User login
Recombinant IL-2 shows potential in atopic dermatitis
BERLIN – A novel regulatory T cell–stimulating therapy appears to significantly improve atopic dermatitis in patients with moderate to severe disease and may even benefit quality of life, suggest results from a phase 1b trial.
The research was presented at the annual congress of the European Academy of Dermatology and Venereology.
, after which responders were observed out to 48 weeks. The higher dosage was associated with significant improvements in Eczema Area and Severity Index (EASI) and Body Surface Area (BSA) scores, which were maintained over the course of the study, as well as trends for improved patient-reported outcomes.
“This is the first study to demonstrate the therapeutic potential of rezpegaldesleukin,” said presenter Jonathan Silverberg, MD, PhD, MPH, professor of dermatology and director of clinical research at George Washington University, Washington. He added, “These may be some of the most compelling data to date for the field, proving that, at a high level, if you causally increase regulator T cells, you will take down inflammation and improve a disease state.
“For me, this is proof of concept for so many things, and it gets me very excited.”
Dr. Silverberg noted that with the response maintained out to 48 weeks, despite stopping therapy at week 12, the “hope” with the approach of inducing regulator T cells “is that we could induce tolerance and that we could have some potential for disease modification.”
He continued, “Maybe I daren’t use the word ‘cure,’ but can we at least get to something that is truly remitted, where they can stop the drug and maintain that response?”
Dr. Silverberg said rezpegaldesleukin is now being evaluated in a phase 2b study for moderate to severe atopic dermatitis, and a phase 2b trial for alopecia areata is in development.
Tiago dos Reis Matos, MD, PhD, MSc, Amsterdam University Medical Centers, who was not involved in the study, told this news organization that “recombinant human interleukin-2 is an original therapy.”
Instead of blocking or inhibiting inflammation, it stimulates the patient’s immune system to “restore a healthy balance.”
He explained that it “stimulates regulatory T cells, which can be seen as the Peace Corps of the immune system, responsible for maintaining the equilibrium and avoiding uncontrolled inflammation.”
At the meeting, Dr. Silverberg told the audience that although they are the “beneficiaries of riches of new advances” in atopic dermatitis, “still, many observational studies have shown that the majority of patients do not achieve adequate control by the end of their induction periods and clinical trials, in the real world,” with currently available treatments.
Moreover, “there are challenges that come up with any of the different therapies,” he said, with adverse effects an important issue. For example, biologic therapies are associated with conjunctivitis, facial erythema, and arthralgia, and there are boxed warnings for Janus kinase inhibitors.
Dr. Silverberg continued, “Even patients with a favorable response can experience a loss of disease control when they come off therapy.” Consequently, “new strategies are certainly welcome that could potentially induce both deep and potentially therapy-free remission.”
To those ends, he explained that regulatory T cells play a central role in immune homeostasis but have not been “therapeutically relevant until very recently,” when it was posited that increasing their function can “induce that homeostasis, to normalize the inflammatory cascades” seen in a range of conditions, including atopic dermatitis.
Rezpegaldesleukin has high selectivity for regulatory T cells, without causing activation of effector T cells, and has been shown to increase cell numbers in a dose-dependent manner that is sustained for up to 30 days.
The current study involved patients aged 18-70 years with moderate to severe atopic dermatitis and a history of inadequate responses or intolerance to topical medications, and an EASI score ≥ 16.
Participants were randomly assigned to receive subcutaneous rezpegaldesleukin 12 mcg/kg or 24 mcg/kg or placebo every 2 weeks for 12 weeks. They then discontinued treatment and were followed up until week 19, when responders, defined as having a reduction in EASI score ≥ 50%, continued follow-up out to week 48.
Seventeen patients were randomized to higher-dose rezpegaldesleukin, whereas 16 received the lower dose and 10 were assigned to placebo. Dr. Silverberg said that the three groups were “fairly well balanced,” with “fairly good representation” across age, race, and ethnicity groups.
The mean baseline EASI score was between 21.9 and 23.7, and the Validated Investigator Global Assessment for Atopic Dermatitis (vIGA-AD) suggested that there was an even split between moderate and severe atopic dermatitis, although the higher-dose rezpegaldesleukin group had more patients with moderate disease.
By week 12, rezpegaldesleukin was associated with significantly greater improvements in EASI scores vs. placebo. Patients on the higher dose had a mean 83% improvement over baseline vs. 65% with the lower dose and 47% with placebo (P = .002 for the higher dose vs. placebo).
Crucially, these differences were maintained up to week 48 in patients, particularly in the higher-dose group.
There was also a nonsignificant increase in the proportion of patients who achieved a reduction in EASI scores ≥ 75% over baseline with the active drug: 41% at week 12 with higher-dose rezpegaldesleukin, 25% with the lower dose, and 20% with placebo. Again, the benefit was maintained up to week 48.
The mean improvement in BSA score from baseline with rezpegaldesleukin was significantly greater than that seen with placebo, at 72% with the higher dose, 55% with the lower dose, and 36% with placebo (P = .0158 for the higher dose vs. placebo).
Although improvements in vIGA-AD scores over baseline with rezpegaldesleukin were not substantial at week 12, by week 48 there was a marked difference between higher-dose rezpegaldesleukin and placebo, with 40.0% of patients responding to the drug vs. 0% in the latter group.
A similar pattern was seen for the Itch Numeric Rating Scale, in which 55.6% of patients treated with higher-dose rezpegaldesleukin responding by week 48, compared with 0% of those who received placebo.
Greater improvements in the Dermatology Life Quality Index (DLQI) and Patient Oriented Eczema Measure (POEM) over baseline with higher-dose rezpegaldesleukin vs. plain placebo were also noted, despite a strong response in the latter group.
Dr. Silverberg reported that all treatment-emergent adverse effects in the two rezpegaldesleukin treatment arms were mild to moderate, with no severe or serious events observed.
The most common adverse events were mild to moderate injection-site reactions, seen in 75.0% of the lower-dose rezpegaldesleukin group and 58.8% the of higher-dose group. There were no cases of conjunctivitis.
The study was sponsored by Eli Lilly and Company in collaboration with Nektar Therapeutics.
Dr. Silverberg declares relationships with AbbVie, Alamar, Aldena, Amgen, AOBiome, Arcutis, Arena, Asana, ASLAN, BioMX, Biosion, Bodewell, Boehringer-Ingelheim, Bristol-Myers Squibb, Cara, Castle Biosciences, Celgene, Connect Biopharma, CorEvitas, Dermavant, DermTech, Eli Lilly, Galderma, GlaxoSmithKline, Incyte, Kiniksa, LEO Pharma, Nektar, Novartis, Optum, Pfizer, RAPT, Recludix, Regeneron, Sanofi-Genzyme, Shaperon, Target RWE, Union, and UpToDate.
A version of this article appeared on Medscape.com.
BERLIN – A novel regulatory T cell–stimulating therapy appears to significantly improve atopic dermatitis in patients with moderate to severe disease and may even benefit quality of life, suggest results from a phase 1b trial.
The research was presented at the annual congress of the European Academy of Dermatology and Venereology.
, after which responders were observed out to 48 weeks. The higher dosage was associated with significant improvements in Eczema Area and Severity Index (EASI) and Body Surface Area (BSA) scores, which were maintained over the course of the study, as well as trends for improved patient-reported outcomes.
“This is the first study to demonstrate the therapeutic potential of rezpegaldesleukin,” said presenter Jonathan Silverberg, MD, PhD, MPH, professor of dermatology and director of clinical research at George Washington University, Washington. He added, “These may be some of the most compelling data to date for the field, proving that, at a high level, if you causally increase regulator T cells, you will take down inflammation and improve a disease state.
“For me, this is proof of concept for so many things, and it gets me very excited.”
Dr. Silverberg noted that with the response maintained out to 48 weeks, despite stopping therapy at week 12, the “hope” with the approach of inducing regulator T cells “is that we could induce tolerance and that we could have some potential for disease modification.”
He continued, “Maybe I daren’t use the word ‘cure,’ but can we at least get to something that is truly remitted, where they can stop the drug and maintain that response?”
Dr. Silverberg said rezpegaldesleukin is now being evaluated in a phase 2b study for moderate to severe atopic dermatitis, and a phase 2b trial for alopecia areata is in development.
Tiago dos Reis Matos, MD, PhD, MSc, Amsterdam University Medical Centers, who was not involved in the study, told this news organization that “recombinant human interleukin-2 is an original therapy.”
Instead of blocking or inhibiting inflammation, it stimulates the patient’s immune system to “restore a healthy balance.”
He explained that it “stimulates regulatory T cells, which can be seen as the Peace Corps of the immune system, responsible for maintaining the equilibrium and avoiding uncontrolled inflammation.”
At the meeting, Dr. Silverberg told the audience that although they are the “beneficiaries of riches of new advances” in atopic dermatitis, “still, many observational studies have shown that the majority of patients do not achieve adequate control by the end of their induction periods and clinical trials, in the real world,” with currently available treatments.
Moreover, “there are challenges that come up with any of the different therapies,” he said, with adverse effects an important issue. For example, biologic therapies are associated with conjunctivitis, facial erythema, and arthralgia, and there are boxed warnings for Janus kinase inhibitors.
Dr. Silverberg continued, “Even patients with a favorable response can experience a loss of disease control when they come off therapy.” Consequently, “new strategies are certainly welcome that could potentially induce both deep and potentially therapy-free remission.”
To those ends, he explained that regulatory T cells play a central role in immune homeostasis but have not been “therapeutically relevant until very recently,” when it was posited that increasing their function can “induce that homeostasis, to normalize the inflammatory cascades” seen in a range of conditions, including atopic dermatitis.
Rezpegaldesleukin has high selectivity for regulatory T cells, without causing activation of effector T cells, and has been shown to increase cell numbers in a dose-dependent manner that is sustained for up to 30 days.
The current study involved patients aged 18-70 years with moderate to severe atopic dermatitis and a history of inadequate responses or intolerance to topical medications, and an EASI score ≥ 16.
Participants were randomly assigned to receive subcutaneous rezpegaldesleukin 12 mcg/kg or 24 mcg/kg or placebo every 2 weeks for 12 weeks. They then discontinued treatment and were followed up until week 19, when responders, defined as having a reduction in EASI score ≥ 50%, continued follow-up out to week 48.
Seventeen patients were randomized to higher-dose rezpegaldesleukin, whereas 16 received the lower dose and 10 were assigned to placebo. Dr. Silverberg said that the three groups were “fairly well balanced,” with “fairly good representation” across age, race, and ethnicity groups.
The mean baseline EASI score was between 21.9 and 23.7, and the Validated Investigator Global Assessment for Atopic Dermatitis (vIGA-AD) suggested that there was an even split between moderate and severe atopic dermatitis, although the higher-dose rezpegaldesleukin group had more patients with moderate disease.
By week 12, rezpegaldesleukin was associated with significantly greater improvements in EASI scores vs. placebo. Patients on the higher dose had a mean 83% improvement over baseline vs. 65% with the lower dose and 47% with placebo (P = .002 for the higher dose vs. placebo).
Crucially, these differences were maintained up to week 48 in patients, particularly in the higher-dose group.
There was also a nonsignificant increase in the proportion of patients who achieved a reduction in EASI scores ≥ 75% over baseline with the active drug: 41% at week 12 with higher-dose rezpegaldesleukin, 25% with the lower dose, and 20% with placebo. Again, the benefit was maintained up to week 48.
The mean improvement in BSA score from baseline with rezpegaldesleukin was significantly greater than that seen with placebo, at 72% with the higher dose, 55% with the lower dose, and 36% with placebo (P = .0158 for the higher dose vs. placebo).
Although improvements in vIGA-AD scores over baseline with rezpegaldesleukin were not substantial at week 12, by week 48 there was a marked difference between higher-dose rezpegaldesleukin and placebo, with 40.0% of patients responding to the drug vs. 0% in the latter group.
A similar pattern was seen for the Itch Numeric Rating Scale, in which 55.6% of patients treated with higher-dose rezpegaldesleukin responding by week 48, compared with 0% of those who received placebo.
Greater improvements in the Dermatology Life Quality Index (DLQI) and Patient Oriented Eczema Measure (POEM) over baseline with higher-dose rezpegaldesleukin vs. plain placebo were also noted, despite a strong response in the latter group.
Dr. Silverberg reported that all treatment-emergent adverse effects in the two rezpegaldesleukin treatment arms were mild to moderate, with no severe or serious events observed.
The most common adverse events were mild to moderate injection-site reactions, seen in 75.0% of the lower-dose rezpegaldesleukin group and 58.8% the of higher-dose group. There were no cases of conjunctivitis.
The study was sponsored by Eli Lilly and Company in collaboration with Nektar Therapeutics.
Dr. Silverberg declares relationships with AbbVie, Alamar, Aldena, Amgen, AOBiome, Arcutis, Arena, Asana, ASLAN, BioMX, Biosion, Bodewell, Boehringer-Ingelheim, Bristol-Myers Squibb, Cara, Castle Biosciences, Celgene, Connect Biopharma, CorEvitas, Dermavant, DermTech, Eli Lilly, Galderma, GlaxoSmithKline, Incyte, Kiniksa, LEO Pharma, Nektar, Novartis, Optum, Pfizer, RAPT, Recludix, Regeneron, Sanofi-Genzyme, Shaperon, Target RWE, Union, and UpToDate.
A version of this article appeared on Medscape.com.
BERLIN – A novel regulatory T cell–stimulating therapy appears to significantly improve atopic dermatitis in patients with moderate to severe disease and may even benefit quality of life, suggest results from a phase 1b trial.
The research was presented at the annual congress of the European Academy of Dermatology and Venereology.
, after which responders were observed out to 48 weeks. The higher dosage was associated with significant improvements in Eczema Area and Severity Index (EASI) and Body Surface Area (BSA) scores, which were maintained over the course of the study, as well as trends for improved patient-reported outcomes.
“This is the first study to demonstrate the therapeutic potential of rezpegaldesleukin,” said presenter Jonathan Silverberg, MD, PhD, MPH, professor of dermatology and director of clinical research at George Washington University, Washington. He added, “These may be some of the most compelling data to date for the field, proving that, at a high level, if you causally increase regulator T cells, you will take down inflammation and improve a disease state.
“For me, this is proof of concept for so many things, and it gets me very excited.”
Dr. Silverberg noted that with the response maintained out to 48 weeks, despite stopping therapy at week 12, the “hope” with the approach of inducing regulator T cells “is that we could induce tolerance and that we could have some potential for disease modification.”
He continued, “Maybe I daren’t use the word ‘cure,’ but can we at least get to something that is truly remitted, where they can stop the drug and maintain that response?”
Dr. Silverberg said rezpegaldesleukin is now being evaluated in a phase 2b study for moderate to severe atopic dermatitis, and a phase 2b trial for alopecia areata is in development.
Tiago dos Reis Matos, MD, PhD, MSc, Amsterdam University Medical Centers, who was not involved in the study, told this news organization that “recombinant human interleukin-2 is an original therapy.”
Instead of blocking or inhibiting inflammation, it stimulates the patient’s immune system to “restore a healthy balance.”
He explained that it “stimulates regulatory T cells, which can be seen as the Peace Corps of the immune system, responsible for maintaining the equilibrium and avoiding uncontrolled inflammation.”
At the meeting, Dr. Silverberg told the audience that although they are the “beneficiaries of riches of new advances” in atopic dermatitis, “still, many observational studies have shown that the majority of patients do not achieve adequate control by the end of their induction periods and clinical trials, in the real world,” with currently available treatments.
Moreover, “there are challenges that come up with any of the different therapies,” he said, with adverse effects an important issue. For example, biologic therapies are associated with conjunctivitis, facial erythema, and arthralgia, and there are boxed warnings for Janus kinase inhibitors.
Dr. Silverberg continued, “Even patients with a favorable response can experience a loss of disease control when they come off therapy.” Consequently, “new strategies are certainly welcome that could potentially induce both deep and potentially therapy-free remission.”
To those ends, he explained that regulatory T cells play a central role in immune homeostasis but have not been “therapeutically relevant until very recently,” when it was posited that increasing their function can “induce that homeostasis, to normalize the inflammatory cascades” seen in a range of conditions, including atopic dermatitis.
Rezpegaldesleukin has high selectivity for regulatory T cells, without causing activation of effector T cells, and has been shown to increase cell numbers in a dose-dependent manner that is sustained for up to 30 days.
The current study involved patients aged 18-70 years with moderate to severe atopic dermatitis and a history of inadequate responses or intolerance to topical medications, and an EASI score ≥ 16.
Participants were randomly assigned to receive subcutaneous rezpegaldesleukin 12 mcg/kg or 24 mcg/kg or placebo every 2 weeks for 12 weeks. They then discontinued treatment and were followed up until week 19, when responders, defined as having a reduction in EASI score ≥ 50%, continued follow-up out to week 48.
Seventeen patients were randomized to higher-dose rezpegaldesleukin, whereas 16 received the lower dose and 10 were assigned to placebo. Dr. Silverberg said that the three groups were “fairly well balanced,” with “fairly good representation” across age, race, and ethnicity groups.
The mean baseline EASI score was between 21.9 and 23.7, and the Validated Investigator Global Assessment for Atopic Dermatitis (vIGA-AD) suggested that there was an even split between moderate and severe atopic dermatitis, although the higher-dose rezpegaldesleukin group had more patients with moderate disease.
By week 12, rezpegaldesleukin was associated with significantly greater improvements in EASI scores vs. placebo. Patients on the higher dose had a mean 83% improvement over baseline vs. 65% with the lower dose and 47% with placebo (P = .002 for the higher dose vs. placebo).
Crucially, these differences were maintained up to week 48 in patients, particularly in the higher-dose group.
There was also a nonsignificant increase in the proportion of patients who achieved a reduction in EASI scores ≥ 75% over baseline with the active drug: 41% at week 12 with higher-dose rezpegaldesleukin, 25% with the lower dose, and 20% with placebo. Again, the benefit was maintained up to week 48.
The mean improvement in BSA score from baseline with rezpegaldesleukin was significantly greater than that seen with placebo, at 72% with the higher dose, 55% with the lower dose, and 36% with placebo (P = .0158 for the higher dose vs. placebo).
Although improvements in vIGA-AD scores over baseline with rezpegaldesleukin were not substantial at week 12, by week 48 there was a marked difference between higher-dose rezpegaldesleukin and placebo, with 40.0% of patients responding to the drug vs. 0% in the latter group.
A similar pattern was seen for the Itch Numeric Rating Scale, in which 55.6% of patients treated with higher-dose rezpegaldesleukin responding by week 48, compared with 0% of those who received placebo.
Greater improvements in the Dermatology Life Quality Index (DLQI) and Patient Oriented Eczema Measure (POEM) over baseline with higher-dose rezpegaldesleukin vs. plain placebo were also noted, despite a strong response in the latter group.
Dr. Silverberg reported that all treatment-emergent adverse effects in the two rezpegaldesleukin treatment arms were mild to moderate, with no severe or serious events observed.
The most common adverse events were mild to moderate injection-site reactions, seen in 75.0% of the lower-dose rezpegaldesleukin group and 58.8% the of higher-dose group. There were no cases of conjunctivitis.
The study was sponsored by Eli Lilly and Company in collaboration with Nektar Therapeutics.
Dr. Silverberg declares relationships with AbbVie, Alamar, Aldena, Amgen, AOBiome, Arcutis, Arena, Asana, ASLAN, BioMX, Biosion, Bodewell, Boehringer-Ingelheim, Bristol-Myers Squibb, Cara, Castle Biosciences, Celgene, Connect Biopharma, CorEvitas, Dermavant, DermTech, Eli Lilly, Galderma, GlaxoSmithKline, Incyte, Kiniksa, LEO Pharma, Nektar, Novartis, Optum, Pfizer, RAPT, Recludix, Regeneron, Sanofi-Genzyme, Shaperon, Target RWE, Union, and UpToDate.
A version of this article appeared on Medscape.com.
AT THE EADV CONGRESS
Study reveals potentially unnecessary CRC screening in older adults
TOPLINE:
Older adults with limited life expectancy are just as likely to undergo colorectal cancer (CRC) screening as those with longer life expectancy, a new study shows.
METHODOLOGY:
- Researchers used national survey data to estimate the prevalence and factors associated with CRC screening in 25,888 community-dwelling adults aged 65-84 according to their predicted 10-year mortality risk.
- They estimated 10-year mortality risk using a validated index. From the lowest to highest quintiles, mortality risk was 12%, 24%, 39%, 58%, and 79%, respectively.
- Investigators determined the proportion of screening performed in adults with life expectancy less than 10 years, defined as 10-year mortality risk ≥ 50% (that is, quintiles 4 and 5).
TAKEAWAY:
- In this cohort of older adults previously not up to date with CRC screening, the overall prevalence of past-year screening was 38.5%.
- The prevalence of past-year CRC screening decreased with advancing age but did not differ significantly by 10-year mortality risk. From lowest to highest quintile, prevalence was 39.5%, 40.6%, 38.7%, 36.4%, and 35.4%, respectively.
- The likelihood of CRC screening did not differ between adults in the lowest vs. highest quintile of 10-year mortality risk (adjusted odds ratio, 1.05).
- More than one-quarter (27.9%) of past-year screening occurred in adults with life expectancy less than 10 years, and 50.7% of adults aged 75-84 years had life expectancy less than 10 years at the time of screening.
- Paradoxically, the prevalence of invasive screening increased with lowered life expectancy among adults aged 70-79 years.
IN PRACTICE:
“Our results suggest that health status and life expectancy may be overlooked in current CRC screening programs, and personalized screening incorporating individual life expectancy may improve the value of screening,” the authors write.
SOURCE:
The study, with first author Po-Hong Liu, MD, MPH, division of digestive and liver diseases, University of Texas Southwestern Medical Center, Dallas, was published online in the American Journal of Gastroenterology.
LIMITATIONS:
The survey data were self-reported and were not validated by medical records. The data did not include information to identify individuals who were at higher risk for CRC or to trace prior CRC screening history. It was not possible to reliably classify test indication (screening vs. surveillance vs. diagnostic).
DISCLOSURES:
The study was supported by the National Institutes of Health. One author disclosed serving as a consultant or on advisory boards for Exact Sciences, Universal Dx, Roche, and Freenome. Another disclosed consulting for Freenome.
A version of this article first appeared on Medscape.com.
TOPLINE:
Older adults with limited life expectancy are just as likely to undergo colorectal cancer (CRC) screening as those with longer life expectancy, a new study shows.
METHODOLOGY:
- Researchers used national survey data to estimate the prevalence and factors associated with CRC screening in 25,888 community-dwelling adults aged 65-84 according to their predicted 10-year mortality risk.
- They estimated 10-year mortality risk using a validated index. From the lowest to highest quintiles, mortality risk was 12%, 24%, 39%, 58%, and 79%, respectively.
- Investigators determined the proportion of screening performed in adults with life expectancy less than 10 years, defined as 10-year mortality risk ≥ 50% (that is, quintiles 4 and 5).
TAKEAWAY:
- In this cohort of older adults previously not up to date with CRC screening, the overall prevalence of past-year screening was 38.5%.
- The prevalence of past-year CRC screening decreased with advancing age but did not differ significantly by 10-year mortality risk. From lowest to highest quintile, prevalence was 39.5%, 40.6%, 38.7%, 36.4%, and 35.4%, respectively.
