User login
Lack of after care leaves cancer patients in ‘survivorship abyss’
Although prostate cancer is the second most common cancer in men worldwide, it is not a lethal cancer: Improvements in early detection and treatment have boosted the 10-year relative survival rate to 98%.
But for many men, life after treatment is an ongoing struggle.
One of the first qualitative survey studies of long-term prostate cancer survivorship in Australia found that many survivors are living with adverse effects such as urinary incontinence and sexual dysfunction and that they continue to have heightened feelings of distress.
Many of the patients surveyed said that they had not received follow-up care and felt they had been “abandoned” by their health care professionals.
One man called it “the survivorship abyss.”
“As the prevalence of prostate cancer survivors continues to grow globally, the absence of integrated shared survivorship care models into clinical practice, such as survivorship care guidelines/plans and/or interventions, will perpetuate the sense of abandonment and the overwhelming burden of care of men lost in the PC [prostate cancer] ‘survivorship abyss,’” say the authors.
The report was published online in Psycho-Oncology.
“The good news is that more men than ever before are surviving prostate cancer,” commented lead author Carolyn G. Mazariego, PhD, a research fellow at the Daffodil Center of the Cancer Council New South Wales and the University of Sydney.
“As our population grows and ages, an increasing number of men are facing these survivorship challenges, and the need for clear survivorship care guidelines becomes increasingly vital,” Dr. Mazariego told this news organization.
Details of the survey findings
To find participants for their study, the team drew upon a cohort of 578 men who were included in the 15-year follow-up phase of the longitudinal New South Wales Prostate Cancer Care and Outcomes Study (PCOS).
The researchers interviewed 37 men for the study. The majority (88.6%) had been diagnosed with localized disease, and just over half (54%) had undergone radical prostatectomy as their primary treatment.
Some expressed regret over having had surgery. One respondent, a 15-year survivor, commented: “I really didn’t know how intrusive [surgery] was as far as losing the length of my penis and its functions. To this day, I sometimes can’t believe it’s happened. It’s devastating.”
The survey also found that most survivors viewed active treatment as the only way to avoid death.
In hindsight, some questioned whether radical treatment was necessary and whether they might have been better served by active surveillance.
Many said they were never given a chance to discuss sexual dysfunction, and others said their questions sparked an awkward, limited conversation. Many said they suffered in silence.
“We know that there is a sort of ‘cycle of silence’ between patients and health care providers about sexual issues, and that was particularly true for the men we spoke to,” Dr. Mazariego said. “This cycle of silence can stem from confusion and ambiguity as to who men should speak with regarding these ongoing issues.”
“It’s just like being part of a secret society,” said one survivor. “Like you don’t know about it until you’re in it ... I don’t think people want to know if they have it [prostate cancer] or want it known. It’s all hush hush.”
Prostate cancer patients often feel uncomfortable talking about sexual function, Dr. Mazariego pointed out. “Many men instead internalized these thoughts or concerns and just ‘got on’ with life.”
One survey participant said: “Well, you just gotta deal with it [issues relating to prostate cancer]. Just got to try and wipe out the thoughts, that’s all you can do. Suck it up and carry on.”
Discussions must be part of standard of care
Dr. Mazariego emphasized that for prostate cancer survivorship to improve, conversations about the psychosocial needs of patients must be normalized and made routine. Discussions about post-treatment side effects that cause functional impairments and are stressful to relationships must be embedded into the standards of care, she added. This will allow physicians to use these kinds of conversations “as a springboard for referrals to appropriate care.”
“Patients of all ages will have concerns related to sex and sexual function, whether you ask about them or not,” said Brad Zebrack, PhD, MSW, MPH, professor at the University of Michigan School of Social Work, Ann Arbor, who was approached for comment.
At the very least, physicians should be prepared to “acknowledge and describe possible effects of therapy on sex and sexual function and follow up by describing available supports for education and either individual or couples counseling,” said Dr. Zebrack, who is also a member of the health behavior and outcomes research program at the Rogel Cancer Center.
Physicians can also refer patients to evidence-based resources and toolkits, he said. He noted that Will2Love offers self-help programs for cancer-related sexual problems and is “an outstanding resource.”
Distress screening needed
Universal psychosocial distress screening is needed to identify men with prostate cancer who have high levels of distress, argues Jeff Dunn, AO, PhD, who is CEO of the Prostate Cancer Foundation of Australia (PCFA), in Sydney.
Without this, men will not seek help for their unmet needs, Dr. Dunn noted in a 2019 editorial in the European Journal of Cancer Care.
The unmet psychosocial needs of prostate cancer patients and their partners “are highly prevalent,” said Dr. Dunn and co-author Suzanne K. Chambers, AO, PhD, dean of the Faculty of Health at the University of Technology Sydney. “...[F]or many prostate cancer survivors, the physical, social, psychological and relationship challenges will be long term, if not lifelong,” they write.
Even in Australia, where 1 in every 6 men are expected to be diagnosed with prostate cancer by age 85, efforts to improve survivorship care have not produced the desired results, they note.
In 2019, the PCFA published a monograph in which the organization recommended routine distress screenings and referrals to evidence-based psychosocial care for prostate cancer survivors. The foundation predicted that it would be “a game-changer for every Australian man impacted by the disease.”
“Yet, we still do not have a national survivorship care plan for prostate cancer survivors in Australia,” Dr. Mazariego said.
Left untreated, the psychosocial effects of prostate cancer “are considerable and certainly factors that should be considered as a threat to well-being,” she emphasized.
“Certainly, accumulation of unmet psychosocial needs increases risks for depression and suicide, which is true in both cancer and noncancer populations,” said Dr. Zebrack.
Data back this up. One study of patients with prostate cancer found that after diagnosis, 1 in 4 experienced anxiety, and 1 in 5 experienced depression. Another study found that the risk for suicide was higher among men with prostate cancer during the first year after diagnosis than among men with other solid-organ malignancies.
More recently, a 2018 population-based Australian cohort study of men in New South Wales revealed that the risk for death by suicide was 70% higher among men who had been diagnosed with prostate cancer compared with men in the general population. This risk was higher within the first year following diagnosis and was higher in men with nonlocalized disease, those who were single, those who were living in a major city, and those who were unmarried.
Dr. Mazariego and the team reporting the survey found that men who received supportive care had a greater chance of reconciling living with functional impairments. “Receiving adequate survivorship care and trusting patient-clinician relationships appeared to be associated with greater resilience and positivity in the men’s acceptance of cancer-related, long-term challenges and personal limitations,” they note.
Developing postcancer identity
Survivors also appeared to have developed a post-cancer identity that was more invested in personal relationships or in taking a more active role in their own health.
“Treating my prostate cancer gave me a second chance,” said one survivor. “Yeah, I’m a survivor, but more importantly, I’m a loving husband now. I know I wasn’t as giving back then.”
Another man admitted that before his diagnosis, he never went to the doctor. “I go much more often now,” he said. “You need to check up on yourself, at least once a year. Could have caught the cancer earlier if I was doing that.”
These comments appear to be borne out by data released last year by the American Cancer Society (ACS), which found that the number of number of cancer-related suicides in the United States was on the decline, as reported by this news organization.
Some of the biggest decreases occurred in men with prostate cancer, although prostate cancer was associated with 15% of cancer-related suicides. Only lung cancer was associated with more cancer-related suicides, at 18%.
A factor in the decrease in cancer-related suicides was likely to be an increase in the use of supportive care services, the ACS researchers commented.
“Although no causal relationship can be established, our findings suggest an evolving role of psycho-oncology care and palliative and hospice care given the promotion and increased utilization of these services among cancer patients during this period,” they commented.
The study was funded by the Cancer Institute NSW. Dr. Mazariego and colleagues have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Although prostate cancer is the second most common cancer in men worldwide, it is not a lethal cancer: Improvements in early detection and treatment have boosted the 10-year relative survival rate to 98%.
But for many men, life after treatment is an ongoing struggle.
One of the first qualitative survey studies of long-term prostate cancer survivorship in Australia found that many survivors are living with adverse effects such as urinary incontinence and sexual dysfunction and that they continue to have heightened feelings of distress.
Many of the patients surveyed said that they had not received follow-up care and felt they had been “abandoned” by their health care professionals.
One man called it “the survivorship abyss.”
“As the prevalence of prostate cancer survivors continues to grow globally, the absence of integrated shared survivorship care models into clinical practice, such as survivorship care guidelines/plans and/or interventions, will perpetuate the sense of abandonment and the overwhelming burden of care of men lost in the PC [prostate cancer] ‘survivorship abyss,’” say the authors.
The report was published online in Psycho-Oncology.
“The good news is that more men than ever before are surviving prostate cancer,” commented lead author Carolyn G. Mazariego, PhD, a research fellow at the Daffodil Center of the Cancer Council New South Wales and the University of Sydney.
“As our population grows and ages, an increasing number of men are facing these survivorship challenges, and the need for clear survivorship care guidelines becomes increasingly vital,” Dr. Mazariego told this news organization.
Details of the survey findings
To find participants for their study, the team drew upon a cohort of 578 men who were included in the 15-year follow-up phase of the longitudinal New South Wales Prostate Cancer Care and Outcomes Study (PCOS).
The researchers interviewed 37 men for the study. The majority (88.6%) had been diagnosed with localized disease, and just over half (54%) had undergone radical prostatectomy as their primary treatment.
Some expressed regret over having had surgery. One respondent, a 15-year survivor, commented: “I really didn’t know how intrusive [surgery] was as far as losing the length of my penis and its functions. To this day, I sometimes can’t believe it’s happened. It’s devastating.”
The survey also found that most survivors viewed active treatment as the only way to avoid death.
In hindsight, some questioned whether radical treatment was necessary and whether they might have been better served by active surveillance.
Many said they were never given a chance to discuss sexual dysfunction, and others said their questions sparked an awkward, limited conversation. Many said they suffered in silence.
“We know that there is a sort of ‘cycle of silence’ between patients and health care providers about sexual issues, and that was particularly true for the men we spoke to,” Dr. Mazariego said. “This cycle of silence can stem from confusion and ambiguity as to who men should speak with regarding these ongoing issues.”
“It’s just like being part of a secret society,” said one survivor. “Like you don’t know about it until you’re in it ... I don’t think people want to know if they have it [prostate cancer] or want it known. It’s all hush hush.”
Prostate cancer patients often feel uncomfortable talking about sexual function, Dr. Mazariego pointed out. “Many men instead internalized these thoughts or concerns and just ‘got on’ with life.”
One survey participant said: “Well, you just gotta deal with it [issues relating to prostate cancer]. Just got to try and wipe out the thoughts, that’s all you can do. Suck it up and carry on.”
Discussions must be part of standard of care
Dr. Mazariego emphasized that for prostate cancer survivorship to improve, conversations about the psychosocial needs of patients must be normalized and made routine. Discussions about post-treatment side effects that cause functional impairments and are stressful to relationships must be embedded into the standards of care, she added. This will allow physicians to use these kinds of conversations “as a springboard for referrals to appropriate care.”
“Patients of all ages will have concerns related to sex and sexual function, whether you ask about them or not,” said Brad Zebrack, PhD, MSW, MPH, professor at the University of Michigan School of Social Work, Ann Arbor, who was approached for comment.
At the very least, physicians should be prepared to “acknowledge and describe possible effects of therapy on sex and sexual function and follow up by describing available supports for education and either individual or couples counseling,” said Dr. Zebrack, who is also a member of the health behavior and outcomes research program at the Rogel Cancer Center.
Physicians can also refer patients to evidence-based resources and toolkits, he said. He noted that Will2Love offers self-help programs for cancer-related sexual problems and is “an outstanding resource.”
Distress screening needed
Universal psychosocial distress screening is needed to identify men with prostate cancer who have high levels of distress, argues Jeff Dunn, AO, PhD, who is CEO of the Prostate Cancer Foundation of Australia (PCFA), in Sydney.
Without this, men will not seek help for their unmet needs, Dr. Dunn noted in a 2019 editorial in the European Journal of Cancer Care.
The unmet psychosocial needs of prostate cancer patients and their partners “are highly prevalent,” said Dr. Dunn and co-author Suzanne K. Chambers, AO, PhD, dean of the Faculty of Health at the University of Technology Sydney. “...[F]or many prostate cancer survivors, the physical, social, psychological and relationship challenges will be long term, if not lifelong,” they write.
Even in Australia, where 1 in every 6 men are expected to be diagnosed with prostate cancer by age 85, efforts to improve survivorship care have not produced the desired results, they note.
In 2019, the PCFA published a monograph in which the organization recommended routine distress screenings and referrals to evidence-based psychosocial care for prostate cancer survivors. The foundation predicted that it would be “a game-changer for every Australian man impacted by the disease.”
“Yet, we still do not have a national survivorship care plan for prostate cancer survivors in Australia,” Dr. Mazariego said.
Left untreated, the psychosocial effects of prostate cancer “are considerable and certainly factors that should be considered as a threat to well-being,” she emphasized.
“Certainly, accumulation of unmet psychosocial needs increases risks for depression and suicide, which is true in both cancer and noncancer populations,” said Dr. Zebrack.
Data back this up. One study of patients with prostate cancer found that after diagnosis, 1 in 4 experienced anxiety, and 1 in 5 experienced depression. Another study found that the risk for suicide was higher among men with prostate cancer during the first year after diagnosis than among men with other solid-organ malignancies.
More recently, a 2018 population-based Australian cohort study of men in New South Wales revealed that the risk for death by suicide was 70% higher among men who had been diagnosed with prostate cancer compared with men in the general population. This risk was higher within the first year following diagnosis and was higher in men with nonlocalized disease, those who were single, those who were living in a major city, and those who were unmarried.
Dr. Mazariego and the team reporting the survey found that men who received supportive care had a greater chance of reconciling living with functional impairments. “Receiving adequate survivorship care and trusting patient-clinician relationships appeared to be associated with greater resilience and positivity in the men’s acceptance of cancer-related, long-term challenges and personal limitations,” they note.
Developing postcancer identity
Survivors also appeared to have developed a post-cancer identity that was more invested in personal relationships or in taking a more active role in their own health.
“Treating my prostate cancer gave me a second chance,” said one survivor. “Yeah, I’m a survivor, but more importantly, I’m a loving husband now. I know I wasn’t as giving back then.”
Another man admitted that before his diagnosis, he never went to the doctor. “I go much more often now,” he said. “You need to check up on yourself, at least once a year. Could have caught the cancer earlier if I was doing that.”
These comments appear to be borne out by data released last year by the American Cancer Society (ACS), which found that the number of number of cancer-related suicides in the United States was on the decline, as reported by this news organization.
Some of the biggest decreases occurred in men with prostate cancer, although prostate cancer was associated with 15% of cancer-related suicides. Only lung cancer was associated with more cancer-related suicides, at 18%.
A factor in the decrease in cancer-related suicides was likely to be an increase in the use of supportive care services, the ACS researchers commented.
“Although no causal relationship can be established, our findings suggest an evolving role of psycho-oncology care and palliative and hospice care given the promotion and increased utilization of these services among cancer patients during this period,” they commented.
The study was funded by the Cancer Institute NSW. Dr. Mazariego and colleagues have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Although prostate cancer is the second most common cancer in men worldwide, it is not a lethal cancer: Improvements in early detection and treatment have boosted the 10-year relative survival rate to 98%.
But for many men, life after treatment is an ongoing struggle.
One of the first qualitative survey studies of long-term prostate cancer survivorship in Australia found that many survivors are living with adverse effects such as urinary incontinence and sexual dysfunction and that they continue to have heightened feelings of distress.
Many of the patients surveyed said that they had not received follow-up care and felt they had been “abandoned” by their health care professionals.
One man called it “the survivorship abyss.”
“As the prevalence of prostate cancer survivors continues to grow globally, the absence of integrated shared survivorship care models into clinical practice, such as survivorship care guidelines/plans and/or interventions, will perpetuate the sense of abandonment and the overwhelming burden of care of men lost in the PC [prostate cancer] ‘survivorship abyss,’” say the authors.
The report was published online in Psycho-Oncology.
“The good news is that more men than ever before are surviving prostate cancer,” commented lead author Carolyn G. Mazariego, PhD, a research fellow at the Daffodil Center of the Cancer Council New South Wales and the University of Sydney.
“As our population grows and ages, an increasing number of men are facing these survivorship challenges, and the need for clear survivorship care guidelines becomes increasingly vital,” Dr. Mazariego told this news organization.
Details of the survey findings
To find participants for their study, the team drew upon a cohort of 578 men who were included in the 15-year follow-up phase of the longitudinal New South Wales Prostate Cancer Care and Outcomes Study (PCOS).
The researchers interviewed 37 men for the study. The majority (88.6%) had been diagnosed with localized disease, and just over half (54%) had undergone radical prostatectomy as their primary treatment.
Some expressed regret over having had surgery. One respondent, a 15-year survivor, commented: “I really didn’t know how intrusive [surgery] was as far as losing the length of my penis and its functions. To this day, I sometimes can’t believe it’s happened. It’s devastating.”
The survey also found that most survivors viewed active treatment as the only way to avoid death.
In hindsight, some questioned whether radical treatment was necessary and whether they might have been better served by active surveillance.
Many said they were never given a chance to discuss sexual dysfunction, and others said their questions sparked an awkward, limited conversation. Many said they suffered in silence.
“We know that there is a sort of ‘cycle of silence’ between patients and health care providers about sexual issues, and that was particularly true for the men we spoke to,” Dr. Mazariego said. “This cycle of silence can stem from confusion and ambiguity as to who men should speak with regarding these ongoing issues.”
“It’s just like being part of a secret society,” said one survivor. “Like you don’t know about it until you’re in it ... I don’t think people want to know if they have it [prostate cancer] or want it known. It’s all hush hush.”
Prostate cancer patients often feel uncomfortable talking about sexual function, Dr. Mazariego pointed out. “Many men instead internalized these thoughts or concerns and just ‘got on’ with life.”
One survey participant said: “Well, you just gotta deal with it [issues relating to prostate cancer]. Just got to try and wipe out the thoughts, that’s all you can do. Suck it up and carry on.”
Discussions must be part of standard of care
Dr. Mazariego emphasized that for prostate cancer survivorship to improve, conversations about the psychosocial needs of patients must be normalized and made routine. Discussions about post-treatment side effects that cause functional impairments and are stressful to relationships must be embedded into the standards of care, she added. This will allow physicians to use these kinds of conversations “as a springboard for referrals to appropriate care.”
