User login
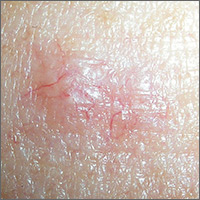
Lesion with vessels

The FP performed a shave biopsy with a sharp razor blade after using local anesthesia (lidocaine and epinephrine), and pathology confirmed the suspected diagnosis of a nodular basal cell carcinoma (BCC). While this case of BCC was diagnosed with naked eye examination, dermoscopic examination would have revealed shiny white structures and branching vessels. This would increase the FP’s confidence in a diagnosis of BCC before a biopsy was even performed.
The FP was experienced with skin surgery and performed an elliptical excision with 4 mm margins. The ellipse was oriented horizontally across the patient’s forehead, so that the healing incision would be hidden among her wrinkle lines. A 2-layer closure was employed using absorbable 4-0 Vicryl for the deep sutures and running 5-0 Prolene for the epidermal layer.
At follow-up 6 days later, the incision was healing well without signs of infection and the external sutures were removed. Pathology showed that the margins were clear of tumor. The FP suggested a total body skin exam to make sure there were no other skin cancers in hiding. The patient agreed, and the remainder of the skin exam was clear. The FP also talked to the patient about sun avoidance and protection. A follow-up was scheduled for 6 months later to recheck the skin, since the diagnosis of one BCC increases the risk for additional skin cancers.
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Smith M. Sebaceous hyperplasia. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013: 931-934.
To learn more about the Color Atlas of Family Medicine, see: www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/
You can now get the second edition of the Color Atlas of Family Medicine as an app by clicking on this link: usatinemedia.com

The FP performed a shave biopsy with a sharp razor blade after using local anesthesia (lidocaine and epinephrine), and pathology confirmed the suspected diagnosis of a nodular basal cell carcinoma (BCC). While this case of BCC was diagnosed with naked eye examination, dermoscopic examination would have revealed shiny white structures and branching vessels. This would increase the FP’s confidence in a diagnosis of BCC before a biopsy was even performed.
The FP was experienced with skin surgery and performed an elliptical excision with 4 mm margins. The ellipse was oriented horizontally across the patient’s forehead, so that the healing incision would be hidden among her wrinkle lines. A 2-layer closure was employed using absorbable 4-0 Vicryl for the deep sutures and running 5-0 Prolene for the epidermal layer.
At follow-up 6 days later, the incision was healing well without signs of infection and the external sutures were removed. Pathology showed that the margins were clear of tumor. The FP suggested a total body skin exam to make sure there were no other skin cancers in hiding. The patient agreed, and the remainder of the skin exam was clear. The FP also talked to the patient about sun avoidance and protection. A follow-up was scheduled for 6 months later to recheck the skin, since the diagnosis of one BCC increases the risk for additional skin cancers.
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Smith M. Sebaceous hyperplasia. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013: 931-934.
To learn more about the Color Atlas of Family Medicine, see: www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/
You can now get the second edition of the Color Atlas of Family Medicine as an app by clicking on this link: usatinemedia.com

The FP performed a shave biopsy with a sharp razor blade after using local anesthesia (lidocaine and epinephrine), and pathology confirmed the suspected diagnosis of a nodular basal cell carcinoma (BCC). While this case of BCC was diagnosed with naked eye examination, dermoscopic examination would have revealed shiny white structures and branching vessels. This would increase the FP’s confidence in a diagnosis of BCC before a biopsy was even performed.
The FP was experienced with skin surgery and performed an elliptical excision with 4 mm margins. The ellipse was oriented horizontally across the patient’s forehead, so that the healing incision would be hidden among her wrinkle lines. A 2-layer closure was employed using absorbable 4-0 Vicryl for the deep sutures and running 5-0 Prolene for the epidermal layer.
At follow-up 6 days later, the incision was healing well without signs of infection and the external sutures were removed. Pathology showed that the margins were clear of tumor. The FP suggested a total body skin exam to make sure there were no other skin cancers in hiding. The patient agreed, and the remainder of the skin exam was clear. The FP also talked to the patient about sun avoidance and protection. A follow-up was scheduled for 6 months later to recheck the skin, since the diagnosis of one BCC increases the risk for additional skin cancers.
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Smith M. Sebaceous hyperplasia. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013: 931-934.
To learn more about the Color Atlas of Family Medicine, see: www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/
You can now get the second edition of the Color Atlas of Family Medicine as an app by clicking on this link: usatinemedia.com
Can You Treat These Feet?
ANSWER
The item that does not belong is tinea corporis (ringworm; choice “c”). There are several reasons this presumed, “obvious” diagnosis does not belong: First, there was no known source (human or animal) from which the patient could have contracted such an infection. Second, what should have been adequate treatment for a fungal infection had no effect. And finally, cutaneous fungal infections almost always disrupt the outer layer of skin; the relevant signs (eg, scaling, vesiculation, follicular granulomas) were absent in this case.
The correct diagnosis is granuloma annulare (GA; choice “a”), an extremely common, benign condition that is often misdiagnosed and treated as fungal infection. Histologically, GA is characterized by palisading (row-like) collections of cells that group together to form granulomas.
Similar patterns can be seen with sarcoidosis (choice “b”) and cutaneous mycobacterial infection (choice “d”), but additional distinguishing histologic features must be sought to confirm those diagnoses.
DISCUSSION
Virtually every medical provider has fallen for this clinical canard, referring an alleged “fungal infection” to dermatology when it fails to respond to treatment. This case was archetypical of GA, a condition most commonly found on the feet of young women.
It manifests on the extensor surfaces of the extremities as brownish red, round-to-oval, intradermal plaques devoid of surface disruption. The borders of the lesions are often raised enough to produce an apparent valley (delling) in the center.
There is a rather wide spectrum of GA variants (eg, generalized, su
Many treatments have been used (including topical or intralesional steroids and liquid nitrogen), but none are particularly effective. Fortunately, most cases eventually clear on their own and do not involve associated morbidity.
ANSWER
The item that does not belong is tinea corporis (ringworm; choice “c”). There are several reasons this presumed, “obvious” diagnosis does not belong: First, there was no known source (human or animal) from which the patient could have contracted such an infection. Second, what should have been adequate treatment for a fungal infection had no effect. And finally, cutaneous fungal infections almost always disrupt the outer layer of skin; the relevant signs (eg, scaling, vesiculation, follicular granulomas) were absent in this case.
The correct diagnosis is granuloma annulare (GA; choice “a”), an extremely common, benign condition that is often misdiagnosed and treated as fungal infection. Histologically, GA is characterized by palisading (row-like) collections of cells that group together to form granulomas.
Similar patterns can be seen with sarcoidosis (choice “b”) and cutaneous mycobacterial infection (choice “d”), but additional distinguishing histologic features must be sought to confirm those diagnoses.
DISCUSSION
Virtually every medical provider has fallen for this clinical canard, referring an alleged “fungal infection” to dermatology when it fails to respond to treatment. This case was archetypical of GA, a condition most commonly found on the feet of young women.
It manifests on the extensor surfaces of the extremities as brownish red, round-to-oval, intradermal plaques devoid of surface disruption. The borders of the lesions are often raised enough to produce an apparent valley (delling) in the center.
There is a rather wide spectrum of GA variants (eg, generalized, su
Many treatments have been used (including topical or intralesional steroids and liquid nitrogen), but none are particularly effective. Fortunately, most cases eventually clear on their own and do not involve associated morbidity.
ANSWER
The item that does not belong is tinea corporis (ringworm; choice “c”). There are several reasons this presumed, “obvious” diagnosis does not belong: First, there was no known source (human or animal) from which the patient could have contracted such an infection. Second, what should have been adequate treatment for a fungal infection had no effect. And finally, cutaneous fungal infections almost always disrupt the outer layer of skin; the relevant signs (eg, scaling, vesiculation, follicular granulomas) were absent in this case.
The correct diagnosis is granuloma annulare (GA; choice “a”), an extremely common, benign condition that is often misdiagnosed and treated as fungal infection. Histologically, GA is characterized by palisading (row-like) collections of cells that group together to form granulomas.
Similar patterns can be seen with sarcoidosis (choice “b”) and cutaneous mycobacterial infection (choice “d”), but additional distinguishing histologic features must be sought to confirm those diagnoses.
DISCUSSION
Virtually every medical provider has fallen for this clinical canard, referring an alleged “fungal infection” to dermatology when it fails to respond to treatment. This case was archetypical of GA, a condition most commonly found on the feet of young women.
It manifests on the extensor surfaces of the extremities as brownish red, round-to-oval, intradermal plaques devoid of surface disruption. The borders of the lesions are often raised enough to produce an apparent valley (delling) in the center.
There is a rather wide spectrum of GA variants (eg, generalized, su
Many treatments have been used (including topical or intralesional steroids and liquid nitrogen), but none are particularly effective. Fortunately, most cases eventually clear on their own and do not involve associated morbidity.
