User login
Twice-daily tofacitinib induces ulcerative colitis remission
A 10-mg dose of tofacitinib twice daily was significantly more effective than placebo for inducing remission in ulcerative colitis patients, based on data from a group of three randomized trials totaling approximately 1,500 adults. The findings were published online May 3 in the New England Journal of Medicine (2017;376:1723-36).
The series of OCTAVE trials (Oral Clinical Trials for Tofacitinib in Ulcerative Colitis) included adults with moderately to severely active ulcerative colitis (UC). Patients were randomized to 10 mg of tofacitinib, 5 mg tofacitinib, or placebo. The studies were conducted over a 4-year period, at 144 sites for OCTAVE 1, 169 sites for OCTAVE 2, and 297 sites for OCTAVE Sustain.
In both OCTAVE 1 and OCTAVE 2, the remission rates at 8 weeks were significantly higher in the 10-mg tofacitinib groups, compared with the placebo groups (18.5% vs. 8.2%, respectively; 16.6% vs. 3.6%, respectively). The rate of remission at 52 weeks was significantly higher in the 5-mg and 10-mg tofacitinib groups (34.3% and 40.6%, respectively) than in the placebo group (11.1%) in the OCTAVE Sustain trial.
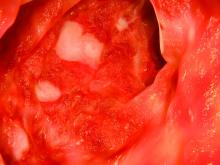
In addition, rates of mucosal healing were greater in the tofacitinib group than in the placebo group at 8 weeks and 52 weeks.
In the OCTAVE 1 trial, serious adverse events occurred in 4.2% and 8.0% of patients in the 10-mg and placebo groups, respectively. In the OCTAVE 2 trial, they occured in 3.4% and 4.1% of the 10-mg and placebo groups, respectively. The rate of serious adverse events in the OCTAVE Sustain trial was 5.1%, 5.6%, and 6.6% in the 10-mg, 5-mg, and placebo groups, respectively. Tofacitinib was associated with increased lipid levels, as well as higher rates of overall infection and herpes zoster infection, compared with placebo.
The study was supported by Pfizer. Lead author Dr. Sandborn and several coauthors disclosed financial relationships with multiple companies including Pfizer.
“This report is the culmination of an international effort,” over a 4-year period, wrote Sonia Friedman, MD, of Harvard University in an accompanying editorial.
“This study has all the elements of a high-quality trial: a large, international cohort of patients and investigators; reasonable enrollment criteria that would apply to many of my own patients with moderate-to-severe ulcerative colitis; rigorous and unbiased scoring for response, remission, and mucosal healing; fair adjudication of adverse events; and meticulous reporting of all meaningful outcomes and laboratory test results,” she said. Tofacitinib has proven its efficacy – its exact role will be determined by additional research, she noted.
“Only a continued combination of human ingenuity, worldwide cooperation, and enthusiastic funding will allow investigators to further explore the mechanisms by which JAK inhibition ameliorates inflammation in patients with ulcerative colitis and ... identify the specific subsets of patients who will most likely benefit from this new therapy,” Dr. Friedman emphasized (N. Engl. J. Med. 2017;376:1792-3).
Dr. Friedman is affiliated with Harvard University, Boston, Mass., and Brigham and Women’s Hospital Center for Crohn’s and Colitis, Chestnut Hill, Mass. She disclosed receiving personal fees from Boston University.
“This report is the culmination of an international effort,” over a 4-year period, wrote Sonia Friedman, MD, of Harvard University in an accompanying editorial.
“This study has all the elements of a high-quality trial: a large, international cohort of patients and investigators; reasonable enrollment criteria that would apply to many of my own patients with moderate-to-severe ulcerative colitis; rigorous and unbiased scoring for response, remission, and mucosal healing; fair adjudication of adverse events; and meticulous reporting of all meaningful outcomes and laboratory test results,” she said. Tofacitinib has proven its efficacy – its exact role will be determined by additional research, she noted.
“Only a continued combination of human ingenuity, worldwide cooperation, and enthusiastic funding will allow investigators to further explore the mechanisms by which JAK inhibition ameliorates inflammation in patients with ulcerative colitis and ... identify the specific subsets of patients who will most likely benefit from this new therapy,” Dr. Friedman emphasized (N. Engl. J. Med. 2017;376:1792-3).
Dr. Friedman is affiliated with Harvard University, Boston, Mass., and Brigham and Women’s Hospital Center for Crohn’s and Colitis, Chestnut Hill, Mass. She disclosed receiving personal fees from Boston University.
“This report is the culmination of an international effort,” over a 4-year period, wrote Sonia Friedman, MD, of Harvard University in an accompanying editorial.
“This study has all the elements of a high-quality trial: a large, international cohort of patients and investigators; reasonable enrollment criteria that would apply to many of my own patients with moderate-to-severe ulcerative colitis; rigorous and unbiased scoring for response, remission, and mucosal healing; fair adjudication of adverse events; and meticulous reporting of all meaningful outcomes and laboratory test results,” she said. Tofacitinib has proven its efficacy – its exact role will be determined by additional research, she noted.
“Only a continued combination of human ingenuity, worldwide cooperation, and enthusiastic funding will allow investigators to further explore the mechanisms by which JAK inhibition ameliorates inflammation in patients with ulcerative colitis and ... identify the specific subsets of patients who will most likely benefit from this new therapy,” Dr. Friedman emphasized (N. Engl. J. Med. 2017;376:1792-3).
Dr. Friedman is affiliated with Harvard University, Boston, Mass., and Brigham and Women’s Hospital Center for Crohn’s and Colitis, Chestnut Hill, Mass. She disclosed receiving personal fees from Boston University.
A 10-mg dose of tofacitinib twice daily was significantly more effective than placebo for inducing remission in ulcerative colitis patients, based on data from a group of three randomized trials totaling approximately 1,500 adults. The findings were published online May 3 in the New England Journal of Medicine (2017;376:1723-36).
The series of OCTAVE trials (Oral Clinical Trials for Tofacitinib in Ulcerative Colitis) included adults with moderately to severely active ulcerative colitis (UC). Patients were randomized to 10 mg of tofacitinib, 5 mg tofacitinib, or placebo. The studies were conducted over a 4-year period, at 144 sites for OCTAVE 1, 169 sites for OCTAVE 2, and 297 sites for OCTAVE Sustain.
In both OCTAVE 1 and OCTAVE 2, the remission rates at 8 weeks were significantly higher in the 10-mg tofacitinib groups, compared with the placebo groups (18.5% vs. 8.2%, respectively; 16.6% vs. 3.6%, respectively). The rate of remission at 52 weeks was significantly higher in the 5-mg and 10-mg tofacitinib groups (34.3% and 40.6%, respectively) than in the placebo group (11.1%) in the OCTAVE Sustain trial.
In addition, rates of mucosal healing were greater in the tofacitinib group than in the placebo group at 8 weeks and 52 weeks.
In the OCTAVE 1 trial, serious adverse events occurred in 4.2% and 8.0% of patients in the 10-mg and placebo groups, respectively. In the OCTAVE 2 trial, they occured in 3.4% and 4.1% of the 10-mg and placebo groups, respectively. The rate of serious adverse events in the OCTAVE Sustain trial was 5.1%, 5.6%, and 6.6% in the 10-mg, 5-mg, and placebo groups, respectively. Tofacitinib was associated with increased lipid levels, as well as higher rates of overall infection and herpes zoster infection, compared with placebo.
The study was supported by Pfizer. Lead author Dr. Sandborn and several coauthors disclosed financial relationships with multiple companies including Pfizer.
