User login
Role of Phototherapy in Patients with Skin of Color
Zain U. Syed, MD, and Iltefat H. Hamzavi, MD
Phototherapy has proven to be one of the most versatile and effective treatment options for a variety of inflammatory and pigmentary skin diseases. However, the use of these treatment modalities in patients of color requires some special considerations. The modality chosen, the dosing of the treatment and duration of treatment are all issues to be considered for patients of color treated with ultraviolet phototherapy. In addition, there are some diseases which are more commonly seen in patients of color. These diseases may have better treatment outcomes using newer phototherapeutic options such as the long pulsed Nd:YAG laser or UVA1. As our population in the United States becomes more diverse it would behoove all dermatologists to acquaint themselves with the special circumstances of treating ethnic patients with phototherapy.
*For a PDF of the full article, click on the link to the left of this introduction.
Zain U. Syed, MD, and Iltefat H. Hamzavi, MD
Phototherapy has proven to be one of the most versatile and effective treatment options for a variety of inflammatory and pigmentary skin diseases. However, the use of these treatment modalities in patients of color requires some special considerations. The modality chosen, the dosing of the treatment and duration of treatment are all issues to be considered for patients of color treated with ultraviolet phototherapy. In addition, there are some diseases which are more commonly seen in patients of color. These diseases may have better treatment outcomes using newer phototherapeutic options such as the long pulsed Nd:YAG laser or UVA1. As our population in the United States becomes more diverse it would behoove all dermatologists to acquaint themselves with the special circumstances of treating ethnic patients with phototherapy.
*For a PDF of the full article, click on the link to the left of this introduction.
Zain U. Syed, MD, and Iltefat H. Hamzavi, MD
Phototherapy has proven to be one of the most versatile and effective treatment options for a variety of inflammatory and pigmentary skin diseases. However, the use of these treatment modalities in patients of color requires some special considerations. The modality chosen, the dosing of the treatment and duration of treatment are all issues to be considered for patients of color treated with ultraviolet phototherapy. In addition, there are some diseases which are more commonly seen in patients of color. These diseases may have better treatment outcomes using newer phototherapeutic options such as the long pulsed Nd:YAG laser or UVA1. As our population in the United States becomes more diverse it would behoove all dermatologists to acquaint themselves with the special circumstances of treating ethnic patients with phototherapy.
*For a PDF of the full article, click on the link to the left of this introduction.
Phototherapy in the Age of Biologics
Daniel Walker, BS, and Heidi Jacobe, MD, MSCS
Dermatologists are presented with a diversity of therapeutic modalities for the treatment of inflammatory, sclerosing, and neoplastic conditions, but with the development of various new irradiation devices that utilize specific parts of the electromagnetic spectrum, phototherapy has become a more viable, accessible, and efficacious option in the treatment of these conditions. The ultraviolet (UV) range (10-400 nm) is further subdivided into UVA and UVB, each of which has been particularly useful in a number of skin conditions. The most commonly used forms of UV irradiation are UVA1, psoralen plus UVA (PUVA), and narrowband (NB) UVB. Each of these modalities differ in their mechanism of action, indications, and side effect profiles, and it is important that clinicians be familiar with these differences. Today, phototherapy is a valuable option in the treatment of many nonpsoriatic conditions including atopic dermatitis, sclerosing skin conditions such as morphea, vitiligo, and mycosis fungoides. Due to its relative safety, phototherapy may be used in most populations, including children and pregnant women. However, contraindications and side effects are known and should be considered before patients begin a phototherapeutic regimen.
*For a PDF of the full article, click on the link to the left of this introduction.
Daniel Walker, BS, and Heidi Jacobe, MD, MSCS
Dermatologists are presented with a diversity of therapeutic modalities for the treatment of inflammatory, sclerosing, and neoplastic conditions, but with the development of various new irradiation devices that utilize specific parts of the electromagnetic spectrum, phototherapy has become a more viable, accessible, and efficacious option in the treatment of these conditions. The ultraviolet (UV) range (10-400 nm) is further subdivided into UVA and UVB, each of which has been particularly useful in a number of skin conditions. The most commonly used forms of UV irradiation are UVA1, psoralen plus UVA (PUVA), and narrowband (NB) UVB. Each of these modalities differ in their mechanism of action, indications, and side effect profiles, and it is important that clinicians be familiar with these differences. Today, phototherapy is a valuable option in the treatment of many nonpsoriatic conditions including atopic dermatitis, sclerosing skin conditions such as morphea, vitiligo, and mycosis fungoides. Due to its relative safety, phototherapy may be used in most populations, including children and pregnant women. However, contraindications and side effects are known and should be considered before patients begin a phototherapeutic regimen.
*For a PDF of the full article, click on the link to the left of this introduction.
Daniel Walker, BS, and Heidi Jacobe, MD, MSCS
Dermatologists are presented with a diversity of therapeutic modalities for the treatment of inflammatory, sclerosing, and neoplastic conditions, but with the development of various new irradiation devices that utilize specific parts of the electromagnetic spectrum, phototherapy has become a more viable, accessible, and efficacious option in the treatment of these conditions. The ultraviolet (UV) range (10-400 nm) is further subdivided into UVA and UVB, each of which has been particularly useful in a number of skin conditions. The most commonly used forms of UV irradiation are UVA1, psoralen plus UVA (PUVA), and narrowband (NB) UVB. Each of these modalities differ in their mechanism of action, indications, and side effect profiles, and it is important that clinicians be familiar with these differences. Today, phototherapy is a valuable option in the treatment of many nonpsoriatic conditions including atopic dermatitis, sclerosing skin conditions such as morphea, vitiligo, and mycosis fungoides. Due to its relative safety, phototherapy may be used in most populations, including children and pregnant women. However, contraindications and side effects are known and should be considered before patients begin a phototherapeutic regimen.
*For a PDF of the full article, click on the link to the left of this introduction.
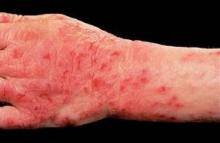
Alitretinoin for Hand Eczema Slashes Sick Days in Half
LISBON – Physicians outside the United States are turning cartwheels over the outcomes they're obtaining with oral alitretinoin for chronic hand eczema.
New data from the postmarketing observational TOCCATA trial demonstrate that oral alitretinoin reduced eczema-related work absences by 50% in German workers, Dr. Thomas Diepgen reported at the annual congress of the European Academy of Dermatology and Venereology.
The TOCCATA study involved 680 German patients with chronic hand eczema rated as severe in two-thirds of participants and moderate in the remainder. TOCCATA was designed to determine whether alitretinoin’s performance in real-world clinical practice is similar to that in the pivotal 1,032-patient randomized BACH (Benefits of Alitretinoin in Chronic Hand Eczema) trial, which resulted in European approval of the novel retinoid (Br. J. Dermatol. 2008;158:808-17).
TOCCATA participants received either 10 mg or 30 mg of alitretinoin per day at their physician’s discretion for up to 24 weeks, with follow-up evaluations at 4-week intervals. Treatment outcomes in TOCCATA proved comparable to those in the BACH trial: a 56.7% rating of clear or almost clear by Physician Global Assessment, as compared with 47.7% in BACH.
As in BACH, the greatest response in TOCCATA was in patients with the hyperkeratotic rhagadiform form of hand eczema, with a 59.2% rate of clear or almost clear. But all the morphologic types showed a favorable response: a 47.9% clear or almost clear rate in dyshidrosiform hand eczema, and a 52.2% rate in fingertip eczema.
In TOCCATA, 522 participants were employed, mostly as steel or other metal workers, or in food processing. At baseline, 80 reported a work absence because of their chronic hand eczema within the previous 4 weeks. By week 8, this number had dropped to 53 workers. At weeks 12 and 16 it was 43 workers, at week 20 it was 41, and by week 24 only 37 TOCCATA participants had missed work during the previous 4 weeks, according to Dr. Diepgen, director of the department of social medicine, occupational, and environmental dermatology at the University of Heidelberg (Germany).
Not only was the number of workers taking sick leave reduced by slightly more than half, but total sick days were even more dramatically impacted. At baseline, workers who had taken hand eczema-related sick leave within the prior 4 weeks had missed an average of 17.6 work days during that period. By week 8, that figure had dropped to an average 10.7 days of absence in the last 4 weeks. At week 24, it was 7.6 days, meaning that after 6 months of daily alitretinoin workers who were off the job because of their hand eczema were taking 57% fewer sick days.
The reduction in work absenteeism in TOCCATA was paralleled by the clinical improvement. It took about 4 weeks of alitretinoin therapy to see a significant impact on Physician Global Assessment ratings. The bulk of the clinical improvement was achieved by week 12, Dr. Diepgen noted.
The most common adverse events in TOCCATA were mild to moderate mucocutaneous reactions, seen in about 10% of patients, which is a lower rate than reported with other retinoids. Headache occurred in 8% of patients, and flushing in 1%.
Alitretinoin is a potent teratogen, like other retinoids. However, its relatively short half-life of 2-10 hours means that women of childbearing potential must continue on contraception for 1 month posttreatment, as compared to 3 years with acitretin.
Asked how much oral alitretinoin costs, Dr. Diepgen said it’s about 600 euros (US $811) per month in Germany. But he added that in another study, he and his coworkers calculated that the yearly cost of severe chronic hand eczema was about 9,000 euros (US $12,170), mostly from sick leave and resultant lost workplace productivity. And that’s a conservative figure, he added; the indirect costs of severe hand eczema run nearly twice as high in expertly skilled, higher-paid workers.
The U.K. National Institute for Health and Clinical Excellence guidelines recommend oral 9-cis-retinoic acid as first-line therapy for patients who fail to respond to potent topical corticosteroids, as do Italian and Canadian guidelines and a German dermatology association. A phase III clinical trial (HANDEL) is currently underway in the United States.
Dr. Diepgen is an adviser to Basilea Pharmaceutica, which markets oral alitretinoin.
LISBON – Physicians outside the United States are turning cartwheels over the outcomes they're obtaining with oral alitretinoin for chronic hand eczema.
New data from the postmarketing observational TOCCATA trial demonstrate that oral alitretinoin reduced eczema-related work absences by 50% in German workers, Dr. Thomas Diepgen reported at the annual congress of the European Academy of Dermatology and Venereology.
The TOCCATA study involved 680 German patients with chronic hand eczema rated as severe in two-thirds of participants and moderate in the remainder. TOCCATA was designed to determine whether alitretinoin’s performance in real-world clinical practice is similar to that in the pivotal 1,032-patient randomized BACH (Benefits of Alitretinoin in Chronic Hand Eczema) trial, which resulted in European approval of the novel retinoid (Br. J. Dermatol. 2008;158:808-17).
TOCCATA participants received either 10 mg or 30 mg of alitretinoin per day at their physician’s discretion for up to 24 weeks, with follow-up evaluations at 4-week intervals. Treatment outcomes in TOCCATA proved comparable to those in the BACH trial: a 56.7% rating of clear or almost clear by Physician Global Assessment, as compared with 47.7% in BACH.
As in BACH, the greatest response in TOCCATA was in patients with the hyperkeratotic rhagadiform form of hand eczema, with a 59.2% rate of clear or almost clear. But all the morphologic types showed a favorable response: a 47.9% clear or almost clear rate in dyshidrosiform hand eczema, and a 52.2% rate in fingertip eczema.
