User login
Cardiology News is an independent news source that provides cardiologists with timely and relevant news and commentary about clinical developments and the impact of health care policy on cardiology and the cardiologist's practice. Cardiology News Digital Network is the online destination and multimedia properties of Cardiology News, the independent news publication for cardiologists. Cardiology news is the leading source of news and commentary about clinical developments in cardiology as well as health care policy and regulations that affect the cardiologist's practice. Cardiology News Digital Network is owned by Frontline Medical Communications.
Skin manifestations are emerging in the coronavirus pandemic
Dermatologists there were pulled from their usual duty to help with the pandemic and looked at what was going on with the skin in 148 COVID-19 inpatients. They excluded 60 who had started new drugs within 15 days to rule out acute drug reactions, then reported what they saw (J Eur Acad Dermatol Venereol. 2020 Mar 26. doi: 10.1111/jdv.16387).
Of the 88 COVID-19 patients, 20.5% developed skin manifestations. Eight of the 18 (44%) had skin eruptions at symptom onset, and the rest after hospitalization. Fourteen (78%) had red rashes, three had widespread urticaria, and one had chickenpox-like vesicles. The most commonly affected area was the trunk. Itching was mild or absent, and lesions usually healed up in a few days. Most importantly, skin manifestations did not correlate with disease severity.
These skin manifestations “are similar to cutaneous involvement occurring during common viral infections,” said the author of the report, Sebastiano Recalcati, MD, a dermatologist at Alessandro Manzoni Hospital.
COVID-19 skin manifestations can cloud the diagnosis, according to the authors of another report from Thailand, where the first case of COVID-19 outside of China was reported.
They described a case of a COVID-19 infection in a Bangkok hospital that masqueraded as dengue fever. A person there presented with only a skin rash, petechiae, and a low platelet count, and was diagnosed with Dengue because that’s exactly what it looked like, the authors wrote (J Am Acad Dermatol. 2020 Mar 22. pii: S0190-9622[20]30454-0. doi: 10.1016/j.jaad.2020.03.036).
The correct diagnosis, COVID-19, was made at a tertiary care center after the patient was admitted with respiratory problems.
“There is a possibility that a COVID-19 patient might initially present with a skin rash that can be misdiagnosed as another common disease. ... The practitioner should recognize the possibility that the patient might have only a skin rash” at first, said the lead author of that report, Beuy Joob, PhD, of the Sanitation1 Medical Academic Center, Bangkok, and a coauthor.
There are similar reports in the United States, too. “Many have wondered if COVID-19 presents with any particular skin changes. The answer is yes,” said Randy Jacobs, MD, an assistant clinical professor of dermatology at the University of California, Riverside, who also has a private practice in southern California.
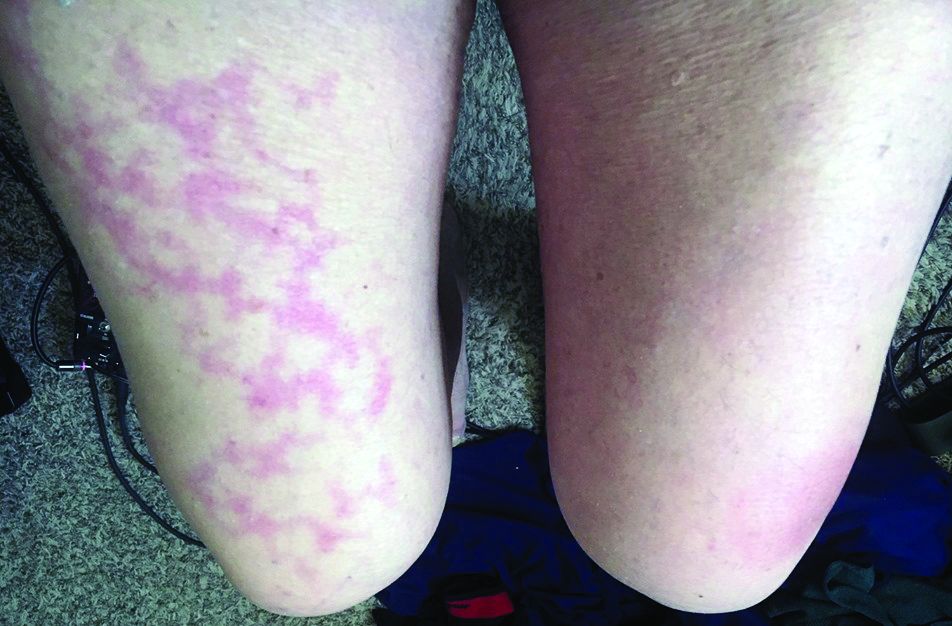
“COVID-19 can feature signs of small blood vessel occlusion. These can be petechiae or tiny bruises, and transient livedoid eruptions,” he said in an interview.
Dr. Jacobs had a 67-year-old patient who presented with a low fever, nasal congestion, postnasal drip, and a wet cough but no shortness of breath. It looked like a common cold. But a week later, the man had a nonpruritic blanching livedoid vascular eruption on his right anterior thigh, and blood in his urine, and he felt weak. The vascular eruption and bloody urine resolved in 24 hours, but the COVID-19 test came back positive and his cough became dry and hacking, and the weakness persisted. He’s in a hospital now and on oxygen, but not ventilated so far.
“Another dermatologist friend of mine also reported a similar transient COVID-19 unilateral livedoid eruption,” Dr. Jacobs said.
It suggests vaso-occlusion. Whether it’s neurogenic, microthrombotic, or immune complex mediated is unknown, but it’s “a skin finding that can help clinicians as they work up their patients with COVID-19 symptoms,” he noted.
Dr. Jacobs and the authors of the studies had no disclosures.
Dermatologists there were pulled from their usual duty to help with the pandemic and looked at what was going on with the skin in 148 COVID-19 inpatients. They excluded 60 who had started new drugs within 15 days to rule out acute drug reactions, then reported what they saw (J Eur Acad Dermatol Venereol. 2020 Mar 26. doi: 10.1111/jdv.16387).
Of the 88 COVID-19 patients, 20.5% developed skin manifestations. Eight of the 18 (44%) had skin eruptions at symptom onset, and the rest after hospitalization. Fourteen (78%) had red rashes, three had widespread urticaria, and one had chickenpox-like vesicles. The most commonly affected area was the trunk. Itching was mild or absent, and lesions usually healed up in a few days. Most importantly, skin manifestations did not correlate with disease severity.
These skin manifestations “are similar to cutaneous involvement occurring during common viral infections,” said the author of the report, Sebastiano Recalcati, MD, a dermatologist at Alessandro Manzoni Hospital.
COVID-19 skin manifestations can cloud the diagnosis, according to the authors of another report from Thailand, where the first case of COVID-19 outside of China was reported.
They described a case of a COVID-19 infection in a Bangkok hospital that masqueraded as dengue fever. A person there presented with only a skin rash, petechiae, and a low platelet count, and was diagnosed with Dengue because that’s exactly what it looked like, the authors wrote (J Am Acad Dermatol. 2020 Mar 22. pii: S0190-9622[20]30454-0. doi: 10.1016/j.jaad.2020.03.036).
The correct diagnosis, COVID-19, was made at a tertiary care center after the patient was admitted with respiratory problems.
“There is a possibility that a COVID-19 patient might initially present with a skin rash that can be misdiagnosed as another common disease. ... The practitioner should recognize the possibility that the patient might have only a skin rash” at first, said the lead author of that report, Beuy Joob, PhD, of the Sanitation1 Medical Academic Center, Bangkok, and a coauthor.
There are similar reports in the United States, too. “Many have wondered if COVID-19 presents with any particular skin changes. The answer is yes,” said Randy Jacobs, MD, an assistant clinical professor of dermatology at the University of California, Riverside, who also has a private practice in southern California.
“COVID-19 can feature signs of small blood vessel occlusion. These can be petechiae or tiny bruises, and transient livedoid eruptions,” he said in an interview.
Dr. Jacobs had a 67-year-old patient who presented with a low fever, nasal congestion, postnasal drip, and a wet cough but no shortness of breath. It looked like a common cold. But a week later, the man had a nonpruritic blanching livedoid vascular eruption on his right anterior thigh, and blood in his urine, and he felt weak. The vascular eruption and bloody urine resolved in 24 hours, but the COVID-19 test came back positive and his cough became dry and hacking, and the weakness persisted. He’s in a hospital now and on oxygen, but not ventilated so far.
“Another dermatologist friend of mine also reported a similar transient COVID-19 unilateral livedoid eruption,” Dr. Jacobs said.
It suggests vaso-occlusion. Whether it’s neurogenic, microthrombotic, or immune complex mediated is unknown, but it’s “a skin finding that can help clinicians as they work up their patients with COVID-19 symptoms,” he noted.
Dr. Jacobs and the authors of the studies had no disclosures.
Dermatologists there were pulled from their usual duty to help with the pandemic and looked at what was going on with the skin in 148 COVID-19 inpatients. They excluded 60 who had started new drugs within 15 days to rule out acute drug reactions, then reported what they saw (J Eur Acad Dermatol Venereol. 2020 Mar 26. doi: 10.1111/jdv.16387).
Of the 88 COVID-19 patients, 20.5% developed skin manifestations. Eight of the 18 (44%) had skin eruptions at symptom onset, and the rest after hospitalization. Fourteen (78%) had red rashes, three had widespread urticaria, and one had chickenpox-like vesicles. The most commonly affected area was the trunk. Itching was mild or absent, and lesions usually healed up in a few days. Most importantly, skin manifestations did not correlate with disease severity.
These skin manifestations “are similar to cutaneous involvement occurring during common viral infections,” said the author of the report, Sebastiano Recalcati, MD, a dermatologist at Alessandro Manzoni Hospital.
COVID-19 skin manifestations can cloud the diagnosis, according to the authors of another report from Thailand, where the first case of COVID-19 outside of China was reported.
They described a case of a COVID-19 infection in a Bangkok hospital that masqueraded as dengue fever. A person there presented with only a skin rash, petechiae, and a low platelet count, and was diagnosed with Dengue because that’s exactly what it looked like, the authors wrote (J Am Acad Dermatol. 2020 Mar 22. pii: S0190-9622[20]30454-0. doi: 10.1016/j.jaad.2020.03.036).
The correct diagnosis, COVID-19, was made at a tertiary care center after the patient was admitted with respiratory problems.
“There is a possibility that a COVID-19 patient might initially present with a skin rash that can be misdiagnosed as another common disease. ... The practitioner should recognize the possibility that the patient might have only a skin rash” at first, said the lead author of that report, Beuy Joob, PhD, of the Sanitation1 Medical Academic Center, Bangkok, and a coauthor.
There are similar reports in the United States, too. “Many have wondered if COVID-19 presents with any particular skin changes. The answer is yes,” said Randy Jacobs, MD, an assistant clinical professor of dermatology at the University of California, Riverside, who also has a private practice in southern California.
“COVID-19 can feature signs of small blood vessel occlusion. These can be petechiae or tiny bruises, and transient livedoid eruptions,” he said in an interview.
Dr. Jacobs had a 67-year-old patient who presented with a low fever, nasal congestion, postnasal drip, and a wet cough but no shortness of breath. It looked like a common cold. But a week later, the man had a nonpruritic blanching livedoid vascular eruption on his right anterior thigh, and blood in his urine, and he felt weak. The vascular eruption and bloody urine resolved in 24 hours, but the COVID-19 test came back positive and his cough became dry and hacking, and the weakness persisted. He’s in a hospital now and on oxygen, but not ventilated so far.
“Another dermatologist friend of mine also reported a similar transient COVID-19 unilateral livedoid eruption,” Dr. Jacobs said.
It suggests vaso-occlusion. Whether it’s neurogenic, microthrombotic, or immune complex mediated is unknown, but it’s “a skin finding that can help clinicians as they work up their patients with COVID-19 symptoms,” he noted.
Dr. Jacobs and the authors of the studies had no disclosures.
VOYAGER PAD: Clopidogrel adds no benefit to rivaroxaban plus aspirin after PAD interventions
The VOYAGER PAD results from more than 6,500 patients created the biggest evidence base by far ever collected from patients with symptomatic peripheral artery disease (PAD) who underwent a vascular intervention, and showed that the combination of twice-daily rivaroxaban and once-daily aspirin was safe and more effective than aspirin alone for reducing future thrombotic and ischemic events.
Following that report on March 28, a prespecified subgroup analysis presented the next day showed that adding clopidogrel to this two-drug combination produced no added efficacy but caused additional bleeding episodes, suggesting that the common practice of using clopidogrel plus aspirin in these patients, especially those who receive a stent in a peripheral artery, should either fall by the wayside or be used very briefly.
“In the absence of clear benefit, clopidogrel exposure along with aspirin and rivaroxaban should be minimized or avoided to reduce this risk,” William R. Hiatt, MD, said at the joint scientific sessions of the American College of Cardiology and the World Heart Federation. The meeting was conducted online after its cancellation because of the COVID-19 pandemic. But he also cautioned that “we did not control for clopidogrel use, and so the patients who received clopidogrel look different [from patients who did not receive clopidogrel]. We must be cautious in interpreting differences between patients on or off clopidogrel,” warned Dr. Hiatt, a lead investigator for VOYAGER PAD, professor for cardiovascular research at the University of Colorado at Denver in Aurora and president of the affiliated Colorado Prevention Center.
In addition to this substantial caveat, the finding that clopidogrel appeared to add no extra benefit to the rivaroxaban/aspirin regimen “contradicts some dogmas that have been in the field for decades,” Dr. Hiatt said. Use of dual-antiplatelet therapy (DAPT), in this setting usually aspirin and clopidogrel, in patients who have just undergone lower-extremity revascularization is “current dogma,” even though it is not based on any direct evidence for efficacy, but instead came on the scene as “an extrapolation from the coronary artery literature, where it does have some benefit, particularly after percutaneous coronary intervention,” he explained.
The only reported study results to examine use of DAPT in patients who underwent peripheral artery revascularization focused entirely on patients who had a surgical procedure and showed no added benefit from DAPT over aspirin only in a multicenter, randomized trial with 851 patients (J Vasc Surg. 2010 Oct;52[4]:825-33), Dr. Hiatt noted. In VOYAGER PAD, two-thirds of all patients underwent an endovascular, not surgical, peripheral intervention, and among those treated with clopidogrel, 91% had endovascular treatment.
“We’re not saying don’t use DAPT, but patients on three drugs are at higher bleeding risk than patients on two drugs. I think our data also suggest starting rivaroxaban immediately after a procedure [as was done in VOYAGER PAD], and not waiting to complete a course of DAPT,” Dr. Hiatt said.
Other experts embraced Dr. Hiatt’s take on these findings, while warning that it may take some time for the message to penetrate into practice.
The overall VOYAGER PAD results “are practice changing for vascular interventions; it was by an order of magnitude the largest vascular intervention trial ever conducted,” commented Sahil A. Parikh, MD, a designated discussant, interventional cardiologist, and director of endovascular services at New York–Presbyterian Medical Center. “The data suggest that the value of clopidogrel is questionable, but the added hazard is not questionable” when given to patients on top of rivaroxaban and aspirin. The results “certainly beg the question of whether one should use DAPT at all, and if so, for how long.”
Use of DAPT in patients undergoing peripheral revascularization, especially patients receiving a stent, has been “dogma,” Dr. Parikh agreed. “It’s been pounded into our heads that DAPT is standard care, so it will take some time to penetrate into the practicing community.”
“Could there be patients who could benefit from triple therapy? That’s possible, but it needs testing,” commented Mark A. Creager, MD, professor of medicine and director of the Heart and Vascular Center at Dartmouth-Hitchcock Medical Center in Lebanon, N.H. “We’ve made terrific strides with the results from VOYAGER PAD,” and from the earlier COMPASS trial, which proved the benefit of rivaroxaban and aspirin in patients with stable atherosclerotic vascular disease including many PAD patients (N Engl J Med. 2017 Oct 5;377[14]:1319-30). Use of rivaroxaban and aspirin in PAD patients based on the COMPASS results “is beginning to make an impact, but has a long way to go,” Dr. Creager said in an interview.
In late 2018, the Food and Drug Administration gave rivaroxaban a revised labeling that included an indication for patients with PAD based on the COMPASS findings. The VOYAGER PAD and COMPASS trials are especially noteworthy because “they opened a whole area [of study] in patients with peripheral vascular disease, ” he added.
The prespecified analysis that Dr. Hiatt reported analyzed outcomes among the 51% of patients enrolled in VOYAGER PAD (Vascular Outcomes Study of Acetylsalicylic Acid Along With Rivaroxaban in Endovascular or Surgical Limb Revascularization for Peripheral Artery Disease) who received clopidogrel during follow-up at the discretion of their treating physician and the outcomes among the remainder who did not. The two subgroups showed several statistically significant differences in the prevalence of various comorbidities and in some baseline demographic and clinical metrics, and the analyses that Dr. Hiatt reported did not attempt to correct for these differences. Patients who received clopidogrel had the drug on board for a median of 29 days, and about 58% received it for 30 days or less.
The main finding of his analysis was that “adding clopidogrel did not modify benefit at all” from the perspective of the primary endpoint of VOYAGER PAD, the incidence of a five-item list of adverse events (acute limb ischemia, major amputation for vascular cause, myocardial infarction, ischemic stroke, and cardiovascular death) during a median follow-up of 28 months (N Engl J Med. 2020 Mar 28. doi: 10.1056/NEJMoa2000052), said Dr. Hiatt. Among patients on clopidogrel, those treated with both rivaroxaban and aspirin had a 16.0% incidence of the primary endpoint, compared with an 18.3% rate among patients on aspirin only, for a 15% relative risk reduction, identical to the study’s primary result. Among patients not on clopidogrel, the primary endpoint occurred in 18.7% of patients on rivaroxaban plus aspirin and in 21.5% of those on aspirin only, a 14% relative risk reduction. The analyses also showed that adding clopidogrel appeared to increase the rate of bleeding episodes, particularly the incidence of major bleeds by the criteria of the International Society on Thrombosis and Haemostasis (ISTH), which rose among patients on aspirin alone from 3.3% without clopidogrel treatment to 4.9% with clopidogrel, and in patients on rivaroxaban plus aspirin these major bleeds increased from 5.4% with no clopidogrel to 6.5% with clopidogrel.
An especially revealing further analysis showed that, among those who also received rivaroxaban and aspirin, clopidogrel treatment for more than 30 days led to substantially more bleeding problems, compared with patients who received the drug for 30 days or less. Patients who received clopidogrel for more than 30 days as part of a triple-drug regimen had a 3.0% rate of major ISTH bleeds during 180 days of follow-up, compared with a 0.9% rate for patients in the aspirin-alone group who also received clopidogrel, a 2.1% between-group difference. In contrast, the difference in major ISTH bleeds between the two treatment arms in the subgroup who received clopidogrel for 30 days or less was 0.7%.
