps available at the time. It shows that there’s a real disconnect between what the end users – the doctors and the patients – want from these solutions and what’s actually being provided.
There’s a flood of different solutions that are out there, and there really isn’t a streamlined way to know, as a clinician or as a patient, which ones really make a difference clinically and which ones are going to be helpful for you. And that’s been the focus of my research – understanding ways to evaluate technologies that are not so burdensome as to be purely in the realm of academics, but to be pragmatic.
Q: Who has had the strongest influence on your life?
A: I would say my spouse. She’s an academic physician at Hopkins. One of the things she has shown me is the importance of finding alignment in what you do professionally with the sort of goals that you have or the values that you hold as an individual. That’s why I’ve done some nontraditional things in my academic career. It’s really been in search of finding that alignment that matches my interests and goals, as opposed to just doing something because it’s a popular thing to do.
Lightning Round
Favorite sport: Soccer
What song do you have to sing along with when you hear it? 80s pop music
Introvert or extrovert? Introvert
Favorite holiday: Christmas
Optimist or pessimist? Realist
Dr. Mathews is on LinkedIn . His health tech blog is Digital Differential.
“It’s influenced the way I see medicine and the work that I do around identifying quality, not in the conventional context in a hospital or a clinic, but applying that lens to the world of technology,” said Dr. Mathews, assistant professor of medicine at Johns Hopkins Medicine in Baltimore.
Bringing greater visibility to digital health technologies is part of his life’s work.
“There is now an expectation that high quality must be part of the development process of these new technologies,” said Dr. Mathews.
In particular, he’d like to see noninvasive diagnostic technologies in the gastroenterology world become more patient-centric.
Bringing somebody into the hospital is often inconvenient and disruptive. The field is heading toward technologies that can be used in the home or in an outpatient setting. “I have some research in that area, and I’d love to see it ultimately reach the patient at the bedside, if possible.”
Dr. Mathews is a member of the AGA Center for GI Innovation and Technology and a previous mentee in the Future Leaders Program.
In an interview, Dr. Mathews discussed his push to validate health technologies in the GI field and to make them more transparent to physicians and patients.
Question: Why did you choose GI?
Answer: I think the world of gastroenterology offers a tremendous amount of diversity in the way we manage and treat patients. There’s a huge spectrum of disease. There’s also the procedural aspect, which is very different from a lot of other medical specialties. For me particularly, there’s the opportunity to work on technology as it relates to GI, as well as research in that space.
Q: It seems like gastroenterology involves a lot of detective work. Would you say that’s true?
A: When you think of something like abdominal pain or GI symptoms, any place in the body can cause those symptoms to be present. You have to think broadly about all of the contributing factors, the whole patient as it relates to travel, pets, exposures, food, diet. You really can’t be myopic when you think about all the potential causes.
The name of the game is to provide answers whenever possible, but I will settle for getting someone feeling better, even if we don’t have the answer etched in stone.
Q: What gives you the most joy in your day-to-day practice?
A: I work in an academic institution at Johns Hopkins. I really enjoy the direct connection with patients. I’ve switched mostly to a hospital-based practice, which means I’m getting patients at their sickest. It’s really a privilege to provide an opportunity for improvement or support in that context. I also enjoy the teaching and training of the next generation of folks that are going into this field. There’s so much to learn, and I think trying to set that example and teach by doing is a great opportunity, and I really enjoy that as well.
Q: Describe your biggest practice-related challenge and what you’re doing to address it.A: One of my focus areas on the research front is about providing greater transparency and validation around health technologies. How do patients know which health technologies to use? How do doctors know which ones to recommend or advocate for?
Q: Can you give an example of a technology of concern?
A: Looking at oncology and mobile apps, one study I coauthored in 2021 found that well over half did not meet physician or patient expectations. These were the most popular and highest rated apps available at the time. It shows that there’s a real disconnect between what the end users – the doctors and the patients – want from these solutions and what’s actually being provided.
There’s a flood of different solutions that are out there, and there really isn’t a streamlined way to know, as a clinician or as a patient, which ones really make a difference clinically and which ones are going to be helpful for you. And that’s been the focus of my research – understanding ways to evaluate technologies that are not so burdensome as to be purely in the realm of academics, but to be pragmatic.
