User login
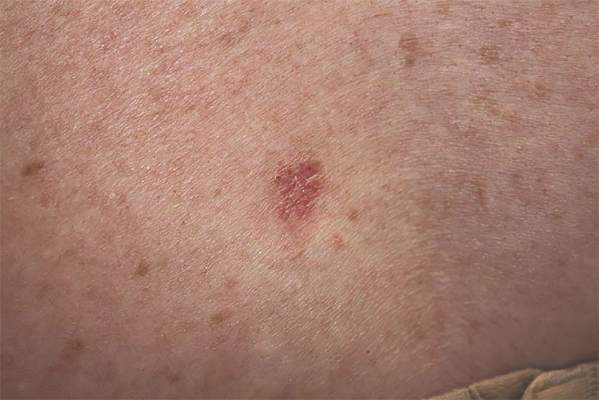
Annual U.S. incidence of BCC pegged at 2 million
Approximately 2 million basal cell carcinomas occur in the United States each year, a number that has increased only modestly during the past 15 years, according to a report published online June 3 in JAMA Dermatology.
The epidemiology of BCCs has been difficult to pin down because these tumors are excluded from cancer registries and national cancer surveillance programs, and because when they are tracked they are usually lumped together with squamous cell carcinomas. The most recent National Cancer Institute–funded survey of BCC was done more than 30 years ago.
So the current incidence of BCC “is not well characterized.” Nevertheless. some researchers have posited that the incidence has risen 80%-200% during the past 10-20 years, said Dr. Maryam M. Asgari of Kaiser Permanente Northern California, Oakland, and the department of dermatology at the University of California, San Francisco.
To estimate incidence more accurately, Dr. Asgari and her associates analyzed data from every electronic pathology report in a registry covering the 3.2 million participants in the HMO from 1998 through 2012. They identified 221,624 cases of BCC in patients aged 2-105 years. The annual incidence increased from 513 to 600 cases per 100,000 population during the study period – a 17% rise that was deemed “not remarkable.”
“In extrapolating our data to the United States, we estimate that approximately 2 million individuals develop at least one BCC in the U.S. in a given year,” Dr. Asgari and her associates wrote (JAMA Dermatol. 2015 June 3 [doi:10.1001/jamadermatol.2015.1188]).
This total is higher than that cited on the National Institutes of Health website, which estimates the annual incidence of all nonmelanoma skin cancers, not just BCC, at 2 million per year.
Males were at higher risk than were females for developing BCC (incidence rate ratio, 1.65), and risk increased with increasing patient age. As expected, whites were at 8- to 70-fold greater risk than were Hispanics, Asians, or blacks. Contrary to one previous report, the incidence of BCC did not increase among Hispanics during the study period.
The National Cancer Institute and the National Institutes of Health supported the study. Dr. Asgari reported receiving research grants from Kaiser Permanente, Pfizer, and Valeant Pharmaceuticals, but not for this project.
Approximately 2 million basal cell carcinomas occur in the United States each year, a number that has increased only modestly during the past 15 years, according to a report published online June 3 in JAMA Dermatology.
The epidemiology of BCCs has been difficult to pin down because these tumors are excluded from cancer registries and national cancer surveillance programs, and because when they are tracked they are usually lumped together with squamous cell carcinomas. The most recent National Cancer Institute–funded survey of BCC was done more than 30 years ago.
So the current incidence of BCC “is not well characterized.” Nevertheless. some researchers have posited that the incidence has risen 80%-200% during the past 10-20 years, said Dr. Maryam M. Asgari of Kaiser Permanente Northern California, Oakland, and the department of dermatology at the University of California, San Francisco.
To estimate incidence more accurately, Dr. Asgari and her associates analyzed data from every electronic pathology report in a registry covering the 3.2 million participants in the HMO from 1998 through 2012. They identified 221,624 cases of BCC in patients aged 2-105 years. The annual incidence increased from 513 to 600 cases per 100,000 population during the study period – a 17% rise that was deemed “not remarkable.”
“In extrapolating our data to the United States, we estimate that approximately 2 million individuals develop at least one BCC in the U.S. in a given year,” Dr. Asgari and her associates wrote (JAMA Dermatol. 2015 June 3 [doi:10.1001/jamadermatol.2015.1188]).
This total is higher than that cited on the National Institutes of Health website, which estimates the annual incidence of all nonmelanoma skin cancers, not just BCC, at 2 million per year.
Males were at higher risk than were females for developing BCC (incidence rate ratio, 1.65), and risk increased with increasing patient age. As expected, whites were at 8- to 70-fold greater risk than were Hispanics, Asians, or blacks. Contrary to one previous report, the incidence of BCC did not increase among Hispanics during the study period.
The National Cancer Institute and the National Institutes of Health supported the study. Dr. Asgari reported receiving research grants from Kaiser Permanente, Pfizer, and Valeant Pharmaceuticals, but not for this project.
Approximately 2 million basal cell carcinomas occur in the United States each year, a number that has increased only modestly during the past 15 years, according to a report published online June 3 in JAMA Dermatology.
The epidemiology of BCCs has been difficult to pin down because these tumors are excluded from cancer registries and national cancer surveillance programs, and because when they are tracked they are usually lumped together with squamous cell carcinomas. The most recent National Cancer Institute–funded survey of BCC was done more than 30 years ago.
So the current incidence of BCC “is not well characterized.” Nevertheless. some researchers have posited that the incidence has risen 80%-200% during the past 10-20 years, said Dr. Maryam M. Asgari of Kaiser Permanente Northern California, Oakland, and the department of dermatology at the University of California, San Francisco.
To estimate incidence more accurately, Dr. Asgari and her associates analyzed data from every electronic pathology report in a registry covering the 3.2 million participants in the HMO from 1998 through 2012. They identified 221,624 cases of BCC in patients aged 2-105 years. The annual incidence increased from 513 to 600 cases per 100,000 population during the study period – a 17% rise that was deemed “not remarkable.”
“In extrapolating our data to the United States, we estimate that approximately 2 million individuals develop at least one BCC in the U.S. in a given year,” Dr. Asgari and her associates wrote (JAMA Dermatol. 2015 June 3 [doi:10.1001/jamadermatol.2015.1188]).
This total is higher than that cited on the National Institutes of Health website, which estimates the annual incidence of all nonmelanoma skin cancers, not just BCC, at 2 million per year.
Males were at higher risk than were females for developing BCC (incidence rate ratio, 1.65), and risk increased with increasing patient age. As expected, whites were at 8- to 70-fold greater risk than were Hispanics, Asians, or blacks. Contrary to one previous report, the incidence of BCC did not increase among Hispanics during the study period.
The National Cancer Institute and the National Institutes of Health supported the study. Dr. Asgari reported receiving research grants from Kaiser Permanente, Pfizer, and Valeant Pharmaceuticals, but not for this project.
Key clinical point: The annual incidence of basal cell carcinoma is estimated to be 2 million in the United States.
Major finding: The annual incidence of BCC increased from 513 to 600 cases per 100,000 population during the study period – a 17% rise that was deemed “not remarkable.”
Data source: A retrospective cohort study involving 147,093 patients with BCC treated at a northern California HMO during 1998-2012.
Disclosures: The National Cancer Institute and the National Institutes of Health supported the study. Dr. Asgari reported receiving research grants from Kaiser Permanente, Pfizer, and Valeant Pharmaceuticals, but not for this project.
High-flow oxygen benefits acute hypoxemic respiratory failure
High-flow oxygen delivered via nasal cannula significantly decreased mortality and improved comfort for ICU patients with nonhypercapnic acute hypoxemic respiratory failure, according to a report published online June 4 in the New England Journal of Medicine.
High-flow oxygen didn’t reduce endotracheal 1-month intubation rates, however, as compared with standard oxygen delivery or noninvasive ventilation in a prospective randomized controlled trial comparing the three techniques at 23 ICUs across France and Belgium, said Dr. Jean-Pierre Frat of Centre Hospitalier Universitaire de Poitiers (France) and his associates.
The 2-year study included 310 adults with nonhypercapnic acute hypoxemic respiratory failure, which was usually the result of community-acquired pneumonia. Patients were randomly assigned to receive high-flow oxygen delivered continuously through large-bore nasal prongs (106 patients), standard oxygen therapy delivered continuously through a nonrebreather face mask (94 patients), or noninvasive ventilation delivered through a face mask connected to an ICU ventilator (110 patients).
Intubation rates at 30 days were 38% for high-flow oxygen, 47% for standard oxygen, and 50% for noninvasive ventilation, which are nonsignificant differences. The hazard ratio for death at 90 days was 2.01 for standard oxygen and 2.50 for noninvasive ventilation, as compared with high-flow oxygen. And the number of ventilator-free days at 1 month was significantly greater with high-flow oxygen (24 days) than with either of the other techniques (22 days and 19 days, respectively), the researchers said.
High-flow oxygen also reduced the intensity of respiratory discomfort at 1 hour to a significantly greater degree than did either of the other forms of oxygen delivery and decreased the dyspnea score as well. “These findings might result from the heating and humidification of inspired gases, which prevented thick secretions and subsequent atelectasis, but also from low levels of PEEP [positive end-expiratory pressure] generated by a high gas flow rate and flushing of upper-airway dead space,” they added (N. Engl. J. Med. 2015 June 4 [doi:10.1056/NEJMoa1503326]). Rates of complications were similar among the three study groups.
The study was supported by the French Ministry of Health’s Programme Hospitalier de Recherche Clinique Interregional 2010. Dr. Frat reported receiving travel fees from Fisher & Paykel Healthcare and personal fees from SOS Oxygene. Fisher & Paykel Healthcare donated face masks, heated humidifiers, and cannulas and provided air-oxygen blenders to the participating ICUs.
High-flow oxygen delivered via nasal cannula significantly decreased mortality and improved comfort for ICU patients with nonhypercapnic acute hypoxemic respiratory failure, according to a report published online June 4 in the New England Journal of Medicine.
High-flow oxygen didn’t reduce endotracheal 1-month intubation rates, however, as compared with standard oxygen delivery or noninvasive ventilation in a prospective randomized controlled trial comparing the three techniques at 23 ICUs across France and Belgium, said Dr. Jean-Pierre Frat of Centre Hospitalier Universitaire de Poitiers (France) and his associates.
The 2-year study included 310 adults with nonhypercapnic acute hypoxemic respiratory failure, which was usually the result of community-acquired pneumonia. Patients were randomly assigned to receive high-flow oxygen delivered continuously through large-bore nasal prongs (106 patients), standard oxygen therapy delivered continuously through a nonrebreather face mask (94 patients), or noninvasive ventilation delivered through a face mask connected to an ICU ventilator (110 patients).
