User login
Shared medical appointments: Increasing patient access without increasing physician hours
Recurrent, Localized Urticaria and Erythema Multiforme: A Review and Management of Cutaneous Anthrax Vaccine–Related Events
The October 2001 domestic anthrax attacks affected 22 people, resulting in 5 fatalities. The added global terrorist threats have created an increasing need for homeland protection, as well as protection of our widely deployed forces battling terrorism. It is now relevant for physicians to be familiar with both clinical anthrax and adverse vaccine-related events associated with the resumption of the anthrax vaccine program. Dermatologists played a lead role in the initial response to the anthrax attack. We must be the lead providers most familiar with the cutaneous reactions that may be seen with the preventive vaccination. This article reviews the latest recommended evaluation and management of anthrax vaccine adverse events.
Case Reports Patient 1—A 36-year-old white male active duty military fighter pilot developed recurrent, localized urticaria after receiving his sixth anthrax vaccination (Figure 1). Results of a skin biopsy showed a superficial perivascular dermatitis with eosinophils consistent with urticaria. The urticaria continues to recur 21/2 years after his last vaccination and remains localized to the vaccinated arm.
Patient 2—A 33-year-old black male military member developed erythema multiforme one day after receiving his fifth anthrax vaccination. He had been treated for pharyngitis with a 10-day course of oral penicillin, which had been completed 2 days prior to receiving the vaccination. Target lesions were present on both arms and hands but were more prominent on the arm that received the vaccination (Figure 2). Results of a skin biopsy revealed a superficial perivascular and interface lymphocytic dermatitis, with vacuolar changes along the dermoepidermal junction compatible with erythema multiforme.
Patient 3—A 28-year-old white male military member presented with a pruritic rash that had developed on his face approximately 12 hours after receiving his fifth anthrax vaccination. The rash had spread to his torso (Figure 3) and lower extremities. Results of a punch biopsy revealed a superficial and deep lymphocytic infiltrate with interface changes and some extravasated red blood cells, findings felt to be consistent with an erythema multiforme reaction (Figure 4). The patient was treated with a 2-week course of prednisone and intramuscular diphenhydramine (Benadryl®), and clearing of symptoms was noted within 10 days.
Comment
The threat of anthrax is deadly and real, as shown by the domestic attacks via the US Postal Service in October 2001. In all, there were 11 confirmed cases of inhalation anthrax, resulting in 5 fatalities. In addition, there were 7 confirmed cases and 4 suspected cases of cutaneous anthrax. Twenty of the 22 cases were unquestionably linked to mail contaminated with a single strain of Bacillus anthracis.1 Anthrax is easy and cheap to produce and can be stored for prolonged periods, with spores survivable for decades in ambient conditions.2 The spores are resistant to dryness, heat, UV light, gamma radiation, and many disinfectants.3 In addition, anthrax is odorless, colorless, tasteless, and difficult to detect, thus making it a likely choice for future biological attacks. After the first gulf war, Iraq admitted to producing and deploying weaponized anthrax in missiles.4 The Sverdlovsk anthrax outbreak in the former Soviet Union occurred after the accidental release of aerosolized anthrax spores from a bioweapons facility and resulted in as many as 250 cases with 100 deaths.2 Fortunately, we have a vaccine that has been judged safe and effective by the US Food and Drug Administration (FDA), Centers for Disease Control and Prevention, and National Academy of Sciences. Protecting the health of US military forces who defend our vital interests is a national obligation.5 The trade-off for force protection of our military personnel involves a small incidence of vaccine-related adverse events (AEs), the most common being local type injection site reactions or skin reactions.
Natural cutaneous anthrax manifests within a few days as a painless, pruritic papule that progresses to a blister and evolves to a painless ulcer, with a black central eschar and surrounding local edema. In contrast, vaccine-related events manifest differently, and the vaccine cannot cause clinical anthrax infections. An algorithm for the evaluation of suspected cutaneous anthrax has been published by the American Academy of Dermatology Ad Hoc Task Force on Bioterrorism.6 Additional guidelines for clinical and laboratory diagnoses, specimen handling, and postexposure prophylaxis are available from the US Centers for Disease Control and Prevention.7
The vaccine itself is made from a noninfectious, cell-free sterile filtrate of an attenuated, nonencapsulated, nonproteolytic strain of B anthracis.8 It is considered an inactivated vaccine and is unable to cause infection. The anthrax vaccine has been approved by the FDA since 1970 and is safely administered to veterinarians, laboratory workers, woolen mill workers, and livestock handlers.8 In 1997, it was mandated that all US military personnel receive it. Full protection requires a schedule of 6 injections over 18 months (specifically, at 0, 2, and 4 weeks and 6, 12, and 18 months), with an annual booster thereafter. In the event of anthrax exposure, the vaccine also can be offered as postexposure prophylaxis with 3 doses at 2-week intervals, along with postexposure antibiotics.2 Contraindications to the anthrax vaccine include hypersensitivity reaction to a prior dose or vaccine component, human immunodeficiency virus positivity or immune suppression (active corticosteroid or other immunosuppressive treatment), any active infection or acute illness, pregnancy (confirmed or suspected), and age younger than 18 years or older than 65 years.
Efficacy and Safety
The vaccine's efficacy against aerosolized anthrax was shown in studies on nonhuman primates. Sixty-two (95%) of the 65 primates vaccinated with the anthrax vaccine adsorbed (AVA) survived a lethal aerosol challenge, whereas all 18 unvaccinated controls died.8 In actively monitored studies on the safety of AVA, mild local reactions occurred in 3% to 20% of doses, moderate reactions in 1% to 3% of doses, and severe reactions in less than 1% of doses.8 Acute systemic reactions were reported in 0.06% of doses and consisted of transient symptoms of fever, chills, nausea, and general body aches.8
The current system for reporting AEs is the Vaccine Adverse Event Reporting System (VAERS), and the FDA reviews 100% of these reports. In addition, a US Department of Defense directive requires its military providers to initiate a report for any event following AVA that results in hospitalization, any loss of duty of more than 24 hours, or for suspected vaccine contamination.9 Reporting of other reactions suspected because of vaccination is encouraged, especially those that are clinically significant or unusual. The form can be obtained on the Web at http://www.vaers.org or via telephone at 800-822-7967. Electronic reporting is available on the Web at http://secure.vaers.org/VaersDataEntryintro.htm. The VAERS is a passive surveillance system, and determining causal associations between vaccines and AEs is not always possible.10 Other concurrent infections or exposures may precipitate a given symptom that may simply coincide with the receipt of a vaccine.11 For example, patient 2 may have had vaccine-associated erythema multiforme but because he had recently completed a course of penicillin, we cannot exclude the possibility of a concurrent antibiotic association.
The Anthrax Vaccine Expert Committee reviewed 602 VAERS reports filed from 1998 through 1999.12 Nearly one half of reports noted a local injection site AE, 33% of which were noted to be moderate to large. A subcutaneous nodule was cited in 5.3% of reports. Although three fourths of reports noted a "systemic" AE, these covered a broad spectrum, with 34 types cited at a frequency of more than 1%. The most common AEs, in declining order of incidence, were flulike symptoms, 20.8%; malaise, 13.3%; rash, 14.2%; arthralgia, 12%; headache, 10.1%; with the remainder of AEs all affecting fewer than 10% of patients. Among the reported 45 total "serious or medically important AEs," one report of each of the following was noted: systemic lupus erythematosus, angioedema, anaphylactoid reaction, and toxic epidermal necrolysis. None of these AEs were judged to be causally (defined as likely, certain, or probable) related to the vaccine itself.12 According to Friedlander et al,8 the "FDA continues to view the anthrax vaccine as safe and effective for individuals at risk of exposure to anthrax."
Management of Adverse Events
Adverse reactions after vaccination can be divided into local and systemic.
Cutaneous Reactions—The cutaneous manifestations and the latest recommendations from the Walter Reed National Vaccine healthcare center network9 are summarized partially in Tables 1 and 2.
Local reactions involve the injection site or have contiguous spread and are graded based on the measured size of the local redness or swelling (Table 1). Most local anthrax vaccine reactions require no treatment and resolve within 72 hours, though topical or oral steroids and oral antihistamines can be used to help manage symptoms. Unless the local reaction is very large or complicated, the patient can usually proceed with subsequent doses. Although some of these reactions may mimic cellulitis, antibiotic therapy for postvaccination inflammation is not warranted. Allergy consultation is recommended for a large or complicated reaction, especially if this occurs after the second dose. In this instance, the patient may be immune (a hyperresponder) and may not require further series (with the exception of the yearly booster).9 When a significant local type reaction has occurred, pretreatment to help prevent future large local reactions is indicated.
Systemic Reactions—These commonly include flulike symptoms, such as fever, anorexia, nausea, arthralgia, myalgia, or malaise. Treatment of mild to moderate systemic events is symptomatic (Table 2). Pretreatment also may be given with the next vaccine in patients who have had these symptoms on prior AVA vaccinations. If symptoms are clinically consistent with serum sickness or are severe and prolonged, the patient may benefit from a short course of oral prednisone. Vaccine-related AEs may warrant temporary delay from the schedule. When resumed, this does not require starting over but rather simply continuing from the last dose.9
For a generalized maculopapular rash or target lesions, a skin biopsy should be performed, especially if the rash is suggestive of early erythema multiforme, Stevens-Johnson syndrome, or toxic epidermal necrolysis. In these cases, temporary exemption from further vaccinations and VAERS reporting are indicated. The possibility exists that additional doses may result in a more serious skin reaction and should be given with caution only after expert evaluation and consideration of the risk:benefit ratio. The dermatologist should provide a clinical histopathologic diagnosis to help the allergist or expert in the vaccination program decide the best course for continuation or exemption from the full anthrax series. These cases may warrant permanent exemption from further vaccination series. No apparent safety data for challenge dosing or desensitization in these potentially life-threatening skin reactions exist. In patient 2 with erythema multiforme, further vaccinations for anthrax were waived permanently. Similarly, deferral from further anthrax vaccinations was recommended in patient 3.
In those cases of severe urticaria or angioedema, temporary exemption may be granted while requesting allergy consultation. Additional doses should be given with caution only after expert evaluation and consideration of the risk:benefit ratio. Permanent exemption may be required for those with anaphylaxis or sudden onset angioedema. In patient 1 with recurrent localized urticaria, the allergist recommended that a formal skin-prick test to future vaccine lots be performed before he received any further vaccine in the series. Although this local allergic-type reaction may be due to some component of the vaccine, we are unable to define the specific cause at this time. This is a rather unusual manifestation, with recurrence of the urticaria still persisting 21/2 years later and restricted only to the vaccinated arm.
Conclusion
There are ongoing studies to evaluate whether a reduced number of anthrax vaccinations will provide the same immunity. In addition, other ongoing studies are comparing intramuscular administration versus the current usual subcutaneous route. Preliminary reports have shown that local reactions are less common in patients who received the vaccine via the intramuscular route than in those who received the vaccine via the subcutaneous route.13 This change in route of administration could reduce the number of adverse cutaneous reactions in the future. For further expert advice or clinical consultations, contact the Walter Reed National Vaccine Healthcare Center via telephone: 202-782-0411; fax: 202-782-4658; or e-mail: [email protected].
Since the domestic anthrax attacks in October 2001 and in the presence of continued worldwide threats to our armed forces, force protection remains a top priority. As dermatologists, we should be familiar with the current anthrax vaccine
program and be able to recognize and treat anthrax vaccine–related AEs.
- Bartlett JG, Inglesby TV, Borio L. Management of anthrax. Clin Infect Dis. 2002;35:851-858.
- Inglesby TV, O'Toole T, Henderson DA, et al. Anthrax as a biological weapon, 2002: updated recommendations for management. JAMA. 2002;287:2236-2252.
- Dixon TC, Meselson M, Guillemin J, et al. Anthrax. N Engl J Med. 1999;341:815-826.
- Swartz MN. Recognition and management of anthrax—an update. N Engl J Med. 2001;345:1621-1626.
- Mazzuchi JF, Claypool RG, Hyams KC, et al. Protecting the health of U.S. military forces: a national obligation. Aviat Space Environ Med. 2000;71:260-265.
- Carucci JA, McGovern TW, Norton SA, et al. Cutaneous anthrax management algorithm. J Am Acad Dermatol. 2002;47:766-769.
- Centers for Disease Control and Prevention. Guidelines for comprehensive procedures for collecting environmental samples for culturing Bacillus anthracis (revised April 2002) and anthrax: exposure management/prophylaxis (preventing transmission). Atlanta, Ga: Centers for Disease Control and Prevention Web sites. Available at: http://www.bt.cdc.gov. Accessed August 18, 2003.
- Friedlander AM, Pittman PR, Parker GW. Anthrax vaccine: evidence for safety and efficacy against inhalational anthrax. JAMA. 1999;282:2104-2106.
- Clinical guidelines for the management of adverse events after vaccination (official AVIP version). August 2002 Web site. Available at: http://www.deploymenthealth.mil/VHC/providers_management.htm. Accessed August 18, 2003.
- Centers for Disease Control and Prevention. Surveillance for safety after immunization: Vaccine Adverse Event Reporting System (VAERS)—United States, 1991-2000. MMWR Morb Mortal Wkly Rep. 2003;52:1-19.
- Halsey NA. Anthrax vaccine and causality assessment from individual case reports. Pharmacoepidemiol Drug Saf. 2002;11:185-187.
- Sever JL, Brenner AI, Gale AD, et al. Safety of anthrax vaccine: a review by the Anthrax Vaccine Expert Committee (AVEC) of adverse events reported to the Vaccine Adverse Event Reporting System (VAERS). Pharmacoepidemiol Drug Saf. 2002;11:189-202.
- Use of anthrax vaccine in the United States. Recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR Morb Mortal Wkly Rep. 2000;49:1-20.
The October 2001 domestic anthrax attacks affected 22 people, resulting in 5 fatalities. The added global terrorist threats have created an increasing need for homeland protection, as well as protection of our widely deployed forces battling terrorism. It is now relevant for physicians to be familiar with both clinical anthrax and adverse vaccine-related events associated with the resumption of the anthrax vaccine program. Dermatologists played a lead role in the initial response to the anthrax attack. We must be the lead providers most familiar with the cutaneous reactions that may be seen with the preventive vaccination. This article reviews the latest recommended evaluation and management of anthrax vaccine adverse events.
Case Reports Patient 1—A 36-year-old white male active duty military fighter pilot developed recurrent, localized urticaria after receiving his sixth anthrax vaccination (Figure 1). Results of a skin biopsy showed a superficial perivascular dermatitis with eosinophils consistent with urticaria. The urticaria continues to recur 21/2 years after his last vaccination and remains localized to the vaccinated arm.
Patient 2—A 33-year-old black male military member developed erythema multiforme one day after receiving his fifth anthrax vaccination. He had been treated for pharyngitis with a 10-day course of oral penicillin, which had been completed 2 days prior to receiving the vaccination. Target lesions were present on both arms and hands but were more prominent on the arm that received the vaccination (Figure 2). Results of a skin biopsy revealed a superficial perivascular and interface lymphocytic dermatitis, with vacuolar changes along the dermoepidermal junction compatible with erythema multiforme.
Patient 3—A 28-year-old white male military member presented with a pruritic rash that had developed on his face approximately 12 hours after receiving his fifth anthrax vaccination. The rash had spread to his torso (Figure 3) and lower extremities. Results of a punch biopsy revealed a superficial and deep lymphocytic infiltrate with interface changes and some extravasated red blood cells, findings felt to be consistent with an erythema multiforme reaction (Figure 4). The patient was treated with a 2-week course of prednisone and intramuscular diphenhydramine (Benadryl®), and clearing of symptoms was noted within 10 days.
Comment
The threat of anthrax is deadly and real, as shown by the domestic attacks via the US Postal Service in October 2001. In all, there were 11 confirmed cases of inhalation anthrax, resulting in 5 fatalities. In addition, there were 7 confirmed cases and 4 suspected cases of cutaneous anthrax. Twenty of the 22 cases were unquestionably linked to mail contaminated with a single strain of Bacillus anthracis.1 Anthrax is easy and cheap to produce and can be stored for prolonged periods, with spores survivable for decades in ambient conditions.2 The spores are resistant to dryness, heat, UV light, gamma radiation, and many disinfectants.3 In addition, anthrax is odorless, colorless, tasteless, and difficult to detect, thus making it a likely choice for future biological attacks. After the first gulf war, Iraq admitted to producing and deploying weaponized anthrax in missiles.4 The Sverdlovsk anthrax outbreak in the former Soviet Union occurred after the accidental release of aerosolized anthrax spores from a bioweapons facility and resulted in as many as 250 cases with 100 deaths.2 Fortunately, we have a vaccine that has been judged safe and effective by the US Food and Drug Administration (FDA), Centers for Disease Control and Prevention, and National Academy of Sciences. Protecting the health of US military forces who defend our vital interests is a national obligation.5 The trade-off for force protection of our military personnel involves a small incidence of vaccine-related adverse events (AEs), the most common being local type injection site reactions or skin reactions.
Natural cutaneous anthrax manifests within a few days as a painless, pruritic papule that progresses to a blister and evolves to a painless ulcer, with a black central eschar and surrounding local edema. In contrast, vaccine-related events manifest differently, and the vaccine cannot cause clinical anthrax infections. An algorithm for the evaluation of suspected cutaneous anthrax has been published by the American Academy of Dermatology Ad Hoc Task Force on Bioterrorism.6 Additional guidelines for clinical and laboratory diagnoses, specimen handling, and postexposure prophylaxis are available from the US Centers for Disease Control and Prevention.7
The vaccine itself is made from a noninfectious, cell-free sterile filtrate of an attenuated, nonencapsulated, nonproteolytic strain of B anthracis.8 It is considered an inactivated vaccine and is unable to cause infection. The anthrax vaccine has been approved by the FDA since 1970 and is safely administered to veterinarians, laboratory workers, woolen mill workers, and livestock handlers.8 In 1997, it was mandated that all US military personnel receive it. Full protection requires a schedule of 6 injections over 18 months (specifically, at 0, 2, and 4 weeks and 6, 12, and 18 months), with an annual booster thereafter. In the event of anthrax exposure, the vaccine also can be offered as postexposure prophylaxis with 3 doses at 2-week intervals, along with postexposure antibiotics.2 Contraindications to the anthrax vaccine include hypersensitivity reaction to a prior dose or vaccine component, human immunodeficiency virus positivity or immune suppression (active corticosteroid or other immunosuppressive treatment), any active infection or acute illness, pregnancy (confirmed or suspected), and age younger than 18 years or older than 65 years.
Efficacy and Safety
The vaccine's efficacy against aerosolized anthrax was shown in studies on nonhuman primates. Sixty-two (95%) of the 65 primates vaccinated with the anthrax vaccine adsorbed (AVA) survived a lethal aerosol challenge, whereas all 18 unvaccinated controls died.8 In actively monitored studies on the safety of AVA, mild local reactions occurred in 3% to 20% of doses, moderate reactions in 1% to 3% of doses, and severe reactions in less than 1% of doses.8 Acute systemic reactions were reported in 0.06% of doses and consisted of transient symptoms of fever, chills, nausea, and general body aches.8
The current system for reporting AEs is the Vaccine Adverse Event Reporting System (VAERS), and the FDA reviews 100% of these reports. In addition, a US Department of Defense directive requires its military providers to initiate a report for any event following AVA that results in hospitalization, any loss of duty of more than 24 hours, or for suspected vaccine contamination.9 Reporting of other reactions suspected because of vaccination is encouraged, especially those that are clinically significant or unusual. The form can be obtained on the Web at http://www.vaers.org or via telephone at 800-822-7967. Electronic reporting is available on the Web at http://secure.vaers.org/VaersDataEntryintro.htm. The VAERS is a passive surveillance system, and determining causal associations between vaccines and AEs is not always possible.10 Other concurrent infections or exposures may precipitate a given symptom that may simply coincide with the receipt of a vaccine.11 For example, patient 2 may have had vaccine-associated erythema multiforme but because he had recently completed a course of penicillin, we cannot exclude the possibility of a concurrent antibiotic association.
