User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
Powered by CHEST Physician, Clinician Reviews, MDedge Family Medicine, Internal Medicine News, and The Journal of Clinical Outcomes Management.
Different OSA subtypes respond differently to therapy
Patients with obstructive sleep apnea can be grouped into distinct clinical subtypes that differ in response to positive airway pressure treatment, according to two studies published in the March issue of the journal Sleep.
In the first study, investigators evaluated whether patients in different clinical clusters responded differently to positive airway pressure (PAP) treatment. Authors identified 706 patients with moderate to severe obstructive sleep apnea (OSA) from the Icelandic Sleep Apnea Cohort. All patients completed a sleep study prior to starting PAP treatment, and completed questionnaires to assess symptoms. Patients were grouped into one of three clusters based on symptomatology: disturbed sleep, minimally symptomatic, or sleepy, wrote Grace W. Pien, MD, of the division of pulmonary and critical care medicine at Johns Hopkins University, Baltimore, and her coauthors.
Patients in the minimally symptomatic cluster reported symptoms at lower rates than patients in the other clusters at baseline, and they remained relatively asymptomatic at follow-up, the authors noted. By comparison, patients in the sleepy group reported the highest Epworth Sleepiness Scale scores at baseline (16.0 plus or minus 3.4), which fell by five points at follow-up (mean change, −5.3; 95% confidence interval, −5.8 to −4.8). Also, patients in the sleepy group reported higher rates of drowsy driving (37.8%) at baseline, which dropped to 8.1% at follow-up (odds ratio, 0.06; 95% CI, 0.03-0.14).
At baseline, the disturbed-sleep group reported mainly insomnia-related symptoms, including difficulty falling asleep (43.2%), waking often at night (90.8%), restless sleep (74.2%), and waking up early (62.3%). At follow-up, improvements in the frequency of insomnia-related symptoms ranged from 0.28 to 1.25 points, and Epworth Sleepiness Scale scores fell significantly (−2.06; 95% CI, −2.64 to −1.48). Reductions in the proportion of patients with insomnia symptoms ranged from 13.1% (OR, 0.35; 95% CI, 0.20-0.59) for difficulty falling asleep to 39.0% (OR, 0.08; 95% CI, 0.04-0.14) for restless sleep, Dr. Pien and her colleagues reported.
The results “demonstrate that although symptoms improved overall among each of the three clinical phenotypes of moderate to severe OSA, patterns of treatment response … varied based on initial clinical presentation,” the authors wrote. “Our findings underscore the need to consider initial OSA phenotype when designing future trials.”
In the second study, also published in Sleep, investigators confirmed the three clinical OSA subtypes previously identified in the Icelandic Sleep Apnea Cohort. In analysis of an international sample, they also expanded these clusters to include two additional disease subtypes. One of these subtypes consisted of patients with symptoms dominated by indications of upper airway obstruction. The other new subtype, sleepiness dominant OSA, included patients who had excessive sleepiness but no symptoms of upper airway obstruction.
The study authors performed a cluster analysis using data from 972 patients from the Sleep Apnea Global Interdisciplinary Consortium with moderate to severe OSA, with 215 of these patients being from Iceland.
In total, 688 (70.8%) patients were diagnosed using laboratory-based polysomnography and 284 (29.2%) with home-based sleep studies. Patients completed questionnaires related to symptoms including sleepiness, insomnia, sleep disturbance, abnormal behaviors during sleep, upper airway symptoms, and other symptoms such as headaches and excessive sweating, wrote Brendan T. Keenan, of the University of Pennsylvania, Philadelphia, and his coauthors.
In the Icelandic group, results identified 72 (33.5%) patients in the disturbed-sleep cluster, 62 (28.8%) in the minimally symptomatic cluster, and 81 (37.7%) in the excessively sleepy cluster, similar to prior research. The three subtypes were found in the international sample of patients as well, with 150 (19.8%) in the disturbed-sleep cluster, 306 (40.4%) in the minimally symptomatic cluster, and 301 (39.8%) in the excessively sleepy cluster.
“Overall, this study provides a novel approach to better characterize patients with OSA presenting at sleep clinics worldwide,” wrote the authors of the second study. “This information can help inform personalized medicine approaches to OSA treatment by allowing clinicians to focus interventions on the most relevant OSA symptoms and consequences within an individual patient.”
Both studies were funded by the National Institutes of Health.
SOURCES: Pien GW et al. Sleep. 2018 Mar. doi: 10.1093/sleep/zsx201; Keenan BT et al. Sleep. 2018 Mar. doi: 10.1093/sleep/zsx214.
The results of these studies “advance the personalization of sleep apnea care by validating distinct symptom-based groups that generalize across nations and assessing how members of these clinical phenotypes respond to therapy,” wrote Vishesh K. Kapur, MD, of the division of pulmonary, critical care and sleep medicine at the University of Washington, Seattle, in an editorial published in the March issue of Sleep (2018 Mar. doi: 10.1093/sleep/zsy042).
“Patients with OSA differ in their presenting symptoms,” he said, and future studies should aim to “elucidate whether the proposed phenotypes will enable a more personalized paradigm of sleep apnea care that results in better tailored and more effective care.”
Dr. Kapur did not report any relevant disclosures.
The results of these studies “advance the personalization of sleep apnea care by validating distinct symptom-based groups that generalize across nations and assessing how members of these clinical phenotypes respond to therapy,” wrote Vishesh K. Kapur, MD, of the division of pulmonary, critical care and sleep medicine at the University of Washington, Seattle, in an editorial published in the March issue of Sleep (2018 Mar. doi: 10.1093/sleep/zsy042).
“Patients with OSA differ in their presenting symptoms,” he said, and future studies should aim to “elucidate whether the proposed phenotypes will enable a more personalized paradigm of sleep apnea care that results in better tailored and more effective care.”
Dr. Kapur did not report any relevant disclosures.
The results of these studies “advance the personalization of sleep apnea care by validating distinct symptom-based groups that generalize across nations and assessing how members of these clinical phenotypes respond to therapy,” wrote Vishesh K. Kapur, MD, of the division of pulmonary, critical care and sleep medicine at the University of Washington, Seattle, in an editorial published in the March issue of Sleep (2018 Mar. doi: 10.1093/sleep/zsy042).
“Patients with OSA differ in their presenting symptoms,” he said, and future studies should aim to “elucidate whether the proposed phenotypes will enable a more personalized paradigm of sleep apnea care that results in better tailored and more effective care.”
Dr. Kapur did not report any relevant disclosures.
Patients with obstructive sleep apnea can be grouped into distinct clinical subtypes that differ in response to positive airway pressure treatment, according to two studies published in the March issue of the journal Sleep.
In the first study, investigators evaluated whether patients in different clinical clusters responded differently to positive airway pressure (PAP) treatment. Authors identified 706 patients with moderate to severe obstructive sleep apnea (OSA) from the Icelandic Sleep Apnea Cohort. All patients completed a sleep study prior to starting PAP treatment, and completed questionnaires to assess symptoms. Patients were grouped into one of three clusters based on symptomatology: disturbed sleep, minimally symptomatic, or sleepy, wrote Grace W. Pien, MD, of the division of pulmonary and critical care medicine at Johns Hopkins University, Baltimore, and her coauthors.
Patients in the minimally symptomatic cluster reported symptoms at lower rates than patients in the other clusters at baseline, and they remained relatively asymptomatic at follow-up, the authors noted. By comparison, patients in the sleepy group reported the highest Epworth Sleepiness Scale scores at baseline (16.0 plus or minus 3.4), which fell by five points at follow-up (mean change, −5.3; 95% confidence interval, −5.8 to −4.8). Also, patients in the sleepy group reported higher rates of drowsy driving (37.8%) at baseline, which dropped to 8.1% at follow-up (odds ratio, 0.06; 95% CI, 0.03-0.14).
At baseline, the disturbed-sleep group reported mainly insomnia-related symptoms, including difficulty falling asleep (43.2%), waking often at night (90.8%), restless sleep (74.2%), and waking up early (62.3%). At follow-up, improvements in the frequency of insomnia-related symptoms ranged from 0.28 to 1.25 points, and Epworth Sleepiness Scale scores fell significantly (−2.06; 95% CI, −2.64 to −1.48). Reductions in the proportion of patients with insomnia symptoms ranged from 13.1% (OR, 0.35; 95% CI, 0.20-0.59) for difficulty falling asleep to 39.0% (OR, 0.08; 95% CI, 0.04-0.14) for restless sleep, Dr. Pien and her colleagues reported.
The results “demonstrate that although symptoms improved overall among each of the three clinical phenotypes of moderate to severe OSA, patterns of treatment response … varied based on initial clinical presentation,” the authors wrote. “Our findings underscore the need to consider initial OSA phenotype when designing future trials.”
In the second study, also published in Sleep, investigators confirmed the three clinical OSA subtypes previously identified in the Icelandic Sleep Apnea Cohort. In analysis of an international sample, they also expanded these clusters to include two additional disease subtypes. One of these subtypes consisted of patients with symptoms dominated by indications of upper airway obstruction. The other new subtype, sleepiness dominant OSA, included patients who had excessive sleepiness but no symptoms of upper airway obstruction.
The study authors performed a cluster analysis using data from 972 patients from the Sleep Apnea Global Interdisciplinary Consortium with moderate to severe OSA, with 215 of these patients being from Iceland.
In total, 688 (70.8%) patients were diagnosed using laboratory-based polysomnography and 284 (29.2%) with home-based sleep studies. Patients completed questionnaires related to symptoms including sleepiness, insomnia, sleep disturbance, abnormal behaviors during sleep, upper airway symptoms, and other symptoms such as headaches and excessive sweating, wrote Brendan T. Keenan, of the University of Pennsylvania, Philadelphia, and his coauthors.
In the Icelandic group, results identified 72 (33.5%) patients in the disturbed-sleep cluster, 62 (28.8%) in the minimally symptomatic cluster, and 81 (37.7%) in the excessively sleepy cluster, similar to prior research. The three subtypes were found in the international sample of patients as well, with 150 (19.8%) in the disturbed-sleep cluster, 306 (40.4%) in the minimally symptomatic cluster, and 301 (39.8%) in the excessively sleepy cluster.
“Overall, this study provides a novel approach to better characterize patients with OSA presenting at sleep clinics worldwide,” wrote the authors of the second study. “This information can help inform personalized medicine approaches to OSA treatment by allowing clinicians to focus interventions on the most relevant OSA symptoms and consequences within an individual patient.”
Both studies were funded by the National Institutes of Health.
SOURCES: Pien GW et al. Sleep. 2018 Mar. doi: 10.1093/sleep/zsx201; Keenan BT et al. Sleep. 2018 Mar. doi: 10.1093/sleep/zsx214.
Patients with obstructive sleep apnea can be grouped into distinct clinical subtypes that differ in response to positive airway pressure treatment, according to two studies published in the March issue of the journal Sleep.
In the first study, investigators evaluated whether patients in different clinical clusters responded differently to positive airway pressure (PAP) treatment. Authors identified 706 patients with moderate to severe obstructive sleep apnea (OSA) from the Icelandic Sleep Apnea Cohort. All patients completed a sleep study prior to starting PAP treatment, and completed questionnaires to assess symptoms. Patients were grouped into one of three clusters based on symptomatology: disturbed sleep, minimally symptomatic, or sleepy, wrote Grace W. Pien, MD, of the division of pulmonary and critical care medicine at Johns Hopkins University, Baltimore, and her coauthors.
Patients in the minimally symptomatic cluster reported symptoms at lower rates than patients in the other clusters at baseline, and they remained relatively asymptomatic at follow-up, the authors noted. By comparison, patients in the sleepy group reported the highest Epworth Sleepiness Scale scores at baseline (16.0 plus or minus 3.4), which fell by five points at follow-up (mean change, −5.3; 95% confidence interval, −5.8 to −4.8). Also, patients in the sleepy group reported higher rates of drowsy driving (37.8%) at baseline, which dropped to 8.1% at follow-up (odds ratio, 0.06; 95% CI, 0.03-0.14).
At baseline, the disturbed-sleep group reported mainly insomnia-related symptoms, including difficulty falling asleep (43.2%), waking often at night (90.8%), restless sleep (74.2%), and waking up early (62.3%). At follow-up, improvements in the frequency of insomnia-related symptoms ranged from 0.28 to 1.25 points, and Epworth Sleepiness Scale scores fell significantly (−2.06; 95% CI, −2.64 to −1.48). Reductions in the proportion of patients with insomnia symptoms ranged from 13.1% (OR, 0.35; 95% CI, 0.20-0.59) for difficulty falling asleep to 39.0% (OR, 0.08; 95% CI, 0.04-0.14) for restless sleep, Dr. Pien and her colleagues reported.
