User login
Older age at primary progressive MS onset predicted faster disability accumulation
In patients with primary progressive multiple sclerosis, older age and bilateral motor symptoms at disease onset predicted faster disability progression in a retrospective analysis of prospectively collected data.
Age was the most important predictor, but both factors seemed to affect disability accumulation throughout the course of primary progressive multiple sclerosis (PPMS), in contrast to the distinct stages and risk factors that characterize relapsing-remitting disease, said Dr. Marcus W. Koch and his associates at the University of Calgary (Alta.).
Primary progressive disease affects about 10%-20% of MS patients. To study its natural history, the investigators analyzed data on 446 patients with PPMS who were followed for a median of 14 years from disease onset (J. Neurol. Neurosurg. Psychiatry 2014 Aug. 4 [doi:10.1136/jnnp-2014-307948]).
Patients reached Expanded Disability Status Scale (EDSS) scores of 4 and 6 a median of 5 and 9 years after disease onset, the researchers said. Median age at EDSS = 4 was 51 years, and median age at EDSS = 6 was 55 years, they added. For each 1-year increase in age at disease onset, time to progression to EDSS = 4 decreased by 3% (hazard ratio per 1-year increase, 1.03; 95% confidence interval, 1.02-1.04), and time from onset to EDSS = 6 decreased by 4% (HR, 1.04; 95% CI, 1.02-1.05), the researchers reported.
Patients with bilateral motor onset symptoms also progressed to EDSS scores of 4 and 6 significantly faster than did patients with unilateral onset motor symptoms (P = .005 and .03, respectively), the investigators reported.
The researchers excluded some patients from analyses because of missing data, and these patients were significantly more likely to be female and to have a younger age at onset than were the patients who were included in analyses. They also did not subgroup PPMS patients by disease course because the criteria for these subcategories were not published until after the study began, they said (Neurology 2014;83:278-86).
Funding information for the study was not available. The authors reported no conflicts of interest.
In patients with primary progressive multiple sclerosis, older age and bilateral motor symptoms at disease onset predicted faster disability progression in a retrospective analysis of prospectively collected data.
Age was the most important predictor, but both factors seemed to affect disability accumulation throughout the course of primary progressive multiple sclerosis (PPMS), in contrast to the distinct stages and risk factors that characterize relapsing-remitting disease, said Dr. Marcus W. Koch and his associates at the University of Calgary (Alta.).
Primary progressive disease affects about 10%-20% of MS patients. To study its natural history, the investigators analyzed data on 446 patients with PPMS who were followed for a median of 14 years from disease onset (J. Neurol. Neurosurg. Psychiatry 2014 Aug. 4 [doi:10.1136/jnnp-2014-307948]).
Patients reached Expanded Disability Status Scale (EDSS) scores of 4 and 6 a median of 5 and 9 years after disease onset, the researchers said. Median age at EDSS = 4 was 51 years, and median age at EDSS = 6 was 55 years, they added. For each 1-year increase in age at disease onset, time to progression to EDSS = 4 decreased by 3% (hazard ratio per 1-year increase, 1.03; 95% confidence interval, 1.02-1.04), and time from onset to EDSS = 6 decreased by 4% (HR, 1.04; 95% CI, 1.02-1.05), the researchers reported.
Patients with bilateral motor onset symptoms also progressed to EDSS scores of 4 and 6 significantly faster than did patients with unilateral onset motor symptoms (P = .005 and .03, respectively), the investigators reported.
The researchers excluded some patients from analyses because of missing data, and these patients were significantly more likely to be female and to have a younger age at onset than were the patients who were included in analyses. They also did not subgroup PPMS patients by disease course because the criteria for these subcategories were not published until after the study began, they said (Neurology 2014;83:278-86).
Funding information for the study was not available. The authors reported no conflicts of interest.
In patients with primary progressive multiple sclerosis, older age and bilateral motor symptoms at disease onset predicted faster disability progression in a retrospective analysis of prospectively collected data.
Age was the most important predictor, but both factors seemed to affect disability accumulation throughout the course of primary progressive multiple sclerosis (PPMS), in contrast to the distinct stages and risk factors that characterize relapsing-remitting disease, said Dr. Marcus W. Koch and his associates at the University of Calgary (Alta.).
Primary progressive disease affects about 10%-20% of MS patients. To study its natural history, the investigators analyzed data on 446 patients with PPMS who were followed for a median of 14 years from disease onset (J. Neurol. Neurosurg. Psychiatry 2014 Aug. 4 [doi:10.1136/jnnp-2014-307948]).
Patients reached Expanded Disability Status Scale (EDSS) scores of 4 and 6 a median of 5 and 9 years after disease onset, the researchers said. Median age at EDSS = 4 was 51 years, and median age at EDSS = 6 was 55 years, they added. For each 1-year increase in age at disease onset, time to progression to EDSS = 4 decreased by 3% (hazard ratio per 1-year increase, 1.03; 95% confidence interval, 1.02-1.04), and time from onset to EDSS = 6 decreased by 4% (HR, 1.04; 95% CI, 1.02-1.05), the researchers reported.
Patients with bilateral motor onset symptoms also progressed to EDSS scores of 4 and 6 significantly faster than did patients with unilateral onset motor symptoms (P = .005 and .03, respectively), the investigators reported.
The researchers excluded some patients from analyses because of missing data, and these patients were significantly more likely to be female and to have a younger age at onset than were the patients who were included in analyses. They also did not subgroup PPMS patients by disease course because the criteria for these subcategories were not published until after the study began, they said (Neurology 2014;83:278-86).
Funding information for the study was not available. The authors reported no conflicts of interest.
FROM JOURNAL OF NEUROLOGY, NEUROSURGERY & PSYCHIATRY
Key clinical point: Older age at disease onset predicted faster disability accumulation in patients with primary progressive multiple sclerosis.
Major finding: For each 1-year increase in age at disease onset, time to progression to EDSS = 4 fell by 3% (HR per 1-year increase, 1.03; 95% CI, 1.02-1.04), and time to EDSS = 6 dropped by 4% (HR, 1.04; 95% CI, 1.02-1.05).
Data source: A retrospective analysis of prospectively collected data on 446 patients with primary progressive multiple sclerosis who were followed for a median of 14 years from disease onset.
Disclosures: Funding information was not available. The authors reported no conflicts of interest.
Study identified predictors of ICU survival in lung cancer patients
Intensive care units can provide meaningful survival for patients with lung cancer who have good performance status and nonrecurrent disease, even if they have severe complications such as sepsis or multiple organ failure, authors of a multicenter observational cohort study reported online in Annals of Oncology.
Mortality rates, however, were "very high" in ICU patients with poor performance status who were deemed unfit for lung cancer treatment, indicating that palliative care may be their best option, said Dr. Marcio Soares of the Instituto Nacional de Câncer and the D’Or Institute for Research and Education, Rio de Janeiro, and his associates.
Patients with lung cancer often are seen as having poor ICU outcomes, even though survival data and multicenter studies for these patients are lacking, the investigators said. They carried out a prospective, multicenter observational cohort study of 449 adults with lung cancer who were admitted to 22 intensive care units in six European and South American countries. A total of 394 (88%) patients had non–small cell lung cancer and the rest had small cell disease (Ann. Oncol. 2014 June 20 [doi:10.1093/annonc/mdu234]).
In all, 28% of patients died in the ICU: 41% of those died within 30 days of admission and 55% died within 6 months – rates that resemble those for unselected ICU cancer patients from prior multicenter studies. Most 6-month survivors were living at home. After the researchers controlled for medical versus surgical ICU admission and early decisions to limit treatment, predictors of 30-day and 6-month mortality included poor performance status; presence of recurrent or progressive disease; cancer complications such as airway compromise, deep vein thrombosis, and superior vena cava syndrome; and severity of acute organ dysfunction, Dr. Soares and his associates reported.
"Importantly, admission to high-volume centers was associated with lower mortality. This effect may be related to expertise, closer collaboration between oncologists and intensivists, or more efficient ICU triage policies," the investigators added.
The study was based on a convenience sample of ICUs, and the researchers said that they did not collect data on quality of life or follow patients beyond 6 months after ICU admission.
The authors reported no conflicts of interest. The study was supported by the National Council for Scientific and Technological Development and Fundação Carlos Chagas Filho de Amparo à Pesquisa do Estado do Rio de Janeiro, and by departmental funds from the D’Or Institute for Research and Education and Instituto Nacional de Câncer in Brazil.
Intensive care units can provide meaningful survival for patients with lung cancer who have good performance status and nonrecurrent disease, even if they have severe complications such as sepsis or multiple organ failure, authors of a multicenter observational cohort study reported online in Annals of Oncology.
Mortality rates, however, were "very high" in ICU patients with poor performance status who were deemed unfit for lung cancer treatment, indicating that palliative care may be their best option, said Dr. Marcio Soares of the Instituto Nacional de Câncer and the D’Or Institute for Research and Education, Rio de Janeiro, and his associates.
Patients with lung cancer often are seen as having poor ICU outcomes, even though survival data and multicenter studies for these patients are lacking, the investigators said. They carried out a prospective, multicenter observational cohort study of 449 adults with lung cancer who were admitted to 22 intensive care units in six European and South American countries. A total of 394 (88%) patients had non–small cell lung cancer and the rest had small cell disease (Ann. Oncol. 2014 June 20 [doi:10.1093/annonc/mdu234]).
In all, 28% of patients died in the ICU: 41% of those died within 30 days of admission and 55% died within 6 months – rates that resemble those for unselected ICU cancer patients from prior multicenter studies. Most 6-month survivors were living at home. After the researchers controlled for medical versus surgical ICU admission and early decisions to limit treatment, predictors of 30-day and 6-month mortality included poor performance status; presence of recurrent or progressive disease; cancer complications such as airway compromise, deep vein thrombosis, and superior vena cava syndrome; and severity of acute organ dysfunction, Dr. Soares and his associates reported.
"Importantly, admission to high-volume centers was associated with lower mortality. This effect may be related to expertise, closer collaboration between oncologists and intensivists, or more efficient ICU triage policies," the investigators added.
The study was based on a convenience sample of ICUs, and the researchers said that they did not collect data on quality of life or follow patients beyond 6 months after ICU admission.
The authors reported no conflicts of interest. The study was supported by the National Council for Scientific and Technological Development and Fundação Carlos Chagas Filho de Amparo à Pesquisa do Estado do Rio de Janeiro, and by departmental funds from the D’Or Institute for Research and Education and Instituto Nacional de Câncer in Brazil.
Intensive care units can provide meaningful survival for patients with lung cancer who have good performance status and nonrecurrent disease, even if they have severe complications such as sepsis or multiple organ failure, authors of a multicenter observational cohort study reported online in Annals of Oncology.
Mortality rates, however, were "very high" in ICU patients with poor performance status who were deemed unfit for lung cancer treatment, indicating that palliative care may be their best option, said Dr. Marcio Soares of the Instituto Nacional de Câncer and the D’Or Institute for Research and Education, Rio de Janeiro, and his associates.
Patients with lung cancer often are seen as having poor ICU outcomes, even though survival data and multicenter studies for these patients are lacking, the investigators said. They carried out a prospective, multicenter observational cohort study of 449 adults with lung cancer who were admitted to 22 intensive care units in six European and South American countries. A total of 394 (88%) patients had non–small cell lung cancer and the rest had small cell disease (Ann. Oncol. 2014 June 20 [doi:10.1093/annonc/mdu234]).
In all, 28% of patients died in the ICU: 41% of those died within 30 days of admission and 55% died within 6 months – rates that resemble those for unselected ICU cancer patients from prior multicenter studies. Most 6-month survivors were living at home. After the researchers controlled for medical versus surgical ICU admission and early decisions to limit treatment, predictors of 30-day and 6-month mortality included poor performance status; presence of recurrent or progressive disease; cancer complications such as airway compromise, deep vein thrombosis, and superior vena cava syndrome; and severity of acute organ dysfunction, Dr. Soares and his associates reported.
"Importantly, admission to high-volume centers was associated with lower mortality. This effect may be related to expertise, closer collaboration between oncologists and intensivists, or more efficient ICU triage policies," the investigators added.
The study was based on a convenience sample of ICUs, and the researchers said that they did not collect data on quality of life or follow patients beyond 6 months after ICU admission.
The authors reported no conflicts of interest. The study was supported by the National Council for Scientific and Technological Development and Fundação Carlos Chagas Filho de Amparo à Pesquisa do Estado do Rio de Janeiro, and by departmental funds from the D’Or Institute for Research and Education and Instituto Nacional de Câncer in Brazil.