The Anthrax Vaccine Expert Committee reviewed 602 VAERS reports filed from 1998 through 1999.12 Nearly one half of reports noted a local injection site AE, 33% of which were noted to be moderate to large. A subcutaneous nodule was cited in 5.3% of reports. Although three fourths of reports noted a "systemic" AE, these covered a broad spectrum, with 34 types cited at a frequency of more than 1%. The most common AEs, in declining order of incidence, were flulike symptoms, 20.8%; malaise, 13.3%; rash, 14.2%; arthralgia, 12%; headache, 10.1%; with the remainder of AEs all affecting fewer than 10% of patients. Among the reported 45 total "serious or medically important AEs," one report of each of the following was noted: systemic lupus erythematosus, angioedema, anaphylactoid reaction, and toxic epidermal necrolysis. None of these AEs were judged to be causally (defined as likely, certain, or probable) related to the vaccine itself.12 According to Friedlander et al,8 the "FDA continues to view the anthrax vaccine as safe and effective for individuals at risk of exposure to anthrax."
Management of Adverse Events
Adverse reactions after vaccination can be divided into local and systemic.
Cutaneous Reactions—The cutaneous manifestations and the latest recommendations from the Walter Reed National Vaccine healthcare center network9 are summarized partially in Tables 1 and 2.
Local reactions involve the injection site or have contiguous spread and are graded based on the measured size of the local redness or swelling (Table 1). Most local anthrax vaccine reactions require no treatment and resolve within 72 hours, though topical or oral steroids and oral antihistamines can be used to help manage symptoms. Unless the local reaction is very large or complicated, the patient can usually proceed with subsequent doses. Although some of these reactions may mimic cellulitis, antibiotic therapy for postvaccination inflammation is not warranted. Allergy consultation is recommended for a large or complicated reaction, especially if this occurs after the second dose. In this instance, the patient may be immune (a hyperresponder) and may not require further series (with the exception of the yearly booster).9 When a significant local type reaction has occurred, pretreatment to help prevent future large local reactions is indicated.
Systemic Reactions—These commonly include flulike symptoms, such as fever, anorexia, nausea, arthralgia, myalgia, or malaise. Treatment of mild to moderate systemic events is symptomatic (Table 2). Pretreatment also may be given with the next vaccine in patients who have had these symptoms on prior AVA vaccinations. If symptoms are clinically consistent with serum sickness or are severe and prolonged, the patient may benefit from a short course of oral prednisone. Vaccine-related AEs may warrant temporary delay from the schedule. When resumed, this does not require starting over but rather simply continuing from the last dose.9
For a generalized maculopapular rash or target lesions, a skin biopsy should be performed, especially if the rash is suggestive of early erythema multiforme, Stevens-Johnson syndrome, or toxic epidermal necrolysis. In these cases, temporary exemption from further vaccinations and VAERS reporting are indicated. The possibility exists that additional doses may result in a more serious skin reaction and should be given with caution only after expert evaluation and consideration of the risk:benefit ratio. The dermatologist should provide a clinical histopathologic diagnosis to help the allergist or expert in the vaccination program decide the best course for continuation or exemption from the full anthrax series. These cases may warrant permanent exemption from further vaccination series. No apparent safety data for challenge dosing or desensitization in these potentially life-threatening skin reactions exist. In patient 2 with erythema multiforme, further vaccinations for anthrax were waived permanently. Similarly, deferral from further anthrax vaccinations was recommended in patient 3.
In those cases of severe urticaria or angioedema, temporary exemption may be granted while requesting allergy consultation. Additional doses should be given with caution only after expert evaluation and consideration of the risk:benefit ratio. Permanent exemption may be required for those with anaphylaxis or sudden onset angioedema. In patient 1 with recurrent localized urticaria, the allergist recommended that a formal skin-prick test to future vaccine lots be performed before he received any further vaccine in the series. Although this local allergic-type reaction may be due to some component of the vaccine, we are unable to define the specific cause at this time. This is a rather unusual manifestation, with recurrence of the urticaria still persisting 21/2 years later and restricted only to the vaccinated arm.
Conclusion
There are ongoing studies to evaluate whether a reduced number of anthrax vaccinations will provide the same immunity. In addition, other ongoing studies are comparing intramuscular administration versus the current usual subcutaneous route. Preliminary reports have shown that local reactions are less common in patients who received the vaccine via the intramuscular route than in those who received the vaccine via the subcutaneous route.13 This change in route of administration could reduce the number of adverse cutaneous reactions in the future. For further expert advice or clinical consultations, contact the Walter Reed National Vaccine Healthcare Center via telephone: 202-782-0411; fax: 202-782-4658; or e-mail: [email protected].
Since the domestic anthrax attacks in October 2001 and in the presence of continued worldwide threats to our armed forces, force protection remains a top priority. As dermatologists, we should be familiar with the current anthrax vaccine
program and be able to recognize and treat anthrax vaccine–related AEs.
The October 2001 domestic anthrax attacks affected 22 people, resulting in 5 fatalities. The added global terrorist threats have created an increasing need for homeland protection, as well as protection of our widely deployed forces battling terrorism. It is now relevant for physicians to be familiar with both clinical anthrax and adverse vaccine-related events associated with the resumption of the anthrax vaccine program. Dermatologists played a lead role in the initial response to the anthrax attack. We must be the lead providers most familiar with the cutaneous reactions that may be seen with the preventive vaccination. This article reviews the latest recommended evaluation and management of anthrax vaccine adverse events.
Case Reports Patient 1—A 36-year-old white male active duty military fighter pilot developed recurrent, localized urticaria after receiving his sixth anthrax vaccination (Figure 1). Results of a skin biopsy showed a superficial perivascular dermatitis with eosinophils consistent with urticaria. The urticaria continues to recur 21/2 years after his last vaccination and remains localized to the vaccinated arm.
Patient 2—A 33-year-old black male military member developed erythema multiforme one day after receiving his fifth anthrax vaccination. He had been treated for pharyngitis with a 10-day course of oral penicillin, which had been completed 2 days prior to receiving the vaccination. Target lesions were present on both arms and hands but were more prominent on the arm that received the vaccination (Figure 2). Results of a skin biopsy revealed a superficial perivascular and interface lymphocytic dermatitis, with vacuolar changes along the dermoepidermal junction compatible with erythema multiforme.
Patient 3—A 28-year-old white male military member presented with a pruritic rash that had developed on his face approximately 12 hours after receiving his fifth anthrax vaccination. The rash had spread to his torso (Figure 3) and lower extremities. Results of a punch biopsy revealed a superficial and deep lymphocytic infiltrate with interface changes and some extravasated red blood cells, findings felt to be consistent with an erythema multiforme reaction (Figure 4). The patient was treated with a 2-week course of prednisone and intramuscular diphenhydramine (Benadryl®), and clearing of symptoms was noted within 10 days.
Comment
The threat of anthrax is deadly and real, as shown by the domestic attacks via the US Postal Service in October 2001. In all, there were 11 confirmed cases of inhalation anthrax, resulting in 5 fatalities. In addition, there were 7 confirmed cases and 4 suspected cases of cutaneous anthrax. Twenty of the 22 cases were unquestionably linked to mail contaminated with a single strain of Bacillus anthracis.1 Anthrax is easy and cheap to produce and can be stored for prolonged periods, with spores survivable for decades in ambient conditions.2 The spores are resistant to dryness, heat, UV light, gamma radiation, and many disinfectants.3 In addition, anthrax is odorless, colorless, tasteless, and difficult to detect, thus making it a likely choice for future biological attacks. After the first gulf war, Iraq admitted to producing and deploying weaponized anthrax in missiles.4 The Sverdlovsk anthrax outbreak in the former Soviet Union occurred after the accidental release of aerosolized anthrax spores from a bioweapons facility and resulted in as many as 250 cases with 100 deaths.2 Fortunately, we have a vaccine that has been judged safe and effective by the US Food and Drug Administration (FDA), Centers for Disease Control and Prevention, and National Academy of Sciences. Protecting the health of US military forces who defend our vital interests is a national obligation.5 The trade-off for force protection of our military personnel involves a small incidence of vaccine-related adverse events (AEs), the most common being local type injection site reactions or skin reactions.
Natural cutaneous anthrax manifests within a few days as a painless, pruritic papule that progresses to a blister and evolves to a painless ulcer, with a black central eschar and surrounding local edema. In contrast, vaccine-related events manifest differently, and the vaccine cannot cause clinical anthrax infections. An algorithm for the evaluation of suspected cutaneous anthrax has been published by the American Academy of Dermatology Ad Hoc Task Force on Bioterrorism.6 Additional guidelines for clinical and laboratory diagnoses, specimen handling, and postexposure prophylaxis are available from the US Centers for Disease Control and Prevention.7
The vaccine itself is made from a noninfectious, cell-free sterile filtrate of an attenuated, nonencapsulated, nonproteolytic strain of B anthracis.8 It is considered an inactivated vaccine and is unable to cause infection. The anthrax vaccine has been approved by the FDA since 1970 and is safely administered to veterinarians, laboratory workers, woolen mill workers, and livestock handlers.8 In 1997, it was mandated that all US military personnel receive it. Full protection requires a schedule of 6 injections over 18 months (specifically, at 0, 2, and 4 weeks and 6, 12, and 18 months), with an annual booster thereafter. In the event of anthrax exposure, the vaccine also can be offered as postexposure prophylaxis with 3 doses at 2-week intervals, along with postexposure antibiotics.2 Contraindications to the anthrax vaccine include hypersensitivity reaction to a prior dose or vaccine component, human immunodeficiency virus positivity or immune suppression (active corticosteroid or other immunosuppressive treatment), any active infection or acute illness, pregnancy (confirmed or suspected), and age younger than 18 years or older than 65 years.
Efficacy and Safety
The vaccine's efficacy against aerosolized anthrax was shown in studies on nonhuman primates. Sixty-two (95%) of the 65 primates vaccinated with the anthrax vaccine adsorbed (AVA) survived a lethal aerosol challenge, whereas all 18 unvaccinated controls died.8 In actively monitored studies on the safety of AVA, mild local reactions occurred in 3% to 20% of doses, moderate reactions in 1% to 3% of doses, and severe reactions in less than 1% of doses.8 Acute systemic reactions were reported in 0.06% of doses and consisted of transient symptoms of fever, chills, nausea, and general body aches.8
The current system for reporting AEs is the Vaccine Adverse Event Reporting System (VAERS), and the FDA reviews 100% of these reports. In addition, a US Department of Defense directive requires its military providers to initiate a report for any event following AVA that results in hospitalization, any loss of duty of more than 24 hours, or for suspected vaccine contamination.9 Reporting of other reactions suspected because of vaccination is encouraged, especially those that are clinically significant or unusual. The form can be obtained on the Web at http://www.vaers.org or via telephone at 800-822-7967. Electronic reporting is available on the Web at http://secure.vaers.org/VaersDataEntryintro.htm. The VAERS is a passive surveillance system, and determining causal associations between vaccines and AEs is not always possible.10 Other concurrent infections or exposures may precipitate a given symptom that may simply coincide with the receipt of a vaccine.11 For example, patient 2 may have had vaccine-associated erythema multiforme but because he had recently completed a course of penicillin, we cannot exclude the possibility of a concurrent antibiotic association.
The Anthrax Vaccine Expert Committee reviewed 602 VAERS reports filed from 1998 through 1999.12 Nearly one half of reports noted a local injection site AE, 33% of which were noted to be moderate to large. A subcutaneous nodule was cited in 5.3% of reports. Although three fourths of reports noted a "systemic" AE, these covered a broad spectrum, with 34 types cited at a frequency of more than 1%. The most common AEs, in declining order of incidence, were flulike symptoms, 20.8%; malaise, 13.3%; rash, 14.2%; arthralgia, 12%; headache, 10.1%; with the remainder of AEs all affecting fewer than 10% of patients. Among the reported 45 total "serious or medically important AEs," one report of each of the following was noted: systemic lupus erythematosus, angioedema, anaphylactoid reaction, and toxic epidermal necrolysis. None of these AEs were judged to be causally (defined as likely, certain, or probable) related to the vaccine itself.12 According to Friedlander et al,8 the "FDA continues to view the anthrax vaccine as safe and effective for individuals at risk of exposure to anthrax."
Management of Adverse Events
Adverse reactions after vaccination can be divided into local and systemic.
Cutaneous Reactions—The cutaneous manifestations and the latest recommendations from the Walter Reed National Vaccine healthcare center network9 are summarized partially in Tables 1 and 2.
Local reactions involve the injection site or have contiguous spread and are graded based on the measured size of the local redness or swelling (Table 1). Most local anthrax vaccine reactions require no treatment and resolve within 72 hours, though topical or oral steroids and oral antihistamines can be used to help manage symptoms. Unless the local reaction is very large or complicated, the patient can usually proceed with subsequent doses. Although some of these reactions may mimic cellulitis, antibiotic therapy for postvaccination inflammation is not warranted. Allergy consultation is recommended for a large or complicated reaction, especially if this occurs after the second dose. In this instance, the patient may be immune (a hyperresponder) and may not require further series (with the exception of the yearly booster).9 When a significant local type reaction has occurred, pretreatment to help prevent future large local reactions is indicated.
Systemic Reactions—These commonly include flulike symptoms, such as fever, anorexia, nausea, arthralgia, myalgia, or malaise. Treatment of mild to moderate systemic events is symptomatic (Table 2). Pretreatment also may be given with the next vaccine in patients who have had these symptoms on prior AVA vaccinations. If symptoms are clinically consistent with serum sickness or are severe and prolonged, the patient may benefit from a short course of oral prednisone. Vaccine-related AEs may warrant temporary delay from the schedule. When resumed, this does not require starting over but rather simply continuing from the last dose.9
For a generalized maculopapular rash or target lesions, a skin biopsy should be performed, especially if the rash is suggestive of early erythema multiforme, Stevens-Johnson syndrome, or toxic epidermal necrolysis. In these cases, temporary exemption from further vaccinations and VAERS reporting are indicated. The possibility exists that additional doses may result in a more serious skin reaction and should be given with caution only after expert evaluation and consideration of the risk:benefit ratio. The dermatologist should provide a clinical histopathologic diagnosis to help the allergist or expert in the vaccination program decide the best course for continuation or exemption from the full anthrax series. These cases may warrant permanent exemption from further vaccination series. No apparent safety data for challenge dosing or desensitization in these potentially life-threatening skin reactions exist. In patient 2 with erythema multiforme, further vaccinations for anthrax were waived permanently. Similarly, deferral from further anthrax vaccinations was recommended in patient 3.
In those cases of severe urticaria or angioedema, temporary exemption may be granted while requesting allergy consultation. Additional doses should be given with caution only after expert evaluation and consideration of the risk:benefit ratio. Permanent exemption may be required for those with anaphylaxis or sudden onset angioedema. In patient 1 with recurrent localized urticaria, the allergist recommended that a formal skin-prick test to future vaccine lots be performed before he received any further vaccine in the series. Although this local allergic-type reaction may be due to some component of the vaccine, we are unable to define the specific cause at this time. This is a rather unusual manifestation, with recurrence of the urticaria still persisting 21/2 years later and restricted only to the vaccinated arm.
Conclusion
There are ongoing studies to evaluate whether a reduced number of anthrax vaccinations will provide the same immunity. In addition, other ongoing studies are comparing intramuscular administration versus the current usual subcutaneous route. Preliminary reports have shown that local reactions are less common in patients who received the vaccine via the intramuscular route than in those who received the vaccine via the subcutaneous route.13 This change in route of administration could reduce the number of adverse cutaneous reactions in the future. For further expert advice or clinical consultations, contact the Walter Reed National Vaccine Healthcare Center via telephone: 202-782-0411; fax: 202-782-4658; or e-mail: [email protected].
Since the domestic anthrax attacks in October 2001 and in the presence of continued worldwide threats to our armed forces, force protection remains a top priority. As dermatologists, we should be familiar with the current anthrax vaccine
program and be able to recognize and treat anthrax vaccine–related AEs.
- Bartlett JG, Inglesby TV, Borio L. Management of anthrax. Clin Infect Dis. 2002;35:851-858.
- Inglesby TV, O'Toole T, Henderson DA, et al. Anthrax as a biological weapon, 2002: updated recommendations for management. JAMA. 2002;287:2236-2252.
- Dixon TC, Meselson M, Guillemin J, et al. Anthrax. N Engl J Med. 1999;341:815-826.
- Swartz MN. Recognition and management of anthrax—an update. N Engl J Med. 2001;345:1621-1626.
- Mazzuchi JF, Claypool RG, Hyams KC, et al. Protecting the health of U.S. military forces: a national obligation. Aviat Space Environ Med. 2000;71:260-265.
- Carucci JA, McGovern TW, Norton SA, et al. Cutaneous anthrax management algorithm. J Am Acad Dermatol. 2002;47:766-769.
- Centers for Disease Control and Prevention. Guidelines for comprehensive procedures for collecting environmental samples for culturing Bacillus anthracis (revised April 2002) and anthrax: exposure management/prophylaxis (preventing transmission). Atlanta, Ga: Centers for Disease Control and Prevention Web sites. Available at: http://www.bt.cdc.gov. Accessed August 18, 2003.
- Friedlander AM, Pittman PR, Parker GW. Anthrax vaccine: evidence for safety and efficacy against inhalational anthrax. JAMA. 1999;282:2104-2106.
- Clinical guidelines for the management of adverse events after vaccination (official AVIP version). August 2002 Web site. Available at: http://www.deploymenthealth.mil/VHC/providers_management.htm. Accessed August 18, 2003.
- Centers for Disease Control and Prevention. Surveillance for safety after immunization: Vaccine Adverse Event Reporting System (VAERS)—United States, 1991-2000. MMWR Morb Mortal Wkly Rep. 2003;52:1-19.
- Halsey NA. Anthrax vaccine and causality assessment from individual case reports. Pharmacoepidemiol Drug Saf. 2002;11:185-187.
- Sever JL, Brenner AI, Gale AD, et al. Safety of anthrax vaccine: a review by the Anthrax Vaccine Expert Committee (AVEC) of adverse events reported to the Vaccine Adverse Event Reporting System (VAERS). Pharmacoepidemiol Drug Saf. 2002;11:189-202.
- Use of anthrax vaccine in the United States. Recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR Morb Mortal Wkly Rep. 2000;49:1-20.
- Bartlett JG, Inglesby TV, Borio L. Management of anthrax. Clin Infect Dis. 2002;35:851-858.
- Inglesby TV, O'Toole T, Henderson DA, et al. Anthrax as a biological weapon, 2002: updated recommendations for management. JAMA. 2002;287:2236-2252.
- Dixon TC, Meselson M, Guillemin J, et al. Anthrax. N Engl J Med. 1999;341:815-826.
- Swartz MN. Recognition and management of anthrax—an update. N Engl J Med. 2001;345:1621-1626.
- Mazzuchi JF, Claypool RG, Hyams KC, et al. Protecting the health of U.S. military forces: a national obligation. Aviat Space Environ Med. 2000;71:260-265.
- Carucci JA, McGovern TW, Norton SA, et al. Cutaneous anthrax management algorithm. J Am Acad Dermatol. 2002;47:766-769.
- Centers for Disease Control and Prevention. Guidelines for comprehensive procedures for collecting environmental samples for culturing Bacillus anthracis (revised April 2002) and anthrax: exposure management/prophylaxis (preventing transmission). Atlanta, Ga: Centers for Disease Control and Prevention Web sites. Available at: http://www.bt.cdc.gov. Accessed August 18, 2003.
- Friedlander AM, Pittman PR, Parker GW. Anthrax vaccine: evidence for safety and efficacy against inhalational anthrax. JAMA. 1999;282:2104-2106.
- Clinical guidelines for the management of adverse events after vaccination (official AVIP version). August 2002 Web site. Available at: http://www.deploymenthealth.mil/VHC/providers_management.htm. Accessed August 18, 2003.
- Centers for Disease Control and Prevention. Surveillance for safety after immunization: Vaccine Adverse Event Reporting System (VAERS)—United States, 1991-2000. MMWR Morb Mortal Wkly Rep. 2003;52:1-19.
- Halsey NA. Anthrax vaccine and causality assessment from individual case reports. Pharmacoepidemiol Drug Saf. 2002;11:185-187.
- Sever JL, Brenner AI, Gale AD, et al. Safety of anthrax vaccine: a review by the Anthrax Vaccine Expert Committee (AVEC) of adverse events reported to the Vaccine Adverse Event Reporting System (VAERS). Pharmacoepidemiol Drug Saf. 2002;11:189-202.