“Patients of all ages will have concerns related to sex and sexual function, whether you ask about them or not,” said Brad Zebrack, PhD, MSW, MPH, professor at the University of Michigan School of Social Work, Ann Arbor, who was approached for comment.
At the very least, physicians should be prepared to “acknowledge and describe possible effects of therapy on sex and sexual function and follow up by describing available supports for education and either individual or couples counseling,” said Dr. Zebrack, who is also a member of the health behavior and outcomes research program at the Rogel Cancer Center.
Physicians can also refer patients to evidence-based resources and toolkits, he said. He noted that Will2Love offers self-help programs for cancer-related sexual problems and is “an outstanding resource.”
Distress screening needed
Universal psychosocial distress screening is needed to identify men with prostate cancer who have high levels of distress, argues Jeff Dunn, AO, PhD, who is CEO of the Prostate Cancer Foundation of Australia (PCFA), in Sydney.
Without this, men will not seek help for their unmet needs, Dr. Dunn noted in a 2019 editorial in the European Journal of Cancer Care.
The unmet psychosocial needs of prostate cancer patients and their partners “are highly prevalent,” said Dr. Dunn and co-author Suzanne K. Chambers, AO, PhD, dean of the Faculty of Health at the University of Technology Sydney. “...[F]or many prostate cancer survivors, the physical, social, psychological and relationship challenges will be long term, if not lifelong,” they write.
Even in Australia, where 1 in every 6 men are expected to be diagnosed with prostate cancer by age 85, efforts to improve survivorship care have not produced the desired results, they note.
In 2019, the PCFA published a monograph in which the organization recommended routine distress screenings and referrals to evidence-based psychosocial care for prostate cancer survivors. The foundation predicted that it would be “a game-changer for every Australian man impacted by the disease.”
“Yet, we still do not have a national survivorship care plan for prostate cancer survivors in Australia,” Dr. Mazariego said.
Left untreated, the psychosocial effects of prostate cancer “are considerable and certainly factors that should be considered as a threat to well-being,” she emphasized.
“Certainly, accumulation of unmet psychosocial needs increases risks for depression and suicide, which is true in both cancer and noncancer populations,” said Dr. Zebrack.
Data back this up. One study of patients with prostate cancer found that after diagnosis, 1 in 4 experienced anxiety, and 1 in 5 experienced depression. Another study found that the risk for suicide was higher among men with prostate cancer during the first year after diagnosis than among men with other solid-organ malignancies.
More recently, a 2018 population-based Australian cohort study of men in New South Wales revealed that the risk for death by suicide was 70% higher among men who had been diagnosed with prostate cancer compared with men in the general population. This risk was higher within the first year following diagnosis and was higher in men with nonlocalized disease, those who were single, those who were living in a major city, and those who were unmarried.
Dr. Mazariego and the team reporting the survey found that men who received supportive care had a greater chance of reconciling living with functional impairments. “Receiving adequate survivorship care and trusting patient-clinician relationships appeared to be associated with greater resilience and positivity in the men’s acceptance of cancer-related, long-term challenges and personal limitations,” they note.
Developing postcancer identity
Survivors also appeared to have developed a post-cancer identity that was more invested in personal relationships or in taking a more active role in their own health.
“Treating my prostate cancer gave me a second chance,” said one survivor. “Yeah, I’m a survivor, but more importantly, I’m a loving husband now. I know I wasn’t as giving back then.”
Another man admitted that before his diagnosis, he never went to the doctor. “I go much more often now,” he said. “You need to check up on yourself, at least once a year. Could have caught the cancer earlier if I was doing that.”
These comments appear to be borne out by data released last year by the American Cancer Society (ACS), which found that the number of number of cancer-related suicides in the United States was on the decline, as reported by this news organization.
Some of the biggest decreases occurred in men with prostate cancer, although prostate cancer was associated with 15% of cancer-related suicides. Only lung cancer was associated with more cancer-related suicides, at 18%.
A factor in the decrease in cancer-related suicides was likely to be an increase in the use of supportive care services, the ACS researchers commented.
“Although no causal relationship can be established, our findings suggest an evolving role of psycho-oncology care and palliative and hospice care given the promotion and increased utilization of these services among cancer patients during this period,” they commented.
The study was funded by the Cancer Institute NSW. Dr. Mazariego and colleagues have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
FDA OKs odevixibat for pruritus associated with rare liver disease
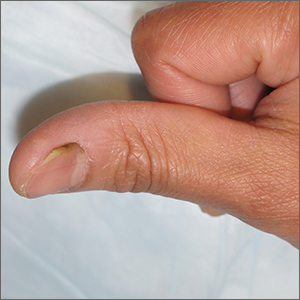
The U.S. Food and Drug Administration has approved odevixibat (Bylvay, Albireo Pharma), the first treatment for pruritus associated with all types of progressive familial intrahepatic cholestasis (PFIC).
PFIC is a rare disorder affecting an estimated one to two people per 100,000. The disorder usually appears within the first few months of life and causes progressive, life-threatening liver disease, often leading to cirrhosis and liver failure before age 10.
In PFIC, liver cells are unable to drain bile acids, leading to the buildup of toxic substances in the liver. While the precise cause of severe itching in patients with PFIC is unknown, it may involve increased levels of bile acids in the body and skin.
Odevixibat is a potent, nonsystemic ileal bile acid transport inhibitor that does not need refrigeration and is given as a once-daily capsule or opened and sprinkled onto soft foods, the company said in a news release announcing the approval.
There are at least three types of PFIC; all are inherited genetic conditions caused by gene mutations. Odevixibat is indicated to treat all subtypes.
“Treating children with PFIC can be difficult and frustrating given the current treatment options. Bylvay gives us a nonsurgical option and will change how we treat PFIC,” Richard Thompson, MD, principal investigator for the two trials that led to the approval, said in the news release.
“With this approval, my colleagues and I now have the opportunity to revisit how PFIC patients are being managed, and we are hopeful for better outcomes for these children,” said Dr. Thompson, professor of molecular hepatology at King’s College London.
The approval of odevixibat was supported by data from the PEDFIC 1 and PEDFIC 2 trials.
PEDFIC 1 enrolled 62 children with PFIC and severe itching, with 20 assigned to placebo and 42 to odevixibat, given once daily with a meal in the morning. Odevixibat met both of its primary endpoints, with the drug improving pruritus (P = .004) and reducing serum bile acid responses (P = .003).
In PEDFIC 2, a long-term, open-label extension study, the effects of odevixibat on pruritis and serum bile acids were sustained up to 48 weeks.
Odevixibat was well tolerated in both trials, with the most common treatment-related gastrointestinal adverse events being diarrhea/frequent stools. There were no serious treatment-related adverse events.
Children taking the drug should undergo liver test monitoring periodically during treatment, the FDA said when announcing the approval. Odevixibat may affect absorption of fat-soluble vitamins such as A, D, E, and K. Patients should be monitored for fat-soluble vitamin deficiency while taking the drug.
Full prescribing information is available online.
“Until now, invasive surgery was the only approved treatment option. With the approval of Bylvay, parents may find hope in having a less invasive treatment option available,” Emily Ventura, leader of the PFIC Advocacy and Resource Network and mother to a child with PFIC, said in the news release.
The company said it will launch odevixibat “immediately” to accelerate availability for patients and families affected by PFIC.
Odevixibat is also being studied in other rare pediatric cholestatic liver diseases, including biliary atresia and Alagille syndrome.
A version of this article first appeared on Medscape.com.
The U.S. Food and Drug Administration has approved odevixibat (Bylvay, Albireo Pharma), the first treatment for pruritus associated with all types of progressive familial intrahepatic cholestasis (PFIC).
PFIC is a rare disorder affecting an estimated one to two people per 100,000. The disorder usually appears within the first few months of life and causes progressive, life-threatening liver disease, often leading to cirrhosis and liver failure before age 10.
In PFIC, liver cells are unable to drain bile acids, leading to the buildup of toxic substances in the liver. While the precise cause of severe itching in patients with PFIC is unknown, it may involve increased levels of bile acids in the body and skin.
Odevixibat is a potent, nonsystemic ileal bile acid transport inhibitor that does not need refrigeration and is given as a once-daily capsule or opened and sprinkled onto soft foods, the company said in a news release announcing the approval.
There are at least three types of PFIC; all are inherited genetic conditions caused by gene mutations. Odevixibat is indicated to treat all subtypes.
“Treating children with PFIC can be difficult and frustrating given the current treatment options. Bylvay gives us a nonsurgical option and will change how we treat PFIC,” Richard Thompson, MD, principal investigator for the two trials that led to the approval, said in the news release.
“With this approval, my colleagues and I now have the opportunity to revisit how PFIC patients are being managed, and we are hopeful for better outcomes for these children,” said Dr. Thompson, professor of molecular hepatology at King’s College London.
The approval of odevixibat was supported by data from the PEDFIC 1 and PEDFIC 2 trials.
PEDFIC 1 enrolled 62 children with PFIC and severe itching, with 20 assigned to placebo and 42 to odevixibat, given once daily with a meal in the morning. Odevixibat met both of its primary endpoints, with the drug improving pruritus (P = .004) and reducing serum bile acid responses (P = .003).
In PEDFIC 2, a long-term, open-label extension study, the effects of odevixibat on pruritis and serum bile acids were sustained up to 48 weeks.
Odevixibat was well tolerated in both trials, with the most common treatment-related gastrointestinal adverse events being diarrhea/frequent stools. There were no serious treatment-related adverse events.
Children taking the drug should undergo liver test monitoring periodically during treatment, the FDA said when announcing the approval. Odevixibat may affect absorption of fat-soluble vitamins such as A, D, E, and K. Patients should be monitored for fat-soluble vitamin deficiency while taking the drug.
Full prescribing information is available online.
“Until now, invasive surgery was the only approved treatment option. With the approval of Bylvay, parents may find hope in having a less invasive treatment option available,” Emily Ventura, leader of the PFIC Advocacy and Resource Network and mother to a child with PFIC, said in the news release.
The company said it will launch odevixibat “immediately” to accelerate availability for patients and families affected by PFIC.
Odevixibat is also being studied in other rare pediatric cholestatic liver diseases, including biliary atresia and Alagille syndrome.
A version of this article first appeared on Medscape.com.
The U.S. Food and Drug Administration has approved odevixibat (Bylvay, Albireo Pharma), the first treatment for pruritus associated with all types of progressive familial intrahepatic cholestasis (PFIC).
PFIC is a rare disorder affecting an estimated one to two people per 100,000. The disorder usually appears within the first few months of life and causes progressive, life-threatening liver disease, often leading to cirrhosis and liver failure before age 10.
In PFIC, liver cells are unable to drain bile acids, leading to the buildup of toxic substances in the liver. While the precise cause of severe itching in patients with PFIC is unknown, it may involve increased levels of bile acids in the body and skin.
Odevixibat is a potent, nonsystemic ileal bile acid transport inhibitor that does not need refrigeration and is given as a once-daily capsule or opened and sprinkled onto soft foods, the company said in a news release announcing the approval.
There are at least three types of PFIC; all are inherited genetic conditions caused by gene mutations. Odevixibat is indicated to treat all subtypes.
“Treating children with PFIC can be difficult and frustrating given the current treatment options. Bylvay gives us a nonsurgical option and will change how we treat PFIC,” Richard Thompson, MD, principal investigator for the two trials that led to the approval, said in the news release.
“With this approval, my colleagues and I now have the opportunity to revisit how PFIC patients are being managed, and we are hopeful for better outcomes for these children,” said Dr. Thompson, professor of molecular hepatology at King’s College London.
The approval of odevixibat was supported by data from the PEDFIC 1 and PEDFIC 2 trials.
PEDFIC 1 enrolled 62 children with PFIC and severe itching, with 20 assigned to placebo and 42 to odevixibat, given once daily with a meal in the morning. Odevixibat met both of its primary endpoints, with the drug improving pruritus (P = .004) and reducing serum bile acid responses (P = .003).
In PEDFIC 2, a long-term, open-label extension study, the effects of odevixibat on pruritis and serum bile acids were sustained up to 48 weeks.
Odevixibat was well tolerated in both trials, with the most common treatment-related gastrointestinal adverse events being diarrhea/frequent stools. There were no serious treatment-related adverse events.
Children taking the drug should undergo liver test monitoring periodically during treatment, the FDA said when announcing the approval. Odevixibat may affect absorption of fat-soluble vitamins such as A, D, E, and K. Patients should be monitored for fat-soluble vitamin deficiency while taking the drug.
Full prescribing information is available online.
“Until now, invasive surgery was the only approved treatment option. With the approval of Bylvay, parents may find hope in having a less invasive treatment option available,” Emily Ventura, leader of the PFIC Advocacy and Resource Network and mother to a child with PFIC, said in the news release.
The company said it will launch odevixibat “immediately” to accelerate availability for patients and families affected by PFIC.
Odevixibat is also being studied in other rare pediatric cholestatic liver diseases, including biliary atresia and Alagille syndrome.
A version of this article first appeared on Medscape.com.
FM diversity has increased, but more physicians of color needed
The specialty has been on the path to a racially diverse workforce over the past few decades. Since family medicine is a discipline where doctors look not just at individual patients, but also at the health of the community, some family physicians see working in their specialty as a way to integrate public health with medicine to curb health inequities.
Maria Harsha Wusu, MD, MSEd, is an example of such a family physician.
Dr. Wusu, who is Black and of Japanese descent, chose to practice family medicine to address health in communities of color “which we know in the United States experience health inequities due to structural racism,” she said in an interview.
“It’s a discipline where you look at the health of the entire family and the community and you really look at the environmental, the political, the historical factors that are influencing the health of the community,” explained Dr. Wusu, who is currently the director of health equity at Morehouse School of Medicine, Atlanta. Family physicians are not just asking: “Does a patient have hypertension?” but also whether a patient has access to healthy food, green space and other things.
While the field of family medicine is more diverse in the 21st century than it was at its beginning, Dr. Wusu, who completed her residency in 2016, still faced challenges to achieving her goal of helping communities of color. These specifically stemmed from a lack of diversity among the people in the places where she studied to become a doctor and family physician.
There were moments when Dr. Wusu felt isolated while in medical school and residency, because so few students and faculty members she saw looked like her.
Plus, studies have shown that a racially and ethnically diverse physician workforce is necessary to address health inequities. Research published in 2018 in the Journal of Health Care for the Poor and Underserved, for example, found that underrepresented physicians are more likely to practice in underserved areas than their White peers.
“I went to medical school at a historically White institution, and so there were very few people who identified as what we would say are underrepresented minorities in medicine,” Dr. Wusu explained. “There are issues with both implicit and explicit racism, which I think could be echoed by colleagues across the country that are additional challenges that I think medical students, particularly students of color, experience during what is an already kind of challenging time of medical school and the rigorous training of residency.”
Ada Stewart, MD, FAAFP, president of the American Academy of Family Physicians, echoed Dr. Wusu’s medical school experience. Dr. Stewart, who finished her residency in 2003, said that, out of the 120 students in her graduating medical class, only 10 were Black.
Marginalized groups are still underrepresented in residences. According to data compiled by the Association of American Medical Colleges, only 9.3% of Black people, 10% of Latino, and 0.3% of Native Hawaiian or other Pacific Islanders are residents in family medicine residency programs in 2019-2020. Meanwhile, White residents make up 50.8% of the residency program.
“We really need to do all that we can to increase diversity within our medical schools and residencies,” Dr. Stewart said.
In regards to gender, there has been an increasing number of women in the family medicine specialty. A 2021 study found that the proportion of female physicians in family medicine has grown from 33.9% 2010 to 41.9% in 2020.
“There’s still room for growth and we have to change the system and those structures that created these problems,” noted Dr. Stewart.
The social responsibility of family medicine
The family medicine specialty was born during an era of protest of social change, alongside the Civil Rights Movement, the peace movement, and counterculture protests. In April 1966, 3 years before American Boards approved family practice as a new specialty; the National Commission on Community Health stated that every person should have a personal physician who is the “central point for the integration and continuity of all medical services to his patient.” They also said such physicians should be aware of the “many and varied social, emotional and environmental factors that influence the health of his patient and family.”
While the diversity of family medicine specialty has significantly increased since its beginnings, it continues to lag behind the general U.S. population. A 2018 study published in the Journal of the American Board of Family Medicine, which aggregated data from 1987 to 2017, found that the proportion of Black and Latino board certified family physicians increased from 1.3% to 7.8% and 2.3% to 9.1%, respectively, in 30 years.
A 2014 study included 2 decades worth of data from the U.S. Census and the Association of American Medical Colleges to examine trends in racial and ethnic composition among family medicine residents. The U.S. population increased from 9% to 17% for Latinos, 11.7% to 12.2% for Blacks/African Americans, and 0.87% to 0.89% for Native Americans from 1990 to 2012. Meanwhile, minority representation in family residencies increased 4.9% to 9.4% for Hispanics/Latinos, from 4.2% to 7.9% for Blacks/African Americans, and from 0.7% to 0.9% for Native Americans.
Furthermore, 13.4% of the U.S. population is Black and 18.5% of the population is Latino, while only 7.8% of family medicine residents in 2019 were Black and 9.1% of family medicine residents were Latino, according to a recent study published in Family Medicine.
Recruiting a diverse physician workforce
The AAFP has launched a few initiatives to increase diversity within the specialty. In 2017, the AAFP established the Center for Diversity and Health Equity, a center to address social determinants of health. The EveryONE Project, an initiative that’s part of the AAFP’s center, offers members education and resources to promote workforce diversity. Some of those resources include “The Ladder Program,” an initiative founded by an AAFP member which involves monthly meetings and events for students as young as 9 years old to introduce them to medicine at a young age.
“You can’t see what you don’t see,” noted Dr. Stewart, who is the first Black, female president of the AAFP, and the fourth woman in the role. “I really have seen how important it is to be a mentor and to be out there so that individuals who look like me can see that they too can become a family physician and be that member of their community.”
In addition to The Ladder Program, some other resources aimed at increasing diversity among family physicians include Tour for Diversity in Medicine and the Doctors Back to School Program.
The Tour for Diversity in Medicine involves a team of physicians, other clinicians and students hosting events nationwide for minority students to help them see a path to medicine and other health professions. Meanwhile, the AAFP’s Doctors Back to School Program involves family physicians visiting children at schools, clubs, community organizations, and other places to raise childhood awareness of family medicine and help them see their own potential in health care careers.
Dr. Stewart said these programs have been successful in increasing underrepresented groups.
“We are trying to see how best to measure their success,” the AAFP president said. “Looking at the high numbers of individuals who chose the specialty of family medicine last year is what I would deem a success.”
