User login
Today’s Product Theaters
12:30 - 1:30 p.m., Product Theater 1
Expert Conversations in Heart Failure: Connecting the Pieces
Thomas Arne, Jr., DO
Sergey Kachur, MDSponsored by Novartis Pharmaceuticals
12:30 - 1:30 p.m., Product Theater 2 Opioid-Induced Constipation
Jeff Gudin, MD
Director, Pain and Palliative Care
Englewood Hospital and Medical Center
Englewood, NJ
Sponsored by Salix Pharmaceuticals
12:30 - 1:30 p.m., Product Theater 3
Challenges of Treating DVT and PE in the Hospital and After Discharge
Dr. Andrew Miller, Emergency Medicine, Lehigh Valley Hospital, Allentown, PA
Sponsored by Pfizer
12:30 - 1:30 p.m., Product Theater 1
Expert Conversations in Heart Failure: Connecting the Pieces
Thomas Arne, Jr., DO
Sergey Kachur, MDSponsored by Novartis Pharmaceuticals
12:30 - 1:30 p.m., Product Theater 2 Opioid-Induced Constipation
Jeff Gudin, MD
Director, Pain and Palliative Care
Englewood Hospital and Medical Center
Englewood, NJ
Sponsored by Salix Pharmaceuticals
12:30 - 1:30 p.m., Product Theater 3
Challenges of Treating DVT and PE in the Hospital and After Discharge
Dr. Andrew Miller, Emergency Medicine, Lehigh Valley Hospital, Allentown, PA
Sponsored by Pfizer
12:30 - 1:30 p.m., Product Theater 1
Expert Conversations in Heart Failure: Connecting the Pieces
Thomas Arne, Jr., DO
Sergey Kachur, MDSponsored by Novartis Pharmaceuticals
12:30 - 1:30 p.m., Product Theater 2 Opioid-Induced Constipation
Jeff Gudin, MD
Director, Pain and Palliative Care
Englewood Hospital and Medical Center
Englewood, NJ
Sponsored by Salix Pharmaceuticals
12:30 - 1:30 p.m., Product Theater 3
Challenges of Treating DVT and PE in the Hospital and After Discharge
Dr. Andrew Miller, Emergency Medicine, Lehigh Valley Hospital, Allentown, PA
Sponsored by Pfizer
April 2018: Click for Credit
Here are 4 articles in the April issue of Journal of Clinical Outcomes Management.
1. Young Adult HIV Patients May Be At Increased Risk of Hypertension
2. Written Exposure Therapy Rivals Cognitive Processing Therapy For PTSD
3. Large Database Analysis Suggests Safety of Bariatric Surgery in Seniors
4. Who Fares Best After Successful ECT?
Here are 4 articles in the April issue of Journal of Clinical Outcomes Management.
1. Young Adult HIV Patients May Be At Increased Risk of Hypertension
2. Written Exposure Therapy Rivals Cognitive Processing Therapy For PTSD
3. Large Database Analysis Suggests Safety of Bariatric Surgery in Seniors
4. Who Fares Best After Successful ECT?
Here are 4 articles in the April issue of Journal of Clinical Outcomes Management.
1. Young Adult HIV Patients May Be At Increased Risk of Hypertension
2. Written Exposure Therapy Rivals Cognitive Processing Therapy For PTSD
3. Large Database Analysis Suggests Safety of Bariatric Surgery in Seniors
4. Who Fares Best After Successful ECT?
SHM CEO to highlight need to prepare for change
If there’s one thing hospital medicine is not, it’s static. And that’s truer today than it’s ever been in the more than 20 years since the field came into existence: As the role of hospitalists continue to expand, it’s now in the setting of a rapidly changing health care scene.
So when Society of Hospital Medicine CEO Larry Wellikson, MD, MHM, takes the annual conference podium this morning for his talk on “Future Challenges for Hospital Medicine,” he’ll have a lot to cover.
His overall message, though, will boil down to this: Learn the skills you’ll need.
With hospitalists managing acute and palliative care and being involved in surgical comanagement, many may need additional training.
“There’s a blurring of our role as we link to the emergency department or critical care units, or even a blurring of where does inpatient care end and outpatient care begin?” he said. “Many of these roles hospitalists haven’t been completely trained for.” He’ll also remind the audience that one of SHM’s main roles is to help provide that training.
He said the urgency of learning new skills is only intensified by the health care field’s transition from volume-based payment to value-based payment and by consolidation of previously separate pieces of the landscape, such as the acquisition of Aetna by CVS, with its nearly 10,000 pharmacy locations and more than 1,000 MinuteClinics.
“The real cost for them is hospitalization,” Dr. Wellikson said. “Any money they spend on hospitalization is money they don’t have left over. That puts pressure on hospitalists.”
And it could mean a role shift.
“Maybe our role now becomes that we see that patient after they leave the hospital to make sure that we complete their hospital care and keep them moving in the right direction, because we don’t want them to bounce back into our hospital,” he said.
On whether all the changes in health care are good or bad for hospitalists, Dr. Wellikson said that “good is a relative term.”
“The most important thing in life is to be relevant and to be needed,” he said. “As you add on new things, you have to acquire those competencies. That’s the challenge.”
Dr. Wellikson will also discuss the expansion of hospital medicine and SHM internationally.
“We’re now working with hospitalists in Japan, in Brazil, in Holland, in Canada,” he said. “We’re working in England and Singapore. And each of these places is different.”
His talk will dovetail with a theme that is more prominent in the annual conference program this year: helping hospitalists in mid-career navigate new opportunities.
“The good news on career development is you have so many different directions you can go,” said Dr. Wellikson, pointing to hospitalists who’ve become CEOs and CMOs. But he added that these opportunities require new skills, which goes back to the importance of training.
As a hospitalist, he said, you have to “make sure that you have the ability to gather the new skills to meet new challenges. Just because you become a manager doesn’t mean that magically you know how to manage. How do you keep your skills up as your scope expands or your opportunities grow? What happens more often in hospital medicine is that hospitalists get promoted into a position that can be overwhelming, which leads to burnout or career problems.”
Future Challenges for Hospital Medicine
Tuesday, 9:35-10:00 a.m.
Palms Ballroom
If there’s one thing hospital medicine is not, it’s static. And that’s truer today than it’s ever been in the more than 20 years since the field came into existence: As the role of hospitalists continue to expand, it’s now in the setting of a rapidly changing health care scene.
So when Society of Hospital Medicine CEO Larry Wellikson, MD, MHM, takes the annual conference podium this morning for his talk on “Future Challenges for Hospital Medicine,” he’ll have a lot to cover.
His overall message, though, will boil down to this: Learn the skills you’ll need.
With hospitalists managing acute and palliative care and being involved in surgical comanagement, many may need additional training.
“There’s a blurring of our role as we link to the emergency department or critical care units, or even a blurring of where does inpatient care end and outpatient care begin?” he said. “Many of these roles hospitalists haven’t been completely trained for.” He’ll also remind the audience that one of SHM’s main roles is to help provide that training.
