User login
LISTEN NOW: Highlights of the December 2014 issue of The Hospitalist newsmagazine
[audio mp3="http://www.the-hospitalist.org/wp-content/uploads/2014/12/2014-December-Hospitalist-Highlights.mp3"][/audio]
[audio mp3="http://www.the-hospitalist.org/wp-content/uploads/2014/12/2014-December-Hospitalist-Highlights.mp3"][/audio]
[audio mp3="http://www.the-hospitalist.org/wp-content/uploads/2014/12/2014-December-Hospitalist-Highlights.mp3"][/audio]
Hospitalists’ Role in Health Reform Evolves
“We’ve gone through an interesting 15 years where hospitals needed to build hospital medicine programs,” said Dr. Wachter, chief of the division of hospital medicine at the University of California at San Francisco, to conference attendees in San Francisco in October. “In the beginning, we were young and had to try to lead, even though we didn’t understand how organizations worked. We had a good voice at the table even before we were ready for it. Now we’re more mature and better leaders, but the problems are harder.”
Asked to name the reform trends most important to hospitalists, Dr. Wachter replied, “Cost pressures, one, two, and three. The system is going to push us to deliver higher-value care at lower cost, with greater standardization and elimination of waste.”
That means adhering to medical guidelines, avoiding unnecessary care, and managing hospital lengths of stay. Likewise, Dr. Wachter anticipates that clinicians will be pushed to practice at the top of their licensure, with new and interesting roles for nurse practitioners and physician assistants.
“But I think the market for hospitalists is good. Those hospitals that survive will all have hospitalists,” he said.
How can hospitalists prepare for healthcare reform?

—Dr. Wachter
“Some of it is to make yourself indispensable, so that when hard decisions come up about whether to spend resources on you or something else [in the hospital], people will say, ‘We get a lot of bang for our buck spending on hospitalists,’” Dr. Wachter added. “And now and then, you’ll need to pull out your copy of Machiavelli,” he noted, referring to the Italian diplomat’s classic book, The Prince, for its maxims on the art of retaining and wielding political power.
Dr. Wachter also has a particular interest in healthcare information technology (IT) and how it is reshaping medical practice, having taken a sabbatical to write a book on the subject, The Digital Doctor: Hope, Hype & Harm at the Dawn of Medicine’s Computer Age, scheduled for publication on March 15.
Acknowledging the problems many hospitalists have experienced with electronic health records, Dr. Wachter predicts some positive changes.
“I think it will get better pretty quickly. Many of us were quite naïve to think that IT would make care safer. We didn’t give enough attention to how technology changes everything, from workflow to personal relationships,” he said. “Now that these systems are in place, we need to ask: Are they really doing the things we want and not doing the things we don’t want? And how do we leverage these systems to get maximum value?”
Larry Beresford is a freelance writer in Alameda, Calif.
“We’ve gone through an interesting 15 years where hospitals needed to build hospital medicine programs,” said Dr. Wachter, chief of the division of hospital medicine at the University of California at San Francisco, to conference attendees in San Francisco in October. “In the beginning, we were young and had to try to lead, even though we didn’t understand how organizations worked. We had a good voice at the table even before we were ready for it. Now we’re more mature and better leaders, but the problems are harder.”
Asked to name the reform trends most important to hospitalists, Dr. Wachter replied, “Cost pressures, one, two, and three. The system is going to push us to deliver higher-value care at lower cost, with greater standardization and elimination of waste.”
That means adhering to medical guidelines, avoiding unnecessary care, and managing hospital lengths of stay. Likewise, Dr. Wachter anticipates that clinicians will be pushed to practice at the top of their licensure, with new and interesting roles for nurse practitioners and physician assistants.
“But I think the market for hospitalists is good. Those hospitals that survive will all have hospitalists,” he said.
How can hospitalists prepare for healthcare reform?

—Dr. Wachter
“Some of it is to make yourself indispensable, so that when hard decisions come up about whether to spend resources on you or something else [in the hospital], people will say, ‘We get a lot of bang for our buck spending on hospitalists,’” Dr. Wachter added. “And now and then, you’ll need to pull out your copy of Machiavelli,” he noted, referring to the Italian diplomat’s classic book, The Prince, for its maxims on the art of retaining and wielding political power.
Dr. Wachter also has a particular interest in healthcare information technology (IT) and how it is reshaping medical practice, having taken a sabbatical to write a book on the subject, The Digital Doctor: Hope, Hype & Harm at the Dawn of Medicine’s Computer Age, scheduled for publication on March 15.
Acknowledging the problems many hospitalists have experienced with electronic health records, Dr. Wachter predicts some positive changes.
“I think it will get better pretty quickly. Many of us were quite naïve to think that IT would make care safer. We didn’t give enough attention to how technology changes everything, from workflow to personal relationships,” he said. “Now that these systems are in place, we need to ask: Are they really doing the things we want and not doing the things we don’t want? And how do we leverage these systems to get maximum value?”
Larry Beresford is a freelance writer in Alameda, Calif.
“We’ve gone through an interesting 15 years where hospitals needed to build hospital medicine programs,” said Dr. Wachter, chief of the division of hospital medicine at the University of California at San Francisco, to conference attendees in San Francisco in October. “In the beginning, we were young and had to try to lead, even though we didn’t understand how organizations worked. We had a good voice at the table even before we were ready for it. Now we’re more mature and better leaders, but the problems are harder.”
Asked to name the reform trends most important to hospitalists, Dr. Wachter replied, “Cost pressures, one, two, and three. The system is going to push us to deliver higher-value care at lower cost, with greater standardization and elimination of waste.”
That means adhering to medical guidelines, avoiding unnecessary care, and managing hospital lengths of stay. Likewise, Dr. Wachter anticipates that clinicians will be pushed to practice at the top of their licensure, with new and interesting roles for nurse practitioners and physician assistants.
“But I think the market for hospitalists is good. Those hospitals that survive will all have hospitalists,” he said.
How can hospitalists prepare for healthcare reform?

—Dr. Wachter
“Some of it is to make yourself indispensable, so that when hard decisions come up about whether to spend resources on you or something else [in the hospital], people will say, ‘We get a lot of bang for our buck spending on hospitalists,’” Dr. Wachter added. “And now and then, you’ll need to pull out your copy of Machiavelli,” he noted, referring to the Italian diplomat’s classic book, The Prince, for its maxims on the art of retaining and wielding political power.
