User login
Food Allergic Infants More Likely to Have Vitamin D Insufficiency
ORLANDO – Vitamin D insufficiency at age 1 year was associated with a nearly fourfold increased prevalence of a food allergy in a case-control study of 269 children.
The finding appears consistent with prior reports that linked the prevalence of food allergies to the latitude gradients for where people lived, Dr. Katrina J. Allen and her associates reported in a poster at the annual meeting of the American Academy of Allergy, Asthma, and Immunology. Those reports had suggested that the further people lived from the equator, the higher their rate of hospitalizations for food-allergy related events, said Dr. Allen, a pediatric allergist and gastroenterologist at Royal Children’s Hospital Melbourne, and her associates.
The study involved 5,276 12-month old infants from the Melbourne area enrolled in the Health Nuts population-based study. All infants had skin prick tests to egg white, peanut, and sesame; 1,005 developed at least a 1 mm wheal to at least one of these foods. Of the 834 food-sensitized infants who returned to the clinic for an oral food challenge with egg, peanut, and sesame, 351 were identified as food allergic with at least three non-contact hives or areas of urticaria that persisted for at least 5 minutes; perioral or periorbital angioedema; or severe and persistent vomiting or anaphylaxis (J. Allergy Clin. Immunol. 2012;129[suppl.]:AB141).
The researchers then drew blood specimens from 165 of the food-allergic infants and 104 control infants without food allergy or sensitivity, and measured their serum level of 25-hydroxyvitamin D.
In all, 92 of the control infants (88%) were vitamin D sufficient, with a serum level greater than 50 nM, corresponding to a level greater than 20 ng/mL. Among the infants with a food allergy, 118 (72%) were vitamin D sufficient (N. Engl. J. Med. 2011;364:248-54).
Vitamin D insufficiency, defined as a serum level of 26-50 nM (10 ng/mL to 20 ng/mL), occurred in 11% (11) of the control infants and in 25% (42) of the infants with a food allergy.
The remainder of the infants in the study, one in the control group and five in the food-allergy group, were vitamin D deficient, with a serum level of 25 nM or less (less than 10 ng/mL), but the numbers in this subgroup were too limited to allow a meaningful statistical analysis.
In a multiple logistical regression model that adjusted for diet (breast fed or formula fed), level of prior egg consumption, number of siblings, the presence of a pet dog, and ambient UV radiation exposure at the time of the blood draw, vitamin D insufficiency was linked with a statistically significant, 3.8-fold increased rate of food allergy, compared with the infants who were vitamin D sufficient, the researchers reported.
Dr. Allen and her associates said that they had no relevant financial disclosures.
ORLANDO – Vitamin D insufficiency at age 1 year was associated with a nearly fourfold increased prevalence of a food allergy in a case-control study of 269 children.
The finding appears consistent with prior reports that linked the prevalence of food allergies to the latitude gradients for where people lived, Dr. Katrina J. Allen and her associates reported in a poster at the annual meeting of the American Academy of Allergy, Asthma, and Immunology. Those reports had suggested that the further people lived from the equator, the higher their rate of hospitalizations for food-allergy related events, said Dr. Allen, a pediatric allergist and gastroenterologist at Royal Children’s Hospital Melbourne, and her associates.
The study involved 5,276 12-month old infants from the Melbourne area enrolled in the Health Nuts population-based study. All infants had skin prick tests to egg white, peanut, and sesame; 1,005 developed at least a 1 mm wheal to at least one of these foods. Of the 834 food-sensitized infants who returned to the clinic for an oral food challenge with egg, peanut, and sesame, 351 were identified as food allergic with at least three non-contact hives or areas of urticaria that persisted for at least 5 minutes; perioral or periorbital angioedema; or severe and persistent vomiting or anaphylaxis (J. Allergy Clin. Immunol. 2012;129[suppl.]:AB141).
The researchers then drew blood specimens from 165 of the food-allergic infants and 104 control infants without food allergy or sensitivity, and measured their serum level of 25-hydroxyvitamin D.
In all, 92 of the control infants (88%) were vitamin D sufficient, with a serum level greater than 50 nM, corresponding to a level greater than 20 ng/mL. Among the infants with a food allergy, 118 (72%) were vitamin D sufficient (N. Engl. J. Med. 2011;364:248-54).
Vitamin D insufficiency, defined as a serum level of 26-50 nM (10 ng/mL to 20 ng/mL), occurred in 11% (11) of the control infants and in 25% (42) of the infants with a food allergy.
The remainder of the infants in the study, one in the control group and five in the food-allergy group, were vitamin D deficient, with a serum level of 25 nM or less (less than 10 ng/mL), but the numbers in this subgroup were too limited to allow a meaningful statistical analysis.
In a multiple logistical regression model that adjusted for diet (breast fed or formula fed), level of prior egg consumption, number of siblings, the presence of a pet dog, and ambient UV radiation exposure at the time of the blood draw, vitamin D insufficiency was linked with a statistically significant, 3.8-fold increased rate of food allergy, compared with the infants who were vitamin D sufficient, the researchers reported.
Dr. Allen and her associates said that they had no relevant financial disclosures.
ORLANDO – Vitamin D insufficiency at age 1 year was associated with a nearly fourfold increased prevalence of a food allergy in a case-control study of 269 children.
The finding appears consistent with prior reports that linked the prevalence of food allergies to the latitude gradients for where people lived, Dr. Katrina J. Allen and her associates reported in a poster at the annual meeting of the American Academy of Allergy, Asthma, and Immunology. Those reports had suggested that the further people lived from the equator, the higher their rate of hospitalizations for food-allergy related events, said Dr. Allen, a pediatric allergist and gastroenterologist at Royal Children’s Hospital Melbourne, and her associates.
The study involved 5,276 12-month old infants from the Melbourne area enrolled in the Health Nuts population-based study. All infants had skin prick tests to egg white, peanut, and sesame; 1,005 developed at least a 1 mm wheal to at least one of these foods. Of the 834 food-sensitized infants who returned to the clinic for an oral food challenge with egg, peanut, and sesame, 351 were identified as food allergic with at least three non-contact hives or areas of urticaria that persisted for at least 5 minutes; perioral or periorbital angioedema; or severe and persistent vomiting or anaphylaxis (J. Allergy Clin. Immunol. 2012;129[suppl.]:AB141).
The researchers then drew blood specimens from 165 of the food-allergic infants and 104 control infants without food allergy or sensitivity, and measured their serum level of 25-hydroxyvitamin D.
In all, 92 of the control infants (88%) were vitamin D sufficient, with a serum level greater than 50 nM, corresponding to a level greater than 20 ng/mL. Among the infants with a food allergy, 118 (72%) were vitamin D sufficient (N. Engl. J. Med. 2011;364:248-54).
Vitamin D insufficiency, defined as a serum level of 26-50 nM (10 ng/mL to 20 ng/mL), occurred in 11% (11) of the control infants and in 25% (42) of the infants with a food allergy.
The remainder of the infants in the study, one in the control group and five in the food-allergy group, were vitamin D deficient, with a serum level of 25 nM or less (less than 10 ng/mL), but the numbers in this subgroup were too limited to allow a meaningful statistical analysis.
In a multiple logistical regression model that adjusted for diet (breast fed or formula fed), level of prior egg consumption, number of siblings, the presence of a pet dog, and ambient UV radiation exposure at the time of the blood draw, vitamin D insufficiency was linked with a statistically significant, 3.8-fold increased rate of food allergy, compared with the infants who were vitamin D sufficient, the researchers reported.
Dr. Allen and her associates said that they had no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE AMERICAN ACADEMY OF ALLERGY, ASTHMA, AND IMMUNOLOGY
Major Finding: Vitamin D–insufficient infants were 3.8-fold more likely to have a food allergy than controls.
Data Source: Findings were from an adjusted, case-control analysis of 165 12-month-old infants with a proven food allergy and 104 control infants with no food allergy or food sensitivity.
Disclosures: Dr. Allen and her associates said that they had no disclosures.
Food Allergy Exacerbates Pediatric Asthma Severity
ORLANDO – School children with asthma who also have a food allergy have a significantly increased need for controller drugs and hospitalization, compared with similar asthmatic children without a food allergy, based on data collected from 302 U.S. patients.
