User login
The perils of CA-125 as a diagnostic tool in patients with adnexal masses
CA-125, or cancer antigen 125, is an epitope (antigen) on the transmembrane glycoprotein MUC16, or mucin 16. This protein is expressed on the surface of tissue derived from embryonic coelomic and Müllerian epithelium including the reproductive tract. CA-125 is also expressed in other tissue such as the pleura, lungs, pericardium, intestines, and kidneys. MUC16 plays an important role in tumor proliferation, invasiveness, and cell motility.1 In patients with epithelial ovarian cancer (EOC), CA-125 may be found on the surface of ovarian cancer cells. It is shed in the bloodstream and can be quantified using a serum test.
There are a number of CA-125 assays in commercial use, and although none have been deemed to be clinically superior, there can be some differences between assays. It is important, if possible, to use the same assay when following serial CA-125 values. Most frequently, this will mean getting the test through the same laboratory.
CA-125 has Food and Drug Administration approval for use in patients with a current or prior diagnosis of ovarian cancer to monitor treatment response, progression of disease, or disease recurrence.
It is frequently used off label in the workup of adnexal masses, while not FDA approved. CA-125 and other serum biomarkers may help determine the etiology of an adnexal mass; however, they are not diagnostic and should be used thoughtfully. It is important to have conversations with patients before ordering a CA-125 (or other serum biomarkers) about potential results and their effect on diagnosis and treatment. This will lessen some patient anxiety when tests results become available, especially in the setting of autoreleasing results under the Cures Act.
One of the reasons that CA-125 can be difficult to interpret when used as a diagnostic tool is the number of nonmalignant disease processes that can result in CA-125 elevations. CA-125 can be elevated in inflammatory and infectious disease states, including but not limited to, chronic obstructive pulmonary disease, pelvic inflammatory disease, diverticulitis, and pneumonia. Severe/critical COVID-19 infection has recently been found to be associated with increased levels of CA-125.2 It is important to obtain a complete medical history and to take specific note of any current or recent flares in inflammatory or infectious processes that could contribute to CA-125 elevations.
Special caution should be taken in premenopausal patients. The sensitivity and specificity of CA-125 are lower in this cohort of patients compared to postmenopausal women. This is multifactorial but in part due to gynecologic conditions that can increase CA-125, such as uterine fibroids and endometriosis, and the higher incidence of nonepithelial ovarian cancers (which frequently have different serum biomarkers) in younger patients. A patient’s gynecologic history, her age, and ultrasound or other imaging findings should help determine what, if any, serum biomarkers are appropriate for workup of an adnexal mass rather than the default ordering of CA-125 to determine need for referral to gynecologic oncology. If the decision has been made to take the patient to the operating room, CA-125 is not approved as a triage tool to guide who best to perform the surgery. In this case, one of two serum tumor marker panel tests that has received FDA approval for triage after the decision for surgery has been made (the multivariate index assay or the risk of ovarian malignancy algorithm) should be used.
When considering its ability to serve as a diagnostic test for ovarian cancer, the sensitivity of CA-125 is affected by the number of patients with epithelial ovarian cancer who have a test result that falls within the normal range (up to 50% of patients with stage I disease).3 The specificity of CA-125 is affected by the large number of nonmalignant conditions that can cause its elevation. Depending on the age of the patient, her menopausal status, comorbid conditions, and reason for obtaining serum biomarkers (e.g., decision for surgery has already been made), CA-125 (or CA-125 alone) may not be the best tool to use in the workup of an adnexal mass and can cause significant patient anxiety. In the setting of acute disease, such as COVID-19 infection, it may be better to delay obtaining serum biomarkers for the work-up of an adnexal mass. If delay is not feasible, then repeat serum biomarkers once the acute phase of illness has passed.
Dr. Tucker is assistant professor of gynecologic oncology at the University of North Carolina at Chapel Hill.
References
1. Thériault C et al. Gynecol Oncol. 2011 Jun 1;121(3):434-43.
2. Wei X et al. J Med Virol. 2020;92(10):2036-41.
3. Zurawski VR Jr et al. Int J Cancer. 1988;42:677-80.
CA-125, or cancer antigen 125, is an epitope (antigen) on the transmembrane glycoprotein MUC16, or mucin 16. This protein is expressed on the surface of tissue derived from embryonic coelomic and Müllerian epithelium including the reproductive tract. CA-125 is also expressed in other tissue such as the pleura, lungs, pericardium, intestines, and kidneys. MUC16 plays an important role in tumor proliferation, invasiveness, and cell motility.1 In patients with epithelial ovarian cancer (EOC), CA-125 may be found on the surface of ovarian cancer cells. It is shed in the bloodstream and can be quantified using a serum test.
There are a number of CA-125 assays in commercial use, and although none have been deemed to be clinically superior, there can be some differences between assays. It is important, if possible, to use the same assay when following serial CA-125 values. Most frequently, this will mean getting the test through the same laboratory.
CA-125 has Food and Drug Administration approval for use in patients with a current or prior diagnosis of ovarian cancer to monitor treatment response, progression of disease, or disease recurrence.
It is frequently used off label in the workup of adnexal masses, while not FDA approved. CA-125 and other serum biomarkers may help determine the etiology of an adnexal mass; however, they are not diagnostic and should be used thoughtfully. It is important to have conversations with patients before ordering a CA-125 (or other serum biomarkers) about potential results and their effect on diagnosis and treatment. This will lessen some patient anxiety when tests results become available, especially in the setting of autoreleasing results under the Cures Act.
One of the reasons that CA-125 can be difficult to interpret when used as a diagnostic tool is the number of nonmalignant disease processes that can result in CA-125 elevations. CA-125 can be elevated in inflammatory and infectious disease states, including but not limited to, chronic obstructive pulmonary disease, pelvic inflammatory disease, diverticulitis, and pneumonia. Severe/critical COVID-19 infection has recently been found to be associated with increased levels of CA-125.2 It is important to obtain a complete medical history and to take specific note of any current or recent flares in inflammatory or infectious processes that could contribute to CA-125 elevations.
Special caution should be taken in premenopausal patients. The sensitivity and specificity of CA-125 are lower in this cohort of patients compared to postmenopausal women. This is multifactorial but in part due to gynecologic conditions that can increase CA-125, such as uterine fibroids and endometriosis, and the higher incidence of nonepithelial ovarian cancers (which frequently have different serum biomarkers) in younger patients. A patient’s gynecologic history, her age, and ultrasound or other imaging findings should help determine what, if any, serum biomarkers are appropriate for workup of an adnexal mass rather than the default ordering of CA-125 to determine need for referral to gynecologic oncology. If the decision has been made to take the patient to the operating room, CA-125 is not approved as a triage tool to guide who best to perform the surgery. In this case, one of two serum tumor marker panel tests that has received FDA approval for triage after the decision for surgery has been made (the multivariate index assay or the risk of ovarian malignancy algorithm) should be used.
When considering its ability to serve as a diagnostic test for ovarian cancer, the sensitivity of CA-125 is affected by the number of patients with epithelial ovarian cancer who have a test result that falls within the normal range (up to 50% of patients with stage I disease).3 The specificity of CA-125 is affected by the large number of nonmalignant conditions that can cause its elevation. Depending on the age of the patient, her menopausal status, comorbid conditions, and reason for obtaining serum biomarkers (e.g., decision for surgery has already been made), CA-125 (or CA-125 alone) may not be the best tool to use in the workup of an adnexal mass and can cause significant patient anxiety. In the setting of acute disease, such as COVID-19 infection, it may be better to delay obtaining serum biomarkers for the work-up of an adnexal mass. If delay is not feasible, then repeat serum biomarkers once the acute phase of illness has passed.
Dr. Tucker is assistant professor of gynecologic oncology at the University of North Carolina at Chapel Hill.
References
1. Thériault C et al. Gynecol Oncol. 2011 Jun 1;121(3):434-43.
2. Wei X et al. J Med Virol. 2020;92(10):2036-41.
3. Zurawski VR Jr et al. Int J Cancer. 1988;42:677-80.
CA-125, or cancer antigen 125, is an epitope (antigen) on the transmembrane glycoprotein MUC16, or mucin 16. This protein is expressed on the surface of tissue derived from embryonic coelomic and Müllerian epithelium including the reproductive tract. CA-125 is also expressed in other tissue such as the pleura, lungs, pericardium, intestines, and kidneys. MUC16 plays an important role in tumor proliferation, invasiveness, and cell motility.1 In patients with epithelial ovarian cancer (EOC), CA-125 may be found on the surface of ovarian cancer cells. It is shed in the bloodstream and can be quantified using a serum test.
There are a number of CA-125 assays in commercial use, and although none have been deemed to be clinically superior, there can be some differences between assays. It is important, if possible, to use the same assay when following serial CA-125 values. Most frequently, this will mean getting the test through the same laboratory.
CA-125 has Food and Drug Administration approval for use in patients with a current or prior diagnosis of ovarian cancer to monitor treatment response, progression of disease, or disease recurrence.
It is frequently used off label in the workup of adnexal masses, while not FDA approved. CA-125 and other serum biomarkers may help determine the etiology of an adnexal mass; however, they are not diagnostic and should be used thoughtfully. It is important to have conversations with patients before ordering a CA-125 (or other serum biomarkers) about potential results and their effect on diagnosis and treatment. This will lessen some patient anxiety when tests results become available, especially in the setting of autoreleasing results under the Cures Act.
One of the reasons that CA-125 can be difficult to interpret when used as a diagnostic tool is the number of nonmalignant disease processes that can result in CA-125 elevations. CA-125 can be elevated in inflammatory and infectious disease states, including but not limited to, chronic obstructive pulmonary disease, pelvic inflammatory disease, diverticulitis, and pneumonia. Severe/critical COVID-19 infection has recently been found to be associated with increased levels of CA-125.2 It is important to obtain a complete medical history and to take specific note of any current or recent flares in inflammatory or infectious processes that could contribute to CA-125 elevations.
Special caution should be taken in premenopausal patients. The sensitivity and specificity of CA-125 are lower in this cohort of patients compared to postmenopausal women. This is multifactorial but in part due to gynecologic conditions that can increase CA-125, such as uterine fibroids and endometriosis, and the higher incidence of nonepithelial ovarian cancers (which frequently have different serum biomarkers) in younger patients. A patient’s gynecologic history, her age, and ultrasound or other imaging findings should help determine what, if any, serum biomarkers are appropriate for workup of an adnexal mass rather than the default ordering of CA-125 to determine need for referral to gynecologic oncology. If the decision has been made to take the patient to the operating room, CA-125 is not approved as a triage tool to guide who best to perform the surgery. In this case, one of two serum tumor marker panel tests that has received FDA approval for triage after the decision for surgery has been made (the multivariate index assay or the risk of ovarian malignancy algorithm) should be used.
When considering its ability to serve as a diagnostic test for ovarian cancer, the sensitivity of CA-125 is affected by the number of patients with epithelial ovarian cancer who have a test result that falls within the normal range (up to 50% of patients with stage I disease).3 The specificity of CA-125 is affected by the large number of nonmalignant conditions that can cause its elevation. Depending on the age of the patient, her menopausal status, comorbid conditions, and reason for obtaining serum biomarkers (e.g., decision for surgery has already been made), CA-125 (or CA-125 alone) may not be the best tool to use in the workup of an adnexal mass and can cause significant patient anxiety. In the setting of acute disease, such as COVID-19 infection, it may be better to delay obtaining serum biomarkers for the work-up of an adnexal mass. If delay is not feasible, then repeat serum biomarkers once the acute phase of illness has passed.
Dr. Tucker is assistant professor of gynecologic oncology at the University of North Carolina at Chapel Hill.
References
1. Thériault C et al. Gynecol Oncol. 2011 Jun 1;121(3):434-43.
2. Wei X et al. J Med Virol. 2020;92(10):2036-41.
3. Zurawski VR Jr et al. Int J Cancer. 1988;42:677-80.
Downtime? Enjoy it
Everything in medicine, and pretty much the universe, is based on averages. Average reduction of seizures, average blood levels, average response to treatment, average insurance reimbursement, average time spent with a new consult.
Statistics are helpful in working through large amounts of data, but on a smaller scale, like my practice, statistics aren’t quite as helpful.
I see, on average, maybe 10 patients per day, consisting of new ones, follow-ups, and electromyography and nerve conduction velocity (EMG/NCV) studies. That is, by far, a smaller number of patients than my colleagues in primary care see, and probably other neurology practices as well. But it works for me.
But that’s on averages and not always. Sometimes we all hit slumps. Who knows why? Everyone is on vacation, or the holidays are coming, or they’ve been abducted by aliens. Whatever the reason, I get the occasional week where I’m pretty bored. Maybe one or two patients in a day. I start to feel like the lonely Maytag repairman behind my desk. I check to see if any drug samples have expired. I wonder if people are actually reading my online reviews and going elsewhere.
Years ago weeks like that terrified me. I was worried my little practice might fail (granted, it still could). But as years – and cycles that make up the averages – go by, they don’t bother me as much.
After 23 years I’ve learned that it’s just part of the normal fluctuations that make up an average. One morning I’ll roll the phones and the lines will explode (figuratively, I hope) with calls. At times like these my secretary seems to grow another pair of arms as she frantically schedules callers, puts others on hold, copies insurance cards, and gives the evil eye to drug reps who step in and ask her if she’s busy.
Then my schedule gets packed. My secretary crams patients in my emergency slots of 7:00, 8:00, and 12:00. MRI results come in that require me to see people sooner rather than later. My “average” of 10 patients per day suddenly doesn’t exist. I go home with a pile of dictations to do and work away into the night to catch up.
With experience we learn to take this in stride. Now, when I hit a slow patch, I remind myself that it’s not the average, and to enjoy it while I can. Read a book, take a long lunch, go home early and nap.
Worrying about where the patients are isn’t productive, or good for your mental health. They know where I am, and will find me when they need me.
. Enjoy the slow times while you can.
Dr. Block has a solo neurology practice in Scottsdale, Ariz.
Everything in medicine, and pretty much the universe, is based on averages. Average reduction of seizures, average blood levels, average response to treatment, average insurance reimbursement, average time spent with a new consult.
Statistics are helpful in working through large amounts of data, but on a smaller scale, like my practice, statistics aren’t quite as helpful.
I see, on average, maybe 10 patients per day, consisting of new ones, follow-ups, and electromyography and nerve conduction velocity (EMG/NCV) studies. That is, by far, a smaller number of patients than my colleagues in primary care see, and probably other neurology practices as well. But it works for me.
But that’s on averages and not always. Sometimes we all hit slumps. Who knows why? Everyone is on vacation, or the holidays are coming, or they’ve been abducted by aliens. Whatever the reason, I get the occasional week where I’m pretty bored. Maybe one or two patients in a day. I start to feel like the lonely Maytag repairman behind my desk. I check to see if any drug samples have expired. I wonder if people are actually reading my online reviews and going elsewhere.
Years ago weeks like that terrified me. I was worried my little practice might fail (granted, it still could). But as years – and cycles that make up the averages – go by, they don’t bother me as much.
After 23 years I’ve learned that it’s just part of the normal fluctuations that make up an average. One morning I’ll roll the phones and the lines will explode (figuratively, I hope) with calls. At times like these my secretary seems to grow another pair of arms as she frantically schedules callers, puts others on hold, copies insurance cards, and gives the evil eye to drug reps who step in and ask her if she’s busy.
Then my schedule gets packed. My secretary crams patients in my emergency slots of 7:00, 8:00, and 12:00. MRI results come in that require me to see people sooner rather than later. My “average” of 10 patients per day suddenly doesn’t exist. I go home with a pile of dictations to do and work away into the night to catch up.
With experience we learn to take this in stride. Now, when I hit a slow patch, I remind myself that it’s not the average, and to enjoy it while I can. Read a book, take a long lunch, go home early and nap.
Worrying about where the patients are isn’t productive, or good for your mental health. They know where I am, and will find me when they need me.
. Enjoy the slow times while you can.
Dr. Block has a solo neurology practice in Scottsdale, Ariz.
Everything in medicine, and pretty much the universe, is based on averages. Average reduction of seizures, average blood levels, average response to treatment, average insurance reimbursement, average time spent with a new consult.