A 10-mg dose of tofacitinib twice daily was significantly more effective than placebo for inducing remission in ulcerative colitis patients, based on data from a group of three randomized trials totaling approximately 1,500 adults. The findings were published online May 3 in the New England Journal of Medicine (2017;376:1723-36).
The series of OCTAVE trials (Oral Clinical Trials for Tofacitinib in Ulcerative Colitis) included adults with moderately to severely active ulcerative colitis (UC). Patients were randomized to 10 mg of tofacitinib, 5 mg tofacitinib, or placebo. The studies were conducted over a 4-year period, at 144 sites for OCTAVE 1, 169 sites for OCTAVE 2, and 297 sites for OCTAVE Sustain.
In both OCTAVE 1 and OCTAVE 2, the remission rates at 8 weeks were significantly higher in the 10-mg tofacitinib groups, compared with the placebo groups (18.5% vs. 8.2%, respectively; 16.6% vs. 3.6%, respectively). The rate of remission at 52 weeks was significantly higher in the 5-mg and 10-mg tofacitinib groups (34.3% and 40.6%, respectively) than in the placebo group (11.1%) in the OCTAVE Sustain trial.
In addition, rates of mucosal healing were greater in the tofacitinib group than in the placebo group at 8 weeks and 52 weeks.
In the OCTAVE 1 trial, serious adverse events occurred in 4.2% and 8.0% of patients in the 10-mg and placebo groups, respectively. In the OCTAVE 2 trial, they occured in 3.4% and 4.1% of the 10-mg and placebo groups, respectively. The rate of serious adverse events in the OCTAVE Sustain trial was 5.1%, 5.6%, and 6.6% in the 10-mg, 5-mg, and placebo groups, respectively. Tofacitinib was associated with increased lipid levels, as well as higher rates of overall infection and herpes zoster infection, compared with placebo.
The study was supported by Pfizer. Lead author Dr. Sandborn and several coauthors disclosed financial relationships with multiple companies including Pfizer.
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Key clinical point: Tofacitinib, a JAK inhibitor, was a significantly more effective induction and maintenance therapy for patients with moderate to severe ulcerative colitis compared with placebo.
Major finding: Tofacitinib dosed at 10 mg twice daily yielded a remission rate of 41% at 52 weeks, compared with 11% in a placebo group.
Data source: The OCTAVE series of three randomized trials totaled approximately 1,500 adults with moderate to severely active ulcerative colitis.
Disclosures: The study was supported by Pfizer. Lead author Dr. Sandborn and several coauthors disclosed financial relationships with multiple companies, including Pfizer.
SJS, TEN occur less frequently in children than adults
Although incidences of Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) are lower in children than in adults, the increased costs, lengths of stay, and mortality still pose a substantial health burden, said Derek Y. Hsu, of Northwestern University, Chicago, and his associates.
Using data from the 2009-2012 Nationwide Inpatient Sample of 1,687,172 pediatric admissions, “estimated frequencies per million children ranged from 4.3 to 5.8 for SJS, 0.6 to 1.4 for SJS/TEN, and 0 to 0.7 for TEN,” the study researchers reported. In adults, those numbers are 9.3, 1.9, and 1.6 per million adults per year, according to a 2016 study by the authors (J Invest Dermatol. 2016 Jul;136[7]:1387-97).
Pediatric SJS, SJS/TEN, and TEN mean hospital costs were $24,947, $63,787, and $102,243, respectively, compared with $10,496 for the control group.
The mean length of stay for patients with SJS, SJS/TEN, and TEN was 9.4 days, 15.7 days, and 20.4 days, compared with 4.6 days in children without these disorders, respectively, and they most often were discharged to their home or to other self-care.
“One in 10 children with SJS, SJS/TEN, and TEN underwent mechanical ventilation,” Mr. Hsu and his associates reported.
Mortality was 0% for SJS, 4% for SJS/TEN, and 16% for TEN.
Read more at the Journal of the American Academy of Dermatology (2017 May;76[5]:811-7).
Although incidences of Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) are lower in children than in adults, the increased costs, lengths of stay, and mortality still pose a substantial health burden, said Derek Y. Hsu, of Northwestern University, Chicago, and his associates.
Using data from the 2009-2012 Nationwide Inpatient Sample of 1,687,172 pediatric admissions, “estimated frequencies per million children ranged from 4.3 to 5.8 for SJS, 0.6 to 1.4 for SJS/TEN, and 0 to 0.7 for TEN,” the study researchers reported. In adults, those numbers are 9.3, 1.9, and 1.6 per million adults per year, according to a 2016 study by the authors (J Invest Dermatol. 2016 Jul;136[7]:1387-97).
Pediatric SJS, SJS/TEN, and TEN mean hospital costs were $24,947, $63,787, and $102,243, respectively, compared with $10,496 for the control group.
The mean length of stay for patients with SJS, SJS/TEN, and TEN was 9.4 days, 15.7 days, and 20.4 days, compared with 4.6 days in children without these disorders, respectively, and they most often were discharged to their home or to other self-care.
“One in 10 children with SJS, SJS/TEN, and TEN underwent mechanical ventilation,” Mr. Hsu and his associates reported.
Mortality was 0% for SJS, 4% for SJS/TEN, and 16% for TEN.
Read more at the Journal of the American Academy of Dermatology (2017 May;76[5]:811-7).
Although incidences of Stevens-Johnson syndrome (SJS) and toxic epidermal necrolysis (TEN) are lower in children than in adults, the increased costs, lengths of stay, and mortality still pose a substantial health burden, said Derek Y. Hsu, of Northwestern University, Chicago, and his associates.
Using data from the 2009-2012 Nationwide Inpatient Sample of 1,687,172 pediatric admissions, “estimated frequencies per million children ranged from 4.3 to 5.8 for SJS, 0.6 to 1.4 for SJS/TEN, and 0 to 0.7 for TEN,” the study researchers reported. In adults, those numbers are 9.3, 1.9, and 1.6 per million adults per year, according to a 2016 study by the authors (J Invest Dermatol. 2016 Jul;136[7]:1387-97).
Pediatric SJS, SJS/TEN, and TEN mean hospital costs were $24,947, $63,787, and $102,243, respectively, compared with $10,496 for the control group.
The mean length of stay for patients with SJS, SJS/TEN, and TEN was 9.4 days, 15.7 days, and 20.4 days, compared with 4.6 days in children without these disorders, respectively, and they most often were discharged to their home or to other self-care.
“One in 10 children with SJS, SJS/TEN, and TEN underwent mechanical ventilation,” Mr. Hsu and his associates reported.
Mortality was 0% for SJS, 4% for SJS/TEN, and 16% for TEN.
Read more at the Journal of the American Academy of Dermatology (2017 May;76[5]:811-7).
Foresight and hard work – not inevitability – shaped HM, CEO says
So, the changing currents in medicine made it inevitable that the hospital medicine movement – and SHM – would have happened no matter what, right?
Not so much, said Laurence Wellikson, MD, MHM, chief executive officer of the Society of Hospital Medicine.
“How did Netflix pop up and not Blockbuster? Why did Sears not become Amazon?” he asked. “I think that SHM is very proud that we – very early on, when there were just a couple hundred hospitalists – saw the potential for this specialty.” At the same time, he said, “many of the other medical associations that were hundreds of years old not only did not see the potential for our specialty but, in many ways, were [also] somewhat contrary to the kinds of things that all of you have been doing over the last 20 years.”