Intubation rates at 30 days were 38% for high-flow oxygen, 47% for standard oxygen, and 50% for noninvasive ventilation, which are nonsignificant differences. The hazard ratio for death at 90 days was 2.01 for standard oxygen and 2.50 for noninvasive ventilation, as compared with high-flow oxygen. And the number of ventilator-free days at 1 month was significantly greater with high-flow oxygen (24 days) than with either of the other techniques (22 days and 19 days, respectively), the researchers said.
High-flow oxygen also reduced the intensity of respiratory discomfort at 1 hour to a significantly greater degree than did either of the other forms of oxygen delivery and decreased the dyspnea score as well. “These findings might result from the heating and humidification of inspired gases, which prevented thick secretions and subsequent atelectasis, but also from low levels of PEEP [positive end-expiratory pressure] generated by a high gas flow rate and flushing of upper-airway dead space,” they added (N. Engl. J. Med. 2015 June 4 [doi:10.1056/NEJMoa1503326]). Rates of complications were similar among the three study groups.
The study was supported by the French Ministry of Health’s Programme Hospitalier de Recherche Clinique Interregional 2010. Dr. Frat reported receiving travel fees from Fisher & Paykel Healthcare and personal fees from SOS Oxygene. Fisher & Paykel Healthcare donated face masks, heated humidifiers, and cannulas and provided air-oxygen blenders to the participating ICUs.
High-flow oxygen delivered via nasal cannula significantly decreased mortality and improved comfort for ICU patients with nonhypercapnic acute hypoxemic respiratory failure, according to a report published online June 4 in the New England Journal of Medicine.
High-flow oxygen didn’t reduce endotracheal 1-month intubation rates, however, as compared with standard oxygen delivery or noninvasive ventilation in a prospective randomized controlled trial comparing the three techniques at 23 ICUs across France and Belgium, said Dr. Jean-Pierre Frat of Centre Hospitalier Universitaire de Poitiers (France) and his associates.
The 2-year study included 310 adults with nonhypercapnic acute hypoxemic respiratory failure, which was usually the result of community-acquired pneumonia. Patients were randomly assigned to receive high-flow oxygen delivered continuously through large-bore nasal prongs (106 patients), standard oxygen therapy delivered continuously through a nonrebreather face mask (94 patients), or noninvasive ventilation delivered through a face mask connected to an ICU ventilator (110 patients).
Intubation rates at 30 days were 38% for high-flow oxygen, 47% for standard oxygen, and 50% for noninvasive ventilation, which are nonsignificant differences. The hazard ratio for death at 90 days was 2.01 for standard oxygen and 2.50 for noninvasive ventilation, as compared with high-flow oxygen. And the number of ventilator-free days at 1 month was significantly greater with high-flow oxygen (24 days) than with either of the other techniques (22 days and 19 days, respectively), the researchers said.
High-flow oxygen also reduced the intensity of respiratory discomfort at 1 hour to a significantly greater degree than did either of the other forms of oxygen delivery and decreased the dyspnea score as well. “These findings might result from the heating and humidification of inspired gases, which prevented thick secretions and subsequent atelectasis, but also from low levels of PEEP [positive end-expiratory pressure] generated by a high gas flow rate and flushing of upper-airway dead space,” they added (N. Engl. J. Med. 2015 June 4 [doi:10.1056/NEJMoa1503326]). Rates of complications were similar among the three study groups.
The study was supported by the French Ministry of Health’s Programme Hospitalier de Recherche Clinique Interregional 2010. Dr. Frat reported receiving travel fees from Fisher & Paykel Healthcare and personal fees from SOS Oxygene. Fisher & Paykel Healthcare donated face masks, heated humidifiers, and cannulas and provided air-oxygen blenders to the participating ICUs.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Key clinical point: High-flow oxygen through a nasal cannula reduced 90-day mortality in patients with nonhypercapnic acute hypoxemic respiratory failure, as compared with standard oxygen delivery or noninvasive ventilation.
Major finding: The hazard ratio for death at 90 days was 2.01 for standard oxygen and 2.50 for noninvasive ventilation, as compared with high-flow oxygen.
Data source: A prospective multicenter open-label randomized controlled trial involving 310 adult ICU patients in France and Belgium.
Disclosures: The study was supported by the French Ministry of Health’s Programme Hospitalier de Recherche Clinique Interregional 2010. Dr. Frat reported receiving travel fees from Fisher & Paykel Healthcare and personal fees from SOS Oxygene. Fisher & Paykel Healthcare donated face masks, heated humidifiers, and cannulas and provided air-oxygen blenders to the participating ICUs.
Tight glycemic control: Somewhat fewer CV events, same mortality
Tight glycemic control modestly reduced the rate of major cardiovascular events but didn’t improve mortality in an extended follow-up of a clinical trial involving 1,791 veterans with type 2 diabetes, which was published online June 3 in the New England Journal of Medicine.
At the conclusion of the treatment phase of the Veteran Affairs Diabetes Trial in 2008, the primary outcome – the rate of a first major CV event – was nonsignificantly lower with intensive glycemic control than with standard glycemic control. Researchers now report the findings after an additional 7.5 years of follow-up of 92% of the participants in that multicenter unblended randomized controlled trial.
During the treatment phase of the study, median glycated hemoglobin level differed by 1.5 percentage points between patients who received intensive therapy (6.9%) and patients who received standard therapy (8.4%). During follow-up, this difference declined to only 0.2-0.3 percentage points. “Even with the support of a dedicated research team, only approximately half the participants [achieved] a glycated hemoglobin level of less than 7%,” said Dr. Rodney A. Hayward of the VA Center for Clinical Management Research, VA Ann Arbor (Mich.) Healthcare System, and his associates.
During extended follow-up, there were 253 major CV events in the group randomly assigned to intensive therapy and 288 in the group assigned to standard therapy. Tight glycemic control using a multidrug regimen was associated with a significant, though modest, 17% relative reduction in a the primary composite outcome of heart attack, stroke, new or worsening congestive heart failure, death from CV causes, or amputation due to ischemic gangrene. This represents 8.6 CV events prevented per 1,000 person-years.
However, there was no evidence of any reduction in either cardiovascular or all-cause mortality. In addition, treatment effects were no different between patients at high and those at low cardiovascular risk, the investigators said (N. Engl. J. Med. 2015 June 3 [doi:10.1056/NEJMoa1414266]).
“In the absence of a reduction in total mortality, a small to moderate reduction in the rate of CV events needs to be weighed against potential harm due to overly aggressive care and the burden, long-term safety profile, and side effects of treatment, including weight gain and hypoglycemia,” they added.
Tight glycemic control modestly reduced the rate of major cardiovascular events but didn’t improve mortality in an extended follow-up of a clinical trial involving 1,791 veterans with type 2 diabetes, which was published online June 3 in the New England Journal of Medicine.
At the conclusion of the treatment phase of the Veteran Affairs Diabetes Trial in 2008, the primary outcome – the rate of a first major CV event – was nonsignificantly lower with intensive glycemic control than with standard glycemic control. Researchers now report the findings after an additional 7.5 years of follow-up of 92% of the participants in that multicenter unblended randomized controlled trial.
During the treatment phase of the study, median glycated hemoglobin level differed by 1.5 percentage points between patients who received intensive therapy (6.9%) and patients who received standard therapy (8.4%). During follow-up, this difference declined to only 0.2-0.3 percentage points. “Even with the support of a dedicated research team, only approximately half the participants [achieved] a glycated hemoglobin level of less than 7%,” said Dr. Rodney A. Hayward of the VA Center for Clinical Management Research, VA Ann Arbor (Mich.) Healthcare System, and his associates.
During extended follow-up, there were 253 major CV events in the group randomly assigned to intensive therapy and 288 in the group assigned to standard therapy. Tight glycemic control using a multidrug regimen was associated with a significant, though modest, 17% relative reduction in a the primary composite outcome of heart attack, stroke, new or worsening congestive heart failure, death from CV causes, or amputation due to ischemic gangrene. This represents 8.6 CV events prevented per 1,000 person-years.
However, there was no evidence of any reduction in either cardiovascular or all-cause mortality. In addition, treatment effects were no different between patients at high and those at low cardiovascular risk, the investigators said (N. Engl. J. Med. 2015 June 3 [doi:10.1056/NEJMoa1414266]).
“In the absence of a reduction in total mortality, a small to moderate reduction in the rate of CV events needs to be weighed against potential harm due to overly aggressive care and the burden, long-term safety profile, and side effects of treatment, including weight gain and hypoglycemia,” they added.
Tight glycemic control modestly reduced the rate of major cardiovascular events but didn’t improve mortality in an extended follow-up of a clinical trial involving 1,791 veterans with type 2 diabetes, which was published online June 3 in the New England Journal of Medicine.
At the conclusion of the treatment phase of the Veteran Affairs Diabetes Trial in 2008, the primary outcome – the rate of a first major CV event – was nonsignificantly lower with intensive glycemic control than with standard glycemic control. Researchers now report the findings after an additional 7.5 years of follow-up of 92% of the participants in that multicenter unblended randomized controlled trial.
During the treatment phase of the study, median glycated hemoglobin level differed by 1.5 percentage points between patients who received intensive therapy (6.9%) and patients who received standard therapy (8.4%). During follow-up, this difference declined to only 0.2-0.3 percentage points. “Even with the support of a dedicated research team, only approximately half the participants [achieved] a glycated hemoglobin level of less than 7%,” said Dr. Rodney A. Hayward of the VA Center for Clinical Management Research, VA Ann Arbor (Mich.) Healthcare System, and his associates.
During extended follow-up, there were 253 major CV events in the group randomly assigned to intensive therapy and 288 in the group assigned to standard therapy. Tight glycemic control using a multidrug regimen was associated with a significant, though modest, 17% relative reduction in a the primary composite outcome of heart attack, stroke, new or worsening congestive heart failure, death from CV causes, or amputation due to ischemic gangrene. This represents 8.6 CV events prevented per 1,000 person-years.
However, there was no evidence of any reduction in either cardiovascular or all-cause mortality. In addition, treatment effects were no different between patients at high and those at low cardiovascular risk, the investigators said (N. Engl. J. Med. 2015 June 3 [doi:10.1056/NEJMoa1414266]).
“In the absence of a reduction in total mortality, a small to moderate reduction in the rate of CV events needs to be weighed against potential harm due to overly aggressive care and the burden, long-term safety profile, and side effects of treatment, including weight gain and hypoglycemia,” they added.
Key clinical point: Tight glycemic control cut the rate of major cardiovascular events by 17% but didn’t improve mortality in patients with type 2 diabetes.
Major finding: Compared with standard glycemic control, tight glycemic control prevented 8.6 CV events per 1,000 person-years.
Data source: Extended follow-up of an unblinded, multicenter, randomized, controlled trial involving 1,791 veterans with type 2 diabetes.
