User login
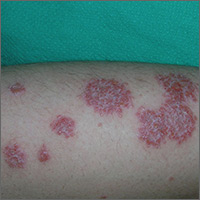
Coin-shaped lesions on arm
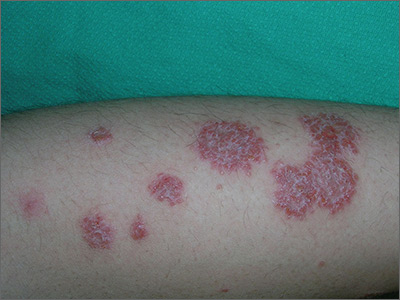
The FP noted the coin-like shape of the lesions and made a presumptive diagnosis of nummular eczema (nummular dermatitis). He was also concerned about a possible bacterial superinfection because yellow crusting was visible. However, upon further inquiry, the FP learned that the patient had just completed a 10-day course of doxycycline that was given to him by doctors in the emergency room, who suspected that this was a case of impetigo; the lesions had not improved. The patient also indicated that when the rash first erupted, he had tried an over-the-counter antifungal cream, but it had not helped. The FP still went ahead, though, and scraped the skin for a potassium hydroxide (KOH) preparation. (See a video on how to perform a KOH preparation here: http://www.mdedge.com/jfponline/article/100603/dermatology/koh-preparation.)
Since the patient hadn’t seen any improvement with either the antibiotic or the antifungal cream, the FP felt confident that this was a case of nummular eczema and not impetigo or tinea corporis. He believed that the vesicles, oozing, and crusting were all secondary to the inflammatory process. (And the KOH prep subsequently came back negative.)
Nummular eczema is a type of eczema characterized by circular or oval-shaped scaling plaques with well-defined borders. (“Nummus” is Latin for “coin.”) Nummular eczema produces multiple lesions that are most commonly found on the dorsa of the hands, arms, and legs.
Secondary morphology includes excoriations from scratching, weeping and crusting after the vesicles leak, and scaling and lichenification in more chronic lesions. Excessive weeping and crusting may indicate secondary bacterial infection, but this weeping is often part of the primary inflammatory dermatosis.
In this case, the FP prescribed a high-potency corticosteroid ointment to be applied twice daily. One month later, the patient’s skin was more than 95% improved. Some post-inflammatory hyperpigmentation remained, but the FP reassured the patient that this would likely fade over time. He also explained that the nummular eczema could return and that the steroid could be used again if that were to happen.
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Wah Y, Usatine R. Eczema. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013.
To learn more about the Color Atlas of Family Medicine, see: www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/
You can now get the second edition of the Color Atlas of Family Medicine as an app by clicking on this link: usatinemedia.com

The FP noted the coin-like shape of the lesions and made a presumptive diagnosis of nummular eczema (nummular dermatitis). He was also concerned about a possible bacterial superinfection because yellow crusting was visible. However, upon further inquiry, the FP learned that the patient had just completed a 10-day course of doxycycline that was given to him by doctors in the emergency room, who suspected that this was a case of impetigo; the lesions had not improved. The patient also indicated that when the rash first erupted, he had tried an over-the-counter antifungal cream, but it had not helped. The FP still went ahead, though, and scraped the skin for a potassium hydroxide (KOH) preparation. (See a video on how to perform a KOH preparation here: http://www.mdedge.com/jfponline/article/100603/dermatology/koh-preparation.)
Since the patient hadn’t seen any improvement with either the antibiotic or the antifungal cream, the FP felt confident that this was a case of nummular eczema and not impetigo or tinea corporis. He believed that the vesicles, oozing, and crusting were all secondary to the inflammatory process. (And the KOH prep subsequently came back negative.)
Nummular eczema is a type of eczema characterized by circular or oval-shaped scaling plaques with well-defined borders. (“Nummus” is Latin for “coin.”) Nummular eczema produces multiple lesions that are most commonly found on the dorsa of the hands, arms, and legs.
Secondary morphology includes excoriations from scratching, weeping and crusting after the vesicles leak, and scaling and lichenification in more chronic lesions. Excessive weeping and crusting may indicate secondary bacterial infection, but this weeping is often part of the primary inflammatory dermatosis.
In this case, the FP prescribed a high-potency corticosteroid ointment to be applied twice daily. One month later, the patient’s skin was more than 95% improved. Some post-inflammatory hyperpigmentation remained, but the FP reassured the patient that this would likely fade over time. He also explained that the nummular eczema could return and that the steroid could be used again if that were to happen.
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Wah Y, Usatine R. Eczema. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013.
To learn more about the Color Atlas of Family Medicine, see: www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/
You can now get the second edition of the Color Atlas of Family Medicine as an app by clicking on this link: usatinemedia.com

The FP noted the coin-like shape of the lesions and made a presumptive diagnosis of nummular eczema (nummular dermatitis). He was also concerned about a possible bacterial superinfection because yellow crusting was visible. However, upon further inquiry, the FP learned that the patient had just completed a 10-day course of doxycycline that was given to him by doctors in the emergency room, who suspected that this was a case of impetigo; the lesions had not improved. The patient also indicated that when the rash first erupted, he had tried an over-the-counter antifungal cream, but it had not helped. The FP still went ahead, though, and scraped the skin for a potassium hydroxide (KOH) preparation. (See a video on how to perform a KOH preparation here: http://www.mdedge.com/jfponline/article/100603/dermatology/koh-preparation.)
Since the patient hadn’t seen any improvement with either the antibiotic or the antifungal cream, the FP felt confident that this was a case of nummular eczema and not impetigo or tinea corporis. He believed that the vesicles, oozing, and crusting were all secondary to the inflammatory process. (And the KOH prep subsequently came back negative.)
Nummular eczema is a type of eczema characterized by circular or oval-shaped scaling plaques with well-defined borders. (“Nummus” is Latin for “coin.”) Nummular eczema produces multiple lesions that are most commonly found on the dorsa of the hands, arms, and legs.
Secondary morphology includes excoriations from scratching, weeping and crusting after the vesicles leak, and scaling and lichenification in more chronic lesions. Excessive weeping and crusting may indicate secondary bacterial infection, but this weeping is often part of the primary inflammatory dermatosis.
In this case, the FP prescribed a high-potency corticosteroid ointment to be applied twice daily. One month later, the patient’s skin was more than 95% improved. Some post-inflammatory hyperpigmentation remained, but the FP reassured the patient that this would likely fade over time. He also explained that the nummular eczema could return and that the steroid could be used again if that were to happen.
Photos and text for Photo Rounds Friday courtesy of Richard P. Usatine, MD. This case was adapted from: Wah Y, Usatine R. Eczema. In: Usatine R, Smith M, Mayeaux EJ, et al, eds. Color Atlas of Family Medicine. 2nd ed. New York, NY: McGraw-Hill; 2013.
To learn more about the Color Atlas of Family Medicine, see: www.amazon.com/Color-Family-Medicine-Richard-Usatine/dp/0071769641/
You can now get the second edition of the Color Atlas of Family Medicine as an app by clicking on this link: usatinemedia.com
Clearing the Air
The month of May marks peak season for asthma and allergies. Coincidentally, May is also Asthma and Allergy Awareness and Clean Air month. Seems a perfect match, don’t you agree? Air quality plays a menacing role in the manifestation of asthma and allergies. Let’s take a closer look at that synergy of poor air quality and respiratory sequelae and discuss approaches to mitigate these problems.
Clean air has a natural balance of gases (ie, oxygen, nitrogen, carbon dioxide) and does not contain pollutants or allergens.1 The Environmental Protection Agency (EPA), whose mission is to protect human health and the environment, identifies six common air pollutants: particulate matter (eg, dust, dirt, soot, smoke), photochemical oxidants (including ozone), carbon monoxide, sulfur dioxide, nitrogen dioxide, and lead.2 The EPA has five goals in their strategic plan, the first of which is “Addressing Climate Change and Improving Air Quality.”3 The agency is working with a multitude of stakeholders to achieve its mission of reducing air pollution. One major way we can contribute to this goal is to use public transportation, walk, or ride a bike instead of driving a car.
As we know, pollutants have detrimental consequences not only on air quality, but the environment as a whole. Pollutants infiltrate our lakes and rivers and can also damage plants and trees. Recall from your early science classes the role that plants and trees have as natural air cleaners—scrubbers, if you will. They rid the air of carbon dioxide and can also remove formaldehyde, benzene, and a host of other toxins. Trees can eradicate gaseous pollutants and airborne particles.4 But these natural air scrubbers are slowly being destroyed by the overwhelming amount of pollutants—and our short- and long-term health will ultimately pay the price. These pollutants contribute to the risk for cardiovascular and respiratory diseases, primarily asthma.5
Surveillance data show the deadly, disruptive, and costly impact asthma has on the nation.6 Asthma is a serious, potentially life-threatening chronic respiratory disease that affects quality of life in more than 24 million Americans, including an estimated six million children.7 Moreover, it is one of the most common diseases associated with poor air quality. Environmental asthma triggers include pollen, chemicals, extreme weather changes, and smoke. Educating patients with asthma on how to avoid these triggers will help them manage their disease and lessen the disruption it can cause. Additionally, a concerted effort to minimize our contribution to air pollution will assist in reducing the incidence of asthma caused by external factors.
Creating an “asthma-friendly environment” is recommended by the American Lung Association. Some might view this as a major undertaking, but simple steps such as avoiding use of aerosol products, changing the air filter in HVAC units, and dusting and vacuuming the house frequently are low-cost, effective approaches to clean the air. Avoiding perfumes and perfumed products is another way to reduce indoor triggers.
In addition to trigger avoidance, proper management of asthma is essential. Vigilance in screening for early indicators of asthma and prompt initiation of treatment can decrease or eliminate the development of long-term consequences, such as COPD and asthma-COPD overlap syndrome.8
Allergies, which affect more than 50 million people in the US, can also result from poor air quality.9 In some cases, allergies are food-based and therefore fairly easy to evade. But others are induced by pollen, pet dander, and other air-based allergens. How do we manage these pesky allergens so we can breathe easy? While the field of allergy research continues to grow, we rely heavily on allergen-specific immunotherapy as a potentially curative treat
In order for a house to be allergen-free, it should also be plant-free, right? Contrary to popular belief, this is not the case! Not all plants are problematic. A houseplant can remove formaldehyde, benzene, and a multitude of other toxins that typically reside in indoor air. Plants such as areca palm, pothos (known as Mother-in-Law’s Tongue), and the Money Plant have been shown to improve air quality.10 Additionally, decreasing or eliminating the use of room deodorizers and other allergen-containing products can reduce flare-ups. More and more frequently, we see notices in offices and at conferences to avoid the use of perfumes; this is an effective measure for the safety and comfort of those with allergies.
Alas, outdoor allergens are a bit more difficult to manage. Airborne allergens exist in such high quantities that they are nearly impossible to elude when in season.11 Keeping windows closed, wiping down surfaces where pollen and dust collects, and avoiding flowering plants can help reduce contact with allergens.
Lowering the incidence of air pollution and the symptoms of allergies and asthma can improve quality of life. By implementing these approaches to contribute to cleaner air and reduce triggers, we can help our patients and ourselves.
