User login
Sleeping on animal skins might protect against childhood asthma, hay fever
Babies who slept on animal skins during their first 3 months of life were almost 40% less likely to have asthma by the time they were 10 years old, according to a population-based cohort study.
Sleeping on animal skins during infancy also was linked to lower odds of wheezing and hay fever, but did not seem to affect eczema or sensitivity to airborne antigens, Dr. Christina Tischer reported at the annual meeting of the European Respiratory Society.
"Early exposure to animal fur could be a simple, cheap, and effective way to resemble an environment with higher microbial exposure," said Dr. Tischer, a researcher at the German Institute for Environmental Health in Neuherberg, Germany. "It might follow similar protective mechanisms in relation to asthma and allergy as it has been observed in farm and rural environments."
The investigators studied 2,441 children in Germany who were up to 10 years old; parents answered a series of questionnaires about asthma and respiratory risk factors and health outcomes. In all, 55% of the children slept on animal skins or animal furs during their first 3 months of life, Dr. Tischer and her associates reported.
By age 10 years, children who slept on animal skins or animal fur as infants had a 25% lower odds of ever having wheezed (adjusted odds ratio, 0.75), a 38% lower odds of having been diagnosed with asthma (aOR, 0.62), and a 35% lower odds of having been diagnosed with hay fever (aOR, 0.65) compared with children who did not sleep on animals skins or furs as infants, the investigators reported.
Funding information for the study was not available. Dr. Tischer reported no conflicts of interest.
Sleeping on animal skins or fur in the first 3 months of life may decrease the risk of childhood atopy BUT increases the risk of death related to Sudden Infant Death Syndrome (SIDS). This study is from Germany, which may explain cultural differences regarding bedding for infants, but there are reports of cultural diversity regarding bedding for infants even in the United States.
The journal Pediatrics published a study looking at data in 2011 discussing African American parental decisions about infant bedding and sleep surfaces (Pediatrics 2011;128;494).The American Academy of Pediatrics (AAP) supports the policy that infants should sleep on firm bedding. Specifically, infants should not be placed on soft bedding, including blankets, pillows, or sheepskin, for example. In addition, crib bumpers should not be used. Finally, once the AAP promoted the “Back to Sleep” program (meaning babies should NOT be placed on their tummies to sleep), SIDS deaths in the United States decreased.
Sleeping on animal skins or fur in the first 3 months of life may decrease the risk of childhood atopy BUT increases the risk of death related to Sudden Infant Death Syndrome (SIDS). This study is from Germany, which may explain cultural differences regarding bedding for infants, but there are reports of cultural diversity regarding bedding for infants even in the United States.
The journal Pediatrics published a study looking at data in 2011 discussing African American parental decisions about infant bedding and sleep surfaces (Pediatrics 2011;128;494).The American Academy of Pediatrics (AAP) supports the policy that infants should sleep on firm bedding. Specifically, infants should not be placed on soft bedding, including blankets, pillows, or sheepskin, for example. In addition, crib bumpers should not be used. Finally, once the AAP promoted the “Back to Sleep” program (meaning babies should NOT be placed on their tummies to sleep), SIDS deaths in the United States decreased.
Sleeping on animal skins or fur in the first 3 months of life may decrease the risk of childhood atopy BUT increases the risk of death related to Sudden Infant Death Syndrome (SIDS). This study is from Germany, which may explain cultural differences regarding bedding for infants, but there are reports of cultural diversity regarding bedding for infants even in the United States.
The journal Pediatrics published a study looking at data in 2011 discussing African American parental decisions about infant bedding and sleep surfaces (Pediatrics 2011;128;494).The American Academy of Pediatrics (AAP) supports the policy that infants should sleep on firm bedding. Specifically, infants should not be placed on soft bedding, including blankets, pillows, or sheepskin, for example. In addition, crib bumpers should not be used. Finally, once the AAP promoted the “Back to Sleep” program (meaning babies should NOT be placed on their tummies to sleep), SIDS deaths in the United States decreased.
Babies who slept on animal skins during their first 3 months of life were almost 40% less likely to have asthma by the time they were 10 years old, according to a population-based cohort study.
Sleeping on animal skins during infancy also was linked to lower odds of wheezing and hay fever, but did not seem to affect eczema or sensitivity to airborne antigens, Dr. Christina Tischer reported at the annual meeting of the European Respiratory Society.
"Early exposure to animal fur could be a simple, cheap, and effective way to resemble an environment with higher microbial exposure," said Dr. Tischer, a researcher at the German Institute for Environmental Health in Neuherberg, Germany. "It might follow similar protective mechanisms in relation to asthma and allergy as it has been observed in farm and rural environments."
The investigators studied 2,441 children in Germany who were up to 10 years old; parents answered a series of questionnaires about asthma and respiratory risk factors and health outcomes. In all, 55% of the children slept on animal skins or animal furs during their first 3 months of life, Dr. Tischer and her associates reported.
By age 10 years, children who slept on animal skins or animal fur as infants had a 25% lower odds of ever having wheezed (adjusted odds ratio, 0.75), a 38% lower odds of having been diagnosed with asthma (aOR, 0.62), and a 35% lower odds of having been diagnosed with hay fever (aOR, 0.65) compared with children who did not sleep on animals skins or furs as infants, the investigators reported.
Funding information for the study was not available. Dr. Tischer reported no conflicts of interest.
Babies who slept on animal skins during their first 3 months of life were almost 40% less likely to have asthma by the time they were 10 years old, according to a population-based cohort study.
Sleeping on animal skins during infancy also was linked to lower odds of wheezing and hay fever, but did not seem to affect eczema or sensitivity to airborne antigens, Dr. Christina Tischer reported at the annual meeting of the European Respiratory Society.
"Early exposure to animal fur could be a simple, cheap, and effective way to resemble an environment with higher microbial exposure," said Dr. Tischer, a researcher at the German Institute for Environmental Health in Neuherberg, Germany. "It might follow similar protective mechanisms in relation to asthma and allergy as it has been observed in farm and rural environments."
The investigators studied 2,441 children in Germany who were up to 10 years old; parents answered a series of questionnaires about asthma and respiratory risk factors and health outcomes. In all, 55% of the children slept on animal skins or animal furs during their first 3 months of life, Dr. Tischer and her associates reported.
By age 10 years, children who slept on animal skins or animal fur as infants had a 25% lower odds of ever having wheezed (adjusted odds ratio, 0.75), a 38% lower odds of having been diagnosed with asthma (aOR, 0.62), and a 35% lower odds of having been diagnosed with hay fever (aOR, 0.65) compared with children who did not sleep on animals skins or furs as infants, the investigators reported.
Funding information for the study was not available. Dr. Tischer reported no conflicts of interest.
FROM THE EUROPEAN RESPIRATORY SOCIETY INTERNATIONAL CONGRESS
Key clinical point: Sleeping on animals skins during infancy might protect against wheezing, asthma, and hay fever.
Major finding: Children who slept on animal skins during the first 3 months of life had 25% lower odds of wheezing, 38% lower odds of asthma, and 35% lower odds of hay fever at up to 10 years of age, compared with children who did not sleep on skins as infants.
Data source: Population-based cohort study of 2,441 children up to age 10 years in Germany.
Disclosures: Funding information for the study was not available. Dr. Tischer reported no conflicts of interest.
Psoriatic arthritis patients often changed or stopped treatment
Patients with psoriatic arthritis who began taking disease-modifying antirheumatic drugs often changed regimens soon afterward, especially if they had started with nonbiologic treatments, researchers reported online in Arthritis Research and Therapy.
Only 31% of patients who started methotrexate or another nonbiologic disease-modifying antirheumatic drug (DMARD) for psoriatic arthritis stayed with their initial treatment for the next year, compared with 54% of patients who started on a biologic DMARD such as etanercept, infliximab, or golimumab, said Dr. Huabin F. Zhang at Celgene in Summit, N.J., and his associates.