Dr. Wachter also has a particular interest in healthcare information technology (IT) and how it is reshaping medical practice, having taken a sabbatical to write a book on the subject, The Digital Doctor: Hope, Hype & Harm at the Dawn of Medicine’s Computer Age, scheduled for publication on March 15.
Acknowledging the problems many hospitalists have experienced with electronic health records, Dr. Wachter predicts some positive changes.
“I think it will get better pretty quickly. Many of us were quite naïve to think that IT would make care safer. We didn’t give enough attention to how technology changes everything, from workflow to personal relationships,” he said. “Now that these systems are in place, we need to ask: Are they really doing the things we want and not doing the things we don’t want? And how do we leverage these systems to get maximum value?”
Larry Beresford is a freelance writer in Alameda, Calif.
Ebola Outbreak Reminds Hospitalists How To Prepare for Infectious Disease
When the outbreak first started, and in the months that followed, Ebola virus dominated American headlines. The disease made its way from West Africa, infecting nurses in Spain and the U.S., and questions arose over how to keep healthcare providers and the public safe.
The answers to these questions are not limited to Ebola. Hospitalists and other providers work in the face of infectious disease on a routine basis, particularly in an era of widespread antibiotic resistance and emerging infections caused by such viruses as chikungunya, enterovirus D68, and MERS (Middle East Respiratory Syndrome) coronavirus.
The key to adequate preparation, says Joshua Lenchus, DO, RPh, FACP, SFHM, associate director of the Center for Patient Safety at the University of Miami-Jackson Memorial Hospital, is “information, the ability to implement relevant protocols and procedures when necessary, and, when possible, simulated exercises.”
Hospitalists can play a key role in ensuring their hospitals are prepared.
“I am constantly being reminded by my Society of Hospital Medicine colleagues that many facilities may not have an infectious disease specialist or an infectious disease program,” says Abbigail Tumpey, MPH, CHES, associate director for communications science in the CDC’s Division of Healthcare Quality Promotion.
It starts at the front door of the hospital, Tumpey and Dr. Lenchus say, with appropriate triage, screening, and isolation of potentially infectious patients.
“We diligently draft screening procedures for our frontline staff, clinic personnel, and appointment line phone operators to adequately and quickly evaluate patients so that those affected are provided the appropriate level of care,” says Dr. Lenchus, also a hospitalist and associate professor of clinical medicine and anesthesiology at the University of Miami Miller School of Medicine.

“We diligently draft screening procedures for our frontline staff, clinic personnel, and appointment line phone operators to adequately and quickly evaluate patients so that those affected are provided the appropriate level of care.”–Dr. Lenchus
These screening and management procedures originate with the CDC and state health departments and are often informed by outbreaks occurring in other locales.
“When an outbreak occurs elsewhere in the world, it is simply a matter of time before we may be faced with it in the United States,” Dr. Lenchus says, “so it behooves us to begin the research process and work with our hospital, local, and state personnel.”
The second line of defense, says Tumpey, is having in place the proper administrative controls to ensure that providers have time to don the appropriate personal protective equipment, or PPE. This means not just having access to PPE, but also the ability to put it on and take it off appropriately.
According to The New York Times, European officials investigated whether the Spanish nurse became infected with Ebola by accidentally touching her face while removing her PPE, and officials in the U.S. investigated whether the Dallas nurse who contracted Ebola while treating an infected Liberian patient also breached protocol. In Spain, investigators determined the layout of the hospital’s cramped Ebola ward could lead to accidents. In Dallas, rapidly changing conditions and poor preparation may have played a role, according to some reports. For just these kinds of reasons, Tumpey and Dr. Lenchus suggest hospitals engage in simulations and drills of outbreak events whenever possible.
“The facilities we’ve seen do this have found information they didn’t realize or a way of handling things that was surprising to them,” Tumpey says. “Certainly, there are some things that come up in those drills that highlight potential flaws and show opportunities where you can improve.”
For instance, simulations might reveal problems with the storage or disposal of PPE, lead to changes in hand hygiene locations, or highlight the need for better communication among healthcare workers.
Calm, Cool, Collected
Proper infection control procedures—hand hygiene, injection safety, appropriate cleanup, and careful waste handling—are a third line of defense in preventing the spread of infectious disease, Tumpey says.
Dr. Lenchus says that, particularly in light of diseases like Ebola, hospitalists should present concerned patients with valid information in a “calm, cool, and collected manner” that “helps allay the fear, misconception, and hysteria from generalizations, emotional responses, and anecdotal hearsay.”
These conversations present hospitalists with an opportunity to highlight the protocols, procedures, and patient safety programs in place at their institutions. They also provide a forum to discuss common cold and influenza viruses, which spread more easily than Ebola.
Of course, in the face of new rules for admissions, packed EDs, mounting metrics, and sometimes nonintuitive electronic health records, staying abreast of the latest information and catching every patient with symptoms that may or may not be related to an infectious disease may be easier said than done.
The CDC is redoubling its outreach efforts, Tumpey says, and will offer webinars and trainings for health providers.
“Our hope is that increased awareness can improve triage, early recognition, and appropriate infection control and could help for other things like MRSA, the endemic threats we face every day in U.S. healthcare facilities, even emerging diseases like MERS and carbapenem-resistant Enterobacteriaceae,” says Tumpey. “Awareness of proper infection control could help with many disease threats.”
Kelly April Tyrrell is a freelance writer in Madison, Wis.
When the outbreak first started, and in the months that followed, Ebola virus dominated American headlines. The disease made its way from West Africa, infecting nurses in Spain and the U.S., and questions arose over how to keep healthcare providers and the public safe.
The answers to these questions are not limited to Ebola. Hospitalists and other providers work in the face of infectious disease on a routine basis, particularly in an era of widespread antibiotic resistance and emerging infections caused by such viruses as chikungunya, enterovirus D68, and MERS (Middle East Respiratory Syndrome) coronavirus.
The key to adequate preparation, says Joshua Lenchus, DO, RPh, FACP, SFHM, associate director of the Center for Patient Safety at the University of Miami-Jackson Memorial Hospital, is “information, the ability to implement relevant protocols and procedures when necessary, and, when possible, simulated exercises.”
Hospitalists can play a key role in ensuring their hospitals are prepared.
“I am constantly being reminded by my Society of Hospital Medicine colleagues that many facilities may not have an infectious disease specialist or an infectious disease program,” says Abbigail Tumpey, MPH, CHES, associate director for communications science in the CDC’s Division of Healthcare Quality Promotion.