Disclosures: This study was supported by the VA Cooperative Studies Program, the National Institute of Diabetes and Digestive and Kidney Diseases, and the National Institutes of Health. Dr. Hayward reported having no relevant financial disclosures; two of his associates reported ties to Amgen, AstraZeneca, Merck, and Novo Nordisk.
Newborn’s pulmonary hypertension risk up slightly after SSRI exposure in pregnancy
Exposure to selective serotonin reuptake inhibitor therapy in the last trimester of pregnancy may raise the risk of persistent pulmonary hypertension of the newborn, but that risk is smaller than previous studies have suggested, according to a report published June 2 in JAMA.
Persistent pulmonary hypertension of the newborn (PPHN) is grave, with up to 20% of affected infants dying from the disorder and survivors facing serious long-term sequelae such as chronic lung disease, seizures, and neurodevelopmental problems. The Food and Drug Administration released a public health advisory in 2006 warning that SSRI exposure during late pregnancy may raise the risk of PPHN, based on a single epidemiologic study. Subsequent studies with conflicting findings prompted an update of the advisory in 2011, which concluded that it is not yet possible to determine whether such a link exists.
To examine the possible association, researchers analyzed information concerning 3,789,330 eligible pregnancies during a 10-year period in a Medicaid database covering 46 states and the District of Columbia. A total of 128,950 of these mothers (3.4%) used an antidepressant in the final trimester: 102,179 used an SSRI and 26,771 used a non-SSRI.
After the data were adjusted to account for the substantial differences between women who used antidepressants and women who did not, the adjusted odds ratio for having a neonate with PPHN was 1.10 for women who used SSRIs and 1.02 for those who used non-SSRIs, compared with nonusers.
This indicates that SSRI exposure “may be” associated with an increased risk of PPHN, but the magnitude of that risk – if present – is smaller than previous studies have reported, Krista F. Huybrechts, Ph.D., of the division of pharmacoepidemiology and pharmacoeconomics at Brigham and Women’s Hospital and of Harvard Medical School, both in Boston, and her associates reported (JAMA 2015;313:2142-51 [doi:10.1001/jama.2015.5605]).
“Clinicians and patients need to balance the potential small increase in the risk of PPHN, along with other risks that have been attributed to SSRI use during pregnancy, with the benefits attributable to these drugs in improving maternal health and well-being,” they wrote.
This study was supported by the Agency for Healthcare Research and Quality and the National Institutes of Health. The researchers reported having no financial disclosures.
Exposure to selective serotonin reuptake inhibitor therapy in the last trimester of pregnancy may raise the risk of persistent pulmonary hypertension of the newborn, but that risk is smaller than previous studies have suggested, according to a report published June 2 in JAMA.
Persistent pulmonary hypertension of the newborn (PPHN) is grave, with up to 20% of affected infants dying from the disorder and survivors facing serious long-term sequelae such as chronic lung disease, seizures, and neurodevelopmental problems. The Food and Drug Administration released a public health advisory in 2006 warning that SSRI exposure during late pregnancy may raise the risk of PPHN, based on a single epidemiologic study. Subsequent studies with conflicting findings prompted an update of the advisory in 2011, which concluded that it is not yet possible to determine whether such a link exists.
To examine the possible association, researchers analyzed information concerning 3,789,330 eligible pregnancies during a 10-year period in a Medicaid database covering 46 states and the District of Columbia. A total of 128,950 of these mothers (3.4%) used an antidepressant in the final trimester: 102,179 used an SSRI and 26,771 used a non-SSRI.
After the data were adjusted to account for the substantial differences between women who used antidepressants and women who did not, the adjusted odds ratio for having a neonate with PPHN was 1.10 for women who used SSRIs and 1.02 for those who used non-SSRIs, compared with nonusers.
This indicates that SSRI exposure “may be” associated with an increased risk of PPHN, but the magnitude of that risk – if present – is smaller than previous studies have reported, Krista F. Huybrechts, Ph.D., of the division of pharmacoepidemiology and pharmacoeconomics at Brigham and Women’s Hospital and of Harvard Medical School, both in Boston, and her associates reported (JAMA 2015;313:2142-51 [doi:10.1001/jama.2015.5605]).
“Clinicians and patients need to balance the potential small increase in the risk of PPHN, along with other risks that have been attributed to SSRI use during pregnancy, with the benefits attributable to these drugs in improving maternal health and well-being,” they wrote.
This study was supported by the Agency for Healthcare Research and Quality and the National Institutes of Health. The researchers reported having no financial disclosures.
Exposure to selective serotonin reuptake inhibitor therapy in the last trimester of pregnancy may raise the risk of persistent pulmonary hypertension of the newborn, but that risk is smaller than previous studies have suggested, according to a report published June 2 in JAMA.
Persistent pulmonary hypertension of the newborn (PPHN) is grave, with up to 20% of affected infants dying from the disorder and survivors facing serious long-term sequelae such as chronic lung disease, seizures, and neurodevelopmental problems. The Food and Drug Administration released a public health advisory in 2006 warning that SSRI exposure during late pregnancy may raise the risk of PPHN, based on a single epidemiologic study. Subsequent studies with conflicting findings prompted an update of the advisory in 2011, which concluded that it is not yet possible to determine whether such a link exists.
To examine the possible association, researchers analyzed information concerning 3,789,330 eligible pregnancies during a 10-year period in a Medicaid database covering 46 states and the District of Columbia. A total of 128,950 of these mothers (3.4%) used an antidepressant in the final trimester: 102,179 used an SSRI and 26,771 used a non-SSRI.
After the data were adjusted to account for the substantial differences between women who used antidepressants and women who did not, the adjusted odds ratio for having a neonate with PPHN was 1.10 for women who used SSRIs and 1.02 for those who used non-SSRIs, compared with nonusers.
This indicates that SSRI exposure “may be” associated with an increased risk of PPHN, but the magnitude of that risk – if present – is smaller than previous studies have reported, Krista F. Huybrechts, Ph.D., of the division of pharmacoepidemiology and pharmacoeconomics at Brigham and Women’s Hospital and of Harvard Medical School, both in Boston, and her associates reported (JAMA 2015;313:2142-51 [doi:10.1001/jama.2015.5605]).
“Clinicians and patients need to balance the potential small increase in the risk of PPHN, along with other risks that have been attributed to SSRI use during pregnancy, with the benefits attributable to these drugs in improving maternal health and well-being,” they wrote.
This study was supported by the Agency for Healthcare Research and Quality and the National Institutes of Health. The researchers reported having no financial disclosures.
FROM JAMA
Key clinical point: Exposure to SSRI therapy in the last trimester may raise the risk of persistent pulmonary hypertension of the newborn, but only to a small degree.
Major finding: The adjusted odds ratio for having a neonate with PPHN was 1.10 for women who used SSRIs and 1.02 for those who used non-SSRIs, compared with nonusers.
Data source: A large cohort study involving 3,789,330 completed pregnancies in 46 states during a 10-year period.
Disclosures: This study was supported by the Agency for Healthcare Research and Quality and the National Institutes of Health. The researchers reported having no financial disclosures.
ED revisits twice as frequent as expected
The rate of adult revisits to emergency departments is more than twice as high as has been reported previously – 8% at 3 days and 20% at 30 days – in large part because until now researchers have failed to account for revisits to different hospitals, according to a report published online June 1 in Annals of Internal Medicine.
Little is known about returns to an emergency department following an index ED visit because most studies have assessed only visits to a single institution or to hospitals within a single state or insurance plan. Now researchers have performed a broader examination of the issue by analyzing newly available multistate longitudinal data from the Healthcare Cost and Utilization Project, which allowed them to identify returns to any ED or acute-care hospital. They focused on acute-care revisits after 57,530,239 initial ED visits by adults in six states (Arizona, California, Florida, Nebraska, Utah, and Hawaii) during 2006-2010.
At 3 days after an initial ED visit, the overall revisit rate was 8.2%, with one-third of these revisits occurring at a medical facility different from that of the initial visit. Previously, estimates of 3-day revisits have ranged from 2.7% to 3.4%. At 30 days, the revisit rate was 20%, and approximately one-third of these revisits involved a different facility. Revisits to different institutions “may have special clinical and financial implications because fragmentation of care increases the likelihood of duplication of services and problems with care transitions,” said Dr. Reena Duseja of the department of emergency medicine, University of California, San Francisco, and her associates.
“The scope of revisits to outside institutions is much greater than previously suspected, which suggests that improving communication infrastructure across institutions (such as health information exchanges) may improve care and allow individual institutions to get a more accurate picture of their revisit rates,” they noted (Ann. Intern. Med. 2015 June 1 [doi:10.7326/M14-1616]).
Revisit rates varied substantially according to diagnosis. “Skin and subcutaneous tissue infection”accounted for 23% of revisits. “Abdominal pain” was the diagnosis with the next highest revisit rate (10%). The most frequent diagnosis among patients who revisited a different hospital was back pain (2.6%), and nonspecific chest pain was the diagnosis with the highest rate of later admission to a different hospital (1.1%).
Financial data from the Florida facilities showed that revisits accounted for more of the total costs of ED care than initial visits did. This demonstrates that revisits are a major, and unaccounted for, component of emergency care costs, Dr. Duseja and her associates said.
Because of insufficient data, they could not determine whether these revisits reflected inadequate access to primary care, patient nonadherence to treatment recommendations, poor quality of care at the initial visit, or other factors, the researchers noted.
The findings of Duseja et al. highlight an underappreciated problem and also raise important questions.
To what extent do ED revisits represent gaps in quality as opposed to reasonable strategies that prevent admissions? How often are revisits due to failures of transitional care, suboptimal patient education, or lack of timely follow-up? And why do patients so often seek care at different institutions? Are they dissatisfied with their initial encounter, exercising greater discretion in choosing a facility the second time around, or doing something else?
Dr. Kumar Dharmarajan and Dr. Harlan M. Krumholz are at the Center for Outcomes Research and Evaluation, Yale University, New Haven Conn. Dr. Dharmarajan reported receiving grant support from the National Institute on Aging and the American Federation for Aging Research. Dr. Krumholz reported receiving grant support from the National Heart, Lung, and Blood Institute and the Center for Cardiovascular Outcomes Research at Yale. The investigators made these remarks in an editorial accompanying Dr. Duseja’s report (Ann. Intern. Med. 2015 June 1 [doi:10.7326/M15-0878]).
The findings of Duseja et al. highlight an underappreciated problem and also raise important questions.
To what extent do ED revisits represent gaps in quality as opposed to reasonable strategies that prevent admissions? How often are revisits due to failures of transitional care, suboptimal patient education, or lack of timely follow-up? And why do patients so often seek care at different institutions? Are they dissatisfied with their initial encounter, exercising greater discretion in choosing a facility the second time around, or doing something else?