Statistics are helpful in working through large amounts of data, but on a smaller scale, like my practice, statistics aren’t quite as helpful.
I see, on average, maybe 10 patients per day, consisting of new ones, follow-ups, and electromyography and nerve conduction velocity (EMG/NCV) studies. That is, by far, a smaller number of patients than my colleagues in primary care see, and probably other neurology practices as well. But it works for me.
But that’s on averages and not always. Sometimes we all hit slumps. Who knows why? Everyone is on vacation, or the holidays are coming, or they’ve been abducted by aliens. Whatever the reason, I get the occasional week where I’m pretty bored. Maybe one or two patients in a day. I start to feel like the lonely Maytag repairman behind my desk. I check to see if any drug samples have expired. I wonder if people are actually reading my online reviews and going elsewhere.
Years ago weeks like that terrified me. I was worried my little practice might fail (granted, it still could). But as years – and cycles that make up the averages – go by, they don’t bother me as much.
After 23 years I’ve learned that it’s just part of the normal fluctuations that make up an average. One morning I’ll roll the phones and the lines will explode (figuratively, I hope) with calls. At times like these my secretary seems to grow another pair of arms as she frantically schedules callers, puts others on hold, copies insurance cards, and gives the evil eye to drug reps who step in and ask her if she’s busy.
Then my schedule gets packed. My secretary crams patients in my emergency slots of 7:00, 8:00, and 12:00. MRI results come in that require me to see people sooner rather than later. My “average” of 10 patients per day suddenly doesn’t exist. I go home with a pile of dictations to do and work away into the night to catch up.
With experience we learn to take this in stride. Now, when I hit a slow patch, I remind myself that it’s not the average, and to enjoy it while I can. Read a book, take a long lunch, go home early and nap.
Worrying about where the patients are isn’t productive, or good for your mental health. They know where I am, and will find me when they need me.
. Enjoy the slow times while you can.
Dr. Block has a solo neurology practice in Scottsdale, Ariz.
Fever after a tropical trip: A guide to differential diagnosis
After 2 years of a pandemic in which traveling was barely possible, tropical diseases are becoming important once more. At a 2022 conference for internal medicine specialists, tropical medicine specialist Fritz Holst, MD, of the Center for Tropical and Travel Medicine in Marburg, Germany, explained what questions you should be asking travelers with a fever at your practice and how to proceed with a suspected case.
The following article is based on the lecture: “Differential Diagnosis of Fever After a Trip to the Tropics,” which Dr. Holst gave at the 128th conference of the German Society of Internal Medicine.
A meta-analysis of studies concerning the topic, “returnee travelers from the tropics with fever,” was published in 2020. According to the analysis, purely tropical infections make up a third (33%) of fever diagnoses worldwide following an exotic trip. Malaria accounts for a fifth (22%), 5% are dengue fever, and 2.2% are typhoid (enteric fever).
In 26% of the returnee travelers investigated, nontropical infections were the cause of the fever. Acute gastroenteritis was responsible for 14%, and respiratory infections were responsible for 13%. In 18% of the cases, the cause of the fever remained unclear.
In Germany, the number of malaria cases has increased, said Dr. Holst. In Hessen, for example, there was recently a malaria fatality. “What we should do has been forgotten again,” he warned. More attention should also be paid once more to prophylaxis.
How to proceed
Dr. Holst described the following steps for treating recently returned travelers who are sick:
- Severely ill or not: If there are signs of a severe disease, such as dyspnea, signs of bleeding, hypotension, or central nervous system symptoms, the patient should be referred to a clinic. A diagnosis should be made within 1 day and treatment should be started.
- Transmissible or dangerous disease: This question should be quickly clarified to protect health care personnel, especially those treating patients. By using a thorough medical history (discussed below), a range of diseases may be clarified.
- Disease outbreak in destination country: Find out about possible disease outbreaks in the country that the traveler visited.
- Malaria? Immediate diagnostics: Malaria should always be excluded in patients at the practice on the same day by using a thick blood smear, even if no fever is present. If this is not possible because of time constraints, the affected person should be transferred directly to the clinic.
- Fever independent of the travel? Exclude other causes of the fever (for example, endocarditis).
- Involve tropical medicine specialists in a timely manner.
Nine mandatory questions
Dr. Holst also listed nine questions that clinicians should ask this patient population.
Where were you exactly?
Depending on the regional prevalence of tropical diseases, certain pathogens can be excluded quickly. Approximately 35% of travelers returning from Africa have malaria, whereas typhoid is much rarer. In contrast, typhoid and dengue fever are much more widespread in Southeast Asia. In Latin America, this is the case for both dengue fever and leptospirosis.
When did you travel?
By using the incubation time of the pathogen in question, as well as the time of return journey, you can determine which diseases are possible and which are not. In one patient who visited the practice 4 weeks after his return, dengue or typhoid were excluded.
Where did you stay overnight?
Whether in an unhygienic bed or under the stars, the question regarding how and where travelers stayed overnight provides important evidence of the following nocturnal vectors:
- Sandflies: Leishmaniasis
- Kissing bugs: Chagas disease
- Fleas: Spotted fever, bubonic plague
- Mosquitoes: Malaria, dengue, filariasis
What did you eat?
Many infections can be attributed to careless eating. For example, when eating fish, crabs, crawfish, or frogs, especially if raw, liver fluke, lung fluke, or ciguatera should be considered. Mussel toxins have been found on the coast of Kenya and even in the south of France. In North African countries, you should be cautious when eating nonpasteurized milk products (for example, camel milk). They can transmit the pathogens for brucellosis and tuberculosis. In beef or pork that has not been cooked thoroughly, there is the risk of trichinosis or of a tapeworm. Even vegetarians need to be careful. Infections with the common liver fluke are possible after eating watercress.
What have you been doing?
You can only get some diseases through certain activities, said Dr. Holst. If long-distance travelers tell you about the following excursions, prick up your ears:
- Freshwater contact: Schistosomiasis, leptospirosis
- Caving: Histoplasmosis, rabies
- Excavations: Anthrax, coccidioidomycosis
- Camel tour: MERS coronavirus (Do not mount a sniffling camel!)
- Walking around barefoot: Strongyloides, hookworm
Was there contact with animals?
Because of the risk of rabies following contact with cats or biting apes, Dr. Holst advised long-distance travelers to get vaccinated.
Were there new sexual partners?
In the event of new sexual contacts, tests for hepatitis A, B, C, and HIV should be performed.
Are you undergoing medical treatment?
The patient may already be under medical supervision because of having a disease.
What prophylactic measures did you take before traveling?
To progress in the differential diagnosis, questions should also be asked regarding prophylactic measures. Vaccination against hepatitis A provides very efficient infection protection, whereas vaccines against typhoid offer a much lower level of protection.
Diagnostic tests
As long as there are no abnormalities, such as meningism or heart murmurs, further diagnostics include routine infectiologic laboratory investigations (C-reactive protein, blood count, etc), blood culture (aerobic, anaerobic), a urine dipstick test, and rapid tests for malaria and dengue.
To exclude malaria, a thick blood smear should always be performed on the same day, said Dr. Holst. “The rapid test is occasionally negative. But you often only detect tertian malaria in the thick blood smear. And you have to repeat the diagnostics the following day.” For this, it is important to know that a single test result does not exclude malaria right away. In contrast, detecting malaria antibodies is obsolete. Depending on the result, further tests include serologies, antigen investigations, and polymerase chain reaction.
Treat early
A complete set of results is not always available promptly. Experts recommend that, “if you already have a hunch, then start the therapy, even without a definite diagnosis.” This applies in particular for the suspected diagnoses in the following table.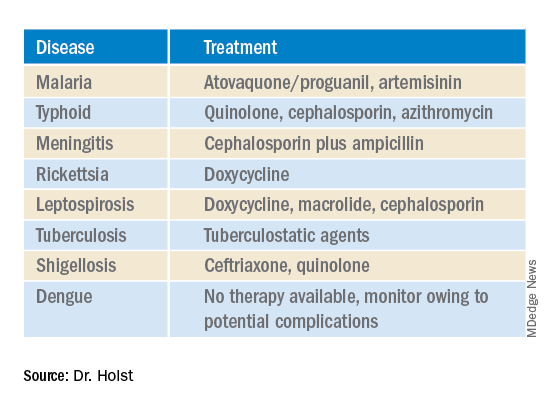
This article was translated from Coliquio. A version of this article appeared on Medscape.com.
After 2 years of a pandemic in which traveling was barely possible, tropical diseases are becoming important once more. At a 2022 conference for internal medicine specialists, tropical medicine specialist Fritz Holst, MD, of the Center for Tropical and Travel Medicine in Marburg, Germany, explained what questions you should be asking travelers with a fever at your practice and how to proceed with a suspected case.
The following article is based on the lecture: “Differential Diagnosis of Fever After a Trip to the Tropics,” which Dr. Holst gave at the 128th conference of the German Society of Internal Medicine.
A meta-analysis of studies concerning the topic, “returnee travelers from the tropics with fever,” was published in 2020. According to the analysis, purely tropical infections make up a third (33%) of fever diagnoses worldwide following an exotic trip. Malaria accounts for a fifth (22%), 5% are dengue fever, and 2.2% are typhoid (enteric fever).
In 26% of the returnee travelers investigated, nontropical infections were the cause of the fever. Acute gastroenteritis was responsible for 14%, and respiratory infections were responsible for 13%. In 18% of the cases, the cause of the fever remained unclear.
In Germany, the number of malaria cases has increased, said Dr. Holst. In Hessen, for example, there was recently a malaria fatality. “What we should do has been forgotten again,” he warned. More attention should also be paid once more to prophylaxis.
How to proceed
Dr. Holst described the following steps for treating recently returned travelers who are sick:
- Severely ill or not: If there are signs of a severe disease, such as dyspnea, signs of bleeding, hypotension, or central nervous system symptoms, the patient should be referred to a clinic. A diagnosis should be made within 1 day and treatment should be started.
- Transmissible or dangerous disease: This question should be quickly clarified to protect health care personnel, especially those treating patients. By using a thorough medical history (discussed below), a range of diseases may be clarified.
- Disease outbreak in destination country: Find out about possible disease outbreaks in the country that the traveler visited.
- Malaria? Immediate diagnostics: Malaria should always be excluded in patients at the practice on the same day by using a thick blood smear, even if no fever is present. If this is not possible because of time constraints, the affected person should be transferred directly to the clinic.
- Fever independent of the travel? Exclude other causes of the fever (for example, endocarditis).
- Involve tropical medicine specialists in a timely manner.
Nine mandatory questions
Dr. Holst also listed nine questions that clinicians should ask this patient population.
Where were you exactly?
Depending on the regional prevalence of tropical diseases, certain pathogens can be excluded quickly. Approximately 35% of travelers returning from Africa have malaria, whereas typhoid is much rarer. In contrast, typhoid and dengue fever are much more widespread in Southeast Asia. In Latin America, this is the case for both dengue fever and leptospirosis.
When did you travel?
By using the incubation time of the pathogen in question, as well as the time of return journey, you can determine which diseases are possible and which are not. In one patient who visited the practice 4 weeks after his return, dengue or typhoid were excluded.
Where did you stay overnight?
Whether in an unhygienic bed or under the stars, the question regarding how and where travelers stayed overnight provides important evidence of the following nocturnal vectors:
- Sandflies: Leishmaniasis
- Kissing bugs: Chagas disease
- Fleas: Spotted fever, bubonic plague
- Mosquitoes: Malaria, dengue, filariasis
What did you eat?
Many infections can be attributed to careless eating. For example, when eating fish, crabs, crawfish, or frogs, especially if raw, liver fluke, lung fluke, or ciguatera should be considered. Mussel toxins have been found on the coast of Kenya and even in the south of France. In North African countries, you should be cautious when eating nonpasteurized milk products (for example, camel milk). They can transmit the pathogens for brucellosis and tuberculosis. In beef or pork that has not been cooked thoroughly, there is the risk of trichinosis or of a tapeworm. Even vegetarians need to be careful. Infections with the common liver fluke are possible after eating watercress.
What have you been doing?
You can only get some diseases through certain activities, said Dr. Holst. If long-distance travelers tell you about the following excursions, prick up your ears:
- Freshwater contact: Schistosomiasis, leptospirosis
- Caving: Histoplasmosis, rabies
- Excavations: Anthrax, coccidioidomycosis
- Camel tour: MERS coronavirus (Do not mount a sniffling camel!)
- Walking around barefoot: Strongyloides, hookworm
Was there contact with animals?
Because of the risk of rabies following contact with cats or biting apes, Dr. Holst advised long-distance travelers to get vaccinated.
Were there new sexual partners?
In the event of new sexual contacts, tests for hepatitis A, B, C, and HIV should be performed.
Are you undergoing medical treatment?
The patient may already be under medical supervision because of having a disease.
What prophylactic measures did you take before traveling?
To progress in the differential diagnosis, questions should also be asked regarding prophylactic measures. Vaccination against hepatitis A provides very efficient infection protection, whereas vaccines against typhoid offer a much lower level of protection.
Diagnostic tests
As long as there are no abnormalities, such as meningism or heart murmurs, further diagnostics include routine infectiologic laboratory investigations (C-reactive protein, blood count, etc), blood culture (aerobic, anaerobic), a urine dipstick test, and rapid tests for malaria and dengue.
To exclude malaria, a thick blood smear should always be performed on the same day, said Dr. Holst. “The rapid test is occasionally negative. But you often only detect tertian malaria in the thick blood smear. And you have to repeat the diagnostics the following day.” For this, it is important to know that a single test result does not exclude malaria right away. In contrast, detecting malaria antibodies is obsolete. Depending on the result, further tests include serologies, antigen investigations, and polymerase chain reaction.
Treat early
A complete set of results is not always available promptly. Experts recommend that, “if you already have a hunch, then start the therapy, even without a definite diagnosis.” This applies in particular for the suspected diagnoses in the following table.
This article was translated from Coliquio. A version of this article appeared on Medscape.com.
After 2 years of a pandemic in which traveling was barely possible, tropical diseases are becoming important once more. At a 2022 conference for internal medicine specialists, tropical medicine specialist Fritz Holst, MD, of the Center for Tropical and Travel Medicine in Marburg, Germany, explained what questions you should be asking travelers with a fever at your practice and how to proceed with a suspected case.
The following article is based on the lecture: “Differential Diagnosis of Fever After a Trip to the Tropics,” which Dr. Holst gave at the 128th conference of the German Society of Internal Medicine.
A meta-analysis of studies concerning the topic, “returnee travelers from the tropics with fever,” was published in 2020. According to the analysis, purely tropical infections make up a third (33%) of fever diagnoses worldwide following an exotic trip. Malaria accounts for a fifth (22%), 5% are dengue fever, and 2.2% are typhoid (enteric fever).
In 26% of the returnee travelers investigated, nontropical infections were the cause of the fever. Acute gastroenteritis was responsible for 14%, and respiratory infections were responsible for 13%. In 18% of the cases, the cause of the fever remained unclear.
In Germany, the number of malaria cases has increased, said Dr. Holst. In Hessen, for example, there was recently a malaria fatality. “What we should do has been forgotten again,” he warned. More attention should also be paid once more to prophylaxis.
How to proceed
Dr. Holst described the following steps for treating recently returned travelers who are sick:
- Severely ill or not: If there are signs of a severe disease, such as dyspnea, signs of bleeding, hypotension, or central nervous system symptoms, the patient should be referred to a clinic. A diagnosis should be made within 1 day and treatment should be started.
- Transmissible or dangerous disease: This question should be quickly clarified to protect health care personnel, especially those treating patients. By using a thorough medical history (discussed below), a range of diseases may be clarified.
- Disease outbreak in destination country: Find out about possible disease outbreaks in the country that the traveler visited.
- Malaria? Immediate diagnostics: Malaria should always be excluded in patients at the practice on the same day by using a thick blood smear, even if no fever is present. If this is not possible because of time constraints, the affected person should be transferred directly to the clinic.
- Fever independent of the travel? Exclude other causes of the fever (for example, endocarditis).
- Involve tropical medicine specialists in a timely manner.
Nine mandatory questions
Dr. Holst also listed nine questions that clinicians should ask this patient population.
