User login
Adding Antithrombotic to tPA Does Not Improve Stroke Outcome
PHOENIX — , results of new research show.
“Ultimately, we found no benefit for either medication added to standard-of-care thrombolysis in terms of improving stroke outcomes,” said lead study author Opeolu M. Adeoye, MD, professor of emergency medicine and department chair, Washington University School of Medicine, St. Louis, Missouri.
The results were surprising and disappointing for Dr. Adeoye. “We went into the trial hopeful and thinking we would be able to benefit patients in reducing disability from stroke,” he said.
The Multi-Arm Optimization of Stroke Thrombolysis (MOST) trial was stopped early because of futility following recommendations from the data and safety monitoring board.
The findings were presented at the International Stroke Conference presented by the American Stroke Association, a division of the American Heart Association.
A thrombolytic drug alone doesn’t help all patients, particularly those with larger clots. “Clots can open; they can reform; they can re-occlude, etc.,” said another author, Andrew D. Barreto, MD, associate professor, Department of Neurology, University of Texas Health Science Center, Houston. “The thought was that adding additional medications that thin the blood, like argatroban or eptifibatide, would amplify the effects of the clot-busting drug.”
Indeed, this approach has had success in cardiology in terms of blood vessel opening, said Dr. Adeoye, adding that some preclinical data suggest that antithrombotic drugs may be neuroprotective.
Six phase 2 studies going back over a dozen years suggested that these drugs are safe in stroke patients. Although these studies weren’t powered for efficacy, “we did see a signal that adding them would be better than just the clot-busting drug alone.” These findings prompted the current phase 3 trial, said Dr. Barreto.
The three-arm, single-blind MOST trial included 514 adult patients with acute ischemic stroke and a National Institutes of Health Stroke Scale (NIHSS) score of 6 or greater at 57 US centers. In the study cohort the mean age was about 68 years, 70% White/25% Black, and with about equal numbers of female and male patients.
All received standard stroke care including thrombolysis within 3 hours of symptom onset. Initially, researchers used intravenous alteplase (0.9 mg/kg), but as the standard of care changed over time, they began using tenecteplase (0.25 mg/kg).
Study patients were also randomly assigned to receive placebo or either argatroban (100 mcg/kg bolus followed by 3 mcg/kg per minute for 12 hours) or eptifibatide (135 mcg/kg bolus followed by 0.75 mcg/kg/min infusion for 2 hours). These treatments were initiated within 75 minutes of thrombolysis.
Two Different Mechanisms
The drugs have different mechanisms of action. Argatroban is an anticoagulant, a direct inhibitor of thrombin, while the antiplatelet eptifibatide blocks the glycoprotein IIb/IIIa receptor and was specifically developed to ensure rapid inhibition of platelet aggregation.
Patients could also receive endovascular thrombectomy as part of their usual care. In this study, about 44% of patients received this treatment.
The primary endpoint was 90-day utility weighted modified Rankin Scale (uw-mRS) scores, where the worst outcome is 0 and the best outcome is 10.
The study used a response-adaptive randomization design, where the randomization switches from a drug that doesn’t appear to have a chance of working to the arm more likely to be beneficial.
Of the 514 patients, the analysis included 228 in the placebo, 59 in the argatroban, and 227 in eptifibatide groups. Of the total, 421 completed the study.
The mean 90-day uw-mRS was 6.8 in the placebo group, 5.2 in the argatroban group, and 6.3 in the eptifibatide group.
The probability of argatroban being better than placebo was 0.2%; the probability of eptifibatide being better than placebo was 0.9%. The futility threshold was enrollment of 500 and less than a 20% chance of benefit, thus the decision to stop the trial.
In all subgroup analyses, which looked at age, stroke severity, the two thrombolytic drugs, and use of endovascular therapy, “we didn’t really see much of a signal that would suggest that’s the group we would need to be testing further,” said Dr. Barreto.
No Increased ICH Risk
The primary safety outcome was symptomatic intracranial hemorrhage within 36 hours of randomization. The researchers found no significant increase in rates of this outcome.
The argatroban cohort had significantly lower odds of favorable outcomes compared with placebo, noted Dr. Adeoye. For example, it had more all-cause deaths, although none were related to the study drug.
Speculating on why the intervention didn’t work, Dr. Barreto pointed to changes in standard of care between the earlier trials and the current one, including the incorporation of endovascular therapy and switch to tenecteplase.
Although the results were disappointing, Dr. Adeoye sees a bright side. “What we’re very proud of, and excited about, is the fact that we have a definitive answer on these two drugs, and we did it in one trial as opposed to sequential, separate ongoing trials.”
But he stressed that more work needs to be done, especially given that even with endovascular therapy, half of stroke patients don’t achieve independence.
“In this trial, we established that argatroban and eptifibatide added to thrombolysis did not work, but that doesn’t address the fact that we need to continue to see what we can do to improve the total proportion of stroke patients who, after our treatments, are functionally independent 90 days after the stroke.”
Down the Rabbit Hole
Commenting on the research, Larry B. Goldstein, MD, professor and chair, Department of Neurology, University of Kentucky, Lexington, praised the study’s adaptive design, noted that the hypothesis the study was based on was “reasonable” given the concern about additional thromboses, and found the results useful.
“The goal is not only to see what works but also what doesn’t work so we don’t go down that rabbit hole.”
He also pointed out that because the two blood-thinning drugs studied have very different mechanisms of action, it’s unlikely that another antithrombotic would add benefit to thrombolysis, “but you never say never.”
Dr. Adeoye and Dr. Barreto report research funding from the National Institutes of Health/National Institute of Neurological Disorders and Stroke. Dr. Adeoye also reports an executive role, receiving royalties/being a patent beneficiary, Sense Diagnostics, Inc. Dr. Goldstein has no relevant conflicts of interest.
A version of this article appeared on Medscape.com.
PHOENIX — , results of new research show.
“Ultimately, we found no benefit for either medication added to standard-of-care thrombolysis in terms of improving stroke outcomes,” said lead study author Opeolu M. Adeoye, MD, professor of emergency medicine and department chair, Washington University School of Medicine, St. Louis, Missouri.
The results were surprising and disappointing for Dr. Adeoye. “We went into the trial hopeful and thinking we would be able to benefit patients in reducing disability from stroke,” he said.
The Multi-Arm Optimization of Stroke Thrombolysis (MOST) trial was stopped early because of futility following recommendations from the data and safety monitoring board.
The findings were presented at the International Stroke Conference presented by the American Stroke Association, a division of the American Heart Association.
A thrombolytic drug alone doesn’t help all patients, particularly those with larger clots. “Clots can open; they can reform; they can re-occlude, etc.,” said another author, Andrew D. Barreto, MD, associate professor, Department of Neurology, University of Texas Health Science Center, Houston. “The thought was that adding additional medications that thin the blood, like argatroban or eptifibatide, would amplify the effects of the clot-busting drug.”
Indeed, this approach has had success in cardiology in terms of blood vessel opening, said Dr. Adeoye, adding that some preclinical data suggest that antithrombotic drugs may be neuroprotective.
Six phase 2 studies going back over a dozen years suggested that these drugs are safe in stroke patients. Although these studies weren’t powered for efficacy, “we did see a signal that adding them would be better than just the clot-busting drug alone.” These findings prompted the current phase 3 trial, said Dr. Barreto.
The three-arm, single-blind MOST trial included 514 adult patients with acute ischemic stroke and a National Institutes of Health Stroke Scale (NIHSS) score of 6 or greater at 57 US centers. In the study cohort the mean age was about 68 years, 70% White/25% Black, and with about equal numbers of female and male patients.
All received standard stroke care including thrombolysis within 3 hours of symptom onset. Initially, researchers used intravenous alteplase (0.9 mg/kg), but as the standard of care changed over time, they began using tenecteplase (0.25 mg/kg).
Study patients were also randomly assigned to receive placebo or either argatroban (100 mcg/kg bolus followed by 3 mcg/kg per minute for 12 hours) or eptifibatide (135 mcg/kg bolus followed by 0.75 mcg/kg/min infusion for 2 hours). These treatments were initiated within 75 minutes of thrombolysis.
Two Different Mechanisms
The drugs have different mechanisms of action. Argatroban is an anticoagulant, a direct inhibitor of thrombin, while the antiplatelet eptifibatide blocks the glycoprotein IIb/IIIa receptor and was specifically developed to ensure rapid inhibition of platelet aggregation.
Patients could also receive endovascular thrombectomy as part of their usual care. In this study, about 44% of patients received this treatment.
The primary endpoint was 90-day utility weighted modified Rankin Scale (uw-mRS) scores, where the worst outcome is 0 and the best outcome is 10.
The study used a response-adaptive randomization design, where the randomization switches from a drug that doesn’t appear to have a chance of working to the arm more likely to be beneficial.
Of the 514 patients, the analysis included 228 in the placebo, 59 in the argatroban, and 227 in eptifibatide groups. Of the total, 421 completed the study.
The mean 90-day uw-mRS was 6.8 in the placebo group, 5.2 in the argatroban group, and 6.3 in the eptifibatide group.
The probability of argatroban being better than placebo was 0.2%; the probability of eptifibatide being better than placebo was 0.9%. The futility threshold was enrollment of 500 and less than a 20% chance of benefit, thus the decision to stop the trial.
In all subgroup analyses, which looked at age, stroke severity, the two thrombolytic drugs, and use of endovascular therapy, “we didn’t really see much of a signal that would suggest that’s the group we would need to be testing further,” said Dr. Barreto.
No Increased ICH Risk
The primary safety outcome was symptomatic intracranial hemorrhage within 36 hours of randomization. The researchers found no significant increase in rates of this outcome.
The argatroban cohort had significantly lower odds of favorable outcomes compared with placebo, noted Dr. Adeoye. For example, it had more all-cause deaths, although none were related to the study drug.
Speculating on why the intervention didn’t work, Dr. Barreto pointed to changes in standard of care between the earlier trials and the current one, including the incorporation of endovascular therapy and switch to tenecteplase.
Although the results were disappointing, Dr. Adeoye sees a bright side. “What we’re very proud of, and excited about, is the fact that we have a definitive answer on these two drugs, and we did it in one trial as opposed to sequential, separate ongoing trials.”
But he stressed that more work needs to be done, especially given that even with endovascular therapy, half of stroke patients don’t achieve independence.
“In this trial, we established that argatroban and eptifibatide added to thrombolysis did not work, but that doesn’t address the fact that we need to continue to see what we can do to improve the total proportion of stroke patients who, after our treatments, are functionally independent 90 days after the stroke.”
Down the Rabbit Hole
Commenting on the research, Larry B. Goldstein, MD, professor and chair, Department of Neurology, University of Kentucky, Lexington, praised the study’s adaptive design, noted that the hypothesis the study was based on was “reasonable” given the concern about additional thromboses, and found the results useful.
“The goal is not only to see what works but also what doesn’t work so we don’t go down that rabbit hole.”
He also pointed out that because the two blood-thinning drugs studied have very different mechanisms of action, it’s unlikely that another antithrombotic would add benefit to thrombolysis, “but you never say never.”
