User login
Lower olanzapine dose just as effective for chemotherapy-induced nausea, vomiting
SAN ANTONIO —
Although it’s highly effective in combination with standard antiemetic therapy, olanzapine at the standard dose of 10 mg makes people too drowsy. “This has prevented its widespread use in clinical practice,” medical oncologist Jyoti Bajpai, DM, of Tata Memorial Cancer Centre, Mumbai, India, explained at the San Antonio Breast Cancer Symposium.
She and her colleagues had a simple idea: Reduce the dose to 2.5 mg instead of 10 mg to prevent the problem. In a randomized trial with 267 patients that Dr. Bajpai presented at the meeting, they found that the lower dose was just as effective for nausea and vomiting prophylaxis, and it greatly reduced daytime somnolence.
“This merits consideration as an antiemetic regimen of choice for highly emetogenic chemotherapy.” The findings are “practice changing,” Dr. Bajpai, the lead investigator, said.
Laura Huppert, MD, a breast oncologist at the University of California, San Francisco, wasn’t surprised by the finding.
She said she and her colleagues at UCSF use a lot of olanzapine for nausea and vomiting prophylaxis. Like the team in India, they have found that 2.5 mg is effective and causes far less sleepiness. Some patients require 5 mg, but the full 10-mg dose is rarely needed.
Although the approach is familiar at UCSF, Dr. Huppert said she doesn’t think a lot of oncologists outside of academic centers know that olanzapine is “really helpful” and that “you don’t need a high dose.” It’s “a very good clinical pearl” and “definitely a new message for some,” she said in an interview.
Over 90% of the subjects in the study were women with breast cancer. Other cancers included sarcoma, germ cell tumors, and head and neck cancer. Subjects were scheduled for their first chemotherapy session with anthracycline-cyclophosphamide and high-dose cisplatin.
The trial randomized 135 patients to 10 mg of olanzapine and 132 to 2.5mg for 5 days, starting the day of their session. They were also on standard triple-antiemetic therapy (selective serotonin receptor (5-HT3) antagonist, neurokinin-1 receptor antagonist, and single-dose dexamethasone).
There were no significant differences between the two arms regarding nausea and vomiting, which patients tracked in daily journals using symptom severity and visual analog scales.
For instance, 44.7% in the 2.5-mg arm and 43.7% in the 10-mg arm reported no vomiting, no use of rescue medications, and no or only mild nausea (P = .87). Results were similar in the first 24 hours as well as on subsequent days.
There was also no difference in the proportion of patients who did have an emetic episode or needed rescue medication: 49.2% in the 2.5-mg arm versus 48.9% with 10 mg (P = .954).
Where the two groups split was on the incidence of daytime somnolence, which was reported by 65.2% of patients in the low-dose arm but 89.6% in the standard-dose group (P < .001). During the first 24 hours, 4.5% of low-dose patients reported severe somnolence versus 40% with 10-mg dosing (P < .001).
The overall incidence declined over the remaining study days, but the differences between the two groups were comparable. On day 5, for instance, 0.8% of low-dose patients but 8.1% of standard-dose patients reported severe somnolence (P = .004).
Low-dose patients also reported less appetite suppression.
The work was supported by the Progressive Ladies Welfare Association. Dr. Bajpai didn’t have any disclosures. Dr. Huppert is an adviser for AstraZeneca.
SAN ANTONIO —
Although it’s highly effective in combination with standard antiemetic therapy, olanzapine at the standard dose of 10 mg makes people too drowsy. “This has prevented its widespread use in clinical practice,” medical oncologist Jyoti Bajpai, DM, of Tata Memorial Cancer Centre, Mumbai, India, explained at the San Antonio Breast Cancer Symposium.
She and her colleagues had a simple idea: Reduce the dose to 2.5 mg instead of 10 mg to prevent the problem. In a randomized trial with 267 patients that Dr. Bajpai presented at the meeting, they found that the lower dose was just as effective for nausea and vomiting prophylaxis, and it greatly reduced daytime somnolence.
“This merits consideration as an antiemetic regimen of choice for highly emetogenic chemotherapy.” The findings are “practice changing,” Dr. Bajpai, the lead investigator, said.
Laura Huppert, MD, a breast oncologist at the University of California, San Francisco, wasn’t surprised by the finding.
She said she and her colleagues at UCSF use a lot of olanzapine for nausea and vomiting prophylaxis. Like the team in India, they have found that 2.5 mg is effective and causes far less sleepiness. Some patients require 5 mg, but the full 10-mg dose is rarely needed.
Although the approach is familiar at UCSF, Dr. Huppert said she doesn’t think a lot of oncologists outside of academic centers know that olanzapine is “really helpful” and that “you don’t need a high dose.” It’s “a very good clinical pearl” and “definitely a new message for some,” she said in an interview.
Over 90% of the subjects in the study were women with breast cancer. Other cancers included sarcoma, germ cell tumors, and head and neck cancer. Subjects were scheduled for their first chemotherapy session with anthracycline-cyclophosphamide and high-dose cisplatin.
The trial randomized 135 patients to 10 mg of olanzapine and 132 to 2.5mg for 5 days, starting the day of their session. They were also on standard triple-antiemetic therapy (selective serotonin receptor (5-HT3) antagonist, neurokinin-1 receptor antagonist, and single-dose dexamethasone).
There were no significant differences between the two arms regarding nausea and vomiting, which patients tracked in daily journals using symptom severity and visual analog scales.
For instance, 44.7% in the 2.5-mg arm and 43.7% in the 10-mg arm reported no vomiting, no use of rescue medications, and no or only mild nausea (P = .87). Results were similar in the first 24 hours as well as on subsequent days.
There was also no difference in the proportion of patients who did have an emetic episode or needed rescue medication: 49.2% in the 2.5-mg arm versus 48.9% with 10 mg (P = .954).
Where the two groups split was on the incidence of daytime somnolence, which was reported by 65.2% of patients in the low-dose arm but 89.6% in the standard-dose group (P < .001). During the first 24 hours, 4.5% of low-dose patients reported severe somnolence versus 40% with 10-mg dosing (P < .001).
The overall incidence declined over the remaining study days, but the differences between the two groups were comparable. On day 5, for instance, 0.8% of low-dose patients but 8.1% of standard-dose patients reported severe somnolence (P = .004).
Low-dose patients also reported less appetite suppression.
The work was supported by the Progressive Ladies Welfare Association. Dr. Bajpai didn’t have any disclosures. Dr. Huppert is an adviser for AstraZeneca.
SAN ANTONIO —
Although it’s highly effective in combination with standard antiemetic therapy, olanzapine at the standard dose of 10 mg makes people too drowsy. “This has prevented its widespread use in clinical practice,” medical oncologist Jyoti Bajpai, DM, of Tata Memorial Cancer Centre, Mumbai, India, explained at the San Antonio Breast Cancer Symposium.
She and her colleagues had a simple idea: Reduce the dose to 2.5 mg instead of 10 mg to prevent the problem. In a randomized trial with 267 patients that Dr. Bajpai presented at the meeting, they found that the lower dose was just as effective for nausea and vomiting prophylaxis, and it greatly reduced daytime somnolence.
“This merits consideration as an antiemetic regimen of choice for highly emetogenic chemotherapy.” The findings are “practice changing,” Dr. Bajpai, the lead investigator, said.
Laura Huppert, MD, a breast oncologist at the University of California, San Francisco, wasn’t surprised by the finding.
She said she and her colleagues at UCSF use a lot of olanzapine for nausea and vomiting prophylaxis. Like the team in India, they have found that 2.5 mg is effective and causes far less sleepiness. Some patients require 5 mg, but the full 10-mg dose is rarely needed.
Although the approach is familiar at UCSF, Dr. Huppert said she doesn’t think a lot of oncologists outside of academic centers know that olanzapine is “really helpful” and that “you don’t need a high dose.” It’s “a very good clinical pearl” and “definitely a new message for some,” she said in an interview.
Over 90% of the subjects in the study were women with breast cancer. Other cancers included sarcoma, germ cell tumors, and head and neck cancer. Subjects were scheduled for their first chemotherapy session with anthracycline-cyclophosphamide and high-dose cisplatin.
The trial randomized 135 patients to 10 mg of olanzapine and 132 to 2.5mg for 5 days, starting the day of their session. They were also on standard triple-antiemetic therapy (selective serotonin receptor (5-HT3) antagonist, neurokinin-1 receptor antagonist, and single-dose dexamethasone).
There were no significant differences between the two arms regarding nausea and vomiting, which patients tracked in daily journals using symptom severity and visual analog scales.
For instance, 44.7% in the 2.5-mg arm and 43.7% in the 10-mg arm reported no vomiting, no use of rescue medications, and no or only mild nausea (P = .87). Results were similar in the first 24 hours as well as on subsequent days.
There was also no difference in the proportion of patients who did have an emetic episode or needed rescue medication: 49.2% in the 2.5-mg arm versus 48.9% with 10 mg (P = .954).
Where the two groups split was on the incidence of daytime somnolence, which was reported by 65.2% of patients in the low-dose arm but 89.6% in the standard-dose group (P < .001). During the first 24 hours, 4.5% of low-dose patients reported severe somnolence versus 40% with 10-mg dosing (P < .001).
The overall incidence declined over the remaining study days, but the differences between the two groups were comparable. On day 5, for instance, 0.8% of low-dose patients but 8.1% of standard-dose patients reported severe somnolence (P = .004).
Low-dose patients also reported less appetite suppression.
The work was supported by the Progressive Ladies Welfare Association. Dr. Bajpai didn’t have any disclosures. Dr. Huppert is an adviser for AstraZeneca.
AT SABCS 2023
PsA Imaging
COVID Strain JN.1 Is Now a ‘Variant of Interest,’ WHO Says
the global health agency has announced.
JN.1 was previously grouped with its relative, BA.2.86, but has increased so much in the past 4 weeks that the WHO moved it to standalone status, according to a summary published by the agency. The prevalence of JN.1 worldwide jumped from 3% for the week ending November 5 to 27% for the week ending December 3. During that same period, JN.1 rose from 1% to 66% of cases in the Western Pacific, which stretches across 37 countries, from China and Mongolia to Australia and New Zealand.
In the United States, JN.1 has been increasing rapidly. The variant accounted for an estimated 21% of cases for the 2-week period ending December 9, up from 8% during the 2 weeks prior.
SARS-CoV-2 is the virus that causes COVID, and like other viruses, it evolves over time, sometimes changing how the virus affects people or how well existing treatments and vaccines work against it.
The WHO and CDC have said the current COVID vaccine appears to protect people against severe symptoms due to JN.1, and the WHO called the rising variant’s public health risk “low.”
“As we observe the rise of the JN.1 variant, it’s important to note that while it may be spreading more widely, there is currently no significant evidence suggesting it is more severe or that it poses a substantial public health risk,” John Brownstein, PhD, chief innovation officer at Boston Children’s Hospital, told ABC News.
In its recent risk analysis, the WHO did acknowledge that it’s not certain whether JN.1 has a higher risk of evading immunity or causing more severe symptoms than other strains. The WHO advised countries to further study how much JN.1 can evade existing antibodies and whether the variant results in more severe disease.
The latest CDC data show that 11% of COVID tests reported to the agency are positive, and 23,432 people were hospitalized with severe symptoms within a 7-day period. The CDC urgently asked people to get vaccinated against respiratory illnesses like the flu and COVID-19 ahead of the holidays as cases rise nationwide.
“Getting vaccinated now can help prevent hospitalizations and save lives,” the agency advised.
A version of this article originally appeared on WebMD.com.
the global health agency has announced.
JN.1 was previously grouped with its relative, BA.2.86, but has increased so much in the past 4 weeks that the WHO moved it to standalone status, according to a summary published by the agency. The prevalence of JN.1 worldwide jumped from 3% for the week ending November 5 to 27% for the week ending December 3. During that same period, JN.1 rose from 1% to 66% of cases in the Western Pacific, which stretches across 37 countries, from China and Mongolia to Australia and New Zealand.
In the United States, JN.1 has been increasing rapidly. The variant accounted for an estimated 21% of cases for the 2-week period ending December 9, up from 8% during the 2 weeks prior.
SARS-CoV-2 is the virus that causes COVID, and like other viruses, it evolves over time, sometimes changing how the virus affects people or how well existing treatments and vaccines work against it.
The WHO and CDC have said the current COVID vaccine appears to protect people against severe symptoms due to JN.1, and the WHO called the rising variant’s public health risk “low.”
“As we observe the rise of the JN.1 variant, it’s important to note that while it may be spreading more widely, there is currently no significant evidence suggesting it is more severe or that it poses a substantial public health risk,” John Brownstein, PhD, chief innovation officer at Boston Children’s Hospital, told ABC News.
In its recent risk analysis, the WHO did acknowledge that it’s not certain whether JN.1 has a higher risk of evading immunity or causing more severe symptoms than other strains. The WHO advised countries to further study how much JN.1 can evade existing antibodies and whether the variant results in more severe disease.
The latest CDC data show that 11% of COVID tests reported to the agency are positive, and 23,432 people were hospitalized with severe symptoms within a 7-day period. The CDC urgently asked people to get vaccinated against respiratory illnesses like the flu and COVID-19 ahead of the holidays as cases rise nationwide.
“Getting vaccinated now can help prevent hospitalizations and save lives,” the agency advised.
A version of this article originally appeared on WebMD.com.
the global health agency has announced.
JN.1 was previously grouped with its relative, BA.2.86, but has increased so much in the past 4 weeks that the WHO moved it to standalone status, according to a summary published by the agency. The prevalence of JN.1 worldwide jumped from 3% for the week ending November 5 to 27% for the week ending December 3. During that same period, JN.1 rose from 1% to 66% of cases in the Western Pacific, which stretches across 37 countries, from China and Mongolia to Australia and New Zealand.
In the United States, JN.1 has been increasing rapidly. The variant accounted for an estimated 21% of cases for the 2-week period ending December 9, up from 8% during the 2 weeks prior.
SARS-CoV-2 is the virus that causes COVID, and like other viruses, it evolves over time, sometimes changing how the virus affects people or how well existing treatments and vaccines work against it.
The WHO and CDC have said the current COVID vaccine appears to protect people against severe symptoms due to JN.1, and the WHO called the rising variant’s public health risk “low.”
“As we observe the rise of the JN.1 variant, it’s important to note that while it may be spreading more widely, there is currently no significant evidence suggesting it is more severe or that it poses a substantial public health risk,” John Brownstein, PhD, chief innovation officer at Boston Children’s Hospital, told ABC News.
In its recent risk analysis, the WHO did acknowledge that it’s not certain whether JN.1 has a higher risk of evading immunity or causing more severe symptoms than other strains. The WHO advised countries to further study how much JN.1 can evade existing antibodies and whether the variant results in more severe disease.
The latest CDC data show that 11% of COVID tests reported to the agency are positive, and 23,432 people were hospitalized with severe symptoms within a 7-day period. The CDC urgently asked people to get vaccinated against respiratory illnesses like the flu and COVID-19 ahead of the holidays as cases rise nationwide.
“Getting vaccinated now can help prevent hospitalizations and save lives,” the agency advised.
A version of this article originally appeared on WebMD.com.
Christmas: A Time for Love and... Penile Fractures
A power outage, like the 1977 blackout in New York City, can lead to an increase in violent crime. However, complete darkness can also have an upside, as it can encourage intimacy and subsequently boost birth rates. The Christmas season, sometimes called the festival of love, appears to stimulate human interactions. Yet this, also, has its downsides, as recently reported by Dr. Nikolaos Pyrgidis and other urologists at Ludwig Maximilian University of Munich in Germany.
The team found that the Christmas period, in particular, is that bit more risky for this injury after they evaluated data from about 3400 men (average age 42) treated for penile fractures between 2005 and 2021. The data was provided by Germany’s Federal Bureau of Statistics.
Out of the 3400 penile fractures that were reported during this period, 40 (1.2%) occurred over 51 Christmas days (from 24th to 26th December each year). The daily incidence rate of penile fractures during the Christmas period was 0.78, with an incidence rate ratio (IRR) of 1.43. The authors note that, if every day were like Christmas, there would have been a 43% increase in penile fractures in Germany since 2005. Interestingly, only 28 (0.82%) penile fractures were reported during the New Year (from 31 December to 2 January in the period between 2005 and 2021), with an IRR of 0.98.
More generally, most patients with penile fractures were admitted to the hospital over the weekend (n=1322; IRR 1.58). Notably, Sunday saw the most admissions due to this injury, followed by Saturday. This suggests that men engaging in sexual activities on Saturday night bear the highest risk of penile fractures, followed by those active on Friday nights.
Penile fractures also increased in the summer months (n=929; IRR 1.11). But the COVID-19 pandemic (n=385; IRR 1.06) and the lockdowns (n=93; IRR 1.95%) did not impact the frequency of this injury.
Rare, Painful, and an Emergency
Penile fractures are a rare urological emergency. The tunica albuginea of one or both corpora cavernosa must tear to be considered problematic, as another team of authors reported in a recent publication. Involvement of the urethra and corpus spongiosum is also possible.
