User login
Richard Franki is the associate editor who writes and creates graphs. He started with the company in 1987, when it was known as the International Medical News Group. In his years as a journalist, Richard has worked for Cap Cities/ABC, Disney, Harcourt, Elsevier, Quadrant, Frontline, and Internet Brands. In the 1990s, he was a contributor to the ill-fated Indications column, predecessor of Livin' on the MDedge.
Cancer survival still lower for African Americans
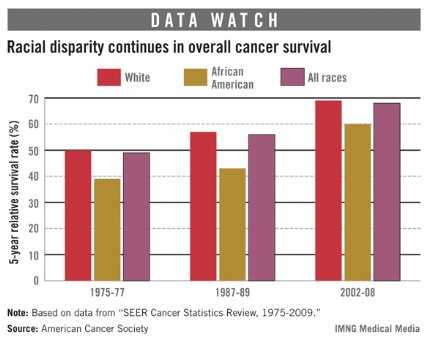
The 5-year cancer survival rate for African Americans has risen 54% since the 1970s, but continues to be lower than that of whites, according to a report from the American Cancer Society.
Data from the Surveillance, Epidemiology, and End Results (SEER) database show that the 5-year relative survival rate in 2002-2008 was 60% for blacks, 69% for whites, and 68% for all races. Those numbers are all up significantly since 1975-77, when the rates for all cancers were 39% for African Americans, 50% for whites, and 49% for all races, the ACS reported.
The differences between blacks and whites varied among specific cancer sites. In 2002-2008, the 5-year survival for melanoma was 70% for blacks and 93% for whites. For colon cancer, the rate was 55% for blacks and 66% for whites. For kidney and renal pelvis cancer, however, the rates were much closer: 70% for blacks and 72% for whites. The only sites for which African Americans had higher survival rates were the brain (41%, compared with 34%) and the stomach (28%, compared with 27%), the ACS said.
The 5-year cancer survival rate for African Americans has risen 54% since the 1970s, but continues to be lower than that of whites, according to a report from the American Cancer Society.
Data from the Surveillance, Epidemiology, and End Results (SEER) database show that the 5-year relative survival rate in 2002-2008 was 60% for blacks, 69% for whites, and 68% for all races. Those numbers are all up significantly since 1975-77, when the rates for all cancers were 39% for African Americans, 50% for whites, and 49% for all races, the ACS reported.
The differences between blacks and whites varied among specific cancer sites. In 2002-2008, the 5-year survival for melanoma was 70% for blacks and 93% for whites. For colon cancer, the rate was 55% for blacks and 66% for whites. For kidney and renal pelvis cancer, however, the rates were much closer: 70% for blacks and 72% for whites. The only sites for which African Americans had higher survival rates were the brain (41%, compared with 34%) and the stomach (28%, compared with 27%), the ACS said.
The 5-year cancer survival rate for African Americans has risen 54% since the 1970s, but continues to be lower than that of whites, according to a report from the American Cancer Society.
Data from the Surveillance, Epidemiology, and End Results (SEER) database show that the 5-year relative survival rate in 2002-2008 was 60% for blacks, 69% for whites, and 68% for all races. Those numbers are all up significantly since 1975-77, when the rates for all cancers were 39% for African Americans, 50% for whites, and 49% for all races, the ACS reported.
The differences between blacks and whites varied among specific cancer sites. In 2002-2008, the 5-year survival for melanoma was 70% for blacks and 93% for whites. For colon cancer, the rate was 55% for blacks and 66% for whites. For kidney and renal pelvis cancer, however, the rates were much closer: 70% for blacks and 72% for whites. The only sites for which African Americans had higher survival rates were the brain (41%, compared with 34%) and the stomach (28%, compared with 27%), the ACS said.