Food allergies are also "highly prevalent" among U.S. school children with asthma in inner-city neighborhoods, affecting a quarter of the children enrolled in the School Inner City Asthma Study, Dr. James L. Friedlander said at the annual meeting of the American Academy of Allergy, Asthma, and Immunology.
Multiple food allergies produced even more pronounced exacerbations, linking with "a higher risk of more severe asthma morbidity and more resource use," said Dr. Friedlander, an allergy and immunology physician at Children’s Hospital Boston.
The School Inner City Asthma Study enrolled 302 children aged 5-13 from about 20 schools in the northeastern United States. All children had physician-diagnosed asthma, plus at least one of these three markers of significant disease: at least one wheezing episode during the prior 12 months, need for daily preventive medical treatment, or at least one unscheduled visit to a physicians for asthma during the prior 12 months. The average age of the enrolled children was 8, and they divided equally as boys and girls. About a third of the children were black, a third were Hispanic, 5% were white, and the remainder were other racial and ethnic groups. Nearly three quarters came from households with an annual income of less than $45,000, and 80% had a family history of asthma (J. Allergy Clin. Immunol. 2012;129[suppl.]:AB132).
In all, 75 of the children (25%) had a food allergy documented by testing at their entry into the study, and 36 of these children were allergic to more than one food. The most common food allergy was to peanut (43%), followed by tree nut (29%), fruit (25%), shellfish (21%), egg (17%), milk (15%), soy (10%), and fish (10%).
About half of the children also had a diagnosis of eczema. Among the children with a food allergy, symptoms generally appeared within an hour of eating the allergic food. This resulted in urticaria in 60%, mouth or throat itching in 44%, and swelling in 40%. But many of the children also displayed respiratory symptoms as their allergic response to food, with 33% having difficulty breathing, 31% experiencing throat tightening, 29% wheezing, and 28% coughing.
Questionnaire replies from the children’s parents identified several features of exacerbated asthma in the children with food allergies. Among those with a food allergy, 73% used a controller medication, compared with a 58% rate among the children without a food allergy, a statistically significant difference. The food-allergic children had a 63% lifetime rate of having been hospitalized at least once, compared with a 40% rate among the children without a food allergy, a statistically significant difference.
Among the 36 children with two or more food allergies, 78% had a history of hospitalization, and 78% used controller medications. Also among the kids with multiple food allergies, 17% had been hospitalized within the 12 months prior to the survey of their parents, compared with a 7% rate among the children with asthma and no food allergy.
Other statistically significant indications of worse asthma morbidity in the children with multiple food allergies included 42% with at least 3 days of asthma symptoms during the preceding 2 weeks, compared with 22% among the children with no food allergy, and a mean number of 5.8 clinic or emergency department visits during the prior 12 months, compared with an average of 4.1 visits among the children with no food allergies.
Dr. Friedlander said that he had no relevant financial disclosures.
ORLANDO – School children with asthma who also have a food allergy have a significantly increased need for controller drugs and hospitalization, compared with similar asthmatic children without a food allergy, based on data collected from 302 U.S. patients.
Food allergies are also "highly prevalent" among U.S. school children with asthma in inner-city neighborhoods, affecting a quarter of the children enrolled in the School Inner City Asthma Study, Dr. James L. Friedlander said at the annual meeting of the American Academy of Allergy, Asthma, and Immunology.
Multiple food allergies produced even more pronounced exacerbations, linking with "a higher risk of more severe asthma morbidity and more resource use," said Dr. Friedlander, an allergy and immunology physician at Children’s Hospital Boston.
The School Inner City Asthma Study enrolled 302 children aged 5-13 from about 20 schools in the northeastern United States. All children had physician-diagnosed asthma, plus at least one of these three markers of significant disease: at least one wheezing episode during the prior 12 months, need for daily preventive medical treatment, or at least one unscheduled visit to a physicians for asthma during the prior 12 months. The average age of the enrolled children was 8, and they divided equally as boys and girls. About a third of the children were black, a third were Hispanic, 5% were white, and the remainder were other racial and ethnic groups. Nearly three quarters came from households with an annual income of less than $45,000, and 80% had a family history of asthma (J. Allergy Clin. Immunol. 2012;129[suppl.]:AB132).
In all, 75 of the children (25%) had a food allergy documented by testing at their entry into the study, and 36 of these children were allergic to more than one food. The most common food allergy was to peanut (43%), followed by tree nut (29%), fruit (25%), shellfish (21%), egg (17%), milk (15%), soy (10%), and fish (10%).
About half of the children also had a diagnosis of eczema. Among the children with a food allergy, symptoms generally appeared within an hour of eating the allergic food. This resulted in urticaria in 60%, mouth or throat itching in 44%, and swelling in 40%. But many of the children also displayed respiratory symptoms as their allergic response to food, with 33% having difficulty breathing, 31% experiencing throat tightening, 29% wheezing, and 28% coughing.
Questionnaire replies from the children’s parents identified several features of exacerbated asthma in the children with food allergies. Among those with a food allergy, 73% used a controller medication, compared with a 58% rate among the children without a food allergy, a statistically significant difference. The food-allergic children had a 63% lifetime rate of having been hospitalized at least once, compared with a 40% rate among the children without a food allergy, a statistically significant difference.
Among the 36 children with two or more food allergies, 78% had a history of hospitalization, and 78% used controller medications. Also among the kids with multiple food allergies, 17% had been hospitalized within the 12 months prior to the survey of their parents, compared with a 7% rate among the children with asthma and no food allergy.
Other statistically significant indications of worse asthma morbidity in the children with multiple food allergies included 42% with at least 3 days of asthma symptoms during the preceding 2 weeks, compared with 22% among the children with no food allergy, and a mean number of 5.8 clinic or emergency department visits during the prior 12 months, compared with an average of 4.1 visits among the children with no food allergies.
Dr. Friedlander said that he had no relevant financial disclosures.
ORLANDO – School children with asthma who also have a food allergy have a significantly increased need for controller drugs and hospitalization, compared with similar asthmatic children without a food allergy, based on data collected from 302 U.S. patients.
Food allergies are also "highly prevalent" among U.S. school children with asthma in inner-city neighborhoods, affecting a quarter of the children enrolled in the School Inner City Asthma Study, Dr. James L. Friedlander said at the annual meeting of the American Academy of Allergy, Asthma, and Immunology.
Multiple food allergies produced even more pronounced exacerbations, linking with "a higher risk of more severe asthma morbidity and more resource use," said Dr. Friedlander, an allergy and immunology physician at Children’s Hospital Boston.
The School Inner City Asthma Study enrolled 302 children aged 5-13 from about 20 schools in the northeastern United States. All children had physician-diagnosed asthma, plus at least one of these three markers of significant disease: at least one wheezing episode during the prior 12 months, need for daily preventive medical treatment, or at least one unscheduled visit to a physicians for asthma during the prior 12 months. The average age of the enrolled children was 8, and they divided equally as boys and girls. About a third of the children were black, a third were Hispanic, 5% were white, and the remainder were other racial and ethnic groups. Nearly three quarters came from households with an annual income of less than $45,000, and 80% had a family history of asthma (J. Allergy Clin. Immunol. 2012;129[suppl.]:AB132).
In all, 75 of the children (25%) had a food allergy documented by testing at their entry into the study, and 36 of these children were allergic to more than one food. The most common food allergy was to peanut (43%), followed by tree nut (29%), fruit (25%), shellfish (21%), egg (17%), milk (15%), soy (10%), and fish (10%).
About half of the children also had a diagnosis of eczema. Among the children with a food allergy, symptoms generally appeared within an hour of eating the allergic food. This resulted in urticaria in 60%, mouth or throat itching in 44%, and swelling in 40%. But many of the children also displayed respiratory symptoms as their allergic response to food, with 33% having difficulty breathing, 31% experiencing throat tightening, 29% wheezing, and 28% coughing.
Questionnaire replies from the children’s parents identified several features of exacerbated asthma in the children with food allergies. Among those with a food allergy, 73% used a controller medication, compared with a 58% rate among the children without a food allergy, a statistically significant difference. The food-allergic children had a 63% lifetime rate of having been hospitalized at least once, compared with a 40% rate among the children without a food allergy, a statistically significant difference.
