User login
The Official Newspaper of the American Association for Thoracic Surgery
Nivolumab plus ipilimumab shines as first-line in advanced NSCLC
VIENNA – The combination of nivolumab and ipilimumab as first-line therapy in patients with advanced non–small cell lung cancer (NSCLC) doubled median progression-free survival time compared with nivolumab monotherapy in updated results from the CheckMate 012 trial, Scott N. Gettinger, MD, reported at the World Congress on Lung Cancer.
This doubling of progression-free survival (PFS) applied to all comers regardless of whether or not their tumor expressed programmed death-ligand 1 (PD-L1). In those patients with any degree of PD-L1 expression – even if just 1% of tumor cells stained positive – combination therapy didn’t just double median PFS, it tripled it, compared with nivolumab alone, added Dr. Gettinger of the Yale Cancer Center in New Haven, Conn.
CheckMate 012 is a phase I study of nivolumab as first-line therapy for advanced NSCLC with numerous treatment arms. Dr. Gettinger presented updated results for 52 patients who received intravenous nivolumab monotherapy at a dose of 3 mg/kg every 2 weeks, 36 patients on nivolumab plus intravenous ipilimumab at 1 mg/kg every 12 weeks, and 39 who received nivolumab plus ipilimumab every 6 weeks. None of the participants had prior chemotherapy for their advanced stage IIIb or IV NSCLC.
Median PFS in the overall study population was 3.6 months with nivolumab monotherapy and 8.0 months with combination therapy. In the roughly 70% of participants who had any degree of tumor PD-L1 expression, median PFS was 3.5 months with monotherapy, compared with 12.7 months in the combined dual therapy arms. And, in the roughly one-quarter of patients whose tumor showed at least 50% PD-L1 expression, median PFS rose to 8.3 months with nivolumab monotherapy and hasn’t yet been reached in patients on combination therapy.
The 1-year overall survival rate in patients on nivolumab monotherapy was 73% in all treated patients, 69% in those with any detectable tumor PD-L1 expression, and 83% in patients with at least 50% PD-L1 expression. In patients on combination therapy, the corresponding figures were higher at 76%, 87%, and 100%.
The clearly enhanced efficacy achieved with the combination of nivolumab plus ipilimumab was accomplished with only a modest increase in toxicity compared with nivolumab alone. At a median follow-up of 22 months in the nivolumab monotherapy group and 16 months for combination therapy, the rate of any treatment-related adverse event leading to study withdrawal was 12% with monotherapy and 18% with combination therapy.
The combination of nivolumab (Opdivo), a PD-L1 immune checkpoint inhibitor, and ipilimumab (Yervoy), a cytotoxic T-lymphocyte–associated protein 4 immune checkpoint inhibitor, is biologically attractive: “The ipilimumab primes the immune system by inducing tumor infiltration of effector T cells while depleting the number of myeloid-derived suppressor cells and suppressive regulatory T cells within the tumor microenvironment,” Dr. Gettinger explained.
Nivolumab is approved for treatment of advanced NSCLC that has progressed despite platinum-based chemotherapy. Of the various toxicities associated with the drug, only dermatologic and GI adverse events occurred more frequently with combination therapy than nivolumab alone.
There were five complete responses in the nivolumab monotherapy group and six with combination therapy. Of note, four of these complete responses occurred in patients without any measurable tumor PD-L1 expression.
Based upon these encouraging results from CheckMate 012, a phase III randomized clinical trial of nivolumab as first-line therapy in patients with advanced NSCLC is underway. In the CheckMate 227 trial, patients with any detectable PD-L1 expression are randomized to nivolumab at 3mg/kg every 2 weeks plus ipilimumab at 1 mg/kg every 6 weeks, nivolumab monotherapy at 240 mg every 2 weeks, or standard platinum-based chemotherapy. Patients with no PD-L1 expression in their tumor are assigned to the nivolumab/ipilimumab combination, or nivolumab at 360 mg every 3 weeks plus chemotherapy, or chemotherapy alone.
“I think we should be cautious despite the excitement about the combination,” argued Dr. Garon, director of thoracic oncology at the University of California, Los Angeles.
He noted that various iterations of the large CheckMate 012 phase I program have been presented repeatedly at major meetings, and the shifting data have raised concerns in his mind about possible patient selection bias stemming from the study design.
“From my perspective, until we see randomized data that can control for these biases, I will remain hopeful but not yet extremely confident that this combination will be the new frontline therapy for metastatic non–small cell lung cancer,” Dr. Garon said.
Dr. Gettinger reported serving as a consultant to Bristol-Myers Squibb, which markets nivolumab.
Dr. Garon reported that his institution receives funding from Bristol-Myers Squibb as well as AstraZeneca, Boehringer Ingelheim, Eli Lilly, Genentech, Mirati, Merck, Pfizer, and Novartis.
VIENNA – The combination of nivolumab and ipilimumab as first-line therapy in patients with advanced non–small cell lung cancer (NSCLC) doubled median progression-free survival time compared with nivolumab monotherapy in updated results from the CheckMate 012 trial, Scott N. Gettinger, MD, reported at the World Congress on Lung Cancer.
This doubling of progression-free survival (PFS) applied to all comers regardless of whether or not their tumor expressed programmed death-ligand 1 (PD-L1). In those patients with any degree of PD-L1 expression – even if just 1% of tumor cells stained positive – combination therapy didn’t just double median PFS, it tripled it, compared with nivolumab alone, added Dr. Gettinger of the Yale Cancer Center in New Haven, Conn.
CheckMate 012 is a phase I study of nivolumab as first-line therapy for advanced NSCLC with numerous treatment arms. Dr. Gettinger presented updated results for 52 patients who received intravenous nivolumab monotherapy at a dose of 3 mg/kg every 2 weeks, 36 patients on nivolumab plus intravenous ipilimumab at 1 mg/kg every 12 weeks, and 39 who received nivolumab plus ipilimumab every 6 weeks. None of the participants had prior chemotherapy for their advanced stage IIIb or IV NSCLC.
Median PFS in the overall study population was 3.6 months with nivolumab monotherapy and 8.0 months with combination therapy. In the roughly 70% of participants who had any degree of tumor PD-L1 expression, median PFS was 3.5 months with monotherapy, compared with 12.7 months in the combined dual therapy arms. And, in the roughly one-quarter of patients whose tumor showed at least 50% PD-L1 expression, median PFS rose to 8.3 months with nivolumab monotherapy and hasn’t yet been reached in patients on combination therapy.
The 1-year overall survival rate in patients on nivolumab monotherapy was 73% in all treated patients, 69% in those with any detectable tumor PD-L1 expression, and 83% in patients with at least 50% PD-L1 expression. In patients on combination therapy, the corresponding figures were higher at 76%, 87%, and 100%.
The clearly enhanced efficacy achieved with the combination of nivolumab plus ipilimumab was accomplished with only a modest increase in toxicity compared with nivolumab alone. At a median follow-up of 22 months in the nivolumab monotherapy group and 16 months for combination therapy, the rate of any treatment-related adverse event leading to study withdrawal was 12% with monotherapy and 18% with combination therapy.
The combination of nivolumab (Opdivo), a PD-L1 immune checkpoint inhibitor, and ipilimumab (Yervoy), a cytotoxic T-lymphocyte–associated protein 4 immune checkpoint inhibitor, is biologically attractive: “The ipilimumab primes the immune system by inducing tumor infiltration of effector T cells while depleting the number of myeloid-derived suppressor cells and suppressive regulatory T cells within the tumor microenvironment,” Dr. Gettinger explained.
Nivolumab is approved for treatment of advanced NSCLC that has progressed despite platinum-based chemotherapy. Of the various toxicities associated with the drug, only dermatologic and GI adverse events occurred more frequently with combination therapy than nivolumab alone.
There were five complete responses in the nivolumab monotherapy group and six with combination therapy. Of note, four of these complete responses occurred in patients without any measurable tumor PD-L1 expression.
Based upon these encouraging results from CheckMate 012, a phase III randomized clinical trial of nivolumab as first-line therapy in patients with advanced NSCLC is underway. In the CheckMate 227 trial, patients with any detectable PD-L1 expression are randomized to nivolumab at 3mg/kg every 2 weeks plus ipilimumab at 1 mg/kg every 6 weeks, nivolumab monotherapy at 240 mg every 2 weeks, or standard platinum-based chemotherapy. Patients with no PD-L1 expression in their tumor are assigned to the nivolumab/ipilimumab combination, or nivolumab at 360 mg every 3 weeks plus chemotherapy, or chemotherapy alone.
“I think we should be cautious despite the excitement about the combination,” argued Dr. Garon, director of thoracic oncology at the University of California, Los Angeles.
He noted that various iterations of the large CheckMate 012 phase I program have been presented repeatedly at major meetings, and the shifting data have raised concerns in his mind about possible patient selection bias stemming from the study design.
“From my perspective, until we see randomized data that can control for these biases, I will remain hopeful but not yet extremely confident that this combination will be the new frontline therapy for metastatic non–small cell lung cancer,” Dr. Garon said.
Dr. Gettinger reported serving as a consultant to Bristol-Myers Squibb, which markets nivolumab.
Dr. Garon reported that his institution receives funding from Bristol-Myers Squibb as well as AstraZeneca, Boehringer Ingelheim, Eli Lilly, Genentech, Mirati, Merck, Pfizer, and Novartis.
VIENNA – The combination of nivolumab and ipilimumab as first-line therapy in patients with advanced non–small cell lung cancer (NSCLC) doubled median progression-free survival time compared with nivolumab monotherapy in updated results from the CheckMate 012 trial, Scott N. Gettinger, MD, reported at the World Congress on Lung Cancer.
This doubling of progression-free survival (PFS) applied to all comers regardless of whether or not their tumor expressed programmed death-ligand 1 (PD-L1). In those patients with any degree of PD-L1 expression – even if just 1% of tumor cells stained positive – combination therapy didn’t just double median PFS, it tripled it, compared with nivolumab alone, added Dr. Gettinger of the Yale Cancer Center in New Haven, Conn.
CheckMate 012 is a phase I study of nivolumab as first-line therapy for advanced NSCLC with numerous treatment arms. Dr. Gettinger presented updated results for 52 patients who received intravenous nivolumab monotherapy at a dose of 3 mg/kg every 2 weeks, 36 patients on nivolumab plus intravenous ipilimumab at 1 mg/kg every 12 weeks, and 39 who received nivolumab plus ipilimumab every 6 weeks. None of the participants had prior chemotherapy for their advanced stage IIIb or IV NSCLC.
Median PFS in the overall study population was 3.6 months with nivolumab monotherapy and 8.0 months with combination therapy. In the roughly 70% of participants who had any degree of tumor PD-L1 expression, median PFS was 3.5 months with monotherapy, compared with 12.7 months in the combined dual therapy arms. And, in the roughly one-quarter of patients whose tumor showed at least 50% PD-L1 expression, median PFS rose to 8.3 months with nivolumab monotherapy and hasn’t yet been reached in patients on combination therapy.
The 1-year overall survival rate in patients on nivolumab monotherapy was 73% in all treated patients, 69% in those with any detectable tumor PD-L1 expression, and 83% in patients with at least 50% PD-L1 expression. In patients on combination therapy, the corresponding figures were higher at 76%, 87%, and 100%.
The clearly enhanced efficacy achieved with the combination of nivolumab plus ipilimumab was accomplished with only a modest increase in toxicity compared with nivolumab alone. At a median follow-up of 22 months in the nivolumab monotherapy group and 16 months for combination therapy, the rate of any treatment-related adverse event leading to study withdrawal was 12% with monotherapy and 18% with combination therapy.
The combination of nivolumab (Opdivo), a PD-L1 immune checkpoint inhibitor, and ipilimumab (Yervoy), a cytotoxic T-lymphocyte–associated protein 4 immune checkpoint inhibitor, is biologically attractive: “The ipilimumab primes the immune system by inducing tumor infiltration of effector T cells while depleting the number of myeloid-derived suppressor cells and suppressive regulatory T cells within the tumor microenvironment,” Dr. Gettinger explained.
Nivolumab is approved for treatment of advanced NSCLC that has progressed despite platinum-based chemotherapy. Of the various toxicities associated with the drug, only dermatologic and GI adverse events occurred more frequently with combination therapy than nivolumab alone.
There were five complete responses in the nivolumab monotherapy group and six with combination therapy. Of note, four of these complete responses occurred in patients without any measurable tumor PD-L1 expression.
Based upon these encouraging results from CheckMate 012, a phase III randomized clinical trial of nivolumab as first-line therapy in patients with advanced NSCLC is underway. In the CheckMate 227 trial, patients with any detectable PD-L1 expression are randomized to nivolumab at 3mg/kg every 2 weeks plus ipilimumab at 1 mg/kg every 6 weeks, nivolumab monotherapy at 240 mg every 2 weeks, or standard platinum-based chemotherapy. Patients with no PD-L1 expression in their tumor are assigned to the nivolumab/ipilimumab combination, or nivolumab at 360 mg every 3 weeks plus chemotherapy, or chemotherapy alone.
“I think we should be cautious despite the excitement about the combination,” argued Dr. Garon, director of thoracic oncology at the University of California, Los Angeles.
He noted that various iterations of the large CheckMate 012 phase I program have been presented repeatedly at major meetings, and the shifting data have raised concerns in his mind about possible patient selection bias stemming from the study design.
“From my perspective, until we see randomized data that can control for these biases, I will remain hopeful but not yet extremely confident that this combination will be the new frontline therapy for metastatic non–small cell lung cancer,” Dr. Garon said.
Dr. Gettinger reported serving as a consultant to Bristol-Myers Squibb, which markets nivolumab.
Dr. Garon reported that his institution receives funding from Bristol-Myers Squibb as well as AstraZeneca, Boehringer Ingelheim, Eli Lilly, Genentech, Mirati, Merck, Pfizer, and Novartis.
AT WCLC 2016
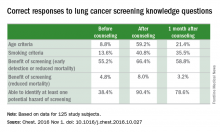
Key clinical point: A combination of two immunotherapy agents with different mechanisms of action produced impressive efficacy and acceptable toxicities as first-line therapy in patients with chemotherapy-naive advanced non–small cell lung cancer.
Major finding: in patients with any detectable tumor PD-L1 expression.
Data source: This analysis from a larger phase I study included 127 patients with no prior chemotherapy for advanced NSCLC.
Disclosures: The study presenter is a consultant to Bristol-Myers Squibb, which sponsored the CheckMate 012 trial.
TAVR valve durability supported in large follow-up
WASHINGTON – First-generation, balloon-expandable transcatheter aortic valves had a less than 1% rate of valve failure in planned echocardiography examinations during follow-up that extended as long as 5 years after valve placement in more than 2,400 patients, a demonstration of durability that experts uniformly called “reassuring.”
This finding from patients who underwent transcatheter aortic valve replacement (TAVR) in the first U.S. pivotal trial for these devices, PARTNER 1 parts A and B, and during the subsequent continued-access program at PARTNER 1 study sites, represents the largest and longest systematic ultrasound follow-up of TAVR patients, Pamela S. Douglas, MD, said at the Transcatheter Cardiovascular Therapeutics annual meeting.
This evaluation of 2,404 TAVR patients in the PARTNER 1 trial examined by echocardiography and encompassing 6,493 patient-years of follow-up is the “largest core-lab based study of transcatheter heart valves to date. These data demonstrate excellent durability of transcatheter heart valves, suggesting that the low 5-year survival observed in this cohort is not related to adverse hemodynamics or transcatheter heart valve deterioration,” said Dr. Douglas, professor of medicine at Duke University, Durham, N.C.
Her findings showed that out of the 2,482 patients treated with TAVR (and including those without echo follow-up) either in the trial or during the continued access program and followed for a median of 2.9 years and an average of 2.6 years, 20 patients (0.8%) required a reintervention. Four of these 20 patients (0.2% of the total cohort) showed a “classic pattern” of aortic valve deterioration marked by an increased valve pressure gradient and a reduced valve area, she reported.
“Reintervention was rare, became less frequent over time, and was usually not due to structural deterioration of the transcatheter heart valve,” she said. But Dr. Douglas also cautioned that among the patients who received the first-generation, balloon expandable Sapien valve in this cohort, just 39% survived to 5 years, and a mere 282 patients (11%) actually underwent echocardiographic examination at 5 years.
“This is one of several steps we need to take to figure out the durability of transcatheter valves,” said Jeffrey J. Popma, MD, professor of medicine and an interventional cardiologist at Beth Israel Deaconess Medical Center, Boston. He noted that data are needed from follow-up periods of 8 or 10 years, but these data will not be available until intermediate- or low-risk patients undergo TAVR in controlled circumstances and have long-term follow-up.