States spend little tobacco revenue on prevention
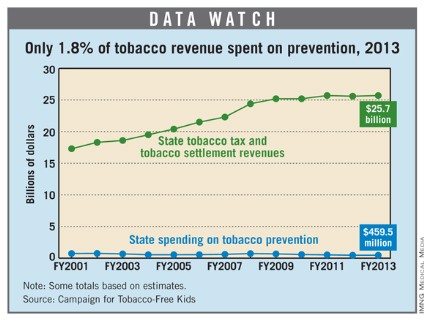
States’ spending on tobacco prevention for 2013 will total $459.5 million, or 1.8% of the $25.7 billion they will receive in revenue from tobacco taxes and the 1998 tobacco settlement, according to a report from the Campaign for Tobacco-Free Kids.
The revenue collected is the largest for a single fiscal year, while the amount spent is the second lowest since states started to receive tobacco settlement funds in 1999, the report noted.
Since 2001, the annual tobacco-related revenue collected by the states has gone up by almost 49%, but spending on tobacco prevention and cessation programs has dropped by nearly 37%, according to the report, which was also sponsored by the American Heart Association, the American Cancer Society Cancer Action Network, the American Lung Association, the Robert Wood Johnson Foundation, and Americans for Nonsmokers’ Rights.
States’ spending on tobacco prevention for 2013 will total $459.5 million, or 1.8% of the $25.7 billion they will receive in revenue from tobacco taxes and the 1998 tobacco settlement, according to a report from the Campaign for Tobacco-Free Kids.
The revenue collected is the largest for a single fiscal year, while the amount spent is the second lowest since states started to receive tobacco settlement funds in 1999, the report noted.
Since 2001, the annual tobacco-related revenue collected by the states has gone up by almost 49%, but spending on tobacco prevention and cessation programs has dropped by nearly 37%, according to the report, which was also sponsored by the American Heart Association, the American Cancer Society Cancer Action Network, the American Lung Association, the Robert Wood Johnson Foundation, and Americans for Nonsmokers’ Rights.
States’ spending on tobacco prevention for 2013 will total $459.5 million, or 1.8% of the $25.7 billion they will receive in revenue from tobacco taxes and the 1998 tobacco settlement, according to a report from the Campaign for Tobacco-Free Kids.
The revenue collected is the largest for a single fiscal year, while the amount spent is the second lowest since states started to receive tobacco settlement funds in 1999, the report noted.
Since 2001, the annual tobacco-related revenue collected by the states has gone up by almost 49%, but spending on tobacco prevention and cessation programs has dropped by nearly 37%, according to the report, which was also sponsored by the American Heart Association, the American Cancer Society Cancer Action Network, the American Lung Association, the Robert Wood Johnson Foundation, and Americans for Nonsmokers’ Rights.
Medicaid's share of state budgets nears 24%
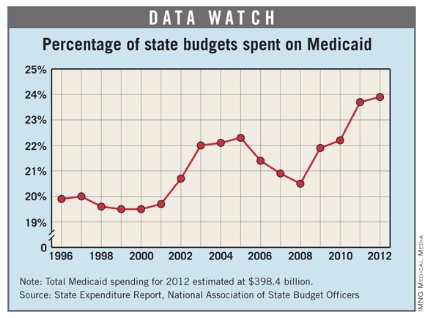
In fiscal 2012, total state spending on Medicaid rose to an estimated $398.4 billion, bringing the program’s average share of state budgets to 23.9%, according to a report from the National Association of State Budget Officers.
Medicaid has accounted for the single largest portion of states’ total spending each year since 2009, outpacing elementary/secondary education, the association’s data show.
The increase in total spending from 2011 to 2012 was 1.2%, which is considerably less than the 9.6% increase from 2010 to 2011 and "significantly below historical trends," the report noted.

In fiscal 2012, total state spending on Medicaid rose to an estimated $398.4 billion, bringing the program’s average share of state budgets to 23.9%, according to a report from the National Association of State Budget Officers.
Medicaid has accounted for the single largest portion of states’ total spending each year since 2009, outpacing elementary/secondary education, the association’s data show.
The increase in total spending from 2011 to 2012 was 1.2%, which is considerably less than the 9.6% increase from 2010 to 2011 and "significantly below historical trends," the report noted.

In fiscal 2012, total state spending on Medicaid rose to an estimated $398.4 billion, bringing the program’s average share of state budgets to 23.9%, according to a report from the National Association of State Budget Officers.
