User login
Peppermint and menthol
Mentha piperita, better known as peppermint, is used worldwide in many ways. Its use for culinary and medical purposes dates back to the ancient Greek and Roman civilizations. Peppermint is used in numerous forms (i.e., oil, leaf, leaf extract, and leaf water), with the oil as the most versatile (Dermatitis 2010;21:327-9). Peppermint has long been known for its beneficial gastrointestinal effects, and it has a well-established record of antimicrobial, antifungal, and analgesic activity (Mills S., Bone K. Principles and Practice of Phytotherapy: Modern Herbal Medicine. [London: Churchill Livingstone, 2000, pp 507-13]; J. Environ. Biol. 2011;32:23-9).
Menthol (C10H20O) is a naturally occurring monocyclic terpene alcohol derived from Mentha piperita as well as other mint oils (Skin Therapy Lett. 2010;15:5-9), and has been associated with several health benefits. Recently, anticancer properties have been ascribed to menthol (Biochim. Biophys. Acta 2009;1792:33-8). This column will discuss recent findings regarding the actual or potential cutaneous benefits of peppermint and menthol.
Various Mentha species, including M. piperita, have exhibited significant antioxidant activity (Toxicol. Ind. Health. 2012;28:83-9; Nat. Prod. Commun. 2009;4:1107-12; Nat. Prod. Commun. 2009;4:535-42). In a 2010 study of the antioxidant activity of the essential oils of six popular herbs, including lavender (Lavendular angustifolia), peppermint (M. piperita), rosemary (Rosmarius officinalis), lemon (Citrus limon), grapefruit (C. paradise), and frankincense (Boswellia carteri), investigators found, in testing free radical-scavenging capacity and lipid peroxidation in the linoleic acid system, that peppermint essential oil exhibited the greatest radical-scavenging activity against the 2,2\'-azinobis-(3-ethylbenzothiazoline-6-sulfonic acid) ABTS radical (Nat. Prod. Res. 2010;24:140-51).
In 2010, Baliga and Rao showed that M. piperita and M. arvensis (wild mint) protected mice against gamma-radiation–induced morbidity and mortality. Specifically, M. piperita protected murine testes as well as gastrointestinal and hemopoietic systems (J. Cancer Res. Ther. 2010;6:255-62).
Anticancer activity
Investigations by Jain et al. into the molecular mechanisms supporting the anticarcinogenic potential of M. piperita leaf extracts on six human cancer cell lines (HeLa, MCF-7, Jurkat, T24, HT-29, MIAPaCa-2) in 2011 revealed that chloroform and ethyl acetate extracts dose- and time-dependently displayed anticarcinogenic activity leading to G1 cell cycle arrest and mitochondrial-mediated apoptosis among the cascade of effects. The investigators identified their findings as the first evidence of direct anticarcinogenic activity of Mentha leaf extracts and suggested that future work might focus on isolating active constituents as a foundation for mechanistic and translational studies leading to new anticancer drugs, alone or in combination, to prevent and treat human cancers (Int. J. Toxicol. 2011;30:225-36).
Topical benefits of menthol
In a recent examination of the antibacterial and antifungal properties, as well as speculated anti-inflammatory activity of menthol as a topical treatment for diaper dermatitis, investigators conducted a pilot clinical trial in a hospital setting. The study involved 84 neonates with diagnosed candidal diaper dermatitis who required no critical care or systemic antifungal and anti-inflammatory medications. The menthol group (n = 42) received topical clotrimazole and topically applied menthol drops and the control group (n = 42) received topical clotrimazole and a placebo. Thirty-five infants in each group completed the study. The researchers found that complete healing was shorter in the menthol group, with significant relief of erythema and pustules observed in this group. They concluded that topically-applied menthol may be an effective agent in the treatment of candidal diaper dermatitis (World J. Pediatr. 2011;7:167-70).
In 2011, Qiu et al. showed, through various assays, that menthol, in low concentrations, could significantly suppress the expression of alpha-hemolysin, enterotoxins A and B, and toxic shock syndrome toxin 1 in Staphylococcus aureus. The investigators concluded that menthol may warrant inclusion in the armamentarium against S. aureus when combined with beta-lactam antibiotics, which, at subinhibitory concentrations, can actually augment S. aureus toxin secretion. They added that menthol may also have possible uses in novel anti-virulence drugs (Appl. Microbiol. Biotechnol. 2011;90:705-12). It should be noted that menthol is considered safe and effective, with concentrations up to 16% approved in OTC external products by the Food and Drug Administration (J. Am. Acad. Dermatol. 2007;57:873-8).
Pruritus, TRPM8, and melanoma
Topically applied menthol, in concentrations of 1%-3%, is often used to treat pruritus, particularly in the elderly (Skin Therapy Lett. 2010;15:5-9). In addition, recent evidence suggests that the presence of menthol can facilitate penetration of other agents in topical products (Int. J. Toxicol. 2001;20 Suppl 3:61-73; J. Am. Acad. Dermatol. 2007;57:873-8). Patel and Yosipovitch suggest that elderly patients who report diminished pruritus with cooling may stand to benefit from menthol-containing topical therapies (J. Am. Acad. Dermatol. 2007;57:873-8; Skin Therapy Lett. 2010;15:5-9). Interestingly, menthol, via the transient receptor potential melastatin subfamily 8 (TRPM8) receptor, a member of a family of excitatory ion channels, engenders the same cooling sensation as low temperature, though menthol is not linked to a reduction in skin temperature (J. Am. Acad. Dermatol. 2007;57:873-8; Skin Therapy Lett. 2010;15:5-9).
Although the exact mechanism by which menthol exerts its antipruritic and analgesic effects has yet to be determined, the discovery that the TRPM8 is its underlying receptor is proving to be significant, particularly in understanding the cooling effect of the botanical (J. Am. Acad. Dermatol. 2007;57:873-8). There are also indications that menthol has therapeutic potential for melanoma. Specifically, melanoma expresses TRPM8 receptors, the activation of which inhibits melanoma viability. Menthol appears to mediate this response through an influx of extracellular calcium ions (Am. J. Physiol. Cell Physiol. 2008;295:C296-301; Am. J. Physiol. Cell Physiol. 2008;295:C293-5).
Peppermint oil
In 2003, Schuhmacher et al. investigated the virucidal effect of peppermint oil and found that it had a direct effect against herpes simplex virus type 1 (HSV-1) and herpes simplex virus type 2 (HSV-2) as well as an acyclovir-resistant HSV-1 strain. The investigators concluded, noting the lipophilic nature of peppermint oil, that it might be an appropriate topical treatment for recurrent herpes outbreaks (Phytomedicine 2003;10:504-10).
Because of its flavor, aroma, and cooling qualities, peppermint oil is used in a wide range of products, including cosmeceuticals, personal hygiene products (e.g., bath preparations, mouthwashes, toothpastes, and topical formulations), foods, pharmaceutical products, and aromatherapy. Topical indications include pruritus, irritation, and inflammation. Peppermint oil can act as a skin sensitizer, though, particularly in impaired and sensitive skin (Dermatitis 2010;21:327-9). Although peppermint oil has been reported to be a sensitizer in isolated cases, peppermint oil 8% was not found to be a sensitizer in a recent test using a maximization protocol and the various forms of peppermint (i.e., oil, extract, leaves, and water) are considered to be safe in cosmetic formulations. In rinse-off products, peppermint oil is used in concentrations up to 3% and up to 0.2% in leave-on formulations (Int. J. Toxicol. 2001;20 Suppl 3:61-73).
Conclusion
Peppermint and menthol, its naturally occurring monocyclic terpene alcohol derivative, have long been used for medical purposes. Contemporary practice and continuing research continue to support various uses of M. piperita in the medical armamentarium, with specific and additional uses continually being found in the dermatologic realm.
Dr. Baumann is chief executive officer of the Baumann Cosmetic & Research Institute in Miami Beach. She founded the cosmetic dermatology center at the University of Miami in 1997. Dr. Baumann wrote the textbook "Cosmetic Dermatology: Principles and Practice" (McGraw-Hill, April 2002), and a book for consumers, "The Skin Type Solution" (Bantam, 2006). She has contributed to the Cosmeceutical Critique column in Skin & Allergy News since January 2001 and joined the editorial advisory board in 2004. Dr. Baumann has received funding for clinical grants from Allergan, Aveeno, Avon Products, Galderma, Mary Kay, Medicis Pharmaceuticals, Neutrogena, Philosophy, Stiefel, Topix Pharmaceuticals, and Unilever.
Mentha piperita, better known as peppermint, is used worldwide in many ways. Its use for culinary and medical purposes dates back to the ancient Greek and Roman civilizations. Peppermint is used in numerous forms (i.e., oil, leaf, leaf extract, and leaf water), with the oil as the most versatile (Dermatitis 2010;21:327-9). Peppermint has long been known for its beneficial gastrointestinal effects, and it has a well-established record of antimicrobial, antifungal, and analgesic activity (Mills S., Bone K. Principles and Practice of Phytotherapy: Modern Herbal Medicine. [London: Churchill Livingstone, 2000, pp 507-13]; J. Environ. Biol. 2011;32:23-9).
Menthol (C10H20O) is a naturally occurring monocyclic terpene alcohol derived from Mentha piperita as well as other mint oils (Skin Therapy Lett. 2010;15:5-9), and has been associated with several health benefits. Recently, anticancer properties have been ascribed to menthol (Biochim. Biophys. Acta 2009;1792:33-8). This column will discuss recent findings regarding the actual or potential cutaneous benefits of peppermint and menthol.
Various Mentha species, including M. piperita, have exhibited significant antioxidant activity (Toxicol. Ind. Health. 2012;28:83-9; Nat. Prod. Commun. 2009;4:1107-12; Nat. Prod. Commun. 2009;4:535-42). In a 2010 study of the antioxidant activity of the essential oils of six popular herbs, including lavender (Lavendular angustifolia), peppermint (M. piperita), rosemary (Rosmarius officinalis), lemon (Citrus limon), grapefruit (C. paradise), and frankincense (Boswellia carteri), investigators found, in testing free radical-scavenging capacity and lipid peroxidation in the linoleic acid system, that peppermint essential oil exhibited the greatest radical-scavenging activity against the 2,2\'-azinobis-(3-ethylbenzothiazoline-6-sulfonic acid) ABTS radical (Nat. Prod. Res. 2010;24:140-51).
In 2010, Baliga and Rao showed that M. piperita and M. arvensis (wild mint) protected mice against gamma-radiation–induced morbidity and mortality. Specifically, M. piperita protected murine testes as well as gastrointestinal and hemopoietic systems (J. Cancer Res. Ther. 2010;6:255-62).
Anticancer activity
Investigations by Jain et al. into the molecular mechanisms supporting the anticarcinogenic potential of M. piperita leaf extracts on six human cancer cell lines (HeLa, MCF-7, Jurkat, T24, HT-29, MIAPaCa-2) in 2011 revealed that chloroform and ethyl acetate extracts dose- and time-dependently displayed anticarcinogenic activity leading to G1 cell cycle arrest and mitochondrial-mediated apoptosis among the cascade of effects. The investigators identified their findings as the first evidence of direct anticarcinogenic activity of Mentha leaf extracts and suggested that future work might focus on isolating active constituents as a foundation for mechanistic and translational studies leading to new anticancer drugs, alone or in combination, to prevent and treat human cancers (Int. J. Toxicol. 2011;30:225-36).
Topical benefits of menthol
In a recent examination of the antibacterial and antifungal properties, as well as speculated anti-inflammatory activity of menthol as a topical treatment for diaper dermatitis, investigators conducted a pilot clinical trial in a hospital setting. The study involved 84 neonates with diagnosed candidal diaper dermatitis who required no critical care or systemic antifungal and anti-inflammatory medications. The menthol group (n = 42) received topical clotrimazole and topically applied menthol drops and the control group (n = 42) received topical clotrimazole and a placebo. Thirty-five infants in each group completed the study. The researchers found that complete healing was shorter in the menthol group, with significant relief of erythema and pustules observed in this group. They concluded that topically-applied menthol may be an effective agent in the treatment of candidal diaper dermatitis (World J. Pediatr. 2011;7:167-70).