Injuries often occur during an erection because it makes the tunica albuginea stiffer and thinner than when the penis is flaccid. Patients report hearing a snap when the penis is forced into an angle during sexual activity. This was reportedly the case with German singer-song writer Dieter Bohlen, whose ex-girlfriend Nadja Abd El Farrag is said to have written in her book “Ungelogen”, or “Honestly”, that there was a sudden snap during an intimate moment one December night (Christmas?), after which she called the fire brigade in her distress.
Multiple Causes Possible
Other factors contributing to penile fractures include rolling over in bed onto an erect penis, forced bending to achieve detumescence, and blunt external traumas like kicks.
Some penile fractures can be caused by patients “kneading and ripping” their erect penis to quickly reduce swelling. In an Iranian study, 269 out of 352 patients (76%) who underwent this process, known as “ taqaandan” in Iran, suffered a penile fracture.
Penile fractures can also occur in children, as evidenced by the case history of a 7-year-old boy described a few years ago in the journal Urology where the cause was a fall onto the penis.
Immediate Action Required
The treatment of choice for a fresh penile fracture is surgical repair of the tunica albuginea defect and, if necessary, the urethra. Timely surgical intervention yields significantly better long-term outcomes than conservative therapy regarding late complications such as erectile dysfunction and penile curvature. It also reduces the rate of early complications, such as severe corporal infections. Conservative therapy should be reserved for patients who explicitly refuse surgical intervention after thorough consultation.
This article was translated from Univadis Germany using ChatGPT followed by human editing.
A version of this article appeared on Medscape.com.
A power outage, like the 1977 blackout in New York City, can lead to an increase in violent crime. However, complete darkness can also have an upside, as it can encourage intimacy and subsequently boost birth rates. The Christmas season, sometimes called the festival of love, appears to stimulate human interactions. Yet this, also, has its downsides, as recently reported by Dr. Nikolaos Pyrgidis and other urologists at Ludwig Maximilian University of Munich in Germany.
The team found that the Christmas period, in particular, is that bit more risky for this injury after they evaluated data from about 3400 men (average age 42) treated for penile fractures between 2005 and 2021. The data was provided by Germany’s Federal Bureau of Statistics.
Out of the 3400 penile fractures that were reported during this period, 40 (1.2%) occurred over 51 Christmas days (from 24th to 26th December each year). The daily incidence rate of penile fractures during the Christmas period was 0.78, with an incidence rate ratio (IRR) of 1.43. The authors note that, if every day were like Christmas, there would have been a 43% increase in penile fractures in Germany since 2005. Interestingly, only 28 (0.82%) penile fractures were reported during the New Year (from 31 December to 2 January in the period between 2005 and 2021), with an IRR of 0.98.
More generally, most patients with penile fractures were admitted to the hospital over the weekend (n=1322; IRR 1.58). Notably, Sunday saw the most admissions due to this injury, followed by Saturday. This suggests that men engaging in sexual activities on Saturday night bear the highest risk of penile fractures, followed by those active on Friday nights.
Penile fractures also increased in the summer months (n=929; IRR 1.11). But the COVID-19 pandemic (n=385; IRR 1.06) and the lockdowns (n=93; IRR 1.95%) did not impact the frequency of this injury.
Rare, Painful, and an Emergency
Penile fractures are a rare urological emergency. The tunica albuginea of one or both corpora cavernosa must tear to be considered problematic, as another team of authors reported in a recent publication. Involvement of the urethra and corpus spongiosum is also possible.
Injuries often occur during an erection because it makes the tunica albuginea stiffer and thinner than when the penis is flaccid. Patients report hearing a snap when the penis is forced into an angle during sexual activity. This was reportedly the case with German singer-song writer Dieter Bohlen, whose ex-girlfriend Nadja Abd El Farrag is said to have written in her book “Ungelogen”, or “Honestly”, that there was a sudden snap during an intimate moment one December night (Christmas?), after which she called the fire brigade in her distress.
Multiple Causes Possible
Other factors contributing to penile fractures include rolling over in bed onto an erect penis, forced bending to achieve detumescence, and blunt external traumas like kicks.
Some penile fractures can be caused by patients “kneading and ripping” their erect penis to quickly reduce swelling. In an Iranian study, 269 out of 352 patients (76%) who underwent this process, known as “ taqaandan” in Iran, suffered a penile fracture.
Penile fractures can also occur in children, as evidenced by the case history of a 7-year-old boy described a few years ago in the journal Urology where the cause was a fall onto the penis.
Immediate Action Required
The treatment of choice for a fresh penile fracture is surgical repair of the tunica albuginea defect and, if necessary, the urethra. Timely surgical intervention yields significantly better long-term outcomes than conservative therapy regarding late complications such as erectile dysfunction and penile curvature. It also reduces the rate of early complications, such as severe corporal infections. Conservative therapy should be reserved for patients who explicitly refuse surgical intervention after thorough consultation.
This article was translated from Univadis Germany using ChatGPT followed by human editing.
A version of this article appeared on Medscape.com.
A power outage, like the 1977 blackout in New York City, can lead to an increase in violent crime. However, complete darkness can also have an upside, as it can encourage intimacy and subsequently boost birth rates. The Christmas season, sometimes called the festival of love, appears to stimulate human interactions. Yet this, also, has its downsides, as recently reported by Dr. Nikolaos Pyrgidis and other urologists at Ludwig Maximilian University of Munich in Germany.
The team found that the Christmas period, in particular, is that bit more risky for this injury after they evaluated data from about 3400 men (average age 42) treated for penile fractures between 2005 and 2021. The data was provided by Germany’s Federal Bureau of Statistics.
Out of the 3400 penile fractures that were reported during this period, 40 (1.2%) occurred over 51 Christmas days (from 24th to 26th December each year). The daily incidence rate of penile fractures during the Christmas period was 0.78, with an incidence rate ratio (IRR) of 1.43. The authors note that, if every day were like Christmas, there would have been a 43% increase in penile fractures in Germany since 2005. Interestingly, only 28 (0.82%) penile fractures were reported during the New Year (from 31 December to 2 January in the period between 2005 and 2021), with an IRR of 0.98.
More generally, most patients with penile fractures were admitted to the hospital over the weekend (n=1322; IRR 1.58). Notably, Sunday saw the most admissions due to this injury, followed by Saturday. This suggests that men engaging in sexual activities on Saturday night bear the highest risk of penile fractures, followed by those active on Friday nights.
Penile fractures also increased in the summer months (n=929; IRR 1.11). But the COVID-19 pandemic (n=385; IRR 1.06) and the lockdowns (n=93; IRR 1.95%) did not impact the frequency of this injury.
Rare, Painful, and an Emergency
Penile fractures are a rare urological emergency. The tunica albuginea of one or both corpora cavernosa must tear to be considered problematic, as another team of authors reported in a recent publication. Involvement of the urethra and corpus spongiosum is also possible.
Injuries often occur during an erection because it makes the tunica albuginea stiffer and thinner than when the penis is flaccid. Patients report hearing a snap when the penis is forced into an angle during sexual activity. This was reportedly the case with German singer-song writer Dieter Bohlen, whose ex-girlfriend Nadja Abd El Farrag is said to have written in her book “Ungelogen”, or “Honestly”, that there was a sudden snap during an intimate moment one December night (Christmas?), after which she called the fire brigade in her distress.
Multiple Causes Possible
Other factors contributing to penile fractures include rolling over in bed onto an erect penis, forced bending to achieve detumescence, and blunt external traumas like kicks.
Some penile fractures can be caused by patients “kneading and ripping” their erect penis to quickly reduce swelling. In an Iranian study, 269 out of 352 patients (76%) who underwent this process, known as “ taqaandan” in Iran, suffered a penile fracture.
Penile fractures can also occur in children, as evidenced by the case history of a 7-year-old boy described a few years ago in the journal Urology where the cause was a fall onto the penis.
Immediate Action Required
The treatment of choice for a fresh penile fracture is surgical repair of the tunica albuginea defect and, if necessary, the urethra. Timely surgical intervention yields significantly better long-term outcomes than conservative therapy regarding late complications such as erectile dysfunction and penile curvature. It also reduces the rate of early complications, such as severe corporal infections. Conservative therapy should be reserved for patients who explicitly refuse surgical intervention after thorough consultation.
This article was translated from Univadis Germany using ChatGPT followed by human editing.
A version of this article appeared on Medscape.com.
Spending the Holidays With GLP-1 Receptor Agonists: 5 Things to Know
As an endocrinologist, I treat many patients who have diabetes, obesity, or both. Antiobesity medications, particularly the class of glucagon-like peptide-1 receptor agonists (GLP-1 RAs), are our first support tools when nutrition and physical activity aren’t enough.
1. Be mindful of fullness cues.
GLP-1 RAs increase satiety; they help patients feel fuller sooner within a meal and longer in between meals. This means consuming the “usual” at a holiday gathering makes them feel as if they ate too much, and often this will result in more side effects, such as nausea and reflux.
Patient tip: A good rule of thumb is to anticipate feeling full with half of your usual portion. Start with half a plate and reassess your hunger level after finishing.
2. Distinguish between hunger and “food noise.”
Ask your patients, “Do you ever find yourself eating even when you’re not hungry?” Many people eat because of emotions (eg, stress, anxiety, happiness), social situations, or cultural expectations. This type of food consumption is what scientists call “hedonic food intake” and may be driven by the “food noise” that patients describe as persistent thoughts about food in the absence of physiologic hunger. Semaglutide (Ozempic, Wegovy) has been found to reduce cravings, though other research has shown that emotional eating may blunt the effect of GLP-1 RAs.
Patient tip: Recognize when you might be seeking food for reasons other than hunger, and try a different way to address the cue (eg, chat with a friend or family member, go for a walk).
3. Be careful with alcohol.
GLP-1 RAs are being researched as potential treatments for alcohol use disorder. Many patients report less interest in alcohol and a lower tolerance to alcohol when they are taking a GLP-1 RA. Additionally, GLP-1 RAs may be a risk factor for pancreatitis, which can be caused by consuming too much alcohol.
Patient tip: The standard recommendation remains true: If drinking alcohol, limit to one to two servings per day, but also know that reduced intake or interest is normal when taking a GLP-1 RA.
4. Be aware of sickness vs side effects.
With holiday travel and the winter season, it is common for people to catch a cold or a stomach bug. Symptoms of common illnesses might include fatigue, loss of appetite, or diarrhea. These symptoms overlap with side effects of antiobesity medications like semaglutide and tirzepatide.
Patient tip: If you are experiencing constitutional or gastrointestinal symptoms due to illness, speak with your board-certified obesity medicine doctor, who may recommend a temporary medication adjustment to avoid excess side effects.
5. Stay strong against weight stigma.
The holiday season can be a stressful time, especially as patients are reconnecting with people who have not been a part of their health or weight loss journey. Unfortunately, weight bias and weight stigma remain rampant. Many people don’t understand the biology of obesity and refuse to accept the necessity of medical treatment. They may be surrounded by opinions, often louder and less informed.
Patient tip: Remember that obesity is a medical disease. Tell your nosy cousin that it’s a private health matter and that your decisions are your own.
Dr. Tchang is Assistant Professor, Clinical Medicine, Division of Endocrinology, Diabetes, and Metabolism, Weill Cornell Medicine; Physician, Department of Medicine, Iris Cantor Women’s Health Center, Comprehensive Weight Control Center, New York, NY. She disclosed financial relationships with Gelesis and Novo Nordisk.
A version of this article appeared on Medscape.com.
As an endocrinologist, I treat many patients who have diabetes, obesity, or both. Antiobesity medications, particularly the class of glucagon-like peptide-1 receptor agonists (GLP-1 RAs), are our first support tools when nutrition and physical activity aren’t enough.
1. Be mindful of fullness cues.
GLP-1 RAs increase satiety; they help patients feel fuller sooner within a meal and longer in between meals. This means consuming the “usual” at a holiday gathering makes them feel as if they ate too much, and often this will result in more side effects, such as nausea and reflux.
Patient tip: A good rule of thumb is to anticipate feeling full with half of your usual portion. Start with half a plate and reassess your hunger level after finishing.
2. Distinguish between hunger and “food noise.”
Ask your patients, “Do you ever find yourself eating even when you’re not hungry?” Many people eat because of emotions (eg, stress, anxiety, happiness), social situations, or cultural expectations. This type of food consumption is what scientists call “hedonic food intake” and may be driven by the “food noise” that patients describe as persistent thoughts about food in the absence of physiologic hunger. Semaglutide (Ozempic, Wegovy) has been found to reduce cravings, though other research has shown that emotional eating may blunt the effect of GLP-1 RAs.
Patient tip: Recognize when you might be seeking food for reasons other than hunger, and try a different way to address the cue (eg, chat with a friend or family member, go for a walk).
3. Be careful with alcohol.
GLP-1 RAs are being researched as potential treatments for alcohol use disorder. Many patients report less interest in alcohol and a lower tolerance to alcohol when they are taking a GLP-1 RA. Additionally, GLP-1 RAs may be a risk factor for pancreatitis, which can be caused by consuming too much alcohol.
Patient tip: The standard recommendation remains true: If drinking alcohol, limit to one to two servings per day, but also know that reduced intake or interest is normal when taking a GLP-1 RA.
4. Be aware of sickness vs side effects.
With holiday travel and the winter season, it is common for people to catch a cold or a stomach bug. Symptoms of common illnesses might include fatigue, loss of appetite, or diarrhea. These symptoms overlap with side effects of antiobesity medications like semaglutide and tirzepatide.
Patient tip: If you are experiencing constitutional or gastrointestinal symptoms due to illness, speak with your board-certified obesity medicine doctor, who may recommend a temporary medication adjustment to avoid excess side effects.
5. Stay strong against weight stigma.
The holiday season can be a stressful time, especially as patients are reconnecting with people who have not been a part of their health or weight loss journey. Unfortunately, weight bias and weight stigma remain rampant. Many people don’t understand the biology of obesity and refuse to accept the necessity of medical treatment. They may be surrounded by opinions, often louder and less informed.
Patient tip: Remember that obesity is a medical disease. Tell your nosy cousin that it’s a private health matter and that your decisions are your own.
Dr. Tchang is Assistant Professor, Clinical Medicine, Division of Endocrinology, Diabetes, and Metabolism, Weill Cornell Medicine; Physician, Department of Medicine, Iris Cantor Women’s Health Center, Comprehensive Weight Control Center, New York, NY. She disclosed financial relationships with Gelesis and Novo Nordisk.
A version of this article appeared on Medscape.com.
As an endocrinologist, I treat many patients who have diabetes, obesity, or both. Antiobesity medications, particularly the class of glucagon-like peptide-1 receptor agonists (GLP-1 RAs), are our first support tools when nutrition and physical activity aren’t enough.
1. Be mindful of fullness cues.
GLP-1 RAs increase satiety; they help patients feel fuller sooner within a meal and longer in between meals. This means consuming the “usual” at a holiday gathering makes them feel as if they ate too much, and often this will result in more side effects, such as nausea and reflux.
Patient tip: A good rule of thumb is to anticipate feeling full with half of your usual portion. Start with half a plate and reassess your hunger level after finishing.
2. Distinguish between hunger and “food noise.”
Ask your patients, “Do you ever find yourself eating even when you’re not hungry?” Many people eat because of emotions (eg, stress, anxiety, happiness), social situations, or cultural expectations. This type of food consumption is what scientists call “hedonic food intake” and may be driven by the “food noise” that patients describe as persistent thoughts about food in the absence of physiologic hunger. Semaglutide (Ozempic, Wegovy) has been found to reduce cravings, though other research has shown that emotional eating may blunt the effect of GLP-1 RAs.
Patient tip: Recognize when you might be seeking food for reasons other than hunger, and try a different way to address the cue (eg, chat with a friend or family member, go for a walk).
3. Be careful with alcohol.
GLP-1 RAs are being researched as potential treatments for alcohol use disorder. Many patients report less interest in alcohol and a lower tolerance to alcohol when they are taking a GLP-1 RA. Additionally, GLP-1 RAs may be a risk factor for pancreatitis, which can be caused by consuming too much alcohol.
Patient tip: The standard recommendation remains true: If drinking alcohol, limit to one to two servings per day, but also know that reduced intake or interest is normal when taking a GLP-1 RA.
4. Be aware of sickness vs side effects.
With holiday travel and the winter season, it is common for people to catch a cold or a stomach bug. Symptoms of common illnesses might include fatigue, loss of appetite, or diarrhea. These symptoms overlap with side effects of antiobesity medications like semaglutide and tirzepatide.
Patient tip: If you are experiencing constitutional or gastrointestinal symptoms due to illness, speak with your board-certified obesity medicine doctor, who may recommend a temporary medication adjustment to avoid excess side effects.
5. Stay strong against weight stigma.
The holiday season can be a stressful time, especially as patients are reconnecting with people who have not been a part of their health or weight loss journey. Unfortunately, weight bias and weight stigma remain rampant. Many people don’t understand the biology of obesity and refuse to accept the necessity of medical treatment. They may be surrounded by opinions, often louder and less informed.
