User login
Plan helped atrial fibrillation patients safely switch oral anticoagulants
A detailed transition plan protected most atrial fibrillation patients from strokes and major bleeding when they switched oral anticoagulants, researchers reported in the August issue of the Journal of the American College of Cardiology.
Following such a plan could help patients safely switch anticoagulants in clinical practice, said Dr. Christian Ruff at Harvard Medical School in Boston and his associates.
They reported an analysis from the ENGAGE AF-TIMI 48 (Effective Anticoagulation With Factor Xa Next Generation in Atrial Fibrillation–Thrombolysis in Myocardial Infarction 48) trial, which randomized more than 21,000 AF patients at high risk of stroke to either the investigational factor Xa inhibitor edoxaban or warfarin. Edoxaban was shown noninferior to warfarin in preventing stroke or systemic embolism (N. Engl. J. Med. 2013; 369:2093-104).
In the past, researchers from the ROCKET AF and ARISTOTLE trials reported excess strokes and bleeding events after patients were switched from blinded factor Xa inhibitors to open-label antithrombotics, the investigators said.
In response, ENGAGE AF-TIMI 48 patients and their physicians decided together whether to switch to an open-label vitamin K antagonist (VKA) or a newer oral anticoagulant at the end of the trial, the researchers said. Patients then received a transition kit with a 14-day supply of either a half-dose edoxaban for patients switching from blinded edoxaban to open warfarin, or a placebo for patients switching from blinded to open warfarin. Patients also underwent at least three international normalized ratio (INR) tests during the first 2 weeks of the transition period and were dosed based on a VKA titration algorithm designed to quickly reach therapeutic INR, they said.
Among 13,642 ENGAGE AF-TIMI patients alive at the end of the trial, 68.2% transitioned to a VKA and 31.2% to a new oral anticoagulant, said the researchers.
Thirty days later, rates of therapeutic INR, stroke, and bleeding events were similar regardless of whether patients had taken low-dose edoxaban, high-dose edoxaban, or warfarin during the trial, they reported. In all, 98.7% of patients switched from high-dose edoxaban had at least one INR of 2 or more, compared with 98.9% of patients switched from low-dose edoxaban and 99.4% of patients switched from warfarin, they said (J. Am. Coll. Cardiol. 2014;64:576-84).
Post-transition rates of strokes (1.85% to 1.90% per year) and major bleeding (2.69% to 4.76% per year) also were similar among the three trial groups, they added.
The excess ischemic events in earlier trials probably resulted from relative delays in achieving a therapeutic INR when patients were switched from a newer oral anticoagulant to an open-label VKA, the researchers noted, adding that "VKAs are effective as long as a therapeutic INR can be rapidly reached and maintained."
Daiichi Sankyo funded the ENGAGE AF-TIMI trial. Dr. Ruff reported having been a consultant and receiving honoraria from Daiichi Sankyo. Two coauthors reported financial relationships, six reported having received grant support, and two reported employment with Daiichi Sankyo.
These results appear to set a new standard for managing patients switching from a new oral anticoagulant to open-label warfarin at the end of blinded anticoagulation trials.
The data reveal ways to manage patients who need their anticoagulation interrupted. Bridging anticoagulation can prevent thromboembolic events when combined with rigorous INR monitoring and algorithm-based warfarin dosing.
Furthermore, the lack of excess bleeding with the half-dose edoxaban bridging regimen raises the possibility that lowering the dose of the anticoagulant can improve safety without compromising efficacy. In past observational studies, bridging with a fast-acting parenteral anticoagulant until INR reached 2.0 increased the risk of bleeding probably because of dose overlap between the bridging agent and warfarin. Also, annualized stroke rates during the transition phase slightly exceeded those during the rest of the trial, reminding clinicians that even when carefully managed, switching from one anticoagulant to another is not without risk.
Remaining questions include whether to apply bridging uniformly, whether a half-dose of edoxaban is sufficient, and whether results for lower edoxaban dosing can be extrapolated to other new oral anticoagulants, said the researchers. Finally, evaluation of the transition kit in the ENGAGE AF-TIMI 48 trial was not randomized, and our conclusions regarding the efficacy and safety of this approach compared with no bridging or a more limited bridging strategy are based on indirect comparisons across trials and cannot be considered definitive. In the meantime several large ongoing trials are evaluating bridging regimens for surgical patients who need their warfarin therapy interrupted.
Dr. John Eikelboom, Dr. Thomas. Vanassche, and Dr. Stuart Connolly, are cardiologists with Hamilton General Hospital and McMaster University in Ontario, Canada. Dr. Eikelboom has received financial support from companies that make and market non–vitamin K antagonist oral anticoagulants, including Bayer HealthCare, Boehringer Ingelheim, Bristol-Myers Squibb, Janssen, and Pfizer. Dr. Connolly has been an adviser, consultant, or speaker for Bayer HealthCare Pharmaceuticals, BI, BMS, Pfizer, and Portola Pharmaceuticals. Dr. Vanassche reported no financial conflicts of interest. These remarks were excerpted from their editorial accompanying Dr. Ruff’s report (J. Am. Coll. Cardiol. 2014;64:585-7).
These results appear to set a new standard for managing patients switching from a new oral anticoagulant to open-label warfarin at the end of blinded anticoagulation trials.
The data reveal ways to manage patients who need their anticoagulation interrupted. Bridging anticoagulation can prevent thromboembolic events when combined with rigorous INR monitoring and algorithm-based warfarin dosing.
Furthermore, the lack of excess bleeding with the half-dose edoxaban bridging regimen raises the possibility that lowering the dose of the anticoagulant can improve safety without compromising efficacy. In past observational studies, bridging with a fast-acting parenteral anticoagulant until INR reached 2.0 increased the risk of bleeding probably because of dose overlap between the bridging agent and warfarin. Also, annualized stroke rates during the transition phase slightly exceeded those during the rest of the trial, reminding clinicians that even when carefully managed, switching from one anticoagulant to another is not without risk.
Remaining questions include whether to apply bridging uniformly, whether a half-dose of edoxaban is sufficient, and whether results for lower edoxaban dosing can be extrapolated to other new oral anticoagulants, said the researchers. Finally, evaluation of the transition kit in the ENGAGE AF-TIMI 48 trial was not randomized, and our conclusions regarding the efficacy and safety of this approach compared with no bridging or a more limited bridging strategy are based on indirect comparisons across trials and cannot be considered definitive. In the meantime several large ongoing trials are evaluating bridging regimens for surgical patients who need their warfarin therapy interrupted.
Dr. John Eikelboom, Dr. Thomas. Vanassche, and Dr. Stuart Connolly, are cardiologists with Hamilton General Hospital and McMaster University in Ontario, Canada. Dr. Eikelboom has received financial support from companies that make and market non–vitamin K antagonist oral anticoagulants, including Bayer HealthCare, Boehringer Ingelheim, Bristol-Myers Squibb, Janssen, and Pfizer. Dr. Connolly has been an adviser, consultant, or speaker for Bayer HealthCare Pharmaceuticals, BI, BMS, Pfizer, and Portola Pharmaceuticals. Dr. Vanassche reported no financial conflicts of interest. These remarks were excerpted from their editorial accompanying Dr. Ruff’s report (J. Am. Coll. Cardiol. 2014;64:585-7).
These results appear to set a new standard for managing patients switching from a new oral anticoagulant to open-label warfarin at the end of blinded anticoagulation trials.
The data reveal ways to manage patients who need their anticoagulation interrupted. Bridging anticoagulation can prevent thromboembolic events when combined with rigorous INR monitoring and algorithm-based warfarin dosing.
Furthermore, the lack of excess bleeding with the half-dose edoxaban bridging regimen raises the possibility that lowering the dose of the anticoagulant can improve safety without compromising efficacy. In past observational studies, bridging with a fast-acting parenteral anticoagulant until INR reached 2.0 increased the risk of bleeding probably because of dose overlap between the bridging agent and warfarin. Also, annualized stroke rates during the transition phase slightly exceeded those during the rest of the trial, reminding clinicians that even when carefully managed, switching from one anticoagulant to another is not without risk.
Remaining questions include whether to apply bridging uniformly, whether a half-dose of edoxaban is sufficient, and whether results for lower edoxaban dosing can be extrapolated to other new oral anticoagulants, said the researchers. Finally, evaluation of the transition kit in the ENGAGE AF-TIMI 48 trial was not randomized, and our conclusions regarding the efficacy and safety of this approach compared with no bridging or a more limited bridging strategy are based on indirect comparisons across trials and cannot be considered definitive. In the meantime several large ongoing trials are evaluating bridging regimens for surgical patients who need their warfarin therapy interrupted.
Dr. John Eikelboom, Dr. Thomas. Vanassche, and Dr. Stuart Connolly, are cardiologists with Hamilton General Hospital and McMaster University in Ontario, Canada. Dr. Eikelboom has received financial support from companies that make and market non–vitamin K antagonist oral anticoagulants, including Bayer HealthCare, Boehringer Ingelheim, Bristol-Myers Squibb, Janssen, and Pfizer. Dr. Connolly has been an adviser, consultant, or speaker for Bayer HealthCare Pharmaceuticals, BI, BMS, Pfizer, and Portola Pharmaceuticals. Dr. Vanassche reported no financial conflicts of interest. These remarks were excerpted from their editorial accompanying Dr. Ruff’s report (J. Am. Coll. Cardiol. 2014;64:585-7).