- The likelihood of CRC screening did not differ between adults in the lowest vs. highest quintile of 10-year mortality risk (adjusted odds ratio, 1.05).
- More than one-quarter (27.9%) of past-year screening occurred in adults with life expectancy less than 10 years, and 50.7% of adults aged 75-84 years had life expectancy less than 10 years at the time of screening.
- Paradoxically, the prevalence of invasive screening increased with lowered life expectancy among adults aged 70-79 years.
IN PRACTICE:
“Our results suggest that health status and life expectancy may be overlooked in current CRC screening programs, and personalized screening incorporating individual life expectancy may improve the value of screening,” the authors write.
SOURCE:
The study, with first author Po-Hong Liu, MD, MPH, division of digestive and liver diseases, University of Texas Southwestern Medical Center, Dallas, was published online in the American Journal of Gastroenterology.
LIMITATIONS:
The survey data were self-reported and were not validated by medical records. The data did not include information to identify individuals who were at higher risk for CRC or to trace prior CRC screening history. It was not possible to reliably classify test indication (screening vs. surveillance vs. diagnostic).
DISCLOSURES:
The study was supported by the National Institutes of Health. One author disclosed serving as a consultant or on advisory boards for Exact Sciences, Universal Dx, Roche, and Freenome. Another disclosed consulting for Freenome.
A version of this article first appeared on Medscape.com.
TOPLINE:
Older adults with limited life expectancy are just as likely to undergo colorectal cancer (CRC) screening as those with longer life expectancy, a new study shows.
METHODOLOGY:
- Researchers used national survey data to estimate the prevalence and factors associated with CRC screening in 25,888 community-dwelling adults aged 65-84 according to their predicted 10-year mortality risk.
- They estimated 10-year mortality risk using a validated index. From the lowest to highest quintiles, mortality risk was 12%, 24%, 39%, 58%, and 79%, respectively.
- Investigators determined the proportion of screening performed in adults with life expectancy less than 10 years, defined as 10-year mortality risk ≥ 50% (that is, quintiles 4 and 5).
TAKEAWAY:
- In this cohort of older adults previously not up to date with CRC screening, the overall prevalence of past-year screening was 38.5%.
- The prevalence of past-year CRC screening decreased with advancing age but did not differ significantly by 10-year mortality risk. From lowest to highest quintile, prevalence was 39.5%, 40.6%, 38.7%, 36.4%, and 35.4%, respectively.
- The likelihood of CRC screening did not differ between adults in the lowest vs. highest quintile of 10-year mortality risk (adjusted odds ratio, 1.05).
- More than one-quarter (27.9%) of past-year screening occurred in adults with life expectancy less than 10 years, and 50.7% of adults aged 75-84 years had life expectancy less than 10 years at the time of screening.
- Paradoxically, the prevalence of invasive screening increased with lowered life expectancy among adults aged 70-79 years.
IN PRACTICE:
“Our results suggest that health status and life expectancy may be overlooked in current CRC screening programs, and personalized screening incorporating individual life expectancy may improve the value of screening,” the authors write.
SOURCE:
The study, with first author Po-Hong Liu, MD, MPH, division of digestive and liver diseases, University of Texas Southwestern Medical Center, Dallas, was published online in the American Journal of Gastroenterology.
LIMITATIONS:
The survey data were self-reported and were not validated by medical records. The data did not include information to identify individuals who were at higher risk for CRC or to trace prior CRC screening history. It was not possible to reliably classify test indication (screening vs. surveillance vs. diagnostic).
DISCLOSURES:
The study was supported by the National Institutes of Health. One author disclosed serving as a consultant or on advisory boards for Exact Sciences, Universal Dx, Roche, and Freenome. Another disclosed consulting for Freenome.
A version of this article first appeared on Medscape.com.
Here’s how to help Black smokers quit
Black Americans attempt to quit smoking more often than their White counterparts but are less likely to succeed, and they pay the health consequences.
This knowledge has driven Kevin Choi, MD, acting scientific director of the National Institute on Minority Health and Health Disparities in Bethesda, Md., to dedicate his career to studying the patterns and disparities of smoking among these patients.
Dr. Choi wants primary care clinicians to know not just that they have the potential to educate patients on the harms of smoking – most patients already know smoking is unhealthy – but that aiding them will likely necessitate more assertive follow-up.
To do so, “we need to understand the bigger backdrop of racial and sociological stress experienced by the Black population, which stems from both interpersonal and structural racism,” Dr. Choi said.
Not only are Black smokers more likely to try to quit, but they also tend to smoke fewer cigarettes per day than other racial groups. Yet they experience higher rates of smoking-related mortality.
The reasons behind the attempts
Multiple factors play into Black smokers’ lower rates of successful quitting attempts than Asian, Hispanic, White, and Native American individuals.
One reason: An estimated 85% of Black smokers smoke highly addictive menthol cigarettes. According to Dr. Choi and other experts, the tobacco industry engages in targeted marketing of menthols by sponsoring community events in predominantly Black neighborhoods and colleges with historically Black populations and by using Black culture in advertising.
“The built environment really drives a change in behavior, and we have seen that chronically in the African American population being overly targeted and now being overly addicted to nicotine,” said Daniel Kortsch, MD, a family medicine physician and chair of the Tobacco Cessation Workgroup at Denver Health.
Menthol cigarettes are more addictive than traditional cigarettes, in part because they provide a less harsh feeling in the respiratory system, owing to anti-tussive, anti-irritant, and cooling properties that act as a cough suppressant and mask irritation and pain.
“You do not feel like you’re smoking that much or that it’s dangerous, and that’s exactly the reason why it’s harder to quit,” said Julia Adamian, MD, section chief of general internal medicine and clinical innovation at NYU Langone Tisch Hospital.
In addition, menthol cigarettes interact with the body in complex ways that make quitting harder, according to a study published in Nicotine & Tobacco Research. Menthol increases the amount of nicotine that the body absorbs and thus increases the risk of dependence on the drug.
According to Dr. Choi, rates of cigar and cigarillo use are higher among Black Americans, compared with other races, and these products are often left out of cessation programs. Smokers, regardless of race, may have a misguided belief that cigars and cigarillos are less harmful than cigarettes.
Research published in 2021 found that Black cigar smokers who were interested in cessation had not been asked by their health care provider if they smoked cigars, and those who were asked reported a lack of support for cessation.
Primary care providers should work to remove any misconceptions a patient has regarding the safety of cigarillos and cigars, Dr. Choi said.
These smokers are also at a disadvantage regarding cessation success because of the neighborhoods they may live in, according to Dr. Choi. Black Americans are more likely to earn less and to live in neighborhoods with lower housing values than other racial groups. Areas with more low-income households tend to have a higher density of tobacco outlets.
“If you’re trying to quit smoking, but you walk by three, four, or five gas stations, convenience stores, and other tobacco outlets with signs that advertise sales, it’s not going to make quitting easy,” Dr. Choi said.
Tailoring treatment to Black smokers
Considering the unique challenges Black patients may face in quitting, clinicians should provide more follow-up and consistent support, according to Dr. Adamian. The higher risk of tobacco-related death among Black smokers means clinicians need to be more aggressive in recommending every treatment possible if one treatment fails.
Pharmacotherapy, nicotine replacement therapy, and counseling are evidence-based options to help patients stop smoking.
Dr. Kortsch considers pharmacotherapy to be the most effective and evidence-based treatment for nicotine addiction. However, Black Americans are less likely than White smokers to try smoking cessation medications, and they express more suspicion about efficacy and potential addiction to the tools.
“African American populations simply do not use pharmacotherapy to the extent that other populations do to help them quit smoking; this is a problem,” Dr. Kortsch said.
Dr. Kortsch recommends the use of varenicline for all patients with nicotine addiction. He recommends varenicline in combination with tobacco replacement products such as lozenges, patches, gums, or inhalers if the patient is a heavy smoker as opposed to someone who has a few cigarettes on the weekends.
If a patient has anxiety or depression, Dr. Adamian advises initiating a pharmacologic treatment such as bupropion or varenicline more quickly, because mood disorders can hinder cessation.
Cessation counseling is another option, but clinicians may need to more thoroughly explain what it entails. According to Dr. Choi, Black patients may be more reluctant to try cessation counseling because of the negative stigma associated with the term “counseling.” But this treatment is not therapy – it involves identifying and coming up with strategies to manage smoking triggers and providing encouragement. Clinicians can eliminate any confusion patients may have between psychological therapy and cessation counseling.
“ ‘Counseling’ tends to have a somewhat negative connotation among racial minority populations, like you go to counseling because you’re crazy,” Dr. Choi said. “That needs to change.”
Clinicians also must clarify how each cessation tool works. For example, some patients may not realize that the nicotine patch isn’t an instant fix for a craving and that hours may pass before the user feels its effects, according to Dr. Choi.
Move past the ‘advise’ stage
While recommending to patients various forms of cessation, clinicians should be mindful of the U.S. Preventive Services Task Force’s guidelines for providers who treat patients who smoke. Those guidelines include a five-step process: Ask, Advise, Assess, Assist, and Arrange.
Dr. Choi said most providers stop at the “Advise” stage. In steps one and two, providers ask patients whether they smoke, then advise them to quit. Stage three involves asking whether or not a patient is ready to quit and where they are in their journey.
Clinicians shouldn’t give up when patients say they do not currently plan to quit. Instead, they can use the conversation to create an ongoing dialogue about the patient’s readiness to quit in future visits. Follow-up phone calls or text messages should be made 2-4 weeks after a patient makes an attempt to quit and at the same interval thereafter, Dr. Adamian advised.
“It takes a concerted effort on behalf of all people to be successful, and it is really uncommon for someone to be successful with only one attempt,” Dr. Kortsch said.
In a recent study published in the Journal of the American Medical Association, researchers identified three key factors that influence a Black smoker’s ability to stop smoking in early attempts. These factors have been shown to increase the chances of long-term cessation: fewer cigarettes per day, nonuse of other tobacco products, and lower levels of cotinine (a nicotine metabolite) at baseline.
“Using these predictors of early treatment response could allow providers to anticipate which smokers may benefit from a minimal, low-cost intervention and who may benefit from more intensive treatment,” said Eleanor Leavens, PhD, assistant professor in the department of population health at the University of Kansas School of Medicine, Kansas City, who led the study.
Dr. Leavens’ research also confirmed that early abstinence predicts long-term cessation success. Smokers who were able to forgo cigarettes within 2 weeks of their quit date were almost four times more likely to remain abstinent over the long term.
A quick phone call or message from the clinician or a staff member can help patients achieve early progress, enable changes in approach to quitting, and build a relationship with the patient, Dr. Adamian said.
“Have more empathy for what Black patients are going through,” Dr. Choi said. “Continue to cheer them on and to be a supporter of their smoking cessation journey.”
A version of this article first appeared on Medscape.com.
Black Americans attempt to quit smoking more often than their White counterparts but are less likely to succeed, and they pay the health consequences.
This knowledge has driven Kevin Choi, MD, acting scientific director of the National Institute on Minority Health and Health Disparities in Bethesda, Md., to dedicate his career to studying the patterns and disparities of smoking among these patients.
Dr. Choi wants primary care clinicians to know not just that they have the potential to educate patients on the harms of smoking – most patients already know smoking is unhealthy – but that aiding them will likely necessitate more assertive follow-up.
To do so, “we need to understand the bigger backdrop of racial and sociological stress experienced by the Black population, which stems from both interpersonal and structural racism,” Dr. Choi said.
Not only are Black smokers more likely to try to quit, but they also tend to smoke fewer cigarettes per day than other racial groups. Yet they experience higher rates of smoking-related mortality.
The reasons behind the attempts
Multiple factors play into Black smokers’ lower rates of successful quitting attempts than Asian, Hispanic, White, and Native American individuals.
One reason: An estimated 85% of Black smokers smoke highly addictive menthol cigarettes. According to Dr. Choi and other experts, the tobacco industry engages in targeted marketing of menthols by sponsoring community events in predominantly Black neighborhoods and colleges with historically Black populations and by using Black culture in advertising.
“The built environment really drives a change in behavior, and we have seen that chronically in the African American population being overly targeted and now being overly addicted to nicotine,” said Daniel Kortsch, MD, a family medicine physician and chair of the Tobacco Cessation Workgroup at Denver Health.
Menthol cigarettes are more addictive than traditional cigarettes, in part because they provide a less harsh feeling in the respiratory system, owing to anti-tussive, anti-irritant, and cooling properties that act as a cough suppressant and mask irritation and pain.
“You do not feel like you’re smoking that much or that it’s dangerous, and that’s exactly the reason why it’s harder to quit,” said Julia Adamian, MD, section chief of general internal medicine and clinical innovation at NYU Langone Tisch Hospital.
In addition, menthol cigarettes interact with the body in complex ways that make quitting harder, according to a study published in Nicotine & Tobacco Research. Menthol increases the amount of nicotine that the body absorbs and thus increases the risk of dependence on the drug.
According to Dr. Choi, rates of cigar and cigarillo use are higher among Black Americans, compared with other races, and these products are often left out of cessation programs. Smokers, regardless of race, may have a misguided belief that cigars and cigarillos are less harmful than cigarettes.
Research published in 2021 found that Black cigar smokers who were interested in cessation had not been asked by their health care provider if they smoked cigars, and those who were asked reported a lack of support for cessation.
Primary care providers should work to remove any misconceptions a patient has regarding the safety of cigarillos and cigars, Dr. Choi said.
These smokers are also at a disadvantage regarding cessation success because of the neighborhoods they may live in, according to Dr. Choi. Black Americans are more likely to earn less and to live in neighborhoods with lower housing values than other racial groups. Areas with more low-income households tend to have a higher density of tobacco outlets.
“If you’re trying to quit smoking, but you walk by three, four, or five gas stations, convenience stores, and other tobacco outlets with signs that advertise sales, it’s not going to make quitting easy,” Dr. Choi said.
Tailoring treatment to Black smokers
Considering the unique challenges Black patients may face in quitting, clinicians should provide more follow-up and consistent support, according to Dr. Adamian. The higher risk of tobacco-related death among Black smokers means clinicians need to be more aggressive in recommending every treatment possible if one treatment fails.
Pharmacotherapy, nicotine replacement therapy, and counseling are evidence-based options to help patients stop smoking.
Dr. Kortsch considers pharmacotherapy to be the most effective and evidence-based treatment for nicotine addiction. However, Black Americans are less likely than White smokers to try smoking cessation medications, and they express more suspicion about efficacy and potential addiction to the tools.
“African American populations simply do not use pharmacotherapy to the extent that other populations do to help them quit smoking; this is a problem,” Dr. Kortsch said.
Dr. Kortsch recommends the use of varenicline for all patients with nicotine addiction. He recommends varenicline in combination with tobacco replacement products such as lozenges, patches, gums, or inhalers if the patient is a heavy smoker as opposed to someone who has a few cigarettes on the weekends.
If a patient has anxiety or depression, Dr. Adamian advises initiating a pharmacologic treatment such as bupropion or varenicline more quickly, because mood disorders can hinder cessation.
Cessation counseling is another option, but clinicians may need to more thoroughly explain what it entails. According to Dr. Choi, Black patients may be more reluctant to try cessation counseling because of the negative stigma associated with the term “counseling.” But this treatment is not therapy – it involves identifying and coming up with strategies to manage smoking triggers and providing encouragement. Clinicians can eliminate any confusion patients may have between psychological therapy and cessation counseling.
“ ‘Counseling’ tends to have a somewhat negative connotation among racial minority populations, like you go to counseling because you’re crazy,” Dr. Choi said. “That needs to change.”
Clinicians also must clarify how each cessation tool works. For example, some patients may not realize that the nicotine patch isn’t an instant fix for a craving and that hours may pass before the user feels its effects, according to Dr. Choi.
Move past the ‘advise’ stage
While recommending to patients various forms of cessation, clinicians should be mindful of the U.S. Preventive Services Task Force’s guidelines for providers who treat patients who smoke. Those guidelines include a five-step process: Ask, Advise, Assess, Assist, and Arrange.
Dr. Choi said most providers stop at the “Advise” stage. In steps one and two, providers ask patients whether they smoke, then advise them to quit. Stage three involves asking whether or not a patient is ready to quit and where they are in their journey.
Clinicians shouldn’t give up when patients say they do not currently plan to quit. Instead, they can use the conversation to create an ongoing dialogue about the patient’s readiness to quit in future visits. Follow-up phone calls or text messages should be made 2-4 weeks after a patient makes an attempt to quit and at the same interval thereafter, Dr. Adamian advised.
“It takes a concerted effort on behalf of all people to be successful, and it is really uncommon for someone to be successful with only one attempt,” Dr. Kortsch said.
In a recent study published in the Journal of the American Medical Association, researchers identified three key factors that influence a Black smoker’s ability to stop smoking in early attempts. These factors have been shown to increase the chances of long-term cessation: fewer cigarettes per day, nonuse of other tobacco products, and lower levels of cotinine (a nicotine metabolite) at baseline.
“Using these predictors of early treatment response could allow providers to anticipate which smokers may benefit from a minimal, low-cost intervention and who may benefit from more intensive treatment,” said Eleanor Leavens, PhD, assistant professor in the department of population health at the University of Kansas School of Medicine, Kansas City, who led the study.
Dr. Leavens’ research also confirmed that early abstinence predicts long-term cessation success. Smokers who were able to forgo cigarettes within 2 weeks of their quit date were almost four times more likely to remain abstinent over the long term.
A quick phone call or message from the clinician or a staff member can help patients achieve early progress, enable changes in approach to quitting, and build a relationship with the patient, Dr. Adamian said.
“Have more empathy for what Black patients are going through,” Dr. Choi said. “Continue to cheer them on and to be a supporter of their smoking cessation journey.”
A version of this article first appeared on Medscape.com.
Black Americans attempt to quit smoking more often than their White counterparts but are less likely to succeed, and they pay the health consequences.
This knowledge has driven Kevin Choi, MD, acting scientific director of the National Institute on Minority Health and Health Disparities in Bethesda, Md., to dedicate his career to studying the patterns and disparities of smoking among these patients.
Dr. Choi wants primary care clinicians to know not just that they have the potential to educate patients on the harms of smoking – most patients already know smoking is unhealthy – but that aiding them will likely necessitate more assertive follow-up.
To do so, “we need to understand the bigger backdrop of racial and sociological stress experienced by the Black population, which stems from both interpersonal and structural racism,” Dr. Choi said.
Not only are Black smokers more likely to try to quit, but they also tend to smoke fewer cigarettes per day than other racial groups. Yet they experience higher rates of smoking-related mortality.
The reasons behind the attempts
Multiple factors play into Black smokers’ lower rates of successful quitting attempts than Asian, Hispanic, White, and Native American individuals.
One reason: An estimated 85% of Black smokers smoke highly addictive menthol cigarettes. According to Dr. Choi and other experts, the tobacco industry engages in targeted marketing of menthols by sponsoring community events in predominantly Black neighborhoods and colleges with historically Black populations and by using Black culture in advertising.
“The built environment really drives a change in behavior, and we have seen that chronically in the African American population being overly targeted and now being overly addicted to nicotine,” said Daniel Kortsch, MD, a family medicine physician and chair of the Tobacco Cessation Workgroup at Denver Health.
Menthol cigarettes are more addictive than traditional cigarettes, in part because they provide a less harsh feeling in the respiratory system, owing to anti-tussive, anti-irritant, and cooling properties that act as a cough suppressant and mask irritation and pain.
“You do not feel like you’re smoking that much or that it’s dangerous, and that’s exactly the reason why it’s harder to quit,” said Julia Adamian, MD, section chief of general internal medicine and clinical innovation at NYU Langone Tisch Hospital.
In addition, menthol cigarettes interact with the body in complex ways that make quitting harder, according to a study published in Nicotine & Tobacco Research. Menthol increases the amount of nicotine that the body absorbs and thus increases the risk of dependence on the drug.
According to Dr. Choi, rates of cigar and cigarillo use are higher among Black Americans, compared with other races, and these products are often left out of cessation programs. Smokers, regardless of race, may have a misguided belief that cigars and cigarillos are less harmful than cigarettes.
Research published in 2021 found that Black cigar smokers who were interested in cessation had not been asked by their health care provider if they smoked cigars, and those who were asked reported a lack of support for cessation.
Primary care providers should work to remove any misconceptions a patient has regarding the safety of cigarillos and cigars, Dr. Choi said.
These smokers are also at a disadvantage regarding cessation success because of the neighborhoods they may live in, according to Dr. Choi. Black Americans are more likely to earn less and to live in neighborhoods with lower housing values than other racial groups. Areas with more low-income households tend to have a higher density of tobacco outlets.
“If you’re trying to quit smoking, but you walk by three, four, or five gas stations, convenience stores, and other tobacco outlets with signs that advertise sales, it’s not going to make quitting easy,” Dr. Choi said.
Tailoring treatment to Black smokers
Considering the unique challenges Black patients may face in quitting, clinicians should provide more follow-up and consistent support, according to Dr. Adamian. The higher risk of tobacco-related death among Black smokers means clinicians need to be more aggressive in recommending every treatment possible if one treatment fails.
Pharmacotherapy, nicotine replacement therapy, and counseling are evidence-based options to help patients stop smoking.
Dr. Kortsch considers pharmacotherapy to be the most effective and evidence-based treatment for nicotine addiction. However, Black Americans are less likely than White smokers to try smoking cessation medications, and they express more suspicion about efficacy and potential addiction to the tools.
“African American populations simply do not use pharmacotherapy to the extent that other populations do to help them quit smoking; this is a problem,” Dr. Kortsch said.
Dr. Kortsch recommends the use of varenicline for all patients with nicotine addiction. He recommends varenicline in combination with tobacco replacement products such as lozenges, patches, gums, or inhalers if the patient is a heavy smoker as opposed to someone who has a few cigarettes on the weekends.
If a patient has anxiety or depression, Dr. Adamian advises initiating a pharmacologic treatment such as bupropion or varenicline more quickly, because mood disorders can hinder cessation.
Cessation counseling is another option, but clinicians may need to more thoroughly explain what it entails. According to Dr. Choi, Black patients may be more reluctant to try cessation counseling because of the negative stigma associated with the term “counseling.” But this treatment is not therapy – it involves identifying and coming up with strategies to manage smoking triggers and providing encouragement. Clinicians can eliminate any confusion patients may have between psychological therapy and cessation counseling.
“ ‘Counseling’ tends to have a somewhat negative connotation among racial minority populations, like you go to counseling because you’re crazy,” Dr. Choi said. “That needs to change.”
Clinicians also must clarify how each cessation tool works. For example, some patients may not realize that the nicotine patch isn’t an instant fix for a craving and that hours may pass before the user feels its effects, according to Dr. Choi.
Move past the ‘advise’ stage
While recommending to patients various forms of cessation, clinicians should be mindful of the U.S. Preventive Services Task Force’s guidelines for providers who treat patients who smoke. Those guidelines include a five-step process: Ask, Advise, Assess, Assist, and Arrange.
Dr. Choi said most providers stop at the “Advise” stage. In steps one and two, providers ask patients whether they smoke, then advise them to quit. Stage three involves asking whether or not a patient is ready to quit and where they are in their journey.