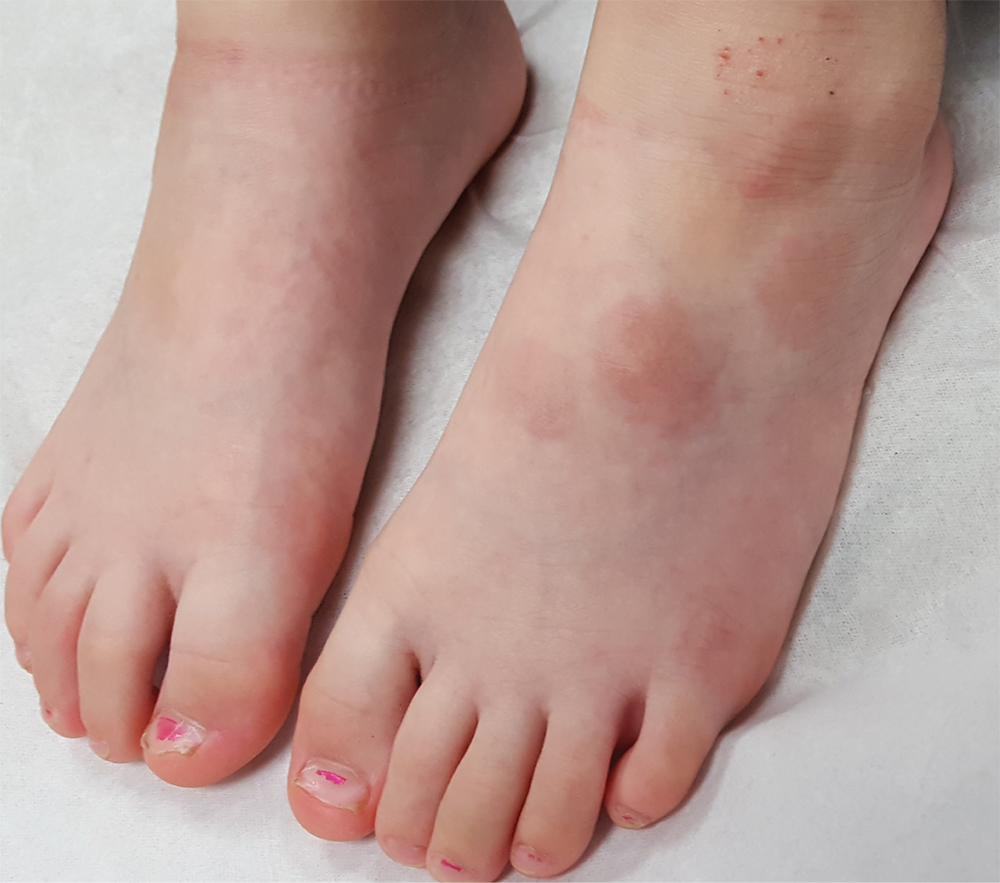
Two years ago, asymptomatic lesions appeared on this 17-year-old girl’s left foot. Diagnosed as “ringworm” by primary care, the spots have not responded to topical econazole or oral terbinafine and have instead grown and darkened.
Five intradermal plaques are found on the dorsal aspect of the patient’s left foot. Round and reddish brown, they measure 3 to 4 cm each. There is modest induration on palpation, but no increased warmth or tenderness. None of the lesions have an epidermal component (ie, scaling, vesiculation); in short, there is nothing to scrape for KOH examination.
The patient has no lesions elsewhere and denies any other health problems. Her mother, who is present, is certain that no one else in the family has had similar lesions. There are no pets in the house.
Budesonide fails to cut deaths in preemies
The administration of inhaled budesonide to extremely preterm infants did not increase the risk of neurodevelopmental disability, but did increase mortality, in a study by Dirk Bassler, MD, of the University of Zürich and his associates.
An older study led by Dr. Bassler and published in the New England Journal of Medicine showed that inhaled budesonide significantly reduced the incidence of bronchopulmonary dysplasia, which has been linked to higher mortality and chronic respiratory and cardiovascular impairment (N Engl J Med. 2015;373:1497-506).
Systemic glucocorticoids have been linked to greater risk of neurodevelopmental disability, but only a few studies have examined the effect of inhaled glucocorticoids, such as budesonide, in preterm infants. These studies, including the earlier one by Dr. Bassler and his colleagues, were either small, covered a short period of time or involved late administering of the drug.
In the two studies by Dr. Bassler and his colleagues, 863 preterm infants between 23 weeks’ and just under 28 weeks’ gestation who required any form of positive-pressure respiratory support were randomized to receive inhaled budesonide (two puffs, 200 mcg per puff) or placebo every 12 hours. They began within 24 hours of birth and continued for the first 14 days of life. Following that, patients received 1 puff every 12 hours until they no longer required supplemental oxygen and positive-pressure support, or reached a postmenstrual age of 32 weeks.
The treatment resulted in a significant reduction in bronchopulmonary dysplasia at a postmenstrual age of 36 weeks (28.2% in the budesonide group vs. 37.4%; P = .01), in the older study.
In the new study, which was also published in the New England Journal of Medicine, Dr. Bassler and his associates found higher mortality (19.9% vs. 14.5%; relative risk, 1.37; 95% confidence interval, 1.01-1.86; P = .04) in the group of patients who had received inhaled budesonide. Additionally, at a corrected age of 18-22 months, surviving infants who received inhaled budesonide had a similar risk of neurodevelopmental disability as those patients who took the placebo.
Broadly speaking, 48.1% of infants who received budesonide had a neurodevelopmental disability, compared with 51.4% of infants who received placebo (RR adjusted for gestational age, 0.93; 95% CI, 0.80-1.09; P = .40). The two groups also had no statistically significant differences in their frequencies of cerebral palsy, blindness, hearing loss, or cognitive delay.
“There was no significant difference between the groups in adverse long-term outcomes in our study. However, the fact that fewer infants died in the placebo group than in the budesonide group complicates the interpretation of the treatment of budesonide,” the researchers wrote.
Supported by a grant from the European Union and by Chiesi Farmaceutici. Disclosure forms provided by the authors are available with the full text of this article at NEJM.org.
SOURCE: N Engl J Med. 2018;378:148-57.
This is an important study regarding bronchopulmonary dysplasia prevention. The study suggests starting budesonide within 24 hours of life resulted in a lower rate of bronchopulmonary dysplasia than placebo but fewer infants died in the placebo group. A bigger question for me is “what is the evidence for starting inhaled steroids prior to neonatal intensive care unit discharge?” Pediatric pulmonologists would like to know if it decreases subsequent respiratory-related ER visits and readmissions.
This is an important study regarding bronchopulmonary dysplasia prevention. The study suggests starting budesonide within 24 hours of life resulted in a lower rate of bronchopulmonary dysplasia than placebo but fewer infants died in the placebo group. A bigger question for me is “what is the evidence for starting inhaled steroids prior to neonatal intensive care unit discharge?” Pediatric pulmonologists would like to know if it decreases subsequent respiratory-related ER visits and readmissions.
This is an important study regarding bronchopulmonary dysplasia prevention. The study suggests starting budesonide within 24 hours of life resulted in a lower rate of bronchopulmonary dysplasia than placebo but fewer infants died in the placebo group. A bigger question for me is “what is the evidence for starting inhaled steroids prior to neonatal intensive care unit discharge?” Pediatric pulmonologists would like to know if it decreases subsequent respiratory-related ER visits and readmissions.
The administration of inhaled budesonide to extremely preterm infants did not increase the risk of neurodevelopmental disability, but did increase mortality, in a study by Dirk Bassler, MD, of the University of Zürich and his associates.
An older study led by Dr. Bassler and published in the New England Journal of Medicine showed that inhaled budesonide significantly reduced the incidence of bronchopulmonary dysplasia, which has been linked to higher mortality and chronic respiratory and cardiovascular impairment (N Engl J Med. 2015;373:1497-506).
Systemic glucocorticoids have been linked to greater risk of neurodevelopmental disability, but only a few studies have examined the effect of inhaled glucocorticoids, such as budesonide, in preterm infants. These studies, including the earlier one by Dr. Bassler and his colleagues, were either small, covered a short period of time or involved late administering of the drug.
In the two studies by Dr. Bassler and his colleagues, 863 preterm infants between 23 weeks’ and just under 28 weeks’ gestation who required any form of positive-pressure respiratory support were randomized to receive inhaled budesonide (two puffs, 200 mcg per puff) or placebo every 12 hours. They began within 24 hours of birth and continued for the first 14 days of life. Following that, patients received 1 puff every 12 hours until they no longer required supplemental oxygen and positive-pressure support, or reached a postmenstrual age of 32 weeks.
The treatment resulted in a significant reduction in bronchopulmonary dysplasia at a postmenstrual age of 36 weeks (28.2% in the budesonide group vs. 37.4%; P = .01), in the older study.
In the new study, which was also published in the New England Journal of Medicine, Dr. Bassler and his associates found higher mortality (19.9% vs. 14.5%; relative risk, 1.37; 95% confidence interval, 1.01-1.86; P = .04) in the group of patients who had received inhaled budesonide. Additionally, at a corrected age of 18-22 months, surviving infants who received inhaled budesonide had a similar risk of neurodevelopmental disability as those patients who took the placebo.
Broadly speaking, 48.1% of infants who received budesonide had a neurodevelopmental disability, compared with 51.4% of infants who received placebo (RR adjusted for gestational age, 0.93; 95% CI, 0.80-1.09; P = .40). The two groups also had no statistically significant differences in their frequencies of cerebral palsy, blindness, hearing loss, or cognitive delay.
“There was no significant difference between the groups in adverse long-term outcomes in our study. However, the fact that fewer infants died in the placebo group than in the budesonide group complicates the interpretation of the treatment of budesonide,” the researchers wrote.
Supported by a grant from the European Union and by Chiesi Farmaceutici. Disclosure forms provided by the authors are available with the full text of this article at NEJM.org.
SOURCE: N Engl J Med. 2018;378:148-57.
The administration of inhaled budesonide to extremely preterm infants did not increase the risk of neurodevelopmental disability, but did increase mortality, in a study by Dirk Bassler, MD, of the University of Zürich and his associates.
An older study led by Dr. Bassler and published in the New England Journal of Medicine showed that inhaled budesonide significantly reduced the incidence of bronchopulmonary dysplasia, which has been linked to higher mortality and chronic respiratory and cardiovascular impairment (N Engl J Med. 2015;373:1497-506).
Systemic glucocorticoids have been linked to greater risk of neurodevelopmental disability, but only a few studies have examined the effect of inhaled glucocorticoids, such as budesonide, in preterm infants. These studies, including the earlier one by Dr. Bassler and his colleagues, were either small, covered a short period of time or involved late administering of the drug.
