User login
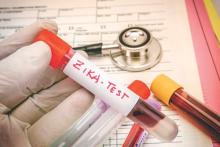
Zika virus RNA detected in serum beyond previously estimated time frame
Zika virus RNA was detected in the serum of five pregnant women beyond previously estimated time frames, according to a new case series study.
“This report adds to the existing evidence that Zika virus RNA in serum may be detected longer than previously expected, an observation now reported among at least eight pregnant women,” reported Dr. Dana Meaney-Delman of the Centers for Disease Control & Prevention, and her colleagues wrote. (Obstet Gynecol. 2016. doi: 10.1097/AOG.0000000000001625).
Five pregnant women who had traveled to or lived in one or more countries with active Zika virus transmission and had prolonged detection of Zika virus RNA in serum were reported to the U.S. Zika Pregnancy Registry, an enhanced surveillance initiative developed by the CDC to collect information on maternal exposure history, clinical presentation, laboratory testing, prenatal imaging, pregnancy screening and complications, fetal and neonatal outcomes, and infant development through the first year of life.
Prolonged detection was defined as the presence of Zika virus RNA detected in serum by real-time reverse transcription-polymerase chain reaction at 14 or more days after symptom onset for symptomatic pregnant women or 21 or more days after last possible exposure to Zika virus for asymptomatic pregnant women. A previous study reported a mean Zika viral RNA duration of 9.9 days, with 14 days being the longest duration of Zika virus RNA detection in a nonpregnant person.
Among the four symptomatic pregnant women, Zika virus RNA was detected in the serum at 17, 23, 44, and 46 days following symptom onset. In the one asymptomatic pregnant woman, Zika virus RNA was detected in serum at 53 days after her travel from an area with active Zika transmission.
Among the five pregnancies, one is ongoing, one was aborted and the fetus tested positive for fetal Zika virus infection, and three resulted in live births of healthy neonates with no reported abnormalities.
“Several questions remain regarding the findings of prolonged detection of Zika virus RNA. Most notably, the duration of Zika virus RNA in serum requires further investigation to determine whether there is a correlation between prolonged viral RNA detection and the presence of infectious virus,” the researchers wrote.
Read the study results here.
On Twitter @jessnicolecraig
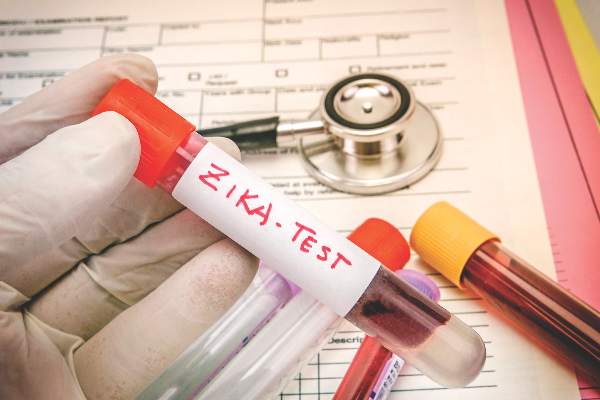
Zika virus RNA was detected in the serum of five pregnant women beyond previously estimated time frames, according to a new case series study.
“This report adds to the existing evidence that Zika virus RNA in serum may be detected longer than previously expected, an observation now reported among at least eight pregnant women,” reported Dr. Dana Meaney-Delman of the Centers for Disease Control & Prevention, and her colleagues wrote. (Obstet Gynecol. 2016. doi: 10.1097/AOG.0000000000001625).
Five pregnant women who had traveled to or lived in one or more countries with active Zika virus transmission and had prolonged detection of Zika virus RNA in serum were reported to the U.S. Zika Pregnancy Registry, an enhanced surveillance initiative developed by the CDC to collect information on maternal exposure history, clinical presentation, laboratory testing, prenatal imaging, pregnancy screening and complications, fetal and neonatal outcomes, and infant development through the first year of life.
Prolonged detection was defined as the presence of Zika virus RNA detected in serum by real-time reverse transcription-polymerase chain reaction at 14 or more days after symptom onset for symptomatic pregnant women or 21 or more days after last possible exposure to Zika virus for asymptomatic pregnant women. A previous study reported a mean Zika viral RNA duration of 9.9 days, with 14 days being the longest duration of Zika virus RNA detection in a nonpregnant person.
Among the four symptomatic pregnant women, Zika virus RNA was detected in the serum at 17, 23, 44, and 46 days following symptom onset. In the one asymptomatic pregnant woman, Zika virus RNA was detected in serum at 53 days after her travel from an area with active Zika transmission.
Among the five pregnancies, one is ongoing, one was aborted and the fetus tested positive for fetal Zika virus infection, and three resulted in live births of healthy neonates with no reported abnormalities.
“Several questions remain regarding the findings of prolonged detection of Zika virus RNA. Most notably, the duration of Zika virus RNA in serum requires further investigation to determine whether there is a correlation between prolonged viral RNA detection and the presence of infectious virus,” the researchers wrote.
Read the study results here.
On Twitter @jessnicolecraig
Zika virus RNA was detected in the serum of five pregnant women beyond previously estimated time frames, according to a new case series study.
“This report adds to the existing evidence that Zika virus RNA in serum may be detected longer than previously expected, an observation now reported among at least eight pregnant women,” reported Dr. Dana Meaney-Delman of the Centers for Disease Control & Prevention, and her colleagues wrote. (Obstet Gynecol. 2016. doi: 10.1097/AOG.0000000000001625).
Five pregnant women who had traveled to or lived in one or more countries with active Zika virus transmission and had prolonged detection of Zika virus RNA in serum were reported to the U.S. Zika Pregnancy Registry, an enhanced surveillance initiative developed by the CDC to collect information on maternal exposure history, clinical presentation, laboratory testing, prenatal imaging, pregnancy screening and complications, fetal and neonatal outcomes, and infant development through the first year of life.
Prolonged detection was defined as the presence of Zika virus RNA detected in serum by real-time reverse transcription-polymerase chain reaction at 14 or more days after symptom onset for symptomatic pregnant women or 21 or more days after last possible exposure to Zika virus for asymptomatic pregnant women. A previous study reported a mean Zika viral RNA duration of 9.9 days, with 14 days being the longest duration of Zika virus RNA detection in a nonpregnant person.
Among the four symptomatic pregnant women, Zika virus RNA was detected in the serum at 17, 23, 44, and 46 days following symptom onset. In the one asymptomatic pregnant woman, Zika virus RNA was detected in serum at 53 days after her travel from an area with active Zika transmission.
Among the five pregnancies, one is ongoing, one was aborted and the fetus tested positive for fetal Zika virus infection, and three resulted in live births of healthy neonates with no reported abnormalities.
“Several questions remain regarding the findings of prolonged detection of Zika virus RNA. Most notably, the duration of Zika virus RNA in serum requires further investigation to determine whether there is a correlation between prolonged viral RNA detection and the presence of infectious virus,” the researchers wrote.
Read the study results here.
On Twitter @jessnicolecraig
FROM OBSTETRICS & GYNECOLOGY
Oocyte donation may up risk of preterm birth
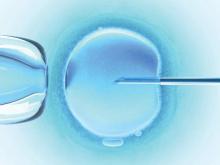
HELSINKI – The risk of preterm birth and low birth weight is higher following oocyte donation for in vitro fertilization, compared with autologous IVF, according to a review of more than 100,000 singleton live births.
The findings could help in counseling women and when managing pregnancies resulting from oocyte donation IVF, Mohan S. Kamath, MBBS, reported at the annual meeting of the European Society of Human Reproduction and Embryology.
In a review of 100,092 singleton live births among women who underwent either fresh donor oocyte or autologous IVF, the rates of several outcomes were increased among the donor recipients. For example, preterm birth, defined as live birth before 37 weeks’ gestation, occurred in 14.8% vs. 9.4% of patients in the groups, respectively (odds ratio, 1.68), early preterm birth (live birth before 32 weeks’ gestation) occurred in 2.1% and 1.8% of patients (OR, 1.77), low birth weight (less than 2,500 g), occurred in 13.8% vs. 9.5% of patients (OR, 1.53), and very low birth weight (less than 1,500 g) occurred in 2.65% vs. 1.9% of patients (OR, 1.42).
The differences between the groups were statistically significant, said Dr. Kamath of Christian Medical College and Hospital, Vellore, India.
After adjusting for potential confounders, including female age, treatment duration, previous live birth, number of embryos transferred, single vs. multiple pregnancies resulting in singleton birth, and day of embryo transfer (before 5 days vs. 5 days or later), the increase in the risk of adverse perinatal outcomes of preterm birth, early preterm birth, and low birth weight remained significant (adjusted OR, 1.56, 1.41, and 1.43, respectively), he said.
The findings are important because the burden of poor ovarian response following IVF has been increasing, likely as a result of delayed childbearing and thus advanced age among those seeking IVF, Dr. Kamath said. However, little information is available regarding maternal or infant outcomes following oocyte donation, and the data that do exist have been conflicting, he said.
The increased risk of pregnancy complications following assisted reproductive technology, compared with spontaneously conceived pregnancies, has been largely attributed to the underlying infertility itself or to embryo-specific epigenetic modifications because of the in vitro fertilization techniques. The current study was conducted to determine whether use of donor oocytes affects obstetric and perinatal outcomes when compared with pregnancies that follow autologous IVF.
Anonymous data were obtained from the Human Fertilisation & Embryology Authority of the United Kingdom, which has collected data on all assisted reproductive treatment in the United Kingdom since 1991. For the current analysis, data from 1991 to 2011, including all singleton live births following fresh oocyte donor and autologous IVF cycles, were evaluated.
Although the dataset did not include information on potential confounders, such as smoking, body mass index, and medical history during pregnancy, the findings provide important insight into potential outcomes, Dr. Kamath said.
Dr. Kamath reported having no financial disclosures.
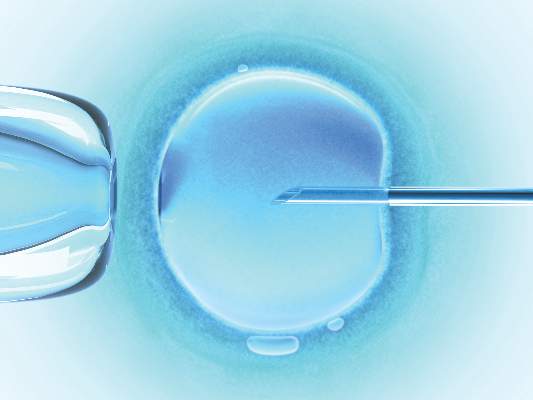
HELSINKI – The risk of preterm birth and low birth weight is higher following oocyte donation for in vitro fertilization, compared with autologous IVF, according to a review of more than 100,000 singleton live births.
The findings could help in counseling women and when managing pregnancies resulting from oocyte donation IVF, Mohan S. Kamath, MBBS, reported at the annual meeting of the European Society of Human Reproduction and Embryology.
In a review of 100,092 singleton live births among women who underwent either fresh donor oocyte or autologous IVF, the rates of several outcomes were increased among the donor recipients. For example, preterm birth, defined as live birth before 37 weeks’ gestation, occurred in 14.8% vs. 9.4% of patients in the groups, respectively (odds ratio, 1.68), early preterm birth (live birth before 32 weeks’ gestation) occurred in 2.1% and 1.8% of patients (OR, 1.77), low birth weight (less than 2,500 g), occurred in 13.8% vs. 9.5% of patients (OR, 1.53), and very low birth weight (less than 1,500 g) occurred in 2.65% vs. 1.9% of patients (OR, 1.42).
The differences between the groups were statistically significant, said Dr. Kamath of Christian Medical College and Hospital, Vellore, India.
After adjusting for potential confounders, including female age, treatment duration, previous live birth, number of embryos transferred, single vs. multiple pregnancies resulting in singleton birth, and day of embryo transfer (before 5 days vs. 5 days or later), the increase in the risk of adverse perinatal outcomes of preterm birth, early preterm birth, and low birth weight remained significant (adjusted OR, 1.56, 1.41, and 1.43, respectively), he said.
