User login
Bringing you the latest news, research and reviews, exclusive interviews, podcasts, quizzes, and more.
div[contains(@class, 'header__large-screen')]
div[contains(@class, 'read-next-article')]
div[contains(@class, 'nav-primary')]
nav[contains(@class, 'nav-primary')]
section[contains(@class, 'footer-nav-section-wrapper')]
footer[@id='footer']
div[contains(@class, 'main-prefix')]
section[contains(@class, 'nav-hidden')]
div[contains(@class, 'ce-card-content')]
nav[contains(@class, 'nav-ce-stack')]
The compass that points toward food
The new breakfast of champions
We love a good ranking system here at LOTME world headquarters, especially the food-based ones. Luckily for us (and our readers), a new study published in Nature Food offers a food-based ranking system.
Sadly, unlike the last food-related ranking we covered, the Food Compass doesn’t tell you how much life you gain or lose from each food you eat down to the precise minute. Instead, it favors a more simple rating system from 1 to 100, with healthier foods scoring higher, and even incorporates mixed foods, not just single ingredients. This makes it better at assessing and comparing food combinations, rather than trying to mix and match the many ingredients that go into even relatively simple recipes.
The top and bottom of the rankings contain the usual suspects. Legumes and nuts, at 78.6, had the highest average score among the broad food groups, followed by fruits and then vegetables. Rounding out the bottom were sweets and savory snacks at 16.4. Among the individual foods, there were perfect scores in both directions: 100 for raw raspberries, while instant noodle soup and nonchocolate, ready-to-eat, nonfat pudding (very specific there) each earned a 1.
There are a few surprises in between. Nonfat cappuccino received a green light from the investigators, great news for the coffee drinkers out there. A serving of sweet potato chips scored better than a simple grilled chicken breast, and a slice of pizza, loaded up with extra meat and a thick crust, is still more nutritious than a bowl of corn flakes.
Neither is good for you, of course, but we’re still going to take this as a sign that pizza is the ideal breakfast food. Add that to your morning coffee, and you’re ready to start the day. Move over Wheaties, there’s a new breakfast of champions.
COVID-19 resisters, please step forward
Some people have all the luck with good genes, both inside and out.
Genetically speaking, humans are 99.9% the same, but that 0.1% is where things get interesting. Because of that 0.1% difference, some people are more likely to contract diseases such as HIV, while others might be more resistant. These small differences in genetic code could be the key to finding treatments for COVID-19.
“The introduction of SARS-CoV-2 to a naive population, on a global scale, has provided yet another demonstration of the remarkable clinical variability between individuals in the course of infection, ranging from asymptomatic infections to life-threatening disease,” the researchers said in Nature Immunology.
The investigators have been scouring the world to find people who might be resistant to SARS-CoV-2 and have enrolled over 400 individuals in a “dedicated resistance study cohort,” according to ScienceAlert.
The investigators are looking at households in which families were infected but one member did not show severe symptoms, or for individuals who have been around the virus multiple times and haven’t contracted it. They are also looking at blood types.
Enrollment is ongoing, so if you’ve been in contact with COVID-19 multiple times and have not gotten sick, scientists would like to hear from you.
Better living through parasitization
How would you like to triple your life span, while maintaining a youthful appearance and gaining special social standing and privileges?
Sounds pretty good, right, so what’s the catch? Well, you have to be infected with a tapeworm ... and you have to be an ant.
If you are an ant, here’s the deal: Workers of the species Temnothorax nylanderi that have tapeworms live much longer than uninfected workers, and while living out those longer lives they do less work and receive gifts of food.
In a study conducted at Johannes Gutenberg University in Mainz, Germany, infected ants’ metabolic rates and lipid levels were similar to those of younger ants, and they appeared to remain in a permanent juvenile stage as a result of the infection, the investigators reported.
They tracked Temnothorax colonies for 3 years, at which point 95% of the uninfected workers had died but over half of the infected ants were still alive. Pretty great, right? Wrong. There was no joy in antville, for the uninfected workers had struck out. “Strained by the additional burden of their wormed-up nestmates, they seemed to be shunting care away from their queen. They were dying sooner than they might have if the colonies had remained parasite-free,” according to an article in the Atlantic.
Does this situation seem just a wee bit familiar? A small group lives longer, healthier lives and enjoys special privileges while the majority of that society works harder to support them? We’ll put it into the form of a chicken-and-egg argument: Which came first, the tapeworms or the one-percenters?
Laughing the pandemic stress away
Doomscrolling on social media has become one of the world’s favorite pastimes during the pandemic, but research shows that those memes about COVID-19 might combat the doom and gloom of the outside world.
A study recently published in Psychology of Popular Media showed that viewing memes, specifically those that were COVID-19 related, actually lessened the stress of the pandemic.
The researchers conducted a survey of 748 people aged 18-88 years. Each participant viewed three memes with text or three memes with text but no images. All three memes had similar cuteness levels (baby or adult), subject (animal or human), and caption (COVID-19–related or not). The participants were then asked to report on their stress levels and feelings before and after the memes.
The people who looked at memes felt less stressed and a higher humor level, especially the participants who received the COVID-19 memes. Study Finds said that they had more “pandemic-coping confidence” than those who got regular memes.
“While the World Health Organization recommended that people avoid too much COVID-related media for the benefit of their mental health, our research reveals that memes about COVID-19 could help people feel more confident in their ability to deal with the pandemic,” lead author Jessica Gall Myrick, PhD, said in a written statement. “The positive emotions associated with this type of content may make people feel psychologically safer and therefore better able to pay attention to the underlying messages related to health threats.”
So if you think you’ve been wasting time looking at memes during this pandemic, think again. It actually might keep you sane. Keep on scrolling!
Giving the gift of stress reduction
It’s a big week here at LOTME. You’ve just read our 100th edition, and to help celebrate that milestone – along with Count Your Buttons Day, Celebration of the Mind Day, and the International Day of the Nacho – we’re presenting an extra-special bonus feature, courtesy of Sad and Useless: The most depressive humor site on the Internet.
We hope you’ll stop your doomscrolling long enough to enjoy this stress-reducing meme. Thanks for reading!
The new breakfast of champions
We love a good ranking system here at LOTME world headquarters, especially the food-based ones. Luckily for us (and our readers), a new study published in Nature Food offers a food-based ranking system.
Sadly, unlike the last food-related ranking we covered, the Food Compass doesn’t tell you how much life you gain or lose from each food you eat down to the precise minute. Instead, it favors a more simple rating system from 1 to 100, with healthier foods scoring higher, and even incorporates mixed foods, not just single ingredients. This makes it better at assessing and comparing food combinations, rather than trying to mix and match the many ingredients that go into even relatively simple recipes.
The top and bottom of the rankings contain the usual suspects. Legumes and nuts, at 78.6, had the highest average score among the broad food groups, followed by fruits and then vegetables. Rounding out the bottom were sweets and savory snacks at 16.4. Among the individual foods, there were perfect scores in both directions: 100 for raw raspberries, while instant noodle soup and nonchocolate, ready-to-eat, nonfat pudding (very specific there) each earned a 1.
There are a few surprises in between. Nonfat cappuccino received a green light from the investigators, great news for the coffee drinkers out there. A serving of sweet potato chips scored better than a simple grilled chicken breast, and a slice of pizza, loaded up with extra meat and a thick crust, is still more nutritious than a bowl of corn flakes.
Neither is good for you, of course, but we’re still going to take this as a sign that pizza is the ideal breakfast food. Add that to your morning coffee, and you’re ready to start the day. Move over Wheaties, there’s a new breakfast of champions.
COVID-19 resisters, please step forward
Some people have all the luck with good genes, both inside and out.
Genetically speaking, humans are 99.9% the same, but that 0.1% is where things get interesting. Because of that 0.1% difference, some people are more likely to contract diseases such as HIV, while others might be more resistant. These small differences in genetic code could be the key to finding treatments for COVID-19.
“The introduction of SARS-CoV-2 to a naive population, on a global scale, has provided yet another demonstration of the remarkable clinical variability between individuals in the course of infection, ranging from asymptomatic infections to life-threatening disease,” the researchers said in Nature Immunology.
The investigators have been scouring the world to find people who might be resistant to SARS-CoV-2 and have enrolled over 400 individuals in a “dedicated resistance study cohort,” according to ScienceAlert.
The investigators are looking at households in which families were infected but one member did not show severe symptoms, or for individuals who have been around the virus multiple times and haven’t contracted it. They are also looking at blood types.
Enrollment is ongoing, so if you’ve been in contact with COVID-19 multiple times and have not gotten sick, scientists would like to hear from you.
Better living through parasitization
How would you like to triple your life span, while maintaining a youthful appearance and gaining special social standing and privileges?
Sounds pretty good, right, so what’s the catch? Well, you have to be infected with a tapeworm ... and you have to be an ant.
If you are an ant, here’s the deal: Workers of the species Temnothorax nylanderi that have tapeworms live much longer than uninfected workers, and while living out those longer lives they do less work and receive gifts of food.
In a study conducted at Johannes Gutenberg University in Mainz, Germany, infected ants’ metabolic rates and lipid levels were similar to those of younger ants, and they appeared to remain in a permanent juvenile stage as a result of the infection, the investigators reported.
They tracked Temnothorax colonies for 3 years, at which point 95% of the uninfected workers had died but over half of the infected ants were still alive. Pretty great, right? Wrong. There was no joy in antville, for the uninfected workers had struck out. “Strained by the additional burden of their wormed-up nestmates, they seemed to be shunting care away from their queen. They were dying sooner than they might have if the colonies had remained parasite-free,” according to an article in the Atlantic.
Does this situation seem just a wee bit familiar? A small group lives longer, healthier lives and enjoys special privileges while the majority of that society works harder to support them? We’ll put it into the form of a chicken-and-egg argument: Which came first, the tapeworms or the one-percenters?
Laughing the pandemic stress away
Doomscrolling on social media has become one of the world’s favorite pastimes during the pandemic, but research shows that those memes about COVID-19 might combat the doom and gloom of the outside world.
A study recently published in Psychology of Popular Media showed that viewing memes, specifically those that were COVID-19 related, actually lessened the stress of the pandemic.
The researchers conducted a survey of 748 people aged 18-88 years. Each participant viewed three memes with text or three memes with text but no images. All three memes had similar cuteness levels (baby or adult), subject (animal or human), and caption (COVID-19–related or not). The participants were then asked to report on their stress levels and feelings before and after the memes.
The people who looked at memes felt less stressed and a higher humor level, especially the participants who received the COVID-19 memes. Study Finds said that they had more “pandemic-coping confidence” than those who got regular memes.
“While the World Health Organization recommended that people avoid too much COVID-related media for the benefit of their mental health, our research reveals that memes about COVID-19 could help people feel more confident in their ability to deal with the pandemic,” lead author Jessica Gall Myrick, PhD, said in a written statement. “The positive emotions associated with this type of content may make people feel psychologically safer and therefore better able to pay attention to the underlying messages related to health threats.”
So if you think you’ve been wasting time looking at memes during this pandemic, think again. It actually might keep you sane. Keep on scrolling!
Giving the gift of stress reduction
It’s a big week here at LOTME. You’ve just read our 100th edition, and to help celebrate that milestone – along with Count Your Buttons Day, Celebration of the Mind Day, and the International Day of the Nacho – we’re presenting an extra-special bonus feature, courtesy of Sad and Useless: The most depressive humor site on the Internet.
We hope you’ll stop your doomscrolling long enough to enjoy this stress-reducing meme. Thanks for reading!
The new breakfast of champions
We love a good ranking system here at LOTME world headquarters, especially the food-based ones. Luckily for us (and our readers), a new study published in Nature Food offers a food-based ranking system.
Sadly, unlike the last food-related ranking we covered, the Food Compass doesn’t tell you how much life you gain or lose from each food you eat down to the precise minute. Instead, it favors a more simple rating system from 1 to 100, with healthier foods scoring higher, and even incorporates mixed foods, not just single ingredients. This makes it better at assessing and comparing food combinations, rather than trying to mix and match the many ingredients that go into even relatively simple recipes.
The top and bottom of the rankings contain the usual suspects. Legumes and nuts, at 78.6, had the highest average score among the broad food groups, followed by fruits and then vegetables. Rounding out the bottom were sweets and savory snacks at 16.4. Among the individual foods, there were perfect scores in both directions: 100 for raw raspberries, while instant noodle soup and nonchocolate, ready-to-eat, nonfat pudding (very specific there) each earned a 1.
There are a few surprises in between. Nonfat cappuccino received a green light from the investigators, great news for the coffee drinkers out there. A serving of sweet potato chips scored better than a simple grilled chicken breast, and a slice of pizza, loaded up with extra meat and a thick crust, is still more nutritious than a bowl of corn flakes.
Neither is good for you, of course, but we’re still going to take this as a sign that pizza is the ideal breakfast food. Add that to your morning coffee, and you’re ready to start the day. Move over Wheaties, there’s a new breakfast of champions.
COVID-19 resisters, please step forward
Some people have all the luck with good genes, both inside and out.
Genetically speaking, humans are 99.9% the same, but that 0.1% is where things get interesting. Because of that 0.1% difference, some people are more likely to contract diseases such as HIV, while others might be more resistant. These small differences in genetic code could be the key to finding treatments for COVID-19.
“The introduction of SARS-CoV-2 to a naive population, on a global scale, has provided yet another demonstration of the remarkable clinical variability between individuals in the course of infection, ranging from asymptomatic infections to life-threatening disease,” the researchers said in Nature Immunology.
The investigators have been scouring the world to find people who might be resistant to SARS-CoV-2 and have enrolled over 400 individuals in a “dedicated resistance study cohort,” according to ScienceAlert.
The investigators are looking at households in which families were infected but one member did not show severe symptoms, or for individuals who have been around the virus multiple times and haven’t contracted it. They are also looking at blood types.
Enrollment is ongoing, so if you’ve been in contact with COVID-19 multiple times and have not gotten sick, scientists would like to hear from you.
Better living through parasitization
How would you like to triple your life span, while maintaining a youthful appearance and gaining special social standing and privileges?
Sounds pretty good, right, so what’s the catch? Well, you have to be infected with a tapeworm ... and you have to be an ant.
If you are an ant, here’s the deal: Workers of the species Temnothorax nylanderi that have tapeworms live much longer than uninfected workers, and while living out those longer lives they do less work and receive gifts of food.
In a study conducted at Johannes Gutenberg University in Mainz, Germany, infected ants’ metabolic rates and lipid levels were similar to those of younger ants, and they appeared to remain in a permanent juvenile stage as a result of the infection, the investigators reported.
They tracked Temnothorax colonies for 3 years, at which point 95% of the uninfected workers had died but over half of the infected ants were still alive. Pretty great, right? Wrong. There was no joy in antville, for the uninfected workers had struck out. “Strained by the additional burden of their wormed-up nestmates, they seemed to be shunting care away from their queen. They were dying sooner than they might have if the colonies had remained parasite-free,” according to an article in the Atlantic.
Does this situation seem just a wee bit familiar? A small group lives longer, healthier lives and enjoys special privileges while the majority of that society works harder to support them? We’ll put it into the form of a chicken-and-egg argument: Which came first, the tapeworms or the one-percenters?
Laughing the pandemic stress away
Doomscrolling on social media has become one of the world’s favorite pastimes during the pandemic, but research shows that those memes about COVID-19 might combat the doom and gloom of the outside world.
A study recently published in Psychology of Popular Media showed that viewing memes, specifically those that were COVID-19 related, actually lessened the stress of the pandemic.
The researchers conducted a survey of 748 people aged 18-88 years. Each participant viewed three memes with text or three memes with text but no images. All three memes had similar cuteness levels (baby or adult), subject (animal or human), and caption (COVID-19–related or not). The participants were then asked to report on their stress levels and feelings before and after the memes.
The people who looked at memes felt less stressed and a higher humor level, especially the participants who received the COVID-19 memes. Study Finds said that they had more “pandemic-coping confidence” than those who got regular memes.
“While the World Health Organization recommended that people avoid too much COVID-related media for the benefit of their mental health, our research reveals that memes about COVID-19 could help people feel more confident in their ability to deal with the pandemic,” lead author Jessica Gall Myrick, PhD, said in a written statement. “The positive emotions associated with this type of content may make people feel psychologically safer and therefore better able to pay attention to the underlying messages related to health threats.”
So if you think you’ve been wasting time looking at memes during this pandemic, think again. It actually might keep you sane. Keep on scrolling!
Giving the gift of stress reduction
It’s a big week here at LOTME. You’ve just read our 100th edition, and to help celebrate that milestone – along with Count Your Buttons Day, Celebration of the Mind Day, and the International Day of the Nacho – we’re presenting an extra-special bonus feature, courtesy of Sad and Useless: The most depressive humor site on the Internet.
We hope you’ll stop your doomscrolling long enough to enjoy this stress-reducing meme. Thanks for reading!
Racial disparities found in treatment of tubal pregnancies
Black and Latina women are more likely to have an open surgery compared with a minimally invasive procedure to treat ectopic pregnancy, according to research presented at the American Society for Reproductive Medicine’s 2021 meeting.
The researchers found that Black and Latina women had 50% lesser odds of undergoing laparoscopic surgery, a minimally invasive procedure, compared to their White peers.
“We see these disparities in minority populations, [especially in] women with regard to so many other aspects of [gynecologic] surgery,” study author Alexandra Huttler, MD, said in an interview. “The fact that these disparities exist [in the treatment of tubal pregnancies] was unfortunately not surprising to us.”
Dr. Huttler and her team analyzed data from the American College of Surgeons’ National Surgical Quality Improvement Program, which followed more than 9,000 patients who had undergone surgical management of a tubal ectopic pregnancy between 2010 and 2019. Of the group, 85% underwent laparoscopic surgery while 14% had open surgery, which requires a longer recovery time.
The proportion of cases performed laparoscopically increased from 81% in 2010 to 91% in 2019. However, a disproportionate number of Black and Latina women underwent open surgery to treat ectopic pregnancies during this time. Because they are more invasive, open surgeries are associated with longer operative times, hospital stays, and increased complications, Dr. Huttler said. They are typically associated with more pain and patients are more likely to be admitted to the hospital for postoperative care.
On the other hand, minimally invasive surgeries are associated with decreased operative time, “less recovery and less pain,” Dr. Huttler explained.
The researchers also looked at trends of the related surgical procedure salpingectomy, which is surgical removal of one or both fallopian tubes versus salpingostomy, a surgical unblocking of the tube. Of the group, 91% underwent salpingectomy and 9% underwent salpingostomy.
Researchers found that Black and Latina women had 78% and 54% greater odds, respectively, of receiving a salpingectomy. However, the clinical significance of these findings are unclear because there are “many factors” that are patient and case specific, Dr. Huttler said.
The study is important and adds to a litany of studies that have shown that women of color do not receive optimal care, said Ruben Alvero, MD, who was not involved in the study.
“Women of color in general have seen compromises in their care at many levels in the system,” Dr. Alvero, professor of obstetrics and gynecology at Stanford (Calif.) University, said in an interview. “We really have to do a massive overhaul of how we treat women of color so they get the same level of treatment that all other populations receive.”
While the factors contributing to these health disparities can be complicated, Dr. Alvero said that one reason for this multivariate discrepancy could be that Black and Latina women tend to seek care at, or only have access to, underresourced hospitals.
Dr. Huttler said she hopes her findings prompt further discussion of these disparities.
“There really are disparities at all levels of care here and figuring out what the root of this is certainly requires further research,” Dr. Huttler said.
The experts interviewed disclosed no conflicts on interests.
Black and Latina women are more likely to have an open surgery compared with a minimally invasive procedure to treat ectopic pregnancy, according to research presented at the American Society for Reproductive Medicine’s 2021 meeting.
The researchers found that Black and Latina women had 50% lesser odds of undergoing laparoscopic surgery, a minimally invasive procedure, compared to their White peers.
“We see these disparities in minority populations, [especially in] women with regard to so many other aspects of [gynecologic] surgery,” study author Alexandra Huttler, MD, said in an interview. “The fact that these disparities exist [in the treatment of tubal pregnancies] was unfortunately not surprising to us.”
Dr. Huttler and her team analyzed data from the American College of Surgeons’ National Surgical Quality Improvement Program, which followed more than 9,000 patients who had undergone surgical management of a tubal ectopic pregnancy between 2010 and 2019. Of the group, 85% underwent laparoscopic surgery while 14% had open surgery, which requires a longer recovery time.
The proportion of cases performed laparoscopically increased from 81% in 2010 to 91% in 2019. However, a disproportionate number of Black and Latina women underwent open surgery to treat ectopic pregnancies during this time. Because they are more invasive, open surgeries are associated with longer operative times, hospital stays, and increased complications, Dr. Huttler said. They are typically associated with more pain and patients are more likely to be admitted to the hospital for postoperative care.
On the other hand, minimally invasive surgeries are associated with decreased operative time, “less recovery and less pain,” Dr. Huttler explained.
The researchers also looked at trends of the related surgical procedure salpingectomy, which is surgical removal of one or both fallopian tubes versus salpingostomy, a surgical unblocking of the tube. Of the group, 91% underwent salpingectomy and 9% underwent salpingostomy.