He acknowledged that there were some “winds at our back” – it was clear that many physicians were wanting to leave the hospital – but he said the hospital medicine movement and the society nonetheless had to push up against resistance to change.
The movement continues to grow, he noted. As proof, there are 57,000 hospitalists, according to American Hospital Association surveys, and 15,000 SHM members.
In a note of caution, he recognized the many roles hospitalists are being asked to fill – from patient-safety projects to perioperative work – and said “hospitalists are more likely to say ‘yes’ when they should probably say ‘maybe.’ ” At the same time, he praised hospitalists for their openness to new ways of thinking and their willingness to partner.
Despite uncertainty, he said the future of health care is right up SHM’s alley.
“The future fits what hospital medicine is all about: We’re about value, we’re about creating the new future,” he said. “We’re about being accountable for what we do, being measured, and improving off those measures. ... We understand that we need to give up some of our autonomy and be in an integrated process to benefit from the expertise and the energies of other people.”
He touted the vital role that hospitalists will play.
“As we stand here today, we are not just large. We are not just the fastest-growing medical specialty of all time,” he said. “We are the answer to many of the questions going forward.”
So, the changing currents in medicine made it inevitable that the hospital medicine movement – and SHM – would have happened no matter what, right?
Not so much, said Laurence Wellikson, MD, MHM, chief executive officer of the Society of Hospital Medicine.
“How did Netflix pop up and not Blockbuster? Why did Sears not become Amazon?” he asked. “I think that SHM is very proud that we – very early on, when there were just a couple hundred hospitalists – saw the potential for this specialty.” At the same time, he said, “many of the other medical associations that were hundreds of years old not only did not see the potential for our specialty but, in many ways, were [also] somewhat contrary to the kinds of things that all of you have been doing over the last 20 years.”
He acknowledged that there were some “winds at our back” – it was clear that many physicians were wanting to leave the hospital – but he said the hospital medicine movement and the society nonetheless had to push up against resistance to change.
The movement continues to grow, he noted. As proof, there are 57,000 hospitalists, according to American Hospital Association surveys, and 15,000 SHM members.
In a note of caution, he recognized the many roles hospitalists are being asked to fill – from patient-safety projects to perioperative work – and said “hospitalists are more likely to say ‘yes’ when they should probably say ‘maybe.’ ” At the same time, he praised hospitalists for their openness to new ways of thinking and their willingness to partner.
Despite uncertainty, he said the future of health care is right up SHM’s alley.
“The future fits what hospital medicine is all about: We’re about value, we’re about creating the new future,” he said. “We’re about being accountable for what we do, being measured, and improving off those measures. ... We understand that we need to give up some of our autonomy and be in an integrated process to benefit from the expertise and the energies of other people.”
He touted the vital role that hospitalists will play.
“As we stand here today, we are not just large. We are not just the fastest-growing medical specialty of all time,” he said. “We are the answer to many of the questions going forward.”
So, the changing currents in medicine made it inevitable that the hospital medicine movement – and SHM – would have happened no matter what, right?
Not so much, said Laurence Wellikson, MD, MHM, chief executive officer of the Society of Hospital Medicine.
“How did Netflix pop up and not Blockbuster? Why did Sears not become Amazon?” he asked. “I think that SHM is very proud that we – very early on, when there were just a couple hundred hospitalists – saw the potential for this specialty.” At the same time, he said, “many of the other medical associations that were hundreds of years old not only did not see the potential for our specialty but, in many ways, were [also] somewhat contrary to the kinds of things that all of you have been doing over the last 20 years.”
He acknowledged that there were some “winds at our back” – it was clear that many physicians were wanting to leave the hospital – but he said the hospital medicine movement and the society nonetheless had to push up against resistance to change.
The movement continues to grow, he noted. As proof, there are 57,000 hospitalists, according to American Hospital Association surveys, and 15,000 SHM members.
In a note of caution, he recognized the many roles hospitalists are being asked to fill – from patient-safety projects to perioperative work – and said “hospitalists are more likely to say ‘yes’ when they should probably say ‘maybe.’ ” At the same time, he praised hospitalists for their openness to new ways of thinking and their willingness to partner.
Despite uncertainty, he said the future of health care is right up SHM’s alley.
“The future fits what hospital medicine is all about: We’re about value, we’re about creating the new future,” he said. “We’re about being accountable for what we do, being measured, and improving off those measures. ... We understand that we need to give up some of our autonomy and be in an integrated process to benefit from the expertise and the energies of other people.”
He touted the vital role that hospitalists will play.
“As we stand here today, we are not just large. We are not just the fastest-growing medical specialty of all time,” he said. “We are the answer to many of the questions going forward.”
Conway says health care payment, quality reform to continue
Keynote speaker Patrick Conway, MD, MSc, MHM, told hospitalists at HM17 Wednesday that, while there is a seemingly endless stream of punditry about the fate of the Affordable Care Act, health care will continue its trajectory to higher value, lower costs, and improved quality for patients.
“Health system transformation, innovation, delivery system reform, accountability, the work that you all do each and every day ... is a bipartisan ideal,” he said. The work “on value, the work on accountability, the work on bundled payments ... will continue and will continue to be important to you and the patients you serve.”
He also echoed Tuesday’s keynote address from Karen DeSalvo, MD, former Acting Assistant Secretary for Health in the U.S. Department of Health & Human Services, that hospital medicine needs to look at health care more holistically to help work on social issues. Dr. Conway, who still moonlights as a pediatric academic hospitalist on weekends, knows the problem first-hand as he often sees children on Medicaid who have multiple chronic conditions.
“I can tell you our system still does not have a highly reliable, whole health system for those children and their families,” he said. “Every weekend, I have a family that I can’t discharge because they don’t have the social and home-based supports for them to go home. So, they literally sit in the hospital until Monday. That makes no sense for our overall health system.”
Dr. Conway said that the gravitation away from fee-for-service toward alternative payment models would ideally lead to better patient outcomes, more coordinated care, and financial savings. He urged hospitalists to continue to help design new payment and care-delivery systems.
“You know what you’re passionate about and where you want to drive better care,” he said. “If the army of people in this room and all the places you are working [at] are the driver of better quality, better safety, coordinated care for patients ... that’s what it’s all about.”
Keynote speaker Patrick Conway, MD, MSc, MHM, told hospitalists at HM17 Wednesday that, while there is a seemingly endless stream of punditry about the fate of the Affordable Care Act, health care will continue its trajectory to higher value, lower costs, and improved quality for patients.
“Health system transformation, innovation, delivery system reform, accountability, the work that you all do each and every day ... is a bipartisan ideal,” he said. The work “on value, the work on accountability, the work on bundled payments ... will continue and will continue to be important to you and the patients you serve.”
He also echoed Tuesday’s keynote address from Karen DeSalvo, MD, former Acting Assistant Secretary for Health in the U.S. Department of Health & Human Services, that hospital medicine needs to look at health care more holistically to help work on social issues. Dr. Conway, who still moonlights as a pediatric academic hospitalist on weekends, knows the problem first-hand as he often sees children on Medicaid who have multiple chronic conditions.
“I can tell you our system still does not have a highly reliable, whole health system for those children and their families,” he said. “Every weekend, I have a family that I can’t discharge because they don’t have the social and home-based supports for them to go home. So, they literally sit in the hospital until Monday. That makes no sense for our overall health system.”
Dr. Conway said that the gravitation away from fee-for-service toward alternative payment models would ideally lead to better patient outcomes, more coordinated care, and financial savings. He urged hospitalists to continue to help design new payment and care-delivery systems.