Medicaid has accounted for the single largest portion of states’ total spending each year since 2009, outpacing elementary/secondary education, the association’s data show.
The increase in total spending from 2011 to 2012 was 1.2%, which is considerably less than the 9.6% increase from 2010 to 2011 and "significantly below historical trends," the report noted.

States fall short on tobacco prevention
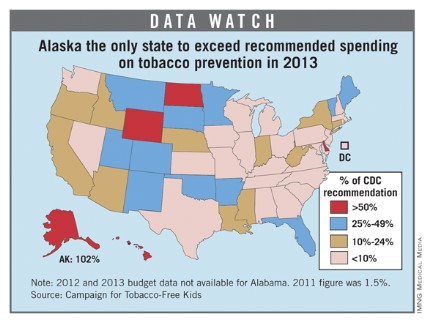
Alaska is the only state exceeding the Centers for Disease Control and Prevention’s recommended level of spending on tobacco prevention programs, according to a report from the Campaign for Tobacco-Free Kids.
In fiscal year 2013, Alaska will spend almost 102% of the $10.7 million recommended by the CDC. The next state, North Dakota at 88%, reaches the recommended level if both state and federal funding is counted. Only three other states – Delaware, Wyoming, and Hawaii – provide even half of the CDC recommendation, the report said.
California is ranked 22nd, spending 14.1% ($62 million) of the $442 million recommended by the CDC. Texas, the second-most populous state, ranks 41st, with funding at 2.4% of the CDC’s target of $266 million.
For 2013, the CDC recommended that the states spend $3.7 billion on tobacco prevention. Actual state spending for the fiscal year will total $459.5 million, or 12.4% of the CDC target, according to the report, which was also sponsored by the American Heart Association, the American Cancer Society Cancer Action Network, the American Lung Association, the Robert Wood Johnson Foundation, and Americans for Nonsmokers’ Rights.
Alaska is the only state exceeding the Centers for Disease Control and Prevention’s recommended level of spending on tobacco prevention programs, according to a report from the Campaign for Tobacco-Free Kids.
In fiscal year 2013, Alaska will spend almost 102% of the $10.7 million recommended by the CDC. The next state, North Dakota at 88%, reaches the recommended level if both state and federal funding is counted. Only three other states – Delaware, Wyoming, and Hawaii – provide even half of the CDC recommendation, the report said.
California is ranked 22nd, spending 14.1% ($62 million) of the $442 million recommended by the CDC. Texas, the second-most populous state, ranks 41st, with funding at 2.4% of the CDC’s target of $266 million.
For 2013, the CDC recommended that the states spend $3.7 billion on tobacco prevention. Actual state spending for the fiscal year will total $459.5 million, or 12.4% of the CDC target, according to the report, which was also sponsored by the American Heart Association, the American Cancer Society Cancer Action Network, the American Lung Association, the Robert Wood Johnson Foundation, and Americans for Nonsmokers’ Rights.
Alaska is the only state exceeding the Centers for Disease Control and Prevention’s recommended level of spending on tobacco prevention programs, according to a report from the Campaign for Tobacco-Free Kids.
In fiscal year 2013, Alaska will spend almost 102% of the $10.7 million recommended by the CDC. The next state, North Dakota at 88%, reaches the recommended level if both state and federal funding is counted. Only three other states – Delaware, Wyoming, and Hawaii – provide even half of the CDC recommendation, the report said.
California is ranked 22nd, spending 14.1% ($62 million) of the $442 million recommended by the CDC. Texas, the second-most populous state, ranks 41st, with funding at 2.4% of the CDC’s target of $266 million.
For 2013, the CDC recommended that the states spend $3.7 billion on tobacco prevention. Actual state spending for the fiscal year will total $459.5 million, or 12.4% of the CDC target, according to the report, which was also sponsored by the American Heart Association, the American Cancer Society Cancer Action Network, the American Lung Association, the Robert Wood Johnson Foundation, and Americans for Nonsmokers’ Rights.
