User login
Formerly Skin & Allergy News
ass lick
assault rifle
balls
ballsac
black jack
bleach
Boko Haram
bondage
causas
cheap
child abuse
cocaine
compulsive behaviors
cost of miracles
cunt
Daech
display network stats
drug paraphernalia
explosion
fart
fda and death
fda AND warn
fda AND warning
fda AND warns
feom
fuck
gambling
gfc
gun
human trafficking
humira AND expensive
illegal
ISIL
ISIS
Islamic caliphate
Islamic state
madvocate
masturbation
mixed martial arts
MMA
molestation
national rifle association
NRA
nsfw
nuccitelli
pedophile
pedophilia
poker
porn
porn
pornography
psychedelic drug
recreational drug
sex slave rings
shit
slot machine
snort
substance abuse
terrorism
terrorist
texarkana
Texas hold 'em
UFC
section[contains(@class, 'nav-hidden')]
section[contains(@class, 'nav-hidden active')]
The leading independent newspaper covering dermatology news and commentary.
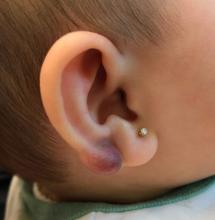
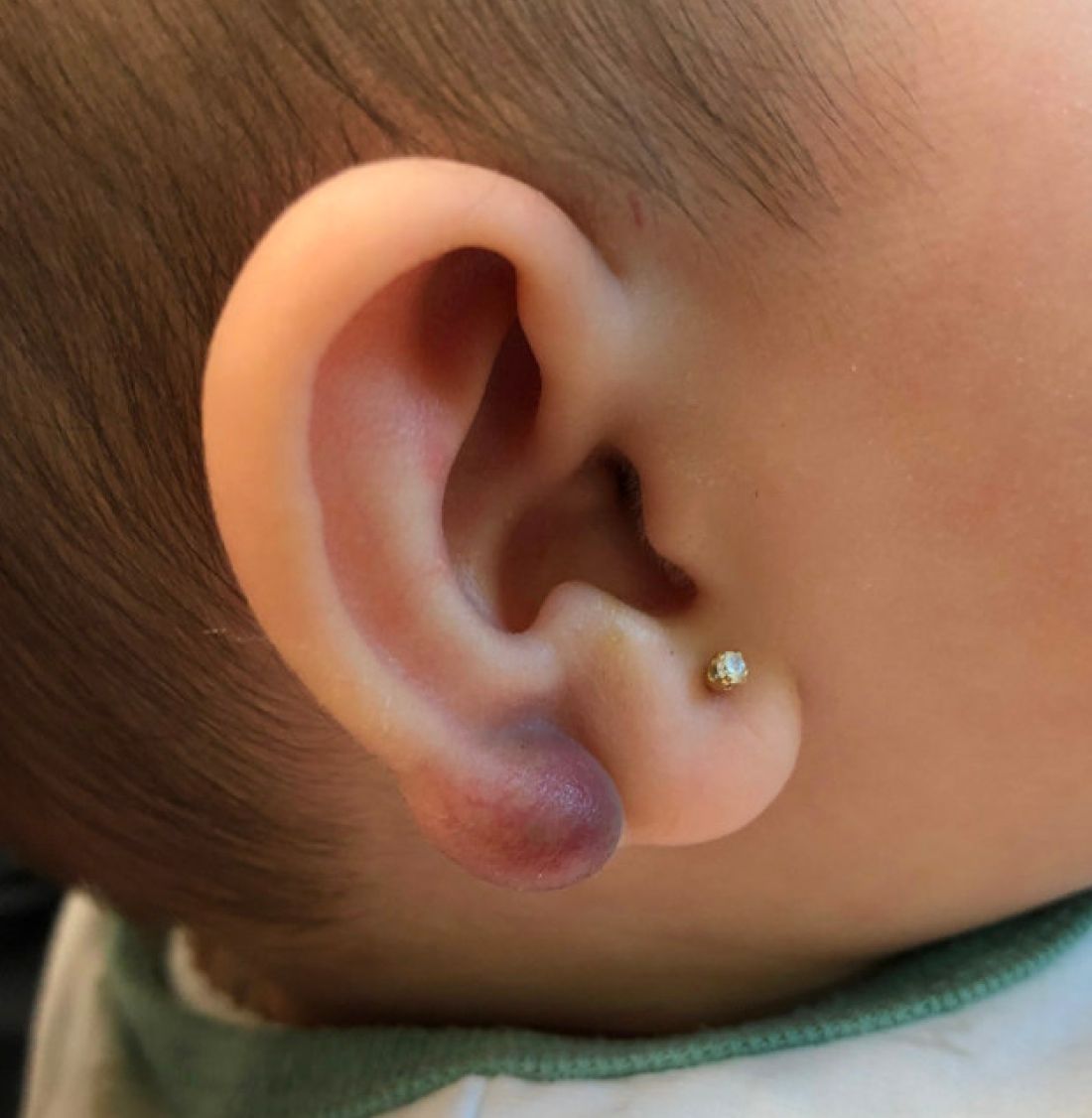
An infant with a tender bump on her ear
A biopsy of the lesion was performed that showed a well-defined nodulocystic tumor composed of nests of basaloid cells that are undergoing trichilemmal keratinization. Shadow cells are seen as well as small areas of calcification. There is also a histiocytic infiltrate with multinucleated giant cells. The histologic diagnosis is of a pilomatrixoma.
Pilomatrixoma, also known as calcifying epithelioma of Malherbe, was first described in 1880, as a tumor of sebaceous gland origin. Later, in 1961, Robert Forbis Jr, MD, and Elson B. Helwig, MD, coined the term pilomatrixoma to describe the hair follicle matrix as the source of the tumor. Pilomatrixomas are commonly seen in the pediatric population, usually in children between 8 and 13 years of age. Our patient is one of the youngest described. The lesions are commonly seen on the face and neck in about 70% of the cases followed by the upper extremities, back, and legs. Clinically, the lesions appear as a firm dermal papule or nodule, which moves freely and may have associated erythema on the skin surface or a blueish gray hue on the underlying skin.
Most pilomatrixomas that have been studied have shown a mutation in Exon 3 of the beta-catenin gene (CTNNB1). The beta-catenin molecule is a subunit of the cadherin protein, which is part of an important pathway in the terminal hair follicle differentiation. Beta-catenin also plays an important role in the Wnt pathway, which regulates cell fate as well as early embryonic patterning. Beta-catenin is responsible for forming adhesion junctions among cells. There have also been immunohistochemical studies that have shown a BCL2 proto-oncogene overexpression to pilomatrixoma.
There are several genetic syndromes that have been associated with the presence of pilomatrixomas: Turner syndrome (XO chromosome abnormality associated with short stature and cardiac defects), Gardner syndrome (polyposis coli and colon and rectal cancer), myotonic dystrophy, Rubinstein-Taybi syndrome (characterized by broad thumbs and toes, short stature, distinctive facial features, and varying degrees of intellectual disability), and trisomy 9. On physical examination our patient didn’t present with any of the typical features or history that could suggest any of these syndromes. A close follow-up and evaluation by a geneticist was recommended because after the initial visit she developed a second lesion on the forehead.
The differential diagnosis for this lesion includes other cysts that may occur on the ear such as epidermal inclusion cyst or dermoid cysts, though these lesions do not tend to be as firm as pilomatrixomas are, which can help with the diagnosis. Dermoid cysts are made of dermal and epidermal components. They are usually present at birth and are commonly seen on the scalp and the periorbital face.
Keloids are rubbery nodules of scar tissue that can form on sites of trauma, and although the lesion occurred after she had her ears pierced, the consistency and rapid growth of the lesion as well as the pathological description made this benign fibrous growth less likely.
When pilomatrixomas are inflamed they can be confused with vascular growths: in this particular case, a hemangioma or another vascular tumor such as a tufted angioma or kaposiform hemangioendothelioma. An ultrasound of the lesion could have helped in the differential diagnosis of the lesion.
Pilomatrixomas can grow significantly and in some cases get inflamed or infected. Surgical management of pilomatrixomas is often required because the lesions do not regress spontaneously.
Dr. Matiz is a pediatric dermatologist at Southern California Permanente Medical Group, San Diego.
References
Forbis R Jr and Helwig EB. Arch Dermatol 1961;83:606-18.
Schwarz Y et al. Int J Pediatr Otorhinolaryngol. 2016 Jun;85:148-53.
A biopsy of the lesion was performed that showed a well-defined nodulocystic tumor composed of nests of basaloid cells that are undergoing trichilemmal keratinization. Shadow cells are seen as well as small areas of calcification. There is also a histiocytic infiltrate with multinucleated giant cells. The histologic diagnosis is of a pilomatrixoma.
Pilomatrixoma, also known as calcifying epithelioma of Malherbe, was first described in 1880, as a tumor of sebaceous gland origin. Later, in 1961, Robert Forbis Jr, MD, and Elson B. Helwig, MD, coined the term pilomatrixoma to describe the hair follicle matrix as the source of the tumor. Pilomatrixomas are commonly seen in the pediatric population, usually in children between 8 and 13 years of age. Our patient is one of the youngest described. The lesions are commonly seen on the face and neck in about 70% of the cases followed by the upper extremities, back, and legs. Clinically, the lesions appear as a firm dermal papule or nodule, which moves freely and may have associated erythema on the skin surface or a blueish gray hue on the underlying skin.
Most pilomatrixomas that have been studied have shown a mutation in Exon 3 of the beta-catenin gene (CTNNB1). The beta-catenin molecule is a subunit of the cadherin protein, which is part of an important pathway in the terminal hair follicle differentiation. Beta-catenin also plays an important role in the Wnt pathway, which regulates cell fate as well as early embryonic patterning. Beta-catenin is responsible for forming adhesion junctions among cells. There have also been immunohistochemical studies that have shown a BCL2 proto-oncogene overexpression to pilomatrixoma.
There are several genetic syndromes that have been associated with the presence of pilomatrixomas: Turner syndrome (XO chromosome abnormality associated with short stature and cardiac defects), Gardner syndrome (polyposis coli and colon and rectal cancer), myotonic dystrophy, Rubinstein-Taybi syndrome (characterized by broad thumbs and toes, short stature, distinctive facial features, and varying degrees of intellectual disability), and trisomy 9. On physical examination our patient didn’t present with any of the typical features or history that could suggest any of these syndromes. A close follow-up and evaluation by a geneticist was recommended because after the initial visit she developed a second lesion on the forehead.
The differential diagnosis for this lesion includes other cysts that may occur on the ear such as epidermal inclusion cyst or dermoid cysts, though these lesions do not tend to be as firm as pilomatrixomas are, which can help with the diagnosis. Dermoid cysts are made of dermal and epidermal components. They are usually present at birth and are commonly seen on the scalp and the periorbital face.
Keloids are rubbery nodules of scar tissue that can form on sites of trauma, and although the lesion occurred after she had her ears pierced, the consistency and rapid growth of the lesion as well as the pathological description made this benign fibrous growth less likely.
When pilomatrixomas are inflamed they can be confused with vascular growths: in this particular case, a hemangioma or another vascular tumor such as a tufted angioma or kaposiform hemangioendothelioma. An ultrasound of the lesion could have helped in the differential diagnosis of the lesion.
Pilomatrixomas can grow significantly and in some cases get inflamed or infected. Surgical management of pilomatrixomas is often required because the lesions do not regress spontaneously.
Dr. Matiz is a pediatric dermatologist at Southern California Permanente Medical Group, San Diego.
References
Forbis R Jr and Helwig EB. Arch Dermatol 1961;83:606-18.
Schwarz Y et al. Int J Pediatr Otorhinolaryngol. 2016 Jun;85:148-53.
A biopsy of the lesion was performed that showed a well-defined nodulocystic tumor composed of nests of basaloid cells that are undergoing trichilemmal keratinization. Shadow cells are seen as well as small areas of calcification. There is also a histiocytic infiltrate with multinucleated giant cells. The histologic diagnosis is of a pilomatrixoma.
Pilomatrixoma, also known as calcifying epithelioma of Malherbe, was first described in 1880, as a tumor of sebaceous gland origin. Later, in 1961, Robert Forbis Jr, MD, and Elson B. Helwig, MD, coined the term pilomatrixoma to describe the hair follicle matrix as the source of the tumor. Pilomatrixomas are commonly seen in the pediatric population, usually in children between 8 and 13 years of age. Our patient is one of the youngest described. The lesions are commonly seen on the face and neck in about 70% of the cases followed by the upper extremities, back, and legs. Clinically, the lesions appear as a firm dermal papule or nodule, which moves freely and may have associated erythema on the skin surface or a blueish gray hue on the underlying skin.
Most pilomatrixomas that have been studied have shown a mutation in Exon 3 of the beta-catenin gene (CTNNB1). The beta-catenin molecule is a subunit of the cadherin protein, which is part of an important pathway in the terminal hair follicle differentiation. Beta-catenin also plays an important role in the Wnt pathway, which regulates cell fate as well as early embryonic patterning. Beta-catenin is responsible for forming adhesion junctions among cells. There have also been immunohistochemical studies that have shown a BCL2 proto-oncogene overexpression to pilomatrixoma.
There are several genetic syndromes that have been associated with the presence of pilomatrixomas: Turner syndrome (XO chromosome abnormality associated with short stature and cardiac defects), Gardner syndrome (polyposis coli and colon and rectal cancer), myotonic dystrophy, Rubinstein-Taybi syndrome (characterized by broad thumbs and toes, short stature, distinctive facial features, and varying degrees of intellectual disability), and trisomy 9. On physical examination our patient didn’t present with any of the typical features or history that could suggest any of these syndromes. A close follow-up and evaluation by a geneticist was recommended because after the initial visit she developed a second lesion on the forehead.
The differential diagnosis for this lesion includes other cysts that may occur on the ear such as epidermal inclusion cyst or dermoid cysts, though these lesions do not tend to be as firm as pilomatrixomas are, which can help with the diagnosis. Dermoid cysts are made of dermal and epidermal components. They are usually present at birth and are commonly seen on the scalp and the periorbital face.
Keloids are rubbery nodules of scar tissue that can form on sites of trauma, and although the lesion occurred after she had her ears pierced, the consistency and rapid growth of the lesion as well as the pathological description made this benign fibrous growth less likely.
When pilomatrixomas are inflamed they can be confused with vascular growths: in this particular case, a hemangioma or another vascular tumor such as a tufted angioma or kaposiform hemangioendothelioma. An ultrasound of the lesion could have helped in the differential diagnosis of the lesion.
Pilomatrixomas can grow significantly and in some cases get inflamed or infected. Surgical management of pilomatrixomas is often required because the lesions do not regress spontaneously.
Dr. Matiz is a pediatric dermatologist at Southern California Permanente Medical Group, San Diego.
References
Forbis R Jr and Helwig EB. Arch Dermatol 1961;83:606-18.
Schwarz Y et al. Int J Pediatr Otorhinolaryngol. 2016 Jun;85:148-53.
A 4-month-old female was referred to our clinic for evaluation of a bump on the right ear. The lesion was first noted at 2 months of age as a little pimple. She was evaluated by her pediatrician and was treated with topical and oral antibiotics without resolution of the lesion. The bump continued to grow and seemed tender to palpation, so she was referred to dermatology for evaluation.
She was born via normal vaginal delivery at 40 weeks. Her mother has no medical conditions and the pregnancy was uneventful. She has been growing and developing well. She takes vitamin D and is currently breast fed.
There have been no other family members with similar lesions. She had her ears pierced at a month of age without any complications.
On skin examination she has a firm red nodule on the right ear that appears slightly tender to touch. She has no other skin lesions of concern. She has normal muscle tone and there are no other abnormalities noted on the physical exam. She has no hepatomegaly, splenomegaly, or lymphadenopathy.
Poor evidence for vaginal laser therapy
Despite a lack of evidence and high cost, laser therapy continues to attract many women seeking “vaginal rejuvenation” to help reverse the physical symptoms of menopause.
Recent reviews of the medical literature continue to show that laser treatment appears to be less effective than estrogen at improving vaginal dryness and pain during sex, according to Cheryl B. Iglesia, MD, a professor of ob.gyn. and urology at Georgetown University, Washington.
“Laser for GSM [genitourinary syndrome of menopause] is showing some promise, but patients need to be offered [Food and Drug Administration]–approved treatments prior to considering laser, and users need to know how to do speculum and pelvic exams and understand vulvovaginal anatomy and pathology,” Dr. Iglesia, who directs the section of female pelvic medicine and reconstructive surgery at MedStar Washington Hospital Center, said in an interview, adding that patients should avoid “vaginal rejuvenation” treatments offered at med-spas.
Dr. Iglesia reviewed how these lasers work and then discussed the controversy over their marketing and the evidence for their use at the annual meeting of the North American Menopause Society.
By 3 years after menopause, more than half of women experience atrophy in their vagina resulting from a lack of estrogen. Marked by a thinning of the epithelium, reduced blood supply, and loss of glycogen, vulvovaginal atrophy is to blame for GSM.
Vaginal laser therapy has been a popular option for women for the last decade, despite a lack of evidence supporting its use or approval from regulators.
The FDA has issued broad clearance for laser therapy for incision, ablation, vaporization, and coagulation of body soft tissues, such as dysplasia, vulvar or anal neoplasia, endometriosis, condylomas, and other disorders. However, the agency has not approved the use of laser therapy for vulvovaginal atrophy, GSM, vaginal dryness, or dyspareunia.
Evidence regarding vaginal laser therapy
According to Dr. Iglesia, the evidence for vaginal laser therapy is mixed and of generally low quality. A systematic review published in the Journal of Sexual Medicine (2022 Jan 29. doi: 10.1016/j.jsxm.2021.12.010) presented mostly low-quality evidence from 25 studies and found promising data for genitourinary symptoms but not enough to justify its use for genitourinary symptoms just yet. Dr. Iglesia discussed her own small, multisite study of 62 participants, which compared vaginal laser with vaginal estrogen and found no differences between the two for multiple outcomes. (The study would have been larger if not for interruption from an FDA warning for an Investigational Device Exemption.)
A JAMA study from Australia found no difference between laser therapy and sham laser therapy, but the most recent systematic review, from JAMA Network Open, found no significant difference between vaginal laser and vaginal estrogen for vaginal and sexual function symptoms. This review, however, covered only the six existing randomized controlled trials, including Dr. Iglesia’s, which were small and had a follow-up period of only 3-6 months.