“You know what you’re passionate about and where you want to drive better care,” he said. “If the army of people in this room and all the places you are working [at] are the driver of better quality, better safety, coordinated care for patients ... that’s what it’s all about.”
Keynote speaker Patrick Conway, MD, MSc, MHM, told hospitalists at HM17 Wednesday that, while there is a seemingly endless stream of punditry about the fate of the Affordable Care Act, health care will continue its trajectory to higher value, lower costs, and improved quality for patients.
“Health system transformation, innovation, delivery system reform, accountability, the work that you all do each and every day ... is a bipartisan ideal,” he said. The work “on value, the work on accountability, the work on bundled payments ... will continue and will continue to be important to you and the patients you serve.”
He also echoed Tuesday’s keynote address from Karen DeSalvo, MD, former Acting Assistant Secretary for Health in the U.S. Department of Health & Human Services, that hospital medicine needs to look at health care more holistically to help work on social issues. Dr. Conway, who still moonlights as a pediatric academic hospitalist on weekends, knows the problem first-hand as he often sees children on Medicaid who have multiple chronic conditions.
“I can tell you our system still does not have a highly reliable, whole health system for those children and their families,” he said. “Every weekend, I have a family that I can’t discharge because they don’t have the social and home-based supports for them to go home. So, they literally sit in the hospital until Monday. That makes no sense for our overall health system.”
Dr. Conway said that the gravitation away from fee-for-service toward alternative payment models would ideally lead to better patient outcomes, more coordinated care, and financial savings. He urged hospitalists to continue to help design new payment and care-delivery systems.
“You know what you’re passionate about and where you want to drive better care,” he said. “If the army of people in this room and all the places you are working [at] are the driver of better quality, better safety, coordinated care for patients ... that’s what it’s all about.”
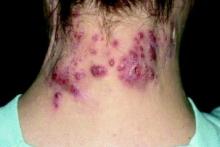
Hidradenitis suppurativa diagnosis typically delayed in children
WASHINGTON – Children with hidradenitis suppurativa (HS) may suffer with symptoms for an average of 7 years before they are diagnosed, according to pediatric dermatologist Anna Yasmine Kirkorian, MD.
Data from a 2015 study showed that 73% of pediatric patients with HS were diagnosed more than 2 years after the onset of symptoms, said Dr. Kirkorian of the department of dermatology at Children’s National Health System and George Washington University, Washington. (Br J Dermatol. 2015 Dec;173[6]:1546-9).
Genetics can play a role in HS, likely via mutations in the gamma-secretase protein that leads to epidermal differentiation and immune regulation, Dr. Kirkorian said. Most of her patients with HS are black, and a recent study described a gamma-secretase mutation in a black family of a proband and four family members, she noted (JAMA Dermatol. 2015 Jun;151[6]:668-70). Gamma-secretase mutations also have been identified in Han Chinese populations, she said.
HS also is associated with precocious puberty. However, defining the age of onset of puberty can be difficulty because pubertal onset may vary between different ethnicities, noted Dr. Kirkorian. “Prepubertal children presenting with HS warrant an endocrinologic evaluation,” she said.
Dr. Kirkorian added that more research is needed to pinpoint the possible genetic component of HS and to identify genetic susceptibility that could lead to targeted treatment strategies.
The optimal treatment plan for pediatric HS is multimodal and addresses the comorbidities common with the condition, she said, and she predicted that specialized clinic or treatment centers that bring together areas, including psychiatry, wound care, pain management, surgery, endocrinology, and genetics, will evolve to serve these patients. To support these collaborative efforts, Dr. Kirkorian is a member of the Pediatric Dermatology Research Alliance (PeDRA), an organization formed to accelerate research on skin diseases in children.
The symposium was sponsored by AbbVie. Dr. Kirkorian had no financial conflicts to disclose. She is on the editorial board of Dermatology News.
WASHINGTON – Children with hidradenitis suppurativa (HS) may suffer with symptoms for an average of 7 years before they are diagnosed, according to pediatric dermatologist Anna Yasmine Kirkorian, MD.
Data from a 2015 study showed that 73% of pediatric patients with HS were diagnosed more than 2 years after the onset of symptoms, said Dr. Kirkorian of the department of dermatology at Children’s National Health System and George Washington University, Washington. (Br J Dermatol. 2015 Dec;173[6]:1546-9).
Genetics can play a role in HS, likely via mutations in the gamma-secretase protein that leads to epidermal differentiation and immune regulation, Dr. Kirkorian said. Most of her patients with HS are black, and a recent study described a gamma-secretase mutation in a black family of a proband and four family members, she noted (JAMA Dermatol. 2015 Jun;151[6]:668-70). Gamma-secretase mutations also have been identified in Han Chinese populations, she said.
HS also is associated with precocious puberty. However, defining the age of onset of puberty can be difficulty because pubertal onset may vary between different ethnicities, noted Dr. Kirkorian. “Prepubertal children presenting with HS warrant an endocrinologic evaluation,” she said.
Dr. Kirkorian added that more research is needed to pinpoint the possible genetic component of HS and to identify genetic susceptibility that could lead to targeted treatment strategies.
The optimal treatment plan for pediatric HS is multimodal and addresses the comorbidities common with the condition, she said, and she predicted that specialized clinic or treatment centers that bring together areas, including psychiatry, wound care, pain management, surgery, endocrinology, and genetics, will evolve to serve these patients. To support these collaborative efforts, Dr. Kirkorian is a member of the Pediatric Dermatology Research Alliance (PeDRA), an organization formed to accelerate research on skin diseases in children.
The symposium was sponsored by AbbVie. Dr. Kirkorian had no financial conflicts to disclose. She is on the editorial board of Dermatology News.
WASHINGTON – Children with hidradenitis suppurativa (HS) may suffer with symptoms for an average of 7 years before they are diagnosed, according to pediatric dermatologist Anna Yasmine Kirkorian, MD.
Data from a 2015 study showed that 73% of pediatric patients with HS were diagnosed more than 2 years after the onset of symptoms, said Dr. Kirkorian of the department of dermatology at Children’s National Health System and George Washington University, Washington. (Br J Dermatol. 2015 Dec;173[6]:1546-9).
Genetics can play a role in HS, likely via mutations in the gamma-secretase protein that leads to epidermal differentiation and immune regulation, Dr. Kirkorian said. Most of her patients with HS are black, and a recent study described a gamma-secretase mutation in a black family of a proband and four family members, she noted (JAMA Dermatol. 2015 Jun;151[6]:668-70). Gamma-secretase mutations also have been identified in Han Chinese populations, she said.
HS also is associated with precocious puberty. However, defining the age of onset of puberty can be difficulty because pubertal onset may vary between different ethnicities, noted Dr. Kirkorian. “Prepubertal children presenting with HS warrant an endocrinologic evaluation,” she said.
Dr. Kirkorian added that more research is needed to pinpoint the possible genetic component of HS and to identify genetic susceptibility that could lead to targeted treatment strategies.
The optimal treatment plan for pediatric HS is multimodal and addresses the comorbidities common with the condition, she said, and she predicted that specialized clinic or treatment centers that bring together areas, including psychiatry, wound care, pain management, surgery, endocrinology, and genetics, will evolve to serve these patients. To support these collaborative efforts, Dr. Kirkorian is a member of the Pediatric Dermatology Research Alliance (PeDRA), an organization formed to accelerate research on skin diseases in children.
The symposium was sponsored by AbbVie. Dr. Kirkorian had no financial conflicts to disclose. She is on the editorial board of Dermatology News.