The findings are important because the burden of poor ovarian response following IVF has been increasing, likely as a result of delayed childbearing and thus advanced age among those seeking IVF, Dr. Kamath said. However, little information is available regarding maternal or infant outcomes following oocyte donation, and the data that do exist have been conflicting, he said.
The increased risk of pregnancy complications following assisted reproductive technology, compared with spontaneously conceived pregnancies, has been largely attributed to the underlying infertility itself or to embryo-specific epigenetic modifications because of the in vitro fertilization techniques. The current study was conducted to determine whether use of donor oocytes affects obstetric and perinatal outcomes when compared with pregnancies that follow autologous IVF.
Anonymous data were obtained from the Human Fertilisation & Embryology Authority of the United Kingdom, which has collected data on all assisted reproductive treatment in the United Kingdom since 1991. For the current analysis, data from 1991 to 2011, including all singleton live births following fresh oocyte donor and autologous IVF cycles, were evaluated.
Although the dataset did not include information on potential confounders, such as smoking, body mass index, and medical history during pregnancy, the findings provide important insight into potential outcomes, Dr. Kamath said.
Dr. Kamath reported having no financial disclosures.
HELSINKI – The risk of preterm birth and low birth weight is higher following oocyte donation for in vitro fertilization, compared with autologous IVF, according to a review of more than 100,000 singleton live births.
The findings could help in counseling women and when managing pregnancies resulting from oocyte donation IVF, Mohan S. Kamath, MBBS, reported at the annual meeting of the European Society of Human Reproduction and Embryology.
In a review of 100,092 singleton live births among women who underwent either fresh donor oocyte or autologous IVF, the rates of several outcomes were increased among the donor recipients. For example, preterm birth, defined as live birth before 37 weeks’ gestation, occurred in 14.8% vs. 9.4% of patients in the groups, respectively (odds ratio, 1.68), early preterm birth (live birth before 32 weeks’ gestation) occurred in 2.1% and 1.8% of patients (OR, 1.77), low birth weight (less than 2,500 g), occurred in 13.8% vs. 9.5% of patients (OR, 1.53), and very low birth weight (less than 1,500 g) occurred in 2.65% vs. 1.9% of patients (OR, 1.42).
The differences between the groups were statistically significant, said Dr. Kamath of Christian Medical College and Hospital, Vellore, India.
After adjusting for potential confounders, including female age, treatment duration, previous live birth, number of embryos transferred, single vs. multiple pregnancies resulting in singleton birth, and day of embryo transfer (before 5 days vs. 5 days or later), the increase in the risk of adverse perinatal outcomes of preterm birth, early preterm birth, and low birth weight remained significant (adjusted OR, 1.56, 1.41, and 1.43, respectively), he said.
The findings are important because the burden of poor ovarian response following IVF has been increasing, likely as a result of delayed childbearing and thus advanced age among those seeking IVF, Dr. Kamath said. However, little information is available regarding maternal or infant outcomes following oocyte donation, and the data that do exist have been conflicting, he said.
The increased risk of pregnancy complications following assisted reproductive technology, compared with spontaneously conceived pregnancies, has been largely attributed to the underlying infertility itself or to embryo-specific epigenetic modifications because of the in vitro fertilization techniques. The current study was conducted to determine whether use of donor oocytes affects obstetric and perinatal outcomes when compared with pregnancies that follow autologous IVF.
Anonymous data were obtained from the Human Fertilisation & Embryology Authority of the United Kingdom, which has collected data on all assisted reproductive treatment in the United Kingdom since 1991. For the current analysis, data from 1991 to 2011, including all singleton live births following fresh oocyte donor and autologous IVF cycles, were evaluated.
Although the dataset did not include information on potential confounders, such as smoking, body mass index, and medical history during pregnancy, the findings provide important insight into potential outcomes, Dr. Kamath said.
Dr. Kamath reported having no financial disclosures.
AT ESHRE 2016
Key clinical point: Risk for preterm birth and low birth weight was increased with oocyte donation, compared with autologous IVF.
Major finding: With oocyte donation, the risk of preterm birth, early preterm birth, and low birth weight were significantly increased (adjusted OR, 1.56, 1.41, and 1.43, respectively), compared with autologous IVF.
Data source: A review of data on 100,092 singleton live births.
Disclosures: Dr. Kamath reported having no financial disclosures.
Abatacept fails to provide benefit in relapsing-remitting MS
Results from the double-blind, randomized, placebo-controlled phase II ACCLAIM study indicate that abatacept has no effect on reducing the number of new gadolinium-enhancing lesions on MRI in patients with relapsing-remitting multiple sclerosis, according to Samia J. Khoury, MD, of Brigham and Women’s Hospital, Boston, and her colleagues from the Immune Tolerance Network.
In the ACCLAIM (A Cooperative Clinical Study of Abatacept in Multiple Sclerosis) study, 42 patients who received abatacept (Orencia) developed a mean of 0.43 new gadolinium-enhancing lesions by week 24, compared with 1.66 for 20 placebo-treated patients (P = .87). None of the secondary MRI endpoints (lesion volume change and percent brain volume change) and clinical endpoints (changes in Multiple Sclerosis Functional Composite score, Expanded Disability Status Scale [EDSS], and annualized relapse rate) at 24 weeks differed significantly between the groups. The rate of patients who met criteria for no evidence of disease activity or its components (no EDSS progression, no clinical exacerbations, and no new gadolinium-enhancing MRI lesion) from week 8 and before week 28 did not differ between the groups.
During a 28-week extension phase in which the groups switched treatments, patients who switched from abatacept to placebo had a greater number of gadolinium-enhancing lesions than did those who switched from placebo to abatacept (1.25 vs. 0.60, respectively), but the difference was not statistically significant.
Abatacept, which is approved for the treatment of rheumatoid arthritis and juvenile idiopathic arthritis, is a CTLA4 immunoglobulin fusion protein that inhibits the activation of T lymphocytes by targeting the adaptive arm of the immune system by blocking the CD28-B7 costimulatory pathway. It was thought to have potential to reduce immune-mediated disease activity in relapsing-remitting multiple sclerosis because T lymphocytes have been implicated in its pathogenesis.
The investigators closed enrollment for the trial early because of slow accrual. The 65 total patients who enrolled in the trial were about half of the number designated in the trial design (n = 123) in order to demonstrate a treatment effect of 50% reduction of new gadolinium-enhancing MRI lesions.
The number of participants “was too small to demonstrate efficacy at the 50% level,” the investigators wrote, and “low numbers of new gadolinium-enhancing MRI lesions in the study population reduced the chances of demonstrating a treatment effect for abatacept.”
A prior phase II trial of abatacept that was stopped early due to safety events yielded inconclusive results because of an imbalance in the baseline disease activity of participants.
Read the full report online in Multiple Sclerosis Journal (Mult Scler J. 2016 Aug 1. doi: 10.1177/1352458516662727).
Results from the double-blind, randomized, placebo-controlled phase II ACCLAIM study indicate that abatacept has no effect on reducing the number of new gadolinium-enhancing lesions on MRI in patients with relapsing-remitting multiple sclerosis, according to Samia J. Khoury, MD, of Brigham and Women’s Hospital, Boston, and her colleagues from the Immune Tolerance Network.
In the ACCLAIM (A Cooperative Clinical Study of Abatacept in Multiple Sclerosis) study, 42 patients who received abatacept (Orencia) developed a mean of 0.43 new gadolinium-enhancing lesions by week 24, compared with 1.66 for 20 placebo-treated patients (P = .87). None of the secondary MRI endpoints (lesion volume change and percent brain volume change) and clinical endpoints (changes in Multiple Sclerosis Functional Composite score, Expanded Disability Status Scale [EDSS], and annualized relapse rate) at 24 weeks differed significantly between the groups. The rate of patients who met criteria for no evidence of disease activity or its components (no EDSS progression, no clinical exacerbations, and no new gadolinium-enhancing MRI lesion) from week 8 and before week 28 did not differ between the groups.
During a 28-week extension phase in which the groups switched treatments, patients who switched from abatacept to placebo had a greater number of gadolinium-enhancing lesions than did those who switched from placebo to abatacept (1.25 vs. 0.60, respectively), but the difference was not statistically significant.
Abatacept, which is approved for the treatment of rheumatoid arthritis and juvenile idiopathic arthritis, is a CTLA4 immunoglobulin fusion protein that inhibits the activation of T lymphocytes by targeting the adaptive arm of the immune system by blocking the CD28-B7 costimulatory pathway. It was thought to have potential to reduce immune-mediated disease activity in relapsing-remitting multiple sclerosis because T lymphocytes have been implicated in its pathogenesis.
The investigators closed enrollment for the trial early because of slow accrual. The 65 total patients who enrolled in the trial were about half of the number designated in the trial design (n = 123) in order to demonstrate a treatment effect of 50% reduction of new gadolinium-enhancing MRI lesions.
The number of participants “was too small to demonstrate efficacy at the 50% level,” the investigators wrote, and “low numbers of new gadolinium-enhancing MRI lesions in the study population reduced the chances of demonstrating a treatment effect for abatacept.”
A prior phase II trial of abatacept that was stopped early due to safety events yielded inconclusive results because of an imbalance in the baseline disease activity of participants.
Read the full report online in Multiple Sclerosis Journal (Mult Scler J. 2016 Aug 1. doi: 10.1177/1352458516662727).
Results from the double-blind, randomized, placebo-controlled phase II ACCLAIM study indicate that abatacept has no effect on reducing the number of new gadolinium-enhancing lesions on MRI in patients with relapsing-remitting multiple sclerosis, according to Samia J. Khoury, MD, of Brigham and Women’s Hospital, Boston, and her colleagues from the Immune Tolerance Network.
In the ACCLAIM (A Cooperative Clinical Study of Abatacept in Multiple Sclerosis) study, 42 patients who received abatacept (Orencia) developed a mean of 0.43 new gadolinium-enhancing lesions by week 24, compared with 1.66 for 20 placebo-treated patients (P = .87). None of the secondary MRI endpoints (lesion volume change and percent brain volume change) and clinical endpoints (changes in Multiple Sclerosis Functional Composite score, Expanded Disability Status Scale [EDSS], and annualized relapse rate) at 24 weeks differed significantly between the groups. The rate of patients who met criteria for no evidence of disease activity or its components (no EDSS progression, no clinical exacerbations, and no new gadolinium-enhancing MRI lesion) from week 8 and before week 28 did not differ between the groups.
During a 28-week extension phase in which the groups switched treatments, patients who switched from abatacept to placebo had a greater number of gadolinium-enhancing lesions than did those who switched from placebo to abatacept (1.25 vs. 0.60, respectively), but the difference was not statistically significant.
Abatacept, which is approved for the treatment of rheumatoid arthritis and juvenile idiopathic arthritis, is a CTLA4 immunoglobulin fusion protein that inhibits the activation of T lymphocytes by targeting the adaptive arm of the immune system by blocking the CD28-B7 costimulatory pathway. It was thought to have potential to reduce immune-mediated disease activity in relapsing-remitting multiple sclerosis because T lymphocytes have been implicated in its pathogenesis.
The investigators closed enrollment for the trial early because of slow accrual. The 65 total patients who enrolled in the trial were about half of the number designated in the trial design (n = 123) in order to demonstrate a treatment effect of 50% reduction of new gadolinium-enhancing MRI lesions.
The number of participants “was too small to demonstrate efficacy at the 50% level,” the investigators wrote, and “low numbers of new gadolinium-enhancing MRI lesions in the study population reduced the chances of demonstrating a treatment effect for abatacept.”
A prior phase II trial of abatacept that was stopped early due to safety events yielded inconclusive results because of an imbalance in the baseline disease activity of participants.
Read the full report online in Multiple Sclerosis Journal (Mult Scler J. 2016 Aug 1. doi: 10.1177/1352458516662727).