- Use of anthrax vaccine in the United States. Recommendations of the Advisory Committee on Immunization Practices (ACIP). MMWR Morb Mortal Wkly Rep. 2000;49:1-20.
Posttraumatic stress disorder: Nature and nurture?
Posttraumatic stress disorder (PTSD) can be one of the most frustrating anxiety disorders for both the patient and clinician. Asymptomatic persons become haunted by an experience they can’t forget. Their resulting anxiety can sour what were once healthy relationships or disable someone who previously was productive.
In some cases, despite aggressive psychopharmacology and psychotherapy, the patient remains incapacitated by inappropriate and unremitting fear. The trauma seems to have broken something—changed something inside the brain—that can’t be fixed.
Brain imaging studies of patients with PTSD—combat veterans and women with histories of childhood sexual abuse—have shown smaller hippocampal volumes compared with patients without PTSD.1,2 This finding has led to speculation that stress hormones (glucocorticoids) adversely affect the hippocampus (Figure 1).
This line of reasoning suggests that prolonged stress causes increased production of glucocorticoids that are neurotoxic to the hippocampus, resulting in hippocampal atrophy.3 Studies of rodents and patients with Cushing’s syndrome support this hypothesis. The hippocampus, therefore, may have been irreversibly damaged in patients with severe PTSD.
Figure 1
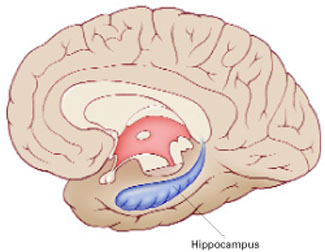
The hippocampus, a specialized type of cortex, is key to memory and emotion. As this medial view shows, it extends along the lateral ventricle floor on each side of the brain.
Illustration for Current Psychiatry by Marcia Hartsock, CMI Hippocampus
Intuitively, this theory makes sense, as the hippocampus is crucial for memory and emotion. However, a recent study of identical twins raises doubts.
Surprising evidence
Gilbertson et al recruited 40 pairs of twins, in which one was a Vietnam combat veteran and the other stayed home.4 Using MRI, the researchers measured hippocampal volume in each twin and assessed the presence and severity of PTSD in the combat-exposed twin.
Consistent with earlier reports, the authors found smaller hippocampal volumes in combat-exposed individuals diagnosed with PTSD. However, they found an almost identical correlation between the noncombat-exposed twin’s hippocampal volume and the combat-exposed twin’s PTSD score (Figure 2). In other words, the twin’s hippocampus size was a better predictor of the veteran’s hippocampus size than was the veteran’s trauma exposure or PTSD symptoms.
This finding puts a new spin on the association between small hippocampal volume and PTSD. The authors stated, “these data indicate that smaller hippocampi in PTSD represents a pre-existing, familial vulnerability factor rather than the neurotoxic product of trauma exposure per se.” Put another way, the small hippocampus is not created by stress and trauma but is a preexisting condition. Further, this study suggests that a larger hippocampus may protect a person from developing PTSD.
This study may help explain why different individuals exposed to the same trauma are frequently left with different symptoms.5,6 PTSD would seem to be an excellent example of the combined effects of nature (small hippocampus) and nurture (traumatic experience).
Figure 2 Hippocampal volume correlates with posttraumatic symptoms
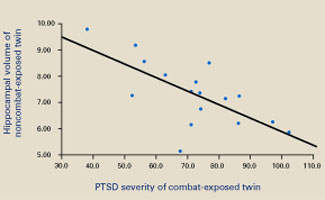
Smaller hippocampal volume in identical twins not exposed to combat was related to more-severe PTSD symptoms in their combat-exposed brothers (P = 0.002). Symptom severity was measured using Clinician-Administered PTSD Scale (CAPS) total scores.
Source: Reprinted with permission from Gilbertson MW, Shenton ME, Ciszewski A, et al. Smaller hippocampal volume predicts pathologic vulnerability to psychological trauma. Nature Neurosci 2002;5:1242-7.
1. Bremner JD, Randall P, Scott TM, et al. MRI-based measurement of hippocampal volume in patients with combat-related posttraumatic stress disorder. Am J Psychiatry 1995;152:973-81.
2. Bremner JD, Vythilingam M, Vermetten E, et al. MRI and PET study of deficits in hippocampal structure and function in women with childhood sexual abuse and posttraumatic stress disorder. Am J Psychiatry 2003;160:924-32.
3. Sapolsky RM. Glucocorticoids and hippocampal atrophy in neuropsychiatric disorders. Arch Gen Psychiatry 2000;57:925-35.
4. Gilbertson MW, Shenton ME, Ciszewski A, et al. Smaller hippocampal volume predicts pathologic vulnerability to psychological trauma. Nat Neurosci 2002;5:1242-7.
5. Macklin ML, Metzger LJ, Litz BT, et al. Lower precombat intelligence is a risk factor for posttraumatic stress disorder. J Consult Clin Psychol 1998;66:323-6.
6. Schlenger WE, Caddell JM, Ebert L, et al. Psychological reactions to terrorist attacks: findings from the National Study of Americans’ Reactions to September 11. JAMA 2002;288:581-8.
Posttraumatic stress disorder (PTSD) can be one of the most frustrating anxiety disorders for both the patient and clinician. Asymptomatic persons become haunted by an experience they can’t forget. Their resulting anxiety can sour what were once healthy relationships or disable someone who previously was productive.
In some cases, despite aggressive psychopharmacology and psychotherapy, the patient remains incapacitated by inappropriate and unremitting fear. The trauma seems to have broken something—changed something inside the brain—that can’t be fixed.
Brain imaging studies of patients with PTSD—combat veterans and women with histories of childhood sexual abuse—have shown smaller hippocampal volumes compared with patients without PTSD.1,2 This finding has led to speculation that stress hormones (glucocorticoids) adversely affect the hippocampus (Figure 1).
This line of reasoning suggests that prolonged stress causes increased production of glucocorticoids that are neurotoxic to the hippocampus, resulting in hippocampal atrophy.3 Studies of rodents and patients with Cushing’s syndrome support this hypothesis. The hippocampus, therefore, may have been irreversibly damaged in patients with severe PTSD.
Figure 1

The hippocampus, a specialized type of cortex, is key to memory and emotion. As this medial view shows, it extends along the lateral ventricle floor on each side of the brain.
Illustration for Current Psychiatry by Marcia Hartsock, CMI Hippocampus
Intuitively, this theory makes sense, as the hippocampus is crucial for memory and emotion. However, a recent study of identical twins raises doubts.
Surprising evidence
Gilbertson et al recruited 40 pairs of twins, in which one was a Vietnam combat veteran and the other stayed home.4 Using MRI, the researchers measured hippocampal volume in each twin and assessed the presence and severity of PTSD in the combat-exposed twin.
Consistent with earlier reports, the authors found smaller hippocampal volumes in combat-exposed individuals diagnosed with PTSD. However, they found an almost identical correlation between the noncombat-exposed twin’s hippocampal volume and the combat-exposed twin’s PTSD score (Figure 2). In other words, the twin’s hippocampus size was a better predictor of the veteran’s hippocampus size than was the veteran’s trauma exposure or PTSD symptoms.
This finding puts a new spin on the association between small hippocampal volume and PTSD. The authors stated, “these data indicate that smaller hippocampi in PTSD represents a pre-existing, familial vulnerability factor rather than the neurotoxic product of trauma exposure per se.” Put another way, the small hippocampus is not created by stress and trauma but is a preexisting condition. Further, this study suggests that a larger hippocampus may protect a person from developing PTSD.
This study may help explain why different individuals exposed to the same trauma are frequently left with different symptoms.5,6 PTSD would seem to be an excellent example of the combined effects of nature (small hippocampus) and nurture (traumatic experience).
Figure 2 Hippocampal volume correlates with posttraumatic symptoms

Smaller hippocampal volume in identical twins not exposed to combat was related to more-severe PTSD symptoms in their combat-exposed brothers (P = 0.002). Symptom severity was measured using Clinician-Administered PTSD Scale (CAPS) total scores.
Source: Reprinted with permission from Gilbertson MW, Shenton ME, Ciszewski A, et al. Smaller hippocampal volume predicts pathologic vulnerability to psychological trauma. Nature Neurosci 2002;5:1242-7.
Posttraumatic stress disorder (PTSD) can be one of the most frustrating anxiety disorders for both the patient and clinician. Asymptomatic persons become haunted by an experience they can’t forget. Their resulting anxiety can sour what were once healthy relationships or disable someone who previously was productive.
In some cases, despite aggressive psychopharmacology and psychotherapy, the patient remains incapacitated by inappropriate and unremitting fear. The trauma seems to have broken something—changed something inside the brain—that can’t be fixed.
Brain imaging studies of patients with PTSD—combat veterans and women with histories of childhood sexual abuse—have shown smaller hippocampal volumes compared with patients without PTSD.1,2 This finding has led to speculation that stress hormones (glucocorticoids) adversely affect the hippocampus (Figure 1).
This line of reasoning suggests that prolonged stress causes increased production of glucocorticoids that are neurotoxic to the hippocampus, resulting in hippocampal atrophy.3 Studies of rodents and patients with Cushing’s syndrome support this hypothesis. The hippocampus, therefore, may have been irreversibly damaged in patients with severe PTSD.
Figure 1

The hippocampus, a specialized type of cortex, is key to memory and emotion. As this medial view shows, it extends along the lateral ventricle floor on each side of the brain.
Illustration for Current Psychiatry by Marcia Hartsock, CMI Hippocampus
Intuitively, this theory makes sense, as the hippocampus is crucial for memory and emotion. However, a recent study of identical twins raises doubts.
Surprising evidence
Gilbertson et al recruited 40 pairs of twins, in which one was a Vietnam combat veteran and the other stayed home.4 Using MRI, the researchers measured hippocampal volume in each twin and assessed the presence and severity of PTSD in the combat-exposed twin.
Consistent with earlier reports, the authors found smaller hippocampal volumes in combat-exposed individuals diagnosed with PTSD. However, they found an almost identical correlation between the noncombat-exposed twin’s hippocampal volume and the combat-exposed twin’s PTSD score (Figure 2). In other words, the twin’s hippocampus size was a better predictor of the veteran’s hippocampus size than was the veteran’s trauma exposure or PTSD symptoms.
This finding puts a new spin on the association between small hippocampal volume and PTSD. The authors stated, “these data indicate that smaller hippocampi in PTSD represents a pre-existing, familial vulnerability factor rather than the neurotoxic product of trauma exposure per se.” Put another way, the small hippocampus is not created by stress and trauma but is a preexisting condition. Further, this study suggests that a larger hippocampus may protect a person from developing PTSD.
This study may help explain why different individuals exposed to the same trauma are frequently left with different symptoms.5,6 PTSD would seem to be an excellent example of the combined effects of nature (small hippocampus) and nurture (traumatic experience).
Figure 2 Hippocampal volume correlates with posttraumatic symptoms

Smaller hippocampal volume in identical twins not exposed to combat was related to more-severe PTSD symptoms in their combat-exposed brothers (P = 0.002). Symptom severity was measured using Clinician-Administered PTSD Scale (CAPS) total scores.
Source: Reprinted with permission from Gilbertson MW, Shenton ME, Ciszewski A, et al. Smaller hippocampal volume predicts pathologic vulnerability to psychological trauma. Nature Neurosci 2002;5:1242-7.
1. Bremner JD, Randall P, Scott TM, et al. MRI-based measurement of hippocampal volume in patients with combat-related posttraumatic stress disorder. Am J Psychiatry 1995;152:973-81.
2. Bremner JD, Vythilingam M, Vermetten E, et al. MRI and PET study of deficits in hippocampal structure and function in women with childhood sexual abuse and posttraumatic stress disorder. Am J Psychiatry 2003;160:924-32.
3. Sapolsky RM. Glucocorticoids and hippocampal atrophy in neuropsychiatric disorders. Arch Gen Psychiatry 2000;57:925-35.
4. Gilbertson MW, Shenton ME, Ciszewski A, et al. Smaller hippocampal volume predicts pathologic vulnerability to psychological trauma. Nat Neurosci 2002;5:1242-7.
5. Macklin ML, Metzger LJ, Litz BT, et al. Lower precombat intelligence is a risk factor for posttraumatic stress disorder. J Consult Clin Psychol 1998;66:323-6.
6. Schlenger WE, Caddell JM, Ebert L, et al. Psychological reactions to terrorist attacks: findings from the National Study of Americans’ Reactions to September 11. JAMA 2002;288:581-8.
1. Bremner JD, Randall P, Scott TM, et al. MRI-based measurement of hippocampal volume in patients with combat-related posttraumatic stress disorder. Am J Psychiatry 1995;152:973-81.
2. Bremner JD, Vythilingam M, Vermetten E, et al. MRI and PET study of deficits in hippocampal structure and function in women with childhood sexual abuse and posttraumatic stress disorder. Am J Psychiatry 2003;160:924-32.
3. Sapolsky RM. Glucocorticoids and hippocampal atrophy in neuropsychiatric disorders. Arch Gen Psychiatry 2000;57:925-35.
4. Gilbertson MW, Shenton ME, Ciszewski A, et al. Smaller hippocampal volume predicts pathologic vulnerability to psychological trauma. Nat Neurosci 2002;5:1242-7.
5. Macklin ML, Metzger LJ, Litz BT, et al. Lower precombat intelligence is a risk factor for posttraumatic stress disorder. J Consult Clin Psychol 1998;66:323-6.
6. Schlenger WE, Caddell JM, Ebert L, et al. Psychological reactions to terrorist attacks: findings from the National Study of Americans’ Reactions to September 11. JAMA 2002;288:581-8.
Skin picking: one teenager’s struggle
I am most grateful for “Captive of the mirror” (Current Psychiatry, December 2003) by Drs. Jon Grant and Katharine Phillips.
I am a 19-year-old female college student who has been diagnosed with depression, anxiety, and trichotillomania. I have bitten my nails all my life, have been taking SSRIs since age 12, and have had numerous problems related to skin-picking. Since adolescence I have obsessively picked and squeezed at acne and miniscule bumps on my face, causing redness, bruising and—in some cases—bleeding. I would then hide from the world, sometimes for days, until the wounds healed.
Until now, I didn’t know skin picking was a recognized disorder, let alone common. Your article is a detailed, clear, evidence-based summary of the problem and possible treatments, most of which I never knew existed. After having tried many things with limited success, I am taking the article to a psychiatrist so that I can discuss options. For the first time in months, I am filled with hope.
I am most grateful for “Captive of the mirror” (Current Psychiatry, December 2003) by Drs. Jon Grant and Katharine Phillips.
I am a 19-year-old female college student who has been diagnosed with depression, anxiety, and trichotillomania. I have bitten my nails all my life, have been taking SSRIs since age 12, and have had numerous problems related to skin-picking. Since adolescence I have obsessively picked and squeezed at acne and miniscule bumps on my face, causing redness, bruising and—in some cases—bleeding. I would then hide from the world, sometimes for days, until the wounds healed.
Until now, I didn’t know skin picking was a recognized disorder, let alone common. Your article is a detailed, clear, evidence-based summary of the problem and possible treatments, most of which I never knew existed. After having tried many things with limited success, I am taking the article to a psychiatrist so that I can discuss options. For the first time in months, I am filled with hope.
I am most grateful for “Captive of the mirror” (Current Psychiatry, December 2003) by Drs. Jon Grant and Katharine Phillips.
I am a 19-year-old female college student who has been diagnosed with depression, anxiety, and trichotillomania. I have bitten my nails all my life, have been taking SSRIs since age 12, and have had numerous problems related to skin-picking. Since adolescence I have obsessively picked and squeezed at acne and miniscule bumps on my face, causing redness, bruising and—in some cases—bleeding. I would then hide from the world, sometimes for days, until the wounds healed.
Until now, I didn’t know skin picking was a recognized disorder, let alone common. Your article is a detailed, clear, evidence-based summary of the problem and possible treatments, most of which I never knew existed. After having tried many things with limited success, I am taking the article to a psychiatrist so that I can discuss options. For the first time in months, I am filled with hope.
Psychological first aid: Emergency care for terrorism and disaster survivors
The night started like any other for Dr. Z. Kids in bed (too late) by 10:30, dog out by 11, fell asleep reading journal by 11:15. Sirens jolt her out of a solid stage 4. Her eyes widen, pulse quickens, mouth dries as she follows the glow of the TV into the living room. On TV, fire frames shots of tearful faces, body bags, and firefighters in protective suits. She catches the announcer’s voice: “…explosion at City Power and Light nuclear facility at 3:10 AM today. Fifty-five are known dead, and thousands are being told to evacuate. The blast’s cause is unknown, but terrorism is suspected.”
As her numbness slowly ebbs, Dr. Z’s questions rise insistently. How can I help the survivors? My patients? My children? What if the media call me? How could I have been better prepared for this?
Disaster shakes us to our human and biological core. More than any other clinical encounter, it reminds us that psychiatrists share the vulnerabilities of those we seek to help. Yet it also reminds us that even simple concepts and interventions can mobilize the healing process.
Are you ready to provide emergency psychiatric care following a disaster in your community—be it a nuclear accident, tornado, airplane crash, or terrorist act? Here is evidence—some counterintuitive—that can help you prepare.
Table 1
‘Psychological first aid’ for disaster survivors
Re-create sense of safety
|
Encourage social support
|
Re-establish sense of efficacy
|
Disaster’s psychobiology
Human reactions to disaster are often conceptualized as the mammalian survival response: flight, fight, and fright (freezing). In most cases, these reactions are adaptive and dissipate after safety is restored. Posttraumatic stress disorder (PTSD) develops in about 5% of natural disaster victims and 33% of mass shooting victims.1
Responses that do go awry appear to be associated with abnormally low cortisol and persistent adrenergic activation, leading to sensitization of the fear response.2 Reminders of trauma or persistent stressors—such as pain, problems with finances or housing, or bereavement—may exacerbate sensitization. On the other hand, preclinical studies suggest that social support3,4 and active coping5 mitigate physiologic stress responses, confirming numerous clinical observations that associate lack of social support and avoidant coping with eventual PTSD development.
Three basics. Just as our emergency medicine colleagues must often revert to life-support basics, we must remind ourselves of biology’s three basics for psychic resilience:
- safety (including—as much as possible—protection from reminders of trauma and ongoing stress)
- meaningful social connection
- re-establishing a sense of efficacy to overcome helplessness (Table 1).
Like the stress response, these protective factors seem hard-wired into our biological make-up. They form the foundation for all phases of disaster psychiatry interventions, from planning to immediate interventions through longterm follow-up.
Disaster planning
As a mental health professional, plan to operate within established disaster plans and agencies, not only for the sake of efficiency but also because structure and support are paramount in disaster situations. Check with the American Psychiatric Association’s local branch to determine if a disaster mental health plan exists. If not, explore how to work directly with local American Red Cross chapters and hospitals, which recruit personnel for the Disaster Medical Assistance Teams mobilized by the public health service.
Table 2
Normal reactions to disaster for adults and children
| All ages | |
| Emotional | Shock, fear, grief, anger, guilt, shame, helplessness, hopelessness, numbness, emptiness Decreased ability to feel interest, pleasure, love |
| Cognitive | Confusion, disorientation, indecisiveness, worry, shortened attention span, poor concentration, memory difficulties, unwanted memories, self-blame |
| Physical | Tension, fatigue, edginess, insomnia, generalized aches and pains, startling easily, rapid heartbeat, nausea, decreased appetite and sex drive |
| Interpersonal | Difficulties being intimate, being over-controlling, feeling rejected or abandoned |
| Children’s age-specific disaster responses | |
| Preschool | Separation fears, regression, fussiness, temper tantrums, somatization Sleep disturbances including nightmares, somnambulism, night terrors |
| School-age | May still have the above, as well as excessive guilt and worries about others’ safety, poor concentration and loss of school performance, repetitious re-telling or play related to trauma |
| Adolescent | Depression, acting out, wish for revenge, sleeping and eating disturbances, altered view of the future |
Immediate disaster mental health plans vary in detail according to local needs and resources but should at least address:
- providing on-site interventions
- disseminating information about responses to trauma
- identifying and publicizing local mental health resources.
