User login
Intermediate alleles may confer mild, late-onset Huntington-like symptoms
Asymptomatic people who carry an intermediate number (27-35) of CAG repeats on the huntingtin gene – that is, the range just below the Huntington’s disease threshold of 36 CAG repeats – may be at increased risk for mild, late-onset symptoms, according to the first report to definitely associate intermediate alleles with such symptoms.
The prevalence of this distinct category of alleles for the huntingtin (HTT) gene, termed IA (for intermediate alleles), ranges from 1.5% to 5.8% both in the general population and in affected families. The clinical manifestations of Huntington’s disease associated with IAs have remain hidden until now in part because asymptomatic family members often decline to undergo genetic testing for the disorder and so are not identified as having IAs. Emerging evidence suggests that some people with IAs are more likely than those with a smaller number of CAG repeats to develop Huntington-like neuropathologic effects, but the data are sparse, and the question is controversial, said Esther Cubo, MD, PhD, of the department of neurology, Hospital Universitario Burgos (Spain) and her associates on behalf of the European Huntington’s Disease Network (Neurology. 2016 Jul 8. doi: 10.1212/WNL.0000000000002944).
To examine this issue in a large cohort of at-risk individuals, the investigators assessed clinical and sociodemographic factors for 657 people enrolled in the European Huntington’s Disease Registry, which tracks the natural course of the disease in patients and family members treated in 1998 through 2014 at 140 medical centers in 17 European and 3 other countries. They focused on individuals who were asymptomatic at baseline: 76 (11.6%) men and women who had IAs (cases) and 581 (88.4%) who had fewer than 27 CAG repeats (controls). The two groups were similar in age, body mass index, educational background, socioeconomic status, tobacco and alcohol use, and medication use, and they scored similarly on measures of health-related quality of life, functional capacity, and the Unified Huntington’s Disease Rating Scale (UHDRS) for motor, behavioral, and cognitive status.
IA status was not associated with any significant differences between cases and controls who were younger than age 60. However, after age 60, participants with IAs had higher median total UHDRS motor scores (13.0 vs. 2.0) and were more likely to show mild gait abnormalities, chorea, and bradykinesia. In the small subgroup of patients who were followed longitudinally for up to 2 years, those with IAs showed faster cognitive decline over time; however, longer follow-up of larger groups of participants is needed to confirm this trend, the investigators said.
In addition, study participants with IAs reported lower quality of life and a greater degree of apathy than those without IAs, but these differences did not reach statistical significance. Whether apathy and poor quality of life reflect Huntington’s disease or simply correlate with normal aging could not be determined.
This study was limited by the relatively small number of participants with IAs, but the findings suggest that IAs “could produce a mild phenotype” of Huntington’s disease in some carriers after age 60. Alternatively, “clinical manifestations of Huntington’s disease in patents with IA might also be potentially accelerated by medical conditions, treatments, and environmental factors” associated with normal aging, Dr. Cubo and her associates added.
This study was supported by the European Huntington’s Disease Registry. Dr. Cubo reported receiving consulting fees from UCB, Allergan, and AbbVie.
These findings are limited by the study’s small cohort size and short follow-up, but they suggest that younger IA carriers will develop few if any signs of Huntington’s disease while older IA carriers may develop a very mild phenotype late in life.
Young IA carriers and carriers who have a low number of CAG repeats (fewer than 27) on the longer allele have “not too much to worry about.” Older IA carriers may develop some mild motor symptoms and a slightly faster cognitive decline as they age. All carriers should remain as fit and healthy as possible, as they have always been advised, and should look to their family members’ experiences as a good yardstick of what might happen to them.
Patrick J. Morrison, MD, DSc, is in the department of genetic medicine at Belfast HSC Trust and the Centre for Cancer Research and Cell Biology at Queens University of Belfast (Northern Ireland). Julián Benito-León, MD, PhD, is in the department of neurology at University Hospital “12 de Octubre” and in the department of medicine at Complutense University, both in Madrid. They reported no targeted funding for this work. Dr. Morrison and Dr. Benito-León made these remarks in an editorial accompanying Dr. Cubo’s report (Neurology. 2016 Jul 8. doi: 10.1212/WNL.0000000000002958).
These findings are limited by the study’s small cohort size and short follow-up, but they suggest that younger IA carriers will develop few if any signs of Huntington’s disease while older IA carriers may develop a very mild phenotype late in life.
Young IA carriers and carriers who have a low number of CAG repeats (fewer than 27) on the longer allele have “not too much to worry about.” Older IA carriers may develop some mild motor symptoms and a slightly faster cognitive decline as they age. All carriers should remain as fit and healthy as possible, as they have always been advised, and should look to their family members’ experiences as a good yardstick of what might happen to them.
Patrick J. Morrison, MD, DSc, is in the department of genetic medicine at Belfast HSC Trust and the Centre for Cancer Research and Cell Biology at Queens University of Belfast (Northern Ireland). Julián Benito-León, MD, PhD, is in the department of neurology at University Hospital “12 de Octubre” and in the department of medicine at Complutense University, both in Madrid. They reported no targeted funding for this work. Dr. Morrison and Dr. Benito-León made these remarks in an editorial accompanying Dr. Cubo’s report (Neurology. 2016 Jul 8. doi: 10.1212/WNL.0000000000002958).
These findings are limited by the study’s small cohort size and short follow-up, but they suggest that younger IA carriers will develop few if any signs of Huntington’s disease while older IA carriers may develop a very mild phenotype late in life.
Young IA carriers and carriers who have a low number of CAG repeats (fewer than 27) on the longer allele have “not too much to worry about.” Older IA carriers may develop some mild motor symptoms and a slightly faster cognitive decline as they age. All carriers should remain as fit and healthy as possible, as they have always been advised, and should look to their family members’ experiences as a good yardstick of what might happen to them.
Patrick J. Morrison, MD, DSc, is in the department of genetic medicine at Belfast HSC Trust and the Centre for Cancer Research and Cell Biology at Queens University of Belfast (Northern Ireland). Julián Benito-León, MD, PhD, is in the department of neurology at University Hospital “12 de Octubre” and in the department of medicine at Complutense University, both in Madrid. They reported no targeted funding for this work. Dr. Morrison and Dr. Benito-León made these remarks in an editorial accompanying Dr. Cubo’s report (Neurology. 2016 Jul 8. doi: 10.1212/WNL.0000000000002958).
Asymptomatic people who carry an intermediate number (27-35) of CAG repeats on the huntingtin gene – that is, the range just below the Huntington’s disease threshold of 36 CAG repeats – may be at increased risk for mild, late-onset symptoms, according to the first report to definitely associate intermediate alleles with such symptoms.
The prevalence of this distinct category of alleles for the huntingtin (HTT) gene, termed IA (for intermediate alleles), ranges from 1.5% to 5.8% both in the general population and in affected families. The clinical manifestations of Huntington’s disease associated with IAs have remain hidden until now in part because asymptomatic family members often decline to undergo genetic testing for the disorder and so are not identified as having IAs. Emerging evidence suggests that some people with IAs are more likely than those with a smaller number of CAG repeats to develop Huntington-like neuropathologic effects, but the data are sparse, and the question is controversial, said Esther Cubo, MD, PhD, of the department of neurology, Hospital Universitario Burgos (Spain) and her associates on behalf of the European Huntington’s Disease Network (Neurology. 2016 Jul 8. doi: 10.1212/WNL.0000000000002944).
To examine this issue in a large cohort of at-risk individuals, the investigators assessed clinical and sociodemographic factors for 657 people enrolled in the European Huntington’s Disease Registry, which tracks the natural course of the disease in patients and family members treated in 1998 through 2014 at 140 medical centers in 17 European and 3 other countries. They focused on individuals who were asymptomatic at baseline: 76 (11.6%) men and women who had IAs (cases) and 581 (88.4%) who had fewer than 27 CAG repeats (controls). The two groups were similar in age, body mass index, educational background, socioeconomic status, tobacco and alcohol use, and medication use, and they scored similarly on measures of health-related quality of life, functional capacity, and the Unified Huntington’s Disease Rating Scale (UHDRS) for motor, behavioral, and cognitive status.
IA status was not associated with any significant differences between cases and controls who were younger than age 60. However, after age 60, participants with IAs had higher median total UHDRS motor scores (13.0 vs. 2.0) and were more likely to show mild gait abnormalities, chorea, and bradykinesia. In the small subgroup of patients who were followed longitudinally for up to 2 years, those with IAs showed faster cognitive decline over time; however, longer follow-up of larger groups of participants is needed to confirm this trend, the investigators said.
In addition, study participants with IAs reported lower quality of life and a greater degree of apathy than those without IAs, but these differences did not reach statistical significance. Whether apathy and poor quality of life reflect Huntington’s disease or simply correlate with normal aging could not be determined.
This study was limited by the relatively small number of participants with IAs, but the findings suggest that IAs “could produce a mild phenotype” of Huntington’s disease in some carriers after age 60. Alternatively, “clinical manifestations of Huntington’s disease in patents with IA might also be potentially accelerated by medical conditions, treatments, and environmental factors” associated with normal aging, Dr. Cubo and her associates added.
This study was supported by the European Huntington’s Disease Registry. Dr. Cubo reported receiving consulting fees from UCB, Allergan, and AbbVie.
Asymptomatic people who carry an intermediate number (27-35) of CAG repeats on the huntingtin gene – that is, the range just below the Huntington’s disease threshold of 36 CAG repeats – may be at increased risk for mild, late-onset symptoms, according to the first report to definitely associate intermediate alleles with such symptoms.
The prevalence of this distinct category of alleles for the huntingtin (HTT) gene, termed IA (for intermediate alleles), ranges from 1.5% to 5.8% both in the general population and in affected families. The clinical manifestations of Huntington’s disease associated with IAs have remain hidden until now in part because asymptomatic family members often decline to undergo genetic testing for the disorder and so are not identified as having IAs. Emerging evidence suggests that some people with IAs are more likely than those with a smaller number of CAG repeats to develop Huntington-like neuropathologic effects, but the data are sparse, and the question is controversial, said Esther Cubo, MD, PhD, of the department of neurology, Hospital Universitario Burgos (Spain) and her associates on behalf of the European Huntington’s Disease Network (Neurology. 2016 Jul 8. doi: 10.1212/WNL.0000000000002944).
To examine this issue in a large cohort of at-risk individuals, the investigators assessed clinical and sociodemographic factors for 657 people enrolled in the European Huntington’s Disease Registry, which tracks the natural course of the disease in patients and family members treated in 1998 through 2014 at 140 medical centers in 17 European and 3 other countries. They focused on individuals who were asymptomatic at baseline: 76 (11.6%) men and women who had IAs (cases) and 581 (88.4%) who had fewer than 27 CAG repeats (controls). The two groups were similar in age, body mass index, educational background, socioeconomic status, tobacco and alcohol use, and medication use, and they scored similarly on measures of health-related quality of life, functional capacity, and the Unified Huntington’s Disease Rating Scale (UHDRS) for motor, behavioral, and cognitive status.