Marijuana Use, Perceptions Changing in 12th Graders
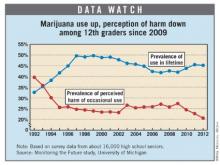
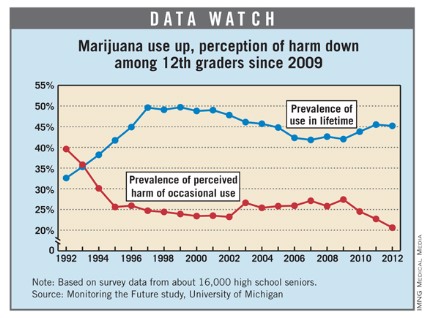
After remaining fairly steady for 14 years, the number of high school seniors who believe there is great risk associated with occasional marijuana use has dropped each year since 2009, according to the Monitoring the Future study.
That drop was accompanied by an increase in use. The prevalence of marijuana use in those 12th graders’ lifetimes has gone up 7.6% since 2009, halting a decline that lasted over a decade, the study shows.
There were approximately 16,000 seniors among the 45,449 students who took part in the Monitoring the Future survey in 2012. The survey is funded by the National Institute on Drug Abuse and conducted by University of Michigan investigators.
After remaining fairly steady for 14 years, the number of high school seniors who believe there is great risk associated with occasional marijuana use has dropped each year since 2009, according to the Monitoring the Future study.
That drop was accompanied by an increase in use. The prevalence of marijuana use in those 12th graders’ lifetimes has gone up 7.6% since 2009, halting a decline that lasted over a decade, the study shows.
There were approximately 16,000 seniors among the 45,449 students who took part in the Monitoring the Future survey in 2012. The survey is funded by the National Institute on Drug Abuse and conducted by University of Michigan investigators.
After remaining fairly steady for 14 years, the number of high school seniors who believe there is great risk associated with occasional marijuana use has dropped each year since 2009, according to the Monitoring the Future study.
That drop was accompanied by an increase in use. The prevalence of marijuana use in those 12th graders’ lifetimes has gone up 7.6% since 2009, halting a decline that lasted over a decade, the study shows.
There were approximately 16,000 seniors among the 45,449 students who took part in the Monitoring the Future survey in 2012. The survey is funded by the National Institute on Drug Abuse and conducted by University of Michigan investigators.
Vermont tops 'America's Health Rankings' for 2012
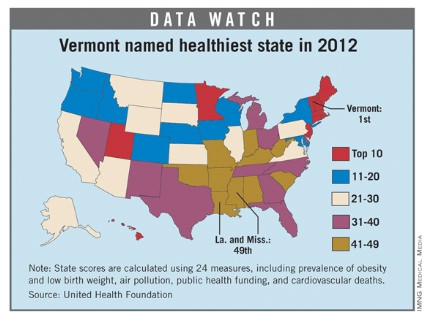
For the fourth consecutive year, Vermont earned the top health rating in the United States, according to the 2012 edition of "America’s Health Rankings."
Hawaii, which has never finished out of the top six since the rankings began in 1990, was second, followed by New Hampshire, Massachusetts, and Minnesota. Mississippi and Louisiana were tied for 49th as the least healthy states, with Arkansas, West Virginia, and South Carolina making up the rest of the bottom five.
The states that showed the greatest improvement since last year were Alaska (up seven places) and Oklahoma (up five slots). The states that fell the furthest in the rankings from 2011 were Michigan (down seven) and West Virginia (down six), according to the report.
"America’s Health Rankings" is published jointly by United Health Foundation, the American Public Health Association, and the Partnership for Prevention. The private, not-for-profit United Health Foundation was founded in 1999 by UnitedHealth Group, which operates UnitedHealthcare.
For the fourth consecutive year, Vermont earned the top health rating in the United States, according to the 2012 edition of "America’s Health Rankings."
Hawaii, which has never finished out of the top six since the rankings began in 1990, was second, followed by New Hampshire, Massachusetts, and Minnesota. Mississippi and Louisiana were tied for 49th as the least healthy states, with Arkansas, West Virginia, and South Carolina making up the rest of the bottom five.