Dr. Kumar Dharmarajan and Dr. Harlan M. Krumholz are at the Center for Outcomes Research and Evaluation, Yale University, New Haven Conn. Dr. Dharmarajan reported receiving grant support from the National Institute on Aging and the American Federation for Aging Research. Dr. Krumholz reported receiving grant support from the National Heart, Lung, and Blood Institute and the Center for Cardiovascular Outcomes Research at Yale. The investigators made these remarks in an editorial accompanying Dr. Duseja’s report (Ann. Intern. Med. 2015 June 1 [doi:10.7326/M15-0878]).
The findings of Duseja et al. highlight an underappreciated problem and also raise important questions.
To what extent do ED revisits represent gaps in quality as opposed to reasonable strategies that prevent admissions? How often are revisits due to failures of transitional care, suboptimal patient education, or lack of timely follow-up? And why do patients so often seek care at different institutions? Are they dissatisfied with their initial encounter, exercising greater discretion in choosing a facility the second time around, or doing something else?
Dr. Kumar Dharmarajan and Dr. Harlan M. Krumholz are at the Center for Outcomes Research and Evaluation, Yale University, New Haven Conn. Dr. Dharmarajan reported receiving grant support from the National Institute on Aging and the American Federation for Aging Research. Dr. Krumholz reported receiving grant support from the National Heart, Lung, and Blood Institute and the Center for Cardiovascular Outcomes Research at Yale. The investigators made these remarks in an editorial accompanying Dr. Duseja’s report (Ann. Intern. Med. 2015 June 1 [doi:10.7326/M15-0878]).
The rate of adult revisits to emergency departments is more than twice as high as has been reported previously – 8% at 3 days and 20% at 30 days – in large part because until now researchers have failed to account for revisits to different hospitals, according to a report published online June 1 in Annals of Internal Medicine.
Little is known about returns to an emergency department following an index ED visit because most studies have assessed only visits to a single institution or to hospitals within a single state or insurance plan. Now researchers have performed a broader examination of the issue by analyzing newly available multistate longitudinal data from the Healthcare Cost and Utilization Project, which allowed them to identify returns to any ED or acute-care hospital. They focused on acute-care revisits after 57,530,239 initial ED visits by adults in six states (Arizona, California, Florida, Nebraska, Utah, and Hawaii) during 2006-2010.
At 3 days after an initial ED visit, the overall revisit rate was 8.2%, with one-third of these revisits occurring at a medical facility different from that of the initial visit. Previously, estimates of 3-day revisits have ranged from 2.7% to 3.4%. At 30 days, the revisit rate was 20%, and approximately one-third of these revisits involved a different facility. Revisits to different institutions “may have special clinical and financial implications because fragmentation of care increases the likelihood of duplication of services and problems with care transitions,” said Dr. Reena Duseja of the department of emergency medicine, University of California, San Francisco, and her associates.
“The scope of revisits to outside institutions is much greater than previously suspected, which suggests that improving communication infrastructure across institutions (such as health information exchanges) may improve care and allow individual institutions to get a more accurate picture of their revisit rates,” they noted (Ann. Intern. Med. 2015 June 1 [doi:10.7326/M14-1616]).
Revisit rates varied substantially according to diagnosis. “Skin and subcutaneous tissue infection”accounted for 23% of revisits. “Abdominal pain” was the diagnosis with the next highest revisit rate (10%). The most frequent diagnosis among patients who revisited a different hospital was back pain (2.6%), and nonspecific chest pain was the diagnosis with the highest rate of later admission to a different hospital (1.1%).
Financial data from the Florida facilities showed that revisits accounted for more of the total costs of ED care than initial visits did. This demonstrates that revisits are a major, and unaccounted for, component of emergency care costs, Dr. Duseja and her associates said.
Because of insufficient data, they could not determine whether these revisits reflected inadequate access to primary care, patient nonadherence to treatment recommendations, poor quality of care at the initial visit, or other factors, the researchers noted.
The rate of adult revisits to emergency departments is more than twice as high as has been reported previously – 8% at 3 days and 20% at 30 days – in large part because until now researchers have failed to account for revisits to different hospitals, according to a report published online June 1 in Annals of Internal Medicine.
Little is known about returns to an emergency department following an index ED visit because most studies have assessed only visits to a single institution or to hospitals within a single state or insurance plan. Now researchers have performed a broader examination of the issue by analyzing newly available multistate longitudinal data from the Healthcare Cost and Utilization Project, which allowed them to identify returns to any ED or acute-care hospital. They focused on acute-care revisits after 57,530,239 initial ED visits by adults in six states (Arizona, California, Florida, Nebraska, Utah, and Hawaii) during 2006-2010.
At 3 days after an initial ED visit, the overall revisit rate was 8.2%, with one-third of these revisits occurring at a medical facility different from that of the initial visit. Previously, estimates of 3-day revisits have ranged from 2.7% to 3.4%. At 30 days, the revisit rate was 20%, and approximately one-third of these revisits involved a different facility. Revisits to different institutions “may have special clinical and financial implications because fragmentation of care increases the likelihood of duplication of services and problems with care transitions,” said Dr. Reena Duseja of the department of emergency medicine, University of California, San Francisco, and her associates.
“The scope of revisits to outside institutions is much greater than previously suspected, which suggests that improving communication infrastructure across institutions (such as health information exchanges) may improve care and allow individual institutions to get a more accurate picture of their revisit rates,” they noted (Ann. Intern. Med. 2015 June 1 [doi:10.7326/M14-1616]).
Revisit rates varied substantially according to diagnosis. “Skin and subcutaneous tissue infection”accounted for 23% of revisits. “Abdominal pain” was the diagnosis with the next highest revisit rate (10%). The most frequent diagnosis among patients who revisited a different hospital was back pain (2.6%), and nonspecific chest pain was the diagnosis with the highest rate of later admission to a different hospital (1.1%).
Financial data from the Florida facilities showed that revisits accounted for more of the total costs of ED care than initial visits did. This demonstrates that revisits are a major, and unaccounted for, component of emergency care costs, Dr. Duseja and her associates said.
Because of insufficient data, they could not determine whether these revisits reflected inadequate access to primary care, patient nonadherence to treatment recommendations, poor quality of care at the initial visit, or other factors, the researchers noted.
Key clinical point: Revisits to the emergency department were twice as frequent as previously reported: 8% at 3 days and 20% at 30 days.
Major finding: At 3 days after an initial ED visit, the overall revisit rate was 8.2%, and at 30 days it was 20%, with one-third of these revisits occurring at a medical facility different from that of the initial visit.
Data source: A longitudinal, population-based study of adult revisits to the ED after 57,530,239 initial visits in six states during 2006-2010.
Disclosures: This study was supported by the U.S. Agency for Healthcare Research and Quality. The researchers’ financial disclosures are available at www.acponline.org
Oral device reduced obstructive sleep apnea, not sleepiness
An oral appliance that advances a patient’s lower jaw reduced episodes of obstructive sleep apnea, snoring, and restless legs symptoms, according to a report published online June 1 in JAMA Internal Medicine.
The device, however, failed to improve daytime sleepiness or quality of life in a Swedish study of adults who had daytime sleepiness and either snoring or mild to moderate sleep apnea, said Marie Marklund, Ph.D., D.D.S., of the department of odontology at Umeå (Sweden) University and her associates (JAMA Intern. Med. 2015 June 1 [doi:10.1001/jamainternmed.2015.2051]).
Previous studies of oral appliances have focused on patients with more severe sleep apnea and have yielded conflicting results, particularly regarding daytime sleepiness.
A total of 91 patients who were randomly assigned to receive either a placebo device (46 patients) or an oral appliance individually made by a dental technician using separate plaster casts of the upper and lower teeth (45 participants) completed the study. The device’s elastomer pieces fitted over the teeth and were connected with a screw that allowed continuous gradual advancement of the lower jaw by 6-7 mm. Holding the lower mandible forward improves breathing during sleep.
After 4 months of follow-up, at-home overnight polysomnography showed “a clear, significant treatment effect”: the mean apnea-hypopnea index (AHI) was 6.7 in the active-treatment group, compared with 16.7 in the placebo group. A total of 49% of the patients receiving active treatment had an AHI lower than 5, compared with only 11% of those using the placebo device, for an odds ratio of 7.8 and a number needed to treat of 3.
Snoring and symptoms of restless legs also were significantly less frequent with the active treatment, Dr. Marklund and her associates said.
In addition, 73% of patients who used oral appliances said that their expectations of treatment were either “totally” or “sufficiently” fulfilled, compared with only 11% of those who used placebo devices. And 89% of patients who used oral appliances said they would continue the treatment after completing the study, compared with only 52% of those who used the sham device.
However, daytime sleepiness, measured subjectively using the Epworth Sleepiness Scale and the Karolinska Sleepiness Scale and measured objectively using the Oxford Sleep Resistance test, did not differ significantly between the two study groups. The number of days with headaches, the intensity of headaches, the presence of nasal congestion, difficulty falling asleep, nighttime awakenings, nightmares, and reaction times also were not significantly different, nor were scores on a quality of life measure.
The study was supported by grants from the Swedish Research Council, the Swedish Heart and Lung Foundation, and the County Council of Vasterbotten. Dr. Marklund and her associates reported no conflicts of interest.
It appears that patients generally prefer these devices to continuous positive airway pressure (CPAP) therapy. Better adherence to an oral appliance may outweigh the fact that it is not as effective as CPAP. Long-term studies comparing the two approaches are warranted.
The benefits of the mandibular advancement devices used in this study cannot be translated automatically to other devices, because there is a huge variety of these appliances on the market.
The extent of the protrusion of the lower jaw, the stability of the material, and the structural design of the devices vary widely. Several experts currently recommend avoiding the less sophisticated appliances that are not tailored to the individual’s jaw and oral cavity and instead using only customized adjustable appliances made by a trained specialist.
Dr. Winfried J. Randerath is with the pneumonology clinic and the Allergology Center for Sleep Medicine and Respiratory Care at Bethanien Hospital in Solingen, Germany. He reported having no relevant financial disclosures. He has, however, received speaking fees and research funds from companies that produce positive airway pressure devices: Heinen und Lowenstein, Resmed, Respironics, and Weinmann. Dr. Randerath made these remarks in an invited commentary (JAMA Intern. Med. 2015 June 1 [doi:10.1001/jamainternmed.2015.2059]).
It appears that patients generally prefer these devices to continuous positive airway pressure (CPAP) therapy. Better adherence to an oral appliance may outweigh the fact that it is not as effective as CPAP. Long-term studies comparing the two approaches are warranted.
The benefits of the mandibular advancement devices used in this study cannot be translated automatically to other devices, because there is a huge variety of these appliances on the market.
