User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
div[contains(@class, 'main-prefix')]
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
‘Gold cards’ allow Texas docs to skip prior authorizations
The law was passed in June and will take effect in September. It excuses physicians from having to obtain prior authorization if, during the previous 6 months, 90% of their treatments met medical necessity criteria by the health insurer. Through this law, doctors in the state will spend less time getting approvals for treatments for their patients.
Automatic approval of authorizations for treatments – or what the Texas Medical Association (TMA) calls a “gold card” – “allows patients to get the care they need in a more timely fashion,” says Debra Patt, MD, an Austin, Tex.–based oncologist and former chair of the council on legislation for the TMA.
Eighty-seven percent of Texas physicians reported a “drastic increase over the past five years in the burden of prior authorization on their patients and their practices,” per a 2020 survey by the TMA. Nearly half (48%) of Texas physicians have hired staff whose work focuses on processing requests for prior authorization, according to the survey.
Jack Resneck Jr., MD, a San Francisco–based dermatologist and president-elect of the American Medical Association (AMA), said other states have investigated ways to ease the impact of prior authorizations on physicians, but no other state has passed such a law.
Administrative burdens plague physicians around the country. The Medscape Physician Compensation Report 2021 found that physicians spend on average 15.6 hours per week on paperwork and administrative duties.
Better outcomes, less anxiety for patients
Dr. Patt, who testified in support of the law’s passage in the Texas legislature, says automatic approval of authorizations “is better for patients because it reduces their anxiety about whether they’re able to get the treatments they need now, and they will have better outcomes if they’re able to receive more timely care.”
Recently, a chemotherapy treatment Dr. Patt prescribed for one of her patients was not authorized by an insurer. The result is “a lot of anxiety and potentially health problems” for the patient, said Dr. Patt.
She expects that automatic approval for treatments will be based on prescribing patterns during the preceding 6 months. “It means that when I order a test today, the [health insurer] looks back at my record 6 months previously,” she said. Still, Dr. Patt awaits guidance from the Texas Department of Insurance, which regulates health insurers in the state, regarding the law.
Dr. Resneck said the pharmacy counter is where most patients encounter prior authorization delays. “That’s when the pharmacist looks at them and says, ‘Actually, this isn’t covered by your health insurer’s formulary,’ or it isn’t covered fully on their formulary.”
One of Dr. Resneck’s patients had a life-altering case of eczema that lasted many years. Because of the condition, the patient couldn’t work or maintain meaningful bonds with family members. A biologic treatment transformed his patient’s life. The patient was able to return to work and to re-engage with family, said Dr. Resneck. But a year after his patient started the treatment, the health insurer wouldn’t authorize the treatment because the patient wasn’t experiencing the same symptoms.
The patient didn’t have the same symptoms because the biologic treatment worked, said Dr. Resneck.
Kristine Grow, a spokesperson for America’s Health Insurance Plans, a national association for health insurers, said, “The use of prior authorization is relatively small – typically, less than 15% – and can help ensure safer opioid prescribing, help prevent dangerous drug interactions, and help protect patients from unnecessary exposure to potentially harmful radiation for inappropriate diagnostic imaging. Numerous studies show that Americans frequently receive inappropriate care, and 25% of unnecessary treatments are associated with complications or adverse events.”
Medical management tools, such as prior authorization, are an “an important way” to deliver “safe, high-quality care” to patients, she added.
State and federal efforts to curb prior authorization
In addition to efforts to curb prior authorization in other states, the AMA supports the Improving Seniors’ Timely Access to Care Act (HR 3173). The act includes a provision related to “gold-carding,” said Robert Mills, an AMA spokesperson.
The bill establishes requirements and standards for prior authorization processes related to Medicare Advantage (MA) plans. The requirements and standards for MA plans include the following:
- Establishing an electronic prior authorization program that meets specific standards, such as the ability to provide real-time decisions in response to requests for items and services that are routinely approved.
- Publishing on an annual basis specific prior authorization information, including the percentage of requests approved and the average response time.
- Meeting standards set by the Centers for Medicare & Medicaid Services related to the quality and timeliness of prior authorization determinations.
The act was introduced to the U.S. House of Representatives in May, after which it was referred to two committees for consideration.
A version of this article first appeared on Medscape.com.
The law was passed in June and will take effect in September. It excuses physicians from having to obtain prior authorization if, during the previous 6 months, 90% of their treatments met medical necessity criteria by the health insurer. Through this law, doctors in the state will spend less time getting approvals for treatments for their patients.
Automatic approval of authorizations for treatments – or what the Texas Medical Association (TMA) calls a “gold card” – “allows patients to get the care they need in a more timely fashion,” says Debra Patt, MD, an Austin, Tex.–based oncologist and former chair of the council on legislation for the TMA.
Eighty-seven percent of Texas physicians reported a “drastic increase over the past five years in the burden of prior authorization on their patients and their practices,” per a 2020 survey by the TMA. Nearly half (48%) of Texas physicians have hired staff whose work focuses on processing requests for prior authorization, according to the survey.
Jack Resneck Jr., MD, a San Francisco–based dermatologist and president-elect of the American Medical Association (AMA), said other states have investigated ways to ease the impact of prior authorizations on physicians, but no other state has passed such a law.
Administrative burdens plague physicians around the country. The Medscape Physician Compensation Report 2021 found that physicians spend on average 15.6 hours per week on paperwork and administrative duties.
Better outcomes, less anxiety for patients
Dr. Patt, who testified in support of the law’s passage in the Texas legislature, says automatic approval of authorizations “is better for patients because it reduces their anxiety about whether they’re able to get the treatments they need now, and they will have better outcomes if they’re able to receive more timely care.”
Recently, a chemotherapy treatment Dr. Patt prescribed for one of her patients was not authorized by an insurer. The result is “a lot of anxiety and potentially health problems” for the patient, said Dr. Patt.
She expects that automatic approval for treatments will be based on prescribing patterns during the preceding 6 months. “It means that when I order a test today, the [health insurer] looks back at my record 6 months previously,” she said. Still, Dr. Patt awaits guidance from the Texas Department of Insurance, which regulates health insurers in the state, regarding the law.
Dr. Resneck said the pharmacy counter is where most patients encounter prior authorization delays. “That’s when the pharmacist looks at them and says, ‘Actually, this isn’t covered by your health insurer’s formulary,’ or it isn’t covered fully on their formulary.”
One of Dr. Resneck’s patients had a life-altering case of eczema that lasted many years. Because of the condition, the patient couldn’t work or maintain meaningful bonds with family members. A biologic treatment transformed his patient’s life. The patient was able to return to work and to re-engage with family, said Dr. Resneck. But a year after his patient started the treatment, the health insurer wouldn’t authorize the treatment because the patient wasn’t experiencing the same symptoms.
The patient didn’t have the same symptoms because the biologic treatment worked, said Dr. Resneck.
Kristine Grow, a spokesperson for America’s Health Insurance Plans, a national association for health insurers, said, “The use of prior authorization is relatively small – typically, less than 15% – and can help ensure safer opioid prescribing, help prevent dangerous drug interactions, and help protect patients from unnecessary exposure to potentially harmful radiation for inappropriate diagnostic imaging. Numerous studies show that Americans frequently receive inappropriate care, and 25% of unnecessary treatments are associated with complications or adverse events.”
Medical management tools, such as prior authorization, are an “an important way” to deliver “safe, high-quality care” to patients, she added.
State and federal efforts to curb prior authorization
In addition to efforts to curb prior authorization in other states, the AMA supports the Improving Seniors’ Timely Access to Care Act (HR 3173). The act includes a provision related to “gold-carding,” said Robert Mills, an AMA spokesperson.
The bill establishes requirements and standards for prior authorization processes related to Medicare Advantage (MA) plans. The requirements and standards for MA plans include the following:
- Establishing an electronic prior authorization program that meets specific standards, such as the ability to provide real-time decisions in response to requests for items and services that are routinely approved.
- Publishing on an annual basis specific prior authorization information, including the percentage of requests approved and the average response time.
- Meeting standards set by the Centers for Medicare & Medicaid Services related to the quality and timeliness of prior authorization determinations.
The act was introduced to the U.S. House of Representatives in May, after which it was referred to two committees for consideration.
A version of this article first appeared on Medscape.com.
The law was passed in June and will take effect in September. It excuses physicians from having to obtain prior authorization if, during the previous 6 months, 90% of their treatments met medical necessity criteria by the health insurer. Through this law, doctors in the state will spend less time getting approvals for treatments for their patients.
Automatic approval of authorizations for treatments – or what the Texas Medical Association (TMA) calls a “gold card” – “allows patients to get the care they need in a more timely fashion,” says Debra Patt, MD, an Austin, Tex.–based oncologist and former chair of the council on legislation for the TMA.
Eighty-seven percent of Texas physicians reported a “drastic increase over the past five years in the burden of prior authorization on their patients and their practices,” per a 2020 survey by the TMA. Nearly half (48%) of Texas physicians have hired staff whose work focuses on processing requests for prior authorization, according to the survey.
Jack Resneck Jr., MD, a San Francisco–based dermatologist and president-elect of the American Medical Association (AMA), said other states have investigated ways to ease the impact of prior authorizations on physicians, but no other state has passed such a law.
Administrative burdens plague physicians around the country. The Medscape Physician Compensation Report 2021 found that physicians spend on average 15.6 hours per week on paperwork and administrative duties.
Better outcomes, less anxiety for patients
Dr. Patt, who testified in support of the law’s passage in the Texas legislature, says automatic approval of authorizations “is better for patients because it reduces their anxiety about whether they’re able to get the treatments they need now, and they will have better outcomes if they’re able to receive more timely care.”
Recently, a chemotherapy treatment Dr. Patt prescribed for one of her patients was not authorized by an insurer. The result is “a lot of anxiety and potentially health problems” for the patient, said Dr. Patt.
She expects that automatic approval for treatments will be based on prescribing patterns during the preceding 6 months. “It means that when I order a test today, the [health insurer] looks back at my record 6 months previously,” she said. Still, Dr. Patt awaits guidance from the Texas Department of Insurance, which regulates health insurers in the state, regarding the law.
Dr. Resneck said the pharmacy counter is where most patients encounter prior authorization delays. “That’s when the pharmacist looks at them and says, ‘Actually, this isn’t covered by your health insurer’s formulary,’ or it isn’t covered fully on their formulary.”
One of Dr. Resneck’s patients had a life-altering case of eczema that lasted many years. Because of the condition, the patient couldn’t work or maintain meaningful bonds with family members. A biologic treatment transformed his patient’s life. The patient was able to return to work and to re-engage with family, said Dr. Resneck. But a year after his patient started the treatment, the health insurer wouldn’t authorize the treatment because the patient wasn’t experiencing the same symptoms.
The patient didn’t have the same symptoms because the biologic treatment worked, said Dr. Resneck.
Kristine Grow, a spokesperson for America’s Health Insurance Plans, a national association for health insurers, said, “The use of prior authorization is relatively small – typically, less than 15% – and can help ensure safer opioid prescribing, help prevent dangerous drug interactions, and help protect patients from unnecessary exposure to potentially harmful radiation for inappropriate diagnostic imaging. Numerous studies show that Americans frequently receive inappropriate care, and 25% of unnecessary treatments are associated with complications or adverse events.”
Medical management tools, such as prior authorization, are an “an important way” to deliver “safe, high-quality care” to patients, she added.
State and federal efforts to curb prior authorization
In addition to efforts to curb prior authorization in other states, the AMA supports the Improving Seniors’ Timely Access to Care Act (HR 3173). The act includes a provision related to “gold-carding,” said Robert Mills, an AMA spokesperson.
The bill establishes requirements and standards for prior authorization processes related to Medicare Advantage (MA) plans. The requirements and standards for MA plans include the following:
- Establishing an electronic prior authorization program that meets specific standards, such as the ability to provide real-time decisions in response to requests for items and services that are routinely approved.
- Publishing on an annual basis specific prior authorization information, including the percentage of requests approved and the average response time.
- Meeting standards set by the Centers for Medicare & Medicaid Services related to the quality and timeliness of prior authorization determinations.
The act was introduced to the U.S. House of Representatives in May, after which it was referred to two committees for consideration.
A version of this article first appeared on Medscape.com.
Mindfulness benefits kids with ADHD, and their families
Meditation, yoga, breathing exercises, and other mindfulness activities can help children with attention-deficit/hyperactivity disorder, but it’s not just the kids who benefit.
When families of children with ADHD complete a mindfulness program together, a new study suggests, children and parents can profit, with potential boosts to self-control, self-compassion, and psychological symptoms.
The findings do not suggest children should ditch medication in favor of focusing on the present moment. Instead, the study adds to growing evidence that mindfulness can be a helpful tool along with other strategies for children and adults with ADHD, said John Mitchell, PhD, a psychologist at Duke University, Durham, N.C., who was not involved with the new study. Mindfulness might help families ease stress and improve quality of life.
“We talk about ADHD because one person has that diagnosis, but we don’t live in bubbles,” he said. “We’re all interconnected and impact one another. And having treatments that acknowledge that and measuring that in the scientific literature is pretty important.”
Mindfulness training, which has its roots in Eastern traditions, generally aims to teach people how to be present in the moment and let go of judgment. Over the last couple of decades, researchers working on depression and other conditions have gathered evidence that practicing mindfulness can help in a variety of ways, including with the self-regulation of attention and emotions. It didn’t take long for those findings to draw interest from researchers who study ADHD, Dr. Mitchell said.
Research on mindfulness for ADHD started with adults, and results have been encouraging, Dr. Mitchell said. People who complete a mindfulness program tend to show some improvement in focus, impulsivity, and hyperactivity, studies show. In one small pilot study, Dr. Mitchell and colleagues reported improvements in symptoms and executive function in adults with ADHD.
Studies with children have lagged behind, but recent work has been promising. When looking at data from a number of studies, researchers have found small reductions in inattentiveness, hyperactivity, and impulsivity in young people with ADHD. Several randomized, controlled trials have also shown a reduction in symptoms as rated by parents and teachers.
Greater understanding, acceptance
In related research, there was a noticed reduction in stress among parents who get mindfulness training that teaches them to listen with their full attention, accept and develop compassion for themselves and their children, and regulate themselves within the relationship with their kids.
Still, first-line treatment for children with ADHD usually includes a combination of medication, cognitive behavioral therapy, and education, even though those strategies don’t always work well for everyone, says Corina Greven, PhD, a psychologist at Radboud (the Netherlands) University Medical Centre and Karakter Child and Adolescent Psychiatry.
Despite suggestive results, the data on mindfulness remains murky, in part because early studies that looked at mindfulness training for children with ADHD have been small. Few trials of mindfulness treatment for ADHD, Dr. Greven said, have included parents.
To fill in some of the gaps, Dr. Greven and colleagues conducted a trial with 103 families who had a child with ADHD between ages 8 and 16. Half of the families were randomly assigned simply to continue care as usual, which included medication for most.
The other half continued their usual care and also took part in a program called MYMind, which used mindfulness-based cognitive therapy for children and mindful parenting training for parents.
Families attended 90-minute group sessions once a week for 8 weeks, with an extra session 2 months later. The mindfulness group also completed homework every day that took about 30-45 minutes for parents and 15 minutes for children. Homework included workbooks and guided meditations.
In the short term, the team reported, children who received the mindfulness intervention showed small improvements in ADHD symptoms, anxiety, autistic symptoms, and problems falling asleep. One-third children who received mindfulness training improved on measures of self-control, Dr. Greven added, compared with just 1 in 10 who got only their usual care.
Benefits were larger and longer-lasting for parents. Compared with parents who didn’t get mindfulness training, those assigned to the mindfulness group improved in self-control, self-compassion, depression, anxiety, stress, well-being, and their own ADHD symptoms. Given a large genetic component to the disorder, it is common for parents of children with ADHD to have a diagnosis or ADHD symptoms as well. In addition, Dr. Greven said, families who completed the mindfulness-based intervention reported improvements in their relationships as well as acceptance of ADHD.