Clinicians shouldn’t give up when patients say they do not currently plan to quit. Instead, they can use the conversation to create an ongoing dialogue about the patient’s readiness to quit in future visits. Follow-up phone calls or text messages should be made 2-4 weeks after a patient makes an attempt to quit and at the same interval thereafter, Dr. Adamian advised.
“It takes a concerted effort on behalf of all people to be successful, and it is really uncommon for someone to be successful with only one attempt,” Dr. Kortsch said.
In a recent study published in the Journal of the American Medical Association, researchers identified three key factors that influence a Black smoker’s ability to stop smoking in early attempts. These factors have been shown to increase the chances of long-term cessation: fewer cigarettes per day, nonuse of other tobacco products, and lower levels of cotinine (a nicotine metabolite) at baseline.
“Using these predictors of early treatment response could allow providers to anticipate which smokers may benefit from a minimal, low-cost intervention and who may benefit from more intensive treatment,” said Eleanor Leavens, PhD, assistant professor in the department of population health at the University of Kansas School of Medicine, Kansas City, who led the study.
Dr. Leavens’ research also confirmed that early abstinence predicts long-term cessation success. Smokers who were able to forgo cigarettes within 2 weeks of their quit date were almost four times more likely to remain abstinent over the long term.
A quick phone call or message from the clinician or a staff member can help patients achieve early progress, enable changes in approach to quitting, and build a relationship with the patient, Dr. Adamian said.
“Have more empathy for what Black patients are going through,” Dr. Choi said. “Continue to cheer them on and to be a supporter of their smoking cessation journey.”
A version of this article first appeared on Medscape.com.
Fathers’ postpartum depression linked to children’s adversity
WASHINGTON – , according to research presented at the annual meeting of the American Academy of Pediatrics.
The findings held even after taking into account postpartum depression in the child’s mother and other factors that might increase risk of adverse childhood experiences, reported Kristine H. Schmitz, MD, an assistant professor of pediatrics at Robert Wood Johnson Medical School, New Brunswick, N.J.
Paternal postpartum depression has not been studied very well, so it’s difficult to pin down its prevalence, but some research has found rates as high as 25%, Dr. Schmitz told attendees.
”We recognize that it’s very under-recognized and often under-reported, but we also know that it has lots of downstream effects on child outcomes, including difficulties with parenting, difficulties with child behavior, as well as school performance and school attainment and employment,” Dr. Schmitz said.
Paternal depression and adverse childhood experiences
The study involved an analysis of six waves of data from the Future of Families & Child Wellbeing Study, which follows a national cohort of children born in large U.S. cities between 1998 and 2000. The cohort includes an intentional over-representation of unmarried mothers, who make up about 75% of the overall population.
The researchers used the World Health Organization’s Composite International Diagnosis Interview Short Form (CIDI-SF) to assess fathers’ depression when their children were 1 year old. Then the researchers looked at the number of adverse childhood experiences (ACEs) children had at 5 years old.
The analysis was adjusted to account for the child’s sex and the father’s age, race/ethnicity, and education as well as whether he was born inside or outside the United States. The findings were also adjusted for the whether the child’s parents were married or cohabiting, whether the child had low birth weight, whether the birth was covered by Medicaid, and whether the mother had postpartum depression.
Among the 1,933 pairs of fathers and children in the analysis, nearly half the fathers were non-Hispanic Black (48%) and more than half (64%) had a high school education or lower level of education. Medicaid paid for half the children’s births.
Nine percent of the fathers experienced depression during their child’s first year, and 70% of the children had at least one ACE at 5 years old. Two in five children (39%) had two ACEs at age 5, and 21% of children had three ACEs.
Children were twice as likely to have three ACEs at 5 years old if their father had depression during the child’s first year (adjusted odds ratio, 2.04; 95% confidence interval, 1.42-2.93). Paternal depression was also significantly associated with children having one ACE (OR, 2.35; 95% CI, 1.45-3.81) and two ACES (OR, 1.89; 95% CI, 1.35-2.63) at age 5.
The ACE with the highest association with paternal depression was the father’s absence from children’s lives (aOR, 2.65; 95% CI, 1.74-4.04). In addition, children of fathers with depression had 60% greater odds of exposure to substance use (aOR, 1.6; 95% CI, 1.08-2.34).
Children also had greater odds of child maltreatment at age 5 if their father had depression in their child’s first year. Odds were greater for psychological maltreatment (aOR, 1.55; 95% CI, 1.02-2.34), neglect (aOR, 1.63; 95% CI, 1.08-2.46), and physical maltreatment (aOR, 1.56; 95% CI, 1.04-2.35). The researchers did not find any association between paternal depression and the ACEs of sexual maltreatment, maternal depression, incarceration of someone in the home, or violence toward the mother.
”We know that dads play a critical role in the family,” Dr. Schmitz said. “We as pediatricians have a really unique position with families, and we should capitalize on that opportunity to engage with fathers just like we do with mothers and postpartum depression. Hopefully by doing that, we’ll reduce hardships for children and families down the road.”
Dr. Schmitz also said it’s important for pediatricians to advocate at a policy level “to really include dads more explicitly in maternal and child health policy and advocate for better father-focused interventions from father-focused research.” She further acknowledged the stigma that exists around men’s mental health in general and the need to find out the best ways to help overcome that stigma.
‘Concerning’ findings may suggest a need for screening
Jason Terk, MD, a pediatrician practicing in north Texas and past president of the Texas Pediatric Society, was not surprised to see a link between depression in fathers and adversity in their children. Dr. Terk was not involved in the research but noted that the 9% rate of paternal depression seen in the study is similar to national rates of depression in U.S. adults.
“I think that the presence of paternal depression being associated with ACEs in their children in their first 5 years of life is certainly concerning and worthy of intervention for both the fathers and their children,” Dr. Terk said. “The key take-home message for clinicians who care for infants and small children is that the presence of paternal depression should increase awareness of adverse effects on those children. We need to consider screening for this at 12 months of age in much the same way we screen for maternal depression for younger infants.”
Dr. Terk noted one limitation of the study was that it didn’t suggest any specific risk factors pediatricians might look for to increase surveillance of potential depression in fathers.
“Also, unlike maternal depression, in which moms may be connected with their obstetricians if they screen positive on an Edinburgh questionnaire, we will be hard-pressed to know where to refer dads who are found to be depressed when their babies are 12 months old,” Dr. Terk said. “Screening must lead to helpful responses if the screening reveals a problem.”
The research was funded by the Robert Wood Johnson Foundation, the National Institutes of Health, and the Health Resources and Services Administration. Dr. Schmitz had no disclosures. Dr. Terk has been a speaker for Sanofi on a topic unrelated to this research.
WASHINGTON – , according to research presented at the annual meeting of the American Academy of Pediatrics.
The findings held even after taking into account postpartum depression in the child’s mother and other factors that might increase risk of adverse childhood experiences, reported Kristine H. Schmitz, MD, an assistant professor of pediatrics at Robert Wood Johnson Medical School, New Brunswick, N.J.
Paternal postpartum depression has not been studied very well, so it’s difficult to pin down its prevalence, but some research has found rates as high as 25%, Dr. Schmitz told attendees.
”We recognize that it’s very under-recognized and often under-reported, but we also know that it has lots of downstream effects on child outcomes, including difficulties with parenting, difficulties with child behavior, as well as school performance and school attainment and employment,” Dr. Schmitz said.
Paternal depression and adverse childhood experiences
The study involved an analysis of six waves of data from the Future of Families & Child Wellbeing Study, which follows a national cohort of children born in large U.S. cities between 1998 and 2000. The cohort includes an intentional over-representation of unmarried mothers, who make up about 75% of the overall population.
The researchers used the World Health Organization’s Composite International Diagnosis Interview Short Form (CIDI-SF) to assess fathers’ depression when their children were 1 year old. Then the researchers looked at the number of adverse childhood experiences (ACEs) children had at 5 years old.
The analysis was adjusted to account for the child’s sex and the father’s age, race/ethnicity, and education as well as whether he was born inside or outside the United States. The findings were also adjusted for the whether the child’s parents were married or cohabiting, whether the child had low birth weight, whether the birth was covered by Medicaid, and whether the mother had postpartum depression.
Among the 1,933 pairs of fathers and children in the analysis, nearly half the fathers were non-Hispanic Black (48%) and more than half (64%) had a high school education or lower level of education. Medicaid paid for half the children’s births.
Nine percent of the fathers experienced depression during their child’s first year, and 70% of the children had at least one ACE at 5 years old. Two in five children (39%) had two ACEs at age 5, and 21% of children had three ACEs.
Children were twice as likely to have three ACEs at 5 years old if their father had depression during the child’s first year (adjusted odds ratio, 2.04; 95% confidence interval, 1.42-2.93). Paternal depression was also significantly associated with children having one ACE (OR, 2.35; 95% CI, 1.45-3.81) and two ACES (OR, 1.89; 95% CI, 1.35-2.63) at age 5.
The ACE with the highest association with paternal depression was the father’s absence from children’s lives (aOR, 2.65; 95% CI, 1.74-4.04). In addition, children of fathers with depression had 60% greater odds of exposure to substance use (aOR, 1.6; 95% CI, 1.08-2.34).
Children also had greater odds of child maltreatment at age 5 if their father had depression in their child’s first year. Odds were greater for psychological maltreatment (aOR, 1.55; 95% CI, 1.02-2.34), neglect (aOR, 1.63; 95% CI, 1.08-2.46), and physical maltreatment (aOR, 1.56; 95% CI, 1.04-2.35). The researchers did not find any association between paternal depression and the ACEs of sexual maltreatment, maternal depression, incarceration of someone in the home, or violence toward the mother.
”We know that dads play a critical role in the family,” Dr. Schmitz said. “We as pediatricians have a really unique position with families, and we should capitalize on that opportunity to engage with fathers just like we do with mothers and postpartum depression. Hopefully by doing that, we’ll reduce hardships for children and families down the road.”
Dr. Schmitz also said it’s important for pediatricians to advocate at a policy level “to really include dads more explicitly in maternal and child health policy and advocate for better father-focused interventions from father-focused research.” She further acknowledged the stigma that exists around men’s mental health in general and the need to find out the best ways to help overcome that stigma.
‘Concerning’ findings may suggest a need for screening
Jason Terk, MD, a pediatrician practicing in north Texas and past president of the Texas Pediatric Society, was not surprised to see a link between depression in fathers and adversity in their children. Dr. Terk was not involved in the research but noted that the 9% rate of paternal depression seen in the study is similar to national rates of depression in U.S. adults.
“I think that the presence of paternal depression being associated with ACEs in their children in their first 5 years of life is certainly concerning and worthy of intervention for both the fathers and their children,” Dr. Terk said. “The key take-home message for clinicians who care for infants and small children is that the presence of paternal depression should increase awareness of adverse effects on those children. We need to consider screening for this at 12 months of age in much the same way we screen for maternal depression for younger infants.”
Dr. Terk noted one limitation of the study was that it didn’t suggest any specific risk factors pediatricians might look for to increase surveillance of potential depression in fathers.
“Also, unlike maternal depression, in which moms may be connected with their obstetricians if they screen positive on an Edinburgh questionnaire, we will be hard-pressed to know where to refer dads who are found to be depressed when their babies are 12 months old,” Dr. Terk said. “Screening must lead to helpful responses if the screening reveals a problem.”
The research was funded by the Robert Wood Johnson Foundation, the National Institutes of Health, and the Health Resources and Services Administration. Dr. Schmitz had no disclosures. Dr. Terk has been a speaker for Sanofi on a topic unrelated to this research.
WASHINGTON – , according to research presented at the annual meeting of the American Academy of Pediatrics.
The findings held even after taking into account postpartum depression in the child’s mother and other factors that might increase risk of adverse childhood experiences, reported Kristine H. Schmitz, MD, an assistant professor of pediatrics at Robert Wood Johnson Medical School, New Brunswick, N.J.
Paternal postpartum depression has not been studied very well, so it’s difficult to pin down its prevalence, but some research has found rates as high as 25%, Dr. Schmitz told attendees.
”We recognize that it’s very under-recognized and often under-reported, but we also know that it has lots of downstream effects on child outcomes, including difficulties with parenting, difficulties with child behavior, as well as school performance and school attainment and employment,” Dr. Schmitz said.
Paternal depression and adverse childhood experiences
The study involved an analysis of six waves of data from the Future of Families & Child Wellbeing Study, which follows a national cohort of children born in large U.S. cities between 1998 and 2000. The cohort includes an intentional over-representation of unmarried mothers, who make up about 75% of the overall population.
The researchers used the World Health Organization’s Composite International Diagnosis Interview Short Form (CIDI-SF) to assess fathers’ depression when their children were 1 year old. Then the researchers looked at the number of adverse childhood experiences (ACEs) children had at 5 years old.
The analysis was adjusted to account for the child’s sex and the father’s age, race/ethnicity, and education as well as whether he was born inside or outside the United States. The findings were also adjusted for the whether the child’s parents were married or cohabiting, whether the child had low birth weight, whether the birth was covered by Medicaid, and whether the mother had postpartum depression.
Among the 1,933 pairs of fathers and children in the analysis, nearly half the fathers were non-Hispanic Black (48%) and more than half (64%) had a high school education or lower level of education. Medicaid paid for half the children’s births.
Nine percent of the fathers experienced depression during their child’s first year, and 70% of the children had at least one ACE at 5 years old. Two in five children (39%) had two ACEs at age 5, and 21% of children had three ACEs.
Children were twice as likely to have three ACEs at 5 years old if their father had depression during the child’s first year (adjusted odds ratio, 2.04; 95% confidence interval, 1.42-2.93). Paternal depression was also significantly associated with children having one ACE (OR, 2.35; 95% CI, 1.45-3.81) and two ACES (OR, 1.89; 95% CI, 1.35-2.63) at age 5.
The ACE with the highest association with paternal depression was the father’s absence from children’s lives (aOR, 2.65; 95% CI, 1.74-4.04). In addition, children of fathers with depression had 60% greater odds of exposure to substance use (aOR, 1.6; 95% CI, 1.08-2.34).
Children also had greater odds of child maltreatment at age 5 if their father had depression in their child’s first year. Odds were greater for psychological maltreatment (aOR, 1.55; 95% CI, 1.02-2.34), neglect (aOR, 1.63; 95% CI, 1.08-2.46), and physical maltreatment (aOR, 1.56; 95% CI, 1.04-2.35). The researchers did not find any association between paternal depression and the ACEs of sexual maltreatment, maternal depression, incarceration of someone in the home, or violence toward the mother.
”We know that dads play a critical role in the family,” Dr. Schmitz said. “We as pediatricians have a really unique position with families, and we should capitalize on that opportunity to engage with fathers just like we do with mothers and postpartum depression. Hopefully by doing that, we’ll reduce hardships for children and families down the road.”
Dr. Schmitz also said it’s important for pediatricians to advocate at a policy level “to really include dads more explicitly in maternal and child health policy and advocate for better father-focused interventions from father-focused research.” She further acknowledged the stigma that exists around men’s mental health in general and the need to find out the best ways to help overcome that stigma.
‘Concerning’ findings may suggest a need for screening
Jason Terk, MD, a pediatrician practicing in north Texas and past president of the Texas Pediatric Society, was not surprised to see a link between depression in fathers and adversity in their children. Dr. Terk was not involved in the research but noted that the 9% rate of paternal depression seen in the study is similar to national rates of depression in U.S. adults.
“I think that the presence of paternal depression being associated with ACEs in their children in their first 5 years of life is certainly concerning and worthy of intervention for both the fathers and their children,” Dr. Terk said. “The key take-home message for clinicians who care for infants and small children is that the presence of paternal depression should increase awareness of adverse effects on those children. We need to consider screening for this at 12 months of age in much the same way we screen for maternal depression for younger infants.”
Dr. Terk noted one limitation of the study was that it didn’t suggest any specific risk factors pediatricians might look for to increase surveillance of potential depression in fathers.
“Also, unlike maternal depression, in which moms may be connected with their obstetricians if they screen positive on an Edinburgh questionnaire, we will be hard-pressed to know where to refer dads who are found to be depressed when their babies are 12 months old,” Dr. Terk said. “Screening must lead to helpful responses if the screening reveals a problem.”
The research was funded by the Robert Wood Johnson Foundation, the National Institutes of Health, and the Health Resources and Services Administration. Dr. Schmitz had no disclosures. Dr. Terk has been a speaker for Sanofi on a topic unrelated to this research.
AT AAP 2023
GI docs’ nutrition education deficit may shortchange patients
Yevgenia Pashinsky, MD, has seen her share of patients who have bounced from one gastroenterologist to the next after becoming frustrated when food elimination, supplements, or medications don’t alleviate their gastrointestinal symptoms.
In most cases, their decision to switch gastroenterologists comes down to a simple fact: No one dissected their diets.
The situation underscores how essential it is for gastroenterologists to be comfortable with nutrition concepts, said Dr. Pashinsky, a gastroenterologist with New York Gastroenterology Associates and affiliated with Mount Sinai Hospital in New York.
“There should be a focus in recognizing patterns that will help the physician pinpoint triggers, thereby helping identify the underlying disorder and guide further diagnostic and treatment options,” she said.
Although many common digestive diseases and their corresponding outcomes are linked to dietary quality and are complicated by poor nutrition and/or obesity, nutrition often gets pushed to the wayside in GI education, write Carolyn Newberry, MD, Brandon Sprung, MD, and Octavia Pickett-Blakely, MD, MHS, in a recent analysis.
“Gastroenterology fellows report limited exposure to nutrition topics leading to knowledge deficit on assessment,” they add.
One 2022 studybased on a survey of 279 GI clinicians treating patients with irritable bowel syndrome (IBS) reported that only 56% felt that they were trained to provide nutrition education, and 46% said that they sometimes, rarely, or never offered to help patients with their menu planning, label reading, or grocery shopping. And 77% said that they spent 10 minutes or less counseling patients on nutrition. Though almost all respondents (91%) said that having access to a dietitian would help them better manage patients with IBS, 42% said that they lack access to one.
But some gastroenterology professors are working to incorporate nutrition into GI training and integrating dietitians in their work with fellows as well as collaborating with dietitians to improve care in their own practices.
Nutrition overlooked in procedure-heavy specialty
In 1985, the National Academies of Sciences, Engineering, and Medicine made recommendations to upgrade nutrition education programs in U.S. medical schools.
Still, medical schools often don’t have the faculty or infrastructure to integrate and teach foundational nutrition concepts. These topics include clinical concepts, such as protein, carbohydrate and fat digestion/absorption, weight loss/gain, and symptoms related to food intake, as well as physical examination, which can help identify nutritional risks, said Dr. Pickett-Blakely, an associate professor of clinical medicine at the University of Pennsylvania and director of the Penn Center for GI Nutrition, both in Philadelphia.
Standardized medical exams include only about five questions on nutrition, and they’re all geared toward pathology, Dr. Pashinsky noted.
GI training, which includes 3 years of internal medicine residency and 3 years of GI fellowship, typically doesn’t focus on nutrition beyond total and peripheral parenteral nutrition and nutritional deficiencies, Dr. Pashinsky said. Instead, it focuses on the recognition, diagnosis, and medical management of GI diseases.
The Accreditation Council for Graduate Medical Education requires that fellows demonstrate core competency in nutrition and in the prevention, evaluation, and management of disorders of nutrient assimilation. The council also has incorporated the opportunity to interact with and learn from dietitians in its requirements for GI fellowship programs. Fellows in the dual GI/transplant hepatology pathway, created in 2021, must show competency in nutritional support for patients with chronic liver disease and in the factors involved in nutrition and malnutrition and their management.
Despite these requirements, the education that fellows receive often falls short for several reasons, said Dr. Sprung, an associate professor of medicine at the University of Rochester Medical Center’s gastroenterology and hepatology division in New York.
Gastroenterology faculties have generally shown a lack of interest in nutrition, translating into fewer faculty members able to train the future generations of physicians, he said. Training institutions have limited nutrition and obesity resources, staff, and support.
Gastroenterology is also a very procedure-focused specialty, and many students and trainees come to fellowships for procedural training, Dr. Sprung noted. Nutrition and obesity training don’t fit as well into what is traditionally an organ- or disease-specific style of education and training and, as a result, are superseded, he added.
It is possible that some fellowships are just not teaching these core concepts, Dr. Pickett-Blakely said. “The depth and breath of coverage of these concepts varies from program to program,” she added.
Exacerbating the problem is the growth of numerous subspecialties, including inflammatory bowel diseases, hepatobiliary disease, neurogastroenterology, and gastrointestinal motility, Dr. Pickett-Blakely said. Emphasis has dwindled over time on an in-depth understanding of core gastrointestinal functions, like digestion and absorption, and how these functions can be supported for optimal wellness and are affected by diseases.
“With the loss of those with the ability to educate trainees, nutrition sort of falls out of curricula, and trainees aren’t able to be exposed to those educational concepts,” she said.
It would be ideal if foundational concepts of nutrition were integrated into the subspecialty GI fellowships, which are 1-year fellowships that take place before or after the 3-year traditional fellowship, Dr. Pickett-Blakely said.
GI fellows interested in incorporating nutrition and obesity in their clinical practice on a routine basis could investigate getting board certified in nutrition, Dr. Sprung said. The National Board of Physician Nutrition Specialists, the National Board for Nutrition Support, and several other organizations offer certifications in nutrition.
If more physicians became board certified in nutritional or obesity specialties, teaching faculty numbers would increase, and that could help training grow, he noted.
Weaving more nutrition into training
To further increase knowledge, Dr. Sprung and Dr. Newberry, who is an assistant professor and director of GI nutrition at Weill Cornell Medicine’s Innovative Center for Health and Nutrition in Gastroenterology in New York, have created a free online resource covering core nutrition and obesity concepts that is available to GI fellowship programs.
Key components of the curriculum include online pre- and postlearning tests, self-directed reading materials, virtual recorded lectures, and case-based learning modules. It also provides a section on care coordination with a GI dietitian.
“Because the curriculum spans all facets of gastroenterology practice, the information can enhance clinical care experiences on general rotations,” write Dr. Newberry and colleagues in their recent analysis in Gastroenterology.
GI fellows can look at the content at their own pace and complete the curriculum as part of a formal elective.
The developers can see who’s taken the tests, and test participation indicates that several GI programs across the country are already using the program, Dr. Sprung said.
But it hasn’t been as widely adopted as hoped, he said.
“We’re trying to put some spotlight on it through articles, presentations during Digestive Disease Week, and emails to program directors, things like that,” Dr. Sprung said. “So it’s great to spread the word and get the message out there.”
Collaboration in practice
Ultimately, helping a patient with functional GI problems takes a village, and many practices are now including multidisciplinary teams.
Having these dietitians available to them, as well as seeing the benefit to their patients first-hand, has helped encourage the attending gastroenterologists’ interest, said Nancee Jaffe, RD, MS, who is senior supervisor for the GI nutrition program at UCLA Health’s Vatche & Tamar Manoukian Division of Digestive Diseases in Beverly Hills, Calif.
“We all subspecialize, which allows both doctors and patients access to the best nutrition information for a myriad of GI conditions,” Ms. Jaffe said.
In the spirit of teamwork, the university also has an integrative digestive health and wellness program, which is inclusive of doctors, dietitians, and psychologists. These teams meet monthly to discuss cases involving disorders of gut-brain interaction using a multicentered approach, she said.
