User login
Unplanned Pregnancy With Weight Loss Drugs: Fact or Fiction?
Claudia* was a charming 27-year-old newlywed. She and her husband wanted to start a family — with one small catch. She had recently gained 30 pounds. During COVID, she and her husband spent 18 months camped out in her parents’ guest room in upstate New York and had eaten their emotions with abandon. They ate when they were happy and ate more when they were sad. They ate when they felt isolated and again when they felt anxious. It didn’t help that her mother was a Culinary Institute–trained amateur chef. They both worked from home and logged long hours on Zoom calls. Because there was no home gym, they replaced their usual fitness club workouts in the city with leisurely strolls around the local lake. When I met her, Claudia categorically refused to entertain the notion of pregnancy until she reached her pre-COVID weight.
At the time, this all seemed quite reasonable to me. We outlined a plan including semaglutide (Wegovy) until she reached her target weight and then a minimum of 2 months off Wegovy prior to conception. We also lined up sessions with a dietitian and trainer and renewed her birth control pill. There was one detail I failed to mention to her: Birth control pills are less effective while on incretin hormones like semaglutide. The reason for my omission is that the medical community at large wasn’t yet aware of this issue.
About 12 weeks into treatment, Claudia had lost 20 of the 30 pounds. She had canceled several appointments with the trainer and dietitian due to work conflicts. She messaged me over the weekend in a panic. Her period was late, and her pregnancy test was positive.
She had three pressing questions for me:
Q: How had this happened while she had taken the birth control pills faithfully?
A: I answered that the scientific reasons for the decrease in efficacy of birth control pills while on semaglutide medications are threefold:
- Weight loss can improve menstrual cycle irregularities and improve fertility. In fact, I have been using semaglutide-like medications to treat polycystic ovary syndrome for decades, well before these medications became mainstream.
- The delayed gastric emptying inherent to incretins leads to decreased absorption of birth control pills.
- Finally, while this did not apply to Claudia, no medicine is particularly efficacious if vomited up shortly after taking. Wegovy is known to cause nausea and vomiting in a sizable percentage of patients.
Q: Would she have a healthy pregnancy given the lingering effects of Wegovy?
A: The short answer is: most likely yes. A review of the package insert revealed something fascinating. It was not strictly contraindicated. It advised doctors to weigh the risks and benefits of the medication during pregnancy. Animal studies have shown that semaglutide increases the risk for fetal death, birth defects, and growth issues, but this is probably due to restrictive eating patterns rather than a direct effect of the medication. A recent study of health records of more than 50,000 women with diabetes who had been inadvertently taking these medications in early pregnancy showed no increase in birth defects when compared with women who took insulin.
Q: What would happen to her weight loss efforts?
A: To address her third concern, I tried to offset the risk for rebound weight gain by stopping Wegovy and giving her metformin in the second and third trimesters. Considered a safe medication in pregnancy, metformin is thought to support weight loss, but it proved to be ineffective against the rebound weight gain from stopping Wegovy. Claudia had not resumed regular exercise and quickly fell into the age-old eating-for-two trap. She gained nearly 50 pounds over the course of her pregnancy.
After a short and unfulfilling attempt at nursing, Claudia restarted Wegovy, this time in conjunction with a Mediterranean meal plan and regular sessions at a fitness club. After losing the pregnancy weight, she has been able to successfully maintain her ideal body weight for the past year, and her baby is perfectly healthy and beautiful.
*Patient’s name changed.
A version of this article appeared on Medscape.com.
Claudia* was a charming 27-year-old newlywed. She and her husband wanted to start a family — with one small catch. She had recently gained 30 pounds. During COVID, she and her husband spent 18 months camped out in her parents’ guest room in upstate New York and had eaten their emotions with abandon. They ate when they were happy and ate more when they were sad. They ate when they felt isolated and again when they felt anxious. It didn’t help that her mother was a Culinary Institute–trained amateur chef. They both worked from home and logged long hours on Zoom calls. Because there was no home gym, they replaced their usual fitness club workouts in the city with leisurely strolls around the local lake. When I met her, Claudia categorically refused to entertain the notion of pregnancy until she reached her pre-COVID weight.
At the time, this all seemed quite reasonable to me. We outlined a plan including semaglutide (Wegovy) until she reached her target weight and then a minimum of 2 months off Wegovy prior to conception. We also lined up sessions with a dietitian and trainer and renewed her birth control pill. There was one detail I failed to mention to her: Birth control pills are less effective while on incretin hormones like semaglutide. The reason for my omission is that the medical community at large wasn’t yet aware of this issue.
About 12 weeks into treatment, Claudia had lost 20 of the 30 pounds. She had canceled several appointments with the trainer and dietitian due to work conflicts. She messaged me over the weekend in a panic. Her period was late, and her pregnancy test was positive.
She had three pressing questions for me:
Q: How had this happened while she had taken the birth control pills faithfully?
A: I answered that the scientific reasons for the decrease in efficacy of birth control pills while on semaglutide medications are threefold:
- Weight loss can improve menstrual cycle irregularities and improve fertility. In fact, I have been using semaglutide-like medications to treat polycystic ovary syndrome for decades, well before these medications became mainstream.
- The delayed gastric emptying inherent to incretins leads to decreased absorption of birth control pills.
- Finally, while this did not apply to Claudia, no medicine is particularly efficacious if vomited up shortly after taking. Wegovy is known to cause nausea and vomiting in a sizable percentage of patients.
Q: Would she have a healthy pregnancy given the lingering effects of Wegovy?
A: The short answer is: most likely yes. A review of the package insert revealed something fascinating. It was not strictly contraindicated. It advised doctors to weigh the risks and benefits of the medication during pregnancy. Animal studies have shown that semaglutide increases the risk for fetal death, birth defects, and growth issues, but this is probably due to restrictive eating patterns rather than a direct effect of the medication. A recent study of health records of more than 50,000 women with diabetes who had been inadvertently taking these medications in early pregnancy showed no increase in birth defects when compared with women who took insulin.
Q: What would happen to her weight loss efforts?
A: To address her third concern, I tried to offset the risk for rebound weight gain by stopping Wegovy and giving her metformin in the second and third trimesters. Considered a safe medication in pregnancy, metformin is thought to support weight loss, but it proved to be ineffective against the rebound weight gain from stopping Wegovy. Claudia had not resumed regular exercise and quickly fell into the age-old eating-for-two trap. She gained nearly 50 pounds over the course of her pregnancy.
After a short and unfulfilling attempt at nursing, Claudia restarted Wegovy, this time in conjunction with a Mediterranean meal plan and regular sessions at a fitness club. After losing the pregnancy weight, she has been able to successfully maintain her ideal body weight for the past year, and her baby is perfectly healthy and beautiful.
*Patient’s name changed.
A version of this article appeared on Medscape.com.
Claudia* was a charming 27-year-old newlywed. She and her husband wanted to start a family — with one small catch. She had recently gained 30 pounds. During COVID, she and her husband spent 18 months camped out in her parents’ guest room in upstate New York and had eaten their emotions with abandon. They ate when they were happy and ate more when they were sad. They ate when they felt isolated and again when they felt anxious. It didn’t help that her mother was a Culinary Institute–trained amateur chef. They both worked from home and logged long hours on Zoom calls. Because there was no home gym, they replaced their usual fitness club workouts in the city with leisurely strolls around the local lake. When I met her, Claudia categorically refused to entertain the notion of pregnancy until she reached her pre-COVID weight.
At the time, this all seemed quite reasonable to me. We outlined a plan including semaglutide (Wegovy) until she reached her target weight and then a minimum of 2 months off Wegovy prior to conception. We also lined up sessions with a dietitian and trainer and renewed her birth control pill. There was one detail I failed to mention to her: Birth control pills are less effective while on incretin hormones like semaglutide. The reason for my omission is that the medical community at large wasn’t yet aware of this issue.
About 12 weeks into treatment, Claudia had lost 20 of the 30 pounds. She had canceled several appointments with the trainer and dietitian due to work conflicts. She messaged me over the weekend in a panic. Her period was late, and her pregnancy test was positive.
She had three pressing questions for me:
Q: How had this happened while she had taken the birth control pills faithfully?
A: I answered that the scientific reasons for the decrease in efficacy of birth control pills while on semaglutide medications are threefold:
- Weight loss can improve menstrual cycle irregularities and improve fertility. In fact, I have been using semaglutide-like medications to treat polycystic ovary syndrome for decades, well before these medications became mainstream.
- The delayed gastric emptying inherent to incretins leads to decreased absorption of birth control pills.
- Finally, while this did not apply to Claudia, no medicine is particularly efficacious if vomited up shortly after taking. Wegovy is known to cause nausea and vomiting in a sizable percentage of patients.
Q: Would she have a healthy pregnancy given the lingering effects of Wegovy?
A: The short answer is: most likely yes. A review of the package insert revealed something fascinating. It was not strictly contraindicated. It advised doctors to weigh the risks and benefits of the medication during pregnancy. Animal studies have shown that semaglutide increases the risk for fetal death, birth defects, and growth issues, but this is probably due to restrictive eating patterns rather than a direct effect of the medication. A recent study of health records of more than 50,000 women with diabetes who had been inadvertently taking these medications in early pregnancy showed no increase in birth defects when compared with women who took insulin.
Q: What would happen to her weight loss efforts?
A: To address her third concern, I tried to offset the risk for rebound weight gain by stopping Wegovy and giving her metformin in the second and third trimesters. Considered a safe medication in pregnancy, metformin is thought to support weight loss, but it proved to be ineffective against the rebound weight gain from stopping Wegovy. Claudia had not resumed regular exercise and quickly fell into the age-old eating-for-two trap. She gained nearly 50 pounds over the course of her pregnancy.
After a short and unfulfilling attempt at nursing, Claudia restarted Wegovy, this time in conjunction with a Mediterranean meal plan and regular sessions at a fitness club. After losing the pregnancy weight, she has been able to successfully maintain her ideal body weight for the past year, and her baby is perfectly healthy and beautiful.
*Patient’s name changed.
A version of this article appeared on Medscape.com.
Nocturnal Hot Flashes and Alzheimer’s Risk
In a recent article in the American Journal of Obstetrics & Gynecology, Rebecca C. Thurston, PhD, and Pauline Maki, PhD, leading scientists in the area of menopause’s impact on brain function, presented data from their assessment of 248 late perimenopausal and postmenopausal women who reported hot flashes, also known as vasomotor symptoms (VMS).
Hot flashes are known to be associated with changes in brain white matter, carotid atherosclerosis, brain function, and memory. Dr. Thurston and colleagues objectively measured VMS over 24 hours, using skin conductance monitoring. Plasma concentrations of Alzheimer’s disease biomarkers, including the amyloid beta 42–to–amyloid beta 40 ratio, were assessed. The mean age of study participants was 59 years, and they experienced a mean of five objective VMS daily.
A key finding was that VMS, particularly those occurring during sleep, were associated with a significantly lower amyloid beta 42–to–beta 40 ratio. This finding suggests that nighttime VMS may be a marker of risk for Alzheimer’s disease.
Previous research has found that menopausal hormone therapy is associated with favorable changes in Alzheimer’s disease biomarkers. Likewise, large observational studies have shown a lower incidence of Alzheimer’s disease among women who initiate hormone therapy in their late perimenopausal or early postmenopausal years and continue such therapy long term.
The findings of this important study by Thurston and colleagues provide further evidence to support the tantalizing possibility that agents that reduce nighttime hot flashes (including hormone therapy) may lower the subsequent incidence of Alzheimer’s disease in high-risk women.
Dr. Kaunitz is a tenured professor and associate chair in the department of obstetrics and gynecology at the University of Florida College of Medicine–Jacksonville, and medical director and director of menopause and gynecologic ultrasound services at the University of Florida Southside Women’s Health, Jacksonville. He disclosed ties to Sumitomo Pharma America, Mithra, Viatris, Bayer, Merck, Mylan (Viatris), and UpToDate.
A version of this article appeared on Medscape.com.
In a recent article in the American Journal of Obstetrics & Gynecology, Rebecca C. Thurston, PhD, and Pauline Maki, PhD, leading scientists in the area of menopause’s impact on brain function, presented data from their assessment of 248 late perimenopausal and postmenopausal women who reported hot flashes, also known as vasomotor symptoms (VMS).
Hot flashes are known to be associated with changes in brain white matter, carotid atherosclerosis, brain function, and memory. Dr. Thurston and colleagues objectively measured VMS over 24 hours, using skin conductance monitoring. Plasma concentrations of Alzheimer’s disease biomarkers, including the amyloid beta 42–to–amyloid beta 40 ratio, were assessed. The mean age of study participants was 59 years, and they experienced a mean of five objective VMS daily.
A key finding was that VMS, particularly those occurring during sleep, were associated with a significantly lower amyloid beta 42–to–beta 40 ratio. This finding suggests that nighttime VMS may be a marker of risk for Alzheimer’s disease.
Previous research has found that menopausal hormone therapy is associated with favorable changes in Alzheimer’s disease biomarkers. Likewise, large observational studies have shown a lower incidence of Alzheimer’s disease among women who initiate hormone therapy in their late perimenopausal or early postmenopausal years and continue such therapy long term.
The findings of this important study by Thurston and colleagues provide further evidence to support the tantalizing possibility that agents that reduce nighttime hot flashes (including hormone therapy) may lower the subsequent incidence of Alzheimer’s disease in high-risk women.
Dr. Kaunitz is a tenured professor and associate chair in the department of obstetrics and gynecology at the University of Florida College of Medicine–Jacksonville, and medical director and director of menopause and gynecologic ultrasound services at the University of Florida Southside Women’s Health, Jacksonville. He disclosed ties to Sumitomo Pharma America, Mithra, Viatris, Bayer, Merck, Mylan (Viatris), and UpToDate.
A version of this article appeared on Medscape.com.
In a recent article in the American Journal of Obstetrics & Gynecology, Rebecca C. Thurston, PhD, and Pauline Maki, PhD, leading scientists in the area of menopause’s impact on brain function, presented data from their assessment of 248 late perimenopausal and postmenopausal women who reported hot flashes, also known as vasomotor symptoms (VMS).
Hot flashes are known to be associated with changes in brain white matter, carotid atherosclerosis, brain function, and memory. Dr. Thurston and colleagues objectively measured VMS over 24 hours, using skin conductance monitoring. Plasma concentrations of Alzheimer’s disease biomarkers, including the amyloid beta 42–to–amyloid beta 40 ratio, were assessed. The mean age of study participants was 59 years, and they experienced a mean of five objective VMS daily.
A key finding was that VMS, particularly those occurring during sleep, were associated with a significantly lower amyloid beta 42–to–beta 40 ratio. This finding suggests that nighttime VMS may be a marker of risk for Alzheimer’s disease.
Previous research has found that menopausal hormone therapy is associated with favorable changes in Alzheimer’s disease biomarkers. Likewise, large observational studies have shown a lower incidence of Alzheimer’s disease among women who initiate hormone therapy in their late perimenopausal or early postmenopausal years and continue such therapy long term.
The findings of this important study by Thurston and colleagues provide further evidence to support the tantalizing possibility that agents that reduce nighttime hot flashes (including hormone therapy) may lower the subsequent incidence of Alzheimer’s disease in high-risk women.
Dr. Kaunitz is a tenured professor and associate chair in the department of obstetrics and gynecology at the University of Florida College of Medicine–Jacksonville, and medical director and director of menopause and gynecologic ultrasound services at the University of Florida Southside Women’s Health, Jacksonville. He disclosed ties to Sumitomo Pharma America, Mithra, Viatris, Bayer, Merck, Mylan (Viatris), and UpToDate.
A version of this article appeared on Medscape.com.
Why Incorporating Obstetric History Matters for CVD Risk Management in Autoimmune Diseases
NEW YORK — Systemic autoimmune disease is well-recognized as a major risk factor for cardiovascular disease (CVD), but less recognized as a cardiovascular risk factor is a history of pregnancy complications, including preeclampsia, and cardiologists and rheumatologists need to include an obstetric history when managing patients with autoimmune diseases, a specialist in reproductive health in rheumatology told attendees at the 4th Annual Cardiometabolic Risk in Inflammatory Conditions conference.