A new therapy?
The findings suggest new potential treatment options for children with ADHD, and for their parents, Dr. Greven said, as well as a need to study the condition more broadly. “Although parents of children with ADHD often have elevated parenting stress, anxiety, or their own ADHD symptoms, usual interventions for children with ADHD do not typically target parental mental health,” she said. “As researchers, we need to go broader than just looking at whether an intervention reduces symptoms and include additional outcomes that families find important.”
It will take more research to find out who is most likely to benefit from mindfulness training and how long those benefits last, but the new study is a useful starting point, experts say.
“Mindfulness training had potentially short-term and long-term beneficial effects to children with ADHD and their parents,” says Samuel Wong, MD, director of the JC School of Public Health and Primary Care at the Chinese University of Hong Kong. He says mindfulness is more likely to become an add-on than a replacement for other kinds of therapies.
“Clinicians may consider combining or adding family-based mindfulness training with current practice for children with ADHD who have residual symptoms with their current treatment,” he said.
Mindfulness training may help with issues beyond the classic symptoms that come with ADHD, Dr. Mitchell said, helping make family life better overall, even when some features of the disorder don’t budge much.
“With this study in particular, we see that we have some pretty promising effects that there may be something that will be beneficial above and beyond the core 18 DSM symptoms,” he said. “This is an important study, because it’s going to be a basis for the continuing evolution of the scientific research on this topic. It’s something to feel excited about.”
A version of this article first appeared on WebMD.com.
Meditation, yoga, breathing exercises, and other mindfulness activities can help children with attention-deficit/hyperactivity disorder, but it’s not just the kids who benefit.
When families of children with ADHD complete a mindfulness program together, a new study suggests, children and parents can profit, with potential boosts to self-control, self-compassion, and psychological symptoms.
The findings do not suggest children should ditch medication in favor of focusing on the present moment. Instead, the study adds to growing evidence that mindfulness can be a helpful tool along with other strategies for children and adults with ADHD, said John Mitchell, PhD, a psychologist at Duke University, Durham, N.C., who was not involved with the new study. Mindfulness might help families ease stress and improve quality of life.
“We talk about ADHD because one person has that diagnosis, but we don’t live in bubbles,” he said. “We’re all interconnected and impact one another. And having treatments that acknowledge that and measuring that in the scientific literature is pretty important.”
Mindfulness training, which has its roots in Eastern traditions, generally aims to teach people how to be present in the moment and let go of judgment. Over the last couple of decades, researchers working on depression and other conditions have gathered evidence that practicing mindfulness can help in a variety of ways, including with the self-regulation of attention and emotions. It didn’t take long for those findings to draw interest from researchers who study ADHD, Dr. Mitchell said.
Research on mindfulness for ADHD started with adults, and results have been encouraging, Dr. Mitchell said. People who complete a mindfulness program tend to show some improvement in focus, impulsivity, and hyperactivity, studies show. In one small pilot study, Dr. Mitchell and colleagues reported improvements in symptoms and executive function in adults with ADHD.
Studies with children have lagged behind, but recent work has been promising. When looking at data from a number of studies, researchers have found small reductions in inattentiveness, hyperactivity, and impulsivity in young people with ADHD. Several randomized, controlled trials have also shown a reduction in symptoms as rated by parents and teachers.
Greater understanding, acceptance
In related research, there was a noticed reduction in stress among parents who get mindfulness training that teaches them to listen with their full attention, accept and develop compassion for themselves and their children, and regulate themselves within the relationship with their kids.
Still, first-line treatment for children with ADHD usually includes a combination of medication, cognitive behavioral therapy, and education, even though those strategies don’t always work well for everyone, says Corina Greven, PhD, a psychologist at Radboud (the Netherlands) University Medical Centre and Karakter Child and Adolescent Psychiatry.
Despite suggestive results, the data on mindfulness remains murky, in part because early studies that looked at mindfulness training for children with ADHD have been small. Few trials of mindfulness treatment for ADHD, Dr. Greven said, have included parents.
To fill in some of the gaps, Dr. Greven and colleagues conducted a trial with 103 families who had a child with ADHD between ages 8 and 16. Half of the families were randomly assigned simply to continue care as usual, which included medication for most.
The other half continued their usual care and also took part in a program called MYMind, which used mindfulness-based cognitive therapy for children and mindful parenting training for parents.
Families attended 90-minute group sessions once a week for 8 weeks, with an extra session 2 months later. The mindfulness group also completed homework every day that took about 30-45 minutes for parents and 15 minutes for children. Homework included workbooks and guided meditations.
In the short term, the team reported, children who received the mindfulness intervention showed small improvements in ADHD symptoms, anxiety, autistic symptoms, and problems falling asleep. One-third children who received mindfulness training improved on measures of self-control, Dr. Greven added, compared with just 1 in 10 who got only their usual care.
Benefits were larger and longer-lasting for parents. Compared with parents who didn’t get mindfulness training, those assigned to the mindfulness group improved in self-control, self-compassion, depression, anxiety, stress, well-being, and their own ADHD symptoms. Given a large genetic component to the disorder, it is common for parents of children with ADHD to have a diagnosis or ADHD symptoms as well. In addition, Dr. Greven said, families who completed the mindfulness-based intervention reported improvements in their relationships as well as acceptance of ADHD.
A new therapy?
The findings suggest new potential treatment options for children with ADHD, and for their parents, Dr. Greven said, as well as a need to study the condition more broadly. “Although parents of children with ADHD often have elevated parenting stress, anxiety, or their own ADHD symptoms, usual interventions for children with ADHD do not typically target parental mental health,” she said. “As researchers, we need to go broader than just looking at whether an intervention reduces symptoms and include additional outcomes that families find important.”
It will take more research to find out who is most likely to benefit from mindfulness training and how long those benefits last, but the new study is a useful starting point, experts say.
“Mindfulness training had potentially short-term and long-term beneficial effects to children with ADHD and their parents,” says Samuel Wong, MD, director of the JC School of Public Health and Primary Care at the Chinese University of Hong Kong. He says mindfulness is more likely to become an add-on than a replacement for other kinds of therapies.
“Clinicians may consider combining or adding family-based mindfulness training with current practice for children with ADHD who have residual symptoms with their current treatment,” he said.
Mindfulness training may help with issues beyond the classic symptoms that come with ADHD, Dr. Mitchell said, helping make family life better overall, even when some features of the disorder don’t budge much.
“With this study in particular, we see that we have some pretty promising effects that there may be something that will be beneficial above and beyond the core 18 DSM symptoms,” he said. “This is an important study, because it’s going to be a basis for the continuing evolution of the scientific research on this topic. It’s something to feel excited about.”
A version of this article first appeared on WebMD.com.
Meditation, yoga, breathing exercises, and other mindfulness activities can help children with attention-deficit/hyperactivity disorder, but it’s not just the kids who benefit.
When families of children with ADHD complete a mindfulness program together, a new study suggests, children and parents can profit, with potential boosts to self-control, self-compassion, and psychological symptoms.
The findings do not suggest children should ditch medication in favor of focusing on the present moment. Instead, the study adds to growing evidence that mindfulness can be a helpful tool along with other strategies for children and adults with ADHD, said John Mitchell, PhD, a psychologist at Duke University, Durham, N.C., who was not involved with the new study. Mindfulness might help families ease stress and improve quality of life.
“We talk about ADHD because one person has that diagnosis, but we don’t live in bubbles,” he said. “We’re all interconnected and impact one another. And having treatments that acknowledge that and measuring that in the scientific literature is pretty important.”
Mindfulness training, which has its roots in Eastern traditions, generally aims to teach people how to be present in the moment and let go of judgment. Over the last couple of decades, researchers working on depression and other conditions have gathered evidence that practicing mindfulness can help in a variety of ways, including with the self-regulation of attention and emotions. It didn’t take long for those findings to draw interest from researchers who study ADHD, Dr. Mitchell said.
Research on mindfulness for ADHD started with adults, and results have been encouraging, Dr. Mitchell said. People who complete a mindfulness program tend to show some improvement in focus, impulsivity, and hyperactivity, studies show. In one small pilot study, Dr. Mitchell and colleagues reported improvements in symptoms and executive function in adults with ADHD.
Studies with children have lagged behind, but recent work has been promising. When looking at data from a number of studies, researchers have found small reductions in inattentiveness, hyperactivity, and impulsivity in young people with ADHD. Several randomized, controlled trials have also shown a reduction in symptoms as rated by parents and teachers.
Greater understanding, acceptance
In related research, there was a noticed reduction in stress among parents who get mindfulness training that teaches them to listen with their full attention, accept and develop compassion for themselves and their children, and regulate themselves within the relationship with their kids.
Still, first-line treatment for children with ADHD usually includes a combination of medication, cognitive behavioral therapy, and education, even though those strategies don’t always work well for everyone, says Corina Greven, PhD, a psychologist at Radboud (the Netherlands) University Medical Centre and Karakter Child and Adolescent Psychiatry.
Despite suggestive results, the data on mindfulness remains murky, in part because early studies that looked at mindfulness training for children with ADHD have been small. Few trials of mindfulness treatment for ADHD, Dr. Greven said, have included parents.
To fill in some of the gaps, Dr. Greven and colleagues conducted a trial with 103 families who had a child with ADHD between ages 8 and 16. Half of the families were randomly assigned simply to continue care as usual, which included medication for most.
The other half continued their usual care and also took part in a program called MYMind, which used mindfulness-based cognitive therapy for children and mindful parenting training for parents.
Families attended 90-minute group sessions once a week for 8 weeks, with an extra session 2 months later. The mindfulness group also completed homework every day that took about 30-45 minutes for parents and 15 minutes for children. Homework included workbooks and guided meditations.
In the short term, the team reported, children who received the mindfulness intervention showed small improvements in ADHD symptoms, anxiety, autistic symptoms, and problems falling asleep. One-third children who received mindfulness training improved on measures of self-control, Dr. Greven added, compared with just 1 in 10 who got only their usual care.
Benefits were larger and longer-lasting for parents. Compared with parents who didn’t get mindfulness training, those assigned to the mindfulness group improved in self-control, self-compassion, depression, anxiety, stress, well-being, and their own ADHD symptoms. Given a large genetic component to the disorder, it is common for parents of children with ADHD to have a diagnosis or ADHD symptoms as well. In addition, Dr. Greven said, families who completed the mindfulness-based intervention reported improvements in their relationships as well as acceptance of ADHD.
A new therapy?
The findings suggest new potential treatment options for children with ADHD, and for their parents, Dr. Greven said, as well as a need to study the condition more broadly. “Although parents of children with ADHD often have elevated parenting stress, anxiety, or their own ADHD symptoms, usual interventions for children with ADHD do not typically target parental mental health,” she said. “As researchers, we need to go broader than just looking at whether an intervention reduces symptoms and include additional outcomes that families find important.”
It will take more research to find out who is most likely to benefit from mindfulness training and how long those benefits last, but the new study is a useful starting point, experts say.
“Mindfulness training had potentially short-term and long-term beneficial effects to children with ADHD and their parents,” says Samuel Wong, MD, director of the JC School of Public Health and Primary Care at the Chinese University of Hong Kong. He says mindfulness is more likely to become an add-on than a replacement for other kinds of therapies.
“Clinicians may consider combining or adding family-based mindfulness training with current practice for children with ADHD who have residual symptoms with their current treatment,” he said.
Mindfulness training may help with issues beyond the classic symptoms that come with ADHD, Dr. Mitchell said, helping make family life better overall, even when some features of the disorder don’t budge much.
“With this study in particular, we see that we have some pretty promising effects that there may be something that will be beneficial above and beyond the core 18 DSM symptoms,” he said. “This is an important study, because it’s going to be a basis for the continuing evolution of the scientific research on this topic. It’s something to feel excited about.”
A version of this article first appeared on WebMD.com.
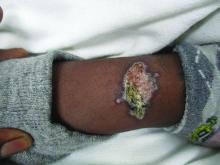
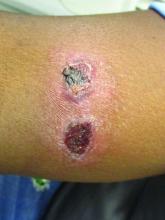
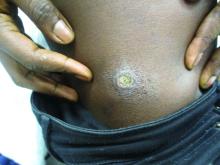
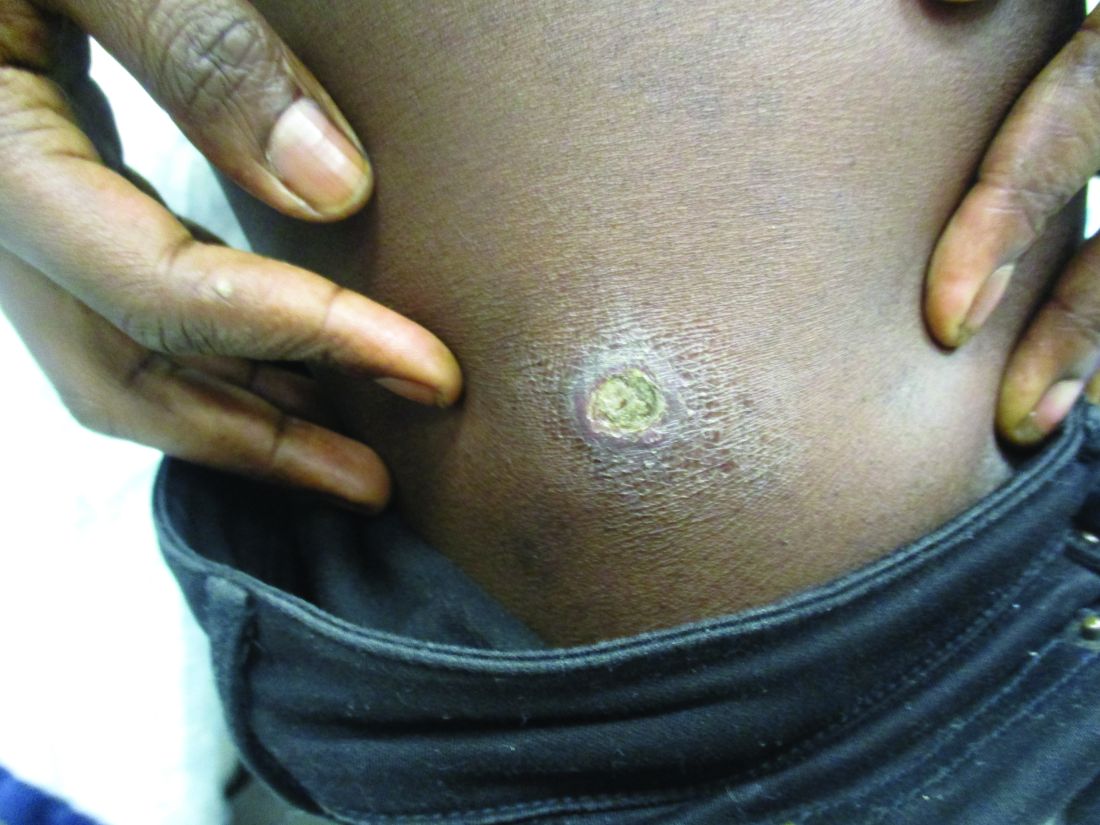
A healthy family who had been living in Brazil presented with crusted plaques on their extremities
Trypanosomatidae
Leishmaniasis is caused by protozoa of the family Trypanosomatidae, called Leishmania. The vector is a sandfly infected with the protozoa.1
The three main forms of leishmaniasis – cutaneous, mucocutaneous, or visceral – varies with the species of organism involved, the geographic distribution, and the immune response of the patient. A majority of the cases seen in the United States are from patients who contracted the disease elsewhere, particularly from Peru and Brazil.2
Lesions can vary from asymptomatic to severe. The initial lesion typically develops within weeks or months, and presents as an erythematous papule that is seen at the bite site.3 The papule evolves into a nodule or plaque that may ulcerate and crust.3 The ulcer can be distinguished by a raised and distinct border. In older stages, atrophic scarring may be seen. In some cases, the lesions may present years after exposure, because of immunosuppression or trauma.