“What’s inarguable is that the course of clopidogrel should be as short as possible, probably not more than 30 days unless there is a real extenuating rationale,” commented designated discussant Gregory Piazza, MD, a cardiologist at Brigham and Women’s Hospital in Boston.
VOYAGER PAD was sponsored by Bayer and Janssen, the companies that market rivaroxaban (Xarelto). The institution that Dr. Hiatt leads has received research funding from Bayer and Janssen and from Amgen. Dr. Parikh has been a consultant to Terumo; has received research funding from Shockwave, Surmodics, and Trireme; has worked on trial monitoring for Boston Scientific and Silk Road; and has had other financial relationships with Abbott, Boston Scientific, and Medtronic. Dr. Creager had no disclosures. Dr. Piazza has received research grants from Bayer and Janssen, as well as Bristol-Myers Squibb, Diiachi, EKOS, and Portola, and he has been a consultant to Optum, Pfizer, and Thrombolex.
SOURCE: Hiatt WR et al. ACC 20, Abstract 406-13.
The VOYAGER PAD results from more than 6,500 patients created the biggest evidence base by far ever collected from patients with symptomatic peripheral artery disease (PAD) who underwent a vascular intervention, and showed that the combination of twice-daily rivaroxaban and once-daily aspirin was safe and more effective than aspirin alone for reducing future thrombotic and ischemic events.
Following that report on March 28, a prespecified subgroup analysis presented the next day showed that adding clopidogrel to this two-drug combination produced no added efficacy but caused additional bleeding episodes, suggesting that the common practice of using clopidogrel plus aspirin in these patients, especially those who receive a stent in a peripheral artery, should either fall by the wayside or be used very briefly.
“In the absence of clear benefit, clopidogrel exposure along with aspirin and rivaroxaban should be minimized or avoided to reduce this risk,” William R. Hiatt, MD, said at the joint scientific sessions of the American College of Cardiology and the World Heart Federation. The meeting was conducted online after its cancellation because of the COVID-19 pandemic. But he also cautioned that “we did not control for clopidogrel use, and so the patients who received clopidogrel look different [from patients who did not receive clopidogrel]. We must be cautious in interpreting differences between patients on or off clopidogrel,” warned Dr. Hiatt, a lead investigator for VOYAGER PAD, professor for cardiovascular research at the University of Colorado at Denver in Aurora and president of the affiliated Colorado Prevention Center.
In addition to this substantial caveat, the finding that clopidogrel appeared to add no extra benefit to the rivaroxaban/aspirin regimen “contradicts some dogmas that have been in the field for decades,” Dr. Hiatt said. Use of dual-antiplatelet therapy (DAPT), in this setting usually aspirin and clopidogrel, in patients who have just undergone lower-extremity revascularization is “current dogma,” even though it is not based on any direct evidence for efficacy, but instead came on the scene as “an extrapolation from the coronary artery literature, where it does have some benefit, particularly after percutaneous coronary intervention,” he explained.
The only reported study results to examine use of DAPT in patients who underwent peripheral artery revascularization focused entirely on patients who had a surgical procedure and showed no added benefit from DAPT over aspirin only in a multicenter, randomized trial with 851 patients (J Vasc Surg. 2010 Oct;52[4]:825-33), Dr. Hiatt noted. In VOYAGER PAD, two-thirds of all patients underwent an endovascular, not surgical, peripheral intervention, and among those treated with clopidogrel, 91% had endovascular treatment.
“We’re not saying don’t use DAPT, but patients on three drugs are at higher bleeding risk than patients on two drugs. I think our data also suggest starting rivaroxaban immediately after a procedure [as was done in VOYAGER PAD], and not waiting to complete a course of DAPT,” Dr. Hiatt said.
Other experts embraced Dr. Hiatt’s take on these findings, while warning that it may take some time for the message to penetrate into practice.
The overall VOYAGER PAD results “are practice changing for vascular interventions; it was by an order of magnitude the largest vascular intervention trial ever conducted,” commented Sahil A. Parikh, MD, a designated discussant, interventional cardiologist, and director of endovascular services at New York–Presbyterian Medical Center. “The data suggest that the value of clopidogrel is questionable, but the added hazard is not questionable” when given to patients on top of rivaroxaban and aspirin. The results “certainly beg the question of whether one should use DAPT at all, and if so, for how long.”
Use of DAPT in patients undergoing peripheral revascularization, especially patients receiving a stent, has been “dogma,” Dr. Parikh agreed. “It’s been pounded into our heads that DAPT is standard care, so it will take some time to penetrate into the practicing community.”
“Could there be patients who could benefit from triple therapy? That’s possible, but it needs testing,” commented Mark A. Creager, MD, professor of medicine and director of the Heart and Vascular Center at Dartmouth-Hitchcock Medical Center in Lebanon, N.H. “We’ve made terrific strides with the results from VOYAGER PAD,” and from the earlier COMPASS trial, which proved the benefit of rivaroxaban and aspirin in patients with stable atherosclerotic vascular disease including many PAD patients (N Engl J Med. 2017 Oct 5;377[14]:1319-30). Use of rivaroxaban and aspirin in PAD patients based on the COMPASS results “is beginning to make an impact, but has a long way to go,” Dr. Creager said in an interview.
In late 2018, the Food and Drug Administration gave rivaroxaban a revised labeling that included an indication for patients with PAD based on the COMPASS findings. The VOYAGER PAD and COMPASS trials are especially noteworthy because “they opened a whole area [of study] in patients with peripheral vascular disease, ” he added.
The prespecified analysis that Dr. Hiatt reported analyzed outcomes among the 51% of patients enrolled in VOYAGER PAD (Vascular Outcomes Study of Acetylsalicylic Acid Along With Rivaroxaban in Endovascular or Surgical Limb Revascularization for Peripheral Artery Disease) who received clopidogrel during follow-up at the discretion of their treating physician and the outcomes among the remainder who did not. The two subgroups showed several statistically significant differences in the prevalence of various comorbidities and in some baseline demographic and clinical metrics, and the analyses that Dr. Hiatt reported did not attempt to correct for these differences. Patients who received clopidogrel had the drug on board for a median of 29 days, and about 58% received it for 30 days or less.
The main finding of his analysis was that “adding clopidogrel did not modify benefit at all” from the perspective of the primary endpoint of VOYAGER PAD, the incidence of a five-item list of adverse events (acute limb ischemia, major amputation for vascular cause, myocardial infarction, ischemic stroke, and cardiovascular death) during a median follow-up of 28 months (N Engl J Med. 2020 Mar 28. doi: 10.1056/NEJMoa2000052), said Dr. Hiatt. Among patients on clopidogrel, those treated with both rivaroxaban and aspirin had a 16.0% incidence of the primary endpoint, compared with an 18.3% rate among patients on aspirin only, for a 15% relative risk reduction, identical to the study’s primary result. Among patients not on clopidogrel, the primary endpoint occurred in 18.7% of patients on rivaroxaban plus aspirin and in 21.5% of those on aspirin only, a 14% relative risk reduction. The analyses also showed that adding clopidogrel appeared to increase the rate of bleeding episodes, particularly the incidence of major bleeds by the criteria of the International Society on Thrombosis and Haemostasis (ISTH), which rose among patients on aspirin alone from 3.3% without clopidogrel treatment to 4.9% with clopidogrel, and in patients on rivaroxaban plus aspirin these major bleeds increased from 5.4% with no clopidogrel to 6.5% with clopidogrel.
An especially revealing further analysis showed that, among those who also received rivaroxaban and aspirin, clopidogrel treatment for more than 30 days led to substantially more bleeding problems, compared with patients who received the drug for 30 days or less. Patients who received clopidogrel for more than 30 days as part of a triple-drug regimen had a 3.0% rate of major ISTH bleeds during 180 days of follow-up, compared with a 0.9% rate for patients in the aspirin-alone group who also received clopidogrel, a 2.1% between-group difference. In contrast, the difference in major ISTH bleeds between the two treatment arms in the subgroup who received clopidogrel for 30 days or less was 0.7%.
“What’s inarguable is that the course of clopidogrel should be as short as possible, probably not more than 30 days unless there is a real extenuating rationale,” commented designated discussant Gregory Piazza, MD, a cardiologist at Brigham and Women’s Hospital in Boston.
VOYAGER PAD was sponsored by Bayer and Janssen, the companies that market rivaroxaban (Xarelto). The institution that Dr. Hiatt leads has received research funding from Bayer and Janssen and from Amgen. Dr. Parikh has been a consultant to Terumo; has received research funding from Shockwave, Surmodics, and Trireme; has worked on trial monitoring for Boston Scientific and Silk Road; and has had other financial relationships with Abbott, Boston Scientific, and Medtronic. Dr. Creager had no disclosures. Dr. Piazza has received research grants from Bayer and Janssen, as well as Bristol-Myers Squibb, Diiachi, EKOS, and Portola, and he has been a consultant to Optum, Pfizer, and Thrombolex.
SOURCE: Hiatt WR et al. ACC 20, Abstract 406-13.
The VOYAGER PAD results from more than 6,500 patients created the biggest evidence base by far ever collected from patients with symptomatic peripheral artery disease (PAD) who underwent a vascular intervention, and showed that the combination of twice-daily rivaroxaban and once-daily aspirin was safe and more effective than aspirin alone for reducing future thrombotic and ischemic events.
Following that report on March 28, a prespecified subgroup analysis presented the next day showed that adding clopidogrel to this two-drug combination produced no added efficacy but caused additional bleeding episodes, suggesting that the common practice of using clopidogrel plus aspirin in these patients, especially those who receive a stent in a peripheral artery, should either fall by the wayside or be used very briefly.
“In the absence of clear benefit, clopidogrel exposure along with aspirin and rivaroxaban should be minimized or avoided to reduce this risk,” William R. Hiatt, MD, said at the joint scientific sessions of the American College of Cardiology and the World Heart Federation. The meeting was conducted online after its cancellation because of the COVID-19 pandemic. But he also cautioned that “we did not control for clopidogrel use, and so the patients who received clopidogrel look different [from patients who did not receive clopidogrel]. We must be cautious in interpreting differences between patients on or off clopidogrel,” warned Dr. Hiatt, a lead investigator for VOYAGER PAD, professor for cardiovascular research at the University of Colorado at Denver in Aurora and president of the affiliated Colorado Prevention Center.
In addition to this substantial caveat, the finding that clopidogrel appeared to add no extra benefit to the rivaroxaban/aspirin regimen “contradicts some dogmas that have been in the field for decades,” Dr. Hiatt said. Use of dual-antiplatelet therapy (DAPT), in this setting usually aspirin and clopidogrel, in patients who have just undergone lower-extremity revascularization is “current dogma,” even though it is not based on any direct evidence for efficacy, but instead came on the scene as “an extrapolation from the coronary artery literature, where it does have some benefit, particularly after percutaneous coronary intervention,” he explained.
The only reported study results to examine use of DAPT in patients who underwent peripheral artery revascularization focused entirely on patients who had a surgical procedure and showed no added benefit from DAPT over aspirin only in a multicenter, randomized trial with 851 patients (J Vasc Surg. 2010 Oct;52[4]:825-33), Dr. Hiatt noted. In VOYAGER PAD, two-thirds of all patients underwent an endovascular, not surgical, peripheral intervention, and among those treated with clopidogrel, 91% had endovascular treatment.
“We’re not saying don’t use DAPT, but patients on three drugs are at higher bleeding risk than patients on two drugs. I think our data also suggest starting rivaroxaban immediately after a procedure [as was done in VOYAGER PAD], and not waiting to complete a course of DAPT,” Dr. Hiatt said.
Other experts embraced Dr. Hiatt’s take on these findings, while warning that it may take some time for the message to penetrate into practice.
The overall VOYAGER PAD results “are practice changing for vascular interventions; it was by an order of magnitude the largest vascular intervention trial ever conducted,” commented Sahil A. Parikh, MD, a designated discussant, interventional cardiologist, and director of endovascular services at New York–Presbyterian Medical Center. “The data suggest that the value of clopidogrel is questionable, but the added hazard is not questionable” when given to patients on top of rivaroxaban and aspirin. The results “certainly beg the question of whether one should use DAPT at all, and if so, for how long.”
Use of DAPT in patients undergoing peripheral revascularization, especially patients receiving a stent, has been “dogma,” Dr. Parikh agreed. “It’s been pounded into our heads that DAPT is standard care, so it will take some time to penetrate into the practicing community.”
“Could there be patients who could benefit from triple therapy? That’s possible, but it needs testing,” commented Mark A. Creager, MD, professor of medicine and director of the Heart and Vascular Center at Dartmouth-Hitchcock Medical Center in Lebanon, N.H. “We’ve made terrific strides with the results from VOYAGER PAD,” and from the earlier COMPASS trial, which proved the benefit of rivaroxaban and aspirin in patients with stable atherosclerotic vascular disease including many PAD patients (N Engl J Med. 2017 Oct 5;377[14]:1319-30). Use of rivaroxaban and aspirin in PAD patients based on the COMPASS results “is beginning to make an impact, but has a long way to go,” Dr. Creager said in an interview.
In late 2018, the Food and Drug Administration gave rivaroxaban a revised labeling that included an indication for patients with PAD based on the COMPASS findings. The VOYAGER PAD and COMPASS trials are especially noteworthy because “they opened a whole area [of study] in patients with peripheral vascular disease, ” he added.
The prespecified analysis that Dr. Hiatt reported analyzed outcomes among the 51% of patients enrolled in VOYAGER PAD (Vascular Outcomes Study of Acetylsalicylic Acid Along With Rivaroxaban in Endovascular or Surgical Limb Revascularization for Peripheral Artery Disease) who received clopidogrel during follow-up at the discretion of their treating physician and the outcomes among the remainder who did not. The two subgroups showed several statistically significant differences in the prevalence of various comorbidities and in some baseline demographic and clinical metrics, and the analyses that Dr. Hiatt reported did not attempt to correct for these differences. Patients who received clopidogrel had the drug on board for a median of 29 days, and about 58% received it for 30 days or less.
The main finding of his analysis was that “adding clopidogrel did not modify benefit at all” from the perspective of the primary endpoint of VOYAGER PAD, the incidence of a five-item list of adverse events (acute limb ischemia, major amputation for vascular cause, myocardial infarction, ischemic stroke, and cardiovascular death) during a median follow-up of 28 months (N Engl J Med. 2020 Mar 28. doi: 10.1056/NEJMoa2000052), said Dr. Hiatt. Among patients on clopidogrel, those treated with both rivaroxaban and aspirin had a 16.0% incidence of the primary endpoint, compared with an 18.3% rate among patients on aspirin only, for a 15% relative risk reduction, identical to the study’s primary result. Among patients not on clopidogrel, the primary endpoint occurred in 18.7% of patients on rivaroxaban plus aspirin and in 21.5% of those on aspirin only, a 14% relative risk reduction. The analyses also showed that adding clopidogrel appeared to increase the rate of bleeding episodes, particularly the incidence of major bleeds by the criteria of the International Society on Thrombosis and Haemostasis (ISTH), which rose among patients on aspirin alone from 3.3% without clopidogrel treatment to 4.9% with clopidogrel, and in patients on rivaroxaban plus aspirin these major bleeds increased from 5.4% with no clopidogrel to 6.5% with clopidogrel.
An especially revealing further analysis showed that, among those who also received rivaroxaban and aspirin, clopidogrel treatment for more than 30 days led to substantially more bleeding problems, compared with patients who received the drug for 30 days or less. Patients who received clopidogrel for more than 30 days as part of a triple-drug regimen had a 3.0% rate of major ISTH bleeds during 180 days of follow-up, compared with a 0.9% rate for patients in the aspirin-alone group who also received clopidogrel, a 2.1% between-group difference. In contrast, the difference in major ISTH bleeds between the two treatment arms in the subgroup who received clopidogrel for 30 days or less was 0.7%.
“What’s inarguable is that the course of clopidogrel should be as short as possible, probably not more than 30 days unless there is a real extenuating rationale,” commented designated discussant Gregory Piazza, MD, a cardiologist at Brigham and Women’s Hospital in Boston.
VOYAGER PAD was sponsored by Bayer and Janssen, the companies that market rivaroxaban (Xarelto). The institution that Dr. Hiatt leads has received research funding from Bayer and Janssen and from Amgen. Dr. Parikh has been a consultant to Terumo; has received research funding from Shockwave, Surmodics, and Trireme; has worked on trial monitoring for Boston Scientific and Silk Road; and has had other financial relationships with Abbott, Boston Scientific, and Medtronic. Dr. Creager had no disclosures. Dr. Piazza has received research grants from Bayer and Janssen, as well as Bristol-Myers Squibb, Diiachi, EKOS, and Portola, and he has been a consultant to Optum, Pfizer, and Thrombolex.
SOURCE: Hiatt WR et al. ACC 20, Abstract 406-13.
FROM ACC 2020
COVID-19: Mental health pros come to the aid of frontline comrades
Frontline COVID-19 healthcare workers across North America are dealing with unprecedented stress, but mental health therapists in both Canada and the US are doing their part to ensure the psychological well-being of their colleagues on the frontlines of the pandemic.
Over the past few weeks, thousands of licensed psychologists, psychotherapists, and social workers have signed up to offer free therapy sessions to healthcare professionals who find themselves psychologically overwhelmed by the pandemic’s economic, social, and financial fallout.
In Canada, the movement was started by Toronto psychotherapist Karen Dougherty, MA, who saw a social media post from someone in New York asking mental health workers to volunteer their time.
Inspired by this, Dougherty reached out to some of her close colleagues with a social media post of her own. A few days later, 450 people had signed up to volunteer and Ontario COVID-19 Therapists was born.
The sessions are provided by licensed Canadian psychotherapists and are free of charge to healthcare workers providing frontline COVID-19 care. After signing up online, users can choose from one of three therapists who will provide up to five free phone sessions.
In New York state, a similar initiative — which is not limited to healthcare workers — has gained incredible momentum. On March 21, Gov. Andrew Cuomo announced the creation of a statewide hotline [844-863-9314] to provide free mental health services to individuals sheltering at home who may be experiencing stress and anxiety as a result of COVID-19.
The governor called on mental-health professionals to volunteer their time and provide telephone and/or telehealth counseling. The New York State Psychiatric Association quickly got on board and encouraged its members to participate.
Just four days later, more than 6,000 mental health workers had volunteered their services, making New York the first state to address the mental health consequences of the pandemic in this way.
Self-care is vital for healthcare workers during the COVID-19 pandemic, particularly as stress mounts and workdays become longer and grimmer. Dougherty recommended that frontline workers manage overwhelming thoughts by limiting their intake of information about the virus.