“There have only been a few randomized controlled trials comparing laser to vaginal estrogen therapy, and most of those did not include a placebo or sham arm,” Monica Christmas, MD, director of the Center for Women’s Integrated Health at the University of Chicago Medicine, said in an interview. “This is extremely important, as most of the trials that did include a sham arm did not find that laser was better than the sham.” Dr. Christmas was not a part of the presentation but attended it at NAMS.
The bottom line, she said, is that “current evidence is not sufficient to make conclusions on long-term safety or sustainability, nor is there compelling evidence to make claims on equivalence to vaginal estrogen therapy.” Currently, committee opinions from a half-dozen medical societies, including NAMS, oppose using vaginal laser therapy until rigorous, robust trials on long-term safety and efficacy have been conducted. The International Continence Society and International Society for the Study of Vulvovaginal Disease issued a joint statement in 2018 that emphasized that histologic changes from lasers do not necessarily equate with changes in function. The statement noted the lack of evidence for laser treatment of incontinence and prolapse and stated that it should not be used for vulvodynia or lichen sclerosus.
A 2020 statement from NAMS found “insufficient placebo-controlled trials of energy-based therapies, including laser, to draw conclusions of efficacy or safety or to make treatment recommendations.” A slightly more optimistic statement from the American Urogynecologic Society concluded that energy-based devices have shown short-term efficacy for menopause-related vaginal atrophy and dyspareunia, including effects lasting up to 1 year from fractionated laser for treat dyspareunia, but also noted that studies up to that time were small and measure various outcomes.
Recommendations on vaginal laser therapy
Given this landscape of uneven and poor-quality evidence, Dr. Iglesia provided several “common sense” recommendations for energy-based therapies, starting with the need for any practitioner to have working knowledge of vulvovaginal anatomy. Contraindications for laser therapy include any malignancy – especially gynecologic – undiagnosed bleeding, active herpes or other infections, radiation, and vaginal mesh, particularly transvaginal mesh. The provider also must discuss the limited data on long-term function and treatment alternatives, including FDA-approved therapies like topical estrogen, dehydroepiandrosterone sulfate (DHEA-S), ospemifene, and moisturizers, Dr. Iglesia said.
Adverse events associated with laser therapy, such as scarring or burning, are rare but do occur, and cost remains an issue, Dr. Iglesia said.
“Vaginal estrogen therapy is well established as a safe and effective treatment option based on high quality evidence,” Dr. Christmas said. “This is not the case for laser therapy. Rare, but serious harms are reported with vaginal laser, including burns, scarring, dyspareunia, pain, and potential irreversible damage.”
Dr. Iglesia also cautioned that clinicians should take extra care with vulnerable populations, particularly cancer patients and others with contraindications for estrogen treatment.
For those in whom vaginal estrogen is contraindicated, Dr. Christmas recommended vaginal moisturizers, lubricants, dilators, and physical therapy for the pelvic floor.
“In patients who fail those nonhormonal approaches, short courses of vaginal estrogen therapy or DHEA-S suppository may be employed with approval from their oncologist,” Dr. Christmas said.
Dr. Iglesia finally reviewed the major research questions that remain with laser therapy:
- What are outcomes for laser versus sham studies?
- What are long-term outcomes (beyond 6 months)
- What pretreatment is necessary?
- Could laser be used as a drug delivery mechanism for estrogen, and could this provide a synergistic effect?
- What is the optimal number and interval for laser treatments?
Dr. Iglesia had no industry disclosures but received honoraria for consulting at UpToDate. Dr. Christmas is a consultant for Materna. The presentation did not rely on any external funding.
Despite a lack of evidence and high cost, laser therapy continues to attract many women seeking “vaginal rejuvenation” to help reverse the physical symptoms of menopause.
Recent reviews of the medical literature continue to show that laser treatment appears to be less effective than estrogen at improving vaginal dryness and pain during sex, according to Cheryl B. Iglesia, MD, a professor of ob.gyn. and urology at Georgetown University, Washington.
“Laser for GSM [genitourinary syndrome of menopause] is showing some promise, but patients need to be offered [Food and Drug Administration]–approved treatments prior to considering laser, and users need to know how to do speculum and pelvic exams and understand vulvovaginal anatomy and pathology,” Dr. Iglesia, who directs the section of female pelvic medicine and reconstructive surgery at MedStar Washington Hospital Center, said in an interview, adding that patients should avoid “vaginal rejuvenation” treatments offered at med-spas.
Dr. Iglesia reviewed how these lasers work and then discussed the controversy over their marketing and the evidence for their use at the annual meeting of the North American Menopause Society.
By 3 years after menopause, more than half of women experience atrophy in their vagina resulting from a lack of estrogen. Marked by a thinning of the epithelium, reduced blood supply, and loss of glycogen, vulvovaginal atrophy is to blame for GSM.
Vaginal laser therapy has been a popular option for women for the last decade, despite a lack of evidence supporting its use or approval from regulators.
The FDA has issued broad clearance for laser therapy for incision, ablation, vaporization, and coagulation of body soft tissues, such as dysplasia, vulvar or anal neoplasia, endometriosis, condylomas, and other disorders. However, the agency has not approved the use of laser therapy for vulvovaginal atrophy, GSM, vaginal dryness, or dyspareunia.
Evidence regarding vaginal laser therapy
According to Dr. Iglesia, the evidence for vaginal laser therapy is mixed and of generally low quality. A systematic review published in the Journal of Sexual Medicine (2022 Jan 29. doi: 10.1016/j.jsxm.2021.12.010) presented mostly low-quality evidence from 25 studies and found promising data for genitourinary symptoms but not enough to justify its use for genitourinary symptoms just yet. Dr. Iglesia discussed her own small, multisite study of 62 participants, which compared vaginal laser with vaginal estrogen and found no differences between the two for multiple outcomes. (The study would have been larger if not for interruption from an FDA warning for an Investigational Device Exemption.)
A JAMA study from Australia found no difference between laser therapy and sham laser therapy, but the most recent systematic review, from JAMA Network Open, found no significant difference between vaginal laser and vaginal estrogen for vaginal and sexual function symptoms. This review, however, covered only the six existing randomized controlled trials, including Dr. Iglesia’s, which were small and had a follow-up period of only 3-6 months.
“There have only been a few randomized controlled trials comparing laser to vaginal estrogen therapy, and most of those did not include a placebo or sham arm,” Monica Christmas, MD, director of the Center for Women’s Integrated Health at the University of Chicago Medicine, said in an interview. “This is extremely important, as most of the trials that did include a sham arm did not find that laser was better than the sham.” Dr. Christmas was not a part of the presentation but attended it at NAMS.
The bottom line, she said, is that “current evidence is not sufficient to make conclusions on long-term safety or sustainability, nor is there compelling evidence to make claims on equivalence to vaginal estrogen therapy.” Currently, committee opinions from a half-dozen medical societies, including NAMS, oppose using vaginal laser therapy until rigorous, robust trials on long-term safety and efficacy have been conducted. The International Continence Society and International Society for the Study of Vulvovaginal Disease issued a joint statement in 2018 that emphasized that histologic changes from lasers do not necessarily equate with changes in function. The statement noted the lack of evidence for laser treatment of incontinence and prolapse and stated that it should not be used for vulvodynia or lichen sclerosus.
A 2020 statement from NAMS found “insufficient placebo-controlled trials of energy-based therapies, including laser, to draw conclusions of efficacy or safety or to make treatment recommendations.” A slightly more optimistic statement from the American Urogynecologic Society concluded that energy-based devices have shown short-term efficacy for menopause-related vaginal atrophy and dyspareunia, including effects lasting up to 1 year from fractionated laser for treat dyspareunia, but also noted that studies up to that time were small and measure various outcomes.
Recommendations on vaginal laser therapy
Given this landscape of uneven and poor-quality evidence, Dr. Iglesia provided several “common sense” recommendations for energy-based therapies, starting with the need for any practitioner to have working knowledge of vulvovaginal anatomy. Contraindications for laser therapy include any malignancy – especially gynecologic – undiagnosed bleeding, active herpes or other infections, radiation, and vaginal mesh, particularly transvaginal mesh. The provider also must discuss the limited data on long-term function and treatment alternatives, including FDA-approved therapies like topical estrogen, dehydroepiandrosterone sulfate (DHEA-S), ospemifene, and moisturizers, Dr. Iglesia said.
Adverse events associated with laser therapy, such as scarring or burning, are rare but do occur, and cost remains an issue, Dr. Iglesia said.
“Vaginal estrogen therapy is well established as a safe and effective treatment option based on high quality evidence,” Dr. Christmas said. “This is not the case for laser therapy. Rare, but serious harms are reported with vaginal laser, including burns, scarring, dyspareunia, pain, and potential irreversible damage.”
Dr. Iglesia also cautioned that clinicians should take extra care with vulnerable populations, particularly cancer patients and others with contraindications for estrogen treatment.
For those in whom vaginal estrogen is contraindicated, Dr. Christmas recommended vaginal moisturizers, lubricants, dilators, and physical therapy for the pelvic floor.
“In patients who fail those nonhormonal approaches, short courses of vaginal estrogen therapy or DHEA-S suppository may be employed with approval from their oncologist,” Dr. Christmas said.
Dr. Iglesia finally reviewed the major research questions that remain with laser therapy:
- What are outcomes for laser versus sham studies?
- What are long-term outcomes (beyond 6 months)
- What pretreatment is necessary?
- Could laser be used as a drug delivery mechanism for estrogen, and could this provide a synergistic effect?
- What is the optimal number and interval for laser treatments?
Dr. Iglesia had no industry disclosures but received honoraria for consulting at UpToDate. Dr. Christmas is a consultant for Materna. The presentation did not rely on any external funding.
Despite a lack of evidence and high cost, laser therapy continues to attract many women seeking “vaginal rejuvenation” to help reverse the physical symptoms of menopause.
Recent reviews of the medical literature continue to show that laser treatment appears to be less effective than estrogen at improving vaginal dryness and pain during sex, according to Cheryl B. Iglesia, MD, a professor of ob.gyn. and urology at Georgetown University, Washington.
“Laser for GSM [genitourinary syndrome of menopause] is showing some promise, but patients need to be offered [Food and Drug Administration]–approved treatments prior to considering laser, and users need to know how to do speculum and pelvic exams and understand vulvovaginal anatomy and pathology,” Dr. Iglesia, who directs the section of female pelvic medicine and reconstructive surgery at MedStar Washington Hospital Center, said in an interview, adding that patients should avoid “vaginal rejuvenation” treatments offered at med-spas.
Dr. Iglesia reviewed how these lasers work and then discussed the controversy over their marketing and the evidence for their use at the annual meeting of the North American Menopause Society.
By 3 years after menopause, more than half of women experience atrophy in their vagina resulting from a lack of estrogen. Marked by a thinning of the epithelium, reduced blood supply, and loss of glycogen, vulvovaginal atrophy is to blame for GSM.
Vaginal laser therapy has been a popular option for women for the last decade, despite a lack of evidence supporting its use or approval from regulators.
The FDA has issued broad clearance for laser therapy for incision, ablation, vaporization, and coagulation of body soft tissues, such as dysplasia, vulvar or anal neoplasia, endometriosis, condylomas, and other disorders. However, the agency has not approved the use of laser therapy for vulvovaginal atrophy, GSM, vaginal dryness, or dyspareunia.
Evidence regarding vaginal laser therapy
According to Dr. Iglesia, the evidence for vaginal laser therapy is mixed and of generally low quality. A systematic review published in the Journal of Sexual Medicine (2022 Jan 29. doi: 10.1016/j.jsxm.2021.12.010) presented mostly low-quality evidence from 25 studies and found promising data for genitourinary symptoms but not enough to justify its use for genitourinary symptoms just yet. Dr. Iglesia discussed her own small, multisite study of 62 participants, which compared vaginal laser with vaginal estrogen and found no differences between the two for multiple outcomes. (The study would have been larger if not for interruption from an FDA warning for an Investigational Device Exemption.)
A JAMA study from Australia found no difference between laser therapy and sham laser therapy, but the most recent systematic review, from JAMA Network Open, found no significant difference between vaginal laser and vaginal estrogen for vaginal and sexual function symptoms. This review, however, covered only the six existing randomized controlled trials, including Dr. Iglesia’s, which were small and had a follow-up period of only 3-6 months.
“There have only been a few randomized controlled trials comparing laser to vaginal estrogen therapy, and most of those did not include a placebo or sham arm,” Monica Christmas, MD, director of the Center for Women’s Integrated Health at the University of Chicago Medicine, said in an interview. “This is extremely important, as most of the trials that did include a sham arm did not find that laser was better than the sham.” Dr. Christmas was not a part of the presentation but attended it at NAMS.
The bottom line, she said, is that “current evidence is not sufficient to make conclusions on long-term safety or sustainability, nor is there compelling evidence to make claims on equivalence to vaginal estrogen therapy.” Currently, committee opinions from a half-dozen medical societies, including NAMS, oppose using vaginal laser therapy until rigorous, robust trials on long-term safety and efficacy have been conducted. The International Continence Society and International Society for the Study of Vulvovaginal Disease issued a joint statement in 2018 that emphasized that histologic changes from lasers do not necessarily equate with changes in function. The statement noted the lack of evidence for laser treatment of incontinence and prolapse and stated that it should not be used for vulvodynia or lichen sclerosus.
A 2020 statement from NAMS found “insufficient placebo-controlled trials of energy-based therapies, including laser, to draw conclusions of efficacy or safety or to make treatment recommendations.” A slightly more optimistic statement from the American Urogynecologic Society concluded that energy-based devices have shown short-term efficacy for menopause-related vaginal atrophy and dyspareunia, including effects lasting up to 1 year from fractionated laser for treat dyspareunia, but also noted that studies up to that time were small and measure various outcomes.
Recommendations on vaginal laser therapy
Given this landscape of uneven and poor-quality evidence, Dr. Iglesia provided several “common sense” recommendations for energy-based therapies, starting with the need for any practitioner to have working knowledge of vulvovaginal anatomy. Contraindications for laser therapy include any malignancy – especially gynecologic – undiagnosed bleeding, active herpes or other infections, radiation, and vaginal mesh, particularly transvaginal mesh. The provider also must discuss the limited data on long-term function and treatment alternatives, including FDA-approved therapies like topical estrogen, dehydroepiandrosterone sulfate (DHEA-S), ospemifene, and moisturizers, Dr. Iglesia said.
Adverse events associated with laser therapy, such as scarring or burning, are rare but do occur, and cost remains an issue, Dr. Iglesia said.
“Vaginal estrogen therapy is well established as a safe and effective treatment option based on high quality evidence,” Dr. Christmas said. “This is not the case for laser therapy. Rare, but serious harms are reported with vaginal laser, including burns, scarring, dyspareunia, pain, and potential irreversible damage.”
Dr. Iglesia also cautioned that clinicians should take extra care with vulnerable populations, particularly cancer patients and others with contraindications for estrogen treatment.
For those in whom vaginal estrogen is contraindicated, Dr. Christmas recommended vaginal moisturizers, lubricants, dilators, and physical therapy for the pelvic floor.
“In patients who fail those nonhormonal approaches, short courses of vaginal estrogen therapy or DHEA-S suppository may be employed with approval from their oncologist,” Dr. Christmas said.
Dr. Iglesia finally reviewed the major research questions that remain with laser therapy:
- What are outcomes for laser versus sham studies?
- What are long-term outcomes (beyond 6 months)
- What pretreatment is necessary?
- Could laser be used as a drug delivery mechanism for estrogen, and could this provide a synergistic effect?
- What is the optimal number and interval for laser treatments?
Dr. Iglesia had no industry disclosures but received honoraria for consulting at UpToDate. Dr. Christmas is a consultant for Materna. The presentation did not rely on any external funding.
FROM NAMS 2022
Vaccinium myrtillus (bilberry seed oil) extract
A member of the Ericaceae family, bilberry (Vaccinium myrtillus) is native to northern Europe and North America, and its fruit is known to contain myriad polyphenols that display potent antioxidant and anti-inflammatory activity.1,2 Also known as European blueberry or whortleberry, this perennial deciduous shrub is also one of the richest sources of the polyphenolic pigments anthocyanins.3-5 Indeed, anthocyanins impart the blue/black color to bilberries and other berries and are thought to be the primary bioactive constituents of berries associated with numerous health benefits.3,6 They are also known to confer anti-allergic, anticancer, and wound healing activity.4 Overall, bilberry has also been reported to exert anti-inflammatory, lipid-lowering, and antimicrobial activity.3 In this column, the focus will be on the chemical constituents and properties of V. myrtillus that indicate potential or applicability for skin care.