The researchers analyzed U. S. health care claims data for 1,698 adults with psoriatic arthritis who were started on oral nonbiologic DMARDs and for 3,263 patients started on biologic DMARDs. In all, 69% of patients who started nonbiologic DMARDs and 46% of those who started biologic DMARDs discontinued, switched, or added on to their treatment within a year of starting therapy, they found. Patients most often switched to or added a biologic as opposed to a nonbiologic DMARD, the investigators said. Those who started on nonbiologics primarily took methotrexate, and "patient persistence with treatment was generally low and relatively brief," they said. Other studies have shown that use of nonbiologic DMARDs "erodes rapidly and progressively over time," they said (Arthritis Res. Ther. 2014 Aug. 22 [doi:10.1186/s13075-014-0420-5]).
Health insurance companies often require patients to take one or two nonbiologics before they will reimburse for a biologic DMARD, which could partially explain these findings, the researchers said. But the retrospective observational study did not capture data on side effects, safety concerns, or other reasons for treatment changes, they noted.
Celgene funded the study and employs Dr. Zhang. The other three coauthors reported receiving consultancy fees from Celgene.
Patients with psoriatic arthritis who began taking disease-modifying antirheumatic drugs often changed regimens soon afterward, especially if they had started with nonbiologic treatments, researchers reported online in Arthritis Research and Therapy.
Only 31% of patients who started methotrexate or another nonbiologic disease-modifying antirheumatic drug (DMARD) for psoriatic arthritis stayed with their initial treatment for the next year, compared with 54% of patients who started on a biologic DMARD such as etanercept, infliximab, or golimumab, said Dr. Huabin F. Zhang at Celgene in Summit, N.J., and his associates.
The researchers analyzed U. S. health care claims data for 1,698 adults with psoriatic arthritis who were started on oral nonbiologic DMARDs and for 3,263 patients started on biologic DMARDs. In all, 69% of patients who started nonbiologic DMARDs and 46% of those who started biologic DMARDs discontinued, switched, or added on to their treatment within a year of starting therapy, they found. Patients most often switched to or added a biologic as opposed to a nonbiologic DMARD, the investigators said. Those who started on nonbiologics primarily took methotrexate, and "patient persistence with treatment was generally low and relatively brief," they said. Other studies have shown that use of nonbiologic DMARDs "erodes rapidly and progressively over time," they said (Arthritis Res. Ther. 2014 Aug. 22 [doi:10.1186/s13075-014-0420-5]).
Health insurance companies often require patients to take one or two nonbiologics before they will reimburse for a biologic DMARD, which could partially explain these findings, the researchers said. But the retrospective observational study did not capture data on side effects, safety concerns, or other reasons for treatment changes, they noted.
Celgene funded the study and employs Dr. Zhang. The other three coauthors reported receiving consultancy fees from Celgene.
Patients with psoriatic arthritis who began taking disease-modifying antirheumatic drugs often changed regimens soon afterward, especially if they had started with nonbiologic treatments, researchers reported online in Arthritis Research and Therapy.
Only 31% of patients who started methotrexate or another nonbiologic disease-modifying antirheumatic drug (DMARD) for psoriatic arthritis stayed with their initial treatment for the next year, compared with 54% of patients who started on a biologic DMARD such as etanercept, infliximab, or golimumab, said Dr. Huabin F. Zhang at Celgene in Summit, N.J., and his associates.
The researchers analyzed U. S. health care claims data for 1,698 adults with psoriatic arthritis who were started on oral nonbiologic DMARDs and for 3,263 patients started on biologic DMARDs. In all, 69% of patients who started nonbiologic DMARDs and 46% of those who started biologic DMARDs discontinued, switched, or added on to their treatment within a year of starting therapy, they found. Patients most often switched to or added a biologic as opposed to a nonbiologic DMARD, the investigators said. Those who started on nonbiologics primarily took methotrexate, and "patient persistence with treatment was generally low and relatively brief," they said. Other studies have shown that use of nonbiologic DMARDs "erodes rapidly and progressively over time," they said (Arthritis Res. Ther. 2014 Aug. 22 [doi:10.1186/s13075-014-0420-5]).
Health insurance companies often require patients to take one or two nonbiologics before they will reimburse for a biologic DMARD, which could partially explain these findings, the researchers said. But the retrospective observational study did not capture data on side effects, safety concerns, or other reasons for treatment changes, they noted.
Celgene funded the study and employs Dr. Zhang. The other three coauthors reported receiving consultancy fees from Celgene.
FROM ARTHRITIS RESEARCH AND THERAPY
Key clinical point: Patients with psoriatic arthritis who started taking a nonbiologic disease-modifying antirheumatic drug often changed therapies within a year, frequently by switching to or adding on a biologic DMARD.
Major finding: In all, 69% of patients who started nonbiologic DMARDs and 46% of those who started biologic DMARDs discontinued, switched, or added on to their treatment within a year of starting therapy.
Data source: Retrospective observational study of health claims data from 1,698 adults with psoriatic arthritis who started oral nonbiologic DMARDs and 3,263 patients who started biologic DMARDs.
Disclosures: Celgene funded the study and employs Dr. Zhang. The other three coauthors reported receiving consultancy fees from Celgene.
Anti-inflammatory treatment could slow bone loss in early rheumatoid arthritis
Aggressive anti-inflammatory treatment correlated with slowed bone loss in patients with early rheumatoid arthritis, according to findings from a prospective cohort study.
The results show that "modern aggressive treatment" can reduce osteoporosis in patients with RA, said Dr. Glenn Haugeberg of the rheumatology department at the Hospital of Southern Norway Trust in Kristiansand and his associates.
In all, 18.5% of patients with RA used biologic disease-modifying antirheumatic drugs during the first 2 years of the study, while 62.6% used these drugs during the next 8 years, at the same time that average bone mineral density loss slowed substantially, the researchers said.
The average yearly rate of bone loss at 2 years and 10 years slowed from –1.00% to –0.56% for the femoral neck, from –0.96% to –0.41% for total spine, and from –0.42% to 0.00% for the L1-L4 vertebrae, the researchers reported (BMC Musculoskelet. Disord. 2014 Sept. 2 [doi: 10.1186/1471-2474-15-289]).
The study included 92 patients (mean age, 50.9 years) with RA, of whom about two-thirds were women, and 80% had their bone mineral densities assessed at 10 years. Patients had experienced symptoms for a mean of 12.4 months.
Contrary to findings from some prior studies, glucocorticoid use was linked to bone loss during only the first 2 years of the study period and only for total hip measurements, the researchers said.
Almost half the patients had missing baseline data on bone mineral density. The study also lacked matched controls and did not assess the prevalence or incidence of vertebral fractures, the authors added.
Funding information for the study was not available. The authors reported having no conflicts of interest.
Aggressive anti-inflammatory treatment correlated with slowed bone loss in patients with early rheumatoid arthritis, according to findings from a prospective cohort study.
The results show that "modern aggressive treatment" can reduce osteoporosis in patients with RA, said Dr. Glenn Haugeberg of the rheumatology department at the Hospital of Southern Norway Trust in Kristiansand and his associates.
In all, 18.5% of patients with RA used biologic disease-modifying antirheumatic drugs during the first 2 years of the study, while 62.6% used these drugs during the next 8 years, at the same time that average bone mineral density loss slowed substantially, the researchers said.
The average yearly rate of bone loss at 2 years and 10 years slowed from –1.00% to –0.56% for the femoral neck, from –0.96% to –0.41% for total spine, and from –0.42% to 0.00% for the L1-L4 vertebrae, the researchers reported (BMC Musculoskelet. Disord. 2014 Sept. 2 [doi: 10.1186/1471-2474-15-289]).
The study included 92 patients (mean age, 50.9 years) with RA, of whom about two-thirds were women, and 80% had their bone mineral densities assessed at 10 years. Patients had experienced symptoms for a mean of 12.4 months.
Contrary to findings from some prior studies, glucocorticoid use was linked to bone loss during only the first 2 years of the study period and only for total hip measurements, the researchers said.