Self-Care a “Selfless Act”
Clinicians need to balance the need to stay informed with the potential for information overload, which can contribute to anxiety, she said.
She also recommended that individuals continue to connect with loved ones while practicing social distancing. Equally important is talking to someone about the struggles people may be facing at work.
For Amin Azzam MD, MA, the benefits of these initiatives are obvious.
“There is always value in providing additional mental health services and tending to psychological well-being,” Azzam, adjunct professor of psychiatry, University of California, San Francisco and UC Berkeley, told Medscape Medical News.
“If there ever were a time when we can use all the emotional support possible, then it would be during a global pandemic,” added Azzam, who is also director of Open Learning Initiatives at Osmosis, a nonprofit health education company.
Azzam urged healthcare professionals to avail themselves of such resources as often as necessary.
“Taking care of ourselves is not a selfish act. When the oxygen masks come down on airplanes we are always instructed to put our own masks on first before helping those in need. It’s a sign of strength, not weakness, to seek emotional support,” he said.
However, it isn’t always easy. The longstanding stigma associated with seeking help for mental health issues has not stopped for COVID-19. Even workers who are in close daily contact with people infected with the virus are finding they’re not immune to the stigma associated with seeking mental health treatment, Azzam added.
“Nevertheless, the burden these frontline workers are facing is real…and often crushing. Some Ontario doctors have reported pretraumatic stress disorder, which they attribute to having watched the virus wreak havoc in other countries, and knowing that similar difficulties are headed their way,” he said.
A Growing Movement
Doris Grinspun, PhD, MSN, the CEO of Registered Nurses’ Association of Ontario (RNAO), said the province’s nurses are under intense pressure at work, then fear infecting family members once they come home. Some are even staying at hotels to ensure they don’t infect others, as reported by CBC News.
However, she added, most recognize the important role that psychotherapy can play, especially since many frontline healthcare workers find it difficult to speak with their families about the issues they face at work, for fear of adding stress to their family life as well.
“None of us are superhuman and immune to stress. When healthcare workers are facing workplace challenges never before seen in their lifetimes, they need opportunities to decompress to maintain their own health and well-being. This will help them pace themselves for the marathon — not sprint — to continue doing the important work of helping others,” said Azzam.
Given the attention it has garnered in such a short time, Azzam is hopeful that the free therapy movement will spread.
In Canada, mental health professionals in other provinces have already reached out to Dougherty, lending credence to the notion of a pan-Canadian network of therapists offering free services to healthcare workers during the outbreak.
In the US, other local initiatives are already underway.
“The one that I’m personally aware of is at my home institution at the University of California, San Francisco,” Azzam said. “We have a Care for the Caregiver program that is being greatly expanded at this time. As part of that initiative, the institution’s psychiatry department has solicited licensed mental health care providers to volunteer their time to provide those additional services.”
Azzam has also worked with colleagues developing a series of mental health tools that Osmosis has made available free of charge.
These include a central site with educational material about COVID-19, a video about supporting educators’ mental health during high-stress periods; a video about managing students’ mental health during public health emergencies; a summary of recommended resources for psychological health in distressing times; and a YouTube Live event he held regarding tips for maximizing psychological health during stressful times.
This article first appeared on Medscape.com.
Frontline COVID-19 healthcare workers across North America are dealing with unprecedented stress, but mental health therapists in both Canada and the US are doing their part to ensure the psychological well-being of their colleagues on the frontlines of the pandemic.
Over the past few weeks, thousands of licensed psychologists, psychotherapists, and social workers have signed up to offer free therapy sessions to healthcare professionals who find themselves psychologically overwhelmed by the pandemic’s economic, social, and financial fallout.
In Canada, the movement was started by Toronto psychotherapist Karen Dougherty, MA, who saw a social media post from someone in New York asking mental health workers to volunteer their time.
Inspired by this, Dougherty reached out to some of her close colleagues with a social media post of her own. A few days later, 450 people had signed up to volunteer and Ontario COVID-19 Therapists was born.
The sessions are provided by licensed Canadian psychotherapists and are free of charge to healthcare workers providing frontline COVID-19 care. After signing up online, users can choose from one of three therapists who will provide up to five free phone sessions.
In New York state, a similar initiative — which is not limited to healthcare workers — has gained incredible momentum. On March 21, Gov. Andrew Cuomo announced the creation of a statewide hotline [844-863-9314] to provide free mental health services to individuals sheltering at home who may be experiencing stress and anxiety as a result of COVID-19.
The governor called on mental-health professionals to volunteer their time and provide telephone and/or telehealth counseling. The New York State Psychiatric Association quickly got on board and encouraged its members to participate.
Just four days later, more than 6,000 mental health workers had volunteered their services, making New York the first state to address the mental health consequences of the pandemic in this way.
Self-care is vital for healthcare workers during the COVID-19 pandemic, particularly as stress mounts and workdays become longer and grimmer. Dougherty recommended that frontline workers manage overwhelming thoughts by limiting their intake of information about the virus.
Self-Care a “Selfless Act”
Clinicians need to balance the need to stay informed with the potential for information overload, which can contribute to anxiety, she said.
She also recommended that individuals continue to connect with loved ones while practicing social distancing. Equally important is talking to someone about the struggles people may be facing at work.
For Amin Azzam MD, MA, the benefits of these initiatives are obvious.
“There is always value in providing additional mental health services and tending to psychological well-being,” Azzam, adjunct professor of psychiatry, University of California, San Francisco and UC Berkeley, told Medscape Medical News.
“If there ever were a time when we can use all the emotional support possible, then it would be during a global pandemic,” added Azzam, who is also director of Open Learning Initiatives at Osmosis, a nonprofit health education company.
Azzam urged healthcare professionals to avail themselves of such resources as often as necessary.
“Taking care of ourselves is not a selfish act. When the oxygen masks come down on airplanes we are always instructed to put our own masks on first before helping those in need. It’s a sign of strength, not weakness, to seek emotional support,” he said.
However, it isn’t always easy. The longstanding stigma associated with seeking help for mental health issues has not stopped for COVID-19. Even workers who are in close daily contact with people infected with the virus are finding they’re not immune to the stigma associated with seeking mental health treatment, Azzam added.
“Nevertheless, the burden these frontline workers are facing is real…and often crushing. Some Ontario doctors have reported pretraumatic stress disorder, which they attribute to having watched the virus wreak havoc in other countries, and knowing that similar difficulties are headed their way,” he said.
A Growing Movement
Doris Grinspun, PhD, MSN, the CEO of Registered Nurses’ Association of Ontario (RNAO), said the province’s nurses are under intense pressure at work, then fear infecting family members once they come home. Some are even staying at hotels to ensure they don’t infect others, as reported by CBC News.
However, she added, most recognize the important role that psychotherapy can play, especially since many frontline healthcare workers find it difficult to speak with their families about the issues they face at work, for fear of adding stress to their family life as well.
“None of us are superhuman and immune to stress. When healthcare workers are facing workplace challenges never before seen in their lifetimes, they need opportunities to decompress to maintain their own health and well-being. This will help them pace themselves for the marathon — not sprint — to continue doing the important work of helping others,” said Azzam.
Given the attention it has garnered in such a short time, Azzam is hopeful that the free therapy movement will spread.
In Canada, mental health professionals in other provinces have already reached out to Dougherty, lending credence to the notion of a pan-Canadian network of therapists offering free services to healthcare workers during the outbreak.
In the US, other local initiatives are already underway.
“The one that I’m personally aware of is at my home institution at the University of California, San Francisco,” Azzam said. “We have a Care for the Caregiver program that is being greatly expanded at this time. As part of that initiative, the institution’s psychiatry department has solicited licensed mental health care providers to volunteer their time to provide those additional services.”
Azzam has also worked with colleagues developing a series of mental health tools that Osmosis has made available free of charge.
These include a central site with educational material about COVID-19, a video about supporting educators’ mental health during high-stress periods; a video about managing students’ mental health during public health emergencies; a summary of recommended resources for psychological health in distressing times; and a YouTube Live event he held regarding tips for maximizing psychological health during stressful times.
This article first appeared on Medscape.com.
Frontline COVID-19 healthcare workers across North America are dealing with unprecedented stress, but mental health therapists in both Canada and the US are doing their part to ensure the psychological well-being of their colleagues on the frontlines of the pandemic.
Over the past few weeks, thousands of licensed psychologists, psychotherapists, and social workers have signed up to offer free therapy sessions to healthcare professionals who find themselves psychologically overwhelmed by the pandemic’s economic, social, and financial fallout.
In Canada, the movement was started by Toronto psychotherapist Karen Dougherty, MA, who saw a social media post from someone in New York asking mental health workers to volunteer their time.
Inspired by this, Dougherty reached out to some of her close colleagues with a social media post of her own. A few days later, 450 people had signed up to volunteer and Ontario COVID-19 Therapists was born.
The sessions are provided by licensed Canadian psychotherapists and are free of charge to healthcare workers providing frontline COVID-19 care. After signing up online, users can choose from one of three therapists who will provide up to five free phone sessions.
In New York state, a similar initiative — which is not limited to healthcare workers — has gained incredible momentum. On March 21, Gov. Andrew Cuomo announced the creation of a statewide hotline [844-863-9314] to provide free mental health services to individuals sheltering at home who may be experiencing stress and anxiety as a result of COVID-19.
The governor called on mental-health professionals to volunteer their time and provide telephone and/or telehealth counseling. The New York State Psychiatric Association quickly got on board and encouraged its members to participate.
Just four days later, more than 6,000 mental health workers had volunteered their services, making New York the first state to address the mental health consequences of the pandemic in this way.
Self-care is vital for healthcare workers during the COVID-19 pandemic, particularly as stress mounts and workdays become longer and grimmer. Dougherty recommended that frontline workers manage overwhelming thoughts by limiting their intake of information about the virus.
Self-Care a “Selfless Act”
Clinicians need to balance the need to stay informed with the potential for information overload, which can contribute to anxiety, she said.
She also recommended that individuals continue to connect with loved ones while practicing social distancing. Equally important is talking to someone about the struggles people may be facing at work.
For Amin Azzam MD, MA, the benefits of these initiatives are obvious.
“There is always value in providing additional mental health services and tending to psychological well-being,” Azzam, adjunct professor of psychiatry, University of California, San Francisco and UC Berkeley, told Medscape Medical News.
“If there ever were a time when we can use all the emotional support possible, then it would be during a global pandemic,” added Azzam, who is also director of Open Learning Initiatives at Osmosis, a nonprofit health education company.
Azzam urged healthcare professionals to avail themselves of such resources as often as necessary.
“Taking care of ourselves is not a selfish act. When the oxygen masks come down on airplanes we are always instructed to put our own masks on first before helping those in need. It’s a sign of strength, not weakness, to seek emotional support,” he said.
However, it isn’t always easy. The longstanding stigma associated with seeking help for mental health issues has not stopped for COVID-19. Even workers who are in close daily contact with people infected with the virus are finding they’re not immune to the stigma associated with seeking mental health treatment, Azzam added.
“Nevertheless, the burden these frontline workers are facing is real…and often crushing. Some Ontario doctors have reported pretraumatic stress disorder, which they attribute to having watched the virus wreak havoc in other countries, and knowing that similar difficulties are headed their way,” he said.
A Growing Movement
Doris Grinspun, PhD, MSN, the CEO of Registered Nurses’ Association of Ontario (RNAO), said the province’s nurses are under intense pressure at work, then fear infecting family members once they come home. Some are even staying at hotels to ensure they don’t infect others, as reported by CBC News.
However, she added, most recognize the important role that psychotherapy can play, especially since many frontline healthcare workers find it difficult to speak with their families about the issues they face at work, for fear of adding stress to their family life as well.
“None of us are superhuman and immune to stress. When healthcare workers are facing workplace challenges never before seen in their lifetimes, they need opportunities to decompress to maintain their own health and well-being. This will help them pace themselves for the marathon — not sprint — to continue doing the important work of helping others,” said Azzam.
Given the attention it has garnered in such a short time, Azzam is hopeful that the free therapy movement will spread.
In Canada, mental health professionals in other provinces have already reached out to Dougherty, lending credence to the notion of a pan-Canadian network of therapists offering free services to healthcare workers during the outbreak.
In the US, other local initiatives are already underway.
“The one that I’m personally aware of is at my home institution at the University of California, San Francisco,” Azzam said. “We have a Care for the Caregiver program that is being greatly expanded at this time. As part of that initiative, the institution’s psychiatry department has solicited licensed mental health care providers to volunteer their time to provide those additional services.”
Azzam has also worked with colleagues developing a series of mental health tools that Osmosis has made available free of charge.
These include a central site with educational material about COVID-19, a video about supporting educators’ mental health during high-stress periods; a video about managing students’ mental health during public health emergencies; a summary of recommended resources for psychological health in distressing times; and a YouTube Live event he held regarding tips for maximizing psychological health during stressful times.
This article first appeared on Medscape.com.
COVID-19 transmission can occur before symptom onset
based on clinical and epidemiologic data for all cases reported in the country by March 16.
As of that date, there had been 243 cases of COVID-19, of which 157 were locally acquired. Among those 157 were 10 cases (6.4%) that involved probable presymptomatic transmission, Wycliffe E. Wei, MPH, and associates said April 1 in the Morbidity and Mortality Weekly Report.
They defined presymptomatic transmission “as the transmission of SARS-CoV-2 from an infected person (source patient) to a secondary patient before the source patient developed symptoms, as ascertained by exposure and symptom onset dates, with no evidence that the secondary patient had been exposed to anyone else with COVID-19.”
Investigation of all 243 cases in Singapore identified seven clusters, each involving two to five patients, as sources of presymptomatic transmission. In four of the clusters, the “exposure occurred 1-3 days before the source patient developed symptoms,” said Mr. Wei of the Singapore Ministry of Health and associates.
These findings, along with evidence from Chinese studies – one of which reported presymptomatic transmission in 12.6% of cases – support “the likelihood that viral shedding can occur in the absence of symptoms and before symptom onset,” they said.
SOURCE: Wei WE et al. MMWR. 2020 Apr 1;69(ePub):1-5. doi: 10.15585/mmwr.mm6914e1.
based on clinical and epidemiologic data for all cases reported in the country by March 16.
As of that date, there had been 243 cases of COVID-19, of which 157 were locally acquired. Among those 157 were 10 cases (6.4%) that involved probable presymptomatic transmission, Wycliffe E. Wei, MPH, and associates said April 1 in the Morbidity and Mortality Weekly Report.
They defined presymptomatic transmission “as the transmission of SARS-CoV-2 from an infected person (source patient) to a secondary patient before the source patient developed symptoms, as ascertained by exposure and symptom onset dates, with no evidence that the secondary patient had been exposed to anyone else with COVID-19.”
Investigation of all 243 cases in Singapore identified seven clusters, each involving two to five patients, as sources of presymptomatic transmission. In four of the clusters, the “exposure occurred 1-3 days before the source patient developed symptoms,” said Mr. Wei of the Singapore Ministry of Health and associates.
These findings, along with evidence from Chinese studies – one of which reported presymptomatic transmission in 12.6% of cases – support “the likelihood that viral shedding can occur in the absence of symptoms and before symptom onset,” they said.
SOURCE: Wei WE et al. MMWR. 2020 Apr 1;69(ePub):1-5. doi: 10.15585/mmwr.mm6914e1.
based on clinical and epidemiologic data for all cases reported in the country by March 16.
As of that date, there had been 243 cases of COVID-19, of which 157 were locally acquired. Among those 157 were 10 cases (6.4%) that involved probable presymptomatic transmission, Wycliffe E. Wei, MPH, and associates said April 1 in the Morbidity and Mortality Weekly Report.
They defined presymptomatic transmission “as the transmission of SARS-CoV-2 from an infected person (source patient) to a secondary patient before the source patient developed symptoms, as ascertained by exposure and symptom onset dates, with no evidence that the secondary patient had been exposed to anyone else with COVID-19.”
Investigation of all 243 cases in Singapore identified seven clusters, each involving two to five patients, as sources of presymptomatic transmission. In four of the clusters, the “exposure occurred 1-3 days before the source patient developed symptoms,” said Mr. Wei of the Singapore Ministry of Health and associates.
These findings, along with evidence from Chinese studies – one of which reported presymptomatic transmission in 12.6% of cases – support “the likelihood that viral shedding can occur in the absence of symptoms and before symptom onset,” they said.
SOURCE: Wei WE et al. MMWR. 2020 Apr 1;69(ePub):1-5. doi: 10.15585/mmwr.mm6914e1.
FROM MMWR
Advice from the front lines: How cancer centers can cope with COVID-19
according to the medical director of a cancer care alliance in the first U.S. epicenter of the coronavirus outbreak.
Jennie R. Crews, MD, the medical director of the Seattle Cancer Care Alliance (SCCA), discussed the SCCA experience and offered advice for other cancer centers in a webinar hosted by the Association of Community Cancer Centers.
Dr. Crews highlighted the SCCA’s use of algorithms to predict which patients can be managed via telehealth and which require face-to-face visits, human resource issues that arose at SCCA, screening and testing procedures, and the importance of communication with patients, caregivers, and staff.
Communication
Dr. Crews stressed the value of clear, regular, and internally consistent staff communication in a variety of formats. SCCA sends daily email blasts to their personnel regarding policies and procedures, which are archived on the SCCA intranet site.
SCCA also holds weekly town hall meetings at which leaders respond to staff questions regarding practical matters they have encountered and future plans. Providers’ up-to-the-minute familiarity with policies and procedures enables all team members to uniformly and clearly communicate to patients and caregivers.
Dr. Crews emphasized the value of consistency and “over-communication” in projecting confidence and preparedness to patients and caregivers during an unsettling time. SCCA has developed fact sheets, posted current information on the SCCA website, and provided education during doorway screenings.
Screening and testing
All SCCA staff members are screened daily at the practice entrance so they have personal experience with the process utilized for patients. Because symptoms associated with coronavirus infection may overlap with cancer treatment–related complaints, SCCA clinicians have expanded the typical coronavirus screening questionnaire for patients on cancer treatment.
Patients with ambiguous symptoms are masked, taken to a physically separate area of the SCCA clinics, and screened further by an advanced practice provider. The patients are then triaged to either the clinic for treatment or to the emergency department for further triage and care.
Although testing processes and procedures have been modified, Dr. Crews advised codifying those policies and procedures, including notification of results and follow-up for both patients and staff. Dr. Crews also stressed the importance of clearly articulated return-to-work policies for staff who have potential exposure and/or positive test results.
At the University of Washington’s virology laboratory, they have a test turnaround time of less than 12 hours.
Planning ahead
Dr. Crews highlighted the importance of community-based surge planning, utilizing predictive models to assess inpatient capacity requirements and potential repurposing of providers.