Among the 36 children with two or more food allergies, 78% had a history of hospitalization, and 78% used controller medications. Also among the kids with multiple food allergies, 17% had been hospitalized within the 12 months prior to the survey of their parents, compared with a 7% rate among the children with asthma and no food allergy.
Other statistically significant indications of worse asthma morbidity in the children with multiple food allergies included 42% with at least 3 days of asthma symptoms during the preceding 2 weeks, compared with 22% among the children with no food allergy, and a mean number of 5.8 clinic or emergency department visits during the prior 12 months, compared with an average of 4.1 visits among the children with no food allergies.
Dr. Friedlander said that he had no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE AMERICAN ACADEMY OF ALLERGY, ASTHMA, AND IMMUNOLOGY
Major Finding:
Among asthmatic children in the U.S.,
73% with a food allergy used controller medication vs. 58% of those without a
food allergy.
Data Source: Data
came from 302 school children with asthma enrolled in the School Inner City
Asthma Study.
Disclosures: Dr.
Friedlander said that he had no disclosures.
Antibiotics Lead Outpatient Cutaneous Adverse Drug Events
SAN DIEGO – Antimicrobial agents were the most common identifiable causes of outpatient cutaneous adverse drug events, with amoxicillin being the most frequent single causative substance, in a study of data collected from 1995 to 2005.
Those are the key findings from the analysis of data from the National Ambulatory Medical Care Survey (NAMC) and the National Hospital and Ambulatory Medical Care Survey (NHAMCS).
While cutaneous reactions are thought to account for 16%-30% of reported adverse drug events, "there is limited information in the medical literature regarding the frequency of outpatient CADEs," Dr. Cheryl L. Gustafson wrote in a poster presented at the annual meeting of the American Academy of Dermatology.
Dr. Gustafson of the department of dermatology at Wake Forest University, Winston-Salem, N.C., and her associates queried the NAMCS and the NHAMC for data regarding CADEs (cutaneous adverse drug events) reported between 1995 and 2005. They used sample weights to estimate the national annual incidence of outpatient CADEs in the United States.
During the time period studied, a total of 635,982 CADE-related visits occurred, which translated into an annual incidence of 2.26 CADEs per 1,000 persons. Patients took an average of 2.2 medications in addition to the one causing the CADE. The incidence of CADEs increased with age, with a peak rate occurring in those aged 70-79 years.
Antibiotics were the most commonly implicated drug class (23%, chiefly amoxicillin), followed by cardiovascular agents (7%) and agents primarily affecting the skin and mucous membranes (6%). Unspecified or unknown agents accounted for a quarter of all CADEs.
Dermatitis and urticaria were the most common skin reactions reported (71% vs. 13%).
"We also found that patients with a dermatologic diagnosis experienced a CADE caused by a drug treating the initial skin condition in 11% of cases," Dr. Gustafson said in an interview.
Dr. Gustafson reported no relevant financial disclosures.
SAN DIEGO – Antimicrobial agents were the most common identifiable causes of outpatient cutaneous adverse drug events, with amoxicillin being the most frequent single causative substance, in a study of data collected from 1995 to 2005.
Those are the key findings from the analysis of data from the National Ambulatory Medical Care Survey (NAMC) and the National Hospital and Ambulatory Medical Care Survey (NHAMCS).
While cutaneous reactions are thought to account for 16%-30% of reported adverse drug events, "there is limited information in the medical literature regarding the frequency of outpatient CADEs," Dr. Cheryl L. Gustafson wrote in a poster presented at the annual meeting of the American Academy of Dermatology.
Dr. Gustafson of the department of dermatology at Wake Forest University, Winston-Salem, N.C., and her associates queried the NAMCS and the NHAMC for data regarding CADEs (cutaneous adverse drug events) reported between 1995 and 2005. They used sample weights to estimate the national annual incidence of outpatient CADEs in the United States.
During the time period studied, a total of 635,982 CADE-related visits occurred, which translated into an annual incidence of 2.26 CADEs per 1,000 persons. Patients took an average of 2.2 medications in addition to the one causing the CADE. The incidence of CADEs increased with age, with a peak rate occurring in those aged 70-79 years.
Antibiotics were the most commonly implicated drug class (23%, chiefly amoxicillin), followed by cardiovascular agents (7%) and agents primarily affecting the skin and mucous membranes (6%). Unspecified or unknown agents accounted for a quarter of all CADEs.
Dermatitis and urticaria were the most common skin reactions reported (71% vs. 13%).
"We also found that patients with a dermatologic diagnosis experienced a CADE caused by a drug treating the initial skin condition in 11% of cases," Dr. Gustafson said in an interview.
Dr. Gustafson reported no relevant financial disclosures.
SAN DIEGO – Antimicrobial agents were the most common identifiable causes of outpatient cutaneous adverse drug events, with amoxicillin being the most frequent single causative substance, in a study of data collected from 1995 to 2005.
Those are the key findings from the analysis of data from the National Ambulatory Medical Care Survey (NAMC) and the National Hospital and Ambulatory Medical Care Survey (NHAMCS).
While cutaneous reactions are thought to account for 16%-30% of reported adverse drug events, "there is limited information in the medical literature regarding the frequency of outpatient CADEs," Dr. Cheryl L. Gustafson wrote in a poster presented at the annual meeting of the American Academy of Dermatology.
Dr. Gustafson of the department of dermatology at Wake Forest University, Winston-Salem, N.C., and her associates queried the NAMCS and the NHAMC for data regarding CADEs (cutaneous adverse drug events) reported between 1995 and 2005. They used sample weights to estimate the national annual incidence of outpatient CADEs in the United States.
During the time period studied, a total of 635,982 CADE-related visits occurred, which translated into an annual incidence of 2.26 CADEs per 1,000 persons. Patients took an average of 2.2 medications in addition to the one causing the CADE. The incidence of CADEs increased with age, with a peak rate occurring in those aged 70-79 years.
Antibiotics were the most commonly implicated drug class (23%, chiefly amoxicillin), followed by cardiovascular agents (7%) and agents primarily affecting the skin and mucous membranes (6%). Unspecified or unknown agents accounted for a quarter of all CADEs.
Dermatitis and urticaria were the most common skin reactions reported (71% vs. 13%).
"We also found that patients with a dermatologic diagnosis experienced a CADE caused by a drug treating the initial skin condition in 11% of cases," Dr. Gustafson said in an interview.
Dr. Gustafson reported no relevant financial disclosures.
FROM THE ANNUAL MEETING OF THE AMERICAN ACADEMY OF DERMATOLOGY
Major Finding: Antibiotics caused the most cutaneous adverse drug events (23%), followed by cardiovascular agents (7%) and agents primarily affecting the skin and mucous membranes (6%).
Data Source: A study of outpatient CADEs occurring between 1995 and 2005 was conducted using data from the National Ambulatory Medical Care Survey and the National Hospital and Ambulatory Medical Care Survey.
Disclosures: Dr. Gustafson said that she had no relevant financial disclosures.
Antibiotics Are Top Contact Allergens Among Medications
SAN DIEGO – Antibiotics are the greatest contributor to allergic contact dermatitis among topical medications, according to a retrospective study of 100 patients.
"Neomycin and bacitracin are the worst offenders," said Dr. Shanna Spring, who presented the study at the annual meeting of the American Contact Dermatitis Society.
The most common positive patch test was for bacitracin (44 tests), followed by neomycin (29) and tixocortol-21-pivalate (19). Notably, 14% of individuals tested positive for both neomycin and bacitracin.
The researchers conducted a retrospective file review from the Ottawa Patch Test Clinic between January 2000 and September 2010. They randomly selected 100 patient files from the “interesting case database” compiled by the clinic staff.
Patients were eligible for the study if they had at least one positive patch test result to a topical medication; those whose patch test read as an irritant, macular erythema, or equivocal were excluded. Three-quarter of patients (74%) were older than 40 years, 68% were female and 34% were atopic, said Dr. Spring of the University of Ottawa.
