User login
Time-Based Physician Services Require Proper Documentation
Providers typically rely on the “key components” (history, exam, medical decision-making) when documenting in the medical record, and they often misunderstand the use of time when selecting visit levels. Sometimes providers may report a lower service level than warranted because they didn’t feel that they spent the required amount of time with the patient; however, the duration of the visit is an ancillary factor and does not control the level of service to be billed unless more than 50% of the face-to-face time (for non-inpatient services) or more than 50% of the floor time (for inpatient services) is spent providing counseling or coordination of care (C/CC).1 In these instances, providers may choose to document only a brief history and exam, or none at all. They should update the medical decision-making based on the discussion.
Consider the hospitalization of an elderly patient who is newly diagnosed with diabetes. In addition to stabilizing the patient’s glucose levels and devising the appropriate care plan, the patient and/or caregivers also require extensive counseling regarding disease management, lifestyle modification, and medication regime. Coordination of care for outpatient programs and resources is also crucial. To make sure that this qualifies as a time-based service, ensure that the documentation contains the duration, the issues addressed, and the signature of the service provider.
Duration of Counseling and/or Coordination of Care
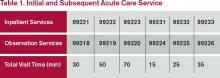
Time is not used for visit level selection if C/CC is minimal (<50%) or absent from the patient encounter. For inpatient services, total visit time is identified as provider face-to-face time (i.e., at the bedside) combined with time spent on the patient’s unit/floor performing services that are directly related to that patient, such as reviewing data, obtaining relevant patient information, and discussing the case with other involved healthcare providers.
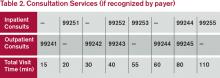
Time associated with activities performed in locations other than the patient’s unit/floor (e.g. reviewing current results or images from the physician’s office) is not allowable in calculating the total visit time. Time associated with teaching students/interns is also excluded, because this doesn’t reflect patient care activities. Once the provider documents all services rendered on a given calendar date, the provider selects the visit level that corresponds with the cumulative visit time documented in the chart (see Tables 1 and 2).
Issues Addressed
When counseling and/or coordination of care dominate more than 50% of the time a physician spends with a patient during an evaluation and management (E/M) service, then time may be considered as the controlling factor to qualify the E/M service for a particular level of care.2 The following must be documented in the patient’s medical record in order to report an E/M service based on time:
- The total length of time of the E/M visit;
- Evidence that more than half of the total length of time of the E/M visit was spent in counseling and coordinating of care; and
- The content of the counseling and coordination of care provided during the E/M visit.
History and exam, if performed or updated, should also be documented, along with the patient response or comprehension of information. An acceptable C/CC time entry may be noted as, “Total visit time = 35 minutes; > 50% spent counseling/coordinating care” or “20 of 35 minutes spent counseling/coordinating care.”
A payer may prefer one documentation style over another. It is always best to query payer policy and review local documentation standards to ensure compliance. Please remember that while this example constitutes the required elements for the notation of time, documentation must also include the details of counseling, care plan revisions, and any information that is pertinent to patient care and communication with other healthcare professionals.
Family Discussions
Family discussions are a typical event involved in taking care of patients and are appropriate to count as C/CC time. Special circumstances are considered when discussions must take place without the patient present. This type of counseling time is recognized but only counts towards C/CC time if the following criteria are met and documented:
- The patient is unable or clinically incompetent to participate in discussions;
- The time is spent on the unit/floor with the family members or surrogate decision makers obtaining a medical history, reviewing the patient’s condition or prognosis, or discussing treatment or limitation(s) of treatment; and
- The conversation bears directly on the management of the patient.3
Time cannot be counted if the discussion takes place in an area outside of the patient’s unit/floor (e.g. in the physician’s office) or if the time is spent counseling the family members through their grieving process.
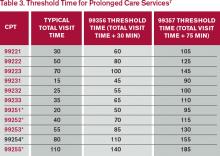
It is fairly common for the family discussion to take place later in the day, after the physician has completed morning rounds. If the earlier encounter involved C/CC, the physician would report the cumulative time spent for that service date. If the earlier encounter was a typical patient assessment incorporating the components of an evaluation (i.e., history update and physical) and management (i.e., care plan review/revision) service, the meeting time may qualify for prolonged care services.
Service Provider
Be sure to count only the physician’s time spent in C/CC. Counseling time by the nursing staff, the social worker, or the resident cannot contribute toward the physician’s total visit time. When more than one physician is involved in services throughout the day, the physicians should select a level of service representative of the combined visits and submit the appropriate code for that level under one physician’s name.4
Consider the following example: The hospitalist takes a brief history about overnight events and reviews some of the pertinent information with the patient. He/she then leaves the room to coordinate the patient’s ongoing care in anticipation that the patient will be discharged over the next few days (25 minutes). The resident is asked to continue the assessment and counsel the patient on the patient’s current disease process (20 minutes).
In the above scenario, the hospitalist is only able to report 99232, because the time spent by the resident is “nonbillable time.”
Carol Pohlig is a billing and coding expert with the University of Pennsylvania Medical Center, Philadelphia. She is also on the faculty of SHM’s inpatient coding course.
References
- Centers for Medicare and Medicaid Services. Medicare Claims Processing Manual: Chapter 12: Physicians/Nonphysician Practitioners, Section 30.6.1B. Available at: www.cms.gov/manuals/downloads/clm104c12.pdf. Accessed December 11, 2014.
- Novitas Solutions, Inc. Frequently Asked Questions: Evaluation and Management Services (Part B). Available at: http://www.novitas-solutions.com/webcenter/faces/oracle/webcenter/page/scopedMD/sad78b265_6797_4ed0_a02f_81627913bc78/Page57.jspx?wc.contextURL=%2Fspaces%2FMedicareJH&wc.originURL=%2Fspaces%2FMedicareJH%2Fpage%2Fpagebyid&contentId=00005056&_afrLoop=1728453012371000#%40%3F_afrLoop%3D1728453012371000%26wc.originURL%3D%252Fspaces%252FMedicareJH%252Fpage%252Fpagebyid%26contentId%3D00005056%26wc.contextURL%3D%252Fspaces%252FMedicareJH%26_adf.ctrl-state%3D610bhasa4_134. Accessed on December 11, 2014.
- Centers for Medicare and Medicaid Services. Medicare National Coverage Determinations Manual: Chapter 1, Part 1: Coverage Determinations, Section 70.1. Available at: www.cms.gov/manuals/downloads/ncd103c1_Part1.pdf. Accessed December 11, 2014.
- Centers for Medicare and Medicaid Services. Medicare Claims Processing Manual: Chapter 12: Physicians/Nonphysician Practitioners, Section 30.6.5. Available at: www.cms.gov/manuals/downloads/clm104c12.pdf. Accessed December 11, 2014.
- Abraham M, Ahlman JT, Boudreau AJ, Connelly J, Levreau-Davis L. Current Procedural Terminology 2014 Professional Edition. Chicago: American Medical Association Press; 2013:1-32.
- Centers for Medicare and Medicaid Services. Medicare Claims Processing Manual: Chapter 12: Physicians/Nonphysician Practitioners, Section 30.6.1C. Available at: www.cms.gov/manuals/downloads/clm104c12.pdf. Accessed December 11, 2014.
- Centers for Medicare and Medicaid Services. Medicare Claims Processing Manual: Chapter 12: Physicians/Nonphysician Practitioners, Section 30.6.15.1G. Available at: www.cms.gov/manuals/downloads/clm104c12.pdf.
Providers typically rely on the “key components” (history, exam, medical decision-making) when documenting in the medical record, and they often misunderstand the use of time when selecting visit levels. Sometimes providers may report a lower service level than warranted because they didn’t feel that they spent the required amount of time with the patient; however, the duration of the visit is an ancillary factor and does not control the level of service to be billed unless more than 50% of the face-to-face time (for non-inpatient services) or more than 50% of the floor time (for inpatient services) is spent providing counseling or coordination of care (C/CC).1 In these instances, providers may choose to document only a brief history and exam, or none at all. They should update the medical decision-making based on the discussion.
Consider the hospitalization of an elderly patient who is newly diagnosed with diabetes. In addition to stabilizing the patient’s glucose levels and devising the appropriate care plan, the patient and/or caregivers also require extensive counseling regarding disease management, lifestyle modification, and medication regime. Coordination of care for outpatient programs and resources is also crucial. To make sure that this qualifies as a time-based service, ensure that the documentation contains the duration, the issues addressed, and the signature of the service provider.
Duration of Counseling and/or Coordination of Care
Time is not used for visit level selection if C/CC is minimal (<50%) or absent from the patient encounter. For inpatient services, total visit time is identified as provider face-to-face time (i.e., at the bedside) combined with time spent on the patient’s unit/floor performing services that are directly related to that patient, such as reviewing data, obtaining relevant patient information, and discussing the case with other involved healthcare providers.
Time associated with activities performed in locations other than the patient’s unit/floor (e.g. reviewing current results or images from the physician’s office) is not allowable in calculating the total visit time. Time associated with teaching students/interns is also excluded, because this doesn’t reflect patient care activities. Once the provider documents all services rendered on a given calendar date, the provider selects the visit level that corresponds with the cumulative visit time documented in the chart (see Tables 1 and 2).
Issues Addressed
When counseling and/or coordination of care dominate more than 50% of the time a physician spends with a patient during an evaluation and management (E/M) service, then time may be considered as the controlling factor to qualify the E/M service for a particular level of care.2 The following must be documented in the patient’s medical record in order to report an E/M service based on time:
- The total length of time of the E/M visit;
- Evidence that more than half of the total length of time of the E/M visit was spent in counseling and coordinating of care; and
- The content of the counseling and coordination of care provided during the E/M visit.
History and exam, if performed or updated, should also be documented, along with the patient response or comprehension of information. An acceptable C/CC time entry may be noted as, “Total visit time = 35 minutes; > 50% spent counseling/coordinating care” or “20 of 35 minutes spent counseling/coordinating care.”
A payer may prefer one documentation style over another. It is always best to query payer policy and review local documentation standards to ensure compliance. Please remember that while this example constitutes the required elements for the notation of time, documentation must also include the details of counseling, care plan revisions, and any information that is pertinent to patient care and communication with other healthcare professionals.
Family Discussions
Family discussions are a typical event involved in taking care of patients and are appropriate to count as C/CC time. Special circumstances are considered when discussions must take place without the patient present. This type of counseling time is recognized but only counts towards C/CC time if the following criteria are met and documented:
- The patient is unable or clinically incompetent to participate in discussions;
- The time is spent on the unit/floor with the family members or surrogate decision makers obtaining a medical history, reviewing the patient’s condition or prognosis, or discussing treatment or limitation(s) of treatment; and
- The conversation bears directly on the management of the patient.3
Time cannot be counted if the discussion takes place in an area outside of the patient’s unit/floor (e.g. in the physician’s office) or if the time is spent counseling the family members through their grieving process.
It is fairly common for the family discussion to take place later in the day, after the physician has completed morning rounds. If the earlier encounter involved C/CC, the physician would report the cumulative time spent for that service date. If the earlier encounter was a typical patient assessment incorporating the components of an evaluation (i.e., history update and physical) and management (i.e., care plan review/revision) service, the meeting time may qualify for prolonged care services.
Service Provider
Be sure to count only the physician’s time spent in C/CC. Counseling time by the nursing staff, the social worker, or the resident cannot contribute toward the physician’s total visit time. When more than one physician is involved in services throughout the day, the physicians should select a level of service representative of the combined visits and submit the appropriate code for that level under one physician’s name.4
Consider the following example: The hospitalist takes a brief history about overnight events and reviews some of the pertinent information with the patient. He/she then leaves the room to coordinate the patient’s ongoing care in anticipation that the patient will be discharged over the next few days (25 minutes). The resident is asked to continue the assessment and counsel the patient on the patient’s current disease process (20 minutes).
In the above scenario, the hospitalist is only able to report 99232, because the time spent by the resident is “nonbillable time.”
Carol Pohlig is a billing and coding expert with the University of Pennsylvania Medical Center, Philadelphia. She is also on the faculty of SHM’s inpatient coding course.
References
- Centers for Medicare and Medicaid Services. Medicare Claims Processing Manual: Chapter 12: Physicians/Nonphysician Practitioners, Section 30.6.1B. Available at: www.cms.gov/manuals/downloads/clm104c12.pdf. Accessed December 11, 2014.
- Novitas Solutions, Inc. Frequently Asked Questions: Evaluation and Management Services (Part B). Available at: http://www.novitas-solutions.com/webcenter/faces/oracle/webcenter/page/scopedMD/sad78b265_6797_4ed0_a02f_81627913bc78/Page57.jspx?wc.contextURL=%2Fspaces%2FMedicareJH&wc.originURL=%2Fspaces%2FMedicareJH%2Fpage%2Fpagebyid&contentId=00005056&_afrLoop=1728453012371000#%40%3F_afrLoop%3D1728453012371000%26wc.originURL%3D%252Fspaces%252FMedicareJH%252Fpage%252Fpagebyid%26contentId%3D00005056%26wc.contextURL%3D%252Fspaces%252FMedicareJH%26_adf.ctrl-state%3D610bhasa4_134. Accessed on December 11, 2014.