The results “demonstrate that although symptoms improved overall among each of the three clinical phenotypes of moderate to severe OSA, patterns of treatment response … varied based on initial clinical presentation,” the authors wrote. “Our findings underscore the need to consider initial OSA phenotype when designing future trials.”
In the second study, also published in Sleep, investigators confirmed the three clinical OSA subtypes previously identified in the Icelandic Sleep Apnea Cohort. In analysis of an international sample, they also expanded these clusters to include two additional disease subtypes. One of these subtypes consisted of patients with symptoms dominated by indications of upper airway obstruction. The other new subtype, sleepiness dominant OSA, included patients who had excessive sleepiness but no symptoms of upper airway obstruction.
The study authors performed a cluster analysis using data from 972 patients from the Sleep Apnea Global Interdisciplinary Consortium with moderate to severe OSA, with 215 of these patients being from Iceland.
In total, 688 (70.8%) patients were diagnosed using laboratory-based polysomnography and 284 (29.2%) with home-based sleep studies. Patients completed questionnaires related to symptoms including sleepiness, insomnia, sleep disturbance, abnormal behaviors during sleep, upper airway symptoms, and other symptoms such as headaches and excessive sweating, wrote Brendan T. Keenan, of the University of Pennsylvania, Philadelphia, and his coauthors.
In the Icelandic group, results identified 72 (33.5%) patients in the disturbed-sleep cluster, 62 (28.8%) in the minimally symptomatic cluster, and 81 (37.7%) in the excessively sleepy cluster, similar to prior research. The three subtypes were found in the international sample of patients as well, with 150 (19.8%) in the disturbed-sleep cluster, 306 (40.4%) in the minimally symptomatic cluster, and 301 (39.8%) in the excessively sleepy cluster.
“Overall, this study provides a novel approach to better characterize patients with OSA presenting at sleep clinics worldwide,” wrote the authors of the second study. “This information can help inform personalized medicine approaches to OSA treatment by allowing clinicians to focus interventions on the most relevant OSA symptoms and consequences within an individual patient.”
Both studies were funded by the National Institutes of Health.
SOURCES: Pien GW et al. Sleep. 2018 Mar. doi: 10.1093/sleep/zsx201; Keenan BT et al. Sleep. 2018 Mar. doi: 10.1093/sleep/zsx214.
FROM SLEEP
Key clinical point: Obstructive sleep apnea patients can be grouped into distinct subtypes depending on disease presentation, and these clusters differ in their responses to positive air pressure treatment.
Major finding: Though improvements were seen in all groups, presentation and changes in symptoms varied widely across clusters; for instance, patients in the sleepy group reported the highest Epworth Sleepiness Scale scores at baseline (16.0 plus or minus 3.4), which fell by five points at follow-up (mean change, −5.3; 95% CI, −5.8 to −4.8); whereas the disturbed-sleep group reported mainly insomnia-related symptoms including difficulty falling asleep (43.2%), waking often at night (90.8%), restless sleep (74.2%), and waking up early (62.3%).
Study details: A study of 706 patients with moderate to severe OSA from the Icelandic Sleep Apnea Cohort, and a study of 972 patients from the Sleep Apnea Global Interdisciplinary Consortium with moderate to severe OSA.
Disclosures: Both studies were funded by the National Institutes of Health.
Sources: Pien GW et al. Sleep. 2018 Mar. doi: 10.1093/sleep/zsx201; Keenan B et al. Sleep. 2018 Mar. doi: 10.1093/sleep/zsx214.
Novel oral immunotherapy increased peanut tolerance in children, adults
ORLANDO – compared with those receiving placebo, according to research results.
Stacie M. Jones, MD, of the University of Arkansas and Arkansas Children’s Hospital, Little Rock, presented the late-breaking results from the pivotal PALISADE trial at the joint congress of the American Academy of Allergy, Asthma, and Immunology and the World Asthma Organization, in which Dr. Jones and her colleagues sought to examine the safety and efficacy of the novel oral immunotherapy AR101 for patients with peanut allergy.
At 12 months, 67% of patients who received AR101 tolerated 600 mg or more of peanut protein, compared with 4% of control patients (P less than .00001). The tolerance benefit for AR101 appeared to continue when the researchers evaluated 1,000 mg of peanut protein. A dose of 1,000 mg or more was tolerated by 50% of patients in the AR101 group, compared with 2.4% of patients in the control group (P less than .00001).
“Tolerance at 600 mg should indicate, not prove, but indicate that this therapy should be able to provide protection for the vast majority of individuals treated,” Dr. Jones said in an interview.
The majority of patients in the study experienced an adverse event; however, those who received AR101 experienced more events, and more events that were considered serious, she said. Patients in the treatment arm also experienced more treatment-related hypersensitivity, compared with patients in the placebo arm (14.5% vs. 3.2%), nearly all of which were mild to moderate.
It is important to note two key safety outcomes regarding AR101, Dr. Jones said. First, that one patient was diagnosed with eosinophilic esophagitis (EoE) during the study. “EoE has been a recurring theme with oral immunotherapy. Previous data showed EoE diagnoses in as many as 2%-5% of patients, and although one is certainly less than that, it is still important.”
Secondly, she pointed out that 6.7% of patients in the treatment group withdrew as a result of gastrointestinal adverse events. “This is a lower percentage than previously published data, but I don’t think you can understate this safety concern,” Dr. Jones said.
The efficacy of AR101 has prompted energy and hope for children with a peanut allergy. In the weeks following her presentation at AAAAI/WAO, Dr. Jones said she has been inundated with emails and calls from allergists asking for these data. However, she called for caution and patience, saying that it is important for the therapy to clear the appropriate steps in the process.
“This should not change clinical care that much in the next 12-18 months,” Dr. Jones said. “But it is very hopeful that this will be a new therapy on the market.”
The PALISADE trial was funded by Aimmune Therapeutics, and Dr. Jones reported holding an advisory board position for Aimmune Therapeutics, as well as having received other forms of support from biotech, pharmaceutical, and governmental organizations.
SOURCE: Jones SM et al. AAAAI/WAO Joint Congress, Abstract L6.
ORLANDO – compared with those receiving placebo, according to research results.
Stacie M. Jones, MD, of the University of Arkansas and Arkansas Children’s Hospital, Little Rock, presented the late-breaking results from the pivotal PALISADE trial at the joint congress of the American Academy of Allergy, Asthma, and Immunology and the World Asthma Organization, in which Dr. Jones and her colleagues sought to examine the safety and efficacy of the novel oral immunotherapy AR101 for patients with peanut allergy.
At 12 months, 67% of patients who received AR101 tolerated 600 mg or more of peanut protein, compared with 4% of control patients (P less than .00001). The tolerance benefit for AR101 appeared to continue when the researchers evaluated 1,000 mg of peanut protein. A dose of 1,000 mg or more was tolerated by 50% of patients in the AR101 group, compared with 2.4% of patients in the control group (P less than .00001).
“Tolerance at 600 mg should indicate, not prove, but indicate that this therapy should be able to provide protection for the vast majority of individuals treated,” Dr. Jones said in an interview.
The majority of patients in the study experienced an adverse event; however, those who received AR101 experienced more events, and more events that were considered serious, she said. Patients in the treatment arm also experienced more treatment-related hypersensitivity, compared with patients in the placebo arm (14.5% vs. 3.2%), nearly all of which were mild to moderate.
It is important to note two key safety outcomes regarding AR101, Dr. Jones said. First, that one patient was diagnosed with eosinophilic esophagitis (EoE) during the study. “EoE has been a recurring theme with oral immunotherapy. Previous data showed EoE diagnoses in as many as 2%-5% of patients, and although one is certainly less than that, it is still important.”
Secondly, she pointed out that 6.7% of patients in the treatment group withdrew as a result of gastrointestinal adverse events. “This is a lower percentage than previously published data, but I don’t think you can understate this safety concern,” Dr. Jones said.
The efficacy of AR101 has prompted energy and hope for children with a peanut allergy. In the weeks following her presentation at AAAAI/WAO, Dr. Jones said she has been inundated with emails and calls from allergists asking for these data. However, she called for caution and patience, saying that it is important for the therapy to clear the appropriate steps in the process.
“This should not change clinical care that much in the next 12-18 months,” Dr. Jones said. “But it is very hopeful that this will be a new therapy on the market.”
The PALISADE trial was funded by Aimmune Therapeutics, and Dr. Jones reported holding an advisory board position for Aimmune Therapeutics, as well as having received other forms of support from biotech, pharmaceutical, and governmental organizations.
SOURCE: Jones SM et al. AAAAI/WAO Joint Congress, Abstract L6.
ORLANDO – compared with those receiving placebo, according to research results.
Stacie M. Jones, MD, of the University of Arkansas and Arkansas Children’s Hospital, Little Rock, presented the late-breaking results from the pivotal PALISADE trial at the joint congress of the American Academy of Allergy, Asthma, and Immunology and the World Asthma Organization, in which Dr. Jones and her colleagues sought to examine the safety and efficacy of the novel oral immunotherapy AR101 for patients with peanut allergy.
At 12 months, 67% of patients who received AR101 tolerated 600 mg or more of peanut protein, compared with 4% of control patients (P less than .00001). The tolerance benefit for AR101 appeared to continue when the researchers evaluated 1,000 mg of peanut protein. A dose of 1,000 mg or more was tolerated by 50% of patients in the AR101 group, compared with 2.4% of patients in the control group (P less than .00001).
“Tolerance at 600 mg should indicate, not prove, but indicate that this therapy should be able to provide protection for the vast majority of individuals treated,” Dr. Jones said in an interview.
The majority of patients in the study experienced an adverse event; however, those who received AR101 experienced more events, and more events that were considered serious, she said. Patients in the treatment arm also experienced more treatment-related hypersensitivity, compared with patients in the placebo arm (14.5% vs. 3.2%), nearly all of which were mild to moderate.
It is important to note two key safety outcomes regarding AR101, Dr. Jones said. First, that one patient was diagnosed with eosinophilic esophagitis (EoE) during the study. “EoE has been a recurring theme with oral immunotherapy. Previous data showed EoE diagnoses in as many as 2%-5% of patients, and although one is certainly less than that, it is still important.”
Secondly, she pointed out that 6.7% of patients in the treatment group withdrew as a result of gastrointestinal adverse events. “This is a lower percentage than previously published data, but I don’t think you can understate this safety concern,” Dr. Jones said.
The efficacy of AR101 has prompted energy and hope for children with a peanut allergy. In the weeks following her presentation at AAAAI/WAO, Dr. Jones said she has been inundated with emails and calls from allergists asking for these data. However, she called for caution and patience, saying that it is important for the therapy to clear the appropriate steps in the process.
“This should not change clinical care that much in the next 12-18 months,” Dr. Jones said. “But it is very hopeful that this will be a new therapy on the market.”
The PALISADE trial was funded by Aimmune Therapeutics, and Dr. Jones reported holding an advisory board position for Aimmune Therapeutics, as well as having received other forms of support from biotech, pharmaceutical, and governmental organizations.
SOURCE: Jones SM et al. AAAAI/WAO Joint Congress, Abstract L6.
FROM AAAAI/WAO JOINT CONGRESS 2018
Key clinical point: A novel oral immunotherapy significantly improved peanut tolerance in children and adults with peanut allergy.
Major finding: Two-thirds of patients who received AR101 tolerated 600 mg or more of peanut protein, compared with 4% of patients who did not receive the novel oral immunotherapy.
Data source: The randomized, phase 3, double-blind, placebo-controlled PALISADE trial.
Disclosures: The study was funded by Aimmune Therapeutics. Dr. Jones reported holding an advisory board position with Aimmune Therapeutics.
Source: Jones SM et al. AAAAI/WAO Joint Congress, Abstract L6.
FDA wants data on role of flavored tobacco products in youth initiation
The Food and Drug Administration is seeking data on the role that flavors, including menthol, in tobacco products play in the initiation, use, and cessation of tobacco products, with an emphasis on how flavoring impacts young people.