He said the urgency of learning new skills is only intensified by the health care field’s transition from volume-based payment to value-based payment and by consolidation of previously separate pieces of the landscape, such as the acquisition of Aetna by CVS, with its nearly 10,000 pharmacy locations and more than 1,000 MinuteClinics.
“The real cost for them is hospitalization,” Dr. Wellikson said. “Any money they spend on hospitalization is money they don’t have left over. That puts pressure on hospitalists.”
And it could mean a role shift.
“Maybe our role now becomes that we see that patient after they leave the hospital to make sure that we complete their hospital care and keep them moving in the right direction, because we don’t want them to bounce back into our hospital,” he said.
On whether all the changes in health care are good or bad for hospitalists, Dr. Wellikson said that “good is a relative term.”
“The most important thing in life is to be relevant and to be needed,” he said. “As you add on new things, you have to acquire those competencies. That’s the challenge.”
Dr. Wellikson will also discuss the expansion of hospital medicine and SHM internationally.
“We’re now working with hospitalists in Japan, in Brazil, in Holland, in Canada,” he said. “We’re working in England and Singapore. And each of these places is different.”
His talk will dovetail with a theme that is more prominent in the annual conference program this year: helping hospitalists in mid-career navigate new opportunities.
“The good news on career development is you have so many different directions you can go,” said Dr. Wellikson, pointing to hospitalists who’ve become CEOs and CMOs. But he added that these opportunities require new skills, which goes back to the importance of training.
As a hospitalist, he said, you have to “make sure that you have the ability to gather the new skills to meet new challenges. Just because you become a manager doesn’t mean that magically you know how to manage. How do you keep your skills up as your scope expands or your opportunities grow? What happens more often in hospital medicine is that hospitalists get promoted into a position that can be overwhelming, which leads to burnout or career problems.”
Future Challenges for Hospital Medicine
Tuesday, 9:35-10:00 a.m.
Palms Ballroom
If there’s one thing hospital medicine is not, it’s static. And that’s truer today than it’s ever been in the more than 20 years since the field came into existence: As the role of hospitalists continue to expand, it’s now in the setting of a rapidly changing health care scene.
So when Society of Hospital Medicine CEO Larry Wellikson, MD, MHM, takes the annual conference podium this morning for his talk on “Future Challenges for Hospital Medicine,” he’ll have a lot to cover.
His overall message, though, will boil down to this: Learn the skills you’ll need.
With hospitalists managing acute and palliative care and being involved in surgical comanagement, many may need additional training.
“There’s a blurring of our role as we link to the emergency department or critical care units, or even a blurring of where does inpatient care end and outpatient care begin?” he said. “Many of these roles hospitalists haven’t been completely trained for.” He’ll also remind the audience that one of SHM’s main roles is to help provide that training.
He said the urgency of learning new skills is only intensified by the health care field’s transition from volume-based payment to value-based payment and by consolidation of previously separate pieces of the landscape, such as the acquisition of Aetna by CVS, with its nearly 10,000 pharmacy locations and more than 1,000 MinuteClinics.
“The real cost for them is hospitalization,” Dr. Wellikson said. “Any money they spend on hospitalization is money they don’t have left over. That puts pressure on hospitalists.”
And it could mean a role shift.
“Maybe our role now becomes that we see that patient after they leave the hospital to make sure that we complete their hospital care and keep them moving in the right direction, because we don’t want them to bounce back into our hospital,” he said.
On whether all the changes in health care are good or bad for hospitalists, Dr. Wellikson said that “good is a relative term.”
“The most important thing in life is to be relevant and to be needed,” he said. “As you add on new things, you have to acquire those competencies. That’s the challenge.”
Dr. Wellikson will also discuss the expansion of hospital medicine and SHM internationally.
“We’re now working with hospitalists in Japan, in Brazil, in Holland, in Canada,” he said. “We’re working in England and Singapore. And each of these places is different.”
His talk will dovetail with a theme that is more prominent in the annual conference program this year: helping hospitalists in mid-career navigate new opportunities.
“The good news on career development is you have so many different directions you can go,” said Dr. Wellikson, pointing to hospitalists who’ve become CEOs and CMOs. But he added that these opportunities require new skills, which goes back to the importance of training.
As a hospitalist, he said, you have to “make sure that you have the ability to gather the new skills to meet new challenges. Just because you become a manager doesn’t mean that magically you know how to manage. How do you keep your skills up as your scope expands or your opportunities grow? What happens more often in hospital medicine is that hospitalists get promoted into a position that can be overwhelming, which leads to burnout or career problems.”
Future Challenges for Hospital Medicine
Tuesday, 9:35-10:00 a.m.
Palms Ballroom
Culture change can improve NP, PA practice
Creating an atmosphere conducive to productive teamwork can help maximize nurse practitioners’ and physician assistants’ potential, say experts presenting at the Tuesday session “How Best NP/PA and MD Hospitalists Can Work Together.”
Session leaders Brian Wolfe, MD, FHM, a general internist at the University of Michigan, Ann Arbor, and Tracy Cardin, ACNP-BC,SFHM, the associate director of clinical integration at Adfinitas Health, Hanover, Md., will break down strategies to help incorporate different perspectives into your practice to improve its culture.
“I think culture beats strategy any day of the week, and the cultural threads we can draw from our different experiences are a lot more powerful, and a lot more translatable, across different institutions,” Dr. Wolfe said in an interview. “The purpose of this session is to get away from saying ‘Well, this is the way we do it,’ and instead say, ‘This is what kind of cultural vision we have for our NPs and PAs, and this is where we succeed, and these are the ways we fail.’ ”
Attendees will learn about what PAs and NPs are looking for in their work, what some providers are doing to change their hospital culture, and the business data behind those decisions.
“NPs and PAs are looking for autonomy, mastery, and purpose,” said Dr. Wolfe. “While some of that comes from where you work and how long your hours are, a lot of it has to do with how the culture treats you as a nurse practitioner or physician assistant and where your place is.”
Following Dr. Wolfe’s initial presentation, the facilitators will analyze cases with evident structural problems in order to uncover the underlying cultural issues.
By hearing about concrete, everyday examples, attendees will be able to recognize some of the problems within their own networks that they might deal with on a regular basis and come away with long-term solutions.
“Nobody really acknowledges these issues on a day-to-day basis, but they can be extremely influential,” Ms. Cardin said in an interview. “Once you’re aware of the cultural impacts on the functionality of your group, then you can begin chipping away at them and altering culture to provide for a more successful path.”
Attendees will leave the session with solutions that can boost productivity and spending, according to Dr. Wolfe.
“As a physician leader, you want to recruit and retain high-level people who can operate at the top of their licenses and can push your practice beyond its structures,” said Dr. Wolfe. “The other piece is that there is no defined cost for retraining, and if you don’t address the issues that will drive your PAs and NPs to leave, you’ll be stuck with a constant turnover, which leads to lower performance and less efficiency.”
How Best NP/PA and MD Hospitalists Can Work Together:
Incorporating NPs/PAs into the workforce and Workplace Culture
Tuesday, 4:30-6 p.m.
