User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
Powered by CHEST Physician, Clinician Reviews, MDedge Family Medicine, Internal Medicine News, and The Journal of Clinical Outcomes Management.
CDC: Flu remains widespread; antivirals underutilized
The approximate midpoint of the 2014-2015 flu season has been reached, disease remains widespread, and antiviral flu medications remain underutilized, according to the Centers for Disease Control and Prevention.
As predicted, this season is proving particularly severe due to the predominance of antigenically drifted H3N2 virus strains, and the CDC is urging clinicians to maintain a high index of suspicion for flu and to prescribe antivirals earlier and more aggressively for patients presenting with flulike illness – especially young children, those over age 65 years, and those with underlying conditions, even if their symptoms are mild, CDC Director Thomas R. Frieden said during a press briefing.
A health advisory on the topic was issued Jan. 9, he noted.
“The CDC has recommended the use of antiviral drugs as an adjunct to vaccination. They are the only medicines that can specifically treat influenza illness, and in the context of an H3N2 predominant season with a less effective vaccine, treatment with antiflu drugs is even more important than usual,” he said, referring to the two neuraminidase inhibitors currently approved for treating influenza: oseltamivir and zanamivir.
About two-thirds of the H3N2 viruses analyzed this season are different from the H3N2 virus included in this year’s vaccine, which is why the vaccine is expected to have reduced effectiveness, he explained.
This makes early antiviral treatment all the more important, he added, noting that treatment within 2 days of symptom onset is optimal, but later treatment can also offer benefit.
“CDC scientists have looked very carefully at the use of influenza drugs in the clinical setting, and the conclusion is clear: They work, but they aren’t being used nearly enough. They can reduce symptoms, shorten duration of illness, and prevent serious complications,” he said.
Early treatment may help patients avoid hospitalization and could be life saving, he added.
Many patients are unaware that effective prescription treatments exist, and many doctors are not using the treatments as recommended. In one study, fewer than one in five eligible high-risk patients received treatment.
“So we’re expanding our efforts to reach clinicians about reminders about the importance of these drugs,” he said, noting that if high-risk patients with underlying conditions such as asthma, sickle cell disease, renal disease, or diabetes were treated, “tens of thousands of hospitalizations, and thousands of deaths could potentially be prevented.”
Dr. Frieden suggested that clinicians consider phone triage lines for high-risk patients to discuss symptoms over the phone and to “facilitate early initiation of treatment.”
An antiviral prescription can be provided without testing and before an office visit, he added.
The typical flu season lasts about 13 weeks on average, and the season began about 7 weeks ago. The continued high rate of H3N2 disease has had the greatest impact on older adults; that is typical of such seasons, which often involve a higher rate of hospitalizations and deaths.
In fact, hospitalization rates in the over 65 age group are rising sharply, Dr. Frieden said.
Last week the rate was 52 per 100,000 population, and this week the rate was 92 per 100,000 population. The cumulative rate 2 years ago when H3N2 viruses last predominated was 183 per 100,000, he noted.
“We wouldn’t be surprised to see something very similar this year,” he said.
Young children are also severely affected; thus far in the season there have been 26 reported pediatric flu-related deaths.
However, there are early signs that infection rates are declining in areas where the season started earlier, such as the Southeast, and the number of patients presenting to a doctor with flulike symptoms has also declined slightly, but it is too soon to tell whether disease activity has peaked, he said, stressing that “we still have several weeks of flu activity ahead.”
It’s not too late to get vaccinated, and despite the reduced efficacy of this year’s vaccine against the circulating H3N2 strains, vaccination may still offer some benefit.
“There are other strains out there as well,” he said, noting that a proportion of cases from other strains, such as influenza B, tend to occur late in the season, and this year’s vaccine offers a good match for influenza B viruses.
Pneumococcal vaccination is also important, particularly for older adults and those at high risk , he said.
Last September the CDC announced a new recommendation that all adults over age 65 years should get two different pneumococcal vaccines. Such vaccination may help prevent flu-related pneumonia.
Patients with the flu or flulike illness should be advised to cover their cough and to stay home from work or school to protect those who are most vulnerable to the flu, he said.
The approximate midpoint of the 2014-2015 flu season has been reached, disease remains widespread, and antiviral flu medications remain underutilized, according to the Centers for Disease Control and Prevention.
As predicted, this season is proving particularly severe due to the predominance of antigenically drifted H3N2 virus strains, and the CDC is urging clinicians to maintain a high index of suspicion for flu and to prescribe antivirals earlier and more aggressively for patients presenting with flulike illness – especially young children, those over age 65 years, and those with underlying conditions, even if their symptoms are mild, CDC Director Thomas R. Frieden said during a press briefing.
A health advisory on the topic was issued Jan. 9, he noted.
“The CDC has recommended the use of antiviral drugs as an adjunct to vaccination. They are the only medicines that can specifically treat influenza illness, and in the context of an H3N2 predominant season with a less effective vaccine, treatment with antiflu drugs is even more important than usual,” he said, referring to the two neuraminidase inhibitors currently approved for treating influenza: oseltamivir and zanamivir.
About two-thirds of the H3N2 viruses analyzed this season are different from the H3N2 virus included in this year’s vaccine, which is why the vaccine is expected to have reduced effectiveness, he explained.
This makes early antiviral treatment all the more important, he added, noting that treatment within 2 days of symptom onset is optimal, but later treatment can also offer benefit.
“CDC scientists have looked very carefully at the use of influenza drugs in the clinical setting, and the conclusion is clear: They work, but they aren’t being used nearly enough. They can reduce symptoms, shorten duration of illness, and prevent serious complications,” he said.
Early treatment may help patients avoid hospitalization and could be life saving, he added.
Many patients are unaware that effective prescription treatments exist, and many doctors are not using the treatments as recommended. In one study, fewer than one in five eligible high-risk patients received treatment.
“So we’re expanding our efforts to reach clinicians about reminders about the importance of these drugs,” he said, noting that if high-risk patients with underlying conditions such as asthma, sickle cell disease, renal disease, or diabetes were treated, “tens of thousands of hospitalizations, and thousands of deaths could potentially be prevented.”
Dr. Frieden suggested that clinicians consider phone triage lines for high-risk patients to discuss symptoms over the phone and to “facilitate early initiation of treatment.”
An antiviral prescription can be provided without testing and before an office visit, he added.
The typical flu season lasts about 13 weeks on average, and the season began about 7 weeks ago. The continued high rate of H3N2 disease has had the greatest impact on older adults; that is typical of such seasons, which often involve a higher rate of hospitalizations and deaths.
In fact, hospitalization rates in the over 65 age group are rising sharply, Dr. Frieden said.
Last week the rate was 52 per 100,000 population, and this week the rate was 92 per 100,000 population. The cumulative rate 2 years ago when H3N2 viruses last predominated was 183 per 100,000, he noted.
“We wouldn’t be surprised to see something very similar this year,” he said.
Young children are also severely affected; thus far in the season there have been 26 reported pediatric flu-related deaths.
However, there are early signs that infection rates are declining in areas where the season started earlier, such as the Southeast, and the number of patients presenting to a doctor with flulike symptoms has also declined slightly, but it is too soon to tell whether disease activity has peaked, he said, stressing that “we still have several weeks of flu activity ahead.”
It’s not too late to get vaccinated, and despite the reduced efficacy of this year’s vaccine against the circulating H3N2 strains, vaccination may still offer some benefit.
“There are other strains out there as well,” he said, noting that a proportion of cases from other strains, such as influenza B, tend to occur late in the season, and this year’s vaccine offers a good match for influenza B viruses.
Pneumococcal vaccination is also important, particularly for older adults and those at high risk , he said.
Last September the CDC announced a new recommendation that all adults over age 65 years should get two different pneumococcal vaccines. Such vaccination may help prevent flu-related pneumonia.
Patients with the flu or flulike illness should be advised to cover their cough and to stay home from work or school to protect those who are most vulnerable to the flu, he said.
The approximate midpoint of the 2014-2015 flu season has been reached, disease remains widespread, and antiviral flu medications remain underutilized, according to the Centers for Disease Control and Prevention.
As predicted, this season is proving particularly severe due to the predominance of antigenically drifted H3N2 virus strains, and the CDC is urging clinicians to maintain a high index of suspicion for flu and to prescribe antivirals earlier and more aggressively for patients presenting with flulike illness – especially young children, those over age 65 years, and those with underlying conditions, even if their symptoms are mild, CDC Director Thomas R. Frieden said during a press briefing.
A health advisory on the topic was issued Jan. 9, he noted.
“The CDC has recommended the use of antiviral drugs as an adjunct to vaccination. They are the only medicines that can specifically treat influenza illness, and in the context of an H3N2 predominant season with a less effective vaccine, treatment with antiflu drugs is even more important than usual,” he said, referring to the two neuraminidase inhibitors currently approved for treating influenza: oseltamivir and zanamivir.
About two-thirds of the H3N2 viruses analyzed this season are different from the H3N2 virus included in this year’s vaccine, which is why the vaccine is expected to have reduced effectiveness, he explained.
This makes early antiviral treatment all the more important, he added, noting that treatment within 2 days of symptom onset is optimal, but later treatment can also offer benefit.
“CDC scientists have looked very carefully at the use of influenza drugs in the clinical setting, and the conclusion is clear: They work, but they aren’t being used nearly enough. They can reduce symptoms, shorten duration of illness, and prevent serious complications,” he said.
Early treatment may help patients avoid hospitalization and could be life saving, he added.
Many patients are unaware that effective prescription treatments exist, and many doctors are not using the treatments as recommended. In one study, fewer than one in five eligible high-risk patients received treatment.
“So we’re expanding our efforts to reach clinicians about reminders about the importance of these drugs,” he said, noting that if high-risk patients with underlying conditions such as asthma, sickle cell disease, renal disease, or diabetes were treated, “tens of thousands of hospitalizations, and thousands of deaths could potentially be prevented.”
Dr. Frieden suggested that clinicians consider phone triage lines for high-risk patients to discuss symptoms over the phone and to “facilitate early initiation of treatment.”
An antiviral prescription can be provided without testing and before an office visit, he added.
The typical flu season lasts about 13 weeks on average, and the season began about 7 weeks ago. The continued high rate of H3N2 disease has had the greatest impact on older adults; that is typical of such seasons, which often involve a higher rate of hospitalizations and deaths.
In fact, hospitalization rates in the over 65 age group are rising sharply, Dr. Frieden said.
Last week the rate was 52 per 100,000 population, and this week the rate was 92 per 100,000 population. The cumulative rate 2 years ago when H3N2 viruses last predominated was 183 per 100,000, he noted.
“We wouldn’t be surprised to see something very similar this year,” he said.
Young children are also severely affected; thus far in the season there have been 26 reported pediatric flu-related deaths.
However, there are early signs that infection rates are declining in areas where the season started earlier, such as the Southeast, and the number of patients presenting to a doctor with flulike symptoms has also declined slightly, but it is too soon to tell whether disease activity has peaked, he said, stressing that “we still have several weeks of flu activity ahead.”
It’s not too late to get vaccinated, and despite the reduced efficacy of this year’s vaccine against the circulating H3N2 strains, vaccination may still offer some benefit.
“There are other strains out there as well,” he said, noting that a proportion of cases from other strains, such as influenza B, tend to occur late in the season, and this year’s vaccine offers a good match for influenza B viruses.
Pneumococcal vaccination is also important, particularly for older adults and those at high risk , he said.