In TOCCATA, 522 participants were employed, mostly as steel or other metal workers, or in food processing. At baseline, 80 reported a work absence because of their chronic hand eczema within the previous 4 weeks. By week 8, this number had dropped to 53 workers. At weeks 12 and 16 it was 43 workers, at week 20 it was 41, and by week 24 only 37 TOCCATA participants had missed work during the previous 4 weeks, according to Dr. Diepgen, director of the department of social medicine, occupational, and environmental dermatology at the University of Heidelberg (Germany).
Not only was the number of workers taking sick leave reduced by slightly more than half, but total sick days were even more dramatically impacted. At baseline, workers who had taken hand eczema-related sick leave within the prior 4 weeks had missed an average of 17.6 work days during that period. By week 8, that figure had dropped to an average 10.7 days of absence in the last 4 weeks. At week 24, it was 7.6 days, meaning that after 6 months of daily alitretinoin workers who were off the job because of their hand eczema were taking 57% fewer sick days.
The reduction in work absenteeism in TOCCATA was paralleled by the clinical improvement. It took about 4 weeks of alitretinoin therapy to see a significant impact on Physician Global Assessment ratings. The bulk of the clinical improvement was achieved by week 12, Dr. Diepgen noted.
The most common adverse events in TOCCATA were mild to moderate mucocutaneous reactions, seen in about 10% of patients, which is a lower rate than reported with other retinoids. Headache occurred in 8% of patients, and flushing in 1%.
Alitretinoin is a potent teratogen, like other retinoids. However, its relatively short half-life of 2-10 hours means that women of childbearing potential must continue on contraception for 1 month posttreatment, as compared to 3 years with acitretin.
Asked how much oral alitretinoin costs, Dr. Diepgen said it’s about 600 euros (US $811) per month in Germany. But he added that in another study, he and his coworkers calculated that the yearly cost of severe chronic hand eczema was about 9,000 euros (US $12,170), mostly from sick leave and resultant lost workplace productivity. And that’s a conservative figure, he added; the indirect costs of severe hand eczema run nearly twice as high in expertly skilled, higher-paid workers.
The U.K. National Institute for Health and Clinical Excellence guidelines recommend oral 9-cis-retinoic acid as first-line therapy for patients who fail to respond to potent topical corticosteroids, as do Italian and Canadian guidelines and a German dermatology association. A phase III clinical trial (HANDEL) is currently underway in the United States.
Dr. Diepgen is an adviser to Basilea Pharmaceutica, which markets oral alitretinoin.
LISBON – Physicians outside the United States are turning cartwheels over the outcomes they're obtaining with oral alitretinoin for chronic hand eczema.
New data from the postmarketing observational TOCCATA trial demonstrate that oral alitretinoin reduced eczema-related work absences by 50% in German workers, Dr. Thomas Diepgen reported at the annual congress of the European Academy of Dermatology and Venereology.
The TOCCATA study involved 680 German patients with chronic hand eczema rated as severe in two-thirds of participants and moderate in the remainder. TOCCATA was designed to determine whether alitretinoin’s performance in real-world clinical practice is similar to that in the pivotal 1,032-patient randomized BACH (Benefits of Alitretinoin in Chronic Hand Eczema) trial, which resulted in European approval of the novel retinoid (Br. J. Dermatol. 2008;158:808-17).
TOCCATA participants received either 10 mg or 30 mg of alitretinoin per day at their physician’s discretion for up to 24 weeks, with follow-up evaluations at 4-week intervals. Treatment outcomes in TOCCATA proved comparable to those in the BACH trial: a 56.7% rating of clear or almost clear by Physician Global Assessment, as compared with 47.7% in BACH.
As in BACH, the greatest response in TOCCATA was in patients with the hyperkeratotic rhagadiform form of hand eczema, with a 59.2% rate of clear or almost clear. But all the morphologic types showed a favorable response: a 47.9% clear or almost clear rate in dyshidrosiform hand eczema, and a 52.2% rate in fingertip eczema.
In TOCCATA, 522 participants were employed, mostly as steel or other metal workers, or in food processing. At baseline, 80 reported a work absence because of their chronic hand eczema within the previous 4 weeks. By week 8, this number had dropped to 53 workers. At weeks 12 and 16 it was 43 workers, at week 20 it was 41, and by week 24 only 37 TOCCATA participants had missed work during the previous 4 weeks, according to Dr. Diepgen, director of the department of social medicine, occupational, and environmental dermatology at the University of Heidelberg (Germany).
Not only was the number of workers taking sick leave reduced by slightly more than half, but total sick days were even more dramatically impacted. At baseline, workers who had taken hand eczema-related sick leave within the prior 4 weeks had missed an average of 17.6 work days during that period. By week 8, that figure had dropped to an average 10.7 days of absence in the last 4 weeks. At week 24, it was 7.6 days, meaning that after 6 months of daily alitretinoin workers who were off the job because of their hand eczema were taking 57% fewer sick days.
The reduction in work absenteeism in TOCCATA was paralleled by the clinical improvement. It took about 4 weeks of alitretinoin therapy to see a significant impact on Physician Global Assessment ratings. The bulk of the clinical improvement was achieved by week 12, Dr. Diepgen noted.
The most common adverse events in TOCCATA were mild to moderate mucocutaneous reactions, seen in about 10% of patients, which is a lower rate than reported with other retinoids. Headache occurred in 8% of patients, and flushing in 1%.
Alitretinoin is a potent teratogen, like other retinoids. However, its relatively short half-life of 2-10 hours means that women of childbearing potential must continue on contraception for 1 month posttreatment, as compared to 3 years with acitretin.
Asked how much oral alitretinoin costs, Dr. Diepgen said it’s about 600 euros (US $811) per month in Germany. But he added that in another study, he and his coworkers calculated that the yearly cost of severe chronic hand eczema was about 9,000 euros (US $12,170), mostly from sick leave and resultant lost workplace productivity. And that’s a conservative figure, he added; the indirect costs of severe hand eczema run nearly twice as high in expertly skilled, higher-paid workers.
The U.K. National Institute for Health and Clinical Excellence guidelines recommend oral 9-cis-retinoic acid as first-line therapy for patients who fail to respond to potent topical corticosteroids, as do Italian and Canadian guidelines and a German dermatology association. A phase III clinical trial (HANDEL) is currently underway in the United States.
Dr. Diepgen is an adviser to Basilea Pharmaceutica, which markets oral alitretinoin.
FROM THE ANNUAL CONGRESS OF THE EUROPEAN ACADEMY OF DERMATOLOGY AND VENEREOLOGY
Major Finding: The number of German workers who took sick leave for their chronic hand eczema was reduced by half after they went on daily therapy with oral alliteration.
Data Source: The observational 680-patient TOCCATA study.
Disclosures: The study was funded by Basilea Pharmaceuticals, which markets oral alitretinoin in Europe and Canada. Dr. Diepgen is an adviser to the company.
Translating 'Crazy Fungus:' The Skinny Podcast
'In this month's podcast, Reporter Sherry Boschert talks to Dr. Libby Edwards about how best to manage genital itching in female patients, while Reporter Jeff Evans catches up with Dr. Darrell Rigel on what dermatologists can expect now that MelaFind has received FDA approval.
Vincent DeLeo reminds dermatologists that they need to tell patients how much sunscreen to use during application because most aren't using enough.
And last but not least, Dr. Alan Rockoff shows off his ability to say "fungus" in multiple languages.
Don't miss another episode of The Skinny Podcast; subscribe on iTunes!
'In this month's podcast, Reporter Sherry Boschert talks to Dr. Libby Edwards about how best to manage genital itching in female patients, while Reporter Jeff Evans catches up with Dr. Darrell Rigel on what dermatologists can expect now that MelaFind has received FDA approval.
Vincent DeLeo reminds dermatologists that they need to tell patients how much sunscreen to use during application because most aren't using enough.
And last but not least, Dr. Alan Rockoff shows off his ability to say "fungus" in multiple languages.
Don't miss another episode of The Skinny Podcast; subscribe on iTunes!
'In this month's podcast, Reporter Sherry Boschert talks to Dr. Libby Edwards about how best to manage genital itching in female patients, while Reporter Jeff Evans catches up with Dr. Darrell Rigel on what dermatologists can expect now that MelaFind has received FDA approval.
Vincent DeLeo reminds dermatologists that they need to tell patients how much sunscreen to use during application because most aren't using enough.
And last but not least, Dr. Alan Rockoff shows off his ability to say "fungus" in multiple languages.
Don't miss another episode of The Skinny Podcast; subscribe on iTunes!
Edelweiss
Leontopodium alpinum, better known as edelweiss (German for noble whiteness and understood as noble purity) is a European mountain flower and member of the sunflower family long honored symbolically in national currency, badges, song, and other forms of national pride. It is also the national flower of Switzerland. Of medical interest, the plant has been used in traditional folk medicine to treat abdominal and respiratory disorders.
In 2003, Dobner et al. assessed the antimicrobial activity of extracts and various individual constituents of edelweiss. Using agar diffusion assays as well as the microbroth dilution method to determine minimum inhibitory concentrations, they observed significant antimicrobial activities exhibited against Enterococcus faecium, Escherichia coli, Pseudomonas aeruginosa, Staphylococcus aureus, Streptococcus pneumoniae, and Streptococcus pyogenes strains. The investigators concluded that their findings buttress the previously observed traditional folk medicine approaches to abdominal and respiratory conditions (J. Ethnopharmacol. 2003;89:301-3).
Dermatologic Applications
In 2004, some of the same researchers conducted a study using Leontopodium alpinum that offered dermatologic implications. Specifically, they examined the aerial (that is, capitula, inflorescence leaves, stems, stem leaves and leaves of the basal rosette; Phytochem. Anal. 2006;17:291-8) parts of edelweiss for their in vivo topical anti-inflammatory activity on Croton oil–induced ear dermatitis in mice. They found that dichloromethane extract yielded a dose-dependent decrease in edema, with the extract imparting greater activity than methanol and 70% aqueous methanol extracts. Dichloromethane extracts from the aerial parts of the plant were also found to be more active than dichloromethane root extracts. The investigators noted that fatty acids contribute significantly to the anti-edema effect of the aerial dichloromethane extract while the anti-inflammatory activity of the root extract could be attributed to bisabolane sesquiterpenes, tricyclic sesquiterpenes, coumarins and lignans (Planta Med. 2004;70:502-8).
In May 2006, some of the same researchers assessed the anti-inflammatory and analgesic effects of the dichloromethane, methanolic and carbon dioxide extracts of the aerial parts and roots of edelweiss after oral administration to rats and mice. In pretreated specimens, histologic examination of the paws of rats revealed significant decreases in inflammation. In the rats’ paw edema assay, the most activity was seen in the lipophilic extracts of the aerial plant parts, with swelling diminished by 80% from the dichloromethane extract and 72% from the carbon dioxide extract. Analgesic effects were more salient in association with treatment from the root extracts, compared with the aerial parts, which the authors suggested was indicative of varying mechanisms of action. Also, they evaluated the antioxidant properties of some of the extracts to ascertain any correlations with the observed anti-inflammatory characteristics (J. Ethnopharmacol. 2006;105:421-6).