IA status was not associated with any significant differences between cases and controls who were younger than age 60. However, after age 60, participants with IAs had higher median total UHDRS motor scores (13.0 vs. 2.0) and were more likely to show mild gait abnormalities, chorea, and bradykinesia. In the small subgroup of patients who were followed longitudinally for up to 2 years, those with IAs showed faster cognitive decline over time; however, longer follow-up of larger groups of participants is needed to confirm this trend, the investigators said.
In addition, study participants with IAs reported lower quality of life and a greater degree of apathy than those without IAs, but these differences did not reach statistical significance. Whether apathy and poor quality of life reflect Huntington’s disease or simply correlate with normal aging could not be determined.
This study was limited by the relatively small number of participants with IAs, but the findings suggest that IAs “could produce a mild phenotype” of Huntington’s disease in some carriers after age 60. Alternatively, “clinical manifestations of Huntington’s disease in patents with IA might also be potentially accelerated by medical conditions, treatments, and environmental factors” associated with normal aging, Dr. Cubo and her associates added.
This study was supported by the European Huntington’s Disease Registry. Dr. Cubo reported receiving consulting fees from UCB, Allergan, and AbbVie.
FROM NEUROLOGY
Key clinical point: Asymptomatic people who carry an intermediate number (27-35) of CAG repeats on the huntingtin gene may be at increased risk for mild symptoms after age 60.
Major finding: After age 60, people with intermediate alleles had higher median UHDRS motor scores (13.0) than did people with fewer CAG repeats (2.0).
Data source: A retrospective, international, observational study involving 76 asymptomatic adults with 27-35 CAG repeats and 581 with fewer than 27 CAG repeats.
Disclosures: This study was supported by the European Huntington’s Disease Registry. Dr. Cubo reported receiving consulting fees from UCB, Allergan, and AbbVie.
Ceritinib effective when NSCLC progresses despite crizotinib
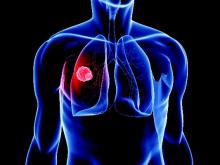
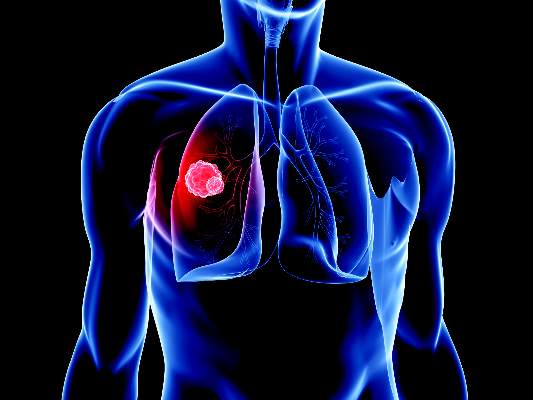
Ceritinib produced clinically meaningful, durable responses in patients who had advanced non–small-cell lung cancer and a history of multiple treatments with chemotherapies and crizotinib, according to investigators.
Ceritinib was effective even in patients with brain metastases, and it both reduced a high tumor burden and improved lung symptoms, said Lucio Crino, MD, of the University Medical School of Perugia (Italy) and his associates.
They assessed ceritinib in a single-arm, open-label, phase II trial involving 140 adults with advanced ALK-rearranged non–small-cell lung cancer at 51 sites worldwide who had received at least two lines of antineoplastic chemotherapy and had progressed while taking crizotinib. A total of 100 patients (72%) had brain metastases.
After a median follow-up of 11 months (range, 0-19 months), the overall response rate was 38.6% and the disease control rate was 77.1%. Tumor burden was significantly reduced in 75.2% of patients. Treatment response was rapid, occurring at a median of 1.8 months, and durable, lasting for a median of 9.7 months. Median progression-free survival was 5.7 months, median overall survival was 14.9 months, and the 1-year overall survival rate was 63.8%.
Treatment response was similar in the subgroup of patients who had brain metastases at baseline: Their overall response rate was 33.0%, the disease control rate was 74.0%, the median duration of response was 9.2 months, and median progression-free survival was 5.4 months (J Clin Oncol. 2016 July 17. doi: 10.1200/JCO.2015.65.5936).
No new or unexpected adverse events occurred. All patients reported at least one adverse event, most commonly nausea, diarrhea, and vomiting. Most adverse events were managed without dose interruption or reduction. There was a trend toward improvement in lung symptoms such as cough, pain, and dyspnea, and both health-related quality of life and functional capacity were generally maintained throughout ceritinib treatment, Dr. Crino and his associates said.
Ceritinib produced clinically meaningful, durable responses in patients who had advanced non–small-cell lung cancer and a history of multiple treatments with chemotherapies and crizotinib, according to investigators.
Ceritinib was effective even in patients with brain metastases, and it both reduced a high tumor burden and improved lung symptoms, said Lucio Crino, MD, of the University Medical School of Perugia (Italy) and his associates.
They assessed ceritinib in a single-arm, open-label, phase II trial involving 140 adults with advanced ALK-rearranged non–small-cell lung cancer at 51 sites worldwide who had received at least two lines of antineoplastic chemotherapy and had progressed while taking crizotinib. A total of 100 patients (72%) had brain metastases.
After a median follow-up of 11 months (range, 0-19 months), the overall response rate was 38.6% and the disease control rate was 77.1%. Tumor burden was significantly reduced in 75.2% of patients. Treatment response was rapid, occurring at a median of 1.8 months, and durable, lasting for a median of 9.7 months. Median progression-free survival was 5.7 months, median overall survival was 14.9 months, and the 1-year overall survival rate was 63.8%.
Treatment response was similar in the subgroup of patients who had brain metastases at baseline: Their overall response rate was 33.0%, the disease control rate was 74.0%, the median duration of response was 9.2 months, and median progression-free survival was 5.4 months (J Clin Oncol. 2016 July 17. doi: 10.1200/JCO.2015.65.5936).
No new or unexpected adverse events occurred. All patients reported at least one adverse event, most commonly nausea, diarrhea, and vomiting. Most adverse events were managed without dose interruption or reduction. There was a trend toward improvement in lung symptoms such as cough, pain, and dyspnea, and both health-related quality of life and functional capacity were generally maintained throughout ceritinib treatment, Dr. Crino and his associates said.
Ceritinib produced clinically meaningful, durable responses in patients who had advanced non–small-cell lung cancer and a history of multiple treatments with chemotherapies and crizotinib, according to investigators.
Ceritinib was effective even in patients with brain metastases, and it both reduced a high tumor burden and improved lung symptoms, said Lucio Crino, MD, of the University Medical School of Perugia (Italy) and his associates.
They assessed ceritinib in a single-arm, open-label, phase II trial involving 140 adults with advanced ALK-rearranged non–small-cell lung cancer at 51 sites worldwide who had received at least two lines of antineoplastic chemotherapy and had progressed while taking crizotinib. A total of 100 patients (72%) had brain metastases.
After a median follow-up of 11 months (range, 0-19 months), the overall response rate was 38.6% and the disease control rate was 77.1%. Tumor burden was significantly reduced in 75.2% of patients. Treatment response was rapid, occurring at a median of 1.8 months, and durable, lasting for a median of 9.7 months. Median progression-free survival was 5.7 months, median overall survival was 14.9 months, and the 1-year overall survival rate was 63.8%.
Treatment response was similar in the subgroup of patients who had brain metastases at baseline: Their overall response rate was 33.0%, the disease control rate was 74.0%, the median duration of response was 9.2 months, and median progression-free survival was 5.4 months (J Clin Oncol. 2016 July 17. doi: 10.1200/JCO.2015.65.5936).
No new or unexpected adverse events occurred. All patients reported at least one adverse event, most commonly nausea, diarrhea, and vomiting. Most adverse events were managed without dose interruption or reduction. There was a trend toward improvement in lung symptoms such as cough, pain, and dyspnea, and both health-related quality of life and functional capacity were generally maintained throughout ceritinib treatment, Dr. Crino and his associates said.
FROM JOURNAL OF CLINICAL ONCOLOGY
Key clinical point: Ceritinib produced meaningful, durable responses in heavily pretreated patients with NSCLC who had advanced disease, including brain metastases.
Major finding: After a median follow-up of 11 months (range, 0-19 months), the overall response rate was 38.6%, the disease control rate was 77.1%, and the overall survival rate was 63.8%.
Data source: A single-arm open-label multicenter phase II trial involving 140 patients whose NSCLC progressed despite multiple treatments including crizotinib.
Disclosures: Novartis supported the study. Dr. Crino reported receiving honoraria from and consulting for Novartis, Eli Lilly, AstraZeneca, Pfizer, and Roche; his associates reported ties to numerous industry sources.
‘Clarion call’ to screen for, treat aldosteronism
The Endocrine Society’s updated Clinical Practice Guideline for managing primary aldosteronism is “a clarion call” for physicians to recognize the impact of this substantial public health problem and dramatically ramp up their screening and treatment efforts and was published in the Journal of Clinical Endocrinology and Metabolism.
This update differs from the previous (2008) version of the guideline in “the explicit recognition of primary aldosteronism as a major public health issue and not merely a matter of case detection, diagnosis, and treatment of individual patients,” wrote John W. Funder, MD, and his associates on the task force that compiled the guideline.
Many physicians in current practice were taught that the disorder “is a rare and benign cause of hypertension, [and] thus merely a footnote to the management of hypertension as a whole. Cardiologists usually write guidelines for hypertension with some input from nephrologists and clinical pharmacologists [but] little or none from endocrinologists,” they noted.
As a result, most patients with hypertension and occult aldosteronism are never screened for the disorder and receive suboptimal care. Primary care providers must be “made keenly aware” that the proportion of people with hypertension who have aldosteronism is much higher than previously thought (at roughly 10%), that another 20% of hypertensive people have “inappropriate aldosterone secretion,” and that both groups respond remarkably well to medical therapy, particularly to mineralocorticoid-receptor antagonists. This is critical because hypertensive patients with aldosteronism are at much greater risk for cardiovascular morbidity and mortality than their age-, sex-, and BP-matched counterparts who don’t have aldosteronism, said Dr. Funder of the Hudson Institute of Medical Research, Clayton (VIC), Australia, and his associates.
In addition to recommendations regarding screening and treatment and summaries of the evidence on which those recommendations are based, the new guideline offers a remarks section for each recommendation, which includes technical suggestions to help clinicians implement them in real-world practice.
Among the Guideline’s recommendations:
• Screen for primary aldosteronism all patients who have sustained BP above 150/100 mm Hg, hypertension resistant to three conventional antihypertensive drugs, hypertension that requires four or more drugs to control it, hypertension plus hypokalemia, hypertension plus adrenal incidentaloma, hypertension plus sleep apnea, hypertension plus a family history of early-onset hypertension or stroke at a young age, and hypertension plus a first-degree relative with primary aldosteronism.