Patient tip: Remember that obesity is a medical disease. Tell your nosy cousin that it’s a private health matter and that your decisions are your own.
Dr. Tchang is Assistant Professor, Clinical Medicine, Division of Endocrinology, Diabetes, and Metabolism, Weill Cornell Medicine; Physician, Department of Medicine, Iris Cantor Women’s Health Center, Comprehensive Weight Control Center, New York, NY. She disclosed financial relationships with Gelesis and Novo Nordisk.
A version of this article appeared on Medscape.com.
A New Test Could Save Arthritis Patients Time, Money, and Pain. But Will It Be Used?
Erinn Maury, MD, knew Remicade wasn’t the right drug for Patti Schulte, a patient with rheumatoid arthritis the physician saw at her Millersville, Maryland, practice. Schulte’s swollen, painful joints hadn’t responded to Enbrel or Humira, two drugs in the same class.
But the insurer insisted, so Schulte went on Remicade. It didn’t work either.
What’s more, Schulte suffered a severe allergic reaction to the infusion therapy, requiring a heavy dose of prednisone, a steroid with grave side effects if used at high doses for too long.
After 18 months, her insurer finally approved Maury’s drug of choice, Orencia. By then, Schulte’s vertebrae, weakened by prednisone, had started cracking. She was only 60.
It’s also a story of how doctors are steered by pharmacy benefit managers — the middlemen of the drug market — as well as by insurers.
Once people with inflammatory conditions such as rheumatoid arthritis reach a certain stage, the first prescription offered is typically Humira, the best-selling drug in history, and part of a class known as tumor necrosis factor inhibitors, or TNFis, which fail to significantly help about half of the patients who take it.
“We practice rheumatology without any help,” said Vibeke Strand, a rheumatologist and adjunct clinical professor at Stanford. She bemoaned the lack of tools available to choose the right drug while bristling at corporate intervention in the decision. “We are told by the insurer what to prescribe to the patient. After they fail methotrexate, it’s a TNF inhibitor, almost always Humira. And that’s not OK.”
If there’s a shred of hope in this story, it’s that a blood test, PrismRA, may herald an era of improved care for patients with rheumatoid arthritis and other autoimmune conditions. But first, it must be embraced by insurers.
PrismRA employs a predictive model that combines clinical factors, blood tests, and 19 gene patterns to identify the roughly 60% of patients who are very unlikely to respond to a TNFi drug.
Over the past 25 years, drug companies have introduced five new classes of autoimmune drugs. TNFis were the first to market, starting in the late 1990s.
Some 1.3 million Americans have rheumatoid arthritis, a disease in which a person’s immune system attacks their joints, causing crippling pain and, if improperly treated, disfigurement. The newer drugs, mostly so-called biologics, are also used by some of the 25 million or more Americans with other autoimmune diseases, such as lupus, Crohn’s disease, and psoriasis. Typically costing tens of thousands of dollars annually, the drugs are prescribed after a patient fails to respond to older, cheaper drugs like methotrexate.
Until recently, rheumatologists have had few ways to predict which of the new drugs would work best on which patients. Often, “it’s a coin flip whether I prescribe drug A or B,” said Jeffrey Curtis, MD, a rheumatology professor at the University of Alabama-Birmingham.
Yet about 90% of the patients who are given one of these advanced drugs start on a TNFi, although there’s often no reason to think a TNFi will work better than another type.
Under these puzzling circumstances, it’s often the insurer rather than the doctor who chooses the patient’s drug. Insurers lean toward TNFis such as adalimumab, commonly sold as brand name Humira, in part because they get large rebates from manufacturers for using them. Although the size of such payments is a trade secret, AbbVie is said to be offering rebates to insurers of up to 60% of Humira’s price. That has enabled it to control 98.5% of the US adalimumab market, even though it has eight biosimilar competitors.
PrismRA’s developer, Scipher Medicine, has provided more than 26,000 test results, rarely covered by insurance. But on October 15, the Centers for Medicare & Medicaid began reimbursing for the test, and its use is expected to rise. At least two other companies are developing drug-matching tests for patients with rheumatoid arthritis.
Although critics say PrismRA is not always useful, it is likely to be the first in a series of diagnostics anticipated over the next decade that could reduce the time that patients with autoimmune disease suffer on the wrong drug.
Academics, small biotechs, and large pharmaceutical companies are investing in methods to distinguish the biological pathways involved in these diseases and the best way to treat each one. This approach, called precision medicine, has existed for years in cancer medicine, in which it’s routine to test the genetics of patients’ tumors to determine the appropriate drug treatment.
“You wouldn’t give Herceptin to a breast cancer patient without knowing whether her tumor was HER2-positive,” said Costantino Pitzalis, MD, a rheumatology professor at the William Harvey Research Institute in London, England. He was speaking before a well-attended session at an American College of Rheumatology conference in San Diego in November. “Why do we not use biopsies or seek molecular markers in rheumatoid arthritis?”
It’s not only patients and doctors who have a stake in which drugs work best for a given person.
When Remicade failed and Schulte waited for the insurer to approve Orencia, she insisted on keeping her job as an accountant. But as her prednisone-related spinal problems worsened, Schulte was forced to retire, go on Medicaid, and seek disability, something she had always sworn to avoid.
Now taxpayers, rather than the insurer, are covering Schulte’s medical bills, Dr. Maury noted.
Precision medicine hasn’t seemed like a priority for large makers of autoimmune drugs, which presumably have some knowledge of which patients are most likely to benefit from their drugs, because they have tested and sold millions of doses over the years. By offering rebate incentives to insurers, companies like AbbVie, which makes Humira, can guarantee theirs are the drugs of choice with insurers.
“If you were AbbVie,” Dr. Curtis said, “why would you ever want to publish data showing who’s not going to do well on your drug, if, in the absence of the test, everyone will start with your drug first?”
What Testing Could Do
Medicare and commercial insurers haven’t yet set a price for PrismRA, but it could save insurers thousands of dollars a year for each patient it helps, according to Krishna Patel, PharmD, Scipher’s associate director of medical affairs.
“If the test cost $750, I still only need it once, and it costs less than a month of whatever drug is not going to work very well for you,” said Dr. Curtis, a coauthor of some studies of the test. “The economics of a biomarker that’s anything but worthless is pretty favorable because our biologics and targeted drugs are so expensive.”
Patients are enthusiastic about the test because so many have had to take TNFis that didn’t work. Many insurers require patients to try a second TNFi and sometimes a third.
Jen Weaver, a patient advocate and mother of three, got little benefit from hydroxychloroquine, sulfasalazine, methotrexate, and Orencia, a non-TNFi biologic therapy, before finding some relief in another, Actemra. But she was taken off that drug when her white blood cells plunged, and the next three drugs she tried — all TNFis — caused allergic reactions, culminating with an outbreak of pus-filled sores. Another drug, Otezla, eventually seemed to help heal the sores, and she’s been stable on it since in combination with methotrexate, Ms. Weaver said.
“What is needed is to substantially shorten this trial-and-error period for patients,” said Shilpa Venkatachalam, PhD, herself a patient and the director of research operations at the Global Healthy Living Foundation. “There’s a lot of anxiety and frustration, weeks in pain wondering whether a drug is going to work for you and what to do if it doesn’t.” A survey by her group found that 91% of patients worried their medications would stop working. And there is evidence that the longer it takes to resolve arthritis symptoms, the less chance they will ever stop.
How insurers will respond to the availability of tests isn’t clear, partly because the arrival of new biosimilar drugs — essentially generic versions — is making TNFis cheaper for insurance plans. While Humira still dominates, AbbVie has increased rebates to insurers, in effect lowering its cost. Lower prices make the PrismRA test less appealing to insurers because widespread use of the test could cut TNFi prescriptions by up to a third.
However, rheumatologist John B. Boone, MD, in Louisville, Kentucky, found to his surprise that insurers mostly accepted alternative prescriptions for 41 patients whom the test showed unlikely to respond to TNFis as part of a clinical trial. Dr. Boone receives consulting fees from Scipher.
Although the test didn’t guarantee good outcomes, he said, the few patients given TNFis despite the test results almost all did poorly on that regimen.
Scientists from AbbVie, which makes several rheumatology drugs in addition to Humira, presented a study at the San Diego conference examining biomarkers that might show which patients would respond to Rinvoq, a new immune-suppressing drug in a class known as the JAK inhibitors. When asked about its use of precision medicine, AbbVie declined to comment.
Over two decades, Humira has been a blockbuster drug for AbbVie. The company sold more than $3.5 billion worth of Humira in the third quarter of 2023, 36% less than a year ago. Sales of Rinvoq, which AbbVie is marketing as a treatment for patients failed by Humira and its class, jumped 60% to $1.1 billion.
What Patients Want
Shannan O’Hara-Levi, a 38-year-old in Monroe, New York, has been on scores of drugs and supplements since being diagnosed with juvenile arthritis at age 3. She’s been nauseated, fatigued, and short of breath and has suffered allergic reactions, but she says the worst part of it was finding a drug that worked and then losing access because of insurance. This happened shortly after she gave birth to a daughter in 2022 and then endured intense joint pain.
“If I could take a blood test that tells me not to waste months or years of my life — absolutely,” she said. “If I could have started my current drug last fall and saved many months of not being able to engage with my baby on the floor — absolutely.”
This article originally appeared on KFFHealthNews.org. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF — the independent source for health policy research, polling, and journalism.
Erinn Maury, MD, knew Remicade wasn’t the right drug for Patti Schulte, a patient with rheumatoid arthritis the physician saw at her Millersville, Maryland, practice. Schulte’s swollen, painful joints hadn’t responded to Enbrel or Humira, two drugs in the same class.
But the insurer insisted, so Schulte went on Remicade. It didn’t work either.
What’s more, Schulte suffered a severe allergic reaction to the infusion therapy, requiring a heavy dose of prednisone, a steroid with grave side effects if used at high doses for too long.
After 18 months, her insurer finally approved Maury’s drug of choice, Orencia. By then, Schulte’s vertebrae, weakened by prednisone, had started cracking. She was only 60.
It’s also a story of how doctors are steered by pharmacy benefit managers — the middlemen of the drug market — as well as by insurers.
Once people with inflammatory conditions such as rheumatoid arthritis reach a certain stage, the first prescription offered is typically Humira, the best-selling drug in history, and part of a class known as tumor necrosis factor inhibitors, or TNFis, which fail to significantly help about half of the patients who take it.
“We practice rheumatology without any help,” said Vibeke Strand, a rheumatologist and adjunct clinical professor at Stanford. She bemoaned the lack of tools available to choose the right drug while bristling at corporate intervention in the decision. “We are told by the insurer what to prescribe to the patient. After they fail methotrexate, it’s a TNF inhibitor, almost always Humira. And that’s not OK.”
If there’s a shred of hope in this story, it’s that a blood test, PrismRA, may herald an era of improved care for patients with rheumatoid arthritis and other autoimmune conditions. But first, it must be embraced by insurers.
PrismRA employs a predictive model that combines clinical factors, blood tests, and 19 gene patterns to identify the roughly 60% of patients who are very unlikely to respond to a TNFi drug.
Over the past 25 years, drug companies have introduced five new classes of autoimmune drugs. TNFis were the first to market, starting in the late 1990s.
Some 1.3 million Americans have rheumatoid arthritis, a disease in which a person’s immune system attacks their joints, causing crippling pain and, if improperly treated, disfigurement. The newer drugs, mostly so-called biologics, are also used by some of the 25 million or more Americans with other autoimmune diseases, such as lupus, Crohn’s disease, and psoriasis. Typically costing tens of thousands of dollars annually, the drugs are prescribed after a patient fails to respond to older, cheaper drugs like methotrexate.
Until recently, rheumatologists have had few ways to predict which of the new drugs would work best on which patients. Often, “it’s a coin flip whether I prescribe drug A or B,” said Jeffrey Curtis, MD, a rheumatology professor at the University of Alabama-Birmingham.
Yet about 90% of the patients who are given one of these advanced drugs start on a TNFi, although there’s often no reason to think a TNFi will work better than another type.
Under these puzzling circumstances, it’s often the insurer rather than the doctor who chooses the patient’s drug. Insurers lean toward TNFis such as adalimumab, commonly sold as brand name Humira, in part because they get large rebates from manufacturers for using them. Although the size of such payments is a trade secret, AbbVie is said to be offering rebates to insurers of up to 60% of Humira’s price. That has enabled it to control 98.5% of the US adalimumab market, even though it has eight biosimilar competitors.
PrismRA’s developer, Scipher Medicine, has provided more than 26,000 test results, rarely covered by insurance. But on October 15, the Centers for Medicare & Medicaid began reimbursing for the test, and its use is expected to rise. At least two other companies are developing drug-matching tests for patients with rheumatoid arthritis.
Although critics say PrismRA is not always useful, it is likely to be the first in a series of diagnostics anticipated over the next decade that could reduce the time that patients with autoimmune disease suffer on the wrong drug.
Academics, small biotechs, and large pharmaceutical companies are investing in methods to distinguish the biological pathways involved in these diseases and the best way to treat each one. This approach, called precision medicine, has existed for years in cancer medicine, in which it’s routine to test the genetics of patients’ tumors to determine the appropriate drug treatment.
“You wouldn’t give Herceptin to a breast cancer patient without knowing whether her tumor was HER2-positive,” said Costantino Pitzalis, MD, a rheumatology professor at the William Harvey Research Institute in London, England. He was speaking before a well-attended session at an American College of Rheumatology conference in San Diego in November. “Why do we not use biopsies or seek molecular markers in rheumatoid arthritis?”
It’s not only patients and doctors who have a stake in which drugs work best for a given person.
When Remicade failed and Schulte waited for the insurer to approve Orencia, she insisted on keeping her job as an accountant. But as her prednisone-related spinal problems worsened, Schulte was forced to retire, go on Medicaid, and seek disability, something she had always sworn to avoid.
Now taxpayers, rather than the insurer, are covering Schulte’s medical bills, Dr. Maury noted.
Precision medicine hasn’t seemed like a priority for large makers of autoimmune drugs, which presumably have some knowledge of which patients are most likely to benefit from their drugs, because they have tested and sold millions of doses over the years. By offering rebate incentives to insurers, companies like AbbVie, which makes Humira, can guarantee theirs are the drugs of choice with insurers.
“If you were AbbVie,” Dr. Curtis said, “why would you ever want to publish data showing who’s not going to do well on your drug, if, in the absence of the test, everyone will start with your drug first?”
What Testing Could Do
Medicare and commercial insurers haven’t yet set a price for PrismRA, but it could save insurers thousands of dollars a year for each patient it helps, according to Krishna Patel, PharmD, Scipher’s associate director of medical affairs.
“If the test cost $750, I still only need it once, and it costs less than a month of whatever drug is not going to work very well for you,” said Dr. Curtis, a coauthor of some studies of the test. “The economics of a biomarker that’s anything but worthless is pretty favorable because our biologics and targeted drugs are so expensive.”
Patients are enthusiastic about the test because so many have had to take TNFis that didn’t work. Many insurers require patients to try a second TNFi and sometimes a third.
Jen Weaver, a patient advocate and mother of three, got little benefit from hydroxychloroquine, sulfasalazine, methotrexate, and Orencia, a non-TNFi biologic therapy, before finding some relief in another, Actemra. But she was taken off that drug when her white blood cells plunged, and the next three drugs she tried — all TNFis — caused allergic reactions, culminating with an outbreak of pus-filled sores. Another drug, Otezla, eventually seemed to help heal the sores, and she’s been stable on it since in combination with methotrexate, Ms. Weaver said.
“What is needed is to substantially shorten this trial-and-error period for patients,” said Shilpa Venkatachalam, PhD, herself a patient and the director of research operations at the Global Healthy Living Foundation. “There’s a lot of anxiety and frustration, weeks in pain wondering whether a drug is going to work for you and what to do if it doesn’t.” A survey by her group found that 91% of patients worried their medications would stop working. And there is evidence that the longer it takes to resolve arthritis symptoms, the less chance they will ever stop.
How insurers will respond to the availability of tests isn’t clear, partly because the arrival of new biosimilar drugs — essentially generic versions — is making TNFis cheaper for insurance plans. While Humira still dominates, AbbVie has increased rebates to insurers, in effect lowering its cost. Lower prices make the PrismRA test less appealing to insurers because widespread use of the test could cut TNFi prescriptions by up to a third.
However, rheumatologist John B. Boone, MD, in Louisville, Kentucky, found to his surprise that insurers mostly accepted alternative prescriptions for 41 patients whom the test showed unlikely to respond to TNFis as part of a clinical trial. Dr. Boone receives consulting fees from Scipher.
Although the test didn’t guarantee good outcomes, he said, the few patients given TNFis despite the test results almost all did poorly on that regimen.
Scientists from AbbVie, which makes several rheumatology drugs in addition to Humira, presented a study at the San Diego conference examining biomarkers that might show which patients would respond to Rinvoq, a new immune-suppressing drug in a class known as the JAK inhibitors. When asked about its use of precision medicine, AbbVie declined to comment.