Dr. Adeoye and Dr. Barreto report research funding from the National Institutes of Health/National Institute of Neurological Disorders and Stroke. Dr. Adeoye also reports an executive role, receiving royalties/being a patent beneficiary, Sense Diagnostics, Inc. Dr. Goldstein has no relevant conflicts of interest.
A version of this article appeared on Medscape.com.
PHOENIX — , results of new research show.
“Ultimately, we found no benefit for either medication added to standard-of-care thrombolysis in terms of improving stroke outcomes,” said lead study author Opeolu M. Adeoye, MD, professor of emergency medicine and department chair, Washington University School of Medicine, St. Louis, Missouri.
The results were surprising and disappointing for Dr. Adeoye. “We went into the trial hopeful and thinking we would be able to benefit patients in reducing disability from stroke,” he said.
The Multi-Arm Optimization of Stroke Thrombolysis (MOST) trial was stopped early because of futility following recommendations from the data and safety monitoring board.
The findings were presented at the International Stroke Conference presented by the American Stroke Association, a division of the American Heart Association.
A thrombolytic drug alone doesn’t help all patients, particularly those with larger clots. “Clots can open; they can reform; they can re-occlude, etc.,” said another author, Andrew D. Barreto, MD, associate professor, Department of Neurology, University of Texas Health Science Center, Houston. “The thought was that adding additional medications that thin the blood, like argatroban or eptifibatide, would amplify the effects of the clot-busting drug.”
Indeed, this approach has had success in cardiology in terms of blood vessel opening, said Dr. Adeoye, adding that some preclinical data suggest that antithrombotic drugs may be neuroprotective.
Six phase 2 studies going back over a dozen years suggested that these drugs are safe in stroke patients. Although these studies weren’t powered for efficacy, “we did see a signal that adding them would be better than just the clot-busting drug alone.” These findings prompted the current phase 3 trial, said Dr. Barreto.
The three-arm, single-blind MOST trial included 514 adult patients with acute ischemic stroke and a National Institutes of Health Stroke Scale (NIHSS) score of 6 or greater at 57 US centers. In the study cohort the mean age was about 68 years, 70% White/25% Black, and with about equal numbers of female and male patients.
All received standard stroke care including thrombolysis within 3 hours of symptom onset. Initially, researchers used intravenous alteplase (0.9 mg/kg), but as the standard of care changed over time, they began using tenecteplase (0.25 mg/kg).
Study patients were also randomly assigned to receive placebo or either argatroban (100 mcg/kg bolus followed by 3 mcg/kg per minute for 12 hours) or eptifibatide (135 mcg/kg bolus followed by 0.75 mcg/kg/min infusion for 2 hours). These treatments were initiated within 75 minutes of thrombolysis.
Two Different Mechanisms
The drugs have different mechanisms of action. Argatroban is an anticoagulant, a direct inhibitor of thrombin, while the antiplatelet eptifibatide blocks the glycoprotein IIb/IIIa receptor and was specifically developed to ensure rapid inhibition of platelet aggregation.
Patients could also receive endovascular thrombectomy as part of their usual care. In this study, about 44% of patients received this treatment.
The primary endpoint was 90-day utility weighted modified Rankin Scale (uw-mRS) scores, where the worst outcome is 0 and the best outcome is 10.
The study used a response-adaptive randomization design, where the randomization switches from a drug that doesn’t appear to have a chance of working to the arm more likely to be beneficial.
Of the 514 patients, the analysis included 228 in the placebo, 59 in the argatroban, and 227 in eptifibatide groups. Of the total, 421 completed the study.
The mean 90-day uw-mRS was 6.8 in the placebo group, 5.2 in the argatroban group, and 6.3 in the eptifibatide group.
The probability of argatroban being better than placebo was 0.2%; the probability of eptifibatide being better than placebo was 0.9%. The futility threshold was enrollment of 500 and less than a 20% chance of benefit, thus the decision to stop the trial.
In all subgroup analyses, which looked at age, stroke severity, the two thrombolytic drugs, and use of endovascular therapy, “we didn’t really see much of a signal that would suggest that’s the group we would need to be testing further,” said Dr. Barreto.
No Increased ICH Risk
The primary safety outcome was symptomatic intracranial hemorrhage within 36 hours of randomization. The researchers found no significant increase in rates of this outcome.
The argatroban cohort had significantly lower odds of favorable outcomes compared with placebo, noted Dr. Adeoye. For example, it had more all-cause deaths, although none were related to the study drug.
Speculating on why the intervention didn’t work, Dr. Barreto pointed to changes in standard of care between the earlier trials and the current one, including the incorporation of endovascular therapy and switch to tenecteplase.
Although the results were disappointing, Dr. Adeoye sees a bright side. “What we’re very proud of, and excited about, is the fact that we have a definitive answer on these two drugs, and we did it in one trial as opposed to sequential, separate ongoing trials.”
But he stressed that more work needs to be done, especially given that even with endovascular therapy, half of stroke patients don’t achieve independence.
“In this trial, we established that argatroban and eptifibatide added to thrombolysis did not work, but that doesn’t address the fact that we need to continue to see what we can do to improve the total proportion of stroke patients who, after our treatments, are functionally independent 90 days after the stroke.”
Down the Rabbit Hole
Commenting on the research, Larry B. Goldstein, MD, professor and chair, Department of Neurology, University of Kentucky, Lexington, praised the study’s adaptive design, noted that the hypothesis the study was based on was “reasonable” given the concern about additional thromboses, and found the results useful.
“The goal is not only to see what works but also what doesn’t work so we don’t go down that rabbit hole.”
He also pointed out that because the two blood-thinning drugs studied have very different mechanisms of action, it’s unlikely that another antithrombotic would add benefit to thrombolysis, “but you never say never.”
Dr. Adeoye and Dr. Barreto report research funding from the National Institutes of Health/National Institute of Neurological Disorders and Stroke. Dr. Adeoye also reports an executive role, receiving royalties/being a patent beneficiary, Sense Diagnostics, Inc. Dr. Goldstein has no relevant conflicts of interest.
A version of this article appeared on Medscape.com.
FROM ISC 2024
Dermatologic Reactions Following COVID-19 Vaccination: A Case Series
Cutaneous reactions associated with the Pfizer-BioNTech COVID-19 vaccine have been reported worldwide since December 2020. Local injection site reactions (<1%) such as erythema, swelling, delayed local reactions (1%–10%), morbilliform rash, urticarial reactions, pityriasis rosea, Rowell syndrome, and lichen planus have been reported following the Pfizer-BioNTech COVID-19 vaccine.1 Cutaneous reactions reported in association with the Sinovac-Coronavac COVID-19 vaccine include swelling, redness, itching, discoloration, induration (1%–10%), urticaria, petechial rash, and exacerbation of psoriasis at the local injection site (<1%).2
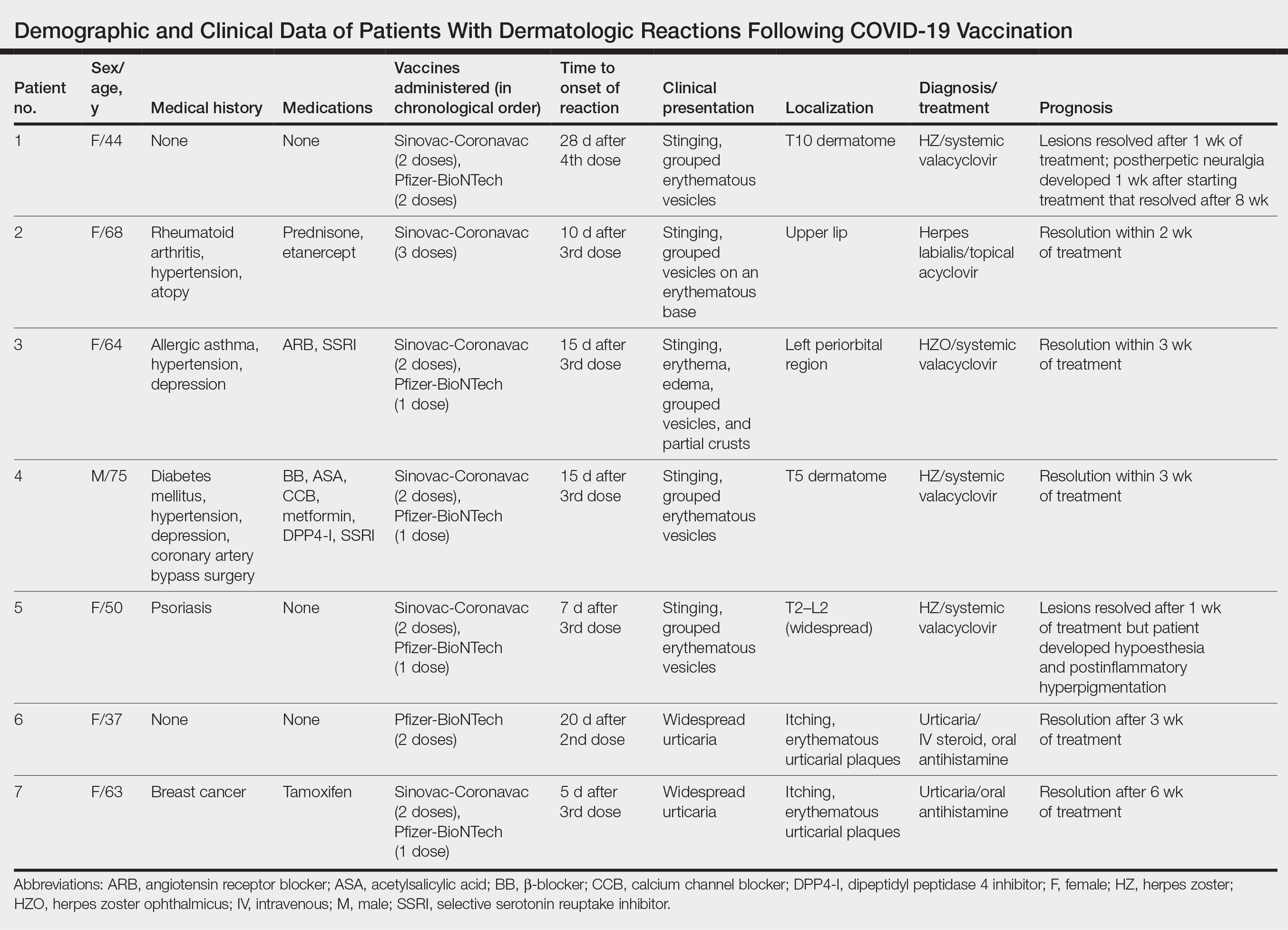
We describe 7 patients from Turkey who presented with various dermatologic problems 5 to 28 days after COVID-19 vaccination, highlighting the possibility of early and late cutaneous reactions related to the vaccine (Table).
Case Reports
Patient 1—A 44-year-old woman was admitted to the dermatology clinic with painful lesions on the trunk of 3 days’ duration. Dermatologic examination revealed grouped erythematous vesicles showing dermatomal spread in the right thoracolumbar (dermatome T10) region. The patient reported that she had received 2 doses of the Sinovac-Coronavac vaccine (doses 1 and 2) and 2 doses of the BioNTech COVID-19 vaccine (doses 3 and 4); the rash had developed 28 days after she received the 4th dose. Her medical history was unremarkable. The lesions regressed after 1 week of treatment with oral valacyclovir 1000 mg 3 times daily, but she developed postherpetic neuralgia 1 week after starting treatment, which resolved after 8 weeks.