In New York, one of the first things Dr. Newberry, who is also a clinical gastroenterologist with advanced training in nutrition and obesity sciences, did when she accepted her job at Weill Cornell was to advocate for a multidisciplinary team. At the Innovative Center for Health and Nutrition in Gastroenterology, she works with a group of dietitians, a hepatologist, an endocrinologist, and a team of surgeons to take care of patients. The focus is on treating patients’ GI issues while helping them lose weight.
The clinic sees a lot of patients with reflux disease and fatty liver disease. When patients come in, they’ll see the gastroenterologist, the dietitian, the endocrinologist, and possibly the bariatric surgeon. The team approach, which calls for constant communication among the physicians, improves outcomes, Dr. Newberry said.
It has been shown in the literature that multidisciplinary teams are effective for chronic diseases like nonalcoholic fatty liver disease (now known as metabolic dysfunction-associated steatotic liver disease) and inflammatory bowel disease, she added.
At the University of Rochester, Dr. Sprung and his fellow gastroenterologists coordinate with dietitians and nutrition experts for nutrition support services, as well as liver and transplant nutritional services.
We have nurse practitioners and physician assistants who run our nutritional support services for people who need such specialized care, such as total parenteral nutrition or tube feeds, or for those who need advanced therapies, like for short-gut syndrome, he said.
At NYGA, Dr. Pashinsky works with a team of registered dietitians who have specialized in gastroenterology. The dietitians help with identifying which foods in a patient’s diet are problematic and making recommendations to replace them with nutritionally equivalent staples to avoid dietary gaps, she said.
Dietitians inform patient care because they’re trained in food compounds and how foods pass through the GI tract, said Tamara Duker Freuman, RD, MS, CDN, who leads the group of registered dietitians at NYGA. Ms. Freuman comanages many patients with Dr. Pashinsky.
Oftentimes, the patient provides insights they never tell the doctor, and the dietitian gets a better idea of the patient’s life and eating habits, she said. “We’re able to spend more time with patients than physicians are, and we ask different questions.”
“Any detective work I do informs any future diagnostics [Dr. Pashinsky] does. It’s a team sport,” Ms. Freuman said.Dr. Pickett-Blakely has been a consultant for Novo Nordisk and WebMD. Dr. Newberry has received a speaking honorarium for Baxter and InBody. Dr. Sprung, Dr. Pashinsky, Ms. Freuman, and Ms. Jaffe reported no disclosures.
A version of this article first appeared on Medscape.com.
Yevgenia Pashinsky, MD, has seen her share of patients who have bounced from one gastroenterologist to the next after becoming frustrated when food elimination, supplements, or medications don’t alleviate their gastrointestinal symptoms.
In most cases, their decision to switch gastroenterologists comes down to a simple fact: No one dissected their diets.
The situation underscores how essential it is for gastroenterologists to be comfortable with nutrition concepts, said Dr. Pashinsky, a gastroenterologist with New York Gastroenterology Associates and affiliated with Mount Sinai Hospital in New York.
“There should be a focus in recognizing patterns that will help the physician pinpoint triggers, thereby helping identify the underlying disorder and guide further diagnostic and treatment options,” she said.
Although many common digestive diseases and their corresponding outcomes are linked to dietary quality and are complicated by poor nutrition and/or obesity, nutrition often gets pushed to the wayside in GI education, write Carolyn Newberry, MD, Brandon Sprung, MD, and Octavia Pickett-Blakely, MD, MHS, in a recent analysis.
“Gastroenterology fellows report limited exposure to nutrition topics leading to knowledge deficit on assessment,” they add.
One 2022 studybased on a survey of 279 GI clinicians treating patients with irritable bowel syndrome (IBS) reported that only 56% felt that they were trained to provide nutrition education, and 46% said that they sometimes, rarely, or never offered to help patients with their menu planning, label reading, or grocery shopping. And 77% said that they spent 10 minutes or less counseling patients on nutrition. Though almost all respondents (91%) said that having access to a dietitian would help them better manage patients with IBS, 42% said that they lack access to one.
But some gastroenterology professors are working to incorporate nutrition into GI training and integrating dietitians in their work with fellows as well as collaborating with dietitians to improve care in their own practices.
Nutrition overlooked in procedure-heavy specialty
In 1985, the National Academies of Sciences, Engineering, and Medicine made recommendations to upgrade nutrition education programs in U.S. medical schools.
Still, medical schools often don’t have the faculty or infrastructure to integrate and teach foundational nutrition concepts. These topics include clinical concepts, such as protein, carbohydrate and fat digestion/absorption, weight loss/gain, and symptoms related to food intake, as well as physical examination, which can help identify nutritional risks, said Dr. Pickett-Blakely, an associate professor of clinical medicine at the University of Pennsylvania and director of the Penn Center for GI Nutrition, both in Philadelphia.
Standardized medical exams include only about five questions on nutrition, and they’re all geared toward pathology, Dr. Pashinsky noted.
GI training, which includes 3 years of internal medicine residency and 3 years of GI fellowship, typically doesn’t focus on nutrition beyond total and peripheral parenteral nutrition and nutritional deficiencies, Dr. Pashinsky said. Instead, it focuses on the recognition, diagnosis, and medical management of GI diseases.
The Accreditation Council for Graduate Medical Education requires that fellows demonstrate core competency in nutrition and in the prevention, evaluation, and management of disorders of nutrient assimilation. The council also has incorporated the opportunity to interact with and learn from dietitians in its requirements for GI fellowship programs. Fellows in the dual GI/transplant hepatology pathway, created in 2021, must show competency in nutritional support for patients with chronic liver disease and in the factors involved in nutrition and malnutrition and their management.
Despite these requirements, the education that fellows receive often falls short for several reasons, said Dr. Sprung, an associate professor of medicine at the University of Rochester Medical Center’s gastroenterology and hepatology division in New York.
Gastroenterology faculties have generally shown a lack of interest in nutrition, translating into fewer faculty members able to train the future generations of physicians, he said. Training institutions have limited nutrition and obesity resources, staff, and support.
Gastroenterology is also a very procedure-focused specialty, and many students and trainees come to fellowships for procedural training, Dr. Sprung noted. Nutrition and obesity training don’t fit as well into what is traditionally an organ- or disease-specific style of education and training and, as a result, are superseded, he added.
It is possible that some fellowships are just not teaching these core concepts, Dr. Pickett-Blakely said. “The depth and breath of coverage of these concepts varies from program to program,” she added.
Exacerbating the problem is the growth of numerous subspecialties, including inflammatory bowel diseases, hepatobiliary disease, neurogastroenterology, and gastrointestinal motility, Dr. Pickett-Blakely said. Emphasis has dwindled over time on an in-depth understanding of core gastrointestinal functions, like digestion and absorption, and how these functions can be supported for optimal wellness and are affected by diseases.
“With the loss of those with the ability to educate trainees, nutrition sort of falls out of curricula, and trainees aren’t able to be exposed to those educational concepts,” she said.
It would be ideal if foundational concepts of nutrition were integrated into the subspecialty GI fellowships, which are 1-year fellowships that take place before or after the 3-year traditional fellowship, Dr. Pickett-Blakely said.
GI fellows interested in incorporating nutrition and obesity in their clinical practice on a routine basis could investigate getting board certified in nutrition, Dr. Sprung said. The National Board of Physician Nutrition Specialists, the National Board for Nutrition Support, and several other organizations offer certifications in nutrition.
If more physicians became board certified in nutritional or obesity specialties, teaching faculty numbers would increase, and that could help training grow, he noted.
Weaving more nutrition into training
To further increase knowledge, Dr. Sprung and Dr. Newberry, who is an assistant professor and director of GI nutrition at Weill Cornell Medicine’s Innovative Center for Health and Nutrition in Gastroenterology in New York, have created a free online resource covering core nutrition and obesity concepts that is available to GI fellowship programs.
Key components of the curriculum include online pre- and postlearning tests, self-directed reading materials, virtual recorded lectures, and case-based learning modules. It also provides a section on care coordination with a GI dietitian.
“Because the curriculum spans all facets of gastroenterology practice, the information can enhance clinical care experiences on general rotations,” write Dr. Newberry and colleagues in their recent analysis in Gastroenterology.
GI fellows can look at the content at their own pace and complete the curriculum as part of a formal elective.
The developers can see who’s taken the tests, and test participation indicates that several GI programs across the country are already using the program, Dr. Sprung said.
But it hasn’t been as widely adopted as hoped, he said.
“We’re trying to put some spotlight on it through articles, presentations during Digestive Disease Week, and emails to program directors, things like that,” Dr. Sprung said. “So it’s great to spread the word and get the message out there.”
Collaboration in practice
Ultimately, helping a patient with functional GI problems takes a village, and many practices are now including multidisciplinary teams.
Having these dietitians available to them, as well as seeing the benefit to their patients first-hand, has helped encourage the attending gastroenterologists’ interest, said Nancee Jaffe, RD, MS, who is senior supervisor for the GI nutrition program at UCLA Health’s Vatche & Tamar Manoukian Division of Digestive Diseases in Beverly Hills, Calif.
“We all subspecialize, which allows both doctors and patients access to the best nutrition information for a myriad of GI conditions,” Ms. Jaffe said.
In the spirit of teamwork, the university also has an integrative digestive health and wellness program, which is inclusive of doctors, dietitians, and psychologists. These teams meet monthly to discuss cases involving disorders of gut-brain interaction using a multicentered approach, she said.
In New York, one of the first things Dr. Newberry, who is also a clinical gastroenterologist with advanced training in nutrition and obesity sciences, did when she accepted her job at Weill Cornell was to advocate for a multidisciplinary team. At the Innovative Center for Health and Nutrition in Gastroenterology, she works with a group of dietitians, a hepatologist, an endocrinologist, and a team of surgeons to take care of patients. The focus is on treating patients’ GI issues while helping them lose weight.
The clinic sees a lot of patients with reflux disease and fatty liver disease. When patients come in, they’ll see the gastroenterologist, the dietitian, the endocrinologist, and possibly the bariatric surgeon. The team approach, which calls for constant communication among the physicians, improves outcomes, Dr. Newberry said.
It has been shown in the literature that multidisciplinary teams are effective for chronic diseases like nonalcoholic fatty liver disease (now known as metabolic dysfunction-associated steatotic liver disease) and inflammatory bowel disease, she added.
At the University of Rochester, Dr. Sprung and his fellow gastroenterologists coordinate with dietitians and nutrition experts for nutrition support services, as well as liver and transplant nutritional services.
We have nurse practitioners and physician assistants who run our nutritional support services for people who need such specialized care, such as total parenteral nutrition or tube feeds, or for those who need advanced therapies, like for short-gut syndrome, he said.
At NYGA, Dr. Pashinsky works with a team of registered dietitians who have specialized in gastroenterology. The dietitians help with identifying which foods in a patient’s diet are problematic and making recommendations to replace them with nutritionally equivalent staples to avoid dietary gaps, she said.
Dietitians inform patient care because they’re trained in food compounds and how foods pass through the GI tract, said Tamara Duker Freuman, RD, MS, CDN, who leads the group of registered dietitians at NYGA. Ms. Freuman comanages many patients with Dr. Pashinsky.
Oftentimes, the patient provides insights they never tell the doctor, and the dietitian gets a better idea of the patient’s life and eating habits, she said. “We’re able to spend more time with patients than physicians are, and we ask different questions.”
“Any detective work I do informs any future diagnostics [Dr. Pashinsky] does. It’s a team sport,” Ms. Freuman said.Dr. Pickett-Blakely has been a consultant for Novo Nordisk and WebMD. Dr. Newberry has received a speaking honorarium for Baxter and InBody. Dr. Sprung, Dr. Pashinsky, Ms. Freuman, and Ms. Jaffe reported no disclosures.
A version of this article first appeared on Medscape.com.
Yevgenia Pashinsky, MD, has seen her share of patients who have bounced from one gastroenterologist to the next after becoming frustrated when food elimination, supplements, or medications don’t alleviate their gastrointestinal symptoms.
In most cases, their decision to switch gastroenterologists comes down to a simple fact: No one dissected their diets.
The situation underscores how essential it is for gastroenterologists to be comfortable with nutrition concepts, said Dr. Pashinsky, a gastroenterologist with New York Gastroenterology Associates and affiliated with Mount Sinai Hospital in New York.
“There should be a focus in recognizing patterns that will help the physician pinpoint triggers, thereby helping identify the underlying disorder and guide further diagnostic and treatment options,” she said.
Although many common digestive diseases and their corresponding outcomes are linked to dietary quality and are complicated by poor nutrition and/or obesity, nutrition often gets pushed to the wayside in GI education, write Carolyn Newberry, MD, Brandon Sprung, MD, and Octavia Pickett-Blakely, MD, MHS, in a recent analysis.
“Gastroenterology fellows report limited exposure to nutrition topics leading to knowledge deficit on assessment,” they add.
One 2022 studybased on a survey of 279 GI clinicians treating patients with irritable bowel syndrome (IBS) reported that only 56% felt that they were trained to provide nutrition education, and 46% said that they sometimes, rarely, or never offered to help patients with their menu planning, label reading, or grocery shopping. And 77% said that they spent 10 minutes or less counseling patients on nutrition. Though almost all respondents (91%) said that having access to a dietitian would help them better manage patients with IBS, 42% said that they lack access to one.
But some gastroenterology professors are working to incorporate nutrition into GI training and integrating dietitians in their work with fellows as well as collaborating with dietitians to improve care in their own practices.
Nutrition overlooked in procedure-heavy specialty
In 1985, the National Academies of Sciences, Engineering, and Medicine made recommendations to upgrade nutrition education programs in U.S. medical schools.
Still, medical schools often don’t have the faculty or infrastructure to integrate and teach foundational nutrition concepts. These topics include clinical concepts, such as protein, carbohydrate and fat digestion/absorption, weight loss/gain, and symptoms related to food intake, as well as physical examination, which can help identify nutritional risks, said Dr. Pickett-Blakely, an associate professor of clinical medicine at the University of Pennsylvania and director of the Penn Center for GI Nutrition, both in Philadelphia.
Standardized medical exams include only about five questions on nutrition, and they’re all geared toward pathology, Dr. Pashinsky noted.
GI training, which includes 3 years of internal medicine residency and 3 years of GI fellowship, typically doesn’t focus on nutrition beyond total and peripheral parenteral nutrition and nutritional deficiencies, Dr. Pashinsky said. Instead, it focuses on the recognition, diagnosis, and medical management of GI diseases.
The Accreditation Council for Graduate Medical Education requires that fellows demonstrate core competency in nutrition and in the prevention, evaluation, and management of disorders of nutrient assimilation. The council also has incorporated the opportunity to interact with and learn from dietitians in its requirements for GI fellowship programs. Fellows in the dual GI/transplant hepatology pathway, created in 2021, must show competency in nutritional support for patients with chronic liver disease and in the factors involved in nutrition and malnutrition and their management.
Despite these requirements, the education that fellows receive often falls short for several reasons, said Dr. Sprung, an associate professor of medicine at the University of Rochester Medical Center’s gastroenterology and hepatology division in New York.
Gastroenterology faculties have generally shown a lack of interest in nutrition, translating into fewer faculty members able to train the future generations of physicians, he said. Training institutions have limited nutrition and obesity resources, staff, and support.
Gastroenterology is also a very procedure-focused specialty, and many students and trainees come to fellowships for procedural training, Dr. Sprung noted. Nutrition and obesity training don’t fit as well into what is traditionally an organ- or disease-specific style of education and training and, as a result, are superseded, he added.
It is possible that some fellowships are just not teaching these core concepts, Dr. Pickett-Blakely said. “The depth and breath of coverage of these concepts varies from program to program,” she added.
Exacerbating the problem is the growth of numerous subspecialties, including inflammatory bowel diseases, hepatobiliary disease, neurogastroenterology, and gastrointestinal motility, Dr. Pickett-Blakely said. Emphasis has dwindled over time on an in-depth understanding of core gastrointestinal functions, like digestion and absorption, and how these functions can be supported for optimal wellness and are affected by diseases.
“With the loss of those with the ability to educate trainees, nutrition sort of falls out of curricula, and trainees aren’t able to be exposed to those educational concepts,” she said.
It would be ideal if foundational concepts of nutrition were integrated into the subspecialty GI fellowships, which are 1-year fellowships that take place before or after the 3-year traditional fellowship, Dr. Pickett-Blakely said.
GI fellows interested in incorporating nutrition and obesity in their clinical practice on a routine basis could investigate getting board certified in nutrition, Dr. Sprung said. The National Board of Physician Nutrition Specialists, the National Board for Nutrition Support, and several other organizations offer certifications in nutrition.
If more physicians became board certified in nutritional or obesity specialties, teaching faculty numbers would increase, and that could help training grow, he noted.
Weaving more nutrition into training
To further increase knowledge, Dr. Sprung and Dr. Newberry, who is an assistant professor and director of GI nutrition at Weill Cornell Medicine’s Innovative Center for Health and Nutrition in Gastroenterology in New York, have created a free online resource covering core nutrition and obesity concepts that is available to GI fellowship programs.
Key components of the curriculum include online pre- and postlearning tests, self-directed reading materials, virtual recorded lectures, and case-based learning modules. It also provides a section on care coordination with a GI dietitian.
“Because the curriculum spans all facets of gastroenterology practice, the information can enhance clinical care experiences on general rotations,” write Dr. Newberry and colleagues in their recent analysis in Gastroenterology.
GI fellows can look at the content at their own pace and complete the curriculum as part of a formal elective.
The developers can see who’s taken the tests, and test participation indicates that several GI programs across the country are already using the program, Dr. Sprung said.
But it hasn’t been as widely adopted as hoped, he said.
“We’re trying to put some spotlight on it through articles, presentations during Digestive Disease Week, and emails to program directors, things like that,” Dr. Sprung said. “So it’s great to spread the word and get the message out there.”
Collaboration in practice
Ultimately, helping a patient with functional GI problems takes a village, and many practices are now including multidisciplinary teams.
Having these dietitians available to them, as well as seeing the benefit to their patients first-hand, has helped encourage the attending gastroenterologists’ interest, said Nancee Jaffe, RD, MS, who is senior supervisor for the GI nutrition program at UCLA Health’s Vatche & Tamar Manoukian Division of Digestive Diseases in Beverly Hills, Calif.
“We all subspecialize, which allows both doctors and patients access to the best nutrition information for a myriad of GI conditions,” Ms. Jaffe said.
In the spirit of teamwork, the university also has an integrative digestive health and wellness program, which is inclusive of doctors, dietitians, and psychologists. These teams meet monthly to discuss cases involving disorders of gut-brain interaction using a multicentered approach, she said.
In New York, one of the first things Dr. Newberry, who is also a clinical gastroenterologist with advanced training in nutrition and obesity sciences, did when she accepted her job at Weill Cornell was to advocate for a multidisciplinary team. At the Innovative Center for Health and Nutrition in Gastroenterology, she works with a group of dietitians, a hepatologist, an endocrinologist, and a team of surgeons to take care of patients. The focus is on treating patients’ GI issues while helping them lose weight.
The clinic sees a lot of patients with reflux disease and fatty liver disease. When patients come in, they’ll see the gastroenterologist, the dietitian, the endocrinologist, and possibly the bariatric surgeon. The team approach, which calls for constant communication among the physicians, improves outcomes, Dr. Newberry said.
It has been shown in the literature that multidisciplinary teams are effective for chronic diseases like nonalcoholic fatty liver disease (now known as metabolic dysfunction-associated steatotic liver disease) and inflammatory bowel disease, she added.
At the University of Rochester, Dr. Sprung and his fellow gastroenterologists coordinate with dietitians and nutrition experts for nutrition support services, as well as liver and transplant nutritional services.
We have nurse practitioners and physician assistants who run our nutritional support services for people who need such specialized care, such as total parenteral nutrition or tube feeds, or for those who need advanced therapies, like for short-gut syndrome, he said.
At NYGA, Dr. Pashinsky works with a team of registered dietitians who have specialized in gastroenterology. The dietitians help with identifying which foods in a patient’s diet are problematic and making recommendations to replace them with nutritionally equivalent staples to avoid dietary gaps, she said.
Dietitians inform patient care because they’re trained in food compounds and how foods pass through the GI tract, said Tamara Duker Freuman, RD, MS, CDN, who leads the group of registered dietitians at NYGA. Ms. Freuman comanages many patients with Dr. Pashinsky.
Oftentimes, the patient provides insights they never tell the doctor, and the dietitian gets a better idea of the patient’s life and eating habits, she said. “We’re able to spend more time with patients than physicians are, and we ask different questions.”
“Any detective work I do informs any future diagnostics [Dr. Pashinsky] does. It’s a team sport,” Ms. Freuman said.Dr. Pickett-Blakely has been a consultant for Novo Nordisk and WebMD. Dr. Newberry has received a speaking honorarium for Baxter and InBody. Dr. Sprung, Dr. Pashinsky, Ms. Freuman, and Ms. Jaffe reported no disclosures.
A version of this article first appeared on Medscape.com.
In ILD, ECMO linked to good outcomes as bridge to transplant
Extracorporeal membrane oxygen support appears to be beneficial in patients with advanced interstitial lung disease (ILD), according to a new meta-analysis. Specifically, , although the confidence in the finding was low.
ECMO has been used increasingly in ILD patients over the past 10-15 years for acute decompensation as well as a bridge to lung transplant, according to Prasanth Balasubramanian, MD, but clinical evidence for its use is limited to case series or short-term retrospective studies. “We don’t have robust evidence on whether it really helps with the outcome, and which mode is better, so that’s why we decided to do a study on this,” said Dr. Balasubramanian, who is a fellow in pulmonary critical care at Mayo Clinic (Jacksonville, Fla.). He presented the new research at the annual meeting of the American College of Chest Physicians (CHEST).
The results were encouraging, according to the study’s lead author Pramod Guru, MD. “I think what we take from this analysis is that ECMO should not be considered as a contraindication for people you are considering for lung transplant. If we have this population of people who are very sick, but we have the opportunity to solve them with VA ECMO and then give the transplantation possibly, that may be the way,” said Dr. Guru, who is a critical care specialist at Mayo Clinic, Jacksonville, Fla. He acknowledged that more work needs to be done to determine whether VA or VV is best in specific patient populations.
The meta-analysis included 18 studies with a total of 1,341 patients, who were a mean age of 55.89 years and 61.08% of whom were male. Most procedures (75.3%) were VV. The overall mortality was 52.6%, including 59.7% for VV ECMO and 34.2% for VA ECMO. The survival difference did not reach statistical significance (odds ratio, 0.48; P = .11). There was also no significant difference in survival between patients who underwent ECMO and those who did not undergo ECMO (OR, 0.48; P = .43).
The researchers also analyzed 13 studies with 1,002 patients that looked at ECMO as a bridge to transplant (mean age, 52.1; 52.2% male; 49.3% VV, 31.1% VA, 32.4% cardiopulmonary bypass). Mortality was lower in the VA group than in the VV group (odds ratio, 0.62; P = .04).
“VA ECMO is generally for sicker patients, so it’s odd that the patients who are on the more aggressive support had lower mortality. But it’s good, it says it works,” said Chris Carroll, MD, an intensivist at the University of Florida, Jacksonville, who was asked to comment on the study.