Researchers found that Black and Latina women had 78% and 54% greater odds, respectively, of receiving a salpingectomy. However, the clinical significance of these findings are unclear because there are “many factors” that are patient and case specific, Dr. Huttler said.
The study is important and adds to a litany of studies that have shown that women of color do not receive optimal care, said Ruben Alvero, MD, who was not involved in the study.
“Women of color in general have seen compromises in their care at many levels in the system,” Dr. Alvero, professor of obstetrics and gynecology at Stanford (Calif.) University, said in an interview. “We really have to do a massive overhaul of how we treat women of color so they get the same level of treatment that all other populations receive.”
While the factors contributing to these health disparities can be complicated, Dr. Alvero said that one reason for this multivariate discrepancy could be that Black and Latina women tend to seek care at, or only have access to, underresourced hospitals.
Dr. Huttler said she hopes her findings prompt further discussion of these disparities.
“There really are disparities at all levels of care here and figuring out what the root of this is certainly requires further research,” Dr. Huttler said.
The experts interviewed disclosed no conflicts on interests.
Black and Latina women are more likely to have an open surgery compared with a minimally invasive procedure to treat ectopic pregnancy, according to research presented at the American Society for Reproductive Medicine’s 2021 meeting.
The researchers found that Black and Latina women had 50% lesser odds of undergoing laparoscopic surgery, a minimally invasive procedure, compared to their White peers.
“We see these disparities in minority populations, [especially in] women with regard to so many other aspects of [gynecologic] surgery,” study author Alexandra Huttler, MD, said in an interview. “The fact that these disparities exist [in the treatment of tubal pregnancies] was unfortunately not surprising to us.”
Dr. Huttler and her team analyzed data from the American College of Surgeons’ National Surgical Quality Improvement Program, which followed more than 9,000 patients who had undergone surgical management of a tubal ectopic pregnancy between 2010 and 2019. Of the group, 85% underwent laparoscopic surgery while 14% had open surgery, which requires a longer recovery time.
The proportion of cases performed laparoscopically increased from 81% in 2010 to 91% in 2019. However, a disproportionate number of Black and Latina women underwent open surgery to treat ectopic pregnancies during this time. Because they are more invasive, open surgeries are associated with longer operative times, hospital stays, and increased complications, Dr. Huttler said. They are typically associated with more pain and patients are more likely to be admitted to the hospital for postoperative care.
On the other hand, minimally invasive surgeries are associated with decreased operative time, “less recovery and less pain,” Dr. Huttler explained.
The researchers also looked at trends of the related surgical procedure salpingectomy, which is surgical removal of one or both fallopian tubes versus salpingostomy, a surgical unblocking of the tube. Of the group, 91% underwent salpingectomy and 9% underwent salpingostomy.
Researchers found that Black and Latina women had 78% and 54% greater odds, respectively, of receiving a salpingectomy. However, the clinical significance of these findings are unclear because there are “many factors” that are patient and case specific, Dr. Huttler said.
The study is important and adds to a litany of studies that have shown that women of color do not receive optimal care, said Ruben Alvero, MD, who was not involved in the study.
“Women of color in general have seen compromises in their care at many levels in the system,” Dr. Alvero, professor of obstetrics and gynecology at Stanford (Calif.) University, said in an interview. “We really have to do a massive overhaul of how we treat women of color so they get the same level of treatment that all other populations receive.”
While the factors contributing to these health disparities can be complicated, Dr. Alvero said that one reason for this multivariate discrepancy could be that Black and Latina women tend to seek care at, or only have access to, underresourced hospitals.
Dr. Huttler said she hopes her findings prompt further discussion of these disparities.
“There really are disparities at all levels of care here and figuring out what the root of this is certainly requires further research,” Dr. Huttler said.
The experts interviewed disclosed no conflicts on interests.
FROM ASRM 2021
Painful lumps in the axilla
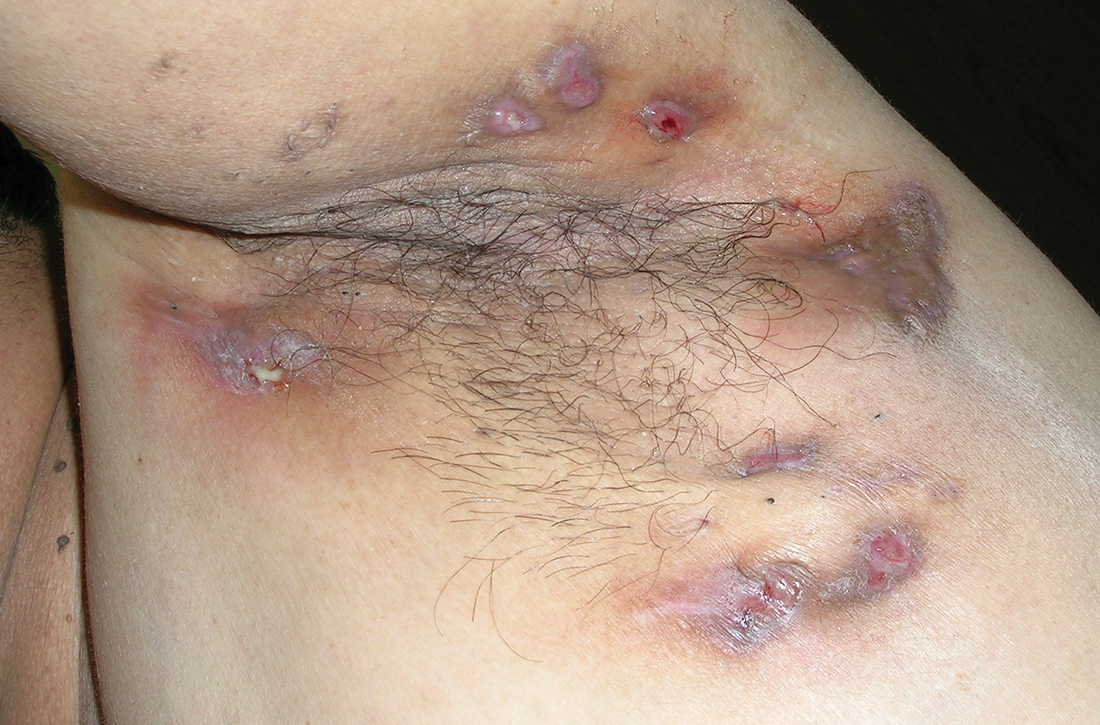
A 30-year-old man presented to the clinic with a complaint of small painful lumps in his armpit. He stated that he initially experienced some itching and discomfort, but after a while he noticed some red, tender, swollen areas. He also mentioned an odorous yellow fluid that would sometimes drain from the lumps. Since first noticing them 2 years earlier, he reported that the nodules had disappeared and reappeared on their own several times.
On physical exam, several small red subcutaneous nodules were present in the axilla and tender to palpation (FIGURE 1A). The patient also had comedonal acne on his back (FIGURE 1B). The patient’s body mass index was 31, and he was a nonsmoker.
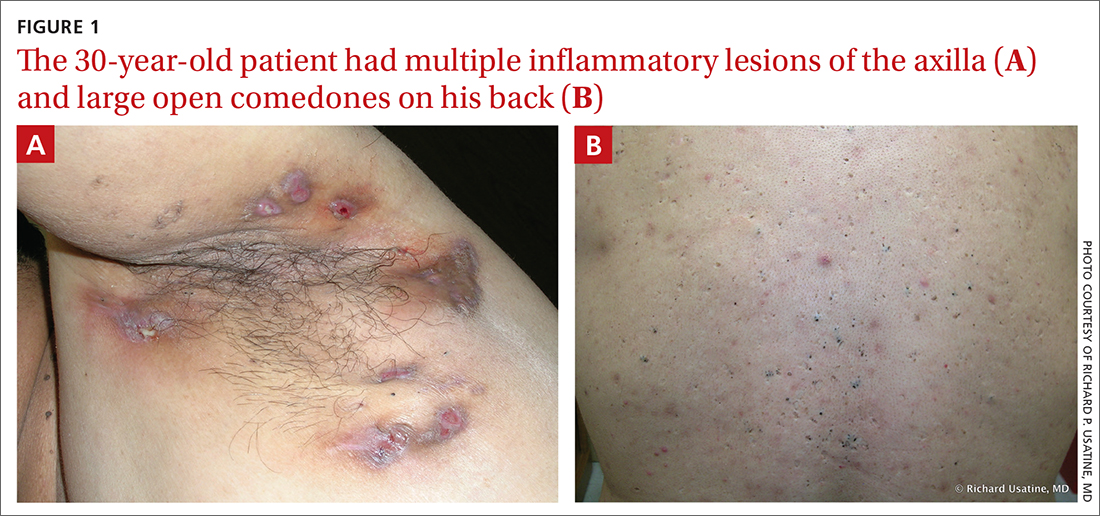
WHAT IS YOUR DIAGNOSIS?
HOW WOULD YOU TREAT THIS PATIENT?
Diagnosis: Hidradenitis suppurativa
The characteristic location and morphology of the lesions, along with the chronicity and odor, were critical in arriving at a diagnosis of hidradenitis suppurativa (HS).
HS is a chronic, inflammatory skin condition that normally manifests in areas of apocrine sweat glands, including the axilla, groin, and perianal, perineal, and inframammary locations.1 It begins when an abnormal hair follicle gets occluded and ruptures, spilling keratin and bacteria into the dermis. An inflammatory response can ensue with surrounding neutrophils and lymphocytes, which leads to abscess formation and destruction of the pilosebaceous unit. Sinus tracts form between the lesions, and a cycle of scarring, fistulas, and contractures can occur.
In this case, the comedones from acne conglobata on the patient’s back indicated a more global follicular occlusion disorder. The characteristic triad is hidradenitis suppurativa, acne conglobata, and dissecting cellulitis of the scalp—of which the patient had 2.
Other potential causes of the pathology include abnormal secretion of apocrine glands, abnormal antimicrobial peptides, deficient numbers of sebaceous glands, and abnormal invaginations of the epidermis.2 Increased levels of tumor necrosis factor alpha and other cytokines have been detected in HS lesions and are a potential target for therapy.
The prevalence of HS in the United States is approximately 0.1%.3 The condition typically begins between the ages of 18 and 39 years. The ratio of women to men affected by the condition is 3:1.2 There is no evident racial or ethnic predilection. There is an association with diabetes and Crohn disease.3 Obesity and smoking are risk factors.1
Continue to: The differential includes an array of common skin conditions
The differential includes an array of common skin conditions
The differential diagnosis in this case included carbuncles, cysts, acne, and abscesses.
A furuncle or carbuncle can result from an infection of hair follicles that can manifest as individual (furuncle) or clusters of (carbuncle) red, painful boils. They form on parts of the skin where hair grows, including the face, neck, armpits, shoulders, and buttocks. They respond well to treatment with antibiotics and incision and drainage. They can be recurrent but usually don’t cluster together in apocrine-rich areas, as seen with HS.
Epidermal inclusion cysts are keratin-filled inclusion cysts with epithelial-lined cyst walls. The cysts are subcutaneous and occasionally more superficial. They can occur almost anywhere but are most often found on the back, scalp, neck, face, and chest. They are usually solitary; however, when there are multiple cysts, they are not linked by sinus tracts as found in HS.
Inflammatory acne lesions tend to form on the face, neck, back, chest, and shoulders, while HS lesions appear most often in apocrine-rich intertriginous areas.
Skin abscesses are local deep infections of the skin caused by bacterial pathogens. The most common agent is Staphylococcus aureus (frequently methicillin resistant). Injection drug use and immunosuppression are risk factors. Although bacteria do not cause HS lesions, bacteria can exacerbate HS through colonization.
Continue to: No lab test needed to diagnosis hidradenitis suppurativa
No lab test needed to diagnose hidradenitis suppurativa
Diagnosis of HS is largely clinical and based on a patient’s history and physical exam findings.2 No specific laboratory test is needed.
Although the patient in this case did have comedonal acne on his back, the lesions that prompted his visit were in an apocrine-rich area, were recurrent, and broke open on their own to release foul-smelling contents—all typical characteristics of HS.
Treatment depends on the severity of the condition
There are 3 stages of HS: Hurley stage I involves abscess formation without tracts or scars. Hurley stage II involves recurrent abscesses with sinus tracts and scarring. Hurley stage III has diffuse involvement with multiple interconnected sinus tracts and abscesses across an entire area.2 Our patient fits into Hurley stage III.
Evidence-based treatment of mild disease (Hurley stage I) includes topical clindamycin 1% solution/gel bid or doxycycline 100 mg bid for widespread disease (Hurley stage II or resistant stage I).2 Chlorhexidine and benzoyl peroxide washes are also often recommended.3 If a patient does not respond to this treatment or the condition is moderate to severe, then clindamycin 300 po bid (with or without rifampin 600/d po) for 10 weeks should be considered.4,5 In a randomized placebo-controlled trial that compared the efficacy of oral clindamycin vs clindamycin plus rifampin in patients with HS, both therapeutic options were statistically equivalent.5 One small, randomized controlled study of patients with mild-to-moderate HS showed that tetracycline 500 mg bid for 3 months resulted in fewer abscesses and nodules but was not superior to topical clindamycin.3
If the patient doesn’t show improvement (Hurley stage III), then adalimumab is an option, as follows: 160 mg subcutaneously at Week 0, 80 mg at Week 2, and then 40 mg weekly, if needed.4 Adalimumab is currently the only FDA-approved treatment for HS. Infliximab by IV infusion can be effective in improving pain, disease severity, and quality of life in patients with moderate-to-severe HS.3 This patient was also a candidate for treatment with systemic retinoids (isotretinoin or acitretin), which could have helped both the HS and the acne conglobata.
Continue to: Intralesional steroid injectiosn with triamcinolone
Intralesional steroid injections with triamcinolone 10 mg/mL can reduce local pain and inflammation rapidly. Pain management is also critical, as HS is painful. First-line therapy includes nonsteroidal anti-inflammatory drugs, acetaminophen, atypical anticonvulsants, and serotonin and norepinephrine reuptake inhibitors.2 Opiate analgesics may be needed for breakthrough pain in patients with severe disease. Avoiding tight clothing, harsh products, and adhesive dressings, as well as using clear petroleum jelly, can prevent skin trauma and help with healing. Weight loss and smoking cessation are also associated with better outcomes.6,7
If medical management fails …
If there is no improvement with medical management, it may be time to consider local procedures such as unroofing/deroofing, punch debridement, skin-tissue-sparing excision with electrosurgical peeling, and laser excision. Incision and drainage may be necessary for acutely inflamed, painful abscesses but should not be routinely performed because lesions can recur.3
Referral to a plastic surgeon is necessary when patients are considering wide excisions of largely affected areas. Even when surgical excisions are performed, medical treatment is needed to prevent new lesions and recurrences.
Our patient was treated initially with oral doxycycline 100 mg bid and intralesional triamcinolone (10 mg/mL) in the most tender lesions. He was also provided with a prescription for ibuprofen 800 mg tid to be taken with meals. The family physician encouraged the patient to lose weight. The patient derived some benefit from treatment but continued to experience new painful lesions.
The physician prescribed oral clindamycin 300 mg bid at a follow-up visit to replace the oral doxycycline. When this failed, the patient was sent for labs to determine if he would be a candidate for adalimumab. When the screening labs were normal, a prescription for adalimumab was provided: 160 mg subcutaneously at Week 0, 80 mg at Week 2, and then 40 mg weekly.4
1. Napolitano M, Megna M, Timoshchuk EA, et al. Hidradenitis suppurativa: from pathogenesis to diagnosis and treatment. Clin Cosmet Investig Dermatol. 2017;10:105-115. doi: 10.2147/CCID.S111019
2. Ballard K, Shuman VL. Hidradenitis Suppurativa. StatPearls Publishing; 2021.
3. Wipperman J, Bragg DA, Litzner B. Hidradenitis suppurativa: rapid evidence review. Am Fam Physician. 2019;100:562-569.
4. Alikhan A, Lymch PJ, Eisen DB. Hidradenitis suppurativa: a comprehensive review. J Am Acad Dermatol. 2009;60:539-561. doi:10.10126/j.jaad.2008.11.911
5. Caro RDC, Cannizzaro MV, Botti E, et al. Clindamycin versus clindamycin plus rifampicin in hidradenitis suppurativa treatment: clinical and ultrasound observations. J Am Acad Dermatol. 2019;80:1314-1321. doi: 10.1016/j.jaad.2018.11.035
6. Hendricks AJ, Hirt PA, Sekhon S, et al. Non-pharmacologic approaches for hidradenitis suppurativa - a systematic review. J Dermatolog Treat. 2021;32:11-18. doi: 10.1080/09546634.2019.1621981
7. Alikhan A, Sayed C, Alavi A, et al. North American clinical management guidelines for hidradenitis suppurativa: a publication from the United States and Canadian Hidradenitis Suppurativa Foundations: part I: diagnosis, evaluation, and the use of complementary and procedural management. J Am Acad Dermatol. 2019;81:76-90. doi: 10.1016/j.jaad.2019.02.067
A 30-year-old man presented to the clinic with a complaint of small painful lumps in his armpit. He stated that he initially experienced some itching and discomfort, but after a while he noticed some red, tender, swollen areas. He also mentioned an odorous yellow fluid that would sometimes drain from the lumps. Since first noticing them 2 years earlier, he reported that the nodules had disappeared and reappeared on their own several times.
On physical exam, several small red subcutaneous nodules were present in the axilla and tender to palpation (FIGURE 1A). The patient also had comedonal acne on his back (FIGURE 1B). The patient’s body mass index was 31, and he was a nonsmoker.

WHAT IS YOUR DIAGNOSIS?
HOW WOULD YOU TREAT THIS PATIENT?
Diagnosis: Hidradenitis suppurativa
The characteristic location and morphology of the lesions, along with the chronicity and odor, were critical in arriving at a diagnosis of hidradenitis suppurativa (HS).
HS is a chronic, inflammatory skin condition that normally manifests in areas of apocrine sweat glands, including the axilla, groin, and perianal, perineal, and inframammary locations.1 It begins when an abnormal hair follicle gets occluded and ruptures, spilling keratin and bacteria into the dermis. An inflammatory response can ensue with surrounding neutrophils and lymphocytes, which leads to abscess formation and destruction of the pilosebaceous unit. Sinus tracts form between the lesions, and a cycle of scarring, fistulas, and contractures can occur.
In this case, the comedones from acne conglobata on the patient’s back indicated a more global follicular occlusion disorder. The characteristic triad is hidradenitis suppurativa, acne conglobata, and dissecting cellulitis of the scalp—of which the patient had 2.
Other potential causes of the pathology include abnormal secretion of apocrine glands, abnormal antimicrobial peptides, deficient numbers of sebaceous glands, and abnormal invaginations of the epidermis.2 Increased levels of tumor necrosis factor alpha and other cytokines have been detected in HS lesions and are a potential target for therapy.
The prevalence of HS in the United States is approximately 0.1%.3 The condition typically begins between the ages of 18 and 39 years. The ratio of women to men affected by the condition is 3:1.2 There is no evident racial or ethnic predilection. There is an association with diabetes and Crohn disease.3 Obesity and smoking are risk factors.1
Continue to: The differential includes an array of common skin conditions
The differential includes an array of common skin conditions
The differential diagnosis in this case included carbuncles, cysts, acne, and abscesses.
A furuncle or carbuncle can result from an infection of hair follicles that can manifest as individual (furuncle) or clusters of (carbuncle) red, painful boils. They form on parts of the skin where hair grows, including the face, neck, armpits, shoulders, and buttocks. They respond well to treatment with antibiotics and incision and drainage. They can be recurrent but usually don’t cluster together in apocrine-rich areas, as seen with HS.
Epidermal inclusion cysts are keratin-filled inclusion cysts with epithelial-lined cyst walls. The cysts are subcutaneous and occasionally more superficial. They can occur almost anywhere but are most often found on the back, scalp, neck, face, and chest. They are usually solitary; however, when there are multiple cysts, they are not linked by sinus tracts as found in HS.
Inflammatory acne lesions tend to form on the face, neck, back, chest, and shoulders, while HS lesions appear most often in apocrine-rich intertriginous areas.
Skin abscesses are local deep infections of the skin caused by bacterial pathogens. The most common agent is Staphylococcus aureus (frequently methicillin resistant). Injection drug use and immunosuppression are risk factors. Although bacteria do not cause HS lesions, bacteria can exacerbate HS through colonization.
Continue to: No lab test needed to diagnosis hidradenitis suppurativa
No lab test needed to diagnose hidradenitis suppurativa
Diagnosis of HS is largely clinical and based on a patient’s history and physical exam findings.2 No specific laboratory test is needed.
Although the patient in this case did have comedonal acne on his back, the lesions that prompted his visit were in an apocrine-rich area, were recurrent, and broke open on their own to release foul-smelling contents—all typical characteristics of HS.
Treatment depends on the severity of the condition
There are 3 stages of HS: Hurley stage I involves abscess formation without tracts or scars. Hurley stage II involves recurrent abscesses with sinus tracts and scarring. Hurley stage III has diffuse involvement with multiple interconnected sinus tracts and abscesses across an entire area.2 Our patient fits into Hurley stage III.