Grand Ballroom 1-3
Creating an atmosphere conducive to productive teamwork can help maximize nurse practitioners’ and physician assistants’ potential, say experts presenting at the Tuesday session “How Best NP/PA and MD Hospitalists Can Work Together.”
Session leaders Brian Wolfe, MD, FHM, a general internist at the University of Michigan, Ann Arbor, and Tracy Cardin, ACNP-BC,SFHM, the associate director of clinical integration at Adfinitas Health, Hanover, Md., will break down strategies to help incorporate different perspectives into your practice to improve its culture.
“I think culture beats strategy any day of the week, and the cultural threads we can draw from our different experiences are a lot more powerful, and a lot more translatable, across different institutions,” Dr. Wolfe said in an interview. “The purpose of this session is to get away from saying ‘Well, this is the way we do it,’ and instead say, ‘This is what kind of cultural vision we have for our NPs and PAs, and this is where we succeed, and these are the ways we fail.’ ”
Attendees will learn about what PAs and NPs are looking for in their work, what some providers are doing to change their hospital culture, and the business data behind those decisions.
“NPs and PAs are looking for autonomy, mastery, and purpose,” said Dr. Wolfe. “While some of that comes from where you work and how long your hours are, a lot of it has to do with how the culture treats you as a nurse practitioner or physician assistant and where your place is.”
Following Dr. Wolfe’s initial presentation, the facilitators will analyze cases with evident structural problems in order to uncover the underlying cultural issues.
By hearing about concrete, everyday examples, attendees will be able to recognize some of the problems within their own networks that they might deal with on a regular basis and come away with long-term solutions.
“Nobody really acknowledges these issues on a day-to-day basis, but they can be extremely influential,” Ms. Cardin said in an interview. “Once you’re aware of the cultural impacts on the functionality of your group, then you can begin chipping away at them and altering culture to provide for a more successful path.”
Attendees will leave the session with solutions that can boost productivity and spending, according to Dr. Wolfe.
“As a physician leader, you want to recruit and retain high-level people who can operate at the top of their licenses and can push your practice beyond its structures,” said Dr. Wolfe. “The other piece is that there is no defined cost for retraining, and if you don’t address the issues that will drive your PAs and NPs to leave, you’ll be stuck with a constant turnover, which leads to lower performance and less efficiency.”
How Best NP/PA and MD Hospitalists Can Work Together:
Incorporating NPs/PAs into the workforce and Workplace Culture
Tuesday, 4:30-6 p.m.
Grand Ballroom 1-3
Creating an atmosphere conducive to productive teamwork can help maximize nurse practitioners’ and physician assistants’ potential, say experts presenting at the Tuesday session “How Best NP/PA and MD Hospitalists Can Work Together.”
Session leaders Brian Wolfe, MD, FHM, a general internist at the University of Michigan, Ann Arbor, and Tracy Cardin, ACNP-BC,SFHM, the associate director of clinical integration at Adfinitas Health, Hanover, Md., will break down strategies to help incorporate different perspectives into your practice to improve its culture.
“I think culture beats strategy any day of the week, and the cultural threads we can draw from our different experiences are a lot more powerful, and a lot more translatable, across different institutions,” Dr. Wolfe said in an interview. “The purpose of this session is to get away from saying ‘Well, this is the way we do it,’ and instead say, ‘This is what kind of cultural vision we have for our NPs and PAs, and this is where we succeed, and these are the ways we fail.’ ”
Attendees will learn about what PAs and NPs are looking for in their work, what some providers are doing to change their hospital culture, and the business data behind those decisions.
“NPs and PAs are looking for autonomy, mastery, and purpose,” said Dr. Wolfe. “While some of that comes from where you work and how long your hours are, a lot of it has to do with how the culture treats you as a nurse practitioner or physician assistant and where your place is.”
Following Dr. Wolfe’s initial presentation, the facilitators will analyze cases with evident structural problems in order to uncover the underlying cultural issues.
By hearing about concrete, everyday examples, attendees will be able to recognize some of the problems within their own networks that they might deal with on a regular basis and come away with long-term solutions.
“Nobody really acknowledges these issues on a day-to-day basis, but they can be extremely influential,” Ms. Cardin said in an interview. “Once you’re aware of the cultural impacts on the functionality of your group, then you can begin chipping away at them and altering culture to provide for a more successful path.”
Attendees will leave the session with solutions that can boost productivity and spending, according to Dr. Wolfe.
“As a physician leader, you want to recruit and retain high-level people who can operate at the top of their licenses and can push your practice beyond its structures,” said Dr. Wolfe. “The other piece is that there is no defined cost for retraining, and if you don’t address the issues that will drive your PAs and NPs to leave, you’ll be stuck with a constant turnover, which leads to lower performance and less efficiency.”
How Best NP/PA and MD Hospitalists Can Work Together:
Incorporating NPs/PAs into the workforce and Workplace Culture
Tuesday, 4:30-6 p.m.
Grand Ballroom 1-3
‘Update in HM’ to highlight practice pearls
Barbara Slawski, MD, MS, SFHM, and Cynthia Cooper, MD, hadn’t met in person until early 2018. But that doesn’t mean they haven’t spent a lot of time together.
Once a month, the two hospitalists checked in with one another through wide-ranging phone calls. Together, they have combed the medical literature and conferred over the past year, making long lists of candidate studies for the “Top 20” journal articles of the year for practicing hospitalists.
The two physicians will comoderate Tuesday’s “Update in Hospital Medicine” session, where they will summarize research findings of these “Top 20” articles. Their hope is to present research that each attendee can bring home to improve patient outcomes on a daily basis, while making for a smoother and more efficient practice.
Dr. Slawski, chief of the section of perioperative medicine at the Medical College of Wisconsin in Milwaukee, said the presentations will not simply summarize study results but also will help attendees focus on the key findings – the clinical pearls – that represent real opportunities to update practice.
Since hospital medicine crosses so many disciplines, each physician said, in separate interviews, that doing justice to the literature has been time consuming and intellectually challenging – but worthwhile.
Dr. Cooper, a hospitalist at Massachusetts General Hospital, Boston, said that, although she and Dr. Slawski practice in geographically diverse areas, their practice settings – academic medical centers – have many similarities. She said that, as she reviewed the medical literature over the past year, she gave considerable thought to the particular challenges and demands of hospitalists who practice in community hospitals and rural settings, where the level of support and access to subspecialty consults might be very different from the academic milieu.
“We hope that our unique approaches lend more breadth to the session,” said Dr. Slawski. “We want to make sure we have a good representation of SHM’s constituency, and that we present high-impact studies.”
To hit the mark of articles that are relevant for all, Dr. Cooper said she wants to make sure to focus on the practicalities of hospital-based practice – possible topics include prediction scores, hepatic encephalopathy, and the management of sepsis.
Neither Dr. Slawski nor Dr. Cooper reported any relevant conflicts of interest.
Update in Hospital Medicine
Tuesday, 1:40-2:40 p.m.
