User login
FDA expands belimumab indication to adults with lupus nephritis
The U.S. Food and Drug Administration has expanded the indication for belimumab (Benlysta) to adults with active lupus nephritis who are receiving standard therapy.
Roughly 40% of patients with systemic lupus erythematosus (SLE) develop lupus nephritis (LN), which causes inflammation in the kidneys and can lead to end-stage kidney disease.
“Benlysta is the first medicine approved to treat systemic lupus and adults with active lupus nephritis, an important treatment advance for patients with this incurable autoimmune disease,” Hal Barron, MD, GlaxoSmithKline’s chief scientific officer and president of research and development, said in a company news release.
Belimumab IV infusion was first approved in the United States in March 2011 for adults with SLE. The FDA approved belimumab IV infusion for use in children as young as age 5 years with SLE in 2019.
Both the IV and subcutaneous formulations are now indicated in the United States for adults with SLE and LN.
Belimumab is a B-lymphocyte stimulator protein inhibitor that is thought to decrease the amount of abnormal B cells; the latter are thought to play a role in lupus.
The expanded indication for belimumab for patients with LN is based on findings from the BLISS-LN phase 3 trial, published in The New England Journal of Medicine in September.
“Neutralizing B-cell activating factor and down-regulating autoreactive B-cell function in kidneys” represents a “compelling therapeutic approach to lupus nephritis,” the lead investigator of BLISS-LN, Richard Furie, MD, told the online annual Perspectives in Rheumatic Diseases meeting recently.
“In the 4 decades I have been caring for people with lupus, we have not been able to achieve remission in more than just one-third of patients with lupus nephritis, and despite all of our efforts, 10%-30% of patients with lupus kidney disease still progress to end-stage kidney disease,” Dr. Furie, who is chief of the division of rheumatology at Northwell Health, notes in the GSK statement.
“The data from the BLISS-LN study show that Benlysta added to standard therapy not only increased response rates over 2 years, but it also prevented worsening of kidney disease in patients with active lupus nephritis, compared to standard therapy alone,” he added.
BLISS-LN study: Belimumab effect seen mostly in those on MMF
BLISS-LN enrolled 448 adults with biopsy-confirmed active LN. Half were randomly allocated to receive IV belimumab (10 mg/kg) plus standard therapy (mycophenolate mofetil for induction and maintenance or cyclophosphamide for induction followed by azathioprine for maintenance, with steroids) and half to receive placebo plus standard therapy.
At 2 years, significantly more patients in the belimumab group than in the placebo group had a primary efficacy renal response (43% vs. 32%; odds ratio, 1.6; 95% confidence interval, 1.0- 2.3; P = .03).
This primary endpoint was defined as a ratio of urinary protein to creatinine of ≤0.7, an estimated glomerular filtration rate that was no worse than 20% below the value before the renal flare or ≥60 mL per minute per 1.73 m2 of body surface area, without use of rescue therapy.
The risk for a renal-related event or death was also significantly lower among patients who received belimumab than among those who received placebo (hazard ratio, 0.51; P = .001). The safety profile of belimumab was consistent with that observed in prior studies.
But in a commentary that accompanied the publication of BLISS-LN, editorialists noted that “most of the treatment effect was seen in patients who had received mycophenolate mofetil. No benefit was present in the subgroup of patients who received cyclophosphamide-azathioprine.”
In addition, induction treatment was not randomly assigned, editorialists Michael Ward, MD, MPH, and Maria Tektonidou, MD, PhD, noted.
“If patients with more severe nephritis were preferentially treated with cyclophosphamide, a likely inclination among most physicians, the trial may be telling us that belimumab enhances responses only among less severely affected patients,” observed Dr. Ward, who is with the National Institutes of Health, and Dr. Tektonidou, of the National and Kopodistrian University, in Athens.
A version of this article first appeared on Medscape.com.
The U.S. Food and Drug Administration has expanded the indication for belimumab (Benlysta) to adults with active lupus nephritis who are receiving standard therapy.
Roughly 40% of patients with systemic lupus erythematosus (SLE) develop lupus nephritis (LN), which causes inflammation in the kidneys and can lead to end-stage kidney disease.
“Benlysta is the first medicine approved to treat systemic lupus and adults with active lupus nephritis, an important treatment advance for patients with this incurable autoimmune disease,” Hal Barron, MD, GlaxoSmithKline’s chief scientific officer and president of research and development, said in a company news release.
Belimumab IV infusion was first approved in the United States in March 2011 for adults with SLE. The FDA approved belimumab IV infusion for use in children as young as age 5 years with SLE in 2019.
Both the IV and subcutaneous formulations are now indicated in the United States for adults with SLE and LN.
Belimumab is a B-lymphocyte stimulator protein inhibitor that is thought to decrease the amount of abnormal B cells; the latter are thought to play a role in lupus.
The expanded indication for belimumab for patients with LN is based on findings from the BLISS-LN phase 3 trial, published in The New England Journal of Medicine in September.
“Neutralizing B-cell activating factor and down-regulating autoreactive B-cell function in kidneys” represents a “compelling therapeutic approach to lupus nephritis,” the lead investigator of BLISS-LN, Richard Furie, MD, told the online annual Perspectives in Rheumatic Diseases meeting recently.
“In the 4 decades I have been caring for people with lupus, we have not been able to achieve remission in more than just one-third of patients with lupus nephritis, and despite all of our efforts, 10%-30% of patients with lupus kidney disease still progress to end-stage kidney disease,” Dr. Furie, who is chief of the division of rheumatology at Northwell Health, notes in the GSK statement.
“The data from the BLISS-LN study show that Benlysta added to standard therapy not only increased response rates over 2 years, but it also prevented worsening of kidney disease in patients with active lupus nephritis, compared to standard therapy alone,” he added.
BLISS-LN study: Belimumab effect seen mostly in those on MMF
BLISS-LN enrolled 448 adults with biopsy-confirmed active LN. Half were randomly allocated to receive IV belimumab (10 mg/kg) plus standard therapy (mycophenolate mofetil for induction and maintenance or cyclophosphamide for induction followed by azathioprine for maintenance, with steroids) and half to receive placebo plus standard therapy.
At 2 years, significantly more patients in the belimumab group than in the placebo group had a primary efficacy renal response (43% vs. 32%; odds ratio, 1.6; 95% confidence interval, 1.0- 2.3; P = .03).
This primary endpoint was defined as a ratio of urinary protein to creatinine of ≤0.7, an estimated glomerular filtration rate that was no worse than 20% below the value before the renal flare or ≥60 mL per minute per 1.73 m2 of body surface area, without use of rescue therapy.
The risk for a renal-related event or death was also significantly lower among patients who received belimumab than among those who received placebo (hazard ratio, 0.51; P = .001). The safety profile of belimumab was consistent with that observed in prior studies.
But in a commentary that accompanied the publication of BLISS-LN, editorialists noted that “most of the treatment effect was seen in patients who had received mycophenolate mofetil. No benefit was present in the subgroup of patients who received cyclophosphamide-azathioprine.”
In addition, induction treatment was not randomly assigned, editorialists Michael Ward, MD, MPH, and Maria Tektonidou, MD, PhD, noted.
“If patients with more severe nephritis were preferentially treated with cyclophosphamide, a likely inclination among most physicians, the trial may be telling us that belimumab enhances responses only among less severely affected patients,” observed Dr. Ward, who is with the National Institutes of Health, and Dr. Tektonidou, of the National and Kopodistrian University, in Athens.
A version of this article first appeared on Medscape.com.
The U.S. Food and Drug Administration has expanded the indication for belimumab (Benlysta) to adults with active lupus nephritis who are receiving standard therapy.
Roughly 40% of patients with systemic lupus erythematosus (SLE) develop lupus nephritis (LN), which causes inflammation in the kidneys and can lead to end-stage kidney disease.
“Benlysta is the first medicine approved to treat systemic lupus and adults with active lupus nephritis, an important treatment advance for patients with this incurable autoimmune disease,” Hal Barron, MD, GlaxoSmithKline’s chief scientific officer and president of research and development, said in a company news release.
Belimumab IV infusion was first approved in the United States in March 2011 for adults with SLE. The FDA approved belimumab IV infusion for use in children as young as age 5 years with SLE in 2019.
Both the IV and subcutaneous formulations are now indicated in the United States for adults with SLE and LN.
Belimumab is a B-lymphocyte stimulator protein inhibitor that is thought to decrease the amount of abnormal B cells; the latter are thought to play a role in lupus.
The expanded indication for belimumab for patients with LN is based on findings from the BLISS-LN phase 3 trial, published in The New England Journal of Medicine in September.
“Neutralizing B-cell activating factor and down-regulating autoreactive B-cell function in kidneys” represents a “compelling therapeutic approach to lupus nephritis,” the lead investigator of BLISS-LN, Richard Furie, MD, told the online annual Perspectives in Rheumatic Diseases meeting recently.
“In the 4 decades I have been caring for people with lupus, we have not been able to achieve remission in more than just one-third of patients with lupus nephritis, and despite all of our efforts, 10%-30% of patients with lupus kidney disease still progress to end-stage kidney disease,” Dr. Furie, who is chief of the division of rheumatology at Northwell Health, notes in the GSK statement.
“The data from the BLISS-LN study show that Benlysta added to standard therapy not only increased response rates over 2 years, but it also prevented worsening of kidney disease in patients with active lupus nephritis, compared to standard therapy alone,” he added.
BLISS-LN study: Belimumab effect seen mostly in those on MMF
BLISS-LN enrolled 448 adults with biopsy-confirmed active LN. Half were randomly allocated to receive IV belimumab (10 mg/kg) plus standard therapy (mycophenolate mofetil for induction and maintenance or cyclophosphamide for induction followed by azathioprine for maintenance, with steroids) and half to receive placebo plus standard therapy.
At 2 years, significantly more patients in the belimumab group than in the placebo group had a primary efficacy renal response (43% vs. 32%; odds ratio, 1.6; 95% confidence interval, 1.0- 2.3; P = .03).
This primary endpoint was defined as a ratio of urinary protein to creatinine of ≤0.7, an estimated glomerular filtration rate that was no worse than 20% below the value before the renal flare or ≥60 mL per minute per 1.73 m2 of body surface area, without use of rescue therapy.
The risk for a renal-related event or death was also significantly lower among patients who received belimumab than among those who received placebo (hazard ratio, 0.51; P = .001). The safety profile of belimumab was consistent with that observed in prior studies.
But in a commentary that accompanied the publication of BLISS-LN, editorialists noted that “most of the treatment effect was seen in patients who had received mycophenolate mofetil. No benefit was present in the subgroup of patients who received cyclophosphamide-azathioprine.”
In addition, induction treatment was not randomly assigned, editorialists Michael Ward, MD, MPH, and Maria Tektonidou, MD, PhD, noted.
“If patients with more severe nephritis were preferentially treated with cyclophosphamide, a likely inclination among most physicians, the trial may be telling us that belimumab enhances responses only among less severely affected patients,” observed Dr. Ward, who is with the National Institutes of Health, and Dr. Tektonidou, of the National and Kopodistrian University, in Athens.
A version of this article first appeared on Medscape.com.
FDA panel puts spironolactone in play for HF with preserved EF
A Food and Drug Administration advisory committee lit a long-standing fuse, recommending that evidence from the controversial TOPCAT trial can be used to support a new indication for spironolactone.
The generic aldosterone blocker is already approved for the treatment of heart failure with reduced ejection fraction (HFrEF).
Hopes that it could be the first therapy to show improved outcomes in HF with preserved EF (HFpEF) were dashed in 2013 when TOPCAT failed to show a significant benefit over placebo for the primary endpoint of cardiovascular (CV) death, HF hospitalization, or aborted cardiac arrest.
Regional differences in the data, however, aroused concerns about the findings early on. Patients enrolled in Russia and the Republic of Georgia were younger, less likely to qualify on the basis of elevated natriuretic peptide levels, and had more evidence of ischemic heart disease than those in the Americas.
Event rates were also substantially lower in Russia/Georgia than in the Americas and in previous HFpEF trials, suggesting that many of these patients may not have had heart failure, the trialists argued.
In the Americas, results for the primary endpoint favor spironolactone over placebo (10.4 vs. 12.6 events per 100 patient-years; P = .026), whereas the rate in Russia/Georgia was much lower than in the Americas and slightly favors placebo (2.5 vs. 2.3 events/100 patient-years).
Medication noncompliance also may have been more common in Russia/Georgia based on pharmacodynamic studies and a 2017 analysis showing undetectable levels of canrenone, an active metabolite of spironolactone, in 30% of Russian versus 3% of North American patients who reported using the drug at 1 year.
TOPCAT investigator Marc Pfeffer, MD, PhD, from Brigham and Women’s Hospital and Harvard Medical School, Boston, said no trial is without flaws but that the observations represent serious misconduct. “Really we’re talking about a cancer, a cancer that has clear margins. The margins are Russia, Georgia that warrant censoring their data.”
The FDA’s own review of the National Institutes of Health–sponsored study, however, showed no significant interaction between treatment and region (P = .12) and “insufficient evidence to conclude the two regions are different enough such that overall results should not be considered,” said FDA statistician Ququan Liu, MD, MS.
She cautioned against removing data from a whole region that constituted almost half the study population and said it would set a precedent on what is considered substantial evidence for approval.
Several advisors concurred but, ultimately, the Cardiovascular and Renal Drugs Advisory Committee voted 8 to 4, with 1 abstention, that TOPCAT provides “sufficient evidence to support any indication.”
The same committee voted yesterday in support of an expanded role for sacubitril/valsartan (Entresto, Novartis) in select patients with HFpEF. In casting a “no” vote, panelist Steven E. Nissen, MD, from the Cleveland Clinic, said that decisions made by the panel set precedent.
“If the pharmaceutical industry came to us with a study like this and said the P value was .14 but we think a bunch of our sites weren’t very good and so we’re going to throw those data out and just look at the sites we like, the FDA would not have even brought that before us,” he said. “I cannot hold other sponsors, including our own government, to a different standard.”
Dr. Nissen argued that the primary endpoint failed by a significant margin (P = .138), the study was marginally powered, there was a troubling amount of missing data in the two regions, and spironolactone is also not without side effects. “Poor study conduct cannot be an excuse for a result we don’t like.”
Panel chair Julia B. Lewis, MD, from Vanderbilt University Medical Center in Nashville, Tenn., said she would love to support a cheap, generic drug to keep HF patients out of the hospital but was troubled by the egregious conduct of the trial and concerns about cherry-picking results. “My heart says this would be a great place for us to go but I can’t say that my head thinks this is an acceptable body of data.”
Several panelists, however, highlighted the benefits with spironolactone over placebo in the Americas including an 18% reduction in hospitalization for HF (21% vs. 25%; hazard ratio, 0.82; P = .04) and a 25% reduction in cumulative HF hospitalizations (361 vs. 438 events; incidence rate ratio, 0.75; P = .024).
There was also a reduction in CV mortality with spironolactone (11% vs. 14%; HR, 0.74; P = .027) – something, it was noted, not observed during the prior day’s proceeding on sacubitril/valsartan.
Panelist Christopher M. O’Connor, MD, from Inova Heart and Vascular Institute in Falls Church, Va., and Duke University, Durham, N.C., said he voted “yes” because of the totality of the information and that the investigators provided “compelling evidence” with or without the Russia/Georgia cohort on the efficacy on HF hospitalization reduction. “I think this is the augmented sweet spot of this data set.”
C. Michael Gibson, MD, said his decision to vote yes was not based on analyses that excluded half the patients but rather on the totality of the evidence, particularly the benefit on cumulative HF hospitalizations and in those with an EF lower than 56%.
Several panelists and members of the public cited for treatments among patients with HFpEF. Edward K. Kasper, MD, from Johns Hopkins University, Baltimore, said he found both sides of the argument persuasive but that he already uses spironolactone in this setting. “Somehow I’ve become convinced that this drug worked, so I voted yes.”
Dr. Kasper said the FDA may ultimately find there isn’t an indication for spironolactone in HFpEF but that it will likely move from a IIb to IIa recommendation in the next iteration of the American College of Cardiology guidelines.
Paul Ridker, MD, MPH, from Brigham and Women’s Hospital and Harvard Medical School, said he shared concerns about the precedent of dropping half the data, “even though, in this case, I believe half the data is wrong.”
Dr. Ridker noted that he would have been comfortable using the secondary endpoint of HF reduction as an indication in patients with mildly reduced EF but abstained because that data was not presented today, although it may be available from TOPCAT and the RALES trial.
The panel took up other nonvoting questions, including what additional data would be needed to augment support for approval. Suggestions ranged from additional analyses to a new trial, with TOPCAT serving as “pilot data,” but no recommendation was made.
A version of this article first appeared on Medscape.com.
A Food and Drug Administration advisory committee lit a long-standing fuse, recommending that evidence from the controversial TOPCAT trial can be used to support a new indication for spironolactone.
The generic aldosterone blocker is already approved for the treatment of heart failure with reduced ejection fraction (HFrEF).
Hopes that it could be the first therapy to show improved outcomes in HF with preserved EF (HFpEF) were dashed in 2013 when TOPCAT failed to show a significant benefit over placebo for the primary endpoint of cardiovascular (CV) death, HF hospitalization, or aborted cardiac arrest.
Regional differences in the data, however, aroused concerns about the findings early on. Patients enrolled in Russia and the Republic of Georgia were younger, less likely to qualify on the basis of elevated natriuretic peptide levels, and had more evidence of ischemic heart disease than those in the Americas.