The researchers were able to identify present relevant sensitizers in 80 patients. The most common sensitizers were antibiotics (59 patients), followed by steroids (31), anesthetics (6) and antifungals (6).
Most patients (64) had only one positive patch test; 20 had two positive tests. Eight patients had five positive patch tests.
In terms of co-reactions, 14 patients had more than one positive patch test for antibiotics. “This is not unexpected, as we know that aminoglycosides cross react,” said Dr. Spring. Eight patients had co-reactions of antibiotics and anesthetics; five patients had co-reactions to steroids only.
Dr. Spring reported that she has no relevant disclosures.
SAN DIEGO – Antibiotics are the greatest contributor to allergic contact dermatitis among topical medications, according to a retrospective study of 100 patients.
"Neomycin and bacitracin are the worst offenders," said Dr. Shanna Spring, who presented the study at the annual meeting of the American Contact Dermatitis Society.
The most common positive patch test was for bacitracin (44 tests), followed by neomycin (29) and tixocortol-21-pivalate (19). Notably, 14% of individuals tested positive for both neomycin and bacitracin.
The researchers conducted a retrospective file review from the Ottawa Patch Test Clinic between January 2000 and September 2010. They randomly selected 100 patient files from the “interesting case database” compiled by the clinic staff.
Patients were eligible for the study if they had at least one positive patch test result to a topical medication; those whose patch test read as an irritant, macular erythema, or equivocal were excluded. Three-quarter of patients (74%) were older than 40 years, 68% were female and 34% were atopic, said Dr. Spring of the University of Ottawa.
The researchers were able to identify present relevant sensitizers in 80 patients. The most common sensitizers were antibiotics (59 patients), followed by steroids (31), anesthetics (6) and antifungals (6).
Most patients (64) had only one positive patch test; 20 had two positive tests. Eight patients had five positive patch tests.
In terms of co-reactions, 14 patients had more than one positive patch test for antibiotics. “This is not unexpected, as we know that aminoglycosides cross react,” said Dr. Spring. Eight patients had co-reactions of antibiotics and anesthetics; five patients had co-reactions to steroids only.
Dr. Spring reported that she has no relevant disclosures.
SAN DIEGO – Antibiotics are the greatest contributor to allergic contact dermatitis among topical medications, according to a retrospective study of 100 patients.
"Neomycin and bacitracin are the worst offenders," said Dr. Shanna Spring, who presented the study at the annual meeting of the American Contact Dermatitis Society.
The most common positive patch test was for bacitracin (44 tests), followed by neomycin (29) and tixocortol-21-pivalate (19). Notably, 14% of individuals tested positive for both neomycin and bacitracin.
The researchers conducted a retrospective file review from the Ottawa Patch Test Clinic between January 2000 and September 2010. They randomly selected 100 patient files from the “interesting case database” compiled by the clinic staff.
Patients were eligible for the study if they had at least one positive patch test result to a topical medication; those whose patch test read as an irritant, macular erythema, or equivocal were excluded. Three-quarter of patients (74%) were older than 40 years, 68% were female and 34% were atopic, said Dr. Spring of the University of Ottawa.
The researchers were able to identify present relevant sensitizers in 80 patients. The most common sensitizers were antibiotics (59 patients), followed by steroids (31), anesthetics (6) and antifungals (6).
Most patients (64) had only one positive patch test; 20 had two positive tests. Eight patients had five positive patch tests.
In terms of co-reactions, 14 patients had more than one positive patch test for antibiotics. “This is not unexpected, as we know that aminoglycosides cross react,” said Dr. Spring. Eight patients had co-reactions of antibiotics and anesthetics; five patients had co-reactions to steroids only.
Dr. Spring reported that she has no relevant disclosures.
FROM THE ANNUAL MEETING OF THE AMERICAN CONTACT DERMATITIS SOCIETY
Major Finding: The most common positive patch test was for bacitracin
(44), followed by neomycin (29), and tixocortol-21-pivalate (19).
Notably, 14% of individuals tested positive for both neomycin and
bacitracin.
Data Source: A retrospective review of 100 randomly
selected cases from the Ottawa Patch Test Clinic between January 2000
and September 2010. The files were selected from the “interesting case
database” compiled by the clinic staff.
Disclosures: Dr. Spring reported that she has no relevant disclosures.
Acrylates Named Contact Allergen of the Year
SAN DIEGO – The ubiquitous acrylates take home the Contact Allergen of the Year title for 2012.
"We chose them because acrylates are everywhere in the environment," said Dr. Donald V. Belsito, who announced this year’s winner at the annual meeting of the American Contact Dermatitis Society.
Acrylates are plastic materials that are formed by the polymerization of monomers derived from acrylic or methacrylic acid. First used in Plexiglas, these compounds have a wide range of applications, including: paints, adhesives, dental composite resins, printing inks, and artificial nails. Acrylates also are used in a number of medical devices, including contact lenses, hearing aids, and bone cement for orthopedic endoprostheses.
While monomers are very strong irritants and allergens, fully polymerized acrylates are relatively inert. "Patch testing is tricky, and I think that’s something that we’re just finding out about the acrylates," said Dr. Belsito, a professor of clinical dermatology at Columbia University in New York. "They’re very volatile. The stability of the [patch test] allergens is a major issue, and they should be frozen or refrigerated."
In addition, the concentration necessary to reveal allergic sensitization is close to the irritancy threshold. These molecules also can induce active sensitization.
The North American Standard Series (Chemotechnique screening series) has been found to identify many cases of acrylate allergy caused by the inclusion of methyl methacrylate and ethyl acrylate in the series. However, clinicians should not rule out acrylate allergy even if the initial screening is negative. (Dermatitis 2011;22:98-101).
When patch tested, acrylate-allergic patients often display multiple positive tests. Previously, this was thought to be caused by cross-reaction. However, more recent analyses have shown that most acrylate-based industrial products contain many other acrylates as impurities – and thus are not included on the material safety data sheets.
"Many of the so-called cross reactions could in fact be concomitant reactions," noted Dr. Denis Sasseville in his article on acrylates, published in the January/February issue of Dermatitis (2012;23:6-16 [doi:10.1097/DER.obo13e31823d1b81]).
Methacrylates are tested at 2%, acrylates at 0.1%, and cyanoacrylates at 10%, according to Dr. Sasseville, who is a researcher in the division of dermatology at McGill University, Montreal. It is believed that patch testing with methyl methacrylate, 2-hydrorxymethyl methacrylate, ethyl acrylate, ethylene dimethacrylate, triethylene glycol diacrylate, and ethyl cyanoacrylate will identify most acrylate allergies.
The occupational exposure for dentists in particular is quite high; classic dental acrylics (including methyl acrylate) will cross through latex and vinyl gloves within minutes. Double gloving is suggested.
In one Finnish study of dental personnel, dentists and other dental personnel were most commonly exposed to 2-hydroxyethyl methacrylate, triethylene glycol dimethacrylate, and 3,3-bis[4-(2-hydroxy-3-methacryoxypropoxy) phenyl] propane (Contact Dermatitis 2007;57:324-30).
Both Dr. Belsito and Dr. Sasseville reported that they have no relevant disclosures.
SAN DIEGO – The ubiquitous acrylates take home the Contact Allergen of the Year title for 2012.
"We chose them because acrylates are everywhere in the environment," said Dr. Donald V. Belsito, who announced this year’s winner at the annual meeting of the American Contact Dermatitis Society.
Acrylates are plastic materials that are formed by the polymerization of monomers derived from acrylic or methacrylic acid. First used in Plexiglas, these compounds have a wide range of applications, including: paints, adhesives, dental composite resins, printing inks, and artificial nails. Acrylates also are used in a number of medical devices, including contact lenses, hearing aids, and bone cement for orthopedic endoprostheses.
While monomers are very strong irritants and allergens, fully polymerized acrylates are relatively inert. "Patch testing is tricky, and I think that’s something that we’re just finding out about the acrylates," said Dr. Belsito, a professor of clinical dermatology at Columbia University in New York. "They’re very volatile. The stability of the [patch test] allergens is a major issue, and they should be frozen or refrigerated."
In addition, the concentration necessary to reveal allergic sensitization is close to the irritancy threshold. These molecules also can induce active sensitization.