In 2011, Qiu et al. showed, through various assays, that menthol, in low concentrations, could significantly suppress the expression of alpha-hemolysin, enterotoxins A and B, and toxic shock syndrome toxin 1 in Staphylococcus aureus. The investigators concluded that menthol may warrant inclusion in the armamentarium against S. aureus when combined with beta-lactam antibiotics, which, at subinhibitory concentrations, can actually augment S. aureus toxin secretion. They added that menthol may also have possible uses in novel anti-virulence drugs (Appl. Microbiol. Biotechnol. 2011;90:705-12). It should be noted that menthol is considered safe and effective, with concentrations up to 16% approved in OTC external products by the Food and Drug Administration (J. Am. Acad. Dermatol. 2007;57:873-8).
Pruritus, TRPM8, and melanoma
Topically applied menthol, in concentrations of 1%-3%, is often used to treat pruritus, particularly in the elderly (Skin Therapy Lett. 2010;15:5-9). In addition, recent evidence suggests that the presence of menthol can facilitate penetration of other agents in topical products (Int. J. Toxicol. 2001;20 Suppl 3:61-73; J. Am. Acad. Dermatol. 2007;57:873-8). Patel and Yosipovitch suggest that elderly patients who report diminished pruritus with cooling may stand to benefit from menthol-containing topical therapies (J. Am. Acad. Dermatol. 2007;57:873-8; Skin Therapy Lett. 2010;15:5-9). Interestingly, menthol, via the transient receptor potential melastatin subfamily 8 (TRPM8) receptor, a member of a family of excitatory ion channels, engenders the same cooling sensation as low temperature, though menthol is not linked to a reduction in skin temperature (J. Am. Acad. Dermatol. 2007;57:873-8; Skin Therapy Lett. 2010;15:5-9).
Although the exact mechanism by which menthol exerts its antipruritic and analgesic effects has yet to be determined, the discovery that the TRPM8 is its underlying receptor is proving to be significant, particularly in understanding the cooling effect of the botanical (J. Am. Acad. Dermatol. 2007;57:873-8). There are also indications that menthol has therapeutic potential for melanoma. Specifically, melanoma expresses TRPM8 receptors, the activation of which inhibits melanoma viability. Menthol appears to mediate this response through an influx of extracellular calcium ions (Am. J. Physiol. Cell Physiol. 2008;295:C296-301; Am. J. Physiol. Cell Physiol. 2008;295:C293-5).
Peppermint oil
In 2003, Schuhmacher et al. investigated the virucidal effect of peppermint oil and found that it had a direct effect against herpes simplex virus type 1 (HSV-1) and herpes simplex virus type 2 (HSV-2) as well as an acyclovir-resistant HSV-1 strain. The investigators concluded, noting the lipophilic nature of peppermint oil, that it might be an appropriate topical treatment for recurrent herpes outbreaks (Phytomedicine 2003;10:504-10).
Because of its flavor, aroma, and cooling qualities, peppermint oil is used in a wide range of products, including cosmeceuticals, personal hygiene products (e.g., bath preparations, mouthwashes, toothpastes, and topical formulations), foods, pharmaceutical products, and aromatherapy. Topical indications include pruritus, irritation, and inflammation. Peppermint oil can act as a skin sensitizer, though, particularly in impaired and sensitive skin (Dermatitis 2010;21:327-9). Although peppermint oil has been reported to be a sensitizer in isolated cases, peppermint oil 8% was not found to be a sensitizer in a recent test using a maximization protocol and the various forms of peppermint (i.e., oil, extract, leaves, and water) are considered to be safe in cosmetic formulations. In rinse-off products, peppermint oil is used in concentrations up to 3% and up to 0.2% in leave-on formulations (Int. J. Toxicol. 2001;20 Suppl 3:61-73).
Conclusion
Peppermint and menthol, its naturally occurring monocyclic terpene alcohol derivative, have long been used for medical purposes. Contemporary practice and continuing research continue to support various uses of M. piperita in the medical armamentarium, with specific and additional uses continually being found in the dermatologic realm.
Dr. Baumann is chief executive officer of the Baumann Cosmetic & Research Institute in Miami Beach. She founded the cosmetic dermatology center at the University of Miami in 1997. Dr. Baumann wrote the textbook "Cosmetic Dermatology: Principles and Practice" (McGraw-Hill, April 2002), and a book for consumers, "The Skin Type Solution" (Bantam, 2006). She has contributed to the Cosmeceutical Critique column in Skin & Allergy News since January 2001 and joined the editorial advisory board in 2004. Dr. Baumann has received funding for clinical grants from Allergan, Aveeno, Avon Products, Galderma, Mary Kay, Medicis Pharmaceuticals, Neutrogena, Philosophy, Stiefel, Topix Pharmaceuticals, and Unilever.
Mentha piperita, better known as peppermint, is used worldwide in many ways. Its use for culinary and medical purposes dates back to the ancient Greek and Roman civilizations. Peppermint is used in numerous forms (i.e., oil, leaf, leaf extract, and leaf water), with the oil as the most versatile (Dermatitis 2010;21:327-9). Peppermint has long been known for its beneficial gastrointestinal effects, and it has a well-established record of antimicrobial, antifungal, and analgesic activity (Mills S., Bone K. Principles and Practice of Phytotherapy: Modern Herbal Medicine. [London: Churchill Livingstone, 2000, pp 507-13]; J. Environ. Biol. 2011;32:23-9).
Menthol (C10H20O) is a naturally occurring monocyclic terpene alcohol derived from Mentha piperita as well as other mint oils (Skin Therapy Lett. 2010;15:5-9), and has been associated with several health benefits. Recently, anticancer properties have been ascribed to menthol (Biochim. Biophys. Acta 2009;1792:33-8). This column will discuss recent findings regarding the actual or potential cutaneous benefits of peppermint and menthol.
Various Mentha species, including M. piperita, have exhibited significant antioxidant activity (Toxicol. Ind. Health. 2012;28:83-9; Nat. Prod. Commun. 2009;4:1107-12; Nat. Prod. Commun. 2009;4:535-42). In a 2010 study of the antioxidant activity of the essential oils of six popular herbs, including lavender (Lavendular angustifolia), peppermint (M. piperita), rosemary (Rosmarius officinalis), lemon (Citrus limon), grapefruit (C. paradise), and frankincense (Boswellia carteri), investigators found, in testing free radical-scavenging capacity and lipid peroxidation in the linoleic acid system, that peppermint essential oil exhibited the greatest radical-scavenging activity against the 2,2\'-azinobis-(3-ethylbenzothiazoline-6-sulfonic acid) ABTS radical (Nat. Prod. Res. 2010;24:140-51).
In 2010, Baliga and Rao showed that M. piperita and M. arvensis (wild mint) protected mice against gamma-radiation–induced morbidity and mortality. Specifically, M. piperita protected murine testes as well as gastrointestinal and hemopoietic systems (J. Cancer Res. Ther. 2010;6:255-62).
Anticancer activity
Investigations by Jain et al. into the molecular mechanisms supporting the anticarcinogenic potential of M. piperita leaf extracts on six human cancer cell lines (HeLa, MCF-7, Jurkat, T24, HT-29, MIAPaCa-2) in 2011 revealed that chloroform and ethyl acetate extracts dose- and time-dependently displayed anticarcinogenic activity leading to G1 cell cycle arrest and mitochondrial-mediated apoptosis among the cascade of effects. The investigators identified their findings as the first evidence of direct anticarcinogenic activity of Mentha leaf extracts and suggested that future work might focus on isolating active constituents as a foundation for mechanistic and translational studies leading to new anticancer drugs, alone or in combination, to prevent and treat human cancers (Int. J. Toxicol. 2011;30:225-36).
Topical benefits of menthol
In a recent examination of the antibacterial and antifungal properties, as well as speculated anti-inflammatory activity of menthol as a topical treatment for diaper dermatitis, investigators conducted a pilot clinical trial in a hospital setting. The study involved 84 neonates with diagnosed candidal diaper dermatitis who required no critical care or systemic antifungal and anti-inflammatory medications. The menthol group (n = 42) received topical clotrimazole and topically applied menthol drops and the control group (n = 42) received topical clotrimazole and a placebo. Thirty-five infants in each group completed the study. The researchers found that complete healing was shorter in the menthol group, with significant relief of erythema and pustules observed in this group. They concluded that topically-applied menthol may be an effective agent in the treatment of candidal diaper dermatitis (World J. Pediatr. 2011;7:167-70).
In 2011, Qiu et al. showed, through various assays, that menthol, in low concentrations, could significantly suppress the expression of alpha-hemolysin, enterotoxins A and B, and toxic shock syndrome toxin 1 in Staphylococcus aureus. The investigators concluded that menthol may warrant inclusion in the armamentarium against S. aureus when combined with beta-lactam antibiotics, which, at subinhibitory concentrations, can actually augment S. aureus toxin secretion. They added that menthol may also have possible uses in novel anti-virulence drugs (Appl. Microbiol. Biotechnol. 2011;90:705-12). It should be noted that menthol is considered safe and effective, with concentrations up to 16% approved in OTC external products by the Food and Drug Administration (J. Am. Acad. Dermatol. 2007;57:873-8).
Pruritus, TRPM8, and melanoma
Topically applied menthol, in concentrations of 1%-3%, is often used to treat pruritus, particularly in the elderly (Skin Therapy Lett. 2010;15:5-9). In addition, recent evidence suggests that the presence of menthol can facilitate penetration of other agents in topical products (Int. J. Toxicol. 2001;20 Suppl 3:61-73; J. Am. Acad. Dermatol. 2007;57:873-8). Patel and Yosipovitch suggest that elderly patients who report diminished pruritus with cooling may stand to benefit from menthol-containing topical therapies (J. Am. Acad. Dermatol. 2007;57:873-8; Skin Therapy Lett. 2010;15:5-9). Interestingly, menthol, via the transient receptor potential melastatin subfamily 8 (TRPM8) receptor, a member of a family of excitatory ion channels, engenders the same cooling sensation as low temperature, though menthol is not linked to a reduction in skin temperature (J. Am. Acad. Dermatol. 2007;57:873-8; Skin Therapy Lett. 2010;15:5-9).
Although the exact mechanism by which menthol exerts its antipruritic and analgesic effects has yet to be determined, the discovery that the TRPM8 is its underlying receptor is proving to be significant, particularly in understanding the cooling effect of the botanical (J. Am. Acad. Dermatol. 2007;57:873-8). There are also indications that menthol has therapeutic potential for melanoma. Specifically, melanoma expresses TRPM8 receptors, the activation of which inhibits melanoma viability. Menthol appears to mediate this response through an influx of extracellular calcium ions (Am. J. Physiol. Cell Physiol. 2008;295:C296-301; Am. J. Physiol. Cell Physiol. 2008;295:C293-5).
Peppermint oil
In 2003, Schuhmacher et al. investigated the virucidal effect of peppermint oil and found that it had a direct effect against herpes simplex virus type 1 (HSV-1) and herpes simplex virus type 2 (HSV-2) as well as an acyclovir-resistant HSV-1 strain. The investigators concluded, noting the lipophilic nature of peppermint oil, that it might be an appropriate topical treatment for recurrent herpes outbreaks (Phytomedicine 2003;10:504-10).
Because of its flavor, aroma, and cooling qualities, peppermint oil is used in a wide range of products, including cosmeceuticals, personal hygiene products (e.g., bath preparations, mouthwashes, toothpastes, and topical formulations), foods, pharmaceutical products, and aromatherapy. Topical indications include pruritus, irritation, and inflammation. Peppermint oil can act as a skin sensitizer, though, particularly in impaired and sensitive skin (Dermatitis 2010;21:327-9). Although peppermint oil has been reported to be a sensitizer in isolated cases, peppermint oil 8% was not found to be a sensitizer in a recent test using a maximization protocol and the various forms of peppermint (i.e., oil, extract, leaves, and water) are considered to be safe in cosmetic formulations. In rinse-off products, peppermint oil is used in concentrations up to 3% and up to 0.2% in leave-on formulations (Int. J. Toxicol. 2001;20 Suppl 3:61-73).
Conclusion
Peppermint and menthol, its naturally occurring monocyclic terpene alcohol derivative, have long been used for medical purposes. Contemporary practice and continuing research continue to support various uses of M. piperita in the medical armamentarium, with specific and additional uses continually being found in the dermatologic realm.