A detailed transition plan protected most atrial fibrillation patients from strokes and major bleeding when they switched oral anticoagulants, researchers reported in the August issue of the Journal of the American College of Cardiology.
Following such a plan could help patients safely switch anticoagulants in clinical practice, said Dr. Christian Ruff at Harvard Medical School in Boston and his associates.
They reported an analysis from the ENGAGE AF-TIMI 48 (Effective Anticoagulation With Factor Xa Next Generation in Atrial Fibrillation–Thrombolysis in Myocardial Infarction 48) trial, which randomized more than 21,000 AF patients at high risk of stroke to either the investigational factor Xa inhibitor edoxaban or warfarin. Edoxaban was shown noninferior to warfarin in preventing stroke or systemic embolism (N. Engl. J. Med. 2013; 369:2093-104).
In the past, researchers from the ROCKET AF and ARISTOTLE trials reported excess strokes and bleeding events after patients were switched from blinded factor Xa inhibitors to open-label antithrombotics, the investigators said.
In response, ENGAGE AF-TIMI 48 patients and their physicians decided together whether to switch to an open-label vitamin K antagonist (VKA) or a newer oral anticoagulant at the end of the trial, the researchers said. Patients then received a transition kit with a 14-day supply of either a half-dose edoxaban for patients switching from blinded edoxaban to open warfarin, or a placebo for patients switching from blinded to open warfarin. Patients also underwent at least three international normalized ratio (INR) tests during the first 2 weeks of the transition period and were dosed based on a VKA titration algorithm designed to quickly reach therapeutic INR, they said.
Among 13,642 ENGAGE AF-TIMI patients alive at the end of the trial, 68.2% transitioned to a VKA and 31.2% to a new oral anticoagulant, said the researchers.
Thirty days later, rates of therapeutic INR, stroke, and bleeding events were similar regardless of whether patients had taken low-dose edoxaban, high-dose edoxaban, or warfarin during the trial, they reported. In all, 98.7% of patients switched from high-dose edoxaban had at least one INR of 2 or more, compared with 98.9% of patients switched from low-dose edoxaban and 99.4% of patients switched from warfarin, they said (J. Am. Coll. Cardiol. 2014;64:576-84).
Post-transition rates of strokes (1.85% to 1.90% per year) and major bleeding (2.69% to 4.76% per year) also were similar among the three trial groups, they added.
The excess ischemic events in earlier trials probably resulted from relative delays in achieving a therapeutic INR when patients were switched from a newer oral anticoagulant to an open-label VKA, the researchers noted, adding that "VKAs are effective as long as a therapeutic INR can be rapidly reached and maintained."
Daiichi Sankyo funded the ENGAGE AF-TIMI trial. Dr. Ruff reported having been a consultant and receiving honoraria from Daiichi Sankyo. Two coauthors reported financial relationships, six reported having received grant support, and two reported employment with Daiichi Sankyo.
A detailed transition plan protected most atrial fibrillation patients from strokes and major bleeding when they switched oral anticoagulants, researchers reported in the August issue of the Journal of the American College of Cardiology.
Following such a plan could help patients safely switch anticoagulants in clinical practice, said Dr. Christian Ruff at Harvard Medical School in Boston and his associates.
They reported an analysis from the ENGAGE AF-TIMI 48 (Effective Anticoagulation With Factor Xa Next Generation in Atrial Fibrillation–Thrombolysis in Myocardial Infarction 48) trial, which randomized more than 21,000 AF patients at high risk of stroke to either the investigational factor Xa inhibitor edoxaban or warfarin. Edoxaban was shown noninferior to warfarin in preventing stroke or systemic embolism (N. Engl. J. Med. 2013; 369:2093-104).
In the past, researchers from the ROCKET AF and ARISTOTLE trials reported excess strokes and bleeding events after patients were switched from blinded factor Xa inhibitors to open-label antithrombotics, the investigators said.
In response, ENGAGE AF-TIMI 48 patients and their physicians decided together whether to switch to an open-label vitamin K antagonist (VKA) or a newer oral anticoagulant at the end of the trial, the researchers said. Patients then received a transition kit with a 14-day supply of either a half-dose edoxaban for patients switching from blinded edoxaban to open warfarin, or a placebo for patients switching from blinded to open warfarin. Patients also underwent at least three international normalized ratio (INR) tests during the first 2 weeks of the transition period and were dosed based on a VKA titration algorithm designed to quickly reach therapeutic INR, they said.
Among 13,642 ENGAGE AF-TIMI patients alive at the end of the trial, 68.2% transitioned to a VKA and 31.2% to a new oral anticoagulant, said the researchers.
Thirty days later, rates of therapeutic INR, stroke, and bleeding events were similar regardless of whether patients had taken low-dose edoxaban, high-dose edoxaban, or warfarin during the trial, they reported. In all, 98.7% of patients switched from high-dose edoxaban had at least one INR of 2 or more, compared with 98.9% of patients switched from low-dose edoxaban and 99.4% of patients switched from warfarin, they said (J. Am. Coll. Cardiol. 2014;64:576-84).
Post-transition rates of strokes (1.85% to 1.90% per year) and major bleeding (2.69% to 4.76% per year) also were similar among the three trial groups, they added.
The excess ischemic events in earlier trials probably resulted from relative delays in achieving a therapeutic INR when patients were switched from a newer oral anticoagulant to an open-label VKA, the researchers noted, adding that "VKAs are effective as long as a therapeutic INR can be rapidly reached and maintained."
Daiichi Sankyo funded the ENGAGE AF-TIMI trial. Dr. Ruff reported having been a consultant and receiving honoraria from Daiichi Sankyo. Two coauthors reported financial relationships, six reported having received grant support, and two reported employment with Daiichi Sankyo.
FROM THE JOURNAL OF THE AMERICAN COLLEGE OF CARDIOLOGY
Key clinical point: Following a prescribed transition plan when switching oral anticoagulants protected most AF patients from strokes and major bleeding.
Major finding: Thirty days after transitioning to a new oral anticoagulant, 98.7% of patients who were switched from high-dose edoxaban had at least one therapeutic INR, compared with 98.9% of patients switched from low-dose edoxaban and 99.4% of patients switched from warfarin. Post-transition rates of stroke and major bleeding also were similar among all three groups.
Data source: Randomized, open-label study of 13,642 patients with AF from the ENGAGE AF-TIMI 48 trial. At the end of the trial, 68.2% of patients transitioned to an open-label vitamin K antagonist, and 31.2% were switched to new oral anticoagulant.
Disclosures: Daiichi Sankyo funded the ENGAGE AF-TIMI trial. Dr. Ruff reported having been a consultant and receiving honoraria from Daiichi Sankyo. Two coauthors reported financial relationships, six reported having received grant support, and two reported employment with Daiichi Sankyo.
Gemtuzumab-ozogamicin improves event-free survival in pediatric AML
In children and young adults with acute myeloid leukemia, the addition of the anti-CD33 antibody gemtuzumab-ozogamicin to standard chemotherapy cut 3-year risk of relapse by 17% and significantly improved event-free survival, according to a study published Aug. 4 in the Journal of Clinical Oncology.
The results contradict those from the controversial Southwest Oncology Group’s trial (SWOG) S0106, which led to the voluntary withdrawal of gemtuzumab-ozogamicin (GO) in 2010, said Dr. Alan Gamis of Children’s Mercy Hospitals and Clinics in Kansas City, Mo., and associates.
For the trial, the researchers randomized 1,022 children, adolescents, and young adults aged less than 1-29 years to receive either standard five-course chemotherapy alone, or standard treatment plus 3 mg/m2 of GO given once during induction course 1 and once during intensification course 2 (J. Clin. Onc. 2014 Aug. 4 [doi: 10.1200/JCO.2014.55.3628]).
Three-year event-free survival was 53.1% for the GO group, compared with 46.9% for the control group (hazard ratio, 0.83; 95% confidence interval, 0.70 to 0.99; P =.04), the investigators reported. In a post hoc analysis, 3-year risk of relapse was 32.8% for the intervention group, compared with 41.3% for controls (HR, 0.73; 95% CI, 0.58-0.91; P = 0.006), they said.
However, GO did not significantly affect 3-year overall survival (69.4% compared with 65.4% for the control arm; HR, 0.91; 95% CI, 0.74 to 1.13; P = .39), the investigators reported. Grade 3-5 adverse events were similar between the study arms, they added.
The trial did not find a statistically significant improvement in event-free survival for all risk subgroups – an increasingly common challenge as the biologic heterogeneity of AML has led to smaller study cohorts, the researchers said.
The results align with published trials in adults with low-risk and moderate-risk AML, wrote the investigators, who said more studies are needed to determine the best ways to administer GO and other CD33-targeted agents.
The study was funded by the National Cancer Institute. The authors reported no financial conflicts of interest.
In children and young adults with acute myeloid leukemia, the addition of the anti-CD33 antibody gemtuzumab-ozogamicin to standard chemotherapy cut 3-year risk of relapse by 17% and significantly improved event-free survival, according to a study published Aug. 4 in the Journal of Clinical Oncology.
The results contradict those from the controversial Southwest Oncology Group’s trial (SWOG) S0106, which led to the voluntary withdrawal of gemtuzumab-ozogamicin (GO) in 2010, said Dr. Alan Gamis of Children’s Mercy Hospitals and Clinics in Kansas City, Mo., and associates.