Over two decades, Humira has been a blockbuster drug for AbbVie. The company sold more than $3.5 billion worth of Humira in the third quarter of 2023, 36% less than a year ago. Sales of Rinvoq, which AbbVie is marketing as a treatment for patients failed by Humira and its class, jumped 60% to $1.1 billion.
What Patients Want
Shannan O’Hara-Levi, a 38-year-old in Monroe, New York, has been on scores of drugs and supplements since being diagnosed with juvenile arthritis at age 3. She’s been nauseated, fatigued, and short of breath and has suffered allergic reactions, but she says the worst part of it was finding a drug that worked and then losing access because of insurance. This happened shortly after she gave birth to a daughter in 2022 and then endured intense joint pain.
“If I could take a blood test that tells me not to waste months or years of my life — absolutely,” she said. “If I could have started my current drug last fall and saved many months of not being able to engage with my baby on the floor — absolutely.”
This article originally appeared on KFFHealthNews.org. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF — the independent source for health policy research, polling, and journalism.
Erinn Maury, MD, knew Remicade wasn’t the right drug for Patti Schulte, a patient with rheumatoid arthritis the physician saw at her Millersville, Maryland, practice. Schulte’s swollen, painful joints hadn’t responded to Enbrel or Humira, two drugs in the same class.
But the insurer insisted, so Schulte went on Remicade. It didn’t work either.
What’s more, Schulte suffered a severe allergic reaction to the infusion therapy, requiring a heavy dose of prednisone, a steroid with grave side effects if used at high doses for too long.
After 18 months, her insurer finally approved Maury’s drug of choice, Orencia. By then, Schulte’s vertebrae, weakened by prednisone, had started cracking. She was only 60.
It’s also a story of how doctors are steered by pharmacy benefit managers — the middlemen of the drug market — as well as by insurers.
Once people with inflammatory conditions such as rheumatoid arthritis reach a certain stage, the first prescription offered is typically Humira, the best-selling drug in history, and part of a class known as tumor necrosis factor inhibitors, or TNFis, which fail to significantly help about half of the patients who take it.
“We practice rheumatology without any help,” said Vibeke Strand, a rheumatologist and adjunct clinical professor at Stanford. She bemoaned the lack of tools available to choose the right drug while bristling at corporate intervention in the decision. “We are told by the insurer what to prescribe to the patient. After they fail methotrexate, it’s a TNF inhibitor, almost always Humira. And that’s not OK.”
If there’s a shred of hope in this story, it’s that a blood test, PrismRA, may herald an era of improved care for patients with rheumatoid arthritis and other autoimmune conditions. But first, it must be embraced by insurers.
PrismRA employs a predictive model that combines clinical factors, blood tests, and 19 gene patterns to identify the roughly 60% of patients who are very unlikely to respond to a TNFi drug.
Over the past 25 years, drug companies have introduced five new classes of autoimmune drugs. TNFis were the first to market, starting in the late 1990s.
Some 1.3 million Americans have rheumatoid arthritis, a disease in which a person’s immune system attacks their joints, causing crippling pain and, if improperly treated, disfigurement. The newer drugs, mostly so-called biologics, are also used by some of the 25 million or more Americans with other autoimmune diseases, such as lupus, Crohn’s disease, and psoriasis. Typically costing tens of thousands of dollars annually, the drugs are prescribed after a patient fails to respond to older, cheaper drugs like methotrexate.
Until recently, rheumatologists have had few ways to predict which of the new drugs would work best on which patients. Often, “it’s a coin flip whether I prescribe drug A or B,” said Jeffrey Curtis, MD, a rheumatology professor at the University of Alabama-Birmingham.
Yet about 90% of the patients who are given one of these advanced drugs start on a TNFi, although there’s often no reason to think a TNFi will work better than another type.
Under these puzzling circumstances, it’s often the insurer rather than the doctor who chooses the patient’s drug. Insurers lean toward TNFis such as adalimumab, commonly sold as brand name Humira, in part because they get large rebates from manufacturers for using them. Although the size of such payments is a trade secret, AbbVie is said to be offering rebates to insurers of up to 60% of Humira’s price. That has enabled it to control 98.5% of the US adalimumab market, even though it has eight biosimilar competitors.
PrismRA’s developer, Scipher Medicine, has provided more than 26,000 test results, rarely covered by insurance. But on October 15, the Centers for Medicare & Medicaid began reimbursing for the test, and its use is expected to rise. At least two other companies are developing drug-matching tests for patients with rheumatoid arthritis.
Although critics say PrismRA is not always useful, it is likely to be the first in a series of diagnostics anticipated over the next decade that could reduce the time that patients with autoimmune disease suffer on the wrong drug.
Academics, small biotechs, and large pharmaceutical companies are investing in methods to distinguish the biological pathways involved in these diseases and the best way to treat each one. This approach, called precision medicine, has existed for years in cancer medicine, in which it’s routine to test the genetics of patients’ tumors to determine the appropriate drug treatment.
“You wouldn’t give Herceptin to a breast cancer patient without knowing whether her tumor was HER2-positive,” said Costantino Pitzalis, MD, a rheumatology professor at the William Harvey Research Institute in London, England. He was speaking before a well-attended session at an American College of Rheumatology conference in San Diego in November. “Why do we not use biopsies or seek molecular markers in rheumatoid arthritis?”
It’s not only patients and doctors who have a stake in which drugs work best for a given person.
When Remicade failed and Schulte waited for the insurer to approve Orencia, she insisted on keeping her job as an accountant. But as her prednisone-related spinal problems worsened, Schulte was forced to retire, go on Medicaid, and seek disability, something she had always sworn to avoid.
Now taxpayers, rather than the insurer, are covering Schulte’s medical bills, Dr. Maury noted.
Precision medicine hasn’t seemed like a priority for large makers of autoimmune drugs, which presumably have some knowledge of which patients are most likely to benefit from their drugs, because they have tested and sold millions of doses over the years. By offering rebate incentives to insurers, companies like AbbVie, which makes Humira, can guarantee theirs are the drugs of choice with insurers.
“If you were AbbVie,” Dr. Curtis said, “why would you ever want to publish data showing who’s not going to do well on your drug, if, in the absence of the test, everyone will start with your drug first?”
What Testing Could Do
Medicare and commercial insurers haven’t yet set a price for PrismRA, but it could save insurers thousands of dollars a year for each patient it helps, according to Krishna Patel, PharmD, Scipher’s associate director of medical affairs.
“If the test cost $750, I still only need it once, and it costs less than a month of whatever drug is not going to work very well for you,” said Dr. Curtis, a coauthor of some studies of the test. “The economics of a biomarker that’s anything but worthless is pretty favorable because our biologics and targeted drugs are so expensive.”
Patients are enthusiastic about the test because so many have had to take TNFis that didn’t work. Many insurers require patients to try a second TNFi and sometimes a third.
Jen Weaver, a patient advocate and mother of three, got little benefit from hydroxychloroquine, sulfasalazine, methotrexate, and Orencia, a non-TNFi biologic therapy, before finding some relief in another, Actemra. But she was taken off that drug when her white blood cells plunged, and the next three drugs she tried — all TNFis — caused allergic reactions, culminating with an outbreak of pus-filled sores. Another drug, Otezla, eventually seemed to help heal the sores, and she’s been stable on it since in combination with methotrexate, Ms. Weaver said.
“What is needed is to substantially shorten this trial-and-error period for patients,” said Shilpa Venkatachalam, PhD, herself a patient and the director of research operations at the Global Healthy Living Foundation. “There’s a lot of anxiety and frustration, weeks in pain wondering whether a drug is going to work for you and what to do if it doesn’t.” A survey by her group found that 91% of patients worried their medications would stop working. And there is evidence that the longer it takes to resolve arthritis symptoms, the less chance they will ever stop.
How insurers will respond to the availability of tests isn’t clear, partly because the arrival of new biosimilar drugs — essentially generic versions — is making TNFis cheaper for insurance plans. While Humira still dominates, AbbVie has increased rebates to insurers, in effect lowering its cost. Lower prices make the PrismRA test less appealing to insurers because widespread use of the test could cut TNFi prescriptions by up to a third.
However, rheumatologist John B. Boone, MD, in Louisville, Kentucky, found to his surprise that insurers mostly accepted alternative prescriptions for 41 patients whom the test showed unlikely to respond to TNFis as part of a clinical trial. Dr. Boone receives consulting fees from Scipher.
Although the test didn’t guarantee good outcomes, he said, the few patients given TNFis despite the test results almost all did poorly on that regimen.
Scientists from AbbVie, which makes several rheumatology drugs in addition to Humira, presented a study at the San Diego conference examining biomarkers that might show which patients would respond to Rinvoq, a new immune-suppressing drug in a class known as the JAK inhibitors. When asked about its use of precision medicine, AbbVie declined to comment.
Over two decades, Humira has been a blockbuster drug for AbbVie. The company sold more than $3.5 billion worth of Humira in the third quarter of 2023, 36% less than a year ago. Sales of Rinvoq, which AbbVie is marketing as a treatment for patients failed by Humira and its class, jumped 60% to $1.1 billion.
What Patients Want
Shannan O’Hara-Levi, a 38-year-old in Monroe, New York, has been on scores of drugs and supplements since being diagnosed with juvenile arthritis at age 3. She’s been nauseated, fatigued, and short of breath and has suffered allergic reactions, but she says the worst part of it was finding a drug that worked and then losing access because of insurance. This happened shortly after she gave birth to a daughter in 2022 and then endured intense joint pain.
“If I could take a blood test that tells me not to waste months or years of my life — absolutely,” she said. “If I could have started my current drug last fall and saved many months of not being able to engage with my baby on the floor — absolutely.”
This article originally appeared on KFFHealthNews.org. KFF Health News is a national newsroom that produces in-depth journalism about health issues and is one of the core operating programs at KFF — the independent source for health policy research, polling, and journalism.
Monitoring Tech for Pulmonary Disorders Moving Beyond Wearables
, but, as with any emergent technology, pitfalls come along with the promise and potential.
Meanwhile, technology to remotely monitor respiratory diseases is advancing into other modalities. In recent months, researchers have reported on an artificial intelligence–aided home stethoscope to monitor asthma exacerbations and an ingestible electronic capsule, which has shown some facility for continuous, remote monitoring of sleep apnea and opioid induced respiratory depression.
“Smartphones and wearable technology in health care are here to stay,” Mariam Louis, MD, pulmonologist and sleep medicine physician at the University of Florida Health and chair of the nonrespiratory sleep section of the Sleep Medicine Network with the American College of Chest Physicians, said in an interview.
“It is an exciting field, as it encourages patients to be actively involved in their medical care and can potentially offer more real-time feedback regarding the patient’s medical conditions,” she said. “There are currently many apps that are being used to monitor sleep and other diseases. However, the technology is still rudimentary, and much more research is needed to see if these apps are accurate and dependable.”
Studies in the past few months have reported on the accuracy of 18 wearable sleep-tracker devices, finding they overestimated sleep duration by 19 minutes on average (Sleep. 2023 Nov 8. doi: 10.1093/sleep/zsad288). Researchers in the United States also recently reported on the first human trial of an ingestible pill for monitoring sleep apnea that sends data to a receiving device up to six feet away (Device. 2023 Nov 17. doi: 10.1016/j.device.2023.100125), and a group in Poland reported than an AI-aided home stethoscope provided reliable information on asthma exacerbations in 149 patients (Ann Fam Med. 2023;21:517-25).
Targeting Challenges With Polysomnography
All of these technologies aim to overcome challenges with traditional devices, such as polysomnography (PSG) for evaluating sleep. Jaques Reifman, PhD, a senior research scientist at the U.S. Army Medical Research and Development Command in Fort Detrick, Maryland, led the study of 18 wearable sleep trackers. “Both polysomnography and sleep tracking devices in a sense are attempting to reach the same goal: they’re trying to estimate certain sleep parameters,” Dr. Reifman said in an interview.
“But they use very different signals,” he added, noting that PSG uses electroencephalography (EEG) to measure electrical signals in the skull whereas most sleep trackers used an accelerometer to measure body movement. “As your wrist moves around, it determines if you are moving or not,” Dr. Reifman said.
“Each of them have their plusses and minuses,” he added. PSG, while it’s considered the gold standard for measuring sleep, isn’t a consumer product. “It generally requires a very sophisticated data acquisition system; they are laden with motion artifacts and you have to have software to remove them before you analyze the data,” Dr. Reifman said. “They generally require an expert to interpret the results, although lately there are a few AI-based algorithms that you can provide the EEG signals to and it does score those stages for you”
Sleep trackers, on the other hand, are consumer products. “They can be used outside the lab, and you can use them to record for long periods of time, which is not really possible with PSG,” Dr. Reifman said. “They are low cost, they are easy to use, small size, and folks have developed algorithms that can directly tell the consumer you slept seven hours last night.
“In that sense, they’re comfortable to use as opposed to using an almost-like shower cap with the EEG and face sensors as part of the PSG montage.”
However, what sleep trackers offer in convenience, they lack in accuracy. “There are things they just cannot do based on the limitations of the signals that they use,” Dr. Reifman said.
The study was actually a meta-analysis of 14 different studies that evaluated 18 different sleep-tracking devices in 364 patients. The meta-analysis found wide variability in accuracy between devices; for example, a 75-minute overestimation of sleep with one device and a one-minute overestimation with another.
And different studies reported variations with the same tracker or different models of a tracker. The Fitbit Charge 2, for example, was found to underestimate sleep by 12 minutes in one study and overestimate sleep by 9 minutes in another, while the Fitbit HR Charge was found to overestimate sleep by 52 minutes in a third study.
The meta-analysis found while sleep trackers have high sensitivity (>90%), they had a relatively low specificity (<50%), Dr. Reifman noted.
“Because they are mainly based on the acceleration of your wrist, if you are laying down in bed and motionless after a few minutes the device is going to think you’re asleep when in reality you’re just motionless, daydreaming or trying to go to sleep but not sleeping, so the specificity to sleep is not that high,” he said.
These types of devices still have obstacles to overcome before they’re more widely used, Dr. Louis said. “All of these technologies are proprietary,” she said. “As such, little is known about the algorithms used to come up with the diagnosis or other conclusions. In addition, the majority of the data cannot be analyzed independently by the providers, limiting some of the usage of these devices for now.”
Early Study of Ingestible Capsule
To overcome some of those challenges with collecting data from wearables, researchers from the Massachusetts Institute of Technology and West Virginia University have worked with Celero Systems to develop a pill-sized capsule the patient swallows and which then collects vitals data from inside the gastrointestinal tract. The first in-human study evaluated the device, called the vitals-monitoring (VM) pill, in 10 patients. The study reported the data captured by the pill aligned with that gathered with standard sleep metrics and that it could detect sleep apnea episodes.
The study described the pill as a wireless device that uses a custom configuration of four off-the shelf integrated circuits — a microcontroller, accelerometer, memory component and radio signal — and electronic sensors for ballistic measurements from within the GI tract. The accelerometer measures movement of the abdomen during breathing.
Ingestible devices have actually been around for a couple of decades. The most common, the PillCam, is mostly used by gastroenterologists to capture images of the small intestine.
In the VM pill study, 3 of the 10 human volunteers had a diagnosis of either central or obstructive sleep apnea and wore a continuous positive airway pressure device during the study. The patients also had PSG. The study found that the heart rate accuracy of the VM pill was within 2.5 beats per minute of the PSG measure. The study found no significant difference in the ability of the VM pill to accurately measure respiratory rate with or without CPAP.
Since study completion, the device has been evaluated in another 10 patients, Ben Pless, CEO of Celero Systems, the company developing the VM pill and a coauthor of the study, said in an interview. All patients passed the capsule without any adverse events, he said.
The capsule carries the advantages of an implantable device without the surgery, Mr. Pless said. “In addition to the product being inside body, it is very good at measuring core temperature and, of course, there are diurnal variations in core temperature,” he said. “Even though this was not in the paper, we found the combination of monitoring respiration and core temperature is a very powerful way to do sleep staging in a completely unobtrusive and discrete way.”
The first study evaluated the overnight use of the VM pill, but future studies will evaluate longer duration of the device, first up to a week and then extending out to a month, with the goal of collecting data through the entire duration, Mr. Pless said.
“If you want to do ongoing monitoring for events that may have a low incidence, for example COPD exacerbations or some asthma which does not occur every day and you want to do long-term monitoring, an ingestible format where you ultimately take one capsule and you’re monitored for a month in a completely unobtrusive way would be a great way to do patient monitoring,” he said.
This platform could also collect multinight data for sleep studies, he added.
“While this is an exciting technology, there is much more to diagnosing sleep apnea than just heart rate and breathing,” Dr. Louis said. “During a sleep study, we look at oxygen levels, snoring, and many other variables.”
AI-Aided Stethoscope
The AI-aided stethoscope demonstrated an ability to collect reliable information on asthma exacerbations, the study in Poland found. “The parameters provided are effective for children, especially those younger than 5 years of age,” the study authors wrote.