Histology of CL reveals tuberculoid granulomas with parasitized histiocytes present. Amastigotes with distinct nuclei and kinetoplasts characterize Leishmania.2 In addition to histology, the biopsy may be sent for the press-imprint-smear method (PIS). In a study of 75 patients, the PIS method showed a higher sensitivity, as well as being a less costly and more rapid option for diagnosis.5
The treatment depends on the severity of the lesion and the species of the Leishmania genus. Mild lesions may resolve spontaneously. Topical imiquimod, cryotherapy, photodynamic therapy, and heat therapy may aid in the healing process.5 Systemic azole antifungal medications, miltefosine, and amphotericin B, and pentamidine may be used for more persistent lesions. In very severe cases, pentavalent antimonials (sodium stibogluconate, Pentostam) may be administered intravenously, although there is a high occurrence of recorded side effects.2
This case and the photos were submitted by Sabrina Liao, BS, University of California, San Diego; and Brooke Resh Sateesh, MD, San Diego Family Dermatology The case was edited by Donna Bilu Martin, MD.
References
1. Leishmaniasis – Resources for Health Professionals. Centers for Disease Control and Prevention. 2021 Jun 3.
2. Stark CG. Leishmaniasis. Medscape. 2020 Feb 18.
3. Markle WH and Makhoul K. Am Fam Physician. 2004 Mar 15;69(6):1455-604.
4. Ngan V. Leishmaniasis. DermNet NZ. 2017 Jan. 7.
5. Sousa AQ et al. Am J Trop Med Hyg. 2014 Nov;91(5):905-7.
Trypanosomatidae
Leishmaniasis is caused by protozoa of the family Trypanosomatidae, called Leishmania. The vector is a sandfly infected with the protozoa.1
The three main forms of leishmaniasis – cutaneous, mucocutaneous, or visceral – varies with the species of organism involved, the geographic distribution, and the immune response of the patient. A majority of the cases seen in the United States are from patients who contracted the disease elsewhere, particularly from Peru and Brazil.2
Lesions can vary from asymptomatic to severe. The initial lesion typically develops within weeks or months, and presents as an erythematous papule that is seen at the bite site.3 The papule evolves into a nodule or plaque that may ulcerate and crust.3 The ulcer can be distinguished by a raised and distinct border. In older stages, atrophic scarring may be seen. In some cases, the lesions may present years after exposure, because of immunosuppression or trauma.
Histology of CL reveals tuberculoid granulomas with parasitized histiocytes present. Amastigotes with distinct nuclei and kinetoplasts characterize Leishmania.2 In addition to histology, the biopsy may be sent for the press-imprint-smear method (PIS). In a study of 75 patients, the PIS method showed a higher sensitivity, as well as being a less costly and more rapid option for diagnosis.5
The treatment depends on the severity of the lesion and the species of the Leishmania genus. Mild lesions may resolve spontaneously. Topical imiquimod, cryotherapy, photodynamic therapy, and heat therapy may aid in the healing process.5 Systemic azole antifungal medications, miltefosine, and amphotericin B, and pentamidine may be used for more persistent lesions. In very severe cases, pentavalent antimonials (sodium stibogluconate, Pentostam) may be administered intravenously, although there is a high occurrence of recorded side effects.2
This case and the photos were submitted by Sabrina Liao, BS, University of California, San Diego; and Brooke Resh Sateesh, MD, San Diego Family Dermatology The case was edited by Donna Bilu Martin, MD.
References
1. Leishmaniasis – Resources for Health Professionals. Centers for Disease Control and Prevention. 2021 Jun 3.
2. Stark CG. Leishmaniasis. Medscape. 2020 Feb 18.
3. Markle WH and Makhoul K. Am Fam Physician. 2004 Mar 15;69(6):1455-604.
4. Ngan V. Leishmaniasis. DermNet NZ. 2017 Jan. 7.
5. Sousa AQ et al. Am J Trop Med Hyg. 2014 Nov;91(5):905-7.
Trypanosomatidae
Leishmaniasis is caused by protozoa of the family Trypanosomatidae, called Leishmania. The vector is a sandfly infected with the protozoa.1
The three main forms of leishmaniasis – cutaneous, mucocutaneous, or visceral – varies with the species of organism involved, the geographic distribution, and the immune response of the patient. A majority of the cases seen in the United States are from patients who contracted the disease elsewhere, particularly from Peru and Brazil.2
Lesions can vary from asymptomatic to severe. The initial lesion typically develops within weeks or months, and presents as an erythematous papule that is seen at the bite site.3 The papule evolves into a nodule or plaque that may ulcerate and crust.3 The ulcer can be distinguished by a raised and distinct border. In older stages, atrophic scarring may be seen. In some cases, the lesions may present years after exposure, because of immunosuppression or trauma.
Histology of CL reveals tuberculoid granulomas with parasitized histiocytes present. Amastigotes with distinct nuclei and kinetoplasts characterize Leishmania.2 In addition to histology, the biopsy may be sent for the press-imprint-smear method (PIS). In a study of 75 patients, the PIS method showed a higher sensitivity, as well as being a less costly and more rapid option for diagnosis.5
The treatment depends on the severity of the lesion and the species of the Leishmania genus. Mild lesions may resolve spontaneously. Topical imiquimod, cryotherapy, photodynamic therapy, and heat therapy may aid in the healing process.5 Systemic azole antifungal medications, miltefosine, and amphotericin B, and pentamidine may be used for more persistent lesions. In very severe cases, pentavalent antimonials (sodium stibogluconate, Pentostam) may be administered intravenously, although there is a high occurrence of recorded side effects.2
This case and the photos were submitted by Sabrina Liao, BS, University of California, San Diego; and Brooke Resh Sateesh, MD, San Diego Family Dermatology The case was edited by Donna Bilu Martin, MD.
References
1. Leishmaniasis – Resources for Health Professionals. Centers for Disease Control and Prevention. 2021 Jun 3.
2. Stark CG. Leishmaniasis. Medscape. 2020 Feb 18.
3. Markle WH and Makhoul K. Am Fam Physician. 2004 Mar 15;69(6):1455-604.
4. Ngan V. Leishmaniasis. DermNet NZ. 2017 Jan. 7.
5. Sousa AQ et al. Am J Trop Med Hyg. 2014 Nov;91(5):905-7.
Admissions for eating disorders double in pandemic
Medical admissions for adolescents with restrictive eating disorders more than doubled at one hospital during the first 12 months of the COVID-19 pandemic, relative to the average number of admissions in prior years, a new study shows.
Doctors are seeing similar increases across the United States and in other countries.
Providers and health care systems “may need to rapidly adapt in response to increasing demands for care during the COVID-19 pandemic,” the researchers said in their study, which was published online in Pediatrics.
To assess whether admission patterns among adolescents with restrictive eating disorders changed during the pandemic, Alana K. Otto, MD, MPH, with the division of adolescent medicine at the University of Michigan, Ann Arbor, and colleagues reviewed the charts of patients admitted to C.S. Mott Children’s Hospital, also in Ann Arbor.
Their analysis included 297 admissions among 248 patients aged 10-23 years between March 1, 2017, and March 31, 2021. Patients had an average age of about 15 years. Approximately 90% were female, and most had a diagnosis of anorexia nervosa or atypical anorexia nervosa.
Indications for medical admission included physiological instability (for example, heart rate less than 50 beats per minute while awake or blood pressure less than 90/40 mm Hg), electrolyte derangements, and acute medical complications of malnutrition such as syncope. Other possible indications included uncontrolled purging, body mass index less than 75% of the median for age and sex, acute food refusal, and failure of outpatient treatment.
Eating disorder–related admissions per month were stable prior to the pandemic. Admissions then decreased in April 2020, but subsequently increased significantly throughout the study period. In all, there were 125 admissions between April 1, 2020, and March 31, 2021. During the previous 3 years, the average number of admissions per year was 56.
Patients’ insurance status was one factor that differed before and during the pandemic. Prepandemic, about 20% of admissions were for adolescents with public insurance. During the pandemic, however, the proportion with public insurance was approximately 9%, the researchers noted. Other characteristics were generally similar.
The study was retrospective and relatively small and only looked at patients with restrictive eating disorders who were severely ill and admitted for medical stabilization. It does not reflect adolescents with eating disorders in different settings, the authors noted.
Primary care pediatricians should be familiar with indications for medical admission, such as severe bradycardia, as outlined by the Society for Adolescent Health and Medicine, they said.
Consistent trends
Unfortunately, the trend seems consistent across the nation, said Michaela M. Voss, MD, director of the the Eating Disorders Center at Children’s Mercy in Kansas City, Mo. “Our outpatient setting went from availability to get in immediately to a 6-month wait list.”
As in Michigan, Dr. Voss noted a drop in admissions as lockdowns started, followed by a spike in treatment demand that has not let up.
Dr. Voss described two of the more common presentations. In one, parents might note that their child had been getting into healthy eating and exercise before the pandemic and seemed fine. “But then COVID came, the lockdown happened, and they became overly obsessed with those things,” Dr. Voss said.
In the other presentation, kids with anxiety, depression, or OCD who lost access to their usual coping strategies and outlets developed eating disorders during the pandemic. “They focused on one of the few things they could during the lockdown, which was their own body, and then their anxiety, depression, [obsessive-compulsive disorder], and other mental health comorbidities presented as an eating disorder,” Dr. Voss said.
The increasing need for treatment over the course of the pandemic may reflect the time that it has taken for the disorders to develop, as well as the time that it takes parents to recognize the problem.
Not only are doctors seeing more cases, but patients are arriving sicker than usual, Dr. Voss said.
Major medical concerns for patients in starvation mode center on the heart, brain, and bones. In addition, refeeding syndrome poses an extreme risk, Dr. Voss noted.
The Academy for Eating Disorders has created a guide to help doctors recognize and manage risks for patients with eating disorders, which may be useful for primary care providers while they are trying to get a patient into more intensive treatment, Dr. Voss suggested. The American Academy of Pediatrics recently published a clinical report on the identification and management of eating disorders in children and adolescents.
At Johns Hopkins Hospital Children’s Center in Baltimore, “we have seen a pretty remarkable increase in the number of eating disorders in the child and adolescent space since COVID,” said Jennifer Leah Goetz, MD, a psychiatrist and medical director of the child and adolescent inpatient unit. “We have seen increasing numbers of kids presenting for acute medical stabilization and refeeding and for specific treatment for the eating disorder.”
It could be that, for people with a genetic predisposition to eating disorders, a confluence of factors related to the pandemic unmasked it. For example, children may have spent more time looking at themselves on virtual meeting platforms, which could stir lingering body image and appearance-related concerns in those who are vulnerable. And some teens who were not able to participate in athletics as usual started to watch what they eat more closely, Dr. Goetz said.
A treatment bottleneck
Patients with eating disorders “can be quite ill from a psychiatric and general medical perspective,” Dr. Goetz said. “Most psychiatrists are not particularly comfortable with the medical complications, and most internists or pediatricians are not particularly comfortable with the psychiatric complications. You end up with a patient population that can only see a really highly specialized group of individuals for care. And it is a problem. It was a problem before the pandemic, and it has been really exacerbated by what we have been going through with COVID.”
Natalie Muth, MD, MPH, RDN, a pediatrician at Children’s Primary Care Medical Group La Costa in Carlsbad, Calif., has also noticed the increase in eating disorders since COVID.
In-patient colleagues “have longer wait lists and more severe cases than they have ever seen previously,” said Dr. Muth, who chairs the American Academy of Pediatrics Section on Obesity and is an adjunct assistant professor at the University of California, Los Angeles. “In primary care, we are all having to better educate and prepare ourselves for identifying and managing patients with eating disorders.”
That could mean connecting with mental health professionals, registered dietitians, and higher levels of care. But that may be a challenge. “Accessing these resources has been more difficult due to the increasing incidence of eating disorders recently,” Dr. Muth said.
Dr. Voss acknowledged that childhood obesity is another concern for pediatricians. “However, there are appropriate and healthy and safe ways to address that,” she said. A patient with overweight or obesity who loses weight may not be doing so in a healthy way.
Clinicians should wonder if a patient’s weight is decreasing too fast. And they should ask patients questions that could help identify a problem, such as: What are they doing to cause the weight loss? Why do they want to lose the weight?
Dr. Voss added that eating disorders “do not discriminate.” While there may be a perception that all patients with eating disorders are White, upper middle–class females who are thin, “that is not the case,” Dr. Voss said. They “come in all genders, all races, all weight classes, and all ages,” she said, “and we see that variety.”
In general, there may be a need to shift how weight is discussed in clinics and society more broadly, Dr. Goetz said. Weight is an incredibly personal thing, and everyone’s genetics, metabolism, and life circumstances vary. At the same time, body mass index is not necessarily the best measure of a person’s health.
Asking a child, teen, or even an adult to go on a diet is not a benign intervention, Dr. Goetz noted. In addition, dieting is unlikely to help in the long term.
Emerging from lockdown, pressure to lose “COVID pounds” is a dangerous message for people with eating disorders, Dr. Goetz said. It also could be a dangerous message for people without eating disorders. “There are so many more interesting things about each one of us than our weight,” she added.
The study authors, Dr. Voss, Dr. Goetz, and Dr. Muth had no relevant disclosures.
Medical admissions for adolescents with restrictive eating disorders more than doubled at one hospital during the first 12 months of the COVID-19 pandemic, relative to the average number of admissions in prior years, a new study shows.
Doctors are seeing similar increases across the United States and in other countries.
Providers and health care systems “may need to rapidly adapt in response to increasing demands for care during the COVID-19 pandemic,” the researchers said in their study, which was published online in Pediatrics.
To assess whether admission patterns among adolescents with restrictive eating disorders changed during the pandemic, Alana K. Otto, MD, MPH, with the division of adolescent medicine at the University of Michigan, Ann Arbor, and colleagues reviewed the charts of patients admitted to C.S. Mott Children’s Hospital, also in Ann Arbor.
Their analysis included 297 admissions among 248 patients aged 10-23 years between March 1, 2017, and March 31, 2021. Patients had an average age of about 15 years. Approximately 90% were female, and most had a diagnosis of anorexia nervosa or atypical anorexia nervosa.
Indications for medical admission included physiological instability (for example, heart rate less than 50 beats per minute while awake or blood pressure less than 90/40 mm Hg), electrolyte derangements, and acute medical complications of malnutrition such as syncope. Other possible indications included uncontrolled purging, body mass index less than 75% of the median for age and sex, acute food refusal, and failure of outpatient treatment.
Eating disorder–related admissions per month were stable prior to the pandemic. Admissions then decreased in April 2020, but subsequently increased significantly throughout the study period. In all, there were 125 admissions between April 1, 2020, and March 31, 2021. During the previous 3 years, the average number of admissions per year was 56.
Patients’ insurance status was one factor that differed before and during the pandemic. Prepandemic, about 20% of admissions were for adolescents with public insurance. During the pandemic, however, the proportion with public insurance was approximately 9%, the researchers noted. Other characteristics were generally similar.
The study was retrospective and relatively small and only looked at patients with restrictive eating disorders who were severely ill and admitted for medical stabilization. It does not reflect adolescents with eating disorders in different settings, the authors noted.
Primary care pediatricians should be familiar with indications for medical admission, such as severe bradycardia, as outlined by the Society for Adolescent Health and Medicine, they said.
Consistent trends
Unfortunately, the trend seems consistent across the nation, said Michaela M. Voss, MD, director of the the Eating Disorders Center at Children’s Mercy in Kansas City, Mo. “Our outpatient setting went from availability to get in immediately to a 6-month wait list.”
As in Michigan, Dr. Voss noted a drop in admissions as lockdowns started, followed by a spike in treatment demand that has not let up.
Dr. Voss described two of the more common presentations. In one, parents might note that their child had been getting into healthy eating and exercise before the pandemic and seemed fine. “But then COVID came, the lockdown happened, and they became overly obsessed with those things,” Dr. Voss said.
