User login
Adolescents’ acute care use for eating disorders has risen
In a repeated cross-sectional study that examined population-based data from January 2017 through August 2022, ED visits increased by 121% above expected levels, and hospital admissions increased by 54% above expected among patients aged 10-17 years during the pandemic.
“We are hoping this study continues to heighten awareness of the importance of eating disorders, and also to bolster support for eating disorder programs so that we can adequately care for patients and address the increasing demand for treatment and services,” lead author Alene Toulany, MD, adolescent medicine specialist and researcher at the Hospital for Sick Children in Toronto, told this news organization.
The study was published in the Canadian Medical Association Journal.
‘A pressing concern’
The researchers used linked health administrative databases that included all patients in Ontario who were eligible for the Ontario Health Insurance Plan, which is publicly funded. They compared observed and expected rates of ED visits and hospitalizations for eating disorders between a prepandemic period (Jan. 1, 2017, to Feb. 29, 2020) and a pandemic period (Mar. 1, 2020, to Aug. 31, 2022). The researchers examined the following four age categories: adolescents (aged 10-17 years), young adults (aged 18-26 years), adults (aged 27-40 years), and older adults (aged 41-105 years).
Among adolescents, the observed rate of ED visits during the 30 pandemic months studied was 7.38 per 100,000 population, compared with 3.33 per 100,000 before the pandemic (incidence rate ratio [IRR], 2.21).
The rate of ED visits among young adults increased by 13% above the expected rate. It reached 2.79 per 100,000, compared with 2.46 per 100,000 in the prepandemic period (IRR, 1.13).
Among older adults, ED visits increased from 0.11 per 100,000 in the prepandemic period to 0.14 per 100,000 in the pandemic period (IRR, 1.15). The rate of ED visits among adults remained approximately the same.
The rate of hospital admissions among adolescents increased by 54% above the expected rate during the pandemic. The observed rate of hospital admissions before the pandemic was 5.74 per 100,000, vs. 8.82 per 100,000 during the pandemic (IRR, 1.54). Hospital admissions remained stable or decreased for the other age groups.
“Eating disorders have increased globally in children and adolescents during COVID,” said Dr. Toulany. “There are a number of risk factors contributing to this pandemic rise, including isolation, more time on social media, decreased access to care (as many in-person services were not available due to the pandemic), as well as fear of getting infected. All of these could contribute to an increased risk of developing an eating disorder or of making an existing one worse.”
Regardless of the cause, more investment in eating disorders research and eating disorder programs for adolescents and adults is needed, she said.
“The pandemic served as a catalyst, because it started to shed light on the prevalence of eating disorders, especially in young people. But it’s very important that we recognize that this has been a long-standing issue and a pressing concern that has been consistently overlooked and underfunded,” said Dr. Toulany.
Surging eating disorders
Commenting on the findings, Victor Fornari, MD, director of child and adolescent psychiatry at Zucker Hillside Hospital/Northwell Health in Glen Oaks, N.Y., said, “Our experience in the United States parallels what is described in this Canadian paper. This was a surge of eating disorders the likes of which I had not experienced in my career.” Dr. Fornari did not participate in the current study.
“I’ve been here for over 40 years, and the average number of our inpatients in our eating disorder program has been three to five and about a dozen patients in our day clinic at any one time. But in the spring of 2020, we surged to 20 inpatients and over 20 day patients,” Dr. Fornari said.
“We can speculate as to the reasons for this,” he continued. “Kids were isolated. School was closed. They spent more time on social media and the Internet. Their sports activities were curtailed. There was anxiety because the guidance that we were all offered to prevent contagion was increasing people’s anxiety about safety and danger. So, I think we saw dramatic rises in eating disorders in the same way we saw dramatic rises in anxiety and depression in adolescents, as well.”
Dr. Fornari cited social media as an important contributing factor to eating disorders, especially among vulnerable teenagers. “Many of these vulnerable kids are looking at pictures of people who are very thin and comparing themselves, feeling inadequate, feeling sad. Social media is one of the reasons why the rates of psychopathology amongst teens has skyrocketed in the last decade. The surgeon general recently said we should delay access to social media until age 16 because the younger kids are impressionable and vulnerable. I think there is wisdom there, but it is very hard to actually put into practice.”
Worsening mental health
“I thought this was very relevant research and an important contribution to our understanding of eating disorders during pandemic times,” said Simon Sherry, PhD, professor of psychology and neuroscience at Dalhousie University in Halifax, Nova Scotia. “It also dovetails with my own experience as a practitioner.” Dr. Sherry was not involved in the research.
The pandemic has been difficult for people with disordered eating for many reasons, Dr. Sherry said. “There was a massive disruption or ‘loss of normal’ around food. Restaurants closed, grocery shopping was disrupted, scarcity of food occurred, hoarding of food occurred. That meant that eating was difficult for all of us, but especially for individuals who were rigid and controlling around the consumption of food. In this COVID era, you would need flexibility and acceptance around eating, but if you had a narrow range of preferred foods and preferred shopping locations, no doubt the pandemic made this a lot worse.”
Certain forms of disordered eating would be much more likely during the pandemic, Dr. Sherry noted. “For example, binge eating is often triggered by psychological, social, and environmental events,” and those triggers were abundant at the beginning of the pandemic. Boredom, anxiety, depression, stress, loneliness, confinement, and isolation are among the triggers. “COVID-19-related stress was and is very fertile ground for the growth of emotional eating, binge eating, or turning to food to cope. Eating disorders tend to fester amid silence and isolation and inactivity, and that was very much our experience during the lockdown phase of the pandemic,” he said.
Dr. Sherry agrees with the need for more funding for eating disorders research. “We know in Canada that eating disorders are a very important and deadly issue that is chronically underfunded. We are not funding disordered eating in proportion to its prevalence or in proportion to the amount of harm and destruction it creates for individuals, their family members, and our society at large. The authors are absolutely correct to advocate for care in proportion to the prevalence and the damage associated with eating disorders,” he said.
The study was supported by ICES, which is funded by an annual grant from the Ontario Ministry of Health, the Ministry of Long-Term Care, and the Canadian Institutes of Health Research (CIHR). Dr. Toulany, Dr. Fornari, and Dr. Sherry reported no relevant financial relationships. One study author reported receiving personal fees from the BMJ Group’s Archives of Diseases in Childhood and grants from CIHR, the Ontario Ministry of Health, the Centre for Addiction and Mental Health, and the Hospital for Sick Children. A second author reported funding from CIHR.
A version of this article first appeared on Medscape.com.
In a repeated cross-sectional study that examined population-based data from January 2017 through August 2022, ED visits increased by 121% above expected levels, and hospital admissions increased by 54% above expected among patients aged 10-17 years during the pandemic.
“We are hoping this study continues to heighten awareness of the importance of eating disorders, and also to bolster support for eating disorder programs so that we can adequately care for patients and address the increasing demand for treatment and services,” lead author Alene Toulany, MD, adolescent medicine specialist and researcher at the Hospital for Sick Children in Toronto, told this news organization.
The study was published in the Canadian Medical Association Journal.
‘A pressing concern’
The researchers used linked health administrative databases that included all patients in Ontario who were eligible for the Ontario Health Insurance Plan, which is publicly funded. They compared observed and expected rates of ED visits and hospitalizations for eating disorders between a prepandemic period (Jan. 1, 2017, to Feb. 29, 2020) and a pandemic period (Mar. 1, 2020, to Aug. 31, 2022). The researchers examined the following four age categories: adolescents (aged 10-17 years), young adults (aged 18-26 years), adults (aged 27-40 years), and older adults (aged 41-105 years).
Among adolescents, the observed rate of ED visits during the 30 pandemic months studied was 7.38 per 100,000 population, compared with 3.33 per 100,000 before the pandemic (incidence rate ratio [IRR], 2.21).
The rate of ED visits among young adults increased by 13% above the expected rate. It reached 2.79 per 100,000, compared with 2.46 per 100,000 in the prepandemic period (IRR, 1.13).
Among older adults, ED visits increased from 0.11 per 100,000 in the prepandemic period to 0.14 per 100,000 in the pandemic period (IRR, 1.15). The rate of ED visits among adults remained approximately the same.
The rate of hospital admissions among adolescents increased by 54% above the expected rate during the pandemic. The observed rate of hospital admissions before the pandemic was 5.74 per 100,000, vs. 8.82 per 100,000 during the pandemic (IRR, 1.54). Hospital admissions remained stable or decreased for the other age groups.
“Eating disorders have increased globally in children and adolescents during COVID,” said Dr. Toulany. “There are a number of risk factors contributing to this pandemic rise, including isolation, more time on social media, decreased access to care (as many in-person services were not available due to the pandemic), as well as fear of getting infected. All of these could contribute to an increased risk of developing an eating disorder or of making an existing one worse.”
Regardless of the cause, more investment in eating disorders research and eating disorder programs for adolescents and adults is needed, she said.
“The pandemic served as a catalyst, because it started to shed light on the prevalence of eating disorders, especially in young people. But it’s very important that we recognize that this has been a long-standing issue and a pressing concern that has been consistently overlooked and underfunded,” said Dr. Toulany.
Surging eating disorders
Commenting on the findings, Victor Fornari, MD, director of child and adolescent psychiatry at Zucker Hillside Hospital/Northwell Health in Glen Oaks, N.Y., said, “Our experience in the United States parallels what is described in this Canadian paper. This was a surge of eating disorders the likes of which I had not experienced in my career.” Dr. Fornari did not participate in the current study.
“I’ve been here for over 40 years, and the average number of our inpatients in our eating disorder program has been three to five and about a dozen patients in our day clinic at any one time. But in the spring of 2020, we surged to 20 inpatients and over 20 day patients,” Dr. Fornari said.
“We can speculate as to the reasons for this,” he continued. “Kids were isolated. School was closed. They spent more time on social media and the Internet. Their sports activities were curtailed. There was anxiety because the guidance that we were all offered to prevent contagion was increasing people’s anxiety about safety and danger. So, I think we saw dramatic rises in eating disorders in the same way we saw dramatic rises in anxiety and depression in adolescents, as well.”
Dr. Fornari cited social media as an important contributing factor to eating disorders, especially among vulnerable teenagers. “Many of these vulnerable kids are looking at pictures of people who are very thin and comparing themselves, feeling inadequate, feeling sad. Social media is one of the reasons why the rates of psychopathology amongst teens has skyrocketed in the last decade. The surgeon general recently said we should delay access to social media until age 16 because the younger kids are impressionable and vulnerable. I think there is wisdom there, but it is very hard to actually put into practice.”
Worsening mental health
“I thought this was very relevant research and an important contribution to our understanding of eating disorders during pandemic times,” said Simon Sherry, PhD, professor of psychology and neuroscience at Dalhousie University in Halifax, Nova Scotia. “It also dovetails with my own experience as a practitioner.” Dr. Sherry was not involved in the research.
The pandemic has been difficult for people with disordered eating for many reasons, Dr. Sherry said. “There was a massive disruption or ‘loss of normal’ around food. Restaurants closed, grocery shopping was disrupted, scarcity of food occurred, hoarding of food occurred. That meant that eating was difficult for all of us, but especially for individuals who were rigid and controlling around the consumption of food. In this COVID era, you would need flexibility and acceptance around eating, but if you had a narrow range of preferred foods and preferred shopping locations, no doubt the pandemic made this a lot worse.”
Certain forms of disordered eating would be much more likely during the pandemic, Dr. Sherry noted. “For example, binge eating is often triggered by psychological, social, and environmental events,” and those triggers were abundant at the beginning of the pandemic. Boredom, anxiety, depression, stress, loneliness, confinement, and isolation are among the triggers. “COVID-19-related stress was and is very fertile ground for the growth of emotional eating, binge eating, or turning to food to cope. Eating disorders tend to fester amid silence and isolation and inactivity, and that was very much our experience during the lockdown phase of the pandemic,” he said.
Dr. Sherry agrees with the need for more funding for eating disorders research. “We know in Canada that eating disorders are a very important and deadly issue that is chronically underfunded. We are not funding disordered eating in proportion to its prevalence or in proportion to the amount of harm and destruction it creates for individuals, their family members, and our society at large. The authors are absolutely correct to advocate for care in proportion to the prevalence and the damage associated with eating disorders,” he said.
The study was supported by ICES, which is funded by an annual grant from the Ontario Ministry of Health, the Ministry of Long-Term Care, and the Canadian Institutes of Health Research (CIHR). Dr. Toulany, Dr. Fornari, and Dr. Sherry reported no relevant financial relationships. One study author reported receiving personal fees from the BMJ Group’s Archives of Diseases in Childhood and grants from CIHR, the Ontario Ministry of Health, the Centre for Addiction and Mental Health, and the Hospital for Sick Children. A second author reported funding from CIHR.
A version of this article first appeared on Medscape.com.
In a repeated cross-sectional study that examined population-based data from January 2017 through August 2022, ED visits increased by 121% above expected levels, and hospital admissions increased by 54% above expected among patients aged 10-17 years during the pandemic.
“We are hoping this study continues to heighten awareness of the importance of eating disorders, and also to bolster support for eating disorder programs so that we can adequately care for patients and address the increasing demand for treatment and services,” lead author Alene Toulany, MD, adolescent medicine specialist and researcher at the Hospital for Sick Children in Toronto, told this news organization.
The study was published in the Canadian Medical Association Journal.
‘A pressing concern’
The researchers used linked health administrative databases that included all patients in Ontario who were eligible for the Ontario Health Insurance Plan, which is publicly funded. They compared observed and expected rates of ED visits and hospitalizations for eating disorders between a prepandemic period (Jan. 1, 2017, to Feb. 29, 2020) and a pandemic period (Mar. 1, 2020, to Aug. 31, 2022). The researchers examined the following four age categories: adolescents (aged 10-17 years), young adults (aged 18-26 years), adults (aged 27-40 years), and older adults (aged 41-105 years).
Among adolescents, the observed rate of ED visits during the 30 pandemic months studied was 7.38 per 100,000 population, compared with 3.33 per 100,000 before the pandemic (incidence rate ratio [IRR], 2.21).
The rate of ED visits among young adults increased by 13% above the expected rate. It reached 2.79 per 100,000, compared with 2.46 per 100,000 in the prepandemic period (IRR, 1.13).
Among older adults, ED visits increased from 0.11 per 100,000 in the prepandemic period to 0.14 per 100,000 in the pandemic period (IRR, 1.15). The rate of ED visits among adults remained approximately the same.
The rate of hospital admissions among adolescents increased by 54% above the expected rate during the pandemic. The observed rate of hospital admissions before the pandemic was 5.74 per 100,000, vs. 8.82 per 100,000 during the pandemic (IRR, 1.54). Hospital admissions remained stable or decreased for the other age groups.
“Eating disorders have increased globally in children and adolescents during COVID,” said Dr. Toulany. “There are a number of risk factors contributing to this pandemic rise, including isolation, more time on social media, decreased access to care (as many in-person services were not available due to the pandemic), as well as fear of getting infected. All of these could contribute to an increased risk of developing an eating disorder or of making an existing one worse.”
Regardless of the cause, more investment in eating disorders research and eating disorder programs for adolescents and adults is needed, she said.
“The pandemic served as a catalyst, because it started to shed light on the prevalence of eating disorders, especially in young people. But it’s very important that we recognize that this has been a long-standing issue and a pressing concern that has been consistently overlooked and underfunded,” said Dr. Toulany.
Surging eating disorders
Commenting on the findings, Victor Fornari, MD, director of child and adolescent psychiatry at Zucker Hillside Hospital/Northwell Health in Glen Oaks, N.Y., said, “Our experience in the United States parallels what is described in this Canadian paper. This was a surge of eating disorders the likes of which I had not experienced in my career.” Dr. Fornari did not participate in the current study.
“I’ve been here for over 40 years, and the average number of our inpatients in our eating disorder program has been three to five and about a dozen patients in our day clinic at any one time. But in the spring of 2020, we surged to 20 inpatients and over 20 day patients,” Dr. Fornari said.
“We can speculate as to the reasons for this,” he continued. “Kids were isolated. School was closed. They spent more time on social media and the Internet. Their sports activities were curtailed. There was anxiety because the guidance that we were all offered to prevent contagion was increasing people’s anxiety about safety and danger. So, I think we saw dramatic rises in eating disorders in the same way we saw dramatic rises in anxiety and depression in adolescents, as well.”
Dr. Fornari cited social media as an important contributing factor to eating disorders, especially among vulnerable teenagers. “Many of these vulnerable kids are looking at pictures of people who are very thin and comparing themselves, feeling inadequate, feeling sad. Social media is one of the reasons why the rates of psychopathology amongst teens has skyrocketed in the last decade. The surgeon general recently said we should delay access to social media until age 16 because the younger kids are impressionable and vulnerable. I think there is wisdom there, but it is very hard to actually put into practice.”
Worsening mental health
“I thought this was very relevant research and an important contribution to our understanding of eating disorders during pandemic times,” said Simon Sherry, PhD, professor of psychology and neuroscience at Dalhousie University in Halifax, Nova Scotia. “It also dovetails with my own experience as a practitioner.” Dr. Sherry was not involved in the research.
The pandemic has been difficult for people with disordered eating for many reasons, Dr. Sherry said. “There was a massive disruption or ‘loss of normal’ around food. Restaurants closed, grocery shopping was disrupted, scarcity of food occurred, hoarding of food occurred. That meant that eating was difficult for all of us, but especially for individuals who were rigid and controlling around the consumption of food. In this COVID era, you would need flexibility and acceptance around eating, but if you had a narrow range of preferred foods and preferred shopping locations, no doubt the pandemic made this a lot worse.”