“In the spirit of our commitment to preventing kids from using tobacco, we are taking a closer look at flavors in tobacco products to better understand their level of impact on youth initiation,” FDA Commissioner Scott Gottlieb, MD, said in statement. It is important “that we also explore how flavors, under a properly regulated framework that protects youth, may also be helping some currently addicted adult cigarette smokers switch to certain noncombustible forms of tobacco products.”
“Youth consistently report product flavoring as a leading reason for using tobacco products,” Dr. Gottlieb noted. “In fact, there is evidence indicating that youth tobacco users who reported their first tobacco was flavored had a higher prevalence of current tobacco product use, compared to youth whose product was not flavored.”
The advance notice calls for information across a number of areas, including the role of flavors other than tobacco in tobacco products; flavors and initiation and patterns of tobacco product use, particularly among youths and young adults; and flavors and cessation, dual-use, and relapse among current and former tobacco product users.
It also is seeking comment on whether standards should be set on tobacco flavoring, including whether there should a prohibition or restriction on flavors and to which types of products these standards should apply. The notice specifically asks about menthol and its role in cigarette initiation and whether limitations on menthol could lead to use of other tobacco products.
“Because almost 90% of adult smokers started smoking by the age of 18, it’s imperative we look at new ways we can ensure that kids don’t progress from experimentation to regular use,” Commissioner Gottlieb said.
The American Heart Association called the action “long overdue.”
“We encourage the FDA to quickly move beyond information gathering and develop a strong flavoring product standard,” CEO Nancy Brown said in a statement. “There is already clear evidence that flavored tobacco products, including menthol, harm the public health. To make it worse, fruit- and candy-flavored e-cigarettes, cigars, and other tobacco products are highly attractive to kids and make it more likely that they will take up this addiction.”
The action comes less than a week after FDA published an advance notice seeking information comments on reducing nicotine levels in cigarettes to help combat nicotine addiction.
The advance notice will be published March 21 in the Federal Register; comments will be accepted at www.regulations.gov for 90 days.
The Food and Drug Administration is seeking data on the role that flavors, including menthol, in tobacco products play in the initiation, use, and cessation of tobacco products, with an emphasis on how flavoring impacts young people.
“In the spirit of our commitment to preventing kids from using tobacco, we are taking a closer look at flavors in tobacco products to better understand their level of impact on youth initiation,” FDA Commissioner Scott Gottlieb, MD, said in statement. It is important “that we also explore how flavors, under a properly regulated framework that protects youth, may also be helping some currently addicted adult cigarette smokers switch to certain noncombustible forms of tobacco products.”
“Youth consistently report product flavoring as a leading reason for using tobacco products,” Dr. Gottlieb noted. “In fact, there is evidence indicating that youth tobacco users who reported their first tobacco was flavored had a higher prevalence of current tobacco product use, compared to youth whose product was not flavored.”
The advance notice calls for information across a number of areas, including the role of flavors other than tobacco in tobacco products; flavors and initiation and patterns of tobacco product use, particularly among youths and young adults; and flavors and cessation, dual-use, and relapse among current and former tobacco product users.
It also is seeking comment on whether standards should be set on tobacco flavoring, including whether there should a prohibition or restriction on flavors and to which types of products these standards should apply. The notice specifically asks about menthol and its role in cigarette initiation and whether limitations on menthol could lead to use of other tobacco products.
“Because almost 90% of adult smokers started smoking by the age of 18, it’s imperative we look at new ways we can ensure that kids don’t progress from experimentation to regular use,” Commissioner Gottlieb said.
The American Heart Association called the action “long overdue.”
“We encourage the FDA to quickly move beyond information gathering and develop a strong flavoring product standard,” CEO Nancy Brown said in a statement. “There is already clear evidence that flavored tobacco products, including menthol, harm the public health. To make it worse, fruit- and candy-flavored e-cigarettes, cigars, and other tobacco products are highly attractive to kids and make it more likely that they will take up this addiction.”
The action comes less than a week after FDA published an advance notice seeking information comments on reducing nicotine levels in cigarettes to help combat nicotine addiction.
The advance notice will be published March 21 in the Federal Register; comments will be accepted at www.regulations.gov for 90 days.
The Food and Drug Administration is seeking data on the role that flavors, including menthol, in tobacco products play in the initiation, use, and cessation of tobacco products, with an emphasis on how flavoring impacts young people.
“In the spirit of our commitment to preventing kids from using tobacco, we are taking a closer look at flavors in tobacco products to better understand their level of impact on youth initiation,” FDA Commissioner Scott Gottlieb, MD, said in statement. It is important “that we also explore how flavors, under a properly regulated framework that protects youth, may also be helping some currently addicted adult cigarette smokers switch to certain noncombustible forms of tobacco products.”
“Youth consistently report product flavoring as a leading reason for using tobacco products,” Dr. Gottlieb noted. “In fact, there is evidence indicating that youth tobacco users who reported their first tobacco was flavored had a higher prevalence of current tobacco product use, compared to youth whose product was not flavored.”
The advance notice calls for information across a number of areas, including the role of flavors other than tobacco in tobacco products; flavors and initiation and patterns of tobacco product use, particularly among youths and young adults; and flavors and cessation, dual-use, and relapse among current and former tobacco product users.
It also is seeking comment on whether standards should be set on tobacco flavoring, including whether there should a prohibition or restriction on flavors and to which types of products these standards should apply. The notice specifically asks about menthol and its role in cigarette initiation and whether limitations on menthol could lead to use of other tobacco products.
“Because almost 90% of adult smokers started smoking by the age of 18, it’s imperative we look at new ways we can ensure that kids don’t progress from experimentation to regular use,” Commissioner Gottlieb said.
The American Heart Association called the action “long overdue.”
“We encourage the FDA to quickly move beyond information gathering and develop a strong flavoring product standard,” CEO Nancy Brown said in a statement. “There is already clear evidence that flavored tobacco products, including menthol, harm the public health. To make it worse, fruit- and candy-flavored e-cigarettes, cigars, and other tobacco products are highly attractive to kids and make it more likely that they will take up this addiction.”
The action comes less than a week after FDA published an advance notice seeking information comments on reducing nicotine levels in cigarettes to help combat nicotine addiction.
The advance notice will be published March 21 in the Federal Register; comments will be accepted at www.regulations.gov for 90 days.
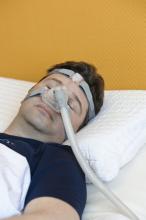
Effectiveness, adherence similar for nasal pillows and standard masks
according to results of a study.
In a retrospective observational study of 144 patients with obstructive sleep apnea, respiratory measures including apnea-hypopnea index (AHI), oxygen desaturation index, mean oxygen saturation, and Epworth Sleepiness scale scores did not differ between the two treatment groups at baseline and during a 12-month follow-up appointment. Treatment adherence was also similar between the two groups, reported Andrea Lanza of the Sleep Medicine Center at Niguarda Hospital in Milan, Italy, and coauthors in Sleep Medicine.
Patients received continuous positive airway pressure (CPAP) treatment between May 2012 and September 2014, and were assigned to one of two groups based on their choice of treatment. Initially, 102 opted for nasal pillows (Group P), and 42 chose the standard nasal mask (Group N). Patients who either changed masks or added a new one during titration or follow-up were assigned to a third group, Group C.
AHI did not differ significantly between groups at baseline or follow-up. In Group P, mean AHI at titration was 1.2 events per hour, compared with 1.8 in Group N and 1.9 in Group C (P = .109). At follow-up, AHI was 0.7 in Group P, 1.1 in Group N, and 0.9 in Group C (P = .172). Oxygen desaturation index and oxygen saturation also remained similar between the groups at baseline and follow-up, the investigators reported.
Additionally, long-term adherence did not differ significantly between the groups, with mean daily CPAP usage of 5.5 hours per night in Group P, 5.3 in Group N, and 5.6 in Group C. Mean usage was less than 4 hours per night for 11.6% in group P, 18.5% in group N, and 13.9% in group C, the authors added.
The frequency of side effects occurring in patients in two of the groups were similar (49% in Group P, vs. 61% in Group N; P = .212), though the nature of the side effects differed. Nostril pain or burning was reported only by patients in the nasal pillows group, and skin breakdown was reported only in the nasal mask group.
Though nasal pillows have typically been reserved for patients who do not tolerate the standard mask, the results of this study suggest that “nasal pillows could be safely prescribed as first-line interfaces,” the authors wrote. “They seem to be efficacious for CPAP titration and long-term treatment, ensuring a good rate of adherence.”
All of the authors reported having no disclosures.
SOURCE: Lanza A et al. Sleep Med. 2018 Jan;41:94-9
These results add to the body of evidence about the efficacy of nasal pillows and nasal masks. Future research should address the need for retitration when changing mask type, said Matthew R. Ebben, PhD, associate clinical professor at Cornell University, New York, in an editorial published with the study in Sleep Medicine.
“Many working in the field of sleep medicine continue to be unaware that differences in efficacy exist between mask styles, particularly in cases of moderate to severe obstructive sleep apnea,” he wrote.
“New clinical practice guidelines are needed to promote the necessity for PAP [positive airway pressure] retitration when changes in mask style are required,” he added. “Ensuring that PAP therapy is as effective as possible will reduce the need for patients and clinicians to investigate other treatment options for obstructive sleep apnea, which may be both less effective and have an inferior side effect profile compared to PAP treatment.”
These results add to the body of evidence about the efficacy of nasal pillows and nasal masks. Future research should address the need for retitration when changing mask type, said Matthew R. Ebben, PhD, associate clinical professor at Cornell University, New York, in an editorial published with the study in Sleep Medicine.
“Many working in the field of sleep medicine continue to be unaware that differences in efficacy exist between mask styles, particularly in cases of moderate to severe obstructive sleep apnea,” he wrote.
“New clinical practice guidelines are needed to promote the necessity for PAP [positive airway pressure] retitration when changes in mask style are required,” he added. “Ensuring that PAP therapy is as effective as possible will reduce the need for patients and clinicians to investigate other treatment options for obstructive sleep apnea, which may be both less effective and have an inferior side effect profile compared to PAP treatment.”
These results add to the body of evidence about the efficacy of nasal pillows and nasal masks. Future research should address the need for retitration when changing mask type, said Matthew R. Ebben, PhD, associate clinical professor at Cornell University, New York, in an editorial published with the study in Sleep Medicine.
“Many working in the field of sleep medicine continue to be unaware that differences in efficacy exist between mask styles, particularly in cases of moderate to severe obstructive sleep apnea,” he wrote.
“New clinical practice guidelines are needed to promote the necessity for PAP [positive airway pressure] retitration when changes in mask style are required,” he added. “Ensuring that PAP therapy is as effective as possible will reduce the need for patients and clinicians to investigate other treatment options for obstructive sleep apnea, which may be both less effective and have an inferior side effect profile compared to PAP treatment.”
according to results of a study.
In a retrospective observational study of 144 patients with obstructive sleep apnea, respiratory measures including apnea-hypopnea index (AHI), oxygen desaturation index, mean oxygen saturation, and Epworth Sleepiness scale scores did not differ between the two treatment groups at baseline and during a 12-month follow-up appointment. Treatment adherence was also similar between the two groups, reported Andrea Lanza of the Sleep Medicine Center at Niguarda Hospital in Milan, Italy, and coauthors in Sleep Medicine.
Patients received continuous positive airway pressure (CPAP) treatment between May 2012 and September 2014, and were assigned to one of two groups based on their choice of treatment. Initially, 102 opted for nasal pillows (Group P), and 42 chose the standard nasal mask (Group N). Patients who either changed masks or added a new one during titration or follow-up were assigned to a third group, Group C.
AHI did not differ significantly between groups at baseline or follow-up. In Group P, mean AHI at titration was 1.2 events per hour, compared with 1.8 in Group N and 1.9 in Group C (P = .109). At follow-up, AHI was 0.7 in Group P, 1.1 in Group N, and 0.9 in Group C (P = .172). Oxygen desaturation index and oxygen saturation also remained similar between the groups at baseline and follow-up, the investigators reported.
Additionally, long-term adherence did not differ significantly between the groups, with mean daily CPAP usage of 5.5 hours per night in Group P, 5.3 in Group N, and 5.6 in Group C. Mean usage was less than 4 hours per night for 11.6% in group P, 18.5% in group N, and 13.9% in group C, the authors added.
The frequency of side effects occurring in patients in two of the groups were similar (49% in Group P, vs. 61% in Group N; P = .212), though the nature of the side effects differed. Nostril pain or burning was reported only by patients in the nasal pillows group, and skin breakdown was reported only in the nasal mask group.