1. Clean air month 2017. www.whathealth.com/awareness/event/cleanairmonth.html. Accessed April 4, 2017.
2. United States Environmental Protection Agency (EPA). Particulate matter (PM) pollution. www.epa.gov/pm-pollution. Accessed April 19, 2017.
3. United States Environmental Protection Agency (EPA). EPA strategic plan. www.epa.gov/planandbudget/strategicplan. Accessed April 4, 2017.
4. Downing A. Air: what’s a tree got to do with it? www.ecology.com/2011/09/02/air-and-trees. Accessed April 4, 2017.
5. World Health Organization. Ambient (outdoor) air quality and health. www.who.int/mediacentre/factsheets/fs313/en. Ac-cessed April 4, 2017.
6. CDC. Asthma’s impact on the nation. www.cdc.gov/asthma/impacts_nation/default.htm. Accessed April 4, 2017.
7. CDC. Asthma. www.cdc.gov/asthma/default.htm. Accessed April 4, 2017.
8. Bui DS, Burgess JA, Lowe AJ, et al. Childhood lung function predicts adult COPD and asthma-COPD overlap syndrome (ACOS). Am J Respir Crit Care Med. 2017 Feb 1. [Epub ahead of print]
9. Doheny K. Living with severe allergies. www.webmd.com/allergies/features/severe-allergies#1. Accessed April 4, 2017.
10. Gromicko N, Tarasenko K. Plants and indoor air quality. www.nachi.org/plants-indoor-air-quality.htm. Accessed April 4, 2017.
11. Asthma and Allergy Foundation of America. Fight the cause of allergy. http://fightthecauseofallergy.org/page/fight. Accessed April 4, 2017.
The month of May marks peak season for asthma and allergies. Coincidentally, May is also Asthma and Allergy Awareness and Clean Air month. Seems a perfect match, don’t you agree? Air quality plays a menacing role in the manifestation of asthma and allergies. Let’s take a closer look at that synergy of poor air quality and respiratory sequelae and discuss approaches to mitigate these problems.
Clean air has a natural balance of gases (ie, oxygen, nitrogen, carbon dioxide) and does not contain pollutants or allergens.1 The Environmental Protection Agency (EPA), whose mission is to protect human health and the environment, identifies six common air pollutants: particulate matter (eg, dust, dirt, soot, smoke), photochemical oxidants (including ozone), carbon monoxide, sulfur dioxide, nitrogen dioxide, and lead.2 The EPA has five goals in their strategic plan, the first of which is “Addressing Climate Change and Improving Air Quality.”3 The agency is working with a multitude of stakeholders to achieve its mission of reducing air pollution. One major way we can contribute to this goal is to use public transportation, walk, or ride a bike instead of driving a car.
As we know, pollutants have detrimental consequences not only on air quality, but the environment as a whole. Pollutants infiltrate our lakes and rivers and can also damage plants and trees. Recall from your early science classes the role that plants and trees have as natural air cleaners—scrubbers, if you will. They rid the air of carbon dioxide and can also remove formaldehyde, benzene, and a host of other toxins. Trees can eradicate gaseous pollutants and airborne particles.4 But these natural air scrubbers are slowly being destroyed by the overwhelming amount of pollutants—and our short- and long-term health will ultimately pay the price. These pollutants contribute to the risk for cardiovascular and respiratory diseases, primarily asthma.5
Surveillance data show the deadly, disruptive, and costly impact asthma has on the nation.6 Asthma is a serious, potentially life-threatening chronic respiratory disease that affects quality of life in more than 24 million Americans, including an estimated six million children.7 Moreover, it is one of the most common diseases associated with poor air quality. Environmental asthma triggers include pollen, chemicals, extreme weather changes, and smoke. Educating patients with asthma on how to avoid these triggers will help them manage their disease and lessen the disruption it can cause. Additionally, a concerted effort to minimize our contribution to air pollution will assist in reducing the incidence of asthma caused by external factors.
Creating an “asthma-friendly environment” is recommended by the American Lung Association. Some might view this as a major undertaking, but simple steps such as avoiding use of aerosol products, changing the air filter in HVAC units, and dusting and vacuuming the house frequently are low-cost, effective approaches to clean the air. Avoiding perfumes and perfumed products is another way to reduce indoor triggers.
In addition to trigger avoidance, proper management of asthma is essential. Vigilance in screening for early indicators of asthma and prompt initiation of treatment can decrease or eliminate the development of long-term consequences, such as COPD and asthma-COPD overlap syndrome.8
Allergies, which affect more than 50 million people in the US, can also result from poor air quality.9 In some cases, allergies are food-based and therefore fairly easy to evade. But others are induced by pollen, pet dander, and other air-based allergens. How do we manage these pesky allergens so we can breathe easy? While the field of allergy research continues to grow, we rely heavily on allergen-specific immunotherapy as a potentially curative treat
In order for a house to be allergen-free, it should also be plant-free, right? Contrary to popular belief, this is not the case! Not all plants are problematic. A houseplant can remove formaldehyde, benzene, and a multitude of other toxins that typically reside in indoor air. Plants such as areca palm, pothos (known as Mother-in-Law’s Tongue), and the Money Plant have been shown to improve air quality.10 Additionally, decreasing or eliminating the use of room deodorizers and other allergen-containing products can reduce flare-ups. More and more frequently, we see notices in offices and at conferences to avoid the use of perfumes; this is an effective measure for the safety and comfort of those with allergies.
Alas, outdoor allergens are a bit more difficult to manage. Airborne allergens exist in such high quantities that they are nearly impossible to elude when in season.11 Keeping windows closed, wiping down surfaces where pollen and dust collects, and avoiding flowering plants can help reduce contact with allergens.
Lowering the incidence of air pollution and the symptoms of allergies and asthma can improve quality of life. By implementing these approaches to contribute to cleaner air and reduce triggers, we can help our patients and ourselves.
The month of May marks peak season for asthma and allergies. Coincidentally, May is also Asthma and Allergy Awareness and Clean Air month. Seems a perfect match, don’t you agree? Air quality plays a menacing role in the manifestation of asthma and allergies. Let’s take a closer look at that synergy of poor air quality and respiratory sequelae and discuss approaches to mitigate these problems.
Clean air has a natural balance of gases (ie, oxygen, nitrogen, carbon dioxide) and does not contain pollutants or allergens.1 The Environmental Protection Agency (EPA), whose mission is to protect human health and the environment, identifies six common air pollutants: particulate matter (eg, dust, dirt, soot, smoke), photochemical oxidants (including ozone), carbon monoxide, sulfur dioxide, nitrogen dioxide, and lead.2 The EPA has five goals in their strategic plan, the first of which is “Addressing Climate Change and Improving Air Quality.”3 The agency is working with a multitude of stakeholders to achieve its mission of reducing air pollution. One major way we can contribute to this goal is to use public transportation, walk, or ride a bike instead of driving a car.
As we know, pollutants have detrimental consequences not only on air quality, but the environment as a whole. Pollutants infiltrate our lakes and rivers and can also damage plants and trees. Recall from your early science classes the role that plants and trees have as natural air cleaners—scrubbers, if you will. They rid the air of carbon dioxide and can also remove formaldehyde, benzene, and a host of other toxins. Trees can eradicate gaseous pollutants and airborne particles.4 But these natural air scrubbers are slowly being destroyed by the overwhelming amount of pollutants—and our short- and long-term health will ultimately pay the price. These pollutants contribute to the risk for cardiovascular and respiratory diseases, primarily asthma.5
Surveillance data show the deadly, disruptive, and costly impact asthma has on the nation.6 Asthma is a serious, potentially life-threatening chronic respiratory disease that affects quality of life in more than 24 million Americans, including an estimated six million children.7 Moreover, it is one of the most common diseases associated with poor air quality. Environmental asthma triggers include pollen, chemicals, extreme weather changes, and smoke. Educating patients with asthma on how to avoid these triggers will help them manage their disease and lessen the disruption it can cause. Additionally, a concerted effort to minimize our contribution to air pollution will assist in reducing the incidence of asthma caused by external factors.
Creating an “asthma-friendly environment” is recommended by the American Lung Association. Some might view this as a major undertaking, but simple steps such as avoiding use of aerosol products, changing the air filter in HVAC units, and dusting and vacuuming the house frequently are low-cost, effective approaches to clean the air. Avoiding perfumes and perfumed products is another way to reduce indoor triggers.
In addition to trigger avoidance, proper management of asthma is essential. Vigilance in screening for early indicators of asthma and prompt initiation of treatment can decrease or eliminate the development of long-term consequences, such as COPD and asthma-COPD overlap syndrome.8
Allergies, which affect more than 50 million people in the US, can also result from poor air quality.9 In some cases, allergies are food-based and therefore fairly easy to evade. But others are induced by pollen, pet dander, and other air-based allergens. How do we manage these pesky allergens so we can breathe easy? While the field of allergy research continues to grow, we rely heavily on allergen-specific immunotherapy as a potentially curative treat
In order for a house to be allergen-free, it should also be plant-free, right? Contrary to popular belief, this is not the case! Not all plants are problematic. A houseplant can remove formaldehyde, benzene, and a multitude of other toxins that typically reside in indoor air. Plants such as areca palm, pothos (known as Mother-in-Law’s Tongue), and the Money Plant have been shown to improve air quality.10 Additionally, decreasing or eliminating the use of room deodorizers and other allergen-containing products can reduce flare-ups. More and more frequently, we see notices in offices and at conferences to avoid the use of perfumes; this is an effective measure for the safety and comfort of those with allergies.
Alas, outdoor allergens are a bit more difficult to manage. Airborne allergens exist in such high quantities that they are nearly impossible to elude when in season.11 Keeping windows closed, wiping down surfaces where pollen and dust collects, and avoiding flowering plants can help reduce contact with allergens.
Lowering the incidence of air pollution and the symptoms of allergies and asthma can improve quality of life. By implementing these approaches to contribute to cleaner air and reduce triggers, we can help our patients and ourselves.
1. Clean air month 2017. www.whathealth.com/awareness/event/cleanairmonth.html. Accessed April 4, 2017.
2. United States Environmental Protection Agency (EPA). Particulate matter (PM) pollution. www.epa.gov/pm-pollution. Accessed April 19, 2017.
3. United States Environmental Protection Agency (EPA). EPA strategic plan. www.epa.gov/planandbudget/strategicplan. Accessed April 4, 2017.
4. Downing A. Air: what’s a tree got to do with it? www.ecology.com/2011/09/02/air-and-trees. Accessed April 4, 2017.
5. World Health Organization. Ambient (outdoor) air quality and health. www.who.int/mediacentre/factsheets/fs313/en. Ac-cessed April 4, 2017.
6. CDC. Asthma’s impact on the nation. www.cdc.gov/asthma/impacts_nation/default.htm. Accessed April 4, 2017.
7. CDC. Asthma. www.cdc.gov/asthma/default.htm. Accessed April 4, 2017.
8. Bui DS, Burgess JA, Lowe AJ, et al. Childhood lung function predicts adult COPD and asthma-COPD overlap syndrome (ACOS). Am J Respir Crit Care Med. 2017 Feb 1. [Epub ahead of print]
9. Doheny K. Living with severe allergies. www.webmd.com/allergies/features/severe-allergies#1. Accessed April 4, 2017.
10. Gromicko N, Tarasenko K. Plants and indoor air quality. www.nachi.org/plants-indoor-air-quality.htm. Accessed April 4, 2017.