Use the plasma aldosterone/renin ratio for this screening.
• Do one or more confirmatory tests to definitively confirm the diagnosis before proceeding to subtype classification. The exception to this recommendation is patients who develop spontaneous hypokalemia.
• Do adrenal CT as the initial step in subtype classification, to exclude large masses that may signal adrenocortical carcinoma and to help interventional radiologists and surgeons make anatomic assessments.
Before surgery, an experienced radiologist should determine whether adrenal disease is unilateral or bilateral using adrenal venous sampling.
Order genetic testing for patients with disease onset before age 20 years and for those who have a family history of either aldosteronism or early stroke.
• Laparoscopic adrenalectomy is the surgery of choice for most patients with unilateral adrenal disease. For patients unwilling or unable to undergo surgery or further investigations, prescribe a mineralocorticoid-receptor antagonist.
Medical therapy is the treatment of choice for bilateral adrenal disease. Spironolactone is the first-line agent, and eplerenone is an alternative agent to offer. This guideline is intended to be revised further as management evolves over the next 5 years. It is likely that by then, a rapid, inexpensive confirmatory test will be available to definitively establish the diagnosis and that third- and perhaps fourth-generation mineralocorticoid-receptor antagonists will be available for treatment. Simpler and more accurate methods of measuring plasma aldosterone concentration and direct renin concentration, which “would be a game changer for the primary care physician,” are currently being developed, Dr. Funder and his associates said (J. Clin. Endocrinol. Metab. 2016 May;101:1889-916).
In the meantime, “the main strategy is to convince primary-care physicians to screen for primary aldosteronism in all at-risk hypertensive patients,” they noted.
Copies of the full Guideline are available at [email protected] or by calling 202-971-3636.
The Endocrine Society’s updated Clinical Practice Guideline for managing primary aldosteronism is “a clarion call” for physicians to recognize the impact of this substantial public health problem and dramatically ramp up their screening and treatment efforts and was published in the Journal of Clinical Endocrinology and Metabolism.
This update differs from the previous (2008) version of the guideline in “the explicit recognition of primary aldosteronism as a major public health issue and not merely a matter of case detection, diagnosis, and treatment of individual patients,” wrote John W. Funder, MD, and his associates on the task force that compiled the guideline.
Many physicians in current practice were taught that the disorder “is a rare and benign cause of hypertension, [and] thus merely a footnote to the management of hypertension as a whole. Cardiologists usually write guidelines for hypertension with some input from nephrologists and clinical pharmacologists [but] little or none from endocrinologists,” they noted.
As a result, most patients with hypertension and occult aldosteronism are never screened for the disorder and receive suboptimal care. Primary care providers must be “made keenly aware” that the proportion of people with hypertension who have aldosteronism is much higher than previously thought (at roughly 10%), that another 20% of hypertensive people have “inappropriate aldosterone secretion,” and that both groups respond remarkably well to medical therapy, particularly to mineralocorticoid-receptor antagonists. This is critical because hypertensive patients with aldosteronism are at much greater risk for cardiovascular morbidity and mortality than their age-, sex-, and BP-matched counterparts who don’t have aldosteronism, said Dr. Funder of the Hudson Institute of Medical Research, Clayton (VIC), Australia, and his associates.
In addition to recommendations regarding screening and treatment and summaries of the evidence on which those recommendations are based, the new guideline offers a remarks section for each recommendation, which includes technical suggestions to help clinicians implement them in real-world practice.
Among the Guideline’s recommendations:
• Screen for primary aldosteronism all patients who have sustained BP above 150/100 mm Hg, hypertension resistant to three conventional antihypertensive drugs, hypertension that requires four or more drugs to control it, hypertension plus hypokalemia, hypertension plus adrenal incidentaloma, hypertension plus sleep apnea, hypertension plus a family history of early-onset hypertension or stroke at a young age, and hypertension plus a first-degree relative with primary aldosteronism.
Use the plasma aldosterone/renin ratio for this screening.
• Do one or more confirmatory tests to definitively confirm the diagnosis before proceeding to subtype classification. The exception to this recommendation is patients who develop spontaneous hypokalemia.
• Do adrenal CT as the initial step in subtype classification, to exclude large masses that may signal adrenocortical carcinoma and to help interventional radiologists and surgeons make anatomic assessments.
Before surgery, an experienced radiologist should determine whether adrenal disease is unilateral or bilateral using adrenal venous sampling.
Order genetic testing for patients with disease onset before age 20 years and for those who have a family history of either aldosteronism or early stroke.
• Laparoscopic adrenalectomy is the surgery of choice for most patients with unilateral adrenal disease. For patients unwilling or unable to undergo surgery or further investigations, prescribe a mineralocorticoid-receptor antagonist.
Medical therapy is the treatment of choice for bilateral adrenal disease. Spironolactone is the first-line agent, and eplerenone is an alternative agent to offer. This guideline is intended to be revised further as management evolves over the next 5 years. It is likely that by then, a rapid, inexpensive confirmatory test will be available to definitively establish the diagnosis and that third- and perhaps fourth-generation mineralocorticoid-receptor antagonists will be available for treatment. Simpler and more accurate methods of measuring plasma aldosterone concentration and direct renin concentration, which “would be a game changer for the primary care physician,” are currently being developed, Dr. Funder and his associates said (J. Clin. Endocrinol. Metab. 2016 May;101:1889-916).
In the meantime, “the main strategy is to convince primary-care physicians to screen for primary aldosteronism in all at-risk hypertensive patients,” they noted.
Copies of the full Guideline are available at [email protected] or by calling 202-971-3636.
The Endocrine Society’s updated Clinical Practice Guideline for managing primary aldosteronism is “a clarion call” for physicians to recognize the impact of this substantial public health problem and dramatically ramp up their screening and treatment efforts and was published in the Journal of Clinical Endocrinology and Metabolism.
This update differs from the previous (2008) version of the guideline in “the explicit recognition of primary aldosteronism as a major public health issue and not merely a matter of case detection, diagnosis, and treatment of individual patients,” wrote John W. Funder, MD, and his associates on the task force that compiled the guideline.
Many physicians in current practice were taught that the disorder “is a rare and benign cause of hypertension, [and] thus merely a footnote to the management of hypertension as a whole. Cardiologists usually write guidelines for hypertension with some input from nephrologists and clinical pharmacologists [but] little or none from endocrinologists,” they noted.
As a result, most patients with hypertension and occult aldosteronism are never screened for the disorder and receive suboptimal care. Primary care providers must be “made keenly aware” that the proportion of people with hypertension who have aldosteronism is much higher than previously thought (at roughly 10%), that another 20% of hypertensive people have “inappropriate aldosterone secretion,” and that both groups respond remarkably well to medical therapy, particularly to mineralocorticoid-receptor antagonists. This is critical because hypertensive patients with aldosteronism are at much greater risk for cardiovascular morbidity and mortality than their age-, sex-, and BP-matched counterparts who don’t have aldosteronism, said Dr. Funder of the Hudson Institute of Medical Research, Clayton (VIC), Australia, and his associates.
In addition to recommendations regarding screening and treatment and summaries of the evidence on which those recommendations are based, the new guideline offers a remarks section for each recommendation, which includes technical suggestions to help clinicians implement them in real-world practice.
Among the Guideline’s recommendations:
• Screen for primary aldosteronism all patients who have sustained BP above 150/100 mm Hg, hypertension resistant to three conventional antihypertensive drugs, hypertension that requires four or more drugs to control it, hypertension plus hypokalemia, hypertension plus adrenal incidentaloma, hypertension plus sleep apnea, hypertension plus a family history of early-onset hypertension or stroke at a young age, and hypertension plus a first-degree relative with primary aldosteronism.
Use the plasma aldosterone/renin ratio for this screening.
• Do one or more confirmatory tests to definitively confirm the diagnosis before proceeding to subtype classification. The exception to this recommendation is patients who develop spontaneous hypokalemia.
• Do adrenal CT as the initial step in subtype classification, to exclude large masses that may signal adrenocortical carcinoma and to help interventional radiologists and surgeons make anatomic assessments.
Before surgery, an experienced radiologist should determine whether adrenal disease is unilateral or bilateral using adrenal venous sampling.
Order genetic testing for patients with disease onset before age 20 years and for those who have a family history of either aldosteronism or early stroke.
• Laparoscopic adrenalectomy is the surgery of choice for most patients with unilateral adrenal disease. For patients unwilling or unable to undergo surgery or further investigations, prescribe a mineralocorticoid-receptor antagonist.
Medical therapy is the treatment of choice for bilateral adrenal disease. Spironolactone is the first-line agent, and eplerenone is an alternative agent to offer. This guideline is intended to be revised further as management evolves over the next 5 years. It is likely that by then, a rapid, inexpensive confirmatory test will be available to definitively establish the diagnosis and that third- and perhaps fourth-generation mineralocorticoid-receptor antagonists will be available for treatment. Simpler and more accurate methods of measuring plasma aldosterone concentration and direct renin concentration, which “would be a game changer for the primary care physician,” are currently being developed, Dr. Funder and his associates said (J. Clin. Endocrinol. Metab. 2016 May;101:1889-916).
In the meantime, “the main strategy is to convince primary-care physicians to screen for primary aldosteronism in all at-risk hypertensive patients,” they noted.
Copies of the full Guideline are available at [email protected] or by calling 202-971-3636.
FROM THE JOURNAL OF CLINICAL ENDOCRINOLOGY AND METABOLISM
Key clinical point: The Endocrine Society’s updated Clinical Practice Guideline for managing primary aldosteronism is “a clarion call” for physicians to ramp up screening for and treatment of this major public health problem.
Major finding: Primary care physicians must be convinced to screen all at-risk hypertensive patients for primary aldosteronism.
Data source: A comprehensive review of the literature and detailed update of a Clinical Practice Guideline for managing primary aldosteronism.
Disclosures: The Endocrine Society provided all the support for this Guideline. Dr. Funder’s and his associates’ conflicts of interest are available from the Endocrine Society.
July 2016: Click for Credit
Here are 4 articles in the July issue of Clinician Reviews (individual articles are valid for one year from date of publication—expiration dates below):
1. Pregnancy Alters Pharmacodynamics of Anti-TNF Agents in Women With IBD
To take the posttest, go to: http://bit.ly/1VQFIHf
Expires May 24, 2017
VITALS
Key clinical point: Blood levels of infliximab rose during pregnancy, while adalimumab levels remained stable, even after researchers accounted for changes in albumin, body mass index, and C-reactive protein levels.