Evidence-based treatment of mild disease (Hurley stage I) includes topical clindamycin 1% solution/gel bid or doxycycline 100 mg bid for widespread disease (Hurley stage II or resistant stage I).2 Chlorhexidine and benzoyl peroxide washes are also often recommended.3 If a patient does not respond to this treatment or the condition is moderate to severe, then clindamycin 300 po bid (with or without rifampin 600/d po) for 10 weeks should be considered.4,5 In a randomized placebo-controlled trial that compared the efficacy of oral clindamycin vs clindamycin plus rifampin in patients with HS, both therapeutic options were statistically equivalent.5 One small, randomized controlled study of patients with mild-to-moderate HS showed that tetracycline 500 mg bid for 3 months resulted in fewer abscesses and nodules but was not superior to topical clindamycin.3
If the patient doesn’t show improvement (Hurley stage III), then adalimumab is an option, as follows: 160 mg subcutaneously at Week 0, 80 mg at Week 2, and then 40 mg weekly, if needed.4 Adalimumab is currently the only FDA-approved treatment for HS. Infliximab by IV infusion can be effective in improving pain, disease severity, and quality of life in patients with moderate-to-severe HS.3 This patient was also a candidate for treatment with systemic retinoids (isotretinoin or acitretin), which could have helped both the HS and the acne conglobata.
Continue to: Intralesional steroid injectiosn with triamcinolone
Intralesional steroid injections with triamcinolone 10 mg/mL can reduce local pain and inflammation rapidly. Pain management is also critical, as HS is painful. First-line therapy includes nonsteroidal anti-inflammatory drugs, acetaminophen, atypical anticonvulsants, and serotonin and norepinephrine reuptake inhibitors.2 Opiate analgesics may be needed for breakthrough pain in patients with severe disease. Avoiding tight clothing, harsh products, and adhesive dressings, as well as using clear petroleum jelly, can prevent skin trauma and help with healing. Weight loss and smoking cessation are also associated with better outcomes.6,7
If medical management fails …
If there is no improvement with medical management, it may be time to consider local procedures such as unroofing/deroofing, punch debridement, skin-tissue-sparing excision with electrosurgical peeling, and laser excision. Incision and drainage may be necessary for acutely inflamed, painful abscesses but should not be routinely performed because lesions can recur.3
Referral to a plastic surgeon is necessary when patients are considering wide excisions of largely affected areas. Even when surgical excisions are performed, medical treatment is needed to prevent new lesions and recurrences.
Our patient was treated initially with oral doxycycline 100 mg bid and intralesional triamcinolone (10 mg/mL) in the most tender lesions. He was also provided with a prescription for ibuprofen 800 mg tid to be taken with meals. The family physician encouraged the patient to lose weight. The patient derived some benefit from treatment but continued to experience new painful lesions.
The physician prescribed oral clindamycin 300 mg bid at a follow-up visit to replace the oral doxycycline. When this failed, the patient was sent for labs to determine if he would be a candidate for adalimumab. When the screening labs were normal, a prescription for adalimumab was provided: 160 mg subcutaneously at Week 0, 80 mg at Week 2, and then 40 mg weekly.4
A 30-year-old man presented to the clinic with a complaint of small painful lumps in his armpit. He stated that he initially experienced some itching and discomfort, but after a while he noticed some red, tender, swollen areas. He also mentioned an odorous yellow fluid that would sometimes drain from the lumps. Since first noticing them 2 years earlier, he reported that the nodules had disappeared and reappeared on their own several times.
On physical exam, several small red subcutaneous nodules were present in the axilla and tender to palpation (FIGURE 1A). The patient also had comedonal acne on his back (FIGURE 1B). The patient’s body mass index was 31, and he was a nonsmoker.

WHAT IS YOUR DIAGNOSIS?
HOW WOULD YOU TREAT THIS PATIENT?
Diagnosis: Hidradenitis suppurativa
The characteristic location and morphology of the lesions, along with the chronicity and odor, were critical in arriving at a diagnosis of hidradenitis suppurativa (HS).
HS is a chronic, inflammatory skin condition that normally manifests in areas of apocrine sweat glands, including the axilla, groin, and perianal, perineal, and inframammary locations.1 It begins when an abnormal hair follicle gets occluded and ruptures, spilling keratin and bacteria into the dermis. An inflammatory response can ensue with surrounding neutrophils and lymphocytes, which leads to abscess formation and destruction of the pilosebaceous unit. Sinus tracts form between the lesions, and a cycle of scarring, fistulas, and contractures can occur.
In this case, the comedones from acne conglobata on the patient’s back indicated a more global follicular occlusion disorder. The characteristic triad is hidradenitis suppurativa, acne conglobata, and dissecting cellulitis of the scalp—of which the patient had 2.
Other potential causes of the pathology include abnormal secretion of apocrine glands, abnormal antimicrobial peptides, deficient numbers of sebaceous glands, and abnormal invaginations of the epidermis.2 Increased levels of tumor necrosis factor alpha and other cytokines have been detected in HS lesions and are a potential target for therapy.
The prevalence of HS in the United States is approximately 0.1%.3 The condition typically begins between the ages of 18 and 39 years. The ratio of women to men affected by the condition is 3:1.2 There is no evident racial or ethnic predilection. There is an association with diabetes and Crohn disease.3 Obesity and smoking are risk factors.1
Continue to: The differential includes an array of common skin conditions
The differential includes an array of common skin conditions
The differential diagnosis in this case included carbuncles, cysts, acne, and abscesses.
A furuncle or carbuncle can result from an infection of hair follicles that can manifest as individual (furuncle) or clusters of (carbuncle) red, painful boils. They form on parts of the skin where hair grows, including the face, neck, armpits, shoulders, and buttocks. They respond well to treatment with antibiotics and incision and drainage. They can be recurrent but usually don’t cluster together in apocrine-rich areas, as seen with HS.
Epidermal inclusion cysts are keratin-filled inclusion cysts with epithelial-lined cyst walls. The cysts are subcutaneous and occasionally more superficial. They can occur almost anywhere but are most often found on the back, scalp, neck, face, and chest. They are usually solitary; however, when there are multiple cysts, they are not linked by sinus tracts as found in HS.
Inflammatory acne lesions tend to form on the face, neck, back, chest, and shoulders, while HS lesions appear most often in apocrine-rich intertriginous areas.
Skin abscesses are local deep infections of the skin caused by bacterial pathogens. The most common agent is Staphylococcus aureus (frequently methicillin resistant). Injection drug use and immunosuppression are risk factors. Although bacteria do not cause HS lesions, bacteria can exacerbate HS through colonization.
Continue to: No lab test needed to diagnosis hidradenitis suppurativa
No lab test needed to diagnose hidradenitis suppurativa
Diagnosis of HS is largely clinical and based on a patient’s history and physical exam findings.2 No specific laboratory test is needed.
Although the patient in this case did have comedonal acne on his back, the lesions that prompted his visit were in an apocrine-rich area, were recurrent, and broke open on their own to release foul-smelling contents—all typical characteristics of HS.
Treatment depends on the severity of the condition
There are 3 stages of HS: Hurley stage I involves abscess formation without tracts or scars. Hurley stage II involves recurrent abscesses with sinus tracts and scarring. Hurley stage III has diffuse involvement with multiple interconnected sinus tracts and abscesses across an entire area.2 Our patient fits into Hurley stage III.
Evidence-based treatment of mild disease (Hurley stage I) includes topical clindamycin 1% solution/gel bid or doxycycline 100 mg bid for widespread disease (Hurley stage II or resistant stage I).2 Chlorhexidine and benzoyl peroxide washes are also often recommended.3 If a patient does not respond to this treatment or the condition is moderate to severe, then clindamycin 300 po bid (with or without rifampin 600/d po) for 10 weeks should be considered.4,5 In a randomized placebo-controlled trial that compared the efficacy of oral clindamycin vs clindamycin plus rifampin in patients with HS, both therapeutic options were statistically equivalent.5 One small, randomized controlled study of patients with mild-to-moderate HS showed that tetracycline 500 mg bid for 3 months resulted in fewer abscesses and nodules but was not superior to topical clindamycin.3
If the patient doesn’t show improvement (Hurley stage III), then adalimumab is an option, as follows: 160 mg subcutaneously at Week 0, 80 mg at Week 2, and then 40 mg weekly, if needed.4 Adalimumab is currently the only FDA-approved treatment for HS. Infliximab by IV infusion can be effective in improving pain, disease severity, and quality of life in patients with moderate-to-severe HS.3 This patient was also a candidate for treatment with systemic retinoids (isotretinoin or acitretin), which could have helped both the HS and the acne conglobata.
Continue to: Intralesional steroid injectiosn with triamcinolone
Intralesional steroid injections with triamcinolone 10 mg/mL can reduce local pain and inflammation rapidly. Pain management is also critical, as HS is painful. First-line therapy includes nonsteroidal anti-inflammatory drugs, acetaminophen, atypical anticonvulsants, and serotonin and norepinephrine reuptake inhibitors.2 Opiate analgesics may be needed for breakthrough pain in patients with severe disease. Avoiding tight clothing, harsh products, and adhesive dressings, as well as using clear petroleum jelly, can prevent skin trauma and help with healing. Weight loss and smoking cessation are also associated with better outcomes.6,7
If medical management fails …
If there is no improvement with medical management, it may be time to consider local procedures such as unroofing/deroofing, punch debridement, skin-tissue-sparing excision with electrosurgical peeling, and laser excision. Incision and drainage may be necessary for acutely inflamed, painful abscesses but should not be routinely performed because lesions can recur.3
Referral to a plastic surgeon is necessary when patients are considering wide excisions of largely affected areas. Even when surgical excisions are performed, medical treatment is needed to prevent new lesions and recurrences.
Our patient was treated initially with oral doxycycline 100 mg bid and intralesional triamcinolone (10 mg/mL) in the most tender lesions. He was also provided with a prescription for ibuprofen 800 mg tid to be taken with meals. The family physician encouraged the patient to lose weight. The patient derived some benefit from treatment but continued to experience new painful lesions.
The physician prescribed oral clindamycin 300 mg bid at a follow-up visit to replace the oral doxycycline. When this failed, the patient was sent for labs to determine if he would be a candidate for adalimumab. When the screening labs were normal, a prescription for adalimumab was provided: 160 mg subcutaneously at Week 0, 80 mg at Week 2, and then 40 mg weekly.4
1. Napolitano M, Megna M, Timoshchuk EA, et al. Hidradenitis suppurativa: from pathogenesis to diagnosis and treatment. Clin Cosmet Investig Dermatol. 2017;10:105-115. doi: 10.2147/CCID.S111019
2. Ballard K, Shuman VL. Hidradenitis Suppurativa. StatPearls Publishing; 2021.
3. Wipperman J, Bragg DA, Litzner B. Hidradenitis suppurativa: rapid evidence review. Am Fam Physician. 2019;100:562-569.
4. Alikhan A, Lymch PJ, Eisen DB. Hidradenitis suppurativa: a comprehensive review. J Am Acad Dermatol. 2009;60:539-561. doi:10.10126/j.jaad.2008.11.911
5. Caro RDC, Cannizzaro MV, Botti E, et al. Clindamycin versus clindamycin plus rifampicin in hidradenitis suppurativa treatment: clinical and ultrasound observations. J Am Acad Dermatol. 2019;80:1314-1321. doi: 10.1016/j.jaad.2018.11.035
6. Hendricks AJ, Hirt PA, Sekhon S, et al. Non-pharmacologic approaches for hidradenitis suppurativa - a systematic review. J Dermatolog Treat. 2021;32:11-18. doi: 10.1080/09546634.2019.1621981
7. Alikhan A, Sayed C, Alavi A, et al. North American clinical management guidelines for hidradenitis suppurativa: a publication from the United States and Canadian Hidradenitis Suppurativa Foundations: part I: diagnosis, evaluation, and the use of complementary and procedural management. J Am Acad Dermatol. 2019;81:76-90. doi: 10.1016/j.jaad.2019.02.067
1. Napolitano M, Megna M, Timoshchuk EA, et al. Hidradenitis suppurativa: from pathogenesis to diagnosis and treatment. Clin Cosmet Investig Dermatol. 2017;10:105-115. doi: 10.2147/CCID.S111019
2. Ballard K, Shuman VL. Hidradenitis Suppurativa. StatPearls Publishing; 2021.
3. Wipperman J, Bragg DA, Litzner B. Hidradenitis suppurativa: rapid evidence review. Am Fam Physician. 2019;100:562-569.
4. Alikhan A, Lymch PJ, Eisen DB. Hidradenitis suppurativa: a comprehensive review. J Am Acad Dermatol. 2009;60:539-561. doi:10.10126/j.jaad.2008.11.911
5. Caro RDC, Cannizzaro MV, Botti E, et al. Clindamycin versus clindamycin plus rifampicin in hidradenitis suppurativa treatment: clinical and ultrasound observations. J Am Acad Dermatol. 2019;80:1314-1321. doi: 10.1016/j.jaad.2018.11.035
6. Hendricks AJ, Hirt PA, Sekhon S, et al. Non-pharmacologic approaches for hidradenitis suppurativa - a systematic review. J Dermatolog Treat. 2021;32:11-18. doi: 10.1080/09546634.2019.1621981
7. Alikhan A, Sayed C, Alavi A, et al. North American clinical management guidelines for hidradenitis suppurativa: a publication from the United States and Canadian Hidradenitis Suppurativa Foundations: part I: diagnosis, evaluation, and the use of complementary and procedural management. J Am Acad Dermatol. 2019;81:76-90. doi: 10.1016/j.jaad.2019.02.067
FDA approves combo pill for severe, acute pain
enough to require an opioid analgesic and for which alternative treatments fail to provide adequate pain relief.
Celecoxib is a nonsteroidal anti-inflammatory drug and tramadol is an opioid agonist. Seglentis contains 56 mg of celecoxib and 44 mg of tramadol.
“The unique co-crystal formulation of Seglentis provides effective pain relief via a multimodal approach,” Craig A. Sponseller, MD, chief medical officer of Kowa Pharmaceuticals America, said in a news release.
Esteve Pharmaceuticals has entered into an agreement with Kowa Pharmaceuticals America to commercialize the pain medicine in the United States, with a launch planned for early 2022.
“Seglentis uses four different and complementary mechanisms of analgesia and offers healthcare providers an important option to treat acute pain in adults that is severe enough to require opioid treatment and for which alternative treatments are inadequate,” Dr. Sponseller said.
Because of the risks of addiction, abuse, and misuse with opioids, even at recommended doses, the FDA will require a Risk Evaluation and Mitigation Strategy (REMS) for Seglentis.
The label states that the drug should be initiated as two tablets every 12 hours as needed and should be prescribed for the shortest duration consistent with individual patient treatment goals.
Patients should be monitored for respiratory depression, especially within the first 24 to 72 hours of initiating therapy with Seglentis.
Prescribers should discuss naloxone (Narcan) with patients and consider prescribing the opioid antagonist naloxone based on the patient’s risk factors for overdose.
Full prescribing information is available online.
A version of this article was first published on Medscape.com.
enough to require an opioid analgesic and for which alternative treatments fail to provide adequate pain relief.
Celecoxib is a nonsteroidal anti-inflammatory drug and tramadol is an opioid agonist. Seglentis contains 56 mg of celecoxib and 44 mg of tramadol.
“The unique co-crystal formulation of Seglentis provides effective pain relief via a multimodal approach,” Craig A. Sponseller, MD, chief medical officer of Kowa Pharmaceuticals America, said in a news release.
Esteve Pharmaceuticals has entered into an agreement with Kowa Pharmaceuticals America to commercialize the pain medicine in the United States, with a launch planned for early 2022.
“Seglentis uses four different and complementary mechanisms of analgesia and offers healthcare providers an important option to treat acute pain in adults that is severe enough to require opioid treatment and for which alternative treatments are inadequate,” Dr. Sponseller said.
Because of the risks of addiction, abuse, and misuse with opioids, even at recommended doses, the FDA will require a Risk Evaluation and Mitigation Strategy (REMS) for Seglentis.
The label states that the drug should be initiated as two tablets every 12 hours as needed and should be prescribed for the shortest duration consistent with individual patient treatment goals.
Patients should be monitored for respiratory depression, especially within the first 24 to 72 hours of initiating therapy with Seglentis.
Prescribers should discuss naloxone (Narcan) with patients and consider prescribing the opioid antagonist naloxone based on the patient’s risk factors for overdose.
Full prescribing information is available online.
A version of this article was first published on Medscape.com.
enough to require an opioid analgesic and for which alternative treatments fail to provide adequate pain relief.
Celecoxib is a nonsteroidal anti-inflammatory drug and tramadol is an opioid agonist. Seglentis contains 56 mg of celecoxib and 44 mg of tramadol.
“The unique co-crystal formulation of Seglentis provides effective pain relief via a multimodal approach,” Craig A. Sponseller, MD, chief medical officer of Kowa Pharmaceuticals America, said in a news release.
Esteve Pharmaceuticals has entered into an agreement with Kowa Pharmaceuticals America to commercialize the pain medicine in the United States, with a launch planned for early 2022.
“Seglentis uses four different and complementary mechanisms of analgesia and offers healthcare providers an important option to treat acute pain in adults that is severe enough to require opioid treatment and for which alternative treatments are inadequate,” Dr. Sponseller said.
Because of the risks of addiction, abuse, and misuse with opioids, even at recommended doses, the FDA will require a Risk Evaluation and Mitigation Strategy (REMS) for Seglentis.
The label states that the drug should be initiated as two tablets every 12 hours as needed and should be prescribed for the shortest duration consistent with individual patient treatment goals.
Patients should be monitored for respiratory depression, especially within the first 24 to 72 hours of initiating therapy with Seglentis.
Prescribers should discuss naloxone (Narcan) with patients and consider prescribing the opioid antagonist naloxone based on the patient’s risk factors for overdose.
Full prescribing information is available online.
A version of this article was first published on Medscape.com.
5 years out, sleeve safer than gastric bypass
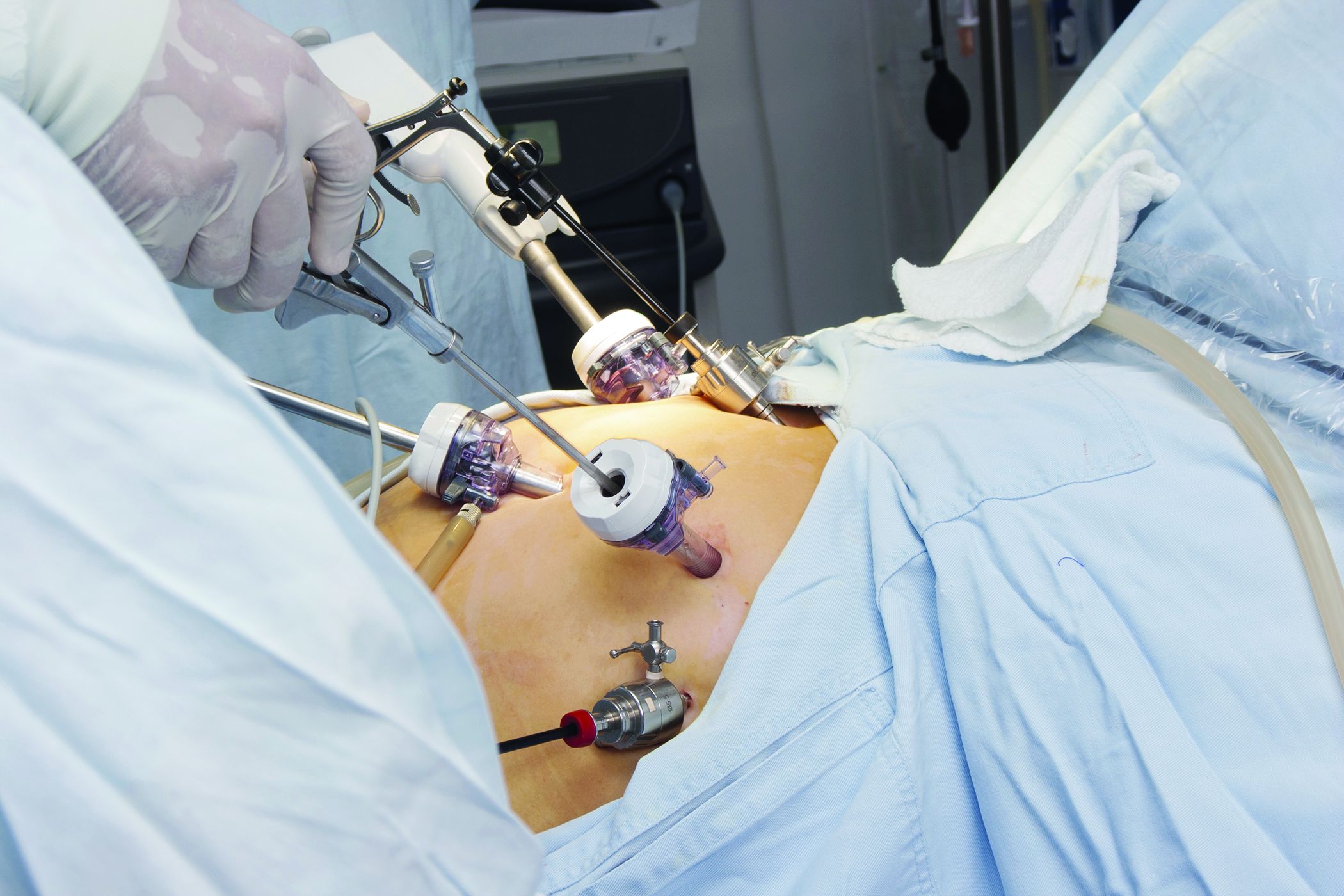
Five years out, sleeve gastrectomy had a lower risk of mortality, complications, and reinterventions than gastric bypass, but there was a higher risk of surgical revision, including conversion to another bariatric surgery, gastrectomy, or anastomotic revision, according to a new analysis.