“Autoimmune diseases, lupus in particular, increase the risk for both cardiovascular disease and maternal placental syndromes,” Lisa R. Sammaritano, MD, a professor at Hospital for Special Surgery in New York City and a specialist in reproductive health issues in rheumatology patients, told attendees. “For those patients who have complications during pregnancy, it further increases their already increased risk for later cardiovascular disease.”
CVD Risk Double Whammy
A history of systemic lupus erythematosus (SLE) and problematic pregnancy can be a double whammy for CVD risk. Dr. Sammaritano cited a 2022 meta-analysis that showed patients with SLE had a 2.5 times greater risk for stroke and almost three times greater risk for myocardial infarction than people without SLE.
Maternal placental syndromes include pregnancy loss, restricted fetal growth, preeclampsia, premature membrane rupture, placental abruption, and intrauterine fetal demise, Dr. Sammaritano said. Hypertensive disorders of pregnancy, formerly called adverse pregnancy outcomes, she noted, include gestational hypertension, preeclampsia, and eclampsia.
Pregnancy complications can have an adverse effect on the mother’s postpartum cardiovascular health, Dr. Sammaritano noted, a fact borne out by the cardiovascular health after maternal placental syndromes population-based retrospective cohort study and a 2007 meta-analysis that found a history of preeclampsia doubles the risk for venous thromboembolism, stroke, and ischemic heart disease up to 15 years after pregnancy.
“It is always important to obtain a reproductive health history from patients with autoimmune diseases,” Dr. Sammaritano told this news organization in an interview. “This is an integral part of any medical history. In the usual setting, this includes not only pregnancy history but also use of contraception in reproductive-aged women. Unplanned pregnancy can lead to adverse outcomes in the setting of active or severe autoimmune disease or when teratogenic medications are used.”
Pregnancy history can be a factor in a woman’s cardiovascular health more than 15 years postpartum, even if a woman is no longer planning a pregnancy or is menopausal. “As such, this history is important in assessing every woman’s risk profile for CVD in addition to usual traditional risk factors,” Dr. Sammaritano said.
“It is even more important for women with autoimmune disorders, who have been shown to have an already increased risk for CVD independent of their pregnancy history, likely related to a chronic inflammatory state and other autoimmune-related factors such as presence of antiphospholipid antibodies [aPL] or use of corticosteroids.”
Timing of disease onset is also an issue, she said. “In patients with SLE, for example, onset of CVD is much earlier than in the general population,” Dr. Sammaritano said. “As a result, these patients should likely be assessed for risk — both traditional and other risk factors — earlier than the general population, especially if an adverse obstetric history is present.”
At the younger end of the age continuum, women with autoimmune disease, including SLE and antiphospholipid syndrome, who are pregnant should be put on guideline-directed low-dose aspirin preeclampsia prophylaxis, Dr. Sammaritano said. “Whether every patient with SLE needs this is still uncertain, but certainly, those with a history of renal disease, hypertension, or aPL antibody clearly do,” she added.
The evidence supporting hydroxychloroquine (HCQ) in these patients is controversial, but Dr. Sammaritano noted two meta-analyses, one in 2022 and the other in 2023, that showed that HCQ lowered the risk for preeclampsia in women.
“The clear benefit of HCQ in preventing maternal disease complications, including flare, means we recommend it regardless for all patients with SLE at baseline and during pregnancy [if tolerated],” Dr. Sammaritano said. “The benefit or optimal use of these medications in other autoimmune diseases is less studied and less certain.”
Dr. Sammaritano added in her presentation, “We really need better therapies and, hopefully, those will be on the way, but I think the takeaway message, particularly for practicing rheumatologists and cardiologists, is to ask the question about obstetric history. Many of us don’t. It doesn’t seem relevant in the moment, but it really is in terms of the patient’s long-term risk for cardiovascular disease.”
The Case for Treatment During Pregnancy
Prophylaxis against pregnancy complications in patients with autoimmune disease may be achievable, Taryn Youngstein, MBBS, consultant rheumatologist and codirector of the Centre of Excellence in Vasculitis Research, Imperial College London, London, England, told this news organization after Dr. Sammaritano’s presentation. At the 2023 American College of Rheumatology Annual Meeting, her group reported the safety and effectiveness of continuing tocilizumab in pregnant women with Takayasu arteritis, a large-vessel vasculitis predominantly affecting women of reproductive age.
“What traditionally happens is you would stop the biologic particularly before the third trimester because of safety and concerns that the monoclonal antibody is actively transported across the placenta, which means the baby gets much more concentration of the drug than the mum,” Dr. Youngstein said.
It’s a situation physicians must monitor closely, she said. “The mum is donating their immune system to the baby, but they’re also donating drug.”
“In high-risk patients, we would share decision-making with the patient,” Dr. Youngstein continued. “We have decided it’s too high of a risk for us to stop the drug, so we have been continuing the interleukin-6 [IL-6] inhibitor throughout the entire pregnancy.”
The data from Dr. Youngstein’s group showed that pregnant women with Takayasu arteritis who continued IL-6 inhibition therapy all carried to term with healthy births.
“We’ve shown that it’s relatively safe to do that, but you have to be very careful in monitoring the baby,” she said. This includes not giving the infant any live vaccines at birth because it will have the high levels of IL-6 inhibition, she said.
Dr. Sammaritano and Dr. Youngstein had no relevant financial relationships to disclose.
A version of this article appeared on Medscape.com.
NEW YORK — Systemic autoimmune disease is well-recognized as a major risk factor for cardiovascular disease (CVD), but less recognized as a cardiovascular risk factor is a history of pregnancy complications, including preeclampsia, and cardiologists and rheumatologists need to include an obstetric history when managing patients with autoimmune diseases, a specialist in reproductive health in rheumatology told attendees at the 4th Annual Cardiometabolic Risk in Inflammatory Conditions conference.
“Autoimmune diseases, lupus in particular, increase the risk for both cardiovascular disease and maternal placental syndromes,” Lisa R. Sammaritano, MD, a professor at Hospital for Special Surgery in New York City and a specialist in reproductive health issues in rheumatology patients, told attendees. “For those patients who have complications during pregnancy, it further increases their already increased risk for later cardiovascular disease.”
CVD Risk Double Whammy
A history of systemic lupus erythematosus (SLE) and problematic pregnancy can be a double whammy for CVD risk. Dr. Sammaritano cited a 2022 meta-analysis that showed patients with SLE had a 2.5 times greater risk for stroke and almost three times greater risk for myocardial infarction than people without SLE.
Maternal placental syndromes include pregnancy loss, restricted fetal growth, preeclampsia, premature membrane rupture, placental abruption, and intrauterine fetal demise, Dr. Sammaritano said. Hypertensive disorders of pregnancy, formerly called adverse pregnancy outcomes, she noted, include gestational hypertension, preeclampsia, and eclampsia.
Pregnancy complications can have an adverse effect on the mother’s postpartum cardiovascular health, Dr. Sammaritano noted, a fact borne out by the cardiovascular health after maternal placental syndromes population-based retrospective cohort study and a 2007 meta-analysis that found a history of preeclampsia doubles the risk for venous thromboembolism, stroke, and ischemic heart disease up to 15 years after pregnancy.
“It is always important to obtain a reproductive health history from patients with autoimmune diseases,” Dr. Sammaritano told this news organization in an interview. “This is an integral part of any medical history. In the usual setting, this includes not only pregnancy history but also use of contraception in reproductive-aged women. Unplanned pregnancy can lead to adverse outcomes in the setting of active or severe autoimmune disease or when teratogenic medications are used.”
Pregnancy history can be a factor in a woman’s cardiovascular health more than 15 years postpartum, even if a woman is no longer planning a pregnancy or is menopausal. “As such, this history is important in assessing every woman’s risk profile for CVD in addition to usual traditional risk factors,” Dr. Sammaritano said.
“It is even more important for women with autoimmune disorders, who have been shown to have an already increased risk for CVD independent of their pregnancy history, likely related to a chronic inflammatory state and other autoimmune-related factors such as presence of antiphospholipid antibodies [aPL] or use of corticosteroids.”
Timing of disease onset is also an issue, she said. “In patients with SLE, for example, onset of CVD is much earlier than in the general population,” Dr. Sammaritano said. “As a result, these patients should likely be assessed for risk — both traditional and other risk factors — earlier than the general population, especially if an adverse obstetric history is present.”
At the younger end of the age continuum, women with autoimmune disease, including SLE and antiphospholipid syndrome, who are pregnant should be put on guideline-directed low-dose aspirin preeclampsia prophylaxis, Dr. Sammaritano said. “Whether every patient with SLE needs this is still uncertain, but certainly, those with a history of renal disease, hypertension, or aPL antibody clearly do,” she added.
The evidence supporting hydroxychloroquine (HCQ) in these patients is controversial, but Dr. Sammaritano noted two meta-analyses, one in 2022 and the other in 2023, that showed that HCQ lowered the risk for preeclampsia in women.
“The clear benefit of HCQ in preventing maternal disease complications, including flare, means we recommend it regardless for all patients with SLE at baseline and during pregnancy [if tolerated],” Dr. Sammaritano said. “The benefit or optimal use of these medications in other autoimmune diseases is less studied and less certain.”
Dr. Sammaritano added in her presentation, “We really need better therapies and, hopefully, those will be on the way, but I think the takeaway message, particularly for practicing rheumatologists and cardiologists, is to ask the question about obstetric history. Many of us don’t. It doesn’t seem relevant in the moment, but it really is in terms of the patient’s long-term risk for cardiovascular disease.”
The Case for Treatment During Pregnancy
Prophylaxis against pregnancy complications in patients with autoimmune disease may be achievable, Taryn Youngstein, MBBS, consultant rheumatologist and codirector of the Centre of Excellence in Vasculitis Research, Imperial College London, London, England, told this news organization after Dr. Sammaritano’s presentation. At the 2023 American College of Rheumatology Annual Meeting, her group reported the safety and effectiveness of continuing tocilizumab in pregnant women with Takayasu arteritis, a large-vessel vasculitis predominantly affecting women of reproductive age.
“What traditionally happens is you would stop the biologic particularly before the third trimester because of safety and concerns that the monoclonal antibody is actively transported across the placenta, which means the baby gets much more concentration of the drug than the mum,” Dr. Youngstein said.
It’s a situation physicians must monitor closely, she said. “The mum is donating their immune system to the baby, but they’re also donating drug.”
“In high-risk patients, we would share decision-making with the patient,” Dr. Youngstein continued. “We have decided it’s too high of a risk for us to stop the drug, so we have been continuing the interleukin-6 [IL-6] inhibitor throughout the entire pregnancy.”
The data from Dr. Youngstein’s group showed that pregnant women with Takayasu arteritis who continued IL-6 inhibition therapy all carried to term with healthy births.
“We’ve shown that it’s relatively safe to do that, but you have to be very careful in monitoring the baby,” she said. This includes not giving the infant any live vaccines at birth because it will have the high levels of IL-6 inhibition, she said.
Dr. Sammaritano and Dr. Youngstein had no relevant financial relationships to disclose.
A version of this article appeared on Medscape.com.
NEW YORK — Systemic autoimmune disease is well-recognized as a major risk factor for cardiovascular disease (CVD), but less recognized as a cardiovascular risk factor is a history of pregnancy complications, including preeclampsia, and cardiologists and rheumatologists need to include an obstetric history when managing patients with autoimmune diseases, a specialist in reproductive health in rheumatology told attendees at the 4th Annual Cardiometabolic Risk in Inflammatory Conditions conference.
“Autoimmune diseases, lupus in particular, increase the risk for both cardiovascular disease and maternal placental syndromes,” Lisa R. Sammaritano, MD, a professor at Hospital for Special Surgery in New York City and a specialist in reproductive health issues in rheumatology patients, told attendees. “For those patients who have complications during pregnancy, it further increases their already increased risk for later cardiovascular disease.”
CVD Risk Double Whammy
A history of systemic lupus erythematosus (SLE) and problematic pregnancy can be a double whammy for CVD risk. Dr. Sammaritano cited a 2022 meta-analysis that showed patients with SLE had a 2.5 times greater risk for stroke and almost three times greater risk for myocardial infarction than people without SLE.
Maternal placental syndromes include pregnancy loss, restricted fetal growth, preeclampsia, premature membrane rupture, placental abruption, and intrauterine fetal demise, Dr. Sammaritano said. Hypertensive disorders of pregnancy, formerly called adverse pregnancy outcomes, she noted, include gestational hypertension, preeclampsia, and eclampsia.
Pregnancy complications can have an adverse effect on the mother’s postpartum cardiovascular health, Dr. Sammaritano noted, a fact borne out by the cardiovascular health after maternal placental syndromes population-based retrospective cohort study and a 2007 meta-analysis that found a history of preeclampsia doubles the risk for venous thromboembolism, stroke, and ischemic heart disease up to 15 years after pregnancy.
“It is always important to obtain a reproductive health history from patients with autoimmune diseases,” Dr. Sammaritano told this news organization in an interview. “This is an integral part of any medical history. In the usual setting, this includes not only pregnancy history but also use of contraception in reproductive-aged women. Unplanned pregnancy can lead to adverse outcomes in the setting of active or severe autoimmune disease or when teratogenic medications are used.”
Pregnancy history can be a factor in a woman’s cardiovascular health more than 15 years postpartum, even if a woman is no longer planning a pregnancy or is menopausal. “As such, this history is important in assessing every woman’s risk profile for CVD in addition to usual traditional risk factors,” Dr. Sammaritano said.
“It is even more important for women with autoimmune disorders, who have been shown to have an already increased risk for CVD independent of their pregnancy history, likely related to a chronic inflammatory state and other autoimmune-related factors such as presence of antiphospholipid antibodies [aPL] or use of corticosteroids.”
Timing of disease onset is also an issue, she said. “In patients with SLE, for example, onset of CVD is much earlier than in the general population,” Dr. Sammaritano said. “As a result, these patients should likely be assessed for risk — both traditional and other risk factors — earlier than the general population, especially if an adverse obstetric history is present.”
At the younger end of the age continuum, women with autoimmune disease, including SLE and antiphospholipid syndrome, who are pregnant should be put on guideline-directed low-dose aspirin preeclampsia prophylaxis, Dr. Sammaritano said. “Whether every patient with SLE needs this is still uncertain, but certainly, those with a history of renal disease, hypertension, or aPL antibody clearly do,” she added.
The evidence supporting hydroxychloroquine (HCQ) in these patients is controversial, but Dr. Sammaritano noted two meta-analyses, one in 2022 and the other in 2023, that showed that HCQ lowered the risk for preeclampsia in women.
“The clear benefit of HCQ in preventing maternal disease complications, including flare, means we recommend it regardless for all patients with SLE at baseline and during pregnancy [if tolerated],” Dr. Sammaritano said. “The benefit or optimal use of these medications in other autoimmune diseases is less studied and less certain.”
Dr. Sammaritano added in her presentation, “We really need better therapies and, hopefully, those will be on the way, but I think the takeaway message, particularly for practicing rheumatologists and cardiologists, is to ask the question about obstetric history. Many of us don’t. It doesn’t seem relevant in the moment, but it really is in terms of the patient’s long-term risk for cardiovascular disease.”
The Case for Treatment During Pregnancy
Prophylaxis against pregnancy complications in patients with autoimmune disease may be achievable, Taryn Youngstein, MBBS, consultant rheumatologist and codirector of the Centre of Excellence in Vasculitis Research, Imperial College London, London, England, told this news organization after Dr. Sammaritano’s presentation. At the 2023 American College of Rheumatology Annual Meeting, her group reported the safety and effectiveness of continuing tocilizumab in pregnant women with Takayasu arteritis, a large-vessel vasculitis predominantly affecting women of reproductive age.
“What traditionally happens is you would stop the biologic particularly before the third trimester because of safety and concerns that the monoclonal antibody is actively transported across the placenta, which means the baby gets much more concentration of the drug than the mum,” Dr. Youngstein said.
It’s a situation physicians must monitor closely, she said. “The mum is donating their immune system to the baby, but they’re also donating drug.”
“In high-risk patients, we would share decision-making with the patient,” Dr. Youngstein continued. “We have decided it’s too high of a risk for us to stop the drug, so we have been continuing the interleukin-6 [IL-6] inhibitor throughout the entire pregnancy.”