In the other presentation, kids with anxiety, depression, or OCD who lost access to their usual coping strategies and outlets developed eating disorders during the pandemic. “They focused on one of the few things they could during the lockdown, which was their own body, and then their anxiety, depression, [obsessive-compulsive disorder], and other mental health comorbidities presented as an eating disorder,” Dr. Voss said.
The increasing need for treatment over the course of the pandemic may reflect the time that it has taken for the disorders to develop, as well as the time that it takes parents to recognize the problem.
Not only are doctors seeing more cases, but patients are arriving sicker than usual, Dr. Voss said.
Major medical concerns for patients in starvation mode center on the heart, brain, and bones. In addition, refeeding syndrome poses an extreme risk, Dr. Voss noted.
The Academy for Eating Disorders has created a guide to help doctors recognize and manage risks for patients with eating disorders, which may be useful for primary care providers while they are trying to get a patient into more intensive treatment, Dr. Voss suggested. The American Academy of Pediatrics recently published a clinical report on the identification and management of eating disorders in children and adolescents.
At Johns Hopkins Hospital Children’s Center in Baltimore, “we have seen a pretty remarkable increase in the number of eating disorders in the child and adolescent space since COVID,” said Jennifer Leah Goetz, MD, a psychiatrist and medical director of the child and adolescent inpatient unit. “We have seen increasing numbers of kids presenting for acute medical stabilization and refeeding and for specific treatment for the eating disorder.”
It could be that, for people with a genetic predisposition to eating disorders, a confluence of factors related to the pandemic unmasked it. For example, children may have spent more time looking at themselves on virtual meeting platforms, which could stir lingering body image and appearance-related concerns in those who are vulnerable. And some teens who were not able to participate in athletics as usual started to watch what they eat more closely, Dr. Goetz said.
A treatment bottleneck
Patients with eating disorders “can be quite ill from a psychiatric and general medical perspective,” Dr. Goetz said. “Most psychiatrists are not particularly comfortable with the medical complications, and most internists or pediatricians are not particularly comfortable with the psychiatric complications. You end up with a patient population that can only see a really highly specialized group of individuals for care. And it is a problem. It was a problem before the pandemic, and it has been really exacerbated by what we have been going through with COVID.”
Natalie Muth, MD, MPH, RDN, a pediatrician at Children’s Primary Care Medical Group La Costa in Carlsbad, Calif., has also noticed the increase in eating disorders since COVID.
In-patient colleagues “have longer wait lists and more severe cases than they have ever seen previously,” said Dr. Muth, who chairs the American Academy of Pediatrics Section on Obesity and is an adjunct assistant professor at the University of California, Los Angeles. “In primary care, we are all having to better educate and prepare ourselves for identifying and managing patients with eating disorders.”
That could mean connecting with mental health professionals, registered dietitians, and higher levels of care. But that may be a challenge. “Accessing these resources has been more difficult due to the increasing incidence of eating disorders recently,” Dr. Muth said.
Dr. Voss acknowledged that childhood obesity is another concern for pediatricians. “However, there are appropriate and healthy and safe ways to address that,” she said. A patient with overweight or obesity who loses weight may not be doing so in a healthy way.
Clinicians should wonder if a patient’s weight is decreasing too fast. And they should ask patients questions that could help identify a problem, such as: What are they doing to cause the weight loss? Why do they want to lose the weight?
Dr. Voss added that eating disorders “do not discriminate.” While there may be a perception that all patients with eating disorders are White, upper middle–class females who are thin, “that is not the case,” Dr. Voss said. They “come in all genders, all races, all weight classes, and all ages,” she said, “and we see that variety.”
In general, there may be a need to shift how weight is discussed in clinics and society more broadly, Dr. Goetz said. Weight is an incredibly personal thing, and everyone’s genetics, metabolism, and life circumstances vary. At the same time, body mass index is not necessarily the best measure of a person’s health.
Asking a child, teen, or even an adult to go on a diet is not a benign intervention, Dr. Goetz noted. In addition, dieting is unlikely to help in the long term.
Emerging from lockdown, pressure to lose “COVID pounds” is a dangerous message for people with eating disorders, Dr. Goetz said. It also could be a dangerous message for people without eating disorders. “There are so many more interesting things about each one of us than our weight,” she added.
The study authors, Dr. Voss, Dr. Goetz, and Dr. Muth had no relevant disclosures.
Medical admissions for adolescents with restrictive eating disorders more than doubled at one hospital during the first 12 months of the COVID-19 pandemic, relative to the average number of admissions in prior years, a new study shows.
Doctors are seeing similar increases across the United States and in other countries.
Providers and health care systems “may need to rapidly adapt in response to increasing demands for care during the COVID-19 pandemic,” the researchers said in their study, which was published online in Pediatrics.
To assess whether admission patterns among adolescents with restrictive eating disorders changed during the pandemic, Alana K. Otto, MD, MPH, with the division of adolescent medicine at the University of Michigan, Ann Arbor, and colleagues reviewed the charts of patients admitted to C.S. Mott Children’s Hospital, also in Ann Arbor.
Their analysis included 297 admissions among 248 patients aged 10-23 years between March 1, 2017, and March 31, 2021. Patients had an average age of about 15 years. Approximately 90% were female, and most had a diagnosis of anorexia nervosa or atypical anorexia nervosa.
Indications for medical admission included physiological instability (for example, heart rate less than 50 beats per minute while awake or blood pressure less than 90/40 mm Hg), electrolyte derangements, and acute medical complications of malnutrition such as syncope. Other possible indications included uncontrolled purging, body mass index less than 75% of the median for age and sex, acute food refusal, and failure of outpatient treatment.
Eating disorder–related admissions per month were stable prior to the pandemic. Admissions then decreased in April 2020, but subsequently increased significantly throughout the study period. In all, there were 125 admissions between April 1, 2020, and March 31, 2021. During the previous 3 years, the average number of admissions per year was 56.
Patients’ insurance status was one factor that differed before and during the pandemic. Prepandemic, about 20% of admissions were for adolescents with public insurance. During the pandemic, however, the proportion with public insurance was approximately 9%, the researchers noted. Other characteristics were generally similar.
The study was retrospective and relatively small and only looked at patients with restrictive eating disorders who were severely ill and admitted for medical stabilization. It does not reflect adolescents with eating disorders in different settings, the authors noted.
Primary care pediatricians should be familiar with indications for medical admission, such as severe bradycardia, as outlined by the Society for Adolescent Health and Medicine, they said.
Consistent trends
Unfortunately, the trend seems consistent across the nation, said Michaela M. Voss, MD, director of the the Eating Disorders Center at Children’s Mercy in Kansas City, Mo. “Our outpatient setting went from availability to get in immediately to a 6-month wait list.”
As in Michigan, Dr. Voss noted a drop in admissions as lockdowns started, followed by a spike in treatment demand that has not let up.
Dr. Voss described two of the more common presentations. In one, parents might note that their child had been getting into healthy eating and exercise before the pandemic and seemed fine. “But then COVID came, the lockdown happened, and they became overly obsessed with those things,” Dr. Voss said.
In the other presentation, kids with anxiety, depression, or OCD who lost access to their usual coping strategies and outlets developed eating disorders during the pandemic. “They focused on one of the few things they could during the lockdown, which was their own body, and then their anxiety, depression, [obsessive-compulsive disorder], and other mental health comorbidities presented as an eating disorder,” Dr. Voss said.
The increasing need for treatment over the course of the pandemic may reflect the time that it has taken for the disorders to develop, as well as the time that it takes parents to recognize the problem.
Not only are doctors seeing more cases, but patients are arriving sicker than usual, Dr. Voss said.
Major medical concerns for patients in starvation mode center on the heart, brain, and bones. In addition, refeeding syndrome poses an extreme risk, Dr. Voss noted.
The Academy for Eating Disorders has created a guide to help doctors recognize and manage risks for patients with eating disorders, which may be useful for primary care providers while they are trying to get a patient into more intensive treatment, Dr. Voss suggested. The American Academy of Pediatrics recently published a clinical report on the identification and management of eating disorders in children and adolescents.
At Johns Hopkins Hospital Children’s Center in Baltimore, “we have seen a pretty remarkable increase in the number of eating disorders in the child and adolescent space since COVID,” said Jennifer Leah Goetz, MD, a psychiatrist and medical director of the child and adolescent inpatient unit. “We have seen increasing numbers of kids presenting for acute medical stabilization and refeeding and for specific treatment for the eating disorder.”
It could be that, for people with a genetic predisposition to eating disorders, a confluence of factors related to the pandemic unmasked it. For example, children may have spent more time looking at themselves on virtual meeting platforms, which could stir lingering body image and appearance-related concerns in those who are vulnerable. And some teens who were not able to participate in athletics as usual started to watch what they eat more closely, Dr. Goetz said.
A treatment bottleneck
Patients with eating disorders “can be quite ill from a psychiatric and general medical perspective,” Dr. Goetz said. “Most psychiatrists are not particularly comfortable with the medical complications, and most internists or pediatricians are not particularly comfortable with the psychiatric complications. You end up with a patient population that can only see a really highly specialized group of individuals for care. And it is a problem. It was a problem before the pandemic, and it has been really exacerbated by what we have been going through with COVID.”
Natalie Muth, MD, MPH, RDN, a pediatrician at Children’s Primary Care Medical Group La Costa in Carlsbad, Calif., has also noticed the increase in eating disorders since COVID.
In-patient colleagues “have longer wait lists and more severe cases than they have ever seen previously,” said Dr. Muth, who chairs the American Academy of Pediatrics Section on Obesity and is an adjunct assistant professor at the University of California, Los Angeles. “In primary care, we are all having to better educate and prepare ourselves for identifying and managing patients with eating disorders.”
That could mean connecting with mental health professionals, registered dietitians, and higher levels of care. But that may be a challenge. “Accessing these resources has been more difficult due to the increasing incidence of eating disorders recently,” Dr. Muth said.
Dr. Voss acknowledged that childhood obesity is another concern for pediatricians. “However, there are appropriate and healthy and safe ways to address that,” she said. A patient with overweight or obesity who loses weight may not be doing so in a healthy way.
Clinicians should wonder if a patient’s weight is decreasing too fast. And they should ask patients questions that could help identify a problem, such as: What are they doing to cause the weight loss? Why do they want to lose the weight?
Dr. Voss added that eating disorders “do not discriminate.” While there may be a perception that all patients with eating disorders are White, upper middle–class females who are thin, “that is not the case,” Dr. Voss said. They “come in all genders, all races, all weight classes, and all ages,” she said, “and we see that variety.”
In general, there may be a need to shift how weight is discussed in clinics and society more broadly, Dr. Goetz said. Weight is an incredibly personal thing, and everyone’s genetics, metabolism, and life circumstances vary. At the same time, body mass index is not necessarily the best measure of a person’s health.
Asking a child, teen, or even an adult to go on a diet is not a benign intervention, Dr. Goetz noted. In addition, dieting is unlikely to help in the long term.
Emerging from lockdown, pressure to lose “COVID pounds” is a dangerous message for people with eating disorders, Dr. Goetz said. It also could be a dangerous message for people without eating disorders. “There are so many more interesting things about each one of us than our weight,” she added.
The study authors, Dr. Voss, Dr. Goetz, and Dr. Muth had no relevant disclosures.
FROM PEDIATRICS
Stop using Neutrogena and Aveeno spray sunscreen, J&J warns
Benzene is not an ingredient of sunscreen, and should not be present in these products. The levels detected were low and would not be expected to have an adverse effect on health, but the company says it is recalling the products anyway “out of an abundance of caution.”
The sunscreen products that have been recalled are:
- NEUTROGENA® Beach Defense® aerosol sunscreen.
- NEUTROGENA® Cool Dry Sport aerosol sunscreen.
- NEUTROGENA® Invisible Daily™ defense aerosol sunscreen.
- NEUTROGENA® Ultra Sheer® aerosol sunscreen.
- AVEENO® Protect + Refresh aerosol sunscreen.
These products were distributed nationwide through a variety of retail stores. Consumers should stop using these products and throw them away, the company said.
At the same time, it emphasized the importance of using alternative sunscreen products to protect the skin from excessive sun exposure, which can lead to skin cancer including melanoma.
Johnson & Johnson has launched an investigation into how benzene got into these products.
One of the company’s other spray sunscreen products, Neutrogena Wet Skin, was not included in the recall.
Recently, benzene was found in 78 widely-used sunscreen products in tests conducted by the online pharmacy and laboratory Valisure. Most of the products were aerosol sprays, and the company called on the Food and Drug Administration to recall them all.
That petition suggested that the finding of benzene was the result of contamination somewhere in the manufacturing process.
“This isn’t a sunscreen issue, it’s a manufacturing issue,” said Adam Friedman, MD, professor and chief of dermatology at George Washington University. “We don’t want those things to be blurred.”
There is a risk that people take away the wrong message from these findings.
“People already have ambivalence about sunscreen, and this is just going to make that worse,” Dr. Friedman said in an interview.
He pointed out that benzene is present in car exhaust, second-hand smoke, and elsewhere. Inhalation exposure has been the primary focus of toxicology investigations, as has exposure from things such as contaminated drinking water – not via topical application. “We don’t know how effectively [benzene] gets through the skin, if it gets absorbed systemically, and how that then behaves downstream,” he noted.
On the other hand, ultraviolet radiation is a well-established carcinogen. Avoiding an effective preventive measure such as sunscreen could prove more harmful than exposure to trace amounts of benzene, he said.
A version of this article first appeared on WebMD.com.
Benzene is not an ingredient of sunscreen, and should not be present in these products. The levels detected were low and would not be expected to have an adverse effect on health, but the company says it is recalling the products anyway “out of an abundance of caution.”
The sunscreen products that have been recalled are:
- NEUTROGENA® Beach Defense® aerosol sunscreen.
- NEUTROGENA® Cool Dry Sport aerosol sunscreen.
- NEUTROGENA® Invisible Daily™ defense aerosol sunscreen.
- NEUTROGENA® Ultra Sheer® aerosol sunscreen.
- AVEENO® Protect + Refresh aerosol sunscreen.
These products were distributed nationwide through a variety of retail stores. Consumers should stop using these products and throw them away, the company said.
At the same time, it emphasized the importance of using alternative sunscreen products to protect the skin from excessive sun exposure, which can lead to skin cancer including melanoma.
Johnson & Johnson has launched an investigation into how benzene got into these products.
One of the company’s other spray sunscreen products, Neutrogena Wet Skin, was not included in the recall.
Recently, benzene was found in 78 widely-used sunscreen products in tests conducted by the online pharmacy and laboratory Valisure. Most of the products were aerosol sprays, and the company called on the Food and Drug Administration to recall them all.
That petition suggested that the finding of benzene was the result of contamination somewhere in the manufacturing process.
“This isn’t a sunscreen issue, it’s a manufacturing issue,” said Adam Friedman, MD, professor and chief of dermatology at George Washington University. “We don’t want those things to be blurred.”
There is a risk that people take away the wrong message from these findings.
“People already have ambivalence about sunscreen, and this is just going to make that worse,” Dr. Friedman said in an interview.
He pointed out that benzene is present in car exhaust, second-hand smoke, and elsewhere. Inhalation exposure has been the primary focus of toxicology investigations, as has exposure from things such as contaminated drinking water – not via topical application. “We don’t know how effectively [benzene] gets through the skin, if it gets absorbed systemically, and how that then behaves downstream,” he noted.
On the other hand, ultraviolet radiation is a well-established carcinogen. Avoiding an effective preventive measure such as sunscreen could prove more harmful than exposure to trace amounts of benzene, he said.
A version of this article first appeared on WebMD.com.
Benzene is not an ingredient of sunscreen, and should not be present in these products. The levels detected were low and would not be expected to have an adverse effect on health, but the company says it is recalling the products anyway “out of an abundance of caution.”
The sunscreen products that have been recalled are:
- NEUTROGENA® Beach Defense® aerosol sunscreen.
- NEUTROGENA® Cool Dry Sport aerosol sunscreen.
- NEUTROGENA® Invisible Daily™ defense aerosol sunscreen.