Immediate interventions
Immediately following a disaster, psychiatrists are frequently asked to assist with on-site crisis and medical interventions, evaluate survivors with unusual or intense reactions, and provide public education about psychological reactions to disaster.
On-site response. All responders, regardless of discipline, should provide disaster survivors with “psychological first aid,” which is directed at reestablishing safety, connection, and efficacy. Basic crisis intervention principles are useful when support and reassurance are not enough.6
For example, relaxation exercises can reduce anxiety and improve sleep. Use focused, structured relaxation tools—such as progressive muscle relaxation and breathing training—as unstructured exercises can exacerbate dissociation and re-experiencing. Grounding techniques, by which survivors learn to focus all senses on immediate surroundings, often alleviate dissociation and flashbacks.
Care for children. Because children’s reactions to disaster greatly depend on their caregivers’ responses (social referencing), focus acute interventions for children on:
- re-connecting them with their families
- reducing caregivers’ distress
- educating caregivers about providing age appropriate information and support (see Related resources).
Medical care. As physicians, psychiatrists may be called upon to intervene medically. Although it is generally advisable to stay within our usual practice, medical personnel may be in short supply. Fortunately, Good Samaritan laws exist in every state, and the potential for a successful malpractice suit against a physician responding in a disaster is almost zero, unless the physician’s performance is grossly negligent (such as moving the neck of a patient with obvious head or neck injuries).7
Principles regarding informed consent and right to refuse treatment—along with the usual exceptions—apply during disasters.
Evaluating survivors in shelters and hospitals requires knowing the normal and abnormal responses to disaster, being able to differentially diagnose changes in mental status, and understanding risk factors for trauma’s psychiatric sequelae. Aside from PTSD, trauma’s long-term effects include other anxiety disorders, depression, substance abuse, and eating disorders. In addition to the usual components of a psychiatric evaluation, assessments must address event-related factors such as proximity to the disaster, loss of significant others or property, physical injuries, immediate needs, and social support.8
Normal stress reactions. Frequently described as “a normal response to an abnormal situation,” the normal stress reaction is multidimensional and depends on the person’s developmental level (Table 2). About 10% to 25% of survivors experience intense affect and dissociation, whereas a similar number may appear unusually calm.
Interventions beyond the“first aid” described above are not usually needed unless individuals:
- are a danger to themselves or others
- are psychotic
- have no social supports
- cannot perform tasks necessary for self-care and to begin the recovery process.
Always re-assess when there is any question about a survivor’s immediate reaction to trauma.
In DSM-IV-TR’s trauma-related diagnoses, the symptom clusters often do not capture many disaster survivors’ subjective experience: the shattering of fundamental beliefs regarding themselves (invulnerability), the world (predictability, safety), and others (trust, benevolence).9 By empathizing with these responses, you can help survivors feel less isolated and estranged.
Differential diagnosis. Survivors’ mental status changes may be manifestations of the stress response, but they also may represent:
- exacerbations of pre-existing psychiatric or general medical conditions
- hypoxemia, hypovolemia, or CNS trauma from physical injury
- responses to medications used for resuscitation or pain control, such as atropine, epinephrine, lidocaine, or morphine.
Effects of bioterrorism agents must also be considered. For example, organophosphorus compounds such as the nerve agents sarin and soman can cause impaired concentration, depression, and anxiety. Anthrax can cause rapidly progressing meningitis.10 Delirium must be differentiated from dissociation; patients with dissociation can be re-oriented, and changes will resolve with time rather than fluctuate.11
Psychopathology risk factors. Multiple studies have addressed risk factors for post-disaster psychiatric sequelae (usually PTSD). In general, risk increases with repeated trauma exposure (including TV viewing), prior trauma, lack of social support, injury, pre-existing psychiatric problems, traumatic bereavement (having witnessed the violent death of a loved one), avoidant coping, and having strong negative beliefs about the meanings of normal stress reactions such as tearfulness, anxiety, and insomnia.
Because a recent meta-analysis supports these observations,12 follow-up evaluation for signs of PTSD is recommended for:
- survivors with one or more of the risk factors discussed above
- vulnerable groups such as rescue workers, children, and dependent individuals
- survivors whose symptoms persist after 2 months.13
Decompensation immediately after a disaster seems to be the exception for psychiatric patients, despite their longer-term vulnerability. One psychiatrist who in 1989 survived Hurricane Hugo—the most intense storm to strike the Mid-Atlantic region in 100 years—noted that demand for inpatient psychiatric services did not increase in the storm’s aftermath. The only patient calls she received were inquiries about her own physical safety.14
Caregivers and rescue workers—including psychi-atrists—are also disaster survivors, and you need to tend to your needs for safety and support. Consult frequently with colleagues within and outside the disaster area, as much for support as for information and guidance.15 Remember also that rescue workers are occasionally targets for victims’ rage at their circumstances. Anticipating and explaining this displacement reduces its toxicity.
Using medications
Uses psychotropics judiciously in the first 48 hours of trauma. Medication effects may interfere with neurologic assessment of the injured, and monitoring and follow-up may not be possible.
However, drug therapy should start quickly when survivors are acutely psychotic or their behavior endangers themselves, others, or the milieu. Medications usually include a fast-acting benzodiazepine and/or an antipsychotic, as described in guidelines for managing agitation.16 Always provide structure and supervision for medicated patients.
No guidelines exist for using medications to manage distressing—but less-severe—acute stress-related symptoms. Some experts advocate using adrenergic antagonists such as clonidine, guanfacine, and beta blockers to reduce excessive arousal. These drugs have not been adequately studied in this setting, however, and may harm those with cardiovascular instability from preexisting conditions or injuries.
Table 3
Psychoeducation: Simple messages for workers and trauma survivors
| Get adequate rest, food, sleep |
| Avoid exposure to trauma cues, including TV images |
| Seek support from loved ones and peers |
| Talk about events and feelings only if this feels comfortable and helpful |
| Return to normal routine as much as possible |
| Take action to rebuild, but at a reasonable pace |
| Reach out to others who may need assistance |
Get help:
|
Short-term (<1 week) benzodiazepine use for panic symptoms and severe insomnia is acceptable, but longer-term use may increase PTSD risk.17 A selective serotonin reuptake inhibitor may help individuals with pre-existing PTSD or depression, if you can arrange follow-up.
In the aftermath
‘Debriefing.’ Critical incident stress debriefing (CISD) is a structured, one-session group intervention in which survivors’ experiences and emotional reactions are discussed and education and follow-up recommendations are provided. Developed by Mitchell in 1983,18 CISD was widely used until systematic evaluations revealed that it did not alleviate psychological distress or prevent PTSD.19
Table 4
How to interact with news media during and after a disaster
| For organizations Identify a spokesperson with media experience beforehand Ensure that the spokesperson is well-informed about all aspects of the disaster |
| For spokespersons |
Always
|
Never
|
Thus, although survivor meetings may provide information, education, screening, and support, avoid detailed discussions of events and emotions. Any meetings should be conducted by mental health clinicians and should not be mandatory. Reserve the term “debriefing” for operational reviews by rescue personnel.20
Public education. Educate survivors, rescue workers, health care providers, teachers, and relief agency workers. Provide concise, simple messages as suggested in Table 3. News media provide our most effective means of reaching out to survivors, which is why having a pre-existing relationship is so important. Some guidelines for working with the media are presented in Table 4.
Outreach. Numerous educational resources are available for survivors and their caregivers (see Related resources). Other potentially useful outreach tools include:
- meetings with teachers’ organizations
- continuing medical education activities for primary care providers
- telephone hot lines.
Legal and ethical issues
Disaster scenes are chaotic and informal, and professionals must be flexible, often providing general support and information rather than specific clinical interventions. However, it is important in each encounter to decide whether a patient-physician relationship has begun.
As a general rule, a physician-patient relationship is established whenever diagnosis or treatment is discussed. Once that happens, briefly document:
- signs and symptoms
- working diagnosis
- suicide or violence potential
- treatment and/or follow-up plans.
Confidentiality may be difficult to preserve in chaotic situations involving workers from many agencies. Even in disasters, however, you must obtain permission before sharing information unless the individual’s situation is emergent.
Table 5
Keys to effective disaster psychiatry
Be prepared
|
Care for survivors
|
Care for yourself
|
Long-term interventions
Longer-term disaster interventions include continued outreach and education and needed follow-up services. Existing structures may provide effective follow-up, but additional resources are often needed.
Federal programs. Following a presidentialdeclared disaster, the Federal Emergency Management Agency (FEMA) provides funding for crisis counseling. Programs are typically funded for 9 to 15 months and administered through the emergency services and disaster relief branch of the Substance Abuse and Mental Health Services Administration (SAMHSA) and community mental health organizations. Examples include Project Heartland following the 1995 Oklahoma City federal building bombing and Project COPE following California’s 1989 Loma Prieta earthquake.
Cognitive-behavioral therapy. For adult survivors with acute stress disorder, specific cognitive-behavioral therapy (CBT) provided by trained therapists may prevent PTSD and other trauma sequelae, such as depression.21 CBT interventions may begin as early as 2 weeks after trauma and focus sequentially on anxiety management, cognitive restructuring, imaginal exposure followed by in vivo exposure, and relapse prevention.
Three controlled trials found 6-month PTSD rates of 14% to 20% among acute stress disorder patients treated with CBT, compared with 58% to 67% with supportive counseling.22-24 Although studies of interventions immediately following trauma are lacking, trauma-focused CBT is also recommended for children.25 Evidence-based treatments for PTSD are discussed in detail elsewhere.26
Not unprepared after all
With some reflection, Dr. Z realized she had the tools to help her community. Her feelings of helplessness receded as she envisioned how she could help survivors understand their experiences, re-create a sense of safety, restore important connections to loved ones, and begin to rebuild their lives (Table 5).
For clinicians
- Young BH, Ford JD, Ruzek JI, et al. Disaster mental health: a guidebook for clinicians and administrators. Washington, DC: National Center for Post-Traumatic Stress Disorder, 1998. http://ncptsd.org/publications/disaster/index.html
- Hillman JL. Crisis intervention and trauma: new approaches to evidence-based practice. New York: Kluwer Academic/Plenum Publishers, 2002.
- Office of the Surgeon General Web site on medical aspects of nuclear, biological, and chemical warfare. http://www.nbc-med.org
For survivors and clinicians
- National Center for Post-Traumatic Stress Disorder. Disaster mental health: Dealing with the aftereffects of terrorism. http://www.ncptsd.org/terrorism/index.html
- Substance Abuse and Mental Health Services Administration. Emergency mental health and traumatic stress. http://www.mentalhealth.org/cmhs/EmergencyServices/default.asp
- American Academy of Child and Adolescent Psychiatry. Talking to children about terrorism and war. http://www.aacap.org/publications/factsFam/87.htm
Drug brand names
- Clonidine • Catapres
- Guanfacine • Tenex
Disclosure
The authors report no financial relationship with any company whose products are mentioned in this article or with manufacturers of competing products.
1. Effects of traumatic stress in a disaster situation. Washington, DC: National Center for Post-Traumatic Stress Disorder. Department of Veterans Affairs, September 12, 2001 (Accessed March 31, 2004 at http://www.ncptsd.org/facts/disasters/fs_effects_disaster.html).
2. Yehuda R, McFarlane AC, Shalev AY. Predicting the development of post-traumatic stress disorder from the acute response to a traumatic event. Biol Psychiatry 1998;44:1305-13.
3. Levine S, Lyons DM, Schatzberg AF. Psychobiological consequences of social relationships. Ann NY Acad Sci 1997;807:210-18.
4. Uchino BN, Garvey TS. The availability of social support reduces cardiovascular reactivity to acute psychological stress. J Behav Med 1997;20:15-27.
5. LeDoux JE, Gorman JM. A call to action: overcoming anxiety through active coping. Am J Psychiatry 2001;158:1953-5.
6. Hillman JL. Crisis intervention and trauma: new approaches to evidence-based practice. New York: Kluwer Academic/Plenum Publishers, 2002.
7. Daniels G. Good Samaritan acts. Emerg Med Clin North Am 1999;17:491-504.
8. Mental-health intervention for disasters. Washington, DC: National Center for Post-Traumatic Stress Disorder, Department of Veterans Affairs, Sept. 12, 2001. (Accessed March 31, 2004 at http://www.ncptsd.org/facts/disasters/fs_treatment_disaster.html.)
9. Difede J, Apfeldorf WJ, Cloitre M, et al. Acute psychiatric responses to the explosion at the World Trade Center: a case series. J Nerv Ment Dis 1997;185:519-22.
10. DiGiovanni C. Domestic terrorism with chemical or biological agents: psychiatric aspects. Am J Psychiatry 1999;156:1500-5.
11. Rundle JR. Psychiatric issues in medical-surgical disaster casualties: consultation-liaison approach. Psychiatr Q 2000;71:245-58.
12. Brewin CR, Andrews B, Valentine JD. Meta-analysis of risk factors for post-traumatic stress disorder in trauma-exposed adults. J Consult Clin Psychol 2000;68:748-66.
13. Mental health and mass violence: evidence-based early psychological intervention for victims/survivors of mass violence. Washington, DC: National Institute of Mental Health, Nov. 1, 2002 (Accessed Oct. 29, 2003 at http://www.nimh.nih.gov/research/massviolence.pdf.)
14. Austin LS. Organizing a disaster response program in one’s home community. In: Austin LS (ed). Responding to disaster: a guide for mental health professionals. Washington, DC: American Psychiatric Publishing, 1992;53-68.
15. Rousseau AW. Notes from Oklahoma City’s recovery. In: Hall RCW, Norwood AE (eds). Disaster psychiatry handbook. Washington, DC: American Psychiatric Association Committee on Psychiatric Dimensions of Disaster, undated:3-11. (Accessed Oct. 29, 2003 at http://www.psych.org/disasterpsych/pdfs/apadisasterhandbk.pdf.)
16. Yildiz A, Sachs GS, Turgay A. Pharmacological management of agitation in emergency settings. Emerg Med J 2003;20:339-46.
17. Gelpin E, Bonne O, Peri T, et al. Treatment of recent trauma survivors with benzodiazepines: a prospective study. J Clin Psychiatry 1996;57:390-4.
18. Mitchell JT. When disaster strikes. J Em Med Serv 1983;8:36-9.
19. Rose S, Bisson J, Wessely S. Psychological debriefing for preventing posttraumatic stress disorder (PTSD). Cochrane Database Syst Rev 2002;(2):CD000560.-
20. Black J. Forming the libidinal cocoon: the Dallas airplane crashes, the Guadalupe river drownings, and Hurricane Hugo in the Virgin Islands. In: Austin LS (ed). Responding to disaster: a guide for mental health professionals. Washington DC: American Psychiatric Publishing, 1992;169:84.-
21. Ehlers A, Clark DM. Early psychological interventions for adult survivors of trauma: a review. Biol Psychiatry 2003;53:817-26.
22. Bryant RA, Moulds M, Guthrie R, Nixon RD. Treating acute stress disorder following mild traumatic brain injury. Am J Psychiatry 2003;160:585-7.
23. Bryant RA, Sackville T, Dang ST, et al. Treating acute stress disorder: an evaluation of cognitive behavior therapy and supportive counseling techniques. Am J Psychiatry 1999;156:1780-6.
24. Bryant RA, Harvey AG, Dang ST, et al. Treatment of acute stress disorder: a comparison of cognitive-behavioral therapy and supportive counseling. J Consult Clin Psychol 1998;66:862-6.
25. Cohen JA. Treating acute posttraumatic reactions in children and adolescents. Biol Psychiatry 2003;53:827-33.
26. Foa EB, Keane TM, Friedman MJ. Effective treatments for PTSD. New York: Guilford Press, 2000.
The night started like any other for Dr. Z. Kids in bed (too late) by 10:30, dog out by 11, fell asleep reading journal by 11:15. Sirens jolt her out of a solid stage 4. Her eyes widen, pulse quickens, mouth dries as she follows the glow of the TV into the living room. On TV, fire frames shots of tearful faces, body bags, and firefighters in protective suits. She catches the announcer’s voice: “…explosion at City Power and Light nuclear facility at 3:10 AM today. Fifty-five are known dead, and thousands are being told to evacuate. The blast’s cause is unknown, but terrorism is suspected.”
As her numbness slowly ebbs, Dr. Z’s questions rise insistently. How can I help the survivors? My patients? My children? What if the media call me? How could I have been better prepared for this?
Disaster shakes us to our human and biological core. More than any other clinical encounter, it reminds us that psychiatrists share the vulnerabilities of those we seek to help. Yet it also reminds us that even simple concepts and interventions can mobilize the healing process.
Are you ready to provide emergency psychiatric care following a disaster in your community—be it a nuclear accident, tornado, airplane crash, or terrorist act? Here is evidence—some counterintuitive—that can help you prepare.
Table 1
‘Psychological first aid’ for disaster survivors
Re-create sense of safety
|
Encourage social support
|
Re-establish sense of efficacy
|
Disaster’s psychobiology
Human reactions to disaster are often conceptualized as the mammalian survival response: flight, fight, and fright (freezing). In most cases, these reactions are adaptive and dissipate after safety is restored. Posttraumatic stress disorder (PTSD) develops in about 5% of natural disaster victims and 33% of mass shooting victims.1
Responses that do go awry appear to be associated with abnormally low cortisol and persistent adrenergic activation, leading to sensitization of the fear response.2 Reminders of trauma or persistent stressors—such as pain, problems with finances or housing, or bereavement—may exacerbate sensitization. On the other hand, preclinical studies suggest that social support3,4 and active coping5 mitigate physiologic stress responses, confirming numerous clinical observations that associate lack of social support and avoidant coping with eventual PTSD development.
Three basics. Just as our emergency medicine colleagues must often revert to life-support basics, we must remind ourselves of biology’s three basics for psychic resilience:
- safety (including—as much as possible—protection from reminders of trauma and ongoing stress)
- meaningful social connection
- re-establishing a sense of efficacy to overcome helplessness (Table 1).
Like the stress response, these protective factors seem hard-wired into our biological make-up. They form the foundation for all phases of disaster psychiatry interventions, from planning to immediate interventions through longterm follow-up.
Disaster planning
As a mental health professional, plan to operate within established disaster plans and agencies, not only for the sake of efficiency but also because structure and support are paramount in disaster situations. Check with the American Psychiatric Association’s local branch to determine if a disaster mental health plan exists. If not, explore how to work directly with local American Red Cross chapters and hospitals, which recruit personnel for the Disaster Medical Assistance Teams mobilized by the public health service.
Table 2
Normal reactions to disaster for adults and children
| All ages | |
| Emotional | Shock, fear, grief, anger, guilt, shame, helplessness, hopelessness, numbness, emptiness Decreased ability to feel interest, pleasure, love |
| Cognitive | Confusion, disorientation, indecisiveness, worry, shortened attention span, poor concentration, memory difficulties, unwanted memories, self-blame |
| Physical | Tension, fatigue, edginess, insomnia, generalized aches and pains, startling easily, rapid heartbeat, nausea, decreased appetite and sex drive |
| Interpersonal | Difficulties being intimate, being over-controlling, feeling rejected or abandoned |
| Children’s age-specific disaster responses | |
| Preschool | Separation fears, regression, fussiness, temper tantrums, somatization Sleep disturbances including nightmares, somnambulism, night terrors |
| School-age | May still have the above, as well as excessive guilt and worries about others’ safety, poor concentration and loss of school performance, repetitious re-telling or play related to trauma |
| Adolescent | Depression, acting out, wish for revenge, sleeping and eating disturbances, altered view of the future |
Immediate disaster mental health plans vary in detail according to local needs and resources but should at least address:
- providing on-site interventions
- disseminating information about responses to trauma
- identifying and publicizing local mental health resources.
Immediate interventions
Immediately following a disaster, psychiatrists are frequently asked to assist with on-site crisis and medical interventions, evaluate survivors with unusual or intense reactions, and provide public education about psychological reactions to disaster.
On-site response. All responders, regardless of discipline, should provide disaster survivors with “psychological first aid,” which is directed at reestablishing safety, connection, and efficacy. Basic crisis intervention principles are useful when support and reassurance are not enough.6
For example, relaxation exercises can reduce anxiety and improve sleep. Use focused, structured relaxation tools—such as progressive muscle relaxation and breathing training—as unstructured exercises can exacerbate dissociation and re-experiencing. Grounding techniques, by which survivors learn to focus all senses on immediate surroundings, often alleviate dissociation and flashbacks.
