User login
Coronary Disease, Stroke to Drop Below Cancer as Top Killer
ORLANDO – After 100 years as America’s No. 1 killer, the combination of coronary disease and stroke is about to fall below cancer as the nation’s top cause of mortality.
The changeover occurred 3 years ago, in 2008, for the approximately 1.9 million adults enrolled in Kaiser Permanente of Northern California, and the ascendancy of cancer over coronary disease and stroke will happen throughout the United States sometime before the end of this decade, Dr. Stephen Sidney said while presenting a poster at the annual scientific sessions of the American Heart Association.*
The main driver of this shift is the huge progress made in curbing coronary and stroke deaths during the past half century, especially since 2000, said Dr. Sidney, associate director for clinical research of Kaiser Permanente of Northern California in Oakland.
"It’s a huge public health success from multifactorial interventions for primary prevention and secondary prevention," he said in an interview. During the 2000s alone, coronary disease mortality among Kaiser adults at least 30 years old fell by 27%, and stroke mortality plunged by 42%. In contrast, cancer mortality among adult members of Kaiser Permanente of Northern California dropped by 11%. "We’ve made huge progress and policy makers need to start thinking that [coronary disease and stroke] are not the biggest causes of mortality," he said.
Coronary disease first topped America’s killer list in 1910 and stayed in place for decades, but then started a trajectory of substantial decline by about 1970, he said. As recently as 2000, among adult members of Kaiser Permanente of Northern California, coronary disease alone accounted for about 300 deaths per 100,000 person-years, putting it on par with cancer, whereas coronary disease plus stroke together sat atop the killer list with a rate of about 400 deaths per 100,000 person-years in 2000. By 2008, coronary deaths alone had fallen to 200 per 100,000 person-years, while coronary and stroke deaths together dropped just below the 270 per 100,000 person-years level that cancer reached that year.
Although the crossing of the cardiovascular and cancer mortality rates has not yet happened throughout the United States, similar trends are at work. During 2000-2007, the gap in age-adjusted death rates between coronary disease and cancer fell by 88%, he said.
Dr. Sidney cited two Kaiser programs begun during the 2000s that he believes led to the big cardiovascular mortality drop of that era.
One was a concerted effort to diagnose and treat hypertension, a prime cardiovascular-event risk factor. As recently as 2001, only 38% of hypertensive patients in Kaiser Permanente of Northern California had their blood pressure controlled. Kaiser physicians perceived this as a major shortcoming, and launched a campaign to address it, so that by 2010 the percentage of controlled hypertensives had risen to 80%, he said.
The other initiative was a Kaiser program to treat all patients with coronary disease, cerebrovascular disease, peripheral arterial disease, chronic kidney disease, and those with an abdominal aortic aneurysm with aspirin, a statin, and an angiotensin-converting enzyme inhibitor.
Parallel efforts to bring the cancer rate down are much harder, because cancer is "a diverse set of etiologically distinct diseases with a myriad of interventions, making implementation of population-based approaches more complex, resulting in a slower rate of mortality decline," Dr. Sidney said in his poster.
Dr. Sidney said that he had no disclosures.
*Correction, 12/16/2011: An earlier version of this story misstated the number of adults enrolled in Kaiser Permanente of Northern California.
ORLANDO – After 100 years as America’s No. 1 killer, the combination of coronary disease and stroke is about to fall below cancer as the nation’s top cause of mortality.
The changeover occurred 3 years ago, in 2008, for the approximately 1.9 million adults enrolled in Kaiser Permanente of Northern California, and the ascendancy of cancer over coronary disease and stroke will happen throughout the United States sometime before the end of this decade, Dr. Stephen Sidney said while presenting a poster at the annual scientific sessions of the American Heart Association.*
The main driver of this shift is the huge progress made in curbing coronary and stroke deaths during the past half century, especially since 2000, said Dr. Sidney, associate director for clinical research of Kaiser Permanente of Northern California in Oakland.
"It’s a huge public health success from multifactorial interventions for primary prevention and secondary prevention," he said in an interview. During the 2000s alone, coronary disease mortality among Kaiser adults at least 30 years old fell by 27%, and stroke mortality plunged by 42%. In contrast, cancer mortality among adult members of Kaiser Permanente of Northern California dropped by 11%. "We’ve made huge progress and policy makers need to start thinking that [coronary disease and stroke] are not the biggest causes of mortality," he said.
Coronary disease first topped America’s killer list in 1910 and stayed in place for decades, but then started a trajectory of substantial decline by about 1970, he said. As recently as 2000, among adult members of Kaiser Permanente of Northern California, coronary disease alone accounted for about 300 deaths per 100,000 person-years, putting it on par with cancer, whereas coronary disease plus stroke together sat atop the killer list with a rate of about 400 deaths per 100,000 person-years in 2000. By 2008, coronary deaths alone had fallen to 200 per 100,000 person-years, while coronary and stroke deaths together dropped just below the 270 per 100,000 person-years level that cancer reached that year.
Although the crossing of the cardiovascular and cancer mortality rates has not yet happened throughout the United States, similar trends are at work. During 2000-2007, the gap in age-adjusted death rates between coronary disease and cancer fell by 88%, he said.
Dr. Sidney cited two Kaiser programs begun during the 2000s that he believes led to the big cardiovascular mortality drop of that era.
One was a concerted effort to diagnose and treat hypertension, a prime cardiovascular-event risk factor. As recently as 2001, only 38% of hypertensive patients in Kaiser Permanente of Northern California had their blood pressure controlled. Kaiser physicians perceived this as a major shortcoming, and launched a campaign to address it, so that by 2010 the percentage of controlled hypertensives had risen to 80%, he said.
The other initiative was a Kaiser program to treat all patients with coronary disease, cerebrovascular disease, peripheral arterial disease, chronic kidney disease, and those with an abdominal aortic aneurysm with aspirin, a statin, and an angiotensin-converting enzyme inhibitor.
Parallel efforts to bring the cancer rate down are much harder, because cancer is "a diverse set of etiologically distinct diseases with a myriad of interventions, making implementation of population-based approaches more complex, resulting in a slower rate of mortality decline," Dr. Sidney said in his poster.
Dr. Sidney said that he had no disclosures.
*Correction, 12/16/2011: An earlier version of this story misstated the number of adults enrolled in Kaiser Permanente of Northern California.
ORLANDO – After 100 years as America’s No. 1 killer, the combination of coronary disease and stroke is about to fall below cancer as the nation’s top cause of mortality.
The changeover occurred 3 years ago, in 2008, for the approximately 1.9 million adults enrolled in Kaiser Permanente of Northern California, and the ascendancy of cancer over coronary disease and stroke will happen throughout the United States sometime before the end of this decade, Dr. Stephen Sidney said while presenting a poster at the annual scientific sessions of the American Heart Association.*
The main driver of this shift is the huge progress made in curbing coronary and stroke deaths during the past half century, especially since 2000, said Dr. Sidney, associate director for clinical research of Kaiser Permanente of Northern California in Oakland.
"It’s a huge public health success from multifactorial interventions for primary prevention and secondary prevention," he said in an interview. During the 2000s alone, coronary disease mortality among Kaiser adults at least 30 years old fell by 27%, and stroke mortality plunged by 42%. In contrast, cancer mortality among adult members of Kaiser Permanente of Northern California dropped by 11%. "We’ve made huge progress and policy makers need to start thinking that [coronary disease and stroke] are not the biggest causes of mortality," he said.
Coronary disease first topped America’s killer list in 1910 and stayed in place for decades, but then started a trajectory of substantial decline by about 1970, he said. As recently as 2000, among adult members of Kaiser Permanente of Northern California, coronary disease alone accounted for about 300 deaths per 100,000 person-years, putting it on par with cancer, whereas coronary disease plus stroke together sat atop the killer list with a rate of about 400 deaths per 100,000 person-years in 2000. By 2008, coronary deaths alone had fallen to 200 per 100,000 person-years, while coronary and stroke deaths together dropped just below the 270 per 100,000 person-years level that cancer reached that year.
Although the crossing of the cardiovascular and cancer mortality rates has not yet happened throughout the United States, similar trends are at work. During 2000-2007, the gap in age-adjusted death rates between coronary disease and cancer fell by 88%, he said.
Dr. Sidney cited two Kaiser programs begun during the 2000s that he believes led to the big cardiovascular mortality drop of that era.
One was a concerted effort to diagnose and treat hypertension, a prime cardiovascular-event risk factor. As recently as 2001, only 38% of hypertensive patients in Kaiser Permanente of Northern California had their blood pressure controlled. Kaiser physicians perceived this as a major shortcoming, and launched a campaign to address it, so that by 2010 the percentage of controlled hypertensives had risen to 80%, he said.
The other initiative was a Kaiser program to treat all patients with coronary disease, cerebrovascular disease, peripheral arterial disease, chronic kidney disease, and those with an abdominal aortic aneurysm with aspirin, a statin, and an angiotensin-converting enzyme inhibitor.
Parallel efforts to bring the cancer rate down are much harder, because cancer is "a diverse set of etiologically distinct diseases with a myriad of interventions, making implementation of population-based approaches more complex, resulting in a slower rate of mortality decline," Dr. Sidney said in his poster.
Dr. Sidney said that he had no disclosures.
*Correction, 12/16/2011: An earlier version of this story misstated the number of adults enrolled in Kaiser Permanente of Northern California.
FROM THE ANNUAL SCIENTIFIC SESSIONS OF THE AMERICAN HEART ASSOCIATION
Major Finding: In 2008, the combined rate of deaths caused by coronary disease and stroke fell for the first time below the rate of deaths caused by cancer, among adult members of Kaiser Permanente of Northern California.
Data Source: Review of age-adjusted mortality rates among people aged 30 years or older who belonged to Kaiser Permanente of Northern California during 2000-2008.
Disclosures: Dr. Sidney said that he had no disclosures.
Novel Hep C Treatment Excludes Peginterferon Alfa
Therapy with a novel nonnucleoside polymerase inhibitor, in combination with a protease inhibitor and ribavirin, achieved a 100% virologic response rate at 29 days among patients with hepatitis C genotype 1, Dr. Stefan Zeuzem and colleagues reported in the December issue of Gastroenterology.