FROM ANNALS OF ONCOLOGY
Key clinical point: Palliative care may be a better option than ICU admission for lung cancer patients deemed unfit for anticancer treatment who have poor performance status.
Major finding: Predictors of 30-day and 6-month mortality included recurrent or progressive cancer, acute organ dysfunction, poor performance status, and cancer-related complications.
Data source: Prospective observational cohort study of 449 adults with lung cancer who were admitted to 22 intensive care units in six European and South American countries. A total of 394 (88%) patients had non–small cell lung cancer and the rest had small cell disease.
Disclosures: The authors reported no conflicts of interest. The study was supported by the National Council for Scientific and Technological Development and Fundação Carlos Chagas Filho de Amparo à Pesquisa do Estado do Rio de Janeiro, and by departmental funds from the D’Or Institute for Research and Education and Instituto Nacional de Câncer in Brazil.
Chikungunya Vaccine Safe, Immunogenic in Phase I Trial
A novel chikungunya virus vaccine caused no serious adverse effects and was about as immunogenic as natural infection, authors of a phase I trial reported in the Lancet.
Eleven months after receiving the noninfectious viruslike particle (VLP) vaccine, trial participants had neutralizing antibody titers that resembled those seen in natural infection, said Dr. Lee-Jah Chang and associates at the National Institutes of Health in Bethesda, Md. (Lancet 2014 Aug. 15 [doi: 10.1016/S0140-6736(14)61185-5]).
Chikungunya virus infection is rarely fatal, but it causes fever and severe arthritis. The mosquito-born pathogen spread to the Americas in 2013, is now epidemic in the Caribbean, and has no approved vaccine or treatment.
To test a novel VLP vaccine candidate, researchers enrolled 25 healthy adults into a phase I, open-label, dose-escalation trial with doses of 10, 20, or 40 mcg administered at weeks 0, 4, and 20, the investigators reported. Participants were followed for 44 weeks after enrollment.
All groups had detectable neutralizing antibodies on ELISA (enzyme-linked immunosorbent assay) after the second dose, with geometric mean titers of the half-maximum inhibitory concentration of 2,688 in the 10-mcg group, 1,775 in the 20-mcg group, and 7,246 in the 40-mcg group. Antibody levels after the second dose substantially exceeded those measured after the first dose, with P values for differences ranging from .07 for the 10-mcg group to less than .0001 for the 40-mcg group, the investigators said. And titers did not significantly differ 4 weeks after the second and third doses, they added.
Participants reported no arthralgias or other serious adverse effects. Mild to moderate side effects occurred in four participants, and consisted of transient neutropenia (three cases) and transient increases in alanine aminotransferase (four cases), all of which resolved without clinical consequences, the investigators said.
"These clinical data represent an important step in vaccine development to combat this rapidly emerging pathogen," the researchers said. The next step is to test the vaccine in larger studies that include persons at risk of chikungunya virus infection, they added.
The trial was funded by the Intramural Research Program of the Vaccine Research Center, National Institute of Allergy and Infectious Diseases; and the National Institutes of Health. The authors declared no competing interests.
"Although this VLP vaccine candidate exhibits a range of properties that suggest it would be a good vaccine option, there is always concern about whether a vaccine for a vector-borne virus will be licensed," said Dr. Ann M. Powers. "Development of vaccines for orphan agents is challenging, because the market might not be large enough to justify the investment."
Developing a vaccine in the United States costs an estimated $200-$500 million; nonetheless, vaccines are the most cost-effective way to prevent disease, she said. "In view of the burden of chikungunya outbreaks, which have affected up to 63% of local populations in a matter of months, the continued development of this VLP vaccine candidate, along with other vaccine options, should be encouraged."
A VLP contains the outer structural proteins of the virus that the immune system typically recognizes, Dr. Powers added. But it does not contain live genetic material, which confers a safety and manufacturing advantage because high-containment facilities are not needed for production.
Dr. Powers is with the division of vector-borne diseases at the U.S. Centers for Disease Control and Prevention. She declared that she had no competing interests. These remarks were excerpted from her editorial accompanying Dr. Chang’s report (Lancet 2014 Aug. 15 [doi: 10.1016/S0140-6736(14)61290-3]).
"Although this VLP vaccine candidate exhibits a range of properties that suggest it would be a good vaccine option, there is always concern about whether a vaccine for a vector-borne virus will be licensed," said Dr. Ann M. Powers. "Development of vaccines for orphan agents is challenging, because the market might not be large enough to justify the investment."
Developing a vaccine in the United States costs an estimated $200-$500 million; nonetheless, vaccines are the most cost-effective way to prevent disease, she said. "In view of the burden of chikungunya outbreaks, which have affected up to 63% of local populations in a matter of months, the continued development of this VLP vaccine candidate, along with other vaccine options, should be encouraged."
A VLP contains the outer structural proteins of the virus that the immune system typically recognizes, Dr. Powers added. But it does not contain live genetic material, which confers a safety and manufacturing advantage because high-containment facilities are not needed for production.
Dr. Powers is with the division of vector-borne diseases at the U.S. Centers for Disease Control and Prevention. She declared that she had no competing interests. These remarks were excerpted from her editorial accompanying Dr. Chang’s report (Lancet 2014 Aug. 15 [doi: 10.1016/S0140-6736(14)61290-3]).
"Although this VLP vaccine candidate exhibits a range of properties that suggest it would be a good vaccine option, there is always concern about whether a vaccine for a vector-borne virus will be licensed," said Dr. Ann M. Powers. "Development of vaccines for orphan agents is challenging, because the market might not be large enough to justify the investment."
Developing a vaccine in the United States costs an estimated $200-$500 million; nonetheless, vaccines are the most cost-effective way to prevent disease, she said. "In view of the burden of chikungunya outbreaks, which have affected up to 63% of local populations in a matter of months, the continued development of this VLP vaccine candidate, along with other vaccine options, should be encouraged."
A VLP contains the outer structural proteins of the virus that the immune system typically recognizes, Dr. Powers added. But it does not contain live genetic material, which confers a safety and manufacturing advantage because high-containment facilities are not needed for production.
Dr. Powers is with the division of vector-borne diseases at the U.S. Centers for Disease Control and Prevention. She declared that she had no competing interests. These remarks were excerpted from her editorial accompanying Dr. Chang’s report (Lancet 2014 Aug. 15 [doi: 10.1016/S0140-6736(14)61290-3]).
A novel chikungunya virus vaccine caused no serious adverse effects and was about as immunogenic as natural infection, authors of a phase I trial reported in the Lancet.
Eleven months after receiving the noninfectious viruslike particle (VLP) vaccine, trial participants had neutralizing antibody titers that resembled those seen in natural infection, said Dr. Lee-Jah Chang and associates at the National Institutes of Health in Bethesda, Md. (Lancet 2014 Aug. 15 [doi: 10.1016/S0140-6736(14)61185-5]).
Chikungunya virus infection is rarely fatal, but it causes fever and severe arthritis. The mosquito-born pathogen spread to the Americas in 2013, is now epidemic in the Caribbean, and has no approved vaccine or treatment.
To test a novel VLP vaccine candidate, researchers enrolled 25 healthy adults into a phase I, open-label, dose-escalation trial with doses of 10, 20, or 40 mcg administered at weeks 0, 4, and 20, the investigators reported. Participants were followed for 44 weeks after enrollment.
All groups had detectable neutralizing antibodies on ELISA (enzyme-linked immunosorbent assay) after the second dose, with geometric mean titers of the half-maximum inhibitory concentration of 2,688 in the 10-mcg group, 1,775 in the 20-mcg group, and 7,246 in the 40-mcg group. Antibody levels after the second dose substantially exceeded those measured after the first dose, with P values for differences ranging from .07 for the 10-mcg group to less than .0001 for the 40-mcg group, the investigators said. And titers did not significantly differ 4 weeks after the second and third doses, they added.
Participants reported no arthralgias or other serious adverse effects. Mild to moderate side effects occurred in four participants, and consisted of transient neutropenia (three cases) and transient increases in alanine aminotransferase (four cases), all of which resolved without clinical consequences, the investigators said.
"These clinical data represent an important step in vaccine development to combat this rapidly emerging pathogen," the researchers said. The next step is to test the vaccine in larger studies that include persons at risk of chikungunya virus infection, they added.
The trial was funded by the Intramural Research Program of the Vaccine Research Center, National Institute of Allergy and Infectious Diseases; and the National Institutes of Health. The authors declared no competing interests.
A novel chikungunya virus vaccine caused no serious adverse effects and was about as immunogenic as natural infection, authors of a phase I trial reported in the Lancet.
Eleven months after receiving the noninfectious viruslike particle (VLP) vaccine, trial participants had neutralizing antibody titers that resembled those seen in natural infection, said Dr. Lee-Jah Chang and associates at the National Institutes of Health in Bethesda, Md. (Lancet 2014 Aug. 15 [doi: 10.1016/S0140-6736(14)61185-5]).
Chikungunya virus infection is rarely fatal, but it causes fever and severe arthritis. The mosquito-born pathogen spread to the Americas in 2013, is now epidemic in the Caribbean, and has no approved vaccine or treatment.
To test a novel VLP vaccine candidate, researchers enrolled 25 healthy adults into a phase I, open-label, dose-escalation trial with doses of 10, 20, or 40 mcg administered at weeks 0, 4, and 20, the investigators reported. Participants were followed for 44 weeks after enrollment.
All groups had detectable neutralizing antibodies on ELISA (enzyme-linked immunosorbent assay) after the second dose, with geometric mean titers of the half-maximum inhibitory concentration of 2,688 in the 10-mcg group, 1,775 in the 20-mcg group, and 7,246 in the 40-mcg group. Antibody levels after the second dose substantially exceeded those measured after the first dose, with P values for differences ranging from .07 for the 10-mcg group to less than .0001 for the 40-mcg group, the investigators said. And titers did not significantly differ 4 weeks after the second and third doses, they added.
Participants reported no arthralgias or other serious adverse effects. Mild to moderate side effects occurred in four participants, and consisted of transient neutropenia (three cases) and transient increases in alanine aminotransferase (four cases), all of which resolved without clinical consequences, the investigators said.
"These clinical data represent an important step in vaccine development to combat this rapidly emerging pathogen," the researchers said. The next step is to test the vaccine in larger studies that include persons at risk of chikungunya virus infection, they added.
The trial was funded by the Intramural Research Program of the Vaccine Research Center, National Institute of Allergy and Infectious Diseases; and the National Institutes of Health. The authors declared no competing interests.
FROM THE LANCET
Chikungunya vaccine safe, immunogenic in phase I trial
A novel chikungunya virus vaccine caused no serious adverse effects and was about as immunogenic as natural infection, authors of a phase I trial reported in the Lancet.
Eleven months after receiving the noninfectious viruslike particle (VLP) vaccine, trial participants had neutralizing antibody titers that resembled those seen in natural infection, said Dr. Lee-Jah Chang and associates at the National Institutes of Health in Bethesda, Md. (Lancet 2014 Aug. 15 [doi: 10.1016/S0140-6736(14)61185-5]).
Chikungunya virus infection is rarely fatal, but it causes fever and severe arthritis. The mosquito-born pathogen spread to the Americas in 2013, is now epidemic in the Caribbean, and has no approved vaccine or treatment.
To test a novel VLP vaccine candidate, researchers enrolled 25 healthy adults into a phase I, open-label, dose-escalation trial with doses of 10, 20, or 40 mcg administered at weeks 0, 4, and 20, the investigators reported. Participants were followed for 44 weeks after enrollment.
All groups had detectable neutralizing antibodies on ELISA (enzyme-linked immunosorbent assay) after the second dose, with geometric mean titers of the half-maximum inhibitory concentration of 2,688 in the 10-mcg group, 1,775 in the 20-mcg group, and 7,246 in the 40-mcg group. Antibody levels after the second dose substantially exceeded those measured after the first dose, with P values for differences ranging from .07 for the 10-mcg group to less than .0001 for the 40-mcg group, the investigators said. And titers did not significantly differ 4 weeks after the second and third doses, they added.
Participants reported no arthralgias or other serious adverse effects. Mild to moderate side effects occurred in four participants, and consisted of transient neutropenia (three cases) and transient increases in alanine aminotransferase (four cases), all of which resolved without clinical consequences, the investigators said.
"These clinical data represent an important step in vaccine development to combat this rapidly emerging pathogen," the researchers said. The next step is to test the vaccine in larger studies that include persons at risk of chikungunya virus infection, they added.
The trial was funded by the Intramural Research Program of the Vaccine Research Center, National Institute of Allergy and Infectious Diseases; and the National Institutes of Health. The authors declared no competing interests.