Care for children. Because children’s reactions to disaster greatly depend on their caregivers’ responses (social referencing), focus acute interventions for children on:
- re-connecting them with their families
- reducing caregivers’ distress
- educating caregivers about providing age appropriate information and support (see Related resources).
Medical care. As physicians, psychiatrists may be called upon to intervene medically. Although it is generally advisable to stay within our usual practice, medical personnel may be in short supply. Fortunately, Good Samaritan laws exist in every state, and the potential for a successful malpractice suit against a physician responding in a disaster is almost zero, unless the physician’s performance is grossly negligent (such as moving the neck of a patient with obvious head or neck injuries).7
Principles regarding informed consent and right to refuse treatment—along with the usual exceptions—apply during disasters.
Evaluating survivors in shelters and hospitals requires knowing the normal and abnormal responses to disaster, being able to differentially diagnose changes in mental status, and understanding risk factors for trauma’s psychiatric sequelae. Aside from PTSD, trauma’s long-term effects include other anxiety disorders, depression, substance abuse, and eating disorders. In addition to the usual components of a psychiatric evaluation, assessments must address event-related factors such as proximity to the disaster, loss of significant others or property, physical injuries, immediate needs, and social support.8
Normal stress reactions. Frequently described as “a normal response to an abnormal situation,” the normal stress reaction is multidimensional and depends on the person’s developmental level (Table 2). About 10% to 25% of survivors experience intense affect and dissociation, whereas a similar number may appear unusually calm.
Interventions beyond the“first aid” described above are not usually needed unless individuals:
- are a danger to themselves or others
- are psychotic
- have no social supports
- cannot perform tasks necessary for self-care and to begin the recovery process.
Always re-assess when there is any question about a survivor’s immediate reaction to trauma.
In DSM-IV-TR’s trauma-related diagnoses, the symptom clusters often do not capture many disaster survivors’ subjective experience: the shattering of fundamental beliefs regarding themselves (invulnerability), the world (predictability, safety), and others (trust, benevolence).9 By empathizing with these responses, you can help survivors feel less isolated and estranged.
Differential diagnosis. Survivors’ mental status changes may be manifestations of the stress response, but they also may represent:
- exacerbations of pre-existing psychiatric or general medical conditions
- hypoxemia, hypovolemia, or CNS trauma from physical injury
- responses to medications used for resuscitation or pain control, such as atropine, epinephrine, lidocaine, or morphine.
Effects of bioterrorism agents must also be considered. For example, organophosphorus compounds such as the nerve agents sarin and soman can cause impaired concentration, depression, and anxiety. Anthrax can cause rapidly progressing meningitis.10 Delirium must be differentiated from dissociation; patients with dissociation can be re-oriented, and changes will resolve with time rather than fluctuate.11
Psychopathology risk factors. Multiple studies have addressed risk factors for post-disaster psychiatric sequelae (usually PTSD). In general, risk increases with repeated trauma exposure (including TV viewing), prior trauma, lack of social support, injury, pre-existing psychiatric problems, traumatic bereavement (having witnessed the violent death of a loved one), avoidant coping, and having strong negative beliefs about the meanings of normal stress reactions such as tearfulness, anxiety, and insomnia.
Because a recent meta-analysis supports these observations,12 follow-up evaluation for signs of PTSD is recommended for:
- survivors with one or more of the risk factors discussed above
- vulnerable groups such as rescue workers, children, and dependent individuals
- survivors whose symptoms persist after 2 months.13
Decompensation immediately after a disaster seems to be the exception for psychiatric patients, despite their longer-term vulnerability. One psychiatrist who in 1989 survived Hurricane Hugo—the most intense storm to strike the Mid-Atlantic region in 100 years—noted that demand for inpatient psychiatric services did not increase in the storm’s aftermath. The only patient calls she received were inquiries about her own physical safety.14
Caregivers and rescue workers—including psychi-atrists—are also disaster survivors, and you need to tend to your needs for safety and support. Consult frequently with colleagues within and outside the disaster area, as much for support as for information and guidance.15 Remember also that rescue workers are occasionally targets for victims’ rage at their circumstances. Anticipating and explaining this displacement reduces its toxicity.
Using medications
Uses psychotropics judiciously in the first 48 hours of trauma. Medication effects may interfere with neurologic assessment of the injured, and monitoring and follow-up may not be possible.
However, drug therapy should start quickly when survivors are acutely psychotic or their behavior endangers themselves, others, or the milieu. Medications usually include a fast-acting benzodiazepine and/or an antipsychotic, as described in guidelines for managing agitation.16 Always provide structure and supervision for medicated patients.
No guidelines exist for using medications to manage distressing—but less-severe—acute stress-related symptoms. Some experts advocate using adrenergic antagonists such as clonidine, guanfacine, and beta blockers to reduce excessive arousal. These drugs have not been adequately studied in this setting, however, and may harm those with cardiovascular instability from preexisting conditions or injuries.
Table 3
Psychoeducation: Simple messages for workers and trauma survivors
| Get adequate rest, food, sleep |
| Avoid exposure to trauma cues, including TV images |
| Seek support from loved ones and peers |
| Talk about events and feelings only if this feels comfortable and helpful |
| Return to normal routine as much as possible |
| Take action to rebuild, but at a reasonable pace |
| Reach out to others who may need assistance |
Get help:
|
Short-term (<1 week) benzodiazepine use for panic symptoms and severe insomnia is acceptable, but longer-term use may increase PTSD risk.17 A selective serotonin reuptake inhibitor may help individuals with pre-existing PTSD or depression, if you can arrange follow-up.
In the aftermath
‘Debriefing.’ Critical incident stress debriefing (CISD) is a structured, one-session group intervention in which survivors’ experiences and emotional reactions are discussed and education and follow-up recommendations are provided. Developed by Mitchell in 1983,18 CISD was widely used until systematic evaluations revealed that it did not alleviate psychological distress or prevent PTSD.19
Table 4
How to interact with news media during and after a disaster
| For organizations Identify a spokesperson with media experience beforehand Ensure that the spokesperson is well-informed about all aspects of the disaster |
| For spokespersons |
Always
|
Never
|
Thus, although survivor meetings may provide information, education, screening, and support, avoid detailed discussions of events and emotions. Any meetings should be conducted by mental health clinicians and should not be mandatory. Reserve the term “debriefing” for operational reviews by rescue personnel.20
Public education. Educate survivors, rescue workers, health care providers, teachers, and relief agency workers. Provide concise, simple messages as suggested in Table 3. News media provide our most effective means of reaching out to survivors, which is why having a pre-existing relationship is so important. Some guidelines for working with the media are presented in Table 4.
Outreach. Numerous educational resources are available for survivors and their caregivers (see Related resources). Other potentially useful outreach tools include:
- meetings with teachers’ organizations
- continuing medical education activities for primary care providers
- telephone hot lines.
Legal and ethical issues
Disaster scenes are chaotic and informal, and professionals must be flexible, often providing general support and information rather than specific clinical interventions. However, it is important in each encounter to decide whether a patient-physician relationship has begun.
As a general rule, a physician-patient relationship is established whenever diagnosis or treatment is discussed. Once that happens, briefly document:
- signs and symptoms
- working diagnosis
- suicide or violence potential
- treatment and/or follow-up plans.
Confidentiality may be difficult to preserve in chaotic situations involving workers from many agencies. Even in disasters, however, you must obtain permission before sharing information unless the individual’s situation is emergent.
Table 5
Keys to effective disaster psychiatry
Be prepared
|
Care for survivors
|
Care for yourself
|
Long-term interventions
Longer-term disaster interventions include continued outreach and education and needed follow-up services. Existing structures may provide effective follow-up, but additional resources are often needed.
Federal programs. Following a presidentialdeclared disaster, the Federal Emergency Management Agency (FEMA) provides funding for crisis counseling. Programs are typically funded for 9 to 15 months and administered through the emergency services and disaster relief branch of the Substance Abuse and Mental Health Services Administration (SAMHSA) and community mental health organizations. Examples include Project Heartland following the 1995 Oklahoma City federal building bombing and Project COPE following California’s 1989 Loma Prieta earthquake.
Cognitive-behavioral therapy. For adult survivors with acute stress disorder, specific cognitive-behavioral therapy (CBT) provided by trained therapists may prevent PTSD and other trauma sequelae, such as depression.21 CBT interventions may begin as early as 2 weeks after trauma and focus sequentially on anxiety management, cognitive restructuring, imaginal exposure followed by in vivo exposure, and relapse prevention.
Three controlled trials found 6-month PTSD rates of 14% to 20% among acute stress disorder patients treated with CBT, compared with 58% to 67% with supportive counseling.22-24 Although studies of interventions immediately following trauma are lacking, trauma-focused CBT is also recommended for children.25 Evidence-based treatments for PTSD are discussed in detail elsewhere.26
Not unprepared after all
With some reflection, Dr. Z realized she had the tools to help her community. Her feelings of helplessness receded as she envisioned how she could help survivors understand their experiences, re-create a sense of safety, restore important connections to loved ones, and begin to rebuild their lives (Table 5).
For clinicians
- Young BH, Ford JD, Ruzek JI, et al. Disaster mental health: a guidebook for clinicians and administrators. Washington, DC: National Center for Post-Traumatic Stress Disorder, 1998. http://ncptsd.org/publications/disaster/index.html
- Hillman JL. Crisis intervention and trauma: new approaches to evidence-based practice. New York: Kluwer Academic/Plenum Publishers, 2002.
- Office of the Surgeon General Web site on medical aspects of nuclear, biological, and chemical warfare. http://www.nbc-med.org
For survivors and clinicians
- National Center for Post-Traumatic Stress Disorder. Disaster mental health: Dealing with the aftereffects of terrorism. http://www.ncptsd.org/terrorism/index.html
- Substance Abuse and Mental Health Services Administration. Emergency mental health and traumatic stress. http://www.mentalhealth.org/cmhs/EmergencyServices/default.asp
- American Academy of Child and Adolescent Psychiatry. Talking to children about terrorism and war. http://www.aacap.org/publications/factsFam/87.htm
Drug brand names
- Clonidine • Catapres
- Guanfacine • Tenex
Disclosure
The authors report no financial relationship with any company whose products are mentioned in this article or with manufacturers of competing products.
The night started like any other for Dr. Z. Kids in bed (too late) by 10:30, dog out by 11, fell asleep reading journal by 11:15. Sirens jolt her out of a solid stage 4. Her eyes widen, pulse quickens, mouth dries as she follows the glow of the TV into the living room. On TV, fire frames shots of tearful faces, body bags, and firefighters in protective suits. She catches the announcer’s voice: “…explosion at City Power and Light nuclear facility at 3:10 AM today. Fifty-five are known dead, and thousands are being told to evacuate. The blast’s cause is unknown, but terrorism is suspected.”
As her numbness slowly ebbs, Dr. Z’s questions rise insistently. How can I help the survivors? My patients? My children? What if the media call me? How could I have been better prepared for this?
Disaster shakes us to our human and biological core. More than any other clinical encounter, it reminds us that psychiatrists share the vulnerabilities of those we seek to help. Yet it also reminds us that even simple concepts and interventions can mobilize the healing process.
Are you ready to provide emergency psychiatric care following a disaster in your community—be it a nuclear accident, tornado, airplane crash, or terrorist act? Here is evidence—some counterintuitive—that can help you prepare.
Table 1
‘Psychological first aid’ for disaster survivors
Re-create sense of safety
|
Encourage social support
|
Re-establish sense of efficacy
|
Disaster’s psychobiology
Human reactions to disaster are often conceptualized as the mammalian survival response: flight, fight, and fright (freezing). In most cases, these reactions are adaptive and dissipate after safety is restored. Posttraumatic stress disorder (PTSD) develops in about 5% of natural disaster victims and 33% of mass shooting victims.1
Responses that do go awry appear to be associated with abnormally low cortisol and persistent adrenergic activation, leading to sensitization of the fear response.2 Reminders of trauma or persistent stressors—such as pain, problems with finances or housing, or bereavement—may exacerbate sensitization. On the other hand, preclinical studies suggest that social support3,4 and active coping5 mitigate physiologic stress responses, confirming numerous clinical observations that associate lack of social support and avoidant coping with eventual PTSD development.
Three basics. Just as our emergency medicine colleagues must often revert to life-support basics, we must remind ourselves of biology’s three basics for psychic resilience:
- safety (including—as much as possible—protection from reminders of trauma and ongoing stress)
- meaningful social connection
- re-establishing a sense of efficacy to overcome helplessness (Table 1).
Like the stress response, these protective factors seem hard-wired into our biological make-up. They form the foundation for all phases of disaster psychiatry interventions, from planning to immediate interventions through longterm follow-up.
Disaster planning
As a mental health professional, plan to operate within established disaster plans and agencies, not only for the sake of efficiency but also because structure and support are paramount in disaster situations. Check with the American Psychiatric Association’s local branch to determine if a disaster mental health plan exists. If not, explore how to work directly with local American Red Cross chapters and hospitals, which recruit personnel for the Disaster Medical Assistance Teams mobilized by the public health service.
Table 2
Normal reactions to disaster for adults and children
| All ages | |
| Emotional | Shock, fear, grief, anger, guilt, shame, helplessness, hopelessness, numbness, emptiness Decreased ability to feel interest, pleasure, love |
| Cognitive | Confusion, disorientation, indecisiveness, worry, shortened attention span, poor concentration, memory difficulties, unwanted memories, self-blame |
| Physical | Tension, fatigue, edginess, insomnia, generalized aches and pains, startling easily, rapid heartbeat, nausea, decreased appetite and sex drive |
| Interpersonal | Difficulties being intimate, being over-controlling, feeling rejected or abandoned |
| Children’s age-specific disaster responses | |
| Preschool | Separation fears, regression, fussiness, temper tantrums, somatization Sleep disturbances including nightmares, somnambulism, night terrors |
| School-age | May still have the above, as well as excessive guilt and worries about others’ safety, poor concentration and loss of school performance, repetitious re-telling or play related to trauma |
| Adolescent | Depression, acting out, wish for revenge, sleeping and eating disturbances, altered view of the future |
Immediate disaster mental health plans vary in detail according to local needs and resources but should at least address:
- providing on-site interventions
- disseminating information about responses to trauma
- identifying and publicizing local mental health resources.
Immediate interventions
Immediately following a disaster, psychiatrists are frequently asked to assist with on-site crisis and medical interventions, evaluate survivors with unusual or intense reactions, and provide public education about psychological reactions to disaster.
On-site response. All responders, regardless of discipline, should provide disaster survivors with “psychological first aid,” which is directed at reestablishing safety, connection, and efficacy. Basic crisis intervention principles are useful when support and reassurance are not enough.6
For example, relaxation exercises can reduce anxiety and improve sleep. Use focused, structured relaxation tools—such as progressive muscle relaxation and breathing training—as unstructured exercises can exacerbate dissociation and re-experiencing. Grounding techniques, by which survivors learn to focus all senses on immediate surroundings, often alleviate dissociation and flashbacks.
Care for children. Because children’s reactions to disaster greatly depend on their caregivers’ responses (social referencing), focus acute interventions for children on:
- re-connecting them with their families
- reducing caregivers’ distress
- educating caregivers about providing age appropriate information and support (see Related resources).
Medical care. As physicians, psychiatrists may be called upon to intervene medically. Although it is generally advisable to stay within our usual practice, medical personnel may be in short supply. Fortunately, Good Samaritan laws exist in every state, and the potential for a successful malpractice suit against a physician responding in a disaster is almost zero, unless the physician’s performance is grossly negligent (such as moving the neck of a patient with obvious head or neck injuries).7
Principles regarding informed consent and right to refuse treatment—along with the usual exceptions—apply during disasters.
Evaluating survivors in shelters and hospitals requires knowing the normal and abnormal responses to disaster, being able to differentially diagnose changes in mental status, and understanding risk factors for trauma’s psychiatric sequelae. Aside from PTSD, trauma’s long-term effects include other anxiety disorders, depression, substance abuse, and eating disorders. In addition to the usual components of a psychiatric evaluation, assessments must address event-related factors such as proximity to the disaster, loss of significant others or property, physical injuries, immediate needs, and social support.8
Normal stress reactions. Frequently described as “a normal response to an abnormal situation,” the normal stress reaction is multidimensional and depends on the person’s developmental level (Table 2). About 10% to 25% of survivors experience intense affect and dissociation, whereas a similar number may appear unusually calm.
Interventions beyond the“first aid” described above are not usually needed unless individuals:
- are a danger to themselves or others
- are psychotic
- have no social supports
- cannot perform tasks necessary for self-care and to begin the recovery process.
Always re-assess when there is any question about a survivor’s immediate reaction to trauma.
In DSM-IV-TR’s trauma-related diagnoses, the symptom clusters often do not capture many disaster survivors’ subjective experience: the shattering of fundamental beliefs regarding themselves (invulnerability), the world (predictability, safety), and others (trust, benevolence).9 By empathizing with these responses, you can help survivors feel less isolated and estranged.
Differential diagnosis. Survivors’ mental status changes may be manifestations of the stress response, but they also may represent:
- exacerbations of pre-existing psychiatric or general medical conditions
- hypoxemia, hypovolemia, or CNS trauma from physical injury
- responses to medications used for resuscitation or pain control, such as atropine, epinephrine, lidocaine, or morphine.
Effects of bioterrorism agents must also be considered. For example, organophosphorus compounds such as the nerve agents sarin and soman can cause impaired concentration, depression, and anxiety. Anthrax can cause rapidly progressing meningitis.10 Delirium must be differentiated from dissociation; patients with dissociation can be re-oriented, and changes will resolve with time rather than fluctuate.11
Psychopathology risk factors. Multiple studies have addressed risk factors for post-disaster psychiatric sequelae (usually PTSD). In general, risk increases with repeated trauma exposure (including TV viewing), prior trauma, lack of social support, injury, pre-existing psychiatric problems, traumatic bereavement (having witnessed the violent death of a loved one), avoidant coping, and having strong negative beliefs about the meanings of normal stress reactions such as tearfulness, anxiety, and insomnia.
Because a recent meta-analysis supports these observations,12 follow-up evaluation for signs of PTSD is recommended for:
- survivors with one or more of the risk factors discussed above
- vulnerable groups such as rescue workers, children, and dependent individuals
- survivors whose symptoms persist after 2 months.13
Decompensation immediately after a disaster seems to be the exception for psychiatric patients, despite their longer-term vulnerability. One psychiatrist who in 1989 survived Hurricane Hugo—the most intense storm to strike the Mid-Atlantic region in 100 years—noted that demand for inpatient psychiatric services did not increase in the storm’s aftermath. The only patient calls she received were inquiries about her own physical safety.14
Caregivers and rescue workers—including psychi-atrists—are also disaster survivors, and you need to tend to your needs for safety and support. Consult frequently with colleagues within and outside the disaster area, as much for support as for information and guidance.15 Remember also that rescue workers are occasionally targets for victims’ rage at their circumstances. Anticipating and explaining this displacement reduces its toxicity.
Using medications
Uses psychotropics judiciously in the first 48 hours of trauma. Medication effects may interfere with neurologic assessment of the injured, and monitoring and follow-up may not be possible.
However, drug therapy should start quickly when survivors are acutely psychotic or their behavior endangers themselves, others, or the milieu. Medications usually include a fast-acting benzodiazepine and/or an antipsychotic, as described in guidelines for managing agitation.16 Always provide structure and supervision for medicated patients.
No guidelines exist for using medications to manage distressing—but less-severe—acute stress-related symptoms. Some experts advocate using adrenergic antagonists such as clonidine, guanfacine, and beta blockers to reduce excessive arousal. These drugs have not been adequately studied in this setting, however, and may harm those with cardiovascular instability from preexisting conditions or injuries.
Table 3
Psychoeducation: Simple messages for workers and trauma survivors
| Get adequate rest, food, sleep |
| Avoid exposure to trauma cues, including TV images |
| Seek support from loved ones and peers |
| Talk about events and feelings only if this feels comfortable and helpful |
| Return to normal routine as much as possible |
| Take action to rebuild, but at a reasonable pace |
| Reach out to others who may need assistance |
Get help:
|
Short-term (<1 week) benzodiazepine use for panic symptoms and severe insomnia is acceptable, but longer-term use may increase PTSD risk.17 A selective serotonin reuptake inhibitor may help individuals with pre-existing PTSD or depression, if you can arrange follow-up.