From idea to abstract, RIV posters highlight novel thinking
Masih Shinwa, MD, stood beside a half-circle of judges Tuesday night at SHM’s annual Research, Innovations and Clinical Vignettes (RIV) poster competition and argued why his entry, already a finalist, should win. And to think, his poster, “Please ‘THINK’ Before You Order: A Multidisciplinary Approach to Decreasing Overutilization of Daily Labs,” was born simply of a group of medical students who incredulously said they were amazed patients would be woken in the middle of the night for laboratory tests.
Eighteen months later, the poster drew hundreds of questions from passersby on how a team approach could help generate fewer labs and chemistry testing. Now, the work could serve as a potential guide for other hospitals seeking to reduce unnecessary tests, a focal point of SHM and the ABIM Foundation’s Choosing Wisely campaign.
“This is a way to make it national,” he said. “You may have affected the lives of the patients in your hospital, but unless you attend these types of national meetings, it’s hard to get that perspective across [the country].”
That level of personal and professional collaboration is the purpose of the RIV, one of the best-attended events of SHM’s annual meeting. The event has become so popular that submissions this year tallied 1,712, nearly triple the number of submissions at the 2010 event.
“One of the amazing things is everyone has their own poster. They are doing their work,” said Margaret Fang, MD, MPH, FHM, program chair for HM17’s scientific abstracts competition, the formal name for the poster contest. “But then they start up conversations with the people next to them. ... seeing the organic networking and the discussions that arise from that is really exciting. RIV really serves as a way of connecting people together who might not have known the other person was doing that kind of work.”
Dr. Shinwa said that the specialty’s focus on research is important. He said it positions the field to be leaders, not just for patient care, but for hospitals and institutions.
“We are physicians. Our role is taking care of patients,” he said. “[But] knowing that there are people who are not just focusing on taking care of specific patients, but are actually there to improve the entire system and the process, that is really gratifying.”
Masih Shinwa, MD, stood beside a half-circle of judges Tuesday night at SHM’s annual Research, Innovations and Clinical Vignettes (RIV) poster competition and argued why his entry, already a finalist, should win. And to think, his poster, “Please ‘THINK’ Before You Order: A Multidisciplinary Approach to Decreasing Overutilization of Daily Labs,” was born simply of a group of medical students who incredulously said they were amazed patients would be woken in the middle of the night for laboratory tests.
Eighteen months later, the poster drew hundreds of questions from passersby on how a team approach could help generate fewer labs and chemistry testing. Now, the work could serve as a potential guide for other hospitals seeking to reduce unnecessary tests, a focal point of SHM and the ABIM Foundation’s Choosing Wisely campaign.
“This is a way to make it national,” he said. “You may have affected the lives of the patients in your hospital, but unless you attend these types of national meetings, it’s hard to get that perspective across [the country].”
That level of personal and professional collaboration is the purpose of the RIV, one of the best-attended events of SHM’s annual meeting. The event has become so popular that submissions this year tallied 1,712, nearly triple the number of submissions at the 2010 event.
“One of the amazing things is everyone has their own poster. They are doing their work,” said Margaret Fang, MD, MPH, FHM, program chair for HM17’s scientific abstracts competition, the formal name for the poster contest. “But then they start up conversations with the people next to them. ... seeing the organic networking and the discussions that arise from that is really exciting. RIV really serves as a way of connecting people together who might not have known the other person was doing that kind of work.”
Dr. Shinwa said that the specialty’s focus on research is important. He said it positions the field to be leaders, not just for patient care, but for hospitals and institutions.
“We are physicians. Our role is taking care of patients,” he said. “[But] knowing that there are people who are not just focusing on taking care of specific patients, but are actually there to improve the entire system and the process, that is really gratifying.”
Masih Shinwa, MD, stood beside a half-circle of judges Tuesday night at SHM’s annual Research, Innovations and Clinical Vignettes (RIV) poster competition and argued why his entry, already a finalist, should win. And to think, his poster, “Please ‘THINK’ Before You Order: A Multidisciplinary Approach to Decreasing Overutilization of Daily Labs,” was born simply of a group of medical students who incredulously said they were amazed patients would be woken in the middle of the night for laboratory tests.
Eighteen months later, the poster drew hundreds of questions from passersby on how a team approach could help generate fewer labs and chemistry testing. Now, the work could serve as a potential guide for other hospitals seeking to reduce unnecessary tests, a focal point of SHM and the ABIM Foundation’s Choosing Wisely campaign.
“This is a way to make it national,” he said. “You may have affected the lives of the patients in your hospital, but unless you attend these types of national meetings, it’s hard to get that perspective across [the country].”
That level of personal and professional collaboration is the purpose of the RIV, one of the best-attended events of SHM’s annual meeting. The event has become so popular that submissions this year tallied 1,712, nearly triple the number of submissions at the 2010 event.
“One of the amazing things is everyone has their own poster. They are doing their work,” said Margaret Fang, MD, MPH, FHM, program chair for HM17’s scientific abstracts competition, the formal name for the poster contest. “But then they start up conversations with the people next to them. ... seeing the organic networking and the discussions that arise from that is really exciting. RIV really serves as a way of connecting people together who might not have known the other person was doing that kind of work.”
Dr. Shinwa said that the specialty’s focus on research is important. He said it positions the field to be leaders, not just for patient care, but for hospitals and institutions.
“We are physicians. Our role is taking care of patients,” he said. “[But] knowing that there are people who are not just focusing on taking care of specific patients, but are actually there to improve the entire system and the process, that is really gratifying.”
No increase in hand osteoarthritis seen in Sjögren’s syndrome
LAS VEGAS – Patients with Sjögren’s syndrome do not have an increased prevalence of hand osteoarthritis, but they are strongly predisposed to have a history of hypothyroidism, Jeremie Sellam, MD, reported at the World Congress on Osteoarthritis.
Both of these findings in his small case-control study were unexpected, he added at the congress sponsored by the Osteoarthritis Research Society International.
The study included 34 women with primary Sjögren’s syndrome according to the 2002 American-European Consensus Group criteria and 54 female controls with sicca syndrome but no autoantibodies and no Sjögren’s syndrome. All subjects were evaluated at a specialized tertiary Sjögren’s syndrome clinic. The controls were referred there to ascertain whether they had Sjögren’s syndrome.
Among the Sjögren’s syndrome patients, 41% had radiographic evidence of hand osteoarthritis, 12% had symptomatic hand osteoarthritis, and 9% had erosive hand osteoarthritis. In the sicca syndrome–only patients, the rates were similar at 52%, 28%, and 9%, respectively.
Looking for commonalities and differences between the Sjögren’s syndrome patients and controls, Dr. Sellam and his coinvestigators noted that the Sjögren’s syndrome patients were significantly older, with an average age of 64 years, compared with 48.5 years in the controls.
Impressively, two-thirds of the 15 Sjögren’s syndrome patients with hand osteoarthritis had a history of hypothyroidism, compared with just 15% of the 27 non-autoimmune sicca syndrome patients with hand osteoarthritis and one-quarter of the Sjögren’s syndrome patients without hand osteoarthritis. This suggests a possible interaction between Sjögren’s syndrome, hand osteoarthritis, and a history of hypothyroidism which merits further study, according to the rheumatologist.
Because of the relatively small patient numbers in the French study, Dr. Sellam and coworkers ran a crosscheck with data from the Framingham Osteoarthritis Study and found hand osteoarthritis prevalence rates comparable to their own findings. For example, the prevalences of radiographic and erosive hand osteoarthritis in the French Sjögren’s syndrome and non-autoimmune sicca syndrome groups were similar to the 44% and 10% figures, respectively, in the general population of age-matched Framingham women (Ann Rheum Dis. 2011 Sep;70[9]:1581-6).
