User login
Official Newspaper of the American College of Surgeons
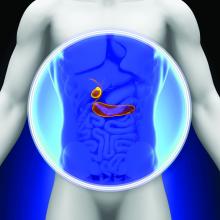
Proceed cautiously with liver cancer resection in elderly patients
MIAMI BEACH – A decision to proceed with major hepatectomy in patients 75 and older with perihilar cholangiocarcinoma should be made on a case-by-case basis following strict selection, Thuy Tran, MD, said, based on a study of 210 patients.
“As the U.S. population ages, an increasing number of elderly patients are being evaluated for resection of GI malignancies,” Dr. Tran said at the annual meeting of the Americas Hepato-Pancreato-Biliary Association.
“Advanced age has been regarded as contraindication to resection for complex hepatobiliary malignancies,” she explained, with concerns that “it may be too risky, and the survival benefit is limited in elderly populations. However, the oncologic benefit of aggressive surgical strategies in perihilar cholangiocarcinoma remains a subject of debate.”
Dr. Tran and her colleagues identified patients who underwent curative resection for perihilar cholangiocarcinoma (CCA) in the U.S. Extrahepatic Biliary Malignancy Consortium database. They compared outcomes of those younger than 75 years versus patients 75 years and older. A total of 59% of the cohort were men, 20% were 75 years and older, and the median age was 66 years.
CCA is a rare and aggressive malignancy, often presenting with obstructive jaundice, said Dr. Tran, a postdoctoral research fellow in general surgery at Stanford (Calif.) University.
Preoperative characteristics were similar in the groups, except that cardiac morbidity was higher in the older cohort. In addition, pathology characteristics did not differ significantly between age groups, including tumor stage, nodal status, grade, size, and margin status.
The in-hospital mortality was double for the older patients, 15% versus 8%, despite the similarities, Dr. Tran said. “This supports the notion that it is more difficult to salvage older patients when they run into a complication,” she added.
Postoperative morbidity was also higher in older patients, 78% versus 68%, but did not reach statistical significance (P = .34).
The 90-day mortality rate was 22% in patients 75 years and older, compared with 10% in younger patients, a nonsignificant difference (P = .09).
Five-year survival was 15% in the older cohort and 22% for the younger patients (P = .003). There was a “more significant drop in the survival curves in the older age group, but then they get closer,” Dr. Tran said. The disease-specific survival did not differ significantly at 46 months versus 37 months, respectively.
Advanced-stage cancer and elevated CA 19-9 tumor marker levels were independent predictors of survival in a multivariate analysis, but age was not. Higher body mass index was associated with a higher perioperative mortality in older patients, but sex, cardiac morbidity, and ASA status were not. Dr. Tran said, “Lower BMI may be a useful tool to select elderly patients,” she noted.
“Elderly patients have double the mortality following major hepatectomy for perihilar cholangiocarcinoma,” Dr. Tran said. “However, the long-term, cancer-specific outcome appears similar to that of younger patients.” Physiologically robust older patients may be better candidates for surgery, she suggested.
Of the six patients who died in the 75 and older group, two patients died from liver failure, one from sepsis, one intraoperatively, one from unknown causes, and one died who required reoperation for postop bleeding, Dr. Tran said. “We did not find patients dying from MI or pneumonia, probably due to the small number of patients.”
Dr. Tran said that 2.5% of the older group and 5% of the younger group received neoadjuvant chemotherapy, which was not a statistically significant difference.
A meeting attendee asked if left versus right hepatectomy made a difference, and why the researchers chose 75 years as the cutoff age between younger and older groups.
“Left vs. right laterality does not seem to make an impact in terms of survival,” Dr. Tran said. “The median age was 66 years, and we used the upper limit of standard deviation, which was 75.”
Dr. Tran had no relevant financial disclosures.
MIAMI BEACH – A decision to proceed with major hepatectomy in patients 75 and older with perihilar cholangiocarcinoma should be made on a case-by-case basis following strict selection, Thuy Tran, MD, said, based on a study of 210 patients.
“As the U.S. population ages, an increasing number of elderly patients are being evaluated for resection of GI malignancies,” Dr. Tran said at the annual meeting of the Americas Hepato-Pancreato-Biliary Association.
“Advanced age has been regarded as contraindication to resection for complex hepatobiliary malignancies,” she explained, with concerns that “it may be too risky, and the survival benefit is limited in elderly populations. However, the oncologic benefit of aggressive surgical strategies in perihilar cholangiocarcinoma remains a subject of debate.”
Dr. Tran and her colleagues identified patients who underwent curative resection for perihilar cholangiocarcinoma (CCA) in the U.S. Extrahepatic Biliary Malignancy Consortium database. They compared outcomes of those younger than 75 years versus patients 75 years and older. A total of 59% of the cohort were men, 20% were 75 years and older, and the median age was 66 years.
CCA is a rare and aggressive malignancy, often presenting with obstructive jaundice, said Dr. Tran, a postdoctoral research fellow in general surgery at Stanford (Calif.) University.
Preoperative characteristics were similar in the groups, except that cardiac morbidity was higher in the older cohort. In addition, pathology characteristics did not differ significantly between age groups, including tumor stage, nodal status, grade, size, and margin status.
The in-hospital mortality was double for the older patients, 15% versus 8%, despite the similarities, Dr. Tran said. “This supports the notion that it is more difficult to salvage older patients when they run into a complication,” she added.
Postoperative morbidity was also higher in older patients, 78% versus 68%, but did not reach statistical significance (P = .34).
The 90-day mortality rate was 22% in patients 75 years and older, compared with 10% in younger patients, a nonsignificant difference (P = .09).
Five-year survival was 15% in the older cohort and 22% for the younger patients (P = .003). There was a “more significant drop in the survival curves in the older age group, but then they get closer,” Dr. Tran said. The disease-specific survival did not differ significantly at 46 months versus 37 months, respectively.
Advanced-stage cancer and elevated CA 19-9 tumor marker levels were independent predictors of survival in a multivariate analysis, but age was not. Higher body mass index was associated with a higher perioperative mortality in older patients, but sex, cardiac morbidity, and ASA status were not. Dr. Tran said, “Lower BMI may be a useful tool to select elderly patients,” she noted.
“Elderly patients have double the mortality following major hepatectomy for perihilar cholangiocarcinoma,” Dr. Tran said. “However, the long-term, cancer-specific outcome appears similar to that of younger patients.” Physiologically robust older patients may be better candidates for surgery, she suggested.
Of the six patients who died in the 75 and older group, two patients died from liver failure, one from sepsis, one intraoperatively, one from unknown causes, and one died who required reoperation for postop bleeding, Dr. Tran said. “We did not find patients dying from MI or pneumonia, probably due to the small number of patients.”
Dr. Tran said that 2.5% of the older group and 5% of the younger group received neoadjuvant chemotherapy, which was not a statistically significant difference.
A meeting attendee asked if left versus right hepatectomy made a difference, and why the researchers chose 75 years as the cutoff age between younger and older groups.
“Left vs. right laterality does not seem to make an impact in terms of survival,” Dr. Tran said. “The median age was 66 years, and we used the upper limit of standard deviation, which was 75.”
Dr. Tran had no relevant financial disclosures.
MIAMI BEACH – A decision to proceed with major hepatectomy in patients 75 and older with perihilar cholangiocarcinoma should be made on a case-by-case basis following strict selection, Thuy Tran, MD, said, based on a study of 210 patients.
“As the U.S. population ages, an increasing number of elderly patients are being evaluated for resection of GI malignancies,” Dr. Tran said at the annual meeting of the Americas Hepato-Pancreato-Biliary Association.
“Advanced age has been regarded as contraindication to resection for complex hepatobiliary malignancies,” she explained, with concerns that “it may be too risky, and the survival benefit is limited in elderly populations. However, the oncologic benefit of aggressive surgical strategies in perihilar cholangiocarcinoma remains a subject of debate.”
Dr. Tran and her colleagues identified patients who underwent curative resection for perihilar cholangiocarcinoma (CCA) in the U.S. Extrahepatic Biliary Malignancy Consortium database. They compared outcomes of those younger than 75 years versus patients 75 years and older. A total of 59% of the cohort were men, 20% were 75 years and older, and the median age was 66 years.
CCA is a rare and aggressive malignancy, often presenting with obstructive jaundice, said Dr. Tran, a postdoctoral research fellow in general surgery at Stanford (Calif.) University.
Preoperative characteristics were similar in the groups, except that cardiac morbidity was higher in the older cohort. In addition, pathology characteristics did not differ significantly between age groups, including tumor stage, nodal status, grade, size, and margin status.
The in-hospital mortality was double for the older patients, 15% versus 8%, despite the similarities, Dr. Tran said. “This supports the notion that it is more difficult to salvage older patients when they run into a complication,” she added.
Postoperative morbidity was also higher in older patients, 78% versus 68%, but did not reach statistical significance (P = .34).
The 90-day mortality rate was 22% in patients 75 years and older, compared with 10% in younger patients, a nonsignificant difference (P = .09).
Five-year survival was 15% in the older cohort and 22% for the younger patients (P = .003). There was a “more significant drop in the survival curves in the older age group, but then they get closer,” Dr. Tran said. The disease-specific survival did not differ significantly at 46 months versus 37 months, respectively.
Advanced-stage cancer and elevated CA 19-9 tumor marker levels were independent predictors of survival in a multivariate analysis, but age was not. Higher body mass index was associated with a higher perioperative mortality in older patients, but sex, cardiac morbidity, and ASA status were not. Dr. Tran said, “Lower BMI may be a useful tool to select elderly patients,” she noted.
“Elderly patients have double the mortality following major hepatectomy for perihilar cholangiocarcinoma,” Dr. Tran said. “However, the long-term, cancer-specific outcome appears similar to that of younger patients.” Physiologically robust older patients may be better candidates for surgery, she suggested.
Of the six patients who died in the 75 and older group, two patients died from liver failure, one from sepsis, one intraoperatively, one from unknown causes, and one died who required reoperation for postop bleeding, Dr. Tran said. “We did not find patients dying from MI or pneumonia, probably due to the small number of patients.”
Dr. Tran said that 2.5% of the older group and 5% of the younger group received neoadjuvant chemotherapy, which was not a statistically significant difference.
A meeting attendee asked if left versus right hepatectomy made a difference, and why the researchers chose 75 years as the cutoff age between younger and older groups.
“Left vs. right laterality does not seem to make an impact in terms of survival,” Dr. Tran said. “The median age was 66 years, and we used the upper limit of standard deviation, which was 75.”
Dr. Tran had no relevant financial disclosures.
Key clinical point: Patients 75 years and older undergoing hepatectomy for perihilar cholangiocarcinoma trended toward higher mortality but experienced cancer-specific outcomes similar to younger patients.
Major finding: 90-day mortality was 22% in patients 75 years and older versus 10% in younger patients (nonsignificant, P = .09).
Data source: Retrospective database study of 210 people who had curative intent resection for perihilar cholangiocarcinoma.
Disclosures: Dr. Tran had no relevant financial disclosures.