Palms Ballroom
Barbara Slawski, MD, MS, SFHM, and Cynthia Cooper, MD, hadn’t met in person until early 2018. But that doesn’t mean they haven’t spent a lot of time together.
Once a month, the two hospitalists checked in with one another through wide-ranging phone calls. Together, they have combed the medical literature and conferred over the past year, making long lists of candidate studies for the “Top 20” journal articles of the year for practicing hospitalists.
The two physicians will comoderate Tuesday’s “Update in Hospital Medicine” session, where they will summarize research findings of these “Top 20” articles. Their hope is to present research that each attendee can bring home to improve patient outcomes on a daily basis, while making for a smoother and more efficient practice.
Dr. Slawski, chief of the section of perioperative medicine at the Medical College of Wisconsin in Milwaukee, said the presentations will not simply summarize study results but also will help attendees focus on the key findings – the clinical pearls – that represent real opportunities to update practice.
Since hospital medicine crosses so many disciplines, each physician said, in separate interviews, that doing justice to the literature has been time consuming and intellectually challenging – but worthwhile.
Dr. Cooper, a hospitalist at Massachusetts General Hospital, Boston, said that, although she and Dr. Slawski practice in geographically diverse areas, their practice settings – academic medical centers – have many similarities. She said that, as she reviewed the medical literature over the past year, she gave considerable thought to the particular challenges and demands of hospitalists who practice in community hospitals and rural settings, where the level of support and access to subspecialty consults might be very different from the academic milieu.
“We hope that our unique approaches lend more breadth to the session,” said Dr. Slawski. “We want to make sure we have a good representation of SHM’s constituency, and that we present high-impact studies.”
To hit the mark of articles that are relevant for all, Dr. Cooper said she wants to make sure to focus on the practicalities of hospital-based practice – possible topics include prediction scores, hepatic encephalopathy, and the management of sepsis.
Neither Dr. Slawski nor Dr. Cooper reported any relevant conflicts of interest.
Update in Hospital Medicine
Tuesday, 1:40-2:40 p.m.
Palms Ballroom
Barbara Slawski, MD, MS, SFHM, and Cynthia Cooper, MD, hadn’t met in person until early 2018. But that doesn’t mean they haven’t spent a lot of time together.
Once a month, the two hospitalists checked in with one another through wide-ranging phone calls. Together, they have combed the medical literature and conferred over the past year, making long lists of candidate studies for the “Top 20” journal articles of the year for practicing hospitalists.
The two physicians will comoderate Tuesday’s “Update in Hospital Medicine” session, where they will summarize research findings of these “Top 20” articles. Their hope is to present research that each attendee can bring home to improve patient outcomes on a daily basis, while making for a smoother and more efficient practice.
Dr. Slawski, chief of the section of perioperative medicine at the Medical College of Wisconsin in Milwaukee, said the presentations will not simply summarize study results but also will help attendees focus on the key findings – the clinical pearls – that represent real opportunities to update practice.
Since hospital medicine crosses so many disciplines, each physician said, in separate interviews, that doing justice to the literature has been time consuming and intellectually challenging – but worthwhile.
Dr. Cooper, a hospitalist at Massachusetts General Hospital, Boston, said that, although she and Dr. Slawski practice in geographically diverse areas, their practice settings – academic medical centers – have many similarities. She said that, as she reviewed the medical literature over the past year, she gave considerable thought to the particular challenges and demands of hospitalists who practice in community hospitals and rural settings, where the level of support and access to subspecialty consults might be very different from the academic milieu.
“We hope that our unique approaches lend more breadth to the session,” said Dr. Slawski. “We want to make sure we have a good representation of SHM’s constituency, and that we present high-impact studies.”
To hit the mark of articles that are relevant for all, Dr. Cooper said she wants to make sure to focus on the practicalities of hospital-based practice – possible topics include prediction scores, hepatic encephalopathy, and the management of sepsis.
Neither Dr. Slawski nor Dr. Cooper reported any relevant conflicts of interest.
Update in Hospital Medicine
Tuesday, 1:40-2:40 p.m.
Palms Ballroom
Welcome to Day 2 of HM18!
I hope all of you enjoyed Day 1 as much as I did. The quality and variety of the presentations yesterday were stellar, and I am sure today will be the same.
The day begins with the Best of Research and Innovations, where the cream of the crop from the hundreds of submitted projects will be presented and recognized. Following that will be the Awards of Excellence, Society of Hospital Medicine’s annual celebration of the very best of our members for their years of stellar contributions in areas such as teaching, clinical excellence, and service to hospital medicine. You will be inspired by the accomplishments of our colleagues who are receiving these awards. They demonstrate to all of us how our specialty improves the health care delivered in our nation’s hospitals.
Our plenary speaker of the morning will be our very own Larry Wellikson, MD, MHM, who will give us his own perspectives on “Future Challenges for Hospital Medicine,” calling on his more than 2 decades of experience as the creative and accomplished CEO of SHM.
After the morning sessions, please join us for a real treat at noon when we have the honor of hearing from our visiting colleagues from the Japanese Society of Hospital General Medicine who will talk to us about hospital medicine in Japan. As much as we come to HM18 to learn from our U.S. colleagues who are doing extraordinary things here at home, this is a unique opportunity to learn from the leaders of one of our international partners how they are shaping the rapidly growing hospitalist movement in Japan.
That will be closely followed by the can’t-miss “Update in Hospital Medicine,” presented this year by Cindy Cooper, MD, and Barbara Slawski, MD, MS, SFHM. And especially important to our students, residents, and younger members, there is an evening session entitled, “Mastering the Job Interview,” a workshop for those who should always be looking to hone the nonclinical skills essential to long-term career success.
Like Day 1, this is a day chockfull of clinical and management presentations to meet everyone’s needs. There are too many to call out, but allow me to pick my personal favorite titles of the day, starting with “Waiting in Line for ‘It’s a Small World’ and Other Things We Do for No Reason” and “Let It Flow: CPAP, BIPAP, and High-Flow Oxygen.”
Yesterday kicked off HM18 with aplomb, and tomorrow we wrap up. So make the most of Day 2 today, and take advantage of the terrific work of our fellow hospitalists. During the breaks, visit the Exhibit Hall to explore, mingle, and thank our exhibitors for supporting our society and our conference.
Please stop by to greet the SHM staff who have made this conference another great success at the SHM Pavilion in the Exhibit Hall. While you’re there, take a chance to meet and chat with SHM board members who will be there throughout the conference.
Enjoy!
Dr. Greeno is president of the Society of Hospital Medicine and chief strategy officer at IPC Healthcare.
I hope all of you enjoyed Day 1 as much as I did. The quality and variety of the presentations yesterday were stellar, and I am sure today will be the same.
The day begins with the Best of Research and Innovations, where the cream of the crop from the hundreds of submitted projects will be presented and recognized. Following that will be the Awards of Excellence, Society of Hospital Medicine’s annual celebration of the very best of our members for their years of stellar contributions in areas such as teaching, clinical excellence, and service to hospital medicine. You will be inspired by the accomplishments of our colleagues who are receiving these awards. They demonstrate to all of us how our specialty improves the health care delivered in our nation’s hospitals.