Certain forms of disordered eating would be much more likely during the pandemic, Dr. Sherry noted. “For example, binge eating is often triggered by psychological, social, and environmental events,” and those triggers were abundant at the beginning of the pandemic. Boredom, anxiety, depression, stress, loneliness, confinement, and isolation are among the triggers. “COVID-19-related stress was and is very fertile ground for the growth of emotional eating, binge eating, or turning to food to cope. Eating disorders tend to fester amid silence and isolation and inactivity, and that was very much our experience during the lockdown phase of the pandemic,” he said.
Dr. Sherry agrees with the need for more funding for eating disorders research. “We know in Canada that eating disorders are a very important and deadly issue that is chronically underfunded. We are not funding disordered eating in proportion to its prevalence or in proportion to the amount of harm and destruction it creates for individuals, their family members, and our society at large. The authors are absolutely correct to advocate for care in proportion to the prevalence and the damage associated with eating disorders,” he said.
The study was supported by ICES, which is funded by an annual grant from the Ontario Ministry of Health, the Ministry of Long-Term Care, and the Canadian Institutes of Health Research (CIHR). Dr. Toulany, Dr. Fornari, and Dr. Sherry reported no relevant financial relationships. One study author reported receiving personal fees from the BMJ Group’s Archives of Diseases in Childhood and grants from CIHR, the Ontario Ministry of Health, the Centre for Addiction and Mental Health, and the Hospital for Sick Children. A second author reported funding from CIHR.
A version of this article first appeared on Medscape.com.
FROM THE CANADIAN MEDICAL ASSOCIATION JOURNAL
Hyperbaric oxygen therapy for traumatic brain injury: Promising or wishful thinking?
A recent review by Hadanny and colleagues recommends hyperbaric oxygen therapy (HBOT) for acute moderate to severe traumatic brain injury (TBI) and selected patients with prolonged postconcussive syndrome.
This article piqued my curiosity because I trained in HBOT more than 20 years ago. As a passionate scuba diver, my motivation was to master treatment for air embolism and decompression illness. Thankfully, these diving accidents are rare. However, I used HBOT for nonhealing wounds, and its efficacy was sometimes remarkable.
Paradoxical results with oxygen therapy
Although it may seem self-evident that “more oxygen is better” for medical illness, this is not necessarily true. I recently interviewed Ola Didrik Saugstad, MD, who demonstrated that the traditional practice of resuscitating newborns with 100% oxygen was more toxic than resuscitation with air (which contains 21% oxygen). His counterintuitive discovery led to a lifesaving change in the international newborn resuscitation guidelines.
The Food and Drug Administration has approved HBOT for a wide variety of conditions, but some practitioners enthusiastically promote it for off-label indications. These include antiaging, autism, multiple sclerosis, and the aforementioned TBI.
More than 50 years ago, HBOT was proposed for stroke, another disorder where the brain has been deprived of oxygen. Despite obvious logic, clinical trials have been unconvincing. The FDA has not approved HBOT for stroke.
HBOT in practice
During HBOT, the patient breathes 100% oxygen while the whole body is pressurized within a hyperbaric chamber. The chamber’s construction allows pressures above normal sea level of 1.0 atmosphere absolute (ATA). For example, The U.S. Navy Treatment Table for decompression sickness recommends 100% oxygen at 2.8 ATA. Chambers may hold one or more patients at a time.
The frequency of therapy varies but often consists of 20-60 sessions lasting 90-120 minutes. For off-label use like TBI, patients usually pay out of pocket. Given the multiple treatments, costs can add up.
Inconsistent evidence and sham controls
The unwieldy 33-page evidence review by Hadanny and colleagues cites multiple studies supporting HBOT for TBI. However, many, if not all, suffer from methodological flaws. These include vague inclusion criteria, lack of a control group, small patient numbers, treatment at different times since injury, poorly defined or varying HBOT protocols, varying outcome measures, and superficial results analysis.
A sham or control arm is essential for HBOT research trials, given the potential placebo effect of placing a human being inside a large, high-tech, sealed tube for an hour or more. In some sham-controlled studies, which consisted of low-pressure oxygen (that is, 1.3 ATA as sham vs. 2.4 ATA as treatment), all groups experienced symptom improvement. The review authors argue that the low-dose HBOT sham arms were biologically active and that the improvements seen mean that both high- and low-dose HBOT is therapeutic. The alternative explanation is that the placebo effect accounted for improvement in both groups.
The late Michael Bennett, a world authority on hyperbaric and underwater medicine, doubted that conventional HBOT sham controls could genuinely have a therapeutic effect, and I agree. The upcoming HOT-POCS trial (discussed below) should answer the question more definitively.
Mechanisms of action and safety
Mechanisms of benefit for HBOT include increased oxygen availability and angiogenesis. Animal research suggests that it may reduce secondary cell death from TBI, through stabilization of the blood-brain barrier and inflammation reduction.
HBOT is generally safe and well tolerated. A retrospective analysis of 1.5 million outpatient hyperbaric treatments revealed that less than 1% were associated with adverse events. The most common were ear and sinus barotrauma. Because HBOT uses increased air pressure, patients must equalize their ears and sinuses. Those who cannot because of altered consciousness, anatomical defects, or congestion must undergo myringotomy or terminate therapy. Claustrophobia was the second most common adverse effect. Convulsions and tension pneumocephalus were rare.
Perhaps the most concerning risk of HBOT for patients with TBI is the potential waste of human and financial resources.
Desperate physicians and patients
As a neurologist who regularly treats patients with TBI, I share the review authors’ frustration regarding the limited efficacy of available treatments. However, the suboptimal efficacy of currently available therapy is insufficient justification to recommend HBOT.
With respect to chronic TBI, it is difficult to imagine how HBOT could reverse brain injury that has been present for months or years. No other therapy exists that reliably encourages neuronal regeneration or prevents the development of posttraumatic epilepsy.
Frank Conidi, MD, a board-certified sports neurologist and headache specialist, shared his thoughts via email. He agrees that HBOT may have a role in TBI, but after reviewing Hadanny and colleagues’ paper, he concluded that there is insufficient evidence for the use of HBOT in all forms of TBI. He would like to see large multicenter, well-designed studies with standardized pressures and duration and a standard definition of the various types of head injury.
Ongoing research
There are at least five ongoing trials on HBOT for TBI or postconcussive syndrome, including the well-designed placebo-controlled HOT-POCS study. The latter has a novel placebo gas system that addresses Hadanny and colleagues’ contention that even low-dose HBOT might be effective.
The placebo arm in HOT-POCS mimics the HBO environment but provides only 0.21 ATA of oxygen, the same as room air. The active arm provides 100% oxygen at 2.0 ATA. If patients in both arms improve, the benefit will be caused by a placebo response, not HBOT.
Conflict of interest
Another concern with the review is that all three authors are affiliated with Aviv Scientific. This company has an exclusive partnership with the world’s largest hyperbaric medicine and research facility, the Sagol Center at Shamir Medical Center in Be’er Ya’akov, Israel.
This conflict of interest does not a priori invalidate their conclusions. However, official HBOT guidelines from a leading organization like the Undersea and Hyperbaric Medicine Society or the American Academy of Neurology would be preferable.
Conclusion
There is an urgent unmet need for more effective treatments for postconcussive syndrome and chronic TBI.
The review authors’ recommendations for HBOT seem premature. They are arguably a disservice to the many desperate patients and their families who will be tempted to expend valuable resources of time and money for an appealing but unproven therapy. Appropriately designed placebo-controlled studies such as HOT-POCS will help separate fact from wishful thinking.
Dr. Wilner is associate professor of neurology at University of Tennessee Health Science Center, Memphis. He reported a conflict of interest with Accordant Health Services.
A version of this article first appeared on Medscape.com.
A recent review by Hadanny and colleagues recommends hyperbaric oxygen therapy (HBOT) for acute moderate to severe traumatic brain injury (TBI) and selected patients with prolonged postconcussive syndrome.
This article piqued my curiosity because I trained in HBOT more than 20 years ago. As a passionate scuba diver, my motivation was to master treatment for air embolism and decompression illness. Thankfully, these diving accidents are rare. However, I used HBOT for nonhealing wounds, and its efficacy was sometimes remarkable.
Paradoxical results with oxygen therapy
Although it may seem self-evident that “more oxygen is better” for medical illness, this is not necessarily true. I recently interviewed Ola Didrik Saugstad, MD, who demonstrated that the traditional practice of resuscitating newborns with 100% oxygen was more toxic than resuscitation with air (which contains 21% oxygen). His counterintuitive discovery led to a lifesaving change in the international newborn resuscitation guidelines.
The Food and Drug Administration has approved HBOT for a wide variety of conditions, but some practitioners enthusiastically promote it for off-label indications. These include antiaging, autism, multiple sclerosis, and the aforementioned TBI.
More than 50 years ago, HBOT was proposed for stroke, another disorder where the brain has been deprived of oxygen. Despite obvious logic, clinical trials have been unconvincing. The FDA has not approved HBOT for stroke.
HBOT in practice
During HBOT, the patient breathes 100% oxygen while the whole body is pressurized within a hyperbaric chamber. The chamber’s construction allows pressures above normal sea level of 1.0 atmosphere absolute (ATA). For example, The U.S. Navy Treatment Table for decompression sickness recommends 100% oxygen at 2.8 ATA. Chambers may hold one or more patients at a time.
The frequency of therapy varies but often consists of 20-60 sessions lasting 90-120 minutes. For off-label use like TBI, patients usually pay out of pocket. Given the multiple treatments, costs can add up.
Inconsistent evidence and sham controls
The unwieldy 33-page evidence review by Hadanny and colleagues cites multiple studies supporting HBOT for TBI. However, many, if not all, suffer from methodological flaws. These include vague inclusion criteria, lack of a control group, small patient numbers, treatment at different times since injury, poorly defined or varying HBOT protocols, varying outcome measures, and superficial results analysis.
A sham or control arm is essential for HBOT research trials, given the potential placebo effect of placing a human being inside a large, high-tech, sealed tube for an hour or more. In some sham-controlled studies, which consisted of low-pressure oxygen (that is, 1.3 ATA as sham vs. 2.4 ATA as treatment), all groups experienced symptom improvement. The review authors argue that the low-dose HBOT sham arms were biologically active and that the improvements seen mean that both high- and low-dose HBOT is therapeutic. The alternative explanation is that the placebo effect accounted for improvement in both groups.
The late Michael Bennett, a world authority on hyperbaric and underwater medicine, doubted that conventional HBOT sham controls could genuinely have a therapeutic effect, and I agree. The upcoming HOT-POCS trial (discussed below) should answer the question more definitively.
Mechanisms of action and safety
Mechanisms of benefit for HBOT include increased oxygen availability and angiogenesis. Animal research suggests that it may reduce secondary cell death from TBI, through stabilization of the blood-brain barrier and inflammation reduction.
HBOT is generally safe and well tolerated. A retrospective analysis of 1.5 million outpatient hyperbaric treatments revealed that less than 1% were associated with adverse events. The most common were ear and sinus barotrauma. Because HBOT uses increased air pressure, patients must equalize their ears and sinuses. Those who cannot because of altered consciousness, anatomical defects, or congestion must undergo myringotomy or terminate therapy. Claustrophobia was the second most common adverse effect. Convulsions and tension pneumocephalus were rare.
Perhaps the most concerning risk of HBOT for patients with TBI is the potential waste of human and financial resources.
Desperate physicians and patients
As a neurologist who regularly treats patients with TBI, I share the review authors’ frustration regarding the limited efficacy of available treatments. However, the suboptimal efficacy of currently available therapy is insufficient justification to recommend HBOT.
With respect to chronic TBI, it is difficult to imagine how HBOT could reverse brain injury that has been present for months or years. No other therapy exists that reliably encourages neuronal regeneration or prevents the development of posttraumatic epilepsy.
Frank Conidi, MD, a board-certified sports neurologist and headache specialist, shared his thoughts via email. He agrees that HBOT may have a role in TBI, but after reviewing Hadanny and colleagues’ paper, he concluded that there is insufficient evidence for the use of HBOT in all forms of TBI. He would like to see large multicenter, well-designed studies with standardized pressures and duration and a standard definition of the various types of head injury.
Ongoing research
There are at least five ongoing trials on HBOT for TBI or postconcussive syndrome, including the well-designed placebo-controlled HOT-POCS study. The latter has a novel placebo gas system that addresses Hadanny and colleagues’ contention that even low-dose HBOT might be effective.
The placebo arm in HOT-POCS mimics the HBO environment but provides only 0.21 ATA of oxygen, the same as room air. The active arm provides 100% oxygen at 2.0 ATA. If patients in both arms improve, the benefit will be caused by a placebo response, not HBOT.
Conflict of interest
Another concern with the review is that all three authors are affiliated with Aviv Scientific. This company has an exclusive partnership with the world’s largest hyperbaric medicine and research facility, the Sagol Center at Shamir Medical Center in Be’er Ya’akov, Israel.
This conflict of interest does not a priori invalidate their conclusions. However, official HBOT guidelines from a leading organization like the Undersea and Hyperbaric Medicine Society or the American Academy of Neurology would be preferable.
Conclusion
There is an urgent unmet need for more effective treatments for postconcussive syndrome and chronic TBI.
The review authors’ recommendations for HBOT seem premature. They are arguably a disservice to the many desperate patients and their families who will be tempted to expend valuable resources of time and money for an appealing but unproven therapy. Appropriately designed placebo-controlled studies such as HOT-POCS will help separate fact from wishful thinking.
Dr. Wilner is associate professor of neurology at University of Tennessee Health Science Center, Memphis. He reported a conflict of interest with Accordant Health Services.
A version of this article first appeared on Medscape.com.
A recent review by Hadanny and colleagues recommends hyperbaric oxygen therapy (HBOT) for acute moderate to severe traumatic brain injury (TBI) and selected patients with prolonged postconcussive syndrome.
This article piqued my curiosity because I trained in HBOT more than 20 years ago. As a passionate scuba diver, my motivation was to master treatment for air embolism and decompression illness. Thankfully, these diving accidents are rare. However, I used HBOT for nonhealing wounds, and its efficacy was sometimes remarkable.
Paradoxical results with oxygen therapy
Although it may seem self-evident that “more oxygen is better” for medical illness, this is not necessarily true. I recently interviewed Ola Didrik Saugstad, MD, who demonstrated that the traditional practice of resuscitating newborns with 100% oxygen was more toxic than resuscitation with air (which contains 21% oxygen). His counterintuitive discovery led to a lifesaving change in the international newborn resuscitation guidelines.
The Food and Drug Administration has approved HBOT for a wide variety of conditions, but some practitioners enthusiastically promote it for off-label indications. These include antiaging, autism, multiple sclerosis, and the aforementioned TBI.
More than 50 years ago, HBOT was proposed for stroke, another disorder where the brain has been deprived of oxygen. Despite obvious logic, clinical trials have been unconvincing. The FDA has not approved HBOT for stroke.
HBOT in practice
During HBOT, the patient breathes 100% oxygen while the whole body is pressurized within a hyperbaric chamber. The chamber’s construction allows pressures above normal sea level of 1.0 atmosphere absolute (ATA). For example, The U.S. Navy Treatment Table for decompression sickness recommends 100% oxygen at 2.8 ATA. Chambers may hold one or more patients at a time.
The frequency of therapy varies but often consists of 20-60 sessions lasting 90-120 minutes. For off-label use like TBI, patients usually pay out of pocket. Given the multiple treatments, costs can add up.
Inconsistent evidence and sham controls
The unwieldy 33-page evidence review by Hadanny and colleagues cites multiple studies supporting HBOT for TBI. However, many, if not all, suffer from methodological flaws. These include vague inclusion criteria, lack of a control group, small patient numbers, treatment at different times since injury, poorly defined or varying HBOT protocols, varying outcome measures, and superficial results analysis.
A sham or control arm is essential for HBOT research trials, given the potential placebo effect of placing a human being inside a large, high-tech, sealed tube for an hour or more. In some sham-controlled studies, which consisted of low-pressure oxygen (that is, 1.3 ATA as sham vs. 2.4 ATA as treatment), all groups experienced symptom improvement. The review authors argue that the low-dose HBOT sham arms were biologically active and that the improvements seen mean that both high- and low-dose HBOT is therapeutic. The alternative explanation is that the placebo effect accounted for improvement in both groups.
The late Michael Bennett, a world authority on hyperbaric and underwater medicine, doubted that conventional HBOT sham controls could genuinely have a therapeutic effect, and I agree. The upcoming HOT-POCS trial (discussed below) should answer the question more definitively.
Mechanisms of action and safety
Mechanisms of benefit for HBOT include increased oxygen availability and angiogenesis. Animal research suggests that it may reduce secondary cell death from TBI, through stabilization of the blood-brain barrier and inflammation reduction.
HBOT is generally safe and well tolerated. A retrospective analysis of 1.5 million outpatient hyperbaric treatments revealed that less than 1% were associated with adverse events. The most common were ear and sinus barotrauma. Because HBOT uses increased air pressure, patients must equalize their ears and sinuses. Those who cannot because of altered consciousness, anatomical defects, or congestion must undergo myringotomy or terminate therapy. Claustrophobia was the second most common adverse effect. Convulsions and tension pneumocephalus were rare.
Perhaps the most concerning risk of HBOT for patients with TBI is the potential waste of human and financial resources.
Desperate physicians and patients
As a neurologist who regularly treats patients with TBI, I share the review authors’ frustration regarding the limited efficacy of available treatments. However, the suboptimal efficacy of currently available therapy is insufficient justification to recommend HBOT.
With respect to chronic TBI, it is difficult to imagine how HBOT could reverse brain injury that has been present for months or years. No other therapy exists that reliably encourages neuronal regeneration or prevents the development of posttraumatic epilepsy.