Dr. Wusu also believes outreach to children in elementary schools is important when it comes to increasing diversity in the family medicine specialty.
One organization that’s proving such outreach is the Student National Medical Association, a branch of the National Medical Association, which is a professional organization of Black physicians. This group’s initiative, the Health Professions Recruitment Exposure Programs, exposes teens to science-related activities while introducing them to careers in health professions. Another SMNA program, called Youth Science Enrichment Program, targets elementary and junior high school students.
Dr. Wusu led a 2019 project that focused on creating a more diverse family medicine residency program by developing and implementing a strategic plan for diversity recruitment, which involved increasing outreach to marginalized groups and revising interviews to minimize bias. In a paper published on the results of the initiative, Dr. Wusu and coauthors noted that, between 2014 and 2017, the total number of underrepresented minority applicants to the Boston Medical Center Family Medicine Residency Program increased by 80%. Before the intervention, the percentage of applicants who were part of an underrepresented group ranged from 0% to 20%. During the intervention, that range jumped to 25% to 50%, according to the paper.
While Dr. Wusu considers these programs to be beneficial for the specialty, she doesn’t believe they should be done in isolation. There should also be efforts to tackle lack of opportunities and structural racism.
“With any inequity, you have to address it on multiple levels,” Dr. Wusu explained. “It’s great that there has been recognition for a need for diversity in family medicine, but my hope is that the call for equity would reach beyond that.”
Fostering an inclusive environment
While family medicine has come a long way with regards to increasing the amount of underrepresented groups in its specialty, Stephen Richmond, MD, MPH, believes there also needs to be a focus on the infrastructure of support to help retain these physicians.
“The problem of diversity within family medicine and largely in other specialties cannot be summed up simply as a matter of poor representation. We must do be better to understand the lived experience of physicians of color, in particular Black physicians, once they arrive in the medical professional environment. Doing so will help institutions to provide that infrastructure of support – including antiracism policies and practices – that will enhance wellness and representation,” said Dr. Richmond, clinical assistant professor of medicine in the division of primary care and population health at Stanford (Calif.) University.
Dr. Wusu also suggested establishing an explicitly antiracist environment. This can be done in multiple ways, including by holding programs that acknowledge the impact of structural racism on both the patients, medical students and faculty, and by educating staff about the history of racism, she said.
Dr. Stewart and Dr. Wusu think the specialty has improved in its representation of minorities, but that it has a “long way to go.”
“I think family medicine is really one of the more inclusive specialties. I mean, it has higher numbers of Black and Brown residents and physicians than other specialties,” Dr. Wusu said. “We still have a very long way to go to be at numbers that match the general population. But I think, in that way, family medicine is a place where a lot of Black and Brown physicians can find a home.”
The specialty has been on the path to a racially diverse workforce over the past few decades. Since family medicine is a discipline where doctors look not just at individual patients, but also at the health of the community, some family physicians see working in their specialty as a way to integrate public health with medicine to curb health inequities.
Maria Harsha Wusu, MD, MSEd, is an example of such a family physician.
Dr. Wusu, who is Black and of Japanese descent, chose to practice family medicine to address health in communities of color “which we know in the United States experience health inequities due to structural racism,” she said in an interview.
“It’s a discipline where you look at the health of the entire family and the community and you really look at the environmental, the political, the historical factors that are influencing the health of the community,” explained Dr. Wusu, who is currently the director of health equity at Morehouse School of Medicine, Atlanta. Family physicians are not just asking: “Does a patient have hypertension?” but also whether a patient has access to healthy food, green space and other things.
While the field of family medicine is more diverse in the 21st century than it was at its beginning, Dr. Wusu, who completed her residency in 2016, still faced challenges to achieving her goal of helping communities of color. These specifically stemmed from a lack of diversity among the people in the places where she studied to become a doctor and family physician.
There were moments when Dr. Wusu felt isolated while in medical school and residency, because so few students and faculty members she saw looked like her.
Plus, studies have shown that a racially and ethnically diverse physician workforce is necessary to address health inequities. Research published in 2018 in the Journal of Health Care for the Poor and Underserved, for example, found that underrepresented physicians are more likely to practice in underserved areas than their White peers.
“I went to medical school at a historically White institution, and so there were very few people who identified as what we would say are underrepresented minorities in medicine,” Dr. Wusu explained. “There are issues with both implicit and explicit racism, which I think could be echoed by colleagues across the country that are additional challenges that I think medical students, particularly students of color, experience during what is an already kind of challenging time of medical school and the rigorous training of residency.”
Ada Stewart, MD, FAAFP, president of the American Academy of Family Physicians, echoed Dr. Wusu’s medical school experience. Dr. Stewart, who finished her residency in 2003, said that, out of the 120 students in her graduating medical class, only 10 were Black.
Marginalized groups are still underrepresented in residences. According to data compiled by the Association of American Medical Colleges, only 9.3% of Black people, 10% of Latino, and 0.3% of Native Hawaiian or other Pacific Islanders are residents in family medicine residency programs in 2019-2020. Meanwhile, White residents make up 50.8% of the residency program.
“We really need to do all that we can to increase diversity within our medical schools and residencies,” Dr. Stewart said.
In regards to gender, there has been an increasing number of women in the family medicine specialty. A 2021 study found that the proportion of female physicians in family medicine has grown from 33.9% 2010 to 41.9% in 2020.
“There’s still room for growth and we have to change the system and those structures that created these problems,” noted Dr. Stewart.
The social responsibility of family medicine
The family medicine specialty was born during an era of protest of social change, alongside the Civil Rights Movement, the peace movement, and counterculture protests. In April 1966, 3 years before American Boards approved family practice as a new specialty; the National Commission on Community Health stated that every person should have a personal physician who is the “central point for the integration and continuity of all medical services to his patient.” They also said such physicians should be aware of the “many and varied social, emotional and environmental factors that influence the health of his patient and family.”
While the diversity of family medicine specialty has significantly increased since its beginnings, it continues to lag behind the general U.S. population. A 2018 study published in the Journal of the American Board of Family Medicine, which aggregated data from 1987 to 2017, found that the proportion of Black and Latino board certified family physicians increased from 1.3% to 7.8% and 2.3% to 9.1%, respectively, in 30 years.
A 2014 study included 2 decades worth of data from the U.S. Census and the Association of American Medical Colleges to examine trends in racial and ethnic composition among family medicine residents. The U.S. population increased from 9% to 17% for Latinos, 11.7% to 12.2% for Blacks/African Americans, and 0.87% to 0.89% for Native Americans from 1990 to 2012. Meanwhile, minority representation in family residencies increased 4.9% to 9.4% for Hispanics/Latinos, from 4.2% to 7.9% for Blacks/African Americans, and from 0.7% to 0.9% for Native Americans.
Furthermore, 13.4% of the U.S. population is Black and 18.5% of the population is Latino, while only 7.8% of family medicine residents in 2019 were Black and 9.1% of family medicine residents were Latino, according to a recent study published in Family Medicine.
Recruiting a diverse physician workforce
The AAFP has launched a few initiatives to increase diversity within the specialty. In 2017, the AAFP established the Center for Diversity and Health Equity, a center to address social determinants of health. The EveryONE Project, an initiative that’s part of the AAFP’s center, offers members education and resources to promote workforce diversity. Some of those resources include “The Ladder Program,” an initiative founded by an AAFP member which involves monthly meetings and events for students as young as 9 years old to introduce them to medicine at a young age.
“You can’t see what you don’t see,” noted Dr. Stewart, who is the first Black, female president of the AAFP, and the fourth woman in the role. “I really have seen how important it is to be a mentor and to be out there so that individuals who look like me can see that they too can become a family physician and be that member of their community.”
In addition to The Ladder Program, some other resources aimed at increasing diversity among family physicians include Tour for Diversity in Medicine and the Doctors Back to School Program.
The Tour for Diversity in Medicine involves a team of physicians, other clinicians and students hosting events nationwide for minority students to help them see a path to medicine and other health professions. Meanwhile, the AAFP’s Doctors Back to School Program involves family physicians visiting children at schools, clubs, community organizations, and other places to raise childhood awareness of family medicine and help them see their own potential in health care careers.
Dr. Stewart said these programs have been successful in increasing underrepresented groups.
“We are trying to see how best to measure their success,” the AAFP president said. “Looking at the high numbers of individuals who chose the specialty of family medicine last year is what I would deem a success.”
Dr. Wusu also believes outreach to children in elementary schools is important when it comes to increasing diversity in the family medicine specialty.
One organization that’s proving such outreach is the Student National Medical Association, a branch of the National Medical Association, which is a professional organization of Black physicians. This group’s initiative, the Health Professions Recruitment Exposure Programs, exposes teens to science-related activities while introducing them to careers in health professions. Another SMNA program, called Youth Science Enrichment Program, targets elementary and junior high school students.
Dr. Wusu led a 2019 project that focused on creating a more diverse family medicine residency program by developing and implementing a strategic plan for diversity recruitment, which involved increasing outreach to marginalized groups and revising interviews to minimize bias. In a paper published on the results of the initiative, Dr. Wusu and coauthors noted that, between 2014 and 2017, the total number of underrepresented minority applicants to the Boston Medical Center Family Medicine Residency Program increased by 80%. Before the intervention, the percentage of applicants who were part of an underrepresented group ranged from 0% to 20%. During the intervention, that range jumped to 25% to 50%, according to the paper.
While Dr. Wusu considers these programs to be beneficial for the specialty, she doesn’t believe they should be done in isolation. There should also be efforts to tackle lack of opportunities and structural racism.
“With any inequity, you have to address it on multiple levels,” Dr. Wusu explained. “It’s great that there has been recognition for a need for diversity in family medicine, but my hope is that the call for equity would reach beyond that.”
Fostering an inclusive environment
While family medicine has come a long way with regards to increasing the amount of underrepresented groups in its specialty, Stephen Richmond, MD, MPH, believes there also needs to be a focus on the infrastructure of support to help retain these physicians.
“The problem of diversity within family medicine and largely in other specialties cannot be summed up simply as a matter of poor representation. We must do be better to understand the lived experience of physicians of color, in particular Black physicians, once they arrive in the medical professional environment. Doing so will help institutions to provide that infrastructure of support – including antiracism policies and practices – that will enhance wellness and representation,” said Dr. Richmond, clinical assistant professor of medicine in the division of primary care and population health at Stanford (Calif.) University.
Dr. Wusu also suggested establishing an explicitly antiracist environment. This can be done in multiple ways, including by holding programs that acknowledge the impact of structural racism on both the patients, medical students and faculty, and by educating staff about the history of racism, she said.
Dr. Stewart and Dr. Wusu think the specialty has improved in its representation of minorities, but that it has a “long way to go.”
“I think family medicine is really one of the more inclusive specialties. I mean, it has higher numbers of Black and Brown residents and physicians than other specialties,” Dr. Wusu said. “We still have a very long way to go to be at numbers that match the general population. But I think, in that way, family medicine is a place where a lot of Black and Brown physicians can find a home.”
The specialty has been on the path to a racially diverse workforce over the past few decades. Since family medicine is a discipline where doctors look not just at individual patients, but also at the health of the community, some family physicians see working in their specialty as a way to integrate public health with medicine to curb health inequities.
Maria Harsha Wusu, MD, MSEd, is an example of such a family physician.
Dr. Wusu, who is Black and of Japanese descent, chose to practice family medicine to address health in communities of color “which we know in the United States experience health inequities due to structural racism,” she said in an interview.
“It’s a discipline where you look at the health of the entire family and the community and you really look at the environmental, the political, the historical factors that are influencing the health of the community,” explained Dr. Wusu, who is currently the director of health equity at Morehouse School of Medicine, Atlanta. Family physicians are not just asking: “Does a patient have hypertension?” but also whether a patient has access to healthy food, green space and other things.
While the field of family medicine is more diverse in the 21st century than it was at its beginning, Dr. Wusu, who completed her residency in 2016, still faced challenges to achieving her goal of helping communities of color. These specifically stemmed from a lack of diversity among the people in the places where she studied to become a doctor and family physician.
There were moments when Dr. Wusu felt isolated while in medical school and residency, because so few students and faculty members she saw looked like her.
Plus, studies have shown that a racially and ethnically diverse physician workforce is necessary to address health inequities. Research published in 2018 in the Journal of Health Care for the Poor and Underserved, for example, found that underrepresented physicians are more likely to practice in underserved areas than their White peers.
“I went to medical school at a historically White institution, and so there were very few people who identified as what we would say are underrepresented minorities in medicine,” Dr. Wusu explained. “There are issues with both implicit and explicit racism, which I think could be echoed by colleagues across the country that are additional challenges that I think medical students, particularly students of color, experience during what is an already kind of challenging time of medical school and the rigorous training of residency.”
Ada Stewart, MD, FAAFP, president of the American Academy of Family Physicians, echoed Dr. Wusu’s medical school experience. Dr. Stewart, who finished her residency in 2003, said that, out of the 120 students in her graduating medical class, only 10 were Black.
Marginalized groups are still underrepresented in residences. According to data compiled by the Association of American Medical Colleges, only 9.3% of Black people, 10% of Latino, and 0.3% of Native Hawaiian or other Pacific Islanders are residents in family medicine residency programs in 2019-2020. Meanwhile, White residents make up 50.8% of the residency program.
“We really need to do all that we can to increase diversity within our medical schools and residencies,” Dr. Stewart said.
In regards to gender, there has been an increasing number of women in the family medicine specialty. A 2021 study found that the proportion of female physicians in family medicine has grown from 33.9% 2010 to 41.9% in 2020.
“There’s still room for growth and we have to change the system and those structures that created these problems,” noted Dr. Stewart.
The social responsibility of family medicine
The family medicine specialty was born during an era of protest of social change, alongside the Civil Rights Movement, the peace movement, and counterculture protests. In April 1966, 3 years before American Boards approved family practice as a new specialty; the National Commission on Community Health stated that every person should have a personal physician who is the “central point for the integration and continuity of all medical services to his patient.” They also said such physicians should be aware of the “many and varied social, emotional and environmental factors that influence the health of his patient and family.”
While the diversity of family medicine specialty has significantly increased since its beginnings, it continues to lag behind the general U.S. population. A 2018 study published in the Journal of the American Board of Family Medicine, which aggregated data from 1987 to 2017, found that the proportion of Black and Latino board certified family physicians increased from 1.3% to 7.8% and 2.3% to 9.1%, respectively, in 30 years.
A 2014 study included 2 decades worth of data from the U.S. Census and the Association of American Medical Colleges to examine trends in racial and ethnic composition among family medicine residents. The U.S. population increased from 9% to 17% for Latinos, 11.7% to 12.2% for Blacks/African Americans, and 0.87% to 0.89% for Native Americans from 1990 to 2012. Meanwhile, minority representation in family residencies increased 4.9% to 9.4% for Hispanics/Latinos, from 4.2% to 7.9% for Blacks/African Americans, and from 0.7% to 0.9% for Native Americans.
Furthermore, 13.4% of the U.S. population is Black and 18.5% of the population is Latino, while only 7.8% of family medicine residents in 2019 were Black and 9.1% of family medicine residents were Latino, according to a recent study published in Family Medicine.
Recruiting a diverse physician workforce
The AAFP has launched a few initiatives to increase diversity within the specialty. In 2017, the AAFP established the Center for Diversity and Health Equity, a center to address social determinants of health. The EveryONE Project, an initiative that’s part of the AAFP’s center, offers members education and resources to promote workforce diversity. Some of those resources include “The Ladder Program,” an initiative founded by an AAFP member which involves monthly meetings and events for students as young as 9 years old to introduce them to medicine at a young age.
“You can’t see what you don’t see,” noted Dr. Stewart, who is the first Black, female president of the AAFP, and the fourth woman in the role. “I really have seen how important it is to be a mentor and to be out there so that individuals who look like me can see that they too can become a family physician and be that member of their community.”
In addition to The Ladder Program, some other resources aimed at increasing diversity among family physicians include Tour for Diversity in Medicine and the Doctors Back to School Program.
The Tour for Diversity in Medicine involves a team of physicians, other clinicians and students hosting events nationwide for minority students to help them see a path to medicine and other health professions. Meanwhile, the AAFP’s Doctors Back to School Program involves family physicians visiting children at schools, clubs, community organizations, and other places to raise childhood awareness of family medicine and help them see their own potential in health care careers.
Dr. Stewart said these programs have been successful in increasing underrepresented groups.
“We are trying to see how best to measure their success,” the AAFP president said. “Looking at the high numbers of individuals who chose the specialty of family medicine last year is what I would deem a success.”
Dr. Wusu also believes outreach to children in elementary schools is important when it comes to increasing diversity in the family medicine specialty.
One organization that’s proving such outreach is the Student National Medical Association, a branch of the National Medical Association, which is a professional organization of Black physicians. This group’s initiative, the Health Professions Recruitment Exposure Programs, exposes teens to science-related activities while introducing them to careers in health professions. Another SMNA program, called Youth Science Enrichment Program, targets elementary and junior high school students.
Dr. Wusu led a 2019 project that focused on creating a more diverse family medicine residency program by developing and implementing a strategic plan for diversity recruitment, which involved increasing outreach to marginalized groups and revising interviews to minimize bias. In a paper published on the results of the initiative, Dr. Wusu and coauthors noted that, between 2014 and 2017, the total number of underrepresented minority applicants to the Boston Medical Center Family Medicine Residency Program increased by 80%. Before the intervention, the percentage of applicants who were part of an underrepresented group ranged from 0% to 20%. During the intervention, that range jumped to 25% to 50%, according to the paper.
While Dr. Wusu considers these programs to be beneficial for the specialty, she doesn’t believe they should be done in isolation. There should also be efforts to tackle lack of opportunities and structural racism.
“With any inequity, you have to address it on multiple levels,” Dr. Wusu explained. “It’s great that there has been recognition for a need for diversity in family medicine, but my hope is that the call for equity would reach beyond that.”
Fostering an inclusive environment
While family medicine has come a long way with regards to increasing the amount of underrepresented groups in its specialty, Stephen Richmond, MD, MPH, believes there also needs to be a focus on the infrastructure of support to help retain these physicians.
“The problem of diversity within family medicine and largely in other specialties cannot be summed up simply as a matter of poor representation. We must do be better to understand the lived experience of physicians of color, in particular Black physicians, once they arrive in the medical professional environment. Doing so will help institutions to provide that infrastructure of support – including antiracism policies and practices – that will enhance wellness and representation,” said Dr. Richmond, clinical assistant professor of medicine in the division of primary care and population health at Stanford (Calif.) University.