In the two studies by Dr. Bassler and his colleagues, 863 preterm infants between 23 weeks’ and just under 28 weeks’ gestation who required any form of positive-pressure respiratory support were randomized to receive inhaled budesonide (two puffs, 200 mcg per puff) or placebo every 12 hours. They began within 24 hours of birth and continued for the first 14 days of life. Following that, patients received 1 puff every 12 hours until they no longer required supplemental oxygen and positive-pressure support, or reached a postmenstrual age of 32 weeks.
The treatment resulted in a significant reduction in bronchopulmonary dysplasia at a postmenstrual age of 36 weeks (28.2% in the budesonide group vs. 37.4%; P = .01), in the older study.
In the new study, which was also published in the New England Journal of Medicine, Dr. Bassler and his associates found higher mortality (19.9% vs. 14.5%; relative risk, 1.37; 95% confidence interval, 1.01-1.86; P = .04) in the group of patients who had received inhaled budesonide. Additionally, at a corrected age of 18-22 months, surviving infants who received inhaled budesonide had a similar risk of neurodevelopmental disability as those patients who took the placebo.
Broadly speaking, 48.1% of infants who received budesonide had a neurodevelopmental disability, compared with 51.4% of infants who received placebo (RR adjusted for gestational age, 0.93; 95% CI, 0.80-1.09; P = .40). The two groups also had no statistically significant differences in their frequencies of cerebral palsy, blindness, hearing loss, or cognitive delay.
“There was no significant difference between the groups in adverse long-term outcomes in our study. However, the fact that fewer infants died in the placebo group than in the budesonide group complicates the interpretation of the treatment of budesonide,” the researchers wrote.
Supported by a grant from the European Union and by Chiesi Farmaceutici. Disclosure forms provided by the authors are available with the full text of this article at NEJM.org.
SOURCE: N Engl J Med. 2018;378:148-57.
FROM NEW ENGLAND JOURNAL OF MEDICINE
Key clinical point:
Major finding: Nearly 20% of infants in the budesonide group died, compared with 14.5% of the placebo group.
Data source: Randomized, controlled trial of 863 extremely preterm infants.
Disclosures: Supported by a grant from the European Union and by Chiesi Farmaceutici. Disclosure forms provided by the authors are available with the full text of this article at NEJM.org.
Source: N Engl J Med. 2018;378:148-57.
Non-PCOS IVF: Two trials show no benefit with frozen embryo transfer
Contrary to findings in women with polycystic ovary syndrome (PCOS), the transfer of frozen vs. fresh embryos does not lead to significantly higher live birth or ongoing pregnancy rates in women with non-PCOS infertility who undergo in vitro fertilization, according to findings from two randomized trials.
Frozen embryo transfer did, however, result in a lower risk of ovarian hyperstimulation syndrome in one of the trials. In that multicenter study, 2,157 women undergoing their first in vitro fertilization (IVF) cycle were randomized to undergo either fresh embryo transfer or embryo cryopreservation followed by frozen embryo transfer, with up to two cleavage-stage embryos transferred, Yuhua Shi, MD, of Shandong University, Jinan, China, and colleagues reported Jan. 11 in the New England Journal of Medicine. The live birth rate, defined as delivery of a viable neonate at 28 weeks of gestation or greater, was 50.2% and 48.7% in the fresh embryo and frozen embryo groups, respectively (relative risk, 0.97). The rate of ovarian hyperstimulation syndrome was 2.0% and 0.6% in the groups, respectively (RR, 0.32), the investigators reported.
Of note, the rates of implantation, clinical pregnancy, overall pregnancy loss, and ongoing pregnancy did not differ between the groups, but in a post hoc analysis, the rate of second-trimester pregnancy loss was lower with frozen embryo transfer (4.7% vs. 1.5%; RR, 0.33). However, the authors urged caution regarding the latter finding because of the post hoc setting and because the overall rates of pregnancy loss did not differ between the groups.
In the second study, 782 women without PCOS who were undergoing a first or second IVF cycle at a single center were randomized to receive either fresh or frozen embryo transfer with up to two embryos transferred.
After the first complete cycle, the ongoing pregnancy rate – the primary outcome in the study, defined as pregnancy with a detectable heart rate after 12 weeks of gestation – was 34.5% in the fresh embryo group and 36.3% in the frozen embryo group (RR in frozen embryo group, 1.05), Lan N. Vuong, MD, of My Duc Hospital, Ho Chi Minh City, Vietnam, and colleagues reported.
The live birth rates after the first transfer were 31.5% and 33.8%, respectively (risk ratio, 1.07). There also were no differences in rates of implantation or clinical pregnancy, or in rates of ectopic pregnancy, miscarriage, multiple pregnancy, ovarian hyperstimulation syndrome in the primary cycle, or pregnancy complications.
The findings of both studies contrast with those from prior studies showing a higher live-birth rate among anovulatory women with PCOS who undergo frozen embryo transfer, compared with those who undergo fresh embryo transfer.
For example, Dr. Shi and associates found in a prior study of women with PCOS that the live birth rate was higher with frozen embryo transfer (42% vs. 49%), and they concluded that this was largely explained by a lower rate of pregnancy loss (N Engl J Med. 2016;375:523-33).
“However, patients with the polycystic ovary syndrome have a different reproductive, metabolic milieu than do other women with infertility; it is characterized by hyperandrogenism and insulin resistance, and these patients typically have a greater ovarian response to gonadotropin stimulation than do ovulatory women undergoing IVF,” they wrote in the current paper.
The findings of the current studies suggest the benefits of frozen vs. fresh embryo transfer, with respect to the primary outcome measures in the studies, do not apply in women with non-PCOS infertility.
Dr. Shi and colleagues speculated that “the difference is due to the unfavorable uterine environment after fresh embryo transfer in women with the polycystic ovary syndrome, as shown by a much lower rate of live birth overall in the previous trial than in the present trial.”
The “altered hormonal milieu” in women with PCOS, along with a need for ovarian stimulation cycle initiation with oral contraceptives or progestin may adversely affect endometrial receptivity after fresh embryo transfer, they explained.
Dr. Vuong and colleagues noted that their findings are not necessarily inconsistent with those reported in women with PCOS, because “the 95% confidence intervals around the risk ratios for live birth that were associated with frozen embryo transfer in our trial overlap with the 95% confidence intervals in that report,” adding that another contributing factor to the different results might be the timing of freezing, which differed in the studies.
They also said that a small difference in the time to conception, which was 1.4 months shorter in the fresh embryo group, could be “a relevant factor for some patients in terms of the overall treatment duration and both the direct and indirect costs of IVF.”
The study by Dr. Shi and associates was supported by grants from the National Key Research and Development Program of China, the Major Program of the National Natural Science Foundation of China, and the State Key Program of the National Natural Science Foundation of China. Dr. Shi reported having no conflicts of interest. One coauthor, Richard S. Legro, MD, reported receiving consulting fees from Ogeda, KinDex Pharmaceuticals, Fractyl Laboratories, Bayer, and AbbVie, and receiving grant support from Ferring Pharmaceuticals. The study by Dr. Vuong and associates was supported by My Duc Hospital. Author disclosures for that study are available with the full text of the article at NEJM.org.
SOURCES: Shi Y et al. N Engl J Med. 2018;378(2):126-36; Vuong N et al. N Engl J Med. 2018;378(2):137-47.
Contrary to findings in women with polycystic ovary syndrome (PCOS), the transfer of frozen vs. fresh embryos does not lead to significantly higher live birth or ongoing pregnancy rates in women with non-PCOS infertility who undergo in vitro fertilization, according to findings from two randomized trials.
Frozen embryo transfer did, however, result in a lower risk of ovarian hyperstimulation syndrome in one of the trials. In that multicenter study, 2,157 women undergoing their first in vitro fertilization (IVF) cycle were randomized to undergo either fresh embryo transfer or embryo cryopreservation followed by frozen embryo transfer, with up to two cleavage-stage embryos transferred, Yuhua Shi, MD, of Shandong University, Jinan, China, and colleagues reported Jan. 11 in the New England Journal of Medicine. The live birth rate, defined as delivery of a viable neonate at 28 weeks of gestation or greater, was 50.2% and 48.7% in the fresh embryo and frozen embryo groups, respectively (relative risk, 0.97). The rate of ovarian hyperstimulation syndrome was 2.0% and 0.6% in the groups, respectively (RR, 0.32), the investigators reported.
Of note, the rates of implantation, clinical pregnancy, overall pregnancy loss, and ongoing pregnancy did not differ between the groups, but in a post hoc analysis, the rate of second-trimester pregnancy loss was lower with frozen embryo transfer (4.7% vs. 1.5%; RR, 0.33). However, the authors urged caution regarding the latter finding because of the post hoc setting and because the overall rates of pregnancy loss did not differ between the groups.
In the second study, 782 women without PCOS who were undergoing a first or second IVF cycle at a single center were randomized to receive either fresh or frozen embryo transfer with up to two embryos transferred.
After the first complete cycle, the ongoing pregnancy rate – the primary outcome in the study, defined as pregnancy with a detectable heart rate after 12 weeks of gestation – was 34.5% in the fresh embryo group and 36.3% in the frozen embryo group (RR in frozen embryo group, 1.05), Lan N. Vuong, MD, of My Duc Hospital, Ho Chi Minh City, Vietnam, and colleagues reported.
The live birth rates after the first transfer were 31.5% and 33.8%, respectively (risk ratio, 1.07). There also were no differences in rates of implantation or clinical pregnancy, or in rates of ectopic pregnancy, miscarriage, multiple pregnancy, ovarian hyperstimulation syndrome in the primary cycle, or pregnancy complications.
The findings of both studies contrast with those from prior studies showing a higher live-birth rate among anovulatory women with PCOS who undergo frozen embryo transfer, compared with those who undergo fresh embryo transfer.