Sleeve gastrectomy has gained rapid popularity, and now represents 60% of all bariatric procedures. It has demonstrated good efficacy and short-term safety, it is easier to perform than laparoscopic Roux-en-Y gastric bypass, and it is a safe option for high-risk patients, authors led by Ryan Howard, MD, of University of Michigan, Ann Arbor, wrote in JAMA Surgery.
Still, there are few comparative data on the long-term efficacy of the two procedures. Randomized, controlled trials have conducted long-term follow-up, but their small size has made it difficult to detect differences in rare outcomes. Observational studies are limited by the potential for bias. A novel approach to limiting bias is instrumental variables analysis, which controls for possible confounding using a factor that impacts treatment choice, but not patient outcome, to control for possible confounders. Studies using this approach confirmed the superior safety profile of sleeve gastrectomy in the short term.
The current study’s authors, used that method to examined 5-year outcomes in a Medicare population, in which obesity and its complications are especially frequent. Partly because of that lack of data, the Medical Evidence Development and Coverage Committee has called for more data in older patients and in patients with disabilities.
The researchers analyzed data from 95,405 Medicare claims between 2012 and 2018, using state-level variation in sleeve gastrectomy as the instrumental variable.
At 5 years, sleeve gastrectomy was associated with a lower cumulative frequency of mortality (4.27%; 95% confidence interval, 4.25%-4.30% vs. 5.67%; 95% CI, 5.63%-5.69%]), complications (22.10%; 95% CI, 22.06%-22.13% vs. 29.03%; 95% CI, 28.99%-29.08%), and reintervention (25.23%; 95% CI, 25.19%-25.27% vs. 33.57%; 95% CI, 33.52%-33.63%). At 5 years, surgical revision was more common in the sleeve gastrectomy group (2.91%; 95% CI, 2.90%-2.93% vs. 1.46%; 95% CI, 1.45%-1.47%).
The sleeve gastrectomy group had lower odds of all-cause hospitalization at 1 year (adjusted hazard ratio, 0.83; 95% CI, 0.80-0.86) and 3 years (aHR, 0.94; 95% CI, 0.90-0.98), as well as emergency department use at 1 year (aHR, 0.87; 95% CI, 0.84-0.90) and 3 years (aHR, 0.93; 95% CI, 0.90-0.97). There was no significant difference between the two groups at 5 years with respect to either outcome.
The effort to understand long-term outcomes of these two procedures has been challenging because follow-up is often incomplete, and because reporting isn’t always standardized, according Anita P. Courcoulas, MD, MPH, and Bestoun Ahmed, MD, in an accompanying editorial in JAMA Surgery. They noted that the differences in mortality is a new finding and the difference in surgical revisions confirmed something often seen in clinical practice. “Overall, these novel methods, which creatively balance unmeasured factors, have succeeded in providing important incremental findings about the long-term comparative safety outcomes between bariatric procedures that will be helpful in clinical practice,” the editorial authors wrote.
The complications discussed in the study are also difficult to interpret, according to Ali Aminian, MD, who is a professor of surgery and director of Bariatric and Metabolic Institute at Cleveland Clinic. They may be related to the surgery, or they may be complications that accrue as patients age. “So that doesn’t mean those were surgical complications, but [the findings are] in line with the other literature that [gastric sleeve] may be safer than gastric bypass, but in a different cohort of patients,” said Dr. Aminian, who was asked to comment.
“I thought it validated that which many of us in clinical practice see on a day to day basis,” said Shanu Kothari, MD, chair of surgery at Prisma Health, and the current president of American Society for Bariatric and Metabolic Surgery. He pointed out that the study was limited by its reliance on administrative claims, which makes it impossible to know the reduction in weight and obesity-related comorbid conditions following the procedures, as well as factors driving individual decisions: A surgeon might offer sleeve to a patient at higher risk of complications, but a gastric bypass to someone with more comorbidities. “What we don’t know is how to interpret this 35,000-foot view of Medicare data to that conversation with the patient sitting right in front of you,” said Dr. Kothari.
The authors similarly cited the “lack of clinical granularity in administrative claims data” among study limitations, as well as how the use of instrumental variables may leave the findings less applicable to patients more strongly indicated for one procedure over the other.
“Longer-term randomized clinical trials and observational studies are warranted to confirm these findings,” the study authors concluded. “Understanding the risk profile of various bariatric operations may further help patients and surgeons make the most appropriate decisions regarding plans of care.”
The study was funded by the National Institute of Diabetes and Digestive and Kidney Diseases. Some study authors and editorialists reported funding from various groups and institutions, such as the National Institutes of Health and the VA Ann Arbor Health System. Dr. Kothari and Dr. Aminian have no relevant financial disclosures.
Five years out, sleeve gastrectomy had a lower risk of mortality, complications, and reinterventions than gastric bypass, but there was a higher risk of surgical revision, including conversion to another bariatric surgery, gastrectomy, or anastomotic revision, according to a new analysis.
Sleeve gastrectomy has gained rapid popularity, and now represents 60% of all bariatric procedures. It has demonstrated good efficacy and short-term safety, it is easier to perform than laparoscopic Roux-en-Y gastric bypass, and it is a safe option for high-risk patients, authors led by Ryan Howard, MD, of University of Michigan, Ann Arbor, wrote in JAMA Surgery.
Still, there are few comparative data on the long-term efficacy of the two procedures. Randomized, controlled trials have conducted long-term follow-up, but their small size has made it difficult to detect differences in rare outcomes. Observational studies are limited by the potential for bias. A novel approach to limiting bias is instrumental variables analysis, which controls for possible confounding using a factor that impacts treatment choice, but not patient outcome, to control for possible confounders. Studies using this approach confirmed the superior safety profile of sleeve gastrectomy in the short term.
The current study’s authors, used that method to examined 5-year outcomes in a Medicare population, in which obesity and its complications are especially frequent. Partly because of that lack of data, the Medical Evidence Development and Coverage Committee has called for more data in older patients and in patients with disabilities.
The researchers analyzed data from 95,405 Medicare claims between 2012 and 2018, using state-level variation in sleeve gastrectomy as the instrumental variable.
At 5 years, sleeve gastrectomy was associated with a lower cumulative frequency of mortality (4.27%; 95% confidence interval, 4.25%-4.30% vs. 5.67%; 95% CI, 5.63%-5.69%]), complications (22.10%; 95% CI, 22.06%-22.13% vs. 29.03%; 95% CI, 28.99%-29.08%), and reintervention (25.23%; 95% CI, 25.19%-25.27% vs. 33.57%; 95% CI, 33.52%-33.63%). At 5 years, surgical revision was more common in the sleeve gastrectomy group (2.91%; 95% CI, 2.90%-2.93% vs. 1.46%; 95% CI, 1.45%-1.47%).
The sleeve gastrectomy group had lower odds of all-cause hospitalization at 1 year (adjusted hazard ratio, 0.83; 95% CI, 0.80-0.86) and 3 years (aHR, 0.94; 95% CI, 0.90-0.98), as well as emergency department use at 1 year (aHR, 0.87; 95% CI, 0.84-0.90) and 3 years (aHR, 0.93; 95% CI, 0.90-0.97). There was no significant difference between the two groups at 5 years with respect to either outcome.
The effort to understand long-term outcomes of these two procedures has been challenging because follow-up is often incomplete, and because reporting isn’t always standardized, according Anita P. Courcoulas, MD, MPH, and Bestoun Ahmed, MD, in an accompanying editorial in JAMA Surgery. They noted that the differences in mortality is a new finding and the difference in surgical revisions confirmed something often seen in clinical practice. “Overall, these novel methods, which creatively balance unmeasured factors, have succeeded in providing important incremental findings about the long-term comparative safety outcomes between bariatric procedures that will be helpful in clinical practice,” the editorial authors wrote.
The complications discussed in the study are also difficult to interpret, according to Ali Aminian, MD, who is a professor of surgery and director of Bariatric and Metabolic Institute at Cleveland Clinic. They may be related to the surgery, or they may be complications that accrue as patients age. “So that doesn’t mean those were surgical complications, but [the findings are] in line with the other literature that [gastric sleeve] may be safer than gastric bypass, but in a different cohort of patients,” said Dr. Aminian, who was asked to comment.
“I thought it validated that which many of us in clinical practice see on a day to day basis,” said Shanu Kothari, MD, chair of surgery at Prisma Health, and the current president of American Society for Bariatric and Metabolic Surgery. He pointed out that the study was limited by its reliance on administrative claims, which makes it impossible to know the reduction in weight and obesity-related comorbid conditions following the procedures, as well as factors driving individual decisions: A surgeon might offer sleeve to a patient at higher risk of complications, but a gastric bypass to someone with more comorbidities. “What we don’t know is how to interpret this 35,000-foot view of Medicare data to that conversation with the patient sitting right in front of you,” said Dr. Kothari.
The authors similarly cited the “lack of clinical granularity in administrative claims data” among study limitations, as well as how the use of instrumental variables may leave the findings less applicable to patients more strongly indicated for one procedure over the other.
“Longer-term randomized clinical trials and observational studies are warranted to confirm these findings,” the study authors concluded. “Understanding the risk profile of various bariatric operations may further help patients and surgeons make the most appropriate decisions regarding plans of care.”
The study was funded by the National Institute of Diabetes and Digestive and Kidney Diseases. Some study authors and editorialists reported funding from various groups and institutions, such as the National Institutes of Health and the VA Ann Arbor Health System. Dr. Kothari and Dr. Aminian have no relevant financial disclosures.
Five years out, sleeve gastrectomy had a lower risk of mortality, complications, and reinterventions than gastric bypass, but there was a higher risk of surgical revision, including conversion to another bariatric surgery, gastrectomy, or anastomotic revision, according to a new analysis.
Sleeve gastrectomy has gained rapid popularity, and now represents 60% of all bariatric procedures. It has demonstrated good efficacy and short-term safety, it is easier to perform than laparoscopic Roux-en-Y gastric bypass, and it is a safe option for high-risk patients, authors led by Ryan Howard, MD, of University of Michigan, Ann Arbor, wrote in JAMA Surgery.
Still, there are few comparative data on the long-term efficacy of the two procedures. Randomized, controlled trials have conducted long-term follow-up, but their small size has made it difficult to detect differences in rare outcomes. Observational studies are limited by the potential for bias. A novel approach to limiting bias is instrumental variables analysis, which controls for possible confounding using a factor that impacts treatment choice, but not patient outcome, to control for possible confounders. Studies using this approach confirmed the superior safety profile of sleeve gastrectomy in the short term.
The current study’s authors, used that method to examined 5-year outcomes in a Medicare population, in which obesity and its complications are especially frequent. Partly because of that lack of data, the Medical Evidence Development and Coverage Committee has called for more data in older patients and in patients with disabilities.
The researchers analyzed data from 95,405 Medicare claims between 2012 and 2018, using state-level variation in sleeve gastrectomy as the instrumental variable.
At 5 years, sleeve gastrectomy was associated with a lower cumulative frequency of mortality (4.27%; 95% confidence interval, 4.25%-4.30% vs. 5.67%; 95% CI, 5.63%-5.69%]), complications (22.10%; 95% CI, 22.06%-22.13% vs. 29.03%; 95% CI, 28.99%-29.08%), and reintervention (25.23%; 95% CI, 25.19%-25.27% vs. 33.57%; 95% CI, 33.52%-33.63%). At 5 years, surgical revision was more common in the sleeve gastrectomy group (2.91%; 95% CI, 2.90%-2.93% vs. 1.46%; 95% CI, 1.45%-1.47%).
The sleeve gastrectomy group had lower odds of all-cause hospitalization at 1 year (adjusted hazard ratio, 0.83; 95% CI, 0.80-0.86) and 3 years (aHR, 0.94; 95% CI, 0.90-0.98), as well as emergency department use at 1 year (aHR, 0.87; 95% CI, 0.84-0.90) and 3 years (aHR, 0.93; 95% CI, 0.90-0.97). There was no significant difference between the two groups at 5 years with respect to either outcome.
The effort to understand long-term outcomes of these two procedures has been challenging because follow-up is often incomplete, and because reporting isn’t always standardized, according Anita P. Courcoulas, MD, MPH, and Bestoun Ahmed, MD, in an accompanying editorial in JAMA Surgery. They noted that the differences in mortality is a new finding and the difference in surgical revisions confirmed something often seen in clinical practice. “Overall, these novel methods, which creatively balance unmeasured factors, have succeeded in providing important incremental findings about the long-term comparative safety outcomes between bariatric procedures that will be helpful in clinical practice,” the editorial authors wrote.
The complications discussed in the study are also difficult to interpret, according to Ali Aminian, MD, who is a professor of surgery and director of Bariatric and Metabolic Institute at Cleveland Clinic. They may be related to the surgery, or they may be complications that accrue as patients age. “So that doesn’t mean those were surgical complications, but [the findings are] in line with the other literature that [gastric sleeve] may be safer than gastric bypass, but in a different cohort of patients,” said Dr. Aminian, who was asked to comment.
“I thought it validated that which many of us in clinical practice see on a day to day basis,” said Shanu Kothari, MD, chair of surgery at Prisma Health, and the current president of American Society for Bariatric and Metabolic Surgery. He pointed out that the study was limited by its reliance on administrative claims, which makes it impossible to know the reduction in weight and obesity-related comorbid conditions following the procedures, as well as factors driving individual decisions: A surgeon might offer sleeve to a patient at higher risk of complications, but a gastric bypass to someone with more comorbidities. “What we don’t know is how to interpret this 35,000-foot view of Medicare data to that conversation with the patient sitting right in front of you,” said Dr. Kothari.
The authors similarly cited the “lack of clinical granularity in administrative claims data” among study limitations, as well as how the use of instrumental variables may leave the findings less applicable to patients more strongly indicated for one procedure over the other.
“Longer-term randomized clinical trials and observational studies are warranted to confirm these findings,” the study authors concluded. “Understanding the risk profile of various bariatric operations may further help patients and surgeons make the most appropriate decisions regarding plans of care.”
The study was funded by the National Institute of Diabetes and Digestive and Kidney Diseases. Some study authors and editorialists reported funding from various groups and institutions, such as the National Institutes of Health and the VA Ann Arbor Health System. Dr. Kothari and Dr. Aminian have no relevant financial disclosures.
FROM JAMA SURGERY
No advantages to using ADM in implant-based breast reconstruction
A European study involving 155 women found that the use of acellular dermal matrix (ADM) did not lead to fewer reoperations, nor was it superior in terms of health-related quality of life or patient-reported cosmetic outcomes.
“We feel that women considering implant-based reconstructions for breast cancer should be informed about the lack of evidence supporting its advantage,” said lead author Fredrik Lohmander MD, department of breast and endocrine surgery, section of breast urgery, Karolinska University Hospital, Stockholm.
It is difficult to say generally whether ADM should be used in IBBR, he noted. “We can only conclude from our trial that there is no hard evidence that ADM is beneficial when performing breast reconstructions with implants,” he said in an interview. “In selected patients, ADM might be indicated.”
The study was conducted in Sweden and the United Kingdom. “Mostly because of high costs, ADM in implant-based breast reconstructions in Sweden is not frequently used,” Dr. Lohmander said. “It is slightly more common in the U.K., but much more common in the U.S.A.”
Although biological meshes have received regulatory approval by the U.S. Food and Drug Administration for reconstructive purposes, ADM has not been approved for use in breast reconstruction surgery, and its use in this setting is off label.
The study was published online October 1 in JAMA Network Open.
Any advantage to using mesh device?
Previous studies of ADMs suggested that the mesh device conferred several benefits, including superior cosmetic results, less need for tissue expanders, fewer elective reoperations, and less capsular contracture. The use of a mesh device also enlarges the subpectoral pocket, which allows for larger fixed-volume implants, the authors note.
However, these suggested advantages have not been universally accepted, and the authors note that there have been reports of associated harm, such as higher rates of infection and implant loss.
The new study included 135 women from five centers in Sweden and the United Kingdom. The patients had breast cancer and had planned to undergo mastectomy and immediate IBBR between 2014 and May 2017.
The primary endpoint was the number of repeat surgeries at 2 years.
At the 2-year follow-up, 31 patients (48%) in the ADM group had undergone at least one reoperation on the ipsilateral side, vs 35 (54%) in the control group (P = .54). Results were similar for the contralateral side: 34 (53%) vs 31 (48%).
Two patients in the ADM group and three patients in the control group underwent a risk-reducing mastectomy on the contralateral side. These five surgeries were included in the final analysis.
For nine patients (14%) in the ADM arm, the implant was removed. Four of the removals took place within 6 months after early surgical complications. In the control group, seven patients (11%) underwent implant removal; four were removed within 6 months, owing to early surgical complications.
The secondary endpoint was postoperative health-related quality of life, including perception of body image and satisfaction with cosmetic outcome. There were no significant differences between the two groups.
Some questions remain
Approached for comment on the study, Sameer A. Patel, MD, FACS, chief of plastic and reconstructive surgery at Fox Chase Cancer Center, Philadelphia, noted that the practice of using AMD for breast reconstruction is quite common in the United States, so these data are informative and add to the current understanding of the value of ADM in breast reconstruction. “The study hypothesized that the use of ADM would reduce the number of reoperations within the first 24 months, which it did not,” he said. “This is despite the fact that the ADM group had a significantly higher number of direct-to-implant reconstructions.”
Importantly, the study showed that patient-reported outcomes, as opposed to surgeon’s evaluation of outcomes, were also not different for the most part between the two groups, Dr. Patel pointed out. “The only exception of small favorable advantage in the ADM group was for fitting bras,” he said.
However, there were limitations to the study’s endpoint. “I would add that there are some purported advantages of using ADM, such as reduction in postoperative pain and reduction in length of hospital stay, which are not evaluated by this study,” Patel explained. “Also, I am not certain that they can conclude from this study that capsular contracture is not reduced, because it is not designed to evaluate that.”
But the biggest limitation is one that study authors point out in their discussion at the end of the article, he added. “The use of prepectoral reconstruction is rapidly replacing the dual plane reconstruction that this paper used in the ADM group,” Dr. Patel said. “The role of ADM in prepectoral reconstruction is somewhat different than in the dual plane reconstruction, and so these results may not necessarily be extrapolated to prepectoral reconstruction.”
The study was funded with grants from the Swedish Breast Cancer Association and Stockholm City Council. The trial was initiated by Karolinska University Hospital and Karolinska Institutet. Acelity (an Allergan company) supplied the study with acellular dermal matrix meshes. Dr. Lohmander and Dr. Patel have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
A European study involving 155 women found that the use of acellular dermal matrix (ADM) did not lead to fewer reoperations, nor was it superior in terms of health-related quality of life or patient-reported cosmetic outcomes.
“We feel that women considering implant-based reconstructions for breast cancer should be informed about the lack of evidence supporting its advantage,” said lead author Fredrik Lohmander MD, department of breast and endocrine surgery, section of breast urgery, Karolinska University Hospital, Stockholm.
It is difficult to say generally whether ADM should be used in IBBR, he noted. “We can only conclude from our trial that there is no hard evidence that ADM is beneficial when performing breast reconstructions with implants,” he said in an interview. “In selected patients, ADM might be indicated.”
The study was conducted in Sweden and the United Kingdom. “Mostly because of high costs, ADM in implant-based breast reconstructions in Sweden is not frequently used,” Dr. Lohmander said. “It is slightly more common in the U.K., but much more common in the U.S.A.”
Although biological meshes have received regulatory approval by the U.S. Food and Drug Administration for reconstructive purposes, ADM has not been approved for use in breast reconstruction surgery, and its use in this setting is off label.
The study was published online October 1 in JAMA Network Open.
Any advantage to using mesh device?
Previous studies of ADMs suggested that the mesh device conferred several benefits, including superior cosmetic results, less need for tissue expanders, fewer elective reoperations, and less capsular contracture. The use of a mesh device also enlarges the subpectoral pocket, which allows for larger fixed-volume implants, the authors note.
However, these suggested advantages have not been universally accepted, and the authors note that there have been reports of associated harm, such as higher rates of infection and implant loss.
The new study included 135 women from five centers in Sweden and the United Kingdom. The patients had breast cancer and had planned to undergo mastectomy and immediate IBBR between 2014 and May 2017.
The primary endpoint was the number of repeat surgeries at 2 years.
At the 2-year follow-up, 31 patients (48%) in the ADM group had undergone at least one reoperation on the ipsilateral side, vs 35 (54%) in the control group (P = .54). Results were similar for the contralateral side: 34 (53%) vs 31 (48%).
Two patients in the ADM group and three patients in the control group underwent a risk-reducing mastectomy on the contralateral side. These five surgeries were included in the final analysis.
For nine patients (14%) in the ADM arm, the implant was removed. Four of the removals took place within 6 months after early surgical complications. In the control group, seven patients (11%) underwent implant removal; four were removed within 6 months, owing to early surgical complications.