Almost half the patients had missing baseline data on bone mineral density. The study also lacked matched controls and did not assess the prevalence or incidence of vertebral fractures, the authors added.
Funding information for the study was not available. The authors reported having no conflicts of interest.
Aggressive anti-inflammatory treatment correlated with slowed bone loss in patients with early rheumatoid arthritis, according to findings from a prospective cohort study.
The results show that "modern aggressive treatment" can reduce osteoporosis in patients with RA, said Dr. Glenn Haugeberg of the rheumatology department at the Hospital of Southern Norway Trust in Kristiansand and his associates.
In all, 18.5% of patients with RA used biologic disease-modifying antirheumatic drugs during the first 2 years of the study, while 62.6% used these drugs during the next 8 years, at the same time that average bone mineral density loss slowed substantially, the researchers said.
The average yearly rate of bone loss at 2 years and 10 years slowed from –1.00% to –0.56% for the femoral neck, from –0.96% to –0.41% for total spine, and from –0.42% to 0.00% for the L1-L4 vertebrae, the researchers reported (BMC Musculoskelet. Disord. 2014 Sept. 2 [doi: 10.1186/1471-2474-15-289]).
The study included 92 patients (mean age, 50.9 years) with RA, of whom about two-thirds were women, and 80% had their bone mineral densities assessed at 10 years. Patients had experienced symptoms for a mean of 12.4 months.
Contrary to findings from some prior studies, glucocorticoid use was linked to bone loss during only the first 2 years of the study period and only for total hip measurements, the researchers said.
Almost half the patients had missing baseline data on bone mineral density. The study also lacked matched controls and did not assess the prevalence or incidence of vertebral fractures, the authors added.
Funding information for the study was not available. The authors reported having no conflicts of interest.
FROM BMC MUSCULOSKELETAL DISORDERS
Key clinical point: Aggressive anti-inflammatory treatment correlated with slowed bone loss in patients with early rheumatoid arthritis.
Major finding: Average use of biologic disease-modifying antirheumatic drugs rose from 18.5% during the first 2 years to 62.6% during the next 8 years, while average bone loss slowed substantially (from –1.00% to –0.56% for the femoral neck, from –0.96% to –0.41% for the total spine, and from –0.42% to 0.00% for the L1-L4 vertebrae).
Data source: Prospective cohort study of 92 patients with rheumatoid arthritis followed for up to 10 years.
Disclosures: Funding information for the study was not available. The authors reported having no conflicts of interest.
Risk factors identified for occult cancers found at risk-reducing salpingo-oophorectomy
Older, postmenopausal women with BRCA1 or BRCA2 mutations and abnormal baseline tests were most likely to have occult cancers at risk-reducing salpingo-oophorectomy, investigators reported online in the Journal of Clinical Oncology.
Pathology results showed that 2.6% of women who underwent the surgery had occult ovarian, tubal, or peritoneal cancers, including 4.6% of BRCA1 mutation carriers, 3.5% of BRCA2 carriers, and 0.5% of women who lacked either mutation, said Dr. Mark Sherman of the National Cancer Institute and his associates. These rates resembled findings from other recent studies, the researchers said.
The investigators studied 966 high-risk women who chose risk-reducing salpingo-oophorectomy (RRSO) as part of a nonrandomized prospective clinical trial (Gynecologic Oncology Group 0199, or GOG 0199) of the National Ovarian Cancer Prevention and Early Detection Study. Cancers rates were similar to those from other recent analyses, the researchers reported. Women were more likely to have occult cancer at RRSO if they had BRCA1/2 mutations (odds ratio, 11.3; 95% confidence interval, 1.4-87.9), abnormal baseline transovarian ultrasound or CA-125 levels (OR, 6.5; 95% CI, 1.8-24.3), or were postmenopausal (OR, 4.0; 95% CI, 1.2-13.3), the investigators wrote (J. Clin. Onc. 2014 Sept. 8 [doi:10.1200/JCO.2013.54.1987]).
All the women with occult cancers were at least 42 years old, and their median age was more than 52 years, compared with 47 years for surgical patients who had benign pathology (P less than .001), said the investigators. Postmenopausal women had an almost fourfold greater cancer rate than that of premenopausal women (P less than .003), they added.
But more than half of patients with occult ovarian or tubal cancer had serous tubal intraepithelial cancer or stage I or II invasive cancer, suggesting a better prognosis than that for patients with overt signs of cancer at surgery, said the researchers.
The National Cancer Institute funded the study. One coauthor reported having served as a paid consultant for Pfizer and the rest reported no conflicts of interest.
Older, postmenopausal women with BRCA1 or BRCA2 mutations and abnormal baseline tests were most likely to have occult cancers at risk-reducing salpingo-oophorectomy, investigators reported online in the Journal of Clinical Oncology.
Pathology results showed that 2.6% of women who underwent the surgery had occult ovarian, tubal, or peritoneal cancers, including 4.6% of BRCA1 mutation carriers, 3.5% of BRCA2 carriers, and 0.5% of women who lacked either mutation, said Dr. Mark Sherman of the National Cancer Institute and his associates. These rates resembled findings from other recent studies, the researchers said.
The investigators studied 966 high-risk women who chose risk-reducing salpingo-oophorectomy (RRSO) as part of a nonrandomized prospective clinical trial (Gynecologic Oncology Group 0199, or GOG 0199) of the National Ovarian Cancer Prevention and Early Detection Study. Cancers rates were similar to those from other recent analyses, the researchers reported. Women were more likely to have occult cancer at RRSO if they had BRCA1/2 mutations (odds ratio, 11.3; 95% confidence interval, 1.4-87.9), abnormal baseline transovarian ultrasound or CA-125 levels (OR, 6.5; 95% CI, 1.8-24.3), or were postmenopausal (OR, 4.0; 95% CI, 1.2-13.3), the investigators wrote (J. Clin. Onc. 2014 Sept. 8 [doi:10.1200/JCO.2013.54.1987]).
All the women with occult cancers were at least 42 years old, and their median age was more than 52 years, compared with 47 years for surgical patients who had benign pathology (P less than .001), said the investigators. Postmenopausal women had an almost fourfold greater cancer rate than that of premenopausal women (P less than .003), they added.
But more than half of patients with occult ovarian or tubal cancer had serous tubal intraepithelial cancer or stage I or II invasive cancer, suggesting a better prognosis than that for patients with overt signs of cancer at surgery, said the researchers.
The National Cancer Institute funded the study. One coauthor reported having served as a paid consultant for Pfizer and the rest reported no conflicts of interest.
Older, postmenopausal women with BRCA1 or BRCA2 mutations and abnormal baseline tests were most likely to have occult cancers at risk-reducing salpingo-oophorectomy, investigators reported online in the Journal of Clinical Oncology.
Pathology results showed that 2.6% of women who underwent the surgery had occult ovarian, tubal, or peritoneal cancers, including 4.6% of BRCA1 mutation carriers, 3.5% of BRCA2 carriers, and 0.5% of women who lacked either mutation, said Dr. Mark Sherman of the National Cancer Institute and his associates. These rates resembled findings from other recent studies, the researchers said.
The investigators studied 966 high-risk women who chose risk-reducing salpingo-oophorectomy (RRSO) as part of a nonrandomized prospective clinical trial (Gynecologic Oncology Group 0199, or GOG 0199) of the National Ovarian Cancer Prevention and Early Detection Study. Cancers rates were similar to those from other recent analyses, the researchers reported. Women were more likely to have occult cancer at RRSO if they had BRCA1/2 mutations (odds ratio, 11.3; 95% confidence interval, 1.4-87.9), abnormal baseline transovarian ultrasound or CA-125 levels (OR, 6.5; 95% CI, 1.8-24.3), or were postmenopausal (OR, 4.0; 95% CI, 1.2-13.3), the investigators wrote (J. Clin. Onc. 2014 Sept. 8 [doi:10.1200/JCO.2013.54.1987]).