Major finding: Median infliximab concentrations rose from 8.5 mcg/mL in the first trimester to a peak of 21 mcg/mL during the middle of the third trimester (P = .04). Median adalimumab levels ranged between 8.6 and 12.2 mcg/mL during pregnancy.
Data source: A prospective study of 25 pregnant women with ulcerative colitis or Crohn's disease.
Disclosures: Dr. Seow disclosed ties with Janssen, AbbVie, Takeda, Shire, and Actavis.
2. Vascular Disease Linked to Sight Loss in Giant Cell Arteritis
To take the posttest, go to: http://bit.ly/1UqLuu5
Expires May 10, 2017
VITALS
Key clinical point: Patients with vascular disease who develop giant cell arteritis may require careful monitoring for sight loss.
Major finding: Overall, 42.9% of patients had some visual disturbance at first clinic review; 7.9% were blind at 6 months.
Data source: Analysis of 433 patients newly diagnosed with GCA participating in the Diagnostic and Classification Criteria in Vasculitis Study (DCVAS).
Disclosures: The DCVAS study is supported by the American College of Rheumatology and is funded by the European League Against Rheumatism and the Vasculitis Foundation. Dr. Yates reported that he had no relevant disclosures.
3. Pediatric and Adolescent Mental Health
Part 1: Diagnoses, drug prescribing vary widely
To take the posttest, go to: http://bit.ly/24FHTxY
Expires April 1, 2017
VITALS
Key clinical point: A lack of psychiatrists only partially accounted for substantial variations in rates of mental illness diagnosis and prescriptions for psychotropic medications given in practices nationwide, a study has shown.
Major finding: Nationwide, 15% of pediatric patients received a mental health diagnosis, and 14% were prescribed psychotropic medications in primary care, regardless of colocated mental health services.
Data source: A retrospective study of electronic health records for 294,748 patients aged 4-18 years.
Disclosures: Dr. Alexander G. Fiks is an investigator for Pfizer; the other researchers said they had no relevant financial disclosures. This study was funded by the National Institutes of Health and the National Institute of Child Health and Human Development under the Best Pharmaceuticals for Children Act.
Part 2: Disorders prevalent in young transgender women
To take the posttest, go to: http://bit.ly/24FCDdq
Expires March 21, 2017
VITALS
Key clinical point: Young transgender women have a high prevalence of psychiatric disorders that is two to four times higher than that in the general population.
Major finding: 41.5% of the study participants had at least one psychiatric disorder, such as major depressive disorder, suicidality, generalized anxiety, PTSD, and alcohol or substance dependence.
Data source: An observational cohort study involving 298 transgender women aged 16-29 years residing in Chicago and Boston.
Disclosures: This study was supported by the National Institute of Mental Health. Dr. Reisner and his associates reported having no relevant financial disclosures.
Here are 4 articles in the July issue of Clinician Reviews (individual articles are valid for one year from date of publication—expiration dates below):
1. Pregnancy Alters Pharmacodynamics of Anti-TNF Agents in Women With IBD
To take the posttest, go to: http://bit.ly/1VQFIHf
Expires May 24, 2017
VITALS
Key clinical point: Blood levels of infliximab rose during pregnancy, while adalimumab levels remained stable, even after researchers accounted for changes in albumin, body mass index, and C-reactive protein levels.
Major finding: Median infliximab concentrations rose from 8.5 mcg/mL in the first trimester to a peak of 21 mcg/mL during the middle of the third trimester (P = .04). Median adalimumab levels ranged between 8.6 and 12.2 mcg/mL during pregnancy.
Data source: A prospective study of 25 pregnant women with ulcerative colitis or Crohn's disease.
Disclosures: Dr. Seow disclosed ties with Janssen, AbbVie, Takeda, Shire, and Actavis.
2. Vascular Disease Linked to Sight Loss in Giant Cell Arteritis
To take the posttest, go to: http://bit.ly/1UqLuu5
Expires May 10, 2017
VITALS
Key clinical point: Patients with vascular disease who develop giant cell arteritis may require careful monitoring for sight loss.
Major finding: Overall, 42.9% of patients had some visual disturbance at first clinic review; 7.9% were blind at 6 months.
Data source: Analysis of 433 patients newly diagnosed with GCA participating in the Diagnostic and Classification Criteria in Vasculitis Study (DCVAS).
Disclosures: The DCVAS study is supported by the American College of Rheumatology and is funded by the European League Against Rheumatism and the Vasculitis Foundation. Dr. Yates reported that he had no relevant disclosures.
3. Pediatric and Adolescent Mental Health
Part 1: Diagnoses, drug prescribing vary widely
To take the posttest, go to: http://bit.ly/24FHTxY
Expires April 1, 2017
VITALS
Key clinical point: A lack of psychiatrists only partially accounted for substantial variations in rates of mental illness diagnosis and prescriptions for psychotropic medications given in practices nationwide, a study has shown.
Major finding: Nationwide, 15% of pediatric patients received a mental health diagnosis, and 14% were prescribed psychotropic medications in primary care, regardless of colocated mental health services.
Data source: A retrospective study of electronic health records for 294,748 patients aged 4-18 years.
Disclosures: Dr. Alexander G. Fiks is an investigator for Pfizer; the other researchers said they had no relevant financial disclosures. This study was funded by the National Institutes of Health and the National Institute of Child Health and Human Development under the Best Pharmaceuticals for Children Act.
Part 2: Disorders prevalent in young transgender women
To take the posttest, go to: http://bit.ly/24FCDdq
Expires March 21, 2017
VITALS
Key clinical point: Young transgender women have a high prevalence of psychiatric disorders that is two to four times higher than that in the general population.
Major finding: 41.5% of the study participants had at least one psychiatric disorder, such as major depressive disorder, suicidality, generalized anxiety, PTSD, and alcohol or substance dependence.
Data source: An observational cohort study involving 298 transgender women aged 16-29 years residing in Chicago and Boston.
Disclosures: This study was supported by the National Institute of Mental Health. Dr. Reisner and his associates reported having no relevant financial disclosures.
Here are 4 articles in the July issue of Clinician Reviews (individual articles are valid for one year from date of publication—expiration dates below):
1. Pregnancy Alters Pharmacodynamics of Anti-TNF Agents in Women With IBD
To take the posttest, go to: http://bit.ly/1VQFIHf
Expires May 24, 2017
VITALS
Key clinical point: Blood levels of infliximab rose during pregnancy, while adalimumab levels remained stable, even after researchers accounted for changes in albumin, body mass index, and C-reactive protein levels.
Major finding: Median infliximab concentrations rose from 8.5 mcg/mL in the first trimester to a peak of 21 mcg/mL during the middle of the third trimester (P = .04). Median adalimumab levels ranged between 8.6 and 12.2 mcg/mL during pregnancy.
Data source: A prospective study of 25 pregnant women with ulcerative colitis or Crohn's disease.
Disclosures: Dr. Seow disclosed ties with Janssen, AbbVie, Takeda, Shire, and Actavis.
2. Vascular Disease Linked to Sight Loss in Giant Cell Arteritis
To take the posttest, go to: http://bit.ly/1UqLuu5
Expires May 10, 2017
VITALS
Key clinical point: Patients with vascular disease who develop giant cell arteritis may require careful monitoring for sight loss.
Major finding: Overall, 42.9% of patients had some visual disturbance at first clinic review; 7.9% were blind at 6 months.
Data source: Analysis of 433 patients newly diagnosed with GCA participating in the Diagnostic and Classification Criteria in Vasculitis Study (DCVAS).
Disclosures: The DCVAS study is supported by the American College of Rheumatology and is funded by the European League Against Rheumatism and the Vasculitis Foundation. Dr. Yates reported that he had no relevant disclosures.
3. Pediatric and Adolescent Mental Health
Part 1: Diagnoses, drug prescribing vary widely
To take the posttest, go to: http://bit.ly/24FHTxY
Expires April 1, 2017
VITALS
Key clinical point: A lack of psychiatrists only partially accounted for substantial variations in rates of mental illness diagnosis and prescriptions for psychotropic medications given in practices nationwide, a study has shown.
Major finding: Nationwide, 15% of pediatric patients received a mental health diagnosis, and 14% were prescribed psychotropic medications in primary care, regardless of colocated mental health services.
Data source: A retrospective study of electronic health records for 294,748 patients aged 4-18 years.
Disclosures: Dr. Alexander G. Fiks is an investigator for Pfizer; the other researchers said they had no relevant financial disclosures. This study was funded by the National Institutes of Health and the National Institute of Child Health and Human Development under the Best Pharmaceuticals for Children Act.
Part 2: Disorders prevalent in young transgender women
To take the posttest, go to: http://bit.ly/24FCDdq
Expires March 21, 2017
VITALS
Key clinical point: Young transgender women have a high prevalence of psychiatric disorders that is two to four times higher than that in the general population.
Major finding: 41.5% of the study participants had at least one psychiatric disorder, such as major depressive disorder, suicidality, generalized anxiety, PTSD, and alcohol or substance dependence.
Data source: An observational cohort study involving 298 transgender women aged 16-29 years residing in Chicago and Boston.
Disclosures: This study was supported by the National Institute of Mental Health. Dr. Reisner and his associates reported having no relevant financial disclosures.
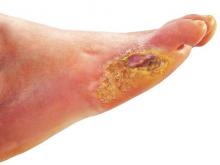
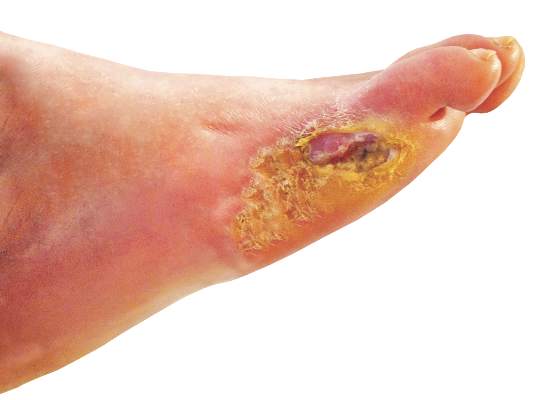
Diabetic Foot Ulcers Linked to Cognitive Decline
Among patients with type 2 diabetes, those with foot ulcers show cognitive impairment across all domains when compared with those without, according to a report published in Diabetes Care.
In what they described as one of the first studies to examine cognitive function in people with diabetic foot ulcers, researchers found that these patients “remember less, have decreased ability to concentrate, and more difficulty with learning, less inhibition, slower cognitive and psychomotor responses, and less verbal fluency” than patients with diabetes that does not include foot involvement.
Although this study had a cross-sectional design that precluded drawing conclusions about causality, an analysis that estimated the participants’ premorbid and postmorbid cognitive abilities suggested that people with diabetic foot ulcers had experienced a recent significant cognitive decline, while those without foot ulcers had not, said Rachel Natovich, Ph.D., of the department of public health, Ben-Gurion University of the Negev, Be’er Sheva (Israel) and the Endocrinology Institute, Sheba Medical Center, Ramat Gan (Israel) and her associates. These findings indicate that patients with diabetic foot ulcers – the very patients who face the greatest self-treatment challenges – are the ones who have the weakest cognitive resources to do so, they noted.