Avoid hysterectomy in POP repairs
SAN ANTONIO – The Systematic Review Group of the Society of Gynecologic Surgeons is suggesting uterine preservation, when not contraindicated, for most pelvic organ prolapse repairs to decrease mesh erosion, operating room time, and blood loss.
The advice is based on a review of 94 original studies, including 12 randomized controlled trials (RCTs) and 41 nonrandomized comparative studies, winnowed down to the strongest work from an original review of 7,324 abstracts through January 2017.
Short-term prolapse outcomes – 12-30 months in most of the studies – “are usually not clinically significant due to uterine preservation,” with the one exception of vaginal hysterectomy with native tissue reconstruction, which the group recommended over laparoscopic sacrohysteropexy, Kate Meriwether, MD, a gynecologic surgeon at the University of Louisville, Ky., said at the annual scientific meeting of the Society of Gynecologic Surgeons.
Hysterectomy for prolapse surgery is common: More than 74,000 hysterectomies are done in the United States each year with prolapse as the main indication. Even so, it’s not always necessary to take out the uterus, and perhaps more than a third of women would prefer to keep theirs, Dr. Meriwether said, speaking on behalf of the SGS Systematic Review Group.
The recommendations from the Systematic Review Group must be sent to the SGS board and the full membership before they can be approved as guidelines.*
The Review Group made a grade A recommendation for vaginal hysterectomy with native tissue reconstruction over laparoscopic sacrohysteropexy, meaning it was based on high-quality evidence. The rest of the advice came in the form of suggestions, based on moderate grade B evidence, often nonrandomized comparative studies and case reviews.
The Review Group suggested uterine preservation during laparoscopic native tissue prolapse repair to reduce operating room (OR) time and blood loss, and preserve vaginal length, based on four nonrandomized comparison studies using various approaches, with a total of 446 women and up to 3 years’ follow-up. There might be a higher risk of apical recurrence without hysterectomy, but without worsening of prolapse symptoms.
The Review Group also suggested uterine preservation in transvaginal mesh reconstruction for prolapse, based on four RCTs and nine comparison studies with 1,381 women and up to 30 months’ follow-up. The studies found a decreased risk of mesh erosion, reoperating for mesh erosion, blood loss, and postop bleeding, and improved posterior and apical Pelvic Organ Prolapse Quantification scores when women keep their uterus.
However, “the patient should be counseled that there may be increased de novo stress incontinence, overactive bladder,” postop constipation, and shorter vaginal length, Dr. Meriwether said.
Also, “we suggest preservation of the uterus in transvaginal apical native tissue repair of prolapse, as it does not worsen any outcomes and slightly reduces OR time and estimated blood loss,” based on 13 studies, including four RCTs, and a total of 1,449 women followed for up to 26 months, she said.
The Review Group also came out in favor of the Manchester procedure, when available, over vaginal hysterectomy with native tissue suspension, based on one RCT and five nonrandomized studies involving 1,126 women and up to 61 months’ follow-up. The Manchester procedure pushed back the time to prolapse reoperation 9 months in one study, and also decreased transfusions, OR time, and blood loss. It also better preserved perineal length.
The group suggested uterine preservation when considering mesh sacrocolpopexy versus mesh sacrohysteropexy, to reduce mesh erosion, OR time, blood loss, hospital stay, and surgery costs, although there might be a slight worsening of Pelvic Floor Distress Inventory and Pelvic Floor Impact scores. The advice was based on nine nonrandomized comparison studies involving 745 women followed for up to 39 months. There was no difference in prolapse resolution between the two techniques.
The one grade A recommendation, for vaginal hysterectomy with native tissue reconstruction over laparoscopic sacrohysteropexy, was based on two RCTs with 182 women followed for up to 12 months.
Hysterectomy in those studies significantly reduced the risk of repeat surgery for prolapse and urinary symptoms, shortened OR time, and improved quality of life scores. However, the benefits came at the cost of slightly shorter vaginal length, worse Pelvic Organ Prolapse Quantification point C scores, greater blood loss, and up to a day longer spent in the hospital.
Dr. Meriwether reported having no relevant financial disclosures.
*Correction, 6/8/2017: An earlier version of this story misstated the status of the Systematic Review Group's recommendations. The recommendations have not been approved as official SGS guidelines. Also, the meeting sponsor information was updated.
SAN ANTONIO – The Systematic Review Group of the Society of Gynecologic Surgeons is suggesting uterine preservation, when not contraindicated, for most pelvic organ prolapse repairs to decrease mesh erosion, operating room time, and blood loss.
The advice is based on a review of 94 original studies, including 12 randomized controlled trials (RCTs) and 41 nonrandomized comparative studies, winnowed down to the strongest work from an original review of 7,324 abstracts through January 2017.
Short-term prolapse outcomes – 12-30 months in most of the studies – “are usually not clinically significant due to uterine preservation,” with the one exception of vaginal hysterectomy with native tissue reconstruction, which the group recommended over laparoscopic sacrohysteropexy, Kate Meriwether, MD, a gynecologic surgeon at the University of Louisville, Ky., said at the annual scientific meeting of the Society of Gynecologic Surgeons.
Hysterectomy for prolapse surgery is common: More than 74,000 hysterectomies are done in the United States each year with prolapse as the main indication. Even so, it’s not always necessary to take out the uterus, and perhaps more than a third of women would prefer to keep theirs, Dr. Meriwether said, speaking on behalf of the SGS Systematic Review Group.
The recommendations from the Systematic Review Group must be sent to the SGS board and the full membership before they can be approved as guidelines.*
The Review Group made a grade A recommendation for vaginal hysterectomy with native tissue reconstruction over laparoscopic sacrohysteropexy, meaning it was based on high-quality evidence. The rest of the advice came in the form of suggestions, based on moderate grade B evidence, often nonrandomized comparative studies and case reviews.
The Review Group suggested uterine preservation during laparoscopic native tissue prolapse repair to reduce operating room (OR) time and blood loss, and preserve vaginal length, based on four nonrandomized comparison studies using various approaches, with a total of 446 women and up to 3 years’ follow-up. There might be a higher risk of apical recurrence without hysterectomy, but without worsening of prolapse symptoms.
The Review Group also suggested uterine preservation in transvaginal mesh reconstruction for prolapse, based on four RCTs and nine comparison studies with 1,381 women and up to 30 months’ follow-up. The studies found a decreased risk of mesh erosion, reoperating for mesh erosion, blood loss, and postop bleeding, and improved posterior and apical Pelvic Organ Prolapse Quantification scores when women keep their uterus.
However, “the patient should be counseled that there may be increased de novo stress incontinence, overactive bladder,” postop constipation, and shorter vaginal length, Dr. Meriwether said.
Also, “we suggest preservation of the uterus in transvaginal apical native tissue repair of prolapse, as it does not worsen any outcomes and slightly reduces OR time and estimated blood loss,” based on 13 studies, including four RCTs, and a total of 1,449 women followed for up to 26 months, she said.
The Review Group also came out in favor of the Manchester procedure, when available, over vaginal hysterectomy with native tissue suspension, based on one RCT and five nonrandomized studies involving 1,126 women and up to 61 months’ follow-up. The Manchester procedure pushed back the time to prolapse reoperation 9 months in one study, and also decreased transfusions, OR time, and blood loss. It also better preserved perineal length.
The group suggested uterine preservation when considering mesh sacrocolpopexy versus mesh sacrohysteropexy, to reduce mesh erosion, OR time, blood loss, hospital stay, and surgery costs, although there might be a slight worsening of Pelvic Floor Distress Inventory and Pelvic Floor Impact scores. The advice was based on nine nonrandomized comparison studies involving 745 women followed for up to 39 months. There was no difference in prolapse resolution between the two techniques.
The one grade A recommendation, for vaginal hysterectomy with native tissue reconstruction over laparoscopic sacrohysteropexy, was based on two RCTs with 182 women followed for up to 12 months.
Hysterectomy in those studies significantly reduced the risk of repeat surgery for prolapse and urinary symptoms, shortened OR time, and improved quality of life scores. However, the benefits came at the cost of slightly shorter vaginal length, worse Pelvic Organ Prolapse Quantification point C scores, greater blood loss, and up to a day longer spent in the hospital.
Dr. Meriwether reported having no relevant financial disclosures.
*Correction, 6/8/2017: An earlier version of this story misstated the status of the Systematic Review Group's recommendations. The recommendations have not been approved as official SGS guidelines. Also, the meeting sponsor information was updated.
SAN ANTONIO – The Systematic Review Group of the Society of Gynecologic Surgeons is suggesting uterine preservation, when not contraindicated, for most pelvic organ prolapse repairs to decrease mesh erosion, operating room time, and blood loss.
The advice is based on a review of 94 original studies, including 12 randomized controlled trials (RCTs) and 41 nonrandomized comparative studies, winnowed down to the strongest work from an original review of 7,324 abstracts through January 2017.
Short-term prolapse outcomes – 12-30 months in most of the studies – “are usually not clinically significant due to uterine preservation,” with the one exception of vaginal hysterectomy with native tissue reconstruction, which the group recommended over laparoscopic sacrohysteropexy, Kate Meriwether, MD, a gynecologic surgeon at the University of Louisville, Ky., said at the annual scientific meeting of the Society of Gynecologic Surgeons.
Hysterectomy for prolapse surgery is common: More than 74,000 hysterectomies are done in the United States each year with prolapse as the main indication. Even so, it’s not always necessary to take out the uterus, and perhaps more than a third of women would prefer to keep theirs, Dr. Meriwether said, speaking on behalf of the SGS Systematic Review Group.
The recommendations from the Systematic Review Group must be sent to the SGS board and the full membership before they can be approved as guidelines.*
The Review Group made a grade A recommendation for vaginal hysterectomy with native tissue reconstruction over laparoscopic sacrohysteropexy, meaning it was based on high-quality evidence. The rest of the advice came in the form of suggestions, based on moderate grade B evidence, often nonrandomized comparative studies and case reviews.
The Review Group suggested uterine preservation during laparoscopic native tissue prolapse repair to reduce operating room (OR) time and blood loss, and preserve vaginal length, based on four nonrandomized comparison studies using various approaches, with a total of 446 women and up to 3 years’ follow-up. There might be a higher risk of apical recurrence without hysterectomy, but without worsening of prolapse symptoms.
The Review Group also suggested uterine preservation in transvaginal mesh reconstruction for prolapse, based on four RCTs and nine comparison studies with 1,381 women and up to 30 months’ follow-up. The studies found a decreased risk of mesh erosion, reoperating for mesh erosion, blood loss, and postop bleeding, and improved posterior and apical Pelvic Organ Prolapse Quantification scores when women keep their uterus.
However, “the patient should be counseled that there may be increased de novo stress incontinence, overactive bladder,” postop constipation, and shorter vaginal length, Dr. Meriwether said.
Also, “we suggest preservation of the uterus in transvaginal apical native tissue repair of prolapse, as it does not worsen any outcomes and slightly reduces OR time and estimated blood loss,” based on 13 studies, including four RCTs, and a total of 1,449 women followed for up to 26 months, she said.