Q: Who has had the strongest influence on your life?
A: I would say my spouse. She’s an academic physician at Hopkins. One of the things she has shown me is the importance of finding alignment in what you do professionally with the sort of goals that you have or the values that you hold as an individual. That’s why I’ve done some nontraditional things in my academic career. It’s really been in search of finding that alignment that matches my interests and goals, as opposed to just doing something because it’s a popular thing to do.
Lightning Round
Favorite sport: Soccer
What song do you have to sing along with when you hear it? 80s pop music
Introvert or extrovert? Introvert
Favorite holiday: Christmas
Optimist or pessimist? Realist
Dr. Mathews is on LinkedIn . His health tech blog is Digital Differential.
Difficulty fitting family into career: Female oncologists
In a survey of just over 1,000 female oncologists, 95% said their career plans were at least somewhat associated with the timing of when to start a family.
The most striking finding was that one third of respondents had miscarried and another one third reported difficulty with infertility that required fertility counseling and/or treatment.
One third reported experiencing discrimination during pregnancy, and another third said they experienced discrimination for taking maternity leave, and having more than one child increased the likelihood of this.
The most common negative factor associated with family planning was long work hours and heavy workload (66.6%),
These findings suggest there are systemic changes needed not only in the healthcare setting but in society as a whole around women in the workplace and their choices of childbearing, say the authors.
The study was published online in JAMA Network Open and led by Anna Lee MD, MPH, from the department of radiation oncology, University of Texas MD Anderson Cancer Center, Houston.
In an invited commentary, Mona Saleh, MD, and Stephanie Blank, MD, from the department of obstetrics, gynecology, and reproductive science at the Icahn School of Medicine at Mount Sinai in New York, suggest that cultural changes are needed that go beyond women in medicine.
“These cultural values are so deeply pervasive (one could also say invasive) that they affect even these most educated and wealthy professional women, such as those who participated in this survey,” the editorialists write.
“[The researchers] advocate for early education on assisted reproductive technology (ART) risks, benefits, and success rates, but this is not getting at the underlying issue: Pregnancy discrimination and unfair distribution of childbearing responsibilities are a reflection of a larger problematic culture rather than an issue specific to women in medicine,” they add.
Survey details
The survey comprised a novel 39-item questionnaire distributed to 1,004 U.S. female oncologists from May 7 to June 30, 2020, via email and social media channels.
Most respondents (84.4%) were married, and 71% were currently working full-time.
About one-third (35%) worked in radiation oncology, another third (34.3%) in medical oncology, 18.4% in surgical oncology, and 9.1% in pediatric oncology.
A total of 768 respondents (76.5%) had children, and of these, 415 (41.3%) first gave birth during postgraduate training and 275 (27.4%) gave birth in years 1-5 as an attending physician.
Of all respondents who had been pregnant, approximately two-thirds (65.7%) had some type of pregnancy complication. About one-third of respondents (31.7%) reported having experienced a miscarriage after a confirmed pregnancy; of those, 61.6% reported one miscarriage, while the remainder had two or more miscarriages (38.4%).
Approximately one-third (31.4%) of respondents reported difficulty with infertility that required fertility counseling and/or treatment.
The questionnaire also asked about assisted reproductive technology, and 164 participants (16.3%) reported the use of fertility medications, and 53 (5.3%) reported cryopreservation of eggs. Nearly 13% reported the use of intrauterine insemination and 13.2% reported the use of in vivo fertilization. Among those who experienced fertility concerns, 36.6% (232 of 634) reported facing financial burdens because of fertility or pregnancy that was in some way associated with their career choice.
When asked on the survey if fertility preservation should be discussed with women during medical school and/or residency, 65.7% of respondents stated that it should.
However, the editorialists suggest that “encouraging formal and directed education regarding the infertility risks specifically toward female physicians (which Lee et al. recommend) could be perceived as a blanket recommendation that it is best for women in medicine to delay childbearing and pursue ART.”
“Medical schools and residency and fellowship training programs should instead focus their energy on creating a framework and culture that normalizes conception during these points in training while also subsidizing and supporting trainees and physicians who prefer to use ART and delay fertility until after training,” they suggest.