- Centers for Medicare and Medicaid Services. Medicare National Coverage Determinations Manual: Chapter 1, Part 1: Coverage Determinations, Section 70.1. Available at: www.cms.gov/manuals/downloads/ncd103c1_Part1.pdf. Accessed December 11, 2014.
- Centers for Medicare and Medicaid Services. Medicare Claims Processing Manual: Chapter 12: Physicians/Nonphysician Practitioners, Section 30.6.5. Available at: www.cms.gov/manuals/downloads/clm104c12.pdf. Accessed December 11, 2014.
- Abraham M, Ahlman JT, Boudreau AJ, Connelly J, Levreau-Davis L. Current Procedural Terminology 2014 Professional Edition. Chicago: American Medical Association Press; 2013:1-32.
- Centers for Medicare and Medicaid Services. Medicare Claims Processing Manual: Chapter 12: Physicians/Nonphysician Practitioners, Section 30.6.1C. Available at: www.cms.gov/manuals/downloads/clm104c12.pdf. Accessed December 11, 2014.
- Centers for Medicare and Medicaid Services. Medicare Claims Processing Manual: Chapter 12: Physicians/Nonphysician Practitioners, Section 30.6.15.1G. Available at: www.cms.gov/manuals/downloads/clm104c12.pdf.
Providers typically rely on the “key components” (history, exam, medical decision-making) when documenting in the medical record, and they often misunderstand the use of time when selecting visit levels. Sometimes providers may report a lower service level than warranted because they didn’t feel that they spent the required amount of time with the patient; however, the duration of the visit is an ancillary factor and does not control the level of service to be billed unless more than 50% of the face-to-face time (for non-inpatient services) or more than 50% of the floor time (for inpatient services) is spent providing counseling or coordination of care (C/CC).1 In these instances, providers may choose to document only a brief history and exam, or none at all. They should update the medical decision-making based on the discussion.
Consider the hospitalization of an elderly patient who is newly diagnosed with diabetes. In addition to stabilizing the patient’s glucose levels and devising the appropriate care plan, the patient and/or caregivers also require extensive counseling regarding disease management, lifestyle modification, and medication regime. Coordination of care for outpatient programs and resources is also crucial. To make sure that this qualifies as a time-based service, ensure that the documentation contains the duration, the issues addressed, and the signature of the service provider.
Duration of Counseling and/or Coordination of Care
Time is not used for visit level selection if C/CC is minimal (<50%) or absent from the patient encounter. For inpatient services, total visit time is identified as provider face-to-face time (i.e., at the bedside) combined with time spent on the patient’s unit/floor performing services that are directly related to that patient, such as reviewing data, obtaining relevant patient information, and discussing the case with other involved healthcare providers.
Time associated with activities performed in locations other than the patient’s unit/floor (e.g. reviewing current results or images from the physician’s office) is not allowable in calculating the total visit time. Time associated with teaching students/interns is also excluded, because this doesn’t reflect patient care activities. Once the provider documents all services rendered on a given calendar date, the provider selects the visit level that corresponds with the cumulative visit time documented in the chart (see Tables 1 and 2).
Issues Addressed
When counseling and/or coordination of care dominate more than 50% of the time a physician spends with a patient during an evaluation and management (E/M) service, then time may be considered as the controlling factor to qualify the E/M service for a particular level of care.2 The following must be documented in the patient’s medical record in order to report an E/M service based on time:
- The total length of time of the E/M visit;
- Evidence that more than half of the total length of time of the E/M visit was spent in counseling and coordinating of care; and
- The content of the counseling and coordination of care provided during the E/M visit.
History and exam, if performed or updated, should also be documented, along with the patient response or comprehension of information. An acceptable C/CC time entry may be noted as, “Total visit time = 35 minutes; > 50% spent counseling/coordinating care” or “20 of 35 minutes spent counseling/coordinating care.”
A payer may prefer one documentation style over another. It is always best to query payer policy and review local documentation standards to ensure compliance. Please remember that while this example constitutes the required elements for the notation of time, documentation must also include the details of counseling, care plan revisions, and any information that is pertinent to patient care and communication with other healthcare professionals.
Family Discussions
Family discussions are a typical event involved in taking care of patients and are appropriate to count as C/CC time. Special circumstances are considered when discussions must take place without the patient present. This type of counseling time is recognized but only counts towards C/CC time if the following criteria are met and documented:
- The patient is unable or clinically incompetent to participate in discussions;
- The time is spent on the unit/floor with the family members or surrogate decision makers obtaining a medical history, reviewing the patient’s condition or prognosis, or discussing treatment or limitation(s) of treatment; and
- The conversation bears directly on the management of the patient.3
Time cannot be counted if the discussion takes place in an area outside of the patient’s unit/floor (e.g. in the physician’s office) or if the time is spent counseling the family members through their grieving process.
It is fairly common for the family discussion to take place later in the day, after the physician has completed morning rounds. If the earlier encounter involved C/CC, the physician would report the cumulative time spent for that service date. If the earlier encounter was a typical patient assessment incorporating the components of an evaluation (i.e., history update and physical) and management (i.e., care plan review/revision) service, the meeting time may qualify for prolonged care services.
Service Provider
Be sure to count only the physician’s time spent in C/CC. Counseling time by the nursing staff, the social worker, or the resident cannot contribute toward the physician’s total visit time. When more than one physician is involved in services throughout the day, the physicians should select a level of service representative of the combined visits and submit the appropriate code for that level under one physician’s name.4
Consider the following example: The hospitalist takes a brief history about overnight events and reviews some of the pertinent information with the patient. He/she then leaves the room to coordinate the patient’s ongoing care in anticipation that the patient will be discharged over the next few days (25 minutes). The resident is asked to continue the assessment and counsel the patient on the patient’s current disease process (20 minutes).
In the above scenario, the hospitalist is only able to report 99232, because the time spent by the resident is “nonbillable time.”
Carol Pohlig is a billing and coding expert with the University of Pennsylvania Medical Center, Philadelphia. She is also on the faculty of SHM’s inpatient coding course.
References
- Centers for Medicare and Medicaid Services. Medicare Claims Processing Manual: Chapter 12: Physicians/Nonphysician Practitioners, Section 30.6.1B. Available at: www.cms.gov/manuals/downloads/clm104c12.pdf. Accessed December 11, 2014.
- Novitas Solutions, Inc. Frequently Asked Questions: Evaluation and Management Services (Part B). Available at: http://www.novitas-solutions.com/webcenter/faces/oracle/webcenter/page/scopedMD/sad78b265_6797_4ed0_a02f_81627913bc78/Page57.jspx?wc.contextURL=%2Fspaces%2FMedicareJH&wc.originURL=%2Fspaces%2FMedicareJH%2Fpage%2Fpagebyid&contentId=00005056&_afrLoop=1728453012371000#%40%3F_afrLoop%3D1728453012371000%26wc.originURL%3D%252Fspaces%252FMedicareJH%252Fpage%252Fpagebyid%26contentId%3D00005056%26wc.contextURL%3D%252Fspaces%252FMedicareJH%26_adf.ctrl-state%3D610bhasa4_134. Accessed on December 11, 2014.
- Centers for Medicare and Medicaid Services. Medicare National Coverage Determinations Manual: Chapter 1, Part 1: Coverage Determinations, Section 70.1. Available at: www.cms.gov/manuals/downloads/ncd103c1_Part1.pdf. Accessed December 11, 2014.
- Centers for Medicare and Medicaid Services. Medicare Claims Processing Manual: Chapter 12: Physicians/Nonphysician Practitioners, Section 30.6.5. Available at: www.cms.gov/manuals/downloads/clm104c12.pdf. Accessed December 11, 2014.
- Abraham M, Ahlman JT, Boudreau AJ, Connelly J, Levreau-Davis L. Current Procedural Terminology 2014 Professional Edition. Chicago: American Medical Association Press; 2013:1-32.
- Centers for Medicare and Medicaid Services. Medicare Claims Processing Manual: Chapter 12: Physicians/Nonphysician Practitioners, Section 30.6.1C. Available at: www.cms.gov/manuals/downloads/clm104c12.pdf. Accessed December 11, 2014.
- Centers for Medicare and Medicaid Services. Medicare Claims Processing Manual: Chapter 12: Physicians/Nonphysician Practitioners, Section 30.6.15.1G. Available at: www.cms.gov/manuals/downloads/clm104c12.pdf.
Vermont Hospital Honored for Reducing Healthcare-Associated Infections
The University of Vermont Medical Center (UVMC), a 562-bed academic facility in Burlington, has been honored with a Partnership in Prevention award for sustainable improvements to eliminate healthcare-associated infections (HAIs). The award, sponsored by the U.S. Department of Health and Human Services, the Association for Professionals in Infection Control and Epidemiology, and the Society for Healthcare Epidemiology of America, recognizes the concepts of the National Action Plan to Prevent Healthcare-Associated Infections: Roadmap to Elimination of the federal Office of Disease Prevention and Health Promotion.
UVMC was honored for creating a culture of safety and collaboration across ranks and disciplines, with a team of infection prevention advocates from the hospital, ambulatory clinics, and dialysis center, along with multi-disciplinary teams focused on infection prevention and control initiatives. The hospital posted a 77% reduction in reported central line-associated blood stream infections (CLABSI) in its medical ICU, and its neonatal ICU went 36 months without a CLABSI. Two surgeon-directed initiatives reduced surgical site infection rates for total knee and hip joint replacements by 81%—with 1,677 consecutive infection-free total knee arthroplasties.
UVMC also joined the Centers for Disease Control and Prevention’s Dialysis Bloodstream Infection Prevention Collaborative in 2009 and has since reduced dialysis-related bloodstream infections by 83%.
One key to its success, according to Anna Noonan, vice president of the Jeffords Institute for Quality and Operational Effectiveness at UVMC, is the fact that executive leadership, infection prevention specialists, clinicians, and quality experts are working together and using data to drive improvement. For example, the medical center implemented protocols for inserting central lines and offered mentored support in its simulation lab for clinicians—including hospitalists—to learn and practice correct insertion techniques.
For more information about UVMC’s award-winning commitment to zero infections, e-mail Noonan at [email protected].
The University of Vermont Medical Center (UVMC), a 562-bed academic facility in Burlington, has been honored with a Partnership in Prevention award for sustainable improvements to eliminate healthcare-associated infections (HAIs). The award, sponsored by the U.S. Department of Health and Human Services, the Association for Professionals in Infection Control and Epidemiology, and the Society for Healthcare Epidemiology of America, recognizes the concepts of the National Action Plan to Prevent Healthcare-Associated Infections: Roadmap to Elimination of the federal Office of Disease Prevention and Health Promotion.
UVMC was honored for creating a culture of safety and collaboration across ranks and disciplines, with a team of infection prevention advocates from the hospital, ambulatory clinics, and dialysis center, along with multi-disciplinary teams focused on infection prevention and control initiatives. The hospital posted a 77% reduction in reported central line-associated blood stream infections (CLABSI) in its medical ICU, and its neonatal ICU went 36 months without a CLABSI. Two surgeon-directed initiatives reduced surgical site infection rates for total knee and hip joint replacements by 81%—with 1,677 consecutive infection-free total knee arthroplasties.
UVMC also joined the Centers for Disease Control and Prevention’s Dialysis Bloodstream Infection Prevention Collaborative in 2009 and has since reduced dialysis-related bloodstream infections by 83%.
One key to its success, according to Anna Noonan, vice president of the Jeffords Institute for Quality and Operational Effectiveness at UVMC, is the fact that executive leadership, infection prevention specialists, clinicians, and quality experts are working together and using data to drive improvement. For example, the medical center implemented protocols for inserting central lines and offered mentored support in its simulation lab for clinicians—including hospitalists—to learn and practice correct insertion techniques.
For more information about UVMC’s award-winning commitment to zero infections, e-mail Noonan at [email protected].
The University of Vermont Medical Center (UVMC), a 562-bed academic facility in Burlington, has been honored with a Partnership in Prevention award for sustainable improvements to eliminate healthcare-associated infections (HAIs). The award, sponsored by the U.S. Department of Health and Human Services, the Association for Professionals in Infection Control and Epidemiology, and the Society for Healthcare Epidemiology of America, recognizes the concepts of the National Action Plan to Prevent Healthcare-Associated Infections: Roadmap to Elimination of the federal Office of Disease Prevention and Health Promotion.
UVMC was honored for creating a culture of safety and collaboration across ranks and disciplines, with a team of infection prevention advocates from the hospital, ambulatory clinics, and dialysis center, along with multi-disciplinary teams focused on infection prevention and control initiatives. The hospital posted a 77% reduction in reported central line-associated blood stream infections (CLABSI) in its medical ICU, and its neonatal ICU went 36 months without a CLABSI. Two surgeon-directed initiatives reduced surgical site infection rates for total knee and hip joint replacements by 81%—with 1,677 consecutive infection-free total knee arthroplasties.