Last September the CDC announced a new recommendation that all adults over age 65 years should get two different pneumococcal vaccines. Such vaccination may help prevent flu-related pneumonia.
Patients with the flu or flulike illness should be advised to cover their cough and to stay home from work or school to protect those who are most vulnerable to the flu, he said.
Edoxaban approved for atrial fib, DVT, and PE indications
Edoxaban, a selective factor Xa-inhibitor, has been approved by the Food and Drug Administration for reducing the risk of stroke and systemic embolism in patients with nonvalvular atrial fibrillation, with a statement in the boxed warning that it should not be used in patients with normal renal function.
The warning reflects the results of a subgroup analysis in the pivotal trial, which found that the 60-mg dose was superior to warfarin in terms of reducing the stroke risk in mildly renally impaired patients, but was worse in patients with normal renal function. This was the main focus of a meeting of the FDA’s Cardiovascular and Renal Drugs Advisory Panel meeting in October, in which the panel voted 9-1 to recommend approval of edoxaban for this indication, but had mixed opinions on whether approval should be limited to patients with mild to moderate renal impairment.
The approved prescribing information recommends that a patient’s creatinine clearance should be checked before edoxaban is prescribed. “Patients with creatinine clearance greater than 95 mL/min have an increased risk of stroke, compared to similar patients given warfarin,” and should be treated with another anticoagulant, the FDA said in the Jan. 9 statement announcing the approval. The recommended dose for those with a creatinine clearance between 50 mL/min and 95 mL/min is 60 mg once a day; for those with a creatinine clearance of 15-50 mL/min, the recommended dose is 30 mg once a day, according to the prescribing information.
Edoxaban, the fourth novel oral anticoagulant drug approved by the FDA, will be marketed as Savaysa by Daiichi Sankyo. It was also approved to treat deep vein thrombosis and pulmonary embolism following 5-10 days of initial therapy with a parenteral anticoagulant. The recommended dose for this indication is 60 mg once a day. For patients with a creatinine clearance of 15-50 mL/min, or who weigh up to 60 kg (about 132 pounds), or who are taking “certain P-glycoprotein inhibitors,” the 30-mg/day dose is recommended.
Approval for the nonvalvular AF indication was based on ENGAGE AF-TIMI 48 (Effective Anticoagulation with Factor Xa Next Generation in Atrial Fibrillation) study, comparing once-daily edoxaban (60 mg and 30 mg) to warfarin in 21,015 patients with nonvalvular AF, at a moderate to high risk of thromboembolic events (N. Engl. J. Med. 2013;369:2093-104). Over a median of almost 3 years, both doses were noninferior to warfarin in the primary efficacy endpoint, the occurrence of first stroke or of a systemic embolic event. Overall, major bleeding events were significantly lower among those on the 60-mg and 30-mg doses, compared with those on warfarin. However, the rate of ischemic stroke was higher relative to warfarin in patients with a creatinine clearance over 95 mL/min.
About half of the edoxaban dose is eliminated by the kidneys, and patients with a creatinine clearance above 95 mL/min have lower plasma edoxaban levels, according to a statement in the clinical trials section of the prescribing information, which adds: “Given the clear relationship of dose and blood levels to effectiveness in the ENGAGE AF-TIMI 48 study, it could be anticipated that patients with better renal function would show a smaller effect of Savaysa, compared to warfarin than would patients with mildly impaired renal function, and this was in fact observed.”
Approval of the DVT and PE indication was based on the Hokusai-VTE study of about 8,200 people comparing edoxaban to warfarin, which found that the edoxaban 60 mg once a day was noninferior to warfarin in the rate of symptomatic venous thromboembolism (3.2% vs. 3.5% in those on warfarin). The rate of major or clinically relevant nonmajor bleeding events was 8.5% among those on edoxaban vs. 10.3% in those on warfarin (N. Engl. J. Med. 2013;369:1406-15).
Bleeding and anemia were the most common adverse events among patients with nonvalvular atrial fibrillation in clinical trials, and “as with other FDA-approved anticlotting drugs, bleeding, including life-threatening bleeding, is the most serious risk with Savaysa,” the FDA statement said. Among those treated for DVT and PE, the most common adverse events were bleeding, rash, abnormal liver function tests, and anemia.
Savaysa is the fourth novel oral anticoagulant to be cleared by the FDA, after dabigatran (Pradaxa), rivaroxaban (Xarelto), and apixaban (Eliquis).
Serious adverse events associated with edoxaban should be reported to the FDA’s MedWatch program or at 800-332-1088.
A precedent does not come readily to mind where one restricts the use of a drug to patients with mild to moderately impaired renal function to optimize the benefit-risk balance. Typically, one avoids the drug or reduces the dose in such subgroups. For this reason, I think the drug is likely going to be a “nonstarter” for many clinicians.
During the FDA Advisory Committee panel meeting on edoxaban, the emphasis was on excluding patients with a creatinine clearance greater than 80 mL/min (representing about 37% of patients in the pivotal trial). The FDA approval used a cut-off of 95 mL/min (representing about 22% of patients in the pivotal trial). Even though the latter increases the eligible pool of patients for edoxaban, the major challenge is going to be clinical acceptability and marketability, especially given no unique advantage of this drug over other approved novel anticoagulants.
The CrCl cut off of 95mL/min applies to nonvalvular atrial fibrillation indication, and not to the venous thromboembolism (DVT/PE) indication. However, the latter indication requires 5-10 days of parenteral anticoagulant therapy, which puts it at a disadvantage compared with rivaroxaban or apixaban.
It is interesting to note that active pathological bleeding qualifies as a contraindication, but use in patients with normal renal function does not. There is a twofold increased risk of overall stroke or systemic embolism (primary endpoint) and ischemic stroke in patients with normal renal function (CrCl > 95 mL/min) along with an attenuation of the hemorrhagic risk advantage in this subgroup. Even though adjudicated major bleeding is still favorable for edoxaban in this subgroup, in my opinion the ischemic stroke risk outweighs the major bleeding advantage.
Sanjay Kaul, M.D., is professor of medicine at the University of California, Los Angeles. He was a member of the FDA’s Cardiovascular and Renal Drugs Advisory Committee that reviewed edoxaban at a meeting on Oct. 30, 2014.
A precedent does not come readily to mind where one restricts the use of a drug to patients with mild to moderately impaired renal function to optimize the benefit-risk balance. Typically, one avoids the drug or reduces the dose in such subgroups. For this reason, I think the drug is likely going to be a “nonstarter” for many clinicians.
During the FDA Advisory Committee panel meeting on edoxaban, the emphasis was on excluding patients with a creatinine clearance greater than 80 mL/min (representing about 37% of patients in the pivotal trial). The FDA approval used a cut-off of 95 mL/min (representing about 22% of patients in the pivotal trial). Even though the latter increases the eligible pool of patients for edoxaban, the major challenge is going to be clinical acceptability and marketability, especially given no unique advantage of this drug over other approved novel anticoagulants.
The CrCl cut off of 95mL/min applies to nonvalvular atrial fibrillation indication, and not to the venous thromboembolism (DVT/PE) indication. However, the latter indication requires 5-10 days of parenteral anticoagulant therapy, which puts it at a disadvantage compared with rivaroxaban or apixaban.
It is interesting to note that active pathological bleeding qualifies as a contraindication, but use in patients with normal renal function does not. There is a twofold increased risk of overall stroke or systemic embolism (primary endpoint) and ischemic stroke in patients with normal renal function (CrCl > 95 mL/min) along with an attenuation of the hemorrhagic risk advantage in this subgroup. Even though adjudicated major bleeding is still favorable for edoxaban in this subgroup, in my opinion the ischemic stroke risk outweighs the major bleeding advantage.
Sanjay Kaul, M.D., is professor of medicine at the University of California, Los Angeles. He was a member of the FDA’s Cardiovascular and Renal Drugs Advisory Committee that reviewed edoxaban at a meeting on Oct. 30, 2014.
A precedent does not come readily to mind where one restricts the use of a drug to patients with mild to moderately impaired renal function to optimize the benefit-risk balance. Typically, one avoids the drug or reduces the dose in such subgroups. For this reason, I think the drug is likely going to be a “nonstarter” for many clinicians.
During the FDA Advisory Committee panel meeting on edoxaban, the emphasis was on excluding patients with a creatinine clearance greater than 80 mL/min (representing about 37% of patients in the pivotal trial). The FDA approval used a cut-off of 95 mL/min (representing about 22% of patients in the pivotal trial). Even though the latter increases the eligible pool of patients for edoxaban, the major challenge is going to be clinical acceptability and marketability, especially given no unique advantage of this drug over other approved novel anticoagulants.
The CrCl cut off of 95mL/min applies to nonvalvular atrial fibrillation indication, and not to the venous thromboembolism (DVT/PE) indication. However, the latter indication requires 5-10 days of parenteral anticoagulant therapy, which puts it at a disadvantage compared with rivaroxaban or apixaban.
It is interesting to note that active pathological bleeding qualifies as a contraindication, but use in patients with normal renal function does not. There is a twofold increased risk of overall stroke or systemic embolism (primary endpoint) and ischemic stroke in patients with normal renal function (CrCl > 95 mL/min) along with an attenuation of the hemorrhagic risk advantage in this subgroup. Even though adjudicated major bleeding is still favorable for edoxaban in this subgroup, in my opinion the ischemic stroke risk outweighs the major bleeding advantage.
Sanjay Kaul, M.D., is professor of medicine at the University of California, Los Angeles. He was a member of the FDA’s Cardiovascular and Renal Drugs Advisory Committee that reviewed edoxaban at a meeting on Oct. 30, 2014.
Edoxaban, a selective factor Xa-inhibitor, has been approved by the Food and Drug Administration for reducing the risk of stroke and systemic embolism in patients with nonvalvular atrial fibrillation, with a statement in the boxed warning that it should not be used in patients with normal renal function.
The warning reflects the results of a subgroup analysis in the pivotal trial, which found that the 60-mg dose was superior to warfarin in terms of reducing the stroke risk in mildly renally impaired patients, but was worse in patients with normal renal function. This was the main focus of a meeting of the FDA’s Cardiovascular and Renal Drugs Advisory Panel meeting in October, in which the panel voted 9-1 to recommend approval of edoxaban for this indication, but had mixed opinions on whether approval should be limited to patients with mild to moderate renal impairment.
The approved prescribing information recommends that a patient’s creatinine clearance should be checked before edoxaban is prescribed. “Patients with creatinine clearance greater than 95 mL/min have an increased risk of stroke, compared to similar patients given warfarin,” and should be treated with another anticoagulant, the FDA said in the Jan. 9 statement announcing the approval. The recommended dose for those with a creatinine clearance between 50 mL/min and 95 mL/min is 60 mg once a day; for those with a creatinine clearance of 15-50 mL/min, the recommended dose is 30 mg once a day, according to the prescribing information.
Edoxaban, the fourth novel oral anticoagulant drug approved by the FDA, will be marketed as Savaysa by Daiichi Sankyo. It was also approved to treat deep vein thrombosis and pulmonary embolism following 5-10 days of initial therapy with a parenteral anticoagulant. The recommended dose for this indication is 60 mg once a day. For patients with a creatinine clearance of 15-50 mL/min, or who weigh up to 60 kg (about 132 pounds), or who are taking “certain P-glycoprotein inhibitors,” the 30-mg/day dose is recommended.
