User login
Atopic dermatitis treated with experimental microbial therapy
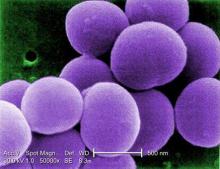
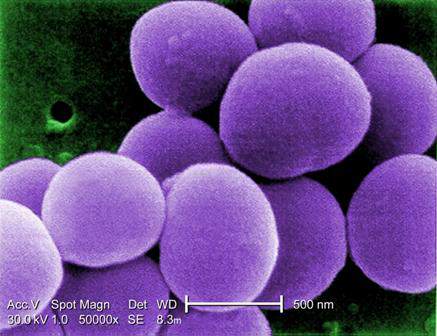
HOUSTON – New science suggests that the skin microbial environment may be manipulated in patients with atopic dermatitis in a way that could quell overgrowth of Staphylococcus aureus – meaning that the first microbiome-based therapies for AD might not be far away.
Dr. Richard L. Gallo, professor of medicine and pediatrics at the University of California, San Diego, described preliminary findings that the skin microbiome functions differently in patients with AD than in those without.
Dr. Gallo and his colleagues took skin sloughs from 50 AD patients and 30 non-AD controls. Most of the Staphylococcus aureus bacteria on sloughs from AD patients were alive, while most were dead on sloughs from patients without AD. Normal subjects had skin biomes that were able to kill S. aureus, Dr. Gallo said in a plenary talk at the annual meeting of the American Academy of Allergy, Asthma, and Immunology.
The investigators looked at the few species of normally occurring skin bacteria that can kill S. aureus, focusing on Staphylococcus hominis, which, they found, produces an antimicrobial peptide very effective against S. aureus. After mouse experiments showed S. hominis effective against S. aureus infection, Dr. Gallo and his colleagues began investigating its activity in a human patient. They isolated S. hominis from the skin of a patient, cultured it, and applied it in a topical cream. The result was a 1,000-fold drop in S. aureus colonization in the same patient. Dr. Gallo did not say how long the effect lasted or whether clinical symptoms abated.
“The pharmaceutical industry has been looking for antimicrobials in the jungles and the deep sea,” Dr. Gallo said. “We just swabbed an arm and found one that was really effective.” The findings suggest, he said, that “perhaps there are some therapeutic opportunities using the skin microbiome that aren’t 5 years away.” He added that his team has funding from NIH to continue this work as well as for a larger study using a similar approach that will be applicable in larger populations.
Dr. Gallo also mentioned new research showing that the skin microbiome goes quite a bit deeper than commonly understood, with immune-mediating bacteria found in the dermis and even the adipose layers. “We have to start thinking about skin in a different way,” he said. “These are not absolute barriers but highly evolved filters that permit selected microbes to interact.” Dr. Gallo has received research support from Galderma and Bayer and is listed on several patents for potential therapies held by his institution.
HOUSTON – New science suggests that the skin microbial environment may be manipulated in patients with atopic dermatitis in a way that could quell overgrowth of Staphylococcus aureus – meaning that the first microbiome-based therapies for AD might not be far away.
Dr. Richard L. Gallo, professor of medicine and pediatrics at the University of California, San Diego, described preliminary findings that the skin microbiome functions differently in patients with AD than in those without.
Dr. Gallo and his colleagues took skin sloughs from 50 AD patients and 30 non-AD controls. Most of the Staphylococcus aureus bacteria on sloughs from AD patients were alive, while most were dead on sloughs from patients without AD. Normal subjects had skin biomes that were able to kill S. aureus, Dr. Gallo said in a plenary talk at the annual meeting of the American Academy of Allergy, Asthma, and Immunology.
The investigators looked at the few species of normally occurring skin bacteria that can kill S. aureus, focusing on Staphylococcus hominis, which, they found, produces an antimicrobial peptide very effective against S. aureus. After mouse experiments showed S. hominis effective against S. aureus infection, Dr. Gallo and his colleagues began investigating its activity in a human patient. They isolated S. hominis from the skin of a patient, cultured it, and applied it in a topical cream. The result was a 1,000-fold drop in S. aureus colonization in the same patient. Dr. Gallo did not say how long the effect lasted or whether clinical symptoms abated.
“The pharmaceutical industry has been looking for antimicrobials in the jungles and the deep sea,” Dr. Gallo said. “We just swabbed an arm and found one that was really effective.” The findings suggest, he said, that “perhaps there are some therapeutic opportunities using the skin microbiome that aren’t 5 years away.” He added that his team has funding from NIH to continue this work as well as for a larger study using a similar approach that will be applicable in larger populations.
Dr. Gallo also mentioned new research showing that the skin microbiome goes quite a bit deeper than commonly understood, with immune-mediating bacteria found in the dermis and even the adipose layers. “We have to start thinking about skin in a different way,” he said. “These are not absolute barriers but highly evolved filters that permit selected microbes to interact.” Dr. Gallo has received research support from Galderma and Bayer and is listed on several patents for potential therapies held by his institution.
HOUSTON – New science suggests that the skin microbial environment may be manipulated in patients with atopic dermatitis in a way that could quell overgrowth of Staphylococcus aureus – meaning that the first microbiome-based therapies for AD might not be far away.
Dr. Richard L. Gallo, professor of medicine and pediatrics at the University of California, San Diego, described preliminary findings that the skin microbiome functions differently in patients with AD than in those without.
Dr. Gallo and his colleagues took skin sloughs from 50 AD patients and 30 non-AD controls. Most of the Staphylococcus aureus bacteria on sloughs from AD patients were alive, while most were dead on sloughs from patients without AD. Normal subjects had skin biomes that were able to kill S. aureus, Dr. Gallo said in a plenary talk at the annual meeting of the American Academy of Allergy, Asthma, and Immunology.
The investigators looked at the few species of normally occurring skin bacteria that can kill S. aureus, focusing on Staphylococcus hominis, which, they found, produces an antimicrobial peptide very effective against S. aureus. After mouse experiments showed S. hominis effective against S. aureus infection, Dr. Gallo and his colleagues began investigating its activity in a human patient. They isolated S. hominis from the skin of a patient, cultured it, and applied it in a topical cream. The result was a 1,000-fold drop in S. aureus colonization in the same patient. Dr. Gallo did not say how long the effect lasted or whether clinical symptoms abated.
“The pharmaceutical industry has been looking for antimicrobials in the jungles and the deep sea,” Dr. Gallo said. “We just swabbed an arm and found one that was really effective.” The findings suggest, he said, that “perhaps there are some therapeutic opportunities using the skin microbiome that aren’t 5 years away.” He added that his team has funding from NIH to continue this work as well as for a larger study using a similar approach that will be applicable in larger populations.
Dr. Gallo also mentioned new research showing that the skin microbiome goes quite a bit deeper than commonly understood, with immune-mediating bacteria found in the dermis and even the adipose layers. “We have to start thinking about skin in a different way,” he said. “These are not absolute barriers but highly evolved filters that permit selected microbes to interact.” Dr. Gallo has received research support from Galderma and Bayer and is listed on several patents for potential therapies held by his institution.
AT 2015 AAAAI ANNUAL MEETING
Get the baby a dog: Infants’ gut biota seen to affect allergy risk
HOUSTON – The specific bacterial composition of infants’ gut biomes may be key to their developing or not developing allergic disease in early childhood, supporting what researchers called “a gut-airway axis” for allergic disease.
In preliminary, unpublished findings, Susan V. Lynch, Ph.D., of the department of medicine at the University of California, San Francisco, and her colleagues looked at stool samples from 298 infants aged between 0 and 11 months. They measured gut bacterial diversity, distribution, and richness at 1, 3, 6, 9, and 12 months. Gut bacteria diversified rapidly and steadily during this time, the researchers found.
"The dramatic diversification that occurs during the first year of life is the peak period of plasticity of microbial accumulation," Dr. Lynch said at the annual meeting of the American Academy of Allergy, Asthma, and Immunology. The composition of the gut microbiomes was significantly related to the age of the infants.