- NEUTROGENA® Ultra Sheer® aerosol sunscreen.
- AVEENO® Protect + Refresh aerosol sunscreen.
These products were distributed nationwide through a variety of retail stores. Consumers should stop using these products and throw them away, the company said.
At the same time, it emphasized the importance of using alternative sunscreen products to protect the skin from excessive sun exposure, which can lead to skin cancer including melanoma.
Johnson & Johnson has launched an investigation into how benzene got into these products.
One of the company’s other spray sunscreen products, Neutrogena Wet Skin, was not included in the recall.
Recently, benzene was found in 78 widely-used sunscreen products in tests conducted by the online pharmacy and laboratory Valisure. Most of the products were aerosol sprays, and the company called on the Food and Drug Administration to recall them all.
That petition suggested that the finding of benzene was the result of contamination somewhere in the manufacturing process.
“This isn’t a sunscreen issue, it’s a manufacturing issue,” said Adam Friedman, MD, professor and chief of dermatology at George Washington University. “We don’t want those things to be blurred.”
There is a risk that people take away the wrong message from these findings.
“People already have ambivalence about sunscreen, and this is just going to make that worse,” Dr. Friedman said in an interview.
He pointed out that benzene is present in car exhaust, second-hand smoke, and elsewhere. Inhalation exposure has been the primary focus of toxicology investigations, as has exposure from things such as contaminated drinking water – not via topical application. “We don’t know how effectively [benzene] gets through the skin, if it gets absorbed systemically, and how that then behaves downstream,” he noted.
On the other hand, ultraviolet radiation is a well-established carcinogen. Avoiding an effective preventive measure such as sunscreen could prove more harmful than exposure to trace amounts of benzene, he said.
A version of this article first appeared on WebMD.com.
Tennessee fires top vaccine official as COVID cases increase
Tennessee officials have fired the state’s top vaccination manager, who faced recent criticism from Republican lawmakers about her efforts to vaccinate teens against COVID-19.
Michelle Fiscus, MD, the medical director for vaccine-preventable diseases and immunization programs at the Tennessee Department of Health, was terminated on July 12. The termination letter doesn’t explain the reason for her dismissal, according to the newspaper, which received a copy of the letter.
“It was my job to provide evidence-based education and vaccine access so that Tennesseans could protect themselves against COVID-19,” Dr. Fiscus told the Tennessean. “I have now been terminated for doing exactly that.”
In May, Dr. Fiscus sent a memo to medical providers that described the state’s “Mature Minor Doctrine,” a legal mechanism established in 1987 that allows some minors between the ages if 14 and 17 years to receive medical care without parental consent. Tennessee is one of five states that allows health care providers to decide if a minor has the capacity to consent to care, according to CNN.
Dr. Fiscus said she sent the letter in response to providers’ questions and that it contained no new information. She also said the wording was approved by the health department’s attorney and the governor’s office, the newspaper reported.
At a June 16 hearing of the state’s Joint Government Operations Committee, however, Republican officials criticized the memo and Dr. Fiscus, saying that the state misinterpreted its legal authority. During the meeting, some lawmakers discussed dissolving the state health department to stop it from promoting vaccines to teens, the newspaper reported.
Since then, the health department has backed down from promoting vaccines to teens by deleting social media posts that recommended vaccines to anyone over age 12. Internal emails, which were obtained by the Tennessean, showed that department leaders ordered county-level employees to avoid holding vaccine events targeted toward adolescents.
Dr. Fiscus’s firing comes as vaccination efforts lag in the state. About 38% of residents have been fully vaccinated. At the current pace, Tennessee won’t pass the 50% mark until next March, according to an internal report obtained by the newspaper.
COVID-19 cases are beginning to climb again, particularly with the Delta variant circulating among unvaccinated residents. After months of a decline in cases, the average of daily cases has more than doubled since the end of June. The state’s test positivity rate has increased from 2% to 4.5% during that time as well.
In a long written statement, Dr. Fiscus said she was the 25th of 64 state and territorial immunization program directors to leave their positions during the pandemic, whether through resignation or termination. With a loss of institutional knowledge and leadership, COVID-19 vaccine efforts will fall behind.
“Each of us should be waking up every morning with one question on our minds: ‘What can I do protect the people of Tennessee against COVID-19?’ ” she wrote. “Instead, our leaders are putting barriers in place to ensure the people of Tennessee remain at risk, even with the Delta variant bearing down upon us.”
A version of this article first appeared on WebMD.com.
Tennessee officials have fired the state’s top vaccination manager, who faced recent criticism from Republican lawmakers about her efforts to vaccinate teens against COVID-19.
Michelle Fiscus, MD, the medical director for vaccine-preventable diseases and immunization programs at the Tennessee Department of Health, was terminated on July 12. The termination letter doesn’t explain the reason for her dismissal, according to the newspaper, which received a copy of the letter.
“It was my job to provide evidence-based education and vaccine access so that Tennesseans could protect themselves against COVID-19,” Dr. Fiscus told the Tennessean. “I have now been terminated for doing exactly that.”
In May, Dr. Fiscus sent a memo to medical providers that described the state’s “Mature Minor Doctrine,” a legal mechanism established in 1987 that allows some minors between the ages if 14 and 17 years to receive medical care without parental consent. Tennessee is one of five states that allows health care providers to decide if a minor has the capacity to consent to care, according to CNN.
Dr. Fiscus said she sent the letter in response to providers’ questions and that it contained no new information. She also said the wording was approved by the health department’s attorney and the governor’s office, the newspaper reported.
At a June 16 hearing of the state’s Joint Government Operations Committee, however, Republican officials criticized the memo and Dr. Fiscus, saying that the state misinterpreted its legal authority. During the meeting, some lawmakers discussed dissolving the state health department to stop it from promoting vaccines to teens, the newspaper reported.
Since then, the health department has backed down from promoting vaccines to teens by deleting social media posts that recommended vaccines to anyone over age 12. Internal emails, which were obtained by the Tennessean, showed that department leaders ordered county-level employees to avoid holding vaccine events targeted toward adolescents.
Dr. Fiscus’s firing comes as vaccination efforts lag in the state. About 38% of residents have been fully vaccinated. At the current pace, Tennessee won’t pass the 50% mark until next March, according to an internal report obtained by the newspaper.
COVID-19 cases are beginning to climb again, particularly with the Delta variant circulating among unvaccinated residents. After months of a decline in cases, the average of daily cases has more than doubled since the end of June. The state’s test positivity rate has increased from 2% to 4.5% during that time as well.
In a long written statement, Dr. Fiscus said she was the 25th of 64 state and territorial immunization program directors to leave their positions during the pandemic, whether through resignation or termination. With a loss of institutional knowledge and leadership, COVID-19 vaccine efforts will fall behind.
“Each of us should be waking up every morning with one question on our minds: ‘What can I do protect the people of Tennessee against COVID-19?’ ” she wrote. “Instead, our leaders are putting barriers in place to ensure the people of Tennessee remain at risk, even with the Delta variant bearing down upon us.”
A version of this article first appeared on WebMD.com.
Tennessee officials have fired the state’s top vaccination manager, who faced recent criticism from Republican lawmakers about her efforts to vaccinate teens against COVID-19.
Michelle Fiscus, MD, the medical director for vaccine-preventable diseases and immunization programs at the Tennessee Department of Health, was terminated on July 12. The termination letter doesn’t explain the reason for her dismissal, according to the newspaper, which received a copy of the letter.
“It was my job to provide evidence-based education and vaccine access so that Tennesseans could protect themselves against COVID-19,” Dr. Fiscus told the Tennessean. “I have now been terminated for doing exactly that.”
In May, Dr. Fiscus sent a memo to medical providers that described the state’s “Mature Minor Doctrine,” a legal mechanism established in 1987 that allows some minors between the ages if 14 and 17 years to receive medical care without parental consent. Tennessee is one of five states that allows health care providers to decide if a minor has the capacity to consent to care, according to CNN.
Dr. Fiscus said she sent the letter in response to providers’ questions and that it contained no new information. She also said the wording was approved by the health department’s attorney and the governor’s office, the newspaper reported.
At a June 16 hearing of the state’s Joint Government Operations Committee, however, Republican officials criticized the memo and Dr. Fiscus, saying that the state misinterpreted its legal authority. During the meeting, some lawmakers discussed dissolving the state health department to stop it from promoting vaccines to teens, the newspaper reported.
Since then, the health department has backed down from promoting vaccines to teens by deleting social media posts that recommended vaccines to anyone over age 12. Internal emails, which were obtained by the Tennessean, showed that department leaders ordered county-level employees to avoid holding vaccine events targeted toward adolescents.
Dr. Fiscus’s firing comes as vaccination efforts lag in the state. About 38% of residents have been fully vaccinated. At the current pace, Tennessee won’t pass the 50% mark until next March, according to an internal report obtained by the newspaper.
COVID-19 cases are beginning to climb again, particularly with the Delta variant circulating among unvaccinated residents. After months of a decline in cases, the average of daily cases has more than doubled since the end of June. The state’s test positivity rate has increased from 2% to 4.5% during that time as well.
In a long written statement, Dr. Fiscus said she was the 25th of 64 state and territorial immunization program directors to leave their positions during the pandemic, whether through resignation or termination. With a loss of institutional knowledge and leadership, COVID-19 vaccine efforts will fall behind.
“Each of us should be waking up every morning with one question on our minds: ‘What can I do protect the people of Tennessee against COVID-19?’ ” she wrote. “Instead, our leaders are putting barriers in place to ensure the people of Tennessee remain at risk, even with the Delta variant bearing down upon us.”
A version of this article first appeared on WebMD.com.
Bullying in academic medicine rife, underreported
Bullying in academic medicine, especially among women, is rife, underreported, and remains largely unaddressed, new research suggests.
Investigators reviewed close to 70 studies, encompassing over 82,000 medical consultants or trainees in academic medical settings, and found that men were identified as the most common perpetrators – close to 70% of respondents – whereas women were the most common victims (56%).
Collectively, respondents in all of the studies identified the most common bullies to be consultants (54%), followed by residents (22%), and nurses (15%).
Disturbingly, less than one-third of victims overall reported that they were bullied, and close to 60% who formally reported the abuse said they did not have a positive outcome.
“We found that bullies are commonly men and senior consultants, while more than half of their victims are women,” senior author Harriette G.C. Van Spall, MD, MPH, associate professor of medicine and director of e-health and virtual care, Division of Cardiology, McMaster University, Hamilton, Ont., said in an interview.
“The greatest barriers to addressing academic bullying are the fear of reprisal, lack of impact of reporting, and non-enforcement of anti-bullying policies,” she added.
The study was published online July 12 in BMJ Open.
Personal experience
“Some behaviors were excruciating to deal with, protesting against them would bring more on, and every day was filled with dread. It took sheer will to show up at work to care for patients, to complete research I was leading, and to have hope, and my academic output, income, and personal well-being dropped during those years,” she added.
Dr. Van Spall thought the subject “merited research because our performance as clinicians, researchers, and educators relies on our work environment.”
To investigate, the researchers reviewed 68 studies (n = 82,349 respondents) conducted between 1999 and 2021 in academic medical settings, in which victims were either consultants or trainees. Many of the studies (31) were conducted in the U.S.
Other countries included the United Kingdom, Canada, Australia, Pakistan, Egypt, Iran, Turkey, New Zealand, Lithuania, Greece, India, Germany, Nigeria, Oman, and Finland.
Studies were required to describe the method and impact of bullying; characteristics of the perpetrators and victims; or interventions that were used to address the bullying.
“Bullying” was defined as “the abuse of authority by a perpetrator who targets the victim in an academic setting through punishing behaviors that include overwork, destabilization, and isolation in order to impede the education or career of the target.”
Systemic sexism
Bullying behaviors, reported in 28 studies (n = 35,779 respondents), were grouped into destabilization, threats to professional status, overwork, and isolation, with overwork found to be the most common form of bullying.
The most common impact of being bullied was psychological distress, reported by 39.1% of respondents in 14 studies, followed by considerations of quitting (35.9%; 7 studies), and worsening of clinical performance (34.6%, 8 studies).
“Among demographic groups, men were identified as the most common perpetrators (67.2% of 4,722 respondents in 5 studies) and women the most common victims (56.2% of 15,246 respondents in 27 studies),” the authors report.
“Academic medicine in many institutions is encumbered by systemic sexism that is evident in processes around remuneration, recognition, opportunities for advancement, and leadership positions,” said Dr. Van Spall.
“There are fewer women at decision-making tables in academic medicine, the climb is uphill at the best of times, and women are likely easier targets for bullies, as their voices are easier to drown out,” she added.
She noted that many men do “exhibit wonderful attributes of professionalism and decency,” but “some in positions of power are given impunity by virtue of other accomplishments.”
Multiple deterrents
Thirty-one studies (n = 15,868) described characteristics of the bullies and showed the most common to be consultants (53.6% [30 studies]), residents (22% [22 studies]), and nurses (14.9% [21 studies]).
Only a minority of victims (28.9% of 9,410 victims [10 studies]) formally reported the bullying. The researchers identified multiple deterrents to reporting.
When a formal complaint was submitted (n = 1,139 respondents), it most frequently had no perceived effect (35.6%); more than one-fifth (21.9%) experienced worsening of the bullying, and only 13.7% reported improvement.
The common institutional facilitators of bullying, described in 25 studies, included lack of enforcement of anti-bullying policies (13 studies), the hierarchical structure of medicine (7 studies), and normalization of bullying (10 studies).
Forty-nine studies looked at strategies to address academic bullying, including anti-bullying policies, mandatory workshops on mistreatment, establishing an anti-bullying oversight committee, and institutional support for victims. However, the studies testing the effectiveness of these interventions “had a high risk of bias.”
Support available
Commenting on the research for this news organization, Roberta Gebhard, DO, past president of the American Medical Women’s Association (AMWA) and a member of the advisory board for Physician Just Equity, called it a “good study, large, international, and well-written.”
Dr. Gebhard, a member of the Governing Council for the American Medical Association Women Physician Section, was not associated with this study but said she is currently researching women who left medical school and residency.
“A common reason for leaving is being bullied. Bullying is often not reported and if reported, often not addressed. Or, if addressed, the person who reports it is often retaliated against, which is a common experience, especially in women.”
She advised female physicians who are bullied to get support from other female physicians – for example, by joining the AMWA, which has an online women’s leadership group.
“Having other women physicians throughout the country you can call for advice and support can be helpful,” said Dr. Gebhard, a family practice physician based in Grand Island, New York.
Dr. Van Spall receives support from the Canadian Institutes of Health Research, the Heart and Stroke Foundation, the Women As One Escalator Award, and McMaster Department of Medicine. The study authors and Dr. Gebhard have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Bullying in academic medicine, especially among women, is rife, underreported, and remains largely unaddressed, new research suggests.
Investigators reviewed close to 70 studies, encompassing over 82,000 medical consultants or trainees in academic medical settings, and found that men were identified as the most common perpetrators – close to 70% of respondents – whereas women were the most common victims (56%).
Collectively, respondents in all of the studies identified the most common bullies to be consultants (54%), followed by residents (22%), and nurses (15%).
Disturbingly, less than one-third of victims overall reported that they were bullied, and close to 60% who formally reported the abuse said they did not have a positive outcome.
“We found that bullies are commonly men and senior consultants, while more than half of their victims are women,” senior author Harriette G.C. Van Spall, MD, MPH, associate professor of medicine and director of e-health and virtual care, Division of Cardiology, McMaster University, Hamilton, Ont., said in an interview.
“The greatest barriers to addressing academic bullying are the fear of reprisal, lack of impact of reporting, and non-enforcement of anti-bullying policies,” she added.
The study was published online July 12 in BMJ Open.
Personal experience
“Some behaviors were excruciating to deal with, protesting against them would bring more on, and every day was filled with dread. It took sheer will to show up at work to care for patients, to complete research I was leading, and to have hope, and my academic output, income, and personal well-being dropped during those years,” she added.