Approval for the nonvalvular AF indication was based on ENGAGE AF-TIMI 48 (Effective Anticoagulation with Factor Xa Next Generation in Atrial Fibrillation) study, comparing once-daily edoxaban (60 mg and 30 mg) to warfarin in 21,015 patients with nonvalvular AF, at a moderate to high risk of thromboembolic events (N. Engl. J. Med. 2013;369:2093-104). Over a median of almost 3 years, both doses were noninferior to warfarin in the primary efficacy endpoint, the occurrence of first stroke or of a systemic embolic event. Overall, major bleeding events were significantly lower among those on the 60-mg and 30-mg doses, compared with those on warfarin. However, the rate of ischemic stroke was higher relative to warfarin in patients with a creatinine clearance over 95 mL/min.
About half of the edoxaban dose is eliminated by the kidneys, and patients with a creatinine clearance above 95 mL/min have lower plasma edoxaban levels, according to a statement in the clinical trials section of the prescribing information, which adds: “Given the clear relationship of dose and blood levels to effectiveness in the ENGAGE AF-TIMI 48 study, it could be anticipated that patients with better renal function would show a smaller effect of Savaysa, compared to warfarin than would patients with mildly impaired renal function, and this was in fact observed.”
Approval of the DVT and PE indication was based on the Hokusai-VTE study of about 8,200 people comparing edoxaban to warfarin, which found that the edoxaban 60 mg once a day was noninferior to warfarin in the rate of symptomatic venous thromboembolism (3.2% vs. 3.5% in those on warfarin). The rate of major or clinically relevant nonmajor bleeding events was 8.5% among those on edoxaban vs. 10.3% in those on warfarin (N. Engl. J. Med. 2013;369:1406-15).
Bleeding and anemia were the most common adverse events among patients with nonvalvular atrial fibrillation in clinical trials, and “as with other FDA-approved anticlotting drugs, bleeding, including life-threatening bleeding, is the most serious risk with Savaysa,” the FDA statement said. Among those treated for DVT and PE, the most common adverse events were bleeding, rash, abnormal liver function tests, and anemia.
Savaysa is the fourth novel oral anticoagulant to be cleared by the FDA, after dabigatran (Pradaxa), rivaroxaban (Xarelto), and apixaban (Eliquis).
Serious adverse events associated with edoxaban should be reported to the FDA’s MedWatch program or at 800-332-1088.
Edoxaban, a selective factor Xa-inhibitor, has been approved by the Food and Drug Administration for reducing the risk of stroke and systemic embolism in patients with nonvalvular atrial fibrillation, with a statement in the boxed warning that it should not be used in patients with normal renal function.
The warning reflects the results of a subgroup analysis in the pivotal trial, which found that the 60-mg dose was superior to warfarin in terms of reducing the stroke risk in mildly renally impaired patients, but was worse in patients with normal renal function. This was the main focus of a meeting of the FDA’s Cardiovascular and Renal Drugs Advisory Panel meeting in October, in which the panel voted 9-1 to recommend approval of edoxaban for this indication, but had mixed opinions on whether approval should be limited to patients with mild to moderate renal impairment.
The approved prescribing information recommends that a patient’s creatinine clearance should be checked before edoxaban is prescribed. “Patients with creatinine clearance greater than 95 mL/min have an increased risk of stroke, compared to similar patients given warfarin,” and should be treated with another anticoagulant, the FDA said in the Jan. 9 statement announcing the approval. The recommended dose for those with a creatinine clearance between 50 mL/min and 95 mL/min is 60 mg once a day; for those with a creatinine clearance of 15-50 mL/min, the recommended dose is 30 mg once a day, according to the prescribing information.
Edoxaban, the fourth novel oral anticoagulant drug approved by the FDA, will be marketed as Savaysa by Daiichi Sankyo. It was also approved to treat deep vein thrombosis and pulmonary embolism following 5-10 days of initial therapy with a parenteral anticoagulant. The recommended dose for this indication is 60 mg once a day. For patients with a creatinine clearance of 15-50 mL/min, or who weigh up to 60 kg (about 132 pounds), or who are taking “certain P-glycoprotein inhibitors,” the 30-mg/day dose is recommended.
Approval for the nonvalvular AF indication was based on ENGAGE AF-TIMI 48 (Effective Anticoagulation with Factor Xa Next Generation in Atrial Fibrillation) study, comparing once-daily edoxaban (60 mg and 30 mg) to warfarin in 21,015 patients with nonvalvular AF, at a moderate to high risk of thromboembolic events (N. Engl. J. Med. 2013;369:2093-104). Over a median of almost 3 years, both doses were noninferior to warfarin in the primary efficacy endpoint, the occurrence of first stroke or of a systemic embolic event. Overall, major bleeding events were significantly lower among those on the 60-mg and 30-mg doses, compared with those on warfarin. However, the rate of ischemic stroke was higher relative to warfarin in patients with a creatinine clearance over 95 mL/min.
About half of the edoxaban dose is eliminated by the kidneys, and patients with a creatinine clearance above 95 mL/min have lower plasma edoxaban levels, according to a statement in the clinical trials section of the prescribing information, which adds: “Given the clear relationship of dose and blood levels to effectiveness in the ENGAGE AF-TIMI 48 study, it could be anticipated that patients with better renal function would show a smaller effect of Savaysa, compared to warfarin than would patients with mildly impaired renal function, and this was in fact observed.”
Approval of the DVT and PE indication was based on the Hokusai-VTE study of about 8,200 people comparing edoxaban to warfarin, which found that the edoxaban 60 mg once a day was noninferior to warfarin in the rate of symptomatic venous thromboembolism (3.2% vs. 3.5% in those on warfarin). The rate of major or clinically relevant nonmajor bleeding events was 8.5% among those on edoxaban vs. 10.3% in those on warfarin (N. Engl. J. Med. 2013;369:1406-15).
Bleeding and anemia were the most common adverse events among patients with nonvalvular atrial fibrillation in clinical trials, and “as with other FDA-approved anticlotting drugs, bleeding, including life-threatening bleeding, is the most serious risk with Savaysa,” the FDA statement said. Among those treated for DVT and PE, the most common adverse events were bleeding, rash, abnormal liver function tests, and anemia.
Savaysa is the fourth novel oral anticoagulant to be cleared by the FDA, after dabigatran (Pradaxa), rivaroxaban (Xarelto), and apixaban (Eliquis).
Serious adverse events associated with edoxaban should be reported to the FDA’s MedWatch program or at 800-332-1088.
RSV peaks linked to increased pneumococcal pneumonia
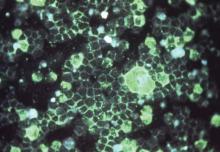
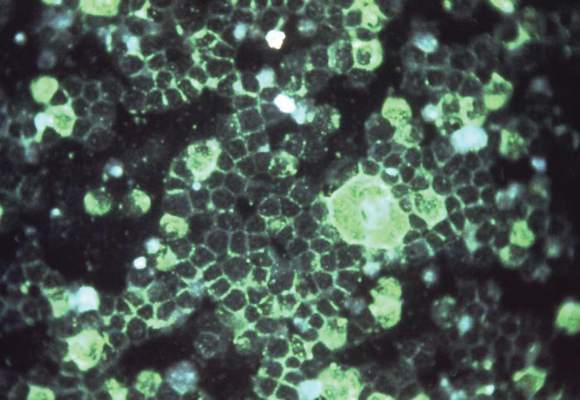
The incidence of pneumococcal pneumonia in young children is significantly associated with seasonal peaks of respiratory syncytial and influenza viruses, although this relationship has been attenuated by introduction of the 7-valent pneumococcal conjugate vaccine, new data suggest.
Analysis of data from the State Inpatient Databases from 1992 to 2009 showed a distinct spatiotemporal association between respiratory syncytial virus (RSV) and pneumococcal pneumonia peaks; RSV peaks were linked to a significant 20.3% increase in pneumococcal pneumonia incidence in children aged under 1 year, and a 10.1% increase in children aged 1-2 years.
Influenza peaks were associated with a smaller effect, with a 3.2% overall increase in pneumococcal pneumonia in children aged 1-2 years.
The introduction of the 7-valent pneumococcal conjugate vaccine was accompanied by an 18% drop in RSV-coded hospitalizations in children aged less than 1 year when the 3 years after introduction of the vaccine were compared with the 3 years prior to its introduction, according to a study published online Jan. 6 inPLOS Medicine(2014 [doi:10.1371/journal.pmed.1001776]).
“These results, obtained from population-based epidemiological data, suggest that RSV might increase the risk for pneumococcal infections and that a subset of hospitalized RSV cases might have a mixed viral-bacterial etiology,” wrote Dr. Daniel M. Weinberger of the Yale School of Public Health, New Haven, Conn., and his colleagues.
The study was partly supported by the U.S. National Institutes of Health, the Yale University School of Medicine, the Yale Center for Clinical Investigation, the Bill & Melinda Gates Foundation, RAPIDD (Research and Policy for Infectious Disease Dynamic), and the Fogarty International Center. Three authors declared unrelated research support from Pfizer and Merck, and one author is a member of the PLOS Medicine editorial board.
The incidence of pneumococcal pneumonia in young children is significantly associated with seasonal peaks of respiratory syncytial and influenza viruses, although this relationship has been attenuated by introduction of the 7-valent pneumococcal conjugate vaccine, new data suggest.
Analysis of data from the State Inpatient Databases from 1992 to 2009 showed a distinct spatiotemporal association between respiratory syncytial virus (RSV) and pneumococcal pneumonia peaks; RSV peaks were linked to a significant 20.3% increase in pneumococcal pneumonia incidence in children aged under 1 year, and a 10.1% increase in children aged 1-2 years.
Influenza peaks were associated with a smaller effect, with a 3.2% overall increase in pneumococcal pneumonia in children aged 1-2 years.
The introduction of the 7-valent pneumococcal conjugate vaccine was accompanied by an 18% drop in RSV-coded hospitalizations in children aged less than 1 year when the 3 years after introduction of the vaccine were compared with the 3 years prior to its introduction, according to a study published online Jan. 6 inPLOS Medicine(2014 [doi:10.1371/journal.pmed.1001776]).
“These results, obtained from population-based epidemiological data, suggest that RSV might increase the risk for pneumococcal infections and that a subset of hospitalized RSV cases might have a mixed viral-bacterial etiology,” wrote Dr. Daniel M. Weinberger of the Yale School of Public Health, New Haven, Conn., and his colleagues.
The study was partly supported by the U.S. National Institutes of Health, the Yale University School of Medicine, the Yale Center for Clinical Investigation, the Bill & Melinda Gates Foundation, RAPIDD (Research and Policy for Infectious Disease Dynamic), and the Fogarty International Center. Three authors declared unrelated research support from Pfizer and Merck, and one author is a member of the PLOS Medicine editorial board.
The incidence of pneumococcal pneumonia in young children is significantly associated with seasonal peaks of respiratory syncytial and influenza viruses, although this relationship has been attenuated by introduction of the 7-valent pneumococcal conjugate vaccine, new data suggest.
Analysis of data from the State Inpatient Databases from 1992 to 2009 showed a distinct spatiotemporal association between respiratory syncytial virus (RSV) and pneumococcal pneumonia peaks; RSV peaks were linked to a significant 20.3% increase in pneumococcal pneumonia incidence in children aged under 1 year, and a 10.1% increase in children aged 1-2 years.
Influenza peaks were associated with a smaller effect, with a 3.2% overall increase in pneumococcal pneumonia in children aged 1-2 years.