Dr. Baumann is chief executive officer of the Baumann Cosmetic & Research Institute in Miami Beach. She founded the cosmetic dermatology center at the University of Miami in 1997. Dr. Baumann wrote the textbook "Cosmetic Dermatology: Principles and Practice" (McGraw-Hill, April 2002), and a book for consumers, "The Skin Type Solution" (Bantam, 2006). She has contributed to the Cosmeceutical Critique column in Skin & Allergy News since January 2001 and joined the editorial advisory board in 2004. Dr. Baumann has received funding for clinical grants from Allergan, Aveeno, Avon Products, Galderma, Mary Kay, Medicis Pharmaceuticals, Neutrogena, Philosophy, Stiefel, Topix Pharmaceuticals, and Unilever.
Wet dressings work for pruritus when other options fail
LAS VEGAS – Wet dressing, a technique forgotten in most places but in continual use at the Mayo Clinic for more than 80 years, knocks out intractable pruritus – whatever its cause – in children and adults, according to Dr. Mark Davis, chair of the division of clinical dermatology at the clinic in Rochester, Minn.
"It’s a simple technique that works extraordinarily well for any itchy condition from head to toe, and has virtually no side effects. It stops itching reliably, when nothing else has worked," including prednisone, methotrexate, phototherapy, and elimination diets, among other strategies, he said at Skin Disease Education Foundation’s annual Las Vegas dermatology seminar.
Even so, "there’s remarkably little on this in the literature, and what’s published is mostly just in kids, but in adults it works brilliantly, too, particularly for atopic dermatitis. We use it when people come in itching from anything, like psoriasis," he said (J. Am. Acad. Dermatol. 2009;60:792-800).
"The commonest question [we hear from people] is ‘I’ve been going to doctors for years. Why didn’t anybody tell me about this?’ " said Dr. Davis.
If their pruritus is severe enough, patients will be admitted to the Mayo Clinic and have wet cloths applied to wherever the itch happens to be – above the waist, below the waist, the feet, or even the entire body, including the face – with a dry blanket on top if needed to ward of the chill. Patients can get up from bed for a bathroom break when the dressings are changed every 3 hours.
Topical steroids are used with the dressings up to three times a day; 1% percent hydrocortisone for the face or genitals, 0.1% or 0.05% triamcinolone elsewhere. The Mayo Clinic has never had a case of hypothalamic-pituitary-adrenal axis suppression with the technique, and insurance usually covers the cost for 3 days, Dr. Davis said.
When outpatient treatment is sufficient, pruritic patients are instructed to put on wet pajamas or long johns, or hop into the shower in dry ones, and then leave them on for 30 minutes to an hour, 3-4 times a day. Nurses, with the help of handouts and videos, teach patients how to do this, and call them every 24 hours to see how they are getting along.
Hospital patients get the same instructions at discharge. "Initially, they have to do [it] at least once a day for a number of weeks, and then they can use [the technique] on an as-needed basis, maybe once or twice a week," Dr. Davis said.
"Wet dressings went out of favor" in most places because "they are just so much trouble," he said. At present, the technique is "largely unknown," as is the reason why it works, he added.
Dr. Davis has no relevant disclosures. SDEF and this news organization are owned by Frontline Medical Communications.
LAS VEGAS – Wet dressing, a technique forgotten in most places but in continual use at the Mayo Clinic for more than 80 years, knocks out intractable pruritus – whatever its cause – in children and adults, according to Dr. Mark Davis, chair of the division of clinical dermatology at the clinic in Rochester, Minn.
"It’s a simple technique that works extraordinarily well for any itchy condition from head to toe, and has virtually no side effects. It stops itching reliably, when nothing else has worked," including prednisone, methotrexate, phototherapy, and elimination diets, among other strategies, he said at Skin Disease Education Foundation’s annual Las Vegas dermatology seminar.
Even so, "there’s remarkably little on this in the literature, and what’s published is mostly just in kids, but in adults it works brilliantly, too, particularly for atopic dermatitis. We use it when people come in itching from anything, like psoriasis," he said (J. Am. Acad. Dermatol. 2009;60:792-800).
"The commonest question [we hear from people] is ‘I’ve been going to doctors for years. Why didn’t anybody tell me about this?’ " said Dr. Davis.
If their pruritus is severe enough, patients will be admitted to the Mayo Clinic and have wet cloths applied to wherever the itch happens to be – above the waist, below the waist, the feet, or even the entire body, including the face – with a dry blanket on top if needed to ward of the chill. Patients can get up from bed for a bathroom break when the dressings are changed every 3 hours.
Topical steroids are used with the dressings up to three times a day; 1% percent hydrocortisone for the face or genitals, 0.1% or 0.05% triamcinolone elsewhere. The Mayo Clinic has never had a case of hypothalamic-pituitary-adrenal axis suppression with the technique, and insurance usually covers the cost for 3 days, Dr. Davis said.
When outpatient treatment is sufficient, pruritic patients are instructed to put on wet pajamas or long johns, or hop into the shower in dry ones, and then leave them on for 30 minutes to an hour, 3-4 times a day. Nurses, with the help of handouts and videos, teach patients how to do this, and call them every 24 hours to see how they are getting along.
Hospital patients get the same instructions at discharge. "Initially, they have to do [it] at least once a day for a number of weeks, and then they can use [the technique] on an as-needed basis, maybe once or twice a week," Dr. Davis said.
"Wet dressings went out of favor" in most places because "they are just so much trouble," he said. At present, the technique is "largely unknown," as is the reason why it works, he added.
Dr. Davis has no relevant disclosures. SDEF and this news organization are owned by Frontline Medical Communications.
LAS VEGAS – Wet dressing, a technique forgotten in most places but in continual use at the Mayo Clinic for more than 80 years, knocks out intractable pruritus – whatever its cause – in children and adults, according to Dr. Mark Davis, chair of the division of clinical dermatology at the clinic in Rochester, Minn.
"It’s a simple technique that works extraordinarily well for any itchy condition from head to toe, and has virtually no side effects. It stops itching reliably, when nothing else has worked," including prednisone, methotrexate, phototherapy, and elimination diets, among other strategies, he said at Skin Disease Education Foundation’s annual Las Vegas dermatology seminar.
Even so, "there’s remarkably little on this in the literature, and what’s published is mostly just in kids, but in adults it works brilliantly, too, particularly for atopic dermatitis. We use it when people come in itching from anything, like psoriasis," he said (J. Am. Acad. Dermatol. 2009;60:792-800).
"The commonest question [we hear from people] is ‘I’ve been going to doctors for years. Why didn’t anybody tell me about this?’ " said Dr. Davis.
If their pruritus is severe enough, patients will be admitted to the Mayo Clinic and have wet cloths applied to wherever the itch happens to be – above the waist, below the waist, the feet, or even the entire body, including the face – with a dry blanket on top if needed to ward of the chill. Patients can get up from bed for a bathroom break when the dressings are changed every 3 hours.
Topical steroids are used with the dressings up to three times a day; 1% percent hydrocortisone for the face or genitals, 0.1% or 0.05% triamcinolone elsewhere. The Mayo Clinic has never had a case of hypothalamic-pituitary-adrenal axis suppression with the technique, and insurance usually covers the cost for 3 days, Dr. Davis said.
When outpatient treatment is sufficient, pruritic patients are instructed to put on wet pajamas or long johns, or hop into the shower in dry ones, and then leave them on for 30 minutes to an hour, 3-4 times a day. Nurses, with the help of handouts and videos, teach patients how to do this, and call them every 24 hours to see how they are getting along.
Hospital patients get the same instructions at discharge. "Initially, they have to do [it] at least once a day for a number of weeks, and then they can use [the technique] on an as-needed basis, maybe once or twice a week," Dr. Davis said.
"Wet dressings went out of favor" in most places because "they are just so much trouble," he said. At present, the technique is "largely unknown," as is the reason why it works, he added.
Dr. Davis has no relevant disclosures. SDEF and this news organization are owned by Frontline Medical Communications.
AT SDEF LAS VEGAS DERMATOLOGY SEMINAR
Lower serum IgE level tied to better treatment response in atopic dermatitis
ISTANBUL – Baseline total serum immunoglobulin E shows promise as a biomarker predictive of long-term treatment outcomes in atopic dermatitis patients.
In a retrospective study involving 175 Finnish patients with atopic dermatitis followed for a mean of 4.2 years, total clearance was achieved in 54% of patients with a baseline total serum IgE below 1,000 IU/mL, 38% of those with a baseline value of 1,000-10,000 IU/mL, and in a mere 8.3% with a baseline total serum IgE in excess of 10,000 IU/mL, Dr. Ville Kiiski reported at the annual congress of the European Academy of Dermatology and Venereology.
Similarly, treatment response, a lower bar as an endpoint in that it was defined as a lasting reduction in atopic dermatitis severity but not necessarily total clearance, occurred in 93% of those with a baseline total serum IgE below 1,000 IU/mL, compared with 64% of patients with a baseline of 1,000-10,000 IU/mL and 13% with a baseline level greater than 10,000 IU/mL, added Dr. Kiiski of Helsinki University.
Of note, this was largely an adult patient population, with a mean age of 32 years, although the range was 3-78 years. And these patients had atopic dermatitis of sufficient severity that it brought them to a specialized outpatient atopic dermatitis clinic at the Helsinki Skin and Allergy Hospital, where their baseline total serum IgE was measured.
Maintenance therapy during more than 4 years of follow-up was topical tacrolimus (Protopic) in 122 patients and topical corticosteroids and tacrolimus in 53.
Treatment had only a modest effect on total serum IgE levels over time. The median value was 1,472 IU/mL at baseline and 1,114 IU/mL more than 4 years later.
This retrospective study was free of commercial sponsorship, and Dr. Kiiski reported having no financial conflicts of interest.
ISTANBUL – Baseline total serum immunoglobulin E shows promise as a biomarker predictive of long-term treatment outcomes in atopic dermatitis patients.
In a retrospective study involving 175 Finnish patients with atopic dermatitis followed for a mean of 4.2 years, total clearance was achieved in 54% of patients with a baseline total serum IgE below 1,000 IU/mL, 38% of those with a baseline value of 1,000-10,000 IU/mL, and in a mere 8.3% with a baseline total serum IgE in excess of 10,000 IU/mL, Dr. Ville Kiiski reported at the annual congress of the European Academy of Dermatology and Venereology.
Similarly, treatment response, a lower bar as an endpoint in that it was defined as a lasting reduction in atopic dermatitis severity but not necessarily total clearance, occurred in 93% of those with a baseline total serum IgE below 1,000 IU/mL, compared with 64% of patients with a baseline of 1,000-10,000 IU/mL and 13% with a baseline level greater than 10,000 IU/mL, added Dr. Kiiski of Helsinki University.
Of note, this was largely an adult patient population, with a mean age of 32 years, although the range was 3-78 years. And these patients had atopic dermatitis of sufficient severity that it brought them to a specialized outpatient atopic dermatitis clinic at the Helsinki Skin and Allergy Hospital, where their baseline total serum IgE was measured.
Maintenance therapy during more than 4 years of follow-up was topical tacrolimus (Protopic) in 122 patients and topical corticosteroids and tacrolimus in 53.
Treatment had only a modest effect on total serum IgE levels over time. The median value was 1,472 IU/mL at baseline and 1,114 IU/mL more than 4 years later.
This retrospective study was free of commercial sponsorship, and Dr. Kiiski reported having no financial conflicts of interest.
ISTANBUL – Baseline total serum immunoglobulin E shows promise as a biomarker predictive of long-term treatment outcomes in atopic dermatitis patients.
In a retrospective study involving 175 Finnish patients with atopic dermatitis followed for a mean of 4.2 years, total clearance was achieved in 54% of patients with a baseline total serum IgE below 1,000 IU/mL, 38% of those with a baseline value of 1,000-10,000 IU/mL, and in a mere 8.3% with a baseline total serum IgE in excess of 10,000 IU/mL, Dr. Ville Kiiski reported at the annual congress of the European Academy of Dermatology and Venereology.
Similarly, treatment response, a lower bar as an endpoint in that it was defined as a lasting reduction in atopic dermatitis severity but not necessarily total clearance, occurred in 93% of those with a baseline total serum IgE below 1,000 IU/mL, compared with 64% of patients with a baseline of 1,000-10,000 IU/mL and 13% with a baseline level greater than 10,000 IU/mL, added Dr. Kiiski of Helsinki University.