Though nasal pillows have typically been reserved for patients who do not tolerate the standard mask, the results of this study suggest that “nasal pillows could be safely prescribed as first-line interfaces,” the authors wrote. “They seem to be efficacious for CPAP titration and long-term treatment, ensuring a good rate of adherence.”
All of the authors reported having no disclosures.
SOURCE: Lanza A et al. Sleep Med. 2018 Jan;41:94-9
according to results of a study.
In a retrospective observational study of 144 patients with obstructive sleep apnea, respiratory measures including apnea-hypopnea index (AHI), oxygen desaturation index, mean oxygen saturation, and Epworth Sleepiness scale scores did not differ between the two treatment groups at baseline and during a 12-month follow-up appointment. Treatment adherence was also similar between the two groups, reported Andrea Lanza of the Sleep Medicine Center at Niguarda Hospital in Milan, Italy, and coauthors in Sleep Medicine.
Patients received continuous positive airway pressure (CPAP) treatment between May 2012 and September 2014, and were assigned to one of two groups based on their choice of treatment. Initially, 102 opted for nasal pillows (Group P), and 42 chose the standard nasal mask (Group N). Patients who either changed masks or added a new one during titration or follow-up were assigned to a third group, Group C.
AHI did not differ significantly between groups at baseline or follow-up. In Group P, mean AHI at titration was 1.2 events per hour, compared with 1.8 in Group N and 1.9 in Group C (P = .109). At follow-up, AHI was 0.7 in Group P, 1.1 in Group N, and 0.9 in Group C (P = .172). Oxygen desaturation index and oxygen saturation also remained similar between the groups at baseline and follow-up, the investigators reported.
Additionally, long-term adherence did not differ significantly between the groups, with mean daily CPAP usage of 5.5 hours per night in Group P, 5.3 in Group N, and 5.6 in Group C. Mean usage was less than 4 hours per night for 11.6% in group P, 18.5% in group N, and 13.9% in group C, the authors added.
The frequency of side effects occurring in patients in two of the groups were similar (49% in Group P, vs. 61% in Group N; P = .212), though the nature of the side effects differed. Nostril pain or burning was reported only by patients in the nasal pillows group, and skin breakdown was reported only in the nasal mask group.
Though nasal pillows have typically been reserved for patients who do not tolerate the standard mask, the results of this study suggest that “nasal pillows could be safely prescribed as first-line interfaces,” the authors wrote. “They seem to be efficacious for CPAP titration and long-term treatment, ensuring a good rate of adherence.”
All of the authors reported having no disclosures.
SOURCE: Lanza A et al. Sleep Med. 2018 Jan;41:94-9
FROM SLEEP MEDICINE
Key clinical point: Nasal pillows showed equal long-term efficacy as standard nasal masks in obstructive sleep apnea patients treated with continuous positive airway pressure.
Major finding: Long-term adherence did not differ significantly between the groups, with mean daily CPAP usage of 5.5 hours per night with nasal pillows and 5.3 hours per night with standard nasal masks; respiratory measures including AHI, oxygen desaturation index, and oxygen saturation also remained similar between the groups at baseline and follow-up.
Data source: A retrospective observational study of 144 OSA patients treated with nasal pillows or standard nasal masks.
Disclosures: All of the authors reported having no disclosures.
Source: Lanza A et al. Sleep Med. 2018 Jan. doi: 10.1016/j.sleep.2017/.08.024.
FDA proposes lower nicotine levels in cigarettes
Nicotine levels in cigarettes could see a significant reduction under regulatory options being considered by the Food and Drug Administration.
Cigarettes “are the only legal consumer product that, when used as intended, will kill half all long-term users,” FDA Commissioner Scott Gottlieb, MD, said in a statement announcing the effort.
The agency is seeking comment on a proposed regulation regarding “a potential maximum nicotine level that would be appropriate for the protection of public health, in light of scientific evidence about the addictive properties of nicotine in cigarettes.” An advance notice of proposed rule making was posted online March 15 and is scheduled for publication in the Federal Register on March 16.
The FDA also is seeking comments on a number of other areas to help inform potential regulatory action down the road, including whether a new standard for lower nicotine levels should be implemented at once or whether a phased-in approach should be taken; whether FDA should specify a method for manufacturers to use in order to detect nicotine levels in their products; and whether the proposed lower level is technically achievable.
The agency also is seeking comment on potential unintended effects of lowering the amount of nicotine in cigarettes, such as turning to other combustible tobacco products such as cigars in conjunction with or as a replacement for cigarette use; increasing the number of cigarettes smoked, or seeking comparable nicotine from noncombustible tobacco sources.
At this time, FDA is not suggesting what the target might be on a specific nicotine level. While the advanced notice asks specifically about the “merits of nicotine levels like 0.3, 0.4, and 0.5 mg nicotine/g of tobacco filler,” it is not suggesting that this is the range being considered.
[polldaddy:9960560]
“Not to prejudge any possible proposed rule that we would do or any possible level, that is the purpose of an advanced proposed rule making, but we share all the science that we are aware of, and we characterize the studies that have been done to date in trying to find out what that right level is,” Mitch Zeller, director of the FDA Center for Tobacco Products, said during a March 15 press call.
He said that the FDA aiming to make sure the level is low enough that it cannot be compensated for by smoking more or inhaling deeper and holding the breath in longer, much like how smokers compensated when they smoked “light” cigarettes in the unregulated market.
Mr. Zeller said that seeking comments on those levels is based on the scientific evidence that is laid out in the advanced notice, but it is not necessarily foreshadowing where the standard will be set.
Drastically reducing the amount of nicotine in cigarettes is expected to significantly lower not only the number of people addicted to cigarettes but also as the negative health effects of nicotine addiction, FDA experts wrote in a perspective piece published March 15 in the New England Journal of Medicine (doi: 10.1065/NEJMsr1714617).
“Our findings show that reducing the nicotine level in cigarettes has the potential to substantially reduce the enormous burden of smoking-related death and disease,” Benjamin J. Apelberg, PhD, director of the Division of Population Health Science, Office of Science, within the FDA Center for Tobacco Products, and his colleagues, wrote in the report.
Modeling for the implementation of a lower nicotine level policy suggests that smoking prevalence will decline from a median of 12.8% in baseline scenario to a median of 10.8% within a year of implementation, with the increase related to smoking cessation.
“We estimate that approximately 5 million additional smokers would quit smoking within a year after implementation of the hypothetical policy,” Dr. Apelberg and his colleagues wrote. “By 2060, smoking prevalence drops from 7.9% in the baseline scenario to 1.4% in the policy scenario.”
Their analysis is based on a nicotine level that is “so low that there would not be enough nicotine available in cigarette tobacco for smokers to sustain addiction,” they noted.
The FDA plans to release two more advanced notices of proposed rule making related to using regulatory levers to reduce cigarette smoking, including one that addresses flavoring in tobacco and one related to the regulation of premium cigars. Other than the 90-day comment period related to the advanced notices, the agency has not set any deadlines on when it will act.
“Legally, we are not going to prejudge how long this will take or what will happen,” Mr. Zeller said. “This is an early step in what could be a potential rule-making process using the product standard authority. We will take a long and hard look at all the comments that come in over the next 90 days and based upon our review of all the information, all the comments that come in, all the feedback that we have, we will then make a decision about taking the next step in the rule-making process.”
Nicotine levels in cigarettes could see a significant reduction under regulatory options being considered by the Food and Drug Administration.
Cigarettes “are the only legal consumer product that, when used as intended, will kill half all long-term users,” FDA Commissioner Scott Gottlieb, MD, said in a statement announcing the effort.
The agency is seeking comment on a proposed regulation regarding “a potential maximum nicotine level that would be appropriate for the protection of public health, in light of scientific evidence about the addictive properties of nicotine in cigarettes.” An advance notice of proposed rule making was posted online March 15 and is scheduled for publication in the Federal Register on March 16.
The FDA also is seeking comments on a number of other areas to help inform potential regulatory action down the road, including whether a new standard for lower nicotine levels should be implemented at once or whether a phased-in approach should be taken; whether FDA should specify a method for manufacturers to use in order to detect nicotine levels in their products; and whether the proposed lower level is technically achievable.
The agency also is seeking comment on potential unintended effects of lowering the amount of nicotine in cigarettes, such as turning to other combustible tobacco products such as cigars in conjunction with or as a replacement for cigarette use; increasing the number of cigarettes smoked, or seeking comparable nicotine from noncombustible tobacco sources.
At this time, FDA is not suggesting what the target might be on a specific nicotine level. While the advanced notice asks specifically about the “merits of nicotine levels like 0.3, 0.4, and 0.5 mg nicotine/g of tobacco filler,” it is not suggesting that this is the range being considered.
[polldaddy:9960560]
“Not to prejudge any possible proposed rule that we would do or any possible level, that is the purpose of an advanced proposed rule making, but we share all the science that we are aware of, and we characterize the studies that have been done to date in trying to find out what that right level is,” Mitch Zeller, director of the FDA Center for Tobacco Products, said during a March 15 press call.
He said that the FDA aiming to make sure the level is low enough that it cannot be compensated for by smoking more or inhaling deeper and holding the breath in longer, much like how smokers compensated when they smoked “light” cigarettes in the unregulated market.
Mr. Zeller said that seeking comments on those levels is based on the scientific evidence that is laid out in the advanced notice, but it is not necessarily foreshadowing where the standard will be set.
Drastically reducing the amount of nicotine in cigarettes is expected to significantly lower not only the number of people addicted to cigarettes but also as the negative health effects of nicotine addiction, FDA experts wrote in a perspective piece published March 15 in the New England Journal of Medicine (doi: 10.1065/NEJMsr1714617).
“Our findings show that reducing the nicotine level in cigarettes has the potential to substantially reduce the enormous burden of smoking-related death and disease,” Benjamin J. Apelberg, PhD, director of the Division of Population Health Science, Office of Science, within the FDA Center for Tobacco Products, and his colleagues, wrote in the report.
Modeling for the implementation of a lower nicotine level policy suggests that smoking prevalence will decline from a median of 12.8% in baseline scenario to a median of 10.8% within a year of implementation, with the increase related to smoking cessation.
“We estimate that approximately 5 million additional smokers would quit smoking within a year after implementation of the hypothetical policy,” Dr. Apelberg and his colleagues wrote. “By 2060, smoking prevalence drops from 7.9% in the baseline scenario to 1.4% in the policy scenario.”
Their analysis is based on a nicotine level that is “so low that there would not be enough nicotine available in cigarette tobacco for smokers to sustain addiction,” they noted.
The FDA plans to release two more advanced notices of proposed rule making related to using regulatory levers to reduce cigarette smoking, including one that addresses flavoring in tobacco and one related to the regulation of premium cigars. Other than the 90-day comment period related to the advanced notices, the agency has not set any deadlines on when it will act.
“Legally, we are not going to prejudge how long this will take or what will happen,” Mr. Zeller said. “This is an early step in what could be a potential rule-making process using the product standard authority. We will take a long and hard look at all the comments that come in over the next 90 days and based upon our review of all the information, all the comments that come in, all the feedback that we have, we will then make a decision about taking the next step in the rule-making process.”
Nicotine levels in cigarettes could see a significant reduction under regulatory options being considered by the Food and Drug Administration.
Cigarettes “are the only legal consumer product that, when used as intended, will kill half all long-term users,” FDA Commissioner Scott Gottlieb, MD, said in a statement announcing the effort.
The agency is seeking comment on a proposed regulation regarding “a potential maximum nicotine level that would be appropriate for the protection of public health, in light of scientific evidence about the addictive properties of nicotine in cigarettes.” An advance notice of proposed rule making was posted online March 15 and is scheduled for publication in the Federal Register on March 16.
The FDA also is seeking comments on a number of other areas to help inform potential regulatory action down the road, including whether a new standard for lower nicotine levels should be implemented at once or whether a phased-in approach should be taken; whether FDA should specify a method for manufacturers to use in order to detect nicotine levels in their products; and whether the proposed lower level is technically achievable.
The agency also is seeking comment on potential unintended effects of lowering the amount of nicotine in cigarettes, such as turning to other combustible tobacco products such as cigars in conjunction with or as a replacement for cigarette use; increasing the number of cigarettes smoked, or seeking comparable nicotine from noncombustible tobacco sources.