FROM MULTIPLE SCLEROSIS JOURNAL
As Zika Looms, Are LARCs the Answer?
In U.S. states where mosquito-borne Zika virus transmission is possible, adult women at risk for unintended pregnancy and sexually active high school girls are primarily using moderately effective and less effective contraceptive methods, according to a report from the Centers for Disease Control & Prevention.
Long-acting reversible contraceptives (LARCs) – considered a highly effective method – are used by fewer than a quarter of nonpregnant women, about one-third of recently postpartum women, and fewer than one-tenth of sexually active high school girls, according to a report published Aug. 2 in the Morbidity and Mortality Weekly Report (doi: 10.15585/mmwr.mm6530e2).
With locally transmitted cases of Zika virus infection increasing rapidly in Florida, the CDC is urging that the full range of FDA-approved contraceptive methods should be readily available and accessible to women who want to avoid or delay pregnancy.
“Given low rates of LARC use, states can implement strategies to remove barriers to the access and availability of LARC including high device costs, limited provider reimbursement, lack of training for providers serving women and adolescents on insertion and removal of LARC, provider lack of knowledge and misperceptions about LARC, limited availability of youth-friendly services that address adolescent confidentiality concerns, inadequate client-centered counseling, and low consumer awareness of the range of contraceptive methods available,” the CDC scientists wrote in the MMWR report.
Among nonpregnant women and recently postpartum women, the proportion not using any contraception ranged from 3.5% to 34.3%. Among sexually active high school girls, the proportion using no contraception ranged from 7.3% to 22.8%. The estimates of contraceptive use are based on 2011-2013 and 2015 survey data from four state-based surveillance systems.
The full MMWR report is available here.
In U.S. states where mosquito-borne Zika virus transmission is possible, adult women at risk for unintended pregnancy and sexually active high school girls are primarily using moderately effective and less effective contraceptive methods, according to a report from the Centers for Disease Control & Prevention.
Long-acting reversible contraceptives (LARCs) – considered a highly effective method – are used by fewer than a quarter of nonpregnant women, about one-third of recently postpartum women, and fewer than one-tenth of sexually active high school girls, according to a report published Aug. 2 in the Morbidity and Mortality Weekly Report (doi: 10.15585/mmwr.mm6530e2).
With locally transmitted cases of Zika virus infection increasing rapidly in Florida, the CDC is urging that the full range of FDA-approved contraceptive methods should be readily available and accessible to women who want to avoid or delay pregnancy.
“Given low rates of LARC use, states can implement strategies to remove barriers to the access and availability of LARC including high device costs, limited provider reimbursement, lack of training for providers serving women and adolescents on insertion and removal of LARC, provider lack of knowledge and misperceptions about LARC, limited availability of youth-friendly services that address adolescent confidentiality concerns, inadequate client-centered counseling, and low consumer awareness of the range of contraceptive methods available,” the CDC scientists wrote in the MMWR report.
Among nonpregnant women and recently postpartum women, the proportion not using any contraception ranged from 3.5% to 34.3%. Among sexually active high school girls, the proportion using no contraception ranged from 7.3% to 22.8%. The estimates of contraceptive use are based on 2011-2013 and 2015 survey data from four state-based surveillance systems.
The full MMWR report is available here.
In U.S. states where mosquito-borne Zika virus transmission is possible, adult women at risk for unintended pregnancy and sexually active high school girls are primarily using moderately effective and less effective contraceptive methods, according to a report from the Centers for Disease Control & Prevention.
Long-acting reversible contraceptives (LARCs) – considered a highly effective method – are used by fewer than a quarter of nonpregnant women, about one-third of recently postpartum women, and fewer than one-tenth of sexually active high school girls, according to a report published Aug. 2 in the Morbidity and Mortality Weekly Report (doi: 10.15585/mmwr.mm6530e2).
With locally transmitted cases of Zika virus infection increasing rapidly in Florida, the CDC is urging that the full range of FDA-approved contraceptive methods should be readily available and accessible to women who want to avoid or delay pregnancy.
“Given low rates of LARC use, states can implement strategies to remove barriers to the access and availability of LARC including high device costs, limited provider reimbursement, lack of training for providers serving women and adolescents on insertion and removal of LARC, provider lack of knowledge and misperceptions about LARC, limited availability of youth-friendly services that address adolescent confidentiality concerns, inadequate client-centered counseling, and low consumer awareness of the range of contraceptive methods available,” the CDC scientists wrote in the MMWR report.
Among nonpregnant women and recently postpartum women, the proportion not using any contraception ranged from 3.5% to 34.3%. Among sexually active high school girls, the proportion using no contraception ranged from 7.3% to 22.8%. The estimates of contraceptive use are based on 2011-2013 and 2015 survey data from four state-based surveillance systems.
The full MMWR report is available here.
FROM MMWR
As Zika looms, are LARCs the answer?
In U.S. states where mosquito-borne Zika virus transmission is possible, adult women at risk for unintended pregnancy and sexually active high school girls are primarily using moderately effective and less effective contraceptive methods, according to a report from the Centers for Disease Control & Prevention.
Long-acting reversible contraceptives (LARCs) – considered a highly effective method – are used by fewer than a quarter of nonpregnant women, about one-third of recently postpartum women, and fewer than one-tenth of sexually active high school girls, according to a report published Aug. 2 in the Morbidity and Mortality Weekly Report (doi: 10.15585/mmwr.mm6530e2).
With locally transmitted cases of Zika virus infection increasing rapidly in Florida, the CDC is urging that the full range of FDA-approved contraceptive methods should be readily available and accessible to women who want to avoid or delay pregnancy.
“Given low rates of LARC use, states can implement strategies to remove barriers to the access and availability of LARC including high device costs, limited provider reimbursement, lack of training for providers serving women and adolescents on insertion and removal of LARC, provider lack of knowledge and misperceptions about LARC, limited availability of youth-friendly services that address adolescent confidentiality concerns, inadequate client-centered counseling, and low consumer awareness of the range of contraceptive methods available,” the CDC scientists wrote in the MMWR report.
Among nonpregnant women and recently postpartum women, the proportion not using any contraception ranged from 3.5% to 34.3%. Among sexually active high school girls, the proportion using no contraception ranged from 7.3% to 22.8%. The estimates of contraceptive use are based on 2011-2013 and 2015 survey data from four state-based surveillance systems.
The full MMWR report is available here.
On Twitter @maryellenny
In U.S. states where mosquito-borne Zika virus transmission is possible, adult women at risk for unintended pregnancy and sexually active high school girls are primarily using moderately effective and less effective contraceptive methods, according to a report from the Centers for Disease Control & Prevention.
Long-acting reversible contraceptives (LARCs) – considered a highly effective method – are used by fewer than a quarter of nonpregnant women, about one-third of recently postpartum women, and fewer than one-tenth of sexually active high school girls, according to a report published Aug. 2 in the Morbidity and Mortality Weekly Report (doi: 10.15585/mmwr.mm6530e2).
With locally transmitted cases of Zika virus infection increasing rapidly in Florida, the CDC is urging that the full range of FDA-approved contraceptive methods should be readily available and accessible to women who want to avoid or delay pregnancy.
“Given low rates of LARC use, states can implement strategies to remove barriers to the access and availability of LARC including high device costs, limited provider reimbursement, lack of training for providers serving women and adolescents on insertion and removal of LARC, provider lack of knowledge and misperceptions about LARC, limited availability of youth-friendly services that address adolescent confidentiality concerns, inadequate client-centered counseling, and low consumer awareness of the range of contraceptive methods available,” the CDC scientists wrote in the MMWR report.
Among nonpregnant women and recently postpartum women, the proportion not using any contraception ranged from 3.5% to 34.3%. Among sexually active high school girls, the proportion using no contraception ranged from 7.3% to 22.8%. The estimates of contraceptive use are based on 2011-2013 and 2015 survey data from four state-based surveillance systems.
The full MMWR report is available here.
On Twitter @maryellenny
In U.S. states where mosquito-borne Zika virus transmission is possible, adult women at risk for unintended pregnancy and sexually active high school girls are primarily using moderately effective and less effective contraceptive methods, according to a report from the Centers for Disease Control & Prevention.
Long-acting reversible contraceptives (LARCs) – considered a highly effective method – are used by fewer than a quarter of nonpregnant women, about one-third of recently postpartum women, and fewer than one-tenth of sexually active high school girls, according to a report published Aug. 2 in the Morbidity and Mortality Weekly Report (doi: 10.15585/mmwr.mm6530e2).
With locally transmitted cases of Zika virus infection increasing rapidly in Florida, the CDC is urging that the full range of FDA-approved contraceptive methods should be readily available and accessible to women who want to avoid or delay pregnancy.
“Given low rates of LARC use, states can implement strategies to remove barriers to the access and availability of LARC including high device costs, limited provider reimbursement, lack of training for providers serving women and adolescents on insertion and removal of LARC, provider lack of knowledge and misperceptions about LARC, limited availability of youth-friendly services that address adolescent confidentiality concerns, inadequate client-centered counseling, and low consumer awareness of the range of contraceptive methods available,” the CDC scientists wrote in the MMWR report.
Among nonpregnant women and recently postpartum women, the proportion not using any contraception ranged from 3.5% to 34.3%. Among sexually active high school girls, the proportion using no contraception ranged from 7.3% to 22.8%. The estimates of contraceptive use are based on 2011-2013 and 2015 survey data from four state-based surveillance systems.
The full MMWR report is available here.
On Twitter @maryellenny
FROM MMWR
Race and America’s future
The issues of racial tensions have surfaced in plain sight in America. These are very trying times for our nation, and I fear some of my European American colleagues may not “get it.”
I recall a decade ago when I was involved with the Committee of Black Psychiatrists in crafting the American Psychiatric Association’s position statement, “Resolution Against Racism and Racial Discrimination and Their Adverse Impacts on Mental Health.” There was great concern that some of our European American colleagues would not get it, so in the preamble to the position statement, we explained that African Americans and European Americans had similar and different experiences in America, and that those differences made dialogue between both groups difficult.
Specifically, both groups believed that in America, people should be judged by the content of their character and not the color of their skin; after all, that is a basic value of the United States – it is one of our ideals. So, when a European American is accused of racism, the person often replies: “No, I am not; I believe in the American ideal of not being prejudiced.”
Unfortunately, the experiences of African Americans too often indicate that they are being judged by the color of our skin and not by our character. Most of the gross societal outcome indicators illustrate those disparities. So, African Americans, although occasionally experience the ideal that makes America great, all too often experience the reality of racial discrimination – including, but not limited to, phenomena the founder of the Black Psychiatrists of America, Chester M. Pierce, MD, coined “microinsults” and “microaggressions.” Women, too, experience these subtle and not-so-subtle put-downs by men all the time.
Accordingly, when we come together to dialogue about racial issues in our nation, many European Americans are focused on the ideal, and African Americans are focused on our reality, leaving the two groups on different pages. Having put everyone on the same page with this preface, I am told by members of the APA’s assembly that the position statement passed easily as a result of this understanding.
The problem is that being European American often prevents absorbing the perspective from the other side. So I thought it would be a good idea to share some personal experiences to help illuminate why so many African Americans feel the way they do about law enforcement.
I clearly recall being around 9 years old and being instructed that when running from the police, we should run zigzag, so it would be more difficult for them to shoot and kill us. We were instructed that running around corners worked better, because bullets fly straight and do not turn corners.
Of course, there also was the occasional experience (about two or three times each year) of sitting on a fence with a few of my friends of the same age, talking about what we were going to do when we grew up. A police car would drive up to the curb, and a police officer would call one of us over to talk. I recall clearly once when I got called over – of course, I took my sweet time, as I was not doing anything wrong, other than being 9 years old and black. The police officer got angry that I had tried to preserve my dignity by cruising over to the car. I remember his threat: Since I thought I was smart, he would drive me down to the police station, and he would not be surprised if my hand accidentally got broken in the car door during my transportation. I was 9 years old! Obviously, that abuse of power might have ruined my future career as a physician, but he let me go.