"Although this VLP vaccine candidate exhibits a range of properties that suggest it would be a good vaccine option, there is always concern about whether a vaccine for a vector-borne virus will be licensed," said Dr. Ann M. Powers. "Development of vaccines for orphan agents is challenging, because the market might not be large enough to justify the investment."
Developing a vaccine in the United States costs an estimated $200-$500 million; nonetheless, vaccines are the most cost-effective way to prevent disease, she said. "In view of the burden of chikungunya outbreaks, which have affected up to 63% of local populations in a matter of months, the continued development of this VLP vaccine candidate, along with other vaccine options, should be encouraged."
A VLP contains the outer structural proteins of the virus that the immune system typically recognizes, Dr. Powers added. But it does not contain live genetic material, which confers a safety and manufacturing advantage because high-containment facilities are not needed for production.
Dr. Powers is with the division of vector-borne diseases at the U.S. Centers for Disease Control and Prevention. She declared that she had no competing interests. These remarks were excerpted from her editorial accompanying Dr. Chang’s report (Lancet 2014 Aug. 15 [doi: 10.1016/S0140-6736(14)61290-3]).
"Although this VLP vaccine candidate exhibits a range of properties that suggest it would be a good vaccine option, there is always concern about whether a vaccine for a vector-borne virus will be licensed," said Dr. Ann M. Powers. "Development of vaccines for orphan agents is challenging, because the market might not be large enough to justify the investment."
Developing a vaccine in the United States costs an estimated $200-$500 million; nonetheless, vaccines are the most cost-effective way to prevent disease, she said. "In view of the burden of chikungunya outbreaks, which have affected up to 63% of local populations in a matter of months, the continued development of this VLP vaccine candidate, along with other vaccine options, should be encouraged."
A VLP contains the outer structural proteins of the virus that the immune system typically recognizes, Dr. Powers added. But it does not contain live genetic material, which confers a safety and manufacturing advantage because high-containment facilities are not needed for production.
Dr. Powers is with the division of vector-borne diseases at the U.S. Centers for Disease Control and Prevention. She declared that she had no competing interests. These remarks were excerpted from her editorial accompanying Dr. Chang’s report (Lancet 2014 Aug. 15 [doi: 10.1016/S0140-6736(14)61290-3]).
"Although this VLP vaccine candidate exhibits a range of properties that suggest it would be a good vaccine option, there is always concern about whether a vaccine for a vector-borne virus will be licensed," said Dr. Ann M. Powers. "Development of vaccines for orphan agents is challenging, because the market might not be large enough to justify the investment."
Developing a vaccine in the United States costs an estimated $200-$500 million; nonetheless, vaccines are the most cost-effective way to prevent disease, she said. "In view of the burden of chikungunya outbreaks, which have affected up to 63% of local populations in a matter of months, the continued development of this VLP vaccine candidate, along with other vaccine options, should be encouraged."
A VLP contains the outer structural proteins of the virus that the immune system typically recognizes, Dr. Powers added. But it does not contain live genetic material, which confers a safety and manufacturing advantage because high-containment facilities are not needed for production.
Dr. Powers is with the division of vector-borne diseases at the U.S. Centers for Disease Control and Prevention. She declared that she had no competing interests. These remarks were excerpted from her editorial accompanying Dr. Chang’s report (Lancet 2014 Aug. 15 [doi: 10.1016/S0140-6736(14)61290-3]).
A novel chikungunya virus vaccine caused no serious adverse effects and was about as immunogenic as natural infection, authors of a phase I trial reported in the Lancet.
Eleven months after receiving the noninfectious viruslike particle (VLP) vaccine, trial participants had neutralizing antibody titers that resembled those seen in natural infection, said Dr. Lee-Jah Chang and associates at the National Institutes of Health in Bethesda, Md. (Lancet 2014 Aug. 15 [doi: 10.1016/S0140-6736(14)61185-5]).
Chikungunya virus infection is rarely fatal, but it causes fever and severe arthritis. The mosquito-born pathogen spread to the Americas in 2013, is now epidemic in the Caribbean, and has no approved vaccine or treatment.
To test a novel VLP vaccine candidate, researchers enrolled 25 healthy adults into a phase I, open-label, dose-escalation trial with doses of 10, 20, or 40 mcg administered at weeks 0, 4, and 20, the investigators reported. Participants were followed for 44 weeks after enrollment.
All groups had detectable neutralizing antibodies on ELISA (enzyme-linked immunosorbent assay) after the second dose, with geometric mean titers of the half-maximum inhibitory concentration of 2,688 in the 10-mcg group, 1,775 in the 20-mcg group, and 7,246 in the 40-mcg group. Antibody levels after the second dose substantially exceeded those measured after the first dose, with P values for differences ranging from .07 for the 10-mcg group to less than .0001 for the 40-mcg group, the investigators said. And titers did not significantly differ 4 weeks after the second and third doses, they added.
Participants reported no arthralgias or other serious adverse effects. Mild to moderate side effects occurred in four participants, and consisted of transient neutropenia (three cases) and transient increases in alanine aminotransferase (four cases), all of which resolved without clinical consequences, the investigators said.
"These clinical data represent an important step in vaccine development to combat this rapidly emerging pathogen," the researchers said. The next step is to test the vaccine in larger studies that include persons at risk of chikungunya virus infection, they added.
The trial was funded by the Intramural Research Program of the Vaccine Research Center, National Institute of Allergy and Infectious Diseases; and the National Institutes of Health. The authors declared no competing interests.
A novel chikungunya virus vaccine caused no serious adverse effects and was about as immunogenic as natural infection, authors of a phase I trial reported in the Lancet.
Eleven months after receiving the noninfectious viruslike particle (VLP) vaccine, trial participants had neutralizing antibody titers that resembled those seen in natural infection, said Dr. Lee-Jah Chang and associates at the National Institutes of Health in Bethesda, Md. (Lancet 2014 Aug. 15 [doi: 10.1016/S0140-6736(14)61185-5]).
Chikungunya virus infection is rarely fatal, but it causes fever and severe arthritis. The mosquito-born pathogen spread to the Americas in 2013, is now epidemic in the Caribbean, and has no approved vaccine or treatment.
To test a novel VLP vaccine candidate, researchers enrolled 25 healthy adults into a phase I, open-label, dose-escalation trial with doses of 10, 20, or 40 mcg administered at weeks 0, 4, and 20, the investigators reported. Participants were followed for 44 weeks after enrollment.
All groups had detectable neutralizing antibodies on ELISA (enzyme-linked immunosorbent assay) after the second dose, with geometric mean titers of the half-maximum inhibitory concentration of 2,688 in the 10-mcg group, 1,775 in the 20-mcg group, and 7,246 in the 40-mcg group. Antibody levels after the second dose substantially exceeded those measured after the first dose, with P values for differences ranging from .07 for the 10-mcg group to less than .0001 for the 40-mcg group, the investigators said. And titers did not significantly differ 4 weeks after the second and third doses, they added.
Participants reported no arthralgias or other serious adverse effects. Mild to moderate side effects occurred in four participants, and consisted of transient neutropenia (three cases) and transient increases in alanine aminotransferase (four cases), all of which resolved without clinical consequences, the investigators said.
"These clinical data represent an important step in vaccine development to combat this rapidly emerging pathogen," the researchers said. The next step is to test the vaccine in larger studies that include persons at risk of chikungunya virus infection, they added.
The trial was funded by the Intramural Research Program of the Vaccine Research Center, National Institute of Allergy and Infectious Diseases; and the National Institutes of Health. The authors declared no competing interests.
FROM THE LANCET
Key clinical point: A novel, noninfectious vaccine for chikungunya virus was highly immunogenic and caused no serious adverse effects in a phase I trial.
Major finding: All dosing groups developed detectable neutralizing antibodies after a second vaccination with a chikungunya virus vaccine (geometric mean titers of the half-maximum inhibitory concentration: 2,688 in the 10-mcg group, 1,775 in the 20-mcg group, and 7,246 in the 40-mcg group).
Data source: Phase I, dose-escalation, open-label clinical trial of noninfectious viruslike particle chikungunya vaccine in 25 healthy adults.
Disclosures: Funding sources included the Intramural Research Program of the Vaccine Research Center, the National Institute of Allergy and Infectious Diseases, and the National Institutes of Health. The authors declared no competing interests.
Review finds sparse evidence for sleep/wake drugs in shift workers
Shift workers often use drugs to try to sleep during the day or stay awake at night, but limited evidence supports the efficacy of these agents, according to a Cochrane Database review of 15 placebo-controlled studies.
"The evidence was of low quality and mostly from small trials," said Dr. Juha Liira of the Finnish Institute of Occupational Health in Helsinki and her associates. "Both sleep- and alertness-promoting agents have potentially serious adverse effects. Therefore, we need more trials to determine the beneficial and harmful effects of these drugs."
The strongest evidence was for the ability of modafinil and armodafinil to promote wakefulness during shift work, but these drugs can pose substantial risks, the authors said.
The review uncovered low-quality evidence for melatonin as a daytime sleep promoter and for caffeine to enhance nighttime wakefulness, the authors said, adding that hypnotics did not affect sleep length or quality after night work.
For the study, reviewers searched the CENTRAL, MEDLINE, EMBASE, PubMed, and PsycINFO databases through September 2013 and ClinicalTrials.gov up to July 2013. They included all randomized, controlled trials, including crossover trials, of pharmacologic agents in shift workers, whether or not the subjects had sleep problems (Cochrane Database Syst. Rev. 2014 Aug. 12 [doi:10.1002/14651858.CD009776.pub2]) They excluded trials that simulated shift work tasks, noting that such studies probably do not approximate shift work in real life. They also excluded studies of airline and military personnel because melatonin has already been reviewed for jet lag (Cochrane Database Syst. Rev. 2002;2:CD001520).
The search yielded 15 randomized, placebo-controlled trials with a total of 718 participants. Nine trials assessed melatonin, two examined hypnotics, three looked at modafinil or armodafinil, and one assessed caffeine, they reported.
Modafinil (200 mg) and armodafinil (150 mg) improved wakefulness and alertness during night shifts at 3-month follow-up, compared with placebo, the researchers said. But armodafinil cut sleepiness by a mean of just one point on the Karolinska Sleepiness Scale (KSS) (range, 1-9 points; 95% confidence interval, -1.32 to -0.67), and improved reaction time by only 50 ms (95% CI, -85.5 to -15.5 ms), they added. "Modafinil probably has similar effects on sleepiness," the reviewers concluded, noting that the drug decreased sleepiness by 0.9 points on the KSS (95% CI, -1.45 to -0.35) while also heightening alertness in a psychomotor vigilance test.
Armodafinil and modafinil also have been linked to serious skin disorders in postmarketing reports, the researchers emphasized. And the drugs caused headache, nausea, and increased blood pressure in clinical trials, they said.
Caffeine at a dose of 300 mg or 4 mg/kg improved alertness during night shifts when combined with a preshift nap, the reviewers said. But the effect size in the single trial was small, with a mean improvement of only 0.63 points on the KSS (95% CI, -1.09 to -0.17), they added.
Melatonin had only low-quality evidence as a sleep promoter, the reviewers said. A dose of 1-10 mg lengthened daytime sleep by an average of 24 minutes, compared with placebo in seven trials of 263 shift workers (95% CI, 9.82-38.86), and added 17 minutes to nighttime sleep in three trials of 234 participants (95% CI, 3.71-30.22), but did not significantly affect other sleep parameters such as sleep latency, they reported.
The only trial of the hypnotic drug zopiclone (7.5 mg) included just 28 participants and found that the agent did not lengthen daytime sleep significantly more than did placebo (mean difference, 44 minutes; 95% CI, -22.67-110.67), while no trials examined adverse effects of hypnotics in shift workers, the reviewers said.
"We need more and better quality trials on the beneficial and adverse effects and costs of all pharmacological agents that induce sleep or promote alertness in shift workers, both with and without a diagnosis of shift work sleep disorder," Dr. Liira and associates concluded. "We also need systematic reviews of their adverse effects."
Most of the melatonin trials had a high risk of bias, so the reviewers downgraded their rating from a high to a low level of quality, they said. They similarly downgraded trials for armodafinil, modafinil, caffeine, and hypnotics.
The Finnish Institute of Occupational Health pays the salary of Dr. Liira and four coauthors. There were no external funding sources or conflicts of interest.
Shift workers often use drugs to try to sleep during the day or stay awake at night, but limited evidence supports the efficacy of these agents, according to a Cochrane Database review of 15 placebo-controlled studies.