Our plenary speaker of the morning will be our very own Larry Wellikson, MD, MHM, who will give us his own perspectives on “Future Challenges for Hospital Medicine,” calling on his more than 2 decades of experience as the creative and accomplished CEO of SHM.
After the morning sessions, please join us for a real treat at noon when we have the honor of hearing from our visiting colleagues from the Japanese Society of Hospital General Medicine who will talk to us about hospital medicine in Japan. As much as we come to HM18 to learn from our U.S. colleagues who are doing extraordinary things here at home, this is a unique opportunity to learn from the leaders of one of our international partners how they are shaping the rapidly growing hospitalist movement in Japan.
That will be closely followed by the can’t-miss “Update in Hospital Medicine,” presented this year by Cindy Cooper, MD, and Barbara Slawski, MD, MS, SFHM. And especially important to our students, residents, and younger members, there is an evening session entitled, “Mastering the Job Interview,” a workshop for those who should always be looking to hone the nonclinical skills essential to long-term career success.
Like Day 1, this is a day chockfull of clinical and management presentations to meet everyone’s needs. There are too many to call out, but allow me to pick my personal favorite titles of the day, starting with “Waiting in Line for ‘It’s a Small World’ and Other Things We Do for No Reason” and “Let It Flow: CPAP, BIPAP, and High-Flow Oxygen.”
Yesterday kicked off HM18 with aplomb, and tomorrow we wrap up. So make the most of Day 2 today, and take advantage of the terrific work of our fellow hospitalists. During the breaks, visit the Exhibit Hall to explore, mingle, and thank our exhibitors for supporting our society and our conference.
Please stop by to greet the SHM staff who have made this conference another great success at the SHM Pavilion in the Exhibit Hall. While you’re there, take a chance to meet and chat with SHM board members who will be there throughout the conference.
Enjoy!
Dr. Greeno is president of the Society of Hospital Medicine and chief strategy officer at IPC Healthcare.
I hope all of you enjoyed Day 1 as much as I did. The quality and variety of the presentations yesterday were stellar, and I am sure today will be the same.
The day begins with the Best of Research and Innovations, where the cream of the crop from the hundreds of submitted projects will be presented and recognized. Following that will be the Awards of Excellence, Society of Hospital Medicine’s annual celebration of the very best of our members for their years of stellar contributions in areas such as teaching, clinical excellence, and service to hospital medicine. You will be inspired by the accomplishments of our colleagues who are receiving these awards. They demonstrate to all of us how our specialty improves the health care delivered in our nation’s hospitals.
Our plenary speaker of the morning will be our very own Larry Wellikson, MD, MHM, who will give us his own perspectives on “Future Challenges for Hospital Medicine,” calling on his more than 2 decades of experience as the creative and accomplished CEO of SHM.
After the morning sessions, please join us for a real treat at noon when we have the honor of hearing from our visiting colleagues from the Japanese Society of Hospital General Medicine who will talk to us about hospital medicine in Japan. As much as we come to HM18 to learn from our U.S. colleagues who are doing extraordinary things here at home, this is a unique opportunity to learn from the leaders of one of our international partners how they are shaping the rapidly growing hospitalist movement in Japan.
That will be closely followed by the can’t-miss “Update in Hospital Medicine,” presented this year by Cindy Cooper, MD, and Barbara Slawski, MD, MS, SFHM. And especially important to our students, residents, and younger members, there is an evening session entitled, “Mastering the Job Interview,” a workshop for those who should always be looking to hone the nonclinical skills essential to long-term career success.
Like Day 1, this is a day chockfull of clinical and management presentations to meet everyone’s needs. There are too many to call out, but allow me to pick my personal favorite titles of the day, starting with “Waiting in Line for ‘It’s a Small World’ and Other Things We Do for No Reason” and “Let It Flow: CPAP, BIPAP, and High-Flow Oxygen.”
Yesterday kicked off HM18 with aplomb, and tomorrow we wrap up. So make the most of Day 2 today, and take advantage of the terrific work of our fellow hospitalists. During the breaks, visit the Exhibit Hall to explore, mingle, and thank our exhibitors for supporting our society and our conference.
Please stop by to greet the SHM staff who have made this conference another great success at the SHM Pavilion in the Exhibit Hall. While you’re there, take a chance to meet and chat with SHM board members who will be there throughout the conference.
Enjoy!
Dr. Greeno is president of the Society of Hospital Medicine and chief strategy officer at IPC Healthcare.
Tuesday’s satellite symposia schedule, information
Valuable Strategies to Reduce the Risk for and Clinical Impact of Hyperkalemia
7:30 – 9:30 p.m. – Canary Room 1-2
Dinner provided at 7:30 p.m.
Presenters: Biff F. Palmer, MD, professor of internal medicine, University of Texas Southwestern Medical Center, Dallas; Robert Toto, MD, associate dean, clinical and translational research, director, Center for Translational Medicine, UT Southwestern Medical Center, Dallas.
Overview: The goal of the case-based symposium is to highlight patients at increased risk of recurrent or sustained hyperkalemia and how these patients may be managed with evidence-based treatment so that they are able to continue renin-angiotensin-aldosterone system inhibitor therapy, if appropriate. The presenters will share their experiences in managing these patients, including suggestions for the hospitalist’s role in continued care.
Accreditation: This activity has been approved for AMA PRA Category 1 Credit(s)™. See final CE activity announcement for specific details.
This activity is supported by an educational grant from Relypsa Inc.
Hepatology News Tonight: Managing Complication of Cirrhosis
7:30 – 9:30 p.m. – Canary Room 3-4
Registration will be at 7:00 p.m.
Dinner provided at 7:30 p.m.
Presenters: Naoky Tsai, MD, clinical professor of medicine, John A. Burns School of Medicine, University of Hawaii, Manoa, Honolulu; Ashwani K. Singal MD, MS, associate professor of medicine and director of UAB Porphyria Center, division of gastroenterology and hepatology, University of Alabama at Birmingham.
Overview: This educational update will highlight the most clinically relevant advances in the management of patients with cirrhosis and hepatic encephalopathy (HE). The symposium will deliver emerging science and incorporate expert opinions on best practices for the diagnosis and management of patients with cirrhosis and HE.
Target audience: This activity has been designed to meet the educational needs of physicians, advanced practice providers, and allied health professionals who provide care for hospitalized patients with liver disease.
Learning objectives:
- Understand the complications and the consequences of chronic liver disease.
- Describe the economic, patient, and caregiver burdens associated with cirrhosis and HE.
- Demonstrate the ability to properly treat HE patients and prevent recurrence of disease.
Accredited by: Rehoboth McKindley Christian Health Care Services
Provided by: Chronic Liver Disease Foundation (CLDF)
Register: http://www.chronicliverdisease.org/
Supported by an educational grant from Salix Pharmaceuticals.
Valuable Strategies to Reduce the Risk for and Clinical Impact of Hyperkalemia
7:30 – 9:30 p.m. – Canary Room 1-2
Dinner provided at 7:30 p.m.