The North American Standard Series (Chemotechnique screening series) has been found to identify many cases of acrylate allergy caused by the inclusion of methyl methacrylate and ethyl acrylate in the series. However, clinicians should not rule out acrylate allergy even if the initial screening is negative. (Dermatitis 2011;22:98-101).
When patch tested, acrylate-allergic patients often display multiple positive tests. Previously, this was thought to be caused by cross-reaction. However, more recent analyses have shown that most acrylate-based industrial products contain many other acrylates as impurities – and thus are not included on the material safety data sheets.
"Many of the so-called cross reactions could in fact be concomitant reactions," noted Dr. Denis Sasseville in his article on acrylates, published in the January/February issue of Dermatitis (2012;23:6-16 [doi:10.1097/DER.obo13e31823d1b81]).
Methacrylates are tested at 2%, acrylates at 0.1%, and cyanoacrylates at 10%, according to Dr. Sasseville, who is a researcher in the division of dermatology at McGill University, Montreal. It is believed that patch testing with methyl methacrylate, 2-hydrorxymethyl methacrylate, ethyl acrylate, ethylene dimethacrylate, triethylene glycol diacrylate, and ethyl cyanoacrylate will identify most acrylate allergies.
The occupational exposure for dentists in particular is quite high; classic dental acrylics (including methyl acrylate) will cross through latex and vinyl gloves within minutes. Double gloving is suggested.
In one Finnish study of dental personnel, dentists and other dental personnel were most commonly exposed to 2-hydroxyethyl methacrylate, triethylene glycol dimethacrylate, and 3,3-bis[4-(2-hydroxy-3-methacryoxypropoxy) phenyl] propane (Contact Dermatitis 2007;57:324-30).
Both Dr. Belsito and Dr. Sasseville reported that they have no relevant disclosures.
SAN DIEGO – The ubiquitous acrylates take home the Contact Allergen of the Year title for 2012.
"We chose them because acrylates are everywhere in the environment," said Dr. Donald V. Belsito, who announced this year’s winner at the annual meeting of the American Contact Dermatitis Society.
Acrylates are plastic materials that are formed by the polymerization of monomers derived from acrylic or methacrylic acid. First used in Plexiglas, these compounds have a wide range of applications, including: paints, adhesives, dental composite resins, printing inks, and artificial nails. Acrylates also are used in a number of medical devices, including contact lenses, hearing aids, and bone cement for orthopedic endoprostheses.
While monomers are very strong irritants and allergens, fully polymerized acrylates are relatively inert. "Patch testing is tricky, and I think that’s something that we’re just finding out about the acrylates," said Dr. Belsito, a professor of clinical dermatology at Columbia University in New York. "They’re very volatile. The stability of the [patch test] allergens is a major issue, and they should be frozen or refrigerated."
In addition, the concentration necessary to reveal allergic sensitization is close to the irritancy threshold. These molecules also can induce active sensitization.
The North American Standard Series (Chemotechnique screening series) has been found to identify many cases of acrylate allergy caused by the inclusion of methyl methacrylate and ethyl acrylate in the series. However, clinicians should not rule out acrylate allergy even if the initial screening is negative. (Dermatitis 2011;22:98-101).
When patch tested, acrylate-allergic patients often display multiple positive tests. Previously, this was thought to be caused by cross-reaction. However, more recent analyses have shown that most acrylate-based industrial products contain many other acrylates as impurities – and thus are not included on the material safety data sheets.
"Many of the so-called cross reactions could in fact be concomitant reactions," noted Dr. Denis Sasseville in his article on acrylates, published in the January/February issue of Dermatitis (2012;23:6-16 [doi:10.1097/DER.obo13e31823d1b81]).
Methacrylates are tested at 2%, acrylates at 0.1%, and cyanoacrylates at 10%, according to Dr. Sasseville, who is a researcher in the division of dermatology at McGill University, Montreal. It is believed that patch testing with methyl methacrylate, 2-hydrorxymethyl methacrylate, ethyl acrylate, ethylene dimethacrylate, triethylene glycol diacrylate, and ethyl cyanoacrylate will identify most acrylate allergies.
The occupational exposure for dentists in particular is quite high; classic dental acrylics (including methyl acrylate) will cross through latex and vinyl gloves within minutes. Double gloving is suggested.
In one Finnish study of dental personnel, dentists and other dental personnel were most commonly exposed to 2-hydroxyethyl methacrylate, triethylene glycol dimethacrylate, and 3,3-bis[4-(2-hydroxy-3-methacryoxypropoxy) phenyl] propane (Contact Dermatitis 2007;57:324-30).
Both Dr. Belsito and Dr. Sasseville reported that they have no relevant disclosures.
FROM THE ANNUAL MEETING OF THE AMERICAN CONTACT DERMATITIS SOCIETY
Advances in Management of Atopic Dermatitis: New Therapies and Novel Uses of Existing Treatments
Elizabeth P. Chase, MD, and April W. Armstrong, MD, MPH
Atopic dermatitis (AD) is a chronic inflammatory skin condition marked by intensely pruritic, eczematous changes. First-line therapy includes topical corticosteroids during an exacerbation and long-term emollient use, followed by topical calcineurin inhibitors, phototherapy, and systemic therapy in more difficult cases. The need for more effective AD therapies with safer side effect profiles has pushed researchers to devise new therapies and to recycle traditional treatments for use in a novel manner. Innovative therapies include barrier therapy, novel antistaphylococcal treatments, new immunomodulatory agents, unconventional antipruritic agents, exclusionary diets, and probiotics. Advancements in these options have paved the way for a targeted approach to AD therapy. We will review the latest clinical research exploring these cutting-edge AD treatment modalities and discuss forward-thinking therapy strategies that use conventional AD medications in a novel manner.
*For a PDF of the full article, click on the link to the left of this introduction.
Elizabeth P. Chase, MD, and April W. Armstrong, MD, MPH
Atopic dermatitis (AD) is a chronic inflammatory skin condition marked by intensely pruritic, eczematous changes. First-line therapy includes topical corticosteroids during an exacerbation and long-term emollient use, followed by topical calcineurin inhibitors, phototherapy, and systemic therapy in more difficult cases. The need for more effective AD therapies with safer side effect profiles has pushed researchers to devise new therapies and to recycle traditional treatments for use in a novel manner. Innovative therapies include barrier therapy, novel antistaphylococcal treatments, new immunomodulatory agents, unconventional antipruritic agents, exclusionary diets, and probiotics. Advancements in these options have paved the way for a targeted approach to AD therapy. We will review the latest clinical research exploring these cutting-edge AD treatment modalities and discuss forward-thinking therapy strategies that use conventional AD medications in a novel manner.
*For a PDF of the full article, click on the link to the left of this introduction.
Elizabeth P. Chase, MD, and April W. Armstrong, MD, MPH
Atopic dermatitis (AD) is a chronic inflammatory skin condition marked by intensely pruritic, eczematous changes. First-line therapy includes topical corticosteroids during an exacerbation and long-term emollient use, followed by topical calcineurin inhibitors, phototherapy, and systemic therapy in more difficult cases. The need for more effective AD therapies with safer side effect profiles has pushed researchers to devise new therapies and to recycle traditional treatments for use in a novel manner. Innovative therapies include barrier therapy, novel antistaphylococcal treatments, new immunomodulatory agents, unconventional antipruritic agents, exclusionary diets, and probiotics. Advancements in these options have paved the way for a targeted approach to AD therapy. We will review the latest clinical research exploring these cutting-edge AD treatment modalities and discuss forward-thinking therapy strategies that use conventional AD medications in a novel manner.
*For a PDF of the full article, click on the link to the left of this introduction.
We will discuss advancements made in the areas of barrier therapy, antistaphylococcal regimens, and immunomodulatory treatments, including both topical and systemic agents. Additionally, we will cover novel antipruritic modalities and discuss the use of diet and probiotics for treatment of AD. We will conclude with a discussion of novel uses of traditional AD medications.