Where were you exactly?
Depending on the regional prevalence of tropical diseases, certain pathogens can be excluded quickly. Approximately 35% of travelers returning from Africa have malaria, whereas typhoid is much rarer. In contrast, typhoid and dengue fever are much more widespread in Southeast Asia. In Latin America, this is the case for both dengue fever and leptospirosis.
When did you travel?
By using the incubation time of the pathogen in question, as well as the time of return journey, you can determine which diseases are possible and which are not. In one patient who visited the practice 4 weeks after his return, dengue or typhoid were excluded.
Where did you stay overnight?
Whether in an unhygienic bed or under the stars, the question regarding how and where travelers stayed overnight provides important evidence of the following nocturnal vectors:
- Sandflies: Leishmaniasis
- Kissing bugs: Chagas disease
- Fleas: Spotted fever, bubonic plague
- Mosquitoes: Malaria, dengue, filariasis
What did you eat?
Many infections can be attributed to careless eating. For example, when eating fish, crabs, crawfish, or frogs, especially if raw, liver fluke, lung fluke, or ciguatera should be considered. Mussel toxins have been found on the coast of Kenya and even in the south of France. In North African countries, you should be cautious when eating nonpasteurized milk products (for example, camel milk). They can transmit the pathogens for brucellosis and tuberculosis. In beef or pork that has not been cooked thoroughly, there is the risk of trichinosis or of a tapeworm. Even vegetarians need to be careful. Infections with the common liver fluke are possible after eating watercress.
What have you been doing?
You can only get some diseases through certain activities, said Dr. Holst. If long-distance travelers tell you about the following excursions, prick up your ears:
- Freshwater contact: Schistosomiasis, leptospirosis
- Caving: Histoplasmosis, rabies
- Excavations: Anthrax, coccidioidomycosis
- Camel tour: MERS coronavirus (Do not mount a sniffling camel!)
- Walking around barefoot: Strongyloides, hookworm
Was there contact with animals?
Because of the risk of rabies following contact with cats or biting apes, Dr. Holst advised long-distance travelers to get vaccinated.
Were there new sexual partners?
In the event of new sexual contacts, tests for hepatitis A, B, C, and HIV should be performed.
Are you undergoing medical treatment?
The patient may already be under medical supervision because of having a disease.
What prophylactic measures did you take before traveling?
To progress in the differential diagnosis, questions should also be asked regarding prophylactic measures. Vaccination against hepatitis A provides very efficient infection protection, whereas vaccines against typhoid offer a much lower level of protection.
Diagnostic tests
As long as there are no abnormalities, such as meningism or heart murmurs, further diagnostics include routine infectiologic laboratory investigations (C-reactive protein, blood count, etc), blood culture (aerobic, anaerobic), a urine dipstick test, and rapid tests for malaria and dengue.
To exclude malaria, a thick blood smear should always be performed on the same day, said Dr. Holst. “The rapid test is occasionally negative. But you often only detect tertian malaria in the thick blood smear. And you have to repeat the diagnostics the following day.” For this, it is important to know that a single test result does not exclude malaria right away. In contrast, detecting malaria antibodies is obsolete. Depending on the result, further tests include serologies, antigen investigations, and polymerase chain reaction.
Treat early
A complete set of results is not always available promptly. Experts recommend that, “if you already have a hunch, then start the therapy, even without a definite diagnosis.” This applies in particular for the suspected diagnoses in the following table.
This article was translated from Coliquio. A version of this article appeared on Medscape.com.
Does COVID-19 raise the risk for diabetes?
This transcript has been edited for clarity.
Does having had a COVID-19 infection increase your risk for the development of diabetes subsequently? Some data say yes and other data say no. No matter what, it’s obviously important to screen people for diabetes routinely, pandemic or not. Remember, screening should start at age 35.
For over a decade, we have known that SARS-type viruses bind to beta cells. This could cause either direct damage to the beta cell or in some way trigger beta cell autoimmunity. We also know that COVID-19 infection increases the levels of inflammatory mediators, which could cause damage to beta cells and potentially to insulin receptors. There is a potential that having had a COVID-19 infection could increase rates of developing type 1 and/or type 2 diabetes.
However, there are other possible causes for people to develop diabetes after having a COVID-19 infection. A COVID-19 infection could cause one to seek medical care, unmasking latent type 1 and/or type 2 diabetes by causing infection-related insulin resistance and worsening preexisting mild hypoglycemia. In addition, people could have sought more medical care in the years since the pandemic has been ebbing, which may make it look like cases have increased.
For example, during the worst of the pandemic, I had multiple referrals for “COVID-19–caused new-onset diabetes” only to find that the patient had an A1c level above 10% and a history of mildly elevated blood glucose levels. This suggests to me that COVID-19 did not cause the diabetes per se but rather worsened an underlying glucose abnormality.
Since the pandemic has improved, I have also seen people diagnosed with type 2 diabetes that I think is associated with pandemic-related weight gain and inactivity.
The bigger issue is what is happening to people after COVID-19 infection who lack risk factors. What about those who we didn’t think were at high risk to get diabetes to begin with and didn’t have prediabetes?
An article by Xie and Al-Aly in The Lancet Diabetes & Endocrinology showed an increase in rates of diabetes in a large VA cohort among those who had a COVID-19 infection compared with both a contemporaneous control who did not have COVID-19 and a historical control. The researchers looked at the patient data 1 year after they’d had COVID-19, so it wasn’t the immediate post–COVID-19 phase but several months later.
They found that the risk for incident type 2 diabetes development was increased by 40% after adjusting for many risk factors. This included individuals who didn’t have traditional risk factors before they developed type 2 diabetes.
What does this mean clinically? First, pandemic or not, people need screening for diabetes and encouragement to have a healthy lifestyle. There may be an increased risk for the diagnosis of type 2 diabetes after COVID-19 infection due to a variety of different mechanisms.
As for people with type 1 diabetes, we also don’t know if having a COVID-19 infection increases their risk. We do know that there was an increase in the severity of diabetic ketoacidosis presentation during the pandemic, so we need to be sure that we reinforce sick-day rules with our patients with type 1 diabetes and that all individuals with type 1 diabetes have the ability to test their ketone levels at home.
In people with new-onset diabetes, whether type 1 or type 2, caused by COVID-19 or not, we need to treat appropriately based on their clinical situation.
Data from registries started during the pandemic will provide more definitive answers and help us find out if there is a relationship between having had COVID-19 infection and developing diabetes.
Perhaps that can help us better understand the mechanisms behind the development of diabetes overall.
Dr. Peters is professor of medicine at the University of Southern California, Los Angeles, and director of the USC clinical diabetes programs. She disclosed ties with Abbott Diabetes Care, AstraZeneca, Becton Dickinson, Boehringer Ingelheim Pharmaceuticals, Dexcom, Eli Lilly, Lexicon Pharmaceuticals, Livongo, MannKind Corporation, Medscape, Merck, Novo Nordisk, Omada Health, OptumHealth, Sanofi, and Zafgen. A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
Does having had a COVID-19 infection increase your risk for the development of diabetes subsequently? Some data say yes and other data say no. No matter what, it’s obviously important to screen people for diabetes routinely, pandemic or not. Remember, screening should start at age 35.
For over a decade, we have known that SARS-type viruses bind to beta cells. This could cause either direct damage to the beta cell or in some way trigger beta cell autoimmunity. We also know that COVID-19 infection increases the levels of inflammatory mediators, which could cause damage to beta cells and potentially to insulin receptors. There is a potential that having had a COVID-19 infection could increase rates of developing type 1 and/or type 2 diabetes.
However, there are other possible causes for people to develop diabetes after having a COVID-19 infection. A COVID-19 infection could cause one to seek medical care, unmasking latent type 1 and/or type 2 diabetes by causing infection-related insulin resistance and worsening preexisting mild hypoglycemia. In addition, people could have sought more medical care in the years since the pandemic has been ebbing, which may make it look like cases have increased.
For example, during the worst of the pandemic, I had multiple referrals for “COVID-19–caused new-onset diabetes” only to find that the patient had an A1c level above 10% and a history of mildly elevated blood glucose levels. This suggests to me that COVID-19 did not cause the diabetes per se but rather worsened an underlying glucose abnormality.
Since the pandemic has improved, I have also seen people diagnosed with type 2 diabetes that I think is associated with pandemic-related weight gain and inactivity.
The bigger issue is what is happening to people after COVID-19 infection who lack risk factors. What about those who we didn’t think were at high risk to get diabetes to begin with and didn’t have prediabetes?
An article by Xie and Al-Aly in The Lancet Diabetes & Endocrinology showed an increase in rates of diabetes in a large VA cohort among those who had a COVID-19 infection compared with both a contemporaneous control who did not have COVID-19 and a historical control. The researchers looked at the patient data 1 year after they’d had COVID-19, so it wasn’t the immediate post–COVID-19 phase but several months later.
They found that the risk for incident type 2 diabetes development was increased by 40% after adjusting for many risk factors. This included individuals who didn’t have traditional risk factors before they developed type 2 diabetes.
What does this mean clinically? First, pandemic or not, people need screening for diabetes and encouragement to have a healthy lifestyle. There may be an increased risk for the diagnosis of type 2 diabetes after COVID-19 infection due to a variety of different mechanisms.
As for people with type 1 diabetes, we also don’t know if having a COVID-19 infection increases their risk. We do know that there was an increase in the severity of diabetic ketoacidosis presentation during the pandemic, so we need to be sure that we reinforce sick-day rules with our patients with type 1 diabetes and that all individuals with type 1 diabetes have the ability to test their ketone levels at home.
In people with new-onset diabetes, whether type 1 or type 2, caused by COVID-19 or not, we need to treat appropriately based on their clinical situation.
Data from registries started during the pandemic will provide more definitive answers and help us find out if there is a relationship between having had COVID-19 infection and developing diabetes.
Perhaps that can help us better understand the mechanisms behind the development of diabetes overall.
Dr. Peters is professor of medicine at the University of Southern California, Los Angeles, and director of the USC clinical diabetes programs. She disclosed ties with Abbott Diabetes Care, AstraZeneca, Becton Dickinson, Boehringer Ingelheim Pharmaceuticals, Dexcom, Eli Lilly, Lexicon Pharmaceuticals, Livongo, MannKind Corporation, Medscape, Merck, Novo Nordisk, Omada Health, OptumHealth, Sanofi, and Zafgen. A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
Does having had a COVID-19 infection increase your risk for the development of diabetes subsequently? Some data say yes and other data say no. No matter what, it’s obviously important to screen people for diabetes routinely, pandemic or not. Remember, screening should start at age 35.
For over a decade, we have known that SARS-type viruses bind to beta cells. This could cause either direct damage to the beta cell or in some way trigger beta cell autoimmunity. We also know that COVID-19 infection increases the levels of inflammatory mediators, which could cause damage to beta cells and potentially to insulin receptors. There is a potential that having had a COVID-19 infection could increase rates of developing type 1 and/or type 2 diabetes.
However, there are other possible causes for people to develop diabetes after having a COVID-19 infection. A COVID-19 infection could cause one to seek medical care, unmasking latent type 1 and/or type 2 diabetes by causing infection-related insulin resistance and worsening preexisting mild hypoglycemia. In addition, people could have sought more medical care in the years since the pandemic has been ebbing, which may make it look like cases have increased.
For example, during the worst of the pandemic, I had multiple referrals for “COVID-19–caused new-onset diabetes” only to find that the patient had an A1c level above 10% and a history of mildly elevated blood glucose levels. This suggests to me that COVID-19 did not cause the diabetes per se but rather worsened an underlying glucose abnormality.
Since the pandemic has improved, I have also seen people diagnosed with type 2 diabetes that I think is associated with pandemic-related weight gain and inactivity.
The bigger issue is what is happening to people after COVID-19 infection who lack risk factors. What about those who we didn’t think were at high risk to get diabetes to begin with and didn’t have prediabetes?
An article by Xie and Al-Aly in The Lancet Diabetes & Endocrinology showed an increase in rates of diabetes in a large VA cohort among those who had a COVID-19 infection compared with both a contemporaneous control who did not have COVID-19 and a historical control. The researchers looked at the patient data 1 year after they’d had COVID-19, so it wasn’t the immediate post–COVID-19 phase but several months later.
They found that the risk for incident type 2 diabetes development was increased by 40% after adjusting for many risk factors. This included individuals who didn’t have traditional risk factors before they developed type 2 diabetes.
What does this mean clinically? First, pandemic or not, people need screening for diabetes and encouragement to have a healthy lifestyle. There may be an increased risk for the diagnosis of type 2 diabetes after COVID-19 infection due to a variety of different mechanisms.
As for people with type 1 diabetes, we also don’t know if having a COVID-19 infection increases their risk. We do know that there was an increase in the severity of diabetic ketoacidosis presentation during the pandemic, so we need to be sure that we reinforce sick-day rules with our patients with type 1 diabetes and that all individuals with type 1 diabetes have the ability to test their ketone levels at home.
In people with new-onset diabetes, whether type 1 or type 2, caused by COVID-19 or not, we need to treat appropriately based on their clinical situation.
Data from registries started during the pandemic will provide more definitive answers and help us find out if there is a relationship between having had COVID-19 infection and developing diabetes.
Perhaps that can help us better understand the mechanisms behind the development of diabetes overall.
Dr. Peters is professor of medicine at the University of Southern California, Los Angeles, and director of the USC clinical diabetes programs. She disclosed ties with Abbott Diabetes Care, AstraZeneca, Becton Dickinson, Boehringer Ingelheim Pharmaceuticals, Dexcom, Eli Lilly, Lexicon Pharmaceuticals, Livongo, MannKind Corporation, Medscape, Merck, Novo Nordisk, Omada Health, OptumHealth, Sanofi, and Zafgen. A version of this article first appeared on Medscape.com.
20th anniversary and history of cosmetic botulinum toxin type A
The timeline of botulinum toxin discovery began with deadly outbreaks related to contaminated food across Europe in the late 1700s, the largest of which occurred in 1793 in Wildebrad, in southern Germany. In 1811, “prussic acid” was named as the culprit in what was referred to as sausage poisoning. Between 1817 and 1822, German physician Justinus Kerner noted that the active substance interrupted signals from motor nerves to muscles, but spared sensory and cognitive abilities, accurately describing botulism. He hypothesized that this substance could possibly be used as treatment for medical conditions when ingested orally. It wasn’t until 1895 that microbiologist Emile Pierre Van Ermengem, a professor of bacteriology in Belgium, identified the bacterium responsible as Bacillus botulinus, later renamed C. botulinum.
In 1905, it was discovered that C. botulinum produced a substance that affected neurotransmitter function, and between 1895 and 1915, seven toxin serotypes were recognized. In 1928, Herman Sommer, PhD, at the Hooper Foundation, at the University of California, San Francisco, isolated the most potent serotype: botulinum toxin type A (BoNT-A).
In 1946, Carl Lamanna and James Duff developed concentration and crystallization techniques that were subsequently used by Edward Schantz, PhD, at Fort Detrick, Md., for a possible biologic weapon. In 1972, Dr. Schantz took his research to the University of Wisconsin, where he produced a large batch of BoNT-A that remained in clinical use until December 1997.
In the late 1960s and early 1970s, an ophthalmologist in San Francisco, Alan Scott, MD, began animal studies with BoNT-A supplied by Dr. Schantz, as a possible treatment for strabismus, publishing his first report of BoNT-A in primates in 1973. In 1978, the Food and Drug Administration granted approval to begin testing small amounts of the toxin in human volunteers. In 1980, a landmark paper was published demonstrating that BoNT-A corrects gaze misalignment in humans. By 1989, it was approved as Oculinum by the FDA for the treatment of strabismus and blepharospasm.
Keen clinical observation and a serendipitous discovery led to botulinum toxin’s first uses for cosmetic purposes. In the mid-1980s, Jean Carruthers, MD, an ophthalmologist in Vancouver, noted an unexpected concomitant improvement of glabellar rhytids in a patient treated with BoNT for blepharospasm. The result of the treatment was a more serene, untroubled expression. Dr. Carruthers discussed the observation with her dermatologist spouse, Alastair Carruthers, MD, who was attempting to use soft tissue–augmenting agents available at the time to soften forehead wrinkles. Intrigued by the possibilities, the Carruthers subsequently injected a small amount of BoNT-A between the eyebrows of their assistant, Cathy Bickerton Swann, also now known as “patient zero” and awaited the results.