Dr. Lynch's group found that in infants less than 6 months of age gut biomes were dominated by Bifidobacteriaceae (70 infants), Enterobacteriaceae (49), or codominated by both (11). Gut composition related to the types of microbial exposures in the home and was affected by the presence or absence of furred pets, particularly dogs, Dr. Lynch said.
Infants without pets in the home were most likely to have a codominated biome, with a relative risk of multiple sensitization of 2.94 when compared with infants with a Bifidobacteriaeae biome and 2.06 compared with those with a Enterobacteriaceae-dominated biome.
“We asked is there a clinical correlate? Yes. That codominated community runs the highest risk of allergic disease development at age 2, having a significantly increased risk ratio, compared with either of the singly dominated communities,” Dr. Lynch said.
Moreover, the different bacterial profiles were responsible for observed differences in gut function. “We find very dramatic differences in carbohydrate and fatty acid metabolism in these communities for which atopy risk is highest,” Dr. Lynch said. “Perhaps the foundation for atopic development in childhood is associated with a compositionally distinct and highly dysfunctional neonatal gut.”
The potential for intervention is highest in the first year of life when the microbiome is most plastic, Dr. Lynch said; however, she declined to speculate what such interventions might amount to, noting that it was too early.
At the same talk, Dr. Erika Von Mutius, medical director of the asthma and allergy clinic at the University of Munich in Germany, described her work with children growing up on European farms, whom decades worth of studies have shown to have both higher diversity and frequency of microbial exposure and also lower risk of asthma and allergies than children raised in non-farm environments.
Dr. Von Mutius reported that her research group is beginning to pinpoint the protective microbes detected in these children’s’ environments and also their respiratory tracts.
A handful of organisms appear to work in concert as a microbial cocktail that predicts lower asthma and allergy rates. “What we’re seeing here is not the needle in the haystack, it’s not the one thing that will protect [from disease]. The question is, is the more the better, or is it like a soup, in which certain components are more important?’ We think it’s more like a soup,” she said.
The way in which these microbes work in the body to become protective is unknown, said Dr. Von Mutius, whose current research is looking at nose and throat samples from children. Dr. Von Mutius and her colleagues found more than fourfold more microbial diversity in farm children’s noses than their throats, though, she said, they did not yet understand why.
“The more diversity in the nose, the less asthma these children had,” she said, adding that it remained to be learned “whether you can do something in the nose to affect asthma” or whether lower respiratory and/or gut processes were key to mediating asthma risk. Dr. Lynch has received support or other funding from Second Genome, Janssen, Regeneron, and KaloBios. Dr. Von Mutius has received fees or support from ALK, Nestle, Airsonett, Protectimmun, and Novartis.
HOUSTON – The specific bacterial composition of infants’ gut biomes may be key to their developing or not developing allergic disease in early childhood, supporting what researchers called “a gut-airway axis” for allergic disease.
In preliminary, unpublished findings, Susan V. Lynch, Ph.D., of the department of medicine at the University of California, San Francisco, and her colleagues looked at stool samples from 298 infants aged between 0 and 11 months. They measured gut bacterial diversity, distribution, and richness at 1, 3, 6, 9, and 12 months. Gut bacteria diversified rapidly and steadily during this time, the researchers found.
"The dramatic diversification that occurs during the first year of life is the peak period of plasticity of microbial accumulation," Dr. Lynch said at the annual meeting of the American Academy of Allergy, Asthma, and Immunology. The composition of the gut microbiomes was significantly related to the age of the infants.
Dr. Lynch's group found that in infants less than 6 months of age gut biomes were dominated by Bifidobacteriaceae (70 infants), Enterobacteriaceae (49), or codominated by both (11). Gut composition related to the types of microbial exposures in the home and was affected by the presence or absence of furred pets, particularly dogs, Dr. Lynch said.
Infants without pets in the home were most likely to have a codominated biome, with a relative risk of multiple sensitization of 2.94 when compared with infants with a Bifidobacteriaeae biome and 2.06 compared with those with a Enterobacteriaceae-dominated biome.
“We asked is there a clinical correlate? Yes. That codominated community runs the highest risk of allergic disease development at age 2, having a significantly increased risk ratio, compared with either of the singly dominated communities,” Dr. Lynch said.
Moreover, the different bacterial profiles were responsible for observed differences in gut function. “We find very dramatic differences in carbohydrate and fatty acid metabolism in these communities for which atopy risk is highest,” Dr. Lynch said. “Perhaps the foundation for atopic development in childhood is associated with a compositionally distinct and highly dysfunctional neonatal gut.”
The potential for intervention is highest in the first year of life when the microbiome is most plastic, Dr. Lynch said; however, she declined to speculate what such interventions might amount to, noting that it was too early.
At the same talk, Dr. Erika Von Mutius, medical director of the asthma and allergy clinic at the University of Munich in Germany, described her work with children growing up on European farms, whom decades worth of studies have shown to have both higher diversity and frequency of microbial exposure and also lower risk of asthma and allergies than children raised in non-farm environments.
Dr. Von Mutius reported that her research group is beginning to pinpoint the protective microbes detected in these children’s’ environments and also their respiratory tracts.
A handful of organisms appear to work in concert as a microbial cocktail that predicts lower asthma and allergy rates. “What we’re seeing here is not the needle in the haystack, it’s not the one thing that will protect [from disease]. The question is, is the more the better, or is it like a soup, in which certain components are more important?’ We think it’s more like a soup,” she said.
The way in which these microbes work in the body to become protective is unknown, said Dr. Von Mutius, whose current research is looking at nose and throat samples from children. Dr. Von Mutius and her colleagues found more than fourfold more microbial diversity in farm children’s noses than their throats, though, she said, they did not yet understand why.
“The more diversity in the nose, the less asthma these children had,” she said, adding that it remained to be learned “whether you can do something in the nose to affect asthma” or whether lower respiratory and/or gut processes were key to mediating asthma risk. Dr. Lynch has received support or other funding from Second Genome, Janssen, Regeneron, and KaloBios. Dr. Von Mutius has received fees or support from ALK, Nestle, Airsonett, Protectimmun, and Novartis.
HOUSTON – The specific bacterial composition of infants’ gut biomes may be key to their developing or not developing allergic disease in early childhood, supporting what researchers called “a gut-airway axis” for allergic disease.
In preliminary, unpublished findings, Susan V. Lynch, Ph.D., of the department of medicine at the University of California, San Francisco, and her colleagues looked at stool samples from 298 infants aged between 0 and 11 months. They measured gut bacterial diversity, distribution, and richness at 1, 3, 6, 9, and 12 months. Gut bacteria diversified rapidly and steadily during this time, the researchers found.
"The dramatic diversification that occurs during the first year of life is the peak period of plasticity of microbial accumulation," Dr. Lynch said at the annual meeting of the American Academy of Allergy, Asthma, and Immunology. The composition of the gut microbiomes was significantly related to the age of the infants.
Dr. Lynch's group found that in infants less than 6 months of age gut biomes were dominated by Bifidobacteriaceae (70 infants), Enterobacteriaceae (49), or codominated by both (11). Gut composition related to the types of microbial exposures in the home and was affected by the presence or absence of furred pets, particularly dogs, Dr. Lynch said.
Infants without pets in the home were most likely to have a codominated biome, with a relative risk of multiple sensitization of 2.94 when compared with infants with a Bifidobacteriaeae biome and 2.06 compared with those with a Enterobacteriaceae-dominated biome.
“We asked is there a clinical correlate? Yes. That codominated community runs the highest risk of allergic disease development at age 2, having a significantly increased risk ratio, compared with either of the singly dominated communities,” Dr. Lynch said.
Moreover, the different bacterial profiles were responsible for observed differences in gut function. “We find very dramatic differences in carbohydrate and fatty acid metabolism in these communities for which atopy risk is highest,” Dr. Lynch said. “Perhaps the foundation for atopic development in childhood is associated with a compositionally distinct and highly dysfunctional neonatal gut.”
The potential for intervention is highest in the first year of life when the microbiome is most plastic, Dr. Lynch said; however, she declined to speculate what such interventions might amount to, noting that it was too early.