Presenters: Biff F. Palmer, MD, professor of internal medicine, University of Texas Southwestern Medical Center, Dallas; Robert Toto, MD, associate dean, clinical and translational research, director, Center for Translational Medicine, UT Southwestern Medical Center, Dallas.
Overview: The goal of the case-based symposium is to highlight patients at increased risk of recurrent or sustained hyperkalemia and how these patients may be managed with evidence-based treatment so that they are able to continue renin-angiotensin-aldosterone system inhibitor therapy, if appropriate. The presenters will share their experiences in managing these patients, including suggestions for the hospitalist’s role in continued care.
Accreditation: This activity has been approved for AMA PRA Category 1 Credit(s)™. See final CE activity announcement for specific details.
This activity is supported by an educational grant from Relypsa Inc.
Hepatology News Tonight: Managing Complication of Cirrhosis
7:30 – 9:30 p.m. – Canary Room 3-4
Registration will be at 7:00 p.m.
Dinner provided at 7:30 p.m.
Presenters: Naoky Tsai, MD, clinical professor of medicine, John A. Burns School of Medicine, University of Hawaii, Manoa, Honolulu; Ashwani K. Singal MD, MS, associate professor of medicine and director of UAB Porphyria Center, division of gastroenterology and hepatology, University of Alabama at Birmingham.
Overview: This educational update will highlight the most clinically relevant advances in the management of patients with cirrhosis and hepatic encephalopathy (HE). The symposium will deliver emerging science and incorporate expert opinions on best practices for the diagnosis and management of patients with cirrhosis and HE.
Target audience: This activity has been designed to meet the educational needs of physicians, advanced practice providers, and allied health professionals who provide care for hospitalized patients with liver disease.
Learning objectives:
- Understand the complications and the consequences of chronic liver disease.
- Describe the economic, patient, and caregiver burdens associated with cirrhosis and HE.
- Demonstrate the ability to properly treat HE patients and prevent recurrence of disease.
Accredited by: Rehoboth McKindley Christian Health Care Services
Provided by: Chronic Liver Disease Foundation (CLDF)
Register: http://www.chronicliverdisease.org/
Supported by an educational grant from Salix Pharmaceuticals.
Valuable Strategies to Reduce the Risk for and Clinical Impact of Hyperkalemia
7:30 – 9:30 p.m. – Canary Room 1-2
Dinner provided at 7:30 p.m.
Presenters: Biff F. Palmer, MD, professor of internal medicine, University of Texas Southwestern Medical Center, Dallas; Robert Toto, MD, associate dean, clinical and translational research, director, Center for Translational Medicine, UT Southwestern Medical Center, Dallas.
Overview: The goal of the case-based symposium is to highlight patients at increased risk of recurrent or sustained hyperkalemia and how these patients may be managed with evidence-based treatment so that they are able to continue renin-angiotensin-aldosterone system inhibitor therapy, if appropriate. The presenters will share their experiences in managing these patients, including suggestions for the hospitalist’s role in continued care.
Accreditation: This activity has been approved for AMA PRA Category 1 Credit(s)™. See final CE activity announcement for specific details.
This activity is supported by an educational grant from Relypsa Inc.
Hepatology News Tonight: Managing Complication of Cirrhosis
7:30 – 9:30 p.m. – Canary Room 3-4
Registration will be at 7:00 p.m.
Dinner provided at 7:30 p.m.
Presenters: Naoky Tsai, MD, clinical professor of medicine, John A. Burns School of Medicine, University of Hawaii, Manoa, Honolulu; Ashwani K. Singal MD, MS, associate professor of medicine and director of UAB Porphyria Center, division of gastroenterology and hepatology, University of Alabama at Birmingham.
Overview: This educational update will highlight the most clinically relevant advances in the management of patients with cirrhosis and hepatic encephalopathy (HE). The symposium will deliver emerging science and incorporate expert opinions on best practices for the diagnosis and management of patients with cirrhosis and HE.
Target audience: This activity has been designed to meet the educational needs of physicians, advanced practice providers, and allied health professionals who provide care for hospitalized patients with liver disease.
Learning objectives:
- Understand the complications and the consequences of chronic liver disease.
- Describe the economic, patient, and caregiver burdens associated with cirrhosis and HE.
- Demonstrate the ability to properly treat HE patients and prevent recurrence of disease.
Accredited by: Rehoboth McKindley Christian Health Care Services
Provided by: Chronic Liver Disease Foundation (CLDF)
Register: http://www.chronicliverdisease.org/
Supported by an educational grant from Salix Pharmaceuticals.
RIV plenary showcases best research
The best research in hospital medicine will be front and center today in the “Best of Research and Innovations in 2018” part of this morning’s plenary session.
New research also will figure prominently in the second “Clinical Vignettes Poster Competition” at lunchtime today.
During the plenary session, investigators will present the top-rated research among hundreds of submissions, said Ethan Cumbler, MD, FHM, chair of the Research, Innovations, Vignettes (RIV) competition and professor of medicine and medical director of the University of Colorado Acute Care Center for the Elderly, Denver, unit. Three independent, blinded reviewers chose the abstracts for oral presentation after rating them based on originality, scientific rigor, and importance to hospital medicine, he said. These oral presentations are meant not only to provide information to other hospitalists but also to inspire hospitalists to engage in research themselves.
“I think about it as a collective celebration of how far the field of hospital medicine has advanced in the last year and its potential moving forward,” Dr. Cumbler said. “My fundamental view is every hospitalist can and should be examining what they’re doing, thinking about how to do it better, and, by God, sharing it with the rest of us when they figure out that something can work better.”
Even as a veteran hospitalist, Dr. Cumbler said he still gets inspired by research presented in the RIV.
“When I see the RIV posters or come to hear the oral presentations, I get inspired, because I get to see what other people are doing in their local microenvironments, in their laboratories, in their hospitals,” he said. “And often I think ... ‘We could be doing stuff just that exciting.’ Often, it’s a chance to collaborate with the people whose work is inspiring you, or to take a great idea and run with it.”
At the Clinical Vignettes competition, research will focus on lessons learned from specific cases, Dr. Cumbler said.
“A typical clinical vignette would be a case presentation, maybe a diagnostic image or a description of the test that clinched the diagnosis, and then, most importantly, the lessons from that case, which are more widely applicable,” he said. “One of the things I love about Clinical Vignettes is it gives you a chance to highlight your best catches, but it also lets you, with humility, share your misses so that other people can learn from your experience.”
He said he hopes the sharing of research in formal oral presentations – and in the poster hall – continues to advance the hospital medicine literature.
“It’s come an incredible distance over the last 10 years, 15 years,” he said. “When I look at where we are heading next, I think it is into more multicenter research, multiple-institution quality improvement. I really see us graduating from proof-of-concept and pilot work into the kind of trials which answer questions – the big questions that face medicine.”
Best of Research and Innovations in 2018
8-9 a.m., Palms Ballroom
Clinical Vignettes #2
Poster Competition
12-1:30 p.m., Cypress Ballroom
The best research in hospital medicine will be front and center today in the “Best of Research and Innovations in 2018” part of this morning’s plenary session.