The study enrolled patients of various ages with asthma, using the AI-aided stethoscope to monitor asthma-related physiologic parameters at home for six months. The stethoscope recorded auscultatory sounds from standard chest point and sent them to a dedicated mobile phone application in which an AI module automatically analyzed the recordings and displayed the results. The researchers trained the AI module using more than 10,000 recordings of respiratory sounds.
The study showed that a host of parameters — wheezes, rhonchi, coarse and fine crackles, heart rate, respiratory rate and inspiration-to-expiration duration ration — measured with the AI-aided stethoscope can detect asthma exacerbations without the need for obtaining peak expiratory flow measurements. It also showed a potential to make asthma diagnosis more straightforward in younger children.
“As we learn more and refine these technologies, we will be able to offer more patient centered and precise medicine to our patients, tailored specifically to their needs,” Dr. Louis said. “AI will certainly play a part in the future.”
Dr. Louis and Dr. Reifman have no relevant relationships to disclose. Mr. Pless is CEO of Celero Systems, a privately held company in Lincoln, Mass.
, but, as with any emergent technology, pitfalls come along with the promise and potential.
Meanwhile, technology to remotely monitor respiratory diseases is advancing into other modalities. In recent months, researchers have reported on an artificial intelligence–aided home stethoscope to monitor asthma exacerbations and an ingestible electronic capsule, which has shown some facility for continuous, remote monitoring of sleep apnea and opioid induced respiratory depression.
“Smartphones and wearable technology in health care are here to stay,” Mariam Louis, MD, pulmonologist and sleep medicine physician at the University of Florida Health and chair of the nonrespiratory sleep section of the Sleep Medicine Network with the American College of Chest Physicians, said in an interview.
“It is an exciting field, as it encourages patients to be actively involved in their medical care and can potentially offer more real-time feedback regarding the patient’s medical conditions,” she said. “There are currently many apps that are being used to monitor sleep and other diseases. However, the technology is still rudimentary, and much more research is needed to see if these apps are accurate and dependable.”
Studies in the past few months have reported on the accuracy of 18 wearable sleep-tracker devices, finding they overestimated sleep duration by 19 minutes on average (Sleep. 2023 Nov 8. doi: 10.1093/sleep/zsad288). Researchers in the United States also recently reported on the first human trial of an ingestible pill for monitoring sleep apnea that sends data to a receiving device up to six feet away (Device. 2023 Nov 17. doi: 10.1016/j.device.2023.100125), and a group in Poland reported than an AI-aided home stethoscope provided reliable information on asthma exacerbations in 149 patients (Ann Fam Med. 2023;21:517-25).
Targeting Challenges With Polysomnography
All of these technologies aim to overcome challenges with traditional devices, such as polysomnography (PSG) for evaluating sleep. Jaques Reifman, PhD, a senior research scientist at the U.S. Army Medical Research and Development Command in Fort Detrick, Maryland, led the study of 18 wearable sleep trackers. “Both polysomnography and sleep tracking devices in a sense are attempting to reach the same goal: they’re trying to estimate certain sleep parameters,” Dr. Reifman said in an interview.
“But they use very different signals,” he added, noting that PSG uses electroencephalography (EEG) to measure electrical signals in the skull whereas most sleep trackers used an accelerometer to measure body movement. “As your wrist moves around, it determines if you are moving or not,” Dr. Reifman said.
“Each of them have their plusses and minuses,” he added. PSG, while it’s considered the gold standard for measuring sleep, isn’t a consumer product. “It generally requires a very sophisticated data acquisition system; they are laden with motion artifacts and you have to have software to remove them before you analyze the data,” Dr. Reifman said. “They generally require an expert to interpret the results, although lately there are a few AI-based algorithms that you can provide the EEG signals to and it does score those stages for you”
Sleep trackers, on the other hand, are consumer products. “They can be used outside the lab, and you can use them to record for long periods of time, which is not really possible with PSG,” Dr. Reifman said. “They are low cost, they are easy to use, small size, and folks have developed algorithms that can directly tell the consumer you slept seven hours last night.
“In that sense, they’re comfortable to use as opposed to using an almost-like shower cap with the EEG and face sensors as part of the PSG montage.”
However, what sleep trackers offer in convenience, they lack in accuracy. “There are things they just cannot do based on the limitations of the signals that they use,” Dr. Reifman said.
The study was actually a meta-analysis of 14 different studies that evaluated 18 different sleep-tracking devices in 364 patients. The meta-analysis found wide variability in accuracy between devices; for example, a 75-minute overestimation of sleep with one device and a one-minute overestimation with another.
And different studies reported variations with the same tracker or different models of a tracker. The Fitbit Charge 2, for example, was found to underestimate sleep by 12 minutes in one study and overestimate sleep by 9 minutes in another, while the Fitbit HR Charge was found to overestimate sleep by 52 minutes in a third study.
The meta-analysis found while sleep trackers have high sensitivity (>90%), they had a relatively low specificity (<50%), Dr. Reifman noted.
“Because they are mainly based on the acceleration of your wrist, if you are laying down in bed and motionless after a few minutes the device is going to think you’re asleep when in reality you’re just motionless, daydreaming or trying to go to sleep but not sleeping, so the specificity to sleep is not that high,” he said.
These types of devices still have obstacles to overcome before they’re more widely used, Dr. Louis said. “All of these technologies are proprietary,” she said. “As such, little is known about the algorithms used to come up with the diagnosis or other conclusions. In addition, the majority of the data cannot be analyzed independently by the providers, limiting some of the usage of these devices for now.”
Early Study of Ingestible Capsule
To overcome some of those challenges with collecting data from wearables, researchers from the Massachusetts Institute of Technology and West Virginia University have worked with Celero Systems to develop a pill-sized capsule the patient swallows and which then collects vitals data from inside the gastrointestinal tract. The first in-human study evaluated the device, called the vitals-monitoring (VM) pill, in 10 patients. The study reported the data captured by the pill aligned with that gathered with standard sleep metrics and that it could detect sleep apnea episodes.
The study described the pill as a wireless device that uses a custom configuration of four off-the shelf integrated circuits — a microcontroller, accelerometer, memory component and radio signal — and electronic sensors for ballistic measurements from within the GI tract. The accelerometer measures movement of the abdomen during breathing.
Ingestible devices have actually been around for a couple of decades. The most common, the PillCam, is mostly used by gastroenterologists to capture images of the small intestine.
In the VM pill study, 3 of the 10 human volunteers had a diagnosis of either central or obstructive sleep apnea and wore a continuous positive airway pressure device during the study. The patients also had PSG. The study found that the heart rate accuracy of the VM pill was within 2.5 beats per minute of the PSG measure. The study found no significant difference in the ability of the VM pill to accurately measure respiratory rate with or without CPAP.
Since study completion, the device has been evaluated in another 10 patients, Ben Pless, CEO of Celero Systems, the company developing the VM pill and a coauthor of the study, said in an interview. All patients passed the capsule without any adverse events, he said.
The capsule carries the advantages of an implantable device without the surgery, Mr. Pless said. “In addition to the product being inside body, it is very good at measuring core temperature and, of course, there are diurnal variations in core temperature,” he said. “Even though this was not in the paper, we found the combination of monitoring respiration and core temperature is a very powerful way to do sleep staging in a completely unobtrusive and discrete way.”
The first study evaluated the overnight use of the VM pill, but future studies will evaluate longer duration of the device, first up to a week and then extending out to a month, with the goal of collecting data through the entire duration, Mr. Pless said.
“If you want to do ongoing monitoring for events that may have a low incidence, for example COPD exacerbations or some asthma which does not occur every day and you want to do long-term monitoring, an ingestible format where you ultimately take one capsule and you’re monitored for a month in a completely unobtrusive way would be a great way to do patient monitoring,” he said.
This platform could also collect multinight data for sleep studies, he added.
“While this is an exciting technology, there is much more to diagnosing sleep apnea than just heart rate and breathing,” Dr. Louis said. “During a sleep study, we look at oxygen levels, snoring, and many other variables.”
AI-Aided Stethoscope
The AI-aided stethoscope demonstrated an ability to collect reliable information on asthma exacerbations, the study in Poland found. “The parameters provided are effective for children, especially those younger than 5 years of age,” the study authors wrote.
The study enrolled patients of various ages with asthma, using the AI-aided stethoscope to monitor asthma-related physiologic parameters at home for six months. The stethoscope recorded auscultatory sounds from standard chest point and sent them to a dedicated mobile phone application in which an AI module automatically analyzed the recordings and displayed the results. The researchers trained the AI module using more than 10,000 recordings of respiratory sounds.
The study showed that a host of parameters — wheezes, rhonchi, coarse and fine crackles, heart rate, respiratory rate and inspiration-to-expiration duration ration — measured with the AI-aided stethoscope can detect asthma exacerbations without the need for obtaining peak expiratory flow measurements. It also showed a potential to make asthma diagnosis more straightforward in younger children.
“As we learn more and refine these technologies, we will be able to offer more patient centered and precise medicine to our patients, tailored specifically to their needs,” Dr. Louis said. “AI will certainly play a part in the future.”
Dr. Louis and Dr. Reifman have no relevant relationships to disclose. Mr. Pless is CEO of Celero Systems, a privately held company in Lincoln, Mass.
, but, as with any emergent technology, pitfalls come along with the promise and potential.
Meanwhile, technology to remotely monitor respiratory diseases is advancing into other modalities. In recent months, researchers have reported on an artificial intelligence–aided home stethoscope to monitor asthma exacerbations and an ingestible electronic capsule, which has shown some facility for continuous, remote monitoring of sleep apnea and opioid induced respiratory depression.
“Smartphones and wearable technology in health care are here to stay,” Mariam Louis, MD, pulmonologist and sleep medicine physician at the University of Florida Health and chair of the nonrespiratory sleep section of the Sleep Medicine Network with the American College of Chest Physicians, said in an interview.
“It is an exciting field, as it encourages patients to be actively involved in their medical care and can potentially offer more real-time feedback regarding the patient’s medical conditions,” she said. “There are currently many apps that are being used to monitor sleep and other diseases. However, the technology is still rudimentary, and much more research is needed to see if these apps are accurate and dependable.”
Studies in the past few months have reported on the accuracy of 18 wearable sleep-tracker devices, finding they overestimated sleep duration by 19 minutes on average (Sleep. 2023 Nov 8. doi: 10.1093/sleep/zsad288). Researchers in the United States also recently reported on the first human trial of an ingestible pill for monitoring sleep apnea that sends data to a receiving device up to six feet away (Device. 2023 Nov 17. doi: 10.1016/j.device.2023.100125), and a group in Poland reported than an AI-aided home stethoscope provided reliable information on asthma exacerbations in 149 patients (Ann Fam Med. 2023;21:517-25).
Targeting Challenges With Polysomnography
All of these technologies aim to overcome challenges with traditional devices, such as polysomnography (PSG) for evaluating sleep. Jaques Reifman, PhD, a senior research scientist at the U.S. Army Medical Research and Development Command in Fort Detrick, Maryland, led the study of 18 wearable sleep trackers. “Both polysomnography and sleep tracking devices in a sense are attempting to reach the same goal: they’re trying to estimate certain sleep parameters,” Dr. Reifman said in an interview.
“But they use very different signals,” he added, noting that PSG uses electroencephalography (EEG) to measure electrical signals in the skull whereas most sleep trackers used an accelerometer to measure body movement. “As your wrist moves around, it determines if you are moving or not,” Dr. Reifman said.
“Each of them have their plusses and minuses,” he added. PSG, while it’s considered the gold standard for measuring sleep, isn’t a consumer product. “It generally requires a very sophisticated data acquisition system; they are laden with motion artifacts and you have to have software to remove them before you analyze the data,” Dr. Reifman said. “They generally require an expert to interpret the results, although lately there are a few AI-based algorithms that you can provide the EEG signals to and it does score those stages for you”
Sleep trackers, on the other hand, are consumer products. “They can be used outside the lab, and you can use them to record for long periods of time, which is not really possible with PSG,” Dr. Reifman said. “They are low cost, they are easy to use, small size, and folks have developed algorithms that can directly tell the consumer you slept seven hours last night.
“In that sense, they’re comfortable to use as opposed to using an almost-like shower cap with the EEG and face sensors as part of the PSG montage.”
However, what sleep trackers offer in convenience, they lack in accuracy. “There are things they just cannot do based on the limitations of the signals that they use,” Dr. Reifman said.
The study was actually a meta-analysis of 14 different studies that evaluated 18 different sleep-tracking devices in 364 patients. The meta-analysis found wide variability in accuracy between devices; for example, a 75-minute overestimation of sleep with one device and a one-minute overestimation with another.
And different studies reported variations with the same tracker or different models of a tracker. The Fitbit Charge 2, for example, was found to underestimate sleep by 12 minutes in one study and overestimate sleep by 9 minutes in another, while the Fitbit HR Charge was found to overestimate sleep by 52 minutes in a third study.
The meta-analysis found while sleep trackers have high sensitivity (>90%), they had a relatively low specificity (<50%), Dr. Reifman noted.
“Because they are mainly based on the acceleration of your wrist, if you are laying down in bed and motionless after a few minutes the device is going to think you’re asleep when in reality you’re just motionless, daydreaming or trying to go to sleep but not sleeping, so the specificity to sleep is not that high,” he said.
These types of devices still have obstacles to overcome before they’re more widely used, Dr. Louis said. “All of these technologies are proprietary,” she said. “As such, little is known about the algorithms used to come up with the diagnosis or other conclusions. In addition, the majority of the data cannot be analyzed independently by the providers, limiting some of the usage of these devices for now.”
Early Study of Ingestible Capsule
To overcome some of those challenges with collecting data from wearables, researchers from the Massachusetts Institute of Technology and West Virginia University have worked with Celero Systems to develop a pill-sized capsule the patient swallows and which then collects vitals data from inside the gastrointestinal tract. The first in-human study evaluated the device, called the vitals-monitoring (VM) pill, in 10 patients. The study reported the data captured by the pill aligned with that gathered with standard sleep metrics and that it could detect sleep apnea episodes.
The study described the pill as a wireless device that uses a custom configuration of four off-the shelf integrated circuits — a microcontroller, accelerometer, memory component and radio signal — and electronic sensors for ballistic measurements from within the GI tract. The accelerometer measures movement of the abdomen during breathing.
Ingestible devices have actually been around for a couple of decades. The most common, the PillCam, is mostly used by gastroenterologists to capture images of the small intestine.
In the VM pill study, 3 of the 10 human volunteers had a diagnosis of either central or obstructive sleep apnea and wore a continuous positive airway pressure device during the study. The patients also had PSG. The study found that the heart rate accuracy of the VM pill was within 2.5 beats per minute of the PSG measure. The study found no significant difference in the ability of the VM pill to accurately measure respiratory rate with or without CPAP.
Since study completion, the device has been evaluated in another 10 patients, Ben Pless, CEO of Celero Systems, the company developing the VM pill and a coauthor of the study, said in an interview. All patients passed the capsule without any adverse events, he said.
The capsule carries the advantages of an implantable device without the surgery, Mr. Pless said. “In addition to the product being inside body, it is very good at measuring core temperature and, of course, there are diurnal variations in core temperature,” he said. “Even though this was not in the paper, we found the combination of monitoring respiration and core temperature is a very powerful way to do sleep staging in a completely unobtrusive and discrete way.”
The first study evaluated the overnight use of the VM pill, but future studies will evaluate longer duration of the device, first up to a week and then extending out to a month, with the goal of collecting data through the entire duration, Mr. Pless said.
“If you want to do ongoing monitoring for events that may have a low incidence, for example COPD exacerbations or some asthma which does not occur every day and you want to do long-term monitoring, an ingestible format where you ultimately take one capsule and you’re monitored for a month in a completely unobtrusive way would be a great way to do patient monitoring,” he said.
This platform could also collect multinight data for sleep studies, he added.
“While this is an exciting technology, there is much more to diagnosing sleep apnea than just heart rate and breathing,” Dr. Louis said. “During a sleep study, we look at oxygen levels, snoring, and many other variables.”
AI-Aided Stethoscope
The AI-aided stethoscope demonstrated an ability to collect reliable information on asthma exacerbations, the study in Poland found. “The parameters provided are effective for children, especially those younger than 5 years of age,” the study authors wrote.
The study enrolled patients of various ages with asthma, using the AI-aided stethoscope to monitor asthma-related physiologic parameters at home for six months. The stethoscope recorded auscultatory sounds from standard chest point and sent them to a dedicated mobile phone application in which an AI module automatically analyzed the recordings and displayed the results. The researchers trained the AI module using more than 10,000 recordings of respiratory sounds.
The study showed that a host of parameters — wheezes, rhonchi, coarse and fine crackles, heart rate, respiratory rate and inspiration-to-expiration duration ration — measured with the AI-aided stethoscope can detect asthma exacerbations without the need for obtaining peak expiratory flow measurements. It also showed a potential to make asthma diagnosis more straightforward in younger children.
“As we learn more and refine these technologies, we will be able to offer more patient centered and precise medicine to our patients, tailored specifically to their needs,” Dr. Louis said. “AI will certainly play a part in the future.”
Dr. Louis and Dr. Reifman have no relevant relationships to disclose. Mr. Pless is CEO of Celero Systems, a privately held company in Lincoln, Mass.