Seventeen additional patients followed, aged 34-51, who collectively, would become part of the first report on the efficacy of BoNT-A for cosmetic use – for the treatment of glabellar frown lines – published in 1992.
Between 1992 and 1997, the popularity of off-label use of BoNT-A grew so rapidly that Allergan’s supply temporarily ran out. By 2002, safety and efficacy profiles of use in medical conditions such as strabismus, blepharospasm, hemifacial spasm, cervical dystonia, cerebral palsy, poststroke spasticity, hyperhidrosis, headache, and back pain had been well-established, facilitating the comfort and use for cosmetic purposes.
By 2002, open-label studies of more than 800 patients confirmed the efficacy and safety of BoNT for the treatment of dynamic facial rhytids. And in April 2002, the FDA granted approval of BoNT for the nonsurgical reduction of glabellar rhytids. The rest, some would say, is history. On this 20th-year anniversary of the approval of botulinum toxin for cosmetic use, special recognition is given here for the physicians and scientists who were astute enough to make this discovery, as botulinum toxin use remains one of the most popular and effective nonsurgical cosmetic procedures today.
Dr. Wesley and Dr. Lily Talakoub are cocontributors to this column. Dr. Wesley practices dermatology in Beverly Hills, Calif. Dr. Talakoub is in private practice in McLean, Va. This month’s column is by Dr. Wesley. Write to them at [email protected]. Dr. Wesley disclosed that she has been a clinical investigator and consultant for Botox manufacturer Allergan in the past, and manufacturers of other brands of botulinum toxins available for cosmetic use; Dysport (Galderma), Xeomin (Merz), and Jeuveau (Evolus). Dr. Talakoub had no disclosures.
Reference
“Botulinum Toxin: Procedures in Cosmetic Dermatology Series 3rd Edition” (Philadelphia: Saunders Elsevier, 2013)
The timeline of botulinum toxin discovery began with deadly outbreaks related to contaminated food across Europe in the late 1700s, the largest of which occurred in 1793 in Wildebrad, in southern Germany. In 1811, “prussic acid” was named as the culprit in what was referred to as sausage poisoning. Between 1817 and 1822, German physician Justinus Kerner noted that the active substance interrupted signals from motor nerves to muscles, but spared sensory and cognitive abilities, accurately describing botulism. He hypothesized that this substance could possibly be used as treatment for medical conditions when ingested orally. It wasn’t until 1895 that microbiologist Emile Pierre Van Ermengem, a professor of bacteriology in Belgium, identified the bacterium responsible as Bacillus botulinus, later renamed C. botulinum.
In 1905, it was discovered that C. botulinum produced a substance that affected neurotransmitter function, and between 1895 and 1915, seven toxin serotypes were recognized. In 1928, Herman Sommer, PhD, at the Hooper Foundation, at the University of California, San Francisco, isolated the most potent serotype: botulinum toxin type A (BoNT-A).
In 1946, Carl Lamanna and James Duff developed concentration and crystallization techniques that were subsequently used by Edward Schantz, PhD, at Fort Detrick, Md., for a possible biologic weapon. In 1972, Dr. Schantz took his research to the University of Wisconsin, where he produced a large batch of BoNT-A that remained in clinical use until December 1997.
In the late 1960s and early 1970s, an ophthalmologist in San Francisco, Alan Scott, MD, began animal studies with BoNT-A supplied by Dr. Schantz, as a possible treatment for strabismus, publishing his first report of BoNT-A in primates in 1973. In 1978, the Food and Drug Administration granted approval to begin testing small amounts of the toxin in human volunteers. In 1980, a landmark paper was published demonstrating that BoNT-A corrects gaze misalignment in humans. By 1989, it was approved as Oculinum by the FDA for the treatment of strabismus and blepharospasm.
Keen clinical observation and a serendipitous discovery led to botulinum toxin’s first uses for cosmetic purposes. In the mid-1980s, Jean Carruthers, MD, an ophthalmologist in Vancouver, noted an unexpected concomitant improvement of glabellar rhytids in a patient treated with BoNT for blepharospasm. The result of the treatment was a more serene, untroubled expression. Dr. Carruthers discussed the observation with her dermatologist spouse, Alastair Carruthers, MD, who was attempting to use soft tissue–augmenting agents available at the time to soften forehead wrinkles. Intrigued by the possibilities, the Carruthers subsequently injected a small amount of BoNT-A between the eyebrows of their assistant, Cathy Bickerton Swann, also now known as “patient zero” and awaited the results.
Seventeen additional patients followed, aged 34-51, who collectively, would become part of the first report on the efficacy of BoNT-A for cosmetic use – for the treatment of glabellar frown lines – published in 1992.
Between 1992 and 1997, the popularity of off-label use of BoNT-A grew so rapidly that Allergan’s supply temporarily ran out. By 2002, safety and efficacy profiles of use in medical conditions such as strabismus, blepharospasm, hemifacial spasm, cervical dystonia, cerebral palsy, poststroke spasticity, hyperhidrosis, headache, and back pain had been well-established, facilitating the comfort and use for cosmetic purposes.
By 2002, open-label studies of more than 800 patients confirmed the efficacy and safety of BoNT for the treatment of dynamic facial rhytids. And in April 2002, the FDA granted approval of BoNT for the nonsurgical reduction of glabellar rhytids. The rest, some would say, is history. On this 20th-year anniversary of the approval of botulinum toxin for cosmetic use, special recognition is given here for the physicians and scientists who were astute enough to make this discovery, as botulinum toxin use remains one of the most popular and effective nonsurgical cosmetic procedures today.
Dr. Wesley and Dr. Lily Talakoub are cocontributors to this column. Dr. Wesley practices dermatology in Beverly Hills, Calif. Dr. Talakoub is in private practice in McLean, Va. This month’s column is by Dr. Wesley. Write to them at [email protected]. Dr. Wesley disclosed that she has been a clinical investigator and consultant for Botox manufacturer Allergan in the past, and manufacturers of other brands of botulinum toxins available for cosmetic use; Dysport (Galderma), Xeomin (Merz), and Jeuveau (Evolus). Dr. Talakoub had no disclosures.
Reference
“Botulinum Toxin: Procedures in Cosmetic Dermatology Series 3rd Edition” (Philadelphia: Saunders Elsevier, 2013)
The timeline of botulinum toxin discovery began with deadly outbreaks related to contaminated food across Europe in the late 1700s, the largest of which occurred in 1793 in Wildebrad, in southern Germany. In 1811, “prussic acid” was named as the culprit in what was referred to as sausage poisoning. Between 1817 and 1822, German physician Justinus Kerner noted that the active substance interrupted signals from motor nerves to muscles, but spared sensory and cognitive abilities, accurately describing botulism. He hypothesized that this substance could possibly be used as treatment for medical conditions when ingested orally. It wasn’t until 1895 that microbiologist Emile Pierre Van Ermengem, a professor of bacteriology in Belgium, identified the bacterium responsible as Bacillus botulinus, later renamed C. botulinum.
In 1905, it was discovered that C. botulinum produced a substance that affected neurotransmitter function, and between 1895 and 1915, seven toxin serotypes were recognized. In 1928, Herman Sommer, PhD, at the Hooper Foundation, at the University of California, San Francisco, isolated the most potent serotype: botulinum toxin type A (BoNT-A).
In 1946, Carl Lamanna and James Duff developed concentration and crystallization techniques that were subsequently used by Edward Schantz, PhD, at Fort Detrick, Md., for a possible biologic weapon. In 1972, Dr. Schantz took his research to the University of Wisconsin, where he produced a large batch of BoNT-A that remained in clinical use until December 1997.
In the late 1960s and early 1970s, an ophthalmologist in San Francisco, Alan Scott, MD, began animal studies with BoNT-A supplied by Dr. Schantz, as a possible treatment for strabismus, publishing his first report of BoNT-A in primates in 1973. In 1978, the Food and Drug Administration granted approval to begin testing small amounts of the toxin in human volunteers. In 1980, a landmark paper was published demonstrating that BoNT-A corrects gaze misalignment in humans. By 1989, it was approved as Oculinum by the FDA for the treatment of strabismus and blepharospasm.
Keen clinical observation and a serendipitous discovery led to botulinum toxin’s first uses for cosmetic purposes. In the mid-1980s, Jean Carruthers, MD, an ophthalmologist in Vancouver, noted an unexpected concomitant improvement of glabellar rhytids in a patient treated with BoNT for blepharospasm. The result of the treatment was a more serene, untroubled expression. Dr. Carruthers discussed the observation with her dermatologist spouse, Alastair Carruthers, MD, who was attempting to use soft tissue–augmenting agents available at the time to soften forehead wrinkles. Intrigued by the possibilities, the Carruthers subsequently injected a small amount of BoNT-A between the eyebrows of their assistant, Cathy Bickerton Swann, also now known as “patient zero” and awaited the results.
Seventeen additional patients followed, aged 34-51, who collectively, would become part of the first report on the efficacy of BoNT-A for cosmetic use – for the treatment of glabellar frown lines – published in 1992.
Between 1992 and 1997, the popularity of off-label use of BoNT-A grew so rapidly that Allergan’s supply temporarily ran out. By 2002, safety and efficacy profiles of use in medical conditions such as strabismus, blepharospasm, hemifacial spasm, cervical dystonia, cerebral palsy, poststroke spasticity, hyperhidrosis, headache, and back pain had been well-established, facilitating the comfort and use for cosmetic purposes.
By 2002, open-label studies of more than 800 patients confirmed the efficacy and safety of BoNT for the treatment of dynamic facial rhytids. And in April 2002, the FDA granted approval of BoNT for the nonsurgical reduction of glabellar rhytids. The rest, some would say, is history. On this 20th-year anniversary of the approval of botulinum toxin for cosmetic use, special recognition is given here for the physicians and scientists who were astute enough to make this discovery, as botulinum toxin use remains one of the most popular and effective nonsurgical cosmetic procedures today.
Dr. Wesley and Dr. Lily Talakoub are cocontributors to this column. Dr. Wesley practices dermatology in Beverly Hills, Calif. Dr. Talakoub is in private practice in McLean, Va. This month’s column is by Dr. Wesley. Write to them at [email protected]. Dr. Wesley disclosed that she has been a clinical investigator and consultant for Botox manufacturer Allergan in the past, and manufacturers of other brands of botulinum toxins available for cosmetic use; Dysport (Galderma), Xeomin (Merz), and Jeuveau (Evolus). Dr. Talakoub had no disclosures.
Reference
“Botulinum Toxin: Procedures in Cosmetic Dermatology Series 3rd Edition” (Philadelphia: Saunders Elsevier, 2013)
Climate change, medical education, and dermatology
The recent article on including the impact of climate on health in medical education programs shines an important light on the challenge – and urgent need – of integrating climate change training into medical education. These nascent efforts are just getting underway across the country, with some programs – notably Harvard’s C-CHANGE (Center for Climate, Health, and the Global Environment) program, mentioned in the article, and others, such as the University of Colorado’s Climate Medicine diploma course – leading the way. A number of publications, such as the editorial titled “A planetary health curriculum for medicine” published in 2021 in the BMJ, offer a roadmap to do so.
Medical schools, residency programs, and other medical specialty programs – including those for advanced practice providers, dentists, nurses, and more – should be incorporating climate change and its myriad of health impacts into their training pathways. The medical student group, Medical Students for a Sustainable Future, has put forth a planetary health report card that evaluates training programs on the strength of their focus on the intersections between climate and health.
While the article did not specifically focus on dermatology, these impacts are true in our field as well. The article notes that “at least one medical journal has recently ramped up its efforts to educate physicians on the links between health issues and climate change.” Notably in dermatology, the International Journal of Women’s Dermatology devoted an entire 124-page themed issue to climate change and dermatology in January, 2021, while JAMA Dermatology editor Kanade Shinkai, MD, PhD, called out climate change as one of the journal’s priorities in her annual editorial, stating, “Another priority for the journal is to better understand the effect of climate change on human health, specifically skin disease.”
The impacts of climate change in dermatology range from heat-related illness (a major cause of climate-associated mortality, with the skin serving as an essential thermoregulatory organ) to changing patterns of vector-borne illnesses to pollution and wildfire smoke flaring inflammatory skin diseases, to an increase in skin cancer, and more. While incorporation of health issues relating to climate change is important at a medical school level, it is also critical at the residency training – and board exam/certification – level as well.
Beyond the importance of building climate education into undergraduate and graduate medical education, it is also important that practicing physicians, post-residency training, remain up to date and keep abreast of changing patterns of disease in our rapidly changing climate. Lyme disease now occurs in Canada – and both earlier and later in the year even in places that are geographically used to seeing it. Early recognition is essential, but unprepared physicians may miss the early erythema migrans rash, and patients may suffer more severe sequelae as a result.
Finally, it’s important that medical organizations are aware of not just the health implications of climate change, but also potential policy impacts. Health care is a major emitter of CO2, and assistant secretary for health for the U.S. Department of Health and Human Services, Admiral Rachel L. Levine, MD, with the National Academy of Medicine, has appropriately pledged to reduce health care carbon emissions as part of the necessary steps that we must all take to avert the worst impacts of a warming world. The field of medicine and individual providers should educate themselves and actively work toward sustainability in health care, to improve the health of their patients, populations, and future generations.
Dr. Rosenbach is associate professor of dermatology and medicine at the University of Pennsylvania, Philadelphia, and is the founder and cochair of the American Academy of Dermatology Expert Resource Group for Climate Change and Environmental Issues. Dr. Rosenbach is speaking on behalf of himself and not the AAD.
The recent article on including the impact of climate on health in medical education programs shines an important light on the challenge – and urgent need – of integrating climate change training into medical education. These nascent efforts are just getting underway across the country, with some programs – notably Harvard’s C-CHANGE (Center for Climate, Health, and the Global Environment) program, mentioned in the article, and others, such as the University of Colorado’s Climate Medicine diploma course – leading the way. A number of publications, such as the editorial titled “A planetary health curriculum for medicine” published in 2021 in the BMJ, offer a roadmap to do so.
Medical schools, residency programs, and other medical specialty programs – including those for advanced practice providers, dentists, nurses, and more – should be incorporating climate change and its myriad of health impacts into their training pathways. The medical student group, Medical Students for a Sustainable Future, has put forth a planetary health report card that evaluates training programs on the strength of their focus on the intersections between climate and health.
While the article did not specifically focus on dermatology, these impacts are true in our field as well. The article notes that “at least one medical journal has recently ramped up its efforts to educate physicians on the links between health issues and climate change.” Notably in dermatology, the International Journal of Women’s Dermatology devoted an entire 124-page themed issue to climate change and dermatology in January, 2021, while JAMA Dermatology editor Kanade Shinkai, MD, PhD, called out climate change as one of the journal’s priorities in her annual editorial, stating, “Another priority for the journal is to better understand the effect of climate change on human health, specifically skin disease.”
The impacts of climate change in dermatology range from heat-related illness (a major cause of climate-associated mortality, with the skin serving as an essential thermoregulatory organ) to changing patterns of vector-borne illnesses to pollution and wildfire smoke flaring inflammatory skin diseases, to an increase in skin cancer, and more. While incorporation of health issues relating to climate change is important at a medical school level, it is also critical at the residency training – and board exam/certification – level as well.
Beyond the importance of building climate education into undergraduate and graduate medical education, it is also important that practicing physicians, post-residency training, remain up to date and keep abreast of changing patterns of disease in our rapidly changing climate. Lyme disease now occurs in Canada – and both earlier and later in the year even in places that are geographically used to seeing it. Early recognition is essential, but unprepared physicians may miss the early erythema migrans rash, and patients may suffer more severe sequelae as a result.
Finally, it’s important that medical organizations are aware of not just the health implications of climate change, but also potential policy impacts. Health care is a major emitter of CO2, and assistant secretary for health for the U.S. Department of Health and Human Services, Admiral Rachel L. Levine, MD, with the National Academy of Medicine, has appropriately pledged to reduce health care carbon emissions as part of the necessary steps that we must all take to avert the worst impacts of a warming world. The field of medicine and individual providers should educate themselves and actively work toward sustainability in health care, to improve the health of their patients, populations, and future generations.