Dr. Wusu also suggested establishing an explicitly antiracist environment. This can be done in multiple ways, including by holding programs that acknowledge the impact of structural racism on both the patients, medical students and faculty, and by educating staff about the history of racism, she said.
Dr. Stewart and Dr. Wusu think the specialty has improved in its representation of minorities, but that it has a “long way to go.”
“I think family medicine is really one of the more inclusive specialties. I mean, it has higher numbers of Black and Brown residents and physicians than other specialties,” Dr. Wusu said. “We still have a very long way to go to be at numbers that match the general population. But I think, in that way, family medicine is a place where a lot of Black and Brown physicians can find a home.”
On a scale of 1-5 ... How frustrating is this?
Like most American doctors, I take a variety of insurances and insurance plans.
Some of these, particularly HMOs, require a referring physician to send me a written, insurance-approved, referral (AKA authorization) before the visit, to submit with my bill.
Medical visits of all kinds are generally billed on a scale from 1 (brief/simple issue) to 5 (lots of time needed/very complicated).
After 23 years, I’m used to this.
But recently a new wrinkle has emerged.
In the last month I’ve gotten two referrals (both from the same internist), except these state, very clearly, that charges for any visit cannot exceed level 3.
And they’re telling me this before I’ve ever seen the patients, or have any idea how complicated they are, or how long a list of questions they and/or their families will have.
No.
I faxed them back asking for a referral allowing me to bill up to level 5 if needed. I might charge less than that, but none of us know how complicated or long a visit will be until someone comes in. There’s no crystal ball in medicine.
I’m sure someone will say I’m a money-grubbing doctor who couldn’t care less about the patient.
That’s far from the truth. I’m here for the patients. I like helping them. It’s why I do this.
But I can’t help anyone if I can’t afford to keep the office lights on, either.
I never heard back from them. Maybe they decided the patients didn’t need me that much. Maybe they sent them to another neurologist and took my name off their referral list. Maybe they never even noticed my return fax.
What will happen now, I have no idea. Maybe this was something that office tried, to see if I noticed. Maybe it’s the start of the next wave of medical cutbacks. Maybe it was a staff error at the other end.
But either way, This isn’t an amusement park or thrift store. People with problems need time, and time costs money. I need to pay my staff, my rent, and my mortgage. If I can’t do those things, I won’t be able to help anyone.
That’s just, for better or worse, the way it is.
Dr. Block has a solo neurology practice in Scottsdale, Ariz.
Like most American doctors, I take a variety of insurances and insurance plans.
Some of these, particularly HMOs, require a referring physician to send me a written, insurance-approved, referral (AKA authorization) before the visit, to submit with my bill.
Medical visits of all kinds are generally billed on a scale from 1 (brief/simple issue) to 5 (lots of time needed/very complicated).
After 23 years, I’m used to this.
But recently a new wrinkle has emerged.
In the last month I’ve gotten two referrals (both from the same internist), except these state, very clearly, that charges for any visit cannot exceed level 3.
And they’re telling me this before I’ve ever seen the patients, or have any idea how complicated they are, or how long a list of questions they and/or their families will have.
No.
I faxed them back asking for a referral allowing me to bill up to level 5 if needed. I might charge less than that, but none of us know how complicated or long a visit will be until someone comes in. There’s no crystal ball in medicine.
I’m sure someone will say I’m a money-grubbing doctor who couldn’t care less about the patient.
That’s far from the truth. I’m here for the patients. I like helping them. It’s why I do this.
But I can’t help anyone if I can’t afford to keep the office lights on, either.
I never heard back from them. Maybe they decided the patients didn’t need me that much. Maybe they sent them to another neurologist and took my name off their referral list. Maybe they never even noticed my return fax.
What will happen now, I have no idea. Maybe this was something that office tried, to see if I noticed. Maybe it’s the start of the next wave of medical cutbacks. Maybe it was a staff error at the other end.
But either way, This isn’t an amusement park or thrift store. People with problems need time, and time costs money. I need to pay my staff, my rent, and my mortgage. If I can’t do those things, I won’t be able to help anyone.
That’s just, for better or worse, the way it is.
Dr. Block has a solo neurology practice in Scottsdale, Ariz.
Like most American doctors, I take a variety of insurances and insurance plans.
Some of these, particularly HMOs, require a referring physician to send me a written, insurance-approved, referral (AKA authorization) before the visit, to submit with my bill.
Medical visits of all kinds are generally billed on a scale from 1 (brief/simple issue) to 5 (lots of time needed/very complicated).
After 23 years, I’m used to this.
But recently a new wrinkle has emerged.
In the last month I’ve gotten two referrals (both from the same internist), except these state, very clearly, that charges for any visit cannot exceed level 3.
And they’re telling me this before I’ve ever seen the patients, or have any idea how complicated they are, or how long a list of questions they and/or their families will have.
No.
I faxed them back asking for a referral allowing me to bill up to level 5 if needed. I might charge less than that, but none of us know how complicated or long a visit will be until someone comes in. There’s no crystal ball in medicine.
I’m sure someone will say I’m a money-grubbing doctor who couldn’t care less about the patient.
That’s far from the truth. I’m here for the patients. I like helping them. It’s why I do this.
But I can’t help anyone if I can’t afford to keep the office lights on, either.
I never heard back from them. Maybe they decided the patients didn’t need me that much. Maybe they sent them to another neurologist and took my name off their referral list. Maybe they never even noticed my return fax.
What will happen now, I have no idea. Maybe this was something that office tried, to see if I noticed. Maybe it’s the start of the next wave of medical cutbacks. Maybe it was a staff error at the other end.
But either way, This isn’t an amusement park or thrift store. People with problems need time, and time costs money. I need to pay my staff, my rent, and my mortgage. If I can’t do those things, I won’t be able to help anyone.
That’s just, for better or worse, the way it is.
Dr. Block has a solo neurology practice in Scottsdale, Ariz.
Hematologic cancer increases risk of delivery complications
The risk of in-hospital complications and poor birth outcomes were greater in pregnant women with current or historical cancer diagnoses, new research suggests.
The study, published in Mayo Clinic Proceedings, found that women with current and historical cancer diagnoses had an increased risk of death, kidney injury, and stroke during delivery hospitalizations, compared with those with no cancer. When it came to delivery outcomes, this group also had a higher risk for preterm birth and postpartum hemorrhage. Those with a current cancer diagnoses had a 1.7-fold increase in odds for a preterm birth, compared with women without cancer.
“Our study found that metastases increased the odds of mortality, cesarean delivery, preterm birth, and stillbirth,” the researchers noted. “Coupled with previous research reporting that pregnant women are more likely to be diagnosed with advanced disease, this implies that pregnant women with newly diagnosed cancer have poor prognoses.”
However, although women with prior cancer had increased odds of mortality, the researchers said it was not statistically significant.
“The study really did not show an increase of mortality [for women with prior cancer diagnosis],” said Justin Chura, MD, a specialist in gynecologic oncology who was not involved in the study. “And the reason might be because there is not or the reason might be because it’s such a rare event. You would need 100 million births to assess that. So I would actually use caution in that interpretation.”
Researchers analyzed more than 43 million delivery hospitalizations of women with or without current or historical cancer diagnoses between January 2004 and December 2014. They found that the most common cancer diagnoses were hematologic, thyroid, cervical, skin, and breast.
Of the five most common cancers, the prevalence of all maternal complications and negative delivery outcomes was the highest among women with hematologic cancers. They were more likely to experience peripartum cardiomyopathy, acute kidney injury, and arrhythmia, compared with other cancers. Postpartum hemorrhage, maternal mortality, and placental abruption was also more likely to occur in those with this type of cancer.
“I was surprised that it was the hematologic cancers that were worse when they did it by cancer type,” said Dr. Chura, who is the chief of surgery and the director of gynecologic oncology and robotic surgery at the Cancer Treatment Centers of America’s Eastern Regional Medical Center in Philadelphia. “I think this is a useful bit of information for counseling our patients and also to identify the cohort with the highest risk.”
The findings also suggested that those with skin cancer had the highest odds for stroke, while women with cervical and breast cancers were more likely to experience acute kidney injury and preterm birth.
Dr. Chura said cancer treatments can have an impact on a woman’s health when she’s giving birth. For example, if a woman is diagnosed with cervical cancer, doctors may perform a cone biopsy on her where they remove a large portion of the cervix and still leave them with the ability to conceive and become pregnant. However, those patients are left with a higher risk of a preterm delivery.
For women with a hematologic cancer like non-Hodgkin’s lymphoma, chest radiation may cause some subsequent damage to their heart muscles “and now the stress of pregnancy puts more demand on the heart that can lead to cardiac complications for that patient,” Dr. Chura said.
“There are potential long-term effects from radiation and chemotherapy,” Dr. Chura said.
Previous studies have shown that chemotherapy may affect pregnancy and delivery. A 2019 study published in the Journal of Cancer also found that 59 pregnant women with cancer had increased mortality compared with those without the long-term illness. Meanwhile, another 2018 study published in Cancer found that women who conceived less than a year after starting chemotherapy had higher risks of preterm birth in comparison with those who conceived more than a year after starting chemotherapy. The study also found that cancer survivors who conceived more than a year after finishing chemotherapy with or without radiation had no higher risk of a preterm birth than those without cancer.
Dr. Chura said the new study could force doctors to think about the long-term effects of their cancer therapies and make them more apt to think about how to make cancer therapy less toxic with less long-term health consequences, while still curing patients.
“Most oncologists, when dealing with younger patients, are very focused on curing the cancer at hand, but not necessarily thinking 5 or 10 years down the road,” Dr. Chura said. “[This study] could help inform or at least make us aware of the long-term consequences of our cancer therapies.”
Dr. Chura had no relevant financial disclosures.
The risk of in-hospital complications and poor birth outcomes were greater in pregnant women with current or historical cancer diagnoses, new research suggests.
The study, published in Mayo Clinic Proceedings, found that women with current and historical cancer diagnoses had an increased risk of death, kidney injury, and stroke during delivery hospitalizations, compared with those with no cancer. When it came to delivery outcomes, this group also had a higher risk for preterm birth and postpartum hemorrhage. Those with a current cancer diagnoses had a 1.7-fold increase in odds for a preterm birth, compared with women without cancer.
“Our study found that metastases increased the odds of mortality, cesarean delivery, preterm birth, and stillbirth,” the researchers noted. “Coupled with previous research reporting that pregnant women are more likely to be diagnosed with advanced disease, this implies that pregnant women with newly diagnosed cancer have poor prognoses.”
However, although women with prior cancer had increased odds of mortality, the researchers said it was not statistically significant.
“The study really did not show an increase of mortality [for women with prior cancer diagnosis],” said Justin Chura, MD, a specialist in gynecologic oncology who was not involved in the study. “And the reason might be because there is not or the reason might be because it’s such a rare event. You would need 100 million births to assess that. So I would actually use caution in that interpretation.”
Researchers analyzed more than 43 million delivery hospitalizations of women with or without current or historical cancer diagnoses between January 2004 and December 2014. They found that the most common cancer diagnoses were hematologic, thyroid, cervical, skin, and breast.
Of the five most common cancers, the prevalence of all maternal complications and negative delivery outcomes was the highest among women with hematologic cancers. They were more likely to experience peripartum cardiomyopathy, acute kidney injury, and arrhythmia, compared with other cancers. Postpartum hemorrhage, maternal mortality, and placental abruption was also more likely to occur in those with this type of cancer.
“I was surprised that it was the hematologic cancers that were worse when they did it by cancer type,” said Dr. Chura, who is the chief of surgery and the director of gynecologic oncology and robotic surgery at the Cancer Treatment Centers of America’s Eastern Regional Medical Center in Philadelphia. “I think this is a useful bit of information for counseling our patients and also to identify the cohort with the highest risk.”
The findings also suggested that those with skin cancer had the highest odds for stroke, while women with cervical and breast cancers were more likely to experience acute kidney injury and preterm birth.
Dr. Chura said cancer treatments can have an impact on a woman’s health when she’s giving birth. For example, if a woman is diagnosed with cervical cancer, doctors may perform a cone biopsy on her where they remove a large portion of the cervix and still leave them with the ability to conceive and become pregnant. However, those patients are left with a higher risk of a preterm delivery.
For women with a hematologic cancer like non-Hodgkin’s lymphoma, chest radiation may cause some subsequent damage to their heart muscles “and now the stress of pregnancy puts more demand on the heart that can lead to cardiac complications for that patient,” Dr. Chura said.
“There are potential long-term effects from radiation and chemotherapy,” Dr. Chura said.
Previous studies have shown that chemotherapy may affect pregnancy and delivery. A 2019 study published in the Journal of Cancer also found that 59 pregnant women with cancer had increased mortality compared with those without the long-term illness. Meanwhile, another 2018 study published in Cancer found that women who conceived less than a year after starting chemotherapy had higher risks of preterm birth in comparison with those who conceived more than a year after starting chemotherapy. The study also found that cancer survivors who conceived more than a year after finishing chemotherapy with or without radiation had no higher risk of a preterm birth than those without cancer.
Dr. Chura said the new study could force doctors to think about the long-term effects of their cancer therapies and make them more apt to think about how to make cancer therapy less toxic with less long-term health consequences, while still curing patients.
“Most oncologists, when dealing with younger patients, are very focused on curing the cancer at hand, but not necessarily thinking 5 or 10 years down the road,” Dr. Chura said. “[This study] could help inform or at least make us aware of the long-term consequences of our cancer therapies.”
Dr. Chura had no relevant financial disclosures.
The risk of in-hospital complications and poor birth outcomes were greater in pregnant women with current or historical cancer diagnoses, new research suggests.
The study, published in Mayo Clinic Proceedings, found that women with current and historical cancer diagnoses had an increased risk of death, kidney injury, and stroke during delivery hospitalizations, compared with those with no cancer. When it came to delivery outcomes, this group also had a higher risk for preterm birth and postpartum hemorrhage. Those with a current cancer diagnoses had a 1.7-fold increase in odds for a preterm birth, compared with women without cancer.
“Our study found that metastases increased the odds of mortality, cesarean delivery, preterm birth, and stillbirth,” the researchers noted. “Coupled with previous research reporting that pregnant women are more likely to be diagnosed with advanced disease, this implies that pregnant women with newly diagnosed cancer have poor prognoses.”
However, although women with prior cancer had increased odds of mortality, the researchers said it was not statistically significant.
“The study really did not show an increase of mortality [for women with prior cancer diagnosis],” said Justin Chura, MD, a specialist in gynecologic oncology who was not involved in the study. “And the reason might be because there is not or the reason might be because it’s such a rare event. You would need 100 million births to assess that. So I would actually use caution in that interpretation.”
Researchers analyzed more than 43 million delivery hospitalizations of women with or without current or historical cancer diagnoses between January 2004 and December 2014. They found that the most common cancer diagnoses were hematologic, thyroid, cervical, skin, and breast.
Of the five most common cancers, the prevalence of all maternal complications and negative delivery outcomes was the highest among women with hematologic cancers. They were more likely to experience peripartum cardiomyopathy, acute kidney injury, and arrhythmia, compared with other cancers. Postpartum hemorrhage, maternal mortality, and placental abruption was also more likely to occur in those with this type of cancer.
“I was surprised that it was the hematologic cancers that were worse when they did it by cancer type,” said Dr. Chura, who is the chief of surgery and the director of gynecologic oncology and robotic surgery at the Cancer Treatment Centers of America’s Eastern Regional Medical Center in Philadelphia. “I think this is a useful bit of information for counseling our patients and also to identify the cohort with the highest risk.”
The findings also suggested that those with skin cancer had the highest odds for stroke, while women with cervical and breast cancers were more likely to experience acute kidney injury and preterm birth.
Dr. Chura said cancer treatments can have an impact on a woman’s health when she’s giving birth. For example, if a woman is diagnosed with cervical cancer, doctors may perform a cone biopsy on her where they remove a large portion of the cervix and still leave them with the ability to conceive and become pregnant. However, those patients are left with a higher risk of a preterm delivery.
For women with a hematologic cancer like non-Hodgkin’s lymphoma, chest radiation may cause some subsequent damage to their heart muscles “and now the stress of pregnancy puts more demand on the heart that can lead to cardiac complications for that patient,” Dr. Chura said.
“There are potential long-term effects from radiation and chemotherapy,” Dr. Chura said.
Previous studies have shown that chemotherapy may affect pregnancy and delivery. A 2019 study published in the Journal of Cancer also found that 59 pregnant women with cancer had increased mortality compared with those without the long-term illness. Meanwhile, another 2018 study published in Cancer found that women who conceived less than a year after starting chemotherapy had higher risks of preterm birth in comparison with those who conceived more than a year after starting chemotherapy. The study also found that cancer survivors who conceived more than a year after finishing chemotherapy with or without radiation had no higher risk of a preterm birth than those without cancer.
Dr. Chura said the new study could force doctors to think about the long-term effects of their cancer therapies and make them more apt to think about how to make cancer therapy less toxic with less long-term health consequences, while still curing patients.
“Most oncologists, when dealing with younger patients, are very focused on curing the cancer at hand, but not necessarily thinking 5 or 10 years down the road,” Dr. Chura said. “[This study] could help inform or at least make us aware of the long-term consequences of our cancer therapies.”
Dr. Chura had no relevant financial disclosures.
FROM MAYO CLINIC PROCEEDINGS
Lucid abductions and Candy Crush addiction
I dream of alien abductions
There he goes! It’s lunchtime and your colleague Tom is going on and on again about that time he was abducted by aliens. It sounds ridiculous, but he does make some convincing arguments. Tom thinks it was real, but could it have all just been in his head?
Lucid dreaming may help explain alleged alien abductions. During a lucid dream, people know that they’re dreaming, and can also have some control over how the dreams play out. During some dream states, a person can feel intense sensations, such as terror and paralysis, so it’s no wonder these dreams feel so real.
In a recent study, scientists encouraged 152 participants who had self-identified as lucid dreamers to dream about aliens. Many (75%) of the participants were able to dream about alien encounters, and 15% “achieved relatively realistic experiences,” the investigators reported.
So cut Tom some slack. He’s not crazy, he might just have lucid dreaming privileges. Tell him he should dream about something more fun, like a vacation in the Bahamas.
Follow your heart: Drink more coffee
It seems like the world is divided into coffee drinkers and non–coffee drinkers. Then there’s decaf and regular drinkers. Whichever camp you fall into, know this: The widespread belief that caffeine consumption has an effect on your heart is all beans.