UVMC also joined the Centers for Disease Control and Prevention’s Dialysis Bloodstream Infection Prevention Collaborative in 2009 and has since reduced dialysis-related bloodstream infections by 83%.
One key to its success, according to Anna Noonan, vice president of the Jeffords Institute for Quality and Operational Effectiveness at UVMC, is the fact that executive leadership, infection prevention specialists, clinicians, and quality experts are working together and using data to drive improvement. For example, the medical center implemented protocols for inserting central lines and offered mentored support in its simulation lab for clinicians—including hospitalists—to learn and practice correct insertion techniques.
For more information about UVMC’s award-winning commitment to zero infections, e-mail Noonan at [email protected].
Hospitals Preparing for Climate Change Win Support from White House
On Dec. 15 at a White House Roundtable, the U.S. Department of Health and Human Services (HHS) unveiled its Sustainable and Climate Resilient Health Care Facilities Initiative [PDF], with a new guide to help health facilities enhance their resilience to extreme weather events. Part of the President’s Climate Action Plan, the guide offers a planning framework, case studies of responses to historical extreme weather events, and emerging practices for improving infrastructure resilience. A best practices document and accompanying web-based toolkit are planned for 2015.
HHS considers climate change one of the top public health challenges of our time, and hospitals are an essential part of the country’s responsiveness to the negative impacts of heat waves, floods, wildfires, worsened air pollution, and extreme storms and their aftermath. Damage to hospitals themselves is another key issue, one that was dramatically illustrated by the ravages of Hurricane Katrina in 2005. Climate change is expected to increase the severity of some extreme weather and could alter the range and intensity of infectious diseases, according to the HHS report.
Steps for building a climate-resilient healthcare sector, outlined in the new guide, start with raising awareness among health professionals about climate-related health impacts, particular issues in their regions, and specific resilience strategies. The guide also recommends assessing the vulnerabilities of health facilities, communities, and at-risk populations; building partnerships with energy, transportation, and other sectors of the community; and developing robust communication channels.
On Dec. 15 at a White House Roundtable, the U.S. Department of Health and Human Services (HHS) unveiled its Sustainable and Climate Resilient Health Care Facilities Initiative [PDF], with a new guide to help health facilities enhance their resilience to extreme weather events. Part of the President’s Climate Action Plan, the guide offers a planning framework, case studies of responses to historical extreme weather events, and emerging practices for improving infrastructure resilience. A best practices document and accompanying web-based toolkit are planned for 2015.
HHS considers climate change one of the top public health challenges of our time, and hospitals are an essential part of the country’s responsiveness to the negative impacts of heat waves, floods, wildfires, worsened air pollution, and extreme storms and their aftermath. Damage to hospitals themselves is another key issue, one that was dramatically illustrated by the ravages of Hurricane Katrina in 2005. Climate change is expected to increase the severity of some extreme weather and could alter the range and intensity of infectious diseases, according to the HHS report.
Steps for building a climate-resilient healthcare sector, outlined in the new guide, start with raising awareness among health professionals about climate-related health impacts, particular issues in their regions, and specific resilience strategies. The guide also recommends assessing the vulnerabilities of health facilities, communities, and at-risk populations; building partnerships with energy, transportation, and other sectors of the community; and developing robust communication channels.
On Dec. 15 at a White House Roundtable, the U.S. Department of Health and Human Services (HHS) unveiled its Sustainable and Climate Resilient Health Care Facilities Initiative [PDF], with a new guide to help health facilities enhance their resilience to extreme weather events. Part of the President’s Climate Action Plan, the guide offers a planning framework, case studies of responses to historical extreme weather events, and emerging practices for improving infrastructure resilience. A best practices document and accompanying web-based toolkit are planned for 2015.
HHS considers climate change one of the top public health challenges of our time, and hospitals are an essential part of the country’s responsiveness to the negative impacts of heat waves, floods, wildfires, worsened air pollution, and extreme storms and their aftermath. Damage to hospitals themselves is another key issue, one that was dramatically illustrated by the ravages of Hurricane Katrina in 2005. Climate change is expected to increase the severity of some extreme weather and could alter the range and intensity of infectious diseases, according to the HHS report.
Steps for building a climate-resilient healthcare sector, outlined in the new guide, start with raising awareness among health professionals about climate-related health impacts, particular issues in their regions, and specific resilience strategies. The guide also recommends assessing the vulnerabilities of health facilities, communities, and at-risk populations; building partnerships with energy, transportation, and other sectors of the community; and developing robust communication channels.
Pediatric Hospitals Identify Patient Care Benchmarks
Citing a lack of accepted benchmarks for quality improvement in pediatric hospital care, researchers described in Pediatrics their process of establishing benchmarks for the treatment of asthma, bronchiolitis, and pneumonia, three common conditions treated by pediatric hospitalists that together amount to 10% of all pediatric hospital admissions. Despite the existence of evidence-based guidelines for these conditions, there is wide variation in adherence by U.S. hospitals.
The researchers, led by Kavita Parikh, MD, MSHM, a pediatric hospitalist at Children’s National Health System and assistant professor of pediatrics at George Washington University School of Medicine and Health Sciences, both in Washington, D.C., measured 2012 performance in freestanding children’s hospitals using recognized clinical quality indicators and data reported to the Pediatric Health Information System of the Children’s Hospital Association to construct what they call “achievable benchmarks of care,” or ABC. The ABCs are calculated from performance averages at the high-performing children’s hospitals.
“In other words, we identified the best measured performance for each quality indicator, based on actual data reflecting the intricacies of real-world pediatric care,” Dr. Parikh recently told Medscape.
The ABCs also emphasize avoiding the overuse of certain treatments that have a potential risk for adverse events. “High performers did not overutilize nonrecommended services,” Dr. Kavikh says.
Citing a lack of accepted benchmarks for quality improvement in pediatric hospital care, researchers described in Pediatrics their process of establishing benchmarks for the treatment of asthma, bronchiolitis, and pneumonia, three common conditions treated by pediatric hospitalists that together amount to 10% of all pediatric hospital admissions. Despite the existence of evidence-based guidelines for these conditions, there is wide variation in adherence by U.S. hospitals.
The researchers, led by Kavita Parikh, MD, MSHM, a pediatric hospitalist at Children’s National Health System and assistant professor of pediatrics at George Washington University School of Medicine and Health Sciences, both in Washington, D.C., measured 2012 performance in freestanding children’s hospitals using recognized clinical quality indicators and data reported to the Pediatric Health Information System of the Children’s Hospital Association to construct what they call “achievable benchmarks of care,” or ABC. The ABCs are calculated from performance averages at the high-performing children’s hospitals.
“In other words, we identified the best measured performance for each quality indicator, based on actual data reflecting the intricacies of real-world pediatric care,” Dr. Parikh recently told Medscape.
The ABCs also emphasize avoiding the overuse of certain treatments that have a potential risk for adverse events. “High performers did not overutilize nonrecommended services,” Dr. Kavikh says.
Citing a lack of accepted benchmarks for quality improvement in pediatric hospital care, researchers described in Pediatrics their process of establishing benchmarks for the treatment of asthma, bronchiolitis, and pneumonia, three common conditions treated by pediatric hospitalists that together amount to 10% of all pediatric hospital admissions. Despite the existence of evidence-based guidelines for these conditions, there is wide variation in adherence by U.S. hospitals.
The researchers, led by Kavita Parikh, MD, MSHM, a pediatric hospitalist at Children’s National Health System and assistant professor of pediatrics at George Washington University School of Medicine and Health Sciences, both in Washington, D.C., measured 2012 performance in freestanding children’s hospitals using recognized clinical quality indicators and data reported to the Pediatric Health Information System of the Children’s Hospital Association to construct what they call “achievable benchmarks of care,” or ABC. The ABCs are calculated from performance averages at the high-performing children’s hospitals.
“In other words, we identified the best measured performance for each quality indicator, based on actual data reflecting the intricacies of real-world pediatric care,” Dr. Parikh recently told Medscape.
The ABCs also emphasize avoiding the overuse of certain treatments that have a potential risk for adverse events. “High performers did not overutilize nonrecommended services,” Dr. Kavikh says.
Fewer Hospital-Acquired Conditions Saves Estimated 50,000 Lives
Estimated total number of saved lives from 2011 to 2013 as a result of reductions in the incidence of hospital-acquired conditions (HACs) in U.S. hospitals, compared with HAC rates in 2010, according to the U.S. Department of Health and Human Services (HHS). In 1999, the Institute of Medicine estimated that as many as 98,000 deaths per year resulted from avoidable hospital errors, such as central line-associated blood stream infections, adverse drug events, falls, and bedsores. Rates of avoidable medical errors fell by 17% between 2010 and 2013, (HHS) reports, which resulted in 1.3 million fewer HACs than expected and overall savings of $12 billion for the healthcare system.
Estimated total number of saved lives from 2011 to 2013 as a result of reductions in the incidence of hospital-acquired conditions (HACs) in U.S. hospitals, compared with HAC rates in 2010, according to the U.S. Department of Health and Human Services (HHS). In 1999, the Institute of Medicine estimated that as many as 98,000 deaths per year resulted from avoidable hospital errors, such as central line-associated blood stream infections, adverse drug events, falls, and bedsores. Rates of avoidable medical errors fell by 17% between 2010 and 2013, (HHS) reports, which resulted in 1.3 million fewer HACs than expected and overall savings of $12 billion for the healthcare system.
Estimated total number of saved lives from 2011 to 2013 as a result of reductions in the incidence of hospital-acquired conditions (HACs) in U.S. hospitals, compared with HAC rates in 2010, according to the U.S. Department of Health and Human Services (HHS). In 1999, the Institute of Medicine estimated that as many as 98,000 deaths per year resulted from avoidable hospital errors, such as central line-associated blood stream infections, adverse drug events, falls, and bedsores. Rates of avoidable medical errors fell by 17% between 2010 and 2013, (HHS) reports, which resulted in 1.3 million fewer HACs than expected and overall savings of $12 billion for the healthcare system.
Society of Hospital Medicine's 2015 Annual Meeting Adds Focus on Early Career Hospitalists
I recall my first time at a national physicians conference. Moving from room to room amongst a sea of medical professionals from across the nation, I felt a bit lost. Which sessions should I attend? How could I maximize learning in my limited time there? Should I enter the cavernous hall for the plenary session?
There were so many offerings, and who knew what might be relevant for me at that early stage of training? (I remember thinking, what the heck is an “RVU”?)
Fear not, future and early career hospitalists: SHM has created a dedicated track and special sessions at HM15 with your issues and concerns in mind.
For the first time, SHM’s annual meeting is offering an educational track specifically tailored to medical students, residents, and early career hospitalists. The “Young Hospitalist” track will be delivered by speakers from the Physicians in Training Committee and will be enhanced by a special luncheon for students and residents, followed by the afternoon Research, Innovations, and Clinical Vignettes abstract presentations.
This month’s “Future Hospitalist” column provides a sneak peek at all of the content in this track. All sessions will be on Monday, March 30, at the Gaylord National Resort and Conference Center in National Harbor, Md. (www.hospitalmedicine2015.org).
“Career Pathways in Hospital Medicine: Getting Your Ideal Job–One Job at a Time”
10:35 a.m. to 11:15 a.m.
This session will explore the many avenues a hospitalist’s career may take, including clinical medicine, administration, hospital leadership, and academic hospital medicine. It will highlight the value of being open to different opportunities and explain how such opportunities can ignite and shape one’s career over the long term.
Through the stories and career trajectories of real hospitalists, the faculty will demonstrate how teaching students and residents, getting involved in patient-related projects, and joining local or national committees can open the door to further opportunities.
Discussion will highlight the ways in which incorporating any one or more of these hospital medicine “extras” into your ongoing responsibilities might be the crucial ingredient to help you find, achieve, and/or create your ideal job.
“How to Stand Out: Being the Best Applicant You Can Be”
11:20 a.m. to noon
This session will focus on the practical skills and information needed to embark on a fulfilling career in hospital medicine. Topics covered in this session will include effective ways to search for a job and maximize the impression you make on potential employers. We will help you identify which mentors can guide you through this process. You will learn how to leverage what you’ve done in training, or just out of training, to make yourself an attractive applicant. We will cover the do’s and don’ts of correspondence with prospective employers and essential questions to ask during interviews.
“Getting to the Top of the Pile: How to Write the Best CV”
1:10 p.m. to 1:50 p.m.
A good CV can be a gateway to a great career in hospital medicine, but a poorly formatted CV can underrepresent a strong future hospitalist, limiting opportunities. This session will provide detailed information about what hospitalist leaders look for in a CV, and dissect good and bad CVs. You will hear strategies for ensuring that your CV will be both attention grabbing and effective.
“Quality and Patient Safety for Residents and Students”
1:55 p.m. to 2:25 p.m.