The introduction of the 7-valent pneumococcal conjugate vaccine was accompanied by an 18% drop in RSV-coded hospitalizations in children aged less than 1 year when the 3 years after introduction of the vaccine were compared with the 3 years prior to its introduction, according to a study published online Jan. 6 inPLOS Medicine(2014 [doi:10.1371/journal.pmed.1001776]).
“These results, obtained from population-based epidemiological data, suggest that RSV might increase the risk for pneumococcal infections and that a subset of hospitalized RSV cases might have a mixed viral-bacterial etiology,” wrote Dr. Daniel M. Weinberger of the Yale School of Public Health, New Haven, Conn., and his colleagues.
The study was partly supported by the U.S. National Institutes of Health, the Yale University School of Medicine, the Yale Center for Clinical Investigation, the Bill & Melinda Gates Foundation, RAPIDD (Research and Policy for Infectious Disease Dynamic), and the Fogarty International Center. Three authors declared unrelated research support from Pfizer and Merck, and one author is a member of the PLOS Medicine editorial board.
FROM PLOS MEDICINE
Key clinical point: The incidence of pneumococcal pneumonia in young children is associated with seasonal peaks of respiratory syncytial and influenza viruses.
Major finding: RSV peaks were linked to a significant 20.3% increase in pneumococcal pneumonia incidence in children aged under 1 year, and 10.1% increase in children aged 1-2 years.
Data source: Analysis of data from the State Inpatient Databases from 1992-2009.
Disclosures: The study was partly supported by the U.S. National Institutes of Health, the Yale University School of Medicine, the Yale Center for Clinical Investigation, the Bill & Melinda Gates Foundation, RAPIDD (Research and Policy for Infectious Disease Dynamic), and the Fogarty International Center. Three authors declared unrelated research support from Pfizer and Merck, and one author is a member of the PLOS Medicine editorial board.
Burn injury risk doubles in HOT patients who smoke
AUSTIN, TEX. – Smokers offered home oxygen therapy were found to be at twice the risk for burn injuries, based on data from a retrospective study.
Even so, almost all the home oxygen therapy (HOT) burn victims were discharged with a prescription for oxygen, including the 15% of patients who had incurred similar injuries at least once, and in some cases, three times.
“I have a problem with this,” said Dr. Mary Baker, a critical care fellow at Indiana University and a medical ethics fellow at the university’s Richard M. Fairbanks Burn Center at Wishard-Eskenazi Health, both in Indianapolis. Dr. Baker presented the findings at the annual meeting of the American College of Chest Physicians.
“Should we be prescribing oxygen to patients who smoke? Maybe the bigger question is [whether] it is ever ethically defensible to take oxygen away once someone has sustained a combustion injury from smoking while using HOT,” she said.
Dr. Baker and her colleagues conducted a chart review of patients admitted to a single site for home oxygen–related burns between 2008 and 2013. They found that 55 of all such burn unit admissions were smokers, representing 4% of the center’s annual admissions rate and twice that of the national burn rate for smokers in general. Nearly all the patients, a balance of men and women with a median age of 61 years, were using HOT for chronic obstructive pulmonary disease.
“The location of the burns, probably not surprisingly, was the face. Probably the most common was the nasal cannula,” Dr. Baker said.
Although nearly three-quarters of the 55-member cohort had less than a 5% total body surface–area burn, Dr. Baker said that in a patient population with baseline respiratory compromise and respiratory failure, this was an alarming rate of morbidity, particularly since half of the injured were intubated, and bronchonscopic exam revealed a third of these patients also had inhalation injuries.
“And here’s the kicker,” said Dr. Baker. “Eight deaths over 5 years. This is huge. So when these [individuals] get burned, it’s often really bad. Several of them had house fires, and we were able to find in the chart where other people [in the home] were burned and admitted to the hospital.”
Still, after a median 5-day stay, almost all the patients who survived were discharged with prescriptions for HOT, including the so-called “repeat offenders.” Because nearly half of all surviving smoking-related HOT patients were discharged to a higher level of care, this cohort tended to have higher health care utilization rates as well, Dr. Baker noted.
A surprise finding was that more than a quarter of the cohort had either current or concomitant problems with substance abuse. “We were not expecting that, and it has not been previously reported,” Dr. Baker said.
The data demonstrate a need for the screening of HOT patients as to whether they smoke and whether they have substance use issues, she said. If either condition applies, then faster follow-up and, potentially, counseling could be offered, including better education about the risks of oxygen therapy. “Currently, we have no formalized way to educate patients on the dangers of those tanks in the home,” said Dr. Baker.
The data raise questions about the risk-benefit ratio of prescribing any breathing aid to COPD patients who are also smokers.
“I don’t know how much sense it makes to keep throwing these inhalers, which cost hundreds of dollars a month, at people who continue to smoke,” Dr. Baker said in an interview. “We take all comers, and we think oxygen therapy helps, and prolongs life, but when you factor in smoking, we don’t really know what the risks and benefits are.”
A large study population would be needed to determine the risks and benefits, she added.
On Twitter @whitneymcknight
AUSTIN, TEX. – Smokers offered home oxygen therapy were found to be at twice the risk for burn injuries, based on data from a retrospective study.
Even so, almost all the home oxygen therapy (HOT) burn victims were discharged with a prescription for oxygen, including the 15% of patients who had incurred similar injuries at least once, and in some cases, three times.
“I have a problem with this,” said Dr. Mary Baker, a critical care fellow at Indiana University and a medical ethics fellow at the university’s Richard M. Fairbanks Burn Center at Wishard-Eskenazi Health, both in Indianapolis. Dr. Baker presented the findings at the annual meeting of the American College of Chest Physicians.
“Should we be prescribing oxygen to patients who smoke? Maybe the bigger question is [whether] it is ever ethically defensible to take oxygen away once someone has sustained a combustion injury from smoking while using HOT,” she said.
Dr. Baker and her colleagues conducted a chart review of patients admitted to a single site for home oxygen–related burns between 2008 and 2013. They found that 55 of all such burn unit admissions were smokers, representing 4% of the center’s annual admissions rate and twice that of the national burn rate for smokers in general. Nearly all the patients, a balance of men and women with a median age of 61 years, were using HOT for chronic obstructive pulmonary disease.
“The location of the burns, probably not surprisingly, was the face. Probably the most common was the nasal cannula,” Dr. Baker said.
Although nearly three-quarters of the 55-member cohort had less than a 5% total body surface–area burn, Dr. Baker said that in a patient population with baseline respiratory compromise and respiratory failure, this was an alarming rate of morbidity, particularly since half of the injured were intubated, and bronchonscopic exam revealed a third of these patients also had inhalation injuries.
“And here’s the kicker,” said Dr. Baker. “Eight deaths over 5 years. This is huge. So when these [individuals] get burned, it’s often really bad. Several of them had house fires, and we were able to find in the chart where other people [in the home] were burned and admitted to the hospital.”
Still, after a median 5-day stay, almost all the patients who survived were discharged with prescriptions for HOT, including the so-called “repeat offenders.” Because nearly half of all surviving smoking-related HOT patients were discharged to a higher level of care, this cohort tended to have higher health care utilization rates as well, Dr. Baker noted.
A surprise finding was that more than a quarter of the cohort had either current or concomitant problems with substance abuse. “We were not expecting that, and it has not been previously reported,” Dr. Baker said.
The data demonstrate a need for the screening of HOT patients as to whether they smoke and whether they have substance use issues, she said. If either condition applies, then faster follow-up and, potentially, counseling could be offered, including better education about the risks of oxygen therapy. “Currently, we have no formalized way to educate patients on the dangers of those tanks in the home,” said Dr. Baker.
The data raise questions about the risk-benefit ratio of prescribing any breathing aid to COPD patients who are also smokers.
“I don’t know how much sense it makes to keep throwing these inhalers, which cost hundreds of dollars a month, at people who continue to smoke,” Dr. Baker said in an interview. “We take all comers, and we think oxygen therapy helps, and prolongs life, but when you factor in smoking, we don’t really know what the risks and benefits are.”
A large study population would be needed to determine the risks and benefits, she added.
On Twitter @whitneymcknight
AUSTIN, TEX. – Smokers offered home oxygen therapy were found to be at twice the risk for burn injuries, based on data from a retrospective study.
Even so, almost all the home oxygen therapy (HOT) burn victims were discharged with a prescription for oxygen, including the 15% of patients who had incurred similar injuries at least once, and in some cases, three times.
“I have a problem with this,” said Dr. Mary Baker, a critical care fellow at Indiana University and a medical ethics fellow at the university’s Richard M. Fairbanks Burn Center at Wishard-Eskenazi Health, both in Indianapolis. Dr. Baker presented the findings at the annual meeting of the American College of Chest Physicians.
“Should we be prescribing oxygen to patients who smoke? Maybe the bigger question is [whether] it is ever ethically defensible to take oxygen away once someone has sustained a combustion injury from smoking while using HOT,” she said.
Dr. Baker and her colleagues conducted a chart review of patients admitted to a single site for home oxygen–related burns between 2008 and 2013. They found that 55 of all such burn unit admissions were smokers, representing 4% of the center’s annual admissions rate and twice that of the national burn rate for smokers in general. Nearly all the patients, a balance of men and women with a median age of 61 years, were using HOT for chronic obstructive pulmonary disease.
“The location of the burns, probably not surprisingly, was the face. Probably the most common was the nasal cannula,” Dr. Baker said.
Although nearly three-quarters of the 55-member cohort had less than a 5% total body surface–area burn, Dr. Baker said that in a patient population with baseline respiratory compromise and respiratory failure, this was an alarming rate of morbidity, particularly since half of the injured were intubated, and bronchonscopic exam revealed a third of these patients also had inhalation injuries.
“And here’s the kicker,” said Dr. Baker. “Eight deaths over 5 years. This is huge. So when these [individuals] get burned, it’s often really bad. Several of them had house fires, and we were able to find in the chart where other people [in the home] were burned and admitted to the hospital.”
Still, after a median 5-day stay, almost all the patients who survived were discharged with prescriptions for HOT, including the so-called “repeat offenders.” Because nearly half of all surviving smoking-related HOT patients were discharged to a higher level of care, this cohort tended to have higher health care utilization rates as well, Dr. Baker noted.
A surprise finding was that more than a quarter of the cohort had either current or concomitant problems with substance abuse. “We were not expecting that, and it has not been previously reported,” Dr. Baker said.
The data demonstrate a need for the screening of HOT patients as to whether they smoke and whether they have substance use issues, she said. If either condition applies, then faster follow-up and, potentially, counseling could be offered, including better education about the risks of oxygen therapy. “Currently, we have no formalized way to educate patients on the dangers of those tanks in the home,” said Dr. Baker.
The data raise questions about the risk-benefit ratio of prescribing any breathing aid to COPD patients who are also smokers.
“I don’t know how much sense it makes to keep throwing these inhalers, which cost hundreds of dollars a month, at people who continue to smoke,” Dr. Baker said in an interview. “We take all comers, and we think oxygen therapy helps, and prolongs life, but when you factor in smoking, we don’t really know what the risks and benefits are.”
A large study population would be needed to determine the risks and benefits, she added.
On Twitter @whitneymcknight
AT CHEST 2014
Key clinical point: Counsel patients on the elevated risk of mortality and morbidity when HOT and smoking are combined.
Major finding: The burn injury rate for smokers with COPD using HOT was 4%, compared with 2% in smokers not using HOT.
Data source: Retrospective analysis of single site burn injury admissions beween 2008 and 2013.