The investigators examined this issue after noting that recent consensus guidelines require patients with diabetic foot ulcers to take on even more self-management than is already required for the diabetes. This demands “applying complex cognitive abilities in learning, understanding, and remembering new information; planning and initiating self-care practices; adopting behavioral changes that involve psychomotor abilities; and maintaining these behaviors while controlling and repressing impulses.” So Dr. Natovich and her associates assessed whether the cognitive profile of patients who have diabetic foot problems differs from that of patients who don’t, using a case-control study design.
The 194 study participants were aged 45-75 years. The 99 subjects who had at least one diabetic foot ulcer (cases) were matched for age and duration of diabetes with 95 subjects who did not (controls). All underwent a comprehensive battery of neuropsychological tests assessing general intelligence, short- and long-term memory, attention and concentration, psychomotor efficiency, reaction time, executive function, nonverbal IQ, visual-motor speed, coordination, capacity for learning, verbal production, semantic memory, and language. All were also assessed for depression via the Patient Health Questionnaire.
After scores were standardized according to the expected performance by age and education level, patients with diabetic foot ulcers showed significantly lower scores in all the domains tested, compared with the patients without foot ulcers. This difference persisted after the data were adjusted to account for possible confounding factors such as smoking status, hemoglobin A1c level, presence or absence of depressive symptoms, and presence or absence of macrovascular disease (Diab Care. 2016 May. doi:10.2337/dc15-2838).
The estimated premorbid cognitive function was similar between the two study groups, but current cognitive function declined significantly in the patients with foot ulcers while remaining relatively constant in the patients without foot ulcers. Prospective studies are needed to explore the timing of cognitive decline and the possibility of causation, Dr. Natovich and her associates said.
The study results “highlight the importance of focusing on cognitive functioning, a less-studied area in diabetic foot research,” they added.
“We feel that it is important to screen the cognitive status of these patients regularly and to take cognitive abilities into consideration in treatment-planning recommendations and follow-up.”
Among patients with type 2 diabetes, those with foot ulcers show cognitive impairment across all domains when compared with those without, according to a report published in Diabetes Care.
In what they described as one of the first studies to examine cognitive function in people with diabetic foot ulcers, researchers found that these patients “remember less, have decreased ability to concentrate, and more difficulty with learning, less inhibition, slower cognitive and psychomotor responses, and less verbal fluency” than patients with diabetes that does not include foot involvement.
Although this study had a cross-sectional design that precluded drawing conclusions about causality, an analysis that estimated the participants’ premorbid and postmorbid cognitive abilities suggested that people with diabetic foot ulcers had experienced a recent significant cognitive decline, while those without foot ulcers had not, said Rachel Natovich, Ph.D., of the department of public health, Ben-Gurion University of the Negev, Be’er Sheva (Israel) and the Endocrinology Institute, Sheba Medical Center, Ramat Gan (Israel) and her associates. These findings indicate that patients with diabetic foot ulcers – the very patients who face the greatest self-treatment challenges – are the ones who have the weakest cognitive resources to do so, they noted.
The investigators examined this issue after noting that recent consensus guidelines require patients with diabetic foot ulcers to take on even more self-management than is already required for the diabetes. This demands “applying complex cognitive abilities in learning, understanding, and remembering new information; planning and initiating self-care practices; adopting behavioral changes that involve psychomotor abilities; and maintaining these behaviors while controlling and repressing impulses.” So Dr. Natovich and her associates assessed whether the cognitive profile of patients who have diabetic foot problems differs from that of patients who don’t, using a case-control study design.
The 194 study participants were aged 45-75 years. The 99 subjects who had at least one diabetic foot ulcer (cases) were matched for age and duration of diabetes with 95 subjects who did not (controls). All underwent a comprehensive battery of neuropsychological tests assessing general intelligence, short- and long-term memory, attention and concentration, psychomotor efficiency, reaction time, executive function, nonverbal IQ, visual-motor speed, coordination, capacity for learning, verbal production, semantic memory, and language. All were also assessed for depression via the Patient Health Questionnaire.
After scores were standardized according to the expected performance by age and education level, patients with diabetic foot ulcers showed significantly lower scores in all the domains tested, compared with the patients without foot ulcers. This difference persisted after the data were adjusted to account for possible confounding factors such as smoking status, hemoglobin A1c level, presence or absence of depressive symptoms, and presence or absence of macrovascular disease (Diab Care. 2016 May. doi:10.2337/dc15-2838).
The estimated premorbid cognitive function was similar between the two study groups, but current cognitive function declined significantly in the patients with foot ulcers while remaining relatively constant in the patients without foot ulcers. Prospective studies are needed to explore the timing of cognitive decline and the possibility of causation, Dr. Natovich and her associates said.
The study results “highlight the importance of focusing on cognitive functioning, a less-studied area in diabetic foot research,” they added.
“We feel that it is important to screen the cognitive status of these patients regularly and to take cognitive abilities into consideration in treatment-planning recommendations and follow-up.”
Among patients with type 2 diabetes, those with foot ulcers show cognitive impairment across all domains when compared with those without, according to a report published in Diabetes Care.
In what they described as one of the first studies to examine cognitive function in people with diabetic foot ulcers, researchers found that these patients “remember less, have decreased ability to concentrate, and more difficulty with learning, less inhibition, slower cognitive and psychomotor responses, and less verbal fluency” than patients with diabetes that does not include foot involvement.
Although this study had a cross-sectional design that precluded drawing conclusions about causality, an analysis that estimated the participants’ premorbid and postmorbid cognitive abilities suggested that people with diabetic foot ulcers had experienced a recent significant cognitive decline, while those without foot ulcers had not, said Rachel Natovich, Ph.D., of the department of public health, Ben-Gurion University of the Negev, Be’er Sheva (Israel) and the Endocrinology Institute, Sheba Medical Center, Ramat Gan (Israel) and her associates. These findings indicate that patients with diabetic foot ulcers – the very patients who face the greatest self-treatment challenges – are the ones who have the weakest cognitive resources to do so, they noted.
The investigators examined this issue after noting that recent consensus guidelines require patients with diabetic foot ulcers to take on even more self-management than is already required for the diabetes. This demands “applying complex cognitive abilities in learning, understanding, and remembering new information; planning and initiating self-care practices; adopting behavioral changes that involve psychomotor abilities; and maintaining these behaviors while controlling and repressing impulses.” So Dr. Natovich and her associates assessed whether the cognitive profile of patients who have diabetic foot problems differs from that of patients who don’t, using a case-control study design.
The 194 study participants were aged 45-75 years. The 99 subjects who had at least one diabetic foot ulcer (cases) were matched for age and duration of diabetes with 95 subjects who did not (controls). All underwent a comprehensive battery of neuropsychological tests assessing general intelligence, short- and long-term memory, attention and concentration, psychomotor efficiency, reaction time, executive function, nonverbal IQ, visual-motor speed, coordination, capacity for learning, verbal production, semantic memory, and language. All were also assessed for depression via the Patient Health Questionnaire.
After scores were standardized according to the expected performance by age and education level, patients with diabetic foot ulcers showed significantly lower scores in all the domains tested, compared with the patients without foot ulcers. This difference persisted after the data were adjusted to account for possible confounding factors such as smoking status, hemoglobin A1c level, presence or absence of depressive symptoms, and presence or absence of macrovascular disease (Diab Care. 2016 May. doi:10.2337/dc15-2838).
The estimated premorbid cognitive function was similar between the two study groups, but current cognitive function declined significantly in the patients with foot ulcers while remaining relatively constant in the patients without foot ulcers. Prospective studies are needed to explore the timing of cognitive decline and the possibility of causation, Dr. Natovich and her associates said.
The study results “highlight the importance of focusing on cognitive functioning, a less-studied area in diabetic foot research,” they added.
“We feel that it is important to screen the cognitive status of these patients regularly and to take cognitive abilities into consideration in treatment-planning recommendations and follow-up.”
FROM DIABETES CARE
Diabetic foot ulcers linked to cognitive decline
Among patients with type 2 diabetes, those with foot ulcers show cognitive impairment across all domains when compared with those without, according to a report published in Diabetes Care.
In what they described as one of the first studies to examine cognitive function in people with diabetic foot ulcers, researchers found that these patients “remember less, have decreased ability to concentrate, and more difficulty with learning, less inhibition, slower cognitive and psychomotor responses, and less verbal fluency” than patients with diabetes that does not include foot involvement.
Although this study had a cross-sectional design that precluded drawing conclusions about causality, an analysis that estimated the participants’ premorbid and postmorbid cognitive abilities suggested that people with diabetic foot ulcers had experienced a recent significant cognitive decline, while those without foot ulcers had not, said Rachel Natovich, Ph.D., of the department of public health, Ben-Gurion University of the Negev, Be’er Sheva (Israel) and the Endocrinology Institute, Sheba Medical Center, Ramat Gan (Israel) and her associates. These findings indicate that patients with diabetic foot ulcers – the very patients who face the greatest self-treatment challenges – are the ones who have the weakest cognitive resources to do so, they noted.
The investigators examined this issue after noting that recent consensus guidelines require patients with diabetic foot ulcers to take on even more self-management than is already required for the diabetes. This demands “applying complex cognitive abilities in learning, understanding, and remembering new information; planning and initiating self-care practices; adopting behavioral changes that involve psychomotor abilities; and maintaining these behaviors while controlling and repressing impulses.” So Dr. Natovich and her associates assessed whether the cognitive profile of patients who have diabetic foot problems differs from that of patients who don’t, using a case-control study design.
The 194 study participants were aged 45-75 years. The 99 subjects who had at least one diabetic foot ulcer (cases) were matched for age and duration of diabetes with 95 subjects who did not (controls). All underwent a comprehensive battery of neuropsychological tests assessing general intelligence, short- and long-term memory, attention and concentration, psychomotor efficiency, reaction time, executive function, nonverbal IQ, visual-motor speed, coordination, capacity for learning, verbal production, semantic memory, and language. All were also assessed for depression via the Patient Health Questionnaire.
After scores were standardized according to the expected performance by age and education level, patients with diabetic foot ulcers showed significantly lower scores in all the domains tested, compared with the patients without foot ulcers. This difference persisted after the data were adjusted to account for possible confounding factors such as smoking status, hemoglobin A1c level, presence or absence of depressive symptoms, and presence or absence of macrovascular disease (Diab Care. 2016 May. doi:10.2337/dc15-2838).