Dr. Van Spall thought the subject “merited research because our performance as clinicians, researchers, and educators relies on our work environment.”
To investigate, the researchers reviewed 68 studies (n = 82,349 respondents) conducted between 1999 and 2021 in academic medical settings, in which victims were either consultants or trainees. Many of the studies (31) were conducted in the U.S.
Other countries included the United Kingdom, Canada, Australia, Pakistan, Egypt, Iran, Turkey, New Zealand, Lithuania, Greece, India, Germany, Nigeria, Oman, and Finland.
Studies were required to describe the method and impact of bullying; characteristics of the perpetrators and victims; or interventions that were used to address the bullying.
“Bullying” was defined as “the abuse of authority by a perpetrator who targets the victim in an academic setting through punishing behaviors that include overwork, destabilization, and isolation in order to impede the education or career of the target.”
Systemic sexism
Bullying behaviors, reported in 28 studies (n = 35,779 respondents), were grouped into destabilization, threats to professional status, overwork, and isolation, with overwork found to be the most common form of bullying.
The most common impact of being bullied was psychological distress, reported by 39.1% of respondents in 14 studies, followed by considerations of quitting (35.9%; 7 studies), and worsening of clinical performance (34.6%, 8 studies).
“Among demographic groups, men were identified as the most common perpetrators (67.2% of 4,722 respondents in 5 studies) and women the most common victims (56.2% of 15,246 respondents in 27 studies),” the authors report.
“Academic medicine in many institutions is encumbered by systemic sexism that is evident in processes around remuneration, recognition, opportunities for advancement, and leadership positions,” said Dr. Van Spall.
“There are fewer women at decision-making tables in academic medicine, the climb is uphill at the best of times, and women are likely easier targets for bullies, as their voices are easier to drown out,” she added.
She noted that many men do “exhibit wonderful attributes of professionalism and decency,” but “some in positions of power are given impunity by virtue of other accomplishments.”
Multiple deterrents
Thirty-one studies (n = 15,868) described characteristics of the bullies and showed the most common to be consultants (53.6% [30 studies]), residents (22% [22 studies]), and nurses (14.9% [21 studies]).
Only a minority of victims (28.9% of 9,410 victims [10 studies]) formally reported the bullying. The researchers identified multiple deterrents to reporting.
When a formal complaint was submitted (n = 1,139 respondents), it most frequently had no perceived effect (35.6%); more than one-fifth (21.9%) experienced worsening of the bullying, and only 13.7% reported improvement.
The common institutional facilitators of bullying, described in 25 studies, included lack of enforcement of anti-bullying policies (13 studies), the hierarchical structure of medicine (7 studies), and normalization of bullying (10 studies).
Forty-nine studies looked at strategies to address academic bullying, including anti-bullying policies, mandatory workshops on mistreatment, establishing an anti-bullying oversight committee, and institutional support for victims. However, the studies testing the effectiveness of these interventions “had a high risk of bias.”
Support available
Commenting on the research for this news organization, Roberta Gebhard, DO, past president of the American Medical Women’s Association (AMWA) and a member of the advisory board for Physician Just Equity, called it a “good study, large, international, and well-written.”
Dr. Gebhard, a member of the Governing Council for the American Medical Association Women Physician Section, was not associated with this study but said she is currently researching women who left medical school and residency.
“A common reason for leaving is being bullied. Bullying is often not reported and if reported, often not addressed. Or, if addressed, the person who reports it is often retaliated against, which is a common experience, especially in women.”
She advised female physicians who are bullied to get support from other female physicians – for example, by joining the AMWA, which has an online women’s leadership group.
“Having other women physicians throughout the country you can call for advice and support can be helpful,” said Dr. Gebhard, a family practice physician based in Grand Island, New York.
Dr. Van Spall receives support from the Canadian Institutes of Health Research, the Heart and Stroke Foundation, the Women As One Escalator Award, and McMaster Department of Medicine. The study authors and Dr. Gebhard have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Bullying in academic medicine, especially among women, is rife, underreported, and remains largely unaddressed, new research suggests.
Investigators reviewed close to 70 studies, encompassing over 82,000 medical consultants or trainees in academic medical settings, and found that men were identified as the most common perpetrators – close to 70% of respondents – whereas women were the most common victims (56%).
Collectively, respondents in all of the studies identified the most common bullies to be consultants (54%), followed by residents (22%), and nurses (15%).
Disturbingly, less than one-third of victims overall reported that they were bullied, and close to 60% who formally reported the abuse said they did not have a positive outcome.
“We found that bullies are commonly men and senior consultants, while more than half of their victims are women,” senior author Harriette G.C. Van Spall, MD, MPH, associate professor of medicine and director of e-health and virtual care, Division of Cardiology, McMaster University, Hamilton, Ont., said in an interview.
“The greatest barriers to addressing academic bullying are the fear of reprisal, lack of impact of reporting, and non-enforcement of anti-bullying policies,” she added.
The study was published online July 12 in BMJ Open.
Personal experience
“Some behaviors were excruciating to deal with, protesting against them would bring more on, and every day was filled with dread. It took sheer will to show up at work to care for patients, to complete research I was leading, and to have hope, and my academic output, income, and personal well-being dropped during those years,” she added.
Dr. Van Spall thought the subject “merited research because our performance as clinicians, researchers, and educators relies on our work environment.”
To investigate, the researchers reviewed 68 studies (n = 82,349 respondents) conducted between 1999 and 2021 in academic medical settings, in which victims were either consultants or trainees. Many of the studies (31) were conducted in the U.S.
Other countries included the United Kingdom, Canada, Australia, Pakistan, Egypt, Iran, Turkey, New Zealand, Lithuania, Greece, India, Germany, Nigeria, Oman, and Finland.
Studies were required to describe the method and impact of bullying; characteristics of the perpetrators and victims; or interventions that were used to address the bullying.
“Bullying” was defined as “the abuse of authority by a perpetrator who targets the victim in an academic setting through punishing behaviors that include overwork, destabilization, and isolation in order to impede the education or career of the target.”
Systemic sexism
Bullying behaviors, reported in 28 studies (n = 35,779 respondents), were grouped into destabilization, threats to professional status, overwork, and isolation, with overwork found to be the most common form of bullying.
The most common impact of being bullied was psychological distress, reported by 39.1% of respondents in 14 studies, followed by considerations of quitting (35.9%; 7 studies), and worsening of clinical performance (34.6%, 8 studies).
“Among demographic groups, men were identified as the most common perpetrators (67.2% of 4,722 respondents in 5 studies) and women the most common victims (56.2% of 15,246 respondents in 27 studies),” the authors report.
“Academic medicine in many institutions is encumbered by systemic sexism that is evident in processes around remuneration, recognition, opportunities for advancement, and leadership positions,” said Dr. Van Spall.
“There are fewer women at decision-making tables in academic medicine, the climb is uphill at the best of times, and women are likely easier targets for bullies, as their voices are easier to drown out,” she added.
She noted that many men do “exhibit wonderful attributes of professionalism and decency,” but “some in positions of power are given impunity by virtue of other accomplishments.”
Multiple deterrents
Thirty-one studies (n = 15,868) described characteristics of the bullies and showed the most common to be consultants (53.6% [30 studies]), residents (22% [22 studies]), and nurses (14.9% [21 studies]).
Only a minority of victims (28.9% of 9,410 victims [10 studies]) formally reported the bullying. The researchers identified multiple deterrents to reporting.
When a formal complaint was submitted (n = 1,139 respondents), it most frequently had no perceived effect (35.6%); more than one-fifth (21.9%) experienced worsening of the bullying, and only 13.7% reported improvement.
The common institutional facilitators of bullying, described in 25 studies, included lack of enforcement of anti-bullying policies (13 studies), the hierarchical structure of medicine (7 studies), and normalization of bullying (10 studies).
Forty-nine studies looked at strategies to address academic bullying, including anti-bullying policies, mandatory workshops on mistreatment, establishing an anti-bullying oversight committee, and institutional support for victims. However, the studies testing the effectiveness of these interventions “had a high risk of bias.”
Support available
Commenting on the research for this news organization, Roberta Gebhard, DO, past president of the American Medical Women’s Association (AMWA) and a member of the advisory board for Physician Just Equity, called it a “good study, large, international, and well-written.”
Dr. Gebhard, a member of the Governing Council for the American Medical Association Women Physician Section, was not associated with this study but said she is currently researching women who left medical school and residency.
“A common reason for leaving is being bullied. Bullying is often not reported and if reported, often not addressed. Or, if addressed, the person who reports it is often retaliated against, which is a common experience, especially in women.”
She advised female physicians who are bullied to get support from other female physicians – for example, by joining the AMWA, which has an online women’s leadership group.
“Having other women physicians throughout the country you can call for advice and support can be helpful,” said Dr. Gebhard, a family practice physician based in Grand Island, New York.
Dr. Van Spall receives support from the Canadian Institutes of Health Research, the Heart and Stroke Foundation, the Women As One Escalator Award, and McMaster Department of Medicine. The study authors and Dr. Gebhard have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Dupilumab safe, effective in kids 6-11 with moderate-to-severe asthma
Dupilumab (Dupixent, Sanofi and Regeneron) significantly reduced exacerbations compared with placebo in children ages 6-11 years who had moderate-to-severe asthma in a phase 3 trial.
A fully human monoclonal antibody, dupilumab also improved lung function versus placebo by week 12, an improvement that lasted the length of the 52-week trial.
Dupilumab previously had been shown to be safe and effective in adolescents and adults with moderate-to-severe asthma, patients 6 years and older with moderate-to-severe atopic dermatitis, and adults with chronic rhinosinusitis with nasal polyposis, but its safety and effectiveness for moderate-to-severe asthma in the 6-11 years age group was not known.
Results from the randomized, double-blind VOYAGE study conducted across several countries were presented Saturday, July 10, at the European Academy of Allergy and Clinical Immunology (EAACI) Hybrid Congress 2021.
Leonard B. Bacharier, MD, professor of pediatrics, allergy/immunology/pulmonary medicine at Vanderbilt University Medical Center in Nashville, Tennessee, presented the results from the trial, which was funded by Sanofi/Regeneron.
Researchers enrolled 408 children ages 6-11 years with uncontrolled moderate-to-severe asthma. Children on high-dose inhaled corticosteroids (ICS) alone or medium-to-high–dose ICS with a second controller were randomly assigned either to add-on subcutaneous dupilumab 100 mg or 200 mg, based on body weight at study start, or to placebo every 2 weeks for 52 weeks.
Analyses were done in two populations: 350 patients with markers of type 2 inflammation (baseline blood eosinophils ≥150 cells/μl or fractional exhaled nitric oxide [FeNO] ≥20 ppb) and 259 patients with baseline blood eosinophils ≥300 cells/µl.
“The primary endpoint was the annualized rate of severe asthma exacerbations,” Dr. Bacharier said. “The key secondary endpoint was change in percent predicted prebronchodilator FEV1 [forced expiratory volume at 1 second] from baseline to week 12.”
At week 12, the annualized severe asthma exacerbation rate was reduced by 59% (P < .0001) in children with blood eosinophils ≥300 cells/µL and results were similar in those with the type 2 inflammatory phenotype compared with placebo.
Results also indicate a favorable safety profile for dupilumab.
James M. Tracy, DO, an expert with the American College of Allergy, Asthma, and Immunology, told this news organization that adding the dupilumab option for children in the 6-11 age group is “huge.”
Dr. Tracy, who was not involved with the study, said although omalizumab (Xolair, Genentech) is also available for these children, dupilumab stands out because of the range of comorbidities it can treat.
“[Children] don’t have the same rhinosinusitis and polyposis that adults would have, but a lot of them have eczema, and this drug with multiple prongs is incredibly useful and addresses a broad array of allergic conditions,” Dr. Tracy said.
More than 90% of children in the study had at least one concurrent type 2 inflammatory condition, including atopic dermatitis and eosinophilic esophagitis. Dupilumab blocks the shared receptor for interleukin (IL)-4/IL-13, which are key drivers of type 2 inflammation in multiple diseases.
Dr. Tracy said that while dupilumab is not the only drug available to treat children 6-11 years with moderate-to-severe asthma, it is “a significant and unique addition to the armamentarium of the individual practitioner taking care of these very severe asthmatics in the 6-11 age group.”
Dupilumab also led to rapid and sustained improvement in lung function. At 12 weeks, children assigned dupilumab improved their lung function as measured by FEV1 by 5.21% (P = .0009), and that continued through the 52-week study period.
“What we know is the [improved lung function] effect is sustained. What we don’t know is how long you have to keep on the drug for a more permanent effect, which is an issue for all these biologics,” Tracy said.
Dr. Bacharier reported speaker fees and research support from Sanofi/Regeneron. Dr. Tracy has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Dupilumab (Dupixent, Sanofi and Regeneron) significantly reduced exacerbations compared with placebo in children ages 6-11 years who had moderate-to-severe asthma in a phase 3 trial.
A fully human monoclonal antibody, dupilumab also improved lung function versus placebo by week 12, an improvement that lasted the length of the 52-week trial.
Dupilumab previously had been shown to be safe and effective in adolescents and adults with moderate-to-severe asthma, patients 6 years and older with moderate-to-severe atopic dermatitis, and adults with chronic rhinosinusitis with nasal polyposis, but its safety and effectiveness for moderate-to-severe asthma in the 6-11 years age group was not known.
Results from the randomized, double-blind VOYAGE study conducted across several countries were presented Saturday, July 10, at the European Academy of Allergy and Clinical Immunology (EAACI) Hybrid Congress 2021.
Leonard B. Bacharier, MD, professor of pediatrics, allergy/immunology/pulmonary medicine at Vanderbilt University Medical Center in Nashville, Tennessee, presented the results from the trial, which was funded by Sanofi/Regeneron.
Researchers enrolled 408 children ages 6-11 years with uncontrolled moderate-to-severe asthma. Children on high-dose inhaled corticosteroids (ICS) alone or medium-to-high–dose ICS with a second controller were randomly assigned either to add-on subcutaneous dupilumab 100 mg or 200 mg, based on body weight at study start, or to placebo every 2 weeks for 52 weeks.
Analyses were done in two populations: 350 patients with markers of type 2 inflammation (baseline blood eosinophils ≥150 cells/μl or fractional exhaled nitric oxide [FeNO] ≥20 ppb) and 259 patients with baseline blood eosinophils ≥300 cells/µl.
“The primary endpoint was the annualized rate of severe asthma exacerbations,” Dr. Bacharier said. “The key secondary endpoint was change in percent predicted prebronchodilator FEV1 [forced expiratory volume at 1 second] from baseline to week 12.”
At week 12, the annualized severe asthma exacerbation rate was reduced by 59% (P < .0001) in children with blood eosinophils ≥300 cells/µL and results were similar in those with the type 2 inflammatory phenotype compared with placebo.
Results also indicate a favorable safety profile for dupilumab.
James M. Tracy, DO, an expert with the American College of Allergy, Asthma, and Immunology, told this news organization that adding the dupilumab option for children in the 6-11 age group is “huge.”
Dr. Tracy, who was not involved with the study, said although omalizumab (Xolair, Genentech) is also available for these children, dupilumab stands out because of the range of comorbidities it can treat.
“[Children] don’t have the same rhinosinusitis and polyposis that adults would have, but a lot of them have eczema, and this drug with multiple prongs is incredibly useful and addresses a broad array of allergic conditions,” Dr. Tracy said.
More than 90% of children in the study had at least one concurrent type 2 inflammatory condition, including atopic dermatitis and eosinophilic esophagitis. Dupilumab blocks the shared receptor for interleukin (IL)-4/IL-13, which are key drivers of type 2 inflammation in multiple diseases.
Dr. Tracy said that while dupilumab is not the only drug available to treat children 6-11 years with moderate-to-severe asthma, it is “a significant and unique addition to the armamentarium of the individual practitioner taking care of these very severe asthmatics in the 6-11 age group.”
Dupilumab also led to rapid and sustained improvement in lung function. At 12 weeks, children assigned dupilumab improved their lung function as measured by FEV1 by 5.21% (P = .0009), and that continued through the 52-week study period.