For example, Dr. Shi and associates found in a prior study of women with PCOS that the live birth rate was higher with frozen embryo transfer (42% vs. 49%), and they concluded that this was largely explained by a lower rate of pregnancy loss (N Engl J Med. 2016;375:523-33).
“However, patients with the polycystic ovary syndrome have a different reproductive, metabolic milieu than do other women with infertility; it is characterized by hyperandrogenism and insulin resistance, and these patients typically have a greater ovarian response to gonadotropin stimulation than do ovulatory women undergoing IVF,” they wrote in the current paper.
The findings of the current studies suggest the benefits of frozen vs. fresh embryo transfer, with respect to the primary outcome measures in the studies, do not apply in women with non-PCOS infertility.
Dr. Shi and colleagues speculated that “the difference is due to the unfavorable uterine environment after fresh embryo transfer in women with the polycystic ovary syndrome, as shown by a much lower rate of live birth overall in the previous trial than in the present trial.”
The “altered hormonal milieu” in women with PCOS, along with a need for ovarian stimulation cycle initiation with oral contraceptives or progestin may adversely affect endometrial receptivity after fresh embryo transfer, they explained.
Dr. Vuong and colleagues noted that their findings are not necessarily inconsistent with those reported in women with PCOS, because “the 95% confidence intervals around the risk ratios for live birth that were associated with frozen embryo transfer in our trial overlap with the 95% confidence intervals in that report,” adding that another contributing factor to the different results might be the timing of freezing, which differed in the studies.
They also said that a small difference in the time to conception, which was 1.4 months shorter in the fresh embryo group, could be “a relevant factor for some patients in terms of the overall treatment duration and both the direct and indirect costs of IVF.”
The study by Dr. Shi and associates was supported by grants from the National Key Research and Development Program of China, the Major Program of the National Natural Science Foundation of China, and the State Key Program of the National Natural Science Foundation of China. Dr. Shi reported having no conflicts of interest. One coauthor, Richard S. Legro, MD, reported receiving consulting fees from Ogeda, KinDex Pharmaceuticals, Fractyl Laboratories, Bayer, and AbbVie, and receiving grant support from Ferring Pharmaceuticals. The study by Dr. Vuong and associates was supported by My Duc Hospital. Author disclosures for that study are available with the full text of the article at NEJM.org.
SOURCES: Shi Y et al. N Engl J Med. 2018;378(2):126-36; Vuong N et al. N Engl J Med. 2018;378(2):137-47.
Contrary to findings in women with polycystic ovary syndrome (PCOS), the transfer of frozen vs. fresh embryos does not lead to significantly higher live birth or ongoing pregnancy rates in women with non-PCOS infertility who undergo in vitro fertilization, according to findings from two randomized trials.
Frozen embryo transfer did, however, result in a lower risk of ovarian hyperstimulation syndrome in one of the trials. In that multicenter study, 2,157 women undergoing their first in vitro fertilization (IVF) cycle were randomized to undergo either fresh embryo transfer or embryo cryopreservation followed by frozen embryo transfer, with up to two cleavage-stage embryos transferred, Yuhua Shi, MD, of Shandong University, Jinan, China, and colleagues reported Jan. 11 in the New England Journal of Medicine. The live birth rate, defined as delivery of a viable neonate at 28 weeks of gestation or greater, was 50.2% and 48.7% in the fresh embryo and frozen embryo groups, respectively (relative risk, 0.97). The rate of ovarian hyperstimulation syndrome was 2.0% and 0.6% in the groups, respectively (RR, 0.32), the investigators reported.
Of note, the rates of implantation, clinical pregnancy, overall pregnancy loss, and ongoing pregnancy did not differ between the groups, but in a post hoc analysis, the rate of second-trimester pregnancy loss was lower with frozen embryo transfer (4.7% vs. 1.5%; RR, 0.33). However, the authors urged caution regarding the latter finding because of the post hoc setting and because the overall rates of pregnancy loss did not differ between the groups.
In the second study, 782 women without PCOS who were undergoing a first or second IVF cycle at a single center were randomized to receive either fresh or frozen embryo transfer with up to two embryos transferred.
After the first complete cycle, the ongoing pregnancy rate – the primary outcome in the study, defined as pregnancy with a detectable heart rate after 12 weeks of gestation – was 34.5% in the fresh embryo group and 36.3% in the frozen embryo group (RR in frozen embryo group, 1.05), Lan N. Vuong, MD, of My Duc Hospital, Ho Chi Minh City, Vietnam, and colleagues reported.
The live birth rates after the first transfer were 31.5% and 33.8%, respectively (risk ratio, 1.07). There also were no differences in rates of implantation or clinical pregnancy, or in rates of ectopic pregnancy, miscarriage, multiple pregnancy, ovarian hyperstimulation syndrome in the primary cycle, or pregnancy complications.
The findings of both studies contrast with those from prior studies showing a higher live-birth rate among anovulatory women with PCOS who undergo frozen embryo transfer, compared with those who undergo fresh embryo transfer.
For example, Dr. Shi and associates found in a prior study of women with PCOS that the live birth rate was higher with frozen embryo transfer (42% vs. 49%), and they concluded that this was largely explained by a lower rate of pregnancy loss (N Engl J Med. 2016;375:523-33).
“However, patients with the polycystic ovary syndrome have a different reproductive, metabolic milieu than do other women with infertility; it is characterized by hyperandrogenism and insulin resistance, and these patients typically have a greater ovarian response to gonadotropin stimulation than do ovulatory women undergoing IVF,” they wrote in the current paper.
The findings of the current studies suggest the benefits of frozen vs. fresh embryo transfer, with respect to the primary outcome measures in the studies, do not apply in women with non-PCOS infertility.
Dr. Shi and colleagues speculated that “the difference is due to the unfavorable uterine environment after fresh embryo transfer in women with the polycystic ovary syndrome, as shown by a much lower rate of live birth overall in the previous trial than in the present trial.”
The “altered hormonal milieu” in women with PCOS, along with a need for ovarian stimulation cycle initiation with oral contraceptives or progestin may adversely affect endometrial receptivity after fresh embryo transfer, they explained.
Dr. Vuong and colleagues noted that their findings are not necessarily inconsistent with those reported in women with PCOS, because “the 95% confidence intervals around the risk ratios for live birth that were associated with frozen embryo transfer in our trial overlap with the 95% confidence intervals in that report,” adding that another contributing factor to the different results might be the timing of freezing, which differed in the studies.
They also said that a small difference in the time to conception, which was 1.4 months shorter in the fresh embryo group, could be “a relevant factor for some patients in terms of the overall treatment duration and both the direct and indirect costs of IVF.”
The study by Dr. Shi and associates was supported by grants from the National Key Research and Development Program of China, the Major Program of the National Natural Science Foundation of China, and the State Key Program of the National Natural Science Foundation of China. Dr. Shi reported having no conflicts of interest. One coauthor, Richard S. Legro, MD, reported receiving consulting fees from Ogeda, KinDex Pharmaceuticals, Fractyl Laboratories, Bayer, and AbbVie, and receiving grant support from Ferring Pharmaceuticals. The study by Dr. Vuong and associates was supported by My Duc Hospital. Author disclosures for that study are available with the full text of the article at NEJM.org.
SOURCES: Shi Y et al. N Engl J Med. 2018;378(2):126-36; Vuong N et al. N Engl J Med. 2018;378(2):137-47.
FROM NEW ENGLAND JOURNAL OF MEDICINE
Key clinical point:
Major finding: The live birth rate was similar with fresh vs. frozen transfer (50.2% and 48.7% in one study; relative risk, 0.97).
Study details: Randomized trials including 2,157 and 782 women, respectively.
Disclosures: The study by Shi et al. was supported by grants from the National Key Research and Development Program of China, the Major Program of the National Natural Science Foundation of China, and the State Key Program of the National Natural Science Foundation of China. Dr. Shi reported having no conflicts of interest. One coauthor, Richard S. Legro, MD, reported receiving consulting fees from Ogeda, KinDex Pharmaceuticals, Fractyl Laboratories, Bayer, and AbbVie, and receiving grant support from Ferring Pharmaceuticals. The study by Vuong et al. was supported by My Duc Hospital. Author disclosures for that study are available with the full text of the article at NEJM.org.
Sources: Shi Y et al. N Engl J Med. 2018;378(2):126-36; Vuong N et al. N Engl J Med. 2018;378(2):137-47.
CMS launches advanced APM focused on bundled payments
The Centers for Medicare & Medicaid Services is launching a new voluntary bundled payment demonstration project that for the first time will qualify as an advanced alternative payment model under the Quality Payment Program.
The Bundled Payments for Care Improvement Advanced (BPCI Advanced) “builds on the earlier success of bundled payment models and is an important step in the move away from fee-for-service and towards paying for value,” CMS Administrator Seema Verma said in a statement. “Under this model, providers will have an incentive to deliver high-quality care.”
Both categories of participants may enter into agreements with individual physicians and nonphysician providers to furnish care under the bundled payment model.
It will cover 29 in-patient episodes and three outpatient clinical episodes. Payment will be tied to performance on quality measures.
The 29 in-patient clinical episodes cover a range of conditions, including liver disorders (excluding malignancy, cirrhosis, and alcoholic hepatitis); various cardiac conditions; chronic obstructive pulmonary disease, bronchitis, and asthma; spinal fusion; joint replacements; femur, hip, or pelvis fractures; gastrointestinal hemorrhage or obstruction; renal failure; sepsis; simple pneumonia and respiratory infections; stroke; and urinary tract infections.
The three outpatient clinical episodes include percutaneous coronary intervention, cardiac defibrillator implantation, and back and neck surgery except spinal fusion.
Seven quality measures will be tracked as part of the payment. For all clinical episodes, measurement of all-cause hospital readmissions and advance care plan will be required.
The other five will be applied to the payment when appropriate, as follows:
- Perioperative care: selection of prophylactic antibiotic: first- or second-generation cephalosporin.