Disclosures: Dr. Baker reported that she had no relevant disclosures.
Insomnia and e-books
Seems that none of my patients sleeps, or at least not very well. Indeed, population-based studies suggest that almost one-third of adults report difficulty initiating or maintaining sleep, waking up too early, and/or nonrestorative or poor quality of sleep.
Light-emitting electronic “e-readers” or “e-books” have exploded as a favorite medium for reading. Many of my patients tell me that when they are unable to sleep, they read. Much of this reading occurs on e-books. But artificial light can produce alerting effects and suppress melatonin. This might be causing or worsening the national insomnia epidemic.
Dr. Anne-Marie Chang and colleagues conducted a randomized, crossover study evaluating the impact of an e-book and a traditional book on sleep (PNAS 2014 Dec. 22 [doi:10.1073/pnas.1418490112]). In the study, 12 healthy young adults were randomized to two conditions: 1) reading an e-book for 4 hours before bedtime; or 2) reading a printed book for 4 hours before bedtime on 5 consecutive evenings. Participants then switched conditions.
The e-book suppressed evening levels of melatonin by 55%, whereas the printed book showed no suppression, and the e-book shifted the melatonin onset to more than 1.5 hours later. Compared with the printed book, the e-book also significantly increased sleep latency (10 minutes longer), decreased REM sleep by11 minutes, decreased evening sleepiness, and increased morning sleepiness.
But not all e-book readers are created equal. Screens of devices used in the current study emit blue light (wavelength 452 nm), the type of light most implicated in melatonin suppression. Newer “e-ink” readers do not emit this light and are “front lit,” with light cast inward rather than outward.
People struggling with insomnia should be encouraged to explore the e-ink options. The table included in the study can provide some guidance as to the type of e-book that may be most beneficial to our sleepy patients.
Dr. Ebbert is professor of medicine, a general internist at the Mayo Clinic in Rochester, Minn., and a diplomate of the American Board of Addiction Medicine. The opinions expressed are those of the author. The opinions expressed in this article should not be used to diagnose or treat any medical condition nor should they be used as a substitute for medical advice from a qualified, board-certified practicing clinician.
Seems that none of my patients sleeps, or at least not very well. Indeed, population-based studies suggest that almost one-third of adults report difficulty initiating or maintaining sleep, waking up too early, and/or nonrestorative or poor quality of sleep.
Light-emitting electronic “e-readers” or “e-books” have exploded as a favorite medium for reading. Many of my patients tell me that when they are unable to sleep, they read. Much of this reading occurs on e-books. But artificial light can produce alerting effects and suppress melatonin. This might be causing or worsening the national insomnia epidemic.
Dr. Anne-Marie Chang and colleagues conducted a randomized, crossover study evaluating the impact of an e-book and a traditional book on sleep (PNAS 2014 Dec. 22 [doi:10.1073/pnas.1418490112]). In the study, 12 healthy young adults were randomized to two conditions: 1) reading an e-book for 4 hours before bedtime; or 2) reading a printed book for 4 hours before bedtime on 5 consecutive evenings. Participants then switched conditions.
The e-book suppressed evening levels of melatonin by 55%, whereas the printed book showed no suppression, and the e-book shifted the melatonin onset to more than 1.5 hours later. Compared with the printed book, the e-book also significantly increased sleep latency (10 minutes longer), decreased REM sleep by11 minutes, decreased evening sleepiness, and increased morning sleepiness.
But not all e-book readers are created equal. Screens of devices used in the current study emit blue light (wavelength 452 nm), the type of light most implicated in melatonin suppression. Newer “e-ink” readers do not emit this light and are “front lit,” with light cast inward rather than outward.
People struggling with insomnia should be encouraged to explore the e-ink options. The table included in the study can provide some guidance as to the type of e-book that may be most beneficial to our sleepy patients.
Dr. Ebbert is professor of medicine, a general internist at the Mayo Clinic in Rochester, Minn., and a diplomate of the American Board of Addiction Medicine. The opinions expressed are those of the author. The opinions expressed in this article should not be used to diagnose or treat any medical condition nor should they be used as a substitute for medical advice from a qualified, board-certified practicing clinician.
Seems that none of my patients sleeps, or at least not very well. Indeed, population-based studies suggest that almost one-third of adults report difficulty initiating or maintaining sleep, waking up too early, and/or nonrestorative or poor quality of sleep.
Light-emitting electronic “e-readers” or “e-books” have exploded as a favorite medium for reading. Many of my patients tell me that when they are unable to sleep, they read. Much of this reading occurs on e-books. But artificial light can produce alerting effects and suppress melatonin. This might be causing or worsening the national insomnia epidemic.
Dr. Anne-Marie Chang and colleagues conducted a randomized, crossover study evaluating the impact of an e-book and a traditional book on sleep (PNAS 2014 Dec. 22 [doi:10.1073/pnas.1418490112]). In the study, 12 healthy young adults were randomized to two conditions: 1) reading an e-book for 4 hours before bedtime; or 2) reading a printed book for 4 hours before bedtime on 5 consecutive evenings. Participants then switched conditions.
The e-book suppressed evening levels of melatonin by 55%, whereas the printed book showed no suppression, and the e-book shifted the melatonin onset to more than 1.5 hours later. Compared with the printed book, the e-book also significantly increased sleep latency (10 minutes longer), decreased REM sleep by11 minutes, decreased evening sleepiness, and increased morning sleepiness.
But not all e-book readers are created equal. Screens of devices used in the current study emit blue light (wavelength 452 nm), the type of light most implicated in melatonin suppression. Newer “e-ink” readers do not emit this light and are “front lit,” with light cast inward rather than outward.
People struggling with insomnia should be encouraged to explore the e-ink options. The table included in the study can provide some guidance as to the type of e-book that may be most beneficial to our sleepy patients.
Dr. Ebbert is professor of medicine, a general internist at the Mayo Clinic in Rochester, Minn., and a diplomate of the American Board of Addiction Medicine. The opinions expressed are those of the author. The opinions expressed in this article should not be used to diagnose or treat any medical condition nor should they be used as a substitute for medical advice from a qualified, board-certified practicing clinician.
Sorting out optimal TB testing can be tricky
LAS VEGAS – In the clinical opinion of Dr. Andi L. Shane, tuberculin skin testing and interferon gamma release assay diagnostics and surveillance for Mycobacterium tuberculosis infection are game-changers in the ongoing effort to reduce the rates of TB infection nationwide.
“From 1982 to 2013, we’ve had a very nice decline in the number of TB cases. However, we still have quite a bit of work to do,” Dr. Shane said at a pediatric update sponsored by the American Academy of Pediatrics California District 9.
Reported case rates are especially high in California, Nevada, Texas, Florida, New York, Washington, New Jersey, and the District of Columbia. By age group, those under 5 years old and those aged 15-24 years are more likely to be affected.
“It’s really important to identify TB as soon as possible, especially in children,” said Dr. Shane of the department of pediatrics, division of infectious diseases, Emory University, Atlanta. “An interferon gamma release assay (IGRA) or a tuberculin skin test (TST) may be used in situation where assessment for MTB [M. tuberculosis] exposure is indicated. IGRA is preferred in persons who received BCG vaccine and who have low rates of test completion, while TST is preferred for testing of children younger than age 5.”
TB disease in people younger than age 15 years is a marker for transmission of TB, usually from an adult. “So when we identify a case of TB in children, that requires a contact investigation,” she said. “We’re more concerned with children under the age of 5 with TB because they are more likely to have disseminated disease.”
Latent TB means that the patient has been exposed to the disease but that his or her body has been able to control the infection; no systemic manifestations of infection are present. “It’s very important to identify the difference between latent tuberculosis infection (LTBI) and actual tuberculosis disease,” she said. “This is one of the most challenging aspects to explain to families when you’re giving your diagnosis. The reason this is important is that children or adults who have LTBI are not infectious to other people, whereas someone who has pulmonary or laryngeal TB is considered to be an infectious risk to other individuals.”
Dr. Shane went on to discuss limitations of the TST in diagnosing TB. For one, the test may be placed incorrectly, resulting in an inflammatory response or no response, “and there is reader variability,” she said. “The other issue is that the reading needs to occur 48-72 hours after placement of the test. So, if you place it on a Thursday, that means you really are not going to read it at the optimal time unless the child comes to you on a weekend or the test is read by somebody else.”
As an alternative, two IGRAs have been developed that measure how the immune system reacts to MTB. One is QuantiFERON, which is widely used in the United States; the other is the T-SPOT.TB test, which is widely used in Europe. A positive result on either test indicates that there has been interaction with MTB bacteria but it does not differentiate between LTBI and active TB disease.
“A negative IGRA tells you there is no reaction to the test and MTB is not likely, while an indeterminate result is when you’re unable to interpret the result due to low positive [mitogen] or increased negative control [nil] compared to TB response,” Dr. Shane said. “This usually indicates that there’s some problem with the assay itself. It can also indicate that the individual may not have an immune system that can respond to and produce the interferon gamma that’s needed.”
Assessment of IGRA accuracy is challenged by a lack of a standard for the diagnosis of LTBI and active TB, especially in children. “The reason is, we just don’t have a lot of good data from resource-endowed settings,” Dr. Shane explained. “We have good data from areas where TB is prevalent.” According to the Centers for Disease Control and Prevention and the AAP, IGRAs are probably reliable in children over the age of 5 years, but a TST is still recommended in children under the age of 5.
“The nice thing about the IGRAs is that their specificity is much higher” than TSTs, Dr. Shane said. “However, in some cases a TST might be more sensitive for detecting more remote MTB infections than an IGRA, but IGRAs may be better at detecting a recent infection. Like the TST, an IGRA also shows that if you’re infected with TB you have 5-10% chance of developing active TB in your lifetime.”
She also pointed out that a significant amount of blood is required to perform an IGRA. “That might not always be optimal, especially in a young child,” Dr. Shane said. “Low CD4 counts and other immunodeficiencies have also been associated with false-negative TST and indeterminate/false-negative IGRA results.”
For contact investigations, IGRAs offer increased specificity, are completed during a single visit, and their response is not boosted if an additional evaluation is needed 8-10 weeks after exposure. For periodic screening of health care workers, IGRA offers “technical and logistical advantages, and two-step testing is not required,” she said.
If the TST or IGRA is positive, additional diagnostic efforts are needed “to differentiate between LTBI and active MTB,” said Dr. Shane, who recommended the Curry International Tuberculosis Center as a resource for clinicians. “Your clinical history, chest radiography, [and results of] sputum/gastric aspirates will help,” she added.
If the TST or IGRA is negative, “it’s not sufficient to exclude MTB infection. If you have a discordant TST and IGRA result, consider history and epidemiologic risk factors. Treat with clinical suspicion or risk of a poor outcome (those younger than age 5 and those infected with HIV).”
Dr. Shane reported having no relevant financial disclosures.
On Twitter @dougbrunk
LAS VEGAS – In the clinical opinion of Dr. Andi L. Shane, tuberculin skin testing and interferon gamma release assay diagnostics and surveillance for Mycobacterium tuberculosis infection are game-changers in the ongoing effort to reduce the rates of TB infection nationwide.
“From 1982 to 2013, we’ve had a very nice decline in the number of TB cases. However, we still have quite a bit of work to do,” Dr. Shane said at a pediatric update sponsored by the American Academy of Pediatrics California District 9.