In what is the largest investigation of its kind, researchers from the University of California, San Francisco, looked into whether drinking caffeinated coffee was linked to a risk for heart arrhythmia. They also researched whether patients with genetic variants that affect their metabolism could change that association. Almost 400,000 people with a mean age of 56 years participated in the study. More than half of the participants were women.
The investigators analyzed the participants’ self-reported coffee consumption using a technique called Mendelian randomization to leverage genetic data with the participants’ relationship with caffeine, making it an even field and not relying on the participant consumption self-reporting for outcomes as in previous studies.
What they found, after the 4-year follow up, was nothing short of myth busting.
“We found no evidence that caffeine consumption leads to a greater risk of arrhythmias,” said senior and corresponding author Gregory Marcus, MD. “Our population-based study provides reassurance that common prohibitions against caffeine to reduce arrhythmia risk are likely unwarranted.”
There was no evidence of a heightened risk of arrhythmias in participants who were genetically predisposed to metabolize caffeine differently from those who were not. And, there was a 3% reduction of arrhythmias in patients who consumed higher amounts of coffee.
We are not lobbying for Big Caffeine, but this study adds to the reported health benefits linked to coffee, which already include reduced risk for cancer, diabetes, and Parkinson’s disease, with an added bonus of anti-inflammatory benefits. So, the next time you’re hesitant to pour that second cup of Joe, just go for it. Your heart can take it.
Bored? Feeling down? Don’t play Candy Crush
Now hang on, aren’t those the perfect times to play video games? If there’s nothing else to do, why not open Candy Crush and mindlessly power through the levels?
Because, according to a study by a group of Canadian researchers, it’s actually the worst thing you can do. Well, maybe not literally, but it’s not helpful. Researchers recruited 60 Candy Crush players who were at various levels in the game. They had the participants play early levels that were far too easy or levels balanced with their gameplay abilities.
Players in the easy-level group got bored and quit far earlier than did those in the advanced-level group. The group playing to their abilities were able to access a “flow” state and focus all their attention on the game. While this is all well and good for their gaming performance, according to the researchers, it confirms the theory that playing to escape boredom or negative emotions is more likely to lead to addiction. As with all addictions, the temporary high can give way to a self-repeating loop, causing patients to ignore real life and deepen depression.
The researchers hope their findings will encourage game developers to “consider implementing responsible video gaming tools directly within their games.” Comedy gold. Perhaps Canadians’ idea of capitalism is a little different from that of those south of the border.
Hiccups and vaccine refusal
Tonight, LOTME News dives into the fetid cesspool that is international politics and comes out with … hiccups?
But first, a word from our sponsor, Fearless Boxing Club of South Etobicoke, Ontario.
Are you looking to flout public health restrictions? Do you want to spend time in an enclosed space with other people who haven’t gotten the COVID-19 vaccine? Do you “feel safer waiting until more research is done on the side effects being discovered right now”? (We are not making this up.)
Then join the Fearless Boxing Club, because we “will not be accepting any vaccinated members.” Our founders, Mohammed Abedeen and Krystal Glazier-Roscoe, are working hard to exclude “those who received the experimental COVID vaccine.” (Still not making it up.)
And now, back to the news.
Brazilian president Jair Bolsonaro was hospitalized recently for a severe case of hiccups that may have been related to a stab wound he received in 2018. [Nope, didn’t make that up, either.]
Mr. Bolsonaro had been hiccuping for 10 days, and was experiencing abdominal pain and difficulty speaking, when he entered the hospital on July 14. Since being stabbed while on the campaign trail, he has undergone several operations, which may have led to the partial intestinal obstruction that caused his latest symptoms.
His medical team advised Mr. Bolsonaro to go on a diet to aid his recovery, but when he was released on July 18 he said, “I hope in 10 days I’ll be eating barbecued ribs.” (Maybe this is all just a lucid dream. Probably shouldn’t have had ribs right before bed.)
I dream of alien abductions
There he goes! It’s lunchtime and your colleague Tom is going on and on again about that time he was abducted by aliens. It sounds ridiculous, but he does make some convincing arguments. Tom thinks it was real, but could it have all just been in his head?
Lucid dreaming may help explain alleged alien abductions. During a lucid dream, people know that they’re dreaming, and can also have some control over how the dreams play out. During some dream states, a person can feel intense sensations, such as terror and paralysis, so it’s no wonder these dreams feel so real.
In a recent study, scientists encouraged 152 participants who had self-identified as lucid dreamers to dream about aliens. Many (75%) of the participants were able to dream about alien encounters, and 15% “achieved relatively realistic experiences,” the investigators reported.
So cut Tom some slack. He’s not crazy, he might just have lucid dreaming privileges. Tell him he should dream about something more fun, like a vacation in the Bahamas.
Follow your heart: Drink more coffee
It seems like the world is divided into coffee drinkers and non–coffee drinkers. Then there’s decaf and regular drinkers. Whichever camp you fall into, know this: The widespread belief that caffeine consumption has an effect on your heart is all beans.
In what is the largest investigation of its kind, researchers from the University of California, San Francisco, looked into whether drinking caffeinated coffee was linked to a risk for heart arrhythmia. They also researched whether patients with genetic variants that affect their metabolism could change that association. Almost 400,000 people with a mean age of 56 years participated in the study. More than half of the participants were women.
The investigators analyzed the participants’ self-reported coffee consumption using a technique called Mendelian randomization to leverage genetic data with the participants’ relationship with caffeine, making it an even field and not relying on the participant consumption self-reporting for outcomes as in previous studies.
What they found, after the 4-year follow up, was nothing short of myth busting.
“We found no evidence that caffeine consumption leads to a greater risk of arrhythmias,” said senior and corresponding author Gregory Marcus, MD. “Our population-based study provides reassurance that common prohibitions against caffeine to reduce arrhythmia risk are likely unwarranted.”
There was no evidence of a heightened risk of arrhythmias in participants who were genetically predisposed to metabolize caffeine differently from those who were not. And, there was a 3% reduction of arrhythmias in patients who consumed higher amounts of coffee.
We are not lobbying for Big Caffeine, but this study adds to the reported health benefits linked to coffee, which already include reduced risk for cancer, diabetes, and Parkinson’s disease, with an added bonus of anti-inflammatory benefits. So, the next time you’re hesitant to pour that second cup of Joe, just go for it. Your heart can take it.
Bored? Feeling down? Don’t play Candy Crush
Now hang on, aren’t those the perfect times to play video games? If there’s nothing else to do, why not open Candy Crush and mindlessly power through the levels?
Because, according to a study by a group of Canadian researchers, it’s actually the worst thing you can do. Well, maybe not literally, but it’s not helpful. Researchers recruited 60 Candy Crush players who were at various levels in the game. They had the participants play early levels that were far too easy or levels balanced with their gameplay abilities.
Players in the easy-level group got bored and quit far earlier than did those in the advanced-level group. The group playing to their abilities were able to access a “flow” state and focus all their attention on the game. While this is all well and good for their gaming performance, according to the researchers, it confirms the theory that playing to escape boredom or negative emotions is more likely to lead to addiction. As with all addictions, the temporary high can give way to a self-repeating loop, causing patients to ignore real life and deepen depression.
The researchers hope their findings will encourage game developers to “consider implementing responsible video gaming tools directly within their games.” Comedy gold. Perhaps Canadians’ idea of capitalism is a little different from that of those south of the border.
Hiccups and vaccine refusal
Tonight, LOTME News dives into the fetid cesspool that is international politics and comes out with … hiccups?
But first, a word from our sponsor, Fearless Boxing Club of South Etobicoke, Ontario.
Are you looking to flout public health restrictions? Do you want to spend time in an enclosed space with other people who haven’t gotten the COVID-19 vaccine? Do you “feel safer waiting until more research is done on the side effects being discovered right now”? (We are not making this up.)
Then join the Fearless Boxing Club, because we “will not be accepting any vaccinated members.” Our founders, Mohammed Abedeen and Krystal Glazier-Roscoe, are working hard to exclude “those who received the experimental COVID vaccine.” (Still not making it up.)
And now, back to the news.
Brazilian president Jair Bolsonaro was hospitalized recently for a severe case of hiccups that may have been related to a stab wound he received in 2018. [Nope, didn’t make that up, either.]
Mr. Bolsonaro had been hiccuping for 10 days, and was experiencing abdominal pain and difficulty speaking, when he entered the hospital on July 14. Since being stabbed while on the campaign trail, he has undergone several operations, which may have led to the partial intestinal obstruction that caused his latest symptoms.
His medical team advised Mr. Bolsonaro to go on a diet to aid his recovery, but when he was released on July 18 he said, “I hope in 10 days I’ll be eating barbecued ribs.” (Maybe this is all just a lucid dream. Probably shouldn’t have had ribs right before bed.)
I dream of alien abductions
There he goes! It’s lunchtime and your colleague Tom is going on and on again about that time he was abducted by aliens. It sounds ridiculous, but he does make some convincing arguments. Tom thinks it was real, but could it have all just been in his head?
Lucid dreaming may help explain alleged alien abductions. During a lucid dream, people know that they’re dreaming, and can also have some control over how the dreams play out. During some dream states, a person can feel intense sensations, such as terror and paralysis, so it’s no wonder these dreams feel so real.
In a recent study, scientists encouraged 152 participants who had self-identified as lucid dreamers to dream about aliens. Many (75%) of the participants were able to dream about alien encounters, and 15% “achieved relatively realistic experiences,” the investigators reported.
So cut Tom some slack. He’s not crazy, he might just have lucid dreaming privileges. Tell him he should dream about something more fun, like a vacation in the Bahamas.
Follow your heart: Drink more coffee
It seems like the world is divided into coffee drinkers and non–coffee drinkers. Then there’s decaf and regular drinkers. Whichever camp you fall into, know this: The widespread belief that caffeine consumption has an effect on your heart is all beans.
In what is the largest investigation of its kind, researchers from the University of California, San Francisco, looked into whether drinking caffeinated coffee was linked to a risk for heart arrhythmia. They also researched whether patients with genetic variants that affect their metabolism could change that association. Almost 400,000 people with a mean age of 56 years participated in the study. More than half of the participants were women.
The investigators analyzed the participants’ self-reported coffee consumption using a technique called Mendelian randomization to leverage genetic data with the participants’ relationship with caffeine, making it an even field and not relying on the participant consumption self-reporting for outcomes as in previous studies.
What they found, after the 4-year follow up, was nothing short of myth busting.
“We found no evidence that caffeine consumption leads to a greater risk of arrhythmias,” said senior and corresponding author Gregory Marcus, MD. “Our population-based study provides reassurance that common prohibitions against caffeine to reduce arrhythmia risk are likely unwarranted.”
There was no evidence of a heightened risk of arrhythmias in participants who were genetically predisposed to metabolize caffeine differently from those who were not. And, there was a 3% reduction of arrhythmias in patients who consumed higher amounts of coffee.
We are not lobbying for Big Caffeine, but this study adds to the reported health benefits linked to coffee, which already include reduced risk for cancer, diabetes, and Parkinson’s disease, with an added bonus of anti-inflammatory benefits. So, the next time you’re hesitant to pour that second cup of Joe, just go for it. Your heart can take it.
Bored? Feeling down? Don’t play Candy Crush
Now hang on, aren’t those the perfect times to play video games? If there’s nothing else to do, why not open Candy Crush and mindlessly power through the levels?
Because, according to a study by a group of Canadian researchers, it’s actually the worst thing you can do. Well, maybe not literally, but it’s not helpful. Researchers recruited 60 Candy Crush players who were at various levels in the game. They had the participants play early levels that were far too easy or levels balanced with their gameplay abilities.
Players in the easy-level group got bored and quit far earlier than did those in the advanced-level group. The group playing to their abilities were able to access a “flow” state and focus all their attention on the game. While this is all well and good for their gaming performance, according to the researchers, it confirms the theory that playing to escape boredom or negative emotions is more likely to lead to addiction. As with all addictions, the temporary high can give way to a self-repeating loop, causing patients to ignore real life and deepen depression.
The researchers hope their findings will encourage game developers to “consider implementing responsible video gaming tools directly within their games.” Comedy gold. Perhaps Canadians’ idea of capitalism is a little different from that of those south of the border.
Hiccups and vaccine refusal
Tonight, LOTME News dives into the fetid cesspool that is international politics and comes out with … hiccups?
But first, a word from our sponsor, Fearless Boxing Club of South Etobicoke, Ontario.
Are you looking to flout public health restrictions? Do you want to spend time in an enclosed space with other people who haven’t gotten the COVID-19 vaccine? Do you “feel safer waiting until more research is done on the side effects being discovered right now”? (We are not making this up.)
Then join the Fearless Boxing Club, because we “will not be accepting any vaccinated members.” Our founders, Mohammed Abedeen and Krystal Glazier-Roscoe, are working hard to exclude “those who received the experimental COVID vaccine.” (Still not making it up.)
And now, back to the news.
Brazilian president Jair Bolsonaro was hospitalized recently for a severe case of hiccups that may have been related to a stab wound he received in 2018. [Nope, didn’t make that up, either.]
Mr. Bolsonaro had been hiccuping for 10 days, and was experiencing abdominal pain and difficulty speaking, when he entered the hospital on July 14. Since being stabbed while on the campaign trail, he has undergone several operations, which may have led to the partial intestinal obstruction that caused his latest symptoms.
His medical team advised Mr. Bolsonaro to go on a diet to aid his recovery, but when he was released on July 18 he said, “I hope in 10 days I’ll be eating barbecued ribs.” (Maybe this is all just a lucid dream. Probably shouldn’t have had ribs right before bed.)
Separation and discoloration of thumb nail
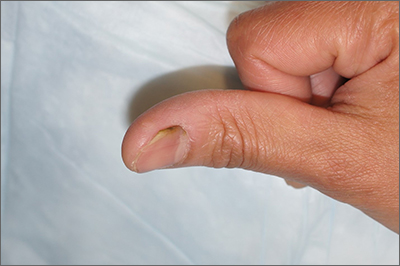
The color change in this case is subtle, but consistent with green nail syndrome also termed chloronychia.
Green nail syndrome is a form of chronic paronychia caused by Pseudomonas aeruginosa and is associated with frequent water exposure. Pseudomonas expresses pyocyanin and pyoverdine, leading to the characteristic blue or green coloration. A Woods lamp may reveal neon green fluorescence.
Risk factors include frequent water exposure, use of an instrument to relieve symptoms of an ingrown nail, and chronic immunosuppression. In this case, frequent hand washing being performed by this patient during the COVID-19 pandemic was the likely culprit.
The differential diagnosis includes simple structural onycholysis, onychomycosis, and nail psoriasis. Polymicrobial infection can occur. When in doubt, culture or pathologic examination of nail clippings with Grocott methenamine silver and periodic acid–Schiff can identify coincident fungal infection.1 While systemic pseudomonas infection could also occur with green nail syndrome, the latter is usually only a mild nuisance and not associated with severe disease.
Treatment consists of avoidance of water and instrumentation. Topical sodium hypochlorite 2% solution applied to the nail or acetic acid soaks for 2 to 3 weeks is often curative. Antibiotic therapy may also be used. Topical tobramycin or gentamicin are available as otic or ophthalmic drops and can be applied just under the nail.
The patient was advised to meticulously dry her hands after washing them and to apply 1 drop of topical gentamicin solution 0.3% tid for 3 weeks. The green discoloration cleared in 3 weeks and the onycholysis resolved within 4 months.
Text courtesy of Jonathan Karnes, MD, medical director, MDFMR Dermatology Services, Augusta, ME. Photos courtesy of Jonathan Karnes, MD (copyright retained).
1. Ohn J, Yu D-A, Park H, et al. Green nail syndrome: analysis of the association with onychomycosis. J Am Acad Dermatol. 2020;83:940-942. doi: 10.1016/j.jaad.2020.01.040

The color change in this case is subtle, but consistent with green nail syndrome also termed chloronychia.
Green nail syndrome is a form of chronic paronychia caused by Pseudomonas aeruginosa and is associated with frequent water exposure. Pseudomonas expresses pyocyanin and pyoverdine, leading to the characteristic blue or green coloration. A Woods lamp may reveal neon green fluorescence.
Risk factors include frequent water exposure, use of an instrument to relieve symptoms of an ingrown nail, and chronic immunosuppression. In this case, frequent hand washing being performed by this patient during the COVID-19 pandemic was the likely culprit.
The differential diagnosis includes simple structural onycholysis, onychomycosis, and nail psoriasis. Polymicrobial infection can occur. When in doubt, culture or pathologic examination of nail clippings with Grocott methenamine silver and periodic acid–Schiff can identify coincident fungal infection.1 While systemic pseudomonas infection could also occur with green nail syndrome, the latter is usually only a mild nuisance and not associated with severe disease.
Treatment consists of avoidance of water and instrumentation. Topical sodium hypochlorite 2% solution applied to the nail or acetic acid soaks for 2 to 3 weeks is often curative. Antibiotic therapy may also be used. Topical tobramycin or gentamicin are available as otic or ophthalmic drops and can be applied just under the nail.
The patient was advised to meticulously dry her hands after washing them and to apply 1 drop of topical gentamicin solution 0.3% tid for 3 weeks. The green discoloration cleared in 3 weeks and the onycholysis resolved within 4 months.
Text courtesy of Jonathan Karnes, MD, medical director, MDFMR Dermatology Services, Augusta, ME. Photos courtesy of Jonathan Karnes, MD (copyright retained).

The color change in this case is subtle, but consistent with green nail syndrome also termed chloronychia.
Green nail syndrome is a form of chronic paronychia caused by Pseudomonas aeruginosa and is associated with frequent water exposure. Pseudomonas expresses pyocyanin and pyoverdine, leading to the characteristic blue or green coloration. A Woods lamp may reveal neon green fluorescence.
Risk factors include frequent water exposure, use of an instrument to relieve symptoms of an ingrown nail, and chronic immunosuppression. In this case, frequent hand washing being performed by this patient during the COVID-19 pandemic was the likely culprit.
The differential diagnosis includes simple structural onycholysis, onychomycosis, and nail psoriasis. Polymicrobial infection can occur. When in doubt, culture or pathologic examination of nail clippings with Grocott methenamine silver and periodic acid–Schiff can identify coincident fungal infection.1 While systemic pseudomonas infection could also occur with green nail syndrome, the latter is usually only a mild nuisance and not associated with severe disease.
Treatment consists of avoidance of water and instrumentation. Topical sodium hypochlorite 2% solution applied to the nail or acetic acid soaks for 2 to 3 weeks is often curative. Antibiotic therapy may also be used. Topical tobramycin or gentamicin are available as otic or ophthalmic drops and can be applied just under the nail.