Patient 2—A 68-year-old woman presented to the dermatology clinic for evaluation of painful sores on the upper lip of 1 day’s duration. She had a history of rheumatoid arthritis, hypertension, and atopy and was currently taking prednisone and etanercept. Dermatologic examination revealed grouped vesicles on an erythematous base on the upper lip. A diagnosis of herpes labialis was made. The patient reported that she had received a third dose of the Sinovac-Coronavac vaccine 10 days prior to the appearance of the lesions. Her symptoms resolved completely within 2 weeks of treatment with topical acyclovir.
Patient 3—A 64-year-old woman was admitted to the hospital with pain, redness, and watery sores on and around the left eyelid of 2 days’ duration. Dermatologic evaluation revealed the erythematous surface of the left eyelid and periorbital area showed partial crusts, clustered vesicles, erythema, and edema. Additionally, the conjunctiva was purulent and erythematous. The patient’s medical history was notable for allergic asthma, hypertension, anxiety, and depression. For this reason, the patient was prescribed an angiotensin receptor blocker and a selective serotonin reuptake inhibitor. She noted that a similar rash had developed around the left eye 6 years prior that was diagnosed as herpes zoster (HZ). She also reported that she had received 2 doses of the Sinovac-Coronavac COVID-19 vaccine followed by 1 dose of the BioNTech COVID-19 vaccine, which she had received 2 weeks before the rash developed. The patient was treated at the eye clinic and was found to have ocular involvement. Ophthalmology was consulted and a diagnosis of herpes zoster ophthalmicus (HZO) was made. Systemic valacyclovir treatment was initiated, resulting in clinical improvement within 3 weeks.
Patient 4—A 75-year-old man was admitted to the hospital with chest and back pain and widespread muscle pain of several days’ duration. His medical history was remarkable for diabetes mellitus, hypertension, depression, and coronary artery bypass surgery. A medication history revealed treatment with a β-blocker, acetylsalicylic acid, a calcium channel blocker, a dipeptidyl peptidase 4 inhibitor, and a selective serotonin reuptake inhibitor. Dermatologic examination revealed grouped vesicles on an erythematous background in dermatome T5 on the right chest and back. A diagnosis of HZ was made. The patient reported that he had received 2 doses of the Sinovac-Coronavac vaccine followed by 1 dose of the Pfizer-BioNTech vaccine 2 weeks prior to the current presentation. He was treated with valacyclovir for 1 week, and his symptoms resolved entirely within 3 weeks.
Patient 5—A 50-year-old woman presented to the hospital for evaluation of painful sores on the back, chest, groin, and abdomen of 10 days’ duration. The lesions initially had developed 7 days after receiving the BioNTech COVID-19 vaccine; she previously had received 2 doses of the Sinovac-Coronavac vaccine. The patient had a history of untreated psoriasis. Dermatologic examination revealed grouped vesicles on an erythematous background in the T2–L2 dermatomes on the left side of the trunk. A diagnosis of HZ was made. The lesions resolved after 1 week of treatment with systemic valacyclovir; however, she subsequently developed postherpetic neuralgia, hypoesthesia, and postinflammatory hyperpigmentation in the affected regions.
Patient 6—A 37-year-old woman presented to the hospital with redness, swelling, and itching all over the body of 3 days’ duration. The patient noted that the rash would subside and reappear throughout the day. Her medical history was unremarkable, except for COVID-19 infection 6 months prior. She had received a second dose of the BioNTech vaccine 20 days prior to development of symptoms. Dermatologic examination revealed widespread erythematous urticarial plaques. A diagnosis of acute urticaria was made. The patient recovered completely after 1 week of treatment with a systemic steroid and 3 weeks of antihistamine treatment.
Patient 7—A 63-year-old woman presented to the hospital with widespread itching and rash that appeared 5 days after the first dose of the BioNTech COVID-19 vaccine. The patient reported that the rash resolved spontaneously within a few hours but then reappeared. Her medical history revealed that she was taking tamoxifen for breast cancer and that she previously had received 2 doses of the Sinovac-Coronavac vaccine. Dermatologic examination revealed erythematous urticarial plaques on the trunk and arms. A diagnosis of urticaria was made, and her symptoms resolved after 6 weeks of antihistamine treatment.
Comment
Skin lesions associated with COVID-19 infection have been reported worldwide3,4 as well as dermatologic reactions following COVID-19 vaccination. In one case from Turkey, HZ infection was reported in a 68-year-old man 5 days after he received a second dose of the COVID-19 vaccine.5 In another case, HZ infection developed in a 78-year-old man 5 days after COVID-19 vaccination.6 Numerous cases of HZ infection developing within 1 to 26 days of COVID-19 vaccination have been reported worldwide.7-9
In a study conducted in the United States, 40 skin reactions associated with the COVID-19 vaccine were investigated; of these cases, 87.5% (35/40) were reported as varicella-zoster virus, and 12.5% (5/40) were reported as herpes simplex reactivation; 54% (19/35) and 80% (4/5) of these cases, respectively, were associated with the Pfizer-BioNTech vaccine.10 The average age of patients who developed a skin reaction was 46 years, and 70% (28/40) were women. The time to onset of the reaction was 2 to 13 days after vaccination, and symptoms were reported to improve within 7 days on average.10
Another study from Spain examined 405 vaccine-related skin reactions, 40.2% of which were related to the Pfizer-BioNTech vaccine. Among them, 80.2% occurred in women; 13.8% of cases were diagnosed as varicella-zoster virus or HZ virus reactivation, and 14.6% were urticaria. Eighty reactions (21%) were classified as severe/very severe and 81% required treatment.11 One study reported 414 skin reactions from the COVID-19 vaccine from December 2020 to February 2021; of these cases, 83% occurred after the Moderna vaccine, which is not available in Turkey, and 17% occurred after the Pfizer-BioNTech vaccine.12A systematic review of 91 patients who developed HZ infection after COVID-19 vaccination reported that 10% (9/91) of cases were receiving immunosuppressive therapy and 13% (12/91) had an autoimmune disease.7 In our case series, it is known that at least 2 of the patients (patients 2 and 5), including 1 patient with rheumatoid arthritis (patient 2) who was on immunosuppressive treatment, had autoimmune disorders. However, reports in the literature indicate that most patients with autoimmune inflammatory rheumatic diseases remain stable after vaccination.13
Herpes zoster ophthalmicus is a rare form of HZ caused by involvement of the ophthalmic branch of the trigeminal nerve that manifests as vesicular lesions and retinitis, uveitis, keratitis, conjunctivitis, and pain on an erythematous background. Two cases of women who developed HZO infection after Pfizer-BioNTech vaccination were reported in the literature.14 Although patient 3 in our case series had a history of HZO 6 years prior, the possibility of the Pfizer-BioNTech vaccine triggering HZO should be taken into consideration.
Although cutaneous reactions after the Sinovac-Coronavac vaccine were observed in only 1 of 7 patients in our case series, skin reactions after Sinovac-Coronavac (an inactivated viral vaccine) have been reported in the literature. In one study, after a total of 35,229 injections, the incidence of cutaneous adverse events due to Sinovac-Coronavac was reported to be 0.94% and 0.70% after the first and second doses, respectively.15 Therefore, further study results are needed to directly attribute the reactions to COVID-19 vaccination.
Conclusion
Our case series highlights that clinicians should be vigilant in diagnosing cutaneous reactions following COVID-19 vaccination early to prevent potential complications. Early recognition of reactions is crucial, and the prognosis can be improved with appropriate treatment. Despite the potential dermatologic adverse effects of the COVID-19 vaccine, the most effective way to protect against serious COVID-19 infection is to continue to be vaccinated.
- Polack FP, Thomas SJ, Kitchin N, et al. Safety and efficacy of the BNT162b2 mRNA COVID-19 vaccine. N Engl J Med. 2020;383:2603-2615.
- Zhang Y, Zeng G, Pan H, et al. Safety, tolerability, and immunogenicity of an inactivated SARS-CoV-2 vaccine in healthy adults aged 18–59 years: a randomised, double-blind, placebo-controlled, phase 1/2 clinical trial. Lancet Infect Dis. 2021;21:181-192.
- Tan SW, Tam YC, Oh CC. Skin manifestations of COVID-19: a worldwide review. JAAD Int. 2021;2:119-133.
- Singh H, Kaur H, Singh K, et al. Cutaneous manifestations of COVID-19: a systematic review. advances in wound care. 2021;10:51-80.
- Aksu SB, Öztürk GZ. A rare case of shingles after COVID-19 vaccine: is it a possible adverse effect? clinical and experimental vaccine research. 2021;10:198-201.
- Bostan E, Yalici-Armagan B. Herpes zoster following inactivated COVID-19 vaccine: a coexistence or coincidence? J Cosmet Dermatol. 2021;20:1566-1567.
- Katsikas Triantafyllidis K, Giannos P, Mian IT, et al. Varicella zoster virus reactivation following COVID-19 vaccination: a systematic review of case reports. Vaccines (Basel). 2021;9:1013. doi:10.3390/vaccines9091013
- Rodríguez-Jiménez P, Chicharro P, Cabrera LM, et al. Varicella-zoster virus reactivation after SARS-CoV-2 BNT162b2 mRNA vaccination: report of 5 cases. JAAD Case Rep. 2021;12:58-59. doi:10.1016/j.jdcr.2021.04.014
- Lee C, Cotter D, Basa J, et al. 20 Post-COVID-19 vaccine-related shingles cases seen at the Las Vegas Dermatology clinic and sent to us via social media. J Cosmet Dermatol. 2021;20:1960-1964.
- Fathy RA, McMahon DE, Lee C, et al. Varicella-zoster and herpes simplex virus reactivation post-COVID-19 vaccination: a review of 40 cases in an International Dermatology Registry. J Eur Acad Dermatol Venerol. 2022;36:E6-E9.
- Català A, Muñoz-Santos C, Galván-Casas C, et al. Cutaneous reactions after SARS-CoV-2 vaccination: a cross-sectional Spanish nationwide study of 405 cases. Br J Dermatol. 2022;186:142-152.
- McMahon DE, Amerson E, Rosenbach M, et al. Cutaneous reactions reported after Moderna and Pfizer COVID-19 vaccination: a registry-based study of 414 cases. J Am Acad Dermatol. 2021;85:46-55.
- Furer V, Eviatar T, Zisman D, et al. Immunogenicity and safety of the BNT162b2 mRNA COVID-19 vaccine in adult patients with autoimmune inflammatory rheumatic diseases and in the general population: a multicentre study. Ann Rheum Dis. 2021;80:1330-1338.
- Bernardini N, Skroza N, Mambrin A, et al. Herpes zoster ophthalmicus in two women after Pfizer-BioNTech (BNT162b2) vaccine. J Med Virol. 2022;94:817-818.
- Rerknimitr P, Puaratanaarunkon T, Wongtada C, et al. Cutaneous adverse reactions from 35,229 doses of Sinovac and AstraZeneca COVID-19 vaccination: a prospective cohort study in healthcare workers. J Eur Acad Dermatol Venereol. 2022;36:E158-E161.