The states that showed the greatest improvement since last year were Alaska (up seven places) and Oklahoma (up five slots). The states that fell the furthest in the rankings from 2011 were Michigan (down seven) and West Virginia (down six), according to the report.
"America’s Health Rankings" is published jointly by United Health Foundation, the American Public Health Association, and the Partnership for Prevention. The private, not-for-profit United Health Foundation was founded in 1999 by UnitedHealth Group, which operates UnitedHealthcare.
For the fourth consecutive year, Vermont earned the top health rating in the United States, according to the 2012 edition of "America’s Health Rankings."
Hawaii, which has never finished out of the top six since the rankings began in 1990, was second, followed by New Hampshire, Massachusetts, and Minnesota. Mississippi and Louisiana were tied for 49th as the least healthy states, with Arkansas, West Virginia, and South Carolina making up the rest of the bottom five.
The states that showed the greatest improvement since last year were Alaska (up seven places) and Oklahoma (up five slots). The states that fell the furthest in the rankings from 2011 were Michigan (down seven) and West Virginia (down six), according to the report.
"America’s Health Rankings" is published jointly by United Health Foundation, the American Public Health Association, and the Partnership for Prevention. The private, not-for-profit United Health Foundation was founded in 1999 by UnitedHealth Group, which operates UnitedHealthcare.
Long-term income growth slow for physicians
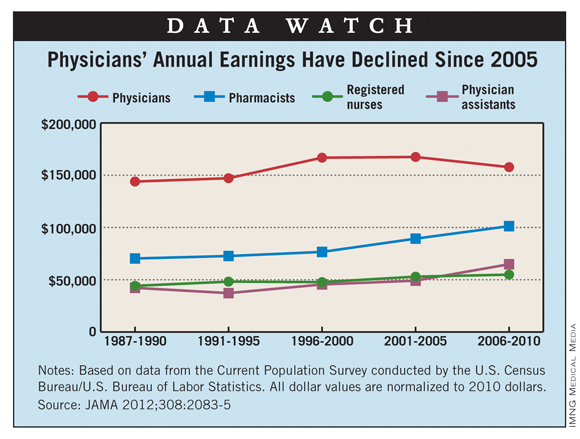
Since 1987, physicians’ income growth has been exceeded by other health care professionals, according to an analysis of survey data from the Census Bureau and the Bureau of Labor Statistics.
Data from the Current Population Survey show that adjusted annual income for physicians rose 9.6% from 1987-1990 to 2006-2010, compared with increases of 54% for physician assistants, 44% for pharmacists, and 24% for registered nurses, said Seth A. Seabury, Ph.D., of the Rand Corp. in Santa Monica, Calif., and his associates.
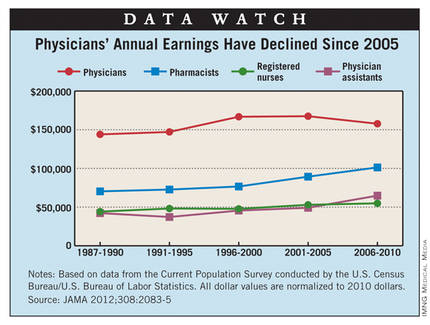
Since the 2001-2005 survey, median annual earnings for physicians have declined from $167,478 to $157,751, they reported.
The sample for this study was 30,556 respondents who identified themselves as health professionals, including 6,258 physicians. The analysis was limited to workers older than 35 years of age.
Since 1987, physicians’ income growth has been exceeded by other health care professionals, according to an analysis of survey data from the Census Bureau and the Bureau of Labor Statistics.
Data from the Current Population Survey show that adjusted annual income for physicians rose 9.6% from 1987-1990 to 2006-2010, compared with increases of 54% for physician assistants, 44% for pharmacists, and 24% for registered nurses, said Seth A. Seabury, Ph.D., of the Rand Corp. in Santa Monica, Calif., and his associates.

Since the 2001-2005 survey, median annual earnings for physicians have declined from $167,478 to $157,751, they reported.