The data from Dr. Youngstein’s group showed that pregnant women with Takayasu arteritis who continued IL-6 inhibition therapy all carried to term with healthy births.
“We’ve shown that it’s relatively safe to do that, but you have to be very careful in monitoring the baby,” she said. This includes not giving the infant any live vaccines at birth because it will have the high levels of IL-6 inhibition, she said.
Dr. Sammaritano and Dr. Youngstein had no relevant financial relationships to disclose.
A version of this article appeared on Medscape.com.
Tool May Help Prioritize High-Risk Patients for Hysteroscopy
Hysteroscopy is a crucial examination for the diagnosis of endometrial cancer. In Brazil, women with postmenopausal bleeding who need to undergo this procedure in the public health system wait in line alongside patients with less severe complaints. Until now, there has been no system to prioritize patients at high risk for cancer. But this situation may change, thanks to a Brazilian study published in February in the Journal of Clinical Medicine.
Researchers from the Municipal Hospital of Vila Santa Catarina in São Paulo, a public unit managed by Hospital Israelita Albert Einstein, have developed the Endometrial Malignancy Prediction System (EMPS), a nomogram to identify patients at high risk for endometrial cancer and prioritize them in the hysteroscopy waiting list.
Bruna Bottura, MD, a gynecologist and obstetrician at Hospital Israelita Albert Einstein and the study’s lead author, told this news organization that the idea to create the nomogram arose during the COVID-19 pandemic. “We noticed that ... when outpatient clinics resumed, we were seeing many patients for intrauterine device (IUD) removal. We thought it was unfair for a patient with postmenopausal bleeding, who has a chance of having cancer, to have to wait in the same line as a patient needing IUD removal,” she said. This realization motivated the development of the tool, which was overseen by Renato Moretti-Marques, MD, PhD.
The EMPS Score
The team conducted a retrospective case-control study involving 1945 patients with suspected endometrial cancer who had undergone diagnostic hysteroscopy at Hospital Israelita Albert Einstein between March 2019 and March 2022. Among these patients, 107 were diagnosed with precursor lesions or endometrial cancer on the basis of biopsy. The other 1838 participants, who had had cancer ruled out by biopsy, formed the control group.
Through bivariate and multivariate linear regression analysis, the authors determined that the presence or absence of hypertension, diabetes, postmenopausal bleeding, endometrial polyps, uterine volume, number of pregnancies, body mass index, age, and endometrial thickness were the main risk factors for endometrial cancer diagnosis.
On the basis of these data, the group developed the EMPS nomogram. Physicians can use it to classify the patient’s risk according to the sum of the scores assigned to each of these factors.
The Table shows the classification system. The scoring tables available in the supplemental materials of the article can be accessed here.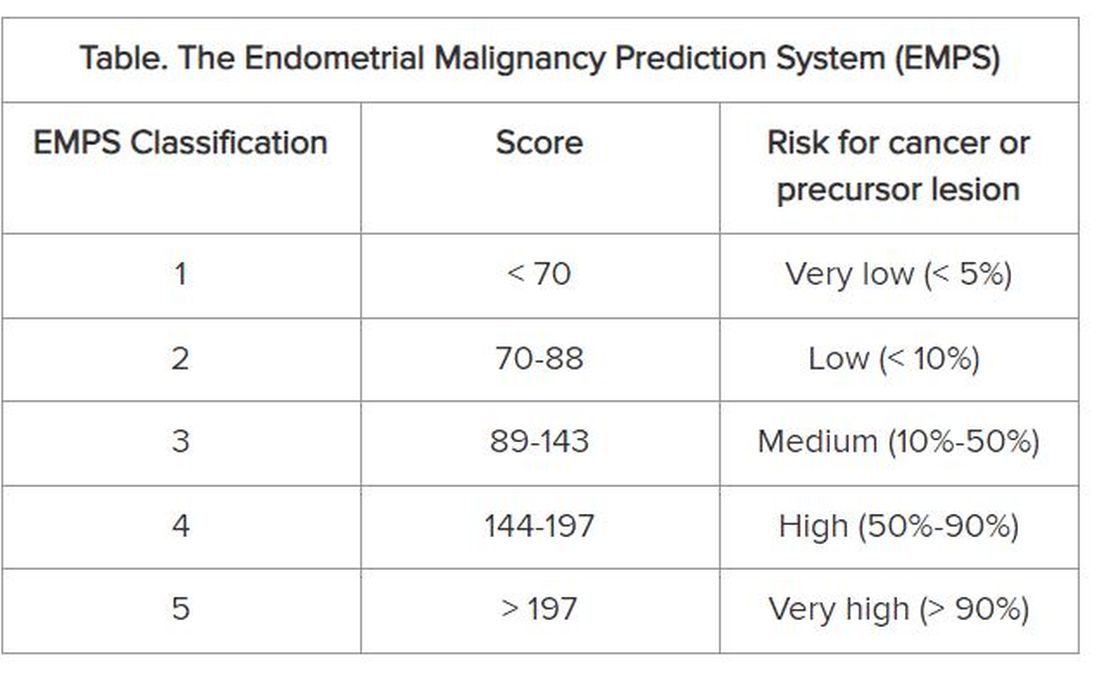
Focus on Primary Care
The goal is not to remove patients classified as low risk from the hysteroscopy waiting list, but rather to prioritize those classified as high risk to get the examination, according to Dr. Bottura.
At the Municipal Hospital of Vila Santa Catarina, the average wait time for hysteroscopy was 120 days. But because the unit is focused on oncologic patients and has a high level of organization, this time is much shorter than observed in other parts of Brazil’s National Health Service, said Dr. Bottura. “Many patients are on the hysteroscopy waiting list for 2 years. Considering patients in more advanced stages [of endometrial cancer], it makes a difference,” she said.
Although the nomogram was developed in tertiary care, it is aimed at professionals working in primary care. The reason is that physicians from primary care health units refer women with clinical indications for hysteroscopy to specialized national health services, such as the Municipal Hospital of Vila Santa Catarina. “Our goal is the primary sector, to enable the clinic to refer this high-risk patient sooner. By the time you reach the tertiary sector, where hysteroscopies are performed, all patients will undergo the procedure. Usually, it is not the hospitals that predetermine the line, but rather the health clinics,” she explained.
The researchers hope to continue the research, starting with a prospective study. “We intend to apply and evaluate the tool within our own service to observe whether any patient with a high [EMPS] score patient ended up waiting too long to be referred. In fact, this will be a system validation step,” said Dr. Bottura.
In parallel, the team has a proposal to take the tool to health clinics in the same region as the study hospital. “We know this involves changing the protocol at a national level, so it’s more challenging,” said Dr. Bottura. She added that the final goal is to create a calculator, possibly an app, that allows primary care doctors to calculate the risk score in the office. This calculator could enable risk classification to be linked to patient referrals.
This story was translated from the Medscape Portuguese edition using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
Hysteroscopy is a crucial examination for the diagnosis of endometrial cancer. In Brazil, women with postmenopausal bleeding who need to undergo this procedure in the public health system wait in line alongside patients with less severe complaints. Until now, there has been no system to prioritize patients at high risk for cancer. But this situation may change, thanks to a Brazilian study published in February in the Journal of Clinical Medicine.
Researchers from the Municipal Hospital of Vila Santa Catarina in São Paulo, a public unit managed by Hospital Israelita Albert Einstein, have developed the Endometrial Malignancy Prediction System (EMPS), a nomogram to identify patients at high risk for endometrial cancer and prioritize them in the hysteroscopy waiting list.
Bruna Bottura, MD, a gynecologist and obstetrician at Hospital Israelita Albert Einstein and the study’s lead author, told this news organization that the idea to create the nomogram arose during the COVID-19 pandemic. “We noticed that ... when outpatient clinics resumed, we were seeing many patients for intrauterine device (IUD) removal. We thought it was unfair for a patient with postmenopausal bleeding, who has a chance of having cancer, to have to wait in the same line as a patient needing IUD removal,” she said. This realization motivated the development of the tool, which was overseen by Renato Moretti-Marques, MD, PhD.
The EMPS Score
The team conducted a retrospective case-control study involving 1945 patients with suspected endometrial cancer who had undergone diagnostic hysteroscopy at Hospital Israelita Albert Einstein between March 2019 and March 2022. Among these patients, 107 were diagnosed with precursor lesions or endometrial cancer on the basis of biopsy. The other 1838 participants, who had had cancer ruled out by biopsy, formed the control group.
Through bivariate and multivariate linear regression analysis, the authors determined that the presence or absence of hypertension, diabetes, postmenopausal bleeding, endometrial polyps, uterine volume, number of pregnancies, body mass index, age, and endometrial thickness were the main risk factors for endometrial cancer diagnosis.
On the basis of these data, the group developed the EMPS nomogram. Physicians can use it to classify the patient’s risk according to the sum of the scores assigned to each of these factors.
The Table shows the classification system. The scoring tables available in the supplemental materials of the article can be accessed here.
Focus on Primary Care
The goal is not to remove patients classified as low risk from the hysteroscopy waiting list, but rather to prioritize those classified as high risk to get the examination, according to Dr. Bottura.
At the Municipal Hospital of Vila Santa Catarina, the average wait time for hysteroscopy was 120 days. But because the unit is focused on oncologic patients and has a high level of organization, this time is much shorter than observed in other parts of Brazil’s National Health Service, said Dr. Bottura. “Many patients are on the hysteroscopy waiting list for 2 years. Considering patients in more advanced stages [of endometrial cancer], it makes a difference,” she said.
Although the nomogram was developed in tertiary care, it is aimed at professionals working in primary care. The reason is that physicians from primary care health units refer women with clinical indications for hysteroscopy to specialized national health services, such as the Municipal Hospital of Vila Santa Catarina. “Our goal is the primary sector, to enable the clinic to refer this high-risk patient sooner. By the time you reach the tertiary sector, where hysteroscopies are performed, all patients will undergo the procedure. Usually, it is not the hospitals that predetermine the line, but rather the health clinics,” she explained.
The researchers hope to continue the research, starting with a prospective study. “We intend to apply and evaluate the tool within our own service to observe whether any patient with a high [EMPS] score patient ended up waiting too long to be referred. In fact, this will be a system validation step,” said Dr. Bottura.
In parallel, the team has a proposal to take the tool to health clinics in the same region as the study hospital. “We know this involves changing the protocol at a national level, so it’s more challenging,” said Dr. Bottura. She added that the final goal is to create a calculator, possibly an app, that allows primary care doctors to calculate the risk score in the office. This calculator could enable risk classification to be linked to patient referrals.
This story was translated from the Medscape Portuguese edition using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
Hysteroscopy is a crucial examination for the diagnosis of endometrial cancer. In Brazil, women with postmenopausal bleeding who need to undergo this procedure in the public health system wait in line alongside patients with less severe complaints. Until now, there has been no system to prioritize patients at high risk for cancer. But this situation may change, thanks to a Brazilian study published in February in the Journal of Clinical Medicine.
Researchers from the Municipal Hospital of Vila Santa Catarina in São Paulo, a public unit managed by Hospital Israelita Albert Einstein, have developed the Endometrial Malignancy Prediction System (EMPS), a nomogram to identify patients at high risk for endometrial cancer and prioritize them in the hysteroscopy waiting list.
Bruna Bottura, MD, a gynecologist and obstetrician at Hospital Israelita Albert Einstein and the study’s lead author, told this news organization that the idea to create the nomogram arose during the COVID-19 pandemic. “We noticed that ... when outpatient clinics resumed, we were seeing many patients for intrauterine device (IUD) removal. We thought it was unfair for a patient with postmenopausal bleeding, who has a chance of having cancer, to have to wait in the same line as a patient needing IUD removal,” she said. This realization motivated the development of the tool, which was overseen by Renato Moretti-Marques, MD, PhD.
The EMPS Score
The team conducted a retrospective case-control study involving 1945 patients with suspected endometrial cancer who had undergone diagnostic hysteroscopy at Hospital Israelita Albert Einstein between March 2019 and March 2022. Among these patients, 107 were diagnosed with precursor lesions or endometrial cancer on the basis of biopsy. The other 1838 participants, who had had cancer ruled out by biopsy, formed the control group.
Through bivariate and multivariate linear regression analysis, the authors determined that the presence or absence of hypertension, diabetes, postmenopausal bleeding, endometrial polyps, uterine volume, number of pregnancies, body mass index, age, and endometrial thickness were the main risk factors for endometrial cancer diagnosis.
On the basis of these data, the group developed the EMPS nomogram. Physicians can use it to classify the patient’s risk according to the sum of the scores assigned to each of these factors.
The Table shows the classification system. The scoring tables available in the supplemental materials of the article can be accessed here.
Focus on Primary Care
The goal is not to remove patients classified as low risk from the hysteroscopy waiting list, but rather to prioritize those classified as high risk to get the examination, according to Dr. Bottura.
At the Municipal Hospital of Vila Santa Catarina, the average wait time for hysteroscopy was 120 days. But because the unit is focused on oncologic patients and has a high level of organization, this time is much shorter than observed in other parts of Brazil’s National Health Service, said Dr. Bottura. “Many patients are on the hysteroscopy waiting list for 2 years. Considering patients in more advanced stages [of endometrial cancer], it makes a difference,” she said.
Although the nomogram was developed in tertiary care, it is aimed at professionals working in primary care. The reason is that physicians from primary care health units refer women with clinical indications for hysteroscopy to specialized national health services, such as the Municipal Hospital of Vila Santa Catarina. “Our goal is the primary sector, to enable the clinic to refer this high-risk patient sooner. By the time you reach the tertiary sector, where hysteroscopies are performed, all patients will undergo the procedure. Usually, it is not the hospitals that predetermine the line, but rather the health clinics,” she explained.
The researchers hope to continue the research, starting with a prospective study. “We intend to apply and evaluate the tool within our own service to observe whether any patient with a high [EMPS] score patient ended up waiting too long to be referred. In fact, this will be a system validation step,” said Dr. Bottura.
In parallel, the team has a proposal to take the tool to health clinics in the same region as the study hospital. “We know this involves changing the protocol at a national level, so it’s more challenging,” said Dr. Bottura. She added that the final goal is to create a calculator, possibly an app, that allows primary care doctors to calculate the risk score in the office. This calculator could enable risk classification to be linked to patient referrals.
This story was translated from the Medscape Portuguese edition using several editorial tools, including AI, as part of the process. Human editors reviewed this content before publication. A version of this article first appeared on Medscape.com.
Clinicians Call for Easing FDA Warnings on Low-Dose Estrogen
Charles Powell, MD, said he sometimes has a hard time persuading patients to start on low-dose vaginal estrogen, which can help prevent urinary tract infections and ease other symptoms of menopause.
Many women fear taking these vaginal products because of what Dr. Powell considers excessively strong warnings about the risk for cancer and cardiovascular disease linked to daily estrogen pills that were issued in the early 2000s.
He is advocating for the US Food and Drug Administration (FDA) to remove the boxed warning on low-dose estrogen. His efforts are separate from his roles as an associate professor of urology at the Indiana University School of Medicine, and as a member of the American Urological Association (AUA), Dr. Powell said.
In his quest to find out how to change labeling, Dr. Powell has gained a quick education about drug regulation. He has enlisted Representative Jim Baird (R-IN) and Senator Mike Braun (R-IN) to contact the FDA on his behalf, while congressional staff guided him through the hurdles of getting the warning label changed. For instance, a manufacturer of low-dose estrogen may need to become involved.
“You don’t learn this in med school,” Dr. Powell said in an interview.
With this work, Dr. Powell is wading into a long-standing argument between the FDA and some clinicians and researchers about the potential harms of low-dose estrogen.
He is doing so at a time of increased interest in understanding genitourinary syndrome of menopause (GSM), a term coined a decade ago by the International Society for the Study of Women’s Sexual Health and the North American Menopause Society to cover “a constellation of conditions” related to urogenital atrophy.
Symptoms of GSM include vaginal dryness and burning and recurrent urinary tract infections.
The federal government in 2022 began a project budgeted with nearly $1 million to review evidence on treatments, including vaginal and low-dose estrogen. The aim is to eventually help the AUA develop clinical guidelines for addressing GSM.