New research also will figure prominently in the second “Clinical Vignettes Poster Competition” at lunchtime today.
During the plenary session, investigators will present the top-rated research among hundreds of submissions, said Ethan Cumbler, MD, FHM, chair of the Research, Innovations, Vignettes (RIV) competition and professor of medicine and medical director of the University of Colorado Acute Care Center for the Elderly, Denver, unit. Three independent, blinded reviewers chose the abstracts for oral presentation after rating them based on originality, scientific rigor, and importance to hospital medicine, he said. These oral presentations are meant not only to provide information to other hospitalists but also to inspire hospitalists to engage in research themselves.
“I think about it as a collective celebration of how far the field of hospital medicine has advanced in the last year and its potential moving forward,” Dr. Cumbler said. “My fundamental view is every hospitalist can and should be examining what they’re doing, thinking about how to do it better, and, by God, sharing it with the rest of us when they figure out that something can work better.”
Even as a veteran hospitalist, Dr. Cumbler said he still gets inspired by research presented in the RIV.
“When I see the RIV posters or come to hear the oral presentations, I get inspired, because I get to see what other people are doing in their local microenvironments, in their laboratories, in their hospitals,” he said. “And often I think ... ‘We could be doing stuff just that exciting.’ Often, it’s a chance to collaborate with the people whose work is inspiring you, or to take a great idea and run with it.”
At the Clinical Vignettes competition, research will focus on lessons learned from specific cases, Dr. Cumbler said.
“A typical clinical vignette would be a case presentation, maybe a diagnostic image or a description of the test that clinched the diagnosis, and then, most importantly, the lessons from that case, which are more widely applicable,” he said. “One of the things I love about Clinical Vignettes is it gives you a chance to highlight your best catches, but it also lets you, with humility, share your misses so that other people can learn from your experience.”
He said he hopes the sharing of research in formal oral presentations – and in the poster hall – continues to advance the hospital medicine literature.
“It’s come an incredible distance over the last 10 years, 15 years,” he said. “When I look at where we are heading next, I think it is into more multicenter research, multiple-institution quality improvement. I really see us graduating from proof-of-concept and pilot work into the kind of trials which answer questions – the big questions that face medicine.”
Best of Research and Innovations in 2018
8-9 a.m., Palms Ballroom
Clinical Vignettes #2
Poster Competition
12-1:30 p.m., Cypress Ballroom
The best research in hospital medicine will be front and center today in the “Best of Research and Innovations in 2018” part of this morning’s plenary session.
New research also will figure prominently in the second “Clinical Vignettes Poster Competition” at lunchtime today.
During the plenary session, investigators will present the top-rated research among hundreds of submissions, said Ethan Cumbler, MD, FHM, chair of the Research, Innovations, Vignettes (RIV) competition and professor of medicine and medical director of the University of Colorado Acute Care Center for the Elderly, Denver, unit. Three independent, blinded reviewers chose the abstracts for oral presentation after rating them based on originality, scientific rigor, and importance to hospital medicine, he said. These oral presentations are meant not only to provide information to other hospitalists but also to inspire hospitalists to engage in research themselves.
“I think about it as a collective celebration of how far the field of hospital medicine has advanced in the last year and its potential moving forward,” Dr. Cumbler said. “My fundamental view is every hospitalist can and should be examining what they’re doing, thinking about how to do it better, and, by God, sharing it with the rest of us when they figure out that something can work better.”
Even as a veteran hospitalist, Dr. Cumbler said he still gets inspired by research presented in the RIV.
“When I see the RIV posters or come to hear the oral presentations, I get inspired, because I get to see what other people are doing in their local microenvironments, in their laboratories, in their hospitals,” he said. “And often I think ... ‘We could be doing stuff just that exciting.’ Often, it’s a chance to collaborate with the people whose work is inspiring you, or to take a great idea and run with it.”
At the Clinical Vignettes competition, research will focus on lessons learned from specific cases, Dr. Cumbler said.
“A typical clinical vignette would be a case presentation, maybe a diagnostic image or a description of the test that clinched the diagnosis, and then, most importantly, the lessons from that case, which are more widely applicable,” he said. “One of the things I love about Clinical Vignettes is it gives you a chance to highlight your best catches, but it also lets you, with humility, share your misses so that other people can learn from your experience.”
He said he hopes the sharing of research in formal oral presentations – and in the poster hall – continues to advance the hospital medicine literature.
“It’s come an incredible distance over the last 10 years, 15 years,” he said. “When I look at where we are heading next, I think it is into more multicenter research, multiple-institution quality improvement. I really see us graduating from proof-of-concept and pilot work into the kind of trials which answer questions – the big questions that face medicine.”
Best of Research and Innovations in 2018
8-9 a.m., Palms Ballroom
Clinical Vignettes #2
Poster Competition
12-1:30 p.m., Cypress Ballroom
Genes, Cigarettes, and Blood Pressure: a Revealing Relationship
Using a technique called “gene-environment interaction analysis,” National Institutes of Health researchers zeroed in on areas of the genome associated with blood pressure. Cigarette smoking, known to raise blood pressure (BP), was an environmental “marker.”
The researchers tested different points of the genome in > 610,000 people from 5 ancestry groups to find where cigarette smoking and BP interacted.
They confirmed 56 known genetic regions and identified 83 new ones. Ten of the newly discovered genes seemed to have a much larger impact on smokers’ BP vs that of nonsmokers, the researchers say—levels were as much as 8 times higher.
Previous genetic studies have identified genes and genetic regions associated with BP but have not explored the interplay between genes and environmental factors, the researchers say. Moreover, the broad cohort of the new study makes the findings widely useful. Most of the known genetic regions linked to BP were identified through European descendants. In this study, several novel regions were identified through African ancestry analysis, “highlighting the importance of pursuing genetic studies in diverse populations.”
Using a technique called “gene-environment interaction analysis,” National Institutes of Health researchers zeroed in on areas of the genome associated with blood pressure. Cigarette smoking, known to raise blood pressure (BP), was an environmental “marker.”
The researchers tested different points of the genome in > 610,000 people from 5 ancestry groups to find where cigarette smoking and BP interacted.
They confirmed 56 known genetic regions and identified 83 new ones. Ten of the newly discovered genes seemed to have a much larger impact on smokers’ BP vs that of nonsmokers, the researchers say—levels were as much as 8 times higher.
Previous genetic studies have identified genes and genetic regions associated with BP but have not explored the interplay between genes and environmental factors, the researchers say. Moreover, the broad cohort of the new study makes the findings widely useful. Most of the known genetic regions linked to BP were identified through European descendants. In this study, several novel regions were identified through African ancestry analysis, “highlighting the importance of pursuing genetic studies in diverse populations.”
Using a technique called “gene-environment interaction analysis,” National Institutes of Health researchers zeroed in on areas of the genome associated with blood pressure. Cigarette smoking, known to raise blood pressure (BP), was an environmental “marker.”