Dr. Rosenbach is associate professor of dermatology and medicine at the University of Pennsylvania, Philadelphia, and is the founder and cochair of the American Academy of Dermatology Expert Resource Group for Climate Change and Environmental Issues. Dr. Rosenbach is speaking on behalf of himself and not the AAD.
The recent article on including the impact of climate on health in medical education programs shines an important light on the challenge – and urgent need – of integrating climate change training into medical education. These nascent efforts are just getting underway across the country, with some programs – notably Harvard’s C-CHANGE (Center for Climate, Health, and the Global Environment) program, mentioned in the article, and others, such as the University of Colorado’s Climate Medicine diploma course – leading the way. A number of publications, such as the editorial titled “A planetary health curriculum for medicine” published in 2021 in the BMJ, offer a roadmap to do so.
Medical schools, residency programs, and other medical specialty programs – including those for advanced practice providers, dentists, nurses, and more – should be incorporating climate change and its myriad of health impacts into their training pathways. The medical student group, Medical Students for a Sustainable Future, has put forth a planetary health report card that evaluates training programs on the strength of their focus on the intersections between climate and health.
While the article did not specifically focus on dermatology, these impacts are true in our field as well. The article notes that “at least one medical journal has recently ramped up its efforts to educate physicians on the links between health issues and climate change.” Notably in dermatology, the International Journal of Women’s Dermatology devoted an entire 124-page themed issue to climate change and dermatology in January, 2021, while JAMA Dermatology editor Kanade Shinkai, MD, PhD, called out climate change as one of the journal’s priorities in her annual editorial, stating, “Another priority for the journal is to better understand the effect of climate change on human health, specifically skin disease.”
The impacts of climate change in dermatology range from heat-related illness (a major cause of climate-associated mortality, with the skin serving as an essential thermoregulatory organ) to changing patterns of vector-borne illnesses to pollution and wildfire smoke flaring inflammatory skin diseases, to an increase in skin cancer, and more. While incorporation of health issues relating to climate change is important at a medical school level, it is also critical at the residency training – and board exam/certification – level as well.
Beyond the importance of building climate education into undergraduate and graduate medical education, it is also important that practicing physicians, post-residency training, remain up to date and keep abreast of changing patterns of disease in our rapidly changing climate. Lyme disease now occurs in Canada – and both earlier and later in the year even in places that are geographically used to seeing it. Early recognition is essential, but unprepared physicians may miss the early erythema migrans rash, and patients may suffer more severe sequelae as a result.
Finally, it’s important that medical organizations are aware of not just the health implications of climate change, but also potential policy impacts. Health care is a major emitter of CO2, and assistant secretary for health for the U.S. Department of Health and Human Services, Admiral Rachel L. Levine, MD, with the National Academy of Medicine, has appropriately pledged to reduce health care carbon emissions as part of the necessary steps that we must all take to avert the worst impacts of a warming world. The field of medicine and individual providers should educate themselves and actively work toward sustainability in health care, to improve the health of their patients, populations, and future generations.
Dr. Rosenbach is associate professor of dermatology and medicine at the University of Pennsylvania, Philadelphia, and is the founder and cochair of the American Academy of Dermatology Expert Resource Group for Climate Change and Environmental Issues. Dr. Rosenbach is speaking on behalf of himself and not the AAD.
Finding ‘bright lights’: Why family physician continues to love practicing mid-career
A few years ago I tracked down my medical school interviewer to thank him for giving me the opportunity to do what I felt I was called to do. I was surprised that, after 15 years, he actually remembered me and remembered details like walking to the courtyard to meet my father who’d driven me to the interview.
Sharing my gratitude and letting him know I was happy felt important to me.
Choosing to practice family medicine has a lot to do with why I am happy in my career today.
One of my frustrations with health care had been its emphasis on treatment of sickness, rather than a broader one that incorporated prevention of sickness. During my third year of medical school, I was following a family and sports medicine faculty member who was focusing on aspects of lifestyle medicine to help a patient remain active and age gracefully. Seeing opportunities to practice preventative medicine in family medicine made me realize the specialty was the perfect fit for me.
Food as medicine
While participating in rotations I also realized you can find a subspecialty within family medicine.
During my fourth year of medical school, I followed an attending who was seeing a patient for hypertension, prediabetes and hypercholesterolemia. The attending told the patient to eat “healthier,” gave her a handout, and scheduled a follow up appointment for 6 months later.
My thoughts were: “That’s it? That’s how we counsel patients to improve their dietary habits?”
As the patient was leaving the exam room, I asked her what type of oil she cooked with, and I proceeded to share culinary tips from my mother – who was a self-taught and early adopter of the food-as-medicine movement.
Once I started my residency, I knew I’d want to incorporate lifestyle and dietary approaches at many of my patient visits.
I scheduled patients every month to monitor their weight, follow up on chronic conditions, but more importantly, to engage them in their health and empower them to make small lifestyle changes each month and report their efforts. I felt like I was their health coach and cheerleader.
My career in family medicine
Entering the job market allowed me to form my philosophy of treating patients with a mind, body, and spirit approach. I chose to practice value-based care, which aligns with my lifestyle and preventative medicine approach .
I currently practice in a small family medicine–only clinic that is part of a larger multispecialty system. Primary care specialties in my organization are valued, respected and central to a patient’s well being and care. We are encouraged to spend time with patients, assess barriers to care and work collaboratively with our healthcare team, so that preventative medicine approaches take the lead in a patient’s health. This supportive culture and environment is one where my passion for food as medicine has thrived.
One day I forgot to pack a lunch and instead brought a grocery bag of items to make a salad. When I realized I made too much, I sent an email to my staff to get some “free salad in my office.” This serendipitous moment started an informal office “salad club” each week. Continued support from my staff and leadership, allowed me to consider further extending this teaching to my patients and my colleagues.
Three years ago, I helped adopt a sustainable plant-forward menu for our physician meetings, complete with a recipe from the menu for physicians to replicate at home or give to their patients.
I also pursued adoption of shared medical appointments for our medical group. These appointments apply the “see one, do one, teach one” model in medicine, but with culinary medicine as the focus.
Knowing that my patients are all connected to their families through food, I sought this as an opportunity to dive in further with wellness opportunities at their next meal. After almost 2 years of working on this project, I was able to host my first shared medical appointment with a group of patients on March 12, 2020. The next day schools closed, lockdowns occurred, and the world changed.
Opportunities highlighted by the pandemic
We always knew health care was broken but adding the increasingly longer hours and COVID vaccine–hesitant patients that the pandemic brought made everything look dark at times. What has helped me stay hopeful and energetic for system changes is feeling gratitude and seeking bright lights.
My experiences seeing patients in telehealth visits are examples of some of the bright lights I found in the pandemic. During these visits, patients showed me something from their pantry, and we’d go over nutritional labels together.
Additionally, my patients became engaged with their own conditions and wanted to improve them because of news articles highlighting risk factors for COVID-19, such as obesity. I had an active audience when it came to talking about food-as-medicine approaches to improving risk factors and immunity. And since everyone was listening, I didn’t stop at food. I also talked about physical health, stress resiliency, planetary diets, sleep, connections, and lastly vaccines!
Once the vaccines were distributed, I naturally gravitated to having those conversations with patients and colleagues and on social media. Plus, the pandemic gave us moments of simple times to slow down, take more rests, be less overscheduled, consider work-life priorities, and, lastly, to be okay with not being totally okay.
In practicing primary care, we have a unique role in seeing medicine from a whole body, whole person, whole family perspective. There is an opportunity to highlight what is broken in medicine and aim to make it whole.
I’m currently looking at shared medical appointments as a new standard way to provide care to all patients, because it improves access, provides better quality visits and aligns my values, mission, and purpose.
In the midst of the pandemic, I helped advocate for a sustainable plant-forward menu that was launched throughout four different hospitals in the Sharp HealthCare system, in California, in 2020. Knowing that patients were served a menu I played a role in, gave me solace.
As part of the hospital food and nutrition team, I am grateful for the opportunity I have to work on a broader mission to address social determinants of health and seek opportunities to help the system work for our patients.
Public health communication has been lacking in the pandemic, but another bright light is that we were still the trusted messengers to our patients and our communities. I’m continually honored and humbled to be trusted with a whole family’s health.
Dr. Neison practices family medicine and culinary medicine at Sharp Rees-Stealy Medical Group in San Diego, and is cochair of climate and planetary health for SRS Medical Group. You can follow her on Instagram, LinkedIn, and Facebook @Flavors4WellnessMD.
A few years ago I tracked down my medical school interviewer to thank him for giving me the opportunity to do what I felt I was called to do. I was surprised that, after 15 years, he actually remembered me and remembered details like walking to the courtyard to meet my father who’d driven me to the interview.
Sharing my gratitude and letting him know I was happy felt important to me.
Choosing to practice family medicine has a lot to do with why I am happy in my career today.
One of my frustrations with health care had been its emphasis on treatment of sickness, rather than a broader one that incorporated prevention of sickness. During my third year of medical school, I was following a family and sports medicine faculty member who was focusing on aspects of lifestyle medicine to help a patient remain active and age gracefully. Seeing opportunities to practice preventative medicine in family medicine made me realize the specialty was the perfect fit for me.
Food as medicine
While participating in rotations I also realized you can find a subspecialty within family medicine.
During my fourth year of medical school, I followed an attending who was seeing a patient for hypertension, prediabetes and hypercholesterolemia. The attending told the patient to eat “healthier,” gave her a handout, and scheduled a follow up appointment for 6 months later.
My thoughts were: “That’s it? That’s how we counsel patients to improve their dietary habits?”
As the patient was leaving the exam room, I asked her what type of oil she cooked with, and I proceeded to share culinary tips from my mother – who was a self-taught and early adopter of the food-as-medicine movement.
Once I started my residency, I knew I’d want to incorporate lifestyle and dietary approaches at many of my patient visits.
I scheduled patients every month to monitor their weight, follow up on chronic conditions, but more importantly, to engage them in their health and empower them to make small lifestyle changes each month and report their efforts. I felt like I was their health coach and cheerleader.
My career in family medicine
Entering the job market allowed me to form my philosophy of treating patients with a mind, body, and spirit approach. I chose to practice value-based care, which aligns with my lifestyle and preventative medicine approach .
I currently practice in a small family medicine–only clinic that is part of a larger multispecialty system. Primary care specialties in my organization are valued, respected and central to a patient’s well being and care. We are encouraged to spend time with patients, assess barriers to care and work collaboratively with our healthcare team, so that preventative medicine approaches take the lead in a patient’s health. This supportive culture and environment is one where my passion for food as medicine has thrived.
One day I forgot to pack a lunch and instead brought a grocery bag of items to make a salad. When I realized I made too much, I sent an email to my staff to get some “free salad in my office.” This serendipitous moment started an informal office “salad club” each week. Continued support from my staff and leadership, allowed me to consider further extending this teaching to my patients and my colleagues.
Three years ago, I helped adopt a sustainable plant-forward menu for our physician meetings, complete with a recipe from the menu for physicians to replicate at home or give to their patients.
I also pursued adoption of shared medical appointments for our medical group. These appointments apply the “see one, do one, teach one” model in medicine, but with culinary medicine as the focus.
Knowing that my patients are all connected to their families through food, I sought this as an opportunity to dive in further with wellness opportunities at their next meal. After almost 2 years of working on this project, I was able to host my first shared medical appointment with a group of patients on March 12, 2020. The next day schools closed, lockdowns occurred, and the world changed.
Opportunities highlighted by the pandemic
We always knew health care was broken but adding the increasingly longer hours and COVID vaccine–hesitant patients that the pandemic brought made everything look dark at times. What has helped me stay hopeful and energetic for system changes is feeling gratitude and seeking bright lights.
My experiences seeing patients in telehealth visits are examples of some of the bright lights I found in the pandemic. During these visits, patients showed me something from their pantry, and we’d go over nutritional labels together.
Additionally, my patients became engaged with their own conditions and wanted to improve them because of news articles highlighting risk factors for COVID-19, such as obesity. I had an active audience when it came to talking about food-as-medicine approaches to improving risk factors and immunity. And since everyone was listening, I didn’t stop at food. I also talked about physical health, stress resiliency, planetary diets, sleep, connections, and lastly vaccines!
Once the vaccines were distributed, I naturally gravitated to having those conversations with patients and colleagues and on social media. Plus, the pandemic gave us moments of simple times to slow down, take more rests, be less overscheduled, consider work-life priorities, and, lastly, to be okay with not being totally okay.
In practicing primary care, we have a unique role in seeing medicine from a whole body, whole person, whole family perspective. There is an opportunity to highlight what is broken in medicine and aim to make it whole.
I’m currently looking at shared medical appointments as a new standard way to provide care to all patients, because it improves access, provides better quality visits and aligns my values, mission, and purpose.
In the midst of the pandemic, I helped advocate for a sustainable plant-forward menu that was launched throughout four different hospitals in the Sharp HealthCare system, in California, in 2020. Knowing that patients were served a menu I played a role in, gave me solace.
As part of the hospital food and nutrition team, I am grateful for the opportunity I have to work on a broader mission to address social determinants of health and seek opportunities to help the system work for our patients.
Public health communication has been lacking in the pandemic, but another bright light is that we were still the trusted messengers to our patients and our communities. I’m continually honored and humbled to be trusted with a whole family’s health.
Dr. Neison practices family medicine and culinary medicine at Sharp Rees-Stealy Medical Group in San Diego, and is cochair of climate and planetary health for SRS Medical Group. You can follow her on Instagram, LinkedIn, and Facebook @Flavors4WellnessMD.
A few years ago I tracked down my medical school interviewer to thank him for giving me the opportunity to do what I felt I was called to do. I was surprised that, after 15 years, he actually remembered me and remembered details like walking to the courtyard to meet my father who’d driven me to the interview.
Sharing my gratitude and letting him know I was happy felt important to me.
Choosing to practice family medicine has a lot to do with why I am happy in my career today.
One of my frustrations with health care had been its emphasis on treatment of sickness, rather than a broader one that incorporated prevention of sickness. During my third year of medical school, I was following a family and sports medicine faculty member who was focusing on aspects of lifestyle medicine to help a patient remain active and age gracefully. Seeing opportunities to practice preventative medicine in family medicine made me realize the specialty was the perfect fit for me.
Food as medicine
While participating in rotations I also realized you can find a subspecialty within family medicine.
During my fourth year of medical school, I followed an attending who was seeing a patient for hypertension, prediabetes and hypercholesterolemia. The attending told the patient to eat “healthier,” gave her a handout, and scheduled a follow up appointment for 6 months later.
My thoughts were: “That’s it? That’s how we counsel patients to improve their dietary habits?”
As the patient was leaving the exam room, I asked her what type of oil she cooked with, and I proceeded to share culinary tips from my mother – who was a self-taught and early adopter of the food-as-medicine movement.
Once I started my residency, I knew I’d want to incorporate lifestyle and dietary approaches at many of my patient visits.
I scheduled patients every month to monitor their weight, follow up on chronic conditions, but more importantly, to engage them in their health and empower them to make small lifestyle changes each month and report their efforts. I felt like I was their health coach and cheerleader.
My career in family medicine
Entering the job market allowed me to form my philosophy of treating patients with a mind, body, and spirit approach. I chose to practice value-based care, which aligns with my lifestyle and preventative medicine approach .
I currently practice in a small family medicine–only clinic that is part of a larger multispecialty system. Primary care specialties in my organization are valued, respected and central to a patient’s well being and care. We are encouraged to spend time with patients, assess barriers to care and work collaboratively with our healthcare team, so that preventative medicine approaches take the lead in a patient’s health. This supportive culture and environment is one where my passion for food as medicine has thrived.
One day I forgot to pack a lunch and instead brought a grocery bag of items to make a salad. When I realized I made too much, I sent an email to my staff to get some “free salad in my office.” This serendipitous moment started an informal office “salad club” each week. Continued support from my staff and leadership, allowed me to consider further extending this teaching to my patients and my colleagues.