Frank Conidi, MD, a board-certified sports neurologist and headache specialist, shared his thoughts via email. He agrees that HBOT may have a role in TBI, but after reviewing Hadanny and colleagues’ paper, he concluded that there is insufficient evidence for the use of HBOT in all forms of TBI. He would like to see large multicenter, well-designed studies with standardized pressures and duration and a standard definition of the various types of head injury.
Ongoing research
There are at least five ongoing trials on HBOT for TBI or postconcussive syndrome, including the well-designed placebo-controlled HOT-POCS study. The latter has a novel placebo gas system that addresses Hadanny and colleagues’ contention that even low-dose HBOT might be effective.
The placebo arm in HOT-POCS mimics the HBO environment but provides only 0.21 ATA of oxygen, the same as room air. The active arm provides 100% oxygen at 2.0 ATA. If patients in both arms improve, the benefit will be caused by a placebo response, not HBOT.
Conflict of interest
Another concern with the review is that all three authors are affiliated with Aviv Scientific. This company has an exclusive partnership with the world’s largest hyperbaric medicine and research facility, the Sagol Center at Shamir Medical Center in Be’er Ya’akov, Israel.
This conflict of interest does not a priori invalidate their conclusions. However, official HBOT guidelines from a leading organization like the Undersea and Hyperbaric Medicine Society or the American Academy of Neurology would be preferable.
Conclusion
There is an urgent unmet need for more effective treatments for postconcussive syndrome and chronic TBI.
The review authors’ recommendations for HBOT seem premature. They are arguably a disservice to the many desperate patients and their families who will be tempted to expend valuable resources of time and money for an appealing but unproven therapy. Appropriately designed placebo-controlled studies such as HOT-POCS will help separate fact from wishful thinking.
Dr. Wilner is associate professor of neurology at University of Tennessee Health Science Center, Memphis. He reported a conflict of interest with Accordant Health Services.
A version of this article first appeared on Medscape.com.
The future for the primary care physician?
“The doctor won’t see you now.”
The editor of the alumni magazine had succeeded in getting my attention. The shock value of the headline hooked me and I was drawn in to chase down the research. A study by a team of researchers at Harvard Medical School has published a study in the British Medical Journal revealing that “from 2013 to 2019 the share of U.S. health care visits delivered by nonphysicians such as nurse practitioners or physician assistants increased from 14% to 26%.” In other words, at more than a quarter of the health care visits in this country the patient is not seen by a physician. The percent seen by advanced-practice providers varied by complaint and specialty. For example, 47% of patients with a respiratory complaint saw a nurse practitioner or physicians assistant, while for an eye condition only 13% were seen by an advanced-practice provider. However, overall the increase was dramatic.
It doesn’t require much deep thinking to come up with some explanations for this shift in provider involvement. It boils down to supply and demand. Compared with other similar nations, we have fewer physicians. Physicians are leaving the profession for a variety of reasons, including disappointment with their work-life balance and a sense that too much of their day is devoted to meaningless work with user unfriendly computer systems.
The number of nurse practitioners and physician assistants is growing faster than that of physicians. In fact it has been predicted that over the next 2 decades advanced-practice providers will increase by more than 50% while the physician pool will grow by less than 5%.
We can mull over the how-we-got-here ad infinitum, but this recent study suggests that we had better hustle and invest some time rethinking the role of a physician and how we should adapt our education system to better prepare for those choosing the path through medical school. This mirror gazing is particularly critical for those of us doing primary care.
While in years past I often heard a discontented grumble from patients that “I was ‘only’ seen by the nurse practitioner,” this complaint has become much less frequent as patients have gained more experience with advanced-practice providers and have begun to accept the new reality and see the change as inevitable.
When someone tells me that their daughter or nephew or second cousin is planning on becoming a doctor, I pause and listen patiently as they go on proudly about it before asking if the young person has considered becoming a physician assistant. I say, “Ya know, if I were 60 years younger I think I would bypass medical school and become a nurse practitioner because they get to do all the cool things that I enjoyed about seeing patients. Sure, my mother wouldn’t have been able to introduce me as her son the doctor. But, my parents and I would have spent less time and money on my training, and I would have had less administrative hassle heaped on me once I went into practice.”
The essence of good primary care is Availability, Continuity, and Expertise. The first two attributes aren’t taught in medical school and rely on commitment and having enough bodies to deliver the care. When it comes to expertise, how important is the broad and deep education of traditional medical school when the provider is seeing the relatively narrow spectrum of bread-and-butter everyday complaints that fill the day for most primary care providers? Particularly, when the population has already been preselected by age, geography, and socioeconomic factors.
The usual argument against my assertion is that a higher-priced and more arduous education pathway better provides the physician with the tools to deal with the outliers, the diagnostic enigmas. My reply is that any good provider regardless of his or her years spent in training is taught to first admit what they don’t know. When faced with an enigma, call a consultant or, in the near future, access a Chatbot.
If the natural market and economic forces continue to drive the growth of advanced-practice providers, what role(s) remains for the medical school–trained primary care provider? Does she or he remain the leader of a team of providers? Does she or he still see patients and somehow remain the first among equals?
While patients seem to be warming to the notion of seeing a nonphysician provider, I often still hear the complaint but “I see a different provider every time I go to the office.” Continuity is one of those three keystones of quality primary care. It is not incompatible with a team concept of care delivery, but it does require a commitment to the concept and creative scheduling that allows the patient to see the same provider at almost every visit. I’m not sure where having a first-among-equals provider fits into that scheme. Is it just one more “different” provider?
Maybe the medical school–trained provider becomes a consultant physician, much as the British and Canadian systems seem to work. She or he would see patients only after the advanced primary care provider has done an evaluation and is unsure of the next step. Would this be at the same site or electronically? Is there a time lag? In my old-school interpretation, if the visit is not the same day or maybe the next day then it doesn’t satisfy my Availability requirement of primary care.
Primarily an educator who generally doesn’t see patients but instead trains advanced primary care providers, organizes them into teams that function to provide care in a timely fashion that emphasizes Continuity, and then performs ongoing, real time assessments to assure that care provided is at the highest level of Expertise.
It sounds like an interesting and challenging job description requiring a deep and broad education. Just not one that appeals to me. I would rather be a nurse practitioner or physician’s assistant who is on the front line and hands on.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at [email protected]
“The doctor won’t see you now.”
The editor of the alumni magazine had succeeded in getting my attention. The shock value of the headline hooked me and I was drawn in to chase down the research. A study by a team of researchers at Harvard Medical School has published a study in the British Medical Journal revealing that “from 2013 to 2019 the share of U.S. health care visits delivered by nonphysicians such as nurse practitioners or physician assistants increased from 14% to 26%.” In other words, at more than a quarter of the health care visits in this country the patient is not seen by a physician. The percent seen by advanced-practice providers varied by complaint and specialty. For example, 47% of patients with a respiratory complaint saw a nurse practitioner or physicians assistant, while for an eye condition only 13% were seen by an advanced-practice provider. However, overall the increase was dramatic.
It doesn’t require much deep thinking to come up with some explanations for this shift in provider involvement. It boils down to supply and demand. Compared with other similar nations, we have fewer physicians. Physicians are leaving the profession for a variety of reasons, including disappointment with their work-life balance and a sense that too much of their day is devoted to meaningless work with user unfriendly computer systems.
The number of nurse practitioners and physician assistants is growing faster than that of physicians. In fact it has been predicted that over the next 2 decades advanced-practice providers will increase by more than 50% while the physician pool will grow by less than 5%.
We can mull over the how-we-got-here ad infinitum, but this recent study suggests that we had better hustle and invest some time rethinking the role of a physician and how we should adapt our education system to better prepare for those choosing the path through medical school. This mirror gazing is particularly critical for those of us doing primary care.
While in years past I often heard a discontented grumble from patients that “I was ‘only’ seen by the nurse practitioner,” this complaint has become much less frequent as patients have gained more experience with advanced-practice providers and have begun to accept the new reality and see the change as inevitable.
When someone tells me that their daughter or nephew or second cousin is planning on becoming a doctor, I pause and listen patiently as they go on proudly about it before asking if the young person has considered becoming a physician assistant. I say, “Ya know, if I were 60 years younger I think I would bypass medical school and become a nurse practitioner because they get to do all the cool things that I enjoyed about seeing patients. Sure, my mother wouldn’t have been able to introduce me as her son the doctor. But, my parents and I would have spent less time and money on my training, and I would have had less administrative hassle heaped on me once I went into practice.”
The essence of good primary care is Availability, Continuity, and Expertise. The first two attributes aren’t taught in medical school and rely on commitment and having enough bodies to deliver the care. When it comes to expertise, how important is the broad and deep education of traditional medical school when the provider is seeing the relatively narrow spectrum of bread-and-butter everyday complaints that fill the day for most primary care providers? Particularly, when the population has already been preselected by age, geography, and socioeconomic factors.
The usual argument against my assertion is that a higher-priced and more arduous education pathway better provides the physician with the tools to deal with the outliers, the diagnostic enigmas. My reply is that any good provider regardless of his or her years spent in training is taught to first admit what they don’t know. When faced with an enigma, call a consultant or, in the near future, access a Chatbot.
If the natural market and economic forces continue to drive the growth of advanced-practice providers, what role(s) remains for the medical school–trained primary care provider? Does she or he remain the leader of a team of providers? Does she or he still see patients and somehow remain the first among equals?
While patients seem to be warming to the notion of seeing a nonphysician provider, I often still hear the complaint but “I see a different provider every time I go to the office.” Continuity is one of those three keystones of quality primary care. It is not incompatible with a team concept of care delivery, but it does require a commitment to the concept and creative scheduling that allows the patient to see the same provider at almost every visit. I’m not sure where having a first-among-equals provider fits into that scheme. Is it just one more “different” provider?
Maybe the medical school–trained provider becomes a consultant physician, much as the British and Canadian systems seem to work. She or he would see patients only after the advanced primary care provider has done an evaluation and is unsure of the next step. Would this be at the same site or electronically? Is there a time lag? In my old-school interpretation, if the visit is not the same day or maybe the next day then it doesn’t satisfy my Availability requirement of primary care.
Primarily an educator who generally doesn’t see patients but instead trains advanced primary care providers, organizes them into teams that function to provide care in a timely fashion that emphasizes Continuity, and then performs ongoing, real time assessments to assure that care provided is at the highest level of Expertise.
It sounds like an interesting and challenging job description requiring a deep and broad education. Just not one that appeals to me. I would rather be a nurse practitioner or physician’s assistant who is on the front line and hands on.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at [email protected]
“The doctor won’t see you now.”
The editor of the alumni magazine had succeeded in getting my attention. The shock value of the headline hooked me and I was drawn in to chase down the research. A study by a team of researchers at Harvard Medical School has published a study in the British Medical Journal revealing that “from 2013 to 2019 the share of U.S. health care visits delivered by nonphysicians such as nurse practitioners or physician assistants increased from 14% to 26%.” In other words, at more than a quarter of the health care visits in this country the patient is not seen by a physician. The percent seen by advanced-practice providers varied by complaint and specialty. For example, 47% of patients with a respiratory complaint saw a nurse practitioner or physicians assistant, while for an eye condition only 13% were seen by an advanced-practice provider. However, overall the increase was dramatic.
It doesn’t require much deep thinking to come up with some explanations for this shift in provider involvement. It boils down to supply and demand. Compared with other similar nations, we have fewer physicians. Physicians are leaving the profession for a variety of reasons, including disappointment with their work-life balance and a sense that too much of their day is devoted to meaningless work with user unfriendly computer systems.
The number of nurse practitioners and physician assistants is growing faster than that of physicians. In fact it has been predicted that over the next 2 decades advanced-practice providers will increase by more than 50% while the physician pool will grow by less than 5%.
We can mull over the how-we-got-here ad infinitum, but this recent study suggests that we had better hustle and invest some time rethinking the role of a physician and how we should adapt our education system to better prepare for those choosing the path through medical school. This mirror gazing is particularly critical for those of us doing primary care.
While in years past I often heard a discontented grumble from patients that “I was ‘only’ seen by the nurse practitioner,” this complaint has become much less frequent as patients have gained more experience with advanced-practice providers and have begun to accept the new reality and see the change as inevitable.
When someone tells me that their daughter or nephew or second cousin is planning on becoming a doctor, I pause and listen patiently as they go on proudly about it before asking if the young person has considered becoming a physician assistant. I say, “Ya know, if I were 60 years younger I think I would bypass medical school and become a nurse practitioner because they get to do all the cool things that I enjoyed about seeing patients. Sure, my mother wouldn’t have been able to introduce me as her son the doctor. But, my parents and I would have spent less time and money on my training, and I would have had less administrative hassle heaped on me once I went into practice.”
The essence of good primary care is Availability, Continuity, and Expertise. The first two attributes aren’t taught in medical school and rely on commitment and having enough bodies to deliver the care. When it comes to expertise, how important is the broad and deep education of traditional medical school when the provider is seeing the relatively narrow spectrum of bread-and-butter everyday complaints that fill the day for most primary care providers? Particularly, when the population has already been preselected by age, geography, and socioeconomic factors.
The usual argument against my assertion is that a higher-priced and more arduous education pathway better provides the physician with the tools to deal with the outliers, the diagnostic enigmas. My reply is that any good provider regardless of his or her years spent in training is taught to first admit what they don’t know. When faced with an enigma, call a consultant or, in the near future, access a Chatbot.
If the natural market and economic forces continue to drive the growth of advanced-practice providers, what role(s) remains for the medical school–trained primary care provider? Does she or he remain the leader of a team of providers? Does she or he still see patients and somehow remain the first among equals?
While patients seem to be warming to the notion of seeing a nonphysician provider, I often still hear the complaint but “I see a different provider every time I go to the office.” Continuity is one of those three keystones of quality primary care. It is not incompatible with a team concept of care delivery, but it does require a commitment to the concept and creative scheduling that allows the patient to see the same provider at almost every visit. I’m not sure where having a first-among-equals provider fits into that scheme. Is it just one more “different” provider?
Maybe the medical school–trained provider becomes a consultant physician, much as the British and Canadian systems seem to work. She or he would see patients only after the advanced primary care provider has done an evaluation and is unsure of the next step. Would this be at the same site or electronically? Is there a time lag? In my old-school interpretation, if the visit is not the same day or maybe the next day then it doesn’t satisfy my Availability requirement of primary care.
Primarily an educator who generally doesn’t see patients but instead trains advanced primary care providers, organizes them into teams that function to provide care in a timely fashion that emphasizes Continuity, and then performs ongoing, real time assessments to assure that care provided is at the highest level of Expertise.
It sounds like an interesting and challenging job description requiring a deep and broad education. Just not one that appeals to me. I would rather be a nurse practitioner or physician’s assistant who is on the front line and hands on.