Event rates were also substantially lower in Russia/Georgia than in the Americas and in previous HFpEF trials, suggesting that many of these patients may not have had heart failure, the trialists argued.
In the Americas, results for the primary endpoint favor spironolactone over placebo (10.4 vs. 12.6 events per 100 patient-years; P = .026), whereas the rate in Russia/Georgia was much lower than in the Americas and slightly favors placebo (2.5 vs. 2.3 events/100 patient-years).
Medication noncompliance also may have been more common in Russia/Georgia based on pharmacodynamic studies and a 2017 analysis showing undetectable levels of canrenone, an active metabolite of spironolactone, in 30% of Russian versus 3% of North American patients who reported using the drug at 1 year.
TOPCAT investigator Marc Pfeffer, MD, PhD, from Brigham and Women’s Hospital and Harvard Medical School, Boston, said no trial is without flaws but that the observations represent serious misconduct. “Really we’re talking about a cancer, a cancer that has clear margins. The margins are Russia, Georgia that warrant censoring their data.”
The FDA’s own review of the National Institutes of Health–sponsored study, however, showed no significant interaction between treatment and region (P = .12) and “insufficient evidence to conclude the two regions are different enough such that overall results should not be considered,” said FDA statistician Ququan Liu, MD, MS.
She cautioned against removing data from a whole region that constituted almost half the study population and said it would set a precedent on what is considered substantial evidence for approval.
Several advisors concurred but, ultimately, the Cardiovascular and Renal Drugs Advisory Committee voted 8 to 4, with 1 abstention, that TOPCAT provides “sufficient evidence to support any indication.”
The same committee voted yesterday in support of an expanded role for sacubitril/valsartan (Entresto, Novartis) in select patients with HFpEF. In casting a “no” vote, panelist Steven E. Nissen, MD, from the Cleveland Clinic, said that decisions made by the panel set precedent.
“If the pharmaceutical industry came to us with a study like this and said the P value was .14 but we think a bunch of our sites weren’t very good and so we’re going to throw those data out and just look at the sites we like, the FDA would not have even brought that before us,” he said. “I cannot hold other sponsors, including our own government, to a different standard.”
Dr. Nissen argued that the primary endpoint failed by a significant margin (P = .138), the study was marginally powered, there was a troubling amount of missing data in the two regions, and spironolactone is also not without side effects. “Poor study conduct cannot be an excuse for a result we don’t like.”
Panel chair Julia B. Lewis, MD, from Vanderbilt University Medical Center in Nashville, Tenn., said she would love to support a cheap, generic drug to keep HF patients out of the hospital but was troubled by the egregious conduct of the trial and concerns about cherry-picking results. “My heart says this would be a great place for us to go but I can’t say that my head thinks this is an acceptable body of data.”
Several panelists, however, highlighted the benefits with spironolactone over placebo in the Americas including an 18% reduction in hospitalization for HF (21% vs. 25%; hazard ratio, 0.82; P = .04) and a 25% reduction in cumulative HF hospitalizations (361 vs. 438 events; incidence rate ratio, 0.75; P = .024).
There was also a reduction in CV mortality with spironolactone (11% vs. 14%; HR, 0.74; P = .027) – something, it was noted, not observed during the prior day’s proceeding on sacubitril/valsartan.
Panelist Christopher M. O’Connor, MD, from Inova Heart and Vascular Institute in Falls Church, Va., and Duke University, Durham, N.C., said he voted “yes” because of the totality of the information and that the investigators provided “compelling evidence” with or without the Russia/Georgia cohort on the efficacy on HF hospitalization reduction. “I think this is the augmented sweet spot of this data set.”
C. Michael Gibson, MD, said his decision to vote yes was not based on analyses that excluded half the patients but rather on the totality of the evidence, particularly the benefit on cumulative HF hospitalizations and in those with an EF lower than 56%.
Several panelists and members of the public cited for treatments among patients with HFpEF. Edward K. Kasper, MD, from Johns Hopkins University, Baltimore, said he found both sides of the argument persuasive but that he already uses spironolactone in this setting. “Somehow I’ve become convinced that this drug worked, so I voted yes.”
Dr. Kasper said the FDA may ultimately find there isn’t an indication for spironolactone in HFpEF but that it will likely move from a IIb to IIa recommendation in the next iteration of the American College of Cardiology guidelines.
Paul Ridker, MD, MPH, from Brigham and Women’s Hospital and Harvard Medical School, said he shared concerns about the precedent of dropping half the data, “even though, in this case, I believe half the data is wrong.”
Dr. Ridker noted that he would have been comfortable using the secondary endpoint of HF reduction as an indication in patients with mildly reduced EF but abstained because that data was not presented today, although it may be available from TOPCAT and the RALES trial.
The panel took up other nonvoting questions, including what additional data would be needed to augment support for approval. Suggestions ranged from additional analyses to a new trial, with TOPCAT serving as “pilot data,” but no recommendation was made.
A version of this article first appeared on Medscape.com.
A Food and Drug Administration advisory committee lit a long-standing fuse, recommending that evidence from the controversial TOPCAT trial can be used to support a new indication for spironolactone.
The generic aldosterone blocker is already approved for the treatment of heart failure with reduced ejection fraction (HFrEF).
Hopes that it could be the first therapy to show improved outcomes in HF with preserved EF (HFpEF) were dashed in 2013 when TOPCAT failed to show a significant benefit over placebo for the primary endpoint of cardiovascular (CV) death, HF hospitalization, or aborted cardiac arrest.
Regional differences in the data, however, aroused concerns about the findings early on. Patients enrolled in Russia and the Republic of Georgia were younger, less likely to qualify on the basis of elevated natriuretic peptide levels, and had more evidence of ischemic heart disease than those in the Americas.
Event rates were also substantially lower in Russia/Georgia than in the Americas and in previous HFpEF trials, suggesting that many of these patients may not have had heart failure, the trialists argued.
In the Americas, results for the primary endpoint favor spironolactone over placebo (10.4 vs. 12.6 events per 100 patient-years; P = .026), whereas the rate in Russia/Georgia was much lower than in the Americas and slightly favors placebo (2.5 vs. 2.3 events/100 patient-years).
Medication noncompliance also may have been more common in Russia/Georgia based on pharmacodynamic studies and a 2017 analysis showing undetectable levels of canrenone, an active metabolite of spironolactone, in 30% of Russian versus 3% of North American patients who reported using the drug at 1 year.
TOPCAT investigator Marc Pfeffer, MD, PhD, from Brigham and Women’s Hospital and Harvard Medical School, Boston, said no trial is without flaws but that the observations represent serious misconduct. “Really we’re talking about a cancer, a cancer that has clear margins. The margins are Russia, Georgia that warrant censoring their data.”
The FDA’s own review of the National Institutes of Health–sponsored study, however, showed no significant interaction between treatment and region (P = .12) and “insufficient evidence to conclude the two regions are different enough such that overall results should not be considered,” said FDA statistician Ququan Liu, MD, MS.
She cautioned against removing data from a whole region that constituted almost half the study population and said it would set a precedent on what is considered substantial evidence for approval.
Several advisors concurred but, ultimately, the Cardiovascular and Renal Drugs Advisory Committee voted 8 to 4, with 1 abstention, that TOPCAT provides “sufficient evidence to support any indication.”
The same committee voted yesterday in support of an expanded role for sacubitril/valsartan (Entresto, Novartis) in select patients with HFpEF. In casting a “no” vote, panelist Steven E. Nissen, MD, from the Cleveland Clinic, said that decisions made by the panel set precedent.
“If the pharmaceutical industry came to us with a study like this and said the P value was .14 but we think a bunch of our sites weren’t very good and so we’re going to throw those data out and just look at the sites we like, the FDA would not have even brought that before us,” he said. “I cannot hold other sponsors, including our own government, to a different standard.”
Dr. Nissen argued that the primary endpoint failed by a significant margin (P = .138), the study was marginally powered, there was a troubling amount of missing data in the two regions, and spironolactone is also not without side effects. “Poor study conduct cannot be an excuse for a result we don’t like.”
Panel chair Julia B. Lewis, MD, from Vanderbilt University Medical Center in Nashville, Tenn., said she would love to support a cheap, generic drug to keep HF patients out of the hospital but was troubled by the egregious conduct of the trial and concerns about cherry-picking results. “My heart says this would be a great place for us to go but I can’t say that my head thinks this is an acceptable body of data.”
Several panelists, however, highlighted the benefits with spironolactone over placebo in the Americas including an 18% reduction in hospitalization for HF (21% vs. 25%; hazard ratio, 0.82; P = .04) and a 25% reduction in cumulative HF hospitalizations (361 vs. 438 events; incidence rate ratio, 0.75; P = .024).
There was also a reduction in CV mortality with spironolactone (11% vs. 14%; HR, 0.74; P = .027) – something, it was noted, not observed during the prior day’s proceeding on sacubitril/valsartan.
Panelist Christopher M. O’Connor, MD, from Inova Heart and Vascular Institute in Falls Church, Va., and Duke University, Durham, N.C., said he voted “yes” because of the totality of the information and that the investigators provided “compelling evidence” with or without the Russia/Georgia cohort on the efficacy on HF hospitalization reduction. “I think this is the augmented sweet spot of this data set.”
C. Michael Gibson, MD, said his decision to vote yes was not based on analyses that excluded half the patients but rather on the totality of the evidence, particularly the benefit on cumulative HF hospitalizations and in those with an EF lower than 56%.
Several panelists and members of the public cited for treatments among patients with HFpEF. Edward K. Kasper, MD, from Johns Hopkins University, Baltimore, said he found both sides of the argument persuasive but that he already uses spironolactone in this setting. “Somehow I’ve become convinced that this drug worked, so I voted yes.”
Dr. Kasper said the FDA may ultimately find there isn’t an indication for spironolactone in HFpEF but that it will likely move from a IIb to IIa recommendation in the next iteration of the American College of Cardiology guidelines.
Paul Ridker, MD, MPH, from Brigham and Women’s Hospital and Harvard Medical School, said he shared concerns about the precedent of dropping half the data, “even though, in this case, I believe half the data is wrong.”
Dr. Ridker noted that he would have been comfortable using the secondary endpoint of HF reduction as an indication in patients with mildly reduced EF but abstained because that data was not presented today, although it may be available from TOPCAT and the RALES trial.
The panel took up other nonvoting questions, including what additional data would be needed to augment support for approval. Suggestions ranged from additional analyses to a new trial, with TOPCAT serving as “pilot data,” but no recommendation was made.
A version of this article first appeared on Medscape.com.
Caregiver burden of outpatient ASCT for multiple myeloma comparable with inpatient transplant
Tending to patients who opt for outpatient autologous stem cell transplants is well tolerated by caregivers, so long as they have the resources and support necessary, according to a recent Italian report.
Investigators surveyed the primary caregivers – most often the spouse – of 25 multiple myeloma patients who, in consultation with their caregiver, opted for an outpatient procedure and 71 others who chose standard inpatient treatment, and compared the results. Outpatients were discharged a day after transplant with twice-weekly clinic visits until sustained hematologic recovery as reported in Clinical Lymphoma, Myeloma and Leukemia.
The teams used portions of the Caregiver Reaction Assessment survey that focused on self-reported sense of family support plus affect on daily activities and general health. Surveys were taken a week before transplant and 3 months afterwards.
Results did not differ significantly between outpatient and inpatient caregivers at either point, and there was no meaningful change in responses over time.
“The outpatient model neither improves nor impairs global caregivers’ burden, compared with” inpatient transplant. Outpatient caregivers “do not show that they suffer from a greater burden of responsibility as compared to those belonging to the inpatient’s arm,” said investigators led by Massimo Martino, MD, director of stem cell transplants at the Great Metropolitan Hospital in Reggio Calabria, Italy, where the patients were treated.
The relatively short-lasting neutropenia and the limited nonhematologic toxicity of high-dose melphalan make multiple myeloma good candidates for outpatient programs. Indeed, the incidence rate of mucositis, fever, chemotherapy-induced nausea and vomiting, and other adverse events did not differ between in and outpatients, which is in keeping with previous reports supporting the feasibility and safety of outpatient programs.
However, the burden on loved ones is considerable. At least during the aplastic phase, outpatient caregivers are on call around the clock and spend most of their time with the patient. Homes have to be kept meticulously clean, vital signs checked, medications administered, and ins and outs monitored, among other duties normally handled by inpatient staff.
The main limit of the study was that outpatients were a self-selected group. They and their caregivers may simply have had the resources and support needed for successful outpatient transplants, while other patients did not. As the investigators put it, “we cannot exclude the problem of residual confounding due to unmeasured variables” such as “factors underlying patients’ preference, which could potentially impact the study results.”
Administering the follow-up survey 3 months after transplant might also have missed the acute impact on outpatient caregivers. It’s been “reported that the quality of life of patients undergoing an” outpatient procedure decreases immediately post treatment but bounces back by 6 months. “The same result can probably be observed in caregivers,” the team said.
The outpatient and inpatient groups were comparable, with a majority of men and a mean age of about 60 years in both. The number of infused stem cells, engraftment kinetics, and hematopoietic cell transplantation–comorbidity index scores did not differ significantly between the two groups.
There was no funding for the work, and the investigators reported that they didn’t have any conflicts of interest.
SOURCE: Martino M et al. Clin Lymphoma Myeloma Leuk. 2020 Nov 19. doi: 10.1016/j.clml.2020.11.011.
Tending to patients who opt for outpatient autologous stem cell transplants is well tolerated by caregivers, so long as they have the resources and support necessary, according to a recent Italian report.
Investigators surveyed the primary caregivers – most often the spouse – of 25 multiple myeloma patients who, in consultation with their caregiver, opted for an outpatient procedure and 71 others who chose standard inpatient treatment, and compared the results. Outpatients were discharged a day after transplant with twice-weekly clinic visits until sustained hematologic recovery as reported in Clinical Lymphoma, Myeloma and Leukemia.
The teams used portions of the Caregiver Reaction Assessment survey that focused on self-reported sense of family support plus affect on daily activities and general health. Surveys were taken a week before transplant and 3 months afterwards.
Results did not differ significantly between outpatient and inpatient caregivers at either point, and there was no meaningful change in responses over time.
“The outpatient model neither improves nor impairs global caregivers’ burden, compared with” inpatient transplant. Outpatient caregivers “do not show that they suffer from a greater burden of responsibility as compared to those belonging to the inpatient’s arm,” said investigators led by Massimo Martino, MD, director of stem cell transplants at the Great Metropolitan Hospital in Reggio Calabria, Italy, where the patients were treated.
The relatively short-lasting neutropenia and the limited nonhematologic toxicity of high-dose melphalan make multiple myeloma good candidates for outpatient programs. Indeed, the incidence rate of mucositis, fever, chemotherapy-induced nausea and vomiting, and other adverse events did not differ between in and outpatients, which is in keeping with previous reports supporting the feasibility and safety of outpatient programs.
However, the burden on loved ones is considerable. At least during the aplastic phase, outpatient caregivers are on call around the clock and spend most of their time with the patient. Homes have to be kept meticulously clean, vital signs checked, medications administered, and ins and outs monitored, among other duties normally handled by inpatient staff.
The main limit of the study was that outpatients were a self-selected group. They and their caregivers may simply have had the resources and support needed for successful outpatient transplants, while other patients did not. As the investigators put it, “we cannot exclude the problem of residual confounding due to unmeasured variables” such as “factors underlying patients’ preference, which could potentially impact the study results.”
Administering the follow-up survey 3 months after transplant might also have missed the acute impact on outpatient caregivers. It’s been “reported that the quality of life of patients undergoing an” outpatient procedure decreases immediately post treatment but bounces back by 6 months. “The same result can probably be observed in caregivers,” the team said.
The outpatient and inpatient groups were comparable, with a majority of men and a mean age of about 60 years in both. The number of infused stem cells, engraftment kinetics, and hematopoietic cell transplantation–comorbidity index scores did not differ significantly between the two groups.
There was no funding for the work, and the investigators reported that they didn’t have any conflicts of interest.
SOURCE: Martino M et al. Clin Lymphoma Myeloma Leuk. 2020 Nov 19. doi: 10.1016/j.clml.2020.11.011.
Tending to patients who opt for outpatient autologous stem cell transplants is well tolerated by caregivers, so long as they have the resources and support necessary, according to a recent Italian report.
Investigators surveyed the primary caregivers – most often the spouse – of 25 multiple myeloma patients who, in consultation with their caregiver, opted for an outpatient procedure and 71 others who chose standard inpatient treatment, and compared the results. Outpatients were discharged a day after transplant with twice-weekly clinic visits until sustained hematologic recovery as reported in Clinical Lymphoma, Myeloma and Leukemia.
The teams used portions of the Caregiver Reaction Assessment survey that focused on self-reported sense of family support plus affect on daily activities and general health. Surveys were taken a week before transplant and 3 months afterwards.
Results did not differ significantly between outpatient and inpatient caregivers at either point, and there was no meaningful change in responses over time.
“The outpatient model neither improves nor impairs global caregivers’ burden, compared with” inpatient transplant. Outpatient caregivers “do not show that they suffer from a greater burden of responsibility as compared to those belonging to the inpatient’s arm,” said investigators led by Massimo Martino, MD, director of stem cell transplants at the Great Metropolitan Hospital in Reggio Calabria, Italy, where the patients were treated.