"The evidence was of low quality and mostly from small trials," said Dr. Juha Liira of the Finnish Institute of Occupational Health in Helsinki and her associates. "Both sleep- and alertness-promoting agents have potentially serious adverse effects. Therefore, we need more trials to determine the beneficial and harmful effects of these drugs."
The strongest evidence was for the ability of modafinil and armodafinil to promote wakefulness during shift work, but these drugs can pose substantial risks, the authors said.
The review uncovered low-quality evidence for melatonin as a daytime sleep promoter and for caffeine to enhance nighttime wakefulness, the authors said, adding that hypnotics did not affect sleep length or quality after night work.
For the study, reviewers searched the CENTRAL, MEDLINE, EMBASE, PubMed, and PsycINFO databases through September 2013 and ClinicalTrials.gov up to July 2013. They included all randomized, controlled trials, including crossover trials, of pharmacologic agents in shift workers, whether or not the subjects had sleep problems (Cochrane Database Syst. Rev. 2014 Aug. 12 [doi:10.1002/14651858.CD009776.pub2]) They excluded trials that simulated shift work tasks, noting that such studies probably do not approximate shift work in real life. They also excluded studies of airline and military personnel because melatonin has already been reviewed for jet lag (Cochrane Database Syst. Rev. 2002;2:CD001520).
The search yielded 15 randomized, placebo-controlled trials with a total of 718 participants. Nine trials assessed melatonin, two examined hypnotics, three looked at modafinil or armodafinil, and one assessed caffeine, they reported.
Modafinil (200 mg) and armodafinil (150 mg) improved wakefulness and alertness during night shifts at 3-month follow-up, compared with placebo, the researchers said. But armodafinil cut sleepiness by a mean of just one point on the Karolinska Sleepiness Scale (KSS) (range, 1-9 points; 95% confidence interval, -1.32 to -0.67), and improved reaction time by only 50 ms (95% CI, -85.5 to -15.5 ms), they added. "Modafinil probably has similar effects on sleepiness," the reviewers concluded, noting that the drug decreased sleepiness by 0.9 points on the KSS (95% CI, -1.45 to -0.35) while also heightening alertness in a psychomotor vigilance test.
Armodafinil and modafinil also have been linked to serious skin disorders in postmarketing reports, the researchers emphasized. And the drugs caused headache, nausea, and increased blood pressure in clinical trials, they said.
Caffeine at a dose of 300 mg or 4 mg/kg improved alertness during night shifts when combined with a preshift nap, the reviewers said. But the effect size in the single trial was small, with a mean improvement of only 0.63 points on the KSS (95% CI, -1.09 to -0.17), they added.
Melatonin had only low-quality evidence as a sleep promoter, the reviewers said. A dose of 1-10 mg lengthened daytime sleep by an average of 24 minutes, compared with placebo in seven trials of 263 shift workers (95% CI, 9.82-38.86), and added 17 minutes to nighttime sleep in three trials of 234 participants (95% CI, 3.71-30.22), but did not significantly affect other sleep parameters such as sleep latency, they reported.
The only trial of the hypnotic drug zopiclone (7.5 mg) included just 28 participants and found that the agent did not lengthen daytime sleep significantly more than did placebo (mean difference, 44 minutes; 95% CI, -22.67-110.67), while no trials examined adverse effects of hypnotics in shift workers, the reviewers said.
"We need more and better quality trials on the beneficial and adverse effects and costs of all pharmacological agents that induce sleep or promote alertness in shift workers, both with and without a diagnosis of shift work sleep disorder," Dr. Liira and associates concluded. "We also need systematic reviews of their adverse effects."
Most of the melatonin trials had a high risk of bias, so the reviewers downgraded their rating from a high to a low level of quality, they said. They similarly downgraded trials for armodafinil, modafinil, caffeine, and hypnotics.
The Finnish Institute of Occupational Health pays the salary of Dr. Liira and four coauthors. There were no external funding sources or conflicts of interest.
Shift workers often use drugs to try to sleep during the day or stay awake at night, but limited evidence supports the efficacy of these agents, according to a Cochrane Database review of 15 placebo-controlled studies.
"The evidence was of low quality and mostly from small trials," said Dr. Juha Liira of the Finnish Institute of Occupational Health in Helsinki and her associates. "Both sleep- and alertness-promoting agents have potentially serious adverse effects. Therefore, we need more trials to determine the beneficial and harmful effects of these drugs."
The strongest evidence was for the ability of modafinil and armodafinil to promote wakefulness during shift work, but these drugs can pose substantial risks, the authors said.
The review uncovered low-quality evidence for melatonin as a daytime sleep promoter and for caffeine to enhance nighttime wakefulness, the authors said, adding that hypnotics did not affect sleep length or quality after night work.
For the study, reviewers searched the CENTRAL, MEDLINE, EMBASE, PubMed, and PsycINFO databases through September 2013 and ClinicalTrials.gov up to July 2013. They included all randomized, controlled trials, including crossover trials, of pharmacologic agents in shift workers, whether or not the subjects had sleep problems (Cochrane Database Syst. Rev. 2014 Aug. 12 [doi:10.1002/14651858.CD009776.pub2]) They excluded trials that simulated shift work tasks, noting that such studies probably do not approximate shift work in real life. They also excluded studies of airline and military personnel because melatonin has already been reviewed for jet lag (Cochrane Database Syst. Rev. 2002;2:CD001520).
The search yielded 15 randomized, placebo-controlled trials with a total of 718 participants. Nine trials assessed melatonin, two examined hypnotics, three looked at modafinil or armodafinil, and one assessed caffeine, they reported.
Modafinil (200 mg) and armodafinil (150 mg) improved wakefulness and alertness during night shifts at 3-month follow-up, compared with placebo, the researchers said. But armodafinil cut sleepiness by a mean of just one point on the Karolinska Sleepiness Scale (KSS) (range, 1-9 points; 95% confidence interval, -1.32 to -0.67), and improved reaction time by only 50 ms (95% CI, -85.5 to -15.5 ms), they added. "Modafinil probably has similar effects on sleepiness," the reviewers concluded, noting that the drug decreased sleepiness by 0.9 points on the KSS (95% CI, -1.45 to -0.35) while also heightening alertness in a psychomotor vigilance test.
Armodafinil and modafinil also have been linked to serious skin disorders in postmarketing reports, the researchers emphasized. And the drugs caused headache, nausea, and increased blood pressure in clinical trials, they said.
Caffeine at a dose of 300 mg or 4 mg/kg improved alertness during night shifts when combined with a preshift nap, the reviewers said. But the effect size in the single trial was small, with a mean improvement of only 0.63 points on the KSS (95% CI, -1.09 to -0.17), they added.
Melatonin had only low-quality evidence as a sleep promoter, the reviewers said. A dose of 1-10 mg lengthened daytime sleep by an average of 24 minutes, compared with placebo in seven trials of 263 shift workers (95% CI, 9.82-38.86), and added 17 minutes to nighttime sleep in three trials of 234 participants (95% CI, 3.71-30.22), but did not significantly affect other sleep parameters such as sleep latency, they reported.
The only trial of the hypnotic drug zopiclone (7.5 mg) included just 28 participants and found that the agent did not lengthen daytime sleep significantly more than did placebo (mean difference, 44 minutes; 95% CI, -22.67-110.67), while no trials examined adverse effects of hypnotics in shift workers, the reviewers said.
"We need more and better quality trials on the beneficial and adverse effects and costs of all pharmacological agents that induce sleep or promote alertness in shift workers, both with and without a diagnosis of shift work sleep disorder," Dr. Liira and associates concluded. "We also need systematic reviews of their adverse effects."
Most of the melatonin trials had a high risk of bias, so the reviewers downgraded their rating from a high to a low level of quality, they said. They similarly downgraded trials for armodafinil, modafinil, caffeine, and hypnotics.
The Finnish Institute of Occupational Health pays the salary of Dr. Liira and four coauthors. There were no external funding sources or conflicts of interest.
FROM COCHRANE DATABASE OF SYSTEMATIC REVIEWS
Key clinical point: Sparse evidence supports the use of sleep- and wakefulness-promoting drugs in shift workers, and both sleep- and wakefulness-promoting agents pose risks of adverse effects.
Major finding: Melatonin improved sleep duration after a night shift but did not affect other measures of sleep quality; modafinil and armodafinil somewhat improved alertness and wakefulness in patients with shift work sleep disorder; caffeine and naps appeared to cut night shift sleepiness; and hypnotics did not improve sleep length and quality after night work.
Data source: A review of 15 randomized, placebo-controlled trials involving 718 shift workers.
Disclosures: The Finnish Institute of Occupational Health pays the salary of Dr. Liira and three coauthors. There were no external funding sources or conflicts of interest.
Diabetes, hypertension drive higher CVD risk in blacks and women
Risk factors for cardiovascular disease have disproportionately affected women and blacks, and while the gender gap has narrowed over time, black-white disparities have widened, reported authors of a large 10-year cohort study published Aug. 11 in the journal Circulation.
The study showed that factors such as high cholesterol and smoking account for less cardiovascular disease (CVD) risk than in the past, said Dr. Susan Cheng of Harvard Medical School in Boston and her associates. "However, the combined contribution of all traditional risk factors has remained substantially higher in women, compared with men, and in blacks, compared with whites," the investigators said. "These sex- and race-based differences continue to be especially pronounced for hypertension and diabetes mellitus."
The researchers calculated the population-attributable risks (PARs) of five major modifiable risk factors – smoking, hypercholesterolemia, hypertension, diabetes, and obesity – for the 10-year incidence of CVD among 13,541 participants in the Atherosclerosis Risk in Communities (ARIC) study. The cohort was 56% female, 26% black, and aged 52-66 years when examined during the time periods 1987-1989, 1990-1992, or 1996-1998, the investigators said (Circulation 2014 Aug. 11 [doi:10.1161/circulationaha.113.008506]).
The contribution of smoking and high cholesterol to CVD risk fell, (from 0.15 to 0.13 and from 0.18 to 0.09, respectively) during the study period, and the contribution of obesity stayed the same at 0.06, the researchers reported.
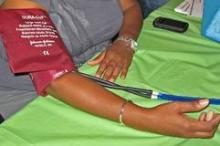
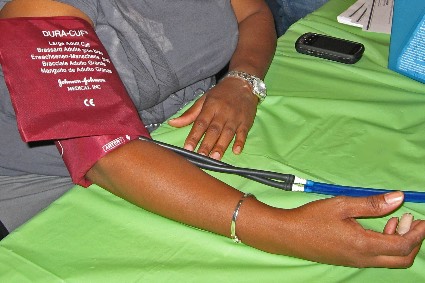
But by 1996-1998, diabetes mellitus accounted for significantly more CVD risk in blacks than whites (0.28 vs. 0.13), and the same was true for hypertension (0.36 vs. 0.21; P = .08) and all risk factors combined (0.67 vs. 0.48; P = .002), the researchers said. Similarly, PARs for women surpassed those for men for diabetes (0.21 vs. 0.14; P less than .0001) and hypertension (0.32 vs. 0.19; P = .02), they reported.
The racial differences suggest that prevention efforts based on traditional risk factors have benefited whites more than blacks, the researchers added. However, most blacks in the study were from the ARIC study center located in Jackson, Miss., so the race-based findings might be specific to that area, they noted.
"The reasons for persistent sex differences in attributable CVD risks over time are not yet clear," said Dr. Cheng and associates. They added that sex-based differences could stem from clustering; underrecognition or undertreatment of risk factors in women; biological differences that are not yet understood; or nontraditional risk factors in men.
The National Heart, Lung, and Blood Institute funded the study. Dr. Cheng also received funding from the Ellison Foundation. The authors reported no conflicts of interest.
Risk factors for cardiovascular disease have disproportionately affected women and blacks, and while the gender gap has narrowed over time, black-white disparities have widened, reported authors of a large 10-year cohort study published Aug. 11 in the journal Circulation.
The study showed that factors such as high cholesterol and smoking account for less cardiovascular disease (CVD) risk than in the past, said Dr. Susan Cheng of Harvard Medical School in Boston and her associates. "However, the combined contribution of all traditional risk factors has remained substantially higher in women, compared with men, and in blacks, compared with whites," the investigators said. "These sex- and race-based differences continue to be especially pronounced for hypertension and diabetes mellitus."