Active ingredients of bilberry
Bilberry seed oil contains unsaturated fatty acids such as linoleic acid and alpha-linolenic acid, which exhibit anti-inflammatory activity and contribute to the suppression of tyrosinase. For instance, Ando et al. showed, in 1998, that linoleic and alpha-linolenic acids lighten UV-induced skin hyperpigmentation. Their in vitro experiments using cultured murine melanoma cells and in vivo study of the topical application of either acid to the UV-induced hyperpigmented dorsal skin of guinea pigs revealed pigment-lightening effects that they partly ascribed to inhibited melanin synthesis by active melanocytes and accelerated desquamation of epidermal melanin pigment.7
A 2009 comparative study of the anthocyanin composition as well as antimicrobial and antioxidant activities delivered by bilberry and blueberry fruits and their skins by Burdulis et al. revealed robust functions in both fruits. Cyanidin was found to be an active anthocyanidin in bilberry. Cultivars of both fruits demonstrated antimicrobial and antioxidant activity, with bilberry fruit skin demonstrating potent antiradical activity.8
The anthocyanins of V. myrtillus are reputed to impart protection against cardiovascular disorders, age-induced oxidative stress, inflammatory responses, and various degenerative conditions, as well ameliorate neuronal and cognitive brain functions and ocular health.6
In 2012, Bornsek et al. demonstrated that bilberry (and blueberry) anthocyanins function as potent intracellular antioxidants, which may account for their noted health benefits despite relatively low bioavailability.9
Six years later, a chemical composition study of wild bilberry found in Montenegro, Brasanac-Vukanovic et al. determined that chlorogenic acid was the most prevalent phenolic constituent, followed by protocatechuic acid, with resveratrol, isoquercetin, quercetin, and hyperoside also found to be abundant. In vitro assays indicated significant antioxidant activity exhibited by these compounds.10
Activity against allergic contact dermatitis
Yamaura et al. used a mouse model, in 2011, to determine that the anthocyanins from a bilberry extract attenuated various symptoms of chronic allergic contact dermatitis, particularly alleviating pruritus.8 A year later, Yamaura et al. used a BALB/c mouse model of allergic contact dermatitis to compare the antipruritic effect of anthocyanin-rich quality-controlled bilberry extract and anthocyanidin-rich degraded extract. The investigators found that anthocyanins, but not anthocyanidins, derived from bilberry exert an antipruritic effect, likely through their inhibitory action on mast cell degranulation. They concluded that anthocyanin-rich bilberry extract could act as an effective oral supplement to treat pruritic symptoms of skin disorders such as chronic allergic contact dermatitis and atopic dermatitis.11
Antioxidant and anti-inflammatory activity
Bilberries, consumed since ancient times, are reputed to function as potent antioxidants because of a wide array of phenolic constituents, and this fruit is gaining interest for use in pharmaceuticals.12
In 2008, Svobodová et al. assessed possible UVA preventive properties of V. myrtillus fruit extract in a human keratinocyte cell line (HaCaT), finding that pre- or posttreatment mitigated UVA-induced harm. They also observed a significant decrease in UVA-caused reactive oxygen species (ROS) formation and the prevention or attenuation of UVA-stimulated peroxidation of membrane lipids. Intracellular glutathione was also protected. The investigators attributed the array of cytoprotective effects conferred by V. myrtillus extract primarily to its constituent anthocyanins.2 A year later, they found that the phenolic fraction of V. myrtillus fruits inhibited UVB-induced damage to HaCaT keratinocytes in vitro.13
In 2014, Calò and Marabini used HaCaT keratinocytes to ascertain whether a water-soluble V. myrtillus extract could mitigate UVA- and UVB-induced damage. They found that the extract diminished UVB-induced cytotoxicity and genotoxicity at lower doses, decreasing lipid peroxidation but exerting no effect on reactive oxygen species generated by UVB. The extract attenuated genotoxicity induced by UVA as well as ROS and apoptosis. Overall, the investigators concluded that V. myrtillus extract demonstrated antioxidant activity, particularly against UVA exposure.14
Four years later, Bucci et al. developed nanoberries, an ultradeformable liposome carrying V. myrtillus ethanolic extract, and determined that the preparation could penetrate the stratum corneum safely and suggested potential for yielding protection against photodamage.15
Skin preparations
In 2021, Tadic et al. developed an oil-in-water (O/W) cream containing wild bilberry leaf extracts and seed oil. The leaves contained copious phenolic acids (particularly chlorogenic acid), flavonoids (especially isoquercetin), and resveratrol. The seed oil was rife with alpha-linolenic, linoleic, and oleic acids. The investigators conducted an in vivo study over 30 days in 25 healthy volunteers (20 women, 5 men; mean age 23.36 ± 0.64 years). They found that the O/W cream successfully increased stratum corneum hydration, enhanced skin barrier function, and maintained skin pH after topical application. The cream was also well tolerated. In vitro assays also indicated that the bilberry isolates displayed notable antioxidant capacity (stronger in the case of the leaves). Tadic et al. suggested that skin disorders characterized by oxidative stress and/or xerosis may be appropriate targets for topically applied bilberry cream.1
Early in 2022, Ruscinc et al. reported on their efforts to incorporate V. myrtillus extract into a multifunctional sunscreen. In vitro and in vivo tests revealed that while sun protection factor was lowered in the presence of the extract, the samples were safe and photostable. The researchers concluded that further study is necessary to elucidate the effect of V. myrtillus extract on photoprotection.16
V. myrtillus has been consumed by human beings for many generations. Skin care formulations based on this ingredient have not been associated with adverse events. Notably, the Environmental Working Group has rated V. myrtillus (bilberry seed) oil as very safe.17
Summary
While research, particularly in the form of randomized controlled trials, is called for, because the fatty acids it contains have been shown to suppress tyrosinase. Currently, this botanical agent seems to be most suited for sensitive, aging skin and for skin with an uneven tone, particularly postinflammatory pigmentation and melasma.
Dr. Baumann is a private practice dermatologist, researcher, author, and entrepreneur in Miami. She founded the division of cosmetic dermatology at the University of Miami in 1997. The third edition of her bestselling textbook, “Cosmetic Dermatology,” was published in 2022. Dr. Baumann has received funding for advisory boards and/or clinical research trials from Allergan, Galderma, Johnson & Johnson, and Burt’s Bees. She is the CEO of Skin Type Solutions, an SaaS company used to generate skin care routines in office and as an ecommerce solution. Write to her at [email protected].
References
1. Tadic VM et al. Antioxidants (Basel). 2021 Mar 16;10(3):465.
2. Svobodová A et al. Biofactors. 2008;33(4):249-66.
3. Chu WK et al. Bilberry (Vaccinium myrtillus L.), in Benzie IFF, Wachtel-Galor S, eds., “Herbal Medicine: Biomolecular and Clinical Aspects,” 2nd ed. (Boca Raton, Fla.: CRC Press/Taylor & Francis, 2011, Chapter 4).
4. Yamaura K et al. Pharmacognosy Res. 2011 Jul;3(3):173-7.
5. Stefanescu BE et al. Molecules. 2019 May 29;24(11):2046.
6. Smeriglio A et al. Mini Rev Med Chem. 2014;14(7):567-84.
7. Ando H et al. Arch Dermatol Res. 1998 Jul;290(7):375-81.
8. Burdulis D et al. Acta Pol Pharm. 2009 Jul-Aug;66(4):399-408.
9. Bornsek SM et al. Food Chem. 2012 Oct 15;134(4):1878-84.
10. Brasanac-Vukanovic S et al. Molecules. 2018 Jul 26;23(8):1864.
11. Yamaura K et al. J Food Sci. 2012 Dec;77(12):H262-7.
12. Pires TCSP et al. Curr Pharm Des. 2020;26(16):1917-28.
13. Svobodová A et al. J Dermatol Sci. 2009 Dec;56(3):196-204.
14. Calò R, Marabini L. J Photochem Photobiol B. 2014 Mar 5;132:27-35.
15. Bucci P et al. J Cosmet Dermatol. 2018 Oct;17(5):889-99.
16. Ruscinc N et al. J Cosmet Dermatol. 2022 Jan 13.
17. Environmental Working Group’s Skin Deep website. Vaccinium Myrtillus Bilberry Seed Oil. Accessed October 18, 2022.
A member of the Ericaceae family, bilberry (Vaccinium myrtillus) is native to northern Europe and North America, and its fruit is known to contain myriad polyphenols that display potent antioxidant and anti-inflammatory activity.1,2 Also known as European blueberry or whortleberry, this perennial deciduous shrub is also one of the richest sources of the polyphenolic pigments anthocyanins.3-5 Indeed, anthocyanins impart the blue/black color to bilberries and other berries and are thought to be the primary bioactive constituents of berries associated with numerous health benefits.3,6 They are also known to confer anti-allergic, anticancer, and wound healing activity.4 Overall, bilberry has also been reported to exert anti-inflammatory, lipid-lowering, and antimicrobial activity.3 In this column, the focus will be on the chemical constituents and properties of V. myrtillus that indicate potential or applicability for skin care.
Active ingredients of bilberry
Bilberry seed oil contains unsaturated fatty acids such as linoleic acid and alpha-linolenic acid, which exhibit anti-inflammatory activity and contribute to the suppression of tyrosinase. For instance, Ando et al. showed, in 1998, that linoleic and alpha-linolenic acids lighten UV-induced skin hyperpigmentation. Their in vitro experiments using cultured murine melanoma cells and in vivo study of the topical application of either acid to the UV-induced hyperpigmented dorsal skin of guinea pigs revealed pigment-lightening effects that they partly ascribed to inhibited melanin synthesis by active melanocytes and accelerated desquamation of epidermal melanin pigment.7
A 2009 comparative study of the anthocyanin composition as well as antimicrobial and antioxidant activities delivered by bilberry and blueberry fruits and their skins by Burdulis et al. revealed robust functions in both fruits. Cyanidin was found to be an active anthocyanidin in bilberry. Cultivars of both fruits demonstrated antimicrobial and antioxidant activity, with bilberry fruit skin demonstrating potent antiradical activity.8
The anthocyanins of V. myrtillus are reputed to impart protection against cardiovascular disorders, age-induced oxidative stress, inflammatory responses, and various degenerative conditions, as well ameliorate neuronal and cognitive brain functions and ocular health.6
In 2012, Bornsek et al. demonstrated that bilberry (and blueberry) anthocyanins function as potent intracellular antioxidants, which may account for their noted health benefits despite relatively low bioavailability.9
Six years later, a chemical composition study of wild bilberry found in Montenegro, Brasanac-Vukanovic et al. determined that chlorogenic acid was the most prevalent phenolic constituent, followed by protocatechuic acid, with resveratrol, isoquercetin, quercetin, and hyperoside also found to be abundant. In vitro assays indicated significant antioxidant activity exhibited by these compounds.10
Activity against allergic contact dermatitis
Yamaura et al. used a mouse model, in 2011, to determine that the anthocyanins from a bilberry extract attenuated various symptoms of chronic allergic contact dermatitis, particularly alleviating pruritus.8 A year later, Yamaura et al. used a BALB/c mouse model of allergic contact dermatitis to compare the antipruritic effect of anthocyanin-rich quality-controlled bilberry extract and anthocyanidin-rich degraded extract. The investigators found that anthocyanins, but not anthocyanidins, derived from bilberry exert an antipruritic effect, likely through their inhibitory action on mast cell degranulation. They concluded that anthocyanin-rich bilberry extract could act as an effective oral supplement to treat pruritic symptoms of skin disorders such as chronic allergic contact dermatitis and atopic dermatitis.11
Antioxidant and anti-inflammatory activity
Bilberries, consumed since ancient times, are reputed to function as potent antioxidants because of a wide array of phenolic constituents, and this fruit is gaining interest for use in pharmaceuticals.12
In 2008, Svobodová et al. assessed possible UVA preventive properties of V. myrtillus fruit extract in a human keratinocyte cell line (HaCaT), finding that pre- or posttreatment mitigated UVA-induced harm. They also observed a significant decrease in UVA-caused reactive oxygen species (ROS) formation and the prevention or attenuation of UVA-stimulated peroxidation of membrane lipids. Intracellular glutathione was also protected. The investigators attributed the array of cytoprotective effects conferred by V. myrtillus extract primarily to its constituent anthocyanins.2 A year later, they found that the phenolic fraction of V. myrtillus fruits inhibited UVB-induced damage to HaCaT keratinocytes in vitro.13
In 2014, Calò and Marabini used HaCaT keratinocytes to ascertain whether a water-soluble V. myrtillus extract could mitigate UVA- and UVB-induced damage. They found that the extract diminished UVB-induced cytotoxicity and genotoxicity at lower doses, decreasing lipid peroxidation but exerting no effect on reactive oxygen species generated by UVB. The extract attenuated genotoxicity induced by UVA as well as ROS and apoptosis. Overall, the investigators concluded that V. myrtillus extract demonstrated antioxidant activity, particularly against UVA exposure.14
Four years later, Bucci et al. developed nanoberries, an ultradeformable liposome carrying V. myrtillus ethanolic extract, and determined that the preparation could penetrate the stratum corneum safely and suggested potential for yielding protection against photodamage.15
Skin preparations
In 2021, Tadic et al. developed an oil-in-water (O/W) cream containing wild bilberry leaf extracts and seed oil. The leaves contained copious phenolic acids (particularly chlorogenic acid), flavonoids (especially isoquercetin), and resveratrol. The seed oil was rife with alpha-linolenic, linoleic, and oleic acids. The investigators conducted an in vivo study over 30 days in 25 healthy volunteers (20 women, 5 men; mean age 23.36 ± 0.64 years). They found that the O/W cream successfully increased stratum corneum hydration, enhanced skin barrier function, and maintained skin pH after topical application. The cream was also well tolerated. In vitro assays also indicated that the bilberry isolates displayed notable antioxidant capacity (stronger in the case of the leaves). Tadic et al. suggested that skin disorders characterized by oxidative stress and/or xerosis may be appropriate targets for topically applied bilberry cream.1
Early in 2022, Ruscinc et al. reported on their efforts to incorporate V. myrtillus extract into a multifunctional sunscreen. In vitro and in vivo tests revealed that while sun protection factor was lowered in the presence of the extract, the samples were safe and photostable. The researchers concluded that further study is necessary to elucidate the effect of V. myrtillus extract on photoprotection.16
V. myrtillus has been consumed by human beings for many generations. Skin care formulations based on this ingredient have not been associated with adverse events. Notably, the Environmental Working Group has rated V. myrtillus (bilberry seed) oil as very safe.17
Summary
While research, particularly in the form of randomized controlled trials, is called for, because the fatty acids it contains have been shown to suppress tyrosinase. Currently, this botanical agent seems to be most suited for sensitive, aging skin and for skin with an uneven tone, particularly postinflammatory pigmentation and melasma.
Dr. Baumann is a private practice dermatologist, researcher, author, and entrepreneur in Miami. She founded the division of cosmetic dermatology at the University of Miami in 1997. The third edition of her bestselling textbook, “Cosmetic Dermatology,” was published in 2022. Dr. Baumann has received funding for advisory boards and/or clinical research trials from Allergan, Galderma, Johnson & Johnson, and Burt’s Bees. She is the CEO of Skin Type Solutions, an SaaS company used to generate skin care routines in office and as an ecommerce solution. Write to her at [email protected].
References
1. Tadic VM et al. Antioxidants (Basel). 2021 Mar 16;10(3):465.
2. Svobodová A et al. Biofactors. 2008;33(4):249-66.
3. Chu WK et al. Bilberry (Vaccinium myrtillus L.), in Benzie IFF, Wachtel-Galor S, eds., “Herbal Medicine: Biomolecular and Clinical Aspects,” 2nd ed. (Boca Raton, Fla.: CRC Press/Taylor & Francis, 2011, Chapter 4).
4. Yamaura K et al. Pharmacognosy Res. 2011 Jul;3(3):173-7.
5. Stefanescu BE et al. Molecules. 2019 May 29;24(11):2046.
6. Smeriglio A et al. Mini Rev Med Chem. 2014;14(7):567-84.
7. Ando H et al. Arch Dermatol Res. 1998 Jul;290(7):375-81.
8. Burdulis D et al. Acta Pol Pharm. 2009 Jul-Aug;66(4):399-408.
9. Bornsek SM et al. Food Chem. 2012 Oct 15;134(4):1878-84.
10. Brasanac-Vukanovic S et al. Molecules. 2018 Jul 26;23(8):1864.
11. Yamaura K et al. J Food Sci. 2012 Dec;77(12):H262-7.
12. Pires TCSP et al. Curr Pharm Des. 2020;26(16):1917-28.
13. Svobodová A et al. J Dermatol Sci. 2009 Dec;56(3):196-204.
14. Calò R, Marabini L. J Photochem Photobiol B. 2014 Mar 5;132:27-35.
15. Bucci P et al. J Cosmet Dermatol. 2018 Oct;17(5):889-99.
16. Ruscinc N et al. J Cosmet Dermatol. 2022 Jan 13.
17. Environmental Working Group’s Skin Deep website. Vaccinium Myrtillus Bilberry Seed Oil. Accessed October 18, 2022.
A member of the Ericaceae family, bilberry (Vaccinium myrtillus) is native to northern Europe and North America, and its fruit is known to contain myriad polyphenols that display potent antioxidant and anti-inflammatory activity.1,2 Also known as European blueberry or whortleberry, this perennial deciduous shrub is also one of the richest sources of the polyphenolic pigments anthocyanins.3-5 Indeed, anthocyanins impart the blue/black color to bilberries and other berries and are thought to be the primary bioactive constituents of berries associated with numerous health benefits.3,6 They are also known to confer anti-allergic, anticancer, and wound healing activity.4 Overall, bilberry has also been reported to exert anti-inflammatory, lipid-lowering, and antimicrobial activity.3 In this column, the focus will be on the chemical constituents and properties of V. myrtillus that indicate potential or applicability for skin care.