All the women with occult cancers were at least 42 years old, and their median age was more than 52 years, compared with 47 years for surgical patients who had benign pathology (P less than .001), said the investigators. Postmenopausal women had an almost fourfold greater cancer rate than that of premenopausal women (P less than .003), they added.
But more than half of patients with occult ovarian or tubal cancer had serous tubal intraepithelial cancer or stage I or II invasive cancer, suggesting a better prognosis than that for patients with overt signs of cancer at surgery, said the researchers.
The National Cancer Institute funded the study. One coauthor reported having served as a paid consultant for Pfizer and the rest reported no conflicts of interest.
FROM JOURNAL OF CLINICAL ONCOLOGY
Key clinical point: Older postmenopausal women, BRCA 1/2 mutation carriers, and women with abnormal cancer 125 (CA-125) serum levels or transovarian ultrasound results were significantly more likely to have occult invasive cancers diagnosed when they underwent RRSO.
Major finding: Significant predictors of invasive cancer at the time of RRSO included BRCA 1/2 mutations (odds ratio, 11.3; 95% confidence interval, 1.4 to 87.9), abnormal baseline CA-125 or transovarian ultrasound results (OR, 6.5; 95% CI, 1.8-24.3), and postmenopausal status (OR, 4.0; 95% CI, 1.2-13.3).
Data source: Analysis of data from 996 high-risk women who chose RRSO as part of a nonrandomized prospective clinical trial (Gynecologic Oncology Group 0199, or GOG 0199) of the National Ovarian Cancer Prevention and Early Detection Study.
Disclosures: The National Cancer Institute funded the study. One coauthor reported having served as a paid consultant for Pfizer, and the rest reported no conflicts of interest.
Sleep disruption, gas exchange abnormalities common in CF
Sleep is an issue for many patients with cystic fibrosis, but noninvasive measures can ease at least some of the problem, according to Dr. Eliot Katz of Harvard Medical School, Boston.
A host of factors can disrupt sleep for patients with CF, including chronic cough, hypoventilation, musculoskeletal pain, gastrointestinal reflux, abdominal discomfort, depression, and the need for frequent defecation, Dr. Katz noted. Children with CF may also have obstructive sleep apnea caused by factors such as adenotonsillar hypertrophy and chronic rhinosinusitis. Some patients also take medications that disrupt sleep or struggle to sleep because they receive overnight enteral feeding, he added (Clin. Chest. Med. 2014 [doi:10.1016/j.ccm.2014.06.005]).
Patients also may develop nocturnal hypercapnia and hypoxemia during sleep. Although nocturnal hypoxemia is most common in patients with advanced lung disease (FEV1 less than 65%), it can also affect patients with milder lung disease, Dr. Katz said. "Hypoxemia is not usually associated with arousal from sleep and, therefore, may be unrecognized," he noted.
As their lung disease progresses, patients with CF develop hypercapnia and subsequent dyspnea, which can be relieved, at least in the short term, by noninvasive ventilation to increase tidal volume and minute ventilation during sleep, Dr. Katz said. He noted that in a study of patients with advanced lung disease, minute ventilation was 22% lower during REM sleep than when patients were awake breathing room air, but was only 14% lower when sleeping patients received noninvasive ventilation (Am. J. Respir. Crit. Care. Med. 2001;163;129-34).
Dr. Katz reported no funding sources and had no disclosures.
Sleep is an issue for many patients with cystic fibrosis, but noninvasive measures can ease at least some of the problem, according to Dr. Eliot Katz of Harvard Medical School, Boston.
A host of factors can disrupt sleep for patients with CF, including chronic cough, hypoventilation, musculoskeletal pain, gastrointestinal reflux, abdominal discomfort, depression, and the need for frequent defecation, Dr. Katz noted. Children with CF may also have obstructive sleep apnea caused by factors such as adenotonsillar hypertrophy and chronic rhinosinusitis. Some patients also take medications that disrupt sleep or struggle to sleep because they receive overnight enteral feeding, he added (Clin. Chest. Med. 2014 [doi:10.1016/j.ccm.2014.06.005]).
Patients also may develop nocturnal hypercapnia and hypoxemia during sleep. Although nocturnal hypoxemia is most common in patients with advanced lung disease (FEV1 less than 65%), it can also affect patients with milder lung disease, Dr. Katz said. "Hypoxemia is not usually associated with arousal from sleep and, therefore, may be unrecognized," he noted.
As their lung disease progresses, patients with CF develop hypercapnia and subsequent dyspnea, which can be relieved, at least in the short term, by noninvasive ventilation to increase tidal volume and minute ventilation during sleep, Dr. Katz said. He noted that in a study of patients with advanced lung disease, minute ventilation was 22% lower during REM sleep than when patients were awake breathing room air, but was only 14% lower when sleeping patients received noninvasive ventilation (Am. J. Respir. Crit. Care. Med. 2001;163;129-34).
Dr. Katz reported no funding sources and had no disclosures.
Sleep is an issue for many patients with cystic fibrosis, but noninvasive measures can ease at least some of the problem, according to Dr. Eliot Katz of Harvard Medical School, Boston.
A host of factors can disrupt sleep for patients with CF, including chronic cough, hypoventilation, musculoskeletal pain, gastrointestinal reflux, abdominal discomfort, depression, and the need for frequent defecation, Dr. Katz noted. Children with CF may also have obstructive sleep apnea caused by factors such as adenotonsillar hypertrophy and chronic rhinosinusitis. Some patients also take medications that disrupt sleep or struggle to sleep because they receive overnight enteral feeding, he added (Clin. Chest. Med. 2014 [doi:10.1016/j.ccm.2014.06.005]).
Patients also may develop nocturnal hypercapnia and hypoxemia during sleep. Although nocturnal hypoxemia is most common in patients with advanced lung disease (FEV1 less than 65%), it can also affect patients with milder lung disease, Dr. Katz said. "Hypoxemia is not usually associated with arousal from sleep and, therefore, may be unrecognized," he noted.
As their lung disease progresses, patients with CF develop hypercapnia and subsequent dyspnea, which can be relieved, at least in the short term, by noninvasive ventilation to increase tidal volume and minute ventilation during sleep, Dr. Katz said. He noted that in a study of patients with advanced lung disease, minute ventilation was 22% lower during REM sleep than when patients were awake breathing room air, but was only 14% lower when sleeping patients received noninvasive ventilation (Am. J. Respir. Crit. Care. Med. 2001;163;129-34).
Dr. Katz reported no funding sources and had no disclosures.
FROM CLINICS IN CHEST MEDICINE
Key clinical point: Noninvasive ventilation and supplemental oxygen can mitigate gas exchange abnormalities in patients with cystic fibrosis who have advanced lung disease.
Major finding: Chronic cough, hypoventilation, musculoskeletal pain, gastrointestinal reflux, abdominal discomfort, depression, and the need for frequent defecation all can disrupt sleep for patients with CF.
Data source: A review of 82 articles on cystic fibrosis and sleep.
Disclosures: Dr. Katz reported no funding sources and had no disclosures.
Assess patient’s body clock before treating circadian rhythm sleep disorders
Clinicians should measure dim light melatonin onset before treating patients with circadian rhythm sleep disorders, according to Dr. Henry Keijzer of the University Maastricht (the Netherlands) and his associates.
The test enables clinicians to assess patients’ individual circadian timing, the reviewers said. At least 17 of the 90 scientific studies they reviewed support the use of the test in this context, and it can be performed by collecting saliva at home if in-clinic testing is not feasible, they added.
Although patients are often told to take exogenous melatonin 1-2 hours before bedtime, this generalized approach can lead to adverse phase-shifting effects, the reviewers said (Sleep Med. Rev. 2014;18:333-9).
"Therefore, we believe that the use of melatonin in patients with chronic sleep problems should occur only after their baseline circadian timing information is known, and should be supervised by a health care professional who is familiar with melatonin and its phase-dependent effects," they wrote.
The authors expressed concern that "melatonin is increasingly recommended for patients with insomnia or used by such patients as an over-the-counter self-care medicine."
The investigators reported no funding sources or conflicts of interest.