At the same talk, Dr. Erika Von Mutius, medical director of the asthma and allergy clinic at the University of Munich in Germany, described her work with children growing up on European farms, whom decades worth of studies have shown to have both higher diversity and frequency of microbial exposure and also lower risk of asthma and allergies than children raised in non-farm environments.
Dr. Von Mutius reported that her research group is beginning to pinpoint the protective microbes detected in these children’s’ environments and also their respiratory tracts.
A handful of organisms appear to work in concert as a microbial cocktail that predicts lower asthma and allergy rates. “What we’re seeing here is not the needle in the haystack, it’s not the one thing that will protect [from disease]. The question is, is the more the better, or is it like a soup, in which certain components are more important?’ We think it’s more like a soup,” she said.
The way in which these microbes work in the body to become protective is unknown, said Dr. Von Mutius, whose current research is looking at nose and throat samples from children. Dr. Von Mutius and her colleagues found more than fourfold more microbial diversity in farm children’s noses than their throats, though, she said, they did not yet understand why.
“The more diversity in the nose, the less asthma these children had,” she said, adding that it remained to be learned “whether you can do something in the nose to affect asthma” or whether lower respiratory and/or gut processes were key to mediating asthma risk. Dr. Lynch has received support or other funding from Second Genome, Janssen, Regeneron, and KaloBios. Dr. Von Mutius has received fees or support from ALK, Nestle, Airsonett, Protectimmun, and Novartis.
AT 2015 AAAAI ANNUAL MEETING
Childhood atopic dermatitis linked to central obesity, high BP
Pediatric atopic dermatitis was linked with key features of metabolic syndrome, including central obesity and high blood pressure, in a multicenter prospective case-control study.
Given the findings, clinicians should routinely measure body mass index and waist circumference in children with atopic dermatitis (AD), said Dr. Jonathan I. Silverberg of Northwestern University, Chicago, and his associates. “In addition, blood pressure should be assessed in children with moderate to severe AD, even those who are a healthy weight with moderate disease and who are not receiving systemic therapy.”
Past studies have linked AD with risk factors for metabolic syndrome, such as chronic inflammation and sleep and mental health problems. To further explore the link between AD and metabolic disease, Dr. Silverberg and his associates studied 132 children with active, moderate to severe AD and 143 healthy controls matched by sex and race/ethnicity (JAMA Dermatol. 2015;151;144-152).
Compared with controls, children with AD were significantly more likely to have BMI in at least the 97th percentile for age and sex (odds ratio, 2.64, P = .02), waist circumference in at least the 85th percentile (OR, 3.92, P = .005), and waist-to-height ratio of a least 0.5 (OR, 2.22; P = .02). Atopic dermatitis was linked with systolic blood pressure in at least the 90th percentile (OR, 2.06, P = .03), even after the researchers accounted for age, sex, race, use of cyclosporine or prednisone, BMI, and waist circumference. Those results conflict with a study in Japanese adults linking AD with low blood pressure, and indicate that more studies are need to confirm and characterize the association between blood pressure and AD, they said.
Dr. Silverberg and his associates did not record blood lipid levels, so they could not determine whether children met criteria for metabolic syndrome. They also measured blood pressure with a single reading, and the controls were significantly older than were the children with AD (P = .03).
The International Psoriasis Council supported the study. The authors reported having no relevant conflicts of interest.
Pediatric atopic dermatitis was linked with key features of metabolic syndrome, including central obesity and high blood pressure, in a multicenter prospective case-control study.
Given the findings, clinicians should routinely measure body mass index and waist circumference in children with atopic dermatitis (AD), said Dr. Jonathan I. Silverberg of Northwestern University, Chicago, and his associates. “In addition, blood pressure should be assessed in children with moderate to severe AD, even those who are a healthy weight with moderate disease and who are not receiving systemic therapy.”
Past studies have linked AD with risk factors for metabolic syndrome, such as chronic inflammation and sleep and mental health problems. To further explore the link between AD and metabolic disease, Dr. Silverberg and his associates studied 132 children with active, moderate to severe AD and 143 healthy controls matched by sex and race/ethnicity (JAMA Dermatol. 2015;151;144-152).
Compared with controls, children with AD were significantly more likely to have BMI in at least the 97th percentile for age and sex (odds ratio, 2.64, P = .02), waist circumference in at least the 85th percentile (OR, 3.92, P = .005), and waist-to-height ratio of a least 0.5 (OR, 2.22; P = .02). Atopic dermatitis was linked with systolic blood pressure in at least the 90th percentile (OR, 2.06, P = .03), even after the researchers accounted for age, sex, race, use of cyclosporine or prednisone, BMI, and waist circumference. Those results conflict with a study in Japanese adults linking AD with low blood pressure, and indicate that more studies are need to confirm and characterize the association between blood pressure and AD, they said.
Dr. Silverberg and his associates did not record blood lipid levels, so they could not determine whether children met criteria for metabolic syndrome. They also measured blood pressure with a single reading, and the controls were significantly older than were the children with AD (P = .03).
The International Psoriasis Council supported the study. The authors reported having no relevant conflicts of interest.
Pediatric atopic dermatitis was linked with key features of metabolic syndrome, including central obesity and high blood pressure, in a multicenter prospective case-control study.
Given the findings, clinicians should routinely measure body mass index and waist circumference in children with atopic dermatitis (AD), said Dr. Jonathan I. Silverberg of Northwestern University, Chicago, and his associates. “In addition, blood pressure should be assessed in children with moderate to severe AD, even those who are a healthy weight with moderate disease and who are not receiving systemic therapy.”
Past studies have linked AD with risk factors for metabolic syndrome, such as chronic inflammation and sleep and mental health problems. To further explore the link between AD and metabolic disease, Dr. Silverberg and his associates studied 132 children with active, moderate to severe AD and 143 healthy controls matched by sex and race/ethnicity (JAMA Dermatol. 2015;151;144-152).
Compared with controls, children with AD were significantly more likely to have BMI in at least the 97th percentile for age and sex (odds ratio, 2.64, P = .02), waist circumference in at least the 85th percentile (OR, 3.92, P = .005), and waist-to-height ratio of a least 0.5 (OR, 2.22; P = .02). Atopic dermatitis was linked with systolic blood pressure in at least the 90th percentile (OR, 2.06, P = .03), even after the researchers accounted for age, sex, race, use of cyclosporine or prednisone, BMI, and waist circumference. Those results conflict with a study in Japanese adults linking AD with low blood pressure, and indicate that more studies are need to confirm and characterize the association between blood pressure and AD, they said.
Dr. Silverberg and his associates did not record blood lipid levels, so they could not determine whether children met criteria for metabolic syndrome. They also measured blood pressure with a single reading, and the controls were significantly older than were the children with AD (P = .03).
The International Psoriasis Council supported the study. The authors reported having no relevant conflicts of interest.
Key clinical point: Childhood atopic dermatitis was associated with central obesity and high systolic blood pressure.
Major finding: Pediatric AD was linked with waist circumference in at least the 85th percentile (OR, 3.92, P = .005), waist-to-height ratio of a least 0.5 (OR, 2.22; P = .02), and systolic blood pressure in at least the 90th percentile for age, sex, and height (OR, 2.06, P = .03).
Data source: Case-control study of 132 children with moderate to severe active AD and 143 healthy controls.
Disclosures: The International Psoriasis Council supported the study. The authors declared no conflicts of interest.
Skin microbiota studies fill research gaps
Critical appraisal of studies involving skin microbiomes may lead to development of new treatments for skin diseases such as atopic dermatitis and psoriasis, according to David Sanchez, a student at Howard University College of Medicine in Washington, D.C., and his associates at Albert Einstein College of Medicine, New York.
Studies involving atopic dermatitis underscore the importance of robust immune function for the skin’s ability to effectively balance transient microbial intruders and resident skin commensals in chronic inflammatory diseases.
While studies involving microbiota in psoriasis have delivered conflicting results, they may provide an impetus for researchers to standardize biopsies when obtaining human skin microbial samples. Some evidence has emerged linking psoriatic arthritis to an introduction of antibiotics into a population.
“Underscoring the current crisis involving antimicrobial resistance, filling the gaps in our knowledge base concerning the microbiome’s role in skin disease may ultimately help reduce antimicrobial use in exchange for agents that help manipulate the composition of a patient’s microbiome,” the investigators wrote. Read the article online at Journal of Drugs in Dermatology (2015;14:127-30).