Three years ago, I helped adopt a sustainable plant-forward menu for our physician meetings, complete with a recipe from the menu for physicians to replicate at home or give to their patients.
I also pursued adoption of shared medical appointments for our medical group. These appointments apply the “see one, do one, teach one” model in medicine, but with culinary medicine as the focus.
Knowing that my patients are all connected to their families through food, I sought this as an opportunity to dive in further with wellness opportunities at their next meal. After almost 2 years of working on this project, I was able to host my first shared medical appointment with a group of patients on March 12, 2020. The next day schools closed, lockdowns occurred, and the world changed.
Opportunities highlighted by the pandemic
We always knew health care was broken but adding the increasingly longer hours and COVID vaccine–hesitant patients that the pandemic brought made everything look dark at times. What has helped me stay hopeful and energetic for system changes is feeling gratitude and seeking bright lights.
My experiences seeing patients in telehealth visits are examples of some of the bright lights I found in the pandemic. During these visits, patients showed me something from their pantry, and we’d go over nutritional labels together.
Additionally, my patients became engaged with their own conditions and wanted to improve them because of news articles highlighting risk factors for COVID-19, such as obesity. I had an active audience when it came to talking about food-as-medicine approaches to improving risk factors and immunity. And since everyone was listening, I didn’t stop at food. I also talked about physical health, stress resiliency, planetary diets, sleep, connections, and lastly vaccines!
Once the vaccines were distributed, I naturally gravitated to having those conversations with patients and colleagues and on social media. Plus, the pandemic gave us moments of simple times to slow down, take more rests, be less overscheduled, consider work-life priorities, and, lastly, to be okay with not being totally okay.
In practicing primary care, we have a unique role in seeing medicine from a whole body, whole person, whole family perspective. There is an opportunity to highlight what is broken in medicine and aim to make it whole.
I’m currently looking at shared medical appointments as a new standard way to provide care to all patients, because it improves access, provides better quality visits and aligns my values, mission, and purpose.
In the midst of the pandemic, I helped advocate for a sustainable plant-forward menu that was launched throughout four different hospitals in the Sharp HealthCare system, in California, in 2020. Knowing that patients were served a menu I played a role in, gave me solace.
As part of the hospital food and nutrition team, I am grateful for the opportunity I have to work on a broader mission to address social determinants of health and seek opportunities to help the system work for our patients.
Public health communication has been lacking in the pandemic, but another bright light is that we were still the trusted messengers to our patients and our communities. I’m continually honored and humbled to be trusted with a whole family’s health.
Dr. Neison practices family medicine and culinary medicine at Sharp Rees-Stealy Medical Group in San Diego, and is cochair of climate and planetary health for SRS Medical Group. You can follow her on Instagram, LinkedIn, and Facebook @Flavors4WellnessMD.
Productively working together
Recently, some liberal colleagues urged a boycott of a conference in Orlando, Fla., because of various actions by its Republican state governor. At the same time, conservative colleagues advocated the boycott because business actions of Disney have become too leftist. Concerns about spreading COVID-19 at the national gathering have become small, compared with the desire to virtue-signal political viewpoints.
The 1960s in the United States were a time of social upheaval and polarization with many similarities to modern America. One difference is that, after a few years of social revolution, society emphasized bridging the differences. Politicians talked about reaching across the aisle. Religious groups sought ecumenical and interfaith ventures. Business and educational institutions promoted equal opportunity programs. The emphasis was finding common ground.
A half century later, the polarized work environment of medical organizations in 2022 has led to emphasis on cancel culture, litmus tests, and finding reasons not to work with others and to silence dissent. A professional working in a polarized environment faces frequent challenges that pit ethical and political principles against the pragmatic need to set and accomplish team goals that productively care for patients and support staff. One of the worst things societies can do for children’s health is to perpetuate the paralyzing divisiveness of modern politics.
As Justice Stephen Breyer nears retirement from the Supreme Court, I reflect back to 1994 when, on the day of his nomination to the court by President Clinton, Justice Breyer at a press conference said, “What [the law is] supposed to do seen as a whole is allow all people, all people, to live together in a society where they have so many different views, so many different needs, but to live together in a way that is more harmonious, that is better so that they can work productively together.”
I generally reject secondary boycotts and the hatred they spew. True inclusivity does not divide. True inclusivity is very messy. It rejects tyrants who insist on litmus tests to prove wokeness. Every red state has Democrats and every blue state has Republicans. If you are dedicated to loving your neighbor, I think it is necessary professionally to focus on who you will work with to improve the world. If woke extremism says you can only work with someone who echoes the same end of the blue or red political spectrum as yourself, that is not loving, not inclusive, and not productive.
My advice is to focus on the values, goals, and pathways you share with colleagues rather than using political or social differences to prejudice you against working with someone toward a common goal. The old adage is that politics makes strange bedfellows. People with diverse, divergent, and even opposed life views can work together to build schools and roads that benefit the community, contrary to the polarized examples that have flooded Washington, D.C., for the past 2 decades. (Generation Z: Take this as testimony from a Boomer who saw how politics used to work, especially in small towns.)
My other advice is to believe in free speech, but it requires a long civics lesson to understand what that means. Facebook promulgating unvetted posts as news feeds is not free speech. Facebook creating profiles so the app creates tailored echo chambers of misinformation is not free speech. President Obama ignoring the problem for 8 years as the iPhone became ubiquitous did not help. President Trump’s outreach to the masses via Twitter did not model responsible free speech. Surreptitiously promoting certain political viewpoints in math textbooks is not responsible behavior and has generated mistrust and the replacement of boards of education. Elon Musk wanting to buy Twitter is an unknown.
I won’t attempt to offer any pearls of wisdom on free speech in this column. It is a complex subject. I will suggest that doing a better job with free speech will save far more lives than eliminating crib bumpers.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at [email protected].
Recently, some liberal colleagues urged a boycott of a conference in Orlando, Fla., because of various actions by its Republican state governor. At the same time, conservative colleagues advocated the boycott because business actions of Disney have become too leftist. Concerns about spreading COVID-19 at the national gathering have become small, compared with the desire to virtue-signal political viewpoints.
The 1960s in the United States were a time of social upheaval and polarization with many similarities to modern America. One difference is that, after a few years of social revolution, society emphasized bridging the differences. Politicians talked about reaching across the aisle. Religious groups sought ecumenical and interfaith ventures. Business and educational institutions promoted equal opportunity programs. The emphasis was finding common ground.
A half century later, the polarized work environment of medical organizations in 2022 has led to emphasis on cancel culture, litmus tests, and finding reasons not to work with others and to silence dissent. A professional working in a polarized environment faces frequent challenges that pit ethical and political principles against the pragmatic need to set and accomplish team goals that productively care for patients and support staff. One of the worst things societies can do for children’s health is to perpetuate the paralyzing divisiveness of modern politics.
As Justice Stephen Breyer nears retirement from the Supreme Court, I reflect back to 1994 when, on the day of his nomination to the court by President Clinton, Justice Breyer at a press conference said, “What [the law is] supposed to do seen as a whole is allow all people, all people, to live together in a society where they have so many different views, so many different needs, but to live together in a way that is more harmonious, that is better so that they can work productively together.”
I generally reject secondary boycotts and the hatred they spew. True inclusivity does not divide. True inclusivity is very messy. It rejects tyrants who insist on litmus tests to prove wokeness. Every red state has Democrats and every blue state has Republicans. If you are dedicated to loving your neighbor, I think it is necessary professionally to focus on who you will work with to improve the world. If woke extremism says you can only work with someone who echoes the same end of the blue or red political spectrum as yourself, that is not loving, not inclusive, and not productive.
My advice is to focus on the values, goals, and pathways you share with colleagues rather than using political or social differences to prejudice you against working with someone toward a common goal. The old adage is that politics makes strange bedfellows. People with diverse, divergent, and even opposed life views can work together to build schools and roads that benefit the community, contrary to the polarized examples that have flooded Washington, D.C., for the past 2 decades. (Generation Z: Take this as testimony from a Boomer who saw how politics used to work, especially in small towns.)
My other advice is to believe in free speech, but it requires a long civics lesson to understand what that means. Facebook promulgating unvetted posts as news feeds is not free speech. Facebook creating profiles so the app creates tailored echo chambers of misinformation is not free speech. President Obama ignoring the problem for 8 years as the iPhone became ubiquitous did not help. President Trump’s outreach to the masses via Twitter did not model responsible free speech. Surreptitiously promoting certain political viewpoints in math textbooks is not responsible behavior and has generated mistrust and the replacement of boards of education. Elon Musk wanting to buy Twitter is an unknown.
I won’t attempt to offer any pearls of wisdom on free speech in this column. It is a complex subject. I will suggest that doing a better job with free speech will save far more lives than eliminating crib bumpers.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at [email protected].
Recently, some liberal colleagues urged a boycott of a conference in Orlando, Fla., because of various actions by its Republican state governor. At the same time, conservative colleagues advocated the boycott because business actions of Disney have become too leftist. Concerns about spreading COVID-19 at the national gathering have become small, compared with the desire to virtue-signal political viewpoints.
The 1960s in the United States were a time of social upheaval and polarization with many similarities to modern America. One difference is that, after a few years of social revolution, society emphasized bridging the differences. Politicians talked about reaching across the aisle. Religious groups sought ecumenical and interfaith ventures. Business and educational institutions promoted equal opportunity programs. The emphasis was finding common ground.
A half century later, the polarized work environment of medical organizations in 2022 has led to emphasis on cancel culture, litmus tests, and finding reasons not to work with others and to silence dissent. A professional working in a polarized environment faces frequent challenges that pit ethical and political principles against the pragmatic need to set and accomplish team goals that productively care for patients and support staff. One of the worst things societies can do for children’s health is to perpetuate the paralyzing divisiveness of modern politics.
As Justice Stephen Breyer nears retirement from the Supreme Court, I reflect back to 1994 when, on the day of his nomination to the court by President Clinton, Justice Breyer at a press conference said, “What [the law is] supposed to do seen as a whole is allow all people, all people, to live together in a society where they have so many different views, so many different needs, but to live together in a way that is more harmonious, that is better so that they can work productively together.”
I generally reject secondary boycotts and the hatred they spew. True inclusivity does not divide. True inclusivity is very messy. It rejects tyrants who insist on litmus tests to prove wokeness. Every red state has Democrats and every blue state has Republicans. If you are dedicated to loving your neighbor, I think it is necessary professionally to focus on who you will work with to improve the world. If woke extremism says you can only work with someone who echoes the same end of the blue or red political spectrum as yourself, that is not loving, not inclusive, and not productive.
My advice is to focus on the values, goals, and pathways you share with colleagues rather than using political or social differences to prejudice you against working with someone toward a common goal. The old adage is that politics makes strange bedfellows. People with diverse, divergent, and even opposed life views can work together to build schools and roads that benefit the community, contrary to the polarized examples that have flooded Washington, D.C., for the past 2 decades. (Generation Z: Take this as testimony from a Boomer who saw how politics used to work, especially in small towns.)
My other advice is to believe in free speech, but it requires a long civics lesson to understand what that means. Facebook promulgating unvetted posts as news feeds is not free speech. Facebook creating profiles so the app creates tailored echo chambers of misinformation is not free speech. President Obama ignoring the problem for 8 years as the iPhone became ubiquitous did not help. President Trump’s outreach to the masses via Twitter did not model responsible free speech. Surreptitiously promoting certain political viewpoints in math textbooks is not responsible behavior and has generated mistrust and the replacement of boards of education. Elon Musk wanting to buy Twitter is an unknown.
I won’t attempt to offer any pearls of wisdom on free speech in this column. It is a complex subject. I will suggest that doing a better job with free speech will save far more lives than eliminating crib bumpers.
Dr. Powell is a pediatric hospitalist and clinical ethics consultant living in St. Louis. Email him at [email protected].
When burnout is moral injury
Several years have passed since I stood among a cohort of eager medical students wearing regalia that signaled a new beginning. Four years of grueling study culminated in a cacophony of unified voices, each reciting a pledge that I had longed to take since early adolescence. Together we celebrated, triumphant despite innumerable exams and various iterations of the Socratic method – all under the guise of assessing knowledge while in truth seeking to insidiously erode the crowd of prospective physicians. Yet our anxiety and uncertainty melted away as names were called, hands firmly clasped, and tassels transposed. For a moment in time, we stood on the precipice of victory, enthusiastic albeit oblivious of the tremendous obstacles that loomed ahead.
Wistfully I reminisce about the unequivocal joy that abounds within the protective shield of naiveté. Specifically, I think about that time when the edict of medicine and the art of being a physician felt congruent. Yet, reality is fickle and often supersedes expectation. Occasionally my thoughts drift to the early days of residency – a time during which the emotional weight of caring for vulnerable patients while learning to master my chosen specialty felt woefully insurmountable. I recall wading blindly through each rotation attempting to emulate the competent and compassionate care so effortlessly demonstrated by senior physicians as they moved through the health care system with apparent ease. They stepped fluidly, as I watched in awe through rose-tinted glasses.
As months passed into years, my perception cleared. What I initially viewed as graceful patient care belied a complex tapestry of health care workers often pressured into arduous decisions, not necessarily in service of a well-constructed treatment plan. Gradually, formidable barriers emerged, guidelines and restrictions embedded within a confining path that suffocated those who dared to cross it. As a result, a field built on the foundations of autonomy, benevolence, and nonmaleficence was slowly engulfed by a system fraught with contrivances. Amid such stressors, physical and psychological health grows tenuous. Classically, this overwhelming feeling of distress is recognized as burnout. Studies reformulated this malady to that which was first described in Vietnam war veterans, a condition known as “moral injury.”
The impact of burnout
To explain the development – and explore the complexities – of moral injury, we must return to 1975 when the term burnout was initially formulated by Herbert Freudenberger, PhD, a psychologist renowned for his work in substance use disorders, psychoanalysis, and clinical education.1 Dr. Freudenberger’s studies noted incidences of heightened emotional and physical distress in his colleagues working in substance abuse and other clinics. He sought to define these experiences as well as understand his own battle with malaise, apathy, and frustration.1 Ultimately, Dr. Freudenberger described burnout as “Becoming exhausted by making excessive demands on energy, strength, or resources in the workplace.”2 Although it characteristically overlaps with depression and anxiety, burnout is conceptualized as a separate entity specifically forged within a context of perfectionism, integrity, and self-sacrifice.2 Such qualities are integral in health care and, as a result, physicians are particularly vulnerable.
Since Dr. Freudenberger published “Burnout: The High Cost of Achievement” in 1980, immense research has assisted in not only identifying critical factors that contribute to its development but also the detrimental effects it has on physiological health.3 These include exhaustion from poor work conditions and extreme commitment to employee responsibilities that in turn precipitate mood destabilization and impaired work performance.3 Furthermore, research has also demonstrated that burnout triggers alterations in neural circuitry via the prefrontal cortex and the amygdala, structures critical for emotional regulation.4 To combat the ill effects of burnout while maintaining productivity and maximizing profit, several high-profile corporations instituted changes focusing on self-care, wellness, benefits, and incentives. Although these modifications are effective in decreasing the rate of employee turnover, such strategies are not easily transferable to health care. In fact, the rate of physician burnout has steadily increased over the past two decades as the business of medicine shifts towards longer hours, decreased reimbursement rates, and inexhaustible insurance stipulations.2,5 Consequently, occupational dissatisfaction increases the risk of cynicism, frustration with patients, internalization of failure, and likelihood of early retirement.5 Moreover, burnout may also fracture interpersonal relationships as well as precipitate errors, negative patient outcomes, malpractice, and development of severe mental health conditions associated with high morbidity and mortality.5,8
Although the concept of burnout is critical in understanding the side effects of stereotypical workplace culture, critics of the concept bemoan a suggestion of individual blame.6,8 In essence, they argue that burnout is explained as a side effect of toxic workplace conditions, but covertly represents a lack of resilience, motivation, and ambition to thrive in a physically or emotionally taxing occupational setting.6,8 Thus, the responsibility of acclimation lies upon the impacted individuals rather than the employer. For this reason, many strategies to ameliorate burnout are focused on the individual, including meditation, wellness retreats, creating or adjusting self-care regimens, or in some cases psychotherapy and psychopharmacology.6 Whereas burnout may respond (at least partially) to such interventions, without altering the causal factors, it is unlikely to remit. This is especially the case in health care, where systemic constraints lie beyond the control of an individual physician. Rather than promoting or specifically relying upon personal improvement and recovery, amendments are needed on multiple levels to affect meaningful change.