For the trial, the researchers randomized 1,022 children, adolescents, and young adults aged less than 1-29 years to receive either standard five-course chemotherapy alone, or standard treatment plus 3 mg/m2 of GO given once during induction course 1 and once during intensification course 2 (J. Clin. Onc. 2014 Aug. 4 [doi: 10.1200/JCO.2014.55.3628]).
Three-year event-free survival was 53.1% for the GO group, compared with 46.9% for the control group (hazard ratio, 0.83; 95% confidence interval, 0.70 to 0.99; P =.04), the investigators reported. In a post hoc analysis, 3-year risk of relapse was 32.8% for the intervention group, compared with 41.3% for controls (HR, 0.73; 95% CI, 0.58-0.91; P = 0.006), they said.
However, GO did not significantly affect 3-year overall survival (69.4% compared with 65.4% for the control arm; HR, 0.91; 95% CI, 0.74 to 1.13; P = .39), the investigators reported. Grade 3-5 adverse events were similar between the study arms, they added.
The trial did not find a statistically significant improvement in event-free survival for all risk subgroups – an increasingly common challenge as the biologic heterogeneity of AML has led to smaller study cohorts, the researchers said.
The results align with published trials in adults with low-risk and moderate-risk AML, wrote the investigators, who said more studies are needed to determine the best ways to administer GO and other CD33-targeted agents.
The study was funded by the National Cancer Institute. The authors reported no financial conflicts of interest.
In children and young adults with acute myeloid leukemia, the addition of the anti-CD33 antibody gemtuzumab-ozogamicin to standard chemotherapy cut 3-year risk of relapse by 17% and significantly improved event-free survival, according to a study published Aug. 4 in the Journal of Clinical Oncology.
The results contradict those from the controversial Southwest Oncology Group’s trial (SWOG) S0106, which led to the voluntary withdrawal of gemtuzumab-ozogamicin (GO) in 2010, said Dr. Alan Gamis of Children’s Mercy Hospitals and Clinics in Kansas City, Mo., and associates.
For the trial, the researchers randomized 1,022 children, adolescents, and young adults aged less than 1-29 years to receive either standard five-course chemotherapy alone, or standard treatment plus 3 mg/m2 of GO given once during induction course 1 and once during intensification course 2 (J. Clin. Onc. 2014 Aug. 4 [doi: 10.1200/JCO.2014.55.3628]).
Three-year event-free survival was 53.1% for the GO group, compared with 46.9% for the control group (hazard ratio, 0.83; 95% confidence interval, 0.70 to 0.99; P =.04), the investigators reported. In a post hoc analysis, 3-year risk of relapse was 32.8% for the intervention group, compared with 41.3% for controls (HR, 0.73; 95% CI, 0.58-0.91; P = 0.006), they said.
However, GO did not significantly affect 3-year overall survival (69.4% compared with 65.4% for the control arm; HR, 0.91; 95% CI, 0.74 to 1.13; P = .39), the investigators reported. Grade 3-5 adverse events were similar between the study arms, they added.
The trial did not find a statistically significant improvement in event-free survival for all risk subgroups – an increasingly common challenge as the biologic heterogeneity of AML has led to smaller study cohorts, the researchers said.
The results align with published trials in adults with low-risk and moderate-risk AML, wrote the investigators, who said more studies are needed to determine the best ways to administer GO and other CD33-targeted agents.
The study was funded by the National Cancer Institute. The authors reported no financial conflicts of interest.
FROM JOURNAL OF CLINICAL ONCOLOGY
Key clinical point: In children, adolescents, and young adults with AML, the addition of gemtuzumab-ozogamicin (GO) to standard chemotherapy significantly improved event-free survival by cutting the risk of relapse.
Major finding: Three-year event-free survival was 53.1% for the GO group, compared with 46.9% for the control group (hazard ratio, 0.83; 95% confidence interval, 0.70 to 0.99; P = .04).
Data source: Randomized trial of 1,022 patients aged 0 to 29 years with AML. Patients received standard five-course chemotherapy, alone or with 3 mg/m2 gemtuzumab-ozogamicin given once during induction course 1 and once during intensification course 2.
Disclosures: The study was funded by the National Cancer Institute. The authors reported no financial conflicts of interest.
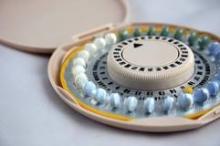
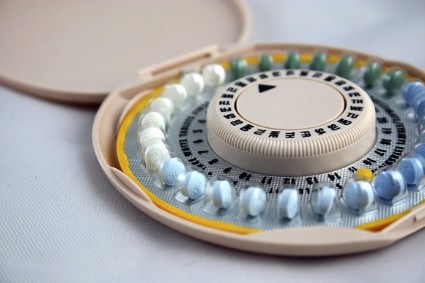
Recent use of oral contraceptives linked to breast cancer
Women who recently used oral contraceptives had a 50% greater chance of developing breast cancer than that of women who formerly used or never used oral contraceptives, according to a case-control study published Aug. 1 in Cancer Research.
For the nested case-control study, the researchers compared 1,102 women aged 20-49 years who had been diagnosed with invasive breast cancer from 1990 to 2009 with 21, 755 controls sampled from the same health care delivery system, matched for age, year, enrollment length, and medical chart availability.
Oral contraceptive use within the prior year was associated with an increased breast cancer risk (odds ratio, 1.5; 95% confidence interval, 1.3-1.9) relative to never or former use of oral contraceptives, reported Dr. Elisabeth Beaber at the University of Washington, Seattle, and her associates.
Their findings suggest that risk may vary by oral contraceptive formulation. The investigators found significant associations between breast cancer and recent use of oral contraceptives involving high-dose estrogen (OR, 2.7; 95% CI, 1.1-6.2), ethynodiol diacetate (OR, 2.6; 95% CI, 1.4-4.7), or triphasic dosing with an average of 0.75 mg of norethindrone (OR, 3.1; 95% CI, 1.9-5.1). But other types of oral birth control, including low-dose estrogen oral contraceptives, were not associated with breast cancer (OR, 1.0; 95% CI, 0.6-1.7), Dr. Beaber and her associates noted (Cancer Res. 2014;74:4078-89).
"If confirmed, consideration of the breast cancer risk associated with different oral contraceptive types could impact discussions weighing recognized health benefits and potential risks," they concluded.
The study was funded by the National Cancer Institute. The authors reported no financial conflicts of interest.
Women who recently used oral contraceptives had a 50% greater chance of developing breast cancer than that of women who formerly used or never used oral contraceptives, according to a case-control study published Aug. 1 in Cancer Research.
For the nested case-control study, the researchers compared 1,102 women aged 20-49 years who had been diagnosed with invasive breast cancer from 1990 to 2009 with 21, 755 controls sampled from the same health care delivery system, matched for age, year, enrollment length, and medical chart availability.
Oral contraceptive use within the prior year was associated with an increased breast cancer risk (odds ratio, 1.5; 95% confidence interval, 1.3-1.9) relative to never or former use of oral contraceptives, reported Dr. Elisabeth Beaber at the University of Washington, Seattle, and her associates.
Their findings suggest that risk may vary by oral contraceptive formulation. The investigators found significant associations between breast cancer and recent use of oral contraceptives involving high-dose estrogen (OR, 2.7; 95% CI, 1.1-6.2), ethynodiol diacetate (OR, 2.6; 95% CI, 1.4-4.7), or triphasic dosing with an average of 0.75 mg of norethindrone (OR, 3.1; 95% CI, 1.9-5.1). But other types of oral birth control, including low-dose estrogen oral contraceptives, were not associated with breast cancer (OR, 1.0; 95% CI, 0.6-1.7), Dr. Beaber and her associates noted (Cancer Res. 2014;74:4078-89).
"If confirmed, consideration of the breast cancer risk associated with different oral contraceptive types could impact discussions weighing recognized health benefits and potential risks," they concluded.
The study was funded by the National Cancer Institute. The authors reported no financial conflicts of interest.
Women who recently used oral contraceptives had a 50% greater chance of developing breast cancer than that of women who formerly used or never used oral contraceptives, according to a case-control study published Aug. 1 in Cancer Research.
For the nested case-control study, the researchers compared 1,102 women aged 20-49 years who had been diagnosed with invasive breast cancer from 1990 to 2009 with 21, 755 controls sampled from the same health care delivery system, matched for age, year, enrollment length, and medical chart availability.
Oral contraceptive use within the prior year was associated with an increased breast cancer risk (odds ratio, 1.5; 95% confidence interval, 1.3-1.9) relative to never or former use of oral contraceptives, reported Dr. Elisabeth Beaber at the University of Washington, Seattle, and her associates.
Their findings suggest that risk may vary by oral contraceptive formulation. The investigators found significant associations between breast cancer and recent use of oral contraceptives involving high-dose estrogen (OR, 2.7; 95% CI, 1.1-6.2), ethynodiol diacetate (OR, 2.6; 95% CI, 1.4-4.7), or triphasic dosing with an average of 0.75 mg of norethindrone (OR, 3.1; 95% CI, 1.9-5.1). But other types of oral birth control, including low-dose estrogen oral contraceptives, were not associated with breast cancer (OR, 1.0; 95% CI, 0.6-1.7), Dr. Beaber and her associates noted (Cancer Res. 2014;74:4078-89).
"If confirmed, consideration of the breast cancer risk associated with different oral contraceptive types could impact discussions weighing recognized health benefits and potential risks," they concluded.
The study was funded by the National Cancer Institute. The authors reported no financial conflicts of interest.