The patient was advised to meticulously dry her hands after washing them and to apply 1 drop of topical gentamicin solution 0.3% tid for 3 weeks. The green discoloration cleared in 3 weeks and the onycholysis resolved within 4 months.
Text courtesy of Jonathan Karnes, MD, medical director, MDFMR Dermatology Services, Augusta, ME. Photos courtesy of Jonathan Karnes, MD (copyright retained).
1. Ohn J, Yu D-A, Park H, et al. Green nail syndrome: analysis of the association with onychomycosis. J Am Acad Dermatol. 2020;83:940-942. doi: 10.1016/j.jaad.2020.01.040
1. Ohn J, Yu D-A, Park H, et al. Green nail syndrome: analysis of the association with onychomycosis. J Am Acad Dermatol. 2020;83:940-942. doi: 10.1016/j.jaad.2020.01.040
Sickle cell disease, trait may up risk for poor COVID outcomes
Sickle cell disease (SCD) was associated with a greater than fourfold excess risk for COVID-19–related hospitalization and a greater than twofold risk for COVID-19–related death, according to a big-data analysis from the United Kingdom.
SCD was associated with an adjusted hazard ratio (HR) of 4.11 (95% confidence interval, 2.98-5.66) for admission to hospital and an HR of 2.55 (95% CI, 1.36-4.75) for death, report Ashley K. Clift, MBBS, a clinical research fellow at the University of Oxford, and colleagues. The results were published online July 20 in Annals of Internal Medicine.
Even those who carry just one copy of the sickle cell gene – the carrier status for sickle cell disease – appeared to be at heightened risk for these outcomes (HR for hospitalization, 1.38; 95% CI, 1.12-1.70; HR for death, 1.51; 95% CI, 1.13-2.00).
“Given the well-known ethnic patterning of sickle cell disorders, the predisposition they pose to other infections, and early evidence from smaller registries, we thought this would be an important analysis to run at the population level,” Dr. Clift said in an interview.
in terms of vaccination strategies and advice on nonpharmacological interventions,” he said.
“The best course of action for managing risk in this group is vaccination,” said Enrico M. Novelli, MD, director of the adult sickle cell program at the University of Pittsburgh Medical Center. Dr. Novelli, who is also section chief of benign hematology in the university’s School of Medicine, was not involved in the study. “To date, there are no specific studies of the effect of COVID-19 vaccination in patients with SCD, but there is no reason to believe it would be less effective or more risky in this patient population,” he said.
In addition, common-sense measures, such as masking and physical distancing, particularly at large, indoor gatherings, should be encouraged, Dr. Novelli added. Keeping SCD under good control with available treatments is also important. “Any patient with SCD who contracts COVID-19 should undergo close, outpatient monitoring with pulse oxygen measurements. If sick, they should be hospitalized in a center familiar with the care of SCD patients.”
The U.K. results are in line with and expand on earlier evidence from specialist centers and registries, but the association with sickle cell trait has been unclear and is notable in these findings, Dr. Clift said.
“The finding of the association with sickle cell trait is somewhat unexpected,” pediatric hematologist/oncologist Rabi Hanna, MD, director of pediatric bone marrow transplantation at Cleveland Clinic Children’s, told this news organization. “But I would question the accuracy of the numbers, since not all people with the trait realize they have it. In other respects, the study confirms earlier hypotheses and data from single-center studies.” Dr. Hanna did not participate in the U.K. study.
Study details
The SCD cohort consisted of 5,059 persons with SCD and 25,682 carriers, those with just one copy of the trait. Data were drawn from the United Kingdom’s large primary-care QResearch database. Follow-up for hospitalizations was conducted from Jan. 24, 2020 to Sept. 30, 2020; follow-up for deaths was conducted from Jan. 24, 2020 to Jan. 18, 2021. Among adults with SCD, there were 40 hospitalizations and 10 deaths. Among those with sickle cell trait, there were 98 hospitalizations and 50 deaths. No children died, and only a few (<5) required hospitalization.
Previous registry research showed similarly elevated risks for severe disease and fatality among patients with SCD who were infected with SARS-CoV-2.
Because SCD affects 8 to 12 million people globally – 100,000 in the United States – the authors say their results are important for policymakers and for prioritizing vaccination. They also note that trait carriers may be underdiagnosed.
“While SCD is part of newborn screening, there may be undiagnosed older people with the trait in the general population, but it’s difficult to quantify how much this is undiagnosed,” Dr. Clift said. “But now we have these results, it’s not that surprising that sickle cell trait is also associated with increased risk, albeit to a lower extent. This could suggest an almost dose-like effect of the sickle mutations on COVID hospitalization risk.”
Neonatal screening for the most common form of SCD is currently mandatory in the United States, but the Centers for Disease Control and Prevention has no clear data on how many people are aware they are carriers, Dr. Hanna said. “The states didn’t all begin screening at the same time – some started in the 1990s, others started in the 2000s – so many young adults may be unaware they have the trait,” he said.
Dr. Clift said the multiorgan complications of SCD, such as cardiac and immune problems, may be contributing to the heightened risk in individuals infected with SARS-CoV-2. “For example, we know that people with sickle cell disease are more susceptible to other viral infections. There is also some pathophysiological overlap between SCD disease and severe COVID, such as clotting dysfunction, so that may be worth further exploration,” he said.
The overlapping clotting problems associated with both COVID-19 and SCD could increase the risk for severe venous thromboembolism. In addition, experts noted that patients with SCD often have pre-COVID endothelial damage and baseline inflammation and are very sensitive to hypoxia; as well, a sizable proportion have lung disease.
The message to patients and physicians counseling patients is twofold, said Dr. Hanna: “SCD patients are at higher risk of COVID complications, and these are preventable with vaccination.”
The study was supported by the UK Medical Research Council. Dr. Clift is supported by Cancer Research UK. Coauthor Dr. Hippisley-Cox has received fees from ClinRisk and nonfinancial support from QResearch outside of the submitted work. Dr. Hanna has disclosed no relevant financial relationships. Dr. Novelli is a consultant for Novartis.
A version of this article first appeared on Medscape.com.
Sickle cell disease (SCD) was associated with a greater than fourfold excess risk for COVID-19–related hospitalization and a greater than twofold risk for COVID-19–related death, according to a big-data analysis from the United Kingdom.
SCD was associated with an adjusted hazard ratio (HR) of 4.11 (95% confidence interval, 2.98-5.66) for admission to hospital and an HR of 2.55 (95% CI, 1.36-4.75) for death, report Ashley K. Clift, MBBS, a clinical research fellow at the University of Oxford, and colleagues. The results were published online July 20 in Annals of Internal Medicine.
Even those who carry just one copy of the sickle cell gene – the carrier status for sickle cell disease – appeared to be at heightened risk for these outcomes (HR for hospitalization, 1.38; 95% CI, 1.12-1.70; HR for death, 1.51; 95% CI, 1.13-2.00).
“Given the well-known ethnic patterning of sickle cell disorders, the predisposition they pose to other infections, and early evidence from smaller registries, we thought this would be an important analysis to run at the population level,” Dr. Clift said in an interview.
in terms of vaccination strategies and advice on nonpharmacological interventions,” he said.
“The best course of action for managing risk in this group is vaccination,” said Enrico M. Novelli, MD, director of the adult sickle cell program at the University of Pittsburgh Medical Center. Dr. Novelli, who is also section chief of benign hematology in the university’s School of Medicine, was not involved in the study. “To date, there are no specific studies of the effect of COVID-19 vaccination in patients with SCD, but there is no reason to believe it would be less effective or more risky in this patient population,” he said.
In addition, common-sense measures, such as masking and physical distancing, particularly at large, indoor gatherings, should be encouraged, Dr. Novelli added. Keeping SCD under good control with available treatments is also important. “Any patient with SCD who contracts COVID-19 should undergo close, outpatient monitoring with pulse oxygen measurements. If sick, they should be hospitalized in a center familiar with the care of SCD patients.”
The U.K. results are in line with and expand on earlier evidence from specialist centers and registries, but the association with sickle cell trait has been unclear and is notable in these findings, Dr. Clift said.
“The finding of the association with sickle cell trait is somewhat unexpected,” pediatric hematologist/oncologist Rabi Hanna, MD, director of pediatric bone marrow transplantation at Cleveland Clinic Children’s, told this news organization. “But I would question the accuracy of the numbers, since not all people with the trait realize they have it. In other respects, the study confirms earlier hypotheses and data from single-center studies.” Dr. Hanna did not participate in the U.K. study.
Study details
The SCD cohort consisted of 5,059 persons with SCD and 25,682 carriers, those with just one copy of the trait. Data were drawn from the United Kingdom’s large primary-care QResearch database. Follow-up for hospitalizations was conducted from Jan. 24, 2020 to Sept. 30, 2020; follow-up for deaths was conducted from Jan. 24, 2020 to Jan. 18, 2021. Among adults with SCD, there were 40 hospitalizations and 10 deaths. Among those with sickle cell trait, there were 98 hospitalizations and 50 deaths. No children died, and only a few (<5) required hospitalization.
Previous registry research showed similarly elevated risks for severe disease and fatality among patients with SCD who were infected with SARS-CoV-2.
Because SCD affects 8 to 12 million people globally – 100,000 in the United States – the authors say their results are important for policymakers and for prioritizing vaccination. They also note that trait carriers may be underdiagnosed.
“While SCD is part of newborn screening, there may be undiagnosed older people with the trait in the general population, but it’s difficult to quantify how much this is undiagnosed,” Dr. Clift said. “But now we have these results, it’s not that surprising that sickle cell trait is also associated with increased risk, albeit to a lower extent. This could suggest an almost dose-like effect of the sickle mutations on COVID hospitalization risk.”
Neonatal screening for the most common form of SCD is currently mandatory in the United States, but the Centers for Disease Control and Prevention has no clear data on how many people are aware they are carriers, Dr. Hanna said. “The states didn’t all begin screening at the same time – some started in the 1990s, others started in the 2000s – so many young adults may be unaware they have the trait,” he said.
Dr. Clift said the multiorgan complications of SCD, such as cardiac and immune problems, may be contributing to the heightened risk in individuals infected with SARS-CoV-2. “For example, we know that people with sickle cell disease are more susceptible to other viral infections. There is also some pathophysiological overlap between SCD disease and severe COVID, such as clotting dysfunction, so that may be worth further exploration,” he said.
The overlapping clotting problems associated with both COVID-19 and SCD could increase the risk for severe venous thromboembolism. In addition, experts noted that patients with SCD often have pre-COVID endothelial damage and baseline inflammation and are very sensitive to hypoxia; as well, a sizable proportion have lung disease.
The message to patients and physicians counseling patients is twofold, said Dr. Hanna: “SCD patients are at higher risk of COVID complications, and these are preventable with vaccination.”
The study was supported by the UK Medical Research Council. Dr. Clift is supported by Cancer Research UK. Coauthor Dr. Hippisley-Cox has received fees from ClinRisk and nonfinancial support from QResearch outside of the submitted work. Dr. Hanna has disclosed no relevant financial relationships. Dr. Novelli is a consultant for Novartis.
A version of this article first appeared on Medscape.com.
Sickle cell disease (SCD) was associated with a greater than fourfold excess risk for COVID-19–related hospitalization and a greater than twofold risk for COVID-19–related death, according to a big-data analysis from the United Kingdom.
SCD was associated with an adjusted hazard ratio (HR) of 4.11 (95% confidence interval, 2.98-5.66) for admission to hospital and an HR of 2.55 (95% CI, 1.36-4.75) for death, report Ashley K. Clift, MBBS, a clinical research fellow at the University of Oxford, and colleagues. The results were published online July 20 in Annals of Internal Medicine.
Even those who carry just one copy of the sickle cell gene – the carrier status for sickle cell disease – appeared to be at heightened risk for these outcomes (HR for hospitalization, 1.38; 95% CI, 1.12-1.70; HR for death, 1.51; 95% CI, 1.13-2.00).
“Given the well-known ethnic patterning of sickle cell disorders, the predisposition they pose to other infections, and early evidence from smaller registries, we thought this would be an important analysis to run at the population level,” Dr. Clift said in an interview.
in terms of vaccination strategies and advice on nonpharmacological interventions,” he said.
“The best course of action for managing risk in this group is vaccination,” said Enrico M. Novelli, MD, director of the adult sickle cell program at the University of Pittsburgh Medical Center. Dr. Novelli, who is also section chief of benign hematology in the university’s School of Medicine, was not involved in the study. “To date, there are no specific studies of the effect of COVID-19 vaccination in patients with SCD, but there is no reason to believe it would be less effective or more risky in this patient population,” he said.
In addition, common-sense measures, such as masking and physical distancing, particularly at large, indoor gatherings, should be encouraged, Dr. Novelli added. Keeping SCD under good control with available treatments is also important. “Any patient with SCD who contracts COVID-19 should undergo close, outpatient monitoring with pulse oxygen measurements. If sick, they should be hospitalized in a center familiar with the care of SCD patients.”
The U.K. results are in line with and expand on earlier evidence from specialist centers and registries, but the association with sickle cell trait has been unclear and is notable in these findings, Dr. Clift said.
“The finding of the association with sickle cell trait is somewhat unexpected,” pediatric hematologist/oncologist Rabi Hanna, MD, director of pediatric bone marrow transplantation at Cleveland Clinic Children’s, told this news organization. “But I would question the accuracy of the numbers, since not all people with the trait realize they have it. In other respects, the study confirms earlier hypotheses and data from single-center studies.” Dr. Hanna did not participate in the U.K. study.
Study details
The SCD cohort consisted of 5,059 persons with SCD and 25,682 carriers, those with just one copy of the trait. Data were drawn from the United Kingdom’s large primary-care QResearch database. Follow-up for hospitalizations was conducted from Jan. 24, 2020 to Sept. 30, 2020; follow-up for deaths was conducted from Jan. 24, 2020 to Jan. 18, 2021. Among adults with SCD, there were 40 hospitalizations and 10 deaths. Among those with sickle cell trait, there were 98 hospitalizations and 50 deaths. No children died, and only a few (<5) required hospitalization.
Previous registry research showed similarly elevated risks for severe disease and fatality among patients with SCD who were infected with SARS-CoV-2.
Because SCD affects 8 to 12 million people globally – 100,000 in the United States – the authors say their results are important for policymakers and for prioritizing vaccination. They also note that trait carriers may be underdiagnosed.
“While SCD is part of newborn screening, there may be undiagnosed older people with the trait in the general population, but it’s difficult to quantify how much this is undiagnosed,” Dr. Clift said. “But now we have these results, it’s not that surprising that sickle cell trait is also associated with increased risk, albeit to a lower extent. This could suggest an almost dose-like effect of the sickle mutations on COVID hospitalization risk.”
Neonatal screening for the most common form of SCD is currently mandatory in the United States, but the Centers for Disease Control and Prevention has no clear data on how many people are aware they are carriers, Dr. Hanna said. “The states didn’t all begin screening at the same time – some started in the 1990s, others started in the 2000s – so many young adults may be unaware they have the trait,” he said.
Dr. Clift said the multiorgan complications of SCD, such as cardiac and immune problems, may be contributing to the heightened risk in individuals infected with SARS-CoV-2. “For example, we know that people with sickle cell disease are more susceptible to other viral infections. There is also some pathophysiological overlap between SCD disease and severe COVID, such as clotting dysfunction, so that may be worth further exploration,” he said.
The overlapping clotting problems associated with both COVID-19 and SCD could increase the risk for severe venous thromboembolism. In addition, experts noted that patients with SCD often have pre-COVID endothelial damage and baseline inflammation and are very sensitive to hypoxia; as well, a sizable proportion have lung disease.
The message to patients and physicians counseling patients is twofold, said Dr. Hanna: “SCD patients are at higher risk of COVID complications, and these are preventable with vaccination.”
The study was supported by the UK Medical Research Council. Dr. Clift is supported by Cancer Research UK. Coauthor Dr. Hippisley-Cox has received fees from ClinRisk and nonfinancial support from QResearch outside of the submitted work. Dr. Hanna has disclosed no relevant financial relationships. Dr. Novelli is a consultant for Novartis.
A version of this article first appeared on Medscape.com.
Statins again linked to lower COVID-19 mortality
Among patients hospitalized for COVID-19, those who had been taking statins had a substantially lower risk of death in a new large observational study.
Results showed that use of statins prior to admission was linked to a greater than 40% reduction in mortality and a greater than 25% reduction in risk of developing a severe outcome.
The findings come an analysis of data from the American Heart Association’s COVID-19 Cardiovascular Disease Registry on more than 10,000 patients hospitalized with COVID-19 at 104 hospitals across the United States published in PLoS One.
While several other studies have suggested benefits of statins in COVID-19, this is by far the largest study so far on this topic.
“I would say this is the most reliable study on statins in COVID-19 to date, with the results adjusted for many confounders, including socioeconomic factors and insurance type,” lead author Lori B. Daniels, MD, told this news organization. “However, it still an observational study and therefore falls short of a randomized study. But I would think a randomized study of statins in COVID-19 is probably not feasible, so this study provides excellent data at an observational level.”
After propensity matching for cardiovascular disease, results showed that most of the benefit of statins occurred in patients with known cardiovascular disease.
“While most patients taking statins will have cardiovascular disease, there are also many patients who take these drugs who don’t have heart disease but do have cardiovascular risk factors, such as those with raised cholesterol, or a family history of cardiovascular disease. For [such patients], the effect of statins was also in the same direction but it was not significant. This doesn’t exclude an effect,” noted Dr. Daniels, who is professor of medicine and director of cardiovascular intensive care at the University of California, San Diego.
“We are not saying that everyone should rush out and take a statin if they do not have risk factors for cardiovascular in order to lower their risk of dying from COVID. But if individuals do have an indication for a statin and are not taking one of these dugs this is another good reason to start taking them now,” she added.
The investigators embarked on the study because, although previous observational studies have found that statins may reduce the severity of COVID-19 infection, these studies have been limited in size with mostly single-center or regional studies, and some results have been conflicting. They therefore conducted the current, much larger analysis, in the AHA COVID-19 CVD Registry which systematically collected hospitalized patient–level data in a broad and diverse hospital and patient population across the United States.
For the analysis, the researchers analyzed data from 10,541 patients hospitalized with COVID-19 through September 2020 at 104 U.S. hospitals enrolled in the AHA registry to evaluate the associations between statin use and outcomes.
Most patients (71%) had either cardiovascular disease, hypertension, or both. Prior to admission, 42% of subjects used statins, with 7% being on statins alone and 35% on statins plus antihypertensives. Death (or discharge to hospice) occurred in 2,212 subjects (21%).