The estimated premorbid cognitive function was similar between the two study groups, but current cognitive function declined significantly in the patients with foot ulcers while remaining relatively constant in the patients without foot ulcers. Prospective studies are needed to explore the timing of cognitive decline and the possibility of causation, Dr. Natovich and her associates said.
The study results “highlight the importance of focusing on cognitive functioning, a less-studied area in diabetic foot research,” they added.
“We feel that it is important to screen the cognitive status of these patients regularly and to take cognitive abilities into consideration in treatment-planning recommendations and follow-up.”
Among patients with type 2 diabetes, those with foot ulcers show cognitive impairment across all domains when compared with those without, according to a report published in Diabetes Care.
In what they described as one of the first studies to examine cognitive function in people with diabetic foot ulcers, researchers found that these patients “remember less, have decreased ability to concentrate, and more difficulty with learning, less inhibition, slower cognitive and psychomotor responses, and less verbal fluency” than patients with diabetes that does not include foot involvement.
Although this study had a cross-sectional design that precluded drawing conclusions about causality, an analysis that estimated the participants’ premorbid and postmorbid cognitive abilities suggested that people with diabetic foot ulcers had experienced a recent significant cognitive decline, while those without foot ulcers had not, said Rachel Natovich, Ph.D., of the department of public health, Ben-Gurion University of the Negev, Be’er Sheva (Israel) and the Endocrinology Institute, Sheba Medical Center, Ramat Gan (Israel) and her associates. These findings indicate that patients with diabetic foot ulcers – the very patients who face the greatest self-treatment challenges – are the ones who have the weakest cognitive resources to do so, they noted.
The investigators examined this issue after noting that recent consensus guidelines require patients with diabetic foot ulcers to take on even more self-management than is already required for the diabetes. This demands “applying complex cognitive abilities in learning, understanding, and remembering new information; planning and initiating self-care practices; adopting behavioral changes that involve psychomotor abilities; and maintaining these behaviors while controlling and repressing impulses.” So Dr. Natovich and her associates assessed whether the cognitive profile of patients who have diabetic foot problems differs from that of patients who don’t, using a case-control study design.
The 194 study participants were aged 45-75 years. The 99 subjects who had at least one diabetic foot ulcer (cases) were matched for age and duration of diabetes with 95 subjects who did not (controls). All underwent a comprehensive battery of neuropsychological tests assessing general intelligence, short- and long-term memory, attention and concentration, psychomotor efficiency, reaction time, executive function, nonverbal IQ, visual-motor speed, coordination, capacity for learning, verbal production, semantic memory, and language. All were also assessed for depression via the Patient Health Questionnaire.
After scores were standardized according to the expected performance by age and education level, patients with diabetic foot ulcers showed significantly lower scores in all the domains tested, compared with the patients without foot ulcers. This difference persisted after the data were adjusted to account for possible confounding factors such as smoking status, hemoglobin A1c level, presence or absence of depressive symptoms, and presence or absence of macrovascular disease (Diab Care. 2016 May. doi:10.2337/dc15-2838).
The estimated premorbid cognitive function was similar between the two study groups, but current cognitive function declined significantly in the patients with foot ulcers while remaining relatively constant in the patients without foot ulcers. Prospective studies are needed to explore the timing of cognitive decline and the possibility of causation, Dr. Natovich and her associates said.
The study results “highlight the importance of focusing on cognitive functioning, a less-studied area in diabetic foot research,” they added.
“We feel that it is important to screen the cognitive status of these patients regularly and to take cognitive abilities into consideration in treatment-planning recommendations and follow-up.”
Among patients with type 2 diabetes, those with foot ulcers show cognitive impairment across all domains when compared with those without, according to a report published in Diabetes Care.
In what they described as one of the first studies to examine cognitive function in people with diabetic foot ulcers, researchers found that these patients “remember less, have decreased ability to concentrate, and more difficulty with learning, less inhibition, slower cognitive and psychomotor responses, and less verbal fluency” than patients with diabetes that does not include foot involvement.
Although this study had a cross-sectional design that precluded drawing conclusions about causality, an analysis that estimated the participants’ premorbid and postmorbid cognitive abilities suggested that people with diabetic foot ulcers had experienced a recent significant cognitive decline, while those without foot ulcers had not, said Rachel Natovich, Ph.D., of the department of public health, Ben-Gurion University of the Negev, Be’er Sheva (Israel) and the Endocrinology Institute, Sheba Medical Center, Ramat Gan (Israel) and her associates. These findings indicate that patients with diabetic foot ulcers – the very patients who face the greatest self-treatment challenges – are the ones who have the weakest cognitive resources to do so, they noted.
The investigators examined this issue after noting that recent consensus guidelines require patients with diabetic foot ulcers to take on even more self-management than is already required for the diabetes. This demands “applying complex cognitive abilities in learning, understanding, and remembering new information; planning and initiating self-care practices; adopting behavioral changes that involve psychomotor abilities; and maintaining these behaviors while controlling and repressing impulses.” So Dr. Natovich and her associates assessed whether the cognitive profile of patients who have diabetic foot problems differs from that of patients who don’t, using a case-control study design.
The 194 study participants were aged 45-75 years. The 99 subjects who had at least one diabetic foot ulcer (cases) were matched for age and duration of diabetes with 95 subjects who did not (controls). All underwent a comprehensive battery of neuropsychological tests assessing general intelligence, short- and long-term memory, attention and concentration, psychomotor efficiency, reaction time, executive function, nonverbal IQ, visual-motor speed, coordination, capacity for learning, verbal production, semantic memory, and language. All were also assessed for depression via the Patient Health Questionnaire.
After scores were standardized according to the expected performance by age and education level, patients with diabetic foot ulcers showed significantly lower scores in all the domains tested, compared with the patients without foot ulcers. This difference persisted after the data were adjusted to account for possible confounding factors such as smoking status, hemoglobin A1c level, presence or absence of depressive symptoms, and presence or absence of macrovascular disease (Diab Care. 2016 May. doi:10.2337/dc15-2838).
The estimated premorbid cognitive function was similar between the two study groups, but current cognitive function declined significantly in the patients with foot ulcers while remaining relatively constant in the patients without foot ulcers. Prospective studies are needed to explore the timing of cognitive decline and the possibility of causation, Dr. Natovich and her associates said.
The study results “highlight the importance of focusing on cognitive functioning, a less-studied area in diabetic foot research,” they added.
“We feel that it is important to screen the cognitive status of these patients regularly and to take cognitive abilities into consideration in treatment-planning recommendations and follow-up.”
FROM DIABETES CARE
Key clinical point: Among patients with type 2 diabetes, those with foot ulcers show cognitive impairment, compared with those who don’t have foot ulcers.
Major finding: Ninety-nine patients with at least one diabetic foot showed significantly lower scores in all cognitive domains tested compared with the 95 patients without foot ulcers.
Data source: A cross-sectional case-control study comparing cognitive performance between 99 patients with and 95 patients without diabetic foot ulcers.
Disclosures: No sponsor of this study was identified. Dr. Natovich and her associates reported having no relevant disclosures.
Smoking linked to longer hospital stay
Current and former cigarette smoking were associated with a longer hospital stay for patients with lung cancer, chronic obstructive pulmonary disease, or ischemic heart disease, according to a report published in Hospital Practice.
Researchers assessed factors influencing hospital length of stay (LOS) as a first step toward shortening that measure, improving inpatient services, and cutting hospital costs in Iran, where this issue has not been studied previously. The overall prevalence of smoking in Iran is 12.5%, and it is much more common among men than women, said Satar Rezaei, Ph.D., of the Research Centre for Environmental Determinants of Health, Kermanshah (Iran) University of Medical Sciences, and his associates.
They assessed LOS in 1,271 patients aged 35-93 years (mean age, 63 years) who were hospitalized at 11 Tehran medical centers during a 1-year period. Slightly more than half (54%) of these patients had never smoked, while 34% were current smokers and 12% were former smokers. A total of 415 (32%) had lung cancer, 427 (34%) had COPD, and 429 (34%) had ischemic heart disease. The overall mean LOS was 7.3 days, with a range from 1 to 45 days.
The mean LOS was 48% longer among current smokers and 15% longer among former smokers than among nonsmokers. It was 9.4 days for current smokers and 7.3 days for former smokers, compared with 6.0 days for nonsmokers, Dr. Rezaei and his associates said (Hosp. Pract. 2016. doi: 10.1080/21548331.2016.1178579).
Patient cigarette smoking imposes a heavy financial burden on these hospitals and contributes to their shortage of resources. Hospital-based smoking cessation programs would be useful in shortening LOS and sparing hospital resources, the researchers added.
This study was supported by Tehran University of Medical Sciences. Dr. Rezaei and his associates reported having no relevant financial disclosures.
Current and former cigarette smoking were associated with a longer hospital stay for patients with lung cancer, chronic obstructive pulmonary disease, or ischemic heart disease, according to a report published in Hospital Practice.
Researchers assessed factors influencing hospital length of stay (LOS) as a first step toward shortening that measure, improving inpatient services, and cutting hospital costs in Iran, where this issue has not been studied previously. The overall prevalence of smoking in Iran is 12.5%, and it is much more common among men than women, said Satar Rezaei, Ph.D., of the Research Centre for Environmental Determinants of Health, Kermanshah (Iran) University of Medical Sciences, and his associates.
They assessed LOS in 1,271 patients aged 35-93 years (mean age, 63 years) who were hospitalized at 11 Tehran medical centers during a 1-year period. Slightly more than half (54%) of these patients had never smoked, while 34% were current smokers and 12% were former smokers. A total of 415 (32%) had lung cancer, 427 (34%) had COPD, and 429 (34%) had ischemic heart disease. The overall mean LOS was 7.3 days, with a range from 1 to 45 days.
The mean LOS was 48% longer among current smokers and 15% longer among former smokers than among nonsmokers. It was 9.4 days for current smokers and 7.3 days for former smokers, compared with 6.0 days for nonsmokers, Dr. Rezaei and his associates said (Hosp. Pract. 2016. doi: 10.1080/21548331.2016.1178579).
Patient cigarette smoking imposes a heavy financial burden on these hospitals and contributes to their shortage of resources. Hospital-based smoking cessation programs would be useful in shortening LOS and sparing hospital resources, the researchers added.
This study was supported by Tehran University of Medical Sciences. Dr. Rezaei and his associates reported having no relevant financial disclosures.
Current and former cigarette smoking were associated with a longer hospital stay for patients with lung cancer, chronic obstructive pulmonary disease, or ischemic heart disease, according to a report published in Hospital Practice.
Researchers assessed factors influencing hospital length of stay (LOS) as a first step toward shortening that measure, improving inpatient services, and cutting hospital costs in Iran, where this issue has not been studied previously. The overall prevalence of smoking in Iran is 12.5%, and it is much more common among men than women, said Satar Rezaei, Ph.D., of the Research Centre for Environmental Determinants of Health, Kermanshah (Iran) University of Medical Sciences, and his associates.
