User login
Does private equity ensure survival of GI practices?
CHICAGO – In this age of corporate megamergers, private practice gastroenterologists are increasingly weighing the pros and cons of selling their practices to private equity firms.
It’s becoming more difficult for solo or small group practices to go it alone. While there may be advantages in selling a medical practice to a private equity firm, physicians could be trading a degree of freedom for financial certainty and relief from administrative burdens, according to Klaus Mergener, MD, PhD, MBA, AGAF, a clinical gastroenterologist, affiliate professor of medicine at the University of Washington, Seattle, and chief medical officer of Pentax Medical’s Lifecare Division.
“Over the last decades, and ongoing, there have been massive downward pressures on reimbursements and costs are rising. Practices have tried to compensate, and they’ve added ancillary revenue streams, and they’ve tried to cut costs internally. It’s fair to say that depending on the local market, many practices find that one of the last viable options is essentially to spread overhead costs – meaning you have to get larger and you have to merge into larger entities,” he said on May 6 during a presentation at the annual Digestive Diseases Week® meeting.
The first independent gastroenterology practice was purchased by a private equity firm in 2016. Today, more than 1,000 gastroenterologists have been acquired by private equity firms, which amounts to a total value in excess of $1 billion.
The pace at which private equity firms are buying private medical practices is accelerating. On April 26, Kaiser Permanente – with 39 hospitals and 24,000 physicians – announced that it had acquired Geisinger Health System, a regional health care provider in Pennsylvania with 10 hospitals, forming a new entity called Risant Health.
Dr. Mergener likened the situation to the story of David and Goliath. David famously defeated the much larger and more powerful Goliath, but the metaphor is imperfect, because small private practices are running out of rocks to sling at the big guys.
In some small, rural markets with no significant competition, it may be possible for small practices to survive through mergers, “but in most U.S. markets, it’s fair to say that ... practices have found it hard to merge without external help. There are egos involved, there are many hurdles, and this is where private equity has essentially moved in as catalyst,” Dr. Mergener said.
Employees of large entities
Other physicians, however, say that while acquisition may seem inevitable, private equity is an option for survival.
“I don’t think this means the demise of private practice,“ said Lawrence R. Kosinski, MD, MBA, AGAF , chief medical officer at SonarMD, a Chicago-based company that specializes in facilitating managing the care of patients with chronic conditions.
“I think that private equity is just another way of aggregating GI doctors into an employment situation,” he said. “It’s just a different tool, and we can argue all day as to whether it’s the right tool, but it’s a tool no different than employment by a hospital. You can work for a hospital or you can work for a private equity funded group, but in the end, you’re an employee of a large entity.”
Michael Weinstein, MD, AGAF, president and CEO of Capital Digestive Care, a practice in Washington, and managing partner of the Metropolitan Gastroenterology Group Division, a medical group practice in Silver Spring, Md., advised taking a long and hard look before taking the leap into the hands of private equity.
“You have to have a strategy, but you have to know what you have and what you need. Ask yourself whether private equity is what you really need. They’re not in the business of making you a better practice,” he said. “Once you do it, you’re no longer in control of your future. Somebody else is in control of your future.”
Private equity firms sell a bill of goods
“They say, ‘We’re going to improve your services, we’re going to bring you tech, we’re going to negotiate better contracts and do all these things for you.’ Ninety percent of it is a lie, because that’s not what they’re going to do. They’re just going to try to increase the bottom line, bolt down a few more practices, increase the gross revenue, and thereby increase the net profit from where it was before, not necessarily because they’re making better lives for the individual providers. They’re just adding more cows to the field, but every cow is the same as far as they’re concerned. They really don’t care about the production of milk,” Dr. Weinstein said.
A few years ago, his practice considered whether private equity would be a good option. His practice, he said, needed to be bigger and more effective and efficient. Instead, his practice formed a partnership with PE GI Solutions (formerly Physicians Endoscopy), a developer and manager of endoscopic ambulatory surgery centers.
In Dallas, private equity firms have increased reimbursements for Texas Digestive Disease Consultants.
“Our practice went through mergers, acquisitions, and now, with private equity coming onto the scene, it’s completely different,” said Kimberly M. Persley, MD, AGAF, a partner with Texas Digestive Disease Consultants and a member of the GI & Hepatology News board of editors.
“We were a five-person independent group negotiating contracts, getting cut every other year by some payer because they negotiated a better price with someone else. And having to go through that process every year when all we really want to do is take care of patients. Private equity adds to our group practice by having someone dedicated to negotiating these contracts, and getting reimbursed far more than we ever did prior to our involvement with private equity,” she said.
How it works
In the typical model, a private equity partner purchases the practice and creates a management services organization (MSO), which provides nonclinical services to the practice, theoretically freeing the physicians from the administrative burdens of day-to-day practice.
The practice then becomes the care center managed by the MSO, and the physicians in the practice at the time of the acquisition get stock in the MSO. “They sell a portion of their annual income, so going forward they’re making less money initially, until some of that is being recovered by higher efficiencies. They get an upfront check at a multiple of the income they just sold, and that provides the initial incentive. Then the entity is grown by adding other practices through the same mechanism,” Dr. Mergener said.
After about 5 years, the private equity partner typically sells the MSO to another, probably even larger buyer, and the cycle starts again.
In addition to the upfront incentive that makes practice mergers and consolidation work, the arrangement gives the GI practice access to top-notch administrators, as well as access to capital for investments such as information technology infrastructure, digital health, and data analytics.
He cautioned that it’s crucial for practices to enter the marriage with eyes wide open and be very careful in choosing the private equity partner.
“The goal is to find a partner that has values and a vision that matches the practice’s. In theory, they should be pulling on the same side of the rope, because if it’s a high-quality practice and efficiencies are being improved, more practices should be more likely to join,” which will benefit physicians, patients, and the private equity partner alike, Dr. Mergener said.
Although the private equity construct has been successful in the short term for many practices, it’s less clear what will happen long-term. There is a risk that after 5 years there won’t be a buyer for the MSO at the expected price, which may result in complex financial transactions that could leave the MSO in debt. In such a scenario, physician employees would not be personally liable, but might suffer the consequences of a failing or unsuccessful operation, Dr. Mergener said.
Dr. Mergener’s talk was presented as part of a an ASGE Presidential Plenary held during DDW 2023. He disclosed consulting, honoraria, advisory board activity or stock options from various corporations, but reported having no relationships with private equity.
DDW is sponsored by the American Association for the Study of Liver Diseases (AASLD), the American Gastroenterological Association (AGA), the American Society for Gastrointestinal Endoscopy (ASGE) and The Society for Surgery of the Alimentary Tract (SSAT).
CHICAGO – In this age of corporate megamergers, private practice gastroenterologists are increasingly weighing the pros and cons of selling their practices to private equity firms.
It’s becoming more difficult for solo or small group practices to go it alone. While there may be advantages in selling a medical practice to a private equity firm, physicians could be trading a degree of freedom for financial certainty and relief from administrative burdens, according to Klaus Mergener, MD, PhD, MBA, AGAF, a clinical gastroenterologist, affiliate professor of medicine at the University of Washington, Seattle, and chief medical officer of Pentax Medical’s Lifecare Division.
“Over the last decades, and ongoing, there have been massive downward pressures on reimbursements and costs are rising. Practices have tried to compensate, and they’ve added ancillary revenue streams, and they’ve tried to cut costs internally. It’s fair to say that depending on the local market, many practices find that one of the last viable options is essentially to spread overhead costs – meaning you have to get larger and you have to merge into larger entities,” he said on May 6 during a presentation at the annual Digestive Diseases Week® meeting.
The first independent gastroenterology practice was purchased by a private equity firm in 2016. Today, more than 1,000 gastroenterologists have been acquired by private equity firms, which amounts to a total value in excess of $1 billion.
The pace at which private equity firms are buying private medical practices is accelerating. On April 26, Kaiser Permanente – with 39 hospitals and 24,000 physicians – announced that it had acquired Geisinger Health System, a regional health care provider in Pennsylvania with 10 hospitals, forming a new entity called Risant Health.
Dr. Mergener likened the situation to the story of David and Goliath. David famously defeated the much larger and more powerful Goliath, but the metaphor is imperfect, because small private practices are running out of rocks to sling at the big guys.
In some small, rural markets with no significant competition, it may be possible for small practices to survive through mergers, “but in most U.S. markets, it’s fair to say that ... practices have found it hard to merge without external help. There are egos involved, there are many hurdles, and this is where private equity has essentially moved in as catalyst,” Dr. Mergener said.
Employees of large entities
Other physicians, however, say that while acquisition may seem inevitable, private equity is an option for survival.
“I don’t think this means the demise of private practice,“ said Lawrence R. Kosinski, MD, MBA, AGAF , chief medical officer at SonarMD, a Chicago-based company that specializes in facilitating managing the care of patients with chronic conditions.
“I think that private equity is just another way of aggregating GI doctors into an employment situation,” he said. “It’s just a different tool, and we can argue all day as to whether it’s the right tool, but it’s a tool no different than employment by a hospital. You can work for a hospital or you can work for a private equity funded group, but in the end, you’re an employee of a large entity.”
Michael Weinstein, MD, AGAF, president and CEO of Capital Digestive Care, a practice in Washington, and managing partner of the Metropolitan Gastroenterology Group Division, a medical group practice in Silver Spring, Md., advised taking a long and hard look before taking the leap into the hands of private equity.
“You have to have a strategy, but you have to know what you have and what you need. Ask yourself whether private equity is what you really need. They’re not in the business of making you a better practice,” he said. “Once you do it, you’re no longer in control of your future. Somebody else is in control of your future.”
Private equity firms sell a bill of goods
“They say, ‘We’re going to improve your services, we’re going to bring you tech, we’re going to negotiate better contracts and do all these things for you.’ Ninety percent of it is a lie, because that’s not what they’re going to do. They’re just going to try to increase the bottom line, bolt down a few more practices, increase the gross revenue, and thereby increase the net profit from where it was before, not necessarily because they’re making better lives for the individual providers. They’re just adding more cows to the field, but every cow is the same as far as they’re concerned. They really don’t care about the production of milk,” Dr. Weinstein said.
A few years ago, his practice considered whether private equity would be a good option. His practice, he said, needed to be bigger and more effective and efficient. Instead, his practice formed a partnership with PE GI Solutions (formerly Physicians Endoscopy), a developer and manager of endoscopic ambulatory surgery centers.
In Dallas, private equity firms have increased reimbursements for Texas Digestive Disease Consultants.
“Our practice went through mergers, acquisitions, and now, with private equity coming onto the scene, it’s completely different,” said Kimberly M. Persley, MD, AGAF, a partner with Texas Digestive Disease Consultants and a member of the GI & Hepatology News board of editors.
“We were a five-person independent group negotiating contracts, getting cut every other year by some payer because they negotiated a better price with someone else. And having to go through that process every year when all we really want to do is take care of patients. Private equity adds to our group practice by having someone dedicated to negotiating these contracts, and getting reimbursed far more than we ever did prior to our involvement with private equity,” she said.
How it works
In the typical model, a private equity partner purchases the practice and creates a management services organization (MSO), which provides nonclinical services to the practice, theoretically freeing the physicians from the administrative burdens of day-to-day practice.
The practice then becomes the care center managed by the MSO, and the physicians in the practice at the time of the acquisition get stock in the MSO. “They sell a portion of their annual income, so going forward they’re making less money initially, until some of that is being recovered by higher efficiencies. They get an upfront check at a multiple of the income they just sold, and that provides the initial incentive. Then the entity is grown by adding other practices through the same mechanism,” Dr. Mergener said.
After about 5 years, the private equity partner typically sells the MSO to another, probably even larger buyer, and the cycle starts again.
In addition to the upfront incentive that makes practice mergers and consolidation work, the arrangement gives the GI practice access to top-notch administrators, as well as access to capital for investments such as information technology infrastructure, digital health, and data analytics.
He cautioned that it’s crucial for practices to enter the marriage with eyes wide open and be very careful in choosing the private equity partner.
“The goal is to find a partner that has values and a vision that matches the practice’s. In theory, they should be pulling on the same side of the rope, because if it’s a high-quality practice and efficiencies are being improved, more practices should be more likely to join,” which will benefit physicians, patients, and the private equity partner alike, Dr. Mergener said.
Although the private equity construct has been successful in the short term for many practices, it’s less clear what will happen long-term. There is a risk that after 5 years there won’t be a buyer for the MSO at the expected price, which may result in complex financial transactions that could leave the MSO in debt. In such a scenario, physician employees would not be personally liable, but might suffer the consequences of a failing or unsuccessful operation, Dr. Mergener said.
Dr. Mergener’s talk was presented as part of a an ASGE Presidential Plenary held during DDW 2023. He disclosed consulting, honoraria, advisory board activity or stock options from various corporations, but reported having no relationships with private equity.
DDW is sponsored by the American Association for the Study of Liver Diseases (AASLD), the American Gastroenterological Association (AGA), the American Society for Gastrointestinal Endoscopy (ASGE) and The Society for Surgery of the Alimentary Tract (SSAT).
CHICAGO – In this age of corporate megamergers, private practice gastroenterologists are increasingly weighing the pros and cons of selling their practices to private equity firms.
It’s becoming more difficult for solo or small group practices to go it alone. While there may be advantages in selling a medical practice to a private equity firm, physicians could be trading a degree of freedom for financial certainty and relief from administrative burdens, according to Klaus Mergener, MD, PhD, MBA, AGAF, a clinical gastroenterologist, affiliate professor of medicine at the University of Washington, Seattle, and chief medical officer of Pentax Medical’s Lifecare Division.