Cutaneous reactions associated with the Pfizer-BioNTech COVID-19 vaccine have been reported worldwide since December 2020. Local injection site reactions (<1%) such as erythema, swelling, delayed local reactions (1%–10%), morbilliform rash, urticarial reactions, pityriasis rosea, Rowell syndrome, and lichen planus have been reported following the Pfizer-BioNTech COVID-19 vaccine.1 Cutaneous reactions reported in association with the Sinovac-Coronavac COVID-19 vaccine include swelling, redness, itching, discoloration, induration (1%–10%), urticaria, petechial rash, and exacerbation of psoriasis at the local injection site (<1%).2
We describe 7 patients from Turkey who presented with various dermatologic problems 5 to 28 days after COVID-19 vaccination, highlighting the possibility of early and late cutaneous reactions related to the vaccine (Table).

Case Reports
Patient 1—A 44-year-old woman was admitted to the dermatology clinic with painful lesions on the trunk of 3 days’ duration. Dermatologic examination revealed grouped erythematous vesicles showing dermatomal spread in the right thoracolumbar (dermatome T10) region. The patient reported that she had received 2 doses of the Sinovac-Coronavac vaccine (doses 1 and 2) and 2 doses of the BioNTech COVID-19 vaccine (doses 3 and 4); the rash had developed 28 days after she received the 4th dose. Her medical history was unremarkable. The lesions regressed after 1 week of treatment with oral valacyclovir 1000 mg 3 times daily, but she developed postherpetic neuralgia 1 week after starting treatment, which resolved after 8 weeks.
Patient 2—A 68-year-old woman presented to the dermatology clinic for evaluation of painful sores on the upper lip of 1 day’s duration. She had a history of rheumatoid arthritis, hypertension, and atopy and was currently taking prednisone and etanercept. Dermatologic examination revealed grouped vesicles on an erythematous base on the upper lip. A diagnosis of herpes labialis was made. The patient reported that she had received a third dose of the Sinovac-Coronavac vaccine 10 days prior to the appearance of the lesions. Her symptoms resolved completely within 2 weeks of treatment with topical acyclovir.
Patient 3—A 64-year-old woman was admitted to the hospital with pain, redness, and watery sores on and around the left eyelid of 2 days’ duration. Dermatologic evaluation revealed the erythematous surface of the left eyelid and periorbital area showed partial crusts, clustered vesicles, erythema, and edema. Additionally, the conjunctiva was purulent and erythematous. The patient’s medical history was notable for allergic asthma, hypertension, anxiety, and depression. For this reason, the patient was prescribed an angiotensin receptor blocker and a selective serotonin reuptake inhibitor. She noted that a similar rash had developed around the left eye 6 years prior that was diagnosed as herpes zoster (HZ). She also reported that she had received 2 doses of the Sinovac-Coronavac COVID-19 vaccine followed by 1 dose of the BioNTech COVID-19 vaccine, which she had received 2 weeks before the rash developed. The patient was treated at the eye clinic and was found to have ocular involvement. Ophthalmology was consulted and a diagnosis of herpes zoster ophthalmicus (HZO) was made. Systemic valacyclovir treatment was initiated, resulting in clinical improvement within 3 weeks.
Patient 4—A 75-year-old man was admitted to the hospital with chest and back pain and widespread muscle pain of several days’ duration. His medical history was remarkable for diabetes mellitus, hypertension, depression, and coronary artery bypass surgery. A medication history revealed treatment with a β-blocker, acetylsalicylic acid, a calcium channel blocker, a dipeptidyl peptidase 4 inhibitor, and a selective serotonin reuptake inhibitor. Dermatologic examination revealed grouped vesicles on an erythematous background in dermatome T5 on the right chest and back. A diagnosis of HZ was made. The patient reported that he had received 2 doses of the Sinovac-Coronavac vaccine followed by 1 dose of the Pfizer-BioNTech vaccine 2 weeks prior to the current presentation. He was treated with valacyclovir for 1 week, and his symptoms resolved entirely within 3 weeks.
Patient 5—A 50-year-old woman presented to the hospital for evaluation of painful sores on the back, chest, groin, and abdomen of 10 days’ duration. The lesions initially had developed 7 days after receiving the BioNTech COVID-19 vaccine; she previously had received 2 doses of the Sinovac-Coronavac vaccine. The patient had a history of untreated psoriasis. Dermatologic examination revealed grouped vesicles on an erythematous background in the T2–L2 dermatomes on the left side of the trunk. A diagnosis of HZ was made. The lesions resolved after 1 week of treatment with systemic valacyclovir; however, she subsequently developed postherpetic neuralgia, hypoesthesia, and postinflammatory hyperpigmentation in the affected regions.
Patient 6—A 37-year-old woman presented to the hospital with redness, swelling, and itching all over the body of 3 days’ duration. The patient noted that the rash would subside and reappear throughout the day. Her medical history was unremarkable, except for COVID-19 infection 6 months prior. She had received a second dose of the BioNTech vaccine 20 days prior to development of symptoms. Dermatologic examination revealed widespread erythematous urticarial plaques. A diagnosis of acute urticaria was made. The patient recovered completely after 1 week of treatment with a systemic steroid and 3 weeks of antihistamine treatment.
Patient 7—A 63-year-old woman presented to the hospital with widespread itching and rash that appeared 5 days after the first dose of the BioNTech COVID-19 vaccine. The patient reported that the rash resolved spontaneously within a few hours but then reappeared. Her medical history revealed that she was taking tamoxifen for breast cancer and that she previously had received 2 doses of the Sinovac-Coronavac vaccine. Dermatologic examination revealed erythematous urticarial plaques on the trunk and arms. A diagnosis of urticaria was made, and her symptoms resolved after 6 weeks of antihistamine treatment.
Comment
Skin lesions associated with COVID-19 infection have been reported worldwide3,4 as well as dermatologic reactions following COVID-19 vaccination. In one case from Turkey, HZ infection was reported in a 68-year-old man 5 days after he received a second dose of the COVID-19 vaccine.5 In another case, HZ infection developed in a 78-year-old man 5 days after COVID-19 vaccination.6 Numerous cases of HZ infection developing within 1 to 26 days of COVID-19 vaccination have been reported worldwide.7-9
In a study conducted in the United States, 40 skin reactions associated with the COVID-19 vaccine were investigated; of these cases, 87.5% (35/40) were reported as varicella-zoster virus, and 12.5% (5/40) were reported as herpes simplex reactivation; 54% (19/35) and 80% (4/5) of these cases, respectively, were associated with the Pfizer-BioNTech vaccine.10 The average age of patients who developed a skin reaction was 46 years, and 70% (28/40) were women. The time to onset of the reaction was 2 to 13 days after vaccination, and symptoms were reported to improve within 7 days on average.10
Another study from Spain examined 405 vaccine-related skin reactions, 40.2% of which were related to the Pfizer-BioNTech vaccine. Among them, 80.2% occurred in women; 13.8% of cases were diagnosed as varicella-zoster virus or HZ virus reactivation, and 14.6% were urticaria. Eighty reactions (21%) were classified as severe/very severe and 81% required treatment.11 One study reported 414 skin reactions from the COVID-19 vaccine from December 2020 to February 2021; of these cases, 83% occurred after the Moderna vaccine, which is not available in Turkey, and 17% occurred after the Pfizer-BioNTech vaccine.12A systematic review of 91 patients who developed HZ infection after COVID-19 vaccination reported that 10% (9/91) of cases were receiving immunosuppressive therapy and 13% (12/91) had an autoimmune disease.7 In our case series, it is known that at least 2 of the patients (patients 2 and 5), including 1 patient with rheumatoid arthritis (patient 2) who was on immunosuppressive treatment, had autoimmune disorders. However, reports in the literature indicate that most patients with autoimmune inflammatory rheumatic diseases remain stable after vaccination.13
Herpes zoster ophthalmicus is a rare form of HZ caused by involvement of the ophthalmic branch of the trigeminal nerve that manifests as vesicular lesions and retinitis, uveitis, keratitis, conjunctivitis, and pain on an erythematous background. Two cases of women who developed HZO infection after Pfizer-BioNTech vaccination were reported in the literature.14 Although patient 3 in our case series had a history of HZO 6 years prior, the possibility of the Pfizer-BioNTech vaccine triggering HZO should be taken into consideration.
Although cutaneous reactions after the Sinovac-Coronavac vaccine were observed in only 1 of 7 patients in our case series, skin reactions after Sinovac-Coronavac (an inactivated viral vaccine) have been reported in the literature. In one study, after a total of 35,229 injections, the incidence of cutaneous adverse events due to Sinovac-Coronavac was reported to be 0.94% and 0.70% after the first and second doses, respectively.15 Therefore, further study results are needed to directly attribute the reactions to COVID-19 vaccination.
Conclusion
Our case series highlights that clinicians should be vigilant in diagnosing cutaneous reactions following COVID-19 vaccination early to prevent potential complications. Early recognition of reactions is crucial, and the prognosis can be improved with appropriate treatment. Despite the potential dermatologic adverse effects of the COVID-19 vaccine, the most effective way to protect against serious COVID-19 infection is to continue to be vaccinated.
Cutaneous reactions associated with the Pfizer-BioNTech COVID-19 vaccine have been reported worldwide since December 2020. Local injection site reactions (<1%) such as erythema, swelling, delayed local reactions (1%–10%), morbilliform rash, urticarial reactions, pityriasis rosea, Rowell syndrome, and lichen planus have been reported following the Pfizer-BioNTech COVID-19 vaccine.1 Cutaneous reactions reported in association with the Sinovac-Coronavac COVID-19 vaccine include swelling, redness, itching, discoloration, induration (1%–10%), urticaria, petechial rash, and exacerbation of psoriasis at the local injection site (<1%).2
We describe 7 patients from Turkey who presented with various dermatologic problems 5 to 28 days after COVID-19 vaccination, highlighting the possibility of early and late cutaneous reactions related to the vaccine (Table).

Case Reports
Patient 1—A 44-year-old woman was admitted to the dermatology clinic with painful lesions on the trunk of 3 days’ duration. Dermatologic examination revealed grouped erythematous vesicles showing dermatomal spread in the right thoracolumbar (dermatome T10) region. The patient reported that she had received 2 doses of the Sinovac-Coronavac vaccine (doses 1 and 2) and 2 doses of the BioNTech COVID-19 vaccine (doses 3 and 4); the rash had developed 28 days after she received the 4th dose. Her medical history was unremarkable. The lesions regressed after 1 week of treatment with oral valacyclovir 1000 mg 3 times daily, but she developed postherpetic neuralgia 1 week after starting treatment, which resolved after 8 weeks.
Patient 2—A 68-year-old woman presented to the dermatology clinic for evaluation of painful sores on the upper lip of 1 day’s duration. She had a history of rheumatoid arthritis, hypertension, and atopy and was currently taking prednisone and etanercept. Dermatologic examination revealed grouped vesicles on an erythematous base on the upper lip. A diagnosis of herpes labialis was made. The patient reported that she had received a third dose of the Sinovac-Coronavac vaccine 10 days prior to the appearance of the lesions. Her symptoms resolved completely within 2 weeks of treatment with topical acyclovir.