At this time, FDA is not suggesting what the target might be on a specific nicotine level. While the advanced notice asks specifically about the “merits of nicotine levels like 0.3, 0.4, and 0.5 mg nicotine/g of tobacco filler,” it is not suggesting that this is the range being considered.
[polldaddy:9960560]
“Not to prejudge any possible proposed rule that we would do or any possible level, that is the purpose of an advanced proposed rule making, but we share all the science that we are aware of, and we characterize the studies that have been done to date in trying to find out what that right level is,” Mitch Zeller, director of the FDA Center for Tobacco Products, said during a March 15 press call.
He said that the FDA aiming to make sure the level is low enough that it cannot be compensated for by smoking more or inhaling deeper and holding the breath in longer, much like how smokers compensated when they smoked “light” cigarettes in the unregulated market.
Mr. Zeller said that seeking comments on those levels is based on the scientific evidence that is laid out in the advanced notice, but it is not necessarily foreshadowing where the standard will be set.
Drastically reducing the amount of nicotine in cigarettes is expected to significantly lower not only the number of people addicted to cigarettes but also as the negative health effects of nicotine addiction, FDA experts wrote in a perspective piece published March 15 in the New England Journal of Medicine (doi: 10.1065/NEJMsr1714617).
“Our findings show that reducing the nicotine level in cigarettes has the potential to substantially reduce the enormous burden of smoking-related death and disease,” Benjamin J. Apelberg, PhD, director of the Division of Population Health Science, Office of Science, within the FDA Center for Tobacco Products, and his colleagues, wrote in the report.
Modeling for the implementation of a lower nicotine level policy suggests that smoking prevalence will decline from a median of 12.8% in baseline scenario to a median of 10.8% within a year of implementation, with the increase related to smoking cessation.
“We estimate that approximately 5 million additional smokers would quit smoking within a year after implementation of the hypothetical policy,” Dr. Apelberg and his colleagues wrote. “By 2060, smoking prevalence drops from 7.9% in the baseline scenario to 1.4% in the policy scenario.”
Their analysis is based on a nicotine level that is “so low that there would not be enough nicotine available in cigarette tobacco for smokers to sustain addiction,” they noted.
The FDA plans to release two more advanced notices of proposed rule making related to using regulatory levers to reduce cigarette smoking, including one that addresses flavoring in tobacco and one related to the regulation of premium cigars. Other than the 90-day comment period related to the advanced notices, the agency has not set any deadlines on when it will act.
“Legally, we are not going to prejudge how long this will take or what will happen,” Mr. Zeller said. “This is an early step in what could be a potential rule-making process using the product standard authority. We will take a long and hard look at all the comments that come in over the next 90 days and based upon our review of all the information, all the comments that come in, all the feedback that we have, we will then make a decision about taking the next step in the rule-making process.”
Good definitions, research lacking for COPD-asthma overlap
ORLANDO – to give clinicians data they can actually use.
The topic is even more pressing given the growing interest and research into biological treatments for asthma and consideration of their possible use in COPD, experts said at the joint congress of the American Academy of Allergy, Asthma, and Immunology and the World Asthma Organization. Their remarks came in what was ostensibly a “debate” on whether ACOS is a distinct entity requiring special treatment but largely turned into a discussion about gaps in knowledge on the topic.
“The problem here is that it has not been defined in a way that everyone agrees on – that does create a problem because, if there’s no consensus on the diagnostic criteria, then it may be difficult to study this overlap,” said Donald Tashkin, MD, director of the pulmonary function laboratories at the University of California, Los Angeles. “Because there is no agreement on how to diagnose ACOS, it hasn’t been studied with respect to its responsiveness to different treatment options.”R. Stokes Peebles Jr., MD, professor of allergy, pulmonary, and critical care medicine at Vanderbilt University Medical Center, Nashville, Tenn., said that, although the number of published articles on ACOS has skyrocketed over the last several years, review articles have outnumbered original research articles.
There is disagreement in published definitions: One set of definitions includes a criterion of fractional exhaled nitric oxide not seen in any other definitions, whereas some other definitions require a history of smoking while others don’t, he said.
“How does one manage a disease without a definition and without clinical studies? It’s impossible for me to know,” Dr. Peebles said.
Jeffrey Drazen, MD, the Distinguished Parker B. Francis Professor of Medicine at Harvard Medical School, Boston, and the editor of the New England Journal of Medicine, also lamented the polar nature of the research.
“We all treat patients in the middle, everybody does, all the time – and we would love more guidance,” he said. “One of the reasons the number of articles has gone up is that there have been lots of case definitions. But we can’t get consensus. So who do we have to bring to the table to get a consensus definition so we can get the funding we need from the drug companies or governmental bodies to do the research that we all want?”
Dr. Tashkin said the way forward could be to draw on the points of consensus that do exist on certain criteria.
Dr. Peebles said an international panel is needed to draw up a consensus guideline, with the panel including both pulmonologists and allergists – “people experienced with clinical trials, who take care of a lot of patients.”
ORLANDO – to give clinicians data they can actually use.
The topic is even more pressing given the growing interest and research into biological treatments for asthma and consideration of their possible use in COPD, experts said at the joint congress of the American Academy of Allergy, Asthma, and Immunology and the World Asthma Organization. Their remarks came in what was ostensibly a “debate” on whether ACOS is a distinct entity requiring special treatment but largely turned into a discussion about gaps in knowledge on the topic.
“The problem here is that it has not been defined in a way that everyone agrees on – that does create a problem because, if there’s no consensus on the diagnostic criteria, then it may be difficult to study this overlap,” said Donald Tashkin, MD, director of the pulmonary function laboratories at the University of California, Los Angeles. “Because there is no agreement on how to diagnose ACOS, it hasn’t been studied with respect to its responsiveness to different treatment options.”R. Stokes Peebles Jr., MD, professor of allergy, pulmonary, and critical care medicine at Vanderbilt University Medical Center, Nashville, Tenn., said that, although the number of published articles on ACOS has skyrocketed over the last several years, review articles have outnumbered original research articles.
There is disagreement in published definitions: One set of definitions includes a criterion of fractional exhaled nitric oxide not seen in any other definitions, whereas some other definitions require a history of smoking while others don’t, he said.
“How does one manage a disease without a definition and without clinical studies? It’s impossible for me to know,” Dr. Peebles said.
Jeffrey Drazen, MD, the Distinguished Parker B. Francis Professor of Medicine at Harvard Medical School, Boston, and the editor of the New England Journal of Medicine, also lamented the polar nature of the research.
“We all treat patients in the middle, everybody does, all the time – and we would love more guidance,” he said. “One of the reasons the number of articles has gone up is that there have been lots of case definitions. But we can’t get consensus. So who do we have to bring to the table to get a consensus definition so we can get the funding we need from the drug companies or governmental bodies to do the research that we all want?”
Dr. Tashkin said the way forward could be to draw on the points of consensus that do exist on certain criteria.
Dr. Peebles said an international panel is needed to draw up a consensus guideline, with the panel including both pulmonologists and allergists – “people experienced with clinical trials, who take care of a lot of patients.”
ORLANDO – to give clinicians data they can actually use.
The topic is even more pressing given the growing interest and research into biological treatments for asthma and consideration of their possible use in COPD, experts said at the joint congress of the American Academy of Allergy, Asthma, and Immunology and the World Asthma Organization. Their remarks came in what was ostensibly a “debate” on whether ACOS is a distinct entity requiring special treatment but largely turned into a discussion about gaps in knowledge on the topic.
“The problem here is that it has not been defined in a way that everyone agrees on – that does create a problem because, if there’s no consensus on the diagnostic criteria, then it may be difficult to study this overlap,” said Donald Tashkin, MD, director of the pulmonary function laboratories at the University of California, Los Angeles. “Because there is no agreement on how to diagnose ACOS, it hasn’t been studied with respect to its responsiveness to different treatment options.”R. Stokes Peebles Jr., MD, professor of allergy, pulmonary, and critical care medicine at Vanderbilt University Medical Center, Nashville, Tenn., said that, although the number of published articles on ACOS has skyrocketed over the last several years, review articles have outnumbered original research articles.
There is disagreement in published definitions: One set of definitions includes a criterion of fractional exhaled nitric oxide not seen in any other definitions, whereas some other definitions require a history of smoking while others don’t, he said.
“How does one manage a disease without a definition and without clinical studies? It’s impossible for me to know,” Dr. Peebles said.
Jeffrey Drazen, MD, the Distinguished Parker B. Francis Professor of Medicine at Harvard Medical School, Boston, and the editor of the New England Journal of Medicine, also lamented the polar nature of the research.
“We all treat patients in the middle, everybody does, all the time – and we would love more guidance,” he said. “One of the reasons the number of articles has gone up is that there have been lots of case definitions. But we can’t get consensus. So who do we have to bring to the table to get a consensus definition so we can get the funding we need from the drug companies or governmental bodies to do the research that we all want?”
Dr. Tashkin said the way forward could be to draw on the points of consensus that do exist on certain criteria.
Dr. Peebles said an international panel is needed to draw up a consensus guideline, with the panel including both pulmonologists and allergists – “people experienced with clinical trials, who take care of a lot of patients.”
EXPERT ANALYSIS FROM AAAAI/WAO JOINT CONGRESS
Swamp coolers not linked to dust mite sensitization in atopic children
ORLANDO – Swamp coolers – a low-cost alternative to air-conditioning in dry regions – weren’t found to increase sensitization to house dust mites or mold in atopic pediatric patients, researchers reported.
Neema Izadi, MD, and his associates say the findings, seen in a pediatric Colorado population in a study evaluating data over 10 years, could mean that not everyone at risk of dust mite and mold sensitization needs to avoid these cooling systems.
“Evaporative coolers have been shown to raise relative humidity by about 10%,” said Dr. Izadi, a pediatric allergy and immunology fellow at National Jewish Health, Denver, presenting at the joint congress of the American Academy of Asthma, Allergy and Immunology and the World Asthma Organization. “They work best in environments where the air is very warm and dry.”
House dust mites and mold thrive in higher humidity. Small studies performed in Colorado, Utah, and other locations have shown that the swamp coolers increase house dust mite allergen content, but there have been very few studies that have looked at actual sensitization. One smaller study in Nevada did find that the coolers increased sensitization to dust mites and mold.
In this study – thought to be the largest ever to look at this question – Dr. Izadi and his colleagues assessed data on patients aged 21 years and younger who were seen at National Jewish Health during 2008-2017 and who had at least one positive environmental skin-prick test. The average age was about 9 years. The cohort included 8,503 patients with sensitization to house dust mites and 9,286 with sensitization to mold. Researchers examined data on swamp coolers in their homes.
The researchers found that 29% of those with swamp coolers were dust-mite positive on skin testing, and 28% of those without one were positive. This was not a significant difference (P = .85). They found that 45% of those with the coolers were positive for sensitization to any mold, compared with 44% without one – also not a significant difference (P = .43).
They also found no difference according to age group, sex, or individually for atopic dermatitis, asthma, or allergic rhinitis.
He acknowledged that the study had no way to reliably account for patients who were transplants to Colorado, having moved there from somewhere else. The study also didn’t examine the age of homes, whether it had carpeting, or other factors.
He noted that the amount of time the coolers were run in the home was not examined and that “it might matter how much it is on.” This, he said, might account for differences in these results, compared with the Nevada study that did find a sensitization increase cause by the coolers.
“Evaporative coolers or swamp coolers are a great low-cost alternative in semiarid and arid environments – they can cut costs from 15%-35%,” Dr. Izadi said. “These data may indicate that it may be unnecessary to recommend that patients remove their swamp cooler, at least from a dust-mite and mold-sensitization standpoint.”
Dr. Izadi had no relevant financial disclosures.
SOURCE: Izadi N et al. AAAAI/WAO Joint Congress, Abstract 586
Susan Millard, MD, FCCP, comments: Swamp coolers are used in semi-arid and arid climates like Arizona, where I did my fellowship training but they didn't work well to keep apartments and homes cool enough if over about 100°F outside! The system is cheaper than air conditioning. So it is great to know that this type of cooling system does not cause more mold and dust mite allergies.
Susan Millard, MD, FCCP, comments: Swamp coolers are used in semi-arid and arid climates like Arizona, where I did my fellowship training but they didn't work well to keep apartments and homes cool enough if over about 100°F outside! The system is cheaper than air conditioning. So it is great to know that this type of cooling system does not cause more mold and dust mite allergies.