“What we know is the [improved lung function] effect is sustained. What we don’t know is how long you have to keep on the drug for a more permanent effect, which is an issue for all these biologics,” Tracy said.
Dr. Bacharier reported speaker fees and research support from Sanofi/Regeneron. Dr. Tracy has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Dupilumab (Dupixent, Sanofi and Regeneron) significantly reduced exacerbations compared with placebo in children ages 6-11 years who had moderate-to-severe asthma in a phase 3 trial.
A fully human monoclonal antibody, dupilumab also improved lung function versus placebo by week 12, an improvement that lasted the length of the 52-week trial.
Dupilumab previously had been shown to be safe and effective in adolescents and adults with moderate-to-severe asthma, patients 6 years and older with moderate-to-severe atopic dermatitis, and adults with chronic rhinosinusitis with nasal polyposis, but its safety and effectiveness for moderate-to-severe asthma in the 6-11 years age group was not known.
Results from the randomized, double-blind VOYAGE study conducted across several countries were presented Saturday, July 10, at the European Academy of Allergy and Clinical Immunology (EAACI) Hybrid Congress 2021.
Leonard B. Bacharier, MD, professor of pediatrics, allergy/immunology/pulmonary medicine at Vanderbilt University Medical Center in Nashville, Tennessee, presented the results from the trial, which was funded by Sanofi/Regeneron.
Researchers enrolled 408 children ages 6-11 years with uncontrolled moderate-to-severe asthma. Children on high-dose inhaled corticosteroids (ICS) alone or medium-to-high–dose ICS with a second controller were randomly assigned either to add-on subcutaneous dupilumab 100 mg or 200 mg, based on body weight at study start, or to placebo every 2 weeks for 52 weeks.
Analyses were done in two populations: 350 patients with markers of type 2 inflammation (baseline blood eosinophils ≥150 cells/μl or fractional exhaled nitric oxide [FeNO] ≥20 ppb) and 259 patients with baseline blood eosinophils ≥300 cells/µl.
“The primary endpoint was the annualized rate of severe asthma exacerbations,” Dr. Bacharier said. “The key secondary endpoint was change in percent predicted prebronchodilator FEV1 [forced expiratory volume at 1 second] from baseline to week 12.”
At week 12, the annualized severe asthma exacerbation rate was reduced by 59% (P < .0001) in children with blood eosinophils ≥300 cells/µL and results were similar in those with the type 2 inflammatory phenotype compared with placebo.
Results also indicate a favorable safety profile for dupilumab.
James M. Tracy, DO, an expert with the American College of Allergy, Asthma, and Immunology, told this news organization that adding the dupilumab option for children in the 6-11 age group is “huge.”
Dr. Tracy, who was not involved with the study, said although omalizumab (Xolair, Genentech) is also available for these children, dupilumab stands out because of the range of comorbidities it can treat.
“[Children] don’t have the same rhinosinusitis and polyposis that adults would have, but a lot of them have eczema, and this drug with multiple prongs is incredibly useful and addresses a broad array of allergic conditions,” Dr. Tracy said.
More than 90% of children in the study had at least one concurrent type 2 inflammatory condition, including atopic dermatitis and eosinophilic esophagitis. Dupilumab blocks the shared receptor for interleukin (IL)-4/IL-13, which are key drivers of type 2 inflammation in multiple diseases.
Dr. Tracy said that while dupilumab is not the only drug available to treat children 6-11 years with moderate-to-severe asthma, it is “a significant and unique addition to the armamentarium of the individual practitioner taking care of these very severe asthmatics in the 6-11 age group.”
Dupilumab also led to rapid and sustained improvement in lung function. At 12 weeks, children assigned dupilumab improved their lung function as measured by FEV1 by 5.21% (P = .0009), and that continued through the 52-week study period.
“What we know is the [improved lung function] effect is sustained. What we don’t know is how long you have to keep on the drug for a more permanent effect, which is an issue for all these biologics,” Tracy said.
Dr. Bacharier reported speaker fees and research support from Sanofi/Regeneron. Dr. Tracy has disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Vaccine mandates, passports, and Kant
Houston Methodist Hospital in June 2021 enforced an April mandate that all its employees, about 26,000 of them, must be vaccinated against COVID-19. In the following weeks, many other large health care systems adopted a similar employer mandate.
Compliance with Houston Methodist’s mandate has been very high at nearly 99%. There were some deferrals, mostly because of pregnancy. There were some “medical and personal” exemptions for less than 1% of employees. The reasons for those personal exemptions have not been made public. A lawsuit by 117 employees objecting to the vaccine mandate was dismissed by a federal district judge on June 12.
Objections to the vaccine mandate have rarely involved religious-based conscientious objections, which need to be accommodated differently, legally and ethically. The objections have been disagreements on the science. As a politician said decades ago: “People are entitled to their own opinions, but not their own facts.” A medical institution is an excellent organization for determining the risks and benefits of vaccination. The judge dismissing the case was very critical of the characterizations used by the plaintiffs.
The vaccine mandate has strong ethical support from both the universalizability principle of Kant and a consequentialist analysis. The U.S. Equal Employment Opportunity Commission on May 28, 2021, released technical assistance that has generally been interpreted to support an employer’s right to set vaccine requirements. HIPAA does not forbid an employer from asking about vaccination, but the EEOC guidance reminds employers that if they do ask, employers have legal obligations to protect the health information and keep it separate from other personnel files.
In the past few years, many hospitals and clinics have adopted mandates for influenza vaccines. In many children’s hospitals staff have been required to have chicken pox vaccines (or, as in my case, titers showing immunity from the real thing – I’m old) since the early 2000s. Measles titers (again, mine were acquired naturally – I still remember the illness and recommend against that) and TB status are occasionally required for locum tenens positions. I keep copies of these labs alongside copies of my diplomas. To me, the COVID-19 mandate is not capricious.
Some people have pointed out that the COVID-19 vaccines are not fully Food and Drug Administration approved. They are used under an emergency use authorization. Any traction that distinction might have had ethically and scientifically in November 2020 has disappeared with the experience of 9 months and 300 million doses in the United States. Dr. Fauci on July 11, 2021, said: “These vaccines are as good as officially approved with all the I’s dotted and the T’s crossed.”
On July 12, 2021, French President Macron, facing a resurgence of the pandemic because of the delta variant, announced a national vaccine mandate for all health care workers. He also announced plans to require proof of vaccination (or prior disease) in order to enter amusement parks, restaurants, and other public facilities. The ethics of his plans have been debated by ethicists and politicians for months under the rubric of a “vaccine passport.” England has required proof of vaccination or a recent negative COVID-19 test before entering soccer stadiums. In the United States, some localities, particularly those where the local politicians are against the vaccine, have passed laws proscribing the creation of these passport-like restrictions. Elsewhere, many businesses have already started to exclude customers who are not vaccinated. Airlines, hotels, and cruise ships are at the forefront of this. Society has started to create consequences for not getting the vaccine. President Macron indicated that the goal was now to put restrictions on the unvaccinated rather than on everyone.
Pediatricians are experts on the importance of consequences for misbehavior and refusals. It is a frequent topic of conversation with parents of toddlers and teenagers. Consequences are ethical, just, and effective ways of promoting safe and fair behavior. At this point, the public has been educated about the disease and the vaccines. In the United States, there has been ample access to the vaccine. It is time to enforce consequences.
Daily vaccination rates in the United States have slowed to 25% of the peak rates. The reasons for hesitancy have been analyzed in many publications. Further public education hasn’t been productive, so empathic listening has been urged to overcome hesitancy. (A similar program has long been advocated to deal with hesitancy for teenage HPV vaccines.) President Biden on July 6, 2021, proposed a program of going door to door to overcome resistance.
The world is in a race between vaccines and the delta variant. The Delta variant is moving the finish line, with some French epidemiologists advising President Macron that this more contagious variant may require a 90% vaccination level to achieve herd immunity. Israel has started giving a third booster shot in select situations and Pfizer is considering the idea. I agree with providing education, using empathic listening, and improving access. Those are all reasonable, even necessary, strategies. But at this point, I anchor my suggestions with the same advice pediatricians have long given to parents. Set rules and create consequences for misbehavior.
Dr. Powell is a retired pediatric hospitalist and clinical ethics consultant living in St. Louis. He has no financial disclosures. Email him at [email protected].
Houston Methodist Hospital in June 2021 enforced an April mandate that all its employees, about 26,000 of them, must be vaccinated against COVID-19. In the following weeks, many other large health care systems adopted a similar employer mandate.
Compliance with Houston Methodist’s mandate has been very high at nearly 99%. There were some deferrals, mostly because of pregnancy. There were some “medical and personal” exemptions for less than 1% of employees. The reasons for those personal exemptions have not been made public. A lawsuit by 117 employees objecting to the vaccine mandate was dismissed by a federal district judge on June 12.
Objections to the vaccine mandate have rarely involved religious-based conscientious objections, which need to be accommodated differently, legally and ethically. The objections have been disagreements on the science. As a politician said decades ago: “People are entitled to their own opinions, but not their own facts.” A medical institution is an excellent organization for determining the risks and benefits of vaccination. The judge dismissing the case was very critical of the characterizations used by the plaintiffs.
The vaccine mandate has strong ethical support from both the universalizability principle of Kant and a consequentialist analysis. The U.S. Equal Employment Opportunity Commission on May 28, 2021, released technical assistance that has generally been interpreted to support an employer’s right to set vaccine requirements. HIPAA does not forbid an employer from asking about vaccination, but the EEOC guidance reminds employers that if they do ask, employers have legal obligations to protect the health information and keep it separate from other personnel files.
In the past few years, many hospitals and clinics have adopted mandates for influenza vaccines. In many children’s hospitals staff have been required to have chicken pox vaccines (or, as in my case, titers showing immunity from the real thing – I’m old) since the early 2000s. Measles titers (again, mine were acquired naturally – I still remember the illness and recommend against that) and TB status are occasionally required for locum tenens positions. I keep copies of these labs alongside copies of my diplomas. To me, the COVID-19 mandate is not capricious.
Some people have pointed out that the COVID-19 vaccines are not fully Food and Drug Administration approved. They are used under an emergency use authorization. Any traction that distinction might have had ethically and scientifically in November 2020 has disappeared with the experience of 9 months and 300 million doses in the United States. Dr. Fauci on July 11, 2021, said: “These vaccines are as good as officially approved with all the I’s dotted and the T’s crossed.”
On July 12, 2021, French President Macron, facing a resurgence of the pandemic because of the delta variant, announced a national vaccine mandate for all health care workers. He also announced plans to require proof of vaccination (or prior disease) in order to enter amusement parks, restaurants, and other public facilities. The ethics of his plans have been debated by ethicists and politicians for months under the rubric of a “vaccine passport.” England has required proof of vaccination or a recent negative COVID-19 test before entering soccer stadiums. In the United States, some localities, particularly those where the local politicians are against the vaccine, have passed laws proscribing the creation of these passport-like restrictions. Elsewhere, many businesses have already started to exclude customers who are not vaccinated. Airlines, hotels, and cruise ships are at the forefront of this. Society has started to create consequences for not getting the vaccine. President Macron indicated that the goal was now to put restrictions on the unvaccinated rather than on everyone.
Pediatricians are experts on the importance of consequences for misbehavior and refusals. It is a frequent topic of conversation with parents of toddlers and teenagers. Consequences are ethical, just, and effective ways of promoting safe and fair behavior. At this point, the public has been educated about the disease and the vaccines. In the United States, there has been ample access to the vaccine. It is time to enforce consequences.
Daily vaccination rates in the United States have slowed to 25% of the peak rates. The reasons for hesitancy have been analyzed in many publications. Further public education hasn’t been productive, so empathic listening has been urged to overcome hesitancy. (A similar program has long been advocated to deal with hesitancy for teenage HPV vaccines.) President Biden on July 6, 2021, proposed a program of going door to door to overcome resistance.
The world is in a race between vaccines and the delta variant. The Delta variant is moving the finish line, with some French epidemiologists advising President Macron that this more contagious variant may require a 90% vaccination level to achieve herd immunity. Israel has started giving a third booster shot in select situations and Pfizer is considering the idea. I agree with providing education, using empathic listening, and improving access. Those are all reasonable, even necessary, strategies. But at this point, I anchor my suggestions with the same advice pediatricians have long given to parents. Set rules and create consequences for misbehavior.
Dr. Powell is a retired pediatric hospitalist and clinical ethics consultant living in St. Louis. He has no financial disclosures. Email him at [email protected].
Houston Methodist Hospital in June 2021 enforced an April mandate that all its employees, about 26,000 of them, must be vaccinated against COVID-19. In the following weeks, many other large health care systems adopted a similar employer mandate.
Compliance with Houston Methodist’s mandate has been very high at nearly 99%. There were some deferrals, mostly because of pregnancy. There were some “medical and personal” exemptions for less than 1% of employees. The reasons for those personal exemptions have not been made public. A lawsuit by 117 employees objecting to the vaccine mandate was dismissed by a federal district judge on June 12.
Objections to the vaccine mandate have rarely involved religious-based conscientious objections, which need to be accommodated differently, legally and ethically. The objections have been disagreements on the science. As a politician said decades ago: “People are entitled to their own opinions, but not their own facts.” A medical institution is an excellent organization for determining the risks and benefits of vaccination. The judge dismissing the case was very critical of the characterizations used by the plaintiffs.
The vaccine mandate has strong ethical support from both the universalizability principle of Kant and a consequentialist analysis. The U.S. Equal Employment Opportunity Commission on May 28, 2021, released technical assistance that has generally been interpreted to support an employer’s right to set vaccine requirements. HIPAA does not forbid an employer from asking about vaccination, but the EEOC guidance reminds employers that if they do ask, employers have legal obligations to protect the health information and keep it separate from other personnel files.
In the past few years, many hospitals and clinics have adopted mandates for influenza vaccines. In many children’s hospitals staff have been required to have chicken pox vaccines (or, as in my case, titers showing immunity from the real thing – I’m old) since the early 2000s. Measles titers (again, mine were acquired naturally – I still remember the illness and recommend against that) and TB status are occasionally required for locum tenens positions. I keep copies of these labs alongside copies of my diplomas. To me, the COVID-19 mandate is not capricious.
Some people have pointed out that the COVID-19 vaccines are not fully Food and Drug Administration approved. They are used under an emergency use authorization. Any traction that distinction might have had ethically and scientifically in November 2020 has disappeared with the experience of 9 months and 300 million doses in the United States. Dr. Fauci on July 11, 2021, said: “These vaccines are as good as officially approved with all the I’s dotted and the T’s crossed.”
On July 12, 2021, French President Macron, facing a resurgence of the pandemic because of the delta variant, announced a national vaccine mandate for all health care workers. He also announced plans to require proof of vaccination (or prior disease) in order to enter amusement parks, restaurants, and other public facilities. The ethics of his plans have been debated by ethicists and politicians for months under the rubric of a “vaccine passport.” England has required proof of vaccination or a recent negative COVID-19 test before entering soccer stadiums. In the United States, some localities, particularly those where the local politicians are against the vaccine, have passed laws proscribing the creation of these passport-like restrictions. Elsewhere, many businesses have already started to exclude customers who are not vaccinated. Airlines, hotels, and cruise ships are at the forefront of this. Society has started to create consequences for not getting the vaccine. President Macron indicated that the goal was now to put restrictions on the unvaccinated rather than on everyone.
Pediatricians are experts on the importance of consequences for misbehavior and refusals. It is a frequent topic of conversation with parents of toddlers and teenagers. Consequences are ethical, just, and effective ways of promoting safe and fair behavior. At this point, the public has been educated about the disease and the vaccines. In the United States, there has been ample access to the vaccine. It is time to enforce consequences.
Daily vaccination rates in the United States have slowed to 25% of the peak rates. The reasons for hesitancy have been analyzed in many publications. Further public education hasn’t been productive, so empathic listening has been urged to overcome hesitancy. (A similar program has long been advocated to deal with hesitancy for teenage HPV vaccines.) President Biden on July 6, 2021, proposed a program of going door to door to overcome resistance.