11. Asthma and Allergy Foundation of America. Fight the cause of allergy. http://fightthecauseofallergy.org/page/fight. Accessed April 4, 2017.
1. Clean air month 2017. www.whathealth.com/awareness/event/cleanairmonth.html. Accessed April 4, 2017.
2. United States Environmental Protection Agency (EPA). Particulate matter (PM) pollution. www.epa.gov/pm-pollution. Accessed April 19, 2017.
3. United States Environmental Protection Agency (EPA). EPA strategic plan. www.epa.gov/planandbudget/strategicplan. Accessed April 4, 2017.
4. Downing A. Air: what’s a tree got to do with it? www.ecology.com/2011/09/02/air-and-trees. Accessed April 4, 2017.
5. World Health Organization. Ambient (outdoor) air quality and health. www.who.int/mediacentre/factsheets/fs313/en. Ac-cessed April 4, 2017.
6. CDC. Asthma’s impact on the nation. www.cdc.gov/asthma/impacts_nation/default.htm. Accessed April 4, 2017.
7. CDC. Asthma. www.cdc.gov/asthma/default.htm. Accessed April 4, 2017.
8. Bui DS, Burgess JA, Lowe AJ, et al. Childhood lung function predicts adult COPD and asthma-COPD overlap syndrome (ACOS). Am J Respir Crit Care Med. 2017 Feb 1. [Epub ahead of print]
9. Doheny K. Living with severe allergies. www.webmd.com/allergies/features/severe-allergies#1. Accessed April 4, 2017.
10. Gromicko N, Tarasenko K. Plants and indoor air quality. www.nachi.org/plants-indoor-air-quality.htm. Accessed April 4, 2017.
11. Asthma and Allergy Foundation of America. Fight the cause of allergy. http://fightthecauseofallergy.org/page/fight. Accessed April 4, 2017.
Antipsychotics ineffective for symptoms of delirium in palliative care
CLINICAL QUESTION: Do antipsychotics provide symptomatic benefit for delirium in palliative care?
BACKGROUND: Antipsychotics are frequently used for the treatment of delirium and guideline recommended for delirium-associated distress. However, a 2016 meta-analysis found antipsychotics are not associated with change in delirium duration or severity. Antipsychotics for palliative management of delirium at end of life is not well studied.
STUDY DESIGN: Double-blind randomized controlled trial with placebo, haloperidol, and risperidone arms.
SETTING: Eleven Australian inpatient hospice or palliative care services.
SYNOPSIS: 247 patients (mean age, 74.9 years; 88.3% with cancer) with advanced incurable disease and active delirium were studied. Most had mild-moderate severity delirium. All received nonpharmacological measures and plan to address reversible precipitants. Patients were randomized to placebo (84), haloperidol (81), or risperidone (82) for 72 hours. Dose titration was allowed based on delirium symptoms. In intention to treat analysis the delirium severity scores were statistically higher in haloperidol and risperidone arms, compared with placebo. This reached statistical significance although less than the minimum clinically significant difference. Mortality, use of rescue medicines, and extrapyramidal symptoms were higher in antipsychotic groups.
BOTTOM LINE: Antipsychotics cause side effects without efficacy in palliation of symptoms of delirium.
CITATIONS: Agar MR, Lawlor PG, Quinn S, et al. Efficacy of oral risperidone, haloperidol, or placebo for symptoms of delirium among patients in palliative care: a randomized clinical trial. JAMA Intern Med. 2017 Jan;177:34-42.
Dr. Cumbler is the associate chief of hospital medicine, Division of Hospital Medicine, University of Colorado School of Medicine, Aurora.
CLINICAL QUESTION: Do antipsychotics provide symptomatic benefit for delirium in palliative care?
BACKGROUND: Antipsychotics are frequently used for the treatment of delirium and guideline recommended for delirium-associated distress. However, a 2016 meta-analysis found antipsychotics are not associated with change in delirium duration or severity. Antipsychotics for palliative management of delirium at end of life is not well studied.
STUDY DESIGN: Double-blind randomized controlled trial with placebo, haloperidol, and risperidone arms.
SETTING: Eleven Australian inpatient hospice or palliative care services.
SYNOPSIS: 247 patients (mean age, 74.9 years; 88.3% with cancer) with advanced incurable disease and active delirium were studied. Most had mild-moderate severity delirium. All received nonpharmacological measures and plan to address reversible precipitants. Patients were randomized to placebo (84), haloperidol (81), or risperidone (82) for 72 hours. Dose titration was allowed based on delirium symptoms. In intention to treat analysis the delirium severity scores were statistically higher in haloperidol and risperidone arms, compared with placebo. This reached statistical significance although less than the minimum clinically significant difference. Mortality, use of rescue medicines, and extrapyramidal symptoms were higher in antipsychotic groups.
BOTTOM LINE: Antipsychotics cause side effects without efficacy in palliation of symptoms of delirium.
CITATIONS: Agar MR, Lawlor PG, Quinn S, et al. Efficacy of oral risperidone, haloperidol, or placebo for symptoms of delirium among patients in palliative care: a randomized clinical trial. JAMA Intern Med. 2017 Jan;177:34-42.
Dr. Cumbler is the associate chief of hospital medicine, Division of Hospital Medicine, University of Colorado School of Medicine, Aurora.
CLINICAL QUESTION: Do antipsychotics provide symptomatic benefit for delirium in palliative care?
BACKGROUND: Antipsychotics are frequently used for the treatment of delirium and guideline recommended for delirium-associated distress. However, a 2016 meta-analysis found antipsychotics are not associated with change in delirium duration or severity. Antipsychotics for palliative management of delirium at end of life is not well studied.
STUDY DESIGN: Double-blind randomized controlled trial with placebo, haloperidol, and risperidone arms.
SETTING: Eleven Australian inpatient hospice or palliative care services.
SYNOPSIS: 247 patients (mean age, 74.9 years; 88.3% with cancer) with advanced incurable disease and active delirium were studied. Most had mild-moderate severity delirium. All received nonpharmacological measures and plan to address reversible precipitants. Patients were randomized to placebo (84), haloperidol (81), or risperidone (82) for 72 hours. Dose titration was allowed based on delirium symptoms. In intention to treat analysis the delirium severity scores were statistically higher in haloperidol and risperidone arms, compared with placebo. This reached statistical significance although less than the minimum clinically significant difference. Mortality, use of rescue medicines, and extrapyramidal symptoms were higher in antipsychotic groups.
BOTTOM LINE: Antipsychotics cause side effects without efficacy in palliation of symptoms of delirium.
CITATIONS: Agar MR, Lawlor PG, Quinn S, et al. Efficacy of oral risperidone, haloperidol, or placebo for symptoms of delirium among patients in palliative care: a randomized clinical trial. JAMA Intern Med. 2017 Jan;177:34-42.
Dr. Cumbler is the associate chief of hospital medicine, Division of Hospital Medicine, University of Colorado School of Medicine, Aurora.
Stump the Professor event entertains, educates
Gurpreet Dhaliwal, MD, professor of medicine at the University of California, San Francisco, joked that participating in a “Stump the Professor” event is “like taking an oral exam in front of 300 or 400 people.”
Dr. Dhaliwal passed his “exam” with flying colors on Wednesday at HM17, correctly making a diagnosis of a case of leptospirosis described by his co-presenter Daniel Brotman, MD, SFHM, professor of medicine and director of the hospitalist program at Johns Hopkins University, Baltimore.
While the format is intended to be fun and entertaining, he said that there is no doubt that learning is taking place – both by him and by the audience.
“The most important goal by far and away is to put our most important procedure on display, which is thinking,” he said. “We don’t always make our thinking explicit, and we don’t often open it to scrutiny. So the goal of this session is to do both.”
Talking through his uncertainty can be one of the most interesting aspects of the session, Dr. Dhaliwal told attendees.
“If I can’t say something insightful, let me try to capture my uncertainty and crystallize that for you so you recognize that as a real part of medicine,” he said.
The HM17 audience seemed to enjoy trying to solve the case and thinking through the clinical reasoning as Dr. Dhaliwal did the same. The diagnosis of leptospirosis in Wednesday’s case surprised the audience, many of whom shook their heads in amazement.
“I pick cases based on being dramatic and/or unusual enough to provide some clinical excitement and diagnostic challenge,” he said.
An “important bonus,” Dr. Dhaliwal said, is that the audience would learn something about the disease that’s being discussed.
“I suspect I learn the most, especially if I get the case wrong,” he told attendees. “After living it on stage, there’s a lot that I upload in my memory for the next time I see something like this in real life.”
He said he’s probably batting about 0.500 on getting the cases right.
“I’ve had plenty of experiences where I’ve pulled the rabbit out of the hat at the last minute, and it’s been glorious, and I’ve had plenty of experiences where I’ve fallen flat on my face, and I didn’t have a prayer of knowing it, either, because my thinking was off, my knowledge was deficient, or it was something I had never heard of before,” he said. “The one thing that’s always rewarding is that people are always very appreciative that I shared my thinking, whether it’s a flash of insight or a total stumble or an uncertainty that I have.”
It might seem that the event has more of a potential downside than upside: If he gets a case right, he’s doing what he should do; if he gets one wrong, it might be embarrassing. He doesn’t see it that way, he told the crowd.
“It’s a total joy to be up here,” Dr. Dhaliwal said. “There’s no doubt that standing in front of a crowd induces a little bit of anxiety, but it is a lot of fun to do. And I had mentors who did this, and then I started to learn it myself, and at some point, you get past the anxiety of being right or wrong, and you just enjoy being up there.”
Gurpreet Dhaliwal, MD, professor of medicine at the University of California, San Francisco, joked that participating in a “Stump the Professor” event is “like taking an oral exam in front of 300 or 400 people.”
Dr. Dhaliwal passed his “exam” with flying colors on Wednesday at HM17, correctly making a diagnosis of a case of leptospirosis described by his co-presenter Daniel Brotman, MD, SFHM, professor of medicine and director of the hospitalist program at Johns Hopkins University, Baltimore.
While the format is intended to be fun and entertaining, he said that there is no doubt that learning is taking place – both by him and by the audience.
“The most important goal by far and away is to put our most important procedure on display, which is thinking,” he said. “We don’t always make our thinking explicit, and we don’t often open it to scrutiny. So the goal of this session is to do both.”
Talking through his uncertainty can be one of the most interesting aspects of the session, Dr. Dhaliwal told attendees.
“If I can’t say something insightful, let me try to capture my uncertainty and crystallize that for you so you recognize that as a real part of medicine,” he said.
The HM17 audience seemed to enjoy trying to solve the case and thinking through the clinical reasoning as Dr. Dhaliwal did the same. The diagnosis of leptospirosis in Wednesday’s case surprised the audience, many of whom shook their heads in amazement.
“I pick cases based on being dramatic and/or unusual enough to provide some clinical excitement and diagnostic challenge,” he said.