Burkitt Lymphoma in a Child With Atopic Dermatitis and a 7-Year History of Regular Topical Tacrolimus Use
Tips for Spotting Dermatoses in Children With Darker Skin
MIAMI – Some hallmark signs of dermatologic problems in children – especially erythema and hyperpigmentation – often are less obvious in children with skin of color and can require more clinical detective work to diagnose.
Dr. Patricia A. Treadwell narrowed down the most likely dermatoses a pediatrician will encounter in this patient population at a pediatric update sponsored by Miami Children’s Hospital. Atopic and contact dermatitis, phytophotodermatitis, transient neonatal pustular melanosis, and neonatal lupus erythematosus are among the noteworthy clinical challenges, she said at the meeting.
"Children with increased pigmentation in their skin may end up testing your knowledge in terms of looking at their dermatitis and being able to diagnose that. Keep in mind it may be a little bit different in terms of the clinical presentation, but it’s important to identify it and start the proper treatment," said Dr. Treadwell, a pediatric dermatologist at Indiana University Health and Riley Hospital for Children in Indianapolis.
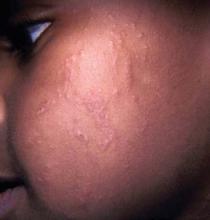
Overcoming this "masking" of a condition by skin pigmentation can be important, Dr. Treadwell said. She cited a patient born with a port-wine stain that went undiagnosed. The infant had subtle erythema and some asymmetry related to the overgrowth of the lesion. "This was not diagnosed based on the fact that the erythema was not apparent. The patient later developed a pyogenic granuloma, which is a complication that can be seen in patients with port-wine stains as they get older."
Erythema can be missed in children of color with atopic dermatitis as well. For this reason, atopic dermatitis may be underdiagnosed in this population overall, she said. Another challenge is the common practice of grading the severity of atopic dermatitis in lighter-skinned patients based on the degree of erythema. "In children with a fair amount of pigmentation in their skin, the erythema may not be noted and the severity will not be recognized."
Similarly, you might need a higher index of clinical suspicion to diagnose a child of color with contact dermatitis. Again, the erythema can be subtle. In contrast, "contact dermatitis can be very clear in a Caucasian patient. But the lesions are the same – linear, asymmetrical, and occurring on exposed areas," Dr. Treadwell said. Pruritus is common, and edema and swelling also occur. Watch for development of vesiculobullous lesions.
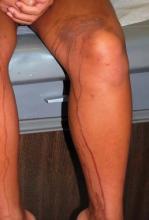
Phytophotodermatitis is another dermatologic condition that may require some additional detective work in children of color. Dr. Treadwell described a girl with a unique hyperpigmentation pattern on her legs and arms. She was referred following a vacation in Cancun, Mexico, with her family, and there was a concern about an autoimmune process. "They asked if she needed blood work. I said no, she was eating a mango and went out in the sun." Some of the mango juice splashed on her legs and arms.
Phytophotodermatitis occurs when furocoumarins from tropical fruit, citrus, celery, fennel, or parsnip come into contact with skin subsequently exposed to the sun.
"This condition can have a fairly bizarre pattern of presentation," Dr. Treadwell said. "Again, if there is more pigment in the skin, hyperpigmentation can present in a less common way than might be expected."
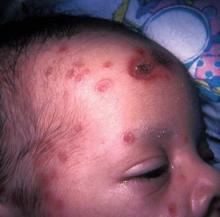
Some dermatoses are noted more commonly in children of color, she said. For example, the hyperpigmented macules or pustules that characterize transient neonatal pustular melanosis are reported in 4.4% of African American infants and 0.2% of Caucasian infants. "The percentages here may be related to the pigmentation in the skin. This does occur in Caucasian infants, but it may not be as noticeable."
The condition can be present at birth. The macules and pustules can appear anywhere on the body, but most often on the chin, neck, upper chest, and/or lower back. The good news is they fade over time and are benign, so no treatment is necessary. The differential diagnosis from such conditions as herpes simplex and erythema toxicum is important, however, said Dr. Treadwell. One tip is to check for lesions on the palms and soles, which can be diagnostic in transient neonatal pustular melanosis, but not for erythema toxicum. A biopsy can confirm your clinical suspicions.
The cutaneous manifestations of neonatal lupus erythematosus can tip you off to this condition, she said. Skin lesions can be annular, discoid, or atrophic. Some children present with "raccoon eyes." Because this condition is related to maternal antibodies passed through the placenta during gestation, lesions generally clear by 6 months to 1 year of age.
The mother may have a diagnosis of an autoimmune disease, or she may be completely asymptomatic. In one instance, a mother brought her newborn to Dr. Treadwell’s clinic. He had annular lesions on his forehead with some erythema. The lesions were more edematous around the edges. He actually got some sun exposure between his first and second visits, and developed more-discoid lesions in his sun-exposed areas. He also presented with lesions in non–sun exposed areas.
"The mother had a positive ANA [antinuclear antibody] test. I told her she should go to her doctor for urine and blood pressure monitoring," Dr. Treadwell said. "She had no symptoms and thought I didn’t know what I was talking about." Two years later, the woman returned with a newborn daughter who also had neonatal lupus with lesions on her face and some patchy alopecia on her scalp.
"The brother came back in, ... and he had telangiectasias already present at age 2 years."
Your evaluation can be more family centered. Consider testing the parent and affected children for anti-Rho, anti-La, and anti-RNP.
"I usually treat them with sun avoidance, sun protection, and possibly hydrocortisone," Dr. Treadwell said. She also recommends one electrocardiogram to rule out any cardiac consequences.
Dr. Treadwell reported that she had no relevant financial disclosures.
MIAMI – Some hallmark signs of dermatologic problems in children – especially erythema and hyperpigmentation – often are less obvious in children with skin of color and can require more clinical detective work to diagnose.
Dr. Patricia A. Treadwell narrowed down the most likely dermatoses a pediatrician will encounter in this patient population at a pediatric update sponsored by Miami Children’s Hospital. Atopic and contact dermatitis, phytophotodermatitis, transient neonatal pustular melanosis, and neonatal lupus erythematosus are among the noteworthy clinical challenges, she said at the meeting.
"Children with increased pigmentation in their skin may end up testing your knowledge in terms of looking at their dermatitis and being able to diagnose that. Keep in mind it may be a little bit different in terms of the clinical presentation, but it’s important to identify it and start the proper treatment," said Dr. Treadwell, a pediatric dermatologist at Indiana University Health and Riley Hospital for Children in Indianapolis.
Overcoming this "masking" of a condition by skin pigmentation can be important, Dr. Treadwell said. She cited a patient born with a port-wine stain that went undiagnosed. The infant had subtle erythema and some asymmetry related to the overgrowth of the lesion. "This was not diagnosed based on the fact that the erythema was not apparent. The patient later developed a pyogenic granuloma, which is a complication that can be seen in patients with port-wine stains as they get older."
Erythema can be missed in children of color with atopic dermatitis as well. For this reason, atopic dermatitis may be underdiagnosed in this population overall, she said. Another challenge is the common practice of grading the severity of atopic dermatitis in lighter-skinned patients based on the degree of erythema. "In children with a fair amount of pigmentation in their skin, the erythema may not be noted and the severity will not be recognized."
Similarly, you might need a higher index of clinical suspicion to diagnose a child of color with contact dermatitis. Again, the erythema can be subtle. In contrast, "contact dermatitis can be very clear in a Caucasian patient. But the lesions are the same – linear, asymmetrical, and occurring on exposed areas," Dr. Treadwell said. Pruritus is common, and edema and swelling also occur. Watch for development of vesiculobullous lesions.
Phytophotodermatitis is another dermatologic condition that may require some additional detective work in children of color. Dr. Treadwell described a girl with a unique hyperpigmentation pattern on her legs and arms. She was referred following a vacation in Cancun, Mexico, with her family, and there was a concern about an autoimmune process. "They asked if she needed blood work. I said no, she was eating a mango and went out in the sun." Some of the mango juice splashed on her legs and arms.
Phytophotodermatitis occurs when furocoumarins from tropical fruit, citrus, celery, fennel, or parsnip come into contact with skin subsequently exposed to the sun.
"This condition can have a fairly bizarre pattern of presentation," Dr. Treadwell said. "Again, if there is more pigment in the skin, hyperpigmentation can present in a less common way than might be expected."