- Hospital-level risk-standardized complication rate following elective primary total hip arthroplasty and/or total knee arthroplasty.
- Hospital 30-day, all-cause, risk-standardized mortality rate following coronary artery bypass graft surgery.
- Excess days in acute care after hospitalization for acute myocardial infarction; and AHRQ patient safety indicators.
CMS has scheduled an open-door forum for those interested in participating in BPCI Advanced on Jan. 30.
Applications for participation will be accepted through March 12.
The Centers for Medicare & Medicaid Services is launching a new voluntary bundled payment demonstration project that for the first time will qualify as an advanced alternative payment model under the Quality Payment Program.
The Bundled Payments for Care Improvement Advanced (BPCI Advanced) “builds on the earlier success of bundled payment models and is an important step in the move away from fee-for-service and towards paying for value,” CMS Administrator Seema Verma said in a statement. “Under this model, providers will have an incentive to deliver high-quality care.”
Both categories of participants may enter into agreements with individual physicians and nonphysician providers to furnish care under the bundled payment model.
It will cover 29 in-patient episodes and three outpatient clinical episodes. Payment will be tied to performance on quality measures.
The 29 in-patient clinical episodes cover a range of conditions, including liver disorders (excluding malignancy, cirrhosis, and alcoholic hepatitis); various cardiac conditions; chronic obstructive pulmonary disease, bronchitis, and asthma; spinal fusion; joint replacements; femur, hip, or pelvis fractures; gastrointestinal hemorrhage or obstruction; renal failure; sepsis; simple pneumonia and respiratory infections; stroke; and urinary tract infections.
The three outpatient clinical episodes include percutaneous coronary intervention, cardiac defibrillator implantation, and back and neck surgery except spinal fusion.
Seven quality measures will be tracked as part of the payment. For all clinical episodes, measurement of all-cause hospital readmissions and advance care plan will be required.
The other five will be applied to the payment when appropriate, as follows:
- Perioperative care: selection of prophylactic antibiotic: first- or second-generation cephalosporin.
- Hospital-level risk-standardized complication rate following elective primary total hip arthroplasty and/or total knee arthroplasty.
- Hospital 30-day, all-cause, risk-standardized mortality rate following coronary artery bypass graft surgery.
- Excess days in acute care after hospitalization for acute myocardial infarction; and AHRQ patient safety indicators.
CMS has scheduled an open-door forum for those interested in participating in BPCI Advanced on Jan. 30.
Applications for participation will be accepted through March 12.
The Centers for Medicare & Medicaid Services is launching a new voluntary bundled payment demonstration project that for the first time will qualify as an advanced alternative payment model under the Quality Payment Program.
The Bundled Payments for Care Improvement Advanced (BPCI Advanced) “builds on the earlier success of bundled payment models and is an important step in the move away from fee-for-service and towards paying for value,” CMS Administrator Seema Verma said in a statement. “Under this model, providers will have an incentive to deliver high-quality care.”
Both categories of participants may enter into agreements with individual physicians and nonphysician providers to furnish care under the bundled payment model.
It will cover 29 in-patient episodes and three outpatient clinical episodes. Payment will be tied to performance on quality measures.
The 29 in-patient clinical episodes cover a range of conditions, including liver disorders (excluding malignancy, cirrhosis, and alcoholic hepatitis); various cardiac conditions; chronic obstructive pulmonary disease, bronchitis, and asthma; spinal fusion; joint replacements; femur, hip, or pelvis fractures; gastrointestinal hemorrhage or obstruction; renal failure; sepsis; simple pneumonia and respiratory infections; stroke; and urinary tract infections.
The three outpatient clinical episodes include percutaneous coronary intervention, cardiac defibrillator implantation, and back and neck surgery except spinal fusion.
Seven quality measures will be tracked as part of the payment. For all clinical episodes, measurement of all-cause hospital readmissions and advance care plan will be required.
The other five will be applied to the payment when appropriate, as follows:
- Perioperative care: selection of prophylactic antibiotic: first- or second-generation cephalosporin.
- Hospital-level risk-standardized complication rate following elective primary total hip arthroplasty and/or total knee arthroplasty.
- Hospital 30-day, all-cause, risk-standardized mortality rate following coronary artery bypass graft surgery.
- Excess days in acute care after hospitalization for acute myocardial infarction; and AHRQ patient safety indicators.
CMS has scheduled an open-door forum for those interested in participating in BPCI Advanced on Jan. 30.
Applications for participation will be accepted through March 12.
Pain after breast surgery may not be caused by the operation
, according to a study of almost 2,000 women recruited from the Mastectomy Reconstructive Outcomes Consortium (MROC).
In the February issue of The Breast, investigators from the University of Michigan, Ann Arbor and Memorial Sloan Kettering Cancer Center, New York, wrote that almost half of the study subjects had some level of pain before their operations and that, at 2 years afterward, their pain had increased but not in a clinically meaningful way. This finding is consistent with earlier research, which investigators noted found that “one-fourth to one-half of women who undergo postmastectomy report persistent pain months and years after surgery.”
“Average clinical pain severity was strikingly similar for preoperative and postoperative assessments,” said lead author Randy S. Roth, PhD, of the University of Michigan, and his coauthors. “Postoperative levels of pain, acute postoperative pain and (marginally) level of depression held consistent relationship at 2-year follow-up with all outcome measures.”
The prospective, multicenter cohort study of 1,996 women was undertaken over 5 years. Most patients had immediate (92.7%) and bilateral (53.8%) reconstruction; 47.6% had sentinel lymph node biopsy and 25.9% had axillary lymph node dissection. Most had no adjuvant therapy: 70.3% received no radiation and 52.7% no chemotherapy.
At 2 years, the Numerical Pain Rating Scale (NPRS) measured what Dr. Roth and his coauthors called a “significant increase in pain intensity” – from an average rating of 1.1 to 1.2, an increase of 9%. However, the absolute change and standard deviation (1.7 for both intervals) “suggest that this was not a clinically meaningful change.” The researchers also recorded more complaints of bodily discomfort after 2 years, “but the statistical parameters again indicate little clinically meaningful differences from preoperative status.”
Pain ratings measured with the McGill Pain Questionnaire showed a significant decrease in the MPQ affective pain rating, from 1.6 preoperatively to 0.8 at 2 years (P less than .001), and virtually no change in the MPQ sensory rating, from 3.2 to 3.1.
The researchers drew some conclusions about demographic profiles and pain after breast reconstruction. Older age was associated with more severe pain on NPRS, and higher body mass index was linked with chronic postsurgical pain for the MPQ sensory rating, NPRS score, and body discomfort scores.
Treatment characteristics associated with chronic postsurgical pain (CPSP) include radiation therapy during or after reconstruction and chemotherapy before reconstruction. Chemotherapy during or after reconstruction was associated with higher MPQ affective rating scores at 2 years (P = .011), as was chemotherapy both before and during or after reconstruction (P = .001). The latter also was linked to higher NPRS scores (P = .0015).
The type of surgery also was a factor in CPSP, the researchers wrote. Both MPQ sensory and affective ratings were higher in women who had free transverse flap surgery, or deep or superficial inferior epigastric perforator surgery than in women who had tissue expander/implant reconstruction. Lymph node status and timing of surgery had no impact on chronic pain.
One noteworthy finding, Dr. Roth and his coauthors wrote, is that “careful examination of our data suggests that CPSP following breast reconstruction may be of less clinical concern as a direct consequence of breast reconstruction than suggested by previous investigations of major surgery, including mastectomy and breast reconstruction.” Future studies of chronic postsurgical pain in breast reconstruction “will require greater methodological rigor” to reach more sound conclusions to use in patient counseling.
Dr. Roth and his coauthors had no financial relationships to disclose.
SOURCE: Roth RS et al. Breast 2018;37:119-25.
, according to a study of almost 2,000 women recruited from the Mastectomy Reconstructive Outcomes Consortium (MROC).
In the February issue of The Breast, investigators from the University of Michigan, Ann Arbor and Memorial Sloan Kettering Cancer Center, New York, wrote that almost half of the study subjects had some level of pain before their operations and that, at 2 years afterward, their pain had increased but not in a clinically meaningful way. This finding is consistent with earlier research, which investigators noted found that “one-fourth to one-half of women who undergo postmastectomy report persistent pain months and years after surgery.”
“Average clinical pain severity was strikingly similar for preoperative and postoperative assessments,” said lead author Randy S. Roth, PhD, of the University of Michigan, and his coauthors. “Postoperative levels of pain, acute postoperative pain and (marginally) level of depression held consistent relationship at 2-year follow-up with all outcome measures.”
The prospective, multicenter cohort study of 1,996 women was undertaken over 5 years. Most patients had immediate (92.7%) and bilateral (53.8%) reconstruction; 47.6% had sentinel lymph node biopsy and 25.9% had axillary lymph node dissection. Most had no adjuvant therapy: 70.3% received no radiation and 52.7% no chemotherapy.
At 2 years, the Numerical Pain Rating Scale (NPRS) measured what Dr. Roth and his coauthors called a “significant increase in pain intensity” – from an average rating of 1.1 to 1.2, an increase of 9%. However, the absolute change and standard deviation (1.7 for both intervals) “suggest that this was not a clinically meaningful change.” The researchers also recorded more complaints of bodily discomfort after 2 years, “but the statistical parameters again indicate little clinically meaningful differences from preoperative status.”
Pain ratings measured with the McGill Pain Questionnaire showed a significant decrease in the MPQ affective pain rating, from 1.6 preoperatively to 0.8 at 2 years (P less than .001), and virtually no change in the MPQ sensory rating, from 3.2 to 3.1.
The researchers drew some conclusions about demographic profiles and pain after breast reconstruction. Older age was associated with more severe pain on NPRS, and higher body mass index was linked with chronic postsurgical pain for the MPQ sensory rating, NPRS score, and body discomfort scores.