Active ingredients of bilberry
Bilberry seed oil contains unsaturated fatty acids such as linoleic acid and alpha-linolenic acid, which exhibit anti-inflammatory activity and contribute to the suppression of tyrosinase. For instance, Ando et al. showed, in 1998, that linoleic and alpha-linolenic acids lighten UV-induced skin hyperpigmentation. Their in vitro experiments using cultured murine melanoma cells and in vivo study of the topical application of either acid to the UV-induced hyperpigmented dorsal skin of guinea pigs revealed pigment-lightening effects that they partly ascribed to inhibited melanin synthesis by active melanocytes and accelerated desquamation of epidermal melanin pigment.7
A 2009 comparative study of the anthocyanin composition as well as antimicrobial and antioxidant activities delivered by bilberry and blueberry fruits and their skins by Burdulis et al. revealed robust functions in both fruits. Cyanidin was found to be an active anthocyanidin in bilberry. Cultivars of both fruits demonstrated antimicrobial and antioxidant activity, with bilberry fruit skin demonstrating potent antiradical activity.8
The anthocyanins of V. myrtillus are reputed to impart protection against cardiovascular disorders, age-induced oxidative stress, inflammatory responses, and various degenerative conditions, as well ameliorate neuronal and cognitive brain functions and ocular health.6
In 2012, Bornsek et al. demonstrated that bilberry (and blueberry) anthocyanins function as potent intracellular antioxidants, which may account for their noted health benefits despite relatively low bioavailability.9
Six years later, a chemical composition study of wild bilberry found in Montenegro, Brasanac-Vukanovic et al. determined that chlorogenic acid was the most prevalent phenolic constituent, followed by protocatechuic acid, with resveratrol, isoquercetin, quercetin, and hyperoside also found to be abundant. In vitro assays indicated significant antioxidant activity exhibited by these compounds.10
Activity against allergic contact dermatitis
Yamaura et al. used a mouse model, in 2011, to determine that the anthocyanins from a bilberry extract attenuated various symptoms of chronic allergic contact dermatitis, particularly alleviating pruritus.8 A year later, Yamaura et al. used a BALB/c mouse model of allergic contact dermatitis to compare the antipruritic effect of anthocyanin-rich quality-controlled bilberry extract and anthocyanidin-rich degraded extract. The investigators found that anthocyanins, but not anthocyanidins, derived from bilberry exert an antipruritic effect, likely through their inhibitory action on mast cell degranulation. They concluded that anthocyanin-rich bilberry extract could act as an effective oral supplement to treat pruritic symptoms of skin disorders such as chronic allergic contact dermatitis and atopic dermatitis.11
Antioxidant and anti-inflammatory activity
Bilberries, consumed since ancient times, are reputed to function as potent antioxidants because of a wide array of phenolic constituents, and this fruit is gaining interest for use in pharmaceuticals.12
In 2008, Svobodová et al. assessed possible UVA preventive properties of V. myrtillus fruit extract in a human keratinocyte cell line (HaCaT), finding that pre- or posttreatment mitigated UVA-induced harm. They also observed a significant decrease in UVA-caused reactive oxygen species (ROS) formation and the prevention or attenuation of UVA-stimulated peroxidation of membrane lipids. Intracellular glutathione was also protected. The investigators attributed the array of cytoprotective effects conferred by V. myrtillus extract primarily to its constituent anthocyanins.2 A year later, they found that the phenolic fraction of V. myrtillus fruits inhibited UVB-induced damage to HaCaT keratinocytes in vitro.13
In 2014, Calò and Marabini used HaCaT keratinocytes to ascertain whether a water-soluble V. myrtillus extract could mitigate UVA- and UVB-induced damage. They found that the extract diminished UVB-induced cytotoxicity and genotoxicity at lower doses, decreasing lipid peroxidation but exerting no effect on reactive oxygen species generated by UVB. The extract attenuated genotoxicity induced by UVA as well as ROS and apoptosis. Overall, the investigators concluded that V. myrtillus extract demonstrated antioxidant activity, particularly against UVA exposure.14
Four years later, Bucci et al. developed nanoberries, an ultradeformable liposome carrying V. myrtillus ethanolic extract, and determined that the preparation could penetrate the stratum corneum safely and suggested potential for yielding protection against photodamage.15
Skin preparations
In 2021, Tadic et al. developed an oil-in-water (O/W) cream containing wild bilberry leaf extracts and seed oil. The leaves contained copious phenolic acids (particularly chlorogenic acid), flavonoids (especially isoquercetin), and resveratrol. The seed oil was rife with alpha-linolenic, linoleic, and oleic acids. The investigators conducted an in vivo study over 30 days in 25 healthy volunteers (20 women, 5 men; mean age 23.36 ± 0.64 years). They found that the O/W cream successfully increased stratum corneum hydration, enhanced skin barrier function, and maintained skin pH after topical application. The cream was also well tolerated. In vitro assays also indicated that the bilberry isolates displayed notable antioxidant capacity (stronger in the case of the leaves). Tadic et al. suggested that skin disorders characterized by oxidative stress and/or xerosis may be appropriate targets for topically applied bilberry cream.1
Early in 2022, Ruscinc et al. reported on their efforts to incorporate V. myrtillus extract into a multifunctional sunscreen. In vitro and in vivo tests revealed that while sun protection factor was lowered in the presence of the extract, the samples were safe and photostable. The researchers concluded that further study is necessary to elucidate the effect of V. myrtillus extract on photoprotection.16
V. myrtillus has been consumed by human beings for many generations. Skin care formulations based on this ingredient have not been associated with adverse events. Notably, the Environmental Working Group has rated V. myrtillus (bilberry seed) oil as very safe.17
Summary
While research, particularly in the form of randomized controlled trials, is called for, because the fatty acids it contains have been shown to suppress tyrosinase. Currently, this botanical agent seems to be most suited for sensitive, aging skin and for skin with an uneven tone, particularly postinflammatory pigmentation and melasma.
Dr. Baumann is a private practice dermatologist, researcher, author, and entrepreneur in Miami. She founded the division of cosmetic dermatology at the University of Miami in 1997. The third edition of her bestselling textbook, “Cosmetic Dermatology,” was published in 2022. Dr. Baumann has received funding for advisory boards and/or clinical research trials from Allergan, Galderma, Johnson & Johnson, and Burt’s Bees. She is the CEO of Skin Type Solutions, an SaaS company used to generate skin care routines in office and as an ecommerce solution. Write to her at [email protected].
References
1. Tadic VM et al. Antioxidants (Basel). 2021 Mar 16;10(3):465.
2. Svobodová A et al. Biofactors. 2008;33(4):249-66.
3. Chu WK et al. Bilberry (Vaccinium myrtillus L.), in Benzie IFF, Wachtel-Galor S, eds., “Herbal Medicine: Biomolecular and Clinical Aspects,” 2nd ed. (Boca Raton, Fla.: CRC Press/Taylor & Francis, 2011, Chapter 4).
4. Yamaura K et al. Pharmacognosy Res. 2011 Jul;3(3):173-7.
5. Stefanescu BE et al. Molecules. 2019 May 29;24(11):2046.
6. Smeriglio A et al. Mini Rev Med Chem. 2014;14(7):567-84.
7. Ando H et al. Arch Dermatol Res. 1998 Jul;290(7):375-81.
8. Burdulis D et al. Acta Pol Pharm. 2009 Jul-Aug;66(4):399-408.
9. Bornsek SM et al. Food Chem. 2012 Oct 15;134(4):1878-84.
10. Brasanac-Vukanovic S et al. Molecules. 2018 Jul 26;23(8):1864.
11. Yamaura K et al. J Food Sci. 2012 Dec;77(12):H262-7.
12. Pires TCSP et al. Curr Pharm Des. 2020;26(16):1917-28.
13. Svobodová A et al. J Dermatol Sci. 2009 Dec;56(3):196-204.
14. Calò R, Marabini L. J Photochem Photobiol B. 2014 Mar 5;132:27-35.
15. Bucci P et al. J Cosmet Dermatol. 2018 Oct;17(5):889-99.
16. Ruscinc N et al. J Cosmet Dermatol. 2022 Jan 13.
17. Environmental Working Group’s Skin Deep website. Vaccinium Myrtillus Bilberry Seed Oil. Accessed October 18, 2022.
The ‘root cause’ visit
“How did we miss out on that?” “What?” my physician friend replied as we stood in line at the coffee cart. “Root cause. I mean, we invented this idea and now all these naturopaths and functional medicine quacks are gettin’ rich off it.” “Take it easy,” he says. “Just order a coffee.”
It’s hard not to be indignant. I had a morning clinic with three patients insisting I find the “root cause” of their problem. Now, if one had flagellate dermatitis after eating Asian mushroom soup, I’d have said “Root cause? Shiitake mushrooms!” and walked out like Costanza in Seinfeld, “All right, that’s it for me! Be good everybody!”
Alas no. They had perioral dermatitis, alopecia areata, eczema – no satisfying “roots” for walk-off answers.
There is a universal desire to find the proximal cause for problems. Patients often want to know it so that we address the root of their trouble and not just cut off the branches. This is deeply gratifying for those who want not only to know why, but also to have agency in how to control their disease. For example, if they believe the root cause of perioral dermatitis was excess yeast, then eating a “candida diet’’ should do the trick! Food sensitivities, hormones, and heavy metals round out the top suspects that root cause patients want to talk about.
Of course, patients have been asking about this for a long time, but lately, the root cause visit seems to be on trend. Check out any hip primary care start-up such as One Medical or any hot direct-to-consumer virtual offering such as ParsleyHealth and you will see root-cause everywhere. Our patients are expecting us to address it, or it seems they will find someone cooler who will.
Yet, it wasn’t the slick marketing team at ParsleyHeath who invented the “root cause doctor visit.” We did. It’s an idea that started with our Greek physician ancestors. Breaking from the diviners and priests, we were the first “naturalists” positing that there was a natural, not a divine cause for illness. The cardinal concept in the Hippocratic Corpus was that health was an equilibrium and illness an imbalance. They didn’t have dehydroepiandrosterone tests or mercury levels, but did have bodily fluids. Yellow bile, black bile, blood, and phlegm, were the root of all root causes. A physician simply had to identify which was in excess or deficient and fix that to cure the disease. Interestingly, the word “diagnosis” appears only once in the Corpus. The word “Diagignoskein” appears occasionally but this describes studying thoroughly, not naming a diagnosis as we understand it.
Advances in chemistry in the 17th century meant physicians could add new theories, and new root causes. Now alkaline or other chemical elixirs were added to cure at the source. Since there was no verifiable evidence to prove causes, theories were adopted to provide some rational direction to treatment. In the 18th century, physicians such as Dr. Benjamin Rush, one of the original faculty at the University of Pennsylvania school of medicine, taught that spasms of the arteries were the root cause of illnesses. “Heroic” treatments such as extreme bloodletting were the cure. (Note, those patients who survived us kept coming back to us for more).
Scientific knowledge and diagnostic technologies led to more and more complex and abstruse causes. Yet, as we became more precise and effective, our explanations became less satisfying to our patients. I can diagnose and readily treat perioral dermatitis, yet I’m hard pressed to give an answer to its root cause. “Root cause? Yes. Just apply this pimecrolimus cream for a couple of weeks and it’ll be better! All right, that’s it for me! Be good everybody!”
You’ll have to do better, George.
Dr. Benabio is director of Healthcare Transformation and chief of dermatology at Kaiser Permanente San Diego. The opinions expressed in this column are his own and do not represent those of Kaiser Permanente. Dr. Benabio is @Dermdoc on Twitter. Write to him at [email protected]
“How did we miss out on that?” “What?” my physician friend replied as we stood in line at the coffee cart. “Root cause. I mean, we invented this idea and now all these naturopaths and functional medicine quacks are gettin’ rich off it.” “Take it easy,” he says. “Just order a coffee.”
It’s hard not to be indignant. I had a morning clinic with three patients insisting I find the “root cause” of their problem. Now, if one had flagellate dermatitis after eating Asian mushroom soup, I’d have said “Root cause? Shiitake mushrooms!” and walked out like Costanza in Seinfeld, “All right, that’s it for me! Be good everybody!”
Alas no. They had perioral dermatitis, alopecia areata, eczema – no satisfying “roots” for walk-off answers.
There is a universal desire to find the proximal cause for problems. Patients often want to know it so that we address the root of their trouble and not just cut off the branches. This is deeply gratifying for those who want not only to know why, but also to have agency in how to control their disease. For example, if they believe the root cause of perioral dermatitis was excess yeast, then eating a “candida diet’’ should do the trick! Food sensitivities, hormones, and heavy metals round out the top suspects that root cause patients want to talk about.
Of course, patients have been asking about this for a long time, but lately, the root cause visit seems to be on trend. Check out any hip primary care start-up such as One Medical or any hot direct-to-consumer virtual offering such as ParsleyHealth and you will see root-cause everywhere. Our patients are expecting us to address it, or it seems they will find someone cooler who will.
Yet, it wasn’t the slick marketing team at ParsleyHeath who invented the “root cause doctor visit.” We did. It’s an idea that started with our Greek physician ancestors. Breaking from the diviners and priests, we were the first “naturalists” positing that there was a natural, not a divine cause for illness. The cardinal concept in the Hippocratic Corpus was that health was an equilibrium and illness an imbalance. They didn’t have dehydroepiandrosterone tests or mercury levels, but did have bodily fluids. Yellow bile, black bile, blood, and phlegm, were the root of all root causes. A physician simply had to identify which was in excess or deficient and fix that to cure the disease. Interestingly, the word “diagnosis” appears only once in the Corpus. The word “Diagignoskein” appears occasionally but this describes studying thoroughly, not naming a diagnosis as we understand it.
Advances in chemistry in the 17th century meant physicians could add new theories, and new root causes. Now alkaline or other chemical elixirs were added to cure at the source. Since there was no verifiable evidence to prove causes, theories were adopted to provide some rational direction to treatment. In the 18th century, physicians such as Dr. Benjamin Rush, one of the original faculty at the University of Pennsylvania school of medicine, taught that spasms of the arteries were the root cause of illnesses. “Heroic” treatments such as extreme bloodletting were the cure. (Note, those patients who survived us kept coming back to us for more).
Scientific knowledge and diagnostic technologies led to more and more complex and abstruse causes. Yet, as we became more precise and effective, our explanations became less satisfying to our patients. I can diagnose and readily treat perioral dermatitis, yet I’m hard pressed to give an answer to its root cause. “Root cause? Yes. Just apply this pimecrolimus cream for a couple of weeks and it’ll be better! All right, that’s it for me! Be good everybody!”
You’ll have to do better, George.
Dr. Benabio is director of Healthcare Transformation and chief of dermatology at Kaiser Permanente San Diego. The opinions expressed in this column are his own and do not represent those of Kaiser Permanente. Dr. Benabio is @Dermdoc on Twitter. Write to him at [email protected]
“How did we miss out on that?” “What?” my physician friend replied as we stood in line at the coffee cart. “Root cause. I mean, we invented this idea and now all these naturopaths and functional medicine quacks are gettin’ rich off it.” “Take it easy,” he says. “Just order a coffee.”
It’s hard not to be indignant. I had a morning clinic with three patients insisting I find the “root cause” of their problem. Now, if one had flagellate dermatitis after eating Asian mushroom soup, I’d have said “Root cause? Shiitake mushrooms!” and walked out like Costanza in Seinfeld, “All right, that’s it for me! Be good everybody!”
Alas no. They had perioral dermatitis, alopecia areata, eczema – no satisfying “roots” for walk-off answers.
There is a universal desire to find the proximal cause for problems. Patients often want to know it so that we address the root of their trouble and not just cut off the branches. This is deeply gratifying for those who want not only to know why, but also to have agency in how to control their disease. For example, if they believe the root cause of perioral dermatitis was excess yeast, then eating a “candida diet’’ should do the trick! Food sensitivities, hormones, and heavy metals round out the top suspects that root cause patients want to talk about.
Of course, patients have been asking about this for a long time, but lately, the root cause visit seems to be on trend. Check out any hip primary care start-up such as One Medical or any hot direct-to-consumer virtual offering such as ParsleyHealth and you will see root-cause everywhere. Our patients are expecting us to address it, or it seems they will find someone cooler who will.
Yet, it wasn’t the slick marketing team at ParsleyHeath who invented the “root cause doctor visit.” We did. It’s an idea that started with our Greek physician ancestors. Breaking from the diviners and priests, we were the first “naturalists” positing that there was a natural, not a divine cause for illness. The cardinal concept in the Hippocratic Corpus was that health was an equilibrium and illness an imbalance. They didn’t have dehydroepiandrosterone tests or mercury levels, but did have bodily fluids. Yellow bile, black bile, blood, and phlegm, were the root of all root causes. A physician simply had to identify which was in excess or deficient and fix that to cure the disease. Interestingly, the word “diagnosis” appears only once in the Corpus. The word “Diagignoskein” appears occasionally but this describes studying thoroughly, not naming a diagnosis as we understand it.
Advances in chemistry in the 17th century meant physicians could add new theories, and new root causes. Now alkaline or other chemical elixirs were added to cure at the source. Since there was no verifiable evidence to prove causes, theories were adopted to provide some rational direction to treatment. In the 18th century, physicians such as Dr. Benjamin Rush, one of the original faculty at the University of Pennsylvania school of medicine, taught that spasms of the arteries were the root cause of illnesses. “Heroic” treatments such as extreme bloodletting were the cure. (Note, those patients who survived us kept coming back to us for more).
Scientific knowledge and diagnostic technologies led to more and more complex and abstruse causes. Yet, as we became more precise and effective, our explanations became less satisfying to our patients. I can diagnose and readily treat perioral dermatitis, yet I’m hard pressed to give an answer to its root cause. “Root cause? Yes. Just apply this pimecrolimus cream for a couple of weeks and it’ll be better! All right, that’s it for me! Be good everybody!”
You’ll have to do better, George.
Dr. Benabio is director of Healthcare Transformation and chief of dermatology at Kaiser Permanente San Diego. The opinions expressed in this column are his own and do not represent those of Kaiser Permanente. Dr. Benabio is @Dermdoc on Twitter. Write to him at [email protected]
Are doctors savers or spenders?
In a poll that ran from August 30 to Sept. 21, conducted by Medscape, physicians were asked if they lived within their means. They were asked whether they pay their bills on time, save at least 20% of their monthly income toward retirement, pay down student loan debt, and contribute to their kids’ college savings or a rainy-day emergency fund.
Medscape polled 468 U.S. physicians and 159 living outside of the United States. Eighty-nine percent of U.S. respondents report living within their means, while only 11% said they don’t.
Medscape’s Physician Wealth & Debt Report 2022 similarly reported that of 13,000 physicians in more than 29 specialties, 94% said they live at or below their means.
For example, over half of physicians have a net worth above $1 million. In contrast, according to Credit Suisse’s Global Wealth Report, less than 7% of the general population has a seven-figure net worth.
So just how do physicians stack up financially?
Habits of physician super savers
Physicians who consider themselves savers likely have money habits that correlate. They buy things on sale, are DIYers for home projects and maintenance, and wait to buy luxury or large expenses when the timing is right, an item is on sale, or they’ve saved for it.
For example, when it comes to life’s luxuries like buying a new car or dining out, overall, physicians seem to be more frugal, as 43% of those who buy cars said they only buy a new car every 10 years; 30% said they buy a new vehicle every 6-7 years, and 22% said every 4-5 years.
When asked about weekly dine-out or delivery habits, 82% of those polled who said they dine out, or order takeout, do so a nominal 1-2 times per week. That’s on par with the Centers for Disease Control, which reports that 3 in 5 Americans eat out once weekly. Another 14% of polled physicians said they dine out 3-5 nights per week. Only 4% revealed they eat out or grab to-go food more than 5 nights a week.
When hiring for essential home maintenance, like house cleaning and pool or lawn service, almost a third of physicians we polled who require such maintenance employ a service for these tasks, and 23% hire out often while 21% hire out only sometimes. However, 14% say they rarely hire out for home maintenance, and 11% never do.
Since physicians are typically tight on time, they tend to favor outsourcing things like housecleaning, lawn service, landscaping, maintenance, and even cooking. So, the fact that a quarter of physicians polled rarely or never hire out for household help is somewhat surprising.
Most physicians also prioritize saving. When asked how important it is to save money consistently, 93% think it’s either extremely or very important, while only 6% think it’s somewhat important.
Barriers to wealth
When asked what barriers prevent them from saving at least 20% of their monthly income, physician respondents who said they live within their means and encountered barriers reported that family necessities (35%), student loan debt (19%), and mortgage sizes (18%) were the top reasons. The average doctor earns five times as much as the average American, according to the Global Wealth Report.
“What prevents me from saving is holding too much debt, responsibilities at home, bills, being unprepared for what is coming, and making excuses to spend even when it’s not necessary,” says Sean Ormond, MD, a dual board-certified physician in Anesthesiology and Pain Management in Phoenix.
When physician respondents who said they didn’t live within their means were asked about the barriers preventing them from saving at least 20% of their monthly income, they cited the cost of family necessities (49%), the size of their mortgage (47%), credit card debt (30%), student loan debt (21%), other loans (15%), and car lease/loan (13%).
“My most significant financial splurge is vacation, since I always choose the best, and the best comes at an extra cost,” says Dr. Ormond.