The SCCA is prepared to close selected community sites and shift personnel to other locations if personnel needs cannot be met because of illness or quarantine. Contingency plans include specialized pharmacy services for patients requiring chemotherapy.
The SCCA has not yet experienced shortages of personal protective equipment (PPE). However, Dr. Crews said staff require detailed education regarding the use of PPE in order to safeguard the supply while providing maximal staff protection.
Helping the helpers
During the pandemic, SCCA has dealt with a variety of challenging human resource issues, including:
- Extending sick time beyond what was previously “stored” in staff members’ earned time off.
- Childcare during an extended hiatus in school and daycare schedules.
- Programs to maintain and/or restore employee wellness (including staff-centered support services, spiritual care, mindfulness exercises, and town halls).
Dr. Crews also discussed recruitment of community resources to provide meals for staff from local restaurants with restricted hours and transportation resources for staff and patients, as visitors are restricted (currently one per patient).
Managing care
Dr. Crews noted that the University of Washington had a foundational structure for a telehealth program prior to the pandemic. Their telehealth committee enabled SCCA to scale up the service quickly with their academic partners, including training modules for and certification of providers, outfitting off-site personnel with dedicated lines and hardware, and provision of personal Zoom accounts.
SCCA also devised algorithms for determining when face-to-face visits, remote management, or deferred visits are appropriate in various scenarios. The algorithms were developed by disease-specialized teams.
As a general rule, routine chemotherapy and radiation are administered on schedule. On-treatment and follow-up office visits are conducted via telehealth if possible. In some cases, initiation of chemotherapy and radiation has been delayed, and screening services have been suspended.
In response to questions about palliative care during the pandemic, Dr. Crews said SCCA has encouraged their patients to complete, review, or update their advance directives. The SCCA has not had the need to resuscitate a coronavirus-infected outpatient but has instituted policies for utilizing full PPE on any patient requiring resuscitation.
In her closing remarks, Dr. Crews stressed that the response to COVID-19 in Washington state has required an intense collaboration among colleagues, the community, and government leaders, as the actions required extended far beyond medical decision makers alone.
Dr. Lyss was a community-based medical oncologist and clinical researcher for more than 35 years before his recent retirement. His clinical and research interests were focused on breast and lung cancers as well as expanding clinical trial access to medically underserved populations. He is based in St. Louis. He has no conflicts of interest.
according to the medical director of a cancer care alliance in the first U.S. epicenter of the coronavirus outbreak.
Jennie R. Crews, MD, the medical director of the Seattle Cancer Care Alliance (SCCA), discussed the SCCA experience and offered advice for other cancer centers in a webinar hosted by the Association of Community Cancer Centers.
Dr. Crews highlighted the SCCA’s use of algorithms to predict which patients can be managed via telehealth and which require face-to-face visits, human resource issues that arose at SCCA, screening and testing procedures, and the importance of communication with patients, caregivers, and staff.
Communication
Dr. Crews stressed the value of clear, regular, and internally consistent staff communication in a variety of formats. SCCA sends daily email blasts to their personnel regarding policies and procedures, which are archived on the SCCA intranet site.
SCCA also holds weekly town hall meetings at which leaders respond to staff questions regarding practical matters they have encountered and future plans. Providers’ up-to-the-minute familiarity with policies and procedures enables all team members to uniformly and clearly communicate to patients and caregivers.
Dr. Crews emphasized the value of consistency and “over-communication” in projecting confidence and preparedness to patients and caregivers during an unsettling time. SCCA has developed fact sheets, posted current information on the SCCA website, and provided education during doorway screenings.
Screening and testing
All SCCA staff members are screened daily at the practice entrance so they have personal experience with the process utilized for patients. Because symptoms associated with coronavirus infection may overlap with cancer treatment–related complaints, SCCA clinicians have expanded the typical coronavirus screening questionnaire for patients on cancer treatment.
Patients with ambiguous symptoms are masked, taken to a physically separate area of the SCCA clinics, and screened further by an advanced practice provider. The patients are then triaged to either the clinic for treatment or to the emergency department for further triage and care.
Although testing processes and procedures have been modified, Dr. Crews advised codifying those policies and procedures, including notification of results and follow-up for both patients and staff. Dr. Crews also stressed the importance of clearly articulated return-to-work policies for staff who have potential exposure and/or positive test results.
At the University of Washington’s virology laboratory, they have a test turnaround time of less than 12 hours.
Planning ahead
Dr. Crews highlighted the importance of community-based surge planning, utilizing predictive models to assess inpatient capacity requirements and potential repurposing of providers.
The SCCA is prepared to close selected community sites and shift personnel to other locations if personnel needs cannot be met because of illness or quarantine. Contingency plans include specialized pharmacy services for patients requiring chemotherapy.
The SCCA has not yet experienced shortages of personal protective equipment (PPE). However, Dr. Crews said staff require detailed education regarding the use of PPE in order to safeguard the supply while providing maximal staff protection.
Helping the helpers
During the pandemic, SCCA has dealt with a variety of challenging human resource issues, including:
- Extending sick time beyond what was previously “stored” in staff members’ earned time off.
- Childcare during an extended hiatus in school and daycare schedules.
- Programs to maintain and/or restore employee wellness (including staff-centered support services, spiritual care, mindfulness exercises, and town halls).
Dr. Crews also discussed recruitment of community resources to provide meals for staff from local restaurants with restricted hours and transportation resources for staff and patients, as visitors are restricted (currently one per patient).
Managing care
Dr. Crews noted that the University of Washington had a foundational structure for a telehealth program prior to the pandemic. Their telehealth committee enabled SCCA to scale up the service quickly with their academic partners, including training modules for and certification of providers, outfitting off-site personnel with dedicated lines and hardware, and provision of personal Zoom accounts.
SCCA also devised algorithms for determining when face-to-face visits, remote management, or deferred visits are appropriate in various scenarios. The algorithms were developed by disease-specialized teams.
As a general rule, routine chemotherapy and radiation are administered on schedule. On-treatment and follow-up office visits are conducted via telehealth if possible. In some cases, initiation of chemotherapy and radiation has been delayed, and screening services have been suspended.
In response to questions about palliative care during the pandemic, Dr. Crews said SCCA has encouraged their patients to complete, review, or update their advance directives. The SCCA has not had the need to resuscitate a coronavirus-infected outpatient but has instituted policies for utilizing full PPE on any patient requiring resuscitation.
In her closing remarks, Dr. Crews stressed that the response to COVID-19 in Washington state has required an intense collaboration among colleagues, the community, and government leaders, as the actions required extended far beyond medical decision makers alone.
Dr. Lyss was a community-based medical oncologist and clinical researcher for more than 35 years before his recent retirement. His clinical and research interests were focused on breast and lung cancers as well as expanding clinical trial access to medically underserved populations. He is based in St. Louis. He has no conflicts of interest.
according to the medical director of a cancer care alliance in the first U.S. epicenter of the coronavirus outbreak.
Jennie R. Crews, MD, the medical director of the Seattle Cancer Care Alliance (SCCA), discussed the SCCA experience and offered advice for other cancer centers in a webinar hosted by the Association of Community Cancer Centers.
Dr. Crews highlighted the SCCA’s use of algorithms to predict which patients can be managed via telehealth and which require face-to-face visits, human resource issues that arose at SCCA, screening and testing procedures, and the importance of communication with patients, caregivers, and staff.
Communication
Dr. Crews stressed the value of clear, regular, and internally consistent staff communication in a variety of formats. SCCA sends daily email blasts to their personnel regarding policies and procedures, which are archived on the SCCA intranet site.
SCCA also holds weekly town hall meetings at which leaders respond to staff questions regarding practical matters they have encountered and future plans. Providers’ up-to-the-minute familiarity with policies and procedures enables all team members to uniformly and clearly communicate to patients and caregivers.
Dr. Crews emphasized the value of consistency and “over-communication” in projecting confidence and preparedness to patients and caregivers during an unsettling time. SCCA has developed fact sheets, posted current information on the SCCA website, and provided education during doorway screenings.
Screening and testing
All SCCA staff members are screened daily at the practice entrance so they have personal experience with the process utilized for patients. Because symptoms associated with coronavirus infection may overlap with cancer treatment–related complaints, SCCA clinicians have expanded the typical coronavirus screening questionnaire for patients on cancer treatment.
Patients with ambiguous symptoms are masked, taken to a physically separate area of the SCCA clinics, and screened further by an advanced practice provider. The patients are then triaged to either the clinic for treatment or to the emergency department for further triage and care.
Although testing processes and procedures have been modified, Dr. Crews advised codifying those policies and procedures, including notification of results and follow-up for both patients and staff. Dr. Crews also stressed the importance of clearly articulated return-to-work policies for staff who have potential exposure and/or positive test results.
At the University of Washington’s virology laboratory, they have a test turnaround time of less than 12 hours.
Planning ahead
Dr. Crews highlighted the importance of community-based surge planning, utilizing predictive models to assess inpatient capacity requirements and potential repurposing of providers.
The SCCA is prepared to close selected community sites and shift personnel to other locations if personnel needs cannot be met because of illness or quarantine. Contingency plans include specialized pharmacy services for patients requiring chemotherapy.
The SCCA has not yet experienced shortages of personal protective equipment (PPE). However, Dr. Crews said staff require detailed education regarding the use of PPE in order to safeguard the supply while providing maximal staff protection.
Helping the helpers
During the pandemic, SCCA has dealt with a variety of challenging human resource issues, including:
- Extending sick time beyond what was previously “stored” in staff members’ earned time off.
- Childcare during an extended hiatus in school and daycare schedules.
- Programs to maintain and/or restore employee wellness (including staff-centered support services, spiritual care, mindfulness exercises, and town halls).
Dr. Crews also discussed recruitment of community resources to provide meals for staff from local restaurants with restricted hours and transportation resources for staff and patients, as visitors are restricted (currently one per patient).
Managing care
Dr. Crews noted that the University of Washington had a foundational structure for a telehealth program prior to the pandemic. Their telehealth committee enabled SCCA to scale up the service quickly with their academic partners, including training modules for and certification of providers, outfitting off-site personnel with dedicated lines and hardware, and provision of personal Zoom accounts.
SCCA also devised algorithms for determining when face-to-face visits, remote management, or deferred visits are appropriate in various scenarios. The algorithms were developed by disease-specialized teams.
As a general rule, routine chemotherapy and radiation are administered on schedule. On-treatment and follow-up office visits are conducted via telehealth if possible. In some cases, initiation of chemotherapy and radiation has been delayed, and screening services have been suspended.
In response to questions about palliative care during the pandemic, Dr. Crews said SCCA has encouraged their patients to complete, review, or update their advance directives. The SCCA has not had the need to resuscitate a coronavirus-infected outpatient but has instituted policies for utilizing full PPE on any patient requiring resuscitation.
In her closing remarks, Dr. Crews stressed that the response to COVID-19 in Washington state has required an intense collaboration among colleagues, the community, and government leaders, as the actions required extended far beyond medical decision makers alone.
Dr. Lyss was a community-based medical oncologist and clinical researcher for more than 35 years before his recent retirement. His clinical and research interests were focused on breast and lung cancers as well as expanding clinical trial access to medically underserved populations. He is based in St. Louis. He has no conflicts of interest.
NYU med student joins COVID fight: ‘Time to step up’
On the evening of March 24, I got the email. When the bolded letters “We ask for your help” flashed across my screen, I knew exactly what was being asked of me: to graduate early and join the fight against COVID-19.
For the 120 fourth-year medical students in my class at NYU Grossman School of Medicine, the arrival of that email was always more a question of when than if. Similar moves had already been made in Italy as well as the United Kingdom, where the surge in patients with COVID-19 has devastated hospitals and left healthcare workers dead or drained. The New York hospitals where I’ve trained, places I have grown to love over the past 4 years, are now experiencing similar horrors. Residents and attending doctors – mentors and teachers – are burned out and exhausted. They need help.
Like most medical students, I chose to pursue medicine out of a desire to help. On both my medical school and residency applications, I spoke about my resolve to bear witness to and provide support to those suffering. Yet, being recruited to the front lines of a global pandemic felt deeply unsettling. Is this how I want to finally enter the world of medicine? The scope of what is actually being asked of me was immense.
Given the onslaught of bad news coming in on every device I had cozied up to during my social distancing, how could I want to do this? I’ve seen the death toll climb in Italy, with dozens of doctors dead. I’ve seen the photos of faces marred by masks worn for 12-16 hours at a time. I’ve been repeatedly reminded that we are just behind Italy. Things are certainly going to get worse.
It sounds selfish and petty, but I feel like COVID-19 has already robbed me of so much. Yet that was my first thought when I received the email. The end of fourth year in medical school is supposed to be a joyous, celebratory time. We have worked years for this moment. So many of us have fought burnout to reach this time, a brief moment of rest between being a medical student and becoming a full-fledged physician.
I matched into residency just 4 days before being asked to join the front lines of the pandemic. I found out my match results without the usual fanfare, sitting on a bench in Madison Square Park, FaceTiming my dad and safely social-distanced from my mom. They both cried tears of joy. Like so many people around the world right now, I couldn’t even embrace my parents. Would they want me to volunteer?
I reached out to my classmates. I thought that some of them would certainly share my worries. I thought they also had to be carrying this uncomfortable kind of grief, a heavy and acidic feeling of dreams collapsing into a moral duty. I received a unanimous reply: “We are needed. It’s our time to step up.” No matter how many “what ifs” I voiced, they wouldn’t crack or waver. Still, even if they never admitted it to me, I wondered whether they privately shared some of my concerns and fears.
Everyone knows information is shared instantly in our Twitter-centric world, but I was still shocked and unprepared for how quickly I was at the center of a major news story. Within an hour of that email, I was contacted by an old acquaintance from elementary school, now a journalist. He had found me through Facebook and asked, “Will you be one of the NYU students graduating early? Would love to get a comment.” Another friend texted me a photo of the leaked email, quipping, “Are you going to save us from the pandemic, Dr. Gabe?!” “It’s not a small decision!” I snapped back.
I went through something like the seven stages of grief in rapid succession. I found that with each excuse I made why I shouldn’t volunteer, I somehow became increasingly more anxious. To my surprise, when I decided I would join 50 of my peers at NYU, graduate early, and volunteer, my mind settled. The more I thought about it, the more I was overtaken by the selfless beauty of the profession I’m entering. This is what it means to be a doctor. I recalled a key part of the Hippocratic Oath: “I will remember that I remain a member of society, with special obligations to all my fellow human beings, those sound of mind and body as well as the infirm.”
I am going to fulfill my special obligations.
The fear is still there. I’m scared of COVID. I’m scared to infect others. I’m scared of winding up paralyzed and intubated. But I have also realized that all we have is each other. Healthcare workers supporting healthcare workers. New Yorkers supporting New Yorkers. Citizens of the world supporting citizens of the world. This is my time to be there for others, unwaveringly.
Logistical details continue to roll in, although they feel trivial in relation to the decision I have already made. The paperwork tells me that I will be onboarded to NYU’s internal medicine residency program. I will be compensated and protected under a similar contract to what current NYU residents sign. I have been promised that I will remain insured until I start my official residency program in July. My student loans won’t begin accruing interest until my normally planned graduation date. I am told that I will have personal protective equipment in line with the Centers for Disease Control and Prevention recommendations.
Questions still linger. Is it safe for me and my newly minted physician peers to continue living with our spouses, children, and friends? How long will I need to quarantine after my contract ends? Will there be a virtual graduation ceremony for my parents and loved ones to enjoy? In these challenging times, each day gives me a little more clarity about what exactly I am signing up for, but there are still so many uncertainties.
Am I naive to say that I do feel prepared? Or at least as prepared as anyone can be. With respect to my training, I have completed the requirements to graduate, which is why I am being permitted to graduate early in the first place. Our faculty points to our professionalism as the most promising indicator of our preparedness. They are heartened that we have embraced this truest test: our duty to others.
There is an eerie calm to New York City that contradicts what is shown on the news. With stores closed and streets quiet, it almost feels like Christmas morning here. Yet, inside the hospital, a fire rages. All the metaphors being used right now speak about violence, devastation, and immeasurable human suffering. “A war is being fought.” Or so I have heard. I guess I am about to find out.
Gabriel Redel-Traub is a fourth-year medical student at NYU Grossman School of Medicine. He will be starting residency in internal medicine at Columbia Presbyterian this summer. He is the former editor-in-chief of Dartmouth College’s Mouth Magazine, an editor of NYU’s LitMed Database, and has published most recently in the Hasting’s Center Magazine. Gabriel Redel-Traub has disclosed no relevant financial relationships.
This article first appeared on Medscape.com.
On the evening of March 24, I got the email. When the bolded letters “We ask for your help” flashed across my screen, I knew exactly what was being asked of me: to graduate early and join the fight against COVID-19.
For the 120 fourth-year medical students in my class at NYU Grossman School of Medicine, the arrival of that email was always more a question of when than if. Similar moves had already been made in Italy as well as the United Kingdom, where the surge in patients with COVID-19 has devastated hospitals and left healthcare workers dead or drained. The New York hospitals where I’ve trained, places I have grown to love over the past 4 years, are now experiencing similar horrors. Residents and attending doctors – mentors and teachers – are burned out and exhausted. They need help.
Like most medical students, I chose to pursue medicine out of a desire to help. On both my medical school and residency applications, I spoke about my resolve to bear witness to and provide support to those suffering. Yet, being recruited to the front lines of a global pandemic felt deeply unsettling. Is this how I want to finally enter the world of medicine? The scope of what is actually being asked of me was immense.
Given the onslaught of bad news coming in on every device I had cozied up to during my social distancing, how could I want to do this? I’ve seen the death toll climb in Italy, with dozens of doctors dead. I’ve seen the photos of faces marred by masks worn for 12-16 hours at a time. I’ve been repeatedly reminded that we are just behind Italy. Things are certainly going to get worse.
It sounds selfish and petty, but I feel like COVID-19 has already robbed me of so much. Yet that was my first thought when I received the email. The end of fourth year in medical school is supposed to be a joyous, celebratory time. We have worked years for this moment. So many of us have fought burnout to reach this time, a brief moment of rest between being a medical student and becoming a full-fledged physician.
I matched into residency just 4 days before being asked to join the front lines of the pandemic. I found out my match results without the usual fanfare, sitting on a bench in Madison Square Park, FaceTiming my dad and safely social-distanced from my mom. They both cried tears of joy. Like so many people around the world right now, I couldn’t even embrace my parents. Would they want me to volunteer?