The sample for this study was 30,556 respondents who identified themselves as health professionals, including 6,258 physicians. The analysis was limited to workers older than 35 years of age.
Since 1987, physicians’ income growth has been exceeded by other health care professionals, according to an analysis of survey data from the Census Bureau and the Bureau of Labor Statistics.
Data from the Current Population Survey show that adjusted annual income for physicians rose 9.6% from 1987-1990 to 2006-2010, compared with increases of 54% for physician assistants, 44% for pharmacists, and 24% for registered nurses, said Seth A. Seabury, Ph.D., of the Rand Corp. in Santa Monica, Calif., and his associates.

Since the 2001-2005 survey, median annual earnings for physicians have declined from $167,478 to $157,751, they reported.
The sample for this study was 30,556 respondents who identified themselves as health professionals, including 6,258 physicians. The analysis was limited to workers older than 35 years of age.
States' Plans for Insurance Exchanges: Latest Info
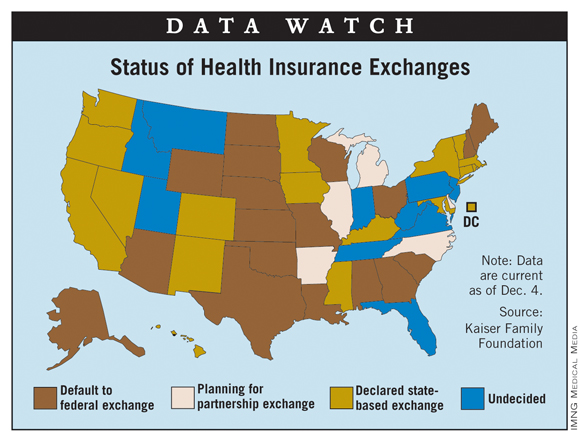
As of Dec. 4, a total of 17 states and the District of Columbia had indicated that they will establish the state-based insurance exchanges mandated by the Affordable Care Act, according to the Kaiser Family Foundation.
California and New York are the largest states to commit to creating their own exchanges, but Texas and Ohio are among the 18 states that have indicated their intention to default to federally facilitated exchanges. Five states, including Illinois and Michigan, are planning to partner with the federal government to operate their exchanges; 10 states, Florida and Pennsylvania among them, are still undecided, Kaiser reported.

As of Dec. 4, a total of 17 states and the District of Columbia had indicated that they will establish the state-based insurance exchanges mandated by the Affordable Care Act, according to the Kaiser Family Foundation.
California and New York are the largest states to commit to creating their own exchanges, but Texas and Ohio are among the 18 states that have indicated their intention to default to federally facilitated exchanges. Five states, including Illinois and Michigan, are planning to partner with the federal government to operate their exchanges; 10 states, Florida and Pennsylvania among them, are still undecided, Kaiser reported.

As of Dec. 4, a total of 17 states and the District of Columbia had indicated that they will establish the state-based insurance exchanges mandated by the Affordable Care Act, according to the Kaiser Family Foundation.
California and New York are the largest states to commit to creating their own exchanges, but Texas and Ohio are among the 18 states that have indicated their intention to default to federally facilitated exchanges. Five states, including Illinois and Michigan, are planning to partner with the federal government to operate their exchanges; 10 states, Florida and Pennsylvania among them, are still undecided, Kaiser reported.

Kentucky Leads U.S. in Adult COPD Prevalence
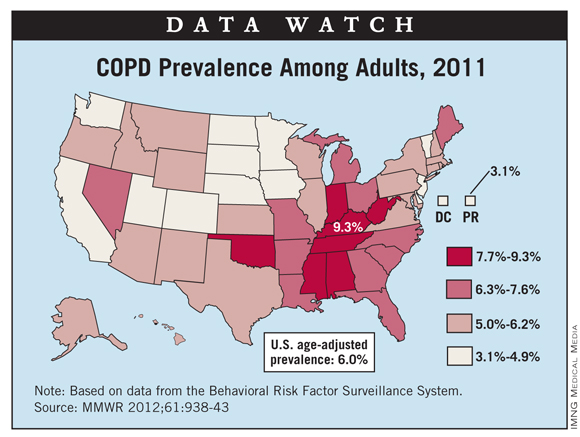
Kentucky had the highest prevalence of chronic obstructive pulmonary disease in adults, 9.3%, in 2011, according to a study in Morbidity and Mortality Weekly Report.