Years later as a teenager, I learned from my brother, a Chicago police officer, that the police are taught to take control of situations and assert their authority to prevent any potential conflicts. My brother also told me that the police were unofficially taught to carry “drop guns” in case they shot an unarmed suspect.
The idea was that they could drop the gun on the person, in other words, plant it and say the person had a gun after they had killed him. (It was always better in these accidents to leave the person dead, so he could not tell his side of the story.)
I often wonder where my brother would stand on this issue in 2016, but unfortunately as a police officer, while in plain clothes, he tried to help some fellow white officers intervene in a robbery. After identifying himself as a Chicago police officer, he and the other two white officers gave chase, but he outran them and trapped the suspect in a vestibule of a Southside Chicago apartment building. While my brother and the suspect were exchanging gunfire, two newer white Chicago police officers came upon a black man (my brother) with a gun, and he was promptly shot and killed. Of course, exactly what happened is murky, but I have my suspicions. Of course, the suspect also was killed during this shootout, so neither of the two black men involved was left alive to tell his side of the story.
Then there was the time I was in college being advised by my white guidance counselor that I should seek a career in something like auto mechanics. Little did he know that my African American grandfather obtained his PhD from Yale in 1924, and my father, like his father, had a couple of PhDs. What caused him to think I could accomplish only blue-collar goals? Charles Pinderhughes, MD, (another wise black psychiatrist) did an excellent dissertation in the American Journal of Psychiatry on “stereotyping,” that explained much of the reason (1979 Jan;136[1]33-7).
Because I was from Chicago and a psychiatrist, I was called in to evaluate several of the more than 100 innocent black men whom Jon Burge (a former Chicago police commander) allegedly tortured to get them to confess to murders they did not commit. Officer Burge was never found guilty of this crime, but he was sent to federal prison for three counts of obstruction of justice and perjury for lying about police torture.
Accordingly, in Chicago we have a saying, “The police hunt black men.” Of course, this statement rang true when a white Chicago police officer was caught on film shooting a 17-year-old child who may have had a developmental disability – Laquan McDonald – 16 times in October 2014.
Until the perceptions of race are viewed from both sides of the equation, there will continue to be racial strife, and America will not be as strong as it could be. I have tried to present some of the perspectives many black people experience as their reality. Of course, there is another side we as Americans believe in – justice and equality for all.
This election places America at a pivotal crossroads – which path will we take? Will we seek a more perfect union – or a country divided?
Dr. Bell is staff psychiatrist at Jackson Park Hospital Family Medicine Clinic in Chicago; clinical psychiatrist emeritus, department of psychiatry at the University of Illinois at Chicago; former president/CEO of Community Mental Health Council; and former director of the Institute for Juvenile Research (birthplace of child psychiatry), also in Chicago.
The issues of racial tensions have surfaced in plain sight in America. These are very trying times for our nation, and I fear some of my European American colleagues may not “get it.”
I recall a decade ago when I was involved with the Committee of Black Psychiatrists in crafting the American Psychiatric Association’s position statement, “Resolution Against Racism and Racial Discrimination and Their Adverse Impacts on Mental Health.” There was great concern that some of our European American colleagues would not get it, so in the preamble to the position statement, we explained that African Americans and European Americans had similar and different experiences in America, and that those differences made dialogue between both groups difficult.
Specifically, both groups believed that in America, people should be judged by the content of their character and not the color of their skin; after all, that is a basic value of the United States – it is one of our ideals. So, when a European American is accused of racism, the person often replies: “No, I am not; I believe in the American ideal of not being prejudiced.”
Unfortunately, the experiences of African Americans too often indicate that they are being judged by the color of our skin and not by our character. Most of the gross societal outcome indicators illustrate those disparities. So, African Americans, although occasionally experience the ideal that makes America great, all too often experience the reality of racial discrimination – including, but not limited to, phenomena the founder of the Black Psychiatrists of America, Chester M. Pierce, MD, coined “microinsults” and “microaggressions.” Women, too, experience these subtle and not-so-subtle put-downs by men all the time.
Accordingly, when we come together to dialogue about racial issues in our nation, many European Americans are focused on the ideal, and African Americans are focused on our reality, leaving the two groups on different pages. Having put everyone on the same page with this preface, I am told by members of the APA’s assembly that the position statement passed easily as a result of this understanding.
The problem is that being European American often prevents absorbing the perspective from the other side. So I thought it would be a good idea to share some personal experiences to help illuminate why so many African Americans feel the way they do about law enforcement.
I clearly recall being around 9 years old and being instructed that when running from the police, we should run zigzag, so it would be more difficult for them to shoot and kill us. We were instructed that running around corners worked better, because bullets fly straight and do not turn corners.
Of course, there also was the occasional experience (about two or three times each year) of sitting on a fence with a few of my friends of the same age, talking about what we were going to do when we grew up. A police car would drive up to the curb, and a police officer would call one of us over to talk. I recall clearly once when I got called over – of course, I took my sweet time, as I was not doing anything wrong, other than being 9 years old and black. The police officer got angry that I had tried to preserve my dignity by cruising over to the car. I remember his threat: Since I thought I was smart, he would drive me down to the police station, and he would not be surprised if my hand accidentally got broken in the car door during my transportation. I was 9 years old! Obviously, that abuse of power might have ruined my future career as a physician, but he let me go.
Years later as a teenager, I learned from my brother, a Chicago police officer, that the police are taught to take control of situations and assert their authority to prevent any potential conflicts. My brother also told me that the police were unofficially taught to carry “drop guns” in case they shot an unarmed suspect.
The idea was that they could drop the gun on the person, in other words, plant it and say the person had a gun after they had killed him. (It was always better in these accidents to leave the person dead, so he could not tell his side of the story.)
I often wonder where my brother would stand on this issue in 2016, but unfortunately as a police officer, while in plain clothes, he tried to help some fellow white officers intervene in a robbery. After identifying himself as a Chicago police officer, he and the other two white officers gave chase, but he outran them and trapped the suspect in a vestibule of a Southside Chicago apartment building. While my brother and the suspect were exchanging gunfire, two newer white Chicago police officers came upon a black man (my brother) with a gun, and he was promptly shot and killed. Of course, exactly what happened is murky, but I have my suspicions. Of course, the suspect also was killed during this shootout, so neither of the two black men involved was left alive to tell his side of the story.
Then there was the time I was in college being advised by my white guidance counselor that I should seek a career in something like auto mechanics. Little did he know that my African American grandfather obtained his PhD from Yale in 1924, and my father, like his father, had a couple of PhDs. What caused him to think I could accomplish only blue-collar goals? Charles Pinderhughes, MD, (another wise black psychiatrist) did an excellent dissertation in the American Journal of Psychiatry on “stereotyping,” that explained much of the reason (1979 Jan;136[1]33-7).
Because I was from Chicago and a psychiatrist, I was called in to evaluate several of the more than 100 innocent black men whom Jon Burge (a former Chicago police commander) allegedly tortured to get them to confess to murders they did not commit. Officer Burge was never found guilty of this crime, but he was sent to federal prison for three counts of obstruction of justice and perjury for lying about police torture.
Accordingly, in Chicago we have a saying, “The police hunt black men.” Of course, this statement rang true when a white Chicago police officer was caught on film shooting a 17-year-old child who may have had a developmental disability – Laquan McDonald – 16 times in October 2014.
Until the perceptions of race are viewed from both sides of the equation, there will continue to be racial strife, and America will not be as strong as it could be. I have tried to present some of the perspectives many black people experience as their reality. Of course, there is another side we as Americans believe in – justice and equality for all.
This election places America at a pivotal crossroads – which path will we take? Will we seek a more perfect union – or a country divided?
Dr. Bell is staff psychiatrist at Jackson Park Hospital Family Medicine Clinic in Chicago; clinical psychiatrist emeritus, department of psychiatry at the University of Illinois at Chicago; former president/CEO of Community Mental Health Council; and former director of the Institute for Juvenile Research (birthplace of child psychiatry), also in Chicago.
The issues of racial tensions have surfaced in plain sight in America. These are very trying times for our nation, and I fear some of my European American colleagues may not “get it.”
I recall a decade ago when I was involved with the Committee of Black Psychiatrists in crafting the American Psychiatric Association’s position statement, “Resolution Against Racism and Racial Discrimination and Their Adverse Impacts on Mental Health.” There was great concern that some of our European American colleagues would not get it, so in the preamble to the position statement, we explained that African Americans and European Americans had similar and different experiences in America, and that those differences made dialogue between both groups difficult.
Specifically, both groups believed that in America, people should be judged by the content of their character and not the color of their skin; after all, that is a basic value of the United States – it is one of our ideals. So, when a European American is accused of racism, the person often replies: “No, I am not; I believe in the American ideal of not being prejudiced.”
Unfortunately, the experiences of African Americans too often indicate that they are being judged by the color of our skin and not by our character. Most of the gross societal outcome indicators illustrate those disparities. So, African Americans, although occasionally experience the ideal that makes America great, all too often experience the reality of racial discrimination – including, but not limited to, phenomena the founder of the Black Psychiatrists of America, Chester M. Pierce, MD, coined “microinsults” and “microaggressions.” Women, too, experience these subtle and not-so-subtle put-downs by men all the time.
Accordingly, when we come together to dialogue about racial issues in our nation, many European Americans are focused on the ideal, and African Americans are focused on our reality, leaving the two groups on different pages. Having put everyone on the same page with this preface, I am told by members of the APA’s assembly that the position statement passed easily as a result of this understanding.
The problem is that being European American often prevents absorbing the perspective from the other side. So I thought it would be a good idea to share some personal experiences to help illuminate why so many African Americans feel the way they do about law enforcement.
I clearly recall being around 9 years old and being instructed that when running from the police, we should run zigzag, so it would be more difficult for them to shoot and kill us. We were instructed that running around corners worked better, because bullets fly straight and do not turn corners.
Of course, there also was the occasional experience (about two or three times each year) of sitting on a fence with a few of my friends of the same age, talking about what we were going to do when we grew up. A police car would drive up to the curb, and a police officer would call one of us over to talk. I recall clearly once when I got called over – of course, I took my sweet time, as I was not doing anything wrong, other than being 9 years old and black. The police officer got angry that I had tried to preserve my dignity by cruising over to the car. I remember his threat: Since I thought I was smart, he would drive me down to the police station, and he would not be surprised if my hand accidentally got broken in the car door during my transportation. I was 9 years old! Obviously, that abuse of power might have ruined my future career as a physician, but he let me go.
Years later as a teenager, I learned from my brother, a Chicago police officer, that the police are taught to take control of situations and assert their authority to prevent any potential conflicts. My brother also told me that the police were unofficially taught to carry “drop guns” in case they shot an unarmed suspect.
The idea was that they could drop the gun on the person, in other words, plant it and say the person had a gun after they had killed him. (It was always better in these accidents to leave the person dead, so he could not tell his side of the story.)
I often wonder where my brother would stand on this issue in 2016, but unfortunately as a police officer, while in plain clothes, he tried to help some fellow white officers intervene in a robbery. After identifying himself as a Chicago police officer, he and the other two white officers gave chase, but he outran them and trapped the suspect in a vestibule of a Southside Chicago apartment building. While my brother and the suspect were exchanging gunfire, two newer white Chicago police officers came upon a black man (my brother) with a gun, and he was promptly shot and killed. Of course, exactly what happened is murky, but I have my suspicions. Of course, the suspect also was killed during this shootout, so neither of the two black men involved was left alive to tell his side of the story.
Then there was the time I was in college being advised by my white guidance counselor that I should seek a career in something like auto mechanics. Little did he know that my African American grandfather obtained his PhD from Yale in 1924, and my father, like his father, had a couple of PhDs. What caused him to think I could accomplish only blue-collar goals? Charles Pinderhughes, MD, (another wise black psychiatrist) did an excellent dissertation in the American Journal of Psychiatry on “stereotyping,” that explained much of the reason (1979 Jan;136[1]33-7).