Of note, this was largely an adult patient population, with a mean age of 32 years, although the range was 3-78 years. And these patients had atopic dermatitis of sufficient severity that it brought them to a specialized outpatient atopic dermatitis clinic at the Helsinki Skin and Allergy Hospital, where their baseline total serum IgE was measured.
Maintenance therapy during more than 4 years of follow-up was topical tacrolimus (Protopic) in 122 patients and topical corticosteroids and tacrolimus in 53.
Treatment had only a modest effect on total serum IgE levels over time. The median value was 1,472 IU/mL at baseline and 1,114 IU/mL more than 4 years later.
This retrospective study was free of commercial sponsorship, and Dr. Kiiski reported having no financial conflicts of interest.
AT THE EADV CONGRESS
Major finding: A reduction in atopic dermatitis severity during 4.2 years of topical therapy occurred in 93% of patients with a baseline total serum IgE level below 1,000 IU/mL, compared with 64% of those with a baseline IgE of 1,000-10,000 IU/mL, and just 13% of patients with a baseline value greater than 10,000 IU/mL.
Data source: This was a retrospective study involving 175 patients with atopic dermatitis followed for a mean of 4.2 years of treatment.
Disclosures: This retrospective study was free of commercial sponsorship, and Dr. Kiiski reported having no financial conflicts of interest.
Hives from showering? Think aquagenic urticaria
SAN DIEGO – If a patient presents to your office with hives triggered by contact with water, think aquagenic urticaria.
"Aquagenic urticaria is a very rare disorder, with only about 100 cases reported in the medical literature," Patrick Coleman, a second-year medical student at the Uniformed Services University of the Health Sciences, Bethesda, Md., said in an interview. "Water is the inciting trigger. It’s followed by a wheal and flare response within 10-13 minutes. Sometimes it’s associated with pruritus. If it’s left untreated, it can resolve within an hour."
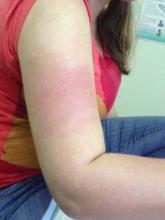
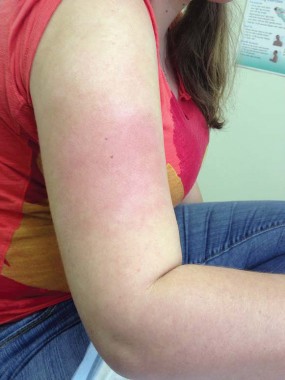
At the annual meeting of the American Academy of Family Physicians, Mr. Coleman and his colleagues discussed the case of a 24-year-old woman who presented to Dr. Robert P. Lennon at the department of family medicine at the U.S. Naval Hospital in Okinawa, Japan, with skin discoloration on her upper arms and legs, hives, and severe global pruritus after showering. Water challenge testing was positive, and the patient was successfully treated with a daily H1 antihistamine.
The hallmark feature of aquagenic urticaria is that the reaction is independent of water temperature. "So whether the water is cold or hot, the reaction will still occur," Mr. Coleman said. The pathogenesis of the condition is unclear, but may involve histamine release from the degranulation of mast cells. "Our patient was treated with an H1 antihistamine and she benefitted," said Mr. Coleman. "For other patients, the care may not be the same. You may need to try different antihistamines to see if they will control it."
In their poster, the researchers noted that urticarias affect 20% of people in the United States. Of these, 25% have urticarias that last more than 6 weeks. Only 10%-20% of urticarias have an identifiable trigger.
The researchers stated that they had no relevant financial disclosures.
SAN DIEGO – If a patient presents to your office with hives triggered by contact with water, think aquagenic urticaria.
"Aquagenic urticaria is a very rare disorder, with only about 100 cases reported in the medical literature," Patrick Coleman, a second-year medical student at the Uniformed Services University of the Health Sciences, Bethesda, Md., said in an interview. "Water is the inciting trigger. It’s followed by a wheal and flare response within 10-13 minutes. Sometimes it’s associated with pruritus. If it’s left untreated, it can resolve within an hour."
At the annual meeting of the American Academy of Family Physicians, Mr. Coleman and his colleagues discussed the case of a 24-year-old woman who presented to Dr. Robert P. Lennon at the department of family medicine at the U.S. Naval Hospital in Okinawa, Japan, with skin discoloration on her upper arms and legs, hives, and severe global pruritus after showering. Water challenge testing was positive, and the patient was successfully treated with a daily H1 antihistamine.
The hallmark feature of aquagenic urticaria is that the reaction is independent of water temperature. "So whether the water is cold or hot, the reaction will still occur," Mr. Coleman said. The pathogenesis of the condition is unclear, but may involve histamine release from the degranulation of mast cells. "Our patient was treated with an H1 antihistamine and she benefitted," said Mr. Coleman. "For other patients, the care may not be the same. You may need to try different antihistamines to see if they will control it."
In their poster, the researchers noted that urticarias affect 20% of people in the United States. Of these, 25% have urticarias that last more than 6 weeks. Only 10%-20% of urticarias have an identifiable trigger.
The researchers stated that they had no relevant financial disclosures.
SAN DIEGO – If a patient presents to your office with hives triggered by contact with water, think aquagenic urticaria.
"Aquagenic urticaria is a very rare disorder, with only about 100 cases reported in the medical literature," Patrick Coleman, a second-year medical student at the Uniformed Services University of the Health Sciences, Bethesda, Md., said in an interview. "Water is the inciting trigger. It’s followed by a wheal and flare response within 10-13 minutes. Sometimes it’s associated with pruritus. If it’s left untreated, it can resolve within an hour."
At the annual meeting of the American Academy of Family Physicians, Mr. Coleman and his colleagues discussed the case of a 24-year-old woman who presented to Dr. Robert P. Lennon at the department of family medicine at the U.S. Naval Hospital in Okinawa, Japan, with skin discoloration on her upper arms and legs, hives, and severe global pruritus after showering. Water challenge testing was positive, and the patient was successfully treated with a daily H1 antihistamine.
The hallmark feature of aquagenic urticaria is that the reaction is independent of water temperature. "So whether the water is cold or hot, the reaction will still occur," Mr. Coleman said. The pathogenesis of the condition is unclear, but may involve histamine release from the degranulation of mast cells. "Our patient was treated with an H1 antihistamine and she benefitted," said Mr. Coleman. "For other patients, the care may not be the same. You may need to try different antihistamines to see if they will control it."
In their poster, the researchers noted that urticarias affect 20% of people in the United States. Of these, 25% have urticarias that last more than 6 weeks. Only 10%-20% of urticarias have an identifiable trigger.
The researchers stated that they had no relevant financial disclosures.
AT THE AAFP SCIENTIFIC ASSEMBLY
Add education, vitamin D to eczema management
SAN FRANCISCO – Treatment for severe eczema should begin with education rather than first-line agents, according to Dr. Timothy G. Berger.
Data reported within the past year from a Japanese study convinced Dr. Berger to modify his therapeutic ladder for severe eczema, he said.
He now starts with greater patient and parental education before prescribing first-line treatments and checks vitamin D levels in patients with severe eczema and frequent infection. He chooses among systemic immunomodulators based on a recent practice update. And as a last resort, for the most difficult cases, he uses omalizumab or photophoresis, he said.
Dr. Berger described his treatment ladder approach at the annual meeting of the Pacific Dermatologic Association:
• First rung: education. He used to start up the therapeutic ladder by prescribing topical steroids, moisturization, and antihistamines. Data from the Japanese study persuaded him to insert more intensive education before sending patients and parents on their way.
The study randomized the mothers of 59 children with moderate to severe atopic dermatitis to attend a 2-day parental education program about managing the disease or to receive a booklet about the disease and conventional care. Six months later, patients in the education group had "dramatically better scores" on the Scoring Atopic Dermatitis (SCORAD) tool and on measures of itching, sleeplessness, and family impact, said Dr. Berger, professor of clinical dermatology at the University of California, San Francisco.
SCORAD scores improved in the education group from 40 at baseline to 15 after treatment, compared with a change from 42 to 27 in the control group (Pediatr. Dermatol. 2013;30:438-43). Parents in the education group also reported less anxiety about steroid use. The patients ranged in age from 6 months to 6 years.
"I think that education is really critical," Dr. Berger said.
• Second rung: first-line treatments. With this foundation of education, Dr. Berger starts patients on topical steroids, moisturizers, and antihistamines.
• Third rung: checking vitamin D levels. A comparison of 95 patients with atopic dermatitis and 58 control patients in another study found that low levels of vitamin D were no more likely in one group than in the other, but frequent skin infections were more likely in the subgroup of patients with atopic dermatitis and low vitamin D levels compared with patients who had the disease and normal vitamin D levels. Vitamin D supplementation in the patients with atopic dermatitis and low vitamin D levels significantly improved SCORAD scores (J. Am. Acad. Dermatol. 2013;69:238-44).
In that study, more than 80% of patients with atopic dermatitis and levels of 25-hydroxyvitamin D below 30 ng/mL developed skin infections compared with less than 20% of patients with atopic dermatitis whose vitamin D levels were above 30 ng/mL, Dr. Berger said. That 30-ng/mL cutoff is the dividing line between normal and abnormal or "insufficient" vitamin D levels, "which I’m not so sure how to interpret," he said. In general, levels below 20 ng/mL are considered vitamin D deficiency.
Now when Dr. Berger sees a patient with atopic dermatitis and frequent infections, he checks vitamin D and looks for levels that are deficient or even close to 10 ng/mL. These patients improve on vitamin D supplementation, he said. Vitamin D is required to deliver antimicrobial peptides to the skin surface, which is the presumed mechanism by which this helps.
He recently used this strategy in a patient with refractory lupus, frequent skin infections, and low vitamin D, he said. Both her lupus and skin infections improved with vitamin D supplementation.
• Fourth, fifth, and sixth rungs. Next he prescribes soak and smear, the conventional therapy of skin hydration and smearing on of topical corticosteroids. Beyond that, phototherapy and then possibly day treatment with ultraviolet light and application of coal tar remain options on his therapeutic ladder. "Day treatment with tar and light works very well for a patient that doesn’t have bullous pemphigoid," he said.
• Seventh rung: systemic immunomodulators. Guidance for choosing among these agents comes from a recent practice update from the American Academy of Allergy, Asthma, and Immunology; the American College of Allergy, Asthma, and Immunology; and the Joint Council of Allergy, Asthma, and Immunology (J. Allergy Clin. Immunol. 2013;131:295-9).
Cyclosporine works fastest, especially if started at higher doses, the recommendations say, but "my experience is that in older patients, it’s hard to use," Dr. Berger added. Oral tacrolimus also works, according to the Dr. Berger, as well as the guidelines.
Beyond that, methotrexate and azathioprine appear to be equally effective, with approximately 80% of patients responding in 3-6 weeks. Ordering an assay to detect deficiency of the thiopurine methyltransferase enzyme helps avoid toxicity from the drug in some patients. Because one study showed that increasing the dose of methotrexate does not help if the patient fails to respond to 15 mg/wk, Dr. Berger said he tries to get to 15 mg/wk for 4-6 weeks and holds that dose if there’s a response.
Another study showed that eczema cleared or almost cleared in around 60% of patients treated with mycophenolate mofetil. "I certainly have used it, but it’s unpredictable and it takes longer to start," he said. "You wait a couple of months to see if it’s going to work and then 20%-30% of the time it’s not going to be good enough."
• Final rung: newer agents. The same practice update recommends a list of newer agents "if you can afford it," Dr. Berger said. Approximately 60% of patients respond, slowly but steadily, to treatment with subcutaneous omalizumab 150-450 mg every 2 weeks. Some patients in studies managed to get off unsustainable levels of systemic steroids with the help of omalizumab. "There really isn’t a rebound" flare when omalizumab is stopped, as happens with cyclosporine, Dr. Berger said. "You kind of get better, then creep along. So if the quality of life is moderately bad, you get to less bad."
Tumor necrosis factor inhibitors work as induction therapy but not for maintenance, so they’re "probably not useful," he said. Anecdotal reports suggest that high-dose intravenous immunoglobulin may help.
For the most refractory patients, extracorporeal photophoresis can improve SCORAD scores by 50%. "The itch and SCORAD drop pretty quickly, but you have to maintain it" with omalizumab or another strategy, Dr. Berger said.
"If everything absolutely fails, that’s a backup," he said. "It does suggest that there will be new ways to manage patients that we don’t have available now."
Dr. Berger reported having no relevant financial disclosures.