The Review Group also came out in favor of the Manchester procedure, when available, over vaginal hysterectomy with native tissue suspension, based on one RCT and five nonrandomized studies involving 1,126 women and up to 61 months’ follow-up. The Manchester procedure pushed back the time to prolapse reoperation 9 months in one study, and also decreased transfusions, OR time, and blood loss. It also better preserved perineal length.
The group suggested uterine preservation when considering mesh sacrocolpopexy versus mesh sacrohysteropexy, to reduce mesh erosion, OR time, blood loss, hospital stay, and surgery costs, although there might be a slight worsening of Pelvic Floor Distress Inventory and Pelvic Floor Impact scores. The advice was based on nine nonrandomized comparison studies involving 745 women followed for up to 39 months. There was no difference in prolapse resolution between the two techniques.
The one grade A recommendation, for vaginal hysterectomy with native tissue reconstruction over laparoscopic sacrohysteropexy, was based on two RCTs with 182 women followed for up to 12 months.
Hysterectomy in those studies significantly reduced the risk of repeat surgery for prolapse and urinary symptoms, shortened OR time, and improved quality of life scores. However, the benefits came at the cost of slightly shorter vaginal length, worse Pelvic Organ Prolapse Quantification point C scores, greater blood loss, and up to a day longer spent in the hospital.
Dr. Meriwether reported having no relevant financial disclosures.
*Correction, 6/8/2017: An earlier version of this story misstated the status of the Systematic Review Group's recommendations. The recommendations have not been approved as official SGS guidelines. Also, the meeting sponsor information was updated.
Neoadjuvant therapy timing may impact pancreatic cancer outcomes
SEATTLE – In patients with pancreatic cancer, an interval of 8 weeks between receiving neoadjuvant chemoradiation and surgical resection may improve resection margins, according to findings presented at the annual Society of Surgical Oncology Cancer Symposium.
The delay in resection did not negatively impact outcomes, and there was a modest improvement in overall survival among patients who had an 8-10 week interval between treatments.
“Attention should be focused on the treatment interval to time of resection in prospective studies,” said lead study author Raphael J. Louie, MD, of Dartmouth (N.H.) Hitchcock Norris Cotton Cancer Center.
Dr. Louie explained that for patients with pancreatic adenocarcinoma who receive neoadjuvant chemoradiation, it is unclear how long the optimal interval should be between therapy completion and surgical resection.
For this study, Dr. Louie and his colleagues sought to determine the optimal interval between neoadjuvant therapy and surgery to maximize response and oncologic outcomes.
“We hypothesized that there may be benefit to a delay,” he said.
The retrospective analysis included 637 patients who had been diagnosed with pancreatic adenocarcinoma at the Norris Cotton Cancer Center, and who had completed neoadjuvant chemoradiation and underwent R0 surgical resection between Jan. 1, 2004, and Dec. 31, 2015.
Of this group, 195 patients had metastatic disease, 28 underwent upfront surgical exploration, and 94 were lost to follow-up or had a poor performance status and were not included in the final analysis.
The cohort was grouped according to time from chemoradiation completion to surgery: 6-8 weeks, 8-10 weeks, and more than 10 weeks.
A total of 320 patients received neoadjuvant chemoradiation and 288 completed the full course. Of this group, 128 were evaluable by pathologic review.
Among patients with a 6- to 8-week interval, 61% had an R0 resection margin. This percentage rose to 72% for those who had an 8- to 10-week interval, and in similar fashion, 70% for those who had a 10- to 13-week interval (P = .6)
However, there was no statistical difference when the three groups were compared collectively.
Of 26 patients who were resected within 6-8 weeks of chemoradiation, 11% achieved a complete response (CR), 27% had a partial response (PR), and 61% had recurrence for an average disease-free survival of 20 months.
In the group (n = 58) of patients who were resected within 8-10 weeks, 7% had CR, 71% had PR, and 62% had recurrence, for an average disease-free survival of 17 months. Finally, the 44 patients who were resected within 10-13 weeks had similar outcomes; 5% had CR, 61% had PR, and 61% of patients had recurrence for an average disease-free survival of 14 months.
Dr. Louie noted that even though they observed improved PR in the 8- to 10-week group, there was no statistical significance in disease-free survival (P = .71) or overall survival (P = .19).
“Allowing more time from neoadjuvant therapy completion to surgical resection may improve the pathologic response,” said Dr. Louie. “Larger studies are needed to determine if the time interval to surgical resection has oncologic benefit for these patients.”
Dr. Louie has no disclosures.
SEATTLE – In patients with pancreatic cancer, an interval of 8 weeks between receiving neoadjuvant chemoradiation and surgical resection may improve resection margins, according to findings presented at the annual Society of Surgical Oncology Cancer Symposium.
The delay in resection did not negatively impact outcomes, and there was a modest improvement in overall survival among patients who had an 8-10 week interval between treatments.
“Attention should be focused on the treatment interval to time of resection in prospective studies,” said lead study author Raphael J. Louie, MD, of Dartmouth (N.H.) Hitchcock Norris Cotton Cancer Center.
Dr. Louie explained that for patients with pancreatic adenocarcinoma who receive neoadjuvant chemoradiation, it is unclear how long the optimal interval should be between therapy completion and surgical resection.
For this study, Dr. Louie and his colleagues sought to determine the optimal interval between neoadjuvant therapy and surgery to maximize response and oncologic outcomes.
“We hypothesized that there may be benefit to a delay,” he said.
The retrospective analysis included 637 patients who had been diagnosed with pancreatic adenocarcinoma at the Norris Cotton Cancer Center, and who had completed neoadjuvant chemoradiation and underwent R0 surgical resection between Jan. 1, 2004, and Dec. 31, 2015.
Of this group, 195 patients had metastatic disease, 28 underwent upfront surgical exploration, and 94 were lost to follow-up or had a poor performance status and were not included in the final analysis.
The cohort was grouped according to time from chemoradiation completion to surgery: 6-8 weeks, 8-10 weeks, and more than 10 weeks.
A total of 320 patients received neoadjuvant chemoradiation and 288 completed the full course. Of this group, 128 were evaluable by pathologic review.
Among patients with a 6- to 8-week interval, 61% had an R0 resection margin. This percentage rose to 72% for those who had an 8- to 10-week interval, and in similar fashion, 70% for those who had a 10- to 13-week interval (P = .6)
However, there was no statistical difference when the three groups were compared collectively.
Of 26 patients who were resected within 6-8 weeks of chemoradiation, 11% achieved a complete response (CR), 27% had a partial response (PR), and 61% had recurrence for an average disease-free survival of 20 months.
In the group (n = 58) of patients who were resected within 8-10 weeks, 7% had CR, 71% had PR, and 62% had recurrence, for an average disease-free survival of 17 months. Finally, the 44 patients who were resected within 10-13 weeks had similar outcomes; 5% had CR, 61% had PR, and 61% of patients had recurrence for an average disease-free survival of 14 months.
Dr. Louie noted that even though they observed improved PR in the 8- to 10-week group, there was no statistical significance in disease-free survival (P = .71) or overall survival (P = .19).
“Allowing more time from neoadjuvant therapy completion to surgical resection may improve the pathologic response,” said Dr. Louie. “Larger studies are needed to determine if the time interval to surgical resection has oncologic benefit for these patients.”
Dr. Louie has no disclosures.
SEATTLE – In patients with pancreatic cancer, an interval of 8 weeks between receiving neoadjuvant chemoradiation and surgical resection may improve resection margins, according to findings presented at the annual Society of Surgical Oncology Cancer Symposium.
The delay in resection did not negatively impact outcomes, and there was a modest improvement in overall survival among patients who had an 8-10 week interval between treatments.
“Attention should be focused on the treatment interval to time of resection in prospective studies,” said lead study author Raphael J. Louie, MD, of Dartmouth (N.H.) Hitchcock Norris Cotton Cancer Center.
Dr. Louie explained that for patients with pancreatic adenocarcinoma who receive neoadjuvant chemoradiation, it is unclear how long the optimal interval should be between therapy completion and surgical resection.
For this study, Dr. Louie and his colleagues sought to determine the optimal interval between neoadjuvant therapy and surgery to maximize response and oncologic outcomes.
“We hypothesized that there may be benefit to a delay,” he said.
The retrospective analysis included 637 patients who had been diagnosed with pancreatic adenocarcinoma at the Norris Cotton Cancer Center, and who had completed neoadjuvant chemoradiation and underwent R0 surgical resection between Jan. 1, 2004, and Dec. 31, 2015.
Of this group, 195 patients had metastatic disease, 28 underwent upfront surgical exploration, and 94 were lost to follow-up or had a poor performance status and were not included in the final analysis.
The cohort was grouped according to time from chemoradiation completion to surgery: 6-8 weeks, 8-10 weeks, and more than 10 weeks.
A total of 320 patients received neoadjuvant chemoradiation and 288 completed the full course. Of this group, 128 were evaluable by pathologic review.
Among patients with a 6- to 8-week interval, 61% had an R0 resection margin. This percentage rose to 72% for those who had an 8- to 10-week interval, and in similar fashion, 70% for those who had a 10- to 13-week interval (P = .6)
However, there was no statistical difference when the three groups were compared collectively.
Of 26 patients who were resected within 6-8 weeks of chemoradiation, 11% achieved a complete response (CR), 27% had a partial response (PR), and 61% had recurrence for an average disease-free survival of 20 months.
In the group (n = 58) of patients who were resected within 8-10 weeks, 7% had CR, 71% had PR, and 62% had recurrence, for an average disease-free survival of 17 months. Finally, the 44 patients who were resected within 10-13 weeks had similar outcomes; 5% had CR, 61% had PR, and 61% of patients had recurrence for an average disease-free survival of 14 months.
Dr. Louie noted that even though they observed improved PR in the 8- to 10-week group, there was no statistical significance in disease-free survival (P = .71) or overall survival (P = .19).
“Allowing more time from neoadjuvant therapy completion to surgical resection may improve the pathologic response,” said Dr. Louie. “Larger studies are needed to determine if the time interval to surgical resection has oncologic benefit for these patients.”
Dr. Louie has no disclosures.
AT SSO 2017
Key clinical point: A longer interval between neoadjuvant therapy and surgical resection could improve some outcomes in pancreatic cancer.
Major finding: Resection after 8 weeks may improve resection margins and may provide a modest improvement in survival for some patients.
Data source: Retrospective cohort study of 128 evaluable patients with biopsy-proven pancreatic adenocarcinoma who received neoadjuvant chemoradiation.
Disclosures: Dr. Louie has no disclosures.
Debulking called reasonable for unresectable liver cancer
MIAMI BEACH – Cytoreductive debulking surgery for neuroendocrine liver metastases provides a lower but “reasonable” long-term survival, compared with curative intent surgery, according to results of a study presented at the annual meeting of the Americas Hepatico-Pancreato-Biliary Association.
Liver debulking for patients with grossly unresectable disease is therefore an option that may extend survival, the study researchers said.