Treatment characteristics associated with chronic postsurgical pain (CPSP) include radiation therapy during or after reconstruction and chemotherapy before reconstruction. Chemotherapy during or after reconstruction was associated with higher MPQ affective rating scores at 2 years (P = .011), as was chemotherapy both before and during or after reconstruction (P = .001). The latter also was linked to higher NPRS scores (P = .0015).
The type of surgery also was a factor in CPSP, the researchers wrote. Both MPQ sensory and affective ratings were higher in women who had free transverse flap surgery, or deep or superficial inferior epigastric perforator surgery than in women who had tissue expander/implant reconstruction. Lymph node status and timing of surgery had no impact on chronic pain.
One noteworthy finding, Dr. Roth and his coauthors wrote, is that “careful examination of our data suggests that CPSP following breast reconstruction may be of less clinical concern as a direct consequence of breast reconstruction than suggested by previous investigations of major surgery, including mastectomy and breast reconstruction.” Future studies of chronic postsurgical pain in breast reconstruction “will require greater methodological rigor” to reach more sound conclusions to use in patient counseling.
Dr. Roth and his coauthors had no financial relationships to disclose.
SOURCE: Roth RS et al. Breast 2018;37:119-25.
, according to a study of almost 2,000 women recruited from the Mastectomy Reconstructive Outcomes Consortium (MROC).
In the February issue of The Breast, investigators from the University of Michigan, Ann Arbor and Memorial Sloan Kettering Cancer Center, New York, wrote that almost half of the study subjects had some level of pain before their operations and that, at 2 years afterward, their pain had increased but not in a clinically meaningful way. This finding is consistent with earlier research, which investigators noted found that “one-fourth to one-half of women who undergo postmastectomy report persistent pain months and years after surgery.”
“Average clinical pain severity was strikingly similar for preoperative and postoperative assessments,” said lead author Randy S. Roth, PhD, of the University of Michigan, and his coauthors. “Postoperative levels of pain, acute postoperative pain and (marginally) level of depression held consistent relationship at 2-year follow-up with all outcome measures.”
The prospective, multicenter cohort study of 1,996 women was undertaken over 5 years. Most patients had immediate (92.7%) and bilateral (53.8%) reconstruction; 47.6% had sentinel lymph node biopsy and 25.9% had axillary lymph node dissection. Most had no adjuvant therapy: 70.3% received no radiation and 52.7% no chemotherapy.
At 2 years, the Numerical Pain Rating Scale (NPRS) measured what Dr. Roth and his coauthors called a “significant increase in pain intensity” – from an average rating of 1.1 to 1.2, an increase of 9%. However, the absolute change and standard deviation (1.7 for both intervals) “suggest that this was not a clinically meaningful change.” The researchers also recorded more complaints of bodily discomfort after 2 years, “but the statistical parameters again indicate little clinically meaningful differences from preoperative status.”
Pain ratings measured with the McGill Pain Questionnaire showed a significant decrease in the MPQ affective pain rating, from 1.6 preoperatively to 0.8 at 2 years (P less than .001), and virtually no change in the MPQ sensory rating, from 3.2 to 3.1.
The researchers drew some conclusions about demographic profiles and pain after breast reconstruction. Older age was associated with more severe pain on NPRS, and higher body mass index was linked with chronic postsurgical pain for the MPQ sensory rating, NPRS score, and body discomfort scores.
Treatment characteristics associated with chronic postsurgical pain (CPSP) include radiation therapy during or after reconstruction and chemotherapy before reconstruction. Chemotherapy during or after reconstruction was associated with higher MPQ affective rating scores at 2 years (P = .011), as was chemotherapy both before and during or after reconstruction (P = .001). The latter also was linked to higher NPRS scores (P = .0015).
The type of surgery also was a factor in CPSP, the researchers wrote. Both MPQ sensory and affective ratings were higher in women who had free transverse flap surgery, or deep or superficial inferior epigastric perforator surgery than in women who had tissue expander/implant reconstruction. Lymph node status and timing of surgery had no impact on chronic pain.
One noteworthy finding, Dr. Roth and his coauthors wrote, is that “careful examination of our data suggests that CPSP following breast reconstruction may be of less clinical concern as a direct consequence of breast reconstruction than suggested by previous investigations of major surgery, including mastectomy and breast reconstruction.” Future studies of chronic postsurgical pain in breast reconstruction “will require greater methodological rigor” to reach more sound conclusions to use in patient counseling.
Dr. Roth and his coauthors had no financial relationships to disclose.
SOURCE: Roth RS et al. Breast 2018;37:119-25.
FROM THE BREAST
Key clinical point: Breast reconstruction surgery may not be the cause of persistent pain afterward.
Major finding: McGill Pain Questionnaire affective pain rating decreased from 1.6 preoperatively to 0.8 at 2 years.
Data source: Five-year prospective multicenter cohort study of 1,966 women recruited for the Mastectomy Reconstruction Outcomes Consortium.
Disclosures: Dr. Roth and his coauthors reported having no financial disclosures.
Source: Roth RS et al. Breast 2018;37:119-25.
Early psychotherapy may predict buprenorphine treatment retention
SAN DIEGO – an observational study found.
“Opioid use disorder and overdose deaths are devastating many communities across the country,” lead study author Ajay Manhapra, MD, said at the annual meeting and scientific symposium of the American Academy of Addiction Psychiatry. “We know that engagement in opioid agonist treatment with buprenorphine/methadone is associated with a two-thirds reduction in mortality and lower morbidity. However, 1-year retention rates are generally less than 50%.”
As part of a larger study on 3-year buprenorphine retention, Dr. Manhapra and his associates set out to investigate what factors predict long-term retention in buprenorphine treatment. From patients with an OUD diagnosis in the Marketscan database, they identified 16,190 individuals who filled their prescription of buprenorphine after the first 60 days of 2011 as new starts and calculated the treatment retention period as the time between the date of their first prescription to the last prescription until the end of 2014. The researchers used CPT codes to identify the receipt of any outpatient psychotherapy and multivariate Cox survival analysis to examine the effect of psychotherapy receipt on buprenorphine retention.
Dr. Manhapra reported that of the 16,190 patients, 15% were engaged in buprenorphine treatment for 30 days or fewer, 40% were engaged for 31 days to 1 year, 31% were engaged between 1 and 3 years, and 14% were engaged for more than 3 years. The mean duration of retention was 1.23 years. At the same time, the outpatient psychotherapy receipt rate in 2011 was 30.29% among those retained for 0-30 days, 35.30% among those retained for 31-364 days, 37.59% among those retained for 1-3 years, and 39.20% among those retained for more than 3 years.
Multivariate Cox survival analysis revealed that receipt of any psychotherapy in 2011 was associated with a lower risk of discontinuation of buprenorphine treatment (hazard ratio, 0.86; P less than .0001). “Is this a direct effect of psychotherapy? I don’t know,” said Dr. Manhapra, who also practices at the Hampton (Virginia) VA Medical Center. “Is this a selection bias not accounted for by the variables available? That is, those who have a better chance of sustained retention might have been selected for or chosen to receive psychotherapy. Those are possibilities. We need further observational and qualitative studies, and maybe more randomized trials.”
Dr. Manhapra disclosed that he has received support from the VA Interprofessional Fellowship in Addiction Treatment and from Research in Addiction Medicine Scholars.
SOURCE: Manhapra A et al. AAAP 2017. Paper session A5.
SAN DIEGO – an observational study found.
“Opioid use disorder and overdose deaths are devastating many communities across the country,” lead study author Ajay Manhapra, MD, said at the annual meeting and scientific symposium of the American Academy of Addiction Psychiatry. “We know that engagement in opioid agonist treatment with buprenorphine/methadone is associated with a two-thirds reduction in mortality and lower morbidity. However, 1-year retention rates are generally less than 50%.”
As part of a larger study on 3-year buprenorphine retention, Dr. Manhapra and his associates set out to investigate what factors predict long-term retention in buprenorphine treatment. From patients with an OUD diagnosis in the Marketscan database, they identified 16,190 individuals who filled their prescription of buprenorphine after the first 60 days of 2011 as new starts and calculated the treatment retention period as the time between the date of their first prescription to the last prescription until the end of 2014. The researchers used CPT codes to identify the receipt of any outpatient psychotherapy and multivariate Cox survival analysis to examine the effect of psychotherapy receipt on buprenorphine retention.
Dr. Manhapra reported that of the 16,190 patients, 15% were engaged in buprenorphine treatment for 30 days or fewer, 40% were engaged for 31 days to 1 year, 31% were engaged between 1 and 3 years, and 14% were engaged for more than 3 years. The mean duration of retention was 1.23 years. At the same time, the outpatient psychotherapy receipt rate in 2011 was 30.29% among those retained for 0-30 days, 35.30% among those retained for 31-364 days, 37.59% among those retained for 1-3 years, and 39.20% among those retained for more than 3 years.
Multivariate Cox survival analysis revealed that receipt of any psychotherapy in 2011 was associated with a lower risk of discontinuation of buprenorphine treatment (hazard ratio, 0.86; P less than .0001). “Is this a direct effect of psychotherapy? I don’t know,” said Dr. Manhapra, who also practices at the Hampton (Virginia) VA Medical Center. “Is this a selection bias not accounted for by the variables available? That is, those who have a better chance of sustained retention might have been selected for or chosen to receive psychotherapy. Those are possibilities. We need further observational and qualitative studies, and maybe more randomized trials.”
Dr. Manhapra disclosed that he has received support from the VA Interprofessional Fellowship in Addiction Treatment and from Research in Addiction Medicine Scholars.
SOURCE: Manhapra A et al. AAAP 2017. Paper session A5.
SAN DIEGO – an observational study found.