Critical appraisal of studies involving skin microbiomes may lead to development of new treatments for skin diseases such as atopic dermatitis and psoriasis, according to David Sanchez, a student at Howard University College of Medicine in Washington, D.C., and his associates at Albert Einstein College of Medicine, New York.
Studies involving atopic dermatitis underscore the importance of robust immune function for the skin’s ability to effectively balance transient microbial intruders and resident skin commensals in chronic inflammatory diseases.
While studies involving microbiota in psoriasis have delivered conflicting results, they may provide an impetus for researchers to standardize biopsies when obtaining human skin microbial samples. Some evidence has emerged linking psoriatic arthritis to an introduction of antibiotics into a population.
“Underscoring the current crisis involving antimicrobial resistance, filling the gaps in our knowledge base concerning the microbiome’s role in skin disease may ultimately help reduce antimicrobial use in exchange for agents that help manipulate the composition of a patient’s microbiome,” the investigators wrote. Read the article online at Journal of Drugs in Dermatology (2015;14:127-30).
Critical appraisal of studies involving skin microbiomes may lead to development of new treatments for skin diseases such as atopic dermatitis and psoriasis, according to David Sanchez, a student at Howard University College of Medicine in Washington, D.C., and his associates at Albert Einstein College of Medicine, New York.
Studies involving atopic dermatitis underscore the importance of robust immune function for the skin’s ability to effectively balance transient microbial intruders and resident skin commensals in chronic inflammatory diseases.
While studies involving microbiota in psoriasis have delivered conflicting results, they may provide an impetus for researchers to standardize biopsies when obtaining human skin microbial samples. Some evidence has emerged linking psoriatic arthritis to an introduction of antibiotics into a population.
“Underscoring the current crisis involving antimicrobial resistance, filling the gaps in our knowledge base concerning the microbiome’s role in skin disease may ultimately help reduce antimicrobial use in exchange for agents that help manipulate the composition of a patient’s microbiome,” the investigators wrote. Read the article online at Journal of Drugs in Dermatology (2015;14:127-30).
Teledermatology as effective as visits for atopic dermatitis management
Patients with atopic dermatitis who participated in a direct-access online model for delivering following-up care achieved equivalent improvements in disease severity compared with those whose disease was managed through in-person visits, according to a study of 156 children and adults published in JAMA Dermatology (doi:10.1001/jamadermatol.2014.2299).
As assessed by patient-oriented eczema measure (POEM) and investigator global assessment (IGA), patients in the direct-access online group whose disease was managed through the direct-access online model over the 12-month study period improved their POEM scores from a mean (SD) baseline of 13.04 (5.32) to 7.94 (4.55) at 12 months.
Dr. April W. Armstrong of the University of Colorado, Denver, and her associates noted that the direct-access online specialty-care delivery model used in the study could be used for other chronic conditions where regular access to specialists is critical to patient outcomes, such as psoriasis and wound management.
Read the entire article here.
Patients with atopic dermatitis who participated in a direct-access online model for delivering following-up care achieved equivalent improvements in disease severity compared with those whose disease was managed through in-person visits, according to a study of 156 children and adults published in JAMA Dermatology (doi:10.1001/jamadermatol.2014.2299).
As assessed by patient-oriented eczema measure (POEM) and investigator global assessment (IGA), patients in the direct-access online group whose disease was managed through the direct-access online model over the 12-month study period improved their POEM scores from a mean (SD) baseline of 13.04 (5.32) to 7.94 (4.55) at 12 months.
Dr. April W. Armstrong of the University of Colorado, Denver, and her associates noted that the direct-access online specialty-care delivery model used in the study could be used for other chronic conditions where regular access to specialists is critical to patient outcomes, such as psoriasis and wound management.
Read the entire article here.
Patients with atopic dermatitis who participated in a direct-access online model for delivering following-up care achieved equivalent improvements in disease severity compared with those whose disease was managed through in-person visits, according to a study of 156 children and adults published in JAMA Dermatology (doi:10.1001/jamadermatol.2014.2299).
As assessed by patient-oriented eczema measure (POEM) and investigator global assessment (IGA), patients in the direct-access online group whose disease was managed through the direct-access online model over the 12-month study period improved their POEM scores from a mean (SD) baseline of 13.04 (5.32) to 7.94 (4.55) at 12 months.
Dr. April W. Armstrong of the University of Colorado, Denver, and her associates noted that the direct-access online specialty-care delivery model used in the study could be used for other chronic conditions where regular access to specialists is critical to patient outcomes, such as psoriasis and wound management.
Read the entire article here.
Atopiclair cheap, effective for atopic dermatitis
Atopiclair, a nonsteroidal topical barrier cream, is more cost effective than regular emollients for mild to moderate pediatric atopic dermatitis, according to a cost-effectiveness study by Mark B.Y. Tang at the National Skin Centre in Singapore and his associates.
While Atopiclair performs slightly better than regular emollients for severe atopic dermatitis (AD), it was much more effective at treating mild and moderate AD, with 72% of patients clear of the disease, compared with only 22% of those using a regular emollient in an evaluation of published trials. Atopiclair also cost less in a study of 12 Asian countries, with high-income countries saving $786 per year, mid-income countries saving $500 per year, and low-income countries saving $289 per year.
“These results provide further insight into the use of [specialized nonsteroidal topical barrier-protection creams] in clinical practice and suggest that cost-effectiveness outcomes should be considered when evaluating treatment options for AD patients,” the investigators concluded.
Read the full article at the Journal of Drugs in Dermatology (2015;14:169-75).
Atopiclair, a nonsteroidal topical barrier cream, is more cost effective than regular emollients for mild to moderate pediatric atopic dermatitis, according to a cost-effectiveness study by Mark B.Y. Tang at the National Skin Centre in Singapore and his associates.
While Atopiclair performs slightly better than regular emollients for severe atopic dermatitis (AD), it was much more effective at treating mild and moderate AD, with 72% of patients clear of the disease, compared with only 22% of those using a regular emollient in an evaluation of published trials. Atopiclair also cost less in a study of 12 Asian countries, with high-income countries saving $786 per year, mid-income countries saving $500 per year, and low-income countries saving $289 per year.
“These results provide further insight into the use of [specialized nonsteroidal topical barrier-protection creams] in clinical practice and suggest that cost-effectiveness outcomes should be considered when evaluating treatment options for AD patients,” the investigators concluded.
Read the full article at the Journal of Drugs in Dermatology (2015;14:169-75).
Atopiclair, a nonsteroidal topical barrier cream, is more cost effective than regular emollients for mild to moderate pediatric atopic dermatitis, according to a cost-effectiveness study by Mark B.Y. Tang at the National Skin Centre in Singapore and his associates.
While Atopiclair performs slightly better than regular emollients for severe atopic dermatitis (AD), it was much more effective at treating mild and moderate AD, with 72% of patients clear of the disease, compared with only 22% of those using a regular emollient in an evaluation of published trials. Atopiclair also cost less in a study of 12 Asian countries, with high-income countries saving $786 per year, mid-income countries saving $500 per year, and low-income countries saving $289 per year.
“These results provide further insight into the use of [specialized nonsteroidal topical barrier-protection creams] in clinical practice and suggest that cost-effectiveness outcomes should be considered when evaluating treatment options for AD patients,” the investigators concluded.
Read the full article at the Journal of Drugs in Dermatology (2015;14:169-75).
Guideline clarifies first-line treatment for allergic rhinitis
First-line treatment for allergic rhinitis should include intranasal steroids, as well as less-sedating second-generation oral antihistamines for patients whose primary complaints are sneezing and itching, according to a new clinical practice guideline published online Feb. 2 in Otolaryngology–Head and Neck Surgery.
In contrast, sinonasal imaging should not be routine when patients first present with symptoms consistent with allergic rhinitis, and oral leukotriene receptor antagonists are not recommended as first-line therapy, said Dr. Michael D. Seidman of Henry Ford West Bloomfield (Mich.) Hospital and chair of the guideline working group, and his associates.