The relatively short-lasting neutropenia and the limited nonhematologic toxicity of high-dose melphalan make multiple myeloma good candidates for outpatient programs. Indeed, the incidence rate of mucositis, fever, chemotherapy-induced nausea and vomiting, and other adverse events did not differ between in and outpatients, which is in keeping with previous reports supporting the feasibility and safety of outpatient programs.
However, the burden on loved ones is considerable. At least during the aplastic phase, outpatient caregivers are on call around the clock and spend most of their time with the patient. Homes have to be kept meticulously clean, vital signs checked, medications administered, and ins and outs monitored, among other duties normally handled by inpatient staff.
The main limit of the study was that outpatients were a self-selected group. They and their caregivers may simply have had the resources and support needed for successful outpatient transplants, while other patients did not. As the investigators put it, “we cannot exclude the problem of residual confounding due to unmeasured variables” such as “factors underlying patients’ preference, which could potentially impact the study results.”
Administering the follow-up survey 3 months after transplant might also have missed the acute impact on outpatient caregivers. It’s been “reported that the quality of life of patients undergoing an” outpatient procedure decreases immediately post treatment but bounces back by 6 months. “The same result can probably be observed in caregivers,” the team said.
The outpatient and inpatient groups were comparable, with a majority of men and a mean age of about 60 years in both. The number of infused stem cells, engraftment kinetics, and hematopoietic cell transplantation–comorbidity index scores did not differ significantly between the two groups.
There was no funding for the work, and the investigators reported that they didn’t have any conflicts of interest.
SOURCE: Martino M et al. Clin Lymphoma Myeloma Leuk. 2020 Nov 19. doi: 10.1016/j.clml.2020.11.011.
FROM CLINICAL LYMPHOMA, MYELOMA AND LEUKEMIA
Flattening the hierarchy
What fellows can learn about leadership from aircraft crews
Fellowship is a time of great growth for pediatric hospital medicine fellows as clinicians, educators, scholars, and as leaders. Leadership is a crucial skill for hospitalists that is cultivated throughout fellowship. As fellows, we step into the role of clinical team leader for the first time and it is our responsibility to create a clinical and educational environment that is safe, inviting and engaging.
For possibly the first time in our careers, pediatric hospital medicine fellows are expected to make final decisions, big and small. We are faced with high-pressure situations almost daily, whether it is a rapid response on a patient, tough diagnostic and therapeutic decisions, difficult conversations with families, or dealing with challenging team members.
Soon after starting fellowship I was faced with a such a situation. The patient was a 6-month-old infant with trisomy 21 who was admitted because of feeding difficulties. They were working on oral feeds but required nasogastric (NG) feeds to meet caloric needs. On my first day on service, the residents indicated that the medical team desired the patient to have a gastrostomy tube (G-tube) placed. I was hoping to send the patient home for a few weeks with the NG tube to see if they were making progress on their oral feeds before deciding on the need for a G-tube. However, the patient’s parents pulled me aside in the hallway and said they were considering a third possibility.
The parents felt strongly about a trial period of a few weeks without the NG tube to see if the patient was able to maintain adequate weight gain with just oral feeds. The bedside nurse reiterated that the family felt their concerns had not been considered up until this point. As the fellow and team leader, it was my job to navigate between my resident team, myself, and the family in order to make a final decision. Through a bedside meeting and shared decision making, we were able to compromise and negotiate a decision, allowing the patient to go home on just oral feeds with close follow-up with their pediatrician. Afterwards, I found myself searching for strategies to be a better leader in these situations.
I found a potential answer in a recent article from the Harvard Business Review titled “What Aircraft Crews Know About Managing High-Pressure Situations.”1 The article discusses crew resource management (CRM), which was developed in the 1980s and is used in civil and military aviation worldwide. CRM is based on two principles to improve crisis management: The hierarchy on the flight deck must be flattened, and crew members must be actively integrated into the flight’s work flows and decision-making processes.
The authors of the article conducted two different studies to further understand CRM and its effects. The first study included observing 11 flight crews in emergency simulations. In the study, the flight crew had to react to an emergency, and then conduct a landing of the aircraft. What the authors found was that the captain’s style of communication had a major impact on crew performance in two major ways: Crews performed consistently better under times of pressure when the copilot was included in the decision-making process, and captains who asked open-ended questions (“How do you assess the situation”) came up with better solutions than captains who asked “yes or no” questions.
The authors conclude that “involving colleagues as equal decision partners by asking them questions…aids constructive, factual information exchange.” The second study consisted of conducting 61 interviews with flight crew members to better understand crisis management. In the interviews, the same theme occurred, that open-ended questions are vital in all decision-making processes and may be preventative against dangerous or imperfect outcomes. As fellows and team leaders we can learn from CRM and these studies. We need to flatten the hierarchy and ask open-ended questions.
To flatten the hierarchy, we should value the thoughts and opinions of all our team members. Now more than ever in this current COVID-19 pandemic with many hospitals instituting telehealth/telerounding for some or all team members, it is essential to utilize our entire “flight crew” (physicians, nurses, therapists, subspecialists, social worker, case managers, etc.) during routine decisions and high-stake decisions. We should make sure our flight crew, especially the bedside nurse is part of the decision-making process.2 This means we need to ensure they are present and given a voice on clinical rounds. To flatten the hierarchy, we must take pride in eliciting other team member’s opinions. We must realize that we alone do not have all the answers, and other team members may have different frameworks in which they process a decision.
Finally, in medicine, our patients and families are included in our flight crew. They too must have a voice in the decision-making process. Previous studies have shown that patients and families desire to be included in the decision-making process, and opportunities exist to improve shared decision-making in pediatrics.3-5 Lastly, we should commit to asking open-ended questions from our team and our patients. We should value their input and use their answers and frameworks to make the best decision for our patients.
I wasn’t aware at the time, but I was using some of the principles of CRM while navigating my high-pressure situation. A bedside meeting with all team members and the patient’s family helped to flatten the hierarchy by understanding and valuing each team member’s input. Asking open-ended questions of the different team members led to a more inviting and engaging clinical and learning environment. These strategies helped to lead our team into a clinical decision that wasn’t entirely clear at first but ended up being the best decision for the patient, as they are now thriving without ever requiring supplemental nutrition after discharge.
As physicians, we have learned a lot from the airline industry about wellness and the effect of fatigue on performance. It is clear now that we can also learn from them about clinical decision-making and leadership strategies. When adopted for health care, CRM principles have been shown to result in a culture of safety and long-term behavioral change.6,7 If we can model ourselves after the airline industry by following the principles of CRM, then we will be better clinicians, educators, and leaders.
Dr. Palmer is a second-year pediatric hospital medicine fellow at Children’s Hospital Los Angeles and is working toward a masters in academic medicine at the University of Southern California, Los Angeles, with a focus on curriculum development and educational scholarship production.
References
1. Hagan J et al. What Aircraft Crews Know About Managing High-Pressure Situations. Harvard Business Review. 2019 Dec. https://hbr.org/2019/12/what-aircraft-crews-know-about-managing-high-pressure-situations
2. Erickson J. Bedside nurse involvement in end-of-life decision-making: A brief review of the literature. Dimens Crit Care Nurs. 2013;32(2):65-8.
3. Richards CA et al. Physicians perceptions of shared decision-making in neonatal and pediatric critical care. Am J Hosp Palliat Care. 2018;35(4):669-76.
4. Boland L et al. Barriers and facilitators of pediatric shared decision-making: A systematic review. Implement Sci. 2019 Jan 18. doi: 10.1186/s13012-018-0851-5.
5. Blankenburg R et al. Shared decision-making during inpatient rounds: Opportunities for improvement in patient engagement and communication. J Hosp Med. 2018;13(7):453-61.
6. Kemper PF et al. Crew resource management training in the intensive care unit. A multisite controlled before-after study. BMJ Qual Saf. 2016;25(8):577-87.
7. Sax HC et al. Can aviation-based team training elicit sustainable behavioral change? Arch Surg. 2009;144(12):1133-7.
What fellows can learn about leadership from aircraft crews
What fellows can learn about leadership from aircraft crews
Fellowship is a time of great growth for pediatric hospital medicine fellows as clinicians, educators, scholars, and as leaders. Leadership is a crucial skill for hospitalists that is cultivated throughout fellowship. As fellows, we step into the role of clinical team leader for the first time and it is our responsibility to create a clinical and educational environment that is safe, inviting and engaging.
For possibly the first time in our careers, pediatric hospital medicine fellows are expected to make final decisions, big and small. We are faced with high-pressure situations almost daily, whether it is a rapid response on a patient, tough diagnostic and therapeutic decisions, difficult conversations with families, or dealing with challenging team members.
Soon after starting fellowship I was faced with a such a situation. The patient was a 6-month-old infant with trisomy 21 who was admitted because of feeding difficulties. They were working on oral feeds but required nasogastric (NG) feeds to meet caloric needs. On my first day on service, the residents indicated that the medical team desired the patient to have a gastrostomy tube (G-tube) placed. I was hoping to send the patient home for a few weeks with the NG tube to see if they were making progress on their oral feeds before deciding on the need for a G-tube. However, the patient’s parents pulled me aside in the hallway and said they were considering a third possibility.
The parents felt strongly about a trial period of a few weeks without the NG tube to see if the patient was able to maintain adequate weight gain with just oral feeds. The bedside nurse reiterated that the family felt their concerns had not been considered up until this point. As the fellow and team leader, it was my job to navigate between my resident team, myself, and the family in order to make a final decision. Through a bedside meeting and shared decision making, we were able to compromise and negotiate a decision, allowing the patient to go home on just oral feeds with close follow-up with their pediatrician. Afterwards, I found myself searching for strategies to be a better leader in these situations.
I found a potential answer in a recent article from the Harvard Business Review titled “What Aircraft Crews Know About Managing High-Pressure Situations.”1 The article discusses crew resource management (CRM), which was developed in the 1980s and is used in civil and military aviation worldwide. CRM is based on two principles to improve crisis management: The hierarchy on the flight deck must be flattened, and crew members must be actively integrated into the flight’s work flows and decision-making processes.
The authors of the article conducted two different studies to further understand CRM and its effects. The first study included observing 11 flight crews in emergency simulations. In the study, the flight crew had to react to an emergency, and then conduct a landing of the aircraft. What the authors found was that the captain’s style of communication had a major impact on crew performance in two major ways: Crews performed consistently better under times of pressure when the copilot was included in the decision-making process, and captains who asked open-ended questions (“How do you assess the situation”) came up with better solutions than captains who asked “yes or no” questions.
The authors conclude that “involving colleagues as equal decision partners by asking them questions…aids constructive, factual information exchange.” The second study consisted of conducting 61 interviews with flight crew members to better understand crisis management. In the interviews, the same theme occurred, that open-ended questions are vital in all decision-making processes and may be preventative against dangerous or imperfect outcomes. As fellows and team leaders we can learn from CRM and these studies. We need to flatten the hierarchy and ask open-ended questions.
To flatten the hierarchy, we should value the thoughts and opinions of all our team members. Now more than ever in this current COVID-19 pandemic with many hospitals instituting telehealth/telerounding for some or all team members, it is essential to utilize our entire “flight crew” (physicians, nurses, therapists, subspecialists, social worker, case managers, etc.) during routine decisions and high-stake decisions. We should make sure our flight crew, especially the bedside nurse is part of the decision-making process.2 This means we need to ensure they are present and given a voice on clinical rounds. To flatten the hierarchy, we must take pride in eliciting other team member’s opinions. We must realize that we alone do not have all the answers, and other team members may have different frameworks in which they process a decision.
Finally, in medicine, our patients and families are included in our flight crew. They too must have a voice in the decision-making process. Previous studies have shown that patients and families desire to be included in the decision-making process, and opportunities exist to improve shared decision-making in pediatrics.3-5 Lastly, we should commit to asking open-ended questions from our team and our patients. We should value their input and use their answers and frameworks to make the best decision for our patients.
I wasn’t aware at the time, but I was using some of the principles of CRM while navigating my high-pressure situation. A bedside meeting with all team members and the patient’s family helped to flatten the hierarchy by understanding and valuing each team member’s input. Asking open-ended questions of the different team members led to a more inviting and engaging clinical and learning environment. These strategies helped to lead our team into a clinical decision that wasn’t entirely clear at first but ended up being the best decision for the patient, as they are now thriving without ever requiring supplemental nutrition after discharge.
As physicians, we have learned a lot from the airline industry about wellness and the effect of fatigue on performance. It is clear now that we can also learn from them about clinical decision-making and leadership strategies. When adopted for health care, CRM principles have been shown to result in a culture of safety and long-term behavioral change.6,7 If we can model ourselves after the airline industry by following the principles of CRM, then we will be better clinicians, educators, and leaders.
Dr. Palmer is a second-year pediatric hospital medicine fellow at Children’s Hospital Los Angeles and is working toward a masters in academic medicine at the University of Southern California, Los Angeles, with a focus on curriculum development and educational scholarship production.
References
1. Hagan J et al. What Aircraft Crews Know About Managing High-Pressure Situations. Harvard Business Review. 2019 Dec. https://hbr.org/2019/12/what-aircraft-crews-know-about-managing-high-pressure-situations
2. Erickson J. Bedside nurse involvement in end-of-life decision-making: A brief review of the literature. Dimens Crit Care Nurs. 2013;32(2):65-8.
3. Richards CA et al. Physicians perceptions of shared decision-making in neonatal and pediatric critical care. Am J Hosp Palliat Care. 2018;35(4):669-76.
4. Boland L et al. Barriers and facilitators of pediatric shared decision-making: A systematic review. Implement Sci. 2019 Jan 18. doi: 10.1186/s13012-018-0851-5.
5. Blankenburg R et al. Shared decision-making during inpatient rounds: Opportunities for improvement in patient engagement and communication. J Hosp Med. 2018;13(7):453-61.
6. Kemper PF et al. Crew resource management training in the intensive care unit. A multisite controlled before-after study. BMJ Qual Saf. 2016;25(8):577-87.
7. Sax HC et al. Can aviation-based team training elicit sustainable behavioral change? Arch Surg. 2009;144(12):1133-7.
Fellowship is a time of great growth for pediatric hospital medicine fellows as clinicians, educators, scholars, and as leaders. Leadership is a crucial skill for hospitalists that is cultivated throughout fellowship. As fellows, we step into the role of clinical team leader for the first time and it is our responsibility to create a clinical and educational environment that is safe, inviting and engaging.
For possibly the first time in our careers, pediatric hospital medicine fellows are expected to make final decisions, big and small. We are faced with high-pressure situations almost daily, whether it is a rapid response on a patient, tough diagnostic and therapeutic decisions, difficult conversations with families, or dealing with challenging team members.
Soon after starting fellowship I was faced with a such a situation. The patient was a 6-month-old infant with trisomy 21 who was admitted because of feeding difficulties. They were working on oral feeds but required nasogastric (NG) feeds to meet caloric needs. On my first day on service, the residents indicated that the medical team desired the patient to have a gastrostomy tube (G-tube) placed. I was hoping to send the patient home for a few weeks with the NG tube to see if they were making progress on their oral feeds before deciding on the need for a G-tube. However, the patient’s parents pulled me aside in the hallway and said they were considering a third possibility.
The parents felt strongly about a trial period of a few weeks without the NG tube to see if the patient was able to maintain adequate weight gain with just oral feeds. The bedside nurse reiterated that the family felt their concerns had not been considered up until this point. As the fellow and team leader, it was my job to navigate between my resident team, myself, and the family in order to make a final decision. Through a bedside meeting and shared decision making, we were able to compromise and negotiate a decision, allowing the patient to go home on just oral feeds with close follow-up with their pediatrician. Afterwards, I found myself searching for strategies to be a better leader in these situations.
I found a potential answer in a recent article from the Harvard Business Review titled “What Aircraft Crews Know About Managing High-Pressure Situations.”1 The article discusses crew resource management (CRM), which was developed in the 1980s and is used in civil and military aviation worldwide. CRM is based on two principles to improve crisis management: The hierarchy on the flight deck must be flattened, and crew members must be actively integrated into the flight’s work flows and decision-making processes.
The authors of the article conducted two different studies to further understand CRM and its effects. The first study included observing 11 flight crews in emergency simulations. In the study, the flight crew had to react to an emergency, and then conduct a landing of the aircraft. What the authors found was that the captain’s style of communication had a major impact on crew performance in two major ways: Crews performed consistently better under times of pressure when the copilot was included in the decision-making process, and captains who asked open-ended questions (“How do you assess the situation”) came up with better solutions than captains who asked “yes or no” questions.
The authors conclude that “involving colleagues as equal decision partners by asking them questions…aids constructive, factual information exchange.” The second study consisted of conducting 61 interviews with flight crew members to better understand crisis management. In the interviews, the same theme occurred, that open-ended questions are vital in all decision-making processes and may be preventative against dangerous or imperfect outcomes. As fellows and team leaders we can learn from CRM and these studies. We need to flatten the hierarchy and ask open-ended questions.
To flatten the hierarchy, we should value the thoughts and opinions of all our team members. Now more than ever in this current COVID-19 pandemic with many hospitals instituting telehealth/telerounding for some or all team members, it is essential to utilize our entire “flight crew” (physicians, nurses, therapists, subspecialists, social worker, case managers, etc.) during routine decisions and high-stake decisions. We should make sure our flight crew, especially the bedside nurse is part of the decision-making process.2 This means we need to ensure they are present and given a voice on clinical rounds. To flatten the hierarchy, we must take pride in eliciting other team member’s opinions. We must realize that we alone do not have all the answers, and other team members may have different frameworks in which they process a decision.