Clinicians should measure dim light melatonin onset before treating patients with circadian rhythm sleep disorders, according to Dr. Henry Keijzer of the University Maastricht (the Netherlands) and his associates.
The test enables clinicians to assess patients’ individual circadian timing, the reviewers said. At least 17 of the 90 scientific studies they reviewed support the use of the test in this context, and it can be performed by collecting saliva at home if in-clinic testing is not feasible, they added.
Although patients are often told to take exogenous melatonin 1-2 hours before bedtime, this generalized approach can lead to adverse phase-shifting effects, the reviewers said (Sleep Med. Rev. 2014;18:333-9).
"Therefore, we believe that the use of melatonin in patients with chronic sleep problems should occur only after their baseline circadian timing information is known, and should be supervised by a health care professional who is familiar with melatonin and its phase-dependent effects," they wrote.
The authors expressed concern that "melatonin is increasingly recommended for patients with insomnia or used by such patients as an over-the-counter self-care medicine."
The investigators reported no funding sources or conflicts of interest.
Clinicians should measure dim light melatonin onset before treating patients with circadian rhythm sleep disorders, according to Dr. Henry Keijzer of the University Maastricht (the Netherlands) and his associates.
The test enables clinicians to assess patients’ individual circadian timing, the reviewers said. At least 17 of the 90 scientific studies they reviewed support the use of the test in this context, and it can be performed by collecting saliva at home if in-clinic testing is not feasible, they added.
Although patients are often told to take exogenous melatonin 1-2 hours before bedtime, this generalized approach can lead to adverse phase-shifting effects, the reviewers said (Sleep Med. Rev. 2014;18:333-9).
"Therefore, we believe that the use of melatonin in patients with chronic sleep problems should occur only after their baseline circadian timing information is known, and should be supervised by a health care professional who is familiar with melatonin and its phase-dependent effects," they wrote.
The authors expressed concern that "melatonin is increasingly recommended for patients with insomnia or used by such patients as an over-the-counter self-care medicine."
The investigators reported no funding sources or conflicts of interest.
FROM SLEEP MEDICINE REVIEWS
Key clinical point: Clinicians should measure dim light melatonin onset before treating patients with circadian rhythm sleep disorders, and should prescribe melatonin or light therapy based on patients’ individualized DLMO result.
Major finding: Measuring DLMO improves the diagnosis and treatment of circadian rhythm sleep disorders.
Data source: A review of 90 articles on circadian rhythms, sleep disorders, DLMO, and the use of lighting and exogenous melatonin to improve sleep measures.
Disclosures: The authors reported no funding sources or conflicts of interest.
Multiples of median OS predicted actual survival in metastatic colorectal cancer
Clinicians can use simple multiples of median overall survival time in clinical trials to estimate survival percentiles for metastatic colorectal cancer, researchers reported online in Annals of Oncology.
"Previous work has suggested that clinicians often overestimate prognosis, and we hope that this study and others will provide more objective estimates on which to base discussions with patients and their families," said Dr. Matt Williams of Imperial College Healthcare NHS Trust, London, and his associates.
Prior studies of incurable breast and lung cancer have shown that multiples of median overall survival (OS) accurately reflected time points when 90%, 75%, 25%, and 10% of patients were alive, the researchers said. To assess this approach for estimated survival in metastatic colorectal cancer, they analyzed 46 MEDLINE-indexed, randomized, phase III clinical trials of chemotherapeutic agents published between 2000 and 2011 (Ann. Onc. 2014 [doi:10.1093/annonc/mdu372]).
The median OS for the 29,011 patients in the trials was 16.5 months, the researchers said. The investigators then estimated 90%, 75%, 25% and 10% survival times by multiplying the median OS by 0.25, 0.5, 2, and 3, they explained.
The estimated survival time fell within 75%-133% of actual survival time 88% of the time, the researchers reported, adding that the lowest concordance was for the earliest or 90% survival level. The low rate of agreement at the 90% survival time point may be due in part to the narrow time window at this survival point, the investigators speculated. "Our definition of agreement allows for approximately 5 weeks’ difference between the actual and predicted values, which is a narrow time window and thus more susceptible to random variation," they said.
"Taken with previous studies, these findings are likely to be valid across a large range of patients," Dr. Williams and his associates commented. "We would encourage clinicians to think of prognosis as a trajectory and to consider quoting survival ranges instead of point estimates, in discussions with patients."
The findings mirror prior work in breast and lung cancer, even though these cancers have very different survival times, the investigators noted. For this reason, the correlations are likely to hold true even if median OS for metastatic colorectal cancer increases in future trials, they said.
The authors said they received no funding for the work and had no conflicts of interest.
Clinicians can use simple multiples of median overall survival time in clinical trials to estimate survival percentiles for metastatic colorectal cancer, researchers reported online in Annals of Oncology.
"Previous work has suggested that clinicians often overestimate prognosis, and we hope that this study and others will provide more objective estimates on which to base discussions with patients and their families," said Dr. Matt Williams of Imperial College Healthcare NHS Trust, London, and his associates.
Prior studies of incurable breast and lung cancer have shown that multiples of median overall survival (OS) accurately reflected time points when 90%, 75%, 25%, and 10% of patients were alive, the researchers said. To assess this approach for estimated survival in metastatic colorectal cancer, they analyzed 46 MEDLINE-indexed, randomized, phase III clinical trials of chemotherapeutic agents published between 2000 and 2011 (Ann. Onc. 2014 [doi:10.1093/annonc/mdu372]).
The median OS for the 29,011 patients in the trials was 16.5 months, the researchers said. The investigators then estimated 90%, 75%, 25% and 10% survival times by multiplying the median OS by 0.25, 0.5, 2, and 3, they explained.
The estimated survival time fell within 75%-133% of actual survival time 88% of the time, the researchers reported, adding that the lowest concordance was for the earliest or 90% survival level. The low rate of agreement at the 90% survival time point may be due in part to the narrow time window at this survival point, the investigators speculated. "Our definition of agreement allows for approximately 5 weeks’ difference between the actual and predicted values, which is a narrow time window and thus more susceptible to random variation," they said.
"Taken with previous studies, these findings are likely to be valid across a large range of patients," Dr. Williams and his associates commented. "We would encourage clinicians to think of prognosis as a trajectory and to consider quoting survival ranges instead of point estimates, in discussions with patients."
The findings mirror prior work in breast and lung cancer, even though these cancers have very different survival times, the investigators noted. For this reason, the correlations are likely to hold true even if median OS for metastatic colorectal cancer increases in future trials, they said.
The authors said they received no funding for the work and had no conflicts of interest.
Clinicians can use simple multiples of median overall survival time in clinical trials to estimate survival percentiles for metastatic colorectal cancer, researchers reported online in Annals of Oncology.
"Previous work has suggested that clinicians often overestimate prognosis, and we hope that this study and others will provide more objective estimates on which to base discussions with patients and their families," said Dr. Matt Williams of Imperial College Healthcare NHS Trust, London, and his associates.
Prior studies of incurable breast and lung cancer have shown that multiples of median overall survival (OS) accurately reflected time points when 90%, 75%, 25%, and 10% of patients were alive, the researchers said. To assess this approach for estimated survival in metastatic colorectal cancer, they analyzed 46 MEDLINE-indexed, randomized, phase III clinical trials of chemotherapeutic agents published between 2000 and 2011 (Ann. Onc. 2014 [doi:10.1093/annonc/mdu372]).
The median OS for the 29,011 patients in the trials was 16.5 months, the researchers said. The investigators then estimated 90%, 75%, 25% and 10% survival times by multiplying the median OS by 0.25, 0.5, 2, and 3, they explained.
The estimated survival time fell within 75%-133% of actual survival time 88% of the time, the researchers reported, adding that the lowest concordance was for the earliest or 90% survival level. The low rate of agreement at the 90% survival time point may be due in part to the narrow time window at this survival point, the investigators speculated. "Our definition of agreement allows for approximately 5 weeks’ difference between the actual and predicted values, which is a narrow time window and thus more susceptible to random variation," they said.