Dr. Seidman and a panel of 20 experts in otolaryngology, allergy and immunology, internal medicine, family medicine, pediatrics, sleep medicine, advanced practice nursing, complementary and alternative medicine, and consumer advocacy developed the new practice guideline to enable clinicians in all settings to improve patient care and reduce harmful or unnecessary variations in care for allergic rhinitis.
“The guideline is intended to focus on a limited number of quality improvement opportunities deemed most important by the working group and is not intended to be a comprehensive reference for diagnosing and managing allergic rhinitis,” the authors noted.
During the course of 1 year, the working group reviewed 1,605 randomized, controlled trials, 31 existing clinical practice guidelines, and 390 systematic reviews of the literature regarding allergic rhinitis in adults and children older than age 2 years. They then compiled 14 key recommendations that underwent extensive peer review, which have been published online and as a supplement to the February issue (Otolaryngol. Head Neck Surg. 2015;152:S1-S43).
In addition to the recommendations noted above, the guideline advises:
* Clinicians should diagnose allergic rhinitis when patients present with a history and physical exam consistent with the disorder (including clear rhinorrhea, nasal congestion, pale discoloration of the nasal mucosa, and red, watery eyes) plus symptoms of nasal congestion, runny nose, itchy nose, or sneezing.
* Clinicians should perform and interpret (or refer patients for) specific IgE allergy testing for allergic rhinitis that doesn’t respond to empiric treatment, or when the diagnosis is uncertain, or when identifying the specific causative allergen would allow targeted therapy.
* Clinicians should assess diagnosed patients for associated conditions such as asthma, atopic dermatitis, sleep-disordered breathing, conjunctivitis, rhinosinusitis, and otitis media, and should document that in the medical record.
* Clinicians should offer (or refer patients for) sublingual or subcutaneous immunotherapy when allergic rhinitis doesn’t respond adequately to pharmacologic therapy.
* Clinicians may advise avoidance of known allergens or controlling the patient’s environment by such measures as removing pets, using air filtration systems, using dust-mite–reducing covers for bedding, and using acaricides.
* Clinicians may offer intranasal antihistamines for patients with seasonal, perennial or episodic allergic rhinitis.*
* Clinicians may offer (or refer patients for) reduction of the inferior turbinates for patients who have nasal airway obstruction or enlarged turbinates.
* Clinicians may offer (or refer patient for) acupuncture if they are interested in nonpharmacologic therapy.
*Clinicians may offer combination pharmacologic therapy in patients with allergic rhinitis who have inadequate response to pharmacologic monotherapy.
The working group offered no recommendations concerning herbal therapy for allergic rhinitis, because of the limited literature on those substances and concern about their safety.
The full text of the guideline and its supporting data are available free of charge at www.entnet.org. In addition, an algorithm of the guideline’s action statements and a table of common allergic rhinitis clinical scenarios are available as quick reference guides for clinicians.
The American Academy of Otolaryngology–Head and Neck Surgery Foundation funded the guideline. Dr. Seidman reported being medical director of the Scientific Advisory Board of Visalus, founder of the Body Language Vitamin, and holder of six patents related to dietary supplements, aircraft, and middle ear and brain implants. His associates reported ties to Acclarent/Johnson/Johnson, FirstLine Medical, GlaxoSmithKline, Intersect, MEDA, Medtronic, Merck, Mylan, Novartis, TEVA, Transit of Venus, Sanofi, Sunovion Pharmaceuticals, and WellPoint.
*Correction, 2/18/2015: An earlier version of this story misstated the guideline for the use of intranasal antihistamines.
First-line treatment for allergic rhinitis should include intranasal steroids, as well as less-sedating second-generation oral antihistamines for patients whose primary complaints are sneezing and itching, according to a new clinical practice guideline published online Feb. 2 in Otolaryngology–Head and Neck Surgery.
In contrast, sinonasal imaging should not be routine when patients first present with symptoms consistent with allergic rhinitis, and oral leukotriene receptor antagonists are not recommended as first-line therapy, said Dr. Michael D. Seidman of Henry Ford West Bloomfield (Mich.) Hospital and chair of the guideline working group, and his associates.
Dr. Seidman and a panel of 20 experts in otolaryngology, allergy and immunology, internal medicine, family medicine, pediatrics, sleep medicine, advanced practice nursing, complementary and alternative medicine, and consumer advocacy developed the new practice guideline to enable clinicians in all settings to improve patient care and reduce harmful or unnecessary variations in care for allergic rhinitis.
“The guideline is intended to focus on a limited number of quality improvement opportunities deemed most important by the working group and is not intended to be a comprehensive reference for diagnosing and managing allergic rhinitis,” the authors noted.
During the course of 1 year, the working group reviewed 1,605 randomized, controlled trials, 31 existing clinical practice guidelines, and 390 systematic reviews of the literature regarding allergic rhinitis in adults and children older than age 2 years. They then compiled 14 key recommendations that underwent extensive peer review, which have been published online and as a supplement to the February issue (Otolaryngol. Head Neck Surg. 2015;152:S1-S43).
In addition to the recommendations noted above, the guideline advises:
* Clinicians should diagnose allergic rhinitis when patients present with a history and physical exam consistent with the disorder (including clear rhinorrhea, nasal congestion, pale discoloration of the nasal mucosa, and red, watery eyes) plus symptoms of nasal congestion, runny nose, itchy nose, or sneezing.
* Clinicians should perform and interpret (or refer patients for) specific IgE allergy testing for allergic rhinitis that doesn’t respond to empiric treatment, or when the diagnosis is uncertain, or when identifying the specific causative allergen would allow targeted therapy.
* Clinicians should assess diagnosed patients for associated conditions such as asthma, atopic dermatitis, sleep-disordered breathing, conjunctivitis, rhinosinusitis, and otitis media, and should document that in the medical record.
* Clinicians should offer (or refer patients for) sublingual or subcutaneous immunotherapy when allergic rhinitis doesn’t respond adequately to pharmacologic therapy.
* Clinicians may advise avoidance of known allergens or controlling the patient’s environment by such measures as removing pets, using air filtration systems, using dust-mite–reducing covers for bedding, and using acaricides.
* Clinicians may offer intranasal antihistamines for patients with seasonal, perennial or episodic allergic rhinitis.*
* Clinicians may offer (or refer patients for) reduction of the inferior turbinates for patients who have nasal airway obstruction or enlarged turbinates.
* Clinicians may offer (or refer patient for) acupuncture if they are interested in nonpharmacologic therapy.
*Clinicians may offer combination pharmacologic therapy in patients with allergic rhinitis who have inadequate response to pharmacologic monotherapy.
The working group offered no recommendations concerning herbal therapy for allergic rhinitis, because of the limited literature on those substances and concern about their safety.
The full text of the guideline and its supporting data are available free of charge at www.entnet.org. In addition, an algorithm of the guideline’s action statements and a table of common allergic rhinitis clinical scenarios are available as quick reference guides for clinicians.
The American Academy of Otolaryngology–Head and Neck Surgery Foundation funded the guideline. Dr. Seidman reported being medical director of the Scientific Advisory Board of Visalus, founder of the Body Language Vitamin, and holder of six patents related to dietary supplements, aircraft, and middle ear and brain implants. His associates reported ties to Acclarent/Johnson/Johnson, FirstLine Medical, GlaxoSmithKline, Intersect, MEDA, Medtronic, Merck, Mylan, Novartis, TEVA, Transit of Venus, Sanofi, Sunovion Pharmaceuticals, and WellPoint.
*Correction, 2/18/2015: An earlier version of this story misstated the guideline for the use of intranasal antihistamines.
First-line treatment for allergic rhinitis should include intranasal steroids, as well as less-sedating second-generation oral antihistamines for patients whose primary complaints are sneezing and itching, according to a new clinical practice guideline published online Feb. 2 in Otolaryngology–Head and Neck Surgery.
In contrast, sinonasal imaging should not be routine when patients first present with symptoms consistent with allergic rhinitis, and oral leukotriene receptor antagonists are not recommended as first-line therapy, said Dr. Michael D. Seidman of Henry Ford West Bloomfield (Mich.) Hospital and chair of the guideline working group, and his associates.