Dr. Wilkoff practiced primary care pediatrics in Brunswick, Maine, for nearly 40 years. He has authored several books on behavioral pediatrics, including “How to Say No to Your Toddler.” Other than a Littman stethoscope he accepted as a first-year medical student in 1966, Dr. Wilkoff reports having nothing to disclose. Email him at [email protected]
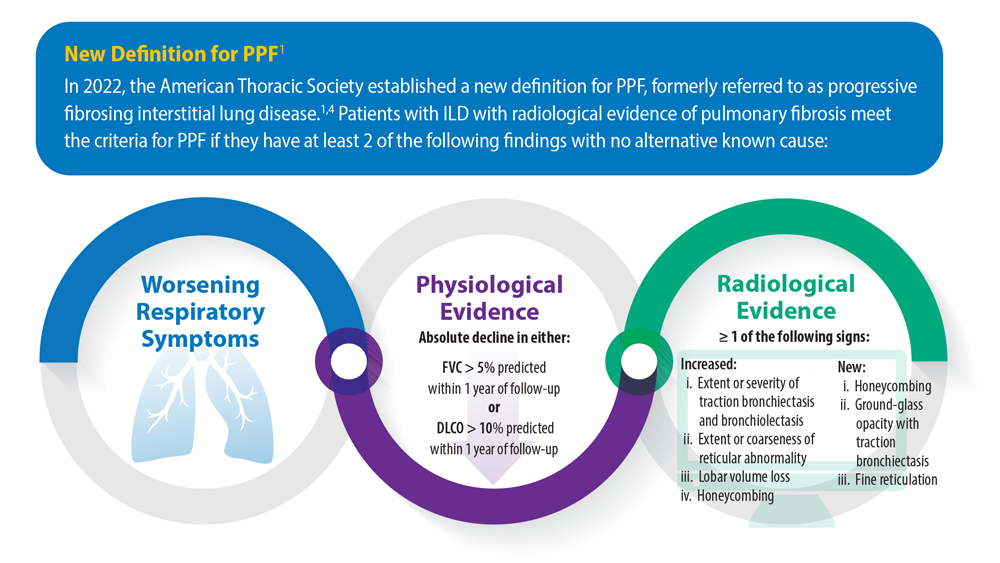
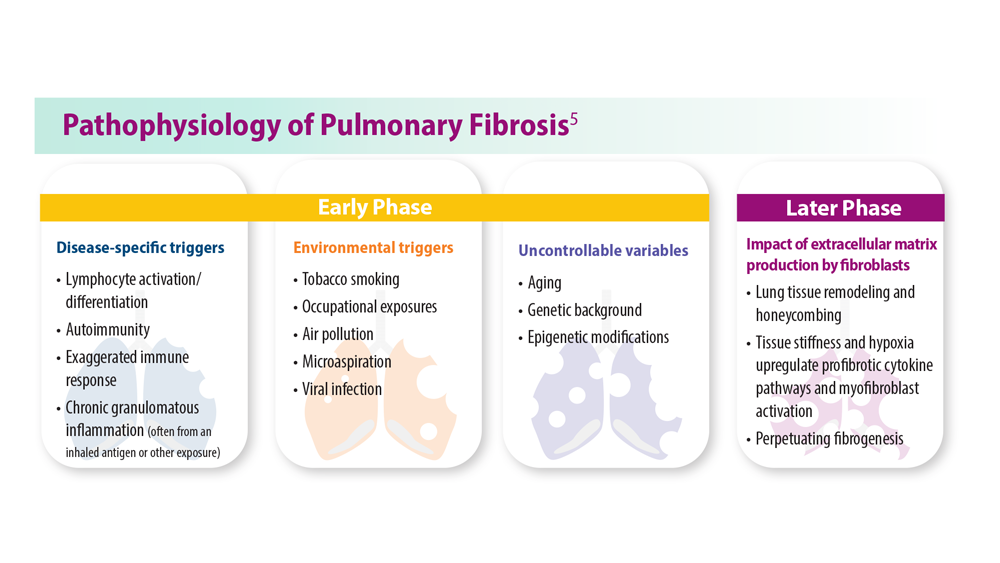
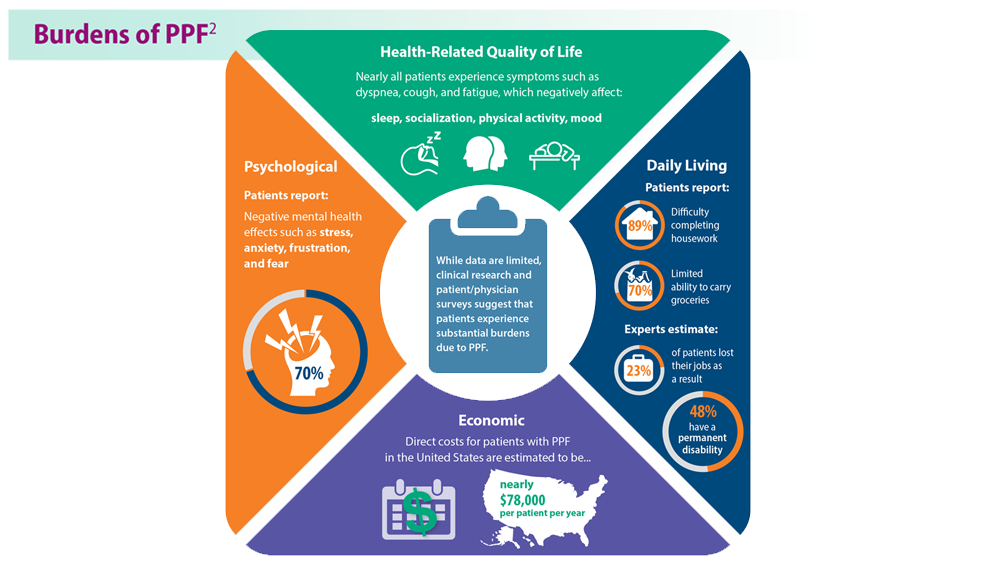
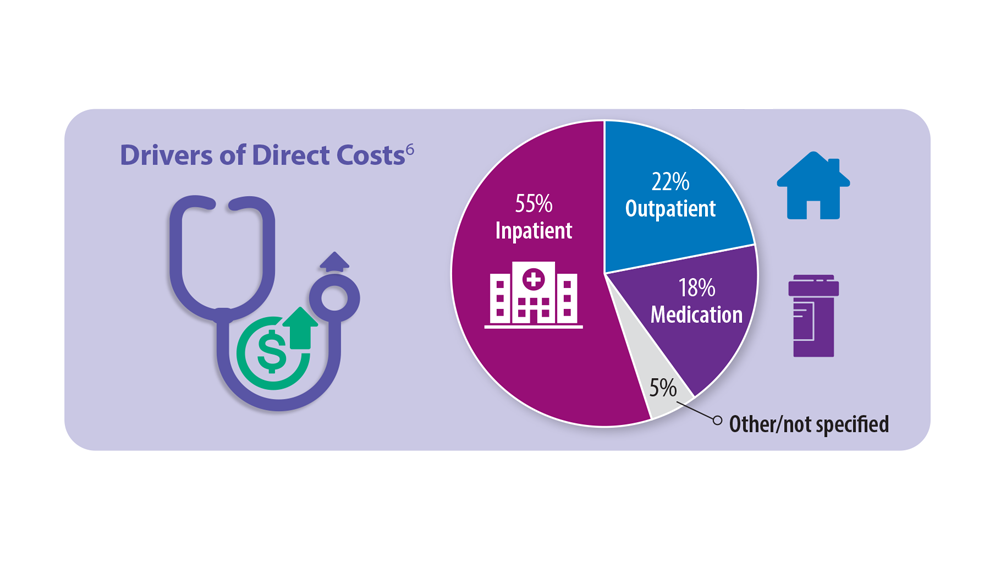
Progressive Pulmonary Fibrosis: Understanding Its Many Forms
- Raghu G et al. Am J Respir Crit Care Med. 2022;205(9):e18-e47. doi:10.1164/rccm.202202-0399ST
- Cottin V et al. Front Med (Lausanne). 2022;9:799912. doi:10.3389/fmed.2022.799912
- Molina-Molina M et al. Expert Rev Respir Med. 2022;16(7):765-774. doi:10.1080/17476348.2022.2107508
- Cottin V. Am J Respir Crit Care Med. 2023;207(1):11-13. doi:10.1164/rccm.202208-1639ED
- Wijsenbeek M, Cottin V. N Engl J Med. 2020;383(10):958-968. doi:10.1056/NEJMra2005230
- Chiu YH et al. Front Med (Lausanne). 2023;10:1106560. doi:10.3389/fmed.2023.1106560
- Wong AW et al. BMC Pulm Med. 2022;22(1):148. doi:10.1186/s12890-022-01922-2
- Raghu G et al. Am J Respir Crit Care Med. 2022;205(9):e18-e47. doi:10.1164/rccm.202202-0399ST
- Cottin V et al. Front Med (Lausanne). 2022;9:799912. doi:10.3389/fmed.2022.799912
- Molina-Molina M et al. Expert Rev Respir Med. 2022;16(7):765-774. doi:10.1080/17476348.2022.2107508
- Cottin V. Am J Respir Crit Care Med. 2023;207(1):11-13. doi:10.1164/rccm.202208-1639ED
- Wijsenbeek M, Cottin V. N Engl J Med. 2020;383(10):958-968. doi:10.1056/NEJMra2005230
- Chiu YH et al. Front Med (Lausanne). 2023;10:1106560. doi:10.3389/fmed.2023.1106560
- Wong AW et al. BMC Pulm Med. 2022;22(1):148. doi:10.1186/s12890-022-01922-2
- Raghu G et al. Am J Respir Crit Care Med. 2022;205(9):e18-e47. doi:10.1164/rccm.202202-0399ST
- Cottin V et al. Front Med (Lausanne). 2022;9:799912. doi:10.3389/fmed.2022.799912
- Molina-Molina M et al. Expert Rev Respir Med. 2022;16(7):765-774. doi:10.1080/17476348.2022.2107508
- Cottin V. Am J Respir Crit Care Med. 2023;207(1):11-13. doi:10.1164/rccm.202208-1639ED
- Wijsenbeek M, Cottin V. N Engl J Med. 2020;383(10):958-968. doi:10.1056/NEJMra2005230
- Chiu YH et al. Front Med (Lausanne). 2023;10:1106560. doi:10.3389/fmed.2023.1106560
- Wong AW et al. BMC Pulm Med. 2022;22(1):148. doi:10.1186/s12890-022-01922-2
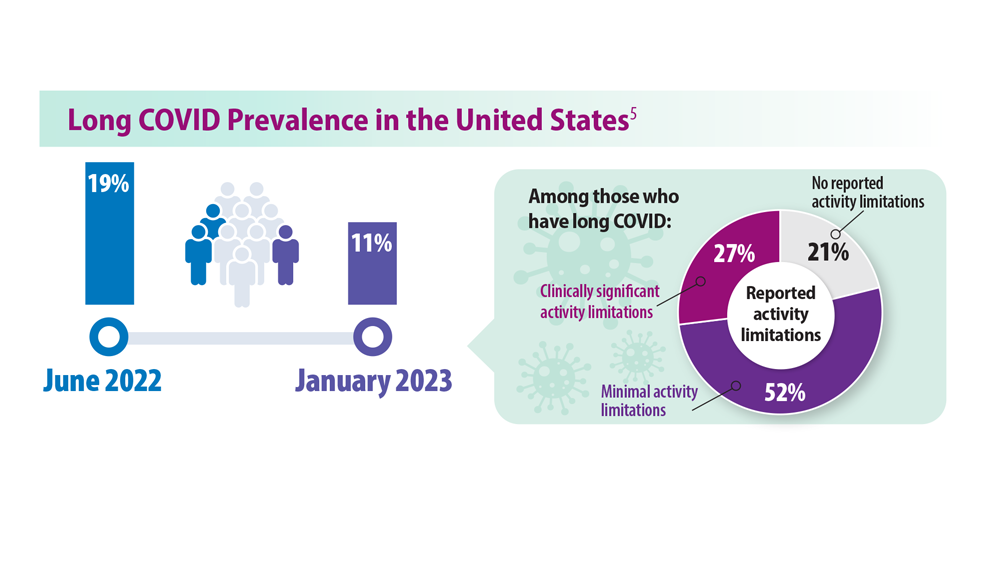
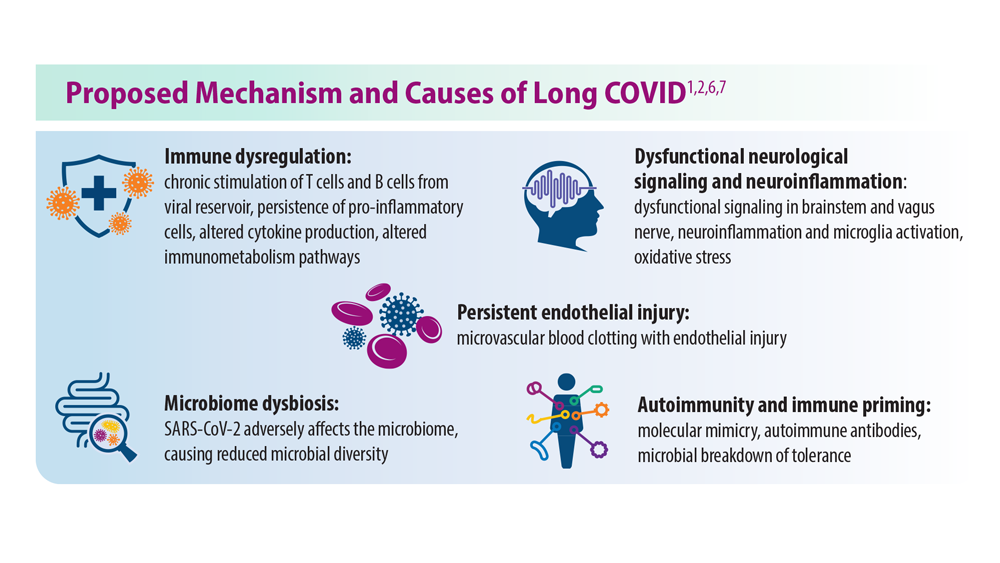
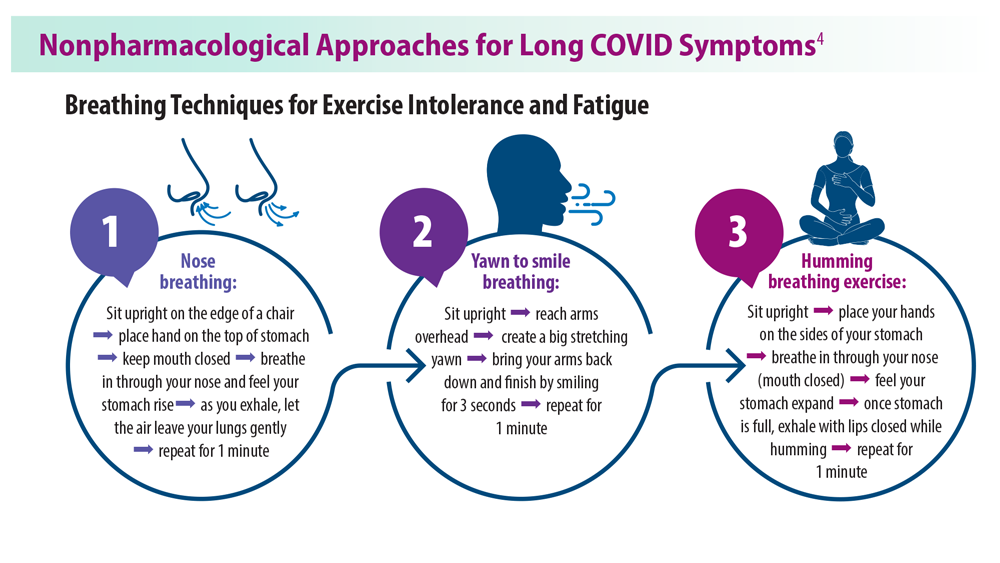
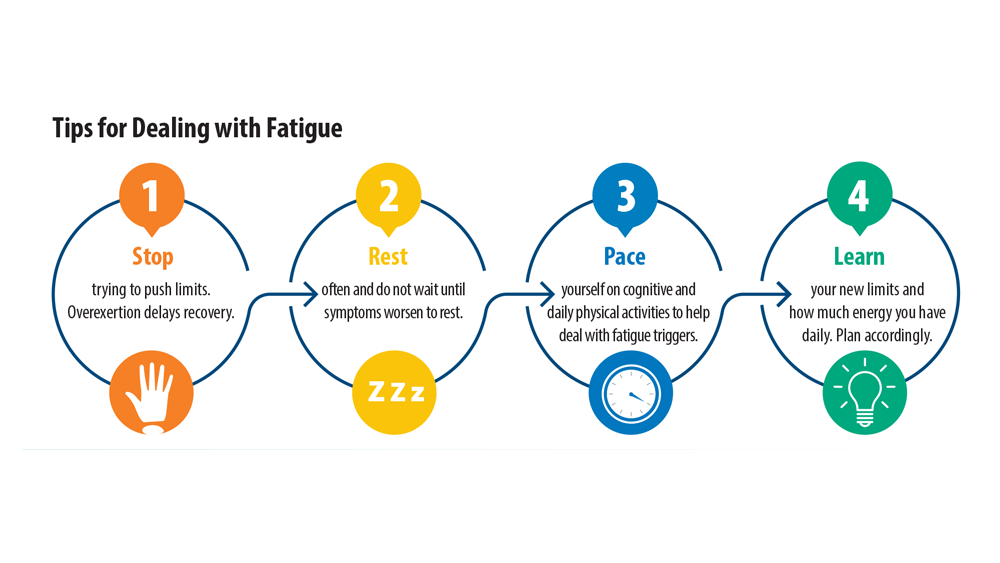
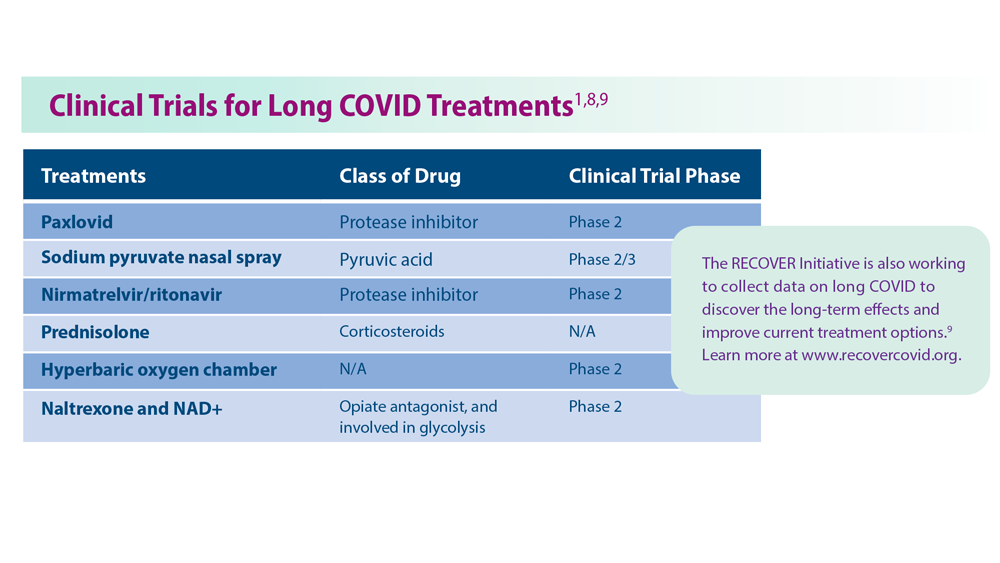
Long COVID: Advocating for Patients and Implementing Effective Techniques
1. Lutchmansingh DD et al. Semin Respir Crit Care Med. 2023;44(1):130-142. doi:10.1055/s-0042-1759568
2. Davis HE et al. Nat Rev Microbiol. 2023;21(3):133-146. doi:10.1038/s41579-022-00846-2
3. Ahmed H et al. J Rehabil Med. 2020;52(5):jrm00063. doi:10.2340/16501977-2694
4. Resources. Long COVID Physio. Accessed May 31, 2023. https://longcovid.physio/resources
5. Long COVID: What do the latest data show? KFF. Published January 26, 2023. Accessed May 31, 2023. https://www.kff.org/policy-watch/long-covid-what-do-latest-data-show/
6. Castanares-Zapatero D et al. Ann Med. 2022;54(1):1473-1487. doi:10.1080/07853890.2022.2076901
7. Mehandru S, Merad M. Nat Immunol. 2022;23(2):194-202. doi:10.1038/s41590-021-01104-y
8. Dhooria S et al. Eur Respir J. 2022;59(2):2102930. doi:10.1183/13993003.02930-2021
9. Researching COVID to enhance recovery. RECOVER. Accessed May 31, 2023. https://recovercovid.org/
1. Lutchmansingh DD et al. Semin Respir Crit Care Med. 2023;44(1):130-142. doi:10.1055/s-0042-1759568
2. Davis HE et al. Nat Rev Microbiol. 2023;21(3):133-146. doi:10.1038/s41579-022-00846-2
3. Ahmed H et al. J Rehabil Med. 2020;52(5):jrm00063. doi:10.2340/16501977-2694
4. Resources. Long COVID Physio. Accessed May 31, 2023. https://longcovid.physio/resources
5. Long COVID: What do the latest data show? KFF. Published January 26, 2023. Accessed May 31, 2023. https://www.kff.org/policy-watch/long-covid-what-do-latest-data-show/
6. Castanares-Zapatero D et al. Ann Med. 2022;54(1):1473-1487. doi:10.1080/07853890.2022.2076901
7. Mehandru S, Merad M. Nat Immunol. 2022;23(2):194-202. doi:10.1038/s41590-021-01104-y
8. Dhooria S et al. Eur Respir J. 2022;59(2):2102930. doi:10.1183/13993003.02930-2021
9. Researching COVID to enhance recovery. RECOVER. Accessed May 31, 2023. https://recovercovid.org/
1. Lutchmansingh DD et al. Semin Respir Crit Care Med. 2023;44(1):130-142. doi:10.1055/s-0042-1759568
2. Davis HE et al. Nat Rev Microbiol. 2023;21(3):133-146. doi:10.1038/s41579-022-00846-2
3. Ahmed H et al. J Rehabil Med. 2020;52(5):jrm00063. doi:10.2340/16501977-2694
4. Resources. Long COVID Physio. Accessed May 31, 2023. https://longcovid.physio/resources
5. Long COVID: What do the latest data show? KFF. Published January 26, 2023. Accessed May 31, 2023. https://www.kff.org/policy-watch/long-covid-what-do-latest-data-show/
6. Castanares-Zapatero D et al. Ann Med. 2022;54(1):1473-1487. doi:10.1080/07853890.2022.2076901
7. Mehandru S, Merad M. Nat Immunol. 2022;23(2):194-202. doi:10.1038/s41590-021-01104-y
8. Dhooria S et al. Eur Respir J. 2022;59(2):2102930. doi:10.1183/13993003.02930-2021
9. Researching COVID to enhance recovery. RECOVER. Accessed May 31, 2023. https://recovercovid.org/
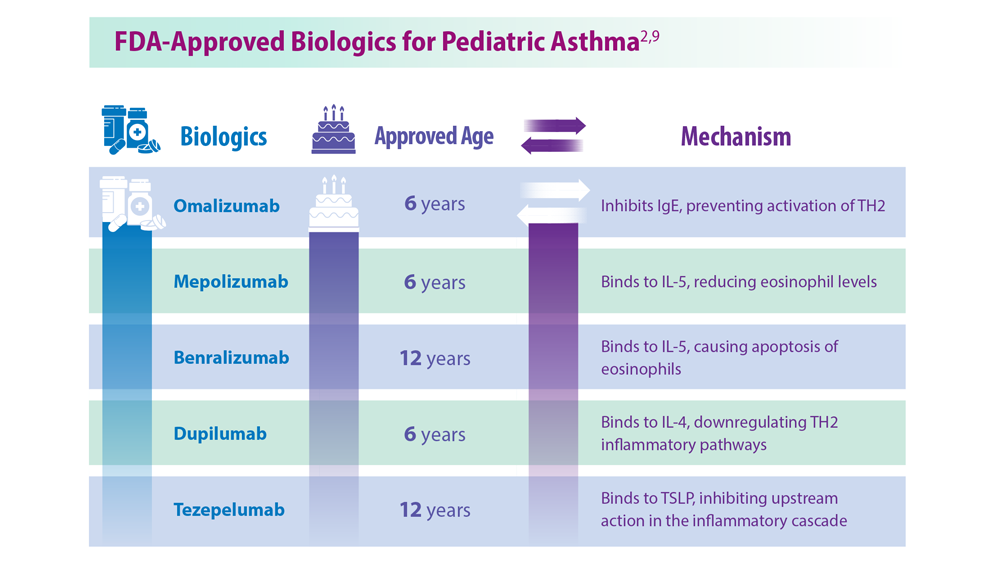
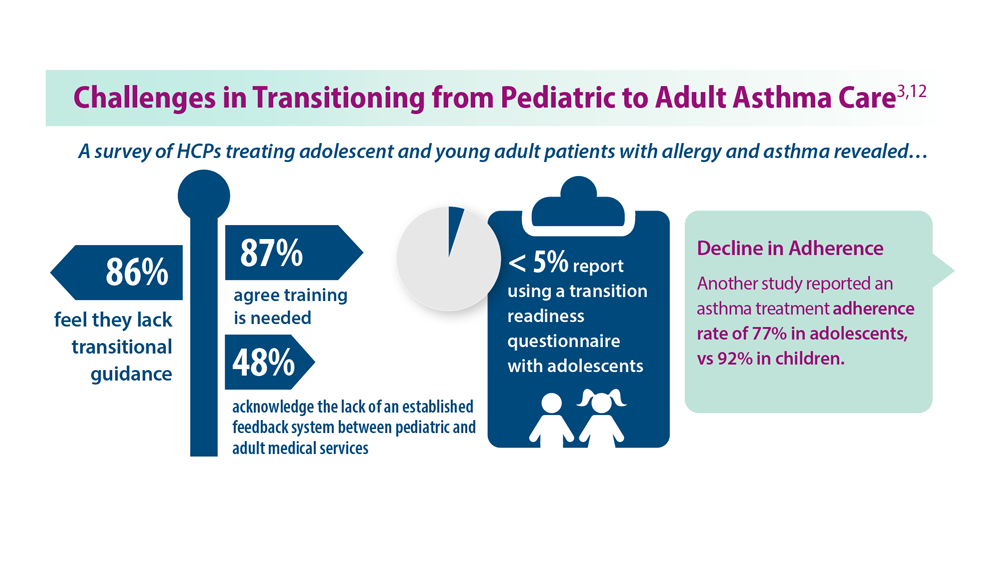
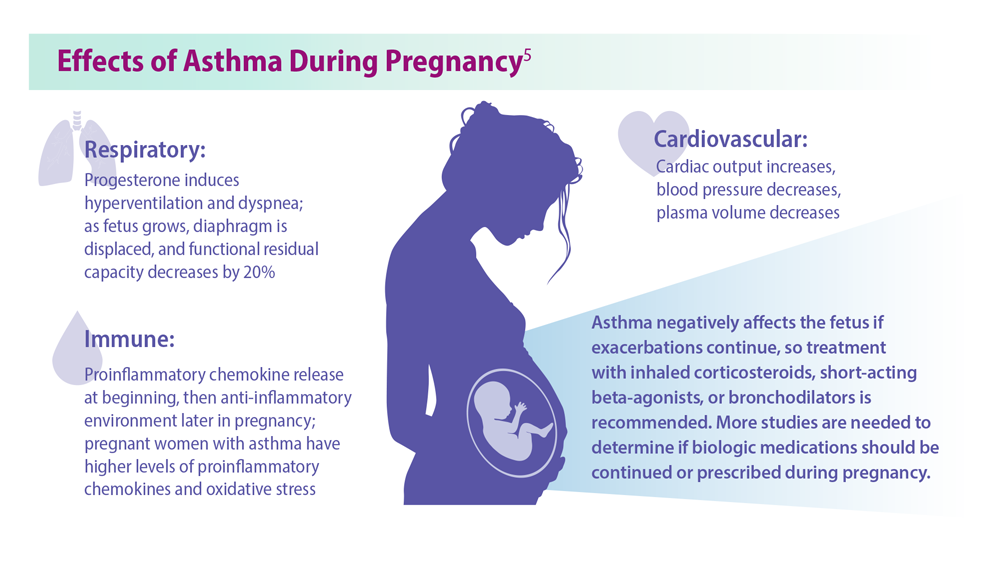
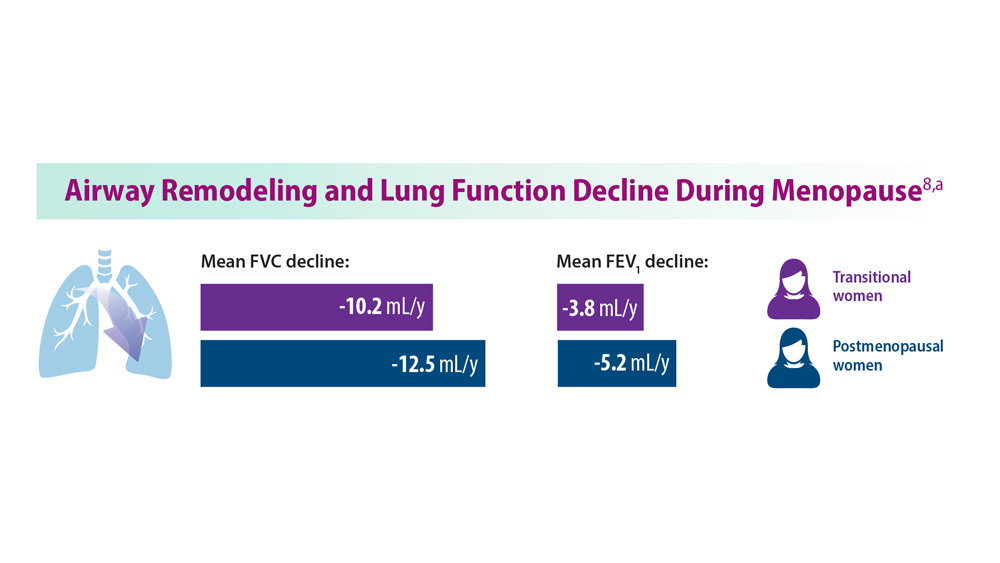
Asthma Across a Woman’s Lifespan
1. Chowdhury NU et al. Eur Respir Rev. 2021;30(162):210067. doi:10.1183/16000617.0067-2021
2. Perikleous EP et al. J Pers Med. 2022;12(6):999. doi:10.3390/jpm12060999
3. Khaleva E et al. Clin Transl Allergy. 2020;10:40. doi:10.1186/s13601-020-00340-z