Reported case rates are especially high in California, Nevada, Texas, Florida, New York, Washington, New Jersey, and the District of Columbia. By age group, those under 5 years old and those aged 15-24 years are more likely to be affected.
“It’s really important to identify TB as soon as possible, especially in children,” said Dr. Shane of the department of pediatrics, division of infectious diseases, Emory University, Atlanta. “An interferon gamma release assay (IGRA) or a tuberculin skin test (TST) may be used in situation where assessment for MTB [M. tuberculosis] exposure is indicated. IGRA is preferred in persons who received BCG vaccine and who have low rates of test completion, while TST is preferred for testing of children younger than age 5.”
TB disease in people younger than age 15 years is a marker for transmission of TB, usually from an adult. “So when we identify a case of TB in children, that requires a contact investigation,” she said. “We’re more concerned with children under the age of 5 with TB because they are more likely to have disseminated disease.”
Latent TB means that the patient has been exposed to the disease but that his or her body has been able to control the infection; no systemic manifestations of infection are present. “It’s very important to identify the difference between latent tuberculosis infection (LTBI) and actual tuberculosis disease,” she said. “This is one of the most challenging aspects to explain to families when you’re giving your diagnosis. The reason this is important is that children or adults who have LTBI are not infectious to other people, whereas someone who has pulmonary or laryngeal TB is considered to be an infectious risk to other individuals.”
Dr. Shane went on to discuss limitations of the TST in diagnosing TB. For one, the test may be placed incorrectly, resulting in an inflammatory response or no response, “and there is reader variability,” she said. “The other issue is that the reading needs to occur 48-72 hours after placement of the test. So, if you place it on a Thursday, that means you really are not going to read it at the optimal time unless the child comes to you on a weekend or the test is read by somebody else.”
As an alternative, two IGRAs have been developed that measure how the immune system reacts to MTB. One is QuantiFERON, which is widely used in the United States; the other is the T-SPOT.TB test, which is widely used in Europe. A positive result on either test indicates that there has been interaction with MTB bacteria but it does not differentiate between LTBI and active TB disease.
“A negative IGRA tells you there is no reaction to the test and MTB is not likely, while an indeterminate result is when you’re unable to interpret the result due to low positive [mitogen] or increased negative control [nil] compared to TB response,” Dr. Shane said. “This usually indicates that there’s some problem with the assay itself. It can also indicate that the individual may not have an immune system that can respond to and produce the interferon gamma that’s needed.”
Assessment of IGRA accuracy is challenged by a lack of a standard for the diagnosis of LTBI and active TB, especially in children. “The reason is, we just don’t have a lot of good data from resource-endowed settings,” Dr. Shane explained. “We have good data from areas where TB is prevalent.” According to the Centers for Disease Control and Prevention and the AAP, IGRAs are probably reliable in children over the age of 5 years, but a TST is still recommended in children under the age of 5.
“The nice thing about the IGRAs is that their specificity is much higher” than TSTs, Dr. Shane said. “However, in some cases a TST might be more sensitive for detecting more remote MTB infections than an IGRA, but IGRAs may be better at detecting a recent infection. Like the TST, an IGRA also shows that if you’re infected with TB you have 5-10% chance of developing active TB in your lifetime.”
She also pointed out that a significant amount of blood is required to perform an IGRA. “That might not always be optimal, especially in a young child,” Dr. Shane said. “Low CD4 counts and other immunodeficiencies have also been associated with false-negative TST and indeterminate/false-negative IGRA results.”
For contact investigations, IGRAs offer increased specificity, are completed during a single visit, and their response is not boosted if an additional evaluation is needed 8-10 weeks after exposure. For periodic screening of health care workers, IGRA offers “technical and logistical advantages, and two-step testing is not required,” she said.
If the TST or IGRA is positive, additional diagnostic efforts are needed “to differentiate between LTBI and active MTB,” said Dr. Shane, who recommended the Curry International Tuberculosis Center as a resource for clinicians. “Your clinical history, chest radiography, [and results of] sputum/gastric aspirates will help,” she added.
If the TST or IGRA is negative, “it’s not sufficient to exclude MTB infection. If you have a discordant TST and IGRA result, consider history and epidemiologic risk factors. Treat with clinical suspicion or risk of a poor outcome (those younger than age 5 and those infected with HIV).”
Dr. Shane reported having no relevant financial disclosures.
On Twitter @dougbrunk
LAS VEGAS – In the clinical opinion of Dr. Andi L. Shane, tuberculin skin testing and interferon gamma release assay diagnostics and surveillance for Mycobacterium tuberculosis infection are game-changers in the ongoing effort to reduce the rates of TB infection nationwide.
“From 1982 to 2013, we’ve had a very nice decline in the number of TB cases. However, we still have quite a bit of work to do,” Dr. Shane said at a pediatric update sponsored by the American Academy of Pediatrics California District 9.
Reported case rates are especially high in California, Nevada, Texas, Florida, New York, Washington, New Jersey, and the District of Columbia. By age group, those under 5 years old and those aged 15-24 years are more likely to be affected.
“It’s really important to identify TB as soon as possible, especially in children,” said Dr. Shane of the department of pediatrics, division of infectious diseases, Emory University, Atlanta. “An interferon gamma release assay (IGRA) or a tuberculin skin test (TST) may be used in situation where assessment for MTB [M. tuberculosis] exposure is indicated. IGRA is preferred in persons who received BCG vaccine and who have low rates of test completion, while TST is preferred for testing of children younger than age 5.”
TB disease in people younger than age 15 years is a marker for transmission of TB, usually from an adult. “So when we identify a case of TB in children, that requires a contact investigation,” she said. “We’re more concerned with children under the age of 5 with TB because they are more likely to have disseminated disease.”
Latent TB means that the patient has been exposed to the disease but that his or her body has been able to control the infection; no systemic manifestations of infection are present. “It’s very important to identify the difference between latent tuberculosis infection (LTBI) and actual tuberculosis disease,” she said. “This is one of the most challenging aspects to explain to families when you’re giving your diagnosis. The reason this is important is that children or adults who have LTBI are not infectious to other people, whereas someone who has pulmonary or laryngeal TB is considered to be an infectious risk to other individuals.”
Dr. Shane went on to discuss limitations of the TST in diagnosing TB. For one, the test may be placed incorrectly, resulting in an inflammatory response or no response, “and there is reader variability,” she said. “The other issue is that the reading needs to occur 48-72 hours after placement of the test. So, if you place it on a Thursday, that means you really are not going to read it at the optimal time unless the child comes to you on a weekend or the test is read by somebody else.”
As an alternative, two IGRAs have been developed that measure how the immune system reacts to MTB. One is QuantiFERON, which is widely used in the United States; the other is the T-SPOT.TB test, which is widely used in Europe. A positive result on either test indicates that there has been interaction with MTB bacteria but it does not differentiate between LTBI and active TB disease.
“A negative IGRA tells you there is no reaction to the test and MTB is not likely, while an indeterminate result is when you’re unable to interpret the result due to low positive [mitogen] or increased negative control [nil] compared to TB response,” Dr. Shane said. “This usually indicates that there’s some problem with the assay itself. It can also indicate that the individual may not have an immune system that can respond to and produce the interferon gamma that’s needed.”
Assessment of IGRA accuracy is challenged by a lack of a standard for the diagnosis of LTBI and active TB, especially in children. “The reason is, we just don’t have a lot of good data from resource-endowed settings,” Dr. Shane explained. “We have good data from areas where TB is prevalent.” According to the Centers for Disease Control and Prevention and the AAP, IGRAs are probably reliable in children over the age of 5 years, but a TST is still recommended in children under the age of 5.
“The nice thing about the IGRAs is that their specificity is much higher” than TSTs, Dr. Shane said. “However, in some cases a TST might be more sensitive for detecting more remote MTB infections than an IGRA, but IGRAs may be better at detecting a recent infection. Like the TST, an IGRA also shows that if you’re infected with TB you have 5-10% chance of developing active TB in your lifetime.”
She also pointed out that a significant amount of blood is required to perform an IGRA. “That might not always be optimal, especially in a young child,” Dr. Shane said. “Low CD4 counts and other immunodeficiencies have also been associated with false-negative TST and indeterminate/false-negative IGRA results.”
For contact investigations, IGRAs offer increased specificity, are completed during a single visit, and their response is not boosted if an additional evaluation is needed 8-10 weeks after exposure. For periodic screening of health care workers, IGRA offers “technical and logistical advantages, and two-step testing is not required,” she said.
If the TST or IGRA is positive, additional diagnostic efforts are needed “to differentiate between LTBI and active MTB,” said Dr. Shane, who recommended the Curry International Tuberculosis Center as a resource for clinicians. “Your clinical history, chest radiography, [and results of] sputum/gastric aspirates will help,” she added.
If the TST or IGRA is negative, “it’s not sufficient to exclude MTB infection. If you have a discordant TST and IGRA result, consider history and epidemiologic risk factors. Treat with clinical suspicion or risk of a poor outcome (those younger than age 5 and those infected with HIV).”
Dr. Shane reported having no relevant financial disclosures.
On Twitter @dougbrunk
EXPERT ANALYSIS FROM A PEDIATRIC UPDATE
Text messages prompt parents to vaccinate their kids
For children who need two doses of influenza vaccine in a season, text messages containing health literacy information are more effective at reminding parents to bring their children in for a second vaccination than are text messages or written messages alone, according to a study published in Pediatrics.
A team of investigators led by Dr. Melissa S. Stockwell of Columbia University Medical Center, New York, found that nearly 73% of children in the educational text message group received a second dose of influenza vaccine by April 30, whereas 67% of those in the conventional text message group received a second dose, and 57% of the written reminder–only group received a second dose (Pediatrics 2015 January [doi/10.1542/peds.2014-2475].
The randomized, controlled trial included 660 families and was conducted during the 2012-2013 influenza season in three community-based pediatric clinics in New York. The majority of the population was categorized as low income, urban, and predominantly Hispanic. Text messages were sent in English or Spanish based on the participants’ preferences.
“The inclusion of health literacy–promoting information in a text message second-dose reminder could potentially increase its efficacy by providing specific information that may compel a family to act overall and in a more timely fashion,” wrote Dr. Stockwell and her associates.
For children who need two doses of influenza vaccine in a season, text messages containing health literacy information are more effective at reminding parents to bring their children in for a second vaccination than are text messages or written messages alone, according to a study published in Pediatrics.
A team of investigators led by Dr. Melissa S. Stockwell of Columbia University Medical Center, New York, found that nearly 73% of children in the educational text message group received a second dose of influenza vaccine by April 30, whereas 67% of those in the conventional text message group received a second dose, and 57% of the written reminder–only group received a second dose (Pediatrics 2015 January [doi/10.1542/peds.2014-2475].
The randomized, controlled trial included 660 families and was conducted during the 2012-2013 influenza season in three community-based pediatric clinics in New York. The majority of the population was categorized as low income, urban, and predominantly Hispanic. Text messages were sent in English or Spanish based on the participants’ preferences.
“The inclusion of health literacy–promoting information in a text message second-dose reminder could potentially increase its efficacy by providing specific information that may compel a family to act overall and in a more timely fashion,” wrote Dr. Stockwell and her associates.
For children who need two doses of influenza vaccine in a season, text messages containing health literacy information are more effective at reminding parents to bring their children in for a second vaccination than are text messages or written messages alone, according to a study published in Pediatrics.