Finally, in medicine, our patients and families are included in our flight crew. They too must have a voice in the decision-making process. Previous studies have shown that patients and families desire to be included in the decision-making process, and opportunities exist to improve shared decision-making in pediatrics.3-5 Lastly, we should commit to asking open-ended questions from our team and our patients. We should value their input and use their answers and frameworks to make the best decision for our patients.
I wasn’t aware at the time, but I was using some of the principles of CRM while navigating my high-pressure situation. A bedside meeting with all team members and the patient’s family helped to flatten the hierarchy by understanding and valuing each team member’s input. Asking open-ended questions of the different team members led to a more inviting and engaging clinical and learning environment. These strategies helped to lead our team into a clinical decision that wasn’t entirely clear at first but ended up being the best decision for the patient, as they are now thriving without ever requiring supplemental nutrition after discharge.
As physicians, we have learned a lot from the airline industry about wellness and the effect of fatigue on performance. It is clear now that we can also learn from them about clinical decision-making and leadership strategies. When adopted for health care, CRM principles have been shown to result in a culture of safety and long-term behavioral change.6,7 If we can model ourselves after the airline industry by following the principles of CRM, then we will be better clinicians, educators, and leaders.
Dr. Palmer is a second-year pediatric hospital medicine fellow at Children’s Hospital Los Angeles and is working toward a masters in academic medicine at the University of Southern California, Los Angeles, with a focus on curriculum development and educational scholarship production.
References
1. Hagan J et al. What Aircraft Crews Know About Managing High-Pressure Situations. Harvard Business Review. 2019 Dec. https://hbr.org/2019/12/what-aircraft-crews-know-about-managing-high-pressure-situations
2. Erickson J. Bedside nurse involvement in end-of-life decision-making: A brief review of the literature. Dimens Crit Care Nurs. 2013;32(2):65-8.
3. Richards CA et al. Physicians perceptions of shared decision-making in neonatal and pediatric critical care. Am J Hosp Palliat Care. 2018;35(4):669-76.
4. Boland L et al. Barriers and facilitators of pediatric shared decision-making: A systematic review. Implement Sci. 2019 Jan 18. doi: 10.1186/s13012-018-0851-5.
5. Blankenburg R et al. Shared decision-making during inpatient rounds: Opportunities for improvement in patient engagement and communication. J Hosp Med. 2018;13(7):453-61.
6. Kemper PF et al. Crew resource management training in the intensive care unit. A multisite controlled before-after study. BMJ Qual Saf. 2016;25(8):577-87.
7. Sax HC et al. Can aviation-based team training elicit sustainable behavioral change? Arch Surg. 2009;144(12):1133-7.
Should I be afraid of getting COVID again?
Is it over or do I have to brace myself for the possibility of a reinfection? Moreover, could the second time potentially be worse than the first?
I was diagnosed with COVID in March of this year. After spending 10 days in the hospital, and one night in the ICU, it took another 2 months for the air-hunger, headaches, and fatigue to completely resolve. Compared with many other unfortunate victims, I did all right – and I am very grateful for the care I received.
Now, as the surge in cases takes new life, I will be on the front lines taking care of patients. Having had an eventful personal encounter with the virus, I now have a unique vantage point and remain fully committed to paying my fortunate circumstances forward. Although I can’t help but have the same question faced by millions of others: Am I safe now?
It is no surprise that studies have shown health care workers comprising 6% of COVID hospital admissions, with one-third of these admissions being nurses. Recently, we heard that over 900 health care workers at Mayo Clinic had acquired the infection in the first 2 weeks of the ongoing second COVID surge. Are these frontline workers protected? Can they return to work with no fear of a rerun? Or, for that matter, anyone who has been afflicted by COVID – are they now forever immune?
There are no clear answers here. But to understand this a little, let’s quickly revisit some basic principles of immunity.
Innate and adaptive immunity
Simply put, there are two forms of immunity: innate and adaptive. Innate immunity encompasses our body’s natural protective mechanisms that come into play almost immediately. This enables recognition of the virus and activates an immediate antiviral defense and attempt at removal of the infective agent. This, however, does not always do the job. Accordingly, a couple weeks after the initial exposure to the pathogen, adaptive immunity is invoked. Circulating white blood cells within our body recognize the virus and set off an immune response, involving the activation of T and B cells that actively attack the infective agent. It is this T- and B-cell–mediated immunity that should protect one against a second infection with the same agent.
What about herd immunity?
Herd immunity is defined as essentially yielding to the virus and letting it spread naturally in order to develop community-wide immunity. By consequence of a large proportion of the population becoming immune after exposure to the disease, person-to-person spread can potentially be mitigated. This does not confer immunity to the virus at the individual level; rather, it reduces the risk of vulnerable people coming in contact with the pathogen.
Unfortunately, depending on herd immunity as a way to deal with COVID-19 has not worked well, even in well-contained countries like Sweden, where a disproportionate number of their most vulnerable populations have died. It is self-evident that containment strategies with vaccination may be our best way forward to achieve herd immunity. Not surrendering to the virus.
Am I safe from reinfection?
In all honesty, we’re not entirely sure. But it is important to recognize a few points when considering your relative safety.
- The immune system is far from perfect. Not everyone has a robust immune response. And in those who do, the immune response can wane over time, potentially allowing for reinfection. While rare, there have already been some clearly documented reinfections, four that have been confirmed and published; two patients (in Nevada and Ecuador) actually fared worse the second time around.
- The virus can mutate and escape detection by the immune system. One could still be susceptible to reinfection from a different strain. (At least, this remains the case with the influenza virus.) There is some evidence that SARS-CoV-2 does not mutate rapidly, and hence this may not be a problem. But we don’t know for certain, at least as of yet.
- Even a vigorous immune response can be overwhelmed by the virus. It is unclear whether the relative length of time and the amount of virus exposure could undermine a previously primed immune system.
A prior infection and a consequent healthy immunity may help you combat a reinfection but it does not prevent you from harboring or carrying the virus. You may be asymptomatic, but you can still be a carrier and spread the infection. I am a strong advocate for limiting your exposure to others no matter your previous exposure status, in order to limit the spread of the virus.
So, what should I do?
I guess the answer is that you can’t be too careful. Not everyone has had their antibody levels tested, and even if positive, it is unclear how well that affords protection. It is best to presume that you are vulnerable for a reinfection and that you can still carry and spread the virus. This may be the safest approach until we actually achieve herd immunity through vaccination.
Even then, for a period of time, there will remain a sense of uncertainty. So, containment strategies inclusive of distancing and masking will and should remain a way of life at least until mid-2021, when we will be in a better position to reassess the landscape.
The surge is back. As I repay my debt and get back to the front line, I will continue to mask up and practice distancing. I am taking no chances of getting reinfected or being an asymptomatic carrier.
I had COVID, I also have antibodies, and I will be taking the vaccine. I implore you all to do the same.
Jag Singh is a physician, scientist, and professor at Harvard. He is passionate about social issues, leadership, digital health, and medical innovations. You can follow him on Twitter @JagSinghMD.
A version of this article first appeared on Medscape.com.
Is it over or do I have to brace myself for the possibility of a reinfection? Moreover, could the second time potentially be worse than the first?
I was diagnosed with COVID in March of this year. After spending 10 days in the hospital, and one night in the ICU, it took another 2 months for the air-hunger, headaches, and fatigue to completely resolve. Compared with many other unfortunate victims, I did all right – and I am very grateful for the care I received.
Now, as the surge in cases takes new life, I will be on the front lines taking care of patients. Having had an eventful personal encounter with the virus, I now have a unique vantage point and remain fully committed to paying my fortunate circumstances forward. Although I can’t help but have the same question faced by millions of others: Am I safe now?
It is no surprise that studies have shown health care workers comprising 6% of COVID hospital admissions, with one-third of these admissions being nurses. Recently, we heard that over 900 health care workers at Mayo Clinic had acquired the infection in the first 2 weeks of the ongoing second COVID surge. Are these frontline workers protected? Can they return to work with no fear of a rerun? Or, for that matter, anyone who has been afflicted by COVID – are they now forever immune?
There are no clear answers here. But to understand this a little, let’s quickly revisit some basic principles of immunity.
Innate and adaptive immunity
Simply put, there are two forms of immunity: innate and adaptive. Innate immunity encompasses our body’s natural protective mechanisms that come into play almost immediately. This enables recognition of the virus and activates an immediate antiviral defense and attempt at removal of the infective agent. This, however, does not always do the job. Accordingly, a couple weeks after the initial exposure to the pathogen, adaptive immunity is invoked. Circulating white blood cells within our body recognize the virus and set off an immune response, involving the activation of T and B cells that actively attack the infective agent. It is this T- and B-cell–mediated immunity that should protect one against a second infection with the same agent.
What about herd immunity?
Herd immunity is defined as essentially yielding to the virus and letting it spread naturally in order to develop community-wide immunity. By consequence of a large proportion of the population becoming immune after exposure to the disease, person-to-person spread can potentially be mitigated. This does not confer immunity to the virus at the individual level; rather, it reduces the risk of vulnerable people coming in contact with the pathogen.
Unfortunately, depending on herd immunity as a way to deal with COVID-19 has not worked well, even in well-contained countries like Sweden, where a disproportionate number of their most vulnerable populations have died. It is self-evident that containment strategies with vaccination may be our best way forward to achieve herd immunity. Not surrendering to the virus.
Am I safe from reinfection?
In all honesty, we’re not entirely sure. But it is important to recognize a few points when considering your relative safety.
- The immune system is far from perfect. Not everyone has a robust immune response. And in those who do, the immune response can wane over time, potentially allowing for reinfection. While rare, there have already been some clearly documented reinfections, four that have been confirmed and published; two patients (in Nevada and Ecuador) actually fared worse the second time around.
- The virus can mutate and escape detection by the immune system. One could still be susceptible to reinfection from a different strain. (At least, this remains the case with the influenza virus.) There is some evidence that SARS-CoV-2 does not mutate rapidly, and hence this may not be a problem. But we don’t know for certain, at least as of yet.
- Even a vigorous immune response can be overwhelmed by the virus. It is unclear whether the relative length of time and the amount of virus exposure could undermine a previously primed immune system.
A prior infection and a consequent healthy immunity may help you combat a reinfection but it does not prevent you from harboring or carrying the virus. You may be asymptomatic, but you can still be a carrier and spread the infection. I am a strong advocate for limiting your exposure to others no matter your previous exposure status, in order to limit the spread of the virus.
So, what should I do?
I guess the answer is that you can’t be too careful. Not everyone has had their antibody levels tested, and even if positive, it is unclear how well that affords protection. It is best to presume that you are vulnerable for a reinfection and that you can still carry and spread the virus. This may be the safest approach until we actually achieve herd immunity through vaccination.
Even then, for a period of time, there will remain a sense of uncertainty. So, containment strategies inclusive of distancing and masking will and should remain a way of life at least until mid-2021, when we will be in a better position to reassess the landscape.
The surge is back. As I repay my debt and get back to the front line, I will continue to mask up and practice distancing. I am taking no chances of getting reinfected or being an asymptomatic carrier.
I had COVID, I also have antibodies, and I will be taking the vaccine. I implore you all to do the same.
Jag Singh is a physician, scientist, and professor at Harvard. He is passionate about social issues, leadership, digital health, and medical innovations. You can follow him on Twitter @JagSinghMD.
A version of this article first appeared on Medscape.com.
Is it over or do I have to brace myself for the possibility of a reinfection? Moreover, could the second time potentially be worse than the first?
I was diagnosed with COVID in March of this year. After spending 10 days in the hospital, and one night in the ICU, it took another 2 months for the air-hunger, headaches, and fatigue to completely resolve. Compared with many other unfortunate victims, I did all right – and I am very grateful for the care I received.
Now, as the surge in cases takes new life, I will be on the front lines taking care of patients. Having had an eventful personal encounter with the virus, I now have a unique vantage point and remain fully committed to paying my fortunate circumstances forward. Although I can’t help but have the same question faced by millions of others: Am I safe now?
It is no surprise that studies have shown health care workers comprising 6% of COVID hospital admissions, with one-third of these admissions being nurses. Recently, we heard that over 900 health care workers at Mayo Clinic had acquired the infection in the first 2 weeks of the ongoing second COVID surge. Are these frontline workers protected? Can they return to work with no fear of a rerun? Or, for that matter, anyone who has been afflicted by COVID – are they now forever immune?
There are no clear answers here. But to understand this a little, let’s quickly revisit some basic principles of immunity.
Innate and adaptive immunity
Simply put, there are two forms of immunity: innate and adaptive. Innate immunity encompasses our body’s natural protective mechanisms that come into play almost immediately. This enables recognition of the virus and activates an immediate antiviral defense and attempt at removal of the infective agent. This, however, does not always do the job. Accordingly, a couple weeks after the initial exposure to the pathogen, adaptive immunity is invoked. Circulating white blood cells within our body recognize the virus and set off an immune response, involving the activation of T and B cells that actively attack the infective agent. It is this T- and B-cell–mediated immunity that should protect one against a second infection with the same agent.
What about herd immunity?
Herd immunity is defined as essentially yielding to the virus and letting it spread naturally in order to develop community-wide immunity. By consequence of a large proportion of the population becoming immune after exposure to the disease, person-to-person spread can potentially be mitigated. This does not confer immunity to the virus at the individual level; rather, it reduces the risk of vulnerable people coming in contact with the pathogen.
Unfortunately, depending on herd immunity as a way to deal with COVID-19 has not worked well, even in well-contained countries like Sweden, where a disproportionate number of their most vulnerable populations have died. It is self-evident that containment strategies with vaccination may be our best way forward to achieve herd immunity. Not surrendering to the virus.
Am I safe from reinfection?
In all honesty, we’re not entirely sure. But it is important to recognize a few points when considering your relative safety.
- The immune system is far from perfect. Not everyone has a robust immune response. And in those who do, the immune response can wane over time, potentially allowing for reinfection. While rare, there have already been some clearly documented reinfections, four that have been confirmed and published; two patients (in Nevada and Ecuador) actually fared worse the second time around.
- The virus can mutate and escape detection by the immune system. One could still be susceptible to reinfection from a different strain. (At least, this remains the case with the influenza virus.) There is some evidence that SARS-CoV-2 does not mutate rapidly, and hence this may not be a problem. But we don’t know for certain, at least as of yet.
- Even a vigorous immune response can be overwhelmed by the virus. It is unclear whether the relative length of time and the amount of virus exposure could undermine a previously primed immune system.
A prior infection and a consequent healthy immunity may help you combat a reinfection but it does not prevent you from harboring or carrying the virus. You may be asymptomatic, but you can still be a carrier and spread the infection. I am a strong advocate for limiting your exposure to others no matter your previous exposure status, in order to limit the spread of the virus.
So, what should I do?
I guess the answer is that you can’t be too careful. Not everyone has had their antibody levels tested, and even if positive, it is unclear how well that affords protection. It is best to presume that you are vulnerable for a reinfection and that you can still carry and spread the virus. This may be the safest approach until we actually achieve herd immunity through vaccination.
Even then, for a period of time, there will remain a sense of uncertainty. So, containment strategies inclusive of distancing and masking will and should remain a way of life at least until mid-2021, when we will be in a better position to reassess the landscape.
The surge is back. As I repay my debt and get back to the front line, I will continue to mask up and practice distancing. I am taking no chances of getting reinfected or being an asymptomatic carrier.
I had COVID, I also have antibodies, and I will be taking the vaccine. I implore you all to do the same.
Jag Singh is a physician, scientist, and professor at Harvard. He is passionate about social issues, leadership, digital health, and medical innovations. You can follow him on Twitter @JagSinghMD.
A version of this article first appeared on Medscape.com.
Generalized pustular eruption
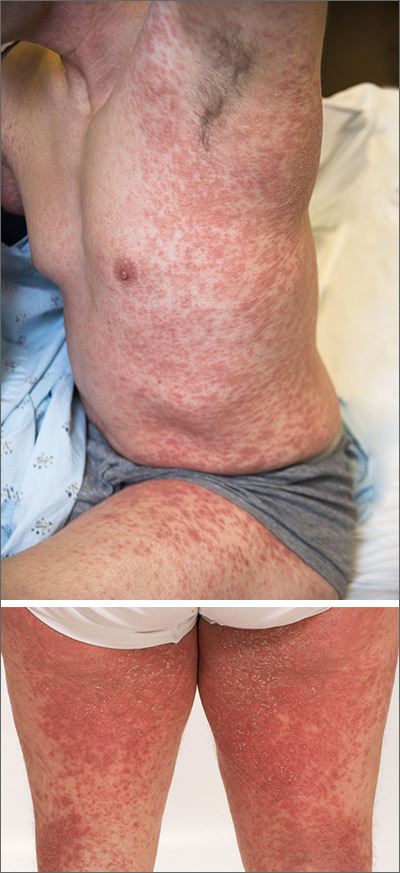
The acute rash with minute pustules and associated leukocytosis with neutrophilia and eosinophilia led to a diagnosis of acute generalized exanthematous pustulosis (AGEP), which may have been triggered by azithromycin—the patient’s only recent medication. AGEP is a severe cutaneous eruption that may be associated with systemic involvement. Medications are usually implicated, and patients often seek urgent evaluation.