The researchers calculated the population-attributable risks (PARs) of five major modifiable risk factors – smoking, hypercholesterolemia, hypertension, diabetes, and obesity – for the 10-year incidence of CVD among 13,541 participants in the Atherosclerosis Risk in Communities (ARIC) study. The cohort was 56% female, 26% black, and aged 52-66 years when examined during the time periods 1987-1989, 1990-1992, or 1996-1998, the investigators said (Circulation 2014 Aug. 11 [doi:10.1161/circulationaha.113.008506]).
The contribution of smoking and high cholesterol to CVD risk fell, (from 0.15 to 0.13 and from 0.18 to 0.09, respectively) during the study period, and the contribution of obesity stayed the same at 0.06, the researchers reported.
But by 1996-1998, diabetes mellitus accounted for significantly more CVD risk in blacks than whites (0.28 vs. 0.13), and the same was true for hypertension (0.36 vs. 0.21; P = .08) and all risk factors combined (0.67 vs. 0.48; P = .002), the researchers said. Similarly, PARs for women surpassed those for men for diabetes (0.21 vs. 0.14; P less than .0001) and hypertension (0.32 vs. 0.19; P = .02), they reported.
The racial differences suggest that prevention efforts based on traditional risk factors have benefited whites more than blacks, the researchers added. However, most blacks in the study were from the ARIC study center located in Jackson, Miss., so the race-based findings might be specific to that area, they noted.
"The reasons for persistent sex differences in attributable CVD risks over time are not yet clear," said Dr. Cheng and associates. They added that sex-based differences could stem from clustering; underrecognition or undertreatment of risk factors in women; biological differences that are not yet understood; or nontraditional risk factors in men.
The National Heart, Lung, and Blood Institute funded the study. Dr. Cheng also received funding from the Ellison Foundation. The authors reported no conflicts of interest.
Risk factors for cardiovascular disease have disproportionately affected women and blacks, and while the gender gap has narrowed over time, black-white disparities have widened, reported authors of a large 10-year cohort study published Aug. 11 in the journal Circulation.
The study showed that factors such as high cholesterol and smoking account for less cardiovascular disease (CVD) risk than in the past, said Dr. Susan Cheng of Harvard Medical School in Boston and her associates. "However, the combined contribution of all traditional risk factors has remained substantially higher in women, compared with men, and in blacks, compared with whites," the investigators said. "These sex- and race-based differences continue to be especially pronounced for hypertension and diabetes mellitus."
The researchers calculated the population-attributable risks (PARs) of five major modifiable risk factors – smoking, hypercholesterolemia, hypertension, diabetes, and obesity – for the 10-year incidence of CVD among 13,541 participants in the Atherosclerosis Risk in Communities (ARIC) study. The cohort was 56% female, 26% black, and aged 52-66 years when examined during the time periods 1987-1989, 1990-1992, or 1996-1998, the investigators said (Circulation 2014 Aug. 11 [doi:10.1161/circulationaha.113.008506]).
The contribution of smoking and high cholesterol to CVD risk fell, (from 0.15 to 0.13 and from 0.18 to 0.09, respectively) during the study period, and the contribution of obesity stayed the same at 0.06, the researchers reported.
But by 1996-1998, diabetes mellitus accounted for significantly more CVD risk in blacks than whites (0.28 vs. 0.13), and the same was true for hypertension (0.36 vs. 0.21; P = .08) and all risk factors combined (0.67 vs. 0.48; P = .002), the researchers said. Similarly, PARs for women surpassed those for men for diabetes (0.21 vs. 0.14; P less than .0001) and hypertension (0.32 vs. 0.19; P = .02), they reported.
The racial differences suggest that prevention efforts based on traditional risk factors have benefited whites more than blacks, the researchers added. However, most blacks in the study were from the ARIC study center located in Jackson, Miss., so the race-based findings might be specific to that area, they noted.
"The reasons for persistent sex differences in attributable CVD risks over time are not yet clear," said Dr. Cheng and associates. They added that sex-based differences could stem from clustering; underrecognition or undertreatment of risk factors in women; biological differences that are not yet understood; or nontraditional risk factors in men.
The National Heart, Lung, and Blood Institute funded the study. Dr. Cheng also received funding from the Ellison Foundation. The authors reported no conflicts of interest.
FROM CIRCULATION
Key clinical point: Cardiovascular risk factors disproportionately affect blacks and women; and while the gender gap has narrowed, the disparity between blacks and whites has increased.
Major finding: By 1996-1998, population attributable risks (PARs) for blacks exceeded those for whites for diabetes (P less than .0001), hypertension (P = .08), and all risk factors combined (P = .002). Among women, PARs surpassed those of men for diabetes (P less than .0001) and hypertension (P = .02).
Data source: Cohort analysis of 13,541 participants in the Atherosclerosis Risk in Communities Study. Participants were 52-66 years old, 56% female, 26% black, and had no cardiovascular disease when examined during 1987-1989, 1990-1992, or 1996-1998.
Disclosures: The study was funded by the National Heart, Lung, and Blood Institute. Dr. Cheng received additional funding from the Ellison Foundation. The authors reported no conflicts of interest.
Twin study confirmed genetic basis of several epilepsy syndromes
A study of twins with seizures confirmed the genetic basis of idiopathic generalized epilepsy, genetic epilepsy with febrile seizures plus, and focal epilepsies, investigators reported online Aug. 8 in Neurology.
The analysis did not support a genetic basis for benign epilepsy with centrotemporal spikes (BECTS), finding no concordance between monozygotic pairs of twins with the disorder, said Dr. Lata Vadlamudi of the University of Queensland in Brisbane, Australia, and her associates.
The researchers calculated casewise concordance estimates for epilepsy syndromes in 558 pairs of twins with suspected epilepsy, 418 of whom had confirmed seizures. They grouped them based on the 2010 ILAE (International League Against Epilepsy) scheme, incorporating molecular data when applicable (Neurology 2014 Aug. 8 [doi: 10.1212/WNL.0000000000000790]).
The estimated concordance for monozygotic twins exceeded that for dizygotic twins for idiopathic generalized epilepsies (0.77 vs. 0.35), genetic epilepsy with febrile seizures plus (0.85 vs. 0.25), and focal epilepsies (0.40 vs. 0.03), the researchers reported.
Applying the 2010 ILAE scheme also confirmed genetic influences for syndromes classified as genetic, and 10.9% of individuals tested had large-effect mutations in known epilepsy genes or had validated susceptibility alleles, the investigators said.
Mutations most often involved the SCN1A gene, which is currently seen as the most clinically relevant gene in epilepsy, they said.
The study also found "striking monozygotic and dizygotic discordance" for BECTS, which has been presumed to have a genetic basis, the researchers said. "Our analysis of the BECTS twins ... highlighted that the etiology and genetics of BECTS are more complicated than initially conceptualized."
For epilepsy patients, the results "highlight the potential to integrate well-established clinical data with molecular genetic findings and pave the way for targeted next-generation sequencing of large cohorts, which is likely to be the next phase in diagnosis, treatment guidance, and genetic counseling," Dr. Vadlamudi and her associates wrote.
The research was supported by the National Health and Medical Research Council of Australia and fellowship funding from the Queensland Department of Health. Dr. Vadlamudi and 11 coauthors reported no disclosures. Two coauthors reported advisory or financial relationships with UCB, Janssen-Cilag EMEA, and other companies.
The most common epilepsy syndromes do not follow a straightforward Mendelian inheritance pattern, but instead involve combinations of large-effect and small-effect alleles and environmental factors. This twin study illuminated the genetic complexities of epilepsy and the influence of genetic variance on complex phenotypes, said Dr. Renzo Guerrini and Dr. Jeffrey Buchhalter.

|
|
The study confirmed the strong genetic component of genetic epilepsy with febrile seizures plus and revealed high monozygotic concordance for the syndrome, they noted. In addition, the analysis found "compelling evidence" for a strong genetic role in generalized epilepsy, corroborating the concept of genetic epilepsy and the role of genes in some nonlesional focal epilepsies.
But it remains unclear whether current classifications for epilepsy reflect the molecular profiles of these syndromes, they said. The category of genetic epilepsy might turn out to be arbitrary, for example, "as what is presumed to be symptomatic today may be revealed as genetic after molecular screening."
The structural/metabolic epilepsy category also is heterogeneous, encompassing generalized and localized brain malformations that are determined by the time of origin of neurons with abnormal migration patterns, they said. "This suggests the need for a category that includes the genetic defect and interposed structural abnormality," they added.
The lack of concordance for monozygotic twins with benign epilepsy with centrotemporal spikes also contradicts prior reports that BECTS is primarily genetic, they noted. But perhaps the current study did not include enough BECTS twins to capture those with rare monozygotic inheritance, or perhaps postzygotic mutations led to genetic discordance in twin pairs, they said.
Dr. Guerrini is a neurologist with the University of Florence in Italy. Dr. Buchhalter is a neurologist with the Alberta Children’s Hospital and the University of Calgary (Alta.). Dr. Guerrini has received honoraria from Biocodex, UCB, and other companies. Dr. Buchhalter has been a consultant to UCB, Upsher-Smith, and Lundbeck. Their remarks were excerpted from their editorial accompanying Dr. Vadlamudi’s report (Neurology 2014 Aug. 8 [doi: 10.1212/WNL.0000000000000802]).
The most common epilepsy syndromes do not follow a straightforward Mendelian inheritance pattern, but instead involve combinations of large-effect and small-effect alleles and environmental factors. This twin study illuminated the genetic complexities of epilepsy and the influence of genetic variance on complex phenotypes, said Dr. Renzo Guerrini and Dr. Jeffrey Buchhalter.

|
|
The study confirmed the strong genetic component of genetic epilepsy with febrile seizures plus and revealed high monozygotic concordance for the syndrome, they noted. In addition, the analysis found "compelling evidence" for a strong genetic role in generalized epilepsy, corroborating the concept of genetic epilepsy and the role of genes in some nonlesional focal epilepsies.
But it remains unclear whether current classifications for epilepsy reflect the molecular profiles of these syndromes, they said. The category of genetic epilepsy might turn out to be arbitrary, for example, "as what is presumed to be symptomatic today may be revealed as genetic after molecular screening."
The structural/metabolic epilepsy category also is heterogeneous, encompassing generalized and localized brain malformations that are determined by the time of origin of neurons with abnormal migration patterns, they said. "This suggests the need for a category that includes the genetic defect and interposed structural abnormality," they added.
The lack of concordance for monozygotic twins with benign epilepsy with centrotemporal spikes also contradicts prior reports that BECTS is primarily genetic, they noted. But perhaps the current study did not include enough BECTS twins to capture those with rare monozygotic inheritance, or perhaps postzygotic mutations led to genetic discordance in twin pairs, they said.
Dr. Guerrini is a neurologist with the University of Florence in Italy. Dr. Buchhalter is a neurologist with the Alberta Children’s Hospital and the University of Calgary (Alta.). Dr. Guerrini has received honoraria from Biocodex, UCB, and other companies. Dr. Buchhalter has been a consultant to UCB, Upsher-Smith, and Lundbeck. Their remarks were excerpted from their editorial accompanying Dr. Vadlamudi’s report (Neurology 2014 Aug. 8 [doi: 10.1212/WNL.0000000000000802]).
The most common epilepsy syndromes do not follow a straightforward Mendelian inheritance pattern, but instead involve combinations of large-effect and small-effect alleles and environmental factors. This twin study illuminated the genetic complexities of epilepsy and the influence of genetic variance on complex phenotypes, said Dr. Renzo Guerrini and Dr. Jeffrey Buchhalter.

|
|
The study confirmed the strong genetic component of genetic epilepsy with febrile seizures plus and revealed high monozygotic concordance for the syndrome, they noted. In addition, the analysis found "compelling evidence" for a strong genetic role in generalized epilepsy, corroborating the concept of genetic epilepsy and the role of genes in some nonlesional focal epilepsies.
But it remains unclear whether current classifications for epilepsy reflect the molecular profiles of these syndromes, they said. The category of genetic epilepsy might turn out to be arbitrary, for example, "as what is presumed to be symptomatic today may be revealed as genetic after molecular screening."
The structural/metabolic epilepsy category also is heterogeneous, encompassing generalized and localized brain malformations that are determined by the time of origin of neurons with abnormal migration patterns, they said. "This suggests the need for a category that includes the genetic defect and interposed structural abnormality," they added.
The lack of concordance for monozygotic twins with benign epilepsy with centrotemporal spikes also contradicts prior reports that BECTS is primarily genetic, they noted. But perhaps the current study did not include enough BECTS twins to capture those with rare monozygotic inheritance, or perhaps postzygotic mutations led to genetic discordance in twin pairs, they said.