FROM CANCER RESEARCH
Key clinical point: Recent use of oral contraceptives may increase breast cancer risk.
Major finding: Oral contraceptive use within the prior year was associated with an increased breast cancer risk (OR, 1.5; 95% CI, 1.3–1.9) relative to never or former use of oral contraceptives.
Data source: Nested case-control study of 1,102 women aged 20-49 years diagnosed with invasive breast cancer, compared with 21,755 controls.
Disclosures: The study was funded by The National Cancer Institute. The authors reported no financial conflicts of interest.
Age, income, ethnicity predicted rheumatoid arthritis drug discontinuation
Some of the same factors that predict patients’ discontinuation of disease-modifying antirheumatic drugs for rheumatoid arthritis also appear to predict their initiation, such as use of oral glucocorticoids and Hispanic ethnicity, according to findings from a longitudinal cohort study.
It was "surprising" to lead investigator Dr. Daniel H. Solomon of Brigham and Women’s Hospital, Boston, and his associates that some of the same variables predicted both starting and stopping RA medication. "These factors may correlate with frequent treatment switches," they wrote. The fact that Hispanics were significantly more likely to start and to stop medication than non-Hispanics might reflect disparities in insurance coverage, differences in the availability of new treatments, or impaired communication about side effects because of language barriers, they added in their report published in Arthritis Care and Research.
Dr. Solomon and his colleagues based their analysis on data from the University of California, San Francisco, RA Panel study, a longitudinal cohort of 1,507 persons with rheumatoid arthritis (RA) who were randomly sampled from rheumatology practices in Northern California (Arthritis Care Res. 2014;66:1152-8). The study used a paired-years analysis to calculate percentages of patients who were on or off RA medications for a year and then either stopped or started medication the next year, the investigators said.
Of 1,974 pairs of years in which people were not on RA medication in year 1, they started medication the next year in 313 (15.9%) of the pairs. And of 7,595 pairs of years in which patients were taking medication in year 1, patients stopped all RA medications the next year in 423 (5.6%) of the pairs, the researchers reported.
In regression analyses, subjects were more likely to start medication when they were younger (odds ratio, 1.30; 95% confidence interval, 1.13-1.50/10-year decrease), Hispanic (OR, 1.88; 95% CI, 1.06-3.33), had RA for a shorter time (OR, 1.11; 95% CI, 1.01-1.22/5-year decrease), or were taking oral glucocorticoids (OR, 1.91; 95% CI, 1.36-2.67), the researchers said. Predictors of stopping RA drugs also included being younger (OR, 0.88; 95% CI, 0.80-0.98/decade decrease) or Hispanic (OR, 1.52; 95% CI, 1.02-2.30) and having the lowest annual income, compared with the highest income (OR, 1.83; 95% CI, 1.13-2.96), according to Dr. Solomon and his associates.
The "noteworthy" drop in RA drug discontinuation during the 23-year course of the study from 9% in 1986 to 3% in 2008 "may correlate with the increasing range of treatment options since the latter half of the 1990s. It may also be that rheumatologists have become less concerned about slightly abnormal laboratory results that occur occasionally by chance, for example, liver function tests among methotrexate users," the investigators suggested.
In contrast, no strong trends could be found for starting disease-modifying antirheumatic drugs during the study period.
"As health systems currently evolve with Medicaid expansions and a greater emphasis on primary care, reducing these barriers to appropriate care for patients with rheumatic disease will be an important goal," they concluded.
The study was funded by grants from the National Institute of Arthritis and Musculoskeletal and Skin Diseases. Some of the investigators reported receiving financial support from Amgen, the Consortium of Rheumatology Researchers of North America, Eli Lilly, and Pfizer.
Some of the same factors that predict patients’ discontinuation of disease-modifying antirheumatic drugs for rheumatoid arthritis also appear to predict their initiation, such as use of oral glucocorticoids and Hispanic ethnicity, according to findings from a longitudinal cohort study.
It was "surprising" to lead investigator Dr. Daniel H. Solomon of Brigham and Women’s Hospital, Boston, and his associates that some of the same variables predicted both starting and stopping RA medication. "These factors may correlate with frequent treatment switches," they wrote. The fact that Hispanics were significantly more likely to start and to stop medication than non-Hispanics might reflect disparities in insurance coverage, differences in the availability of new treatments, or impaired communication about side effects because of language barriers, they added in their report published in Arthritis Care and Research.
Dr. Solomon and his colleagues based their analysis on data from the University of California, San Francisco, RA Panel study, a longitudinal cohort of 1,507 persons with rheumatoid arthritis (RA) who were randomly sampled from rheumatology practices in Northern California (Arthritis Care Res. 2014;66:1152-8). The study used a paired-years analysis to calculate percentages of patients who were on or off RA medications for a year and then either stopped or started medication the next year, the investigators said.
Of 1,974 pairs of years in which people were not on RA medication in year 1, they started medication the next year in 313 (15.9%) of the pairs. And of 7,595 pairs of years in which patients were taking medication in year 1, patients stopped all RA medications the next year in 423 (5.6%) of the pairs, the researchers reported.
In regression analyses, subjects were more likely to start medication when they were younger (odds ratio, 1.30; 95% confidence interval, 1.13-1.50/10-year decrease), Hispanic (OR, 1.88; 95% CI, 1.06-3.33), had RA for a shorter time (OR, 1.11; 95% CI, 1.01-1.22/5-year decrease), or were taking oral glucocorticoids (OR, 1.91; 95% CI, 1.36-2.67), the researchers said. Predictors of stopping RA drugs also included being younger (OR, 0.88; 95% CI, 0.80-0.98/decade decrease) or Hispanic (OR, 1.52; 95% CI, 1.02-2.30) and having the lowest annual income, compared with the highest income (OR, 1.83; 95% CI, 1.13-2.96), according to Dr. Solomon and his associates.
The "noteworthy" drop in RA drug discontinuation during the 23-year course of the study from 9% in 1986 to 3% in 2008 "may correlate with the increasing range of treatment options since the latter half of the 1990s. It may also be that rheumatologists have become less concerned about slightly abnormal laboratory results that occur occasionally by chance, for example, liver function tests among methotrexate users," the investigators suggested.
In contrast, no strong trends could be found for starting disease-modifying antirheumatic drugs during the study period.
"As health systems currently evolve with Medicaid expansions and a greater emphasis on primary care, reducing these barriers to appropriate care for patients with rheumatic disease will be an important goal," they concluded.
The study was funded by grants from the National Institute of Arthritis and Musculoskeletal and Skin Diseases. Some of the investigators reported receiving financial support from Amgen, the Consortium of Rheumatology Researchers of North America, Eli Lilly, and Pfizer.
Some of the same factors that predict patients’ discontinuation of disease-modifying antirheumatic drugs for rheumatoid arthritis also appear to predict their initiation, such as use of oral glucocorticoids and Hispanic ethnicity, according to findings from a longitudinal cohort study.
It was "surprising" to lead investigator Dr. Daniel H. Solomon of Brigham and Women’s Hospital, Boston, and his associates that some of the same variables predicted both starting and stopping RA medication. "These factors may correlate with frequent treatment switches," they wrote. The fact that Hispanics were significantly more likely to start and to stop medication than non-Hispanics might reflect disparities in insurance coverage, differences in the availability of new treatments, or impaired communication about side effects because of language barriers, they added in their report published in Arthritis Care and Research.
Dr. Solomon and his colleagues based their analysis on data from the University of California, San Francisco, RA Panel study, a longitudinal cohort of 1,507 persons with rheumatoid arthritis (RA) who were randomly sampled from rheumatology practices in Northern California (Arthritis Care Res. 2014;66:1152-8). The study used a paired-years analysis to calculate percentages of patients who were on or off RA medications for a year and then either stopped or started medication the next year, the investigators said.
Of 1,974 pairs of years in which people were not on RA medication in year 1, they started medication the next year in 313 (15.9%) of the pairs. And of 7,595 pairs of years in which patients were taking medication in year 1, patients stopped all RA medications the next year in 423 (5.6%) of the pairs, the researchers reported.
In regression analyses, subjects were more likely to start medication when they were younger (odds ratio, 1.30; 95% confidence interval, 1.13-1.50/10-year decrease), Hispanic (OR, 1.88; 95% CI, 1.06-3.33), had RA for a shorter time (OR, 1.11; 95% CI, 1.01-1.22/5-year decrease), or were taking oral glucocorticoids (OR, 1.91; 95% CI, 1.36-2.67), the researchers said. Predictors of stopping RA drugs also included being younger (OR, 0.88; 95% CI, 0.80-0.98/decade decrease) or Hispanic (OR, 1.52; 95% CI, 1.02-2.30) and having the lowest annual income, compared with the highest income (OR, 1.83; 95% CI, 1.13-2.96), according to Dr. Solomon and his associates.
The "noteworthy" drop in RA drug discontinuation during the 23-year course of the study from 9% in 1986 to 3% in 2008 "may correlate with the increasing range of treatment options since the latter half of the 1990s. It may also be that rheumatologists have become less concerned about slightly abnormal laboratory results that occur occasionally by chance, for example, liver function tests among methotrexate users," the investigators suggested.
In contrast, no strong trends could be found for starting disease-modifying antirheumatic drugs during the study period.
"As health systems currently evolve with Medicaid expansions and a greater emphasis on primary care, reducing these barriers to appropriate care for patients with rheumatic disease will be an important goal," they concluded.