The finding may also be an artifact of bias in the retrospective data, according to Joshua Diamond, MD, who comoderated the session where the study was presented. He noted age, physical function, and illness severity, among other factors can play a role in decision-making. “I have a feeling that what you’re seeing is a very carefully selected patient population as opposed to a true mortality benefit with VA versus VV ECMO,” said Dr. Diamond, who is associate medical director of the Penn Lung Transplant Program in Philadelphia.
Another weakness of the study is that ECMO techniques and devices have changed over time, making some of the older data less relevant to current practice. Overall Dr. Diamond described the study as interesting, but “I’d like to see a bit more granularity of data to figure out who makes or doesn’t make a good candidate,” said Dr. Diamond.
Patients with ILD undergoing ECMO as a bridge to transplant had a higher 1-year posttransplant mortality than patients with other causes for transplant (OR, 1.78; P<.01). However, this finding relied on two retrospective studies using the UNOS database at different time points (2001-2012 and 2015-2020), leading to potential confounders and risk of bias.
Dr. Balasubramanian recognized the limitations of the analysis. “We do think that further prospective studies comparing various modalities would be essential, although it would be challenging,” he said.
Nevertheless, Dr. Guru said that his own center is changing its patient selection criteria for ECMO and will begin to collect prospective data: “I would say that in 12 months we’ll have our own data to support what we are doing.”
The study can also inform patients and family who are trying to make a potential end-of-life decision about pursuing aggressive ECMO therapy. “This study says that if you choose to pursue that more aggressive therapy, you may still have a good outcome. A patient might say, ‘Why am I going to go through all this? Is it just prolonging my death, or is there a chance of saving my life? I think what this study shows is that it does have potential of saving their life,” said Dr. Carroll.
Dr. Balasubramanian, Dr. Guru, and Dr. Carroll have no relevant financial disclosures.
Extracorporeal membrane oxygen support appears to be beneficial in patients with advanced interstitial lung disease (ILD), according to a new meta-analysis. Specifically, , although the confidence in the finding was low.
ECMO has been used increasingly in ILD patients over the past 10-15 years for acute decompensation as well as a bridge to lung transplant, according to Prasanth Balasubramanian, MD, but clinical evidence for its use is limited to case series or short-term retrospective studies. “We don’t have robust evidence on whether it really helps with the outcome, and which mode is better, so that’s why we decided to do a study on this,” said Dr. Balasubramanian, who is a fellow in pulmonary critical care at Mayo Clinic (Jacksonville, Fla.). He presented the new research at the annual meeting of the American College of Chest Physicians (CHEST).
The results were encouraging, according to the study’s lead author Pramod Guru, MD. “I think what we take from this analysis is that ECMO should not be considered as a contraindication for people you are considering for lung transplant. If we have this population of people who are very sick, but we have the opportunity to solve them with VA ECMO and then give the transplantation possibly, that may be the way,” said Dr. Guru, who is a critical care specialist at Mayo Clinic, Jacksonville, Fla. He acknowledged that more work needs to be done to determine whether VA or VV is best in specific patient populations.
The meta-analysis included 18 studies with a total of 1,341 patients, who were a mean age of 55.89 years and 61.08% of whom were male. Most procedures (75.3%) were VV. The overall mortality was 52.6%, including 59.7% for VV ECMO and 34.2% for VA ECMO. The survival difference did not reach statistical significance (odds ratio, 0.48; P = .11). There was also no significant difference in survival between patients who underwent ECMO and those who did not undergo ECMO (OR, 0.48; P = .43).
The researchers also analyzed 13 studies with 1,002 patients that looked at ECMO as a bridge to transplant (mean age, 52.1; 52.2% male; 49.3% VV, 31.1% VA, 32.4% cardiopulmonary bypass). Mortality was lower in the VA group than in the VV group (odds ratio, 0.62; P = .04).
“VA ECMO is generally for sicker patients, so it’s odd that the patients who are on the more aggressive support had lower mortality. But it’s good, it says it works,” said Chris Carroll, MD, an intensivist at the University of Florida, Jacksonville, who was asked to comment on the study.
The finding may also be an artifact of bias in the retrospective data, according to Joshua Diamond, MD, who comoderated the session where the study was presented. He noted age, physical function, and illness severity, among other factors can play a role in decision-making. “I have a feeling that what you’re seeing is a very carefully selected patient population as opposed to a true mortality benefit with VA versus VV ECMO,” said Dr. Diamond, who is associate medical director of the Penn Lung Transplant Program in Philadelphia.
Another weakness of the study is that ECMO techniques and devices have changed over time, making some of the older data less relevant to current practice. Overall Dr. Diamond described the study as interesting, but “I’d like to see a bit more granularity of data to figure out who makes or doesn’t make a good candidate,” said Dr. Diamond.
Patients with ILD undergoing ECMO as a bridge to transplant had a higher 1-year posttransplant mortality than patients with other causes for transplant (OR, 1.78; P<.01). However, this finding relied on two retrospective studies using the UNOS database at different time points (2001-2012 and 2015-2020), leading to potential confounders and risk of bias.
Dr. Balasubramanian recognized the limitations of the analysis. “We do think that further prospective studies comparing various modalities would be essential, although it would be challenging,” he said.
Nevertheless, Dr. Guru said that his own center is changing its patient selection criteria for ECMO and will begin to collect prospective data: “I would say that in 12 months we’ll have our own data to support what we are doing.”
The study can also inform patients and family who are trying to make a potential end-of-life decision about pursuing aggressive ECMO therapy. “This study says that if you choose to pursue that more aggressive therapy, you may still have a good outcome. A patient might say, ‘Why am I going to go through all this? Is it just prolonging my death, or is there a chance of saving my life? I think what this study shows is that it does have potential of saving their life,” said Dr. Carroll.
Dr. Balasubramanian, Dr. Guru, and Dr. Carroll have no relevant financial disclosures.
Extracorporeal membrane oxygen support appears to be beneficial in patients with advanced interstitial lung disease (ILD), according to a new meta-analysis. Specifically, , although the confidence in the finding was low.
ECMO has been used increasingly in ILD patients over the past 10-15 years for acute decompensation as well as a bridge to lung transplant, according to Prasanth Balasubramanian, MD, but clinical evidence for its use is limited to case series or short-term retrospective studies. “We don’t have robust evidence on whether it really helps with the outcome, and which mode is better, so that’s why we decided to do a study on this,” said Dr. Balasubramanian, who is a fellow in pulmonary critical care at Mayo Clinic (Jacksonville, Fla.). He presented the new research at the annual meeting of the American College of Chest Physicians (CHEST).
The results were encouraging, according to the study’s lead author Pramod Guru, MD. “I think what we take from this analysis is that ECMO should not be considered as a contraindication for people you are considering for lung transplant. If we have this population of people who are very sick, but we have the opportunity to solve them with VA ECMO and then give the transplantation possibly, that may be the way,” said Dr. Guru, who is a critical care specialist at Mayo Clinic, Jacksonville, Fla. He acknowledged that more work needs to be done to determine whether VA or VV is best in specific patient populations.
The meta-analysis included 18 studies with a total of 1,341 patients, who were a mean age of 55.89 years and 61.08% of whom were male. Most procedures (75.3%) were VV. The overall mortality was 52.6%, including 59.7% for VV ECMO and 34.2% for VA ECMO. The survival difference did not reach statistical significance (odds ratio, 0.48; P = .11). There was also no significant difference in survival between patients who underwent ECMO and those who did not undergo ECMO (OR, 0.48; P = .43).
The researchers also analyzed 13 studies with 1,002 patients that looked at ECMO as a bridge to transplant (mean age, 52.1; 52.2% male; 49.3% VV, 31.1% VA, 32.4% cardiopulmonary bypass). Mortality was lower in the VA group than in the VV group (odds ratio, 0.62; P = .04).
“VA ECMO is generally for sicker patients, so it’s odd that the patients who are on the more aggressive support had lower mortality. But it’s good, it says it works,” said Chris Carroll, MD, an intensivist at the University of Florida, Jacksonville, who was asked to comment on the study.
The finding may also be an artifact of bias in the retrospective data, according to Joshua Diamond, MD, who comoderated the session where the study was presented. He noted age, physical function, and illness severity, among other factors can play a role in decision-making. “I have a feeling that what you’re seeing is a very carefully selected patient population as opposed to a true mortality benefit with VA versus VV ECMO,” said Dr. Diamond, who is associate medical director of the Penn Lung Transplant Program in Philadelphia.
Another weakness of the study is that ECMO techniques and devices have changed over time, making some of the older data less relevant to current practice. Overall Dr. Diamond described the study as interesting, but “I’d like to see a bit more granularity of data to figure out who makes or doesn’t make a good candidate,” said Dr. Diamond.
Patients with ILD undergoing ECMO as a bridge to transplant had a higher 1-year posttransplant mortality than patients with other causes for transplant (OR, 1.78; P<.01). However, this finding relied on two retrospective studies using the UNOS database at different time points (2001-2012 and 2015-2020), leading to potential confounders and risk of bias.
Dr. Balasubramanian recognized the limitations of the analysis. “We do think that further prospective studies comparing various modalities would be essential, although it would be challenging,” he said.
Nevertheless, Dr. Guru said that his own center is changing its patient selection criteria for ECMO and will begin to collect prospective data: “I would say that in 12 months we’ll have our own data to support what we are doing.”
The study can also inform patients and family who are trying to make a potential end-of-life decision about pursuing aggressive ECMO therapy. “This study says that if you choose to pursue that more aggressive therapy, you may still have a good outcome. A patient might say, ‘Why am I going to go through all this? Is it just prolonging my death, or is there a chance of saving my life? I think what this study shows is that it does have potential of saving their life,” said Dr. Carroll.
Dr. Balasubramanian, Dr. Guru, and Dr. Carroll have no relevant financial disclosures.
FROM CHEST 2023
Plaquelike Syringoma Mimicking Microcystic Adnexal Carcinoma: A Potential Histologic Pitfall
To the Editor:
Plaquelike or plaque-type syringoma is a lesser-known variant of syringoma that can appear histologically indistinguishable from the superficial portion of microcystic adnexal carcinoma (MAC). The plaquelike variant of syringoma holds a benign clinical course, and no treatment is necessary. Microcystic adnexal carcinoma is distinguished from plaquelike syringoma by an aggressive growth pattern with a high risk for local invasion and recurrence if inadequately treated. Thus, treatment with Mohs micrographic surgery (MMS) has been recommended as the mainstay for MAC. If superficial biopsy specimens reveal suspicion for MAC and patients are referred for MMS, careful consideration should be made to differentiate MAC and plaquelike syringoma early to prevent unnecessary morbidity.
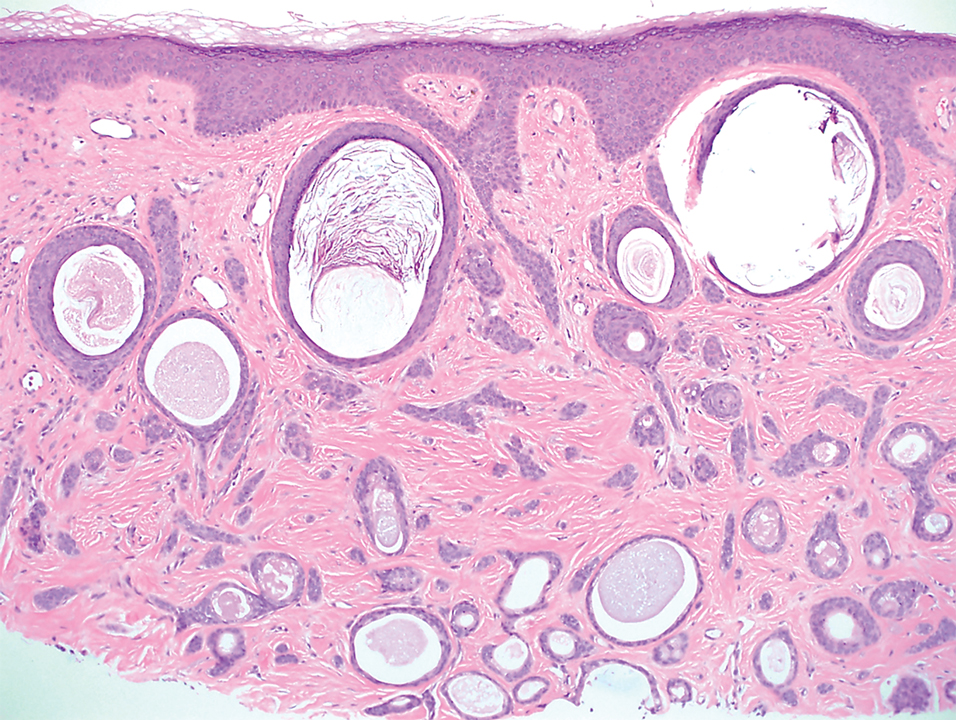
A 78-year-old woman was referred for MMS for a left forehead lesion that was diagnosed via shave biopsy as a desmoplastic and cystic adnexal neoplasm with suspicion for desmoplastic trichoepithelioma or MAC (Figure 1). Upon presentation for MMS, a well-healed, 1.0×0.9-cm scar at the biopsy site on the left forehead was observed (Figure 2A). One stage was obtained by standard MMS technique and sent for intraoperative processing (Figure 2B). Frozen section examination of the first stage demonstrated peripheral margin involvement with syringomatous change confined to the superficial and mid dermis (Figure 3). Before proceeding further, these findings were reviewed with an in-house dermatopathologist, and it was determined that no infiltrative tumor, perineural involvement, or other features to indicate malignancy were noted. A decision was made to refrain from obtaining any additional layers and to send excised Burow triangles for permanent section analysis. A primary linear closure was performed without complication, and the patient was discharged from the ambulatory surgery suite. Histopathologic examination of the Burow triangles later confirmed findings consistent with plaquelike syringoma with no evidence of malignancy (Figure 4).
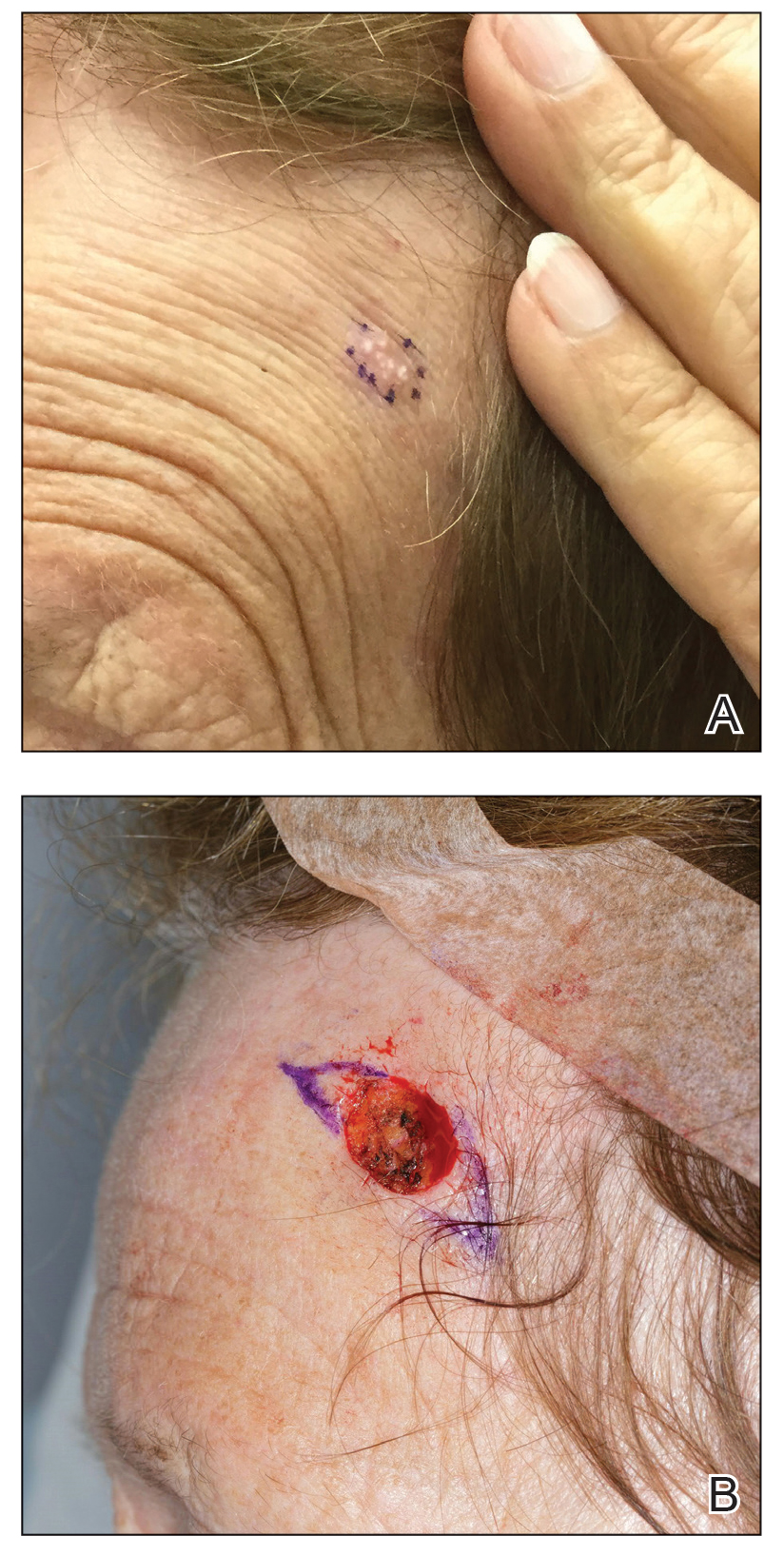
Syringomas present as small flesh-colored papules in the periorbital areas. These benign neoplasms previously have been classified into 4 major clinical variants: localized, generalized, Down syndrome associated, and familial.1 The lesser-known plaquelike variant of syringoma was first described by Kikuchi et al2 in 1979. Aside from our report, a PubMed search of articles indexed for MEDLINE using the terms plaquelike or plaque-type syringoma yielded 16 cases in the literature.2-14 Of these, 6 were referred to or encountered in the MMS setting.8,9,11,12,14 Plaquelike syringoma can be solitary or multiple in presentation.6 It most commonly involves the head and neck but also can present on the trunk, arms, legs, and groin areas. The clinical size of plaquelike syringoma is variable, with the largest reported cases extending several centimeters in diameter.2,6 Similar to reported associations with conventional syringoma, the plaquelike subtype of syringoma has been reported in association with Down syndrome.13
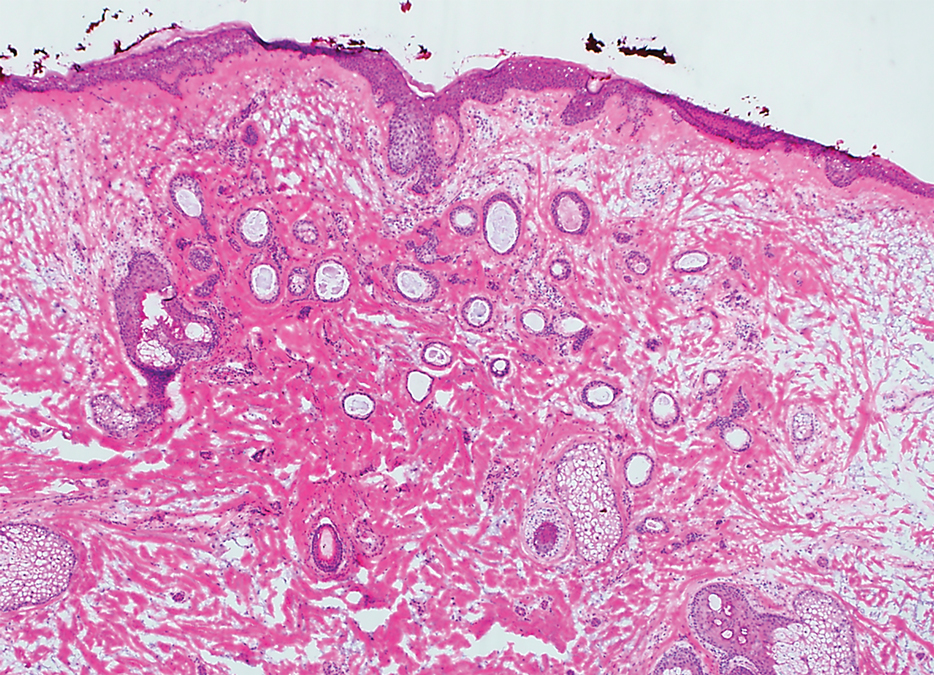
Histopathologically, plaquelike syringoma shares features with MAC as well as desmoplastic trichoepithelioma and desmoplastic basal cell carcinoma. Plaquelike syringoma demonstrates broad proliferations of small tubules morphologically reminiscent of tadpoles confined within the dermis. Ducts typically are lined with 2 or 3 layers of small cuboidal cells. Microcystic adnexal carcinoma typically features asymmetric ductal structures lined with single cells extending from the dermis into the subcutis and even underlying muscle, cartilage, or bone.8 There are no reliable immunohistochemical stains to differentiate between these 2 entities; thus, the primary distinction lies in the depth of involvement. Desmoplastic trichoepithelioma is composed of narrow cords and nests of basaloid cells of follicular origin commonly admixed with small cornifying cysts appearing in the dermis.8 Colonizing Merkel cells positive for cytokeratin 20 often are present in desmoplastic trichoepithelioma and not in syringoma or MAC.15 Desmoplastic basal cell carcinoma demonstrates narrow strands of basaloid cells of follicular origin appearing in the dermis. Desmoplastic trichoepithelioma and desmoplastic basal cell carcinoma are each fundamentally differentiated from plaquelike syringoma in that proliferations of cords and nests are not of eccrine or apocrine origin.