The extent of the protrusion of the lower jaw, the stability of the material, and the structural design of the devices vary widely. Several experts currently recommend avoiding the less sophisticated appliances that are not tailored to the individual’s jaw and oral cavity and instead using only customized adjustable appliances made by a trained specialist.
Dr. Winfried J. Randerath is with the pneumonology clinic and the Allergology Center for Sleep Medicine and Respiratory Care at Bethanien Hospital in Solingen, Germany. He reported having no relevant financial disclosures. He has, however, received speaking fees and research funds from companies that produce positive airway pressure devices: Heinen und Lowenstein, Resmed, Respironics, and Weinmann. Dr. Randerath made these remarks in an invited commentary (JAMA Intern. Med. 2015 June 1 [doi:10.1001/jamainternmed.2015.2059]).
It appears that patients generally prefer these devices to continuous positive airway pressure (CPAP) therapy. Better adherence to an oral appliance may outweigh the fact that it is not as effective as CPAP. Long-term studies comparing the two approaches are warranted.
The benefits of the mandibular advancement devices used in this study cannot be translated automatically to other devices, because there is a huge variety of these appliances on the market.
The extent of the protrusion of the lower jaw, the stability of the material, and the structural design of the devices vary widely. Several experts currently recommend avoiding the less sophisticated appliances that are not tailored to the individual’s jaw and oral cavity and instead using only customized adjustable appliances made by a trained specialist.
Dr. Winfried J. Randerath is with the pneumonology clinic and the Allergology Center for Sleep Medicine and Respiratory Care at Bethanien Hospital in Solingen, Germany. He reported having no relevant financial disclosures. He has, however, received speaking fees and research funds from companies that produce positive airway pressure devices: Heinen und Lowenstein, Resmed, Respironics, and Weinmann. Dr. Randerath made these remarks in an invited commentary (JAMA Intern. Med. 2015 June 1 [doi:10.1001/jamainternmed.2015.2059]).
An oral appliance that advances a patient’s lower jaw reduced episodes of obstructive sleep apnea, snoring, and restless legs symptoms, according to a report published online June 1 in JAMA Internal Medicine.
The device, however, failed to improve daytime sleepiness or quality of life in a Swedish study of adults who had daytime sleepiness and either snoring or mild to moderate sleep apnea, said Marie Marklund, Ph.D., D.D.S., of the department of odontology at Umeå (Sweden) University and her associates (JAMA Intern. Med. 2015 June 1 [doi:10.1001/jamainternmed.2015.2051]).
Previous studies of oral appliances have focused on patients with more severe sleep apnea and have yielded conflicting results, particularly regarding daytime sleepiness.
A total of 91 patients who were randomly assigned to receive either a placebo device (46 patients) or an oral appliance individually made by a dental technician using separate plaster casts of the upper and lower teeth (45 participants) completed the study. The device’s elastomer pieces fitted over the teeth and were connected with a screw that allowed continuous gradual advancement of the lower jaw by 6-7 mm. Holding the lower mandible forward improves breathing during sleep.
After 4 months of follow-up, at-home overnight polysomnography showed “a clear, significant treatment effect”: the mean apnea-hypopnea index (AHI) was 6.7 in the active-treatment group, compared with 16.7 in the placebo group. A total of 49% of the patients receiving active treatment had an AHI lower than 5, compared with only 11% of those using the placebo device, for an odds ratio of 7.8 and a number needed to treat of 3.
Snoring and symptoms of restless legs also were significantly less frequent with the active treatment, Dr. Marklund and her associates said.
In addition, 73% of patients who used oral appliances said that their expectations of treatment were either “totally” or “sufficiently” fulfilled, compared with only 11% of those who used placebo devices. And 89% of patients who used oral appliances said they would continue the treatment after completing the study, compared with only 52% of those who used the sham device.
However, daytime sleepiness, measured subjectively using the Epworth Sleepiness Scale and the Karolinska Sleepiness Scale and measured objectively using the Oxford Sleep Resistance test, did not differ significantly between the two study groups. The number of days with headaches, the intensity of headaches, the presence of nasal congestion, difficulty falling asleep, nighttime awakenings, nightmares, and reaction times also were not significantly different, nor were scores on a quality of life measure.
The study was supported by grants from the Swedish Research Council, the Swedish Heart and Lung Foundation, and the County Council of Vasterbotten. Dr. Marklund and her associates reported no conflicts of interest.
An oral appliance that advances a patient’s lower jaw reduced episodes of obstructive sleep apnea, snoring, and restless legs symptoms, according to a report published online June 1 in JAMA Internal Medicine.
The device, however, failed to improve daytime sleepiness or quality of life in a Swedish study of adults who had daytime sleepiness and either snoring or mild to moderate sleep apnea, said Marie Marklund, Ph.D., D.D.S., of the department of odontology at Umeå (Sweden) University and her associates (JAMA Intern. Med. 2015 June 1 [doi:10.1001/jamainternmed.2015.2051]).
Previous studies of oral appliances have focused on patients with more severe sleep apnea and have yielded conflicting results, particularly regarding daytime sleepiness.
A total of 91 patients who were randomly assigned to receive either a placebo device (46 patients) or an oral appliance individually made by a dental technician using separate plaster casts of the upper and lower teeth (45 participants) completed the study. The device’s elastomer pieces fitted over the teeth and were connected with a screw that allowed continuous gradual advancement of the lower jaw by 6-7 mm. Holding the lower mandible forward improves breathing during sleep.
After 4 months of follow-up, at-home overnight polysomnography showed “a clear, significant treatment effect”: the mean apnea-hypopnea index (AHI) was 6.7 in the active-treatment group, compared with 16.7 in the placebo group. A total of 49% of the patients receiving active treatment had an AHI lower than 5, compared with only 11% of those using the placebo device, for an odds ratio of 7.8 and a number needed to treat of 3.
Snoring and symptoms of restless legs also were significantly less frequent with the active treatment, Dr. Marklund and her associates said.
In addition, 73% of patients who used oral appliances said that their expectations of treatment were either “totally” or “sufficiently” fulfilled, compared with only 11% of those who used placebo devices. And 89% of patients who used oral appliances said they would continue the treatment after completing the study, compared with only 52% of those who used the sham device.
However, daytime sleepiness, measured subjectively using the Epworth Sleepiness Scale and the Karolinska Sleepiness Scale and measured objectively using the Oxford Sleep Resistance test, did not differ significantly between the two study groups. The number of days with headaches, the intensity of headaches, the presence of nasal congestion, difficulty falling asleep, nighttime awakenings, nightmares, and reaction times also were not significantly different, nor were scores on a quality of life measure.
The study was supported by grants from the Swedish Research Council, the Swedish Heart and Lung Foundation, and the County Council of Vasterbotten. Dr. Marklund and her associates reported no conflicts of interest.
FROM JAMA INTERNAL MEDICINE
Key clinical point: An oral appliance to advance the lower jaw reduced apneic episodes, snoring, and restless legs symptoms.
Major finding: Half of the patients receiving active treatment had an apnea-hypopnea index lower than 5, compared with only 11% of those using the placebo device, for an odds ratio of 7.8 and a number-needed-to-treat of 3.
Data source: A randomized, single-blind trial comparing a customized oral appliance against a placebo device in 96 adults with daytime sleepiness and either snoring or mild to moderate obstructive sleep apnea.
Disclosures: This study was supported by grants from the Swedish Research Council, the Swedish Heart and Lung Foundation, and the County Council of Vasterbotten. Dr. Marklund and her associates reported no conflicts of interest.
June 2015: Click for Credit
Here are 6 articles in the June issue of Clinician Reviews (accreditation valid until January 1, 2016):
1. ACCP and CTS Issue Joint Guideline on COPD Exacerbations
To take the posttest, go to: http://bit.ly/1EIadmv
VITALS
Key clinical point: The American College of Chest Physicians and the Canadian Thoracic Society have issued a guideline for prevention of acute exacerbations of COPD.
Major finding: COPD exacerbations are acute, trajectory changing, and often deadly manifestations of a chronic disease.
Data source: A comprehensive literature review on prevention of acute COPD exacerbations and a compilation of 33 recommendations and suggestions for clinicians in clinical practice.
Disclosures: The American College of Chest Physicians, the Canadian Thoracic Society, and the American Thoracic Society supported the project. Dr Criner reported having no relevant financial disclosures; his associates reported ties to numerous industry sources.
2. GI Symptoms Common in Parkinson Disease and Related Disorders
To take the posttest, go to: http://bit.ly/1AZSaXA
VITALS
Key clinical point: GI symptoms were linked with specific motor and nonmotor features of Parkinson disease and related disorders.
Major finding: Constipation was the most common symptom among all three parkinsonian disorders.
Data source: Multicenter, cross-sectional survey of 473 patients with Parkinson disease, atypical parkinsonism, or vascular parkinsonism.
Disclosures: The Collaborative Clinical Research Fund of Boramae Medical Center partially funded the work. The authors declared no relevant conflicts of interest.
3. Aerosolized Measles Vaccine Inferior to Subcutaneous
To take the posttest, go to: http://bit.ly/1RKJizC
VITALS
Key clinical point: An aerosolized measles vaccine was immunogenic but inferior to the subcutaneous vaccine at inducing seropositivity among babies residing in rural India.
Major finding: The primary endpoint—seropositivity for antibodies against measles at 91 days after vaccination—was 85.4% for aerosolized vaccine and 94.6% for subcutaneous.
Data source: An open-label, randomized noninferiority trial comparing aerosolized vs subcutaneous measles vaccination in 2,004 infants ages 9 to 11.9 months in villages in India.
Disclosures: This study was funded by the Bill and Melinda Gates Foundation. The Serum Institute of India provided vaccines free of charge, and Aerogen provided the delivery devices free of charge. Dr Low reported several grants plus monies paid to her institution from the World Health Organization for projects about vaccines and sexually transmitted infections; her associates reported ties to the Serum Institute of India, Aerogen, and Dance Biopharm. One associate has a patent pending on an aerosol device licensed to Novartis and another has a patent pending related to vaccine nebulizers.
4. Unrecognized Diabetes Common in Acute MI
To take the posttest, go to: http://bit.ly/1IB9sC8
VITALS
Key clinical point: Many patients presenting with acute MI had unrecognized diabetes, which, in most cases, remained undiagnosed, untreated, and unrecorded.
Major finding: Of 2,854 (10%) patients enrolled in an MI registry, 287 had A1C levels of 6.5% or higher on routine laboratory testing during hospitalization for acute MI, but treating physicians recognized only 101 of these cases of diabetes (35%).
Data source: A retrospective cohort study involving 2,854 adults presenting with acute MI to 24 US medical centers in a 3.5-year period.
Disclosures: This study was sponsored by the National Heart, Lung, and Blood Institute and supported by a research grant from Genentech. Dr Arnold reported receiving honoraria from Novartis; her associates reported ties to numerous industry sources.