Depression Medications
Navigating Hair Loss in Medical School: Experiences of 2 Young Black Women
As medical students, we often assume we are exempt from the diagnoses we learn about. During the first 2 years of medical school, we learn about alopecia as a condition that may be associated with stress, hormonal imbalances, nutrient deficiencies, and aging. However, our curricula do not explore the subtypes, psychosocial impact, or even the overwhelming number of Black women who are disproportionately affected by alopecia. For Black women, hair is a colossal part of their cultural identity, learning from a young age how to nurture and style natural coils. It becomes devastating when women begin to lose them.
The diagnosis of alopecia subtypes in Black women has been explored in the literature; however, understanding the unique experiences of young Black women is an important part of patient care, as alopecia often is destructive to the patient’s self-image. Therefore, it is important to shed light on these experiences so others feel empowered and supported in their journeys. Herein, we share the experiences of 2 authors (J.D. and C.A.V.O.)—both young Black women—who navigated unexpected hair loss in medical school.
Jewell’s Story
During my first year of medical school, I noticed my hair was shedding more than usual, and my ponytail was not as thick as it once was. I also had an area in my crown that was abnormally thin. My parents suggested that it was a consequence of stress, but I knew something was not right. With only 1 Black dermatologist within 2 hours of Nashville, Tennessee, I remember worrying about seeing a dermatologist who did not understand Black hair. I still scheduled an appointment, but I remember debating if I should straighten my hair or wear my naturally curly Afro. The first dermatologist I saw diagnosed me with seborrheic dermatitis—without even examining my scalp. She told me that I had a “full head of hair” and that I had nothing to worry about. I was unconvinced. Weeks later, I met with another dermatologist who took the time to listen to my concerns. After a scalp biopsy and laboratory work, she diagnosed me with telogen effluvium and androgenetic alopecia. Months later, I had the opportunity to visit the Black dermatologist, and she diagnosed me with central centrifugal cicatricial alopecia. I am grateful for the earlier dermatologists I saw, but I finally feel at ease with my diagnosis and treatment plan after being seen by the latter.
Chidubem’s Story
From a young age, I was conditioned to think my hair was thick, unmanageable, and a nuisance. I grew accustomed to people yanking on my hair, and my gentle whispers of “this hurts” and “the braid is too tight” being ignored. That continued into adulthood. While studying for the US Medical Licensing Examination, I noticed a burning sensation on my scalp. I decided to ignore it. However, as the days progressed, the slight burning sensation turned into intense burning and itching. I still ignored it. Not only did I lack the funds for a dermatology appointment, but my licensing examination was approaching, and it was more important than anything related to my hair. After the examination, I eventually made an appointment with my primary care physician, who attributed my symptoms to the stressors of medical school. “I think you are having migraines,” she told me. So, I continued to ignore my symptoms. A year passed, and a hair braider pointed out that I had 2 well-defined bald patches on my scalp. I remember feeling angry and confused as to how I missed those findings. I could no longer ignore it—it bothered me less when no one else knew about it. I quickly made a dermatology appointment. Although I opted out of a biopsy, we decided to treat my hair loss empirically, and I have experienced drastic improvement.
Final Thoughts
We are 2 Black women living more than 500 miles away from each other at different medical institutions, yet we share the same experience, which many other women unfortunately face alone. It is not uncommon for us to feel unheard, dismissed, or misdiagnosed. We write this for the Black woman sorting through the feelings of confusion and shock as she traces the hairless spot on her scalp. We write this for the medical student ignoring their symptoms until after their examination. We even write this for any nondermatologists uncomfortable with diagnosing and treating textured hair. To improve patient satisfaction and overall health outcomes, physicians must approach patients with both knowledge and cultural competency. Most importantly, dermatologists (and other physicians) should be appropriately trained in not only the structural differences of textured hair but also the unique practices and beliefs among Black women in relation to their hair.
Acknowledgments—Jewell Dinkins is the inaugural recipient of the Janssen–Skin of Color Research Fellowship at Howard University (Washington, DC), and Chidubem A.V. Okeke is the inaugural recipient of the Women’s Dermatologic Society–La Roche-Posay dermatology fellowship at Howard University.
As medical students, we often assume we are exempt from the diagnoses we learn about. During the first 2 years of medical school, we learn about alopecia as a condition that may be associated with stress, hormonal imbalances, nutrient deficiencies, and aging. However, our curricula do not explore the subtypes, psychosocial impact, or even the overwhelming number of Black women who are disproportionately affected by alopecia. For Black women, hair is a colossal part of their cultural identity, learning from a young age how to nurture and style natural coils. It becomes devastating when women begin to lose them.
The diagnosis of alopecia subtypes in Black women has been explored in the literature; however, understanding the unique experiences of young Black women is an important part of patient care, as alopecia often is destructive to the patient’s self-image. Therefore, it is important to shed light on these experiences so others feel empowered and supported in their journeys. Herein, we share the experiences of 2 authors (J.D. and C.A.V.O.)—both young Black women—who navigated unexpected hair loss in medical school.
Jewell’s Story
During my first year of medical school, I noticed my hair was shedding more than usual, and my ponytail was not as thick as it once was. I also had an area in my crown that was abnormally thin. My parents suggested that it was a consequence of stress, but I knew something was not right. With only 1 Black dermatologist within 2 hours of Nashville, Tennessee, I remember worrying about seeing a dermatologist who did not understand Black hair. I still scheduled an appointment, but I remember debating if I should straighten my hair or wear my naturally curly Afro. The first dermatologist I saw diagnosed me with seborrheic dermatitis—without even examining my scalp. She told me that I had a “full head of hair” and that I had nothing to worry about. I was unconvinced. Weeks later, I met with another dermatologist who took the time to listen to my concerns. After a scalp biopsy and laboratory work, she diagnosed me with telogen effluvium and androgenetic alopecia. Months later, I had the opportunity to visit the Black dermatologist, and she diagnosed me with central centrifugal cicatricial alopecia. I am grateful for the earlier dermatologists I saw, but I finally feel at ease with my diagnosis and treatment plan after being seen by the latter.
Chidubem’s Story
From a young age, I was conditioned to think my hair was thick, unmanageable, and a nuisance. I grew accustomed to people yanking on my hair, and my gentle whispers of “this hurts” and “the braid is too tight” being ignored. That continued into adulthood. While studying for the US Medical Licensing Examination, I noticed a burning sensation on my scalp. I decided to ignore it. However, as the days progressed, the slight burning sensation turned into intense burning and itching. I still ignored it. Not only did I lack the funds for a dermatology appointment, but my licensing examination was approaching, and it was more important than anything related to my hair. After the examination, I eventually made an appointment with my primary care physician, who attributed my symptoms to the stressors of medical school. “I think you are having migraines,” she told me. So, I continued to ignore my symptoms. A year passed, and a hair braider pointed out that I had 2 well-defined bald patches on my scalp. I remember feeling angry and confused as to how I missed those findings. I could no longer ignore it—it bothered me less when no one else knew about it. I quickly made a dermatology appointment. Although I opted out of a biopsy, we decided to treat my hair loss empirically, and I have experienced drastic improvement.
Final Thoughts
We are 2 Black women living more than 500 miles away from each other at different medical institutions, yet we share the same experience, which many other women unfortunately face alone. It is not uncommon for us to feel unheard, dismissed, or misdiagnosed. We write this for the Black woman sorting through the feelings of confusion and shock as she traces the hairless spot on her scalp. We write this for the medical student ignoring their symptoms until after their examination. We even write this for any nondermatologists uncomfortable with diagnosing and treating textured hair. To improve patient satisfaction and overall health outcomes, physicians must approach patients with both knowledge and cultural competency. Most importantly, dermatologists (and other physicians) should be appropriately trained in not only the structural differences of textured hair but also the unique practices and beliefs among Black women in relation to their hair.
Acknowledgments—Jewell Dinkins is the inaugural recipient of the Janssen–Skin of Color Research Fellowship at Howard University (Washington, DC), and Chidubem A.V. Okeke is the inaugural recipient of the Women’s Dermatologic Society–La Roche-Posay dermatology fellowship at Howard University.
As medical students, we often assume we are exempt from the diagnoses we learn about. During the first 2 years of medical school, we learn about alopecia as a condition that may be associated with stress, hormonal imbalances, nutrient deficiencies, and aging. However, our curricula do not explore the subtypes, psychosocial impact, or even the overwhelming number of Black women who are disproportionately affected by alopecia. For Black women, hair is a colossal part of their cultural identity, learning from a young age how to nurture and style natural coils. It becomes devastating when women begin to lose them.
The diagnosis of alopecia subtypes in Black women has been explored in the literature; however, understanding the unique experiences of young Black women is an important part of patient care, as alopecia often is destructive to the patient’s self-image. Therefore, it is important to shed light on these experiences so others feel empowered and supported in their journeys. Herein, we share the experiences of 2 authors (J.D. and C.A.V.O.)—both young Black women—who navigated unexpected hair loss in medical school.
Jewell’s Story
During my first year of medical school, I noticed my hair was shedding more than usual, and my ponytail was not as thick as it once was. I also had an area in my crown that was abnormally thin. My parents suggested that it was a consequence of stress, but I knew something was not right. With only 1 Black dermatologist within 2 hours of Nashville, Tennessee, I remember worrying about seeing a dermatologist who did not understand Black hair. I still scheduled an appointment, but I remember debating if I should straighten my hair or wear my naturally curly Afro. The first dermatologist I saw diagnosed me with seborrheic dermatitis—without even examining my scalp. She told me that I had a “full head of hair” and that I had nothing to worry about. I was unconvinced. Weeks later, I met with another dermatologist who took the time to listen to my concerns. After a scalp biopsy and laboratory work, she diagnosed me with telogen effluvium and androgenetic alopecia. Months later, I had the opportunity to visit the Black dermatologist, and she diagnosed me with central centrifugal cicatricial alopecia. I am grateful for the earlier dermatologists I saw, but I finally feel at ease with my diagnosis and treatment plan after being seen by the latter.
Chidubem’s Story
From a young age, I was conditioned to think my hair was thick, unmanageable, and a nuisance. I grew accustomed to people yanking on my hair, and my gentle whispers of “this hurts” and “the braid is too tight” being ignored. That continued into adulthood. While studying for the US Medical Licensing Examination, I noticed a burning sensation on my scalp. I decided to ignore it. However, as the days progressed, the slight burning sensation turned into intense burning and itching. I still ignored it. Not only did I lack the funds for a dermatology appointment, but my licensing examination was approaching, and it was more important than anything related to my hair. After the examination, I eventually made an appointment with my primary care physician, who attributed my symptoms to the stressors of medical school. “I think you are having migraines,” she told me. So, I continued to ignore my symptoms. A year passed, and a hair braider pointed out that I had 2 well-defined bald patches on my scalp. I remember feeling angry and confused as to how I missed those findings. I could no longer ignore it—it bothered me less when no one else knew about it. I quickly made a dermatology appointment. Although I opted out of a biopsy, we decided to treat my hair loss empirically, and I have experienced drastic improvement.
Final Thoughts
We are 2 Black women living more than 500 miles away from each other at different medical institutions, yet we share the same experience, which many other women unfortunately face alone. It is not uncommon for us to feel unheard, dismissed, or misdiagnosed. We write this for the Black woman sorting through the feelings of confusion and shock as she traces the hairless spot on her scalp. We write this for the medical student ignoring their symptoms until after their examination. We even write this for any nondermatologists uncomfortable with diagnosing and treating textured hair. To improve patient satisfaction and overall health outcomes, physicians must approach patients with both knowledge and cultural competency. Most importantly, dermatologists (and other physicians) should be appropriately trained in not only the structural differences of textured hair but also the unique practices and beliefs among Black women in relation to their hair.
Acknowledgments—Jewell Dinkins is the inaugural recipient of the Janssen–Skin of Color Research Fellowship at Howard University (Washington, DC), and Chidubem A.V. Okeke is the inaugural recipient of the Women’s Dermatologic Society–La Roche-Posay dermatology fellowship at Howard University.
Practice Points
- Hair loss is a common dermatologic concern among Black women and can represent a diagnostic challenge to dermatologists who may not be familiar with textured hair.
- Dermatologists should practice cultural sensitivity and provide relevant recommendations to Black patients dealing with hair loss.
Thalidomide Analogue Drug Eruption Along the Lines of Blaschko
To the Editor:
Lenalidomide is a thalidomide analogue used to treat various hematologic malignancies, including non-Hodgkin lymphoma, myelodysplastic syndrome, and multiple myeloma (MM).1 Lenalidomide is referred to as a degrader therapeutic because it induces targeted protein degradation of disease-relevant proteins (eg, Ikaros family zinc finger protein 1 [IKZF1], Ikaros family zinc finger protein 3 [IKZF3], and casein kinase I isoform-α [CK1α]) as its primary mechanism of action.1,2 Although cutaneous adverse events are relatively common among thalidomide analogues, the morphologic and histopathologic descriptions of these drug eruptions have not been fully elucidated.3,4 We report a novel pityriasiform drug eruption followed by a clinical eruption suggestive of blaschkitis in a patient with MM who was being treated with lenalidomide.
A 76-year-old man presented to the dermatology clinic with a progressive, mildly pruritic eruption on the chest and axillae of 1 year’s duration. He had a medical history of chronic hepatitis B, malignant carcinoid tumor of the colon, prostate cancer, and MM. The eruption emerged 1 to 2 weeks after the patient started oral lenalidomide 10 mg/d and oral dexamethasone40 mg/wk following autologous stem cell transplantation for MM. The patient had not received any other therapy for MM.
Physical examination revealed multiple erythematous, hyperpigmented, scaly papules and plaques on the lateral chest and within the axillae (Figure 1). A skin biopsy from the left axilla demonstrated a mild lichenoid and perivascular lymphocytic infiltrate with scattered eosinophils, neutrophils, and extravasated erythrocytes. The overlying epidermis showed spongiosis with parakeratosis in addition to lymphocytic exocytosis (Figure 2). No fungal organisms were highlighted on periodic acid–Schiff staining. After this evaluation, we recommended that the patient discontinue lenalidomide and start taking a topical over-the-counter corticosteroid for 2 weeks. Over time, he noted marked improvement in the eruption and associated pruritus.
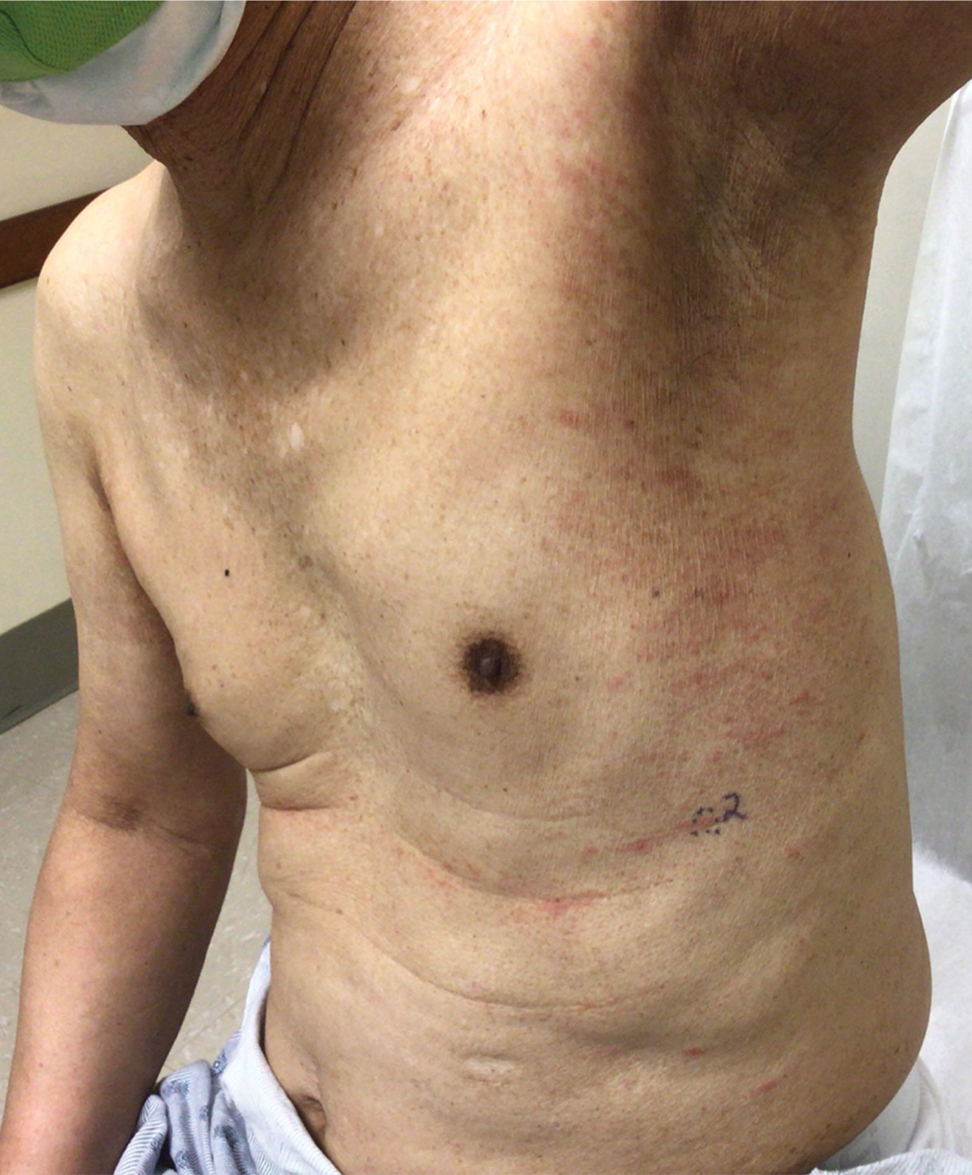
After a drug holiday of 2 months, the patient resumed a maintenance dosage of oral lenalidomide 10 mg/d. Four or 5 days after restarting lenalidomide, a pruritic eruption appeared that involved the axillae and the left lower abdomen, circling around to the left lower back. The axillary eruption resolved with a topical over-the-counter corticosteroid; the abdominal eruption persisted.