The data for the first-ever report of state-specific prevalence of COPD among adults in all 50 states, the District of Columbia, and Puerto Rico come from the Behavioral Risk Factor Surveillance System. Among the 498,225 respondents to the survey, 39,038 reported that they had been told by a physician that they had COPD, for an overall prevalence of 6.3% (age-adjusted to 6%).
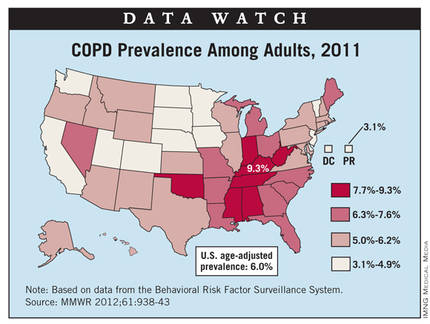
At 3.1%, Puerto Rico had the lowest COPD prevalence in the United States in 2011. The states with the lowest prevalence were Minnesota and Washington, both at 3.9%, according to the report.
Kentucky had the highest prevalence of chronic obstructive pulmonary disease in adults, 9.3%, in 2011, according to a study in Morbidity and Mortality Weekly Report.
The data for the first-ever report of state-specific prevalence of COPD among adults in all 50 states, the District of Columbia, and Puerto Rico come from the Behavioral Risk Factor Surveillance System. Among the 498,225 respondents to the survey, 39,038 reported that they had been told by a physician that they had COPD, for an overall prevalence of 6.3% (age-adjusted to 6%).

At 3.1%, Puerto Rico had the lowest COPD prevalence in the United States in 2011. The states with the lowest prevalence were Minnesota and Washington, both at 3.9%, according to the report.
Kentucky had the highest prevalence of chronic obstructive pulmonary disease in adults, 9.3%, in 2011, according to a study in Morbidity and Mortality Weekly Report.
The data for the first-ever report of state-specific prevalence of COPD among adults in all 50 states, the District of Columbia, and Puerto Rico come from the Behavioral Risk Factor Surveillance System. Among the 498,225 respondents to the survey, 39,038 reported that they had been told by a physician that they had COPD, for an overall prevalence of 6.3% (age-adjusted to 6%).

At 3.1%, Puerto Rico had the lowest COPD prevalence in the United States in 2011. The states with the lowest prevalence were Minnesota and Washington, both at 3.9%, according to the report.
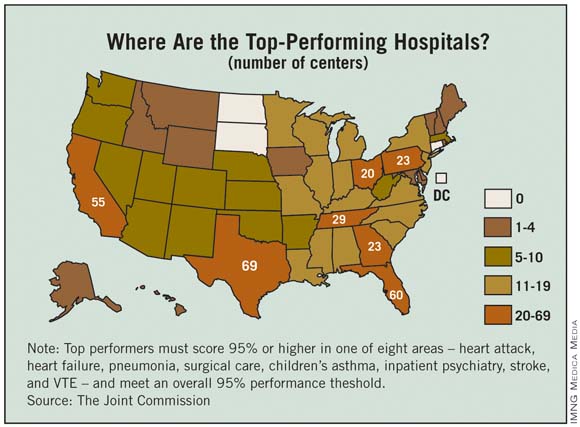
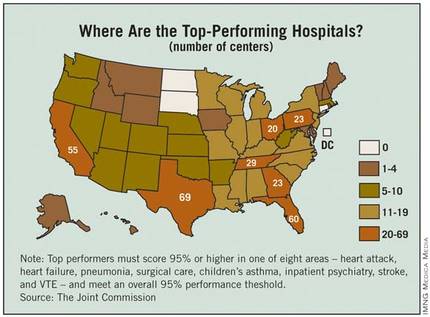
Joint Commission Names Top-Performing Hospitals
The number of hospitals considered to be top performers increased by 53% from 2011 to 2012, according to a report from the Joint Commission.