In the aftermath
‘Debriefing.’ Critical incident stress debriefing (CISD) is a structured, one-session group intervention in which survivors’ experiences and emotional reactions are discussed and education and follow-up recommendations are provided. Developed by Mitchell in 1983,18 CISD was widely used until systematic evaluations revealed that it did not alleviate psychological distress or prevent PTSD.19
Table 4
How to interact with news media during and after a disaster
| For organizations Identify a spokesperson with media experience beforehand Ensure that the spokesperson is well-informed about all aspects of the disaster |
| For spokespersons |
Always
|
Never
|
Thus, although survivor meetings may provide information, education, screening, and support, avoid detailed discussions of events and emotions. Any meetings should be conducted by mental health clinicians and should not be mandatory. Reserve the term “debriefing” for operational reviews by rescue personnel.20
Public education. Educate survivors, rescue workers, health care providers, teachers, and relief agency workers. Provide concise, simple messages as suggested in Table 3. News media provide our most effective means of reaching out to survivors, which is why having a pre-existing relationship is so important. Some guidelines for working with the media are presented in Table 4.
Outreach. Numerous educational resources are available for survivors and their caregivers (see Related resources). Other potentially useful outreach tools include:
- meetings with teachers’ organizations
- continuing medical education activities for primary care providers
- telephone hot lines.
Legal and ethical issues
Disaster scenes are chaotic and informal, and professionals must be flexible, often providing general support and information rather than specific clinical interventions. However, it is important in each encounter to decide whether a patient-physician relationship has begun.
As a general rule, a physician-patient relationship is established whenever diagnosis or treatment is discussed. Once that happens, briefly document:
- signs and symptoms
- working diagnosis
- suicide or violence potential
- treatment and/or follow-up plans.
Confidentiality may be difficult to preserve in chaotic situations involving workers from many agencies. Even in disasters, however, you must obtain permission before sharing information unless the individual’s situation is emergent.
Table 5
Keys to effective disaster psychiatry
Be prepared
|
Care for survivors
|
Care for yourself
|
Long-term interventions
Longer-term disaster interventions include continued outreach and education and needed follow-up services. Existing structures may provide effective follow-up, but additional resources are often needed.
Federal programs. Following a presidentialdeclared disaster, the Federal Emergency Management Agency (FEMA) provides funding for crisis counseling. Programs are typically funded for 9 to 15 months and administered through the emergency services and disaster relief branch of the Substance Abuse and Mental Health Services Administration (SAMHSA) and community mental health organizations. Examples include Project Heartland following the 1995 Oklahoma City federal building bombing and Project COPE following California’s 1989 Loma Prieta earthquake.
Cognitive-behavioral therapy. For adult survivors with acute stress disorder, specific cognitive-behavioral therapy (CBT) provided by trained therapists may prevent PTSD and other trauma sequelae, such as depression.21 CBT interventions may begin as early as 2 weeks after trauma and focus sequentially on anxiety management, cognitive restructuring, imaginal exposure followed by in vivo exposure, and relapse prevention.
Three controlled trials found 6-month PTSD rates of 14% to 20% among acute stress disorder patients treated with CBT, compared with 58% to 67% with supportive counseling.22-24 Although studies of interventions immediately following trauma are lacking, trauma-focused CBT is also recommended for children.25 Evidence-based treatments for PTSD are discussed in detail elsewhere.26
Not unprepared after all
With some reflection, Dr. Z realized she had the tools to help her community. Her feelings of helplessness receded as she envisioned how she could help survivors understand their experiences, re-create a sense of safety, restore important connections to loved ones, and begin to rebuild their lives (Table 5).
For clinicians
- Young BH, Ford JD, Ruzek JI, et al. Disaster mental health: a guidebook for clinicians and administrators. Washington, DC: National Center for Post-Traumatic Stress Disorder, 1998. http://ncptsd.org/publications/disaster/index.html
- Hillman JL. Crisis intervention and trauma: new approaches to evidence-based practice. New York: Kluwer Academic/Plenum Publishers, 2002.
- Office of the Surgeon General Web site on medical aspects of nuclear, biological, and chemical warfare. http://www.nbc-med.org
For survivors and clinicians
- National Center for Post-Traumatic Stress Disorder. Disaster mental health: Dealing with the aftereffects of terrorism. http://www.ncptsd.org/terrorism/index.html
- Substance Abuse and Mental Health Services Administration. Emergency mental health and traumatic stress. http://www.mentalhealth.org/cmhs/EmergencyServices/default.asp
- American Academy of Child and Adolescent Psychiatry. Talking to children about terrorism and war. http://www.aacap.org/publications/factsFam/87.htm
Drug brand names
- Clonidine • Catapres
- Guanfacine • Tenex
Disclosure
The authors report no financial relationship with any company whose products are mentioned in this article or with manufacturers of competing products.
1. Effects of traumatic stress in a disaster situation. Washington, DC: National Center for Post-Traumatic Stress Disorder. Department of Veterans Affairs, September 12, 2001 (Accessed March 31, 2004 at http://www.ncptsd.org/facts/disasters/fs_effects_disaster.html).
2. Yehuda R, McFarlane AC, Shalev AY. Predicting the development of post-traumatic stress disorder from the acute response to a traumatic event. Biol Psychiatry 1998;44:1305-13.
3. Levine S, Lyons DM, Schatzberg AF. Psychobiological consequences of social relationships. Ann NY Acad Sci 1997;807:210-18.
4. Uchino BN, Garvey TS. The availability of social support reduces cardiovascular reactivity to acute psychological stress. J Behav Med 1997;20:15-27.
5. LeDoux JE, Gorman JM. A call to action: overcoming anxiety through active coping. Am J Psychiatry 2001;158:1953-5.
6. Hillman JL. Crisis intervention and trauma: new approaches to evidence-based practice. New York: Kluwer Academic/Plenum Publishers, 2002.
7. Daniels G. Good Samaritan acts. Emerg Med Clin North Am 1999;17:491-504.
8. Mental-health intervention for disasters. Washington, DC: National Center for Post-Traumatic Stress Disorder, Department of Veterans Affairs, Sept. 12, 2001. (Accessed March 31, 2004 at http://www.ncptsd.org/facts/disasters/fs_treatment_disaster.html.)
9. Difede J, Apfeldorf WJ, Cloitre M, et al. Acute psychiatric responses to the explosion at the World Trade Center: a case series. J Nerv Ment Dis 1997;185:519-22.
10. DiGiovanni C. Domestic terrorism with chemical or biological agents: psychiatric aspects. Am J Psychiatry 1999;156:1500-5.
11. Rundle JR. Psychiatric issues in medical-surgical disaster casualties: consultation-liaison approach. Psychiatr Q 2000;71:245-58.
12. Brewin CR, Andrews B, Valentine JD. Meta-analysis of risk factors for post-traumatic stress disorder in trauma-exposed adults. J Consult Clin Psychol 2000;68:748-66.
13. Mental health and mass violence: evidence-based early psychological intervention for victims/survivors of mass violence. Washington, DC: National Institute of Mental Health, Nov. 1, 2002 (Accessed Oct. 29, 2003 at http://www.nimh.nih.gov/research/massviolence.pdf.)
14. Austin LS. Organizing a disaster response program in one’s home community. In: Austin LS (ed). Responding to disaster: a guide for mental health professionals. Washington, DC: American Psychiatric Publishing, 1992;53-68.
15. Rousseau AW. Notes from Oklahoma City’s recovery. In: Hall RCW, Norwood AE (eds). Disaster psychiatry handbook. Washington, DC: American Psychiatric Association Committee on Psychiatric Dimensions of Disaster, undated:3-11. (Accessed Oct. 29, 2003 at http://www.psych.org/disasterpsych/pdfs/apadisasterhandbk.pdf.)
16. Yildiz A, Sachs GS, Turgay A. Pharmacological management of agitation in emergency settings. Emerg Med J 2003;20:339-46.
17. Gelpin E, Bonne O, Peri T, et al. Treatment of recent trauma survivors with benzodiazepines: a prospective study. J Clin Psychiatry 1996;57:390-4.
18. Mitchell JT. When disaster strikes. J Em Med Serv 1983;8:36-9.
19. Rose S, Bisson J, Wessely S. Psychological debriefing for preventing posttraumatic stress disorder (PTSD). Cochrane Database Syst Rev 2002;(2):CD000560.-
20. Black J. Forming the libidinal cocoon: the Dallas airplane crashes, the Guadalupe river drownings, and Hurricane Hugo in the Virgin Islands. In: Austin LS (ed). Responding to disaster: a guide for mental health professionals. Washington DC: American Psychiatric Publishing, 1992;169:84.-
21. Ehlers A, Clark DM. Early psychological interventions for adult survivors of trauma: a review. Biol Psychiatry 2003;53:817-26.
22. Bryant RA, Moulds M, Guthrie R, Nixon RD. Treating acute stress disorder following mild traumatic brain injury. Am J Psychiatry 2003;160:585-7.
23. Bryant RA, Sackville T, Dang ST, et al. Treating acute stress disorder: an evaluation of cognitive behavior therapy and supportive counseling techniques. Am J Psychiatry 1999;156:1780-6.
24. Bryant RA, Harvey AG, Dang ST, et al. Treatment of acute stress disorder: a comparison of cognitive-behavioral therapy and supportive counseling. J Consult Clin Psychol 1998;66:862-6.
25. Cohen JA. Treating acute posttraumatic reactions in children and adolescents. Biol Psychiatry 2003;53:827-33.
26. Foa EB, Keane TM, Friedman MJ. Effective treatments for PTSD. New York: Guilford Press, 2000.
1. Effects of traumatic stress in a disaster situation. Washington, DC: National Center for Post-Traumatic Stress Disorder. Department of Veterans Affairs, September 12, 2001 (Accessed March 31, 2004 at http://www.ncptsd.org/facts/disasters/fs_effects_disaster.html).
2. Yehuda R, McFarlane AC, Shalev AY. Predicting the development of post-traumatic stress disorder from the acute response to a traumatic event. Biol Psychiatry 1998;44:1305-13.
3. Levine S, Lyons DM, Schatzberg AF. Psychobiological consequences of social relationships. Ann NY Acad Sci 1997;807:210-18.
4. Uchino BN, Garvey TS. The availability of social support reduces cardiovascular reactivity to acute psychological stress. J Behav Med 1997;20:15-27.
5. LeDoux JE, Gorman JM. A call to action: overcoming anxiety through active coping. Am J Psychiatry 2001;158:1953-5.
6. Hillman JL. Crisis intervention and trauma: new approaches to evidence-based practice. New York: Kluwer Academic/Plenum Publishers, 2002.
7. Daniels G. Good Samaritan acts. Emerg Med Clin North Am 1999;17:491-504.
8. Mental-health intervention for disasters. Washington, DC: National Center for Post-Traumatic Stress Disorder, Department of Veterans Affairs, Sept. 12, 2001. (Accessed March 31, 2004 at http://www.ncptsd.org/facts/disasters/fs_treatment_disaster.html.)
9. Difede J, Apfeldorf WJ, Cloitre M, et al. Acute psychiatric responses to the explosion at the World Trade Center: a case series. J Nerv Ment Dis 1997;185:519-22.
10. DiGiovanni C. Domestic terrorism with chemical or biological agents: psychiatric aspects. Am J Psychiatry 1999;156:1500-5.
11. Rundle JR. Psychiatric issues in medical-surgical disaster casualties: consultation-liaison approach. Psychiatr Q 2000;71:245-58.
12. Brewin CR, Andrews B, Valentine JD. Meta-analysis of risk factors for post-traumatic stress disorder in trauma-exposed adults. J Consult Clin Psychol 2000;68:748-66.
13. Mental health and mass violence: evidence-based early psychological intervention for victims/survivors of mass violence. Washington, DC: National Institute of Mental Health, Nov. 1, 2002 (Accessed Oct. 29, 2003 at http://www.nimh.nih.gov/research/massviolence.pdf.)
14. Austin LS. Organizing a disaster response program in one’s home community. In: Austin LS (ed). Responding to disaster: a guide for mental health professionals. Washington, DC: American Psychiatric Publishing, 1992;53-68.
15. Rousseau AW. Notes from Oklahoma City’s recovery. In: Hall RCW, Norwood AE (eds). Disaster psychiatry handbook. Washington, DC: American Psychiatric Association Committee on Psychiatric Dimensions of Disaster, undated:3-11. (Accessed Oct. 29, 2003 at http://www.psych.org/disasterpsych/pdfs/apadisasterhandbk.pdf.)
16. Yildiz A, Sachs GS, Turgay A. Pharmacological management of agitation in emergency settings. Emerg Med J 2003;20:339-46.
17. Gelpin E, Bonne O, Peri T, et al. Treatment of recent trauma survivors with benzodiazepines: a prospective study. J Clin Psychiatry 1996;57:390-4.
18. Mitchell JT. When disaster strikes. J Em Med Serv 1983;8:36-9.
19. Rose S, Bisson J, Wessely S. Psychological debriefing for preventing posttraumatic stress disorder (PTSD). Cochrane Database Syst Rev 2002;(2):CD000560.-
20. Black J. Forming the libidinal cocoon: the Dallas airplane crashes, the Guadalupe river drownings, and Hurricane Hugo in the Virgin Islands. In: Austin LS (ed). Responding to disaster: a guide for mental health professionals. Washington DC: American Psychiatric Publishing, 1992;169:84.-
21. Ehlers A, Clark DM. Early psychological interventions for adult survivors of trauma: a review. Biol Psychiatry 2003;53:817-26.
22. Bryant RA, Moulds M, Guthrie R, Nixon RD. Treating acute stress disorder following mild traumatic brain injury. Am J Psychiatry 2003;160:585-7.
23. Bryant RA, Sackville T, Dang ST, et al. Treating acute stress disorder: an evaluation of cognitive behavior therapy and supportive counseling techniques. Am J Psychiatry 1999;156:1780-6.
24. Bryant RA, Harvey AG, Dang ST, et al. Treatment of acute stress disorder: a comparison of cognitive-behavioral therapy and supportive counseling. J Consult Clin Psychol 1998;66:862-6.
25. Cohen JA. Treating acute posttraumatic reactions in children and adolescents. Biol Psychiatry 2003;53:827-33.
26. Foa EB, Keane TM, Friedman MJ. Effective treatments for PTSD. New York: Guilford Press, 2000.
Trichotillomania: A heads-up on severe cases
History: Bald at age 9
Ms. D, age 41, began compulsively pulling out and eating her hair at age 8. When she didn’t get her way at home or was nervous about school, she would sit for hours, pulling and eating a strand or two at a time, ultimately ingesting a clump of hair.
By age 9, Ms. D was bald. In grade school, she often wore hats and scarves to class to avoid teasing from other children about her baldness. In high school, she kept to herself and frequently wore wigs.
Ms. D stops pulling for brief periods and her hair grows out, but she invariably resumes pulling when psychosocial stressors mount. Many of life’s normal anxieties—job interviews, work-related stress, social rejection—trigger episodes.
When she is bald, Ms. D pulls and eats hair off her wig. Over the years, she has spent thousands of dollars on custom-made wigs that mask her baldness while feeding her habit.
Ms. D’s episodes are increasingly interfering with her life. She has been steadily employed as an office assistant, but does not socialize with coworkers. She has not dated in years, and during an exacerbation leaves home only to go to work. She also pulls her eyelashes and eyebrows and picks her nails and cuticles.
Ms. D first presented in 1994 after seeing a television segment I did on trichotillomania. At intake, she was wearing a wig and exhibited anxious mood. She also has Crohn’s disease; a gastroenterologist monitors her closely.
Ms. D reports compulsive counting and checking but denies other similar behaviors. No immediate family members have exhibited obsessive-compulsive or hair-pulling behaviors. Her father abused alcohol and a sister has a stuttering problem, although Ms. D denies that these have affected her psychologically.
Ms. D’s hair-pulling behavior suggests:
- a pica disorder
- an impulse control disorder
- or an obsessive-compulsive disorder?
- Recurrent pulling out of one’s own hair, resulting in noticeable hair loss.
- Increasing tension immediately before pulling out the hair or when attempting to resist the behavior.
- Pleasure, gratification, or relief while pulling out the hair.
- The disturbance is not better explained as another mental disorder and is not caused by a dermatological or other general medical condition.
- The disturbance causes clinically significant distress or impairment in social, occupational, or other important areas of functioning.
Source: Reprinted with permission from the Diagnostic and statistical manual of mental disorders, 4th ed., text revision. Copyright 2000. American Psychiatric Association.
Dr. Lundt’s observations
Trichotillomania, defined as compulsive pulling of hair, usually begins in childhood or adolescence. Scalp hair is most commonly pulled, but some patients also pull their eyelashes, pubic hair, and other body hair. Some, especially children, have reportedly pulled their pets’ hair.
Mansueto et al estimate that trichotillomania afflicts approximately 1.5% of males and 3.5% of females.1 These estimates, however, do not include persons with the disorder who are too embarrassed to seek treatment.
DSM-IV-TR classifies trichotillomania as an impulse control disorder (Box). Although comorbid anxiety and depressive disorders are common, Ms. D did not meet criteria for any other psychiatric disorder.
Trichotillomania often is episodic. Months or years of abstinence is common after periods of exacerbation, usually caused by stress (Figure).
Many clinicians mistakenly consider trichotillomania a benign disorder with few consequences beyond alopecia.2 Some patients, however, progress into trichophagia—ingestion of pulled hair. Trichophagia is a form of pica disorder, typically defined as persistent eating of non-nutritive substances. Patients often harbor tremendous shame over their hair-eating behavior and resist psychiatric or medical treatment.2
The undigested hair can form sometimes massive clumps called trichobezoars, which are most common among children and the developmentally disabled.4 Persons with trichophagia face a 37.5% risk of forming a trichobezoar.5 The mass can cause abdominal pain, nausea, vomiting, and weight loss; complications include GI obstruction, ulceration, perforation, and peritonitis.6 An untreated trichobezoar can be fatal,7 although such deaths are rare among patients being treated for trichotillomania.
Patients with trichotillomania often respond to medications used to treat obsessive-compulsive disorder, such as clomipramine. Some clinicians believe this agent is more effective than selective serotonin reuptake inhibitors (SSRIs) but more difficult to tolerate. For Ms. D, I started with both.
Treatment: ‘I Don’t need medication’
Initial treatments—including fluoxetine, 20 mg/d for 6 months; hypnotherapy; and clomipramine, 25 mg/d—were unsuccessful. Ms. D was only marginally compliant, believing that she did not need medication.
I referred Ms. D to an out-of-state residential behavioral program specializing in trichotillomania, but she refused to go even as her hair-pulling intensified. Clomipramine was gradually increased to 75 mg nightly, briefly decreasing her pulling, then to 100 mg nightly when symptoms re-emerged. Clomipramine blood levels were monitored with each dosage change to guard against CNS and cardiac toxicity and other side effects (GI complaints, dizziness, cardiac arrhythmias, somnolence).
After watching for seasonal patterns, I found that Ms. D’s hair-pulling worsened during the winter, although no seasonal change in mood was detected. Phototherapy produced initial success, but Ms. D continued to pull her eyelashes.
Eight weeks later, however, Ms. D’s symptoms escalated. Clomipramine was increased to 150 mg nightly, resulting in blood levels of 99 ng/mL for clomipramine and 204 ng/mL for the metabolite N-desmethylclomipramine—both within the therapeutic range. As she continued pulling, I added buspirone, 10 mg/d.
At this point, would you:
- continue clomipramine and increase the dosage?
- discontinue clomipramine and start another psychotropic?
- or maintain clomipramine at the same dosage and add another psychotropic?
Dr. Lundt’s observations
Drug treatment of trichotillomania has not been studied extensively or long-term, and no consensus exists. Psychoanalysis, cognitive-behavioral therapy (CBT), and hypnotherapy are usually administered with psychotropics.8 Patients often respond to treatment at first, then reach a plateau and resume pulling their hair.9
Numerous psychotropics are used off-label to treat trichotillomania. Several agents have been shown in clinical trials and case reports to reduce hair pulling/eating behaviors (Table), but these findings are limited by small sample size, lack of control groups, and lack of a standard symptom rating scale.