Dr. Guerrini is a neurologist with the University of Florence in Italy. Dr. Buchhalter is a neurologist with the Alberta Children’s Hospital and the University of Calgary (Alta.). Dr. Guerrini has received honoraria from Biocodex, UCB, and other companies. Dr. Buchhalter has been a consultant to UCB, Upsher-Smith, and Lundbeck. Their remarks were excerpted from their editorial accompanying Dr. Vadlamudi’s report (Neurology 2014 Aug. 8 [doi: 10.1212/WNL.0000000000000802]).
A study of twins with seizures confirmed the genetic basis of idiopathic generalized epilepsy, genetic epilepsy with febrile seizures plus, and focal epilepsies, investigators reported online Aug. 8 in Neurology.
The analysis did not support a genetic basis for benign epilepsy with centrotemporal spikes (BECTS), finding no concordance between monozygotic pairs of twins with the disorder, said Dr. Lata Vadlamudi of the University of Queensland in Brisbane, Australia, and her associates.
The researchers calculated casewise concordance estimates for epilepsy syndromes in 558 pairs of twins with suspected epilepsy, 418 of whom had confirmed seizures. They grouped them based on the 2010 ILAE (International League Against Epilepsy) scheme, incorporating molecular data when applicable (Neurology 2014 Aug. 8 [doi: 10.1212/WNL.0000000000000790]).
The estimated concordance for monozygotic twins exceeded that for dizygotic twins for idiopathic generalized epilepsies (0.77 vs. 0.35), genetic epilepsy with febrile seizures plus (0.85 vs. 0.25), and focal epilepsies (0.40 vs. 0.03), the researchers reported.
Applying the 2010 ILAE scheme also confirmed genetic influences for syndromes classified as genetic, and 10.9% of individuals tested had large-effect mutations in known epilepsy genes or had validated susceptibility alleles, the investigators said.
Mutations most often involved the SCN1A gene, which is currently seen as the most clinically relevant gene in epilepsy, they said.
The study also found "striking monozygotic and dizygotic discordance" for BECTS, which has been presumed to have a genetic basis, the researchers said. "Our analysis of the BECTS twins ... highlighted that the etiology and genetics of BECTS are more complicated than initially conceptualized."
For epilepsy patients, the results "highlight the potential to integrate well-established clinical data with molecular genetic findings and pave the way for targeted next-generation sequencing of large cohorts, which is likely to be the next phase in diagnosis, treatment guidance, and genetic counseling," Dr. Vadlamudi and her associates wrote.
The research was supported by the National Health and Medical Research Council of Australia and fellowship funding from the Queensland Department of Health. Dr. Vadlamudi and 11 coauthors reported no disclosures. Two coauthors reported advisory or financial relationships with UCB, Janssen-Cilag EMEA, and other companies.
A study of twins with seizures confirmed the genetic basis of idiopathic generalized epilepsy, genetic epilepsy with febrile seizures plus, and focal epilepsies, investigators reported online Aug. 8 in Neurology.
The analysis did not support a genetic basis for benign epilepsy with centrotemporal spikes (BECTS), finding no concordance between monozygotic pairs of twins with the disorder, said Dr. Lata Vadlamudi of the University of Queensland in Brisbane, Australia, and her associates.
The researchers calculated casewise concordance estimates for epilepsy syndromes in 558 pairs of twins with suspected epilepsy, 418 of whom had confirmed seizures. They grouped them based on the 2010 ILAE (International League Against Epilepsy) scheme, incorporating molecular data when applicable (Neurology 2014 Aug. 8 [doi: 10.1212/WNL.0000000000000790]).
The estimated concordance for monozygotic twins exceeded that for dizygotic twins for idiopathic generalized epilepsies (0.77 vs. 0.35), genetic epilepsy with febrile seizures plus (0.85 vs. 0.25), and focal epilepsies (0.40 vs. 0.03), the researchers reported.
Applying the 2010 ILAE scheme also confirmed genetic influences for syndromes classified as genetic, and 10.9% of individuals tested had large-effect mutations in known epilepsy genes or had validated susceptibility alleles, the investigators said.
Mutations most often involved the SCN1A gene, which is currently seen as the most clinically relevant gene in epilepsy, they said.
The study also found "striking monozygotic and dizygotic discordance" for BECTS, which has been presumed to have a genetic basis, the researchers said. "Our analysis of the BECTS twins ... highlighted that the etiology and genetics of BECTS are more complicated than initially conceptualized."
For epilepsy patients, the results "highlight the potential to integrate well-established clinical data with molecular genetic findings and pave the way for targeted next-generation sequencing of large cohorts, which is likely to be the next phase in diagnosis, treatment guidance, and genetic counseling," Dr. Vadlamudi and her associates wrote.
The research was supported by the National Health and Medical Research Council of Australia and fellowship funding from the Queensland Department of Health. Dr. Vadlamudi and 11 coauthors reported no disclosures. Two coauthors reported advisory or financial relationships with UCB, Janssen-Cilag EMEA, and other companies.
FROM NEUROLOGY
Key clinical point: A study of pairs of twins confirmed the genetic basis of specific epilepsies.
Major finding: Twin concordance estimates for monozygotic twin pairs exceeded those for dizygotic twins for idiopathic generalized epilepsies (0.77 vs. 0.35), genetic epilepsy with febrile seizures plus (0.85 vs. 0.25), and focal epilepsies (0.40 vs. 0.03).
Data source: Analysis of 558 pairs of twins with suspected epilepsy, of whom 418 had confirmed seizures.
Disclosures: The research was supported by the National Health and Medical Research Council of Australia and fellowship funding from the Queensland Department of Health. Dr. Vadlamudi and 11 coauthors reported no disclosures. Two coauthors reported advisory or financial relationships with UCB, Janssen-Cilag EMEA, and other companies.
Guidelines, quality indicators found lacking for CVD in RA
Rheumatoid arthritis increases cardiovascular risks as much as diabetes does, but guidelines and quality indicators fail to adequately address cardiovascular disease prevention for RA patients, authors of the first systematic review on the topic wrote in Arthritis Care & Research.
To date, only one guideline has focused entirely on the topic, and guidelines are too general to be used in adherence or quality improvement efforts, Dr. Claire Barber of the division of rheumatology at the University of Calgary (Alta.) and her associates reported. Furthermore, just four quality indicators have targeted CVD risk in RA patients, the investigators found (Arthritis Care Res. 2014 July 29 [doi:10.1002/acr.22419]).
The researchers searched MEDLINE, EMBASE, CINAHL, Web of Science, and other sources to find 16,064 abstracts on CVD or RA since 2008 that mentioned guidelines or quality indicators. Of these, they fully reviewed 808 manuscripts, and scored 10 guidelines with the six-domain Appraisal of Guidelines for Research & Evaluation (AGREE) II instrument, they said.
Only two guidelines recommended using a cardiovascular risk score, and only one, from the European League Against Rheumatism, suggested adjusting that score to account for RA, the researchers said. The guidelines also lacked thresholds for treating modifiable risk factors and did not clarify whether such thresholds should be lower than for the general population, they added.
Furthermore, the recommendations did clearly guide clinicians on monitoring or treating side effects of drugs such tocilizumab – which can cause dyslipidemia – and leflunomide, which can cause hypertension, said the investigators.
Levels of supporting evidence for guidelines also varied, and many recommendations lacked high-level evidence, particularly related to diet and exercise, the researchers said.
The four quality indicators included general screening for comorbidities, formal estimation of CVD risk, exercise, and minimizing use of steroids, the investigators said. The measures "did not cover the recognized breadth of CVD preventive care in RA," they added.
Future research should focus on how best to evaluate CVD risk in RA patients and should determine thresholds for lipid-lowering medications and other treatments, the investigators said. In the meantime, they recommended developing quality indicators for preventing CVD in RA based on the guidelines reviewed and on general population recommendations.
The research was supported by grants from Alberta Innovates Health Solutions, UCB Canada, the Canadian Rheumatology Association, and the Arthritis Society. The authors did not disclose conflicts of interest.
Rheumatoid arthritis increases cardiovascular risks as much as diabetes does, but guidelines and quality indicators fail to adequately address cardiovascular disease prevention for RA patients, authors of the first systematic review on the topic wrote in Arthritis Care & Research.
To date, only one guideline has focused entirely on the topic, and guidelines are too general to be used in adherence or quality improvement efforts, Dr. Claire Barber of the division of rheumatology at the University of Calgary (Alta.) and her associates reported. Furthermore, just four quality indicators have targeted CVD risk in RA patients, the investigators found (Arthritis Care Res. 2014 July 29 [doi:10.1002/acr.22419]).
The researchers searched MEDLINE, EMBASE, CINAHL, Web of Science, and other sources to find 16,064 abstracts on CVD or RA since 2008 that mentioned guidelines or quality indicators. Of these, they fully reviewed 808 manuscripts, and scored 10 guidelines with the six-domain Appraisal of Guidelines for Research & Evaluation (AGREE) II instrument, they said.
Only two guidelines recommended using a cardiovascular risk score, and only one, from the European League Against Rheumatism, suggested adjusting that score to account for RA, the researchers said. The guidelines also lacked thresholds for treating modifiable risk factors and did not clarify whether such thresholds should be lower than for the general population, they added.
Furthermore, the recommendations did clearly guide clinicians on monitoring or treating side effects of drugs such tocilizumab – which can cause dyslipidemia – and leflunomide, which can cause hypertension, said the investigators.
Levels of supporting evidence for guidelines also varied, and many recommendations lacked high-level evidence, particularly related to diet and exercise, the researchers said.
The four quality indicators included general screening for comorbidities, formal estimation of CVD risk, exercise, and minimizing use of steroids, the investigators said. The measures "did not cover the recognized breadth of CVD preventive care in RA," they added.
Future research should focus on how best to evaluate CVD risk in RA patients and should determine thresholds for lipid-lowering medications and other treatments, the investigators said. In the meantime, they recommended developing quality indicators for preventing CVD in RA based on the guidelines reviewed and on general population recommendations.
The research was supported by grants from Alberta Innovates Health Solutions, UCB Canada, the Canadian Rheumatology Association, and the Arthritis Society. The authors did not disclose conflicts of interest.
Rheumatoid arthritis increases cardiovascular risks as much as diabetes does, but guidelines and quality indicators fail to adequately address cardiovascular disease prevention for RA patients, authors of the first systematic review on the topic wrote in Arthritis Care & Research.
To date, only one guideline has focused entirely on the topic, and guidelines are too general to be used in adherence or quality improvement efforts, Dr. Claire Barber of the division of rheumatology at the University of Calgary (Alta.) and her associates reported. Furthermore, just four quality indicators have targeted CVD risk in RA patients, the investigators found (Arthritis Care Res. 2014 July 29 [doi:10.1002/acr.22419]).
The researchers searched MEDLINE, EMBASE, CINAHL, Web of Science, and other sources to find 16,064 abstracts on CVD or RA since 2008 that mentioned guidelines or quality indicators. Of these, they fully reviewed 808 manuscripts, and scored 10 guidelines with the six-domain Appraisal of Guidelines for Research & Evaluation (AGREE) II instrument, they said.
Only two guidelines recommended using a cardiovascular risk score, and only one, from the European League Against Rheumatism, suggested adjusting that score to account for RA, the researchers said. The guidelines also lacked thresholds for treating modifiable risk factors and did not clarify whether such thresholds should be lower than for the general population, they added.
Furthermore, the recommendations did clearly guide clinicians on monitoring or treating side effects of drugs such tocilizumab – which can cause dyslipidemia – and leflunomide, which can cause hypertension, said the investigators.
Levels of supporting evidence for guidelines also varied, and many recommendations lacked high-level evidence, particularly related to diet and exercise, the researchers said.
The four quality indicators included general screening for comorbidities, formal estimation of CVD risk, exercise, and minimizing use of steroids, the investigators said. The measures "did not cover the recognized breadth of CVD preventive care in RA," they added.
Future research should focus on how best to evaluate CVD risk in RA patients and should determine thresholds for lipid-lowering medications and other treatments, the investigators said. In the meantime, they recommended developing quality indicators for preventing CVD in RA based on the guidelines reviewed and on general population recommendations.
The research was supported by grants from Alberta Innovates Health Solutions, UCB Canada, the Canadian Rheumatology Association, and the Arthritis Society. The authors did not disclose conflicts of interest.
FROM ARTHRITIS CARE AND RESEARCH
Key clinical point: Guidelines and quality indicators on preventing cardiovascular disease in patients with rheumatoid arthritis (RA) are sparse and nonspecific.
Major finding: Ten guidelines addressed cardiovascular disease prevention in RA patients, but most were not specific enough to measure adherence, and there were only four quality indicators specific to RA.