The researchers tested different points of the genome in > 610,000 people from 5 ancestry groups to find where cigarette smoking and BP interacted.
They confirmed 56 known genetic regions and identified 83 new ones. Ten of the newly discovered genes seemed to have a much larger impact on smokers’ BP vs that of nonsmokers, the researchers say—levels were as much as 8 times higher.
Previous genetic studies have identified genes and genetic regions associated with BP but have not explored the interplay between genes and environmental factors, the researchers say. Moreover, the broad cohort of the new study makes the findings widely useful. Most of the known genetic regions linked to BP were identified through European descendants. In this study, several novel regions were identified through African ancestry analysis, “highlighting the importance of pursuing genetic studies in diverse populations.”
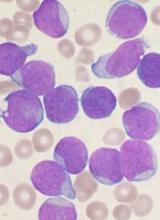
Health Canada approves product for adult ALL
Health Canada has approved inotuzumab ozogamicin (Besponsa™) as monotherapy for adults with relapsed or refractory, CD22-positive, B-cell precursor acute lymphoblastic leukemia (ALL).
Inotuzumab ozogamicin is the first and only CD22-directed antibody-drug conjugate approved for this indication.
The product consists of a monoclonal antibody targeting CD22 and a cytotoxic agent known as calicheamicin.
Health Canada’s approval of inotuzumab ozogamicin is based on results from the phase 3 INO-VATE trial, which were published in NEJM in June 2016.
The trial enrolled 326 adults with relapsed or refractory B-cell precursor ALL.
Patients received inotuzumab ozogamicin or 1 of 3 chemotherapy regimens—high-dose cytarabine; cytarabine plus mitoxantrone; or fludarabine, cytarabine, and granulocyte colony-stimulating factor.
The rate of complete remission, including incomplete hematologic recovery, was 80.7% in the inotuzumab arm and 29.4% in the chemotherapy arm (P<0.001). The median duration of remission was 4.6 months and 3.1 months, respectively (P=0.03).
Forty-one percent of patients treated with inotuzumab and 11% of those who received chemotherapy proceeded to stem cell transplant directly after treatment (P<0.001).
The median progression-free survival was 5.0 months in the inotuzumab arm and 1.8 months in the chemotherapy arm (P<0.001).
The median overall survival was 7.7 months and 6.7 months, respectively (P=0.04). This did not meet the prespecified boundary of significance (P=0.0208).
Liver-related adverse events were more common in the inotuzumab arm than the chemotherapy arm. The most frequent of these were increased aspartate aminotransferase level (20% vs 10%), hyperbilirubinemia (15% vs 10%), and increased alanine aminotransferase level (14% vs 11%).
Veno-occlusive liver disease occurred in 11% of patients in the inotuzumab arm and 1% in the chemotherapy arm.
There were 17 deaths during treatment in the inotuzumab arm and 11 in the chemotherapy arm. Four deaths were considered related to inotuzumab, and 2 were deemed related to chemotherapy.
Health Canada has approved inotuzumab ozogamicin (Besponsa™) as monotherapy for adults with relapsed or refractory, CD22-positive, B-cell precursor acute lymphoblastic leukemia (ALL).
Inotuzumab ozogamicin is the first and only CD22-directed antibody-drug conjugate approved for this indication.
The product consists of a monoclonal antibody targeting CD22 and a cytotoxic agent known as calicheamicin.
Health Canada’s approval of inotuzumab ozogamicin is based on results from the phase 3 INO-VATE trial, which were published in NEJM in June 2016.
The trial enrolled 326 adults with relapsed or refractory B-cell precursor ALL.
Patients received inotuzumab ozogamicin or 1 of 3 chemotherapy regimens—high-dose cytarabine; cytarabine plus mitoxantrone; or fludarabine, cytarabine, and granulocyte colony-stimulating factor.
The rate of complete remission, including incomplete hematologic recovery, was 80.7% in the inotuzumab arm and 29.4% in the chemotherapy arm (P<0.001). The median duration of remission was 4.6 months and 3.1 months, respectively (P=0.03).
Forty-one percent of patients treated with inotuzumab and 11% of those who received chemotherapy proceeded to stem cell transplant directly after treatment (P<0.001).
The median progression-free survival was 5.0 months in the inotuzumab arm and 1.8 months in the chemotherapy arm (P<0.001).
The median overall survival was 7.7 months and 6.7 months, respectively (P=0.04). This did not meet the prespecified boundary of significance (P=0.0208).
Liver-related adverse events were more common in the inotuzumab arm than the chemotherapy arm. The most frequent of these were increased aspartate aminotransferase level (20% vs 10%), hyperbilirubinemia (15% vs 10%), and increased alanine aminotransferase level (14% vs 11%).
Veno-occlusive liver disease occurred in 11% of patients in the inotuzumab arm and 1% in the chemotherapy arm.
There were 17 deaths during treatment in the inotuzumab arm and 11 in the chemotherapy arm. Four deaths were considered related to inotuzumab, and 2 were deemed related to chemotherapy.
Health Canada has approved inotuzumab ozogamicin (Besponsa™) as monotherapy for adults with relapsed or refractory, CD22-positive, B-cell precursor acute lymphoblastic leukemia (ALL).
Inotuzumab ozogamicin is the first and only CD22-directed antibody-drug conjugate approved for this indication.
The product consists of a monoclonal antibody targeting CD22 and a cytotoxic agent known as calicheamicin.
Health Canada’s approval of inotuzumab ozogamicin is based on results from the phase 3 INO-VATE trial, which were published in NEJM in June 2016.
The trial enrolled 326 adults with relapsed or refractory B-cell precursor ALL.
Patients received inotuzumab ozogamicin or 1 of 3 chemotherapy regimens—high-dose cytarabine; cytarabine plus mitoxantrone; or fludarabine, cytarabine, and granulocyte colony-stimulating factor.
The rate of complete remission, including incomplete hematologic recovery, was 80.7% in the inotuzumab arm and 29.4% in the chemotherapy arm (P<0.001). The median duration of remission was 4.6 months and 3.1 months, respectively (P=0.03).
Forty-one percent of patients treated with inotuzumab and 11% of those who received chemotherapy proceeded to stem cell transplant directly after treatment (P<0.001).
The median progression-free survival was 5.0 months in the inotuzumab arm and 1.8 months in the chemotherapy arm (P<0.001).
The median overall survival was 7.7 months and 6.7 months, respectively (P=0.04). This did not meet the prespecified boundary of significance (P=0.0208).
Liver-related adverse events were more common in the inotuzumab arm than the chemotherapy arm. The most frequent of these were increased aspartate aminotransferase level (20% vs 10%), hyperbilirubinemia (15% vs 10%), and increased alanine aminotransferase level (14% vs 11%).
Veno-occlusive liver disease occurred in 11% of patients in the inotuzumab arm and 1% in the chemotherapy arm.
There were 17 deaths during treatment in the inotuzumab arm and 11 in the chemotherapy arm. Four deaths were considered related to inotuzumab, and 2 were deemed related to chemotherapy.