In addition, a bipartisan Senate bill introduced in May calls for authorizing $125 million over 5 years for the National Institutes of Health (NIH) to fund research on menopause. Senator Patty Murray (D-WA), the lead sponsor of the bill, is a longtime advocate for women’s health and serves as chairwoman for the Senate Appropriations Committee, which largely sets the NIH budget.
“The bottom line is, for too long, menopause has been overlooked, underinvested in and left behind,” Sen. Murray said during a May 2 press conference. “It is well past time to stop treating menopause like some kind of secret and start treating it like the major mainstream public health issue it is.”
Evidence Demands
Increased federal funding for menopause research could help efforts to change the warning label on low-dose estrogen, according to JoAnn Manson, MD, chief of preventive medicine at Brigham and Women’s Hospital in Boston.
Dr. Manson was a leader of the Women’s Health Initiative (WHI), a major federally funded research project launched in 1991 to investigate if hormone therapy and diet could protect older women from chronic diseases related to aging.
Before the WHI, clinicians prescribed hormones to prevent cardiovascular disease, based on evidence from earlier research.
But in 2002, a WHI trial that compared estrogen-progestin tablets with placebo was halted early because of disturbing findings, including an association with higher risk for breast cancer and cardiovascular disease.
Compared with placebo, for every 10,000 women taking estrogen plus progestin annually, incidences of cardiovascular disease, stroke, pulmonary embolism, and invasive breast cancer were seven to eight times higher.
In January 2003, the FDA announced it would put a boxed warning about cardiovascular risk and cancer risk on estrogen products, reflecting the WHI finding.
The agency at the time said clinicians should work with patients to assess risks and benefits of these products to manage the effects of menopause.
But more news on the potential harms of estrogen followed in 2004: A WHI study comparing estrogen-only pills with placebo produced signals of a small increased risk for stroke, although it also indicated no excess risk for breast cancer for at least 6.8 years of use.
Dr. Manson and the North American Menopause Society in 2016 filed a petition with the FDA to remove the boxed warning that appears on the front of low-dose estrogen products. The group wanted the information on risks moved to the usual warning section of the label.
Two years later, the FDA rejected the petition, citing the absence of “well-controlled studies,” to prove low-dose topical estrogen poses less risk to women than the high-dose pills studied in the WHI.
The FDA told this news organization that it stands by the decisions in its rejection of the petition.
Persuading the FDA to revise the labels on low-dose estrogen products likely will require evidence from randomized, large-scale studies, Dr. Manson said. The agency has not been satisfied to date with findings from other kinds of studies, including observational research.
“Once that evidence is available that the benefit-risk profile is different for different formulations and the evidence is compelling and definitive, that warning should change,” Dr. Manson told this news organization.
But the warning continues to have a chilling effect on patient willingness to use low-dose vaginal estrogen, even with the FDA’s continued endorsement of estrogen for menopause symptoms, clinicians told this news organization.
Risa Kagan, MD, a gynecologist at Sutter Health in Berkeley, California, said in many cases her patients’ partners also need to be reassured. Dr. Kagan said she still sees women who have had to discontinue sexual intercourse because of pain. In some cases, the patients will bring the medicine home only to find that the warnings frighten their spouses.
“The spouse says, ‘Oh my God, I don’t want you to get dementia, to get breast cancer, it’s not worth it, so let’s keep doing outercourse’,” meaning sexual relations without penetration, Dr. Kagan said.
Difficult Messaging
From the initial unveiling of disappointing WHI results, clinicians and researchers have stressed that women could continue using estrogen products for managing symptoms of menopause, even while advising strongly against their continued use with the intention of preventing heart disease.
Newly published findings from follow-ups of WHI participants may give clinicians and patients even more confidence for the use of estrogen products in early menopause.
According to the study, which Dr. Manson coauthored, younger women have a low risk for cardiovascular disease and other associated conditions when taking hormone therapy. Risks attributed to these drugs were less than one additional adverse event per 1000 women annually. This population may also derive significant quality-of-life benefits for symptom relief.
Dr. Manson told this news organization that estrogen in lower doses and delivered through the skin as a patch or gel may further reduce risks.
“The WHI findings should never be used as a reason to deny hormone therapy to women in early menopause with bothersome menopausal symptoms,” Dr. Manson said. “Many women are good candidates for treatment and, in shared decision-making with their clinicians, should be able to receive appropriate and personalized healthcare for their needs.”
But the current FDA warning label makes it difficult to help women understand the risk and benefits of low-dose estrogen, according to Stephanie Faubion, MD, MBA, medical director at the North American Menopause Society and director of Mayo Clinic’s Center for Women’s Health in Jacksonville, Florida.
Clinicians now must set aside time to explain the warnings to women when they prescribe low-dose estrogen, Dr. Faubion said.
“The package insert is going to look scary: I prepare women for that because otherwise they often won’t even fill it or use it.”
A version of this article appeared on Medscape.com .
Charles Powell, MD, said he sometimes has a hard time persuading patients to start on low-dose vaginal estrogen, which can help prevent urinary tract infections and ease other symptoms of menopause.
Many women fear taking these vaginal products because of what Dr. Powell considers excessively strong warnings about the risk for cancer and cardiovascular disease linked to daily estrogen pills that were issued in the early 2000s.
He is advocating for the US Food and Drug Administration (FDA) to remove the boxed warning on low-dose estrogen. His efforts are separate from his roles as an associate professor of urology at the Indiana University School of Medicine, and as a member of the American Urological Association (AUA), Dr. Powell said.
In his quest to find out how to change labeling, Dr. Powell has gained a quick education about drug regulation. He has enlisted Representative Jim Baird (R-IN) and Senator Mike Braun (R-IN) to contact the FDA on his behalf, while congressional staff guided him through the hurdles of getting the warning label changed. For instance, a manufacturer of low-dose estrogen may need to become involved.
“You don’t learn this in med school,” Dr. Powell said in an interview.
With this work, Dr. Powell is wading into a long-standing argument between the FDA and some clinicians and researchers about the potential harms of low-dose estrogen.
He is doing so at a time of increased interest in understanding genitourinary syndrome of menopause (GSM), a term coined a decade ago by the International Society for the Study of Women’s Sexual Health and the North American Menopause Society to cover “a constellation of conditions” related to urogenital atrophy.
Symptoms of GSM include vaginal dryness and burning and recurrent urinary tract infections.
The federal government in 2022 began a project budgeted with nearly $1 million to review evidence on treatments, including vaginal and low-dose estrogen. The aim is to eventually help the AUA develop clinical guidelines for addressing GSM.
In addition, a bipartisan Senate bill introduced in May calls for authorizing $125 million over 5 years for the National Institutes of Health (NIH) to fund research on menopause. Senator Patty Murray (D-WA), the lead sponsor of the bill, is a longtime advocate for women’s health and serves as chairwoman for the Senate Appropriations Committee, which largely sets the NIH budget.
“The bottom line is, for too long, menopause has been overlooked, underinvested in and left behind,” Sen. Murray said during a May 2 press conference. “It is well past time to stop treating menopause like some kind of secret and start treating it like the major mainstream public health issue it is.”
Evidence Demands
Increased federal funding for menopause research could help efforts to change the warning label on low-dose estrogen, according to JoAnn Manson, MD, chief of preventive medicine at Brigham and Women’s Hospital in Boston.
Dr. Manson was a leader of the Women’s Health Initiative (WHI), a major federally funded research project launched in 1991 to investigate if hormone therapy and diet could protect older women from chronic diseases related to aging.
Before the WHI, clinicians prescribed hormones to prevent cardiovascular disease, based on evidence from earlier research.
But in 2002, a WHI trial that compared estrogen-progestin tablets with placebo was halted early because of disturbing findings, including an association with higher risk for breast cancer and cardiovascular disease.
Compared with placebo, for every 10,000 women taking estrogen plus progestin annually, incidences of cardiovascular disease, stroke, pulmonary embolism, and invasive breast cancer were seven to eight times higher.
In January 2003, the FDA announced it would put a boxed warning about cardiovascular risk and cancer risk on estrogen products, reflecting the WHI finding.
The agency at the time said clinicians should work with patients to assess risks and benefits of these products to manage the effects of menopause.
But more news on the potential harms of estrogen followed in 2004: A WHI study comparing estrogen-only pills with placebo produced signals of a small increased risk for stroke, although it also indicated no excess risk for breast cancer for at least 6.8 years of use.
Dr. Manson and the North American Menopause Society in 2016 filed a petition with the FDA to remove the boxed warning that appears on the front of low-dose estrogen products. The group wanted the information on risks moved to the usual warning section of the label.
Two years later, the FDA rejected the petition, citing the absence of “well-controlled studies,” to prove low-dose topical estrogen poses less risk to women than the high-dose pills studied in the WHI.
The FDA told this news organization that it stands by the decisions in its rejection of the petition.
Persuading the FDA to revise the labels on low-dose estrogen products likely will require evidence from randomized, large-scale studies, Dr. Manson said. The agency has not been satisfied to date with findings from other kinds of studies, including observational research.
“Once that evidence is available that the benefit-risk profile is different for different formulations and the evidence is compelling and definitive, that warning should change,” Dr. Manson told this news organization.
But the warning continues to have a chilling effect on patient willingness to use low-dose vaginal estrogen, even with the FDA’s continued endorsement of estrogen for menopause symptoms, clinicians told this news organization.
Risa Kagan, MD, a gynecologist at Sutter Health in Berkeley, California, said in many cases her patients’ partners also need to be reassured. Dr. Kagan said she still sees women who have had to discontinue sexual intercourse because of pain. In some cases, the patients will bring the medicine home only to find that the warnings frighten their spouses.
“The spouse says, ‘Oh my God, I don’t want you to get dementia, to get breast cancer, it’s not worth it, so let’s keep doing outercourse’,” meaning sexual relations without penetration, Dr. Kagan said.
Difficult Messaging
From the initial unveiling of disappointing WHI results, clinicians and researchers have stressed that women could continue using estrogen products for managing symptoms of menopause, even while advising strongly against their continued use with the intention of preventing heart disease.
Newly published findings from follow-ups of WHI participants may give clinicians and patients even more confidence for the use of estrogen products in early menopause.
According to the study, which Dr. Manson coauthored, younger women have a low risk for cardiovascular disease and other associated conditions when taking hormone therapy. Risks attributed to these drugs were less than one additional adverse event per 1000 women annually. This population may also derive significant quality-of-life benefits for symptom relief.
Dr. Manson told this news organization that estrogen in lower doses and delivered through the skin as a patch or gel may further reduce risks.
“The WHI findings should never be used as a reason to deny hormone therapy to women in early menopause with bothersome menopausal symptoms,” Dr. Manson said. “Many women are good candidates for treatment and, in shared decision-making with their clinicians, should be able to receive appropriate and personalized healthcare for their needs.”
But the current FDA warning label makes it difficult to help women understand the risk and benefits of low-dose estrogen, according to Stephanie Faubion, MD, MBA, medical director at the North American Menopause Society and director of Mayo Clinic’s Center for Women’s Health in Jacksonville, Florida.
Clinicians now must set aside time to explain the warnings to women when they prescribe low-dose estrogen, Dr. Faubion said.
“The package insert is going to look scary: I prepare women for that because otherwise they often won’t even fill it or use it.”
A version of this article appeared on Medscape.com .
Charles Powell, MD, said he sometimes has a hard time persuading patients to start on low-dose vaginal estrogen, which can help prevent urinary tract infections and ease other symptoms of menopause.
Many women fear taking these vaginal products because of what Dr. Powell considers excessively strong warnings about the risk for cancer and cardiovascular disease linked to daily estrogen pills that were issued in the early 2000s.
He is advocating for the US Food and Drug Administration (FDA) to remove the boxed warning on low-dose estrogen. His efforts are separate from his roles as an associate professor of urology at the Indiana University School of Medicine, and as a member of the American Urological Association (AUA), Dr. Powell said.
In his quest to find out how to change labeling, Dr. Powell has gained a quick education about drug regulation. He has enlisted Representative Jim Baird (R-IN) and Senator Mike Braun (R-IN) to contact the FDA on his behalf, while congressional staff guided him through the hurdles of getting the warning label changed. For instance, a manufacturer of low-dose estrogen may need to become involved.
“You don’t learn this in med school,” Dr. Powell said in an interview.
With this work, Dr. Powell is wading into a long-standing argument between the FDA and some clinicians and researchers about the potential harms of low-dose estrogen.
He is doing so at a time of increased interest in understanding genitourinary syndrome of menopause (GSM), a term coined a decade ago by the International Society for the Study of Women’s Sexual Health and the North American Menopause Society to cover “a constellation of conditions” related to urogenital atrophy.
Symptoms of GSM include vaginal dryness and burning and recurrent urinary tract infections.
The federal government in 2022 began a project budgeted with nearly $1 million to review evidence on treatments, including vaginal and low-dose estrogen. The aim is to eventually help the AUA develop clinical guidelines for addressing GSM.
In addition, a bipartisan Senate bill introduced in May calls for authorizing $125 million over 5 years for the National Institutes of Health (NIH) to fund research on menopause. Senator Patty Murray (D-WA), the lead sponsor of the bill, is a longtime advocate for women’s health and serves as chairwoman for the Senate Appropriations Committee, which largely sets the NIH budget.
“The bottom line is, for too long, menopause has been overlooked, underinvested in and left behind,” Sen. Murray said during a May 2 press conference. “It is well past time to stop treating menopause like some kind of secret and start treating it like the major mainstream public health issue it is.”
Evidence Demands
Increased federal funding for menopause research could help efforts to change the warning label on low-dose estrogen, according to JoAnn Manson, MD, chief of preventive medicine at Brigham and Women’s Hospital in Boston.
Dr. Manson was a leader of the Women’s Health Initiative (WHI), a major federally funded research project launched in 1991 to investigate if hormone therapy and diet could protect older women from chronic diseases related to aging.
Before the WHI, clinicians prescribed hormones to prevent cardiovascular disease, based on evidence from earlier research.
But in 2002, a WHI trial that compared estrogen-progestin tablets with placebo was halted early because of disturbing findings, including an association with higher risk for breast cancer and cardiovascular disease.
Compared with placebo, for every 10,000 women taking estrogen plus progestin annually, incidences of cardiovascular disease, stroke, pulmonary embolism, and invasive breast cancer were seven to eight times higher.
In January 2003, the FDA announced it would put a boxed warning about cardiovascular risk and cancer risk on estrogen products, reflecting the WHI finding.
The agency at the time said clinicians should work with patients to assess risks and benefits of these products to manage the effects of menopause.
But more news on the potential harms of estrogen followed in 2004: A WHI study comparing estrogen-only pills with placebo produced signals of a small increased risk for stroke, although it also indicated no excess risk for breast cancer for at least 6.8 years of use.
Dr. Manson and the North American Menopause Society in 2016 filed a petition with the FDA to remove the boxed warning that appears on the front of low-dose estrogen products. The group wanted the information on risks moved to the usual warning section of the label.
Two years later, the FDA rejected the petition, citing the absence of “well-controlled studies,” to prove low-dose topical estrogen poses less risk to women than the high-dose pills studied in the WHI.
The FDA told this news organization that it stands by the decisions in its rejection of the petition.
Persuading the FDA to revise the labels on low-dose estrogen products likely will require evidence from randomized, large-scale studies, Dr. Manson said. The agency has not been satisfied to date with findings from other kinds of studies, including observational research.
“Once that evidence is available that the benefit-risk profile is different for different formulations and the evidence is compelling and definitive, that warning should change,” Dr. Manson told this news organization.
But the warning continues to have a chilling effect on patient willingness to use low-dose vaginal estrogen, even with the FDA’s continued endorsement of estrogen for menopause symptoms, clinicians told this news organization.
Risa Kagan, MD, a gynecologist at Sutter Health in Berkeley, California, said in many cases her patients’ partners also need to be reassured. Dr. Kagan said she still sees women who have had to discontinue sexual intercourse because of pain. In some cases, the patients will bring the medicine home only to find that the warnings frighten their spouses.
“The spouse says, ‘Oh my God, I don’t want you to get dementia, to get breast cancer, it’s not worth it, so let’s keep doing outercourse’,” meaning sexual relations without penetration, Dr. Kagan said.