“Surgical resection offers the best chance for long-term survival but may not be technically feasible for all our patients,” said Fabio Bagante, MD, a resident at the University of Verona (Italy). “Debulking neuroendocrine liver metastases has been proposed as an alternative.”
Dr. Bagante and coinvestigators compared outcomes between 180 patients who had debulking surgery (defined as an R2 outcome) and 449 who underwent curative intent resection (R0 or R1). Patients had surgery between 1990 and 2015 at eight institutions, and the primary outcome was overall survival. The mean follow-up was 51 months; during that time, 174 patients died.
The 5-year overall survival was 72% in the debulking group and 89% in the curative intent group. The 10-year overall survival was 41% in the debulking group and 77% among the curative intent surgery patients.
“Debulking operations for neuroendocrine liver metastases provide lower but reasonable long-term survival, compared with patients who underwent curative intent,” Dr. Bagante said.
“Nearly 3 in 10 patients underwent debulking surgery,” Dr. Bagante said. “It was more common among the elderly, males with symptomatic disease, and patients with greater liver involvement.”
Patients in the liver-debulking groups were also significantly more likely to have high–tumor grade disease, 35%, versus 13% of the curative intent resection group (P less than .001). They were also more likely to have metastatic disease, with an N1 rate of 73% versus 52% (P less than .001).
“Great work. Thanks for presenting this topic. It’s quite a debated topic,” said study discussant Aaron Lee, DO, of the department of general surgery at Cleveland Clinic Florida in Weston. “I looked at your data on asymptomatic patients who had a 5-year survival of 60%; U.K. data show [the] same survival without any intervention.” He asked Dr. Bagante to comment on operating on patients without any symptoms.
“Regarding the role of symptoms as a predictor of survival, there are many papers in the literature debating what are the true predictors of survival,” Dr. Bagante noted. “We don’t think [symptoms have an] impact; our data do not demonstrate that. We think the biologic behavior of the disease, the impact of the progression of the disease, and the grade of the tumor, [indicated by] Ki-67, could have more of a role.”
MIAMI BEACH – Cytoreductive debulking surgery for neuroendocrine liver metastases provides a lower but “reasonable” long-term survival, compared with curative intent surgery, according to results of a study presented at the annual meeting of the Americas Hepatico-Pancreato-Biliary Association.
Liver debulking for patients with grossly unresectable disease is therefore an option that may extend survival, the study researchers said.
“Surgical resection offers the best chance for long-term survival but may not be technically feasible for all our patients,” said Fabio Bagante, MD, a resident at the University of Verona (Italy). “Debulking neuroendocrine liver metastases has been proposed as an alternative.”
Dr. Bagante and coinvestigators compared outcomes between 180 patients who had debulking surgery (defined as an R2 outcome) and 449 who underwent curative intent resection (R0 or R1). Patients had surgery between 1990 and 2015 at eight institutions, and the primary outcome was overall survival. The mean follow-up was 51 months; during that time, 174 patients died.
The 5-year overall survival was 72% in the debulking group and 89% in the curative intent group. The 10-year overall survival was 41% in the debulking group and 77% among the curative intent surgery patients.
“Debulking operations for neuroendocrine liver metastases provide lower but reasonable long-term survival, compared with patients who underwent curative intent,” Dr. Bagante said.
“Nearly 3 in 10 patients underwent debulking surgery,” Dr. Bagante said. “It was more common among the elderly, males with symptomatic disease, and patients with greater liver involvement.”
Patients in the liver-debulking groups were also significantly more likely to have high–tumor grade disease, 35%, versus 13% of the curative intent resection group (P less than .001). They were also more likely to have metastatic disease, with an N1 rate of 73% versus 52% (P less than .001).
“Great work. Thanks for presenting this topic. It’s quite a debated topic,” said study discussant Aaron Lee, DO, of the department of general surgery at Cleveland Clinic Florida in Weston. “I looked at your data on asymptomatic patients who had a 5-year survival of 60%; U.K. data show [the] same survival without any intervention.” He asked Dr. Bagante to comment on operating on patients without any symptoms.
“Regarding the role of symptoms as a predictor of survival, there are many papers in the literature debating what are the true predictors of survival,” Dr. Bagante noted. “We don’t think [symptoms have an] impact; our data do not demonstrate that. We think the biologic behavior of the disease, the impact of the progression of the disease, and the grade of the tumor, [indicated by] Ki-67, could have more of a role.”
MIAMI BEACH – Cytoreductive debulking surgery for neuroendocrine liver metastases provides a lower but “reasonable” long-term survival, compared with curative intent surgery, according to results of a study presented at the annual meeting of the Americas Hepatico-Pancreato-Biliary Association.
Liver debulking for patients with grossly unresectable disease is therefore an option that may extend survival, the study researchers said.
“Surgical resection offers the best chance for long-term survival but may not be technically feasible for all our patients,” said Fabio Bagante, MD, a resident at the University of Verona (Italy). “Debulking neuroendocrine liver metastases has been proposed as an alternative.”
Dr. Bagante and coinvestigators compared outcomes between 180 patients who had debulking surgery (defined as an R2 outcome) and 449 who underwent curative intent resection (R0 or R1). Patients had surgery between 1990 and 2015 at eight institutions, and the primary outcome was overall survival. The mean follow-up was 51 months; during that time, 174 patients died.
The 5-year overall survival was 72% in the debulking group and 89% in the curative intent group. The 10-year overall survival was 41% in the debulking group and 77% among the curative intent surgery patients.
“Debulking operations for neuroendocrine liver metastases provide lower but reasonable long-term survival, compared with patients who underwent curative intent,” Dr. Bagante said.
“Nearly 3 in 10 patients underwent debulking surgery,” Dr. Bagante said. “It was more common among the elderly, males with symptomatic disease, and patients with greater liver involvement.”
Patients in the liver-debulking groups were also significantly more likely to have high–tumor grade disease, 35%, versus 13% of the curative intent resection group (P less than .001). They were also more likely to have metastatic disease, with an N1 rate of 73% versus 52% (P less than .001).
“Great work. Thanks for presenting this topic. It’s quite a debated topic,” said study discussant Aaron Lee, DO, of the department of general surgery at Cleveland Clinic Florida in Weston. “I looked at your data on asymptomatic patients who had a 5-year survival of 60%; U.K. data show [the] same survival without any intervention.” He asked Dr. Bagante to comment on operating on patients without any symptoms.
“Regarding the role of symptoms as a predictor of survival, there are many papers in the literature debating what are the true predictors of survival,” Dr. Bagante noted. “We don’t think [symptoms have an] impact; our data do not demonstrate that. We think the biologic behavior of the disease, the impact of the progression of the disease, and the grade of the tumor, [indicated by] Ki-67, could have more of a role.”
AT AHPBA 2017
Key clinical point:
Major finding: The 10-year overall survival was 77% in the curative intent surgery group, compared with 41% among the debulking patients.
Data source: A retrospective database study of 629 people with neuroendocrine liver metastases.
Disclosures: Dr. Bagante and Dr. Lee had no relevant financial disclosures.
Medicaid reform: Work-based waivers may not fly
The Trump administration may not be able to successfully implement the work requirements and other Medicaid eligibility caveats proffered by Health and Human Services Secretary Tom Price, MD, according to Jane Perkins, legal director for the National Health Law Program.
In March, Secretary Price and Seema Verma, administrator of the Centers for Medicare & Medicaid Services, wrote to state governors, letting them know that the HHS would support states’ efforts to increase employment, community engagement, and work requirements for Medicaid recipients. The letter also was supportive of aligning Medicaid benefits with private insurance via alternative benefits, cost-sharing, and premium payments.
High mandatory premiums, cost sharing, lifetime limits, and drug testing “are of concern to us,” Ms. Perkins said at an April 13 press briefing. “They really change the complexion of Medicaid and Medicaid coverage for low-income people.”
These requirements “are not typically seen in Medicaid programs,” she said.
While Section 1115 of the Social Security Act “allows states to test novel approaches to providing medical assistance” via Medicaid waivers, it does not allow the HHS or the states to “ignore congressional mandates; to cut eligibility, services, or provider payments; or to use section 1115 to save money,” according to an issue brief by Ms. Perkins.
When asked how work requirements harm people, Ms. Perkins responded that adding a work requirement to Medicaid eligibility gets things “backwards,” because a sick person needs health care before being able to return to work.
The work requirement would not save states much money, as nearly 8 in 10 adults on Medicaid are in a household that includes a worker and 59% of recipients work themselves, according to a Kaiser Family Foundation study. The adults affected by the work requirement would make up only a drop in the ocean of Medicaid spending. About two-thirds of that spending goes toward senior citizens, people with disabilities, children, and people in long term care, according to projections from the Congressional Budget Office.
The National Health Law program, which advocates for low-income Medicaid recipients, is following the waivers state-by-state with a network of lawyers who work with people with disabilities in each state.
“With this new openness to flexibility, we are certainly watching what is going on in the states,” Ms. Perkins said.
The Trump administration may not be able to successfully implement the work requirements and other Medicaid eligibility caveats proffered by Health and Human Services Secretary Tom Price, MD, according to Jane Perkins, legal director for the National Health Law Program.
In March, Secretary Price and Seema Verma, administrator of the Centers for Medicare & Medicaid Services, wrote to state governors, letting them know that the HHS would support states’ efforts to increase employment, community engagement, and work requirements for Medicaid recipients. The letter also was supportive of aligning Medicaid benefits with private insurance via alternative benefits, cost-sharing, and premium payments.
High mandatory premiums, cost sharing, lifetime limits, and drug testing “are of concern to us,” Ms. Perkins said at an April 13 press briefing. “They really change the complexion of Medicaid and Medicaid coverage for low-income people.”
These requirements “are not typically seen in Medicaid programs,” she said.
While Section 1115 of the Social Security Act “allows states to test novel approaches to providing medical assistance” via Medicaid waivers, it does not allow the HHS or the states to “ignore congressional mandates; to cut eligibility, services, or provider payments; or to use section 1115 to save money,” according to an issue brief by Ms. Perkins.
When asked how work requirements harm people, Ms. Perkins responded that adding a work requirement to Medicaid eligibility gets things “backwards,” because a sick person needs health care before being able to return to work.
The work requirement would not save states much money, as nearly 8 in 10 adults on Medicaid are in a household that includes a worker and 59% of recipients work themselves, according to a Kaiser Family Foundation study. The adults affected by the work requirement would make up only a drop in the ocean of Medicaid spending. About two-thirds of that spending goes toward senior citizens, people with disabilities, children, and people in long term care, according to projections from the Congressional Budget Office.
The National Health Law program, which advocates for low-income Medicaid recipients, is following the waivers state-by-state with a network of lawyers who work with people with disabilities in each state.
“With this new openness to flexibility, we are certainly watching what is going on in the states,” Ms. Perkins said.
The Trump administration may not be able to successfully implement the work requirements and other Medicaid eligibility caveats proffered by Health and Human Services Secretary Tom Price, MD, according to Jane Perkins, legal director for the National Health Law Program.