Moreover, this novel alternative to the standard peginterferon alfa regimen was safe, with no serious adverse events, and was highly tolerable, the investigators said.
"This indicates that HCV [hepatitis C virus] can be eradicated in chronically infected patients with a PegIFN-free DAA [direct-acting antiviral agent] combination regimen," the authors wrote.
Dr. Zeuzem, of the Johann Wolfgang Goethe University Hospital in Frankfurt, Germany, and colleagues studied 34 adult patients (mean age 51 years) who were naive to interferon, PegIFN, ribavirin, or any DAA for acute or chronic hepatitis C infection.
All patients had plasma HCV RNA levels of at least 100,000 IU/mL at screening and did not have cirrhosis.
Patients with hepatitis B virus, human immunodeficiency virus, previous or ongoing rash or photosensitivity, decompensated liver disease, or hyperbilirubinemia greater than 1.5 times the upper limit of normal were excluded.
Participants were randomized in a 1:1 fashion to receive a thrice-daily 400-mg or 600-mg dose of BI 207127, "an orally bioavailable, reversible, thumb pocket 1 nonnucleoside inhibitor (NNI) of the HCV NS5B polymerase with potent and specific antiviral activity in vitro," according to the authors (Gastroenterology 2011 [doi:10.1053/j.gastro.2011.08.051]).
"This indicates that HCV can be eradicated in chronically infected patients with a PegIFN-free DAA combination regimen."
All participants also received BI 201335, "a second-generation HCV NS3/4A protease inhibitor with highly potent in vitro activity against GT-1a/1b subtypes," wrote the authors, at a dose of 120 mg per day, as well as daily weight-dosed ribavirin, all taken with food, for 4 weeks.
"Drug-resistance studies in cell culture demonstrate that BI 201335 and BI 207127 have different resistance profiles, and previous observations using NS3/4A protease inhibitors and NS5B thumb pocket 1 NNI compounds demonstrate that 2-drug combinations profoundly reduce the selection of drug-resistant variants," explained Dr. Zeuzem.
The researchers found that in the cohort taking the larger, 600-mg doses of the polymerase inhibitor BI 207127, virologic response rates (defined as plasma HCV RNA levels of less than 25 IU/mL) were 18%, 82%, 100%, and 100% at days 8, 15, 22, and 29, respectively.
Slightly less impressive results were seen in the 400-mg group, with rates of 27%, 47%, 67%, and 73% at days 8, 15, 22, and 29 respectively.
Also in the 400-mg cohort, "higher response rates were observed in genotype 1b infected patients, compared with genotype 1a infected patients," wrote the authors, whereas results in the 600 mg group were not contingent on sub-genotypes.
"Most patients in the 600 mg TID [three times a day] dose group even had undetectable HCV RNA at days 22 and 29 (53% and 71%, respectively), while these rates did not exceed 20% in the 400 mg TID dose group," added the investigators.
Looking at safety and tolerability, Dr. Zeuzem and colleagues noted that most patients in both dosing cohorts complained of mild diarrhea, nausea, and vomiting.
Additionally, at the 600-mg dose, 42% developed mild rashes or photosensitivities, they said, and four patients developed "transient and very mild paresthesias of very different localizations."
"However, there were no severe AEs [adverse events], serious AEs or AE-related premature treatment discontinuations within the 4-week study period."
The "crucial next step," according to the investigators, will be achievement of longer-term SVR on the novel peginterferon-free regimen.
"Moreover, eliminating not only PegIFN but also RBV [ribavirin] from future HCV treatment would undoubtedly improve tolerability and would potentially allow for the treatment of patients with RBV contraindications," they added.
Indeed, at the time of this study’s publication, a phase 2b study was ongoing.
Dr. Zeuzem, along with several of his coinvestigators, disclosed financial and consulting relationships with multiple pharmaceutical companies, including the makers of the novel drugs used in this study, Boehringer Ingelheim. Boehringer Ingelheim also funded editorial assistance provided for this article.
Therapy with a novel nonnucleoside polymerase inhibitor, in combination with a protease inhibitor and ribavirin, achieved a 100% virologic response rate at 29 days among patients with hepatitis C genotype 1, Dr. Stefan Zeuzem and colleagues reported in the December issue of Gastroenterology.
Moreover, this novel alternative to the standard peginterferon alfa regimen was safe, with no serious adverse events, and was highly tolerable, the investigators said.
"This indicates that HCV [hepatitis C virus] can be eradicated in chronically infected patients with a PegIFN-free DAA [direct-acting antiviral agent] combination regimen," the authors wrote.
Dr. Zeuzem, of the Johann Wolfgang Goethe University Hospital in Frankfurt, Germany, and colleagues studied 34 adult patients (mean age 51 years) who were naive to interferon, PegIFN, ribavirin, or any DAA for acute or chronic hepatitis C infection.
All patients had plasma HCV RNA levels of at least 100,000 IU/mL at screening and did not have cirrhosis.
Patients with hepatitis B virus, human immunodeficiency virus, previous or ongoing rash or photosensitivity, decompensated liver disease, or hyperbilirubinemia greater than 1.5 times the upper limit of normal were excluded.
Participants were randomized in a 1:1 fashion to receive a thrice-daily 400-mg or 600-mg dose of BI 207127, "an orally bioavailable, reversible, thumb pocket 1 nonnucleoside inhibitor (NNI) of the HCV NS5B polymerase with potent and specific antiviral activity in vitro," according to the authors (Gastroenterology 2011 [doi:10.1053/j.gastro.2011.08.051]).
"This indicates that HCV can be eradicated in chronically infected patients with a PegIFN-free DAA combination regimen."
All participants also received BI 201335, "a second-generation HCV NS3/4A protease inhibitor with highly potent in vitro activity against GT-1a/1b subtypes," wrote the authors, at a dose of 120 mg per day, as well as daily weight-dosed ribavirin, all taken with food, for 4 weeks.
"Drug-resistance studies in cell culture demonstrate that BI 201335 and BI 207127 have different resistance profiles, and previous observations using NS3/4A protease inhibitors and NS5B thumb pocket 1 NNI compounds demonstrate that 2-drug combinations profoundly reduce the selection of drug-resistant variants," explained Dr. Zeuzem.
The researchers found that in the cohort taking the larger, 600-mg doses of the polymerase inhibitor BI 207127, virologic response rates (defined as plasma HCV RNA levels of less than 25 IU/mL) were 18%, 82%, 100%, and 100% at days 8, 15, 22, and 29, respectively.
Slightly less impressive results were seen in the 400-mg group, with rates of 27%, 47%, 67%, and 73% at days 8, 15, 22, and 29 respectively.
Also in the 400-mg cohort, "higher response rates were observed in genotype 1b infected patients, compared with genotype 1a infected patients," wrote the authors, whereas results in the 600 mg group were not contingent on sub-genotypes.
"Most patients in the 600 mg TID [three times a day] dose group even had undetectable HCV RNA at days 22 and 29 (53% and 71%, respectively), while these rates did not exceed 20% in the 400 mg TID dose group," added the investigators.
Looking at safety and tolerability, Dr. Zeuzem and colleagues noted that most patients in both dosing cohorts complained of mild diarrhea, nausea, and vomiting.
Additionally, at the 600-mg dose, 42% developed mild rashes or photosensitivities, they said, and four patients developed "transient and very mild paresthesias of very different localizations."
"However, there were no severe AEs [adverse events], serious AEs or AE-related premature treatment discontinuations within the 4-week study period."
The "crucial next step," according to the investigators, will be achievement of longer-term SVR on the novel peginterferon-free regimen.
"Moreover, eliminating not only PegIFN but also RBV [ribavirin] from future HCV treatment would undoubtedly improve tolerability and would potentially allow for the treatment of patients with RBV contraindications," they added.
Indeed, at the time of this study’s publication, a phase 2b study was ongoing.
Dr. Zeuzem, along with several of his coinvestigators, disclosed financial and consulting relationships with multiple pharmaceutical companies, including the makers of the novel drugs used in this study, Boehringer Ingelheim. Boehringer Ingelheim also funded editorial assistance provided for this article.
Therapy with a novel nonnucleoside polymerase inhibitor, in combination with a protease inhibitor and ribavirin, achieved a 100% virologic response rate at 29 days among patients with hepatitis C genotype 1, Dr. Stefan Zeuzem and colleagues reported in the December issue of Gastroenterology.
Moreover, this novel alternative to the standard peginterferon alfa regimen was safe, with no serious adverse events, and was highly tolerable, the investigators said.
"This indicates that HCV [hepatitis C virus] can be eradicated in chronically infected patients with a PegIFN-free DAA [direct-acting antiviral agent] combination regimen," the authors wrote.
Dr. Zeuzem, of the Johann Wolfgang Goethe University Hospital in Frankfurt, Germany, and colleagues studied 34 adult patients (mean age 51 years) who were naive to interferon, PegIFN, ribavirin, or any DAA for acute or chronic hepatitis C infection.
All patients had plasma HCV RNA levels of at least 100,000 IU/mL at screening and did not have cirrhosis.
Patients with hepatitis B virus, human immunodeficiency virus, previous or ongoing rash or photosensitivity, decompensated liver disease, or hyperbilirubinemia greater than 1.5 times the upper limit of normal were excluded.
Participants were randomized in a 1:1 fashion to receive a thrice-daily 400-mg or 600-mg dose of BI 207127, "an orally bioavailable, reversible, thumb pocket 1 nonnucleoside inhibitor (NNI) of the HCV NS5B polymerase with potent and specific antiviral activity in vitro," according to the authors (Gastroenterology 2011 [doi:10.1053/j.gastro.2011.08.051]).
"This indicates that HCV can be eradicated in chronically infected patients with a PegIFN-free DAA combination regimen."
All participants also received BI 201335, "a second-generation HCV NS3/4A protease inhibitor with highly potent in vitro activity against GT-1a/1b subtypes," wrote the authors, at a dose of 120 mg per day, as well as daily weight-dosed ribavirin, all taken with food, for 4 weeks.
"Drug-resistance studies in cell culture demonstrate that BI 201335 and BI 207127 have different resistance profiles, and previous observations using NS3/4A protease inhibitors and NS5B thumb pocket 1 NNI compounds demonstrate that 2-drug combinations profoundly reduce the selection of drug-resistant variants," explained Dr. Zeuzem.