Later that year, some of the same investigators, led by Schwaiger, identified and measured the major phenolic constituents of edelweiss. They compared retention times, UV, and mass spectra of nearly all separated constituents to commercially available reference compounds or those isolated from the plant using column chromatography. Among the constituent compounds of edelweiss were found several known antioxidants, including quercetin-3-O-beta-D-glucoside, luteolin-7-O-beta-D-glucoside, luteolin-3'-O-beta-D-glucoside, luteolin-4'-O-beta-D-glucoside, apigenin-7-O-beta-D-glucoside, 6-hydroxy-luteolin-7-O-beta-D-glucoside, luteolin-7,4'-di-O-beta-D-glucoside, chrysoeriol-7-O-beta-D-glucoside, leontopodic acid and 3,5-dicaffeoylquinic acid. A new natural product [3,4,5-tri-(E)-caffeoly-D-glucaric acid] was also identified in the process and named leontopodic acid B (Phytochem Anal. 2006;17:291-8).
In 2009, some of the same investigators, led by Costa, assessed the chemopreventive effects of the antioxidant leontopodic acid isolated from Leontopodium alpinum. After pretreatment with leontopodic acid, they assessed different mycotoxins in two different cell lines, aflatoxin B1 on HepG2 cells and deoxynivalenol on U937 cells. Leontopodic acid was shown to have protected U937 cells from deoxynivalenol-induced cell damage; it did not protect HepG2 cells from aflatoxin B1 toxicity. The researchers also found that the edelweiss isolate enhanced glutathione peroxidase activity in U937; it had no such effect on glutathione S-transferase activity in HepG2. They concluded that the primary mechanism of antioxidant-associated chemopreventive activity imparted by leontopodic acid is the elevation of detoxifying enzymes (J. Appl. Toxicol. 2009;29:7-14).
Products
Scar and Stretch Mark Body Cream is a new formulation launched by Dr. H. Bellin Swiss Skin Care that is touted for containing various peptides, hyaluronic acid, some forms of vitamin B, and Swiss edelweiss extract. Edelweiss extract is also a featured ingredient in the company’s new All in One Eye Cream and All in One Face Cream. The company claims that skin cell regeneration is stimulated by edelweiss. The alpine plant is also featured in Fabulous Eye Cream, a new product from MyChelle Dermaceuticals that they tout for its capacity to reduce collagen degradation and loss of skin firmness. Finally, Athanor products offers a line of edelweiss products, including an anti-aging cream, cleansing lotion, anti-aging serum, peeling mask, as well as neck and breast skin care lotions.
Conclusion
A botanical ingredient is always more intriguing when it is associated with a history of traditional folk medicine. In terms of potential dermatologic applications, herbs that have been used to treat various cutaneous conditions are even more compelling. For the many plants and plant constituents gaining favor in research and development, there is a wide range of evidentiary support. But there is a notable dearth of research to support the claims of effectiveness for edelweiss in topical formulations. Much more research is necessary to establish edelweiss as a useful ingredient in skin care, though the scant data available are promising. Much of the research does appear to be coming from a small group of investigators. I would like to see their work duplicated and built on by several more teams.
Leontopodium alpinum, better known as edelweiss (German for noble whiteness and understood as noble purity) is a European mountain flower and member of the sunflower family long honored symbolically in national currency, badges, song, and other forms of national pride. It is also the national flower of Switzerland. Of medical interest, the plant has been used in traditional folk medicine to treat abdominal and respiratory disorders.
In 2003, Dobner et al. assessed the antimicrobial activity of extracts and various individual constituents of edelweiss. Using agar diffusion assays as well as the microbroth dilution method to determine minimum inhibitory concentrations, they observed significant antimicrobial activities exhibited against Enterococcus faecium, Escherichia coli, Pseudomonas aeruginosa, Staphylococcus aureus, Streptococcus pneumoniae, and Streptococcus pyogenes strains. The investigators concluded that their findings buttress the previously observed traditional folk medicine approaches to abdominal and respiratory conditions (J. Ethnopharmacol. 2003;89:301-3).
Dermatologic Applications
In 2004, some of the same researchers conducted a study using Leontopodium alpinum that offered dermatologic implications. Specifically, they examined the aerial (that is, capitula, inflorescence leaves, stems, stem leaves and leaves of the basal rosette; Phytochem. Anal. 2006;17:291-8) parts of edelweiss for their in vivo topical anti-inflammatory activity on Croton oil–induced ear dermatitis in mice. They found that dichloromethane extract yielded a dose-dependent decrease in edema, with the extract imparting greater activity than methanol and 70% aqueous methanol extracts. Dichloromethane extracts from the aerial parts of the plant were also found to be more active than dichloromethane root extracts. The investigators noted that fatty acids contribute significantly to the anti-edema effect of the aerial dichloromethane extract while the anti-inflammatory activity of the root extract could be attributed to bisabolane sesquiterpenes, tricyclic sesquiterpenes, coumarins and lignans (Planta Med. 2004;70:502-8).
In May 2006, some of the same researchers assessed the anti-inflammatory and analgesic effects of the dichloromethane, methanolic and carbon dioxide extracts of the aerial parts and roots of edelweiss after oral administration to rats and mice. In pretreated specimens, histologic examination of the paws of rats revealed significant decreases in inflammation. In the rats’ paw edema assay, the most activity was seen in the lipophilic extracts of the aerial plant parts, with swelling diminished by 80% from the dichloromethane extract and 72% from the carbon dioxide extract. Analgesic effects were more salient in association with treatment from the root extracts, compared with the aerial parts, which the authors suggested was indicative of varying mechanisms of action. Also, they evaluated the antioxidant properties of some of the extracts to ascertain any correlations with the observed anti-inflammatory characteristics (J. Ethnopharmacol. 2006;105:421-6).
Later that year, some of the same investigators, led by Schwaiger, identified and measured the major phenolic constituents of edelweiss. They compared retention times, UV, and mass spectra of nearly all separated constituents to commercially available reference compounds or those isolated from the plant using column chromatography. Among the constituent compounds of edelweiss were found several known antioxidants, including quercetin-3-O-beta-D-glucoside, luteolin-7-O-beta-D-glucoside, luteolin-3'-O-beta-D-glucoside, luteolin-4'-O-beta-D-glucoside, apigenin-7-O-beta-D-glucoside, 6-hydroxy-luteolin-7-O-beta-D-glucoside, luteolin-7,4'-di-O-beta-D-glucoside, chrysoeriol-7-O-beta-D-glucoside, leontopodic acid and 3,5-dicaffeoylquinic acid. A new natural product [3,4,5-tri-(E)-caffeoly-D-glucaric acid] was also identified in the process and named leontopodic acid B (Phytochem Anal. 2006;17:291-8).
In 2009, some of the same investigators, led by Costa, assessed the chemopreventive effects of the antioxidant leontopodic acid isolated from Leontopodium alpinum. After pretreatment with leontopodic acid, they assessed different mycotoxins in two different cell lines, aflatoxin B1 on HepG2 cells and deoxynivalenol on U937 cells. Leontopodic acid was shown to have protected U937 cells from deoxynivalenol-induced cell damage; it did not protect HepG2 cells from aflatoxin B1 toxicity. The researchers also found that the edelweiss isolate enhanced glutathione peroxidase activity in U937; it had no such effect on glutathione S-transferase activity in HepG2. They concluded that the primary mechanism of antioxidant-associated chemopreventive activity imparted by leontopodic acid is the elevation of detoxifying enzymes (J. Appl. Toxicol. 2009;29:7-14).
Products
Scar and Stretch Mark Body Cream is a new formulation launched by Dr. H. Bellin Swiss Skin Care that is touted for containing various peptides, hyaluronic acid, some forms of vitamin B, and Swiss edelweiss extract. Edelweiss extract is also a featured ingredient in the company’s new All in One Eye Cream and All in One Face Cream. The company claims that skin cell regeneration is stimulated by edelweiss. The alpine plant is also featured in Fabulous Eye Cream, a new product from MyChelle Dermaceuticals that they tout for its capacity to reduce collagen degradation and loss of skin firmness. Finally, Athanor products offers a line of edelweiss products, including an anti-aging cream, cleansing lotion, anti-aging serum, peeling mask, as well as neck and breast skin care lotions.
Conclusion
A botanical ingredient is always more intriguing when it is associated with a history of traditional folk medicine. In terms of potential dermatologic applications, herbs that have been used to treat various cutaneous conditions are even more compelling. For the many plants and plant constituents gaining favor in research and development, there is a wide range of evidentiary support. But there is a notable dearth of research to support the claims of effectiveness for edelweiss in topical formulations. Much more research is necessary to establish edelweiss as a useful ingredient in skin care, though the scant data available are promising. Much of the research does appear to be coming from a small group of investigators. I would like to see their work duplicated and built on by several more teams.
Leontopodium alpinum, better known as edelweiss (German for noble whiteness and understood as noble purity) is a European mountain flower and member of the sunflower family long honored symbolically in national currency, badges, song, and other forms of national pride. It is also the national flower of Switzerland. Of medical interest, the plant has been used in traditional folk medicine to treat abdominal and respiratory disorders.
In 2003, Dobner et al. assessed the antimicrobial activity of extracts and various individual constituents of edelweiss. Using agar diffusion assays as well as the microbroth dilution method to determine minimum inhibitory concentrations, they observed significant antimicrobial activities exhibited against Enterococcus faecium, Escherichia coli, Pseudomonas aeruginosa, Staphylococcus aureus, Streptococcus pneumoniae, and Streptococcus pyogenes strains. The investigators concluded that their findings buttress the previously observed traditional folk medicine approaches to abdominal and respiratory conditions (J. Ethnopharmacol. 2003;89:301-3).
Dermatologic Applications
In 2004, some of the same researchers conducted a study using Leontopodium alpinum that offered dermatologic implications. Specifically, they examined the aerial (that is, capitula, inflorescence leaves, stems, stem leaves and leaves of the basal rosette; Phytochem. Anal. 2006;17:291-8) parts of edelweiss for their in vivo topical anti-inflammatory activity on Croton oil–induced ear dermatitis in mice. They found that dichloromethane extract yielded a dose-dependent decrease in edema, with the extract imparting greater activity than methanol and 70% aqueous methanol extracts. Dichloromethane extracts from the aerial parts of the plant were also found to be more active than dichloromethane root extracts. The investigators noted that fatty acids contribute significantly to the anti-edema effect of the aerial dichloromethane extract while the anti-inflammatory activity of the root extract could be attributed to bisabolane sesquiterpenes, tricyclic sesquiterpenes, coumarins and lignans (Planta Med. 2004;70:502-8).
In May 2006, some of the same researchers assessed the anti-inflammatory and analgesic effects of the dichloromethane, methanolic and carbon dioxide extracts of the aerial parts and roots of edelweiss after oral administration to rats and mice. In pretreated specimens, histologic examination of the paws of rats revealed significant decreases in inflammation. In the rats’ paw edema assay, the most activity was seen in the lipophilic extracts of the aerial plant parts, with swelling diminished by 80% from the dichloromethane extract and 72% from the carbon dioxide extract. Analgesic effects were more salient in association with treatment from the root extracts, compared with the aerial parts, which the authors suggested was indicative of varying mechanisms of action. Also, they evaluated the antioxidant properties of some of the extracts to ascertain any correlations with the observed anti-inflammatory characteristics (J. Ethnopharmacol. 2006;105:421-6).