The secondary endpoint was postoperative health-related quality of life, including perception of body image and satisfaction with cosmetic outcome. There were no significant differences between the two groups.
Some questions remain
Approached for comment on the study, Sameer A. Patel, MD, FACS, chief of plastic and reconstructive surgery at Fox Chase Cancer Center, Philadelphia, noted that the practice of using AMD for breast reconstruction is quite common in the United States, so these data are informative and add to the current understanding of the value of ADM in breast reconstruction. “The study hypothesized that the use of ADM would reduce the number of reoperations within the first 24 months, which it did not,” he said. “This is despite the fact that the ADM group had a significantly higher number of direct-to-implant reconstructions.”
Importantly, the study showed that patient-reported outcomes, as opposed to surgeon’s evaluation of outcomes, were also not different for the most part between the two groups, Dr. Patel pointed out. “The only exception of small favorable advantage in the ADM group was for fitting bras,” he said.
However, there were limitations to the study’s endpoint. “I would add that there are some purported advantages of using ADM, such as reduction in postoperative pain and reduction in length of hospital stay, which are not evaluated by this study,” Patel explained. “Also, I am not certain that they can conclude from this study that capsular contracture is not reduced, because it is not designed to evaluate that.”
But the biggest limitation is one that study authors point out in their discussion at the end of the article, he added. “The use of prepectoral reconstruction is rapidly replacing the dual plane reconstruction that this paper used in the ADM group,” Dr. Patel said. “The role of ADM in prepectoral reconstruction is somewhat different than in the dual plane reconstruction, and so these results may not necessarily be extrapolated to prepectoral reconstruction.”
The study was funded with grants from the Swedish Breast Cancer Association and Stockholm City Council. The trial was initiated by Karolinska University Hospital and Karolinska Institutet. Acelity (an Allergan company) supplied the study with acellular dermal matrix meshes. Dr. Lohmander and Dr. Patel have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
A European study involving 155 women found that the use of acellular dermal matrix (ADM) did not lead to fewer reoperations, nor was it superior in terms of health-related quality of life or patient-reported cosmetic outcomes.
“We feel that women considering implant-based reconstructions for breast cancer should be informed about the lack of evidence supporting its advantage,” said lead author Fredrik Lohmander MD, department of breast and endocrine surgery, section of breast urgery, Karolinska University Hospital, Stockholm.
It is difficult to say generally whether ADM should be used in IBBR, he noted. “We can only conclude from our trial that there is no hard evidence that ADM is beneficial when performing breast reconstructions with implants,” he said in an interview. “In selected patients, ADM might be indicated.”
The study was conducted in Sweden and the United Kingdom. “Mostly because of high costs, ADM in implant-based breast reconstructions in Sweden is not frequently used,” Dr. Lohmander said. “It is slightly more common in the U.K., but much more common in the U.S.A.”
Although biological meshes have received regulatory approval by the U.S. Food and Drug Administration for reconstructive purposes, ADM has not been approved for use in breast reconstruction surgery, and its use in this setting is off label.
The study was published online October 1 in JAMA Network Open.
Any advantage to using mesh device?
Previous studies of ADMs suggested that the mesh device conferred several benefits, including superior cosmetic results, less need for tissue expanders, fewer elective reoperations, and less capsular contracture. The use of a mesh device also enlarges the subpectoral pocket, which allows for larger fixed-volume implants, the authors note.
However, these suggested advantages have not been universally accepted, and the authors note that there have been reports of associated harm, such as higher rates of infection and implant loss.
The new study included 135 women from five centers in Sweden and the United Kingdom. The patients had breast cancer and had planned to undergo mastectomy and immediate IBBR between 2014 and May 2017.
The primary endpoint was the number of repeat surgeries at 2 years.
At the 2-year follow-up, 31 patients (48%) in the ADM group had undergone at least one reoperation on the ipsilateral side, vs 35 (54%) in the control group (P = .54). Results were similar for the contralateral side: 34 (53%) vs 31 (48%).
Two patients in the ADM group and three patients in the control group underwent a risk-reducing mastectomy on the contralateral side. These five surgeries were included in the final analysis.
For nine patients (14%) in the ADM arm, the implant was removed. Four of the removals took place within 6 months after early surgical complications. In the control group, seven patients (11%) underwent implant removal; four were removed within 6 months, owing to early surgical complications.
The secondary endpoint was postoperative health-related quality of life, including perception of body image and satisfaction with cosmetic outcome. There were no significant differences between the two groups.
Some questions remain
Approached for comment on the study, Sameer A. Patel, MD, FACS, chief of plastic and reconstructive surgery at Fox Chase Cancer Center, Philadelphia, noted that the practice of using AMD for breast reconstruction is quite common in the United States, so these data are informative and add to the current understanding of the value of ADM in breast reconstruction. “The study hypothesized that the use of ADM would reduce the number of reoperations within the first 24 months, which it did not,” he said. “This is despite the fact that the ADM group had a significantly higher number of direct-to-implant reconstructions.”
Importantly, the study showed that patient-reported outcomes, as opposed to surgeon’s evaluation of outcomes, were also not different for the most part between the two groups, Dr. Patel pointed out. “The only exception of small favorable advantage in the ADM group was for fitting bras,” he said.
However, there were limitations to the study’s endpoint. “I would add that there are some purported advantages of using ADM, such as reduction in postoperative pain and reduction in length of hospital stay, which are not evaluated by this study,” Patel explained. “Also, I am not certain that they can conclude from this study that capsular contracture is not reduced, because it is not designed to evaluate that.”
But the biggest limitation is one that study authors point out in their discussion at the end of the article, he added. “The use of prepectoral reconstruction is rapidly replacing the dual plane reconstruction that this paper used in the ADM group,” Dr. Patel said. “The role of ADM in prepectoral reconstruction is somewhat different than in the dual plane reconstruction, and so these results may not necessarily be extrapolated to prepectoral reconstruction.”
The study was funded with grants from the Swedish Breast Cancer Association and Stockholm City Council. The trial was initiated by Karolinska University Hospital and Karolinska Institutet. Acelity (an Allergan company) supplied the study with acellular dermal matrix meshes. Dr. Lohmander and Dr. Patel have disclosed no relevant financial relationships.
A version of this article first appeared on Medscape.com.
New land mines in your next (and even current) employment contract
Physician employment contracts include some new dangers. This includes physicians taking a new job, but it also includes already-employed doctors who are being asked to resign a new contract that contains new conditions. A number of these new clauses have arisen because of COVID-19. When the pandemic dramatically reduced patient flow, many employers didn’t have enough money to pay doctors and didn’t always have physicians in the right location or practice setting.
Vowing this would never happen again, some employers have rewritten their physician contracts to make it easier to reassign and terminate physicians.
Here are 12 potential land mines in a physician employment contract, some of which were added as a result of the pandemic.
You could be immediately terminated without notice
One outcome of the pandemic is the growing use of “force majeure” clauses, which give the employer the right to reduce your compensation or even terminate you due to a natural disaster, which could include COVID.
“COVID made employers aware of the potential impact of disasters on their operations,” said Dan Shay, a health law attorney at Alice Gosfield & Associates in Philadelphia. “Therefore, even as the threat of COVID abates in many places, employers are continuing to put this provision in the contract.”
What can you do? “One way to get some protection is to rule out a termination without cause in the first year,” said Michael A. Cassidy, a physician contract attorney at Tucker Arensberg in Pittsburgh.
The force majeure clause is less likely to affect salary, but could impact bonus and incentive tied to performance. It’s wise to try to specifically limit how much the force majeure could reduce pay tied to performance, and to be prepared to negotiate that aspect of your contract.
No protections if you’re let go through no fault of your own
You could lose your job if your employer could not generate enough business and has to let some doctors go. This happened quite often in the early days of the COVID pandemic.
In these situations, the doctor has not done anything wrong to prompt the termination, but the restrictive covenant may still apply, meaning that the doctor would have to leave the area to find work.
What can you do? You’re in a good position to get this changed, said Christopher L. Nuland, a solo physician contract attorney in Jacksonville, Fla. “Many employers recognize that it would be draconian to require a restrictive covenant in this case, and they will agree to modify this provision.”
Similarly, the employer may not cover your tail insurance even if you were let go from your work through no fault of your own. Most malpractice policies for employer physicians require buying an extra policy, called a tail, if you leave. In some cases, the employer won’t provide a tail and will make the departing doctor buy it.
In these cases, “try for a compromise, such as stipulating that the party that caused the termination should pay for the tail,” Mr. Nuland said. “The employer may not agree to anything more than that because they want to set up a disincentive against you leaving.”
Employer could unilaterally alter your compensation
Many recent contracts give the employer the option to unilaterally modify compensation, such as changing the base salary or raising the target required for meeting the productivity bonus, said Ericka L. Adler, a physician contract attorney at Roetzel & Andress in Chicago.
Ms. Adler thought this change could have been prompted by employers’ financial problems during the pandemic. In the early months of COVID, many physicians were not making much money for the employer but still had to be paid. So employers added a clause saying they could reduce compensation at any time, she said.
What can you do? Harsh provisions like this often come up in contracts with private equity firms, Mr. Cassidy said. “The contract might say the employer can adjust compensation or even terminate physicians based on productivity or their profitability. And it may say that if they reassign you to a new location and you refuse, they can terminate you.”
“If you can’t get these clauses removed, try to reduce the impact of a termination by providing longer notice periods or by inserting a severance agreement,” Mr. Cassidy said.
Accelerating notice for without-cause terminations
Physicians who are convicted of a felony or other moral issue can usually be terminated immediately. But if you are terminated for other reasons – that is, “without cause” – you are given notice at a certain number of days before you have to leave (typically 60-90 days), so that you have time to find a new job.
Some recent contracts, however, allow for very little notice in without-cause terminations, which allows the employer to fire you in as little as 0 days after providing notice, Ms. Adler said.
“This means that, even if 90 days’ notice is provided in the contract, the employer can decide that your last day will be an earlier date,” she said.
Why is this happening? Ms. Adler said employers want to begin reallocating resources and patients as soon as possible. The problem came to employers’ attention during the COVID pandemic, when they were contractually forced to pay doctors for doing little or nothing during the notice period.
What can you do? Possibly not much, other than attempt to negotiate. “Large employers typically don’t want to drop this provision, but at the least, the doctor needs to understand the risk it creates for them,” she said.
You could be assigned to far-off locations
As patient care needs changed dramatically during the pandemic, employers needed to reassign doctors to new locations.
Some new contracts allow employers to simply inform the doctor that they are changing the work location. However, “you don’t want to be assigned to a new work location that is 50 miles away,” Mr. Nuland said.
What can you do? Mr. Nuland recommended adding new language saying that, if the new assignment is more than 20 miles away, both parties would have to approve it.
You could end up working too many off-hours
“Most employers won’t issue a specific work schedule,” Mr. Nuland said. “They want the flexibility to assign evening or weekend work, and it would be difficult for a young doctor to change this.”
What can you do? Mr. Nuland recommended trying to set some limits. “You can try to limit off-hours work to two times a month or something like that,” she said. And if you need to have a special schedule, such as not working on Fridays, Adler advises that this should be put into the contract.
If you can’t get anything changed in the contract, Mr. Nuland said the next-best thing is to ask employers to tell you specifically what they plan to do with you. “Most employers will give you an informal idea of what’s expected – maybe not an exact schedule, but it’s quite likely they will honor it.”
You wouldn’t be able to work nearby if you left the job
Most contracts have a noncompete clause, also known as a “restrictive covenant,” which prevents employed physicians from working in the area if they left the job.
“Almost every doctor I represent has told me that they’re not concerned about the noncompete clause because, they believe, it is not enforceable anyway,” Ms. Adler said. “This is incorrect.”
Mr. Nuland said the faster pace of job-changing during the pandemic makes it all the more likely that doctors have to deal with a restrictive covenant. At the same time, some employers have been expanding the restriction – either by enlarging the radius where the restriction applies or by making the restriction apply to each of their sites, so that each one has a restricted radius around it.
For example, one contract Mr. Nuland is currently reviewing has a 20-mile radius that in effect becomes a 120-mile radius because the employer is counting four offices.
What can you do? Mr. Nuland advised trying to reduce the impact of the noncompete – for instance, making it apply only to the offices where you worked, or trading more time for less distance. “If you have a 2-year, 20-mile restriction, ask for a 3-year, 10-mile restriction, where the radius could be easier to deal with,” he said.
You might end up with too much call
Contracts rarely detail your call schedule because employers want flexibility to expand call as patient care needs change, but you can try adding some specificity, said Sanja Ord, a physician contract attorney at Greensfelder, Hemker & Gale in St. Louis.
Contracts often use wide-open language to describe call, such as simply making it “subject to the house call policies,” Mr. Cassidy said. Language that is more beneficial to the physician would say that call must be “equal” among “similarly situated” physicians.
But Ms. Ord said even provisions for equal call can turn out to be onerous if there are too few doctors in the call roster, so it’s a good idea to find out just how many doctors will be participating in call.
Still, Adler said even that strategy can’t remove all risk. What happens, she asked, if several physicians participating in call decide to leave? Then you might end up with call every other night.
What can you do? Mr. Cassidy recommends specifying a maximum amount of call – for example, no more frequent than one in four nights.
Physician must pay for reimbursement claw-backs by payers
When auditors for Medicare or other payers find overpayments after the fact, called a ‘claw-back,’ the provider must pay them back. But which provider has to do that – you or your employer?
In many cases, your employer’s billing office may have introduced the error, but there may be a clause in the contract stating that the physician is solely responsible for all claw-backs. That could be costly.
What can you do? Mr. Shay said the clause should state that you have to pay only when it is the result of your own error or omission, and also not when it was made at the direction of the employer.
Some work may be outside of your subspecialty
In some cases, the employer may assign subspecialized doctors to work outside their subspecialty, Mr. Nuland said.
For example, he said he represented an endocrinologist who expected to see only diabetes patients but was assigned to some general internal medicine work as well, and an otolaryngologist client of his who completed a fellowship on facial plastic surgery was expected to do liposuction in a cosmetic surgery group.
What can you do? To prevent this from happening, Mr. Nuland recommends a clause stating that your work will be restricted to your subspecialty.
What the employer promised isn’t in the contract
“Beware of promises that are not in the contract,” Mr. Shay said. “You might feel you can really trust your new boss and what he tells you, but what if that person resigns, or the organization gets a new owner who doesn’t honor unwritten agreements?”
Many contracts have an integration clause, which specifies that the contract constitutes the complete agreement between the two parties, and it nullifies any other oral or written promises made to the physician.
For example, the employer might have promised a relocation bonus and a sign-on bonus, but for some reason it didn’t get into the contract, Ms. Ord said. In those cases, the employer is under no obligation to honor the promise.
What can you do? Mr. Cassidy said it is possible to hold the employer to a commitment made outside the contract. The alternative document, such as an offer letter, has to specifically state that the commitment is protected from the integration clause in the contract, he said, adding: “It is still better to have the commitment put into the contract.”
Contract is simply accepted as is
“Generally, the bigger the employer, the less likely they will alter an agreement just to make you happy,” Mr. Shay said.
But even in these contracts, he said there is still opportunity to fix errors and ambiguities that could harm you later – or even alter a provision if you can’t remove it outright.
The back-and-forth is important, Ms. Adler said. “Negotiation means trying to have some control over your job and your life.”
Mr. Cassidy said a big part of contract review is facing up to the possibility that you may have to resign or be let go.
“Many physicians don’t like to think about leaving when they’re just starting a job, but they need to,” he said. “You need to begin with the end in mind. Think about what would happen if this job didn’t work out.”
A version of this article first appeared on Medscape.com.
Physician employment contracts include some new dangers. This includes physicians taking a new job, but it also includes already-employed doctors who are being asked to resign a new contract that contains new conditions. A number of these new clauses have arisen because of COVID-19. When the pandemic dramatically reduced patient flow, many employers didn’t have enough money to pay doctors and didn’t always have physicians in the right location or practice setting.
Vowing this would never happen again, some employers have rewritten their physician contracts to make it easier to reassign and terminate physicians.
Here are 12 potential land mines in a physician employment contract, some of which were added as a result of the pandemic.
You could be immediately terminated without notice
One outcome of the pandemic is the growing use of “force majeure” clauses, which give the employer the right to reduce your compensation or even terminate you due to a natural disaster, which could include COVID.
“COVID made employers aware of the potential impact of disasters on their operations,” said Dan Shay, a health law attorney at Alice Gosfield & Associates in Philadelphia. “Therefore, even as the threat of COVID abates in many places, employers are continuing to put this provision in the contract.”
What can you do? “One way to get some protection is to rule out a termination without cause in the first year,” said Michael A. Cassidy, a physician contract attorney at Tucker Arensberg in Pittsburgh.
The force majeure clause is less likely to affect salary, but could impact bonus and incentive tied to performance. It’s wise to try to specifically limit how much the force majeure could reduce pay tied to performance, and to be prepared to negotiate that aspect of your contract.
No protections if you’re let go through no fault of your own
You could lose your job if your employer could not generate enough business and has to let some doctors go. This happened quite often in the early days of the COVID pandemic.
In these situations, the doctor has not done anything wrong to prompt the termination, but the restrictive covenant may still apply, meaning that the doctor would have to leave the area to find work.
What can you do? You’re in a good position to get this changed, said Christopher L. Nuland, a solo physician contract attorney in Jacksonville, Fla. “Many employers recognize that it would be draconian to require a restrictive covenant in this case, and they will agree to modify this provision.”
Similarly, the employer may not cover your tail insurance even if you were let go from your work through no fault of your own. Most malpractice policies for employer physicians require buying an extra policy, called a tail, if you leave. In some cases, the employer won’t provide a tail and will make the departing doctor buy it.
In these cases, “try for a compromise, such as stipulating that the party that caused the termination should pay for the tail,” Mr. Nuland said. “The employer may not agree to anything more than that because they want to set up a disincentive against you leaving.”
Employer could unilaterally alter your compensation
Many recent contracts give the employer the option to unilaterally modify compensation, such as changing the base salary or raising the target required for meeting the productivity bonus, said Ericka L. Adler, a physician contract attorney at Roetzel & Andress in Chicago.
Ms. Adler thought this change could have been prompted by employers’ financial problems during the pandemic. In the early months of COVID, many physicians were not making much money for the employer but still had to be paid. So employers added a clause saying they could reduce compensation at any time, she said.
What can you do? Harsh provisions like this often come up in contracts with private equity firms, Mr. Cassidy said. “The contract might say the employer can adjust compensation or even terminate physicians based on productivity or their profitability. And it may say that if they reassign you to a new location and you refuse, they can terminate you.”
“If you can’t get these clauses removed, try to reduce the impact of a termination by providing longer notice periods or by inserting a severance agreement,” Mr. Cassidy said.
Accelerating notice for without-cause terminations
Physicians who are convicted of a felony or other moral issue can usually be terminated immediately. But if you are terminated for other reasons – that is, “without cause” – you are given notice at a certain number of days before you have to leave (typically 60-90 days), so that you have time to find a new job.
Some recent contracts, however, allow for very little notice in without-cause terminations, which allows the employer to fire you in as little as 0 days after providing notice, Ms. Adler said.
“This means that, even if 90 days’ notice is provided in the contract, the employer can decide that your last day will be an earlier date,” she said.
Why is this happening? Ms. Adler said employers want to begin reallocating resources and patients as soon as possible. The problem came to employers’ attention during the COVID pandemic, when they were contractually forced to pay doctors for doing little or nothing during the notice period.
What can you do? Possibly not much, other than attempt to negotiate. “Large employers typically don’t want to drop this provision, but at the least, the doctor needs to understand the risk it creates for them,” she said.
You could be assigned to far-off locations
As patient care needs changed dramatically during the pandemic, employers needed to reassign doctors to new locations.
Some new contracts allow employers to simply inform the doctor that they are changing the work location. However, “you don’t want to be assigned to a new work location that is 50 miles away,” Mr. Nuland said.
What can you do? Mr. Nuland recommended adding new language saying that, if the new assignment is more than 20 miles away, both parties would have to approve it.
You could end up working too many off-hours
“Most employers won’t issue a specific work schedule,” Mr. Nuland said. “They want the flexibility to assign evening or weekend work, and it would be difficult for a young doctor to change this.”
What can you do? Mr. Nuland recommended trying to set some limits. “You can try to limit off-hours work to two times a month or something like that,” she said. And if you need to have a special schedule, such as not working on Fridays, Adler advises that this should be put into the contract.
If you can’t get anything changed in the contract, Mr. Nuland said the next-best thing is to ask employers to tell you specifically what they plan to do with you. “Most employers will give you an informal idea of what’s expected – maybe not an exact schedule, but it’s quite likely they will honor it.”
You wouldn’t be able to work nearby if you left the job
Most contracts have a noncompete clause, also known as a “restrictive covenant,” which prevents employed physicians from working in the area if they left the job.
“Almost every doctor I represent has told me that they’re not concerned about the noncompete clause because, they believe, it is not enforceable anyway,” Ms. Adler said. “This is incorrect.”
Mr. Nuland said the faster pace of job-changing during the pandemic makes it all the more likely that doctors have to deal with a restrictive covenant. At the same time, some employers have been expanding the restriction – either by enlarging the radius where the restriction applies or by making the restriction apply to each of their sites, so that each one has a restricted radius around it.