I reached out to my classmates. I thought that some of them would certainly share my worries. I thought they also had to be carrying this uncomfortable kind of grief, a heavy and acidic feeling of dreams collapsing into a moral duty. I received a unanimous reply: “We are needed. It’s our time to step up.” No matter how many “what ifs” I voiced, they wouldn’t crack or waver. Still, even if they never admitted it to me, I wondered whether they privately shared some of my concerns and fears.
Everyone knows information is shared instantly in our Twitter-centric world, but I was still shocked and unprepared for how quickly I was at the center of a major news story. Within an hour of that email, I was contacted by an old acquaintance from elementary school, now a journalist. He had found me through Facebook and asked, “Will you be one of the NYU students graduating early? Would love to get a comment.” Another friend texted me a photo of the leaked email, quipping, “Are you going to save us from the pandemic, Dr. Gabe?!” “It’s not a small decision!” I snapped back.
I went through something like the seven stages of grief in rapid succession. I found that with each excuse I made why I shouldn’t volunteer, I somehow became increasingly more anxious. To my surprise, when I decided I would join 50 of my peers at NYU, graduate early, and volunteer, my mind settled. The more I thought about it, the more I was overtaken by the selfless beauty of the profession I’m entering. This is what it means to be a doctor. I recalled a key part of the Hippocratic Oath: “I will remember that I remain a member of society, with special obligations to all my fellow human beings, those sound of mind and body as well as the infirm.”
I am going to fulfill my special obligations.
The fear is still there. I’m scared of COVID. I’m scared to infect others. I’m scared of winding up paralyzed and intubated. But I have also realized that all we have is each other. Healthcare workers supporting healthcare workers. New Yorkers supporting New Yorkers. Citizens of the world supporting citizens of the world. This is my time to be there for others, unwaveringly.
Logistical details continue to roll in, although they feel trivial in relation to the decision I have already made. The paperwork tells me that I will be onboarded to NYU’s internal medicine residency program. I will be compensated and protected under a similar contract to what current NYU residents sign. I have been promised that I will remain insured until I start my official residency program in July. My student loans won’t begin accruing interest until my normally planned graduation date. I am told that I will have personal protective equipment in line with the Centers for Disease Control and Prevention recommendations.
Questions still linger. Is it safe for me and my newly minted physician peers to continue living with our spouses, children, and friends? How long will I need to quarantine after my contract ends? Will there be a virtual graduation ceremony for my parents and loved ones to enjoy? In these challenging times, each day gives me a little more clarity about what exactly I am signing up for, but there are still so many uncertainties.
Am I naive to say that I do feel prepared? Or at least as prepared as anyone can be. With respect to my training, I have completed the requirements to graduate, which is why I am being permitted to graduate early in the first place. Our faculty points to our professionalism as the most promising indicator of our preparedness. They are heartened that we have embraced this truest test: our duty to others.
There is an eerie calm to New York City that contradicts what is shown on the news. With stores closed and streets quiet, it almost feels like Christmas morning here. Yet, inside the hospital, a fire rages. All the metaphors being used right now speak about violence, devastation, and immeasurable human suffering. “A war is being fought.” Or so I have heard. I guess I am about to find out.
Gabriel Redel-Traub is a fourth-year medical student at NYU Grossman School of Medicine. He will be starting residency in internal medicine at Columbia Presbyterian this summer. He is the former editor-in-chief of Dartmouth College’s Mouth Magazine, an editor of NYU’s LitMed Database, and has published most recently in the Hasting’s Center Magazine. Gabriel Redel-Traub has disclosed no relevant financial relationships.
This article first appeared on Medscape.com.
On the evening of March 24, I got the email. When the bolded letters “We ask for your help” flashed across my screen, I knew exactly what was being asked of me: to graduate early and join the fight against COVID-19.
For the 120 fourth-year medical students in my class at NYU Grossman School of Medicine, the arrival of that email was always more a question of when than if. Similar moves had already been made in Italy as well as the United Kingdom, where the surge in patients with COVID-19 has devastated hospitals and left healthcare workers dead or drained. The New York hospitals where I’ve trained, places I have grown to love over the past 4 years, are now experiencing similar horrors. Residents and attending doctors – mentors and teachers – are burned out and exhausted. They need help.
Like most medical students, I chose to pursue medicine out of a desire to help. On both my medical school and residency applications, I spoke about my resolve to bear witness to and provide support to those suffering. Yet, being recruited to the front lines of a global pandemic felt deeply unsettling. Is this how I want to finally enter the world of medicine? The scope of what is actually being asked of me was immense.
Given the onslaught of bad news coming in on every device I had cozied up to during my social distancing, how could I want to do this? I’ve seen the death toll climb in Italy, with dozens of doctors dead. I’ve seen the photos of faces marred by masks worn for 12-16 hours at a time. I’ve been repeatedly reminded that we are just behind Italy. Things are certainly going to get worse.
It sounds selfish and petty, but I feel like COVID-19 has already robbed me of so much. Yet that was my first thought when I received the email. The end of fourth year in medical school is supposed to be a joyous, celebratory time. We have worked years for this moment. So many of us have fought burnout to reach this time, a brief moment of rest between being a medical student and becoming a full-fledged physician.
I matched into residency just 4 days before being asked to join the front lines of the pandemic. I found out my match results without the usual fanfare, sitting on a bench in Madison Square Park, FaceTiming my dad and safely social-distanced from my mom. They both cried tears of joy. Like so many people around the world right now, I couldn’t even embrace my parents. Would they want me to volunteer?
I reached out to my classmates. I thought that some of them would certainly share my worries. I thought they also had to be carrying this uncomfortable kind of grief, a heavy and acidic feeling of dreams collapsing into a moral duty. I received a unanimous reply: “We are needed. It’s our time to step up.” No matter how many “what ifs” I voiced, they wouldn’t crack or waver. Still, even if they never admitted it to me, I wondered whether they privately shared some of my concerns and fears.
Everyone knows information is shared instantly in our Twitter-centric world, but I was still shocked and unprepared for how quickly I was at the center of a major news story. Within an hour of that email, I was contacted by an old acquaintance from elementary school, now a journalist. He had found me through Facebook and asked, “Will you be one of the NYU students graduating early? Would love to get a comment.” Another friend texted me a photo of the leaked email, quipping, “Are you going to save us from the pandemic, Dr. Gabe?!” “It’s not a small decision!” I snapped back.
I went through something like the seven stages of grief in rapid succession. I found that with each excuse I made why I shouldn’t volunteer, I somehow became increasingly more anxious. To my surprise, when I decided I would join 50 of my peers at NYU, graduate early, and volunteer, my mind settled. The more I thought about it, the more I was overtaken by the selfless beauty of the profession I’m entering. This is what it means to be a doctor. I recalled a key part of the Hippocratic Oath: “I will remember that I remain a member of society, with special obligations to all my fellow human beings, those sound of mind and body as well as the infirm.”
I am going to fulfill my special obligations.
The fear is still there. I’m scared of COVID. I’m scared to infect others. I’m scared of winding up paralyzed and intubated. But I have also realized that all we have is each other. Healthcare workers supporting healthcare workers. New Yorkers supporting New Yorkers. Citizens of the world supporting citizens of the world. This is my time to be there for others, unwaveringly.
Logistical details continue to roll in, although they feel trivial in relation to the decision I have already made. The paperwork tells me that I will be onboarded to NYU’s internal medicine residency program. I will be compensated and protected under a similar contract to what current NYU residents sign. I have been promised that I will remain insured until I start my official residency program in July. My student loans won’t begin accruing interest until my normally planned graduation date. I am told that I will have personal protective equipment in line with the Centers for Disease Control and Prevention recommendations.
Questions still linger. Is it safe for me and my newly minted physician peers to continue living with our spouses, children, and friends? How long will I need to quarantine after my contract ends? Will there be a virtual graduation ceremony for my parents and loved ones to enjoy? In these challenging times, each day gives me a little more clarity about what exactly I am signing up for, but there are still so many uncertainties.
Am I naive to say that I do feel prepared? Or at least as prepared as anyone can be. With respect to my training, I have completed the requirements to graduate, which is why I am being permitted to graduate early in the first place. Our faculty points to our professionalism as the most promising indicator of our preparedness. They are heartened that we have embraced this truest test: our duty to others.
There is an eerie calm to New York City that contradicts what is shown on the news. With stores closed and streets quiet, it almost feels like Christmas morning here. Yet, inside the hospital, a fire rages. All the metaphors being used right now speak about violence, devastation, and immeasurable human suffering. “A war is being fought.” Or so I have heard. I guess I am about to find out.
Gabriel Redel-Traub is a fourth-year medical student at NYU Grossman School of Medicine. He will be starting residency in internal medicine at Columbia Presbyterian this summer. He is the former editor-in-chief of Dartmouth College’s Mouth Magazine, an editor of NYU’s LitMed Database, and has published most recently in the Hasting’s Center Magazine. Gabriel Redel-Traub has disclosed no relevant financial relationships.
This article first appeared on Medscape.com.
Neurologists navigate unknown territory during COVID-19 pandemic
Neurologic disorders are among the “underlying medical conditions that may increase the risk of serious COVID-19 for individuals of any age,” according to the Centers for Disease Control and Prevention.
Potentially relevant drug interactions, how immunosuppressive medications may influence the risk of COVID-19, and neurologic diseases that may be associated with greater risk are among the questions that experts and groups have addressed.
According to the CDC, neurologic conditions that may heighten the risk of severe COVID-19 include “disorders of the brain, spinal cord, peripheral nerve, and muscle such as cerebral palsy, epilepsy (seizure disorders), stroke, intellectual disability, moderate to severe developmental delay, muscular dystrophy, or spinal cord injury.” Many patients, however, may not have substantially increased risks, neurologists suggest.
“Patients with conditions that do not affect their swallowing or breathing muscles and in whom the immune system is working normally are not considered to be at increased risk from COVID-19,” according to March 26 guidance from the Association of British Neurologists (ABN). “Milder or moderate forms of many of the commoner neurological disorders, such as Parkinson’s disease, multiple sclerosis, epilepsy, are not currently considered to confer increased risk, so long as the breathing and swallowing muscles are functioning well.”
Neurologists should tailor treatment decisions to individual patients, according to the ABN. “Although some neurological conditions or treatments increase the risk of complicated COVID-19, most patients in these groups will overcome the infection,” the association noted.
Interactions with potential COVID-19 treatments
Standard drugs in neurology may interact with potential COVID-19 treatments. For example, “preliminary experience suggests that there is a possible benefit from hydroxychloroquine and azithromycin treatment in COVID-19 infection,” but either of those drugs “may lead to a deterioration in myasthenia gravis,” the ABN notes. “Doctors will have to balance the risks from myasthenia and COVID-19 on a case-by-case basis.” The Liverpool Drug Interactions Group has published tables that describe interactions between potential COVID-19 treatments and anticonvulsants, analgesics, immunosuppressants, and other medication classes.
Many muscle diseases and neuromuscular junction diseases may entail higher risks of complicated COVID-19, the ABN suggested. For patients on immunotherapy, the medication may be a more important consideration for COVID-19 than the underlying disease. Other comorbidities such as hypertension, renal impairment, neutropenia, lymphopenia, liver disease, diabetes mellitus, ischemic heart disease, and lung disease may be important factors, according to the association.
Seizures may not worsen
After the CDC added epilepsy to its list of conditions that entail higher risk of severe COVID-19, M. Scott Perry, MD, medical director of neurology at Cook Children’s Medical Center in Fort Worth, Tex., commented on Twitter that “most healthy people with controlled epilepsy [are] probably at no more risk than others.”
“Those treated with steroids or other immunosuppressive drugs are likely higher risk,” Dr. Perry said. “Likewise, patients with other medical comorbidities such as muscle weakness, swallowing or breathing problems, and other complex cases of epilepsy are likely higher risk. Regardless: be responsible, avoid crowds, wash your hands, avoid sick contacts.”
Doctors in Italy, based on small numbers of cases, have found that seizures are not worse in patients with epilepsy and COVID-19, said Dr. Perry. A few children, including several patients with Dravet syndrome, “had uncomplicated illness and seizures were no worse,” he said. “That is reassuring.”
“Until now, there is no evidence of a direct effect of COVID-19 on seizures or epilepsy,” according to the International League Against Epilepsy (ILAE). “However, patients may experience worsening of seizures due to systemic illnesses, drug interactions, decreased access to antiseizure medications, and increased stress.”
“In younger children, the fever that accompanies COVID-19 may exacerbate seizures, as might any febrile illness,” according to an American Epilepsy Society (AES) resource for epilepsy clinicians. “The main known elevated risk factors related to COVID-19 are age, respiratory disease, and other chronic medical conditions not related to epilepsy. As for all, people with epilepsy should adhere to the CDC recommendations for reducing risk of infection.” Neurologists should review with patients the importance of treatment adherence, update plans for managing breakthrough seizures, and ensure necessary medications are on hand, according to the AES.
The Epilepsy Foundation created a page with information about COVID-19 for patients with epilepsy and recorded a discussion with epilepsy specialists. DEE-P (Developmental Epileptic Encephalopathy–Project) Connections recorded a webinar about protecting medically complex or immune-suppressed children with epilepsy from COVID-19.
MS DMTs and the coronavirus
The National Multiple Sclerosis (MS) Society has provided guidance on the use of disease-modifying therapies (DMTs) during the COVID-19 pandemic. “There are numerous recommendations circulating that attempt to provide clarity and guidance, however, differences among the recommendations have created confusion,” the society says. “DMT decision making varies significantly from country to country, ranging from highly provider-directed to a collaborative decision-making model. ... DMT decisions should be individualized and made collaboratively between the person with MS and his/her healthcare provider.”
Patients with MS and their physicians should weigh risks and benefits before starting cell-depleting DMTs such as alemtuzumab, cladribine, ocrelizumab, or rituximab, according the National MS Society. They also should consider the risks and benefits of DMTs that carry warnings of a potentially severe increase in disability after stopping therapy, such as fingolimod and natalizumab. “We endorse the global advice provided by the MS International Federation (MSIF) – but emphasize that DMT decision making must be individualized and based upon multiple factors,” the National MS Society said.
Neurologists currently lack evidence about how COVID-19 affects patients with MS, according to the MSIF, which based its DMT guidance on advice from MS neurologists and research experts from member organizations. Many DMTs suppress or modify the immune system, and “some MS medications might increase the likelihood of developing complications from a COVID-19 infection but this risk needs to be balanced with the risks of stopping treatment,” according to the federation.
Patients currently taking DMTs should continue treatment, and those who develop symptoms of COVID-19 or test positive for the infection should discuss their DMT with a health care professional familiar with their care, the MSIF recommends. Decisions about starting a DMT should take into account a patient’s disease course, disease activity, and regional COVID-19 risks, according to the federation. For patients due to start DMT, treatments that do not reduce lymphocytes, such as interferons, glatiramer acetate, or natalizumab, should be considered.
Fingolimod, dimethyl fumarate, teriflunomide, and siponimod “may reduce the ability of the immune system to respond to an infection,” and “people should carefully consider the risks and benefits of initiating these treatments during the COVID-19 pandemic,” according to the federation. “People with MS who are currently taking alemtuzumab, cladribine, ocrelizumab, rituximab, fingolimod, dimethyl fumarate, teriflunomide or siponimod and are living in a community with a COVID-19 outbreak should isolate as much as possible to reduce their risk of infection.”
Extended isolation during the COVID-19 outbreak may be warranted for patients with MS who have recently undergone autologous hematopoietic stem cell treatment, which entails intensive chemotherapy, the guidance says. In addition, postponement of this procedure should be considered.
Child neurology, migraine, movement disorders, and stroke
The Child Neurology Foundation (CNF) and Child Neurology Society (CNS) published a joint statement about COVID-19. “Most children who contract COVID-19 appear to exhibit only mild symptoms,” said Scott Pomeroy, MD, president of CNF’s board of directors and chair of the department of neurology at Boston Children’s Hospital, in the statement. “However, if your child is taking a medication such as steroids that can lower their immune system response, there could be an increased risk for more significant symptoms. In addition, children with lung disease, such as asthma, may also be at higher risk. Therefore, it is important to practice preventative precautions. We hope that this information will help to reduce some of the fears that families in our community may be experiencing.”
The American Migraine Foundation shared COVID-19 considerations for patients with migraine from Mia Minen, MD, associate professor of neurology and population health at NYU Langone in New York. Patients with migraine who are otherwise in good health are not expected to be at increased risk of severe COVID-19, according to Dr. Minen. Best practices include having an adequate supply of medicine, considering alternatives to in-person doctor visits, and being “mindful of routine and diet to reduce migraine triggers,” the foundation suggests. In addition, patients should try to limit stress and seek out “alternative methods of social interaction.”
“The relationship between COVID-19 and Parkinson’s disease or other movement disorders remains unknown,” the International Parkinson and Movement Disorder Society said. “In general, we recommend that our movement disorder patients do not assume they are at extreme risks, which for the time being are uncertain. Nevertheless, we strongly recommend following the standard measures strictly to avoid exposures to the virus.”
The American Heart Association (AHA) cautions that older patients with coronary heart disease or hypertension “may be more likely than others to be infected by the coronavirus that causes COVID-19 and to develop more severe symptoms.” In addition, people with a history of stroke “may face a higher risk of complications,” according to the AHA. “As a result, people who have heart disease or another underlying condition should stay home to limit their risk of contracting the virus.”
Several groups emphasized the importance of telemedicine as an option for patients with neurologic conditions during the pandemic. The American Headache Society has hosted discussions on conducting neurologic exams via telemedicine. The American Academy of Neurology also conducted a webinar on telemedicine and COVID-19 and created a page with COVID-19 resources. The journal Neurology is publishing invited commentaries about neurologic aspects of the COVID-19 pandemic.
Neurologic disorders are among the “underlying medical conditions that may increase the risk of serious COVID-19 for individuals of any age,” according to the Centers for Disease Control and Prevention.
Potentially relevant drug interactions, how immunosuppressive medications may influence the risk of COVID-19, and neurologic diseases that may be associated with greater risk are among the questions that experts and groups have addressed.
According to the CDC, neurologic conditions that may heighten the risk of severe COVID-19 include “disorders of the brain, spinal cord, peripheral nerve, and muscle such as cerebral palsy, epilepsy (seizure disorders), stroke, intellectual disability, moderate to severe developmental delay, muscular dystrophy, or spinal cord injury.” Many patients, however, may not have substantially increased risks, neurologists suggest.
“Patients with conditions that do not affect their swallowing or breathing muscles and in whom the immune system is working normally are not considered to be at increased risk from COVID-19,” according to March 26 guidance from the Association of British Neurologists (ABN). “Milder or moderate forms of many of the commoner neurological disorders, such as Parkinson’s disease, multiple sclerosis, epilepsy, are not currently considered to confer increased risk, so long as the breathing and swallowing muscles are functioning well.”