Students and residents are required to have at least some quality and patient safety exposure during their training; however, it is often not until they embark upon their own careers that they realize the critical role quality and safety play in both hospital operations and patient care. In this session, we will use interactive methods and case studies to help students, residents, and early career hospitalists learn how to make the most of opportunities in quality and safety. Through these methods, we will illustrate how hospitalists can effect change within these realms even when they are just starting their careers.
“Time Management”
2:45 p.m. to 3:25 p.m.
Time management can be a challenge for any hospitalist, but it’s especially challenging early in one’s career. This session is taught by experienced hospitalists who have learned how to succeed and thrive in various venues. Presenters will examine a typical hospitalist workday and review clinical practices that help enhance efficiency and organization on the wards.
In addition, presenters will walk through different patient care scenarios and discuss strategies for maximizing the face time spent with patients and our workflow outside the patient’s room. Faculty will use examples but will leave time at the end of the session for Q&A and for sharing of techniques.
“Making the Most of Mentorship”
3:30 p.m. to 4:10 p.m.
A great mentor/mentee relationship can be a springboard to a promising career in hospital medicine. This session will help attendees to understand the importance and impact of mentorship. We will demonstrate how to identify and approach mentors—including project mentors—and to create meaningful relationships that can be both personally and professionally rewarding. Areas of focus will include choosing and planning academic, operational, or clinical projects, as well as evaluating career choices.
In addition to the above session offerings, a cornerstone of our student/resident track will be the special luncheon for medical students and residents. We will have assembled some of the best and the brightest within the field to sit with you and provide career mentoring and advice. Students and residents will have the chance to chat informally with nationally recognized leaders in diverse realms such as HM administration, academia, quality, information technology, and more.
Act now if you are interested in attending; space will be limited, and we ask that you register in advance at www.hospitalmedicine2015.org/program.
We also encourage you to attend the Research, Innovations, and Clinical Vignettes (RIV) abstract competition. Many of the concepts presented in the “Young Hospitalists” track will be illustrated in the work displayed here, and it’s a great chance to see these themes and possibilities played out in more detail. Moreover, this year you can show support for your colleagues who have achieved the new Trainee Award, which will recognize resident and student authors within each category.
The first day of HM15 promises to be an exciting opportunity for budding hospitalists to connect with each other and learn a bit about the job application process and career development. We hope you can join us next month.
Dr. Tad-y is assistant professor of medicine, associate program director of the internal medicine residency program, and associate program director of the hospitalist training program at the University of Colorado School of Medicine in Aurora. Dr. Steinberg is associate professor of medicine, associate chair for education, and residency program director in the Department of Medicine at Mount Sinai Beth Israel Icahn School of Medicine in New York City. Dr. Donahue is assistant professor of medicine in the division of hospital medicine, department of medicine, at the University of Massachusetts Medical School in Boston. Debra Beach is SHM’s manager of membership outreach programs.
All three authors are members of SHM’s Physicians in Training Committee. Other members of the committee also contributed to this report.
I recall my first time at a national physicians conference. Moving from room to room amongst a sea of medical professionals from across the nation, I felt a bit lost. Which sessions should I attend? How could I maximize learning in my limited time there? Should I enter the cavernous hall for the plenary session?
There were so many offerings, and who knew what might be relevant for me at that early stage of training? (I remember thinking, what the heck is an “RVU”?)
Fear not, future and early career hospitalists: SHM has created a dedicated track and special sessions at HM15 with your issues and concerns in mind.
For the first time, SHM’s annual meeting is offering an educational track specifically tailored to medical students, residents, and early career hospitalists. The “Young Hospitalist” track will be delivered by speakers from the Physicians in Training Committee and will be enhanced by a special luncheon for students and residents, followed by the afternoon Research, Innovations, and Clinical Vignettes abstract presentations.
This month’s “Future Hospitalist” column provides a sneak peek at all of the content in this track. All sessions will be on Monday, March 30, at the Gaylord National Resort and Conference Center in National Harbor, Md. (www.hospitalmedicine2015.org).
“Career Pathways in Hospital Medicine: Getting Your Ideal Job–One Job at a Time”
10:35 a.m. to 11:15 a.m.
This session will explore the many avenues a hospitalist’s career may take, including clinical medicine, administration, hospital leadership, and academic hospital medicine. It will highlight the value of being open to different opportunities and explain how such opportunities can ignite and shape one’s career over the long term.
Through the stories and career trajectories of real hospitalists, the faculty will demonstrate how teaching students and residents, getting involved in patient-related projects, and joining local or national committees can open the door to further opportunities.
Discussion will highlight the ways in which incorporating any one or more of these hospital medicine “extras” into your ongoing responsibilities might be the crucial ingredient to help you find, achieve, and/or create your ideal job.
“How to Stand Out: Being the Best Applicant You Can Be”
11:20 a.m. to noon
This session will focus on the practical skills and information needed to embark on a fulfilling career in hospital medicine. Topics covered in this session will include effective ways to search for a job and maximize the impression you make on potential employers. We will help you identify which mentors can guide you through this process. You will learn how to leverage what you’ve done in training, or just out of training, to make yourself an attractive applicant. We will cover the do’s and don’ts of correspondence with prospective employers and essential questions to ask during interviews.
“Getting to the Top of the Pile: How to Write the Best CV”
1:10 p.m. to 1:50 p.m.
A good CV can be a gateway to a great career in hospital medicine, but a poorly formatted CV can underrepresent a strong future hospitalist, limiting opportunities. This session will provide detailed information about what hospitalist leaders look for in a CV, and dissect good and bad CVs. You will hear strategies for ensuring that your CV will be both attention grabbing and effective.
“Quality and Patient Safety for Residents and Students”
1:55 p.m. to 2:25 p.m.
Students and residents are required to have at least some quality and patient safety exposure during their training; however, it is often not until they embark upon their own careers that they realize the critical role quality and safety play in both hospital operations and patient care. In this session, we will use interactive methods and case studies to help students, residents, and early career hospitalists learn how to make the most of opportunities in quality and safety. Through these methods, we will illustrate how hospitalists can effect change within these realms even when they are just starting their careers.
“Time Management”
2:45 p.m. to 3:25 p.m.
Time management can be a challenge for any hospitalist, but it’s especially challenging early in one’s career. This session is taught by experienced hospitalists who have learned how to succeed and thrive in various venues. Presenters will examine a typical hospitalist workday and review clinical practices that help enhance efficiency and organization on the wards.
In addition, presenters will walk through different patient care scenarios and discuss strategies for maximizing the face time spent with patients and our workflow outside the patient’s room. Faculty will use examples but will leave time at the end of the session for Q&A and for sharing of techniques.
“Making the Most of Mentorship”
3:30 p.m. to 4:10 p.m.
A great mentor/mentee relationship can be a springboard to a promising career in hospital medicine. This session will help attendees to understand the importance and impact of mentorship. We will demonstrate how to identify and approach mentors—including project mentors—and to create meaningful relationships that can be both personally and professionally rewarding. Areas of focus will include choosing and planning academic, operational, or clinical projects, as well as evaluating career choices.
In addition to the above session offerings, a cornerstone of our student/resident track will be the special luncheon for medical students and residents. We will have assembled some of the best and the brightest within the field to sit with you and provide career mentoring and advice. Students and residents will have the chance to chat informally with nationally recognized leaders in diverse realms such as HM administration, academia, quality, information technology, and more.
Act now if you are interested in attending; space will be limited, and we ask that you register in advance at www.hospitalmedicine2015.org/program.
We also encourage you to attend the Research, Innovations, and Clinical Vignettes (RIV) abstract competition. Many of the concepts presented in the “Young Hospitalists” track will be illustrated in the work displayed here, and it’s a great chance to see these themes and possibilities played out in more detail. Moreover, this year you can show support for your colleagues who have achieved the new Trainee Award, which will recognize resident and student authors within each category.
The first day of HM15 promises to be an exciting opportunity for budding hospitalists to connect with each other and learn a bit about the job application process and career development. We hope you can join us next month.
Dr. Tad-y is assistant professor of medicine, associate program director of the internal medicine residency program, and associate program director of the hospitalist training program at the University of Colorado School of Medicine in Aurora. Dr. Steinberg is associate professor of medicine, associate chair for education, and residency program director in the Department of Medicine at Mount Sinai Beth Israel Icahn School of Medicine in New York City. Dr. Donahue is assistant professor of medicine in the division of hospital medicine, department of medicine, at the University of Massachusetts Medical School in Boston. Debra Beach is SHM’s manager of membership outreach programs.
All three authors are members of SHM’s Physicians in Training Committee. Other members of the committee also contributed to this report.
I recall my first time at a national physicians conference. Moving from room to room amongst a sea of medical professionals from across the nation, I felt a bit lost. Which sessions should I attend? How could I maximize learning in my limited time there? Should I enter the cavernous hall for the plenary session?
There were so many offerings, and who knew what might be relevant for me at that early stage of training? (I remember thinking, what the heck is an “RVU”?)
Fear not, future and early career hospitalists: SHM has created a dedicated track and special sessions at HM15 with your issues and concerns in mind.
For the first time, SHM’s annual meeting is offering an educational track specifically tailored to medical students, residents, and early career hospitalists. The “Young Hospitalist” track will be delivered by speakers from the Physicians in Training Committee and will be enhanced by a special luncheon for students and residents, followed by the afternoon Research, Innovations, and Clinical Vignettes abstract presentations.
This month’s “Future Hospitalist” column provides a sneak peek at all of the content in this track. All sessions will be on Monday, March 30, at the Gaylord National Resort and Conference Center in National Harbor, Md. (www.hospitalmedicine2015.org).
“Career Pathways in Hospital Medicine: Getting Your Ideal Job–One Job at a Time”
10:35 a.m. to 11:15 a.m.
This session will explore the many avenues a hospitalist’s career may take, including clinical medicine, administration, hospital leadership, and academic hospital medicine. It will highlight the value of being open to different opportunities and explain how such opportunities can ignite and shape one’s career over the long term.
Through the stories and career trajectories of real hospitalists, the faculty will demonstrate how teaching students and residents, getting involved in patient-related projects, and joining local or national committees can open the door to further opportunities.
Discussion will highlight the ways in which incorporating any one or more of these hospital medicine “extras” into your ongoing responsibilities might be the crucial ingredient to help you find, achieve, and/or create your ideal job.
“How to Stand Out: Being the Best Applicant You Can Be”
11:20 a.m. to noon
This session will focus on the practical skills and information needed to embark on a fulfilling career in hospital medicine. Topics covered in this session will include effective ways to search for a job and maximize the impression you make on potential employers. We will help you identify which mentors can guide you through this process. You will learn how to leverage what you’ve done in training, or just out of training, to make yourself an attractive applicant. We will cover the do’s and don’ts of correspondence with prospective employers and essential questions to ask during interviews.
“Getting to the Top of the Pile: How to Write the Best CV”
1:10 p.m. to 1:50 p.m.
A good CV can be a gateway to a great career in hospital medicine, but a poorly formatted CV can underrepresent a strong future hospitalist, limiting opportunities. This session will provide detailed information about what hospitalist leaders look for in a CV, and dissect good and bad CVs. You will hear strategies for ensuring that your CV will be both attention grabbing and effective.
“Quality and Patient Safety for Residents and Students”
1:55 p.m. to 2:25 p.m.
Students and residents are required to have at least some quality and patient safety exposure during their training; however, it is often not until they embark upon their own careers that they realize the critical role quality and safety play in both hospital operations and patient care. In this session, we will use interactive methods and case studies to help students, residents, and early career hospitalists learn how to make the most of opportunities in quality and safety. Through these methods, we will illustrate how hospitalists can effect change within these realms even when they are just starting their careers.
“Time Management”
2:45 p.m. to 3:25 p.m.
Time management can be a challenge for any hospitalist, but it’s especially challenging early in one’s career. This session is taught by experienced hospitalists who have learned how to succeed and thrive in various venues. Presenters will examine a typical hospitalist workday and review clinical practices that help enhance efficiency and organization on the wards.
In addition, presenters will walk through different patient care scenarios and discuss strategies for maximizing the face time spent with patients and our workflow outside the patient’s room. Faculty will use examples but will leave time at the end of the session for Q&A and for sharing of techniques.
“Making the Most of Mentorship”
3:30 p.m. to 4:10 p.m.
A great mentor/mentee relationship can be a springboard to a promising career in hospital medicine. This session will help attendees to understand the importance and impact of mentorship. We will demonstrate how to identify and approach mentors—including project mentors—and to create meaningful relationships that can be both personally and professionally rewarding. Areas of focus will include choosing and planning academic, operational, or clinical projects, as well as evaluating career choices.
In addition to the above session offerings, a cornerstone of our student/resident track will be the special luncheon for medical students and residents. We will have assembled some of the best and the brightest within the field to sit with you and provide career mentoring and advice. Students and residents will have the chance to chat informally with nationally recognized leaders in diverse realms such as HM administration, academia, quality, information technology, and more.
Act now if you are interested in attending; space will be limited, and we ask that you register in advance at www.hospitalmedicine2015.org/program.