On Twitter @sherryboschert
SAN FRANCISCO – Treatment for severe eczema should begin with education rather than first-line agents, according to Dr. Timothy G. Berger.
Data reported within the past year from a Japanese study convinced Dr. Berger to modify his therapeutic ladder for severe eczema, he said.
He now starts with greater patient and parental education before prescribing first-line treatments and checks vitamin D levels in patients with severe eczema and frequent infection. He chooses among systemic immunomodulators based on a recent practice update. And as a last resort, for the most difficult cases, he uses omalizumab or photophoresis, he said.
Dr. Berger described his treatment ladder approach at the annual meeting of the Pacific Dermatologic Association:
• First rung: education. He used to start up the therapeutic ladder by prescribing topical steroids, moisturization, and antihistamines. Data from the Japanese study persuaded him to insert more intensive education before sending patients and parents on their way.
The study randomized the mothers of 59 children with moderate to severe atopic dermatitis to attend a 2-day parental education program about managing the disease or to receive a booklet about the disease and conventional care. Six months later, patients in the education group had "dramatically better scores" on the Scoring Atopic Dermatitis (SCORAD) tool and on measures of itching, sleeplessness, and family impact, said Dr. Berger, professor of clinical dermatology at the University of California, San Francisco.
SCORAD scores improved in the education group from 40 at baseline to 15 after treatment, compared with a change from 42 to 27 in the control group (Pediatr. Dermatol. 2013;30:438-43). Parents in the education group also reported less anxiety about steroid use. The patients ranged in age from 6 months to 6 years.
"I think that education is really critical," Dr. Berger said.
• Second rung: first-line treatments. With this foundation of education, Dr. Berger starts patients on topical steroids, moisturizers, and antihistamines.
• Third rung: checking vitamin D levels. A comparison of 95 patients with atopic dermatitis and 58 control patients in another study found that low levels of vitamin D were no more likely in one group than in the other, but frequent skin infections were more likely in the subgroup of patients with atopic dermatitis and low vitamin D levels compared with patients who had the disease and normal vitamin D levels. Vitamin D supplementation in the patients with atopic dermatitis and low vitamin D levels significantly improved SCORAD scores (J. Am. Acad. Dermatol. 2013;69:238-44).
In that study, more than 80% of patients with atopic dermatitis and levels of 25-hydroxyvitamin D below 30 ng/mL developed skin infections compared with less than 20% of patients with atopic dermatitis whose vitamin D levels were above 30 ng/mL, Dr. Berger said. That 30-ng/mL cutoff is the dividing line between normal and abnormal or "insufficient" vitamin D levels, "which I’m not so sure how to interpret," he said. In general, levels below 20 ng/mL are considered vitamin D deficiency.
Now when Dr. Berger sees a patient with atopic dermatitis and frequent infections, he checks vitamin D and looks for levels that are deficient or even close to 10 ng/mL. These patients improve on vitamin D supplementation, he said. Vitamin D is required to deliver antimicrobial peptides to the skin surface, which is the presumed mechanism by which this helps.
He recently used this strategy in a patient with refractory lupus, frequent skin infections, and low vitamin D, he said. Both her lupus and skin infections improved with vitamin D supplementation.
• Fourth, fifth, and sixth rungs. Next he prescribes soak and smear, the conventional therapy of skin hydration and smearing on of topical corticosteroids. Beyond that, phototherapy and then possibly day treatment with ultraviolet light and application of coal tar remain options on his therapeutic ladder. "Day treatment with tar and light works very well for a patient that doesn’t have bullous pemphigoid," he said.
• Seventh rung: systemic immunomodulators. Guidance for choosing among these agents comes from a recent practice update from the American Academy of Allergy, Asthma, and Immunology; the American College of Allergy, Asthma, and Immunology; and the Joint Council of Allergy, Asthma, and Immunology (J. Allergy Clin. Immunol. 2013;131:295-9).
Cyclosporine works fastest, especially if started at higher doses, the recommendations say, but "my experience is that in older patients, it’s hard to use," Dr. Berger added. Oral tacrolimus also works, according to the Dr. Berger, as well as the guidelines.
Beyond that, methotrexate and azathioprine appear to be equally effective, with approximately 80% of patients responding in 3-6 weeks. Ordering an assay to detect deficiency of the thiopurine methyltransferase enzyme helps avoid toxicity from the drug in some patients. Because one study showed that increasing the dose of methotrexate does not help if the patient fails to respond to 15 mg/wk, Dr. Berger said he tries to get to 15 mg/wk for 4-6 weeks and holds that dose if there’s a response.
Another study showed that eczema cleared or almost cleared in around 60% of patients treated with mycophenolate mofetil. "I certainly have used it, but it’s unpredictable and it takes longer to start," he said. "You wait a couple of months to see if it’s going to work and then 20%-30% of the time it’s not going to be good enough."
• Final rung: newer agents. The same practice update recommends a list of newer agents "if you can afford it," Dr. Berger said. Approximately 60% of patients respond, slowly but steadily, to treatment with subcutaneous omalizumab 150-450 mg every 2 weeks. Some patients in studies managed to get off unsustainable levels of systemic steroids with the help of omalizumab. "There really isn’t a rebound" flare when omalizumab is stopped, as happens with cyclosporine, Dr. Berger said. "You kind of get better, then creep along. So if the quality of life is moderately bad, you get to less bad."
Tumor necrosis factor inhibitors work as induction therapy but not for maintenance, so they’re "probably not useful," he said. Anecdotal reports suggest that high-dose intravenous immunoglobulin may help.
For the most refractory patients, extracorporeal photophoresis can improve SCORAD scores by 50%. "The itch and SCORAD drop pretty quickly, but you have to maintain it" with omalizumab or another strategy, Dr. Berger said.
"If everything absolutely fails, that’s a backup," he said. "It does suggest that there will be new ways to manage patients that we don’t have available now."
Dr. Berger reported having no relevant financial disclosures.
On Twitter @sherryboschert
SAN FRANCISCO – Treatment for severe eczema should begin with education rather than first-line agents, according to Dr. Timothy G. Berger.
Data reported within the past year from a Japanese study convinced Dr. Berger to modify his therapeutic ladder for severe eczema, he said.
He now starts with greater patient and parental education before prescribing first-line treatments and checks vitamin D levels in patients with severe eczema and frequent infection. He chooses among systemic immunomodulators based on a recent practice update. And as a last resort, for the most difficult cases, he uses omalizumab or photophoresis, he said.
Dr. Berger described his treatment ladder approach at the annual meeting of the Pacific Dermatologic Association:
• First rung: education. He used to start up the therapeutic ladder by prescribing topical steroids, moisturization, and antihistamines. Data from the Japanese study persuaded him to insert more intensive education before sending patients and parents on their way.
The study randomized the mothers of 59 children with moderate to severe atopic dermatitis to attend a 2-day parental education program about managing the disease or to receive a booklet about the disease and conventional care. Six months later, patients in the education group had "dramatically better scores" on the Scoring Atopic Dermatitis (SCORAD) tool and on measures of itching, sleeplessness, and family impact, said Dr. Berger, professor of clinical dermatology at the University of California, San Francisco.
SCORAD scores improved in the education group from 40 at baseline to 15 after treatment, compared with a change from 42 to 27 in the control group (Pediatr. Dermatol. 2013;30:438-43). Parents in the education group also reported less anxiety about steroid use. The patients ranged in age from 6 months to 6 years.
"I think that education is really critical," Dr. Berger said.
• Second rung: first-line treatments. With this foundation of education, Dr. Berger starts patients on topical steroids, moisturizers, and antihistamines.
• Third rung: checking vitamin D levels. A comparison of 95 patients with atopic dermatitis and 58 control patients in another study found that low levels of vitamin D were no more likely in one group than in the other, but frequent skin infections were more likely in the subgroup of patients with atopic dermatitis and low vitamin D levels compared with patients who had the disease and normal vitamin D levels. Vitamin D supplementation in the patients with atopic dermatitis and low vitamin D levels significantly improved SCORAD scores (J. Am. Acad. Dermatol. 2013;69:238-44).
In that study, more than 80% of patients with atopic dermatitis and levels of 25-hydroxyvitamin D below 30 ng/mL developed skin infections compared with less than 20% of patients with atopic dermatitis whose vitamin D levels were above 30 ng/mL, Dr. Berger said. That 30-ng/mL cutoff is the dividing line between normal and abnormal or "insufficient" vitamin D levels, "which I’m not so sure how to interpret," he said. In general, levels below 20 ng/mL are considered vitamin D deficiency.
Now when Dr. Berger sees a patient with atopic dermatitis and frequent infections, he checks vitamin D and looks for levels that are deficient or even close to 10 ng/mL. These patients improve on vitamin D supplementation, he said. Vitamin D is required to deliver antimicrobial peptides to the skin surface, which is the presumed mechanism by which this helps.
He recently used this strategy in a patient with refractory lupus, frequent skin infections, and low vitamin D, he said. Both her lupus and skin infections improved with vitamin D supplementation.
• Fourth, fifth, and sixth rungs. Next he prescribes soak and smear, the conventional therapy of skin hydration and smearing on of topical corticosteroids. Beyond that, phototherapy and then possibly day treatment with ultraviolet light and application of coal tar remain options on his therapeutic ladder. "Day treatment with tar and light works very well for a patient that doesn’t have bullous pemphigoid," he said.
• Seventh rung: systemic immunomodulators. Guidance for choosing among these agents comes from a recent practice update from the American Academy of Allergy, Asthma, and Immunology; the American College of Allergy, Asthma, and Immunology; and the Joint Council of Allergy, Asthma, and Immunology (J. Allergy Clin. Immunol. 2013;131:295-9).
Cyclosporine works fastest, especially if started at higher doses, the recommendations say, but "my experience is that in older patients, it’s hard to use," Dr. Berger added. Oral tacrolimus also works, according to the Dr. Berger, as well as the guidelines.
Beyond that, methotrexate and azathioprine appear to be equally effective, with approximately 80% of patients responding in 3-6 weeks. Ordering an assay to detect deficiency of the thiopurine methyltransferase enzyme helps avoid toxicity from the drug in some patients. Because one study showed that increasing the dose of methotrexate does not help if the patient fails to respond to 15 mg/wk, Dr. Berger said he tries to get to 15 mg/wk for 4-6 weeks and holds that dose if there’s a response.
Another study showed that eczema cleared or almost cleared in around 60% of patients treated with mycophenolate mofetil. "I certainly have used it, but it’s unpredictable and it takes longer to start," he said. "You wait a couple of months to see if it’s going to work and then 20%-30% of the time it’s not going to be good enough."
• Final rung: newer agents. The same practice update recommends a list of newer agents "if you can afford it," Dr. Berger said. Approximately 60% of patients respond, slowly but steadily, to treatment with subcutaneous omalizumab 150-450 mg every 2 weeks. Some patients in studies managed to get off unsustainable levels of systemic steroids with the help of omalizumab. "There really isn’t a rebound" flare when omalizumab is stopped, as happens with cyclosporine, Dr. Berger said. "You kind of get better, then creep along. So if the quality of life is moderately bad, you get to less bad."
Tumor necrosis factor inhibitors work as induction therapy but not for maintenance, so they’re "probably not useful," he said. Anecdotal reports suggest that high-dose intravenous immunoglobulin may help.
For the most refractory patients, extracorporeal photophoresis can improve SCORAD scores by 50%. "The itch and SCORAD drop pretty quickly, but you have to maintain it" with omalizumab or another strategy, Dr. Berger said.
"If everything absolutely fails, that’s a backup," he said. "It does suggest that there will be new ways to manage patients that we don’t have available now."
Dr. Berger reported having no relevant financial disclosures.
On Twitter @sherryboschert
EXPERT ANALYSIS FROM THE PDA ANNUAL MEETING
Perioral dermatitis and diet
Perioral dermatitis is a common and frustrating skin condition that is often treatment resistant and recurs when treatment stops. Perioral dermatitis is classified in the rosacea family of skin diseases, and it is often associated with fair skin, light eyes, and marked actinic damage.
Although it is common in white skin, perioral dermatitis is underdiagnosed and an increasing problem in skin of color as well. The condition often begins as a papular, erythematous rash around the mouth. In darker skin types, however, it is often misdiagnosed because the erythema is masked by the skin pigmentation, so it appears as reddish-brown or even hyperpigmented papules around the mouth or eyes.