Data source: Review of 16,064 abstracts and 808 full manuscripts on guidelines or quality indicators for cardiovascular care in patients with RA.
Disclosures: The research was supported by grants from Alberta Innovates Health Solutions, UCB Canada, the Canadian Rheumatology Association, and the Arthritis Society. The authors did not disclose conflicts of interest.
One in six SLE patients readmitted in 30 days
One in six patients with systemic lupus erythematosus was readmitted within 30 days after discharge in a multistate, administrative database study of more than 800 hospitals and 55,000 hospitalizations, and these readmissions occurred more often among black and Hispanic patients than whites.
"These findings suggest potential racial disparities in factors that are known to influence readmissions, such as the quality of care delivered in the hospital or during health care transitions to the outpatient settings," lead author Dr. Jinoos Yazdany, codirector of the lupus clinic at the University of California, San Francisco, said in an interview. "Poor access to high-quality care, both in the hospital and in the outpatient clinic, may be contributing, but further research is needed to prove this."
Patients with systemic lupus erythematosus (SLE) on Medicare or Medicaid also had higher readmission rates than those on private insurance, Dr. Yazdany and her associates reported Aug. 11 in Arthritis & Rheumatology.
Up to 25% of patients with SLE are hospitalized each year, and SLE has the sixth-highest readmission rate of any medical condition in the United States. To better characterize SLE readmissions, the researchers analyzed an administrative dataset representing 31,903 adult patients with SLE admitted at 810 hospitals in California, Florida, New York, Utah, and Washington during 2008-2009 (Arthritis Rheumatol. 2014 Aug. 11 [doi: 10.1002/art.38768]).
Of 55,936 total hospitalizations, 9,244 (16.5%) led to readmission within 30 days, the investigators reported. Patients were more likely to be readmitted if they were younger (odds ratio, 0.98 per year; 95% confidence interval, 0.98-0.98); black (OR, 1.18; 95% CI, 1.09-1.28); Hispanic (OR, 1.12; 95% CI, 1.02-1.22); or had Medicare or Medicaid versus private insurance (OR, 1.57; 95% CI, 1.45-1.69; and OR, 1.53; 95% CI, 1.40-1.67, respectively), the researchers added.
While SLE tends to be worse in younger patients, its greater prevalence and severity in minorities appears to be multifactorial, Dr. Yazdany said. "Environmental, psychosocial, biologic, and health care factors seem to all play a role," she noted. "This means that no one strategy will be enough to eliminate disparities in SLE."
Clinical features of SLE most often associated with readmission included lupus nephritis, serositis, and thrombocytopenia, the researchers added. New York hospitals had significantly lower risk-adjusted readmission rates than did those in California (OR, 0.77; 95% CI, 0.70-0.85), while hospitals in Florida had significantly higher rates (OR, 1.20; 95% CI, 1.11-1.32), compared with California, they reported.
"We should learn more about the systems that New York has in place for SLE patients, including whether the high concentration of dedicated SLE centers helps improve the quality of care," Dr. Yazdany said. Improving discharge planning, hospital transitions, coordination of care, and patient education are known to prevent avoidable hospitalizations in the overall population, she said. "To reduce readmissions in SLE, we need to investigate all of these strategies."
Notably, hospitals with high readmission rates for SLE did not also have higher rates for common chronic diseases such as heart disease or pneumonia, the researchers reported. "This tells us that it is important to look at SLE separately to properly target quality improvement initiatives," Dr. Yazdany said. "SLE requires highly coordinated, interdisciplinary care both in the hospital and during outpatient transitions, and our study implies that some hospital systems are doing a better job than others in caring for these patients."
Using readmissions to grade hospital quality is controversial, Dr. Yazdany noted. "However, readmissions can also serve as an outcome measure to help us identify disparities in care and to target quality improvement initiatives," she said. "Now that we know that there is significant unexplained variation in SLE readmission rates across states, the next step is to develop interventions to improve this outcome, particularly in high-risk patients."
Some states did not report whether admissions were planned, which could have led investigators to misclassify planned rehospitalizations as acute readmissions, they said. The dataset used in the study also had sparse clinical information, making it impossible to determine if readmissions were preventable, they added.
The study was partly funded by the National Institute of Arthritis and Musculoskeletal and Skin Diseases. The authors reported no conflicts of interest.
One in six patients with systemic lupus erythematosus was readmitted within 30 days after discharge in a multistate, administrative database study of more than 800 hospitals and 55,000 hospitalizations, and these readmissions occurred more often among black and Hispanic patients than whites.
"These findings suggest potential racial disparities in factors that are known to influence readmissions, such as the quality of care delivered in the hospital or during health care transitions to the outpatient settings," lead author Dr. Jinoos Yazdany, codirector of the lupus clinic at the University of California, San Francisco, said in an interview. "Poor access to high-quality care, both in the hospital and in the outpatient clinic, may be contributing, but further research is needed to prove this."
Patients with systemic lupus erythematosus (SLE) on Medicare or Medicaid also had higher readmission rates than those on private insurance, Dr. Yazdany and her associates reported Aug. 11 in Arthritis & Rheumatology.
Up to 25% of patients with SLE are hospitalized each year, and SLE has the sixth-highest readmission rate of any medical condition in the United States. To better characterize SLE readmissions, the researchers analyzed an administrative dataset representing 31,903 adult patients with SLE admitted at 810 hospitals in California, Florida, New York, Utah, and Washington during 2008-2009 (Arthritis Rheumatol. 2014 Aug. 11 [doi: 10.1002/art.38768]).
Of 55,936 total hospitalizations, 9,244 (16.5%) led to readmission within 30 days, the investigators reported. Patients were more likely to be readmitted if they were younger (odds ratio, 0.98 per year; 95% confidence interval, 0.98-0.98); black (OR, 1.18; 95% CI, 1.09-1.28); Hispanic (OR, 1.12; 95% CI, 1.02-1.22); or had Medicare or Medicaid versus private insurance (OR, 1.57; 95% CI, 1.45-1.69; and OR, 1.53; 95% CI, 1.40-1.67, respectively), the researchers added.
While SLE tends to be worse in younger patients, its greater prevalence and severity in minorities appears to be multifactorial, Dr. Yazdany said. "Environmental, psychosocial, biologic, and health care factors seem to all play a role," she noted. "This means that no one strategy will be enough to eliminate disparities in SLE."
Clinical features of SLE most often associated with readmission included lupus nephritis, serositis, and thrombocytopenia, the researchers added. New York hospitals had significantly lower risk-adjusted readmission rates than did those in California (OR, 0.77; 95% CI, 0.70-0.85), while hospitals in Florida had significantly higher rates (OR, 1.20; 95% CI, 1.11-1.32), compared with California, they reported.
"We should learn more about the systems that New York has in place for SLE patients, including whether the high concentration of dedicated SLE centers helps improve the quality of care," Dr. Yazdany said. Improving discharge planning, hospital transitions, coordination of care, and patient education are known to prevent avoidable hospitalizations in the overall population, she said. "To reduce readmissions in SLE, we need to investigate all of these strategies."
Notably, hospitals with high readmission rates for SLE did not also have higher rates for common chronic diseases such as heart disease or pneumonia, the researchers reported. "This tells us that it is important to look at SLE separately to properly target quality improvement initiatives," Dr. Yazdany said. "SLE requires highly coordinated, interdisciplinary care both in the hospital and during outpatient transitions, and our study implies that some hospital systems are doing a better job than others in caring for these patients."
Using readmissions to grade hospital quality is controversial, Dr. Yazdany noted. "However, readmissions can also serve as an outcome measure to help us identify disparities in care and to target quality improvement initiatives," she said. "Now that we know that there is significant unexplained variation in SLE readmission rates across states, the next step is to develop interventions to improve this outcome, particularly in high-risk patients."
Some states did not report whether admissions were planned, which could have led investigators to misclassify planned rehospitalizations as acute readmissions, they said. The dataset used in the study also had sparse clinical information, making it impossible to determine if readmissions were preventable, they added.
The study was partly funded by the National Institute of Arthritis and Musculoskeletal and Skin Diseases. The authors reported no conflicts of interest.
One in six patients with systemic lupus erythematosus was readmitted within 30 days after discharge in a multistate, administrative database study of more than 800 hospitals and 55,000 hospitalizations, and these readmissions occurred more often among black and Hispanic patients than whites.
"These findings suggest potential racial disparities in factors that are known to influence readmissions, such as the quality of care delivered in the hospital or during health care transitions to the outpatient settings," lead author Dr. Jinoos Yazdany, codirector of the lupus clinic at the University of California, San Francisco, said in an interview. "Poor access to high-quality care, both in the hospital and in the outpatient clinic, may be contributing, but further research is needed to prove this."
Patients with systemic lupus erythematosus (SLE) on Medicare or Medicaid also had higher readmission rates than those on private insurance, Dr. Yazdany and her associates reported Aug. 11 in Arthritis & Rheumatology.
Up to 25% of patients with SLE are hospitalized each year, and SLE has the sixth-highest readmission rate of any medical condition in the United States. To better characterize SLE readmissions, the researchers analyzed an administrative dataset representing 31,903 adult patients with SLE admitted at 810 hospitals in California, Florida, New York, Utah, and Washington during 2008-2009 (Arthritis Rheumatol. 2014 Aug. 11 [doi: 10.1002/art.38768]).
Of 55,936 total hospitalizations, 9,244 (16.5%) led to readmission within 30 days, the investigators reported. Patients were more likely to be readmitted if they were younger (odds ratio, 0.98 per year; 95% confidence interval, 0.98-0.98); black (OR, 1.18; 95% CI, 1.09-1.28); Hispanic (OR, 1.12; 95% CI, 1.02-1.22); or had Medicare or Medicaid versus private insurance (OR, 1.57; 95% CI, 1.45-1.69; and OR, 1.53; 95% CI, 1.40-1.67, respectively), the researchers added.
While SLE tends to be worse in younger patients, its greater prevalence and severity in minorities appears to be multifactorial, Dr. Yazdany said. "Environmental, psychosocial, biologic, and health care factors seem to all play a role," she noted. "This means that no one strategy will be enough to eliminate disparities in SLE."
Clinical features of SLE most often associated with readmission included lupus nephritis, serositis, and thrombocytopenia, the researchers added. New York hospitals had significantly lower risk-adjusted readmission rates than did those in California (OR, 0.77; 95% CI, 0.70-0.85), while hospitals in Florida had significantly higher rates (OR, 1.20; 95% CI, 1.11-1.32), compared with California, they reported.
"We should learn more about the systems that New York has in place for SLE patients, including whether the high concentration of dedicated SLE centers helps improve the quality of care," Dr. Yazdany said. Improving discharge planning, hospital transitions, coordination of care, and patient education are known to prevent avoidable hospitalizations in the overall population, she said. "To reduce readmissions in SLE, we need to investigate all of these strategies."
Notably, hospitals with high readmission rates for SLE did not also have higher rates for common chronic diseases such as heart disease or pneumonia, the researchers reported. "This tells us that it is important to look at SLE separately to properly target quality improvement initiatives," Dr. Yazdany said. "SLE requires highly coordinated, interdisciplinary care both in the hospital and during outpatient transitions, and our study implies that some hospital systems are doing a better job than others in caring for these patients."
Using readmissions to grade hospital quality is controversial, Dr. Yazdany noted. "However, readmissions can also serve as an outcome measure to help us identify disparities in care and to target quality improvement initiatives," she said. "Now that we know that there is significant unexplained variation in SLE readmission rates across states, the next step is to develop interventions to improve this outcome, particularly in high-risk patients."
Some states did not report whether admissions were planned, which could have led investigators to misclassify planned rehospitalizations as acute readmissions, they said. The dataset used in the study also had sparse clinical information, making it impossible to determine if readmissions were preventable, they added.
The study was partly funded by the National Institute of Arthritis and Musculoskeletal and Skin Diseases. The authors reported no conflicts of interest.
FROM ARTHRITIS & RHEUMATOLOGY
Key clinical point: One in six patients with systemic lupus erythematosus (SLE) was readmitted to the hospital within 30 days of discharge, and the odds of readmission were higher among younger patients and historically underserved groups.
Major finding: The all-cause 30-day readmission rate was 16.5%. Patient factors associated with readmission included younger age (odds ratio, 0.98 per year), black race (OR, 1.18), Hispanic ethnicity (OR, 1.12), and having Medicare or Medicaid versus private insurance (OR, 1.57 and 1.53, respectively).
Data source: Analysis of an administrative dataset from 810 hospitals in five states that included 55,936 hospitalizations among 31,903 adults with SLE.