Later that year, some of the same investigators, led by Schwaiger, identified and measured the major phenolic constituents of edelweiss. They compared retention times, UV, and mass spectra of nearly all separated constituents to commercially available reference compounds or those isolated from the plant using column chromatography. Among the constituent compounds of edelweiss were found several known antioxidants, including quercetin-3-O-beta-D-glucoside, luteolin-7-O-beta-D-glucoside, luteolin-3'-O-beta-D-glucoside, luteolin-4'-O-beta-D-glucoside, apigenin-7-O-beta-D-glucoside, 6-hydroxy-luteolin-7-O-beta-D-glucoside, luteolin-7,4'-di-O-beta-D-glucoside, chrysoeriol-7-O-beta-D-glucoside, leontopodic acid and 3,5-dicaffeoylquinic acid. A new natural product [3,4,5-tri-(E)-caffeoly-D-glucaric acid] was also identified in the process and named leontopodic acid B (Phytochem Anal. 2006;17:291-8).
In 2009, some of the same investigators, led by Costa, assessed the chemopreventive effects of the antioxidant leontopodic acid isolated from Leontopodium alpinum. After pretreatment with leontopodic acid, they assessed different mycotoxins in two different cell lines, aflatoxin B1 on HepG2 cells and deoxynivalenol on U937 cells. Leontopodic acid was shown to have protected U937 cells from deoxynivalenol-induced cell damage; it did not protect HepG2 cells from aflatoxin B1 toxicity. The researchers also found that the edelweiss isolate enhanced glutathione peroxidase activity in U937; it had no such effect on glutathione S-transferase activity in HepG2. They concluded that the primary mechanism of antioxidant-associated chemopreventive activity imparted by leontopodic acid is the elevation of detoxifying enzymes (J. Appl. Toxicol. 2009;29:7-14).
Products
Scar and Stretch Mark Body Cream is a new formulation launched by Dr. H. Bellin Swiss Skin Care that is touted for containing various peptides, hyaluronic acid, some forms of vitamin B, and Swiss edelweiss extract. Edelweiss extract is also a featured ingredient in the company’s new All in One Eye Cream and All in One Face Cream. The company claims that skin cell regeneration is stimulated by edelweiss. The alpine plant is also featured in Fabulous Eye Cream, a new product from MyChelle Dermaceuticals that they tout for its capacity to reduce collagen degradation and loss of skin firmness. Finally, Athanor products offers a line of edelweiss products, including an anti-aging cream, cleansing lotion, anti-aging serum, peeling mask, as well as neck and breast skin care lotions.
Conclusion
A botanical ingredient is always more intriguing when it is associated with a history of traditional folk medicine. In terms of potential dermatologic applications, herbs that have been used to treat various cutaneous conditions are even more compelling. For the many plants and plant constituents gaining favor in research and development, there is a wide range of evidentiary support. But there is a notable dearth of research to support the claims of effectiveness for edelweiss in topical formulations. Much more research is necessary to establish edelweiss as a useful ingredient in skin care, though the scant data available are promising. Much of the research does appear to be coming from a small group of investigators. I would like to see their work duplicated and built on by several more teams.
Metal Orthopedic Implants Unlikely to Trigger Allergy
NAPA, CALIF. – There is little risk that patients with orthopedic metal implants will have a skin reaction or joint pain from the device, said Dr. Joseph F. Fowler.
"I do patch test patients ... who have concerns about a metal allergy or are going to have an implant. I tell them if they have a positive patch test, they may have a skin reaction," said Dr. Fowler. However, there is a small chance they will have a cutaneous reaction, and a smaller chance they will have problems with the joint.
Metals used in orthopedic implants include stainless steel, which is composed of an iron-chromium alloy plus nickel and molybdenum, and sometimes a little chromium and titanium; nitinol (55% nickel and 45% titanium); vitallium (iron cobalt plus chromium 30% and molybdenum 5%); and titanium. Two of the four metals contain nickel, a common contact allergen, noted Dr. Fowler, a dermatologist at the University of Louisville (Ky.).
When it comes to joint pain from implants, findings from a small German study of 15 patients showed that levels of the inflammatory marker interleukin-17 (IL-17) were increased in only those patients with nickel containing replacement joints who both had a positive patch test to nickel and complaints of joint pain. IL-17 levels were not increased in patients with a positive patch test to nickel who did not complain of joint pain (Contact Dermatitis 2010;63:15-22).
In an unpublished study, Dr. James Taylor of the Cleveland Clinic found that 60% of a small group of patients (10) with a metal implant who had a positive patch to metal experienced resolution of joint pain after the metal was replaced. "There is getting to be more and more of a suggestion that metal allergies and joint problems do go hand in hand," said Dr. Fowler.
If you just had to guess what would be the best material to put in a patient who with a chance of a metal allergy, titanium is the best bet, he said. "It comes down to a medical legal question. Will doctors and patients accept a small amount of risk if there is an implant that is better than titanium?"
He said that he will patch test patients if requested by the physician who will be performing the implant surgery, but it is not normally done because there is less than a 1% chance that even if they do have a positive patch test to metal, dermatitis will occur. There have been reports, although rare, that a metal allergy may cause joint failure, but prospective studies are needed, he said.
Dr. Fowler reported financial conflicts of interest with multiple pharmaceutical companies.
NAPA, CALIF. – There is little risk that patients with orthopedic metal implants will have a skin reaction or joint pain from the device, said Dr. Joseph F. Fowler.
"I do patch test patients ... who have concerns about a metal allergy or are going to have an implant. I tell them if they have a positive patch test, they may have a skin reaction," said Dr. Fowler. However, there is a small chance they will have a cutaneous reaction, and a smaller chance they will have problems with the joint.
Metals used in orthopedic implants include stainless steel, which is composed of an iron-chromium alloy plus nickel and molybdenum, and sometimes a little chromium and titanium; nitinol (55% nickel and 45% titanium); vitallium (iron cobalt plus chromium 30% and molybdenum 5%); and titanium. Two of the four metals contain nickel, a common contact allergen, noted Dr. Fowler, a dermatologist at the University of Louisville (Ky.).
When it comes to joint pain from implants, findings from a small German study of 15 patients showed that levels of the inflammatory marker interleukin-17 (IL-17) were increased in only those patients with nickel containing replacement joints who both had a positive patch test to nickel and complaints of joint pain. IL-17 levels were not increased in patients with a positive patch test to nickel who did not complain of joint pain (Contact Dermatitis 2010;63:15-22).
In an unpublished study, Dr. James Taylor of the Cleveland Clinic found that 60% of a small group of patients (10) with a metal implant who had a positive patch to metal experienced resolution of joint pain after the metal was replaced. "There is getting to be more and more of a suggestion that metal allergies and joint problems do go hand in hand," said Dr. Fowler.
If you just had to guess what would be the best material to put in a patient who with a chance of a metal allergy, titanium is the best bet, he said. "It comes down to a medical legal question. Will doctors and patients accept a small amount of risk if there is an implant that is better than titanium?"
He said that he will patch test patients if requested by the physician who will be performing the implant surgery, but it is not normally done because there is less than a 1% chance that even if they do have a positive patch test to metal, dermatitis will occur. There have been reports, although rare, that a metal allergy may cause joint failure, but prospective studies are needed, he said.
Dr. Fowler reported financial conflicts of interest with multiple pharmaceutical companies.
NAPA, CALIF. – There is little risk that patients with orthopedic metal implants will have a skin reaction or joint pain from the device, said Dr. Joseph F. Fowler.
"I do patch test patients ... who have concerns about a metal allergy or are going to have an implant. I tell them if they have a positive patch test, they may have a skin reaction," said Dr. Fowler. However, there is a small chance they will have a cutaneous reaction, and a smaller chance they will have problems with the joint.
Metals used in orthopedic implants include stainless steel, which is composed of an iron-chromium alloy plus nickel and molybdenum, and sometimes a little chromium and titanium; nitinol (55% nickel and 45% titanium); vitallium (iron cobalt plus chromium 30% and molybdenum 5%); and titanium. Two of the four metals contain nickel, a common contact allergen, noted Dr. Fowler, a dermatologist at the University of Louisville (Ky.).
When it comes to joint pain from implants, findings from a small German study of 15 patients showed that levels of the inflammatory marker interleukin-17 (IL-17) were increased in only those patients with nickel containing replacement joints who both had a positive patch test to nickel and complaints of joint pain. IL-17 levels were not increased in patients with a positive patch test to nickel who did not complain of joint pain (Contact Dermatitis 2010;63:15-22).
In an unpublished study, Dr. James Taylor of the Cleveland Clinic found that 60% of a small group of patients (10) with a metal implant who had a positive patch to metal experienced resolution of joint pain after the metal was replaced. "There is getting to be more and more of a suggestion that metal allergies and joint problems do go hand in hand," said Dr. Fowler.
If you just had to guess what would be the best material to put in a patient who with a chance of a metal allergy, titanium is the best bet, he said. "It comes down to a medical legal question. Will doctors and patients accept a small amount of risk if there is an implant that is better than titanium?"
He said that he will patch test patients if requested by the physician who will be performing the implant surgery, but it is not normally done because there is less than a 1% chance that even if they do have a positive patch test to metal, dermatitis will occur. There have been reports, although rare, that a metal allergy may cause joint failure, but prospective studies are needed, he said.
Dr. Fowler reported financial conflicts of interest with multiple pharmaceutical companies.
EXPERT ANALYSIS FROM THE COASTAL DERMATOLOGY SYMPOSIUM
Pharma-Sponsored Comparison Studies Hold Clinical Value
NAPA, CALIF. – "You are almost never going to see a study where the sponsoring company’s product wasn’t at least as good if not better," than the comparator drug, said Dr. Joseph F. Fowler. But that reality does not necessarily mean the study results don’t provide good clinical information.
"Once a drug goes generic, you’re almost never going to see any further study on it."
Most comparison studies are done by pharmaceutical companies and are limited to comparing competing drugs to the company’s branded drugs, explained Dr. Fowler, a dermatologist at the University of Louisville (Ky.). Also, "once a drug goes generic, you’re almost never going to see any further study on it."
Dr. Fowler discussed several comparison studies that run across the dermatology gamut at the meeting, and then asked the audience which drug they prefer.
Ivermectin Vs. Malathion for Lice
In a recent comparison of oral ivermectin to malathion lotion for difficult-to-treat head lice, ivermectin came out slightly on top in terms of clearance at day 15 (95% vs. 85%, respectively), he reported.
In the multicenter trial, 812 patients from 376 households were randomized to receive 400 mcg/kg of body weight of ivermectin or 0.5% malathion lotion on days 1 and 8. The study patients had lice that were not cleared with a topical insecticide 2-6 weeks before study enrollment (N. Engl. J. Med. 2010;362:896-905).
"I tend to use more ivermectin when I see these patients than I ever used to, and I tend to use less topicals," said Dr. Fowler. However, systemic drugs probably have more of a chance of causing toxicity than topicals.
Ivermectin Vs. Permethrin for Scabies
In another comparison of oral ivermectin, this time for scabies, permethrin came out slightly on top. Patients with scabies (n = 85) were randomized to treatment with 200 mcg/kg body weight of ivermectin or a single topical application of 5% permethrin cream. Clearance was seen in 95% of permethrin-treated patients, compared with 70% of ivermectin-treated patients at 8 weeks (J. Am. Acad. Dermatol. 2000;42:236-40).