He reported having no financial conflicts regarding his study, which was conducted free of commercial support.
LAS VEGAS – Patients with Sjögren’s syndrome do not have an increased prevalence of hand osteoarthritis, but they are strongly predisposed to have a history of hypothyroidism, Jeremie Sellam, MD, reported at the World Congress on Osteoarthritis.
Both of these findings in his small case-control study were unexpected, he added at the congress sponsored by the Osteoarthritis Research Society International.
The study included 34 women with primary Sjögren’s syndrome according to the 2002 American-European Consensus Group criteria and 54 female controls with sicca syndrome but no autoantibodies and no Sjögren’s syndrome. All subjects were evaluated at a specialized tertiary Sjögren’s syndrome clinic. The controls were referred there to ascertain whether they had Sjögren’s syndrome.
Among the Sjögren’s syndrome patients, 41% had radiographic evidence of hand osteoarthritis, 12% had symptomatic hand osteoarthritis, and 9% had erosive hand osteoarthritis. In the sicca syndrome–only patients, the rates were similar at 52%, 28%, and 9%, respectively.
Looking for commonalities and differences between the Sjögren’s syndrome patients and controls, Dr. Sellam and his coinvestigators noted that the Sjögren’s syndrome patients were significantly older, with an average age of 64 years, compared with 48.5 years in the controls.
Impressively, two-thirds of the 15 Sjögren’s syndrome patients with hand osteoarthritis had a history of hypothyroidism, compared with just 15% of the 27 non-autoimmune sicca syndrome patients with hand osteoarthritis and one-quarter of the Sjögren’s syndrome patients without hand osteoarthritis. This suggests a possible interaction between Sjögren’s syndrome, hand osteoarthritis, and a history of hypothyroidism which merits further study, according to the rheumatologist.
Because of the relatively small patient numbers in the French study, Dr. Sellam and coworkers ran a crosscheck with data from the Framingham Osteoarthritis Study and found hand osteoarthritis prevalence rates comparable to their own findings. For example, the prevalences of radiographic and erosive hand osteoarthritis in the French Sjögren’s syndrome and non-autoimmune sicca syndrome groups were similar to the 44% and 10% figures, respectively, in the general population of age-matched Framingham women (Ann Rheum Dis. 2011 Sep;70[9]:1581-6).
He reported having no financial conflicts regarding his study, which was conducted free of commercial support.
LAS VEGAS – Patients with Sjögren’s syndrome do not have an increased prevalence of hand osteoarthritis, but they are strongly predisposed to have a history of hypothyroidism, Jeremie Sellam, MD, reported at the World Congress on Osteoarthritis.
Both of these findings in his small case-control study were unexpected, he added at the congress sponsored by the Osteoarthritis Research Society International.
The study included 34 women with primary Sjögren’s syndrome according to the 2002 American-European Consensus Group criteria and 54 female controls with sicca syndrome but no autoantibodies and no Sjögren’s syndrome. All subjects were evaluated at a specialized tertiary Sjögren’s syndrome clinic. The controls were referred there to ascertain whether they had Sjögren’s syndrome.
Among the Sjögren’s syndrome patients, 41% had radiographic evidence of hand osteoarthritis, 12% had symptomatic hand osteoarthritis, and 9% had erosive hand osteoarthritis. In the sicca syndrome–only patients, the rates were similar at 52%, 28%, and 9%, respectively.
Looking for commonalities and differences between the Sjögren’s syndrome patients and controls, Dr. Sellam and his coinvestigators noted that the Sjögren’s syndrome patients were significantly older, with an average age of 64 years, compared with 48.5 years in the controls.
Impressively, two-thirds of the 15 Sjögren’s syndrome patients with hand osteoarthritis had a history of hypothyroidism, compared with just 15% of the 27 non-autoimmune sicca syndrome patients with hand osteoarthritis and one-quarter of the Sjögren’s syndrome patients without hand osteoarthritis. This suggests a possible interaction between Sjögren’s syndrome, hand osteoarthritis, and a history of hypothyroidism which merits further study, according to the rheumatologist.
Because of the relatively small patient numbers in the French study, Dr. Sellam and coworkers ran a crosscheck with data from the Framingham Osteoarthritis Study and found hand osteoarthritis prevalence rates comparable to their own findings. For example, the prevalences of radiographic and erosive hand osteoarthritis in the French Sjögren’s syndrome and non-autoimmune sicca syndrome groups were similar to the 44% and 10% figures, respectively, in the general population of age-matched Framingham women (Ann Rheum Dis. 2011 Sep;70[9]:1581-6).
He reported having no financial conflicts regarding his study, which was conducted free of commercial support.
AT OARSI 2017
Key clinical point:
Major finding: Nine percent of women with Sjögren’s syndrome had erosive hand osteoarthritis, a prevalence identical to that in a group with non-autoimmune sicca syndrome only.
Data source: This case-control study included 34 women with Sjögren’s syndrome and 54 women with non-autoimmune sicca syndrome.
Disclosures: The presenter reported having no financial conflicts regarding the study, which was conducted free of commercial support.
RF, IPL score highest for facial rejuvenation in review
SAN DIEGO – A review of existing research found that newer technologies are safer and more effective at skin rejuvenation than older ones, with two types – intense pulsed laser (IPL) and radiofrequency (RF) – at or near the head of the pack on both fronts.
In addition, 10 types of treatments, including multiple laser technologies, scored higher than facial peels on safety, although the peels beat almost all comers in terms of efficacy, the study’s lead author, Caerwyn Ash, PhD, said in an interview after presenting the results at the annual meeting of the American Society for Laser Medicine and Surgery.
The review is unique because it maps the various treatments on two axes – safety and efficacy – in a chart. Viewers gain an instant perspective on how the individual treatments fare when stacked up against each other. “The study gives credence to the new technologies,” said Dr. Ash, associate professor of medical devices at the University of Wales Trinity Saint David, Swansea. “We’re moving toward safer and more efficacious results.”
He and his colleagues analyzed more than 500 studies published since 1985, which evaluated 15 different types of technology used for facial rejuvenation. They reviewed at least 35 clinical studies per platform. They also reported on the safety and efficacy of facial peels.
The technologies examined included RF, light emitting diode (LED), pulsed dyed laser (PDL), frequency doubled 532-nm potassium-titanyl-phosphate neodymium:YAG laser (which had a low number of clinical studies), 980-nm diode laser, Q-switched Nd:YAG laser, 1320-nm Nd:YAG laser, 1540-nm Erbium:glass laser, 1450-nm diode laser, IPL, long pulsed Nd:YAG laser, plasma, and copper bromide laser.
Another technology reviewed was fractional selective photothermolysis, but studies of this modality were difficult to compare, according to the authors. Also included was the carbon dioxide laser, which the authors described as being hampered by long healing times and discomfort that requires anesthesia.
The review notes that comparisons between studies of the different treatments in the review were limited by such factors as varied beam and tip sizes (even within individual studies), various pulse durations, and different treatment times and intervals.
The researchers mapped the treatments in a single chart on two axes, safety and efficacy.
Three treatments scored the best in terms of efficacy: RF, IPL and chemical peels. However, while RF and IPL scored near the top of all treatments on the safety scale, chemical peels pulled up the rear.
The treatment strategies on the safety scale, ranked from most safe to least safe, were LED, IPL, diode laser, RF, argon laser, PDL and carbon dioxide laser, Nd:YAG, ablative Erbium, plasma, and chemical peel.