“Over the last decades, and ongoing, there have been massive downward pressures on reimbursements and costs are rising. Practices have tried to compensate, and they’ve added ancillary revenue streams, and they’ve tried to cut costs internally. It’s fair to say that depending on the local market, many practices find that one of the last viable options is essentially to spread overhead costs – meaning you have to get larger and you have to merge into larger entities,” he said on May 6 during a presentation at the annual Digestive Diseases Week® meeting.
The first independent gastroenterology practice was purchased by a private equity firm in 2016. Today, more than 1,000 gastroenterologists have been acquired by private equity firms, which amounts to a total value in excess of $1 billion.
The pace at which private equity firms are buying private medical practices is accelerating. On April 26, Kaiser Permanente – with 39 hospitals and 24,000 physicians – announced that it had acquired Geisinger Health System, a regional health care provider in Pennsylvania with 10 hospitals, forming a new entity called Risant Health.
Dr. Mergener likened the situation to the story of David and Goliath. David famously defeated the much larger and more powerful Goliath, but the metaphor is imperfect, because small private practices are running out of rocks to sling at the big guys.
In some small, rural markets with no significant competition, it may be possible for small practices to survive through mergers, “but in most U.S. markets, it’s fair to say that ... practices have found it hard to merge without external help. There are egos involved, there are many hurdles, and this is where private equity has essentially moved in as catalyst,” Dr. Mergener said.
Employees of large entities
Other physicians, however, say that while acquisition may seem inevitable, private equity is an option for survival.
“I don’t think this means the demise of private practice,“ said Lawrence R. Kosinski, MD, MBA, AGAF , chief medical officer at SonarMD, a Chicago-based company that specializes in facilitating managing the care of patients with chronic conditions.
“I think that private equity is just another way of aggregating GI doctors into an employment situation,” he said. “It’s just a different tool, and we can argue all day as to whether it’s the right tool, but it’s a tool no different than employment by a hospital. You can work for a hospital or you can work for a private equity funded group, but in the end, you’re an employee of a large entity.”
Michael Weinstein, MD, AGAF, president and CEO of Capital Digestive Care, a practice in Washington, and managing partner of the Metropolitan Gastroenterology Group Division, a medical group practice in Silver Spring, Md., advised taking a long and hard look before taking the leap into the hands of private equity.
“You have to have a strategy, but you have to know what you have and what you need. Ask yourself whether private equity is what you really need. They’re not in the business of making you a better practice,” he said. “Once you do it, you’re no longer in control of your future. Somebody else is in control of your future.”
Private equity firms sell a bill of goods
“They say, ‘We’re going to improve your services, we’re going to bring you tech, we’re going to negotiate better contracts and do all these things for you.’ Ninety percent of it is a lie, because that’s not what they’re going to do. They’re just going to try to increase the bottom line, bolt down a few more practices, increase the gross revenue, and thereby increase the net profit from where it was before, not necessarily because they’re making better lives for the individual providers. They’re just adding more cows to the field, but every cow is the same as far as they’re concerned. They really don’t care about the production of milk,” Dr. Weinstein said.
A few years ago, his practice considered whether private equity would be a good option. His practice, he said, needed to be bigger and more effective and efficient. Instead, his practice formed a partnership with PE GI Solutions (formerly Physicians Endoscopy), a developer and manager of endoscopic ambulatory surgery centers.
In Dallas, private equity firms have increased reimbursements for Texas Digestive Disease Consultants.
“Our practice went through mergers, acquisitions, and now, with private equity coming onto the scene, it’s completely different,” said Kimberly M. Persley, MD, AGAF, a partner with Texas Digestive Disease Consultants and a member of the GI & Hepatology News board of editors.
“We were a five-person independent group negotiating contracts, getting cut every other year by some payer because they negotiated a better price with someone else. And having to go through that process every year when all we really want to do is take care of patients. Private equity adds to our group practice by having someone dedicated to negotiating these contracts, and getting reimbursed far more than we ever did prior to our involvement with private equity,” she said.
How it works
In the typical model, a private equity partner purchases the practice and creates a management services organization (MSO), which provides nonclinical services to the practice, theoretically freeing the physicians from the administrative burdens of day-to-day practice.
The practice then becomes the care center managed by the MSO, and the physicians in the practice at the time of the acquisition get stock in the MSO. “They sell a portion of their annual income, so going forward they’re making less money initially, until some of that is being recovered by higher efficiencies. They get an upfront check at a multiple of the income they just sold, and that provides the initial incentive. Then the entity is grown by adding other practices through the same mechanism,” Dr. Mergener said.
After about 5 years, the private equity partner typically sells the MSO to another, probably even larger buyer, and the cycle starts again.
In addition to the upfront incentive that makes practice mergers and consolidation work, the arrangement gives the GI practice access to top-notch administrators, as well as access to capital for investments such as information technology infrastructure, digital health, and data analytics.
He cautioned that it’s crucial for practices to enter the marriage with eyes wide open and be very careful in choosing the private equity partner.
“The goal is to find a partner that has values and a vision that matches the practice’s. In theory, they should be pulling on the same side of the rope, because if it’s a high-quality practice and efficiencies are being improved, more practices should be more likely to join,” which will benefit physicians, patients, and the private equity partner alike, Dr. Mergener said.
Although the private equity construct has been successful in the short term for many practices, it’s less clear what will happen long-term. There is a risk that after 5 years there won’t be a buyer for the MSO at the expected price, which may result in complex financial transactions that could leave the MSO in debt. In such a scenario, physician employees would not be personally liable, but might suffer the consequences of a failing or unsuccessful operation, Dr. Mergener said.
Dr. Mergener’s talk was presented as part of a an ASGE Presidential Plenary held during DDW 2023. He disclosed consulting, honoraria, advisory board activity or stock options from various corporations, but reported having no relationships with private equity.
DDW is sponsored by the American Association for the Study of Liver Diseases (AASLD), the American Gastroenterological Association (AGA), the American Society for Gastrointestinal Endoscopy (ASGE) and The Society for Surgery of the Alimentary Tract (SSAT).
AT DDW 2023
Evidence weighed for suicide/self-harm with obesity drugs
Following reports that the European Medicines Agency is looking into instances of suicide or self-harm after patients took the weight loss drugs semaglutide or liraglutide, the manufacturer, Novo Nordisk, issued a statement to this news organization in which it says it “remains confident in the benefit risk profile of the products and remains committed to ensuring patient safety.”
U.S. experts say they haven’t personally seen this adverse effect in any patients except for one isolated case. An increase in suicidal ideation, particularly among younger people, has been reported following bariatric surgery for weight loss.
In the United States, the two drugs – both GLP-1 agonists – already come with a warning about the potential for these adverse effects on the branded versions approved for weight loss, Wegovy and Saxenda. (Years earlier, both drugs, marketed as Ozempic and Victoza, were also approved for treatment of type 2 diabetes.)
Of more than 1,200 reports of adverse reactions with semaglutide, 60 cases of suicidal ideation and 7 suicide attempts have been reported since 2018, according to the Food and Drug Administration’s Adverse Event Reporting System (FAERS) public database. For liraglutide, there were 71 cases of suicidal ideation, 28 suicide attempts, and 25 completed suicides out of more than 35,000 reports of adverse reactions.
The FAERS website cautions users that the data may be duplicated or incomplete, that rates of occurrence cannot be established using the data, that reports have not been verified, and that the existence of a report cannot establish causation.
The EMA is looking into about 150 reports of possible cases of self-injury and suicidal thoughts, according to a press release from the agency.
“It is not yet clear whether the reported cases are linked to the medicines themselves or to the patients’ underlying conditions or other factors,” it says. The medicines are widely used in the European Union, according to the press release.
The review of Ozempic, Saxenda, and Wegovy, which started on July 3, 2023, has been extended to include other GLP-1 receptor agonists, which include dulaglutide, exenatide, and lixisenatide. This review is expected to conclude in November 2023.
In a statement, Novo Nordisk did not directly dispute a potential link between the drugs and suicidal ideation.
“In the U.S., FDA requires medications for chronic weight management that work on the central nervous system, including Wegovy and Saxenda, to carry a warning about suicidal behavior and ideation,” the statement indicates. “This event had been reported in clinical trials with other weight management products.”
It adds: “Novo Nordisk is continuously performing surveillance of the data from ongoing clinical trials and real-world use of its products and collaborates closely with the authorities to ensure patient safety and adequate information to healthcare professionals.”
Important to know the denominator
“What’s important to know is the denominator,” said Holly Lofton, MD, a clinical associate professor of surgery and medicine and the director of the medical weight management program at NYU Langone, New York. “It needs a denominator with the total population on the medication so we can determine if that’s really a significant risk.”
Dr. Lofton described an isolated, anecdotal case of a patient who had no history of depression or mental health problems but developed suicidal thoughts after taking Saxenda for several months. In that case, the 25-year-old was experiencing problems in a personal relationship and with social media.
Two other weight loss specialists contacted by this news organization had not had patients who had experienced suicidal ideation with the drugs. “These are not very common in practice,” Dr. Lofton said in an interview.
The U.S. prescribing information for Saxenda, which contains liraglutide and has been approved as an adjunct to diet and exercise for chronic weight management, recommends monitoring for the emergence of depression and suicidal thoughts. In the clinical trials, 6 of the 3,384 patients who took the drug reported suicidal ideation; none of the 1,941 patients who received placebo did so, according to the FDA.
Similarly, the U.S. prescribing information for Wegovy, which contains semaglutide, recommends monitoring for the emergence of suicidal thoughts or depression, but this recommendation was based on clinical trials of other weight management products. The prescribing information for Ozempic, the brand name for semaglutide for type 2 diabetes, does not include this recommendation.
Is it the weight loss, rather than the meds? Seen with bariatric surgery too
Speculating what the link, if any, might be, Dr. Lofton suggested dopamine release could be playing a role. Small trials in humans as well as animal studies hint at a blunting of dopamine responses to usual triggers – including addictive substances and possibly food – that may also affect mood.
Young people (aged 18-34) who undergo bariatric surgery are at an increased risk of suicide during follow-up compared to their peers who don’t have surgery. And a study found an increase in events involving self-harm after bariatric surgery, especially among patients who already had a mental health disorder.
For a patient who derives comfort from food, not being able to eat in response to a stressful event may lead that patient to act out in more serious ways, according to Dr. Lofton. “That’s why, again, surgical follow-up is so important and their presurgical psychiatric evaluation is so important.”
A version of this article originally appeared on Medscape.com.
Following reports that the European Medicines Agency is looking into instances of suicide or self-harm after patients took the weight loss drugs semaglutide or liraglutide, the manufacturer, Novo Nordisk, issued a statement to this news organization in which it says it “remains confident in the benefit risk profile of the products and remains committed to ensuring patient safety.”
U.S. experts say they haven’t personally seen this adverse effect in any patients except for one isolated case. An increase in suicidal ideation, particularly among younger people, has been reported following bariatric surgery for weight loss.
In the United States, the two drugs – both GLP-1 agonists – already come with a warning about the potential for these adverse effects on the branded versions approved for weight loss, Wegovy and Saxenda. (Years earlier, both drugs, marketed as Ozempic and Victoza, were also approved for treatment of type 2 diabetes.)
Of more than 1,200 reports of adverse reactions with semaglutide, 60 cases of suicidal ideation and 7 suicide attempts have been reported since 2018, according to the Food and Drug Administration’s Adverse Event Reporting System (FAERS) public database. For liraglutide, there were 71 cases of suicidal ideation, 28 suicide attempts, and 25 completed suicides out of more than 35,000 reports of adverse reactions.
The FAERS website cautions users that the data may be duplicated or incomplete, that rates of occurrence cannot be established using the data, that reports have not been verified, and that the existence of a report cannot establish causation.
The EMA is looking into about 150 reports of possible cases of self-injury and suicidal thoughts, according to a press release from the agency.
“It is not yet clear whether the reported cases are linked to the medicines themselves or to the patients’ underlying conditions or other factors,” it says. The medicines are widely used in the European Union, according to the press release.
The review of Ozempic, Saxenda, and Wegovy, which started on July 3, 2023, has been extended to include other GLP-1 receptor agonists, which include dulaglutide, exenatide, and lixisenatide. This review is expected to conclude in November 2023.
In a statement, Novo Nordisk did not directly dispute a potential link between the drugs and suicidal ideation.
“In the U.S., FDA requires medications for chronic weight management that work on the central nervous system, including Wegovy and Saxenda, to carry a warning about suicidal behavior and ideation,” the statement indicates. “This event had been reported in clinical trials with other weight management products.”
It adds: “Novo Nordisk is continuously performing surveillance of the data from ongoing clinical trials and real-world use of its products and collaborates closely with the authorities to ensure patient safety and adequate information to healthcare professionals.”
Important to know the denominator
“What’s important to know is the denominator,” said Holly Lofton, MD, a clinical associate professor of surgery and medicine and the director of the medical weight management program at NYU Langone, New York. “It needs a denominator with the total population on the medication so we can determine if that’s really a significant risk.”
Dr. Lofton described an isolated, anecdotal case of a patient who had no history of depression or mental health problems but developed suicidal thoughts after taking Saxenda for several months. In that case, the 25-year-old was experiencing problems in a personal relationship and with social media.
Two other weight loss specialists contacted by this news organization had not had patients who had experienced suicidal ideation with the drugs. “These are not very common in practice,” Dr. Lofton said in an interview.
The U.S. prescribing information for Saxenda, which contains liraglutide and has been approved as an adjunct to diet and exercise for chronic weight management, recommends monitoring for the emergence of depression and suicidal thoughts. In the clinical trials, 6 of the 3,384 patients who took the drug reported suicidal ideation; none of the 1,941 patients who received placebo did so, according to the FDA.