Patient 3—A 64-year-old woman was admitted to the hospital with pain, redness, and watery sores on and around the left eyelid of 2 days’ duration. Dermatologic evaluation revealed the erythematous surface of the left eyelid and periorbital area showed partial crusts, clustered vesicles, erythema, and edema. Additionally, the conjunctiva was purulent and erythematous. The patient’s medical history was notable for allergic asthma, hypertension, anxiety, and depression. For this reason, the patient was prescribed an angiotensin receptor blocker and a selective serotonin reuptake inhibitor. She noted that a similar rash had developed around the left eye 6 years prior that was diagnosed as herpes zoster (HZ). She also reported that she had received 2 doses of the Sinovac-Coronavac COVID-19 vaccine followed by 1 dose of the BioNTech COVID-19 vaccine, which she had received 2 weeks before the rash developed. The patient was treated at the eye clinic and was found to have ocular involvement. Ophthalmology was consulted and a diagnosis of herpes zoster ophthalmicus (HZO) was made. Systemic valacyclovir treatment was initiated, resulting in clinical improvement within 3 weeks.
Patient 4—A 75-year-old man was admitted to the hospital with chest and back pain and widespread muscle pain of several days’ duration. His medical history was remarkable for diabetes mellitus, hypertension, depression, and coronary artery bypass surgery. A medication history revealed treatment with a β-blocker, acetylsalicylic acid, a calcium channel blocker, a dipeptidyl peptidase 4 inhibitor, and a selective serotonin reuptake inhibitor. Dermatologic examination revealed grouped vesicles on an erythematous background in dermatome T5 on the right chest and back. A diagnosis of HZ was made. The patient reported that he had received 2 doses of the Sinovac-Coronavac vaccine followed by 1 dose of the Pfizer-BioNTech vaccine 2 weeks prior to the current presentation. He was treated with valacyclovir for 1 week, and his symptoms resolved entirely within 3 weeks.
Patient 5—A 50-year-old woman presented to the hospital for evaluation of painful sores on the back, chest, groin, and abdomen of 10 days’ duration. The lesions initially had developed 7 days after receiving the BioNTech COVID-19 vaccine; she previously had received 2 doses of the Sinovac-Coronavac vaccine. The patient had a history of untreated psoriasis. Dermatologic examination revealed grouped vesicles on an erythematous background in the T2–L2 dermatomes on the left side of the trunk. A diagnosis of HZ was made. The lesions resolved after 1 week of treatment with systemic valacyclovir; however, she subsequently developed postherpetic neuralgia, hypoesthesia, and postinflammatory hyperpigmentation in the affected regions.
Patient 6—A 37-year-old woman presented to the hospital with redness, swelling, and itching all over the body of 3 days’ duration. The patient noted that the rash would subside and reappear throughout the day. Her medical history was unremarkable, except for COVID-19 infection 6 months prior. She had received a second dose of the BioNTech vaccine 20 days prior to development of symptoms. Dermatologic examination revealed widespread erythematous urticarial plaques. A diagnosis of acute urticaria was made. The patient recovered completely after 1 week of treatment with a systemic steroid and 3 weeks of antihistamine treatment.
Patient 7—A 63-year-old woman presented to the hospital with widespread itching and rash that appeared 5 days after the first dose of the BioNTech COVID-19 vaccine. The patient reported that the rash resolved spontaneously within a few hours but then reappeared. Her medical history revealed that she was taking tamoxifen for breast cancer and that she previously had received 2 doses of the Sinovac-Coronavac vaccine. Dermatologic examination revealed erythematous urticarial plaques on the trunk and arms. A diagnosis of urticaria was made, and her symptoms resolved after 6 weeks of antihistamine treatment.
Comment
Skin lesions associated with COVID-19 infection have been reported worldwide3,4 as well as dermatologic reactions following COVID-19 vaccination. In one case from Turkey, HZ infection was reported in a 68-year-old man 5 days after he received a second dose of the COVID-19 vaccine.5 In another case, HZ infection developed in a 78-year-old man 5 days after COVID-19 vaccination.6 Numerous cases of HZ infection developing within 1 to 26 days of COVID-19 vaccination have been reported worldwide.7-9
In a study conducted in the United States, 40 skin reactions associated with the COVID-19 vaccine were investigated; of these cases, 87.5% (35/40) were reported as varicella-zoster virus, and 12.5% (5/40) were reported as herpes simplex reactivation; 54% (19/35) and 80% (4/5) of these cases, respectively, were associated with the Pfizer-BioNTech vaccine.10 The average age of patients who developed a skin reaction was 46 years, and 70% (28/40) were women. The time to onset of the reaction was 2 to 13 days after vaccination, and symptoms were reported to improve within 7 days on average.10
Another study from Spain examined 405 vaccine-related skin reactions, 40.2% of which were related to the Pfizer-BioNTech vaccine. Among them, 80.2% occurred in women; 13.8% of cases were diagnosed as varicella-zoster virus or HZ virus reactivation, and 14.6% were urticaria. Eighty reactions (21%) were classified as severe/very severe and 81% required treatment.11 One study reported 414 skin reactions from the COVID-19 vaccine from December 2020 to February 2021; of these cases, 83% occurred after the Moderna vaccine, which is not available in Turkey, and 17% occurred after the Pfizer-BioNTech vaccine.12A systematic review of 91 patients who developed HZ infection after COVID-19 vaccination reported that 10% (9/91) of cases were receiving immunosuppressive therapy and 13% (12/91) had an autoimmune disease.7 In our case series, it is known that at least 2 of the patients (patients 2 and 5), including 1 patient with rheumatoid arthritis (patient 2) who was on immunosuppressive treatment, had autoimmune disorders. However, reports in the literature indicate that most patients with autoimmune inflammatory rheumatic diseases remain stable after vaccination.13
Herpes zoster ophthalmicus is a rare form of HZ caused by involvement of the ophthalmic branch of the trigeminal nerve that manifests as vesicular lesions and retinitis, uveitis, keratitis, conjunctivitis, and pain on an erythematous background. Two cases of women who developed HZO infection after Pfizer-BioNTech vaccination were reported in the literature.14 Although patient 3 in our case series had a history of HZO 6 years prior, the possibility of the Pfizer-BioNTech vaccine triggering HZO should be taken into consideration.
Although cutaneous reactions after the Sinovac-Coronavac vaccine were observed in only 1 of 7 patients in our case series, skin reactions after Sinovac-Coronavac (an inactivated viral vaccine) have been reported in the literature. In one study, after a total of 35,229 injections, the incidence of cutaneous adverse events due to Sinovac-Coronavac was reported to be 0.94% and 0.70% after the first and second doses, respectively.15 Therefore, further study results are needed to directly attribute the reactions to COVID-19 vaccination.
Conclusion
Our case series highlights that clinicians should be vigilant in diagnosing cutaneous reactions following COVID-19 vaccination early to prevent potential complications. Early recognition of reactions is crucial, and the prognosis can be improved with appropriate treatment. Despite the potential dermatologic adverse effects of the COVID-19 vaccine, the most effective way to protect against serious COVID-19 infection is to continue to be vaccinated.
- Polack FP, Thomas SJ, Kitchin N, et al. Safety and efficacy of the BNT162b2 mRNA COVID-19 vaccine. N Engl J Med. 2020;383:2603-2615.
- Zhang Y, Zeng G, Pan H, et al. Safety, tolerability, and immunogenicity of an inactivated SARS-CoV-2 vaccine in healthy adults aged 18–59 years: a randomised, double-blind, placebo-controlled, phase 1/2 clinical trial. Lancet Infect Dis. 2021;21:181-192.
- Tan SW, Tam YC, Oh CC. Skin manifestations of COVID-19: a worldwide review. JAAD Int. 2021;2:119-133.
- Singh H, Kaur H, Singh K, et al. Cutaneous manifestations of COVID-19: a systematic review. advances in wound care. 2021;10:51-80.
- Aksu SB, Öztürk GZ. A rare case of shingles after COVID-19 vaccine: is it a possible adverse effect? clinical and experimental vaccine research. 2021;10:198-201.
- Bostan E, Yalici-Armagan B. Herpes zoster following inactivated COVID-19 vaccine: a coexistence or coincidence? J Cosmet Dermatol. 2021;20:1566-1567.
- Katsikas Triantafyllidis K, Giannos P, Mian IT, et al. Varicella zoster virus reactivation following COVID-19 vaccination: a systematic review of case reports. Vaccines (Basel). 2021;9:1013. doi:10.3390/vaccines9091013
- Rodríguez-Jiménez P, Chicharro P, Cabrera LM, et al. Varicella-zoster virus reactivation after SARS-CoV-2 BNT162b2 mRNA vaccination: report of 5 cases. JAAD Case Rep. 2021;12:58-59. doi:10.1016/j.jdcr.2021.04.014
- Lee C, Cotter D, Basa J, et al. 20 Post-COVID-19 vaccine-related shingles cases seen at the Las Vegas Dermatology clinic and sent to us via social media. J Cosmet Dermatol. 2021;20:1960-1964.
- Fathy RA, McMahon DE, Lee C, et al. Varicella-zoster and herpes simplex virus reactivation post-COVID-19 vaccination: a review of 40 cases in an International Dermatology Registry. J Eur Acad Dermatol Venerol. 2022;36:E6-E9.
- Català A, Muñoz-Santos C, Galván-Casas C, et al. Cutaneous reactions after SARS-CoV-2 vaccination: a cross-sectional Spanish nationwide study of 405 cases. Br J Dermatol. 2022;186:142-152.
- McMahon DE, Amerson E, Rosenbach M, et al. Cutaneous reactions reported after Moderna and Pfizer COVID-19 vaccination: a registry-based study of 414 cases. J Am Acad Dermatol. 2021;85:46-55.
- Furer V, Eviatar T, Zisman D, et al. Immunogenicity and safety of the BNT162b2 mRNA COVID-19 vaccine in adult patients with autoimmune inflammatory rheumatic diseases and in the general population: a multicentre study. Ann Rheum Dis. 2021;80:1330-1338.
- Bernardini N, Skroza N, Mambrin A, et al. Herpes zoster ophthalmicus in two women after Pfizer-BioNTech (BNT162b2) vaccine. J Med Virol. 2022;94:817-818.
- Rerknimitr P, Puaratanaarunkon T, Wongtada C, et al. Cutaneous adverse reactions from 35,229 doses of Sinovac and AstraZeneca COVID-19 vaccination: a prospective cohort study in healthcare workers. J Eur Acad Dermatol Venereol. 2022;36:E158-E161.
- Polack FP, Thomas SJ, Kitchin N, et al. Safety and efficacy of the BNT162b2 mRNA COVID-19 vaccine. N Engl J Med. 2020;383:2603-2615.
- Zhang Y, Zeng G, Pan H, et al. Safety, tolerability, and immunogenicity of an inactivated SARS-CoV-2 vaccine in healthy adults aged 18–59 years: a randomised, double-blind, placebo-controlled, phase 1/2 clinical trial. Lancet Infect Dis. 2021;21:181-192.
- Tan SW, Tam YC, Oh CC. Skin manifestations of COVID-19: a worldwide review. JAAD Int. 2021;2:119-133.