“Ten-year follow-up data will essentially be impossible” for the high-risk or inoperable patients treated with TAVR in the PARTNER 1 trial, which focused on the sickest patients with aortic stenosis, said Dr. Popma, lead investigator for several studies of TAVR using self-expanding aortic valves and marketed as CoreValve devices.
“We obviously need to follow patients longer. The 5-year results look terrific, and so very reassuring, but we need to keep an eye on this as we move TAVR into less sick and younger patients,” said Dr. Robert O. Bonow, professor of cardiology at Northwestern University, Chicago. “Durability is the remaining frontier in terms of moving TAVR into younger patients,” Dr. Bonow said at the meeting, which was sponsored by the Cardiovascular Research Foundation.
These data continue to show that “transcatheter valves have looked hemodynamically superior to surgically-placed valves with respect to the VARC (Valve Academic Research Consortium)–2 criteria” for prosthetic valve function, Dr. Popma noted. “I think the benefits of surgical valves have been overstated and the benefits of transcatheter valves understated,” he said.
“Surgical valves have not been held to the same [very demanding] standard as transcatheter valves,” Dr. Douglas agreed.
The data Dr. Douglas reported contrast with longer-term follow-up reported in May 2016 for 378 patients who underwent TAVR at either of two pioneering centers in a retrospective review. Those data suggested a valve degeneration rate of about 50% after 8 years, Danny Dvir, MD, reported at the annual congress of the European Association of Percutaneous Cardiovascular Interventions. Speaking recently in an interview, Dr. Dvir acknowledged some of the challenges in trying to derive valve durability information from a relatively small number of very-high-risk patients who underwent TAVR very early during development of the procedure.
Some TAVR experts have also questioned the criteria that Dr. Dvir used to identify valve structural valve degeneration for this analysis. “The criteria he used were much more stringent that the criteria we have used to assess surgically-placed valves,” said Michael J. Reardon, MD, professor of cardiovascular surgery at Houston Methodist Hospital. “If surgically-placed aortic valves were subjected to the same criteria Dr. Dvir applied then they would perform even worse,” Dr. Reardon said in an interview.
PARTNER 1 was sponsored by Edwards Lifesciences, the company that had marketed the Sapien first-generation, balloon expandable TAVR system. Dr. Douglas has received research support from Edwards. Dr. Bonow had no disclosures. Dr. Popma has been the lead investigator for several studies of a self-expanding TAVR system sponsored by Medtronic, and he has also received research funding from several other companies, has been a consultant to Boston Scientific and Direct Flow, and owns equity in Direct Flow. Dr. Dvir has been a consultant to and received research support from Edwards, Medtronic, and St. Jude. Dr. Reardon has been a consultant to Medtronic.
[email protected]
On Twitter @mitchelzoler
The data reported by Dr. Douglas are very important and very reassuring. It isn’t easy to evaluate long-term results in patients who underwent TAVR in the early days because that population of patients was old and at very high risk. Even when patients had successful procedures their longevity wasn’t long. Only about 10% of the starting population of 2,482 patients in Dr. Douglas’ study actually had echocardiography done after 5 years. To assess durability you need longer-term echo follow-up, but it will be very challenging to have enough patients to have statistical power to do that.
I am not nervous about long-term durability of TAVR in octogenarian patients, the most typical age for TAVR patients today and since we began using it. Durability is more of an issue for patients who are 75 or younger, and we will need data from 7- to 10-year follow-up of younger patients to have a reasonable answer. Younger patients who undergo TAVR may face more of a threat from valve deterioration simply because of their longer life expectancy. In addition, with surgical valves we know that younger age is one of the strongest predictors of valve degeneration.
Danny Dvir, MD , is an interventional cardiologist at the University of Washington in Seattle. He has been a consultant to and received research support from Edwards, Medtronic, and St. Jude. He made these comments in an interview.
The data reported by Dr. Douglas are very important and very reassuring. It isn’t easy to evaluate long-term results in patients who underwent TAVR in the early days because that population of patients was old and at very high risk. Even when patients had successful procedures their longevity wasn’t long. Only about 10% of the starting population of 2,482 patients in Dr. Douglas’ study actually had echocardiography done after 5 years. To assess durability you need longer-term echo follow-up, but it will be very challenging to have enough patients to have statistical power to do that.
I am not nervous about long-term durability of TAVR in octogenarian patients, the most typical age for TAVR patients today and since we began using it. Durability is more of an issue for patients who are 75 or younger, and we will need data from 7- to 10-year follow-up of younger patients to have a reasonable answer. Younger patients who undergo TAVR may face more of a threat from valve deterioration simply because of their longer life expectancy. In addition, with surgical valves we know that younger age is one of the strongest predictors of valve degeneration.
Danny Dvir, MD , is an interventional cardiologist at the University of Washington in Seattle. He has been a consultant to and received research support from Edwards, Medtronic, and St. Jude. He made these comments in an interview.
The data reported by Dr. Douglas are very important and very reassuring. It isn’t easy to evaluate long-term results in patients who underwent TAVR in the early days because that population of patients was old and at very high risk. Even when patients had successful procedures their longevity wasn’t long. Only about 10% of the starting population of 2,482 patients in Dr. Douglas’ study actually had echocardiography done after 5 years. To assess durability you need longer-term echo follow-up, but it will be very challenging to have enough patients to have statistical power to do that.
I am not nervous about long-term durability of TAVR in octogenarian patients, the most typical age for TAVR patients today and since we began using it. Durability is more of an issue for patients who are 75 or younger, and we will need data from 7- to 10-year follow-up of younger patients to have a reasonable answer. Younger patients who undergo TAVR may face more of a threat from valve deterioration simply because of their longer life expectancy. In addition, with surgical valves we know that younger age is one of the strongest predictors of valve degeneration.
Danny Dvir, MD , is an interventional cardiologist at the University of Washington in Seattle. He has been a consultant to and received research support from Edwards, Medtronic, and St. Jude. He made these comments in an interview.
WASHINGTON – First-generation, balloon-expandable transcatheter aortic valves had a less than 1% rate of valve failure in planned echocardiography examinations during follow-up that extended as long as 5 years after valve placement in more than 2,400 patients, a demonstration of durability that experts uniformly called “reassuring.”
This finding from patients who underwent transcatheter aortic valve replacement (TAVR) in the first U.S. pivotal trial for these devices, PARTNER 1 parts A and B, and during the subsequent continued-access program at PARTNER 1 study sites, represents the largest and longest systematic ultrasound follow-up of TAVR patients, Pamela S. Douglas, MD, said at the Transcatheter Cardiovascular Therapeutics annual meeting.
This evaluation of 2,404 TAVR patients in the PARTNER 1 trial examined by echocardiography and encompassing 6,493 patient-years of follow-up is the “largest core-lab based study of transcatheter heart valves to date. These data demonstrate excellent durability of transcatheter heart valves, suggesting that the low 5-year survival observed in this cohort is not related to adverse hemodynamics or transcatheter heart valve deterioration,” said Dr. Douglas, professor of medicine at Duke University, Durham, N.C.
Her findings showed that out of the 2,482 patients treated with TAVR (and including those without echo follow-up) either in the trial or during the continued access program and followed for a median of 2.9 years and an average of 2.6 years, 20 patients (0.8%) required a reintervention. Four of these 20 patients (0.2% of the total cohort) showed a “classic pattern” of aortic valve deterioration marked by an increased valve pressure gradient and a reduced valve area, she reported.
“Reintervention was rare, became less frequent over time, and was usually not due to structural deterioration of the transcatheter heart valve,” she said. But Dr. Douglas also cautioned that among the patients who received the first-generation, balloon expandable Sapien valve in this cohort, just 39% survived to 5 years, and a mere 282 patients (11%) actually underwent echocardiographic examination at 5 years.
“This is one of several steps we need to take to figure out the durability of transcatheter valves,” said Jeffrey J. Popma, MD, professor of medicine and an interventional cardiologist at Beth Israel Deaconess Medical Center, Boston. He noted that data are needed from follow-up periods of 8 or 10 years, but these data will not be available until intermediate- or low-risk patients undergo TAVR in controlled circumstances and have long-term follow-up.
“Ten-year follow-up data will essentially be impossible” for the high-risk or inoperable patients treated with TAVR in the PARTNER 1 trial, which focused on the sickest patients with aortic stenosis, said Dr. Popma, lead investigator for several studies of TAVR using self-expanding aortic valves and marketed as CoreValve devices.
“We obviously need to follow patients longer. The 5-year results look terrific, and so very reassuring, but we need to keep an eye on this as we move TAVR into less sick and younger patients,” said Dr. Robert O. Bonow, professor of cardiology at Northwestern University, Chicago. “Durability is the remaining frontier in terms of moving TAVR into younger patients,” Dr. Bonow said at the meeting, which was sponsored by the Cardiovascular Research Foundation.
These data continue to show that “transcatheter valves have looked hemodynamically superior to surgically-placed valves with respect to the VARC (Valve Academic Research Consortium)–2 criteria” for prosthetic valve function, Dr. Popma noted. “I think the benefits of surgical valves have been overstated and the benefits of transcatheter valves understated,” he said.
“Surgical valves have not been held to the same [very demanding] standard as transcatheter valves,” Dr. Douglas agreed.
The data Dr. Douglas reported contrast with longer-term follow-up reported in May 2016 for 378 patients who underwent TAVR at either of two pioneering centers in a retrospective review. Those data suggested a valve degeneration rate of about 50% after 8 years, Danny Dvir, MD, reported at the annual congress of the European Association of Percutaneous Cardiovascular Interventions. Speaking recently in an interview, Dr. Dvir acknowledged some of the challenges in trying to derive valve durability information from a relatively small number of very-high-risk patients who underwent TAVR very early during development of the procedure.
Some TAVR experts have also questioned the criteria that Dr. Dvir used to identify valve structural valve degeneration for this analysis. “The criteria he used were much more stringent that the criteria we have used to assess surgically-placed valves,” said Michael J. Reardon, MD, professor of cardiovascular surgery at Houston Methodist Hospital. “If surgically-placed aortic valves were subjected to the same criteria Dr. Dvir applied then they would perform even worse,” Dr. Reardon said in an interview.
PARTNER 1 was sponsored by Edwards Lifesciences, the company that had marketed the Sapien first-generation, balloon expandable TAVR system. Dr. Douglas has received research support from Edwards. Dr. Bonow had no disclosures. Dr. Popma has been the lead investigator for several studies of a self-expanding TAVR system sponsored by Medtronic, and he has also received research funding from several other companies, has been a consultant to Boston Scientific and Direct Flow, and owns equity in Direct Flow. Dr. Dvir has been a consultant to and received research support from Edwards, Medtronic, and St. Jude. Dr. Reardon has been a consultant to Medtronic.
[email protected]
On Twitter @mitchelzoler
WASHINGTON – First-generation, balloon-expandable transcatheter aortic valves had a less than 1% rate of valve failure in planned echocardiography examinations during follow-up that extended as long as 5 years after valve placement in more than 2,400 patients, a demonstration of durability that experts uniformly called “reassuring.”
This finding from patients who underwent transcatheter aortic valve replacement (TAVR) in the first U.S. pivotal trial for these devices, PARTNER 1 parts A and B, and during the subsequent continued-access program at PARTNER 1 study sites, represents the largest and longest systematic ultrasound follow-up of TAVR patients, Pamela S. Douglas, MD, said at the Transcatheter Cardiovascular Therapeutics annual meeting.
This evaluation of 2,404 TAVR patients in the PARTNER 1 trial examined by echocardiography and encompassing 6,493 patient-years of follow-up is the “largest core-lab based study of transcatheter heart valves to date. These data demonstrate excellent durability of transcatheter heart valves, suggesting that the low 5-year survival observed in this cohort is not related to adverse hemodynamics or transcatheter heart valve deterioration,” said Dr. Douglas, professor of medicine at Duke University, Durham, N.C.
Her findings showed that out of the 2,482 patients treated with TAVR (and including those without echo follow-up) either in the trial or during the continued access program and followed for a median of 2.9 years and an average of 2.6 years, 20 patients (0.8%) required a reintervention. Four of these 20 patients (0.2% of the total cohort) showed a “classic pattern” of aortic valve deterioration marked by an increased valve pressure gradient and a reduced valve area, she reported.
“Reintervention was rare, became less frequent over time, and was usually not due to structural deterioration of the transcatheter heart valve,” she said. But Dr. Douglas also cautioned that among the patients who received the first-generation, balloon expandable Sapien valve in this cohort, just 39% survived to 5 years, and a mere 282 patients (11%) actually underwent echocardiographic examination at 5 years.
“This is one of several steps we need to take to figure out the durability of transcatheter valves,” said Jeffrey J. Popma, MD, professor of medicine and an interventional cardiologist at Beth Israel Deaconess Medical Center, Boston. He noted that data are needed from follow-up periods of 8 or 10 years, but these data will not be available until intermediate- or low-risk patients undergo TAVR in controlled circumstances and have long-term follow-up.
“Ten-year follow-up data will essentially be impossible” for the high-risk or inoperable patients treated with TAVR in the PARTNER 1 trial, which focused on the sickest patients with aortic stenosis, said Dr. Popma, lead investigator for several studies of TAVR using self-expanding aortic valves and marketed as CoreValve devices.
“We obviously need to follow patients longer. The 5-year results look terrific, and so very reassuring, but we need to keep an eye on this as we move TAVR into less sick and younger patients,” said Dr. Robert O. Bonow, professor of cardiology at Northwestern University, Chicago. “Durability is the remaining frontier in terms of moving TAVR into younger patients,” Dr. Bonow said at the meeting, which was sponsored by the Cardiovascular Research Foundation.
These data continue to show that “transcatheter valves have looked hemodynamically superior to surgically-placed valves with respect to the VARC (Valve Academic Research Consortium)–2 criteria” for prosthetic valve function, Dr. Popma noted. “I think the benefits of surgical valves have been overstated and the benefits of transcatheter valves understated,” he said.
“Surgical valves have not been held to the same [very demanding] standard as transcatheter valves,” Dr. Douglas agreed.
The data Dr. Douglas reported contrast with longer-term follow-up reported in May 2016 for 378 patients who underwent TAVR at either of two pioneering centers in a retrospective review. Those data suggested a valve degeneration rate of about 50% after 8 years, Danny Dvir, MD, reported at the annual congress of the European Association of Percutaneous Cardiovascular Interventions. Speaking recently in an interview, Dr. Dvir acknowledged some of the challenges in trying to derive valve durability information from a relatively small number of very-high-risk patients who underwent TAVR very early during development of the procedure.
Some TAVR experts have also questioned the criteria that Dr. Dvir used to identify valve structural valve degeneration for this analysis. “The criteria he used were much more stringent that the criteria we have used to assess surgically-placed valves,” said Michael J. Reardon, MD, professor of cardiovascular surgery at Houston Methodist Hospital. “If surgically-placed aortic valves were subjected to the same criteria Dr. Dvir applied then they would perform even worse,” Dr. Reardon said in an interview.
PARTNER 1 was sponsored by Edwards Lifesciences, the company that had marketed the Sapien first-generation, balloon expandable TAVR system. Dr. Douglas has received research support from Edwards. Dr. Bonow had no disclosures. Dr. Popma has been the lead investigator for several studies of a self-expanding TAVR system sponsored by Medtronic, and he has also received research funding from several other companies, has been a consultant to Boston Scientific and Direct Flow, and owns equity in Direct Flow. Dr. Dvir has been a consultant to and received research support from Edwards, Medtronic, and St. Jude. Dr. Reardon has been a consultant to Medtronic.
[email protected]
On Twitter @mitchelzoler
AT TCT 2016
Key clinical point:
Major finding: During median follow-up of 2.9 years, 0.2% of patients had valves with classic hemodynamic signs of valve deterioration.
Data source: A total of 2,482 TAVR patients either enrolled in the PARTNER 1 trial or who underwent TAVR during a continued access program.
Disclosures: PARTNER 1 was sponsored by Edwards Lifesciences, the company that had marketed the Sapien first-generation, balloon expandable TAVR system. Dr. Douglas has received research support from Edwards. Dr. Bonow had no disclosures. Dr. Popma has been the lead investigator for several studies of a self-expanding TAVR system sponsored by Medtronic, and he has also received research funding from several other companies, has been a consultant to Boston Scientific and Direct Flow, and owns equity in Direct Flow. Dr. Dvir has been a consultant to and received research support from Edwards, Medtronic, and St. Jude. Dr. Reardon has been a consultant to Medtronic.
House passes 21st Century Cures bill
A pared-down version of the 21st Century Cures Act passed the House Nov. 30 by an overwhelming 392-26 vote, setting the stage for a quick Senate vote on the compromise legislation.