What’s your financial grade?
Finally, physicians were asked who they considered better at saving money, themselves or their spouse/domestic partner. Forty-four percent think they are the better saver, whereas 41% said that both they and their partner were equally good at saving. Thirteen percent credited their partner with better saving habits, and 2% said neither themselves nor their partner were good at saving money.
More than half (63%) of physicians polled pay off their credit card balance monthly, but 18% carry a $1,000-$5,000 balance, 10% have $5,000-$10,000 in credit card debt, and 6% hold more than $10,000 of credit card debt.
“I would grade myself with a B, because however much I love having the best, I still have a budget, and I always ensure that I follow it to the dot,” says Dr. Ormond.
A version of this article first appeared on Medscape.com.
In a poll that ran from August 30 to Sept. 21, conducted by Medscape, physicians were asked if they lived within their means. They were asked whether they pay their bills on time, save at least 20% of their monthly income toward retirement, pay down student loan debt, and contribute to their kids’ college savings or a rainy-day emergency fund.
Medscape polled 468 U.S. physicians and 159 living outside of the United States. Eighty-nine percent of U.S. respondents report living within their means, while only 11% said they don’t.
Medscape’s Physician Wealth & Debt Report 2022 similarly reported that of 13,000 physicians in more than 29 specialties, 94% said they live at or below their means.
For example, over half of physicians have a net worth above $1 million. In contrast, according to Credit Suisse’s Global Wealth Report, less than 7% of the general population has a seven-figure net worth.
So just how do physicians stack up financially?
Habits of physician super savers
Physicians who consider themselves savers likely have money habits that correlate. They buy things on sale, are DIYers for home projects and maintenance, and wait to buy luxury or large expenses when the timing is right, an item is on sale, or they’ve saved for it.
For example, when it comes to life’s luxuries like buying a new car or dining out, overall, physicians seem to be more frugal, as 43% of those who buy cars said they only buy a new car every 10 years; 30% said they buy a new vehicle every 6-7 years, and 22% said every 4-5 years.
When asked about weekly dine-out or delivery habits, 82% of those polled who said they dine out, or order takeout, do so a nominal 1-2 times per week. That’s on par with the Centers for Disease Control, which reports that 3 in 5 Americans eat out once weekly. Another 14% of polled physicians said they dine out 3-5 nights per week. Only 4% revealed they eat out or grab to-go food more than 5 nights a week.
When hiring for essential home maintenance, like house cleaning and pool or lawn service, almost a third of physicians we polled who require such maintenance employ a service for these tasks, and 23% hire out often while 21% hire out only sometimes. However, 14% say they rarely hire out for home maintenance, and 11% never do.
Since physicians are typically tight on time, they tend to favor outsourcing things like housecleaning, lawn service, landscaping, maintenance, and even cooking. So, the fact that a quarter of physicians polled rarely or never hire out for household help is somewhat surprising.
Most physicians also prioritize saving. When asked how important it is to save money consistently, 93% think it’s either extremely or very important, while only 6% think it’s somewhat important.
Barriers to wealth
When asked what barriers prevent them from saving at least 20% of their monthly income, physician respondents who said they live within their means and encountered barriers reported that family necessities (35%), student loan debt (19%), and mortgage sizes (18%) were the top reasons. The average doctor earns five times as much as the average American, according to the Global Wealth Report.
“What prevents me from saving is holding too much debt, responsibilities at home, bills, being unprepared for what is coming, and making excuses to spend even when it’s not necessary,” says Sean Ormond, MD, a dual board-certified physician in Anesthesiology and Pain Management in Phoenix.
When physician respondents who said they didn’t live within their means were asked about the barriers preventing them from saving at least 20% of their monthly income, they cited the cost of family necessities (49%), the size of their mortgage (47%), credit card debt (30%), student loan debt (21%), other loans (15%), and car lease/loan (13%).
“My most significant financial splurge is vacation, since I always choose the best, and the best comes at an extra cost,” says Dr. Ormond.
What’s your financial grade?
Finally, physicians were asked who they considered better at saving money, themselves or their spouse/domestic partner. Forty-four percent think they are the better saver, whereas 41% said that both they and their partner were equally good at saving. Thirteen percent credited their partner with better saving habits, and 2% said neither themselves nor their partner were good at saving money.
More than half (63%) of physicians polled pay off their credit card balance monthly, but 18% carry a $1,000-$5,000 balance, 10% have $5,000-$10,000 in credit card debt, and 6% hold more than $10,000 of credit card debt.
“I would grade myself with a B, because however much I love having the best, I still have a budget, and I always ensure that I follow it to the dot,” says Dr. Ormond.
A version of this article first appeared on Medscape.com.
In a poll that ran from August 30 to Sept. 21, conducted by Medscape, physicians were asked if they lived within their means. They were asked whether they pay their bills on time, save at least 20% of their monthly income toward retirement, pay down student loan debt, and contribute to their kids’ college savings or a rainy-day emergency fund.
Medscape polled 468 U.S. physicians and 159 living outside of the United States. Eighty-nine percent of U.S. respondents report living within their means, while only 11% said they don’t.
Medscape’s Physician Wealth & Debt Report 2022 similarly reported that of 13,000 physicians in more than 29 specialties, 94% said they live at or below their means.
For example, over half of physicians have a net worth above $1 million. In contrast, according to Credit Suisse’s Global Wealth Report, less than 7% of the general population has a seven-figure net worth.
So just how do physicians stack up financially?
Habits of physician super savers
Physicians who consider themselves savers likely have money habits that correlate. They buy things on sale, are DIYers for home projects and maintenance, and wait to buy luxury or large expenses when the timing is right, an item is on sale, or they’ve saved for it.
For example, when it comes to life’s luxuries like buying a new car or dining out, overall, physicians seem to be more frugal, as 43% of those who buy cars said they only buy a new car every 10 years; 30% said they buy a new vehicle every 6-7 years, and 22% said every 4-5 years.
When asked about weekly dine-out or delivery habits, 82% of those polled who said they dine out, or order takeout, do so a nominal 1-2 times per week. That’s on par with the Centers for Disease Control, which reports that 3 in 5 Americans eat out once weekly. Another 14% of polled physicians said they dine out 3-5 nights per week. Only 4% revealed they eat out or grab to-go food more than 5 nights a week.
When hiring for essential home maintenance, like house cleaning and pool or lawn service, almost a third of physicians we polled who require such maintenance employ a service for these tasks, and 23% hire out often while 21% hire out only sometimes. However, 14% say they rarely hire out for home maintenance, and 11% never do.
Since physicians are typically tight on time, they tend to favor outsourcing things like housecleaning, lawn service, landscaping, maintenance, and even cooking. So, the fact that a quarter of physicians polled rarely or never hire out for household help is somewhat surprising.
Most physicians also prioritize saving. When asked how important it is to save money consistently, 93% think it’s either extremely or very important, while only 6% think it’s somewhat important.
Barriers to wealth
When asked what barriers prevent them from saving at least 20% of their monthly income, physician respondents who said they live within their means and encountered barriers reported that family necessities (35%), student loan debt (19%), and mortgage sizes (18%) were the top reasons. The average doctor earns five times as much as the average American, according to the Global Wealth Report.
“What prevents me from saving is holding too much debt, responsibilities at home, bills, being unprepared for what is coming, and making excuses to spend even when it’s not necessary,” says Sean Ormond, MD, a dual board-certified physician in Anesthesiology and Pain Management in Phoenix.
When physician respondents who said they didn’t live within their means were asked about the barriers preventing them from saving at least 20% of their monthly income, they cited the cost of family necessities (49%), the size of their mortgage (47%), credit card debt (30%), student loan debt (21%), other loans (15%), and car lease/loan (13%).
“My most significant financial splurge is vacation, since I always choose the best, and the best comes at an extra cost,” says Dr. Ormond.
What’s your financial grade?
Finally, physicians were asked who they considered better at saving money, themselves or their spouse/domestic partner. Forty-four percent think they are the better saver, whereas 41% said that both they and their partner were equally good at saving. Thirteen percent credited their partner with better saving habits, and 2% said neither themselves nor their partner were good at saving money.
More than half (63%) of physicians polled pay off their credit card balance monthly, but 18% carry a $1,000-$5,000 balance, 10% have $5,000-$10,000 in credit card debt, and 6% hold more than $10,000 of credit card debt.
“I would grade myself with a B, because however much I love having the best, I still have a budget, and I always ensure that I follow it to the dot,” says Dr. Ormond.
A version of this article first appeared on Medscape.com.
New COVID variant gaining traction in U.S.
, according to the CDC’s latest data.
Just 1 month ago, the variant accounted for less than 1% of cases.
“When you get variants like that, you look at what their rate of increase is as a relative proportion of the variants, and this has a pretty troublesome doubling time,” Anthony Fauci, MD, said in an interview with CBS News. Dr. Fauci is the director of the National Institute of Allergy and Infectious Diseases and also the chief medical adviser to President Joe Biden.
There are also concerning features of the BQ.1 variant, which include mutations that could potentially escape vaccines and treatments for COVID-19.
Currently, the most widespread variant in the U.S. is the Omicron subvariant known as BA.5, which accounts for 68% of all infections. One of the go-to treatments for BA.5 infections is monoclonal antibodies, which may not be as effective when fighting the up-and-coming strains of BQ.1 and its descendant BQ.1.1, according to experts.
“That’s the reason why people are concerned about BQ.1.1, for the double reason of its doubling time and the fact that it seems to elude important monoclonal antibodies,” Dr. Fauci told CBS News.
Currently, BQ.1 and BQ.1.1 appear most widespread in the New York and New Jersey region, accounting for nearly 20% of infections there, according to the CDC.
But because the new variant is a descendant of Omicron, Dr. Fauci said the currently available booster shots are still the best first line of protection against this up-and-coming threat.
“The bad news is that there’s a new variant that’s emerging and that has qualities or characteristics that could evade some of the interventions we have. But, the somewhat encouraging news is that it’s a BA.5 sub-lineage, so there is almost certainly going to be some cross-protection that you can boost up,” he said.
A version of this article first appeared on WebMD.com.
, according to the CDC’s latest data.
Just 1 month ago, the variant accounted for less than 1% of cases.
“When you get variants like that, you look at what their rate of increase is as a relative proportion of the variants, and this has a pretty troublesome doubling time,” Anthony Fauci, MD, said in an interview with CBS News. Dr. Fauci is the director of the National Institute of Allergy and Infectious Diseases and also the chief medical adviser to President Joe Biden.
There are also concerning features of the BQ.1 variant, which include mutations that could potentially escape vaccines and treatments for COVID-19.
Currently, the most widespread variant in the U.S. is the Omicron subvariant known as BA.5, which accounts for 68% of all infections. One of the go-to treatments for BA.5 infections is monoclonal antibodies, which may not be as effective when fighting the up-and-coming strains of BQ.1 and its descendant BQ.1.1, according to experts.
“That’s the reason why people are concerned about BQ.1.1, for the double reason of its doubling time and the fact that it seems to elude important monoclonal antibodies,” Dr. Fauci told CBS News.
Currently, BQ.1 and BQ.1.1 appear most widespread in the New York and New Jersey region, accounting for nearly 20% of infections there, according to the CDC.
But because the new variant is a descendant of Omicron, Dr. Fauci said the currently available booster shots are still the best first line of protection against this up-and-coming threat.
“The bad news is that there’s a new variant that’s emerging and that has qualities or characteristics that could evade some of the interventions we have. But, the somewhat encouraging news is that it’s a BA.5 sub-lineage, so there is almost certainly going to be some cross-protection that you can boost up,” he said.
A version of this article first appeared on WebMD.com.
, according to the CDC’s latest data.
Just 1 month ago, the variant accounted for less than 1% of cases.
“When you get variants like that, you look at what their rate of increase is as a relative proportion of the variants, and this has a pretty troublesome doubling time,” Anthony Fauci, MD, said in an interview with CBS News. Dr. Fauci is the director of the National Institute of Allergy and Infectious Diseases and also the chief medical adviser to President Joe Biden.
There are also concerning features of the BQ.1 variant, which include mutations that could potentially escape vaccines and treatments for COVID-19.
Currently, the most widespread variant in the U.S. is the Omicron subvariant known as BA.5, which accounts for 68% of all infections. One of the go-to treatments for BA.5 infections is monoclonal antibodies, which may not be as effective when fighting the up-and-coming strains of BQ.1 and its descendant BQ.1.1, according to experts.
“That’s the reason why people are concerned about BQ.1.1, for the double reason of its doubling time and the fact that it seems to elude important monoclonal antibodies,” Dr. Fauci told CBS News.
Currently, BQ.1 and BQ.1.1 appear most widespread in the New York and New Jersey region, accounting for nearly 20% of infections there, according to the CDC.
But because the new variant is a descendant of Omicron, Dr. Fauci said the currently available booster shots are still the best first line of protection against this up-and-coming threat.
“The bad news is that there’s a new variant that’s emerging and that has qualities or characteristics that could evade some of the interventions we have. But, the somewhat encouraging news is that it’s a BA.5 sub-lineage, so there is almost certainly going to be some cross-protection that you can boost up,” he said.
A version of this article first appeared on WebMD.com.
‘Not in our lane’: Physicians rebel at idea they should discuss gun safety with patients
The latest NPR/PBS NewsHour/Marist poll shows that that the margin of public opinion in the United States is the widest that it has been during the past 10 years in favor of taking steps to control gun violence; 59% of U.S. adults said it’s more important to control gun violence than to protect gun rights, and 35% said the opposite.
Have physicians’ opinions about gun issues in our country shifted meaningfully during that period? That’s a complex question that can be informed with the basic snapshot provided by doctors› comments to New York University (and Medscape blogger) bioethicist Arthur L. Caplan’s four video blogs on whether physicians should discuss gun safety with their patients. Dr. Caplan’s video blogs appeared on the Medscape website in 2014, 2016, 2018, and 2022.
Hundreds of physicians have posted comments to Dr. Caplan’s arguments that doctors should bring up gun safety when talking to their patients. The great majority of comments opposed his position in 2014, and that remained the case through 2022, regardless of incidents of gun-related violence. Supportive comments have been a small minority that has grown only slightly over his four video blogs.
Physicians’ lack of qualifications
The most prevalent counterarguments expressed against Dr. Caplan’s position are that physicians lack the proper knowledge to discuss gun safety with patients; and the responsibility falls on family members, certified firearms instructors, teachers, and others – but not doctors – to educate people about firearm safety.
“Then there’s a third group that says, ‘I don’t want to do this because I am too busy trying to figure out what is wrong with the patient,’ ” Dr. Caplan says.
Here are a few on-point comments that were posted to his video blogs:
- “Unless physicians become certified firearms instructors like myself, they are not qualified to talk to patients on the subject and should advise patients to find a program and take a course.” – Dr. Ken Long, March 31, 2014
- “Gun safety should be taught in school, just like health and sex education.” – Patricia L., Feb. 11, 2016
- “None of my medical or surgical training or experience qualifies me as a policy expert on gun laws or regulations.” – Dr. Kelly Hyde, Dec. 23, 2018
- “I have the Constitution hanging in my office with an NRA plaque next to it. Most MDs can’t mow their own yard.” – Dr. Brian Anseeuw, June 21, 2022
Do mental health issues trump gun talks?
Another counterargument to discussing gun safety with patients involves mental health issues that many physicians may not be trained to address. Mental health entered comments to Dr. Caplan’s video blogs in 2016 and has shaped much of the discussion since.
- “First of all, two-thirds of gun deaths are suicides. It is foolish to talk about counseling patients about gun safety, etc, and ignore the mental health issues.” – Dr. Jeffrey Jennings, Jan. 25, 2016
- “Suicide victims and those committing mass shootings are mentally ill. ... Blame society, drugs, mental illness, easy access to illegal firearms, and poor recognition of SOS (signs of suicide).” – Dr. Alan DeCarlo, Dec. 24, 2018
- “Yes, we have gun violence, but what is the underlying problem? Bullying? Mental issues? Not enough parental supervision? These and others are the issues I feel need to be discussed.” – T. Deese, June 24, 2022
- “The causes of increased gun violence are mental health, problems with bullying, social media, and normalization of deviant behavior.” – Julie Johng, 2022
Added responsibility is too much
Another theme that has grown over time is that talks of gun safety just heap issues onto physicians’ treatment plates that are already too full.
- “Oh, for God’s sake, is there anything else I can do while I›m at it? Primary care has gotten to be more headache than it’s worth. Thanks for another reason to think about retiring.” – Dr. Kathleen Collins, March 31, 2014
- “THE JOB OF POLICE, COURTS, AND LAW-EDUCATED PROSECUTORS SHOULD NOT BE HANDLED BY PHYSICIANS.” – Dr. Sudarshan Singla, Jan. 25, 2016
- “This is a debate that only those at the academic/ivory tower–level of medicine even have time to lament. The frontline medical providers barely have enough time to adequately address the pertinent.” – Tobin Purslow, Jan. 15, 2016
Other ways to communicate
For his part, Dr. Caplan believes there is a variety of ways physicians can effectively discuss gun safety with patients to help minimize the potential of injury or death.
Acknowledging that other aspects of treatment are often more pressing, he suggested that the gun safety education could be done through educational videos that are shown in waiting rooms, through pamphlets available at the front desk, or throuigh a newsletter sent to patients.
“Everything doesn’t have to happen in conversation. The doctor’s office should become more of an educational site.
“I am 100% more passionate about this than when I first started down this road.”
A version of this article first appeared on Medscape.com.
The latest NPR/PBS NewsHour/Marist poll shows that that the margin of public opinion in the United States is the widest that it has been during the past 10 years in favor of taking steps to control gun violence; 59% of U.S. adults said it’s more important to control gun violence than to protect gun rights, and 35% said the opposite.
Have physicians’ opinions about gun issues in our country shifted meaningfully during that period? That’s a complex question that can be informed with the basic snapshot provided by doctors› comments to New York University (and Medscape blogger) bioethicist Arthur L. Caplan’s four video blogs on whether physicians should discuss gun safety with their patients. Dr. Caplan’s video blogs appeared on the Medscape website in 2014, 2016, 2018, and 2022.
Hundreds of physicians have posted comments to Dr. Caplan’s arguments that doctors should bring up gun safety when talking to their patients. The great majority of comments opposed his position in 2014, and that remained the case through 2022, regardless of incidents of gun-related violence. Supportive comments have been a small minority that has grown only slightly over his four video blogs.
Physicians’ lack of qualifications
The most prevalent counterarguments expressed against Dr. Caplan’s position are that physicians lack the proper knowledge to discuss gun safety with patients; and the responsibility falls on family members, certified firearms instructors, teachers, and others – but not doctors – to educate people about firearm safety.