Results showed that outpatient use of statins, either alone or with antihypertensives, was associated with a 41% reduced risk of death (odds ratio, 0.59; 95% confidence interval, 0.50-0.69), after adjusting for demographic characteristics, underlying conditions, insurance status, hospital site, and concurrent medications. Statin use was also associated with a roughly 25% lower adjusted odds of developing severe disease.
Noting that patients on statins are also likely to be on antihypertensive medication, the researchers found that the statin benefit on mortality was seen in both patients taking a statin alone (OR, 0.54) and in those taking statins with an antihypertensive medication (OR, 0.60).
Use of antihypertensive drugs was associated with a smaller, albeit still substantial, 27% lower odds of death (OR, 0.73; 95% CI, 0.62-0.87).
In propensity-matched analyses, use of statins and/or antihypertensives was tied to a 32% reduced risk of death among those with a history of CVD and/or hypertension (OR, 0.68; 95% CI, 0.58-0.81). An observed 16% reduction in odds of death with statins and/or antihypertensive drugs among those without cardiovascular disease and/or hypertension was not statistically significant (OR, 0.84; 95% CI, 0.58-1.22).
Stabilizing the underlying disease
The researchers pointed out that the results of the propensity matching analysis are consistent with the hypothesis that the major benefit of these medications accrues from treating and/or stabilizing underlying disease.
“Although it is well known that statins improve long-term outcomes among patients with or at elevated risk for cardiovascular disease, the association with a large short-term benefit which accrues in the setting of hospitalization for COVID-19 is a new and intriguing finding,” they said.
They cited several “plausible mechanisms whereby statins could directly mitigate outcomes in COVID-19 beyond treating underlying disease conditions,” including anti-inflammatory effects and a direct inhibitory effect on the SARS-CoV-2 virus.
Dr. Daniels elaborated more on the potential mechanism at play in an interview: “I think what is happening is that the statin is stabilizing the coronary disease so patients are less likely to die from MI or stroke, and this gives them more time and strength to recover from COVID-19.”
She added: “Statins may also have some direct anti-COVID effects such as an anti-inflammatory actions, but I would guess that this is probably not the primary effect behind what we’re seeing here.”
‘Important clinical implications’
The authors say their findings have “important clinical implications.”
They noted that early in the pandemic there was speculation that certain medications, including statins, and the ACE inhibitor/angiotensin receptor blocker (ARB) classes of antihypertensives may confer an increased susceptibility to COVID-19 positivity and/or severity.
“Our study reinforces the AHA and others’ recommendations that not only is it safe to remain on these medications, but they may substantially reduce risk of severe COVID-19 and especially death from COVID-19, particularly statins, and particularly among those with associated underlying conditions,” the authors stressed.
Dr. Daniels added that, although statins are very safe drugs, there are always some patients who prefer not to take medication even if indicated, and others who may have borderline indications and decide not to take a statin at present.
“This study may persuade these patients that taking a statin is the right thing to do. It may give those patients on the cusp of thinking about taking one of these drugs a reason to go ahead,” she said.
‘Provocative but not definitive’
Commenting on the study, Robert Harrington, MD, professor of medicine and chair of the department of medicine at Stanford (Calif.) University, said: “These are interesting observational data but as such have all the limitations of nonrandomized comparisons despite the best attempts to adjust for a variety of potential confounders. For example, is this an effect of statins (perhaps through some anti-inflammatory mechanism) or is it more an effect that can be attributed to the patients who are prescribed and taking a statin, compared with those who are not?”
He added: “The primary clinical benefit of statins, based on many large randomized clinical trials, seems to be derived from their LDL lowering effect. Observational studies have suggested potential benefits from anti-inflammatory effects of statins, but the randomized trials have not confirmed these observations. So, the current data are interesting, even provocative, but ultimately hypothesis generating rather than definitive.”
Also commenting on the study, Steven Nissen, MD, professor of medicine at the Cleveland Clinic, said: “While statins have many established benefits, their role in preventing COVID-19 complications is very speculative. Like all observational studies, the current study must be viewed as hypothesis generating, not definitive evidence of benefit. There are many potential confounders. I’m skeptical.”
The authors of this study received no specific funding for this work and report no competing interests. Dr. Harrington was AHA president when the COVID registry was created and he is still a member of the AHA board, which has oversight over the project.
Among patients hospitalized for COVID-19, those who had been taking statins had a substantially lower risk of death in a new large observational study.
Results showed that use of statins prior to admission was linked to a greater than 40% reduction in mortality and a greater than 25% reduction in risk of developing a severe outcome.
The findings come an analysis of data from the American Heart Association’s COVID-19 Cardiovascular Disease Registry on more than 10,000 patients hospitalized with COVID-19 at 104 hospitals across the United States published in PLoS One.
While several other studies have suggested benefits of statins in COVID-19, this is by far the largest study so far on this topic.
“I would say this is the most reliable study on statins in COVID-19 to date, with the results adjusted for many confounders, including socioeconomic factors and insurance type,” lead author Lori B. Daniels, MD, told this news organization. “However, it still an observational study and therefore falls short of a randomized study. But I would think a randomized study of statins in COVID-19 is probably not feasible, so this study provides excellent data at an observational level.”
After propensity matching for cardiovascular disease, results showed that most of the benefit of statins occurred in patients with known cardiovascular disease.
“While most patients taking statins will have cardiovascular disease, there are also many patients who take these drugs who don’t have heart disease but do have cardiovascular risk factors, such as those with raised cholesterol, or a family history of cardiovascular disease. For [such patients], the effect of statins was also in the same direction but it was not significant. This doesn’t exclude an effect,” noted Dr. Daniels, who is professor of medicine and director of cardiovascular intensive care at the University of California, San Diego.
“We are not saying that everyone should rush out and take a statin if they do not have risk factors for cardiovascular in order to lower their risk of dying from COVID. But if individuals do have an indication for a statin and are not taking one of these dugs this is another good reason to start taking them now,” she added.
The investigators embarked on the study because, although previous observational studies have found that statins may reduce the severity of COVID-19 infection, these studies have been limited in size with mostly single-center or regional studies, and some results have been conflicting. They therefore conducted the current, much larger analysis, in the AHA COVID-19 CVD Registry which systematically collected hospitalized patient–level data in a broad and diverse hospital and patient population across the United States.
For the analysis, the researchers analyzed data from 10,541 patients hospitalized with COVID-19 through September 2020 at 104 U.S. hospitals enrolled in the AHA registry to evaluate the associations between statin use and outcomes.
Most patients (71%) had either cardiovascular disease, hypertension, or both. Prior to admission, 42% of subjects used statins, with 7% being on statins alone and 35% on statins plus antihypertensives. Death (or discharge to hospice) occurred in 2,212 subjects (21%).
Results showed that outpatient use of statins, either alone or with antihypertensives, was associated with a 41% reduced risk of death (odds ratio, 0.59; 95% confidence interval, 0.50-0.69), after adjusting for demographic characteristics, underlying conditions, insurance status, hospital site, and concurrent medications. Statin use was also associated with a roughly 25% lower adjusted odds of developing severe disease.
Noting that patients on statins are also likely to be on antihypertensive medication, the researchers found that the statin benefit on mortality was seen in both patients taking a statin alone (OR, 0.54) and in those taking statins with an antihypertensive medication (OR, 0.60).
Use of antihypertensive drugs was associated with a smaller, albeit still substantial, 27% lower odds of death (OR, 0.73; 95% CI, 0.62-0.87).
In propensity-matched analyses, use of statins and/or antihypertensives was tied to a 32% reduced risk of death among those with a history of CVD and/or hypertension (OR, 0.68; 95% CI, 0.58-0.81). An observed 16% reduction in odds of death with statins and/or antihypertensive drugs among those without cardiovascular disease and/or hypertension was not statistically significant (OR, 0.84; 95% CI, 0.58-1.22).
Stabilizing the underlying disease
The researchers pointed out that the results of the propensity matching analysis are consistent with the hypothesis that the major benefit of these medications accrues from treating and/or stabilizing underlying disease.
“Although it is well known that statins improve long-term outcomes among patients with or at elevated risk for cardiovascular disease, the association with a large short-term benefit which accrues in the setting of hospitalization for COVID-19 is a new and intriguing finding,” they said.
They cited several “plausible mechanisms whereby statins could directly mitigate outcomes in COVID-19 beyond treating underlying disease conditions,” including anti-inflammatory effects and a direct inhibitory effect on the SARS-CoV-2 virus.
Dr. Daniels elaborated more on the potential mechanism at play in an interview: “I think what is happening is that the statin is stabilizing the coronary disease so patients are less likely to die from MI or stroke, and this gives them more time and strength to recover from COVID-19.”
She added: “Statins may also have some direct anti-COVID effects such as an anti-inflammatory actions, but I would guess that this is probably not the primary effect behind what we’re seeing here.”
‘Important clinical implications’
The authors say their findings have “important clinical implications.”
They noted that early in the pandemic there was speculation that certain medications, including statins, and the ACE inhibitor/angiotensin receptor blocker (ARB) classes of antihypertensives may confer an increased susceptibility to COVID-19 positivity and/or severity.
“Our study reinforces the AHA and others’ recommendations that not only is it safe to remain on these medications, but they may substantially reduce risk of severe COVID-19 and especially death from COVID-19, particularly statins, and particularly among those with associated underlying conditions,” the authors stressed.
Dr. Daniels added that, although statins are very safe drugs, there are always some patients who prefer not to take medication even if indicated, and others who may have borderline indications and decide not to take a statin at present.
“This study may persuade these patients that taking a statin is the right thing to do. It may give those patients on the cusp of thinking about taking one of these drugs a reason to go ahead,” she said.
‘Provocative but not definitive’
Commenting on the study, Robert Harrington, MD, professor of medicine and chair of the department of medicine at Stanford (Calif.) University, said: “These are interesting observational data but as such have all the limitations of nonrandomized comparisons despite the best attempts to adjust for a variety of potential confounders. For example, is this an effect of statins (perhaps through some anti-inflammatory mechanism) or is it more an effect that can be attributed to the patients who are prescribed and taking a statin, compared with those who are not?”
He added: “The primary clinical benefit of statins, based on many large randomized clinical trials, seems to be derived from their LDL lowering effect. Observational studies have suggested potential benefits from anti-inflammatory effects of statins, but the randomized trials have not confirmed these observations. So, the current data are interesting, even provocative, but ultimately hypothesis generating rather than definitive.”
Also commenting on the study, Steven Nissen, MD, professor of medicine at the Cleveland Clinic, said: “While statins have many established benefits, their role in preventing COVID-19 complications is very speculative. Like all observational studies, the current study must be viewed as hypothesis generating, not definitive evidence of benefit. There are many potential confounders. I’m skeptical.”
The authors of this study received no specific funding for this work and report no competing interests. Dr. Harrington was AHA president when the COVID registry was created and he is still a member of the AHA board, which has oversight over the project.
Among patients hospitalized for COVID-19, those who had been taking statins had a substantially lower risk of death in a new large observational study.
Results showed that use of statins prior to admission was linked to a greater than 40% reduction in mortality and a greater than 25% reduction in risk of developing a severe outcome.
The findings come an analysis of data from the American Heart Association’s COVID-19 Cardiovascular Disease Registry on more than 10,000 patients hospitalized with COVID-19 at 104 hospitals across the United States published in PLoS One.
While several other studies have suggested benefits of statins in COVID-19, this is by far the largest study so far on this topic.
“I would say this is the most reliable study on statins in COVID-19 to date, with the results adjusted for many confounders, including socioeconomic factors and insurance type,” lead author Lori B. Daniels, MD, told this news organization. “However, it still an observational study and therefore falls short of a randomized study. But I would think a randomized study of statins in COVID-19 is probably not feasible, so this study provides excellent data at an observational level.”
After propensity matching for cardiovascular disease, results showed that most of the benefit of statins occurred in patients with known cardiovascular disease.
“While most patients taking statins will have cardiovascular disease, there are also many patients who take these drugs who don’t have heart disease but do have cardiovascular risk factors, such as those with raised cholesterol, or a family history of cardiovascular disease. For [such patients], the effect of statins was also in the same direction but it was not significant. This doesn’t exclude an effect,” noted Dr. Daniels, who is professor of medicine and director of cardiovascular intensive care at the University of California, San Diego.
“We are not saying that everyone should rush out and take a statin if they do not have risk factors for cardiovascular in order to lower their risk of dying from COVID. But if individuals do have an indication for a statin and are not taking one of these dugs this is another good reason to start taking them now,” she added.
The investigators embarked on the study because, although previous observational studies have found that statins may reduce the severity of COVID-19 infection, these studies have been limited in size with mostly single-center or regional studies, and some results have been conflicting. They therefore conducted the current, much larger analysis, in the AHA COVID-19 CVD Registry which systematically collected hospitalized patient–level data in a broad and diverse hospital and patient population across the United States.
For the analysis, the researchers analyzed data from 10,541 patients hospitalized with COVID-19 through September 2020 at 104 U.S. hospitals enrolled in the AHA registry to evaluate the associations between statin use and outcomes.
Most patients (71%) had either cardiovascular disease, hypertension, or both. Prior to admission, 42% of subjects used statins, with 7% being on statins alone and 35% on statins plus antihypertensives. Death (or discharge to hospice) occurred in 2,212 subjects (21%).
Results showed that outpatient use of statins, either alone or with antihypertensives, was associated with a 41% reduced risk of death (odds ratio, 0.59; 95% confidence interval, 0.50-0.69), after adjusting for demographic characteristics, underlying conditions, insurance status, hospital site, and concurrent medications. Statin use was also associated with a roughly 25% lower adjusted odds of developing severe disease.
Noting that patients on statins are also likely to be on antihypertensive medication, the researchers found that the statin benefit on mortality was seen in both patients taking a statin alone (OR, 0.54) and in those taking statins with an antihypertensive medication (OR, 0.60).
Use of antihypertensive drugs was associated with a smaller, albeit still substantial, 27% lower odds of death (OR, 0.73; 95% CI, 0.62-0.87).
In propensity-matched analyses, use of statins and/or antihypertensives was tied to a 32% reduced risk of death among those with a history of CVD and/or hypertension (OR, 0.68; 95% CI, 0.58-0.81). An observed 16% reduction in odds of death with statins and/or antihypertensive drugs among those without cardiovascular disease and/or hypertension was not statistically significant (OR, 0.84; 95% CI, 0.58-1.22).
Stabilizing the underlying disease
The researchers pointed out that the results of the propensity matching analysis are consistent with the hypothesis that the major benefit of these medications accrues from treating and/or stabilizing underlying disease.
“Although it is well known that statins improve long-term outcomes among patients with or at elevated risk for cardiovascular disease, the association with a large short-term benefit which accrues in the setting of hospitalization for COVID-19 is a new and intriguing finding,” they said.
They cited several “plausible mechanisms whereby statins could directly mitigate outcomes in COVID-19 beyond treating underlying disease conditions,” including anti-inflammatory effects and a direct inhibitory effect on the SARS-CoV-2 virus.
Dr. Daniels elaborated more on the potential mechanism at play in an interview: “I think what is happening is that the statin is stabilizing the coronary disease so patients are less likely to die from MI or stroke, and this gives them more time and strength to recover from COVID-19.”
She added: “Statins may also have some direct anti-COVID effects such as an anti-inflammatory actions, but I would guess that this is probably not the primary effect behind what we’re seeing here.”
‘Important clinical implications’
The authors say their findings have “important clinical implications.”
They noted that early in the pandemic there was speculation that certain medications, including statins, and the ACE inhibitor/angiotensin receptor blocker (ARB) classes of antihypertensives may confer an increased susceptibility to COVID-19 positivity and/or severity.
“Our study reinforces the AHA and others’ recommendations that not only is it safe to remain on these medications, but they may substantially reduce risk of severe COVID-19 and especially death from COVID-19, particularly statins, and particularly among those with associated underlying conditions,” the authors stressed.
Dr. Daniels added that, although statins are very safe drugs, there are always some patients who prefer not to take medication even if indicated, and others who may have borderline indications and decide not to take a statin at present.
“This study may persuade these patients that taking a statin is the right thing to do. It may give those patients on the cusp of thinking about taking one of these drugs a reason to go ahead,” she said.
‘Provocative but not definitive’
Commenting on the study, Robert Harrington, MD, professor of medicine and chair of the department of medicine at Stanford (Calif.) University, said: “These are interesting observational data but as such have all the limitations of nonrandomized comparisons despite the best attempts to adjust for a variety of potential confounders. For example, is this an effect of statins (perhaps through some anti-inflammatory mechanism) or is it more an effect that can be attributed to the patients who are prescribed and taking a statin, compared with those who are not?”
He added: “The primary clinical benefit of statins, based on many large randomized clinical trials, seems to be derived from their LDL lowering effect. Observational studies have suggested potential benefits from anti-inflammatory effects of statins, but the randomized trials have not confirmed these observations. So, the current data are interesting, even provocative, but ultimately hypothesis generating rather than definitive.”
Also commenting on the study, Steven Nissen, MD, professor of medicine at the Cleveland Clinic, said: “While statins have many established benefits, their role in preventing COVID-19 complications is very speculative. Like all observational studies, the current study must be viewed as hypothesis generating, not definitive evidence of benefit. There are many potential confounders. I’m skeptical.”
The authors of this study received no specific funding for this work and report no competing interests. Dr. Harrington was AHA president when the COVID registry was created and he is still a member of the AHA board, which has oversight over the project.
FROM PLOS ONE
Five risk factors may predict thrombus on LAA occlusion implants
, itself an important risk factor for cerebrovascular events, in patients with implants for left atrial appendage occlusion (LAAO), new research suggests.
The identified independent predictors of DRT in the largest dedicated multicenter LAAO-DRT registry to date were presence of a hypercoagulability disorder, pericardial effusion, renal insufficiency, an implantation depth greater than 10 mm from the pulmonary ridge, and presence of nonparoxysmal atrial fibrillation (AFib).
“Unfortunately, most of them are not modifiable, like hypercoaguable disorders or nonparoxysmal atrial fibrillation. But we can avoid deep implants because that’s been associated with creating a little bit of a crater or valley where the clot can form,” senior author Mohamad Alkhouli, MD, said in an interview.
But most important, and “really why we wanted to do this,” he said, is that “we want to give the patient a realistic prediction of adverse events for this procedure.”
LAAO has taken off in recent years for preventing thrombus formation and stroke in patients with AFib. Predicting DRT is a priority for the LAAO field, the authors note, especially given its expansion to younger, lower-risk patients and the increasing procedural volumes.