5. Methotrexate and Biologics Linked to Higher Zoster Risk in Psoriasis
To take the posttest, go to: http://bit.ly/1AZScyF
VITALS
Key clinical point: The combination of methotrexate and biologics for the treatment of psoriasis may increase risk for herpes zoster.
Major finding: Combination therapy with both biologic medications and methotrexate was associated with a significant 66% increase in the incidence of herpes zoster over more than 11 years of follow-up.
Data source: Analysis of medical records for 95,941 patients with psoriasis.
Disclosures: One author reported consultancies and research grants from a range of pharmaceutical companies. There were no other disclosures.
6. ACP: Avoid ECG, MPI Cardiac Screening in Low-risk Patients
To take the posttest, go to: http://bit.ly/1e3NLha
Here are 6 articles in the June issue of Clinician Reviews (accreditation valid until January 1, 2016):
1. ACCP and CTS Issue Joint Guideline on COPD Exacerbations
To take the posttest, go to: http://bit.ly/1EIadmv
VITALS
Key clinical point: The American College of Chest Physicians and the Canadian Thoracic Society have issued a guideline for prevention of acute exacerbations of COPD.
Major finding: COPD exacerbations are acute, trajectory changing, and often deadly manifestations of a chronic disease.
Data source: A comprehensive literature review on prevention of acute COPD exacerbations and a compilation of 33 recommendations and suggestions for clinicians in clinical practice.
Disclosures: The American College of Chest Physicians, the Canadian Thoracic Society, and the American Thoracic Society supported the project. Dr Criner reported having no relevant financial disclosures; his associates reported ties to numerous industry sources.
2. GI Symptoms Common in Parkinson Disease and Related Disorders
To take the posttest, go to: http://bit.ly/1AZSaXA
VITALS
Key clinical point: GI symptoms were linked with specific motor and nonmotor features of Parkinson disease and related disorders.
Major finding: Constipation was the most common symptom among all three parkinsonian disorders.
Data source: Multicenter, cross-sectional survey of 473 patients with Parkinson disease, atypical parkinsonism, or vascular parkinsonism.
Disclosures: The Collaborative Clinical Research Fund of Boramae Medical Center partially funded the work. The authors declared no relevant conflicts of interest.
3. Aerosolized Measles Vaccine Inferior to Subcutaneous
To take the posttest, go to: http://bit.ly/1RKJizC
VITALS
Key clinical point: An aerosolized measles vaccine was immunogenic but inferior to the subcutaneous vaccine at inducing seropositivity among babies residing in rural India.
Major finding: The primary endpoint—seropositivity for antibodies against measles at 91 days after vaccination—was 85.4% for aerosolized vaccine and 94.6% for subcutaneous.
Data source: An open-label, randomized noninferiority trial comparing aerosolized vs subcutaneous measles vaccination in 2,004 infants ages 9 to 11.9 months in villages in India.
Disclosures: This study was funded by the Bill and Melinda Gates Foundation. The Serum Institute of India provided vaccines free of charge, and Aerogen provided the delivery devices free of charge. Dr Low reported several grants plus monies paid to her institution from the World Health Organization for projects about vaccines and sexually transmitted infections; her associates reported ties to the Serum Institute of India, Aerogen, and Dance Biopharm. One associate has a patent pending on an aerosol device licensed to Novartis and another has a patent pending related to vaccine nebulizers.
4. Unrecognized Diabetes Common in Acute MI
To take the posttest, go to: http://bit.ly/1IB9sC8
VITALS
Key clinical point: Many patients presenting with acute MI had unrecognized diabetes, which, in most cases, remained undiagnosed, untreated, and unrecorded.
Major finding: Of 2,854 (10%) patients enrolled in an MI registry, 287 had A1C levels of 6.5% or higher on routine laboratory testing during hospitalization for acute MI, but treating physicians recognized only 101 of these cases of diabetes (35%).
Data source: A retrospective cohort study involving 2,854 adults presenting with acute MI to 24 US medical centers in a 3.5-year period.
Disclosures: This study was sponsored by the National Heart, Lung, and Blood Institute and supported by a research grant from Genentech. Dr Arnold reported receiving honoraria from Novartis; her associates reported ties to numerous industry sources.
5. Methotrexate and Biologics Linked to Higher Zoster Risk in Psoriasis
To take the posttest, go to: http://bit.ly/1AZScyF
VITALS
Key clinical point: The combination of methotrexate and biologics for the treatment of psoriasis may increase risk for herpes zoster.
Major finding: Combination therapy with both biologic medications and methotrexate was associated with a significant 66% increase in the incidence of herpes zoster over more than 11 years of follow-up.
Data source: Analysis of medical records for 95,941 patients with psoriasis.
Disclosures: One author reported consultancies and research grants from a range of pharmaceutical companies. There were no other disclosures.
6. ACP: Avoid ECG, MPI Cardiac Screening in Low-risk Patients
To take the posttest, go to: http://bit.ly/1e3NLha
Here are 6 articles in the June issue of Clinician Reviews (accreditation valid until January 1, 2016):
1. ACCP and CTS Issue Joint Guideline on COPD Exacerbations
To take the posttest, go to: http://bit.ly/1EIadmv
VITALS
Key clinical point: The American College of Chest Physicians and the Canadian Thoracic Society have issued a guideline for prevention of acute exacerbations of COPD.
Major finding: COPD exacerbations are acute, trajectory changing, and often deadly manifestations of a chronic disease.
Data source: A comprehensive literature review on prevention of acute COPD exacerbations and a compilation of 33 recommendations and suggestions for clinicians in clinical practice.
Disclosures: The American College of Chest Physicians, the Canadian Thoracic Society, and the American Thoracic Society supported the project. Dr Criner reported having no relevant financial disclosures; his associates reported ties to numerous industry sources.
2. GI Symptoms Common in Parkinson Disease and Related Disorders
To take the posttest, go to: http://bit.ly/1AZSaXA
VITALS
Key clinical point: GI symptoms were linked with specific motor and nonmotor features of Parkinson disease and related disorders.
Major finding: Constipation was the most common symptom among all three parkinsonian disorders.
Data source: Multicenter, cross-sectional survey of 473 patients with Parkinson disease, atypical parkinsonism, or vascular parkinsonism.
Disclosures: The Collaborative Clinical Research Fund of Boramae Medical Center partially funded the work. The authors declared no relevant conflicts of interest.
3. Aerosolized Measles Vaccine Inferior to Subcutaneous
To take the posttest, go to: http://bit.ly/1RKJizC
VITALS
Key clinical point: An aerosolized measles vaccine was immunogenic but inferior to the subcutaneous vaccine at inducing seropositivity among babies residing in rural India.
Major finding: The primary endpoint—seropositivity for antibodies against measles at 91 days after vaccination—was 85.4% for aerosolized vaccine and 94.6% for subcutaneous.
Data source: An open-label, randomized noninferiority trial comparing aerosolized vs subcutaneous measles vaccination in 2,004 infants ages 9 to 11.9 months in villages in India.
Disclosures: This study was funded by the Bill and Melinda Gates Foundation. The Serum Institute of India provided vaccines free of charge, and Aerogen provided the delivery devices free of charge. Dr Low reported several grants plus monies paid to her institution from the World Health Organization for projects about vaccines and sexually transmitted infections; her associates reported ties to the Serum Institute of India, Aerogen, and Dance Biopharm. One associate has a patent pending on an aerosol device licensed to Novartis and another has a patent pending related to vaccine nebulizers.
4. Unrecognized Diabetes Common in Acute MI
To take the posttest, go to: http://bit.ly/1IB9sC8
VITALS
Key clinical point: Many patients presenting with acute MI had unrecognized diabetes, which, in most cases, remained undiagnosed, untreated, and unrecorded.
Major finding: Of 2,854 (10%) patients enrolled in an MI registry, 287 had A1C levels of 6.5% or higher on routine laboratory testing during hospitalization for acute MI, but treating physicians recognized only 101 of these cases of diabetes (35%).
Data source: A retrospective cohort study involving 2,854 adults presenting with acute MI to 24 US medical centers in a 3.5-year period.
Disclosures: This study was sponsored by the National Heart, Lung, and Blood Institute and supported by a research grant from Genentech. Dr Arnold reported receiving honoraria from Novartis; her associates reported ties to numerous industry sources.
5. Methotrexate and Biologics Linked to Higher Zoster Risk in Psoriasis
To take the posttest, go to: http://bit.ly/1AZScyF
VITALS
Key clinical point: The combination of methotrexate and biologics for the treatment of psoriasis may increase risk for herpes zoster.
Major finding: Combination therapy with both biologic medications and methotrexate was associated with a significant 66% increase in the incidence of herpes zoster over more than 11 years of follow-up.
Data source: Analysis of medical records for 95,941 patients with psoriasis.
Disclosures: One author reported consultancies and research grants from a range of pharmaceutical companies. There were no other disclosures.
6. ACP: Avoid ECG, MPI Cardiac Screening in Low-risk Patients
To take the posttest, go to: http://bit.ly/1e3NLha
Bevacizumab beneficial for Chinese NSCLC patients
Adding bevacixumab to standard first-line carboplatin-plus-paclitaxel therapy extended survival and was well tolerated in Chinese patients with advanced or recurrent nonsquamous non–small-cell lung cancer, as has already been reported in white patients, according to a report published online May 26 in the Journal of Clinical Oncology.
Recent trials have reported that adding bevacixumab prolongs survival in NSCLC, but these studies have involved primarily white patients; data concerning the agents’ efficacy in Asian populations are sparse. So researchers performed an industry-sponsored, double-blind phase III trial involving 276 Chinese adults treated at 16 hospitals across China. These participants (median age, 57 years; range, 23-75 years) were randomly assigned to receive up to six cycles of either standard carboplatin/paclitaxel chemotherapy alone (138 patients) or carboplatin/paclitaxel plus bevacixumab (138 patients) and were followed for approximately 28 months, said Dr. Caicun Zhou, director of oncology at Shanghai (China) Pulmonary Hospital and director of the Cancer Institute at Tongji University, Shanghai, and his associates.
The primary efficacy endpoint, progression-free survival, was extended with the addition of bevacixumab, with an HR of 0.40. The median survival was 9.2 months with bevacixumab and 6.5 months without it, a significant difference. The median overall survival also was significantly longer with bevacixumab (24.3 months) than without it (17.7 months). Other secondary endpoints also were improved by the addition of bevacixumab, including the objective response rate (54% vs. 26%), the disease control rate (94% vs. 89%), and the median duration of treatment response (8.0 months vs. 5.3 months).