"Taken with previous studies, these findings are likely to be valid across a large range of patients," Dr. Williams and his associates commented. "We would encourage clinicians to think of prognosis as a trajectory and to consider quoting survival ranges instead of point estimates, in discussions with patients."
The findings mirror prior work in breast and lung cancer, even though these cancers have very different survival times, the investigators noted. For this reason, the correlations are likely to hold true even if median OS for metastatic colorectal cancer increases in future trials, they said.
The authors said they received no funding for the work and had no conflicts of interest.
FROM ANNALS OF ONCOLOGY
Key clinical point: Clinicians can use simple multiples of median overall survival times from clinical trials to estimate survival percentiles for patients with metastatic colorectal cancer.
Major finding: Multiplying the median overall survival time (16.5 months) by the multiples 0.25, 0.5, 2, and 3 yielded estimated times when 90%, 75%, 25%, and 10% of patients were alive, and these estimates fell within 75%-133% of actual survival times 88% of the time.
Data source: Analysis of 46 phase III randomized clinical trials of chemotherapy agents in 29,011 patients with metastatic colorectal cancer.
Disclosures: The authors said they received no funding for the work and had no conflicts of interest.
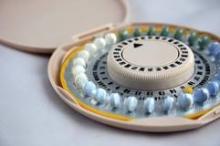
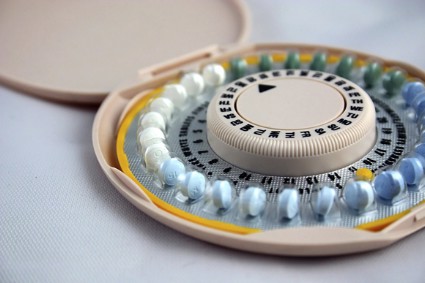
Recent Use of Oral Contraceptives Linked to Breast Cancer
Earn 0.25 hours AMA PRA Category 1 credit: Read this article, and click the link at the end to take the posttest.
Women who recently used oral contraceptives had a 50% greater chance of developing breast cancer than that of women who formerly used or never used oral contraceptives, according to a case-control study published Aug. 1 in Cancer Research.
For the nested case-control study, the researchers compared 1,102 women aged 20-49 years who had been diagnosed with invasive breast cancer from 1990 to 2009 with 21, 755 controls sampled from the same health care delivery system, matched for age, year, enrollment length, and medical chart availability.
Oral contraceptive use within the prior year was associated with an increased breast cancer risk (odds ratio, 1.5; 95% confidence interval, 1.3-1.9) relative to never or former use of oral contraceptives, reported Dr. Elisabeth Beaber at the University of Washington, Seattle, and her associates.
Their findings suggest that risk may vary by oral contraceptive formulation. The investigators found significant associations between breast cancer and recent use of oral contraceptives involving high-dose estrogen (OR, 2.7; 95% CI, 1.1-6.2), ethynodiol diacetate (OR, 2.6; 95% CI, 1.4-4.7), or triphasic dosing with an average of 0.75 mg of norethindrone (OR, 3.1; 95% CI, 1.9-5.1). But other types of oral birth control, including low-dose estrogen oral contraceptives, were not associated with breast cancer (OR, 1.0; 95% CI, 0.6-1.7), Dr. Beaber and her associates noted (Cancer Res. 2014;74:4078-89).
"If confirmed, consideration of the breast cancer risk associated with different oral contraceptive types could impact discussions weighing recognized health benefits and potential risks," they concluded.
The study was funded by the National Cancer Institute. The authors reported no financial conflicts of interest.
To earn 0.25 hours AMA PRA Category 1 credit after reading this article, take the post-test here.
Earn 0.25 hours AMA PRA Category 1 credit: Read this article, and click the link at the end to take the posttest.
Women who recently used oral contraceptives had a 50% greater chance of developing breast cancer than that of women who formerly used or never used oral contraceptives, according to a case-control study published Aug. 1 in Cancer Research.
For the nested case-control study, the researchers compared 1,102 women aged 20-49 years who had been diagnosed with invasive breast cancer from 1990 to 2009 with 21, 755 controls sampled from the same health care delivery system, matched for age, year, enrollment length, and medical chart availability.
Oral contraceptive use within the prior year was associated with an increased breast cancer risk (odds ratio, 1.5; 95% confidence interval, 1.3-1.9) relative to never or former use of oral contraceptives, reported Dr. Elisabeth Beaber at the University of Washington, Seattle, and her associates.
Their findings suggest that risk may vary by oral contraceptive formulation. The investigators found significant associations between breast cancer and recent use of oral contraceptives involving high-dose estrogen (OR, 2.7; 95% CI, 1.1-6.2), ethynodiol diacetate (OR, 2.6; 95% CI, 1.4-4.7), or triphasic dosing with an average of 0.75 mg of norethindrone (OR, 3.1; 95% CI, 1.9-5.1). But other types of oral birth control, including low-dose estrogen oral contraceptives, were not associated with breast cancer (OR, 1.0; 95% CI, 0.6-1.7), Dr. Beaber and her associates noted (Cancer Res. 2014;74:4078-89).
"If confirmed, consideration of the breast cancer risk associated with different oral contraceptive types could impact discussions weighing recognized health benefits and potential risks," they concluded.
The study was funded by the National Cancer Institute. The authors reported no financial conflicts of interest.
To earn 0.25 hours AMA PRA Category 1 credit after reading this article, take the post-test here.
Earn 0.25 hours AMA PRA Category 1 credit: Read this article, and click the link at the end to take the posttest.
Women who recently used oral contraceptives had a 50% greater chance of developing breast cancer than that of women who formerly used or never used oral contraceptives, according to a case-control study published Aug. 1 in Cancer Research.
For the nested case-control study, the researchers compared 1,102 women aged 20-49 years who had been diagnosed with invasive breast cancer from 1990 to 2009 with 21, 755 controls sampled from the same health care delivery system, matched for age, year, enrollment length, and medical chart availability.
Oral contraceptive use within the prior year was associated with an increased breast cancer risk (odds ratio, 1.5; 95% confidence interval, 1.3-1.9) relative to never or former use of oral contraceptives, reported Dr. Elisabeth Beaber at the University of Washington, Seattle, and her associates.
Their findings suggest that risk may vary by oral contraceptive formulation. The investigators found significant associations between breast cancer and recent use of oral contraceptives involving high-dose estrogen (OR, 2.7; 95% CI, 1.1-6.2), ethynodiol diacetate (OR, 2.6; 95% CI, 1.4-4.7), or triphasic dosing with an average of 0.75 mg of norethindrone (OR, 3.1; 95% CI, 1.9-5.1). But other types of oral birth control, including low-dose estrogen oral contraceptives, were not associated with breast cancer (OR, 1.0; 95% CI, 0.6-1.7), Dr. Beaber and her associates noted (Cancer Res. 2014;74:4078-89).
"If confirmed, consideration of the breast cancer risk associated with different oral contraceptive types could impact discussions weighing recognized health benefits and potential risks," they concluded.
The study was funded by the National Cancer Institute. The authors reported no financial conflicts of interest.
To earn 0.25 hours AMA PRA Category 1 credit after reading this article, take the post-test here.
FROM CANCER RESEARCH
Life expectancy approached 40 years for children born with CF in 2010
Mortality in patients with cystic fibrosis fell by almost 2% per year in the United States between 2000 and 2010, authors of a registry-based study reported online August 18 in Annals of Internal Medicine.
Based on the analyses, patients born and diagnosed in 2010 can expect to live almost 40 years if the state of CF care remains static, and about 56 years if treatments progress at the current rate, said Todd MacKenzie, Ph.D., of Dartmouth School of Medicine in Hanover, N.H., and his associates.