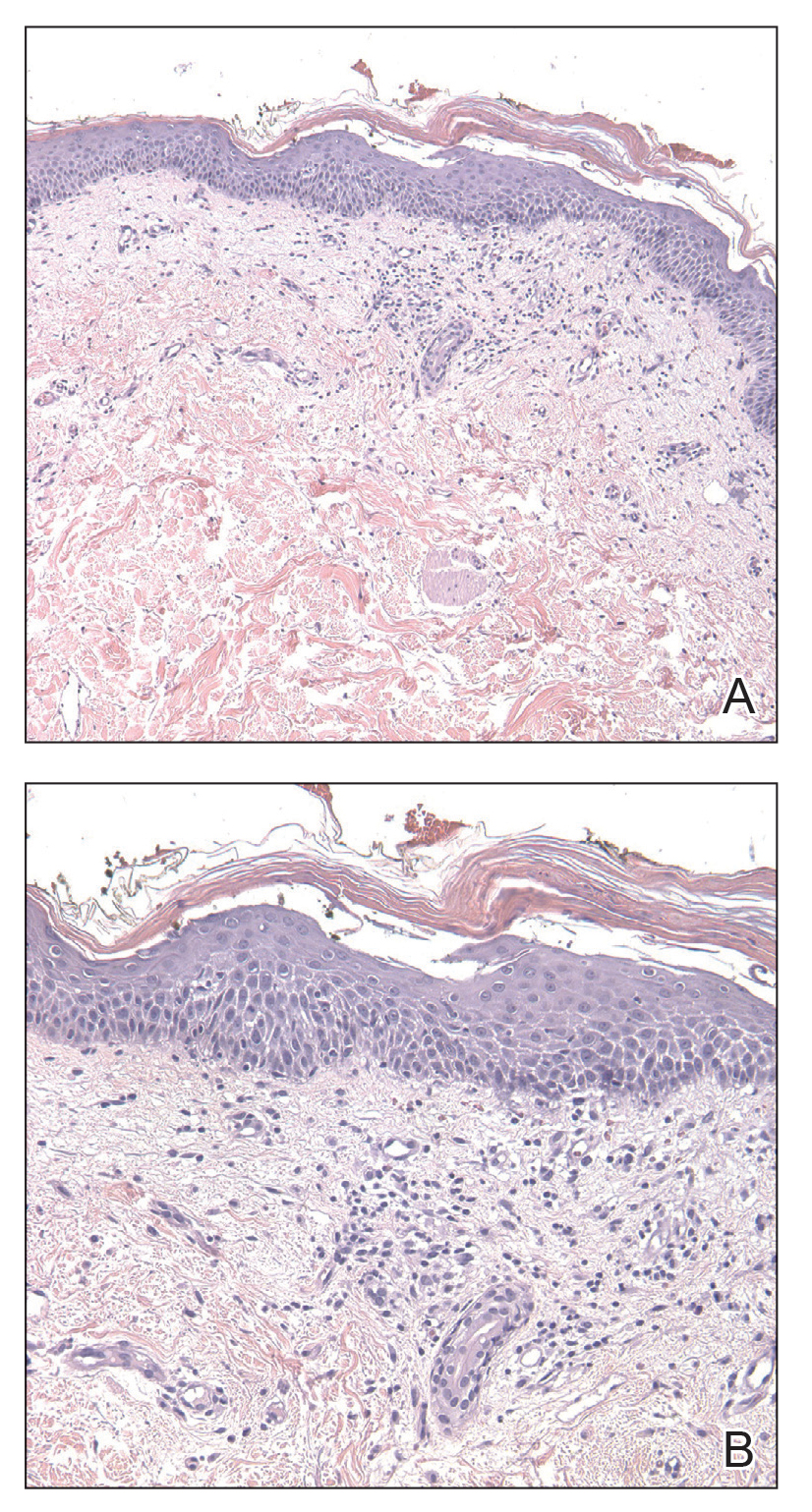
At the 3-month follow-up visit, physical examination revealed erythematous macules and papules that coalesced over a salmon-colored base along the lines of Blaschko extending from the left lower abdominal quadrant, crossing the left flank, and continuing to the left lower back without crossing the midline (Figure 3).
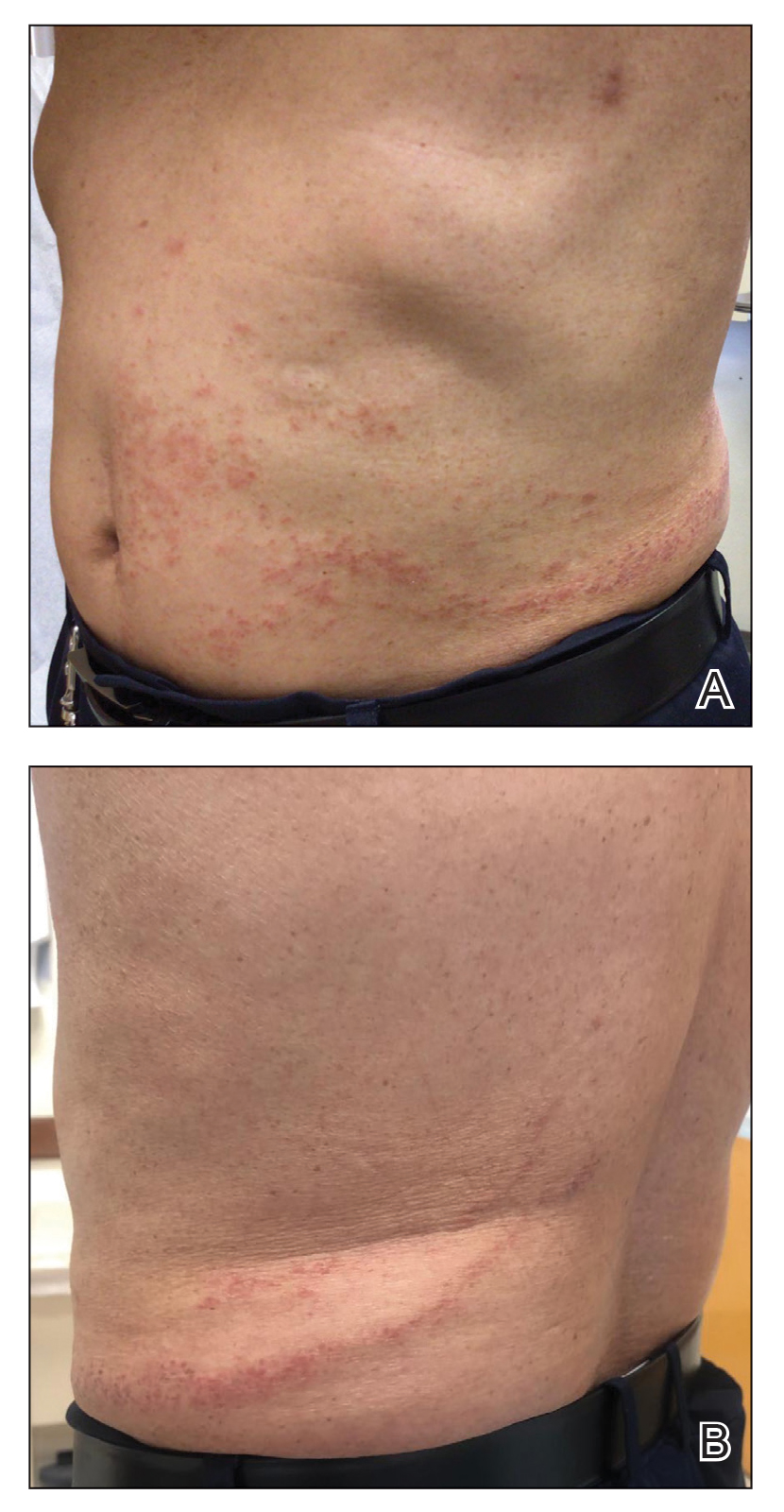
We recommended that the patient continue treatment through this eruption; he was instructed to apply a corticosteroid cream and resume lenalidomide at the maintenance dosage. A month later, he reported that the eruption and associated pruritus resolved with the corticosteroid cream and resumption of the maintenance dose of lenalidomide. The patient noted no further spread of the eruption.
Cutaneous adverse events are common following lenalidomide. In prior trials, the overall incidence of any-grade rash following lenalidomide exposure was 22% to 33%.5 A meta-analysis of 10 trials determined the overall incidence of all-grade and high-grade cutaneous adverse events after exposure to lenalidomide was 27.2% and 3.6%, respectively.6 Our case represents a pityriasiform eruption due to lenalidomide followed by a secondary eruption suggestive of blaschkitis.
The rash due to lenalidomide has been described as morbilliform, urticarial, dermatitic, acneform, and undefined.7 Lenalidomide-induced rash typically develops during the first month of therapy, similar to our patient’s presentation. It has even been observed in the first week of therapy.8 Severe reactions such as Stevens-Johnson syndrome and toxic epidermal necrolysis have been reported.5,6 Risk factors associated with rash secondary to lenalidomide include advanced age (≥70 years), presence of Bence-Jones protein-type MM in urine, and no prior chemotherapy.8 Our patient had 2 of these risk factors: advanced age and no prior chemotherapy for MM. The exact pathogenesis by which lenalidomide leads to a pityriasiform eruption, as in our patient, or to a rash in general is unclear. Studies have hypothesized that a lenalidomide-induced rash could be attributable to a delayed hypersensitivity type IV reaction or to a reaction related to the molecular mechanism of action of the drug.9
At the molecular level, the antimyeloma effects of lenalidomide include promoting degradation of transcription factors IKZF1 and IKZF3, which subsequently increases production of IL-2.1,2,9 Recombinant IL-2 has been associated with an increased incidence of rash in other cancers.9 Overexpression of programmed death 1(PD-1) and its ligand (PD-L1) has been demonstrated in MM; lenalidomide has been shown to downregulate both PD-1 and PD-L1. Patients receiving PD-1 and PD-L1 inhibitors commonly have developed rash.9 However, the association between lenalidomide and its downregulation of PD-1 and PD-L1 leading to rash has not been fully elucidated. Given the multiple malignancies in our patient—MM, prostate cancer, malignant carcinoid tumor—an underlying paraneoplastic phenomenon may be possible. Additionally, because our patient initially received dexamethasone along with lenalidomide, the manifestation of the initial pityriasiform rash may have been less severe due to the steroid use. Although our patient underwent a 2-month drug holiday following the initial pityriasiform eruption, most lenalidomide-induced rashes do not necessitate discontinuation of the drug.5,7
Our patient’s secondary drug eruption was clinically suggestive of lenalidomide-induced blaschkitis. A report of a German patient with plasmacytoma described a unilateral papular exanthem that developed 4 months after lenalidomide was initiated.10 The papular exanthem following the lines of Blaschko lines extended from that patient’s posterior left foot to the calf and on to the thigh and flank,10 which was more extensive than our patient’s eruption. Blaschkitis in this patient resolved with a corticosteroid cream and UV light therapy10; lenalidomide was not discontinued, similar to our patient.
The pathogenesis of our patient’s secondary eruption that preferentially involved the lines of Blaschko is unclear. After the initial pityriasiform eruption, the secondary eruption was blaschkitis. Distinguishing dermatomes from the lines of Blaschko, which are thought to represent pathways of epidermal cell migration and proliferation during embryologic development, is important. Genodermatoses such as incontinentia pigmenti and hypomelanosis of Ito involve the lines of Blaschko11; other disorders in the differential diagnosis of linear configurations include linear lichen planus, linear cutaneous lupus erythematosus, linear morphea, and lichen striatus.11 Notably, drug-induced blaschkitis is rare.
Cutaneous adverse reactions from thalidomide analogues are relatively common. Our case of lenalidomide-associated blaschkitis that developed following an initial pityriasiform drug eruption in a patient with MM highlights that dermatologists need to collaborate with the oncologist regarding the severity of drug eruptions to determine if the patient should continue treatment through the cutaneous eruptions or discontinue a vital medication.
- Jan M, Sperling AS, Ebert BL. Cancer therapies based on targeted protein degradation—lessons learned with lenalidomide. Nat Rev Clin Oncol. 2021;18:401-417. doi:10.1038/s41571-021-00479-z
- Shah UA, Mailankody S. Emerging immunotherapies in multiple myeloma. BMJ. 2020;370:3176. doi:10.1136/BMJ.M3176
- Richardson PG, Blood E, Mitsiades CS, et al. A randomized phase 2 study of lenalidomide therapy for patients with relapsed or relapsed and refractory multiple myeloma. Blood. 2006;108:3458-3464. doi:10.1182/BLOOD-2006-04-015909
- Benboubker L, Dimopoulos MA, Dispenzieri A, et al. Lenalidomide and dexamethasone in transplant-ineligible patients with myeloma. N Engl J Med. 2014;371:906-917. doi:10.1056/NEJMOA1402551
- Tinsley SM, Kurtin SE, Ridgeway JA. Practical management of lenalidomide-related rash. Clin Lymphoma Myeloma Leuk. 2015;15(suppl):S64-S69. doi:10.1016/J.CLML.2015.02.008
- Nardone B, Wu S, Garden BC, et al. Risk of rash associated with lenalidomide in cancer patients: a systematic review of the literature and meta-analysis. Clin Lymphoma Myeloma Leuk. 2013;13:424-429. doi:10.1016/J.CLML.2013.03.006
- Sviggum HP, Davis MDP, Rajkumar SV, et al. Dermatologic adverse effects of lenalidomide therapy for amyloidosis and multiple myeloma. Arch Dermatol. 2006;142:1298-1302. doi:10.1001/ARCHDERM.142.10.1298
- Sugi T, Nishigami Y, Saigo H, et al. Analysis of risk factors for lenalidomide-associated skin rash in patients with multiple myeloma. Leuk Lymphoma. 2021;62:1405-1410. doi:10.1080/10428194.2021.1876867
- Barley K, He W, Agarwal S, et al. Outcomes and management of lenalidomide-associated rash in patients with multiple myeloma. Leuk Lymphoma. 2016;57:2510-2515. doi:10.3109/10428194.2016.1151507
- Grape J, Frosch P. Papular drug eruption along the lines of Blaschko caused by lenalidomide [in German]. Hautarzt. 2011;62:618-620. doi:10.1007/S00105-010-2121-6
- Bolognia JL, Orlow SJ, Glick SA. Lines of Blaschko. J Am Acad Dermatol. 1994;31(2 pt 1):157-190. doi:10.1016/S0190-9622(94)70143-1
To the Editor:
Lenalidomide is a thalidomide analogue used to treat various hematologic malignancies, including non-Hodgkin lymphoma, myelodysplastic syndrome, and multiple myeloma (MM).1 Lenalidomide is referred to as a degrader therapeutic because it induces targeted protein degradation of disease-relevant proteins (eg, Ikaros family zinc finger protein 1 [IKZF1], Ikaros family zinc finger protein 3 [IKZF3], and casein kinase I isoform-α [CK1α]) as its primary mechanism of action.1,2 Although cutaneous adverse events are relatively common among thalidomide analogues, the morphologic and histopathologic descriptions of these drug eruptions have not been fully elucidated.3,4 We report a novel pityriasiform drug eruption followed by a clinical eruption suggestive of blaschkitis in a patient with MM who was being treated with lenalidomide.
A 76-year-old man presented to the dermatology clinic with a progressive, mildly pruritic eruption on the chest and axillae of 1 year’s duration. He had a medical history of chronic hepatitis B, malignant carcinoid tumor of the colon, prostate cancer, and MM. The eruption emerged 1 to 2 weeks after the patient started oral lenalidomide 10 mg/d and oral dexamethasone40 mg/wk following autologous stem cell transplantation for MM. The patient had not received any other therapy for MM.