It starts at the front door of the hospital, Tumpey and Dr. Lenchus say, with appropriate triage, screening, and isolation of potentially infectious patients.
“We diligently draft screening procedures for our frontline staff, clinic personnel, and appointment line phone operators to adequately and quickly evaluate patients so that those affected are provided the appropriate level of care,” says Dr. Lenchus, also a hospitalist and associate professor of clinical medicine and anesthesiology at the University of Miami Miller School of Medicine.

“We diligently draft screening procedures for our frontline staff, clinic personnel, and appointment line phone operators to adequately and quickly evaluate patients so that those affected are provided the appropriate level of care.”–Dr. Lenchus
These screening and management procedures originate with the CDC and state health departments and are often informed by outbreaks occurring in other locales.
“When an outbreak occurs elsewhere in the world, it is simply a matter of time before we may be faced with it in the United States,” Dr. Lenchus says, “so it behooves us to begin the research process and work with our hospital, local, and state personnel.”
The second line of defense, says Tumpey, is having in place the proper administrative controls to ensure that providers have time to don the appropriate personal protective equipment, or PPE. This means not just having access to PPE, but also the ability to put it on and take it off appropriately.
According to The New York Times, European officials investigated whether the Spanish nurse became infected with Ebola by accidentally touching her face while removing her PPE, and officials in the U.S. investigated whether the Dallas nurse who contracted Ebola while treating an infected Liberian patient also breached protocol. In Spain, investigators determined the layout of the hospital’s cramped Ebola ward could lead to accidents. In Dallas, rapidly changing conditions and poor preparation may have played a role, according to some reports. For just these kinds of reasons, Tumpey and Dr. Lenchus suggest hospitals engage in simulations and drills of outbreak events whenever possible.
“The facilities we’ve seen do this have found information they didn’t realize or a way of handling things that was surprising to them,” Tumpey says. “Certainly, there are some things that come up in those drills that highlight potential flaws and show opportunities where you can improve.”
For instance, simulations might reveal problems with the storage or disposal of PPE, lead to changes in hand hygiene locations, or highlight the need for better communication among healthcare workers.
Calm, Cool, Collected
Proper infection control procedures—hand hygiene, injection safety, appropriate cleanup, and careful waste handling—are a third line of defense in preventing the spread of infectious disease, Tumpey says.
Dr. Lenchus says that, particularly in light of diseases like Ebola, hospitalists should present concerned patients with valid information in a “calm, cool, and collected manner” that “helps allay the fear, misconception, and hysteria from generalizations, emotional responses, and anecdotal hearsay.”
These conversations present hospitalists with an opportunity to highlight the protocols, procedures, and patient safety programs in place at their institutions. They also provide a forum to discuss common cold and influenza viruses, which spread more easily than Ebola.
Of course, in the face of new rules for admissions, packed EDs, mounting metrics, and sometimes nonintuitive electronic health records, staying abreast of the latest information and catching every patient with symptoms that may or may not be related to an infectious disease may be easier said than done.
The CDC is redoubling its outreach efforts, Tumpey says, and will offer webinars and trainings for health providers.
“Our hope is that increased awareness can improve triage, early recognition, and appropriate infection control and could help for other things like MRSA, the endemic threats we face every day in U.S. healthcare facilities, even emerging diseases like MERS and carbapenem-resistant Enterobacteriaceae,” says Tumpey. “Awareness of proper infection control could help with many disease threats.”
Kelly April Tyrrell is a freelance writer in Madison, Wis.
When the outbreak first started, and in the months that followed, Ebola virus dominated American headlines. The disease made its way from West Africa, infecting nurses in Spain and the U.S., and questions arose over how to keep healthcare providers and the public safe.
The answers to these questions are not limited to Ebola. Hospitalists and other providers work in the face of infectious disease on a routine basis, particularly in an era of widespread antibiotic resistance and emerging infections caused by such viruses as chikungunya, enterovirus D68, and MERS (Middle East Respiratory Syndrome) coronavirus.
The key to adequate preparation, says Joshua Lenchus, DO, RPh, FACP, SFHM, associate director of the Center for Patient Safety at the University of Miami-Jackson Memorial Hospital, is “information, the ability to implement relevant protocols and procedures when necessary, and, when possible, simulated exercises.”
Hospitalists can play a key role in ensuring their hospitals are prepared.
“I am constantly being reminded by my Society of Hospital Medicine colleagues that many facilities may not have an infectious disease specialist or an infectious disease program,” says Abbigail Tumpey, MPH, CHES, associate director for communications science in the CDC’s Division of Healthcare Quality Promotion.
It starts at the front door of the hospital, Tumpey and Dr. Lenchus say, with appropriate triage, screening, and isolation of potentially infectious patients.
“We diligently draft screening procedures for our frontline staff, clinic personnel, and appointment line phone operators to adequately and quickly evaluate patients so that those affected are provided the appropriate level of care,” says Dr. Lenchus, also a hospitalist and associate professor of clinical medicine and anesthesiology at the University of Miami Miller School of Medicine.

“We diligently draft screening procedures for our frontline staff, clinic personnel, and appointment line phone operators to adequately and quickly evaluate patients so that those affected are provided the appropriate level of care.”–Dr. Lenchus
These screening and management procedures originate with the CDC and state health departments and are often informed by outbreaks occurring in other locales.
“When an outbreak occurs elsewhere in the world, it is simply a matter of time before we may be faced with it in the United States,” Dr. Lenchus says, “so it behooves us to begin the research process and work with our hospital, local, and state personnel.”
The second line of defense, says Tumpey, is having in place the proper administrative controls to ensure that providers have time to don the appropriate personal protective equipment, or PPE. This means not just having access to PPE, but also the ability to put it on and take it off appropriately.
According to The New York Times, European officials investigated whether the Spanish nurse became infected with Ebola by accidentally touching her face while removing her PPE, and officials in the U.S. investigated whether the Dallas nurse who contracted Ebola while treating an infected Liberian patient also breached protocol. In Spain, investigators determined the layout of the hospital’s cramped Ebola ward could lead to accidents. In Dallas, rapidly changing conditions and poor preparation may have played a role, according to some reports. For just these kinds of reasons, Tumpey and Dr. Lenchus suggest hospitals engage in simulations and drills of outbreak events whenever possible.
“The facilities we’ve seen do this have found information they didn’t realize or a way of handling things that was surprising to them,” Tumpey says. “Certainly, there are some things that come up in those drills that highlight potential flaws and show opportunities where you can improve.”