H.R. 34 gained more support on the House floor than did a version of the legislation that passed the House in 2015. In order to gain that additional support and ensure Senate approval, funding for key biomedical research efforts – the BRAIN Initiative, the Cancer Moonshot, and the Precision Medicine Initiative – was reduced from $9.3 billion to $4.8 billion over 10 years. Further, those funds are not guaranteed but will need to be appropriated through the federal budget process.
Other provisions include creation of an NIH program to support new researchers; funds to accelerate improved methods for prevention, diagnosis, and treatment of tick-borne diseases; the development of a national neurologic condition surveillance system; and the establishment of a task force on research specific to pregnant and breastfeeding women.
“More women with chronic diseases are becoming pregnant, yet safe and effective medications to manage these ongoing conditions throughout their pregnancy and beyond are needed,” Mary Norton, MD, president of the Society for Maternal-Fetal Medicine, said in a statement. “This legislation is a great first step toward greater collaboration and communication among federal agencies and public stakeholders.”
The 21st Century Cures bill also “takes concrete steps to help women and families suffering from postpartum depression,” Thomas Gellhaus, MD, president of the American College of Obstetricians and Gynecologists, said in a statement. “Postpartum depression is one of the most common medical complications following pregnancy. ... Cures expands state programs to better identify, treat, and support women and families at risk for or facing postpartum depression.”
The bill provides $500 million to the Food and Drug Administration to help the agency speed up the drug approval process, focusing on identifying biomarkers and developing targeted drugs for rare diseases. It also reauthorizes the pediatric rare disease priority review voucher program; requires drug companies to have a publicly accessible compassionate use policy for drugs treating serious or life-threatening conditions; and provides flexibility to get new antimicrobial drugs to market quickly.
Changes in the drug approval process were contentious during debate on the House floor.
“In its attempt to speed up the drug and device approval process, this legislation neglects the very people whom clinical trials are meant to help, that is, the patients,” Rep. Rosa DeLauro (D-Conn.) said. “Rather than protect those who rely on the health care system, it reduces the already weak regulation on medical devices, allows drugs with only limited evidence of the drug’s safety and efficacy, and rushes the use of new and unproven antibiotics.”
Other legislators expressed disappointment at the bill’s mental health care provisions. Rep. Joseph Kennedy III (D-Mass.) said that his “real concerns with the legislation lie with the mental health reform proposals, which don’t go nearly far enough. Mental health parity is already the law, thanks to the Mental Health Parity and Addiction Equity Act and the Affordable Care Act; but each study we read, Mr. Speaker, and each story we hear proves that insurance companies are skirting those rules.
“We need enforcement and transparency today,” Rep. Kennedy continued. “We need random audits before there have been violations, not after. We need insurers to publicly disclose the rates and reasons for denials in a way that patients and their families can understand, not in away that mental health advocates can’t even obtain. We need to increase Medicaid reimbursements in order to expand access to care, not to reduce them or roll back expansion.”
The pediatric provisions drew mixed reviews from the American Academy of Pediatrics.
“The 21st Century Cures Act includes three new programs that, if funded, would improve infant and child mental health: one that supports behavioral and mental health integration into the pediatric primary care setting, one that increases screening and treatment for maternal depression, and one that enhances infant and early childhood mental health,” AAP President Benard Dreyer, MD, said in a statement. “Of additional note is a provision that incentivizes the certification of health information technology for use by pediatricians, and a provision that ensures children in [psychiatric facilities] receive Medicaid’s early periodic screening, treatment, and diagnosis gold standard of care. Finally, the AAP supports the 21st Century Cures Act’s reauthorization of a bill to prevent underage drinking, which includes a new program to train pediatric health professionals in substance use screening, intervention, and referrals.”
However, Dr. Dreyer noted that more work needs to be done.
“The Family First Prevention Services Act of 2016, a comprehensive, bipartisan effort to improve how the child welfare system serves children and families in adversity, was connected to the 21st Century Cures Act until earlier this week,” he said. “Family First represents more than 2 years of work, and is a pivotal opportunity for a major federal policy shift away from placing children in out-of-home care and toward keeping families together. Removing it from this legislative package could mean losing the chance to pass it at all, an unacceptable and undeserved setback for the nation’s most vulnerable children.”
21st Century Cures also contains health IT-related provisions, mostly aimed at improving the interoperability of electronic health records. It also reduces the documentation burden on providers and establishes the authority for the HHS Office of Inspector General to penalize those engaged in information blocking between EHRs.
The bill also increases the transparency around Medicare local coverage decisions and exempts certain transfers of value from reporting requirements related to continuing education. It sets reimbursement for Medicare Part B drugs infused through durable medical equipment at 106% of average sales price.
Sen. Lamar Alexander, chairman of the Health, Education, Labor and Pensions Committee, said that a vote in that chamber could happen as early as Dec. 5. Upon House passage, President Obama signaled his intention to sign the bill, according to a statement from the White House Press Secretary.
A pared-down version of the 21st Century Cures Act passed the House Nov. 30 by an overwhelming 392-26 vote, setting the stage for a quick Senate vote on the compromise legislation.
H.R. 34 gained more support on the House floor than did a version of the legislation that passed the House in 2015. In order to gain that additional support and ensure Senate approval, funding for key biomedical research efforts – the BRAIN Initiative, the Cancer Moonshot, and the Precision Medicine Initiative – was reduced from $9.3 billion to $4.8 billion over 10 years. Further, those funds are not guaranteed but will need to be appropriated through the federal budget process.
Other provisions include creation of an NIH program to support new researchers; funds to accelerate improved methods for prevention, diagnosis, and treatment of tick-borne diseases; the development of a national neurologic condition surveillance system; and the establishment of a task force on research specific to pregnant and breastfeeding women.
“More women with chronic diseases are becoming pregnant, yet safe and effective medications to manage these ongoing conditions throughout their pregnancy and beyond are needed,” Mary Norton, MD, president of the Society for Maternal-Fetal Medicine, said in a statement. “This legislation is a great first step toward greater collaboration and communication among federal agencies and public stakeholders.”
The 21st Century Cures bill also “takes concrete steps to help women and families suffering from postpartum depression,” Thomas Gellhaus, MD, president of the American College of Obstetricians and Gynecologists, said in a statement. “Postpartum depression is one of the most common medical complications following pregnancy. ... Cures expands state programs to better identify, treat, and support women and families at risk for or facing postpartum depression.”
The bill provides $500 million to the Food and Drug Administration to help the agency speed up the drug approval process, focusing on identifying biomarkers and developing targeted drugs for rare diseases. It also reauthorizes the pediatric rare disease priority review voucher program; requires drug companies to have a publicly accessible compassionate use policy for drugs treating serious or life-threatening conditions; and provides flexibility to get new antimicrobial drugs to market quickly.
Changes in the drug approval process were contentious during debate on the House floor.
“In its attempt to speed up the drug and device approval process, this legislation neglects the very people whom clinical trials are meant to help, that is, the patients,” Rep. Rosa DeLauro (D-Conn.) said. “Rather than protect those who rely on the health care system, it reduces the already weak regulation on medical devices, allows drugs with only limited evidence of the drug’s safety and efficacy, and rushes the use of new and unproven antibiotics.”
Other legislators expressed disappointment at the bill’s mental health care provisions. Rep. Joseph Kennedy III (D-Mass.) said that his “real concerns with the legislation lie with the mental health reform proposals, which don’t go nearly far enough. Mental health parity is already the law, thanks to the Mental Health Parity and Addiction Equity Act and the Affordable Care Act; but each study we read, Mr. Speaker, and each story we hear proves that insurance companies are skirting those rules.
“We need enforcement and transparency today,” Rep. Kennedy continued. “We need random audits before there have been violations, not after. We need insurers to publicly disclose the rates and reasons for denials in a way that patients and their families can understand, not in away that mental health advocates can’t even obtain. We need to increase Medicaid reimbursements in order to expand access to care, not to reduce them or roll back expansion.”
The pediatric provisions drew mixed reviews from the American Academy of Pediatrics.
“The 21st Century Cures Act includes three new programs that, if funded, would improve infant and child mental health: one that supports behavioral and mental health integration into the pediatric primary care setting, one that increases screening and treatment for maternal depression, and one that enhances infant and early childhood mental health,” AAP President Benard Dreyer, MD, said in a statement. “Of additional note is a provision that incentivizes the certification of health information technology for use by pediatricians, and a provision that ensures children in [psychiatric facilities] receive Medicaid’s early periodic screening, treatment, and diagnosis gold standard of care. Finally, the AAP supports the 21st Century Cures Act’s reauthorization of a bill to prevent underage drinking, which includes a new program to train pediatric health professionals in substance use screening, intervention, and referrals.”
However, Dr. Dreyer noted that more work needs to be done.
“The Family First Prevention Services Act of 2016, a comprehensive, bipartisan effort to improve how the child welfare system serves children and families in adversity, was connected to the 21st Century Cures Act until earlier this week,” he said. “Family First represents more than 2 years of work, and is a pivotal opportunity for a major federal policy shift away from placing children in out-of-home care and toward keeping families together. Removing it from this legislative package could mean losing the chance to pass it at all, an unacceptable and undeserved setback for the nation’s most vulnerable children.”
21st Century Cures also contains health IT-related provisions, mostly aimed at improving the interoperability of electronic health records. It also reduces the documentation burden on providers and establishes the authority for the HHS Office of Inspector General to penalize those engaged in information blocking between EHRs.
The bill also increases the transparency around Medicare local coverage decisions and exempts certain transfers of value from reporting requirements related to continuing education. It sets reimbursement for Medicare Part B drugs infused through durable medical equipment at 106% of average sales price.
Sen. Lamar Alexander, chairman of the Health, Education, Labor and Pensions Committee, said that a vote in that chamber could happen as early as Dec. 5. Upon House passage, President Obama signaled his intention to sign the bill, according to a statement from the White House Press Secretary.
A pared-down version of the 21st Century Cures Act passed the House Nov. 30 by an overwhelming 392-26 vote, setting the stage for a quick Senate vote on the compromise legislation.
H.R. 34 gained more support on the House floor than did a version of the legislation that passed the House in 2015. In order to gain that additional support and ensure Senate approval, funding for key biomedical research efforts – the BRAIN Initiative, the Cancer Moonshot, and the Precision Medicine Initiative – was reduced from $9.3 billion to $4.8 billion over 10 years. Further, those funds are not guaranteed but will need to be appropriated through the federal budget process.
Other provisions include creation of an NIH program to support new researchers; funds to accelerate improved methods for prevention, diagnosis, and treatment of tick-borne diseases; the development of a national neurologic condition surveillance system; and the establishment of a task force on research specific to pregnant and breastfeeding women.
“More women with chronic diseases are becoming pregnant, yet safe and effective medications to manage these ongoing conditions throughout their pregnancy and beyond are needed,” Mary Norton, MD, president of the Society for Maternal-Fetal Medicine, said in a statement. “This legislation is a great first step toward greater collaboration and communication among federal agencies and public stakeholders.”
The 21st Century Cures bill also “takes concrete steps to help women and families suffering from postpartum depression,” Thomas Gellhaus, MD, president of the American College of Obstetricians and Gynecologists, said in a statement. “Postpartum depression is one of the most common medical complications following pregnancy. ... Cures expands state programs to better identify, treat, and support women and families at risk for or facing postpartum depression.”
The bill provides $500 million to the Food and Drug Administration to help the agency speed up the drug approval process, focusing on identifying biomarkers and developing targeted drugs for rare diseases. It also reauthorizes the pediatric rare disease priority review voucher program; requires drug companies to have a publicly accessible compassionate use policy for drugs treating serious or life-threatening conditions; and provides flexibility to get new antimicrobial drugs to market quickly.
Changes in the drug approval process were contentious during debate on the House floor.
“In its attempt to speed up the drug and device approval process, this legislation neglects the very people whom clinical trials are meant to help, that is, the patients,” Rep. Rosa DeLauro (D-Conn.) said. “Rather than protect those who rely on the health care system, it reduces the already weak regulation on medical devices, allows drugs with only limited evidence of the drug’s safety and efficacy, and rushes the use of new and unproven antibiotics.”
Other legislators expressed disappointment at the bill’s mental health care provisions. Rep. Joseph Kennedy III (D-Mass.) said that his “real concerns with the legislation lie with the mental health reform proposals, which don’t go nearly far enough. Mental health parity is already the law, thanks to the Mental Health Parity and Addiction Equity Act and the Affordable Care Act; but each study we read, Mr. Speaker, and each story we hear proves that insurance companies are skirting those rules.
“We need enforcement and transparency today,” Rep. Kennedy continued. “We need random audits before there have been violations, not after. We need insurers to publicly disclose the rates and reasons for denials in a way that patients and their families can understand, not in away that mental health advocates can’t even obtain. We need to increase Medicaid reimbursements in order to expand access to care, not to reduce them or roll back expansion.”
The pediatric provisions drew mixed reviews from the American Academy of Pediatrics.
“The 21st Century Cures Act includes three new programs that, if funded, would improve infant and child mental health: one that supports behavioral and mental health integration into the pediatric primary care setting, one that increases screening and treatment for maternal depression, and one that enhances infant and early childhood mental health,” AAP President Benard Dreyer, MD, said in a statement. “Of additional note is a provision that incentivizes the certification of health information technology for use by pediatricians, and a provision that ensures children in [psychiatric facilities] receive Medicaid’s early periodic screening, treatment, and diagnosis gold standard of care. Finally, the AAP supports the 21st Century Cures Act’s reauthorization of a bill to prevent underage drinking, which includes a new program to train pediatric health professionals in substance use screening, intervention, and referrals.”
However, Dr. Dreyer noted that more work needs to be done.
“The Family First Prevention Services Act of 2016, a comprehensive, bipartisan effort to improve how the child welfare system serves children and families in adversity, was connected to the 21st Century Cures Act until earlier this week,” he said. “Family First represents more than 2 years of work, and is a pivotal opportunity for a major federal policy shift away from placing children in out-of-home care and toward keeping families together. Removing it from this legislative package could mean losing the chance to pass it at all, an unacceptable and undeserved setback for the nation’s most vulnerable children.”
21st Century Cures also contains health IT-related provisions, mostly aimed at improving the interoperability of electronic health records. It also reduces the documentation burden on providers and establishes the authority for the HHS Office of Inspector General to penalize those engaged in information blocking between EHRs.
The bill also increases the transparency around Medicare local coverage decisions and exempts certain transfers of value from reporting requirements related to continuing education. It sets reimbursement for Medicare Part B drugs infused through durable medical equipment at 106% of average sales price.
Sen. Lamar Alexander, chairman of the Health, Education, Labor and Pensions Committee, said that a vote in that chamber could happen as early as Dec. 5. Upon House passage, President Obama signaled his intention to sign the bill, according to a statement from the White House Press Secretary.
Slavitt to Trump administration: Keep the CMS Innovation Center
WASHINGTON – Acting Administrator Andy Slavitt has some advice for his successors at the CMS: Keep the Center for Medicare & Medicaid Innovation, even if you trash the Affordable Care Act.
The innovation center is vital to the success of the Quality Payment Program, the value-based payment framework set up by the Medicare Access and CHIP Reauthorization Act (MACRA), Mr. Slavitt said Dec. 1 at the National MACRA MIPS/APM Summit.
“MACRA can’t work as well without a CMS Innovation Center that can move quickly to develop and expand new approaches to paying for care,” Mr. Slavitt said. “With changes to the Innovation Center, the advanced alternative payment approaches could slow significantly. We will have a much narrower path with fewer specialty options and approaches, which take in patient and physician feedback. Medicare and commercial payers would then fall further out of alignment, and more importantly, less patients would have access to innovative care methods.”
Mr. Slavitt offered a few other recommendations to the next regime. First, he called on the Trump administration to ensure that the 20 million people who have obtained health care coverage under the ACA do not lose it as a key to continued delivery system reform.
“Build from a foundation of progress, do not head backwards,” Mr. Slavitt advised. “There can be no delivery system reform without building on the foundation of reaching universal coverage.”
To that end, he advised keeping other key ACA provisions, including no-cost preventive care, the elimination of annual and lifetime coverage caps, and the end of pre-existing condition exclusions.
“If we want to fix how care is delivered, so that we’re providing value, then we must ensure that Americans can afford and access quality care at every point in their lives,” he said. “If we lose even some of the coverage gains made under the ACA, or leave people in limbo, people will lose access to regular care and we will drive up long-term costs.”
He also called for more improvements in the health IT space, including a demand for affordable systems and technologies that can exchange data and support quality health care.