Similarly, the U.S. prescribing information for Wegovy, which contains semaglutide, recommends monitoring for the emergence of suicidal thoughts or depression, but this recommendation was based on clinical trials of other weight management products. The prescribing information for Ozempic, the brand name for semaglutide for type 2 diabetes, does not include this recommendation.
Is it the weight loss, rather than the meds? Seen with bariatric surgery too
Speculating what the link, if any, might be, Dr. Lofton suggested dopamine release could be playing a role. Small trials in humans as well as animal studies hint at a blunting of dopamine responses to usual triggers – including addictive substances and possibly food – that may also affect mood.
Young people (aged 18-34) who undergo bariatric surgery are at an increased risk of suicide during follow-up compared to their peers who don’t have surgery. And a study found an increase in events involving self-harm after bariatric surgery, especially among patients who already had a mental health disorder.
For a patient who derives comfort from food, not being able to eat in response to a stressful event may lead that patient to act out in more serious ways, according to Dr. Lofton. “That’s why, again, surgical follow-up is so important and their presurgical psychiatric evaluation is so important.”
A version of this article originally appeared on Medscape.com.
Following reports that the European Medicines Agency is looking into instances of suicide or self-harm after patients took the weight loss drugs semaglutide or liraglutide, the manufacturer, Novo Nordisk, issued a statement to this news organization in which it says it “remains confident in the benefit risk profile of the products and remains committed to ensuring patient safety.”
U.S. experts say they haven’t personally seen this adverse effect in any patients except for one isolated case. An increase in suicidal ideation, particularly among younger people, has been reported following bariatric surgery for weight loss.
In the United States, the two drugs – both GLP-1 agonists – already come with a warning about the potential for these adverse effects on the branded versions approved for weight loss, Wegovy and Saxenda. (Years earlier, both drugs, marketed as Ozempic and Victoza, were also approved for treatment of type 2 diabetes.)
Of more than 1,200 reports of adverse reactions with semaglutide, 60 cases of suicidal ideation and 7 suicide attempts have been reported since 2018, according to the Food and Drug Administration’s Adverse Event Reporting System (FAERS) public database. For liraglutide, there were 71 cases of suicidal ideation, 28 suicide attempts, and 25 completed suicides out of more than 35,000 reports of adverse reactions.
The FAERS website cautions users that the data may be duplicated or incomplete, that rates of occurrence cannot be established using the data, that reports have not been verified, and that the existence of a report cannot establish causation.
The EMA is looking into about 150 reports of possible cases of self-injury and suicidal thoughts, according to a press release from the agency.
“It is not yet clear whether the reported cases are linked to the medicines themselves or to the patients’ underlying conditions or other factors,” it says. The medicines are widely used in the European Union, according to the press release.
The review of Ozempic, Saxenda, and Wegovy, which started on July 3, 2023, has been extended to include other GLP-1 receptor agonists, which include dulaglutide, exenatide, and lixisenatide. This review is expected to conclude in November 2023.
In a statement, Novo Nordisk did not directly dispute a potential link between the drugs and suicidal ideation.
“In the U.S., FDA requires medications for chronic weight management that work on the central nervous system, including Wegovy and Saxenda, to carry a warning about suicidal behavior and ideation,” the statement indicates. “This event had been reported in clinical trials with other weight management products.”
It adds: “Novo Nordisk is continuously performing surveillance of the data from ongoing clinical trials and real-world use of its products and collaborates closely with the authorities to ensure patient safety and adequate information to healthcare professionals.”
Important to know the denominator
“What’s important to know is the denominator,” said Holly Lofton, MD, a clinical associate professor of surgery and medicine and the director of the medical weight management program at NYU Langone, New York. “It needs a denominator with the total population on the medication so we can determine if that’s really a significant risk.”
Dr. Lofton described an isolated, anecdotal case of a patient who had no history of depression or mental health problems but developed suicidal thoughts after taking Saxenda for several months. In that case, the 25-year-old was experiencing problems in a personal relationship and with social media.
Two other weight loss specialists contacted by this news organization had not had patients who had experienced suicidal ideation with the drugs. “These are not very common in practice,” Dr. Lofton said in an interview.
The U.S. prescribing information for Saxenda, which contains liraglutide and has been approved as an adjunct to diet and exercise for chronic weight management, recommends monitoring for the emergence of depression and suicidal thoughts. In the clinical trials, 6 of the 3,384 patients who took the drug reported suicidal ideation; none of the 1,941 patients who received placebo did so, according to the FDA.
Similarly, the U.S. prescribing information for Wegovy, which contains semaglutide, recommends monitoring for the emergence of suicidal thoughts or depression, but this recommendation was based on clinical trials of other weight management products. The prescribing information for Ozempic, the brand name for semaglutide for type 2 diabetes, does not include this recommendation.
Is it the weight loss, rather than the meds? Seen with bariatric surgery too
Speculating what the link, if any, might be, Dr. Lofton suggested dopamine release could be playing a role. Small trials in humans as well as animal studies hint at a blunting of dopamine responses to usual triggers – including addictive substances and possibly food – that may also affect mood.
Young people (aged 18-34) who undergo bariatric surgery are at an increased risk of suicide during follow-up compared to their peers who don’t have surgery. And a study found an increase in events involving self-harm after bariatric surgery, especially among patients who already had a mental health disorder.
For a patient who derives comfort from food, not being able to eat in response to a stressful event may lead that patient to act out in more serious ways, according to Dr. Lofton. “That’s why, again, surgical follow-up is so important and their presurgical psychiatric evaluation is so important.”
A version of this article originally appeared on Medscape.com.
FDA clears the Tandem Mobi insulin pump
The product is half the size of the company’s t:slim X2 and is now the smallest of the commercially available durable tubed pumps. It is fully controllable from a mobile app through a user’s compatible iPhone.
Features of the Mobi include a 200-unit insulin cartridge and an on-pump button that can be used instead of the phone for bolusing insulin. The device can be clipped to clothing or worn on-body with an adhesive sleeve that is sold separately.
The Mobi is compatible with all existing Tandem-branded infusion sets manufactured by the Convatec Group, and there is a new 5-inch tubing option made just for the Tandem Mobi.
The Mobi is part of a hybrid-closed loop automated delivery system, along with the current Control-IQ technology and a compatible continuous glucose monitor (CGM). The CGM sensor predicts glucose values 30 minutes ahead and adjusts insulin delivery every 5 minutes to prevent highs and lows. Users must still manually bolus for meals. The system can deliver automatic correction boluses for up to 1 hour to prevent hyperglycemia.
Limited release of the Tandem Mobi is expected in late 2023, followed by full commercial availability in early 2024.
A version of this article originally appeared on Medscape.com.
The product is half the size of the company’s t:slim X2 and is now the smallest of the commercially available durable tubed pumps. It is fully controllable from a mobile app through a user’s compatible iPhone.
Features of the Mobi include a 200-unit insulin cartridge and an on-pump button that can be used instead of the phone for bolusing insulin. The device can be clipped to clothing or worn on-body with an adhesive sleeve that is sold separately.
The Mobi is compatible with all existing Tandem-branded infusion sets manufactured by the Convatec Group, and there is a new 5-inch tubing option made just for the Tandem Mobi.
The Mobi is part of a hybrid-closed loop automated delivery system, along with the current Control-IQ technology and a compatible continuous glucose monitor (CGM). The CGM sensor predicts glucose values 30 minutes ahead and adjusts insulin delivery every 5 minutes to prevent highs and lows. Users must still manually bolus for meals. The system can deliver automatic correction boluses for up to 1 hour to prevent hyperglycemia.
Limited release of the Tandem Mobi is expected in late 2023, followed by full commercial availability in early 2024.
A version of this article originally appeared on Medscape.com.
The product is half the size of the company’s t:slim X2 and is now the smallest of the commercially available durable tubed pumps. It is fully controllable from a mobile app through a user’s compatible iPhone.
Features of the Mobi include a 200-unit insulin cartridge and an on-pump button that can be used instead of the phone for bolusing insulin. The device can be clipped to clothing or worn on-body with an adhesive sleeve that is sold separately.
The Mobi is compatible with all existing Tandem-branded infusion sets manufactured by the Convatec Group, and there is a new 5-inch tubing option made just for the Tandem Mobi.
The Mobi is part of a hybrid-closed loop automated delivery system, along with the current Control-IQ technology and a compatible continuous glucose monitor (CGM). The CGM sensor predicts glucose values 30 minutes ahead and adjusts insulin delivery every 5 minutes to prevent highs and lows. Users must still manually bolus for meals. The system can deliver automatic correction boluses for up to 1 hour to prevent hyperglycemia.
Limited release of the Tandem Mobi is expected in late 2023, followed by full commercial availability in early 2024.
A version of this article originally appeared on Medscape.com.
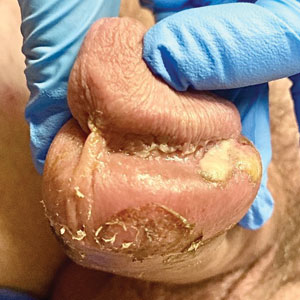
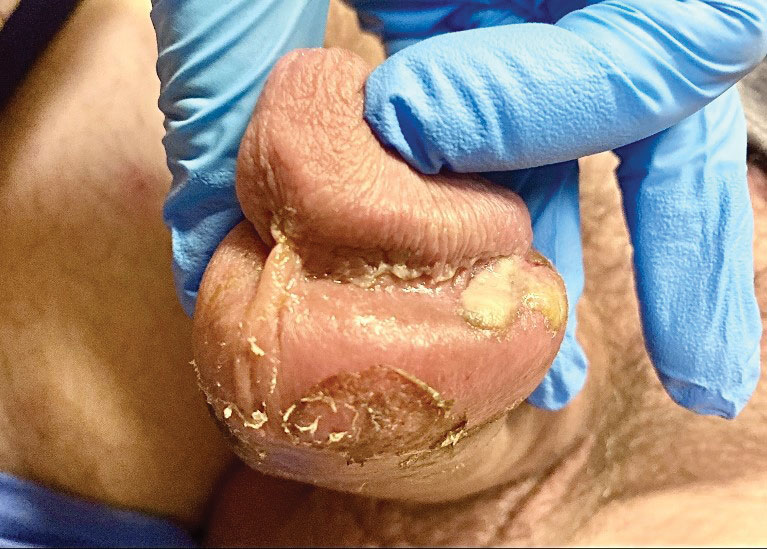
Genital Ulcerations With Swelling
The Diagnosis: Mpox (Monkeypox)
Tests for active herpes simplex virus (HHV), gonorrhea, chlamydia, HIV, and syphilis were negative. Swabs from the penile lesion demonstrated positivity for the West African clade of mpox (monkeypox) virus (MPXV) by polymerase chain reaction. The patient was treated supportively without the addition of antiviral therapy, and he experienced a complete recovery.
Mpox virus was first isolated in 1958 in a research facility and was named after the laboratory animals that were housed there. The first human documentation of the disease occurred in 1970, and it was first documented in the United States in 2003 in an infection that was traced to a shipment of small mammals from Ghana to Texas.1 The disease has always been endemic to Africa; however, the incidence has been increasing.2 A new MPXV outbreak was reported in many countries in early 2022, including the United States.1
The MPXV is a double-stranded DNA virus of the genus Orthopoxvirus, and 2 genetic clades have been identified: clade I (formerly the Central African clade) and clade II (formerly the West African clade). The virus has the capability to infect many mammals; however, its host remains unidentified.1 The exact mechanism of transmission from infected animals to humans largely is unknown; however, direct or indirect contact with infected animals likely is responsible. Human-to-human transmission can occur by many mechanisms including contact with large respiratory droplets, bodily fluids, and contaminated surfaces. The incubation period is 5 to 21 days, and the symptoms last 2 to 5 weeks.1
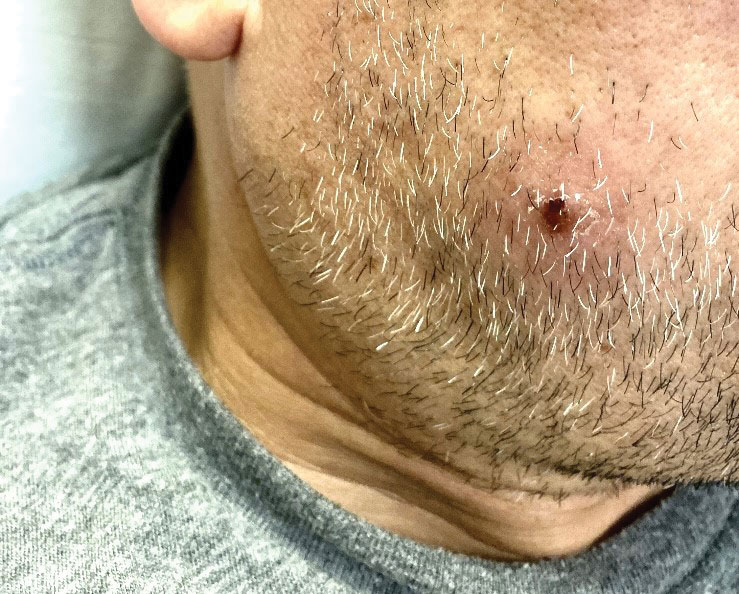
The clinical manifestations of MPXV during the most recent outbreak differ from prior outbreaks. Patients are more likely to experience minimal to no systemic symptoms, and cutaneous lesions can be few and localized to a focal area, especially on the face and in the anogenital region,3 similar to the presentation in our patient (Figure 1). Cutaneous lesions of the most recent MPXV outbreak also include painless ulcerations similar to syphilitic chancres and lesions that are in various stages of healing.3 Lesions often begin as pseudopustules, which are firm white papules with or without a necrotic center that resemble pustules; unlike true pustules, there is no identifiable purulent material within it. Bacterial superinfection of the lesions is not uncommon.4 Over time, a secondary pustular eruption resembling folliculitis also may occur,4 as noted in our patient (Figure 2).