Because I was from Chicago and a psychiatrist, I was called in to evaluate several of the more than 100 innocent black men whom Jon Burge (a former Chicago police commander) allegedly tortured to get them to confess to murders they did not commit. Officer Burge was never found guilty of this crime, but he was sent to federal prison for three counts of obstruction of justice and perjury for lying about police torture.
Accordingly, in Chicago we have a saying, “The police hunt black men.” Of course, this statement rang true when a white Chicago police officer was caught on film shooting a 17-year-old child who may have had a developmental disability – Laquan McDonald – 16 times in October 2014.
Until the perceptions of race are viewed from both sides of the equation, there will continue to be racial strife, and America will not be as strong as it could be. I have tried to present some of the perspectives many black people experience as their reality. Of course, there is another side we as Americans believe in – justice and equality for all.
This election places America at a pivotal crossroads – which path will we take? Will we seek a more perfect union – or a country divided?
Dr. Bell is staff psychiatrist at Jackson Park Hospital Family Medicine Clinic in Chicago; clinical psychiatrist emeritus, department of psychiatry at the University of Illinois at Chicago; former president/CEO of Community Mental Health Council; and former director of the Institute for Juvenile Research (birthplace of child psychiatry), also in Chicago.
UTIs not caused by E. coli more likely in certain children
Certain children are more highly predisposed to contracting a urinary tract infection caused by a pathogen other than Escherichia coli, which is typically the most common cause of UTIs, a study showed.
“It may be clinically important to predict which children have UTIs caused by organisms other than E. coli because these organisms differ in their patterns of antimicrobial susceptibility,” wrote the study authors led by Nader Shaikh, MD, of the University of Pittsburgh. “Furthermore, some guidelines have suggested that screening for vesicoureteral reflux (VUR) with a voiding cystourethrogram (VCUG) should, at least in part, be based on whether an organism other than E. coli is recovered,” they wrote.
Dr. Shaikh and his coinvestigators examined the medical records of children in the Randomized Intervention for Children With Vesicoureteral Reflux (RIVUR) trial and the Careful Urinary Tract Infection Evaluation (CUTIE), both of which were prospective multicenter studies. Children included in both studies were 2-71 months of age; RIVUR subjects had VUR grades 1-4 and presented with either a first or second febrile or symptomatic UTI, while CUTIE subjects presented with either their first or second UTI but not VUR (Ped Inf Dis J. 2016. doi:10.1097/INF.0000000000001301).
In total, 769 children from 19 centers were included from both studies, of which 703 (91%) were female and 596 (78%) were white. Nine percent of all the children had UTIs that were not caused by E. coli. Circumcised males had the highest odds ratio associated with non–E. coli UTIs, with an OR of 5.5 (95% CI, 1.18-17.1; P = .003). significantly higher than the 1.6 odds ratio for uncircumcised males (95% CI, 0.6-4.6; P = .35).
Hispanic children also had a higher risk (OR = 2.3; 95% CI, 1.1-4.6; P = .02) than either non-Hispanic children or females, which were reference cohorts. Other groups found to be at higher-than-normal risk for non–E. coli UTIs were children without fever (OR = 2.8; 95% CI, 1.2-6.6; P = .02) and children with VUR grade 3 or 4 (OR = 2.2; 95% CI, 1.2-4.1; P = .01).
While more than 90% of children’s UTIs were caused by E. coli, the most common pathogens causing UTIs, causative organisms in the other 70 children were Proteus species (21 children, 30%), Klebsiella species (16, 23%), Enterococcus species (14, 20%), Enterobacter species (8, 11%), and “other species” (11, 16%).
“Children with UTIs caused by organisms other than E. coli were twice as likely to have high-grade VUR (grade 3 and 4), which is consistent with prior studies,” Dr. Shaikh and his coauthors noted, adding, “the association between Hispanic ethnicity and non-E. coli pathogens is novel and may be due to differences in genes involved with susceptibility to UTIs.”
There were no disclosures or sources of funding provided.
In this study of almost 800 children in the Pittsburgh area, the investigators sought to identify children at risk for urinary tract infections that more likely would have a bacterial organism not susceptible to standard first-line empiric antibiotic treatment.
They found that circumcised males, children with grade 3-4 vesicoureteral reflux, Hispanic children, and children without fever were more likely to have a UTI caused by organisms other than Escherichia coli and, therefore, less likely to respond to standard first-line antibiotic therapy. These investigators are the preeminent authorities in UTI management for children, so their findings should be viewed in that light.

|
Dr. Michael E. Pichichero |
The advance from the study is not a major one because all children with a suspected UTI should have a suitable culture specimen obtained before starting antibiotics, and the treatment choice continued or changed based on culture results. So really, the findings apply only to a decision about initial empiric treatment while awaiting culture results.
As a guide, if a clinician were to consider the diagnosis of UTI based on history, examination, and urinalysis, and the child was a circumcised male, a child with known grade 3 or 4 vesicoureteral reflux, Hispanic, or without fever, then the empiric antibiotic selected should be broader spectrum while awaiting urine culture results.
Michael E. Pichichero, MD, a specialist in pediatric infectious diseases, is director of the Research Institute, Rochester (N.Y.) General Hospital. He is also a pediatrician at Legacy Pediatrics in Rochester. Dr. Pichichero said he had no relevant financial disclosures.
In this study of almost 800 children in the Pittsburgh area, the investigators sought to identify children at risk for urinary tract infections that more likely would have a bacterial organism not susceptible to standard first-line empiric antibiotic treatment.
They found that circumcised males, children with grade 3-4 vesicoureteral reflux, Hispanic children, and children without fever were more likely to have a UTI caused by organisms other than Escherichia coli and, therefore, less likely to respond to standard first-line antibiotic therapy. These investigators are the preeminent authorities in UTI management for children, so their findings should be viewed in that light.

|
Dr. Michael E. Pichichero |
The advance from the study is not a major one because all children with a suspected UTI should have a suitable culture specimen obtained before starting antibiotics, and the treatment choice continued or changed based on culture results. So really, the findings apply only to a decision about initial empiric treatment while awaiting culture results.
As a guide, if a clinician were to consider the diagnosis of UTI based on history, examination, and urinalysis, and the child was a circumcised male, a child with known grade 3 or 4 vesicoureteral reflux, Hispanic, or without fever, then the empiric antibiotic selected should be broader spectrum while awaiting urine culture results.
Michael E. Pichichero, MD, a specialist in pediatric infectious diseases, is director of the Research Institute, Rochester (N.Y.) General Hospital. He is also a pediatrician at Legacy Pediatrics in Rochester. Dr. Pichichero said he had no relevant financial disclosures.
In this study of almost 800 children in the Pittsburgh area, the investigators sought to identify children at risk for urinary tract infections that more likely would have a bacterial organism not susceptible to standard first-line empiric antibiotic treatment.
They found that circumcised males, children with grade 3-4 vesicoureteral reflux, Hispanic children, and children without fever were more likely to have a UTI caused by organisms other than Escherichia coli and, therefore, less likely to respond to standard first-line antibiotic therapy. These investigators are the preeminent authorities in UTI management for children, so their findings should be viewed in that light.

|
Dr. Michael E. Pichichero |
The advance from the study is not a major one because all children with a suspected UTI should have a suitable culture specimen obtained before starting antibiotics, and the treatment choice continued or changed based on culture results. So really, the findings apply only to a decision about initial empiric treatment while awaiting culture results.
As a guide, if a clinician were to consider the diagnosis of UTI based on history, examination, and urinalysis, and the child was a circumcised male, a child with known grade 3 or 4 vesicoureteral reflux, Hispanic, or without fever, then the empiric antibiotic selected should be broader spectrum while awaiting urine culture results.
Michael E. Pichichero, MD, a specialist in pediatric infectious diseases, is director of the Research Institute, Rochester (N.Y.) General Hospital. He is also a pediatrician at Legacy Pediatrics in Rochester. Dr. Pichichero said he had no relevant financial disclosures.
Certain children are more highly predisposed to contracting a urinary tract infection caused by a pathogen other than Escherichia coli, which is typically the most common cause of UTIs, a study showed.
“It may be clinically important to predict which children have UTIs caused by organisms other than E. coli because these organisms differ in their patterns of antimicrobial susceptibility,” wrote the study authors led by Nader Shaikh, MD, of the University of Pittsburgh. “Furthermore, some guidelines have suggested that screening for vesicoureteral reflux (VUR) with a voiding cystourethrogram (VCUG) should, at least in part, be based on whether an organism other than E. coli is recovered,” they wrote.
Dr. Shaikh and his coinvestigators examined the medical records of children in the Randomized Intervention for Children With Vesicoureteral Reflux (RIVUR) trial and the Careful Urinary Tract Infection Evaluation (CUTIE), both of which were prospective multicenter studies. Children included in both studies were 2-71 months of age; RIVUR subjects had VUR grades 1-4 and presented with either a first or second febrile or symptomatic UTI, while CUTIE subjects presented with either their first or second UTI but not VUR (Ped Inf Dis J. 2016. doi:10.1097/INF.0000000000001301).
In total, 769 children from 19 centers were included from both studies, of which 703 (91%) were female and 596 (78%) were white. Nine percent of all the children had UTIs that were not caused by E. coli. Circumcised males had the highest odds ratio associated with non–E. coli UTIs, with an OR of 5.5 (95% CI, 1.18-17.1; P = .003). significantly higher than the 1.6 odds ratio for uncircumcised males (95% CI, 0.6-4.6; P = .35).
Hispanic children also had a higher risk (OR = 2.3; 95% CI, 1.1-4.6; P = .02) than either non-Hispanic children or females, which were reference cohorts. Other groups found to be at higher-than-normal risk for non–E. coli UTIs were children without fever (OR = 2.8; 95% CI, 1.2-6.6; P = .02) and children with VUR grade 3 or 4 (OR = 2.2; 95% CI, 1.2-4.1; P = .01).
While more than 90% of children’s UTIs were caused by E. coli, the most common pathogens causing UTIs, causative organisms in the other 70 children were Proteus species (21 children, 30%), Klebsiella species (16, 23%), Enterococcus species (14, 20%), Enterobacter species (8, 11%), and “other species” (11, 16%).
“Children with UTIs caused by organisms other than E. coli were twice as likely to have high-grade VUR (grade 3 and 4), which is consistent with prior studies,” Dr. Shaikh and his coauthors noted, adding, “the association between Hispanic ethnicity and non-E. coli pathogens is novel and may be due to differences in genes involved with susceptibility to UTIs.”
There were no disclosures or sources of funding provided.
Certain children are more highly predisposed to contracting a urinary tract infection caused by a pathogen other than Escherichia coli, which is typically the most common cause of UTIs, a study showed.
“It may be clinically important to predict which children have UTIs caused by organisms other than E. coli because these organisms differ in their patterns of antimicrobial susceptibility,” wrote the study authors led by Nader Shaikh, MD, of the University of Pittsburgh. “Furthermore, some guidelines have suggested that screening for vesicoureteral reflux (VUR) with a voiding cystourethrogram (VCUG) should, at least in part, be based on whether an organism other than E. coli is recovered,” they wrote.
Dr. Shaikh and his coinvestigators examined the medical records of children in the Randomized Intervention for Children With Vesicoureteral Reflux (RIVUR) trial and the Careful Urinary Tract Infection Evaluation (CUTIE), both of which were prospective multicenter studies. Children included in both studies were 2-71 months of age; RIVUR subjects had VUR grades 1-4 and presented with either a first or second febrile or symptomatic UTI, while CUTIE subjects presented with either their first or second UTI but not VUR (Ped Inf Dis J. 2016. doi:10.1097/INF.0000000000001301).
In total, 769 children from 19 centers were included from both studies, of which 703 (91%) were female and 596 (78%) were white. Nine percent of all the children had UTIs that were not caused by E. coli. Circumcised males had the highest odds ratio associated with non–E. coli UTIs, with an OR of 5.5 (95% CI, 1.18-17.1; P = .003). significantly higher than the 1.6 odds ratio for uncircumcised males (95% CI, 0.6-4.6; P = .35).