Dr. Seidman and a panel of 20 experts in otolaryngology, allergy and immunology, internal medicine, family medicine, pediatrics, sleep medicine, advanced practice nursing, complementary and alternative medicine, and consumer advocacy developed the new practice guideline to enable clinicians in all settings to improve patient care and reduce harmful or unnecessary variations in care for allergic rhinitis.
“The guideline is intended to focus on a limited number of quality improvement opportunities deemed most important by the working group and is not intended to be a comprehensive reference for diagnosing and managing allergic rhinitis,” the authors noted.
During the course of 1 year, the working group reviewed 1,605 randomized, controlled trials, 31 existing clinical practice guidelines, and 390 systematic reviews of the literature regarding allergic rhinitis in adults and children older than age 2 years. They then compiled 14 key recommendations that underwent extensive peer review, which have been published online and as a supplement to the February issue (Otolaryngol. Head Neck Surg. 2015;152:S1-S43).
In addition to the recommendations noted above, the guideline advises:
* Clinicians should diagnose allergic rhinitis when patients present with a history and physical exam consistent with the disorder (including clear rhinorrhea, nasal congestion, pale discoloration of the nasal mucosa, and red, watery eyes) plus symptoms of nasal congestion, runny nose, itchy nose, or sneezing.
* Clinicians should perform and interpret (or refer patients for) specific IgE allergy testing for allergic rhinitis that doesn’t respond to empiric treatment, or when the diagnosis is uncertain, or when identifying the specific causative allergen would allow targeted therapy.
* Clinicians should assess diagnosed patients for associated conditions such as asthma, atopic dermatitis, sleep-disordered breathing, conjunctivitis, rhinosinusitis, and otitis media, and should document that in the medical record.
* Clinicians should offer (or refer patients for) sublingual or subcutaneous immunotherapy when allergic rhinitis doesn’t respond adequately to pharmacologic therapy.
* Clinicians may advise avoidance of known allergens or controlling the patient’s environment by such measures as removing pets, using air filtration systems, using dust-mite–reducing covers for bedding, and using acaricides.
* Clinicians may offer intranasal antihistamines for patients with seasonal, perennial or episodic allergic rhinitis.*
* Clinicians may offer (or refer patients for) reduction of the inferior turbinates for patients who have nasal airway obstruction or enlarged turbinates.
* Clinicians may offer (or refer patient for) acupuncture if they are interested in nonpharmacologic therapy.
*Clinicians may offer combination pharmacologic therapy in patients with allergic rhinitis who have inadequate response to pharmacologic monotherapy.
The working group offered no recommendations concerning herbal therapy for allergic rhinitis, because of the limited literature on those substances and concern about their safety.
The full text of the guideline and its supporting data are available free of charge at www.entnet.org. In addition, an algorithm of the guideline’s action statements and a table of common allergic rhinitis clinical scenarios are available as quick reference guides for clinicians.
The American Academy of Otolaryngology–Head and Neck Surgery Foundation funded the guideline. Dr. Seidman reported being medical director of the Scientific Advisory Board of Visalus, founder of the Body Language Vitamin, and holder of six patents related to dietary supplements, aircraft, and middle ear and brain implants. His associates reported ties to Acclarent/Johnson/Johnson, FirstLine Medical, GlaxoSmithKline, Intersect, MEDA, Medtronic, Merck, Mylan, Novartis, TEVA, Transit of Venus, Sanofi, Sunovion Pharmaceuticals, and WellPoint.
*Correction, 2/18/2015: An earlier version of this story misstated the guideline for the use of intranasal antihistamines.
FROM OTOLARYNGOLOGY–HEAD AND NECK SURGERY
Key clinical point: First-line treatment for allergic rhinitis should include intranasal steroids and second-generation oral antihistamines, and should not include leukotriene receptor antagonists or sinonasal imaging studies.
Major finding: A panel of 20 experts took 1 year to review the literature and develop action items focusing on a limited number of quality improvement opportunities they deemed most important to improve patient care.
Data source: A review of 1,605 randomized, controlled trials, 31 sets of practice guidelines, and 390 systematic reviews regarding allergic rhinitis, and a compilation of 14 recommendations for managing the disorder.
Disclosures: The American Academy of Otolaryngology–Head and Neck Surgery Foundation funded the guideline. Dr. Seidman reported being medical director of the Scientific Advisory Board of Visalus, founder of the Body Language Vitamin, and holder of six patents related to dietary supplements, aircraft, and middle ear and brain implants. His associates reported ties to Acclarent/Johnson/Johnson, FirstLine Medical, GlaxoSmithKline, Intersect, MEDA, Medtronic, Merck, Mylan, Novartis, TEVA, Transit of Venus, Sanofi, Sunovion Pharmaceuticals, and WellPoint.
Early ANA could predict atopic dermatitis severity in children
Antinuclear antibodies tended to appear earlier in children with atopic dermatitis, according to Dr. Krista Ress of the University of Tartu (Estonia) and her associates.
The researchers compared 346 serum samples from children with active atopic dermatitis to samples from 117 controls with no known skin disease. Although there was no significant difference in the prevalence of antinuclear antibodies (ANA) between the atopic and control groups, the antibodies appeared significantly earlier in children with atopic dermatitis. ANA appeared in children with dermatitis as early as 2 years of age, compared with an average of 4.6 years of age in the control group. Overall ANA prevalence increased with age in both groups.
Active atopic dermatitis during a child’s early years could indicate a more severe form of the disease and could dispose patients toward earlier development of systemic autoreactivity, the researchers said.
Read the full article at the International Journal of Dermatology (Int. J. Dermatol. 2015;54:24-8).
Antinuclear antibodies tended to appear earlier in children with atopic dermatitis, according to Dr. Krista Ress of the University of Tartu (Estonia) and her associates.
The researchers compared 346 serum samples from children with active atopic dermatitis to samples from 117 controls with no known skin disease. Although there was no significant difference in the prevalence of antinuclear antibodies (ANA) between the atopic and control groups, the antibodies appeared significantly earlier in children with atopic dermatitis. ANA appeared in children with dermatitis as early as 2 years of age, compared with an average of 4.6 years of age in the control group. Overall ANA prevalence increased with age in both groups.
Active atopic dermatitis during a child’s early years could indicate a more severe form of the disease and could dispose patients toward earlier development of systemic autoreactivity, the researchers said.
Read the full article at the International Journal of Dermatology (Int. J. Dermatol. 2015;54:24-8).
Antinuclear antibodies tended to appear earlier in children with atopic dermatitis, according to Dr. Krista Ress of the University of Tartu (Estonia) and her associates.
The researchers compared 346 serum samples from children with active atopic dermatitis to samples from 117 controls with no known skin disease. Although there was no significant difference in the prevalence of antinuclear antibodies (ANA) between the atopic and control groups, the antibodies appeared significantly earlier in children with atopic dermatitis. ANA appeared in children with dermatitis as early as 2 years of age, compared with an average of 4.6 years of age in the control group. Overall ANA prevalence increased with age in both groups.
Active atopic dermatitis during a child’s early years could indicate a more severe form of the disease and could dispose patients toward earlier development of systemic autoreactivity, the researchers said.
Read the full article at the International Journal of Dermatology (Int. J. Dermatol. 2015;54:24-8).
Systemic biologics might revolutionize the treatment of atopic dermatitis
The future looks bright for new atopic dermatitis treatments, according to Dr. Charles Ellis, a dermatology professor at the University of Michigan in Ann Arbor.
“I think we are at the point where we were with psoriasis some years ago; if you think back 15 years, we had methotrexate and that was about it” systemically for psoriasis, but then the biologics arrived. “We are at that point now” for atopic dermatitis, with biologics in the pipeline. “I think we’ve turned the corner,” Dr. Ellis said at the meeting sponsored by Global Academy for Medical Education.
It “should make a big difference for patients; there’s an unmet need for systemic treatments. The leading candidate is dupilumab; the data look good,” he said.
Trials of the human monoclonal antibody report that over 80% of patients achieve 50% reductions in Eczema Area and Severity Index scores, versus about a third with placebo (N. Engl. J. Med. 2014;371:130-9). Dupilumab is currently in phase III testing.