The world is in a race between vaccines and the delta variant. The Delta variant is moving the finish line, with some French epidemiologists advising President Macron that this more contagious variant may require a 90% vaccination level to achieve herd immunity. Israel has started giving a third booster shot in select situations and Pfizer is considering the idea. I agree with providing education, using empathic listening, and improving access. Those are all reasonable, even necessary, strategies. But at this point, I anchor my suggestions with the same advice pediatricians have long given to parents. Set rules and create consequences for misbehavior.
Dr. Powell is a retired pediatric hospitalist and clinical ethics consultant living in St. Louis. He has no financial disclosures. Email him at [email protected].
Dogs know their humans, but humans don’t know expiration dates
An extreme price to pay for immortality
We know that men don’t live as long as women, but the reasons aren’t entirely clear. However, some New Zealand scientists have a thought on the subject, thanks to a sheep called Shrek.
The researchers were inspired by a famous old sheep who escaped captivity, but was captured 6 years later at the age of 10. The sheep then lived 6 more years, far beyond the lifespan of a normal sheep, capturing the hearts and minds of Kiwis everywhere. Look, it’s New Zealand, sheep are life, so it’s only natural the country got attached. Scientists from the University of Otago suspected that Shrek lived such a long life because he was castrated.
So they undertook a study of sheep, and lo and behold, sheep that were castrated lived significantly longer than their uncastrated kin, thanks to a slowing of their epigenetic clocks – the DNA aged noticeably slower in the castrated sheep.
Although the research can most immediately be applied to the improvement of the New Zealand sheep industry, the implication for humanity is also apparent. Want to live longer? Get rid of the testosterone. An extreme solution to be sure. As previously reported in this column, researchers wanted to torture our mouths to get us to lose weight, and now they want to castrate people for longer life. What exactly is going on down there in New Zealand?
Man’s best mind reader
There are a lot of reasons why dogs are sometimes called “man’s best friend,” but the root of it may actually have something to do with how easily we communicate with each other. Researchers dug deeper and fetched something that Fido is born with, but his wild wolf cousin isn’t.
That something is known as the “theory of mind” ability. Have you noticed that when you point and tell dogs to grab a leash or toy, they react as if they understood the language you spoke? Researchers from Duke University wondered if this ability is a canine thing or just a domesticated dog thing.
They compared 44 canine puppies and 37 wolf pups between 5 and 18 weeks old. The wolf pups were taken into human homes and raised with a great amount of human interaction, while the dog pups were left with their mothers and raised with less human interaction.
All the puppies were then put through multiple tests. In one test, they were given clues to find a treat under a bowl. In another test, a block of wood was placed next to the treat as a physical marker. During yet another test, researchers pointed to the food directly.
The researchers discovered that the dog puppies knew where the treat was every time, while their wild relatives didn’t.
“This study really solidifies the evidence that the social genius of dogs is a product of domestication,” senior author Brian Hare said in a separate statement.
The domestication hypothesis theorizes that dogs picked up the human social cues through thousands of years of interaction. The more friendly and cooperative a wolf was with humans, the more likely it was to survive and pass on those same traits and practices. Even within the study, the dog puppies were 30 times more likely to approach a stranger than were the wolf pups.
You may think your dog understands everything you say, but it’s actually body language that Fido is most fluent in.
I’m not a dentist, but I play one on TikTok
In last week’s column, it was garlic cloves up the nose to treat a cold. This week, TikTok brings us a new way to whiten teeth.
Familiar with the Mr. Clean Magic Eraser? If not, we’ll save you the trouble of Googling it: Check it out here and here.
Have you heard anything about using it to clean your teeth? No, neither did we, and we did a lot of Googling. Proctor & Gamble, which makes the Magic Eraser, goes so far as to say on the package: “Do not use on skin or other parts of the body. Using on skin will likely cause abrasions.” (The warning is actually in all caps, but we are stylistically forbidden by our editorial overlords to do that.)
But it’s magic, right? How can you not use it on your teeth? Enter TikTok. Heather Dunn posted a video in which she rubbed a bit of a Magic Eraser on her teeth – being careful to avoid her gums, because you can never be too careful – “as the product squeaked back and forth,” the Miami Herald reported. The video has almost 256,000 likes so far.
“Yeah, your teeth are white because you scrubbed all the enamel off them. So don’t do this,” Dr. Benjamin Winters, aka the Bentist, said in a YouTube video that has 105,000 likes.
In this race for common sense, common sense is losing. Please help the Bentist restore sanity to the dental world by liking his video. It would make Mr. Clean happy.
Don’t let an expiration date boss you around
Surely you’ve been there: It’s Taco Tuesday and you’re rummaging through the refrigerator to find that shredded cheese you’re sure you have. Jackpot! You find it, but realize it’s probably been in the refrigerator for a while. You open the bag, it smells and looks fine, but the expiration date was 2 days ago. Now you have a decision to make. Maybe you’ll be fine, or maybe you’ll risk food poisoning right before your brother’s wedding.
But here’s the truth: Americans throw away perfectly good food every day. The average American family throws out $1,365 to $2,275 worth of food a year, according to a 2013 study.
Truthfully, expiration dates are not for buyers, rather they’re for stores to have an idea of their stock’s freshness. Emily Broad Leib, director of the Harvard Law School Food and Policy Clinic and lead author of the 2013 study, told Vox that manufacturers use the dates as a way of “protecting the brand” to keep consumers from eating food that’s just a little past its peak.
With approximately 40 million people in the United States concerned about where their next meal is coming from, the Vox article noted, we need to reevaluate our system. Our national misunderstanding of expiration labels is hurting both suppliers and consumers because perfectly good food is wasted.
Sure, there is always that chance that something might be a little funky after a certain amount of time, but all in all, food probably stays fresh a lot longer than we think. Don’t always judge the shredded cheese by its expiration date.
An extreme price to pay for immortality
We know that men don’t live as long as women, but the reasons aren’t entirely clear. However, some New Zealand scientists have a thought on the subject, thanks to a sheep called Shrek.
The researchers were inspired by a famous old sheep who escaped captivity, but was captured 6 years later at the age of 10. The sheep then lived 6 more years, far beyond the lifespan of a normal sheep, capturing the hearts and minds of Kiwis everywhere. Look, it’s New Zealand, sheep are life, so it’s only natural the country got attached. Scientists from the University of Otago suspected that Shrek lived such a long life because he was castrated.
So they undertook a study of sheep, and lo and behold, sheep that were castrated lived significantly longer than their uncastrated kin, thanks to a slowing of their epigenetic clocks – the DNA aged noticeably slower in the castrated sheep.
Although the research can most immediately be applied to the improvement of the New Zealand sheep industry, the implication for humanity is also apparent. Want to live longer? Get rid of the testosterone. An extreme solution to be sure. As previously reported in this column, researchers wanted to torture our mouths to get us to lose weight, and now they want to castrate people for longer life. What exactly is going on down there in New Zealand?
Man’s best mind reader
There are a lot of reasons why dogs are sometimes called “man’s best friend,” but the root of it may actually have something to do with how easily we communicate with each other. Researchers dug deeper and fetched something that Fido is born with, but his wild wolf cousin isn’t.
That something is known as the “theory of mind” ability. Have you noticed that when you point and tell dogs to grab a leash or toy, they react as if they understood the language you spoke? Researchers from Duke University wondered if this ability is a canine thing or just a domesticated dog thing.
They compared 44 canine puppies and 37 wolf pups between 5 and 18 weeks old. The wolf pups were taken into human homes and raised with a great amount of human interaction, while the dog pups were left with their mothers and raised with less human interaction.
All the puppies were then put through multiple tests. In one test, they were given clues to find a treat under a bowl. In another test, a block of wood was placed next to the treat as a physical marker. During yet another test, researchers pointed to the food directly.
The researchers discovered that the dog puppies knew where the treat was every time, while their wild relatives didn’t.
“This study really solidifies the evidence that the social genius of dogs is a product of domestication,” senior author Brian Hare said in a separate statement.
The domestication hypothesis theorizes that dogs picked up the human social cues through thousands of years of interaction. The more friendly and cooperative a wolf was with humans, the more likely it was to survive and pass on those same traits and practices. Even within the study, the dog puppies were 30 times more likely to approach a stranger than were the wolf pups.
You may think your dog understands everything you say, but it’s actually body language that Fido is most fluent in.
I’m not a dentist, but I play one on TikTok
In last week’s column, it was garlic cloves up the nose to treat a cold. This week, TikTok brings us a new way to whiten teeth.
Familiar with the Mr. Clean Magic Eraser? If not, we’ll save you the trouble of Googling it: Check it out here and here.
Have you heard anything about using it to clean your teeth? No, neither did we, and we did a lot of Googling. Proctor & Gamble, which makes the Magic Eraser, goes so far as to say on the package: “Do not use on skin or other parts of the body. Using on skin will likely cause abrasions.” (The warning is actually in all caps, but we are stylistically forbidden by our editorial overlords to do that.)
But it’s magic, right? How can you not use it on your teeth? Enter TikTok. Heather Dunn posted a video in which she rubbed a bit of a Magic Eraser on her teeth – being careful to avoid her gums, because you can never be too careful – “as the product squeaked back and forth,” the Miami Herald reported. The video has almost 256,000 likes so far.
“Yeah, your teeth are white because you scrubbed all the enamel off them. So don’t do this,” Dr. Benjamin Winters, aka the Bentist, said in a YouTube video that has 105,000 likes.
In this race for common sense, common sense is losing. Please help the Bentist restore sanity to the dental world by liking his video. It would make Mr. Clean happy.
Don’t let an expiration date boss you around
Surely you’ve been there: It’s Taco Tuesday and you’re rummaging through the refrigerator to find that shredded cheese you’re sure you have. Jackpot! You find it, but realize it’s probably been in the refrigerator for a while. You open the bag, it smells and looks fine, but the expiration date was 2 days ago. Now you have a decision to make. Maybe you’ll be fine, or maybe you’ll risk food poisoning right before your brother’s wedding.
But here’s the truth: Americans throw away perfectly good food every day. The average American family throws out $1,365 to $2,275 worth of food a year, according to a 2013 study.
Truthfully, expiration dates are not for buyers, rather they’re for stores to have an idea of their stock’s freshness. Emily Broad Leib, director of the Harvard Law School Food and Policy Clinic and lead author of the 2013 study, told Vox that manufacturers use the dates as a way of “protecting the brand” to keep consumers from eating food that’s just a little past its peak.
With approximately 40 million people in the United States concerned about where their next meal is coming from, the Vox article noted, we need to reevaluate our system. Our national misunderstanding of expiration labels is hurting both suppliers and consumers because perfectly good food is wasted.
Sure, there is always that chance that something might be a little funky after a certain amount of time, but all in all, food probably stays fresh a lot longer than we think. Don’t always judge the shredded cheese by its expiration date.
An extreme price to pay for immortality
We know that men don’t live as long as women, but the reasons aren’t entirely clear. However, some New Zealand scientists have a thought on the subject, thanks to a sheep called Shrek.
The researchers were inspired by a famous old sheep who escaped captivity, but was captured 6 years later at the age of 10. The sheep then lived 6 more years, far beyond the lifespan of a normal sheep, capturing the hearts and minds of Kiwis everywhere. Look, it’s New Zealand, sheep are life, so it’s only natural the country got attached. Scientists from the University of Otago suspected that Shrek lived such a long life because he was castrated.
So they undertook a study of sheep, and lo and behold, sheep that were castrated lived significantly longer than their uncastrated kin, thanks to a slowing of their epigenetic clocks – the DNA aged noticeably slower in the castrated sheep.
Although the research can most immediately be applied to the improvement of the New Zealand sheep industry, the implication for humanity is also apparent. Want to live longer? Get rid of the testosterone. An extreme solution to be sure. As previously reported in this column, researchers wanted to torture our mouths to get us to lose weight, and now they want to castrate people for longer life. What exactly is going on down there in New Zealand?
Man’s best mind reader
There are a lot of reasons why dogs are sometimes called “man’s best friend,” but the root of it may actually have something to do with how easily we communicate with each other. Researchers dug deeper and fetched something that Fido is born with, but his wild wolf cousin isn’t.
That something is known as the “theory of mind” ability. Have you noticed that when you point and tell dogs to grab a leash or toy, they react as if they understood the language you spoke? Researchers from Duke University wondered if this ability is a canine thing or just a domesticated dog thing.
They compared 44 canine puppies and 37 wolf pups between 5 and 18 weeks old. The wolf pups were taken into human homes and raised with a great amount of human interaction, while the dog pups were left with their mothers and raised with less human interaction.
All the puppies were then put through multiple tests. In one test, they were given clues to find a treat under a bowl. In another test, a block of wood was placed next to the treat as a physical marker. During yet another test, researchers pointed to the food directly.
The researchers discovered that the dog puppies knew where the treat was every time, while their wild relatives didn’t.
“This study really solidifies the evidence that the social genius of dogs is a product of domestication,” senior author Brian Hare said in a separate statement.
The domestication hypothesis theorizes that dogs picked up the human social cues through thousands of years of interaction. The more friendly and cooperative a wolf was with humans, the more likely it was to survive and pass on those same traits and practices. Even within the study, the dog puppies were 30 times more likely to approach a stranger than were the wolf pups.
You may think your dog understands everything you say, but it’s actually body language that Fido is most fluent in.
I’m not a dentist, but I play one on TikTok
In last week’s column, it was garlic cloves up the nose to treat a cold. This week, TikTok brings us a new way to whiten teeth.
Familiar with the Mr. Clean Magic Eraser? If not, we’ll save you the trouble of Googling it: Check it out here and here.
Have you heard anything about using it to clean your teeth? No, neither did we, and we did a lot of Googling. Proctor & Gamble, which makes the Magic Eraser, goes so far as to say on the package: “Do not use on skin or other parts of the body. Using on skin will likely cause abrasions.” (The warning is actually in all caps, but we are stylistically forbidden by our editorial overlords to do that.)
But it’s magic, right? How can you not use it on your teeth? Enter TikTok. Heather Dunn posted a video in which she rubbed a bit of a Magic Eraser on her teeth – being careful to avoid her gums, because you can never be too careful – “as the product squeaked back and forth,” the Miami Herald reported. The video has almost 256,000 likes so far.
“Yeah, your teeth are white because you scrubbed all the enamel off them. So don’t do this,” Dr. Benjamin Winters, aka the Bentist, said in a YouTube video that has 105,000 likes.
In this race for common sense, common sense is losing. Please help the Bentist restore sanity to the dental world by liking his video. It would make Mr. Clean happy.
Don’t let an expiration date boss you around
Surely you’ve been there: It’s Taco Tuesday and you’re rummaging through the refrigerator to find that shredded cheese you’re sure you have. Jackpot! You find it, but realize it’s probably been in the refrigerator for a while. You open the bag, it smells and looks fine, but the expiration date was 2 days ago. Now you have a decision to make. Maybe you’ll be fine, or maybe you’ll risk food poisoning right before your brother’s wedding.
But here’s the truth: Americans throw away perfectly good food every day. The average American family throws out $1,365 to $2,275 worth of food a year, according to a 2013 study.
Truthfully, expiration dates are not for buyers, rather they’re for stores to have an idea of their stock’s freshness. Emily Broad Leib, director of the Harvard Law School Food and Policy Clinic and lead author of the 2013 study, told Vox that manufacturers use the dates as a way of “protecting the brand” to keep consumers from eating food that’s just a little past its peak.
With approximately 40 million people in the United States concerned about where their next meal is coming from, the Vox article noted, we need to reevaluate our system. Our national misunderstanding of expiration labels is hurting both suppliers and consumers because perfectly good food is wasted.
Sure, there is always that chance that something might be a little funky after a certain amount of time, but all in all, food probably stays fresh a lot longer than we think. Don’t always judge the shredded cheese by its expiration date.