Physical examination revealed multiple erythematous, hyperpigmented, scaly papules and plaques on the lateral chest and within the axillae (Figure 1). A skin biopsy from the left axilla demonstrated a mild lichenoid and perivascular lymphocytic infiltrate with scattered eosinophils, neutrophils, and extravasated erythrocytes. The overlying epidermis showed spongiosis with parakeratosis in addition to lymphocytic exocytosis (Figure 2). No fungal organisms were highlighted on periodic acid–Schiff staining. After this evaluation, we recommended that the patient discontinue lenalidomide and start taking a topical over-the-counter corticosteroid for 2 weeks. Over time, he noted marked improvement in the eruption and associated pruritus.

After a drug holiday of 2 months, the patient resumed a maintenance dosage of oral lenalidomide 10 mg/d. Four or 5 days after restarting lenalidomide, a pruritic eruption appeared that involved the axillae and the left lower abdomen, circling around to the left lower back. The axillary eruption resolved with a topical over-the-counter corticosteroid; the abdominal eruption persisted.

At the 3-month follow-up visit, physical examination revealed erythematous macules and papules that coalesced over a salmon-colored base along the lines of Blaschko extending from the left lower abdominal quadrant, crossing the left flank, and continuing to the left lower back without crossing the midline (Figure 3).

We recommended that the patient continue treatment through this eruption; he was instructed to apply a corticosteroid cream and resume lenalidomide at the maintenance dosage. A month later, he reported that the eruption and associated pruritus resolved with the corticosteroid cream and resumption of the maintenance dose of lenalidomide. The patient noted no further spread of the eruption.
Cutaneous adverse events are common following lenalidomide. In prior trials, the overall incidence of any-grade rash following lenalidomide exposure was 22% to 33%.5 A meta-analysis of 10 trials determined the overall incidence of all-grade and high-grade cutaneous adverse events after exposure to lenalidomide was 27.2% and 3.6%, respectively.6 Our case represents a pityriasiform eruption due to lenalidomide followed by a secondary eruption suggestive of blaschkitis.
The rash due to lenalidomide has been described as morbilliform, urticarial, dermatitic, acneform, and undefined.7 Lenalidomide-induced rash typically develops during the first month of therapy, similar to our patient’s presentation. It has even been observed in the first week of therapy.8 Severe reactions such as Stevens-Johnson syndrome and toxic epidermal necrolysis have been reported.5,6 Risk factors associated with rash secondary to lenalidomide include advanced age (≥70 years), presence of Bence-Jones protein-type MM in urine, and no prior chemotherapy.8 Our patient had 2 of these risk factors: advanced age and no prior chemotherapy for MM. The exact pathogenesis by which lenalidomide leads to a pityriasiform eruption, as in our patient, or to a rash in general is unclear. Studies have hypothesized that a lenalidomide-induced rash could be attributable to a delayed hypersensitivity type IV reaction or to a reaction related to the molecular mechanism of action of the drug.9
At the molecular level, the antimyeloma effects of lenalidomide include promoting degradation of transcription factors IKZF1 and IKZF3, which subsequently increases production of IL-2.1,2,9 Recombinant IL-2 has been associated with an increased incidence of rash in other cancers.9 Overexpression of programmed death 1(PD-1) and its ligand (PD-L1) has been demonstrated in MM; lenalidomide has been shown to downregulate both PD-1 and PD-L1. Patients receiving PD-1 and PD-L1 inhibitors commonly have developed rash.9 However, the association between lenalidomide and its downregulation of PD-1 and PD-L1 leading to rash has not been fully elucidated. Given the multiple malignancies in our patient—MM, prostate cancer, malignant carcinoid tumor—an underlying paraneoplastic phenomenon may be possible. Additionally, because our patient initially received dexamethasone along with lenalidomide, the manifestation of the initial pityriasiform rash may have been less severe due to the steroid use. Although our patient underwent a 2-month drug holiday following the initial pityriasiform eruption, most lenalidomide-induced rashes do not necessitate discontinuation of the drug.5,7
Our patient’s secondary drug eruption was clinically suggestive of lenalidomide-induced blaschkitis. A report of a German patient with plasmacytoma described a unilateral papular exanthem that developed 4 months after lenalidomide was initiated.10 The papular exanthem following the lines of Blaschko lines extended from that patient’s posterior left foot to the calf and on to the thigh and flank,10 which was more extensive than our patient’s eruption. Blaschkitis in this patient resolved with a corticosteroid cream and UV light therapy10; lenalidomide was not discontinued, similar to our patient.
The pathogenesis of our patient’s secondary eruption that preferentially involved the lines of Blaschko is unclear. After the initial pityriasiform eruption, the secondary eruption was blaschkitis. Distinguishing dermatomes from the lines of Blaschko, which are thought to represent pathways of epidermal cell migration and proliferation during embryologic development, is important. Genodermatoses such as incontinentia pigmenti and hypomelanosis of Ito involve the lines of Blaschko11; other disorders in the differential diagnosis of linear configurations include linear lichen planus, linear cutaneous lupus erythematosus, linear morphea, and lichen striatus.11 Notably, drug-induced blaschkitis is rare.
Cutaneous adverse reactions from thalidomide analogues are relatively common. Our case of lenalidomide-associated blaschkitis that developed following an initial pityriasiform drug eruption in a patient with MM highlights that dermatologists need to collaborate with the oncologist regarding the severity of drug eruptions to determine if the patient should continue treatment through the cutaneous eruptions or discontinue a vital medication.
To the Editor:
Lenalidomide is a thalidomide analogue used to treat various hematologic malignancies, including non-Hodgkin lymphoma, myelodysplastic syndrome, and multiple myeloma (MM).1 Lenalidomide is referred to as a degrader therapeutic because it induces targeted protein degradation of disease-relevant proteins (eg, Ikaros family zinc finger protein 1 [IKZF1], Ikaros family zinc finger protein 3 [IKZF3], and casein kinase I isoform-α [CK1α]) as its primary mechanism of action.1,2 Although cutaneous adverse events are relatively common among thalidomide analogues, the morphologic and histopathologic descriptions of these drug eruptions have not been fully elucidated.3,4 We report a novel pityriasiform drug eruption followed by a clinical eruption suggestive of blaschkitis in a patient with MM who was being treated with lenalidomide.
A 76-year-old man presented to the dermatology clinic with a progressive, mildly pruritic eruption on the chest and axillae of 1 year’s duration. He had a medical history of chronic hepatitis B, malignant carcinoid tumor of the colon, prostate cancer, and MM. The eruption emerged 1 to 2 weeks after the patient started oral lenalidomide 10 mg/d and oral dexamethasone40 mg/wk following autologous stem cell transplantation for MM. The patient had not received any other therapy for MM.
Physical examination revealed multiple erythematous, hyperpigmented, scaly papules and plaques on the lateral chest and within the axillae (Figure 1). A skin biopsy from the left axilla demonstrated a mild lichenoid and perivascular lymphocytic infiltrate with scattered eosinophils, neutrophils, and extravasated erythrocytes. The overlying epidermis showed spongiosis with parakeratosis in addition to lymphocytic exocytosis (Figure 2). No fungal organisms were highlighted on periodic acid–Schiff staining. After this evaluation, we recommended that the patient discontinue lenalidomide and start taking a topical over-the-counter corticosteroid for 2 weeks. Over time, he noted marked improvement in the eruption and associated pruritus.

After a drug holiday of 2 months, the patient resumed a maintenance dosage of oral lenalidomide 10 mg/d. Four or 5 days after restarting lenalidomide, a pruritic eruption appeared that involved the axillae and the left lower abdomen, circling around to the left lower back. The axillary eruption resolved with a topical over-the-counter corticosteroid; the abdominal eruption persisted.

At the 3-month follow-up visit, physical examination revealed erythematous macules and papules that coalesced over a salmon-colored base along the lines of Blaschko extending from the left lower abdominal quadrant, crossing the left flank, and continuing to the left lower back without crossing the midline (Figure 3).

We recommended that the patient continue treatment through this eruption; he was instructed to apply a corticosteroid cream and resume lenalidomide at the maintenance dosage. A month later, he reported that the eruption and associated pruritus resolved with the corticosteroid cream and resumption of the maintenance dose of lenalidomide. The patient noted no further spread of the eruption.
Cutaneous adverse events are common following lenalidomide. In prior trials, the overall incidence of any-grade rash following lenalidomide exposure was 22% to 33%.5 A meta-analysis of 10 trials determined the overall incidence of all-grade and high-grade cutaneous adverse events after exposure to lenalidomide was 27.2% and 3.6%, respectively.6 Our case represents a pityriasiform eruption due to lenalidomide followed by a secondary eruption suggestive of blaschkitis.
The rash due to lenalidomide has been described as morbilliform, urticarial, dermatitic, acneform, and undefined.7 Lenalidomide-induced rash typically develops during the first month of therapy, similar to our patient’s presentation. It has even been observed in the first week of therapy.8 Severe reactions such as Stevens-Johnson syndrome and toxic epidermal necrolysis have been reported.5,6 Risk factors associated with rash secondary to lenalidomide include advanced age (≥70 years), presence of Bence-Jones protein-type MM in urine, and no prior chemotherapy.8 Our patient had 2 of these risk factors: advanced age and no prior chemotherapy for MM. The exact pathogenesis by which lenalidomide leads to a pityriasiform eruption, as in our patient, or to a rash in general is unclear. Studies have hypothesized that a lenalidomide-induced rash could be attributable to a delayed hypersensitivity type IV reaction or to a reaction related to the molecular mechanism of action of the drug.9
At the molecular level, the antimyeloma effects of lenalidomide include promoting degradation of transcription factors IKZF1 and IKZF3, which subsequently increases production of IL-2.1,2,9 Recombinant IL-2 has been associated with an increased incidence of rash in other cancers.9 Overexpression of programmed death 1(PD-1) and its ligand (PD-L1) has been demonstrated in MM; lenalidomide has been shown to downregulate both PD-1 and PD-L1. Patients receiving PD-1 and PD-L1 inhibitors commonly have developed rash.9 However, the association between lenalidomide and its downregulation of PD-1 and PD-L1 leading to rash has not been fully elucidated. Given the multiple malignancies in our patient—MM, prostate cancer, malignant carcinoid tumor—an underlying paraneoplastic phenomenon may be possible. Additionally, because our patient initially received dexamethasone along with lenalidomide, the manifestation of the initial pityriasiform rash may have been less severe due to the steroid use. Although our patient underwent a 2-month drug holiday following the initial pityriasiform eruption, most lenalidomide-induced rashes do not necessitate discontinuation of the drug.5,7
Our patient’s secondary drug eruption was clinically suggestive of lenalidomide-induced blaschkitis. A report of a German patient with plasmacytoma described a unilateral papular exanthem that developed 4 months after lenalidomide was initiated.10 The papular exanthem following the lines of Blaschko lines extended from that patient’s posterior left foot to the calf and on to the thigh and flank,10 which was more extensive than our patient’s eruption. Blaschkitis in this patient resolved with a corticosteroid cream and UV light therapy10; lenalidomide was not discontinued, similar to our patient.
The pathogenesis of our patient’s secondary eruption that preferentially involved the lines of Blaschko is unclear. After the initial pityriasiform eruption, the secondary eruption was blaschkitis. Distinguishing dermatomes from the lines of Blaschko, which are thought to represent pathways of epidermal cell migration and proliferation during embryologic development, is important. Genodermatoses such as incontinentia pigmenti and hypomelanosis of Ito involve the lines of Blaschko11; other disorders in the differential diagnosis of linear configurations include linear lichen planus, linear cutaneous lupus erythematosus, linear morphea, and lichen striatus.11 Notably, drug-induced blaschkitis is rare.
Cutaneous adverse reactions from thalidomide analogues are relatively common. Our case of lenalidomide-associated blaschkitis that developed following an initial pityriasiform drug eruption in a patient with MM highlights that dermatologists need to collaborate with the oncologist regarding the severity of drug eruptions to determine if the patient should continue treatment through the cutaneous eruptions or discontinue a vital medication.
- Jan M, Sperling AS, Ebert BL. Cancer therapies based on targeted protein degradation—lessons learned with lenalidomide. Nat Rev Clin Oncol. 2021;18:401-417. doi:10.1038/s41571-021-00479-z
- Shah UA, Mailankody S. Emerging immunotherapies in multiple myeloma. BMJ. 2020;370:3176. doi:10.1136/BMJ.M3176
- Richardson PG, Blood E, Mitsiades CS, et al. A randomized phase 2 study of lenalidomide therapy for patients with relapsed or relapsed and refractory multiple myeloma. Blood. 2006;108:3458-3464. doi:10.1182/BLOOD-2006-04-015909
- Benboubker L, Dimopoulos MA, Dispenzieri A, et al. Lenalidomide and dexamethasone in transplant-ineligible patients with myeloma. N Engl J Med. 2014;371:906-917. doi:10.1056/NEJMOA1402551
- Tinsley SM, Kurtin SE, Ridgeway JA. Practical management of lenalidomide-related rash. Clin Lymphoma Myeloma Leuk. 2015;15(suppl):S64-S69. doi:10.1016/J.CLML.2015.02.008
- Nardone B, Wu S, Garden BC, et al. Risk of rash associated with lenalidomide in cancer patients: a systematic review of the literature and meta-analysis. Clin Lymphoma Myeloma Leuk. 2013;13:424-429. doi:10.1016/J.CLML.2013.03.006
- Sviggum HP, Davis MDP, Rajkumar SV, et al. Dermatologic adverse effects of lenalidomide therapy for amyloidosis and multiple myeloma. Arch Dermatol. 2006;142:1298-1302. doi:10.1001/ARCHDERM.142.10.1298
- Sugi T, Nishigami Y, Saigo H, et al. Analysis of risk factors for lenalidomide-associated skin rash in patients with multiple myeloma. Leuk Lymphoma. 2021;62:1405-1410. doi:10.1080/10428194.2021.1876867
- Barley K, He W, Agarwal S, et al. Outcomes and management of lenalidomide-associated rash in patients with multiple myeloma. Leuk Lymphoma. 2016;57:2510-2515. doi:10.3109/10428194.2016.1151507
- Grape J, Frosch P. Papular drug eruption along the lines of Blaschko caused by lenalidomide [in German]. Hautarzt. 2011;62:618-620. doi:10.1007/S00105-010-2121-6
- Bolognia JL, Orlow SJ, Glick SA. Lines of Blaschko. J Am Acad Dermatol. 1994;31(2 pt 1):157-190. doi:10.1016/S0190-9622(94)70143-1
- Jan M, Sperling AS, Ebert BL. Cancer therapies based on targeted protein degradation—lessons learned with lenalidomide. Nat Rev Clin Oncol. 2021;18:401-417. doi:10.1038/s41571-021-00479-z
- Shah UA, Mailankody S. Emerging immunotherapies in multiple myeloma. BMJ. 2020;370:3176. doi:10.1136/BMJ.M3176
- Richardson PG, Blood E, Mitsiades CS, et al. A randomized phase 2 study of lenalidomide therapy for patients with relapsed or relapsed and refractory multiple myeloma. Blood. 2006;108:3458-3464. doi:10.1182/BLOOD-2006-04-015909
- Benboubker L, Dimopoulos MA, Dispenzieri A, et al. Lenalidomide and dexamethasone in transplant-ineligible patients with myeloma. N Engl J Med. 2014;371:906-917. doi:10.1056/NEJMOA1402551
- Tinsley SM, Kurtin SE, Ridgeway JA. Practical management of lenalidomide-related rash. Clin Lymphoma Myeloma Leuk. 2015;15(suppl):S64-S69. doi:10.1016/J.CLML.2015.02.008
- Nardone B, Wu S, Garden BC, et al. Risk of rash associated with lenalidomide in cancer patients: a systematic review of the literature and meta-analysis. Clin Lymphoma Myeloma Leuk. 2013;13:424-429. doi:10.1016/J.CLML.2013.03.006
- Sviggum HP, Davis MDP, Rajkumar SV, et al. Dermatologic adverse effects of lenalidomide therapy for amyloidosis and multiple myeloma. Arch Dermatol. 2006;142:1298-1302. doi:10.1001/ARCHDERM.142.10.1298
- Sugi T, Nishigami Y, Saigo H, et al. Analysis of risk factors for lenalidomide-associated skin rash in patients with multiple myeloma. Leuk Lymphoma. 2021;62:1405-1410. doi:10.1080/10428194.2021.1876867
- Barley K, He W, Agarwal S, et al. Outcomes and management of lenalidomide-associated rash in patients with multiple myeloma. Leuk Lymphoma. 2016;57:2510-2515. doi:10.3109/10428194.2016.1151507
- Grape J, Frosch P. Papular drug eruption along the lines of Blaschko caused by lenalidomide [in German]. Hautarzt. 2011;62:618-620. doi:10.1007/S00105-010-2121-6
- Bolognia JL, Orlow SJ, Glick SA. Lines of Blaschko. J Am Acad Dermatol. 1994;31(2 pt 1):157-190. doi:10.1016/S0190-9622(94)70143-1
Practice Points
- Dermatologists should be aware of the variety of cutaneous adverse events that can arise from the use of immunotherapeutic agents for hematologic malignancies.
- Some cutaneous reactions to immunotherapeutic medications, such as pityriasiform eruption and blaschkitis, generally are benign and may not necessitate halting an important therapy.