For example, one contract Mr. Nuland is currently reviewing has a 20-mile radius that in effect becomes a 120-mile radius because the employer is counting four offices.
What can you do? Mr. Nuland advised trying to reduce the impact of the noncompete – for instance, making it apply only to the offices where you worked, or trading more time for less distance. “If you have a 2-year, 20-mile restriction, ask for a 3-year, 10-mile restriction, where the radius could be easier to deal with,” he said.
You might end up with too much call
Contracts rarely detail your call schedule because employers want flexibility to expand call as patient care needs change, but you can try adding some specificity, said Sanja Ord, a physician contract attorney at Greensfelder, Hemker & Gale in St. Louis.
Contracts often use wide-open language to describe call, such as simply making it “subject to the house call policies,” Mr. Cassidy said. Language that is more beneficial to the physician would say that call must be “equal” among “similarly situated” physicians.
But Ms. Ord said even provisions for equal call can turn out to be onerous if there are too few doctors in the call roster, so it’s a good idea to find out just how many doctors will be participating in call.
Still, Adler said even that strategy can’t remove all risk. What happens, she asked, if several physicians participating in call decide to leave? Then you might end up with call every other night.
What can you do? Mr. Cassidy recommends specifying a maximum amount of call – for example, no more frequent than one in four nights.
Physician must pay for reimbursement claw-backs by payers
When auditors for Medicare or other payers find overpayments after the fact, called a ‘claw-back,’ the provider must pay them back. But which provider has to do that – you or your employer?
In many cases, your employer’s billing office may have introduced the error, but there may be a clause in the contract stating that the physician is solely responsible for all claw-backs. That could be costly.
What can you do? Mr. Shay said the clause should state that you have to pay only when it is the result of your own error or omission, and also not when it was made at the direction of the employer.
Some work may be outside of your subspecialty
In some cases, the employer may assign subspecialized doctors to work outside their subspecialty, Mr. Nuland said.
For example, he said he represented an endocrinologist who expected to see only diabetes patients but was assigned to some general internal medicine work as well, and an otolaryngologist client of his who completed a fellowship on facial plastic surgery was expected to do liposuction in a cosmetic surgery group.
What can you do? To prevent this from happening, Mr. Nuland recommends a clause stating that your work will be restricted to your subspecialty.
What the employer promised isn’t in the contract
“Beware of promises that are not in the contract,” Mr. Shay said. “You might feel you can really trust your new boss and what he tells you, but what if that person resigns, or the organization gets a new owner who doesn’t honor unwritten agreements?”
Many contracts have an integration clause, which specifies that the contract constitutes the complete agreement between the two parties, and it nullifies any other oral or written promises made to the physician.
For example, the employer might have promised a relocation bonus and a sign-on bonus, but for some reason it didn’t get into the contract, Ms. Ord said. In those cases, the employer is under no obligation to honor the promise.
What can you do? Mr. Cassidy said it is possible to hold the employer to a commitment made outside the contract. The alternative document, such as an offer letter, has to specifically state that the commitment is protected from the integration clause in the contract, he said, adding: “It is still better to have the commitment put into the contract.”
Contract is simply accepted as is
“Generally, the bigger the employer, the less likely they will alter an agreement just to make you happy,” Mr. Shay said.
But even in these contracts, he said there is still opportunity to fix errors and ambiguities that could harm you later – or even alter a provision if you can’t remove it outright.
The back-and-forth is important, Ms. Adler said. “Negotiation means trying to have some control over your job and your life.”
Mr. Cassidy said a big part of contract review is facing up to the possibility that you may have to resign or be let go.
“Many physicians don’t like to think about leaving when they’re just starting a job, but they need to,” he said. “You need to begin with the end in mind. Think about what would happen if this job didn’t work out.”
A version of this article first appeared on Medscape.com.
Physician employment contracts include some new dangers. This includes physicians taking a new job, but it also includes already-employed doctors who are being asked to resign a new contract that contains new conditions. A number of these new clauses have arisen because of COVID-19. When the pandemic dramatically reduced patient flow, many employers didn’t have enough money to pay doctors and didn’t always have physicians in the right location or practice setting.
Vowing this would never happen again, some employers have rewritten their physician contracts to make it easier to reassign and terminate physicians.
Here are 12 potential land mines in a physician employment contract, some of which were added as a result of the pandemic.
You could be immediately terminated without notice
One outcome of the pandemic is the growing use of “force majeure” clauses, which give the employer the right to reduce your compensation or even terminate you due to a natural disaster, which could include COVID.
“COVID made employers aware of the potential impact of disasters on their operations,” said Dan Shay, a health law attorney at Alice Gosfield & Associates in Philadelphia. “Therefore, even as the threat of COVID abates in many places, employers are continuing to put this provision in the contract.”
What can you do? “One way to get some protection is to rule out a termination without cause in the first year,” said Michael A. Cassidy, a physician contract attorney at Tucker Arensberg in Pittsburgh.
The force majeure clause is less likely to affect salary, but could impact bonus and incentive tied to performance. It’s wise to try to specifically limit how much the force majeure could reduce pay tied to performance, and to be prepared to negotiate that aspect of your contract.
No protections if you’re let go through no fault of your own
You could lose your job if your employer could not generate enough business and has to let some doctors go. This happened quite often in the early days of the COVID pandemic.
In these situations, the doctor has not done anything wrong to prompt the termination, but the restrictive covenant may still apply, meaning that the doctor would have to leave the area to find work.
What can you do? You’re in a good position to get this changed, said Christopher L. Nuland, a solo physician contract attorney in Jacksonville, Fla. “Many employers recognize that it would be draconian to require a restrictive covenant in this case, and they will agree to modify this provision.”
Similarly, the employer may not cover your tail insurance even if you were let go from your work through no fault of your own. Most malpractice policies for employer physicians require buying an extra policy, called a tail, if you leave. In some cases, the employer won’t provide a tail and will make the departing doctor buy it.
In these cases, “try for a compromise, such as stipulating that the party that caused the termination should pay for the tail,” Mr. Nuland said. “The employer may not agree to anything more than that because they want to set up a disincentive against you leaving.”
Employer could unilaterally alter your compensation
Many recent contracts give the employer the option to unilaterally modify compensation, such as changing the base salary or raising the target required for meeting the productivity bonus, said Ericka L. Adler, a physician contract attorney at Roetzel & Andress in Chicago.
Ms. Adler thought this change could have been prompted by employers’ financial problems during the pandemic. In the early months of COVID, many physicians were not making much money for the employer but still had to be paid. So employers added a clause saying they could reduce compensation at any time, she said.
What can you do? Harsh provisions like this often come up in contracts with private equity firms, Mr. Cassidy said. “The contract might say the employer can adjust compensation or even terminate physicians based on productivity or their profitability. And it may say that if they reassign you to a new location and you refuse, they can terminate you.”
“If you can’t get these clauses removed, try to reduce the impact of a termination by providing longer notice periods or by inserting a severance agreement,” Mr. Cassidy said.
Accelerating notice for without-cause terminations
Physicians who are convicted of a felony or other moral issue can usually be terminated immediately. But if you are terminated for other reasons – that is, “without cause” – you are given notice at a certain number of days before you have to leave (typically 60-90 days), so that you have time to find a new job.
Some recent contracts, however, allow for very little notice in without-cause terminations, which allows the employer to fire you in as little as 0 days after providing notice, Ms. Adler said.
“This means that, even if 90 days’ notice is provided in the contract, the employer can decide that your last day will be an earlier date,” she said.
Why is this happening? Ms. Adler said employers want to begin reallocating resources and patients as soon as possible. The problem came to employers’ attention during the COVID pandemic, when they were contractually forced to pay doctors for doing little or nothing during the notice period.
What can you do? Possibly not much, other than attempt to negotiate. “Large employers typically don’t want to drop this provision, but at the least, the doctor needs to understand the risk it creates for them,” she said.
You could be assigned to far-off locations
As patient care needs changed dramatically during the pandemic, employers needed to reassign doctors to new locations.
Some new contracts allow employers to simply inform the doctor that they are changing the work location. However, “you don’t want to be assigned to a new work location that is 50 miles away,” Mr. Nuland said.
What can you do? Mr. Nuland recommended adding new language saying that, if the new assignment is more than 20 miles away, both parties would have to approve it.
You could end up working too many off-hours
“Most employers won’t issue a specific work schedule,” Mr. Nuland said. “They want the flexibility to assign evening or weekend work, and it would be difficult for a young doctor to change this.”
What can you do? Mr. Nuland recommended trying to set some limits. “You can try to limit off-hours work to two times a month or something like that,” she said. And if you need to have a special schedule, such as not working on Fridays, Adler advises that this should be put into the contract.
If you can’t get anything changed in the contract, Mr. Nuland said the next-best thing is to ask employers to tell you specifically what they plan to do with you. “Most employers will give you an informal idea of what’s expected – maybe not an exact schedule, but it’s quite likely they will honor it.”
You wouldn’t be able to work nearby if you left the job
Most contracts have a noncompete clause, also known as a “restrictive covenant,” which prevents employed physicians from working in the area if they left the job.
“Almost every doctor I represent has told me that they’re not concerned about the noncompete clause because, they believe, it is not enforceable anyway,” Ms. Adler said. “This is incorrect.”
Mr. Nuland said the faster pace of job-changing during the pandemic makes it all the more likely that doctors have to deal with a restrictive covenant. At the same time, some employers have been expanding the restriction – either by enlarging the radius where the restriction applies or by making the restriction apply to each of their sites, so that each one has a restricted radius around it.
For example, one contract Mr. Nuland is currently reviewing has a 20-mile radius that in effect becomes a 120-mile radius because the employer is counting four offices.
What can you do? Mr. Nuland advised trying to reduce the impact of the noncompete – for instance, making it apply only to the offices where you worked, or trading more time for less distance. “If you have a 2-year, 20-mile restriction, ask for a 3-year, 10-mile restriction, where the radius could be easier to deal with,” he said.
You might end up with too much call
Contracts rarely detail your call schedule because employers want flexibility to expand call as patient care needs change, but you can try adding some specificity, said Sanja Ord, a physician contract attorney at Greensfelder, Hemker & Gale in St. Louis.
Contracts often use wide-open language to describe call, such as simply making it “subject to the house call policies,” Mr. Cassidy said. Language that is more beneficial to the physician would say that call must be “equal” among “similarly situated” physicians.
But Ms. Ord said even provisions for equal call can turn out to be onerous if there are too few doctors in the call roster, so it’s a good idea to find out just how many doctors will be participating in call.
Still, Adler said even that strategy can’t remove all risk. What happens, she asked, if several physicians participating in call decide to leave? Then you might end up with call every other night.
What can you do? Mr. Cassidy recommends specifying a maximum amount of call – for example, no more frequent than one in four nights.
Physician must pay for reimbursement claw-backs by payers
When auditors for Medicare or other payers find overpayments after the fact, called a ‘claw-back,’ the provider must pay them back. But which provider has to do that – you or your employer?
In many cases, your employer’s billing office may have introduced the error, but there may be a clause in the contract stating that the physician is solely responsible for all claw-backs. That could be costly.
What can you do? Mr. Shay said the clause should state that you have to pay only when it is the result of your own error or omission, and also not when it was made at the direction of the employer.
Some work may be outside of your subspecialty
In some cases, the employer may assign subspecialized doctors to work outside their subspecialty, Mr. Nuland said.
For example, he said he represented an endocrinologist who expected to see only diabetes patients but was assigned to some general internal medicine work as well, and an otolaryngologist client of his who completed a fellowship on facial plastic surgery was expected to do liposuction in a cosmetic surgery group.
What can you do? To prevent this from happening, Mr. Nuland recommends a clause stating that your work will be restricted to your subspecialty.
What the employer promised isn’t in the contract
“Beware of promises that are not in the contract,” Mr. Shay said. “You might feel you can really trust your new boss and what he tells you, but what if that person resigns, or the organization gets a new owner who doesn’t honor unwritten agreements?”
Many contracts have an integration clause, which specifies that the contract constitutes the complete agreement between the two parties, and it nullifies any other oral or written promises made to the physician.
For example, the employer might have promised a relocation bonus and a sign-on bonus, but for some reason it didn’t get into the contract, Ms. Ord said. In those cases, the employer is under no obligation to honor the promise.
What can you do? Mr. Cassidy said it is possible to hold the employer to a commitment made outside the contract. The alternative document, such as an offer letter, has to specifically state that the commitment is protected from the integration clause in the contract, he said, adding: “It is still better to have the commitment put into the contract.”
Contract is simply accepted as is
“Generally, the bigger the employer, the less likely they will alter an agreement just to make you happy,” Mr. Shay said.
But even in these contracts, he said there is still opportunity to fix errors and ambiguities that could harm you later – or even alter a provision if you can’t remove it outright.
The back-and-forth is important, Ms. Adler said. “Negotiation means trying to have some control over your job and your life.”
Mr. Cassidy said a big part of contract review is facing up to the possibility that you may have to resign or be let go.
“Many physicians don’t like to think about leaving when they’re just starting a job, but they need to,” he said. “You need to begin with the end in mind. Think about what would happen if this job didn’t work out.”
A version of this article first appeared on Medscape.com.
Docs: Insurers’ payment delays, downcoding a ‘revenue grab’
Despite reporting record profits during the COVID-19 pandemic, major insurance companies are delaying claims payments and making it more difficult for hospitals and physicians to get paid the full amount of claims, observers and physicians say.
Kaiser Health News recently reported that hospitals, in particular, are affected by the slowdown in claims payments from Anthem Blue Cross, the nation’s second largest health insurer. The investigative piece did not focus on outpatient or independent practices. Research by this news organization shows that the health plans’ new policies are also reducing cash flow and raising costs for ambulatory care groups. In addition, it showed that other payers besides Anthem have engaged in the same practices.
“What we’ve seen is that with complex claims, such as those with -25 modifiers, plans are routinely requiring documentation,” Jim Donohue, senior manager and associate principal at ECG Management Consultants, said in an interview. “It’s not a denial, it’s a request for more information for medical records prior to processing payments. That has the effect of slowing down payments.”
This is exactly what one internal medicine group in the Southeast has noticed. The internist who heads the practice, who asked not to be identified, says that about 4-6 months ago, United, Humana, and other payers started to require documentation for prepayment review on a higher percentage of complex claims such as 99214 (established patient), 99204 (new patient), and claims with -25 modifiers. (The latter are appended to evaluation and management [E/M] claims in which patients had comorbidities that were addressed in the same visit as the main complaint.)
“That’s really frustrating, because you have to print out or take the record for that particular visit and computer fax it to them,” the practice leader notes. “And invariably, they’ll say they didn’t get a certain percentage of them. It’s our fault because they lost the claim.”
In the past, he says, health plans would occasionally ask for the note related to a complex visit where they saw issues, and they’ve always done random postpayment chart audits. But the percentage of prepayment reviews has significantly increased in recent months, he says.
Until a plan does this review, the claim can’t be processed because it’s not regarded as a clean claim. And this has implications for insurers’ compliance with laws that, in most states, require them to pay claims within 30-40 days of submission. (Medicare’s limit is 30 days.) According to Mr. Donohue, the clock doesn’t start ticking on this requirement unless and until a claim is clean. So by requiring documentation on complex claims, the plans can not only justify downcoding a claim, but can also delay payment without triggering state penalties.
Insurer admits ‘challenges’ with claims processing
VCU Health, a health system affiliated with Virginia Commonwealth University, recently filed a complaint against Anthem with Virginia’s insurance commissioner, asking that the Virginia Bureau of Insurance investigate the company’s claims-processing delays. The complaint claimed Anthem owes VCU more than $385 million, of which $171 million is over 90 days old. Much of that consists of commercial claims, which are subject to the state’s 40-day claims payment rule.
VCU cited several problems it said Anthem had created that slowed claims payments:
Any claim over a certain dollar limit requires an itemized bill.
Anthem requests detailed medical records prior to considering payment of even clean claims.
Documents must be uploaded to a web portal that has technical problems, and Anthem has lost some documents as a result.
Claims are being incorrectly processed for some professionals, “resulting in multi-million-dollar underpayments of anesthesia, nurse practitioners, pathology, and behavioral health providers.”
In addition, as the Kaiser Health News article points out, hospitals have blamed the increase in payment delays or denials partly on “preauthorization hurdles for routine procedures and requirements that doctors themselves – not support staffers – speak to insurance gatekeepers.”
In response to an inquiry from this news organization, an Anthem spokesman admitted that some payments to providers have been delayed, partly because of changes in the company’s claims-processing system. “We recognize there have been some challenges as we work with care providers to update claims processing, and readjust and adapt to a new set of dynamics as we continue to manage the pandemic,” said the spokesman.
The Kaiser Health News piece reported that Anthem’s CFO had told stock analysts on a conference call that the company had slowed claims payments to build up its financial reserves during the pandemic – a statement that some physicians called “outrageous.” But the Anthem spokesman told this news organization the quote was taken out of context and that the CFO was talking not about reserves but about “days in claims payable.” The spokesman said, “The payment delays that the article focuses on are not the primary driver or even a material driver of the increase in our overall reserves or DCPs [defined contribution plans] relative to historical levels. In fact, the vast majority of our claims are being processed in a timely manner.”
Some claims routinely downcoded
Even if that were the case, it would not explain why some physicians are seeing their higher-cost claims routinely downcoded. Will Sawyer, MD, a family physician in Cincinnati, told this news organization, “Anthem has been downcoding relentlessly since October 2020.” More often than not, when his office submits a claim with a 99214 code (office visit, 30-39 minutes, moderate medical decision-making), it’s changed to 99213 (office visit, 20-29 minutes, low medical decision-making) before processing, he says.
This has resulted in a significant diminution of his income, he notes. Anthem pays him less than Medicare for E/M visits, and the downcoding reduces his payment from $86 to $68 for a complex visit that may have taken half an hour or more.
In some cases where his office manager has noticed the downcoding, Dr. Sawyer says, she has resubmitted the claim with a copy of the encounter form. But Anthem hasn’t budged. And the refiling effort takes a toll on his solo practice, which doesn’t have sufficient staff, as it is.
Dr. Sawyer acknowledges that he has sent in a higher percentage of complex claims in the past year than he did previously. But much of that is the result of two factors beyond his control: First, many patients avoided coming into the office early in the pandemic, and when they returned, their preventive and chronic care needs were greater. Second, he says, “There are many comorbidities and mental health aspects, which exacerbate many issues and become an issue. We’re not dealing with engines here; they’re human beings. And it takes time.”
In response to Dr. Sawyer’s comments, Anthem said that it uses “analytical tools to review evaluation and management (E/M) codes during the claims adjudication and processing process.” Physicians who believe that certain claims should not have been downcoded can dispute these decisions; they must supply a statement explaining why they disagree with the decision along with documentation to support their statement, the company said. Anthem added that it reviews claims to lower costs for its members.
‘Revenue-grab strategy’
Dr. Sawyer believes that what Anthem is doing to him and other physicians reflects its desire to increase profits by netting extra revenue and keeping physicians’ money while it delays payments to them – a practice known in the trade as “the float.” Moreover, he says, the company depends on many practices not keeping track of their finances during the pandemic.
“When practices are running at warp speed, trying to keep people healthy and getting burned out, they aren’t paying as close attention to the details of payment. It’s an absolute revenue-grab strategy that’s unconscionable,” says Dr. Sawyer.
The Southeast internist also thinks that insurance companies other than Anthem – including United and Humana – are profiting from the float. Besides delaying his payments with gratuitous demands for documentation, he said, they also downcode many claims, forcing the practice to refile the claims and appeal. That forces the practice to pay overtime or bring on more claims staff, which raises administrative costs.
The plans’ strategy, the internist says, is this: “If they downcode millions of claims, a certain number of physicians will give up without appealing, and they’ll raise their profits.”
A United spokesperson said in an interview, “We pay claims appropriately under members’ plans and within the required time frame.” Humana had not responded to this news organization’s request for comment at press time.
Challenge to practice economics
Insurer policies that delay payments or downcode claims, ECG’s Mr. Donohue points out, are especially harmful to primary care and other ambulatory practices that have many small-dollar claims.
“That’s where it’s challenging, because it’s not like a $10,000 case where you add $100 to it [to meet records requests]. You’re talking about something that’s relatively low dollar, where the practice makes a small surplus, and when you add administrative costs, it can change the economics,” he says.
While the economic burden on ambulatory care practices may be greater, Anders Gilberg, senior vice president of government affairs for the Medical Group Management Association (MGMA), said that the payment delays and demands for documentation – along with prior authorization – particularly affect inpatient care. The health plans are questioning big-ticket items more than ever, he said, and most of those services occur in hospitals.
However, the greater level of insurer scrutiny also affects physicians who treat patients in the hospital, including surgeons and emergency department physicians who contract with the facilities, he adds.
Mr. Gilberg views the current situation as an exacerbation of the health plan policies that physicians have long struggled with. “It’s not new to have insurers play the float and not pay claims on time. Unfortunately, this is something that medical practices are used to.”
A version of this article first appeared on Medscape.com.
Despite reporting record profits during the COVID-19 pandemic, major insurance companies are delaying claims payments and making it more difficult for hospitals and physicians to get paid the full amount of claims, observers and physicians say.