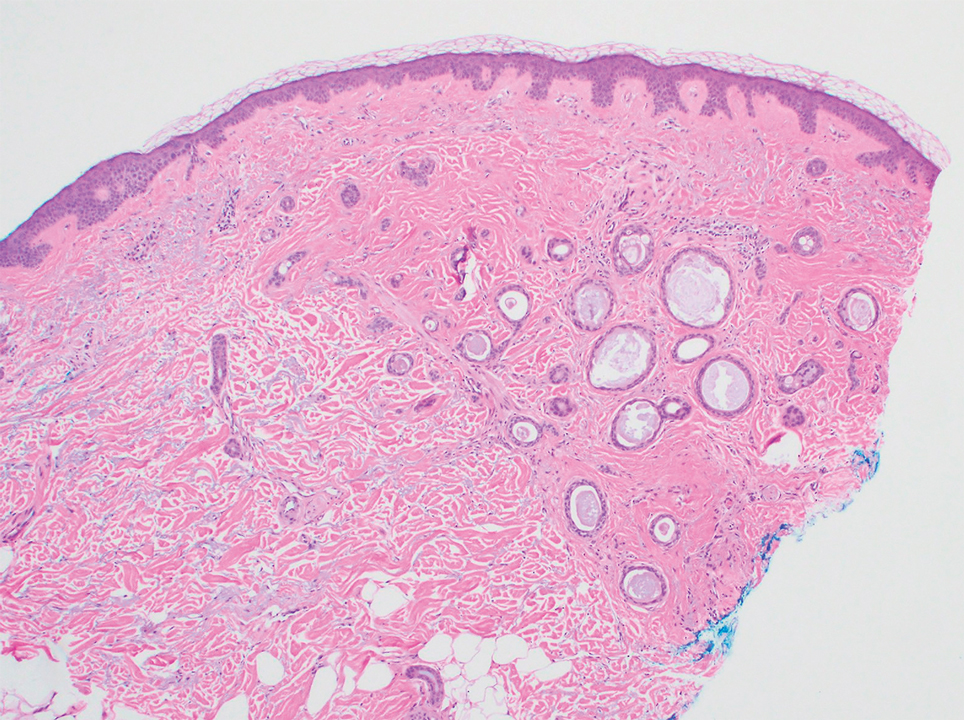
Several cases of plaquelike syringoma have been challenging to distinguish from MAC in performing MMS.8,9,11 Underlying extension of this syringoma variant can be far-reaching, extending to several centimeters in size and involving multiple cosmetic subunits.6,11,14 Inadvertent overtreatment with multiple MMS stages can be avoided with careful recognition of the differentiating histopathologic features. Syringomatous lesions commonly are encountered in MMS and may even be present at the edge of other tumor types. Plaquelike syringoma has been reported as a coexistent entity with nodular basal cell carcinoma.12 Boos et al16 similarly reported the presence of deceptive ductal proliferations along the immediate peripheral margin of MAC, which prompted multiple re-excisions. Pursuit of permanent section analysis in these cases revealed the appearance of small syringomas, and a diagnosis of benign subclinical syringomatous proliferations was made, averting further intervention.16
Our case sheds light on the threat of commission bias in dermatologic surgery, which is the tendency for action rather than inaction.17 In this context, it is important to avoid the perspective that harm to the patient can only be prevented by active intervention. Cognitive bias has been increasingly recognized as a source of medical error, and methods to mitigate bias in medical practice have been well described.17 Microcystic adnexal carcinoma and plaquelike syringoma can be hard to differentiate especially initially, as demonstrated in our case, which particularly illustrates the importance of slowing down a surgical case at the appropriate time, considering and revisiting alternative diagnoses, implementing checklists, and seeking histopathologic collaboration with colleagues when necessary. Our attempted implementation of these principles, especially early collaboration with colleagues, led to intraoperative recognition of plaquelike syringoma within the first stage of MMS.
We seek to raise the index of suspicion for plaquelike syringoma among dermatologists and dermatologic surgeons, especially when syringomatous structures are limited to the superficial dermis. We encourage familiarity with the plaquelike syringoma entity as well as careful consideration of further investigation via scouting biopsies or permanent section analysis when other characteristic features of MAC are unclear or lacking. Adequate sampling as well as collaboration with a dermatopathologist in cases of suspected syringoma can help to reduce the susceptibility to commission bias and prevent histopathologic pitfalls and unwarranted surgical morbidity.
- Friedman SJ, Butler DF. Syringoma presenting as milia. J Am Acad Dermatol. 1987;16:310-314.
- Kikuchi I, Idemori M, Okazaki M. Plaque type syringoma. J Dermatol. 1979;6:329-331.
- Dekio S, Jidoi J. Submammary syringoma—report of a case. J Dermatol. 1988;15:351-352.
- Patrizi A, Neri I, Marzaduri S, et al. Syringoma: a review of twenty-nine cases. Acta Derm Venereol. 1998;78:460-462.
- Nguyen DB, Patterson JW, Wilson BB. Syringoma of the moustache area. J Am Acad Dermatol. 2003;49:337-339.
- Rongioletti F, Semino MT, Rebora A. Unilateral multiple plaque-like syringomas. Br J Dermatol. 1996;135:623-625.
- Chi HI. A case of unusual syringoma: unilateral linear distribution and plaque formation. J Dermatol. 1996;23:505-506.
- Suwatee P, McClelland MC, Huiras EE, et al. Plaque-type syringoma: two cases misdiagnosed as microcystic adnexal carcinoma. J Cutan Pathol. 2008;35:570-574.
- Wallace JS, Bond JS, Seidel GD, et al. An important mimicker: plaque-type syringoma mistakenly diagnosed as microcystic adnexal carcinoma. Dermatol Surg. 2014;40:810-812.
- Mitkov M, Balagula Y, Taube JM, et al. Plaque-like syringoma with involvement of deep reticular dermis. J Am Acad Dermatol. 2014;71:E206-E207.
- Schleich C, Ferringer T, Petrick M. Plaque type syringoma mimicking a microcystic adnexal carcinoma. J Am Acad Dermatol. 2016;74(suppl 1):AB287.
- Yang Y, Srivastava D. Plaque-type syringoma coexisting with basal cell carcinoma. Dermatol Surg. 2018;44:1464-1466.
- Motegi SI, Sekiguchi A, Fujiwara C, et al. Milia-like idiopathic calcinosis cutis and plaque-type syringoma in a girl with Down syndrome. J Dermatol. 2019;46:E136-E137.
- Clark M, Duprey C, Sutton A, et al. Plaque-type syringoma masquerading as microcystic adnexal carcinoma: review of the literature and description of a novel technique that emphasizes lesion architecture to help make the diagnosis. Am J Dermatopathol. 2019;41:E98-E101.
- Abesamis-Cubillan E, El-Shabrawi-Caelen L, LeBoit PE. Merkel cells and sclerosing epithelial neoplasms. Am J Dermatopathol. 2000;22:311-315.
- Boos MD, Elenitsas R, Seykora J, et al. Benign subclinical syringomatous proliferations adjacent to a microcystic adnexal carcinoma: a tumor mimic with significant patient implications. Am J Dermatopathol. 2014;36:174-178.
- O’Sullivan ED, Schofield SJ. Cognitive bias in clinical medicine. J R Coll Physicians Edinb. 2018;48:225-232.
To the Editor:
Plaquelike or plaque-type syringoma is a lesser-known variant of syringoma that can appear histologically indistinguishable from the superficial portion of microcystic adnexal carcinoma (MAC). The plaquelike variant of syringoma holds a benign clinical course, and no treatment is necessary. Microcystic adnexal carcinoma is distinguished from plaquelike syringoma by an aggressive growth pattern with a high risk for local invasion and recurrence if inadequately treated. Thus, treatment with Mohs micrographic surgery (MMS) has been recommended as the mainstay for MAC. If superficial biopsy specimens reveal suspicion for MAC and patients are referred for MMS, careful consideration should be made to differentiate MAC and plaquelike syringoma early to prevent unnecessary morbidity.

A 78-year-old woman was referred for MMS for a left forehead lesion that was diagnosed via shave biopsy as a desmoplastic and cystic adnexal neoplasm with suspicion for desmoplastic trichoepithelioma or MAC (Figure 1). Upon presentation for MMS, a well-healed, 1.0×0.9-cm scar at the biopsy site on the left forehead was observed (Figure 2A). One stage was obtained by standard MMS technique and sent for intraoperative processing (Figure 2B). Frozen section examination of the first stage demonstrated peripheral margin involvement with syringomatous change confined to the superficial and mid dermis (Figure 3). Before proceeding further, these findings were reviewed with an in-house dermatopathologist, and it was determined that no infiltrative tumor, perineural involvement, or other features to indicate malignancy were noted. A decision was made to refrain from obtaining any additional layers and to send excised Burow triangles for permanent section analysis. A primary linear closure was performed without complication, and the patient was discharged from the ambulatory surgery suite. Histopathologic examination of the Burow triangles later confirmed findings consistent with plaquelike syringoma with no evidence of malignancy (Figure 4).

Syringomas present as small flesh-colored papules in the periorbital areas. These benign neoplasms previously have been classified into 4 major clinical variants: localized, generalized, Down syndrome associated, and familial.1 The lesser-known plaquelike variant of syringoma was first described by Kikuchi et al2 in 1979. Aside from our report, a PubMed search of articles indexed for MEDLINE using the terms plaquelike or plaque-type syringoma yielded 16 cases in the literature.2-14 Of these, 6 were referred to or encountered in the MMS setting.8,9,11,12,14 Plaquelike syringoma can be solitary or multiple in presentation.6 It most commonly involves the head and neck but also can present on the trunk, arms, legs, and groin areas. The clinical size of plaquelike syringoma is variable, with the largest reported cases extending several centimeters in diameter.2,6 Similar to reported associations with conventional syringoma, the plaquelike subtype of syringoma has been reported in association with Down syndrome.13

Histopathologically, plaquelike syringoma shares features with MAC as well as desmoplastic trichoepithelioma and desmoplastic basal cell carcinoma. Plaquelike syringoma demonstrates broad proliferations of small tubules morphologically reminiscent of tadpoles confined within the dermis. Ducts typically are lined with 2 or 3 layers of small cuboidal cells. Microcystic adnexal carcinoma typically features asymmetric ductal structures lined with single cells extending from the dermis into the subcutis and even underlying muscle, cartilage, or bone.8 There are no reliable immunohistochemical stains to differentiate between these 2 entities; thus, the primary distinction lies in the depth of involvement. Desmoplastic trichoepithelioma is composed of narrow cords and nests of basaloid cells of follicular origin commonly admixed with small cornifying cysts appearing in the dermis.8 Colonizing Merkel cells positive for cytokeratin 20 often are present in desmoplastic trichoepithelioma and not in syringoma or MAC.15 Desmoplastic basal cell carcinoma demonstrates narrow strands of basaloid cells of follicular origin appearing in the dermis. Desmoplastic trichoepithelioma and desmoplastic basal cell carcinoma are each fundamentally differentiated from plaquelike syringoma in that proliferations of cords and nests are not of eccrine or apocrine origin.

Several cases of plaquelike syringoma have been challenging to distinguish from MAC in performing MMS.8,9,11 Underlying extension of this syringoma variant can be far-reaching, extending to several centimeters in size and involving multiple cosmetic subunits.6,11,14 Inadvertent overtreatment with multiple MMS stages can be avoided with careful recognition of the differentiating histopathologic features. Syringomatous lesions commonly are encountered in MMS and may even be present at the edge of other tumor types. Plaquelike syringoma has been reported as a coexistent entity with nodular basal cell carcinoma.12 Boos et al16 similarly reported the presence of deceptive ductal proliferations along the immediate peripheral margin of MAC, which prompted multiple re-excisions. Pursuit of permanent section analysis in these cases revealed the appearance of small syringomas, and a diagnosis of benign subclinical syringomatous proliferations was made, averting further intervention.16
Our case sheds light on the threat of commission bias in dermatologic surgery, which is the tendency for action rather than inaction.17 In this context, it is important to avoid the perspective that harm to the patient can only be prevented by active intervention. Cognitive bias has been increasingly recognized as a source of medical error, and methods to mitigate bias in medical practice have been well described.17 Microcystic adnexal carcinoma and plaquelike syringoma can be hard to differentiate especially initially, as demonstrated in our case, which particularly illustrates the importance of slowing down a surgical case at the appropriate time, considering and revisiting alternative diagnoses, implementing checklists, and seeking histopathologic collaboration with colleagues when necessary. Our attempted implementation of these principles, especially early collaboration with colleagues, led to intraoperative recognition of plaquelike syringoma within the first stage of MMS.
We seek to raise the index of suspicion for plaquelike syringoma among dermatologists and dermatologic surgeons, especially when syringomatous structures are limited to the superficial dermis. We encourage familiarity with the plaquelike syringoma entity as well as careful consideration of further investigation via scouting biopsies or permanent section analysis when other characteristic features of MAC are unclear or lacking. Adequate sampling as well as collaboration with a dermatopathologist in cases of suspected syringoma can help to reduce the susceptibility to commission bias and prevent histopathologic pitfalls and unwarranted surgical morbidity.
To the Editor:
Plaquelike or plaque-type syringoma is a lesser-known variant of syringoma that can appear histologically indistinguishable from the superficial portion of microcystic adnexal carcinoma (MAC). The plaquelike variant of syringoma holds a benign clinical course, and no treatment is necessary. Microcystic adnexal carcinoma is distinguished from plaquelike syringoma by an aggressive growth pattern with a high risk for local invasion and recurrence if inadequately treated. Thus, treatment with Mohs micrographic surgery (MMS) has been recommended as the mainstay for MAC. If superficial biopsy specimens reveal suspicion for MAC and patients are referred for MMS, careful consideration should be made to differentiate MAC and plaquelike syringoma early to prevent unnecessary morbidity.

A 78-year-old woman was referred for MMS for a left forehead lesion that was diagnosed via shave biopsy as a desmoplastic and cystic adnexal neoplasm with suspicion for desmoplastic trichoepithelioma or MAC (Figure 1). Upon presentation for MMS, a well-healed, 1.0×0.9-cm scar at the biopsy site on the left forehead was observed (Figure 2A). One stage was obtained by standard MMS technique and sent for intraoperative processing (Figure 2B). Frozen section examination of the first stage demonstrated peripheral margin involvement with syringomatous change confined to the superficial and mid dermis (Figure 3). Before proceeding further, these findings were reviewed with an in-house dermatopathologist, and it was determined that no infiltrative tumor, perineural involvement, or other features to indicate malignancy were noted. A decision was made to refrain from obtaining any additional layers and to send excised Burow triangles for permanent section analysis. A primary linear closure was performed without complication, and the patient was discharged from the ambulatory surgery suite. Histopathologic examination of the Burow triangles later confirmed findings consistent with plaquelike syringoma with no evidence of malignancy (Figure 4).

Syringomas present as small flesh-colored papules in the periorbital areas. These benign neoplasms previously have been classified into 4 major clinical variants: localized, generalized, Down syndrome associated, and familial.1 The lesser-known plaquelike variant of syringoma was first described by Kikuchi et al2 in 1979. Aside from our report, a PubMed search of articles indexed for MEDLINE using the terms plaquelike or plaque-type syringoma yielded 16 cases in the literature.2-14 Of these, 6 were referred to or encountered in the MMS setting.8,9,11,12,14 Plaquelike syringoma can be solitary or multiple in presentation.6 It most commonly involves the head and neck but also can present on the trunk, arms, legs, and groin areas. The clinical size of plaquelike syringoma is variable, with the largest reported cases extending several centimeters in diameter.2,6 Similar to reported associations with conventional syringoma, the plaquelike subtype of syringoma has been reported in association with Down syndrome.13

Histopathologically, plaquelike syringoma shares features with MAC as well as desmoplastic trichoepithelioma and desmoplastic basal cell carcinoma. Plaquelike syringoma demonstrates broad proliferations of small tubules morphologically reminiscent of tadpoles confined within the dermis. Ducts typically are lined with 2 or 3 layers of small cuboidal cells. Microcystic adnexal carcinoma typically features asymmetric ductal structures lined with single cells extending from the dermis into the subcutis and even underlying muscle, cartilage, or bone.8 There are no reliable immunohistochemical stains to differentiate between these 2 entities; thus, the primary distinction lies in the depth of involvement. Desmoplastic trichoepithelioma is composed of narrow cords and nests of basaloid cells of follicular origin commonly admixed with small cornifying cysts appearing in the dermis.8 Colonizing Merkel cells positive for cytokeratin 20 often are present in desmoplastic trichoepithelioma and not in syringoma or MAC.15 Desmoplastic basal cell carcinoma demonstrates narrow strands of basaloid cells of follicular origin appearing in the dermis. Desmoplastic trichoepithelioma and desmoplastic basal cell carcinoma are each fundamentally differentiated from plaquelike syringoma in that proliferations of cords and nests are not of eccrine or apocrine origin.

Several cases of plaquelike syringoma have been challenging to distinguish from MAC in performing MMS.8,9,11 Underlying extension of this syringoma variant can be far-reaching, extending to several centimeters in size and involving multiple cosmetic subunits.6,11,14 Inadvertent overtreatment with multiple MMS stages can be avoided with careful recognition of the differentiating histopathologic features. Syringomatous lesions commonly are encountered in MMS and may even be present at the edge of other tumor types. Plaquelike syringoma has been reported as a coexistent entity with nodular basal cell carcinoma.12 Boos et al16 similarly reported the presence of deceptive ductal proliferations along the immediate peripheral margin of MAC, which prompted multiple re-excisions. Pursuit of permanent section analysis in these cases revealed the appearance of small syringomas, and a diagnosis of benign subclinical syringomatous proliferations was made, averting further intervention.16
Our case sheds light on the threat of commission bias in dermatologic surgery, which is the tendency for action rather than inaction.17 In this context, it is important to avoid the perspective that harm to the patient can only be prevented by active intervention. Cognitive bias has been increasingly recognized as a source of medical error, and methods to mitigate bias in medical practice have been well described.17 Microcystic adnexal carcinoma and plaquelike syringoma can be hard to differentiate especially initially, as demonstrated in our case, which particularly illustrates the importance of slowing down a surgical case at the appropriate time, considering and revisiting alternative diagnoses, implementing checklists, and seeking histopathologic collaboration with colleagues when necessary. Our attempted implementation of these principles, especially early collaboration with colleagues, led to intraoperative recognition of plaquelike syringoma within the first stage of MMS.
We seek to raise the index of suspicion for plaquelike syringoma among dermatologists and dermatologic surgeons, especially when syringomatous structures are limited to the superficial dermis. We encourage familiarity with the plaquelike syringoma entity as well as careful consideration of further investigation via scouting biopsies or permanent section analysis when other characteristic features of MAC are unclear or lacking. Adequate sampling as well as collaboration with a dermatopathologist in cases of suspected syringoma can help to reduce the susceptibility to commission bias and prevent histopathologic pitfalls and unwarranted surgical morbidity.
- Friedman SJ, Butler DF. Syringoma presenting as milia. J Am Acad Dermatol. 1987;16:310-314.
- Kikuchi I, Idemori M, Okazaki M. Plaque type syringoma. J Dermatol. 1979;6:329-331.
- Dekio S, Jidoi J. Submammary syringoma—report of a case. J Dermatol. 1988;15:351-352.
- Patrizi A, Neri I, Marzaduri S, et al. Syringoma: a review of twenty-nine cases. Acta Derm Venereol. 1998;78:460-462.
- Nguyen DB, Patterson JW, Wilson BB. Syringoma of the moustache area. J Am Acad Dermatol. 2003;49:337-339.
- Rongioletti F, Semino MT, Rebora A. Unilateral multiple plaque-like syringomas. Br J Dermatol. 1996;135:623-625.
- Chi HI. A case of unusual syringoma: unilateral linear distribution and plaque formation. J Dermatol. 1996;23:505-506.
- Suwatee P, McClelland MC, Huiras EE, et al. Plaque-type syringoma: two cases misdiagnosed as microcystic adnexal carcinoma. J Cutan Pathol. 2008;35:570-574.
- Wallace JS, Bond JS, Seidel GD, et al. An important mimicker: plaque-type syringoma mistakenly diagnosed as microcystic adnexal carcinoma. Dermatol Surg. 2014;40:810-812.
- Mitkov M, Balagula Y, Taube JM, et al. Plaque-like syringoma with involvement of deep reticular dermis. J Am Acad Dermatol. 2014;71:E206-E207.
- Schleich C, Ferringer T, Petrick M. Plaque type syringoma mimicking a microcystic adnexal carcinoma. J Am Acad Dermatol. 2016;74(suppl 1):AB287.
- Yang Y, Srivastava D. Plaque-type syringoma coexisting with basal cell carcinoma. Dermatol Surg. 2018;44:1464-1466.
- Motegi SI, Sekiguchi A, Fujiwara C, et al. Milia-like idiopathic calcinosis cutis and plaque-type syringoma in a girl with Down syndrome. J Dermatol. 2019;46:E136-E137.
- Clark M, Duprey C, Sutton A, et al. Plaque-type syringoma masquerading as microcystic adnexal carcinoma: review of the literature and description of a novel technique that emphasizes lesion architecture to help make the diagnosis. Am J Dermatopathol. 2019;41:E98-E101.
- Abesamis-Cubillan E, El-Shabrawi-Caelen L, LeBoit PE. Merkel cells and sclerosing epithelial neoplasms. Am J Dermatopathol. 2000;22:311-315.
- Boos MD, Elenitsas R, Seykora J, et al. Benign subclinical syringomatous proliferations adjacent to a microcystic adnexal carcinoma: a tumor mimic with significant patient implications. Am J Dermatopathol. 2014;36:174-178.
- O’Sullivan ED, Schofield SJ. Cognitive bias in clinical medicine. J R Coll Physicians Edinb. 2018;48:225-232.
- Friedman SJ, Butler DF. Syringoma presenting as milia. J Am Acad Dermatol. 1987;16:310-314.
- Kikuchi I, Idemori M, Okazaki M. Plaque type syringoma. J Dermatol. 1979;6:329-331.
- Dekio S, Jidoi J. Submammary syringoma—report of a case. J Dermatol. 1988;15:351-352.
- Patrizi A, Neri I, Marzaduri S, et al. Syringoma: a review of twenty-nine cases. Acta Derm Venereol. 1998;78:460-462.
- Nguyen DB, Patterson JW, Wilson BB. Syringoma of the moustache area. J Am Acad Dermatol. 2003;49:337-339.
- Rongioletti F, Semino MT, Rebora A. Unilateral multiple plaque-like syringomas. Br J Dermatol. 1996;135:623-625.
- Chi HI. A case of unusual syringoma: unilateral linear distribution and plaque formation. J Dermatol. 1996;23:505-506.
- Suwatee P, McClelland MC, Huiras EE, et al. Plaque-type syringoma: two cases misdiagnosed as microcystic adnexal carcinoma. J Cutan Pathol. 2008;35:570-574.
- Wallace JS, Bond JS, Seidel GD, et al. An important mimicker: plaque-type syringoma mistakenly diagnosed as microcystic adnexal carcinoma. Dermatol Surg. 2014;40:810-812.
- Mitkov M, Balagula Y, Taube JM, et al. Plaque-like syringoma with involvement of deep reticular dermis. J Am Acad Dermatol. 2014;71:E206-E207.
- Schleich C, Ferringer T, Petrick M. Plaque type syringoma mimicking a microcystic adnexal carcinoma. J Am Acad Dermatol. 2016;74(suppl 1):AB287.
- Yang Y, Srivastava D. Plaque-type syringoma coexisting with basal cell carcinoma. Dermatol Surg. 2018;44:1464-1466.
- Motegi SI, Sekiguchi A, Fujiwara C, et al. Milia-like idiopathic calcinosis cutis and plaque-type syringoma in a girl with Down syndrome. J Dermatol. 2019;46:E136-E137.
- Clark M, Duprey C, Sutton A, et al. Plaque-type syringoma masquerading as microcystic adnexal carcinoma: review of the literature and description of a novel technique that emphasizes lesion architecture to help make the diagnosis. Am J Dermatopathol. 2019;41:E98-E101.
- Abesamis-Cubillan E, El-Shabrawi-Caelen L, LeBoit PE. Merkel cells and sclerosing epithelial neoplasms. Am J Dermatopathol. 2000;22:311-315.
- Boos MD, Elenitsas R, Seykora J, et al. Benign subclinical syringomatous proliferations adjacent to a microcystic adnexal carcinoma: a tumor mimic with significant patient implications. Am J Dermatopathol. 2014;36:174-178.
- O’Sullivan ED, Schofield SJ. Cognitive bias in clinical medicine. J R Coll Physicians Edinb. 2018;48:225-232.
Practice Points
- Dermatologists should familiarize themselves with the plaquelike subtype of syringoma, which can histologically mimic the superficial portion of microcystic adnexal carcinoma (MAC).