For instance, simulations might reveal problems with the storage or disposal of PPE, lead to changes in hand hygiene locations, or highlight the need for better communication among healthcare workers.
Calm, Cool, Collected
Proper infection control procedures—hand hygiene, injection safety, appropriate cleanup, and careful waste handling—are a third line of defense in preventing the spread of infectious disease, Tumpey says.
Dr. Lenchus says that, particularly in light of diseases like Ebola, hospitalists should present concerned patients with valid information in a “calm, cool, and collected manner” that “helps allay the fear, misconception, and hysteria from generalizations, emotional responses, and anecdotal hearsay.”
These conversations present hospitalists with an opportunity to highlight the protocols, procedures, and patient safety programs in place at their institutions. They also provide a forum to discuss common cold and influenza viruses, which spread more easily than Ebola.
Of course, in the face of new rules for admissions, packed EDs, mounting metrics, and sometimes nonintuitive electronic health records, staying abreast of the latest information and catching every patient with symptoms that may or may not be related to an infectious disease may be easier said than done.
The CDC is redoubling its outreach efforts, Tumpey says, and will offer webinars and trainings for health providers.
“Our hope is that increased awareness can improve triage, early recognition, and appropriate infection control and could help for other things like MRSA, the endemic threats we face every day in U.S. healthcare facilities, even emerging diseases like MERS and carbapenem-resistant Enterobacteriaceae,” says Tumpey. “Awareness of proper infection control could help with many disease threats.”
Kelly April Tyrrell is a freelance writer in Madison, Wis.
Hospitalist Tips for Talking to Seriously Ill Patients
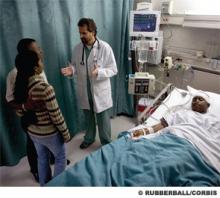
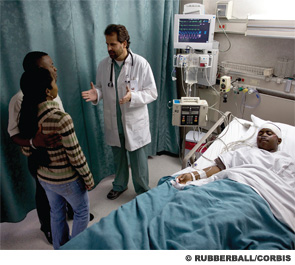
The need to relieve patients’ suffering should not be the reason for withdrawing life-sustaining interventions in the ICU, Steven Z. Pantilat, MD, MHM, medical director of the University of California San Francisco (UCSF) School of Medicine palliative care service, told attendees at the “Management of the Hospitalized Patient” conference in San Francisco.
Patients in the ICU experience a lot of suffering, Dr. Pantilat said during a session on communication about serious illness. He underscored the importance of treating patients in the ICU as human beings, giving attention to their comfort and dignity, and addressing them by name.
“I’m not always sure they can hear me,” he said, “but there’s a humanizing element to it, as much to remind myself as for the patient’s benefit.”
Dr. Pantilat emphasized the importance of family conferences in communicating with patients and families, sometimes in advance of when important treatment decisions need to be made. The meeting should be documented in the EHR, with the note easy to retrieve.
“Resist launching in with what you know [about their case] until you ask what they know,” he advised. Dr. Pantilat tries to avoid expressions like “there’s nothing more we can do.”

—Dr. Pantilat
“[It’s] better to say, ‘I wish there was something we could do to make her lungs get better.’ Or, ‘I worry that your mother’s getting worse,’” he said.
He asks families what the patient was like before getting ill. And he always says, “We’ll take really good care of her.”
Many health professionals still associate palliative care with end-of-life care or withdrawing treatment, he said, rather than its self-defined role of relieving suffering and promoting quality of life for any seriously ill patient. Even so, he sees the hospitalists’ role in palliative care in the hospital growing.
“They are taking care of hospitalized patients who are sick; they are having lots of goals-of-care conversations; they are treating a lot of pain, a lot of dyspnea and nausea, and making referrals to hospice,” he noted. “So we know they are providing palliative care.”
Many hospitalists also work in more formal ways as palliative care consultants.
ICU patients represent 30% of referrals to his service at UCSF, which has initiatives underway to integrate palliative care into the practice of ICU nurses and into the work of the medical center’s advanced heart failure team.
Training in palliative care also is becoming a bigger part of medical education and residency programs, although medical residency graduates could benefit from additional training.
“This is a subtle and difficult skill to get right, particularly the communication piece,” Dr. Pantilat said. “People need practice and more training, just as you’d want to get better at putting in central lines or intubating patients.”
For the hospitalist, providing palliative care and “addressing issues of seriously ill patients around decision-making, talking about prognosis, treating their symptoms, [and] addressing their spiritual concerns, it’s good for the patient. It’s good for the family. It’s actually good for the hospitalist, as well. It’s very rewarding work,” Dr. Pantilat said. “Here’s this opportunity to do something incredibly meaningful that makes a huge difference. And, through your work, renew yourself and renew your commitment to your work while doing it. That’s a rare opportunity in the middle of a busy day.”
The need to relieve patients’ suffering should not be the reason for withdrawing life-sustaining interventions in the ICU, Steven Z. Pantilat, MD, MHM, medical director of the University of California San Francisco (UCSF) School of Medicine palliative care service, told attendees at the “Management of the Hospitalized Patient” conference in San Francisco.
Patients in the ICU experience a lot of suffering, Dr. Pantilat said during a session on communication about serious illness. He underscored the importance of treating patients in the ICU as human beings, giving attention to their comfort and dignity, and addressing them by name.
“I’m not always sure they can hear me,” he said, “but there’s a humanizing element to it, as much to remind myself as for the patient’s benefit.”
Dr. Pantilat emphasized the importance of family conferences in communicating with patients and families, sometimes in advance of when important treatment decisions need to be made. The meeting should be documented in the EHR, with the note easy to retrieve.
“Resist launching in with what you know [about their case] until you ask what they know,” he advised. Dr. Pantilat tries to avoid expressions like “there’s nothing more we can do.”

—Dr. Pantilat
“[It’s] better to say, ‘I wish there was something we could do to make her lungs get better.’ Or, ‘I worry that your mother’s getting worse,’” he said.
He asks families what the patient was like before getting ill. And he always says, “We’ll take really good care of her.”
Many health professionals still associate palliative care with end-of-life care or withdrawing treatment, he said, rather than its self-defined role of relieving suffering and promoting quality of life for any seriously ill patient. Even so, he sees the hospitalists’ role in palliative care in the hospital growing.