Popular treatments for perioral dermatitis include oral doxycycline, topical metronidazole, and topical tacrolimus. Often patients self-treat with topical corticosteroids for quick relief, which can initially improve the condition. However, corticosteroid use can result in exacerbation of the disease once the steroid is stopped, and often leads to recalcitrant cases. In skin of color patients, topical steroids used around the mouth and eyes also cause hypopigmentation of the skin, which further masks the clinical presentation of the disease and contributes to underdiagnosis and improper management.
In my practice, I have seen a consistent link between perioral dermatitis in skin of color patients and diet. Often patients who develop the rash have gluten sensitivity or mild, undiagnosed gluten intolerance. When these patients are switched to a gluten-free diet, their skin condition improves. Similarly, patients with no clinically diagnosed gluten sensitivity but who adopt a carbohydrate-free/low-glycemic-index and high-protein diet have shown dramatic improvement with minimal oral or topical treatments and less recurrence.
Although there are no well-controlled studies – or even case reports – linking carbohydrate or gluten intake to perioral dermatitis, studies have shown a strong link between diet and rosacea. Erythematotelangiectatic and papulopustular rosacea are known to be exacerbated by alcohol, hot or spicy foods, and chocolate. However, the common ingredient in these foods has never been identified as a link to the exacerbation of the disease. As all of the aforementioned foods often contain carbohydrates, could the common link simply be carbs or processed sugar?
Carbohydrates are the most common nutrients in the American diet. Often, emigrants to the United States develop perioral dermatitis or other inflammatory skin conditions such as acne and rosacea that they did not have in their home countries. Perhaps the Paleo or Mediterranean diets that have become popular for weight loss help control both bowel and skin inflammation. More studies are needed to better define the complex relationship and causality between diet and perioral dermatitis. In the meantime, I have been recommending carb-free diets in addition to topical tacrolimus or metronidazole for my skin of color patients with perioral dermatitis to prevent recurrences, and I have seen excellent results.
Dr. Talakoub is in private practice in McLean, Va.
Do you have questions about treating patients with dark skin? If so, send them to [email protected].
Perioral dermatitis is a common and frustrating skin condition that is often treatment resistant and recurs when treatment stops. Perioral dermatitis is classified in the rosacea family of skin diseases, and it is often associated with fair skin, light eyes, and marked actinic damage.
Although it is common in white skin, perioral dermatitis is underdiagnosed and an increasing problem in skin of color as well. The condition often begins as a papular, erythematous rash around the mouth. In darker skin types, however, it is often misdiagnosed because the erythema is masked by the skin pigmentation, so it appears as reddish-brown or even hyperpigmented papules around the mouth or eyes.
Popular treatments for perioral dermatitis include oral doxycycline, topical metronidazole, and topical tacrolimus. Often patients self-treat with topical corticosteroids for quick relief, which can initially improve the condition. However, corticosteroid use can result in exacerbation of the disease once the steroid is stopped, and often leads to recalcitrant cases. In skin of color patients, topical steroids used around the mouth and eyes also cause hypopigmentation of the skin, which further masks the clinical presentation of the disease and contributes to underdiagnosis and improper management.
In my practice, I have seen a consistent link between perioral dermatitis in skin of color patients and diet. Often patients who develop the rash have gluten sensitivity or mild, undiagnosed gluten intolerance. When these patients are switched to a gluten-free diet, their skin condition improves. Similarly, patients with no clinically diagnosed gluten sensitivity but who adopt a carbohydrate-free/low-glycemic-index and high-protein diet have shown dramatic improvement with minimal oral or topical treatments and less recurrence.
Although there are no well-controlled studies – or even case reports – linking carbohydrate or gluten intake to perioral dermatitis, studies have shown a strong link between diet and rosacea. Erythematotelangiectatic and papulopustular rosacea are known to be exacerbated by alcohol, hot or spicy foods, and chocolate. However, the common ingredient in these foods has never been identified as a link to the exacerbation of the disease. As all of the aforementioned foods often contain carbohydrates, could the common link simply be carbs or processed sugar?
Carbohydrates are the most common nutrients in the American diet. Often, emigrants to the United States develop perioral dermatitis or other inflammatory skin conditions such as acne and rosacea that they did not have in their home countries. Perhaps the Paleo or Mediterranean diets that have become popular for weight loss help control both bowel and skin inflammation. More studies are needed to better define the complex relationship and causality between diet and perioral dermatitis. In the meantime, I have been recommending carb-free diets in addition to topical tacrolimus or metronidazole for my skin of color patients with perioral dermatitis to prevent recurrences, and I have seen excellent results.
Dr. Talakoub is in private practice in McLean, Va.
Do you have questions about treating patients with dark skin? If so, send them to [email protected].
Perioral dermatitis is a common and frustrating skin condition that is often treatment resistant and recurs when treatment stops. Perioral dermatitis is classified in the rosacea family of skin diseases, and it is often associated with fair skin, light eyes, and marked actinic damage.
Although it is common in white skin, perioral dermatitis is underdiagnosed and an increasing problem in skin of color as well. The condition often begins as a papular, erythematous rash around the mouth. In darker skin types, however, it is often misdiagnosed because the erythema is masked by the skin pigmentation, so it appears as reddish-brown or even hyperpigmented papules around the mouth or eyes.
Popular treatments for perioral dermatitis include oral doxycycline, topical metronidazole, and topical tacrolimus. Often patients self-treat with topical corticosteroids for quick relief, which can initially improve the condition. However, corticosteroid use can result in exacerbation of the disease once the steroid is stopped, and often leads to recalcitrant cases. In skin of color patients, topical steroids used around the mouth and eyes also cause hypopigmentation of the skin, which further masks the clinical presentation of the disease and contributes to underdiagnosis and improper management.
In my practice, I have seen a consistent link between perioral dermatitis in skin of color patients and diet. Often patients who develop the rash have gluten sensitivity or mild, undiagnosed gluten intolerance. When these patients are switched to a gluten-free diet, their skin condition improves. Similarly, patients with no clinically diagnosed gluten sensitivity but who adopt a carbohydrate-free/low-glycemic-index and high-protein diet have shown dramatic improvement with minimal oral or topical treatments and less recurrence.
Although there are no well-controlled studies – or even case reports – linking carbohydrate or gluten intake to perioral dermatitis, studies have shown a strong link between diet and rosacea. Erythematotelangiectatic and papulopustular rosacea are known to be exacerbated by alcohol, hot or spicy foods, and chocolate. However, the common ingredient in these foods has never been identified as a link to the exacerbation of the disease. As all of the aforementioned foods often contain carbohydrates, could the common link simply be carbs or processed sugar?
Carbohydrates are the most common nutrients in the American diet. Often, emigrants to the United States develop perioral dermatitis or other inflammatory skin conditions such as acne and rosacea that they did not have in their home countries. Perhaps the Paleo or Mediterranean diets that have become popular for weight loss help control both bowel and skin inflammation. More studies are needed to better define the complex relationship and causality between diet and perioral dermatitis. In the meantime, I have been recommending carb-free diets in addition to topical tacrolimus or metronidazole for my skin of color patients with perioral dermatitis to prevent recurrences, and I have seen excellent results.
Dr. Talakoub is in private practice in McLean, Va.
Do you have questions about treating patients with dark skin? If so, send them to [email protected].
Intensive ‘Boot Camp’ protocol improves kids’ atopic dermatitis
NEW YORK – To frustrated parents of children with severe atopic dermatitis, Dr. Sheilagh Maguiness offers a fast and effective remedy: a 2-week intensive treatment she calls Boot Camp. Instead of push-ups, however, this Boot Camp involves bleach baths, wet wraps, steroids, moisturizers, and sometimes oral antibiotics or antihistamines.
During the 2-week period, the treatment plan attempts to address all aspects of the disease – dry skin, itching, inflammation, and infection or colonization – simultaneously.
Dr. Maguiness’ instructions for the severe atopic dermatitis Boot Camp are as follows:
• For 2 weeks, bathe the child nightly in a dilute bleach bath of lukewarm water for 10 minutes. (No soap is needed, or use unscented Dove or Cetaphil for armpits, groin, hands, and feet.) After 2 weeks, use lukewarm water alone.
Data have shown that the baths are safe, said Dr. Maguiness of Harvard University, Boston, and Boston Children’s Hospital. In a recent randomized trial of 31 children, those who underwent regular, dilute bleach baths showed improvement in their atopic dermatitis with no increased susceptibility to infection (Pediatrics 2009;123:e808-14). The recipe for the bleach baths is ¼ to ½ cup of plain Clorox bleach in a full tub of bath water. (With more concentrated forms of Clorox, use 1/3 cup per full tub.) Comfort the worried parents by letting them know that the concentration is similar to that found in a swimming pool, and is safe for head and neck areas, she said in a presentation at the American Academy of Dermatology summer meeting.
• After bathing, pat the skin dry, and within 3 minutes apply triamcinolone (0.1% ointment) to affected areas on the body, and hydrocortisone (2.5% ointment) to the face.
• Follow the bath with a thick moisturizer (Vaseline, Aquaphor, or Hydrolatum ointment). Use the moisturizer on top of the medication twice daily, even if no bath is taken. Avoid lotions.
• Add wet pajama wraps nightly for 1-2 weeks as part of the Boot Camp and/or for acute flares, Dr. Maguiness noted. Studies have shown that wet wraps plus topical corticosteroids are effective, and can promote rapid improvement in the majority of patients, with very few side effects. In a recent retrospective study of 216 pediatric patients who underwent this combination, all of them showed at least 25% improvement, and 45% had 75-100% improvement (J. Am. Acad. Dermatol. 2012;67:100-6).
Advise parents to use long-sleeve cotton pajamas or Onesies for wet wraps, Dr. Maguiness added. Parents should soak the garment in warm water, wring it out until it’s slightly damp, then dress the child, and put on a dry outfit on top of the wet one. They should make sure the room is warm so the child can go to sleep.
In cases of obvious superinfection, prescribe an appropriate oral antibiotic such as cephalexin.
For itching at night, sedating antihistamines such as hydroxyzine 10 mg/5 mL, 30 minutes before bedtime can be helpful, Dr. Maguiness noted. For daytime itching, she suggested fexofenadine or cetirizine in the morning. Have a few "go-to" agents, she advised. For infants, consider fluocinolone oil or triamcinalone 0.025% ointment. For children, consider triamcinalone 0.1% ointment. For teenagers (or for use in more localized areas with younger children), consider stronger agents such as mometasone or fluocinonide ointment.
Limited studies support some systemic therapies for use in pediatric atopic dermatitis, including narrow-band ultraviolet B (nb UVB); cyclosporine and mycophenolate mofetil; and methotrexate and azathioprine, Dr. Maguiness said. Perhaps in the future, biologics such as tocilizumab may emerge as additional treatment options, she added. While cyclosporine can help with the rapid clearance of the disease, methotrexate and mycophenolate mofetil may represent longer-term options, she said.
Meanwhile, don’t be surprised if families resist the Boot Camp at first, Dr. Maguiness said.
"You have to get the families on your side," she said. "They’re terrified of bleach baths, wet pajamas, and topical steroids. Let them know there’s no faster or safer way to improve their child’s condition in 2 weeks or less."
So invest time in the first visit, educate your patients and parents about the treatment plan, and give them printed instructions and handouts, Dr. Maguiness said.
Finally, don’t forget to obtain cultures to rule out possible superinfection, as well as schedule a prompt follow-up visit in about 2 weeks.
At this visit, after following the Boot Camp regimen, the eczematous areas should be mostly cleared, with possible residual hot spots, she said. Begin to taper the topical steroids, bleach baths, and wet wraps at night.
Despite the challenges of treating severe atopic dermatitis in children, she told her audience that treating these young patients has been one of the most rewarding parts of her practice.
Dr. Maguiness had no relevant disclosures.
On Twitter @naseemsmiller
NEW YORK – To frustrated parents of children with severe atopic dermatitis, Dr. Sheilagh Maguiness offers a fast and effective remedy: a 2-week intensive treatment she calls Boot Camp. Instead of push-ups, however, this Boot Camp involves bleach baths, wet wraps, steroids, moisturizers, and sometimes oral antibiotics or antihistamines.
During the 2-week period, the treatment plan attempts to address all aspects of the disease – dry skin, itching, inflammation, and infection or colonization – simultaneously.