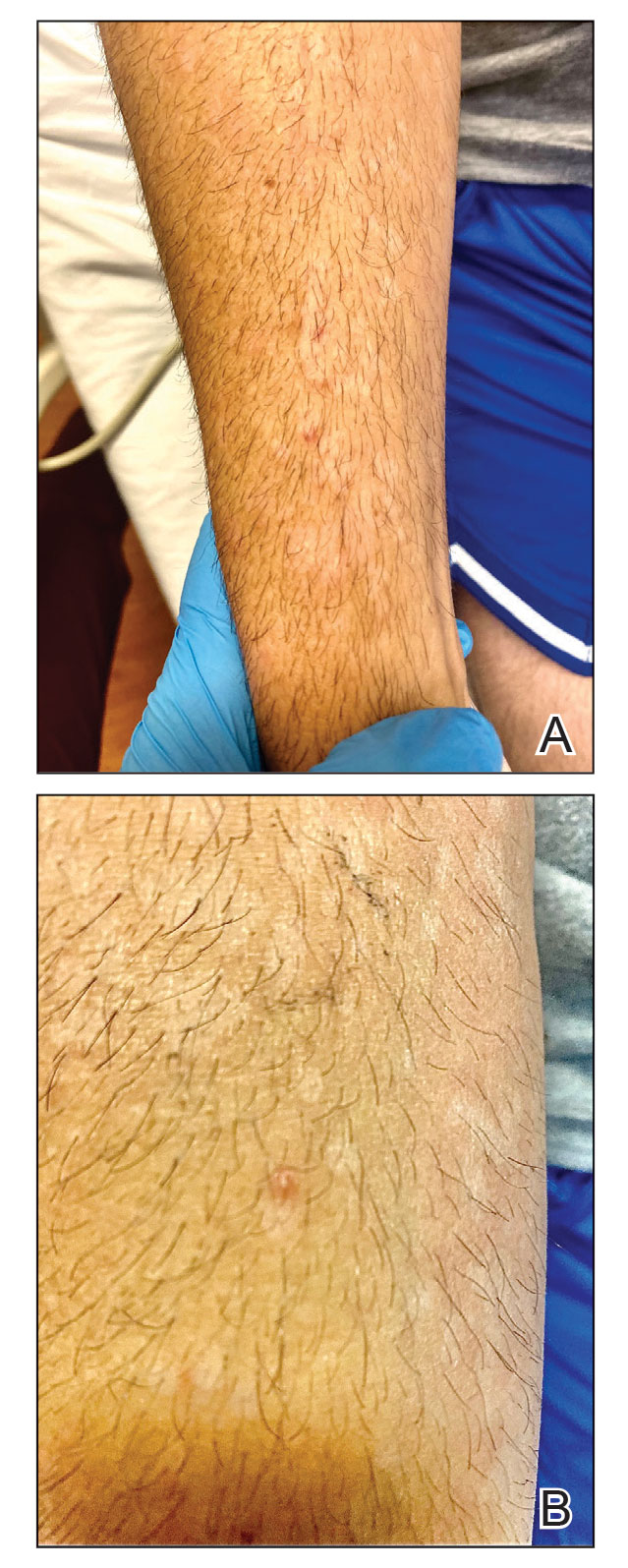
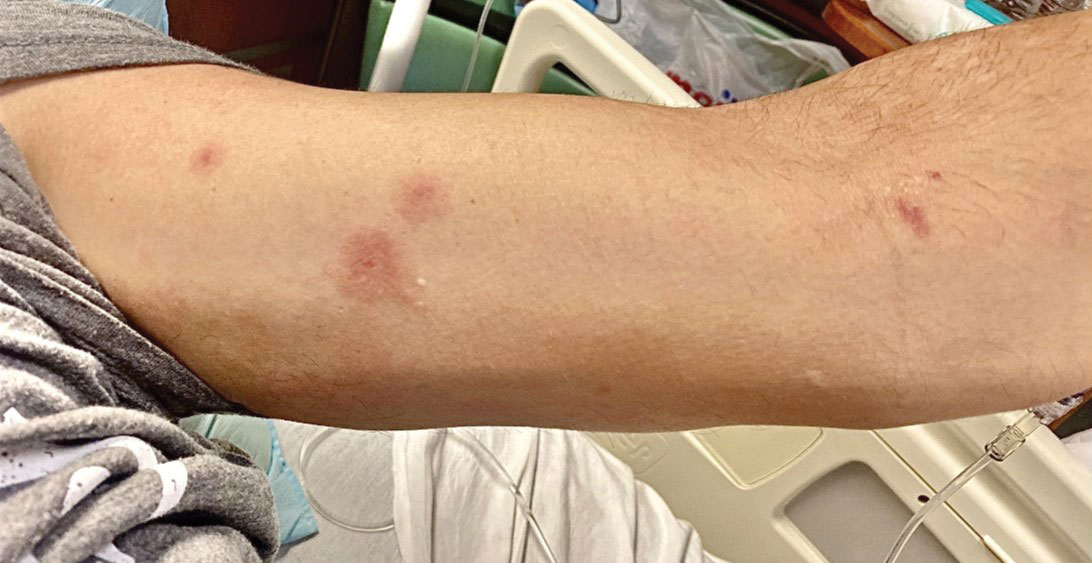
Although we did not have a biopsy to support the diagnosis of associated erythema multiforme (EM) in our patient, features supportive of this diagnosis included the classic clinical appearance of typical, well-defined, targetoid plaques with 3 distinct zones (Figure 3); the association with a known infection; the distribution on the arms with truncal sparing; and self-limited lesions. More than 90% of EM cases are associated with infection, with HHV representing the most common culprit5; therefore, the relationship with a different virus is not an unreasonable suggestion. Additionally, there have been rare reports of EM in association with MPXV.4
Histopathology of MPXV may have distinctive features. Lesions often demonstrate keratinocytic necrosis and basal layer vacuolization with an associated superficial and deep perivascular lymphohistiocytic infiltrate. When the morphology of the lesion is vesicular, histopathology reveals spongiosis and ballooning degeneration with epidermal necrosis. Viral inclusion bodies within keratinocytes may be identified.1 Death rates from MPXV has been reported from 1% to 11%, with increased mortality among high-risk populations including children and immunocompromised individuals. Treatment of the disease largely consists of supportive care and management of any associated complications including bacterial infection, pneumonia, and encephalitis.1
The differential diagnosis of MPXV includes other ulcerative lesions that can occur on the genital skin. Fixed drug eruptions often present on the penis,6 but there was no identifiable inciting drug in our patient. Herpes simplex virus infection was very high on the differential given our patient’s history of recurrent infections and association with a targetoid rash, but HHV type 1 and HHV type 2 testing of the lesion was negative. A syphilitic chancre also may present with the nontender genital ulceration7 that was seen in our patient, but serology did not support this diagnosis. Cutaneous Crohn disease also may manifest with genital ulceration even before a diagnosis of Crohn disease is made, but these lesions often present as linear knife-cut ulcerations of the anogenital region.8
Our case further supports a clinical presentation that diverges from the more traditional cases of MPXV. Additionally, associated EM may be a clue to infection, especially in cases of negative HHV and other sexually transmitted infection testing.
- Bunge EM, Hoet B, Chen L, et al. The changing epidemiology of human monkeypox—a potential threat? a systematic review. PLoS Negl Trop Dis. 2022;16:E0010141.
- Kumar N, Acharya A, Gendelman HE, et al. The 2022 outbreak and the pathobiology of the monkeypox virus. J Autoimmun. 2022;131:102855.
- Eisenstadt R, Liszewski WJ, Nguyen CV. Recognizing minimal cutaneous involvement or systemic symptoms in monkeypox. JAMA Dermatol. 2022;158:1457-1458.
- Català A, Clavo-Escribano P, Riera-Monroig J, et al. Monkeypox outbreak in Spain: clinical and epidemiological findings in a prospective cross-sectional study of 185 cases [published online August 2, 2022]. Br J Dermatol. 2022;187:765-772.
- Sokumbi O, Wetter DA. Clinical features, diagnosis, and treatment of erythema multiforme: a review for the practicing dermatologist. Int J Dermatol. 2012;51:889-902.
- Waleryie-Allanore L, Obeid G, Revuz J. Drug reactions. In: Bolognia J, Schaffer J, Cerroni L, eds. Dermatology. Elsevier; 2018:348-375.
- Stary G, Stary A. Sexually transmitted infections. In: Bolognia J, Schaffer J, Cerroni L, eds. Dermatology. Elsevier; 2018:1447-1469.
- Rosenbach MA, Wanat KA, Reisenauer A, et al. Non-infectious granulomas. In: Bolognia J, Schaffer J, Cerroni L, eds. Dermatology. Elsevier; 2018:1644-1663.
The Diagnosis: Mpox (Monkeypox)
Tests for active herpes simplex virus (HHV), gonorrhea, chlamydia, HIV, and syphilis were negative. Swabs from the penile lesion demonstrated positivity for the West African clade of mpox (monkeypox) virus (MPXV) by polymerase chain reaction. The patient was treated supportively without the addition of antiviral therapy, and he experienced a complete recovery.
Mpox virus was first isolated in 1958 in a research facility and was named after the laboratory animals that were housed there. The first human documentation of the disease occurred in 1970, and it was first documented in the United States in 2003 in an infection that was traced to a shipment of small mammals from Ghana to Texas.1 The disease has always been endemic to Africa; however, the incidence has been increasing.2 A new MPXV outbreak was reported in many countries in early 2022, including the United States.1
The MPXV is a double-stranded DNA virus of the genus Orthopoxvirus, and 2 genetic clades have been identified: clade I (formerly the Central African clade) and clade II (formerly the West African clade). The virus has the capability to infect many mammals; however, its host remains unidentified.1 The exact mechanism of transmission from infected animals to humans largely is unknown; however, direct or indirect contact with infected animals likely is responsible. Human-to-human transmission can occur by many mechanisms including contact with large respiratory droplets, bodily fluids, and contaminated surfaces. The incubation period is 5 to 21 days, and the symptoms last 2 to 5 weeks.1

The clinical manifestations of MPXV during the most recent outbreak differ from prior outbreaks. Patients are more likely to experience minimal to no systemic symptoms, and cutaneous lesions can be few and localized to a focal area, especially on the face and in the anogenital region,3 similar to the presentation in our patient (Figure 1). Cutaneous lesions of the most recent MPXV outbreak also include painless ulcerations similar to syphilitic chancres and lesions that are in various stages of healing.3 Lesions often begin as pseudopustules, which are firm white papules with or without a necrotic center that resemble pustules; unlike true pustules, there is no identifiable purulent material within it. Bacterial superinfection of the lesions is not uncommon.4 Over time, a secondary pustular eruption resembling folliculitis also may occur,4 as noted in our patient (Figure 2).

Although we did not have a biopsy to support the diagnosis of associated erythema multiforme (EM) in our patient, features supportive of this diagnosis included the classic clinical appearance of typical, well-defined, targetoid plaques with 3 distinct zones (Figure 3); the association with a known infection; the distribution on the arms with truncal sparing; and self-limited lesions. More than 90% of EM cases are associated with infection, with HHV representing the most common culprit5; therefore, the relationship with a different virus is not an unreasonable suggestion. Additionally, there have been rare reports of EM in association with MPXV.4

Histopathology of MPXV may have distinctive features. Lesions often demonstrate keratinocytic necrosis and basal layer vacuolization with an associated superficial and deep perivascular lymphohistiocytic infiltrate. When the morphology of the lesion is vesicular, histopathology reveals spongiosis and ballooning degeneration with epidermal necrosis. Viral inclusion bodies within keratinocytes may be identified.1 Death rates from MPXV has been reported from 1% to 11%, with increased mortality among high-risk populations including children and immunocompromised individuals. Treatment of the disease largely consists of supportive care and management of any associated complications including bacterial infection, pneumonia, and encephalitis.1
The differential diagnosis of MPXV includes other ulcerative lesions that can occur on the genital skin. Fixed drug eruptions often present on the penis,6 but there was no identifiable inciting drug in our patient. Herpes simplex virus infection was very high on the differential given our patient’s history of recurrent infections and association with a targetoid rash, but HHV type 1 and HHV type 2 testing of the lesion was negative. A syphilitic chancre also may present with the nontender genital ulceration7 that was seen in our patient, but serology did not support this diagnosis. Cutaneous Crohn disease also may manifest with genital ulceration even before a diagnosis of Crohn disease is made, but these lesions often present as linear knife-cut ulcerations of the anogenital region.8
Our case further supports a clinical presentation that diverges from the more traditional cases of MPXV. Additionally, associated EM may be a clue to infection, especially in cases of negative HHV and other sexually transmitted infection testing.
The Diagnosis: Mpox (Monkeypox)
Tests for active herpes simplex virus (HHV), gonorrhea, chlamydia, HIV, and syphilis were negative. Swabs from the penile lesion demonstrated positivity for the West African clade of mpox (monkeypox) virus (MPXV) by polymerase chain reaction. The patient was treated supportively without the addition of antiviral therapy, and he experienced a complete recovery.