Radiofrequency topped the efficacy scale, followed closely by chemical peel and IPL. Following them, from most efficacious to least efficacious, were carbon dioxide laser, ablative Erbium, plasma treatments, and PDL, Nd:YAG and argon laser, diode laser, and LED.
The study was funded by the University of Wales Trinity Saint David. The authors had no disclosures.
SAN DIEGO – A review of existing research found that newer technologies are safer and more effective at skin rejuvenation than older ones, with two types – intense pulsed laser (IPL) and radiofrequency (RF) – at or near the head of the pack on both fronts.
In addition, 10 types of treatments, including multiple laser technologies, scored higher than facial peels on safety, although the peels beat almost all comers in terms of efficacy, the study’s lead author, Caerwyn Ash, PhD, said in an interview after presenting the results at the annual meeting of the American Society for Laser Medicine and Surgery.
The review is unique because it maps the various treatments on two axes – safety and efficacy – in a chart. Viewers gain an instant perspective on how the individual treatments fare when stacked up against each other. “The study gives credence to the new technologies,” said Dr. Ash, associate professor of medical devices at the University of Wales Trinity Saint David, Swansea. “We’re moving toward safer and more efficacious results.”
He and his colleagues analyzed more than 500 studies published since 1985, which evaluated 15 different types of technology used for facial rejuvenation. They reviewed at least 35 clinical studies per platform. They also reported on the safety and efficacy of facial peels.
The technologies examined included RF, light emitting diode (LED), pulsed dyed laser (PDL), frequency doubled 532-nm potassium-titanyl-phosphate neodymium:YAG laser (which had a low number of clinical studies), 980-nm diode laser, Q-switched Nd:YAG laser, 1320-nm Nd:YAG laser, 1540-nm Erbium:glass laser, 1450-nm diode laser, IPL, long pulsed Nd:YAG laser, plasma, and copper bromide laser.
Another technology reviewed was fractional selective photothermolysis, but studies of this modality were difficult to compare, according to the authors. Also included was the carbon dioxide laser, which the authors described as being hampered by long healing times and discomfort that requires anesthesia.
The review notes that comparisons between studies of the different treatments in the review were limited by such factors as varied beam and tip sizes (even within individual studies), various pulse durations, and different treatment times and intervals.
The researchers mapped the treatments in a single chart on two axes, safety and efficacy.
Three treatments scored the best in terms of efficacy: RF, IPL and chemical peels. However, while RF and IPL scored near the top of all treatments on the safety scale, chemical peels pulled up the rear.
The treatment strategies on the safety scale, ranked from most safe to least safe, were LED, IPL, diode laser, RF, argon laser, PDL and carbon dioxide laser, Nd:YAG, ablative Erbium, plasma, and chemical peel.
Radiofrequency topped the efficacy scale, followed closely by chemical peel and IPL. Following them, from most efficacious to least efficacious, were carbon dioxide laser, ablative Erbium, plasma treatments, and PDL, Nd:YAG and argon laser, diode laser, and LED.
The study was funded by the University of Wales Trinity Saint David. The authors had no disclosures.
SAN DIEGO – A review of existing research found that newer technologies are safer and more effective at skin rejuvenation than older ones, with two types – intense pulsed laser (IPL) and radiofrequency (RF) – at or near the head of the pack on both fronts.
In addition, 10 types of treatments, including multiple laser technologies, scored higher than facial peels on safety, although the peels beat almost all comers in terms of efficacy, the study’s lead author, Caerwyn Ash, PhD, said in an interview after presenting the results at the annual meeting of the American Society for Laser Medicine and Surgery.
The review is unique because it maps the various treatments on two axes – safety and efficacy – in a chart. Viewers gain an instant perspective on how the individual treatments fare when stacked up against each other. “The study gives credence to the new technologies,” said Dr. Ash, associate professor of medical devices at the University of Wales Trinity Saint David, Swansea. “We’re moving toward safer and more efficacious results.”
He and his colleagues analyzed more than 500 studies published since 1985, which evaluated 15 different types of technology used for facial rejuvenation. They reviewed at least 35 clinical studies per platform. They also reported on the safety and efficacy of facial peels.
The technologies examined included RF, light emitting diode (LED), pulsed dyed laser (PDL), frequency doubled 532-nm potassium-titanyl-phosphate neodymium:YAG laser (which had a low number of clinical studies), 980-nm diode laser, Q-switched Nd:YAG laser, 1320-nm Nd:YAG laser, 1540-nm Erbium:glass laser, 1450-nm diode laser, IPL, long pulsed Nd:YAG laser, plasma, and copper bromide laser.
Another technology reviewed was fractional selective photothermolysis, but studies of this modality were difficult to compare, according to the authors. Also included was the carbon dioxide laser, which the authors described as being hampered by long healing times and discomfort that requires anesthesia.
The review notes that comparisons between studies of the different treatments in the review were limited by such factors as varied beam and tip sizes (even within individual studies), various pulse durations, and different treatment times and intervals.
The researchers mapped the treatments in a single chart on two axes, safety and efficacy.
Three treatments scored the best in terms of efficacy: RF, IPL and chemical peels. However, while RF and IPL scored near the top of all treatments on the safety scale, chemical peels pulled up the rear.
The treatment strategies on the safety scale, ranked from most safe to least safe, were LED, IPL, diode laser, RF, argon laser, PDL and carbon dioxide laser, Nd:YAG, ablative Erbium, plasma, and chemical peel.
Radiofrequency topped the efficacy scale, followed closely by chemical peel and IPL. Following them, from most efficacious to least efficacious, were carbon dioxide laser, ablative Erbium, plasma treatments, and PDL, Nd:YAG and argon laser, diode laser, and LED.
The study was funded by the University of Wales Trinity Saint David. The authors had no disclosures.
AT LASER 2017
Key clinical point:
Major finding: IPL and RF were among the modalities that were safer and more effective at skin rejuvenation than were older ones.
Data source: An analysis of more than 500 studies published since 1985 evaluating of 15 different types of technology used for facial rejuvenation, reviewing at least 35 clinical studies per platform.
Disclosures: The study was funded by the University of Wales Trinity Saint David. The authors had no disclosures.
VIDEO: Attaining the tools to start your own quality improvement project
Quality improvement at the program level is a major concern for most hospitalists. That’s exactly why Venkata Dontaraju, MD, MRCP, FHM, attended a Tuesday afternoon HM17 workshop entitled “Adding to Your Toolbox: QI Methodologies.”
Dr. Dontaraju, a hospitalist for 7 years with Rockford Health Physicians in Loves Park, Ill., wants to begin QI projects of his own. He planned to attend a number of QI-focused sessions at the annual meeting, with the toolbox session laying the foundation for such work.
“There is a lot of emphasis on cutting down the waste in health care, and also improving the processes,” he said. “That is where the role of QI comes into place. I want to do QI projects at my own hospital, but I first want to get the tools necessary for a successful project.”
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Quality improvement at the program level is a major concern for most hospitalists. That’s exactly why Venkata Dontaraju, MD, MRCP, FHM, attended a Tuesday afternoon HM17 workshop entitled “Adding to Your Toolbox: QI Methodologies.”
Dr. Dontaraju, a hospitalist for 7 years with Rockford Health Physicians in Loves Park, Ill., wants to begin QI projects of his own. He planned to attend a number of QI-focused sessions at the annual meeting, with the toolbox session laying the foundation for such work.