Dr. Maguiness’ instructions for the severe atopic dermatitis Boot Camp are as follows:
• For 2 weeks, bathe the child nightly in a dilute bleach bath of lukewarm water for 10 minutes. (No soap is needed, or use unscented Dove or Cetaphil for armpits, groin, hands, and feet.) After 2 weeks, use lukewarm water alone.
Data have shown that the baths are safe, said Dr. Maguiness of Harvard University, Boston, and Boston Children’s Hospital. In a recent randomized trial of 31 children, those who underwent regular, dilute bleach baths showed improvement in their atopic dermatitis with no increased susceptibility to infection (Pediatrics 2009;123:e808-14). The recipe for the bleach baths is ¼ to ½ cup of plain Clorox bleach in a full tub of bath water. (With more concentrated forms of Clorox, use 1/3 cup per full tub.) Comfort the worried parents by letting them know that the concentration is similar to that found in a swimming pool, and is safe for head and neck areas, she said in a presentation at the American Academy of Dermatology summer meeting.
• After bathing, pat the skin dry, and within 3 minutes apply triamcinolone (0.1% ointment) to affected areas on the body, and hydrocortisone (2.5% ointment) to the face.
• Follow the bath with a thick moisturizer (Vaseline, Aquaphor, or Hydrolatum ointment). Use the moisturizer on top of the medication twice daily, even if no bath is taken. Avoid lotions.
• Add wet pajama wraps nightly for 1-2 weeks as part of the Boot Camp and/or for acute flares, Dr. Maguiness noted. Studies have shown that wet wraps plus topical corticosteroids are effective, and can promote rapid improvement in the majority of patients, with very few side effects. In a recent retrospective study of 216 pediatric patients who underwent this combination, all of them showed at least 25% improvement, and 45% had 75-100% improvement (J. Am. Acad. Dermatol. 2012;67:100-6).
Advise parents to use long-sleeve cotton pajamas or Onesies for wet wraps, Dr. Maguiness added. Parents should soak the garment in warm water, wring it out until it’s slightly damp, then dress the child, and put on a dry outfit on top of the wet one. They should make sure the room is warm so the child can go to sleep.
In cases of obvious superinfection, prescribe an appropriate oral antibiotic such as cephalexin.
For itching at night, sedating antihistamines such as hydroxyzine 10 mg/5 mL, 30 minutes before bedtime can be helpful, Dr. Maguiness noted. For daytime itching, she suggested fexofenadine or cetirizine in the morning. Have a few "go-to" agents, she advised. For infants, consider fluocinolone oil or triamcinalone 0.025% ointment. For children, consider triamcinalone 0.1% ointment. For teenagers (or for use in more localized areas with younger children), consider stronger agents such as mometasone or fluocinonide ointment.
Limited studies support some systemic therapies for use in pediatric atopic dermatitis, including narrow-band ultraviolet B (nb UVB); cyclosporine and mycophenolate mofetil; and methotrexate and azathioprine, Dr. Maguiness said. Perhaps in the future, biologics such as tocilizumab may emerge as additional treatment options, she added. While cyclosporine can help with the rapid clearance of the disease, methotrexate and mycophenolate mofetil may represent longer-term options, she said.
Meanwhile, don’t be surprised if families resist the Boot Camp at first, Dr. Maguiness said.
"You have to get the families on your side," she said. "They’re terrified of bleach baths, wet pajamas, and topical steroids. Let them know there’s no faster or safer way to improve their child’s condition in 2 weeks or less."
So invest time in the first visit, educate your patients and parents about the treatment plan, and give them printed instructions and handouts, Dr. Maguiness said.
Finally, don’t forget to obtain cultures to rule out possible superinfection, as well as schedule a prompt follow-up visit in about 2 weeks.
At this visit, after following the Boot Camp regimen, the eczematous areas should be mostly cleared, with possible residual hot spots, she said. Begin to taper the topical steroids, bleach baths, and wet wraps at night.
Despite the challenges of treating severe atopic dermatitis in children, she told her audience that treating these young patients has been one of the most rewarding parts of her practice.
Dr. Maguiness had no relevant disclosures.
On Twitter @naseemsmiller
NEW YORK – To frustrated parents of children with severe atopic dermatitis, Dr. Sheilagh Maguiness offers a fast and effective remedy: a 2-week intensive treatment she calls Boot Camp. Instead of push-ups, however, this Boot Camp involves bleach baths, wet wraps, steroids, moisturizers, and sometimes oral antibiotics or antihistamines.
During the 2-week period, the treatment plan attempts to address all aspects of the disease – dry skin, itching, inflammation, and infection or colonization – simultaneously.
Dr. Maguiness’ instructions for the severe atopic dermatitis Boot Camp are as follows:
• For 2 weeks, bathe the child nightly in a dilute bleach bath of lukewarm water for 10 minutes. (No soap is needed, or use unscented Dove or Cetaphil for armpits, groin, hands, and feet.) After 2 weeks, use lukewarm water alone.
Data have shown that the baths are safe, said Dr. Maguiness of Harvard University, Boston, and Boston Children’s Hospital. In a recent randomized trial of 31 children, those who underwent regular, dilute bleach baths showed improvement in their atopic dermatitis with no increased susceptibility to infection (Pediatrics 2009;123:e808-14). The recipe for the bleach baths is ¼ to ½ cup of plain Clorox bleach in a full tub of bath water. (With more concentrated forms of Clorox, use 1/3 cup per full tub.) Comfort the worried parents by letting them know that the concentration is similar to that found in a swimming pool, and is safe for head and neck areas, she said in a presentation at the American Academy of Dermatology summer meeting.
• After bathing, pat the skin dry, and within 3 minutes apply triamcinolone (0.1% ointment) to affected areas on the body, and hydrocortisone (2.5% ointment) to the face.
• Follow the bath with a thick moisturizer (Vaseline, Aquaphor, or Hydrolatum ointment). Use the moisturizer on top of the medication twice daily, even if no bath is taken. Avoid lotions.
• Add wet pajama wraps nightly for 1-2 weeks as part of the Boot Camp and/or for acute flares, Dr. Maguiness noted. Studies have shown that wet wraps plus topical corticosteroids are effective, and can promote rapid improvement in the majority of patients, with very few side effects. In a recent retrospective study of 216 pediatric patients who underwent this combination, all of them showed at least 25% improvement, and 45% had 75-100% improvement (J. Am. Acad. Dermatol. 2012;67:100-6).
Advise parents to use long-sleeve cotton pajamas or Onesies for wet wraps, Dr. Maguiness added. Parents should soak the garment in warm water, wring it out until it’s slightly damp, then dress the child, and put on a dry outfit on top of the wet one. They should make sure the room is warm so the child can go to sleep.
In cases of obvious superinfection, prescribe an appropriate oral antibiotic such as cephalexin.
For itching at night, sedating antihistamines such as hydroxyzine 10 mg/5 mL, 30 minutes before bedtime can be helpful, Dr. Maguiness noted. For daytime itching, she suggested fexofenadine or cetirizine in the morning. Have a few "go-to" agents, she advised. For infants, consider fluocinolone oil or triamcinalone 0.025% ointment. For children, consider triamcinalone 0.1% ointment. For teenagers (or for use in more localized areas with younger children), consider stronger agents such as mometasone or fluocinonide ointment.
Limited studies support some systemic therapies for use in pediatric atopic dermatitis, including narrow-band ultraviolet B (nb UVB); cyclosporine and mycophenolate mofetil; and methotrexate and azathioprine, Dr. Maguiness said. Perhaps in the future, biologics such as tocilizumab may emerge as additional treatment options, she added. While cyclosporine can help with the rapid clearance of the disease, methotrexate and mycophenolate mofetil may represent longer-term options, she said.
Meanwhile, don’t be surprised if families resist the Boot Camp at first, Dr. Maguiness said.
"You have to get the families on your side," she said. "They’re terrified of bleach baths, wet pajamas, and topical steroids. Let them know there’s no faster or safer way to improve their child’s condition in 2 weeks or less."
So invest time in the first visit, educate your patients and parents about the treatment plan, and give them printed instructions and handouts, Dr. Maguiness said.
Finally, don’t forget to obtain cultures to rule out possible superinfection, as well as schedule a prompt follow-up visit in about 2 weeks.
At this visit, after following the Boot Camp regimen, the eczematous areas should be mostly cleared, with possible residual hot spots, she said. Begin to taper the topical steroids, bleach baths, and wet wraps at night.
Despite the challenges of treating severe atopic dermatitis in children, she told her audience that treating these young patients has been one of the most rewarding parts of her practice.
Dr. Maguiness had no relevant disclosures.
On Twitter @naseemsmiller
EXPERT ANALYSIS FROM AAD SUMMER ACADEMY 2013
Dexamethasone improves outcomes for infants with bronchiolitis, atopy history
A 5-day course of dexamethasone significantly shortened hospital stays for infants with bronchiolitis who had eczema or close relatives with asthma.
The randomized, placebo-controlled study suggests that a family history of atopy could identify a subset of babies who would benefit from the addition of a corticosteroid to the usual salbutamol therapy for acute bronchiolitis, according to Dr. Khalid Alansari and colleagues. The report was published in the Sept. 16 issue of Pediatrics.
The researchers examined 7-day outcomes in 200 infants with acute bronchiolitis who were at a high risk of asthma, as determined by having at least one first-degree relative with either asthma or eczema. All of the children (mean age 3.5 months) were admitted to a pediatric hospital for treatment, wrote Dr. Alansari of Weill Cornell Medical College, Doha, Qatar, and coauthors. Infants who received dexamethasone were discharged 8 hours earlier than were those receiving standard treatment. The mean duration of symptoms was 4.5 days (Pediatrics 2013 Sept. 13 [doi: 10.1542/peds.2012-3746]).
The study’s primary outcome was time until discharge. Secondary outcomes included the number of patients who needed epinephrine treatment, readmission for a shorter stay in an infirmary site, and revisiting the emergency department or another clinic for the same illness. A study nurse made daily calls to assess the patients after discharge.
Infants in the dexamethasone group were discharged at a mean of 18.6 hours – significantly sooner than those in the control group (27 hours). Epinephrine was necessary for 19 infants in the dexamethasone group and 31 in the placebo group – again a significant difference.
Similar numbers in each group needed readmission and additional outpatient visits in the week after discharge. During the follow-up week, 22% of the dexamethasone group needed infirmary care and the mean stay was 17 hours, compared with 21% of the placebo group with a mean stay of 18 hours.
Nineteen in the dexamethasone group and 11 in the placebo group made a clinic visit (18.6% vs. 11%); this difference was not significant.
The chest radiograph was normal in about 37% of infants studied. About half showed lesser infiltrates; 15% had a lobar collapse or consolidation.
More than 70% had a full sibling with asthma. About 20% had a parent with the disease; in 5%, both parents had it. About 20% of patients had both eczema and first-degree relative with asthma.
All of the infants received 2.5 mg salbutamol nebulization at baseline and at 30, 60, and 120 minutes, and then every 2 hours until discharge. Nebulized epinephrine (0.5 mL/kg with a maximum dose of 5 mL) was available if needed. In addition, they were randomized to either placebo or to a 5-day course of dexamethasone 1 mg/mL, at a rate of 1 mL/kg on day 1, reduced to 0.6 mL/kg for days 2-5.
The study was sponsored by Hamad Medical Corporation. The authors reported no financial conflicts.
A 5-day course of dexamethasone significantly shortened hospital stays for infants with bronchiolitis who had eczema or close relatives with asthma.
The randomized, placebo-controlled study suggests that a family history of atopy could identify a subset of babies who would benefit from the addition of a corticosteroid to the usual salbutamol therapy for acute bronchiolitis, according to Dr. Khalid Alansari and colleagues. The report was published in the Sept. 16 issue of Pediatrics.
The researchers examined 7-day outcomes in 200 infants with acute bronchiolitis who were at a high risk of asthma, as determined by having at least one first-degree relative with either asthma or eczema. All of the children (mean age 3.5 months) were admitted to a pediatric hospital for treatment, wrote Dr. Alansari of Weill Cornell Medical College, Doha, Qatar, and coauthors. Infants who received dexamethasone were discharged 8 hours earlier than were those receiving standard treatment. The mean duration of symptoms was 4.5 days (Pediatrics 2013 Sept. 13 [doi: 10.1542/peds.2012-3746]).