4. Robijn AL et al. Curr Opin Pulm Med. 2019;25(1):11-17. doi:10.1097/MCP.0000000000000538
5. Bravo-Solarte DC et al. Allergy Asthma Proc. 2023;44(1):24-34. doi:10.2500/aap.2023.44.220077
6. Wang G et al. J Matern Fetal Neonatal Med. 2014;27(9):934-942. doi:10.3109/14767058.2013.847080
7. Hough KP et al. Front Med (Lausanne). 2020;7:191. doi:10.3389/fmed.2020.00191
8. Triebner K et al. Am J Respir Crit Care Med. 2017;195(8):1058-1065. doi:10.1164/rccm.201605-0968OC
9. Bacharier LB, Jackson DJ. J Allergy Clin Immunol. 2023;151(3):581-589. doi:10.1016/j.jaci.2023.01.002
10. An amazing journey: how young lungs develop. American Lung Association. Published May 11, 2018. Accessed June 28, 2023. https://www.lung.org/blog/how-young-lungs-develop
11. Strunk RC et al. J Allergy Clin Immunol. 2006;118(5):1040-1047. doi:10.1016/j.jaci.2006.07.053
12. Kaplan A, Price D. J Asthma Allergy. 2020;13:39-49. doi:10.2147/JAA.S233268
1. Chowdhury NU et al. Eur Respir Rev. 2021;30(162):210067. doi:10.1183/16000617.0067-2021
2. Perikleous EP et al. J Pers Med. 2022;12(6):999. doi:10.3390/jpm12060999
3. Khaleva E et al. Clin Transl Allergy. 2020;10:40. doi:10.1186/s13601-020-00340-z
4. Robijn AL et al. Curr Opin Pulm Med. 2019;25(1):11-17. doi:10.1097/MCP.0000000000000538
5. Bravo-Solarte DC et al. Allergy Asthma Proc. 2023;44(1):24-34. doi:10.2500/aap.2023.44.220077
6. Wang G et al. J Matern Fetal Neonatal Med. 2014;27(9):934-942. doi:10.3109/14767058.2013.847080
7. Hough KP et al. Front Med (Lausanne). 2020;7:191. doi:10.3389/fmed.2020.00191
8. Triebner K et al. Am J Respir Crit Care Med. 2017;195(8):1058-1065. doi:10.1164/rccm.201605-0968OC
9. Bacharier LB, Jackson DJ. J Allergy Clin Immunol. 2023;151(3):581-589. doi:10.1016/j.jaci.2023.01.002
10. An amazing journey: how young lungs develop. American Lung Association. Published May 11, 2018. Accessed June 28, 2023. https://www.lung.org/blog/how-young-lungs-develop
11. Strunk RC et al. J Allergy Clin Immunol. 2006;118(5):1040-1047. doi:10.1016/j.jaci.2006.07.053
12. Kaplan A, Price D. J Asthma Allergy. 2020;13:39-49. doi:10.2147/JAA.S233268
1. Chowdhury NU et al. Eur Respir Rev. 2021;30(162):210067. doi:10.1183/16000617.0067-2021
2. Perikleous EP et al. J Pers Med. 2022;12(6):999. doi:10.3390/jpm12060999
3. Khaleva E et al. Clin Transl Allergy. 2020;10:40. doi:10.1186/s13601-020-00340-z
4. Robijn AL et al. Curr Opin Pulm Med. 2019;25(1):11-17. doi:10.1097/MCP.0000000000000538
5. Bravo-Solarte DC et al. Allergy Asthma Proc. 2023;44(1):24-34. doi:10.2500/aap.2023.44.220077
6. Wang G et al. J Matern Fetal Neonatal Med. 2014;27(9):934-942. doi:10.3109/14767058.2013.847080
7. Hough KP et al. Front Med (Lausanne). 2020;7:191. doi:10.3389/fmed.2020.00191
8. Triebner K et al. Am J Respir Crit Care Med. 2017;195(8):1058-1065. doi:10.1164/rccm.201605-0968OC
9. Bacharier LB, Jackson DJ. J Allergy Clin Immunol. 2023;151(3):581-589. doi:10.1016/j.jaci.2023.01.002
10. An amazing journey: how young lungs develop. American Lung Association. Published May 11, 2018. Accessed June 28, 2023. https://www.lung.org/blog/how-young-lungs-develop
11. Strunk RC et al. J Allergy Clin Immunol. 2006;118(5):1040-1047. doi:10.1016/j.jaci.2006.07.053
12. Kaplan A, Price D. J Asthma Allergy. 2020;13:39-49. doi:10.2147/JAA.S233268
Pulmonology Data Trends 2023 (Slideshow)
CHEST Physician presents the 2023 edition of Pulmonology Data Trends (click to read). This special issue provides updates on hot topics in pulmonology through original infographics and visual storytelling.
In this issue:
Long-Awaited RSV Vaccines Now Available for Older Adults and Pediatric Patients
Burton L. Lesnick, MD, FCCP
Decreasing Pulmonary Embolism-Related Mortality
Parth Rali, MD
Addressing Physician Burnout in Pulmonology and Critical Care
Kelly Vranas, MD, MCR
Updated Guidelines for COPD Management: 2023 GOLD Strategy Report
Muhammad Adrish, MD, MBA, FCCP, FCCM
Progressive Pulmonary Fibrosis: Understanding Its Many Forms
Tejaswini Kulkarni, MD, MPH, FCCP
Sleep Apnea: Comorbidities, Racial Disparities, Weight Guidelines, and Alternatives to CPAP
Lauren Tobias, MD, FCCP
Lung Cancer Screening: A Need for Adjunctive Testing
Eric S. Edell, MD, FCCP
Asthma Across a Woman’s Lifespan
Navitha Ramesh, MD, FCCP
Tuberculosis Management: Returning to Pre-Pandemic Priorities
Patricio Escalante, MD, MSc, FCCP, and Paige K. Marty, MD
Long COVID: Advocating for Patients and Implementing Effective Techniques
Kyle B. Enfield, MD, MS, FSHEA, FCCM
CHEST Physician presents the 2023 edition of Pulmonology Data Trends (click to read). This special issue provides updates on hot topics in pulmonology through original infographics and visual storytelling.
In this issue:
Long-Awaited RSV Vaccines Now Available for Older Adults and Pediatric Patients
Burton L. Lesnick, MD, FCCP
Decreasing Pulmonary Embolism-Related Mortality
Parth Rali, MD
Addressing Physician Burnout in Pulmonology and Critical Care
Kelly Vranas, MD, MCR
Updated Guidelines for COPD Management: 2023 GOLD Strategy Report
Muhammad Adrish, MD, MBA, FCCP, FCCM
Progressive Pulmonary Fibrosis: Understanding Its Many Forms
Tejaswini Kulkarni, MD, MPH, FCCP
Sleep Apnea: Comorbidities, Racial Disparities, Weight Guidelines, and Alternatives to CPAP
Lauren Tobias, MD, FCCP
Lung Cancer Screening: A Need for Adjunctive Testing
Eric S. Edell, MD, FCCP
Asthma Across a Woman’s Lifespan
Navitha Ramesh, MD, FCCP
Tuberculosis Management: Returning to Pre-Pandemic Priorities
Patricio Escalante, MD, MSc, FCCP, and Paige K. Marty, MD
Long COVID: Advocating for Patients and Implementing Effective Techniques
Kyle B. Enfield, MD, MS, FSHEA, FCCM
CHEST Physician presents the 2023 edition of Pulmonology Data Trends (click to read). This special issue provides updates on hot topics in pulmonology through original infographics and visual storytelling.