Adverse effects were consistent with these agents’ established safety profiles, and no new safety concerns were identified. The most common adverse effects were hematologic abnormalities, GI disorders, and alopecia, and the incidence of less serious adverse effects was comparable between the two study groups. The rate of more serious adverse events was higher in the bevacixumab group (11% vs. 2%) and was largely due to hypertension and proteinuria, the investigators reported (J. Clin. Oncol. 2015 May 26 [doi:10.1200/JCO.2014.59.4424]).
“These data have confirmed that bevacixumab has clinically meaningful efficacy and an acceptable safety profile in Asian populations, as well as in global populations,” they added.
Adding bevacixumab to standard first-line carboplatin-plus-paclitaxel therapy extended survival and was well tolerated in Chinese patients with advanced or recurrent nonsquamous non–small-cell lung cancer, as has already been reported in white patients, according to a report published online May 26 in the Journal of Clinical Oncology.
Recent trials have reported that adding bevacixumab prolongs survival in NSCLC, but these studies have involved primarily white patients; data concerning the agents’ efficacy in Asian populations are sparse. So researchers performed an industry-sponsored, double-blind phase III trial involving 276 Chinese adults treated at 16 hospitals across China. These participants (median age, 57 years; range, 23-75 years) were randomly assigned to receive up to six cycles of either standard carboplatin/paclitaxel chemotherapy alone (138 patients) or carboplatin/paclitaxel plus bevacixumab (138 patients) and were followed for approximately 28 months, said Dr. Caicun Zhou, director of oncology at Shanghai (China) Pulmonary Hospital and director of the Cancer Institute at Tongji University, Shanghai, and his associates.
The primary efficacy endpoint, progression-free survival, was extended with the addition of bevacixumab, with an HR of 0.40. The median survival was 9.2 months with bevacixumab and 6.5 months without it, a significant difference. The median overall survival also was significantly longer with bevacixumab (24.3 months) than without it (17.7 months). Other secondary endpoints also were improved by the addition of bevacixumab, including the objective response rate (54% vs. 26%), the disease control rate (94% vs. 89%), and the median duration of treatment response (8.0 months vs. 5.3 months).
Adverse effects were consistent with these agents’ established safety profiles, and no new safety concerns were identified. The most common adverse effects were hematologic abnormalities, GI disorders, and alopecia, and the incidence of less serious adverse effects was comparable between the two study groups. The rate of more serious adverse events was higher in the bevacixumab group (11% vs. 2%) and was largely due to hypertension and proteinuria, the investigators reported (J. Clin. Oncol. 2015 May 26 [doi:10.1200/JCO.2014.59.4424]).
“These data have confirmed that bevacixumab has clinically meaningful efficacy and an acceptable safety profile in Asian populations, as well as in global populations,” they added.
Adding bevacixumab to standard first-line carboplatin-plus-paclitaxel therapy extended survival and was well tolerated in Chinese patients with advanced or recurrent nonsquamous non–small-cell lung cancer, as has already been reported in white patients, according to a report published online May 26 in the Journal of Clinical Oncology.
Recent trials have reported that adding bevacixumab prolongs survival in NSCLC, but these studies have involved primarily white patients; data concerning the agents’ efficacy in Asian populations are sparse. So researchers performed an industry-sponsored, double-blind phase III trial involving 276 Chinese adults treated at 16 hospitals across China. These participants (median age, 57 years; range, 23-75 years) were randomly assigned to receive up to six cycles of either standard carboplatin/paclitaxel chemotherapy alone (138 patients) or carboplatin/paclitaxel plus bevacixumab (138 patients) and were followed for approximately 28 months, said Dr. Caicun Zhou, director of oncology at Shanghai (China) Pulmonary Hospital and director of the Cancer Institute at Tongji University, Shanghai, and his associates.
The primary efficacy endpoint, progression-free survival, was extended with the addition of bevacixumab, with an HR of 0.40. The median survival was 9.2 months with bevacixumab and 6.5 months without it, a significant difference. The median overall survival also was significantly longer with bevacixumab (24.3 months) than without it (17.7 months). Other secondary endpoints also were improved by the addition of bevacixumab, including the objective response rate (54% vs. 26%), the disease control rate (94% vs. 89%), and the median duration of treatment response (8.0 months vs. 5.3 months).
Adverse effects were consistent with these agents’ established safety profiles, and no new safety concerns were identified. The most common adverse effects were hematologic abnormalities, GI disorders, and alopecia, and the incidence of less serious adverse effects was comparable between the two study groups. The rate of more serious adverse events was higher in the bevacixumab group (11% vs. 2%) and was largely due to hypertension and proteinuria, the investigators reported (J. Clin. Oncol. 2015 May 26 [doi:10.1200/JCO.2014.59.4424]).
“These data have confirmed that bevacixumab has clinically meaningful efficacy and an acceptable safety profile in Asian populations, as well as in global populations,” they added.
Key clinical point: Adding bevacizumab to carboplatin plus paclitaxel extends progression-free survival in Chinese patients with advanced or recurrent nonsquamous NSCLC, as in whites.
Major finding: The median survival was 9.2 months with the addition of bevacixumab and 6.5 months without it, a significant difference.
Data source: A multicenter, randomized, double-blind placebo-controlled trial involving 276 Chinese adults with NSCLC who were followed for a median of approximately 28 months.
Disclosures: This trial was supported by Hoffmann-La Roche. Dr. Zhou reported receiving honoraria from Hoffmann-La Roche, Eli Lilly, Boehringer Ingelheim, and AstraZeneca; his associates reported ties to Hoffmann-La Roche, Eli Lilly, AstraZeneca, Pfizer, Sanofi, and Roche (China) Holding.
Additive radiotherapy’s advantages outweigh QOL disadvantages
For locally advanced prostate cancer, adding radiotherapy to androgen-deprivation therapy significantly improves survival and exerts “only modest and transient negative impact” on health-related quality of life, according to a report published online May 26 in the Journal of Clinical Oncology.
In a nonblinded international clinical trial, 1,205 men with locally advanced prostate cancer were randomly assigned to receive either lifelong androgen-deprivation therapy alone (602 patients) or ADT plus radiotherapy (603 patients). Health-related quality of life (QOL) was assessed at 6-month intervals for 2 years and annually thereafter for up to 4 years, using either the European Organisation for Research and Treatment of Cancer core questionnaire plus a prostate cancer–specific checklist (EORTC QLQ-30) or the Functional Assessment of Cancer Therapy-Prostate questionnaire (FACT-P), said Dr. Michael Brundage of Queen’s Cancer Research Institute and the Cancer Centre of Southeastern Ontario, Kingston, and his associates.
Additive radiotherapy produced bowel symptoms and diarrhea and adversely affected urinary function and erectile function, but these effects receded over time and were no longer evident at 2 years. This pattern is consistent with the known toxicity of radiotherapy. Moreover, the proportion of men reporting severe bowel or bladder symptoms at any time was only slightly higher (less than 5% higher) in the radiotherapy group than in the ADT-only group. In contrast, urinary symptoms improved in many men in both treatment groups and overall survival was significantly higher with the addition of radiotherapy, the investigators said (J. Clin. Oncol. 2015 May 25 [doi:10.1200/JCO.2014.57.8724]).
“The adverse impact of radiotherapy overall was modest and temporary and, in our view, not of sufficient magnitude to offset the clear disease-specific and overall survival benefits conferred by curative RT in this setting,” Dr. Brundage and his associates wrote.
They added that treatment has changed somewhat since this study was conducted. Currently, ADT is how administered for a shorter period, rather than the lifelong duration of treatment that was standard practice at that time. In addition, radiotherapy techniques used in the study were “relatively crude” and prescribed doses were lower, compared with current practice, they noted.
This study was supported by the Canadian Cancer Society Research Institute, the U.S. National Cancer Institute, and the United Kingdom Medical Research Council. Dr. Brundage reported having no financial disclosures; two of his associates reported ties to Astellas, Eli Lilly, Janssen-Cilag, Novartis, Pfizer, Dendreon, Ferring Pharmaceuticals, and Sanofi.
For locally advanced prostate cancer, adding radiotherapy to androgen-deprivation therapy significantly improves survival and exerts “only modest and transient negative impact” on health-related quality of life, according to a report published online May 26 in the Journal of Clinical Oncology.
In a nonblinded international clinical trial, 1,205 men with locally advanced prostate cancer were randomly assigned to receive either lifelong androgen-deprivation therapy alone (602 patients) or ADT plus radiotherapy (603 patients). Health-related quality of life (QOL) was assessed at 6-month intervals for 2 years and annually thereafter for up to 4 years, using either the European Organisation for Research and Treatment of Cancer core questionnaire plus a prostate cancer–specific checklist (EORTC QLQ-30) or the Functional Assessment of Cancer Therapy-Prostate questionnaire (FACT-P), said Dr. Michael Brundage of Queen’s Cancer Research Institute and the Cancer Centre of Southeastern Ontario, Kingston, and his associates.
Additive radiotherapy produced bowel symptoms and diarrhea and adversely affected urinary function and erectile function, but these effects receded over time and were no longer evident at 2 years. This pattern is consistent with the known toxicity of radiotherapy. Moreover, the proportion of men reporting severe bowel or bladder symptoms at any time was only slightly higher (less than 5% higher) in the radiotherapy group than in the ADT-only group. In contrast, urinary symptoms improved in many men in both treatment groups and overall survival was significantly higher with the addition of radiotherapy, the investigators said (J. Clin. Oncol. 2015 May 25 [doi:10.1200/JCO.2014.57.8724]).
“The adverse impact of radiotherapy overall was modest and temporary and, in our view, not of sufficient magnitude to offset the clear disease-specific and overall survival benefits conferred by curative RT in this setting,” Dr. Brundage and his associates wrote.
They added that treatment has changed somewhat since this study was conducted. Currently, ADT is how administered for a shorter period, rather than the lifelong duration of treatment that was standard practice at that time. In addition, radiotherapy techniques used in the study were “relatively crude” and prescribed doses were lower, compared with current practice, they noted.
This study was supported by the Canadian Cancer Society Research Institute, the U.S. National Cancer Institute, and the United Kingdom Medical Research Council. Dr. Brundage reported having no financial disclosures; two of his associates reported ties to Astellas, Eli Lilly, Janssen-Cilag, Novartis, Pfizer, Dendreon, Ferring Pharmaceuticals, and Sanofi.
For locally advanced prostate cancer, adding radiotherapy to androgen-deprivation therapy significantly improves survival and exerts “only modest and transient negative impact” on health-related quality of life, according to a report published online May 26 in the Journal of Clinical Oncology.