- Careful recognition of plaquelike syringoma in the Mohs micrographic surgery setting may prevent unnecessary surgical morbidity.
- Further diagnostic investigation is warranted for superficial biopsies suggestive of MAC or when other characteristic features are lacking.
Blue Nodules on the Forearms in an Active-Duty Military Servicemember
The Diagnosis: Glomangiomyoma
A punch biopsy of the right forearm revealed a collection of vascular and smooth muscle components with small and spindled bland cells containing minimal eosinophilic cytoplasm (Figure 1), confirming the diagnosis of glomangiomyoma. Immunohistochemical stains also supported the diagnosis and were positive for smooth muscle actin, desmin, and CD34 (Figure 2). Magnetic resonance imaging from a prior attempt at treatment with sclerotherapy demonstrated scattered vascular malformations with no notable internal derangement. There was no improvement with sclerotherapy. Given the number and vascular nature of the lesions, a trial of pulsed dye laser (PDL) therapy was administered and tolerated by the patient. He subsequently moved to a new military duty station. On follow-up, he reported no noticeable clinical improvement in the lesions after PDL and opted not to continue with laser treatment.

Glomangiomyoma is a rare and benign glomus tumor variant that demonstrates differentiation into the smooth muscle and potentially can result in substantial complications.1 Glomus tumors generally are benign neoplasms of the glomus apparatus, and glomus cells function as thermoregulators in the reticular dermis.2 Glomus tumors comprise less than 2% of soft tissue neoplasms and generally are solitary nodules; only 10% of glomus tumors occur with multiple lesions, and among them, glomangiomyoma is the rarest subtype, presenting in only 15% of cases.2,3 The 3 main subtypes of glomus tumors are solid, glomangioma, and glomangiomyoma.4 Clinically, the lesions may present as small blue nodules with associated pain and cold or pressure sensitivity. Although there appears to be variation of the nomenclature depending on the source in the literature, glomangiomas are characterized by their predominant vascular malformations on biopsy. Glomangiomyomas are a subset of glomus tumors with distinct smooth muscle differentiation.4 Given their pathologic presentation, our patient’s lesions were most consistent with the diagnosis of glomangiomyoma.
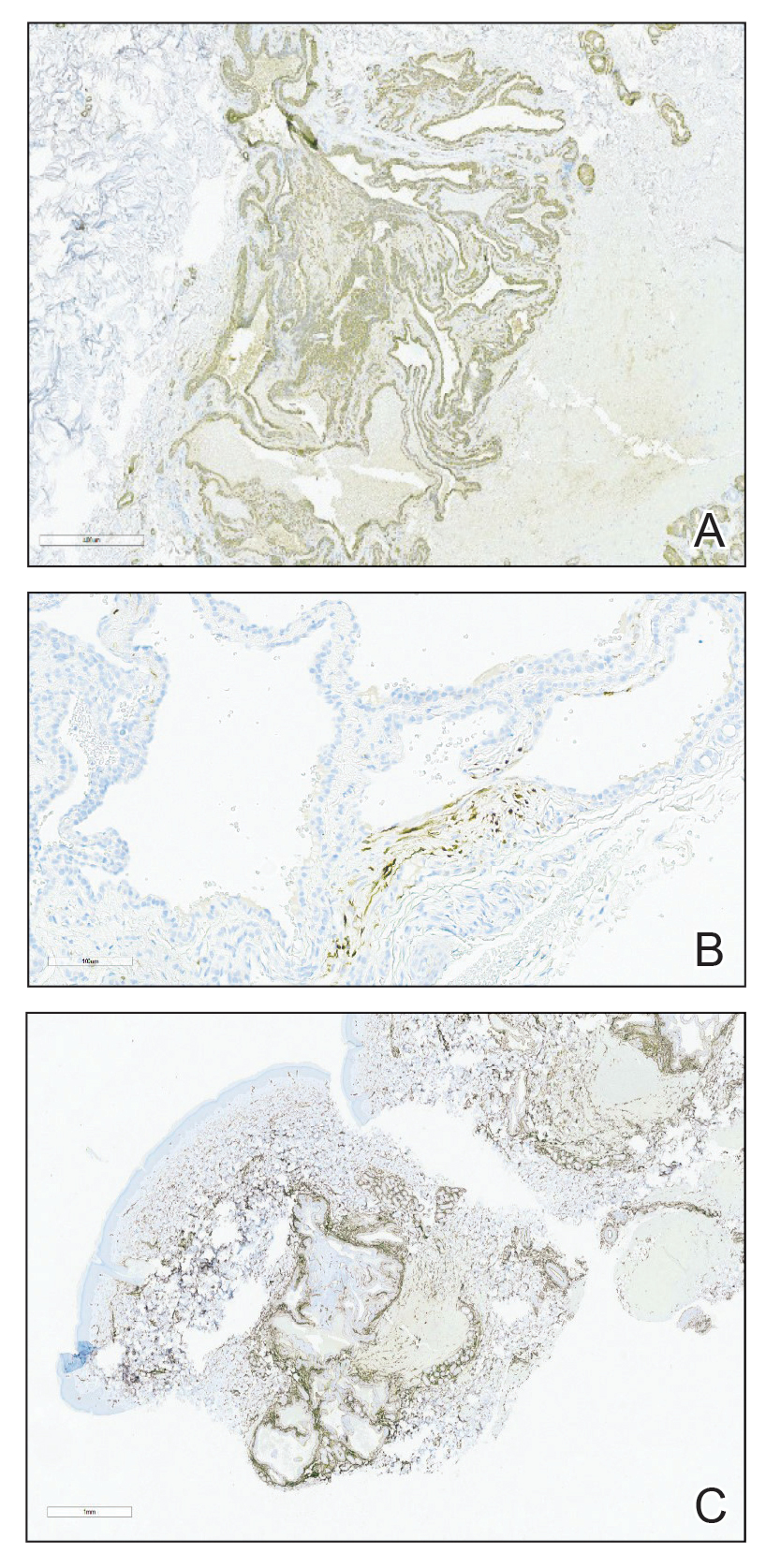
The small size of the lesions may result in difficulty establishing a clinical diagnosis, particularly if there is no hand involvement, where lesions most commonly occur.2 Therefore, histopathologic evaluation is essential and is the best initial step in evaluating glomangiomyomas.4 Biopsy is the most reliable means of confirming a diagnosis2,4,5; however, diagnostic imaging such as a computed tomography also should be performed if considering blue rubber bleb nevus syndrome due to the primary site of involvement. Surgical excision is the treatment of choice after confirming the diagnosis in most cases of symptomatic glomangiomyomas, particularly with painful lesions.6
Neurilemmomas (also known as schwannomas) are benign lesions that generally present as asymptomatic, soft, smooth nodules most often on the neck; however, they also may present on the flexor extremities or in internal organs. Although primarily asymptomatic, the tumors may be associated with pain and paresthesia as they enlarge and affect surrounding structures. Neurilemmomas may occur spontaneously or as part of a syndrome, such as neurofibromatosis type 2 or Carney complex.7
Hereditary hemorrhagic telangiectasia (formerly known as Osler-Weber-Rendu syndrome) is an autosomal-dominant disease that presents with arteriovenous malformations and telangiectases. Patients generally present in the third decade of life, with the main concern generally being epistaxis.8
Kaposi sarcoma is a viral infection secondary to human herpesvirus 8 that results in red-purple lesions commonly on mucocutaneous sites. Kaposi sarcoma can be AIDS associated and non-HIV associated. Although clinically indistinguishable, a few subtle histologic features can assist in differentiating the 2 etiologies. In addition to a potential history of immunodeficiency, evaluating for involvement of the lymphatic system, respiratory tract, or gastrointestinal tract can aid in differentiating this entity from glomus tumors.9
Leiomyomas are smooth muscle lesions divided into 3 subcategories: angioleiomyoma, piloleiomyoma, and genital leiomyoma. The clinical presentation and histopathology will vary depending on the subcategory. Although cutaneous leiomyomas are benign, further workup for piloleiomyoma may be required given the reported association with hereditary leiomyomatosis and renal cell cancer (Reed syndrome).10
Imaging can be helpful when the clinical diagnosis of a glomus tumor vs other painful neoplasms of the skin is unclear, such as in blue rubber bleb nevus syndrome, angioleiomyomas, neuromas, glomus tumors, leiomyomas, eccrine spiradenomas, congenital vascular malformations, schwannomas, or hemangiomas.4 Radiologic findings for glomus tumors may demonstrate cortical or cystic osseous defects. Magnetic resonance imaging and ultrasonography can help provide additional information on the lesion size and depth of involvement.1 Additionally, deeper glomangiomyomas have been associated with malignancy,2 potentially highlighting the benefit of early incorporation of imaging in the workup for this condition. Malignant transformation is rare and has been reported in less than 1% of cases.6
Treatment of glomus tumors predominantly is directed to the patient’s symptoms; asymptomatic lesions may be monitored.4 For symptomatic lesions, therapeutic options include wide local excision; sclerotherapy; and incorporation of various lasers, including Nd:YAG, CO2, and flashlamp tunable dye laser.4,5 One case report documented use of a PDL that successfully eliminated the pain associated with glomangiomyoma; however, the lesion in that report was not biopsy proven.11
Our case highlights the need to consider glomus tumors in patients presenting with multiple small nodules given the potential for misdiagnosis, impact on quality of life with associated psychological distress, and potential utility of incorporating PDL in treatment. Although our patient did not report clinical improvement in the appearance of the lesions with PDL therapy, additional treatment sessions may have helped,11 but he opted to discontinue. Follow-up for persistently symptomatic or changing lesions is necessary, given the minimal risk for malignant transformation.6
- Lee DY, Hwang SC, Jeong ST, et al. The value of diagnostic ultrasonography in the assessment of a glomus tumor of the subcutaneous layer of the forearm mimicking a hemangioma: a case report. J Med Case Rep. 2015;9:191. doi:10.1186/s13256-015-0672-y
- Li L, Bardsley V, Grainger A, et al. Extradigital glomangiomyoma of the forearm mimicking peripheral nerve sheath tumour and thrombosed varicose vein. BMJ Case Rep. 2021;14:E241221. doi: 10.1136 /bcr-2020-241221
- Calduch L, Monteagudo C, Martínez-Ruiz E, et al. Familial generalized multiple glomangiomyoma: report of a new family, with immunohistochemical and ultrastructural studies and review of the literature. Pediatr Dermatol. 2002;19:402-408. doi:10.1046/j.1525-1470.2002.00114.x
- Mohammadi O, Suarez M. Glomus cancer. StatPearls [Internet]. StatPearls Publishing; 2021.
- Maxey ML, Houghton CC, Mastriani KS, et al. Large prepatellar glomangioma: a case report [published online July 10, 2015]. Int J Surg Case Rep. 2015;14:80-84. doi:10.1016/j.ijscr.2015.07.002
- Brathwaite CD, Poppiti RJ Jr. Malignant glomus tumor. a case report of widespread metastases in a patient with multiple glomus body hamartomas. Am J Surg Pathol. 1996;20:233-238. doi:10.1097/00000478-199602000-00012
- Davis DD, Kane SM. Neurilemmoma. StatPearls [Internet]. StatPearls Publishing; 2022.
- Kühnel T, Wirsching K, Wohlgemuth W, et al. Hereditary hemorrhagic telangiectasia. Otolaryngol Clin North Am. 2018;51:237-254. doi:10.1016/j.otc.2017.09.017
- Radu O, Pantanowitz L. Kaposi sarcoma. Arch Pathol Lab Med. 2013;137:289-294. doi:10.5858/arpa.2012-0101-RS
- Bernett CN, Mammino JJ. Cutaneous leiomyomas. StatPearls [Internet]. StatPearls Publishing; 2022.
- Antony FC, Cliff S, Cowley N. Complete pain relief following treatment of a glomangiomyoma with the pulsed dye laser. Clin Exp Dermatol. 2003;28:617-619. doi:10.1046/j.1365-2230.2003.01403.x
The Diagnosis: Glomangiomyoma
A punch biopsy of the right forearm revealed a collection of vascular and smooth muscle components with small and spindled bland cells containing minimal eosinophilic cytoplasm (Figure 1), confirming the diagnosis of glomangiomyoma. Immunohistochemical stains also supported the diagnosis and were positive for smooth muscle actin, desmin, and CD34 (Figure 2). Magnetic resonance imaging from a prior attempt at treatment with sclerotherapy demonstrated scattered vascular malformations with no notable internal derangement. There was no improvement with sclerotherapy. Given the number and vascular nature of the lesions, a trial of pulsed dye laser (PDL) therapy was administered and tolerated by the patient. He subsequently moved to a new military duty station. On follow-up, he reported no noticeable clinical improvement in the lesions after PDL and opted not to continue with laser treatment.

Glomangiomyoma is a rare and benign glomus tumor variant that demonstrates differentiation into the smooth muscle and potentially can result in substantial complications.1 Glomus tumors generally are benign neoplasms of the glomus apparatus, and glomus cells function as thermoregulators in the reticular dermis.2 Glomus tumors comprise less than 2% of soft tissue neoplasms and generally are solitary nodules; only 10% of glomus tumors occur with multiple lesions, and among them, glomangiomyoma is the rarest subtype, presenting in only 15% of cases.2,3 The 3 main subtypes of glomus tumors are solid, glomangioma, and glomangiomyoma.4 Clinically, the lesions may present as small blue nodules with associated pain and cold or pressure sensitivity. Although there appears to be variation of the nomenclature depending on the source in the literature, glomangiomas are characterized by their predominant vascular malformations on biopsy. Glomangiomyomas are a subset of glomus tumors with distinct smooth muscle differentiation.4 Given their pathologic presentation, our patient’s lesions were most consistent with the diagnosis of glomangiomyoma.

The small size of the lesions may result in difficulty establishing a clinical diagnosis, particularly if there is no hand involvement, where lesions most commonly occur.2 Therefore, histopathologic evaluation is essential and is the best initial step in evaluating glomangiomyomas.4 Biopsy is the most reliable means of confirming a diagnosis2,4,5; however, diagnostic imaging such as a computed tomography also should be performed if considering blue rubber bleb nevus syndrome due to the primary site of involvement. Surgical excision is the treatment of choice after confirming the diagnosis in most cases of symptomatic glomangiomyomas, particularly with painful lesions.6
Neurilemmomas (also known as schwannomas) are benign lesions that generally present as asymptomatic, soft, smooth nodules most often on the neck; however, they also may present on the flexor extremities or in internal organs. Although primarily asymptomatic, the tumors may be associated with pain and paresthesia as they enlarge and affect surrounding structures. Neurilemmomas may occur spontaneously or as part of a syndrome, such as neurofibromatosis type 2 or Carney complex.7
Hereditary hemorrhagic telangiectasia (formerly known as Osler-Weber-Rendu syndrome) is an autosomal-dominant disease that presents with arteriovenous malformations and telangiectases. Patients generally present in the third decade of life, with the main concern generally being epistaxis.8
Kaposi sarcoma is a viral infection secondary to human herpesvirus 8 that results in red-purple lesions commonly on mucocutaneous sites. Kaposi sarcoma can be AIDS associated and non-HIV associated. Although clinically indistinguishable, a few subtle histologic features can assist in differentiating the 2 etiologies. In addition to a potential history of immunodeficiency, evaluating for involvement of the lymphatic system, respiratory tract, or gastrointestinal tract can aid in differentiating this entity from glomus tumors.9
Leiomyomas are smooth muscle lesions divided into 3 subcategories: angioleiomyoma, piloleiomyoma, and genital leiomyoma. The clinical presentation and histopathology will vary depending on the subcategory. Although cutaneous leiomyomas are benign, further workup for piloleiomyoma may be required given the reported association with hereditary leiomyomatosis and renal cell cancer (Reed syndrome).10
Imaging can be helpful when the clinical diagnosis of a glomus tumor vs other painful neoplasms of the skin is unclear, such as in blue rubber bleb nevus syndrome, angioleiomyomas, neuromas, glomus tumors, leiomyomas, eccrine spiradenomas, congenital vascular malformations, schwannomas, or hemangiomas.4 Radiologic findings for glomus tumors may demonstrate cortical or cystic osseous defects. Magnetic resonance imaging and ultrasonography can help provide additional information on the lesion size and depth of involvement.1 Additionally, deeper glomangiomyomas have been associated with malignancy,2 potentially highlighting the benefit of early incorporation of imaging in the workup for this condition. Malignant transformation is rare and has been reported in less than 1% of cases.6
Treatment of glomus tumors predominantly is directed to the patient’s symptoms; asymptomatic lesions may be monitored.4 For symptomatic lesions, therapeutic options include wide local excision; sclerotherapy; and incorporation of various lasers, including Nd:YAG, CO2, and flashlamp tunable dye laser.4,5 One case report documented use of a PDL that successfully eliminated the pain associated with glomangiomyoma; however, the lesion in that report was not biopsy proven.11
Our case highlights the need to consider glomus tumors in patients presenting with multiple small nodules given the potential for misdiagnosis, impact on quality of life with associated psychological distress, and potential utility of incorporating PDL in treatment. Although our patient did not report clinical improvement in the appearance of the lesions with PDL therapy, additional treatment sessions may have helped,11 but he opted to discontinue. Follow-up for persistently symptomatic or changing lesions is necessary, given the minimal risk for malignant transformation.6
The Diagnosis: Glomangiomyoma
A punch biopsy of the right forearm revealed a collection of vascular and smooth muscle components with small and spindled bland cells containing minimal eosinophilic cytoplasm (Figure 1), confirming the diagnosis of glomangiomyoma. Immunohistochemical stains also supported the diagnosis and were positive for smooth muscle actin, desmin, and CD34 (Figure 2). Magnetic resonance imaging from a prior attempt at treatment with sclerotherapy demonstrated scattered vascular malformations with no notable internal derangement. There was no improvement with sclerotherapy. Given the number and vascular nature of the lesions, a trial of pulsed dye laser (PDL) therapy was administered and tolerated by the patient. He subsequently moved to a new military duty station. On follow-up, he reported no noticeable clinical improvement in the lesions after PDL and opted not to continue with laser treatment.

Glomangiomyoma is a rare and benign glomus tumor variant that demonstrates differentiation into the smooth muscle and potentially can result in substantial complications.1 Glomus tumors generally are benign neoplasms of the glomus apparatus, and glomus cells function as thermoregulators in the reticular dermis.2 Glomus tumors comprise less than 2% of soft tissue neoplasms and generally are solitary nodules; only 10% of glomus tumors occur with multiple lesions, and among them, glomangiomyoma is the rarest subtype, presenting in only 15% of cases.2,3 The 3 main subtypes of glomus tumors are solid, glomangioma, and glomangiomyoma.4 Clinically, the lesions may present as small blue nodules with associated pain and cold or pressure sensitivity. Although there appears to be variation of the nomenclature depending on the source in the literature, glomangiomas are characterized by their predominant vascular malformations on biopsy. Glomangiomyomas are a subset of glomus tumors with distinct smooth muscle differentiation.4 Given their pathologic presentation, our patient’s lesions were most consistent with the diagnosis of glomangiomyoma.

The small size of the lesions may result in difficulty establishing a clinical diagnosis, particularly if there is no hand involvement, where lesions most commonly occur.2 Therefore, histopathologic evaluation is essential and is the best initial step in evaluating glomangiomyomas.4 Biopsy is the most reliable means of confirming a diagnosis2,4,5; however, diagnostic imaging such as a computed tomography also should be performed if considering blue rubber bleb nevus syndrome due to the primary site of involvement. Surgical excision is the treatment of choice after confirming the diagnosis in most cases of symptomatic glomangiomyomas, particularly with painful lesions.6
Neurilemmomas (also known as schwannomas) are benign lesions that generally present as asymptomatic, soft, smooth nodules most often on the neck; however, they also may present on the flexor extremities or in internal organs. Although primarily asymptomatic, the tumors may be associated with pain and paresthesia as they enlarge and affect surrounding structures. Neurilemmomas may occur spontaneously or as part of a syndrome, such as neurofibromatosis type 2 or Carney complex.7
Hereditary hemorrhagic telangiectasia (formerly known as Osler-Weber-Rendu syndrome) is an autosomal-dominant disease that presents with arteriovenous malformations and telangiectases. Patients generally present in the third decade of life, with the main concern generally being epistaxis.8
Kaposi sarcoma is a viral infection secondary to human herpesvirus 8 that results in red-purple lesions commonly on mucocutaneous sites. Kaposi sarcoma can be AIDS associated and non-HIV associated. Although clinically indistinguishable, a few subtle histologic features can assist in differentiating the 2 etiologies. In addition to a potential history of immunodeficiency, evaluating for involvement of the lymphatic system, respiratory tract, or gastrointestinal tract can aid in differentiating this entity from glomus tumors.9
Leiomyomas are smooth muscle lesions divided into 3 subcategories: angioleiomyoma, piloleiomyoma, and genital leiomyoma. The clinical presentation and histopathology will vary depending on the subcategory. Although cutaneous leiomyomas are benign, further workup for piloleiomyoma may be required given the reported association with hereditary leiomyomatosis and renal cell cancer (Reed syndrome).10
Imaging can be helpful when the clinical diagnosis of a glomus tumor vs other painful neoplasms of the skin is unclear, such as in blue rubber bleb nevus syndrome, angioleiomyomas, neuromas, glomus tumors, leiomyomas, eccrine spiradenomas, congenital vascular malformations, schwannomas, or hemangiomas.4 Radiologic findings for glomus tumors may demonstrate cortical or cystic osseous defects. Magnetic resonance imaging and ultrasonography can help provide additional information on the lesion size and depth of involvement.1 Additionally, deeper glomangiomyomas have been associated with malignancy,2 potentially highlighting the benefit of early incorporation of imaging in the workup for this condition. Malignant transformation is rare and has been reported in less than 1% of cases.6
Treatment of glomus tumors predominantly is directed to the patient’s symptoms; asymptomatic lesions may be monitored.4 For symptomatic lesions, therapeutic options include wide local excision; sclerotherapy; and incorporation of various lasers, including Nd:YAG, CO2, and flashlamp tunable dye laser.4,5 One case report documented use of a PDL that successfully eliminated the pain associated with glomangiomyoma; however, the lesion in that report was not biopsy proven.11
Our case highlights the need to consider glomus tumors in patients presenting with multiple small nodules given the potential for misdiagnosis, impact on quality of life with associated psychological distress, and potential utility of incorporating PDL in treatment. Although our patient did not report clinical improvement in the appearance of the lesions with PDL therapy, additional treatment sessions may have helped,11 but he opted to discontinue. Follow-up for persistently symptomatic or changing lesions is necessary, given the minimal risk for malignant transformation.6
- Lee DY, Hwang SC, Jeong ST, et al. The value of diagnostic ultrasonography in the assessment of a glomus tumor of the subcutaneous layer of the forearm mimicking a hemangioma: a case report. J Med Case Rep. 2015;9:191. doi:10.1186/s13256-015-0672-y
- Li L, Bardsley V, Grainger A, et al. Extradigital glomangiomyoma of the forearm mimicking peripheral nerve sheath tumour and thrombosed varicose vein. BMJ Case Rep. 2021;14:E241221. doi: 10.1136 /bcr-2020-241221
- Calduch L, Monteagudo C, Martínez-Ruiz E, et al. Familial generalized multiple glomangiomyoma: report of a new family, with immunohistochemical and ultrastructural studies and review of the literature. Pediatr Dermatol. 2002;19:402-408. doi:10.1046/j.1525-1470.2002.00114.x
- Mohammadi O, Suarez M. Glomus cancer. StatPearls [Internet]. StatPearls Publishing; 2021.