“MACRA is an opportunity to move the focus away from paperwork and reporting and toward paying for what works,” Mr. Slavitt said. “For a variety of reasons, EHRs became an industry before they became a useful tool. The technology community must be held accountable ... to make room for new innovators and to give clinicians more freedom and more flexibility to focus on their patients, to practice medicine, and deliver better care.”
President-elect Trump has designated Seema Verma, a health care consultant who helped design the Indiana’s ACA Medicaid expansion, to be the next CMS administrator.
WASHINGTON – Acting Administrator Andy Slavitt has some advice for his successors at the CMS: Keep the Center for Medicare & Medicaid Innovation, even if you trash the Affordable Care Act.
The innovation center is vital to the success of the Quality Payment Program, the value-based payment framework set up by the Medicare Access and CHIP Reauthorization Act (MACRA), Mr. Slavitt said Dec. 1 at the National MACRA MIPS/APM Summit.
“MACRA can’t work as well without a CMS Innovation Center that can move quickly to develop and expand new approaches to paying for care,” Mr. Slavitt said. “With changes to the Innovation Center, the advanced alternative payment approaches could slow significantly. We will have a much narrower path with fewer specialty options and approaches, which take in patient and physician feedback. Medicare and commercial payers would then fall further out of alignment, and more importantly, less patients would have access to innovative care methods.”
Mr. Slavitt offered a few other recommendations to the next regime. First, he called on the Trump administration to ensure that the 20 million people who have obtained health care coverage under the ACA do not lose it as a key to continued delivery system reform.
“Build from a foundation of progress, do not head backwards,” Mr. Slavitt advised. “There can be no delivery system reform without building on the foundation of reaching universal coverage.”
To that end, he advised keeping other key ACA provisions, including no-cost preventive care, the elimination of annual and lifetime coverage caps, and the end of pre-existing condition exclusions.
“If we want to fix how care is delivered, so that we’re providing value, then we must ensure that Americans can afford and access quality care at every point in their lives,” he said. “If we lose even some of the coverage gains made under the ACA, or leave people in limbo, people will lose access to regular care and we will drive up long-term costs.”
He also called for more improvements in the health IT space, including a demand for affordable systems and technologies that can exchange data and support quality health care.
“MACRA is an opportunity to move the focus away from paperwork and reporting and toward paying for what works,” Mr. Slavitt said. “For a variety of reasons, EHRs became an industry before they became a useful tool. The technology community must be held accountable ... to make room for new innovators and to give clinicians more freedom and more flexibility to focus on their patients, to practice medicine, and deliver better care.”
President-elect Trump has designated Seema Verma, a health care consultant who helped design the Indiana’s ACA Medicaid expansion, to be the next CMS administrator.
WASHINGTON – Acting Administrator Andy Slavitt has some advice for his successors at the CMS: Keep the Center for Medicare & Medicaid Innovation, even if you trash the Affordable Care Act.
The innovation center is vital to the success of the Quality Payment Program, the value-based payment framework set up by the Medicare Access and CHIP Reauthorization Act (MACRA), Mr. Slavitt said Dec. 1 at the National MACRA MIPS/APM Summit.
“MACRA can’t work as well without a CMS Innovation Center that can move quickly to develop and expand new approaches to paying for care,” Mr. Slavitt said. “With changes to the Innovation Center, the advanced alternative payment approaches could slow significantly. We will have a much narrower path with fewer specialty options and approaches, which take in patient and physician feedback. Medicare and commercial payers would then fall further out of alignment, and more importantly, less patients would have access to innovative care methods.”
Mr. Slavitt offered a few other recommendations to the next regime. First, he called on the Trump administration to ensure that the 20 million people who have obtained health care coverage under the ACA do not lose it as a key to continued delivery system reform.
“Build from a foundation of progress, do not head backwards,” Mr. Slavitt advised. “There can be no delivery system reform without building on the foundation of reaching universal coverage.”
To that end, he advised keeping other key ACA provisions, including no-cost preventive care, the elimination of annual and lifetime coverage caps, and the end of pre-existing condition exclusions.
“If we want to fix how care is delivered, so that we’re providing value, then we must ensure that Americans can afford and access quality care at every point in their lives,” he said. “If we lose even some of the coverage gains made under the ACA, or leave people in limbo, people will lose access to regular care and we will drive up long-term costs.”
He also called for more improvements in the health IT space, including a demand for affordable systems and technologies that can exchange data and support quality health care.
“MACRA is an opportunity to move the focus away from paperwork and reporting and toward paying for what works,” Mr. Slavitt said. “For a variety of reasons, EHRs became an industry before they became a useful tool. The technology community must be held accountable ... to make room for new innovators and to give clinicians more freedom and more flexibility to focus on their patients, to practice medicine, and deliver better care.”
President-elect Trump has designated Seema Verma, a health care consultant who helped design the Indiana’s ACA Medicaid expansion, to be the next CMS administrator.
AT THE NATIONAL MACRA MIPS/APM SUMMIT
GOLD: Base COPD treatment on symptoms, exacerbation risk
The Global Initiative for Chronic Obstructive Lung Disease (GOLD) has uncoupled spirometry results from the ABCD treatment algorithm; this move marks the organization’s first announcing of major COPD guidance since 2011.
Spirometry now stands apart from GOLD’s ABCD symptom/exacerbation risk score with its own grade, with possibilities ranging from 1 to 4. A forced expiratory volume in 1 second (FEV1) of 80% or more of the predicted value rates a 1; the score degrades to 4 with an FEV1 below 30%.
“In previous GOLD documents, recommendations for management of COPD were based solely on spirometric category. However, there is considerable evidence that the level of FEV1 is a poor descriptor of disease status, and, for this reason, the management of stable COPD based on … disease impact (determined mainly by symptom burden and activity limitation) and future risk of disease progression (especially of exacerbations) is recommended. ... ABCD groups are now proposed to be derived exclusively from patient symptoms and their history of exacerbations,” GOLD said.
The clear focus on symptoms and exacerbations is “the major accomplishment” of the new report, which has been downloaded more than 45,000 times since it’s release, a testament to GOLD’s importance to clinicians trying to help COPD patients.
“We are trying to do a better job of personalizing treatment,” said GOLD board member Gerard Criner, MD, chair and professor of thoracic medicine and surgery at Temple University in Philadelphia.
The change “allows you to plan treatment based on symptoms [even] if you don’t have immediate access to spirometry, and then refine treatment once you have spirometry results. It also allows you to escalate and deescalate treatment because you are not boxed into a letter grade group” forced by spirometry. “You can also take a better look at pharmacologic versus nonpharmacologic therapy” when deciding what to do, he said.
In short, “we think it gives more freedom” to manage patients based on what seems best, Dr. Criner said.
GOLD included an example of how the new assessment can help. “Consider two patients,” it said, both with an FEV1 less than 30% and a COPD Assessment Test result of 18, but one with no exacerbations in the past year and the other with three. Both would have scored a GOLD D in the old system, and been treated similarly.
“However, with the new proposed scheme, the subject with three exacerbations ... would be labeled GOLD [spirometry] grade 4, group D,” and their treatment would focus on exacerbations. The no-exacerbation patient would be classified as GOLD grade 4, group B. Treatment would focus on symptoms. Drugs are still an option, but also lung volume reduction and lung transplant, GOLD said. Spirometry, in other words, is less important than how the patient is doing.
The group incorporated “every major study up to the first week of November” in the new report, Dr. Criner said, so there’s more to consider.
For instance, it’s clear now that patients benefit from home oxygen if they are severely hypoxemic while sitting on the couch watching TV, but not if they desaturate only when they get up and walk around, or come into the clinic to exercise. “We did not” know that in 2011, he said.
GOLD also recommended pulmonary rehabilitation and palliative care when indicated, as well as ongoing evaluation to make sure patients are able to use their inhalers, a major problem in COPD.
GOLD said that group A patients - those with few symptoms and low exacerbation risk - should be offered a bronchodilator. Initial therapy for group B - more symptoms, but low exacerbation risk - and group C - higher exacerbation risk but fewer symptoms - “should consist of a single long-acting bronchodilator. There is no evidence to recommend one class of long-acting bronchodilator over another.”
For group D - highly symptomatic with frequent exacerbations - “we recommend starting therapy with a [long-acting beta-2 agonist]/[long-acting antimuscarinic antagonist] combination,” the group said.
There was no industry involvement in GOLD’s report, but numerous authors and board members had pharmaceutical company ties, and GOLD’s treatment advice relies on drug company studies. Dr. Criner reported personal payments from Holaria, and research funding and other nonpersonal payments from AstraZeneca, Boehringer-Ingelheim, GlaxoSmithKline, Johnson and Johnson, and others.
As health care moves toward individualized care plans for patients, the updated GOLD recommendations enhance the possibility of personalized COPD treatment. This means more symptom-focused treatment for patients and, as Dr. Criner points out, more freedom for providers to manage patients based on what seems best.
As health care moves toward individualized care plans for patients, the updated GOLD recommendations enhance the possibility of personalized COPD treatment. This means more symptom-focused treatment for patients and, as Dr. Criner points out, more freedom for providers to manage patients based on what seems best.
As health care moves toward individualized care plans for patients, the updated GOLD recommendations enhance the possibility of personalized COPD treatment. This means more symptom-focused treatment for patients and, as Dr. Criner points out, more freedom for providers to manage patients based on what seems best.
The Global Initiative for Chronic Obstructive Lung Disease (GOLD) has uncoupled spirometry results from the ABCD treatment algorithm; this move marks the organization’s first announcing of major COPD guidance since 2011.
Spirometry now stands apart from GOLD’s ABCD symptom/exacerbation risk score with its own grade, with possibilities ranging from 1 to 4. A forced expiratory volume in 1 second (FEV1) of 80% or more of the predicted value rates a 1; the score degrades to 4 with an FEV1 below 30%.
“In previous GOLD documents, recommendations for management of COPD were based solely on spirometric category. However, there is considerable evidence that the level of FEV1 is a poor descriptor of disease status, and, for this reason, the management of stable COPD based on … disease impact (determined mainly by symptom burden and activity limitation) and future risk of disease progression (especially of exacerbations) is recommended. ... ABCD groups are now proposed to be derived exclusively from patient symptoms and their history of exacerbations,” GOLD said.
The clear focus on symptoms and exacerbations is “the major accomplishment” of the new report, which has been downloaded more than 45,000 times since it’s release, a testament to GOLD’s importance to clinicians trying to help COPD patients.
“We are trying to do a better job of personalizing treatment,” said GOLD board member Gerard Criner, MD, chair and professor of thoracic medicine and surgery at Temple University in Philadelphia.
The change “allows you to plan treatment based on symptoms [even] if you don’t have immediate access to spirometry, and then refine treatment once you have spirometry results. It also allows you to escalate and deescalate treatment because you are not boxed into a letter grade group” forced by spirometry. “You can also take a better look at pharmacologic versus nonpharmacologic therapy” when deciding what to do, he said.
In short, “we think it gives more freedom” to manage patients based on what seems best, Dr. Criner said.
GOLD included an example of how the new assessment can help. “Consider two patients,” it said, both with an FEV1 less than 30% and a COPD Assessment Test result of 18, but one with no exacerbations in the past year and the other with three. Both would have scored a GOLD D in the old system, and been treated similarly.
“However, with the new proposed scheme, the subject with three exacerbations ... would be labeled GOLD [spirometry] grade 4, group D,” and their treatment would focus on exacerbations. The no-exacerbation patient would be classified as GOLD grade 4, group B. Treatment would focus on symptoms. Drugs are still an option, but also lung volume reduction and lung transplant, GOLD said. Spirometry, in other words, is less important than how the patient is doing.
The group incorporated “every major study up to the first week of November” in the new report, Dr. Criner said, so there’s more to consider.
For instance, it’s clear now that patients benefit from home oxygen if they are severely hypoxemic while sitting on the couch watching TV, but not if they desaturate only when they get up and walk around, or come into the clinic to exercise. “We did not” know that in 2011, he said.
GOLD also recommended pulmonary rehabilitation and palliative care when indicated, as well as ongoing evaluation to make sure patients are able to use their inhalers, a major problem in COPD.
GOLD said that group A patients - those with few symptoms and low exacerbation risk - should be offered a bronchodilator. Initial therapy for group B - more symptoms, but low exacerbation risk - and group C - higher exacerbation risk but fewer symptoms - “should consist of a single long-acting bronchodilator. There is no evidence to recommend one class of long-acting bronchodilator over another.”
For group D - highly symptomatic with frequent exacerbations - “we recommend starting therapy with a [long-acting beta-2 agonist]/[long-acting antimuscarinic antagonist] combination,” the group said.
There was no industry involvement in GOLD’s report, but numerous authors and board members had pharmaceutical company ties, and GOLD’s treatment advice relies on drug company studies. Dr. Criner reported personal payments from Holaria, and research funding and other nonpersonal payments from AstraZeneca, Boehringer-Ingelheim, GlaxoSmithKline, Johnson and Johnson, and others.
The Global Initiative for Chronic Obstructive Lung Disease (GOLD) has uncoupled spirometry results from the ABCD treatment algorithm; this move marks the organization’s first announcing of major COPD guidance since 2011.
Spirometry now stands apart from GOLD’s ABCD symptom/exacerbation risk score with its own grade, with possibilities ranging from 1 to 4. A forced expiratory volume in 1 second (FEV1) of 80% or more of the predicted value rates a 1; the score degrades to 4 with an FEV1 below 30%.
“In previous GOLD documents, recommendations for management of COPD were based solely on spirometric category. However, there is considerable evidence that the level of FEV1 is a poor descriptor of disease status, and, for this reason, the management of stable COPD based on … disease impact (determined mainly by symptom burden and activity limitation) and future risk of disease progression (especially of exacerbations) is recommended. ... ABCD groups are now proposed to be derived exclusively from patient symptoms and their history of exacerbations,” GOLD said.
The clear focus on symptoms and exacerbations is “the major accomplishment” of the new report, which has been downloaded more than 45,000 times since it’s release, a testament to GOLD’s importance to clinicians trying to help COPD patients.
“We are trying to do a better job of personalizing treatment,” said GOLD board member Gerard Criner, MD, chair and professor of thoracic medicine and surgery at Temple University in Philadelphia.
The change “allows you to plan treatment based on symptoms [even] if you don’t have immediate access to spirometry, and then refine treatment once you have spirometry results. It also allows you to escalate and deescalate treatment because you are not boxed into a letter grade group” forced by spirometry. “You can also take a better look at pharmacologic versus nonpharmacologic therapy” when deciding what to do, he said.
In short, “we think it gives more freedom” to manage patients based on what seems best, Dr. Criner said.
GOLD included an example of how the new assessment can help. “Consider two patients,” it said, both with an FEV1 less than 30% and a COPD Assessment Test result of 18, but one with no exacerbations in the past year and the other with three. Both would have scored a GOLD D in the old system, and been treated similarly.
“However, with the new proposed scheme, the subject with three exacerbations ... would be labeled GOLD [spirometry] grade 4, group D,” and their treatment would focus on exacerbations. The no-exacerbation patient would be classified as GOLD grade 4, group B. Treatment would focus on symptoms. Drugs are still an option, but also lung volume reduction and lung transplant, GOLD said. Spirometry, in other words, is less important than how the patient is doing.
The group incorporated “every major study up to the first week of November” in the new report, Dr. Criner said, so there’s more to consider.
For instance, it’s clear now that patients benefit from home oxygen if they are severely hypoxemic while sitting on the couch watching TV, but not if they desaturate only when they get up and walk around, or come into the clinic to exercise. “We did not” know that in 2011, he said.
GOLD also recommended pulmonary rehabilitation and palliative care when indicated, as well as ongoing evaluation to make sure patients are able to use their inhalers, a major problem in COPD.
GOLD said that group A patients - those with few symptoms and low exacerbation risk - should be offered a bronchodilator. Initial therapy for group B - more symptoms, but low exacerbation risk - and group C - higher exacerbation risk but fewer symptoms - “should consist of a single long-acting bronchodilator. There is no evidence to recommend one class of long-acting bronchodilator over another.”
For group D - highly symptomatic with frequent exacerbations - “we recommend starting therapy with a [long-acting beta-2 agonist]/[long-acting antimuscarinic antagonist] combination,” the group said.
There was no industry involvement in GOLD’s report, but numerous authors and board members had pharmaceutical company ties, and GOLD’s treatment advice relies on drug company studies. Dr. Criner reported personal payments from Holaria, and research funding and other nonpersonal payments from AstraZeneca, Boehringer-Ingelheim, GlaxoSmithKline, Johnson and Johnson, and others.
In lung cancer screening, patient education works
A counseling and shared decision-making visit improved patient knowledge of the eligibility criteria, benefits, and potential risks of lung cancer screening via a low-radiation chest CT scan.