Figure Trichotillomania: Excessive grooming, habit, or vicious circle?
Most clinicians begin with SSRIs because they are generally well tolerated, even at high dosages. Monotherapy often is not adequate for trichotillomania, however. Medication augmentation is common, although little empiric data support this practice.
When clomipramine did not work initally, I explored serotonergic combination strategies.
Table
Medications shown to benefit patients with trichotillomania
| Drug | Evidence | Dosage range (mg/d) | Potential side effects |
|---|---|---|---|
| First-line | |||
| Tricyclic | |||
| Clomipramine | Swedo et al10 | 50 to 300 | Sedation, weight gain, cardiac arrythmias |
| SSRIs | |||
| Fluoxetine | van Minnen et al11 | 20 to 60 | GI symptoms, insomnia |
| Fluvoxamine | Gabriel12 | 50 to 250 | Sexual dysfunction, weight gain |
| Paroxetine | Ravindran et al13 | 20 to 60 | Sexual dysfunction, weight gain |
| Sertraline | Bradford and Gratzer14 | 50 to 200 | Sexual dysfunction, GI symptoms, insomnia |
| Second-line | |||
| Antipsychotics | |||
| Haloperidol | Van Ameringen et al15 | 0.25 to 2 | Sedation, EPS |
| Olanzapine | Gupta and Gupta16 | 2.5 to 10 | Sedation, weight gain |
| Pimozide | Stein and Hollander17 | 25 to 200 | Restlessness, EPS |
| Quetiapine | Khouzam et al8 | 25 to 200 | Sedation |
| Risperidone | Gabriel12 Senturk and Tanriverdi18 | 0.5 to 4.0 | Sedation, hyperprolactinemia |
| Mood stabilizer | |||
| Lithium | Christenson et al19 | 900 to 1,500 | Increased thirst, weight gain, tremor |
| EPS: extrapyramidal symptoms | |||
Further treatment: Relapse, resection
Ms. D was lost to follow-up for 1 year. She returned in 1996, just after undergoing a laparotomy for removal of a trichobezoar large enough to fill two 2-inch-by-6-inch bags. She also had been treated for pneumonia and a pulmonary embolus.
Riddled with shame and embarrassment, Ms. D had stopped pulling for 10 months, during which time she was off medication. Her pulling behaviors re-emerged, however, and clomipramine was restarted and titrated to 250 mg nightly.
One year later, a second trichobezoar was resected. Her clomipramine/N-desmethylclomipramine level reached 1,535 ng/mL, although an ECG reading was normal. Subsequent clomipramine/N-desmethylclomipramine blood levels were within the therapeutic range. Fluvoxamine, 25 mg/d titrated across 6 weeks to 150 mg/d, was added.
Again, Ms. D stopped taking her medications and was lost to follow-up. Her gastroenterologist began managing her care and started sertraline, dosage unknown, to address her depressed mood. A third trichobezoar was removed.
When Ms. D returned to my practice, I resumed CBT and increased sertraline over 1 month from 100 to 300 mg/d. Adding olanzapine, 2.5 mg/d, diminished her anxiety and markedly decreased her hair pulling.
Months later, her hair-pulling/eating behaviors again intensified, resulting in a small-bowel obstruction and a fourth trichobezoar removal. Olanzapine was increased to 5 mg nightly without significant benefit and with sedating effects.
Clomipramine, 125 mg/d, was reintroduced and her symptoms improved dramatically. On a regimen of sertraline, clomipramine and olanzapine, Ms. D remained stable for 2 years.
Last year, however, a fifth trichobezoar measuring 20 x 15 cm was removed. Subsequent trials of methylphenidate, titrated to 72 mg every morning, and tramadol, titrated to 100 mg/d, were unsuccessful.
After 10 years of medication and psychotherapy with three different providers, Ms. D’s hair-pulling/eating behaviors persist. She is taking ziprasidone, 120 mg bid, and naltrexone, 100 mg bid, to help her impulse control, as well as sertraline, 300 mg/d, and clomipramine, 125 mg/d. Another trichobezoar removal—her sixth in 8 years—is scheduled.
What strategies exist for minimizing Ms. D’s hair-pulling behavior and keeping her in therapy?
Dr. Lundt’s observations
Trichotillomania’s waxing and waning course—and its destructive effects on a patient’s self-esteem—pose a clinical challenge. The disorder’s severity can range from cosmetically annoying to life-threatening, as in Ms. D’s case. Patients embarrassed by their behavior often prematurely leave treatment, desperate to cut off all social contact—including medical appointments.
It is crucial to maintain a nonjudgmental, inviting demeanor to alleviate the patient’s fears and facilitate a return to treatment. Support groups, especially online, can help decrease patients’ isolation and provide a reliable information network (see Related resources).
I have had excellent results with other trichotillomania patients—especially children and adolescents. Simply naming their condition and demystifying the problem can be therapeutic. Many patients have responded to SSRIs combined with CBT.
Not long ago, trichotillomania patients were met with ignorance and disbelief within the medical community as the disorder was poorly understood. We need to break this cycle of shame and continue investigating treatment strategies.
- StopPulling.com, an interactive behavioral program for persons with trichotillomania. www.stoppulling.com.
- Penzel F. The hair pulling problem: a complete guide to trichotillomania. New York: Oxford University Press, 2003.
- Keuthen NJ, Stein DJ, Christenson GA. Help for hair pullers: understanding and coping with trichotillomania. Oakland, CA: New Harbinger Publications, 2001.
Drug brand names
- Amitriptyline • Elavil
- Buspirone • BuSpar
- Clomipramine • Anafranil
- Fluoxetine • Prozac
- Fluvoxamine • Luvox
- Haloperidol • Haldol
- Lithium • Eskalith, others
- Methylphenidate • Concerta, Ritalin
- Naltrexone • ReVia
- Olanzapine • Zyprexa
- Paroxetine • Paxil
- Pimozide • Orap
- Quetiapine • Seroquel
- Risperidone • Risperdal
- Sertraline • Zoloft
- Tramadol • Ultram
- Ziprasidone • Geodon
Disclosure
Dr. Lundt receives research grants from and/or is a speaker for Eli Lilly and Co., Pfizer Inc., GlaxoSmithKline, and Bristol-Myers Squibb Co.
1. Mansueto C, Ninan PT, Rothbaum B. Trichotillomania and its treatment in adults: a guide for clinicians. Available at: (http://www.trich.org/articles/view_default.asp?filename="0305_Cases" aid=22&yd= researchers_intro). Accessed April 13, 2004
2. Bouwer C, Stein DJ. Trichobezoars in trichotillomania. Psychosom Med 1998;60:658-60.
3. Philippopoulos GS. A case of trichotillomania (hair pulling). Doc Geigy Acta Psychosom 1961;9:304-12.
4. Lee J. Bezoars and foreign bodies in the stomach. Gastrointest Endosc 1996;6:605-19.
5. Christenson GA, Crow SJ. The characterization and treatment of trichotillomania. Clin Psychiatry 1996;57(suppl 8):42-7.
6. Lal MM, Dhall JC. Trichobezoar: A collective analysis of 39 cases from India with a case report. Indian J Pediatr 1975;12:351-3.
7. DeBakey M, Ochsner W. Bezoars and concretions: A comprehensive review of the literature with an analysis of 303 collected cases and a presentation of 8 additional cases. Surgery 1939;4:934-63.
8. Khouzam HR, Battista MA, Byers PE. An overview of trichotillomania and its response to treatment with quetiapine. Psychiatry 2002;65:261-70.
9. Keuthen NJ, Fraim C, Deckersbach T, et al. Longitudinal follow-up of naturalistic treatment outcome in patients with trichotillomania. J Clin Psychiatry 2001;62:101-7.
10. Swedo SE, Leonard HL, Rapoport JL, et al. A double-blind comparison of clomipramine and desipramine in the treatment of trichotillomania (hair pulling). N Engl J Med 1989;8:497-501.
11. van Minnen A, Hoogduin KA, Keijsers GP, et al. Treatment of trichotillomania with behavioral therapy or fluoxetine: a randomized, waiting-list controlled study. Arch Gen Psychiatry 2003;60:517-22.
12. Gabriel A. A case of resistant trichotillomania treated with risperidone-augmented fluvoxamine. Can J Psychiatry 2001;46:285-6.
13. Ravindran AV, Lapierre YD, Anisman H. Obsessive-compulsive spectrum disorders: Effective treatment with paroxetine. Can J Psychiatry 1999;44:805-7.
14. Bradford JM, Gratzer TG. A treatment for impulse control disorders and paraphilia: a case report. Can J Psychiatry 1995;40:4-5.
15. Van Ameringen M, Mancini C, Oakman JM, Farvolden p. The potential role of haloperidol in the treatment of trichotillomania. J Affect Disord 1999;56:219-26.
16. Gupta MA, Gupta AK. Olanzapine is effective in the management of some self-induced dermatoses: Three case reports. Cutis 2000;66:143-6.
17. Stein DJ, Hollander E. Low-dose pimozide augmentation of serotonin reuptake blockers in the treatment of trichotillomania. J Clin Psych 1992;53:123-6.
18. Senturk V, Tanriverdi N. Resistant trichotillomania and risperidone. Psychosomatics 2002;43:429-30
19. Christenson GA, Popkin MK, Mackenzie TB, Realmuto GM. Lithium treatment of chronic hair pulling. J Clin Psychiatry 1991;52:116-20.
History: Bald at age 9
Ms. D, age 41, began compulsively pulling out and eating her hair at age 8. When she didn’t get her way at home or was nervous about school, she would sit for hours, pulling and eating a strand or two at a time, ultimately ingesting a clump of hair.
By age 9, Ms. D was bald. In grade school, she often wore hats and scarves to class to avoid teasing from other children about her baldness. In high school, she kept to herself and frequently wore wigs.
Ms. D stops pulling for brief periods and her hair grows out, but she invariably resumes pulling when psychosocial stressors mount. Many of life’s normal anxieties—job interviews, work-related stress, social rejection—trigger episodes.
When she is bald, Ms. D pulls and eats hair off her wig. Over the years, she has spent thousands of dollars on custom-made wigs that mask her baldness while feeding her habit.
Ms. D’s episodes are increasingly interfering with her life. She has been steadily employed as an office assistant, but does not socialize with coworkers. She has not dated in years, and during an exacerbation leaves home only to go to work. She also pulls her eyelashes and eyebrows and picks her nails and cuticles.
Ms. D first presented in 1994 after seeing a television segment I did on trichotillomania. At intake, she was wearing a wig and exhibited anxious mood. She also has Crohn’s disease; a gastroenterologist monitors her closely.
Ms. D reports compulsive counting and checking but denies other similar behaviors. No immediate family members have exhibited obsessive-compulsive or hair-pulling behaviors. Her father abused alcohol and a sister has a stuttering problem, although Ms. D denies that these have affected her psychologically.
Ms. D’s hair-pulling behavior suggests:
- a pica disorder
- an impulse control disorder
- or an obsessive-compulsive disorder?
- Recurrent pulling out of one’s own hair, resulting in noticeable hair loss.
- Increasing tension immediately before pulling out the hair or when attempting to resist the behavior.
- Pleasure, gratification, or relief while pulling out the hair.
- The disturbance is not better explained as another mental disorder and is not caused by a dermatological or other general medical condition.
- The disturbance causes clinically significant distress or impairment in social, occupational, or other important areas of functioning.
Source: Reprinted with permission from the Diagnostic and statistical manual of mental disorders, 4th ed., text revision. Copyright 2000. American Psychiatric Association.
Dr. Lundt’s observations
Trichotillomania, defined as compulsive pulling of hair, usually begins in childhood or adolescence. Scalp hair is most commonly pulled, but some patients also pull their eyelashes, pubic hair, and other body hair. Some, especially children, have reportedly pulled their pets’ hair.
Mansueto et al estimate that trichotillomania afflicts approximately 1.5% of males and 3.5% of females.1 These estimates, however, do not include persons with the disorder who are too embarrassed to seek treatment.
DSM-IV-TR classifies trichotillomania as an impulse control disorder (Box). Although comorbid anxiety and depressive disorders are common, Ms. D did not meet criteria for any other psychiatric disorder.
Trichotillomania often is episodic. Months or years of abstinence is common after periods of exacerbation, usually caused by stress (Figure).
Many clinicians mistakenly consider trichotillomania a benign disorder with few consequences beyond alopecia.2 Some patients, however, progress into trichophagia—ingestion of pulled hair. Trichophagia is a form of pica disorder, typically defined as persistent eating of non-nutritive substances. Patients often harbor tremendous shame over their hair-eating behavior and resist psychiatric or medical treatment.2
The undigested hair can form sometimes massive clumps called trichobezoars, which are most common among children and the developmentally disabled.4 Persons with trichophagia face a 37.5% risk of forming a trichobezoar.5 The mass can cause abdominal pain, nausea, vomiting, and weight loss; complications include GI obstruction, ulceration, perforation, and peritonitis.6 An untreated trichobezoar can be fatal,7 although such deaths are rare among patients being treated for trichotillomania.
Patients with trichotillomania often respond to medications used to treat obsessive-compulsive disorder, such as clomipramine. Some clinicians believe this agent is more effective than selective serotonin reuptake inhibitors (SSRIs) but more difficult to tolerate. For Ms. D, I started with both.
Treatment: ‘I Don’t need medication’
Initial treatments—including fluoxetine, 20 mg/d for 6 months; hypnotherapy; and clomipramine, 25 mg/d—were unsuccessful. Ms. D was only marginally compliant, believing that she did not need medication.
I referred Ms. D to an out-of-state residential behavioral program specializing in trichotillomania, but she refused to go even as her hair-pulling intensified. Clomipramine was gradually increased to 75 mg nightly, briefly decreasing her pulling, then to 100 mg nightly when symptoms re-emerged. Clomipramine blood levels were monitored with each dosage change to guard against CNS and cardiac toxicity and other side effects (GI complaints, dizziness, cardiac arrhythmias, somnolence).
After watching for seasonal patterns, I found that Ms. D’s hair-pulling worsened during the winter, although no seasonal change in mood was detected. Phototherapy produced initial success, but Ms. D continued to pull her eyelashes.
Eight weeks later, however, Ms. D’s symptoms escalated. Clomipramine was increased to 150 mg nightly, resulting in blood levels of 99 ng/mL for clomipramine and 204 ng/mL for the metabolite N-desmethylclomipramine—both within the therapeutic range. As she continued pulling, I added buspirone, 10 mg/d.
At this point, would you:
- continue clomipramine and increase the dosage?
- discontinue clomipramine and start another psychotropic?
- or maintain clomipramine at the same dosage and add another psychotropic?
Dr. Lundt’s observations
Drug treatment of trichotillomania has not been studied extensively or long-term, and no consensus exists. Psychoanalysis, cognitive-behavioral therapy (CBT), and hypnotherapy are usually administered with psychotropics.8 Patients often respond to treatment at first, then reach a plateau and resume pulling their hair.9
Numerous psychotropics are used off-label to treat trichotillomania. Several agents have been shown in clinical trials and case reports to reduce hair pulling/eating behaviors (Table), but these findings are limited by small sample size, lack of control groups, and lack of a standard symptom rating scale.
Figure Trichotillomania: Excessive grooming, habit, or vicious circle?
Most clinicians begin with SSRIs because they are generally well tolerated, even at high dosages. Monotherapy often is not adequate for trichotillomania, however. Medication augmentation is common, although little empiric data support this practice.
When clomipramine did not work initally, I explored serotonergic combination strategies.
Table
Medications shown to benefit patients with trichotillomania
| Drug | Evidence | Dosage range (mg/d) | Potential side effects |
|---|---|---|---|
| First-line | |||
| Tricyclic | |||
| Clomipramine | Swedo et al10 | 50 to 300 | Sedation, weight gain, cardiac arrythmias |
| SSRIs | |||
| Fluoxetine | van Minnen et al11 | 20 to 60 | GI symptoms, insomnia |
| Fluvoxamine | Gabriel12 | 50 to 250 | Sexual dysfunction, weight gain |
| Paroxetine | Ravindran et al13 | 20 to 60 | Sexual dysfunction, weight gain |
| Sertraline | Bradford and Gratzer14 | 50 to 200 | Sexual dysfunction, GI symptoms, insomnia |
| Second-line | |||
| Antipsychotics | |||
| Haloperidol | Van Ameringen et al15 | 0.25 to 2 | Sedation, EPS |
| Olanzapine | Gupta and Gupta16 | 2.5 to 10 | Sedation, weight gain |
| Pimozide | Stein and Hollander17 | 25 to 200 | Restlessness, EPS |
| Quetiapine | Khouzam et al8 | 25 to 200 | Sedation |
| Risperidone | Gabriel12 Senturk and Tanriverdi18 | 0.5 to 4.0 | Sedation, hyperprolactinemia |
| Mood stabilizer | |||
| Lithium | Christenson et al19 | 900 to 1,500 | Increased thirst, weight gain, tremor |
| EPS: extrapyramidal symptoms | |||
Further treatment: Relapse, resection
Ms. D was lost to follow-up for 1 year. She returned in 1996, just after undergoing a laparotomy for removal of a trichobezoar large enough to fill two 2-inch-by-6-inch bags. She also had been treated for pneumonia and a pulmonary embolus.
Riddled with shame and embarrassment, Ms. D had stopped pulling for 10 months, during which time she was off medication. Her pulling behaviors re-emerged, however, and clomipramine was restarted and titrated to 250 mg nightly.
One year later, a second trichobezoar was resected. Her clomipramine/N-desmethylclomipramine level reached 1,535 ng/mL, although an ECG reading was normal. Subsequent clomipramine/N-desmethylclomipramine blood levels were within the therapeutic range. Fluvoxamine, 25 mg/d titrated across 6 weeks to 150 mg/d, was added.
Again, Ms. D stopped taking her medications and was lost to follow-up. Her gastroenterologist began managing her care and started sertraline, dosage unknown, to address her depressed mood. A third trichobezoar was removed.
When Ms. D returned to my practice, I resumed CBT and increased sertraline over 1 month from 100 to 300 mg/d. Adding olanzapine, 2.5 mg/d, diminished her anxiety and markedly decreased her hair pulling.
Months later, her hair-pulling/eating behaviors again intensified, resulting in a small-bowel obstruction and a fourth trichobezoar removal. Olanzapine was increased to 5 mg nightly without significant benefit and with sedating effects.
Clomipramine, 125 mg/d, was reintroduced and her symptoms improved dramatically. On a regimen of sertraline, clomipramine and olanzapine, Ms. D remained stable for 2 years.
Last year, however, a fifth trichobezoar measuring 20 x 15 cm was removed. Subsequent trials of methylphenidate, titrated to 72 mg every morning, and tramadol, titrated to 100 mg/d, were unsuccessful.
After 10 years of medication and psychotherapy with three different providers, Ms. D’s hair-pulling/eating behaviors persist. She is taking ziprasidone, 120 mg bid, and naltrexone, 100 mg bid, to help her impulse control, as well as sertraline, 300 mg/d, and clomipramine, 125 mg/d. Another trichobezoar removal—her sixth in 8 years—is scheduled.
What strategies exist for minimizing Ms. D’s hair-pulling behavior and keeping her in therapy?
Dr. Lundt’s observations
Trichotillomania’s waxing and waning course—and its destructive effects on a patient’s self-esteem—pose a clinical challenge. The disorder’s severity can range from cosmetically annoying to life-threatening, as in Ms. D’s case. Patients embarrassed by their behavior often prematurely leave treatment, desperate to cut off all social contact—including medical appointments.
It is crucial to maintain a nonjudgmental, inviting demeanor to alleviate the patient’s fears and facilitate a return to treatment. Support groups, especially online, can help decrease patients’ isolation and provide a reliable information network (see Related resources).
I have had excellent results with other trichotillomania patients—especially children and adolescents. Simply naming their condition and demystifying the problem can be therapeutic. Many patients have responded to SSRIs combined with CBT.
Not long ago, trichotillomania patients were met with ignorance and disbelief within the medical community as the disorder was poorly understood. We need to break this cycle of shame and continue investigating treatment strategies.