An “important bonus,” Dr. Dhaliwal said, is that the audience would learn something about the disease that’s being discussed.
“I suspect I learn the most, especially if I get the case wrong,” he told attendees. “After living it on stage, there’s a lot that I upload in my memory for the next time I see something like this in real life.”
He said he’s probably batting about 0.500 on getting the cases right.
“I’ve had plenty of experiences where I’ve pulled the rabbit out of the hat at the last minute, and it’s been glorious, and I’ve had plenty of experiences where I’ve fallen flat on my face, and I didn’t have a prayer of knowing it, either, because my thinking was off, my knowledge was deficient, or it was something I had never heard of before,” he said. “The one thing that’s always rewarding is that people are always very appreciative that I shared my thinking, whether it’s a flash of insight or a total stumble or an uncertainty that I have.”
It might seem that the event has more of a potential downside than upside: If he gets a case right, he’s doing what he should do; if he gets one wrong, it might be embarrassing. He doesn’t see it that way, he told the crowd.
“It’s a total joy to be up here,” Dr. Dhaliwal said. “There’s no doubt that standing in front of a crowd induces a little bit of anxiety, but it is a lot of fun to do. And I had mentors who did this, and then I started to learn it myself, and at some point, you get past the anxiety of being right or wrong, and you just enjoy being up there.”
Gurpreet Dhaliwal, MD, professor of medicine at the University of California, San Francisco, joked that participating in a “Stump the Professor” event is “like taking an oral exam in front of 300 or 400 people.”
Dr. Dhaliwal passed his “exam” with flying colors on Wednesday at HM17, correctly making a diagnosis of a case of leptospirosis described by his co-presenter Daniel Brotman, MD, SFHM, professor of medicine and director of the hospitalist program at Johns Hopkins University, Baltimore.
While the format is intended to be fun and entertaining, he said that there is no doubt that learning is taking place – both by him and by the audience.
“The most important goal by far and away is to put our most important procedure on display, which is thinking,” he said. “We don’t always make our thinking explicit, and we don’t often open it to scrutiny. So the goal of this session is to do both.”
Talking through his uncertainty can be one of the most interesting aspects of the session, Dr. Dhaliwal told attendees.
“If I can’t say something insightful, let me try to capture my uncertainty and crystallize that for you so you recognize that as a real part of medicine,” he said.
The HM17 audience seemed to enjoy trying to solve the case and thinking through the clinical reasoning as Dr. Dhaliwal did the same. The diagnosis of leptospirosis in Wednesday’s case surprised the audience, many of whom shook their heads in amazement.
“I pick cases based on being dramatic and/or unusual enough to provide some clinical excitement and diagnostic challenge,” he said.
An “important bonus,” Dr. Dhaliwal said, is that the audience would learn something about the disease that’s being discussed.
“I suspect I learn the most, especially if I get the case wrong,” he told attendees. “After living it on stage, there’s a lot that I upload in my memory for the next time I see something like this in real life.”
He said he’s probably batting about 0.500 on getting the cases right.
“I’ve had plenty of experiences where I’ve pulled the rabbit out of the hat at the last minute, and it’s been glorious, and I’ve had plenty of experiences where I’ve fallen flat on my face, and I didn’t have a prayer of knowing it, either, because my thinking was off, my knowledge was deficient, or it was something I had never heard of before,” he said. “The one thing that’s always rewarding is that people are always very appreciative that I shared my thinking, whether it’s a flash of insight or a total stumble or an uncertainty that I have.”
It might seem that the event has more of a potential downside than upside: If he gets a case right, he’s doing what he should do; if he gets one wrong, it might be embarrassing. He doesn’t see it that way, he told the crowd.
“It’s a total joy to be up here,” Dr. Dhaliwal said. “There’s no doubt that standing in front of a crowd induces a little bit of anxiety, but it is a lot of fun to do. And I had mentors who did this, and then I started to learn it myself, and at some point, you get past the anxiety of being right or wrong, and you just enjoy being up there.”
For bone and joint infections, oral antibiotics match IV, cost less
VIENNA – Oral antibiotic therapy is just as effective as intravenous treatment in curing bone and joint infections, but costs about $3,500 less.
Treating these infections with oral agents also “improves patient autonomy, as it’s not necessary to have IV lines at home,” and represents a generally wiser use of powerful antibiotics, Matthew Scarborough, MD, said at the European Society of Clinical Microbiology and Infectious Diseases annual congress.
OVIVA (Oral vs. Intravenous Antibiotics for Bone and Joint Infection) was conducted at 26 sites in the United Kingdom. It randomized 1,054 adults with bone or joint infections to 6 weeks of either oral or intravenous treatment.
An important aspect of the trial was that both oral and IV treatment choices were made before randomization, Dr. Scarborough said. However, the decisions on what drug to use were left up to the treating physician and depended on the infection site and pathogen.
The primary outcome was definite treatment failure (bacteriologic, histologic, and clinical). Patients were followed for 1 year.
Patients were a median of 60 years old. All had surgical treatment before antibiotic therapy, including debridement and, in those with implants, removal of infected devices. The lower limb was involved in 81%, including hip, knee, and foot. The infection was in an upper limb in 10% and in the spine in 7%.
Staphylococcus aureus was present in 38% of cases, coagulase-negative staphylococci in 27%, and streptococci in 15%. Gram-negative bacteria were found in 22%.
For those patients randomized to IV therapy, glycopeptides and cephalosporins were most commonly employed (41% and 33%, respectively). For oral therapy, quinolones and penicillins were most common (37% and 16%). Most patients (74%) continued antibiotic treatment for more than 6 weeks. Forty patients were lost to follow-up.
In the primary intent-to-treat analysis, the failure rate was 13% for oral therapy and 14% for IV therapy, not a significant difference. Results were similar in the other analyses, including a modified intent to treat with only patients who had complete 1-year data, and a per-protocol analysis. All of the point prevalence numbers favored oral therapy, but crossed the null. Curves in the time-to-treatment-failure analysis were virtually superimposable, as were curves in time to discontinuation of therapy.
Another subgroup analysis examined treatment failure by infective organism; again, there were no significant treatment differences in any of the pathogen subgroups examined (S. aureus, coagulase-negative staph, streptococci species, and other gram-negative bacteria).
Nor did the type of antibiotic significantly affect failure rate, Dr. Scarborough noted. The median length of stay was 14 days for patients on IV treatment and 11 days for those taking oral medications. The incidence of serious adverse events was very similar – about 86% in each group.
On a visual analog scale that assessed health-related quality of life, patients taking oral treatment reported better mobility, self-care, and activity level, and less pain, discomfort, anxiety, and depression than those taking IV medications.
Cost represented the other significant difference between the groups. Over 1 year, the mean IV treatment cost was the equivalent of $17,152, and the mean oral treatment cost was $13,611 – a significant difference of $3,541.
“This represents a potential savings to the National Health Service of 16-25 million pounds sterling ($20.6 million-$32.3 million) per year,” Dr. Scarborough said. “All coming at no expense of good clinical outcomes.”
OVIVA was sponsored by the U.K. National Institute of Health Research. Dr. Scarborough had no financial disclosures.
[email protected]
On Twitter @alz_gal
VIENNA – Oral antibiotic therapy is just as effective as intravenous treatment in curing bone and joint infections, but costs about $3,500 less.
Treating these infections with oral agents also “improves patient autonomy, as it’s not necessary to have IV lines at home,” and represents a generally wiser use of powerful antibiotics, Matthew Scarborough, MD, said at the European Society of Clinical Microbiology and Infectious Diseases annual congress.
OVIVA (Oral vs. Intravenous Antibiotics for Bone and Joint Infection) was conducted at 26 sites in the United Kingdom. It randomized 1,054 adults with bone or joint infections to 6 weeks of either oral or intravenous treatment.
An important aspect of the trial was that both oral and IV treatment choices were made before randomization, Dr. Scarborough said. However, the decisions on what drug to use were left up to the treating physician and depended on the infection site and pathogen.
The primary outcome was definite treatment failure (bacteriologic, histologic, and clinical). Patients were followed for 1 year.
Patients were a median of 60 years old. All had surgical treatment before antibiotic therapy, including debridement and, in those with implants, removal of infected devices. The lower limb was involved in 81%, including hip, knee, and foot. The infection was in an upper limb in 10% and in the spine in 7%.
Staphylococcus aureus was present in 38% of cases, coagulase-negative staphylococci in 27%, and streptococci in 15%. Gram-negative bacteria were found in 22%.
For those patients randomized to IV therapy, glycopeptides and cephalosporins were most commonly employed (41% and 33%, respectively). For oral therapy, quinolones and penicillins were most common (37% and 16%). Most patients (74%) continued antibiotic treatment for more than 6 weeks. Forty patients were lost to follow-up.
In the primary intent-to-treat analysis, the failure rate was 13% for oral therapy and 14% for IV therapy, not a significant difference. Results were similar in the other analyses, including a modified intent to treat with only patients who had complete 1-year data, and a per-protocol analysis. All of the point prevalence numbers favored oral therapy, but crossed the null. Curves in the time-to-treatment-failure analysis were virtually superimposable, as were curves in time to discontinuation of therapy.
Another subgroup analysis examined treatment failure by infective organism; again, there were no significant treatment differences in any of the pathogen subgroups examined (S. aureus, coagulase-negative staph, streptococci species, and other gram-negative bacteria).
Nor did the type of antibiotic significantly affect failure rate, Dr. Scarborough noted. The median length of stay was 14 days for patients on IV treatment and 11 days for those taking oral medications. The incidence of serious adverse events was very similar – about 86% in each group.
On a visual analog scale that assessed health-related quality of life, patients taking oral treatment reported better mobility, self-care, and activity level, and less pain, discomfort, anxiety, and depression than those taking IV medications.
Cost represented the other significant difference between the groups. Over 1 year, the mean IV treatment cost was the equivalent of $17,152, and the mean oral treatment cost was $13,611 – a significant difference of $3,541.
“This represents a potential savings to the National Health Service of 16-25 million pounds sterling ($20.6 million-$32.3 million) per year,” Dr. Scarborough said. “All coming at no expense of good clinical outcomes.”
OVIVA was sponsored by the U.K. National Institute of Health Research. Dr. Scarborough had no financial disclosures.
[email protected]
On Twitter @alz_gal
VIENNA – Oral antibiotic therapy is just as effective as intravenous treatment in curing bone and joint infections, but costs about $3,500 less.
Treating these infections with oral agents also “improves patient autonomy, as it’s not necessary to have IV lines at home,” and represents a generally wiser use of powerful antibiotics, Matthew Scarborough, MD, said at the European Society of Clinical Microbiology and Infectious Diseases annual congress.
OVIVA (Oral vs. Intravenous Antibiotics for Bone and Joint Infection) was conducted at 26 sites in the United Kingdom. It randomized 1,054 adults with bone or joint infections to 6 weeks of either oral or intravenous treatment.
An important aspect of the trial was that both oral and IV treatment choices were made before randomization, Dr. Scarborough said. However, the decisions on what drug to use were left up to the treating physician and depended on the infection site and pathogen.