Susan Millard, MD, FCCP, comments: Swamp coolers are used in semi-arid and arid climates like Arizona, where I did my fellowship training but they didn't work well to keep apartments and homes cool enough if over about 100°F outside! The system is cheaper than air conditioning. So it is great to know that this type of cooling system does not cause more mold and dust mite allergies.
ORLANDO – Swamp coolers – a low-cost alternative to air-conditioning in dry regions – weren’t found to increase sensitization to house dust mites or mold in atopic pediatric patients, researchers reported.
Neema Izadi, MD, and his associates say the findings, seen in a pediatric Colorado population in a study evaluating data over 10 years, could mean that not everyone at risk of dust mite and mold sensitization needs to avoid these cooling systems.
“Evaporative coolers have been shown to raise relative humidity by about 10%,” said Dr. Izadi, a pediatric allergy and immunology fellow at National Jewish Health, Denver, presenting at the joint congress of the American Academy of Asthma, Allergy and Immunology and the World Asthma Organization. “They work best in environments where the air is very warm and dry.”
House dust mites and mold thrive in higher humidity. Small studies performed in Colorado, Utah, and other locations have shown that the swamp coolers increase house dust mite allergen content, but there have been very few studies that have looked at actual sensitization. One smaller study in Nevada did find that the coolers increased sensitization to dust mites and mold.
In this study – thought to be the largest ever to look at this question – Dr. Izadi and his colleagues assessed data on patients aged 21 years and younger who were seen at National Jewish Health during 2008-2017 and who had at least one positive environmental skin-prick test. The average age was about 9 years. The cohort included 8,503 patients with sensitization to house dust mites and 9,286 with sensitization to mold. Researchers examined data on swamp coolers in their homes.
The researchers found that 29% of those with swamp coolers were dust-mite positive on skin testing, and 28% of those without one were positive. This was not a significant difference (P = .85). They found that 45% of those with the coolers were positive for sensitization to any mold, compared with 44% without one – also not a significant difference (P = .43).
They also found no difference according to age group, sex, or individually for atopic dermatitis, asthma, or allergic rhinitis.
He acknowledged that the study had no way to reliably account for patients who were transplants to Colorado, having moved there from somewhere else. The study also didn’t examine the age of homes, whether it had carpeting, or other factors.
He noted that the amount of time the coolers were run in the home was not examined and that “it might matter how much it is on.” This, he said, might account for differences in these results, compared with the Nevada study that did find a sensitization increase cause by the coolers.
“Evaporative coolers or swamp coolers are a great low-cost alternative in semiarid and arid environments – they can cut costs from 15%-35%,” Dr. Izadi said. “These data may indicate that it may be unnecessary to recommend that patients remove their swamp cooler, at least from a dust-mite and mold-sensitization standpoint.”
Dr. Izadi had no relevant financial disclosures.
SOURCE: Izadi N et al. AAAAI/WAO Joint Congress, Abstract 586
ORLANDO – Swamp coolers – a low-cost alternative to air-conditioning in dry regions – weren’t found to increase sensitization to house dust mites or mold in atopic pediatric patients, researchers reported.
Neema Izadi, MD, and his associates say the findings, seen in a pediatric Colorado population in a study evaluating data over 10 years, could mean that not everyone at risk of dust mite and mold sensitization needs to avoid these cooling systems.
“Evaporative coolers have been shown to raise relative humidity by about 10%,” said Dr. Izadi, a pediatric allergy and immunology fellow at National Jewish Health, Denver, presenting at the joint congress of the American Academy of Asthma, Allergy and Immunology and the World Asthma Organization. “They work best in environments where the air is very warm and dry.”
House dust mites and mold thrive in higher humidity. Small studies performed in Colorado, Utah, and other locations have shown that the swamp coolers increase house dust mite allergen content, but there have been very few studies that have looked at actual sensitization. One smaller study in Nevada did find that the coolers increased sensitization to dust mites and mold.
In this study – thought to be the largest ever to look at this question – Dr. Izadi and his colleagues assessed data on patients aged 21 years and younger who were seen at National Jewish Health during 2008-2017 and who had at least one positive environmental skin-prick test. The average age was about 9 years. The cohort included 8,503 patients with sensitization to house dust mites and 9,286 with sensitization to mold. Researchers examined data on swamp coolers in their homes.
The researchers found that 29% of those with swamp coolers were dust-mite positive on skin testing, and 28% of those without one were positive. This was not a significant difference (P = .85). They found that 45% of those with the coolers were positive for sensitization to any mold, compared with 44% without one – also not a significant difference (P = .43).
They also found no difference according to age group, sex, or individually for atopic dermatitis, asthma, or allergic rhinitis.
He acknowledged that the study had no way to reliably account for patients who were transplants to Colorado, having moved there from somewhere else. The study also didn’t examine the age of homes, whether it had carpeting, or other factors.
He noted that the amount of time the coolers were run in the home was not examined and that “it might matter how much it is on.” This, he said, might account for differences in these results, compared with the Nevada study that did find a sensitization increase cause by the coolers.
“Evaporative coolers or swamp coolers are a great low-cost alternative in semiarid and arid environments – they can cut costs from 15%-35%,” Dr. Izadi said. “These data may indicate that it may be unnecessary to recommend that patients remove their swamp cooler, at least from a dust-mite and mold-sensitization standpoint.”
Dr. Izadi had no relevant financial disclosures.
SOURCE: Izadi N et al. AAAAI/WAO Joint Congress, Abstract 586
REPORTING FROM AAAAI/WAO JOINT CONGRESS
Key clinical point:
Major finding: Researchers found that 29% of those with swamp coolers were dust-mite positive on skin testing, and 28% of those without one were as well. This was not a significant difference (P = .85).
Study details: A retrospective review of more than 17,000 cases of atopic children aged 21 years and younger who were seen at National Jewish Health and had a positive environmental skin prick test.
Disclosures: Dr. Izadi had no relevant financial disclosures.
Source: Izadi N et al. AAAAI/WAO Joint Congress, Abstract 586
Teleconference is effective in assessing penicillin allergy
ORLANDO – and resulted in almost every patient having their allergy label removed, researchers reported.
In what the researchers said was the first study showing the utility of telemedicine in evaluating patient-reported penicillin allergies, allergy and immunology physicians did a secure telemedicine consultation with patients after they underwent penicillin skin testing with a physician assistant; an approach which, on average, took 123 minutes fewer each time than if the physician had done the consultation face-to-face. The teleconference can be done on a laptop or smartphone.
She said the approach is sensible and effective, and it is a good alternative to the traditional way of doing these tests. “What this takes out of that is the travel part. Someone else is doing the travel and the technique of testing,” added that people often are labeled in childhood after getting a rash that was thought to be related to penicillin, but actually was just a coincidence that was unrelated. Then the false allergy label is attached to them for life.
“This is so overlabeled,” Dr. Ramsey said. “Ten percent of the population thinks they’re allergic to penicillin, and 90% of them are not.”
A stark difference was found in the types of medicines administered before and after the evaluations, with aminopenicillin therapy jumping from 0 days of use to 188 days, and vancomycin – a more potent, but more costly alternative – dropping from 130 days of use to 16 days (P less than .05 for both).
Dr. Ramsey noted that, in part because of the time-consuming nature of the penicillin skin tests, they often are simply not done, so the false allergy labels are not caught, leading to pointless costs and exposure to more potent and potentially harmful forms of antibiotic therapy.
“Some hospitals don’t have allergists who will come in to do testing,” she said. “Sometimes patients are on medications that may interfere. And then a lot of times it’s just underrecognized – the implications of a penicillin allergy label. That is a very hot topic in our field and also in infectious disease.”
She hopes the telemedicine approach catches on more widely, which would help minimize the multitude of problems linked to penicillin allergy labels.
“Patients that avoid penicillin, they’re on more costly second-line antibiotics that are, in general, less effective, depending on which infection you’re talking about,” Dr. Ramsey said. “The [second-line antibiotics] have more side effects. And there’s data to show that patients with [a] penicillin allergy label have longer hospital stays, more costly hospital stays, are at risk for more resistant infections. And it breeds antimicrobial resistance in the long-term.”
Dr. Ramsey had no relevant financial disclosures.
SOURCE: Ramsey AC et al. AAAAI/WAO Joint Congress, Abstract 104.
ORLANDO – and resulted in almost every patient having their allergy label removed, researchers reported.
In what the researchers said was the first study showing the utility of telemedicine in evaluating patient-reported penicillin allergies, allergy and immunology physicians did a secure telemedicine consultation with patients after they underwent penicillin skin testing with a physician assistant; an approach which, on average, took 123 minutes fewer each time than if the physician had done the consultation face-to-face. The teleconference can be done on a laptop or smartphone.
She said the approach is sensible and effective, and it is a good alternative to the traditional way of doing these tests. “What this takes out of that is the travel part. Someone else is doing the travel and the technique of testing,” added that people often are labeled in childhood after getting a rash that was thought to be related to penicillin, but actually was just a coincidence that was unrelated. Then the false allergy label is attached to them for life.
“This is so overlabeled,” Dr. Ramsey said. “Ten percent of the population thinks they’re allergic to penicillin, and 90% of them are not.”
A stark difference was found in the types of medicines administered before and after the evaluations, with aminopenicillin therapy jumping from 0 days of use to 188 days, and vancomycin – a more potent, but more costly alternative – dropping from 130 days of use to 16 days (P less than .05 for both).
Dr. Ramsey noted that, in part because of the time-consuming nature of the penicillin skin tests, they often are simply not done, so the false allergy labels are not caught, leading to pointless costs and exposure to more potent and potentially harmful forms of antibiotic therapy.
“Some hospitals don’t have allergists who will come in to do testing,” she said. “Sometimes patients are on medications that may interfere. And then a lot of times it’s just underrecognized – the implications of a penicillin allergy label. That is a very hot topic in our field and also in infectious disease.”
She hopes the telemedicine approach catches on more widely, which would help minimize the multitude of problems linked to penicillin allergy labels.
“Patients that avoid penicillin, they’re on more costly second-line antibiotics that are, in general, less effective, depending on which infection you’re talking about,” Dr. Ramsey said. “The [second-line antibiotics] have more side effects. And there’s data to show that patients with [a] penicillin allergy label have longer hospital stays, more costly hospital stays, are at risk for more resistant infections. And it breeds antimicrobial resistance in the long-term.”
Dr. Ramsey had no relevant financial disclosures.
SOURCE: Ramsey AC et al. AAAAI/WAO Joint Congress, Abstract 104.
ORLANDO – and resulted in almost every patient having their allergy label removed, researchers reported.
In what the researchers said was the first study showing the utility of telemedicine in evaluating patient-reported penicillin allergies, allergy and immunology physicians did a secure telemedicine consultation with patients after they underwent penicillin skin testing with a physician assistant; an approach which, on average, took 123 minutes fewer each time than if the physician had done the consultation face-to-face. The teleconference can be done on a laptop or smartphone.
She said the approach is sensible and effective, and it is a good alternative to the traditional way of doing these tests. “What this takes out of that is the travel part. Someone else is doing the travel and the technique of testing,” added that people often are labeled in childhood after getting a rash that was thought to be related to penicillin, but actually was just a coincidence that was unrelated. Then the false allergy label is attached to them for life.
“This is so overlabeled,” Dr. Ramsey said. “Ten percent of the population thinks they’re allergic to penicillin, and 90% of them are not.”
A stark difference was found in the types of medicines administered before and after the evaluations, with aminopenicillin therapy jumping from 0 days of use to 188 days, and vancomycin – a more potent, but more costly alternative – dropping from 130 days of use to 16 days (P less than .05 for both).
Dr. Ramsey noted that, in part because of the time-consuming nature of the penicillin skin tests, they often are simply not done, so the false allergy labels are not caught, leading to pointless costs and exposure to more potent and potentially harmful forms of antibiotic therapy.
“Some hospitals don’t have allergists who will come in to do testing,” she said. “Sometimes patients are on medications that may interfere. And then a lot of times it’s just underrecognized – the implications of a penicillin allergy label. That is a very hot topic in our field and also in infectious disease.”
She hopes the telemedicine approach catches on more widely, which would help minimize the multitude of problems linked to penicillin allergy labels.
“Patients that avoid penicillin, they’re on more costly second-line antibiotics that are, in general, less effective, depending on which infection you’re talking about,” Dr. Ramsey said. “The [second-line antibiotics] have more side effects. And there’s data to show that patients with [a] penicillin allergy label have longer hospital stays, more costly hospital stays, are at risk for more resistant infections. And it breeds antimicrobial resistance in the long-term.”