Difficult Messaging
From the initial unveiling of disappointing WHI results, clinicians and researchers have stressed that women could continue using estrogen products for managing symptoms of menopause, even while advising strongly against their continued use with the intention of preventing heart disease.
Newly published findings from follow-ups of WHI participants may give clinicians and patients even more confidence for the use of estrogen products in early menopause.
According to the study, which Dr. Manson coauthored, younger women have a low risk for cardiovascular disease and other associated conditions when taking hormone therapy. Risks attributed to these drugs were less than one additional adverse event per 1000 women annually. This population may also derive significant quality-of-life benefits for symptom relief.
Dr. Manson told this news organization that estrogen in lower doses and delivered through the skin as a patch or gel may further reduce risks.
“The WHI findings should never be used as a reason to deny hormone therapy to women in early menopause with bothersome menopausal symptoms,” Dr. Manson said. “Many women are good candidates for treatment and, in shared decision-making with their clinicians, should be able to receive appropriate and personalized healthcare for their needs.”
But the current FDA warning label makes it difficult to help women understand the risk and benefits of low-dose estrogen, according to Stephanie Faubion, MD, MBA, medical director at the North American Menopause Society and director of Mayo Clinic’s Center for Women’s Health in Jacksonville, Florida.
Clinicians now must set aside time to explain the warnings to women when they prescribe low-dose estrogen, Dr. Faubion said.
“The package insert is going to look scary: I prepare women for that because otherwise they often won’t even fill it or use it.”
A version of this article appeared on Medscape.com .
Molecular Classification of Endometrial Carcinomas
Historically, endometrial cancer has been classified as type I or type II. Type I endometrial cancers are typically estrogen driven, low grade, with endometrioid histology, and have a more favorable prognosis. In contrast, type II endometrial cancers are typically high grade, have more aggressive histologies (eg, serous or clear cell), and have a poorer prognosis.1
While this system provides a helpful schema for understanding endometrial cancers, it fails to represent the immense variation of biologic behavior and outcomes in endometrial cancers and oversimplifies what has come to be understood as a complex and molecularly diverse disease.
In 2013, The Cancer Genome Atlas (TCGA) performed genomic, transcriptomic, and proteomic characterization of 373 endometrial carcinomas. They identified four categories with distinct genetic profiles corresponding to clinical outcomes: 1) DNA polymerase epsilon (POLE) mutated; 2) mismatch repair deficient; 3) copy number high/p53 abnormal; and 4) copy number low/no specific molecular profile.2 By providing both predictive and prognostic information, these molecular features may be incorporated into treatment planning decisions in the future.
The POLE-mutated subtype are endometrial cancers with recurrent mutations in the POLE gene, which is involved in DNA replication and repair. POLE mutations occur in about 5%-10% of endometrial cancers. Despite some more aggressive histopathologic findings (eg, higher grade, deeper myometrial invasion, positive lymphovascular space invasion), recurrences rarely occur, and patients with POLE mutations have the best prognosis of the four molecular subtypes, with a 5-year recurrence-free survival of 92%-100%.3
The mismatch repair–deficient (MMRd) subtype are endometrial cancers with abnormalities in any of the mismatch repair proteins (MLH1, PMS2, MSH2, MSH6). These alterations may result from hereditary or somatic mutations in any of the MMR genes or epigenetic changes in the MLH1 promoter. Germ-line mutations are associated with Lynch syndrome; thus, patients found to have a germ-line mutation in any of the MMR genes necessitate a genetics referral. The MMRd subtype accounts for about 20%-30% of endometrial cancers, and patients with MMRd tumors have an intermediate prognosis, with a 5-year recurrence-free survival of about 70%.3. These tumors are more responsive to the use of immunotherapy checkpoint inhibitors. Two recent landmark trials showed improved outcomes in patients with advanced MMRd endometrial cancer treated with immune checkpoint inhibitors in addition to standard chemotherapy.4,5
The worst prognosis belongs to the copy number high subgroup, which accounts for approximately 10% of endometrial cancers. Five-year recurrence-free survival is ~50%.3 These tumors often contain TP53 mutations and are composed of aggressive histologies, such as serous, clear cell, high-grade endometrioid, and carcinosarcomas. Recent data suggests that human epidermal growth factor receptor 2 (HER2) amplification may also be prevalent in this subgroup.6
Endometrial cancers that lack any of the above alterations fall into the no specific molecular profile (NSMP) or copy number low subgroup. Mutations in other genes, such as PTEN, PIK3CA, CTNNB1, KRAS, and ARID1A, are often present in these tumors. As the most common subtype, this heterogeneous group accounts for about 50% of all endometrial cancers. These tumors frequently comprise endometrioid histology with estrogen and progesterone receptor positivity, high rates of response to hormonal therapy, and an overall intermediate to favorable prognosis, with a 5-year recurrence-free survival of ~75%.3
The use of whole-genome sequencing in TCGA limits the clinical applicability of testing because of the cost and complex methodologies involved. Multiple algorithms have been developed in the interim that approximate TCGA subtypes using relatively less expensive and more widely available testing methods, such as immunohistochemistry and next-generation sequencing. In the ProMisE algorithm, immunohistochemistry for p53 and MMR proteins is used as a surrogate for copy number high and MMRd tumors, respectively, and targeted sequencing is used to identify POLE mutations.7
Full molecular classification of endometrial tumors provides important prognostic information and allows for incorporation into treatment planning. To this end, the new 2023 International Federation of Gynecology and Obstetrics (FIGO) endometrial cancer staging incorporates an option for the addition of molecular subtype, with the stance that it allows for better prognostic prediction.8 While complete molecular classification is not required, it is encouraged. Furthermore, several clinical trials are currently investigating different treatment regimens based on these distinct molecular profiles.
Dr. Haag is a gynecologic oncology fellow in the Department of Obstetrics and Gynecology, University of North Carolina Hospitals, Chapel Hill. Dr. Tucker is assistant professor of gynecologic oncology at the University of North Carolina at Chapel Hill. They have no conflicts of interest.
References
1. Bokhman JV. Two pathogenetic types of endometrial carcinoma. Gynecologic Oncology. 1983;15(1):10-17.
2. Kandoth C et al. Integrated genomic characterization of endometrial carcinoma. Nature. 2013;497(7447):67-73.
3. León-Castillo A et al. Molecular classification of the PORTEC-3 trial for high-risk endometrial cancer: Impact on prognosis and benefit from adjuvant therapy. J Clin Oncology. 2020;38(29):3388-3397.
4. Mirza MR et al. Dostarlimab for primary advanced or recurrent endometrial cancer. N Engl J Med. 2023;388(23):2145-2158.
5. Eskander RN et al. Pembrolizumab plus chemotherapy in advanced endometrial cancer. N Engl J Med. 2023;388(23):2159-2170.
6. Talia KL et al. The role of HER2 as a therapeutic biomarker in gynaecological malignancy: Potential for use beyond uterine serous carcinoma. Pathology. 2023;55(1):8-18.
7. Kommoss S et al. Final validation of the ProMisE molecular classifier for endometrial carcinoma in a large population-based case series. Annals Oncology. 2018;29(5):1180-1188.
8. Berek JS et al. FIGO staging of endometrial cancer: 2023. Int J Gynaecol Obstet. 2023;162(2):383-394.
Historically, endometrial cancer has been classified as type I or type II. Type I endometrial cancers are typically estrogen driven, low grade, with endometrioid histology, and have a more favorable prognosis. In contrast, type II endometrial cancers are typically high grade, have more aggressive histologies (eg, serous or clear cell), and have a poorer prognosis.1
While this system provides a helpful schema for understanding endometrial cancers, it fails to represent the immense variation of biologic behavior and outcomes in endometrial cancers and oversimplifies what has come to be understood as a complex and molecularly diverse disease.
In 2013, The Cancer Genome Atlas (TCGA) performed genomic, transcriptomic, and proteomic characterization of 373 endometrial carcinomas. They identified four categories with distinct genetic profiles corresponding to clinical outcomes: 1) DNA polymerase epsilon (POLE) mutated; 2) mismatch repair deficient; 3) copy number high/p53 abnormal; and 4) copy number low/no specific molecular profile.2 By providing both predictive and prognostic information, these molecular features may be incorporated into treatment planning decisions in the future.
The POLE-mutated subtype are endometrial cancers with recurrent mutations in the POLE gene, which is involved in DNA replication and repair. POLE mutations occur in about 5%-10% of endometrial cancers. Despite some more aggressive histopathologic findings (eg, higher grade, deeper myometrial invasion, positive lymphovascular space invasion), recurrences rarely occur, and patients with POLE mutations have the best prognosis of the four molecular subtypes, with a 5-year recurrence-free survival of 92%-100%.3
The mismatch repair–deficient (MMRd) subtype are endometrial cancers with abnormalities in any of the mismatch repair proteins (MLH1, PMS2, MSH2, MSH6). These alterations may result from hereditary or somatic mutations in any of the MMR genes or epigenetic changes in the MLH1 promoter. Germ-line mutations are associated with Lynch syndrome; thus, patients found to have a germ-line mutation in any of the MMR genes necessitate a genetics referral. The MMRd subtype accounts for about 20%-30% of endometrial cancers, and patients with MMRd tumors have an intermediate prognosis, with a 5-year recurrence-free survival of about 70%.3. These tumors are more responsive to the use of immunotherapy checkpoint inhibitors. Two recent landmark trials showed improved outcomes in patients with advanced MMRd endometrial cancer treated with immune checkpoint inhibitors in addition to standard chemotherapy.4,5
The worst prognosis belongs to the copy number high subgroup, which accounts for approximately 10% of endometrial cancers. Five-year recurrence-free survival is ~50%.3 These tumors often contain TP53 mutations and are composed of aggressive histologies, such as serous, clear cell, high-grade endometrioid, and carcinosarcomas. Recent data suggests that human epidermal growth factor receptor 2 (HER2) amplification may also be prevalent in this subgroup.6
Endometrial cancers that lack any of the above alterations fall into the no specific molecular profile (NSMP) or copy number low subgroup. Mutations in other genes, such as PTEN, PIK3CA, CTNNB1, KRAS, and ARID1A, are often present in these tumors. As the most common subtype, this heterogeneous group accounts for about 50% of all endometrial cancers. These tumors frequently comprise endometrioid histology with estrogen and progesterone receptor positivity, high rates of response to hormonal therapy, and an overall intermediate to favorable prognosis, with a 5-year recurrence-free survival of ~75%.3
The use of whole-genome sequencing in TCGA limits the clinical applicability of testing because of the cost and complex methodologies involved. Multiple algorithms have been developed in the interim that approximate TCGA subtypes using relatively less expensive and more widely available testing methods, such as immunohistochemistry and next-generation sequencing. In the ProMisE algorithm, immunohistochemistry for p53 and MMR proteins is used as a surrogate for copy number high and MMRd tumors, respectively, and targeted sequencing is used to identify POLE mutations.7
Full molecular classification of endometrial tumors provides important prognostic information and allows for incorporation into treatment planning. To this end, the new 2023 International Federation of Gynecology and Obstetrics (FIGO) endometrial cancer staging incorporates an option for the addition of molecular subtype, with the stance that it allows for better prognostic prediction.8 While complete molecular classification is not required, it is encouraged. Furthermore, several clinical trials are currently investigating different treatment regimens based on these distinct molecular profiles.
Dr. Haag is a gynecologic oncology fellow in the Department of Obstetrics and Gynecology, University of North Carolina Hospitals, Chapel Hill. Dr. Tucker is assistant professor of gynecologic oncology at the University of North Carolina at Chapel Hill. They have no conflicts of interest.
References
1. Bokhman JV. Two pathogenetic types of endometrial carcinoma. Gynecologic Oncology. 1983;15(1):10-17.
2. Kandoth C et al. Integrated genomic characterization of endometrial carcinoma. Nature. 2013;497(7447):67-73.
3. León-Castillo A et al. Molecular classification of the PORTEC-3 trial for high-risk endometrial cancer: Impact on prognosis and benefit from adjuvant therapy. J Clin Oncology. 2020;38(29):3388-3397.
4. Mirza MR et al. Dostarlimab for primary advanced or recurrent endometrial cancer. N Engl J Med. 2023;388(23):2145-2158.
5. Eskander RN et al. Pembrolizumab plus chemotherapy in advanced endometrial cancer. N Engl J Med. 2023;388(23):2159-2170.
6. Talia KL et al. The role of HER2 as a therapeutic biomarker in gynaecological malignancy: Potential for use beyond uterine serous carcinoma. Pathology. 2023;55(1):8-18.
7. Kommoss S et al. Final validation of the ProMisE molecular classifier for endometrial carcinoma in a large population-based case series. Annals Oncology. 2018;29(5):1180-1188.
8. Berek JS et al. FIGO staging of endometrial cancer: 2023. Int J Gynaecol Obstet. 2023;162(2):383-394.
Historically, endometrial cancer has been classified as type I or type II. Type I endometrial cancers are typically estrogen driven, low grade, with endometrioid histology, and have a more favorable prognosis. In contrast, type II endometrial cancers are typically high grade, have more aggressive histologies (eg, serous or clear cell), and have a poorer prognosis.1
While this system provides a helpful schema for understanding endometrial cancers, it fails to represent the immense variation of biologic behavior and outcomes in endometrial cancers and oversimplifies what has come to be understood as a complex and molecularly diverse disease.
In 2013, The Cancer Genome Atlas (TCGA) performed genomic, transcriptomic, and proteomic characterization of 373 endometrial carcinomas. They identified four categories with distinct genetic profiles corresponding to clinical outcomes: 1) DNA polymerase epsilon (POLE) mutated; 2) mismatch repair deficient; 3) copy number high/p53 abnormal; and 4) copy number low/no specific molecular profile.2 By providing both predictive and prognostic information, these molecular features may be incorporated into treatment planning decisions in the future.
The POLE-mutated subtype are endometrial cancers with recurrent mutations in the POLE gene, which is involved in DNA replication and repair. POLE mutations occur in about 5%-10% of endometrial cancers. Despite some more aggressive histopathologic findings (eg, higher grade, deeper myometrial invasion, positive lymphovascular space invasion), recurrences rarely occur, and patients with POLE mutations have the best prognosis of the four molecular subtypes, with a 5-year recurrence-free survival of 92%-100%.3
The mismatch repair–deficient (MMRd) subtype are endometrial cancers with abnormalities in any of the mismatch repair proteins (MLH1, PMS2, MSH2, MSH6). These alterations may result from hereditary or somatic mutations in any of the MMR genes or epigenetic changes in the MLH1 promoter. Germ-line mutations are associated with Lynch syndrome; thus, patients found to have a germ-line mutation in any of the MMR genes necessitate a genetics referral. The MMRd subtype accounts for about 20%-30% of endometrial cancers, and patients with MMRd tumors have an intermediate prognosis, with a 5-year recurrence-free survival of about 70%.3. These tumors are more responsive to the use of immunotherapy checkpoint inhibitors. Two recent landmark trials showed improved outcomes in patients with advanced MMRd endometrial cancer treated with immune checkpoint inhibitors in addition to standard chemotherapy.4,5
The worst prognosis belongs to the copy number high subgroup, which accounts for approximately 10% of endometrial cancers. Five-year recurrence-free survival is ~50%.3 These tumors often contain TP53 mutations and are composed of aggressive histologies, such as serous, clear cell, high-grade endometrioid, and carcinosarcomas. Recent data suggests that human epidermal growth factor receptor 2 (HER2) amplification may also be prevalent in this subgroup.6
Endometrial cancers that lack any of the above alterations fall into the no specific molecular profile (NSMP) or copy number low subgroup. Mutations in other genes, such as PTEN, PIK3CA, CTNNB1, KRAS, and ARID1A, are often present in these tumors. As the most common subtype, this heterogeneous group accounts for about 50% of all endometrial cancers. These tumors frequently comprise endometrioid histology with estrogen and progesterone receptor positivity, high rates of response to hormonal therapy, and an overall intermediate to favorable prognosis, with a 5-year recurrence-free survival of ~75%.3
The use of whole-genome sequencing in TCGA limits the clinical applicability of testing because of the cost and complex methodologies involved. Multiple algorithms have been developed in the interim that approximate TCGA subtypes using relatively less expensive and more widely available testing methods, such as immunohistochemistry and next-generation sequencing. In the ProMisE algorithm, immunohistochemistry for p53 and MMR proteins is used as a surrogate for copy number high and MMRd tumors, respectively, and targeted sequencing is used to identify POLE mutations.7
Full molecular classification of endometrial tumors provides important prognostic information and allows for incorporation into treatment planning. To this end, the new 2023 International Federation of Gynecology and Obstetrics (FIGO) endometrial cancer staging incorporates an option for the addition of molecular subtype, with the stance that it allows for better prognostic prediction.8 While complete molecular classification is not required, it is encouraged. Furthermore, several clinical trials are currently investigating different treatment regimens based on these distinct molecular profiles.