“This is a problem, DRT, that’s been discussed a lot because this is a preventative procedure,” observed Dr. Alkhouli, professor of medicine at Mayo Medical School, Rochester, Minn.
“The actual stroke risk every year – even if you don’t take any blood thinner and you have a CHADsVASc score of 9, the highest – is 11%. So if the chance of having thrombus is close, then that’s not a good tradeoff.”
Previous studies have also identified implantation depth and nonparoxysmal AFib as risk factors for DRT. But most of them have been small, he noted, with one of the largest reporting 65 DRTs in four prospective trials.
To cast a wider net, the investigators, led by Trevor Simard, MD, also from the Mayo Clinic, invited more than 50 international sites to contribute data to the registry. Of these, 37 centers reported on 237 DRTs and 474 device-matched control subjects from the same site.
Three-fourths of patients received a first-generation Watchman or a FLEX device (Boston Scientific).
Medical regimens were similar between the DRT and control cohorts at discharge after LAA closure. Most patients were managed with single (36.3%) or dual antiplatelet therapy (26.2%) at the time of DRT diagnosis.
As reported July 19 in the Journal of the American College of Cardiology, the timing of DRT development varied widely, with 24.9% appearing in the first 45 days, 38.8% between days 45 and 180, 16.0% between days 180 to 365, and 20.3% beyond 1 year. At last known follow-up, one-quarter of patients had DRT.
The odds ratios for DRT associated with the five identified risk factors were:
- 17.50 (95% confidence interval, 3.39-90.45) for hypercoagulability disorder
- 13.45 (95% CI, 1.46-123.52) for pericardial effusion
- 4.02 (95% CI, 1.22-13.25) for renal insufficiency
- 2.41 (95% CI, 1.57-3.69) for implantation depth >10 mm
- 1.90 (95% CI, 1.22-2.97) for nonparoxysmal AFib
The risk for a composite of death, ischemic stroke, and systemic embolization was twofold higher in the DRT cohort than in the control cohort (29.5% vs. 14.4%; hazard ratio, 2.37; 95% CI, 1.58-3.56) and driven by a higher rate of ischemic stroke (16.9% vs. 3.6%; HR, 3.49; 95% CI, 1.35-9.00).
The incidence of bleeding and intracerebral hemorrhage, however, was similar in the DRT and control cohorts.
One of the surprises of the study was that medications prescribed in the short term after LAA closure were not associated with DRT, Dr. Alkhouli said. A previous meta-analysis of 66 studies by the investigators also found that antithrombotic regimen did not explain the heterogeneity of DRT formation.
“I think we’ll have to take that with a grain of salt, because there’s so many variations in the practice, and this is observational data. But that, in my mind, brings up a mechanistic issue,” he said.
It’s often recommended “that we should put patients on blood thinners for 3 months or 6 weeks, or whatever it is, to decrease the chance of thrombus, assuming the patients will have a normal endothelialization of the device,” Dr. Alkhouli said.
“Well, we know that’s not the reality,” he continued. “We know many patients don’t endothelialize, and, even if some patients do, there may be some endothelial damage. So I think the whole mechanism of prescribing a little bit of a blood thinner to avoid that risk may be missing the point. It’s a bit more complex than that, evidenced also by the fact that three-fourths of all the DRTs happened after 45 days, when patients are typically not taking a blood thinner.”
Based on the five independent risk factors, the investigators created a clinical DRT risk score that assigned 1 point for renal insufficiency, implantation depth greater than 10 mm from the pulmonary ridge, and nonparoxysmal AFib; and 4 points for iatrogenic pericardial effusion and for hypercoagulability disorder. Low risk was categorized as 1 point and high risk as 2 or more points.
The presence of one major risk factor or two minor risk factors, for example, led to a 2.1-fold increased risk for DRT, compared with those with no DRT risk factors.
The risk score will require validation in a prospective cohort but is “a step forward in addressing DRT” and triaging patients, Dr. Alkhouli said. The findings highlight the need to avoid deep device implantation and the importance of shared decision-making with patients, especially with those at high risk.
“And third, which is most important, I think, in my mind, is that it tells us not to put a blind eye to this topic and just say with improved devices it will go away,” he said. “That’s a bit unrealistic.”
In an accompanying editorial, Oussama Wazni, MD, Walid Saliba, MD, and Ayman A. Hussein, MD, all from the Cleveland Clinic, write that “the study sheds light on this yet unresolved issue, and the observations may help with risk stratification and optimization of procedural techniques.”
Whereas many of the nonmodifiable risk factors are helpful in shared decision-making decisions, they continue, “knowledge of these risk factors may not preclude implantation in patients who are otherwise at risk of both stroke off anticoagulation and bleeding on anticoagulation.”
Dr. Wazni and colleagues acknowledge that the small number of events in the study limits statistical power for definitive conclusions and say that further studies are needed to clarify the natural history of DRTs and their management, resolution, and impact on cardiovascular events.
Practitioners should also continue to cautiously assess for LAAO clinical indications for implant, according to the editorialists, who point out that the regulatory approval language in the United States was “flexible and nonspecific.”
“As the field grows wider, enhancing LAAO safety with optimal design, implantation, and periprocedural management is critically important, yet the main focus should remain on optimal patient selection for the purpose of achieving safe and successful outcomes,” the editorialists conclude.
Dr. Alkhouli has served as a consultant for Boston Scientific. Coauthor disclosures are listed in the paper. Dr. Wazni and Dr. Hussein have received research grant support from Boston Scientific. Dr. Wazni and Dr. Saliba have been consultants for Boston Scientific.
A version of this article first appeared on Medscape.com.
, itself an important risk factor for cerebrovascular events, in patients with implants for left atrial appendage occlusion (LAAO), new research suggests.
The identified independent predictors of DRT in the largest dedicated multicenter LAAO-DRT registry to date were presence of a hypercoagulability disorder, pericardial effusion, renal insufficiency, an implantation depth greater than 10 mm from the pulmonary ridge, and presence of nonparoxysmal atrial fibrillation (AFib).
“Unfortunately, most of them are not modifiable, like hypercoaguable disorders or nonparoxysmal atrial fibrillation. But we can avoid deep implants because that’s been associated with creating a little bit of a crater or valley where the clot can form,” senior author Mohamad Alkhouli, MD, said in an interview.
But most important, and “really why we wanted to do this,” he said, is that “we want to give the patient a realistic prediction of adverse events for this procedure.”
LAAO has taken off in recent years for preventing thrombus formation and stroke in patients with AFib. Predicting DRT is a priority for the LAAO field, the authors note, especially given its expansion to younger, lower-risk patients and the increasing procedural volumes.
“This is a problem, DRT, that’s been discussed a lot because this is a preventative procedure,” observed Dr. Alkhouli, professor of medicine at Mayo Medical School, Rochester, Minn.
“The actual stroke risk every year – even if you don’t take any blood thinner and you have a CHADsVASc score of 9, the highest – is 11%. So if the chance of having thrombus is close, then that’s not a good tradeoff.”
Previous studies have also identified implantation depth and nonparoxysmal AFib as risk factors for DRT. But most of them have been small, he noted, with one of the largest reporting 65 DRTs in four prospective trials.
To cast a wider net, the investigators, led by Trevor Simard, MD, also from the Mayo Clinic, invited more than 50 international sites to contribute data to the registry. Of these, 37 centers reported on 237 DRTs and 474 device-matched control subjects from the same site.
Three-fourths of patients received a first-generation Watchman or a FLEX device (Boston Scientific).
Medical regimens were similar between the DRT and control cohorts at discharge after LAA closure. Most patients were managed with single (36.3%) or dual antiplatelet therapy (26.2%) at the time of DRT diagnosis.
As reported July 19 in the Journal of the American College of Cardiology, the timing of DRT development varied widely, with 24.9% appearing in the first 45 days, 38.8% between days 45 and 180, 16.0% between days 180 to 365, and 20.3% beyond 1 year. At last known follow-up, one-quarter of patients had DRT.
The odds ratios for DRT associated with the five identified risk factors were:
- 17.50 (95% confidence interval, 3.39-90.45) for hypercoagulability disorder
- 13.45 (95% CI, 1.46-123.52) for pericardial effusion
- 4.02 (95% CI, 1.22-13.25) for renal insufficiency
- 2.41 (95% CI, 1.57-3.69) for implantation depth >10 mm
- 1.90 (95% CI, 1.22-2.97) for nonparoxysmal AFib
The risk for a composite of death, ischemic stroke, and systemic embolization was twofold higher in the DRT cohort than in the control cohort (29.5% vs. 14.4%; hazard ratio, 2.37; 95% CI, 1.58-3.56) and driven by a higher rate of ischemic stroke (16.9% vs. 3.6%; HR, 3.49; 95% CI, 1.35-9.00).
The incidence of bleeding and intracerebral hemorrhage, however, was similar in the DRT and control cohorts.
One of the surprises of the study was that medications prescribed in the short term after LAA closure were not associated with DRT, Dr. Alkhouli said. A previous meta-analysis of 66 studies by the investigators also found that antithrombotic regimen did not explain the heterogeneity of DRT formation.
“I think we’ll have to take that with a grain of salt, because there’s so many variations in the practice, and this is observational data. But that, in my mind, brings up a mechanistic issue,” he said.
It’s often recommended “that we should put patients on blood thinners for 3 months or 6 weeks, or whatever it is, to decrease the chance of thrombus, assuming the patients will have a normal endothelialization of the device,” Dr. Alkhouli said.
“Well, we know that’s not the reality,” he continued. “We know many patients don’t endothelialize, and, even if some patients do, there may be some endothelial damage. So I think the whole mechanism of prescribing a little bit of a blood thinner to avoid that risk may be missing the point. It’s a bit more complex than that, evidenced also by the fact that three-fourths of all the DRTs happened after 45 days, when patients are typically not taking a blood thinner.”
Based on the five independent risk factors, the investigators created a clinical DRT risk score that assigned 1 point for renal insufficiency, implantation depth greater than 10 mm from the pulmonary ridge, and nonparoxysmal AFib; and 4 points for iatrogenic pericardial effusion and for hypercoagulability disorder. Low risk was categorized as 1 point and high risk as 2 or more points.
The presence of one major risk factor or two minor risk factors, for example, led to a 2.1-fold increased risk for DRT, compared with those with no DRT risk factors.
The risk score will require validation in a prospective cohort but is “a step forward in addressing DRT” and triaging patients, Dr. Alkhouli said. The findings highlight the need to avoid deep device implantation and the importance of shared decision-making with patients, especially with those at high risk.
“And third, which is most important, I think, in my mind, is that it tells us not to put a blind eye to this topic and just say with improved devices it will go away,” he said. “That’s a bit unrealistic.”
In an accompanying editorial, Oussama Wazni, MD, Walid Saliba, MD, and Ayman A. Hussein, MD, all from the Cleveland Clinic, write that “the study sheds light on this yet unresolved issue, and the observations may help with risk stratification and optimization of procedural techniques.”
Whereas many of the nonmodifiable risk factors are helpful in shared decision-making decisions, they continue, “knowledge of these risk factors may not preclude implantation in patients who are otherwise at risk of both stroke off anticoagulation and bleeding on anticoagulation.”
Dr. Wazni and colleagues acknowledge that the small number of events in the study limits statistical power for definitive conclusions and say that further studies are needed to clarify the natural history of DRTs and their management, resolution, and impact on cardiovascular events.
Practitioners should also continue to cautiously assess for LAAO clinical indications for implant, according to the editorialists, who point out that the regulatory approval language in the United States was “flexible and nonspecific.”
“As the field grows wider, enhancing LAAO safety with optimal design, implantation, and periprocedural management is critically important, yet the main focus should remain on optimal patient selection for the purpose of achieving safe and successful outcomes,” the editorialists conclude.
Dr. Alkhouli has served as a consultant for Boston Scientific. Coauthor disclosures are listed in the paper. Dr. Wazni and Dr. Hussein have received research grant support from Boston Scientific. Dr. Wazni and Dr. Saliba have been consultants for Boston Scientific.
A version of this article first appeared on Medscape.com.
, itself an important risk factor for cerebrovascular events, in patients with implants for left atrial appendage occlusion (LAAO), new research suggests.
The identified independent predictors of DRT in the largest dedicated multicenter LAAO-DRT registry to date were presence of a hypercoagulability disorder, pericardial effusion, renal insufficiency, an implantation depth greater than 10 mm from the pulmonary ridge, and presence of nonparoxysmal atrial fibrillation (AFib).
“Unfortunately, most of them are not modifiable, like hypercoaguable disorders or nonparoxysmal atrial fibrillation. But we can avoid deep implants because that’s been associated with creating a little bit of a crater or valley where the clot can form,” senior author Mohamad Alkhouli, MD, said in an interview.
But most important, and “really why we wanted to do this,” he said, is that “we want to give the patient a realistic prediction of adverse events for this procedure.”
LAAO has taken off in recent years for preventing thrombus formation and stroke in patients with AFib. Predicting DRT is a priority for the LAAO field, the authors note, especially given its expansion to younger, lower-risk patients and the increasing procedural volumes.
“This is a problem, DRT, that’s been discussed a lot because this is a preventative procedure,” observed Dr. Alkhouli, professor of medicine at Mayo Medical School, Rochester, Minn.
“The actual stroke risk every year – even if you don’t take any blood thinner and you have a CHADsVASc score of 9, the highest – is 11%. So if the chance of having thrombus is close, then that’s not a good tradeoff.”
Previous studies have also identified implantation depth and nonparoxysmal AFib as risk factors for DRT. But most of them have been small, he noted, with one of the largest reporting 65 DRTs in four prospective trials.
To cast a wider net, the investigators, led by Trevor Simard, MD, also from the Mayo Clinic, invited more than 50 international sites to contribute data to the registry. Of these, 37 centers reported on 237 DRTs and 474 device-matched control subjects from the same site.
Three-fourths of patients received a first-generation Watchman or a FLEX device (Boston Scientific).
Medical regimens were similar between the DRT and control cohorts at discharge after LAA closure. Most patients were managed with single (36.3%) or dual antiplatelet therapy (26.2%) at the time of DRT diagnosis.
As reported July 19 in the Journal of the American College of Cardiology, the timing of DRT development varied widely, with 24.9% appearing in the first 45 days, 38.8% between days 45 and 180, 16.0% between days 180 to 365, and 20.3% beyond 1 year. At last known follow-up, one-quarter of patients had DRT.
The odds ratios for DRT associated with the five identified risk factors were:
- 17.50 (95% confidence interval, 3.39-90.45) for hypercoagulability disorder
- 13.45 (95% CI, 1.46-123.52) for pericardial effusion
- 4.02 (95% CI, 1.22-13.25) for renal insufficiency
- 2.41 (95% CI, 1.57-3.69) for implantation depth >10 mm
- 1.90 (95% CI, 1.22-2.97) for nonparoxysmal AFib
The risk for a composite of death, ischemic stroke, and systemic embolization was twofold higher in the DRT cohort than in the control cohort (29.5% vs. 14.4%; hazard ratio, 2.37; 95% CI, 1.58-3.56) and driven by a higher rate of ischemic stroke (16.9% vs. 3.6%; HR, 3.49; 95% CI, 1.35-9.00).
The incidence of bleeding and intracerebral hemorrhage, however, was similar in the DRT and control cohorts.
One of the surprises of the study was that medications prescribed in the short term after LAA closure were not associated with DRT, Dr. Alkhouli said. A previous meta-analysis of 66 studies by the investigators also found that antithrombotic regimen did not explain the heterogeneity of DRT formation.
“I think we’ll have to take that with a grain of salt, because there’s so many variations in the practice, and this is observational data. But that, in my mind, brings up a mechanistic issue,” he said.
It’s often recommended “that we should put patients on blood thinners for 3 months or 6 weeks, or whatever it is, to decrease the chance of thrombus, assuming the patients will have a normal endothelialization of the device,” Dr. Alkhouli said.
“Well, we know that’s not the reality,” he continued. “We know many patients don’t endothelialize, and, even if some patients do, there may be some endothelial damage. So I think the whole mechanism of prescribing a little bit of a blood thinner to avoid that risk may be missing the point. It’s a bit more complex than that, evidenced also by the fact that three-fourths of all the DRTs happened after 45 days, when patients are typically not taking a blood thinner.”
Based on the five independent risk factors, the investigators created a clinical DRT risk score that assigned 1 point for renal insufficiency, implantation depth greater than 10 mm from the pulmonary ridge, and nonparoxysmal AFib; and 4 points for iatrogenic pericardial effusion and for hypercoagulability disorder. Low risk was categorized as 1 point and high risk as 2 or more points.
The presence of one major risk factor or two minor risk factors, for example, led to a 2.1-fold increased risk for DRT, compared with those with no DRT risk factors.
The risk score will require validation in a prospective cohort but is “a step forward in addressing DRT” and triaging patients, Dr. Alkhouli said. The findings highlight the need to avoid deep device implantation and the importance of shared decision-making with patients, especially with those at high risk.
“And third, which is most important, I think, in my mind, is that it tells us not to put a blind eye to this topic and just say with improved devices it will go away,” he said. “That’s a bit unrealistic.”
In an accompanying editorial, Oussama Wazni, MD, Walid Saliba, MD, and Ayman A. Hussein, MD, all from the Cleveland Clinic, write that “the study sheds light on this yet unresolved issue, and the observations may help with risk stratification and optimization of procedural techniques.”
Whereas many of the nonmodifiable risk factors are helpful in shared decision-making decisions, they continue, “knowledge of these risk factors may not preclude implantation in patients who are otherwise at risk of both stroke off anticoagulation and bleeding on anticoagulation.”
Dr. Wazni and colleagues acknowledge that the small number of events in the study limits statistical power for definitive conclusions and say that further studies are needed to clarify the natural history of DRTs and their management, resolution, and impact on cardiovascular events.
Practitioners should also continue to cautiously assess for LAAO clinical indications for implant, according to the editorialists, who point out that the regulatory approval language in the United States was “flexible and nonspecific.”
“As the field grows wider, enhancing LAAO safety with optimal design, implantation, and periprocedural management is critically important, yet the main focus should remain on optimal patient selection for the purpose of achieving safe and successful outcomes,” the editorialists conclude.
Dr. Alkhouli has served as a consultant for Boston Scientific. Coauthor disclosures are listed in the paper. Dr. Wazni and Dr. Hussein have received research grant support from Boston Scientific. Dr. Wazni and Dr. Saliba have been consultants for Boston Scientific.
A version of this article first appeared on Medscape.com.