“Then there’s a third group that says, ‘I don’t want to do this because I am too busy trying to figure out what is wrong with the patient,’ ” Dr. Caplan says.
Here are a few on-point comments that were posted to his video blogs:
- “Unless physicians become certified firearms instructors like myself, they are not qualified to talk to patients on the subject and should advise patients to find a program and take a course.” – Dr. Ken Long, March 31, 2014
- “Gun safety should be taught in school, just like health and sex education.” – Patricia L., Feb. 11, 2016
- “None of my medical or surgical training or experience qualifies me as a policy expert on gun laws or regulations.” – Dr. Kelly Hyde, Dec. 23, 2018
- “I have the Constitution hanging in my office with an NRA plaque next to it. Most MDs can’t mow their own yard.” – Dr. Brian Anseeuw, June 21, 2022
Do mental health issues trump gun talks?
Another counterargument to discussing gun safety with patients involves mental health issues that many physicians may not be trained to address. Mental health entered comments to Dr. Caplan’s video blogs in 2016 and has shaped much of the discussion since.
- “First of all, two-thirds of gun deaths are suicides. It is foolish to talk about counseling patients about gun safety, etc, and ignore the mental health issues.” – Dr. Jeffrey Jennings, Jan. 25, 2016
- “Suicide victims and those committing mass shootings are mentally ill. ... Blame society, drugs, mental illness, easy access to illegal firearms, and poor recognition of SOS (signs of suicide).” – Dr. Alan DeCarlo, Dec. 24, 2018
- “Yes, we have gun violence, but what is the underlying problem? Bullying? Mental issues? Not enough parental supervision? These and others are the issues I feel need to be discussed.” – T. Deese, June 24, 2022
- “The causes of increased gun violence are mental health, problems with bullying, social media, and normalization of deviant behavior.” – Julie Johng, 2022
Added responsibility is too much
Another theme that has grown over time is that talks of gun safety just heap issues onto physicians’ treatment plates that are already too full.
- “Oh, for God’s sake, is there anything else I can do while I›m at it? Primary care has gotten to be more headache than it’s worth. Thanks for another reason to think about retiring.” – Dr. Kathleen Collins, March 31, 2014
- “THE JOB OF POLICE, COURTS, AND LAW-EDUCATED PROSECUTORS SHOULD NOT BE HANDLED BY PHYSICIANS.” – Dr. Sudarshan Singla, Jan. 25, 2016
- “This is a debate that only those at the academic/ivory tower–level of medicine even have time to lament. The frontline medical providers barely have enough time to adequately address the pertinent.” – Tobin Purslow, Jan. 15, 2016
Other ways to communicate
For his part, Dr. Caplan believes there is a variety of ways physicians can effectively discuss gun safety with patients to help minimize the potential of injury or death.
Acknowledging that other aspects of treatment are often more pressing, he suggested that the gun safety education could be done through educational videos that are shown in waiting rooms, through pamphlets available at the front desk, or throuigh a newsletter sent to patients.
“Everything doesn’t have to happen in conversation. The doctor’s office should become more of an educational site.
“I am 100% more passionate about this than when I first started down this road.”
A version of this article first appeared on Medscape.com.
The latest NPR/PBS NewsHour/Marist poll shows that that the margin of public opinion in the United States is the widest that it has been during the past 10 years in favor of taking steps to control gun violence; 59% of U.S. adults said it’s more important to control gun violence than to protect gun rights, and 35% said the opposite.
Have physicians’ opinions about gun issues in our country shifted meaningfully during that period? That’s a complex question that can be informed with the basic snapshot provided by doctors› comments to New York University (and Medscape blogger) bioethicist Arthur L. Caplan’s four video blogs on whether physicians should discuss gun safety with their patients. Dr. Caplan’s video blogs appeared on the Medscape website in 2014, 2016, 2018, and 2022.
Hundreds of physicians have posted comments to Dr. Caplan’s arguments that doctors should bring up gun safety when talking to their patients. The great majority of comments opposed his position in 2014, and that remained the case through 2022, regardless of incidents of gun-related violence. Supportive comments have been a small minority that has grown only slightly over his four video blogs.
Physicians’ lack of qualifications
The most prevalent counterarguments expressed against Dr. Caplan’s position are that physicians lack the proper knowledge to discuss gun safety with patients; and the responsibility falls on family members, certified firearms instructors, teachers, and others – but not doctors – to educate people about firearm safety.
“Then there’s a third group that says, ‘I don’t want to do this because I am too busy trying to figure out what is wrong with the patient,’ ” Dr. Caplan says.
Here are a few on-point comments that were posted to his video blogs:
- “Unless physicians become certified firearms instructors like myself, they are not qualified to talk to patients on the subject and should advise patients to find a program and take a course.” – Dr. Ken Long, March 31, 2014
- “Gun safety should be taught in school, just like health and sex education.” – Patricia L., Feb. 11, 2016
- “None of my medical or surgical training or experience qualifies me as a policy expert on gun laws or regulations.” – Dr. Kelly Hyde, Dec. 23, 2018
- “I have the Constitution hanging in my office with an NRA plaque next to it. Most MDs can’t mow their own yard.” – Dr. Brian Anseeuw, June 21, 2022
Do mental health issues trump gun talks?
Another counterargument to discussing gun safety with patients involves mental health issues that many physicians may not be trained to address. Mental health entered comments to Dr. Caplan’s video blogs in 2016 and has shaped much of the discussion since.
- “First of all, two-thirds of gun deaths are suicides. It is foolish to talk about counseling patients about gun safety, etc, and ignore the mental health issues.” – Dr. Jeffrey Jennings, Jan. 25, 2016
- “Suicide victims and those committing mass shootings are mentally ill. ... Blame society, drugs, mental illness, easy access to illegal firearms, and poor recognition of SOS (signs of suicide).” – Dr. Alan DeCarlo, Dec. 24, 2018
- “Yes, we have gun violence, but what is the underlying problem? Bullying? Mental issues? Not enough parental supervision? These and others are the issues I feel need to be discussed.” – T. Deese, June 24, 2022
- “The causes of increased gun violence are mental health, problems with bullying, social media, and normalization of deviant behavior.” – Julie Johng, 2022
Added responsibility is too much
Another theme that has grown over time is that talks of gun safety just heap issues onto physicians’ treatment plates that are already too full.
- “Oh, for God’s sake, is there anything else I can do while I›m at it? Primary care has gotten to be more headache than it’s worth. Thanks for another reason to think about retiring.” – Dr. Kathleen Collins, March 31, 2014
- “THE JOB OF POLICE, COURTS, AND LAW-EDUCATED PROSECUTORS SHOULD NOT BE HANDLED BY PHYSICIANS.” – Dr. Sudarshan Singla, Jan. 25, 2016
- “This is a debate that only those at the academic/ivory tower–level of medicine even have time to lament. The frontline medical providers barely have enough time to adequately address the pertinent.” – Tobin Purslow, Jan. 15, 2016
Other ways to communicate
For his part, Dr. Caplan believes there is a variety of ways physicians can effectively discuss gun safety with patients to help minimize the potential of injury or death.
Acknowledging that other aspects of treatment are often more pressing, he suggested that the gun safety education could be done through educational videos that are shown in waiting rooms, through pamphlets available at the front desk, or throuigh a newsletter sent to patients.
“Everything doesn’t have to happen in conversation. The doctor’s office should become more of an educational site.
“I am 100% more passionate about this than when I first started down this road.”
A version of this article first appeared on Medscape.com.
You and the skeptical patient: Who’s the doctor here?
“I spoke to him on many occasions about the dangers of COVID, but he just didn’t believe me,” said Dr. Hood, an internist in Lexington, Ky. “He just didn’t give me enough time to help him. He waited to let me know he was ill with COVID and took days to pick up the medicine. Unfortunately, he then passed away.”
The rise of the skeptical patient
It can be extremely frustrating for doctors when patients question or disbelieve their physician’s medical advice and explanations. And many physicians resent the amount of time they spend trying to explain or make their case, especially during a busy day. But patients’ skepticism about the validity of some treatments seems to be increasing.
“Patients are now more likely to have their own medical explanation for their complaint than they used to, and that can be bad for their health,” Dr. Hood said.
Dr. Hood sees medical cynicism as part of Americans’ growing distrust of experts, leveraged by easy access to the internet. “When people Google, they tend to look for support of their opinions, rather than arrive at a fully educated decision.”
Only about half of patients believe their physicians “provide fair and accurate treatment information all or most of the time,” according to a 2019 survey by the Pew Research Center.
Patients’ distrust has become more obvious during the COVID-19 pandemic, said John Schumann, MD, an internist with Oak Street Health, a practice with more than 500 physicians and other providers in 20 states, treating almost exclusively Medicare patients.
“The skeptics became more entrenched during the pandemic,” said Dr. Schumann, who is based in Tulsa, Okla. “They may think the COVID vaccines were approved too quickly, or believe the pandemic itself is a hoax.”
“There’s a lot of antiscience rhetoric now,” Dr. Schumann added. “I’d say about half of my patients are comfortable with science-based decisions and the other half are not.”
What are patients mistrustful about?
Patients’ suspicions of certain therapies began long before the pandemic. In dermatology, for example, some patients refuse to take topical steroids, said Steven R. Feldman, MD, a dermatologist in Winston-Salem, N.C.
“Their distrust is usually based on anecdotal stories they read about,” he noted. “Patients in other specialties are dead set against vaccinations.”
In addition to refusing treatments and inoculations, some patients ask for questionable regimens mentioned in the news. “Some patients have demanded hydroxychloroquine or Noromectin, drugs that are unproven in the treatment of COVID,” Dr. Schumann said. “We refuse to prescribe them.”
Dr. Hood said patients’ reluctance to follow medical advice can often be based on cost. “I have a patient who was more willing to save $20 than to save his life. But when the progression of his test results fit my predictions, he became more willing to take treatments. I had to wait for the opportune moment to convince him.”
Many naysayer patients keep their views to themselves, and physicians may be unaware that the patients are stonewalling. A 2006 study estimated that about 10%-16% of primary care patients actively resist medical authority.
Dr. Schumann cited patients who don’t want to hear an upsetting diagnosis. “Some patients might refuse to take a biopsy to see if they have cancer because they don’t want to know,” he said. “In many cases, they simply won’t get the biopsy and won’t tell the doctor that they didn’t.”
Sometimes skeptics’ arguments have merit
Some patients’ concerns can be valid, such as when they refuse to go on statins, said Zain Hakeem, DO, a physician in Austin, Tex.
“In some cases, I feel that statins are not necessary,” he said. “The science on statins for primary prevention is not strong, although they should be used for exceedingly high-risk patients.”
Certain patients, especially those with chronic conditions, do a great deal of research, using legitimate sources on the Web, and their research is well supported.
However, these patients can be overconfident in their conclusions. Several studies have shown that with just a little experience, people can replace beginners’ caution with a false sense of competence.
For example, “Patients may not weigh the risks correctly,” Dr. Hakeem said. “They can be more concerned about the risk of having their colon perforated during a colonoscopy, while the risk of cancer if they don’t have a colonoscopy is much higher.”
Some highly successful people may be more likely to trust their own medical instincts. When Steve Jobs, the founder of Apple, was diagnosed with pancreatic cancer in 2003, he put off surgery for 9 months while he tried to cure his disease with a vegan diet, acupuncture, herbs, bowel cleansings, and other remedies he read about. He died in 2011. Some experts believe that delay hastened his death.
Of course, not all physicians’ diagnoses or treatments are correct. One study indicated doctors’ diagnostic error rate could be as high as 15%. And just as patients can be overconfident in their conclusions, so can doctors. Another study found that physicians’ stated confidence in their diagnosis was only slightly affected by the inaccuracy of that diagnosis or the difficulty of the case.
Best ways to deal with cynical patients
Patients’ skepticism can frustrate doctors, reduce the efficiency of care delivery, and interfere with recovery. What can doctors do to deal with these problems?
1. Build the patient’s trust in you. “Getting patients to adhere to your advice involves making sure they feel they have a caring doctor whom they trust,” Dr. Feldman said.
“I want to show patients that I am entirely focused on them,” he added. “For example, I may rush to the door of the exam room from my last appointment, but I open the door very slowly and deliberately, because I want the patient to see that I won’t hurry with them.”
2. Spend time with the patient. Familiarity builds trust. Dr. Schumann said doctors at Oak Street Health see their patients an average of six to eight times a year, an unusually high number. “The more patients see their physicians, the more likely they are to trust them.”
3. Keep up to date. “I make sure I’m up to date with the literature, and I try to present a truthful message,” Dr. Hood said. “For instance, my research showed that inflammation played a strong role in developing complications from COVID, so I wrote a detailed treatment protocol aimed at the inflammation and the immune response, which has been very effective.”
4. Confront patients tactfully. Patients who do research on the Web don’t want to be scolded, Dr. Feldman said. In fact, he praises them, even if he doesn’t agree with their findings. “I might say: ‘What a relief to finally find patients who’ve taken the time to educate themselves before coming here.’ ”
Dr. Feldman is careful not to dispute patients’ conclusions. “Debating the issues is not an effective approach to get patients to trust you. The last thing you want to tell a patient is: ‘Listen to me! I’m an expert.’ People just dig in.”
However, it does help to give patients feedback. “I’m a big fan of patients arguing with me,” Dr. Hakeem said. “It means you can straighten out misunderstandings and improve decision-making.”
5. Explain your reasoning. “You need to communicate clearly and show them your thinking,” Dr. Hood said. “For instance, I’ll explain why a patient has a strong risk for heart attack.”
6. Acknowledge uncertainties. “The doctor may present the science as far more certain than it is,” Dr. Hakeem said. “If you don’t acknowledge the uncertainties, you could break the patient’s trust in you.”
7. Don’t use a lot of numbers. “Data is not a good tool to convince patients,” Dr. Feldman said. “The human brain isn’t designed to work that way.”
If you want to use numbers to show clinical risk, Dr. Hakeem advisd using natural frequencies, such as 10 out of 10,000, which is less confusing to the patient than the equivalent percentage of 0.1%.
It can be helpful to refer to familiar concepts. One way to understand a risk is to compare it with risks in daily life, such as the dangers of driving or falling in the shower, Dr. Hakeem added.
Dr. Feldman often refers to another person’s experience when presenting his medical advice. “I might say to the patient: ‘You remind me of another patient I had. They were sitting in the same chair you’re sitting in. They did really well on this drug, and I think it’s probably the best choice for you, too.’ ”
8. Adopt shared decision-making. This approach involves empowering the patient to become an equal partner in medical decisions. The patient is given information through portals and is encouraged to do research. Critics, however, say that most patients don’t want this degree of empowerment and would rather depend on the doctor’s advice.
Conclusion
It’s often impossible to get through to a skeptical patient, which can be disheartening for doctors. “Physicians want to do what is best for the patient, so when the patient doesn’t listen, they may take it personally,” Dr. Hood said. “But you always have to remember, the patient is the one with disease, and it’s up to the patient to open the door.”
Still, some skeptical patients ultimately change their minds. Dr. Schumann said patients who initially declined the COVID vaccine eventually decided to get it. “It often took them more than a year. but it’s never too late.”
A version of this article first appeared on Medscape.com.
“I spoke to him on many occasions about the dangers of COVID, but he just didn’t believe me,” said Dr. Hood, an internist in Lexington, Ky. “He just didn’t give me enough time to help him. He waited to let me know he was ill with COVID and took days to pick up the medicine. Unfortunately, he then passed away.”
The rise of the skeptical patient
It can be extremely frustrating for doctors when patients question or disbelieve their physician’s medical advice and explanations. And many physicians resent the amount of time they spend trying to explain or make their case, especially during a busy day. But patients’ skepticism about the validity of some treatments seems to be increasing.
“Patients are now more likely to have their own medical explanation for their complaint than they used to, and that can be bad for their health,” Dr. Hood said.
Dr. Hood sees medical cynicism as part of Americans’ growing distrust of experts, leveraged by easy access to the internet. “When people Google, they tend to look for support of their opinions, rather than arrive at a fully educated decision.”
Only about half of patients believe their physicians “provide fair and accurate treatment information all or most of the time,” according to a 2019 survey by the Pew Research Center.
Patients’ distrust has become more obvious during the COVID-19 pandemic, said John Schumann, MD, an internist with Oak Street Health, a practice with more than 500 physicians and other providers in 20 states, treating almost exclusively Medicare patients.
“The skeptics became more entrenched during the pandemic,” said Dr. Schumann, who is based in Tulsa, Okla. “They may think the COVID vaccines were approved too quickly, or believe the pandemic itself is a hoax.”
“There’s a lot of antiscience rhetoric now,” Dr. Schumann added. “I’d say about half of my patients are comfortable with science-based decisions and the other half are not.”
What are patients mistrustful about?
Patients’ suspicions of certain therapies began long before the pandemic. In dermatology, for example, some patients refuse to take topical steroids, said Steven R. Feldman, MD, a dermatologist in Winston-Salem, N.C.
“Their distrust is usually based on anecdotal stories they read about,” he noted. “Patients in other specialties are dead set against vaccinations.”
In addition to refusing treatments and inoculations, some patients ask for questionable regimens mentioned in the news. “Some patients have demanded hydroxychloroquine or Noromectin, drugs that are unproven in the treatment of COVID,” Dr. Schumann said. “We refuse to prescribe them.”
Dr. Hood said patients’ reluctance to follow medical advice can often be based on cost. “I have a patient who was more willing to save $20 than to save his life. But when the progression of his test results fit my predictions, he became more willing to take treatments. I had to wait for the opportune moment to convince him.”
Many naysayer patients keep their views to themselves, and physicians may be unaware that the patients are stonewalling. A 2006 study estimated that about 10%-16% of primary care patients actively resist medical authority.
Dr. Schumann cited patients who don’t want to hear an upsetting diagnosis. “Some patients might refuse to take a biopsy to see if they have cancer because they don’t want to know,” he said. “In many cases, they simply won’t get the biopsy and won’t tell the doctor that they didn’t.”
Sometimes skeptics’ arguments have merit
Some patients’ concerns can be valid, such as when they refuse to go on statins, said Zain Hakeem, DO, a physician in Austin, Tex.
“In some cases, I feel that statins are not necessary,” he said. “The science on statins for primary prevention is not strong, although they should be used for exceedingly high-risk patients.”
Certain patients, especially those with chronic conditions, do a great deal of research, using legitimate sources on the Web, and their research is well supported.