The Center for Medicare & Medicaid Services has added the type of visit addressed in this study to Medicare’s preventive services benefits for individuals meeting certain criteria, but no previous study had looked at how the implementation of such a visit impacted a patient’s knowledge and understanding.
The researchers noted significant improvement in all questions before and after a counseling session (P = .03 to P less than .0001). Those improvements lessened at 1 month, but were still higher than precounseling scores.
The percentages of participants who knew the age criteria for lung cancer screening before counseling, immediately after counseling, and 1 month after counseling, for example, were 8.8% (11 patients), 59.2% (74 patients), and 21.4% (24 patients), respectively. The percentage of participants able to identify at least one of the potential hazards of screening increased by a similar amount immediately after receiving counseling, as did the percentage of participants able to identify the age criteria for lung cancer screening immediately after receiving counseling. The percentages of patients able to identify at least one of the potential hazards of screening were 38.4% before counseling and 90.4% immediately after receiving counseling. One month following counseling, the percentage of patients with such knowledge remained fairly high, dropping to 78.6%.
“Showing the value of these visits is very important to encourage policymakers and payers to continue to support the counseling and shared decision-making visit,” Peter J. Mazzone, MD, MPH, who led the study, said in an interview.
These types of conversations are important because of the uncertainties surrounding lung cancer screening, which leads to about a 20% reduction in mortality risk. That translates to the need to screen about 250 people to save 1 life. “I think the public sometimes doesn’t realize that the effectiveness of some of these preventive screenings may not be as large as they think they are,” said David Grossman, vice chair of the US Preventive Services Task Force and a senior investigator at the Group Health Research Institute, Seattle, who was not involved in the study.
The researchers developed a centralized counseling and shared decision-making visit that included a narrated slide show and individualized risk assessment. They approached 423 consecutive patients who had been identified by their primary care provider or a specialist as potential candidates for screening. Of those 423 patients, 125 agreed to participate in the study (Chest. 2016 Nov 1. doi: 10.1016/j.chest.2016.10.027).
The session delivered expected improvements in patient knowledge, but there were some surprises. “The starting point of knowledge was perhaps less than we would have anticipated, and the gains, though very substantial, weren’t perfect,” said Dr. Mazzone, who is also director of the lung cancer screening program at the Cleveland Clinic.
The drop in knowledge at 1 month suggests that the information needs to be reinforced, possibly each time patients come in for an annual screening visit, Dr. Mazzone added.
Counseling sessions can also help convince patients to quit smoking, if tobacco use is a concern. “It’s not appropriate to screen for lung cancer without making a commitment to try to quit,” said Dr. Grossman.
No funding source was disclosed. Dr. Mazzone and Dr. Grossman reported having no financial disclosures.
A counseling and shared decision-making visit improved patient knowledge of the eligibility criteria, benefits, and potential risks of lung cancer screening via a low-radiation chest CT scan.
The Center for Medicare & Medicaid Services has added the type of visit addressed in this study to Medicare’s preventive services benefits for individuals meeting certain criteria, but no previous study had looked at how the implementation of such a visit impacted a patient’s knowledge and understanding.
The researchers noted significant improvement in all questions before and after a counseling session (P = .03 to P less than .0001). Those improvements lessened at 1 month, but were still higher than precounseling scores.
The percentages of participants who knew the age criteria for lung cancer screening before counseling, immediately after counseling, and 1 month after counseling, for example, were 8.8% (11 patients), 59.2% (74 patients), and 21.4% (24 patients), respectively. The percentage of participants able to identify at least one of the potential hazards of screening increased by a similar amount immediately after receiving counseling, as did the percentage of participants able to identify the age criteria for lung cancer screening immediately after receiving counseling. The percentages of patients able to identify at least one of the potential hazards of screening were 38.4% before counseling and 90.4% immediately after receiving counseling. One month following counseling, the percentage of patients with such knowledge remained fairly high, dropping to 78.6%.
“Showing the value of these visits is very important to encourage policymakers and payers to continue to support the counseling and shared decision-making visit,” Peter J. Mazzone, MD, MPH, who led the study, said in an interview.
These types of conversations are important because of the uncertainties surrounding lung cancer screening, which leads to about a 20% reduction in mortality risk. That translates to the need to screen about 250 people to save 1 life. “I think the public sometimes doesn’t realize that the effectiveness of some of these preventive screenings may not be as large as they think they are,” said David Grossman, vice chair of the US Preventive Services Task Force and a senior investigator at the Group Health Research Institute, Seattle, who was not involved in the study.
The researchers developed a centralized counseling and shared decision-making visit that included a narrated slide show and individualized risk assessment. They approached 423 consecutive patients who had been identified by their primary care provider or a specialist as potential candidates for screening. Of those 423 patients, 125 agreed to participate in the study (Chest. 2016 Nov 1. doi: 10.1016/j.chest.2016.10.027).
The session delivered expected improvements in patient knowledge, but there were some surprises. “The starting point of knowledge was perhaps less than we would have anticipated, and the gains, though very substantial, weren’t perfect,” said Dr. Mazzone, who is also director of the lung cancer screening program at the Cleveland Clinic.
The drop in knowledge at 1 month suggests that the information needs to be reinforced, possibly each time patients come in for an annual screening visit, Dr. Mazzone added.
Counseling sessions can also help convince patients to quit smoking, if tobacco use is a concern. “It’s not appropriate to screen for lung cancer without making a commitment to try to quit,” said Dr. Grossman.
No funding source was disclosed. Dr. Mazzone and Dr. Grossman reported having no financial disclosures.
A counseling and shared decision-making visit improved patient knowledge of the eligibility criteria, benefits, and potential risks of lung cancer screening via a low-radiation chest CT scan.
The Center for Medicare & Medicaid Services has added the type of visit addressed in this study to Medicare’s preventive services benefits for individuals meeting certain criteria, but no previous study had looked at how the implementation of such a visit impacted a patient’s knowledge and understanding.
The researchers noted significant improvement in all questions before and after a counseling session (P = .03 to P less than .0001). Those improvements lessened at 1 month, but were still higher than precounseling scores.
The percentages of participants who knew the age criteria for lung cancer screening before counseling, immediately after counseling, and 1 month after counseling, for example, were 8.8% (11 patients), 59.2% (74 patients), and 21.4% (24 patients), respectively. The percentage of participants able to identify at least one of the potential hazards of screening increased by a similar amount immediately after receiving counseling, as did the percentage of participants able to identify the age criteria for lung cancer screening immediately after receiving counseling. The percentages of patients able to identify at least one of the potential hazards of screening were 38.4% before counseling and 90.4% immediately after receiving counseling. One month following counseling, the percentage of patients with such knowledge remained fairly high, dropping to 78.6%.
“Showing the value of these visits is very important to encourage policymakers and payers to continue to support the counseling and shared decision-making visit,” Peter J. Mazzone, MD, MPH, who led the study, said in an interview.
These types of conversations are important because of the uncertainties surrounding lung cancer screening, which leads to about a 20% reduction in mortality risk. That translates to the need to screen about 250 people to save 1 life. “I think the public sometimes doesn’t realize that the effectiveness of some of these preventive screenings may not be as large as they think they are,” said David Grossman, vice chair of the US Preventive Services Task Force and a senior investigator at the Group Health Research Institute, Seattle, who was not involved in the study.
The researchers developed a centralized counseling and shared decision-making visit that included a narrated slide show and individualized risk assessment. They approached 423 consecutive patients who had been identified by their primary care provider or a specialist as potential candidates for screening. Of those 423 patients, 125 agreed to participate in the study (Chest. 2016 Nov 1. doi: 10.1016/j.chest.2016.10.027).
The session delivered expected improvements in patient knowledge, but there were some surprises. “The starting point of knowledge was perhaps less than we would have anticipated, and the gains, though very substantial, weren’t perfect,” said Dr. Mazzone, who is also director of the lung cancer screening program at the Cleveland Clinic.
The drop in knowledge at 1 month suggests that the information needs to be reinforced, possibly each time patients come in for an annual screening visit, Dr. Mazzone added.
Counseling sessions can also help convince patients to quit smoking, if tobacco use is a concern. “It’s not appropriate to screen for lung cancer without making a commitment to try to quit,” said Dr. Grossman.
No funding source was disclosed. Dr. Mazzone and Dr. Grossman reported having no financial disclosures.
FROM CHEST
Key clinical point:
Major finding: Failure to identify potential harm dropped from 61.6% to 21.4%.
Data source: Prospective study of 125 patients.
Disclosures: No funding source was disclosed. Dr. Mazzone and Dr. Grossman reported having no financial disclosures.
Can bioprosthetics work for large airway defects?
Large and complex airway defects that primary repair cannot fully close require alternative surgical approaches and techniques that are far more difficult to perform, but bioprosthetic materials may be an option to repair large tracheal and bronchial defects that has achieved good results, without postoperative death or defect recurrence, in a small cohort of patients at Massachusetts General Hospital, in Boston.
Brooks Udelsman, MD, and his coauthors reported their results of bioprosthetic repair of central airway defects in eight patients in the Journal of Thoracic and Cardiovascular Surgery (2016 Nov;152:1388-97). “Although our results are derived from a limited number of heterogeneous patients, they suggest that closure of noncircumferential large airway defects with bioprosthetic materials is feasible, safe and reliable,” Dr. Udelsman said. He previously reported the results at the annual meeting of the American Association for Thoracic Surgery, May 14-18, 2016, in Baltimore.
These complex defects typically exceed 5 cm and can involve communication with the esophagus. For repair of smaller defects, surgeons can use a more conventional approach that involves neck flexion, laryngeal release, airway mobilization, and hilar release, but in larger defects, these techniques increase the risk of too much tension on the anastomosis and dehiscence along with airway failure. Large and complex defects occur in patients who have had a previous airway operation or radiation exposure, requiring alternative strategies, the researchers wrote. “Patients in this rare category should be referred to a high-volume center for careful evaluation by a surgeon experienced in complex airway reconstruction before the decision to abandon primary repair is made,” he said. Among the advantages that bioprosthetic materials have over synthetic materials for airway defect repair are easier handling, minimal immunogenic response, and potential for tissue ingrowth, Dr. Udelsman and his coauthors said.
All eight patients in this study, who underwent repair from 2008 to 2015, had significant comorbidities, including previous surgery of the trachea, esophagus, or thyroid. The etiology of the airway defect included HIV-AIDS–associated esophagitis, malignancy, mesh erosion, and complications from extended intubation. Three patients had previous radiation therapy to the neck or chest. Five patients had defects localized to the membranous tracheal wall, two had defects of the mainstem bronchus or bronchus intermedius, and one patient had a defect of the anterior wall of the trachea.
Dr. Udelsman and his coauthors used both aortic homograft and acellular dermal matrix to repair large defects. Their experience confirmed previous reports of the formation of granulation tissue with aortic autografts, underscoring the importance of frequent bronchoscopy and debridement when necessary. And while previous reports have claimed human acellular dermis resists granulation formation, that wasn’t the case in this study. “The exact histologic basis of bioprosthetic incorporation and reepithelialization in these patients is still elusive and will require further study,” the researchers said.
This study also employed the controversial muscle buttress repair in six patients, which helped, at least theoretically, to secure the repairs when leaks occur, to separate suture lines when both the airway and esophagus were repaired and to support the bioprosthetic material to prevent tissue softening, Dr. Udelsman and his coauthors said.
Postoperative examinations confirmed that the operations successfully closed the airway defects in all eight patients. Long term, most resumed oral intake, but three did not for various reasons: one had a pharyngostomy; another had neurocognitive issues preoperatively; and a third with a tracheoesophageal fistula repair and cervical esophagostomy could resume oral intake but depended on tube feeds to meet caloric needs.
All patients developed granulation at the repair site, two of whom required further debridement and one who underwent balloon dilation. Pneumonia was the most common complication within 30 days of surgery, occurring in two patients. Three patients died within 120 days from metastatic disease, and a fourth patient progressed to end-stage AIDS 6 years after the operation and eventually died.
Dr. Udelsman and his coauthors reported having no financial disclosures.
In his invited commentary, Raja Flores, MD, of Mount Sinai Health System in New York said this study demonstrated “modest success” with bioprosthetic materials for repair of large airway deficits – the same level of success he ascribes to human studies of other surgical approaches to large airway deficits (J Thorac Cardiovasc Surg. 2016 Nov;152:1233-4).
But progress has been slow and animal studies of large airway deficit repair have been “wastefully repetitive” without any advances. “We must build on what these human studies have taught us and not continue unsuccessfully to reinvent the same malfunctioning [airways],” Dr. Flores said.
When surgeons encounter such patients, surgery isn’t necessary for their survival, Dr. Flores said. “T-tubes work just fine.” The goal is to improve their quality of life. “Unless we can provide a reliable, long-lasting solution, an unpredictable life-threatening experimental surgical intervention is not justified to treat a stable, functional patient,” he said.
And while Dr. Udelsman and his colleagues have shown “some progress” in their study, he cautioned surgeons to heed the words of a tracheal surgery pioneer Hermes Grillo, MD, at Boston’s Massachusetts General Hospital and Harvard Medical School: “Success has been announced episodically over the decades in each of these categories, but thus far no one replacement method has held for the long term in any safe and practicable manner.” Dr. Flores added: “This still holds true today.”
Dr. Flores reported having no financial disclosures.
In his invited commentary, Raja Flores, MD, of Mount Sinai Health System in New York said this study demonstrated “modest success” with bioprosthetic materials for repair of large airway deficits – the same level of success he ascribes to human studies of other surgical approaches to large airway deficits (J Thorac Cardiovasc Surg. 2016 Nov;152:1233-4).
But progress has been slow and animal studies of large airway deficit repair have been “wastefully repetitive” without any advances. “We must build on what these human studies have taught us and not continue unsuccessfully to reinvent the same malfunctioning [airways],” Dr. Flores said.
When surgeons encounter such patients, surgery isn’t necessary for their survival, Dr. Flores said. “T-tubes work just fine.” The goal is to improve their quality of life. “Unless we can provide a reliable, long-lasting solution, an unpredictable life-threatening experimental surgical intervention is not justified to treat a stable, functional patient,” he said.
And while Dr. Udelsman and his colleagues have shown “some progress” in their study, he cautioned surgeons to heed the words of a tracheal surgery pioneer Hermes Grillo, MD, at Boston’s Massachusetts General Hospital and Harvard Medical School: “Success has been announced episodically over the decades in each of these categories, but thus far no one replacement method has held for the long term in any safe and practicable manner.” Dr. Flores added: “This still holds true today.”
Dr. Flores reported having no financial disclosures.
In his invited commentary, Raja Flores, MD, of Mount Sinai Health System in New York said this study demonstrated “modest success” with bioprosthetic materials for repair of large airway deficits – the same level of success he ascribes to human studies of other surgical approaches to large airway deficits (J Thorac Cardiovasc Surg. 2016 Nov;152:1233-4).
But progress has been slow and animal studies of large airway deficit repair have been “wastefully repetitive” without any advances. “We must build on what these human studies have taught us and not continue unsuccessfully to reinvent the same malfunctioning [airways],” Dr. Flores said.
When surgeons encounter such patients, surgery isn’t necessary for their survival, Dr. Flores said. “T-tubes work just fine.” The goal is to improve their quality of life. “Unless we can provide a reliable, long-lasting solution, an unpredictable life-threatening experimental surgical intervention is not justified to treat a stable, functional patient,” he said.
And while Dr. Udelsman and his colleagues have shown “some progress” in their study, he cautioned surgeons to heed the words of a tracheal surgery pioneer Hermes Grillo, MD, at Boston’s Massachusetts General Hospital and Harvard Medical School: “Success has been announced episodically over the decades in each of these categories, but thus far no one replacement method has held for the long term in any safe and practicable manner.” Dr. Flores added: “This still holds true today.”
Dr. Flores reported having no financial disclosures.
Large and complex airway defects that primary repair cannot fully close require alternative surgical approaches and techniques that are far more difficult to perform, but bioprosthetic materials may be an option to repair large tracheal and bronchial defects that has achieved good results, without postoperative death or defect recurrence, in a small cohort of patients at Massachusetts General Hospital, in Boston.
Brooks Udelsman, MD, and his coauthors reported their results of bioprosthetic repair of central airway defects in eight patients in the Journal of Thoracic and Cardiovascular Surgery (2016 Nov;152:1388-97). “Although our results are derived from a limited number of heterogeneous patients, they suggest that closure of noncircumferential large airway defects with bioprosthetic materials is feasible, safe and reliable,” Dr. Udelsman said. He previously reported the results at the annual meeting of the American Association for Thoracic Surgery, May 14-18, 2016, in Baltimore.