- Singh H, Kaur H, Singh K, et al. Cutaneous manifestations of COVID-19: a systematic review. advances in wound care. 2021;10:51-80.
- Aksu SB, Öztürk GZ. A rare case of shingles after COVID-19 vaccine: is it a possible adverse effect? clinical and experimental vaccine research. 2021;10:198-201.
- Bostan E, Yalici-Armagan B. Herpes zoster following inactivated COVID-19 vaccine: a coexistence or coincidence? J Cosmet Dermatol. 2021;20:1566-1567.
- Katsikas Triantafyllidis K, Giannos P, Mian IT, et al. Varicella zoster virus reactivation following COVID-19 vaccination: a systematic review of case reports. Vaccines (Basel). 2021;9:1013. doi:10.3390/vaccines9091013
- Rodríguez-Jiménez P, Chicharro P, Cabrera LM, et al. Varicella-zoster virus reactivation after SARS-CoV-2 BNT162b2 mRNA vaccination: report of 5 cases. JAAD Case Rep. 2021;12:58-59. doi:10.1016/j.jdcr.2021.04.014
- Lee C, Cotter D, Basa J, et al. 20 Post-COVID-19 vaccine-related shingles cases seen at the Las Vegas Dermatology clinic and sent to us via social media. J Cosmet Dermatol. 2021;20:1960-1964.
- Fathy RA, McMahon DE, Lee C, et al. Varicella-zoster and herpes simplex virus reactivation post-COVID-19 vaccination: a review of 40 cases in an International Dermatology Registry. J Eur Acad Dermatol Venerol. 2022;36:E6-E9.
- Català A, Muñoz-Santos C, Galván-Casas C, et al. Cutaneous reactions after SARS-CoV-2 vaccination: a cross-sectional Spanish nationwide study of 405 cases. Br J Dermatol. 2022;186:142-152.
- McMahon DE, Amerson E, Rosenbach M, et al. Cutaneous reactions reported after Moderna and Pfizer COVID-19 vaccination: a registry-based study of 414 cases. J Am Acad Dermatol. 2021;85:46-55.
- Furer V, Eviatar T, Zisman D, et al. Immunogenicity and safety of the BNT162b2 mRNA COVID-19 vaccine in adult patients with autoimmune inflammatory rheumatic diseases and in the general population: a multicentre study. Ann Rheum Dis. 2021;80:1330-1338.
- Bernardini N, Skroza N, Mambrin A, et al. Herpes zoster ophthalmicus in two women after Pfizer-BioNTech (BNT162b2) vaccine. J Med Virol. 2022;94:817-818.
- Rerknimitr P, Puaratanaarunkon T, Wongtada C, et al. Cutaneous adverse reactions from 35,229 doses of Sinovac and AstraZeneca COVID-19 vaccination: a prospective cohort study in healthcare workers. J Eur Acad Dermatol Venereol. 2022;36:E158-E161.
Practice Points
- Cutaneous reactions have been reported following COVID-19 vaccination.
- Herpes infections and urticarial reactions can be associated with COVID-19 vaccination, regardless of the delay in onset between the injection and symptom development.
Determinants of Topical Corticosteroid Effectiveness in Eosinophilic Esophagitis in Real‐World Practice
Key clinical point: Reduced symptom severity and use of budesonide orodispersible tablets and high topical corticosteroid (tC) doses (eg, fluticasone propionate metered dose ≥ 1 mg/day from inhalation devices) are all independent predictors of tC effectiveness in patients with eosinophilic esophagitis (EoE) in the real‐world setting.
Major finding: Corticosteroid treatment proved to be the most important determining factor in achieving clinico-histological remission, with budesonide orodispersible tablets presenting the highest efficacy (adjusted odds ratio [aOR], 18.9; P < .001). High tC doses (aOR, 4.3; P = .03) and lower symptom scores (aOR, 0.9; P = .01) were also significant predictors of tC effectiveness.
Study details: This real-world cross‐sectional analysis of the multicenter EoE CONNECT registry assessed the data on 1456 prescriptions of tC monotherapy used in 866 patients with EoE.
Disclosures: This study did not receive any specific funding. The authors declared no conflicts of interest.
Source: Laserna‐Mendieta EJ, Navarro P, Casabona-Francés S, et al. Swallowed topical corticosteroids for eosinophilic esophagitis: Utilization and real‐world efficacy from the EoE CONNECT registry. United European Gastroenterol J. Published online January 29, 2024. Source
Key clinical point: Reduced symptom severity and use of budesonide orodispersible tablets and high topical corticosteroid (tC) doses (eg, fluticasone propionate metered dose ≥ 1 mg/day from inhalation devices) are all independent predictors of tC effectiveness in patients with eosinophilic esophagitis (EoE) in the real‐world setting.
Major finding: Corticosteroid treatment proved to be the most important determining factor in achieving clinico-histological remission, with budesonide orodispersible tablets presenting the highest efficacy (adjusted odds ratio [aOR], 18.9; P < .001). High tC doses (aOR, 4.3; P = .03) and lower symptom scores (aOR, 0.9; P = .01) were also significant predictors of tC effectiveness.
Study details: This real-world cross‐sectional analysis of the multicenter EoE CONNECT registry assessed the data on 1456 prescriptions of tC monotherapy used in 866 patients with EoE.
Disclosures: This study did not receive any specific funding. The authors declared no conflicts of interest.
Source: Laserna‐Mendieta EJ, Navarro P, Casabona-Francés S, et al. Swallowed topical corticosteroids for eosinophilic esophagitis: Utilization and real‐world efficacy from the EoE CONNECT registry. United European Gastroenterol J. Published online January 29, 2024. Source
Key clinical point: Reduced symptom severity and use of budesonide orodispersible tablets and high topical corticosteroid (tC) doses (eg, fluticasone propionate metered dose ≥ 1 mg/day from inhalation devices) are all independent predictors of tC effectiveness in patients with eosinophilic esophagitis (EoE) in the real‐world setting.
Major finding: Corticosteroid treatment proved to be the most important determining factor in achieving clinico-histological remission, with budesonide orodispersible tablets presenting the highest efficacy (adjusted odds ratio [aOR], 18.9; P < .001). High tC doses (aOR, 4.3; P = .03) and lower symptom scores (aOR, 0.9; P = .01) were also significant predictors of tC effectiveness.
Study details: This real-world cross‐sectional analysis of the multicenter EoE CONNECT registry assessed the data on 1456 prescriptions of tC monotherapy used in 866 patients with EoE.
Disclosures: This study did not receive any specific funding. The authors declared no conflicts of interest.
Source: Laserna‐Mendieta EJ, Navarro P, Casabona-Francés S, et al. Swallowed topical corticosteroids for eosinophilic esophagitis: Utilization and real‐world efficacy from the EoE CONNECT registry. United European Gastroenterol J. Published online January 29, 2024. Source
Salivary Proteins May Have a Diagnostic Potential in Pediatric Eosinophilic Esophagitis
Key clinical point: Children with eosinophilic esophagitis (EoE) have distinct salivary immunoinflammatory protein profiles compared with those without EoE, highlighting the diagnostic potential of salivary proteins in pediatric EoE.
Major finding: Children with EoE were distinguished from those without EoE through a panel of 10 proteins (higher expression levels of C-C motif chemokine-3, macrophage metalloelastase, granulocyte colony-stimulating factor-3, interleukin [IL]-15, pro-transforming growth factor alpha, and oncostatin-M and lower expression levels of IL-18, C-C motif chemokine-2, interstitial collagenase, and macrophage colony-stimulating factor-1), with an accuracy of 0.95 validated through the Least Absolute Shrinkage and Selection Operator regression.
Study details: This cross-sectional study analyzed the saliva samples collected from 40 children aged 6-18 years with (n = 23) or without EoE (n = 17) immediately before their scheduled esophagogastroduodenoscopy with biopsies.
Disclosures: Girish Hiremath and Seesandra V Rajagopala were supported by grants from the US National Institutes of Health. The former declared serving as a consultant for and receiving speaker fees from various organizations.
Source: Hiremath G, Wang Y, Correa H, Sheng Q, Rajagopala SV. Salivary immunoinflammatory proteins identify children with eosinophilic esophagitis. Allergy. 2024 (Jan 29). doi: 10.1111/all.16040 Source
Key clinical point: Children with eosinophilic esophagitis (EoE) have distinct salivary immunoinflammatory protein profiles compared with those without EoE, highlighting the diagnostic potential of salivary proteins in pediatric EoE.
Major finding: Children with EoE were distinguished from those without EoE through a panel of 10 proteins (higher expression levels of C-C motif chemokine-3, macrophage metalloelastase, granulocyte colony-stimulating factor-3, interleukin [IL]-15, pro-transforming growth factor alpha, and oncostatin-M and lower expression levels of IL-18, C-C motif chemokine-2, interstitial collagenase, and macrophage colony-stimulating factor-1), with an accuracy of 0.95 validated through the Least Absolute Shrinkage and Selection Operator regression.
Study details: This cross-sectional study analyzed the saliva samples collected from 40 children aged 6-18 years with (n = 23) or without EoE (n = 17) immediately before their scheduled esophagogastroduodenoscopy with biopsies.
Disclosures: Girish Hiremath and Seesandra V Rajagopala were supported by grants from the US National Institutes of Health. The former declared serving as a consultant for and receiving speaker fees from various organizations.
Source: Hiremath G, Wang Y, Correa H, Sheng Q, Rajagopala SV. Salivary immunoinflammatory proteins identify children with eosinophilic esophagitis. Allergy. 2024 (Jan 29). doi: 10.1111/all.16040 Source
Key clinical point: Children with eosinophilic esophagitis (EoE) have distinct salivary immunoinflammatory protein profiles compared with those without EoE, highlighting the diagnostic potential of salivary proteins in pediatric EoE.
Major finding: Children with EoE were distinguished from those without EoE through a panel of 10 proteins (higher expression levels of C-C motif chemokine-3, macrophage metalloelastase, granulocyte colony-stimulating factor-3, interleukin [IL]-15, pro-transforming growth factor alpha, and oncostatin-M and lower expression levels of IL-18, C-C motif chemokine-2, interstitial collagenase, and macrophage colony-stimulating factor-1), with an accuracy of 0.95 validated through the Least Absolute Shrinkage and Selection Operator regression.
Study details: This cross-sectional study analyzed the saliva samples collected from 40 children aged 6-18 years with (n = 23) or without EoE (n = 17) immediately before their scheduled esophagogastroduodenoscopy with biopsies.
Disclosures: Girish Hiremath and Seesandra V Rajagopala were supported by grants from the US National Institutes of Health. The former declared serving as a consultant for and receiving speaker fees from various organizations.
Source: Hiremath G, Wang Y, Correa H, Sheng Q, Rajagopala SV. Salivary immunoinflammatory proteins identify children with eosinophilic esophagitis. Allergy. 2024 (Jan 29). doi: 10.1111/all.16040 Source
Eosinophilic Esophagitis Alters Eating Behaviors in Children
Key clinical point: Altered eating behaviors, including increased chewing and increased consumption time, observed in children with eosinophilic esophagitis (EoE) correlated with patient-reported symptoms, endoscopic findings, and histologic features.