However, these patients can be overconfident in their conclusions. Several studies have shown that with just a little experience, people can replace beginners’ caution with a false sense of competence.
For example, “Patients may not weigh the risks correctly,” Dr. Hakeem said. “They can be more concerned about the risk of having their colon perforated during a colonoscopy, while the risk of cancer if they don’t have a colonoscopy is much higher.”
Some highly successful people may be more likely to trust their own medical instincts. When Steve Jobs, the founder of Apple, was diagnosed with pancreatic cancer in 2003, he put off surgery for 9 months while he tried to cure his disease with a vegan diet, acupuncture, herbs, bowel cleansings, and other remedies he read about. He died in 2011. Some experts believe that delay hastened his death.
Of course, not all physicians’ diagnoses or treatments are correct. One study indicated doctors’ diagnostic error rate could be as high as 15%. And just as patients can be overconfident in their conclusions, so can doctors. Another study found that physicians’ stated confidence in their diagnosis was only slightly affected by the inaccuracy of that diagnosis or the difficulty of the case.
Best ways to deal with cynical patients
Patients’ skepticism can frustrate doctors, reduce the efficiency of care delivery, and interfere with recovery. What can doctors do to deal with these problems?
1. Build the patient’s trust in you. “Getting patients to adhere to your advice involves making sure they feel they have a caring doctor whom they trust,” Dr. Feldman said.
“I want to show patients that I am entirely focused on them,” he added. “For example, I may rush to the door of the exam room from my last appointment, but I open the door very slowly and deliberately, because I want the patient to see that I won’t hurry with them.”
2. Spend time with the patient. Familiarity builds trust. Dr. Schumann said doctors at Oak Street Health see their patients an average of six to eight times a year, an unusually high number. “The more patients see their physicians, the more likely they are to trust them.”
3. Keep up to date. “I make sure I’m up to date with the literature, and I try to present a truthful message,” Dr. Hood said. “For instance, my research showed that inflammation played a strong role in developing complications from COVID, so I wrote a detailed treatment protocol aimed at the inflammation and the immune response, which has been very effective.”
4. Confront patients tactfully. Patients who do research on the Web don’t want to be scolded, Dr. Feldman said. In fact, he praises them, even if he doesn’t agree with their findings. “I might say: ‘What a relief to finally find patients who’ve taken the time to educate themselves before coming here.’ ”
Dr. Feldman is careful not to dispute patients’ conclusions. “Debating the issues is not an effective approach to get patients to trust you. The last thing you want to tell a patient is: ‘Listen to me! I’m an expert.’ People just dig in.”
However, it does help to give patients feedback. “I’m a big fan of patients arguing with me,” Dr. Hakeem said. “It means you can straighten out misunderstandings and improve decision-making.”
5. Explain your reasoning. “You need to communicate clearly and show them your thinking,” Dr. Hood said. “For instance, I’ll explain why a patient has a strong risk for heart attack.”
6. Acknowledge uncertainties. “The doctor may present the science as far more certain than it is,” Dr. Hakeem said. “If you don’t acknowledge the uncertainties, you could break the patient’s trust in you.”
7. Don’t use a lot of numbers. “Data is not a good tool to convince patients,” Dr. Feldman said. “The human brain isn’t designed to work that way.”
If you want to use numbers to show clinical risk, Dr. Hakeem advisd using natural frequencies, such as 10 out of 10,000, which is less confusing to the patient than the equivalent percentage of 0.1%.
It can be helpful to refer to familiar concepts. One way to understand a risk is to compare it with risks in daily life, such as the dangers of driving or falling in the shower, Dr. Hakeem added.
Dr. Feldman often refers to another person’s experience when presenting his medical advice. “I might say to the patient: ‘You remind me of another patient I had. They were sitting in the same chair you’re sitting in. They did really well on this drug, and I think it’s probably the best choice for you, too.’ ”
8. Adopt shared decision-making. This approach involves empowering the patient to become an equal partner in medical decisions. The patient is given information through portals and is encouraged to do research. Critics, however, say that most patients don’t want this degree of empowerment and would rather depend on the doctor’s advice.
Conclusion
It’s often impossible to get through to a skeptical patient, which can be disheartening for doctors. “Physicians want to do what is best for the patient, so when the patient doesn’t listen, they may take it personally,” Dr. Hood said. “But you always have to remember, the patient is the one with disease, and it’s up to the patient to open the door.”
Still, some skeptical patients ultimately change their minds. Dr. Schumann said patients who initially declined the COVID vaccine eventually decided to get it. “It often took them more than a year. but it’s never too late.”
A version of this article first appeared on Medscape.com.
“I spoke to him on many occasions about the dangers of COVID, but he just didn’t believe me,” said Dr. Hood, an internist in Lexington, Ky. “He just didn’t give me enough time to help him. He waited to let me know he was ill with COVID and took days to pick up the medicine. Unfortunately, he then passed away.”
The rise of the skeptical patient
It can be extremely frustrating for doctors when patients question or disbelieve their physician’s medical advice and explanations. And many physicians resent the amount of time they spend trying to explain or make their case, especially during a busy day. But patients’ skepticism about the validity of some treatments seems to be increasing.
“Patients are now more likely to have their own medical explanation for their complaint than they used to, and that can be bad for their health,” Dr. Hood said.
Dr. Hood sees medical cynicism as part of Americans’ growing distrust of experts, leveraged by easy access to the internet. “When people Google, they tend to look for support of their opinions, rather than arrive at a fully educated decision.”
Only about half of patients believe their physicians “provide fair and accurate treatment information all or most of the time,” according to a 2019 survey by the Pew Research Center.
Patients’ distrust has become more obvious during the COVID-19 pandemic, said John Schumann, MD, an internist with Oak Street Health, a practice with more than 500 physicians and other providers in 20 states, treating almost exclusively Medicare patients.
“The skeptics became more entrenched during the pandemic,” said Dr. Schumann, who is based in Tulsa, Okla. “They may think the COVID vaccines were approved too quickly, or believe the pandemic itself is a hoax.”
“There’s a lot of antiscience rhetoric now,” Dr. Schumann added. “I’d say about half of my patients are comfortable with science-based decisions and the other half are not.”
What are patients mistrustful about?
Patients’ suspicions of certain therapies began long before the pandemic. In dermatology, for example, some patients refuse to take topical steroids, said Steven R. Feldman, MD, a dermatologist in Winston-Salem, N.C.
“Their distrust is usually based on anecdotal stories they read about,” he noted. “Patients in other specialties are dead set against vaccinations.”
In addition to refusing treatments and inoculations, some patients ask for questionable regimens mentioned in the news. “Some patients have demanded hydroxychloroquine or Noromectin, drugs that are unproven in the treatment of COVID,” Dr. Schumann said. “We refuse to prescribe them.”
Dr. Hood said patients’ reluctance to follow medical advice can often be based on cost. “I have a patient who was more willing to save $20 than to save his life. But when the progression of his test results fit my predictions, he became more willing to take treatments. I had to wait for the opportune moment to convince him.”
Many naysayer patients keep their views to themselves, and physicians may be unaware that the patients are stonewalling. A 2006 study estimated that about 10%-16% of primary care patients actively resist medical authority.
Dr. Schumann cited patients who don’t want to hear an upsetting diagnosis. “Some patients might refuse to take a biopsy to see if they have cancer because they don’t want to know,” he said. “In many cases, they simply won’t get the biopsy and won’t tell the doctor that they didn’t.”
Sometimes skeptics’ arguments have merit
Some patients’ concerns can be valid, such as when they refuse to go on statins, said Zain Hakeem, DO, a physician in Austin, Tex.
“In some cases, I feel that statins are not necessary,” he said. “The science on statins for primary prevention is not strong, although they should be used for exceedingly high-risk patients.”
Certain patients, especially those with chronic conditions, do a great deal of research, using legitimate sources on the Web, and their research is well supported.
However, these patients can be overconfident in their conclusions. Several studies have shown that with just a little experience, people can replace beginners’ caution with a false sense of competence.
For example, “Patients may not weigh the risks correctly,” Dr. Hakeem said. “They can be more concerned about the risk of having their colon perforated during a colonoscopy, while the risk of cancer if they don’t have a colonoscopy is much higher.”
Some highly successful people may be more likely to trust their own medical instincts. When Steve Jobs, the founder of Apple, was diagnosed with pancreatic cancer in 2003, he put off surgery for 9 months while he tried to cure his disease with a vegan diet, acupuncture, herbs, bowel cleansings, and other remedies he read about. He died in 2011. Some experts believe that delay hastened his death.
Of course, not all physicians’ diagnoses or treatments are correct. One study indicated doctors’ diagnostic error rate could be as high as 15%. And just as patients can be overconfident in their conclusions, so can doctors. Another study found that physicians’ stated confidence in their diagnosis was only slightly affected by the inaccuracy of that diagnosis or the difficulty of the case.
Best ways to deal with cynical patients
Patients’ skepticism can frustrate doctors, reduce the efficiency of care delivery, and interfere with recovery. What can doctors do to deal with these problems?
1. Build the patient’s trust in you. “Getting patients to adhere to your advice involves making sure they feel they have a caring doctor whom they trust,” Dr. Feldman said.
“I want to show patients that I am entirely focused on them,” he added. “For example, I may rush to the door of the exam room from my last appointment, but I open the door very slowly and deliberately, because I want the patient to see that I won’t hurry with them.”
2. Spend time with the patient. Familiarity builds trust. Dr. Schumann said doctors at Oak Street Health see their patients an average of six to eight times a year, an unusually high number. “The more patients see their physicians, the more likely they are to trust them.”
3. Keep up to date. “I make sure I’m up to date with the literature, and I try to present a truthful message,” Dr. Hood said. “For instance, my research showed that inflammation played a strong role in developing complications from COVID, so I wrote a detailed treatment protocol aimed at the inflammation and the immune response, which has been very effective.”
4. Confront patients tactfully. Patients who do research on the Web don’t want to be scolded, Dr. Feldman said. In fact, he praises them, even if he doesn’t agree with their findings. “I might say: ‘What a relief to finally find patients who’ve taken the time to educate themselves before coming here.’ ”
Dr. Feldman is careful not to dispute patients’ conclusions. “Debating the issues is not an effective approach to get patients to trust you. The last thing you want to tell a patient is: ‘Listen to me! I’m an expert.’ People just dig in.”
However, it does help to give patients feedback. “I’m a big fan of patients arguing with me,” Dr. Hakeem said. “It means you can straighten out misunderstandings and improve decision-making.”
5. Explain your reasoning. “You need to communicate clearly and show them your thinking,” Dr. Hood said. “For instance, I’ll explain why a patient has a strong risk for heart attack.”
6. Acknowledge uncertainties. “The doctor may present the science as far more certain than it is,” Dr. Hakeem said. “If you don’t acknowledge the uncertainties, you could break the patient’s trust in you.”
7. Don’t use a lot of numbers. “Data is not a good tool to convince patients,” Dr. Feldman said. “The human brain isn’t designed to work that way.”
If you want to use numbers to show clinical risk, Dr. Hakeem advisd using natural frequencies, such as 10 out of 10,000, which is less confusing to the patient than the equivalent percentage of 0.1%.
It can be helpful to refer to familiar concepts. One way to understand a risk is to compare it with risks in daily life, such as the dangers of driving or falling in the shower, Dr. Hakeem added.
Dr. Feldman often refers to another person’s experience when presenting his medical advice. “I might say to the patient: ‘You remind me of another patient I had. They were sitting in the same chair you’re sitting in. They did really well on this drug, and I think it’s probably the best choice for you, too.’ ”
8. Adopt shared decision-making. This approach involves empowering the patient to become an equal partner in medical decisions. The patient is given information through portals and is encouraged to do research. Critics, however, say that most patients don’t want this degree of empowerment and would rather depend on the doctor’s advice.
Conclusion
It’s often impossible to get through to a skeptical patient, which can be disheartening for doctors. “Physicians want to do what is best for the patient, so when the patient doesn’t listen, they may take it personally,” Dr. Hood said. “But you always have to remember, the patient is the one with disease, and it’s up to the patient to open the door.”
Still, some skeptical patients ultimately change their minds. Dr. Schumann said patients who initially declined the COVID vaccine eventually decided to get it. “It often took them more than a year. but it’s never too late.”
A version of this article first appeared on Medscape.com.
New deep dive into Paxlovid interactions with CVD meds
Nirmatrelvir/ritonavir (Paxlovid) has been a game changer for high-risk patients with early COVID-19 symptoms but has significant interactions with commonly used cardiovascular medications, a new paper cautions.
COVID-19 patients with cardiovascular disease (CVD) or risk factors such as diabetes, hypertension, and chronic kidney disease are at high risk of severe disease and account for the lion’s share of those receiving Paxlovid. Data from the initial EPIC-HR trial and recent real-world data also suggest they’re among the most likely to benefit from the oral antiviral, regardless of their COVID-19 vaccination status.
“But at the same time, it unfortunately interacts with many very commonly prescribed cardiovascular medications and with many of them in a very clinically meaningful way, which may lead to serious adverse consequences,” senior author Sarju Ganatra, MD, said in an interview. “So, while it’s being prescribed with a good intention to help these people, we may actually end up doing more harm than good.
“We don’t want to deter people from getting their necessary COVID-19 treatment, which is excellent for the most part these days as an outpatient,” he added. “So, we felt the need to make a comprehensive list of cardiac medications and level of interactions with Paxlovid and also to help the clinicians and prescribers at the point of care to make the clinical decision of what modifications they may need to do.”
The paper, published online in the Journal of the American College of Cardiology, details drug-drug interactions with some 80 CV medications including statins, antihypertensive agents, heart failure therapies, and antiplatelet/anticoagulants.
It also includes a color-coded figure denoting whether a drug is safe to coadminister with Paxlovid, may potentially interact and require a dose adjustment or temporary discontinuation, or is contraindicated.
Among the commonly used blood thinners, for example, the paper notes that Paxlovid significantly increases drug levels of the direct oral anticoagulants (DOACs) apixaban, rivaroxaban, edoxaban, and dabigatran and, thus, increases the risk of bleeding.
“It can still be administered, if it’s necessary, but the dose of the DOAC either needs to be reduced or held depending on what they are getting it for, whether they’re getting it for pulmonary embolism or atrial fibrillation, and we adjust for all those things in the table in the paper,” said Dr. Ganatra, from Lahey Hospital and Medical Center, Burlington, Mass.
When the DOAC can’t be interrupted or dose adjusted, however, Paxlovid should not be given, the experts said. The antiviral is safe to use with enoxaparin, a low-molecular-weight heparin, but can increase or decrease levels of warfarin and should be used with close international normalized ratio monitoring.
For patients on antiplatelet agents, clinicians are advised to avoid prescribing nirmatrelvir/ritonavir to those on ticagrelor or clopidogrel unless the agents can be replaced by prasugrel.
Ritonavir – an inhibitor of cytochrome P 450 enzymes, particularly CYP3A4 – poses an increased risk of bleeding when given with ticagrelor, a CYP3A4 substrate, and decreases the active metabolite of clopidogrel, cutting its platelet inhibition by 20%. Although there’s a twofold decrease in the maximum concentration of prasugrel in patients on ritonavir, this does not affect its antiplatelet activity, the paper explains.
Among the lipid-lowering agents, experts suggested temporarily withholding atorvastatin, rosuvastatin, simvastatin, and lovastatin because of an increased risk for myopathy and liver toxicity but say that other statins, fibrates, ezetimibe, and the proprotein convertase subtilisin/kexin type 9 inhibitors evolocumab and alirocumab are safe to coadminister with Paxlovid.
While statins typically leave the body within hours, most of the antiarrhythmic drugs, except for sotalol, are not safe to give with Paxlovid, Dr. Ganatra said. It’s technically not feasible to hold these drugs because most have long half-lives, reaching about 100 days, for example, for amiodarone.
“It’s going to hang around in your system for a long time, so you don’t want to be falsely reassured that you’re holding the drug and it’s going to be fine to go back slowly,” he said. “You need to look for alternative therapies in those scenarios for COVID-19 treatment, which could be other antivirals, or a monoclonal antibody individualized to the patient’s risk.”
Although there’s limited clinical information regarding interaction-related adverse events with Paxlovid, the team used pharmacokinetics and pharmacodynamics data to provide the guidance. Serious adverse events are also well documented for ritonavir, which has been prescribed for years to treat HIV, Dr. Ganatra noted.
The Infectious Disease Society of America also published guidance on the management of potential drug interactions with Paxlovid in May and, earlier in October, the Food and Drug Administration updated its Paxlovid patient eligibility screening checklist.
Still, most prescribers are actually primary care physicians and even pharmacists, who may not be completely attuned, said Dr. Ganatra, who noted that some centers have started programs to help connect primary care physicians with their cardiology colleagues to check on CV drugs in their COVID-19 patients.
“We need to be thinking more broadly and at a system level where the hospital or health care system leverages the electronic health record systems,” he said. “Most of them are sophisticated enough to incorporate simple drug-drug interaction information, so if you try to prescribe someone Paxlovid and it’s a heart transplant patient who is on immunosuppressive therapy or a patient on a blood thinner, then it should give you a warning ... or at least give them a link to our paper or other valuable resources.
“If someone is on a blood thinner and the blood thinner level goes up by ninefold, we can only imagine what we would be dealing with,” Dr. Ganatra said. “So, these interactions should be taken very seriously and I think it’s worth the time and investment.”
The authors reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Nirmatrelvir/ritonavir (Paxlovid) has been a game changer for high-risk patients with early COVID-19 symptoms but has significant interactions with commonly used cardiovascular medications, a new paper cautions.
COVID-19 patients with cardiovascular disease (CVD) or risk factors such as diabetes, hypertension, and chronic kidney disease are at high risk of severe disease and account for the lion’s share of those receiving Paxlovid. Data from the initial EPIC-HR trial and recent real-world data also suggest they’re among the most likely to benefit from the oral antiviral, regardless of their COVID-19 vaccination status.
“But at the same time, it unfortunately interacts with many very commonly prescribed cardiovascular medications and with many of them in a very clinically meaningful way, which may lead to serious adverse consequences,” senior author Sarju Ganatra, MD, said in an interview. “So, while it’s being prescribed with a good intention to help these people, we may actually end up doing more harm than good.
“We don’t want to deter people from getting their necessary COVID-19 treatment, which is excellent for the most part these days as an outpatient,” he added. “So, we felt the need to make a comprehensive list of cardiac medications and level of interactions with Paxlovid and also to help the clinicians and prescribers at the point of care to make the clinical decision of what modifications they may need to do.”