The primary outcome was definite treatment failure (bacteriologic, histologic, and clinical). Patients were followed for 1 year.
Patients were a median of 60 years old. All had surgical treatment before antibiotic therapy, including debridement and, in those with implants, removal of infected devices. The lower limb was involved in 81%, including hip, knee, and foot. The infection was in an upper limb in 10% and in the spine in 7%.
Staphylococcus aureus was present in 38% of cases, coagulase-negative staphylococci in 27%, and streptococci in 15%. Gram-negative bacteria were found in 22%.
For those patients randomized to IV therapy, glycopeptides and cephalosporins were most commonly employed (41% and 33%, respectively). For oral therapy, quinolones and penicillins were most common (37% and 16%). Most patients (74%) continued antibiotic treatment for more than 6 weeks. Forty patients were lost to follow-up.
In the primary intent-to-treat analysis, the failure rate was 13% for oral therapy and 14% for IV therapy, not a significant difference. Results were similar in the other analyses, including a modified intent to treat with only patients who had complete 1-year data, and a per-protocol analysis. All of the point prevalence numbers favored oral therapy, but crossed the null. Curves in the time-to-treatment-failure analysis were virtually superimposable, as were curves in time to discontinuation of therapy.
Another subgroup analysis examined treatment failure by infective organism; again, there were no significant treatment differences in any of the pathogen subgroups examined (S. aureus, coagulase-negative staph, streptococci species, and other gram-negative bacteria).
Nor did the type of antibiotic significantly affect failure rate, Dr. Scarborough noted. The median length of stay was 14 days for patients on IV treatment and 11 days for those taking oral medications. The incidence of serious adverse events was very similar – about 86% in each group.
On a visual analog scale that assessed health-related quality of life, patients taking oral treatment reported better mobility, self-care, and activity level, and less pain, discomfort, anxiety, and depression than those taking IV medications.
Cost represented the other significant difference between the groups. Over 1 year, the mean IV treatment cost was the equivalent of $17,152, and the mean oral treatment cost was $13,611 – a significant difference of $3,541.
“This represents a potential savings to the National Health Service of 16-25 million pounds sterling ($20.6 million-$32.3 million) per year,” Dr. Scarborough said. “All coming at no expense of good clinical outcomes.”
OVIVA was sponsored by the U.K. National Institute of Health Research. Dr. Scarborough had no financial disclosures.
[email protected]
On Twitter @alz_gal
AT ECCMID 2017
Key clinical point:
Major finding: At 1 year, cure rates were identical, but oral treatment cost about $3,500 less than IV treatment.
Data source: The study randomized 1,054 patients.
Disclosures: OVIVA was sponsored by the U.K. National Institute of Health Research. Dr. Scarborough had no financial disclosures.
Declining bullying rates in Maryland study contradict common misconception
Rates of bullying among students in grades 4-12 decreased over the past 10 years in a state study, contradicting a common perception of a rising trend in schools, according to a study.
The rate of self-reported, frequent bullying victimization fell from 28% in 2005 to 13% in 2014, reported Tracy Evian Waasdorp, PhD, at the Children’s Hospital of Philadelphia and the Center for the Prevention of Youth Violence at the Johns Hopkins Bloomberg School of Public Health, Baltimore, and her associates. “These findings do contradict the public’s [mis]perception that bullying is increasing.”
Data collected through a survey of 246,306 students in grades 4-12 from 109 schools in Maryland in 2005-2014 found significant decreases in 10 of 13 bullying indicators (Pediatrics. 2017. doi: 10.1542/peds.2016-2615).
In the survey, students anonymously reported if they had been a frequent victim of bullying – two or more times within the past month – as defined by the World Health Organization and Center for Disease Control and Prevention’s definition: “A person is bullied when he or she is exposed, repeatedly and over time, to negative actions on the part of one or more other persons. Bullying often occurs in situations where there is a power or status difference. Bullying includes actions like threatening, teasing, name-calling, ignoring, rumor spreading, sending hurtful emails and text messages, and leaving someone out on purpose.”
The investigators found victimization decreased across indicators including pushing (beta = –0.03), hitting (beta = –0.03), threats (beta = –0.02), cyberbullying (beta = –0.01), and rumors (beta = –0.02), according to the researchers. All values were determined with a P value less than .001.
“It was hypothesized that cyberbullying might increase, but consistent with the other forms of bullying, cyberbullying also decreased,” the researchers wrote. “However, given the rapid change of technology and new social media platforms used by youth and increasingly at younger ages, the nature and quality of cyberbullying may change.”
Dr. Waasdorp and her colleagues also had children report if and how often they had participated in bullying or had witnessed bullying, both of which also declined, from 21% to 7% of students and 66% to 43% of students, respectively.
Along with bullying, students were asked how safe they felt in school and if adults in their school were doing enough to prevent bullying, both of which sentiments increased over the course of the study. While 80% of students reported feeling safe in the school, the number of those who felt as though they belonged remained relatively unchanged.
While decreases in each category were relatively small from year to year, “some of these changes were fairly substantial across 10 years, as indicated by the effect size estimates comparing the first and last years (average difference = 0.325),” according to the researchers.
In fact, Dr. Waasdorp and her peers found the final year of the study to have the greatest improvement, which they estimate may come from more comprehensive bullying laws and school practices.
Looking across grade levels, Dr. Waasdorp and her colleagues found greater declines in witnessing bullying and school safety in high schoolers than middle schoolers, which they say may indicate more support in middle school systems, where bullying peaks.
Because of the large number of outcomes, significant associations between school levels and bullying indicators were limited. The anonymous nature of the survey limited the ability of the researchers to link student data across years. The investigators also did not collect data on why changes to the bullying indicators occurred.
During the study, the researchers were supported in part by grants from the U.S. Department of Education, the William T. Grant Foundation, and the National Institute of Justice. The authors reported no relevant financial disclosures.
[email protected]
On Twitter @eaztweets
The Waasdorp et al. study is a comprehensive one using a sophisticated longitudinal design and a number of covariates to give a better comprehension of current bullying trends.
While it is encouraging to hear of the declining trends across many forms of bullying, it is important to remember 48% of children still reported bullying as an issue in their lives, with nearly as many reporting witnessing bullying against others.
We must be watchful for instances of bullying and active in getting rid of it both in and out of the classroom.
This means calling on educators to implement programs that not only sound like they will work, but have been tested and proven to be the best choice for the entire community. Programs that build empathy and encourage students to figure out productive conflict-management solutions often are good choices.
The responsibility to end bullying is not just with educators, but with pediatricians as well. Bullying can have serious mental and physical ramifications for patients, and clinicians must be vigilant for signs of victimization, such as anxiety, depression, or social withdrawal. If it seems as though a patient has been the victim or is the perpetrator of bullying, clinicians may want to talk with the child and their parents about finding a counselor at school where bullying might occur most often, encourage the child to talk with his or her parents about any problems at school, build a stronger communication between parents and the school, and help to support at least one peer friendship, which has been found to be a strong buffer against peer victimization.
This study is a good example of the progress made so far, but there is still plenty of work to be done.
Stephen S. Leff, PhD, is a psychologist in the department of child and adolescent psychiatry and behavioral sciences and codirector of the Violence Prevention Initiative at the Children’s Hospital of Philadelphia and Chris Feudtner, MD, PhD, is director of the department of medical ethics at the hospital. This a summary of their comments from an editorial accompanying the report by Waasdorp et al. (Pediatrics. 2017. doi: 10.1542/peds.2017-0504 ) Neither Dr. Leff nor Dr. Feudtner reported any relevant disclosures.
The Waasdorp et al. study is a comprehensive one using a sophisticated longitudinal design and a number of covariates to give a better comprehension of current bullying trends.
While it is encouraging to hear of the declining trends across many forms of bullying, it is important to remember 48% of children still reported bullying as an issue in their lives, with nearly as many reporting witnessing bullying against others.
We must be watchful for instances of bullying and active in getting rid of it both in and out of the classroom.
This means calling on educators to implement programs that not only sound like they will work, but have been tested and proven to be the best choice for the entire community. Programs that build empathy and encourage students to figure out productive conflict-management solutions often are good choices.
The responsibility to end bullying is not just with educators, but with pediatricians as well. Bullying can have serious mental and physical ramifications for patients, and clinicians must be vigilant for signs of victimization, such as anxiety, depression, or social withdrawal. If it seems as though a patient has been the victim or is the perpetrator of bullying, clinicians may want to talk with the child and their parents about finding a counselor at school where bullying might occur most often, encourage the child to talk with his or her parents about any problems at school, build a stronger communication between parents and the school, and help to support at least one peer friendship, which has been found to be a strong buffer against peer victimization.
This study is a good example of the progress made so far, but there is still plenty of work to be done.
Stephen S. Leff, PhD, is a psychologist in the department of child and adolescent psychiatry and behavioral sciences and codirector of the Violence Prevention Initiative at the Children’s Hospital of Philadelphia and Chris Feudtner, MD, PhD, is director of the department of medical ethics at the hospital. This a summary of their comments from an editorial accompanying the report by Waasdorp et al. (Pediatrics. 2017. doi: 10.1542/peds.2017-0504 ) Neither Dr. Leff nor Dr. Feudtner reported any relevant disclosures.
The Waasdorp et al. study is a comprehensive one using a sophisticated longitudinal design and a number of covariates to give a better comprehension of current bullying trends.
While it is encouraging to hear of the declining trends across many forms of bullying, it is important to remember 48% of children still reported bullying as an issue in their lives, with nearly as many reporting witnessing bullying against others.
We must be watchful for instances of bullying and active in getting rid of it both in and out of the classroom.
This means calling on educators to implement programs that not only sound like they will work, but have been tested and proven to be the best choice for the entire community. Programs that build empathy and encourage students to figure out productive conflict-management solutions often are good choices.
The responsibility to end bullying is not just with educators, but with pediatricians as well. Bullying can have serious mental and physical ramifications for patients, and clinicians must be vigilant for signs of victimization, such as anxiety, depression, or social withdrawal. If it seems as though a patient has been the victim or is the perpetrator of bullying, clinicians may want to talk with the child and their parents about finding a counselor at school where bullying might occur most often, encourage the child to talk with his or her parents about any problems at school, build a stronger communication between parents and the school, and help to support at least one peer friendship, which has been found to be a strong buffer against peer victimization.
This study is a good example of the progress made so far, but there is still plenty of work to be done.
Stephen S. Leff, PhD, is a psychologist in the department of child and adolescent psychiatry and behavioral sciences and codirector of the Violence Prevention Initiative at the Children’s Hospital of Philadelphia and Chris Feudtner, MD, PhD, is director of the department of medical ethics at the hospital. This a summary of their comments from an editorial accompanying the report by Waasdorp et al. (Pediatrics. 2017. doi: 10.1542/peds.2017-0504 ) Neither Dr. Leff nor Dr. Feudtner reported any relevant disclosures.
Rates of bullying among students in grades 4-12 decreased over the past 10 years in a state study, contradicting a common perception of a rising trend in schools, according to a study.