“They are taking care of hospitalized patients who are sick; they are having lots of goals-of-care conversations; they are treating a lot of pain, a lot of dyspnea and nausea, and making referrals to hospice,” he noted. “So we know they are providing palliative care.”
Many hospitalists also work in more formal ways as palliative care consultants.
ICU patients represent 30% of referrals to his service at UCSF, which has initiatives underway to integrate palliative care into the practice of ICU nurses and into the work of the medical center’s advanced heart failure team.
Training in palliative care also is becoming a bigger part of medical education and residency programs, although medical residency graduates could benefit from additional training.
“This is a subtle and difficult skill to get right, particularly the communication piece,” Dr. Pantilat said. “People need practice and more training, just as you’d want to get better at putting in central lines or intubating patients.”
For the hospitalist, providing palliative care and “addressing issues of seriously ill patients around decision-making, talking about prognosis, treating their symptoms, [and] addressing their spiritual concerns, it’s good for the patient. It’s good for the family. It’s actually good for the hospitalist, as well. It’s very rewarding work,” Dr. Pantilat said. “Here’s this opportunity to do something incredibly meaningful that makes a huge difference. And, through your work, renew yourself and renew your commitment to your work while doing it. That’s a rare opportunity in the middle of a busy day.”
The need to relieve patients’ suffering should not be the reason for withdrawing life-sustaining interventions in the ICU, Steven Z. Pantilat, MD, MHM, medical director of the University of California San Francisco (UCSF) School of Medicine palliative care service, told attendees at the “Management of the Hospitalized Patient” conference in San Francisco.
Patients in the ICU experience a lot of suffering, Dr. Pantilat said during a session on communication about serious illness. He underscored the importance of treating patients in the ICU as human beings, giving attention to their comfort and dignity, and addressing them by name.
“I’m not always sure they can hear me,” he said, “but there’s a humanizing element to it, as much to remind myself as for the patient’s benefit.”
Dr. Pantilat emphasized the importance of family conferences in communicating with patients and families, sometimes in advance of when important treatment decisions need to be made. The meeting should be documented in the EHR, with the note easy to retrieve.
“Resist launching in with what you know [about their case] until you ask what they know,” he advised. Dr. Pantilat tries to avoid expressions like “there’s nothing more we can do.”

—Dr. Pantilat
“[It’s] better to say, ‘I wish there was something we could do to make her lungs get better.’ Or, ‘I worry that your mother’s getting worse,’” he said.
He asks families what the patient was like before getting ill. And he always says, “We’ll take really good care of her.”
Many health professionals still associate palliative care with end-of-life care or withdrawing treatment, he said, rather than its self-defined role of relieving suffering and promoting quality of life for any seriously ill patient. Even so, he sees the hospitalists’ role in palliative care in the hospital growing.
“They are taking care of hospitalized patients who are sick; they are having lots of goals-of-care conversations; they are treating a lot of pain, a lot of dyspnea and nausea, and making referrals to hospice,” he noted. “So we know they are providing palliative care.”
Many hospitalists also work in more formal ways as palliative care consultants.
ICU patients represent 30% of referrals to his service at UCSF, which has initiatives underway to integrate palliative care into the practice of ICU nurses and into the work of the medical center’s advanced heart failure team.
Training in palliative care also is becoming a bigger part of medical education and residency programs, although medical residency graduates could benefit from additional training.
“This is a subtle and difficult skill to get right, particularly the communication piece,” Dr. Pantilat said. “People need practice and more training, just as you’d want to get better at putting in central lines or intubating patients.”
For the hospitalist, providing palliative care and “addressing issues of seriously ill patients around decision-making, talking about prognosis, treating their symptoms, [and] addressing their spiritual concerns, it’s good for the patient. It’s good for the family. It’s actually good for the hospitalist, as well. It’s very rewarding work,” Dr. Pantilat said. “Here’s this opportunity to do something incredibly meaningful that makes a huge difference. And, through your work, renew yourself and renew your commitment to your work while doing it. That’s a rare opportunity in the middle of a busy day.”
Clarification: Hyponatremia Article Chart Should Have Referenced Hypervolemia, Not Hypovolemia
Dear Editor:
Excellent article on hyponatremia management in the August 2014 issue. I would like to point out a possible error/typo in Figure 2 on page 12. In the flowchart, the third category is described as “HYPOvolemia,” with causes mentioned as congestive heart failure, cirrhosis, nephrotic syndrome. Did the authors mean HYPERvolemia? Thanks again for publishing an article about this common-but-confusing clinical problem.
–Rahul Kumar, MD
San Juan Regional Medical Center
Farmington, N.M.
From the editors:
Dr. Kumar, thanks for the e-mail and attention to detail. Yes, in Figure 2 on page 12 of the August 2014 issue, the third category should read “HYPERvolemia,” not “HYPOvolemia.” Apologies for the error!
Dear Editor:
Excellent article on hyponatremia management in the August 2014 issue. I would like to point out a possible error/typo in Figure 2 on page 12. In the flowchart, the third category is described as “HYPOvolemia,” with causes mentioned as congestive heart failure, cirrhosis, nephrotic syndrome. Did the authors mean HYPERvolemia? Thanks again for publishing an article about this common-but-confusing clinical problem.
–Rahul Kumar, MD
San Juan Regional Medical Center
Farmington, N.M.
From the editors:
Dr. Kumar, thanks for the e-mail and attention to detail. Yes, in Figure 2 on page 12 of the August 2014 issue, the third category should read “HYPERvolemia,” not “HYPOvolemia.” Apologies for the error!
Dear Editor:
Excellent article on hyponatremia management in the August 2014 issue. I would like to point out a possible error/typo in Figure 2 on page 12. In the flowchart, the third category is described as “HYPOvolemia,” with causes mentioned as congestive heart failure, cirrhosis, nephrotic syndrome. Did the authors mean HYPERvolemia? Thanks again for publishing an article about this common-but-confusing clinical problem.
–Rahul Kumar, MD
San Juan Regional Medical Center
Farmington, N.M.
From the editors:
Dr. Kumar, thanks for the e-mail and attention to detail. Yes, in Figure 2 on page 12 of the August 2014 issue, the third category should read “HYPERvolemia,” not “HYPOvolemia.” Apologies for the error!
Society of Hospital Medicine To Offer New Programming, Savings, Opportunities at HM15
Now is the time to register, make travel arrangements, and book hotel rooms before the rush. Starting early means saving money: The deadline for early online registration—$100 savings—is February 2, 2015. Plus, hospitalists staying at the Gaylord National Resort & Convention Center, the official headquarters hotel for HM15, can save another $100 off their registration fees.