- Maxey ML, Houghton CC, Mastriani KS, et al. Large prepatellar glomangioma: a case report [published online July 10, 2015]. Int J Surg Case Rep. 2015;14:80-84. doi:10.1016/j.ijscr.2015.07.002
- Brathwaite CD, Poppiti RJ Jr. Malignant glomus tumor. a case report of widespread metastases in a patient with multiple glomus body hamartomas. Am J Surg Pathol. 1996;20:233-238. doi:10.1097/00000478-199602000-00012
- Davis DD, Kane SM. Neurilemmoma. StatPearls [Internet]. StatPearls Publishing; 2022.
- Kühnel T, Wirsching K, Wohlgemuth W, et al. Hereditary hemorrhagic telangiectasia. Otolaryngol Clin North Am. 2018;51:237-254. doi:10.1016/j.otc.2017.09.017
- Radu O, Pantanowitz L. Kaposi sarcoma. Arch Pathol Lab Med. 2013;137:289-294. doi:10.5858/arpa.2012-0101-RS
- Bernett CN, Mammino JJ. Cutaneous leiomyomas. StatPearls [Internet]. StatPearls Publishing; 2022.
- Antony FC, Cliff S, Cowley N. Complete pain relief following treatment of a glomangiomyoma with the pulsed dye laser. Clin Exp Dermatol. 2003;28:617-619. doi:10.1046/j.1365-2230.2003.01403.x
- Lee DY, Hwang SC, Jeong ST, et al. The value of diagnostic ultrasonography in the assessment of a glomus tumor of the subcutaneous layer of the forearm mimicking a hemangioma: a case report. J Med Case Rep. 2015;9:191. doi:10.1186/s13256-015-0672-y
- Li L, Bardsley V, Grainger A, et al. Extradigital glomangiomyoma of the forearm mimicking peripheral nerve sheath tumour and thrombosed varicose vein. BMJ Case Rep. 2021;14:E241221. doi: 10.1136 /bcr-2020-241221
- Calduch L, Monteagudo C, Martínez-Ruiz E, et al. Familial generalized multiple glomangiomyoma: report of a new family, with immunohistochemical and ultrastructural studies and review of the literature. Pediatr Dermatol. 2002;19:402-408. doi:10.1046/j.1525-1470.2002.00114.x
- Mohammadi O, Suarez M. Glomus cancer. StatPearls [Internet]. StatPearls Publishing; 2021.
- Maxey ML, Houghton CC, Mastriani KS, et al. Large prepatellar glomangioma: a case report [published online July 10, 2015]. Int J Surg Case Rep. 2015;14:80-84. doi:10.1016/j.ijscr.2015.07.002
- Brathwaite CD, Poppiti RJ Jr. Malignant glomus tumor. a case report of widespread metastases in a patient with multiple glomus body hamartomas. Am J Surg Pathol. 1996;20:233-238. doi:10.1097/00000478-199602000-00012
- Davis DD, Kane SM. Neurilemmoma. StatPearls [Internet]. StatPearls Publishing; 2022.
- Kühnel T, Wirsching K, Wohlgemuth W, et al. Hereditary hemorrhagic telangiectasia. Otolaryngol Clin North Am. 2018;51:237-254. doi:10.1016/j.otc.2017.09.017
- Radu O, Pantanowitz L. Kaposi sarcoma. Arch Pathol Lab Med. 2013;137:289-294. doi:10.5858/arpa.2012-0101-RS
- Bernett CN, Mammino JJ. Cutaneous leiomyomas. StatPearls [Internet]. StatPearls Publishing; 2022.
- Antony FC, Cliff S, Cowley N. Complete pain relief following treatment of a glomangiomyoma with the pulsed dye laser. Clin Exp Dermatol. 2003;28:617-619. doi:10.1046/j.1365-2230.2003.01403.x
A 31-year-old active-duty military servicemember presented to the dermatology clinic for evaluation of 0.3- to 2-cm, tender, blue nodules on the wrists and forearms. The lesions first appeared on the right volar wrist secondary to a presumed injury sustained approximately 10 years prior to presentation and spread to the proximal forearm as well as the left wrist and forearm. He denied fevers, chills, chest pain, hematochezia, hematuria, or other skin findings. Physical examination revealed blue-violaceous, firm nodules on the right volar wrist and forearm that were tender to palpation. Blue-violaceous, papulonodular lesions on the left volar wrist and dorsal hand were not tender to palpation. A punch biopsy was performed.
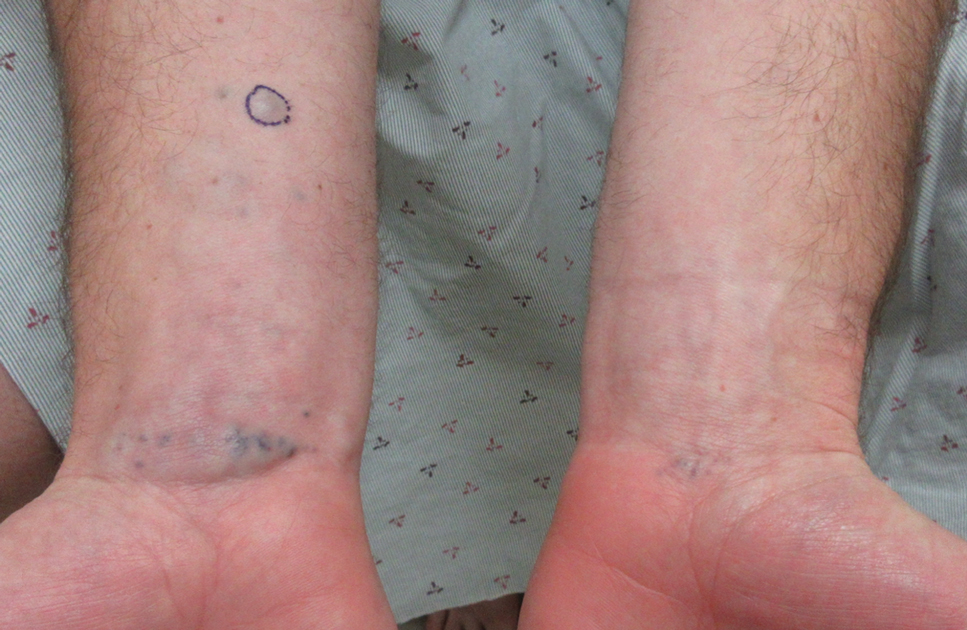
Cold snare polypectomy underused despite recommendations
, shows new research presented this week in Vancouver at the annual meeting of the American College of Gastroenterology.
Polypectomy is a key part of colorectal cancer prevention, but endoscopists’ choice of polypectomy is a major factor in quality, and the characteristics of polypectomies in clinical practice are highly variable, said Seth D. Crockett, MD, of Oregon Health & Science University, Portland, in a presentation at the meeting.
Cold snare polypectomy is preferred for the removal of polyps less than 1 cm because of a high complete resection rate and a strong safety profile, compared to forceps and hot snares, which tend to be associated with high incomplete resection rates, inadequate histopathologic specimens, and/or complication rates. The adherence of endoscopists to the recommendations was not known until now, Dr. Crockett said.
This was a cross-sectional study of 1,589,499 colonoscopies that were conducted between 2019 and 2022 in patients (aged 40-80 years) who underwent a screening or surveillance colonoscopy in which at least one small polyp of less than 1 cm was removed. The final analysis included 3,082 endoscopists. Colonoscopies in which larger polyps were detected, or there was a confirmed case of cancer, were not included.
The mean endoscopist cold snare polypectomy rate (CSPR) was 51.2%, which was “lower than expected based on current guideline recommendations,” Dr. Crockett said.
Higher cold snare polypectomy rates were more common among specialists with training in gastroenterology, and more common among those who practiced in the Midwest (69%), as compared with practitioners in the Northeast who, at 40%, had the lowest rate. Colonoscopy volume, adenoma detection rate (ADR), serrated polyp detection rate (SDR), and cecal intubation rate (CIR), were all associated with a higher CSPR.
CSPR was more than 30% higher for endoscopists with an adenoma detection rate (ADR) of greater than 35%, compared with those with an ADR of less than 25% (58% vs. 27%, respectively; P < .0001). Lower usage rates among endoscopists with low ADRs could compound the problem of interval cancer if polyps are missed, Dr. Crockett said. Endoscopist serrated polyp detection rates of 7% of higher, cecal intubation rates of 95% or higher, and mean withdrawal times greater than 9 minutes were significantly associated with higher CSPR (P < .0001 for all).
The findings suggest a correlation between higher cold snare usage and improved quality metrics, such as adenoma detection rate and cecal intubation rate, said Jonathan A. Leighton, MD, of the Mayo Clinic, Scottsdale, Ariz., in an interview.
“I would agree with the authors that much of the focus on colonoscopy quality has been directed toward polyp detection, and little on the quality of polyp resection, which can be difficult to measure,” he said. “Their results suggest that cold snare polypectomy for removal of small polyps is currently underutilized, but as with any polypectomy, it is important that all of the dysplastic tissue is removed using good technique.”
The results were strengthened by the large sample size and high fidelity of measurements of polyp size, polypectomy tools, and quality measures. But more research is needed to determine the impact of polypectomy technique on outcomes of colonoscopy efficacy and safety. In terms of limitations, small polyps carry a relatively low risk of recurrence, and the associations between an endoscopist’s polypectomy practice and polyp recurrence, interval cancer, and adverse events were not examined, Dr. Crockett said.
The study was supported by a grant from the ACG. Dr. Crockett disclosed relationships with Carelon, Exact Sciences, Freenome, and Guardant.
, shows new research presented this week in Vancouver at the annual meeting of the American College of Gastroenterology.
Polypectomy is a key part of colorectal cancer prevention, but endoscopists’ choice of polypectomy is a major factor in quality, and the characteristics of polypectomies in clinical practice are highly variable, said Seth D. Crockett, MD, of Oregon Health & Science University, Portland, in a presentation at the meeting.
Cold snare polypectomy is preferred for the removal of polyps less than 1 cm because of a high complete resection rate and a strong safety profile, compared to forceps and hot snares, which tend to be associated with high incomplete resection rates, inadequate histopathologic specimens, and/or complication rates. The adherence of endoscopists to the recommendations was not known until now, Dr. Crockett said.
This was a cross-sectional study of 1,589,499 colonoscopies that were conducted between 2019 and 2022 in patients (aged 40-80 years) who underwent a screening or surveillance colonoscopy in which at least one small polyp of less than 1 cm was removed. The final analysis included 3,082 endoscopists. Colonoscopies in which larger polyps were detected, or there was a confirmed case of cancer, were not included.
The mean endoscopist cold snare polypectomy rate (CSPR) was 51.2%, which was “lower than expected based on current guideline recommendations,” Dr. Crockett said.
Higher cold snare polypectomy rates were more common among specialists with training in gastroenterology, and more common among those who practiced in the Midwest (69%), as compared with practitioners in the Northeast who, at 40%, had the lowest rate. Colonoscopy volume, adenoma detection rate (ADR), serrated polyp detection rate (SDR), and cecal intubation rate (CIR), were all associated with a higher CSPR.
CSPR was more than 30% higher for endoscopists with an adenoma detection rate (ADR) of greater than 35%, compared with those with an ADR of less than 25% (58% vs. 27%, respectively; P < .0001). Lower usage rates among endoscopists with low ADRs could compound the problem of interval cancer if polyps are missed, Dr. Crockett said. Endoscopist serrated polyp detection rates of 7% of higher, cecal intubation rates of 95% or higher, and mean withdrawal times greater than 9 minutes were significantly associated with higher CSPR (P < .0001 for all).
The findings suggest a correlation between higher cold snare usage and improved quality metrics, such as adenoma detection rate and cecal intubation rate, said Jonathan A. Leighton, MD, of the Mayo Clinic, Scottsdale, Ariz., in an interview.
“I would agree with the authors that much of the focus on colonoscopy quality has been directed toward polyp detection, and little on the quality of polyp resection, which can be difficult to measure,” he said. “Their results suggest that cold snare polypectomy for removal of small polyps is currently underutilized, but as with any polypectomy, it is important that all of the dysplastic tissue is removed using good technique.”
The results were strengthened by the large sample size and high fidelity of measurements of polyp size, polypectomy tools, and quality measures. But more research is needed to determine the impact of polypectomy technique on outcomes of colonoscopy efficacy and safety. In terms of limitations, small polyps carry a relatively low risk of recurrence, and the associations between an endoscopist’s polypectomy practice and polyp recurrence, interval cancer, and adverse events were not examined, Dr. Crockett said.
The study was supported by a grant from the ACG. Dr. Crockett disclosed relationships with Carelon, Exact Sciences, Freenome, and Guardant.
, shows new research presented this week in Vancouver at the annual meeting of the American College of Gastroenterology.
Polypectomy is a key part of colorectal cancer prevention, but endoscopists’ choice of polypectomy is a major factor in quality, and the characteristics of polypectomies in clinical practice are highly variable, said Seth D. Crockett, MD, of Oregon Health & Science University, Portland, in a presentation at the meeting.
Cold snare polypectomy is preferred for the removal of polyps less than 1 cm because of a high complete resection rate and a strong safety profile, compared to forceps and hot snares, which tend to be associated with high incomplete resection rates, inadequate histopathologic specimens, and/or complication rates. The adherence of endoscopists to the recommendations was not known until now, Dr. Crockett said.
This was a cross-sectional study of 1,589,499 colonoscopies that were conducted between 2019 and 2022 in patients (aged 40-80 years) who underwent a screening or surveillance colonoscopy in which at least one small polyp of less than 1 cm was removed. The final analysis included 3,082 endoscopists. Colonoscopies in which larger polyps were detected, or there was a confirmed case of cancer, were not included.
The mean endoscopist cold snare polypectomy rate (CSPR) was 51.2%, which was “lower than expected based on current guideline recommendations,” Dr. Crockett said.
Higher cold snare polypectomy rates were more common among specialists with training in gastroenterology, and more common among those who practiced in the Midwest (69%), as compared with practitioners in the Northeast who, at 40%, had the lowest rate. Colonoscopy volume, adenoma detection rate (ADR), serrated polyp detection rate (SDR), and cecal intubation rate (CIR), were all associated with a higher CSPR.
CSPR was more than 30% higher for endoscopists with an adenoma detection rate (ADR) of greater than 35%, compared with those with an ADR of less than 25% (58% vs. 27%, respectively; P < .0001). Lower usage rates among endoscopists with low ADRs could compound the problem of interval cancer if polyps are missed, Dr. Crockett said. Endoscopist serrated polyp detection rates of 7% of higher, cecal intubation rates of 95% or higher, and mean withdrawal times greater than 9 minutes were significantly associated with higher CSPR (P < .0001 for all).
The findings suggest a correlation between higher cold snare usage and improved quality metrics, such as adenoma detection rate and cecal intubation rate, said Jonathan A. Leighton, MD, of the Mayo Clinic, Scottsdale, Ariz., in an interview.
“I would agree with the authors that much of the focus on colonoscopy quality has been directed toward polyp detection, and little on the quality of polyp resection, which can be difficult to measure,” he said. “Their results suggest that cold snare polypectomy for removal of small polyps is currently underutilized, but as with any polypectomy, it is important that all of the dysplastic tissue is removed using good technique.”
The results were strengthened by the large sample size and high fidelity of measurements of polyp size, polypectomy tools, and quality measures. But more research is needed to determine the impact of polypectomy technique on outcomes of colonoscopy efficacy and safety. In terms of limitations, small polyps carry a relatively low risk of recurrence, and the associations between an endoscopist’s polypectomy practice and polyp recurrence, interval cancer, and adverse events were not examined, Dr. Crockett said.
The study was supported by a grant from the ACG. Dr. Crockett disclosed relationships with Carelon, Exact Sciences, Freenome, and Guardant.
FROM ACG 2023
FDA approves subcutaneous infliximab for IBD
Infliximab-dyyb is a subcutaneous formulation of Celltrion’s infliximab. The FDA approval provides an alternative administration option for delivering the drug, which blocks the action of tumor necrosis factor alpha.
The new formulation was approved based on phase 3 pivotal trials that evaluated the safety and efficacy of infliximab-dyyb as maintenance therapy in patients with moderately to severely active UC (LIBERTY-UC) and CD (LIBERTY-CD).
In both 54-week trials, infliximab-dyyb demonstrated superiority to placebo in the primary endpoints of clinical remission (UC and CD) and endoscopic response (CD) when given as maintenance therapy after induction therapy with IV infliximab.
The overall safety profile of infliximab-dyyb was similar to that of the placebo during the maintenance period in both studies, with no new safety signals seen.
In the randomized, placebo-controlled, double-blind LIBERTY-UC study, 438 patients with moderately to severely active UC after induction therapy with IV infliximab were randomly assigned at week 10. The rate of clinical remission at week 54 was significantly greater with infliximab-dyyb (43.2%), compared with placebo (20.8%).
The most common adverse events were COVID-19, anemia, arthralgia, injection site reaction, increased alanine aminotransferase, and abdominal pain.
In the similarly designed LIBERTY-CD study, 343 patients with moderately to severely active CD after induction therapy were randomly assigned at week 10. At week 54, the clinical remission rate was greater with infliximab-dyyb (62.3%) than with placebo (32.1%).
In parallel, the endoscopic response rate at week 54 was also greater in the infliximab-dyyb arm than in the placebo arm (51.1% vs. 17.9%, respectively).
The safety profile during the maintenance phase was generally comparable between the two trial arms. The most common adverse events were COVID-19, upper respiratory tract infection, headache, injection site reaction, diarrhea, increased alanine aminotransferase, increased blood creatine phosphokinase, neutropenia, hypertension, urinary tract infection, dizziness, and leukopenia.
Full prescribing information is available online.
“As someone dedicated to improving the lives of patients with IBD, I am excited to see data supporting the efficacy and safety of a new formulation offering convenience and improved access to a well-known and proven drug,” Andres Yarur, MD, of Cedars-Sinai Medical Center, Los Angeles, said in a news release.
The data “validate a convenient treatment option that could allow more patients in the United States to have greater control of their disease management,” added Jean-Frederic Colombel, MD, of Icahn School of Medicine at Mount Sinai, New York.
A version of this article first appeared on Medscape.com.
Infliximab-dyyb is a subcutaneous formulation of Celltrion’s infliximab. The FDA approval provides an alternative administration option for delivering the drug, which blocks the action of tumor necrosis factor alpha.
The new formulation was approved based on phase 3 pivotal trials that evaluated the safety and efficacy of infliximab-dyyb as maintenance therapy in patients with moderately to severely active UC (LIBERTY-UC) and CD (LIBERTY-CD).
In both 54-week trials, infliximab-dyyb demonstrated superiority to placebo in the primary endpoints of clinical remission (UC and CD) and endoscopic response (CD) when given as maintenance therapy after induction therapy with IV infliximab.
The overall safety profile of infliximab-dyyb was similar to that of the placebo during the maintenance period in both studies, with no new safety signals seen.
In the randomized, placebo-controlled, double-blind LIBERTY-UC study, 438 patients with moderately to severely active UC after induction therapy with IV infliximab were randomly assigned at week 10. The rate of clinical remission at week 54 was significantly greater with infliximab-dyyb (43.2%), compared with placebo (20.8%).
The most common adverse events were COVID-19, anemia, arthralgia, injection site reaction, increased alanine aminotransferase, and abdominal pain.
In the similarly designed LIBERTY-CD study, 343 patients with moderately to severely active CD after induction therapy were randomly assigned at week 10. At week 54, the clinical remission rate was greater with infliximab-dyyb (62.3%) than with placebo (32.1%).
In parallel, the endoscopic response rate at week 54 was also greater in the infliximab-dyyb arm than in the placebo arm (51.1% vs. 17.9%, respectively).
The safety profile during the maintenance phase was generally comparable between the two trial arms. The most common adverse events were COVID-19, upper respiratory tract infection, headache, injection site reaction, diarrhea, increased alanine aminotransferase, increased blood creatine phosphokinase, neutropenia, hypertension, urinary tract infection, dizziness, and leukopenia.
Full prescribing information is available online.
“As someone dedicated to improving the lives of patients with IBD, I am excited to see data supporting the efficacy and safety of a new formulation offering convenience and improved access to a well-known and proven drug,” Andres Yarur, MD, of Cedars-Sinai Medical Center, Los Angeles, said in a news release.
The data “validate a convenient treatment option that could allow more patients in the United States to have greater control of their disease management,” added Jean-Frederic Colombel, MD, of Icahn School of Medicine at Mount Sinai, New York.
A version of this article first appeared on Medscape.com.
Infliximab-dyyb is a subcutaneous formulation of Celltrion’s infliximab. The FDA approval provides an alternative administration option for delivering the drug, which blocks the action of tumor necrosis factor alpha.
The new formulation was approved based on phase 3 pivotal trials that evaluated the safety and efficacy of infliximab-dyyb as maintenance therapy in patients with moderately to severely active UC (LIBERTY-UC) and CD (LIBERTY-CD).
In both 54-week trials, infliximab-dyyb demonstrated superiority to placebo in the primary endpoints of clinical remission (UC and CD) and endoscopic response (CD) when given as maintenance therapy after induction therapy with IV infliximab.
The overall safety profile of infliximab-dyyb was similar to that of the placebo during the maintenance period in both studies, with no new safety signals seen.
In the randomized, placebo-controlled, double-blind LIBERTY-UC study, 438 patients with moderately to severely active UC after induction therapy with IV infliximab were randomly assigned at week 10. The rate of clinical remission at week 54 was significantly greater with infliximab-dyyb (43.2%), compared with placebo (20.8%).
The most common adverse events were COVID-19, anemia, arthralgia, injection site reaction, increased alanine aminotransferase, and abdominal pain.
In the similarly designed LIBERTY-CD study, 343 patients with moderately to severely active CD after induction therapy were randomly assigned at week 10. At week 54, the clinical remission rate was greater with infliximab-dyyb (62.3%) than with placebo (32.1%).
In parallel, the endoscopic response rate at week 54 was also greater in the infliximab-dyyb arm than in the placebo arm (51.1% vs. 17.9%, respectively).
The safety profile during the maintenance phase was generally comparable between the two trial arms. The most common adverse events were COVID-19, upper respiratory tract infection, headache, injection site reaction, diarrhea, increased alanine aminotransferase, increased blood creatine phosphokinase, neutropenia, hypertension, urinary tract infection, dizziness, and leukopenia.
Full prescribing information is available online.
“As someone dedicated to improving the lives of patients with IBD, I am excited to see data supporting the efficacy and safety of a new formulation offering convenience and improved access to a well-known and proven drug,” Andres Yarur, MD, of Cedars-Sinai Medical Center, Los Angeles, said in a news release.
The data “validate a convenient treatment option that could allow more patients in the United States to have greater control of their disease management,” added Jean-Frederic Colombel, MD, of Icahn School of Medicine at Mount Sinai, New York.
A version of this article first appeared on Medscape.com.