The rate of self-reported, frequent bullying victimization fell from 28% in 2005 to 13% in 2014, reported Tracy Evian Waasdorp, PhD, at the Children’s Hospital of Philadelphia and the Center for the Prevention of Youth Violence at the Johns Hopkins Bloomberg School of Public Health, Baltimore, and her associates. “These findings do contradict the public’s [mis]perception that bullying is increasing.”
Data collected through a survey of 246,306 students in grades 4-12 from 109 schools in Maryland in 2005-2014 found significant decreases in 10 of 13 bullying indicators (Pediatrics. 2017. doi: 10.1542/peds.2016-2615).
In the survey, students anonymously reported if they had been a frequent victim of bullying – two or more times within the past month – as defined by the World Health Organization and Center for Disease Control and Prevention’s definition: “A person is bullied when he or she is exposed, repeatedly and over time, to negative actions on the part of one or more other persons. Bullying often occurs in situations where there is a power or status difference. Bullying includes actions like threatening, teasing, name-calling, ignoring, rumor spreading, sending hurtful emails and text messages, and leaving someone out on purpose.”
The investigators found victimization decreased across indicators including pushing (beta = –0.03), hitting (beta = –0.03), threats (beta = –0.02), cyberbullying (beta = –0.01), and rumors (beta = –0.02), according to the researchers. All values were determined with a P value less than .001.
“It was hypothesized that cyberbullying might increase, but consistent with the other forms of bullying, cyberbullying also decreased,” the researchers wrote. “However, given the rapid change of technology and new social media platforms used by youth and increasingly at younger ages, the nature and quality of cyberbullying may change.”
Dr. Waasdorp and her colleagues also had children report if and how often they had participated in bullying or had witnessed bullying, both of which also declined, from 21% to 7% of students and 66% to 43% of students, respectively.
Along with bullying, students were asked how safe they felt in school and if adults in their school were doing enough to prevent bullying, both of which sentiments increased over the course of the study. While 80% of students reported feeling safe in the school, the number of those who felt as though they belonged remained relatively unchanged.
While decreases in each category were relatively small from year to year, “some of these changes were fairly substantial across 10 years, as indicated by the effect size estimates comparing the first and last years (average difference = 0.325),” according to the researchers.
In fact, Dr. Waasdorp and her peers found the final year of the study to have the greatest improvement, which they estimate may come from more comprehensive bullying laws and school practices.
Looking across grade levels, Dr. Waasdorp and her colleagues found greater declines in witnessing bullying and school safety in high schoolers than middle schoolers, which they say may indicate more support in middle school systems, where bullying peaks.
Because of the large number of outcomes, significant associations between school levels and bullying indicators were limited. The anonymous nature of the survey limited the ability of the researchers to link student data across years. The investigators also did not collect data on why changes to the bullying indicators occurred.
During the study, the researchers were supported in part by grants from the U.S. Department of Education, the William T. Grant Foundation, and the National Institute of Justice. The authors reported no relevant financial disclosures.
[email protected]
On Twitter @eaztweets
Rates of bullying among students in grades 4-12 decreased over the past 10 years in a state study, contradicting a common perception of a rising trend in schools, according to a study.
The rate of self-reported, frequent bullying victimization fell from 28% in 2005 to 13% in 2014, reported Tracy Evian Waasdorp, PhD, at the Children’s Hospital of Philadelphia and the Center for the Prevention of Youth Violence at the Johns Hopkins Bloomberg School of Public Health, Baltimore, and her associates. “These findings do contradict the public’s [mis]perception that bullying is increasing.”
Data collected through a survey of 246,306 students in grades 4-12 from 109 schools in Maryland in 2005-2014 found significant decreases in 10 of 13 bullying indicators (Pediatrics. 2017. doi: 10.1542/peds.2016-2615).
In the survey, students anonymously reported if they had been a frequent victim of bullying – two or more times within the past month – as defined by the World Health Organization and Center for Disease Control and Prevention’s definition: “A person is bullied when he or she is exposed, repeatedly and over time, to negative actions on the part of one or more other persons. Bullying often occurs in situations where there is a power or status difference. Bullying includes actions like threatening, teasing, name-calling, ignoring, rumor spreading, sending hurtful emails and text messages, and leaving someone out on purpose.”
The investigators found victimization decreased across indicators including pushing (beta = –0.03), hitting (beta = –0.03), threats (beta = –0.02), cyberbullying (beta = –0.01), and rumors (beta = –0.02), according to the researchers. All values were determined with a P value less than .001.
“It was hypothesized that cyberbullying might increase, but consistent with the other forms of bullying, cyberbullying also decreased,” the researchers wrote. “However, given the rapid change of technology and new social media platforms used by youth and increasingly at younger ages, the nature and quality of cyberbullying may change.”
Dr. Waasdorp and her colleagues also had children report if and how often they had participated in bullying or had witnessed bullying, both of which also declined, from 21% to 7% of students and 66% to 43% of students, respectively.
Along with bullying, students were asked how safe they felt in school and if adults in their school were doing enough to prevent bullying, both of which sentiments increased over the course of the study. While 80% of students reported feeling safe in the school, the number of those who felt as though they belonged remained relatively unchanged.
While decreases in each category were relatively small from year to year, “some of these changes were fairly substantial across 10 years, as indicated by the effect size estimates comparing the first and last years (average difference = 0.325),” according to the researchers.
In fact, Dr. Waasdorp and her peers found the final year of the study to have the greatest improvement, which they estimate may come from more comprehensive bullying laws and school practices.
Looking across grade levels, Dr. Waasdorp and her colleagues found greater declines in witnessing bullying and school safety in high schoolers than middle schoolers, which they say may indicate more support in middle school systems, where bullying peaks.
Because of the large number of outcomes, significant associations between school levels and bullying indicators were limited. The anonymous nature of the survey limited the ability of the researchers to link student data across years. The investigators also did not collect data on why changes to the bullying indicators occurred.
During the study, the researchers were supported in part by grants from the U.S. Department of Education, the William T. Grant Foundation, and the National Institute of Justice. The authors reported no relevant financial disclosures.
[email protected]
On Twitter @eaztweets
FROM PEDIATRICS
Key clinical point:
Major finding: Reports of victimization overall among Maryland students in grades 4-12 decreased from 28% to 13% over a decade, with decreases in 10 of 13 bullying indicators in the study.
Data source: Self-reported survey of 246,306 students in grades 4-12 from 109 Maryland schools in 2005-2014, analyzed using a longitudinal hierarchical linear model.
Disclosures: During the study, researchers were supported in part by grants from the U.S. Department of Education, the William T. Grant Foundation, and the National Institute of Justice. The authors reported no relevant financial disclosures.
RIV winners celebrated for their creative use of data
This year’s RIV innovation winners reflect a nascent trend of applying informatics to quality improvement and patient safety initiatives.
“One striking thing is that all three winners used either EHR or Big Data and large collaboratives to achieve their goals,” Margaret Fang, MD, MPH, FHM, program chair for HM17’s scientific abstracts competition, and moderator of the winners’ panel, said in an interview. This year’s winners included a sleep-promoting “nudge” system that Dr. Fang said she expects will help improve sleep and lower rates of delirium and a source code that connects disparate data systems for daily updates on where quality can be improved. The third winner used what Dr. Fang, a hospitalist and the medical director of the anticoagulation clinic at the University of California, San Francisco, called a “classic quality improvement collaborative,” which simplifies the decision tree around venous thromboembolism (VTE) prophylaxis for better patient outcomes.
Calling uninterrupted sleep the “sine qua non” of patient care, RIV award recipient Vineet Arora, MD, an associate professor of medicine at the University of Chicago, described the rationale for her RIV award-winning SIESTA (Sleep for Inpatients: Empowering Staff to Act) program. She and her colleagues surveyed hospitalists, nurses, residents, and patients to determine the most common sleep disrupters in their institution and devised “nudges” to alter how staff performed various tasks that otherwise might interfere with patient sleep. Rather than use overt incentives, nudges are changes in what Dr. Arora called the “choice architecture” of people’s behavior.
Based on survey feedback, Dr. Arora and her colleagues worked with their electronic health record (EHR) vendor to consolidate the performance of certain tasks that were affecting patient sleep. Reminders were added to daily nursing huddles to prompt them to look for ways they could decrease patient interruptions, and empowerment coaching was offered to nurses to encourage patient advocacy when physicians had given orders that would interfere with patients’ sleep.
When tested and measured over the course of a year, SIESTA’s EHR innovations resulted in six fewer nighttime disruptions than before the intervention, compared with controls, a statistically significant difference. The nursing-based interventions resulted in one less nocturnal interruption on average, also a significant change.
“If every patient were admitted into a SIESTA unit, 84% would say they were not disrupted by medications, compared to 57%. For interruptions for vitals, it would be 17% vs. 41%,” Dr. Arora said. In terms of the Hospital Consumer Assessment of Healthcare Providers and Systems) data, this translates into as much as a 25th-percentile performance improvement for hospitals in related domains, according to Dr. Arora.
Nader Najafi, MD, an assistant clinical professor of medicine at UCSF, and his colleagues created Murmur, an open-source code data aggregator, which can be customized to solve a variety of quality improvement issues. RIV award winner Dr. Najafi applied the code to determine how systems failures in their institution were contributing to avoidable inpatient days, for example. At a daily appointed time, Murmur would determine which staff members were scheduled to work that day. Each provider would then receive a brief, customized survey about patients for that day on their cell phone. The data were then collected to create instant reports of where the delays in discharge were occurring.
Testing by gastroenterologists was pinpointed as a “huge source of delays, something we had never been able to quantify before, “ Dr. Najafi said. This led to brainstorming sessions with the department for solutions.
To reduce rates of hospital-associated VTE, 35 California hospitals with varying numbers of beds and locations collaborated on a project led by RIV award recipient Ian Jenkins, MD, SFHM, a health sciences clinical professor at the University of California, San Diego. Key components of the intervention were mentoring at the sites by VTE prophylaxis experts, group webinars in best practices, and a “measure-vention.” Teams were taught how to rate patient risk for VTE and apply specific protocols according to risk rating using the SHM-mentored implementation model. Real-time monitoring of the intervention was used to make any necessary adjustments. When before-and-after data were compared, following the 18-month period during which the intervention was measured, Dr. Jenkins said an average of 330 VTEs were averted annually. “We found the results very gratifying,” said Dr. Jenkins.
“These projects all reflect a broader trend in hospital medicine where we are using the wealth of data we have now for quality improvement and for outcomes research,” Dr. Fang said in the interview.
There were no relevant disclosures.
This year’s RIV innovation winners reflect a nascent trend of applying informatics to quality improvement and patient safety initiatives.
“One striking thing is that all three winners used either EHR or Big Data and large collaboratives to achieve their goals,” Margaret Fang, MD, MPH, FHM, program chair for HM17’s scientific abstracts competition, and moderator of the winners’ panel, said in an interview. This year’s winners included a sleep-promoting “nudge” system that Dr. Fang said she expects will help improve sleep and lower rates of delirium and a source code that connects disparate data systems for daily updates on where quality can be improved. The third winner used what Dr. Fang, a hospitalist and the medical director of the anticoagulation clinic at the University of California, San Francisco, called a “classic quality improvement collaborative,” which simplifies the decision tree around venous thromboembolism (VTE) prophylaxis for better patient outcomes.