“Opioid use disorder and overdose deaths are devastating many communities across the country,” lead study author Ajay Manhapra, MD, said at the annual meeting and scientific symposium of the American Academy of Addiction Psychiatry. “We know that engagement in opioid agonist treatment with buprenorphine/methadone is associated with a two-thirds reduction in mortality and lower morbidity. However, 1-year retention rates are generally less than 50%.”
As part of a larger study on 3-year buprenorphine retention, Dr. Manhapra and his associates set out to investigate what factors predict long-term retention in buprenorphine treatment. From patients with an OUD diagnosis in the Marketscan database, they identified 16,190 individuals who filled their prescription of buprenorphine after the first 60 days of 2011 as new starts and calculated the treatment retention period as the time between the date of their first prescription to the last prescription until the end of 2014. The researchers used CPT codes to identify the receipt of any outpatient psychotherapy and multivariate Cox survival analysis to examine the effect of psychotherapy receipt on buprenorphine retention.
Dr. Manhapra reported that of the 16,190 patients, 15% were engaged in buprenorphine treatment for 30 days or fewer, 40% were engaged for 31 days to 1 year, 31% were engaged between 1 and 3 years, and 14% were engaged for more than 3 years. The mean duration of retention was 1.23 years. At the same time, the outpatient psychotherapy receipt rate in 2011 was 30.29% among those retained for 0-30 days, 35.30% among those retained for 31-364 days, 37.59% among those retained for 1-3 years, and 39.20% among those retained for more than 3 years.
Multivariate Cox survival analysis revealed that receipt of any psychotherapy in 2011 was associated with a lower risk of discontinuation of buprenorphine treatment (hazard ratio, 0.86; P less than .0001). “Is this a direct effect of psychotherapy? I don’t know,” said Dr. Manhapra, who also practices at the Hampton (Virginia) VA Medical Center. “Is this a selection bias not accounted for by the variables available? That is, those who have a better chance of sustained retention might have been selected for or chosen to receive psychotherapy. Those are possibilities. We need further observational and qualitative studies, and maybe more randomized trials.”
Dr. Manhapra disclosed that he has received support from the VA Interprofessional Fellowship in Addiction Treatment and from Research in Addiction Medicine Scholars.
SOURCE: Manhapra A et al. AAAP 2017. Paper session A5.
REPORTING FROM AAAP
Key clinical point: Psychotherapy at the beginning of buprenorphine treatment may affect retention in patients with opioid use disorder.
Major finding: Receipt of any psychotherapy in 2011 was associated with a lower risk of discontinuation of buprenorphine treatment by 2014 (hazard ratio, 0.86; P less than .0001).
Study details: An observational study of 16,190 individuals with OUD.
Disclosures: Dr. Manhapra disclosed that he has received support from the VA Interprofessional Fellowship in Addiction Treatment and from Research in Addiction Medicine Scholars.
Source: Manhapra A et al. AAAP 2017. Paper session A5.
Review: Common gastrointestinal conditions in people living with HIV/AIDS
The two most common gastrointestinal conditions reported by people living with HIV/AIDS are diarrhea and nausea, according to Vincent Hall, PhD.
Diarrhea has been reported in up to 60% of people living with HIV/AIDS, and is generally classified as being infectious or noninfectious. While infectious causes of diarrhea, such as bacteria, fungi, viruses, and protozoa, have declined, noninfectious causes have increased. Common causes of noninfectious diarrhea include HIV enteropathy, diarrhea associated with highly active antiretroviral therapy (HAART), autonomic neuropathy, and chronic pancreatitis.
Prior to the development of HAART, nausea in people living with HIV/AIDS was usually caused by opportunistic infections; however, this has changed. Nausea can come from medication side effects, overlapping drug interactions, and from opportunistic infections in patients with poor immune health. The most common side effect of ART is nausea, and nausea is also the most common cause of ART discontinuation.
“It has been noted that HIV infection can be considered a disease of the GI tract because it is a significant target of infection and because of the side effects HAART can have on the GI system. Therefore, it is important that clinicians have an understanding of the causes of diarrhea and nausea and vomiting in people living with HIV/AIDS and educate patients about potential side effects and treatment options,” Mr. Hall concluded.
Find the full review in Critical Care Nursing Clinics of North America (doi: 10.1016/j.cnc.2017.10.009).
The two most common gastrointestinal conditions reported by people living with HIV/AIDS are diarrhea and nausea, according to Vincent Hall, PhD.
Diarrhea has been reported in up to 60% of people living with HIV/AIDS, and is generally classified as being infectious or noninfectious. While infectious causes of diarrhea, such as bacteria, fungi, viruses, and protozoa, have declined, noninfectious causes have increased. Common causes of noninfectious diarrhea include HIV enteropathy, diarrhea associated with highly active antiretroviral therapy (HAART), autonomic neuropathy, and chronic pancreatitis.
Prior to the development of HAART, nausea in people living with HIV/AIDS was usually caused by opportunistic infections; however, this has changed. Nausea can come from medication side effects, overlapping drug interactions, and from opportunistic infections in patients with poor immune health. The most common side effect of ART is nausea, and nausea is also the most common cause of ART discontinuation.
“It has been noted that HIV infection can be considered a disease of the GI tract because it is a significant target of infection and because of the side effects HAART can have on the GI system. Therefore, it is important that clinicians have an understanding of the causes of diarrhea and nausea and vomiting in people living with HIV/AIDS and educate patients about potential side effects and treatment options,” Mr. Hall concluded.
Find the full review in Critical Care Nursing Clinics of North America (doi: 10.1016/j.cnc.2017.10.009).
The two most common gastrointestinal conditions reported by people living with HIV/AIDS are diarrhea and nausea, according to Vincent Hall, PhD.
Diarrhea has been reported in up to 60% of people living with HIV/AIDS, and is generally classified as being infectious or noninfectious. While infectious causes of diarrhea, such as bacteria, fungi, viruses, and protozoa, have declined, noninfectious causes have increased. Common causes of noninfectious diarrhea include HIV enteropathy, diarrhea associated with highly active antiretroviral therapy (HAART), autonomic neuropathy, and chronic pancreatitis.
Prior to the development of HAART, nausea in people living with HIV/AIDS was usually caused by opportunistic infections; however, this has changed. Nausea can come from medication side effects, overlapping drug interactions, and from opportunistic infections in patients with poor immune health. The most common side effect of ART is nausea, and nausea is also the most common cause of ART discontinuation.
“It has been noted that HIV infection can be considered a disease of the GI tract because it is a significant target of infection and because of the side effects HAART can have on the GI system. Therefore, it is important that clinicians have an understanding of the causes of diarrhea and nausea and vomiting in people living with HIV/AIDS and educate patients about potential side effects and treatment options,” Mr. Hall concluded.
Find the full review in Critical Care Nursing Clinics of North America (doi: 10.1016/j.cnc.2017.10.009).
FROM CRITICAL CARE NURSING CLINICS OF NORTH AMERICA
Disparities persist in infant safe sleep practices
Sleep-related deaths among infants in the United States decreased during the 1990s as a result of recommendations to place babies on their backs to sleep. However, the decline has leveled off in recent years, and health care providers should proactively counsel caregivers about safe sleep practices, wrote Jennifer M. Bombard, MSPH, of the Centers for Disease Control and Prevention and her colleagues in a study published online in the Morbidity and Mortality Weekly Report.
Overall, 22% of respondents from 32 states and New York City in 2015 reported placing babies in a position other than their backs to sleep. In addition, 61% of respondents from 14 states reported bed sharing, and 39% from 13 states and New York City reported using soft bedding, including bumper pads and thick blankets.
Unsafe sleep practices varied by maternal demographics; nonsupine sleep positioning was more likely among non-Hispanic blacks, individuals aged 25 years or younger, those with 12 years or less of education, and those participating in the Special Supplemental Nutrition Program for Women, Infants, and Children.
“These findings highlight the need to implement and evaluate interventions to continue improving safe sleep practices,” Ms. Bombard and her associates said.
They cited the Study of Attitudes and Factors Effecting Infant Care Practices, in which caregivers who received appropriate advice on safe sleep practices were significantly less likely to place infants in a nonsupine position to sleep. “Evidence-based approaches to increase use of safe sleep practices include developing health messages and educational tools for caregivers and educating health and child care professionals on safe sleep practices,” they noted.
The study was limited by several factors, including reliance on self reports and inclusion of only states with Pregnancy Risk Assessment Monitoring System records, the researchers said.
Ms. Bombard and her associates had no relevant financial disclosures.
SOURCE: Bombard J et al. MMWR. 2018 Jan 9. doi: 10.15585/mmwr.mm6701e1.
Sleep-related deaths among infants in the United States decreased during the 1990s as a result of recommendations to place babies on their backs to sleep. However, the decline has leveled off in recent years, and health care providers should proactively counsel caregivers about safe sleep practices, wrote Jennifer M. Bombard, MSPH, of the Centers for Disease Control and Prevention and her colleagues in a study published online in the Morbidity and Mortality Weekly Report.
Overall, 22% of respondents from 32 states and New York City in 2015 reported placing babies in a position other than their backs to sleep. In addition, 61% of respondents from 14 states reported bed sharing, and 39% from 13 states and New York City reported using soft bedding, including bumper pads and thick blankets.
Unsafe sleep practices varied by maternal demographics; nonsupine sleep positioning was more likely among non-Hispanic blacks, individuals aged 25 years or younger, those with 12 years or less of education, and those participating in the Special Supplemental Nutrition Program for Women, Infants, and Children.
“These findings highlight the need to implement and evaluate interventions to continue improving safe sleep practices,” Ms. Bombard and her associates said.
They cited the Study of Attitudes and Factors Effecting Infant Care Practices, in which caregivers who received appropriate advice on safe sleep practices were significantly less likely to place infants in a nonsupine position to sleep. “Evidence-based approaches to increase use of safe sleep practices include developing health messages and educational tools for caregivers and educating health and child care professionals on safe sleep practices,” they noted.