Major finding: Children with vs without EoE demonstrated more chews per bite and increased consumption time with soft solid (P = .031 and P = .002, respectively), chewable (P = .047 and P = .005, respectively), and hard solid (P = .037 and P = .034, respectively) foods. Increased consumption time significantly correlated with a peak eosinophil count (r 0.42; P = .050) and decreased esophageal distensibility (r −0.82; P < .0001).
Study details: This prospective observational study included 27 children with EoE (age 5-17 years) and 25 control children without EoE who consumed four food items, each representing a different texture (puree, soft solid, chewable, and hard solid).
Disclosures: This study was supported by the 2021 American College of Gastroenterology Clinical Research Award and other sources. The authors declared no conflicts of interest.
Source: Kennedy KV, Umeweni CN, Alston M, et al. Esophageal remodeling correlates with eating behaviors in pediatric eosinophilic esophagitis. Am J Gastroenterol. 2024 (Jan 18). doi: 10.14309/ajg.0000000000002661 Source
Key clinical point: Altered eating behaviors, including increased chewing and increased consumption time, observed in children with eosinophilic esophagitis (EoE) correlated with patient-reported symptoms, endoscopic findings, and histologic features.
Major finding: Children with vs without EoE demonstrated more chews per bite and increased consumption time with soft solid (P = .031 and P = .002, respectively), chewable (P = .047 and P = .005, respectively), and hard solid (P = .037 and P = .034, respectively) foods. Increased consumption time significantly correlated with a peak eosinophil count (r 0.42; P = .050) and decreased esophageal distensibility (r −0.82; P < .0001).
Study details: This prospective observational study included 27 children with EoE (age 5-17 years) and 25 control children without EoE who consumed four food items, each representing a different texture (puree, soft solid, chewable, and hard solid).
Disclosures: This study was supported by the 2021 American College of Gastroenterology Clinical Research Award and other sources. The authors declared no conflicts of interest.
Source: Kennedy KV, Umeweni CN, Alston M, et al. Esophageal remodeling correlates with eating behaviors in pediatric eosinophilic esophagitis. Am J Gastroenterol. 2024 (Jan 18). doi: 10.14309/ajg.0000000000002661 Source
Key clinical point: Altered eating behaviors, including increased chewing and increased consumption time, observed in children with eosinophilic esophagitis (EoE) correlated with patient-reported symptoms, endoscopic findings, and histologic features.
Major finding: Children with vs without EoE demonstrated more chews per bite and increased consumption time with soft solid (P = .031 and P = .002, respectively), chewable (P = .047 and P = .005, respectively), and hard solid (P = .037 and P = .034, respectively) foods. Increased consumption time significantly correlated with a peak eosinophil count (r 0.42; P = .050) and decreased esophageal distensibility (r −0.82; P < .0001).
Study details: This prospective observational study included 27 children with EoE (age 5-17 years) and 25 control children without EoE who consumed four food items, each representing a different texture (puree, soft solid, chewable, and hard solid).
Disclosures: This study was supported by the 2021 American College of Gastroenterology Clinical Research Award and other sources. The authors declared no conflicts of interest.
Source: Kennedy KV, Umeweni CN, Alston M, et al. Esophageal remodeling correlates with eating behaviors in pediatric eosinophilic esophagitis. Am J Gastroenterol. 2024 (Jan 18). doi: 10.14309/ajg.0000000000002661 Source
Major Basic Protein Can Distinguish Eosinophilic Esophagitis From IBD-Associated Eosinophilia
Key clinical point: Eosinophilic esophagitis (EoE) can be distinguished from eosinophilia caused by inflammatory bowel diseases (IBD) by measuring the expression levels of the major basic protein (MBP) biomarker.
Major finding: The median MBP staining levels were significantly higher in patients with EoE vs those with IBD-associated eosinophilia (52.8 vs 0.2; P < .001). Based on the MBP cutoff point of 3.49 units that distinguished EoE from non-EoE cases, 100% of patients with EoE were MBP positive compared with 3% of patients with IBD-associated eosinophilia (P < .05).
Study details: This retrospective study included 29 patients with EoE, 27 patients with both EoE and IBD, 29 patients with IBD-associated eosinophilia, 30 patients with IBD, and 30 control individuals without either EoE or IBD.
Disclosures: This study did not report any source of funding. The authors declared no conflicts of interest.
Source: Butzke S, Nasiri-Blomgren S, Corao-Uribe D, He Z, Molle-Rios Z. Major basic protein is a useful marker to distinguish eosinophilic esophagitis from IBD-associated eosinophilia in children. J Pediatr Gastroenterol Nutr. 2024 (Feb 5). doi: 10.1002/jpn3.12143 Source
Key clinical point: Eosinophilic esophagitis (EoE) can be distinguished from eosinophilia caused by inflammatory bowel diseases (IBD) by measuring the expression levels of the major basic protein (MBP) biomarker.
Major finding: The median MBP staining levels were significantly higher in patients with EoE vs those with IBD-associated eosinophilia (52.8 vs 0.2; P < .001). Based on the MBP cutoff point of 3.49 units that distinguished EoE from non-EoE cases, 100% of patients with EoE were MBP positive compared with 3% of patients with IBD-associated eosinophilia (P < .05).
Study details: This retrospective study included 29 patients with EoE, 27 patients with both EoE and IBD, 29 patients with IBD-associated eosinophilia, 30 patients with IBD, and 30 control individuals without either EoE or IBD.
Disclosures: This study did not report any source of funding. The authors declared no conflicts of interest.
Source: Butzke S, Nasiri-Blomgren S, Corao-Uribe D, He Z, Molle-Rios Z. Major basic protein is a useful marker to distinguish eosinophilic esophagitis from IBD-associated eosinophilia in children. J Pediatr Gastroenterol Nutr. 2024 (Feb 5). doi: 10.1002/jpn3.12143 Source
Key clinical point: Eosinophilic esophagitis (EoE) can be distinguished from eosinophilia caused by inflammatory bowel diseases (IBD) by measuring the expression levels of the major basic protein (MBP) biomarker.
Major finding: The median MBP staining levels were significantly higher in patients with EoE vs those with IBD-associated eosinophilia (52.8 vs 0.2; P < .001). Based on the MBP cutoff point of 3.49 units that distinguished EoE from non-EoE cases, 100% of patients with EoE were MBP positive compared with 3% of patients with IBD-associated eosinophilia (P < .05).
Study details: This retrospective study included 29 patients with EoE, 27 patients with both EoE and IBD, 29 patients with IBD-associated eosinophilia, 30 patients with IBD, and 30 control individuals without either EoE or IBD.
Disclosures: This study did not report any source of funding. The authors declared no conflicts of interest.
Source: Butzke S, Nasiri-Blomgren S, Corao-Uribe D, He Z, Molle-Rios Z. Major basic protein is a useful marker to distinguish eosinophilic esophagitis from IBD-associated eosinophilia in children. J Pediatr Gastroenterol Nutr. 2024 (Feb 5). doi: 10.1002/jpn3.12143 Source
Psychosocial Burden in Pediatric Patients with Eosinophilic Esophagitis
Key clinical point: Pediatric patients with a more recent diagnosis of eosinophilic esophagitis (EoE) are likely to have a greater psychosocial burden from their condition, with a higher symptom burden score correlating positively with somatic symptom scores and negatively with quality of life (QoL).
Major finding: Compared with patients with longer disease duration (>12 months), those with shorter disease duration (6-12 months) had higher symptom burden (P = .03), somatic symptom (P < .01), and trait anxiety (P < .01) scores. Furthermore, a higher symptom burden was significantly associated with increased somatic symptoms (adjusted β [aβ] 0.34; 95% CI 0.23-0.45) and decreased QoL (aβ −0.42; 95% CI −0.59 to −0.25).
Study details: Findings are from a cross-sectional study including 87 pediatric patients with EoE, of whom 71 patients had longer disease duration.
Disclosures: This study was supported by a grant from the University of California San Diego (USCD) Academic Senate and US National Institutes of Health K24 and partially supported by the UCSD Altman Clinical and Translational Research Institute (ACTRI). The authors declared no conflicts of interest.
Source: Jensen ET, Chaiboonma K, Ayala O, Proia A, Aceves SS. Sleep, anxiety, somatization, quality of life, and resilience in pediatric patients with eosinophilic esophagitis. Clin Transl Gastroenterol. 2024 (Jan 11). Doi: 10.14309/ctg.0000000000000672 Source
Key clinical point: Pediatric patients with a more recent diagnosis of eosinophilic esophagitis (EoE) are likely to have a greater psychosocial burden from their condition, with a higher symptom burden score correlating positively with somatic symptom scores and negatively with quality of life (QoL).
Major finding: Compared with patients with longer disease duration (>12 months), those with shorter disease duration (6-12 months) had higher symptom burden (P = .03), somatic symptom (P < .01), and trait anxiety (P < .01) scores. Furthermore, a higher symptom burden was significantly associated with increased somatic symptoms (adjusted β [aβ] 0.34; 95% CI 0.23-0.45) and decreased QoL (aβ −0.42; 95% CI −0.59 to −0.25).
Study details: Findings are from a cross-sectional study including 87 pediatric patients with EoE, of whom 71 patients had longer disease duration.
Disclosures: This study was supported by a grant from the University of California San Diego (USCD) Academic Senate and US National Institutes of Health K24 and partially supported by the UCSD Altman Clinical and Translational Research Institute (ACTRI). The authors declared no conflicts of interest.
Source: Jensen ET, Chaiboonma K, Ayala O, Proia A, Aceves SS. Sleep, anxiety, somatization, quality of life, and resilience in pediatric patients with eosinophilic esophagitis. Clin Transl Gastroenterol. 2024 (Jan 11). Doi: 10.14309/ctg.0000000000000672 Source
Key clinical point: Pediatric patients with a more recent diagnosis of eosinophilic esophagitis (EoE) are likely to have a greater psychosocial burden from their condition, with a higher symptom burden score correlating positively with somatic symptom scores and negatively with quality of life (QoL).
Major finding: Compared with patients with longer disease duration (>12 months), those with shorter disease duration (6-12 months) had higher symptom burden (P = .03), somatic symptom (P < .01), and trait anxiety (P < .01) scores. Furthermore, a higher symptom burden was significantly associated with increased somatic symptoms (adjusted β [aβ] 0.34; 95% CI 0.23-0.45) and decreased QoL (aβ −0.42; 95% CI −0.59 to −0.25).
Study details: Findings are from a cross-sectional study including 87 pediatric patients with EoE, of whom 71 patients had longer disease duration.
Disclosures: This study was supported by a grant from the University of California San Diego (USCD) Academic Senate and US National Institutes of Health K24 and partially supported by the UCSD Altman Clinical and Translational Research Institute (ACTRI). The authors declared no conflicts of interest.
Source: Jensen ET, Chaiboonma K, Ayala O, Proia A, Aceves SS. Sleep, anxiety, somatization, quality of life, and resilience in pediatric patients with eosinophilic esophagitis. Clin Transl Gastroenterol. 2024 (Jan 11). Doi: 10.14309/ctg.0000000000000672 Source
Early Clinical Benefits With Dupilumab in Eosinophilic Esophagitis
Key clinical point: Treatment with dupilumab led to histologic remission and clinical benefits in patients with eosinophilic esophagitis (EoE) as early as within 12 weeks.