Kaiser Health News recently reported that hospitals, in particular, are affected by the slowdown in claims payments from Anthem Blue Cross, the nation’s second largest health insurer. The investigative piece did not focus on outpatient or independent practices. Research by this news organization shows that the health plans’ new policies are also reducing cash flow and raising costs for ambulatory care groups. In addition, it showed that other payers besides Anthem have engaged in the same practices.
“What we’ve seen is that with complex claims, such as those with -25 modifiers, plans are routinely requiring documentation,” Jim Donohue, senior manager and associate principal at ECG Management Consultants, said in an interview. “It’s not a denial, it’s a request for more information for medical records prior to processing payments. That has the effect of slowing down payments.”
This is exactly what one internal medicine group in the Southeast has noticed. The internist who heads the practice, who asked not to be identified, says that about 4-6 months ago, United, Humana, and other payers started to require documentation for prepayment review on a higher percentage of complex claims such as 99214 (established patient), 99204 (new patient), and claims with -25 modifiers. (The latter are appended to evaluation and management [E/M] claims in which patients had comorbidities that were addressed in the same visit as the main complaint.)
“That’s really frustrating, because you have to print out or take the record for that particular visit and computer fax it to them,” the practice leader notes. “And invariably, they’ll say they didn’t get a certain percentage of them. It’s our fault because they lost the claim.”
In the past, he says, health plans would occasionally ask for the note related to a complex visit where they saw issues, and they’ve always done random postpayment chart audits. But the percentage of prepayment reviews has significantly increased in recent months, he says.
Until a plan does this review, the claim can’t be processed because it’s not regarded as a clean claim. And this has implications for insurers’ compliance with laws that, in most states, require them to pay claims within 30-40 days of submission. (Medicare’s limit is 30 days.) According to Mr. Donohue, the clock doesn’t start ticking on this requirement unless and until a claim is clean. So by requiring documentation on complex claims, the plans can not only justify downcoding a claim, but can also delay payment without triggering state penalties.
Insurer admits ‘challenges’ with claims processing
VCU Health, a health system affiliated with Virginia Commonwealth University, recently filed a complaint against Anthem with Virginia’s insurance commissioner, asking that the Virginia Bureau of Insurance investigate the company’s claims-processing delays. The complaint claimed Anthem owes VCU more than $385 million, of which $171 million is over 90 days old. Much of that consists of commercial claims, which are subject to the state’s 40-day claims payment rule.
VCU cited several problems it said Anthem had created that slowed claims payments:
Any claim over a certain dollar limit requires an itemized bill.
Anthem requests detailed medical records prior to considering payment of even clean claims.
Documents must be uploaded to a web portal that has technical problems, and Anthem has lost some documents as a result.
Claims are being incorrectly processed for some professionals, “resulting in multi-million-dollar underpayments of anesthesia, nurse practitioners, pathology, and behavioral health providers.”
In addition, as the Kaiser Health News article points out, hospitals have blamed the increase in payment delays or denials partly on “preauthorization hurdles for routine procedures and requirements that doctors themselves – not support staffers – speak to insurance gatekeepers.”
In response to an inquiry from this news organization, an Anthem spokesman admitted that some payments to providers have been delayed, partly because of changes in the company’s claims-processing system. “We recognize there have been some challenges as we work with care providers to update claims processing, and readjust and adapt to a new set of dynamics as we continue to manage the pandemic,” said the spokesman.
The Kaiser Health News piece reported that Anthem’s CFO had told stock analysts on a conference call that the company had slowed claims payments to build up its financial reserves during the pandemic – a statement that some physicians called “outrageous.” But the Anthem spokesman told this news organization the quote was taken out of context and that the CFO was talking not about reserves but about “days in claims payable.” The spokesman said, “The payment delays that the article focuses on are not the primary driver or even a material driver of the increase in our overall reserves or DCPs [defined contribution plans] relative to historical levels. In fact, the vast majority of our claims are being processed in a timely manner.”
Some claims routinely downcoded
Even if that were the case, it would not explain why some physicians are seeing their higher-cost claims routinely downcoded. Will Sawyer, MD, a family physician in Cincinnati, told this news organization, “Anthem has been downcoding relentlessly since October 2020.” More often than not, when his office submits a claim with a 99214 code (office visit, 30-39 minutes, moderate medical decision-making), it’s changed to 99213 (office visit, 20-29 minutes, low medical decision-making) before processing, he says.
This has resulted in a significant diminution of his income, he notes. Anthem pays him less than Medicare for E/M visits, and the downcoding reduces his payment from $86 to $68 for a complex visit that may have taken half an hour or more.
In some cases where his office manager has noticed the downcoding, Dr. Sawyer says, she has resubmitted the claim with a copy of the encounter form. But Anthem hasn’t budged. And the refiling effort takes a toll on his solo practice, which doesn’t have sufficient staff, as it is.
Dr. Sawyer acknowledges that he has sent in a higher percentage of complex claims in the past year than he did previously. But much of that is the result of two factors beyond his control: First, many patients avoided coming into the office early in the pandemic, and when they returned, their preventive and chronic care needs were greater. Second, he says, “There are many comorbidities and mental health aspects, which exacerbate many issues and become an issue. We’re not dealing with engines here; they’re human beings. And it takes time.”
In response to Dr. Sawyer’s comments, Anthem said that it uses “analytical tools to review evaluation and management (E/M) codes during the claims adjudication and processing process.” Physicians who believe that certain claims should not have been downcoded can dispute these decisions; they must supply a statement explaining why they disagree with the decision along with documentation to support their statement, the company said. Anthem added that it reviews claims to lower costs for its members.
‘Revenue-grab strategy’
Dr. Sawyer believes that what Anthem is doing to him and other physicians reflects its desire to increase profits by netting extra revenue and keeping physicians’ money while it delays payments to them – a practice known in the trade as “the float.” Moreover, he says, the company depends on many practices not keeping track of their finances during the pandemic.
“When practices are running at warp speed, trying to keep people healthy and getting burned out, they aren’t paying as close attention to the details of payment. It’s an absolute revenue-grab strategy that’s unconscionable,” says Dr. Sawyer.
The Southeast internist also thinks that insurance companies other than Anthem – including United and Humana – are profiting from the float. Besides delaying his payments with gratuitous demands for documentation, he said, they also downcode many claims, forcing the practice to refile the claims and appeal. That forces the practice to pay overtime or bring on more claims staff, which raises administrative costs.
The plans’ strategy, the internist says, is this: “If they downcode millions of claims, a certain number of physicians will give up without appealing, and they’ll raise their profits.”
A United spokesperson said in an interview, “We pay claims appropriately under members’ plans and within the required time frame.” Humana had not responded to this news organization’s request for comment at press time.
Challenge to practice economics
Insurer policies that delay payments or downcode claims, ECG’s Mr. Donohue points out, are especially harmful to primary care and other ambulatory practices that have many small-dollar claims.
“That’s where it’s challenging, because it’s not like a $10,000 case where you add $100 to it [to meet records requests]. You’re talking about something that’s relatively low dollar, where the practice makes a small surplus, and when you add administrative costs, it can change the economics,” he says.
While the economic burden on ambulatory care practices may be greater, Anders Gilberg, senior vice president of government affairs for the Medical Group Management Association (MGMA), said that the payment delays and demands for documentation – along with prior authorization – particularly affect inpatient care. The health plans are questioning big-ticket items more than ever, he said, and most of those services occur in hospitals.
However, the greater level of insurer scrutiny also affects physicians who treat patients in the hospital, including surgeons and emergency department physicians who contract with the facilities, he adds.
Mr. Gilberg views the current situation as an exacerbation of the health plan policies that physicians have long struggled with. “It’s not new to have insurers play the float and not pay claims on time. Unfortunately, this is something that medical practices are used to.”
A version of this article first appeared on Medscape.com.
Despite reporting record profits during the COVID-19 pandemic, major insurance companies are delaying claims payments and making it more difficult for hospitals and physicians to get paid the full amount of claims, observers and physicians say.
Kaiser Health News recently reported that hospitals, in particular, are affected by the slowdown in claims payments from Anthem Blue Cross, the nation’s second largest health insurer. The investigative piece did not focus on outpatient or independent practices. Research by this news organization shows that the health plans’ new policies are also reducing cash flow and raising costs for ambulatory care groups. In addition, it showed that other payers besides Anthem have engaged in the same practices.
“What we’ve seen is that with complex claims, such as those with -25 modifiers, plans are routinely requiring documentation,” Jim Donohue, senior manager and associate principal at ECG Management Consultants, said in an interview. “It’s not a denial, it’s a request for more information for medical records prior to processing payments. That has the effect of slowing down payments.”
This is exactly what one internal medicine group in the Southeast has noticed. The internist who heads the practice, who asked not to be identified, says that about 4-6 months ago, United, Humana, and other payers started to require documentation for prepayment review on a higher percentage of complex claims such as 99214 (established patient), 99204 (new patient), and claims with -25 modifiers. (The latter are appended to evaluation and management [E/M] claims in which patients had comorbidities that were addressed in the same visit as the main complaint.)
“That’s really frustrating, because you have to print out or take the record for that particular visit and computer fax it to them,” the practice leader notes. “And invariably, they’ll say they didn’t get a certain percentage of them. It’s our fault because they lost the claim.”
In the past, he says, health plans would occasionally ask for the note related to a complex visit where they saw issues, and they’ve always done random postpayment chart audits. But the percentage of prepayment reviews has significantly increased in recent months, he says.
Until a plan does this review, the claim can’t be processed because it’s not regarded as a clean claim. And this has implications for insurers’ compliance with laws that, in most states, require them to pay claims within 30-40 days of submission. (Medicare’s limit is 30 days.) According to Mr. Donohue, the clock doesn’t start ticking on this requirement unless and until a claim is clean. So by requiring documentation on complex claims, the plans can not only justify downcoding a claim, but can also delay payment without triggering state penalties.
Insurer admits ‘challenges’ with claims processing
VCU Health, a health system affiliated with Virginia Commonwealth University, recently filed a complaint against Anthem with Virginia’s insurance commissioner, asking that the Virginia Bureau of Insurance investigate the company’s claims-processing delays. The complaint claimed Anthem owes VCU more than $385 million, of which $171 million is over 90 days old. Much of that consists of commercial claims, which are subject to the state’s 40-day claims payment rule.
VCU cited several problems it said Anthem had created that slowed claims payments:
Any claim over a certain dollar limit requires an itemized bill.
Anthem requests detailed medical records prior to considering payment of even clean claims.
Documents must be uploaded to a web portal that has technical problems, and Anthem has lost some documents as a result.
Claims are being incorrectly processed for some professionals, “resulting in multi-million-dollar underpayments of anesthesia, nurse practitioners, pathology, and behavioral health providers.”
In addition, as the Kaiser Health News article points out, hospitals have blamed the increase in payment delays or denials partly on “preauthorization hurdles for routine procedures and requirements that doctors themselves – not support staffers – speak to insurance gatekeepers.”
In response to an inquiry from this news organization, an Anthem spokesman admitted that some payments to providers have been delayed, partly because of changes in the company’s claims-processing system. “We recognize there have been some challenges as we work with care providers to update claims processing, and readjust and adapt to a new set of dynamics as we continue to manage the pandemic,” said the spokesman.
The Kaiser Health News piece reported that Anthem’s CFO had told stock analysts on a conference call that the company had slowed claims payments to build up its financial reserves during the pandemic – a statement that some physicians called “outrageous.” But the Anthem spokesman told this news organization the quote was taken out of context and that the CFO was talking not about reserves but about “days in claims payable.” The spokesman said, “The payment delays that the article focuses on are not the primary driver or even a material driver of the increase in our overall reserves or DCPs [defined contribution plans] relative to historical levels. In fact, the vast majority of our claims are being processed in a timely manner.”
Some claims routinely downcoded
Even if that were the case, it would not explain why some physicians are seeing their higher-cost claims routinely downcoded. Will Sawyer, MD, a family physician in Cincinnati, told this news organization, “Anthem has been downcoding relentlessly since October 2020.” More often than not, when his office submits a claim with a 99214 code (office visit, 30-39 minutes, moderate medical decision-making), it’s changed to 99213 (office visit, 20-29 minutes, low medical decision-making) before processing, he says.
This has resulted in a significant diminution of his income, he notes. Anthem pays him less than Medicare for E/M visits, and the downcoding reduces his payment from $86 to $68 for a complex visit that may have taken half an hour or more.
In some cases where his office manager has noticed the downcoding, Dr. Sawyer says, she has resubmitted the claim with a copy of the encounter form. But Anthem hasn’t budged. And the refiling effort takes a toll on his solo practice, which doesn’t have sufficient staff, as it is.
Dr. Sawyer acknowledges that he has sent in a higher percentage of complex claims in the past year than he did previously. But much of that is the result of two factors beyond his control: First, many patients avoided coming into the office early in the pandemic, and when they returned, their preventive and chronic care needs were greater. Second, he says, “There are many comorbidities and mental health aspects, which exacerbate many issues and become an issue. We’re not dealing with engines here; they’re human beings. And it takes time.”
In response to Dr. Sawyer’s comments, Anthem said that it uses “analytical tools to review evaluation and management (E/M) codes during the claims adjudication and processing process.” Physicians who believe that certain claims should not have been downcoded can dispute these decisions; they must supply a statement explaining why they disagree with the decision along with documentation to support their statement, the company said. Anthem added that it reviews claims to lower costs for its members.
‘Revenue-grab strategy’
Dr. Sawyer believes that what Anthem is doing to him and other physicians reflects its desire to increase profits by netting extra revenue and keeping physicians’ money while it delays payments to them – a practice known in the trade as “the float.” Moreover, he says, the company depends on many practices not keeping track of their finances during the pandemic.
“When practices are running at warp speed, trying to keep people healthy and getting burned out, they aren’t paying as close attention to the details of payment. It’s an absolute revenue-grab strategy that’s unconscionable,” says Dr. Sawyer.
The Southeast internist also thinks that insurance companies other than Anthem – including United and Humana – are profiting from the float. Besides delaying his payments with gratuitous demands for documentation, he said, they also downcode many claims, forcing the practice to refile the claims and appeal. That forces the practice to pay overtime or bring on more claims staff, which raises administrative costs.
The plans’ strategy, the internist says, is this: “If they downcode millions of claims, a certain number of physicians will give up without appealing, and they’ll raise their profits.”
A United spokesperson said in an interview, “We pay claims appropriately under members’ plans and within the required time frame.” Humana had not responded to this news organization’s request for comment at press time.
Challenge to practice economics
Insurer policies that delay payments or downcode claims, ECG’s Mr. Donohue points out, are especially harmful to primary care and other ambulatory practices that have many small-dollar claims.
“That’s where it’s challenging, because it’s not like a $10,000 case where you add $100 to it [to meet records requests]. You’re talking about something that’s relatively low dollar, where the practice makes a small surplus, and when you add administrative costs, it can change the economics,” he says.
While the economic burden on ambulatory care practices may be greater, Anders Gilberg, senior vice president of government affairs for the Medical Group Management Association (MGMA), said that the payment delays and demands for documentation – along with prior authorization – particularly affect inpatient care. The health plans are questioning big-ticket items more than ever, he said, and most of those services occur in hospitals.
However, the greater level of insurer scrutiny also affects physicians who treat patients in the hospital, including surgeons and emergency department physicians who contract with the facilities, he adds.
Mr. Gilberg views the current situation as an exacerbation of the health plan policies that physicians have long struggled with. “It’s not new to have insurers play the float and not pay claims on time. Unfortunately, this is something that medical practices are used to.”
A version of this article first appeared on Medscape.com.
Watchful waiting sometimes best for asymptomatic basal cell carcinoma
“Patient preferences, treatment goals, and the option for proceeding with a watchful waiting approach should be discussed as part of personalized shared decision-making,” wrote Marieke van Winden, MD, MSc, of Radboud University Medical Center in Nijmegen, the Netherlands, and colleagues. “In patients with a limited life expectancy and asymptomatic low-risk tumors, the time to benefit from treatment might exceed life expectancy, and watchful waiting should be discussed as a potentially appropriate approach.”
As little research has been undertaken on watchful waiting in patients with BCC, the expected tumor growth, progression and the chance of developing symptoms while taking this approach are poorly understood. Patients with limited life expectancy might not live long enough to develop BCC symptoms and may benefit more from watchful waiting than active treatment, authors of the study wrote.
This observational cohort study evaluated the reasons for watchful waiting, along with the natural course of 280 BCCs in 89 patients (53% men, median age 83 years) who chose this approach. Patients had one or more untreated BCCs for at least 3 months and the median follow-up was 9 months. The researchers also looked at the reasons for initiating later treatment.
Patient-related factors, including limited life expectancy, comorbidity prioritizations, and frailty, were the most important reasons to choose watchful waiting in 83% of patients, followed by tumor-related factors in 55% of patients. Of the tumors, 47% increased in size. The estimated tumor diameter increase in 1 year was 4.46 mm for infiltrative/micronodular BCCs and 1.06 mm for nodular, superficial, or clinical BCCs. Tumor growth was not associated with initial tumor size and location.
The most common reasons to initiate active treatment were tumor burden, resolved reasons for watchful waiting, and reevaluation of patient-related factors.
“All patients should be followed up regularly to determine whether a watchful waiting approach is still suited and if patients still prefer watchful waiting to reconsider the consequences of refraining from treatment,” the authors wrote.
In an accompanying editorial, Mackenzie R. Wehner, MD, MPhil, of the University of Texas MD Anderson Cancer Center in Houston, said that, while the observational and retrospective design was a limitation of the study, this allowed the authors to observe patients avoiding or delaying treatment for BCC in real clinical practice.
The study “shows that few patients developed new symptoms, and few patients who decided to treat after a delay had more invasive interventions than originally anticipated, an encouraging result as we continue to study the option and hone the details of active surveillance in BCC,” Dr. Wehner wrote. “It is important to note that the authors did not perform actual active surveillance. This study did not prospectively enroll patients and see them in follow-up at set times, nor did it have prespecified end points for recommending treatment.”
“Before evidence-based active surveillance in BCC can become a viable option, prospective studies of active surveillance, with specified follow-up times and clear outcome measures, are needed,” Dr. Wehner wrote.
Dr. van Winden did not report any conflicts of interest.
“Patient preferences, treatment goals, and the option for proceeding with a watchful waiting approach should be discussed as part of personalized shared decision-making,” wrote Marieke van Winden, MD, MSc, of Radboud University Medical Center in Nijmegen, the Netherlands, and colleagues. “In patients with a limited life expectancy and asymptomatic low-risk tumors, the time to benefit from treatment might exceed life expectancy, and watchful waiting should be discussed as a potentially appropriate approach.”
As little research has been undertaken on watchful waiting in patients with BCC, the expected tumor growth, progression and the chance of developing symptoms while taking this approach are poorly understood. Patients with limited life expectancy might not live long enough to develop BCC symptoms and may benefit more from watchful waiting than active treatment, authors of the study wrote.
This observational cohort study evaluated the reasons for watchful waiting, along with the natural course of 280 BCCs in 89 patients (53% men, median age 83 years) who chose this approach. Patients had one or more untreated BCCs for at least 3 months and the median follow-up was 9 months. The researchers also looked at the reasons for initiating later treatment.
Patient-related factors, including limited life expectancy, comorbidity prioritizations, and frailty, were the most important reasons to choose watchful waiting in 83% of patients, followed by tumor-related factors in 55% of patients. Of the tumors, 47% increased in size. The estimated tumor diameter increase in 1 year was 4.46 mm for infiltrative/micronodular BCCs and 1.06 mm for nodular, superficial, or clinical BCCs. Tumor growth was not associated with initial tumor size and location.
The most common reasons to initiate active treatment were tumor burden, resolved reasons for watchful waiting, and reevaluation of patient-related factors.
“All patients should be followed up regularly to determine whether a watchful waiting approach is still suited and if patients still prefer watchful waiting to reconsider the consequences of refraining from treatment,” the authors wrote.
In an accompanying editorial, Mackenzie R. Wehner, MD, MPhil, of the University of Texas MD Anderson Cancer Center in Houston, said that, while the observational and retrospective design was a limitation of the study, this allowed the authors to observe patients avoiding or delaying treatment for BCC in real clinical practice.
The study “shows that few patients developed new symptoms, and few patients who decided to treat after a delay had more invasive interventions than originally anticipated, an encouraging result as we continue to study the option and hone the details of active surveillance in BCC,” Dr. Wehner wrote. “It is important to note that the authors did not perform actual active surveillance. This study did not prospectively enroll patients and see them in follow-up at set times, nor did it have prespecified end points for recommending treatment.”
“Before evidence-based active surveillance in BCC can become a viable option, prospective studies of active surveillance, with specified follow-up times and clear outcome measures, are needed,” Dr. Wehner wrote.
Dr. van Winden did not report any conflicts of interest.
“Patient preferences, treatment goals, and the option for proceeding with a watchful waiting approach should be discussed as part of personalized shared decision-making,” wrote Marieke van Winden, MD, MSc, of Radboud University Medical Center in Nijmegen, the Netherlands, and colleagues. “In patients with a limited life expectancy and asymptomatic low-risk tumors, the time to benefit from treatment might exceed life expectancy, and watchful waiting should be discussed as a potentially appropriate approach.”