In March, Secretary Price and Seema Verma, administrator of the Centers for Medicare & Medicaid Services, wrote to state governors, letting them know that the HHS would support states’ efforts to increase employment, community engagement, and work requirements for Medicaid recipients. The letter also was supportive of aligning Medicaid benefits with private insurance via alternative benefits, cost-sharing, and premium payments.
High mandatory premiums, cost sharing, lifetime limits, and drug testing “are of concern to us,” Ms. Perkins said at an April 13 press briefing. “They really change the complexion of Medicaid and Medicaid coverage for low-income people.”
These requirements “are not typically seen in Medicaid programs,” she said.
While Section 1115 of the Social Security Act “allows states to test novel approaches to providing medical assistance” via Medicaid waivers, it does not allow the HHS or the states to “ignore congressional mandates; to cut eligibility, services, or provider payments; or to use section 1115 to save money,” according to an issue brief by Ms. Perkins.
When asked how work requirements harm people, Ms. Perkins responded that adding a work requirement to Medicaid eligibility gets things “backwards,” because a sick person needs health care before being able to return to work.
The work requirement would not save states much money, as nearly 8 in 10 adults on Medicaid are in a household that includes a worker and 59% of recipients work themselves, according to a Kaiser Family Foundation study. The adults affected by the work requirement would make up only a drop in the ocean of Medicaid spending. About two-thirds of that spending goes toward senior citizens, people with disabilities, children, and people in long term care, according to projections from the Congressional Budget Office.
The National Health Law program, which advocates for low-income Medicaid recipients, is following the waivers state-by-state with a network of lawyers who work with people with disabilities in each state.
“With this new openness to flexibility, we are certainly watching what is going on in the states,” Ms. Perkins said.
CMS market stabilization efforts useless without subsidies
New final regulations designed to bring stability to the individual health insurance market may not matter if the White House follows through on a threat to kill subsidies paid to insurers to help reduce deductibles and other out-of-pocket costs for low-income patients.
The final rule from the Centers for Medicare & Medicaid Services grants a number of wishes sought by the insurance industry to help bring a level of predictability and flexibility when designing plans for the individual market. Specifically, it does the following:
• Shortens the open enrollment period for the 2018 plan year to 6 weeks running from Nov. 1 to Dec. 15, so that open enrollment closely aligns with Medicare and other private insurance.
• Requires individuals to submit documentation when seeking coverage through a special enrollment period.
• Allows insurers to collect past-due premiums before issuing coverage for a future year.
• Provides more actuarial flexibility to allow for different plan designs.
• Returns network adequacy oversight to states.
The new rules are not expected to alter the existing market dynamic, according to Kelly Brantley, vice president at Avalere Health.
“I would say the rule is nominally helpful, but it’s really unlikely to persuade anyone, particularly those insurers who are already on their way out. I don’t think this a game-changer for them,” she said in an interview.
The American Medical Association, in comments to the CMS when the rule was proposed as a draft, said that if finalized, the rule “would raise premiums, out-of-pocket costs, or both for millions of moderate-income families and would make it more difficult for eligible individuals to enroll in health coverage and access needed care.”
The potential impact of these regulatory changes could be moot if President Trump makes good on his threat to withhold cost-sharing subsidies to insurers. The subsides already are the subject of a lawsuit brought by the House of Representatives against the Obama administration; they continue to be paid while the suit makes its way through the judicial process. President Trump has threatened to cut off the subsidies in an effort to force Congressional Democrats to the negotiating table regarding the repeal and replacement of the Affordable Care Act.
“My take on this is that the [market stabilization] rule as written is not likely to shift the market, really, in terms of access,” Ms. Brantley said. “The bigger question is whether the cost-sharing reductions are going to be paid. I think that has a bigger likelihood of influencing issuer participation and robustness of the market in 2018.”
Even with the changes made by the market stabilization rule, “there is still too much instability and uncertainty in this market,” Marilyn Tavenner, president and CEO of the industry group America’s Health Insurance Plans, said in a statement. “Most urgently, health plans and the consumers they serve need to know that funding for cost-sharing reduction subsidies will continue uninterrupted.”
Ms. Tavenner noted that without the subsidies, more plans are likely to drop out of the health insurance exchanges, leading to premium increases, and “doctors and hospitals will see even greater strains on their ability to care for people.”
The AMA, in an April 12 letter to President Trump, cosigned by America’s Health Insurance Plans, the American Academy of Family Physicians, the American Hospital Association, the Federation of American Hospitals, the American Benefits Council, the Blue Cross Blue Shield Association, and the U.S. Chamber of Commerce, stated that the “most critical action to help stabilize the individual market for 2017 and 2018 is to remove uncertainty about continued funding for cost sharing reductions.”
Ms. Brantley added that if the subsides were cut, “it makes it more challenging to bring any kind of money back into the system at a later point. I think it would be hard for those cost-sharing reductions to go away at this point and then ever come back, but I do think that it’s a possibility that that could happen.”
The CMS released the final rule April 13, 2017, and it is scheduled for publication in the Federal Register on April 18, 2017.
New final regulations designed to bring stability to the individual health insurance market may not matter if the White House follows through on a threat to kill subsidies paid to insurers to help reduce deductibles and other out-of-pocket costs for low-income patients.
The final rule from the Centers for Medicare & Medicaid Services grants a number of wishes sought by the insurance industry to help bring a level of predictability and flexibility when designing plans for the individual market. Specifically, it does the following:
• Shortens the open enrollment period for the 2018 plan year to 6 weeks running from Nov. 1 to Dec. 15, so that open enrollment closely aligns with Medicare and other private insurance.
• Requires individuals to submit documentation when seeking coverage through a special enrollment period.
• Allows insurers to collect past-due premiums before issuing coverage for a future year.
• Provides more actuarial flexibility to allow for different plan designs.
• Returns network adequacy oversight to states.
The new rules are not expected to alter the existing market dynamic, according to Kelly Brantley, vice president at Avalere Health.
“I would say the rule is nominally helpful, but it’s really unlikely to persuade anyone, particularly those insurers who are already on their way out. I don’t think this a game-changer for them,” she said in an interview.
The American Medical Association, in comments to the CMS when the rule was proposed as a draft, said that if finalized, the rule “would raise premiums, out-of-pocket costs, or both for millions of moderate-income families and would make it more difficult for eligible individuals to enroll in health coverage and access needed care.”
The potential impact of these regulatory changes could be moot if President Trump makes good on his threat to withhold cost-sharing subsidies to insurers. The subsides already are the subject of a lawsuit brought by the House of Representatives against the Obama administration; they continue to be paid while the suit makes its way through the judicial process. President Trump has threatened to cut off the subsidies in an effort to force Congressional Democrats to the negotiating table regarding the repeal and replacement of the Affordable Care Act.
“My take on this is that the [market stabilization] rule as written is not likely to shift the market, really, in terms of access,” Ms. Brantley said. “The bigger question is whether the cost-sharing reductions are going to be paid. I think that has a bigger likelihood of influencing issuer participation and robustness of the market in 2018.”
Even with the changes made by the market stabilization rule, “there is still too much instability and uncertainty in this market,” Marilyn Tavenner, president and CEO of the industry group America’s Health Insurance Plans, said in a statement. “Most urgently, health plans and the consumers they serve need to know that funding for cost-sharing reduction subsidies will continue uninterrupted.”
Ms. Tavenner noted that without the subsidies, more plans are likely to drop out of the health insurance exchanges, leading to premium increases, and “doctors and hospitals will see even greater strains on their ability to care for people.”
The AMA, in an April 12 letter to President Trump, cosigned by America’s Health Insurance Plans, the American Academy of Family Physicians, the American Hospital Association, the Federation of American Hospitals, the American Benefits Council, the Blue Cross Blue Shield Association, and the U.S. Chamber of Commerce, stated that the “most critical action to help stabilize the individual market for 2017 and 2018 is to remove uncertainty about continued funding for cost sharing reductions.”
Ms. Brantley added that if the subsides were cut, “it makes it more challenging to bring any kind of money back into the system at a later point. I think it would be hard for those cost-sharing reductions to go away at this point and then ever come back, but I do think that it’s a possibility that that could happen.”
The CMS released the final rule April 13, 2017, and it is scheduled for publication in the Federal Register on April 18, 2017.
New final regulations designed to bring stability to the individual health insurance market may not matter if the White House follows through on a threat to kill subsidies paid to insurers to help reduce deductibles and other out-of-pocket costs for low-income patients.
The final rule from the Centers for Medicare & Medicaid Services grants a number of wishes sought by the insurance industry to help bring a level of predictability and flexibility when designing plans for the individual market. Specifically, it does the following:
• Shortens the open enrollment period for the 2018 plan year to 6 weeks running from Nov. 1 to Dec. 15, so that open enrollment closely aligns with Medicare and other private insurance.
• Requires individuals to submit documentation when seeking coverage through a special enrollment period.
• Allows insurers to collect past-due premiums before issuing coverage for a future year.
• Provides more actuarial flexibility to allow for different plan designs.
• Returns network adequacy oversight to states.
The new rules are not expected to alter the existing market dynamic, according to Kelly Brantley, vice president at Avalere Health.
“I would say the rule is nominally helpful, but it’s really unlikely to persuade anyone, particularly those insurers who are already on their way out. I don’t think this a game-changer for them,” she said in an interview.
The American Medical Association, in comments to the CMS when the rule was proposed as a draft, said that if finalized, the rule “would raise premiums, out-of-pocket costs, or both for millions of moderate-income families and would make it more difficult for eligible individuals to enroll in health coverage and access needed care.”
The potential impact of these regulatory changes could be moot if President Trump makes good on his threat to withhold cost-sharing subsidies to insurers. The subsides already are the subject of a lawsuit brought by the House of Representatives against the Obama administration; they continue to be paid while the suit makes its way through the judicial process. President Trump has threatened to cut off the subsidies in an effort to force Congressional Democrats to the negotiating table regarding the repeal and replacement of the Affordable Care Act.
“My take on this is that the [market stabilization] rule as written is not likely to shift the market, really, in terms of access,” Ms. Brantley said. “The bigger question is whether the cost-sharing reductions are going to be paid. I think that has a bigger likelihood of influencing issuer participation and robustness of the market in 2018.”
Even with the changes made by the market stabilization rule, “there is still too much instability and uncertainty in this market,” Marilyn Tavenner, president and CEO of the industry group America’s Health Insurance Plans, said in a statement. “Most urgently, health plans and the consumers they serve need to know that funding for cost-sharing reduction subsidies will continue uninterrupted.”
Ms. Tavenner noted that without the subsidies, more plans are likely to drop out of the health insurance exchanges, leading to premium increases, and “doctors and hospitals will see even greater strains on their ability to care for people.”
The AMA, in an April 12 letter to President Trump, cosigned by America’s Health Insurance Plans, the American Academy of Family Physicians, the American Hospital Association, the Federation of American Hospitals, the American Benefits Council, the Blue Cross Blue Shield Association, and the U.S. Chamber of Commerce, stated that the “most critical action to help stabilize the individual market for 2017 and 2018 is to remove uncertainty about continued funding for cost sharing reductions.”