Some dermatoses are noted more commonly in children of color, she said. For example, the hyperpigmented macules or pustules that characterize transient neonatal pustular melanosis are reported in 4.4% of African American infants and 0.2% of Caucasian infants. "The percentages here may be related to the pigmentation in the skin. This does occur in Caucasian infants, but it may not be as noticeable."
The condition can be present at birth. The macules and pustules can appear anywhere on the body, but most often on the chin, neck, upper chest, and/or lower back. The good news is they fade over time and are benign, so no treatment is necessary. The differential diagnosis from such conditions as herpes simplex and erythema toxicum is important, however, said Dr. Treadwell. One tip is to check for lesions on the palms and soles, which can be diagnostic in transient neonatal pustular melanosis, but not for erythema toxicum. A biopsy can confirm your clinical suspicions.
The cutaneous manifestations of neonatal lupus erythematosus can tip you off to this condition, she said. Skin lesions can be annular, discoid, or atrophic. Some children present with "raccoon eyes." Because this condition is related to maternal antibodies passed through the placenta during gestation, lesions generally clear by 6 months to 1 year of age.
The mother may have a diagnosis of an autoimmune disease, or she may be completely asymptomatic. In one instance, a mother brought her newborn to Dr. Treadwell’s clinic. He had annular lesions on his forehead with some erythema. The lesions were more edematous around the edges. He actually got some sun exposure between his first and second visits, and developed more-discoid lesions in his sun-exposed areas. He also presented with lesions in non–sun exposed areas.
"The mother had a positive ANA [antinuclear antibody] test. I told her she should go to her doctor for urine and blood pressure monitoring," Dr. Treadwell said. "She had no symptoms and thought I didn’t know what I was talking about." Two years later, the woman returned with a newborn daughter who also had neonatal lupus with lesions on her face and some patchy alopecia on her scalp.
"The brother came back in, ... and he had telangiectasias already present at age 2 years."
Your evaluation can be more family centered. Consider testing the parent and affected children for anti-Rho, anti-La, and anti-RNP.
"I usually treat them with sun avoidance, sun protection, and possibly hydrocortisone," Dr. Treadwell said. She also recommends one electrocardiogram to rule out any cardiac consequences.
Dr. Treadwell reported that she had no relevant financial disclosures.
MIAMI – Some hallmark signs of dermatologic problems in children – especially erythema and hyperpigmentation – often are less obvious in children with skin of color and can require more clinical detective work to diagnose.
Dr. Patricia A. Treadwell narrowed down the most likely dermatoses a pediatrician will encounter in this patient population at a pediatric update sponsored by Miami Children’s Hospital. Atopic and contact dermatitis, phytophotodermatitis, transient neonatal pustular melanosis, and neonatal lupus erythematosus are among the noteworthy clinical challenges, she said at the meeting.
"Children with increased pigmentation in their skin may end up testing your knowledge in terms of looking at their dermatitis and being able to diagnose that. Keep in mind it may be a little bit different in terms of the clinical presentation, but it’s important to identify it and start the proper treatment," said Dr. Treadwell, a pediatric dermatologist at Indiana University Health and Riley Hospital for Children in Indianapolis.
Overcoming this "masking" of a condition by skin pigmentation can be important, Dr. Treadwell said. She cited a patient born with a port-wine stain that went undiagnosed. The infant had subtle erythema and some asymmetry related to the overgrowth of the lesion. "This was not diagnosed based on the fact that the erythema was not apparent. The patient later developed a pyogenic granuloma, which is a complication that can be seen in patients with port-wine stains as they get older."
Erythema can be missed in children of color with atopic dermatitis as well. For this reason, atopic dermatitis may be underdiagnosed in this population overall, she said. Another challenge is the common practice of grading the severity of atopic dermatitis in lighter-skinned patients based on the degree of erythema. "In children with a fair amount of pigmentation in their skin, the erythema may not be noted and the severity will not be recognized."
Similarly, you might need a higher index of clinical suspicion to diagnose a child of color with contact dermatitis. Again, the erythema can be subtle. In contrast, "contact dermatitis can be very clear in a Caucasian patient. But the lesions are the same – linear, asymmetrical, and occurring on exposed areas," Dr. Treadwell said. Pruritus is common, and edema and swelling also occur. Watch for development of vesiculobullous lesions.
Phytophotodermatitis is another dermatologic condition that may require some additional detective work in children of color. Dr. Treadwell described a girl with a unique hyperpigmentation pattern on her legs and arms. She was referred following a vacation in Cancun, Mexico, with her family, and there was a concern about an autoimmune process. "They asked if she needed blood work. I said no, she was eating a mango and went out in the sun." Some of the mango juice splashed on her legs and arms.
Phytophotodermatitis occurs when furocoumarins from tropical fruit, citrus, celery, fennel, or parsnip come into contact with skin subsequently exposed to the sun.
"This condition can have a fairly bizarre pattern of presentation," Dr. Treadwell said. "Again, if there is more pigment in the skin, hyperpigmentation can present in a less common way than might be expected."
Some dermatoses are noted more commonly in children of color, she said. For example, the hyperpigmented macules or pustules that characterize transient neonatal pustular melanosis are reported in 4.4% of African American infants and 0.2% of Caucasian infants. "The percentages here may be related to the pigmentation in the skin. This does occur in Caucasian infants, but it may not be as noticeable."
The condition can be present at birth. The macules and pustules can appear anywhere on the body, but most often on the chin, neck, upper chest, and/or lower back. The good news is they fade over time and are benign, so no treatment is necessary. The differential diagnosis from such conditions as herpes simplex and erythema toxicum is important, however, said Dr. Treadwell. One tip is to check for lesions on the palms and soles, which can be diagnostic in transient neonatal pustular melanosis, but not for erythema toxicum. A biopsy can confirm your clinical suspicions.
The cutaneous manifestations of neonatal lupus erythematosus can tip you off to this condition, she said. Skin lesions can be annular, discoid, or atrophic. Some children present with "raccoon eyes." Because this condition is related to maternal antibodies passed through the placenta during gestation, lesions generally clear by 6 months to 1 year of age.
The mother may have a diagnosis of an autoimmune disease, or she may be completely asymptomatic. In one instance, a mother brought her newborn to Dr. Treadwell’s clinic. He had annular lesions on his forehead with some erythema. The lesions were more edematous around the edges. He actually got some sun exposure between his first and second visits, and developed more-discoid lesions in his sun-exposed areas. He also presented with lesions in non–sun exposed areas.
"The mother had a positive ANA [antinuclear antibody] test. I told her she should go to her doctor for urine and blood pressure monitoring," Dr. Treadwell said. "She had no symptoms and thought I didn’t know what I was talking about." Two years later, the woman returned with a newborn daughter who also had neonatal lupus with lesions on her face and some patchy alopecia on her scalp.
"The brother came back in, ... and he had telangiectasias already present at age 2 years."
Your evaluation can be more family centered. Consider testing the parent and affected children for anti-Rho, anti-La, and anti-RNP.
"I usually treat them with sun avoidance, sun protection, and possibly hydrocortisone," Dr. Treadwell said. She also recommends one electrocardiogram to rule out any cardiac consequences.
Dr. Treadwell reported that she had no relevant financial disclosures.
EXPERT ANALYSIS FROM A PEDIATRIC UPDATE SPONSORED BY MIAMI CHILDREN'S HOSPITAL
Blog: Car Seats Linked to Dermatitis
"Oh my god. I've been missing this," said Dr. Moise L. Levy about a new case series on car seat dermatitis published in the Journal of Pediatric Dermatology.
The case series reported that from 2006-2009 there were 21 cases of dermatitis linked to car seats. Of the reported cases, all of the patients had symmetric dermatitis on their lateral legs, 95% had symmetric dermatitis on their elbows, and some of the case patients presented with the dermatitis on their upper posterior thighs and occipital scalp. An atopic history was present in 12 of 21 of the children.
The report noted: "Over the last several years, our clinic has documented an increasing trend of contact dermatitis presenting in areas that are in direct contact with certain types of car seats composed of a shiny, nylon-like material. Our practice has encountered these cases in both atopic and nonatopic infants, with a seasonal predilection for the warmer months. This brief report highlights some of the key features of this condition and alerts the clinician to this newly described form of contact dermatitis," (Pediatr. Dermatol. 2011;28:321).