The researchers found that in the cohort taking the larger, 600-mg doses of the polymerase inhibitor BI 207127, virologic response rates (defined as plasma HCV RNA levels of less than 25 IU/mL) were 18%, 82%, 100%, and 100% at days 8, 15, 22, and 29, respectively.
Slightly less impressive results were seen in the 400-mg group, with rates of 27%, 47%, 67%, and 73% at days 8, 15, 22, and 29 respectively.
Also in the 400-mg cohort, "higher response rates were observed in genotype 1b infected patients, compared with genotype 1a infected patients," wrote the authors, whereas results in the 600 mg group were not contingent on sub-genotypes.
"Most patients in the 600 mg TID [three times a day] dose group even had undetectable HCV RNA at days 22 and 29 (53% and 71%, respectively), while these rates did not exceed 20% in the 400 mg TID dose group," added the investigators.
Looking at safety and tolerability, Dr. Zeuzem and colleagues noted that most patients in both dosing cohorts complained of mild diarrhea, nausea, and vomiting.
Additionally, at the 600-mg dose, 42% developed mild rashes or photosensitivities, they said, and four patients developed "transient and very mild paresthesias of very different localizations."
"However, there were no severe AEs [adverse events], serious AEs or AE-related premature treatment discontinuations within the 4-week study period."
The "crucial next step," according to the investigators, will be achievement of longer-term SVR on the novel peginterferon-free regimen.
"Moreover, eliminating not only PegIFN but also RBV [ribavirin] from future HCV treatment would undoubtedly improve tolerability and would potentially allow for the treatment of patients with RBV contraindications," they added.
Indeed, at the time of this study’s publication, a phase 2b study was ongoing.
Dr. Zeuzem, along with several of his coinvestigators, disclosed financial and consulting relationships with multiple pharmaceutical companies, including the makers of the novel drugs used in this study, Boehringer Ingelheim. Boehringer Ingelheim also funded editorial assistance provided for this article.
FROM GASTROENTEROLOGY
Major Finding: A novel regimen that did not include peginterferon alfa resulted in a 100% virologic response rate in patients with hepatitis C genotype 1 at 29 days.
Data Source: A phase 1b, multicenter, open-label, randomized trial of 34 treatment-naive hepatitis C patients.
Disclosures: Dr. Zeuzem, along with several of his coinvestigators, disclosed financial and consulting relationships with multiple pharmaceutical companies, including the makers of the novel drugs used in this study, Boehringer Ingelheim. Editorial assistance was also provided by a company that is funded by Boehringer Ingelheim.
Community Oncology Podcast: Everolimus in ER-positive breast cancer
Dr. David Henry is your audio tour guide to the November 2011 issue of Community Oncology. Issue highlights include Community Translations, which addresses the role of everolimus in treating hormone-resistant ER-positive breast cancer; a review of guidelines for screening cancer patients for distress by Amy E. Lowery and Jimmie C. Holland; and original research on the impact of bone metastases and skeletal-related events on healthcare costs in prostate cancer patients on hormonal therapy by May Hagiwara, et.al. Also, reports from recent oncology meetings and regulatory news from Congress and the FDA.
Dr. David Henry is your audio tour guide to the November 2011 issue of Community Oncology. Issue highlights include Community Translations, which addresses the role of everolimus in treating hormone-resistant ER-positive breast cancer; a review of guidelines for screening cancer patients for distress by Amy E. Lowery and Jimmie C. Holland; and original research on the impact of bone metastases and skeletal-related events on healthcare costs in prostate cancer patients on hormonal therapy by May Hagiwara, et.al. Also, reports from recent oncology meetings and regulatory news from Congress and the FDA.
Dr. David Henry is your audio tour guide to the November 2011 issue of Community Oncology. Issue highlights include Community Translations, which addresses the role of everolimus in treating hormone-resistant ER-positive breast cancer; a review of guidelines for screening cancer patients for distress by Amy E. Lowery and Jimmie C. Holland; and original research on the impact of bone metastases and skeletal-related events on healthcare costs in prostate cancer patients on hormonal therapy by May Hagiwara, et.al. Also, reports from recent oncology meetings and regulatory news from Congress and the FDA.
Lymphedema Common After Head & Neck Cancer
SAN FRANCISCO – Lymphedema is highly common and a source of considerable morbidity among patients who undergo treatment for head and neck cancer, finds a cross-sectional study among 103 survivors.
Fully three-fourths had developed some degree of lymphedema, according to results presented at the annual Oncology Congress presented by Reed Medical Education. The more severe it was, the more likely patients were to have symptoms, functional impairments, and poorer quality of life.
Disease and treatment-related factors such as high radiation dose and combined surgery and radiation therapy were risk factors for the development of lymphedema.
"This is the first study that we are aware of in the United States of this depth to systematically examine lymphedema" in this population, noted lead investigator Jie Deng, Ph.D., R.N., O.C.N., a postdoctoral fellow at the Vanderbilt University, Nashville, Tenn.
"Health care professionals should be aware that lymphedema is a frequent late effect in the head and neck cancer population," she advised. "We need to educate patients about the risk of lymphedema prior to treatment, during treatment, and posttreatment, and we need to conduct external and internal examinations to evaluate related signs and symptoms at each clinic visit."
Patients found to have any signs or symptoms should be referred for lymphedema assessment. Furthermore, "it’s very important we have very detailed documentation so we can follow up on patients’ treatment effect and also identify potential issues in this population," Dr. Deng stressed. "An interdisciplinary approach is needed to best manage lymphedema."
She and her colleagues are now evaluating interventions to treat head and neck lymphedema. Manual lymphatic drainage is one possibility. Elevating the head of the bed at night is another, as anecdotal comments suggest that symptoms worsen in the recumbent position.
"Patients will mention in the morning they feel more tightness, more fluid accumulated in the submental area; around noontime or afternoon, they feel it has drained by itself," she explained.
There are more than half a million survivors of head and neck cancer in the United States, according to Dr. Deng. As a result of their disease and its treatment, these patients can develop both external lymphedema, causing symptoms such as facial puffiness, and internal lymphedema, causing issues such as epiglottal swelling.
The investigators studied adult patients treated for head and neck cancer at the Vanderbilt-Ingram Cancer Center who were at least 3 months out from the end of their treatment and had no evidence of cancer. External lymphedema was assessed with a clinical exam, using the Foldi scale. Internal lymphedema was assessed with an endoscopic exam, using the Patterson scale for edema of the larynx and pharynx.
The patients were 60 years old, on average. The majority were male (69%) and white (89%). In terms of health behaviors, 66% had a history of smoking and 38% had a history of alcohol use.
In all, 81% of the patients had had locally advanced cancer, and 90% had received at least two treatment modalities. The median time since end of treatment was 20 months.
Study results, reported at the meeting and also recently published, showed that 75% of the patients overall had lymphedema of the head and neck; of those with lymphedema (61 out of 81), 10% had only the external kind, 39% had only the internal kind, and 51% had both (J. Pain Symptom Manage. 2011 July 29 [doi:10.1016/j.jpainsymman.2011.03.019]).
The type and severity of lymphedema were associated with both physical and psychological symptoms, Dr. Deng reported.
As the severity of lymphedema increased, patients were significantly more likely to report difficulty swallowing, issues with mucus or dry mouth, nutritional problems, pain, and voice problems (P = .001 to P = .047, depending on the type of lymphedema and the specific symptom).
Additionally, increasing severity was associated with poorer body image (P = .028 to P = .049). "However, there was no statistically significant relationship between lymphedema and anxiety and depressive symptoms," she noted.
Lymphedema severity was also associated with hearing deficits, limitation of neck range of motion, and impaired quality of life (P = .004 to P = .045).
Analyses identified certain disease and treatment-related factors to be risk factors for the development of lymphedema, according to Dr. Deng.
Namely, patients were more likely to develop lymphedema if they had pharyngeal tumors; were a shorter time out from the end of treatment; received a high total dose of radiation, mirroring what has been seen in breast cancer; received a greater number of treatment modalities, a marker of treatment intensity; or had combined surgery and radiation therapy – specifically, either surgery plus postoperative radiation, or salvage surgery within the irradiated field – as compared with surgery alone.
The higher risk with shorter time since surgery hints that the lymphatics in the area may undergo regeneration over time, she speculated. "This was identified in the murine tail [model of lymphedema]; however, we didn’t know whether or not this phenomenon or similar exists in the head and neck cancer population."
None of the demographic factors or health behaviors assessed were found to be risk factors for the development of lymphedema. But the lack of association between smoking and alcohol consumption and lymphedema may have been related to the fact that patients were asked whether they smoked or drank but not the intensity, or to the cross-sectional nature of the study, Dr. Deng noted. "In the future, longitudinal study is needed to examine whether or not these are risk factors," she said.
Dr. Deng reported that she had no conflicts of interest related to the study. Reed Medical Education and this news organization are owned by Reed Elsevier.
SAN FRANCISCO – Lymphedema is highly common and a source of considerable morbidity among patients who undergo treatment for head and neck cancer, finds a cross-sectional study among 103 survivors.
Fully three-fourths had developed some degree of lymphedema, according to results presented at the annual Oncology Congress presented by Reed Medical Education. The more severe it was, the more likely patients were to have symptoms, functional impairments, and poorer quality of life.
Disease and treatment-related factors such as high radiation dose and combined surgery and radiation therapy were risk factors for the development of lymphedema.
"This is the first study that we are aware of in the United States of this depth to systematically examine lymphedema" in this population, noted lead investigator Jie Deng, Ph.D., R.N., O.C.N., a postdoctoral fellow at the Vanderbilt University, Nashville, Tenn.
"Health care professionals should be aware that lymphedema is a frequent late effect in the head and neck cancer population," she advised. "We need to educate patients about the risk of lymphedema prior to treatment, during treatment, and posttreatment, and we need to conduct external and internal examinations to evaluate related signs and symptoms at each clinic visit."
Patients found to have any signs or symptoms should be referred for lymphedema assessment. Furthermore, "it’s very important we have very detailed documentation so we can follow up on patients’ treatment effect and also identify potential issues in this population," Dr. Deng stressed. "An interdisciplinary approach is needed to best manage lymphedema."