Disclosures: The study was partly funded by the National Institute of Arthritis and Musculoskeletal and Skin diseases. The authors disclosed no conflicts of interest.
PALB2 mutation increased lifetime risk of breast cancer
Women with inherited loss-of-function mutations in the PALB2 gene were more than nine times as likely to develop breast cancer, compared with the general population, according to a large multicenter study reported Aug. 6 in the New England Journal of Medicine.
The study showed that women with germline loss-of-function PALB2 mutations had a 14% cumulative risk of breast cancer by age 50 years and a 35% risk by age 70, said Antonis C. Antoniou, Ph.D., of the University of Cambridge, England, and his associates.
"On the basis of our estimates, the breast-cancer risk for a PALB2 mutation carrier, even in the absence of a family history of breast cancer, would be classified as high according to various guidelines. This level of risk may justify adding PALB2 to genetic testing for BRCA1 and BRCA2," the researchers said.
Germline PALB2 mutations affect about 0.08% of the population and are a known risk factor for breast cancer. To better characterize lifetime risk in PALB2 mutation carriers, the researchers studied 154 families in the United Kingdom whose 362 members had inherited harmful truncating, splice, or deletion mutations in PALB2 (N. Engl. J. Med. 2014;371:497-506). The cohort included 311 women, of whom 229 had breast cancer, the researchers said.
After controlling for other familial factors, the risk of breast cancer in PALB2 mutation carriers was 9.47 times (95% confidence interval, 7.16-12.57) greater than in the United Kingdom overall between 1993 and 1997, the investigators reported.
Risk correlated inversely with age and also was affected by family history of breast cancer, they found. Women with the mutation whose first-degree relatives were cancer free had a 33% risk of breast cancer at age 70 years (95% CI, 25%-44%), but this risk was 58% if the women had at least two first-degree relatives who developed breast cancer by age 50 years (95% CI, 50%-66%), Dr. Antoniou and his associates said.
"Our study includes most of the reported families with PALB2 mutation carriers, as well as many not previously reported, but it is still based on small numbers," Dr. Antoniou and associates said. As screening for these mutations enters clinical practice, more families with the PALB2 mutation will be identified and risk estimates can be refined, they said, adding that future studies should evaluate whether the heightened breast cancer surveillance that women with BRCA2 mutations receive can affect outcomes in women who carry the PALB2 loss-of-function mutation.
The study was funded by the European Research Council and 25 other nonprofit and governmental entities in Europe, the United States, Canada, and Australia. Two authors reported being listed on patents related to breast cancer susceptibility genes. The authors disclosed no other conflicts of interest.
The results point to new opportunities to pursue the "synthetic lethality of cancer therapy," said Dr. Michele Evans and Dr. Dan Longo.
In synthetic lethality, two related genes simultaneously lose function, which has a cumulative effect and spurs cell death instead of sublethal changes. "Loss of heterozygosity at the PALB2 locus is likely to result in increased sensitivity to cell death with PARP inhibition as well, given that synthetic lethality is seen with other proteins that are involved in homologous recombination," they said.
"The promise of synthetic lethality in breast-cancer treatment through genetic and pharmacologic targeting of the Fanconi’s anemia-breast cancer pathway will lead the way to the examination and exploitation of defective DNA-repair mechanisms in other cancers," they wrote.
Based on the findings, women with germline PALB2 mutations face about the same risk of breast cancer as women who carry the BRCA2 mutation, Dr. Evans and Dr. Longo said. They noted that PALB2 encodes a protein that binds and colocalizes with BRCA2 in cell nuclei, which enables tumor suppression by preventing DNA damage and promoting repair.
The analyses also indicate that risks linked to PALB2 mutations "synergize with unknown environmental, lifestyle, or additional genetic factors," which "highlights the need to use genetic information within the context of family history and lifestyle factors when assessing risk," they added.
Because the study cohort was racially homogeneous, future studies need to characterize PALB2 in other populations, they noted.
Dr. Evans and Dr. Longo are with the National Institute on Aging, Baltimore. These remarks were excerpted from their editorial accompanying Dr. Antoniou’s report (N. Engl. J. Med. 2014;371:566-8 [doi: 10.1056/NEJMe1405784]).
The results point to new opportunities to pursue the "synthetic lethality of cancer therapy," said Dr. Michele Evans and Dr. Dan Longo.
In synthetic lethality, two related genes simultaneously lose function, which has a cumulative effect and spurs cell death instead of sublethal changes. "Loss of heterozygosity at the PALB2 locus is likely to result in increased sensitivity to cell death with PARP inhibition as well, given that synthetic lethality is seen with other proteins that are involved in homologous recombination," they said.
"The promise of synthetic lethality in breast-cancer treatment through genetic and pharmacologic targeting of the Fanconi’s anemia-breast cancer pathway will lead the way to the examination and exploitation of defective DNA-repair mechanisms in other cancers," they wrote.
Based on the findings, women with germline PALB2 mutations face about the same risk of breast cancer as women who carry the BRCA2 mutation, Dr. Evans and Dr. Longo said. They noted that PALB2 encodes a protein that binds and colocalizes with BRCA2 in cell nuclei, which enables tumor suppression by preventing DNA damage and promoting repair.
The analyses also indicate that risks linked to PALB2 mutations "synergize with unknown environmental, lifestyle, or additional genetic factors," which "highlights the need to use genetic information within the context of family history and lifestyle factors when assessing risk," they added.
Because the study cohort was racially homogeneous, future studies need to characterize PALB2 in other populations, they noted.
Dr. Evans and Dr. Longo are with the National Institute on Aging, Baltimore. These remarks were excerpted from their editorial accompanying Dr. Antoniou’s report (N. Engl. J. Med. 2014;371:566-8 [doi: 10.1056/NEJMe1405784]).
The results point to new opportunities to pursue the "synthetic lethality of cancer therapy," said Dr. Michele Evans and Dr. Dan Longo.
In synthetic lethality, two related genes simultaneously lose function, which has a cumulative effect and spurs cell death instead of sublethal changes. "Loss of heterozygosity at the PALB2 locus is likely to result in increased sensitivity to cell death with PARP inhibition as well, given that synthetic lethality is seen with other proteins that are involved in homologous recombination," they said.
"The promise of synthetic lethality in breast-cancer treatment through genetic and pharmacologic targeting of the Fanconi’s anemia-breast cancer pathway will lead the way to the examination and exploitation of defective DNA-repair mechanisms in other cancers," they wrote.
Based on the findings, women with germline PALB2 mutations face about the same risk of breast cancer as women who carry the BRCA2 mutation, Dr. Evans and Dr. Longo said. They noted that PALB2 encodes a protein that binds and colocalizes with BRCA2 in cell nuclei, which enables tumor suppression by preventing DNA damage and promoting repair.
The analyses also indicate that risks linked to PALB2 mutations "synergize with unknown environmental, lifestyle, or additional genetic factors," which "highlights the need to use genetic information within the context of family history and lifestyle factors when assessing risk," they added.
Because the study cohort was racially homogeneous, future studies need to characterize PALB2 in other populations, they noted.
Dr. Evans and Dr. Longo are with the National Institute on Aging, Baltimore. These remarks were excerpted from their editorial accompanying Dr. Antoniou’s report (N. Engl. J. Med. 2014;371:566-8 [doi: 10.1056/NEJMe1405784]).
Women with inherited loss-of-function mutations in the PALB2 gene were more than nine times as likely to develop breast cancer, compared with the general population, according to a large multicenter study reported Aug. 6 in the New England Journal of Medicine.
The study showed that women with germline loss-of-function PALB2 mutations had a 14% cumulative risk of breast cancer by age 50 years and a 35% risk by age 70, said Antonis C. Antoniou, Ph.D., of the University of Cambridge, England, and his associates.
"On the basis of our estimates, the breast-cancer risk for a PALB2 mutation carrier, even in the absence of a family history of breast cancer, would be classified as high according to various guidelines. This level of risk may justify adding PALB2 to genetic testing for BRCA1 and BRCA2," the researchers said.
Germline PALB2 mutations affect about 0.08% of the population and are a known risk factor for breast cancer. To better characterize lifetime risk in PALB2 mutation carriers, the researchers studied 154 families in the United Kingdom whose 362 members had inherited harmful truncating, splice, or deletion mutations in PALB2 (N. Engl. J. Med. 2014;371:497-506). The cohort included 311 women, of whom 229 had breast cancer, the researchers said.
After controlling for other familial factors, the risk of breast cancer in PALB2 mutation carriers was 9.47 times (95% confidence interval, 7.16-12.57) greater than in the United Kingdom overall between 1993 and 1997, the investigators reported.
Risk correlated inversely with age and also was affected by family history of breast cancer, they found. Women with the mutation whose first-degree relatives were cancer free had a 33% risk of breast cancer at age 70 years (95% CI, 25%-44%), but this risk was 58% if the women had at least two first-degree relatives who developed breast cancer by age 50 years (95% CI, 50%-66%), Dr. Antoniou and his associates said.
"Our study includes most of the reported families with PALB2 mutation carriers, as well as many not previously reported, but it is still based on small numbers," Dr. Antoniou and associates said. As screening for these mutations enters clinical practice, more families with the PALB2 mutation will be identified and risk estimates can be refined, they said, adding that future studies should evaluate whether the heightened breast cancer surveillance that women with BRCA2 mutations receive can affect outcomes in women who carry the PALB2 loss-of-function mutation.
The study was funded by the European Research Council and 25 other nonprofit and governmental entities in Europe, the United States, Canada, and Australia. Two authors reported being listed on patents related to breast cancer susceptibility genes. The authors disclosed no other conflicts of interest.
Women with inherited loss-of-function mutations in the PALB2 gene were more than nine times as likely to develop breast cancer, compared with the general population, according to a large multicenter study reported Aug. 6 in the New England Journal of Medicine.
The study showed that women with germline loss-of-function PALB2 mutations had a 14% cumulative risk of breast cancer by age 50 years and a 35% risk by age 70, said Antonis C. Antoniou, Ph.D., of the University of Cambridge, England, and his associates.
"On the basis of our estimates, the breast-cancer risk for a PALB2 mutation carrier, even in the absence of a family history of breast cancer, would be classified as high according to various guidelines. This level of risk may justify adding PALB2 to genetic testing for BRCA1 and BRCA2," the researchers said.
Germline PALB2 mutations affect about 0.08% of the population and are a known risk factor for breast cancer. To better characterize lifetime risk in PALB2 mutation carriers, the researchers studied 154 families in the United Kingdom whose 362 members had inherited harmful truncating, splice, or deletion mutations in PALB2 (N. Engl. J. Med. 2014;371:497-506). The cohort included 311 women, of whom 229 had breast cancer, the researchers said.
After controlling for other familial factors, the risk of breast cancer in PALB2 mutation carriers was 9.47 times (95% confidence interval, 7.16-12.57) greater than in the United Kingdom overall between 1993 and 1997, the investigators reported.
Risk correlated inversely with age and also was affected by family history of breast cancer, they found. Women with the mutation whose first-degree relatives were cancer free had a 33% risk of breast cancer at age 70 years (95% CI, 25%-44%), but this risk was 58% if the women had at least two first-degree relatives who developed breast cancer by age 50 years (95% CI, 50%-66%), Dr. Antoniou and his associates said.
"Our study includes most of the reported families with PALB2 mutation carriers, as well as many not previously reported, but it is still based on small numbers," Dr. Antoniou and associates said. As screening for these mutations enters clinical practice, more families with the PALB2 mutation will be identified and risk estimates can be refined, they said, adding that future studies should evaluate whether the heightened breast cancer surveillance that women with BRCA2 mutations receive can affect outcomes in women who carry the PALB2 loss-of-function mutation.
The study was funded by the European Research Council and 25 other nonprofit and governmental entities in Europe, the United States, Canada, and Australia. Two authors reported being listed on patents related to breast cancer susceptibility genes. The authors disclosed no other conflicts of interest.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Key clinical point: Inherited loss-of-function mutations in PALB2 significantly increase women’s lifetime risk of breast cancer.
Major finding: Women with inherited loss-of-function mutations in the PALB2 gene were 9.47 times more likely to develop breast cancer than the general population.
Data source: Modified segregation analysis of breast cancer risk among 154 families in the United Kingdom whose 362 members had truncating, splice, or deletion mutations in the PALB2 gene.
Disclosures: The study was funded by the European Research Council and 25 other nonprofit and governmental entities in Europe, the United States, Canada, and Australia. Two authors reported having been listed on patents related to breast cancer susceptibility genes. The authors reported no other conflicts of interest.