Topical permethrin was also found to be more effective than topical crotamiton, topical lindane, and oral ivermectin for scabies in a Cochrane database system review (Arch. Dermatol. 2008;144:1638-40).
A show of hands in the audience found that the room was divided on their preferred treatment for head lice and scabies.
Griseofulvin Vs. Terbinafine for Tinea Capitis
A meta-analysis of seven randomized, controlled trials comparing griseofulvin and terbinafine in the treatment of tinea capitis resulted in a draw. However, griseofulvin was found to be slightly better for the Microsporum species, while terbinafine was found to be slightly more effective for the Trichophyton species (J. Am. Acad. Dermatol. 2011;64:663-70).
If cost is an issue, terbinafine is the cheaper drug, noted Dr. Fowler, who said the cost is about $4 in Kentucky. Further, treatment time is shorter with terbinafine at 4 weeks as compared with griseofulvin at 8 weeks. Also, terbinafine appears to be associated with fewer adverse effects than griseofulvin.
The majority of the audience members agreed, via a show of hands, noting their preference for terbinafine to treat children and adults with tinea capitis.
Tazarotene Vs. Adapalene for Acne
In a 16-week, multicenter, randomized, investigator-blinded study, patients treated once a day with tazarotene 0.1% cream had better acne lesion clearance than patients treated with adapalene 0.3% gel. More patients treated with tazarotene had at least a 50% reduction in lesions and less disease severity as compared with adapalene-treated patients (J. Drugs Dermatol. 2010;9:549-58).
However, tazarotene was somewhat less tolerated than adapalene, reported Dr. Fowler. Erythema occurred in 6% of tazarotene patients, dryness in 7%, and peeling in 11%. In the adapalene group, peeling was the only adverse event and was reported by 1% of patients.
By a show of hands, the majority of the audience members prefer adapalene.
Calcitriol Vs. Calcipotriol for Psoriasis
Calcitriol ointment was found to be better tolerated than calcipotriol for treating mild to moderate psoriasis in sensitive areas, such as on the face, around the hairline, and behind the ears (Br. J. Dermatol. 2003;148:326-33).
In the left-to-right, randomized, multicenter, investigator-blinded study, calcitriol 3 mcg ointment was compared with calcipotriol 50 mcg ointment in 75 patients. After 6 weeks, study patients reported preferring calcitriol ointment, which demonstrated "superior" tolerability and equal efficacy, reported Dr. Fowler. Adverse events (contact or irritant dermatitis) occurred in eight patients on the calcipotriol-treated side of their face (one patient reported dermatitis on both sides).
When asked to take cost and possible systemic adverse events into consideration, most audience members noted a preference for calcitriol ointment.
Methotrexate Vs. Azathioprine for Atopy
In the treatment of severe atopic dermatitis, methotrexate and azathioprine were found to be almost equal in efficacy (42% vs. 39%, respectively). Patients (52 completed the study) were randomized to receive 10-22.5 mg of methotrexate per week or 1.5-2.2 mg/kg per day for 12 weeks (J. Allergy Clin. Immunol. 2011;128:353-9). Outcome was assessed by blinded reviewers.
"I think that the adverse event profile of methotrexate in most people is much better, so I tend to disagree with the outcome of this study," said Dr. Fowler.
Dr. Fowler reported financial conflicts of interest with multiple pharmaceutical companies, including many of the products mentioned during his presentation.
NAPA, CALIF. – "You are almost never going to see a study where the sponsoring company’s product wasn’t at least as good if not better," than the comparator drug, said Dr. Joseph F. Fowler. But that reality does not necessarily mean the study results don’t provide good clinical information.
"Once a drug goes generic, you’re almost never going to see any further study on it."
Most comparison studies are done by pharmaceutical companies and are limited to comparing competing drugs to the company’s branded drugs, explained Dr. Fowler, a dermatologist at the University of Louisville (Ky.). Also, "once a drug goes generic, you’re almost never going to see any further study on it."
Dr. Fowler discussed several comparison studies that run across the dermatology gamut at the meeting, and then asked the audience which drug they prefer.
Ivermectin Vs. Malathion for Lice
In a recent comparison of oral ivermectin to malathion lotion for difficult-to-treat head lice, ivermectin came out slightly on top in terms of clearance at day 15 (95% vs. 85%, respectively), he reported.
In the multicenter trial, 812 patients from 376 households were randomized to receive 400 mcg/kg of body weight of ivermectin or 0.5% malathion lotion on days 1 and 8. The study patients had lice that were not cleared with a topical insecticide 2-6 weeks before study enrollment (N. Engl. J. Med. 2010;362:896-905).
"I tend to use more ivermectin when I see these patients than I ever used to, and I tend to use less topicals," said Dr. Fowler. However, systemic drugs probably have more of a chance of causing toxicity than topicals.
Ivermectin Vs. Permethrin for Scabies
In another comparison of oral ivermectin, this time for scabies, permethrin came out slightly on top. Patients with scabies (n = 85) were randomized to treatment with 200 mcg/kg body weight of ivermectin or a single topical application of 5% permethrin cream. Clearance was seen in 95% of permethrin-treated patients, compared with 70% of ivermectin-treated patients at 8 weeks (J. Am. Acad. Dermatol. 2000;42:236-40).
Topical permethrin was also found to be more effective than topical crotamiton, topical lindane, and oral ivermectin for scabies in a Cochrane database system review (Arch. Dermatol. 2008;144:1638-40).
A show of hands in the audience found that the room was divided on their preferred treatment for head lice and scabies.
Griseofulvin Vs. Terbinafine for Tinea Capitis
A meta-analysis of seven randomized, controlled trials comparing griseofulvin and terbinafine in the treatment of tinea capitis resulted in a draw. However, griseofulvin was found to be slightly better for the Microsporum species, while terbinafine was found to be slightly more effective for the Trichophyton species (J. Am. Acad. Dermatol. 2011;64:663-70).
If cost is an issue, terbinafine is the cheaper drug, noted Dr. Fowler, who said the cost is about $4 in Kentucky. Further, treatment time is shorter with terbinafine at 4 weeks as compared with griseofulvin at 8 weeks. Also, terbinafine appears to be associated with fewer adverse effects than griseofulvin.
The majority of the audience members agreed, via a show of hands, noting their preference for terbinafine to treat children and adults with tinea capitis.
Tazarotene Vs. Adapalene for Acne
In a 16-week, multicenter, randomized, investigator-blinded study, patients treated once a day with tazarotene 0.1% cream had better acne lesion clearance than patients treated with adapalene 0.3% gel. More patients treated with tazarotene had at least a 50% reduction in lesions and less disease severity as compared with adapalene-treated patients (J. Drugs Dermatol. 2010;9:549-58).
However, tazarotene was somewhat less tolerated than adapalene, reported Dr. Fowler. Erythema occurred in 6% of tazarotene patients, dryness in 7%, and peeling in 11%. In the adapalene group, peeling was the only adverse event and was reported by 1% of patients.
By a show of hands, the majority of the audience members prefer adapalene.
Calcitriol Vs. Calcipotriol for Psoriasis
Calcitriol ointment was found to be better tolerated than calcipotriol for treating mild to moderate psoriasis in sensitive areas, such as on the face, around the hairline, and behind the ears (Br. J. Dermatol. 2003;148:326-33).
In the left-to-right, randomized, multicenter, investigator-blinded study, calcitriol 3 mcg ointment was compared with calcipotriol 50 mcg ointment in 75 patients. After 6 weeks, study patients reported preferring calcitriol ointment, which demonstrated "superior" tolerability and equal efficacy, reported Dr. Fowler. Adverse events (contact or irritant dermatitis) occurred in eight patients on the calcipotriol-treated side of their face (one patient reported dermatitis on both sides).
When asked to take cost and possible systemic adverse events into consideration, most audience members noted a preference for calcitriol ointment.
Methotrexate Vs. Azathioprine for Atopy
In the treatment of severe atopic dermatitis, methotrexate and azathioprine were found to be almost equal in efficacy (42% vs. 39%, respectively). Patients (52 completed the study) were randomized to receive 10-22.5 mg of methotrexate per week or 1.5-2.2 mg/kg per day for 12 weeks (J. Allergy Clin. Immunol. 2011;128:353-9). Outcome was assessed by blinded reviewers.
"I think that the adverse event profile of methotrexate in most people is much better, so I tend to disagree with the outcome of this study," said Dr. Fowler.
Dr. Fowler reported financial conflicts of interest with multiple pharmaceutical companies, including many of the products mentioned during his presentation.
NAPA, CALIF. – "You are almost never going to see a study where the sponsoring company’s product wasn’t at least as good if not better," than the comparator drug, said Dr. Joseph F. Fowler. But that reality does not necessarily mean the study results don’t provide good clinical information.
"Once a drug goes generic, you’re almost never going to see any further study on it."
Most comparison studies are done by pharmaceutical companies and are limited to comparing competing drugs to the company’s branded drugs, explained Dr. Fowler, a dermatologist at the University of Louisville (Ky.). Also, "once a drug goes generic, you’re almost never going to see any further study on it."
Dr. Fowler discussed several comparison studies that run across the dermatology gamut at the meeting, and then asked the audience which drug they prefer.
Ivermectin Vs. Malathion for Lice
In a recent comparison of oral ivermectin to malathion lotion for difficult-to-treat head lice, ivermectin came out slightly on top in terms of clearance at day 15 (95% vs. 85%, respectively), he reported.
In the multicenter trial, 812 patients from 376 households were randomized to receive 400 mcg/kg of body weight of ivermectin or 0.5% malathion lotion on days 1 and 8. The study patients had lice that were not cleared with a topical insecticide 2-6 weeks before study enrollment (N. Engl. J. Med. 2010;362:896-905).
"I tend to use more ivermectin when I see these patients than I ever used to, and I tend to use less topicals," said Dr. Fowler. However, systemic drugs probably have more of a chance of causing toxicity than topicals.
Ivermectin Vs. Permethrin for Scabies
In another comparison of oral ivermectin, this time for scabies, permethrin came out slightly on top. Patients with scabies (n = 85) were randomized to treatment with 200 mcg/kg body weight of ivermectin or a single topical application of 5% permethrin cream. Clearance was seen in 95% of permethrin-treated patients, compared with 70% of ivermectin-treated patients at 8 weeks (J. Am. Acad. Dermatol. 2000;42:236-40).
Topical permethrin was also found to be more effective than topical crotamiton, topical lindane, and oral ivermectin for scabies in a Cochrane database system review (Arch. Dermatol. 2008;144:1638-40).
A show of hands in the audience found that the room was divided on their preferred treatment for head lice and scabies.
Griseofulvin Vs. Terbinafine for Tinea Capitis
A meta-analysis of seven randomized, controlled trials comparing griseofulvin and terbinafine in the treatment of tinea capitis resulted in a draw. However, griseofulvin was found to be slightly better for the Microsporum species, while terbinafine was found to be slightly more effective for the Trichophyton species (J. Am. Acad. Dermatol. 2011;64:663-70).
If cost is an issue, terbinafine is the cheaper drug, noted Dr. Fowler, who said the cost is about $4 in Kentucky. Further, treatment time is shorter with terbinafine at 4 weeks as compared with griseofulvin at 8 weeks. Also, terbinafine appears to be associated with fewer adverse effects than griseofulvin.