We also encourage you to attend the Research, Innovations, and Clinical Vignettes (RIV) abstract competition. Many of the concepts presented in the “Young Hospitalists” track will be illustrated in the work displayed here, and it’s a great chance to see these themes and possibilities played out in more detail. Moreover, this year you can show support for your colleagues who have achieved the new Trainee Award, which will recognize resident and student authors within each category.
The first day of HM15 promises to be an exciting opportunity for budding hospitalists to connect with each other and learn a bit about the job application process and career development. We hope you can join us next month.
Dr. Tad-y is assistant professor of medicine, associate program director of the internal medicine residency program, and associate program director of the hospitalist training program at the University of Colorado School of Medicine in Aurora. Dr. Steinberg is associate professor of medicine, associate chair for education, and residency program director in the Department of Medicine at Mount Sinai Beth Israel Icahn School of Medicine in New York City. Dr. Donahue is assistant professor of medicine in the division of hospital medicine, department of medicine, at the University of Massachusetts Medical School in Boston. Debra Beach is SHM’s manager of membership outreach programs.
All three authors are members of SHM’s Physicians in Training Committee. Other members of the committee also contributed to this report.
Dr. Peter Pronovost to Speak to Hospitalists About Healthcare Quality at HM15
Type the name Peter Pronovost into Google and try to make it past the “n” before the word “checklist” pops up. That’s because Peter Pronovost, MD, PhD, FCCM, senior vice president for patient safety and quality at Johns Hopkins Medicine in Baltimore, is the “checklist doctor,” widely known for a five-step checklist designed to reduce the incidence of central-line infections and credited by SHM with saving thousands of lives. He was named one of the 100 Most Influential People in the World by Time magazine, and he co-authored a book, “Safe Patients, Smart Hospitals: How One Doctor’s Checklist Can Help Us Change Health Care from the Inside Out.”
Dr. Pronovost is one of three keynote speakers slated to offer their wisdom and insights to thousands of hospitalists attending HM15, scheduled for March 29-April 1 at the Gaylord National Resort and Convention Center in National Harbor, Md.
And before you ask—yes, he smiles when people call him the “checklist guy.”
“These catheter infections, just to give you an example, they used to kill as many people as breast or prostate cancer in the U.S. This isn’t some trivial public health problem,” Dr. Pronovost says. “This is a public health problem the size of breast or prostate cancer. And we virtually eliminated it, [which is] pretty remarkable about what the potential of this approach is in healthcare. That is just one harm. We have a lot of other things to go still.”
Dr. Pronovost, director of the Armstrong Institute for Patient Safety and Quality at Johns Hopkins, has titled his HM15 talk, “Taking Quality to the Next Level.” One of his main beliefs is that intrinsically motivated efforts are much more successful than payment carrots or sticks wielded by the Centers for Medicare and Medicaid Services (CMS).

—Dr. Pronovost
“We tap into this incredibly rich and passionate juice of improvement work,” he says of intrinsic motivation. “Whether it’s through a church or through a club, all of us have felt that when you connect to a community, the energy and the passion that that unleashes. Hospitalists have the wisdom to know what to do and how to do it right, and it’s just so much more effective when you tap into intrinsic motivation.”
His famed checklist was a great start to that, but he says more needs to be done. That work looked at eliminating a single hospital-acquired condition. Now, Dr. Pronovost has reframed the question: Can we eliminate all harms? What if hospitals listed out all harms and then gave each a checklist?
“It quickly gets to well beyond the potential of human memory, because there are about 150 things we have to do,” he says. “So I’m going to be showcasing a new app that we made that gives you real-time compliance with all those checklists. If I’m missing any one of those 150 things, there’s a red box next to the patient’s name, and all I have to go do is click on the red box and see what I’m missing.”
Dr. Pronovost sees that approach as a fundamental shift in how safety is viewed. It can’t be based on “heroism,” when someone remembers to remember something; rather, it needs to be rooted in properly designed systems that leverage technology to achieve desired results.
To look at it another way, consider a conversation Dr. Pronovost had with friends in engineering who previously worked on missions launching satellites into space.
“They said to me, ‘Peter, you guys are thinking about this backwards in healthcare. If we had to put a mission up…it can blow up for 12 reasons. It didn’t blow up for reason No. 1—call it a bloodstream infection—but it did blow up for reasons 2 through 12, do you think we’d be patting ourselves on the back [because] that No. 1 reason didn’t get us?”
In that vein, Dr. Pronovost believes that hospitalists can be a lynchpin in what he calls “change leadership.”
“Hospitalists have an essential role in improving the quality and safety of care for hospitalized patients and for transitions,” he says. “I would say that between quality and safety, and the patient experience as a core competency of a hospitalist role, healthcare organizations need to actively engage them, including providing support for their time to lead these efforts.”
Richard Quinn is a freelance writer in New Jersey.
Type the name Peter Pronovost into Google and try to make it past the “n” before the word “checklist” pops up. That’s because Peter Pronovost, MD, PhD, FCCM, senior vice president for patient safety and quality at Johns Hopkins Medicine in Baltimore, is the “checklist doctor,” widely known for a five-step checklist designed to reduce the incidence of central-line infections and credited by SHM with saving thousands of lives. He was named one of the 100 Most Influential People in the World by Time magazine, and he co-authored a book, “Safe Patients, Smart Hospitals: How One Doctor’s Checklist Can Help Us Change Health Care from the Inside Out.”
Dr. Pronovost is one of three keynote speakers slated to offer their wisdom and insights to thousands of hospitalists attending HM15, scheduled for March 29-April 1 at the Gaylord National Resort and Convention Center in National Harbor, Md.
And before you ask—yes, he smiles when people call him the “checklist guy.”
“These catheter infections, just to give you an example, they used to kill as many people as breast or prostate cancer in the U.S. This isn’t some trivial public health problem,” Dr. Pronovost says. “This is a public health problem the size of breast or prostate cancer. And we virtually eliminated it, [which is] pretty remarkable about what the potential of this approach is in healthcare. That is just one harm. We have a lot of other things to go still.”
Dr. Pronovost, director of the Armstrong Institute for Patient Safety and Quality at Johns Hopkins, has titled his HM15 talk, “Taking Quality to the Next Level.” One of his main beliefs is that intrinsically motivated efforts are much more successful than payment carrots or sticks wielded by the Centers for Medicare and Medicaid Services (CMS).

—Dr. Pronovost
“We tap into this incredibly rich and passionate juice of improvement work,” he says of intrinsic motivation. “Whether it’s through a church or through a club, all of us have felt that when you connect to a community, the energy and the passion that that unleashes. Hospitalists have the wisdom to know what to do and how to do it right, and it’s just so much more effective when you tap into intrinsic motivation.”
His famed checklist was a great start to that, but he says more needs to be done. That work looked at eliminating a single hospital-acquired condition. Now, Dr. Pronovost has reframed the question: Can we eliminate all harms? What if hospitals listed out all harms and then gave each a checklist?
“It quickly gets to well beyond the potential of human memory, because there are about 150 things we have to do,” he says. “So I’m going to be showcasing a new app that we made that gives you real-time compliance with all those checklists. If I’m missing any one of those 150 things, there’s a red box next to the patient’s name, and all I have to go do is click on the red box and see what I’m missing.”
Dr. Pronovost sees that approach as a fundamental shift in how safety is viewed. It can’t be based on “heroism,” when someone remembers to remember something; rather, it needs to be rooted in properly designed systems that leverage technology to achieve desired results.
To look at it another way, consider a conversation Dr. Pronovost had with friends in engineering who previously worked on missions launching satellites into space.
“They said to me, ‘Peter, you guys are thinking about this backwards in healthcare. If we had to put a mission up…it can blow up for 12 reasons. It didn’t blow up for reason No. 1—call it a bloodstream infection—but it did blow up for reasons 2 through 12, do you think we’d be patting ourselves on the back [because] that No. 1 reason didn’t get us?”
In that vein, Dr. Pronovost believes that hospitalists can be a lynchpin in what he calls “change leadership.”
“Hospitalists have an essential role in improving the quality and safety of care for hospitalized patients and for transitions,” he says. “I would say that between quality and safety, and the patient experience as a core competency of a hospitalist role, healthcare organizations need to actively engage them, including providing support for their time to lead these efforts.”
Richard Quinn is a freelance writer in New Jersey.
Type the name Peter Pronovost into Google and try to make it past the “n” before the word “checklist” pops up. That’s because Peter Pronovost, MD, PhD, FCCM, senior vice president for patient safety and quality at Johns Hopkins Medicine in Baltimore, is the “checklist doctor,” widely known for a five-step checklist designed to reduce the incidence of central-line infections and credited by SHM with saving thousands of lives. He was named one of the 100 Most Influential People in the World by Time magazine, and he co-authored a book, “Safe Patients, Smart Hospitals: How One Doctor’s Checklist Can Help Us Change Health Care from the Inside Out.”
Dr. Pronovost is one of three keynote speakers slated to offer their wisdom and insights to thousands of hospitalists attending HM15, scheduled for March 29-April 1 at the Gaylord National Resort and Convention Center in National Harbor, Md.
And before you ask—yes, he smiles when people call him the “checklist guy.”
“These catheter infections, just to give you an example, they used to kill as many people as breast or prostate cancer in the U.S. This isn’t some trivial public health problem,” Dr. Pronovost says. “This is a public health problem the size of breast or prostate cancer. And we virtually eliminated it, [which is] pretty remarkable about what the potential of this approach is in healthcare. That is just one harm. We have a lot of other things to go still.”
Dr. Pronovost, director of the Armstrong Institute for Patient Safety and Quality at Johns Hopkins, has titled his HM15 talk, “Taking Quality to the Next Level.” One of his main beliefs is that intrinsically motivated efforts are much more successful than payment carrots or sticks wielded by the Centers for Medicare and Medicaid Services (CMS).

—Dr. Pronovost
“We tap into this incredibly rich and passionate juice of improvement work,” he says of intrinsic motivation. “Whether it’s through a church or through a club, all of us have felt that when you connect to a community, the energy and the passion that that unleashes. Hospitalists have the wisdom to know what to do and how to do it right, and it’s just so much more effective when you tap into intrinsic motivation.”
His famed checklist was a great start to that, but he says more needs to be done. That work looked at eliminating a single hospital-acquired condition. Now, Dr. Pronovost has reframed the question: Can we eliminate all harms? What if hospitals listed out all harms and then gave each a checklist?
“It quickly gets to well beyond the potential of human memory, because there are about 150 things we have to do,” he says. “So I’m going to be showcasing a new app that we made that gives you real-time compliance with all those checklists. If I’m missing any one of those 150 things, there’s a red box next to the patient’s name, and all I have to go do is click on the red box and see what I’m missing.”
Dr. Pronovost sees that approach as a fundamental shift in how safety is viewed. It can’t be based on “heroism,” when someone remembers to remember something; rather, it needs to be rooted in properly designed systems that leverage technology to achieve desired results.
To look at it another way, consider a conversation Dr. Pronovost had with friends in engineering who previously worked on missions launching satellites into space.
“They said to me, ‘Peter, you guys are thinking about this backwards in healthcare. If we had to put a mission up…it can blow up for 12 reasons. It didn’t blow up for reason No. 1—call it a bloodstream infection—but it did blow up for reasons 2 through 12, do you think we’d be patting ourselves on the back [because] that No. 1 reason didn’t get us?”
In that vein, Dr. Pronovost believes that hospitalists can be a lynchpin in what he calls “change leadership.”
“Hospitalists have an essential role in improving the quality and safety of care for hospitalized patients and for transitions,” he says. “I would say that between quality and safety, and the patient experience as a core competency of a hospitalist role, healthcare organizations need to actively engage them, including providing support for their time to lead these efforts.”
Richard Quinn is a freelance writer in New Jersey.
Tips for Hospitalists Managing Care of High-Profile Patients
Hospitalists around the globe have cared for their share of high profile patients, also known as very important people, or VIPs. Many of us dread the prospect of admitting a VIP to our service, knowing that such patients tend to be demanding and entitled and often want to dictate their care.
The term “VIP syndrome” was coined as early as 1964 by psychiatrist Walter Weintraub, who described how “the treatment of an influential man can be extremely hazardous for both patient and doctor.”1 He found, even back then, that the admission of VIPs to an inpatient setting was “often followed by considerable turmoil within the institution,” which can unfortunately undermine the quality of the care that the patient receives.
Some high profile—and controversial—deaths that have at least partially been attributable to VIP syndrome were those of Michael Jackson and Joan Rivers. In both cases, physicians veered from normal or usual standards to meet the apparent needs of their high profile patients. The Jackson case represented a violation of care standards: Dr. Conrad Murray administered propofol, midazolam, and lorazepam simultaneously without monitoring his patient, and this treatment resulted in cardiac arrest. The death was considered a homicide, and the physician was convicted of involuntary manslaughter and sentenced to two years in prison. In the Rivers case, the entertainer’s private ENT physician was involved in her care at a site in which he was not privileged to practice; it is unclear if the clinic was equipped to handle the complexity of her case, and she died after her airway was lost. Countless other examples of VIP quality care concerns signifying alterations in care standards based on the patient’s social status have resulted in less dramatically poor outcomes.