Mpox virus was first isolated in 1958 in a research facility and was named after the laboratory animals that were housed there. The first human documentation of the disease occurred in 1970, and it was first documented in the United States in 2003 in an infection that was traced to a shipment of small mammals from Ghana to Texas.1 The disease has always been endemic to Africa; however, the incidence has been increasing.2 A new MPXV outbreak was reported in many countries in early 2022, including the United States.1
The MPXV is a double-stranded DNA virus of the genus Orthopoxvirus, and 2 genetic clades have been identified: clade I (formerly the Central African clade) and clade II (formerly the West African clade). The virus has the capability to infect many mammals; however, its host remains unidentified.1 The exact mechanism of transmission from infected animals to humans largely is unknown; however, direct or indirect contact with infected animals likely is responsible. Human-to-human transmission can occur by many mechanisms including contact with large respiratory droplets, bodily fluids, and contaminated surfaces. The incubation period is 5 to 21 days, and the symptoms last 2 to 5 weeks.1

The clinical manifestations of MPXV during the most recent outbreak differ from prior outbreaks. Patients are more likely to experience minimal to no systemic symptoms, and cutaneous lesions can be few and localized to a focal area, especially on the face and in the anogenital region,3 similar to the presentation in our patient (Figure 1). Cutaneous lesions of the most recent MPXV outbreak also include painless ulcerations similar to syphilitic chancres and lesions that are in various stages of healing.3 Lesions often begin as pseudopustules, which are firm white papules with or without a necrotic center that resemble pustules; unlike true pustules, there is no identifiable purulent material within it. Bacterial superinfection of the lesions is not uncommon.4 Over time, a secondary pustular eruption resembling folliculitis also may occur,4 as noted in our patient (Figure 2).

Although we did not have a biopsy to support the diagnosis of associated erythema multiforme (EM) in our patient, features supportive of this diagnosis included the classic clinical appearance of typical, well-defined, targetoid plaques with 3 distinct zones (Figure 3); the association with a known infection; the distribution on the arms with truncal sparing; and self-limited lesions. More than 90% of EM cases are associated with infection, with HHV representing the most common culprit5; therefore, the relationship with a different virus is not an unreasonable suggestion. Additionally, there have been rare reports of EM in association with MPXV.4

Histopathology of MPXV may have distinctive features. Lesions often demonstrate keratinocytic necrosis and basal layer vacuolization with an associated superficial and deep perivascular lymphohistiocytic infiltrate. When the morphology of the lesion is vesicular, histopathology reveals spongiosis and ballooning degeneration with epidermal necrosis. Viral inclusion bodies within keratinocytes may be identified.1 Death rates from MPXV has been reported from 1% to 11%, with increased mortality among high-risk populations including children and immunocompromised individuals. Treatment of the disease largely consists of supportive care and management of any associated complications including bacterial infection, pneumonia, and encephalitis.1
The differential diagnosis of MPXV includes other ulcerative lesions that can occur on the genital skin. Fixed drug eruptions often present on the penis,6 but there was no identifiable inciting drug in our patient. Herpes simplex virus infection was very high on the differential given our patient’s history of recurrent infections and association with a targetoid rash, but HHV type 1 and HHV type 2 testing of the lesion was negative. A syphilitic chancre also may present with the nontender genital ulceration7 that was seen in our patient, but serology did not support this diagnosis. Cutaneous Crohn disease also may manifest with genital ulceration even before a diagnosis of Crohn disease is made, but these lesions often present as linear knife-cut ulcerations of the anogenital region.8
Our case further supports a clinical presentation that diverges from the more traditional cases of MPXV. Additionally, associated EM may be a clue to infection, especially in cases of negative HHV and other sexually transmitted infection testing.
- Bunge EM, Hoet B, Chen L, et al. The changing epidemiology of human monkeypox—a potential threat? a systematic review. PLoS Negl Trop Dis. 2022;16:E0010141.
- Kumar N, Acharya A, Gendelman HE, et al. The 2022 outbreak and the pathobiology of the monkeypox virus. J Autoimmun. 2022;131:102855.
- Eisenstadt R, Liszewski WJ, Nguyen CV. Recognizing minimal cutaneous involvement or systemic symptoms in monkeypox. JAMA Dermatol. 2022;158:1457-1458.
- Català A, Clavo-Escribano P, Riera-Monroig J, et al. Monkeypox outbreak in Spain: clinical and epidemiological findings in a prospective cross-sectional study of 185 cases [published online August 2, 2022]. Br J Dermatol. 2022;187:765-772.
- Sokumbi O, Wetter DA. Clinical features, diagnosis, and treatment of erythema multiforme: a review for the practicing dermatologist. Int J Dermatol. 2012;51:889-902.
- Waleryie-Allanore L, Obeid G, Revuz J. Drug reactions. In: Bolognia J, Schaffer J, Cerroni L, eds. Dermatology. Elsevier; 2018:348-375.
- Stary G, Stary A. Sexually transmitted infections. In: Bolognia J, Schaffer J, Cerroni L, eds. Dermatology. Elsevier; 2018:1447-1469.
- Rosenbach MA, Wanat KA, Reisenauer A, et al. Non-infectious granulomas. In: Bolognia J, Schaffer J, Cerroni L, eds. Dermatology. Elsevier; 2018:1644-1663.
- Bunge EM, Hoet B, Chen L, et al. The changing epidemiology of human monkeypox—a potential threat? a systematic review. PLoS Negl Trop Dis. 2022;16:E0010141.
- Kumar N, Acharya A, Gendelman HE, et al. The 2022 outbreak and the pathobiology of the monkeypox virus. J Autoimmun. 2022;131:102855.
- Eisenstadt R, Liszewski WJ, Nguyen CV. Recognizing minimal cutaneous involvement or systemic symptoms in monkeypox. JAMA Dermatol. 2022;158:1457-1458.
- Català A, Clavo-Escribano P, Riera-Monroig J, et al. Monkeypox outbreak in Spain: clinical and epidemiological findings in a prospective cross-sectional study of 185 cases [published online August 2, 2022]. Br J Dermatol. 2022;187:765-772.
- Sokumbi O, Wetter DA. Clinical features, diagnosis, and treatment of erythema multiforme: a review for the practicing dermatologist. Int J Dermatol. 2012;51:889-902.
- Waleryie-Allanore L, Obeid G, Revuz J. Drug reactions. In: Bolognia J, Schaffer J, Cerroni L, eds. Dermatology. Elsevier; 2018:348-375.
- Stary G, Stary A. Sexually transmitted infections. In: Bolognia J, Schaffer J, Cerroni L, eds. Dermatology. Elsevier; 2018:1447-1469.
- Rosenbach MA, Wanat KA, Reisenauer A, et al. Non-infectious granulomas. In: Bolognia J, Schaffer J, Cerroni L, eds. Dermatology. Elsevier; 2018:1644-1663.
A 50-year-old man with a history of recurrent genital herpes simplex virus infections presented to the hospital with genital lesions and swelling of 5 days’ duration. Prior to admission, the patient was treated with a course of valacyclovir by an urgent care physician without improvement. Physical examination revealed a 3-cm, nontender, shallow, ulcerative plaque with irregular borders and a purulent yellow base distributed on the distal shaft of the penis with extension into the coronal sulcus. A few other scattered erosions were noted on the distal penile shaft. He had associated diffuse nonpitting edema of the penis and scrotum as well as tender bilateral inguinal lymphadenopathy. Three days after the genital ulcerations began, the patient developed a nontender erythematous papule with a necrotic center on the right jaw followed by an eruption of erythematous papulopustules on the arms and trunk. The patient denied dysuria, purulent penile discharge, fevers, chills, headaches, myalgia, arthralgia, nausea, vomiting, or diarrhea. The patient was sexually active exclusively with females and had more than 10 partners in the prior year. Shortly after hospital admission, the patient developed red targetoid plaques on the groin, trunk, and arms. No oral mucosal lesions were identified.
Link between low co-pays for new diabetes drugs and patient adherence
Findings from a recent study indicate that the less U.S. patients pay out of pocket for drugs that often have high co-pays, such as sodium-glucose cotransporter 2 (SGLT2) inhibitors or glucagonlike peptide-1 (GLP-1) agonists, the more they adhere to taking these medications.
The study, led by Utibe R. Essien, MD, from University of California, Los Angeles, and Balvindar Singh, MD, PhD, from University of Pittsburgh, was published online in JAMA Cardiology.
Patient data from Clinformatics Data Mart, a health insurance claims database, was analyzed for the study. The information for 90,041 adults from the United States who had commercial and Medicare health insurance, and who started taking a GLP-1 agonist or SGLT2 inhibitor between 2014 and 2020 was reviewed. Participants had type 2 diabetes, heart failure, or both.
The primary outcome showed patients with a lower drug co-pay had significantly higher odds of 12-month adherence to GLP-1 agonists and SGLT2 inhibitors, compared with those with a higher co-pay. These differences persisted after controlling for patient demographic, clinical, and socioeconomic covariates.
After full adjustments were made and after the 12 months, patients with a high co-pay of $50 per month or more were 53% less likely to adhere to an SGLT2 inhibitor and 32% less likely to adhere to a GLP-1 agonist, compared with patients with a co-pay of less than $10 per month for these agents.
“Lowering high out-of-pocket prescription costs may be key to improving adherence to guideline-recommended therapies and advancing overall quality of care in patients with type 2 diabetes and heart failure,” the authors conclude.
The authors acknowledge the study’s limitations, including the inability to exclude residual confounding, uncertain generalizability for those without health insurance or with public insurance and possible misclassifications of type 2 diabetes and heart failure diagnoses or medical comorbidities. Additionally, this study did not have information on patients’ preferences associated with medication use, including specific reasons for poor adherence, and could not assess how co-payments influenced initial prescription receipt or abandonment at the pharmacy, or other factors including possible price inflation.
The study received no commercial funding. One author (not a lead author) is an adviser to several drug companies including ones that market SGLT2 inhibitors or GLP-1 agonists.
Findings from a recent study indicate that the less U.S. patients pay out of pocket for drugs that often have high co-pays, such as sodium-glucose cotransporter 2 (SGLT2) inhibitors or glucagonlike peptide-1 (GLP-1) agonists, the more they adhere to taking these medications.
The study, led by Utibe R. Essien, MD, from University of California, Los Angeles, and Balvindar Singh, MD, PhD, from University of Pittsburgh, was published online in JAMA Cardiology.
Patient data from Clinformatics Data Mart, a health insurance claims database, was analyzed for the study. The information for 90,041 adults from the United States who had commercial and Medicare health insurance, and who started taking a GLP-1 agonist or SGLT2 inhibitor between 2014 and 2020 was reviewed. Participants had type 2 diabetes, heart failure, or both.
The primary outcome showed patients with a lower drug co-pay had significantly higher odds of 12-month adherence to GLP-1 agonists and SGLT2 inhibitors, compared with those with a higher co-pay. These differences persisted after controlling for patient demographic, clinical, and socioeconomic covariates.
After full adjustments were made and after the 12 months, patients with a high co-pay of $50 per month or more were 53% less likely to adhere to an SGLT2 inhibitor and 32% less likely to adhere to a GLP-1 agonist, compared with patients with a co-pay of less than $10 per month for these agents.
“Lowering high out-of-pocket prescription costs may be key to improving adherence to guideline-recommended therapies and advancing overall quality of care in patients with type 2 diabetes and heart failure,” the authors conclude.
The authors acknowledge the study’s limitations, including the inability to exclude residual confounding, uncertain generalizability for those without health insurance or with public insurance and possible misclassifications of type 2 diabetes and heart failure diagnoses or medical comorbidities. Additionally, this study did not have information on patients’ preferences associated with medication use, including specific reasons for poor adherence, and could not assess how co-payments influenced initial prescription receipt or abandonment at the pharmacy, or other factors including possible price inflation.
The study received no commercial funding. One author (not a lead author) is an adviser to several drug companies including ones that market SGLT2 inhibitors or GLP-1 agonists.
Findings from a recent study indicate that the less U.S. patients pay out of pocket for drugs that often have high co-pays, such as sodium-glucose cotransporter 2 (SGLT2) inhibitors or glucagonlike peptide-1 (GLP-1) agonists, the more they adhere to taking these medications.
The study, led by Utibe R. Essien, MD, from University of California, Los Angeles, and Balvindar Singh, MD, PhD, from University of Pittsburgh, was published online in JAMA Cardiology.
Patient data from Clinformatics Data Mart, a health insurance claims database, was analyzed for the study. The information for 90,041 adults from the United States who had commercial and Medicare health insurance, and who started taking a GLP-1 agonist or SGLT2 inhibitor between 2014 and 2020 was reviewed. Participants had type 2 diabetes, heart failure, or both.
The primary outcome showed patients with a lower drug co-pay had significantly higher odds of 12-month adherence to GLP-1 agonists and SGLT2 inhibitors, compared with those with a higher co-pay. These differences persisted after controlling for patient demographic, clinical, and socioeconomic covariates.
After full adjustments were made and after the 12 months, patients with a high co-pay of $50 per month or more were 53% less likely to adhere to an SGLT2 inhibitor and 32% less likely to adhere to a GLP-1 agonist, compared with patients with a co-pay of less than $10 per month for these agents.
“Lowering high out-of-pocket prescription costs may be key to improving adherence to guideline-recommended therapies and advancing overall quality of care in patients with type 2 diabetes and heart failure,” the authors conclude.
The authors acknowledge the study’s limitations, including the inability to exclude residual confounding, uncertain generalizability for those without health insurance or with public insurance and possible misclassifications of type 2 diabetes and heart failure diagnoses or medical comorbidities. Additionally, this study did not have information on patients’ preferences associated with medication use, including specific reasons for poor adherence, and could not assess how co-payments influenced initial prescription receipt or abandonment at the pharmacy, or other factors including possible price inflation.
The study received no commercial funding. One author (not a lead author) is an adviser to several drug companies including ones that market SGLT2 inhibitors or GLP-1 agonists.