Dr. Ramsey had no relevant financial disclosures.
SOURCE: Ramsey AC et al. AAAAI/WAO Joint Congress, Abstract 104.
REPORTING FROM AAAAI/WAO JOINT CONGRESS
Key clinical point: Teleconferencing to assess patient-reported penicillin allergies saves time and results in 9 out of 10 patients being delabeled.
Major finding: Of 50 patients prospectively assessed with this approach over a 4-month period last year, 46 were delabeled, with $23,000 in direct antibiotic cost savings, or $360 per patient.
Study details: A prospective study conducted over 4 months in 2017.
Disclosures: Dr. Ramsey had no relevant financial disclosures.
Source: Ramsey AC et al. AAAAI/WAO Joint Congress, Abstract 104.
OSA may provide cardioprotection
, according to researchers.
In a study of 127 patients presenting with acute coronary syndromes (ACS), median peak cardiac troponin-I (cTn-I) values were significantly higher in patients without obstructive sleep apnea, compared with OSA patients (10.7; interquartile range: 1.78-40.1, vs. 3.79; IQR: 0.37-24.3, respectively; P = .04 ). The findings were published Feb. 5 in the journal CHEST®.
The study comprised 89 OSA patients and 38 non-OSA patients who were admitted to a hospital for acute coronary syndromes. The OSA group had a median apnea-hypopnea index (AHI) of 32, while the non-OSA group had a median AHI of 4.8. There was no significant difference between the two groups in gender, age, or cardiovascular risk factors such as hypertension, diabetes mellitus, body mass index, dyslipidemia, and smoking.
The cohort was part of the Continuous Positive Airway Pressure (CPAP) in Patients With Acute Coronary Syndrome and Obstructive Sleep Apnea (ISAACC) study, a prior randomized, controlled trial that evaluated the effect of CPAP treatment on new cardiovascular events in patients with an episode of ACS and OSA, reported Alicia Sánchez-de-la-Torre, PhD, of the respiratory department at Hospital Universitari Arnau de Vilanova and Santa Maria in Catalonia, Spain, and her coauthors.
Respiratory polygraphy was performed in the first 24-72 hours after hospital admission, and patients with an AHI of at least 15 events per hour were considered to have OSA. Those with an AHI less than 15 events per hour were included in the non-OSA group.
The OSA patients were randomized to conservative or CPAP treatment. An obstructive apnea “episode” was defined as a complete cessation of airflow for 10 seconds or longer, and an episode of hypopnea was defined as a reduction in airflow for at least 10 seconds associated with a greater than 4% decrease in arterial oxygen saturation.
Blood samples were collected from patients every 6 hours until two consecutive cTn-I measurements showed a decrease, with the highest measurement considered the peak cTn-I value.
Peak cTn-I value was significantly higher in non-OSA patients than in OSA patients. Median infarct size, measured by calculating the area under the cTn-I curve, was significantly different between the two groups (451 for non-OSA patients vs. 143 in OSA patients; P = .049), wrote Dr. Sánchez-de-la-Torre and her colleagues.
As cTn-I levels decreased, there was a trend toward increased OSA severity (P = .058). In the multivariable linear regression model used to assess OSA severity, patients with severe OSA had 61% lower cTn-I levels than non-OSA patients, the authors noted.
“The effects of chronic hypoxia in individual organ systems are not well understood. While chronic sustained hypoxia as seen with COPD may lead to pulmonary hypertension, chronic intermittent hypoxia (CIH) as seen predominantly in sleep apnea has been attributed to causing widespread effects ranging from systemic hypertension to metabolic dysfunction and systemic inflammation,” noted Krishna Sundar, MD, FCCP. “Despite these associations, an increased risk of major cardiovascular events from untreated OSA is yet to be definitively established.”
In this article, a protective effect from OSA on myocardial ischemic events is demonstrated in a group of 127 consecutively admitted patients with acute coronary syndrome (ACS). While it is interesting that a high proportion of those admitted for ACS had OSA, there were no significant differences in the age, sex, BMI, usage of antihypertensive or antiplatelet agents, presence of hypertension, DM, dyslipidemia or smoking status between those with and without OSA. “OSA appeared to confer a protective effect on the size of myocardial injury with those having higher AHI values demonstrating lower peak cardiac troponin values,” said Dr. Sundar, who is an associate clinical professor of pulmonary, critical care and sleep medicine at the University of Utah.“An effect of age (mean age in this study being 64 years) and BMI (mean being 27) on the occurrence of preconditioning effects of OSA is not excluded given deleterious effects of untreated OSA on infarct size in other studies on obese or younger patients with ACS. Further understanding of molecular effects of chronic hypoxia exposure (high altitude, chronic lung disease, OSA) is required before the complex and often contradictory effects of chronic hypoxia can be affirmed as being protective or deleterious,” added Dr. Sundar, who is also medical director of the Sleep-Wake Center at the University of Utah and a member of CHEST Physician’s editorial advisory board.
According to the study’s authors, their findings “suggest that patients with higher AHI are significantly more likely to have low cTn-I levels than patients without evidence of OSA, which could imply that patients with elevated AHI, particularly those with severe OSA, may experience less severe myocardial injury.”Limitations of the study include exclusion of patients with severe ACS, exclusion of sleepy subjects, and assessment of myocardial injury using cTn-I as a biomarker, without further data to determine infarct size.
“The possible role of OSA in cardioprotection should be explored in future studies,” the authors concluded.
The authors disclosed relationships with ResMed, Spanish Ministry of Health, Spanish Respiratory Society, Catalonian Cardiology Society, and ALLER. No other disclosures were reported.
SOURCE: Chest. 2018 Feb 5;153[2]:329-38. doi: 10.1016/j.chest.2017.06.046.
Although this study cannot definitively establish a clinically meaningful protective effect, it does provide important “preliminary evidence supporting the concept of OSA-induced cardioprotection” and challenges existing research, according to an editorial by Doron Aronson, MD, of the department of cardiology at Rambam Medical Center, Haifa, Israel, and coauthors (CHEST. 2018 Feb 153[2]:295-7. doi: 10.1016/j.chest.2017.07.036).
The results should be interpreted with caution, especially since accurate assessment of infarct size poses a challenge, they wrote.
“Myocardial infarct size is highly variable and is influenced by the duration of coronary occlusion, ST-segment elevation or non–ST elevation myocardial infarction, infarct location, residual antegrade infarct-related artery flow, collateral flow, the presence of non–culprit vessel coronary artery disease and myocardial metabolic demand,” they wrote. “Without accounting for these variables in a small study, results may be affected by variation in the characteristics of the patients.”
Though further study is needed, the findings may have “profound clinical implications regarding our therapeutic approach to patients with sleep apnea” if confirmed, the authors concluded.
Although this study cannot definitively establish a clinically meaningful protective effect, it does provide important “preliminary evidence supporting the concept of OSA-induced cardioprotection” and challenges existing research, according to an editorial by Doron Aronson, MD, of the department of cardiology at Rambam Medical Center, Haifa, Israel, and coauthors (CHEST. 2018 Feb 153[2]:295-7. doi: 10.1016/j.chest.2017.07.036).
The results should be interpreted with caution, especially since accurate assessment of infarct size poses a challenge, they wrote.
“Myocardial infarct size is highly variable and is influenced by the duration of coronary occlusion, ST-segment elevation or non–ST elevation myocardial infarction, infarct location, residual antegrade infarct-related artery flow, collateral flow, the presence of non–culprit vessel coronary artery disease and myocardial metabolic demand,” they wrote. “Without accounting for these variables in a small study, results may be affected by variation in the characteristics of the patients.”
Though further study is needed, the findings may have “profound clinical implications regarding our therapeutic approach to patients with sleep apnea” if confirmed, the authors concluded.
Although this study cannot definitively establish a clinically meaningful protective effect, it does provide important “preliminary evidence supporting the concept of OSA-induced cardioprotection” and challenges existing research, according to an editorial by Doron Aronson, MD, of the department of cardiology at Rambam Medical Center, Haifa, Israel, and coauthors (CHEST. 2018 Feb 153[2]:295-7. doi: 10.1016/j.chest.2017.07.036).
The results should be interpreted with caution, especially since accurate assessment of infarct size poses a challenge, they wrote.
“Myocardial infarct size is highly variable and is influenced by the duration of coronary occlusion, ST-segment elevation or non–ST elevation myocardial infarction, infarct location, residual antegrade infarct-related artery flow, collateral flow, the presence of non–culprit vessel coronary artery disease and myocardial metabolic demand,” they wrote. “Without accounting for these variables in a small study, results may be affected by variation in the characteristics of the patients.”
Though further study is needed, the findings may have “profound clinical implications regarding our therapeutic approach to patients with sleep apnea” if confirmed, the authors concluded.
, according to researchers.
In a study of 127 patients presenting with acute coronary syndromes (ACS), median peak cardiac troponin-I (cTn-I) values were significantly higher in patients without obstructive sleep apnea, compared with OSA patients (10.7; interquartile range: 1.78-40.1, vs. 3.79; IQR: 0.37-24.3, respectively; P = .04 ). The findings were published Feb. 5 in the journal CHEST®.
The study comprised 89 OSA patients and 38 non-OSA patients who were admitted to a hospital for acute coronary syndromes. The OSA group had a median apnea-hypopnea index (AHI) of 32, while the non-OSA group had a median AHI of 4.8. There was no significant difference between the two groups in gender, age, or cardiovascular risk factors such as hypertension, diabetes mellitus, body mass index, dyslipidemia, and smoking.
The cohort was part of the Continuous Positive Airway Pressure (CPAP) in Patients With Acute Coronary Syndrome and Obstructive Sleep Apnea (ISAACC) study, a prior randomized, controlled trial that evaluated the effect of CPAP treatment on new cardiovascular events in patients with an episode of ACS and OSA, reported Alicia Sánchez-de-la-Torre, PhD, of the respiratory department at Hospital Universitari Arnau de Vilanova and Santa Maria in Catalonia, Spain, and her coauthors.
Respiratory polygraphy was performed in the first 24-72 hours after hospital admission, and patients with an AHI of at least 15 events per hour were considered to have OSA. Those with an AHI less than 15 events per hour were included in the non-OSA group.
The OSA patients were randomized to conservative or CPAP treatment. An obstructive apnea “episode” was defined as a complete cessation of airflow for 10 seconds or longer, and an episode of hypopnea was defined as a reduction in airflow for at least 10 seconds associated with a greater than 4% decrease in arterial oxygen saturation.
Blood samples were collected from patients every 6 hours until two consecutive cTn-I measurements showed a decrease, with the highest measurement considered the peak cTn-I value.
Peak cTn-I value was significantly higher in non-OSA patients than in OSA patients. Median infarct size, measured by calculating the area under the cTn-I curve, was significantly different between the two groups (451 for non-OSA patients vs. 143 in OSA patients; P = .049), wrote Dr. Sánchez-de-la-Torre and her colleagues.
As cTn-I levels decreased, there was a trend toward increased OSA severity (P = .058). In the multivariable linear regression model used to assess OSA severity, patients with severe OSA had 61% lower cTn-I levels than non-OSA patients, the authors noted.
“The effects of chronic hypoxia in individual organ systems are not well understood. While chronic sustained hypoxia as seen with COPD may lead to pulmonary hypertension, chronic intermittent hypoxia (CIH) as seen predominantly in sleep apnea has been attributed to causing widespread effects ranging from systemic hypertension to metabolic dysfunction and systemic inflammation,” noted Krishna Sundar, MD, FCCP. “Despite these associations, an increased risk of major cardiovascular events from untreated OSA is yet to be definitively established.”
In this article, a protective effect from OSA on myocardial ischemic events is demonstrated in a group of 127 consecutively admitted patients with acute coronary syndrome (ACS). While it is interesting that a high proportion of those admitted for ACS had OSA, there were no significant differences in the age, sex, BMI, usage of antihypertensive or antiplatelet agents, presence of hypertension, DM, dyslipidemia or smoking status between those with and without OSA. “OSA appeared to confer a protective effect on the size of myocardial injury with those having higher AHI values demonstrating lower peak cardiac troponin values,” said Dr. Sundar, who is an associate clinical professor of pulmonary, critical care and sleep medicine at the University of Utah.“An effect of age (mean age in this study being 64 years) and BMI (mean being 27) on the occurrence of preconditioning effects of OSA is not excluded given deleterious effects of untreated OSA on infarct size in other studies on obese or younger patients with ACS. Further understanding of molecular effects of chronic hypoxia exposure (high altitude, chronic lung disease, OSA) is required before the complex and often contradictory effects of chronic hypoxia can be affirmed as being protective or deleterious,” added Dr. Sundar, who is also medical director of the Sleep-Wake Center at the University of Utah and a member of CHEST Physician’s editorial advisory board.