The study was funded by grants from the National Institute of Arthritis and Musculoskeletal and Skin Diseases. Some of the investigators reported receiving financial support from Amgen, the Consortium of Rheumatology Researchers of North America, Eli Lilly, and Pfizer.
FROM ARTHRITIS CARE AND RESEARCH
Key clinical point: Being younger, Hispanic, or having a relatively low income were significant predictors of stopping medication for RA.
Major finding: Predictors of stopping RA drugs included being younger (OR, 0.88; 95% CI, 0.80-0.98 per decade decrease), Hispanic (OR, 1.52; 95% CI, 1.02-2.30), and having the lowest annual income, compared with the highest income (OR, 1.83; 95% CI, 1.13-2.96).
Data source: Analysis of data from 1,507 patients in the University of California, San Francisco, RA Panel study.
Disclosures: The study was funded by grants from the National Institute of Arthritis and Musculoskeletal and Skin Diseases. Some of the investigators reported receiving financial support from Amgen, the Consortium of Rheumatology Researchers of North America, Eli Lilly, and Pfizer.
Measures of lesion volume and brain atrophy predicted outcomes in early MS
Baseline MRI measures of lesion volume and brain atrophy predicted distinct long-term clinical changes in patients with early multiple sclerosis, reported authors of a small study published in Multiple Sclerosis and Related Disorders.
"We have identified several interesting putative biomarkers that are strongly associated with clinical worsening in early MS," wrote Dr. Amir-Hadi Maghzi of the University of California, San Francisco, and his associates.
The study included 43 patients with early MS, of whom 22 completed the 3-year assessment, the researchers said. MRI showed that T2 lesion volume significantly predicted longitudinal changes in the Paced Auditory Serial Addition Test (P = .004), they reported (Mult. Scler. Relat. Disord. 2014 July 23 [doi:10.1016/j.msard.2014.07.003]). The patients had participated in a randomized, double-blind, placebo-controlled trial at two centers that assessed the possible neuroprotective effects of riluzole in combination with intramuscular interferon beta-1a.
In addition, three baseline measures of atrophy – brain parenchymal volume and normal-appearing white and grey matter volumes – predicted longitudinal changes in the MS Functional Composite score and the Timed 25-Foot Walk (all P values less than .041), the researchers said. The different findings for lesion and brain volume could reflect distinct disease processes, the investigators added.
Dr. Maghzi and his colleagues calculated longitudinal changes in brain volume by using the SIENA (Structural Image Evaluation Using Normalization of Atrophy) analysis. They counted T2 and contrast-enhancing lesions by simultaneously visualizing T2 and T1 images before and after enhancement. Most MRI measures did not correlate with clinical outcomes at baseline, they noted.
In longitudinal analyses, every 1% decrease in brain volume was associated with a 1.14-point drop on the Symbol Digit Modalities Test (SDMT; P = .03). For MS patients, a 4- to 5-point decrease in SDMT is associated with job loss, according to the authors.
For every 1% decrease in brain volume, low-contrast letter acuity also declined by an average of nearly 1.5 letters, the investigators said.
The National MS Society and the Multiple Sclerosis International Federation funded the research. Three coauthors reported serving as committee members or receiving consulting fees, honoraria, or free study medication from Biogen Idec, Novartis, Mylan, Roche, Acorda, Bionure, CNS Imaging Consultant, Hoffman-LaRoche, Genzyme, Teva, Sanofi-Aventis, and Genentech.
Baseline MRI measures of lesion volume and brain atrophy predicted distinct long-term clinical changes in patients with early multiple sclerosis, reported authors of a small study published in Multiple Sclerosis and Related Disorders.
"We have identified several interesting putative biomarkers that are strongly associated with clinical worsening in early MS," wrote Dr. Amir-Hadi Maghzi of the University of California, San Francisco, and his associates.
The study included 43 patients with early MS, of whom 22 completed the 3-year assessment, the researchers said. MRI showed that T2 lesion volume significantly predicted longitudinal changes in the Paced Auditory Serial Addition Test (P = .004), they reported (Mult. Scler. Relat. Disord. 2014 July 23 [doi:10.1016/j.msard.2014.07.003]). The patients had participated in a randomized, double-blind, placebo-controlled trial at two centers that assessed the possible neuroprotective effects of riluzole in combination with intramuscular interferon beta-1a.
In addition, three baseline measures of atrophy – brain parenchymal volume and normal-appearing white and grey matter volumes – predicted longitudinal changes in the MS Functional Composite score and the Timed 25-Foot Walk (all P values less than .041), the researchers said. The different findings for lesion and brain volume could reflect distinct disease processes, the investigators added.
Dr. Maghzi and his colleagues calculated longitudinal changes in brain volume by using the SIENA (Structural Image Evaluation Using Normalization of Atrophy) analysis. They counted T2 and contrast-enhancing lesions by simultaneously visualizing T2 and T1 images before and after enhancement. Most MRI measures did not correlate with clinical outcomes at baseline, they noted.
In longitudinal analyses, every 1% decrease in brain volume was associated with a 1.14-point drop on the Symbol Digit Modalities Test (SDMT; P = .03). For MS patients, a 4- to 5-point decrease in SDMT is associated with job loss, according to the authors.
For every 1% decrease in brain volume, low-contrast letter acuity also declined by an average of nearly 1.5 letters, the investigators said.
The National MS Society and the Multiple Sclerosis International Federation funded the research. Three coauthors reported serving as committee members or receiving consulting fees, honoraria, or free study medication from Biogen Idec, Novartis, Mylan, Roche, Acorda, Bionure, CNS Imaging Consultant, Hoffman-LaRoche, Genzyme, Teva, Sanofi-Aventis, and Genentech.
Baseline MRI measures of lesion volume and brain atrophy predicted distinct long-term clinical changes in patients with early multiple sclerosis, reported authors of a small study published in Multiple Sclerosis and Related Disorders.
"We have identified several interesting putative biomarkers that are strongly associated with clinical worsening in early MS," wrote Dr. Amir-Hadi Maghzi of the University of California, San Francisco, and his associates.
The study included 43 patients with early MS, of whom 22 completed the 3-year assessment, the researchers said. MRI showed that T2 lesion volume significantly predicted longitudinal changes in the Paced Auditory Serial Addition Test (P = .004), they reported (Mult. Scler. Relat. Disord. 2014 July 23 [doi:10.1016/j.msard.2014.07.003]). The patients had participated in a randomized, double-blind, placebo-controlled trial at two centers that assessed the possible neuroprotective effects of riluzole in combination with intramuscular interferon beta-1a.
In addition, three baseline measures of atrophy – brain parenchymal volume and normal-appearing white and grey matter volumes – predicted longitudinal changes in the MS Functional Composite score and the Timed 25-Foot Walk (all P values less than .041), the researchers said. The different findings for lesion and brain volume could reflect distinct disease processes, the investigators added.
Dr. Maghzi and his colleagues calculated longitudinal changes in brain volume by using the SIENA (Structural Image Evaluation Using Normalization of Atrophy) analysis. They counted T2 and contrast-enhancing lesions by simultaneously visualizing T2 and T1 images before and after enhancement. Most MRI measures did not correlate with clinical outcomes at baseline, they noted.
In longitudinal analyses, every 1% decrease in brain volume was associated with a 1.14-point drop on the Symbol Digit Modalities Test (SDMT; P = .03). For MS patients, a 4- to 5-point decrease in SDMT is associated with job loss, according to the authors.
For every 1% decrease in brain volume, low-contrast letter acuity also declined by an average of nearly 1.5 letters, the investigators said.
The National MS Society and the Multiple Sclerosis International Federation funded the research. Three coauthors reported serving as committee members or receiving consulting fees, honoraria, or free study medication from Biogen Idec, Novartis, Mylan, Roche, Acorda, Bionure, CNS Imaging Consultant, Hoffman-LaRoche, Genzyme, Teva, Sanofi-Aventis, and Genentech.
FROM MULTIPLE SCLEROSIS AND RELATED DISORDERS
Key clinical point: Baseline MRI measures of lesion volume and brain atrophy predicted long-term clinical outcomes in patients with multiple sclerosis.
Major finding: T2 lesion volume predicted changes in the Paced Auditory Serial Addition Test (P = .004), and three measures of brain atrophy predicted longitudinal changes in the MS Functional Composite score (P values = .016, .040, and .021) and the Timed-25 Foot Walk (P less than .05).
Data source: A 3-year longitudinal study of 43 patients with MS who had disease onset within 12 months.
Disclosures: The National MS Society and the Multiple Sclerosis International Federation funded the research. Three coauthors reported serving as committee members or receiving consulting fees, honoraria, or free study medication from Biogen Idec, Novartis, Mylan, Roche, Acorda, Bionure, CNS Imaging Consultant, Hoffman-LaRoche, Genzyme, Teva, Sanofi-Aventis, and Genentech.
Early low-dose menopausal hormone therapy did not affect atherosclerosis
Two low-dose menopausal hormone regimens improved some cardiovascular parameters in healthy women but did not affect atherosclerosis progression, even when started early and continued for up to 4 years, investigators reported online July 28 in Annals of Internal Medicine.
Neither of the low-dose menopausal hormone therapy (MHT) regimens used in the study affected blood pressure, but both relieved hot flushes, added Dr. S. Mitchell Harman of the Phoenix Veterans Affairs Health Care System in Arizona and his associates.
Follow-up analyses of Women’s Health Initiative data had suggested that MHT might have cardiovascular benefits if started early enough or in younger women, the researchers noted.