FROM JAMA CARDIOLOGY
FDA: No excess mortality risk from paclitaxel stents, balloons for peripheral intervention
, the agency July 11 in a statement to health care providers.
The FDA announcement comes about 4 years after it warned physicians of a “potentially concerning” signal of excess mortality linked to paclitaxel-coated balloons and paclitaxel-eluting stents in published analysis.
The agency’s concerns had been based on a December 2018 meta-analysis in the Journal of the American Heart Association that saw a 68% jump in mortality risk at 2 years and a 93% excess risk at 5 years associated with the paclitaxel devices in the periphery.
The findings, which led an FDA advisory committee to recommend device labeling changes and otherwise upended the practice of peripheral interventions, were followed by an FDA recommendation to limit the use of paclitaxel devices in the periphery to higher-risk cases.
In its July 11 update to providers, the FDA said it was satisfied the devices do not pose an excess mortality risk. It based its conclusion on extensive further evidence review and recently available “additional data” from the randomized controlled trials (RCTs) contributing to the meta-analysis that had ignited the controversy.
“FDA clinicians and statisticians reviewed the study data,” the agency said, “and concluded that the updated RCT meta-analysis does not indicate that the use of paclitaxel-coated devices is associated with a late mortality risk.”
A version of this article originally appeared on Medscape.com.
, the agency July 11 in a statement to health care providers.
The FDA announcement comes about 4 years after it warned physicians of a “potentially concerning” signal of excess mortality linked to paclitaxel-coated balloons and paclitaxel-eluting stents in published analysis.
The agency’s concerns had been based on a December 2018 meta-analysis in the Journal of the American Heart Association that saw a 68% jump in mortality risk at 2 years and a 93% excess risk at 5 years associated with the paclitaxel devices in the periphery.
The findings, which led an FDA advisory committee to recommend device labeling changes and otherwise upended the practice of peripheral interventions, were followed by an FDA recommendation to limit the use of paclitaxel devices in the periphery to higher-risk cases.
In its July 11 update to providers, the FDA said it was satisfied the devices do not pose an excess mortality risk. It based its conclusion on extensive further evidence review and recently available “additional data” from the randomized controlled trials (RCTs) contributing to the meta-analysis that had ignited the controversy.
“FDA clinicians and statisticians reviewed the study data,” the agency said, “and concluded that the updated RCT meta-analysis does not indicate that the use of paclitaxel-coated devices is associated with a late mortality risk.”
A version of this article originally appeared on Medscape.com.
, the agency July 11 in a statement to health care providers.
The FDA announcement comes about 4 years after it warned physicians of a “potentially concerning” signal of excess mortality linked to paclitaxel-coated balloons and paclitaxel-eluting stents in published analysis.
The agency’s concerns had been based on a December 2018 meta-analysis in the Journal of the American Heart Association that saw a 68% jump in mortality risk at 2 years and a 93% excess risk at 5 years associated with the paclitaxel devices in the periphery.
The findings, which led an FDA advisory committee to recommend device labeling changes and otherwise upended the practice of peripheral interventions, were followed by an FDA recommendation to limit the use of paclitaxel devices in the periphery to higher-risk cases.
In its July 11 update to providers, the FDA said it was satisfied the devices do not pose an excess mortality risk. It based its conclusion on extensive further evidence review and recently available “additional data” from the randomized controlled trials (RCTs) contributing to the meta-analysis that had ignited the controversy.
“FDA clinicians and statisticians reviewed the study data,” the agency said, “and concluded that the updated RCT meta-analysis does not indicate that the use of paclitaxel-coated devices is associated with a late mortality risk.”
A version of this article originally appeared on Medscape.com.
FDA approves cognitive-behavioral app for adults with type 2 diabetes
A smartphone-based app designed to deliver cognitive-behavioral therapy (CBT) to adults with type 2 diabetes received marketing approval as a class II medical device from the Food and Drug Administration on July 10, becoming the first digital behavioral therapeutic device for people with diabetes to receive this designation for U.S. patients.
Better Therapeutics representatives said that the app, formerly known as BT-001, will be called AspyreRX, with U.S. sales planned to launch in October-December 2023.
The app will be available to patients exclusively by prescription, with a planned 90-day use duration and an option for a second 90-day prescription. A company official said the price per prescription will be about $500-800, although this is not yet finalized. The app is intended for use in concert with the conventional pillars of glycemic control in people with type 2 diabetes: lifestyle modification and treatment with antidiabetes medications.
Senior staff members of Better Therapeutics acknowledged the critical need for an education program, which they will now launch for clinicians, payers, and patients to get across the message of the potential benefit and safety associated with using the CBT app. Their initial marketing will target patients with type 2 diabetes and poorly controlled hemoglobin A1c levels in five to six U.S. regions with high numbers of these patients. The company will also attempt to make the app available through the Department of Veterans Affairs health system and try to secure coverage by Medicare and commercial health-insurance providers.
Approval based on pivotal trial results
The FDA approval focused on data collected in the BT-001 randomized, controlled trial, which included 669 U.S. adults with poorly controlled type 2 diabetes. Results, published in 2022 in Diabetes Care, showed that after 90 days, people using the app had an average incremental reduction in A1c of 0.39 percentage points, compared with control patients who didn’t use the app, the primary endpoint. Use of the app also appeared safe.
Subsequent meeting presentations of study findings showed that A1c-lowering linked with app use was durable during continued use for a total of 180 days, that the effectiveness of the app in helping to lower A1c levels was “dose dependent” relative to the number of lessons a person completed, and that using the app significantly linked with a reduced need for intensified glycemic control through added medications.
Another finding of the extended-use phase of the study was that 81% of patients assigned to the app-using group continued to regularly use the app after 180 days, a level of durable engagement by patients that “exceeded our expectations,” said Diane Gomez-Thinnes, chief commercial officer of Better Therapeutics, during a press conference.
The company plans to tweak the app prior to its launch based on additional analyses of results from the pivotal study to further improve patient engagement and app ease of use. The company is also planning to expand the range of smartphones that can support the app, although about 90%-95% of U.S. smartphones have this capability.
Better Therapeutics is also actively developing and testing other modifications to the basic CBT app to make it usable by people with other cardiometabolic disorders such as hypertension, obesity, and fatty liver disease.
The BT-001 study was funded by Better Therapeutics.
A version of this article first appeared on Medscape.com.
A smartphone-based app designed to deliver cognitive-behavioral therapy (CBT) to adults with type 2 diabetes received marketing approval as a class II medical device from the Food and Drug Administration on July 10, becoming the first digital behavioral therapeutic device for people with diabetes to receive this designation for U.S. patients.
Better Therapeutics representatives said that the app, formerly known as BT-001, will be called AspyreRX, with U.S. sales planned to launch in October-December 2023.
The app will be available to patients exclusively by prescription, with a planned 90-day use duration and an option for a second 90-day prescription. A company official said the price per prescription will be about $500-800, although this is not yet finalized. The app is intended for use in concert with the conventional pillars of glycemic control in people with type 2 diabetes: lifestyle modification and treatment with antidiabetes medications.
Senior staff members of Better Therapeutics acknowledged the critical need for an education program, which they will now launch for clinicians, payers, and patients to get across the message of the potential benefit and safety associated with using the CBT app. Their initial marketing will target patients with type 2 diabetes and poorly controlled hemoglobin A1c levels in five to six U.S. regions with high numbers of these patients. The company will also attempt to make the app available through the Department of Veterans Affairs health system and try to secure coverage by Medicare and commercial health-insurance providers.
Approval based on pivotal trial results
The FDA approval focused on data collected in the BT-001 randomized, controlled trial, which included 669 U.S. adults with poorly controlled type 2 diabetes. Results, published in 2022 in Diabetes Care, showed that after 90 days, people using the app had an average incremental reduction in A1c of 0.39 percentage points, compared with control patients who didn’t use the app, the primary endpoint. Use of the app also appeared safe.
Subsequent meeting presentations of study findings showed that A1c-lowering linked with app use was durable during continued use for a total of 180 days, that the effectiveness of the app in helping to lower A1c levels was “dose dependent” relative to the number of lessons a person completed, and that using the app significantly linked with a reduced need for intensified glycemic control through added medications.
Another finding of the extended-use phase of the study was that 81% of patients assigned to the app-using group continued to regularly use the app after 180 days, a level of durable engagement by patients that “exceeded our expectations,” said Diane Gomez-Thinnes, chief commercial officer of Better Therapeutics, during a press conference.
The company plans to tweak the app prior to its launch based on additional analyses of results from the pivotal study to further improve patient engagement and app ease of use. The company is also planning to expand the range of smartphones that can support the app, although about 90%-95% of U.S. smartphones have this capability.
Better Therapeutics is also actively developing and testing other modifications to the basic CBT app to make it usable by people with other cardiometabolic disorders such as hypertension, obesity, and fatty liver disease.
The BT-001 study was funded by Better Therapeutics.
A version of this article first appeared on Medscape.com.
A smartphone-based app designed to deliver cognitive-behavioral therapy (CBT) to adults with type 2 diabetes received marketing approval as a class II medical device from the Food and Drug Administration on July 10, becoming the first digital behavioral therapeutic device for people with diabetes to receive this designation for U.S. patients.
Better Therapeutics representatives said that the app, formerly known as BT-001, will be called AspyreRX, with U.S. sales planned to launch in October-December 2023.
The app will be available to patients exclusively by prescription, with a planned 90-day use duration and an option for a second 90-day prescription. A company official said the price per prescription will be about $500-800, although this is not yet finalized. The app is intended for use in concert with the conventional pillars of glycemic control in people with type 2 diabetes: lifestyle modification and treatment with antidiabetes medications.
Senior staff members of Better Therapeutics acknowledged the critical need for an education program, which they will now launch for clinicians, payers, and patients to get across the message of the potential benefit and safety associated with using the CBT app. Their initial marketing will target patients with type 2 diabetes and poorly controlled hemoglobin A1c levels in five to six U.S. regions with high numbers of these patients. The company will also attempt to make the app available through the Department of Veterans Affairs health system and try to secure coverage by Medicare and commercial health-insurance providers.
Approval based on pivotal trial results
The FDA approval focused on data collected in the BT-001 randomized, controlled trial, which included 669 U.S. adults with poorly controlled type 2 diabetes. Results, published in 2022 in Diabetes Care, showed that after 90 days, people using the app had an average incremental reduction in A1c of 0.39 percentage points, compared with control patients who didn’t use the app, the primary endpoint. Use of the app also appeared safe.
Subsequent meeting presentations of study findings showed that A1c-lowering linked with app use was durable during continued use for a total of 180 days, that the effectiveness of the app in helping to lower A1c levels was “dose dependent” relative to the number of lessons a person completed, and that using the app significantly linked with a reduced need for intensified glycemic control through added medications.
Another finding of the extended-use phase of the study was that 81% of patients assigned to the app-using group continued to regularly use the app after 180 days, a level of durable engagement by patients that “exceeded our expectations,” said Diane Gomez-Thinnes, chief commercial officer of Better Therapeutics, during a press conference.
The company plans to tweak the app prior to its launch based on additional analyses of results from the pivotal study to further improve patient engagement and app ease of use. The company is also planning to expand the range of smartphones that can support the app, although about 90%-95% of U.S. smartphones have this capability.
Better Therapeutics is also actively developing and testing other modifications to the basic CBT app to make it usable by people with other cardiometabolic disorders such as hypertension, obesity, and fatty liver disease.
The BT-001 study was funded by Better Therapeutics.
A version of this article first appeared on Medscape.com.
Aging and type 1 diabetes: ‘Complete picture’ 40 years on
SAN DIEGO –
New funding for 2022-2027 for the DCCT long-term observational follow-up study, the Epidemiology of Diabetes Interventions and Complications (EDIC) will go toward investigating aspects of type 1 diabetes that are associated with aging and are also common in type 2 diabetes, including cardiovascular disease, fatty liver disease, and sleep apnea.
The original randomized DCCT clinical trial results, published in 1993 in the New England Journal of Medicine, proved that early intensive glycemic control was the key to preventing or slowing the progression of long-term eye, kidney, and nerve complications of type 1 diabetes. Subsequently, EDIC has yielded many more major findings including that early tight glycemic control also reduces cardiovascular risk and prolongs survival in type 1 diabetes.
And although the phenomenon of metabolic memory initially seen in EDIC means that early glycemic control is important, subsequent EDIC data also have suggested that it is never too late to initiate intensive glycemic control, speakers emphasized during a special symposium commemorating 40 years since the start of DCCT, held during the annual scientific sessions of the American Diabetes Association. As with the 30-year DCCT/EDIC commemorative symposium held in 2013, local study participants were in the audience and were acknowledged with long applause.
Together, DCCT and EDIC – both funded by the National Institutes of Health at 27 sites in the United States and Canada – have changed the standard of care for people with type 1 diabetes and continue to inform clinical practice. Prior to the DCCT, between 1930 and 1970, about a third of people with type 1 diabetes developed vision loss and one in five experienced kidney failure and/or myocardial infarction. Stroke and amputation were also common, DCCT/EDIC chair David M. Nathan, MD, said while introducing the symposium.
“All of the advances in care of type 1 diabetes have developed because this study demonstrated that it was important – continuous glucose monitoring (CGM), new insulins, better [insulin] pumps. ... I think the most profound finding is that mortality in our intensively treated cohort is the same as in the general population. That says it all,” Dr. Nathan said in an interview.
And now, “what we still have yet to contribute is what happens to type 1 diabetes as people get older,” added Dr. Nathan, a professor of medicine at Harvard Medical School and director of the Diabetes Center at Massachusetts General Hospital, both in Boston.