These complex defects typically exceed 5 cm and can involve communication with the esophagus. For repair of smaller defects, surgeons can use a more conventional approach that involves neck flexion, laryngeal release, airway mobilization, and hilar release, but in larger defects, these techniques increase the risk of too much tension on the anastomosis and dehiscence along with airway failure. Large and complex defects occur in patients who have had a previous airway operation or radiation exposure, requiring alternative strategies, the researchers wrote. “Patients in this rare category should be referred to a high-volume center for careful evaluation by a surgeon experienced in complex airway reconstruction before the decision to abandon primary repair is made,” he said. Among the advantages that bioprosthetic materials have over synthetic materials for airway defect repair are easier handling, minimal immunogenic response, and potential for tissue ingrowth, Dr. Udelsman and his coauthors said.
All eight patients in this study, who underwent repair from 2008 to 2015, had significant comorbidities, including previous surgery of the trachea, esophagus, or thyroid. The etiology of the airway defect included HIV-AIDS–associated esophagitis, malignancy, mesh erosion, and complications from extended intubation. Three patients had previous radiation therapy to the neck or chest. Five patients had defects localized to the membranous tracheal wall, two had defects of the mainstem bronchus or bronchus intermedius, and one patient had a defect of the anterior wall of the trachea.
Dr. Udelsman and his coauthors used both aortic homograft and acellular dermal matrix to repair large defects. Their experience confirmed previous reports of the formation of granulation tissue with aortic autografts, underscoring the importance of frequent bronchoscopy and debridement when necessary. And while previous reports have claimed human acellular dermis resists granulation formation, that wasn’t the case in this study. “The exact histologic basis of bioprosthetic incorporation and reepithelialization in these patients is still elusive and will require further study,” the researchers said.
This study also employed the controversial muscle buttress repair in six patients, which helped, at least theoretically, to secure the repairs when leaks occur, to separate suture lines when both the airway and esophagus were repaired and to support the bioprosthetic material to prevent tissue softening, Dr. Udelsman and his coauthors said.
Postoperative examinations confirmed that the operations successfully closed the airway defects in all eight patients. Long term, most resumed oral intake, but three did not for various reasons: one had a pharyngostomy; another had neurocognitive issues preoperatively; and a third with a tracheoesophageal fistula repair and cervical esophagostomy could resume oral intake but depended on tube feeds to meet caloric needs.
All patients developed granulation at the repair site, two of whom required further debridement and one who underwent balloon dilation. Pneumonia was the most common complication within 30 days of surgery, occurring in two patients. Three patients died within 120 days from metastatic disease, and a fourth patient progressed to end-stage AIDS 6 years after the operation and eventually died.
Dr. Udelsman and his coauthors reported having no financial disclosures.
Large and complex airway defects that primary repair cannot fully close require alternative surgical approaches and techniques that are far more difficult to perform, but bioprosthetic materials may be an option to repair large tracheal and bronchial defects that has achieved good results, without postoperative death or defect recurrence, in a small cohort of patients at Massachusetts General Hospital, in Boston.
Brooks Udelsman, MD, and his coauthors reported their results of bioprosthetic repair of central airway defects in eight patients in the Journal of Thoracic and Cardiovascular Surgery (2016 Nov;152:1388-97). “Although our results are derived from a limited number of heterogeneous patients, they suggest that closure of noncircumferential large airway defects with bioprosthetic materials is feasible, safe and reliable,” Dr. Udelsman said. He previously reported the results at the annual meeting of the American Association for Thoracic Surgery, May 14-18, 2016, in Baltimore.
These complex defects typically exceed 5 cm and can involve communication with the esophagus. For repair of smaller defects, surgeons can use a more conventional approach that involves neck flexion, laryngeal release, airway mobilization, and hilar release, but in larger defects, these techniques increase the risk of too much tension on the anastomosis and dehiscence along with airway failure. Large and complex defects occur in patients who have had a previous airway operation or radiation exposure, requiring alternative strategies, the researchers wrote. “Patients in this rare category should be referred to a high-volume center for careful evaluation by a surgeon experienced in complex airway reconstruction before the decision to abandon primary repair is made,” he said. Among the advantages that bioprosthetic materials have over synthetic materials for airway defect repair are easier handling, minimal immunogenic response, and potential for tissue ingrowth, Dr. Udelsman and his coauthors said.
All eight patients in this study, who underwent repair from 2008 to 2015, had significant comorbidities, including previous surgery of the trachea, esophagus, or thyroid. The etiology of the airway defect included HIV-AIDS–associated esophagitis, malignancy, mesh erosion, and complications from extended intubation. Three patients had previous radiation therapy to the neck or chest. Five patients had defects localized to the membranous tracheal wall, two had defects of the mainstem bronchus or bronchus intermedius, and one patient had a defect of the anterior wall of the trachea.
Dr. Udelsman and his coauthors used both aortic homograft and acellular dermal matrix to repair large defects. Their experience confirmed previous reports of the formation of granulation tissue with aortic autografts, underscoring the importance of frequent bronchoscopy and debridement when necessary. And while previous reports have claimed human acellular dermis resists granulation formation, that wasn’t the case in this study. “The exact histologic basis of bioprosthetic incorporation and reepithelialization in these patients is still elusive and will require further study,” the researchers said.
This study also employed the controversial muscle buttress repair in six patients, which helped, at least theoretically, to secure the repairs when leaks occur, to separate suture lines when both the airway and esophagus were repaired and to support the bioprosthetic material to prevent tissue softening, Dr. Udelsman and his coauthors said.
Postoperative examinations confirmed that the operations successfully closed the airway defects in all eight patients. Long term, most resumed oral intake, but three did not for various reasons: one had a pharyngostomy; another had neurocognitive issues preoperatively; and a third with a tracheoesophageal fistula repair and cervical esophagostomy could resume oral intake but depended on tube feeds to meet caloric needs.
All patients developed granulation at the repair site, two of whom required further debridement and one who underwent balloon dilation. Pneumonia was the most common complication within 30 days of surgery, occurring in two patients. Three patients died within 120 days from metastatic disease, and a fourth patient progressed to end-stage AIDS 6 years after the operation and eventually died.
Dr. Udelsman and his coauthors reported having no financial disclosures.
FROM THE JOURNAL OF THORACIC AND CARDIOVASCULAR SURGERY
Key clinical point: Bioprosthetic materials show progress for reconstruction of large airway defects.
Major finding: Airway defects were successfully closed in all patients, with no postoperative deaths or recurrence of airway defect.
Data source: Eight patients who underwent closure of complex central airway defects with bioprosthetic materials between 2008 and 2015.
Disclosures: Dr. Udelsman and coauthors reported having no relevant financial disclosures.
Evaluating Fontan failure risk after arrhythmia
People who have undergone the Fontan procedure have been known to be prone to developing arrhythmias, but few studies have evaluated their prognosis, so researchers from Australia and New Zealand analyzed results of more than 1,000 patients with Fontan circulation and found that two-thirds did not have any arrhythmia at 20 years, and that, among those who did have arrhythmias, almost three-quarters survived 10 years.
“After the first onset of an arrhythmia, close surveillance of ventricular function is required,” Thomas A. Carins, MD, and his colleagues reported (J Thorac Cardiovasc Surg. 2016;152:1355-63). They analyzed data from 1,034 patients who had Fontan procedures from 1975 to 2014 in the Australia and New Zealand Fontan Registry. “The development of an arrhythmia is associated with a heightened risk of subsequent failure of the Fontan circulation,” they wrote.
The study aimed to determine the type of arrhythmias Fontan patients had and what impact that had on long-term outcomes. The most common Fontan approach used in study patients was the extracardiac conduit (555), followed by the lateral tunnel approach (269) and atriopulmonary (210). Those who had the extracardiac Fontan were least likely to develop an arrhythmia, with a hazard ratio of 0.23 (P less than .001), which Dr. Carins and his coauthors noted was in line with previous reports of arrhythmias occurring in patients who had undergone the atriopulmonary connection (Circulation. 2004;109:2319-25; J Thorac Cardiovasc Surg. 1998;115:499-505).
Overall, 195 patients in the study developed arrhythmia, with 162 having tachyarrhythmia, 74 having bradyarrhythmia and 41 having both. “At 20 years, freedom from any arrhythmia, tachyarrhythmia, and bradyarrhythmia was 66%, 69%, and 85%, respectively,” the researchers said.
The following outcomes occurred after the first onset of arrhythmia – tachyarrhythmia in 153 patients and bradyarrhythmia in 42: Thirty-three died; 12 had heart transplants, 30 had a Fontan correction to an extracardiac conduit, three had a Fontan takedown, 12 developed enteropathy, and 25 developed New York Heart Association class III or IV symptoms. Eighty-four patients reached the composite endpoint of Fontan failure.
After they developed arrhythmias, most patients in all three Fontan procedure groups remained free from Fontan failure at 10 years: 67% in the extracardiac conduit group; 54% in the lateral tunnel group; and 51% in the atriopulmonary group.
Medical management of up to four medications was the preferred initial treatment for those with tachyarrhythmias (86%); 101 patients had a single episode of tachyarrhythmia at follow-up intervals of four to 13 years (7.6 year median). “Those who experienced a single versus multiple episodes of tachyarrhythmia showed comparable freedom from Fontan failure at 15 years,” noted Dr. Carins and his coauthors – with rates of 34% and 33%, respectively. Of the 74 patients with bradyarrhythmias, 66 received pacemakers.
“Survival after the onset of an arrhythmia was surprisingly good with 67% and 84% of patients alive at 10 years after the onset of a tachyarrhythmia and bradyarrhythmia, respectively,” the study authors said. “There was no association between occurrence of arrhythmia and survival.”
About 40% of the patients with a tachyarrhythmia or bradyarrhythmia in the study had reduced ventricular function at 10 years after onset, the researchers wrote. “Although the assessment of ventricular function in this study was clearly subjective, we nonetheless believe that these findings suggest that the onset of an arrhythmia is associated with a progressive deterioration in cardiac function,”they noted.
Coauthor Andrew Bullock, MBBS, disclosed receiving consulting fees from Actelion. Dr. Cairns and other coauthors had no financial relationships to disclose.
When interpreting the data that the Australian and New Zealand researchers analyzed, one must be cautious about viewing arrhythmia as an early indicator for Fontan revision, Mark E. Alexander, MD, of Boston Children’s Hospital and Harvard Medical School, said in his invited commentary (J Thorac Cardiovasc Surg. 2016;152:1364-5).
The outcome of a Fontan revision after an arrhythmia “becomes self-fulfilling,” Dr. Alexander said. He questioned what the revision procedure would be when the initial operation was an extracardiac Fontan. “The complex risks of that procedure continue to keep decisions regarding Fontan revisions challenging,” he said. He also noted the study did not analyze the association of ventricular function and arrhythmias “in a substantive way.”
And Dr. Alexander did not interpret the study results as an endorsement of the extracardiac Fontan or a rejection of the lateral tunnel approach. The early adoption of the extracardiac Fontan by the groups the authors represented is itself a limitation of the study, he said. Challenges with follow-up of extracardiac techniques in this and other studies “limit our ability to declare a ‘victor’ in that debate,” he said. “It does remind the electrophysiologist that he or she needs to master the techniques of entering the pulmonary venous atrium in these patients.”
The precision of calculating risk after an operation grows weaker with time, he said, and at 15-20 years morbidity starts to increase and follow-up becomes “more diffuse,” Dr. Alexander said. “That reality means we look forward to this group continuing to enhance our understanding of how our changing management decisions can aid our patients.”
Dr. Alexander had no financial relationships to disclose.
When interpreting the data that the Australian and New Zealand researchers analyzed, one must be cautious about viewing arrhythmia as an early indicator for Fontan revision, Mark E. Alexander, MD, of Boston Children’s Hospital and Harvard Medical School, said in his invited commentary (J Thorac Cardiovasc Surg. 2016;152:1364-5).
The outcome of a Fontan revision after an arrhythmia “becomes self-fulfilling,” Dr. Alexander said. He questioned what the revision procedure would be when the initial operation was an extracardiac Fontan. “The complex risks of that procedure continue to keep decisions regarding Fontan revisions challenging,” he said. He also noted the study did not analyze the association of ventricular function and arrhythmias “in a substantive way.”
And Dr. Alexander did not interpret the study results as an endorsement of the extracardiac Fontan or a rejection of the lateral tunnel approach. The early adoption of the extracardiac Fontan by the groups the authors represented is itself a limitation of the study, he said. Challenges with follow-up of extracardiac techniques in this and other studies “limit our ability to declare a ‘victor’ in that debate,” he said. “It does remind the electrophysiologist that he or she needs to master the techniques of entering the pulmonary venous atrium in these patients.”
The precision of calculating risk after an operation grows weaker with time, he said, and at 15-20 years morbidity starts to increase and follow-up becomes “more diffuse,” Dr. Alexander said. “That reality means we look forward to this group continuing to enhance our understanding of how our changing management decisions can aid our patients.”
Dr. Alexander had no financial relationships to disclose.
When interpreting the data that the Australian and New Zealand researchers analyzed, one must be cautious about viewing arrhythmia as an early indicator for Fontan revision, Mark E. Alexander, MD, of Boston Children’s Hospital and Harvard Medical School, said in his invited commentary (J Thorac Cardiovasc Surg. 2016;152:1364-5).
The outcome of a Fontan revision after an arrhythmia “becomes self-fulfilling,” Dr. Alexander said. He questioned what the revision procedure would be when the initial operation was an extracardiac Fontan. “The complex risks of that procedure continue to keep decisions regarding Fontan revisions challenging,” he said. He also noted the study did not analyze the association of ventricular function and arrhythmias “in a substantive way.”
And Dr. Alexander did not interpret the study results as an endorsement of the extracardiac Fontan or a rejection of the lateral tunnel approach. The early adoption of the extracardiac Fontan by the groups the authors represented is itself a limitation of the study, he said. Challenges with follow-up of extracardiac techniques in this and other studies “limit our ability to declare a ‘victor’ in that debate,” he said. “It does remind the electrophysiologist that he or she needs to master the techniques of entering the pulmonary venous atrium in these patients.”
The precision of calculating risk after an operation grows weaker with time, he said, and at 15-20 years morbidity starts to increase and follow-up becomes “more diffuse,” Dr. Alexander said. “That reality means we look forward to this group continuing to enhance our understanding of how our changing management decisions can aid our patients.”
Dr. Alexander had no financial relationships to disclose.
People who have undergone the Fontan procedure have been known to be prone to developing arrhythmias, but few studies have evaluated their prognosis, so researchers from Australia and New Zealand analyzed results of more than 1,000 patients with Fontan circulation and found that two-thirds did not have any arrhythmia at 20 years, and that, among those who did have arrhythmias, almost three-quarters survived 10 years.
“After the first onset of an arrhythmia, close surveillance of ventricular function is required,” Thomas A. Carins, MD, and his colleagues reported (J Thorac Cardiovasc Surg. 2016;152:1355-63). They analyzed data from 1,034 patients who had Fontan procedures from 1975 to 2014 in the Australia and New Zealand Fontan Registry. “The development of an arrhythmia is associated with a heightened risk of subsequent failure of the Fontan circulation,” they wrote.
The study aimed to determine the type of arrhythmias Fontan patients had and what impact that had on long-term outcomes. The most common Fontan approach used in study patients was the extracardiac conduit (555), followed by the lateral tunnel approach (269) and atriopulmonary (210). Those who had the extracardiac Fontan were least likely to develop an arrhythmia, with a hazard ratio of 0.23 (P less than .001), which Dr. Carins and his coauthors noted was in line with previous reports of arrhythmias occurring in patients who had undergone the atriopulmonary connection (Circulation. 2004;109:2319-25; J Thorac Cardiovasc Surg. 1998;115:499-505).
Overall, 195 patients in the study developed arrhythmia, with 162 having tachyarrhythmia, 74 having bradyarrhythmia and 41 having both. “At 20 years, freedom from any arrhythmia, tachyarrhythmia, and bradyarrhythmia was 66%, 69%, and 85%, respectively,” the researchers said.
The following outcomes occurred after the first onset of arrhythmia – tachyarrhythmia in 153 patients and bradyarrhythmia in 42: Thirty-three died; 12 had heart transplants, 30 had a Fontan correction to an extracardiac conduit, three had a Fontan takedown, 12 developed enteropathy, and 25 developed New York Heart Association class III or IV symptoms. Eighty-four patients reached the composite endpoint of Fontan failure.
After they developed arrhythmias, most patients in all three Fontan procedure groups remained free from Fontan failure at 10 years: 67% in the extracardiac conduit group; 54% in the lateral tunnel group; and 51% in the atriopulmonary group.