AGEP typically begins as an acute eruption in the intertriginous sites of the axilla, groin, and neck, but often becomes more generalized. The diagnosis is strongly suggested by the condition’s key features: fever (97% of cases) and leukocytosis (87%) with neutrophilia (91%) and eosinophilia (30%). Leukocytosis peaks 4 days after pustulosis occurs and lasts for about 12 days. Although common, fever is not always documented in patients with AGEP. (This patient was a case in point.)
In approximately 90% of AGEP cases, medications such as antibiotics and calcium channel blockers are implicated; however, the lack of such an association does not preclude the diagnosis. In cases of drug reactions, the eruption typically develops 1 to 2 days after a medication is begun, and the pustules typically resolve in fewer than 15 days. In 17% of patients, systemic involvement can occur and can include the liver, kidneys, bone marrow, and lungs. A physical exam, review of systems, and a laboratory evaluation can help rule out systemic involvement and guide additional testing.
AGEP has an incidence of 1 to 5 cases per million people per year, affecting women slightly more frequently than men. While the pathophysiology is not well understood, AGEP and its differential diagnoses are categorized as T cell-related inflammatory responses.
There are at least 4 severe cutaneous eruptions that might be confused with AGEP, all of which may be associated with fever. They include a drug reaction with eosinophilia and systemic symptoms, Stevens-Johnson syndrome, toxic epidermal necrolysis, and pustular psoriasis. The clinical features that may help differentiate these conditions from AGEP include timeline, mucocutaneous features, organ system involvement, and histopathologic findings.
Patients who have AGEP, including those with systemic involvement, generally improve after the offending drug is discontinued and treatment with topical corticosteroids is initiated. A brief course of systemic corticosteroids can also be considered for patients with severe skin involvement or systemic involvement.
This patient was prescribed topical corticosteroid wet dressing treatments twice daily for 2 weeks. At the 2-week follow-up visit, the rash had completely cleared and only minimal residual erythema was noted. The patient was instructed to avoid azithromycin.
This case was adapted from: Tolkachjov SN, Wetter DA, Sandefur BJ. Generalized pustular eruption. J Fam Pract. 2018;67:309-310,312.

The acute rash with minute pustules and associated leukocytosis with neutrophilia and eosinophilia led to a diagnosis of acute generalized exanthematous pustulosis (AGEP), which may have been triggered by azithromycin—the patient’s only recent medication. AGEP is a severe cutaneous eruption that may be associated with systemic involvement. Medications are usually implicated, and patients often seek urgent evaluation.
AGEP typically begins as an acute eruption in the intertriginous sites of the axilla, groin, and neck, but often becomes more generalized. The diagnosis is strongly suggested by the condition’s key features: fever (97% of cases) and leukocytosis (87%) with neutrophilia (91%) and eosinophilia (30%). Leukocytosis peaks 4 days after pustulosis occurs and lasts for about 12 days. Although common, fever is not always documented in patients with AGEP. (This patient was a case in point.)
In approximately 90% of AGEP cases, medications such as antibiotics and calcium channel blockers are implicated; however, the lack of such an association does not preclude the diagnosis. In cases of drug reactions, the eruption typically develops 1 to 2 days after a medication is begun, and the pustules typically resolve in fewer than 15 days. In 17% of patients, systemic involvement can occur and can include the liver, kidneys, bone marrow, and lungs. A physical exam, review of systems, and a laboratory evaluation can help rule out systemic involvement and guide additional testing.
AGEP has an incidence of 1 to 5 cases per million people per year, affecting women slightly more frequently than men. While the pathophysiology is not well understood, AGEP and its differential diagnoses are categorized as T cell-related inflammatory responses.
There are at least 4 severe cutaneous eruptions that might be confused with AGEP, all of which may be associated with fever. They include a drug reaction with eosinophilia and systemic symptoms, Stevens-Johnson syndrome, toxic epidermal necrolysis, and pustular psoriasis. The clinical features that may help differentiate these conditions from AGEP include timeline, mucocutaneous features, organ system involvement, and histopathologic findings.
Patients who have AGEP, including those with systemic involvement, generally improve after the offending drug is discontinued and treatment with topical corticosteroids is initiated. A brief course of systemic corticosteroids can also be considered for patients with severe skin involvement or systemic involvement.
This patient was prescribed topical corticosteroid wet dressing treatments twice daily for 2 weeks. At the 2-week follow-up visit, the rash had completely cleared and only minimal residual erythema was noted. The patient was instructed to avoid azithromycin.
This case was adapted from: Tolkachjov SN, Wetter DA, Sandefur BJ. Generalized pustular eruption. J Fam Pract. 2018;67:309-310,312.

The acute rash with minute pustules and associated leukocytosis with neutrophilia and eosinophilia led to a diagnosis of acute generalized exanthematous pustulosis (AGEP), which may have been triggered by azithromycin—the patient’s only recent medication. AGEP is a severe cutaneous eruption that may be associated with systemic involvement. Medications are usually implicated, and patients often seek urgent evaluation.
AGEP typically begins as an acute eruption in the intertriginous sites of the axilla, groin, and neck, but often becomes more generalized. The diagnosis is strongly suggested by the condition’s key features: fever (97% of cases) and leukocytosis (87%) with neutrophilia (91%) and eosinophilia (30%). Leukocytosis peaks 4 days after pustulosis occurs and lasts for about 12 days. Although common, fever is not always documented in patients with AGEP. (This patient was a case in point.)
In approximately 90% of AGEP cases, medications such as antibiotics and calcium channel blockers are implicated; however, the lack of such an association does not preclude the diagnosis. In cases of drug reactions, the eruption typically develops 1 to 2 days after a medication is begun, and the pustules typically resolve in fewer than 15 days. In 17% of patients, systemic involvement can occur and can include the liver, kidneys, bone marrow, and lungs. A physical exam, review of systems, and a laboratory evaluation can help rule out systemic involvement and guide additional testing.
AGEP has an incidence of 1 to 5 cases per million people per year, affecting women slightly more frequently than men. While the pathophysiology is not well understood, AGEP and its differential diagnoses are categorized as T cell-related inflammatory responses.
There are at least 4 severe cutaneous eruptions that might be confused with AGEP, all of which may be associated with fever. They include a drug reaction with eosinophilia and systemic symptoms, Stevens-Johnson syndrome, toxic epidermal necrolysis, and pustular psoriasis. The clinical features that may help differentiate these conditions from AGEP include timeline, mucocutaneous features, organ system involvement, and histopathologic findings.
Patients who have AGEP, including those with systemic involvement, generally improve after the offending drug is discontinued and treatment with topical corticosteroids is initiated. A brief course of systemic corticosteroids can also be considered for patients with severe skin involvement or systemic involvement.
This patient was prescribed topical corticosteroid wet dressing treatments twice daily for 2 weeks. At the 2-week follow-up visit, the rash had completely cleared and only minimal residual erythema was noted. The patient was instructed to avoid azithromycin.
This case was adapted from: Tolkachjov SN, Wetter DA, Sandefur BJ. Generalized pustular eruption. J Fam Pract. 2018;67:309-310,312.
LDL cholesterol not the primary culprit in ASCVD?
Two new studies suggest that LDL cholesterol (LDL-C) may be not the main driver of atherosclerotic cardiovascular disease (ASCVD).
The findings instead implicate remnant cholesterol (remnant-C) and very-low-density lipoprotein (VLDL) cholesterol in the development of cardiovascular disease (CVD) and MI.
The PREDIMED study, conducted in Spain, examined the association of triglycerides and remnant-C with major cardiovascular events (MACE) in older individuals with high CVD risk. It found that levels of triglycerides and remnant-C were associated with MACE independently of other risk factors, but there was no similar association with LDL-C.
“These findings lead [clinicians] to consider in the clinical management of dyslipidemias a greater control of the lipid profiles as a whole, including remnant-cholesterol and/or triglycerides,” Montserrat Fitó Colomer, MD, PhD, of the Cardiovascular Risk and Nutrition Research Group, Hospital del Mar Medical Research Institute, Barcelona, said in an interview.
In a separate analysis, the Copenhagen General Population Study, which focused on 25,000 individuals who were not taking lipid-lowering therapy, looked at the role of VLDL cholesterol and triglycerides in driving MI risk from apolipoprotein B (apoB)–containing lipoproteins.
“Elevated VLDL cholesterol explained a larger fraction of risk than did elevated LDL cholesterol, or elevated VLDL triglycerides,” Børge G. Nordestgaard, MD, DMSc, professor, University of Copenhagen, said in an interview.
Both studies were published online Nov. 30 in the Journal of the American College of Cardiology.
But in an editorial accompanying both reports, John Burnett, MD, PhD, from the University of Western Australia, Perth, and colleagues cautioned that it would be “premature to discard LDL-C based on PREDIMED.”
The findings are “insufficient to offset the mountain of literally hundreds of studies that uphold the value of LDL-C in prediction and intervention of ASCVD,” Dr. Burnett and coauthors wrote.
Similarly, the editorialists cautioned that, although the findings from the study by Dr. Nordestgaard and colleagues indicate that VLDL cholesterol is the “new kid in town for prediction, LDL cholesterol retains predictive power.” Clinical cardiologists should not “shelve LDL cholesterol and embrace VLDL and remnant cholesterol as the new oracles of ASCVD risk.”
In a comment, Dr. Burnett said, “The take-home message for clinicians in both papers is that LDL-C is the main lipid measurement to guide clinical decisions; however, residual risk of atherosclerotic cardiovascular disease remains, even after LCL-C is treated.
“Assessment of residual ASCVD risk with nontraditional lipid biomarkers, including VLDL cholesterol and remnant cholesterol, as well as lipoprotein (a) and apoB, may improve prognostication and help guide preventive treatments,” he added.
“Affordable and inexpensive”
In their report, the PREDIMED study authors explained that atherogenic dyslipidemia is characterized by “an excess of serum triglycerides” contained in VLDL cholesterol, intermediate-density lipoproteins, and their remnants, all of which are called “triglyceride-rich lipoproteins (TRLs).”
TRLs and remnant-C “have the capacity to cross the arterial wall,” and may therefore play a causal role in atherosclerosis development, they wrote.
The main PREDIMED trial compared a low-fat diet with the Mediterranean diet for the primary prevention of CVD in high-risk participants. Those enrolled in the trial “had a high prevalence of diabetes, obesity, and metabolic syndrome, conditions that are associated with insulin resistance, hypertriglyceridemia, and atherogenic dyslipidemia,” the authors wrote. “Thus, this cohort of subjects at high cardiovascular risk was well suited to investigate the association of triglycerides and TRLs with cardiovascular outcomes.”
The researchers investigated the role of triglycerides and remnant-C in incident CVD among these high-risk individuals, particularly those with chronic cardiometabolic disorders (prediabetes, type 2 diabetes, and poorly controlled diabetes), overweight and obesity, metabolic syndrome, and renal failure.
Their 6,901 participants (42.6% male, mean age 67 years, mean BMI 30.0 kg/m2) had a diagnosis of type 2 diabetes or at least three CVD risk factors including current smoking, hypertension, elevated LDL-C levels, low HDL cholesterol levels, elevated body mass index, or family history of premature coronary heart disease.
The primary study endpoint was a composite of adverse cardiovascular events (MACE): MI, stroke, or cardiovascular death. Participants were followed for a mean of 4.8 years, during which there was a total of 263 MACE events.
Multivariable-adjusted analyses showed that levels of triglycerides and remnant-C were both associated with MACE independent of other risk factors (hazard ratio, 1.04; 95% confidence interval, 1.02-1.06; and HR, 1.21; 95% CI, 1.10-1.33 per 10 mg/dl, respectively, both P < .001). Non–HDL cholesterol was also associated with MACE (HR, 1.05; 95% CI, 1.01-1.10 per 10 mg/dl, P = .026).
In particular, elevated remnant-C (≥30 mg/dL), compared with lower concentrations, flagged subjects at a higher risk of MACE, even if their LDL-C levels were at target (defined as ≤ 100 mg/dL).
Levels of LDL-C and HDL cholesterol were not associated with MACE.
“The indirect calculation of remnant-C is an affordable and inexpensive method, which could provide valuable data for clinical management,” Dr. Fitó Colomer said.
“The results of this study suggest that, in individuals at high cardiovascular risk with well-controlled LDL-C, triglycerides and mainly remnant-C should be considered as a treatment target,” she proposed.
New oracles?
Evidence has pointed to triglyceride-rich remnants or VLDL cholesterol as contributing to atherosclerotic CVD, together with LDL-C, but it is “unclear which fraction of risk is explained by, respectively, cholesterol and triglycerides in VLDL,” write the authors of the Copenhagen population study.
Dr. Nordestgaard said their study was motivated by an awareness that “in clinical practice, the focus for lipid-related risk is almost solely on reduction of LDL-C for prevention of ASCVD,” so the current focus needs to be reevaluated because patients with low LDL-C but elevated VLDL cholesterol and plasma triglycerides “may not be offered adequate preventive lipid-lowering therapy in order to prevent future MI and ASCVD.”
His group therefore tested the hypothesis that VLDL cholesterol and triglycerides may each explain part of the MI risk from apoB-containing lipoproteins.
They used measurements of plasma apoB and cholesterol and triglyceride content of VLDL cholesterol, intermediate-density-lipoprotein cholesterol, and LDL-C in the study participants (N = 25,480, median age 61 years, 53% female), who were required to be free of MI and not receiving lipid-lowering therapy at baseline.
During a median 11-year follow-up period, 1,816 participants experienced an MI. They tended to be older, compared with those who did not experience an MI, and also more likely to be male, to smoke, and to have higher systolic blood pressure.
Each 39-mg/dL increase in lipid level was found to be associated with higher MI risk.
The researchers looked at MI-associated risk of specific subfractions of apoB-containing lipoproteins. “VLDL cholesterol explained half of the MI risk from elevated apoB-containing lipoproteins, and [intermediate-density-lipoprotein] and LDL-C together accounted for only 29% of the risk,” Dr. Nordestgaard said.
“If LDL cholesterol is adequately reduced, clinicians need to evaluate possible elevated triglyceride-rich lipoproteins, either as elevated plasma triglycerides, remnant cholesterol, or elevated VLDL cholesterol; and, if elevated, consideration should also be given to reduction of triglyceride-rich lipoproteins,” he advised.
The Copenhagen General Population study was funded by the Danish Heart Foundation and the Novo Nordisk Foundation. Dr. Nordestgaard disclosed consulting for AstraZeneca, Sanofi, Regeneron, Akcea, Amgen, Kowa, Denka Seiken, Amarin, Novartis, Novo Nordisk, and Silence Therapeutrics. PREDIMED was supported by grants from the Instituto de Salud Carlos III- FEDER, Fundació La Marató de TV3, and Agència de Gestió d’Ajuts Universitaris i de Recerca. Dr. Fitó Colomer disclosed no relevant financial relationships. Dr. Burnett disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Two new studies suggest that LDL cholesterol (LDL-C) may be not the main driver of atherosclerotic cardiovascular disease (ASCVD).
The findings instead implicate remnant cholesterol (remnant-C) and very-low-density lipoprotein (VLDL) cholesterol in the development of cardiovascular disease (CVD) and MI.
The PREDIMED study, conducted in Spain, examined the association of triglycerides and remnant-C with major cardiovascular events (MACE) in older individuals with high CVD risk. It found that levels of triglycerides and remnant-C were associated with MACE independently of other risk factors, but there was no similar association with LDL-C.
“These findings lead [clinicians] to consider in the clinical management of dyslipidemias a greater control of the lipid profiles as a whole, including remnant-cholesterol and/or triglycerides,” Montserrat Fitó Colomer, MD, PhD, of the Cardiovascular Risk and Nutrition Research Group, Hospital del Mar Medical Research Institute, Barcelona, said in an interview.
In a separate analysis, the Copenhagen General Population Study, which focused on 25,000 individuals who were not taking lipid-lowering therapy, looked at the role of VLDL cholesterol and triglycerides in driving MI risk from apolipoprotein B (apoB)–containing lipoproteins.
“Elevated VLDL cholesterol explained a larger fraction of risk than did elevated LDL cholesterol, or elevated VLDL triglycerides,” Børge G. Nordestgaard, MD, DMSc, professor, University of Copenhagen, said in an interview.
Both studies were published online Nov. 30 in the Journal of the American College of Cardiology.
But in an editorial accompanying both reports, John Burnett, MD, PhD, from the University of Western Australia, Perth, and colleagues cautioned that it would be “premature to discard LDL-C based on PREDIMED.”
The findings are “insufficient to offset the mountain of literally hundreds of studies that uphold the value of LDL-C in prediction and intervention of ASCVD,” Dr. Burnett and coauthors wrote.
Similarly, the editorialists cautioned that, although the findings from the study by Dr. Nordestgaard and colleagues indicate that VLDL cholesterol is the “new kid in town for prediction, LDL cholesterol retains predictive power.” Clinical cardiologists should not “shelve LDL cholesterol and embrace VLDL and remnant cholesterol as the new oracles of ASCVD risk.”
In a comment, Dr. Burnett said, “The take-home message for clinicians in both papers is that LDL-C is the main lipid measurement to guide clinical decisions; however, residual risk of atherosclerotic cardiovascular disease remains, even after LCL-C is treated.