‘Something that heretofore none of us could have imagined’
The 1,441 DCCT participants had a mean age of 27 years at baseline in 1983, when they were randomized to intensive insulin therapy or usual care. The 1,375 participants (96%) who continued into EDIC in 1994 were an average of 35 years old at that point, when the usual care group was taught intensive glycemic management and all participants returned to their personal health care teams. The 1,075 participants in EDIC today are an average age of 63 years.
Only 11 participants had died at the start of EDIC, and just 250 (17%) have died as of 2023, said study coordinator cochair Gayle Lorenzi, RN, who is a certified diabetes care and education specialist at the University of California, San Diego.
“DCCT/EDIC because of its longevity represents a unique opportunity to explore aging in long duration of type 1 diabetes, something that heretofore none of us could have imagined, especially for those of you in the audience who started your careers in the 70s and 80s,” Ms. Lorenzi commented.
About 36% of the cohort now has overweight and 40% have obesity, mirroring the general population. And they now have a mean hemoglobin A1c of 7.3%.
According to Barbara H. Braffett, PhD, co–principal investigator at the DCCT/EDIC data coordinating center: “The EDIC study is now shifting its focus during the next 5 years to understand the clinical course of type 1 diabetes in the setting of advancing duration and age, as well as increasing adiposity, which has progressively affected individuals with type 1 diabetes and has potential long-term adverse consequences.”
Dr. Braffett outlined the new study approaches added in 2022-2027. Cardiopulmonary exercise testing, two-dimensional Doppler echocardiography, and carotid-femoral pulse wave velocity will be used to quantify functional and structural changes central to heart failure.
Dr. Nathan commented that, although enough cardiovascular events were available in EDIC by 2006 to demonstrate a significant 58% reduction in the intensive therapy group, “now we can start looking at the aging heart. We have a bunch of great cardiologists working with us who will be guiding us on measuring everything.”
Fatty liver disease in the setting of increasing adiposity will also be investigated using transient elastography (FibroScan) and the Fibrosis-4 index, a quantification of liver enzymes and platelet count.
Dr. Nathan noted that the study participants have had “this kind of funny metabolic milieu in their liver for decades. They don’t make insulin in their pancreas, and therefore, the insulin they get is peripheral and then it goes to their liver. Well, what does that do to them?”
Participants will also complete three symptom questionnaires assessing obstructive sleep apnea, aimed at guiding future sleep studies in those found to be at high risk, Dr. Braffett said.
DCCT/EDIC over 40 years: ‘Incredibly complete picture’
As of 2023, the DCCT/EDIC participants have been studied for longer than 60% of their lifespans and for over 80% of their diabetes duration, Dr. Braffett noted.
During the EDIC 2017-2022 cycle, Dr. Braffett and other speakers summarized, prior EDIC efforts had focused on aspects of cognitive function, physical function, and cheiroarthropathy.
Other DCCT/EDIC studies examined the relationship of A1c and diabetes duration in cardiovascular disease risk, the association of microvascular complications with the risk of cardiovascular disease beyond traditional risk factors, and the risk of severe hypoglycemia over the first 30 years of DCCT/EDIC follow-up.
Moreover, the longitudinal eye and kidney assessments over the 40 years have informed screening guidelines for retinopathy and urinary albumin.
Dr. Nathan said: “Today, the number with horrible complications is very few, but we haven’t erased complications entirely. ... We have this incredibly complete picture of type 1 diabetes that allows us to explore everything. We welcome people to come to us with ideas. That’s the value of this research.”
Dr. Nathan, Ms. Lorenzi, and Dr. Braffett reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
SAN DIEGO –
New funding for 2022-2027 for the DCCT long-term observational follow-up study, the Epidemiology of Diabetes Interventions and Complications (EDIC) will go toward investigating aspects of type 1 diabetes that are associated with aging and are also common in type 2 diabetes, including cardiovascular disease, fatty liver disease, and sleep apnea.
The original randomized DCCT clinical trial results, published in 1993 in the New England Journal of Medicine, proved that early intensive glycemic control was the key to preventing or slowing the progression of long-term eye, kidney, and nerve complications of type 1 diabetes. Subsequently, EDIC has yielded many more major findings including that early tight glycemic control also reduces cardiovascular risk and prolongs survival in type 1 diabetes.
And although the phenomenon of metabolic memory initially seen in EDIC means that early glycemic control is important, subsequent EDIC data also have suggested that it is never too late to initiate intensive glycemic control, speakers emphasized during a special symposium commemorating 40 years since the start of DCCT, held during the annual scientific sessions of the American Diabetes Association. As with the 30-year DCCT/EDIC commemorative symposium held in 2013, local study participants were in the audience and were acknowledged with long applause.
Together, DCCT and EDIC – both funded by the National Institutes of Health at 27 sites in the United States and Canada – have changed the standard of care for people with type 1 diabetes and continue to inform clinical practice. Prior to the DCCT, between 1930 and 1970, about a third of people with type 1 diabetes developed vision loss and one in five experienced kidney failure and/or myocardial infarction. Stroke and amputation were also common, DCCT/EDIC chair David M. Nathan, MD, said while introducing the symposium.
“All of the advances in care of type 1 diabetes have developed because this study demonstrated that it was important – continuous glucose monitoring (CGM), new insulins, better [insulin] pumps. ... I think the most profound finding is that mortality in our intensively treated cohort is the same as in the general population. That says it all,” Dr. Nathan said in an interview.
And now, “what we still have yet to contribute is what happens to type 1 diabetes as people get older,” added Dr. Nathan, a professor of medicine at Harvard Medical School and director of the Diabetes Center at Massachusetts General Hospital, both in Boston.
‘Something that heretofore none of us could have imagined’
The 1,441 DCCT participants had a mean age of 27 years at baseline in 1983, when they were randomized to intensive insulin therapy or usual care. The 1,375 participants (96%) who continued into EDIC in 1994 were an average of 35 years old at that point, when the usual care group was taught intensive glycemic management and all participants returned to their personal health care teams. The 1,075 participants in EDIC today are an average age of 63 years.
Only 11 participants had died at the start of EDIC, and just 250 (17%) have died as of 2023, said study coordinator cochair Gayle Lorenzi, RN, who is a certified diabetes care and education specialist at the University of California, San Diego.
“DCCT/EDIC because of its longevity represents a unique opportunity to explore aging in long duration of type 1 diabetes, something that heretofore none of us could have imagined, especially for those of you in the audience who started your careers in the 70s and 80s,” Ms. Lorenzi commented.
About 36% of the cohort now has overweight and 40% have obesity, mirroring the general population. And they now have a mean hemoglobin A1c of 7.3%.
According to Barbara H. Braffett, PhD, co–principal investigator at the DCCT/EDIC data coordinating center: “The EDIC study is now shifting its focus during the next 5 years to understand the clinical course of type 1 diabetes in the setting of advancing duration and age, as well as increasing adiposity, which has progressively affected individuals with type 1 diabetes and has potential long-term adverse consequences.”
Dr. Braffett outlined the new study approaches added in 2022-2027. Cardiopulmonary exercise testing, two-dimensional Doppler echocardiography, and carotid-femoral pulse wave velocity will be used to quantify functional and structural changes central to heart failure.
Dr. Nathan commented that, although enough cardiovascular events were available in EDIC by 2006 to demonstrate a significant 58% reduction in the intensive therapy group, “now we can start looking at the aging heart. We have a bunch of great cardiologists working with us who will be guiding us on measuring everything.”
Fatty liver disease in the setting of increasing adiposity will also be investigated using transient elastography (FibroScan) and the Fibrosis-4 index, a quantification of liver enzymes and platelet count.
Dr. Nathan noted that the study participants have had “this kind of funny metabolic milieu in their liver for decades. They don’t make insulin in their pancreas, and therefore, the insulin they get is peripheral and then it goes to their liver. Well, what does that do to them?”
Participants will also complete three symptom questionnaires assessing obstructive sleep apnea, aimed at guiding future sleep studies in those found to be at high risk, Dr. Braffett said.
DCCT/EDIC over 40 years: ‘Incredibly complete picture’
As of 2023, the DCCT/EDIC participants have been studied for longer than 60% of their lifespans and for over 80% of their diabetes duration, Dr. Braffett noted.
During the EDIC 2017-2022 cycle, Dr. Braffett and other speakers summarized, prior EDIC efforts had focused on aspects of cognitive function, physical function, and cheiroarthropathy.
Other DCCT/EDIC studies examined the relationship of A1c and diabetes duration in cardiovascular disease risk, the association of microvascular complications with the risk of cardiovascular disease beyond traditional risk factors, and the risk of severe hypoglycemia over the first 30 years of DCCT/EDIC follow-up.
Moreover, the longitudinal eye and kidney assessments over the 40 years have informed screening guidelines for retinopathy and urinary albumin.
Dr. Nathan said: “Today, the number with horrible complications is very few, but we haven’t erased complications entirely. ... We have this incredibly complete picture of type 1 diabetes that allows us to explore everything. We welcome people to come to us with ideas. That’s the value of this research.”
Dr. Nathan, Ms. Lorenzi, and Dr. Braffett reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
SAN DIEGO –
New funding for 2022-2027 for the DCCT long-term observational follow-up study, the Epidemiology of Diabetes Interventions and Complications (EDIC) will go toward investigating aspects of type 1 diabetes that are associated with aging and are also common in type 2 diabetes, including cardiovascular disease, fatty liver disease, and sleep apnea.
The original randomized DCCT clinical trial results, published in 1993 in the New England Journal of Medicine, proved that early intensive glycemic control was the key to preventing or slowing the progression of long-term eye, kidney, and nerve complications of type 1 diabetes. Subsequently, EDIC has yielded many more major findings including that early tight glycemic control also reduces cardiovascular risk and prolongs survival in type 1 diabetes.
And although the phenomenon of metabolic memory initially seen in EDIC means that early glycemic control is important, subsequent EDIC data also have suggested that it is never too late to initiate intensive glycemic control, speakers emphasized during a special symposium commemorating 40 years since the start of DCCT, held during the annual scientific sessions of the American Diabetes Association. As with the 30-year DCCT/EDIC commemorative symposium held in 2013, local study participants were in the audience and were acknowledged with long applause.
Together, DCCT and EDIC – both funded by the National Institutes of Health at 27 sites in the United States and Canada – have changed the standard of care for people with type 1 diabetes and continue to inform clinical practice. Prior to the DCCT, between 1930 and 1970, about a third of people with type 1 diabetes developed vision loss and one in five experienced kidney failure and/or myocardial infarction. Stroke and amputation were also common, DCCT/EDIC chair David M. Nathan, MD, said while introducing the symposium.
“All of the advances in care of type 1 diabetes have developed because this study demonstrated that it was important – continuous glucose monitoring (CGM), new insulins, better [insulin] pumps. ... I think the most profound finding is that mortality in our intensively treated cohort is the same as in the general population. That says it all,” Dr. Nathan said in an interview.
And now, “what we still have yet to contribute is what happens to type 1 diabetes as people get older,” added Dr. Nathan, a professor of medicine at Harvard Medical School and director of the Diabetes Center at Massachusetts General Hospital, both in Boston.
‘Something that heretofore none of us could have imagined’
The 1,441 DCCT participants had a mean age of 27 years at baseline in 1983, when they were randomized to intensive insulin therapy or usual care. The 1,375 participants (96%) who continued into EDIC in 1994 were an average of 35 years old at that point, when the usual care group was taught intensive glycemic management and all participants returned to their personal health care teams. The 1,075 participants in EDIC today are an average age of 63 years.
Only 11 participants had died at the start of EDIC, and just 250 (17%) have died as of 2023, said study coordinator cochair Gayle Lorenzi, RN, who is a certified diabetes care and education specialist at the University of California, San Diego.
“DCCT/EDIC because of its longevity represents a unique opportunity to explore aging in long duration of type 1 diabetes, something that heretofore none of us could have imagined, especially for those of you in the audience who started your careers in the 70s and 80s,” Ms. Lorenzi commented.
About 36% of the cohort now has overweight and 40% have obesity, mirroring the general population. And they now have a mean hemoglobin A1c of 7.3%.
According to Barbara H. Braffett, PhD, co–principal investigator at the DCCT/EDIC data coordinating center: “The EDIC study is now shifting its focus during the next 5 years to understand the clinical course of type 1 diabetes in the setting of advancing duration and age, as well as increasing adiposity, which has progressively affected individuals with type 1 diabetes and has potential long-term adverse consequences.”
Dr. Braffett outlined the new study approaches added in 2022-2027. Cardiopulmonary exercise testing, two-dimensional Doppler echocardiography, and carotid-femoral pulse wave velocity will be used to quantify functional and structural changes central to heart failure.
Dr. Nathan commented that, although enough cardiovascular events were available in EDIC by 2006 to demonstrate a significant 58% reduction in the intensive therapy group, “now we can start looking at the aging heart. We have a bunch of great cardiologists working with us who will be guiding us on measuring everything.”
Fatty liver disease in the setting of increasing adiposity will also be investigated using transient elastography (FibroScan) and the Fibrosis-4 index, a quantification of liver enzymes and platelet count.
Dr. Nathan noted that the study participants have had “this kind of funny metabolic milieu in their liver for decades. They don’t make insulin in their pancreas, and therefore, the insulin they get is peripheral and then it goes to their liver. Well, what does that do to them?”
Participants will also complete three symptom questionnaires assessing obstructive sleep apnea, aimed at guiding future sleep studies in those found to be at high risk, Dr. Braffett said.
DCCT/EDIC over 40 years: ‘Incredibly complete picture’
As of 2023, the DCCT/EDIC participants have been studied for longer than 60% of their lifespans and for over 80% of their diabetes duration, Dr. Braffett noted.