Dr. Haag is a gynecologic oncology fellow in the Department of Obstetrics and Gynecology, University of North Carolina Hospitals, Chapel Hill. Dr. Tucker is assistant professor of gynecologic oncology at the University of North Carolina at Chapel Hill. They have no conflicts of interest.
References
1. Bokhman JV. Two pathogenetic types of endometrial carcinoma. Gynecologic Oncology. 1983;15(1):10-17.
2. Kandoth C et al. Integrated genomic characterization of endometrial carcinoma. Nature. 2013;497(7447):67-73.
3. León-Castillo A et al. Molecular classification of the PORTEC-3 trial for high-risk endometrial cancer: Impact on prognosis and benefit from adjuvant therapy. J Clin Oncology. 2020;38(29):3388-3397.
4. Mirza MR et al. Dostarlimab for primary advanced or recurrent endometrial cancer. N Engl J Med. 2023;388(23):2145-2158.
5. Eskander RN et al. Pembrolizumab plus chemotherapy in advanced endometrial cancer. N Engl J Med. 2023;388(23):2159-2170.
6. Talia KL et al. The role of HER2 as a therapeutic biomarker in gynaecological malignancy: Potential for use beyond uterine serous carcinoma. Pathology. 2023;55(1):8-18.
7. Kommoss S et al. Final validation of the ProMisE molecular classifier for endometrial carcinoma in a large population-based case series. Annals Oncology. 2018;29(5):1180-1188.
8. Berek JS et al. FIGO staging of endometrial cancer: 2023. Int J Gynaecol Obstet. 2023;162(2):383-394.
Hypofractionated Radiotherapy Limits Toxic Effects in Cervical Cancer
TOPLINE:
results from the phase 2 POHIM-CCRT trial suggested.
METHODOLOGY:
- To date, no studies have assessed the treatment outcomes and toxic effects of hypofractionated IMRT following radical hysterectomy in patients with cervical cancer undergoing curative radiotherapy.
- The team analyzed outcomes from 79 patients undergoing hypofractionated IMRT for cervical cancer after radical hysterectomy and pelvic lymph node dissection.
- Patients were a median age of 48; 29.5% had stage IB to IIA disease, another 29.5% had stage IIB disease, and 41% had stage III disease. Patients also had at least one of the following criteria following radical hysterectomy and pelvic lymph node dissection: lymph node metastasis (39.7%), parametrial invasion (54.4%), and positive resection margin (5.1%).
- The prescribed dose to the planning target volume was 40 Gy, delivered in 16 fractions to the whole pelvis, with any type of IMRT permitted. Overall, 71 patients also underwent concurrent weekly cisplatin (40 mg/m2 of body surface area for three cycles), and eight received fluorouracil (1000 mg/m2 on days 1-5) with cisplatin (60 mg/m2 for two cycles).
- The primary endpoint was the incidence of acute grade 3 or higher gastrointestinal tract, genitourinary, and hematologic toxic effects during radiotherapy or within 3 months of completing radiotherapy.
TAKEAWAY:
- After radiotherapy, only two patients (2.5%) experienced acute grade 3 or higher toxic effects. One was hospitalized for enterocolitis on the last day of radiotherapy and developed grade 3 anemia 3 months after completing radiotherapy; the other experienced hematologic toxic effects and also developed grade 3 anemia 3 months after completing radiotherapy.
- No patients experienced late grade 3 or higher toxic effects.
- When assessing toxic effects of any grade, acute and late gastrointestinal tract toxicities occurred in 76% and 31.6% of patients, respectively; acute and late genitourinary toxicities, all grade 1, occurred in 19% and 24.1% of patients, respectively; and hematologic toxicities occurred in 29.1% and 6.3% of patients, respectively.
- Overall, at 3 years, 79.3% of patients were disease-free and 98% were alive. After a median follow-up of 43 months, 16 patients (20.3%) experienced disease recurrence, four of whom were salvaged and three of whom died.
IN PRACTICE:
“This nonrandomized controlled trial is the first prospective trial, to our knowledge, to show acceptable acute toxic effects of hypofractionated IMRT for cervical cancer in a postoperative concurrent chemoradiotherapy setting,” the authors said, adding that the rate of grade 3 or higher acute toxic effects of 2.5% reported in this study was “substantially lower than our initial hypothesis of less than 15%.”
However , in an accompanying editorial, Mark E. Bernard, MD, of the University of Kentucky College of Medicine, Lexington, highlighted caveats to the study design and raised two core questions: “Should acute toxic effects be the primary endpoint of a single-group, phase 2 study using hypofractionation with fewer cycles of concurrent chemotherapy? Should the primary endpoint rather have been a cancer control endpoint, such as disease-free survival, overall survival, or local control?”
Still, Dr. Bernard wrote, “This trial does help lay the foundation for future pelvic hypofractionated trials with concurrent chemotherapy, especially for gynecological malignant tumors.”
SOURCE:
The research, led by Won Park, MD, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Republic of Korea, was published in JAMA Oncology.
LIMITATIONS:
The trial is a single-arm study, with a short follow-up time. In the editorial, Bernard listed several limitations, including the fact that patients received fewer cycles of concurrent chemotherapy than what’s typically given in this population.
DISCLOSURES:
No funding or relevant financial relationships were declared.
A version of this article appeared on Medscape.com.
TOPLINE:
results from the phase 2 POHIM-CCRT trial suggested.
METHODOLOGY:
- To date, no studies have assessed the treatment outcomes and toxic effects of hypofractionated IMRT following radical hysterectomy in patients with cervical cancer undergoing curative radiotherapy.
- The team analyzed outcomes from 79 patients undergoing hypofractionated IMRT for cervical cancer after radical hysterectomy and pelvic lymph node dissection.
- Patients were a median age of 48; 29.5% had stage IB to IIA disease, another 29.5% had stage IIB disease, and 41% had stage III disease. Patients also had at least one of the following criteria following radical hysterectomy and pelvic lymph node dissection: lymph node metastasis (39.7%), parametrial invasion (54.4%), and positive resection margin (5.1%).
- The prescribed dose to the planning target volume was 40 Gy, delivered in 16 fractions to the whole pelvis, with any type of IMRT permitted. Overall, 71 patients also underwent concurrent weekly cisplatin (40 mg/m2 of body surface area for three cycles), and eight received fluorouracil (1000 mg/m2 on days 1-5) with cisplatin (60 mg/m2 for two cycles).
- The primary endpoint was the incidence of acute grade 3 or higher gastrointestinal tract, genitourinary, and hematologic toxic effects during radiotherapy or within 3 months of completing radiotherapy.
TAKEAWAY:
- After radiotherapy, only two patients (2.5%) experienced acute grade 3 or higher toxic effects. One was hospitalized for enterocolitis on the last day of radiotherapy and developed grade 3 anemia 3 months after completing radiotherapy; the other experienced hematologic toxic effects and also developed grade 3 anemia 3 months after completing radiotherapy.
- No patients experienced late grade 3 or higher toxic effects.
- When assessing toxic effects of any grade, acute and late gastrointestinal tract toxicities occurred in 76% and 31.6% of patients, respectively; acute and late genitourinary toxicities, all grade 1, occurred in 19% and 24.1% of patients, respectively; and hematologic toxicities occurred in 29.1% and 6.3% of patients, respectively.
- Overall, at 3 years, 79.3% of patients were disease-free and 98% were alive. After a median follow-up of 43 months, 16 patients (20.3%) experienced disease recurrence, four of whom were salvaged and three of whom died.
IN PRACTICE:
“This nonrandomized controlled trial is the first prospective trial, to our knowledge, to show acceptable acute toxic effects of hypofractionated IMRT for cervical cancer in a postoperative concurrent chemoradiotherapy setting,” the authors said, adding that the rate of grade 3 or higher acute toxic effects of 2.5% reported in this study was “substantially lower than our initial hypothesis of less than 15%.”
However , in an accompanying editorial, Mark E. Bernard, MD, of the University of Kentucky College of Medicine, Lexington, highlighted caveats to the study design and raised two core questions: “Should acute toxic effects be the primary endpoint of a single-group, phase 2 study using hypofractionation with fewer cycles of concurrent chemotherapy? Should the primary endpoint rather have been a cancer control endpoint, such as disease-free survival, overall survival, or local control?”
Still, Dr. Bernard wrote, “This trial does help lay the foundation for future pelvic hypofractionated trials with concurrent chemotherapy, especially for gynecological malignant tumors.”
SOURCE:
The research, led by Won Park, MD, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Republic of Korea, was published in JAMA Oncology.
LIMITATIONS:
The trial is a single-arm study, with a short follow-up time. In the editorial, Bernard listed several limitations, including the fact that patients received fewer cycles of concurrent chemotherapy than what’s typically given in this population.
DISCLOSURES:
No funding or relevant financial relationships were declared.
A version of this article appeared on Medscape.com.
TOPLINE:
results from the phase 2 POHIM-CCRT trial suggested.
METHODOLOGY:
- To date, no studies have assessed the treatment outcomes and toxic effects of hypofractionated IMRT following radical hysterectomy in patients with cervical cancer undergoing curative radiotherapy.
- The team analyzed outcomes from 79 patients undergoing hypofractionated IMRT for cervical cancer after radical hysterectomy and pelvic lymph node dissection.
- Patients were a median age of 48; 29.5% had stage IB to IIA disease, another 29.5% had stage IIB disease, and 41% had stage III disease. Patients also had at least one of the following criteria following radical hysterectomy and pelvic lymph node dissection: lymph node metastasis (39.7%), parametrial invasion (54.4%), and positive resection margin (5.1%).
- The prescribed dose to the planning target volume was 40 Gy, delivered in 16 fractions to the whole pelvis, with any type of IMRT permitted. Overall, 71 patients also underwent concurrent weekly cisplatin (40 mg/m2 of body surface area for three cycles), and eight received fluorouracil (1000 mg/m2 on days 1-5) with cisplatin (60 mg/m2 for two cycles).
- The primary endpoint was the incidence of acute grade 3 or higher gastrointestinal tract, genitourinary, and hematologic toxic effects during radiotherapy or within 3 months of completing radiotherapy.
TAKEAWAY:
- After radiotherapy, only two patients (2.5%) experienced acute grade 3 or higher toxic effects. One was hospitalized for enterocolitis on the last day of radiotherapy and developed grade 3 anemia 3 months after completing radiotherapy; the other experienced hematologic toxic effects and also developed grade 3 anemia 3 months after completing radiotherapy.
- No patients experienced late grade 3 or higher toxic effects.
- When assessing toxic effects of any grade, acute and late gastrointestinal tract toxicities occurred in 76% and 31.6% of patients, respectively; acute and late genitourinary toxicities, all grade 1, occurred in 19% and 24.1% of patients, respectively; and hematologic toxicities occurred in 29.1% and 6.3% of patients, respectively.
- Overall, at 3 years, 79.3% of patients were disease-free and 98% were alive. After a median follow-up of 43 months, 16 patients (20.3%) experienced disease recurrence, four of whom were salvaged and three of whom died.
IN PRACTICE:
“This nonrandomized controlled trial is the first prospective trial, to our knowledge, to show acceptable acute toxic effects of hypofractionated IMRT for cervical cancer in a postoperative concurrent chemoradiotherapy setting,” the authors said, adding that the rate of grade 3 or higher acute toxic effects of 2.5% reported in this study was “substantially lower than our initial hypothesis of less than 15%.”
However , in an accompanying editorial, Mark E. Bernard, MD, of the University of Kentucky College of Medicine, Lexington, highlighted caveats to the study design and raised two core questions: “Should acute toxic effects be the primary endpoint of a single-group, phase 2 study using hypofractionation with fewer cycles of concurrent chemotherapy? Should the primary endpoint rather have been a cancer control endpoint, such as disease-free survival, overall survival, or local control?”
Still, Dr. Bernard wrote, “This trial does help lay the foundation for future pelvic hypofractionated trials with concurrent chemotherapy, especially for gynecological malignant tumors.”
SOURCE:
The research, led by Won Park, MD, Samsung Medical Center, Sungkyunkwan University School of Medicine, Seoul, Republic of Korea, was published in JAMA Oncology.
LIMITATIONS:
The trial is a single-arm study, with a short follow-up time. In the editorial, Bernard listed several limitations, including the fact that patients received fewer cycles of concurrent chemotherapy than what’s typically given in this population.
DISCLOSURES:
No funding or relevant financial relationships were declared.
A version of this article appeared on Medscape.com.
US Researchers Call for Robust Studies Into Dequalinium, a Bacterial Vaginosis Therapy Common in Europe
Interest is growing in a standard European treatment for bacterial vaginosis (BV).
In a commentary published in JAMA Network Open, researchers and doctors from the Johns Hopkins University School of Medicine in Baltimore and the University of Maryland, Baltimore, urged clinical trials in the United States to determine if dequalinium chloride — an antiseptic that inhibits the growth of bacteria and fungi — is on par with or better than treatments currently available.
Dequalinium has been used throughout Europe for decades and is recommended as an alternative or second-line BV treatment by the World Health Organization; the International Society for the Study of Vulvovaginal Disease; and the Austrian, German, Portuguese, Spanish, and Swiss Societies of Gynecology and Obstetrics. However, the product has not been approved for clinical use in the United States, no trials studying the drug have been registered on ClinicalTrials.gov, and the US Food and Drug Administration has not received an application for approval, according to agency records.
Treatments in the United States for BV include metronidazole and clindamycin that, while effective, have a recurrence rate of up to 60%.
“Current treatments for bacterial vaginosis often fall short, primarily due to frequent recurrences after treatment,” said Rebecca M. Brotman, PhD, MPH, a professor in the Department of Epidemiology and Public Health at the Institute for Genome Sciences at the University of Maryland School of Medicine, and the corresponding author of the commentary.
More than 40% of people with recurrent BV do not receive adequate treatment, according to Caroline M. Mitchell, MD, MPH, director of the Vulvovaginal Disorders Program at Massachusetts General Hospital Vincent Center for Reproductive Biology, Boston, Massachusetts.
“BV is very disruptive to people’s daily lives and causes significant distress,” said Dr. Mitchell, who was not a coauthor of the new article. “Additionally, BV is associated with higher risk for HPV [human papillomavirus] infection, progression of HPV to cervical dysplasia, as well as risk for acquisition of other sexually transmitted infections.”
Dr. Mitchell said she hopes a recent trial from Europe comparing dequalinium chloride to metronidazole spurs researchers to study its efficacy and safety among women in the United States.
“Dequalinium has some antifungal activity, so it might offer a lower chance of yeast infection after treatment, which is important because posttreatment vulvovaginal candidiasis is one of the downsides to conventional antibiotic treatments,” Dr. Mitchell said.
The recent clinical trial included 147 premenopausal women with BV who received 10 mg of dequalinium per day for 6 days or oral metronidazole (500 mg twice daily for 7 days).
Dr. Brotman said any studies in the United States would need to examine long-term recurrence of vaginosis after treatment with dequalinium chloride and its use during pregnancy.
The study was funded by various grants from the National Institutes of Health and the Gates Foundation. Various authors reported receiving royalties from UpToDate outside the submitted work or receiving a donation of sexually transmitted infection testing kits from Hologic for a study outside the submitted work. No other disclosures were reported.
A version of this article first appeared on Medscape.com.
Interest is growing in a standard European treatment for bacterial vaginosis (BV).
In a commentary published in JAMA Network Open, researchers and doctors from the Johns Hopkins University School of Medicine in Baltimore and the University of Maryland, Baltimore, urged clinical trials in the United States to determine if dequalinium chloride — an antiseptic that inhibits the growth of bacteria and fungi — is on par with or better than treatments currently available.