Neurologists should tailor treatment decisions to individual patients, according to the ABN. “Although some neurological conditions or treatments increase the risk of complicated COVID-19, most patients in these groups will overcome the infection,” the association noted.
Interactions with potential COVID-19 treatments
Standard drugs in neurology may interact with potential COVID-19 treatments. For example, “preliminary experience suggests that there is a possible benefit from hydroxychloroquine and azithromycin treatment in COVID-19 infection,” but either of those drugs “may lead to a deterioration in myasthenia gravis,” the ABN notes. “Doctors will have to balance the risks from myasthenia and COVID-19 on a case-by-case basis.” The Liverpool Drug Interactions Group has published tables that describe interactions between potential COVID-19 treatments and anticonvulsants, analgesics, immunosuppressants, and other medication classes.
Many muscle diseases and neuromuscular junction diseases may entail higher risks of complicated COVID-19, the ABN suggested. For patients on immunotherapy, the medication may be a more important consideration for COVID-19 than the underlying disease. Other comorbidities such as hypertension, renal impairment, neutropenia, lymphopenia, liver disease, diabetes mellitus, ischemic heart disease, and lung disease may be important factors, according to the association.
Seizures may not worsen
After the CDC added epilepsy to its list of conditions that entail higher risk of severe COVID-19, M. Scott Perry, MD, medical director of neurology at Cook Children’s Medical Center in Fort Worth, Tex., commented on Twitter that “most healthy people with controlled epilepsy [are] probably at no more risk than others.”
“Those treated with steroids or other immunosuppressive drugs are likely higher risk,” Dr. Perry said. “Likewise, patients with other medical comorbidities such as muscle weakness, swallowing or breathing problems, and other complex cases of epilepsy are likely higher risk. Regardless: be responsible, avoid crowds, wash your hands, avoid sick contacts.”
Doctors in Italy, based on small numbers of cases, have found that seizures are not worse in patients with epilepsy and COVID-19, said Dr. Perry. A few children, including several patients with Dravet syndrome, “had uncomplicated illness and seizures were no worse,” he said. “That is reassuring.”
“Until now, there is no evidence of a direct effect of COVID-19 on seizures or epilepsy,” according to the International League Against Epilepsy (ILAE). “However, patients may experience worsening of seizures due to systemic illnesses, drug interactions, decreased access to antiseizure medications, and increased stress.”
“In younger children, the fever that accompanies COVID-19 may exacerbate seizures, as might any febrile illness,” according to an American Epilepsy Society (AES) resource for epilepsy clinicians. “The main known elevated risk factors related to COVID-19 are age, respiratory disease, and other chronic medical conditions not related to epilepsy. As for all, people with epilepsy should adhere to the CDC recommendations for reducing risk of infection.” Neurologists should review with patients the importance of treatment adherence, update plans for managing breakthrough seizures, and ensure necessary medications are on hand, according to the AES.
The Epilepsy Foundation created a page with information about COVID-19 for patients with epilepsy and recorded a discussion with epilepsy specialists. DEE-P (Developmental Epileptic Encephalopathy–Project) Connections recorded a webinar about protecting medically complex or immune-suppressed children with epilepsy from COVID-19.
MS DMTs and the coronavirus
The National Multiple Sclerosis (MS) Society has provided guidance on the use of disease-modifying therapies (DMTs) during the COVID-19 pandemic. “There are numerous recommendations circulating that attempt to provide clarity and guidance, however, differences among the recommendations have created confusion,” the society says. “DMT decision making varies significantly from country to country, ranging from highly provider-directed to a collaborative decision-making model. ... DMT decisions should be individualized and made collaboratively between the person with MS and his/her healthcare provider.”
Patients with MS and their physicians should weigh risks and benefits before starting cell-depleting DMTs such as alemtuzumab, cladribine, ocrelizumab, or rituximab, according the National MS Society. They also should consider the risks and benefits of DMTs that carry warnings of a potentially severe increase in disability after stopping therapy, such as fingolimod and natalizumab. “We endorse the global advice provided by the MS International Federation (MSIF) – but emphasize that DMT decision making must be individualized and based upon multiple factors,” the National MS Society said.
Neurologists currently lack evidence about how COVID-19 affects patients with MS, according to the MSIF, which based its DMT guidance on advice from MS neurologists and research experts from member organizations. Many DMTs suppress or modify the immune system, and “some MS medications might increase the likelihood of developing complications from a COVID-19 infection but this risk needs to be balanced with the risks of stopping treatment,” according to the federation.
Patients currently taking DMTs should continue treatment, and those who develop symptoms of COVID-19 or test positive for the infection should discuss their DMT with a health care professional familiar with their care, the MSIF recommends. Decisions about starting a DMT should take into account a patient’s disease course, disease activity, and regional COVID-19 risks, according to the federation. For patients due to start DMT, treatments that do not reduce lymphocytes, such as interferons, glatiramer acetate, or natalizumab, should be considered.
Fingolimod, dimethyl fumarate, teriflunomide, and siponimod “may reduce the ability of the immune system to respond to an infection,” and “people should carefully consider the risks and benefits of initiating these treatments during the COVID-19 pandemic,” according to the federation. “People with MS who are currently taking alemtuzumab, cladribine, ocrelizumab, rituximab, fingolimod, dimethyl fumarate, teriflunomide or siponimod and are living in a community with a COVID-19 outbreak should isolate as much as possible to reduce their risk of infection.”
Extended isolation during the COVID-19 outbreak may be warranted for patients with MS who have recently undergone autologous hematopoietic stem cell treatment, which entails intensive chemotherapy, the guidance says. In addition, postponement of this procedure should be considered.
Child neurology, migraine, movement disorders, and stroke
The Child Neurology Foundation (CNF) and Child Neurology Society (CNS) published a joint statement about COVID-19. “Most children who contract COVID-19 appear to exhibit only mild symptoms,” said Scott Pomeroy, MD, president of CNF’s board of directors and chair of the department of neurology at Boston Children’s Hospital, in the statement. “However, if your child is taking a medication such as steroids that can lower their immune system response, there could be an increased risk for more significant symptoms. In addition, children with lung disease, such as asthma, may also be at higher risk. Therefore, it is important to practice preventative precautions. We hope that this information will help to reduce some of the fears that families in our community may be experiencing.”
The American Migraine Foundation shared COVID-19 considerations for patients with migraine from Mia Minen, MD, associate professor of neurology and population health at NYU Langone in New York. Patients with migraine who are otherwise in good health are not expected to be at increased risk of severe COVID-19, according to Dr. Minen. Best practices include having an adequate supply of medicine, considering alternatives to in-person doctor visits, and being “mindful of routine and diet to reduce migraine triggers,” the foundation suggests. In addition, patients should try to limit stress and seek out “alternative methods of social interaction.”
“The relationship between COVID-19 and Parkinson’s disease or other movement disorders remains unknown,” the International Parkinson and Movement Disorder Society said. “In general, we recommend that our movement disorder patients do not assume they are at extreme risks, which for the time being are uncertain. Nevertheless, we strongly recommend following the standard measures strictly to avoid exposures to the virus.”
The American Heart Association (AHA) cautions that older patients with coronary heart disease or hypertension “may be more likely than others to be infected by the coronavirus that causes COVID-19 and to develop more severe symptoms.” In addition, people with a history of stroke “may face a higher risk of complications,” according to the AHA. “As a result, people who have heart disease or another underlying condition should stay home to limit their risk of contracting the virus.”
Several groups emphasized the importance of telemedicine as an option for patients with neurologic conditions during the pandemic. The American Headache Society has hosted discussions on conducting neurologic exams via telemedicine. The American Academy of Neurology also conducted a webinar on telemedicine and COVID-19 and created a page with COVID-19 resources. The journal Neurology is publishing invited commentaries about neurologic aspects of the COVID-19 pandemic.
Neurologic disorders are among the “underlying medical conditions that may increase the risk of serious COVID-19 for individuals of any age,” according to the Centers for Disease Control and Prevention.
Potentially relevant drug interactions, how immunosuppressive medications may influence the risk of COVID-19, and neurologic diseases that may be associated with greater risk are among the questions that experts and groups have addressed.
According to the CDC, neurologic conditions that may heighten the risk of severe COVID-19 include “disorders of the brain, spinal cord, peripheral nerve, and muscle such as cerebral palsy, epilepsy (seizure disorders), stroke, intellectual disability, moderate to severe developmental delay, muscular dystrophy, or spinal cord injury.” Many patients, however, may not have substantially increased risks, neurologists suggest.
“Patients with conditions that do not affect their swallowing or breathing muscles and in whom the immune system is working normally are not considered to be at increased risk from COVID-19,” according to March 26 guidance from the Association of British Neurologists (ABN). “Milder or moderate forms of many of the commoner neurological disorders, such as Parkinson’s disease, multiple sclerosis, epilepsy, are not currently considered to confer increased risk, so long as the breathing and swallowing muscles are functioning well.”
Neurologists should tailor treatment decisions to individual patients, according to the ABN. “Although some neurological conditions or treatments increase the risk of complicated COVID-19, most patients in these groups will overcome the infection,” the association noted.
Interactions with potential COVID-19 treatments
Standard drugs in neurology may interact with potential COVID-19 treatments. For example, “preliminary experience suggests that there is a possible benefit from hydroxychloroquine and azithromycin treatment in COVID-19 infection,” but either of those drugs “may lead to a deterioration in myasthenia gravis,” the ABN notes. “Doctors will have to balance the risks from myasthenia and COVID-19 on a case-by-case basis.” The Liverpool Drug Interactions Group has published tables that describe interactions between potential COVID-19 treatments and anticonvulsants, analgesics, immunosuppressants, and other medication classes.
Many muscle diseases and neuromuscular junction diseases may entail higher risks of complicated COVID-19, the ABN suggested. For patients on immunotherapy, the medication may be a more important consideration for COVID-19 than the underlying disease. Other comorbidities such as hypertension, renal impairment, neutropenia, lymphopenia, liver disease, diabetes mellitus, ischemic heart disease, and lung disease may be important factors, according to the association.
Seizures may not worsen
After the CDC added epilepsy to its list of conditions that entail higher risk of severe COVID-19, M. Scott Perry, MD, medical director of neurology at Cook Children’s Medical Center in Fort Worth, Tex., commented on Twitter that “most healthy people with controlled epilepsy [are] probably at no more risk than others.”
“Those treated with steroids or other immunosuppressive drugs are likely higher risk,” Dr. Perry said. “Likewise, patients with other medical comorbidities such as muscle weakness, swallowing or breathing problems, and other complex cases of epilepsy are likely higher risk. Regardless: be responsible, avoid crowds, wash your hands, avoid sick contacts.”
Doctors in Italy, based on small numbers of cases, have found that seizures are not worse in patients with epilepsy and COVID-19, said Dr. Perry. A few children, including several patients with Dravet syndrome, “had uncomplicated illness and seizures were no worse,” he said. “That is reassuring.”
“Until now, there is no evidence of a direct effect of COVID-19 on seizures or epilepsy,” according to the International League Against Epilepsy (ILAE). “However, patients may experience worsening of seizures due to systemic illnesses, drug interactions, decreased access to antiseizure medications, and increased stress.”
“In younger children, the fever that accompanies COVID-19 may exacerbate seizures, as might any febrile illness,” according to an American Epilepsy Society (AES) resource for epilepsy clinicians. “The main known elevated risk factors related to COVID-19 are age, respiratory disease, and other chronic medical conditions not related to epilepsy. As for all, people with epilepsy should adhere to the CDC recommendations for reducing risk of infection.” Neurologists should review with patients the importance of treatment adherence, update plans for managing breakthrough seizures, and ensure necessary medications are on hand, according to the AES.
The Epilepsy Foundation created a page with information about COVID-19 for patients with epilepsy and recorded a discussion with epilepsy specialists. DEE-P (Developmental Epileptic Encephalopathy–Project) Connections recorded a webinar about protecting medically complex or immune-suppressed children with epilepsy from COVID-19.
MS DMTs and the coronavirus
The National Multiple Sclerosis (MS) Society has provided guidance on the use of disease-modifying therapies (DMTs) during the COVID-19 pandemic. “There are numerous recommendations circulating that attempt to provide clarity and guidance, however, differences among the recommendations have created confusion,” the society says. “DMT decision making varies significantly from country to country, ranging from highly provider-directed to a collaborative decision-making model. ... DMT decisions should be individualized and made collaboratively between the person with MS and his/her healthcare provider.”
Patients with MS and their physicians should weigh risks and benefits before starting cell-depleting DMTs such as alemtuzumab, cladribine, ocrelizumab, or rituximab, according the National MS Society. They also should consider the risks and benefits of DMTs that carry warnings of a potentially severe increase in disability after stopping therapy, such as fingolimod and natalizumab. “We endorse the global advice provided by the MS International Federation (MSIF) – but emphasize that DMT decision making must be individualized and based upon multiple factors,” the National MS Society said.
Neurologists currently lack evidence about how COVID-19 affects patients with MS, according to the MSIF, which based its DMT guidance on advice from MS neurologists and research experts from member organizations. Many DMTs suppress or modify the immune system, and “some MS medications might increase the likelihood of developing complications from a COVID-19 infection but this risk needs to be balanced with the risks of stopping treatment,” according to the federation.
Patients currently taking DMTs should continue treatment, and those who develop symptoms of COVID-19 or test positive for the infection should discuss their DMT with a health care professional familiar with their care, the MSIF recommends. Decisions about starting a DMT should take into account a patient’s disease course, disease activity, and regional COVID-19 risks, according to the federation. For patients due to start DMT, treatments that do not reduce lymphocytes, such as interferons, glatiramer acetate, or natalizumab, should be considered.
Fingolimod, dimethyl fumarate, teriflunomide, and siponimod “may reduce the ability of the immune system to respond to an infection,” and “people should carefully consider the risks and benefits of initiating these treatments during the COVID-19 pandemic,” according to the federation. “People with MS who are currently taking alemtuzumab, cladribine, ocrelizumab, rituximab, fingolimod, dimethyl fumarate, teriflunomide or siponimod and are living in a community with a COVID-19 outbreak should isolate as much as possible to reduce their risk of infection.”
Extended isolation during the COVID-19 outbreak may be warranted for patients with MS who have recently undergone autologous hematopoietic stem cell treatment, which entails intensive chemotherapy, the guidance says. In addition, postponement of this procedure should be considered.
Child neurology, migraine, movement disorders, and stroke
The Child Neurology Foundation (CNF) and Child Neurology Society (CNS) published a joint statement about COVID-19. “Most children who contract COVID-19 appear to exhibit only mild symptoms,” said Scott Pomeroy, MD, president of CNF’s board of directors and chair of the department of neurology at Boston Children’s Hospital, in the statement. “However, if your child is taking a medication such as steroids that can lower their immune system response, there could be an increased risk for more significant symptoms. In addition, children with lung disease, such as asthma, may also be at higher risk. Therefore, it is important to practice preventative precautions. We hope that this information will help to reduce some of the fears that families in our community may be experiencing.”
The American Migraine Foundation shared COVID-19 considerations for patients with migraine from Mia Minen, MD, associate professor of neurology and population health at NYU Langone in New York. Patients with migraine who are otherwise in good health are not expected to be at increased risk of severe COVID-19, according to Dr. Minen. Best practices include having an adequate supply of medicine, considering alternatives to in-person doctor visits, and being “mindful of routine and diet to reduce migraine triggers,” the foundation suggests. In addition, patients should try to limit stress and seek out “alternative methods of social interaction.”
“The relationship between COVID-19 and Parkinson’s disease or other movement disorders remains unknown,” the International Parkinson and Movement Disorder Society said. “In general, we recommend that our movement disorder patients do not assume they are at extreme risks, which for the time being are uncertain. Nevertheless, we strongly recommend following the standard measures strictly to avoid exposures to the virus.”
The American Heart Association (AHA) cautions that older patients with coronary heart disease or hypertension “may be more likely than others to be infected by the coronavirus that causes COVID-19 and to develop more severe symptoms.” In addition, people with a history of stroke “may face a higher risk of complications,” according to the AHA. “As a result, people who have heart disease or another underlying condition should stay home to limit their risk of contracting the virus.”
Several groups emphasized the importance of telemedicine as an option for patients with neurologic conditions during the pandemic. The American Headache Society has hosted discussions on conducting neurologic exams via telemedicine. The American Academy of Neurology also conducted a webinar on telemedicine and COVID-19 and created a page with COVID-19 resources. The journal Neurology is publishing invited commentaries about neurologic aspects of the COVID-19 pandemic.
Surge in firearm sales tied to COVID-19 fears, uncertainty presents risks
Use gentle assumptions and focus on home access to elicit positive answers.
In the wake of the 2012 shooting at Sandy Hook Elementary, in Newtown, Conn., after 20 children and seven adults were murdered, American gun sales surged on fears of new restrictions.
In the ensuing months, 20 more children and 40 more adults died from unintentional shootings believed to be tied to that surge in gun purchases.1 More recently, American gun sales surged in response to the COVID-19 pandemic with heated legal battles brewing over whether gun sales are essential.2,3 The results of this surge in sales are yet to fully manifest, but I would like to discuss several risks.
The public health risks of firearm access are well established: Nearly every measure of harm, from suicide to negligent injury and death to homicide to shootings of police, increase along with access to firearms.4 That firearms in the home are associated with greater likelihoods of suicide, negligent injury and death, and intrafamilial homicide has been recognized for decades as has the substantially heightened risk in the immediate period after a firearm is brought into the home.5,6 Defensive gun use is rare despite this being the nominal reason for firearm ownership among many.7 Even prior to recent events, there had been concerns of increased unsafe carrying and handling of firearms.8 It seems reasonable to expect such trends not to be diminished by recent events.
Added to this are several stressors, which one can reasonably expect to be associated with increased risks for unsafe use. There are new, broad social stressors from fear and uncertainty about COVID-19. Unemployment rates have skyrocketed, clinical care has been disrupted, and basic necessities have become scant. Children are home from school, unable to play with friends and unable to access mental health services as easily as before; risks of negligent and suicidal injuries and death may ensue. Couples and families are isolated in homes together for longer periods and with fewer avenues for relief; previously peaceful homes may see conflicts increase and homes with abuse have now trapped victims with their assailants. Social isolation is difficult for any person and may be even more traumatic for people with underlying vulnerabilities, including mental illness. The risks of being isolated in a home – struggling with worsening symptoms – with ready access to a firearm are self-evident.
- Consider reassessing for firearm access. Patients may be in new homes, or there may be new firearms in their homes. Use gentle assumptions and focus on home access over personal access to elicit the most true, positive answers, for example: “I understand there have been a lot of changes recently; how many guns are in the home now?”