HM15 is the perfect time to join the hospital medicine movement. Nonmembers who register for HM15 will receive free SHM membership for one year.
HM15 course director Efrén Manjarrez, MD, says that HM15 will bring many new angles and topics for conference veterans and will attract other members of the “big tent” of hospital medicine.
“For the first time, the American Academy of Family Physicians is endorsing the meeting, so we are excited to welcome even more family physicians to the meeting, many of whom might not have considered coming to an SHM meeting in the past,” he says.
For long-time meeting attendees, Dr. Manjarrez suggests taking a look at the new content for maintenance of certification (MOC) and patient experience. He is equally interested in welcoming residents and medical students to the meeting.
“We are meeting [past president] Eric Howell’s mission to increase the pipeline of future hospitalists,” Dr. Manjarrez says. “I’m personally challenging every single academic hospitalist to bring at least one medical student or resident with them to HM15.”
A First Step
As part of an effort to include even more medical school students and residents in the HM movement, SHM has created the first “young hospitalist” educational track. Designed for med students, residents, and even hospitalists freshly out of residency, the six courses in the “young hospitalist” track cover many of the topics never touched in med school or resident training, such as how to write a CV and how to create a meaningful relationship with a resident.
“The track will bring faculty and young hospitalists together to learn about and discuss topics that are critical in this part of a hospitalist’s career,” says Darlene Tad-y, MD, chair of SHM’s Physicians in Training Committee. “Attendees can expect a great deal of hands-on interaction with the faculty and advice on getting their hospitalist career off to a running start.”
Students and residents will have new opportunities for visibility and networking at HM15. SHM has created a Trainee Award category within its awards program and a career fair during the popular poster session to help introduce new hospitalists to staffing companies and recruiters. Students and residents will have a chance to meet the leaders of the specialty face to face during the luncheon and forum organized specifically for them.
Let Your Voice Be Heard in Congress
With hospitalists testifying before Congress on important patient care issues and rising to the highest levels of CMS, the voice of the hospitalist has never been more important in Washington, D.C. And you can add your voice to the movement.
On Wednesday, April 1, 2015, SHM will bring dozens of hospitalists to the halls of Capitol Hill to talk with legislators and staffers about patient and policy issues, including observation status, quality improvement, accountable care organizations (ACOs), and the impact of the Affordable Care Act on hospitalized patients. At “Hospitalists on the Hill,” hospitalists will talk face to face with policymakers and provide the kind of personal and professional perspective that they need to make decisions that affect millions of hospitalized patients every year.
Brendon Shank is SHM’s associate vice president of communications.
Now is the time to register, make travel arrangements, and book hotel rooms before the rush. Starting early means saving money: The deadline for early online registration—$100 savings—is February 2, 2015. Plus, hospitalists staying at the Gaylord National Resort & Convention Center, the official headquarters hotel for HM15, can save another $100 off their registration fees.
HM15 is the perfect time to join the hospital medicine movement. Nonmembers who register for HM15 will receive free SHM membership for one year.
HM15 course director Efrén Manjarrez, MD, says that HM15 will bring many new angles and topics for conference veterans and will attract other members of the “big tent” of hospital medicine.
“For the first time, the American Academy of Family Physicians is endorsing the meeting, so we are excited to welcome even more family physicians to the meeting, many of whom might not have considered coming to an SHM meeting in the past,” he says.
For long-time meeting attendees, Dr. Manjarrez suggests taking a look at the new content for maintenance of certification (MOC) and patient experience. He is equally interested in welcoming residents and medical students to the meeting.
“We are meeting [past president] Eric Howell’s mission to increase the pipeline of future hospitalists,” Dr. Manjarrez says. “I’m personally challenging every single academic hospitalist to bring at least one medical student or resident with them to HM15.”
A First Step
As part of an effort to include even more medical school students and residents in the HM movement, SHM has created the first “young hospitalist” educational track. Designed for med students, residents, and even hospitalists freshly out of residency, the six courses in the “young hospitalist” track cover many of the topics never touched in med school or resident training, such as how to write a CV and how to create a meaningful relationship with a resident.
“The track will bring faculty and young hospitalists together to learn about and discuss topics that are critical in this part of a hospitalist’s career,” says Darlene Tad-y, MD, chair of SHM’s Physicians in Training Committee. “Attendees can expect a great deal of hands-on interaction with the faculty and advice on getting their hospitalist career off to a running start.”
Students and residents will have new opportunities for visibility and networking at HM15. SHM has created a Trainee Award category within its awards program and a career fair during the popular poster session to help introduce new hospitalists to staffing companies and recruiters. Students and residents will have a chance to meet the leaders of the specialty face to face during the luncheon and forum organized specifically for them.
Let Your Voice Be Heard in Congress
With hospitalists testifying before Congress on important patient care issues and rising to the highest levels of CMS, the voice of the hospitalist has never been more important in Washington, D.C. And you can add your voice to the movement.
On Wednesday, April 1, 2015, SHM will bring dozens of hospitalists to the halls of Capitol Hill to talk with legislators and staffers about patient and policy issues, including observation status, quality improvement, accountable care organizations (ACOs), and the impact of the Affordable Care Act on hospitalized patients. At “Hospitalists on the Hill,” hospitalists will talk face to face with policymakers and provide the kind of personal and professional perspective that they need to make decisions that affect millions of hospitalized patients every year.
Brendon Shank is SHM’s associate vice president of communications.
Now is the time to register, make travel arrangements, and book hotel rooms before the rush. Starting early means saving money: The deadline for early online registration—$100 savings—is February 2, 2015. Plus, hospitalists staying at the Gaylord National Resort & Convention Center, the official headquarters hotel for HM15, can save another $100 off their registration fees.
HM15 is the perfect time to join the hospital medicine movement. Nonmembers who register for HM15 will receive free SHM membership for one year.
HM15 course director Efrén Manjarrez, MD, says that HM15 will bring many new angles and topics for conference veterans and will attract other members of the “big tent” of hospital medicine.
“For the first time, the American Academy of Family Physicians is endorsing the meeting, so we are excited to welcome even more family physicians to the meeting, many of whom might not have considered coming to an SHM meeting in the past,” he says.
For long-time meeting attendees, Dr. Manjarrez suggests taking a look at the new content for maintenance of certification (MOC) and patient experience. He is equally interested in welcoming residents and medical students to the meeting.