In this issue:
Long-Awaited RSV Vaccines Now Available for Older Adults and Pediatric Patients
Burton L. Lesnick, MD, FCCP
Decreasing Pulmonary Embolism-Related Mortality
Parth Rali, MD
Addressing Physician Burnout in Pulmonology and Critical Care
Kelly Vranas, MD, MCR
Updated Guidelines for COPD Management: 2023 GOLD Strategy Report
Muhammad Adrish, MD, MBA, FCCP, FCCM
Progressive Pulmonary Fibrosis: Understanding Its Many Forms
Tejaswini Kulkarni, MD, MPH, FCCP
Sleep Apnea: Comorbidities, Racial Disparities, Weight Guidelines, and Alternatives to CPAP
Lauren Tobias, MD, FCCP
Lung Cancer Screening: A Need for Adjunctive Testing
Eric S. Edell, MD, FCCP
Asthma Across a Woman’s Lifespan
Navitha Ramesh, MD, FCCP
Tuberculosis Management: Returning to Pre-Pandemic Priorities
Patricio Escalante, MD, MSc, FCCP, and Paige K. Marty, MD
Long COVID: Advocating for Patients and Implementing Effective Techniques
Kyle B. Enfield, MD, MS, FSHEA, FCCM
Higher RT doses can boost lifespan, reduce risk of death in LS-SCLC patients
SAN DIEGO – , according to a new multicenter, open-label, randomized phase III trial.
Among 224 patients in China, aged 18-70, those randomly assigned to receive volumetric-modulated arc radiotherapy of high-dose, hypofractionated thoracic radiotherapy of 54 Gy in 30 fractions had a much higher median overall survival (62.4 months) than those who received the standard dose of 45 Gy in 30 fractions (43.1 months, P = .001), reported Jiayi Yu, PhD, of Beijing University Cancer Hospital and Institute and colleagues at the annual meeting of the American Society for Radiation Oncology.
Median progression-free survival was also higher in the 54 Gy group (30.5 months vs. 16.7 months in the 45 Gy group, P = .044).
Kristin Higgins, MD, of Winship Cancer Institute of Emory University, Atlanta, provided perspective at the ASTRO session following Dr. Yu’s presentation. She noted that the study population is quite different than that of LS-SCLC patients in the United States, where patients are often older and more likely to have a history of smoking.
“We need more technical details to understand how to deliver this regimen in clinical practice, and it may not be applicable for all patients,” she said. Still, she added that “a key takeaway here is that optimizing the radiotherapy component of treatment is very important.”
Both groups received chemotherapy. “Higher-dose thoracic radiation therapy concurrently with chemotherapy is an alternative therapeutic option,” Dr. Yu said at an ASTRO presentation.
As Dr. Yu noted, twice-daily thoracic radiotherapy of 45 Gy in 30 fractions and concurrent chemotherapy has been the standard treatment for LS-SCLC for the last 20 years. Trials failed to show benefits for once-daily 66-Gy (33 fractions) or 70-Gy treatment (35 fractions), but a phase 2 trial published in 2023 did indicate that twice-daily treatment of 60 Gy (40 fractions) improved survival without boosting side effects.
For the new study, researchers tracked 224 patients from 2017 to 2021 who were previously untreated or had received specific chemotherapy treatments and had ECOG performance status scores of 0 or 1; 108 patients were randomly assigned to the 54-Gy arm and 116 to the 45-Gy arm. All were recruited at 16 public hospitals in China.
The median age in the two groups were 60 in the 54-Gy arm and 62 in the 45-Gy arm; the percentages of women were similar (45.4% and 45.7%, respectively). Most were current or former smokers (62.0% and 61.2%, respectively).
The researchers closed the trial in April 2021 because of the survival benefit in the 54-Gy arm, and patients were tracked through January 2023 for a median 45 months.
Nearly three-quarters of patients in the 54-Gy arm survived to 2 years (77.7%) vs. 53.4% in the 45-Gy arm, a 41% reduction in risk of death. Adverse events were similar between the groups, with 1 reported treatment-related death (myocardial infarction), in the 54-Gy group.
In an interview, Kenneth Rosenzweig, MD, chairman of the department of radiation oncology at Icahn School of Medicine at Mount Sinai, New York, praised the study. It’s “no surprise” that higher radiation doses are well-tolerated since “our ability to shield normal tissue has improved” over the years, said Dr. Rosenzweig, who served as a moderator of the ASTRO session where the research was presented.
However, he cautioned that hypofractionation is still “intense” and may not be appropriate for certain patients. And he added that some clinics may not be set up to provide twice-daily treatments.
Information about study funding was not provided. The study authors have no disclosures. Dr. Higgins discloses relationships with AstraZeneca and Regeneron (advisory board), Jazz (funded research), and Janssen and Picture Health (consulting). Dr. Rosenzweig has no disclosures.
SAN DIEGO – , according to a new multicenter, open-label, randomized phase III trial.
Among 224 patients in China, aged 18-70, those randomly assigned to receive volumetric-modulated arc radiotherapy of high-dose, hypofractionated thoracic radiotherapy of 54 Gy in 30 fractions had a much higher median overall survival (62.4 months) than those who received the standard dose of 45 Gy in 30 fractions (43.1 months, P = .001), reported Jiayi Yu, PhD, of Beijing University Cancer Hospital and Institute and colleagues at the annual meeting of the American Society for Radiation Oncology.
Median progression-free survival was also higher in the 54 Gy group (30.5 months vs. 16.7 months in the 45 Gy group, P = .044).
Kristin Higgins, MD, of Winship Cancer Institute of Emory University, Atlanta, provided perspective at the ASTRO session following Dr. Yu’s presentation. She noted that the study population is quite different than that of LS-SCLC patients in the United States, where patients are often older and more likely to have a history of smoking.
“We need more technical details to understand how to deliver this regimen in clinical practice, and it may not be applicable for all patients,” she said. Still, she added that “a key takeaway here is that optimizing the radiotherapy component of treatment is very important.”
Both groups received chemotherapy. “Higher-dose thoracic radiation therapy concurrently with chemotherapy is an alternative therapeutic option,” Dr. Yu said at an ASTRO presentation.
As Dr. Yu noted, twice-daily thoracic radiotherapy of 45 Gy in 30 fractions and concurrent chemotherapy has been the standard treatment for LS-SCLC for the last 20 years. Trials failed to show benefits for once-daily 66-Gy (33 fractions) or 70-Gy treatment (35 fractions), but a phase 2 trial published in 2023 did indicate that twice-daily treatment of 60 Gy (40 fractions) improved survival without boosting side effects.
For the new study, researchers tracked 224 patients from 2017 to 2021 who were previously untreated or had received specific chemotherapy treatments and had ECOG performance status scores of 0 or 1; 108 patients were randomly assigned to the 54-Gy arm and 116 to the 45-Gy arm. All were recruited at 16 public hospitals in China.
The median age in the two groups were 60 in the 54-Gy arm and 62 in the 45-Gy arm; the percentages of women were similar (45.4% and 45.7%, respectively). Most were current or former smokers (62.0% and 61.2%, respectively).
The researchers closed the trial in April 2021 because of the survival benefit in the 54-Gy arm, and patients were tracked through January 2023 for a median 45 months.
Nearly three-quarters of patients in the 54-Gy arm survived to 2 years (77.7%) vs. 53.4% in the 45-Gy arm, a 41% reduction in risk of death. Adverse events were similar between the groups, with 1 reported treatment-related death (myocardial infarction), in the 54-Gy group.
In an interview, Kenneth Rosenzweig, MD, chairman of the department of radiation oncology at Icahn School of Medicine at Mount Sinai, New York, praised the study. It’s “no surprise” that higher radiation doses are well-tolerated since “our ability to shield normal tissue has improved” over the years, said Dr. Rosenzweig, who served as a moderator of the ASTRO session where the research was presented.
However, he cautioned that hypofractionation is still “intense” and may not be appropriate for certain patients. And he added that some clinics may not be set up to provide twice-daily treatments.
Information about study funding was not provided. The study authors have no disclosures. Dr. Higgins discloses relationships with AstraZeneca and Regeneron (advisory board), Jazz (funded research), and Janssen and Picture Health (consulting). Dr. Rosenzweig has no disclosures.
SAN DIEGO – , according to a new multicenter, open-label, randomized phase III trial.
Among 224 patients in China, aged 18-70, those randomly assigned to receive volumetric-modulated arc radiotherapy of high-dose, hypofractionated thoracic radiotherapy of 54 Gy in 30 fractions had a much higher median overall survival (62.4 months) than those who received the standard dose of 45 Gy in 30 fractions (43.1 months, P = .001), reported Jiayi Yu, PhD, of Beijing University Cancer Hospital and Institute and colleagues at the annual meeting of the American Society for Radiation Oncology.
Median progression-free survival was also higher in the 54 Gy group (30.5 months vs. 16.7 months in the 45 Gy group, P = .044).
Kristin Higgins, MD, of Winship Cancer Institute of Emory University, Atlanta, provided perspective at the ASTRO session following Dr. Yu’s presentation. She noted that the study population is quite different than that of LS-SCLC patients in the United States, where patients are often older and more likely to have a history of smoking.
“We need more technical details to understand how to deliver this regimen in clinical practice, and it may not be applicable for all patients,” she said. Still, she added that “a key takeaway here is that optimizing the radiotherapy component of treatment is very important.”
Both groups received chemotherapy. “Higher-dose thoracic radiation therapy concurrently with chemotherapy is an alternative therapeutic option,” Dr. Yu said at an ASTRO presentation.
As Dr. Yu noted, twice-daily thoracic radiotherapy of 45 Gy in 30 fractions and concurrent chemotherapy has been the standard treatment for LS-SCLC for the last 20 years. Trials failed to show benefits for once-daily 66-Gy (33 fractions) or 70-Gy treatment (35 fractions), but a phase 2 trial published in 2023 did indicate that twice-daily treatment of 60 Gy (40 fractions) improved survival without boosting side effects.
For the new study, researchers tracked 224 patients from 2017 to 2021 who were previously untreated or had received specific chemotherapy treatments and had ECOG performance status scores of 0 or 1; 108 patients were randomly assigned to the 54-Gy arm and 116 to the 45-Gy arm. All were recruited at 16 public hospitals in China.
The median age in the two groups were 60 in the 54-Gy arm and 62 in the 45-Gy arm; the percentages of women were similar (45.4% and 45.7%, respectively). Most were current or former smokers (62.0% and 61.2%, respectively).
The researchers closed the trial in April 2021 because of the survival benefit in the 54-Gy arm, and patients were tracked through January 2023 for a median 45 months.
Nearly three-quarters of patients in the 54-Gy arm survived to 2 years (77.7%) vs. 53.4% in the 45-Gy arm, a 41% reduction in risk of death. Adverse events were similar between the groups, with 1 reported treatment-related death (myocardial infarction), in the 54-Gy group.
In an interview, Kenneth Rosenzweig, MD, chairman of the department of radiation oncology at Icahn School of Medicine at Mount Sinai, New York, praised the study. It’s “no surprise” that higher radiation doses are well-tolerated since “our ability to shield normal tissue has improved” over the years, said Dr. Rosenzweig, who served as a moderator of the ASTRO session where the research was presented.
However, he cautioned that hypofractionation is still “intense” and may not be appropriate for certain patients. And he added that some clinics may not be set up to provide twice-daily treatments.
Information about study funding was not provided. The study authors have no disclosures. Dr. Higgins discloses relationships with AstraZeneca and Regeneron (advisory board), Jazz (funded research), and Janssen and Picture Health (consulting). Dr. Rosenzweig has no disclosures.
AT ASTRO 2023
CT simulation not needed in palliative radiotherapy planning
, according to a results from a randomized trial presented at the annual meeting of the American Society for Radiation Oncology.
The aim of this same-day CT scan, called a CT simulation scan, is to optimize radiation targeting by mimicking the conditions under which radiation is delivered using the latest information on the size and location of lesions.
But investigators reported that skipping the CT simulation scan saves patients hours in the clinic, allows patients to experience pain relief faster, and saves radiation oncologists time without compromising dosimetric coverage of cancerous lesions.
“This is huge in a symptomatic patient population,” said Melissa O’Neil, an advanced practice radiation therapist at the London, Ont., Health Sciences Centre and the lead investigator on the trial, dubbed DART (Diagnostic CT-Enabled Radiation Therapy).
“Diagnostic CT-based radiation planning substantially reduces time in the [treatment] center without a detriment in plan deliverability or quality,” Ms. O’Neil said.
In addition, patients are exposed to less radiation, and staff doesn’t have to spend as much time tending to symptomatic patients before treatment. Omitting this scan “should be considered for patients with a recent diagnostic CT scan who are undergoing simple palliative radiation,” Ms. O’Neil said.
CT simulation scans are standard of care in cases involving palliative radiation, but they create bottlenecks in the workflow. When a CT simulation is performed on the day of treatment, patients must wait hours as the results are translated into a treatment plan.
In the DART analysis, 33 patients with 42 treatment sites were randomly assigned to CT simulation planning or diagnostic CT planning.
Patients received up to 30 Gy in up to 10 fractions for bone or soft tissue metastases or primary tumor targets in the thorax, abdomen, pelvis, or proximal limbs. Single-fraction treatments were most common.
Three-quarters of the patients were men (median age, 72 years). Lung cancer was the most common type of primary tumor, followed by prostate and breast cancer.
The eight participants for whom the CT simulation approach was used waited 3-4 hours for treatment planning and overall spent a median of 4.8 hours in the cancer center on their day of treatment.
The 25 patients for whom diagnostic CT planning was used spent a median of 0.4 hours, or about 24 minutes, in the center on their day of treatment because radiation plans were completed before they arrived. The median time between their diagnostic CTs and radiation treatment was 13 days (range, 8-22 days).
Ms. O’Neil and her team found that if the original diagnostic CT was performed within 28 days, lesion anatomy would not have changed enough to warrant a new scan.
On the day of treatment, the study team used surface-guided radiation therapy techniques to ensure patients in the diagnostic CT planning group were positioned within 3 mm of where they were during their diagnostic scans, an essential step to ensure that radiation is delivered to the correct location. Ms. O’Neil noted that other investigators have used anatomic landmarks, a simpler approach, to achieve these results.
Overall, radiation oncologists rated radiation dose distribution as “acceptable” in about 80% of cases in both arms of DART and “acceptable with minor deviation” in the remaining 20% of cases.
Every radiation oncologist and medical physicists in the trial gave the workflow with diagnostic CT planning a 5 out of 5 rating for acceptability, and 90% of patients in this group rated the amount of time they spent for treatment as “acceptable.”
In contrast, only half of patients in the simulation arm said the amount of time spent was acceptable.
These findings align with several previous studies that support the diagnostic approach.
Jacob Scott, MD, a radiation oncologist at the Cleveland Clinic, said, “The comparable results using a recent diagnostic CT in place of a CT simulation for palliative radiation is an exciting step forward in radiation oncology. We may soon be in a world where we no longer need simulations.”
Dr. Scott also noted that combining diagnostic scans with cone beam or surface-guided positioning in lieu of CT simulations could further save “the health system and patients time and money.”
No external funding for the study was reported. The investigators, Ms. O’Neil, and Dr. Scott have disclosed no relevant financial relationships. One investigator reported receiving honoraria from Knight Therapeutics, AbbVie, Tersera, and Eisai and owns stock in Myovant.
A version of this article first appeared on Medscape.com.
, according to a results from a randomized trial presented at the annual meeting of the American Society for Radiation Oncology.
The aim of this same-day CT scan, called a CT simulation scan, is to optimize radiation targeting by mimicking the conditions under which radiation is delivered using the latest information on the size and location of lesions.
But investigators reported that skipping the CT simulation scan saves patients hours in the clinic, allows patients to experience pain relief faster, and saves radiation oncologists time without compromising dosimetric coverage of cancerous lesions.
“This is huge in a symptomatic patient population,” said Melissa O’Neil, an advanced practice radiation therapist at the London, Ont., Health Sciences Centre and the lead investigator on the trial, dubbed DART (Diagnostic CT-Enabled Radiation Therapy).
“Diagnostic CT-based radiation planning substantially reduces time in the [treatment] center without a detriment in plan deliverability or quality,” Ms. O’Neil said.
In addition, patients are exposed to less radiation, and staff doesn’t have to spend as much time tending to symptomatic patients before treatment. Omitting this scan “should be considered for patients with a recent diagnostic CT scan who are undergoing simple palliative radiation,” Ms. O’Neil said.
CT simulation scans are standard of care in cases involving palliative radiation, but they create bottlenecks in the workflow. When a CT simulation is performed on the day of treatment, patients must wait hours as the results are translated into a treatment plan.
In the DART analysis, 33 patients with 42 treatment sites were randomly assigned to CT simulation planning or diagnostic CT planning.
Patients received up to 30 Gy in up to 10 fractions for bone or soft tissue metastases or primary tumor targets in the thorax, abdomen, pelvis, or proximal limbs. Single-fraction treatments were most common.
Three-quarters of the patients were men (median age, 72 years). Lung cancer was the most common type of primary tumor, followed by prostate and breast cancer.
The eight participants for whom the CT simulation approach was used waited 3-4 hours for treatment planning and overall spent a median of 4.8 hours in the cancer center on their day of treatment.