They assessed LOS in 1,271 patients aged 35-93 years (mean age, 63 years) who were hospitalized at 11 Tehran medical centers during a 1-year period. Slightly more than half (54%) of these patients had never smoked, while 34% were current smokers and 12% were former smokers. A total of 415 (32%) had lung cancer, 427 (34%) had COPD, and 429 (34%) had ischemic heart disease. The overall mean LOS was 7.3 days, with a range from 1 to 45 days.
The mean LOS was 48% longer among current smokers and 15% longer among former smokers than among nonsmokers. It was 9.4 days for current smokers and 7.3 days for former smokers, compared with 6.0 days for nonsmokers, Dr. Rezaei and his associates said (Hosp. Pract. 2016. doi: 10.1080/21548331.2016.1178579).
Patient cigarette smoking imposes a heavy financial burden on these hospitals and contributes to their shortage of resources. Hospital-based smoking cessation programs would be useful in shortening LOS and sparing hospital resources, the researchers added.
This study was supported by Tehran University of Medical Sciences. Dr. Rezaei and his associates reported having no relevant financial disclosures.
FROM HOSPITAL PRACTICE
Key clinical point: Current and former cigarette smoking are associated with a longer hospital stay for patients with lung cancer, chronic obstructive pulmonary disease, or ischemic heart disease.
Major finding: The mean LOS was 48% longer among current smokers and 15% longer among former smokers than among nonsmokers.
Data source: A retrospective cohort study involving 1,271 patients hospitalized in Iran during a 1-year period.
Disclosures: This study was supported by Tehran University of Medical Sciences. Dr. Rezaei and his associates reported having no relevant financial disclosures.
Initiative dramatically raises HCV screening, treatment
A hepatitis C awareness initiative dramatically raised the rate of HCV screening and treatment in a large American Indian population – the ethnic group with the highest rate of HCV infection and HCV-related mortality in the United States, according to a report published May 13 in Morbidity and Mortality Weekly Report.
Cherokee Nation Health Services undertook the effort in 2012 to improve detection and management of HCV. It included a reminder in eligible patients’ electronic health records (EHRs) to offer screening; HCV education for primary care physicians and other health care providers; establishment of an HCV registry to monitor the clinical care of patients who initiated antiviral treatment; and outreach efforts by public health nurses to HCV patients, including home visits.
In 2014, an additional initiative was implemented to expand services for the rapidly increasing number of patients diagnosed as having HCV. This allowed a transition from having a single clinic staffed by only one caregiver with expertise in HCV management to five clinics staffed by three physicians, two nurse practitioners, and two pharmacists with HCV expertise, said Dr. Jorge Mera, director of infectious diseases, Cherokee Nation Health Services, Tulsa, Okla., and his associates.
An analysis of deidentified data in the HCV registry and EHRs showed that 92,012 patients aged 20 years and older had at least one visit with Cherokee Nation Health Services after the program was implemented, between October 2012 and July 2015. The proportion of this patient population that was tested for HCV antibodies rose fivefold, from 3.6% to 18.2% during the study period. A total of 715 patients were antibody positive, and 388 of them were found to have chronic HCV infection. Approximately 60% of these patients initiated antiviral treatment, and approximately 90% of them achieved a sustained virologic response and were essentially cured, Dr. Mera and his associates said (MMWR. 2016 May 13;65[18]:461-6).
The program included a component that particularly targeted baby boomers – patients born between 1945 and 1965 – for HCV screening. Across the Indian Health Service clinics in 34 states that adopted this component of the program, such screening increased fourfold in this high-risk population during the study period (MMWR. 2016 May 13;65[18]:467-9).
These efforts, the first of their kind in the United States, may help eliminate hepatitis C as a health disparity for American Indian/Alaska Native populations and also may serve as a model for other health care settings, the investigators added.
A hepatitis C awareness initiative dramatically raised the rate of HCV screening and treatment in a large American Indian population – the ethnic group with the highest rate of HCV infection and HCV-related mortality in the United States, according to a report published May 13 in Morbidity and Mortality Weekly Report.
Cherokee Nation Health Services undertook the effort in 2012 to improve detection and management of HCV. It included a reminder in eligible patients’ electronic health records (EHRs) to offer screening; HCV education for primary care physicians and other health care providers; establishment of an HCV registry to monitor the clinical care of patients who initiated antiviral treatment; and outreach efforts by public health nurses to HCV patients, including home visits.
In 2014, an additional initiative was implemented to expand services for the rapidly increasing number of patients diagnosed as having HCV. This allowed a transition from having a single clinic staffed by only one caregiver with expertise in HCV management to five clinics staffed by three physicians, two nurse practitioners, and two pharmacists with HCV expertise, said Dr. Jorge Mera, director of infectious diseases, Cherokee Nation Health Services, Tulsa, Okla., and his associates.
An analysis of deidentified data in the HCV registry and EHRs showed that 92,012 patients aged 20 years and older had at least one visit with Cherokee Nation Health Services after the program was implemented, between October 2012 and July 2015. The proportion of this patient population that was tested for HCV antibodies rose fivefold, from 3.6% to 18.2% during the study period. A total of 715 patients were antibody positive, and 388 of them were found to have chronic HCV infection. Approximately 60% of these patients initiated antiviral treatment, and approximately 90% of them achieved a sustained virologic response and were essentially cured, Dr. Mera and his associates said (MMWR. 2016 May 13;65[18]:461-6).
The program included a component that particularly targeted baby boomers – patients born between 1945 and 1965 – for HCV screening. Across the Indian Health Service clinics in 34 states that adopted this component of the program, such screening increased fourfold in this high-risk population during the study period (MMWR. 2016 May 13;65[18]:467-9).
These efforts, the first of their kind in the United States, may help eliminate hepatitis C as a health disparity for American Indian/Alaska Native populations and also may serve as a model for other health care settings, the investigators added.
A hepatitis C awareness initiative dramatically raised the rate of HCV screening and treatment in a large American Indian population – the ethnic group with the highest rate of HCV infection and HCV-related mortality in the United States, according to a report published May 13 in Morbidity and Mortality Weekly Report.
Cherokee Nation Health Services undertook the effort in 2012 to improve detection and management of HCV. It included a reminder in eligible patients’ electronic health records (EHRs) to offer screening; HCV education for primary care physicians and other health care providers; establishment of an HCV registry to monitor the clinical care of patients who initiated antiviral treatment; and outreach efforts by public health nurses to HCV patients, including home visits.
In 2014, an additional initiative was implemented to expand services for the rapidly increasing number of patients diagnosed as having HCV. This allowed a transition from having a single clinic staffed by only one caregiver with expertise in HCV management to five clinics staffed by three physicians, two nurse practitioners, and two pharmacists with HCV expertise, said Dr. Jorge Mera, director of infectious diseases, Cherokee Nation Health Services, Tulsa, Okla., and his associates.
An analysis of deidentified data in the HCV registry and EHRs showed that 92,012 patients aged 20 years and older had at least one visit with Cherokee Nation Health Services after the program was implemented, between October 2012 and July 2015. The proportion of this patient population that was tested for HCV antibodies rose fivefold, from 3.6% to 18.2% during the study period. A total of 715 patients were antibody positive, and 388 of them were found to have chronic HCV infection. Approximately 60% of these patients initiated antiviral treatment, and approximately 90% of them achieved a sustained virologic response and were essentially cured, Dr. Mera and his associates said (MMWR. 2016 May 13;65[18]:461-6).
The program included a component that particularly targeted baby boomers – patients born between 1945 and 1965 – for HCV screening. Across the Indian Health Service clinics in 34 states that adopted this component of the program, such screening increased fourfold in this high-risk population during the study period (MMWR. 2016 May 13;65[18]:467-9).
These efforts, the first of their kind in the United States, may help eliminate hepatitis C as a health disparity for American Indian/Alaska Native populations and also may serve as a model for other health care settings, the investigators added.
FROM MORBIDITY and MORTALITY WEEKLY REPORT
Key clinical point: A new program dramatically raised the rate of HCV screening and treatment in a large American Indian population – the ethnic group with the highest rate of HCV infection and HCV-related mortality in the United States.
Major finding: The proportion of adults tested for HCV antibodies rose fivefold, from 3.6% to 18.2%, during the study period.
Data source: An observational cohort study involving 92,012 adults who had at least 1 visit to Cherokee Nation Health Services between October 2012 and July 2015.
Disclosures: The sponsor of this study was not specified, and potential financial conflicts of interest were not provided. The authors were affiliated with Cherokee Nation Health Services, the U.S. Centers for Disease Control and Prevention, the University of Oklahoma Health Sciences Center, the Oklahoma City Veterans Affairs Medical Center, the Indian Health Service, and the Northwest Portland (Ore.) Area Indian Health Board.
ED visits due to anaphylaxis doubled at Canadian children’s hospital
The percentage of emergency department (ED) visits due to anaphylaxis more than doubled from 2011 to 2015 at one Canadian children’s hospital, according to a Research Letter to the Editor published in the Journal of Allergy and Clinical Immunology.
“Our results are limited to one pediatric center, but they suggest a worrisome increase in anaphylaxis rate that is consistent with the worldwide reported increase,” said Dr. Elana Hochstadter of the Hospital for Sick Children, University of Toronto, and her associates. The investigators analyzed longitudinal data in a national registry of anaphylaxis cases to track time trends for the disorder at their hospital. They identified 965 cases presenting to their ED during a 4-year period. The percentage of all ED visits accounted for by anaphylaxis rose from 0.20% to 0.41%. The overall volume of ED visits and the volume of specific ED diagnoses did not change during this interval.
As in other studies of anaphylaxis around the world, food was the most common trigger in this series, responsible for 82% of cases. Peanut was the most common food allergen, accounting for 22% of cases. Most reactions were of moderate severity, and the percentages of mild, moderate, and severe reactions remained relatively stable throughout the study period. The presence of asthma was associated with increased severity of anaphylaxis (odds ratio, 2.3), as was the presence of eczema (OR, 2.1). Only half of the patients who had an epinephrine autoinjector used it before presenting to the ED, Dr. Hochstadter and her associates said (J Allergy Clin Immunol. 2016 doi: 10.1016/j.jaci.2016.02.016). The median age of the patients was 6 years.
The reason for this rapid increase is unknown, but it parallels that reported in studies of anaphylaxis throughout North America and Europe. “An important observation in our study is that administration of epinephrine before arrival in the ED is independently associated with a decreased likelihood of requiring multiple doses of epinephrine in the ED, suggesting that prompt epinephrine administration is beneficial,” they noted.
The Allergy, Genes, and Environment Network Centres of Excellence, Health Canada, and Sanofi funded the study. Dr. Hochstadter and her associates reported having no relevant disclosures.