Ms. Brantley added that if the subsides were cut, “it makes it more challenging to bring any kind of money back into the system at a later point. I think it would be hard for those cost-sharing reductions to go away at this point and then ever come back, but I do think that it’s a possibility that that could happen.”
The CMS released the final rule April 13, 2017, and it is scheduled for publication in the Federal Register on April 18, 2017.
Same-day discharge for lap hiatal procedures found feasible, safe
HOUSTON – Selected patients who need operations, such as paraesophageal hernia repair and Heller myotomy, for benign hiatal diseases can have laparoscopic outpatient procedures with outcomes comparable with those of inpatients, a Canadian retrospective cohort study found.
“When comparing planned day-case patients with those who had planned admissions, we found that postoperative complication was the only statistically significant different outcome. Our data show same-day discharge resulted in no postoperative mortality, and no difference in postoperative morbidity, emergency room visits, and readmissions compared to traditional inpatient care,” said Juan Carlos Molina, MD, of McGill University Health Centre in Montreal, reporting the study results at the annual meeting of the American Society of Gastrointestinal and Endoscopic Surgeons.
The McGill researchers analyzed outcomes for 261 patients who had laparoscopic hiatal procedures from April 2011 to August 2016 – 163 as inpatients, 98 as outpatients, whom the study called planned day-case patients. The outpatient cohort consisted of younger patients (aged 60 vs. 66 years), but otherwise demographics between the two cohorts were similar. Discharge requirements after same-day hiatal procedures were the same as those for other outpatient procedures, Dr. Molina said.
The procedures included primary or revisional paraesophageal hernia repair (PEHR) in 123 (47.1%) patients; Heller myotomy in 94 (36%), 9 of which also underwent resection of an epiphrenic diverticulum; and Nissen fundoplication for gastroesophageal reflux disease in 44 (16.9%), of which 20 (45.5%) had a concomitant type I hiatal hernia. Among PEHR patients, 90% were at least type III.
“We include complex cases, such as revisional surgery, massive paraesophageal hernias, patients who had previous treatments for achalasia before surgery, or concurrent epiphrenic diverticulum resection,” Dr. Molina said. “To our knowledge, this report is the first to describe successful outpatient surgery in these complex patients, with comparable outcomes to admitted patients and to those described for more well-established outpatient procedures.”
The overall success rate of planned day surgery was 81.6%. Of the 18 unplanned admissions, patient preference to stay in the hospital and pain were the most common factors. Dr. Molina-Franjola said, “We identified factors that might be predictors of unplanned admission, and we found that female [sex], intraoperative complication, postoperative complications, and procedure performed in the afternoon were significant risk factors.”
Women accounted for 94.4% of the unplanned admissions after outpatient surgery, and PEHR/fundoplication represented 72.2% of unplanned admissions. No day-case patients with unplanned admission group required a reoperation within 30 days, although one who did not have an unplanned admission did.
With time, the share of outpatient procedures increased, Dr. Molina said. “In 2011, around 10% of procedures were day-case and that increased progressively to 67% in 2016,” he said.
Dr. Molina said that patients were sent home with antinauseates and instructions to call immediately if nausea or vomiting ensued. About 5% of outpatients returned for reflux, nausea, or vomiting, he said.
Dr. Molina reported having no financial disclosures.
HOUSTON – Selected patients who need operations, such as paraesophageal hernia repair and Heller myotomy, for benign hiatal diseases can have laparoscopic outpatient procedures with outcomes comparable with those of inpatients, a Canadian retrospective cohort study found.
“When comparing planned day-case patients with those who had planned admissions, we found that postoperative complication was the only statistically significant different outcome. Our data show same-day discharge resulted in no postoperative mortality, and no difference in postoperative morbidity, emergency room visits, and readmissions compared to traditional inpatient care,” said Juan Carlos Molina, MD, of McGill University Health Centre in Montreal, reporting the study results at the annual meeting of the American Society of Gastrointestinal and Endoscopic Surgeons.
The McGill researchers analyzed outcomes for 261 patients who had laparoscopic hiatal procedures from April 2011 to August 2016 – 163 as inpatients, 98 as outpatients, whom the study called planned day-case patients. The outpatient cohort consisted of younger patients (aged 60 vs. 66 years), but otherwise demographics between the two cohorts were similar. Discharge requirements after same-day hiatal procedures were the same as those for other outpatient procedures, Dr. Molina said.
The procedures included primary or revisional paraesophageal hernia repair (PEHR) in 123 (47.1%) patients; Heller myotomy in 94 (36%), 9 of which also underwent resection of an epiphrenic diverticulum; and Nissen fundoplication for gastroesophageal reflux disease in 44 (16.9%), of which 20 (45.5%) had a concomitant type I hiatal hernia. Among PEHR patients, 90% were at least type III.
“We include complex cases, such as revisional surgery, massive paraesophageal hernias, patients who had previous treatments for achalasia before surgery, or concurrent epiphrenic diverticulum resection,” Dr. Molina said. “To our knowledge, this report is the first to describe successful outpatient surgery in these complex patients, with comparable outcomes to admitted patients and to those described for more well-established outpatient procedures.”
The overall success rate of planned day surgery was 81.6%. Of the 18 unplanned admissions, patient preference to stay in the hospital and pain were the most common factors. Dr. Molina-Franjola said, “We identified factors that might be predictors of unplanned admission, and we found that female [sex], intraoperative complication, postoperative complications, and procedure performed in the afternoon were significant risk factors.”
Women accounted for 94.4% of the unplanned admissions after outpatient surgery, and PEHR/fundoplication represented 72.2% of unplanned admissions. No day-case patients with unplanned admission group required a reoperation within 30 days, although one who did not have an unplanned admission did.
With time, the share of outpatient procedures increased, Dr. Molina said. “In 2011, around 10% of procedures were day-case and that increased progressively to 67% in 2016,” he said.
Dr. Molina said that patients were sent home with antinauseates and instructions to call immediately if nausea or vomiting ensued. About 5% of outpatients returned for reflux, nausea, or vomiting, he said.
Dr. Molina reported having no financial disclosures.
HOUSTON – Selected patients who need operations, such as paraesophageal hernia repair and Heller myotomy, for benign hiatal diseases can have laparoscopic outpatient procedures with outcomes comparable with those of inpatients, a Canadian retrospective cohort study found.
“When comparing planned day-case patients with those who had planned admissions, we found that postoperative complication was the only statistically significant different outcome. Our data show same-day discharge resulted in no postoperative mortality, and no difference in postoperative morbidity, emergency room visits, and readmissions compared to traditional inpatient care,” said Juan Carlos Molina, MD, of McGill University Health Centre in Montreal, reporting the study results at the annual meeting of the American Society of Gastrointestinal and Endoscopic Surgeons.
The McGill researchers analyzed outcomes for 261 patients who had laparoscopic hiatal procedures from April 2011 to August 2016 – 163 as inpatients, 98 as outpatients, whom the study called planned day-case patients. The outpatient cohort consisted of younger patients (aged 60 vs. 66 years), but otherwise demographics between the two cohorts were similar. Discharge requirements after same-day hiatal procedures were the same as those for other outpatient procedures, Dr. Molina said.
The procedures included primary or revisional paraesophageal hernia repair (PEHR) in 123 (47.1%) patients; Heller myotomy in 94 (36%), 9 of which also underwent resection of an epiphrenic diverticulum; and Nissen fundoplication for gastroesophageal reflux disease in 44 (16.9%), of which 20 (45.5%) had a concomitant type I hiatal hernia. Among PEHR patients, 90% were at least type III.
“We include complex cases, such as revisional surgery, massive paraesophageal hernias, patients who had previous treatments for achalasia before surgery, or concurrent epiphrenic diverticulum resection,” Dr. Molina said. “To our knowledge, this report is the first to describe successful outpatient surgery in these complex patients, with comparable outcomes to admitted patients and to those described for more well-established outpatient procedures.”
The overall success rate of planned day surgery was 81.6%. Of the 18 unplanned admissions, patient preference to stay in the hospital and pain were the most common factors. Dr. Molina-Franjola said, “We identified factors that might be predictors of unplanned admission, and we found that female [sex], intraoperative complication, postoperative complications, and procedure performed in the afternoon were significant risk factors.”
Women accounted for 94.4% of the unplanned admissions after outpatient surgery, and PEHR/fundoplication represented 72.2% of unplanned admissions. No day-case patients with unplanned admission group required a reoperation within 30 days, although one who did not have an unplanned admission did.
With time, the share of outpatient procedures increased, Dr. Molina said. “In 2011, around 10% of procedures were day-case and that increased progressively to 67% in 2016,” he said.
Dr. Molina said that patients were sent home with antinauseates and instructions to call immediately if nausea or vomiting ensued. About 5% of outpatients returned for reflux, nausea, or vomiting, he said.
Dr. Molina reported having no financial disclosures.
AT SAGES 2017
Key clinical point: Same-day surgery for benign laparoscopic hiatal procedures have outcomes comparable with those of inpatient procedures.
Major finding: Postoperative complications were 9.2% for outpatient operations vs. 19% for inpatient, and 81.7% of patients who had same-day surgery did not have an unplanned admission.
Data source: Retrospective single-center study of 261 patients who had inpatient and outpatient laparoscopic hiatal procedures from April 2011 to August 2016.
Disclosures: Dr. Molina-Franjola reported having no financial disclosures.
Postsurgical O2 may cut AHI events
Postoperative oxygen therapy in patients with previously undetected obstructive sleep apnea (OSA) led to a reduction in apnea-hypopnea index (AHI) events per hour with no increase in apnea-hypopnea event duration.
The results suggest that postoperative oxygen could be useful in patients with OSA who refuse continuous positive airway pressure (CPAP) therapy, those with newly diagnosed OSA, and those with suspected OSA.
The researchers set out to determine if postoperative oxygen therapy could improve oxygenation in patients with previously undiagnosed OSA, reasoning that the intervention could reduce adverse events.
The study, published in CHEST (2017 March;151[3]:597-611), provided generally good news, but with a caveat: “Essentially we are saying, yes, if you give supplemental oxygen, you improve oxygenation of the patient. But overall we have to be careful because a significant number of patients have significant carbon dioxide retention when receiving supplemental oxygen. So we have to monitor patients – not just oxygen, but we may have to monitor carbon dioxide levels, too,” said lead study author Frances Chung, MBBS, professor of anesthesiology at the University of Toronto and Toronto Western Hospital.
The researchers randomized 123 patients with an AHI of at least five events per hour to postoperative oxygen (3 L/min for 3 nights via nasal prongs) or no postoperative oxygen.
On the third night, the oxygen group had a higher average oxygen saturation than controls (95.2% plus or minus 3.2% vs. 91.4% plus or minus 3.5%; P less than .0001) and a lower oxygen desaturation index (median, 2.3 events per hour vs. median, 18.5; P less than .0001).
A lower number of AHI events per hour occurred in the oxygen group (median, 8.0) than in the control group (median, 15.6; P = .016).