The majority of the audience members agreed, via a show of hands, noting their preference for terbinafine to treat children and adults with tinea capitis.
Tazarotene Vs. Adapalene for Acne
In a 16-week, multicenter, randomized, investigator-blinded study, patients treated once a day with tazarotene 0.1% cream had better acne lesion clearance than patients treated with adapalene 0.3% gel. More patients treated with tazarotene had at least a 50% reduction in lesions and less disease severity as compared with adapalene-treated patients (J. Drugs Dermatol. 2010;9:549-58).
However, tazarotene was somewhat less tolerated than adapalene, reported Dr. Fowler. Erythema occurred in 6% of tazarotene patients, dryness in 7%, and peeling in 11%. In the adapalene group, peeling was the only adverse event and was reported by 1% of patients.
By a show of hands, the majority of the audience members prefer adapalene.
Calcitriol Vs. Calcipotriol for Psoriasis
Calcitriol ointment was found to be better tolerated than calcipotriol for treating mild to moderate psoriasis in sensitive areas, such as on the face, around the hairline, and behind the ears (Br. J. Dermatol. 2003;148:326-33).
In the left-to-right, randomized, multicenter, investigator-blinded study, calcitriol 3 mcg ointment was compared with calcipotriol 50 mcg ointment in 75 patients. After 6 weeks, study patients reported preferring calcitriol ointment, which demonstrated "superior" tolerability and equal efficacy, reported Dr. Fowler. Adverse events (contact or irritant dermatitis) occurred in eight patients on the calcipotriol-treated side of their face (one patient reported dermatitis on both sides).
When asked to take cost and possible systemic adverse events into consideration, most audience members noted a preference for calcitriol ointment.
Methotrexate Vs. Azathioprine for Atopy
In the treatment of severe atopic dermatitis, methotrexate and azathioprine were found to be almost equal in efficacy (42% vs. 39%, respectively). Patients (52 completed the study) were randomized to receive 10-22.5 mg of methotrexate per week or 1.5-2.2 mg/kg per day for 12 weeks (J. Allergy Clin. Immunol. 2011;128:353-9). Outcome was assessed by blinded reviewers.
"I think that the adverse event profile of methotrexate in most people is much better, so I tend to disagree with the outcome of this study," said Dr. Fowler.
Dr. Fowler reported financial conflicts of interest with multiple pharmaceutical companies, including many of the products mentioned during his presentation.
EXPERT ANALYSIS FROM THE COASTAL DERMATOLOGY SYMPOSIUM
Causal Link Between Atopic Dermatitis, ADHD Remains Elusive
Evidence suggests that a strong positive correlation exists between atopic disease and attention-deficit/hyperactivity disorder. But since all studies of the issue to date have been observational, "a causal relationship cannot be inferred," according to a research commentary in the August issue of the Archives of Dermatology.
"Further epidemiologic studies that use consistent and validated measures to more accurately define atopic disease and ADHD and adjust for confounders and disease severity are needed to better elucidate this relationship," said Dr. Sarah N. Gee and Dr. Michael Bigby of the departments of dermatology at Harvard Medical School and Beth Israel Deaconess Medical Center, both in Boston (Arch. Dermatol. 2011;147:967-70).
Dr. Gee and Dr. Bigby commented on a review of the literature presented by Dr. Jochen Schmitt and colleagues in the journal Allergy, which was titled: "Is atopic disease a risk factor for attention-deficit/hyperactivity disorder?" A systematic review (Allergy 2010;65:1506-24). That review covered 20 studies – 1 cohort study, 2 case-control studies, and 17 cross-sectional studies – involving 170,175 patients with eczema, asthma, rhinitis, or atopic dermatitis who also had ADHD symptoms. The studies reviewed had been conducted around the world, including in Germany and in other parts of Europe, and in North America, Australia, and New Zealand. All except one of the studies focused on children and adolescents.
"Four of the six studies that investigated eczema and ADHD found a statistically significant positive association, two with an odds ratio greater than four. Two of the three studies that used multivariate logistic regression for confounding factors found a statistically significant positive relationship between atopic dermatitis and ADHD. [And] with respect to asthma, all 12 studies that investigated asthma and ADHD reported a positive association ([odds ratio], 1.23-2.42)," Dr. Gee and Dr. Bigby said.
However, two studies that examined a possible link between allergic rhinitis and ADHD found no correlations.
The review by Dr. Schmitt fulfilled most of the criteria laid out by the Centre for Evidence-Based Medicine’s guidelines for "a useful and valid review." The choice of articles to include was appropriate, and the data were sufficient to answer the clinical question they posed.
The review was restricted to studies published in English or German, which might have left out some relevant studies. "However, we replicated their search without language restriction and found no additional studies," Dr. Gee and Dr. Bigby reported.
The review included searches of two databases, but Dr. Gee and Dr. Bigby found two additional relevant studies when they searched additional databases. Both of these were observational studies, and both found a significant association between atopic dermatitis and ADHD symptoms, they noted.
The most important criticism of the review by Dr. Schmitt is that assessment of both atopic disease and ADHD was inconsistent across the various studies, and tended to rely on parent reporting rather than physician diagnoses. For example, only 1 of the 20 articles used Diagnostic and Statistical Manual criteria for an ADHD diagnosis.
Such shortcomings should be addressed in any future research of the issue, Dr. Gee and Dr. Bigby said.
No financial conflicts of interest were reported.
Evidence suggests that a strong positive correlation exists between atopic disease and attention-deficit/hyperactivity disorder. But since all studies of the issue to date have been observational, "a causal relationship cannot be inferred," according to a research commentary in the August issue of the Archives of Dermatology.
"Further epidemiologic studies that use consistent and validated measures to more accurately define atopic disease and ADHD and adjust for confounders and disease severity are needed to better elucidate this relationship," said Dr. Sarah N. Gee and Dr. Michael Bigby of the departments of dermatology at Harvard Medical School and Beth Israel Deaconess Medical Center, both in Boston (Arch. Dermatol. 2011;147:967-70).
Dr. Gee and Dr. Bigby commented on a review of the literature presented by Dr. Jochen Schmitt and colleagues in the journal Allergy, which was titled: "Is atopic disease a risk factor for attention-deficit/hyperactivity disorder?" A systematic review (Allergy 2010;65:1506-24). That review covered 20 studies – 1 cohort study, 2 case-control studies, and 17 cross-sectional studies – involving 170,175 patients with eczema, asthma, rhinitis, or atopic dermatitis who also had ADHD symptoms. The studies reviewed had been conducted around the world, including in Germany and in other parts of Europe, and in North America, Australia, and New Zealand. All except one of the studies focused on children and adolescents.
"Four of the six studies that investigated eczema and ADHD found a statistically significant positive association, two with an odds ratio greater than four. Two of the three studies that used multivariate logistic regression for confounding factors found a statistically significant positive relationship between atopic dermatitis and ADHD. [And] with respect to asthma, all 12 studies that investigated asthma and ADHD reported a positive association ([odds ratio], 1.23-2.42)," Dr. Gee and Dr. Bigby said.
However, two studies that examined a possible link between allergic rhinitis and ADHD found no correlations.
The review by Dr. Schmitt fulfilled most of the criteria laid out by the Centre for Evidence-Based Medicine’s guidelines for "a useful and valid review." The choice of articles to include was appropriate, and the data were sufficient to answer the clinical question they posed.
The review was restricted to studies published in English or German, which might have left out some relevant studies. "However, we replicated their search without language restriction and found no additional studies," Dr. Gee and Dr. Bigby reported.
The review included searches of two databases, but Dr. Gee and Dr. Bigby found two additional relevant studies when they searched additional databases. Both of these were observational studies, and both found a significant association between atopic dermatitis and ADHD symptoms, they noted.
The most important criticism of the review by Dr. Schmitt is that assessment of both atopic disease and ADHD was inconsistent across the various studies, and tended to rely on parent reporting rather than physician diagnoses. For example, only 1 of the 20 articles used Diagnostic and Statistical Manual criteria for an ADHD diagnosis.
Such shortcomings should be addressed in any future research of the issue, Dr. Gee and Dr. Bigby said.
No financial conflicts of interest were reported.
Evidence suggests that a strong positive correlation exists between atopic disease and attention-deficit/hyperactivity disorder. But since all studies of the issue to date have been observational, "a causal relationship cannot be inferred," according to a research commentary in the August issue of the Archives of Dermatology.
"Further epidemiologic studies that use consistent and validated measures to more accurately define atopic disease and ADHD and adjust for confounders and disease severity are needed to better elucidate this relationship," said Dr. Sarah N. Gee and Dr. Michael Bigby of the departments of dermatology at Harvard Medical School and Beth Israel Deaconess Medical Center, both in Boston (Arch. Dermatol. 2011;147:967-70).
Dr. Gee and Dr. Bigby commented on a review of the literature presented by Dr. Jochen Schmitt and colleagues in the journal Allergy, which was titled: "Is atopic disease a risk factor for attention-deficit/hyperactivity disorder?" A systematic review (Allergy 2010;65:1506-24). That review covered 20 studies – 1 cohort study, 2 case-control studies, and 17 cross-sectional studies – involving 170,175 patients with eczema, asthma, rhinitis, or atopic dermatitis who also had ADHD symptoms. The studies reviewed had been conducted around the world, including in Germany and in other parts of Europe, and in North America, Australia, and New Zealand. All except one of the studies focused on children and adolescents.
"Four of the six studies that investigated eczema and ADHD found a statistically significant positive association, two with an odds ratio greater than four. Two of the three studies that used multivariate logistic regression for confounding factors found a statistically significant positive relationship between atopic dermatitis and ADHD. [And] with respect to asthma, all 12 studies that investigated asthma and ADHD reported a positive association ([odds ratio], 1.23-2.42)," Dr. Gee and Dr. Bigby said.
However, two studies that examined a possible link between allergic rhinitis and ADHD found no correlations.
The review by Dr. Schmitt fulfilled most of the criteria laid out by the Centre for Evidence-Based Medicine’s guidelines for "a useful and valid review." The choice of articles to include was appropriate, and the data were sufficient to answer the clinical question they posed.
The review was restricted to studies published in English or German, which might have left out some relevant studies. "However, we replicated their search without language restriction and found no additional studies," Dr. Gee and Dr. Bigby reported.
The review included searches of two databases, but Dr. Gee and Dr. Bigby found two additional relevant studies when they searched additional databases. Both of these were observational studies, and both found a significant association between atopic dermatitis and ADHD symptoms, they noted.
The most important criticism of the review by Dr. Schmitt is that assessment of both atopic disease and ADHD was inconsistent across the various studies, and tended to rely on parent reporting rather than physician diagnoses. For example, only 1 of the 20 articles used Diagnostic and Statistical Manual criteria for an ADHD diagnosis.
Such shortcomings should be addressed in any future research of the issue, Dr. Gee and Dr. Bigby said.
No financial conflicts of interest were reported.
FROM THE ARCHIVES OF DERMATOLOGY
Major Finding: Of three studies that examined a possible correlation between atopic dermatitis and ADHD, two found a correlation; of six studies that examined a possible correlation between eczema and ADHD, four found a strong correlation; and of 12 studies that examined a possible correlation between asthma and ADHD, all 12 found a correlation.
Data Source: A commentary on a review of the literature examining the link between atopic disease and ADHD.
Disclosures: No financial conflicts of interest were reported.