To further explore the association, the Kronos Early Estrogen Prevention Study (KEEPS) enrolled 727 healthy women aged 42-58 years who were considered low risk for cardiovascular disease and were within 36 months of their last menses (Ann. Intern. Med. 2014 July 28 [doi: 10.7326/M14-0353]). The women were randomized in a double-blinded fashion to oral progesterone (200 mg for 12 days per month), plus either oral estrogen (conjugated equine estrogen, 0.45 mg per day) or transdermal estrogen (17-beta-estradiol, 50 mcg per day), or to a placebo, the researchers said.
Vascular ultrasonography at baseline and after up to 4 years of treatment revealed no effect of MHT on the progression of atherosclerosis, the researchers said. Average increases in carotid artery intima-media thickness were 0.0076 mm per year and were similar across treatment groups, as were increases in coronary artery calcium scores (17.4% for the oral estrogen group, 18.9% for the transdermal estrogen group, and 21.0% for the placebo group), they reported.
Neither hormone therapy regimen led to changes in blood pressure or interleukin-6 levels, although vasomotor symptoms (hot flushes) improved with both regimens, the investigators said. Lipoprotein cholesterol levels also improved in both treatment groups, and the oral estrogen group had improvements in C-reactive protein and sex hormone–binding globulin. The transdermal estrogen group had improvements in insulin sensitivity.
The study was inadequately powered to allow comparison of clinical events, and power for the coronary artery calcium score also was limited, the researchers noted. The results also might not be generalizable to women who have substantial cardiovascular risk factors, they added.
The Aurora Foundation funded the research, and Abbott Laboratories and Bayer Healthcare donated study medications. Dr. Harman reported no relevant conflicts of interest.
Two low-dose menopausal hormone regimens improved some cardiovascular parameters in healthy women but did not affect atherosclerosis progression, even when started early and continued for up to 4 years, investigators reported online July 28 in Annals of Internal Medicine.
Neither of the low-dose menopausal hormone therapy (MHT) regimens used in the study affected blood pressure, but both relieved hot flushes, added Dr. S. Mitchell Harman of the Phoenix Veterans Affairs Health Care System in Arizona and his associates.
Follow-up analyses of Women’s Health Initiative data had suggested that MHT might have cardiovascular benefits if started early enough or in younger women, the researchers noted.
To further explore the association, the Kronos Early Estrogen Prevention Study (KEEPS) enrolled 727 healthy women aged 42-58 years who were considered low risk for cardiovascular disease and were within 36 months of their last menses (Ann. Intern. Med. 2014 July 28 [doi: 10.7326/M14-0353]). The women were randomized in a double-blinded fashion to oral progesterone (200 mg for 12 days per month), plus either oral estrogen (conjugated equine estrogen, 0.45 mg per day) or transdermal estrogen (17-beta-estradiol, 50 mcg per day), or to a placebo, the researchers said.
Vascular ultrasonography at baseline and after up to 4 years of treatment revealed no effect of MHT on the progression of atherosclerosis, the researchers said. Average increases in carotid artery intima-media thickness were 0.0076 mm per year and were similar across treatment groups, as were increases in coronary artery calcium scores (17.4% for the oral estrogen group, 18.9% for the transdermal estrogen group, and 21.0% for the placebo group), they reported.
Neither hormone therapy regimen led to changes in blood pressure or interleukin-6 levels, although vasomotor symptoms (hot flushes) improved with both regimens, the investigators said. Lipoprotein cholesterol levels also improved in both treatment groups, and the oral estrogen group had improvements in C-reactive protein and sex hormone–binding globulin. The transdermal estrogen group had improvements in insulin sensitivity.
The study was inadequately powered to allow comparison of clinical events, and power for the coronary artery calcium score also was limited, the researchers noted. The results also might not be generalizable to women who have substantial cardiovascular risk factors, they added.
The Aurora Foundation funded the research, and Abbott Laboratories and Bayer Healthcare donated study medications. Dr. Harman reported no relevant conflicts of interest.
Two low-dose menopausal hormone regimens improved some cardiovascular parameters in healthy women but did not affect atherosclerosis progression, even when started early and continued for up to 4 years, investigators reported online July 28 in Annals of Internal Medicine.
Neither of the low-dose menopausal hormone therapy (MHT) regimens used in the study affected blood pressure, but both relieved hot flushes, added Dr. S. Mitchell Harman of the Phoenix Veterans Affairs Health Care System in Arizona and his associates.
Follow-up analyses of Women’s Health Initiative data had suggested that MHT might have cardiovascular benefits if started early enough or in younger women, the researchers noted.
To further explore the association, the Kronos Early Estrogen Prevention Study (KEEPS) enrolled 727 healthy women aged 42-58 years who were considered low risk for cardiovascular disease and were within 36 months of their last menses (Ann. Intern. Med. 2014 July 28 [doi: 10.7326/M14-0353]). The women were randomized in a double-blinded fashion to oral progesterone (200 mg for 12 days per month), plus either oral estrogen (conjugated equine estrogen, 0.45 mg per day) or transdermal estrogen (17-beta-estradiol, 50 mcg per day), or to a placebo, the researchers said.
Vascular ultrasonography at baseline and after up to 4 years of treatment revealed no effect of MHT on the progression of atherosclerosis, the researchers said. Average increases in carotid artery intima-media thickness were 0.0076 mm per year and were similar across treatment groups, as were increases in coronary artery calcium scores (17.4% for the oral estrogen group, 18.9% for the transdermal estrogen group, and 21.0% for the placebo group), they reported.
Neither hormone therapy regimen led to changes in blood pressure or interleukin-6 levels, although vasomotor symptoms (hot flushes) improved with both regimens, the investigators said. Lipoprotein cholesterol levels also improved in both treatment groups, and the oral estrogen group had improvements in C-reactive protein and sex hormone–binding globulin. The transdermal estrogen group had improvements in insulin sensitivity.
The study was inadequately powered to allow comparison of clinical events, and power for the coronary artery calcium score also was limited, the researchers noted. The results also might not be generalizable to women who have substantial cardiovascular risk factors, they added.
The Aurora Foundation funded the research, and Abbott Laboratories and Bayer Healthcare donated study medications. Dr. Harman reported no relevant conflicts of interest.
FROM ANNALS OF INTERNAL MEDICINE
Key clinical point: Low-dose menopausal hormone therapy did not affect the progression of atherosclerosis, even when started early and continued for up to 4 years.
Major finding: Average increases in carotid artery intima-media thickness were 0.0076 mm per year and were similar across treatment groups, as were average changes in coronary artery calcium scores (17.4% for the oral estrogen group, 18.9% for the transdermal estrogen group, and 21.0% for the placebo group).
Data source: Multicenter, double-blind, placebo-controlled, randomized clinical trial of 727 healthy women within 36 months of their last menses. Women were randomized to oral conjugated equine estrogens (0.45 mg per day) and oral progesterone (200 mg for 12 days per month); the same dose of oral progesterone plus transdermal 17-beta-estradiol (50 mcg per day); or placebo.
Disclosures: The Aurora Foundation funded the research, and Abbott Laboratories and Bayer Healthcare donated study medications. Dr. Harman reported no relevant conflicts of interest.
Enteral contrast did not add diagnostic benefit in suspected appendicitis
Enteral contrast did not augment the accuracy of computed tomography in appendectomy patients, compared with intravenous contrast CT alone, according to a large multihospital study published in Annals of Surgery.
"Enteral contrast should be eliminated in IV-enhanced CT scans performed for suspected appendicitis," said Dr. Frederick Drake at the University of Washington Medical Center in Seattle and his associates. "We conclude that IV contrast alone is sufficient for the diagnosis of appendicitis in a wide variety of hospitals, outside of tertiary centers and strict research protocols."
The investigators studied 9,047 adults who underwent nonelective appendectomies at 56 hospitals in the state of Washington during a 2-year period. Patients were identified through the Surgical Care Outcomes and Assessment Program (SCOAP), which is based on direct reviews of clinical records and captures more than 85% of nonelective appendectomies performed in the state, the researchers said (Ann. Surg. 2014;260:311-6).
The primary outcome measure was concordance between a patient’s final pathology and the final radiologic report, they said.
Almost 90% of patients underwent CT before surgery. Among these patients, 54% received only IV contrast and 28.5% received both IV and enteral contrast, said the investigators. After controlling for age, sex, comorbidities, weight, hospital type, and perforation, they found no significant difference in concordance rates for IV-only contrast versus IV with enteral contrast (odds ratio, 0.95; 95% confidence interval, 0.72-1.25). Pathology and radiographic findings correlated in 90% of patients who received IV and enteral contrast, and in 90.4% of patients who received only IV contrast, they added, noting that eliminating enteral contrast could improve patients’ safety and comfort, and the efficiency of emergency departments.
The Life Discovery Fund of Washington State, the Agency for Healthcare Research and Quality, and the National Institutes of Health funded the research. The authors reported having no conflicts of interest.
Enteral contrast did not augment the accuracy of computed tomography in appendectomy patients, compared with intravenous contrast CT alone, according to a large multihospital study published in Annals of Surgery.
"Enteral contrast should be eliminated in IV-enhanced CT scans performed for suspected appendicitis," said Dr. Frederick Drake at the University of Washington Medical Center in Seattle and his associates. "We conclude that IV contrast alone is sufficient for the diagnosis of appendicitis in a wide variety of hospitals, outside of tertiary centers and strict research protocols."