The study’s primary outcome was time until discharge. Secondary outcomes included the number of patients who needed epinephrine treatment, readmission for a shorter stay in an infirmary site, and revisiting the emergency department or another clinic for the same illness. A study nurse made daily calls to assess the patients after discharge.
Infants in the dexamethasone group were discharged at a mean of 18.6 hours – significantly sooner than those in the control group (27 hours). Epinephrine was necessary for 19 infants in the dexamethasone group and 31 in the placebo group – again a significant difference.
Similar numbers in each group needed readmission and additional outpatient visits in the week after discharge. During the follow-up week, 22% of the dexamethasone group needed infirmary care and the mean stay was 17 hours, compared with 21% of the placebo group with a mean stay of 18 hours.
Nineteen in the dexamethasone group and 11 in the placebo group made a clinic visit (18.6% vs. 11%); this difference was not significant.
The chest radiograph was normal in about 37% of infants studied. About half showed lesser infiltrates; 15% had a lobar collapse or consolidation.
More than 70% had a full sibling with asthma. About 20% had a parent with the disease; in 5%, both parents had it. About 20% of patients had both eczema and first-degree relative with asthma.
All of the infants received 2.5 mg salbutamol nebulization at baseline and at 30, 60, and 120 minutes, and then every 2 hours until discharge. Nebulized epinephrine (0.5 mL/kg with a maximum dose of 5 mL) was available if needed. In addition, they were randomized to either placebo or to a 5-day course of dexamethasone 1 mg/mL, at a rate of 1 mL/kg on day 1, reduced to 0.6 mL/kg for days 2-5.
The study was sponsored by Hamad Medical Corporation. The authors reported no financial conflicts.
A 5-day course of dexamethasone significantly shortened hospital stays for infants with bronchiolitis who had eczema or close relatives with asthma.
The randomized, placebo-controlled study suggests that a family history of atopy could identify a subset of babies who would benefit from the addition of a corticosteroid to the usual salbutamol therapy for acute bronchiolitis, according to Dr. Khalid Alansari and colleagues. The report was published in the Sept. 16 issue of Pediatrics.
The researchers examined 7-day outcomes in 200 infants with acute bronchiolitis who were at a high risk of asthma, as determined by having at least one first-degree relative with either asthma or eczema. All of the children (mean age 3.5 months) were admitted to a pediatric hospital for treatment, wrote Dr. Alansari of Weill Cornell Medical College, Doha, Qatar, and coauthors. Infants who received dexamethasone were discharged 8 hours earlier than were those receiving standard treatment. The mean duration of symptoms was 4.5 days (Pediatrics 2013 Sept. 13 [doi: 10.1542/peds.2012-3746]).
The study’s primary outcome was time until discharge. Secondary outcomes included the number of patients who needed epinephrine treatment, readmission for a shorter stay in an infirmary site, and revisiting the emergency department or another clinic for the same illness. A study nurse made daily calls to assess the patients after discharge.
Infants in the dexamethasone group were discharged at a mean of 18.6 hours – significantly sooner than those in the control group (27 hours). Epinephrine was necessary for 19 infants in the dexamethasone group and 31 in the placebo group – again a significant difference.
Similar numbers in each group needed readmission and additional outpatient visits in the week after discharge. During the follow-up week, 22% of the dexamethasone group needed infirmary care and the mean stay was 17 hours, compared with 21% of the placebo group with a mean stay of 18 hours.
Nineteen in the dexamethasone group and 11 in the placebo group made a clinic visit (18.6% vs. 11%); this difference was not significant.
The chest radiograph was normal in about 37% of infants studied. About half showed lesser infiltrates; 15% had a lobar collapse or consolidation.
More than 70% had a full sibling with asthma. About 20% had a parent with the disease; in 5%, both parents had it. About 20% of patients had both eczema and first-degree relative with asthma.
All of the infants received 2.5 mg salbutamol nebulization at baseline and at 30, 60, and 120 minutes, and then every 2 hours until discharge. Nebulized epinephrine (0.5 mL/kg with a maximum dose of 5 mL) was available if needed. In addition, they were randomized to either placebo or to a 5-day course of dexamethasone 1 mg/mL, at a rate of 1 mL/kg on day 1, reduced to 0.6 mL/kg for days 2-5.
The study was sponsored by Hamad Medical Corporation. The authors reported no financial conflicts.
FROM PEDIATRICS
Major finding: Infants with bronchiolitis who had a family history of atopy who received dexamethasone added to salbutamol were discharged significantly sooner than were those receiving usual therapy (18.6 hours vs. 27 hours).
Data source: The randomized, placebo controlled study comprised 200 infants with acute bronchiolitis.
Disclosures: The study was sponsored by Hamad Medical Corporation. The authors reported no financial conflicts.
Antibiotic Use: Yet Another Threat?

The issue of increasing antibiotic resistance has become a serious global threat. The World Health Organization proclaimed that World Health Day 2011 would be dedicated to a comprehensive consolidated strategy to prevent regression to a preantibiotic era when infections were the single leading causes of death. At the 2013 G8 summit, the health ministers of the 8 wealthiest nations in the world proclaimed that antibiotic resistance is the single biggest threat to health security facing the 21st century. In addition to the problem of resistance, the use of antibiotics can lead to long-lasting alterations in the gut flora, making posttraumatic septicemia due to enteric organisms difficult to manage. Antibiotic use also has been associated with the development of inflammatory bowel disease in a number of well-done studies. Acute antibiotic side effects have included dyschromia, photosensitivity, potential hepatic and/or renal dysfunction, gastrointestinal tract distress, and various cutaneous events ranging from morbilliform eruptions to hives and even toxic epidermal necrolysis. All of the foregoing begs for more rational, appropriate, and circumspect use of antibiotic medications by all health care providers.
If the preceding commentary didn’t catch your attention, perhaps the findings from a recent article published online in the British Journal of Dermatology will. In this thoughtful and comprehensive review, a meta-analysis was performed on 20 large-scale observational studies involving individuals aged 0 to 25 years, which assessed the impact of antibiotic exposure in utero or within the first year of life on the subsequent risk for developing eczema. Both cross-sectional and longitudinal studies demonstrated a consistently increased risk (odds ratio, 1.4) of developing atopic eczema associated with postnatal antibiotic exposure. In fact, this association was so reliable that a dose-response association could be determined, suggesting a 7% increased risk for eczema for each additional oral or parenteral antibiotic course received during the first year of life. Why this effect happens remains uncertain, but the association is clear.
What’s the issue?
Think about your use of antibiotics! Do you use open-ended and prolonged courses for acne, rosacea, hidradenitis suppurativa, dissecting cellulitis of the scalp, and other conditions in adults? Are you contributing to the ever-expanding pool of antibiotic-resistant microbes carried by the adult population? When you do utilize antibiotics, do you always verify the presence of infection by culture? Do you always obtain sensitivities on bacterial isolates? Do you explicitly admonish antibiotic recipients or their parents/guardians to finish the antibiotic course and not save or share? This recent article now makes concerns about antibiotic use early in life highly relevant. Do you treat impetigo, for example, with one of the several approved topical agents or still routinely administer oral antibiotics? How would you manage neonatal acne or furunculosis in a young child? This paper from the British Journal of Dermatology supplies us with yet another good reason to evaluate and refine our own prescribing habits when it comes to antibiotics.

The issue of increasing antibiotic resistance has become a serious global threat. The World Health Organization proclaimed that World Health Day 2011 would be dedicated to a comprehensive consolidated strategy to prevent regression to a preantibiotic era when infections were the single leading causes of death. At the 2013 G8 summit, the health ministers of the 8 wealthiest nations in the world proclaimed that antibiotic resistance is the single biggest threat to health security facing the 21st century. In addition to the problem of resistance, the use of antibiotics can lead to long-lasting alterations in the gut flora, making posttraumatic septicemia due to enteric organisms difficult to manage. Antibiotic use also has been associated with the development of inflammatory bowel disease in a number of well-done studies. Acute antibiotic side effects have included dyschromia, photosensitivity, potential hepatic and/or renal dysfunction, gastrointestinal tract distress, and various cutaneous events ranging from morbilliform eruptions to hives and even toxic epidermal necrolysis. All of the foregoing begs for more rational, appropriate, and circumspect use of antibiotic medications by all health care providers.
If the preceding commentary didn’t catch your attention, perhaps the findings from a recent article published online in the British Journal of Dermatology will. In this thoughtful and comprehensive review, a meta-analysis was performed on 20 large-scale observational studies involving individuals aged 0 to 25 years, which assessed the impact of antibiotic exposure in utero or within the first year of life on the subsequent risk for developing eczema. Both cross-sectional and longitudinal studies demonstrated a consistently increased risk (odds ratio, 1.4) of developing atopic eczema associated with postnatal antibiotic exposure. In fact, this association was so reliable that a dose-response association could be determined, suggesting a 7% increased risk for eczema for each additional oral or parenteral antibiotic course received during the first year of life. Why this effect happens remains uncertain, but the association is clear.
What’s the issue?
Think about your use of antibiotics! Do you use open-ended and prolonged courses for acne, rosacea, hidradenitis suppurativa, dissecting cellulitis of the scalp, and other conditions in adults? Are you contributing to the ever-expanding pool of antibiotic-resistant microbes carried by the adult population? When you do utilize antibiotics, do you always verify the presence of infection by culture? Do you always obtain sensitivities on bacterial isolates? Do you explicitly admonish antibiotic recipients or their parents/guardians to finish the antibiotic course and not save or share? This recent article now makes concerns about antibiotic use early in life highly relevant. Do you treat impetigo, for example, with one of the several approved topical agents or still routinely administer oral antibiotics? How would you manage neonatal acne or furunculosis in a young child? This paper from the British Journal of Dermatology supplies us with yet another good reason to evaluate and refine our own prescribing habits when it comes to antibiotics.

The issue of increasing antibiotic resistance has become a serious global threat. The World Health Organization proclaimed that World Health Day 2011 would be dedicated to a comprehensive consolidated strategy to prevent regression to a preantibiotic era when infections were the single leading causes of death. At the 2013 G8 summit, the health ministers of the 8 wealthiest nations in the world proclaimed that antibiotic resistance is the single biggest threat to health security facing the 21st century. In addition to the problem of resistance, the use of antibiotics can lead to long-lasting alterations in the gut flora, making posttraumatic septicemia due to enteric organisms difficult to manage. Antibiotic use also has been associated with the development of inflammatory bowel disease in a number of well-done studies. Acute antibiotic side effects have included dyschromia, photosensitivity, potential hepatic and/or renal dysfunction, gastrointestinal tract distress, and various cutaneous events ranging from morbilliform eruptions to hives and even toxic epidermal necrolysis. All of the foregoing begs for more rational, appropriate, and circumspect use of antibiotic medications by all health care providers.
If the preceding commentary didn’t catch your attention, perhaps the findings from a recent article published online in the British Journal of Dermatology will. In this thoughtful and comprehensive review, a meta-analysis was performed on 20 large-scale observational studies involving individuals aged 0 to 25 years, which assessed the impact of antibiotic exposure in utero or within the first year of life on the subsequent risk for developing eczema. Both cross-sectional and longitudinal studies demonstrated a consistently increased risk (odds ratio, 1.4) of developing atopic eczema associated with postnatal antibiotic exposure. In fact, this association was so reliable that a dose-response association could be determined, suggesting a 7% increased risk for eczema for each additional oral or parenteral antibiotic course received during the first year of life. Why this effect happens remains uncertain, but the association is clear.
What’s the issue?
Think about your use of antibiotics! Do you use open-ended and prolonged courses for acne, rosacea, hidradenitis suppurativa, dissecting cellulitis of the scalp, and other conditions in adults? Are you contributing to the ever-expanding pool of antibiotic-resistant microbes carried by the adult population? When you do utilize antibiotics, do you always verify the presence of infection by culture? Do you always obtain sensitivities on bacterial isolates? Do you explicitly admonish antibiotic recipients or their parents/guardians to finish the antibiotic course and not save or share? This recent article now makes concerns about antibiotic use early in life highly relevant. Do you treat impetigo, for example, with one of the several approved topical agents or still routinely administer oral antibiotics? How would you manage neonatal acne or furunculosis in a young child? This paper from the British Journal of Dermatology supplies us with yet another good reason to evaluate and refine our own prescribing habits when it comes to antibiotics.