The editorialists also emphasized that women may choose to become pregnant at any point during the years that it takes to go from being a medical student to resident/fellow to attending physician, and they should be supported by their workplace on their decisions.
The study was funded by grants from National Institutes of Health/National Cancer Institute Cancer Center.
Dr. Lee and coauthors reported no relevant financial relationships. Dr. Blank reported receiving grants from AstraZeneca, Aravive, Akesobio, GlaxoSmithKline, Merck, and Seattle Genetics outside the submitted work. Dr. Saleh reports no relevant financial relationships.
A version of this article first appeared on Medscape.com.
In a survey of just over 1,000 female oncologists, 95% said their career plans were at least somewhat associated with the timing of when to start a family.
The most striking finding was that one third of respondents had miscarried and another one third reported difficulty with infertility that required fertility counseling and/or treatment.
One third reported experiencing discrimination during pregnancy, and another third said they experienced discrimination for taking maternity leave, and having more than one child increased the likelihood of this.
The most common negative factor associated with family planning was long work hours and heavy workload (66.6%),
These findings suggest there are systemic changes needed not only in the healthcare setting but in society as a whole around women in the workplace and their choices of childbearing, say the authors.
The study was published online in JAMA Network Open and led by Anna Lee MD, MPH, from the department of radiation oncology, University of Texas MD Anderson Cancer Center, Houston.
In an invited commentary, Mona Saleh, MD, and Stephanie Blank, MD, from the department of obstetrics, gynecology, and reproductive science at the Icahn School of Medicine at Mount Sinai in New York, suggest that cultural changes are needed that go beyond women in medicine.
“These cultural values are so deeply pervasive (one could also say invasive) that they affect even these most educated and wealthy professional women, such as those who participated in this survey,” the editorialists write.
“[The researchers] advocate for early education on assisted reproductive technology (ART) risks, benefits, and success rates, but this is not getting at the underlying issue: Pregnancy discrimination and unfair distribution of childbearing responsibilities are a reflection of a larger problematic culture rather than an issue specific to women in medicine,” they add.
Survey details
The survey comprised a novel 39-item questionnaire distributed to 1,004 U.S. female oncologists from May 7 to June 30, 2020, via email and social media channels.
Most respondents (84.4%) were married, and 71% were currently working full-time.
About one-third (35%) worked in radiation oncology, another third (34.3%) in medical oncology, 18.4% in surgical oncology, and 9.1% in pediatric oncology.
A total of 768 respondents (76.5%) had children, and of these, 415 (41.3%) first gave birth during postgraduate training and 275 (27.4%) gave birth in years 1-5 as an attending physician.
Of all respondents who had been pregnant, approximately two-thirds (65.7%) had some type of pregnancy complication. About one-third of respondents (31.7%) reported having experienced a miscarriage after a confirmed pregnancy; of those, 61.6% reported one miscarriage, while the remainder had two or more miscarriages (38.4%).
Approximately one-third (31.4%) of respondents reported difficulty with infertility that required fertility counseling and/or treatment.
The questionnaire also asked about assisted reproductive technology, and 164 participants (16.3%) reported the use of fertility medications, and 53 (5.3%) reported cryopreservation of eggs. Nearly 13% reported the use of intrauterine insemination and 13.2% reported the use of in vivo fertilization. Among those who experienced fertility concerns, 36.6% (232 of 634) reported facing financial burdens because of fertility or pregnancy that was in some way associated with their career choice.
When asked on the survey if fertility preservation should be discussed with women during medical school and/or residency, 65.7% of respondents stated that it should.
However, the editorialists suggest that “encouraging formal and directed education regarding the infertility risks specifically toward female physicians (which Lee et al. recommend) could be perceived as a blanket recommendation that it is best for women in medicine to delay childbearing and pursue ART.”
“Medical schools and residency and fellowship training programs should instead focus their energy on creating a framework and culture that normalizes conception during these points in training while also subsidizing and supporting trainees and physicians who prefer to use ART and delay fertility until after training,” they suggest.
The editorialists also emphasized that women may choose to become pregnant at any point during the years that it takes to go from being a medical student to resident/fellow to attending physician, and they should be supported by their workplace on their decisions.
The study was funded by grants from National Institutes of Health/National Cancer Institute Cancer Center.