Some hospitals have carved out wings or floors to cater to VIP crowds. In these cases, the room and board charges are extraordinary and are billed directly “out of pocket” to the patient, bypassing insurance companies or payers. These wards or units are often staffed “ad hoc” by nurses and other care providers at very low staff-to-patient ratios, so that they can be at the beck and call of the VIP. Some of these admitted patients even bring along their private physicians and nurses, practitioners who are not privileged to practice on site but who may try to dictate the care being delivered.
The real issue, when VIP syndrome is in full swing, is that it violates many codes of medical professionalism, including those found in the Physician Charter of the ABIM Foundation, which emphasizes the guiding principles of patient welfare, autonomy, and social justice.2 Because there exists a whole cadre of patients who qualify as “VIPs” (celebrities, politicians, royalty, local board members, community leaders, and fellow physicians or healthcare administrators), it is extremely likely that each of us will be called upon to care for such a population at some point. As such, we need to have a plan for how we will manage the emotions and care of such patients, without violating any care or professionalism standards.
Roller Coaster of Emotions
My hospital recently had a VIP in for a protracted and complex illness. The patient and family became so demanding and time-consuming that we considered “rotating” them to various other units to give the physicians and staff a break. The typical emotions affiliated with such VIP cases are resentment and frustration, even hostility at times, especially when we recognize the fact that the care we are delivering is not better than average, and may actually be worse. The resentment stems from the fact that we all like to think we deliver the best care possible to all patients, regardless of their personal characteristics, because we all want and deserve the best care, regardless of our bank accounts or public popularity.
So, while none of us can or should avoid taking care of a VIP patient or family, we do have to be thoughtful—in advance—about how we will approach their care. An article from the Cleveland Clinic offers advice to clinicians taking care of these VIPs, in the form of nine guiding principles:3
- Don’t bend the rules: Although VIPs can exert immense pressure to change our practices and procedures to meet their needs, we should resist any temptation to bend to their wishes. Often, practices and procedures are in place for operational or safety reasons, and veering from them can put both practitioners and patients in harm’s way. Practitioners should be explicit in their conversations with VIP patients, explaining that they will be treated within the boundaries of all the usual operational and safety safeguards that are built into the system, for their own good.
- Work as a team: It must be made very clear to the VIP that the attending is in charge of all medical decision-making, and all other providers will be consultants in their care.
- Communicate: Structured, regular, and predictable communication is a must for the patient, family, and all other providers involved in the VIP’s care. While this can seem very time-consuming, it will save time in the end if the patient, providers, and community understand how and when communication will occur. Predictable communication can also set boundaries on how and when it is appropriate for the patient’s family to contact the attending (e.g. cell phone, text, pager, and so on).
- Carefully manage communication with media: Just as with any patient, a VIP’s confidentiality is paramount. Any media coverage should be carefully planned with the hospital’s public relations department, and the only information that should be shared is that which the patient agrees to in advance.
- Resist “chairperson’s syndrome”: This happens when the family insists on being assigned the most senior physician on staff, even when that physician might not be the one best suited for the clinical scenario. VIP care should be as close to “business as usual” as possible, including being staffed by the “best fit” attending and trainees (in teaching hospitals).
- Care should occur where it is most appropriate: This includes care in an “open” ICU, if that is the level of care needed. This conversation should also be undertaken early in the hospital stay, to ensure that the patient and family understand the rationale and need for matching their level of care with the appropriate care setting, while being mindful of privacy and security needs.
- Protect the patient’s security: High profile patients often are heavily pursued by the media, and all measures should be taken to ensure their safety, security, and privacy. These patients should be listed under an alias or as a confidential patient, to reduce the risk of HIPAA breaches by hospital staff or visitors.
- Be careful about accepting or declining gifts: Accepting and declining gifts can both be hazardous; it would be best to avoid accepting any gifts during the hospital stay, but you can offer to accept a reasonable and appropriate gift after the stay has concluded.
- Work with the patient’s personal physicians: In the event the VIP patient has personal physician(s), it is best to invite their input and show them that you value their opinion; however, it must be clear that the attending has ultimate responsibility for the care of the patient during the hospital stay and that all ordering of diagnostics and therapeutics will be done solely by the attending.

References
- Weintraub W. The VIP syndrome: A clinical study in hospital psychiatry. J Nerv Ment Dis. 1964;138(2):181-193.
- ABIM Foundation. Physician charter. Available at: http://www.abimfoundation.org/Professionalism/Physician-Charter.aspx. Accessed January 10, 2015.
- Guzman JA, Sasidhar M, Stoller JK. Caring for VIPs: nine principles. February 2011. Available at: http://www.ccjm.org/fileadmin/content_pdf/ccjm/content_2fd90f2_90.pdf. Accessed January 10, 2015.
Hospitalists around the globe have cared for their share of high profile patients, also known as very important people, or VIPs. Many of us dread the prospect of admitting a VIP to our service, knowing that such patients tend to be demanding and entitled and often want to dictate their care.
The term “VIP syndrome” was coined as early as 1964 by psychiatrist Walter Weintraub, who described how “the treatment of an influential man can be extremely hazardous for both patient and doctor.”1 He found, even back then, that the admission of VIPs to an inpatient setting was “often followed by considerable turmoil within the institution,” which can unfortunately undermine the quality of the care that the patient receives.
Some high profile—and controversial—deaths that have at least partially been attributable to VIP syndrome were those of Michael Jackson and Joan Rivers. In both cases, physicians veered from normal or usual standards to meet the apparent needs of their high profile patients. The Jackson case represented a violation of care standards: Dr. Conrad Murray administered propofol, midazolam, and lorazepam simultaneously without monitoring his patient, and this treatment resulted in cardiac arrest. The death was considered a homicide, and the physician was convicted of involuntary manslaughter and sentenced to two years in prison. In the Rivers case, the entertainer’s private ENT physician was involved in her care at a site in which he was not privileged to practice; it is unclear if the clinic was equipped to handle the complexity of her case, and she died after her airway was lost. Countless other examples of VIP quality care concerns signifying alterations in care standards based on the patient’s social status have resulted in less dramatically poor outcomes.
Some hospitals have carved out wings or floors to cater to VIP crowds. In these cases, the room and board charges are extraordinary and are billed directly “out of pocket” to the patient, bypassing insurance companies or payers. These wards or units are often staffed “ad hoc” by nurses and other care providers at very low staff-to-patient ratios, so that they can be at the beck and call of the VIP. Some of these admitted patients even bring along their private physicians and nurses, practitioners who are not privileged to practice on site but who may try to dictate the care being delivered.
The real issue, when VIP syndrome is in full swing, is that it violates many codes of medical professionalism, including those found in the Physician Charter of the ABIM Foundation, which emphasizes the guiding principles of patient welfare, autonomy, and social justice.2 Because there exists a whole cadre of patients who qualify as “VIPs” (celebrities, politicians, royalty, local board members, community leaders, and fellow physicians or healthcare administrators), it is extremely likely that each of us will be called upon to care for such a population at some point. As such, we need to have a plan for how we will manage the emotions and care of such patients, without violating any care or professionalism standards.
Roller Coaster of Emotions
My hospital recently had a VIP in for a protracted and complex illness. The patient and family became so demanding and time-consuming that we considered “rotating” them to various other units to give the physicians and staff a break. The typical emotions affiliated with such VIP cases are resentment and frustration, even hostility at times, especially when we recognize the fact that the care we are delivering is not better than average, and may actually be worse. The resentment stems from the fact that we all like to think we deliver the best care possible to all patients, regardless of their personal characteristics, because we all want and deserve the best care, regardless of our bank accounts or public popularity.
So, while none of us can or should avoid taking care of a VIP patient or family, we do have to be thoughtful—in advance—about how we will approach their care. An article from the Cleveland Clinic offers advice to clinicians taking care of these VIPs, in the form of nine guiding principles:3
- Don’t bend the rules: Although VIPs can exert immense pressure to change our practices and procedures to meet their needs, we should resist any temptation to bend to their wishes. Often, practices and procedures are in place for operational or safety reasons, and veering from them can put both practitioners and patients in harm’s way. Practitioners should be explicit in their conversations with VIP patients, explaining that they will be treated within the boundaries of all the usual operational and safety safeguards that are built into the system, for their own good.
- Work as a team: It must be made very clear to the VIP that the attending is in charge of all medical decision-making, and all other providers will be consultants in their care.
- Communicate: Structured, regular, and predictable communication is a must for the patient, family, and all other providers involved in the VIP’s care. While this can seem very time-consuming, it will save time in the end if the patient, providers, and community understand how and when communication will occur. Predictable communication can also set boundaries on how and when it is appropriate for the patient’s family to contact the attending (e.g. cell phone, text, pager, and so on).
- Carefully manage communication with media: Just as with any patient, a VIP’s confidentiality is paramount. Any media coverage should be carefully planned with the hospital’s public relations department, and the only information that should be shared is that which the patient agrees to in advance.
- Resist “chairperson’s syndrome”: This happens when the family insists on being assigned the most senior physician on staff, even when that physician might not be the one best suited for the clinical scenario. VIP care should be as close to “business as usual” as possible, including being staffed by the “best fit” attending and trainees (in teaching hospitals).
- Care should occur where it is most appropriate: This includes care in an “open” ICU, if that is the level of care needed. This conversation should also be undertaken early in the hospital stay, to ensure that the patient and family understand the rationale and need for matching their level of care with the appropriate care setting, while being mindful of privacy and security needs.
- Protect the patient’s security: High profile patients often are heavily pursued by the media, and all measures should be taken to ensure their safety, security, and privacy. These patients should be listed under an alias or as a confidential patient, to reduce the risk of HIPAA breaches by hospital staff or visitors.
- Be careful about accepting or declining gifts: Accepting and declining gifts can both be hazardous; it would be best to avoid accepting any gifts during the hospital stay, but you can offer to accept a reasonable and appropriate gift after the stay has concluded.
- Work with the patient’s personal physicians: In the event the VIP patient has personal physician(s), it is best to invite their input and show them that you value their opinion; however, it must be clear that the attending has ultimate responsibility for the care of the patient during the hospital stay and that all ordering of diagnostics and therapeutics will be done solely by the attending.

References
- Weintraub W. The VIP syndrome: A clinical study in hospital psychiatry. J Nerv Ment Dis. 1964;138(2):181-193.
- ABIM Foundation. Physician charter. Available at: http://www.abimfoundation.org/Professionalism/Physician-Charter.aspx. Accessed January 10, 2015.
- Guzman JA, Sasidhar M, Stoller JK. Caring for VIPs: nine principles. February 2011. Available at: http://www.ccjm.org/fileadmin/content_pdf/ccjm/content_2fd90f2_90.pdf. Accessed January 10, 2015.
Hospitalists around the globe have cared for their share of high profile patients, also known as very important people, or VIPs. Many of us dread the prospect of admitting a VIP to our service, knowing that such patients tend to be demanding and entitled and often want to dictate their care.
The term “VIP syndrome” was coined as early as 1964 by psychiatrist Walter Weintraub, who described how “the treatment of an influential man can be extremely hazardous for both patient and doctor.”1 He found, even back then, that the admission of VIPs to an inpatient setting was “often followed by considerable turmoil within the institution,” which can unfortunately undermine the quality of the care that the patient receives.
Some high profile—and controversial—deaths that have at least partially been attributable to VIP syndrome were those of Michael Jackson and Joan Rivers. In both cases, physicians veered from normal or usual standards to meet the apparent needs of their high profile patients. The Jackson case represented a violation of care standards: Dr. Conrad Murray administered propofol, midazolam, and lorazepam simultaneously without monitoring his patient, and this treatment resulted in cardiac arrest. The death was considered a homicide, and the physician was convicted of involuntary manslaughter and sentenced to two years in prison. In the Rivers case, the entertainer’s private ENT physician was involved in her care at a site in which he was not privileged to practice; it is unclear if the clinic was equipped to handle the complexity of her case, and she died after her airway was lost. Countless other examples of VIP quality care concerns signifying alterations in care standards based on the patient’s social status have resulted in less dramatically poor outcomes.
Some hospitals have carved out wings or floors to cater to VIP crowds. In these cases, the room and board charges are extraordinary and are billed directly “out of pocket” to the patient, bypassing insurance companies or payers. These wards or units are often staffed “ad hoc” by nurses and other care providers at very low staff-to-patient ratios, so that they can be at the beck and call of the VIP. Some of these admitted patients even bring along their private physicians and nurses, practitioners who are not privileged to practice on site but who may try to dictate the care being delivered.
The real issue, when VIP syndrome is in full swing, is that it violates many codes of medical professionalism, including those found in the Physician Charter of the ABIM Foundation, which emphasizes the guiding principles of patient welfare, autonomy, and social justice.2 Because there exists a whole cadre of patients who qualify as “VIPs” (celebrities, politicians, royalty, local board members, community leaders, and fellow physicians or healthcare administrators), it is extremely likely that each of us will be called upon to care for such a population at some point. As such, we need to have a plan for how we will manage the emotions and care of such patients, without violating any care or professionalism standards.