Hispanic children also had a higher risk (OR = 2.3; 95% CI, 1.1-4.6; P = .02) than either non-Hispanic children or females, which were reference cohorts. Other groups found to be at higher-than-normal risk for non–E. coli UTIs were children without fever (OR = 2.8; 95% CI, 1.2-6.6; P = .02) and children with VUR grade 3 or 4 (OR = 2.2; 95% CI, 1.2-4.1; P = .01).
While more than 90% of children’s UTIs were caused by E. coli, the most common pathogens causing UTIs, causative organisms in the other 70 children were Proteus species (21 children, 30%), Klebsiella species (16, 23%), Enterococcus species (14, 20%), Enterobacter species (8, 11%), and “other species” (11, 16%).
“Children with UTIs caused by organisms other than E. coli were twice as likely to have high-grade VUR (grade 3 and 4), which is consistent with prior studies,” Dr. Shaikh and his coauthors noted, adding, “the association between Hispanic ethnicity and non-E. coli pathogens is novel and may be due to differences in genes involved with susceptibility to UTIs.”
There were no disclosures or sources of funding provided.
FROM THE PEDIATRIC INFECTIOUS DISEASE JOURNAL
Key clinical point: Non–Escherichia coli urinary tract infections are more likely to occur in children who are uncircumcised, are Hispanic, have no fever, or have grade 3-4 vesicoureteral reflux.
Major finding: Circumcised males had an odds ratio of 5.5 (95% CI, 1.8-17.1; P = .003) of infection by pathogens other than E. coli; the odds ratio for Hispanic children (OR = 2.3; 95% CI, 1.1-4.6; P = .02), children without fever (OR = 2.8; 95% CI, 1.2-6.6; P = .02), and children with grade 3-4 VUR (OR = 2.2; 95% CI, 1.2-4.1; P = .01) also were relatively high.
Data source: A review of data from two prospective multicenter studies involving 769 children with a UTI aged 2-71 months .
Disclosures: Funding sources and individual disclosures were not provided.
In septic shock, vasopressin not better than norepinephrine
Vasopressin was no better than norepinephrine in preventing kidney failure when used as a first-line treatment for septic shock, according to a report published online Aug. 2 in JAMA.
In a multicenter, double-blind, randomized trial comparing the two approaches in 408 ICU patients with septic shock, the early use of vasopressin didn’t reduce the number of days free of kidney failure, compared with standard norepinephrine.
However, “the 95% confidence intervals of the difference between [study] groups has an upper limit of 5 days in favor of vasopressin, which could be clinically important,” said Anthony C. Gordon, MD, of Charing Cross Hospital and Imperial College London, and his associates. “Therefore, these results are still consistent with a potentially clinically important benefit for vasopressin; but a larger trial would be needed to confirm or refute this.”
Norepinephrine is the recommended first-line vasopressor for septic shock, but “there has been a growing interest in the use of vasopressin” ever since researchers described a relative deficiency of vasopressin in the disorder, Dr. Gordon and his associates noted.
“Preclinical and small clinical studies have suggested that vasopressin may be better able to maintain glomerular filtration rate and improve creatinine clearance, compared with norepinephrine,” the investigators said, and other studies have suggested that combining vasopressin with corticosteroids may prevent deterioration in organ function and reduce the duration of shock, thereby improving survival.
To examine those possibilities, they performed the VANISH (Vasopressin vs. Norepinephrine as Initial Therapy in Septic Shock) trial, assessing patients age 16 years and older at 18 general adult ICUs in the United Kingdom during a 2-year period. The study participants were randomly assigned to receive vasopressin plus hydrocortisone (100 patients), vasopressin plus matching placebo (104 patients), norepinephrine plus hydrocortisone (101 patients), or norepinephrine plus matching placebo (103 patients).
The primary outcome measure was the number of days alive and free of kidney failure during the 28 days following randomization. There was no significant difference among the four study groups in the number or the distribution of kidney-failure–free days, the investigators said (JAMA. 2016 Aug 2. doi: 10.1001/jama.2016.10485).
In addition, the percentage of survivors who never developed kidney failure was not significantly different between the two groups who received vasopressin (57.0%) and the two who received norepinephrine (59.2%). And the median number of days free of kidney failure in the subgroup of patients who died or developed kidney failure was not significantly different between those receiving vasopressin (9 days) and those receiving norepinephrine (13 days).
The quantities of IV fluids administered, the total fluid balance, serum lactate levels, and heart rate were all similar across the four study groups. There also was no significant difference in 28-day mortality between patients who received vasopressin (30.9%) and those who received norepinephrine (27.5%). Adverse event profiles also were comparable.
However, the rate of renal replacement therapy was 25.4% with vasopressin, significantly lower than the 35.3% rate in the norepinephrine group. The use of such therapy was not controlled in the trial and was initiated according to the treating physicians’ preference. “It is therefore not possible to know why renal replacement therapy was or was not started,” Dr. Gordon and his associates noted.
The use of renal replacement therapy wasn’t a primary outcome of the trial. Nevertheless, it is an important patient-centered outcome and may be a factor to consider when treating adults who have septic shock, the researchers added.
The study was supported by the U.K. National Institute for Health Research and the U.K. Intensive Care Foundation. Dr. Gordon reported ties to Ferring, HCA International, Orion, and Tenax Therapeutics; his associates reported having no relevant financial disclosures.
Vasopressin was no better than norepinephrine in preventing kidney failure when used as a first-line treatment for septic shock, according to a report published online Aug. 2 in JAMA.
In a multicenter, double-blind, randomized trial comparing the two approaches in 408 ICU patients with septic shock, the early use of vasopressin didn’t reduce the number of days free of kidney failure, compared with standard norepinephrine.
However, “the 95% confidence intervals of the difference between [study] groups has an upper limit of 5 days in favor of vasopressin, which could be clinically important,” said Anthony C. Gordon, MD, of Charing Cross Hospital and Imperial College London, and his associates. “Therefore, these results are still consistent with a potentially clinically important benefit for vasopressin; but a larger trial would be needed to confirm or refute this.”
Norepinephrine is the recommended first-line vasopressor for septic shock, but “there has been a growing interest in the use of vasopressin” ever since researchers described a relative deficiency of vasopressin in the disorder, Dr. Gordon and his associates noted.
“Preclinical and small clinical studies have suggested that vasopressin may be better able to maintain glomerular filtration rate and improve creatinine clearance, compared with norepinephrine,” the investigators said, and other studies have suggested that combining vasopressin with corticosteroids may prevent deterioration in organ function and reduce the duration of shock, thereby improving survival.
To examine those possibilities, they performed the VANISH (Vasopressin vs. Norepinephrine as Initial Therapy in Septic Shock) trial, assessing patients age 16 years and older at 18 general adult ICUs in the United Kingdom during a 2-year period. The study participants were randomly assigned to receive vasopressin plus hydrocortisone (100 patients), vasopressin plus matching placebo (104 patients), norepinephrine plus hydrocortisone (101 patients), or norepinephrine plus matching placebo (103 patients).
The primary outcome measure was the number of days alive and free of kidney failure during the 28 days following randomization. There was no significant difference among the four study groups in the number or the distribution of kidney-failure–free days, the investigators said (JAMA. 2016 Aug 2. doi: 10.1001/jama.2016.10485).
In addition, the percentage of survivors who never developed kidney failure was not significantly different between the two groups who received vasopressin (57.0%) and the two who received norepinephrine (59.2%). And the median number of days free of kidney failure in the subgroup of patients who died or developed kidney failure was not significantly different between those receiving vasopressin (9 days) and those receiving norepinephrine (13 days).
The quantities of IV fluids administered, the total fluid balance, serum lactate levels, and heart rate were all similar across the four study groups. There also was no significant difference in 28-day mortality between patients who received vasopressin (30.9%) and those who received norepinephrine (27.5%). Adverse event profiles also were comparable.
However, the rate of renal replacement therapy was 25.4% with vasopressin, significantly lower than the 35.3% rate in the norepinephrine group. The use of such therapy was not controlled in the trial and was initiated according to the treating physicians’ preference. “It is therefore not possible to know why renal replacement therapy was or was not started,” Dr. Gordon and his associates noted.
The use of renal replacement therapy wasn’t a primary outcome of the trial. Nevertheless, it is an important patient-centered outcome and may be a factor to consider when treating adults who have septic shock, the researchers added.
The study was supported by the U.K. National Institute for Health Research and the U.K. Intensive Care Foundation. Dr. Gordon reported ties to Ferring, HCA International, Orion, and Tenax Therapeutics; his associates reported having no relevant financial disclosures.
Vasopressin was no better than norepinephrine in preventing kidney failure when used as a first-line treatment for septic shock, according to a report published online Aug. 2 in JAMA.
In a multicenter, double-blind, randomized trial comparing the two approaches in 408 ICU patients with septic shock, the early use of vasopressin didn’t reduce the number of days free of kidney failure, compared with standard norepinephrine.
However, “the 95% confidence intervals of the difference between [study] groups has an upper limit of 5 days in favor of vasopressin, which could be clinically important,” said Anthony C. Gordon, MD, of Charing Cross Hospital and Imperial College London, and his associates. “Therefore, these results are still consistent with a potentially clinically important benefit for vasopressin; but a larger trial would be needed to confirm or refute this.”
Norepinephrine is the recommended first-line vasopressor for septic shock, but “there has been a growing interest in the use of vasopressin” ever since researchers described a relative deficiency of vasopressin in the disorder, Dr. Gordon and his associates noted.
“Preclinical and small clinical studies have suggested that vasopressin may be better able to maintain glomerular filtration rate and improve creatinine clearance, compared with norepinephrine,” the investigators said, and other studies have suggested that combining vasopressin with corticosteroids may prevent deterioration in organ function and reduce the duration of shock, thereby improving survival.
To examine those possibilities, they performed the VANISH (Vasopressin vs. Norepinephrine as Initial Therapy in Septic Shock) trial, assessing patients age 16 years and older at 18 general adult ICUs in the United Kingdom during a 2-year period. The study participants were randomly assigned to receive vasopressin plus hydrocortisone (100 patients), vasopressin plus matching placebo (104 patients), norepinephrine plus hydrocortisone (101 patients), or norepinephrine plus matching placebo (103 patients).
The primary outcome measure was the number of days alive and free of kidney failure during the 28 days following randomization. There was no significant difference among the four study groups in the number or the distribution of kidney-failure–free days, the investigators said (JAMA. 2016 Aug 2. doi: 10.1001/jama.2016.10485).
In addition, the percentage of survivors who never developed kidney failure was not significantly different between the two groups who received vasopressin (57.0%) and the two who received norepinephrine (59.2%). And the median number of days free of kidney failure in the subgroup of patients who died or developed kidney failure was not significantly different between those receiving vasopressin (9 days) and those receiving norepinephrine (13 days).
The quantities of IV fluids administered, the total fluid balance, serum lactate levels, and heart rate were all similar across the four study groups. There also was no significant difference in 28-day mortality between patients who received vasopressin (30.9%) and those who received norepinephrine (27.5%). Adverse event profiles also were comparable.
However, the rate of renal replacement therapy was 25.4% with vasopressin, significantly lower than the 35.3% rate in the norepinephrine group. The use of such therapy was not controlled in the trial and was initiated according to the treating physicians’ preference. “It is therefore not possible to know why renal replacement therapy was or was not started,” Dr. Gordon and his associates noted.
The use of renal replacement therapy wasn’t a primary outcome of the trial. Nevertheless, it is an important patient-centered outcome and may be a factor to consider when treating adults who have septic shock, the researchers added.
The study was supported by the U.K. National Institute for Health Research and the U.K. Intensive Care Foundation. Dr. Gordon reported ties to Ferring, HCA International, Orion, and Tenax Therapeutics; his associates reported having no relevant financial disclosures.