Calling uninterrupted sleep the “sine qua non” of patient care, RIV award recipient Vineet Arora, MD, an associate professor of medicine at the University of Chicago, described the rationale for her RIV award-winning SIESTA (Sleep for Inpatients: Empowering Staff to Act) program. She and her colleagues surveyed hospitalists, nurses, residents, and patients to determine the most common sleep disrupters in their institution and devised “nudges” to alter how staff performed various tasks that otherwise might interfere with patient sleep. Rather than use overt incentives, nudges are changes in what Dr. Arora called the “choice architecture” of people’s behavior.
Based on survey feedback, Dr. Arora and her colleagues worked with their electronic health record (EHR) vendor to consolidate the performance of certain tasks that were affecting patient sleep. Reminders were added to daily nursing huddles to prompt them to look for ways they could decrease patient interruptions, and empowerment coaching was offered to nurses to encourage patient advocacy when physicians had given orders that would interfere with patients’ sleep.
When tested and measured over the course of a year, SIESTA’s EHR innovations resulted in six fewer nighttime disruptions than before the intervention, compared with controls, a statistically significant difference. The nursing-based interventions resulted in one less nocturnal interruption on average, also a significant change.
“If every patient were admitted into a SIESTA unit, 84% would say they were not disrupted by medications, compared to 57%. For interruptions for vitals, it would be 17% vs. 41%,” Dr. Arora said. In terms of the Hospital Consumer Assessment of Healthcare Providers and Systems) data, this translates into as much as a 25th-percentile performance improvement for hospitals in related domains, according to Dr. Arora.
Nader Najafi, MD, an assistant clinical professor of medicine at UCSF, and his colleagues created Murmur, an open-source code data aggregator, which can be customized to solve a variety of quality improvement issues. RIV award winner Dr. Najafi applied the code to determine how systems failures in their institution were contributing to avoidable inpatient days, for example. At a daily appointed time, Murmur would determine which staff members were scheduled to work that day. Each provider would then receive a brief, customized survey about patients for that day on their cell phone. The data were then collected to create instant reports of where the delays in discharge were occurring.
Testing by gastroenterologists was pinpointed as a “huge source of delays, something we had never been able to quantify before, “ Dr. Najafi said. This led to brainstorming sessions with the department for solutions.
To reduce rates of hospital-associated VTE, 35 California hospitals with varying numbers of beds and locations collaborated on a project led by RIV award recipient Ian Jenkins, MD, SFHM, a health sciences clinical professor at the University of California, San Diego. Key components of the intervention were mentoring at the sites by VTE prophylaxis experts, group webinars in best practices, and a “measure-vention.” Teams were taught how to rate patient risk for VTE and apply specific protocols according to risk rating using the SHM-mentored implementation model. Real-time monitoring of the intervention was used to make any necessary adjustments. When before-and-after data were compared, following the 18-month period during which the intervention was measured, Dr. Jenkins said an average of 330 VTEs were averted annually. “We found the results very gratifying,” said Dr. Jenkins.
“These projects all reflect a broader trend in hospital medicine where we are using the wealth of data we have now for quality improvement and for outcomes research,” Dr. Fang said in the interview.
There were no relevant disclosures.
This year’s RIV innovation winners reflect a nascent trend of applying informatics to quality improvement and patient safety initiatives.
“One striking thing is that all three winners used either EHR or Big Data and large collaboratives to achieve their goals,” Margaret Fang, MD, MPH, FHM, program chair for HM17’s scientific abstracts competition, and moderator of the winners’ panel, said in an interview. This year’s winners included a sleep-promoting “nudge” system that Dr. Fang said she expects will help improve sleep and lower rates of delirium and a source code that connects disparate data systems for daily updates on where quality can be improved. The third winner used what Dr. Fang, a hospitalist and the medical director of the anticoagulation clinic at the University of California, San Francisco, called a “classic quality improvement collaborative,” which simplifies the decision tree around venous thromboembolism (VTE) prophylaxis for better patient outcomes.
Calling uninterrupted sleep the “sine qua non” of patient care, RIV award recipient Vineet Arora, MD, an associate professor of medicine at the University of Chicago, described the rationale for her RIV award-winning SIESTA (Sleep for Inpatients: Empowering Staff to Act) program. She and her colleagues surveyed hospitalists, nurses, residents, and patients to determine the most common sleep disrupters in their institution and devised “nudges” to alter how staff performed various tasks that otherwise might interfere with patient sleep. Rather than use overt incentives, nudges are changes in what Dr. Arora called the “choice architecture” of people’s behavior.
Based on survey feedback, Dr. Arora and her colleagues worked with their electronic health record (EHR) vendor to consolidate the performance of certain tasks that were affecting patient sleep. Reminders were added to daily nursing huddles to prompt them to look for ways they could decrease patient interruptions, and empowerment coaching was offered to nurses to encourage patient advocacy when physicians had given orders that would interfere with patients’ sleep.
When tested and measured over the course of a year, SIESTA’s EHR innovations resulted in six fewer nighttime disruptions than before the intervention, compared with controls, a statistically significant difference. The nursing-based interventions resulted in one less nocturnal interruption on average, also a significant change.
“If every patient were admitted into a SIESTA unit, 84% would say they were not disrupted by medications, compared to 57%. For interruptions for vitals, it would be 17% vs. 41%,” Dr. Arora said. In terms of the Hospital Consumer Assessment of Healthcare Providers and Systems) data, this translates into as much as a 25th-percentile performance improvement for hospitals in related domains, according to Dr. Arora.
Nader Najafi, MD, an assistant clinical professor of medicine at UCSF, and his colleagues created Murmur, an open-source code data aggregator, which can be customized to solve a variety of quality improvement issues. RIV award winner Dr. Najafi applied the code to determine how systems failures in their institution were contributing to avoidable inpatient days, for example. At a daily appointed time, Murmur would determine which staff members were scheduled to work that day. Each provider would then receive a brief, customized survey about patients for that day on their cell phone. The data were then collected to create instant reports of where the delays in discharge were occurring.
Testing by gastroenterologists was pinpointed as a “huge source of delays, something we had never been able to quantify before, “ Dr. Najafi said. This led to brainstorming sessions with the department for solutions.
To reduce rates of hospital-associated VTE, 35 California hospitals with varying numbers of beds and locations collaborated on a project led by RIV award recipient Ian Jenkins, MD, SFHM, a health sciences clinical professor at the University of California, San Diego. Key components of the intervention were mentoring at the sites by VTE prophylaxis experts, group webinars in best practices, and a “measure-vention.” Teams were taught how to rate patient risk for VTE and apply specific protocols according to risk rating using the SHM-mentored implementation model. Real-time monitoring of the intervention was used to make any necessary adjustments. When before-and-after data were compared, following the 18-month period during which the intervention was measured, Dr. Jenkins said an average of 330 VTEs were averted annually. “We found the results very gratifying,” said Dr. Jenkins.
“These projects all reflect a broader trend in hospital medicine where we are using the wealth of data we have now for quality improvement and for outcomes research,” Dr. Fang said in the interview.
There were no relevant disclosures.
VIDEO: Hospitalists can help improve antibiotic stewardship
Hospitalists can – and should – help curb unnecessary antibiotic use, according to an expert who spoke at HM17.
Nearly three-quarters of patients who have been diagnosed with community acquired pneumonia are receiving antibiotics for longer periods than necessary, either because the severity of their illness doesn’t warrant them or because they do not have pneumonia, according to Valerie M. Vaughn, MD, a research scientist in the division of hospital medicine and the Patient Safety Enhancement Program at Michigan Medicine, Ann Arbor.
“As hospitalists, we have a role to play in antibiotic stewardship,” Dr. Vaughn said in this interview recorded at the meeting.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Hospitalists can – and should – help curb unnecessary antibiotic use, according to an expert who spoke at HM17.
Nearly three-quarters of patients who have been diagnosed with community acquired pneumonia are receiving antibiotics for longer periods than necessary, either because the severity of their illness doesn’t warrant them or because they do not have pneumonia, according to Valerie M. Vaughn, MD, a research scientist in the division of hospital medicine and the Patient Safety Enhancement Program at Michigan Medicine, Ann Arbor.
“As hospitalists, we have a role to play in antibiotic stewardship,” Dr. Vaughn said in this interview recorded at the meeting.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Hospitalists can – and should – help curb unnecessary antibiotic use, according to an expert who spoke at HM17.
Nearly three-quarters of patients who have been diagnosed with community acquired pneumonia are receiving antibiotics for longer periods than necessary, either because the severity of their illness doesn’t warrant them or because they do not have pneumonia, according to Valerie M. Vaughn, MD, a research scientist in the division of hospital medicine and the Patient Safety Enhancement Program at Michigan Medicine, Ann Arbor.
“As hospitalists, we have a role to play in antibiotic stewardship,” Dr. Vaughn said in this interview recorded at the meeting.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
VIDEO: How informatics can help your hospital prevent infections
Hospitalists have a powerful tool to help them fight outbreaks of Clostridium difficile and other infectious agents: electronic health record data.
Sara Murray, MD, an assistant professor of medicine at the University of California, San Francisco, and her colleagues, used EHR data to map temporal and spatial coordinates to determine where patients in their hospital were at highest risk for C. difficile. Patients who’d had a CT scan on a particular machine in the emergency department within 24 hours of an infected person having been scanned there had a threefold higher risk of infection, they found. This information helped the hospital’s infection control team to create a more effective sterilization plan for that specific machine.
“The takeaway is that we should be leveraging our EHR data to inform our quality improvement efforts,” Dr. Murray said in this video interview, recorded during HM17.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Hospitalists have a powerful tool to help them fight outbreaks of Clostridium difficile and other infectious agents: electronic health record data.
Sara Murray, MD, an assistant professor of medicine at the University of California, San Francisco, and her colleagues, used EHR data to map temporal and spatial coordinates to determine where patients in their hospital were at highest risk for C. difficile. Patients who’d had a CT scan on a particular machine in the emergency department within 24 hours of an infected person having been scanned there had a threefold higher risk of infection, they found. This information helped the hospital’s infection control team to create a more effective sterilization plan for that specific machine.
“The takeaway is that we should be leveraging our EHR data to inform our quality improvement efforts,” Dr. Murray said in this video interview, recorded during HM17.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Hospitalists have a powerful tool to help them fight outbreaks of Clostridium difficile and other infectious agents: electronic health record data.
Sara Murray, MD, an assistant professor of medicine at the University of California, San Francisco, and her colleagues, used EHR data to map temporal and spatial coordinates to determine where patients in their hospital were at highest risk for C. difficile. Patients who’d had a CT scan on a particular machine in the emergency department within 24 hours of an infected person having been scanned there had a threefold higher risk of infection, they found. This information helped the hospital’s infection control team to create a more effective sterilization plan for that specific machine.
“The takeaway is that we should be leveraging our EHR data to inform our quality improvement efforts,” Dr. Murray said in this video interview, recorded during HM17.