She and her colleagues are now evaluating interventions to treat head and neck lymphedema. Manual lymphatic drainage is one possibility. Elevating the head of the bed at night is another, as anecdotal comments suggest that symptoms worsen in the recumbent position.
"Patients will mention in the morning they feel more tightness, more fluid accumulated in the submental area; around noontime or afternoon, they feel it has drained by itself," she explained.
There are more than half a million survivors of head and neck cancer in the United States, according to Dr. Deng. As a result of their disease and its treatment, these patients can develop both external lymphedema, causing symptoms such as facial puffiness, and internal lymphedema, causing issues such as epiglottal swelling.
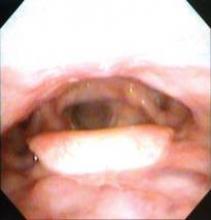
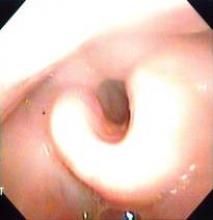
The investigators studied adult patients treated for head and neck cancer at the Vanderbilt-Ingram Cancer Center who were at least 3 months out from the end of their treatment and had no evidence of cancer. External lymphedema was assessed with a clinical exam, using the Foldi scale. Internal lymphedema was assessed with an endoscopic exam, using the Patterson scale for edema of the larynx and pharynx.
The patients were 60 years old, on average. The majority were male (69%) and white (89%). In terms of health behaviors, 66% had a history of smoking and 38% had a history of alcohol use.
In all, 81% of the patients had had locally advanced cancer, and 90% had received at least two treatment modalities. The median time since end of treatment was 20 months.
Study results, reported at the meeting and also recently published, showed that 75% of the patients overall had lymphedema of the head and neck; of those with lymphedema (61 out of 81), 10% had only the external kind, 39% had only the internal kind, and 51% had both (J. Pain Symptom Manage. 2011 July 29 [doi:10.1016/j.jpainsymman.2011.03.019]).
The type and severity of lymphedema were associated with both physical and psychological symptoms, Dr. Deng reported.
As the severity of lymphedema increased, patients were significantly more likely to report difficulty swallowing, issues with mucus or dry mouth, nutritional problems, pain, and voice problems (P = .001 to P = .047, depending on the type of lymphedema and the specific symptom).
Additionally, increasing severity was associated with poorer body image (P = .028 to P = .049). "However, there was no statistically significant relationship between lymphedema and anxiety and depressive symptoms," she noted.
Lymphedema severity was also associated with hearing deficits, limitation of neck range of motion, and impaired quality of life (P = .004 to P = .045).
Analyses identified certain disease and treatment-related factors to be risk factors for the development of lymphedema, according to Dr. Deng.
Namely, patients were more likely to develop lymphedema if they had pharyngeal tumors; were a shorter time out from the end of treatment; received a high total dose of radiation, mirroring what has been seen in breast cancer; received a greater number of treatment modalities, a marker of treatment intensity; or had combined surgery and radiation therapy – specifically, either surgery plus postoperative radiation, or salvage surgery within the irradiated field – as compared with surgery alone.
The higher risk with shorter time since surgery hints that the lymphatics in the area may undergo regeneration over time, she speculated. "This was identified in the murine tail [model of lymphedema]; however, we didn’t know whether or not this phenomenon or similar exists in the head and neck cancer population."
None of the demographic factors or health behaviors assessed were found to be risk factors for the development of lymphedema. But the lack of association between smoking and alcohol consumption and lymphedema may have been related to the fact that patients were asked whether they smoked or drank but not the intensity, or to the cross-sectional nature of the study, Dr. Deng noted. "In the future, longitudinal study is needed to examine whether or not these are risk factors," she said.
Dr. Deng reported that she had no conflicts of interest related to the study. Reed Medical Education and this news organization are owned by Reed Elsevier.
SAN FRANCISCO – Lymphedema is highly common and a source of considerable morbidity among patients who undergo treatment for head and neck cancer, finds a cross-sectional study among 103 survivors.
Fully three-fourths had developed some degree of lymphedema, according to results presented at the annual Oncology Congress presented by Reed Medical Education. The more severe it was, the more likely patients were to have symptoms, functional impairments, and poorer quality of life.
Disease and treatment-related factors such as high radiation dose and combined surgery and radiation therapy were risk factors for the development of lymphedema.
"This is the first study that we are aware of in the United States of this depth to systematically examine lymphedema" in this population, noted lead investigator Jie Deng, Ph.D., R.N., O.C.N., a postdoctoral fellow at the Vanderbilt University, Nashville, Tenn.
"Health care professionals should be aware that lymphedema is a frequent late effect in the head and neck cancer population," she advised. "We need to educate patients about the risk of lymphedema prior to treatment, during treatment, and posttreatment, and we need to conduct external and internal examinations to evaluate related signs and symptoms at each clinic visit."
Patients found to have any signs or symptoms should be referred for lymphedema assessment. Furthermore, "it’s very important we have very detailed documentation so we can follow up on patients’ treatment effect and also identify potential issues in this population," Dr. Deng stressed. "An interdisciplinary approach is needed to best manage lymphedema."
She and her colleagues are now evaluating interventions to treat head and neck lymphedema. Manual lymphatic drainage is one possibility. Elevating the head of the bed at night is another, as anecdotal comments suggest that symptoms worsen in the recumbent position.
"Patients will mention in the morning they feel more tightness, more fluid accumulated in the submental area; around noontime or afternoon, they feel it has drained by itself," she explained.
There are more than half a million survivors of head and neck cancer in the United States, according to Dr. Deng. As a result of their disease and its treatment, these patients can develop both external lymphedema, causing symptoms such as facial puffiness, and internal lymphedema, causing issues such as epiglottal swelling.
The investigators studied adult patients treated for head and neck cancer at the Vanderbilt-Ingram Cancer Center who were at least 3 months out from the end of their treatment and had no evidence of cancer. External lymphedema was assessed with a clinical exam, using the Foldi scale. Internal lymphedema was assessed with an endoscopic exam, using the Patterson scale for edema of the larynx and pharynx.
The patients were 60 years old, on average. The majority were male (69%) and white (89%). In terms of health behaviors, 66% had a history of smoking and 38% had a history of alcohol use.
In all, 81% of the patients had had locally advanced cancer, and 90% had received at least two treatment modalities. The median time since end of treatment was 20 months.
Study results, reported at the meeting and also recently published, showed that 75% of the patients overall had lymphedema of the head and neck; of those with lymphedema (61 out of 81), 10% had only the external kind, 39% had only the internal kind, and 51% had both (J. Pain Symptom Manage. 2011 July 29 [doi:10.1016/j.jpainsymman.2011.03.019]).
The type and severity of lymphedema were associated with both physical and psychological symptoms, Dr. Deng reported.
As the severity of lymphedema increased, patients were significantly more likely to report difficulty swallowing, issues with mucus or dry mouth, nutritional problems, pain, and voice problems (P = .001 to P = .047, depending on the type of lymphedema and the specific symptom).
Additionally, increasing severity was associated with poorer body image (P = .028 to P = .049). "However, there was no statistically significant relationship between lymphedema and anxiety and depressive symptoms," she noted.
Lymphedema severity was also associated with hearing deficits, limitation of neck range of motion, and impaired quality of life (P = .004 to P = .045).
Analyses identified certain disease and treatment-related factors to be risk factors for the development of lymphedema, according to Dr. Deng.
Namely, patients were more likely to develop lymphedema if they had pharyngeal tumors; were a shorter time out from the end of treatment; received a high total dose of radiation, mirroring what has been seen in breast cancer; received a greater number of treatment modalities, a marker of treatment intensity; or had combined surgery and radiation therapy – specifically, either surgery plus postoperative radiation, or salvage surgery within the irradiated field – as compared with surgery alone.
The higher risk with shorter time since surgery hints that the lymphatics in the area may undergo regeneration over time, she speculated. "This was identified in the murine tail [model of lymphedema]; however, we didn’t know whether or not this phenomenon or similar exists in the head and neck cancer population."
None of the demographic factors or health behaviors assessed were found to be risk factors for the development of lymphedema. But the lack of association between smoking and alcohol consumption and lymphedema may have been related to the fact that patients were asked whether they smoked or drank but not the intensity, or to the cross-sectional nature of the study, Dr. Deng noted. "In the future, longitudinal study is needed to examine whether or not these are risk factors," she said.
Dr. Deng reported that she had no conflicts of interest related to the study. Reed Medical Education and this news organization are owned by Reed Elsevier.
FROM THE ANNUAL ONCOLOGY CONGRESS
Major Finding: Fully 75% of patients had lymphedema. The severity of lymphedema was associated with symptoms, functional impairments, and poorer quality of life.
Data Source: A descriptive cross-sectional study among a convenience sample of 103 patients treated for head and neck cancer.
Disclosures: Dr. Deng reported that she had no conflicts of interest related to the study.
Predicting Response to Placebos in Oncology
What is the role of placebos in oncology? What works and what doesn't? And could placebos be more than just controls and be used as an intervention? And if so, which patients would respond to placebos? A panel of experts discuss these questions during a gathering at the 7th annual Chicago Supportive Oncology Conference.
What is the role of placebos in oncology? What works and what doesn't? And could placebos be more than just controls and be used as an intervention? And if so, which patients would respond to placebos? A panel of experts discuss these questions during a gathering at the 7th annual Chicago Supportive Oncology Conference.
What is the role of placebos in oncology? What works and what doesn't? And could placebos be more than just controls and be used as an intervention? And if so, which patients would respond to placebos? A panel of experts discuss these questions during a gathering at the 7th annual Chicago Supportive Oncology Conference.
Discussing End-of-Life Planning with Patients
Talking about end-of-life planning might not be so simple. Data suggests that patients want to know more about their prognosis, but sometimes physicians aren't sure how to bring up the discussion. Four supportive oncology experts discuss the importance and challenges of end-of-life planning during the 7th annual Chicago Supportive Oncology Conference.
Talking about end-of-life planning might not be so simple. Data suggests that patients want to know more about their prognosis, but sometimes physicians aren't sure how to bring up the discussion. Four supportive oncology experts discuss the importance and challenges of end-of-life planning during the 7th annual Chicago Supportive Oncology Conference.