The investigators studied 9,047 adults who underwent nonelective appendectomies at 56 hospitals in the state of Washington during a 2-year period. Patients were identified through the Surgical Care Outcomes and Assessment Program (SCOAP), which is based on direct reviews of clinical records and captures more than 85% of nonelective appendectomies performed in the state, the researchers said (Ann. Surg. 2014;260:311-6).
The primary outcome measure was concordance between a patient’s final pathology and the final radiologic report, they said.
Almost 90% of patients underwent CT before surgery. Among these patients, 54% received only IV contrast and 28.5% received both IV and enteral contrast, said the investigators. After controlling for age, sex, comorbidities, weight, hospital type, and perforation, they found no significant difference in concordance rates for IV-only contrast versus IV with enteral contrast (odds ratio, 0.95; 95% confidence interval, 0.72-1.25). Pathology and radiographic findings correlated in 90% of patients who received IV and enteral contrast, and in 90.4% of patients who received only IV contrast, they added, noting that eliminating enteral contrast could improve patients’ safety and comfort, and the efficiency of emergency departments.
The Life Discovery Fund of Washington State, the Agency for Healthcare Research and Quality, and the National Institutes of Health funded the research. The authors reported having no conflicts of interest.
Enteral contrast did not augment the accuracy of computed tomography in appendectomy patients, compared with intravenous contrast CT alone, according to a large multihospital study published in Annals of Surgery.
"Enteral contrast should be eliminated in IV-enhanced CT scans performed for suspected appendicitis," said Dr. Frederick Drake at the University of Washington Medical Center in Seattle and his associates. "We conclude that IV contrast alone is sufficient for the diagnosis of appendicitis in a wide variety of hospitals, outside of tertiary centers and strict research protocols."
The investigators studied 9,047 adults who underwent nonelective appendectomies at 56 hospitals in the state of Washington during a 2-year period. Patients were identified through the Surgical Care Outcomes and Assessment Program (SCOAP), which is based on direct reviews of clinical records and captures more than 85% of nonelective appendectomies performed in the state, the researchers said (Ann. Surg. 2014;260:311-6).
The primary outcome measure was concordance between a patient’s final pathology and the final radiologic report, they said.
Almost 90% of patients underwent CT before surgery. Among these patients, 54% received only IV contrast and 28.5% received both IV and enteral contrast, said the investigators. After controlling for age, sex, comorbidities, weight, hospital type, and perforation, they found no significant difference in concordance rates for IV-only contrast versus IV with enteral contrast (odds ratio, 0.95; 95% confidence interval, 0.72-1.25). Pathology and radiographic findings correlated in 90% of patients who received IV and enteral contrast, and in 90.4% of patients who received only IV contrast, they added, noting that eliminating enteral contrast could improve patients’ safety and comfort, and the efficiency of emergency departments.
The Life Discovery Fund of Washington State, the Agency for Healthcare Research and Quality, and the National Institutes of Health funded the research. The authors reported having no conflicts of interest.
FROM ANNALS OF SURGERY
Key clinical point: Enteral contrast is not of additional diagnostic benefit in appendectomy patients undergoing intravenous contrast computed tomography.
Major finding: After adjustment for age, sex, comorbidities, weight, hospital type, and perforation, there was no significant difference in rates of pathologic and radiologic concordance for patients who underwent IV-only contrast CT versus IV and enteral contrast CT (odds ratio, 0.95; 95% confidence interval, 0.72-1.25).
Data Source: Prospective cohort study of 9,047 adults who underwent nonelective appendectomies at 56 hospitals in the state of Washington between Jan. 1, 2010, and Dec. 31, 2011.
Disclosures: The Life Discovery Fund of Washington State, the Agency for Healthcare Research and Quality, and the National Institutes of Health funded the research. The authors reported having no conflicts of interest.
Laparoscopy found effective alternative to open IBD surgery
In an urban colorectal surgery department, a near-doubling in the proportion of surgical procedures performed laparoscopically accompanied significant declines in both severe postoperative morbidity and conversions to laparotomy, in a 14-year, single-hospital study reported in Annals of Surgery.
"This study demonstrated that a laparoscopic approach is a safe and effective alternative to open surgery" for management of inflammatory bowel disease (IBD), wrote Dr. León Maggiori and his associates at the Assistance Publique-Hôpitaux de Paris.
"Associated postoperative morbidity was comparable to reported rates after open approach," the researchers added.
Dr. Maggiori and his associates studied 790 consecutive intestinal resections for IBD performed on 633 patients between June 1998 and July 2012. About two-thirds of the procedures were for Crohn’s disease, and one-third were for ulcerative colitis, the investigators said (Ann. Surg. 2014;260:305-10). The proportion of laparoscopically performed procedures rose from 42% to 80% during the study period (P less than .001), and the trend occurred both for Crohn’s and for ulcerative colitis cases, they added.
As surgeons accrued experience, the rate of complex cases performed laparoscopically also approximately doubled (from 16% to 33%; P less than .023), the researchers said. Furthermore, the mean adjusted risk of conversion to open surgery fell significantly (from 18% to 6%; P less than .001), as did the rate of severe postoperative morbidity (from 14% to 8%; P less than .001).
In all, 12% of laparoscopic cases required conversion, most often because of abscesses or fistulas found during surgery or difficulty dissecting adhesions, the investigators said. Thirteen percent of laparoscopies led to severe postoperative morbidity, defined as Clavien-Dindo grade 3 or 4 complications, they added. The single postoperative death occurred in a patient who developed peritonitis and septic shock 3 days after laparoscopic colectomy with ileosigmoidostomy, the researchers said.
The hospital now uses laparoscopy as the standard approach for surgical management of IBD, except in cases of complicated acute colitis, Dr. Maggiori and his associates said.
The limited number of straight open surgical cases meant that they could not directly be compared with laparoscopy, said the investigators, adding that they lacked data on long-term outcomes because many patients underwent surgery in 2008 or later.
The Association François Aupetit partially funded the study. The authors reported having no conflicts of interest.
In an urban colorectal surgery department, a near-doubling in the proportion of surgical procedures performed laparoscopically accompanied significant declines in both severe postoperative morbidity and conversions to laparotomy, in a 14-year, single-hospital study reported in Annals of Surgery.
"This study demonstrated that a laparoscopic approach is a safe and effective alternative to open surgery" for management of inflammatory bowel disease (IBD), wrote Dr. León Maggiori and his associates at the Assistance Publique-Hôpitaux de Paris.
"Associated postoperative morbidity was comparable to reported rates after open approach," the researchers added.
Dr. Maggiori and his associates studied 790 consecutive intestinal resections for IBD performed on 633 patients between June 1998 and July 2012. About two-thirds of the procedures were for Crohn’s disease, and one-third were for ulcerative colitis, the investigators said (Ann. Surg. 2014;260:305-10). The proportion of laparoscopically performed procedures rose from 42% to 80% during the study period (P less than .001), and the trend occurred both for Crohn’s and for ulcerative colitis cases, they added.
As surgeons accrued experience, the rate of complex cases performed laparoscopically also approximately doubled (from 16% to 33%; P less than .023), the researchers said. Furthermore, the mean adjusted risk of conversion to open surgery fell significantly (from 18% to 6%; P less than .001), as did the rate of severe postoperative morbidity (from 14% to 8%; P less than .001).
In all, 12% of laparoscopic cases required conversion, most often because of abscesses or fistulas found during surgery or difficulty dissecting adhesions, the investigators said. Thirteen percent of laparoscopies led to severe postoperative morbidity, defined as Clavien-Dindo grade 3 or 4 complications, they added. The single postoperative death occurred in a patient who developed peritonitis and septic shock 3 days after laparoscopic colectomy with ileosigmoidostomy, the researchers said.
The hospital now uses laparoscopy as the standard approach for surgical management of IBD, except in cases of complicated acute colitis, Dr. Maggiori and his associates said.
The limited number of straight open surgical cases meant that they could not directly be compared with laparoscopy, said the investigators, adding that they lacked data on long-term outcomes because many patients underwent surgery in 2008 or later.
The Association François Aupetit partially funded the study. The authors reported having no conflicts of interest.
In an urban colorectal surgery department, a near-doubling in the proportion of surgical procedures performed laparoscopically accompanied significant declines in both severe postoperative morbidity and conversions to laparotomy, in a 14-year, single-hospital study reported in Annals of Surgery.
"This study demonstrated that a laparoscopic approach is a safe and effective alternative to open surgery" for management of inflammatory bowel disease (IBD), wrote Dr. León Maggiori and his associates at the Assistance Publique-Hôpitaux de Paris.
"Associated postoperative morbidity was comparable to reported rates after open approach," the researchers added.
Dr. Maggiori and his associates studied 790 consecutive intestinal resections for IBD performed on 633 patients between June 1998 and July 2012. About two-thirds of the procedures were for Crohn’s disease, and one-third were for ulcerative colitis, the investigators said (Ann. Surg. 2014;260:305-10). The proportion of laparoscopically performed procedures rose from 42% to 80% during the study period (P less than .001), and the trend occurred both for Crohn’s and for ulcerative colitis cases, they added.
As surgeons accrued experience, the rate of complex cases performed laparoscopically also approximately doubled (from 16% to 33%; P less than .023), the researchers said. Furthermore, the mean adjusted risk of conversion to open surgery fell significantly (from 18% to 6%; P less than .001), as did the rate of severe postoperative morbidity (from 14% to 8%; P less than .001).