“Assessment of residual ASCVD risk with nontraditional lipid biomarkers, including VLDL cholesterol and remnant cholesterol, as well as lipoprotein (a) and apoB, may improve prognostication and help guide preventive treatments,” he added.
“Affordable and inexpensive”
In their report, the PREDIMED study authors explained that atherogenic dyslipidemia is characterized by “an excess of serum triglycerides” contained in VLDL cholesterol, intermediate-density lipoproteins, and their remnants, all of which are called “triglyceride-rich lipoproteins (TRLs).”
TRLs and remnant-C “have the capacity to cross the arterial wall,” and may therefore play a causal role in atherosclerosis development, they wrote.
The main PREDIMED trial compared a low-fat diet with the Mediterranean diet for the primary prevention of CVD in high-risk participants. Those enrolled in the trial “had a high prevalence of diabetes, obesity, and metabolic syndrome, conditions that are associated with insulin resistance, hypertriglyceridemia, and atherogenic dyslipidemia,” the authors wrote. “Thus, this cohort of subjects at high cardiovascular risk was well suited to investigate the association of triglycerides and TRLs with cardiovascular outcomes.”
The researchers investigated the role of triglycerides and remnant-C in incident CVD among these high-risk individuals, particularly those with chronic cardiometabolic disorders (prediabetes, type 2 diabetes, and poorly controlled diabetes), overweight and obesity, metabolic syndrome, and renal failure.
Their 6,901 participants (42.6% male, mean age 67 years, mean BMI 30.0 kg/m2) had a diagnosis of type 2 diabetes or at least three CVD risk factors including current smoking, hypertension, elevated LDL-C levels, low HDL cholesterol levels, elevated body mass index, or family history of premature coronary heart disease.
The primary study endpoint was a composite of adverse cardiovascular events (MACE): MI, stroke, or cardiovascular death. Participants were followed for a mean of 4.8 years, during which there was a total of 263 MACE events.
Multivariable-adjusted analyses showed that levels of triglycerides and remnant-C were both associated with MACE independent of other risk factors (hazard ratio, 1.04; 95% confidence interval, 1.02-1.06; and HR, 1.21; 95% CI, 1.10-1.33 per 10 mg/dl, respectively, both P < .001). Non–HDL cholesterol was also associated with MACE (HR, 1.05; 95% CI, 1.01-1.10 per 10 mg/dl, P = .026).
In particular, elevated remnant-C (≥30 mg/dL), compared with lower concentrations, flagged subjects at a higher risk of MACE, even if their LDL-C levels were at target (defined as ≤ 100 mg/dL).
Levels of LDL-C and HDL cholesterol were not associated with MACE.
“The indirect calculation of remnant-C is an affordable and inexpensive method, which could provide valuable data for clinical management,” Dr. Fitó Colomer said.
“The results of this study suggest that, in individuals at high cardiovascular risk with well-controlled LDL-C, triglycerides and mainly remnant-C should be considered as a treatment target,” she proposed.
New oracles?
Evidence has pointed to triglyceride-rich remnants or VLDL cholesterol as contributing to atherosclerotic CVD, together with LDL-C, but it is “unclear which fraction of risk is explained by, respectively, cholesterol and triglycerides in VLDL,” write the authors of the Copenhagen population study.
Dr. Nordestgaard said their study was motivated by an awareness that “in clinical practice, the focus for lipid-related risk is almost solely on reduction of LDL-C for prevention of ASCVD,” so the current focus needs to be reevaluated because patients with low LDL-C but elevated VLDL cholesterol and plasma triglycerides “may not be offered adequate preventive lipid-lowering therapy in order to prevent future MI and ASCVD.”
His group therefore tested the hypothesis that VLDL cholesterol and triglycerides may each explain part of the MI risk from apoB-containing lipoproteins.
They used measurements of plasma apoB and cholesterol and triglyceride content of VLDL cholesterol, intermediate-density-lipoprotein cholesterol, and LDL-C in the study participants (N = 25,480, median age 61 years, 53% female), who were required to be free of MI and not receiving lipid-lowering therapy at baseline.
During a median 11-year follow-up period, 1,816 participants experienced an MI. They tended to be older, compared with those who did not experience an MI, and also more likely to be male, to smoke, and to have higher systolic blood pressure.
Each 39-mg/dL increase in lipid level was found to be associated with higher MI risk.
The researchers looked at MI-associated risk of specific subfractions of apoB-containing lipoproteins. “VLDL cholesterol explained half of the MI risk from elevated apoB-containing lipoproteins, and [intermediate-density-lipoprotein] and LDL-C together accounted for only 29% of the risk,” Dr. Nordestgaard said.
“If LDL cholesterol is adequately reduced, clinicians need to evaluate possible elevated triglyceride-rich lipoproteins, either as elevated plasma triglycerides, remnant cholesterol, or elevated VLDL cholesterol; and, if elevated, consideration should also be given to reduction of triglyceride-rich lipoproteins,” he advised.
The Copenhagen General Population study was funded by the Danish Heart Foundation and the Novo Nordisk Foundation. Dr. Nordestgaard disclosed consulting for AstraZeneca, Sanofi, Regeneron, Akcea, Amgen, Kowa, Denka Seiken, Amarin, Novartis, Novo Nordisk, and Silence Therapeutrics. PREDIMED was supported by grants from the Instituto de Salud Carlos III- FEDER, Fundació La Marató de TV3, and Agència de Gestió d’Ajuts Universitaris i de Recerca. Dr. Fitó Colomer disclosed no relevant financial relationships. Dr. Burnett disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Two new studies suggest that LDL cholesterol (LDL-C) may be not the main driver of atherosclerotic cardiovascular disease (ASCVD).
The findings instead implicate remnant cholesterol (remnant-C) and very-low-density lipoprotein (VLDL) cholesterol in the development of cardiovascular disease (CVD) and MI.
The PREDIMED study, conducted in Spain, examined the association of triglycerides and remnant-C with major cardiovascular events (MACE) in older individuals with high CVD risk. It found that levels of triglycerides and remnant-C were associated with MACE independently of other risk factors, but there was no similar association with LDL-C.
“These findings lead [clinicians] to consider in the clinical management of dyslipidemias a greater control of the lipid profiles as a whole, including remnant-cholesterol and/or triglycerides,” Montserrat Fitó Colomer, MD, PhD, of the Cardiovascular Risk and Nutrition Research Group, Hospital del Mar Medical Research Institute, Barcelona, said in an interview.
In a separate analysis, the Copenhagen General Population Study, which focused on 25,000 individuals who were not taking lipid-lowering therapy, looked at the role of VLDL cholesterol and triglycerides in driving MI risk from apolipoprotein B (apoB)–containing lipoproteins.
“Elevated VLDL cholesterol explained a larger fraction of risk than did elevated LDL cholesterol, or elevated VLDL triglycerides,” Børge G. Nordestgaard, MD, DMSc, professor, University of Copenhagen, said in an interview.
Both studies were published online Nov. 30 in the Journal of the American College of Cardiology.
But in an editorial accompanying both reports, John Burnett, MD, PhD, from the University of Western Australia, Perth, and colleagues cautioned that it would be “premature to discard LDL-C based on PREDIMED.”
The findings are “insufficient to offset the mountain of literally hundreds of studies that uphold the value of LDL-C in prediction and intervention of ASCVD,” Dr. Burnett and coauthors wrote.
Similarly, the editorialists cautioned that, although the findings from the study by Dr. Nordestgaard and colleagues indicate that VLDL cholesterol is the “new kid in town for prediction, LDL cholesterol retains predictive power.” Clinical cardiologists should not “shelve LDL cholesterol and embrace VLDL and remnant cholesterol as the new oracles of ASCVD risk.”
In a comment, Dr. Burnett said, “The take-home message for clinicians in both papers is that LDL-C is the main lipid measurement to guide clinical decisions; however, residual risk of atherosclerotic cardiovascular disease remains, even after LCL-C is treated.
“Assessment of residual ASCVD risk with nontraditional lipid biomarkers, including VLDL cholesterol and remnant cholesterol, as well as lipoprotein (a) and apoB, may improve prognostication and help guide preventive treatments,” he added.
“Affordable and inexpensive”
In their report, the PREDIMED study authors explained that atherogenic dyslipidemia is characterized by “an excess of serum triglycerides” contained in VLDL cholesterol, intermediate-density lipoproteins, and their remnants, all of which are called “triglyceride-rich lipoproteins (TRLs).”
TRLs and remnant-C “have the capacity to cross the arterial wall,” and may therefore play a causal role in atherosclerosis development, they wrote.
The main PREDIMED trial compared a low-fat diet with the Mediterranean diet for the primary prevention of CVD in high-risk participants. Those enrolled in the trial “had a high prevalence of diabetes, obesity, and metabolic syndrome, conditions that are associated with insulin resistance, hypertriglyceridemia, and atherogenic dyslipidemia,” the authors wrote. “Thus, this cohort of subjects at high cardiovascular risk was well suited to investigate the association of triglycerides and TRLs with cardiovascular outcomes.”
The researchers investigated the role of triglycerides and remnant-C in incident CVD among these high-risk individuals, particularly those with chronic cardiometabolic disorders (prediabetes, type 2 diabetes, and poorly controlled diabetes), overweight and obesity, metabolic syndrome, and renal failure.
Their 6,901 participants (42.6% male, mean age 67 years, mean BMI 30.0 kg/m2) had a diagnosis of type 2 diabetes or at least three CVD risk factors including current smoking, hypertension, elevated LDL-C levels, low HDL cholesterol levels, elevated body mass index, or family history of premature coronary heart disease.
The primary study endpoint was a composite of adverse cardiovascular events (MACE): MI, stroke, or cardiovascular death. Participants were followed for a mean of 4.8 years, during which there was a total of 263 MACE events.
Multivariable-adjusted analyses showed that levels of triglycerides and remnant-C were both associated with MACE independent of other risk factors (hazard ratio, 1.04; 95% confidence interval, 1.02-1.06; and HR, 1.21; 95% CI, 1.10-1.33 per 10 mg/dl, respectively, both P < .001). Non–HDL cholesterol was also associated with MACE (HR, 1.05; 95% CI, 1.01-1.10 per 10 mg/dl, P = .026).
In particular, elevated remnant-C (≥30 mg/dL), compared with lower concentrations, flagged subjects at a higher risk of MACE, even if their LDL-C levels were at target (defined as ≤ 100 mg/dL).
Levels of LDL-C and HDL cholesterol were not associated with MACE.
“The indirect calculation of remnant-C is an affordable and inexpensive method, which could provide valuable data for clinical management,” Dr. Fitó Colomer said.
“The results of this study suggest that, in individuals at high cardiovascular risk with well-controlled LDL-C, triglycerides and mainly remnant-C should be considered as a treatment target,” she proposed.
New oracles?
Evidence has pointed to triglyceride-rich remnants or VLDL cholesterol as contributing to atherosclerotic CVD, together with LDL-C, but it is “unclear which fraction of risk is explained by, respectively, cholesterol and triglycerides in VLDL,” write the authors of the Copenhagen population study.
Dr. Nordestgaard said their study was motivated by an awareness that “in clinical practice, the focus for lipid-related risk is almost solely on reduction of LDL-C for prevention of ASCVD,” so the current focus needs to be reevaluated because patients with low LDL-C but elevated VLDL cholesterol and plasma triglycerides “may not be offered adequate preventive lipid-lowering therapy in order to prevent future MI and ASCVD.”
His group therefore tested the hypothesis that VLDL cholesterol and triglycerides may each explain part of the MI risk from apoB-containing lipoproteins.
They used measurements of plasma apoB and cholesterol and triglyceride content of VLDL cholesterol, intermediate-density-lipoprotein cholesterol, and LDL-C in the study participants (N = 25,480, median age 61 years, 53% female), who were required to be free of MI and not receiving lipid-lowering therapy at baseline.
During a median 11-year follow-up period, 1,816 participants experienced an MI. They tended to be older, compared with those who did not experience an MI, and also more likely to be male, to smoke, and to have higher systolic blood pressure.
Each 39-mg/dL increase in lipid level was found to be associated with higher MI risk.
The researchers looked at MI-associated risk of specific subfractions of apoB-containing lipoproteins. “VLDL cholesterol explained half of the MI risk from elevated apoB-containing lipoproteins, and [intermediate-density-lipoprotein] and LDL-C together accounted for only 29% of the risk,” Dr. Nordestgaard said.
“If LDL cholesterol is adequately reduced, clinicians need to evaluate possible elevated triglyceride-rich lipoproteins, either as elevated plasma triglycerides, remnant cholesterol, or elevated VLDL cholesterol; and, if elevated, consideration should also be given to reduction of triglyceride-rich lipoproteins,” he advised.
The Copenhagen General Population study was funded by the Danish Heart Foundation and the Novo Nordisk Foundation. Dr. Nordestgaard disclosed consulting for AstraZeneca, Sanofi, Regeneron, Akcea, Amgen, Kowa, Denka Seiken, Amarin, Novartis, Novo Nordisk, and Silence Therapeutrics. PREDIMED was supported by grants from the Instituto de Salud Carlos III- FEDER, Fundació La Marató de TV3, and Agència de Gestió d’Ajuts Universitaris i de Recerca. Dr. Fitó Colomer disclosed no relevant financial relationships. Dr. Burnett disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
Antibiotic prescribing: How to manage patient pressures
Inappropriate antibiotic prescribing in the face of growing microbial resistance is a global public health problem, and a major cause is perceived patient pressure.
At the annual meeting of the European Society for Paediatric Infectious Diseases, held virtually this year, Tanya Stivers, PhD, professor of sociology at the University of California, Los Angeles, presented some of her team’s work studying patterns of clinical prescription.
It is widely appreciated that inappropriate prescribing is a common problem that the medical community seems powerless to stop, particularly in primary care. Already, clinicians are running out of effective antibiotics to treat a range of serious infections. Dr. Stivers began by saying that this problem isn’t caused by a lack of understanding about disease causation and microbial resistance or patients overtly demanding antibiotics, which occurs in less than 2% of cases. Instead, the cause appears to lie in doctor-patient interactions during consultations.
In pediatric practice, physicians have previously been found to prescribe antibiotics for a clinically diagnosed respiratory viral infection in 62% of cases when they perceive that this diagnosis was expected by parents, compared with 7% in the absence of such perception. Similarly, associated ear infections were diagnosed three times more often, and sinus infections seven times more often, leading to increased prescribing.
In adult practice, Dr. Stivers reported that patients can exert subtle pressure to prescribe through:
- Priming. Patients help their physician to see the problem as relatively severe (e.g., a sore throat that “feels like a knife”).
- Nudging. Patients redirect physicians back to a bacterial problem (e.g., “I’ve tried all these medicines, and nothing worked”). Nudging was found to occur in 41% of encounters.
- Resisting. Patients contest diagnosis or treatment in 40% of consultations (e.g., “there was pus yesterday”).
Priming or nudging resulted in antibiotic prescribing in 60% of patients without signs of a bacterial infection, compared with 30% where this was not a feature (P < 0.05).
But how can these pressures be countered? Dr. Stivers offered advice based on her original data from 570 video recordings of pediatric encounters. The current findings come from an analysis of 68 adult primary care visits for upper respiratory tract infections in Southern California. Inappropriate prescribing was identified in 37%.
When researching the antibiotic prescribing problem, it is helpful to explore a typical primary care consultation. The acute medical visit structure is a stepwise process involving opening, establishing the problem, gathering information, counseling, and then closing the consultation. It is important is to recognize that patients shape prescribing decisions, and effective communication is vital in influencing the outcome. In Dr. Stivers’ experience, priming, nudging, and resisting result in antibiotic prescribing in 60% of cases in whom clinical signs of bacterial illness are absent, compared with 30% where patient pressure is not a feature.
How can we change practice? Global experience suggests that printed material aimed at physicians is only of marginal benefit. By comparison, patient education does work but needs to be repeated, and there’s always a reason why this consultation should be “special.”
Try a 3-prong communication plan
To counteract these pressures, Dr. Stivers recommends a three-prong communication plan to influence the consultation:
- Foreshadowing, where suggesting that the cause of the patient’s symptoms is likely to be viral is introduced early in the consultation. This approach was found to reduce antibiotic prescribing to 33%, compared with 59% without foreshadowing (P < .05). Resistance may also be reduced.
- Affirmative nonantibiotic treatment plans, where specific positive recommendations given early (e.g., “I’m going to put you on some medicine to try to dry that out”) are less likely to be resisted than is vague negative advice at the end of a consultation.
- Persuasion, which involves explaining the diagnosis and nature of a cough and cold, educating about viral and bacterial differences, and presenting the risks of antibiotics. When persuasion is employed, antibiotic prescribing is reduced to 33%, compared with 63% (P < .05) without persuasion. In general, effective foreshadowing and affirmation should avoid the need for persuasion.
Dr. Stivers’ research suggests that these techniques work, but to do so, they should be delivered naturally as part of routine practice. Interestingly, her data showed that physicians rarely foreshadowed, and when they encountered resistance, they adopted persuasion in 53% of cases. By comparison, affirmative recommendations were used in 89% of cases, but their effects were reduced by the physician being vague and nonspecific.
In conclusion, Dr. Stivers said that addressing inappropriate prescribing requires awareness but that is not enough. The challenge is to reconsider health policies and ways of communicating about antibiotics. There is no downside to foreshadowing a likely viral origin, delivering affirmation, or using persuasion. She added, “If we can make even a 5%-10% reduction [in prescribing], wouldn’t it be worth it?”