FROM JAMA
Key clinical point: Vasopressin didn’t perform better than norepinephrine in preventing kidney failure when used as a first-line treatment for septic shock.
Major finding: The primary outcome measure – the number of days alive and free of kidney failure during the first month of treatment – was not significantly different among the four study groups.
Data source: A multicenter, double-blind, randomized clinical trial involving 408 ICU patients treated in the United Kingdom during a 2-year period.
Disclosures: The study was supported by the U.K. National Institute for Health Research and the U.K. Intensive Care Foundation. Dr. Gordon reported ties to Ferring, HCA International, Orion, and Tenax Therapeutics; his associates reported having no relevant financial disclosures.
Psychiatric disorders often impair antiretroviral adherence in perinatally HIV-infected teens
DURBAN, SOUTH AFRICA – Adolescents who were perinatally infected with HIV have a high prevalence of selected psychiatric disorders that impede their adherence to antiretroviral therapy, Claude Ann Mellins, PhD, reported at the 21st International AIDS Conference.
Those psychiatric diagnoses were predictive of viremia over the ensuing 2-3 years in a new analysis from the ongoing Child and Adolescent Self-Awareness and Health (CASAH) study, according to Dr. Mellins, professor of medical psychology at Columbia University, New York, and codirector of CASAH.
The clinical implications of the CASAH findings are clear, she added. “Assessing and treating specific categories of psychiatric and substance abuse problems may enhance efforts to improve adherence and prevent poor health outcomes in these adolescents and young adults, who are especially vulnerable due to their very challenging circumstances,” Dr. Mellins said.
CASAH is a longitudinal study of perinatally HIV-infected and perinatally HIV-exposed but uninfected New York City youth. They were enrolled during 2003-2008, when they were 9-16 years old. They and their caregivers undergo detailed psychosocial interviews every 12-18 months. The goal is to identify risk factors as well as protective factors influencing their behavioral health outcomes, the clinical psychologist explained.
She reported on 179 perinatally infected adolescents who were at least 13 years old at the first of their three interviews conducted over a 2.7-year period. Of note, 53% of them met Diagnostic Interview Schedule for Children (DISC-IV) criteria for one or more psychiatric diagnoses at all three time points. The pattern of psychopathology was somewhat different from that previously described in adults with HIV, who have been studied much more extensively than perinatally infected teens.
“Much of the literature on adults has focused on depression and mood disorders as predictors of poor health outcomes. Our data suggest that among youth, disruptive behavioral disorders – things like [attention-deficit/hyperactivity disorder], conduct disorder, or oppositional defiant disorder – may be just as important, if not more so. Substance abuse was also a critical factor,” Dr. Mellins said.
In a cross-sectional multivariate logistic regression analysis, a behavior disorder diagnosed at the first interview was associated with a 2.57-fold increased likelihood of contemporaneous viremia as evidenced by a plasma HIV RNA viral load greater than 1,000 copies/mL, and with a threefold increased likelihood of self-reported missed doses of antiretroviral medications during the previous week.
Anxiety disorder was the most common psychiatric diagnosis at the initial interview, followed by disruptive behavior disorder and substance use disorder. A diagnosis of any psychiatric disorder at the time of the first interview was associated with a significantly increased risk of viremia across the next 2.7 years. Forty-seven percent of subjects had viremia at 2.7 years of follow-up, reflective of chronic suboptimal medication adherence.
She noted that the pattern of psychiatric disorders in perinatally infected patients shifts between adolescence and young adulthood.
“By the time perinatally infected adolescents become young adults, I will say that anxiety and mood disorders become much more prevalent. But the number of psychiatric problems actually goes down by young adulthood,” according to Dr. Mellins.
Indeed, in another CASAH analysis she presented at AIDS 2016, this one involving 136 perinatally infected young adults and 86 perinatally exposed but uninfected controls, the vast majority living in impoverished communities, there was no difference between the two groups in rates of psychiatric or substance use disorders, although the 27% prevalence of substance use disorders is higher than that found in the age-matched general population.
Eighty-four percent of the perinatally infected 18- to 28-year-olds had graduated from high school, 94% were in a stable housing situation, 59% were currently working or in school, 54% were paying rent, and 95% reported ever being in a romantic relationship. Rates were similar in the perinatally exposed but uninfected group with the exception that these individuals were less likely to be paying rent.
“In spite of substantive risks, there is a relatively large portion of both groups with positive behavioral health outcomes, achieving normative young adult transition milestones. We need to understand why. Identification of protective factors conferring resilience can inform evidence-based prevention efforts, which are critical given the staggering numbers of children and young adolescents worldwide affected by HIV who will be transitioning to adulthood,” she said.
Dr. Mellins said the CASAH findings constitute a persuasive argument in favor of integrating mental health as a component of HIV care.
“Young people don’t always go to mental health appointments that are separate from medical care, so integrating mental health as a component of HIV care might be one of the most effective ways to identify and treat mental health problems in infected youth while simultaneously improving medication adherence and health outcomes,” Dr. Mellins said.
The ongoing CASAH study is funded by the National Institute of Mental Health. Dr. Mellins reported having no relevant financial conflicts.
DURBAN, SOUTH AFRICA – Adolescents who were perinatally infected with HIV have a high prevalence of selected psychiatric disorders that impede their adherence to antiretroviral therapy, Claude Ann Mellins, PhD, reported at the 21st International AIDS Conference.
Those psychiatric diagnoses were predictive of viremia over the ensuing 2-3 years in a new analysis from the ongoing Child and Adolescent Self-Awareness and Health (CASAH) study, according to Dr. Mellins, professor of medical psychology at Columbia University, New York, and codirector of CASAH.
The clinical implications of the CASAH findings are clear, she added. “Assessing and treating specific categories of psychiatric and substance abuse problems may enhance efforts to improve adherence and prevent poor health outcomes in these adolescents and young adults, who are especially vulnerable due to their very challenging circumstances,” Dr. Mellins said.
CASAH is a longitudinal study of perinatally HIV-infected and perinatally HIV-exposed but uninfected New York City youth. They were enrolled during 2003-2008, when they were 9-16 years old. They and their caregivers undergo detailed psychosocial interviews every 12-18 months. The goal is to identify risk factors as well as protective factors influencing their behavioral health outcomes, the clinical psychologist explained.
She reported on 179 perinatally infected adolescents who were at least 13 years old at the first of their three interviews conducted over a 2.7-year period. Of note, 53% of them met Diagnostic Interview Schedule for Children (DISC-IV) criteria for one or more psychiatric diagnoses at all three time points. The pattern of psychopathology was somewhat different from that previously described in adults with HIV, who have been studied much more extensively than perinatally infected teens.
“Much of the literature on adults has focused on depression and mood disorders as predictors of poor health outcomes. Our data suggest that among youth, disruptive behavioral disorders – things like [attention-deficit/hyperactivity disorder], conduct disorder, or oppositional defiant disorder – may be just as important, if not more so. Substance abuse was also a critical factor,” Dr. Mellins said.
In a cross-sectional multivariate logistic regression analysis, a behavior disorder diagnosed at the first interview was associated with a 2.57-fold increased likelihood of contemporaneous viremia as evidenced by a plasma HIV RNA viral load greater than 1,000 copies/mL, and with a threefold increased likelihood of self-reported missed doses of antiretroviral medications during the previous week.
Anxiety disorder was the most common psychiatric diagnosis at the initial interview, followed by disruptive behavior disorder and substance use disorder. A diagnosis of any psychiatric disorder at the time of the first interview was associated with a significantly increased risk of viremia across the next 2.7 years. Forty-seven percent of subjects had viremia at 2.7 years of follow-up, reflective of chronic suboptimal medication adherence.
She noted that the pattern of psychiatric disorders in perinatally infected patients shifts between adolescence and young adulthood.
“By the time perinatally infected adolescents become young adults, I will say that anxiety and mood disorders become much more prevalent. But the number of psychiatric problems actually goes down by young adulthood,” according to Dr. Mellins.
Indeed, in another CASAH analysis she presented at AIDS 2016, this one involving 136 perinatally infected young adults and 86 perinatally exposed but uninfected controls, the vast majority living in impoverished communities, there was no difference between the two groups in rates of psychiatric or substance use disorders, although the 27% prevalence of substance use disorders is higher than that found in the age-matched general population.
Eighty-four percent of the perinatally infected 18- to 28-year-olds had graduated from high school, 94% were in a stable housing situation, 59% were currently working or in school, 54% were paying rent, and 95% reported ever being in a romantic relationship. Rates were similar in the perinatally exposed but uninfected group with the exception that these individuals were less likely to be paying rent.
“In spite of substantive risks, there is a relatively large portion of both groups with positive behavioral health outcomes, achieving normative young adult transition milestones. We need to understand why. Identification of protective factors conferring resilience can inform evidence-based prevention efforts, which are critical given the staggering numbers of children and young adolescents worldwide affected by HIV who will be transitioning to adulthood,” she said.
Dr. Mellins said the CASAH findings constitute a persuasive argument in favor of integrating mental health as a component of HIV care.
“Young people don’t always go to mental health appointments that are separate from medical care, so integrating mental health as a component of HIV care might be one of the most effective ways to identify and treat mental health problems in infected youth while simultaneously improving medication adherence and health outcomes,” Dr. Mellins said.
The ongoing CASAH study is funded by the National Institute of Mental Health. Dr. Mellins reported having no relevant financial conflicts.
DURBAN, SOUTH AFRICA – Adolescents who were perinatally infected with HIV have a high prevalence of selected psychiatric disorders that impede their adherence to antiretroviral therapy, Claude Ann Mellins, PhD, reported at the 21st International AIDS Conference.
Those psychiatric diagnoses were predictive of viremia over the ensuing 2-3 years in a new analysis from the ongoing Child and Adolescent Self-Awareness and Health (CASAH) study, according to Dr. Mellins, professor of medical psychology at Columbia University, New York, and codirector of CASAH.
The clinical implications of the CASAH findings are clear, she added. “Assessing and treating specific categories of psychiatric and substance abuse problems may enhance efforts to improve adherence and prevent poor health outcomes in these adolescents and young adults, who are especially vulnerable due to their very challenging circumstances,” Dr. Mellins said.
CASAH is a longitudinal study of perinatally HIV-infected and perinatally HIV-exposed but uninfected New York City youth. They were enrolled during 2003-2008, when they were 9-16 years old. They and their caregivers undergo detailed psychosocial interviews every 12-18 months. The goal is to identify risk factors as well as protective factors influencing their behavioral health outcomes, the clinical psychologist explained.
She reported on 179 perinatally infected adolescents who were at least 13 years old at the first of their three interviews conducted over a 2.7-year period. Of note, 53% of them met Diagnostic Interview Schedule for Children (DISC-IV) criteria for one or more psychiatric diagnoses at all three time points. The pattern of psychopathology was somewhat different from that previously described in adults with HIV, who have been studied much more extensively than perinatally infected teens.
“Much of the literature on adults has focused on depression and mood disorders as predictors of poor health outcomes. Our data suggest that among youth, disruptive behavioral disorders – things like [attention-deficit/hyperactivity disorder], conduct disorder, or oppositional defiant disorder – may be just as important, if not more so. Substance abuse was also a critical factor,” Dr. Mellins said.
In a cross-sectional multivariate logistic regression analysis, a behavior disorder diagnosed at the first interview was associated with a 2.57-fold increased likelihood of contemporaneous viremia as evidenced by a plasma HIV RNA viral load greater than 1,000 copies/mL, and with a threefold increased likelihood of self-reported missed doses of antiretroviral medications during the previous week.
Anxiety disorder was the most common psychiatric diagnosis at the initial interview, followed by disruptive behavior disorder and substance use disorder. A diagnosis of any psychiatric disorder at the time of the first interview was associated with a significantly increased risk of viremia across the next 2.7 years. Forty-seven percent of subjects had viremia at 2.7 years of follow-up, reflective of chronic suboptimal medication adherence.