A Food and Drug Administration advisory panel recently and unanimously recommended approval of another human monoclonal antibody, secukinumab, for plaque psoriasis. “It could be useful in atopic dermatitis. It’s certainly something that we want to look into,” Dr. Ellis said.
Both agents are interleukin blockers, and more are in development, along with drugs and biologics with different targets.
Meanwhile, the phosphodiesterase inhibitor apremilast, approved by the FDA in 2014 for plaque psoriasis and psoriatic arthritis, is being studied for atopic dermatitis, although results aren’t due until 2016.
Overall, and at least with current treatments, “I think the main thing that we do” at the University of Michigan “is treat aggressively. When you treat aggressively, you show patients that the therapy works, so they are much more likely to use it,” Dr. Ellis said.
One-percent hydrocortisone cream is the strongest thing that a lot of patients have tried by the time they walk through the doors in Ann Arbor; many are close to losing hope in medical treatment.
Because of that, “we are more likely to use higher-potency topical corticosteroids, and use them more often and under occlusion. We are very likely to try triamcinolone in children and sometimes even more potent corticosteroids in adults. We [also] use a fair amount of methotrexate.” The heightened approach can “make a big difference,” he said.
Customer service is another focus at the university. If patients or parents feel better about their visits – not just with the doctor, but from their appointment phone calls right through to their checkouts – they are more likely to stick with treatments.
Dr. Ellis leads a service excellence program to train physicians, nurses, and ancillary staff to ensure that visits go well and patient needs are met. It’s “similar to what you might find in a fancy hotel chain,” and has proven itself with high patient satisfaction scores, he said.
A thorough history is part of good customer service. One thing to pay attention to is calcium channel blocker and thiazide use in older patients.
Both can cause chronic eczematous eruptions that look like atopic dermatitis, and elderly people might have been on the drugs for so long that the relationship with skin problems is easy to miss.
“If you haven’t contemplated particularly calcium channel blockers as a potential cause, you might not give patients a chance to go off them for a while to see if it helps,” he said.
Global Academy and this news organization are owned by the same parent company.
Dr. Ellis is a consultant for Celgene, Ferndale, Otsuka, and Johnson & Johnson.
The future looks bright for new atopic dermatitis treatments, according to Dr. Charles Ellis, a dermatology professor at the University of Michigan in Ann Arbor.
“I think we are at the point where we were with psoriasis some years ago; if you think back 15 years, we had methotrexate and that was about it” systemically for psoriasis, but then the biologics arrived. “We are at that point now” for atopic dermatitis, with biologics in the pipeline. “I think we’ve turned the corner,” Dr. Ellis said at the meeting sponsored by Global Academy for Medical Education.
It “should make a big difference for patients; there’s an unmet need for systemic treatments. The leading candidate is dupilumab; the data look good,” he said.
Trials of the human monoclonal antibody report that over 80% of patients achieve 50% reductions in Eczema Area and Severity Index scores, versus about a third with placebo (N. Engl. J. Med. 2014;371:130-9). Dupilumab is currently in phase III testing.
A Food and Drug Administration advisory panel recently and unanimously recommended approval of another human monoclonal antibody, secukinumab, for plaque psoriasis. “It could be useful in atopic dermatitis. It’s certainly something that we want to look into,” Dr. Ellis said.
Both agents are interleukin blockers, and more are in development, along with drugs and biologics with different targets.
Meanwhile, the phosphodiesterase inhibitor apremilast, approved by the FDA in 2014 for plaque psoriasis and psoriatic arthritis, is being studied for atopic dermatitis, although results aren’t due until 2016.
Overall, and at least with current treatments, “I think the main thing that we do” at the University of Michigan “is treat aggressively. When you treat aggressively, you show patients that the therapy works, so they are much more likely to use it,” Dr. Ellis said.
One-percent hydrocortisone cream is the strongest thing that a lot of patients have tried by the time they walk through the doors in Ann Arbor; many are close to losing hope in medical treatment.
Because of that, “we are more likely to use higher-potency topical corticosteroids, and use them more often and under occlusion. We are very likely to try triamcinolone in children and sometimes even more potent corticosteroids in adults. We [also] use a fair amount of methotrexate.” The heightened approach can “make a big difference,” he said.
Customer service is another focus at the university. If patients or parents feel better about their visits – not just with the doctor, but from their appointment phone calls right through to their checkouts – they are more likely to stick with treatments.
Dr. Ellis leads a service excellence program to train physicians, nurses, and ancillary staff to ensure that visits go well and patient needs are met. It’s “similar to what you might find in a fancy hotel chain,” and has proven itself with high patient satisfaction scores, he said.
A thorough history is part of good customer service. One thing to pay attention to is calcium channel blocker and thiazide use in older patients.
Both can cause chronic eczematous eruptions that look like atopic dermatitis, and elderly people might have been on the drugs for so long that the relationship with skin problems is easy to miss.
“If you haven’t contemplated particularly calcium channel blockers as a potential cause, you might not give patients a chance to go off them for a while to see if it helps,” he said.
Global Academy and this news organization are owned by the same parent company.
Dr. Ellis is a consultant for Celgene, Ferndale, Otsuka, and Johnson & Johnson.
The future looks bright for new atopic dermatitis treatments, according to Dr. Charles Ellis, a dermatology professor at the University of Michigan in Ann Arbor.
“I think we are at the point where we were with psoriasis some years ago; if you think back 15 years, we had methotrexate and that was about it” systemically for psoriasis, but then the biologics arrived. “We are at that point now” for atopic dermatitis, with biologics in the pipeline. “I think we’ve turned the corner,” Dr. Ellis said at the meeting sponsored by Global Academy for Medical Education.
It “should make a big difference for patients; there’s an unmet need for systemic treatments. The leading candidate is dupilumab; the data look good,” he said.
Trials of the human monoclonal antibody report that over 80% of patients achieve 50% reductions in Eczema Area and Severity Index scores, versus about a third with placebo (N. Engl. J. Med. 2014;371:130-9). Dupilumab is currently in phase III testing.
A Food and Drug Administration advisory panel recently and unanimously recommended approval of another human monoclonal antibody, secukinumab, for plaque psoriasis. “It could be useful in atopic dermatitis. It’s certainly something that we want to look into,” Dr. Ellis said.
Both agents are interleukin blockers, and more are in development, along with drugs and biologics with different targets.
Meanwhile, the phosphodiesterase inhibitor apremilast, approved by the FDA in 2014 for plaque psoriasis and psoriatic arthritis, is being studied for atopic dermatitis, although results aren’t due until 2016.
Overall, and at least with current treatments, “I think the main thing that we do” at the University of Michigan “is treat aggressively. When you treat aggressively, you show patients that the therapy works, so they are much more likely to use it,” Dr. Ellis said.
One-percent hydrocortisone cream is the strongest thing that a lot of patients have tried by the time they walk through the doors in Ann Arbor; many are close to losing hope in medical treatment.
Because of that, “we are more likely to use higher-potency topical corticosteroids, and use them more often and under occlusion. We are very likely to try triamcinolone in children and sometimes even more potent corticosteroids in adults. We [also] use a fair amount of methotrexate.” The heightened approach can “make a big difference,” he said.
Customer service is another focus at the university. If patients or parents feel better about their visits – not just with the doctor, but from their appointment phone calls right through to their checkouts – they are more likely to stick with treatments.
Dr. Ellis leads a service excellence program to train physicians, nurses, and ancillary staff to ensure that visits go well and patient needs are met. It’s “similar to what you might find in a fancy hotel chain,” and has proven itself with high patient satisfaction scores, he said.
A thorough history is part of good customer service. One thing to pay attention to is calcium channel blocker and thiazide use in older patients.
Both can cause chronic eczematous eruptions that look like atopic dermatitis, and elderly people might have been on the drugs for so long that the relationship with skin problems is easy to miss.
“If you haven’t contemplated particularly calcium channel blockers as a potential cause, you might not give patients a chance to go off them for a while to see if it helps,” he said.
Global Academy and this news organization are owned by the same parent company.