Major finding: The median composite symptom score reduced from 5.5 to 0 (P = .000488) and the median peak eosinophil counts decreased from 44.5 eosinophils/high‐power field (eos/hpf) to 2 eos/hpf (P = .000977) in patients who received dupilumab for 0-12 weeks. However, there were no significant differences in changes in median composite symptom score (P = .1350) and peak eosinophil count (P = .0746) among patients who received dupilumab between 0-12, 12-24, and >24 weeks.
Study details: This retrospective study included 79 patients with EoE who received dupilumab for a median period of 22.7 weeks, and of whom 12 patients received dupilumab for 0-12 weeks.
Disclosures: This study did not receive any specific funding. The corresponding author J Leung declared serving as a consultant for several sources.
Source: Sia T, Miller A, Bacchus L, et al. Dupilumab improves clinical and histologic features of eosinophilic esophagitis prior to 12 weeks of treatment. Clin Transl Allergy. 2024;14(1):e12333. Doi: 10.1002/clt2.12333 Source
Key clinical point: Treatment with dupilumab led to histologic remission and clinical benefits in patients with eosinophilic esophagitis (EoE) as early as within 12 weeks.
Major finding: The median composite symptom score reduced from 5.5 to 0 (P = .000488) and the median peak eosinophil counts decreased from 44.5 eosinophils/high‐power field (eos/hpf) to 2 eos/hpf (P = .000977) in patients who received dupilumab for 0-12 weeks. However, there were no significant differences in changes in median composite symptom score (P = .1350) and peak eosinophil count (P = .0746) among patients who received dupilumab between 0-12, 12-24, and >24 weeks.
Study details: This retrospective study included 79 patients with EoE who received dupilumab for a median period of 22.7 weeks, and of whom 12 patients received dupilumab for 0-12 weeks.
Disclosures: This study did not receive any specific funding. The corresponding author J Leung declared serving as a consultant for several sources.
Source: Sia T, Miller A, Bacchus L, et al. Dupilumab improves clinical and histologic features of eosinophilic esophagitis prior to 12 weeks of treatment. Clin Transl Allergy. 2024;14(1):e12333. Doi: 10.1002/clt2.12333 Source
Key clinical point: Treatment with dupilumab led to histologic remission and clinical benefits in patients with eosinophilic esophagitis (EoE) as early as within 12 weeks.
Major finding: The median composite symptom score reduced from 5.5 to 0 (P = .000488) and the median peak eosinophil counts decreased from 44.5 eosinophils/high‐power field (eos/hpf) to 2 eos/hpf (P = .000977) in patients who received dupilumab for 0-12 weeks. However, there were no significant differences in changes in median composite symptom score (P = .1350) and peak eosinophil count (P = .0746) among patients who received dupilumab between 0-12, 12-24, and >24 weeks.
Study details: This retrospective study included 79 patients with EoE who received dupilumab for a median period of 22.7 weeks, and of whom 12 patients received dupilumab for 0-12 weeks.
Disclosures: This study did not receive any specific funding. The corresponding author J Leung declared serving as a consultant for several sources.
Source: Sia T, Miller A, Bacchus L, et al. Dupilumab improves clinical and histologic features of eosinophilic esophagitis prior to 12 weeks of treatment. Clin Transl Allergy. 2024;14(1):e12333. Doi: 10.1002/clt2.12333 Source
Co-Diagnosis of Eosinophilic Esophagitis and IBD Increases Disease Burden
Key clinical point: Patients diagnosed with both eosinophilic esophagitis (EoE) and inflammatory bowel diseases (IBD), like ulcerative colitis (UC) or Crohn’s disease (CD), are found to be more susceptible to immune-mediated comorbidities and IBD-related conditions but less susceptible to food bolus impaction.
Major finding: The risk for IBD-related complications (adjusted hazard ratio [aHR] > 1.1; P < .05) was higher, whereas the risk for food bolus impaction was lower (aHR 0.445; P = .0011), in patients with EoE and a concurrent diagnosis of IBD. The risk for immune-related comorbidities, such as celiac disease, IBD-related inflammatory conditions, eczema, and asthma, was also higher (P < .05) in patients with IBD who did vs did not have EoE.
Study details: Findings are from a retrospective population-based cohort study that included 174,755 patients with CD, 150,774 patients with UC, and 47,615 patients with EoE.
Disclosures: This study did not receive any funding. The authors declared no conflicts of interest.
Source: Malik A, Liu BD, Zhu L, Kaelber D, Song G. A comprehensive global population-based analysis on the coexistence of eosinophilic esophagitis and inflammatory bowel disease. Dig Dis Sci. 2024 (Jan 13). doi: 10.1007/s10620-024-08283-2 Source
Key clinical point: Patients diagnosed with both eosinophilic esophagitis (EoE) and inflammatory bowel diseases (IBD), like ulcerative colitis (UC) or Crohn’s disease (CD), are found to be more susceptible to immune-mediated comorbidities and IBD-related conditions but less susceptible to food bolus impaction.
Major finding: The risk for IBD-related complications (adjusted hazard ratio [aHR] > 1.1; P < .05) was higher, whereas the risk for food bolus impaction was lower (aHR 0.445; P = .0011), in patients with EoE and a concurrent diagnosis of IBD. The risk for immune-related comorbidities, such as celiac disease, IBD-related inflammatory conditions, eczema, and asthma, was also higher (P < .05) in patients with IBD who did vs did not have EoE.
Study details: Findings are from a retrospective population-based cohort study that included 174,755 patients with CD, 150,774 patients with UC, and 47,615 patients with EoE.
Disclosures: This study did not receive any funding. The authors declared no conflicts of interest.
Source: Malik A, Liu BD, Zhu L, Kaelber D, Song G. A comprehensive global population-based analysis on the coexistence of eosinophilic esophagitis and inflammatory bowel disease. Dig Dis Sci. 2024 (Jan 13). doi: 10.1007/s10620-024-08283-2 Source
Key clinical point: Patients diagnosed with both eosinophilic esophagitis (EoE) and inflammatory bowel diseases (IBD), like ulcerative colitis (UC) or Crohn’s disease (CD), are found to be more susceptible to immune-mediated comorbidities and IBD-related conditions but less susceptible to food bolus impaction.
Major finding: The risk for IBD-related complications (adjusted hazard ratio [aHR] > 1.1; P < .05) was higher, whereas the risk for food bolus impaction was lower (aHR 0.445; P = .0011), in patients with EoE and a concurrent diagnosis of IBD. The risk for immune-related comorbidities, such as celiac disease, IBD-related inflammatory conditions, eczema, and asthma, was also higher (P < .05) in patients with IBD who did vs did not have EoE.
Study details: Findings are from a retrospective population-based cohort study that included 174,755 patients with CD, 150,774 patients with UC, and 47,615 patients with EoE.
Disclosures: This study did not receive any funding. The authors declared no conflicts of interest.
Source: Malik A, Liu BD, Zhu L, Kaelber D, Song G. A comprehensive global population-based analysis on the coexistence of eosinophilic esophagitis and inflammatory bowel disease. Dig Dis Sci. 2024 (Jan 13). doi: 10.1007/s10620-024-08283-2 Source
Twice- vs Once-Daily PPI Better Suited to Induce Remission in Eosinophilic Esophagitis
Key clinical point: A twice-daily moderate proton pump inhibitor (PPI) dose (20 mg omeprazole twice daily) induced greater histologic response rates in patients with eosinophilic esophagitis (EoE) than a once-daily moderate PPI dose (40 mg once daily), regardless of the total daily dosage.
Major finding: The rate of histologic remission significantly improved with twice-daily moderate vs once-daily moderate PPI dose (52.8% vs 10.0%; P < .0001). Compared with a standard PPI dose (20 mg omeprazole once daily), twice-daily moderate (adjusted odds ratio [aOR] 6.75; P = .0008) and high (40 mg omeprazole twice daily; aOR 12.8; P < .0001) PPI doses were associated with increased odds of histologic response.
Study details: This retrospective cohort study included 305 newly diagnosed patients with EoE who received standard, once-daily moderate, twice-daily moderate, or high PPI doses for more than 8 weeks.
Disclosures: This study did not disclose the source of any funding. Walter W. Chan declared serving on scientific advisory boards for various organizations, including Sanofi and Regeneron Pharmaceuticals.
Source: Muftah M, Goldin AH, Barshop K, et al. Twice daily PPI induces higher remission rate in eosinophilic esophagitis than once daily regimen regardless of total daily dose. Am J Gastroenterol. 2024 (Feb 5). doi: 10.14309/ajg.0000000000002712 Source
Key clinical point: A twice-daily moderate proton pump inhibitor (PPI) dose (20 mg omeprazole twice daily) induced greater histologic response rates in patients with eosinophilic esophagitis (EoE) than a once-daily moderate PPI dose (40 mg once daily), regardless of the total daily dosage.
Major finding: The rate of histologic remission significantly improved with twice-daily moderate vs once-daily moderate PPI dose (52.8% vs 10.0%; P < .0001). Compared with a standard PPI dose (20 mg omeprazole once daily), twice-daily moderate (adjusted odds ratio [aOR] 6.75; P = .0008) and high (40 mg omeprazole twice daily; aOR 12.8; P < .0001) PPI doses were associated with increased odds of histologic response.
Study details: This retrospective cohort study included 305 newly diagnosed patients with EoE who received standard, once-daily moderate, twice-daily moderate, or high PPI doses for more than 8 weeks.
Disclosures: This study did not disclose the source of any funding. Walter W. Chan declared serving on scientific advisory boards for various organizations, including Sanofi and Regeneron Pharmaceuticals.
Source: Muftah M, Goldin AH, Barshop K, et al. Twice daily PPI induces higher remission rate in eosinophilic esophagitis than once daily regimen regardless of total daily dose. Am J Gastroenterol. 2024 (Feb 5). doi: 10.14309/ajg.0000000000002712 Source
Key clinical point: A twice-daily moderate proton pump inhibitor (PPI) dose (20 mg omeprazole twice daily) induced greater histologic response rates in patients with eosinophilic esophagitis (EoE) than a once-daily moderate PPI dose (40 mg once daily), regardless of the total daily dosage.
Major finding: The rate of histologic remission significantly improved with twice-daily moderate vs once-daily moderate PPI dose (52.8% vs 10.0%; P < .0001). Compared with a standard PPI dose (20 mg omeprazole once daily), twice-daily moderate (adjusted odds ratio [aOR] 6.75; P = .0008) and high (40 mg omeprazole twice daily; aOR 12.8; P < .0001) PPI doses were associated with increased odds of histologic response.
Study details: This retrospective cohort study included 305 newly diagnosed patients with EoE who received standard, once-daily moderate, twice-daily moderate, or high PPI doses for more than 8 weeks.
Disclosures: This study did not disclose the source of any funding. Walter W. Chan declared serving on scientific advisory boards for various organizations, including Sanofi and Regeneron Pharmaceuticals.
Source: Muftah M, Goldin AH, Barshop K, et al. Twice daily PPI induces higher remission rate in eosinophilic esophagitis than once daily regimen regardless of total daily dose. Am J Gastroenterol. 2024 (Feb 5). doi: 10.14309/ajg.0000000000002712 Source