According to the study’s authors, their findings “suggest that patients with higher AHI are significantly more likely to have low cTn-I levels than patients without evidence of OSA, which could imply that patients with elevated AHI, particularly those with severe OSA, may experience less severe myocardial injury.”Limitations of the study include exclusion of patients with severe ACS, exclusion of sleepy subjects, and assessment of myocardial injury using cTn-I as a biomarker, without further data to determine infarct size.
“The possible role of OSA in cardioprotection should be explored in future studies,” the authors concluded.
The authors disclosed relationships with ResMed, Spanish Ministry of Health, Spanish Respiratory Society, Catalonian Cardiology Society, and ALLER. No other disclosures were reported.
SOURCE: Chest. 2018 Feb 5;153[2]:329-38. doi: 10.1016/j.chest.2017.06.046.
, according to researchers.
In a study of 127 patients presenting with acute coronary syndromes (ACS), median peak cardiac troponin-I (cTn-I) values were significantly higher in patients without obstructive sleep apnea, compared with OSA patients (10.7; interquartile range: 1.78-40.1, vs. 3.79; IQR: 0.37-24.3, respectively; P = .04 ). The findings were published Feb. 5 in the journal CHEST®.
The study comprised 89 OSA patients and 38 non-OSA patients who were admitted to a hospital for acute coronary syndromes. The OSA group had a median apnea-hypopnea index (AHI) of 32, while the non-OSA group had a median AHI of 4.8. There was no significant difference between the two groups in gender, age, or cardiovascular risk factors such as hypertension, diabetes mellitus, body mass index, dyslipidemia, and smoking.
The cohort was part of the Continuous Positive Airway Pressure (CPAP) in Patients With Acute Coronary Syndrome and Obstructive Sleep Apnea (ISAACC) study, a prior randomized, controlled trial that evaluated the effect of CPAP treatment on new cardiovascular events in patients with an episode of ACS and OSA, reported Alicia Sánchez-de-la-Torre, PhD, of the respiratory department at Hospital Universitari Arnau de Vilanova and Santa Maria in Catalonia, Spain, and her coauthors.
Respiratory polygraphy was performed in the first 24-72 hours after hospital admission, and patients with an AHI of at least 15 events per hour were considered to have OSA. Those with an AHI less than 15 events per hour were included in the non-OSA group.
The OSA patients were randomized to conservative or CPAP treatment. An obstructive apnea “episode” was defined as a complete cessation of airflow for 10 seconds or longer, and an episode of hypopnea was defined as a reduction in airflow for at least 10 seconds associated with a greater than 4% decrease in arterial oxygen saturation.
Blood samples were collected from patients every 6 hours until two consecutive cTn-I measurements showed a decrease, with the highest measurement considered the peak cTn-I value.
Peak cTn-I value was significantly higher in non-OSA patients than in OSA patients. Median infarct size, measured by calculating the area under the cTn-I curve, was significantly different between the two groups (451 for non-OSA patients vs. 143 in OSA patients; P = .049), wrote Dr. Sánchez-de-la-Torre and her colleagues.
As cTn-I levels decreased, there was a trend toward increased OSA severity (P = .058). In the multivariable linear regression model used to assess OSA severity, patients with severe OSA had 61% lower cTn-I levels than non-OSA patients, the authors noted.
“The effects of chronic hypoxia in individual organ systems are not well understood. While chronic sustained hypoxia as seen with COPD may lead to pulmonary hypertension, chronic intermittent hypoxia (CIH) as seen predominantly in sleep apnea has been attributed to causing widespread effects ranging from systemic hypertension to metabolic dysfunction and systemic inflammation,” noted Krishna Sundar, MD, FCCP. “Despite these associations, an increased risk of major cardiovascular events from untreated OSA is yet to be definitively established.”
In this article, a protective effect from OSA on myocardial ischemic events is demonstrated in a group of 127 consecutively admitted patients with acute coronary syndrome (ACS). While it is interesting that a high proportion of those admitted for ACS had OSA, there were no significant differences in the age, sex, BMI, usage of antihypertensive or antiplatelet agents, presence of hypertension, DM, dyslipidemia or smoking status between those with and without OSA. “OSA appeared to confer a protective effect on the size of myocardial injury with those having higher AHI values demonstrating lower peak cardiac troponin values,” said Dr. Sundar, who is an associate clinical professor of pulmonary, critical care and sleep medicine at the University of Utah.“An effect of age (mean age in this study being 64 years) and BMI (mean being 27) on the occurrence of preconditioning effects of OSA is not excluded given deleterious effects of untreated OSA on infarct size in other studies on obese or younger patients with ACS. Further understanding of molecular effects of chronic hypoxia exposure (high altitude, chronic lung disease, OSA) is required before the complex and often contradictory effects of chronic hypoxia can be affirmed as being protective or deleterious,” added Dr. Sundar, who is also medical director of the Sleep-Wake Center at the University of Utah and a member of CHEST Physician’s editorial advisory board.
According to the study’s authors, their findings “suggest that patients with higher AHI are significantly more likely to have low cTn-I levels than patients without evidence of OSA, which could imply that patients with elevated AHI, particularly those with severe OSA, may experience less severe myocardial injury.”Limitations of the study include exclusion of patients with severe ACS, exclusion of sleepy subjects, and assessment of myocardial injury using cTn-I as a biomarker, without further data to determine infarct size.
“The possible role of OSA in cardioprotection should be explored in future studies,” the authors concluded.
The authors disclosed relationships with ResMed, Spanish Ministry of Health, Spanish Respiratory Society, Catalonian Cardiology Society, and ALLER. No other disclosures were reported.
SOURCE: Chest. 2018 Feb 5;153[2]:329-38. doi: 10.1016/j.chest.2017.06.046.
Unassigned school epinephrine used more than assigned injectors
ORLANDO –
In the 2015-2016 and 2016-2017 school years, epinephrine was administered to students 31 times at schools in the Austin Independent School District, which began to stock unassigned epinephrine in its schools after state legislators approved a law in 2015 allowing, but not requiring, school districts to do so. In 21 of those cases, or 68% of the time, it was the unassigned stockpile that was used, Kathryn Neupert, MD, said at the joint congress of the American Academy of Allergy, Asthma, and Immunology and the World Asthma Organization.
She drew attention to the finding that 22% of the time in the study, the epinephrine use involved the unassigned stock for children with no history of anaphylaxis or allergy.
“It kind of argues that, for those people that we don’t know have anaphylaxis to anything, it’s definitely important to have it available to them,” reported Dr. Neupert, a resident at the University of Texas, Austin.
In 45% of the cases, epinephrine was administered to children who had a known history of allergic reactions but, for whatever reason, did not have an epinephrine injector assigned to them.
Food was the most common trigger for use of epinephrine, accounting for 48% of the injections, with fragrance at 16%, insect stings at 10%, and exercise and overheating at 7%.
Dr. Neupert and her associates said the frequency with which epinephrine was administered after exposure to a fragrance – seen in about the same amount for unassigned and assigned epinephrine – might signal a need for greater education.
She emphasized the importance of follow-up after the use of unassigned injectors. If children get epinephrine that was unassigned and they have known allergies, “be sure that they subsequently get back in with their pediatrician or their allergist [and] that they’re getting their up-to-date epinephrine pens renewed,” she noted.
Carla Davis, MD, a pediatrician at Baylor College of Medicine, Houston, said she hopes more school districts adopt the stock epinephrine policy, despite barriers of cost and education. “I do think that it’s important for these schools to have these, because 20% of children will have their first episode of food allergic reaction – and in some of those cases it will be anaphylaxis – in schools.”
Dr. Neupert had no relevant financial disclosures.
SOURCE: AAAAI/WAO Joint Congress Abstract 465.
ORLANDO –
In the 2015-2016 and 2016-2017 school years, epinephrine was administered to students 31 times at schools in the Austin Independent School District, which began to stock unassigned epinephrine in its schools after state legislators approved a law in 2015 allowing, but not requiring, school districts to do so. In 21 of those cases, or 68% of the time, it was the unassigned stockpile that was used, Kathryn Neupert, MD, said at the joint congress of the American Academy of Allergy, Asthma, and Immunology and the World Asthma Organization.
She drew attention to the finding that 22% of the time in the study, the epinephrine use involved the unassigned stock for children with no history of anaphylaxis or allergy.
“It kind of argues that, for those people that we don’t know have anaphylaxis to anything, it’s definitely important to have it available to them,” reported Dr. Neupert, a resident at the University of Texas, Austin.
In 45% of the cases, epinephrine was administered to children who had a known history of allergic reactions but, for whatever reason, did not have an epinephrine injector assigned to them.
Food was the most common trigger for use of epinephrine, accounting for 48% of the injections, with fragrance at 16%, insect stings at 10%, and exercise and overheating at 7%.
Dr. Neupert and her associates said the frequency with which epinephrine was administered after exposure to a fragrance – seen in about the same amount for unassigned and assigned epinephrine – might signal a need for greater education.
She emphasized the importance of follow-up after the use of unassigned injectors. If children get epinephrine that was unassigned and they have known allergies, “be sure that they subsequently get back in with their pediatrician or their allergist [and] that they’re getting their up-to-date epinephrine pens renewed,” she noted.
Carla Davis, MD, a pediatrician at Baylor College of Medicine, Houston, said she hopes more school districts adopt the stock epinephrine policy, despite barriers of cost and education. “I do think that it’s important for these schools to have these, because 20% of children will have their first episode of food allergic reaction – and in some of those cases it will be anaphylaxis – in schools.”
Dr. Neupert had no relevant financial disclosures.
SOURCE: AAAAI/WAO Joint Congress Abstract 465.
ORLANDO –
In the 2015-2016 and 2016-2017 school years, epinephrine was administered to students 31 times at schools in the Austin Independent School District, which began to stock unassigned epinephrine in its schools after state legislators approved a law in 2015 allowing, but not requiring, school districts to do so. In 21 of those cases, or 68% of the time, it was the unassigned stockpile that was used, Kathryn Neupert, MD, said at the joint congress of the American Academy of Allergy, Asthma, and Immunology and the World Asthma Organization.
She drew attention to the finding that 22% of the time in the study, the epinephrine use involved the unassigned stock for children with no history of anaphylaxis or allergy.
“It kind of argues that, for those people that we don’t know have anaphylaxis to anything, it’s definitely important to have it available to them,” reported Dr. Neupert, a resident at the University of Texas, Austin.
In 45% of the cases, epinephrine was administered to children who had a known history of allergic reactions but, for whatever reason, did not have an epinephrine injector assigned to them.
Food was the most common trigger for use of epinephrine, accounting for 48% of the injections, with fragrance at 16%, insect stings at 10%, and exercise and overheating at 7%.
Dr. Neupert and her associates said the frequency with which epinephrine was administered after exposure to a fragrance – seen in about the same amount for unassigned and assigned epinephrine – might signal a need for greater education.
She emphasized the importance of follow-up after the use of unassigned injectors. If children get epinephrine that was unassigned and they have known allergies, “be sure that they subsequently get back in with their pediatrician or their allergist [and] that they’re getting their up-to-date epinephrine pens renewed,” she noted.
Carla Davis, MD, a pediatrician at Baylor College of Medicine, Houston, said she hopes more school districts adopt the stock epinephrine policy, despite barriers of cost and education. “I do think that it’s important for these schools to have these, because 20% of children will have their first episode of food allergic reaction – and in some of those cases it will be anaphylaxis – in schools.”
Dr. Neupert had no relevant financial disclosures.
SOURCE: AAAAI/WAO Joint Congress Abstract 465.
REPORTING FROM AAAAI/WAO JOINT CONGRESS
Key clinical point: Unassigned epinephrine was used more often in a Texas school district than assigned epinephrine.
Major finding: Over 2 years, 31 epinephrine injections were administered, and in 68% of the cases, it was the unassigned stock that was used.
Study details: A review of nursing records for the Austin Independent School District.
Disclosures: Dr. Kathryn Neupert had no relevant financial disclosures.
Source: Neupert K et al. Abstract 465.