A team of investigators led by Dr. Melissa S. Stockwell of Columbia University Medical Center, New York, found that nearly 73% of children in the educational text message group received a second dose of influenza vaccine by April 30, whereas 67% of those in the conventional text message group received a second dose, and 57% of the written reminder–only group received a second dose (Pediatrics 2015 January [doi/10.1542/peds.2014-2475].
The randomized, controlled trial included 660 families and was conducted during the 2012-2013 influenza season in three community-based pediatric clinics in New York. The majority of the population was categorized as low income, urban, and predominantly Hispanic. Text messages were sent in English or Spanish based on the participants’ preferences.
“The inclusion of health literacy–promoting information in a text message second-dose reminder could potentially increase its efficacy by providing specific information that may compel a family to act overall and in a more timely fashion,” wrote Dr. Stockwell and her associates.
FROM PEDIATRICS
FDA approves pediatric dosage of QNASL
The Food and Drug Administration has approved the 40-mcg dose of QNASL for use in the treatment of nasal symptoms associated with allergic rhinitis in children aged 4-11 years, making it the first waterless nasal allergy spray approved for use in children as young as 4 years old.
“Through the availability of QNASL [beclomethasone dipropionate] 40 mcg, we are aiming to aid children and their caregivers in better managing the burdensome symptoms associated with nasal allergies,” said Dr. Tushar Shah, senior vice president of Teva Global Respiratory Research and Development.
The FDA approved beclomethasone dipropionate 40 mcg based on data from three double-blind, placebo-controlled studies of children aged 4-11 years. In those studies, once-daily beclomethasone dipropionate 40 mcg alleviated allergy symptoms in children with both seasonal and perennial allergic rhinitis with a minimum of adverse effects. The most common side effects were nosebleed and ulcers, which was “consistent with those seen in previous clinical studies of QNASL Nasal Aerosol,” according to a statement from the manufacturer.
QNASL40 mcg is expected to become available in February 2015.
The Food and Drug Administration has approved the 40-mcg dose of QNASL for use in the treatment of nasal symptoms associated with allergic rhinitis in children aged 4-11 years, making it the first waterless nasal allergy spray approved for use in children as young as 4 years old.
“Through the availability of QNASL [beclomethasone dipropionate] 40 mcg, we are aiming to aid children and their caregivers in better managing the burdensome symptoms associated with nasal allergies,” said Dr. Tushar Shah, senior vice president of Teva Global Respiratory Research and Development.
The FDA approved beclomethasone dipropionate 40 mcg based on data from three double-blind, placebo-controlled studies of children aged 4-11 years. In those studies, once-daily beclomethasone dipropionate 40 mcg alleviated allergy symptoms in children with both seasonal and perennial allergic rhinitis with a minimum of adverse effects. The most common side effects were nosebleed and ulcers, which was “consistent with those seen in previous clinical studies of QNASL Nasal Aerosol,” according to a statement from the manufacturer.
QNASL40 mcg is expected to become available in February 2015.
The Food and Drug Administration has approved the 40-mcg dose of QNASL for use in the treatment of nasal symptoms associated with allergic rhinitis in children aged 4-11 years, making it the first waterless nasal allergy spray approved for use in children as young as 4 years old.
“Through the availability of QNASL [beclomethasone dipropionate] 40 mcg, we are aiming to aid children and their caregivers in better managing the burdensome symptoms associated with nasal allergies,” said Dr. Tushar Shah, senior vice president of Teva Global Respiratory Research and Development.
The FDA approved beclomethasone dipropionate 40 mcg based on data from three double-blind, placebo-controlled studies of children aged 4-11 years. In those studies, once-daily beclomethasone dipropionate 40 mcg alleviated allergy symptoms in children with both seasonal and perennial allergic rhinitis with a minimum of adverse effects. The most common side effects were nosebleed and ulcers, which was “consistent with those seen in previous clinical studies of QNASL Nasal Aerosol,” according to a statement from the manufacturer.
QNASL40 mcg is expected to become available in February 2015.
Cheaper cytisine topped nicotine replacement therapy for smoking cessation
Cytisine was more effective than nicotine replacement therapy at helping adults quit smoking, with effect sizes similar to those reported in trials of varenicline, according to a report published online Dec. 18 in the New England Journal of Medicine.
Cytisine is a plant-based alkaloid that, like varenicline, is a partial agonist of nicotinic acetylcholine receptors. It remains relatively unknown outside of Eastern Europe, where it has been used successfully for 50 years, the study authors noted, even though it has proved effective there and is inexpensive. Some in the medical community have called for it to be licensed worldwide as a smoking-cessation aid.
The researchers directly compared cytisine with nicotine replacement therapy in an open-label, randomized, noninferiority trial in New Zealand.
A total of 1,310 adults who contacted New Zealand’s Quitline for assistance in smoking cessation were randomly assigned in equal numbers to receive either 25 days’ worth of cytisine tablets or 8 weeks of nicotine replacement therapy (patch and/or gum) plus brief behavioral counseling. They were followed for 6 months.
Cytisine proved significantly superior to nicotine replacement therapy: 40% of patients who took cytisine reported continuous smoking abstinence at 1 month, compared with 31% of those in the control group, said Natalie Walker, Ph.D., of the National Institute for Health Innovation, University of Auckland (New Zealand), and her associates.
Patients in the cytisine group also reported fewer symptoms of tobacco withdrawal than those in the nicotine replacement group.
Among study participants who resumed smoking after completing treatment, the median time to relapse was significantly longer with cytisine (53 days) than with nicotine replacement (11 days). People in the cytisine group also reported smoking fewer cigarettes per day and found smoking less rewarding than it had been before the study, the investigators said (N. Engl. J. Med. 2014;371:2353-62).
However, self-reported adverse events – most commonly nausea, vomiting, and sleep disorders – were almost twice as frequent in the cytisine group as in the control group. Most adverse events were mild to moderate in severity, and only 5% of the study population discontinued treatment because of adverse events.
The findings show that cytisine “is an effective smoking cessation aid for use as a first-line treatment for tobacco dependence,” Dr. Walker and her associates said.
The Health Research Council of New Zealand supported the study. Sopharma, a manufacturer of cytisine (Tabex), supplied the agent at no cost. Dr. Walker reported having no financial conflicts of interest; one of her associates reported receiving lecture fees from Johnson & Johnson and grant support from Pfizer.
Tobacco use is now the leading preventable cause of death worldwide, and the need for smoking cessation aids is urgent.
The compelling rationale for bringing cytisine to market is not that its efficacy is superior to that of current pharmacotherapies, but that the latter are unavailable to many smokers because of their cost. People in low- and middle-income countries would certainly benefit from a less expensive alternative, as would those in high-income countries who seek to contain health care costs.
Dr. Nancy A. Rigotti is in the department of medicine and the Tobacco Research and Treatment Center at Massachusetts General Hospital and Harvard Medical School, Boston. She reported receiving nonfinancial support from Pfizer unrelated to this work. Dr. Rigotti made these remarks in an editorial accompanying Dr. Walker’s report (N. Engl. J. Med. 2014;371:2429-30).
Tobacco use is now the leading preventable cause of death worldwide, and the need for smoking cessation aids is urgent.
The compelling rationale for bringing cytisine to market is not that its efficacy is superior to that of current pharmacotherapies, but that the latter are unavailable to many smokers because of their cost. People in low- and middle-income countries would certainly benefit from a less expensive alternative, as would those in high-income countries who seek to contain health care costs.
Dr. Nancy A. Rigotti is in the department of medicine and the Tobacco Research and Treatment Center at Massachusetts General Hospital and Harvard Medical School, Boston. She reported receiving nonfinancial support from Pfizer unrelated to this work. Dr. Rigotti made these remarks in an editorial accompanying Dr. Walker’s report (N. Engl. J. Med. 2014;371:2429-30).
Tobacco use is now the leading preventable cause of death worldwide, and the need for smoking cessation aids is urgent.
The compelling rationale for bringing cytisine to market is not that its efficacy is superior to that of current pharmacotherapies, but that the latter are unavailable to many smokers because of their cost. People in low- and middle-income countries would certainly benefit from a less expensive alternative, as would those in high-income countries who seek to contain health care costs.
Dr. Nancy A. Rigotti is in the department of medicine and the Tobacco Research and Treatment Center at Massachusetts General Hospital and Harvard Medical School, Boston. She reported receiving nonfinancial support from Pfizer unrelated to this work. Dr. Rigotti made these remarks in an editorial accompanying Dr. Walker’s report (N. Engl. J. Med. 2014;371:2429-30).
Cytisine was more effective than nicotine replacement therapy at helping adults quit smoking, with effect sizes similar to those reported in trials of varenicline, according to a report published online Dec. 18 in the New England Journal of Medicine.
Cytisine is a plant-based alkaloid that, like varenicline, is a partial agonist of nicotinic acetylcholine receptors. It remains relatively unknown outside of Eastern Europe, where it has been used successfully for 50 years, the study authors noted, even though it has proved effective there and is inexpensive. Some in the medical community have called for it to be licensed worldwide as a smoking-cessation aid.
The researchers directly compared cytisine with nicotine replacement therapy in an open-label, randomized, noninferiority trial in New Zealand.
A total of 1,310 adults who contacted New Zealand’s Quitline for assistance in smoking cessation were randomly assigned in equal numbers to receive either 25 days’ worth of cytisine tablets or 8 weeks of nicotine replacement therapy (patch and/or gum) plus brief behavioral counseling. They were followed for 6 months.
Cytisine proved significantly superior to nicotine replacement therapy: 40% of patients who took cytisine reported continuous smoking abstinence at 1 month, compared with 31% of those in the control group, said Natalie Walker, Ph.D., of the National Institute for Health Innovation, University of Auckland (New Zealand), and her associates.
Patients in the cytisine group also reported fewer symptoms of tobacco withdrawal than those in the nicotine replacement group.
Among study participants who resumed smoking after completing treatment, the median time to relapse was significantly longer with cytisine (53 days) than with nicotine replacement (11 days). People in the cytisine group also reported smoking fewer cigarettes per day and found smoking less rewarding than it had been before the study, the investigators said (N. Engl. J. Med. 2014;371:2353-62).
However, self-reported adverse events – most commonly nausea, vomiting, and sleep disorders – were almost twice as frequent in the cytisine group as in the control group. Most adverse events were mild to moderate in severity, and only 5% of the study population discontinued treatment because of adverse events.
The findings show that cytisine “is an effective smoking cessation aid for use as a first-line treatment for tobacco dependence,” Dr. Walker and her associates said.
The Health Research Council of New Zealand supported the study. Sopharma, a manufacturer of cytisine (Tabex), supplied the agent at no cost. Dr. Walker reported having no financial conflicts of interest; one of her associates reported receiving lecture fees from Johnson & Johnson and grant support from Pfizer.
Cytisine was more effective than nicotine replacement therapy at helping adults quit smoking, with effect sizes similar to those reported in trials of varenicline, according to a report published online Dec. 18 in the New England Journal of Medicine.
Cytisine is a plant-based alkaloid that, like varenicline, is a partial agonist of nicotinic acetylcholine receptors. It remains relatively unknown outside of Eastern Europe, where it has been used successfully for 50 years, the study authors noted, even though it has proved effective there and is inexpensive. Some in the medical community have called for it to be licensed worldwide as a smoking-cessation aid.
The researchers directly compared cytisine with nicotine replacement therapy in an open-label, randomized, noninferiority trial in New Zealand.