- Reinforce safer storage practices. Simple measures, such as storing ammunition separately and using trigger locks or safes, can make a substantial difference in injury risks.
- Do not forget aging clients; suicide risk increases with age, and there may be substantial risks among the geriatric population for suicide and murder-suicide. If using telepsychiatry, realize that the abuser might be in the home or within earshot of any clinical encounter, and this might put the client at heightened risk, during and after telesessions.
- Highlight access to local and national resources, including the Disaster Distress Hotline (800-985-5990) and the National Suicide Prevention Lifeline (800-273-TALK). Promote both numbers, and note that some people may be more comfortable reaching out for help for “distress” than for “suicide.”
References
1. Levine PB and McKnight R. Science. 2017 Dec 8;358(6368):1324-8.
2. Levin D. “Coronavirus and firearms: Are gun shops essential businesses?” The New York Times. 2020 Mar 25.
3. Robertson L. “Neither hurricanes nor 9/11 caused as big a surge in gun sales as coronavirus.” Miami Herald. 2020 Mar 25.
4. Moyer MW. Scientific American. 2017 Oct;317(4):54-63.
5. Kellermann AL et al. J Trauma. 1998 Aug;45(2):263-7.
6. Wintemute GJ et al. New Engl J Med. 1999 Nov 18;341(21):1583-9.
7. Firearm Justifiable Homicides and Non-Fatal Self-Defense Gun Use: An Analysis of Federal Bureau of Investigation and National Crime Victimization Survey Data. Washington: Violence Policy Center; 2019 Jul.
8. Towers S et al. bioRxiv. 2019 Apr 18;613687.
Dr. Rozel is the medical director of resolve Crisis Services at UPMC Western Psychiatric Hospital and president of the American Association for Emergency Psychiatry. He also is associate professor of psychiatry and an adjunct professor of law at the University of Pittsburgh. He has no conflicts of interest but has worked for a gun dealer to teach sales staff how to recognize people in crisis (rather than sell a gun).
Use gentle assumptions and focus on home access to elicit positive answers.
Use gentle assumptions and focus on home access to elicit positive answers.
In the wake of the 2012 shooting at Sandy Hook Elementary, in Newtown, Conn., after 20 children and seven adults were murdered, American gun sales surged on fears of new restrictions.
In the ensuing months, 20 more children and 40 more adults died from unintentional shootings believed to be tied to that surge in gun purchases.1 More recently, American gun sales surged in response to the COVID-19 pandemic with heated legal battles brewing over whether gun sales are essential.2,3 The results of this surge in sales are yet to fully manifest, but I would like to discuss several risks.
The public health risks of firearm access are well established: Nearly every measure of harm, from suicide to negligent injury and death to homicide to shootings of police, increase along with access to firearms.4 That firearms in the home are associated with greater likelihoods of suicide, negligent injury and death, and intrafamilial homicide has been recognized for decades as has the substantially heightened risk in the immediate period after a firearm is brought into the home.5,6 Defensive gun use is rare despite this being the nominal reason for firearm ownership among many.7 Even prior to recent events, there had been concerns of increased unsafe carrying and handling of firearms.8 It seems reasonable to expect such trends not to be diminished by recent events.
Added to this are several stressors, which one can reasonably expect to be associated with increased risks for unsafe use. There are new, broad social stressors from fear and uncertainty about COVID-19. Unemployment rates have skyrocketed, clinical care has been disrupted, and basic necessities have become scant. Children are home from school, unable to play with friends and unable to access mental health services as easily as before; risks of negligent and suicidal injuries and death may ensue. Couples and families are isolated in homes together for longer periods and with fewer avenues for relief; previously peaceful homes may see conflicts increase and homes with abuse have now trapped victims with their assailants. Social isolation is difficult for any person and may be even more traumatic for people with underlying vulnerabilities, including mental illness. The risks of being isolated in a home – struggling with worsening symptoms – with ready access to a firearm are self-evident.
- Consider reassessing for firearm access. Patients may be in new homes, or there may be new firearms in their homes. Use gentle assumptions and focus on home access over personal access to elicit the most true, positive answers, for example: “I understand there have been a lot of changes recently; how many guns are in the home now?”
- Reinforce safer storage practices. Simple measures, such as storing ammunition separately and using trigger locks or safes, can make a substantial difference in injury risks.
- Do not forget aging clients; suicide risk increases with age, and there may be substantial risks among the geriatric population for suicide and murder-suicide. If using telepsychiatry, realize that the abuser might be in the home or within earshot of any clinical encounter, and this might put the client at heightened risk, during and after telesessions.
- Highlight access to local and national resources, including the Disaster Distress Hotline (800-985-5990) and the National Suicide Prevention Lifeline (800-273-TALK). Promote both numbers, and note that some people may be more comfortable reaching out for help for “distress” than for “suicide.”
References
1. Levine PB and McKnight R. Science. 2017 Dec 8;358(6368):1324-8.
2. Levin D. “Coronavirus and firearms: Are gun shops essential businesses?” The New York Times. 2020 Mar 25.
3. Robertson L. “Neither hurricanes nor 9/11 caused as big a surge in gun sales as coronavirus.” Miami Herald. 2020 Mar 25.
4. Moyer MW. Scientific American. 2017 Oct;317(4):54-63.
5. Kellermann AL et al. J Trauma. 1998 Aug;45(2):263-7.
6. Wintemute GJ et al. New Engl J Med. 1999 Nov 18;341(21):1583-9.
7. Firearm Justifiable Homicides and Non-Fatal Self-Defense Gun Use: An Analysis of Federal Bureau of Investigation and National Crime Victimization Survey Data. Washington: Violence Policy Center; 2019 Jul.
8. Towers S et al. bioRxiv. 2019 Apr 18;613687.
Dr. Rozel is the medical director of resolve Crisis Services at UPMC Western Psychiatric Hospital and president of the American Association for Emergency Psychiatry. He also is associate professor of psychiatry and an adjunct professor of law at the University of Pittsburgh. He has no conflicts of interest but has worked for a gun dealer to teach sales staff how to recognize people in crisis (rather than sell a gun).
In the wake of the 2012 shooting at Sandy Hook Elementary, in Newtown, Conn., after 20 children and seven adults were murdered, American gun sales surged on fears of new restrictions.
In the ensuing months, 20 more children and 40 more adults died from unintentional shootings believed to be tied to that surge in gun purchases.1 More recently, American gun sales surged in response to the COVID-19 pandemic with heated legal battles brewing over whether gun sales are essential.2,3 The results of this surge in sales are yet to fully manifest, but I would like to discuss several risks.
The public health risks of firearm access are well established: Nearly every measure of harm, from suicide to negligent injury and death to homicide to shootings of police, increase along with access to firearms.4 That firearms in the home are associated with greater likelihoods of suicide, negligent injury and death, and intrafamilial homicide has been recognized for decades as has the substantially heightened risk in the immediate period after a firearm is brought into the home.5,6 Defensive gun use is rare despite this being the nominal reason for firearm ownership among many.7 Even prior to recent events, there had been concerns of increased unsafe carrying and handling of firearms.8 It seems reasonable to expect such trends not to be diminished by recent events.
Added to this are several stressors, which one can reasonably expect to be associated with increased risks for unsafe use. There are new, broad social stressors from fear and uncertainty about COVID-19. Unemployment rates have skyrocketed, clinical care has been disrupted, and basic necessities have become scant. Children are home from school, unable to play with friends and unable to access mental health services as easily as before; risks of negligent and suicidal injuries and death may ensue. Couples and families are isolated in homes together for longer periods and with fewer avenues for relief; previously peaceful homes may see conflicts increase and homes with abuse have now trapped victims with their assailants. Social isolation is difficult for any person and may be even more traumatic for people with underlying vulnerabilities, including mental illness. The risks of being isolated in a home – struggling with worsening symptoms – with ready access to a firearm are self-evident.
- Consider reassessing for firearm access. Patients may be in new homes, or there may be new firearms in their homes. Use gentle assumptions and focus on home access over personal access to elicit the most true, positive answers, for example: “I understand there have been a lot of changes recently; how many guns are in the home now?”
- Reinforce safer storage practices. Simple measures, such as storing ammunition separately and using trigger locks or safes, can make a substantial difference in injury risks.
- Do not forget aging clients; suicide risk increases with age, and there may be substantial risks among the geriatric population for suicide and murder-suicide. If using telepsychiatry, realize that the abuser might be in the home or within earshot of any clinical encounter, and this might put the client at heightened risk, during and after telesessions.
- Highlight access to local and national resources, including the Disaster Distress Hotline (800-985-5990) and the National Suicide Prevention Lifeline (800-273-TALK). Promote both numbers, and note that some people may be more comfortable reaching out for help for “distress” than for “suicide.”
References
1. Levine PB and McKnight R. Science. 2017 Dec 8;358(6368):1324-8.
2. Levin D. “Coronavirus and firearms: Are gun shops essential businesses?” The New York Times. 2020 Mar 25.
3. Robertson L. “Neither hurricanes nor 9/11 caused as big a surge in gun sales as coronavirus.” Miami Herald. 2020 Mar 25.
4. Moyer MW. Scientific American. 2017 Oct;317(4):54-63.
5. Kellermann AL et al. J Trauma. 1998 Aug;45(2):263-7.
6. Wintemute GJ et al. New Engl J Med. 1999 Nov 18;341(21):1583-9.
7. Firearm Justifiable Homicides and Non-Fatal Self-Defense Gun Use: An Analysis of Federal Bureau of Investigation and National Crime Victimization Survey Data. Washington: Violence Policy Center; 2019 Jul.
8. Towers S et al. bioRxiv. 2019 Apr 18;613687.
Dr. Rozel is the medical director of resolve Crisis Services at UPMC Western Psychiatric Hospital and president of the American Association for Emergency Psychiatry. He also is associate professor of psychiatry and an adjunct professor of law at the University of Pittsburgh. He has no conflicts of interest but has worked for a gun dealer to teach sales staff how to recognize people in crisis (rather than sell a gun).
No staff COVID-19 diagnoses after plan at Chinese cancer center
Short-term results
No staff members or patients were diagnosed with COVID-19 after “strict protective measures” for screening and managing patients were implemented at the National Cancer Center/Cancer Hospital, Chinese Academy of Sciences, in Beijing, according to a report published online April 1 in JAMA Oncology.
However, the time period for the analysis, which included nearly 3000 patients, was short — only about 3 weeks (February 12 to March 3). Also, Beijing is more than 1100 kilometers from Wuhan, the center of the Chinese outbreak of COVID-19.
The Beijing cancer hospital implemented a multipronged safety plan in February in order to “avoid COVID-19 related nosocomial cross-infection between patients and medical staff,” explain the authors, led by medical oncologist Zhijie Wang, MD.
Notably, “all of the measures taken in China are actively being implemented and used in major oncology centers in the United States,” Robert Carlson, MD, chief executive officer, National Comprehensive Cancer Network (NCCN), told Medscape Medical News.
John Greene, MD, section chief, Infectious Disease and Tropical Medicine, Moffitt Cancer Center, Tampa, Florida, pointed out that the Chinese safety plan, which is full of “good measures,” is being largely used at his center. However, he observed that one tool — doing a temperature check at the hospital front door — is not well supported by most of the literature. “It gives good optics and looks like you are doing the most you possibly can, but scientifically it may not be as effective [as other screening measures],” he said.
The Chinese plan consists of four broad elements
First, the above-mentioned on-site temperature tests are performed at the entrances of the hospital, outpatient clinic, and wards. Contact and travel histories related to the Wuhan epidemic area are also established and recorded.
Second, an outpatient appointment scheduling system allows both online scheduling and on-site registration. Online consultation channels are open daily, featuring instruction on medication taking and cancer-related symptom management. These “substantially reduced the flow of people in the hospital,” write the authors. On-site patients must wear a mask and have their own disinfectant.
Third, for patients with cancer preparing to be admitted to hospital, symptoms associated with COVID-19, such as fever and cough, are recorded. Mandatory blood tests and CT scans of the lungs are performed. COVID-19 virus nucleic acid tests are performed for patients with suspected pneumonia on imaging.
Fourth, some anticancer drugs conventionally administered by infusion have been changed to oral administration, such as etoposide and vinorelbine. For adjuvant or maintenance chemotherapy, the infusion intervals were appropriately prolonged depending on patients’ conditions.
Eight out of 2,900 patients had imaging suspicious for infection
The Chinese authors report that a total of 2,944 patients with cancer were seen for clinic consultation and treatment in the wards (2795 outpatients and 149 inpatients).
Patients with cancer are believed to have a higher probability of severe illness and increased mortality compared with the healthy population once infected with COVID-19, point out the authors.
Under the new “strict screening strategy,” 27 patients showed radiologic manifestations of inflammatory changes or multiple-site exudative pneumonia in the lungs, including eight suspected of having COVID-19 infection. “Fortunately, negative results from nucleic acid testing ultimately excluded COVID-19 infection in all these patients,” the authors report.
However, two of these patients “presented with recovered pneumonia after symptomatic treatment.” Commenting on this finding, Moffitt’s Greene said that may mean these two patients were tested and found to be positive but were early in the infection and not yet shedding the virus, or they were infected after the initial negative result.
Greene said his center has implemented some measures not mentioned in the Chinese plan. For example, the Florida center no longer allows inpatient visitation. Also, one third of staff now work from home, resulting in less social interaction. Social distancing in meetings, the cafeteria, and hallways is being observed “aggressively,” and most meetings are now on Zoom, he said.
Moffitt has not been hard hit with COVID-19 and is at level one preparedness, the lowest rung. The center has performed 60 tests to date, with only one positive for the virus (< 2%), Greene told Medscape Medical News.
Currently, in the larger Tampa Bay community setting, about 12% of tests are positive.
The low percentage found among the Moffitt patients “tells you that a lot of cancer patients have fever and respiratory symptoms due to other viruses and, more importantly, other reasons, whether it’s their immunotherapy or chemotherapy or their cancer,” said Greene.
NCCN’s Carlson said the publication of the Chinese data was a good sign in terms of international science.
“This is a strong example of how the global oncology community rapidly shares information and experience whenever it makes a difference in patient care,” he commented.
The authors, as well as Carlson and Greene, have reported no relevant financial relationships.
This article first appeared on Medscape.com.
Short-term results
Short-term results
No staff members or patients were diagnosed with COVID-19 after “strict protective measures” for screening and managing patients were implemented at the National Cancer Center/Cancer Hospital, Chinese Academy of Sciences, in Beijing, according to a report published online April 1 in JAMA Oncology.
However, the time period for the analysis, which included nearly 3000 patients, was short — only about 3 weeks (February 12 to March 3). Also, Beijing is more than 1100 kilometers from Wuhan, the center of the Chinese outbreak of COVID-19.
The Beijing cancer hospital implemented a multipronged safety plan in February in order to “avoid COVID-19 related nosocomial cross-infection between patients and medical staff,” explain the authors, led by medical oncologist Zhijie Wang, MD.
Notably, “all of the measures taken in China are actively being implemented and used in major oncology centers in the United States,” Robert Carlson, MD, chief executive officer, National Comprehensive Cancer Network (NCCN), told Medscape Medical News.
John Greene, MD, section chief, Infectious Disease and Tropical Medicine, Moffitt Cancer Center, Tampa, Florida, pointed out that the Chinese safety plan, which is full of “good measures,” is being largely used at his center. However, he observed that one tool — doing a temperature check at the hospital front door — is not well supported by most of the literature. “It gives good optics and looks like you are doing the most you possibly can, but scientifically it may not be as effective [as other screening measures],” he said.
The Chinese plan consists of four broad elements
First, the above-mentioned on-site temperature tests are performed at the entrances of the hospital, outpatient clinic, and wards. Contact and travel histories related to the Wuhan epidemic area are also established and recorded.
Second, an outpatient appointment scheduling system allows both online scheduling and on-site registration. Online consultation channels are open daily, featuring instruction on medication taking and cancer-related symptom management. These “substantially reduced the flow of people in the hospital,” write the authors. On-site patients must wear a mask and have their own disinfectant.
Third, for patients with cancer preparing to be admitted to hospital, symptoms associated with COVID-19, such as fever and cough, are recorded. Mandatory blood tests and CT scans of the lungs are performed. COVID-19 virus nucleic acid tests are performed for patients with suspected pneumonia on imaging.
Fourth, some anticancer drugs conventionally administered by infusion have been changed to oral administration, such as etoposide and vinorelbine. For adjuvant or maintenance chemotherapy, the infusion intervals were appropriately prolonged depending on patients’ conditions.
Eight out of 2,900 patients had imaging suspicious for infection
The Chinese authors report that a total of 2,944 patients with cancer were seen for clinic consultation and treatment in the wards (2795 outpatients and 149 inpatients).
Patients with cancer are believed to have a higher probability of severe illness and increased mortality compared with the healthy population once infected with COVID-19, point out the authors.
Under the new “strict screening strategy,” 27 patients showed radiologic manifestations of inflammatory changes or multiple-site exudative pneumonia in the lungs, including eight suspected of having COVID-19 infection. “Fortunately, negative results from nucleic acid testing ultimately excluded COVID-19 infection in all these patients,” the authors report.
However, two of these patients “presented with recovered pneumonia after symptomatic treatment.” Commenting on this finding, Moffitt’s Greene said that may mean these two patients were tested and found to be positive but were early in the infection and not yet shedding the virus, or they were infected after the initial negative result.
Greene said his center has implemented some measures not mentioned in the Chinese plan. For example, the Florida center no longer allows inpatient visitation. Also, one third of staff now work from home, resulting in less social interaction. Social distancing in meetings, the cafeteria, and hallways is being observed “aggressively,” and most meetings are now on Zoom, he said.
Moffitt has not been hard hit with COVID-19 and is at level one preparedness, the lowest rung. The center has performed 60 tests to date, with only one positive for the virus (< 2%), Greene told Medscape Medical News.
Currently, in the larger Tampa Bay community setting, about 12% of tests are positive.
The low percentage found among the Moffitt patients “tells you that a lot of cancer patients have fever and respiratory symptoms due to other viruses and, more importantly, other reasons, whether it’s their immunotherapy or chemotherapy or their cancer,” said Greene.
NCCN’s Carlson said the publication of the Chinese data was a good sign in terms of international science.
“This is a strong example of how the global oncology community rapidly shares information and experience whenever it makes a difference in patient care,” he commented.
The authors, as well as Carlson and Greene, have reported no relevant financial relationships.
This article first appeared on Medscape.com.
No staff members or patients were diagnosed with COVID-19 after “strict protective measures” for screening and managing patients were implemented at the National Cancer Center/Cancer Hospital, Chinese Academy of Sciences, in Beijing, according to a report published online April 1 in JAMA Oncology.