The car seat dermatitis rapidly improves with a barrier to the car seat or by changing the car seat's fabric, reported Dr. Levy, chief of pediatric dermatology at Dell Children's Medical Center, Austin, Texas. Topical steroids and oral antibiotics can be used if a secondary infection is present.
"The question is where it is really irritant or allergic," he said at the annual meeting of the Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation.
Discussions with car seat manufacturers are underway to better elucidate details of what could be causing the reactions, such as whether the preservative dimethylfumarate is used, or if the dermatitis could be from a flame retardant.
Dr. Levy had no relevant disclosures. SDEF and this news organization are owned by Elsevier.
-Amy Pfeiffer
"Oh my god. I've been missing this," said Dr. Moise L. Levy about a new case series on car seat dermatitis published in the Journal of Pediatric Dermatology.
The case series reported that from 2006-2009 there were 21 cases of dermatitis linked to car seats. Of the reported cases, all of the patients had symmetric dermatitis on their lateral legs, 95% had symmetric dermatitis on their elbows, and some of the case patients presented with the dermatitis on their upper posterior thighs and occipital scalp. An atopic history was present in 12 of 21 of the children.
The report noted: "Over the last several years, our clinic has documented an increasing trend of contact dermatitis presenting in areas that are in direct contact with certain types of car seats composed of a shiny, nylon-like material. Our practice has encountered these cases in both atopic and nonatopic infants, with a seasonal predilection for the warmer months. This brief report highlights some of the key features of this condition and alerts the clinician to this newly described form of contact dermatitis," (Pediatr. Dermatol. 2011;28:321).
The car seat dermatitis rapidly improves with a barrier to the car seat or by changing the car seat's fabric, reported Dr. Levy, chief of pediatric dermatology at Dell Children's Medical Center, Austin, Texas. Topical steroids and oral antibiotics can be used if a secondary infection is present.
"The question is where it is really irritant or allergic," he said at the annual meeting of the Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation.
Discussions with car seat manufacturers are underway to better elucidate details of what could be causing the reactions, such as whether the preservative dimethylfumarate is used, or if the dermatitis could be from a flame retardant.
Dr. Levy had no relevant disclosures. SDEF and this news organization are owned by Elsevier.
-Amy Pfeiffer
"Oh my god. I've been missing this," said Dr. Moise L. Levy about a new case series on car seat dermatitis published in the Journal of Pediatric Dermatology.
The case series reported that from 2006-2009 there were 21 cases of dermatitis linked to car seats. Of the reported cases, all of the patients had symmetric dermatitis on their lateral legs, 95% had symmetric dermatitis on their elbows, and some of the case patients presented with the dermatitis on their upper posterior thighs and occipital scalp. An atopic history was present in 12 of 21 of the children.
The report noted: "Over the last several years, our clinic has documented an increasing trend of contact dermatitis presenting in areas that are in direct contact with certain types of car seats composed of a shiny, nylon-like material. Our practice has encountered these cases in both atopic and nonatopic infants, with a seasonal predilection for the warmer months. This brief report highlights some of the key features of this condition and alerts the clinician to this newly described form of contact dermatitis," (Pediatr. Dermatol. 2011;28:321).
The car seat dermatitis rapidly improves with a barrier to the car seat or by changing the car seat's fabric, reported Dr. Levy, chief of pediatric dermatology at Dell Children's Medical Center, Austin, Texas. Topical steroids and oral antibiotics can be used if a secondary infection is present.
"The question is where it is really irritant or allergic," he said at the annual meeting of the Hawaii Dermatology Seminar sponsored by Skin Disease Education Foundation.
Discussions with car seat manufacturers are underway to better elucidate details of what could be causing the reactions, such as whether the preservative dimethylfumarate is used, or if the dermatitis could be from a flame retardant.
Dr. Levy had no relevant disclosures. SDEF and this news organization are owned by Elsevier.
-Amy Pfeiffer
Blog: Top Five Most Watched Dermatology Videos
What were dermatologists watching from Skin & Allergy News in 2011? Here's the top five countdown.
5. New Drugs Help Melanoma Patients Live Longer: Dr. Lynn Schuchter puts the studies, which were presented at the 2011 ASCO Annual Meeting in Chicago, in perspective and offers advice to physicians.
4. Laviv May Offer Longer-Term Acne Scarring Tx: Azficel-T, an autologous cellular product, produced significant improvement in acne scarring, compared with placebo, according to study results reported at the annual meeting of the American Society for Dermatologic Surgery. Laviv was approved by the FDA earlier this year for treating wrinkles. We interviewed Dr. Girish Munavalli, a study investigator, at the meeting.
3. How to ID and Treat Fire Ant Bites: Dr. Ronald Rapini offered advice on recognizing and treating fire ant bites at the American Academy of Dermatology's Summer Academy meeting in New York.
2. Eczema and Food Allergies Often Go Hand and Hand: Dr. Lawrence Eichenfield talked about atopic dermatitis, food allergies, and national guidelines at the American Academy of Dermatology's Summer Academy meeting in New York.
Drum roll please…
1. Gel Nail Polish: The Painted Truth: Dr. Richard K. Scher discussed the dangers of gel nail polish, and also gave tips to share with patients on how to have a safe experience at the nail salon at the American Academy of Dermatology's Summer Academy meeting in New York.
What were dermatologists watching from Skin & Allergy News in 2011? Here's the top five countdown.
5. New Drugs Help Melanoma Patients Live Longer: Dr. Lynn Schuchter puts the studies, which were presented at the 2011 ASCO Annual Meeting in Chicago, in perspective and offers advice to physicians.
4. Laviv May Offer Longer-Term Acne Scarring Tx: Azficel-T, an autologous cellular product, produced significant improvement in acne scarring, compared with placebo, according to study results reported at the annual meeting of the American Society for Dermatologic Surgery. Laviv was approved by the FDA earlier this year for treating wrinkles. We interviewed Dr. Girish Munavalli, a study investigator, at the meeting.
3. How to ID and Treat Fire Ant Bites: Dr. Ronald Rapini offered advice on recognizing and treating fire ant bites at the American Academy of Dermatology's Summer Academy meeting in New York.
2. Eczema and Food Allergies Often Go Hand and Hand: Dr. Lawrence Eichenfield talked about atopic dermatitis, food allergies, and national guidelines at the American Academy of Dermatology's Summer Academy meeting in New York.
Drum roll please…
1. Gel Nail Polish: The Painted Truth: Dr. Richard K. Scher discussed the dangers of gel nail polish, and also gave tips to share with patients on how to have a safe experience at the nail salon at the American Academy of Dermatology's Summer Academy meeting in New York.
What were dermatologists watching from Skin & Allergy News in 2011? Here's the top five countdown.
5. New Drugs Help Melanoma Patients Live Longer: Dr. Lynn Schuchter puts the studies, which were presented at the 2011 ASCO Annual Meeting in Chicago, in perspective and offers advice to physicians.
4. Laviv May Offer Longer-Term Acne Scarring Tx: Azficel-T, an autologous cellular product, produced significant improvement in acne scarring, compared with placebo, according to study results reported at the annual meeting of the American Society for Dermatologic Surgery. Laviv was approved by the FDA earlier this year for treating wrinkles. We interviewed Dr. Girish Munavalli, a study investigator, at the meeting.
3. How to ID and Treat Fire Ant Bites: Dr. Ronald Rapini offered advice on recognizing and treating fire ant bites at the American Academy of Dermatology's Summer Academy meeting in New York.
2. Eczema and Food Allergies Often Go Hand and Hand: Dr. Lawrence Eichenfield talked about atopic dermatitis, food allergies, and national guidelines at the American Academy of Dermatology's Summer Academy meeting in New York.
Drum roll please…
1. Gel Nail Polish: The Painted Truth: Dr. Richard K. Scher discussed the dangers of gel nail polish, and also gave tips to share with patients on how to have a safe experience at the nail salon at the American Academy of Dermatology's Summer Academy meeting in New York.