Moral injury
Similar to burnout, moral injury was not initially conceived within the scope of health care. In the 1990s Jonathan Shay, MD, PhD, identified veterans presenting with symptoms mimicking PTSD that failed to respond to standard, well established and efficacious treatments.9-11 With further analysis he determined that veterans who demonstrated minimal improvement reported similar histories of guilt, shame, and disgust following perceived injustices enacted or abetted by immoral leaders.10,11 Ultimately Shay identified three components of moral injury: 1. A betrayal of what is morally right; 2. By someone who holds legitimate priority; 3. In a high stakes situation.10
This definition was further modified in 2007 by Brett Linz, PhD, and colleagues as: “Perpetuating, failing to prevent, or bearing witness to acts that transgress deeply held moral beliefs and expectations.”10,11 By expanding this description to include distress experienced by physicians and health care workers, Wendy Dean and Simon Talbot (in 2018 and 2019 respectively) explored how the health care system leads practitioners to deliver what they identify as substandard treatment.6-8 This results in disillusionment and lays the foundation for ethical and moral dilemmas in clinicians.
Themes of moral injury are repeatedly cited in various surveys and studies as a cause for occupational dissatisfaction. As physicians and other health care professionals reel from the aftermath of COVID-19, the effects of reconfiguring medicine into a business-oriented framework are glaringly conspicuous. Vast hospital nursing shortages, high patient census exacerbated by the political misuse and polarization of science, and insufficient availability of psychiatric beds, have culminated in a deluge of psychological strain in emergency medical physicians. Furthermore, pressure from administrators, mandated patient satisfaction measures, tedious electronic medical record systems, and copious licensing and certification requirements, contribute to physician distress as they attempt to navigate a system that challenges the vows which they swore to uphold.8 Because the cost of pursuing a medical degree frequently necessitates acquisition of loans that, without a physician income, may be difficult to repay,9 many doctors feel trapped within a seemingly endless cycle of misgiving that contributes to emotional exhaustion, pessimism, and low morale.
In my next series of The Myth of the Superdoctor columns, we will explore various factors that potentiate risk of moral injury. From medical school and residency training to corporate infrastructure and insurance obstacles, I will seek to discern and deliberate strategies for repair and rehabilitation. It is my hope that together we will illuminate the myriad complexities within the business of medicine, and become advocates and harbingers of change not only for physicians and health care workers but also for the sake of our patients and their families.
Dr. Thomas is a board-certified adult psychiatrist with interests in chronic illness, women’s behavioral health, and minority mental health. She currently practices in North Kingstown and East Providence, R.I. Dr. Thomas has no conflicts of interest.
References
1. King N. When a Psychologist Succumbed to Stress, He Coined The Term Burnout. 2016 Dec 8. NPR: All Things Considered.
2. Maslach C and Leiter MP. World Psychiatry. 2016 Jun;15(2):103-11. doi: 10.1002/wps.20311.
3. InformedHealth.org and Institute for Quality and Efficiency in Health Care. Depression: What is burnout?. https://www.ncbi.nlm.nih.gov/books/NBK279286/.
4. Michel A. Burnout and the Brain. Observer. 2016 Jan 29. https://www.psychologicalscience.org/observer/burnout-and-the-brain.
5. Patel RS et al. Behav Sci. 2018;8(11):98. doi:10.3390/bs8110098.
6. Dean W and Talbot S. Physicians aren’t ‘burning out.’ They’re suffering from moral injury. Stat. 2018 Jul 26. https://www.statnews.com/2018/07/26/physicians-not-burning-out-they-are-suffering-moral-injury/.
7. Dean W and Talbot S. Moral injury and burnout in medicine: A year of lessons learned. Stat. 2019 Jul 26. https://www.statnews.com/2019/07/26/moral-injury-burnout-medicine-lessons-learned/.
8. Dean W et al. Reframing Clinician Distress: Moral Injury Not Burnout. Fed Pract. 2019 Sep; 36(9):400-2. https://www.mdedge.com/fedprac/article/207458/mental-health/reframing-clinician-distress-moral-injury-not-burnout.
9. Bailey M. Beyond Burnout: Docs Decry ‘Moral Injury’ From Financial Pressures of Health Care. KHN. 2020 Feb 4. https://khn.org/news/beyond-burnout-docs-decry-moral-injury-from-financial-pressures-of-health-care/.
10. Litz B et al. Clin Psychol Rev. 2009 Dec;29(8):695-706. doi: 10.1016/j.cpr.2009.07.003.
11. Norman S and Maguen S. Moral Injury. PTSD: National Center for PTSD. https://www.ptsd.va.gov/professional/treat/cooccurring/moral_injury.asp.
Several years have passed since I stood among a cohort of eager medical students wearing regalia that signaled a new beginning. Four years of grueling study culminated in a cacophony of unified voices, each reciting a pledge that I had longed to take since early adolescence. Together we celebrated, triumphant despite innumerable exams and various iterations of the Socratic method – all under the guise of assessing knowledge while in truth seeking to insidiously erode the crowd of prospective physicians. Yet our anxiety and uncertainty melted away as names were called, hands firmly clasped, and tassels transposed. For a moment in time, we stood on the precipice of victory, enthusiastic albeit oblivious of the tremendous obstacles that loomed ahead.
Wistfully I reminisce about the unequivocal joy that abounds within the protective shield of naiveté. Specifically, I think about that time when the edict of medicine and the art of being a physician felt congruent. Yet, reality is fickle and often supersedes expectation. Occasionally my thoughts drift to the early days of residency – a time during which the emotional weight of caring for vulnerable patients while learning to master my chosen specialty felt woefully insurmountable. I recall wading blindly through each rotation attempting to emulate the competent and compassionate care so effortlessly demonstrated by senior physicians as they moved through the health care system with apparent ease. They stepped fluidly, as I watched in awe through rose-tinted glasses.
As months passed into years, my perception cleared. What I initially viewed as graceful patient care belied a complex tapestry of health care workers often pressured into arduous decisions, not necessarily in service of a well-constructed treatment plan. Gradually, formidable barriers emerged, guidelines and restrictions embedded within a confining path that suffocated those who dared to cross it. As a result, a field built on the foundations of autonomy, benevolence, and nonmaleficence was slowly engulfed by a system fraught with contrivances. Amid such stressors, physical and psychological health grows tenuous. Classically, this overwhelming feeling of distress is recognized as burnout. Studies reformulated this malady to that which was first described in Vietnam war veterans, a condition known as “moral injury.”
The impact of burnout
To explain the development – and explore the complexities – of moral injury, we must return to 1975 when the term burnout was initially formulated by Herbert Freudenberger, PhD, a psychologist renowned for his work in substance use disorders, psychoanalysis, and clinical education.1 Dr. Freudenberger’s studies noted incidences of heightened emotional and physical distress in his colleagues working in substance abuse and other clinics. He sought to define these experiences as well as understand his own battle with malaise, apathy, and frustration.1 Ultimately, Dr. Freudenberger described burnout as “Becoming exhausted by making excessive demands on energy, strength, or resources in the workplace.”2 Although it characteristically overlaps with depression and anxiety, burnout is conceptualized as a separate entity specifically forged within a context of perfectionism, integrity, and self-sacrifice.2 Such qualities are integral in health care and, as a result, physicians are particularly vulnerable.
Since Dr. Freudenberger published “Burnout: The High Cost of Achievement” in 1980, immense research has assisted in not only identifying critical factors that contribute to its development but also the detrimental effects it has on physiological health.3 These include exhaustion from poor work conditions and extreme commitment to employee responsibilities that in turn precipitate mood destabilization and impaired work performance.3 Furthermore, research has also demonstrated that burnout triggers alterations in neural circuitry via the prefrontal cortex and the amygdala, structures critical for emotional regulation.4 To combat the ill effects of burnout while maintaining productivity and maximizing profit, several high-profile corporations instituted changes focusing on self-care, wellness, benefits, and incentives. Although these modifications are effective in decreasing the rate of employee turnover, such strategies are not easily transferable to health care. In fact, the rate of physician burnout has steadily increased over the past two decades as the business of medicine shifts towards longer hours, decreased reimbursement rates, and inexhaustible insurance stipulations.2,5 Consequently, occupational dissatisfaction increases the risk of cynicism, frustration with patients, internalization of failure, and likelihood of early retirement.5 Moreover, burnout may also fracture interpersonal relationships as well as precipitate errors, negative patient outcomes, malpractice, and development of severe mental health conditions associated with high morbidity and mortality.5,8
Although the concept of burnout is critical in understanding the side effects of stereotypical workplace culture, critics of the concept bemoan a suggestion of individual blame.6,8 In essence, they argue that burnout is explained as a side effect of toxic workplace conditions, but covertly represents a lack of resilience, motivation, and ambition to thrive in a physically or emotionally taxing occupational setting.6,8 Thus, the responsibility of acclimation lies upon the impacted individuals rather than the employer. For this reason, many strategies to ameliorate burnout are focused on the individual, including meditation, wellness retreats, creating or adjusting self-care regimens, or in some cases psychotherapy and psychopharmacology.6 Whereas burnout may respond (at least partially) to such interventions, without altering the causal factors, it is unlikely to remit. This is especially the case in health care, where systemic constraints lie beyond the control of an individual physician. Rather than promoting or specifically relying upon personal improvement and recovery, amendments are needed on multiple levels to affect meaningful change.
Moral injury
Similar to burnout, moral injury was not initially conceived within the scope of health care. In the 1990s Jonathan Shay, MD, PhD, identified veterans presenting with symptoms mimicking PTSD that failed to respond to standard, well established and efficacious treatments.9-11 With further analysis he determined that veterans who demonstrated minimal improvement reported similar histories of guilt, shame, and disgust following perceived injustices enacted or abetted by immoral leaders.10,11 Ultimately Shay identified three components of moral injury: 1. A betrayal of what is morally right; 2. By someone who holds legitimate priority; 3. In a high stakes situation.10
This definition was further modified in 2007 by Brett Linz, PhD, and colleagues as: “Perpetuating, failing to prevent, or bearing witness to acts that transgress deeply held moral beliefs and expectations.”10,11 By expanding this description to include distress experienced by physicians and health care workers, Wendy Dean and Simon Talbot (in 2018 and 2019 respectively) explored how the health care system leads practitioners to deliver what they identify as substandard treatment.6-8 This results in disillusionment and lays the foundation for ethical and moral dilemmas in clinicians.
Themes of moral injury are repeatedly cited in various surveys and studies as a cause for occupational dissatisfaction. As physicians and other health care professionals reel from the aftermath of COVID-19, the effects of reconfiguring medicine into a business-oriented framework are glaringly conspicuous. Vast hospital nursing shortages, high patient census exacerbated by the political misuse and polarization of science, and insufficient availability of psychiatric beds, have culminated in a deluge of psychological strain in emergency medical physicians. Furthermore, pressure from administrators, mandated patient satisfaction measures, tedious electronic medical record systems, and copious licensing and certification requirements, contribute to physician distress as they attempt to navigate a system that challenges the vows which they swore to uphold.8 Because the cost of pursuing a medical degree frequently necessitates acquisition of loans that, without a physician income, may be difficult to repay,9 many doctors feel trapped within a seemingly endless cycle of misgiving that contributes to emotional exhaustion, pessimism, and low morale.
In my next series of The Myth of the Superdoctor columns, we will explore various factors that potentiate risk of moral injury. From medical school and residency training to corporate infrastructure and insurance obstacles, I will seek to discern and deliberate strategies for repair and rehabilitation. It is my hope that together we will illuminate the myriad complexities within the business of medicine, and become advocates and harbingers of change not only for physicians and health care workers but also for the sake of our patients and their families.
Dr. Thomas is a board-certified adult psychiatrist with interests in chronic illness, women’s behavioral health, and minority mental health. She currently practices in North Kingstown and East Providence, R.I. Dr. Thomas has no conflicts of interest.
References
1. King N. When a Psychologist Succumbed to Stress, He Coined The Term Burnout. 2016 Dec 8. NPR: All Things Considered.
2. Maslach C and Leiter MP. World Psychiatry. 2016 Jun;15(2):103-11. doi: 10.1002/wps.20311.
3. InformedHealth.org and Institute for Quality and Efficiency in Health Care. Depression: What is burnout?. https://www.ncbi.nlm.nih.gov/books/NBK279286/.
4. Michel A. Burnout and the Brain. Observer. 2016 Jan 29. https://www.psychologicalscience.org/observer/burnout-and-the-brain.
5. Patel RS et al. Behav Sci. 2018;8(11):98. doi:10.3390/bs8110098.
6. Dean W and Talbot S. Physicians aren’t ‘burning out.’ They’re suffering from moral injury. Stat. 2018 Jul 26. https://www.statnews.com/2018/07/26/physicians-not-burning-out-they-are-suffering-moral-injury/.
7. Dean W and Talbot S. Moral injury and burnout in medicine: A year of lessons learned. Stat. 2019 Jul 26. https://www.statnews.com/2019/07/26/moral-injury-burnout-medicine-lessons-learned/.
8. Dean W et al. Reframing Clinician Distress: Moral Injury Not Burnout. Fed Pract. 2019 Sep; 36(9):400-2. https://www.mdedge.com/fedprac/article/207458/mental-health/reframing-clinician-distress-moral-injury-not-burnout.
9. Bailey M. Beyond Burnout: Docs Decry ‘Moral Injury’ From Financial Pressures of Health Care. KHN. 2020 Feb 4. https://khn.org/news/beyond-burnout-docs-decry-moral-injury-from-financial-pressures-of-health-care/.
10. Litz B et al. Clin Psychol Rev. 2009 Dec;29(8):695-706. doi: 10.1016/j.cpr.2009.07.003.
11. Norman S and Maguen S. Moral Injury. PTSD: National Center for PTSD. https://www.ptsd.va.gov/professional/treat/cooccurring/moral_injury.asp.
Several years have passed since I stood among a cohort of eager medical students wearing regalia that signaled a new beginning. Four years of grueling study culminated in a cacophony of unified voices, each reciting a pledge that I had longed to take since early adolescence. Together we celebrated, triumphant despite innumerable exams and various iterations of the Socratic method – all under the guise of assessing knowledge while in truth seeking to insidiously erode the crowd of prospective physicians. Yet our anxiety and uncertainty melted away as names were called, hands firmly clasped, and tassels transposed. For a moment in time, we stood on the precipice of victory, enthusiastic albeit oblivious of the tremendous obstacles that loomed ahead.
Wistfully I reminisce about the unequivocal joy that abounds within the protective shield of naiveté. Specifically, I think about that time when the edict of medicine and the art of being a physician felt congruent. Yet, reality is fickle and often supersedes expectation. Occasionally my thoughts drift to the early days of residency – a time during which the emotional weight of caring for vulnerable patients while learning to master my chosen specialty felt woefully insurmountable. I recall wading blindly through each rotation attempting to emulate the competent and compassionate care so effortlessly demonstrated by senior physicians as they moved through the health care system with apparent ease. They stepped fluidly, as I watched in awe through rose-tinted glasses.
As months passed into years, my perception cleared. What I initially viewed as graceful patient care belied a complex tapestry of health care workers often pressured into arduous decisions, not necessarily in service of a well-constructed treatment plan. Gradually, formidable barriers emerged, guidelines and restrictions embedded within a confining path that suffocated those who dared to cross it. As a result, a field built on the foundations of autonomy, benevolence, and nonmaleficence was slowly engulfed by a system fraught with contrivances. Amid such stressors, physical and psychological health grows tenuous. Classically, this overwhelming feeling of distress is recognized as burnout. Studies reformulated this malady to that which was first described in Vietnam war veterans, a condition known as “moral injury.”