The percentage of emergency department (ED) visits due to anaphylaxis more than doubled from 2011 to 2015 at one Canadian children’s hospital, according to a Research Letter to the Editor published in the Journal of Allergy and Clinical Immunology.
“Our results are limited to one pediatric center, but they suggest a worrisome increase in anaphylaxis rate that is consistent with the worldwide reported increase,” said Dr. Elana Hochstadter of the Hospital for Sick Children, University of Toronto, and her associates. The investigators analyzed longitudinal data in a national registry of anaphylaxis cases to track time trends for the disorder at their hospital. They identified 965 cases presenting to their ED during a 4-year period. The percentage of all ED visits accounted for by anaphylaxis rose from 0.20% to 0.41%. The overall volume of ED visits and the volume of specific ED diagnoses did not change during this interval.
As in other studies of anaphylaxis around the world, food was the most common trigger in this series, responsible for 82% of cases. Peanut was the most common food allergen, accounting for 22% of cases. Most reactions were of moderate severity, and the percentages of mild, moderate, and severe reactions remained relatively stable throughout the study period. The presence of asthma was associated with increased severity of anaphylaxis (odds ratio, 2.3), as was the presence of eczema (OR, 2.1). Only half of the patients who had an epinephrine autoinjector used it before presenting to the ED, Dr. Hochstadter and her associates said (J Allergy Clin Immunol. 2016 doi: 10.1016/j.jaci.2016.02.016). The median age of the patients was 6 years.
The reason for this rapid increase is unknown, but it parallels that reported in studies of anaphylaxis throughout North America and Europe. “An important observation in our study is that administration of epinephrine before arrival in the ED is independently associated with a decreased likelihood of requiring multiple doses of epinephrine in the ED, suggesting that prompt epinephrine administration is beneficial,” they noted.
The Allergy, Genes, and Environment Network Centres of Excellence, Health Canada, and Sanofi funded the study. Dr. Hochstadter and her associates reported having no relevant disclosures.
The percentage of emergency department (ED) visits due to anaphylaxis more than doubled from 2011 to 2015 at one Canadian children’s hospital, according to a Research Letter to the Editor published in the Journal of Allergy and Clinical Immunology.
“Our results are limited to one pediatric center, but they suggest a worrisome increase in anaphylaxis rate that is consistent with the worldwide reported increase,” said Dr. Elana Hochstadter of the Hospital for Sick Children, University of Toronto, and her associates. The investigators analyzed longitudinal data in a national registry of anaphylaxis cases to track time trends for the disorder at their hospital. They identified 965 cases presenting to their ED during a 4-year period. The percentage of all ED visits accounted for by anaphylaxis rose from 0.20% to 0.41%. The overall volume of ED visits and the volume of specific ED diagnoses did not change during this interval.
As in other studies of anaphylaxis around the world, food was the most common trigger in this series, responsible for 82% of cases. Peanut was the most common food allergen, accounting for 22% of cases. Most reactions were of moderate severity, and the percentages of mild, moderate, and severe reactions remained relatively stable throughout the study period. The presence of asthma was associated with increased severity of anaphylaxis (odds ratio, 2.3), as was the presence of eczema (OR, 2.1). Only half of the patients who had an epinephrine autoinjector used it before presenting to the ED, Dr. Hochstadter and her associates said (J Allergy Clin Immunol. 2016 doi: 10.1016/j.jaci.2016.02.016). The median age of the patients was 6 years.
The reason for this rapid increase is unknown, but it parallels that reported in studies of anaphylaxis throughout North America and Europe. “An important observation in our study is that administration of epinephrine before arrival in the ED is independently associated with a decreased likelihood of requiring multiple doses of epinephrine in the ED, suggesting that prompt epinephrine administration is beneficial,” they noted.
The Allergy, Genes, and Environment Network Centres of Excellence, Health Canada, and Sanofi funded the study. Dr. Hochstadter and her associates reported having no relevant disclosures.
FROM JOURNAL OF ALLERGY AND CLINICAL IMMUNOLOGY
Key clinical point: The percentage of ED visits due to anaphylaxis more than doubled at one Canadian children’s hospital between 2011 and 2015.
Major finding: The percentage of all ED visits accounted for by anaphylaxis rose from 0.20% to 0.41% during the 4-year study.
Data source: A single-center longitudinal analysis of 965 ED visits for anaphylaxis.
Disclosures: The Allergy, Genes, and Environment Network Centres of Excellence, Health Canada, and Sanofi funded the study. Dr. Hochstadter and her associates reported having no relevant disclosures.
Hepatitis B vaccine immunogenic, safe in diabetes patients
The hepatitis B vaccine was immunogenic in adults with type 2 diabetes and had a safety profile similar to that of control subjects in a manufacturer-sponsored phase-IV trial published in Human Vaccines & Immunotherapeutics.
Adults with diabetes are at twice the risk for developing acute hepatitis B infection as are nondiabetic adults, and the U.S. Advisory Committee on Immunization Practices recommends the vaccine in this patient population, said Dr. Olivier Van Der Meeren of GlaxoSmithKline, Wavre (Belgium) and his associates.
They performed a prospective study comparing the immunogenicity of the vaccine in 378 people with, and 189 without, type 2 diabetes. These participants were followed at 21 sites in Australia, Canada, New Zealand, and the United States. Control subjects were matched to diabetes patients for age and body mass index.
One month after receiving the final of three doses of the vaccine, the seroprotection rate was 75.4% in the diabetes group and 82.0% in the control group, which was considered comparable. However, in a stepwise regression analysis, older age, higher BMI, female gender, and presence of diabetes were associated with reduced hepatitis B antibody concentrations, suggesting that the vaccine was less immunogenic in diabetic patients than in healthy controls, the investigators noted (Human Vacc Immunother. 2016 April 28. doi: 10.1080/21645515.2016.1164362).
Reactions and adverse events were deemed similar between the two study groups. Grade 3 adverse events developed in 8.4% of the diabetes group and 6.3% of the control group. Serious adverse events developed in 3.8% of the diabetes group and 1.6% of the control group, and none were considered to be related to the vaccine.
“Because increasing age was generally associated with a reduction in seroprotection rates, hepatitis B vaccine should be administered as soon as possible after the diagnosis of diabetes,” Dr. Van Der Meeren and his colleagues said.
Dr. Van Der Meeren is employed by and holds stock options for GlaxoSmithKline, which sponsored the study and was involved in its design, in collecting and analyzing the data, and in publishing the report. His associates reported ties to numerous industry sources.
The hepatitis B vaccine was immunogenic in adults with type 2 diabetes and had a safety profile similar to that of control subjects in a manufacturer-sponsored phase-IV trial published in Human Vaccines & Immunotherapeutics.
Adults with diabetes are at twice the risk for developing acute hepatitis B infection as are nondiabetic adults, and the U.S. Advisory Committee on Immunization Practices recommends the vaccine in this patient population, said Dr. Olivier Van Der Meeren of GlaxoSmithKline, Wavre (Belgium) and his associates.
They performed a prospective study comparing the immunogenicity of the vaccine in 378 people with, and 189 without, type 2 diabetes. These participants were followed at 21 sites in Australia, Canada, New Zealand, and the United States. Control subjects were matched to diabetes patients for age and body mass index.
One month after receiving the final of three doses of the vaccine, the seroprotection rate was 75.4% in the diabetes group and 82.0% in the control group, which was considered comparable. However, in a stepwise regression analysis, older age, higher BMI, female gender, and presence of diabetes were associated with reduced hepatitis B antibody concentrations, suggesting that the vaccine was less immunogenic in diabetic patients than in healthy controls, the investigators noted (Human Vacc Immunother. 2016 April 28. doi: 10.1080/21645515.2016.1164362).
Reactions and adverse events were deemed similar between the two study groups. Grade 3 adverse events developed in 8.4% of the diabetes group and 6.3% of the control group. Serious adverse events developed in 3.8% of the diabetes group and 1.6% of the control group, and none were considered to be related to the vaccine.
“Because increasing age was generally associated with a reduction in seroprotection rates, hepatitis B vaccine should be administered as soon as possible after the diagnosis of diabetes,” Dr. Van Der Meeren and his colleagues said.
Dr. Van Der Meeren is employed by and holds stock options for GlaxoSmithKline, which sponsored the study and was involved in its design, in collecting and analyzing the data, and in publishing the report. His associates reported ties to numerous industry sources.
The hepatitis B vaccine was immunogenic in adults with type 2 diabetes and had a safety profile similar to that of control subjects in a manufacturer-sponsored phase-IV trial published in Human Vaccines & Immunotherapeutics.
Adults with diabetes are at twice the risk for developing acute hepatitis B infection as are nondiabetic adults, and the U.S. Advisory Committee on Immunization Practices recommends the vaccine in this patient population, said Dr. Olivier Van Der Meeren of GlaxoSmithKline, Wavre (Belgium) and his associates.
They performed a prospective study comparing the immunogenicity of the vaccine in 378 people with, and 189 without, type 2 diabetes. These participants were followed at 21 sites in Australia, Canada, New Zealand, and the United States. Control subjects were matched to diabetes patients for age and body mass index.
One month after receiving the final of three doses of the vaccine, the seroprotection rate was 75.4% in the diabetes group and 82.0% in the control group, which was considered comparable. However, in a stepwise regression analysis, older age, higher BMI, female gender, and presence of diabetes were associated with reduced hepatitis B antibody concentrations, suggesting that the vaccine was less immunogenic in diabetic patients than in healthy controls, the investigators noted (Human Vacc Immunother. 2016 April 28. doi: 10.1080/21645515.2016.1164362).
Reactions and adverse events were deemed similar between the two study groups. Grade 3 adverse events developed in 8.4% of the diabetes group and 6.3% of the control group. Serious adverse events developed in 3.8% of the diabetes group and 1.6% of the control group, and none were considered to be related to the vaccine.
“Because increasing age was generally associated with a reduction in seroprotection rates, hepatitis B vaccine should be administered as soon as possible after the diagnosis of diabetes,” Dr. Van Der Meeren and his colleagues said.
Dr. Van Der Meeren is employed by and holds stock options for GlaxoSmithKline, which sponsored the study and was involved in its design, in collecting and analyzing the data, and in publishing the report. His associates reported ties to numerous industry sources.
FROM HUMAN VACCINES & IMMUNOTHERAPEUTICS
Key clinical point: The hepatitis B vaccine is immunogenic in adults with type 2 diabetes and has a safety profile similar to that of other adults.
Major finding: The seroprotection rate was 75.4% in the diabetes group and 82.0% in the control group.
Data source: A manufacturer-sponsored prospective international phase-IV study involving 378 adults with diabetes and 189 controls.
Disclosures: Dr. Van Der Meeren is employed by and holds stock options for GlaxoSmithKline, which sponsored the study and was involved in its design, in collecting and analyzing the data, and in publishing the report. His associates reported ties to numerous industry sources.