She noted that the pattern of psychiatric disorders in perinatally infected patients shifts between adolescence and young adulthood.
“By the time perinatally infected adolescents become young adults, I will say that anxiety and mood disorders become much more prevalent. But the number of psychiatric problems actually goes down by young adulthood,” according to Dr. Mellins.
Indeed, in another CASAH analysis she presented at AIDS 2016, this one involving 136 perinatally infected young adults and 86 perinatally exposed but uninfected controls, the vast majority living in impoverished communities, there was no difference between the two groups in rates of psychiatric or substance use disorders, although the 27% prevalence of substance use disorders is higher than that found in the age-matched general population.
Eighty-four percent of the perinatally infected 18- to 28-year-olds had graduated from high school, 94% were in a stable housing situation, 59% were currently working or in school, 54% were paying rent, and 95% reported ever being in a romantic relationship. Rates were similar in the perinatally exposed but uninfected group with the exception that these individuals were less likely to be paying rent.
“In spite of substantive risks, there is a relatively large portion of both groups with positive behavioral health outcomes, achieving normative young adult transition milestones. We need to understand why. Identification of protective factors conferring resilience can inform evidence-based prevention efforts, which are critical given the staggering numbers of children and young adolescents worldwide affected by HIV who will be transitioning to adulthood,” she said.
Dr. Mellins said the CASAH findings constitute a persuasive argument in favor of integrating mental health as a component of HIV care.
“Young people don’t always go to mental health appointments that are separate from medical care, so integrating mental health as a component of HIV care might be one of the most effective ways to identify and treat mental health problems in infected youth while simultaneously improving medication adherence and health outcomes,” Dr. Mellins said.
The ongoing CASAH study is funded by the National Institute of Mental Health. Dr. Mellins reported having no relevant financial conflicts.
AT AIDS 2016
Key clinical point: Look for and treat psychiatric disorders in perinatally HIV-infected adolescents as a means of optimizing their antiretroviral medication adherence.
Major finding: A majority of perinatally HIV-infected adolescents meet the criteria for at least one psychiatric diagnosis, and they are at significantly increased risk for poor medication adherence and viremia during the next 2-3 years.
Data source: The longitudinal CASAH study involving prospective follow-up of several hundred perinatally HIV-infected and perinatally exposed but uninfected subjects through adolescence and young adulthood.
Disclosures: The ongoing CASAH study is funded by the National Institute of Mental Health. Dr. Mellins reported having no relevant financial conflicts.
A few 20-shot sessions might be enough for deoxycholic acid
NEWPORT BEACH, CALIF. – It’s unclear how well deoxycholic acid (Kybella) will work in the clinic because doctors and patients are generally opting for fewer injections and fewer treatment sessions than were evaluated in phase III studies, according to Lawrence Bass, MD.
The fat cytolytic was approved in 2015 for shrinking double chins, with up to six 50-injection sessions. In trials, patients tended to get more than 40 shots in their first two sessions and more than 30 in subsequent sessions. At that dosing, 40.5% of patients in one trial and 46% in another lost at least 10% of their submental volume on MRI, according to Food and Drug Administration review documents.
However, at the Summit in Aesthetic Medicine, Dr. Bass, a plastic surgeon in New York City, said that, in clinical practice, patients are typically being treated with 20 injections for two or three sessions – partly because of cost. “This product costs $300 for each 2 mL vial, which means in a typical 20-injection treatment, you use $600 of material,” he noted. An average treatment session in Manhattan costs patients about $1,500. In other parts of the country, sessions are probably around $1,200 each, he added.
Also, the necks of patients enrolled in trials “had to be pretty big, but the necks we are probably going to treat with this are the smaller and medium ones. The big ones are just going to do liposuction or something else,” he said. Given all the variables, “we don’t know how well the study experience is going to match clinical experience.”
Dr. Bass treated his first postapproval patient, a 52-year-old woman, with two 20-injection treatment sessions 2 months apart. “The fat definitely cleaned out” and her skin looked a bit tighter, but it’s tough to know if her skin truly tightened or simply draped flatter, he said.
FDA labeling notes that “the safe and effective use of Kybella for the treatment of subcutaneous fat outside the submental region has not been established and is not recommended,” but this advice is unlikely to keep doctors from trying it in off-label areas.
One issue is that “almost every other area is a whole lot bigger” than a double chin, Dr. Bass said. Treating a tummy with 50 injections six to eight times, for example, would cost patients $12,000-$15,000, which is “a whole lot more than lipo,” he added.
Also, administering more than 50 injections at a time for a larger area is not possible because of toxicity. Trying to get around that limit and cut costs by diluting deoxycholic acid or spacing the injections farther apart doesn’t seem to be an option, since phase II testing showed a loss of efficacy with that approach.
Dr. Bass tried deoxycholic acid on a woman with leftover tummy bulges following liposuction. After two 40-injection sessions, “there was still a little shape there, so I don’t think I’ll be doing that again,” he said at the meeting, which is held by Global Academy for Medical Education. Global Academy and this news organization are owned the same company.
Gynecomastia, meanwhile, would probably require too many shots, and the jowl, another potential target, is too close to the marginal mandibular branch of the facial nerve, “so you are not supposed to inject there,” Dr. Bass said. Diluted deoxycholic acid might be an option for bulging periorbital fat, “but I am going to let somebody who is braver than me try that for a while before I go there.”
Dr. Bass is an investigator and speaker for Cynosure, an investigator for Endo Pharmaceuticals and Neothetics, and an advisor to Merz. He participated in phase III testing of deoxycholic acid.
The indication approved for deoxycholic acid is “for improvement in the appearance of moderate to severe convexity or fullness associated with submental fat in adults.”
NEWPORT BEACH, CALIF. – It’s unclear how well deoxycholic acid (Kybella) will work in the clinic because doctors and patients are generally opting for fewer injections and fewer treatment sessions than were evaluated in phase III studies, according to Lawrence Bass, MD.
The fat cytolytic was approved in 2015 for shrinking double chins, with up to six 50-injection sessions. In trials, patients tended to get more than 40 shots in their first two sessions and more than 30 in subsequent sessions. At that dosing, 40.5% of patients in one trial and 46% in another lost at least 10% of their submental volume on MRI, according to Food and Drug Administration review documents.
However, at the Summit in Aesthetic Medicine, Dr. Bass, a plastic surgeon in New York City, said that, in clinical practice, patients are typically being treated with 20 injections for two or three sessions – partly because of cost. “This product costs $300 for each 2 mL vial, which means in a typical 20-injection treatment, you use $600 of material,” he noted. An average treatment session in Manhattan costs patients about $1,500. In other parts of the country, sessions are probably around $1,200 each, he added.
Also, the necks of patients enrolled in trials “had to be pretty big, but the necks we are probably going to treat with this are the smaller and medium ones. The big ones are just going to do liposuction or something else,” he said. Given all the variables, “we don’t know how well the study experience is going to match clinical experience.”
Dr. Bass treated his first postapproval patient, a 52-year-old woman, with two 20-injection treatment sessions 2 months apart. “The fat definitely cleaned out” and her skin looked a bit tighter, but it’s tough to know if her skin truly tightened or simply draped flatter, he said.
FDA labeling notes that “the safe and effective use of Kybella for the treatment of subcutaneous fat outside the submental region has not been established and is not recommended,” but this advice is unlikely to keep doctors from trying it in off-label areas.
One issue is that “almost every other area is a whole lot bigger” than a double chin, Dr. Bass said. Treating a tummy with 50 injections six to eight times, for example, would cost patients $12,000-$15,000, which is “a whole lot more than lipo,” he added.
Also, administering more than 50 injections at a time for a larger area is not possible because of toxicity. Trying to get around that limit and cut costs by diluting deoxycholic acid or spacing the injections farther apart doesn’t seem to be an option, since phase II testing showed a loss of efficacy with that approach.
Dr. Bass tried deoxycholic acid on a woman with leftover tummy bulges following liposuction. After two 40-injection sessions, “there was still a little shape there, so I don’t think I’ll be doing that again,” he said at the meeting, which is held by Global Academy for Medical Education. Global Academy and this news organization are owned the same company.
Gynecomastia, meanwhile, would probably require too many shots, and the jowl, another potential target, is too close to the marginal mandibular branch of the facial nerve, “so you are not supposed to inject there,” Dr. Bass said. Diluted deoxycholic acid might be an option for bulging periorbital fat, “but I am going to let somebody who is braver than me try that for a while before I go there.”
Dr. Bass is an investigator and speaker for Cynosure, an investigator for Endo Pharmaceuticals and Neothetics, and an advisor to Merz. He participated in phase III testing of deoxycholic acid.
The indication approved for deoxycholic acid is “for improvement in the appearance of moderate to severe convexity or fullness associated with submental fat in adults.”
NEWPORT BEACH, CALIF. – It’s unclear how well deoxycholic acid (Kybella) will work in the clinic because doctors and patients are generally opting for fewer injections and fewer treatment sessions than were evaluated in phase III studies, according to Lawrence Bass, MD.
The fat cytolytic was approved in 2015 for shrinking double chins, with up to six 50-injection sessions. In trials, patients tended to get more than 40 shots in their first two sessions and more than 30 in subsequent sessions. At that dosing, 40.5% of patients in one trial and 46% in another lost at least 10% of their submental volume on MRI, according to Food and Drug Administration review documents.
However, at the Summit in Aesthetic Medicine, Dr. Bass, a plastic surgeon in New York City, said that, in clinical practice, patients are typically being treated with 20 injections for two or three sessions – partly because of cost. “This product costs $300 for each 2 mL vial, which means in a typical 20-injection treatment, you use $600 of material,” he noted. An average treatment session in Manhattan costs patients about $1,500. In other parts of the country, sessions are probably around $1,200 each, he added.
Also, the necks of patients enrolled in trials “had to be pretty big, but the necks we are probably going to treat with this are the smaller and medium ones. The big ones are just going to do liposuction or something else,” he said. Given all the variables, “we don’t know how well the study experience is going to match clinical experience.”
Dr. Bass treated his first postapproval patient, a 52-year-old woman, with two 20-injection treatment sessions 2 months apart. “The fat definitely cleaned out” and her skin looked a bit tighter, but it’s tough to know if her skin truly tightened or simply draped flatter, he said.
FDA labeling notes that “the safe and effective use of Kybella for the treatment of subcutaneous fat outside the submental region has not been established and is not recommended,” but this advice is unlikely to keep doctors from trying it in off-label areas.
One issue is that “almost every other area is a whole lot bigger” than a double chin, Dr. Bass said. Treating a tummy with 50 injections six to eight times, for example, would cost patients $12,000-$15,000, which is “a whole lot more than lipo,” he added.
Also, administering more than 50 injections at a time for a larger area is not possible because of toxicity. Trying to get around that limit and cut costs by diluting deoxycholic acid or spacing the injections farther apart doesn’t seem to be an option, since phase II testing showed a loss of efficacy with that approach.
Dr. Bass tried deoxycholic acid on a woman with leftover tummy bulges following liposuction. After two 40-injection sessions, “there was still a little shape there, so I don’t think I’ll be doing that again,” he said at the meeting, which is held by Global Academy for Medical Education. Global Academy and this news organization are owned the same company.
Gynecomastia, meanwhile, would probably require too many shots, and the jowl, another potential target, is too close to the marginal mandibular branch of the facial nerve, “so you are not supposed to inject there,” Dr. Bass said. Diluted deoxycholic acid might be an option for bulging periorbital fat, “but I am going to let somebody who is braver than me try that for a while before I go there.”
Dr. Bass is an investigator and speaker for Cynosure, an investigator for Endo Pharmaceuticals and Neothetics, and an advisor to Merz. He participated in phase III testing of deoxycholic acid.
The indication approved for deoxycholic acid is “for improvement in the appearance of moderate to severe convexity or fullness associated with submental fat in adults.”
EXPERT ANALYSIS FROM THE SUMMIT IN AESTHETIC MEDICINE