The impact of burnout
To explain the development – and explore the complexities – of moral injury, we must return to 1975 when the term burnout was initially formulated by Herbert Freudenberger, PhD, a psychologist renowned for his work in substance use disorders, psychoanalysis, and clinical education.1 Dr. Freudenberger’s studies noted incidences of heightened emotional and physical distress in his colleagues working in substance abuse and other clinics. He sought to define these experiences as well as understand his own battle with malaise, apathy, and frustration.1 Ultimately, Dr. Freudenberger described burnout as “Becoming exhausted by making excessive demands on energy, strength, or resources in the workplace.”2 Although it characteristically overlaps with depression and anxiety, burnout is conceptualized as a separate entity specifically forged within a context of perfectionism, integrity, and self-sacrifice.2 Such qualities are integral in health care and, as a result, physicians are particularly vulnerable.
Since Dr. Freudenberger published “Burnout: The High Cost of Achievement” in 1980, immense research has assisted in not only identifying critical factors that contribute to its development but also the detrimental effects it has on physiological health.3 These include exhaustion from poor work conditions and extreme commitment to employee responsibilities that in turn precipitate mood destabilization and impaired work performance.3 Furthermore, research has also demonstrated that burnout triggers alterations in neural circuitry via the prefrontal cortex and the amygdala, structures critical for emotional regulation.4 To combat the ill effects of burnout while maintaining productivity and maximizing profit, several high-profile corporations instituted changes focusing on self-care, wellness, benefits, and incentives. Although these modifications are effective in decreasing the rate of employee turnover, such strategies are not easily transferable to health care. In fact, the rate of physician burnout has steadily increased over the past two decades as the business of medicine shifts towards longer hours, decreased reimbursement rates, and inexhaustible insurance stipulations.2,5 Consequently, occupational dissatisfaction increases the risk of cynicism, frustration with patients, internalization of failure, and likelihood of early retirement.5 Moreover, burnout may also fracture interpersonal relationships as well as precipitate errors, negative patient outcomes, malpractice, and development of severe mental health conditions associated with high morbidity and mortality.5,8
Although the concept of burnout is critical in understanding the side effects of stereotypical workplace culture, critics of the concept bemoan a suggestion of individual blame.6,8 In essence, they argue that burnout is explained as a side effect of toxic workplace conditions, but covertly represents a lack of resilience, motivation, and ambition to thrive in a physically or emotionally taxing occupational setting.6,8 Thus, the responsibility of acclimation lies upon the impacted individuals rather than the employer. For this reason, many strategies to ameliorate burnout are focused on the individual, including meditation, wellness retreats, creating or adjusting self-care regimens, or in some cases psychotherapy and psychopharmacology.6 Whereas burnout may respond (at least partially) to such interventions, without altering the causal factors, it is unlikely to remit. This is especially the case in health care, where systemic constraints lie beyond the control of an individual physician. Rather than promoting or specifically relying upon personal improvement and recovery, amendments are needed on multiple levels to affect meaningful change.
Moral injury
Similar to burnout, moral injury was not initially conceived within the scope of health care. In the 1990s Jonathan Shay, MD, PhD, identified veterans presenting with symptoms mimicking PTSD that failed to respond to standard, well established and efficacious treatments.9-11 With further analysis he determined that veterans who demonstrated minimal improvement reported similar histories of guilt, shame, and disgust following perceived injustices enacted or abetted by immoral leaders.10,11 Ultimately Shay identified three components of moral injury: 1. A betrayal of what is morally right; 2. By someone who holds legitimate priority; 3. In a high stakes situation.10
This definition was further modified in 2007 by Brett Linz, PhD, and colleagues as: “Perpetuating, failing to prevent, or bearing witness to acts that transgress deeply held moral beliefs and expectations.”10,11 By expanding this description to include distress experienced by physicians and health care workers, Wendy Dean and Simon Talbot (in 2018 and 2019 respectively) explored how the health care system leads practitioners to deliver what they identify as substandard treatment.6-8 This results in disillusionment and lays the foundation for ethical and moral dilemmas in clinicians.
Themes of moral injury are repeatedly cited in various surveys and studies as a cause for occupational dissatisfaction. As physicians and other health care professionals reel from the aftermath of COVID-19, the effects of reconfiguring medicine into a business-oriented framework are glaringly conspicuous. Vast hospital nursing shortages, high patient census exacerbated by the political misuse and polarization of science, and insufficient availability of psychiatric beds, have culminated in a deluge of psychological strain in emergency medical physicians. Furthermore, pressure from administrators, mandated patient satisfaction measures, tedious electronic medical record systems, and copious licensing and certification requirements, contribute to physician distress as they attempt to navigate a system that challenges the vows which they swore to uphold.8 Because the cost of pursuing a medical degree frequently necessitates acquisition of loans that, without a physician income, may be difficult to repay,9 many doctors feel trapped within a seemingly endless cycle of misgiving that contributes to emotional exhaustion, pessimism, and low morale.
In my next series of The Myth of the Superdoctor columns, we will explore various factors that potentiate risk of moral injury. From medical school and residency training to corporate infrastructure and insurance obstacles, I will seek to discern and deliberate strategies for repair and rehabilitation. It is my hope that together we will illuminate the myriad complexities within the business of medicine, and become advocates and harbingers of change not only for physicians and health care workers but also for the sake of our patients and their families.
Dr. Thomas is a board-certified adult psychiatrist with interests in chronic illness, women’s behavioral health, and minority mental health. She currently practices in North Kingstown and East Providence, R.I. Dr. Thomas has no conflicts of interest.
References
1. King N. When a Psychologist Succumbed to Stress, He Coined The Term Burnout. 2016 Dec 8. NPR: All Things Considered.
2. Maslach C and Leiter MP. World Psychiatry. 2016 Jun;15(2):103-11. doi: 10.1002/wps.20311.
3. InformedHealth.org and Institute for Quality and Efficiency in Health Care. Depression: What is burnout?. https://www.ncbi.nlm.nih.gov/books/NBK279286/.
4. Michel A. Burnout and the Brain. Observer. 2016 Jan 29. https://www.psychologicalscience.org/observer/burnout-and-the-brain.
5. Patel RS et al. Behav Sci. 2018;8(11):98. doi:10.3390/bs8110098.
6. Dean W and Talbot S. Physicians aren’t ‘burning out.’ They’re suffering from moral injury. Stat. 2018 Jul 26. https://www.statnews.com/2018/07/26/physicians-not-burning-out-they-are-suffering-moral-injury/.
7. Dean W and Talbot S. Moral injury and burnout in medicine: A year of lessons learned. Stat. 2019 Jul 26. https://www.statnews.com/2019/07/26/moral-injury-burnout-medicine-lessons-learned/.
8. Dean W et al. Reframing Clinician Distress: Moral Injury Not Burnout. Fed Pract. 2019 Sep; 36(9):400-2. https://www.mdedge.com/fedprac/article/207458/mental-health/reframing-clinician-distress-moral-injury-not-burnout.
9. Bailey M. Beyond Burnout: Docs Decry ‘Moral Injury’ From Financial Pressures of Health Care. KHN. 2020 Feb 4. https://khn.org/news/beyond-burnout-docs-decry-moral-injury-from-financial-pressures-of-health-care/.
10. Litz B et al. Clin Psychol Rev. 2009 Dec;29(8):695-706. doi: 10.1016/j.cpr.2009.07.003.
11. Norman S and Maguen S. Moral Injury. PTSD: National Center for PTSD. https://www.ptsd.va.gov/professional/treat/cooccurring/moral_injury.asp.
One weird trick to fight burnout
“Here and now is what counts. So, let’s go to work!” –Walter Orthmann, 100 years old
How long before you retire? If you know the answer in exact years, months, and days, you aren’t alone. For many good reasons, we doctors are more likely to be counting down the years until we retire rather than counting up the years since we started working. For me, if I’m to break the Guinness World Record, I have 69 more years, 3 months and 6 days left to go. That would surpass the current achievement for the longest career at one company, Mr. Walter Orthmann, who has been sitting at the same desk for 84 years. At 100 years old, Mr. Orthmann still shows up every Monday morning, as bright eyed and bushy tailed as a young squirrel. I’ll be 119 when I break his streak, which would also put me past Anthony Mancinelli, a New York barber who at 107 years of age was still brushing off his chair for the next customer. Unbelievable, I know! I wonder, what’s the one weird trick these guys are doing that keeps them going?

Of course, the job itself matters. Some jobs, like being a police officer, aren’t suitable for old people. Or are they? Officer L.C. “Buckshot” Smith was still keeping streets safe from his patrol car at 91 years old. After a bit of searching, I found pretty much any job you can think of has a very long-lasting Energizer Bunny story: A female surgeon who was operating at 90 years old, a 100-year-old rheumatologist who was still teaching at University of California, San Francisco, and a 105-year-old Japanese physician who was still seeing patients. There are plenty of geriatric lawyers, nurses, land surveyors, accountants, judges, you name it. So it seems it’s not the work, but the worker that matters. Why do some older workers recharge daily and carry on while many younger ones say the daily grind is burning them out? What makes the Greatest Generation so great?
We all know colleagues who hung up their white coats early. In my medical group, it’s often financially feasible to retire at 58 and many have chosen that option. Yet, we have loads of Partner Emeritus docs in their 70’s who still log on to EPIC and pitch in everyday.
“So, how do you keep going?” I asked my 105-year-old patient who still walks and manages his affairs. “Just stay healthy,” he advised. A circular argument, yet he’s right. You must both be lucky and also choose to be active mentally and physically. Mr. Mancinelli, who was barbering full time at 107 years old, had no aches and pains and all his teeth. He pruned his own bushes. The data are crystal clear that physical activity adds not only years of life, but also improves cognitive capabilities during those years.
As for beating burnout, it seems the one trick that these ultraworkers do is to focus only on the present. Mr. Orthmann’s pithy advice as quoted by NPR is, “You need to get busy with the present, not the past or the future.” These centenarian employees also frame their work not as stressful but rather as their daily series of problems to be solved.
When I asked my super-geriatric patient how he sleeps so well, he said, “I never worry when I get into bed, I just shut my eyes and sleep. I’ll think about tomorrow when I wake up.” Now if I can do that about 25,000 more times, I’ll have the record.
Dr. Jeff Benabio is director of Healthcare Transformation and chief of dermatology at Kaiser Permanente San Diego. The opinions expressed in this column are his own and do not represent those of Kaiser Permanente. Dr. Benabio is @Dermdoc on Twitter. Write to him at [email protected]
“Here and now is what counts. So, let’s go to work!” –Walter Orthmann, 100 years old
How long before you retire? If you know the answer in exact years, months, and days, you aren’t alone. For many good reasons, we doctors are more likely to be counting down the years until we retire rather than counting up the years since we started working. For me, if I’m to break the Guinness World Record, I have 69 more years, 3 months and 6 days left to go. That would surpass the current achievement for the longest career at one company, Mr. Walter Orthmann, who has been sitting at the same desk for 84 years. At 100 years old, Mr. Orthmann still shows up every Monday morning, as bright eyed and bushy tailed as a young squirrel. I’ll be 119 when I break his streak, which would also put me past Anthony Mancinelli, a New York barber who at 107 years of age was still brushing off his chair for the next customer. Unbelievable, I know! I wonder, what’s the one weird trick these guys are doing that keeps them going?

Of course, the job itself matters. Some jobs, like being a police officer, aren’t suitable for old people. Or are they? Officer L.C. “Buckshot” Smith was still keeping streets safe from his patrol car at 91 years old. After a bit of searching, I found pretty much any job you can think of has a very long-lasting Energizer Bunny story: A female surgeon who was operating at 90 years old, a 100-year-old rheumatologist who was still teaching at University of California, San Francisco, and a 105-year-old Japanese physician who was still seeing patients. There are plenty of geriatric lawyers, nurses, land surveyors, accountants, judges, you name it. So it seems it’s not the work, but the worker that matters. Why do some older workers recharge daily and carry on while many younger ones say the daily grind is burning them out? What makes the Greatest Generation so great?
We all know colleagues who hung up their white coats early. In my medical group, it’s often financially feasible to retire at 58 and many have chosen that option. Yet, we have loads of Partner Emeritus docs in their 70’s who still log on to EPIC and pitch in everyday.
“So, how do you keep going?” I asked my 105-year-old patient who still walks and manages his affairs. “Just stay healthy,” he advised. A circular argument, yet he’s right. You must both be lucky and also choose to be active mentally and physically. Mr. Mancinelli, who was barbering full time at 107 years old, had no aches and pains and all his teeth. He pruned his own bushes. The data are crystal clear that physical activity adds not only years of life, but also improves cognitive capabilities during those years.
As for beating burnout, it seems the one trick that these ultraworkers do is to focus only on the present. Mr. Orthmann’s pithy advice as quoted by NPR is, “You need to get busy with the present, not the past or the future.” These centenarian employees also frame their work not as stressful but rather as their daily series of problems to be solved.
When I asked my super-geriatric patient how he sleeps so well, he said, “I never worry when I get into bed, I just shut my eyes and sleep. I’ll think about tomorrow when I wake up.” Now if I can do that about 25,000 more times, I’ll have the record.
Dr. Jeff Benabio is director of Healthcare Transformation and chief of dermatology at Kaiser Permanente San Diego. The opinions expressed in this column are his own and do not represent those of Kaiser Permanente. Dr. Benabio is @Dermdoc on Twitter. Write to him at [email protected]
“Here and now is what counts. So, let’s go to work!” –Walter Orthmann, 100 years old
How long before you retire? If you know the answer in exact years, months, and days, you aren’t alone. For many good reasons, we doctors are more likely to be counting down the years until we retire rather than counting up the years since we started working. For me, if I’m to break the Guinness World Record, I have 69 more years, 3 months and 6 days left to go. That would surpass the current achievement for the longest career at one company, Mr. Walter Orthmann, who has been sitting at the same desk for 84 years. At 100 years old, Mr. Orthmann still shows up every Monday morning, as bright eyed and bushy tailed as a young squirrel. I’ll be 119 when I break his streak, which would also put me past Anthony Mancinelli, a New York barber who at 107 years of age was still brushing off his chair for the next customer. Unbelievable, I know! I wonder, what’s the one weird trick these guys are doing that keeps them going?

Of course, the job itself matters. Some jobs, like being a police officer, aren’t suitable for old people. Or are they? Officer L.C. “Buckshot” Smith was still keeping streets safe from his patrol car at 91 years old. After a bit of searching, I found pretty much any job you can think of has a very long-lasting Energizer Bunny story: A female surgeon who was operating at 90 years old, a 100-year-old rheumatologist who was still teaching at University of California, San Francisco, and a 105-year-old Japanese physician who was still seeing patients. There are plenty of geriatric lawyers, nurses, land surveyors, accountants, judges, you name it. So it seems it’s not the work, but the worker that matters. Why do some older workers recharge daily and carry on while many younger ones say the daily grind is burning them out? What makes the Greatest Generation so great?
We all know colleagues who hung up their white coats early. In my medical group, it’s often financially feasible to retire at 58 and many have chosen that option. Yet, we have loads of Partner Emeritus docs in their 70’s who still log on to EPIC and pitch in everyday.
“So, how do you keep going?” I asked my 105-year-old patient who still walks and manages his affairs. “Just stay healthy,” he advised. A circular argument, yet he’s right. You must both be lucky and also choose to be active mentally and physically. Mr. Mancinelli, who was barbering full time at 107 years old, had no aches and pains and all his teeth. He pruned his own bushes. The data are crystal clear that physical activity adds not only years of life, but also improves cognitive capabilities during those years.
As for beating burnout, it seems the one trick that these ultraworkers do is to focus only on the present. Mr. Orthmann’s pithy advice as quoted by NPR is, “You need to get busy with the present, not the past or the future.” These centenarian employees also frame their work not as stressful but rather as their daily series of problems to be solved.
When I asked my super-geriatric patient how he sleeps so well, he said, “I never worry when I get into bed, I just shut my eyes and sleep. I’ll think about tomorrow when I wake up.” Now if I can do that about 25,000 more times, I’ll have the record.
Dr. Jeff Benabio is director of Healthcare Transformation and chief of dermatology at Kaiser Permanente San Diego. The opinions expressed in this column are his own and do not represent those of Kaiser Permanente. Dr. Benabio is @Dermdoc on Twitter. Write to him at [email protected]

