Dequalinium has been used throughout Europe for decades and is recommended as an alternative or second-line BV treatment by the World Health Organization; the International Society for the Study of Vulvovaginal Disease; and the Austrian, German, Portuguese, Spanish, and Swiss Societies of Gynecology and Obstetrics. However, the product has not been approved for clinical use in the United States, no trials studying the drug have been registered on ClinicalTrials.gov, and the US Food and Drug Administration has not received an application for approval, according to agency records.
Treatments in the United States for BV include metronidazole and clindamycin that, while effective, have a recurrence rate of up to 60%.
“Current treatments for bacterial vaginosis often fall short, primarily due to frequent recurrences after treatment,” said Rebecca M. Brotman, PhD, MPH, a professor in the Department of Epidemiology and Public Health at the Institute for Genome Sciences at the University of Maryland School of Medicine, and the corresponding author of the commentary.
More than 40% of people with recurrent BV do not receive adequate treatment, according to Caroline M. Mitchell, MD, MPH, director of the Vulvovaginal Disorders Program at Massachusetts General Hospital Vincent Center for Reproductive Biology, Boston, Massachusetts.
“BV is very disruptive to people’s daily lives and causes significant distress,” said Dr. Mitchell, who was not a coauthor of the new article. “Additionally, BV is associated with higher risk for HPV [human papillomavirus] infection, progression of HPV to cervical dysplasia, as well as risk for acquisition of other sexually transmitted infections.”
Dr. Mitchell said she hopes a recent trial from Europe comparing dequalinium chloride to metronidazole spurs researchers to study its efficacy and safety among women in the United States.
“Dequalinium has some antifungal activity, so it might offer a lower chance of yeast infection after treatment, which is important because posttreatment vulvovaginal candidiasis is one of the downsides to conventional antibiotic treatments,” Dr. Mitchell said.
The recent clinical trial included 147 premenopausal women with BV who received 10 mg of dequalinium per day for 6 days or oral metronidazole (500 mg twice daily for 7 days).
Dr. Brotman said any studies in the United States would need to examine long-term recurrence of vaginosis after treatment with dequalinium chloride and its use during pregnancy.
The study was funded by various grants from the National Institutes of Health and the Gates Foundation. Various authors reported receiving royalties from UpToDate outside the submitted work or receiving a donation of sexually transmitted infection testing kits from Hologic for a study outside the submitted work. No other disclosures were reported.
A version of this article first appeared on Medscape.com.
Interest is growing in a standard European treatment for bacterial vaginosis (BV).
In a commentary published in JAMA Network Open, researchers and doctors from the Johns Hopkins University School of Medicine in Baltimore and the University of Maryland, Baltimore, urged clinical trials in the United States to determine if dequalinium chloride — an antiseptic that inhibits the growth of bacteria and fungi — is on par with or better than treatments currently available.
Dequalinium has been used throughout Europe for decades and is recommended as an alternative or second-line BV treatment by the World Health Organization; the International Society for the Study of Vulvovaginal Disease; and the Austrian, German, Portuguese, Spanish, and Swiss Societies of Gynecology and Obstetrics. However, the product has not been approved for clinical use in the United States, no trials studying the drug have been registered on ClinicalTrials.gov, and the US Food and Drug Administration has not received an application for approval, according to agency records.
Treatments in the United States for BV include metronidazole and clindamycin that, while effective, have a recurrence rate of up to 60%.
“Current treatments for bacterial vaginosis often fall short, primarily due to frequent recurrences after treatment,” said Rebecca M. Brotman, PhD, MPH, a professor in the Department of Epidemiology and Public Health at the Institute for Genome Sciences at the University of Maryland School of Medicine, and the corresponding author of the commentary.
More than 40% of people with recurrent BV do not receive adequate treatment, according to Caroline M. Mitchell, MD, MPH, director of the Vulvovaginal Disorders Program at Massachusetts General Hospital Vincent Center for Reproductive Biology, Boston, Massachusetts.
“BV is very disruptive to people’s daily lives and causes significant distress,” said Dr. Mitchell, who was not a coauthor of the new article. “Additionally, BV is associated with higher risk for HPV [human papillomavirus] infection, progression of HPV to cervical dysplasia, as well as risk for acquisition of other sexually transmitted infections.”
Dr. Mitchell said she hopes a recent trial from Europe comparing dequalinium chloride to metronidazole spurs researchers to study its efficacy and safety among women in the United States.
“Dequalinium has some antifungal activity, so it might offer a lower chance of yeast infection after treatment, which is important because posttreatment vulvovaginal candidiasis is one of the downsides to conventional antibiotic treatments,” Dr. Mitchell said.
The recent clinical trial included 147 premenopausal women with BV who received 10 mg of dequalinium per day for 6 days or oral metronidazole (500 mg twice daily for 7 days).
Dr. Brotman said any studies in the United States would need to examine long-term recurrence of vaginosis after treatment with dequalinium chloride and its use during pregnancy.
The study was funded by various grants from the National Institutes of Health and the Gates Foundation. Various authors reported receiving royalties from UpToDate outside the submitted work or receiving a donation of sexually transmitted infection testing kits from Hologic for a study outside the submitted work. No other disclosures were reported.
A version of this article first appeared on Medscape.com.
FROM JAMA NETWORK OPEN
Starting Points if Patient Chooses Medication Abortion
An evolving legal landscape surrounding medication abortion has left physicians with as many questions as patients. A panel of clinicians at the annual meeting of the American College of Physicians offered guidance on how to help patients who choose medication abortion, which is available to women until 10 weeks of gestation.
Approved in 2000, abortion pills have become the most common method for terminating pregnancy in the United States, accounting for 63% of all abortions in 2023. The US Supreme Court is reviewing access to medication abortions, with a decision expected within months.
According to the Guttmacher Institute, 29 states as of February restrict access to medication abortion, either by limiting or banning the use of the drugs or by curtailing who can prescribe them and under what circumstances.
First, Determine Gestational Age
Cynthia Chuang, MD, MSc, an internist and professor of medicine at Penn State College of Medicine in Hershey, Pennsylvania, said in most cases, a woman can pinpoint the date of the first day of her last menstrual period, and the physician can confirm gestational age is 70 days or less. An ultrasound should be performed if the date of the last period is uncertain, she said, or if ectopic pregnancy is suspected, periods are irregular, or ultrasound is legally required in the state.
Women are not eligible for abortion pills if they have a bleeding or clotting disorder, have an intrauterine device, have adrenal insufficiency or chronic steroid use, or have porphyria or hemoglobin levels < 9 g/dL, she said.
“If the person has a known hemoglobin of less than 9, we would suggest that person have a procedural abortion,” Dr. Chuang said.
Components of Medication
Patients first receive 200 mg of oral mifepristone, which separates the pregnancy from the uterine wall. “Typically, people don’t experience side effects from the mifepristone alone,” Dr. Chaung said.
In the next 48 hours, the patient takes 800 mcg of misoprostol, either vaginally or buccally. “Patients can expect heavy cramping and bleeding 1-2 days after taking misoprostol,” she said. The bleeding should gradually subside over the following week or 2, she said. If the gestational age is 9 weeks or more, a second dose of misoprostol can be administered 3-6 hours after the first dose to improve efficacy.
If mifepristone is not available, misoprostol can be used alone in three doses spaced 3 hours apart, Dr. Chuang said.
The failure rate for mifepristone plus misoprostol has been calculated at 2% if the gestational age is less than 7 weeks. For misoprostol alone, the failure rate varies by the study, depending on gestational age and population analyzed, Dr. Chuang said. A 2023 meta-analysis in Contraception put the failure rate at 11%.
When to Call the Clinician
Dr. Chuang said clinicians should instruct women who have taken abortion pills to call the clinic if they are soaking through two sanitary pads an hour for more than 1 hour, if there is little to no bleeding, or if they think the medication isn’t working after taking the full regimen.
Mindy Sobota, MD, MS, an internist and associate professor of medicine at the Warren Alpert Medical School of Brown University in Providence, Rhode Island, recommended a continuing medical education site for evidence-based guidance on how best to talk with women about medication abortions.
She also recommended physicians and patients consult the Plan C website for guidance on telehealth services and price information on receiving abortion pills by mail in every state. “It’s a very reliable and safe clearing house,” Dr. Sobota said.
Internists should let patients know that whatever their choices are around pregnancy, they are open to discussing those choices and helping them through the process, Dr. Sobota said, adding that she makes those statements in annual visits.
Alexandra Bachorik, MD, EdM, director of education in the Women’s Health Unit and assistant professor of medicine at Boston University Chobanian & Avedisian School of Medicine, Boston, Massachusetts, said patients in restrictive states who need financial help related to obtaining abortion services in a less restricted state can visit the National Network of Abortion Funds, which can help people with travel or housing expenses.
Facilitating access to a clinic in a less restrictive state may be helpful to people approaching a gestational age limit, she said.
Adelaide McClintock, MD, an internist and assistant professor of general internal medicine at the University of Washington School of Medicine in Seattle, Washington, noted that even clinicians who cannot legally prescribe abortion pills can support their patients by providing resources and counseling on options before, during, and after pregnancy. Those who live in restrictive states also can provide support to women who have traveled to less restrictive states for an abortion if they have postabortion complications, she said.
She recommended the Reproductive Health Access Project website for a comprehensive guide for evidence-based care and counseling patients about all choices in reproductive healthcare.
Panelists urged clinicians to get familiar with abortion-access resources and keep them at their fingertips in practice. Patient requests for the services are common, she noted, as “one in four women will have an abortion by the age of 45.”
Dr. Chuang, Dr. McClintock, Dr. Sobota, and Dr. Bachorik reported no relevant financial conflicts of interest.
A version of this article appeared on Medscape.com.
An evolving legal landscape surrounding medication abortion has left physicians with as many questions as patients. A panel of clinicians at the annual meeting of the American College of Physicians offered guidance on how to help patients who choose medication abortion, which is available to women until 10 weeks of gestation.
Approved in 2000, abortion pills have become the most common method for terminating pregnancy in the United States, accounting for 63% of all abortions in 2023. The US Supreme Court is reviewing access to medication abortions, with a decision expected within months.
According to the Guttmacher Institute, 29 states as of February restrict access to medication abortion, either by limiting or banning the use of the drugs or by curtailing who can prescribe them and under what circumstances.
First, Determine Gestational Age
Cynthia Chuang, MD, MSc, an internist and professor of medicine at Penn State College of Medicine in Hershey, Pennsylvania, said in most cases, a woman can pinpoint the date of the first day of her last menstrual period, and the physician can confirm gestational age is 70 days or less. An ultrasound should be performed if the date of the last period is uncertain, she said, or if ectopic pregnancy is suspected, periods are irregular, or ultrasound is legally required in the state.
Women are not eligible for abortion pills if they have a bleeding or clotting disorder, have an intrauterine device, have adrenal insufficiency or chronic steroid use, or have porphyria or hemoglobin levels < 9 g/dL, she said.
“If the person has a known hemoglobin of less than 9, we would suggest that person have a procedural abortion,” Dr. Chuang said.
Components of Medication
Patients first receive 200 mg of oral mifepristone, which separates the pregnancy from the uterine wall. “Typically, people don’t experience side effects from the mifepristone alone,” Dr. Chaung said.
In the next 48 hours, the patient takes 800 mcg of misoprostol, either vaginally or buccally. “Patients can expect heavy cramping and bleeding 1-2 days after taking misoprostol,” she said. The bleeding should gradually subside over the following week or 2, she said. If the gestational age is 9 weeks or more, a second dose of misoprostol can be administered 3-6 hours after the first dose to improve efficacy.
If mifepristone is not available, misoprostol can be used alone in three doses spaced 3 hours apart, Dr. Chuang said.
The failure rate for mifepristone plus misoprostol has been calculated at 2% if the gestational age is less than 7 weeks. For misoprostol alone, the failure rate varies by the study, depending on gestational age and population analyzed, Dr. Chuang said. A 2023 meta-analysis in Contraception put the failure rate at 11%.
When to Call the Clinician
Dr. Chuang said clinicians should instruct women who have taken abortion pills to call the clinic if they are soaking through two sanitary pads an hour for more than 1 hour, if there is little to no bleeding, or if they think the medication isn’t working after taking the full regimen.
Mindy Sobota, MD, MS, an internist and associate professor of medicine at the Warren Alpert Medical School of Brown University in Providence, Rhode Island, recommended a continuing medical education site for evidence-based guidance on how best to talk with women about medication abortions.
She also recommended physicians and patients consult the Plan C website for guidance on telehealth services and price information on receiving abortion pills by mail in every state. “It’s a very reliable and safe clearing house,” Dr. Sobota said.
Internists should let patients know that whatever their choices are around pregnancy, they are open to discussing those choices and helping them through the process, Dr. Sobota said, adding that she makes those statements in annual visits.
Alexandra Bachorik, MD, EdM, director of education in the Women’s Health Unit and assistant professor of medicine at Boston University Chobanian & Avedisian School of Medicine, Boston, Massachusetts, said patients in restrictive states who need financial help related to obtaining abortion services in a less restricted state can visit the National Network of Abortion Funds, which can help people with travel or housing expenses.
Facilitating access to a clinic in a less restrictive state may be helpful to people approaching a gestational age limit, she said.
Adelaide McClintock, MD, an internist and assistant professor of general internal medicine at the University of Washington School of Medicine in Seattle, Washington, noted that even clinicians who cannot legally prescribe abortion pills can support their patients by providing resources and counseling on options before, during, and after pregnancy. Those who live in restrictive states also can provide support to women who have traveled to less restrictive states for an abortion if they have postabortion complications, she said.
She recommended the Reproductive Health Access Project website for a comprehensive guide for evidence-based care and counseling patients about all choices in reproductive healthcare.
Panelists urged clinicians to get familiar with abortion-access resources and keep them at their fingertips in practice. Patient requests for the services are common, she noted, as “one in four women will have an abortion by the age of 45.”
Dr. Chuang, Dr. McClintock, Dr. Sobota, and Dr. Bachorik reported no relevant financial conflicts of interest.
A version of this article appeared on Medscape.com.
An evolving legal landscape surrounding medication abortion has left physicians with as many questions as patients. A panel of clinicians at the annual meeting of the American College of Physicians offered guidance on how to help patients who choose medication abortion, which is available to women until 10 weeks of gestation.
Approved in 2000, abortion pills have become the most common method for terminating pregnancy in the United States, accounting for 63% of all abortions in 2023. The US Supreme Court is reviewing access to medication abortions, with a decision expected within months.
According to the Guttmacher Institute, 29 states as of February restrict access to medication abortion, either by limiting or banning the use of the drugs or by curtailing who can prescribe them and under what circumstances.
First, Determine Gestational Age
Cynthia Chuang, MD, MSc, an internist and professor of medicine at Penn State College of Medicine in Hershey, Pennsylvania, said in most cases, a woman can pinpoint the date of the first day of her last menstrual period, and the physician can confirm gestational age is 70 days or less. An ultrasound should be performed if the date of the last period is uncertain, she said, or if ectopic pregnancy is suspected, periods are irregular, or ultrasound is legally required in the state.
Women are not eligible for abortion pills if they have a bleeding or clotting disorder, have an intrauterine device, have adrenal insufficiency or chronic steroid use, or have porphyria or hemoglobin levels < 9 g/dL, she said.
“If the person has a known hemoglobin of less than 9, we would suggest that person have a procedural abortion,” Dr. Chuang said.
Components of Medication
Patients first receive 200 mg of oral mifepristone, which separates the pregnancy from the uterine wall. “Typically, people don’t experience side effects from the mifepristone alone,” Dr. Chaung said.
In the next 48 hours, the patient takes 800 mcg of misoprostol, either vaginally or buccally. “Patients can expect heavy cramping and bleeding 1-2 days after taking misoprostol,” she said. The bleeding should gradually subside over the following week or 2, she said. If the gestational age is 9 weeks or more, a second dose of misoprostol can be administered 3-6 hours after the first dose to improve efficacy.
If mifepristone is not available, misoprostol can be used alone in three doses spaced 3 hours apart, Dr. Chuang said.