Dr. Ellis is a consultant for Celgene, Ferndale, Otsuka, and Johnson & Johnson.
EXPERT ANALYSIS FROM THE CARIBBEAN DERMATOLOGY SYMPOSIUM
Adults with eczema face increased risk of fracture and bone or joint injuries
Eczema in adulthood is directly associated with an increase in incidence of injuries that cause physical limitations, particularly fracture, bone, and joint injuries, according to the results of a prospective study published online in JAMA Dermatology.
“The risk of bone fracture and other injury causing limitation in adults with eczema has been largely unexplored,” noted Dr. Nitin Garg and Dr. Jonathan I. Silverberg of Northwestern University in Chicago.
“Patients with eczema may be at risk of fracture given their use of systemic corticosteroids, which may decrease bone mineral density [and] therefore, studies describing the prevalence of fracture among adults with eczema are needed,” they added (JAMA Dermatol. 2015;151:33-41 [doi:10.1001/jamadermatol.2014.2098]).
Dr. Garg and Dr. Silverberg used data from the 2012 National Health Interview Survey, which was conducted by the National Center for Health Statistics, to create their prospective, questionnaire-based study. The final analysis included 34,500 adults aged 18-85 years. They controlled for factors such as age, sex, race, Hispanic origin, household income, highest level of household education, family structure, and whether or not the subject was born in the United States.
The prevalence of self-reported eczema or skin allergy was 7.2%, the prevalence of any limitation-causing injury was 2.0%, and any limitation-causing injury in the past 12 months among adults was 7.2%. A fracture and bone or joint injury (FBJI) causing limitation was reported by 1.5% of the study population and other types of injury causing limitation were reported by 0.6%. The prevalence of FBJI causing limitation increased gradually with age, to peak in subjects aged 50-69 years, decreasing thereafter.
In a logistic regression analysis, adults with eczema had a 44% increased risk of any injury causing limitation (adjusted odds ratio, 1.44), and a 67% increased risk of FBJI (aOR, 1.67).
Adults with eczema who also reported experiencing fatigue (aOR, 1.59; 95% CI, 1.16-2.19), daytime sleepiness (aOR, 1.81), or insomnia (aOR, 1.74) had higher rates of FBJI than individuals with sleep symptoms but no eczema. Adults with both eczema and psychiatric or behavioral disorders also were more likely to experience FBJI than individuals suffering from eczema alone, or individuals suffering from psychiatric and behavioral disorders, but not eczema.
“Taken together, these data suggest that adult eczema is a previously unrecognized risk factor for fracture and other injury, emphasizing the importance of developing safer and more effective clinical interventions for itch and sleep problems in eczema, as well as preventive measures for injury risk reduction in eczema,” wrote Dr. Garg and Dr. Silverberg. The authors reported no relevant financial disclosures.
Eczema in adulthood is directly associated with an increase in incidence of injuries that cause physical limitations, particularly fracture, bone, and joint injuries, according to the results of a prospective study published online in JAMA Dermatology.
“The risk of bone fracture and other injury causing limitation in adults with eczema has been largely unexplored,” noted Dr. Nitin Garg and Dr. Jonathan I. Silverberg of Northwestern University in Chicago.
“Patients with eczema may be at risk of fracture given their use of systemic corticosteroids, which may decrease bone mineral density [and] therefore, studies describing the prevalence of fracture among adults with eczema are needed,” they added (JAMA Dermatol. 2015;151:33-41 [doi:10.1001/jamadermatol.2014.2098]).
Dr. Garg and Dr. Silverberg used data from the 2012 National Health Interview Survey, which was conducted by the National Center for Health Statistics, to create their prospective, questionnaire-based study. The final analysis included 34,500 adults aged 18-85 years. They controlled for factors such as age, sex, race, Hispanic origin, household income, highest level of household education, family structure, and whether or not the subject was born in the United States.
The prevalence of self-reported eczema or skin allergy was 7.2%, the prevalence of any limitation-causing injury was 2.0%, and any limitation-causing injury in the past 12 months among adults was 7.2%. A fracture and bone or joint injury (FBJI) causing limitation was reported by 1.5% of the study population and other types of injury causing limitation were reported by 0.6%. The prevalence of FBJI causing limitation increased gradually with age, to peak in subjects aged 50-69 years, decreasing thereafter.
In a logistic regression analysis, adults with eczema had a 44% increased risk of any injury causing limitation (adjusted odds ratio, 1.44), and a 67% increased risk of FBJI (aOR, 1.67).
Adults with eczema who also reported experiencing fatigue (aOR, 1.59; 95% CI, 1.16-2.19), daytime sleepiness (aOR, 1.81), or insomnia (aOR, 1.74) had higher rates of FBJI than individuals with sleep symptoms but no eczema. Adults with both eczema and psychiatric or behavioral disorders also were more likely to experience FBJI than individuals suffering from eczema alone, or individuals suffering from psychiatric and behavioral disorders, but not eczema.
“Taken together, these data suggest that adult eczema is a previously unrecognized risk factor for fracture and other injury, emphasizing the importance of developing safer and more effective clinical interventions for itch and sleep problems in eczema, as well as preventive measures for injury risk reduction in eczema,” wrote Dr. Garg and Dr. Silverberg. The authors reported no relevant financial disclosures.
Eczema in adulthood is directly associated with an increase in incidence of injuries that cause physical limitations, particularly fracture, bone, and joint injuries, according to the results of a prospective study published online in JAMA Dermatology.
“The risk of bone fracture and other injury causing limitation in adults with eczema has been largely unexplored,” noted Dr. Nitin Garg and Dr. Jonathan I. Silverberg of Northwestern University in Chicago.
“Patients with eczema may be at risk of fracture given their use of systemic corticosteroids, which may decrease bone mineral density [and] therefore, studies describing the prevalence of fracture among adults with eczema are needed,” they added (JAMA Dermatol. 2015;151:33-41 [doi:10.1001/jamadermatol.2014.2098]).
Dr. Garg and Dr. Silverberg used data from the 2012 National Health Interview Survey, which was conducted by the National Center for Health Statistics, to create their prospective, questionnaire-based study. The final analysis included 34,500 adults aged 18-85 years. They controlled for factors such as age, sex, race, Hispanic origin, household income, highest level of household education, family structure, and whether or not the subject was born in the United States.
The prevalence of self-reported eczema or skin allergy was 7.2%, the prevalence of any limitation-causing injury was 2.0%, and any limitation-causing injury in the past 12 months among adults was 7.2%. A fracture and bone or joint injury (FBJI) causing limitation was reported by 1.5% of the study population and other types of injury causing limitation were reported by 0.6%. The prevalence of FBJI causing limitation increased gradually with age, to peak in subjects aged 50-69 years, decreasing thereafter.
In a logistic regression analysis, adults with eczema had a 44% increased risk of any injury causing limitation (adjusted odds ratio, 1.44), and a 67% increased risk of FBJI (aOR, 1.67).
Adults with eczema who also reported experiencing fatigue (aOR, 1.59; 95% CI, 1.16-2.19), daytime sleepiness (aOR, 1.81), or insomnia (aOR, 1.74) had higher rates of FBJI than individuals with sleep symptoms but no eczema. Adults with both eczema and psychiatric or behavioral disorders also were more likely to experience FBJI than individuals suffering from eczema alone, or individuals suffering from psychiatric and behavioral disorders, but not eczema.
“Taken together, these data suggest that adult eczema is a previously unrecognized risk factor for fracture and other injury, emphasizing the importance of developing safer and more effective clinical interventions for itch and sleep problems in eczema, as well as preventive measures for injury risk reduction in eczema,” wrote Dr. Garg and Dr. Silverberg. The authors reported no relevant financial disclosures.
FROM JAMA DERMATOLOGY
Key clinical point: Eczema in adulthood is associated with an increased risk of limitation-causing injuries.
Major finding: Adults with eczema had a 67% increased risk of fracture and bone or joint injury (FBJI) causing limitation (aOR 1.67).
Data source: Prospective, questionnaire-based, cohort study of 34,500 adults aged 18-85 years from the 2012 National Health Interview Survey.
Disclosures: The authors reported no financial conflicts of interest.