The video associated with this article is no longer available on this site. Please view all of our videos on the MDedge YouTube channel
Twice-daily tofacitinib induces ulcerative colitis remission
A 10-mg dose of tofacitinib twice daily was significantly more effective than placebo for inducing remission in ulcerative colitis patients, based on data from a group of three randomized trials totaling approximately 1,500 adults. The findings were published online May 3 in the New England Journal of Medicine (2017;376:1723-36).
The series of OCTAVE trials (Oral Clinical Trials for Tofacitinib in Ulcerative Colitis) included adults with moderately to severely active ulcerative colitis (UC). Patients were randomized to 10 mg of tofacitinib, 5 mg tofacitinib, or placebo. The studies were conducted over a 4-year period, at 144 sites for OCTAVE 1, 169 sites for OCTAVE 2, and 297 sites for OCTAVE Sustain.
In both OCTAVE 1 and OCTAVE 2, the remission rates at 8 weeks were significantly higher in the 10-mg tofacitinib groups, compared with the placebo groups (18.5% vs. 8.2%, respectively; 16.6% vs. 3.6%, respectively). The rate of remission at 52 weeks was significantly higher in the 5-mg and 10-mg tofacitinib groups (34.3% and 40.6%, respectively) than in the placebo group (11.1%) in the OCTAVE Sustain trial.
“Pharmacokinetic results in the OCTAVE trials did not indicate a decrease in plasma tofacitinib concentrations during the course of treatment at any given dose in individual patients. These results are consistent with the previously established physicochemical characteristics and clearance mechanisms of tofacitinib,” noted William J. Sandborn, MD, of the University of California, San Diego, and his colleagues.
In the OCTAVE 1 trial, serious adverse events occurred in 4.2% and 8.0% of patients in the 10-mg and placebo groups, respectively. In the OCTAVE 2 trial, they occured in 3.4% and 4.1% of the 10-mg and placebo groups, respectively. The rate of serious adverse events in the OCTAVE Sustain trial was 5.1%, 5.6%, and 6.6% in the 10-mg, 5-mg, and placebo groups, respectively. Tofacitinib was associated with increased lipid levels, as well as higher rates of overall infection and herpes zoster infection, compared with placebo.
The study was supported by Pfizer. Lead author Dr. Sandborn and several coauthors disclosed financial relationships with multiple companies including Pfizer.
AGA Resource
AGA offers materials to help you manage patients with Crohn’s disease and ulcerative colitis, and integrate patient education into your practice, including multimedia publications that are accessible and informative. Learn more at http://www.gastro.org/ibd
“This report is the culmination of an international effort,” over a 4-year period, wrote Sonia Friedman, MD, of Harvard University in an accompanying editorial.
“This study has all the elements of a high-quality trial: a large, international cohort of patients and investigators; reasonable enrollment criteria that would apply to many of my own patients with moderate-to-severe ulcerative colitis; rigorous and unbiased scoring for response, remission, and mucosal healing; fair adjudication of adverse events; and meticulous reporting of all meaningful outcomes and laboratory test results,” she said. Tofacitinib has proven its efficacy – its exact role will be determined by additional research, she noted.
“Only a continued combination of human ingenuity, worldwide cooperation, and enthusiastic funding will allow investigators to further explore the mechanisms by which JAK inhibition ameliorates inflammation in patients with ulcerative colitis and ... identify the specific subsets of patients who will most likely benefit from this new therapy,” Dr. Friedman emphasized (N. Engl. J. Med. 2017;376:1792-3).
Dr. Friedman is affiliated with Harvard University, Boston, Mass., and Brigham and Women’s Hospital Center for Crohn’s and Colitis, Chestnut Hill, Mass. She disclosed receiving personal fees from Boston University.
“This report is the culmination of an international effort,” over a 4-year period, wrote Sonia Friedman, MD, of Harvard University in an accompanying editorial.
“This study has all the elements of a high-quality trial: a large, international cohort of patients and investigators; reasonable enrollment criteria that would apply to many of my own patients with moderate-to-severe ulcerative colitis; rigorous and unbiased scoring for response, remission, and mucosal healing; fair adjudication of adverse events; and meticulous reporting of all meaningful outcomes and laboratory test results,” she said. Tofacitinib has proven its efficacy – its exact role will be determined by additional research, she noted.
“Only a continued combination of human ingenuity, worldwide cooperation, and enthusiastic funding will allow investigators to further explore the mechanisms by which JAK inhibition ameliorates inflammation in patients with ulcerative colitis and ... identify the specific subsets of patients who will most likely benefit from this new therapy,” Dr. Friedman emphasized (N. Engl. J. Med. 2017;376:1792-3).
Dr. Friedman is affiliated with Harvard University, Boston, Mass., and Brigham and Women’s Hospital Center for Crohn’s and Colitis, Chestnut Hill, Mass. She disclosed receiving personal fees from Boston University.
“This report is the culmination of an international effort,” over a 4-year period, wrote Sonia Friedman, MD, of Harvard University in an accompanying editorial.
“This study has all the elements of a high-quality trial: a large, international cohort of patients and investigators; reasonable enrollment criteria that would apply to many of my own patients with moderate-to-severe ulcerative colitis; rigorous and unbiased scoring for response, remission, and mucosal healing; fair adjudication of adverse events; and meticulous reporting of all meaningful outcomes and laboratory test results,” she said. Tofacitinib has proven its efficacy – its exact role will be determined by additional research, she noted.
“Only a continued combination of human ingenuity, worldwide cooperation, and enthusiastic funding will allow investigators to further explore the mechanisms by which JAK inhibition ameliorates inflammation in patients with ulcerative colitis and ... identify the specific subsets of patients who will most likely benefit from this new therapy,” Dr. Friedman emphasized (N. Engl. J. Med. 2017;376:1792-3).
Dr. Friedman is affiliated with Harvard University, Boston, Mass., and Brigham and Women’s Hospital Center for Crohn’s and Colitis, Chestnut Hill, Mass. She disclosed receiving personal fees from Boston University.
A 10-mg dose of tofacitinib twice daily was significantly more effective than placebo for inducing remission in ulcerative colitis patients, based on data from a group of three randomized trials totaling approximately 1,500 adults. The findings were published online May 3 in the New England Journal of Medicine (2017;376:1723-36).
The series of OCTAVE trials (Oral Clinical Trials for Tofacitinib in Ulcerative Colitis) included adults with moderately to severely active ulcerative colitis (UC). Patients were randomized to 10 mg of tofacitinib, 5 mg tofacitinib, or placebo. The studies were conducted over a 4-year period, at 144 sites for OCTAVE 1, 169 sites for OCTAVE 2, and 297 sites for OCTAVE Sustain.
In both OCTAVE 1 and OCTAVE 2, the remission rates at 8 weeks were significantly higher in the 10-mg tofacitinib groups, compared with the placebo groups (18.5% vs. 8.2%, respectively; 16.6% vs. 3.6%, respectively). The rate of remission at 52 weeks was significantly higher in the 5-mg and 10-mg tofacitinib groups (34.3% and 40.6%, respectively) than in the placebo group (11.1%) in the OCTAVE Sustain trial.
“Pharmacokinetic results in the OCTAVE trials did not indicate a decrease in plasma tofacitinib concentrations during the course of treatment at any given dose in individual patients. These results are consistent with the previously established physicochemical characteristics and clearance mechanisms of tofacitinib,” noted William J. Sandborn, MD, of the University of California, San Diego, and his colleagues.
In the OCTAVE 1 trial, serious adverse events occurred in 4.2% and 8.0% of patients in the 10-mg and placebo groups, respectively. In the OCTAVE 2 trial, they occured in 3.4% and 4.1% of the 10-mg and placebo groups, respectively. The rate of serious adverse events in the OCTAVE Sustain trial was 5.1%, 5.6%, and 6.6% in the 10-mg, 5-mg, and placebo groups, respectively. Tofacitinib was associated with increased lipid levels, as well as higher rates of overall infection and herpes zoster infection, compared with placebo.
The study was supported by Pfizer. Lead author Dr. Sandborn and several coauthors disclosed financial relationships with multiple companies including Pfizer.
AGA Resource
AGA offers materials to help you manage patients with Crohn’s disease and ulcerative colitis, and integrate patient education into your practice, including multimedia publications that are accessible and informative. Learn more at http://www.gastro.org/ibd
A 10-mg dose of tofacitinib twice daily was significantly more effective than placebo for inducing remission in ulcerative colitis patients, based on data from a group of three randomized trials totaling approximately 1,500 adults. The findings were published online May 3 in the New England Journal of Medicine (2017;376:1723-36).
The series of OCTAVE trials (Oral Clinical Trials for Tofacitinib in Ulcerative Colitis) included adults with moderately to severely active ulcerative colitis (UC). Patients were randomized to 10 mg of tofacitinib, 5 mg tofacitinib, or placebo. The studies were conducted over a 4-year period, at 144 sites for OCTAVE 1, 169 sites for OCTAVE 2, and 297 sites for OCTAVE Sustain.
In both OCTAVE 1 and OCTAVE 2, the remission rates at 8 weeks were significantly higher in the 10-mg tofacitinib groups, compared with the placebo groups (18.5% vs. 8.2%, respectively; 16.6% vs. 3.6%, respectively). The rate of remission at 52 weeks was significantly higher in the 5-mg and 10-mg tofacitinib groups (34.3% and 40.6%, respectively) than in the placebo group (11.1%) in the OCTAVE Sustain trial.
“Pharmacokinetic results in the OCTAVE trials did not indicate a decrease in plasma tofacitinib concentrations during the course of treatment at any given dose in individual patients. These results are consistent with the previously established physicochemical characteristics and clearance mechanisms of tofacitinib,” noted William J. Sandborn, MD, of the University of California, San Diego, and his colleagues.
In the OCTAVE 1 trial, serious adverse events occurred in 4.2% and 8.0% of patients in the 10-mg and placebo groups, respectively. In the OCTAVE 2 trial, they occured in 3.4% and 4.1% of the 10-mg and placebo groups, respectively. The rate of serious adverse events in the OCTAVE Sustain trial was 5.1%, 5.6%, and 6.6% in the 10-mg, 5-mg, and placebo groups, respectively. Tofacitinib was associated with increased lipid levels, as well as higher rates of overall infection and herpes zoster infection, compared with placebo.
The study was supported by Pfizer. Lead author Dr. Sandborn and several coauthors disclosed financial relationships with multiple companies including Pfizer.
AGA Resource
AGA offers materials to help you manage patients with Crohn’s disease and ulcerative colitis, and integrate patient education into your practice, including multimedia publications that are accessible and informative. Learn more at http://www.gastro.org/ibd
FROM THE NEW ENGLAND JOURNAL OF MEDICINE
Key clinical point: Tofacitinib, a JAK inhibitor, was a significantly more effective induction and maintenance therapy for patients with moderate to severe ulcerative colitis compared with placebo.
Major finding: Tofacitinib dosed at 10 mg twice daily yielded a remission rate of 41% at 52 weeks, compared with 11% in a placebo group.
Data source: The OCTAVE series of three randomized trials totaled approximately 1,500 adults with moderate to severely active ulcerative colitis.
Disclosures: The study was supported by Pfizer. Lead author Dr. Sandborn and several coauthors disclosed financial relationships with multiple companies, including Pfizer.