The 25 patients for whom diagnostic CT planning was used spent a median of 0.4 hours, or about 24 minutes, in the center on their day of treatment because radiation plans were completed before they arrived. The median time between their diagnostic CTs and radiation treatment was 13 days (range, 8-22 days).
Ms. O’Neil and her team found that if the original diagnostic CT was performed within 28 days, lesion anatomy would not have changed enough to warrant a new scan.
On the day of treatment, the study team used surface-guided radiation therapy techniques to ensure patients in the diagnostic CT planning group were positioned within 3 mm of where they were during their diagnostic scans, an essential step to ensure that radiation is delivered to the correct location. Ms. O’Neil noted that other investigators have used anatomic landmarks, a simpler approach, to achieve these results.
Overall, radiation oncologists rated radiation dose distribution as “acceptable” in about 80% of cases in both arms of DART and “acceptable with minor deviation” in the remaining 20% of cases.
Every radiation oncologist and medical physicists in the trial gave the workflow with diagnostic CT planning a 5 out of 5 rating for acceptability, and 90% of patients in this group rated the amount of time they spent for treatment as “acceptable.”
In contrast, only half of patients in the simulation arm said the amount of time spent was acceptable.
These findings align with several previous studies that support the diagnostic approach.
Jacob Scott, MD, a radiation oncologist at the Cleveland Clinic, said, “The comparable results using a recent diagnostic CT in place of a CT simulation for palliative radiation is an exciting step forward in radiation oncology. We may soon be in a world where we no longer need simulations.”
Dr. Scott also noted that combining diagnostic scans with cone beam or surface-guided positioning in lieu of CT simulations could further save “the health system and patients time and money.”
No external funding for the study was reported. The investigators, Ms. O’Neil, and Dr. Scott have disclosed no relevant financial relationships. One investigator reported receiving honoraria from Knight Therapeutics, AbbVie, Tersera, and Eisai and owns stock in Myovant.
A version of this article first appeared on Medscape.com.
, according to a results from a randomized trial presented at the annual meeting of the American Society for Radiation Oncology.
The aim of this same-day CT scan, called a CT simulation scan, is to optimize radiation targeting by mimicking the conditions under which radiation is delivered using the latest information on the size and location of lesions.
But investigators reported that skipping the CT simulation scan saves patients hours in the clinic, allows patients to experience pain relief faster, and saves radiation oncologists time without compromising dosimetric coverage of cancerous lesions.
“This is huge in a symptomatic patient population,” said Melissa O’Neil, an advanced practice radiation therapist at the London, Ont., Health Sciences Centre and the lead investigator on the trial, dubbed DART (Diagnostic CT-Enabled Radiation Therapy).
“Diagnostic CT-based radiation planning substantially reduces time in the [treatment] center without a detriment in plan deliverability or quality,” Ms. O’Neil said.
In addition, patients are exposed to less radiation, and staff doesn’t have to spend as much time tending to symptomatic patients before treatment. Omitting this scan “should be considered for patients with a recent diagnostic CT scan who are undergoing simple palliative radiation,” Ms. O’Neil said.
CT simulation scans are standard of care in cases involving palliative radiation, but they create bottlenecks in the workflow. When a CT simulation is performed on the day of treatment, patients must wait hours as the results are translated into a treatment plan.
In the DART analysis, 33 patients with 42 treatment sites were randomly assigned to CT simulation planning or diagnostic CT planning.
Patients received up to 30 Gy in up to 10 fractions for bone or soft tissue metastases or primary tumor targets in the thorax, abdomen, pelvis, or proximal limbs. Single-fraction treatments were most common.
Three-quarters of the patients were men (median age, 72 years). Lung cancer was the most common type of primary tumor, followed by prostate and breast cancer.
The eight participants for whom the CT simulation approach was used waited 3-4 hours for treatment planning and overall spent a median of 4.8 hours in the cancer center on their day of treatment.
The 25 patients for whom diagnostic CT planning was used spent a median of 0.4 hours, or about 24 minutes, in the center on their day of treatment because radiation plans were completed before they arrived. The median time between their diagnostic CTs and radiation treatment was 13 days (range, 8-22 days).
Ms. O’Neil and her team found that if the original diagnostic CT was performed within 28 days, lesion anatomy would not have changed enough to warrant a new scan.
On the day of treatment, the study team used surface-guided radiation therapy techniques to ensure patients in the diagnostic CT planning group were positioned within 3 mm of where they were during their diagnostic scans, an essential step to ensure that radiation is delivered to the correct location. Ms. O’Neil noted that other investigators have used anatomic landmarks, a simpler approach, to achieve these results.
Overall, radiation oncologists rated radiation dose distribution as “acceptable” in about 80% of cases in both arms of DART and “acceptable with minor deviation” in the remaining 20% of cases.
Every radiation oncologist and medical physicists in the trial gave the workflow with diagnostic CT planning a 5 out of 5 rating for acceptability, and 90% of patients in this group rated the amount of time they spent for treatment as “acceptable.”
In contrast, only half of patients in the simulation arm said the amount of time spent was acceptable.
These findings align with several previous studies that support the diagnostic approach.
Jacob Scott, MD, a radiation oncologist at the Cleveland Clinic, said, “The comparable results using a recent diagnostic CT in place of a CT simulation for palliative radiation is an exciting step forward in radiation oncology. We may soon be in a world where we no longer need simulations.”
Dr. Scott also noted that combining diagnostic scans with cone beam or surface-guided positioning in lieu of CT simulations could further save “the health system and patients time and money.”
No external funding for the study was reported. The investigators, Ms. O’Neil, and Dr. Scott have disclosed no relevant financial relationships. One investigator reported receiving honoraria from Knight Therapeutics, AbbVie, Tersera, and Eisai and owns stock in Myovant.
A version of this article first appeared on Medscape.com.
FROM ASTRO 2023
Rheumatoid arthritis: Five things to know
Rheumatoid arthritis (RA) is a chronic systemic inflammatory disease that typically presents as a symmetric inflammatory polyarthritis (synovitis) primarily affecting the hands and feet. Any joint lined by a synovial membrane may be involved; however, extraarticular involvement of various organs can be significant. RA is theorized to develop when a genetically susceptible individual experiences an external trigger (e.g., cigarette smoking, infection, trauma) that precipitates an autoimmune reaction.
Rheumatology is a rapidly advancing, but relatively young, subspecialty. An understanding of the pathophysiology, treatment, and classification of RA is still emerging. Here are five things to know about RA.
1. A healthier lifestyle is associated with a reduced risk of developing RA.
Large epidemiologic studies have identified several factors that increase the incidence of RA; these include an unhealthy diet, smoking, adiposity, low educational level, and low socioeconomic status. A patient’s response to antirheumatic medications can be affected by certain lifestyle habits, which can be associated with worse treatment outcomes; such habits include smoking, insufficient physical activity, and obesity, among others. Although methodologic problems may impede making firm conclusions regarding a causal role for these factors in the disease course and risk of developing RA, current evidence is sufficient to recommend quitting smoking, adopting a healthy diet, preventing obesity, and maintaining a high level of physical activity to support the effectiveness of current antirheumatic drugs.
In the Nurses’ Health Study, biennial questionnaires were used to collect lifestyle and medical information to determine which modifiable risk factors are associated with the risk for RA in women. Patient medical records were used to confirm incident RA and serostatus. The healthy lifestyle index score (HLIS), which includes five modifiable risk factors (smoking, alcohol consumption, body mass index, physical activity, and diet), was used to assess risk. Cox regression, which was adjusted for confounders, was used to model associations between HLIS and the incidence of RA. The study concluded that a healthier lifestyle was associated with a lower risk of developing RA, and a significant number of RA cases may be preventable if patients adopted four or more healthy lifestyle factors.
The Mediterranean diet is one current popular dietary option that appears to have promising evidence in many disease processes, including RA.
2. In pregnant women with RA, the course of the disease can change throughout pregnancy.
The course of RA often changes during pregnancy. About half of pregnant women with RA have low disease activity, and 20%-40% achieve remission by the third trimester; however, nearly 20% have worse or moderate to high disease activity during pregnancy that may require further therapeutic intervention. Postpartum flares of RA also may occur, with studies reporting rates of 39%-90%.
No specific guidelines address obstetric monitoring in patients with RA. Because few data suggest a significantly increased risk for preterm birth, preeclampsia, or fetal growth restriction, no special obstetric monitoring is indicated beyond what is performed for usual obstetric care.
Medications considered to be low risk in pregnancy include low-dose corticosteroids, antimalarial agents, sulfasalazine, and azathioprine. Certain tumor necrosis factor inhibitors are also thought to be relatively safe.
3. A well-designed exercise program can be beneficial in RA.
Regular physical activity has replaced bed rest as the recommended response to the stiffness and pain associated with RA. However, many patients who have RA do not really believe this. Lack of conviction and motivation appear to be the major factors that deter nearly half of patients with RA from moving about enough to help their situation. There is ample evidence about the benefits of physical activity in RA, but little research into why few patients with RA take advantage of it. The extreme physical inactivity of patients with RA becomes a vicious cycle in terms of health and disease progression. Thus, encouraging physical activity is an essential part of the overall treatment of RA.
Findings from randomized controlled trials show that exercise is fundamentally beneficial for patients with RA. The benefits of properly designed physical exercise programs include improved cardiorespiratory fitness and cardiovascular health, increased muscle mass, reduced adiposity, increased strength, and improved physical functioning, all achieved without exacerbation of disease activity or joint damage.
The American College of Rheumatology (ACR) has released recommendations for exercise interventions for RA. The ACR strongly recommends consistent engagement in an exercise program over no exercise. The type of exercise is open to interpretation. An exercise program for patients with rheumatic diseases aims to preserve or restore the range of motion of affected joints, increase muscle strength and endurance, and improve mood and decrease health risks associated with a sedentary lifestyle.
4. RA is a systemic disease that affects multiple organ systems.
Although synovitis is the pathologic hallmark of RA, extraarticular manifestations and comorbidities occur presumably owing to the complex, chronic, inflammatory, and autoimmune features of RA.
The most common cause of death in patients with RA is cardiovascular disease. Compared with the general population, patients with RA have two times the risk of having a myocardial infarction, and they have up to 50% greater cardiovascular mortality risk. Factors identified to play important roles in atherosclerotic damage and incident cardiovascular disease include severe and prolonged disease activity, inflammation (e.g., C-reactive protein, anti–citrullinated protein antibodies (ACPAs), cytokines, matrix-degrading enzymes), and genetics.
Respiratory disease is the second major cause of death in patients with RA; this occurs in 30%-40% of patients with RA. The lung interstitium, airways, and pleurae can all be affected by RA, but pulmonary vascular involvement is less common.
Central and peripheral nervous system involvement is typically attributed to RA-associated small-vessel vasculitis, joint damage, and/or drug toxicity. Evidence also suggests that systemic inflammation causes microvascular cerebral damage that is associated with the development of vascular dementia and Alzheimer’s disease. Finally, some observational studies have suggested that drugs commonly used to treat RA – disease-modifying antirheumatic drugs (DMARDs) and biologics – may reduce the incidence of dementia.
5. As treatment options for RA improve, many controversies have arisen.
In patients without RA symptoms but with biomarkers, experts debate whether early treatment with DMARDs could prevent irreversible joint damage.
There is no clear definition of pre-RA, but it could be defined as having positive markers for RA (e.g., positive rheumatoid factor and anti–cyclic citrullinated peptides) or having joint pain with abnormal ultrasonography findings but not having positive biomarkers. However, not all patients who have positive biomarkers progress to clinical RA, so what exactly determines this progression is unclear. Nevertheless, some clinicians do treat pre-RA. This was a major debate at the ACR’s 2022 meeting.
Studies have shown that early treatment of RA, including during the preclinical phase, can lead to better long-term outcomes. It can help reduce joint inflammation, control disease activity, and prevent or minimize irreversible joint damage. Early treatment also increases the likelihood of achieving remission or low disease activity, which improves quality of life for patients. Lifestyle interventions in these patients, including exercise, weight control, and cardiovascular health, may not prevent disease but may delay the onset of full-blown clinical RA.
The discovery of pre-RA has also underpinned the development of several clinical prevention trials in RA; specifically, the PRAIRI study demonstrated that a single dose of rituximab can delay the onset of clinically apparent RA in at-risk individuals. Additional studies are evaluating the ability of drugs, including abatacept, hydroxychloroquine, and methotrexate, to prevent or delay future RA.
Dual biologics target different pathways – ostensibly boosting efficacy – but unknowns, concerns over safety, and lack of evidence make the practice controversial.
Several randomized controlled trials have assessed the safety and efficacy of dual-biologic treatment of RA, but the results have been mixed, which has raised safety concerns. Overall, there is a paucity of data concerning the safety of the simultaneous use of more than one biologic. Dual therapy may constitute an efficacious and safe add-on treatment to biologic therapy, but properly conducted clinical investigations are needed. In the meantime, dual biologic therapy used at physicians’ discretion requires close monitoring of patients, with an emphasis on the safety profile.
Large language models (artificial intelligence [AI]) are rapidly taking hold in medicine. Many argue that they can enrich patient care, but they come with liability risks.
Large language models, such as AI chatbots or ChatGPT, can increase access to information, help with patient education, and support decision-making. Limitations include lack of personalization, clinical experience, and emotional connection. The use of large language models in health care is fraught with ethical and legal concerns.
Liability issues can arise if errors, inaccuracies, or adverse outcomes result from the use of AI chatbots. Determining liability may involve assessing factors such as the design and development of the AI system, training and deployment of the model, the communication of limitations and disclaimers to users, and the involvement of human healthcare professionals in the decision-making process.
To mitigate liability risks, AI chatbots in rheumatology must comply with applicable regulations and guidelines. Transparency in the capabilities and limitations of the system, clear communication of the boundaries of its advice, and the presence of human oversight are essential. Collaborating with legal experts and following best practices in the development and deployment of AI technologies can help to minimize liability concerns.
The benefits and risks associated with tapering DMARD therapy in patients with RA who have sustained remission of disease should be considered.
Although some patients with well-controlled RA have relapse after tapering or discontinuing DMARDs, some do not, making this treatment strategy a personal decision undertaken with a rheumatologist.
In the RETRO study, German researchers examined the effects of tapering or stopping DMARDs in patients whose RA was in sustained remission. In the phase 3 trial (n = 316), investigators randomized 303 patients with remission for ≥ 6 months who were on stable conventional synthetic or biologic DMARD treatment into three groups: (1) continuation on 100% DMARD dose, (2) tapering to 50% of the DMARD dose, and (3) 50% tapering followed by DMARD withdrawal. The proportion of patients who continued in remission at 1 year was 81.2% in group 1, 58.6% in group 2, and 43.3% in group 3. Predictors for flare-ups were female sex, longer disease duration, rheumatoid factor or ACPA positivity, and higher disease activity scores at baseline.
The abrupt cessation or reduction of DMARDs without medical supervision and guidance can exacerbate symptoms and result in disease flares.
The interplay between long COVID and RA is a recent phenomenon that needs to be considered.
RA shares similar symptoms with long COVID. Patients with a history of RA and a previous diagnosis of COVID-19 who have developed persistent joint or muscle symptoms pose a significant challenge to clinicians. Such patients may be experiencing long COVID or a flare-up of their preexisting rheumatic disease.
Immunosuppressive medications can potentially increase the risk for COVID-19, but it is not clear how they affect disease severity risk. Individuals with RA and long COVID need careful evaluation to balance the management of disease activity while considering the risks associated with immunosuppression and potential susceptibility to viral infections.
Dr. Dombrosky is a staff physician in rheumatology at Central Virginia VA Health Care System in Richmond. He has disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
Rheumatoid arthritis (RA) is a chronic systemic inflammatory disease that typically presents as a symmetric inflammatory polyarthritis (synovitis) primarily affecting the hands and feet. Any joint lined by a synovial membrane may be involved; however, extraarticular involvement of various organs can be significant. RA is theorized to develop when a genetically susceptible individual experiences an external trigger (e.g., cigarette smoking, infection, trauma) that precipitates an autoimmune reaction.
Rheumatology is a rapidly advancing, but relatively young, subspecialty. An understanding of the pathophysiology, treatment, and classification of RA is still emerging. Here are five things to know about RA.
1. A healthier lifestyle is associated with a reduced risk of developing RA.
Large epidemiologic studies have identified several factors that increase the incidence of RA; these include an unhealthy diet, smoking, adiposity, low educational level, and low socioeconomic status. A patient’s response to antirheumatic medications can be affected by certain lifestyle habits, which can be associated with worse treatment outcomes; such habits include smoking, insufficient physical activity, and obesity, among others. Although methodologic problems may impede making firm conclusions regarding a causal role for these factors in the disease course and risk of developing RA, current evidence is sufficient to recommend quitting smoking, adopting a healthy diet, preventing obesity, and maintaining a high level of physical activity to support the effectiveness of current antirheumatic drugs.
In the Nurses’ Health Study, biennial questionnaires were used to collect lifestyle and medical information to determine which modifiable risk factors are associated with the risk for RA in women. Patient medical records were used to confirm incident RA and serostatus. The healthy lifestyle index score (HLIS), which includes five modifiable risk factors (smoking, alcohol consumption, body mass index, physical activity, and diet), was used to assess risk. Cox regression, which was adjusted for confounders, was used to model associations between HLIS and the incidence of RA. The study concluded that a healthier lifestyle was associated with a lower risk of developing RA, and a significant number of RA cases may be preventable if patients adopted four or more healthy lifestyle factors.
The Mediterranean diet is one current popular dietary option that appears to have promising evidence in many disease processes, including RA.