- StopPulling.com, an interactive behavioral program for persons with trichotillomania. www.stoppulling.com.
- Penzel F. The hair pulling problem: a complete guide to trichotillomania. New York: Oxford University Press, 2003.
- Keuthen NJ, Stein DJ, Christenson GA. Help for hair pullers: understanding and coping with trichotillomania. Oakland, CA: New Harbinger Publications, 2001.
Drug brand names
- Amitriptyline • Elavil
- Buspirone • BuSpar
- Clomipramine • Anafranil
- Fluoxetine • Prozac
- Fluvoxamine • Luvox
- Haloperidol • Haldol
- Lithium • Eskalith, others
- Methylphenidate • Concerta, Ritalin
- Naltrexone • ReVia
- Olanzapine • Zyprexa
- Paroxetine • Paxil
- Pimozide • Orap
- Quetiapine • Seroquel
- Risperidone • Risperdal
- Sertraline • Zoloft
- Tramadol • Ultram
- Ziprasidone • Geodon
Disclosure
Dr. Lundt receives research grants from and/or is a speaker for Eli Lilly and Co., Pfizer Inc., GlaxoSmithKline, and Bristol-Myers Squibb Co.
History: Bald at age 9
Ms. D, age 41, began compulsively pulling out and eating her hair at age 8. When she didn’t get her way at home or was nervous about school, she would sit for hours, pulling and eating a strand or two at a time, ultimately ingesting a clump of hair.
By age 9, Ms. D was bald. In grade school, she often wore hats and scarves to class to avoid teasing from other children about her baldness. In high school, she kept to herself and frequently wore wigs.
Ms. D stops pulling for brief periods and her hair grows out, but she invariably resumes pulling when psychosocial stressors mount. Many of life’s normal anxieties—job interviews, work-related stress, social rejection—trigger episodes.
When she is bald, Ms. D pulls and eats hair off her wig. Over the years, she has spent thousands of dollars on custom-made wigs that mask her baldness while feeding her habit.
Ms. D’s episodes are increasingly interfering with her life. She has been steadily employed as an office assistant, but does not socialize with coworkers. She has not dated in years, and during an exacerbation leaves home only to go to work. She also pulls her eyelashes and eyebrows and picks her nails and cuticles.
Ms. D first presented in 1994 after seeing a television segment I did on trichotillomania. At intake, she was wearing a wig and exhibited anxious mood. She also has Crohn’s disease; a gastroenterologist monitors her closely.
Ms. D reports compulsive counting and checking but denies other similar behaviors. No immediate family members have exhibited obsessive-compulsive or hair-pulling behaviors. Her father abused alcohol and a sister has a stuttering problem, although Ms. D denies that these have affected her psychologically.
Ms. D’s hair-pulling behavior suggests:
- a pica disorder
- an impulse control disorder
- or an obsessive-compulsive disorder?
- Recurrent pulling out of one’s own hair, resulting in noticeable hair loss.
- Increasing tension immediately before pulling out the hair or when attempting to resist the behavior.
- Pleasure, gratification, or relief while pulling out the hair.
- The disturbance is not better explained as another mental disorder and is not caused by a dermatological or other general medical condition.
- The disturbance causes clinically significant distress or impairment in social, occupational, or other important areas of functioning.
Source: Reprinted with permission from the Diagnostic and statistical manual of mental disorders, 4th ed., text revision. Copyright 2000. American Psychiatric Association.
Dr. Lundt’s observations
Trichotillomania, defined as compulsive pulling of hair, usually begins in childhood or adolescence. Scalp hair is most commonly pulled, but some patients also pull their eyelashes, pubic hair, and other body hair. Some, especially children, have reportedly pulled their pets’ hair.
Mansueto et al estimate that trichotillomania afflicts approximately 1.5% of males and 3.5% of females.1 These estimates, however, do not include persons with the disorder who are too embarrassed to seek treatment.
DSM-IV-TR classifies trichotillomania as an impulse control disorder (Box). Although comorbid anxiety and depressive disorders are common, Ms. D did not meet criteria for any other psychiatric disorder.
Trichotillomania often is episodic. Months or years of abstinence is common after periods of exacerbation, usually caused by stress (Figure).
Many clinicians mistakenly consider trichotillomania a benign disorder with few consequences beyond alopecia.2 Some patients, however, progress into trichophagia—ingestion of pulled hair. Trichophagia is a form of pica disorder, typically defined as persistent eating of non-nutritive substances. Patients often harbor tremendous shame over their hair-eating behavior and resist psychiatric or medical treatment.2
The undigested hair can form sometimes massive clumps called trichobezoars, which are most common among children and the developmentally disabled.4 Persons with trichophagia face a 37.5% risk of forming a trichobezoar.5 The mass can cause abdominal pain, nausea, vomiting, and weight loss; complications include GI obstruction, ulceration, perforation, and peritonitis.6 An untreated trichobezoar can be fatal,7 although such deaths are rare among patients being treated for trichotillomania.
Patients with trichotillomania often respond to medications used to treat obsessive-compulsive disorder, such as clomipramine. Some clinicians believe this agent is more effective than selective serotonin reuptake inhibitors (SSRIs) but more difficult to tolerate. For Ms. D, I started with both.
Treatment: ‘I Don’t need medication’
Initial treatments—including fluoxetine, 20 mg/d for 6 months; hypnotherapy; and clomipramine, 25 mg/d—were unsuccessful. Ms. D was only marginally compliant, believing that she did not need medication.
I referred Ms. D to an out-of-state residential behavioral program specializing in trichotillomania, but she refused to go even as her hair-pulling intensified. Clomipramine was gradually increased to 75 mg nightly, briefly decreasing her pulling, then to 100 mg nightly when symptoms re-emerged. Clomipramine blood levels were monitored with each dosage change to guard against CNS and cardiac toxicity and other side effects (GI complaints, dizziness, cardiac arrhythmias, somnolence).
After watching for seasonal patterns, I found that Ms. D’s hair-pulling worsened during the winter, although no seasonal change in mood was detected. Phototherapy produced initial success, but Ms. D continued to pull her eyelashes.
Eight weeks later, however, Ms. D’s symptoms escalated. Clomipramine was increased to 150 mg nightly, resulting in blood levels of 99 ng/mL for clomipramine and 204 ng/mL for the metabolite N-desmethylclomipramine—both within the therapeutic range. As she continued pulling, I added buspirone, 10 mg/d.
At this point, would you:
- continue clomipramine and increase the dosage?
- discontinue clomipramine and start another psychotropic?
- or maintain clomipramine at the same dosage and add another psychotropic?
Dr. Lundt’s observations
Drug treatment of trichotillomania has not been studied extensively or long-term, and no consensus exists. Psychoanalysis, cognitive-behavioral therapy (CBT), and hypnotherapy are usually administered with psychotropics.8 Patients often respond to treatment at first, then reach a plateau and resume pulling their hair.9
Numerous psychotropics are used off-label to treat trichotillomania. Several agents have been shown in clinical trials and case reports to reduce hair pulling/eating behaviors (Table), but these findings are limited by small sample size, lack of control groups, and lack of a standard symptom rating scale.
Figure Trichotillomania: Excessive grooming, habit, or vicious circle?
Most clinicians begin with SSRIs because they are generally well tolerated, even at high dosages. Monotherapy often is not adequate for trichotillomania, however. Medication augmentation is common, although little empiric data support this practice.
When clomipramine did not work initally, I explored serotonergic combination strategies.
Table
Medications shown to benefit patients with trichotillomania
| Drug | Evidence | Dosage range (mg/d) | Potential side effects |
|---|---|---|---|
| First-line | |||
| Tricyclic | |||
| Clomipramine | Swedo et al10 | 50 to 300 | Sedation, weight gain, cardiac arrythmias |
| SSRIs | |||
| Fluoxetine | van Minnen et al11 | 20 to 60 | GI symptoms, insomnia |
| Fluvoxamine | Gabriel12 | 50 to 250 | Sexual dysfunction, weight gain |
| Paroxetine | Ravindran et al13 | 20 to 60 | Sexual dysfunction, weight gain |
| Sertraline | Bradford and Gratzer14 | 50 to 200 | Sexual dysfunction, GI symptoms, insomnia |
| Second-line | |||
| Antipsychotics | |||
| Haloperidol | Van Ameringen et al15 | 0.25 to 2 | Sedation, EPS |
| Olanzapine | Gupta and Gupta16 | 2.5 to 10 | Sedation, weight gain |
| Pimozide | Stein and Hollander17 | 25 to 200 | Restlessness, EPS |
| Quetiapine | Khouzam et al8 | 25 to 200 | Sedation |
| Risperidone | Gabriel12 Senturk and Tanriverdi18 | 0.5 to 4.0 | Sedation, hyperprolactinemia |
| Mood stabilizer | |||
| Lithium | Christenson et al19 | 900 to 1,500 | Increased thirst, weight gain, tremor |
| EPS: extrapyramidal symptoms | |||
Further treatment: Relapse, resection
Ms. D was lost to follow-up for 1 year. She returned in 1996, just after undergoing a laparotomy for removal of a trichobezoar large enough to fill two 2-inch-by-6-inch bags. She also had been treated for pneumonia and a pulmonary embolus.
Riddled with shame and embarrassment, Ms. D had stopped pulling for 10 months, during which time she was off medication. Her pulling behaviors re-emerged, however, and clomipramine was restarted and titrated to 250 mg nightly.
One year later, a second trichobezoar was resected. Her clomipramine/N-desmethylclomipramine level reached 1,535 ng/mL, although an ECG reading was normal. Subsequent clomipramine/N-desmethylclomipramine blood levels were within the therapeutic range. Fluvoxamine, 25 mg/d titrated across 6 weeks to 150 mg/d, was added.
Again, Ms. D stopped taking her medications and was lost to follow-up. Her gastroenterologist began managing her care and started sertraline, dosage unknown, to address her depressed mood. A third trichobezoar was removed.
When Ms. D returned to my practice, I resumed CBT and increased sertraline over 1 month from 100 to 300 mg/d. Adding olanzapine, 2.5 mg/d, diminished her anxiety and markedly decreased her hair pulling.
Months later, her hair-pulling/eating behaviors again intensified, resulting in a small-bowel obstruction and a fourth trichobezoar removal. Olanzapine was increased to 5 mg nightly without significant benefit and with sedating effects.
Clomipramine, 125 mg/d, was reintroduced and her symptoms improved dramatically. On a regimen of sertraline, clomipramine and olanzapine, Ms. D remained stable for 2 years.
Last year, however, a fifth trichobezoar measuring 20 x 15 cm was removed. Subsequent trials of methylphenidate, titrated to 72 mg every morning, and tramadol, titrated to 100 mg/d, were unsuccessful.
After 10 years of medication and psychotherapy with three different providers, Ms. D’s hair-pulling/eating behaviors persist. She is taking ziprasidone, 120 mg bid, and naltrexone, 100 mg bid, to help her impulse control, as well as sertraline, 300 mg/d, and clomipramine, 125 mg/d. Another trichobezoar removal—her sixth in 8 years—is scheduled.
What strategies exist for minimizing Ms. D’s hair-pulling behavior and keeping her in therapy?
Dr. Lundt’s observations
Trichotillomania’s waxing and waning course—and its destructive effects on a patient’s self-esteem—pose a clinical challenge. The disorder’s severity can range from cosmetically annoying to life-threatening, as in Ms. D’s case. Patients embarrassed by their behavior often prematurely leave treatment, desperate to cut off all social contact—including medical appointments.
It is crucial to maintain a nonjudgmental, inviting demeanor to alleviate the patient’s fears and facilitate a return to treatment. Support groups, especially online, can help decrease patients’ isolation and provide a reliable information network (see Related resources).
I have had excellent results with other trichotillomania patients—especially children and adolescents. Simply naming their condition and demystifying the problem can be therapeutic. Many patients have responded to SSRIs combined with CBT.
Not long ago, trichotillomania patients were met with ignorance and disbelief within the medical community as the disorder was poorly understood. We need to break this cycle of shame and continue investigating treatment strategies.
- StopPulling.com, an interactive behavioral program for persons with trichotillomania. www.stoppulling.com.
- Penzel F. The hair pulling problem: a complete guide to trichotillomania. New York: Oxford University Press, 2003.
- Keuthen NJ, Stein DJ, Christenson GA. Help for hair pullers: understanding and coping with trichotillomania. Oakland, CA: New Harbinger Publications, 2001.
Drug brand names
- Amitriptyline • Elavil
- Buspirone • BuSpar
- Clomipramine • Anafranil
- Fluoxetine • Prozac
- Fluvoxamine • Luvox
- Haloperidol • Haldol
- Lithium • Eskalith, others
- Methylphenidate • Concerta, Ritalin
- Naltrexone • ReVia
- Olanzapine • Zyprexa
- Paroxetine • Paxil
- Pimozide • Orap
- Quetiapine • Seroquel
- Risperidone • Risperdal
- Sertraline • Zoloft
- Tramadol • Ultram
- Ziprasidone • Geodon
Disclosure
Dr. Lundt receives research grants from and/or is a speaker for Eli Lilly and Co., Pfizer Inc., GlaxoSmithKline, and Bristol-Myers Squibb Co.
1. Mansueto C, Ninan PT, Rothbaum B. Trichotillomania and its treatment in adults: a guide for clinicians. Available at: (http://www.trich.org/articles/view_default.asp?filename="0305_Cases" aid=22&yd= researchers_intro). Accessed April 13, 2004
2. Bouwer C, Stein DJ. Trichobezoars in trichotillomania. Psychosom Med 1998;60:658-60.
3. Philippopoulos GS. A case of trichotillomania (hair pulling). Doc Geigy Acta Psychosom 1961;9:304-12.
4. Lee J. Bezoars and foreign bodies in the stomach. Gastrointest Endosc 1996;6:605-19.
5. Christenson GA, Crow SJ. The characterization and treatment of trichotillomania. Clin Psychiatry 1996;57(suppl 8):42-7.
6. Lal MM, Dhall JC. Trichobezoar: A collective analysis of 39 cases from India with a case report. Indian J Pediatr 1975;12:351-3.
7. DeBakey M, Ochsner W. Bezoars and concretions: A comprehensive review of the literature with an analysis of 303 collected cases and a presentation of 8 additional cases. Surgery 1939;4:934-63.
8. Khouzam HR, Battista MA, Byers PE. An overview of trichotillomania and its response to treatment with quetiapine. Psychiatry 2002;65:261-70.
9. Keuthen NJ, Fraim C, Deckersbach T, et al. Longitudinal follow-up of naturalistic treatment outcome in patients with trichotillomania. J Clin Psychiatry 2001;62:101-7.
10. Swedo SE, Leonard HL, Rapoport JL, et al. A double-blind comparison of clomipramine and desipramine in the treatment of trichotillomania (hair pulling). N Engl J Med 1989;8:497-501.
11. van Minnen A, Hoogduin KA, Keijsers GP, et al. Treatment of trichotillomania with behavioral therapy or fluoxetine: a randomized, waiting-list controlled study. Arch Gen Psychiatry 2003;60:517-22.
12. Gabriel A. A case of resistant trichotillomania treated with risperidone-augmented fluvoxamine. Can J Psychiatry 2001;46:285-6.
13. Ravindran AV, Lapierre YD, Anisman H. Obsessive-compulsive spectrum disorders: Effective treatment with paroxetine. Can J Psychiatry 1999;44:805-7.
14. Bradford JM, Gratzer TG. A treatment for impulse control disorders and paraphilia: a case report. Can J Psychiatry 1995;40:4-5.
15. Van Ameringen M, Mancini C, Oakman JM, Farvolden p. The potential role of haloperidol in the treatment of trichotillomania. J Affect Disord 1999;56:219-26.
16. Gupta MA, Gupta AK. Olanzapine is effective in the management of some self-induced dermatoses: Three case reports. Cutis 2000;66:143-6.
17. Stein DJ, Hollander E. Low-dose pimozide augmentation of serotonin reuptake blockers in the treatment of trichotillomania. J Clin Psych 1992;53:123-6.
18. Senturk V, Tanriverdi N. Resistant trichotillomania and risperidone. Psychosomatics 2002;43:429-30
19. Christenson GA, Popkin MK, Mackenzie TB, Realmuto GM. Lithium treatment of chronic hair pulling. J Clin Psychiatry 1991;52:116-20.
1. Mansueto C, Ninan PT, Rothbaum B. Trichotillomania and its treatment in adults: a guide for clinicians. Available at: (http://www.trich.org/articles/view_default.asp?filename="0305_Cases" aid=22&yd= researchers_intro). Accessed April 13, 2004
2. Bouwer C, Stein DJ. Trichobezoars in trichotillomania. Psychosom Med 1998;60:658-60.
3. Philippopoulos GS. A case of trichotillomania (hair pulling). Doc Geigy Acta Psychosom 1961;9:304-12.
4. Lee J. Bezoars and foreign bodies in the stomach. Gastrointest Endosc 1996;6:605-19.
5. Christenson GA, Crow SJ. The characterization and treatment of trichotillomania. Clin Psychiatry 1996;57(suppl 8):42-7.
6. Lal MM, Dhall JC. Trichobezoar: A collective analysis of 39 cases from India with a case report. Indian J Pediatr 1975;12:351-3.
7. DeBakey M, Ochsner W. Bezoars and concretions: A comprehensive review of the literature with an analysis of 303 collected cases and a presentation of 8 additional cases. Surgery 1939;4:934-63.
8. Khouzam HR, Battista MA, Byers PE. An overview of trichotillomania and its response to treatment with quetiapine. Psychiatry 2002;65:261-70.
9. Keuthen NJ, Fraim C, Deckersbach T, et al. Longitudinal follow-up of naturalistic treatment outcome in patients with trichotillomania. J Clin Psychiatry 2001;62:101-7.
10. Swedo SE, Leonard HL, Rapoport JL, et al. A double-blind comparison of clomipramine and desipramine in the treatment of trichotillomania (hair pulling). N Engl J Med 1989;8:497-501.
11. van Minnen A, Hoogduin KA, Keijsers GP, et al. Treatment of trichotillomania with behavioral therapy or fluoxetine: a randomized, waiting-list controlled study. Arch Gen Psychiatry 2003;60:517-22.
12. Gabriel A. A case of resistant trichotillomania treated with risperidone-augmented fluvoxamine. Can J Psychiatry 2001;46:285-6.
13. Ravindran AV, Lapierre YD, Anisman H. Obsessive-compulsive spectrum disorders: Effective treatment with paroxetine. Can J Psychiatry 1999;44:805-7.
14. Bradford JM, Gratzer TG. A treatment for impulse control disorders and paraphilia: a case report. Can J Psychiatry 1995;40:4-5.
15. Van Ameringen M, Mancini C, Oakman JM, Farvolden p. The potential role of haloperidol in the treatment of trichotillomania. J Affect Disord 1999;56:219-26.
16. Gupta MA, Gupta AK. Olanzapine is effective in the management of some self-induced dermatoses: Three case reports. Cutis 2000;66:143-6.
17. Stein DJ, Hollander E. Low-dose pimozide augmentation of serotonin reuptake blockers in the treatment of trichotillomania. J Clin Psych 1992;53:123-6.
18. Senturk V, Tanriverdi N. Resistant trichotillomania and risperidone. Psychosomatics 2002;43:429-30
19. Christenson GA, Popkin MK, Mackenzie TB, Realmuto GM. Lithium treatment of chronic hair pulling. J Clin Psychiatry 1991;52:116-20.
Annual proteinuria screening not cost-effective
Annual screening of adults to detect proteinuria and prevent end-stage renal disease (ESRD) is not cost-effective unless directed only at high-risk groups (that is, those patients with diabetes and hypertension). Screening every 10 years beginning at the age 60 years, however, is highly cost-effective. (LOE=1b)
Annual screening of adults to detect proteinuria and prevent end-stage renal disease (ESRD) is not cost-effective unless directed only at high-risk groups (that is, those patients with diabetes and hypertension). Screening every 10 years beginning at the age 60 years, however, is highly cost-effective. (LOE=1b)
Annual screening of adults to detect proteinuria and prevent end-stage renal disease (ESRD) is not cost-effective unless directed only at high-risk groups (that is, those patients with diabetes and hypertension). Screening every 10 years beginning at the age 60 years, however, is highly cost-effective. (LOE=1b)