Medical management of up to four medications was the preferred initial treatment for those with tachyarrhythmias (86%); 101 patients had a single episode of tachyarrhythmia at follow-up intervals of four to 13 years (7.6 year median). “Those who experienced a single versus multiple episodes of tachyarrhythmia showed comparable freedom from Fontan failure at 15 years,” noted Dr. Carins and his coauthors – with rates of 34% and 33%, respectively. Of the 74 patients with bradyarrhythmias, 66 received pacemakers.
“Survival after the onset of an arrhythmia was surprisingly good with 67% and 84% of patients alive at 10 years after the onset of a tachyarrhythmia and bradyarrhythmia, respectively,” the study authors said. “There was no association between occurrence of arrhythmia and survival.”
About 40% of the patients with a tachyarrhythmia or bradyarrhythmia in the study had reduced ventricular function at 10 years after onset, the researchers wrote. “Although the assessment of ventricular function in this study was clearly subjective, we nonetheless believe that these findings suggest that the onset of an arrhythmia is associated with a progressive deterioration in cardiac function,”they noted.
Coauthor Andrew Bullock, MBBS, disclosed receiving consulting fees from Actelion. Dr. Cairns and other coauthors had no financial relationships to disclose.
People who have undergone the Fontan procedure have been known to be prone to developing arrhythmias, but few studies have evaluated their prognosis, so researchers from Australia and New Zealand analyzed results of more than 1,000 patients with Fontan circulation and found that two-thirds did not have any arrhythmia at 20 years, and that, among those who did have arrhythmias, almost three-quarters survived 10 years.
“After the first onset of an arrhythmia, close surveillance of ventricular function is required,” Thomas A. Carins, MD, and his colleagues reported (J Thorac Cardiovasc Surg. 2016;152:1355-63). They analyzed data from 1,034 patients who had Fontan procedures from 1975 to 2014 in the Australia and New Zealand Fontan Registry. “The development of an arrhythmia is associated with a heightened risk of subsequent failure of the Fontan circulation,” they wrote.
The study aimed to determine the type of arrhythmias Fontan patients had and what impact that had on long-term outcomes. The most common Fontan approach used in study patients was the extracardiac conduit (555), followed by the lateral tunnel approach (269) and atriopulmonary (210). Those who had the extracardiac Fontan were least likely to develop an arrhythmia, with a hazard ratio of 0.23 (P less than .001), which Dr. Carins and his coauthors noted was in line with previous reports of arrhythmias occurring in patients who had undergone the atriopulmonary connection (Circulation. 2004;109:2319-25; J Thorac Cardiovasc Surg. 1998;115:499-505).
Overall, 195 patients in the study developed arrhythmia, with 162 having tachyarrhythmia, 74 having bradyarrhythmia and 41 having both. “At 20 years, freedom from any arrhythmia, tachyarrhythmia, and bradyarrhythmia was 66%, 69%, and 85%, respectively,” the researchers said.
The following outcomes occurred after the first onset of arrhythmia – tachyarrhythmia in 153 patients and bradyarrhythmia in 42: Thirty-three died; 12 had heart transplants, 30 had a Fontan correction to an extracardiac conduit, three had a Fontan takedown, 12 developed enteropathy, and 25 developed New York Heart Association class III or IV symptoms. Eighty-four patients reached the composite endpoint of Fontan failure.
After they developed arrhythmias, most patients in all three Fontan procedure groups remained free from Fontan failure at 10 years: 67% in the extracardiac conduit group; 54% in the lateral tunnel group; and 51% in the atriopulmonary group.
Medical management of up to four medications was the preferred initial treatment for those with tachyarrhythmias (86%); 101 patients had a single episode of tachyarrhythmia at follow-up intervals of four to 13 years (7.6 year median). “Those who experienced a single versus multiple episodes of tachyarrhythmia showed comparable freedom from Fontan failure at 15 years,” noted Dr. Carins and his coauthors – with rates of 34% and 33%, respectively. Of the 74 patients with bradyarrhythmias, 66 received pacemakers.
“Survival after the onset of an arrhythmia was surprisingly good with 67% and 84% of patients alive at 10 years after the onset of a tachyarrhythmia and bradyarrhythmia, respectively,” the study authors said. “There was no association between occurrence of arrhythmia and survival.”
About 40% of the patients with a tachyarrhythmia or bradyarrhythmia in the study had reduced ventricular function at 10 years after onset, the researchers wrote. “Although the assessment of ventricular function in this study was clearly subjective, we nonetheless believe that these findings suggest that the onset of an arrhythmia is associated with a progressive deterioration in cardiac function,”they noted.
Coauthor Andrew Bullock, MBBS, disclosed receiving consulting fees from Actelion. Dr. Cairns and other coauthors had no financial relationships to disclose.
FROM THE JOURNAL OF THORACIC AND CARDIOVASCULAR SURGERY
Key clinical point: The development of arrhythmia is associated with a heightened risk of failure of Fontan circulation after a Fontan procedure.
Major finding: At 20 years, freedom from any arrhythmia was 66%, and after the onset of any arrhythmia freedom from Fontan failure was 55%.
Data source: 1,034 patients who had undergone a Fontan procedure from 1975 to 2014 as recorded in the Australian and New Zealand Fontan Registry.
Disclosures: Coauthor Andrew Bullock, MBBS, reported receiving consulting fees from Actelion. All other others have no financial relationships to disclose.
Revision technique treats graft dysfunction after esophageal reconstruction
Ingestion of caustic substances like alkali, acid, and bleaches that call for esophageal surgery is relatively rare, and the study of dealing with postsurgery complications even rarer, but a team of surgeons from a large public referral hospital in Paris has collected enough cases over the first years of this century to report that a form of revision surgery in these cases can yield good outcomes with acceptable morbidity, according to a study in the Journal of Thoracic and Cardiovascular Surgery (2016;152:1378-85).
Thibault Voron, MD, and coauthors at Hôpitaux Saint-Louis and the University of Paris performed revision cervicosternolaparotomy (CSLap) on 55 patients from 1999 to 2015. Two patients (4%) died and the severe morbidity rate was 27%, but the long-term functional success rate was 85%. “Of note, these figures compare favorably with results of primary esophageal reconstruction for caustic injuries in the literature,” Dr. Voron and colleagues said. Overall the study authors performed revision surgery on 100 patients, with the remaining 45 undergoing repair through a limited approach. There were no significant differences in characteristics between the two groups.
Primary esophageal reconstruction for caustic injuries can usually be done at referral centers with good results, but up to half of these patients can have late complications, consisting mostly of strictures and redundancy that can cause loss of function, Dr. Voron and coauthors said. Published series have reported revision surgery in 15%-38% of patients (Dis Esophagus. 2008;21:E1-5; Dis Esophagus. 1999;12:7-9), but revision surgery itself is difficult to accomplish.
CSLap involves a large operative field from the jaw to the pubis. It starts with a comprehensive neck exploration through the previous cervical incision or with a median laparotomy to rule out a limited-approach repair. CSLap was undertaken when the graft was too short for a tension-free anastomosis. After the upper part of the graft was dissected from the thoracic inlet, the abdomen was opened for dissection of the abdominal part of the transplant. All scar tissues and strictures were excised after the transplant release, and a new anastomosis was constructed in healthy tissues. In cases involving life-threatening complications, patient survival prevailed over graft preservation and reconstruction of digestive continuity. The operations took up to 10 hours, with 8 hours, 20 minutes the median.
Dr. Voron and coauthors identified two distinct indications for CSLap: graft strictures in 43 (78%) of patients to rescue the primary conduit and reconstruct the cervical anastomosis and a need to access the retrosternal space to treat graft-related complications. “Graft lengthening was definitely not the issue in this situation,” Dr. Voron and colleagues said of the latter indication.
Four patients had emergency revision CSLap for spontaneous graft perforation and complications related to caustic reingestion. None died and one patient had preservation of the primary conduit. “Retrosternal grafts can be quickly removed by blunt dissection in life-threatening circumstances; however, if reasonable chances to recover the transplant exist, CSLap exploration can be justified,” Dr. Voron and coauthors said.
CSLap offers a few advantages in these situations: Transplant release provides significant lengthening of the graft that enables preservation of the primary conduit and redo of the cervical anastomosis in most patients, and it allows direct access to the retrosternal space if needed, Dr. Voron and coauthors said.
Dr. Voron and coauthors had no financial relationships to disclose.
This series by Dr. Voron and coauthors was “truly remarkable,” given the rarity of esophageal caustic injuries and even rarer occasion of revision surgery, Victor A. Ferraris, MD, PhD, of the University of Kentucky, Lexington, said in his invited commentary (J Thorac Cardiovasc Surg. 2016;152:1386-7). He attributed the series size to the authors’ clinical setting in a trauma entry point for Europe’s largest hospital system – the same hospital that received victims of the terrorist attack at the Bataclan concert hall in Paris in November 2015.
“Voron and coauthors clearly have the benefit of a large referral population and vast medical infrastructure in the Assistance Publique-Hôpitaux de Paris,” Dr. Ferraris said. That volume certainly factors into their ability to achieve “very good outcomes,” he said.
“This seems to be an argument in favor of localization of resources to a single center,” Dr. Ferraris said. “Dr. Voron and coauthors have translated their experience into knowledge that can help other surgeons deal with this difficult problem.”
Dr. Ferraris had no financial relationships to disclose.
This series by Dr. Voron and coauthors was “truly remarkable,” given the rarity of esophageal caustic injuries and even rarer occasion of revision surgery, Victor A. Ferraris, MD, PhD, of the University of Kentucky, Lexington, said in his invited commentary (J Thorac Cardiovasc Surg. 2016;152:1386-7). He attributed the series size to the authors’ clinical setting in a trauma entry point for Europe’s largest hospital system – the same hospital that received victims of the terrorist attack at the Bataclan concert hall in Paris in November 2015.
“Voron and coauthors clearly have the benefit of a large referral population and vast medical infrastructure in the Assistance Publique-Hôpitaux de Paris,” Dr. Ferraris said. That volume certainly factors into their ability to achieve “very good outcomes,” he said.
“This seems to be an argument in favor of localization of resources to a single center,” Dr. Ferraris said. “Dr. Voron and coauthors have translated their experience into knowledge that can help other surgeons deal with this difficult problem.”
Dr. Ferraris had no financial relationships to disclose.
This series by Dr. Voron and coauthors was “truly remarkable,” given the rarity of esophageal caustic injuries and even rarer occasion of revision surgery, Victor A. Ferraris, MD, PhD, of the University of Kentucky, Lexington, said in his invited commentary (J Thorac Cardiovasc Surg. 2016;152:1386-7). He attributed the series size to the authors’ clinical setting in a trauma entry point for Europe’s largest hospital system – the same hospital that received victims of the terrorist attack at the Bataclan concert hall in Paris in November 2015.
“Voron and coauthors clearly have the benefit of a large referral population and vast medical infrastructure in the Assistance Publique-Hôpitaux de Paris,” Dr. Ferraris said. That volume certainly factors into their ability to achieve “very good outcomes,” he said.
“This seems to be an argument in favor of localization of resources to a single center,” Dr. Ferraris said. “Dr. Voron and coauthors have translated their experience into knowledge that can help other surgeons deal with this difficult problem.”
Dr. Ferraris had no financial relationships to disclose.
Ingestion of caustic substances like alkali, acid, and bleaches that call for esophageal surgery is relatively rare, and the study of dealing with postsurgery complications even rarer, but a team of surgeons from a large public referral hospital in Paris has collected enough cases over the first years of this century to report that a form of revision surgery in these cases can yield good outcomes with acceptable morbidity, according to a study in the Journal of Thoracic and Cardiovascular Surgery (2016;152:1378-85).
Thibault Voron, MD, and coauthors at Hôpitaux Saint-Louis and the University of Paris performed revision cervicosternolaparotomy (CSLap) on 55 patients from 1999 to 2015. Two patients (4%) died and the severe morbidity rate was 27%, but the long-term functional success rate was 85%. “Of note, these figures compare favorably with results of primary esophageal reconstruction for caustic injuries in the literature,” Dr. Voron and colleagues said. Overall the study authors performed revision surgery on 100 patients, with the remaining 45 undergoing repair through a limited approach. There were no significant differences in characteristics between the two groups.
Primary esophageal reconstruction for caustic injuries can usually be done at referral centers with good results, but up to half of these patients can have late complications, consisting mostly of strictures and redundancy that can cause loss of function, Dr. Voron and coauthors said. Published series have reported revision surgery in 15%-38% of patients (Dis Esophagus. 2008;21:E1-5; Dis Esophagus. 1999;12:7-9), but revision surgery itself is difficult to accomplish.
CSLap involves a large operative field from the jaw to the pubis. It starts with a comprehensive neck exploration through the previous cervical incision or with a median laparotomy to rule out a limited-approach repair. CSLap was undertaken when the graft was too short for a tension-free anastomosis. After the upper part of the graft was dissected from the thoracic inlet, the abdomen was opened for dissection of the abdominal part of the transplant. All scar tissues and strictures were excised after the transplant release, and a new anastomosis was constructed in healthy tissues. In cases involving life-threatening complications, patient survival prevailed over graft preservation and reconstruction of digestive continuity. The operations took up to 10 hours, with 8 hours, 20 minutes the median.
Dr. Voron and coauthors identified two distinct indications for CSLap: graft strictures in 43 (78%) of patients to rescue the primary conduit and reconstruct the cervical anastomosis and a need to access the retrosternal space to treat graft-related complications. “Graft lengthening was definitely not the issue in this situation,” Dr. Voron and colleagues said of the latter indication.
Four patients had emergency revision CSLap for spontaneous graft perforation and complications related to caustic reingestion. None died and one patient had preservation of the primary conduit. “Retrosternal grafts can be quickly removed by blunt dissection in life-threatening circumstances; however, if reasonable chances to recover the transplant exist, CSLap exploration can be justified,” Dr. Voron and coauthors said.
CSLap offers a few advantages in these situations: Transplant release provides significant lengthening of the graft that enables preservation of the primary conduit and redo of the cervical anastomosis in most patients, and it allows direct access to the retrosternal space if needed, Dr. Voron and coauthors said.
Dr. Voron and coauthors had no financial relationships to disclose.
Ingestion of caustic substances like alkali, acid, and bleaches that call for esophageal surgery is relatively rare, and the study of dealing with postsurgery complications even rarer, but a team of surgeons from a large public referral hospital in Paris has collected enough cases over the first years of this century to report that a form of revision surgery in these cases can yield good outcomes with acceptable morbidity, according to a study in the Journal of Thoracic and Cardiovascular Surgery (2016;152:1378-85).
Thibault Voron, MD, and coauthors at Hôpitaux Saint-Louis and the University of Paris performed revision cervicosternolaparotomy (CSLap) on 55 patients from 1999 to 2015. Two patients (4%) died and the severe morbidity rate was 27%, but the long-term functional success rate was 85%. “Of note, these figures compare favorably with results of primary esophageal reconstruction for caustic injuries in the literature,” Dr. Voron and colleagues said. Overall the study authors performed revision surgery on 100 patients, with the remaining 45 undergoing repair through a limited approach. There were no significant differences in characteristics between the two groups.
Primary esophageal reconstruction for caustic injuries can usually be done at referral centers with good results, but up to half of these patients can have late complications, consisting mostly of strictures and redundancy that can cause loss of function, Dr. Voron and coauthors said. Published series have reported revision surgery in 15%-38% of patients (Dis Esophagus. 2008;21:E1-5; Dis Esophagus. 1999;12:7-9), but revision surgery itself is difficult to accomplish.
CSLap involves a large operative field from the jaw to the pubis. It starts with a comprehensive neck exploration through the previous cervical incision or with a median laparotomy to rule out a limited-approach repair. CSLap was undertaken when the graft was too short for a tension-free anastomosis. After the upper part of the graft was dissected from the thoracic inlet, the abdomen was opened for dissection of the abdominal part of the transplant. All scar tissues and strictures were excised after the transplant release, and a new anastomosis was constructed in healthy tissues. In cases involving life-threatening complications, patient survival prevailed over graft preservation and reconstruction of digestive continuity. The operations took up to 10 hours, with 8 hours, 20 minutes the median.
Dr. Voron and coauthors identified two distinct indications for CSLap: graft strictures in 43 (78%) of patients to rescue the primary conduit and reconstruct the cervical anastomosis and a need to access the retrosternal space to treat graft-related complications. “Graft lengthening was definitely not the issue in this situation,” Dr. Voron and colleagues said of the latter indication.
Four patients had emergency revision CSLap for spontaneous graft perforation and complications related to caustic reingestion. None died and one patient had preservation of the primary conduit. “Retrosternal grafts can be quickly removed by blunt dissection in life-threatening circumstances; however, if reasonable chances to recover the transplant exist, CSLap exploration can be justified,” Dr. Voron and coauthors said.