2. In pregnant women with RA, the course of the disease can change throughout pregnancy.
The course of RA often changes during pregnancy. About half of pregnant women with RA have low disease activity, and 20%-40% achieve remission by the third trimester; however, nearly 20% have worse or moderate to high disease activity during pregnancy that may require further therapeutic intervention. Postpartum flares of RA also may occur, with studies reporting rates of 39%-90%.
No specific guidelines address obstetric monitoring in patients with RA. Because few data suggest a significantly increased risk for preterm birth, preeclampsia, or fetal growth restriction, no special obstetric monitoring is indicated beyond what is performed for usual obstetric care.
Medications considered to be low risk in pregnancy include low-dose corticosteroids, antimalarial agents, sulfasalazine, and azathioprine. Certain tumor necrosis factor inhibitors are also thought to be relatively safe.
3. A well-designed exercise program can be beneficial in RA.
Regular physical activity has replaced bed rest as the recommended response to the stiffness and pain associated with RA. However, many patients who have RA do not really believe this. Lack of conviction and motivation appear to be the major factors that deter nearly half of patients with RA from moving about enough to help their situation. There is ample evidence about the benefits of physical activity in RA, but little research into why few patients with RA take advantage of it. The extreme physical inactivity of patients with RA becomes a vicious cycle in terms of health and disease progression. Thus, encouraging physical activity is an essential part of the overall treatment of RA.
Findings from randomized controlled trials show that exercise is fundamentally beneficial for patients with RA. The benefits of properly designed physical exercise programs include improved cardiorespiratory fitness and cardiovascular health, increased muscle mass, reduced adiposity, increased strength, and improved physical functioning, all achieved without exacerbation of disease activity or joint damage.
The American College of Rheumatology (ACR) has released recommendations for exercise interventions for RA. The ACR strongly recommends consistent engagement in an exercise program over no exercise. The type of exercise is open to interpretation. An exercise program for patients with rheumatic diseases aims to preserve or restore the range of motion of affected joints, increase muscle strength and endurance, and improve mood and decrease health risks associated with a sedentary lifestyle.
4. RA is a systemic disease that affects multiple organ systems.
Although synovitis is the pathologic hallmark of RA, extraarticular manifestations and comorbidities occur presumably owing to the complex, chronic, inflammatory, and autoimmune features of RA.
The most common cause of death in patients with RA is cardiovascular disease. Compared with the general population, patients with RA have two times the risk of having a myocardial infarction, and they have up to 50% greater cardiovascular mortality risk. Factors identified to play important roles in atherosclerotic damage and incident cardiovascular disease include severe and prolonged disease activity, inflammation (e.g., C-reactive protein, anti–citrullinated protein antibodies (ACPAs), cytokines, matrix-degrading enzymes), and genetics.
Respiratory disease is the second major cause of death in patients with RA; this occurs in 30%-40% of patients with RA. The lung interstitium, airways, and pleurae can all be affected by RA, but pulmonary vascular involvement is less common.
Central and peripheral nervous system involvement is typically attributed to RA-associated small-vessel vasculitis, joint damage, and/or drug toxicity. Evidence also suggests that systemic inflammation causes microvascular cerebral damage that is associated with the development of vascular dementia and Alzheimer’s disease. Finally, some observational studies have suggested that drugs commonly used to treat RA – disease-modifying antirheumatic drugs (DMARDs) and biologics – may reduce the incidence of dementia.
5. As treatment options for RA improve, many controversies have arisen.
In patients without RA symptoms but with biomarkers, experts debate whether early treatment with DMARDs could prevent irreversible joint damage.
There is no clear definition of pre-RA, but it could be defined as having positive markers for RA (e.g., positive rheumatoid factor and anti–cyclic citrullinated peptides) or having joint pain with abnormal ultrasonography findings but not having positive biomarkers. However, not all patients who have positive biomarkers progress to clinical RA, so what exactly determines this progression is unclear. Nevertheless, some clinicians do treat pre-RA. This was a major debate at the ACR’s 2022 meeting.
Studies have shown that early treatment of RA, including during the preclinical phase, can lead to better long-term outcomes. It can help reduce joint inflammation, control disease activity, and prevent or minimize irreversible joint damage. Early treatment also increases the likelihood of achieving remission or low disease activity, which improves quality of life for patients. Lifestyle interventions in these patients, including exercise, weight control, and cardiovascular health, may not prevent disease but may delay the onset of full-blown clinical RA.
The discovery of pre-RA has also underpinned the development of several clinical prevention trials in RA; specifically, the PRAIRI study demonstrated that a single dose of rituximab can delay the onset of clinically apparent RA in at-risk individuals. Additional studies are evaluating the ability of drugs, including abatacept, hydroxychloroquine, and methotrexate, to prevent or delay future RA.
Dual biologics target different pathways – ostensibly boosting efficacy – but unknowns, concerns over safety, and lack of evidence make the practice controversial.
Several randomized controlled trials have assessed the safety and efficacy of dual-biologic treatment of RA, but the results have been mixed, which has raised safety concerns. Overall, there is a paucity of data concerning the safety of the simultaneous use of more than one biologic. Dual therapy may constitute an efficacious and safe add-on treatment to biologic therapy, but properly conducted clinical investigations are needed. In the meantime, dual biologic therapy used at physicians’ discretion requires close monitoring of patients, with an emphasis on the safety profile.
Large language models (artificial intelligence [AI]) are rapidly taking hold in medicine. Many argue that they can enrich patient care, but they come with liability risks.
Large language models, such as AI chatbots or ChatGPT, can increase access to information, help with patient education, and support decision-making. Limitations include lack of personalization, clinical experience, and emotional connection. The use of large language models in health care is fraught with ethical and legal concerns.
Liability issues can arise if errors, inaccuracies, or adverse outcomes result from the use of AI chatbots. Determining liability may involve assessing factors such as the design and development of the AI system, training and deployment of the model, the communication of limitations and disclaimers to users, and the involvement of human healthcare professionals in the decision-making process.
To mitigate liability risks, AI chatbots in rheumatology must comply with applicable regulations and guidelines. Transparency in the capabilities and limitations of the system, clear communication of the boundaries of its advice, and the presence of human oversight are essential. Collaborating with legal experts and following best practices in the development and deployment of AI technologies can help to minimize liability concerns.
The benefits and risks associated with tapering DMARD therapy in patients with RA who have sustained remission of disease should be considered.
Although some patients with well-controlled RA have relapse after tapering or discontinuing DMARDs, some do not, making this treatment strategy a personal decision undertaken with a rheumatologist.
In the RETRO study, German researchers examined the effects of tapering or stopping DMARDs in patients whose RA was in sustained remission. In the phase 3 trial (n = 316), investigators randomized 303 patients with remission for ≥ 6 months who were on stable conventional synthetic or biologic DMARD treatment into three groups: (1) continuation on 100% DMARD dose, (2) tapering to 50% of the DMARD dose, and (3) 50% tapering followed by DMARD withdrawal. The proportion of patients who continued in remission at 1 year was 81.2% in group 1, 58.6% in group 2, and 43.3% in group 3. Predictors for flare-ups were female sex, longer disease duration, rheumatoid factor or ACPA positivity, and higher disease activity scores at baseline.
The abrupt cessation or reduction of DMARDs without medical supervision and guidance can exacerbate symptoms and result in disease flares.
The interplay between long COVID and RA is a recent phenomenon that needs to be considered.
RA shares similar symptoms with long COVID. Patients with a history of RA and a previous diagnosis of COVID-19 who have developed persistent joint or muscle symptoms pose a significant challenge to clinicians. Such patients may be experiencing long COVID or a flare-up of their preexisting rheumatic disease.
Immunosuppressive medications can potentially increase the risk for COVID-19, but it is not clear how they affect disease severity risk. Individuals with RA and long COVID need careful evaluation to balance the management of disease activity while considering the risks associated with immunosuppression and potential susceptibility to viral infections.
Dr. Dombrosky is a staff physician in rheumatology at Central Virginia VA Health Care System in Richmond. He has disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.
Rheumatoid arthritis (RA) is a chronic systemic inflammatory disease that typically presents as a symmetric inflammatory polyarthritis (synovitis) primarily affecting the hands and feet. Any joint lined by a synovial membrane may be involved; however, extraarticular involvement of various organs can be significant. RA is theorized to develop when a genetically susceptible individual experiences an external trigger (e.g., cigarette smoking, infection, trauma) that precipitates an autoimmune reaction.
Rheumatology is a rapidly advancing, but relatively young, subspecialty. An understanding of the pathophysiology, treatment, and classification of RA is still emerging. Here are five things to know about RA.
1. A healthier lifestyle is associated with a reduced risk of developing RA.
Large epidemiologic studies have identified several factors that increase the incidence of RA; these include an unhealthy diet, smoking, adiposity, low educational level, and low socioeconomic status. A patient’s response to antirheumatic medications can be affected by certain lifestyle habits, which can be associated with worse treatment outcomes; such habits include smoking, insufficient physical activity, and obesity, among others. Although methodologic problems may impede making firm conclusions regarding a causal role for these factors in the disease course and risk of developing RA, current evidence is sufficient to recommend quitting smoking, adopting a healthy diet, preventing obesity, and maintaining a high level of physical activity to support the effectiveness of current antirheumatic drugs.
In the Nurses’ Health Study, biennial questionnaires were used to collect lifestyle and medical information to determine which modifiable risk factors are associated with the risk for RA in women. Patient medical records were used to confirm incident RA and serostatus. The healthy lifestyle index score (HLIS), which includes five modifiable risk factors (smoking, alcohol consumption, body mass index, physical activity, and diet), was used to assess risk. Cox regression, which was adjusted for confounders, was used to model associations between HLIS and the incidence of RA. The study concluded that a healthier lifestyle was associated with a lower risk of developing RA, and a significant number of RA cases may be preventable if patients adopted four or more healthy lifestyle factors.
The Mediterranean diet is one current popular dietary option that appears to have promising evidence in many disease processes, including RA.
2. In pregnant women with RA, the course of the disease can change throughout pregnancy.
The course of RA often changes during pregnancy. About half of pregnant women with RA have low disease activity, and 20%-40% achieve remission by the third trimester; however, nearly 20% have worse or moderate to high disease activity during pregnancy that may require further therapeutic intervention. Postpartum flares of RA also may occur, with studies reporting rates of 39%-90%.
No specific guidelines address obstetric monitoring in patients with RA. Because few data suggest a significantly increased risk for preterm birth, preeclampsia, or fetal growth restriction, no special obstetric monitoring is indicated beyond what is performed for usual obstetric care.
Medications considered to be low risk in pregnancy include low-dose corticosteroids, antimalarial agents, sulfasalazine, and azathioprine. Certain tumor necrosis factor inhibitors are also thought to be relatively safe.
3. A well-designed exercise program can be beneficial in RA.
Regular physical activity has replaced bed rest as the recommended response to the stiffness and pain associated with RA. However, many patients who have RA do not really believe this. Lack of conviction and motivation appear to be the major factors that deter nearly half of patients with RA from moving about enough to help their situation. There is ample evidence about the benefits of physical activity in RA, but little research into why few patients with RA take advantage of it. The extreme physical inactivity of patients with RA becomes a vicious cycle in terms of health and disease progression. Thus, encouraging physical activity is an essential part of the overall treatment of RA.
Findings from randomized controlled trials show that exercise is fundamentally beneficial for patients with RA. The benefits of properly designed physical exercise programs include improved cardiorespiratory fitness and cardiovascular health, increased muscle mass, reduced adiposity, increased strength, and improved physical functioning, all achieved without exacerbation of disease activity or joint damage.
The American College of Rheumatology (ACR) has released recommendations for exercise interventions for RA. The ACR strongly recommends consistent engagement in an exercise program over no exercise. The type of exercise is open to interpretation. An exercise program for patients with rheumatic diseases aims to preserve or restore the range of motion of affected joints, increase muscle strength and endurance, and improve mood and decrease health risks associated with a sedentary lifestyle.
4. RA is a systemic disease that affects multiple organ systems.
Although synovitis is the pathologic hallmark of RA, extraarticular manifestations and comorbidities occur presumably owing to the complex, chronic, inflammatory, and autoimmune features of RA.
The most common cause of death in patients with RA is cardiovascular disease. Compared with the general population, patients with RA have two times the risk of having a myocardial infarction, and they have up to 50% greater cardiovascular mortality risk. Factors identified to play important roles in atherosclerotic damage and incident cardiovascular disease include severe and prolonged disease activity, inflammation (e.g., C-reactive protein, anti–citrullinated protein antibodies (ACPAs), cytokines, matrix-degrading enzymes), and genetics.
Respiratory disease is the second major cause of death in patients with RA; this occurs in 30%-40% of patients with RA. The lung interstitium, airways, and pleurae can all be affected by RA, but pulmonary vascular involvement is less common.
Central and peripheral nervous system involvement is typically attributed to RA-associated small-vessel vasculitis, joint damage, and/or drug toxicity. Evidence also suggests that systemic inflammation causes microvascular cerebral damage that is associated with the development of vascular dementia and Alzheimer’s disease. Finally, some observational studies have suggested that drugs commonly used to treat RA – disease-modifying antirheumatic drugs (DMARDs) and biologics – may reduce the incidence of dementia.
5. As treatment options for RA improve, many controversies have arisen.
In patients without RA symptoms but with biomarkers, experts debate whether early treatment with DMARDs could prevent irreversible joint damage.
There is no clear definition of pre-RA, but it could be defined as having positive markers for RA (e.g., positive rheumatoid factor and anti–cyclic citrullinated peptides) or having joint pain with abnormal ultrasonography findings but not having positive biomarkers. However, not all patients who have positive biomarkers progress to clinical RA, so what exactly determines this progression is unclear. Nevertheless, some clinicians do treat pre-RA. This was a major debate at the ACR’s 2022 meeting.
Studies have shown that early treatment of RA, including during the preclinical phase, can lead to better long-term outcomes. It can help reduce joint inflammation, control disease activity, and prevent or minimize irreversible joint damage. Early treatment also increases the likelihood of achieving remission or low disease activity, which improves quality of life for patients. Lifestyle interventions in these patients, including exercise, weight control, and cardiovascular health, may not prevent disease but may delay the onset of full-blown clinical RA.
The discovery of pre-RA has also underpinned the development of several clinical prevention trials in RA; specifically, the PRAIRI study demonstrated that a single dose of rituximab can delay the onset of clinically apparent RA in at-risk individuals. Additional studies are evaluating the ability of drugs, including abatacept, hydroxychloroquine, and methotrexate, to prevent or delay future RA.
Dual biologics target different pathways – ostensibly boosting efficacy – but unknowns, concerns over safety, and lack of evidence make the practice controversial.
Several randomized controlled trials have assessed the safety and efficacy of dual-biologic treatment of RA, but the results have been mixed, which has raised safety concerns. Overall, there is a paucity of data concerning the safety of the simultaneous use of more than one biologic. Dual therapy may constitute an efficacious and safe add-on treatment to biologic therapy, but properly conducted clinical investigations are needed. In the meantime, dual biologic therapy used at physicians’ discretion requires close monitoring of patients, with an emphasis on the safety profile.
Large language models (artificial intelligence [AI]) are rapidly taking hold in medicine. Many argue that they can enrich patient care, but they come with liability risks.
Large language models, such as AI chatbots or ChatGPT, can increase access to information, help with patient education, and support decision-making. Limitations include lack of personalization, clinical experience, and emotional connection. The use of large language models in health care is fraught with ethical and legal concerns.
Liability issues can arise if errors, inaccuracies, or adverse outcomes result from the use of AI chatbots. Determining liability may involve assessing factors such as the design and development of the AI system, training and deployment of the model, the communication of limitations and disclaimers to users, and the involvement of human healthcare professionals in the decision-making process.
To mitigate liability risks, AI chatbots in rheumatology must comply with applicable regulations and guidelines. Transparency in the capabilities and limitations of the system, clear communication of the boundaries of its advice, and the presence of human oversight are essential. Collaborating with legal experts and following best practices in the development and deployment of AI technologies can help to minimize liability concerns.
The benefits and risks associated with tapering DMARD therapy in patients with RA who have sustained remission of disease should be considered.
Although some patients with well-controlled RA have relapse after tapering or discontinuing DMARDs, some do not, making this treatment strategy a personal decision undertaken with a rheumatologist.
In the RETRO study, German researchers examined the effects of tapering or stopping DMARDs in patients whose RA was in sustained remission. In the phase 3 trial (n = 316), investigators randomized 303 patients with remission for ≥ 6 months who were on stable conventional synthetic or biologic DMARD treatment into three groups: (1) continuation on 100% DMARD dose, (2) tapering to 50% of the DMARD dose, and (3) 50% tapering followed by DMARD withdrawal. The proportion of patients who continued in remission at 1 year was 81.2% in group 1, 58.6% in group 2, and 43.3% in group 3. Predictors for flare-ups were female sex, longer disease duration, rheumatoid factor or ACPA positivity, and higher disease activity scores at baseline.
The abrupt cessation or reduction of DMARDs without medical supervision and guidance can exacerbate symptoms and result in disease flares.
The interplay between long COVID and RA is a recent phenomenon that needs to be considered.
RA shares similar symptoms with long COVID. Patients with a history of RA and a previous diagnosis of COVID-19 who have developed persistent joint or muscle symptoms pose a significant challenge to clinicians. Such patients may be experiencing long COVID or a flare-up of their preexisting rheumatic disease.
Immunosuppressive medications can potentially increase the risk for COVID-19, but it is not clear how they affect disease severity risk. Individuals with RA and long COVID need careful evaluation to balance the management of disease activity while considering the risks associated with immunosuppression and potential susceptibility to viral infections.
Dr. Dombrosky is a staff physician in rheumatology at Central Virginia VA Health Care System in Richmond. He has disclosed no relevant financial relationships.
A version of this article appeared on Medscape.com.