Talking about end-of-life planning might not be so simple. Data suggests that patients want to know more about their prognosis, but sometimes physicians aren't sure how to bring up the discussion. Four supportive oncology experts discuss the importance and challenges of end-of-life planning during the 7th annual Chicago Supportive Oncology Conference.
With Cancer, Communication is Key
n this roundtable discussion from the Chicago Supportive Oncology Conference, Dr. Michael J. Fisch and Dr. Anthony Back discuss the importance of effective communication with cancer patients and some exciting studies that are underway.
n this roundtable discussion from the Chicago Supportive Oncology Conference, Dr. Michael J. Fisch and Dr. Anthony Back discuss the importance of effective communication with cancer patients and some exciting studies that are underway.
n this roundtable discussion from the Chicago Supportive Oncology Conference, Dr. Michael J. Fisch and Dr. Anthony Back discuss the importance of effective communication with cancer patients and some exciting studies that are underway.
Half of Older Cancer Patients Have Unrecognized Medical Problems
PARIS – About half of older cancer patients have unrecognized medical problems that may need to be addressed, according to the results of a prospective, multicenter study being conducted in Belgium.
Initial findings from the ongoing study of 1,347 elderly individuals with a mean age of 77 years and a variety of malignant diseases indicate that 51.4% of patients assessed using a systematic battery of geriatric screening tests had additional problems.
The additional problems reported were reduced physical functioning (20.4%), nutritional deficiencies coupled with fatigue (19.2%), falls (16.6%), depression (14.3%), pain (12.6%), cognitive impairments (8.3%), and a lack of social support or problems linked to their social status (5.3%).
"Forty-two per cent of physicians were not aware of the geriatric assessment results at the time of treatment decision," said Cindy Kenis, R.N., of the University Hospitals Leuven (Belgium).
At the annual meeting of the International Society of Geriatric Oncology, Ms. Kenis emphasized the need for better communication between health care professionals who treat elderly patients, specifically between geriatricians and oncologists.
The goal of the study is to look at the utility of a systemic geriatric assessment at 10 institutions in patients aged 70 years and older who have one of six specific tumor types. Currently, almost 39% of study participants have breast cancer, about 22% have colorectal cancer, 14% have hematologic malignancies, nearly 12% have lung cancer, approximately 8% have prostate cancer, and roughly 5% have ovarian carcinomas.
"You have to screen, you have to perform a geriatric assessment, and you have to do something with the results."
Nearly two-thirds of the patients being evaluated are women, with 65% undergoing systematic geriatric assessment at diagnosis and 35% at progression of their malignant disease.
Patients in the study were first screened with the G8 questionnaire, an eight-item tool that can be easily used by oncologists. If the G8 score was 14 or less out of a total of 17, indicating some possible impairment, a full geriatric assessment was performed. This was done in 72.5% of the study population.
The full geriatric assessment includes the evaluation of Activities of Daily Living, Independent or Instrumental Activities of Daily Living, fall history, Mobility-Tiredness questionnaire, the Mini-Mental State Examination, the four-item Geriatric Depression Scale, the Mini Nutritional Assessment, the Charlson Comorbidity Index, and polypharmacy.
Physicians also completed a questionnaire about their awareness of the results of geriatric assessment and treatment plans.
The results of the geriatric assessment led to interventions being planned to address previously unknown problems in a third of patients, with treatment decisions influenced in 15.5%.
While all of these assessments have been used in the study, which may have some oncologists reeling from the additional work involved, Dr. Stuart M. Lichtman of the 65+ clinical geriatrics program at Memorial Sloan-Kettering Cancer Center in New York commented that geriatric assessment did not need to be as complicated in practice. A variety of tools are available to physicians, but the key thing is to be aware and to ask a few simple questions, advised Dr. Lichtman, professor of medicine at Cornell University, New York, who chaired the meeting’s scientific committee and was not involved in the study.
Ms. Kenis agreed with his observations in an interview. "One of the main things is that we have to do an assessment, and that we don’t just perform the assessment, but we actually do something with it."
The study findings support a "three-step" approach in geriatric oncology, Ms. Kenis said: "You have to screen, you have to perform a geriatric assessment, and you have to do something with the results."
The study is supported by the Belgian government as part of the National Cancer Plan. Ms. Kenis said she had no relevant financial disclosures. The society is also known as the Société Internationale d’Oncologie Gériatrique (SIOG).
PARIS – About half of older cancer patients have unrecognized medical problems that may need to be addressed, according to the results of a prospective, multicenter study being conducted in Belgium.
Initial findings from the ongoing study of 1,347 elderly individuals with a mean age of 77 years and a variety of malignant diseases indicate that 51.4% of patients assessed using a systematic battery of geriatric screening tests had additional problems.
The additional problems reported were reduced physical functioning (20.4%), nutritional deficiencies coupled with fatigue (19.2%), falls (16.6%), depression (14.3%), pain (12.6%), cognitive impairments (8.3%), and a lack of social support or problems linked to their social status (5.3%).
"Forty-two per cent of physicians were not aware of the geriatric assessment results at the time of treatment decision," said Cindy Kenis, R.N., of the University Hospitals Leuven (Belgium).
At the annual meeting of the International Society of Geriatric Oncology, Ms. Kenis emphasized the need for better communication between health care professionals who treat elderly patients, specifically between geriatricians and oncologists.
The goal of the study is to look at the utility of a systemic geriatric assessment at 10 institutions in patients aged 70 years and older who have one of six specific tumor types. Currently, almost 39% of study participants have breast cancer, about 22% have colorectal cancer, 14% have hematologic malignancies, nearly 12% have lung cancer, approximately 8% have prostate cancer, and roughly 5% have ovarian carcinomas.
"You have to screen, you have to perform a geriatric assessment, and you have to do something with the results."
Nearly two-thirds of the patients being evaluated are women, with 65% undergoing systematic geriatric assessment at diagnosis and 35% at progression of their malignant disease.
Patients in the study were first screened with the G8 questionnaire, an eight-item tool that can be easily used by oncologists. If the G8 score was 14 or less out of a total of 17, indicating some possible impairment, a full geriatric assessment was performed. This was done in 72.5% of the study population.
The full geriatric assessment includes the evaluation of Activities of Daily Living, Independent or Instrumental Activities of Daily Living, fall history, Mobility-Tiredness questionnaire, the Mini-Mental State Examination, the four-item Geriatric Depression Scale, the Mini Nutritional Assessment, the Charlson Comorbidity Index, and polypharmacy.
Physicians also completed a questionnaire about their awareness of the results of geriatric assessment and treatment plans.
The results of the geriatric assessment led to interventions being planned to address previously unknown problems in a third of patients, with treatment decisions influenced in 15.5%.
While all of these assessments have been used in the study, which may have some oncologists reeling from the additional work involved, Dr. Stuart M. Lichtman of the 65+ clinical geriatrics program at Memorial Sloan-Kettering Cancer Center in New York commented that geriatric assessment did not need to be as complicated in practice. A variety of tools are available to physicians, but the key thing is to be aware and to ask a few simple questions, advised Dr. Lichtman, professor of medicine at Cornell University, New York, who chaired the meeting’s scientific committee and was not involved in the study.
Ms. Kenis agreed with his observations in an interview. "One of the main things is that we have to do an assessment, and that we don’t just perform the assessment, but we actually do something with it."
The study findings support a "three-step" approach in geriatric oncology, Ms. Kenis said: "You have to screen, you have to perform a geriatric assessment, and you have to do something with the results."
The study is supported by the Belgian government as part of the National Cancer Plan. Ms. Kenis said she had no relevant financial disclosures. The society is also known as the Société Internationale d’Oncologie Gériatrique (SIOG).
PARIS – About half of older cancer patients have unrecognized medical problems that may need to be addressed, according to the results of a prospective, multicenter study being conducted in Belgium.
Initial findings from the ongoing study of 1,347 elderly individuals with a mean age of 77 years and a variety of malignant diseases indicate that 51.4% of patients assessed using a systematic battery of geriatric screening tests had additional problems.
The additional problems reported were reduced physical functioning (20.4%), nutritional deficiencies coupled with fatigue (19.2%), falls (16.6%), depression (14.3%), pain (12.6%), cognitive impairments (8.3%), and a lack of social support or problems linked to their social status (5.3%).
"Forty-two per cent of physicians were not aware of the geriatric assessment results at the time of treatment decision," said Cindy Kenis, R.N., of the University Hospitals Leuven (Belgium).
At the annual meeting of the International Society of Geriatric Oncology, Ms. Kenis emphasized the need for better communication between health care professionals who treat elderly patients, specifically between geriatricians and oncologists.
The goal of the study is to look at the utility of a systemic geriatric assessment at 10 institutions in patients aged 70 years and older who have one of six specific tumor types. Currently, almost 39% of study participants have breast cancer, about 22% have colorectal cancer, 14% have hematologic malignancies, nearly 12% have lung cancer, approximately 8% have prostate cancer, and roughly 5% have ovarian carcinomas.
"You have to screen, you have to perform a geriatric assessment, and you have to do something with the results."
Nearly two-thirds of the patients being evaluated are women, with 65% undergoing systematic geriatric assessment at diagnosis and 35% at progression of their malignant disease.
Patients in the study were first screened with the G8 questionnaire, an eight-item tool that can be easily used by oncologists. If the G8 score was 14 or less out of a total of 17, indicating some possible impairment, a full geriatric assessment was performed. This was done in 72.5% of the study population.
The full geriatric assessment includes the evaluation of Activities of Daily Living, Independent or Instrumental Activities of Daily Living, fall history, Mobility-Tiredness questionnaire, the Mini-Mental State Examination, the four-item Geriatric Depression Scale, the Mini Nutritional Assessment, the Charlson Comorbidity Index, and polypharmacy.
Physicians also completed a questionnaire about their awareness of the results of geriatric assessment and treatment plans.
The results of the geriatric assessment led to interventions being planned to address previously unknown problems in a third of patients, with treatment decisions influenced in 15.5%.