The study included 110 Cystic Fibrosis Foundation–accredited care centers in the United States. Mortality fell by 1.8% per year between 2000 and 2010 (95% confidence interval, 0.5%-2.7%), and males had a 19% lower risk of death than females (95% CI, 13%-24%), the investigators found. The estimated median survival for children born and diagnosed in 2010 was 39 years overall (95% CI, 38-40 years), 37 years for females (95% CI, 35-39 years), and 40 years for males (95% CI, 39-42 years), they reported (Ann. Int. Med. 2014 Aug. 18 [doi:10.7326/M13-0636]).
The results apply only to patients diagnosed in the first year of life, as patients diagnosed later are likely pancreatic-sufficient and therefore have a better prognosis, Dr. MacKenzie and associates noted. Improved survival could partially reflect the increasing diagnosis of patients with less severe phenotypes, they said.
The Cystic Fibrosis Foundation funded the study. Dr. MacKenzie reported no conflicts of interest. Three coauthors reported grant support from the Cystic Fibrosis Foundation.
The findings are "worth celebrating," said Dr. Joseph Pilewski and Dr. Darren Taichman. "However, continuing to ensure the kind of care that has resulted in a growing number of patients with CF living far into adulthood will not be simple or inexpensive."
The patients in the study all were treated at CF Foundation–accredited centers, which provide coordinated, multidisciplinary care, Dr. Pilewski and Dr. Taichman said. And patients with CF often need care from additional specialists for comorbidities such as diabetes, osteoporosis, cancer, depression, and anxiety, they added. "Caring for adults with CF requires a village."
As for other complex primary care scenarios, coordinating and managing the medical and social issues of CF patients can be time-intensive, stressful, and poorly reimbursed, they said. Furthermore, coordinated nursing, social work, nutrition, and respiratory therapy services often are not available outside accredited CF care centers.
"Will the remarkable community support that has enabled progress in CF care and survival continue in an era when growing proportions of patients are no longer children, for whom it may be easier to solicit donations?" Dr. Pilewski and Dr. Taichman asked. "If not, we will need to think hard about other solutions because, although survival of patients with CF has improved, many still suffer and die prematurely."
Dr. Pilewski is codirector of the Adult Cystic Fibrosis program at the University of Pittsburgh Medical Center. Dr. Taichman is executive deputy editor for Annals of Internal Medicine. These remarks were taken from their editorial accompanying Dr. MacKenzie’s report (Ann. Int. Med. 2014 Aug. 18 [doi:10.7326/M14-1534]).
The findings are "worth celebrating," said Dr. Joseph Pilewski and Dr. Darren Taichman. "However, continuing to ensure the kind of care that has resulted in a growing number of patients with CF living far into adulthood will not be simple or inexpensive."
The patients in the study all were treated at CF Foundation–accredited centers, which provide coordinated, multidisciplinary care, Dr. Pilewski and Dr. Taichman said. And patients with CF often need care from additional specialists for comorbidities such as diabetes, osteoporosis, cancer, depression, and anxiety, they added. "Caring for adults with CF requires a village."
As for other complex primary care scenarios, coordinating and managing the medical and social issues of CF patients can be time-intensive, stressful, and poorly reimbursed, they said. Furthermore, coordinated nursing, social work, nutrition, and respiratory therapy services often are not available outside accredited CF care centers.
"Will the remarkable community support that has enabled progress in CF care and survival continue in an era when growing proportions of patients are no longer children, for whom it may be easier to solicit donations?" Dr. Pilewski and Dr. Taichman asked. "If not, we will need to think hard about other solutions because, although survival of patients with CF has improved, many still suffer and die prematurely."
Dr. Pilewski is codirector of the Adult Cystic Fibrosis program at the University of Pittsburgh Medical Center. Dr. Taichman is executive deputy editor for Annals of Internal Medicine. These remarks were taken from their editorial accompanying Dr. MacKenzie’s report (Ann. Int. Med. 2014 Aug. 18 [doi:10.7326/M14-1534]).
The findings are "worth celebrating," said Dr. Joseph Pilewski and Dr. Darren Taichman. "However, continuing to ensure the kind of care that has resulted in a growing number of patients with CF living far into adulthood will not be simple or inexpensive."
The patients in the study all were treated at CF Foundation–accredited centers, which provide coordinated, multidisciplinary care, Dr. Pilewski and Dr. Taichman said. And patients with CF often need care from additional specialists for comorbidities such as diabetes, osteoporosis, cancer, depression, and anxiety, they added. "Caring for adults with CF requires a village."
As for other complex primary care scenarios, coordinating and managing the medical and social issues of CF patients can be time-intensive, stressful, and poorly reimbursed, they said. Furthermore, coordinated nursing, social work, nutrition, and respiratory therapy services often are not available outside accredited CF care centers.
"Will the remarkable community support that has enabled progress in CF care and survival continue in an era when growing proportions of patients are no longer children, for whom it may be easier to solicit donations?" Dr. Pilewski and Dr. Taichman asked. "If not, we will need to think hard about other solutions because, although survival of patients with CF has improved, many still suffer and die prematurely."
Dr. Pilewski is codirector of the Adult Cystic Fibrosis program at the University of Pittsburgh Medical Center. Dr. Taichman is executive deputy editor for Annals of Internal Medicine. These remarks were taken from their editorial accompanying Dr. MacKenzie’s report (Ann. Int. Med. 2014 Aug. 18 [doi:10.7326/M14-1534]).
Mortality in patients with cystic fibrosis fell by almost 2% per year in the United States between 2000 and 2010, authors of a registry-based study reported online August 18 in Annals of Internal Medicine.
Based on the analyses, patients born and diagnosed in 2010 can expect to live almost 40 years if the state of CF care remains static, and about 56 years if treatments progress at the current rate, said Todd MacKenzie, Ph.D., of Dartmouth School of Medicine in Hanover, N.H., and his associates.
The study included 110 Cystic Fibrosis Foundation–accredited care centers in the United States. Mortality fell by 1.8% per year between 2000 and 2010 (95% confidence interval, 0.5%-2.7%), and males had a 19% lower risk of death than females (95% CI, 13%-24%), the investigators found. The estimated median survival for children born and diagnosed in 2010 was 39 years overall (95% CI, 38-40 years), 37 years for females (95% CI, 35-39 years), and 40 years for males (95% CI, 39-42 years), they reported (Ann. Int. Med. 2014 Aug. 18 [doi:10.7326/M13-0636]).
The results apply only to patients diagnosed in the first year of life, as patients diagnosed later are likely pancreatic-sufficient and therefore have a better prognosis, Dr. MacKenzie and associates noted. Improved survival could partially reflect the increasing diagnosis of patients with less severe phenotypes, they said.
The Cystic Fibrosis Foundation funded the study. Dr. MacKenzie reported no conflicts of interest. Three coauthors reported grant support from the Cystic Fibrosis Foundation.
Mortality in patients with cystic fibrosis fell by almost 2% per year in the United States between 2000 and 2010, authors of a registry-based study reported online August 18 in Annals of Internal Medicine.
Based on the analyses, patients born and diagnosed in 2010 can expect to live almost 40 years if the state of CF care remains static, and about 56 years if treatments progress at the current rate, said Todd MacKenzie, Ph.D., of Dartmouth School of Medicine in Hanover, N.H., and his associates.
The study included 110 Cystic Fibrosis Foundation–accredited care centers in the United States. Mortality fell by 1.8% per year between 2000 and 2010 (95% confidence interval, 0.5%-2.7%), and males had a 19% lower risk of death than females (95% CI, 13%-24%), the investigators found. The estimated median survival for children born and diagnosed in 2010 was 39 years overall (95% CI, 38-40 years), 37 years for females (95% CI, 35-39 years), and 40 years for males (95% CI, 39-42 years), they reported (Ann. Int. Med. 2014 Aug. 18 [doi:10.7326/M13-0636]).
The results apply only to patients diagnosed in the first year of life, as patients diagnosed later are likely pancreatic-sufficient and therefore have a better prognosis, Dr. MacKenzie and associates noted. Improved survival could partially reflect the increasing diagnosis of patients with less severe phenotypes, they said.