The paper, published online in the Journal of the American College of Cardiology, details drug-drug interactions with some 80 CV medications including statins, antihypertensive agents, heart failure therapies, and antiplatelet/anticoagulants.
It also includes a color-coded figure denoting whether a drug is safe to coadminister with Paxlovid, may potentially interact and require a dose adjustment or temporary discontinuation, or is contraindicated.
Among the commonly used blood thinners, for example, the paper notes that Paxlovid significantly increases drug levels of the direct oral anticoagulants (DOACs) apixaban, rivaroxaban, edoxaban, and dabigatran and, thus, increases the risk of bleeding.
“It can still be administered, if it’s necessary, but the dose of the DOAC either needs to be reduced or held depending on what they are getting it for, whether they’re getting it for pulmonary embolism or atrial fibrillation, and we adjust for all those things in the table in the paper,” said Dr. Ganatra, from Lahey Hospital and Medical Center, Burlington, Mass.
When the DOAC can’t be interrupted or dose adjusted, however, Paxlovid should not be given, the experts said. The antiviral is safe to use with enoxaparin, a low-molecular-weight heparin, but can increase or decrease levels of warfarin and should be used with close international normalized ratio monitoring.
For patients on antiplatelet agents, clinicians are advised to avoid prescribing nirmatrelvir/ritonavir to those on ticagrelor or clopidogrel unless the agents can be replaced by prasugrel.
Ritonavir – an inhibitor of cytochrome P 450 enzymes, particularly CYP3A4 – poses an increased risk of bleeding when given with ticagrelor, a CYP3A4 substrate, and decreases the active metabolite of clopidogrel, cutting its platelet inhibition by 20%. Although there’s a twofold decrease in the maximum concentration of prasugrel in patients on ritonavir, this does not affect its antiplatelet activity, the paper explains.
Among the lipid-lowering agents, experts suggested temporarily withholding atorvastatin, rosuvastatin, simvastatin, and lovastatin because of an increased risk for myopathy and liver toxicity but say that other statins, fibrates, ezetimibe, and the proprotein convertase subtilisin/kexin type 9 inhibitors evolocumab and alirocumab are safe to coadminister with Paxlovid.
While statins typically leave the body within hours, most of the antiarrhythmic drugs, except for sotalol, are not safe to give with Paxlovid, Dr. Ganatra said. It’s technically not feasible to hold these drugs because most have long half-lives, reaching about 100 days, for example, for amiodarone.
“It’s going to hang around in your system for a long time, so you don’t want to be falsely reassured that you’re holding the drug and it’s going to be fine to go back slowly,” he said. “You need to look for alternative therapies in those scenarios for COVID-19 treatment, which could be other antivirals, or a monoclonal antibody individualized to the patient’s risk.”
Although there’s limited clinical information regarding interaction-related adverse events with Paxlovid, the team used pharmacokinetics and pharmacodynamics data to provide the guidance. Serious adverse events are also well documented for ritonavir, which has been prescribed for years to treat HIV, Dr. Ganatra noted.
The Infectious Disease Society of America also published guidance on the management of potential drug interactions with Paxlovid in May and, earlier in October, the Food and Drug Administration updated its Paxlovid patient eligibility screening checklist.
Still, most prescribers are actually primary care physicians and even pharmacists, who may not be completely attuned, said Dr. Ganatra, who noted that some centers have started programs to help connect primary care physicians with their cardiology colleagues to check on CV drugs in their COVID-19 patients.
“We need to be thinking more broadly and at a system level where the hospital or health care system leverages the electronic health record systems,” he said. “Most of them are sophisticated enough to incorporate simple drug-drug interaction information, so if you try to prescribe someone Paxlovid and it’s a heart transplant patient who is on immunosuppressive therapy or a patient on a blood thinner, then it should give you a warning ... or at least give them a link to our paper or other valuable resources.
“If someone is on a blood thinner and the blood thinner level goes up by ninefold, we can only imagine what we would be dealing with,” Dr. Ganatra said. “So, these interactions should be taken very seriously and I think it’s worth the time and investment.”
The authors reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Nirmatrelvir/ritonavir (Paxlovid) has been a game changer for high-risk patients with early COVID-19 symptoms but has significant interactions with commonly used cardiovascular medications, a new paper cautions.
COVID-19 patients with cardiovascular disease (CVD) or risk factors such as diabetes, hypertension, and chronic kidney disease are at high risk of severe disease and account for the lion’s share of those receiving Paxlovid. Data from the initial EPIC-HR trial and recent real-world data also suggest they’re among the most likely to benefit from the oral antiviral, regardless of their COVID-19 vaccination status.
“But at the same time, it unfortunately interacts with many very commonly prescribed cardiovascular medications and with many of them in a very clinically meaningful way, which may lead to serious adverse consequences,” senior author Sarju Ganatra, MD, said in an interview. “So, while it’s being prescribed with a good intention to help these people, we may actually end up doing more harm than good.
“We don’t want to deter people from getting their necessary COVID-19 treatment, which is excellent for the most part these days as an outpatient,” he added. “So, we felt the need to make a comprehensive list of cardiac medications and level of interactions with Paxlovid and also to help the clinicians and prescribers at the point of care to make the clinical decision of what modifications they may need to do.”
The paper, published online in the Journal of the American College of Cardiology, details drug-drug interactions with some 80 CV medications including statins, antihypertensive agents, heart failure therapies, and antiplatelet/anticoagulants.
It also includes a color-coded figure denoting whether a drug is safe to coadminister with Paxlovid, may potentially interact and require a dose adjustment or temporary discontinuation, or is contraindicated.
Among the commonly used blood thinners, for example, the paper notes that Paxlovid significantly increases drug levels of the direct oral anticoagulants (DOACs) apixaban, rivaroxaban, edoxaban, and dabigatran and, thus, increases the risk of bleeding.
“It can still be administered, if it’s necessary, but the dose of the DOAC either needs to be reduced or held depending on what they are getting it for, whether they’re getting it for pulmonary embolism or atrial fibrillation, and we adjust for all those things in the table in the paper,” said Dr. Ganatra, from Lahey Hospital and Medical Center, Burlington, Mass.
When the DOAC can’t be interrupted or dose adjusted, however, Paxlovid should not be given, the experts said. The antiviral is safe to use with enoxaparin, a low-molecular-weight heparin, but can increase or decrease levels of warfarin and should be used with close international normalized ratio monitoring.
For patients on antiplatelet agents, clinicians are advised to avoid prescribing nirmatrelvir/ritonavir to those on ticagrelor or clopidogrel unless the agents can be replaced by prasugrel.
Ritonavir – an inhibitor of cytochrome P 450 enzymes, particularly CYP3A4 – poses an increased risk of bleeding when given with ticagrelor, a CYP3A4 substrate, and decreases the active metabolite of clopidogrel, cutting its platelet inhibition by 20%. Although there’s a twofold decrease in the maximum concentration of prasugrel in patients on ritonavir, this does not affect its antiplatelet activity, the paper explains.
Among the lipid-lowering agents, experts suggested temporarily withholding atorvastatin, rosuvastatin, simvastatin, and lovastatin because of an increased risk for myopathy and liver toxicity but say that other statins, fibrates, ezetimibe, and the proprotein convertase subtilisin/kexin type 9 inhibitors evolocumab and alirocumab are safe to coadminister with Paxlovid.
While statins typically leave the body within hours, most of the antiarrhythmic drugs, except for sotalol, are not safe to give with Paxlovid, Dr. Ganatra said. It’s technically not feasible to hold these drugs because most have long half-lives, reaching about 100 days, for example, for amiodarone.
“It’s going to hang around in your system for a long time, so you don’t want to be falsely reassured that you’re holding the drug and it’s going to be fine to go back slowly,” he said. “You need to look for alternative therapies in those scenarios for COVID-19 treatment, which could be other antivirals, or a monoclonal antibody individualized to the patient’s risk.”
Although there’s limited clinical information regarding interaction-related adverse events with Paxlovid, the team used pharmacokinetics and pharmacodynamics data to provide the guidance. Serious adverse events are also well documented for ritonavir, which has been prescribed for years to treat HIV, Dr. Ganatra noted.
The Infectious Disease Society of America also published guidance on the management of potential drug interactions with Paxlovid in May and, earlier in October, the Food and Drug Administration updated its Paxlovid patient eligibility screening checklist.
Still, most prescribers are actually primary care physicians and even pharmacists, who may not be completely attuned, said Dr. Ganatra, who noted that some centers have started programs to help connect primary care physicians with their cardiology colleagues to check on CV drugs in their COVID-19 patients.
“We need to be thinking more broadly and at a system level where the hospital or health care system leverages the electronic health record systems,” he said. “Most of them are sophisticated enough to incorporate simple drug-drug interaction information, so if you try to prescribe someone Paxlovid and it’s a heart transplant patient who is on immunosuppressive therapy or a patient on a blood thinner, then it should give you a warning ... or at least give them a link to our paper or other valuable resources.
“If someone is on a blood thinner and the blood thinner level goes up by ninefold, we can only imagine what we would be dealing with,” Dr. Ganatra said. “So, these interactions should be taken very seriously and I think it’s worth the time and investment.”
The authors reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FROM THE JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY
Starting a blog
. Health information is one of the most popular topics people search for online. Starting a physician blog can provide your practice with promotional and marketing benefits that you may have a difficult time finding elsewhere. A blog can be an effective way to drive traffic to your website, establish yourself as an authority or expert in a particular area, and stay on the radar with your patients. However, there are a few things you should think about before you start.
Start by determining what you want to accomplish. Do you want to reach quantitative milestones, like a certain number of followers, or are you looking to increase your website traffic from potential patients? One goal will probably be to augment the health knowledge of your patients. Decide early on what your benchmarks will be and how you will track them.
Next, determine who your potential readers are. Initially, most will probably be local (your existing patient base and their family and friends), but your audience may expand geographically as your blog gains in popularity.
By now, you probably realize that blogging will require a significant commitment, over and above the time needed to write the content. Decide whether you have the time and energy to take this on yourself, or whether help will be needed. Ideally, you should have one person in charge of all your social media efforts, so that everything is consistent and has the same voice. That person can be in-house, or you can outsource to any of the many companies that administer blogs and other media functions. (As always, I have no financial interest in any company or service mentioned in this column.)
The advantage of hiring an outside administrator is that a professionally designed blog will be far more attractive and polished than anything you could build yourself. Furthermore, an experienced designer will employ “search engine optimization” (SEO), meaning that content will be created using key words and phrases that will make it readily visible to search engine users.
You can leave design and SEO to the pros, but don’t delegate the content itself; as captain of the ship you are responsible for all the facts and opinions on your blog. You may not be up to writing everything yourself, but anything you don’t write personally needs to be scrutinized by you personally to make sure that it is factually accurate and reflects your personal view. And remember that, once it’s online, it’s online forever; consider the ramifications of anything you post on any site – yours or others – before hitting the “send” button. “The most damaging item about you,” one consultant told me, “could well be something you post yourself.” Just ask any of several prominent politicians who have famously sabotaged their own careers online.
That said, don’t be shy about creating content. Patients appreciate factual information, but they value your opinions too. Give people content that will be of interest or benefit to them. This can include health-related tips, reminders, suggestions, whatever. If they are interested in it, they will keep reading and may even share it with others. You should also write about subjects – medical and otherwise – that interest you personally. If you have expertise in a particular field, be sure to write about that.
Your practice is a local business, so localize your blog to attract people from your area. Be sure to include local city keywords in your writing. You may also want to post about local events in which your practice is involved.
Try to avoid political diatribes. While most physicians have strong political opinions, and some are not shy about expressing them, there are many venues that are more appropriate for those discussions than medical blogs. Also avoid outright sales pitches. It’s fine to describe procedures that you offer, but aggressive solicitation will only turn readers off.
Keep any medical advice in general terms; don’t use any specific examples that might make a patient identifiable and generate a HIPAA violation.
If you are having trouble growing your readership, use your practice’s Facebook page to push blog updates into patients’ feeds. Additionally, track Twitter hashtags that are relevant to your practice, and use them to find existing online communities with an interest in your blog’s topics.
Dr. Eastern practices dermatology and dermatologic surgery in Belleville, N.J. He is the author of numerous articles and textbook chapters, and is a longtime monthly columnist for Dermatology News. Write to him at [email protected].
*This article was updated 10/17/2022.
. Health information is one of the most popular topics people search for online. Starting a physician blog can provide your practice with promotional and marketing benefits that you may have a difficult time finding elsewhere. A blog can be an effective way to drive traffic to your website, establish yourself as an authority or expert in a particular area, and stay on the radar with your patients. However, there are a few things you should think about before you start.
Start by determining what you want to accomplish. Do you want to reach quantitative milestones, like a certain number of followers, or are you looking to increase your website traffic from potential patients? One goal will probably be to augment the health knowledge of your patients. Decide early on what your benchmarks will be and how you will track them.
Next, determine who your potential readers are. Initially, most will probably be local (your existing patient base and their family and friends), but your audience may expand geographically as your blog gains in popularity.
By now, you probably realize that blogging will require a significant commitment, over and above the time needed to write the content. Decide whether you have the time and energy to take this on yourself, or whether help will be needed. Ideally, you should have one person in charge of all your social media efforts, so that everything is consistent and has the same voice. That person can be in-house, or you can outsource to any of the many companies that administer blogs and other media functions. (As always, I have no financial interest in any company or service mentioned in this column.)
The advantage of hiring an outside administrator is that a professionally designed blog will be far more attractive and polished than anything you could build yourself. Furthermore, an experienced designer will employ “search engine optimization” (SEO), meaning that content will be created using key words and phrases that will make it readily visible to search engine users.
You can leave design and SEO to the pros, but don’t delegate the content itself; as captain of the ship you are responsible for all the facts and opinions on your blog. You may not be up to writing everything yourself, but anything you don’t write personally needs to be scrutinized by you personally to make sure that it is factually accurate and reflects your personal view. And remember that, once it’s online, it’s online forever; consider the ramifications of anything you post on any site – yours or others – before hitting the “send” button. “The most damaging item about you,” one consultant told me, “could well be something you post yourself.” Just ask any of several prominent politicians who have famously sabotaged their own careers online.
That said, don’t be shy about creating content. Patients appreciate factual information, but they value your opinions too. Give people content that will be of interest or benefit to them. This can include health-related tips, reminders, suggestions, whatever. If they are interested in it, they will keep reading and may even share it with others. You should also write about subjects – medical and otherwise – that interest you personally. If you have expertise in a particular field, be sure to write about that.
Your practice is a local business, so localize your blog to attract people from your area. Be sure to include local city keywords in your writing. You may also want to post about local events in which your practice is involved.
Try to avoid political diatribes. While most physicians have strong political opinions, and some are not shy about expressing them, there are many venues that are more appropriate for those discussions than medical blogs. Also avoid outright sales pitches. It’s fine to describe procedures that you offer, but aggressive solicitation will only turn readers off.
Keep any medical advice in general terms; don’t use any specific examples that might make a patient identifiable and generate a HIPAA violation.
If you are having trouble growing your readership, use your practice’s Facebook page to push blog updates into patients’ feeds. Additionally, track Twitter hashtags that are relevant to your practice, and use them to find existing online communities with an interest in your blog’s topics.
Dr. Eastern practices dermatology and dermatologic surgery in Belleville, N.J. He is the author of numerous articles and textbook chapters, and is a longtime monthly columnist for Dermatology News. Write to him at [email protected].
*This article was updated 10/17/2022.
. Health information is one of the most popular topics people search for online. Starting a physician blog can provide your practice with promotional and marketing benefits that you may have a difficult time finding elsewhere. A blog can be an effective way to drive traffic to your website, establish yourself as an authority or expert in a particular area, and stay on the radar with your patients. However, there are a few things you should think about before you start.
Start by determining what you want to accomplish. Do you want to reach quantitative milestones, like a certain number of followers, or are you looking to increase your website traffic from potential patients? One goal will probably be to augment the health knowledge of your patients. Decide early on what your benchmarks will be and how you will track them.
Next, determine who your potential readers are. Initially, most will probably be local (your existing patient base and their family and friends), but your audience may expand geographically as your blog gains in popularity.
By now, you probably realize that blogging will require a significant commitment, over and above the time needed to write the content. Decide whether you have the time and energy to take this on yourself, or whether help will be needed. Ideally, you should have one person in charge of all your social media efforts, so that everything is consistent and has the same voice. That person can be in-house, or you can outsource to any of the many companies that administer blogs and other media functions. (As always, I have no financial interest in any company or service mentioned in this column.)
The advantage of hiring an outside administrator is that a professionally designed blog will be far more attractive and polished than anything you could build yourself. Furthermore, an experienced designer will employ “search engine optimization” (SEO), meaning that content will be created using key words and phrases that will make it readily visible to search engine users.
You can leave design and SEO to the pros, but don’t delegate the content itself; as captain of the ship you are responsible for all the facts and opinions on your blog. You may not be up to writing everything yourself, but anything you don’t write personally needs to be scrutinized by you personally to make sure that it is factually accurate and reflects your personal view. And remember that, once it’s online, it’s online forever; consider the ramifications of anything you post on any site – yours or others – before hitting the “send” button. “The most damaging item about you,” one consultant told me, “could well be something you post yourself.” Just ask any of several prominent politicians who have famously sabotaged their own careers online.
That said, don’t be shy about creating content. Patients appreciate factual information, but they value your opinions too. Give people content that will be of interest or benefit to them. This can include health-related tips, reminders, suggestions, whatever. If they are interested in it, they will keep reading and may even share it with others. You should also write about subjects – medical and otherwise – that interest you personally. If you have expertise in a particular field, be sure to write about that.
Your practice is a local business, so localize your blog to attract people from your area. Be sure to include local city keywords in your writing. You may also want to post about local events in which your practice is involved.
Try to avoid political diatribes. While most physicians have strong political opinions, and some are not shy about expressing them, there are many venues that are more appropriate for those discussions than medical blogs. Also avoid outright sales pitches. It’s fine to describe procedures that you offer, but aggressive solicitation will only turn readers off.
Keep any medical advice in general terms; don’t use any specific examples that might make a patient identifiable and generate a HIPAA violation.
If you are having trouble growing your readership, use your practice’s Facebook page to push blog updates into patients’ feeds. Additionally, track Twitter hashtags that are relevant to your practice, and use them to find existing online communities with an interest in your blog’s topics.
Dr. Eastern practices dermatology and dermatologic surgery in Belleville, N.J. He is the author of numerous articles and textbook chapters, and is a longtime monthly columnist for Dermatology News. Write to him at [email protected].
*This article was updated 10/17/2022.