Dr. Lee and coauthors reported no relevant financial relationships. Dr. Blank reported receiving grants from AstraZeneca, Aravive, Akesobio, GlaxoSmithKline, Merck, and Seattle Genetics outside the submitted work. Dr. Saleh reports no relevant financial relationships.
A version of this article first appeared on Medscape.com.
In a survey of just over 1,000 female oncologists, 95% said their career plans were at least somewhat associated with the timing of when to start a family.
The most striking finding was that one third of respondents had miscarried and another one third reported difficulty with infertility that required fertility counseling and/or treatment.
One third reported experiencing discrimination during pregnancy, and another third said they experienced discrimination for taking maternity leave, and having more than one child increased the likelihood of this.
The most common negative factor associated with family planning was long work hours and heavy workload (66.6%),
These findings suggest there are systemic changes needed not only in the healthcare setting but in society as a whole around women in the workplace and their choices of childbearing, say the authors.
The study was published online in JAMA Network Open and led by Anna Lee MD, MPH, from the department of radiation oncology, University of Texas MD Anderson Cancer Center, Houston.
In an invited commentary, Mona Saleh, MD, and Stephanie Blank, MD, from the department of obstetrics, gynecology, and reproductive science at the Icahn School of Medicine at Mount Sinai in New York, suggest that cultural changes are needed that go beyond women in medicine.
“These cultural values are so deeply pervasive (one could also say invasive) that they affect even these most educated and wealthy professional women, such as those who participated in this survey,” the editorialists write.
“[The researchers] advocate for early education on assisted reproductive technology (ART) risks, benefits, and success rates, but this is not getting at the underlying issue: Pregnancy discrimination and unfair distribution of childbearing responsibilities are a reflection of a larger problematic culture rather than an issue specific to women in medicine,” they add.
Survey details
The survey comprised a novel 39-item questionnaire distributed to 1,004 U.S. female oncologists from May 7 to June 30, 2020, via email and social media channels.
Most respondents (84.4%) were married, and 71% were currently working full-time.
About one-third (35%) worked in radiation oncology, another third (34.3%) in medical oncology, 18.4% in surgical oncology, and 9.1% in pediatric oncology.
A total of 768 respondents (76.5%) had children, and of these, 415 (41.3%) first gave birth during postgraduate training and 275 (27.4%) gave birth in years 1-5 as an attending physician.
Of all respondents who had been pregnant, approximately two-thirds (65.7%) had some type of pregnancy complication. About one-third of respondents (31.7%) reported having experienced a miscarriage after a confirmed pregnancy; of those, 61.6% reported one miscarriage, while the remainder had two or more miscarriages (38.4%).
Approximately one-third (31.4%) of respondents reported difficulty with infertility that required fertility counseling and/or treatment.
The questionnaire also asked about assisted reproductive technology, and 164 participants (16.3%) reported the use of fertility medications, and 53 (5.3%) reported cryopreservation of eggs. Nearly 13% reported the use of intrauterine insemination and 13.2% reported the use of in vivo fertilization. Among those who experienced fertility concerns, 36.6% (232 of 634) reported facing financial burdens because of fertility or pregnancy that was in some way associated with their career choice.
When asked on the survey if fertility preservation should be discussed with women during medical school and/or residency, 65.7% of respondents stated that it should.
However, the editorialists suggest that “encouraging formal and directed education regarding the infertility risks specifically toward female physicians (which Lee et al. recommend) could be perceived as a blanket recommendation that it is best for women in medicine to delay childbearing and pursue ART.”
“Medical schools and residency and fellowship training programs should instead focus their energy on creating a framework and culture that normalizes conception during these points in training while also subsidizing and supporting trainees and physicians who prefer to use ART and delay fertility until after training,” they suggest.
The editorialists also emphasized that women may choose to become pregnant at any point during the years that it takes to go from being a medical student to resident/fellow to attending physician, and they should be supported by their workplace on their decisions.
The study was funded by grants from National Institutes of Health/National Cancer Institute Cancer Center.
Dr. Lee and coauthors reported no relevant financial relationships. Dr. Blank reported receiving grants from AstraZeneca, Aravive, Akesobio, GlaxoSmithKline, Merck, and Seattle Genetics outside the submitted work. Dr. Saleh reports no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM JAMA NETWORK OPEN