The failure rate for mifepristone plus misoprostol has been calculated at 2% if the gestational age is less than 7 weeks. For misoprostol alone, the failure rate varies by the study, depending on gestational age and population analyzed, Dr. Chuang said. A 2023 meta-analysis in Contraception put the failure rate at 11%.
When to Call the Clinician
Dr. Chuang said clinicians should instruct women who have taken abortion pills to call the clinic if they are soaking through two sanitary pads an hour for more than 1 hour, if there is little to no bleeding, or if they think the medication isn’t working after taking the full regimen.
Mindy Sobota, MD, MS, an internist and associate professor of medicine at the Warren Alpert Medical School of Brown University in Providence, Rhode Island, recommended a continuing medical education site for evidence-based guidance on how best to talk with women about medication abortions.
She also recommended physicians and patients consult the Plan C website for guidance on telehealth services and price information on receiving abortion pills by mail in every state. “It’s a very reliable and safe clearing house,” Dr. Sobota said.
Internists should let patients know that whatever their choices are around pregnancy, they are open to discussing those choices and helping them through the process, Dr. Sobota said, adding that she makes those statements in annual visits.
Alexandra Bachorik, MD, EdM, director of education in the Women’s Health Unit and assistant professor of medicine at Boston University Chobanian & Avedisian School of Medicine, Boston, Massachusetts, said patients in restrictive states who need financial help related to obtaining abortion services in a less restricted state can visit the National Network of Abortion Funds, which can help people with travel or housing expenses.
Facilitating access to a clinic in a less restrictive state may be helpful to people approaching a gestational age limit, she said.
Adelaide McClintock, MD, an internist and assistant professor of general internal medicine at the University of Washington School of Medicine in Seattle, Washington, noted that even clinicians who cannot legally prescribe abortion pills can support their patients by providing resources and counseling on options before, during, and after pregnancy. Those who live in restrictive states also can provide support to women who have traveled to less restrictive states for an abortion if they have postabortion complications, she said.
She recommended the Reproductive Health Access Project website for a comprehensive guide for evidence-based care and counseling patients about all choices in reproductive healthcare.
Panelists urged clinicians to get familiar with abortion-access resources and keep them at their fingertips in practice. Patient requests for the services are common, she noted, as “one in four women will have an abortion by the age of 45.”
Dr. Chuang, Dr. McClintock, Dr. Sobota, and Dr. Bachorik reported no relevant financial conflicts of interest.
A version of this article appeared on Medscape.com.
FROM INTERNAL MEDICINE 2024
Intermittent Fasting + HIIT: Fitness Fad or Fix?
Let’s be honest: Although as physicians we have the power of the prescription pad, so much of health, in the end, comes down to lifestyle. Of course, taking a pill is often way easier than changing your longstanding habits. And what’s worse, doesn’t it always seem like the lifestyle stuff that is good for your health is unpleasant?
Two recent lifestyle interventions that I have tried and find really not enjoyable are time-restricted eating (also known as intermittent fasting) and high-intensity interval training, or HIIT. The former leaves me hangry for half the day; the latter is, well, it’s just really hard compared with my usual jog.
But given the rule of unpleasant lifestyle changes, I knew as soon as I saw this recent study what the result would be. What if we combined time-restricted eating with high-intensity interval training?
I’m referring to this study, appearing in PLOS ONE from Ranya Ameur and colleagues, which is a small trial that enrolled otherwise healthy women with a BMI > 30 and randomized them to one of three conditions.
First was time-restricted eating. Women in this group could eat whatever they wanted, but only from 8 a.m. to 4 p.m. daily.
Second: high-intensity functional training. This is a variant of high-intensity interval training which focuses a bit more on resistance exercise than on pure cardiovascular stuff but has the same vibe of doing brief bursts of intensive activity followed by a cool-down period.
Third: a combination of the two. Sounds rough to me.
The study was otherwise straightforward. At baseline, researchers collected data on body composition and dietary intake, and measured blood pressure, glucose, insulin, and lipid biomarkers. A 12-week intervention period followed, after which all of this stuff was measured again.
Now, you may have noticed that there is no control group in this study. We’ll come back to that — a few times.
Let me walk you through some of the outcomes here.
First off, body composition metrics. All three groups lost weight — on average, around 10% of body weight which, for a 12-week intervention, is fairly impressive. BMI and waist circumference went down as well, and, interestingly, much of the weight loss here was in fat mass, not fat-free mass.
Most interventions that lead to weight loss — and I’m including some of the newer drugs here — lead to both fat and muscle loss. That might not be as bad as it sounds; the truth is that muscle mass increases as fat increases because of the simple fact that if you’re carrying more weight when you walk around, your leg muscles get bigger. But to preserve muscle mass in the face of fat loss is sort of a Goldilocks finding, and, based on these results, there’s a suggestion that the high-intensity functional training helps to do just that.
The dietary intake findings were really surprising to me. Across the board, caloric intake decreased. It’s no surprise that time-restricted eating reduces calorie intake. That has been shown many times before and is probably the main reason it induces weight loss — less time to eat means you eat less.
But why would high-intensity functional training lead to lower caloric intake? Most people, myself included, get hungry after they exercise. In fact, one of the reasons it’s hard to lose weight with exercise alone is that we end up eating more calories to make up for what we lost during the exercise. This calorie reduction could be a unique effect of this type of exercise, but honestly this could also be something called the Hawthorne effect. Women in the study kept a food diary to track their intake, and the act of doing that might actually make you eat less. It makes it a little more annoying to snack a bit if you know you have to write it down. This is a situation where I would kill for a control group.
The lipid findings are also pretty striking, with around a 40% reduction in LDL across the board, and evidence of synergistic effects of combined TRE and high-intensity training on total cholesterol and triglycerides. This is like a statin level of effect — pretty impressive. Again, my heart pines for a control group, though.
Same story with glucose and insulin measures: an impressive reduction in fasting glucose and good evidence that the combination of time-restricted eating and high-intensity functional training reduces insulin levels and HOMA-IR as well.
Really the only thing that wasn’t very impressive was the change in blood pressure, with only modest decreases across the board.
Okay, so let’s take a breath after this high-intensity cerebral workout and put this all together. This was a small study, lacking a control group, but with large effect sizes in very relevant clinical areas. It confirms what we know about time-restricted eating — that it makes you eat less calories — and introduces the potential that vigorous exercise can not only magnify the benefits of time-restricted eating but maybe even mitigate some of the risks, like the risk for muscle loss. And of course, it comports with my central hypothesis, which is that the more unpleasant a lifestyle intervention is, the better it is for you. No pain, no gain, right?
Of course, I am being overly dogmatic. There are plenty of caveats. Wrestling bears is quite unpleasant and almost certainly bad for you. And there are even some pleasant things that are pretty good for you — like coffee and sex. And there are even people who find time-restricted eating and high-intensity training pleasurable. They are called masochists.
I’m joking. The truth is that Or, at least, much less painful. The trick is getting over the hump of change. If only there were a pill for that.
Dr. Wilson is associate professor of medicine and public health and director of the Clinical and Translational Research Accelerator at Yale University, New Haven, Connecticut. He has disclosed no relevant financial relationships. This transcript has been edited for clarity.
A version of this article appeared on Medscape.com.
Let’s be honest: Although as physicians we have the power of the prescription pad, so much of health, in the end, comes down to lifestyle. Of course, taking a pill is often way easier than changing your longstanding habits. And what’s worse, doesn’t it always seem like the lifestyle stuff that is good for your health is unpleasant?
Two recent lifestyle interventions that I have tried and find really not enjoyable are time-restricted eating (also known as intermittent fasting) and high-intensity interval training, or HIIT. The former leaves me hangry for half the day; the latter is, well, it’s just really hard compared with my usual jog.
But given the rule of unpleasant lifestyle changes, I knew as soon as I saw this recent study what the result would be. What if we combined time-restricted eating with high-intensity interval training?
I’m referring to this study, appearing in PLOS ONE from Ranya Ameur and colleagues, which is a small trial that enrolled otherwise healthy women with a BMI > 30 and randomized them to one of three conditions.
First was time-restricted eating. Women in this group could eat whatever they wanted, but only from 8 a.m. to 4 p.m. daily.
Second: high-intensity functional training. This is a variant of high-intensity interval training which focuses a bit more on resistance exercise than on pure cardiovascular stuff but has the same vibe of doing brief bursts of intensive activity followed by a cool-down period.
Third: a combination of the two. Sounds rough to me.
The study was otherwise straightforward. At baseline, researchers collected data on body composition and dietary intake, and measured blood pressure, glucose, insulin, and lipid biomarkers. A 12-week intervention period followed, after which all of this stuff was measured again.
Now, you may have noticed that there is no control group in this study. We’ll come back to that — a few times.
Let me walk you through some of the outcomes here.
First off, body composition metrics. All three groups lost weight — on average, around 10% of body weight which, for a 12-week intervention, is fairly impressive. BMI and waist circumference went down as well, and, interestingly, much of the weight loss here was in fat mass, not fat-free mass.
Most interventions that lead to weight loss — and I’m including some of the newer drugs here — lead to both fat and muscle loss. That might not be as bad as it sounds; the truth is that muscle mass increases as fat increases because of the simple fact that if you’re carrying more weight when you walk around, your leg muscles get bigger. But to preserve muscle mass in the face of fat loss is sort of a Goldilocks finding, and, based on these results, there’s a suggestion that the high-intensity functional training helps to do just that.
The dietary intake findings were really surprising to me. Across the board, caloric intake decreased. It’s no surprise that time-restricted eating reduces calorie intake. That has been shown many times before and is probably the main reason it induces weight loss — less time to eat means you eat less.
But why would high-intensity functional training lead to lower caloric intake? Most people, myself included, get hungry after they exercise. In fact, one of the reasons it’s hard to lose weight with exercise alone is that we end up eating more calories to make up for what we lost during the exercise. This calorie reduction could be a unique effect of this type of exercise, but honestly this could also be something called the Hawthorne effect. Women in the study kept a food diary to track their intake, and the act of doing that might actually make you eat less. It makes it a little more annoying to snack a bit if you know you have to write it down. This is a situation where I would kill for a control group.
The lipid findings are also pretty striking, with around a 40% reduction in LDL across the board, and evidence of synergistic effects of combined TRE and high-intensity training on total cholesterol and triglycerides. This is like a statin level of effect — pretty impressive. Again, my heart pines for a control group, though.
Same story with glucose and insulin measures: an impressive reduction in fasting glucose and good evidence that the combination of time-restricted eating and high-intensity functional training reduces insulin levels and HOMA-IR as well.
Really the only thing that wasn’t very impressive was the change in blood pressure, with only modest decreases across the board.
Okay, so let’s take a breath after this high-intensity cerebral workout and put this all together. This was a small study, lacking a control group, but with large effect sizes in very relevant clinical areas. It confirms what we know about time-restricted eating — that it makes you eat less calories — and introduces the potential that vigorous exercise can not only magnify the benefits of time-restricted eating but maybe even mitigate some of the risks, like the risk for muscle loss. And of course, it comports with my central hypothesis, which is that the more unpleasant a lifestyle intervention is, the better it is for you. No pain, no gain, right?
Of course, I am being overly dogmatic. There are plenty of caveats. Wrestling bears is quite unpleasant and almost certainly bad for you. And there are even some pleasant things that are pretty good for you — like coffee and sex. And there are even people who find time-restricted eating and high-intensity training pleasurable. They are called masochists.
I’m joking. The truth is that Or, at least, much less painful. The trick is getting over the hump of change. If only there were a pill for that.
Dr. Wilson is associate professor of medicine and public health and director of the Clinical and Translational Research Accelerator at Yale University, New Haven, Connecticut. He has disclosed no relevant financial relationships. This transcript has been edited for clarity.
A version of this article appeared on Medscape.com.
Let’s be honest: Although as physicians we have the power of the prescription pad, so much of health, in the end, comes down to lifestyle. Of course, taking a pill is often way easier than changing your longstanding habits. And what’s worse, doesn’t it always seem like the lifestyle stuff that is good for your health is unpleasant?
Two recent lifestyle interventions that I have tried and find really not enjoyable are time-restricted eating (also known as intermittent fasting) and high-intensity interval training, or HIIT. The former leaves me hangry for half the day; the latter is, well, it’s just really hard compared with my usual jog.
But given the rule of unpleasant lifestyle changes, I knew as soon as I saw this recent study what the result would be. What if we combined time-restricted eating with high-intensity interval training?
I’m referring to this study, appearing in PLOS ONE from Ranya Ameur and colleagues, which is a small trial that enrolled otherwise healthy women with a BMI > 30 and randomized them to one of three conditions.
First was time-restricted eating. Women in this group could eat whatever they wanted, but only from 8 a.m. to 4 p.m. daily.
Second: high-intensity functional training. This is a variant of high-intensity interval training which focuses a bit more on resistance exercise than on pure cardiovascular stuff but has the same vibe of doing brief bursts of intensive activity followed by a cool-down period.
Third: a combination of the two. Sounds rough to me.
The study was otherwise straightforward. At baseline, researchers collected data on body composition and dietary intake, and measured blood pressure, glucose, insulin, and lipid biomarkers. A 12-week intervention period followed, after which all of this stuff was measured again.
Now, you may have noticed that there is no control group in this study. We’ll come back to that — a few times.
Let me walk you through some of the outcomes here.
First off, body composition metrics. All three groups lost weight — on average, around 10% of body weight which, for a 12-week intervention, is fairly impressive. BMI and waist circumference went down as well, and, interestingly, much of the weight loss here was in fat mass, not fat-free mass.
Most interventions that lead to weight loss — and I’m including some of the newer drugs here — lead to both fat and muscle loss. That might not be as bad as it sounds; the truth is that muscle mass increases as fat increases because of the simple fact that if you’re carrying more weight when you walk around, your leg muscles get bigger. But to preserve muscle mass in the face of fat loss is sort of a Goldilocks finding, and, based on these results, there’s a suggestion that the high-intensity functional training helps to do just that.
The dietary intake findings were really surprising to me. Across the board, caloric intake decreased. It’s no surprise that time-restricted eating reduces calorie intake. That has been shown many times before and is probably the main reason it induces weight loss — less time to eat means you eat less.
But why would high-intensity functional training lead to lower caloric intake? Most people, myself included, get hungry after they exercise. In fact, one of the reasons it’s hard to lose weight with exercise alone is that we end up eating more calories to make up for what we lost during the exercise. This calorie reduction could be a unique effect of this type of exercise, but honestly this could also be something called the Hawthorne effect. Women in the study kept a food diary to track their intake, and the act of doing that might actually make you eat less. It makes it a little more annoying to snack a bit if you know you have to write it down. This is a situation where I would kill for a control group.
The lipid findings are also pretty striking, with around a 40% reduction in LDL across the board, and evidence of synergistic effects of combined TRE and high-intensity training on total cholesterol and triglycerides. This is like a statin level of effect — pretty impressive. Again, my heart pines for a control group, though.
Same story with glucose and insulin measures: an impressive reduction in fasting glucose and good evidence that the combination of time-restricted eating and high-intensity functional training reduces insulin levels and HOMA-IR as well.
Really the only thing that wasn’t very impressive was the change in blood pressure, with only modest decreases across the board.
Okay, so let’s take a breath after this high-intensity cerebral workout and put this all together. This was a small study, lacking a control group, but with large effect sizes in very relevant clinical areas. It confirms what we know about time-restricted eating — that it makes you eat less calories — and introduces the potential that vigorous exercise can not only magnify the benefits of time-restricted eating but maybe even mitigate some of the risks, like the risk for muscle loss. And of course, it comports with my central hypothesis, which is that the more unpleasant a lifestyle intervention is, the better it is for you. No pain, no gain, right?
Of course, I am being overly dogmatic. There are plenty of caveats. Wrestling bears is quite unpleasant and almost certainly bad for you. And there are even some pleasant things that are pretty good for you — like coffee and sex. And there are even people who find time-restricted eating and high-intensity training pleasurable. They are called masochists.
I’m joking. The truth is that Or, at least, much less painful. The trick is getting over the hump of change. If only there were a pill for that.
Dr. Wilson is associate professor of medicine and public health and director of the Clinical and Translational Research Accelerator at Yale University, New Haven, Connecticut. He has disclosed no relevant financial relationships. This transcript has been edited for clarity.
A version of this article appeared on Medscape.com.