“We are meeting [past president] Eric Howell’s mission to increase the pipeline of future hospitalists,” Dr. Manjarrez says. “I’m personally challenging every single academic hospitalist to bring at least one medical student or resident with them to HM15.”
A First Step
As part of an effort to include even more medical school students and residents in the HM movement, SHM has created the first “young hospitalist” educational track. Designed for med students, residents, and even hospitalists freshly out of residency, the six courses in the “young hospitalist” track cover many of the topics never touched in med school or resident training, such as how to write a CV and how to create a meaningful relationship with a resident.
“The track will bring faculty and young hospitalists together to learn about and discuss topics that are critical in this part of a hospitalist’s career,” says Darlene Tad-y, MD, chair of SHM’s Physicians in Training Committee. “Attendees can expect a great deal of hands-on interaction with the faculty and advice on getting their hospitalist career off to a running start.”
Students and residents will have new opportunities for visibility and networking at HM15. SHM has created a Trainee Award category within its awards program and a career fair during the popular poster session to help introduce new hospitalists to staffing companies and recruiters. Students and residents will have a chance to meet the leaders of the specialty face to face during the luncheon and forum organized specifically for them.
Let Your Voice Be Heard in Congress
With hospitalists testifying before Congress on important patient care issues and rising to the highest levels of CMS, the voice of the hospitalist has never been more important in Washington, D.C. And you can add your voice to the movement.
On Wednesday, April 1, 2015, SHM will bring dozens of hospitalists to the halls of Capitol Hill to talk with legislators and staffers about patient and policy issues, including observation status, quality improvement, accountable care organizations (ACOs), and the impact of the Affordable Care Act on hospitalized patients. At “Hospitalists on the Hill,” hospitalists will talk face to face with policymakers and provide the kind of personal and professional perspective that they need to make decisions that affect millions of hospitalized patients every year.
Brendon Shank is SHM’s associate vice president of communications.
Society of Hospital Medicine Adds Young Hospitalist Educational Track at HM15
HM15 now has education sessions targeted to early-career hospitalists, trainees, and medical students. The sessions will take place March 30, 2015. Here are some of the planned sessions:
- Career Pathways in Hospital Medicine;
- How to Stand Out: Being the Best Applicant You Can Be;
- Getting to the Top of the Pile: Writing Your CV;
- Quality and Safety for Residents and Students;
- Time Management; and
- Making the Most of Your Mentoring Relationships.
Student and resident discounts are available. Visit www.hospitalmedicine2015.org for details.
HM15 now has education sessions targeted to early-career hospitalists, trainees, and medical students. The sessions will take place March 30, 2015. Here are some of the planned sessions:
- Career Pathways in Hospital Medicine;
- How to Stand Out: Being the Best Applicant You Can Be;
- Getting to the Top of the Pile: Writing Your CV;
- Quality and Safety for Residents and Students;
- Time Management; and
- Making the Most of Your Mentoring Relationships.
Student and resident discounts are available. Visit www.hospitalmedicine2015.org for details.
HM15 now has education sessions targeted to early-career hospitalists, trainees, and medical students. The sessions will take place March 30, 2015. Here are some of the planned sessions:
- Career Pathways in Hospital Medicine;
- How to Stand Out: Being the Best Applicant You Can Be;
- Getting to the Top of the Pile: Writing Your CV;
- Quality and Safety for Residents and Students;
- Time Management; and
- Making the Most of Your Mentoring Relationships.
Student and resident discounts are available. Visit www.hospitalmedicine2015.org for details.
Physicians-in-Training Committee Chair Outlines SHM's Young Hospitalist Track at HM15
For the first time, SHM’s annual meeting will feature a daylong track specifically designed for young hospitalists: medical students, residents, and hospitalists just starting their career. Darlene Tad-y, MD, chair of SHM’s Physicians in Training (PIT) Committee, explains why young hospitalists are so important to the future of the hospital medicine movement and outlines the new educational track planned for HM15.
Question: Why is the new track for young hospitalists important?
Answer: It’s very exciting to have the new track! Young hospitalists can have different questions and concerns at the beginning of their careers. For hospitalists-in-training, there are still many unanswered questions about getting their first job, the status of the job market, getting involved in quality or scholarly work in the hospital, and other logistical considerations. Also, it is a great way for SHM to welcome and recognize the students, residents, and new hospitalists who are attending our national meeting—and the valuable contribution they make to our organization.
high-quality, efficient inpatient care for patients.”
Q: If I’m a med student or a resident or new hospitalist, what can I expect from this track?
A: The track will bring faculty and young hospitalists together to learn about and discuss topics that are critical in this part of a hospitalist’s career. Attendees can expect a great deal of hands-on interaction with the faculty and also advice on getting their hospitalist career off to a running start.
Q: How were these courses and faculty selected?
A: The PIT committee partnered with the Annual Meeting Committee to select the courses and faculty. Students, residents, and young hospitalists were asked for input on what content would be most useful. Along with some input from clerkship and program directors around the country, the courses were chosen. Faculty were selected through a competitive process.
Q: What are you most excited to do at HM15? What sessions do you plan on attending?
A: I’m always energized by the student/resident forum and also the RIV competition. Meeting the trainees en masse and hearing their ideas about hospital medicine are always eye opening. The poster sessions always are another great way to learn about the future of hospital medicine. I’m always amazed at the innovation and tenacity that our trainees demonstrate in furthering what we know about hospital medicine and providing high-quality, efficient inpatient care for patients.
For the first time, SHM’s annual meeting will feature a daylong track specifically designed for young hospitalists: medical students, residents, and hospitalists just starting their career. Darlene Tad-y, MD, chair of SHM’s Physicians in Training (PIT) Committee, explains why young hospitalists are so important to the future of the hospital medicine movement and outlines the new educational track planned for HM15.
Question: Why is the new track for young hospitalists important?
Answer: It’s very exciting to have the new track! Young hospitalists can have different questions and concerns at the beginning of their careers. For hospitalists-in-training, there are still many unanswered questions about getting their first job, the status of the job market, getting involved in quality or scholarly work in the hospital, and other logistical considerations. Also, it is a great way for SHM to welcome and recognize the students, residents, and new hospitalists who are attending our national meeting—and the valuable contribution they make to our organization.
high-quality, efficient inpatient care for patients.”
Q: If I’m a med student or a resident or new hospitalist, what can I expect from this track?