While all of these assessments have been used in the study, which may have some oncologists reeling from the additional work involved, Dr. Stuart M. Lichtman of the 65+ clinical geriatrics program at Memorial Sloan-Kettering Cancer Center in New York commented that geriatric assessment did not need to be as complicated in practice. A variety of tools are available to physicians, but the key thing is to be aware and to ask a few simple questions, advised Dr. Lichtman, professor of medicine at Cornell University, New York, who chaired the meeting’s scientific committee and was not involved in the study.
Ms. Kenis agreed with his observations in an interview. "One of the main things is that we have to do an assessment, and that we don’t just perform the assessment, but we actually do something with it."
The study findings support a "three-step" approach in geriatric oncology, Ms. Kenis said: "You have to screen, you have to perform a geriatric assessment, and you have to do something with the results."
The study is supported by the Belgian government as part of the National Cancer Plan. Ms. Kenis said she had no relevant financial disclosures. The society is also known as the Société Internationale d’Oncologie Gériatrique (SIOG).
FROM THE ANNUAL MEETING OF THE INTERNATIONAL SOCIETY OF GERIATRIC ONCOLOGY
Major Finding: Additional medical problems, such as reduced physical functioning, nutritional, and other issues, were detected in 51.4% of elderly patients assessed through a systematic battery of geriatric screening tests.
Data Source: 1,347 patients with cancer in an ongoing, prospective, multicenter Belgian study.
Disclosures: The study is supported by the Belgian government as part of the National Cancer Plan. Ms. Kenis said she had no relevant financial disclosures.
Cancer Often Goes Untreated in Nursing Home Residents
PARIS – For elderly nursing home residents, a cancer diagnosis often comes at an advanced stage and fails to trigger appropriate therapy or overall general care, according to data from a study of more than 145,000 nursing home residents in the United States.
Even early-stage cancers are likely to go untreated, and more than 20% of patients in pain receive no medication, regardless of the cancer site or the degree of pain, investigators reported at the annual meeting of the International Society for Geriatric Oncology.
"We saw that late and unstaged cancer was more prevalent in nursing home patients than in other elderly patients," Dr. Giuseppe Colloca, a geriatrician at the Università Cattolica del Sacro Cuore in Rome, told attendees.
"Older age was associated with late-stage diagnosis and death within a few months of diagnosis," Dr. Colloca said, adding that there was "low hospice use and very little cancer-directed treatment – even among patients with early-stage cancer."
The aim of the study was to look at patterns of cancer diagnosis, survival, treatment, and quality of care among elderly individuals recently admitted to nursing homes. In the United States, an estimated 5% of elderly individuals live in nursing homes categorized as offering a high-level of care, with a further 1.5% in residential care that provides lower levels of nursing support, according to Dr. Colloca.
The investigators obtained data on individuals aged 65 years or older whose records were contained with the SAGE (Systematic Assessment of Geriatric Drug Use via Epidemiology) database. This is a multilinked database of clinical care information based on a census of all nursing home residents in the United States.
The study evaluated data on 145,757 elderly individuals who were recently admitted to a nursing home in five U.S. states; of these, 21,064 (14%) had a cancer diagnosis that was made in most cases after admission. Among these residents with cancer, the most common diagnoses were prostate (10.8%) and lung (9%) tumors, with other known cancer types including colon (6.7%), breast (4.5%), bladder (3.1%), anal (2.9%), skin (2.2%), brain (1.6%), pancreas (1.5%), and renal (1.5%).
Analysis of sociodemographic characteristics showed that across all tumor types, the average age was between 75 and 84 years of age but did vary according to the type of tumor. More than 40% of patients with prostate or colon cancer were 85 years or older, while just 13% of lung cancer patients were this old.
Most of the elderly cancer patients were white (83.2%-91.2%), with moderate (49.7%-54.4%) or severe (34.9%-44.1%) limitations in physical function. More than half were moderately (36.4%-44.1%) or severely (7.8%-11.3%) cognitively impaired.
Around a quarter of patients experienced daily symptoms of pain, with other common symptoms including shortness of breath, constipation, unstable cognitive status, edema, and recent falls. "Control of pain symptoms has been shown to be inadequate among nursing home cancer patients," Dr. Colloca said.
"Chemotherapy and radiation treatment were really quite infrequent," he added, noting that while 17.1% of breast cancer patients received chemotherapy, only 2.9% of those with colon cancer received such treatment. Chemotherapy rates also were low among those with lung (3%), prostate (6.3%), and "other" (5.4%) tumors.
Lung cancer patients were more likely to receive radiation with a radiotherapy rate of 10.9%. In the other cancer patients radiotherapy rates ranged from 0.9% for colon cancer to 4.2% for "other." Only 3.8% of breast tumors and 2.9% of prostate cancers were treated with radiation.
A terminal diagnosis of cancer was reported in 8.4% of breast, 8.9% of prostate, 10.5% of colon, 12.4% of "other," and 21.5% of lung tumors. Lung cancer patients also had the highest 1-year mortality rate: 91.9% (lung). But 1-year mortality was high across the board at 80% in breast cancer patients, 78.6% (prostate), 80.9% (colon), and 83.2% ("other’).
Survival time was usually short, at just 54 days for those with lung cancer and 110 days for patients with "other" cancers. The longest survival times were in breast (172 days), prostate (149 days), and colon (142) cancers.
"Cancer appears to be ignored in the nursing home," Dr. Colloca observed in an interview. "Often there is a misdiagnosis of cancer," with patients not being diagnosed with terminal cancer and cancer considered more of a comorbidity." This needs to be addressed, he said.
Dr. Colloca reported no conflicts of interest. The society is also known as the Société Internationale d’Oncologie Gériatrique (SIOG).
Dr. Stuart M. Lichtman, scientific committee chair of the meeting, noted that although a high percentage of patients in this study reported pain, not all pain may be caused by cancer. "The worst pain I see in practice is not due to cancer. The worst pain is usually due to vertebral pain, body collapse, and a lot of people are reluctant to give these old people narcotics, but sometimes that is the best way to go," he said in an interview.
Dr. Lichtman is a professor of medicine at Cornell University and an attending physician with the 65+ Clinical Geriatrics Program at Memorial Sloan-Kettering Cancer Center, both in New York. He was not involved in the study and reported no disclosures.
Dr. Stuart M. Lichtman, scientific committee chair of the meeting, noted that although a high percentage of patients in this study reported pain, not all pain may be caused by cancer. "The worst pain I see in practice is not due to cancer. The worst pain is usually due to vertebral pain, body collapse, and a lot of people are reluctant to give these old people narcotics, but sometimes that is the best way to go," he said in an interview.
Dr. Lichtman is a professor of medicine at Cornell University and an attending physician with the 65+ Clinical Geriatrics Program at Memorial Sloan-Kettering Cancer Center, both in New York. He was not involved in the study and reported no disclosures.
Dr. Stuart M. Lichtman, scientific committee chair of the meeting, noted that although a high percentage of patients in this study reported pain, not all pain may be caused by cancer. "The worst pain I see in practice is not due to cancer. The worst pain is usually due to vertebral pain, body collapse, and a lot of people are reluctant to give these old people narcotics, but sometimes that is the best way to go," he said in an interview.
Dr. Lichtman is a professor of medicine at Cornell University and an attending physician with the 65+ Clinical Geriatrics Program at Memorial Sloan-Kettering Cancer Center, both in New York. He was not involved in the study and reported no disclosures.
PARIS – For elderly nursing home residents, a cancer diagnosis often comes at an advanced stage and fails to trigger appropriate therapy or overall general care, according to data from a study of more than 145,000 nursing home residents in the United States.
Even early-stage cancers are likely to go untreated, and more than 20% of patients in pain receive no medication, regardless of the cancer site or the degree of pain, investigators reported at the annual meeting of the International Society for Geriatric Oncology.
"We saw that late and unstaged cancer was more prevalent in nursing home patients than in other elderly patients," Dr. Giuseppe Colloca, a geriatrician at the Università Cattolica del Sacro Cuore in Rome, told attendees.
"Older age was associated with late-stage diagnosis and death within a few months of diagnosis," Dr. Colloca said, adding that there was "low hospice use and very little cancer-directed treatment – even among patients with early-stage cancer."
The aim of the study was to look at patterns of cancer diagnosis, survival, treatment, and quality of care among elderly individuals recently admitted to nursing homes. In the United States, an estimated 5% of elderly individuals live in nursing homes categorized as offering a high-level of care, with a further 1.5% in residential care that provides lower levels of nursing support, according to Dr. Colloca.
The investigators obtained data on individuals aged 65 years or older whose records were contained with the SAGE (Systematic Assessment of Geriatric Drug Use via Epidemiology) database. This is a multilinked database of clinical care information based on a census of all nursing home residents in the United States.
The study evaluated data on 145,757 elderly individuals who were recently admitted to a nursing home in five U.S. states; of these, 21,064 (14%) had a cancer diagnosis that was made in most cases after admission. Among these residents with cancer, the most common diagnoses were prostate (10.8%) and lung (9%) tumors, with other known cancer types including colon (6.7%), breast (4.5%), bladder (3.1%), anal (2.9%), skin (2.2%), brain (1.6%), pancreas (1.5%), and renal (1.5%).
Analysis of sociodemographic characteristics showed that across all tumor types, the average age was between 75 and 84 years of age but did vary according to the type of tumor. More than 40% of patients with prostate or colon cancer were 85 years or older, while just 13% of lung cancer patients were this old.
Most of the elderly cancer patients were white (83.2%-91.2%), with moderate (49.7%-54.4%) or severe (34.9%-44.1%) limitations in physical function. More than half were moderately (36.4%-44.1%) or severely (7.8%-11.3%) cognitively impaired.
Around a quarter of patients experienced daily symptoms of pain, with other common symptoms including shortness of breath, constipation, unstable cognitive status, edema, and recent falls. "Control of pain symptoms has been shown to be inadequate among nursing home cancer patients," Dr. Colloca said.
"Chemotherapy and radiation treatment were really quite infrequent," he added, noting that while 17.1% of breast cancer patients received chemotherapy, only 2.9% of those with colon cancer received such treatment. Chemotherapy rates also were low among those with lung (3%), prostate (6.3%), and "other" (5.4%) tumors.
Lung cancer patients were more likely to receive radiation with a radiotherapy rate of 10.9%. In the other cancer patients radiotherapy rates ranged from 0.9% for colon cancer to 4.2% for "other." Only 3.8% of breast tumors and 2.9% of prostate cancers were treated with radiation.