Roller Coaster of Emotions
My hospital recently had a VIP in for a protracted and complex illness. The patient and family became so demanding and time-consuming that we considered “rotating” them to various other units to give the physicians and staff a break. The typical emotions affiliated with such VIP cases are resentment and frustration, even hostility at times, especially when we recognize the fact that the care we are delivering is not better than average, and may actually be worse. The resentment stems from the fact that we all like to think we deliver the best care possible to all patients, regardless of their personal characteristics, because we all want and deserve the best care, regardless of our bank accounts or public popularity.
So, while none of us can or should avoid taking care of a VIP patient or family, we do have to be thoughtful—in advance—about how we will approach their care. An article from the Cleveland Clinic offers advice to clinicians taking care of these VIPs, in the form of nine guiding principles:3
- Don’t bend the rules: Although VIPs can exert immense pressure to change our practices and procedures to meet their needs, we should resist any temptation to bend to their wishes. Often, practices and procedures are in place for operational or safety reasons, and veering from them can put both practitioners and patients in harm’s way. Practitioners should be explicit in their conversations with VIP patients, explaining that they will be treated within the boundaries of all the usual operational and safety safeguards that are built into the system, for their own good.
- Work as a team: It must be made very clear to the VIP that the attending is in charge of all medical decision-making, and all other providers will be consultants in their care.
- Communicate: Structured, regular, and predictable communication is a must for the patient, family, and all other providers involved in the VIP’s care. While this can seem very time-consuming, it will save time in the end if the patient, providers, and community understand how and when communication will occur. Predictable communication can also set boundaries on how and when it is appropriate for the patient’s family to contact the attending (e.g. cell phone, text, pager, and so on).
- Carefully manage communication with media: Just as with any patient, a VIP’s confidentiality is paramount. Any media coverage should be carefully planned with the hospital’s public relations department, and the only information that should be shared is that which the patient agrees to in advance.
- Resist “chairperson’s syndrome”: This happens when the family insists on being assigned the most senior physician on staff, even when that physician might not be the one best suited for the clinical scenario. VIP care should be as close to “business as usual” as possible, including being staffed by the “best fit” attending and trainees (in teaching hospitals).
- Care should occur where it is most appropriate: This includes care in an “open” ICU, if that is the level of care needed. This conversation should also be undertaken early in the hospital stay, to ensure that the patient and family understand the rationale and need for matching their level of care with the appropriate care setting, while being mindful of privacy and security needs.
- Protect the patient’s security: High profile patients often are heavily pursued by the media, and all measures should be taken to ensure their safety, security, and privacy. These patients should be listed under an alias or as a confidential patient, to reduce the risk of HIPAA breaches by hospital staff or visitors.
- Be careful about accepting or declining gifts: Accepting and declining gifts can both be hazardous; it would be best to avoid accepting any gifts during the hospital stay, but you can offer to accept a reasonable and appropriate gift after the stay has concluded.
- Work with the patient’s personal physicians: In the event the VIP patient has personal physician(s), it is best to invite their input and show them that you value their opinion; however, it must be clear that the attending has ultimate responsibility for the care of the patient during the hospital stay and that all ordering of diagnostics and therapeutics will be done solely by the attending.

References
- Weintraub W. The VIP syndrome: A clinical study in hospital psychiatry. J Nerv Ment Dis. 1964;138(2):181-193.
- ABIM Foundation. Physician charter. Available at: http://www.abimfoundation.org/Professionalism/Physician-Charter.aspx. Accessed January 10, 2015.
- Guzman JA, Sasidhar M, Stoller JK. Caring for VIPs: nine principles. February 2011. Available at: http://www.ccjm.org/fileadmin/content_pdf/ccjm/content_2fd90f2_90.pdf. Accessed January 10, 2015.
Sightseeing, Activities, Events for Hospitalists, Families Attending HM15
Networking, education, and professional refreshment will keep several thousand hospitalists busy during HM15 workdays next month at the Gaylord National Resort and Conference Center in National Harbor, Md. But what will fill the evenings? And what are families to do while hospitalists attend sessions?
That’s where hospitalist Amit Pahwa, MD, of Johns Hopkins Hospital in Baltimore, can help. He lives in Ellicott City, Md., a bedroom community some 40 miles north of Washington, D.C. Visiting for a day or three at a time is practically a part-time job for him.
First up on his travel itinerary would be the 2015 National Cherry Blossom Festival, which kicks off March 20. In fact, the annual Blossom Kite Festival is set for Saturday, March 28, the day before HM15 pre-courses kick off.
“It’s beautiful,” says Dr. Pahwa, vice president of SHM’s Maryland chapter. “It’s absolutely beautiful. The weather’s getting nicer, everybody’s been inside for a couple of months…it’s really nice.”
While on the National Mall, hospitalists can point at dozens of museums they’d like to visit. Dr. Pahwa’s two young kids often choose for him. Their favorite is the National Museum of Natural History.
“And my son loves the (National) Air and Space Museum,” he says.
For the more adventurous or athletic, he suggests kayaking the Potomac River.
Hospitalists who are a little less adventurous may want to look into Capital Bikeshare, a bike-sharing program that allows visitors to rent a bike at stations around the district and then return them to other stations.
“It’s a cool thing to do to get around the city,” Dr. Pahwa says.
Of course, after all that exercise, even the heartiest hospitalist is bound to be hungry. Dr. Pahwa recommends the following restaurants:
- National Harbor: Rosa Mexicano (guacamole made tableside) and Harrington’s Pub and Kitchen (classic pub grub with a pint of Guinness) are both within walking distance from the convention center.
- Washington: Dukem (1114-1118 U Street NW), an Ethiopian restaurant, is one of his favorites; meats and spices dominate the menu. For Mexican, try Oyamel Cucina Mexicana (401 7th Street NW). Those with a sweeter palate can try Sticky Fingers Sweets & Eats (1370 Park Road NW), a vegan bakery so good Dr. Pahwa almost bought his wedding cake there.
- Old Town Alexandria, Va. Chart House, a national seafood chain whose Old Town location overlooks the Potomac River. “I know it’s a chain, but it’s really good,” he says.
Dr. Pahwa says that hospitalists in Old Town—there’s a water taxi that comes straight from National Harbor—should take the time to walk around. Although national retailers like the Gap have popped up on King Street, the downtown’s main thoroughfare, the area retains its old-time charm.
“There are still a lot of mom and pop areas people can hang out and get some coffee,” he says. “It’s just a nice area to walk around.”
For more visitor information, check out www.washington.org. For information about HM15’s family programs, click here.
Richard Quinn is a freelance writer in New Jersey.
Networking, education, and professional refreshment will keep several thousand hospitalists busy during HM15 workdays next month at the Gaylord National Resort and Conference Center in National Harbor, Md. But what will fill the evenings? And what are families to do while hospitalists attend sessions?
That’s where hospitalist Amit Pahwa, MD, of Johns Hopkins Hospital in Baltimore, can help. He lives in Ellicott City, Md., a bedroom community some 40 miles north of Washington, D.C. Visiting for a day or three at a time is practically a part-time job for him.
First up on his travel itinerary would be the 2015 National Cherry Blossom Festival, which kicks off March 20. In fact, the annual Blossom Kite Festival is set for Saturday, March 28, the day before HM15 pre-courses kick off.
“It’s beautiful,” says Dr. Pahwa, vice president of SHM’s Maryland chapter. “It’s absolutely beautiful. The weather’s getting nicer, everybody’s been inside for a couple of months…it’s really nice.”
While on the National Mall, hospitalists can point at dozens of museums they’d like to visit. Dr. Pahwa’s two young kids often choose for him. Their favorite is the National Museum of Natural History.
“And my son loves the (National) Air and Space Museum,” he says.
For the more adventurous or athletic, he suggests kayaking the Potomac River.
Hospitalists who are a little less adventurous may want to look into Capital Bikeshare, a bike-sharing program that allows visitors to rent a bike at stations around the district and then return them to other stations.
“It’s a cool thing to do to get around the city,” Dr. Pahwa says.
Of course, after all that exercise, even the heartiest hospitalist is bound to be hungry. Dr. Pahwa recommends the following restaurants:
- National Harbor: Rosa Mexicano (guacamole made tableside) and Harrington’s Pub and Kitchen (classic pub grub with a pint of Guinness) are both within walking distance from the convention center.
- Washington: Dukem (1114-1118 U Street NW), an Ethiopian restaurant, is one of his favorites; meats and spices dominate the menu. For Mexican, try Oyamel Cucina Mexicana (401 7th Street NW). Those with a sweeter palate can try Sticky Fingers Sweets & Eats (1370 Park Road NW), a vegan bakery so good Dr. Pahwa almost bought his wedding cake there.
- Old Town Alexandria, Va. Chart House, a national seafood chain whose Old Town location overlooks the Potomac River. “I know it’s a chain, but it’s really good,” he says.
Dr. Pahwa says that hospitalists in Old Town—there’s a water taxi that comes straight from National Harbor—should take the time to walk around. Although national retailers like the Gap have popped up on King Street, the downtown’s main thoroughfare, the area retains its old-time charm.
“There are still a lot of mom and pop areas people can hang out and get some coffee,” he says. “It’s just a nice area to walk around.”
For more visitor information, check out www.washington.org. For information about HM15’s family programs, click here.
Richard Quinn is a freelance writer in New Jersey.
Networking, education, and professional refreshment will keep several thousand hospitalists busy during HM15 workdays next month at the Gaylord National Resort and Conference Center in National Harbor, Md. But what will fill the evenings? And what are families to do while hospitalists attend sessions?
That’s where hospitalist Amit Pahwa, MD, of Johns Hopkins Hospital in Baltimore, can help. He lives in Ellicott City, Md., a bedroom community some 40 miles north of Washington, D.C. Visiting for a day or three at a time is practically a part-time job for him.
First up on his travel itinerary would be the 2015 National Cherry Blossom Festival, which kicks off March 20. In fact, the annual Blossom Kite Festival is set for Saturday, March 28, the day before HM15 pre-courses kick off.
“It’s beautiful,” says Dr. Pahwa, vice president of SHM’s Maryland chapter. “It’s absolutely beautiful. The weather’s getting nicer, everybody’s been inside for a couple of months…it’s really nice.”
While on the National Mall, hospitalists can point at dozens of museums they’d like to visit. Dr. Pahwa’s two young kids often choose for him. Their favorite is the National Museum of Natural History.
“And my son loves the (National) Air and Space Museum,” he says.
For the more adventurous or athletic, he suggests kayaking the Potomac River.
Hospitalists who are a little less adventurous may want to look into Capital Bikeshare, a bike-sharing program that allows visitors to rent a bike at stations around the district and then return them to other stations.
“It’s a cool thing to do to get around the city,” Dr. Pahwa says.
Of course, after all that exercise, even the heartiest hospitalist is bound to be hungry. Dr. Pahwa recommends the following restaurants:
- National Harbor: Rosa Mexicano (guacamole made tableside) and Harrington’s Pub and Kitchen (classic pub grub with a pint of Guinness) are both within walking distance from the convention center.
- Washington: Dukem (1114-1118 U Street NW), an Ethiopian restaurant, is one of his favorites; meats and spices dominate the menu. For Mexican, try Oyamel Cucina Mexicana (401 7th Street NW). Those with a sweeter palate can try Sticky Fingers Sweets & Eats (1370 Park Road NW), a vegan bakery so good Dr. Pahwa almost bought his wedding cake there.
- Old Town Alexandria, Va. Chart House, a national seafood chain whose Old Town location overlooks the Potomac River. “I know it’s a chain, but it’s really good,” he says.
Dr. Pahwa says that hospitalists in Old Town—there’s a water taxi that comes straight from National Harbor—should take the time to walk around. Although national retailers like the Gap have popped up on King Street, the downtown’s main thoroughfare, the area retains its old-time charm.
“There are still a lot of mom and pop areas people can hang out and get some coffee,” he says. “It’s just a nice area to walk around.”
For more visitor information, check out www.washington.org. For information about HM15’s family programs, click here.
Richard Quinn is a freelance writer in New Jersey.
Hospital Medicine Career Perfect Fit for Hands-On Hospitalist Sowmya Kanikkannan
Sowmya Kanikkannan, MD, SFHM, has medicine in her blood. Stories her physician mother told her when she was a child piqued her curiosity. That inquiring mindset led her to volunteer at a hospital, an experience that turned into college studies, which eventually led to a career in hospital medicine.
“It wasn’t until my second year of residency that I started hearing more about hospital medicine,” says Dr. Kanikkannan, one of the newer additions to Team Hospitalist, the volunteer editorial advisory board of The Hospitalist. “By then, I had started to think about what I wanted to do after graduation. The things that I liked about it were the fast pace of hospital work, the higher acuity of medicine that hospitalists practiced, and the collaborative nature of the field.”