A: The track will bring faculty and young hospitalists together to learn about and discuss topics that are critical in this part of a hospitalist’s career. Attendees can expect a great deal of hands-on interaction with the faculty and also advice on getting their hospitalist career off to a running start.
Q: How were these courses and faculty selected?
A: The PIT committee partnered with the Annual Meeting Committee to select the courses and faculty. Students, residents, and young hospitalists were asked for input on what content would be most useful. Along with some input from clerkship and program directors around the country, the courses were chosen. Faculty were selected through a competitive process.
Q: What are you most excited to do at HM15? What sessions do you plan on attending?
A: I’m always energized by the student/resident forum and also the RIV competition. Meeting the trainees en masse and hearing their ideas about hospital medicine are always eye opening. The poster sessions always are another great way to learn about the future of hospital medicine. I’m always amazed at the innovation and tenacity that our trainees demonstrate in furthering what we know about hospital medicine and providing high-quality, efficient inpatient care for patients.
For the first time, SHM’s annual meeting will feature a daylong track specifically designed for young hospitalists: medical students, residents, and hospitalists just starting their career. Darlene Tad-y, MD, chair of SHM’s Physicians in Training (PIT) Committee, explains why young hospitalists are so important to the future of the hospital medicine movement and outlines the new educational track planned for HM15.
Question: Why is the new track for young hospitalists important?
Answer: It’s very exciting to have the new track! Young hospitalists can have different questions and concerns at the beginning of their careers. For hospitalists-in-training, there are still many unanswered questions about getting their first job, the status of the job market, getting involved in quality or scholarly work in the hospital, and other logistical considerations. Also, it is a great way for SHM to welcome and recognize the students, residents, and new hospitalists who are attending our national meeting—and the valuable contribution they make to our organization.
high-quality, efficient inpatient care for patients.”
Q: If I’m a med student or a resident or new hospitalist, what can I expect from this track?
A: The track will bring faculty and young hospitalists together to learn about and discuss topics that are critical in this part of a hospitalist’s career. Attendees can expect a great deal of hands-on interaction with the faculty and also advice on getting their hospitalist career off to a running start.
Q: How were these courses and faculty selected?
A: The PIT committee partnered with the Annual Meeting Committee to select the courses and faculty. Students, residents, and young hospitalists were asked for input on what content would be most useful. Along with some input from clerkship and program directors around the country, the courses were chosen. Faculty were selected through a competitive process.
Q: What are you most excited to do at HM15? What sessions do you plan on attending?
A: I’m always energized by the student/resident forum and also the RIV competition. Meeting the trainees en masse and hearing their ideas about hospital medicine are always eye opening. The poster sessions always are another great way to learn about the future of hospital medicine. I’m always amazed at the innovation and tenacity that our trainees demonstrate in furthering what we know about hospital medicine and providing high-quality, efficient inpatient care for patients.
Society of Hospital Medicine Learning Portal Adds Information on Anticoagulants, Pediatrics
The SHM Learning Portal, the best destination for hospitalist CME, now offers new materials on two important topics: anticoagulants and pediatrics.
In addition to offering free on-demand information that many hospitalists can use on a daily basis, the anticoagulant series will be presented in a new way for the Learning Portal: The presentation will be recorded to individual slides rather than as a recorded webinar.
Later in December, SHM will be posting new pediatric Maintenance of Certification modules.
To access SHM’s Learning Portal, visit www.shmlearningportal.org.
The SHM Learning Portal, the best destination for hospitalist CME, now offers new materials on two important topics: anticoagulants and pediatrics.
In addition to offering free on-demand information that many hospitalists can use on a daily basis, the anticoagulant series will be presented in a new way for the Learning Portal: The presentation will be recorded to individual slides rather than as a recorded webinar.
Later in December, SHM will be posting new pediatric Maintenance of Certification modules.
To access SHM’s Learning Portal, visit www.shmlearningportal.org.
The SHM Learning Portal, the best destination for hospitalist CME, now offers new materials on two important topics: anticoagulants and pediatrics.
In addition to offering free on-demand information that many hospitalists can use on a daily basis, the anticoagulant series will be presented in a new way for the Learning Portal: The presentation will be recorded to individual slides rather than as a recorded webinar.
Later in December, SHM will be posting new pediatric Maintenance of Certification modules.
To access SHM’s Learning Portal, visit www.shmlearningportal.org.
Hospital Medicine Exchange Online Conversation Starter for Hospitalists
From finding the best scheduling software to glycemic control performance measures to staffing to workloads, Hospital Medicine Exchange has become hospitalists’ first stop for questions and answers from other hospitalists on a wide range of topics.
In September, hospitalists posted nearly 250 discussion starters, questions, and answers, including topics like:
- Resources for ABIM Maintenance of Certification for hospitalists;
- Palliative care and discharge;
- Responsibilities for signing death certificates;
- Coverage for rehabilitation and ventricular assist device (VAD) patients;
- Improving length of stay (LOS); and
- Opiate management for hospitalized chronic pain patients.
Do you have a question for SHM’s 12,000 members? Want to share a success story? Visit HMX today at www.HMXchange.org.
From finding the best scheduling software to glycemic control performance measures to staffing to workloads, Hospital Medicine Exchange has become hospitalists’ first stop for questions and answers from other hospitalists on a wide range of topics.
In September, hospitalists posted nearly 250 discussion starters, questions, and answers, including topics like:
- Resources for ABIM Maintenance of Certification for hospitalists;
- Palliative care and discharge;
- Responsibilities for signing death certificates;
- Coverage for rehabilitation and ventricular assist device (VAD) patients;
- Improving length of stay (LOS); and
- Opiate management for hospitalized chronic pain patients.
Do you have a question for SHM’s 12,000 members? Want to share a success story? Visit HMX today at www.HMXchange.org.
From finding the best scheduling software to glycemic control performance measures to staffing to workloads, Hospital Medicine Exchange has become hospitalists’ first stop for questions and answers from other hospitalists on a wide range of topics.
In September, hospitalists posted nearly 250 discussion starters, questions, and answers, including topics like:
- Resources for ABIM Maintenance of Certification for hospitalists;
- Palliative care and discharge;
- Responsibilities for signing death certificates;
- Coverage for rehabilitation and ventricular assist device (VAD) patients;
- Improving length of stay (LOS); and
- Opiate management for hospitalized chronic pain patients.
Do you have a question for SHM’s 12,000 members? Want to share a success story? Visit HMX today at www.HMXchange.org.