A terminal diagnosis of cancer was reported in 8.4% of breast, 8.9% of prostate, 10.5% of colon, 12.4% of "other," and 21.5% of lung tumors. Lung cancer patients also had the highest 1-year mortality rate: 91.9% (lung). But 1-year mortality was high across the board at 80% in breast cancer patients, 78.6% (prostate), 80.9% (colon), and 83.2% ("other’).
Survival time was usually short, at just 54 days for those with lung cancer and 110 days for patients with "other" cancers. The longest survival times were in breast (172 days), prostate (149 days), and colon (142) cancers.
"Cancer appears to be ignored in the nursing home," Dr. Colloca observed in an interview. "Often there is a misdiagnosis of cancer," with patients not being diagnosed with terminal cancer and cancer considered more of a comorbidity." This needs to be addressed, he said.
Dr. Colloca reported no conflicts of interest. The society is also known as the Société Internationale d’Oncologie Gériatrique (SIOG).
PARIS – For elderly nursing home residents, a cancer diagnosis often comes at an advanced stage and fails to trigger appropriate therapy or overall general care, according to data from a study of more than 145,000 nursing home residents in the United States.
Even early-stage cancers are likely to go untreated, and more than 20% of patients in pain receive no medication, regardless of the cancer site or the degree of pain, investigators reported at the annual meeting of the International Society for Geriatric Oncology.
"We saw that late and unstaged cancer was more prevalent in nursing home patients than in other elderly patients," Dr. Giuseppe Colloca, a geriatrician at the Università Cattolica del Sacro Cuore in Rome, told attendees.
"Older age was associated with late-stage diagnosis and death within a few months of diagnosis," Dr. Colloca said, adding that there was "low hospice use and very little cancer-directed treatment – even among patients with early-stage cancer."
The aim of the study was to look at patterns of cancer diagnosis, survival, treatment, and quality of care among elderly individuals recently admitted to nursing homes. In the United States, an estimated 5% of elderly individuals live in nursing homes categorized as offering a high-level of care, with a further 1.5% in residential care that provides lower levels of nursing support, according to Dr. Colloca.
The investigators obtained data on individuals aged 65 years or older whose records were contained with the SAGE (Systematic Assessment of Geriatric Drug Use via Epidemiology) database. This is a multilinked database of clinical care information based on a census of all nursing home residents in the United States.
The study evaluated data on 145,757 elderly individuals who were recently admitted to a nursing home in five U.S. states; of these, 21,064 (14%) had a cancer diagnosis that was made in most cases after admission. Among these residents with cancer, the most common diagnoses were prostate (10.8%) and lung (9%) tumors, with other known cancer types including colon (6.7%), breast (4.5%), bladder (3.1%), anal (2.9%), skin (2.2%), brain (1.6%), pancreas (1.5%), and renal (1.5%).
Analysis of sociodemographic characteristics showed that across all tumor types, the average age was between 75 and 84 years of age but did vary according to the type of tumor. More than 40% of patients with prostate or colon cancer were 85 years or older, while just 13% of lung cancer patients were this old.
Most of the elderly cancer patients were white (83.2%-91.2%), with moderate (49.7%-54.4%) or severe (34.9%-44.1%) limitations in physical function. More than half were moderately (36.4%-44.1%) or severely (7.8%-11.3%) cognitively impaired.
Around a quarter of patients experienced daily symptoms of pain, with other common symptoms including shortness of breath, constipation, unstable cognitive status, edema, and recent falls. "Control of pain symptoms has been shown to be inadequate among nursing home cancer patients," Dr. Colloca said.
"Chemotherapy and radiation treatment were really quite infrequent," he added, noting that while 17.1% of breast cancer patients received chemotherapy, only 2.9% of those with colon cancer received such treatment. Chemotherapy rates also were low among those with lung (3%), prostate (6.3%), and "other" (5.4%) tumors.
Lung cancer patients were more likely to receive radiation with a radiotherapy rate of 10.9%. In the other cancer patients radiotherapy rates ranged from 0.9% for colon cancer to 4.2% for "other." Only 3.8% of breast tumors and 2.9% of prostate cancers were treated with radiation.
A terminal diagnosis of cancer was reported in 8.4% of breast, 8.9% of prostate, 10.5% of colon, 12.4% of "other," and 21.5% of lung tumors. Lung cancer patients also had the highest 1-year mortality rate: 91.9% (lung). But 1-year mortality was high across the board at 80% in breast cancer patients, 78.6% (prostate), 80.9% (colon), and 83.2% ("other’).
Survival time was usually short, at just 54 days for those with lung cancer and 110 days for patients with "other" cancers. The longest survival times were in breast (172 days), prostate (149 days), and colon (142) cancers.
"Cancer appears to be ignored in the nursing home," Dr. Colloca observed in an interview. "Often there is a misdiagnosis of cancer," with patients not being diagnosed with terminal cancer and cancer considered more of a comorbidity." This needs to be addressed, he said.
Dr. Colloca reported no conflicts of interest. The society is also known as the Société Internationale d’Oncologie Gériatrique (SIOG).
FROM A MEETING OF THE INTERNATIONAL SOCIETY OF GERIATRIC ONCOLOGY
Major Finding: Chemotherapy treatment rates ranged from 2.9% of residents with colon cancer to 17.1 % of those diagnosed with breast cancer.
Data Source: Records of than 145,000 elderly individuals newly admitted to nursing homes in the SAGE (Systematic Assessment of Geriatric Drug Use via Epidemiology) database.
Disclosures: Dr. Colloca reported no conflicts of interest.
Fewer Visits Don't Jeopardize Melanoma Patient Care
A novel, less-intensive monitoring schedule for patients with localized primary cutaneous melanoma appears to reduce follow-up visits without affecting the rate of detection of new primary or recurrent melanomas, according to an analysis of data from an inception cohort of 3,081 patients.
Given that follow-up care for melanoma patients in the United States costs up to $500 million per year, the findings could have important implications for cost savings, according to Robin M. Turner, Ph.D., and colleagues.
Using data from the Melanoma Institute Australia on the inception cohort, which included consecutive patients with stage I or II melanoma first diagnosed between January 1985 and December 2009, the investigators modeled the delay in diagnosis of a new primary melanoma or recurrence with two different monitoring schedules.
Schedule one was based on 2008 Australian and New Zealand guidelines, which recommend follow-up every 6 months for 5 years, then annually for 5 years for patients with stage 1A and 1B disease, or every 3 months for 5 years, then annually for 5 years in patients with stages IIA, IIB, or IIC.
Schedule two, the novel monitoring arm, called for annual follow-up for 10 years for patients with stage I disease; every 6 months for 2 years, and then annually for 8 years, for patients with stage IIA disease; and every 4 months for 2 years, every 6 months in year 3, and then annually for 5 years, for patients with stages IIB and IIC disease.
Within 10 years, the total number of recurrences was 229 for every 1,000 patients, and the number of new primary melanomas was 61 for every 1,000 patients.
Compared with the 2008 Australia and New Zealand guidelines for monitoring, the novel schedule, which required almost 3,000 fewer visits per 1,000 patients (8,044 vs. 5,221 visits), resulted in a delay in the detection – by at least 2 months – of an additional 44.9 recurrences per 1,000 patients, and an additional 9.6 new primary melanomas, Robin M. Turner, Ph.D., of the School of Public Health at the University of Sydney, Australia, and colleagues reported online in the Journal of Clinical Oncology (2011 Nov. 7 [doi:10.1200/JCO.2010.34.2956]).
"If we assume self-detection rates based on published estimates [75% for recurrence and 50% for new primary], use of schedule two rather than schedule one results in only a small number of additional patients experiencing a delay in recurrence diagnosis (up to [a] maximum of 3 months; extra 11.3 patients per 1,000 with delay [greater than] 2 months) and even fewer experiencing a delay in new primary diagnosis (up to [a] maximum of 6 months; extra 4.9 per 1,000)," the investigators wrote.
Moreover, if there were no patients lost to follow-up and they attended all visits until diagnosis or 10 years, the total number of visits for schedule one would be 19,546, compared with 12,303 for schedule two.
"Not only would these fewer monitoring visits reduce the burden on patients in terms of time and expense in attendance and possible unnecessary anxiety, but they would also represent substantial savings for the health care system," the investigators wrote.
They also found that the risk of recurrence was greatest in the first year of follow-up; that the most important predictor of recurrence was American Joint Committee on Cancer substage (hazard ratios of 1, 1.12, 0.56, 0.70, and 0.95 for stages IA, IB, IIA, IIB, and IIC, respectively); and that the most important predictors of new primary melanomas were age and date of primary diagnosis after 1992 (hazard ratios of 1.29 and 2.21, respectively).
This study was supported by grants from the Australian National Health and Medical Research Council. The investigators said they had no relevant financial disclosures.
In an accompanying editorial, Dr. Vernon K. Sondak and Dr. Sancy A.
Leachman wrote that the findings of Dr. Turner and colleagues "have
begun to move us down the path toward data-driven, personalized
follow-up guidelines."
This path is an important one, because in
the current era of personalized medicine, too little attention has been
paid to personalizing follow-up for patients after curative treatment of
cancer, including localized cutaneous melanoma, they noted (J. Clin.
Oncol. 2011 Nov. 7 [doi:10.1200/JCO.2011.37.6681]).
Success,
however, will require new partnerships and collaborations. Specifically,
the ultimate solution should involve shared follow-up with physicians
in the community, as well as with the patient and the patient’s family,
through education designed to maximize their ability to identify
recurrent and new melanomas.
Shared follow-up with local
dermatologists of patients with melanoma would address the goal of
detecting recurrences and new primary melanomas while simultaneously
decreasing the frequency of visits to surgical or medical oncologists.
Focusing
the lens of personalized medicine onto follow-up strategies, and
pursuing new partnerships and collaborations, will provide "a golden
opportunity to deliver the right care to the right patients at the right
time and in the right place," they concluded.
Dr. Sondak is with the Moffitt Cancer Center and the University of South Florida, Tampa. Dr. Leachman is with the Huntsman Cancer Institute and the University of Utah, Salt Lake City. Dr. Sondak reported serving as a consultant or adviser to Merck/Schering Plough, and receiving honoraria from Merck. Dr. Leachman reported no relevant financial disclosures.