“There is a lot of emphasis on cutting down the waste in health care, and also improving the processes,” he said. “That is where the role of QI comes into place. I want to do QI projects at my own hospital, but I first want to get the tools necessary for a successful project.”
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Quality improvement at the program level is a major concern for most hospitalists. That’s exactly why Venkata Dontaraju, MD, MRCP, FHM, attended a Tuesday afternoon HM17 workshop entitled “Adding to Your Toolbox: QI Methodologies.”
Dr. Dontaraju, a hospitalist for 7 years with Rockford Health Physicians in Loves Park, Ill., wants to begin QI projects of his own. He planned to attend a number of QI-focused sessions at the annual meeting, with the toolbox session laying the foundation for such work.
“There is a lot of emphasis on cutting down the waste in health care, and also improving the processes,” he said. “That is where the role of QI comes into place. I want to do QI projects at my own hospital, but I first want to get the tools necessary for a successful project.”
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Forum focuses on forging Q.I. connections
Scrounging for information that could help her with quality improvement (Q.I.) projects, Charmaine Lewis, MD, MPH, the quality director with New Hanover Hospitalists in Wilmington, N.C., said she finds herself reviewing posters at the Annual Meeting and squinting at the images to see whether the electronic health records involved match the system she uses back home.
There’s got to be a better way.
Mangla Gulati, MD, SFHM, associate professor of medicine and chief quality officer at the University of Maryland, and Jenna Goldstein, director of SHM’s Center for Hospital Innovation and Improvement, led what grew into a lively, thoughtful discussion about ways for hospitalists to exchange information and to get support with Q.I. efforts at their centers.
The hospitalists who attended brought their experiences and their questions from a diverse range of centers, from Anchorage, Alaska, to southern California to Poughkeepsie, New York. They emphasized the need for easier access to initiatives that mirror what they are trying to do at their own centers, for more mentoring opportunities, and for more SHM chapters outside major metropolitan areas to help with networking. And they offered lessons on what they have already learned.
Remus Popa, MD, FHM, associate professor of medicine at the University of California, Riverside, who has led Q.I. projects on the use of telemetry, said a successful project will likely be more than an idea that blooms inside the head of a hospitalist.
“We have to find something that the institution really needs,” Dr. Popa said. “You have to design a better fit with them. Otherwise, it’s going to be a tough conversation about resources, right?”
Esther Lee, MD, a hospitalist in Anchorage, Alaska, asked whether it might be possible for SHM to host a “mini-conference” specifically on quality improvement. At the Annual Meeting, she said, she often finds herself torn between attending Q.I. sessions and sessions on clinical topics.
SHM’s Goldstein said it was a possibility.
“It is something that we have talked about and will continue to talk about,” she said.
David Lucier, MD, MBA, MPH, Director of Quality and Safety for Hospital Medicine at Massachusetts General Hospital, said that emphasizing the safety aspect of a project can often help push it along.
“I find these [types of projects] to be quite compelling, at least in reordering the priority list,” he said.
Ms. Goldstein said the suggestions were helpful in SHM’s goal of creating a “culture of ‘quality enthusiasts.’”
“We want to be the home for quality for hospitalists,” she said. “So this input is really helpful for all of us in here.”
Scrounging for information that could help her with quality improvement (Q.I.) projects, Charmaine Lewis, MD, MPH, the quality director with New Hanover Hospitalists in Wilmington, N.C., said she finds herself reviewing posters at the Annual Meeting and squinting at the images to see whether the electronic health records involved match the system she uses back home.
There’s got to be a better way.
Mangla Gulati, MD, SFHM, associate professor of medicine and chief quality officer at the University of Maryland, and Jenna Goldstein, director of SHM’s Center for Hospital Innovation and Improvement, led what grew into a lively, thoughtful discussion about ways for hospitalists to exchange information and to get support with Q.I. efforts at their centers.
The hospitalists who attended brought their experiences and their questions from a diverse range of centers, from Anchorage, Alaska, to southern California to Poughkeepsie, New York. They emphasized the need for easier access to initiatives that mirror what they are trying to do at their own centers, for more mentoring opportunities, and for more SHM chapters outside major metropolitan areas to help with networking. And they offered lessons on what they have already learned.
Remus Popa, MD, FHM, associate professor of medicine at the University of California, Riverside, who has led Q.I. projects on the use of telemetry, said a successful project will likely be more than an idea that blooms inside the head of a hospitalist.
“We have to find something that the institution really needs,” Dr. Popa said. “You have to design a better fit with them. Otherwise, it’s going to be a tough conversation about resources, right?”
Esther Lee, MD, a hospitalist in Anchorage, Alaska, asked whether it might be possible for SHM to host a “mini-conference” specifically on quality improvement. At the Annual Meeting, she said, she often finds herself torn between attending Q.I. sessions and sessions on clinical topics.
SHM’s Goldstein said it was a possibility.
“It is something that we have talked about and will continue to talk about,” she said.
David Lucier, MD, MBA, MPH, Director of Quality and Safety for Hospital Medicine at Massachusetts General Hospital, said that emphasizing the safety aspect of a project can often help push it along.
“I find these [types of projects] to be quite compelling, at least in reordering the priority list,” he said.
Ms. Goldstein said the suggestions were helpful in SHM’s goal of creating a “culture of ‘quality enthusiasts.’”
“We want to be the home for quality for hospitalists,” she said. “So this input is really helpful for all of us in here.”
Scrounging for information that could help her with quality improvement (Q.I.) projects, Charmaine Lewis, MD, MPH, the quality director with New Hanover Hospitalists in Wilmington, N.C., said she finds herself reviewing posters at the Annual Meeting and squinting at the images to see whether the electronic health records involved match the system she uses back home.
There’s got to be a better way.
Mangla Gulati, MD, SFHM, associate professor of medicine and chief quality officer at the University of Maryland, and Jenna Goldstein, director of SHM’s Center for Hospital Innovation and Improvement, led what grew into a lively, thoughtful discussion about ways for hospitalists to exchange information and to get support with Q.I. efforts at their centers.
The hospitalists who attended brought their experiences and their questions from a diverse range of centers, from Anchorage, Alaska, to southern California to Poughkeepsie, New York. They emphasized the need for easier access to initiatives that mirror what they are trying to do at their own centers, for more mentoring opportunities, and for more SHM chapters outside major metropolitan areas to help with networking. And they offered lessons on what they have already learned.
Remus Popa, MD, FHM, associate professor of medicine at the University of California, Riverside, who has led Q.I. projects on the use of telemetry, said a successful project will likely be more than an idea that blooms inside the head of a hospitalist.
“We have to find something that the institution really needs,” Dr. Popa said. “You have to design a better fit with them. Otherwise, it’s going to be a tough conversation about resources, right?”
Esther Lee, MD, a hospitalist in Anchorage, Alaska, asked whether it might be possible for SHM to host a “mini-conference” specifically on quality improvement. At the Annual Meeting, she said, she often finds herself torn between attending Q.I. sessions and sessions on clinical topics.
SHM’s Goldstein said it was a possibility.
“It is something that we have talked about and will continue to talk about,” she said.
David Lucier, MD, MBA, MPH, Director of Quality and Safety for Hospital Medicine at Massachusetts General Hospital, said that emphasizing the safety aspect of a project can often help push it along.
“I find these [types of projects] to be quite compelling, at least in reordering the priority list,” he said.
Ms. Goldstein said the suggestions were helpful in SHM’s goal of creating a “culture of ‘quality enthusiasts.’”
“We want to be the home for quality for hospitalists,” she said. “So this input is really helpful for all of us in here.”