AAD: Untangling the Web of Eczema and Food Allergies
NEW YORK – Children with atopic dermatitis have a high risk of food allergies – although these allergies are not always easy to pinpoint.
"In this population, up to 20% of [those] with mild to moderate atopic dermatitis and 30%-40% of the severe patients will have a true food allergy," that can be confirmed with an open food challenge. Dr. Lawrence F. Eichenfield said at the American Academy of Dermatology’s 2010 meeting.
However, he said, positive skin prick testing – a common form of allergen identification – isn’t a very accurate way to detect the allergies. As a result, parents of children with atopic dermatitis (AD) will frequently state that their child has a food allergy, when, in fact, none exists.
A new national guideline helps clarify that issue, he said. Published in late 2010, "Guidelines for the Diagnosis and Management of Food Allergy in the United States," from the National Institute of Allergy and Infectious Diseases, provides some helpful information for dermatologists trying to make the AD/food allergy connection.
The document defines a food allergy as an adverse health effect arising from a specific immune response that occurs reproducibly on exposure to a given food. Skin prick testing, however, can only identify sensitization to a food, which doesn’t necessarily correlate with a clinical event, said Dr. Eichenfield, a professor of clinical pediatrics and dermatology at the University of California, San Diego.
"It’s very clearly written in the guidelines that an individual can develop allergic sensitization without having clinical symptoms on exposure to the food. Therefore, skin testing is not sufficient to say there is a food allergy."
Nevertheless, a common clinical scenario in the pediatric dermatology office is a parent who claims the child is allergic to a given food – most often eggs, soy, milk, wheat, or peanuts – because of a positive skin test. "What people don’t understand is, these tests are neither very sensitive nor specific," he said.
The specificity of skin prick testing hovers at about 85%, while the sensitivity is around 75%. "That means if we assume a 5% true milk allergy in a group of 1,000 people, skin prick testing will identify 42 of the 50 with a true allergy, miss 8 of those with the allergy, and give a false positive result to 238 people without the allergy," he said. "It’s a problem when you start labeling someone as having an allergy with just a positive test, but no clinical indicator."
The national guidelines stress that both family history and AD are risk factors for food allergy. The report suggests that children younger than 5 years who have moderate to severe AD that is uncontrolled despite optimal treatment, should be tested for allergies to milk, egg, peanut, soy and wheat. A positive, reliable history of a clinical reaction immediately after exposure to a specific food is also grounds for an investigation, according to the report.
Oral food challenge is probably the best way to determine a true food allergy, but can only be carried out in an environment set up to cope with severe reactions – usually an allergist’ s office. The good news is that the common overrepresentation of "food allergies" among children with AD means that many can safely consume foods that have been, literally, taken off the table.
A 2010 retrospective study looked at 125 children with atopic dermatitis, 44 of whom had suspected allergies to a variety of foods. All of them underwent oral food challenges. At baseline, there were 111 reports of food avoidance due to positive skin prick testing – foods included egg, fruit, meat, vegetables, milk, soy, wheat, shellfish, oats, and peanuts (J. Pediatr. 2010;158:578-83).
"Except for wheat, 80% or more of the oral food challenges were negative to the foods being avoided," wrote Dr. David M. Fleisher of the University of Colorado, Denver, and colleagues. This study was funded by National Jewish Health and the authors declared no conflicts. The only positive reactions were for egg, banana, peanut, soy, and wheat.
"Depending on the reason for avoidance, 84%-93% of the foods being avoided were successfully reintroduced into the diet," Dr. Eichenfield said.
The new management guidelines have affected the way he assesses AD patients, Dr. Eichenfield added. "Now I ask about food allergy reactions. If I find anything positive, I take a very detailed history, including the type of reaction, the time course, and the consistency of it after exposure to the food. Many times, just by asking, you will uncover a very significant reaction, like contact dermatitis, urticaria, or even anaphylaxis."
The guidelines note that anaphylaxis can be a real - and life-threatening – complication of food allergy. Parents of children with a proven food allergy should be experts in avoiding the food and in emergency management. "The standard management is to write a prescription for an Epi-Pen and make sure they know how to use it," Dr. Eichenfield said.
He’s also more likely to refer children with moderate to severe AD and persistent flares for testing now. "I am more liberal about using the allergist to evaluate these patients, with the understanding that a positive test may not change the eczema, but with the hope that if there is an avenue that might help, it’s one we want to explore."
Dr. Eichenfield had no financial disclosures.
NEW YORK – Children with atopic dermatitis have a high risk of food allergies – although these allergies are not always easy to pinpoint.
"In this population, up to 20% of [those] with mild to moderate atopic dermatitis and 30%-40% of the severe patients will have a true food allergy," that can be confirmed with an open food challenge. Dr. Lawrence F. Eichenfield said at the American Academy of Dermatology’s 2010 meeting.
However, he said, positive skin prick testing – a common form of allergen identification – isn’t a very accurate way to detect the allergies. As a result, parents of children with atopic dermatitis (AD) will frequently state that their child has a food allergy, when, in fact, none exists.
A new national guideline helps clarify that issue, he said. Published in late 2010, "Guidelines for the Diagnosis and Management of Food Allergy in the United States," from the National Institute of Allergy and Infectious Diseases, provides some helpful information for dermatologists trying to make the AD/food allergy connection.
The document defines a food allergy as an adverse health effect arising from a specific immune response that occurs reproducibly on exposure to a given food. Skin prick testing, however, can only identify sensitization to a food, which doesn’t necessarily correlate with a clinical event, said Dr. Eichenfield, a professor of clinical pediatrics and dermatology at the University of California, San Diego.
"It’s very clearly written in the guidelines that an individual can develop allergic sensitization without having clinical symptoms on exposure to the food. Therefore, skin testing is not sufficient to say there is a food allergy."
Nevertheless, a common clinical scenario in the pediatric dermatology office is a parent who claims the child is allergic to a given food – most often eggs, soy, milk, wheat, or peanuts – because of a positive skin test. "What people don’t understand is, these tests are neither very sensitive nor specific," he said.
The specificity of skin prick testing hovers at about 85%, while the sensitivity is around 75%. "That means if we assume a 5% true milk allergy in a group of 1,000 people, skin prick testing will identify 42 of the 50 with a true allergy, miss 8 of those with the allergy, and give a false positive result to 238 people without the allergy," he said. "It’s a problem when you start labeling someone as having an allergy with just a positive test, but no clinical indicator."
The national guidelines stress that both family history and AD are risk factors for food allergy. The report suggests that children younger than 5 years who have moderate to severe AD that is uncontrolled despite optimal treatment, should be tested for allergies to milk, egg, peanut, soy and wheat. A positive, reliable history of a clinical reaction immediately after exposure to a specific food is also grounds for an investigation, according to the report.
Oral food challenge is probably the best way to determine a true food allergy, but can only be carried out in an environment set up to cope with severe reactions – usually an allergist’ s office. The good news is that the common overrepresentation of "food allergies" among children with AD means that many can safely consume foods that have been, literally, taken off the table.
A 2010 retrospective study looked at 125 children with atopic dermatitis, 44 of whom had suspected allergies to a variety of foods. All of them underwent oral food challenges. At baseline, there were 111 reports of food avoidance due to positive skin prick testing – foods included egg, fruit, meat, vegetables, milk, soy, wheat, shellfish, oats, and peanuts (J. Pediatr. 2010;158:578-83).
"Except for wheat, 80% or more of the oral food challenges were negative to the foods being avoided," wrote Dr. David M. Fleisher of the University of Colorado, Denver, and colleagues. This study was funded by National Jewish Health and the authors declared no conflicts. The only positive reactions were for egg, banana, peanut, soy, and wheat.
"Depending on the reason for avoidance, 84%-93% of the foods being avoided were successfully reintroduced into the diet," Dr. Eichenfield said.
The new management guidelines have affected the way he assesses AD patients, Dr. Eichenfield added. "Now I ask about food allergy reactions. If I find anything positive, I take a very detailed history, including the type of reaction, the time course, and the consistency of it after exposure to the food. Many times, just by asking, you will uncover a very significant reaction, like contact dermatitis, urticaria, or even anaphylaxis."
The guidelines note that anaphylaxis can be a real - and life-threatening – complication of food allergy. Parents of children with a proven food allergy should be experts in avoiding the food and in emergency management. "The standard management is to write a prescription for an Epi-Pen and make sure they know how to use it," Dr. Eichenfield said.
He’s also more likely to refer children with moderate to severe AD and persistent flares for testing now. "I am more liberal about using the allergist to evaluate these patients, with the understanding that a positive test may not change the eczema, but with the hope that if there is an avenue that might help, it’s one we want to explore."
Dr. Eichenfield had no financial disclosures.
NEW YORK – Children with atopic dermatitis have a high risk of food allergies – although these allergies are not always easy to pinpoint.
"In this population, up to 20% of [those] with mild to moderate atopic dermatitis and 30%-40% of the severe patients will have a true food allergy," that can be confirmed with an open food challenge. Dr. Lawrence F. Eichenfield said at the American Academy of Dermatology’s 2010 meeting.
However, he said, positive skin prick testing – a common form of allergen identification – isn’t a very accurate way to detect the allergies. As a result, parents of children with atopic dermatitis (AD) will frequently state that their child has a food allergy, when, in fact, none exists.
A new national guideline helps clarify that issue, he said. Published in late 2010, "Guidelines for the Diagnosis and Management of Food Allergy in the United States," from the National Institute of Allergy and Infectious Diseases, provides some helpful information for dermatologists trying to make the AD/food allergy connection.
The document defines a food allergy as an adverse health effect arising from a specific immune response that occurs reproducibly on exposure to a given food. Skin prick testing, however, can only identify sensitization to a food, which doesn’t necessarily correlate with a clinical event, said Dr. Eichenfield, a professor of clinical pediatrics and dermatology at the University of California, San Diego.
"It’s very clearly written in the guidelines that an individual can develop allergic sensitization without having clinical symptoms on exposure to the food. Therefore, skin testing is not sufficient to say there is a food allergy."
Nevertheless, a common clinical scenario in the pediatric dermatology office is a parent who claims the child is allergic to a given food – most often eggs, soy, milk, wheat, or peanuts – because of a positive skin test. "What people don’t understand is, these tests are neither very sensitive nor specific," he said.
The specificity of skin prick testing hovers at about 85%, while the sensitivity is around 75%. "That means if we assume a 5% true milk allergy in a group of 1,000 people, skin prick testing will identify 42 of the 50 with a true allergy, miss 8 of those with the allergy, and give a false positive result to 238 people without the allergy," he said. "It’s a problem when you start labeling someone as having an allergy with just a positive test, but no clinical indicator."
The national guidelines stress that both family history and AD are risk factors for food allergy. The report suggests that children younger than 5 years who have moderate to severe AD that is uncontrolled despite optimal treatment, should be tested for allergies to milk, egg, peanut, soy and wheat. A positive, reliable history of a clinical reaction immediately after exposure to a specific food is also grounds for an investigation, according to the report.
Oral food challenge is probably the best way to determine a true food allergy, but can only be carried out in an environment set up to cope with severe reactions – usually an allergist’ s office. The good news is that the common overrepresentation of "food allergies" among children with AD means that many can safely consume foods that have been, literally, taken off the table.