In a nonblinded international clinical trial, 1,205 men with locally advanced prostate cancer were randomly assigned to receive either lifelong androgen-deprivation therapy alone (602 patients) or ADT plus radiotherapy (603 patients). Health-related quality of life (QOL) was assessed at 6-month intervals for 2 years and annually thereafter for up to 4 years, using either the European Organisation for Research and Treatment of Cancer core questionnaire plus a prostate cancer–specific checklist (EORTC QLQ-30) or the Functional Assessment of Cancer Therapy-Prostate questionnaire (FACT-P), said Dr. Michael Brundage of Queen’s Cancer Research Institute and the Cancer Centre of Southeastern Ontario, Kingston, and his associates.
Additive radiotherapy produced bowel symptoms and diarrhea and adversely affected urinary function and erectile function, but these effects receded over time and were no longer evident at 2 years. This pattern is consistent with the known toxicity of radiotherapy. Moreover, the proportion of men reporting severe bowel or bladder symptoms at any time was only slightly higher (less than 5% higher) in the radiotherapy group than in the ADT-only group. In contrast, urinary symptoms improved in many men in both treatment groups and overall survival was significantly higher with the addition of radiotherapy, the investigators said (J. Clin. Oncol. 2015 May 25 [doi:10.1200/JCO.2014.57.8724]).
“The adverse impact of radiotherapy overall was modest and temporary and, in our view, not of sufficient magnitude to offset the clear disease-specific and overall survival benefits conferred by curative RT in this setting,” Dr. Brundage and his associates wrote.
They added that treatment has changed somewhat since this study was conducted. Currently, ADT is how administered for a shorter period, rather than the lifelong duration of treatment that was standard practice at that time. In addition, radiotherapy techniques used in the study were “relatively crude” and prescribed doses were lower, compared with current practice, they noted.
This study was supported by the Canadian Cancer Society Research Institute, the U.S. National Cancer Institute, and the United Kingdom Medical Research Council. Dr. Brundage reported having no financial disclosures; two of his associates reported ties to Astellas, Eli Lilly, Janssen-Cilag, Novartis, Pfizer, Dendreon, Ferring Pharmaceuticals, and Sanofi.
FROM JOURNAL OF CLINICAL ONCOLOGY
Key clinical point: In locally advanced prostate cancer, adding radiotherapy to androgen-deprivation therapy improves survival with only modest and transient negative effects on QOL.
Major finding: Additive radiotherapy produced bowel symptoms and diarrhea and adversely affected urinary function and erectile function, but these effects receded over time and were no longer evident at 2 years.
Data source: A randomized controlled nonblinded trial comparing QOL outcomes during 3-4 years of follow-up between 602 men assigned to ADT alone and 603 assigned to ADT plus radiotherapy.
Disclosures: This study was supported by the Canadian Cancer Society Research Institute, the U.S. National Cancer Institute, and the United Kingdom Medical Research Council. Dr. Brundage reported having no financial disclosures; two of his associates reported ties to Astellas, Eli Lilly, Janssen-Cilag, Novartis, Pfizer, Dendreon, Ferring Pharmaceuticals, and Sanofi.
Less severe impairment spurs mental health treatment among youths
The recent increase in the use of outpatient mental health treatment among children and adolescents was driven in large part by expansion in care for those who have less severe impairment rather than for the severely impaired, according to a report published online May 21 in the New England Journal of Medicine.
Outpatient mental health treatment of youths is known to have increased in recent years, but the range of impairment in this age group is very wide, from “ostensibly healthy adolescents who seek mental health care to improve their academic performance to children with early-onset schizophrenia. ... Some observers worry that psychotropic and other mental health treatment of young people with less impairing conditions has increased disproportionately as a result of the recent broadening of conceptualizations of child and adolescent psychiatric disorders. Yet this concern has not been subject to empirical evaluation,” said Dr. Mark Olfson of Columbia University and the New York State Psychiatric Institute, both in New York.
Dr. Olfson and his colleagues analyzed time trends in the use of mental health services ascertained in Medical Expenditure Panel Surveys conducted by the U.S. Agency for Healthcare Research and Quality. These questionnaires are completed by nationally representative samples of households each year. The investigators focused on parental assessments of mental health functioning in 53,622 children aged 6-17 years: 15,307 youths assessed in 1996-1998, 19,450 assessed in 2003-2005, and 18,865 assessed in 2010-2012. Mental health impairment was evaluated via the Columbia Impairment Scale, a 13-item measure of interpersonal relations, psychopathologic symptoms, functioning in school, and use of leisure time.
Between the earliest and the most recent surveys, the percentage of youths using any outpatient mental health service increased significantly, as expected. This increase occurred across most subgroups of respondents, involving both children and adolescents, both boys and girls, and both whites and nonwhites. However, the increase was approximately twofold among youths with less severe impairment, rising from 2.74 million uses per year to 4.19 million uses per year. In contrast, the increase was smaller among youths with the most severe impairment, rising from 1.56 million uses per year to 2.28 million uses per year, the investigators said (N. Engl. J. Med. 2015 May 21 [doi:10.1056/NEJMsa1413512]). Some experts suggest that revisions to the DSM and aggressive pharmaceutical marketing have contributed to the increase in treatment of less severely impaired youths. “An increasing public acceptance of psychotropic medications may also have been a contributing factor,” Dr. Olfson and his associates said.
However, it is important to note that children and adolescents with severe impairment were much more likely than were the less severely impaired to use outpatient mental health services. And use of these services increased among all subgroups of severely impaired youths: both children and adolescents, both boys and girls, and both whites and nonwhites, the researchers added.
The recent increase in the use of outpatient mental health treatment among children and adolescents was driven in large part by expansion in care for those who have less severe impairment rather than for the severely impaired, according to a report published online May 21 in the New England Journal of Medicine.
Outpatient mental health treatment of youths is known to have increased in recent years, but the range of impairment in this age group is very wide, from “ostensibly healthy adolescents who seek mental health care to improve their academic performance to children with early-onset schizophrenia. ... Some observers worry that psychotropic and other mental health treatment of young people with less impairing conditions has increased disproportionately as a result of the recent broadening of conceptualizations of child and adolescent psychiatric disorders. Yet this concern has not been subject to empirical evaluation,” said Dr. Mark Olfson of Columbia University and the New York State Psychiatric Institute, both in New York.
Dr. Olfson and his colleagues analyzed time trends in the use of mental health services ascertained in Medical Expenditure Panel Surveys conducted by the U.S. Agency for Healthcare Research and Quality. These questionnaires are completed by nationally representative samples of households each year. The investigators focused on parental assessments of mental health functioning in 53,622 children aged 6-17 years: 15,307 youths assessed in 1996-1998, 19,450 assessed in 2003-2005, and 18,865 assessed in 2010-2012. Mental health impairment was evaluated via the Columbia Impairment Scale, a 13-item measure of interpersonal relations, psychopathologic symptoms, functioning in school, and use of leisure time.
Between the earliest and the most recent surveys, the percentage of youths using any outpatient mental health service increased significantly, as expected. This increase occurred across most subgroups of respondents, involving both children and adolescents, both boys and girls, and both whites and nonwhites. However, the increase was approximately twofold among youths with less severe impairment, rising from 2.74 million uses per year to 4.19 million uses per year. In contrast, the increase was smaller among youths with the most severe impairment, rising from 1.56 million uses per year to 2.28 million uses per year, the investigators said (N. Engl. J. Med. 2015 May 21 [doi:10.1056/NEJMsa1413512]). Some experts suggest that revisions to the DSM and aggressive pharmaceutical marketing have contributed to the increase in treatment of less severely impaired youths. “An increasing public acceptance of psychotropic medications may also have been a contributing factor,” Dr. Olfson and his associates said.
However, it is important to note that children and adolescents with severe impairment were much more likely than were the less severely impaired to use outpatient mental health services. And use of these services increased among all subgroups of severely impaired youths: both children and adolescents, both boys and girls, and both whites and nonwhites, the researchers added.
The recent increase in the use of outpatient mental health treatment among children and adolescents was driven in large part by expansion in care for those who have less severe impairment rather than for the severely impaired, according to a report published online May 21 in the New England Journal of Medicine.
Outpatient mental health treatment of youths is known to have increased in recent years, but the range of impairment in this age group is very wide, from “ostensibly healthy adolescents who seek mental health care to improve their academic performance to children with early-onset schizophrenia. ... Some observers worry that psychotropic and other mental health treatment of young people with less impairing conditions has increased disproportionately as a result of the recent broadening of conceptualizations of child and adolescent psychiatric disorders. Yet this concern has not been subject to empirical evaluation,” said Dr. Mark Olfson of Columbia University and the New York State Psychiatric Institute, both in New York.
Dr. Olfson and his colleagues analyzed time trends in the use of mental health services ascertained in Medical Expenditure Panel Surveys conducted by the U.S. Agency for Healthcare Research and Quality. These questionnaires are completed by nationally representative samples of households each year. The investigators focused on parental assessments of mental health functioning in 53,622 children aged 6-17 years: 15,307 youths assessed in 1996-1998, 19,450 assessed in 2003-2005, and 18,865 assessed in 2010-2012. Mental health impairment was evaluated via the Columbia Impairment Scale, a 13-item measure of interpersonal relations, psychopathologic symptoms, functioning in school, and use of leisure time.
Between the earliest and the most recent surveys, the percentage of youths using any outpatient mental health service increased significantly, as expected. This increase occurred across most subgroups of respondents, involving both children and adolescents, both boys and girls, and both whites and nonwhites. However, the increase was approximately twofold among youths with less severe impairment, rising from 2.74 million uses per year to 4.19 million uses per year. In contrast, the increase was smaller among youths with the most severe impairment, rising from 1.56 million uses per year to 2.28 million uses per year, the investigators said (N. Engl. J. Med. 2015 May 21 [doi:10.1056/NEJMsa1413512]). Some experts suggest that revisions to the DSM and aggressive pharmaceutical marketing have contributed to the increase in treatment of less severely impaired youths. “An increasing public acceptance of psychotropic medications may also have been a contributing factor,” Dr. Olfson and his associates said.
However, it is important to note that children and adolescents with severe impairment were much more likely than were the less severely impaired to use outpatient mental health services. And use of these services increased among all subgroups of severely impaired youths: both children and adolescents, both boys and girls, and both whites and nonwhites, the researchers added.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Key clinical point: Youths with less severe impairment account for most of the recent increase in that age group’s use of outpatient mental health treatment.
Major finding: The use of outpatient mental health treatment approximately doubled over time among youths with less severe impairment, rising from 2.74 million uses per year during 1996-1998 to 4.19 million uses per year in 2010-2012.
Data source: An analysis of nationally representative surveys of U.S. households, focusing on time trends in the use of mental health services by 53,622 family members aged 6-17 years.
Disclosures: The Agency for Healthcare Research and Quality and the New York State Psychiatric Institute supported the study. Dr. Olfson disclosed ties with Johnson & Johnson, and a colleague disclosed ties with Alkermes, Forest, Johnson & Johnson, and Shire.