However, the time period for the analysis, which included nearly 3000 patients, was short — only about 3 weeks (February 12 to March 3). Also, Beijing is more than 1100 kilometers from Wuhan, the center of the Chinese outbreak of COVID-19.
The Beijing cancer hospital implemented a multipronged safety plan in February in order to “avoid COVID-19 related nosocomial cross-infection between patients and medical staff,” explain the authors, led by medical oncologist Zhijie Wang, MD.
Notably, “all of the measures taken in China are actively being implemented and used in major oncology centers in the United States,” Robert Carlson, MD, chief executive officer, National Comprehensive Cancer Network (NCCN), told Medscape Medical News.
John Greene, MD, section chief, Infectious Disease and Tropical Medicine, Moffitt Cancer Center, Tampa, Florida, pointed out that the Chinese safety plan, which is full of “good measures,” is being largely used at his center. However, he observed that one tool — doing a temperature check at the hospital front door — is not well supported by most of the literature. “It gives good optics and looks like you are doing the most you possibly can, but scientifically it may not be as effective [as other screening measures],” he said.
The Chinese plan consists of four broad elements
First, the above-mentioned on-site temperature tests are performed at the entrances of the hospital, outpatient clinic, and wards. Contact and travel histories related to the Wuhan epidemic area are also established and recorded.
Second, an outpatient appointment scheduling system allows both online scheduling and on-site registration. Online consultation channels are open daily, featuring instruction on medication taking and cancer-related symptom management. These “substantially reduced the flow of people in the hospital,” write the authors. On-site patients must wear a mask and have their own disinfectant.
Third, for patients with cancer preparing to be admitted to hospital, symptoms associated with COVID-19, such as fever and cough, are recorded. Mandatory blood tests and CT scans of the lungs are performed. COVID-19 virus nucleic acid tests are performed for patients with suspected pneumonia on imaging.
Fourth, some anticancer drugs conventionally administered by infusion have been changed to oral administration, such as etoposide and vinorelbine. For adjuvant or maintenance chemotherapy, the infusion intervals were appropriately prolonged depending on patients’ conditions.
Eight out of 2,900 patients had imaging suspicious for infection
The Chinese authors report that a total of 2,944 patients with cancer were seen for clinic consultation and treatment in the wards (2795 outpatients and 149 inpatients).
Patients with cancer are believed to have a higher probability of severe illness and increased mortality compared with the healthy population once infected with COVID-19, point out the authors.
Under the new “strict screening strategy,” 27 patients showed radiologic manifestations of inflammatory changes or multiple-site exudative pneumonia in the lungs, including eight suspected of having COVID-19 infection. “Fortunately, negative results from nucleic acid testing ultimately excluded COVID-19 infection in all these patients,” the authors report.
However, two of these patients “presented with recovered pneumonia after symptomatic treatment.” Commenting on this finding, Moffitt’s Greene said that may mean these two patients were tested and found to be positive but were early in the infection and not yet shedding the virus, or they were infected after the initial negative result.
Greene said his center has implemented some measures not mentioned in the Chinese plan. For example, the Florida center no longer allows inpatient visitation. Also, one third of staff now work from home, resulting in less social interaction. Social distancing in meetings, the cafeteria, and hallways is being observed “aggressively,” and most meetings are now on Zoom, he said.
Moffitt has not been hard hit with COVID-19 and is at level one preparedness, the lowest rung. The center has performed 60 tests to date, with only one positive for the virus (< 2%), Greene told Medscape Medical News.
Currently, in the larger Tampa Bay community setting, about 12% of tests are positive.
The low percentage found among the Moffitt patients “tells you that a lot of cancer patients have fever and respiratory symptoms due to other viruses and, more importantly, other reasons, whether it’s their immunotherapy or chemotherapy or their cancer,” said Greene.
NCCN’s Carlson said the publication of the Chinese data was a good sign in terms of international science.
“This is a strong example of how the global oncology community rapidly shares information and experience whenever it makes a difference in patient care,” he commented.
The authors, as well as Carlson and Greene, have reported no relevant financial relationships.
This article first appeared on Medscape.com.
Enhanced team-based CVD care found to benefit diabetes patients
PHOENIX, ARIZ. – Diabetes patients in China who were enrolled in a team-based care intervention with clinical decision support systems significantly reduced their hemoglobin A1c, systolic blood pressure, and LDL cholesterol over 18 months, compared with those who received team-based care alone.
The finding comes from the Diabetes Complication Control in Community Clinics (D4C), a cluster randomized trial conducted in 38 community health centers in Xiamen, China.
“Diabetes has become a major public health challenge worldwide, especially in low- and middle-income countries where populations are large and growing and health care resources are limited,” Jiang He, MD, PhD, said at the Epidemiology and Prevention/Lifestyle and Cardiometabolic Health meeting.
According to Dr. He, chair and professor of epidemiology at Tulane School of Public Health and Tropical Medicine, New Orleans, the prevalence of diabetes has increased rapidly in recent decades in China, from 2.5% in 1994 to 11.6% in 2010. “It was estimated that 114 million Chinese adults had diabetes in 2010,” he said. “Hyperglycemia, high blood pressure, and elevated LDL cholesterol are major risk factors for cardiovascular disease and premature death. The majority of patients with diabetes have multiple uncontrolled CVD risk factors due to suboptimal care. Diabetes and its complications further strain an already overburdened and overwhelmed health care system, especially tertiary care facilities, in China. On the other hand, community health centers are underutilized.”
In D4C, Dr. He and colleagues set out to evaluate changes in CVD risk factors among patients with diabetes after implementing a team-based care model at community health centers in Xiamen, China. They compared the effectiveness of team-based care with clinical decision support systems versus team-based care alone on CVD risk factor control among patients with diabetes at these community health centers.
The study population consisted of 10,942 patients aged 50 years and older with uncontrolled diabetes and at least one of the following three additional CVD risk factors: systolic BP of at least 140 mm Hg and/or diastolic BP of at least 90 mm Hg; LDL cholesterol of at least 100 mg/dL, or clinical atherosclerotic cardiovascular disease (ASCVD). At the intervention clinics, team-based care was delivered by a team of primary care physicians, nurses, and diabetes specialists. The researchers trained the primary care physicians and nurses, and a clinical decision support system was integrated with guideline-based treatment algorithms for controlling glycemia, blood pressure, and lipids.
At the enhanced care control clinics, team-based care was delivered by a team of primary care physicians, nurses, and diabetes specialists. The city health commission trained the primary care physicians and nurses. The intervention lasted for 18 months in both groups.
Dr. He, the D4C study chair, reported findings from 10,942 patients: 5,394 in the intervention group and 5,548 in the enhanced care group. The mean baseline age was similar between the intervention group and the enhanced care group (a mean of 63 years), as was body mass index (a mean of 24.9 kg/m2), hemoglobin A1c (a mean of 8.8 vs. 8.7%, respectively), LDL cholesterol (121.2 vs. 121.1 mg/dL), systolic blood pressure (136.6 vs. 136.9 mm Hg), and diastolic blood pressure (79.7 vs. 79.8 mm Hg).
The researchers found patients in both groups experienced significant reductions in HbA1c, LDL cholesterol, and BP over the 18-month follow-up, but those in the intervention group fared better in all measures. Specifically, the mean change in HbA1c from baseline was –.85% in the intervention group, compared with –.66% in the enhanced care group, while the change in LDL was –19 mg/dL, compared with –12.8 mg/dL, respectively; the change in systolic blood pressure was –8.9 mm Hg vs. –7.7 mm Hg, and the change in 10-year ASCVD risk was .57% vs. .28% (P < .0001 for all associations).
The researchers also observed that the proportions of controlled HbA1c, LDL, and blood pressure at 18 months were higher in the intervention group, compared with the enhanced care group. Specifically, 38% of patients in the intervention group achieved glycemic control, compared with 35% of those in the enhanced care group (P =. 0006), while 48% vs. 39%, respectively, achieved control of LDL cholesterol (P < .0001), and 78% vs. 75% achieved control of blood pressure (P = .0009). In addition, 15% vs. 12% achieved control of all three risk factors at 18 months (P < .0001).
“Implementing team-based care with a clinical decision support system is an effective and sustainable strategy for diabetes control in primary care settings,” Dr. He said at the meeting, which was sponsored by the American Heart Association. “This implementation strategy could be scaled up within primary care settings in China and other low- to middle-income countries to improve CVD risk factor control in patients with diabetes.”
In an interview, session moderator Joshua J. Joseph, MD, of Ohio State University, Columbus, pointed out that since only 12%-15% of study participants achieved control of all three CVD risk factors, “that leaves a great opportunity for [figuring out] how to we get the other 88% or 85% of patients to target levels. That’s going to be important as we think about cardiovascular disease prevention in type 2 diabetes. The more we can use team-based care along with clinical decision support tools, the more we will continue to improve the lives of patients.”
The study was supported by the Xiamen City Health Commission. Dr. He reported having no financial disclosures.
SOURCE: He J et al. EPI/LIFESTYLE 2020, session 7A, abstract 17.
PHOENIX, ARIZ. – Diabetes patients in China who were enrolled in a team-based care intervention with clinical decision support systems significantly reduced their hemoglobin A1c, systolic blood pressure, and LDL cholesterol over 18 months, compared with those who received team-based care alone.
The finding comes from the Diabetes Complication Control in Community Clinics (D4C), a cluster randomized trial conducted in 38 community health centers in Xiamen, China.
“Diabetes has become a major public health challenge worldwide, especially in low- and middle-income countries where populations are large and growing and health care resources are limited,” Jiang He, MD, PhD, said at the Epidemiology and Prevention/Lifestyle and Cardiometabolic Health meeting.
According to Dr. He, chair and professor of epidemiology at Tulane School of Public Health and Tropical Medicine, New Orleans, the prevalence of diabetes has increased rapidly in recent decades in China, from 2.5% in 1994 to 11.6% in 2010. “It was estimated that 114 million Chinese adults had diabetes in 2010,” he said. “Hyperglycemia, high blood pressure, and elevated LDL cholesterol are major risk factors for cardiovascular disease and premature death. The majority of patients with diabetes have multiple uncontrolled CVD risk factors due to suboptimal care. Diabetes and its complications further strain an already overburdened and overwhelmed health care system, especially tertiary care facilities, in China. On the other hand, community health centers are underutilized.”
In D4C, Dr. He and colleagues set out to evaluate changes in CVD risk factors among patients with diabetes after implementing a team-based care model at community health centers in Xiamen, China. They compared the effectiveness of team-based care with clinical decision support systems versus team-based care alone on CVD risk factor control among patients with diabetes at these community health centers.
The study population consisted of 10,942 patients aged 50 years and older with uncontrolled diabetes and at least one of the following three additional CVD risk factors: systolic BP of at least 140 mm Hg and/or diastolic BP of at least 90 mm Hg; LDL cholesterol of at least 100 mg/dL, or clinical atherosclerotic cardiovascular disease (ASCVD). At the intervention clinics, team-based care was delivered by a team of primary care physicians, nurses, and diabetes specialists. The researchers trained the primary care physicians and nurses, and a clinical decision support system was integrated with guideline-based treatment algorithms for controlling glycemia, blood pressure, and lipids.
At the enhanced care control clinics, team-based care was delivered by a team of primary care physicians, nurses, and diabetes specialists. The city health commission trained the primary care physicians and nurses. The intervention lasted for 18 months in both groups.
Dr. He, the D4C study chair, reported findings from 10,942 patients: 5,394 in the intervention group and 5,548 in the enhanced care group. The mean baseline age was similar between the intervention group and the enhanced care group (a mean of 63 years), as was body mass index (a mean of 24.9 kg/m2), hemoglobin A1c (a mean of 8.8 vs. 8.7%, respectively), LDL cholesterol (121.2 vs. 121.1 mg/dL), systolic blood pressure (136.6 vs. 136.9 mm Hg), and diastolic blood pressure (79.7 vs. 79.8 mm Hg).
The researchers found patients in both groups experienced significant reductions in HbA1c, LDL cholesterol, and BP over the 18-month follow-up, but those in the intervention group fared better in all measures. Specifically, the mean change in HbA1c from baseline was –.85% in the intervention group, compared with –.66% in the enhanced care group, while the change in LDL was –19 mg/dL, compared with –12.8 mg/dL, respectively; the change in systolic blood pressure was –8.9 mm Hg vs. –7.7 mm Hg, and the change in 10-year ASCVD risk was .57% vs. .28% (P < .0001 for all associations).
The researchers also observed that the proportions of controlled HbA1c, LDL, and blood pressure at 18 months were higher in the intervention group, compared with the enhanced care group. Specifically, 38% of patients in the intervention group achieved glycemic control, compared with 35% of those in the enhanced care group (P =. 0006), while 48% vs. 39%, respectively, achieved control of LDL cholesterol (P < .0001), and 78% vs. 75% achieved control of blood pressure (P = .0009). In addition, 15% vs. 12% achieved control of all three risk factors at 18 months (P < .0001).
“Implementing team-based care with a clinical decision support system is an effective and sustainable strategy for diabetes control in primary care settings,” Dr. He said at the meeting, which was sponsored by the American Heart Association. “This implementation strategy could be scaled up within primary care settings in China and other low- to middle-income countries to improve CVD risk factor control in patients with diabetes.”
In an interview, session moderator Joshua J. Joseph, MD, of Ohio State University, Columbus, pointed out that since only 12%-15% of study participants achieved control of all three CVD risk factors, “that leaves a great opportunity for [figuring out] how to we get the other 88% or 85% of patients to target levels. That’s going to be important as we think about cardiovascular disease prevention in type 2 diabetes. The more we can use team-based care along with clinical decision support tools, the more we will continue to improve the lives of patients.”
The study was supported by the Xiamen City Health Commission. Dr. He reported having no financial disclosures.
SOURCE: He J et al. EPI/LIFESTYLE 2020, session 7A, abstract 17.
PHOENIX, ARIZ. – Diabetes patients in China who were enrolled in a team-based care intervention with clinical decision support systems significantly reduced their hemoglobin A1c, systolic blood pressure, and LDL cholesterol over 18 months, compared with those who received team-based care alone.
The finding comes from the Diabetes Complication Control in Community Clinics (D4C), a cluster randomized trial conducted in 38 community health centers in Xiamen, China.
“Diabetes has become a major public health challenge worldwide, especially in low- and middle-income countries where populations are large and growing and health care resources are limited,” Jiang He, MD, PhD, said at the Epidemiology and Prevention/Lifestyle and Cardiometabolic Health meeting.
According to Dr. He, chair and professor of epidemiology at Tulane School of Public Health and Tropical Medicine, New Orleans, the prevalence of diabetes has increased rapidly in recent decades in China, from 2.5% in 1994 to 11.6% in 2010. “It was estimated that 114 million Chinese adults had diabetes in 2010,” he said. “Hyperglycemia, high blood pressure, and elevated LDL cholesterol are major risk factors for cardiovascular disease and premature death. The majority of patients with diabetes have multiple uncontrolled CVD risk factors due to suboptimal care. Diabetes and its complications further strain an already overburdened and overwhelmed health care system, especially tertiary care facilities, in China. On the other hand, community health centers are underutilized.”
In D4C, Dr. He and colleagues set out to evaluate changes in CVD risk factors among patients with diabetes after implementing a team-based care model at community health centers in Xiamen, China. They compared the effectiveness of team-based care with clinical decision support systems versus team-based care alone on CVD risk factor control among patients with diabetes at these community health centers.
The study population consisted of 10,942 patients aged 50 years and older with uncontrolled diabetes and at least one of the following three additional CVD risk factors: systolic BP of at least 140 mm Hg and/or diastolic BP of at least 90 mm Hg; LDL cholesterol of at least 100 mg/dL, or clinical atherosclerotic cardiovascular disease (ASCVD). At the intervention clinics, team-based care was delivered by a team of primary care physicians, nurses, and diabetes specialists. The researchers trained the primary care physicians and nurses, and a clinical decision support system was integrated with guideline-based treatment algorithms for controlling glycemia, blood pressure, and lipids.
At the enhanced care control clinics, team-based care was delivered by a team of primary care physicians, nurses, and diabetes specialists. The city health commission trained the primary care physicians and nurses. The intervention lasted for 18 months in both groups.
Dr. He, the D4C study chair, reported findings from 10,942 patients: 5,394 in the intervention group and 5,548 in the enhanced care group. The mean baseline age was similar between the intervention group and the enhanced care group (a mean of 63 years), as was body mass index (a mean of 24.9 kg/m2), hemoglobin A1c (a mean of 8.8 vs. 8.7%, respectively), LDL cholesterol (121.2 vs. 121.1 mg/dL), systolic blood pressure (136.6 vs. 136.9 mm Hg), and diastolic blood pressure (79.7 vs. 79.8 mm Hg).
The researchers found patients in both groups experienced significant reductions in HbA1c, LDL cholesterol, and BP over the 18-month follow-up, but those in the intervention group fared better in all measures. Specifically, the mean change in HbA1c from baseline was –.85% in the intervention group, compared with –.66% in the enhanced care group, while the change in LDL was –19 mg/dL, compared with –12.8 mg/dL, respectively; the change in systolic blood pressure was –8.9 mm Hg vs. –7.7 mm Hg, and the change in 10-year ASCVD risk was .57% vs. .28% (P < .0001 for all associations).
The researchers also observed that the proportions of controlled HbA1c, LDL, and blood pressure at 18 months were higher in the intervention group, compared with the enhanced care group. Specifically, 38% of patients in the intervention group achieved glycemic control, compared with 35% of those in the enhanced care group (P =. 0006), while 48% vs. 39%, respectively, achieved control of LDL cholesterol (P < .0001), and 78% vs. 75% achieved control of blood pressure (P = .0009). In addition, 15% vs. 12% achieved control of all three risk factors at 18 months (P < .0001).
“Implementing team-based care with a clinical decision support system is an effective and sustainable strategy for diabetes control in primary care settings,” Dr. He said at the meeting, which was sponsored by the American Heart Association. “This implementation strategy could be scaled up within primary care settings in China and other low- to middle-income countries to improve CVD risk factor control in patients with diabetes.”
In an interview, session moderator Joshua J. Joseph, MD, of Ohio State University, Columbus, pointed out that since only 12%-15% of study participants achieved control of all three CVD risk factors, “that leaves a great opportunity for [figuring out] how to we get the other 88% or 85% of patients to target levels. That’s going to be important as we think about cardiovascular disease prevention in type 2 diabetes. The more we can use team-based care along with clinical decision support tools, the more we will continue to improve the lives of patients.”
The study was supported by the Xiamen City Health Commission. Dr. He reported having no financial disclosures.
SOURCE: He J et al. EPI/LIFESTYLE 2020, session 7A, abstract 17.
REPORTING FROM EPI/LIFESTYLE 2020