CSLap offers a few advantages in these situations: Transplant release provides significant lengthening of the graft that enables preservation of the primary conduit and redo of the cervical anastomosis in most patients, and it allows direct access to the retrosternal space if needed, Dr. Voron and coauthors said.
Dr. Voron and coauthors had no financial relationships to disclose.
Key clinical point: Cervicosternolaparotomy revision surgery for graft dysfunction after esophageal reconstruction for caustic injuries can achieve good results with acceptable morbidity.
Major finding: Functional success rate after revision CSLap was 85% after a mean follow-up of 4.4 years.
Data source: 55 patients who underwent CSLap revision surgery between 1999 and 2015 at a single center.
Disclosures: Dr. Voron and coauthors had no financial relationships to disclose.
SYNTAX analysis: Making the case for CABG over PCI
Whenever seminal clinical trials report results that challenge conventional thinking, physicians face the challenge of actually applying those findings in the clinic. A team of cardiac surgeons from Baylor University in Plano, Tex., has offered its take on the clinical implications of recent findings from the cause-of-death analysis of the SYNTAX trial that compared coronary artery bypass grafting with stenting: When counseling higher-risk patients with coronary artery disease about revascularization procedures, cardiologists and cardiac surgeons should clearly elucidate the dramatic advantage of coronary artery bypass grafting over stenting that SYNTAX had demonstrated.
Michael Mack, MD, and coauthors made their case in a featured expert opinion in the Journal of Thoracic and Cardiovascular Surgery (2016;152:1237-40).
“In fact, there was a significant survival advantage for CABG in the patients with intermediate and high SYNTAX scores, with the death rate of CABG versus PCI being 9.6% versus 16.3% (P less than .047) and 8.8% versus 17.8% (P less than .02), respectively,” they wrote.
The advantages of surgery “have been most striking for patients with intermediate or high SYNTAX scores, but seem to exist for patients with low scores as well, although requiring more follow-up,” Dr. Mack and colleagues said. But the situation is less clear in other subgroups, particularly in patients with less diffuse distal disease and lower SYNTAX scores, they added.
Complete revascularization after the procedure may explain the better outcomes with CABG, as 43.3% of those in the PCI arm had incomplete revascularization vs. 36.8% in the CABG arm. “Incomplete revascularization was associated with increased risk for major adverse cardiac or cerebrovascular events three years after PCI, but incomplete revascularization in the CABG group could not be identified as a predictor for worse outcomes,” Dr. Mack and colleagues noted.
The expert opinion authors debunk one of the recent criticisms of SYNTAX: that its reliance on first-generation drug-eluting stents is dated and not relevant today. They noted the more recent Bypass Surgery Vs. Everolimus-Eluting Stent Implantation for Multivessel Coronary Artery Disease trial found a similarly higher rate of death, heart attack, and target vessel revascularization occurred more frequently in the PCI group (15.3% vs. 10.6% in the CABG group) (N Engl J Med. 2015;372:1204-12).
Nonetheless, Dr. Mack and coauthors found room for improvement for CABG through increased use of atrial revascularization and appropriate measures to minimize stroke.
The latest SYNTAX findings can inform the approach surgeons take with high-risk patients, they said. This should include “a discussion of these data, particularly in regard to survival.” And physicians should base their therapeutic recommendations on these data. “At present, there are data seeming to indicate that the majority of patients with three-vessel disease receiving invasive treatment in the United States are being treated with PCI, an outcome that is not congruent with these outcome findings,” they said.
Taking into consideration other SYNTAX analyses that have shown that completeness of revascularization is a determining factor in post-PCI outcomes, Dr. Mack and coauthors said that physicians should calculate the degree of coronary artery disease (CAD) left untreated after intervention, “and those patients who are likely to have a high residual SYNTAX score should be strongly considered for CABG.” Doctors should also focus “intensive efforts” on adherence to optimal medical therapy after both CABG and PCI.
“Finally, although there is a strong patient preference for a less-invasive treatment of their CAD, patients with advanced disease should be made aware that the choice of PCI puts them at an increased risk of death relative to CABG, and a full and transparent discussion should occur regarding the implications of their decision,” Dr. Mack and coauthors concluded.
They had no relevant financial relationships to disclose.
In their invited editorial commentary, Saswata Deb, MD, and Stephen E. Fremes, MD, of the Schulich Heart Center at the University of Toronto, concurred with the conclusions of Dr. Mack and colleagues (J Thorac Cardiovasc Surg. 2016;152:1241-2). And Joseph F. Sabik III, MD, of the Cleveland Clinic arrived at a similar conclusion in an accompanying editorial (J. Thorac Cardiovasc Surg. 2016;152:1227-8).
Dr. Deb and Dr. Fremes found noteworthy the point Dr. Mack and coauthors raised about cardiologists and internists continuing to recommend PCI to patients with complex multivessel CAD despite evidence from SYNTAX and other trials. “This raises the importance of having a multidisciplinary heart team,” Dr. Deb and Dr. Fremes said.
But they also raised an important question about the difference in outcomes between CABG and PCI in complex multivessel disease. CABG should be the preferred intervention if the high rates of late fatal myocardial infarction after PCI are due to incomplete revascularization; however, if late stent thrombosis was the cause of this disparity in outcomes, then improvements in PCI could close that gap.
In his editorial, Dr. Sabik attributed the difference in outcomes between PCI and CABG to the ability of the former to both treat existing and prevent future stenosis. PCI can be “difficult, dangerous, and even impossible” when the target vessel is totally occluded or the stenosis is complex, hence leading to incomplete revascularization and residual ischemia. “Performing CABG to these vessels is no more difficult than for an isolated, noncomplex stenosis,” Dr. Sabik said.
Dr. Sabik disclosed he is the principal investigator for an Abbott Laboratories–sponsored trial of left main coronary disease, and is on the scientific advisory board of Medtronic.
Dr. Deb and Dr. Fremes had no relationships to disclose.
In their invited editorial commentary, Saswata Deb, MD, and Stephen E. Fremes, MD, of the Schulich Heart Center at the University of Toronto, concurred with the conclusions of Dr. Mack and colleagues (J Thorac Cardiovasc Surg. 2016;152:1241-2). And Joseph F. Sabik III, MD, of the Cleveland Clinic arrived at a similar conclusion in an accompanying editorial (J. Thorac Cardiovasc Surg. 2016;152:1227-8).
Dr. Deb and Dr. Fremes found noteworthy the point Dr. Mack and coauthors raised about cardiologists and internists continuing to recommend PCI to patients with complex multivessel CAD despite evidence from SYNTAX and other trials. “This raises the importance of having a multidisciplinary heart team,” Dr. Deb and Dr. Fremes said.
But they also raised an important question about the difference in outcomes between CABG and PCI in complex multivessel disease. CABG should be the preferred intervention if the high rates of late fatal myocardial infarction after PCI are due to incomplete revascularization; however, if late stent thrombosis was the cause of this disparity in outcomes, then improvements in PCI could close that gap.
In his editorial, Dr. Sabik attributed the difference in outcomes between PCI and CABG to the ability of the former to both treat existing and prevent future stenosis. PCI can be “difficult, dangerous, and even impossible” when the target vessel is totally occluded or the stenosis is complex, hence leading to incomplete revascularization and residual ischemia. “Performing CABG to these vessels is no more difficult than for an isolated, noncomplex stenosis,” Dr. Sabik said.
Dr. Sabik disclosed he is the principal investigator for an Abbott Laboratories–sponsored trial of left main coronary disease, and is on the scientific advisory board of Medtronic.
Dr. Deb and Dr. Fremes had no relationships to disclose.
In their invited editorial commentary, Saswata Deb, MD, and Stephen E. Fremes, MD, of the Schulich Heart Center at the University of Toronto, concurred with the conclusions of Dr. Mack and colleagues (J Thorac Cardiovasc Surg. 2016;152:1241-2). And Joseph F. Sabik III, MD, of the Cleveland Clinic arrived at a similar conclusion in an accompanying editorial (J. Thorac Cardiovasc Surg. 2016;152:1227-8).
Dr. Deb and Dr. Fremes found noteworthy the point Dr. Mack and coauthors raised about cardiologists and internists continuing to recommend PCI to patients with complex multivessel CAD despite evidence from SYNTAX and other trials. “This raises the importance of having a multidisciplinary heart team,” Dr. Deb and Dr. Fremes said.
But they also raised an important question about the difference in outcomes between CABG and PCI in complex multivessel disease. CABG should be the preferred intervention if the high rates of late fatal myocardial infarction after PCI are due to incomplete revascularization; however, if late stent thrombosis was the cause of this disparity in outcomes, then improvements in PCI could close that gap.
In his editorial, Dr. Sabik attributed the difference in outcomes between PCI and CABG to the ability of the former to both treat existing and prevent future stenosis. PCI can be “difficult, dangerous, and even impossible” when the target vessel is totally occluded or the stenosis is complex, hence leading to incomplete revascularization and residual ischemia. “Performing CABG to these vessels is no more difficult than for an isolated, noncomplex stenosis,” Dr. Sabik said.
Dr. Sabik disclosed he is the principal investigator for an Abbott Laboratories–sponsored trial of left main coronary disease, and is on the scientific advisory board of Medtronic.
Dr. Deb and Dr. Fremes had no relationships to disclose.
Whenever seminal clinical trials report results that challenge conventional thinking, physicians face the challenge of actually applying those findings in the clinic. A team of cardiac surgeons from Baylor University in Plano, Tex., has offered its take on the clinical implications of recent findings from the cause-of-death analysis of the SYNTAX trial that compared coronary artery bypass grafting with stenting: When counseling higher-risk patients with coronary artery disease about revascularization procedures, cardiologists and cardiac surgeons should clearly elucidate the dramatic advantage of coronary artery bypass grafting over stenting that SYNTAX had demonstrated.
Michael Mack, MD, and coauthors made their case in a featured expert opinion in the Journal of Thoracic and Cardiovascular Surgery (2016;152:1237-40).
“In fact, there was a significant survival advantage for CABG in the patients with intermediate and high SYNTAX scores, with the death rate of CABG versus PCI being 9.6% versus 16.3% (P less than .047) and 8.8% versus 17.8% (P less than .02), respectively,” they wrote.
The advantages of surgery “have been most striking for patients with intermediate or high SYNTAX scores, but seem to exist for patients with low scores as well, although requiring more follow-up,” Dr. Mack and colleagues said. But the situation is less clear in other subgroups, particularly in patients with less diffuse distal disease and lower SYNTAX scores, they added.
Complete revascularization after the procedure may explain the better outcomes with CABG, as 43.3% of those in the PCI arm had incomplete revascularization vs. 36.8% in the CABG arm. “Incomplete revascularization was associated with increased risk for major adverse cardiac or cerebrovascular events three years after PCI, but incomplete revascularization in the CABG group could not be identified as a predictor for worse outcomes,” Dr. Mack and colleagues noted.
The expert opinion authors debunk one of the recent criticisms of SYNTAX: that its reliance on first-generation drug-eluting stents is dated and not relevant today. They noted the more recent Bypass Surgery Vs. Everolimus-Eluting Stent Implantation for Multivessel Coronary Artery Disease trial found a similarly higher rate of death, heart attack, and target vessel revascularization occurred more frequently in the PCI group (15.3% vs. 10.6% in the CABG group) (N Engl J Med. 2015;372:1204-12).
Nonetheless, Dr. Mack and coauthors found room for improvement for CABG through increased use of atrial revascularization and appropriate measures to minimize stroke.
The latest SYNTAX findings can inform the approach surgeons take with high-risk patients, they said. This should include “a discussion of these data, particularly in regard to survival.” And physicians should base their therapeutic recommendations on these data. “At present, there are data seeming to indicate that the majority of patients with three-vessel disease receiving invasive treatment in the United States are being treated with PCI, an outcome that is not congruent with these outcome findings,” they said.
Taking into consideration other SYNTAX analyses that have shown that completeness of revascularization is a determining factor in post-PCI outcomes, Dr. Mack and coauthors said that physicians should calculate the degree of coronary artery disease (CAD) left untreated after intervention, “and those patients who are likely to have a high residual SYNTAX score should be strongly considered for CABG.” Doctors should also focus “intensive efforts” on adherence to optimal medical therapy after both CABG and PCI.
“Finally, although there is a strong patient preference for a less-invasive treatment of their CAD, patients with advanced disease should be made aware that the choice of PCI puts them at an increased risk of death relative to CABG, and a full and transparent discussion should occur regarding the implications of their decision,” Dr. Mack and coauthors concluded.
They had no relevant financial relationships to disclose.
Whenever seminal clinical trials report results that challenge conventional thinking, physicians face the challenge of actually applying those findings in the clinic. A team of cardiac surgeons from Baylor University in Plano, Tex., has offered its take on the clinical implications of recent findings from the cause-of-death analysis of the SYNTAX trial that compared coronary artery bypass grafting with stenting: When counseling higher-risk patients with coronary artery disease about revascularization procedures, cardiologists and cardiac surgeons should clearly elucidate the dramatic advantage of coronary artery bypass grafting over stenting that SYNTAX had demonstrated.
Michael Mack, MD, and coauthors made their case in a featured expert opinion in the Journal of Thoracic and Cardiovascular Surgery (2016;152:1237-40).
“In fact, there was a significant survival advantage for CABG in the patients with intermediate and high SYNTAX scores, with the death rate of CABG versus PCI being 9.6% versus 16.3% (P less than .047) and 8.8% versus 17.8% (P less than .02), respectively,” they wrote.
The advantages of surgery “have been most striking for patients with intermediate or high SYNTAX scores, but seem to exist for patients with low scores as well, although requiring more follow-up,” Dr. Mack and colleagues said. But the situation is less clear in other subgroups, particularly in patients with less diffuse distal disease and lower SYNTAX scores, they added.
Complete revascularization after the procedure may explain the better outcomes with CABG, as 43.3% of those in the PCI arm had incomplete revascularization vs. 36.8% in the CABG arm. “Incomplete revascularization was associated with increased risk for major adverse cardiac or cerebrovascular events three years after PCI, but incomplete revascularization in the CABG group could not be identified as a predictor for worse outcomes,” Dr. Mack and colleagues noted.
The expert opinion authors debunk one of the recent criticisms of SYNTAX: that its reliance on first-generation drug-eluting stents is dated and not relevant today. They noted the more recent Bypass Surgery Vs. Everolimus-Eluting Stent Implantation for Multivessel Coronary Artery Disease trial found a similarly higher rate of death, heart attack, and target vessel revascularization occurred more frequently in the PCI group (15.3% vs. 10.6% in the CABG group) (N Engl J Med. 2015;372:1204-12).
Nonetheless, Dr. Mack and coauthors found room for improvement for CABG through increased use of atrial revascularization and appropriate measures to minimize stroke.
The latest SYNTAX findings can inform the approach surgeons take with high-risk patients, they said. This should include “a discussion of these data, particularly in regard to survival.” And physicians should base their therapeutic recommendations on these data. “At present, there are data seeming to indicate that the majority of patients with three-vessel disease receiving invasive treatment in the United States are being treated with PCI, an outcome that is not congruent with these outcome findings,” they said.
Taking into consideration other SYNTAX analyses that have shown that completeness of revascularization is a determining factor in post-PCI outcomes, Dr. Mack and coauthors said that physicians should calculate the degree of coronary artery disease (CAD) left untreated after intervention, “and those patients who are likely to have a high residual SYNTAX score should be strongly considered for CABG.” Doctors should also focus “intensive efforts” on adherence to optimal medical therapy after both CABG and PCI.
“Finally, although there is a strong patient preference for a less-invasive treatment of their CAD, patients with advanced disease should be made aware that the choice of PCI puts them at an increased risk of death relative to CABG, and a full and transparent discussion should occur regarding the implications of their decision,” Dr. Mack and coauthors concluded.
They had no relevant financial relationships to disclose.
FROM THE JOURNAL OF THORACIC AND CARDIOVASCULAR SURGERY
Key clinical point: Physicians should clearly communicate to patients with complex multivessel artery disease the key findings of the SYNTAX trial.
Major finding: The SYNTAX trials showed the risk of cardiac death from myocardial infarction after percutaneous coronary intervention (PCI) is 10 times greater than that after coronary artery bypass grafting in higher-risk patients.
Data source: A post hoc analysis of causes of death in all 3,075 trial and registry patients in the Synergy Between Percutaneous Coronary Intervention With Taxus and Cardiac Surgery (SYNTAX) trial.
Disclosures: Dr. Mack and coauthors reported having no financial disclosures.