In all, 12% of laparoscopic cases required conversion, most often because of abscesses or fistulas found during surgery or difficulty dissecting adhesions, the investigators said. Thirteen percent of laparoscopies led to severe postoperative morbidity, defined as Clavien-Dindo grade 3 or 4 complications, they added. The single postoperative death occurred in a patient who developed peritonitis and septic shock 3 days after laparoscopic colectomy with ileosigmoidostomy, the researchers said.
The hospital now uses laparoscopy as the standard approach for surgical management of IBD, except in cases of complicated acute colitis, Dr. Maggiori and his associates said.
The limited number of straight open surgical cases meant that they could not directly be compared with laparoscopy, said the investigators, adding that they lacked data on long-term outcomes because many patients underwent surgery in 2008 or later.
The Association François Aupetit partially funded the study. The authors reported having no conflicts of interest.
FROM ANNALS OF SURGERY
Key clinical point: Laparoscopic approaches are becoming standard for the surgical management of inflammatory bowel disease (IBD), except in cases of complicated acute colitis.
Major finding: The proportion of IBD procedures performed laparoscopically increased from 42% to 80% (P less than .001). The rate of complex laparoscopies also increased (P = .023), while the mean adjusted risks of conversion and severe postoperative morbidity dropped (P less than .001 for both).
Data source: Prospective analysis of 790 consecutive resections for IBD performed during a 14-year period, including 574 (73%) laparoscopic procedures.
Disclosures: The Association François Aupetit partially funded the study. The authors reported having no conflicts of interest.
Adenotonsillectomy for OSAS led to weight gain, even in overweight children
Adenotonsillectomy for obstructive sleep apnea syndrome led to clinically significant weight gain, even in children who were overweight at baseline, according to a first-in-kind randomized clinical trial published in the August issue of Pediatrics.
More than 52% of overweight children with obstructive sleep apnea syndrome (OSAS) who underwent adenotonsillectomy developed obesity within 7 months, compared with 21% of those randomized to watchful waiting and supportive care (P less than .05), reported Dr. Eliot S. Katz of Boston Children’s Hospital and his associates.
Based on those results, children who undergo adenotonsillectomy for OSAS should be monitored for weight changes, receive nutritional counseling, and be encouraged to exercise, the researchers said (Pediatrics 2014;134:282-9).
For the multicenter, single-blind clinical trial, the investigators randomized 464 children aged 5-9.9 years with OSAS to undergo either early adenotonsillectomy – defined as surgery within 4 weeks of randomization – or watchful waiting and supportive care.
Children classified as failing to thrive at baseline were more likely to attain a normal weight after adenotonsillectomy, compared with watchful waiting, although the difference was not statistically significant, Dr. Katz and his associates said.
The National Institutes of Health funded the study. One coauthor reported having served as a consultant for Zansors and receiving grants from Respironics/Phillips and Fisher-Paykel. The other authors reported no conflicts of interest.
Adenotonsillectomy for obstructive sleep apnea syndrome led to clinically significant weight gain, even in children who were overweight at baseline, according to a first-in-kind randomized clinical trial published in the August issue of Pediatrics.
More than 52% of overweight children with obstructive sleep apnea syndrome (OSAS) who underwent adenotonsillectomy developed obesity within 7 months, compared with 21% of those randomized to watchful waiting and supportive care (P less than .05), reported Dr. Eliot S. Katz of Boston Children’s Hospital and his associates.
Based on those results, children who undergo adenotonsillectomy for OSAS should be monitored for weight changes, receive nutritional counseling, and be encouraged to exercise, the researchers said (Pediatrics 2014;134:282-9).
For the multicenter, single-blind clinical trial, the investigators randomized 464 children aged 5-9.9 years with OSAS to undergo either early adenotonsillectomy – defined as surgery within 4 weeks of randomization – or watchful waiting and supportive care.
Children classified as failing to thrive at baseline were more likely to attain a normal weight after adenotonsillectomy, compared with watchful waiting, although the difference was not statistically significant, Dr. Katz and his associates said.
The National Institutes of Health funded the study. One coauthor reported having served as a consultant for Zansors and receiving grants from Respironics/Phillips and Fisher-Paykel. The other authors reported no conflicts of interest.
Adenotonsillectomy for obstructive sleep apnea syndrome led to clinically significant weight gain, even in children who were overweight at baseline, according to a first-in-kind randomized clinical trial published in the August issue of Pediatrics.
More than 52% of overweight children with obstructive sleep apnea syndrome (OSAS) who underwent adenotonsillectomy developed obesity within 7 months, compared with 21% of those randomized to watchful waiting and supportive care (P less than .05), reported Dr. Eliot S. Katz of Boston Children’s Hospital and his associates.
Based on those results, children who undergo adenotonsillectomy for OSAS should be monitored for weight changes, receive nutritional counseling, and be encouraged to exercise, the researchers said (Pediatrics 2014;134:282-9).
For the multicenter, single-blind clinical trial, the investigators randomized 464 children aged 5-9.9 years with OSAS to undergo either early adenotonsillectomy – defined as surgery within 4 weeks of randomization – or watchful waiting and supportive care.
Children classified as failing to thrive at baseline were more likely to attain a normal weight after adenotonsillectomy, compared with watchful waiting, although the difference was not statistically significant, Dr. Katz and his associates said.
The National Institutes of Health funded the study. One coauthor reported having served as a consultant for Zansors and receiving grants from Respironics/Phillips and Fisher-Paykel. The other authors reported no conflicts of interest.
FROM PEDIATRICS
Key clinical point: Adenotonsillectomy for obstructive sleep apnea syndrome increases the risk of obesity in overweight children.
Major finding: Almost 52% of overweight children randomized to adenotonsillectomy developed obesity in the subsequent 7 months, compared with 21% of overweight children in the control group (P less than .05).
Data source: Multicenter, single-blind, clinical trial of 464 children with OSAS randomized either to early adenotonsillectomy or watchful waiting and supportive care.
Disclosures: The National Institutes of Health funded the study. One coauthor reported having served as a consultant for Zansors and receiving grants from Respironics/Phillips and Fisher-Paykel. The other authors reported no conflicts of interest.
FDA approves opioid tablet designed to deter abuse if crushed
The Food and Drug Administration on July 24 approved an opioid tablet formulated to deter abuse if crushed, the agency announced.
Called Targiniq ER (extended release), the long-acting oxycodone formulation contains naloxone hydrochloride to block euphoric effects if the tablet is crushed and then snorted or injected, according to the FDA.
But Targiniq ER still can be abused if swallowed whole, which is currently the most common form of oxycodone abuse, the FDA said.
The drug is approved for patients who do not respond to or cannot tolerate alternative pain treatments and is not intended for as-needed pain relief, the FDA said.
The approval is based on a clinical trial of 601 patients with chronic low back pain and a safety database of more than 3,000 patients, the FDA said. The drug’s most common side effects were nausea and vomiting, the agency reported.
The FDA said it is requiring postmarketing studies of the potential for abuse, increased pain sensitivity, addiction, overdose, and death should Targiniq ER be used for more than 12 weeks.
The drug’s maker, Purdue Pharma, manufactures several other opioids, including transdermal buprenorphine, injectable and oral hydromorphone, morphine sulfate extended-release tablets, and extended-release oxycodone without naloxone.
The Food and Drug Administration on July 24 approved an opioid tablet formulated to deter abuse if crushed, the agency announced.
Called Targiniq ER (extended release), the long-acting oxycodone formulation contains naloxone hydrochloride to block euphoric effects if the tablet is crushed and then snorted or injected, according to the FDA.
But Targiniq ER still can be abused if swallowed whole, which is currently the most common form of oxycodone abuse, the FDA said.
The drug is approved for patients who do not respond to or cannot tolerate alternative pain treatments and is not intended for as-needed pain relief, the FDA said.
The approval is based on a clinical trial of 601 patients with chronic low back pain and a safety database of more than 3,000 patients, the FDA said. The drug’s most common side effects were nausea and vomiting, the agency reported.
The FDA said it is requiring postmarketing studies of the potential for abuse, increased pain sensitivity, addiction, overdose, and death should Targiniq ER be used for more than 12 weeks.
The drug’s maker, Purdue Pharma, manufactures several other opioids, including transdermal buprenorphine, injectable and oral hydromorphone, morphine sulfate extended-release tablets, and extended-release oxycodone without naloxone.
The Food and Drug Administration on July 24 approved an opioid tablet formulated to deter abuse if crushed, the agency announced.
Called Targiniq ER (extended release), the long-acting oxycodone formulation contains naloxone hydrochloride to block euphoric effects if the tablet is crushed and then snorted or injected, according to the FDA.
But Targiniq ER still can be abused if swallowed whole, which is currently the most common form of oxycodone abuse, the FDA said.
The drug is approved for patients who do not respond to or cannot tolerate alternative pain treatments and is not intended for as-needed pain relief, the FDA said.
The approval is based on a clinical trial of 601 patients with chronic low back pain and a safety database of more than 3,000 patients, the FDA said. The drug’s most common side effects were nausea and vomiting, the agency reported.
The FDA said it is requiring postmarketing studies of the potential for abuse, increased pain sensitivity, addiction, overdose, and death should Targiniq ER be used for more than 12 weeks.
The drug’s maker, Purdue Pharma, manufactures several other opioids, including transdermal buprenorphine, injectable and oral hydromorphone, morphine sulfate extended-release tablets, and extended-release oxycodone without naloxone.