A 2010 retrospective study looked at 125 children with atopic dermatitis, 44 of whom had suspected allergies to a variety of foods. All of them underwent oral food challenges. At baseline, there were 111 reports of food avoidance due to positive skin prick testing – foods included egg, fruit, meat, vegetables, milk, soy, wheat, shellfish, oats, and peanuts (J. Pediatr. 2010;158:578-83).
"Except for wheat, 80% or more of the oral food challenges were negative to the foods being avoided," wrote Dr. David M. Fleisher of the University of Colorado, Denver, and colleagues. This study was funded by National Jewish Health and the authors declared no conflicts. The only positive reactions were for egg, banana, peanut, soy, and wheat.
"Depending on the reason for avoidance, 84%-93% of the foods being avoided were successfully reintroduced into the diet," Dr. Eichenfield said.
The new management guidelines have affected the way he assesses AD patients, Dr. Eichenfield added. "Now I ask about food allergy reactions. If I find anything positive, I take a very detailed history, including the type of reaction, the time course, and the consistency of it after exposure to the food. Many times, just by asking, you will uncover a very significant reaction, like contact dermatitis, urticaria, or even anaphylaxis."
The guidelines note that anaphylaxis can be a real - and life-threatening – complication of food allergy. Parents of children with a proven food allergy should be experts in avoiding the food and in emergency management. "The standard management is to write a prescription for an Epi-Pen and make sure they know how to use it," Dr. Eichenfield said.
He’s also more likely to refer children with moderate to severe AD and persistent flares for testing now. "I am more liberal about using the allergist to evaluate these patients, with the understanding that a positive test may not change the eczema, but with the hope that if there is an avenue that might help, it’s one we want to explore."
Dr. Eichenfield had no financial disclosures.
EXPERT ANALYSIS FROM THE AMERICAN ACADEMY OF DERMATOLOGY'S SUMMER ACADEMY MEETING
Contact Dermatitis May Protect Patients From Cancer
Patients with a history of contact allergies may be less likely to develop nonmelanoma skin cancer, brain cancer, and breast cancer, a study has shown.
In research published online July 11 in BMJ Open (doi:10.1136/bmjopen-2011-000084), investigators conversely found diagnoses of bladder cancer more likely in people with a history of contact allergies.
Any protective effects could possibly be explained by the stimulation of natural killer T (NKT) cells through contact allergic reactions, the observational study’s lead author, Kaare Engkilde, Ph.D., of the national allergy research center at Copenhagen University Hospital, said in an interview. "You would probably think that [contact allergy] could lead to skin cancer, but that is not what we found," Dr. Engkilde said.
Contact allergic reactions are delayed reactions caused by chemicals small enough to penetrate the skin – triggers can include perfumes, hair dyes, cobalt, nickel, and formaldehyde. Animal studies have shown that contact allergens have the ability to increase the number of NKT cells, at least temporarily, Dr. Engkilde said.
For their research, Dr. Engkilde and his colleagues used a database of 16,922 Danish patients patch tested for type IV allergies between 1984 and 2008. Of these, 6,065 (35.8%) had at least one positive reaction (26.1% of men, 41.4% of women). Linkage with the Danish Cancer Registry showed 3,200, or 18.9%, of dermatitis patients had a benign tumor, a malignant cancer diagnosis, or both, and 1,207 (37.7%) of these patients had had a positive patch test reaction.
Dr. Engkilde and his colleagues looked specifically at 15 types of cancers, all of which affected at least 40 people in the study population.
The investigators found an inverse association between diagnosed contact allergy and nonmelanoma skin cancer (OR, 0.82) along with breast cancer (OR, 0.80) among both men and women. Dr. Engkilde and his colleagues also noted an inverse trend for brain cancer among women with contact allergies, though the P value was above.05 (OR, 0.36).
The findings related to nonmelanoma skin cancers were on some level expected, Dr. Engkilde said; however, the researchers said they were surprised not to see any protective effect against melanomas.
Dr. Engkilde said his group had no hypothesis for the inverse breast cancer finding, but noted that an earlier study had found that self-reported perfume allergy, a type IV allergy, was related inversely to brain cancer incidence (Am. J. Epidemiol. 2007;166:941-50).
The positive association between contact allergy and bladder cancer (OR, 1.44) was more likely related to accumulations of chemical metabolites of type IV allergens in the bladder than to an effect on NKT cells or another immune response, the investigators said.
They cautioned that the relationships between type IV reactions and cancers were "uncertain and not necessarily the result of causality," and that future analyses would have to adjust for social class and smoking, as the latter can increase the risk of developing nickel contact allergies and several types of cancer.
Also, they wrote, "studies focusing on specific chemical exposures are required to further our understanding of the role of contact allergies in the development of cancer." However, if the relationships are in fact etiologic, the findings have "implications for understanding how contact allergy can affect cancer development and vice versa," they said.
Dr. Engkilde and his coauthors received research support from Aage Bang’s Foundation and the Capital Region’s Research Foundation, and disclosed no competing interests.
Patients with a history of contact allergies may be less likely to develop nonmelanoma skin cancer, brain cancer, and breast cancer, a study has shown.
In research published online July 11 in BMJ Open (doi:10.1136/bmjopen-2011-000084), investigators conversely found diagnoses of bladder cancer more likely in people with a history of contact allergies.
Any protective effects could possibly be explained by the stimulation of natural killer T (NKT) cells through contact allergic reactions, the observational study’s lead author, Kaare Engkilde, Ph.D., of the national allergy research center at Copenhagen University Hospital, said in an interview. "You would probably think that [contact allergy] could lead to skin cancer, but that is not what we found," Dr. Engkilde said.
Contact allergic reactions are delayed reactions caused by chemicals small enough to penetrate the skin – triggers can include perfumes, hair dyes, cobalt, nickel, and formaldehyde. Animal studies have shown that contact allergens have the ability to increase the number of NKT cells, at least temporarily, Dr. Engkilde said.
For their research, Dr. Engkilde and his colleagues used a database of 16,922 Danish patients patch tested for type IV allergies between 1984 and 2008. Of these, 6,065 (35.8%) had at least one positive reaction (26.1% of men, 41.4% of women). Linkage with the Danish Cancer Registry showed 3,200, or 18.9%, of dermatitis patients had a benign tumor, a malignant cancer diagnosis, or both, and 1,207 (37.7%) of these patients had had a positive patch test reaction.
Dr. Engkilde and his colleagues looked specifically at 15 types of cancers, all of which affected at least 40 people in the study population.
The investigators found an inverse association between diagnosed contact allergy and nonmelanoma skin cancer (OR, 0.82) along with breast cancer (OR, 0.80) among both men and women. Dr. Engkilde and his colleagues also noted an inverse trend for brain cancer among women with contact allergies, though the P value was above.05 (OR, 0.36).
The findings related to nonmelanoma skin cancers were on some level expected, Dr. Engkilde said; however, the researchers said they were surprised not to see any protective effect against melanomas.
Dr. Engkilde said his group had no hypothesis for the inverse breast cancer finding, but noted that an earlier study had found that self-reported perfume allergy, a type IV allergy, was related inversely to brain cancer incidence (Am. J. Epidemiol. 2007;166:941-50).
The positive association between contact allergy and bladder cancer (OR, 1.44) was more likely related to accumulations of chemical metabolites of type IV allergens in the bladder than to an effect on NKT cells or another immune response, the investigators said.
They cautioned that the relationships between type IV reactions and cancers were "uncertain and not necessarily the result of causality," and that future analyses would have to adjust for social class and smoking, as the latter can increase the risk of developing nickel contact allergies and several types of cancer.
Also, they wrote, "studies focusing on specific chemical exposures are required to further our understanding of the role of contact allergies in the development of cancer." However, if the relationships are in fact etiologic, the findings have "implications for understanding how contact allergy can affect cancer development and vice versa," they said.
Dr. Engkilde and his coauthors received research support from Aage Bang’s Foundation and the Capital Region’s Research Foundation, and disclosed no competing interests.
Patients with a history of contact allergies may be less likely to develop nonmelanoma skin cancer, brain cancer, and breast cancer, a study has shown.
In research published online July 11 in BMJ Open (doi:10.1136/bmjopen-2011-000084), investigators conversely found diagnoses of bladder cancer more likely in people with a history of contact allergies.
Any protective effects could possibly be explained by the stimulation of natural killer T (NKT) cells through contact allergic reactions, the observational study’s lead author, Kaare Engkilde, Ph.D., of the national allergy research center at Copenhagen University Hospital, said in an interview. "You would probably think that [contact allergy] could lead to skin cancer, but that is not what we found," Dr. Engkilde said.
Contact allergic reactions are delayed reactions caused by chemicals small enough to penetrate the skin – triggers can include perfumes, hair dyes, cobalt, nickel, and formaldehyde. Animal studies have shown that contact allergens have the ability to increase the number of NKT cells, at least temporarily, Dr. Engkilde said.
For their research, Dr. Engkilde and his colleagues used a database of 16,922 Danish patients patch tested for type IV allergies between 1984 and 2008. Of these, 6,065 (35.8%) had at least one positive reaction (26.1% of men, 41.4% of women). Linkage with the Danish Cancer Registry showed 3,200, or 18.9%, of dermatitis patients had a benign tumor, a malignant cancer diagnosis, or both, and 1,207 (37.7%) of these patients had had a positive patch test reaction.
Dr. Engkilde and his colleagues looked specifically at 15 types of cancers, all of which affected at least 40 people in the study population.
The investigators found an inverse association between diagnosed contact allergy and nonmelanoma skin cancer (OR, 0.82) along with breast cancer (OR, 0.80) among both men and women. Dr. Engkilde and his colleagues also noted an inverse trend for brain cancer among women with contact allergies, though the P value was above.05 (OR, 0.36).
The findings related to nonmelanoma skin cancers were on some level expected, Dr. Engkilde said; however, the researchers said they were surprised not to see any protective effect against melanomas.
Dr. Engkilde said his group had no hypothesis for the inverse breast cancer finding, but noted that an earlier study had found that self-reported perfume allergy, a type IV allergy, was related inversely to brain cancer incidence (Am. J. Epidemiol. 2007;166:941-50).
The positive association between contact allergy and bladder cancer (OR, 1.44) was more likely related to accumulations of chemical metabolites of type IV allergens in the bladder than to an effect on NKT cells or another immune response, the investigators said.
They cautioned that the relationships between type IV reactions and cancers were "uncertain and not necessarily the result of causality," and that future analyses would have to adjust for social class and smoking, as the latter can increase the risk of developing nickel contact allergies and several types of cancer.
Also, they wrote, "studies focusing on specific chemical exposures are required to further our understanding of the role of contact allergies in the development of cancer." However, if the relationships are in fact etiologic, the findings have "implications for understanding how contact allergy can affect cancer development and vice versa," they said.
Dr. Engkilde and his coauthors received research support from Aage Bang’s Foundation and the Capital Region’s Research Foundation, and disclosed no competing interests.
FROM BMJ OPEN
Major Finding: The investigators found an inverse association between diagnosed contact allergy and nonmelanoma skin cancer (OR, 0.82) along with breast cancer (OR, 0.80) among both men and women.
Data Source: A database of 16,922 Danish patients patch tested for type IV allergies between 1984 and 2008.
Disclosures: Dr. Engkilde and his coauthors received research support from Aage Bang's Foundation and the Capital Region’s Research Foundation, and disclosed no competing interests.