In an accompanying editorial, Dr. Vernon K. Sondak and Dr. Sancy A.
Leachman wrote that the findings of Dr. Turner and colleagues "have
begun to move us down the path toward data-driven, personalized
follow-up guidelines."
This path is an important one, because in
the current era of personalized medicine, too little attention has been
paid to personalizing follow-up for patients after curative treatment of
cancer, including localized cutaneous melanoma, they noted (J. Clin.
Oncol. 2011 Nov. 7 [doi:10.1200/JCO.2011.37.6681]).
Success,
however, will require new partnerships and collaborations. Specifically,
the ultimate solution should involve shared follow-up with physicians
in the community, as well as with the patient and the patient’s family,
through education designed to maximize their ability to identify
recurrent and new melanomas.
Shared follow-up with local
dermatologists of patients with melanoma would address the goal of
detecting recurrences and new primary melanomas while simultaneously
decreasing the frequency of visits to surgical or medical oncologists.
Focusing
the lens of personalized medicine onto follow-up strategies, and
pursuing new partnerships and collaborations, will provide "a golden
opportunity to deliver the right care to the right patients at the right
time and in the right place," they concluded.
Dr. Sondak is with the Moffitt Cancer Center and the University of South Florida, Tampa. Dr. Leachman is with the Huntsman Cancer Institute and the University of Utah, Salt Lake City. Dr. Sondak reported serving as a consultant or adviser to Merck/Schering Plough, and receiving honoraria from Merck. Dr. Leachman reported no relevant financial disclosures.
In an accompanying editorial, Dr. Vernon K. Sondak and Dr. Sancy A.
Leachman wrote that the findings of Dr. Turner and colleagues "have
begun to move us down the path toward data-driven, personalized
follow-up guidelines."
This path is an important one, because in
the current era of personalized medicine, too little attention has been
paid to personalizing follow-up for patients after curative treatment of
cancer, including localized cutaneous melanoma, they noted (J. Clin.
Oncol. 2011 Nov. 7 [doi:10.1200/JCO.2011.37.6681]).
Success,
however, will require new partnerships and collaborations. Specifically,
the ultimate solution should involve shared follow-up with physicians
in the community, as well as with the patient and the patient’s family,
through education designed to maximize their ability to identify
recurrent and new melanomas.
Shared follow-up with local
dermatologists of patients with melanoma would address the goal of
detecting recurrences and new primary melanomas while simultaneously
decreasing the frequency of visits to surgical or medical oncologists.
Focusing
the lens of personalized medicine onto follow-up strategies, and
pursuing new partnerships and collaborations, will provide "a golden
opportunity to deliver the right care to the right patients at the right
time and in the right place," they concluded.
Dr. Sondak is with the Moffitt Cancer Center and the University of South Florida, Tampa. Dr. Leachman is with the Huntsman Cancer Institute and the University of Utah, Salt Lake City. Dr. Sondak reported serving as a consultant or adviser to Merck/Schering Plough, and receiving honoraria from Merck. Dr. Leachman reported no relevant financial disclosures.
A novel, less-intensive monitoring schedule for patients with localized primary cutaneous melanoma appears to reduce follow-up visits without affecting the rate of detection of new primary or recurrent melanomas, according to an analysis of data from an inception cohort of 3,081 patients.
Given that follow-up care for melanoma patients in the United States costs up to $500 million per year, the findings could have important implications for cost savings, according to Robin M. Turner, Ph.D., and colleagues.
Using data from the Melanoma Institute Australia on the inception cohort, which included consecutive patients with stage I or II melanoma first diagnosed between January 1985 and December 2009, the investigators modeled the delay in diagnosis of a new primary melanoma or recurrence with two different monitoring schedules.
Schedule one was based on 2008 Australian and New Zealand guidelines, which recommend follow-up every 6 months for 5 years, then annually for 5 years for patients with stage 1A and 1B disease, or every 3 months for 5 years, then annually for 5 years in patients with stages IIA, IIB, or IIC.
Schedule two, the novel monitoring arm, called for annual follow-up for 10 years for patients with stage I disease; every 6 months for 2 years, and then annually for 8 years, for patients with stage IIA disease; and every 4 months for 2 years, every 6 months in year 3, and then annually for 5 years, for patients with stages IIB and IIC disease.
Within 10 years, the total number of recurrences was 229 for every 1,000 patients, and the number of new primary melanomas was 61 for every 1,000 patients.
Compared with the 2008 Australia and New Zealand guidelines for monitoring, the novel schedule, which required almost 3,000 fewer visits per 1,000 patients (8,044 vs. 5,221 visits), resulted in a delay in the detection – by at least 2 months – of an additional 44.9 recurrences per 1,000 patients, and an additional 9.6 new primary melanomas, Robin M. Turner, Ph.D., of the School of Public Health at the University of Sydney, Australia, and colleagues reported online in the Journal of Clinical Oncology (2011 Nov. 7 [doi:10.1200/JCO.2010.34.2956]).
"If we assume self-detection rates based on published estimates [75% for recurrence and 50% for new primary], use of schedule two rather than schedule one results in only a small number of additional patients experiencing a delay in recurrence diagnosis (up to [a] maximum of 3 months; extra 11.3 patients per 1,000 with delay [greater than] 2 months) and even fewer experiencing a delay in new primary diagnosis (up to [a] maximum of 6 months; extra 4.9 per 1,000)," the investigators wrote.
Moreover, if there were no patients lost to follow-up and they attended all visits until diagnosis or 10 years, the total number of visits for schedule one would be 19,546, compared with 12,303 for schedule two.
"Not only would these fewer monitoring visits reduce the burden on patients in terms of time and expense in attendance and possible unnecessary anxiety, but they would also represent substantial savings for the health care system," the investigators wrote.
They also found that the risk of recurrence was greatest in the first year of follow-up; that the most important predictor of recurrence was American Joint Committee on Cancer substage (hazard ratios of 1, 1.12, 0.56, 0.70, and 0.95 for stages IA, IB, IIA, IIB, and IIC, respectively); and that the most important predictors of new primary melanomas were age and date of primary diagnosis after 1992 (hazard ratios of 1.29 and 2.21, respectively).
This study was supported by grants from the Australian National Health and Medical Research Council. The investigators said they had no relevant financial disclosures.
A novel, less-intensive monitoring schedule for patients with localized primary cutaneous melanoma appears to reduce follow-up visits without affecting the rate of detection of new primary or recurrent melanomas, according to an analysis of data from an inception cohort of 3,081 patients.
Given that follow-up care for melanoma patients in the United States costs up to $500 million per year, the findings could have important implications for cost savings, according to Robin M. Turner, Ph.D., and colleagues.
Using data from the Melanoma Institute Australia on the inception cohort, which included consecutive patients with stage I or II melanoma first diagnosed between January 1985 and December 2009, the investigators modeled the delay in diagnosis of a new primary melanoma or recurrence with two different monitoring schedules.
Schedule one was based on 2008 Australian and New Zealand guidelines, which recommend follow-up every 6 months for 5 years, then annually for 5 years for patients with stage 1A and 1B disease, or every 3 months for 5 years, then annually for 5 years in patients with stages IIA, IIB, or IIC.
Schedule two, the novel monitoring arm, called for annual follow-up for 10 years for patients with stage I disease; every 6 months for 2 years, and then annually for 8 years, for patients with stage IIA disease; and every 4 months for 2 years, every 6 months in year 3, and then annually for 5 years, for patients with stages IIB and IIC disease.
Within 10 years, the total number of recurrences was 229 for every 1,000 patients, and the number of new primary melanomas was 61 for every 1,000 patients.
Compared with the 2008 Australia and New Zealand guidelines for monitoring, the novel schedule, which required almost 3,000 fewer visits per 1,000 patients (8,044 vs. 5,221 visits), resulted in a delay in the detection – by at least 2 months – of an additional 44.9 recurrences per 1,000 patients, and an additional 9.6 new primary melanomas, Robin M. Turner, Ph.D., of the School of Public Health at the University of Sydney, Australia, and colleagues reported online in the Journal of Clinical Oncology (2011 Nov. 7 [doi:10.1200/JCO.2010.34.2956]).
"If we assume self-detection rates based on published estimates [75% for recurrence and 50% for new primary], use of schedule two rather than schedule one results in only a small number of additional patients experiencing a delay in recurrence diagnosis (up to [a] maximum of 3 months; extra 11.3 patients per 1,000 with delay [greater than] 2 months) and even fewer experiencing a delay in new primary diagnosis (up to [a] maximum of 6 months; extra 4.9 per 1,000)," the investigators wrote.
Moreover, if there were no patients lost to follow-up and they attended all visits until diagnosis or 10 years, the total number of visits for schedule one would be 19,546, compared with 12,303 for schedule two.
"Not only would these fewer monitoring visits reduce the burden on patients in terms of time and expense in attendance and possible unnecessary anxiety, but they would also represent substantial savings for the health care system," the investigators wrote.
They also found that the risk of recurrence was greatest in the first year of follow-up; that the most important predictor of recurrence was American Joint Committee on Cancer substage (hazard ratios of 1, 1.12, 0.56, 0.70, and 0.95 for stages IA, IB, IIA, IIB, and IIC, respectively); and that the most important predictors of new primary melanomas were age and date of primary diagnosis after 1992 (hazard ratios of 1.29 and 2.21, respectively).
This study was supported by grants from the Australian National Health and Medical Research Council. The investigators said they had no relevant financial disclosures.
FROM THE JOURNAL OF CLINICAL ONCOLOGY
Major Finding: Compared with the 2008 Australia and New Zealand guidelines for monitoring, the novel schedule, which required almost 3,000 fewer visits per 1,000 patients (8,044 vs. 5,221), resulted in a delay in the detection – by at least 2 months – of an additional 44.9 recurrences per 1,000 patients, and an additional 9.6 new primary melanomas.
Data Source: An analysis of data from an inception cohort of more than 3,081 patients with stage I or II melanoma.
Disclosures: This study was supported by grants from the Australian National Health and Medical Research Council. The authors said they had no relevant financial disclosures.