The Cystic Fibrosis Foundation funded the study. Dr. MacKenzie reported no conflicts of interest. Three coauthors reported grant support from the Cystic Fibrosis Foundation.
FROM ANNALS OF INTERNAL MEDICINE
Key clinical point: Patients with cystic fibrosis who are born and diagnosed in 2010 can expect to live almost 40 years if clinical care remains at its current level.
Major finding: Mortality in patients with cystic fibrosis fell by 1.8% per year between 2000 and 2010 (95% confidence interval, 0.5%-2.7%), and patients born and diagnosed in 2010 were projected to survive 39 years given no further improvements in the current state of care (95% CI, 38-40 years).
Data source: Registry-based study of 110 Cystic Fibrosis Foundation–accredited care centers in the United States.
Disclosures: The Cystic Fibrosis Foundation funded the study. Dr. MacKenzie reported no conflicts of interest. Three coauthors reported grant support from the Cystic Fibrosis Foundation.
MS disability linked to abnormalities of spinal cord grey matter
Disability in patients with multiple sclerosis was independently linked to microstructural abnormalities of spinal cord grey matter on diffusion tensor imaging study in a prospective study of healthy controls and patients at various stages of disease.
Spinal cord atrophy and abnormal grey matter radial diffusivity explained 77% of variance in scores on the Expanded Disability Status Scale (EDSS), said Dr. Hugh Kearney of the Queen Square MS Centre at the University College London Institute of Neurology and his associates. Grey matter involvement was already present in patients with relapsing-remitting multiple sclerosis (MS) but was more pronounced in those with secondary progressive disease, the investigators said.
The researchers performed 3 T spinal cord magnetic resonance imaging and diffusion tensor imaging on 113 subjects – 30 healthy controls, 21 individuals with a clinically isolated syndrome, 33 who had relapsing-remitting MS and 29 who had secondary progressive MS (J. Neurol. Neurosurg. Psychiatry 2014 Aug. 5 [doi:10.1136/jnnp-2014-308241]).
Compared with controls and subjects with relapsing-remitting MS, those with secondary progressive disease had significantly worse abnormalities in measures of spinal cord radial diffusivity, fractional anisotropy, and mean diffusivity in the grey matter and posterior columns, the investigators said.
Furthermore, spinal cord grey matter radial diffusivity and cord area were independently associated with EDSS disability scores (beta = 0.33 and P less than .01; beta = –0.45 and P less than .01, respectively), and radial diffusivity was independently linked to scores on a 9-hole peg test (beta = –0.33; P less than .01) and timed walk (beta = –0.20, P = .04), the researchers said.
Based on the findings, grey matter pathology in the spinal cord may underlie physical disability in MS, including the irreversible disability that characterizes secondary progressive disease, Dr. Kearney and his associates said. Investigators should next examine longitudinal changes in diffusion tensor imaging measures of spinal cord grey matter and how these changes relate to clinical progression, they said.
The research was funded by the MS Society of Great Britain and Northern Ireland, UCLH-UCL Biomedical Research Centre, the International Spinal Research Trust, and the Engineering and Physical Sciences Research Council. The authors reported no competing interests.
Disability in patients with multiple sclerosis was independently linked to microstructural abnormalities of spinal cord grey matter on diffusion tensor imaging study in a prospective study of healthy controls and patients at various stages of disease.
Spinal cord atrophy and abnormal grey matter radial diffusivity explained 77% of variance in scores on the Expanded Disability Status Scale (EDSS), said Dr. Hugh Kearney of the Queen Square MS Centre at the University College London Institute of Neurology and his associates. Grey matter involvement was already present in patients with relapsing-remitting multiple sclerosis (MS) but was more pronounced in those with secondary progressive disease, the investigators said.
The researchers performed 3 T spinal cord magnetic resonance imaging and diffusion tensor imaging on 113 subjects – 30 healthy controls, 21 individuals with a clinically isolated syndrome, 33 who had relapsing-remitting MS and 29 who had secondary progressive MS (J. Neurol. Neurosurg. Psychiatry 2014 Aug. 5 [doi:10.1136/jnnp-2014-308241]).
Compared with controls and subjects with relapsing-remitting MS, those with secondary progressive disease had significantly worse abnormalities in measures of spinal cord radial diffusivity, fractional anisotropy, and mean diffusivity in the grey matter and posterior columns, the investigators said.
Furthermore, spinal cord grey matter radial diffusivity and cord area were independently associated with EDSS disability scores (beta = 0.33 and P less than .01; beta = –0.45 and P less than .01, respectively), and radial diffusivity was independently linked to scores on a 9-hole peg test (beta = –0.33; P less than .01) and timed walk (beta = –0.20, P = .04), the researchers said.
Based on the findings, grey matter pathology in the spinal cord may underlie physical disability in MS, including the irreversible disability that characterizes secondary progressive disease, Dr. Kearney and his associates said. Investigators should next examine longitudinal changes in diffusion tensor imaging measures of spinal cord grey matter and how these changes relate to clinical progression, they said.
The research was funded by the MS Society of Great Britain and Northern Ireland, UCLH-UCL Biomedical Research Centre, the International Spinal Research Trust, and the Engineering and Physical Sciences Research Council. The authors reported no competing interests.
Disability in patients with multiple sclerosis was independently linked to microstructural abnormalities of spinal cord grey matter on diffusion tensor imaging study in a prospective study of healthy controls and patients at various stages of disease.
Spinal cord atrophy and abnormal grey matter radial diffusivity explained 77% of variance in scores on the Expanded Disability Status Scale (EDSS), said Dr. Hugh Kearney of the Queen Square MS Centre at the University College London Institute of Neurology and his associates. Grey matter involvement was already present in patients with relapsing-remitting multiple sclerosis (MS) but was more pronounced in those with secondary progressive disease, the investigators said.
The researchers performed 3 T spinal cord magnetic resonance imaging and diffusion tensor imaging on 113 subjects – 30 healthy controls, 21 individuals with a clinically isolated syndrome, 33 who had relapsing-remitting MS and 29 who had secondary progressive MS (J. Neurol. Neurosurg. Psychiatry 2014 Aug. 5 [doi:10.1136/jnnp-2014-308241]).
Compared with controls and subjects with relapsing-remitting MS, those with secondary progressive disease had significantly worse abnormalities in measures of spinal cord radial diffusivity, fractional anisotropy, and mean diffusivity in the grey matter and posterior columns, the investigators said.
Furthermore, spinal cord grey matter radial diffusivity and cord area were independently associated with EDSS disability scores (beta = 0.33 and P less than .01; beta = –0.45 and P less than .01, respectively), and radial diffusivity was independently linked to scores on a 9-hole peg test (beta = –0.33; P less than .01) and timed walk (beta = –0.20, P = .04), the researchers said.
Based on the findings, grey matter pathology in the spinal cord may underlie physical disability in MS, including the irreversible disability that characterizes secondary progressive disease, Dr. Kearney and his associates said. Investigators should next examine longitudinal changes in diffusion tensor imaging measures of spinal cord grey matter and how these changes relate to clinical progression, they said.
The research was funded by the MS Society of Great Britain and Northern Ireland, UCLH-UCL Biomedical Research Centre, the International Spinal Research Trust, and the Engineering and Physical Sciences Research Council. The authors reported no competing interests.
FROM JOURNAL OF NEUROLOGY, NEUROSURGERY & PSYCHIATRY
Key clinical point: Pathology of spinal cord grey matter contributes to disability in MS, especially in patients with secondary-progressive MS.
Major finding: Spinal cord area and radial diffusivity of the spinal cord grey matter together accounted for 77% of variance of scores on the EDSS.
Data source: A prospective study that compared diffusion tensor imaging (DTI) results between 30 controls, 21 patients with a clinically isolated syndrome, 33 with relapsing-remitting MS, and 29 with secondary progressive MS.
Disclosures: The research was funded by the MS Society of Great Britain and Northern Ireland, UCLH-UCL Biomedical Research Centre, the International Spinal Research Trust, and the Engineering and Physical Sciences Research Council. The authors reported no competing interests.