The commission recognized 620 hospitals, compared with 405 last year, as "top performers on key quality measures." Those 620 hospitals represent about 18% of the more than 3,300 that report performance data, with 244 making the list for the second year in a row. 2011 was the first year in which the commission released its list of top hospitals.
The Joint Commission said that it tracks hospital performance "on 45 accountability measures of evidence-based care processes linked to positive patient outcomes."
To be named a top performer, each hospital must achieve performance of 95% or more on a composite score in at least one of eight areas – heart attack, heart failure, pneumonia, surgical care, children’s asthma, inpatient psychiatry, stroke, and venous thromboembolism – including measures with fewer than 30 eligible cases. Each hospital also must meet or exceed "95% performance on every accountability measure for which it reports data," although this requirement excludes measures with fewer than 30 eligible cases, the commission said.
In addition to the top performers, the commission noted that 583 hospitals (17% of those reporting) missed 95% performance on only one measure.
The states with at least 20 top-performing hospitals tended to be the most populous states: Texas (69), Florida (60), California (55), Tennessee (29), Georgia (23), Pennsylvania (23), and Ohio (20). States without any top-performing hospitals tended to be among the lowest in population: North Dakota, South Dakota, and Connecticut (and the District of Columbia).
The number of hospitals considered to be top performers increased by 53% from 2011 to 2012, according to a report from the Joint Commission.
The commission recognized 620 hospitals, compared with 405 last year, as "top performers on key quality measures." Those 620 hospitals represent about 18% of the more than 3,300 that report performance data, with 244 making the list for the second year in a row. 2011 was the first year in which the commission released its list of top hospitals.

The Joint Commission said that it tracks hospital performance "on 45 accountability measures of evidence-based care processes linked to positive patient outcomes."
To be named a top performer, each hospital must achieve performance of 95% or more on a composite score in at least one of eight areas – heart attack, heart failure, pneumonia, surgical care, children’s asthma, inpatient psychiatry, stroke, and venous thromboembolism – including measures with fewer than 30 eligible cases. Each hospital also must meet or exceed "95% performance on every accountability measure for which it reports data," although this requirement excludes measures with fewer than 30 eligible cases, the commission said.
In addition to the top performers, the commission noted that 583 hospitals (17% of those reporting) missed 95% performance on only one measure.
The states with at least 20 top-performing hospitals tended to be the most populous states: Texas (69), Florida (60), California (55), Tennessee (29), Georgia (23), Pennsylvania (23), and Ohio (20). States without any top-performing hospitals tended to be among the lowest in population: North Dakota, South Dakota, and Connecticut (and the District of Columbia).
The number of hospitals considered to be top performers increased by 53% from 2011 to 2012, according to a report from the Joint Commission.
The commission recognized 620 hospitals, compared with 405 last year, as "top performers on key quality measures." Those 620 hospitals represent about 18% of the more than 3,300 that report performance data, with 244 making the list for the second year in a row. 2011 was the first year in which the commission released its list of top hospitals.

The Joint Commission said that it tracks hospital performance "on 45 accountability measures of evidence-based care processes linked to positive patient outcomes."
To be named a top performer, each hospital must achieve performance of 95% or more on a composite score in at least one of eight areas – heart attack, heart failure, pneumonia, surgical care, children’s asthma, inpatient psychiatry, stroke, and venous thromboembolism – including measures with fewer than 30 eligible cases. Each hospital also must meet or exceed "95% performance on every accountability measure for which it reports data," although this requirement excludes measures with fewer than 30 eligible cases, the commission said.
In addition to the top performers, the commission noted that 583 hospitals (17% of those reporting) missed 95% performance on only one measure.
The states with at least 20 top-performing hospitals tended to be the most populous states: Texas (69), Florida (60), California (55), Tennessee (29), Georgia (23), Pennsylvania (23), and Ohio (20). States without any top-performing hospitals tended to be among the lowest in population: North Dakota, South Dakota, and Connecticut (and the District of Columbia).