Questions answered
A question-and-answer session followed Dr. Stivers’ presentation, and points raised included:
- Physicians have a desire to please. Dr. Stivers countered this point by saying that satisfaction is not tied to antibiotic prescription, and that physicians often misjudge what patients want. It’s important to communicate other treatment options because patients often just want “something they can do.”
- Decision fatigue is often a factor. Evidence shows that antibiotic prescription is more frequent toward the end of a shift. Doctors should avoid negotiation because it increases consultation time. Here, foreshadowing early on may help. Setting may also be important – prescription is more frequent in the ED.
- Vaccine-resistant parents often want active treatment. Here, conversations can be challenging. Trying to persuade may be a less successful than giving positive instruction (e.g., “we’ll give you a vaccine today.”) Resistance is likely to be lower.
- Concern was expressed about manipulating patients ahead of a firm diagnosis. Could this lead to missing a serious bacterial infection? Dr. Stivers acknowledged that this was a gamble. She recommended a “neutral” early foreshadowing statement such as “we are seeing a lot of viral infections at the present.”
- Cultural differences can have an effect. In China, for example, the argument between parents and physicians no longer focuses on antibiotics versus nonantibiotics but rather on oral versus intravenous administration.
- Litigation is a factor in prescribing, especially in the United States. Dr. Stivers stated that her proposed approach to prescribing should not interfere with appropriate management. The clinical picture can change, and antibiotics should be prescribed where needed.
- Audits improve prescribing in the short term. These results were based on recorded consultations, and that factor may have influenced management. In unrecorded consultations, inappropriate antibiotic prescription would be higher.
- Increased point-of-care testing can reduce unnecessary prescribing. This has been documented in countries such as Sweden. Evidence from China suggests that many patients will still receive antibiotics even if a bacterial cause is excluded.
When patients dictate treatment, sometimes we must tell them what is best. Dr. Stivers closed her presentation by emphasizing that, “how you say things will matter.”
Louis Bont, MD, PhD, chair of this session and pediatric infectious diseases specialist at the University Medical Center Utrecht (the Netherlands), commented: “Antimicrobial resistance is a global health threat which jeopardizes sustainable health goals. The World Health Organization has declared that antimicrobial resistance is one of the top 10 global public health threats facing humanity. Resistance to ciprofloxacin varies from 8%-93% in Escherichia coli and 4%-80% in Klebsiella pneumoniae. Colistin is the only last-resort treatment for life-threatening infections caused by carbapenem-resistant enterobacteriaceae.”
Dr. Stivers stated that she has nothing to disclose.
Inappropriate antibiotic prescribing in the face of growing microbial resistance is a global public health problem, and a major cause is perceived patient pressure.
At the annual meeting of the European Society for Paediatric Infectious Diseases, held virtually this year, Tanya Stivers, PhD, professor of sociology at the University of California, Los Angeles, presented some of her team’s work studying patterns of clinical prescription.
It is widely appreciated that inappropriate prescribing is a common problem that the medical community seems powerless to stop, particularly in primary care. Already, clinicians are running out of effective antibiotics to treat a range of serious infections. Dr. Stivers began by saying that this problem isn’t caused by a lack of understanding about disease causation and microbial resistance or patients overtly demanding antibiotics, which occurs in less than 2% of cases. Instead, the cause appears to lie in doctor-patient interactions during consultations.
In pediatric practice, physicians have previously been found to prescribe antibiotics for a clinically diagnosed respiratory viral infection in 62% of cases when they perceive that this diagnosis was expected by parents, compared with 7% in the absence of such perception. Similarly, associated ear infections were diagnosed three times more often, and sinus infections seven times more often, leading to increased prescribing.
In adult practice, Dr. Stivers reported that patients can exert subtle pressure to prescribe through:
- Priming. Patients help their physician to see the problem as relatively severe (e.g., a sore throat that “feels like a knife”).
- Nudging. Patients redirect physicians back to a bacterial problem (e.g., “I’ve tried all these medicines, and nothing worked”). Nudging was found to occur in 41% of encounters.
- Resisting. Patients contest diagnosis or treatment in 40% of consultations (e.g., “there was pus yesterday”).
Priming or nudging resulted in antibiotic prescribing in 60% of patients without signs of a bacterial infection, compared with 30% where this was not a feature (P < 0.05).
But how can these pressures be countered? Dr. Stivers offered advice based on her original data from 570 video recordings of pediatric encounters. The current findings come from an analysis of 68 adult primary care visits for upper respiratory tract infections in Southern California. Inappropriate prescribing was identified in 37%.
When researching the antibiotic prescribing problem, it is helpful to explore a typical primary care consultation. The acute medical visit structure is a stepwise process involving opening, establishing the problem, gathering information, counseling, and then closing the consultation. It is important is to recognize that patients shape prescribing decisions, and effective communication is vital in influencing the outcome. In Dr. Stivers’ experience, priming, nudging, and resisting result in antibiotic prescribing in 60% of cases in whom clinical signs of bacterial illness are absent, compared with 30% where patient pressure is not a feature.
How can we change practice? Global experience suggests that printed material aimed at physicians is only of marginal benefit. By comparison, patient education does work but needs to be repeated, and there’s always a reason why this consultation should be “special.”
Try a 3-prong communication plan
To counteract these pressures, Dr. Stivers recommends a three-prong communication plan to influence the consultation:
- Foreshadowing, where suggesting that the cause of the patient’s symptoms is likely to be viral is introduced early in the consultation. This approach was found to reduce antibiotic prescribing to 33%, compared with 59% without foreshadowing (P < .05). Resistance may also be reduced.
- Affirmative nonantibiotic treatment plans, where specific positive recommendations given early (e.g., “I’m going to put you on some medicine to try to dry that out”) are less likely to be resisted than is vague negative advice at the end of a consultation.
- Persuasion, which involves explaining the diagnosis and nature of a cough and cold, educating about viral and bacterial differences, and presenting the risks of antibiotics. When persuasion is employed, antibiotic prescribing is reduced to 33%, compared with 63% (P < .05) without persuasion. In general, effective foreshadowing and affirmation should avoid the need for persuasion.
Dr. Stivers’ research suggests that these techniques work, but to do so, they should be delivered naturally as part of routine practice. Interestingly, her data showed that physicians rarely foreshadowed, and when they encountered resistance, they adopted persuasion in 53% of cases. By comparison, affirmative recommendations were used in 89% of cases, but their effects were reduced by the physician being vague and nonspecific.
In conclusion, Dr. Stivers said that addressing inappropriate prescribing requires awareness but that is not enough. The challenge is to reconsider health policies and ways of communicating about antibiotics. There is no downside to foreshadowing a likely viral origin, delivering affirmation, or using persuasion. She added, “If we can make even a 5%-10% reduction [in prescribing], wouldn’t it be worth it?”
Questions answered
A question-and-answer session followed Dr. Stivers’ presentation, and points raised included:
- Physicians have a desire to please. Dr. Stivers countered this point by saying that satisfaction is not tied to antibiotic prescription, and that physicians often misjudge what patients want. It’s important to communicate other treatment options because patients often just want “something they can do.”
- Decision fatigue is often a factor. Evidence shows that antibiotic prescription is more frequent toward the end of a shift. Doctors should avoid negotiation because it increases consultation time. Here, foreshadowing early on may help. Setting may also be important – prescription is more frequent in the ED.
- Vaccine-resistant parents often want active treatment. Here, conversations can be challenging. Trying to persuade may be a less successful than giving positive instruction (e.g., “we’ll give you a vaccine today.”) Resistance is likely to be lower.
- Concern was expressed about manipulating patients ahead of a firm diagnosis. Could this lead to missing a serious bacterial infection? Dr. Stivers acknowledged that this was a gamble. She recommended a “neutral” early foreshadowing statement such as “we are seeing a lot of viral infections at the present.”
- Cultural differences can have an effect. In China, for example, the argument between parents and physicians no longer focuses on antibiotics versus nonantibiotics but rather on oral versus intravenous administration.
- Litigation is a factor in prescribing, especially in the United States. Dr. Stivers stated that her proposed approach to prescribing should not interfere with appropriate management. The clinical picture can change, and antibiotics should be prescribed where needed.
- Audits improve prescribing in the short term. These results were based on recorded consultations, and that factor may have influenced management. In unrecorded consultations, inappropriate antibiotic prescription would be higher.
- Increased point-of-care testing can reduce unnecessary prescribing. This has been documented in countries such as Sweden. Evidence from China suggests that many patients will still receive antibiotics even if a bacterial cause is excluded.
When patients dictate treatment, sometimes we must tell them what is best. Dr. Stivers closed her presentation by emphasizing that, “how you say things will matter.”
Louis Bont, MD, PhD, chair of this session and pediatric infectious diseases specialist at the University Medical Center Utrecht (the Netherlands), commented: “Antimicrobial resistance is a global health threat which jeopardizes sustainable health goals. The World Health Organization has declared that antimicrobial resistance is one of the top 10 global public health threats facing humanity. Resistance to ciprofloxacin varies from 8%-93% in Escherichia coli and 4%-80% in Klebsiella pneumoniae. Colistin is the only last-resort treatment for life-threatening infections caused by carbapenem-resistant enterobacteriaceae.”
Dr. Stivers stated that she has nothing to disclose.
Inappropriate antibiotic prescribing in the face of growing microbial resistance is a global public health problem, and a major cause is perceived patient pressure.
At the annual meeting of the European Society for Paediatric Infectious Diseases, held virtually this year, Tanya Stivers, PhD, professor of sociology at the University of California, Los Angeles, presented some of her team’s work studying patterns of clinical prescription.
It is widely appreciated that inappropriate prescribing is a common problem that the medical community seems powerless to stop, particularly in primary care. Already, clinicians are running out of effective antibiotics to treat a range of serious infections. Dr. Stivers began by saying that this problem isn’t caused by a lack of understanding about disease causation and microbial resistance or patients overtly demanding antibiotics, which occurs in less than 2% of cases. Instead, the cause appears to lie in doctor-patient interactions during consultations.
In pediatric practice, physicians have previously been found to prescribe antibiotics for a clinically diagnosed respiratory viral infection in 62% of cases when they perceive that this diagnosis was expected by parents, compared with 7% in the absence of such perception. Similarly, associated ear infections were diagnosed three times more often, and sinus infections seven times more often, leading to increased prescribing.
In adult practice, Dr. Stivers reported that patients can exert subtle pressure to prescribe through:
- Priming. Patients help their physician to see the problem as relatively severe (e.g., a sore throat that “feels like a knife”).
- Nudging. Patients redirect physicians back to a bacterial problem (e.g., “I’ve tried all these medicines, and nothing worked”). Nudging was found to occur in 41% of encounters.
- Resisting. Patients contest diagnosis or treatment in 40% of consultations (e.g., “there was pus yesterday”).
Priming or nudging resulted in antibiotic prescribing in 60% of patients without signs of a bacterial infection, compared with 30% where this was not a feature (P < 0.05).
But how can these pressures be countered? Dr. Stivers offered advice based on her original data from 570 video recordings of pediatric encounters. The current findings come from an analysis of 68 adult primary care visits for upper respiratory tract infections in Southern California. Inappropriate prescribing was identified in 37%.
When researching the antibiotic prescribing problem, it is helpful to explore a typical primary care consultation. The acute medical visit structure is a stepwise process involving opening, establishing the problem, gathering information, counseling, and then closing the consultation. It is important is to recognize that patients shape prescribing decisions, and effective communication is vital in influencing the outcome. In Dr. Stivers’ experience, priming, nudging, and resisting result in antibiotic prescribing in 60% of cases in whom clinical signs of bacterial illness are absent, compared with 30% where patient pressure is not a feature.
How can we change practice? Global experience suggests that printed material aimed at physicians is only of marginal benefit. By comparison, patient education does work but needs to be repeated, and there’s always a reason why this consultation should be “special.”
Try a 3-prong communication plan
To counteract these pressures, Dr. Stivers recommends a three-prong communication plan to influence the consultation:
- Foreshadowing, where suggesting that the cause of the patient’s symptoms is likely to be viral is introduced early in the consultation. This approach was found to reduce antibiotic prescribing to 33%, compared with 59% without foreshadowing (P < .05). Resistance may also be reduced.
- Affirmative nonantibiotic treatment plans, where specific positive recommendations given early (e.g., “I’m going to put you on some medicine to try to dry that out”) are less likely to be resisted than is vague negative advice at the end of a consultation.
- Persuasion, which involves explaining the diagnosis and nature of a cough and cold, educating about viral and bacterial differences, and presenting the risks of antibiotics. When persuasion is employed, antibiotic prescribing is reduced to 33%, compared with 63% (P < .05) without persuasion. In general, effective foreshadowing and affirmation should avoid the need for persuasion.
Dr. Stivers’ research suggests that these techniques work, but to do so, they should be delivered naturally as part of routine practice. Interestingly, her data showed that physicians rarely foreshadowed, and when they encountered resistance, they adopted persuasion in 53% of cases. By comparison, affirmative recommendations were used in 89% of cases, but their effects were reduced by the physician being vague and nonspecific.
In conclusion, Dr. Stivers said that addressing inappropriate prescribing requires awareness but that is not enough. The challenge is to reconsider health policies and ways of communicating about antibiotics. There is no downside to foreshadowing a likely viral origin, delivering affirmation, or using persuasion. She added, “If we can make even a 5%-10% reduction [in prescribing], wouldn’t it be worth it?”
Questions answered
A question-and-answer session followed Dr. Stivers’ presentation, and points raised included:
- Physicians have a desire to please. Dr. Stivers countered this point by saying that satisfaction is not tied to antibiotic prescription, and that physicians often misjudge what patients want. It’s important to communicate other treatment options because patients often just want “something they can do.”
- Decision fatigue is often a factor. Evidence shows that antibiotic prescription is more frequent toward the end of a shift. Doctors should avoid negotiation because it increases consultation time. Here, foreshadowing early on may help. Setting may also be important – prescription is more frequent in the ED.
- Vaccine-resistant parents often want active treatment. Here, conversations can be challenging. Trying to persuade may be a less successful than giving positive instruction (e.g., “we’ll give you a vaccine today.”) Resistance is likely to be lower.
- Concern was expressed about manipulating patients ahead of a firm diagnosis. Could this lead to missing a serious bacterial infection? Dr. Stivers acknowledged that this was a gamble. She recommended a “neutral” early foreshadowing statement such as “we are seeing a lot of viral infections at the present.”
- Cultural differences can have an effect. In China, for example, the argument between parents and physicians no longer focuses on antibiotics versus nonantibiotics but rather on oral versus intravenous administration.
- Litigation is a factor in prescribing, especially in the United States. Dr. Stivers stated that her proposed approach to prescribing should not interfere with appropriate management. The clinical picture can change, and antibiotics should be prescribed where needed.
- Audits improve prescribing in the short term. These results were based on recorded consultations, and that factor may have influenced management. In unrecorded consultations, inappropriate antibiotic prescription would be higher.
- Increased point-of-care testing can reduce unnecessary prescribing. This has been documented in countries such as Sweden. Evidence from China suggests that many patients will still receive antibiotics even if a bacterial cause is excluded.
When patients dictate treatment, sometimes we must tell them what is best. Dr. Stivers closed her presentation by emphasizing that, “how you say things will matter.”
Louis Bont, MD, PhD, chair of this session and pediatric infectious diseases specialist at the University Medical Center Utrecht (the Netherlands), commented: “Antimicrobial resistance is a global health threat which jeopardizes sustainable health goals. The World Health Organization has declared that antimicrobial resistance is one of the top 10 global public health threats facing humanity. Resistance to ciprofloxacin varies from 8%-93% in Escherichia coli and 4%-80% in Klebsiella pneumoniae. Colistin is the only last-resort treatment for life-threatening infections caused by carbapenem-resistant enterobacteriaceae.”
Dr. Stivers stated that she has nothing to disclose.
FROM ESPID 2020
Hand hygiene in pediatric ICUs: Identifying areas for improvement
A multidisciplinary team seeking to measure compliance with hand hygiene (HH) practices in pediatric ICUs across Europe found compliance was comparable and relatively high among unit doctors and nurses, but not as high in nonunit doctors and nurses.
Ioannis Kopsidas, MD, presented these results from the RANIN-KIDS Network during the annual meeting of the European Society for Paediatric Infectious Diseases, held virtually this year. RANIN-KIDS (Reducing Antimicrobial Use and Nosocomial Infections in Kids) is a European network with the aim of preventing hospital-associated infections and promoting judicial antimicrobial use in pediatric patients using a common sustainable methodology across Europe.
Infections kill. This is especially the case in pediatric ICUs, where young age and an immunocompromised status make patients particularly vulnerable to infections. Poor HH is a major cause for disease transmission. To reduce the risk, the World Health Organization recommends attention to five moments of hand hygiene and nine steps for hand washing. Various tools are available to improve adherence, but whether these measures are being followed is unclear. The researchers sought to assess the degree of compliance with HH practices in pediatric ICUs and to identify targets for improvement.