On average, the longest apnea-hypopnea event (median, 33.8 seconds) was shorter for a patient on oxygen, compared with a patient who did not receive oxygen (median, 49.6 seconds; P = .002).
But one finding surprised the researchers and led to some concern: Across both groups, 11.4% of patients experienced substantial CO2 retention. Specifically, for at least 10% of 1 of the nights, these patients had a partial pressure of CO2 of at least 55 mm Hg, according to measurements taken with a transcutaneous CO2 monitor. Of the 14 patients who experienced this event, 13 were receiving oxygen.
Dr. Chung said the results argue strongly for postsurgical oxygen in patients with OSA, who are known to be at increased risk for complications. “We are not doing something about it, and we should be doing something. Because one death from a complication is too many,” she said.
The study was funded by the University Health Network Foundation, Toronto, and the University of Toronto. Dr. Chung reported receiving research grant support from Ontario Ministry of Health Innovation Grant, University Health Network Foundation, ResMed Foundation, Acacia, and Medtronic.
Postoperative oxygen therapy in patients with previously undetected obstructive sleep apnea (OSA) led to a reduction in apnea-hypopnea index (AHI) events per hour with no increase in apnea-hypopnea event duration.
The results suggest that postoperative oxygen could be useful in patients with OSA who refuse continuous positive airway pressure (CPAP) therapy, those with newly diagnosed OSA, and those with suspected OSA.
The researchers set out to determine if postoperative oxygen therapy could improve oxygenation in patients with previously undiagnosed OSA, reasoning that the intervention could reduce adverse events.
The study, published in CHEST (2017 March;151[3]:597-611), provided generally good news, but with a caveat: “Essentially we are saying, yes, if you give supplemental oxygen, you improve oxygenation of the patient. But overall we have to be careful because a significant number of patients have significant carbon dioxide retention when receiving supplemental oxygen. So we have to monitor patients – not just oxygen, but we may have to monitor carbon dioxide levels, too,” said lead study author Frances Chung, MBBS, professor of anesthesiology at the University of Toronto and Toronto Western Hospital.
The researchers randomized 123 patients with an AHI of at least five events per hour to postoperative oxygen (3 L/min for 3 nights via nasal prongs) or no postoperative oxygen.
On the third night, the oxygen group had a higher average oxygen saturation than controls (95.2% plus or minus 3.2% vs. 91.4% plus or minus 3.5%; P less than .0001) and a lower oxygen desaturation index (median, 2.3 events per hour vs. median, 18.5; P less than .0001).
A lower number of AHI events per hour occurred in the oxygen group (median, 8.0) than in the control group (median, 15.6; P = .016).
On average, the longest apnea-hypopnea event (median, 33.8 seconds) was shorter for a patient on oxygen, compared with a patient who did not receive oxygen (median, 49.6 seconds; P = .002).
But one finding surprised the researchers and led to some concern: Across both groups, 11.4% of patients experienced substantial CO2 retention. Specifically, for at least 10% of 1 of the nights, these patients had a partial pressure of CO2 of at least 55 mm Hg, according to measurements taken with a transcutaneous CO2 monitor. Of the 14 patients who experienced this event, 13 were receiving oxygen.
Dr. Chung said the results argue strongly for postsurgical oxygen in patients with OSA, who are known to be at increased risk for complications. “We are not doing something about it, and we should be doing something. Because one death from a complication is too many,” she said.
The study was funded by the University Health Network Foundation, Toronto, and the University of Toronto. Dr. Chung reported receiving research grant support from Ontario Ministry of Health Innovation Grant, University Health Network Foundation, ResMed Foundation, Acacia, and Medtronic.
Postoperative oxygen therapy in patients with previously undetected obstructive sleep apnea (OSA) led to a reduction in apnea-hypopnea index (AHI) events per hour with no increase in apnea-hypopnea event duration.
The results suggest that postoperative oxygen could be useful in patients with OSA who refuse continuous positive airway pressure (CPAP) therapy, those with newly diagnosed OSA, and those with suspected OSA.
The researchers set out to determine if postoperative oxygen therapy could improve oxygenation in patients with previously undiagnosed OSA, reasoning that the intervention could reduce adverse events.
The study, published in CHEST (2017 March;151[3]:597-611), provided generally good news, but with a caveat: “Essentially we are saying, yes, if you give supplemental oxygen, you improve oxygenation of the patient. But overall we have to be careful because a significant number of patients have significant carbon dioxide retention when receiving supplemental oxygen. So we have to monitor patients – not just oxygen, but we may have to monitor carbon dioxide levels, too,” said lead study author Frances Chung, MBBS, professor of anesthesiology at the University of Toronto and Toronto Western Hospital.
The researchers randomized 123 patients with an AHI of at least five events per hour to postoperative oxygen (3 L/min for 3 nights via nasal prongs) or no postoperative oxygen.
On the third night, the oxygen group had a higher average oxygen saturation than controls (95.2% plus or minus 3.2% vs. 91.4% plus or minus 3.5%; P less than .0001) and a lower oxygen desaturation index (median, 2.3 events per hour vs. median, 18.5; P less than .0001).
A lower number of AHI events per hour occurred in the oxygen group (median, 8.0) than in the control group (median, 15.6; P = .016).
On average, the longest apnea-hypopnea event (median, 33.8 seconds) was shorter for a patient on oxygen, compared with a patient who did not receive oxygen (median, 49.6 seconds; P = .002).
But one finding surprised the researchers and led to some concern: Across both groups, 11.4% of patients experienced substantial CO2 retention. Specifically, for at least 10% of 1 of the nights, these patients had a partial pressure of CO2 of at least 55 mm Hg, according to measurements taken with a transcutaneous CO2 monitor. Of the 14 patients who experienced this event, 13 were receiving oxygen.
Dr. Chung said the results argue strongly for postsurgical oxygen in patients with OSA, who are known to be at increased risk for complications. “We are not doing something about it, and we should be doing something. Because one death from a complication is too many,” she said.
The study was funded by the University Health Network Foundation, Toronto, and the University of Toronto. Dr. Chung reported receiving research grant support from Ontario Ministry of Health Innovation Grant, University Health Network Foundation, ResMed Foundation, Acacia, and Medtronic.
FROM CHEST
Key clinical point: Postsurgical oxygen may reduce complications in patients with obstructive sleep apnea.
Major finding: For patients receiving oxygen, the longest apnea-hypopnea event duration was 33.8 seconds versus 49.6 for controls.
Data source: A randomized, placebo-controlled study of 123 patients.
Disclosures: The study was funded by the University Health Network Foundation, Toronto, and the University of Toronto. Dr. Chung reported receiving research grant support from various entities.
OSA tool uncovers risks of postoperative complications
High scores on the symptomless multivariable apnea prediction index (sMVAP) showed a strong correlation with increased risk for postsurgery complications, according to a study approved by the University of Pennsylvania, Philadelphia.
This validation helps assert the benefits of using the sMVAP as a tool to screen for obstructive sleep apnea (OSA) before elective inpatient surgeries, a test that is highly underutilized but very important, wrote M. Melanie Lyons, PhD, of the Center for Sleep and Circadian Neurobiology, University of Pennsylvania, Philadelphia, and her colleagues.
“Most patients having elective surgery are not screened for obstructive sleep apnea, even though OSA is a risk factor for postoperative complications,” wrote Dr. Lyons and her colleagues. “We observe that sMVAP correlates with higher risk for OSA, hypertension, and select postoperative complications, particularly in non-bariatric groups without routine preoperative screening for OSA.”
In a retrospective study of 40,432 patients undergoing elective surgery, high sMVAP scores were strongly correlated with postoperative complications including longer hospital stays (OR = 1.83), stays in the ICU (OR = 1.44), and respiratory complications (OR = 1.85) according to the researchers (Sleep. 2017 Jan 6. doi: 10.1093/sleep/zsw081).
Researchers separated participants into 10 categories according to the type of procedure: bariatric, orthopedic, cardiac, gastrointestinal, genitourinary, neurological, otorhinolaryngology/oral-maxillofacial/ear-nose-throat, pulmonary/thoracic, spine, and vascular.
The sMVAP calculates risk factors for OSA based on gender, age and body mass index, the researchers noted.
Those in the highest sMVAP score quintile were predominantly male (58%), with average age of 61 years, and average BMI of 40.9 kg/m2 (indicating morbid obesity). These patients reported the highest prevalence of having been previously diagnosed with OSA (26%). Comparatively, those patients in the lowest sMVAP quintile reported the lowest prevalence of an OSA diagnosis prior to undergoing their surgeries (9.3%).
Among non–bariatric surgery patients, those undergoing orthopedic procedures showed the highest correlation between complications and sMVAP scores.
The orthopedic surgery category reported a higher percentage of ICU-stay compared with bariatric surgery (14.3% vs 5.4%, P less than .0001), despite 23% of the patients who underwent an orthopedic surgery reporting previous OSA, compared with 50% of those who underwent surgery in the bariatric category.
This difference in previously reported OSA, according to Dr. Lyons and her colleagues, shows another example of the need for sMVAP in non–bariatric surgery preoperative procedure as a way to catch potentially undiagnosed OSA.
“[W]ork by Penn Bariatrics suggests that it is logical that the benefits of rigorous preoperative screening and diagnosis for OSA followed by a tailored team approach toward ensuring compliance toward treatment postoperation ... may be effective in limiting the likelihood of select postoperative complications,” the researchers wrote.
With 9.3% of all patients diagnosed with OSA, and a projected 14%-47% increase in specialty surgeries, there is an urgency in implementation of sMVAP and in conducting further studies, they noted.
This test was limited by the sample population, primarily male commercial truck drivers, the researchers noted. In addition, misclassification of OSA based on weight may have occurred in up to 20% of normal weight patients. Finally, data were collected from one hospital network, so generalizability may be limited.
Dr. M. Melanie Lyons and Dr. Junxin Li, another of the study’s authors, receive grants from the National Institutes of Health. The other authors reported no relevant disclosures.
High scores on the symptomless multivariable apnea prediction index (sMVAP) showed a strong correlation with increased risk for postsurgery complications, according to a study approved by the University of Pennsylvania, Philadelphia.
This validation helps assert the benefits of using the sMVAP as a tool to screen for obstructive sleep apnea (OSA) before elective inpatient surgeries, a test that is highly underutilized but very important, wrote M. Melanie Lyons, PhD, of the Center for Sleep and Circadian Neurobiology, University of Pennsylvania, Philadelphia, and her colleagues.
“Most patients having elective surgery are not screened for obstructive sleep apnea, even though OSA is a risk factor for postoperative complications,” wrote Dr. Lyons and her colleagues. “We observe that sMVAP correlates with higher risk for OSA, hypertension, and select postoperative complications, particularly in non-bariatric groups without routine preoperative screening for OSA.”
In a retrospective study of 40,432 patients undergoing elective surgery, high sMVAP scores were strongly correlated with postoperative complications including longer hospital stays (OR = 1.83), stays in the ICU (OR = 1.44), and respiratory complications (OR = 1.85) according to the researchers (Sleep. 2017 Jan 6. doi: 10.1093/sleep/zsw081).