A total of 1,310 adults who contacted New Zealand’s Quitline for assistance in smoking cessation were randomly assigned in equal numbers to receive either 25 days’ worth of cytisine tablets or 8 weeks of nicotine replacement therapy (patch and/or gum) plus brief behavioral counseling. They were followed for 6 months.
Cytisine proved significantly superior to nicotine replacement therapy: 40% of patients who took cytisine reported continuous smoking abstinence at 1 month, compared with 31% of those in the control group, said Natalie Walker, Ph.D., of the National Institute for Health Innovation, University of Auckland (New Zealand), and her associates.
Patients in the cytisine group also reported fewer symptoms of tobacco withdrawal than those in the nicotine replacement group.
Among study participants who resumed smoking after completing treatment, the median time to relapse was significantly longer with cytisine (53 days) than with nicotine replacement (11 days). People in the cytisine group also reported smoking fewer cigarettes per day and found smoking less rewarding than it had been before the study, the investigators said (N. Engl. J. Med. 2014;371:2353-62).
However, self-reported adverse events – most commonly nausea, vomiting, and sleep disorders – were almost twice as frequent in the cytisine group as in the control group. Most adverse events were mild to moderate in severity, and only 5% of the study population discontinued treatment because of adverse events.
The findings show that cytisine “is an effective smoking cessation aid for use as a first-line treatment for tobacco dependence,” Dr. Walker and her associates said.
The Health Research Council of New Zealand supported the study. Sopharma, a manufacturer of cytisine (Tabex), supplied the agent at no cost. Dr. Walker reported having no financial conflicts of interest; one of her associates reported receiving lecture fees from Johnson & Johnson and grant support from Pfizer.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Key clinical point: Cytisine was superior to nicotine replacement therapy for helping adults quit smoking.
Major finding: 40% of patients who took cytisine reported continuous smoking abstinence at 1 month, compared with 31% of patients in the control group.
Data source: An open-label randomized, controlled, noninferiority trial involving 1,310 New Zealand adults followed for 6 months.
Disclosures: The Health Research Council of New Zealand supported the study. Sopharma, a manufacturer of cytisine (Tabex), supplied the agent at no cost. Dr. Walker reported having no financial conflicts of interest; one of her associates reported receiving lecture fees from Johnson & Johnson and grant support from Pfizer.
E-cigarettes with nicotine can be useful for smoking cessation
Electronic cigarettes that contain nicotine are more effective than e-cigarettes without nicotine in helping smokers quit, and smokers attempting to quit are able to achieve a 50% or greater reduction in smoking with the use of e-cigarettes containing nicotine.
About 9% of smokers who used e-cigarettes that contained nicotine were able to stop smoking at up to 1 year, compared with about 4% of smokers who used nicotine-free e-cigarettes, according to a small-scale data review published in the Cochrane Database of Systematic Reviews (2014 Dec. 16:CD010216 [doi:10.1002/14651858.CD010216.pub2]).
“There is evidence from the pooled results of two trials that electronic cigarettes with nicotine, compared with [e-cigarettes without nicotine], helped smokers to stop smoking long-term; they also increased the number of people who did not quit altogether to halve cigarette consumption,” wrote Dr. Hayden McRobbie of the Wolfson Institute of Preventive Medicine, Queen Mary University of London, and his colleagues.
Of the smokers included in the review who were not able to quit conventional cigarettes, 36% who used e-cigarettes with nicotine reported reducing the number of conventional cigarettes consumed by about half, compared with 28% of users who were given e-cigarettes without nicotine.
A team of researchers from New Zealand and the United Kingdom reviewed data from two trials of 662 current smokers to evaluate the efficacy of e-cigarettes use for helping smokers achieve long-term abstinence.
E-cigarettes are electronic vaporizing devices that heat a liquid, usually consisting of propylene glycol and glycerol and often containing nicotine, into an aerosol for inhalation.
There is little clinical information on the amount of nicotine typically ingested from an e-cigarette, as the devices typically are not regulated by government health agencies. No serious adverse effects related to e-cigarette use were reported from either of the studies.
Although this is the first meta-analysis on e-cigarette use and the effects on smoking cessation, the authors said that more data are needed for it to become clinically useful.
“Given the variety of electronic cigarette products on the market and the product evolution, future studies need to select electronic cigarettes with good nicotine delivery that are representative of the best current standard in terms of reliability and user satisfaction,” Dr. McRobbie and his associates wrote.
In addition, data were limited by the small number of trials and the small sample of participants from the studies. Also, there were few biochemical data on the participants or the sensorimotor effects of using electronic cigarettes.
“Data are also needed on the proportions of smokers who successfully quit smoking with the help of [e-cigarettes] and who continue to use [e-cigarettes] long-term and the proportion who eventually become nicotine-free,” the authors concluded.
Dr. Hayden McRobbie has undertaken educational sessions sponsored by Pfizer and Johnson & Johnson. Dr. Chris Bullen and Dr. McRobbie were also investigators on a study of e-cigarettes from an e-cigarette manufacturer (Ruyan Group) funded by the University of Auckland (New Zealand). Dr. Peter Hajek has provided consultancy to GSK, Pfizer, and Johnson & Johnson.
Electronic cigarettes that contain nicotine are more effective than e-cigarettes without nicotine in helping smokers quit, and smokers attempting to quit are able to achieve a 50% or greater reduction in smoking with the use of e-cigarettes containing nicotine.
About 9% of smokers who used e-cigarettes that contained nicotine were able to stop smoking at up to 1 year, compared with about 4% of smokers who used nicotine-free e-cigarettes, according to a small-scale data review published in the Cochrane Database of Systematic Reviews (2014 Dec. 16:CD010216 [doi:10.1002/14651858.CD010216.pub2]).
“There is evidence from the pooled results of two trials that electronic cigarettes with nicotine, compared with [e-cigarettes without nicotine], helped smokers to stop smoking long-term; they also increased the number of people who did not quit altogether to halve cigarette consumption,” wrote Dr. Hayden McRobbie of the Wolfson Institute of Preventive Medicine, Queen Mary University of London, and his colleagues.
Of the smokers included in the review who were not able to quit conventional cigarettes, 36% who used e-cigarettes with nicotine reported reducing the number of conventional cigarettes consumed by about half, compared with 28% of users who were given e-cigarettes without nicotine.
A team of researchers from New Zealand and the United Kingdom reviewed data from two trials of 662 current smokers to evaluate the efficacy of e-cigarettes use for helping smokers achieve long-term abstinence.
E-cigarettes are electronic vaporizing devices that heat a liquid, usually consisting of propylene glycol and glycerol and often containing nicotine, into an aerosol for inhalation.
There is little clinical information on the amount of nicotine typically ingested from an e-cigarette, as the devices typically are not regulated by government health agencies. No serious adverse effects related to e-cigarette use were reported from either of the studies.
Although this is the first meta-analysis on e-cigarette use and the effects on smoking cessation, the authors said that more data are needed for it to become clinically useful.
“Given the variety of electronic cigarette products on the market and the product evolution, future studies need to select electronic cigarettes with good nicotine delivery that are representative of the best current standard in terms of reliability and user satisfaction,” Dr. McRobbie and his associates wrote.
In addition, data were limited by the small number of trials and the small sample of participants from the studies. Also, there were few biochemical data on the participants or the sensorimotor effects of using electronic cigarettes.
“Data are also needed on the proportions of smokers who successfully quit smoking with the help of [e-cigarettes] and who continue to use [e-cigarettes] long-term and the proportion who eventually become nicotine-free,” the authors concluded.
Dr. Hayden McRobbie has undertaken educational sessions sponsored by Pfizer and Johnson & Johnson. Dr. Chris Bullen and Dr. McRobbie were also investigators on a study of e-cigarettes from an e-cigarette manufacturer (Ruyan Group) funded by the University of Auckland (New Zealand). Dr. Peter Hajek has provided consultancy to GSK, Pfizer, and Johnson & Johnson.
Electronic cigarettes that contain nicotine are more effective than e-cigarettes without nicotine in helping smokers quit, and smokers attempting to quit are able to achieve a 50% or greater reduction in smoking with the use of e-cigarettes containing nicotine.
About 9% of smokers who used e-cigarettes that contained nicotine were able to stop smoking at up to 1 year, compared with about 4% of smokers who used nicotine-free e-cigarettes, according to a small-scale data review published in the Cochrane Database of Systematic Reviews (2014 Dec. 16:CD010216 [doi:10.1002/14651858.CD010216.pub2]).
“There is evidence from the pooled results of two trials that electronic cigarettes with nicotine, compared with [e-cigarettes without nicotine], helped smokers to stop smoking long-term; they also increased the number of people who did not quit altogether to halve cigarette consumption,” wrote Dr. Hayden McRobbie of the Wolfson Institute of Preventive Medicine, Queen Mary University of London, and his colleagues.
Of the smokers included in the review who were not able to quit conventional cigarettes, 36% who used e-cigarettes with nicotine reported reducing the number of conventional cigarettes consumed by about half, compared with 28% of users who were given e-cigarettes without nicotine.
A team of researchers from New Zealand and the United Kingdom reviewed data from two trials of 662 current smokers to evaluate the efficacy of e-cigarettes use for helping smokers achieve long-term abstinence.
E-cigarettes are electronic vaporizing devices that heat a liquid, usually consisting of propylene glycol and glycerol and often containing nicotine, into an aerosol for inhalation.
There is little clinical information on the amount of nicotine typically ingested from an e-cigarette, as the devices typically are not regulated by government health agencies. No serious adverse effects related to e-cigarette use were reported from either of the studies.
Although this is the first meta-analysis on e-cigarette use and the effects on smoking cessation, the authors said that more data are needed for it to become clinically useful.
“Given the variety of electronic cigarette products on the market and the product evolution, future studies need to select electronic cigarettes with good nicotine delivery that are representative of the best current standard in terms of reliability and user satisfaction,” Dr. McRobbie and his associates wrote.
In addition, data were limited by the small number of trials and the small sample of participants from the studies. Also, there were few biochemical data on the participants or the sensorimotor effects of using electronic cigarettes.
“Data are also needed on the proportions of smokers who successfully quit smoking with the help of [e-cigarettes] and who continue to use [e-cigarettes] long-term and the proportion who eventually become nicotine-free,” the authors concluded.
Dr. Hayden McRobbie has undertaken educational sessions sponsored by Pfizer and Johnson & Johnson. Dr. Chris Bullen and Dr. McRobbie were also investigators on a study of e-cigarettes from an e-cigarette manufacturer (Ruyan Group) funded by the University of Auckland (New Zealand). Dr. Peter Hajek has provided consultancy to GSK, Pfizer, and Johnson & Johnson.
FROM COCHRANE DATABASE OF SYSTEMATIC REVIEWS
Key clinical point: Electronic cigarettes with nicotine appear to help smokers stop smoking long term, but more data are needed.
Major finding: Smokers who use e-cigarettes containing nicotine are significantly more likely to quit than those who switch to e-cigarettes without nicotine. In addition, smokers who use e-cigarettes with nicotine and do not quit altogether succeed in cutting their cigarette consumption by half.
Data source: A meta-analysis of two randomized controlled trials that analyzed data from 662 current smokers.
Disclosures: Dr. Hayden McRobbie has undertaken educational sessions sponsored by Pfizer and Johnson & Johnson. Dr. Chris Bullen and Dr. McRobbie also were investigators on a study of e-cigarettes from an e-cigarette manufacturer (Ruyan Group) funded by the University of Auckland (New Zealand). Dr. Peter Hajek has provided consultancy to GSK, Pfizer, and Johnson & Johnson.