The study was limited by several factors, including reliance on self reports and inclusion of only states with Pregnancy Risk Assessment Monitoring System records, the researchers said.
Ms. Bombard and her associates had no relevant financial disclosures.
SOURCE: Bombard J et al. MMWR. 2018 Jan 9. doi: 10.15585/mmwr.mm6701e1.
Sleep-related deaths among infants in the United States decreased during the 1990s as a result of recommendations to place babies on their backs to sleep. However, the decline has leveled off in recent years, and health care providers should proactively counsel caregivers about safe sleep practices, wrote Jennifer M. Bombard, MSPH, of the Centers for Disease Control and Prevention and her colleagues in a study published online in the Morbidity and Mortality Weekly Report.
Overall, 22% of respondents from 32 states and New York City in 2015 reported placing babies in a position other than their backs to sleep. In addition, 61% of respondents from 14 states reported bed sharing, and 39% from 13 states and New York City reported using soft bedding, including bumper pads and thick blankets.
Unsafe sleep practices varied by maternal demographics; nonsupine sleep positioning was more likely among non-Hispanic blacks, individuals aged 25 years or younger, those with 12 years or less of education, and those participating in the Special Supplemental Nutrition Program for Women, Infants, and Children.
“These findings highlight the need to implement and evaluate interventions to continue improving safe sleep practices,” Ms. Bombard and her associates said.
They cited the Study of Attitudes and Factors Effecting Infant Care Practices, in which caregivers who received appropriate advice on safe sleep practices were significantly less likely to place infants in a nonsupine position to sleep. “Evidence-based approaches to increase use of safe sleep practices include developing health messages and educational tools for caregivers and educating health and child care professionals on safe sleep practices,” they noted.
The study was limited by several factors, including reliance on self reports and inclusion of only states with Pregnancy Risk Assessment Monitoring System records, the researchers said.
Ms. Bombard and her associates had no relevant financial disclosures.
SOURCE: Bombard J et al. MMWR. 2018 Jan 9. doi: 10.15585/mmwr.mm6701e1.
FROM MMWR
Key clinical point: Health care providers can improve safe sleep for babies by counseling caregivers.
Major finding: Of respondents from 32 states and New York City in 2015, 22% reported placing babies in a position other than their backs to sleep.
Study details: The data come from the 2009-2015 Pregnancy Risk Assessment Monitoring System.
Disclosures: The researchers had no relevant financial disclosures.
Source: Bombard J et al. MMWR 2018 Jan 9. doi: 10.15585/mmwr.mm6701e1.
Prepregnancy obesity linked to bump in severe morbidity
Having a high or low prepregnancy body mass index was associated with a small absolute increase in severe maternal morbidity and mortality in a large, retrospective cohort study.
Some studies have suggested a link between obesity and pregnancy complications such as preeclampsia, gestational diabetes, thromboembolism, and cesarean delivery. But one study suggested no link between higher BMI and risk of severe morbidity.
Adjustment for weight gain had no significant effect on the observed associations, Sarka Lisonkova, MD, PhD, of B.C. Women’s Hospital & Health Centre in Vancouver and her colleagues reported in JAMA.
Compared with normal weight women (BMI 18.5-24.9), women considered underweight (BMI less than 18.5) had an adjusted odds ratio (aOR) for mortality or severity morbidity of 1.2 (95% confidence interval, 1.0-1.3). Women who were overweight (BMI of 25.0-29.9) had an aOR of 1.1 (95% CI, 1.1-1.2).
The risk was also greater for women with class 1 obesity (BMI, 30.0-34.9; aOR, 1.1; 95% CI, 1.1-1.2), class 2 obesity (BMI, 35.0-39.9; aOR, 1.2; 95% CI, 1.1-1.3), and class 3 obesity (BMI, 40 or greater; aOR, 1.4; 95% CI, 1.3-1.5).
In all cases, the absolute increases in mortality and severe morbidity, compared with normal weight women, were small, ranging from adjusted rated differences of 17.6 per 10,000 for overweight women to 61.1 per 10,000 women with class 3 obesity. Underweight women had an increase of 28.8 per 10,000.
Specifically, underweight women had a higher risk for antepartum and postpartum hemorrhage and acute renal failure, whereas women who were obese had increased risks for respiratory morbidity and thromboembolism, the researchers reported.
The study was funded by the Canadian Institutes of Health Research. Dr. Lisonkova is supported by an award from the Michael Smith Foundation for Health Research. No other financial disclosures were reported.
SOURCE: Lisonkova S et al. JAMA. 2017 Nov 14;318(18):1777-86.
Having a high or low prepregnancy body mass index was associated with a small absolute increase in severe maternal morbidity and mortality in a large, retrospective cohort study.
Some studies have suggested a link between obesity and pregnancy complications such as preeclampsia, gestational diabetes, thromboembolism, and cesarean delivery. But one study suggested no link between higher BMI and risk of severe morbidity.
Adjustment for weight gain had no significant effect on the observed associations, Sarka Lisonkova, MD, PhD, of B.C. Women’s Hospital & Health Centre in Vancouver and her colleagues reported in JAMA.
Compared with normal weight women (BMI 18.5-24.9), women considered underweight (BMI less than 18.5) had an adjusted odds ratio (aOR) for mortality or severity morbidity of 1.2 (95% confidence interval, 1.0-1.3). Women who were overweight (BMI of 25.0-29.9) had an aOR of 1.1 (95% CI, 1.1-1.2).
The risk was also greater for women with class 1 obesity (BMI, 30.0-34.9; aOR, 1.1; 95% CI, 1.1-1.2), class 2 obesity (BMI, 35.0-39.9; aOR, 1.2; 95% CI, 1.1-1.3), and class 3 obesity (BMI, 40 or greater; aOR, 1.4; 95% CI, 1.3-1.5).
In all cases, the absolute increases in mortality and severe morbidity, compared with normal weight women, were small, ranging from adjusted rated differences of 17.6 per 10,000 for overweight women to 61.1 per 10,000 women with class 3 obesity. Underweight women had an increase of 28.8 per 10,000.
Specifically, underweight women had a higher risk for antepartum and postpartum hemorrhage and acute renal failure, whereas women who were obese had increased risks for respiratory morbidity and thromboembolism, the researchers reported.
The study was funded by the Canadian Institutes of Health Research. Dr. Lisonkova is supported by an award from the Michael Smith Foundation for Health Research. No other financial disclosures were reported.
SOURCE: Lisonkova S et al. JAMA. 2017 Nov 14;318(18):1777-86.
Having a high or low prepregnancy body mass index was associated with a small absolute increase in severe maternal morbidity and mortality in a large, retrospective cohort study.
Some studies have suggested a link between obesity and pregnancy complications such as preeclampsia, gestational diabetes, thromboembolism, and cesarean delivery. But one study suggested no link between higher BMI and risk of severe morbidity.
Adjustment for weight gain had no significant effect on the observed associations, Sarka Lisonkova, MD, PhD, of B.C. Women’s Hospital & Health Centre in Vancouver and her colleagues reported in JAMA.
Compared with normal weight women (BMI 18.5-24.9), women considered underweight (BMI less than 18.5) had an adjusted odds ratio (aOR) for mortality or severity morbidity of 1.2 (95% confidence interval, 1.0-1.3). Women who were overweight (BMI of 25.0-29.9) had an aOR of 1.1 (95% CI, 1.1-1.2).
The risk was also greater for women with class 1 obesity (BMI, 30.0-34.9; aOR, 1.1; 95% CI, 1.1-1.2), class 2 obesity (BMI, 35.0-39.9; aOR, 1.2; 95% CI, 1.1-1.3), and class 3 obesity (BMI, 40 or greater; aOR, 1.4; 95% CI, 1.3-1.5).
In all cases, the absolute increases in mortality and severe morbidity, compared with normal weight women, were small, ranging from adjusted rated differences of 17.6 per 10,000 for overweight women to 61.1 per 10,000 women with class 3 obesity. Underweight women had an increase of 28.8 per 10,000.
Specifically, underweight women had a higher risk for antepartum and postpartum hemorrhage and acute renal failure, whereas women who were obese had increased risks for respiratory morbidity and thromboembolism, the researchers reported.
The study was funded by the Canadian Institutes of Health Research. Dr. Lisonkova is supported by an award from the Michael Smith Foundation for Health Research. No other financial disclosures were reported.
SOURCE: Lisonkova S et al. JAMA. 2017 Nov 14;318(18):1777-86.
FROM JAMA
Key clinical point: Major finding: Severe morbidity and mortality risk was increased by 20% in women with prepregnancy class 2 obesity and 40% in women with class 3 obesity.
Study details: Retrospective analysis of 743,630 singleton pregnancies in Washington state between 2004 and 2013.
Disclosures: The study was funded by the Canadian Institutes of Health Research. Dr. Lisonkova is supported by an award from the Michael Smith Foundation for Health Research. No other financial disclosures were reported.
Source: Lisonkova S et al. JAMA. 2017 Nov 14;318(18):1777-86.
views
There is a link between obesity and maternal complications during pregnancy, but a causal relationship has not been established. It could be that obese women are inherently at greater risk of mortality, or it could be that physicians have a harder time managing severe conditions in women who are obese.
One way to better understand the problem is to study obesity and severe maternal morbidity in pregnant women because the severe morbidity may precede and add to the increased mortality rates that are being seen among obese pregnant women.
The results of the current study support the idea that the association between class 3 obesity and severe complications in pregnancy may play a role in the increased risk of maternal mortality that was also observed.
The results also suggest that physicians caring for women of childbearing age should emphasize the importance of achieving optimal body mass index in reducing pregnancy complications.
Aaron B. Caughey, MD, PhD, is the chair of the department of obstetrics and gynecology at Oregon Health and Science University, Portland. His comments are adapted from an accompanying editorial (JAMA. 2017;318[18]:1765-6). Dr. Caughey reported having no financial disclosures.