During the EDIC 2017-2022 cycle, Dr. Braffett and other speakers summarized, prior EDIC efforts had focused on aspects of cognitive function, physical function, and cheiroarthropathy.
Other DCCT/EDIC studies examined the relationship of A1c and diabetes duration in cardiovascular disease risk, the association of microvascular complications with the risk of cardiovascular disease beyond traditional risk factors, and the risk of severe hypoglycemia over the first 30 years of DCCT/EDIC follow-up.
Moreover, the longitudinal eye and kidney assessments over the 40 years have informed screening guidelines for retinopathy and urinary albumin.
Dr. Nathan said: “Today, the number with horrible complications is very few, but we haven’t erased complications entirely. ... We have this incredibly complete picture of type 1 diabetes that allows us to explore everything. We welcome people to come to us with ideas. That’s the value of this research.”
Dr. Nathan, Ms. Lorenzi, and Dr. Braffett reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
AT ADA 2023
Is there a link between body image concerns and polycystic ovary syndrome?
This transcript has been edited for clarity.
At ENDO 2023, I presented our systematic review and meta-analysis related to body image concerns in women and individuals with polycystic ovary syndrome (PCOS). PCOS is the most common endocrine condition affecting women worldwide. It’s as common as 10%-15%.
Previously thought to be a benign condition affecting a small proportion of women of reproductive age, it’s changed now. It affects women of all ages, all ethnicities, and throughout the world. Body image concern is an area where one feels uncomfortable with how they look and how they feel. Someone might wonder, why worry about body image concerns? When people have body image concerns, it leads to low self-esteem.
Low self-esteem can lead to depression and anxiety, eventually making you a not-so-productive member of society. Several studies have also shown that body image concerns can lead to eating disorders such as anorexia and bulimia, which can be life threatening. Several studies in the past have shown there is a link between PCOS and body image concerns, but what exactly is the link? We don’t know. How big is the problem? We didn’t know until now.
To answer this, we looked at everything published about PCOS and body image concerns together, be it a randomized study, a cluster study, or any kind of study. We put them all into one place and studied them for evidence. The second objective of our work was that we wanted to share any evidence with the international PCOS guidelines group, who are currently reviewing and revising the guidelines for 2023.
We looked at all the major scientific databases, such as PubMed, PubMed Central, and Medline, for any study that’s been published for polycystic ovary syndrome and body image concerns where they specifically used a validated questionnaire – that’s important, and I’ll come back to that later.
We found 6,221 articles on an initial search. After meticulously looking through all of them, we narrowed it down to 9 articles that were relevant to our work. That’s going from 6,221 articles to 9, which were reviewed by 2 independent researchers. If there was any conflict between them, a third independent researcher resolved the conflict.
We found some studies had used the same questionnaires and some had their own questionnaire. We combined the studies where they used the same questionnaire and we did what we call a meta-analysis. We used their data and combined them to find an additional analysis, which is a combination of the two.
The two most commonly used questionnaires were the Multidimensional Body-Self Relations Questionnaire (MBSRQ) survey and the Body-Esteem Scale for Adolescents and Adults (BESAA). I’m not going into detail, but in simplest terms, the MBSRQ has 69 questions, which breaks down into 5 subscales, and BESAA has 3 subscales, which has 23 questions.
When we combined the results in the MBSRQ questionnaire, women with PCOS fared worse in all the subscales, showing there is a concern about body image in women with PCOS when compared with their colleagues who are healthy and do not have PCOS.
With BESAA, we found a little bit of a mixed picture. There was still a significant difference about weight perception, but how they felt and how they attributed, there was no significant difference. Probably the main reason was that only two studies used it and there was a smaller number of people involved in the study.
Why is this important? We feel that by identifying or diagnosing body image concerns, we will be addressing patient concerns. That is important because we clinicians have our own thoughts of what we need to do to help women with PCOS to prevent long-term risk, but it’s also important to talk to the person sitting in front of you right now. What is their concern?
There’s also been a generational shift where women with PCOS used say, “Oh, I’m worried that I can’t have a kid,” to now say, “I’m worried that I don’t feel well about myself.” We need to address that.
When we shared these findings with the international PCOS guidelines, they said we should probably approach this on an individual case-by-case basis because it will mean that the length of consultation might increase if we spend time with body image concerns.
This is where questionnaires come into play. With a validated questionnaire, a person can complete that before they come into the consultation, thereby minimizing the amount of time spent. If they’re not scoring high on the questionnaire, we don’t need to address that. If they are scoring high, then it can be picked up as a topic to discuss.
As I mentioned, there are a couple of limitations, one being the fewer studies and lower numbers of people in the studies. We need to address this in the future.
Long story short, at the moment, there is evidence to say that body image concerns are quite significantly high in women and individuals with PCOS. This is something we need to address as soon as possible.
We are planning future work to understand how social media comes into play, how society influences body image, and how health care professionals across the world are addressing PCOS and body image concerns. Hopefully, we will be able to share these findings in the near future. Thank you.
Dr. Kempegowda is assistant professor in endocrinology, diabetes, and general medicine at the Institute of Applied Health Research, University of Birmingham, and a consultant in endocrinology, diabetes and acute medicine, Queen Elizabeth Hospital, Birmingham, England, and disclosed no relevant conflicts of interest.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
At ENDO 2023, I presented our systematic review and meta-analysis related to body image concerns in women and individuals with polycystic ovary syndrome (PCOS). PCOS is the most common endocrine condition affecting women worldwide. It’s as common as 10%-15%.
Previously thought to be a benign condition affecting a small proportion of women of reproductive age, it’s changed now. It affects women of all ages, all ethnicities, and throughout the world. Body image concern is an area where one feels uncomfortable with how they look and how they feel. Someone might wonder, why worry about body image concerns? When people have body image concerns, it leads to low self-esteem.
Low self-esteem can lead to depression and anxiety, eventually making you a not-so-productive member of society. Several studies have also shown that body image concerns can lead to eating disorders such as anorexia and bulimia, which can be life threatening. Several studies in the past have shown there is a link between PCOS and body image concerns, but what exactly is the link? We don’t know. How big is the problem? We didn’t know until now.
To answer this, we looked at everything published about PCOS and body image concerns together, be it a randomized study, a cluster study, or any kind of study. We put them all into one place and studied them for evidence. The second objective of our work was that we wanted to share any evidence with the international PCOS guidelines group, who are currently reviewing and revising the guidelines for 2023.
We looked at all the major scientific databases, such as PubMed, PubMed Central, and Medline, for any study that’s been published for polycystic ovary syndrome and body image concerns where they specifically used a validated questionnaire – that’s important, and I’ll come back to that later.
We found 6,221 articles on an initial search. After meticulously looking through all of them, we narrowed it down to 9 articles that were relevant to our work. That’s going from 6,221 articles to 9, which were reviewed by 2 independent researchers. If there was any conflict between them, a third independent researcher resolved the conflict.
We found some studies had used the same questionnaires and some had their own questionnaire. We combined the studies where they used the same questionnaire and we did what we call a meta-analysis. We used their data and combined them to find an additional analysis, which is a combination of the two.
The two most commonly used questionnaires were the Multidimensional Body-Self Relations Questionnaire (MBSRQ) survey and the Body-Esteem Scale for Adolescents and Adults (BESAA). I’m not going into detail, but in simplest terms, the MBSRQ has 69 questions, which breaks down into 5 subscales, and BESAA has 3 subscales, which has 23 questions.
When we combined the results in the MBSRQ questionnaire, women with PCOS fared worse in all the subscales, showing there is a concern about body image in women with PCOS when compared with their colleagues who are healthy and do not have PCOS.
With BESAA, we found a little bit of a mixed picture. There was still a significant difference about weight perception, but how they felt and how they attributed, there was no significant difference. Probably the main reason was that only two studies used it and there was a smaller number of people involved in the study.
Why is this important? We feel that by identifying or diagnosing body image concerns, we will be addressing patient concerns. That is important because we clinicians have our own thoughts of what we need to do to help women with PCOS to prevent long-term risk, but it’s also important to talk to the person sitting in front of you right now. What is their concern?
There’s also been a generational shift where women with PCOS used say, “Oh, I’m worried that I can’t have a kid,” to now say, “I’m worried that I don’t feel well about myself.” We need to address that.
When we shared these findings with the international PCOS guidelines, they said we should probably approach this on an individual case-by-case basis because it will mean that the length of consultation might increase if we spend time with body image concerns.
This is where questionnaires come into play. With a validated questionnaire, a person can complete that before they come into the consultation, thereby minimizing the amount of time spent. If they’re not scoring high on the questionnaire, we don’t need to address that. If they are scoring high, then it can be picked up as a topic to discuss.
As I mentioned, there are a couple of limitations, one being the fewer studies and lower numbers of people in the studies. We need to address this in the future.
Long story short, at the moment, there is evidence to say that body image concerns are quite significantly high in women and individuals with PCOS. This is something we need to address as soon as possible.
We are planning future work to understand how social media comes into play, how society influences body image, and how health care professionals across the world are addressing PCOS and body image concerns. Hopefully, we will be able to share these findings in the near future. Thank you.
Dr. Kempegowda is assistant professor in endocrinology, diabetes, and general medicine at the Institute of Applied Health Research, University of Birmingham, and a consultant in endocrinology, diabetes and acute medicine, Queen Elizabeth Hospital, Birmingham, England, and disclosed no relevant conflicts of interest.
A version of this article first appeared on Medscape.com.
This transcript has been edited for clarity.
At ENDO 2023, I presented our systematic review and meta-analysis related to body image concerns in women and individuals with polycystic ovary syndrome (PCOS). PCOS is the most common endocrine condition affecting women worldwide. It’s as common as 10%-15%.
Previously thought to be a benign condition affecting a small proportion of women of reproductive age, it’s changed now. It affects women of all ages, all ethnicities, and throughout the world. Body image concern is an area where one feels uncomfortable with how they look and how they feel. Someone might wonder, why worry about body image concerns? When people have body image concerns, it leads to low self-esteem.
Low self-esteem can lead to depression and anxiety, eventually making you a not-so-productive member of society. Several studies have also shown that body image concerns can lead to eating disorders such as anorexia and bulimia, which can be life threatening. Several studies in the past have shown there is a link between PCOS and body image concerns, but what exactly is the link? We don’t know. How big is the problem? We didn’t know until now.
To answer this, we looked at everything published about PCOS and body image concerns together, be it a randomized study, a cluster study, or any kind of study. We put them all into one place and studied them for evidence. The second objective of our work was that we wanted to share any evidence with the international PCOS guidelines group, who are currently reviewing and revising the guidelines for 2023.
We looked at all the major scientific databases, such as PubMed, PubMed Central, and Medline, for any study that’s been published for polycystic ovary syndrome and body image concerns where they specifically used a validated questionnaire – that’s important, and I’ll come back to that later.
We found 6,221 articles on an initial search. After meticulously looking through all of them, we narrowed it down to 9 articles that were relevant to our work. That’s going from 6,221 articles to 9, which were reviewed by 2 independent researchers. If there was any conflict between them, a third independent researcher resolved the conflict.
We found some studies had used the same questionnaires and some had their own questionnaire. We combined the studies where they used the same questionnaire and we did what we call a meta-analysis. We used their data and combined them to find an additional analysis, which is a combination of the two.
The two most commonly used questionnaires were the Multidimensional Body-Self Relations Questionnaire (MBSRQ) survey and the Body-Esteem Scale for Adolescents and Adults (BESAA). I’m not going into detail, but in simplest terms, the MBSRQ has 69 questions, which breaks down into 5 subscales, and BESAA has 3 subscales, which has 23 questions.
When we combined the results in the MBSRQ questionnaire, women with PCOS fared worse in all the subscales, showing there is a concern about body image in women with PCOS when compared with their colleagues who are healthy and do not have PCOS.
With BESAA, we found a little bit of a mixed picture. There was still a significant difference about weight perception, but how they felt and how they attributed, there was no significant difference. Probably the main reason was that only two studies used it and there was a smaller number of people involved in the study.
Why is this important? We feel that by identifying or diagnosing body image concerns, we will be addressing patient concerns. That is important because we clinicians have our own thoughts of what we need to do to help women with PCOS to prevent long-term risk, but it’s also important to talk to the person sitting in front of you right now. What is their concern?
There’s also been a generational shift where women with PCOS used say, “Oh, I’m worried that I can’t have a kid,” to now say, “I’m worried that I don’t feel well about myself.” We need to address that.
When we shared these findings with the international PCOS guidelines, they said we should probably approach this on an individual case-by-case basis because it will mean that the length of consultation might increase if we spend time with body image concerns.
This is where questionnaires come into play. With a validated questionnaire, a person can complete that before they come into the consultation, thereby minimizing the amount of time spent. If they’re not scoring high on the questionnaire, we don’t need to address that. If they are scoring high, then it can be picked up as a topic to discuss.
As I mentioned, there are a couple of limitations, one being the fewer studies and lower numbers of people in the studies. We need to address this in the future.
Long story short, at the moment, there is evidence to say that body image concerns are quite significantly high in women and individuals with PCOS. This is something we need to address as soon as possible.
We are planning future work to understand how social media comes into play, how society influences body image, and how health care professionals across the world are addressing PCOS and body image concerns. Hopefully, we will be able to share these findings in the near future. Thank you.
Dr. Kempegowda is assistant professor in endocrinology, diabetes, and general medicine at the Institute of Applied Health Research, University of Birmingham, and a consultant in endocrinology, diabetes and acute medicine, Queen Elizabeth Hospital, Birmingham, England, and disclosed no relevant conflicts of interest.
A version of this article first appeared on Medscape.com.