As little research has been undertaken on watchful waiting in patients with BCC, the expected tumor growth, progression and the chance of developing symptoms while taking this approach are poorly understood. Patients with limited life expectancy might not live long enough to develop BCC symptoms and may benefit more from watchful waiting than active treatment, authors of the study wrote.
This observational cohort study evaluated the reasons for watchful waiting, along with the natural course of 280 BCCs in 89 patients (53% men, median age 83 years) who chose this approach. Patients had one or more untreated BCCs for at least 3 months and the median follow-up was 9 months. The researchers also looked at the reasons for initiating later treatment.
Patient-related factors, including limited life expectancy, comorbidity prioritizations, and frailty, were the most important reasons to choose watchful waiting in 83% of patients, followed by tumor-related factors in 55% of patients. Of the tumors, 47% increased in size. The estimated tumor diameter increase in 1 year was 4.46 mm for infiltrative/micronodular BCCs and 1.06 mm for nodular, superficial, or clinical BCCs. Tumor growth was not associated with initial tumor size and location.
The most common reasons to initiate active treatment were tumor burden, resolved reasons for watchful waiting, and reevaluation of patient-related factors.
“All patients should be followed up regularly to determine whether a watchful waiting approach is still suited and if patients still prefer watchful waiting to reconsider the consequences of refraining from treatment,” the authors wrote.
In an accompanying editorial, Mackenzie R. Wehner, MD, MPhil, of the University of Texas MD Anderson Cancer Center in Houston, said that, while the observational and retrospective design was a limitation of the study, this allowed the authors to observe patients avoiding or delaying treatment for BCC in real clinical practice.
The study “shows that few patients developed new symptoms, and few patients who decided to treat after a delay had more invasive interventions than originally anticipated, an encouraging result as we continue to study the option and hone the details of active surveillance in BCC,” Dr. Wehner wrote. “It is important to note that the authors did not perform actual active surveillance. This study did not prospectively enroll patients and see them in follow-up at set times, nor did it have prespecified end points for recommending treatment.”
“Before evidence-based active surveillance in BCC can become a viable option, prospective studies of active surveillance, with specified follow-up times and clear outcome measures, are needed,” Dr. Wehner wrote.
Dr. van Winden did not report any conflicts of interest.
FROM JAMA DERMATOLOGY
Radiofrequency ablation gains favor for thyroid nodules in U.S.
And in one case, a hospital has taken the unique step of forming a multidisciplinary thyroid nodule RFA tumor board, which helps in the often tricky decision-making process that is involved.
“Our multidisciplinary RFA tumor board has been invaluable in this process, and it is the only one of its kind in the nation that I’m aware of,” James Lim, MD, of the Division of Surgical Oncology, Thyroid, and Parathyroid Center at Oregon Health Sciences University (OHSU), told this news organization.
Dr. Lim reports receiving referrals from “all avenues, some from thyroid specialists and others from nonthyroid specialists such as primary care practitioners or patient self-referrals.”
“Because of this, our centralized process of multidisciplinary review ensures that each patient is evaluated thoroughly through each thyroid specialists’ lens to optimize patient outcomes,” noted Dr. Lim, an assistant professor of endocrine surgery.
The RFA tumor board consists of experts in all specialties involved in thyroid nodule assessment and treatment, including surgeons, interventional radiologists, and endocrinologists.
Just because you can, doesn’t mean you should
However, there should be some caution that although there is enthusiasm regarding this noninvasive alternative to surgery, there is another option, that of mere observation, which is appropriate in many cases of thyroid nodules and should not be overlooked.
“For a number of reasons, the key to keep in mind is that, just because we can do something doesn’t mean we should,” Michael Singer, MD, director of the Division of Thyroid & Parathyroid Surgery, Department of Otolaryngology – Head and Neck Surgery, at the Henry Ford Health System, Detroit, said in an interview.
While emphasizing that he believes RFA to be a promising technology that will likely benefit patients in the future, Dr. Singer voiced concern about the approach becoming an easy choice – particularly if profit is to be had – when observation is a clear alternative. “If RFA becomes seen as an opportunity to create revenue, potential conflicts of interest may arise,” he said.
“As it is not a major procedure with a dramatic risk profile, my concern is that some clinicians [could] adopt the attitude of ‘Why not do it?’ even when the indication is minimal or nonexistent,” he added.
Dr. Lim said he agrees that “any new medical technology requires thoughtful evaluation and appropriate patient selection in order to ensure optimal patient outcomes.”
That’s where the tumor board has been especially beneficial.
“We have found great benefit in reviewing potential RFA cases in a multidisciplinary fashion within our tumor board and would recommend other institutions to consider it,” he noted. In the absence of a tumor board, “at a minimum, a thyroid specialist should be involved in the evaluation of a potential thyroid RFA patient prior to ablation treatment,” he advised.
Tumor board was able to identify a small subset of patients for surgery
In his research presented at the 90th Annual Meeting of the American Thyroid Association (ATA), Dr. Lim and colleagues evaluated the tumor board’s efficacy in altering diagnosis and treatment plans in a retrospective review of cases presented to the board for RFA consideration since its inception in July 2020 through June 2021.
Over the study period, 65 patients with biopsy-proven benign thyroid nodules were newly referred for RFA, with 58 referred for mass effect symptoms and seven for autonomous function.
After the multidisciplinary review, about half of the cases, 37 (56.9%), were approved for RFA.
Of the remainder, 22 (33.8%) were determined to need additional studies, just two (3.0%) were recommended for surgery, and four (6.2%) were recommended to not receive any intervention.
Of the 22 cases recommended for additional studies, 15 were subsequently recommended for RFA and four were recommended to receive surgery due to suspicious clinical findings.
Of those that underwent surgery, two showed thyroid cancer on final pathology.
Among the nodules recommended to RFA, the average nodule volume was 15.1 mL, whereas the average volume for those recommended for surgery was 40.9 mL (P = .08).
No significant complications occurred among patients that underwent RFA or those who had surgery.
“The tumor board’s multidisciplinary review was able to identify high-risk features in some patients with benign biopsies. This led to a change in recommendation from RFA to surgery for possible malignancy in a small subset of patients,” Dr. Lim noted.
In a separate analysis, Dr. Lim and colleagues reported that, among patients treated with RFA (with a mean baseline nodule volume of 11.9 mL), mean nodule volume was 6.4 mL after 1 month, 4.5 mL after 3 months, and 3.8 mL at 6 months, which were all significantly reduced versus baseline (P < .001). Similar improvements were also reported in symptom and cosmetic scores at each timepoint (all P < .001).
There were no cases of postprocedural hypothyroidism or symptomatic thyrotoxicosis.
Underlining that patients can expect noticeable improvement in symptom scores by their 30-day visit, Dr. Lim noted that patients should be warned of some early swelling.
“It is important to inform patients that they may have swelling of their treated nodule immediately after the procedure, but this should subside within a few days,” he said.
Outpatient RFA safe and efficacious
In a separate study also presented at the meeting, three practitioners described their experiences with RFA in their outpatient thyroid practices in San Antonio; Santa Monica, California; and Gettysburg, Pennsylvania.
Overall, there were 68 cases involving benign, class II thyroid nodules, and the authors reported average procedure times of under an hour, with actual RFA time varying from 7 to 22 minutes.
Of note, for nodules larger than 4.5 cm, two procedures were necessary to achieve desired results.
Excluding the larger nodules requiring more than one procedure, there was an average decrease in nodule size of 48% at 1 month and a decrease of 82% after 3 months in more than 80% of cases.
None of the cases required surgery. There were no major complications, and all patients had preserved baseline thyroid function.
“This preliminary study of 68 patients shows how thyroid RFA is safe and efficacious when performed in an endocrine outpatient office practice,” Kathleen Hands, MD, of the Thyroid Center of South Texas, and coauthors concluded.
Insurance coverage an issue in U.S.
Among much larger studies demonstrating the safety and efficacy of RFA for benign nodules, a study of 450 Chinese patients published in January showed RFA to be superior to conventional thyroidectomy in terms of patient satisfaction, postoperative quality of life, and shorter hospital stay, although the caveat was it took longer to achieve nodule volume reduction.
But if RFA use is to become more widespread in the United States, a key obstacle is that insurance companies generally do not cover the procedure. Although patients in Dr. Lim’s analyses did have coverage, it didn’t come easily, he said.
“Thankfully, all of our patients have been approved by insurance, and no one has had to pay by themselves, but this has sometimes required multiple appeals to the insurance company,” Dr. Lim said.
“The American Association of Endocrine Surgeons and Society of Interventional Radiology are both working towards getting this valuable treatment more readily accepted by more insurance companies,” he said.
Dr. Lim and Dr. Singer have reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
And in one case, a hospital has taken the unique step of forming a multidisciplinary thyroid nodule RFA tumor board, which helps in the often tricky decision-making process that is involved.
“Our multidisciplinary RFA tumor board has been invaluable in this process, and it is the only one of its kind in the nation that I’m aware of,” James Lim, MD, of the Division of Surgical Oncology, Thyroid, and Parathyroid Center at Oregon Health Sciences University (OHSU), told this news organization.
Dr. Lim reports receiving referrals from “all avenues, some from thyroid specialists and others from nonthyroid specialists such as primary care practitioners or patient self-referrals.”
“Because of this, our centralized process of multidisciplinary review ensures that each patient is evaluated thoroughly through each thyroid specialists’ lens to optimize patient outcomes,” noted Dr. Lim, an assistant professor of endocrine surgery.
The RFA tumor board consists of experts in all specialties involved in thyroid nodule assessment and treatment, including surgeons, interventional radiologists, and endocrinologists.
Just because you can, doesn’t mean you should
However, there should be some caution that although there is enthusiasm regarding this noninvasive alternative to surgery, there is another option, that of mere observation, which is appropriate in many cases of thyroid nodules and should not be overlooked.
“For a number of reasons, the key to keep in mind is that, just because we can do something doesn’t mean we should,” Michael Singer, MD, director of the Division of Thyroid & Parathyroid Surgery, Department of Otolaryngology – Head and Neck Surgery, at the Henry Ford Health System, Detroit, said in an interview.
While emphasizing that he believes RFA to be a promising technology that will likely benefit patients in the future, Dr. Singer voiced concern about the approach becoming an easy choice – particularly if profit is to be had – when observation is a clear alternative. “If RFA becomes seen as an opportunity to create revenue, potential conflicts of interest may arise,” he said.
“As it is not a major procedure with a dramatic risk profile, my concern is that some clinicians [could] adopt the attitude of ‘Why not do it?’ even when the indication is minimal or nonexistent,” he added.
Dr. Lim said he agrees that “any new medical technology requires thoughtful evaluation and appropriate patient selection in order to ensure optimal patient outcomes.”
That’s where the tumor board has been especially beneficial.
“We have found great benefit in reviewing potential RFA cases in a multidisciplinary fashion within our tumor board and would recommend other institutions to consider it,” he noted. In the absence of a tumor board, “at a minimum, a thyroid specialist should be involved in the evaluation of a potential thyroid RFA patient prior to ablation treatment,” he advised.
Tumor board was able to identify a small subset of patients for surgery
In his research presented at the 90th Annual Meeting of the American Thyroid Association (ATA), Dr. Lim and colleagues evaluated the tumor board’s efficacy in altering diagnosis and treatment plans in a retrospective review of cases presented to the board for RFA consideration since its inception in July 2020 through June 2021.
Over the study period, 65 patients with biopsy-proven benign thyroid nodules were newly referred for RFA, with 58 referred for mass effect symptoms and seven for autonomous function.
After the multidisciplinary review, about half of the cases, 37 (56.9%), were approved for RFA.
Of the remainder, 22 (33.8%) were determined to need additional studies, just two (3.0%) were recommended for surgery, and four (6.2%) were recommended to not receive any intervention.
Of the 22 cases recommended for additional studies, 15 were subsequently recommended for RFA and four were recommended to receive surgery due to suspicious clinical findings.
Of those that underwent surgery, two showed thyroid cancer on final pathology.
Among the nodules recommended to RFA, the average nodule volume was 15.1 mL, whereas the average volume for those recommended for surgery was 40.9 mL (P = .08).
No significant complications occurred among patients that underwent RFA or those who had surgery.
“The tumor board’s multidisciplinary review was able to identify high-risk features in some patients with benign biopsies. This led to a change in recommendation from RFA to surgery for possible malignancy in a small subset of patients,” Dr. Lim noted.
In a separate analysis, Dr. Lim and colleagues reported that, among patients treated with RFA (with a mean baseline nodule volume of 11.9 mL), mean nodule volume was 6.4 mL after 1 month, 4.5 mL after 3 months, and 3.8 mL at 6 months, which were all significantly reduced versus baseline (P < .001). Similar improvements were also reported in symptom and cosmetic scores at each timepoint (all P < .001).
There were no cases of postprocedural hypothyroidism or symptomatic thyrotoxicosis.
Underlining that patients can expect noticeable improvement in symptom scores by their 30-day visit, Dr. Lim noted that patients should be warned of some early swelling.
“It is important to inform patients that they may have swelling of their treated nodule immediately after the procedure, but this should subside within a few days,” he said.
Outpatient RFA safe and efficacious
In a separate study also presented at the meeting, three practitioners described their experiences with RFA in their outpatient thyroid practices in San Antonio; Santa Monica, California; and Gettysburg, Pennsylvania.
Overall, there were 68 cases involving benign, class II thyroid nodules, and the authors reported average procedure times of under an hour, with actual RFA time varying from 7 to 22 minutes.
Of note, for nodules larger than 4.5 cm, two procedures were necessary to achieve desired results.
Excluding the larger nodules requiring more than one procedure, there was an average decrease in nodule size of 48% at 1 month and a decrease of 82% after 3 months in more than 80% of cases.
None of the cases required surgery. There were no major complications, and all patients had preserved baseline thyroid function.
“This preliminary study of 68 patients shows how thyroid RFA is safe and efficacious when performed in an endocrine outpatient office practice,” Kathleen Hands, MD, of the Thyroid Center of South Texas, and coauthors concluded.
Insurance coverage an issue in U.S.
Among much larger studies demonstrating the safety and efficacy of RFA for benign nodules, a study of 450 Chinese patients published in January showed RFA to be superior to conventional thyroidectomy in terms of patient satisfaction, postoperative quality of life, and shorter hospital stay, although the caveat was it took longer to achieve nodule volume reduction.
But if RFA use is to become more widespread in the United States, a key obstacle is that insurance companies generally do not cover the procedure. Although patients in Dr. Lim’s analyses did have coverage, it didn’t come easily, he said.
“Thankfully, all of our patients have been approved by insurance, and no one has had to pay by themselves, but this has sometimes required multiple appeals to the insurance company,” Dr. Lim said.
“The American Association of Endocrine Surgeons and Society of Interventional Radiology are both working towards getting this valuable treatment more readily accepted by more insurance companies,” he said.
Dr. Lim and Dr. Singer have reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.
And in one case, a hospital has taken the unique step of forming a multidisciplinary thyroid nodule RFA tumor board, which helps in the often tricky decision-making process that is involved.
“Our multidisciplinary RFA tumor board has been invaluable in this process, and it is the only one of its kind in the nation that I’m aware of,” James Lim, MD, of the Division of Surgical Oncology, Thyroid, and Parathyroid Center at Oregon Health Sciences University (OHSU), told this news organization.
Dr. Lim reports receiving referrals from “all avenues, some from thyroid specialists and others from nonthyroid specialists such as primary care practitioners or patient self-referrals.”
“Because of this, our centralized process of multidisciplinary review ensures that each patient is evaluated thoroughly through each thyroid specialists’ lens to optimize patient outcomes,” noted Dr. Lim, an assistant professor of endocrine surgery.
The RFA tumor board consists of experts in all specialties involved in thyroid nodule assessment and treatment, including surgeons, interventional radiologists, and endocrinologists.
Just because you can, doesn’t mean you should
However, there should be some caution that although there is enthusiasm regarding this noninvasive alternative to surgery, there is another option, that of mere observation, which is appropriate in many cases of thyroid nodules and should not be overlooked.
“For a number of reasons, the key to keep in mind is that, just because we can do something doesn’t mean we should,” Michael Singer, MD, director of the Division of Thyroid & Parathyroid Surgery, Department of Otolaryngology – Head and Neck Surgery, at the Henry Ford Health System, Detroit, said in an interview.
While emphasizing that he believes RFA to be a promising technology that will likely benefit patients in the future, Dr. Singer voiced concern about the approach becoming an easy choice – particularly if profit is to be had – when observation is a clear alternative. “If RFA becomes seen as an opportunity to create revenue, potential conflicts of interest may arise,” he said.
“As it is not a major procedure with a dramatic risk profile, my concern is that some clinicians [could] adopt the attitude of ‘Why not do it?’ even when the indication is minimal or nonexistent,” he added.
Dr. Lim said he agrees that “any new medical technology requires thoughtful evaluation and appropriate patient selection in order to ensure optimal patient outcomes.”
That’s where the tumor board has been especially beneficial.
“We have found great benefit in reviewing potential RFA cases in a multidisciplinary fashion within our tumor board and would recommend other institutions to consider it,” he noted. In the absence of a tumor board, “at a minimum, a thyroid specialist should be involved in the evaluation of a potential thyroid RFA patient prior to ablation treatment,” he advised.
Tumor board was able to identify a small subset of patients for surgery
In his research presented at the 90th Annual Meeting of the American Thyroid Association (ATA), Dr. Lim and colleagues evaluated the tumor board’s efficacy in altering diagnosis and treatment plans in a retrospective review of cases presented to the board for RFA consideration since its inception in July 2020 through June 2021.
Over the study period, 65 patients with biopsy-proven benign thyroid nodules were newly referred for RFA, with 58 referred for mass effect symptoms and seven for autonomous function.
After the multidisciplinary review, about half of the cases, 37 (56.9%), were approved for RFA.
Of the remainder, 22 (33.8%) were determined to need additional studies, just two (3.0%) were recommended for surgery, and four (6.2%) were recommended to not receive any intervention.
Of the 22 cases recommended for additional studies, 15 were subsequently recommended for RFA and four were recommended to receive surgery due to suspicious clinical findings.
Of those that underwent surgery, two showed thyroid cancer on final pathology.
Among the nodules recommended to RFA, the average nodule volume was 15.1 mL, whereas the average volume for those recommended for surgery was 40.9 mL (P = .08).
No significant complications occurred among patients that underwent RFA or those who had surgery.
“The tumor board’s multidisciplinary review was able to identify high-risk features in some patients with benign biopsies. This led to a change in recommendation from RFA to surgery for possible malignancy in a small subset of patients,” Dr. Lim noted.
In a separate analysis, Dr. Lim and colleagues reported that, among patients treated with RFA (with a mean baseline nodule volume of 11.9 mL), mean nodule volume was 6.4 mL after 1 month, 4.5 mL after 3 months, and 3.8 mL at 6 months, which were all significantly reduced versus baseline (P < .001). Similar improvements were also reported in symptom and cosmetic scores at each timepoint (all P < .001).
There were no cases of postprocedural hypothyroidism or symptomatic thyrotoxicosis.
Underlining that patients can expect noticeable improvement in symptom scores by their 30-day visit, Dr. Lim noted that patients should be warned of some early swelling.
“It is important to inform patients that they may have swelling of their treated nodule immediately after the procedure, but this should subside within a few days,” he said.
Outpatient RFA safe and efficacious
In a separate study also presented at the meeting, three practitioners described their experiences with RFA in their outpatient thyroid practices in San Antonio; Santa Monica, California; and Gettysburg, Pennsylvania.
Overall, there were 68 cases involving benign, class II thyroid nodules, and the authors reported average procedure times of under an hour, with actual RFA time varying from 7 to 22 minutes.
Of note, for nodules larger than 4.5 cm, two procedures were necessary to achieve desired results.
Excluding the larger nodules requiring more than one procedure, there was an average decrease in nodule size of 48% at 1 month and a decrease of 82% after 3 months in more than 80% of cases.
None of the cases required surgery. There were no major complications, and all patients had preserved baseline thyroid function.
“This preliminary study of 68 patients shows how thyroid RFA is safe and efficacious when performed in an endocrine outpatient office practice,” Kathleen Hands, MD, of the Thyroid Center of South Texas, and coauthors concluded.
Insurance coverage an issue in U.S.
Among much larger studies demonstrating the safety and efficacy of RFA for benign nodules, a study of 450 Chinese patients published in January showed RFA to be superior to conventional thyroidectomy in terms of patient satisfaction, postoperative quality of life, and shorter hospital stay, although the caveat was it took longer to achieve nodule volume reduction.
But if RFA use is to become more widespread in the United States, a key obstacle is that insurance companies generally do not cover the procedure. Although patients in Dr. Lim’s analyses did have coverage, it didn’t come easily, he said.
“Thankfully, all of our patients have been approved by insurance, and no one has had to pay by themselves, but this has sometimes required multiple appeals to the insurance company,” Dr. Lim said.
“The American Association of Endocrine Surgeons and Society of Interventional Radiology are both working towards getting this valuable treatment more readily accepted by more insurance companies,” he said.
Dr. Lim and Dr. Singer have reported no relevant financial relationships.
A version of this article first appeared on Medscape.com.