Dr. Kopsidas, of the Center of Clinical Epidemiology and Outcomes Research, the National and Kapodistrian University of Athens, and colleagues examined practices in nine pediatric ICUs across six European countries (Estonia, Germany, Greece, Italy, Spain, and Switzerland) by means of prospective observational study. All organizations were part of the RANIN-KIDS network. Over a 6-month period starting in March 2019, observations were conducted in every unit by observers using a data collection tool developed based on WHO guidelines. Training for observers was provided using a self-paced teaching kit comprising PowerPoint and video presentations, followed by the completion of a test observation form after observing staged hand hygiene exercises. Results were then compared with WHO guidance, and irregularities were explained in order to achieve interrater reliability.
Researchers observed 1,715 HH opportunities. Across all pediatric ICUs, the median HH compliance rate was 82% (interquartile range, 72%-95%). Stratified by type of professional, median compliance was comparable among unit doctors (90%) and nurses (87%), but lower for nonunit doctors and nurses (81%) and also for nondoctors and nonnurses (67%). Alcohol-based hand rub was substantially preferred to soap and water, being used in 84% of the observations (IQR, 69%-87%). Cleaning and drying technique was considered appropriate in a median of 93% of observations (IQR, 86%-96%).
Compliance to moment 5 (after touching patient surroundings) was the lowest across hospitals (median 71%), compared with a median 100% for moment 2 (before clean/aseptic procedures) and a median 93% for moment 3 (after body fluid exposure/risk). For moment 1, median compliance was 87% (before touching a patient), and for moment 4, median compliance was 82% (after touching a patient).
Dr. Kopsidas concluded that the overall level of HH compliance among doctors and nurses working in European pediatric ICUs appears to be high, with moment 5 being the most frequently missed opportunity. Nonunit doctors and nurses and other personnel show lower WHO guidelines adherence. He stated that “these results will be used to design tailor-made interventions in participating units with the aim of reducing HAIs [health care–associated infections] and spread of multidrug resistant infections.”
He also said that “unified surveillance in Europe is possible and achievable, and allows for benchmarking among countries, institutions and wards.”
For some units, improving HH is a missed opportunity. The next stop for the RANIN-KIDS network is to look at the effects of interventions on reducing spread.
Dr. Kopsidas had no relevant financial disclosures.
A multidisciplinary team seeking to measure compliance with hand hygiene (HH) practices in pediatric ICUs across Europe found compliance was comparable and relatively high among unit doctors and nurses, but not as high in nonunit doctors and nurses.
Ioannis Kopsidas, MD, presented these results from the RANIN-KIDS Network during the annual meeting of the European Society for Paediatric Infectious Diseases, held virtually this year. RANIN-KIDS (Reducing Antimicrobial Use and Nosocomial Infections in Kids) is a European network with the aim of preventing hospital-associated infections and promoting judicial antimicrobial use in pediatric patients using a common sustainable methodology across Europe.
Infections kill. This is especially the case in pediatric ICUs, where young age and an immunocompromised status make patients particularly vulnerable to infections. Poor HH is a major cause for disease transmission. To reduce the risk, the World Health Organization recommends attention to five moments of hand hygiene and nine steps for hand washing. Various tools are available to improve adherence, but whether these measures are being followed is unclear. The researchers sought to assess the degree of compliance with HH practices in pediatric ICUs and to identify targets for improvement.
Dr. Kopsidas, of the Center of Clinical Epidemiology and Outcomes Research, the National and Kapodistrian University of Athens, and colleagues examined practices in nine pediatric ICUs across six European countries (Estonia, Germany, Greece, Italy, Spain, and Switzerland) by means of prospective observational study. All organizations were part of the RANIN-KIDS network. Over a 6-month period starting in March 2019, observations were conducted in every unit by observers using a data collection tool developed based on WHO guidelines. Training for observers was provided using a self-paced teaching kit comprising PowerPoint and video presentations, followed by the completion of a test observation form after observing staged hand hygiene exercises. Results were then compared with WHO guidance, and irregularities were explained in order to achieve interrater reliability.
Researchers observed 1,715 HH opportunities. Across all pediatric ICUs, the median HH compliance rate was 82% (interquartile range, 72%-95%). Stratified by type of professional, median compliance was comparable among unit doctors (90%) and nurses (87%), but lower for nonunit doctors and nurses (81%) and also for nondoctors and nonnurses (67%). Alcohol-based hand rub was substantially preferred to soap and water, being used in 84% of the observations (IQR, 69%-87%). Cleaning and drying technique was considered appropriate in a median of 93% of observations (IQR, 86%-96%).
Compliance to moment 5 (after touching patient surroundings) was the lowest across hospitals (median 71%), compared with a median 100% for moment 2 (before clean/aseptic procedures) and a median 93% for moment 3 (after body fluid exposure/risk). For moment 1, median compliance was 87% (before touching a patient), and for moment 4, median compliance was 82% (after touching a patient).
Dr. Kopsidas concluded that the overall level of HH compliance among doctors and nurses working in European pediatric ICUs appears to be high, with moment 5 being the most frequently missed opportunity. Nonunit doctors and nurses and other personnel show lower WHO guidelines adherence. He stated that “these results will be used to design tailor-made interventions in participating units with the aim of reducing HAIs [health care–associated infections] and spread of multidrug resistant infections.”
He also said that “unified surveillance in Europe is possible and achievable, and allows for benchmarking among countries, institutions and wards.”
For some units, improving HH is a missed opportunity. The next stop for the RANIN-KIDS network is to look at the effects of interventions on reducing spread.
Dr. Kopsidas had no relevant financial disclosures.
A multidisciplinary team seeking to measure compliance with hand hygiene (HH) practices in pediatric ICUs across Europe found compliance was comparable and relatively high among unit doctors and nurses, but not as high in nonunit doctors and nurses.
Ioannis Kopsidas, MD, presented these results from the RANIN-KIDS Network during the annual meeting of the European Society for Paediatric Infectious Diseases, held virtually this year. RANIN-KIDS (Reducing Antimicrobial Use and Nosocomial Infections in Kids) is a European network with the aim of preventing hospital-associated infections and promoting judicial antimicrobial use in pediatric patients using a common sustainable methodology across Europe.
Infections kill. This is especially the case in pediatric ICUs, where young age and an immunocompromised status make patients particularly vulnerable to infections. Poor HH is a major cause for disease transmission. To reduce the risk, the World Health Organization recommends attention to five moments of hand hygiene and nine steps for hand washing. Various tools are available to improve adherence, but whether these measures are being followed is unclear. The researchers sought to assess the degree of compliance with HH practices in pediatric ICUs and to identify targets for improvement.
Dr. Kopsidas, of the Center of Clinical Epidemiology and Outcomes Research, the National and Kapodistrian University of Athens, and colleagues examined practices in nine pediatric ICUs across six European countries (Estonia, Germany, Greece, Italy, Spain, and Switzerland) by means of prospective observational study. All organizations were part of the RANIN-KIDS network. Over a 6-month period starting in March 2019, observations were conducted in every unit by observers using a data collection tool developed based on WHO guidelines. Training for observers was provided using a self-paced teaching kit comprising PowerPoint and video presentations, followed by the completion of a test observation form after observing staged hand hygiene exercises. Results were then compared with WHO guidance, and irregularities were explained in order to achieve interrater reliability.
Researchers observed 1,715 HH opportunities. Across all pediatric ICUs, the median HH compliance rate was 82% (interquartile range, 72%-95%). Stratified by type of professional, median compliance was comparable among unit doctors (90%) and nurses (87%), but lower for nonunit doctors and nurses (81%) and also for nondoctors and nonnurses (67%). Alcohol-based hand rub was substantially preferred to soap and water, being used in 84% of the observations (IQR, 69%-87%). Cleaning and drying technique was considered appropriate in a median of 93% of observations (IQR, 86%-96%).
Compliance to moment 5 (after touching patient surroundings) was the lowest across hospitals (median 71%), compared with a median 100% for moment 2 (before clean/aseptic procedures) and a median 93% for moment 3 (after body fluid exposure/risk). For moment 1, median compliance was 87% (before touching a patient), and for moment 4, median compliance was 82% (after touching a patient).
Dr. Kopsidas concluded that the overall level of HH compliance among doctors and nurses working in European pediatric ICUs appears to be high, with moment 5 being the most frequently missed opportunity. Nonunit doctors and nurses and other personnel show lower WHO guidelines adherence. He stated that “these results will be used to design tailor-made interventions in participating units with the aim of reducing HAIs [health care–associated infections] and spread of multidrug resistant infections.”
He also said that “unified surveillance in Europe is possible and achievable, and allows for benchmarking among countries, institutions and wards.”
For some units, improving HH is a missed opportunity. The next stop for the RANIN-KIDS network is to look at the effects of interventions on reducing spread.
Dr. Kopsidas had no relevant financial disclosures.
FROM ESPID 2020
Margetuximab approved for HER2-positive metastatic breast cancer
The new drug is indicated for use in combination with chemotherapy for the treatment of patients with metastatic HER2-positive breast cancer who have already received two or more prior anti-HER2 regimens, with at least one for metastatic disease.
Margetuximab-cmkb is also the first HER2-targeted therapy shown to improve progression-free survival (PFS) as compared with the first-ever HER2-targeted agent, trastuzumab in a head-to-head, phase 3 clinical trial (known as SOPHIA).
“Early detection and treatment have had a positive impact on the survival of patients with breast cancer, but the prognosis for people diagnosed with metastatic breast cancer remains poor, and additional treatments are needed,” said Hope S. Rugo, MD, director of breast oncology and clinical trials education, University of California, San Francisco, Diller Family Comprehensive Cancer Center, in a press release.
“As the only HER2-targeted agent to have shown a PFS improvement versus trastuzumab in a head-to-head phase 3 clinical trial, margetuximab with chemotherapy represents the newest treatment option for patients who have progressed on available HER2-directed therapies,” said Dr. Rugo, who is an investigator in the SOPHIA trial.
Like trastuzumab, margetuximab-cmkb binds HER2 with high specificity and affinity and disrupts signaling that drives cell proliferation and survival, but margetuximab binds with elevated affinity to both the lower- and higher-affinity forms of CD16A, an Fc gamma receptor important for antibody dependent cell-mediated cytotoxicity against tumor cells, according to the manufacturer, MacroGenics.
Details of the pivotal trial
The SOPHIA trial was a randomized, open-label, phase 3 clinical trial that compared margetuximab-cmkb plus chemotherapy with trastuzumab plus chemotherapy in both arms in patients with HER2-positive metastatic breast cancer who had previously been treated with anti–HER2-targeted therapies.
All patients in the cohort had previously received trastuzumab, all but one patient had previously also received pertuzumab, and most of the patients (91%) had also been treated with ado-trastuzumab emtansine, or T-DM1.
The trial randomly assigned 536 patients to receive either margetuximab-cmkb (n = 266) given intravenously at 15 mg/kg every 3 weeks or trastuzumab (n = 270) given intravenously at 6 mg/kg (or 8 mg/kg for loading dose) every 3 weeks in combination with either capecitabine, eribulin, gemcitabine, or vinorelbine, given at the standard doses.
As compared with trastuzumab, margetuximab plus chemotherapy led to a significant 24% reduction in the risk for progression or death (hazard ratio, 0.76).
The median PFS also favored margetuximab (5.8 months vs. 4.9 months), as did the overall response rate (22% vs. 16%).
The final overall survival analysis is expected in the second half of 2021.
Common adverse events associated with the margetuximab regimen included fatigue/asthenia (57%), nausea (33%), diarrhea (25%), and vomiting (21%). Infusion-related reactions occurred in 13% of patients receiving margetuximab, and almost all were grade 1 or 2, with only 1.5% at grade 3.
The product also carries a boxed warning for left ventricular dysfunction and embryo-fetal toxicity.
A version of this article first appeared on Medscape.com.
The new drug is indicated for use in combination with chemotherapy for the treatment of patients with metastatic HER2-positive breast cancer who have already received two or more prior anti-HER2 regimens, with at least one for metastatic disease.
Margetuximab-cmkb is also the first HER2-targeted therapy shown to improve progression-free survival (PFS) as compared with the first-ever HER2-targeted agent, trastuzumab in a head-to-head, phase 3 clinical trial (known as SOPHIA).
“Early detection and treatment have had a positive impact on the survival of patients with breast cancer, but the prognosis for people diagnosed with metastatic breast cancer remains poor, and additional treatments are needed,” said Hope S. Rugo, MD, director of breast oncology and clinical trials education, University of California, San Francisco, Diller Family Comprehensive Cancer Center, in a press release.
“As the only HER2-targeted agent to have shown a PFS improvement versus trastuzumab in a head-to-head phase 3 clinical trial, margetuximab with chemotherapy represents the newest treatment option for patients who have progressed on available HER2-directed therapies,” said Dr. Rugo, who is an investigator in the SOPHIA trial.
Like trastuzumab, margetuximab-cmkb binds HER2 with high specificity and affinity and disrupts signaling that drives cell proliferation and survival, but margetuximab binds with elevated affinity to both the lower- and higher-affinity forms of CD16A, an Fc gamma receptor important for antibody dependent cell-mediated cytotoxicity against tumor cells, according to the manufacturer, MacroGenics.
Details of the pivotal trial
The SOPHIA trial was a randomized, open-label, phase 3 clinical trial that compared margetuximab-cmkb plus chemotherapy with trastuzumab plus chemotherapy in both arms in patients with HER2-positive metastatic breast cancer who had previously been treated with anti–HER2-targeted therapies.
All patients in the cohort had previously received trastuzumab, all but one patient had previously also received pertuzumab, and most of the patients (91%) had also been treated with ado-trastuzumab emtansine, or T-DM1.
The trial randomly assigned 536 patients to receive either margetuximab-cmkb (n = 266) given intravenously at 15 mg/kg every 3 weeks or trastuzumab (n = 270) given intravenously at 6 mg/kg (or 8 mg/kg for loading dose) every 3 weeks in combination with either capecitabine, eribulin, gemcitabine, or vinorelbine, given at the standard doses.
As compared with trastuzumab, margetuximab plus chemotherapy led to a significant 24% reduction in the risk for progression or death (hazard ratio, 0.76).
The median PFS also favored margetuximab (5.8 months vs. 4.9 months), as did the overall response rate (22% vs. 16%).
The final overall survival analysis is expected in the second half of 2021.
Common adverse events associated with the margetuximab regimen included fatigue/asthenia (57%), nausea (33%), diarrhea (25%), and vomiting (21%). Infusion-related reactions occurred in 13% of patients receiving margetuximab, and almost all were grade 1 or 2, with only 1.5% at grade 3.
The product also carries a boxed warning for left ventricular dysfunction and embryo-fetal toxicity.
A version of this article first appeared on Medscape.com.
The new drug is indicated for use in combination with chemotherapy for the treatment of patients with metastatic HER2-positive breast cancer who have already received two or more prior anti-HER2 regimens, with at least one for metastatic disease.
Margetuximab-cmkb is also the first HER2-targeted therapy shown to improve progression-free survival (PFS) as compared with the first-ever HER2-targeted agent, trastuzumab in a head-to-head, phase 3 clinical trial (known as SOPHIA).
“Early detection and treatment have had a positive impact on the survival of patients with breast cancer, but the prognosis for people diagnosed with metastatic breast cancer remains poor, and additional treatments are needed,” said Hope S. Rugo, MD, director of breast oncology and clinical trials education, University of California, San Francisco, Diller Family Comprehensive Cancer Center, in a press release.
“As the only HER2-targeted agent to have shown a PFS improvement versus trastuzumab in a head-to-head phase 3 clinical trial, margetuximab with chemotherapy represents the newest treatment option for patients who have progressed on available HER2-directed therapies,” said Dr. Rugo, who is an investigator in the SOPHIA trial.
Like trastuzumab, margetuximab-cmkb binds HER2 with high specificity and affinity and disrupts signaling that drives cell proliferation and survival, but margetuximab binds with elevated affinity to both the lower- and higher-affinity forms of CD16A, an Fc gamma receptor important for antibody dependent cell-mediated cytotoxicity against tumor cells, according to the manufacturer, MacroGenics.
Details of the pivotal trial
The SOPHIA trial was a randomized, open-label, phase 3 clinical trial that compared margetuximab-cmkb plus chemotherapy with trastuzumab plus chemotherapy in both arms in patients with HER2-positive metastatic breast cancer who had previously been treated with anti–HER2-targeted therapies.
All patients in the cohort had previously received trastuzumab, all but one patient had previously also received pertuzumab, and most of the patients (91%) had also been treated with ado-trastuzumab emtansine, or T-DM1.
The trial randomly assigned 536 patients to receive either margetuximab-cmkb (n = 266) given intravenously at 15 mg/kg every 3 weeks or trastuzumab (n = 270) given intravenously at 6 mg/kg (or 8 mg/kg for loading dose) every 3 weeks in combination with either capecitabine, eribulin, gemcitabine, or vinorelbine, given at the standard doses.
As compared with trastuzumab, margetuximab plus chemotherapy led to a significant 24% reduction in the risk for progression or death (hazard ratio, 0.76).
The median PFS also favored margetuximab (5.8 months vs. 4.9 months), as did the overall response rate (22% vs. 16%).
The final overall survival analysis is expected in the second half of 2021.
Common adverse events associated with the margetuximab regimen included fatigue/asthenia (57%), nausea (33%), diarrhea (25%), and vomiting (21%). Infusion-related reactions occurred in 13% of patients receiving margetuximab, and almost all were grade 1 or 2, with only 1.5% at grade 3.
The product also carries a boxed warning for left ventricular dysfunction and embryo-fetal toxicity.
A version of this article first appeared on Medscape.com.