Researchers separated participants into 10 categories according to the type of procedure: bariatric, orthopedic, cardiac, gastrointestinal, genitourinary, neurological, otorhinolaryngology/oral-maxillofacial/ear-nose-throat, pulmonary/thoracic, spine, and vascular.
The sMVAP calculates risk factors for OSA based on gender, age and body mass index, the researchers noted.
Those in the highest sMVAP score quintile were predominantly male (58%), with average age of 61 years, and average BMI of 40.9 kg/m2 (indicating morbid obesity). These patients reported the highest prevalence of having been previously diagnosed with OSA (26%). Comparatively, those patients in the lowest sMVAP quintile reported the lowest prevalence of an OSA diagnosis prior to undergoing their surgeries (9.3%).
Among non–bariatric surgery patients, those undergoing orthopedic procedures showed the highest correlation between complications and sMVAP scores.
The orthopedic surgery category reported a higher percentage of ICU-stay compared with bariatric surgery (14.3% vs 5.4%, P less than .0001), despite 23% of the patients who underwent an orthopedic surgery reporting previous OSA, compared with 50% of those who underwent surgery in the bariatric category.
This difference in previously reported OSA, according to Dr. Lyons and her colleagues, shows another example of the need for sMVAP in non–bariatric surgery preoperative procedure as a way to catch potentially undiagnosed OSA.
“[W]ork by Penn Bariatrics suggests that it is logical that the benefits of rigorous preoperative screening and diagnosis for OSA followed by a tailored team approach toward ensuring compliance toward treatment postoperation ... may be effective in limiting the likelihood of select postoperative complications,” the researchers wrote.
With 9.3% of all patients diagnosed with OSA, and a projected 14%-47% increase in specialty surgeries, there is an urgency in implementation of sMVAP and in conducting further studies, they noted.
This test was limited by the sample population, primarily male commercial truck drivers, the researchers noted. In addition, misclassification of OSA based on weight may have occurred in up to 20% of normal weight patients. Finally, data were collected from one hospital network, so generalizability may be limited.
Dr. M. Melanie Lyons and Dr. Junxin Li, another of the study’s authors, receive grants from the National Institutes of Health. The other authors reported no relevant disclosures.
High scores on the symptomless multivariable apnea prediction index (sMVAP) showed a strong correlation with increased risk for postsurgery complications, according to a study approved by the University of Pennsylvania, Philadelphia.
This validation helps assert the benefits of using the sMVAP as a tool to screen for obstructive sleep apnea (OSA) before elective inpatient surgeries, a test that is highly underutilized but very important, wrote M. Melanie Lyons, PhD, of the Center for Sleep and Circadian Neurobiology, University of Pennsylvania, Philadelphia, and her colleagues.
“Most patients having elective surgery are not screened for obstructive sleep apnea, even though OSA is a risk factor for postoperative complications,” wrote Dr. Lyons and her colleagues. “We observe that sMVAP correlates with higher risk for OSA, hypertension, and select postoperative complications, particularly in non-bariatric groups without routine preoperative screening for OSA.”
In a retrospective study of 40,432 patients undergoing elective surgery, high sMVAP scores were strongly correlated with postoperative complications including longer hospital stays (OR = 1.83), stays in the ICU (OR = 1.44), and respiratory complications (OR = 1.85) according to the researchers (Sleep. 2017 Jan 6. doi: 10.1093/sleep/zsw081).
Researchers separated participants into 10 categories according to the type of procedure: bariatric, orthopedic, cardiac, gastrointestinal, genitourinary, neurological, otorhinolaryngology/oral-maxillofacial/ear-nose-throat, pulmonary/thoracic, spine, and vascular.
The sMVAP calculates risk factors for OSA based on gender, age and body mass index, the researchers noted.
Those in the highest sMVAP score quintile were predominantly male (58%), with average age of 61 years, and average BMI of 40.9 kg/m2 (indicating morbid obesity). These patients reported the highest prevalence of having been previously diagnosed with OSA (26%). Comparatively, those patients in the lowest sMVAP quintile reported the lowest prevalence of an OSA diagnosis prior to undergoing their surgeries (9.3%).
Among non–bariatric surgery patients, those undergoing orthopedic procedures showed the highest correlation between complications and sMVAP scores.
The orthopedic surgery category reported a higher percentage of ICU-stay compared with bariatric surgery (14.3% vs 5.4%, P less than .0001), despite 23% of the patients who underwent an orthopedic surgery reporting previous OSA, compared with 50% of those who underwent surgery in the bariatric category.
This difference in previously reported OSA, according to Dr. Lyons and her colleagues, shows another example of the need for sMVAP in non–bariatric surgery preoperative procedure as a way to catch potentially undiagnosed OSA.
“[W]ork by Penn Bariatrics suggests that it is logical that the benefits of rigorous preoperative screening and diagnosis for OSA followed by a tailored team approach toward ensuring compliance toward treatment postoperation ... may be effective in limiting the likelihood of select postoperative complications,” the researchers wrote.
With 9.3% of all patients diagnosed with OSA, and a projected 14%-47% increase in specialty surgeries, there is an urgency in implementation of sMVAP and in conducting further studies, they noted.
This test was limited by the sample population, primarily male commercial truck drivers, the researchers noted. In addition, misclassification of OSA based on weight may have occurred in up to 20% of normal weight patients. Finally, data were collected from one hospital network, so generalizability may be limited.
Dr. M. Melanie Lyons and Dr. Junxin Li, another of the study’s authors, receive grants from the National Institutes of Health. The other authors reported no relevant disclosures.
FROM SLEEP
Key clinical point:
Major finding: Patients with high sMVAP scores had increased odds of complications, including extended length of stay (OR = 1.83), ICU stay (OR = 1.44), and respiratory complications (OR = 1.85).
Data source: Retrospective study of 40,432 elective surgery patient records collected from the Hospital of University of Pennsylvania, Pennsylvania Hospital, and Penn Presbyterian Medical Center between July 1, 2011, and June 30, 2014.
Disclosures: Dr. M. Melanie Lyons and Dr. Junxin Li receive grants from the National Institutes of Health. Other authors reported no relevant financial disclosures.
Tapering opioids
The Centers for Disease Control and Prevention guideline for prescribing opioids for chronic pain released in March 2016 suggests that if “patients are found to be receiving high total daily dosages of opioids, clinicians should discuss their safety concerns with the patient [and] consider tapering to a safer dosage...”
All of us who prescribe opioids have had these discussions with patients. They are frequently fraught with hand-wringing and, all-too-often, a “steeling” for battle. We may have a general sense for what these discussions are like from the provider perspective, but what are they like for patients?
Interestingly, patients had an overall low self-perceived risk of opioid overdose. Patients attributed reports of overdose to intent or risky behaviors. Patients rated the importance of treatment of current pain higher than the future potential risk of opioid use and had little faith in nonopioid pain management strategies. Patients reported fear of opioid withdrawal. They also reported the importance of social support and a healthy, trusting relationship with their provider for the facilitation of tapering. None of the patients reported switching providers who had recommended tapering. Patients who had tapered off opioids reported improved quality of life and a level of pain that was largely unchanged.
This work provides critical insight into the fears and reservations of patients facing the prospect of life on lower doses of opioids or life without them altogether. Addressing these fears directly may facilitate the discussions with patients when discussing the tapering of opioids.
Dr. Ebbert is professor of medicine, a general internist at the Mayo Clinic in Rochester, Minn., and a diplomate of the American Board of Addiction Medicine. The opinions expressed are those of the author and do not necessarily represent the views and opinions of the Mayo Clinic. The opinions expressed in this article should not be used to diagnose or treat any medical condition nor should they be used as a substitute for medical advice from a qualified, board-certified practicing clinician. Dr. Ebbert has no relevant financial disclosures about this article.
The Centers for Disease Control and Prevention guideline for prescribing opioids for chronic pain released in March 2016 suggests that if “patients are found to be receiving high total daily dosages of opioids, clinicians should discuss their safety concerns with the patient [and] consider tapering to a safer dosage...”
All of us who prescribe opioids have had these discussions with patients. They are frequently fraught with hand-wringing and, all-too-often, a “steeling” for battle. We may have a general sense for what these discussions are like from the provider perspective, but what are they like for patients?
Interestingly, patients had an overall low self-perceived risk of opioid overdose. Patients attributed reports of overdose to intent or risky behaviors. Patients rated the importance of treatment of current pain higher than the future potential risk of opioid use and had little faith in nonopioid pain management strategies. Patients reported fear of opioid withdrawal. They also reported the importance of social support and a healthy, trusting relationship with their provider for the facilitation of tapering. None of the patients reported switching providers who had recommended tapering. Patients who had tapered off opioids reported improved quality of life and a level of pain that was largely unchanged.
This work provides critical insight into the fears and reservations of patients facing the prospect of life on lower doses of opioids or life without them altogether. Addressing these fears directly may facilitate the discussions with patients when discussing the tapering of opioids.
Dr. Ebbert is professor of medicine, a general internist at the Mayo Clinic in Rochester, Minn., and a diplomate of the American Board of Addiction Medicine. The opinions expressed are those of the author and do not necessarily represent the views and opinions of the Mayo Clinic. The opinions expressed in this article should not be used to diagnose or treat any medical condition nor should they be used as a substitute for medical advice from a qualified, board-certified practicing clinician. Dr. Ebbert has no relevant financial disclosures about this article.
The Centers for Disease Control and Prevention guideline for prescribing opioids for chronic pain released in March 2016 suggests that if “patients are found to be receiving high total daily dosages of opioids, clinicians should discuss their safety concerns with the patient [and] consider tapering to a safer dosage...”
All of us who prescribe opioids have had these discussions with patients. They are frequently fraught with hand-wringing and, all-too-often, a “steeling” for battle. We may have a general sense for what these discussions are like from the provider perspective, but what are they like for patients?
Interestingly, patients had an overall low self-perceived risk of opioid overdose. Patients attributed reports of overdose to intent or risky behaviors. Patients rated the importance of treatment of current pain higher than the future potential risk of opioid use and had little faith in nonopioid pain management strategies. Patients reported fear of opioid withdrawal. They also reported the importance of social support and a healthy, trusting relationship with their provider for the facilitation of tapering. None of the patients reported switching providers who had recommended tapering. Patients who had tapered off opioids reported improved quality of life and a level of pain that was largely unchanged.
This work provides critical insight into the fears and reservations of patients facing the prospect of life on lower doses of opioids or life without them altogether. Addressing these fears directly may facilitate the discussions with patients when discussing the tapering of opioids.
Dr. Ebbert is professor of medicine, a general internist at the Mayo Clinic in Rochester, Minn., and a diplomate of the American Board of Addiction Medicine. The opinions expressed are those of the author and do not necessarily represent the views and opinions of the Mayo Clinic. The opinions expressed in this article should not be used to diagnose or treat any medical condition nor should they be used as a substitute for medical advice from a qualified, board-certified practicing clinician. Dr. Ebbert has no relevant financial disclosures about this article.