The choice is working out just fine.
Last year, Dr. Kanikkannan was named hospitalist medical director for Rowan University School of Osteopathic Medicine in Stratford, N.J. She also is a member of SHM’s national leadership committee and writes for SHM’s blog, “The Hospital Leader”.
Despite her leadership roles, Dr. Kanikkannan believes she must keep direct patient care in her schedule.
“Seeing patients is important to me, since I am a physician at heart,” she says. “As a leader, it is equally important to me to see patients; it keeps me grounded. Being hands on helps me better understand my program and make successful administrative decisions that can be sustained in the long run.”
Question: What do you dislike most about working as a hospitalist?
Answer: There are times when I see frequent fliers get readmitted to the hospital over and over again. Sometimes, this is difficult to deal with and can be frustrating for the hospitalist, because patients either don’t have the resources to take care of themselves when discharged or they don’t take their health seriously enough to make attempts to lead healthier lives. At times like these, I really wish that as hospitalists we could help these patients in some way that is sustainable long-term.
Q: What’s the best advice you ever received?
A: The best advice that I received was from family, and it was to believe in myself and to believe that I can achieve anything that I want to if I put my mind to it and worked hard for it. My high school math teacher also told me that I shouldn’t change because I was so awesome. But then, who wouldn’t like that advice?

Q: What’s the biggest change you’ve seen in hospital medicine in your career?
A: The biggest change would have to be the exponential growth and expansion—not just in the number of hospitalist programs but [also in] the growth of our scope of practice. I have seen the field grow from doctors who practice in the hospital to doctors who are part of the hospital. This is really amazing. I am glad to see that hospitalists are more involved in hospital systems and processes in addition to providing patient care.
Q: What’s the biggest change you would like to see?
A: The biggest change that I would like to see is to solidify hospital medicine as a career and recruit career-hospitalists into our field. As with any new and upcoming field, this is a process that takes some time. I already am starting to see this trend, as residents are entering hospitalist tracks and medical students are beginning to understand the existence of hospital medicine. I’m sure that it’s only a matter of time.
Q: What aspect of patient care is most rewarding?
A: My favorite part is seeing my patients recover quickly. I also enjoy interacting and forming good relationships with my patients and their families, albeit during a short hospital visit. When people are sick, you see them at their most vulnerable. To know that they trust your care during that time is very humbling. Last week, the wife of a patient suddenly hugged me and thanked me for taking care of her husband. It was totally unexpected, but it was also a great feeling that I helped someone get better.
Q: What is your biggest professional challenge?
A: One of my biggest professional challenges is learning how to get diverse and often different groups of medical professionals to come together and collaborate on system changes in the hospital. No matter how many times you do it, each experience is different and presents its own unique challenge.
Q: When you aren’t working, what is important to you?
A: I love spending time with my family and friends. Since I am usually busy during my weeks on service, I catch up with everyone during my weeks off. My husband and I like exploring Philadelphia when we can. We’ve been enjoying the amazing new vegetarian restaurants that have opened in Philly over the last year.
Q: Where do you see yourself in 10 years?
A: I see myself in hospital medicine leadership, since being a leader has given me the opportunity to impact positive change for my hospital, my patients, and the hospitalists in my group.
Q: If you weren’t a doctor, what would you be doing right now?
A: This is a question that I was asked during my medical school interview. I believe that I didn’t have an answer at that time; however, if I really had to pick, I would want to be an artist and a performer in Broadway musicals. I love all forms of dance, especially contemporary dancing, salsa, and bharathnatyam (a classical south Indian dance). I also enjoy singing, although my skills, I’m afraid, have deteriorated due to disuse.
Q: What impact do you feel devices like Apple and Android products have had on your job—and on medicine in a broader sense?
A: I think that the new mobile technology has had a significant and positive impact on healthcare as a whole. The most beneficial is the ease of access to information, both related to patient care and medical resources. The next wave will be the integration of these devices into the actual delivery of patient care.
Richard Quinn is a freelance writer in New Jersey.
Sowmya Kanikkannan, MD, SFHM, has medicine in her blood. Stories her physician mother told her when she was a child piqued her curiosity. That inquiring mindset led her to volunteer at a hospital, an experience that turned into college studies, which eventually led to a career in hospital medicine.
“It wasn’t until my second year of residency that I started hearing more about hospital medicine,” says Dr. Kanikkannan, one of the newer additions to Team Hospitalist, the volunteer editorial advisory board of The Hospitalist. “By then, I had started to think about what I wanted to do after graduation. The things that I liked about it were the fast pace of hospital work, the higher acuity of medicine that hospitalists practiced, and the collaborative nature of the field.”
The choice is working out just fine.
Last year, Dr. Kanikkannan was named hospitalist medical director for Rowan University School of Osteopathic Medicine in Stratford, N.J. She also is a member of SHM’s national leadership committee and writes for SHM’s blog, “The Hospital Leader”.
Despite her leadership roles, Dr. Kanikkannan believes she must keep direct patient care in her schedule.
“Seeing patients is important to me, since I am a physician at heart,” she says. “As a leader, it is equally important to me to see patients; it keeps me grounded. Being hands on helps me better understand my program and make successful administrative decisions that can be sustained in the long run.”
Question: What do you dislike most about working as a hospitalist?
Answer: There are times when I see frequent fliers get readmitted to the hospital over and over again. Sometimes, this is difficult to deal with and can be frustrating for the hospitalist, because patients either don’t have the resources to take care of themselves when discharged or they don’t take their health seriously enough to make attempts to lead healthier lives. At times like these, I really wish that as hospitalists we could help these patients in some way that is sustainable long-term.
Q: What’s the best advice you ever received?
A: The best advice that I received was from family, and it was to believe in myself and to believe that I can achieve anything that I want to if I put my mind to it and worked hard for it. My high school math teacher also told me that I shouldn’t change because I was so awesome. But then, who wouldn’t like that advice?

Q: What’s the biggest change you’ve seen in hospital medicine in your career?
A: The biggest change would have to be the exponential growth and expansion—not just in the number of hospitalist programs but [also in] the growth of our scope of practice. I have seen the field grow from doctors who practice in the hospital to doctors who are part of the hospital. This is really amazing. I am glad to see that hospitalists are more involved in hospital systems and processes in addition to providing patient care.
Q: What’s the biggest change you would like to see?
A: The biggest change that I would like to see is to solidify hospital medicine as a career and recruit career-hospitalists into our field. As with any new and upcoming field, this is a process that takes some time. I already am starting to see this trend, as residents are entering hospitalist tracks and medical students are beginning to understand the existence of hospital medicine. I’m sure that it’s only a matter of time.
Q: What aspect of patient care is most rewarding?
A: My favorite part is seeing my patients recover quickly. I also enjoy interacting and forming good relationships with my patients and their families, albeit during a short hospital visit. When people are sick, you see them at their most vulnerable. To know that they trust your care during that time is very humbling. Last week, the wife of a patient suddenly hugged me and thanked me for taking care of her husband. It was totally unexpected, but it was also a great feeling that I helped someone get better.
Q: What is your biggest professional challenge?
A: One of my biggest professional challenges is learning how to get diverse and often different groups of medical professionals to come together and collaborate on system changes in the hospital. No matter how many times you do it, each experience is different and presents its own unique challenge.
Q: When you aren’t working, what is important to you?
A: I love spending time with my family and friends. Since I am usually busy during my weeks on service, I catch up with everyone during my weeks off. My husband and I like exploring Philadelphia when we can. We’ve been enjoying the amazing new vegetarian restaurants that have opened in Philly over the last year.
Q: Where do you see yourself in 10 years?
A: I see myself in hospital medicine leadership, since being a leader has given me the opportunity to impact positive change for my hospital, my patients, and the hospitalists in my group.
Q: If you weren’t a doctor, what would you be doing right now?
A: This is a question that I was asked during my medical school interview. I believe that I didn’t have an answer at that time; however, if I really had to pick, I would want to be an artist and a performer in Broadway musicals. I love all forms of dance, especially contemporary dancing, salsa, and bharathnatyam (a classical south Indian dance). I also enjoy singing, although my skills, I’m afraid, have deteriorated due to disuse.
Q: What impact do you feel devices like Apple and Android products have had on your job—and on medicine in a broader sense?
A: I think that the new mobile technology has had a significant and positive impact on healthcare as a whole. The most beneficial is the ease of access to information, both related to patient care and medical resources. The next wave will be the integration of these devices into the actual delivery of patient care.
Richard Quinn is a freelance writer in New Jersey.
Sowmya Kanikkannan, MD, SFHM, has medicine in her blood. Stories her physician mother told her when she was a child piqued her curiosity. That inquiring mindset led her to volunteer at a hospital, an experience that turned into college studies, which eventually led to a career in hospital medicine.
“It wasn’t until my second year of residency that I started hearing more about hospital medicine,” says Dr. Kanikkannan, one of the newer additions to Team Hospitalist, the volunteer editorial advisory board of The Hospitalist. “By then, I had started to think about what I wanted to do after graduation. The things that I liked about it were the fast pace of hospital work, the higher acuity of medicine that hospitalists practiced, and the collaborative nature of the field.”
The choice is working out just fine.
Last year, Dr. Kanikkannan was named hospitalist medical director for Rowan University School of Osteopathic Medicine in Stratford, N.J. She also is a member of SHM’s national leadership committee and writes for SHM’s blog, “The Hospital Leader”.
Despite her leadership roles, Dr. Kanikkannan believes she must keep direct patient care in her schedule.
“Seeing patients is important to me, since I am a physician at heart,” she says. “As a leader, it is equally important to me to see patients; it keeps me grounded. Being hands on helps me better understand my program and make successful administrative decisions that can be sustained in the long run.”
Question: What do you dislike most about working as a hospitalist?
Answer: There are times when I see frequent fliers get readmitted to the hospital over and over again. Sometimes, this is difficult to deal with and can be frustrating for the hospitalist, because patients either don’t have the resources to take care of themselves when discharged or they don’t take their health seriously enough to make attempts to lead healthier lives. At times like these, I really wish that as hospitalists we could help these patients in some way that is sustainable long-term.
Q: What’s the best advice you ever received?
A: The best advice that I received was from family, and it was to believe in myself and to believe that I can achieve anything that I want to if I put my mind to it and worked hard for it. My high school math teacher also told me that I shouldn’t change because I was so awesome. But then, who wouldn’t like that advice?

Q: What’s the biggest change you’ve seen in hospital medicine in your career?
A: The biggest change would have to be the exponential growth and expansion—not just in the number of hospitalist programs but [also in] the growth of our scope of practice. I have seen the field grow from doctors who practice in the hospital to doctors who are part of the hospital. This is really amazing. I am glad to see that hospitalists are more involved in hospital systems and processes in addition to providing patient care.
Q: What’s the biggest change you would like to see?
A: The biggest change that I would like to see is to solidify hospital medicine as a career and recruit career-hospitalists into our field. As with any new and upcoming field, this is a process that takes some time. I already am starting to see this trend, as residents are entering hospitalist tracks and medical students are beginning to understand the existence of hospital medicine. I’m sure that it’s only a matter of time.
Q: What aspect of patient care is most rewarding?
A: My favorite part is seeing my patients recover quickly. I also enjoy interacting and forming good relationships with my patients and their families, albeit during a short hospital visit. When people are sick, you see them at their most vulnerable. To know that they trust your care during that time is very humbling. Last week, the wife of a patient suddenly hugged me and thanked me for taking care of her husband. It was totally unexpected, but it was also a great feeling that I helped someone get better.
Q: What is your biggest professional challenge?
A: One of my biggest professional challenges is learning how to get diverse and often different groups of medical professionals to come together and collaborate on system changes in the hospital. No matter how many times you do it, each experience is different and presents its own unique challenge.
Q: When you aren’t working, what is important to you?
A: I love spending time with my family and friends. Since I am usually busy during my weeks on service, I catch up with everyone during my weeks off. My husband and I like exploring Philadelphia when we can. We’ve been enjoying the amazing new vegetarian restaurants that have opened in Philly over the last year.
Q: Where do you see yourself in 10 years?
A: I see myself in hospital medicine leadership, since being a leader has given me the opportunity to impact positive change for my hospital, my patients, and the hospitalists in my group.
Q: If you weren’t a doctor, what would you be doing right now?
A: This is a question that I was asked during my medical school interview. I believe that I didn’t have an answer at that time; however, if I really had to pick, I would want to be an artist and a performer in Broadway musicals. I love all forms of dance, especially contemporary dancing, salsa, and bharathnatyam (a classical south Indian dance). I also enjoy singing, although my skills, I’m afraid, have deteriorated due to disuse.
Q: What impact do you feel devices like Apple and Android products have had on your job—and on medicine in a broader sense?
A: I think that the new mobile technology has had a significant and positive impact on healthcare as a whole. The most beneficial is the ease of access to information, both related to patient care and medical resources. The next wave will be the integration of these devices into the actual delivery of patient care.
Richard Quinn is a freelance writer in New Jersey.